Interpretation of the Experts Consensus on the criteria for the diagnosis and grading of neonatal asphyxia in China
|
|
|
- Clyde Robbins
- 7 years ago
- Views:
Transcription
1 Guidelines Interpretation of the Experts Consensus on the criteria for the diagnosis and grading of neonatal asphyxia in China Zi-Li Chen 1, Jing Liu 2 1 Department of Neonatology, Beihai Maternal and Child Health Care Hospital, Beihai , China; 2 Bayi Children s Hospital, Affiliated to the General Hospital of Chinese PLA Beijing Military Region, Beijing , China Correspondence to: Zi-Li Chen. Department of Neonatology, Beihai Maternal and Child Health Care Hospital, Beihai , China. czl350@yahoo.com.cn. Submitted Mar 05, Accepted for publication Apr 03, doi: /j.issn View this article at: Neonatal asphyxia (NA) refers to a critically ill condition in which there is an acute interruption of gas exchange between mother and fetus via placental blood flow, causing severe fetal hypoxia and acidosis, which can be followed by the depression of respiratory,circulatory and central nervous systems. As a result, the neonates can not promptly gain and maintain normal breathing. However, there is still no relatively objective and scientifically rigorous assessment criteria for NA. Based on the research advances and real conditions in China and following the basic principles of evidence-based medicine, the Neonatal Professional Committee of Chinese Medical Doctor Association summoned a working panel to develop the diagnostic and grading criteria of NA to further standardize its clinical diagnosis and treatment (1). We hereby write this article to help the doctors further understand this Expert Consensus and apply it correctly in their clinical practices. Apgar score often results in a high false positive rate of NA Apgar score has been widely applied for the diagnosis of NA and the assessment of asphyxia degree in the past decades. However, it has many limitations (2); particularly, it has high sensitivity and low specificity, and the false positive rate of Apgar scoring can be up to 50-80% (3-5). Such a high misdiagnosis rate is resulted from the poorly defined diagnostic criteria, and can cause a series of medical, ethical and social issues. Other limitations of Apgar score in diagnosing NA include: (I) Although the Apgar score is useful for identifying the presence of respiratory depression in neonates, it can not indentify its pathophysiological nature and etiology; (II) the Apgar score does not emphasize the role of respiratory depression; rather, it equally assigns the scores to five components with different importance degree; (III) its accuracy in assessing NA is affected by the gestational age; and (IV) it is not feasible for neonates upon endotracheal intubation and positive-pressure ventilation (ETI/PPV). However, since Apgar score can generally reflect the clinical manifestations of neonates with respiration, circulation, and CNS depression, the current Expert Consensus still includes it as a major indicator for assessing NA; together with umbilical arterial ph, the Apgar score can be useful for the diagnosis of NA. During the panel meetings, the experts discussed why Apgar scores 7 at 1 minute after birth should be applied. Several international documents have proposed the use of 1-min Apgar scores 6 or 3, or 5-min Apgar score 7, 6, or 3. However, no clinical evidence has demonstrated that the modification of Apgar scores can improve its specificity without lowering its sensitivity. As we all know, a normal fetus takes the first breath within 2 seconds after delivery, cries within 5 seconds, and establishes the regular respiration within 10 s to 1 min. If an infant fails to establish spontaneous and effective respirations 1 min after birth, the situation can be problematic. Also, a study (3) has shown that 40% of infants with the Apgar scores 7 at 1 minute after birth had hypoxic organ injury. To avoid misdiagnosis, the Expert Consensus still uses failure to establish regular and effective respirations 1 min after birth (respiratory depression and Apgar score 7) as one of the diagnostic critera of NA, including those failure to establish
2 60 Chen and Liu. Interpretation of the Experts Consensus on the criteria regular and effective respirations 5 min after birth and Apgar score 7, or relatively high 1-min Apgar score but the infant experiences respiratory dysfunction with an 5-min Apgar score 7. In addition, for infants without spontaneous respiration or severe respiratory depression (e.g., without spontaneous breathing or with sobbing breaths), active and proper resuscitation may raise the 1-min Apgar score to 7 or higher. However, if the infants meet the other several criteria, they can still be diagnosed as with NA. High rate of missed NA remains problematic in the United States In the history, diagnosis of NA based on Apgar score alone had dramatically increased the diagnosis of NA. Therefore, many developed countries and regions have already ceased the application of Apgar score alone for NA diagnosis since 1990s. The diagnostic criteria (6) jointly released by American College of Obstetricians and Gynecologists (ACOG) and American Academy of Pediatrics (AAP) were once widely accepted. The criteria include (6): (I) umbilical arterial ph <7.00; (II) an Apgar score of 0 to 3 for longer than 5 minutes; (III) neurologic manifestation, e.g., seizure, coma, or hypotonia, and (IV) evidence of multiorgan dysfunction. In fact, diagnoses based on these criteria not only include asphyxia but also hypoxic-ischemic encephalopathy (HIE) and multiorgan dysfunction. However, clinical practices have shown that the rate of missed diagnosis reached 79-88% (7,8). Obviously, the above criteria is not feasible for clinical application. Risk factors of NA Many risk factors can result in NA: (I) Maternal factors: primiparous women aged >35 years or <16 years; hypertensive disorders of pregnancy (including preeclampsia and eclampsia); severe lung disease, asthma, heart disease, primary hypertension, kidney disease, epilepsy, diabetes, or thyroid disease; low urinary estriol; anemia (Hb <100 g/l); isoimmunization; placenta previa or placental abruption; hypotension; premature rupture of membranes; previous history of fetal death/stillbirth, or neonatal death. (II) Delivery-related factors: malposition; assisted deliveries (forceps, vacuum extractor, and internal podalic version); epidural anesthesia; prolonged labor; abnormal uterine contractions; use of oxytocin; or use of morphine-like analgesics and magnesium sulfate. (III) Fetal factors: umbilical cord problems; cephalopelvic disproportion; premature birth; post-term birth; twins & multiple births; abnormality in fetal heart rate or rhythm; decreased fetal movement; amniotic fluid volume abnormalities; meconium stained amniotic fluid; intrauterine growth restriction; macrosomia fetus; fetal acidosis; or fetal anemia (Hb <100 g/l). Research has identified 11 most significant risk factors: abnormal findings of fetal heart monitoring, fetal acidosis, placental abruption, placenta previa, abnormal fetal position, meconium stained amniotic fluid, forceps delivery, prolonged labor, abnormal uterine contraction, premature birth, and maternal asthma (9). Inclusion of the risk factors in the diagnostic criteria helps the doctors to be more alert about NE and take necessary measures to prevent its occurrence and development. For diagnosis, a risk factor just indicates that there is a possibility of NA and do not mean that NA will be unavoidable. In fact, the presence of a risk factor is not a direct evidence of asphyxia. A domestic prospective study involving tens of thousands of subjects showed that although all the NA infants had risk factors, only 1.37% of infants with risk factors suffered from asphyxia (9). Therefore, these risk factors are just used as a minor criterion for explaining the etiology. Umbilical cord arterial blood gas analysis Clinical significance of arterial blood gases In essence, asphyxia is the damaging hypoxemia and metabolic acidosis. Therefore, the diagnosis of NA should be based on more objective indicators to increase its accuracy and reliability. Among these indicators, umbilical cord arterial blood gas analysis provides a simple, accurate, and reliable tool. The results of umbilical cord arterial blood gas analysis at birth is a gold standard that reflects the blood gas and acid-base status immediately before birth (5), meanwhile it provides key evidences for analyzing the perinatal adverse events and neonatal status (5,10,11). Therefore, it has been widely accepted that umbilical cord arterial blood gas analysis should be added for neonates with low Apgar score to increase the accuracy of an NA diagnosis (12-15). The normal findings of umbilical cord arterial blood gas analysis is helpful to rule out the possibility of intrapartum asphyxia and its association with cerebral palsy (5,10,11), so as to avoid misdiagnoses and unnecessary legal disputes. Therefore, this Experts Consensus emphasizes the importance of umbilical cord arterial blood gas analysis
3 Translational Pediatrics, Vol 2, No 2 April 2013 in NA diagnosis. Umbilical blood gas determination and Apgar scoring complement each other Umbilical blood gas determination alone also has its limitations and can not be used as the only indicator for NA diagnosis. As shown in several large-scale domestic studies, except those with low Apgar scores, about 87% of neonates with umbilical arterial ph <7.00 did not have NA. On the contrary, the combination of umbilical arterial ph and Apgar score can overcome their shortcomings (3,4). Clinical significance and pathological threshold values of umbilical arterial blood gas parameters Among the umbilical arterial blood gas parameters, ph is most important. After the influence of maternal acidosis is ruled out, a decreased ph value can reflect the severity of neonatal hypoxia and acidosis. BE and PaCO 2 are helpful to identify the nature of acidosis. PaO 2 is least important, because the levels of PaCO 2 and PaO 2 fluctuate rapidly and dramatically, and can only reflect a transient condition at sampling. On the contrary, ph and BE reflect the outcomes of hypoxia and are more stable. Therefore, ph and/or BE have widely adopted for NA assessment. As shown in a domestic study (4) with an ultra-large sample size, due to the individual differences, the ph values in NA neonates were not at a fixed point but vary within a certain range. The combination of 1-min Apgar score with umbilical arterial ph <7.20 had a sensitivity of 100% for NA diagnosis, but its specificity was only 64.4%. As the ph value declines, its specificity for NA diagnosis gradually increases but the sensitivity decreases. A low 1-min Apgar score with umbilical arterial ph <7.00 yielded a specificity of 99% for diagnosing NA, while the sensitivity was only 41%. In contrast, a low 1-min Apgar score with umbilical arterial ph <7.15 had a sensitivity and specificity of about 80% for NA diagnosis (4). After balancing the sensitivity and specificity, the expert group decided to use ph <7.15 as the umbilical arterial blood gas parameter for NA diagnosis. In NA neonates, the distribution of BE values are more diffuse than that of ph values; thus, ph is superior to BE as an indicator for diagnosing NA. Importance of ruling out other causes The fourth criterion of NA diagnosis urges that other 61 causes of low Apgar score must be ruled out. This has not been seen in other criteria or recommendations on NA diagnosis. These causes include (2-4): (I) congenital malformations of the respiratory system; (II) congenital malformations of the circulation system; (III) congenital malformations of the central nervous system; (IV) neuromuscular disorders; (V) fetal hemorrhagic shock; (VI) fetal hydrops; or (VII) fetal passive drug toxicity from intrapartum high-dosage use of magnesium sulfate or anesthetic/analgesic agents to the mother. In fact, NA remains a major cause of medical disputes in China. All the above mentioned causes, particularly the congenital malformations, can mimic the clinical manifestations of NA. However, the maternal-fetal gas exchange through the placenta shows no disorder, the umbilical cord arterial blood gas remains normal, and there is no relationship with the measures taken by the medical staff during the labor. Therefore, these conditions should be properly diagnosed according to their specific etiologies and should not be misdiagnosed as NA. Therefore, the differential diagnosis added in the Experts Consensus can enhance the scientific rigorousness and accuracy of NA diagnosis, improve the doctor s understanding and management of NA, and avoid or minimize the misdiagnoses and their related medical disputes. Grading of NA Clinical experiences have shown that NA neonates (even without respiration or heart beating at birth) will not necessarily suffer from organ injury if they can gain timely and proper neonatal resuscitation. In recent years, unfortunately, NA-associated deaths in neonates are mainly resulted from various severe complications of NA. Therefore, after a neonate is transferred to the intensive care unit after resuscitation, any potential organ injury (and its severity) must be carefully examined. The grading of NA is helpful to guide the post-resuscitation management for NA infants. The care, monitoring, and treatment should be properly adjusted for infants with or without organ injury aand its severity, it has been shown that the incidence of organ injury is closely related with the severity of acidosis. As the umbilical cord arterial ph value decreased from 7.20 to <7.00, the organ injury rate gradually rose from 0.39% to 13.62%; in contrast, with the BE value dropped from 10 mmol/l to < 20 mmol/l, the organ injury rate gradually increased from 1.24% to 9.05% (4). The vital organs are often protected by some physiological
4 62 Chen and Liu. Interpretation of the Experts Consensus on the criteria mechanisms such as diving reflex in case of hypoxia. While brain is often the last damaged organ, brain injury is often associated with multiple organ dysfunction. However, in a neonate with acute total asphyxia, the body can not provide timely compensation; then, the brain can be damaged first (without multiple organ dysfunction) due to its high oxygen consumption rate and metabolism rate. Hypoxicischemic organ injury is a marker of decompensation during the pathophysiologic process of asphyxia, indicating that the persistent, severe hypoxia has developed from the physiological stress compensation to pathological decompensation. Therefore, it can be used for grading the severity of asphyxia. In the presence of other NA criteria, asphyxia cases without organ injury can be diagnosed as mild and those with organ injury as severe. The diagnosis of organ injury can be based on the criteria proposed by the Subspecialty Group of Neonatology, Pediatric Society, Chinese Medical Association and in the monograph Practical Neonatology (16,17). Key points During the clinical application of the Experts Consensus, the medical staff must pay attention to the following key points: (I) Among these NA diagnostic criteria, the first one is a minor criterion and the others are the major criteria; (II) Once a neonate at high risk of asphyxia is born in the delivery room or operating room, clamp a segment of umbilical cord (near the fetal side) with two sterile hemostats immediately, cut off the umbilical cord from the outer side of the hemostats, and sampling the umbilical cord arterial blood from the cut down umbilical cord for blood gas analysis; (III) For neonates without spontaneous respiration or with severe respiratory depression at birth and/or with low Apgar scores 1 min or longer after birth, umbilical cord arterial blood gas analysis must be conducted; if no such abnormality is found, the cut down umbilical cord specimen can be discarded; (IV) Non-vigorous neonates with low Apgar score at birth should be timely transferred to neonatal intensive care unit after proper resuscitation, in which they should undergo further examinations for the presence of organ injury and differential diagnosis and receive appropriate medical care. In summary, the Experts Consensus on the Criteria for the Diagnosis and Grading of Neonatal Asphyxia in China developed by the Neonatal Professional Committee of Chinese Medical Doctor Association will play an active role in standardize the diagnosis and treatment of NA and avoid/minimize medical disputes. However, since the nature of NA is still poorly understood and the development of medical sciences still has many limitations, this Experts Consensus is still far from perfect and warrants further revisions in the coming years. Acknowledgements None. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. References 1. Neonatal Professional Committee of Chinese Medical Doctor Association. Experts consensus on the criteria for the diagnosis and grading of neonatal asphyxia in China. Zhongguo Dang Dai Er Ke Za Zhi 2013;15:1. 2. American Academy of Pediatrics, Committee on Fetus and Newborn, American College of Obstetricians and Gynecologists and Committee on Obstetric Practice. The Apgar score. Pediatrics 2006;117: Chen ZL, He RZ, Peng Q, et al. Clinical study on improving the diagnostic criteria for neonatal asphyxia. Zhonghua Er Ke Za Zhi 2006;44: Collaborative Study Group of Neonatal Umbilical Cord Blood Gas Parameters. Multicenter clinical study on umbilical cord arterial blood gas parameters for diagnosis of neonatal asphyxia. Zhonghua Er Ke Za Zhi 2010;48: Thorp JA, Rushing RS. Umbilical cord blood gas analysis. Obstet Gynecol Clin North Am 1999;26: Use and abuse of the Apgar score. Committee on Fetus and Newborn, American Academy of Pediatrics, and Committee on Obstetric Practice, American College of Obstetricians and Gynecologists. Pediatrics 1996;98: Korst LM, Phelan JP, Wang YM, et al. Acute fetal asphyxia and permanent brain injury: a retrospective analysis of current indicators. J Matern Fetal Med 1999;8: Murphy-Kaulbeck L, Bland E, Oppenheimer L. Neonatal encephalopathy and asphyxia: revisiting diagnostic criteria. Otawa: Canadian OB/GYN Society, Chen ZL, He RZ, Peng Q, et al. Prenatal risk factors for neonatal asphyxia: how risk for each? Zhongguo Dang Dai
5 Translational Pediatrics, Vol 2, No 2 April Er Ke Za Zhi 2009;11: ACOG Committee on Obstetric Practice. ACOG Committee Opinion No. 348, November 2006: Umbilical cord blood gas and acid-base analysis. Obstet Gynecol 2006;108: Blickstein I, Green T. Umbilical cord blood gases. Clin Perinatol 2007;34: White CR, Doherty DA, Henderson JJ, et al. Benefits of introducing universal umbilical cord blood gas and lactate analysis into an obstetric unit. Aust N Z J Obstet Gynaecol 2010;50: Malin GL, Morris RK, Khan KS. Strength of association between umbilical cord ph and perinatal and long term outcomes: systematic review and meta-analysis. BMJ 2010;340:c Armstrong L, Stenson BJ. Use of umbilical cord blood gas analysis in the assessment of the newborn. Arch Dis Child Fetal Neonatal Ed 2007;92:F Chen ZL. Correct use of umbilical cord arterial blood gas analysis in perinatal medicine. Zhongguo Dang Dai Er Ke Za Zhi 2010;12: Subspecialty Group of Neonatology, Pediatric Society, Chinese Medical Association. Diagnostic criteria of neonatal hypoxic-ischemic brain diseases. Zhongguo Dang Dai Er Ke Za Zhi 2005;7: Yu RJ. Multiorgan injury in neonatal asphysia. In: Shao XM, Ye HM, Qiu XS. eds. Practical Neonatology. 4th edition. Beijing: People s Health Publishing House, 2011: Cite this article as: Chen ZL, Liu J. Interpretation of the Experts Consensus on the criteria for the diagnosis and grading of neonatal asphyxia in China.. doi: /j.issn
A8b. Resuscitation of a Term Infant with Meconium Staining. Session Summary. Session Objectives. References
 A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
CORD BLOOD COLLECTION / ANALYSIS- AT BIRTH
 WOMEN AND NEWBORN HEALTH SERVICE King Edward Memorial Hospital CLINICAL GUIDELINES OBSTETRICS AND MIDWIFERY King Edward Memorial Hospital WOMEN AND NEWBORN HEALTH SERVICE INTRAPARTUM CARE SPECIMEN COLLECTION
WOMEN AND NEWBORN HEALTH SERVICE King Edward Memorial Hospital CLINICAL GUIDELINES OBSTETRICS AND MIDWIFERY King Edward Memorial Hospital WOMEN AND NEWBORN HEALTH SERVICE INTRAPARTUM CARE SPECIMEN COLLECTION
Fetal Acid Base Status and Umbilical Cord Sampling. David Acker, MD
 Fetal Acid Base Status and Umbilical Cord Sampling David Acker, MD Part I: Some Background Intra-uterine Event as Causative of CP Cord ph < 7.00 and base excess of > 12 Early onset neonatal encephalopathy
Fetal Acid Base Status and Umbilical Cord Sampling David Acker, MD Part I: Some Background Intra-uterine Event as Causative of CP Cord ph < 7.00 and base excess of > 12 Early onset neonatal encephalopathy
Cord Blood Erythropoietin and Markers of Fetal Hypoxia
 July 21, 2011 By NeedsFixing [1] To investigating the relationship between cord blood erythropoietin and clinical markers of fetal hypoxia. Abstract Objective: To investigating the relationship between
July 21, 2011 By NeedsFixing [1] To investigating the relationship between cord blood erythropoietin and clinical markers of fetal hypoxia. Abstract Objective: To investigating the relationship between
Physiologic Basis for Fetal Heart Rate Monitoring
 Physiologic Basis for Fetal Heart Rate Monitoring Physiologic Basis for Fetal Heart Rate Monitoring The objective of intrapartum fetal heart rate (FHR) monitoring is to prevent fetal injury that might
Physiologic Basis for Fetal Heart Rate Monitoring Physiologic Basis for Fetal Heart Rate Monitoring The objective of intrapartum fetal heart rate (FHR) monitoring is to prevent fetal injury that might
Newborn outcomes after cesarean section for fetal distress in BC
 Newborn outcomes after cesarean section for fetal distress in BC Patricia Janssen, PhD, UBC School of Population and Public Health Scientist, Child and Family Research Institute Kevin Jenniskens, MSc,
Newborn outcomes after cesarean section for fetal distress in BC Patricia Janssen, PhD, UBC School of Population and Public Health Scientist, Child and Family Research Institute Kevin Jenniskens, MSc,
BIRTH INJURY AND NEWBORN BRAIN DAMAGE
 BIRTH INJURY AND NEWBORN BRAIN DAMAGE ROBERT J. TALASKA 1415 North Loop West Suite 200 Houston, Texas 77008 713.869.1240 713.869.1465 fax State Bar of Texas 15 TH ANNUAL ADVANCED MEDICAL MALPRACTICE COURSE
BIRTH INJURY AND NEWBORN BRAIN DAMAGE ROBERT J. TALASKA 1415 North Loop West Suite 200 Houston, Texas 77008 713.869.1240 713.869.1465 fax State Bar of Texas 15 TH ANNUAL ADVANCED MEDICAL MALPRACTICE COURSE
What do we mean by birth asphyxia
 Neonatal Medicine and brain injury in the Infant at term Andrew Whitelaw Professor of Neonatal Medicine University of Bristol What do we mean by birth asphyxia Interruption in oxygen delivery to the fetus
Neonatal Medicine and brain injury in the Infant at term Andrew Whitelaw Professor of Neonatal Medicine University of Bristol What do we mean by birth asphyxia Interruption in oxygen delivery to the fetus
Cerebral Palsy An Expensive Enigma
 Cerebral Palsy An Expensive Enigma Rhona Mahony National Maternity Hospital A group of permanent disorders of the development of movement and posture, causing activity limitation that are not attributed
Cerebral Palsy An Expensive Enigma Rhona Mahony National Maternity Hospital A group of permanent disorders of the development of movement and posture, causing activity limitation that are not attributed
Brain Injury during Fetal-Neonatal Transition
 Brain Injury during Fetal-Neonatal Transition Adre du Plessis, MBChB Fetal and Transitional Medicine Children s National Medical Center Washington, DC Brain injury during fetal-neonatal transition Injury
Brain Injury during Fetal-Neonatal Transition Adre du Plessis, MBChB Fetal and Transitional Medicine Children s National Medical Center Washington, DC Brain injury during fetal-neonatal transition Injury
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
BIRTH ASPHYXIA The New Consensus Statement
 P.E.L.T. 2015 BIRTH ASPHYXIA The New Consensus Statement Keith Bolton Rahima Moosa Mother & Child Hospital THE HERD IS UNDER THREAT HPCSA CIVIL COURTS CRIMINAL COURTS Background The child with cerebral
P.E.L.T. 2015 BIRTH ASPHYXIA The New Consensus Statement Keith Bolton Rahima Moosa Mother & Child Hospital THE HERD IS UNDER THREAT HPCSA CIVIL COURTS CRIMINAL COURTS Background The child with cerebral
The New England. Copyright 2001 by the Massachusetts Medical Society THE CONTINUING VALUE OF THE APGAR SCORE FOR THE ASSESSMENT OF NEWBORN INFANTS
 The New England Journal of Medicine Copyright 21 by the Massachusetts Medical Society VOLUME 344 F EBRUARY, 21 NUMBER 7 THE CONTINUING VALUE OF THE APGAR SCORE FOR THE ASSESSMENT OF NEWBORN INFANTS BRIAN
The New England Journal of Medicine Copyright 21 by the Massachusetts Medical Society VOLUME 344 F EBRUARY, 21 NUMBER 7 THE CONTINUING VALUE OF THE APGAR SCORE FOR THE ASSESSMENT OF NEWBORN INFANTS BRIAN
Correlation between Umbilical Cord ph and Apgar Score in High Risk Pregnancy
 Original Article Iran J Pediatr Dec 2010; Vol 20 (No 4), Pp:401-406 Correlation between Umbilical Cord ph and Apgar Score in High Risk Pregnancy Mousa Ahmadpour Kacho* 1, MD; Nesa Asnafi 2, MD; Maryam
Original Article Iran J Pediatr Dec 2010; Vol 20 (No 4), Pp:401-406 Correlation between Umbilical Cord ph and Apgar Score in High Risk Pregnancy Mousa Ahmadpour Kacho* 1, MD; Nesa Asnafi 2, MD; Maryam
Identification of peripartum near-miss for perinatal audit
 Facts Views Vis Obgyn, 2014, 6 (4): 177-183 Original paper Identification of peripartum near-miss for perinatal audit C. Kerkhofs 1, C. De Bruyn 1, T. Mesens 1, C. Theyskens 2, M. Vanhoestenberghe 2, E.
Facts Views Vis Obgyn, 2014, 6 (4): 177-183 Original paper Identification of peripartum near-miss for perinatal audit C. Kerkhofs 1, C. De Bruyn 1, T. Mesens 1, C. Theyskens 2, M. Vanhoestenberghe 2, E.
Careful collection, organization and review of medical information
 Preparing Birth Injury Case Prior To Expert Review of Causation Careful collection, organization and review of medical information essential to documentation of injury By RICHARD A. SILVER When analyzing
Preparing Birth Injury Case Prior To Expert Review of Causation Careful collection, organization and review of medical information essential to documentation of injury By RICHARD A. SILVER When analyzing
What percentage of term cerebral palsy cases have a normal head MRI? Cerebral Palsy: Definition. No financial conflicts of interest to report
 Cerebral Palsy: Risk Factors and Etiology No financial conflicts of interest to report William M. Gilbert, MD Regional Medical Director, Women s Services Sutter Health, Sac-Sierra Region What percentage
Cerebral Palsy: Risk Factors and Etiology No financial conflicts of interest to report William M. Gilbert, MD Regional Medical Director, Women s Services Sutter Health, Sac-Sierra Region What percentage
Oregon Birth Outcomes, by Planned Birth Place and Attendant Pursuant to: HB 2380 (2011)
 Oregon Birth Outcomes, by Birth Place and Attendant Pursuant to: HB 2380 (2011) In 2011, the Oregon Legislature passed House Bill 2380, which required the Oregon Public Health Division to add two questions
Oregon Birth Outcomes, by Birth Place and Attendant Pursuant to: HB 2380 (2011) In 2011, the Oregon Legislature passed House Bill 2380, which required the Oregon Public Health Division to add two questions
Rural Health Advisory Committee s Rural Obstetric Services Work Group
 Rural Health Advisory Committee s Rural Obstetric Services Work Group March 15 th webinar topic: Rural Obstetric Patient and Community Issues Audio: 888-742-5095, conference code 6054760826 Rural Obstetric
Rural Health Advisory Committee s Rural Obstetric Services Work Group March 15 th webinar topic: Rural Obstetric Patient and Community Issues Audio: 888-742-5095, conference code 6054760826 Rural Obstetric
A look at continuing developments in the field, including history of fetal monitoring and causation issues
 Medical malpractice: Preparation and trial of birth injury cases A look at continuing developments in the field, including history of fetal monitoring and causation issues BY JAMES BOSTWICK Over the past
Medical malpractice: Preparation and trial of birth injury cases A look at continuing developments in the field, including history of fetal monitoring and causation issues BY JAMES BOSTWICK Over the past
Measurement of fetal scalp lactate to determine fetal well being in labour
 Measurement of fetal scalp lactate to determine fetal well being in labour Clinical question Among women at term in labour is the measurement of fetal scalp lactate superior to fetal scalp ph in predicting
Measurement of fetal scalp lactate to determine fetal well being in labour Clinical question Among women at term in labour is the measurement of fetal scalp lactate superior to fetal scalp ph in predicting
Umbilical Arterial Blood Gas and Perinatal Outcome in the Second Twin according to the Planned Mode of Delivery
 643 Ivyspring International Publisher Research Paper International Journal of Medical Sciences 2011; 8(8):643-648 Umbilical Arterial Blood Gas and Perinatal Outcome in the Second Twin according to the
643 Ivyspring International Publisher Research Paper International Journal of Medical Sciences 2011; 8(8):643-648 Umbilical Arterial Blood Gas and Perinatal Outcome in the Second Twin according to the
TIMING OF ASPHYXIAL INJURY AND BIRTH TRAUMA
 TIMING OF ASPHYXIAL INJURY AND BIRTH TRAUMA Richard C. Halpern, Partner, Thomson Rogers Obstetric Malpractice cases involving asphyxiated newborns present unique challenges to Plaintiffs counsel. Standard
TIMING OF ASPHYXIAL INJURY AND BIRTH TRAUMA Richard C. Halpern, Partner, Thomson Rogers Obstetric Malpractice cases involving asphyxiated newborns present unique challenges to Plaintiffs counsel. Standard
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context
 Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
How To Test For Fetal Blood
 Fetal (FBS) / paired cord blood sampling guideline (GL839) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Mr Mark Selinger, Consultant
Fetal (FBS) / paired cord blood sampling guideline (GL839) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Mr Mark Selinger, Consultant
The importance of acidosis in asphyxia
 The importance of acidosis in asphyxia Janet M Rennie Senior Lecturer in Neonatal Medicine Institute for Women s Health, UCL, London Clinical negligence seminar, 1 Crown Office Row Objectives To review
The importance of acidosis in asphyxia Janet M Rennie Senior Lecturer in Neonatal Medicine Institute for Women s Health, UCL, London Clinical negligence seminar, 1 Crown Office Row Objectives To review
C. P. Noel McCarthy, MD 1936 1936--2009 2009 Risk Reduction Strategies in Risk Obstetrics & Gynecology
 C. P. Noel McCarthy, MD 1936-2009 Risk Reduction Strategies in Obstetrics & Gynecology John F. Rodis, MD Professor of Clinical Obstetrics & Gynecology Columbia University College of Physicians & Surgeons
C. P. Noel McCarthy, MD 1936-2009 Risk Reduction Strategies in Obstetrics & Gynecology John F. Rodis, MD Professor of Clinical Obstetrics & Gynecology Columbia University College of Physicians & Surgeons
Obstetric Guideline 6B ELECTRONIC FETAL MONITORING IN LABOUR, SCALP SAMPLING, & CORD BLOOD GASES
 British Columbia Reproductive Care Program Obstetric Guideline 6B ELECTRONIC FETAL MONITORING IN LABOUR, SCALP SAMPLING, & CORD BLOOD GASES 1. PREAMBLE Meta-analysis of randomized clinical trials 1,2 indicate
British Columbia Reproductive Care Program Obstetric Guideline 6B ELECTRONIC FETAL MONITORING IN LABOUR, SCALP SAMPLING, & CORD BLOOD GASES 1. PREAMBLE Meta-analysis of randomized clinical trials 1,2 indicate
Re-Evaluation of Cord Blood Arterial and Venous Reference Ranges for ph, po 2, pco 2, According to Spontaneous or Cesarean Delivery
 Journal of Clinical Laboratory Analysis 24 : 300 304 (2010) Re-Evaluation of Cord Blood Arterial and Venous Reference Ranges for ph, po 2, pco 2, According to Spontaneous or Cesarean Delivery K. Kotaska,
Journal of Clinical Laboratory Analysis 24 : 300 304 (2010) Re-Evaluation of Cord Blood Arterial and Venous Reference Ranges for ph, po 2, pco 2, According to Spontaneous or Cesarean Delivery K. Kotaska,
Severe Newborn Encephalopathy Unrelated to Intrapartum Hypoxic Events: 3 Case Reports
 653 Severe Newborn Encephalopathy Unrelated to Intrapartum Hypoxic Events: 3 Case Reports T C Tan,*MBBS, T Y T Tan,**M Med (O&G), MRANZCOG, MRCOG, K Y C Kwek,***M Med (O&G), MRACOG, MRCOG, J C S Tee, +
653 Severe Newborn Encephalopathy Unrelated to Intrapartum Hypoxic Events: 3 Case Reports T C Tan,*MBBS, T Y T Tan,**M Med (O&G), MRANZCOG, MRCOG, K Y C Kwek,***M Med (O&G), MRACOG, MRCOG, J C S Tee, +
Advanced Fetal Assessment and Monitoring: Online Program. Advanced Practice Strategies, LLC
 Advanced Fetal Assessment and Monitoring: Online Program Advanced Fetal Assessment and Monitoring: Online Program Comments from the Authors As a physician who does a great deal of medical legal expert
Advanced Fetal Assessment and Monitoring: Online Program Advanced Fetal Assessment and Monitoring: Online Program Comments from the Authors As a physician who does a great deal of medical legal expert
Obstetrical Emergencies
 Date: July 18, 2014 Page 1 of 5 Obstetrical Emergencies Purpose: To provide the process for the assessment and management of the patient with an obstetrical related emergency. Pre-Medical Control 1. Follow
Date: July 18, 2014 Page 1 of 5 Obstetrical Emergencies Purpose: To provide the process for the assessment and management of the patient with an obstetrical related emergency. Pre-Medical Control 1. Follow
ST Segment Analysis (STAN) as an Adjunct to Electronic Fetal Monitoring, Part II: Clinical Studies and Future Directions
 ST Segment Analysis (STAN) as an Adjunct to Electronic Fetal Monitoring, Part II: Clinical Studies and Future Directions Michael A. Belfort, MBBCH, MD, PhD*, George R. Saade, MD KEYWORDS ST segment analysis
ST Segment Analysis (STAN) as an Adjunct to Electronic Fetal Monitoring, Part II: Clinical Studies and Future Directions Michael A. Belfort, MBBCH, MD, PhD*, George R. Saade, MD KEYWORDS ST segment analysis
Umbilical-Cord Blood Gas Analysis in Obstetrical Practice
 Umbilical-Cord Blood Gas Analysis in Obstetrical Practice Webinar - Wednesday, July 1, 2015 Jan Stener Jørgensen, MD, PhD Head of Obstetrics Professor of Clinical Obstetrics Odense University Hospital
Umbilical-Cord Blood Gas Analysis in Obstetrical Practice Webinar - Wednesday, July 1, 2015 Jan Stener Jørgensen, MD, PhD Head of Obstetrics Professor of Clinical Obstetrics Odense University Hospital
Newborn Neurological Injury and Litigation: Medical Legal Challenges to Causation
 Newborn Neurological Injury and Litigation: Medical Legal Challenges to Causation Richard C. Halpern Thomson Rogers July 12, 2011 INTRODUCTION Newborn neurological injury due to trauma occurring in and
Newborn Neurological Injury and Litigation: Medical Legal Challenges to Causation Richard C. Halpern Thomson Rogers July 12, 2011 INTRODUCTION Newborn neurological injury due to trauma occurring in and
Chapter 14. Board of Certified Direct-Entry Midwives.
 Chapter 14. Board of Certified Direct-Entry Midwives. (Words in boldface and underlined indicate language being added; words [CAPITALIZED AND BRACKETED] indicate language being deleted. Complete new sections
Chapter 14. Board of Certified Direct-Entry Midwives. (Words in boldface and underlined indicate language being added; words [CAPITALIZED AND BRACKETED] indicate language being deleted. Complete new sections
Priya Rajan, MD Northwestern University September 13, 2013
 Priya Rajan, MD Northwestern University September 13, 2013 o Study Finds Benefits in Delaying Severing of Umbilical Cord nytimes.com, 7/10/13 o Delay cord clamping for baby health, say experts bbc.com.uk,
Priya Rajan, MD Northwestern University September 13, 2013 o Study Finds Benefits in Delaying Severing of Umbilical Cord nytimes.com, 7/10/13 o Delay cord clamping for baby health, say experts bbc.com.uk,
OET: Listening Part A: Influenza
 Listening Test Part B Time allowed: 23 minutes In this part, you will hear a talk on critical illnesses due to A/H1N1 influenza in pregnant and postpartum women, given by a medical researcher. You will
Listening Test Part B Time allowed: 23 minutes In this part, you will hear a talk on critical illnesses due to A/H1N1 influenza in pregnant and postpartum women, given by a medical researcher. You will
Intrapartum Fetal Heart Rate Monitoring. A Standardized Approach to Interpretation and Management
 Intrapartum Fetal Heart Rate Monitoring A Standardized Approach to Interpretation and Management Lecture Objectives At the end of this program, participants will be able to: Review standardized FHR terminology
Intrapartum Fetal Heart Rate Monitoring A Standardized Approach to Interpretation and Management Lecture Objectives At the end of this program, participants will be able to: Review standardized FHR terminology
CHAPTER 11 FETAL HEALTH SURVEILLANCE IN LABOUR
 CHAPTER 11 FETAL HEALTH SURVEILLANCE IN LABOUR Learning Objectives By the end of this chapter, the participant will: 1. Define and recognize normal (reassuring), atypical and abnormal (non-reassuring)
CHAPTER 11 FETAL HEALTH SURVEILLANCE IN LABOUR Learning Objectives By the end of this chapter, the participant will: 1. Define and recognize normal (reassuring), atypical and abnormal (non-reassuring)
Cord Blood Lactate and ph Values at Term and Perinatal Outcome: A Retrospective Cohort Study
 Article ID: WMC00694 ISSN 2046-1690 Cord Blood Lactate and ph Values at Term and Perinatal Outcome: A Retrospective Cohort Study Author(s):Dr. Qemer Khoshnow, Dr. Max Mongelli Corresponding Author: Dr.
Article ID: WMC00694 ISSN 2046-1690 Cord Blood Lactate and ph Values at Term and Perinatal Outcome: A Retrospective Cohort Study Author(s):Dr. Qemer Khoshnow, Dr. Max Mongelli Corresponding Author: Dr.
Second stage fetal heart rate patterns and neonatal acid-base status Faridah Hanim Zam Zam 1, Nazimah Idris 2, Tham Seng Woh 1
 Original Article IeJSME 2012 6(2): 18-23 Second stage fetal heart rate patterns and neonatal acid-base status Faridah Hanim Zam Zam 1, Nazimah Idris 2, Tham Seng Woh 1 Background: Fetal surveillance in
Original Article IeJSME 2012 6(2): 18-23 Second stage fetal heart rate patterns and neonatal acid-base status Faridah Hanim Zam Zam 1, Nazimah Idris 2, Tham Seng Woh 1 Background: Fetal surveillance in
UMBILICAL CORD CLAMPING FOR TERM INFANTS 37 WEEKS
 UMBILICAL CORD CLAMPING FOR TERM INFANTS 37 WEEKS This guideline refers to umbilical cord clamping in term infants (those 37 weeks gestational age) DEFINITION Immediate (early) cord clamping (ICC): the
UMBILICAL CORD CLAMPING FOR TERM INFANTS 37 WEEKS This guideline refers to umbilical cord clamping in term infants (those 37 weeks gestational age) DEFINITION Immediate (early) cord clamping (ICC): the
Delayed Cord Clamping
 ICEA Position Paper Delayed Cord Clamping Position The International Childbirth Education Association recognizes that the first minutes after birth are crucial to both mother and newborn. Optimal care
ICEA Position Paper Delayed Cord Clamping Position The International Childbirth Education Association recognizes that the first minutes after birth are crucial to both mother and newborn. Optimal care
SWISS SOCIETY OF NEONATOLOGY. Umbilical cord complications in two subsequent pregnancies
 SWISS SOCIETY OF NEONATOLOGY Umbilical cord complications in two subsequent pregnancies June 2006 2 Hetzel PG, Godi E, Bührer C, Department of Neonatology (HPG, BC), University Children s Hospital, Basel,
SWISS SOCIETY OF NEONATOLOGY Umbilical cord complications in two subsequent pregnancies June 2006 2 Hetzel PG, Godi E, Bührer C, Department of Neonatology (HPG, BC), University Children s Hospital, Basel,
Quality of Birth Certificate Data. Daniela Nitcheva, PhD Division of Biostatistics PHSIS
 Quality of Birth Certificate Data Daniela Nitcheva, PhD Division of Biostatistics PHSIS Data Quality SC State Law requires that you file the birth certificate within 5 days of a child s birth. Data needs
Quality of Birth Certificate Data Daniela Nitcheva, PhD Division of Biostatistics PHSIS Data Quality SC State Law requires that you file the birth certificate within 5 days of a child s birth. Data needs
The effect of blood gas and Apgar score on cord blood cardiac Troponin I
 The 2004;16:315 319 Case Report The effect of blood gas and Apgar score on cord blood cardiac Troponin I Gülcan Türker, Kadir Babaoğlu, Can Duman, Ayşe S Gökalp, Emine Zengin and Ayşe Engin Arısoy From
The 2004;16:315 319 Case Report The effect of blood gas and Apgar score on cord blood cardiac Troponin I Gülcan Türker, Kadir Babaoğlu, Can Duman, Ayşe S Gökalp, Emine Zengin and Ayşe Engin Arısoy From
INTRAPARTUM PATHWAYS TO NEONATAL NEUROLOGIC INJURY - A LAWYER S VIEW OF THE MEDICINE
 INTRAPARTUM PATHWAYS TO NEONATAL NEUROLOGIC INJURY - A LAWYER S VIEW OF THE MEDICINE By Richard C. Halpern Partner Thomson Rogers rhalpern@thomsonrogers.com 416-868-3215 November 2013 INTRODUCTION Newborn
INTRAPARTUM PATHWAYS TO NEONATAL NEUROLOGIC INJURY - A LAWYER S VIEW OF THE MEDICINE By Richard C. Halpern Partner Thomson Rogers rhalpern@thomsonrogers.com 416-868-3215 November 2013 INTRODUCTION Newborn
Clinical Policy Title: Home uterine activity monitoring
 Clinical Policy Title: Home uterine activity monitoring Clinical Policy Number: 12.01.01 Effective Date: August 19, 2015 Initial Review Date: July 17, 2013 Most Recent Review Date: July 15, 2015 Next Review
Clinical Policy Title: Home uterine activity monitoring Clinical Policy Number: 12.01.01 Effective Date: August 19, 2015 Initial Review Date: July 17, 2013 Most Recent Review Date: July 15, 2015 Next Review
SOUTHERN WEST MIDLANDS NEWBORN NETWORK
 SOUTHERN WEST MIDLANDS NEWBORN NETWORK Hereford, Worcester, Birmingham, Sandwell & Solihull Title Person Responsible for Review Delayed Umbilical Cord Clamping Dr Andrew Gallagher Date Guideline Agreed:
SOUTHERN WEST MIDLANDS NEWBORN NETWORK Hereford, Worcester, Birmingham, Sandwell & Solihull Title Person Responsible for Review Delayed Umbilical Cord Clamping Dr Andrew Gallagher Date Guideline Agreed:
Doppler Ultrasound in the Management of Fetal Growth Restriction Chukwuma I. Onyeije, M.D. Atlanta Perinatal Associates
 Doppler Ultrasound in the Management of Fetal Growth Restriction Chukwuma I. Onyeije, M.D. Atlanta Perinatal Associates 1 For your convenience a copy of this lecture is available for review and download
Doppler Ultrasound in the Management of Fetal Growth Restriction Chukwuma I. Onyeije, M.D. Atlanta Perinatal Associates 1 For your convenience a copy of this lecture is available for review and download
Neonatal Emergencies. Care of the Neonate. Care of the Neonate. Care of the Neonate. Student Objectives. Student Objectives continued.
 Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
 GUIDELINES FOR HOSPITALS WITH NEONATAL INTENSIVE CARE SERVICE : REGULATION 4 OF THE PRIVATE HOSPITALS AND MEDICAL CLINICS REGULATIONS [CAP 248, Rg 1] I Introduction 1. These Guidelines serve as a guide
GUIDELINES FOR HOSPITALS WITH NEONATAL INTENSIVE CARE SERVICE : REGULATION 4 OF THE PRIVATE HOSPITALS AND MEDICAL CLINICS REGULATIONS [CAP 248, Rg 1] I Introduction 1. These Guidelines serve as a guide
Post - resuscitation management of an asphyxiated neonate
 Post - resuscitation management of an asphyxiated neonate Slide PA 1, 2 Introduction Perinatal asphyxia is a common neonatal problem and contributes significantly to neonatal morbidity and mortality. It
Post - resuscitation management of an asphyxiated neonate Slide PA 1, 2 Introduction Perinatal asphyxia is a common neonatal problem and contributes significantly to neonatal morbidity and mortality. It
Evaluation of cardiotocographic and cord blood changes in induced labor with dinoprostone and misoprostol
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Pandey K et al. Int J Reprod Contracept Obstet Gynecol. 2014 Mar;3(1):199-203 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Pandey K et al. Int J Reprod Contracept Obstet Gynecol. 2014 Mar;3(1):199-203 www.ijrcog.org pissn 2320-1770 eissn 2320-1789
Corporate Reimbursement Policy
 Corporate Reimbursement Policy Guidelines for Global Maternity Reimbursement File Name: Origination: Last Review: Next Review: guidelines_for_global_maternity_reimbursement 10/2003 7/2016 7/2017 Description
Corporate Reimbursement Policy Guidelines for Global Maternity Reimbursement File Name: Origination: Last Review: Next Review: guidelines_for_global_maternity_reimbursement 10/2003 7/2016 7/2017 Description
Cardiovascular Disease and Maternal Mortality what do we know and what are the key questions?
 Cardiovascular Disease and Maternal Mortality what do we know and what are the key questions? AFSHAN HAMEED, MD, FACOG, FACC Associate Clinical Professor Maternal Fetal Medicine and Cardiology University
Cardiovascular Disease and Maternal Mortality what do we know and what are the key questions? AFSHAN HAMEED, MD, FACOG, FACC Associate Clinical Professor Maternal Fetal Medicine and Cardiology University
Pregnancy and Substance Abuse
 Pregnancy and Substance Abuse Introduction When you are pregnant, you are not just "eating for two." You also breathe and drink for two, so it is important to carefully consider what you put into your
Pregnancy and Substance Abuse Introduction When you are pregnant, you are not just "eating for two." You also breathe and drink for two, so it is important to carefully consider what you put into your
How To Compare Pregnancy Complications With Pregnancy And Labor
 Correlation between Intrapartum Cardiotocogram Findings and Cord Blood ph in Term and Preterm Labours Sarah SC CHAN MBBS, MRCOG William WK TO MBBS, MPhil, FRCOG, FHKAM (O&G) Department of Obstetrics and
Correlation between Intrapartum Cardiotocogram Findings and Cord Blood ph in Term and Preterm Labours Sarah SC CHAN MBBS, MRCOG William WK TO MBBS, MPhil, FRCOG, FHKAM (O&G) Department of Obstetrics and
Certified Professional Midwives Caring for Mothers and Babies in Virginia
 Certified Professional Midwives Caring for Mothers and Babies in Virginia Commonwealth Midwives Alliance Certified Professional Midwives in VA Licensed by the BOM since January 2006 5 member Midwifery
Certified Professional Midwives Caring for Mothers and Babies in Virginia Commonwealth Midwives Alliance Certified Professional Midwives in VA Licensed by the BOM since January 2006 5 member Midwifery
Distortions in Fetal Growth Standards
 Pediat. Res. 12: 987-991 (1978) Fetus fetal growth retardation fetal growth standards Distortions in Fetal Growth Standards RICHARD L. NAEYE"" AND JOSEPH B. DIXON Department of Pathology and Research Computing
Pediat. Res. 12: 987-991 (1978) Fetus fetal growth retardation fetal growth standards Distortions in Fetal Growth Standards RICHARD L. NAEYE"" AND JOSEPH B. DIXON Department of Pathology and Research Computing
Diagnosis Codes for Pregnancy and Complications of Pregnancy
 This list is for informational purposes only and is not a binding or definitive list of covered conditions. It is not a guarantee of coverage; coverage depends on the available benefits and eligibility
This list is for informational purposes only and is not a binding or definitive list of covered conditions. It is not a guarantee of coverage; coverage depends on the available benefits and eligibility
FETAL SCALP LACTATE RESEARCH STUDY COMPARISON OF TWO POINT OF CARE METERS
 FETAL SCALP LACTATE RESEARCH STUDY COMPARISON OF TWO POINT OF CARE METERS Presentation to Healthy Mothers, Healthy Babies Conference Perinatal Services BC February 22 nd, 2014 Ivy Fernando, RN BSN, PNC(C)
FETAL SCALP LACTATE RESEARCH STUDY COMPARISON OF TWO POINT OF CARE METERS Presentation to Healthy Mothers, Healthy Babies Conference Perinatal Services BC February 22 nd, 2014 Ivy Fernando, RN BSN, PNC(C)
I.O. Phd International Research Program
 Founders A.W.D. Gavilanes, MD, PhD (Maastricht, The Netherlands) D.S.M. Gazzolo, MD, PhD (Alessandria, Italy) F. van Bel, MD, PhD (Utrecht, The Netherlands) G.H.A. Visser, MD, PhD (Utrecht, The Netherlands)
Founders A.W.D. Gavilanes, MD, PhD (Maastricht, The Netherlands) D.S.M. Gazzolo, MD, PhD (Alessandria, Italy) F. van Bel, MD, PhD (Utrecht, The Netherlands) G.H.A. Visser, MD, PhD (Utrecht, The Netherlands)
1 NCC Monograph, Volume 3, No. 1, 2010
 NICHD Definitions and Classifications: Application to Electronic Fetal Monitoring Interpretation Purpose of this Monograph Safe care for mothers and babies during labor and birth is the goal of all health
NICHD Definitions and Classifications: Application to Electronic Fetal Monitoring Interpretation Purpose of this Monograph Safe care for mothers and babies during labor and birth is the goal of all health
2016 CODING FOR FETAL ALCOHOL SPECTRUM DISORDERS
 2016 CODING FOR FETAL ALCOHOL SPECTRUM DISORDERS Listed below are the most commonly used codes applicable to FASD patient care. Code Description ICD-10-CM Primary Diagnosis P04.3 Newborn (suspected to
2016 CODING FOR FETAL ALCOHOL SPECTRUM DISORDERS Listed below are the most commonly used codes applicable to FASD patient care. Code Description ICD-10-CM Primary Diagnosis P04.3 Newborn (suspected to
ABSTRACT LABOR AND DELIVERY
 ABSTRACT POLICY Prior to fetal viability, intentionally undertaking delivery of a fetus is the equivalent of abortion and is not permissible. After fetal viability has been reached, intentionally undertaking
ABSTRACT POLICY Prior to fetal viability, intentionally undertaking delivery of a fetus is the equivalent of abortion and is not permissible. After fetal viability has been reached, intentionally undertaking
Early Predictions of Hypoxic-Ischemic Encephalopathy by Umbilical Cord Nucleated Red Blood Cells and Lactate
 Med. J. Cairo Univ., Vol. 79, No. 1, December: 625-631, 2011 www.medicaljournalofcairouniversity.com Early Predictions of Hypoxic-Ischemic Encephalopathy by Umbilical Cord Nucleated Red Blood Cells and
Med. J. Cairo Univ., Vol. 79, No. 1, December: 625-631, 2011 www.medicaljournalofcairouniversity.com Early Predictions of Hypoxic-Ischemic Encephalopathy by Umbilical Cord Nucleated Red Blood Cells and
Innovative use of Neonatal Nurse Practitioners in Rural Hawaii
 Innovative use of Neonatal Nurse Practitioners in Rural Hawaii Petri Pate Pieron, MSN, MPH, APRN Rx, CPNP, NNP Presentation was supported by NIH 1 R25 RR019321 Clinical Research Education and Career Development
Innovative use of Neonatal Nurse Practitioners in Rural Hawaii Petri Pate Pieron, MSN, MPH, APRN Rx, CPNP, NNP Presentation was supported by NIH 1 R25 RR019321 Clinical Research Education and Career Development
The Facts about Cerebral Palsy
 The Role of the Obstetrician in preventing Cerebral palsy and protecting oneself from litigation. Prof R. J. PEPPERELL Professor Emeritus,University of Melbourne Previous Professor, Penang Medical College,
The Role of the Obstetrician in preventing Cerebral palsy and protecting oneself from litigation. Prof R. J. PEPPERELL Professor Emeritus,University of Melbourne Previous Professor, Penang Medical College,
CHLAMYDIA SCREENING IN WOMEN
 CHLAMYDIA SCREENING IN WOMEN APPLICATIONS OBJECTIVE Purpose of Measure: ELIGIBLE POPULATION Which members are included? STANDARD OF CARE What screening should be done? NCQA ACCEPTED CODES DOCUMENTATION
CHLAMYDIA SCREENING IN WOMEN APPLICATIONS OBJECTIVE Purpose of Measure: ELIGIBLE POPULATION Which members are included? STANDARD OF CARE What screening should be done? NCQA ACCEPTED CODES DOCUMENTATION
Cord Blood Lactate and ph Values at Term and Perinatal Outcome: A Retrospective Cohort Study
 Article ID: WMC00694 ISSN 2046-1690 Cord Blood Lactate and ph Values at Term and Perinatal Outcome: A Retrospective Cohort Study Corresponding Author: Dr. Max Mongelli, Consultant, Women and Childrens'
Article ID: WMC00694 ISSN 2046-1690 Cord Blood Lactate and ph Values at Term and Perinatal Outcome: A Retrospective Cohort Study Corresponding Author: Dr. Max Mongelli, Consultant, Women and Childrens'
Women's Circle Nurse-Midwife Services Inc. Angela Kreider CNM, MSN 1003 Plumas Street Yuba City, CA 95991 (530)751-2273 FAX (530)751-2274
 Women's Circle Nurse-Midwife Services Inc. Angela Kreider CNM, MSN 1003 Plumas Street Yuba City, CA 95991 (530)751-2273 FAX (530)751-2274 Informed Disclosure and Consent The following consent explains
Women's Circle Nurse-Midwife Services Inc. Angela Kreider CNM, MSN 1003 Plumas Street Yuba City, CA 95991 (530)751-2273 FAX (530)751-2274 Informed Disclosure and Consent The following consent explains
Document Classification
 Document Classification Document Title Document Type Unique Identifier Function(s) (see table) Scope (see table) Target Audience Key words Author(s) Owner (see table) Date first published 2004 Date this
Document Classification Document Title Document Type Unique Identifier Function(s) (see table) Scope (see table) Target Audience Key words Author(s) Owner (see table) Date first published 2004 Date this
Birth Trauma. Position: Relationship of the presenting part to the internal pelvis. ROP: right occiput posterior; or LOA: Left occiput anterior.
 Birth Trauma Position: Relationship of the presenting part to the internal pelvis. ROP: right occiput posterior; or LOA: Left occiput anterior. Engagement: The fetus is engaged if the widest leading part
Birth Trauma Position: Relationship of the presenting part to the internal pelvis. ROP: right occiput posterior; or LOA: Left occiput anterior. Engagement: The fetus is engaged if the widest leading part
Cerebral palsy, neonatal death and stillbirth rates Victoria, 1973-1999
 Cerebral Palsy: Aetiology, Associated Problems and Management Lecture for FRACP candidates July 2010 Definitions and prevalence Risk factors and aetiology Associated problems Management options Cerebral
Cerebral Palsy: Aetiology, Associated Problems and Management Lecture for FRACP candidates July 2010 Definitions and prevalence Risk factors and aetiology Associated problems Management options Cerebral
8/13/2014. Blood, Sweat (and Tears): Delayed Cord Clamping and Delivery Room Temperature. Delayed Cord Clamping
 8/13/2014 Blood, Sweat (and Tears): Delayed Cord Clamping and Delivery Room Temperature James F. Smith, Jr., MD Professor and Chair Obstetrics and Gynecology Creighton University School of Medicine The
8/13/2014 Blood, Sweat (and Tears): Delayed Cord Clamping and Delivery Room Temperature James F. Smith, Jr., MD Professor and Chair Obstetrics and Gynecology Creighton University School of Medicine The
Premature Infant Care
 Premature Infant Care Introduction A premature baby is born before the 37th week of pregnancy. Premature babies are also called preemies. Premature babies may have health problems because their organs
Premature Infant Care Introduction A premature baby is born before the 37th week of pregnancy. Premature babies are also called preemies. Premature babies may have health problems because their organs
Cerebral palsy and clinical negligence litigation: a cohort study
 BJOG: an International Journal of Obstetrics and Gynaecology January 2003, Vol. 110, pp. 6 11 Cerebral palsy and clinical negligence litigation: a cohort study Catherine Greenwood a,b, *, Sally Newman
BJOG: an International Journal of Obstetrics and Gynaecology January 2003, Vol. 110, pp. 6 11 Cerebral palsy and clinical negligence litigation: a cohort study Catherine Greenwood a,b, *, Sally Newman
Guide to Pregnancy and Birth Injury Claims
 Being pregnant, especially for the first time can be a very daunting experience where you often have to put all of your faith in your midwife or doctor. The majority of pregnancies and births occur without
Being pregnant, especially for the first time can be a very daunting experience where you often have to put all of your faith in your midwife or doctor. The majority of pregnancies and births occur without
Prenatal Factors Influencing the Interpretation of Cord Blood Thyroid Stimulating Hormone Levels
 Original Article DOI: 1.17354/ijss/15/115 Prenatal Factors Influencing the Interpretation of Cord Blood Thyroid Stimulating Hormone Levels Divya Durga 1, Sudha Rudrappa 2, Rajendra Kumar 3, SN Manjunath
Original Article DOI: 1.17354/ijss/15/115 Prenatal Factors Influencing the Interpretation of Cord Blood Thyroid Stimulating Hormone Levels Divya Durga 1, Sudha Rudrappa 2, Rajendra Kumar 3, SN Manjunath
PNE 136 Maternal and Child Health Nursing
 Hours Revised: Fall 2015 PNE 136 Maternal and Child Health Nursing Prerequisites: None Course Description: Examines pregnancy, childbirth, postpartum, and newborn care from a family centered approach,
Hours Revised: Fall 2015 PNE 136 Maternal and Child Health Nursing Prerequisites: None Course Description: Examines pregnancy, childbirth, postpartum, and newborn care from a family centered approach,
THE LABOUR ADMISSION CTG An assessment of the test s predictive values, reliability and effect How the test is perceived by practicing midwives
 THE LABOUR ADMISSION CTG An assessment of the test s predictive values, reliability and effect How the test is perceived by practicing midwives Ellen Blix Doctoral thesis at the Nordic School of Public
THE LABOUR ADMISSION CTG An assessment of the test s predictive values, reliability and effect How the test is perceived by practicing midwives Ellen Blix Doctoral thesis at the Nordic School of Public
OXYTOCIN: THE NEW HIGH ALERT MEDICATION. A. Oxytocin Becomes a High Alert Drug
 OXYTOCIN: THE NEW HIGH ALERT MEDICATION A. Oxytocin Becomes a High Alert Drug On August 9, 2007, the Institute for Safe Medication Practices named oxytocin to its list of High-Alert Medications. 1 Institute
OXYTOCIN: THE NEW HIGH ALERT MEDICATION A. Oxytocin Becomes a High Alert Drug On August 9, 2007, the Institute for Safe Medication Practices named oxytocin to its list of High-Alert Medications. 1 Institute
A review of the Condition Present on Admission (CPoA) variable
 A review of the Condition Present on Admission (C) variable Miles Utz, Rachael Wills, Stephanie Callaghan, Taku Endo, Lachlan Mortimer, Sandra Martyn, Trisha Johnston, Corrie Martin Health Statistics Centre,
A review of the Condition Present on Admission (C) variable Miles Utz, Rachael Wills, Stephanie Callaghan, Taku Endo, Lachlan Mortimer, Sandra Martyn, Trisha Johnston, Corrie Martin Health Statistics Centre,
NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS
 NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION 4 TEMPERATURE CONTROL.4 CLEARING THE AIRWAY OF MECONIUM 5
NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION 4 TEMPERATURE CONTROL.4 CLEARING THE AIRWAY OF MECONIUM 5
Inpatient Obstetric Nursing
 NCC believes the individual certified nurse is the best person to determine the specialty code for their CE, as they have the specific content of the CE program. Inpatient Obstetric Nursing NCC Maintenance
NCC believes the individual certified nurse is the best person to determine the specialty code for their CE, as they have the specific content of the CE program. Inpatient Obstetric Nursing NCC Maintenance
Neonatal Hypotonia. Clinical Approach to Floppy Baby
 Neonatal Hypotonia Clinical Approach to Floppy Baby Hypotonia in the newborn is a common presenting feature of systemic illness or neurologic dysfunction at any level of the central or peripheral nervous
Neonatal Hypotonia Clinical Approach to Floppy Baby Hypotonia in the newborn is a common presenting feature of systemic illness or neurologic dysfunction at any level of the central or peripheral nervous
Chapter 31 Obstetrics and Neonatal Care 1137. Scene Size-up. Primary Assessment
 Chapter 31 Obstetrics and Neonatal Care 1137 Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and safe access to the patient. Standard precautions should
Chapter 31 Obstetrics and Neonatal Care 1137 Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and safe access to the patient. Standard precautions should
ANMC Certified-Nurse Midwife Practice Guideline
 Approved by the ANMC MCH CCBG April 2013 Reviewed Nov. 16, 2015 1. Intent of Certified Nurse-Midwife Practice Guideline 1.1. The intent of this practice guideline is to provide guidance for midwifery practice
Approved by the ANMC MCH CCBG April 2013 Reviewed Nov. 16, 2015 1. Intent of Certified Nurse-Midwife Practice Guideline 1.1. The intent of this practice guideline is to provide guidance for midwifery practice
The sensitive marker for glomerular filtration rate (GFR) Estimation of GFR from Serum Cystatin C:
 The sensitive marker for glomerular filtration rate (GFR) Estimation of GFR from Serum Cystatin C: The good correlation allows close estimation of GFR Cystatin C GFR GFR in serum estimated* measured* n
The sensitive marker for glomerular filtration rate (GFR) Estimation of GFR from Serum Cystatin C: The good correlation allows close estimation of GFR Cystatin C GFR GFR in serum estimated* measured* n
Maj Alison Baum. R3, Nellis FMR
 Maj Alison Baum R3, Nellis FMR What are some of your thoughts about birth plans? http://www.youtube.com/watch?v=hh62v0c xf04 Labor: Pain management wishes Doulas Episiotomy Intermittent fetal monitoring
Maj Alison Baum R3, Nellis FMR What are some of your thoughts about birth plans? http://www.youtube.com/watch?v=hh62v0c xf04 Labor: Pain management wishes Doulas Episiotomy Intermittent fetal monitoring
Reference values for umbilical cord diameters in placenta specimens
 1 2 3 Reference values for umbilical cord diameters in placenta specimens H. Pinar 1, Murat Iyigün 2 4 5 6 7 8 9 10 Halit Pinar, MD Brown Medical School Women and Infants Hospital Division of Perinatal
1 2 3 Reference values for umbilical cord diameters in placenta specimens H. Pinar 1, Murat Iyigün 2 4 5 6 7 8 9 10 Halit Pinar, MD Brown Medical School Women and Infants Hospital Division of Perinatal
COMPLICATIONS OF PREGNANCY, CHILDBIRTH AND THE PUERPERIUM
 COMPLICATIONS OF PREGNANCY, CHILDBIRTH AND THE PUERPERIUM PREGNANCY WITH ABORTIVE OUTCOME (630 639.9) 630 HYDATIDIFORM MOLE 631 OTHER ABNORMAL PRODUCT OF CONCEPTION 632 MISSED ABORTION 633 ECTOPIC PREGNANCY
COMPLICATIONS OF PREGNANCY, CHILDBIRTH AND THE PUERPERIUM PREGNANCY WITH ABORTIVE OUTCOME (630 639.9) 630 HYDATIDIFORM MOLE 631 OTHER ABNORMAL PRODUCT OF CONCEPTION 632 MISSED ABORTION 633 ECTOPIC PREGNANCY
http://journals.tbzmed.ac.ir/jarcm,
 Rasooli S., Moslemi F., J Anal Res Clin Med, 2014, 2(1), 11-6. doi: 10.5681/jarcm.2014.002 Original Article Apgar scores and cord blood gas values on neonates from cesarean with general anesthesia and
Rasooli S., Moslemi F., J Anal Res Clin Med, 2014, 2(1), 11-6. doi: 10.5681/jarcm.2014.002 Original Article Apgar scores and cord blood gas values on neonates from cesarean with general anesthesia and
More detailed background information and references can be found at the end of this guideline
 Neonatal Intensive Care Unit Clinical Guideline Oxygen Over the past few years there have been significant changes, based on high quality research, in our understanding of how to give the right amount
Neonatal Intensive Care Unit Clinical Guideline Oxygen Over the past few years there have been significant changes, based on high quality research, in our understanding of how to give the right amount
MANA Home Birth Data 2004-2009: Consumer Considerations
 MANA Home Birth Data 2004-2009: Consumer Considerations By: Lauren Korfine, PhD U.S. maternity care costs continue to rise without evidence of improving outcomes for women or babies. The cesarean section
MANA Home Birth Data 2004-2009: Consumer Considerations By: Lauren Korfine, PhD U.S. maternity care costs continue to rise without evidence of improving outcomes for women or babies. The cesarean section
Wendy Martinez, MPH, CPH County of San Diego, Maternal, Child & Adolescent Health
 Wendy Martinez, MPH, CPH County of San Diego, Maternal, Child & Adolescent Health Describe local trends in birth Identify 3 perinatal health problems Identify 3 leading causes of infant death Age Class
Wendy Martinez, MPH, CPH County of San Diego, Maternal, Child & Adolescent Health Describe local trends in birth Identify 3 perinatal health problems Identify 3 leading causes of infant death Age Class
Obstetrical units should develop a procedure for archiving the fetal monitoring tracings within their own institution.
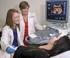 The following guidelines are intended only as a general educational resource for hospitals and clinicians, and are not intended to reflect or establish a standard of care or to replace individual clinician
The following guidelines are intended only as a general educational resource for hospitals and clinicians, and are not intended to reflect or establish a standard of care or to replace individual clinician
Epilepsy 101: Getting Started
 American Epilepsy Society 1 Epilepsy 101 for nurses has been developed by the American Epilepsy Society to prepare professional nurses to understand the general issues, concerns and needs of people with
American Epilepsy Society 1 Epilepsy 101 for nurses has been developed by the American Epilepsy Society to prepare professional nurses to understand the general issues, concerns and needs of people with
