Pressure Ulcers: What You Should Know
|
|
|
- Madeline Hicks
- 10 years ago
- Views:
Transcription
1 SPINAL CORD MEDICINE CONSUMER GUIDE: PRESSURE ULCERS Pressure Ulcers: What You Should Know A Guide for People with Spinal Cord Injury Administrative and financial support provided by Paralyzed Veterans of America
2 PRESSURE ULCERS: What You Should Know Consumer Guide Panel Members Susan L. Garber, MA, OTR, FAOTA (Chair) (Occupational Therapy) Department of Physical Medicine and Rehabilitation Baylor College of Medicine Houston, TX Rehabilitation Medicine Service and Rehabilitation Research and Development Center of Excellence on Healthy Aging with Disabilities Houston VA Medical Center Houston, TX Carla N. Click, RN, MSN, CWOCN, GNP (Nursing) Nursing Service Houston VA Medical Center Houston, TX J. Fred Cowell (Consumer) Paralyzed Veterans of America Washington, DC Theresa L. Gregorio-Torres, MA, OTR (Occupational Therapy) Department of Occupational Therapy The Institute for Rehabilitation and Research Houston, TX Department of Physical Medicine and Rehabilitation Baylor College of Medicine Houston, TX Luther C. Kloth, MS, PT, CWS (Physical Therapy) Department of Physical Therapy Marquette University Milwaukee, WI Daniel P. Lammertse, MD (Physical Medicine and Rehabilitation) Medical Director Craig Hospital Englewood, CO Consumer Focus Group Members J. Fred Cowell (Chair) Paralyzed Veterans of America Washington, DC Ronald P. Amador California Paralyzed Veterans Association, Inc. Long Beach, CA Craig Bash, MD PVA Member Bethesda, MD Robert Herman Paralyzed Vaterans of America Washington, DC Ronald P. Hoskins PVA Delaware-Maryland Chapter Christiana, DE Kenneth C. Huber PVA Michigan Chapter Novi, MI John T. Jackson PVA Virginia Mid-Atlantic Chapter Richmond, VA Consortium Member Organizations American Academy of Orthopedic Surgeons American Academy of Physical Medicine and Rehabilitation American Association of Neurological Surgeons American Association of Spinal Cord Injury Nurses American Association of Spinal Cord Injury Psychologists and Social Workers American College of Emergency Physicians American Congress of Rehabilitation Medicine American Occupational Therapy Association American Paraplegia Society American Physical Therapy Association American Psychological Association American Spinal Injury Association Association of Academic Physiatrists Association of Rehabilitation Nurses Congress of Neurological Surgeons Eastern Paralyzed Veterans Association Insurance Rehabilitation Study Group Paralyzed Veterans of America U.S. Department of Veterans Affairs Copyright 2002 Paralyzed Veterans of America This guide has been prepared based on scientific and professional information found in Pressure Ulcer Prevention and Treatment Following Spinal Cord Injury: A Clinical Practice Guideline for Health-Care Professionals published August Users of this guide should periodically review this material to ensure that the advice herein is consistent with current reasonable clinical practice.
3 A Guide for People with Spinal Cord Injury 1 Contents Who Should Read This Guide?...3 Why Is This Guide Important?...3 What Is a Pressure Ulcer?...4 Figure 1. Layers of Skin and Tissue Who Gets Pressure Ulcers?...4 What Are Other Risk Factors, Besides SCI?...6 Table 1. Risk Factors for Pressure Ulcers and Suggestions for Reducing Risk Where Do Pressure Ulcers Occur?...12 Figure 2. Common Sites of Pressure Ulcers What Do Pressure Ulcers Look Like?...13 Figure 3. Pressure Ulcer Stages What Can I Do to Prevent Pressure Ulcers?...15 Table 2. Strategies to Prevent Pressure Ulcers What Is a Support Surface and Which Ones Should I Use?...18 Beds Figure 4. Hand Check of Bottoming Out Wheelchairs and Seating Systems Table 3. Four Seat Cushion Types: Some Benefits and Limitations What Should I Do if I Get a Pressure Ulcer?...23 What Should I Expect When I Visit My Doctor?...23 What Is the Best Treatment for Me?...25
4 2 PRESSURE ULCERS: What You Should Know What Should I Know About Nonsurgical Treatments?...26 Cleansing Debridement Dressings Monitoring What Should I Know About Surgical Treatments?...28 Before Surgery After Surgery Can Pressure Ulcers Come Back After They Heal?...31 What Are Some Complications of Pressure Ulcers?...32 Infection Poor Nutrition Deconditioning The Wound Depression A Final Note...34 Glossary...35 Appendix A: Resources for People with SCI...38 Medical History...40 Equipment Diary...42 Emergency Information...43 Insurance Information...43 Attendant/Caregiver Information...43 Acknowledgments...44
5 A Guide for People with Spinal Cord Injury 3 Who Should Read This Guide? People with spinal cord injury (SCI). Family, friends, personal care attendants, and others who help you with your care. Health-care providers with whom you come in contact, especially your primary care physician. Your health-care professionals can order a copy of the full clinical practice guideline, Pressure Ulcer Prevention and Treatment Following Spinal Cord Injury, by calling the Paralyzed Veterans of America s Distribution Center toll-free at (888) or download a free copy by visiting the Consortium for Spinal Cord Medicine s web site at SPINAL CORD MEDICINE Pressure Ulcer Prevention and Treatment Following Spinal Cord Injury: A Clinical Practice Guideline for Health-Care Professionals CLINICAL PRACTICE GUIDELINE: PRESSURE ULCER Why Is This Guide Important? This Guide is important because: People with SCI are at lifelong risk for developing pressure ulcers. Pressure ulcers are a serious problem that affects health and well-being. Many pressure ulcers can be prevented. The earlier pressure ulcers are found, the more easily they can be treated. This Guide is intended to help you and those who assist with your care learn how to prevent pressure ulcers. If a pressure ulcer develops, this Guide will help you spot it early so that you can seek appropriate treatment. The more you know about this problem, the better able you will be to participate fully in the decisions that need to be made for treatment. Administrative and financial support provided by Paralyzed Veterans of America *Words in italics are explained in the Glossary on page 35.
6 4 PRESSURE ULCERS: What You Should Know FIGURE 1 What Is a Pressure Ulcer? A pressure ulcer is a lesion/wound or injury, usually caused by unrelieved pressure that results in damage of underlying tissue. Factors other than pressure alone can contribute to the development of a pressure ulcer. These include friction, shear, and moisture (from excessive perspiration or incontinence). Certain parts of the body are more vulnerable to pressure ulcers than others (see Where Do Pressure Ulcers Occur? Page 12). For example, if you lie in bed in one position too long, tissue damage can and will occur if you do not change your position. If you sit in your wheelchair for hours without routinely shifting your weight, you may find a discolored pressure area or a break in the skin on your buttocks. In both cases, the tissue may start to die (necrosis). This is a pressure ulcer. It is important to understand EPIDERMIS DERMIS HYPODERMIS (SUBCUTANEOUS FAT LAYER SUBCUTANEOUS MUSCLE LAYER/FASCIA HAIR FOLLICLE that pressure ulcers do not necessarily start on top of your skin, where you can see them. Instead, they may begin deep inside the tissues of your body, called the fascia, and work their way up, to the outside of your skin (see Figure 1). That makes it hard to find an ulcer early. By the time your skin is discolored or has an open area, called a lesion, the tissue beneath it is already damaged. That is why it is important to learn how to prevent pressure ulcers and how to check your body for signs of them. Who Gets Pressure Ulcers? Anyone who has a condition that impairs mobility (the ability to move) and sensation (the ability to feel) is at risk for the development of pressure ulcers. Because people with spinal cord injury have both impaired mobility and sensation they spend a lot of time either sitting in a wheelchair or reclining in
7 A Guide for People with Spinal Cord Injury 5 bed. This puts continuous pressure on the same parts of the body throughout the day. It is important to understand that when you recline in bed, the pressure exerted between your body and the bed surface is distributed across a broader surface, whereas in the sitting position, the pressures are more concentrated on the buttocks area (ischial tuberosities) and tailbone (coccyx). Another reason people with SCI are prone to pressure ulcers is that the SCI has caused changes in the way their skin functions. Skin is the largest organ of the body. Like any good covering, skin protects its contents muscles, organs, bones, etc. from outside elements. It also helps keep body temperature within a healthy range, in part by sweating (see A Special Note below). The changes in the skin that occur as a result of SCI may continue for three to five years after the SCI, and they may make skin more fragile. The combination of more fragile skin and long periods of time in one position puts people with SCI at especially high risk for pressure ulcers. A Special Note When normal skin heats up to about degrees Centigrade ( Fahrenheit), the body begins to sweat automatically. For people with a complete SCI, as their spinal cord recovers after injury, sweating may return below the level of injury, but without normal regulation. People who have this kind of reflex sweating below their injury level are at added risk for pressure ulcers due to the potential accumulation of moisture. Consequences of overheating are a drop in blood pressure that may cause you to faint, get a headache, or if severe enough, suffer heat stroke. Tips to avoid overheating are: Wear lightweight, breathable clothing, such as cotton. Carry water to spray on your skin. Use cool compresses over you skin. Carry cool water to drink. Stay in shaded areas when outdoors, or move out of direct sunlight when possible.
8 6 PRESSURE ULCERS: What You Should Know What Are Other Risk Factors, Besides SCI? SCI itself puts people at risk for pressure ulcers. But there are other risk factors as well factors that make some people more likely to develop pressure ulcers than others. Some you can control, such as being active and keeping your skin clean and dry; others, such as your age and level of injury, you cannot control or change, but you should know about them. These risk factors are discussed below and in table 1 on page 10. Age As people age, there is a reduction in muscle mass and skin firmness. This results in less padding between their bones and other surfaces. For people with SCI, some of those changes can bring a greater risk for pressure ulcers. Other health problems Multiple health problems are called comorbid conditions, and they also increase the risk of developing pressure ulcers. Several health problems have been linked to pressure ulcers. They include heart disease, diabetes, kidney disease, lung disease, poor nutrition, and frequent urinary tract infections. Smoking Anything that interferes with your circulatory system the network that carries blood throughout your body can affect your skin and put you at risk for pressure ulcers. Smoking impairs circulation. If you were a smoker before your SCI, you were probably advised to quit. Pressure ulcers are just one of the health risks increased by smoking, especially in people with SCI. Severity of SCI The level and completeness of your SCI may increase the risk of developing pressure ulcers. Issues such as the inability to check your skin or perform a weight shift on your own can increase the likelihood that you will develop a pressure ulcer. However, even people with full use of their arms and hands are at risk if they do not take responsibility for doing those things that contribute to healthy skin. Activity Activity means your participation in those things you do every day. This includes activities that are social, work- or school-related, or for leisure. The less active you
9 A Guide for People with Spinal Cord Injury 7 are, the greater your risk for pressure ulcers. Being physically active and involved in your community is good for the body and the mind. In fact, being active can, by itself, improve your overall health. Although there may be times when you need to be alone for a while, do not stay isolated. Reach out let your family, friends, and the world in. Many resources for support are now available for people with SCI. Talk with your health-care providers to identify them (see Appendix A, page 38). Skin moisture In people with SCI, as their spinal cord recovers, sweating frequently returns below the level of injury, but without normal regulation. This is a result of the neurological damage and changes in that part of the nervous system that controls body temperature. People with SCI must be very careful because the body cannot cool itself effectively and can become easily overheated in a hot environment. Damp, moist skin is a natural environment for skin breakdown and infection. It is important to have good bladder and bowel management programs to prevent the skin from being in contact with harmful bodily wastes. (Order a copy of Neurogenic Bowel: What You Should Know by calling toll-free (888) or download a free copy by visiting the Consortium for Spinal Cord Medicine web site at Mental distress Your state of mind (feelings/emotional state) has a lot to do with your overall health. It also affects how you get along with family members, personal care attendants, and others who help you throughout the day. Everyone experiences depression, anxiety, anger, frustration, or a lack of self-esteem, morale, or self-confidence at some point in his or her life. These feelings may be so strong that you are less able to take care of yourself. If these feelings persist, contact your health-care provider for help. (Order a copy of Depression: What You Should Know, available by calling toll-free (888) or download a free copy by visiting the Consortium for Spinal Cord Medicine web site at Adherence In a health context, adherence is following directions and recommendations. Since the onset of your SCI, many health-care providers have given you a great deal of
10 8 PRESSURE ULCERS: What You Should Know information. Most likely, this included the medical aspects of SCI, its complications, and ways to maintain your health and well-being. During your rehabilitation, you were encouraged to take responsibility for as much of your care as possible. It is not uncommon to need reminders (or a refresher course) about a specific aspect of your health. If you develop a pressure ulcer that requires you to visit a health-care provider, ask for written instructions on the treatment program you are to follow at home. Discuss specific problems with the appropriate health-care provider. Wheelchair maintenance or parts are usually discussed with an occupational or physical therapist (an OT or PT) or, at the Department of Veterans Affairs (VA), a kinesiotherapist (KT); wound care products are usually discussed with your physician or nurse. Solutions can be found through team effort. If a family member accompanies you to the clinic or your health-care provider s office, encourage him or her to ask questions. Important: For any health problem, always make sure you understand what you are supposed to do. Do not be embarrassed to ask a doctor, nurse, or therapist to review instructions with you or to explain something that sounds complicated. It is your body, and you have a right to understand what is going on with it. It is also your responsibility to do everything you can to take care of your health. If you cannot do the actual care yourself, learn to direct your care. Your health-care providers need your cooperation and active participation to do their best for you. Illegal drugs and alcohol People who use illegal drugs or alcohol are often careless of their health and are less likely to stick with any prevention routine. This can be a special problem for people with SCI. It is natural to be private about the use of illegal drugs or alcohol. However, if you have a drug or alcohol problem and want help, contact your primary care physician who will direct you to the appropriate resources.
11 A Guide for People with Spinal Cord Injury 9 Autonomic Dysreflexia Autonomic dysreflexia is a serious blood pressure problem for people with SCI who have an injury at or above the T6 level. It is also a major risk factor for pressure ulcers. More important, it can be a life-threatening condition. Learn more about this potentially fatal condition. Order a copy of Autonomic Dysreflexia: What You Should Know by calling toll-free (888) or download a free copy by visiting the Consortium for Spinal Cord Medicine s web site at A Special Note Malnutrition can be a serious problem for individuals with SCI. This may be due to lack of information regarding proper nutrition, lack of financial resources, or inability to prepare a proper diet. People who develop pressure ulcers are sometimes malnourished. If you are malnourished, your health-care provider may suggest you take vitamins or other dietary supplements to boost your nutrition and immune system. Solutions to malnutrition can be sought if identified in a timely manner. Inappropriate, worn-out, or inadequate euipment Equipment wears out with age and daily use. It is important to regularly check all of your requipment to make sure its condition is adequate and appropriate to support you and distribute your weight. Pressure ulcers occur because of a number of factors that may happen individually or in combination. The risk factors described above are intended to alert you to the potential for developing a pressure ulcer. Although all people with SCI are at risk, there are a number of routine activities that will reduce the risk significantly (see Table 1 on page 10). Most important, however, is how much responsibility you take to maintain healthy skin or to direct caregivers on appropriate ways to prevent pressure ulcers. Keeping in touch with your health-care provider who knows about pressure ulcers and SCI is one way of reducing your risk of severe complications. Health-care providers familiar with you can assist you by referring you to needed resources.
12 10 PRESSURE ULCERS: What You Should Know TABLE 1. Risk Factors for Pressure Ulcers and Suggestions for Reducing Risk RISK FACTOR Age SUGGESTIONS Be aware that pressure ulcer risk increases with age, especially as the skin changes after age 40. Focus on prevention. Other health problems Smoking Spinal cord injury Activity Skin moisture Mental distress Monitor your body and health. Work with your health-care team to keep comorbid conditions under control as much as possible. If you smoke, quit. The health benefits are almost immediate and are particularly important to people with SCI. Most smokers try several times before they quit for good. If you have tried before, try again do not give up! Ask your health-care provider if the level and completeness of your SCI put you at greater risk for pressure ulcers (or any other health problem). Make an effort to remain physically active and involved in your community. You will have a more rewarding and healthier life. Follow a skin care plan that keeps your skin dry and clean. An effective bladder and bowel management program is essential not only for preventing pressure ulcers, but for your general health and well-being. Your health-care provider or members of your health-care team will help you design a program that meets your individual needs. Depression and anger are common responses to SCI. If negative feelings seem to be controlling your life long after you have left your rehabilitation program, ask for help! Ask a member of your health-care team for a referral to a mental health professional, and order a copy of Depression: What You Should Know by calling toll-free (888) or download a free copy by visiting the Consortium for Spinal Cord Medicine s web site at
13 A Guide for People with Spinal Cord Injury 11 TABLE 1. continued Adherence Illegal drugs and alcohol Autonomic dysreflexia Malnutrition Cognitive impairments Inappropriate, worn-out, or inadequate equipment Ask for written instructions and any available printed materials that are relevant. Ask questions until you are sure you understand what you are supposed to do. Practice your routines; involve family members and others who help in your daily care. Remember, it is your responsibility to take an active role in preventing pressure ulcers. Tell your health-care provider (or someone else you trust) what drugs you use, how much alcohol and drugs are consumed, and how often. Consider getting help to quit. Learn more about this potentially fatal health problem and its warning signs and share this information with all persons who provide assistance with your care. Order a copy of Autonomic Dysreflexia: What You Should Know by calling toll-free (888) or download a free copy by visiting the Consortium for Spinal Cord Medicine s web site at Eat well-balanced meals and drink plenty of fluids to maintain proper nutrition. Talk to your health-care provider about your diet and what you can do to maintain your intake of calories, protein, and vitamins. Sometimes brain injury or disease can reduce your ability to understand and follow directions. You may need special assistance to understand your condition and to follow instructions. See Adherence (above) and tell your health-care provider, attendant, or family member if you have a problem understanding or following directions. Keep track of the condition of al of your equipment (see Equipment Diary on page 42). Replace any equipment that is worn-out, inadequate for your current needs, or inappropriate to effectively support you and distribute your weight.
14 12 PRESSURE ULCERS: What You Should Know Where Do Pressure Ulcers Occur? Pressure ulcers usually occur over bony prominences. Figure 2 shows the areas of the body where pressure ulcers are likely to develop. Positioning in bed or sitting in a wheelchair will focus the pressure on different parts of your body. When you are lying in bed on your back, pressure is distributed over a greater area than when you are sitting. However, your sacrum (lower end of your spine, just below your waist), your coccyx (tailbone), and your heels are the most vulnerable when lying in bed. In very thin people, their shoulder blades (scapulae) also may be at risk. If you are lying on your side, your hip bone (trochanter) is the most vulnerable. Also, in the side-lying position, if your knees or ankles are touching, they are at risk as well. When you are sitting in your wheelchair (or on any other surface), your seat bones (ischium) are at greatest risk. If you have any problems with your posture such as scoliosis (curvature of the spine), you may sit in a position that puts more pressure on one side of your buttocks than on the other side. An appropriate wheelchair and seating system will help to position you so that your sitting pressure is distributed more evenly. FIGURE 2: COMMON SITES OF PRESSURE ULCERS TROCHANTER ISCHIUM ANKLE ANTERIOR KNEE PERINEUM SHOULDER SIDE OF THE HEAD SHOULDER BLADE RIM OF EAR OCCIPUT SACRUM AND COCCYX ISCHIAL TUBEROSITY POSTERIOR KNEE FOOT HEEL ELBOW DORSAL THORACIC AREA
15 A Guide for People with Spinal Cord Injury 13 What Do Pressure Ulcers Look Like? Pressure ulcers are classified as Stages I IV based on the degree of tissue damage initially observed. The stages are based on which layers of skin and tissue are damaged and how severe that damage is. Health-care providers use these stages to describe pressure ulcers and decide how best to treat them. Stage I This stage is considered mild STAGE I and has the least amount of damage. Because the skin is not broken (remains intact) it may not be thought of as an ulcer in the usual sense. However, some warnings are important signs of an ulcer developing. Compared with other areas of your body, you might find that: The skin is warmer or cooler to the touch. The tissue feels firmer or boggy or mushy as a result of fluid underneath, called edema. The area may hurt or itch. The skin is a different color pink or red in light skin; red, blue, or purple in darker skin. EPIDERMIS Stage I pressures ulcers are often missed because: Changes in skin color can be hard to spot especially in people with dark skin. Many people with SCI, their caregivers, and even some health-care providers may be unfamiliar with the characteristics of a Stage I pressure ulcer. Nevertheless, it is important to detect these ulcers as early as possible. They are the early warning signs that you need better prevention and skin checks. Frequent skin checks will enable you to recognize what normal skin is for you. If you, your family, or others who help you with your
16 14 PRESSURE ULCERS: What You Should Know STAGE II SUBCUTANEOUS FAT care know how your skin looks when it is healthy, you will be more likely to notice when something changes especially if you know the most common pressure ulcer sites (see figure 2 on page 12). STAGE III STAGE IV DEEP FASCIA BONE Stage II At this stage, still considered mild, the ulcer involves only the skin the epidermis, the dermis, or both. The ulcer looks like a scrape, blister, or shallow crater. Stage III At this stage, considered severe, the ulcer extends through both layers of skin and the subcutaneous tissue all the way to, but not completely through, the deep fascia. The ulcer looks like a deep crater with or without evidence of damage to neighboring tissue. Stage IV This is the most severe stage with the deepest levels of damage. In Stage IV, the ulcer extends all the way from the surface of the skin through the fascia to involve muscle and bone and may extend to tendons and joints. The same forces that cause pressure ulcers can make skin thick and leathery. This type of dead, callused skin is called eschar. Because it prevents your health-care provider from seeing the tissues beneath, it is usually removed so that your pressure ulcer can be staged correctly. A qualified health-care provider usually removes eschar by using sterile instruments (scalpel, scissors, etc.).
17 A Guide for People with Spinal Cord Injury 15 What Can I Do to Prevent Pressure Ulcers? Table 2 summarizes actions you can take and tools you can use to prevent pressure ulcers. Work with your health-care team to decide which ones are most important and practical for you. Then, focus on those strategies and check your progress regularly. If something works, stick with it; if it is not effective, ask for help in making changes. TABLE 2. STRATEGY Change positions regularly Strategies to Prevent Pressure Ulcers COMMENTS People with a new injury are usually started on a schedule of turning in bed every 2 hours. Your health-care provider will work with you to cautiously individualize your turning schedule as you recover from your injury. If you need help, encourage those assisting you to use turning aids sheets, a trapeze, or a lift to protect your skin. When lying on your side, try to keep pressure off your trochanter (hip bone). Also, try to keep bony areas, like ankle bones and knees, from touching each other. When seated in a wheelchair, do a weight shift every 15 minutes for 15 seconds if your SCI is at T1 or lower. If you cannot shift your own weight (if your injury is at the cervical level), ask someone to assist you to do a weight shift or use a power mechanism for independent pressure relief every 30 minutes for 30 seconds. Check your skin every day Keep your skin clean and dry Use your eyes and hands to check your skin carefully. This should be done at least twice each day once in the morning and once in the evening. Pay special attention to common sites of pressure ulcers, including use of a long-handled or adaptive mirror for self examination (see Where Do Pressure Ulcers Occur? Page 12). If you need help, make sure those who assist you know what to look for (see What Do Pressure Ulcers Look Like? Page 13). Clean and dry your skin as soon as possible when you have been sweating and after a bowel or bladder accident. Avoid soaps or other products that dry out the skin (such as those that contain alcohol). Avoid very hot water, which can dry out your skin or burn you. Be careful not to rub or press down on your skin too hard. continued on page 16
18 16 PRESSURE ULCERS: What You Should Know TABLE 2. continued Use support When you are lying down: surfaces on your Use a pressure-reducing mattress or overlay. bed and in your Use pillows or foam wedges behind your back and wheelchair (See between your legs. What Is a Use a device that keeps all pressure off your heels (usually Support Surface by raising your heels off the bed). and Which Ones Limit raising the head of your bed to 30 minutes at a time. Should I Use? When you are sitting in your wheelchair: Page 18.) Use a wheelchair cushion that reduces the pressure under the areas at risk and distributes your weight over the greatest area. (See Figure 2 Common Sites of Pressure Ulcers Page 12) If you are in doubt about your cushion, contact the healthcare provider who ordered it. If you did not have a professional person recommend the cushion, contact your primary care physician for a referral for a cushion evaluation. If you travel by car and transfer onto the car seat, use a cushion to protect your skin. Make sure that the cushion is thin enough so that you do not hit your head when going over bumps in the road. Use padded seats on your shower/commode chair or other adaptive equipment. Note: Avoid donut-shaped cushions because they reduce blood flow to surrounding tissues. Check your equipment regularly Even the best equipment wears out with everyday use. Inspect each part of your wheelchair, especially the seat and back, and replace anything that no longer supports you or adequately distributes your weight. Shifting your weight in the chair is good for your body and the seat cushion. Vinyl seat and back upholstery on wheelchairs wears out more quickly than solid/ hard components. All wheelchair cushions wear out, some, such as foam, more quickly than other materials. You can keep track of your equipment by using the Equipment Diary on page 42. Choose Avoid clothes that: appropriate Are too tight, including shoes, socks, braces, splints, clothes, clothing and leg bag straps. Are rough enough to cause skin friction. Have hard studs, fasteners, or double-welted seams. Hold heat (such as nylon or wool); cotton is best. continued on page 17
19 A Guide for People with Spinal Cord Injury 17 TABLE 2. continued Maintain an appropriate weight This can be difficult when physical mobility is limited, but weight control is important to people with SCI. A nutritionist can help develop meal plans for you. An OT, PT, or KT can help develop an exercise plan for you. Monitor your weight Eat a well-balanced diet and drink plenty of fluids If you gain or lose a lot of weight, it may change your size and your wheelchair may no longer fit well and your cushion may not be appropriate. Seats that are too large or too small can contribute to pressure ulcers. Monitor your weight and ask an OT, PT, or KT to check your wheelchair and cushion if your weight changes noticeably. On average, a weight gain or loss of 10% or more warrants assessment by your primary care physician. Proper nutrition is essential for prevention and treatment of pressure ulcers. That means adequate total calories, protein, vitamins (zinc, vitamin C, vitamin A, vitamin E), and fluids. Carefully monitor your intake of caffeine and alcohol as both can dehydrate you and upset the balance of the fluids in your body. If you are having problems sticking to a healthy diet, tell your health-care provider. You may benefit from help with: Meal planning Meal preparation Assistive eating devices A switch to six small meals per day More high-calorie and high-protein foods, like custard, pudding, and cheese Food supplements Be careful about heat Be careful about exposure to heat. Many forms of heat can damage your skin and make pressure ulcers more likely, including: Time spent outdoors on hot, sunny days Cigarettes, cigars, and pipes (hot ashes and burns) Exposed plumbing pipes and heaters Heating pads and electric blankets Ovens, including microwave food containers Hot liquids Car interiors continued on page 18
20 18 PRESSURE ULCERS: What You Should Know TABLE 2. continued Follow a regular exercise program Regular, daily exercise (if approved by your health-care provider) will contribute to your overall health and well-being, including reducing the risk of pressure ulcers. Exercise can help: Strengthen your muscles Improve your heart and lung condition Increase your flexibility Boost your energy What Is a Support Surface and Which Ones Should I Use? A support surface is any bed, mattress, mattress overlay, or seat cushion that is intended to reduce pressure, especially to areas vulnerable to pressure ulcer development. It is important to remember that the wheelchair itself is an important part of the support surface. Support surfaces for the bed and wheelchair reduce the risk of pressure ulcers. They do not heal them. Many of the support surfaces and techniques used to prevent pressure ulcers are also used during the time you are being treated for a pressure ulcer. They may enhance healing, but they are only one component of a prevention or treatment package that contains many parts. If you had rehabilitation in a facility with a special SCI unit, including a medical center, most likely your health-care provider referred you for a wheelchair and cushion evaluation. If you have questions about the recommended equipment, contact either the health-care provider who cared for you during rehabilitation or the therapist who recommended your equipment. If you did not have rehabilitation in a facility with a special SCI unit, contact the healthcare provider who cared for you in the general hospital or other facility. This individual should be able to refer you for assistance with your essential equipment. If you are a veteran, and did not receive rehabilitation at a VA SCI center, contact your local PVA chapter for information and assistance. For more information, see the series of consumer guides Expected Outcomes: What You Should Know available by calling toll-free (888) or download a free copy by
21 A Guide for People with Spinal Cord Injury 19 visitng the Consortium for Spinal Cord Medicine s web site at All equipment should meet your individual needs. Remember, the equipment that was recommended for you during rehabilitation, or shortly thereafter, may not be appropriate later as you increase the amount and types of activities in which you participate. There are a number of factors, other than those associated with your SCI, that determine the type of pressure-reducing equipment that may be recommended for you. The individual assessing your needs should ask the following questions: What are your regular daily activities and life-style (work, school, leisure)? With whom do you live and who assists you on a daily basis? Do you have access to all areas in your residence (doorways, carpet vs. hard flooring)? How do you get around in your community? What is the landscape like around your home? What resources are available to you for replacement and repair of equipment? Do you have any specific preferences regarding your equipment? Do you know whom to contact if you have a problem with your equipment that may be related to your skin? Do you know under what circumstances it would be necessary to contact your health-care provider or other health-care provider (nurse, social worker, or therapist) about your equipment? The result should be equipment that works well for you and those who help in your care. If not, be sure to let your health-care provider know, so that you can try something else. Also, what is right for you right now may not be right for you later in life. Always remember that you are the most important member of the rehabilitation team. It is essential that you
22 20 PRESSURE ULCERS: What You Should Know have enough information, and the right information, about your equipment, and other issues about your SCI, so that you can contribute to the decisions that will result in healthy skin and good health. All questions and concerns are important. Be active in seeking out the facts that will shape your health and well-being. Important: Financial coverage (reimbursement) for support surfaces for the bed and wheelchair differs among insurance companies and other third-party payers. Before you buy anything, check your policy to see what your insurer will cover. If you encounter problems with reimbursement, contact your social worker (or case manager) if you worked with one during your hospitalization. If you did not have a social worker (or case manager) during your hospitalization(s), ask your health-care provider to refer you to an appropriate person. The therapist who ordered the equipment for you may be able to help. However, this individual may not have all the answers regarding your insurance coverage. Beds There are two broad categories of support surfaces for beds: static support surfaces and dynamic support surfaces. Static support surfaces for the bed are either mattresses themselves or mattress overlays. These devices may be air filled or made of foam, a gel material, or a combination. What the device is made of and how it is designed provide the pressure-reducing and pressure-distributing elements of the device. Dynamic support surfaces depend on a power source and change their support features in timed cycles for maximum reduction of pressure. They are used when: You have ulcers on multiple body surfaces. You cannot be positioned without pressure on an ulcer. You cannot be turned or positioned due to other medical conditions (contractures, spasms, etc.). An ulcer is not healing on a static support surface. Some examples are the alternating air pressure mattresses (powered) and the non-powered air displacement mattress.
23 A Guide for People with Spinal Cord Injury 21 Watch Out for Bottoming Out Bottoming out is the term used to describe what happens to support surfaces that no longer provide adequate pressure reduction and support. This may be due to the age of the device, moisture from incontinence or excessive perspiration, inadequate support under the mattress or overlay (bed frame or hospital mattress) or, as in the case of an air-filled wheelchair cushion, a puncture that lets air seep out. Over time, bed and chair surfaces are squashed/compressed and flattened. When this happens, they no longer provide adequate protection against the effects of pressure. (See Equipment Diary Page 42.) It is important to note that foam support surfaces come in a variety of thicknesses and densities (stiffness). Recognizing these variations is essential if pressure ulcers are to be prevented. One easy way to check for bottoming out is to put a hand, palm up, under the support surface at places where vulnerable body parts or a pressure ulcer would rest on it. (See Common Sites of Pressure Ulcers Page 12.) Another way to check is by placing the open hand with palm against the skin or clothing at the bony prominence and estimating the seat cushion or support thickness below by feeling with the fingers (see Figure 4). If the surface is less than an inch thick in those places, it has bottomed out and should be replaced. Mattresses and overlays should be checked at least once a month. Air-filled static mattresses and wheelchair cushions should be checked at least once a week. A more accurate way to check for bottoming out or whether a support surface is the right one for you is to have your physical or occupational therapist evaluate pressures across the support surface using a pressure mapping device. This device uses dozens of sensors linked to a computer that will show a picture of high- and low-pressure areas across your support surface. FIGURE 4: HAND CHECK OF BOTTOMING OUT
24 22 PRESSURE ULCERS: What You Should Know Specialty beds are another type of dynamic pressurereducing device. There are two major types of specialty beds: low-air loss and air fluidized. Generally, these are used in hospitals following pressure ulcer surgery. Rarely are they used in the home because they are very heavy, may be difficult to transfer in and out of, and require high-energy consumption. Some of the newer low-air-loss beds can be used in the home because they are more easily managed than airfluidized beds. A fail-safe system or back-up batteries are needed by home-users in case of power outages. Low-air-loss beds generally reduce pressure and control moisture. Although air-fluidized beds reduce pressure and manage moisture, they can dry out moist dressings prematurely. In addition, they are very expensive and do not allow for changing positions or elevating the head of the bed. Wheelchairs and Seating Systems The wheelchair is the foundation on which the pressurereducing seat cushion is placed. A number of important factors must be considered before a wheelchair cushion or seating system is recommended. The ones that pertain to you, the individual with an SCI, are: Your height, weight, and body build Your sitting posture (Do you sometimes slouch or have any curvature?) Your ability to shift your weight Your level of comfort Your length of time sitting in the wheelchair Your daily activities (types and frequency) Your financial and social resources Factors that pertain to your wheelchair and cushion are: The type of wheelchair that meets your mobility needs (such as manual versus motorized, tilt-in-space versus recliner, solid seat versus sling seat). The cushion s ability to support your body and promote good posture. The cushion s cost, care, and maintenance.
25 A Guide for People with Spinal Cord Injury 23 Table 3 describes some benefits and limitations of four categories of seat cushions. Wheelchairs and seat cushions wear out with use. Get into the habit of inspecting your wheelchair and cushion on a regular basis. If the seat and back upholstery of the wheelchair are vinyl (sling style), inspect them at least twice a year to determine if there is any need for repair or replacement. (See Equipment Diary Page 42.) Remember, the more active you are and the more you sit in your wheelchair, the sooner the materials will wear out. Tires also need to be inspected for safety and function. Wheelchair cushions wear out at different rates. Foam cushions wear out sooner than cushions of other materials. Check the foam for changes in its texture, color, or ability to support you. Replace foam cushions if you notice these changes or if you develop a new red spot anywhere. Air-filled and fluid-filled cushions last longer than foam cushions. Generally, you should consider replacing your air-filled cushion when it develops a leak that cannot be repaired. Fluid-filled cushions should be replaced when its material seems to be becoming more liquid than solid. What Should I Do If I Get a Pressure Ulcer? Pressure ulcers can be treated more easily when detected in their early stages. The earlier you notice a change in your skin, the sooner you can start treatment and reduce your risk for more serious problems. If you or others who help you see a suspicious area on your skin, you should get off of it immediately. If your skin does not return to its normal appearance within 24 hours, call your health-care provider right away. Your health-care provider may ask you to come in and have the area examined. What Should I Expect When I Visit My Doctor? Your health-care provider should: Ask you questions to update your medical history, discuss what help you have at home, inspect the equipment you use, and discuss what caused your ulcer.
26 24 PRESSURE ULCERS: What You Should Know TABLE 3. Four Seat Cushion Types: Some Benefits and Limitations Cushion Category Benefits Limitations Foams Can be shaped to fit the user, Wear out relatively fast for lower pressures and more Retain heat stable support while sitting Hard to clean Lightweight Support features change Lower in cost quickly when exposed to Available in many forms heat or moisture Can be flat or contoured Become hard in cold weather Fluid-filled Covered with easy-to-clean Gel-filled cushions may be Cushions material better shock absorbers (water, Effective for many different users than pressure reducers gel, etc.) Distribute pressure more evenly May be expensive Control skin temperatures better Heavier weight Gel-filled cushions may reduce shear Air Lightweight Tendency to puncture Easy to clean Must be checked Effective for many people frequently for proper air Reduce shear and peak pressures pressure and maintenance Hard to repair May interfere with balance and posture Combination* Tailored to each person by Additional individual combining a variety of materials devices are created by using removable and adjustable parts from cushions with a variety of components such as hip guides, wedges, etc. May be expensive. *May use foams of different densities or combinations of gel, air, and foam.
27 A Guide for People with Spinal Cord Injury 25 Perform a physical examination that includes a thorough inspection of your skin. Order laboratory and other diagnostic tests (i.e., blood or radiology tests) to evaluate the extent of the pressure ulcer and any other possible medical problems that may have contributed to the development of the pressure ulcer. Perform a thorough examination of the pressure ulcer, including measurements of the ulcer and descriptions of other observations, such as color, drainage (exudate), odor, infection, etc. Perform a thorough examination of the area around the ulcer, looking for signs of swelling, warmth, and/or skin damage caused by moisture (maceration) from problems with bladder or bowel management. Discuss next steps in the treatment of your ulcer. Include family member(s), attendant(s), or others who assist you with your care in discussions, if appropriate. What Is the Best Treatment for Me? There is no one-size-fits all treatment for pressure ulcers. Treatments may range from the simple to the very complex. Your health-care provider may: Tell you to get off the area until your skin returns to normal. Use products that cleanse the area, such as normal saline or wound cleansers. Use products or methods that remove dead tissue. Prescribe antibiotics if you have an infection. Change the type of wound dressing as the condition of your ulcer changes. Consider and use other treatment technologies, such as vacuum assisted closure and electrical stimulation. Recommend surgery.
28 26 PRESSURE ULCERS: What You Should Know You and your health-care provider will discuss the best course of action for healing your pressure ulcer. All of the options will be presented to you so that you can make an informed decision regarding the treatment choices. Many things will determine your best treatment, including: What is your current state of health and nutrition? What is the size and stage/severity of your pressure ulcer? Is there any evidence of infection? Do you have other medical problems that might interfere with healing, such as diabetes or circulatory problems? Do you have a prior history of pressure ulcers and pressure ulcer surgery? Do you have adequate insurance coverage? What Should I Know About Nonsurgical Treatments? Nonsurgical treatments are listed below. Remember, your pressure ulcer may require some of the procedures and not others. Cleansing the ulcer. Removing infected and dead tissue from the ulcer (debridement). Using a dressing on the ulcer. Monitoring the ulcer regularly to see if it is healing. Cleansing The first step in treating a pressure ulcer is to clean it. Cleaning removes germs and unhealthy tissues that interfere with healing. Normal saline is the cleansing agent most often used. Your health-care provider will use a normal saline or another wound cleansing product that is not an antiseptic. Do not use products such as hydrogen peroxide as they may be harmful to the tissues. You or those who help you at home will be shown how to clean the ulcer when you change the dressings. It is important to be gentle, so the skin is not stretched and stressed.
29 A Guide for People with Spinal Cord Injury 27 Important: Anyone who helps an individual with a spinal cord injury and a pressure ulcer should remember that when cleansing the pressure ulcer: Always wear gloves to protect the individual being treated as well as yourself against contamination. Always discard cleansing applicators (such as cloths and sponges), used dressings, and gloves in a plastic bag that is tied closed. Debridement Debridement is defined as the removal of dead or infected tissue from a wound. There are several different ways to debride an ulcer. These include autolytic, enzymatic, mechanical, sharp, and surgical debridement. Debridement can be performed either at the bedside or in the operating room. Your health-care provider will assess your pressure ulcer, determine if it needs to be debrided, and determine the most effective debriding method for you. If you have questions about this procedure, ask your health-care provider for an explanation of the types of debridement and why a specific one was chosen for you. Dressings Dressings are products that protect the pressure ulcer from bacteria contamination and trauma. They can be used to apply medication, absorb drainage, or debride the ulcer. Dressings are used to provide a moist wound environment, which promotes healing. There are hundreds of pressure ulcer dressings on the market today. They are grouped together based on what they do when they come in contact with a pressure ulcer. Some of the major categories include: Transparent films Hydrocolloids Hydrogels Hydropolymer Foams Alginates Gauze dressings
30 28 PRESSURE ULCERS: What You Should Know Your health-care providers will select a dressing based on the condition/severity/stage of your ulcer (e.g. presence of drainage, infection, eschar) and the presence of other healthrelated conditions discussed in this guide. They will provide you with information and instructions for using the dressings appropriately. Monitoring Examine your pressure ulcer every time your dressing is changed. If you are unable to see the area, use a hand-held, long-handled mirror or ask the person who helps you with your daily living activities to inspect the ulcer and the area around it. This is very important to determine if your treatment plan is working and the ulcer is healing. Report any additional problems to your physician or other health-care providers including: Pain or discomfort around the ulcer. A change in swelling, skin color, or skin temperature. Fluids seeping through the dressing. A strong smell around the dressing. In general, the ulcer should show signs of healing in two to four weeks. If it does not, your health-care provider will discuss changing your treatment plan. What Should I Know About Surgical Treatments? If you have a deep (Stage III or IV) or a complicated pressure ulcer, your health-care provider may suggest that you see a plastic surgeon. The surgeon will examine you thoroughly, to determine if surgery is the best treatment for your ulcer. Like so many aspects of health care, the best surgical technique for closing your ulcer will depend on factors specific to you. Before Surgery The health issues described below can complicate surgery and its recovery. If you have any of these conditions, your health-care provider will take steps to address and manage them before your surgery.
31 A Guide for People with Spinal Cord Injury 29 Infected pressure ulcer The ulcer will be cleaned thoroughly. Your health-care provider may prescribe antibiotics. Poor nutrition Poor nutrition can make you more prone to pressure ulcers and affect healing. If you are malnourished, vitamins or other dietary supplements may be suggested to boost your nutrition and immune system. Bowel management problems For proper healing, a pressure ulcer must be kept clean after surgery. If you are having problems with bowel management especially if the ulcer is near your anus your healthcare provider will discuss options for preventing contamination. Spasms Severe spasms may contribute to pressure ulcers or cause problems with healing. Problems occur because when you experience a spasm, the surgical area will be put under greater stress, compromising the incision and/or flap. If you have spasms and are on medication, your health-care provider may change either the actual medication or the dose to control the spasms. Other health problems Heart disease, lung disease, and diabetes can interfere with healing. Your health-care provider should be aware of these conditions to make sure they are stable before you have surgery. If you have any concerns about the effect of the surgery on your general health, tell your surgeon so your fears and worries can be addressed. Urinary tract infection People with SCI are prone to urinary tract infections, which increase the risk of infections in other areas of the body. Your health-care provider will want to treat any infections you may have before surgery. Smoking Surgical sites need good blood supply for healing. Smoking narrows blood vessels and can affect blood flow. The health benefits of quitting are many, but timing may be an issue. If you are trying to quit, do not use nicotine patches before surgery! The
32 30 PRESSURE ULCERS: What You Should Know nicotine from patches stays in your body longer than nicotine from cigarettes and can delay healing. After Surgery Your health-care provider will discuss your individual postpressure ulcer surgery recovery plan. Always ask for written instructions on what you are supposed to do and not do. If you have surgery to repair a pressure ulcer, most likely you will be in the hospital for four to eight weeks after surgery. Members of your health-care team (health-care providers, nurses, therapists, etc.) will recommend special bed surfaces and positioning and transfer techniques to keep pressure completely off the surgery site. Your family members or others who will help you during your recovery will be instructed on the best post-operative ways to promote healing. (See What Is a Support Surface and Which Ones Should I Use? Page 18.) For a speedy recovery, make sure you and everyone who helps with your care follow all the team s directions. Remember, do not hesitate to ask questions if you are uncertain about something or do not fully understand the instructions or recommendations. A post-surgery plan will be developed to meet your individual needs. In general it will include: Prolonged bedrest to allow adequate wound healing prior to return to sitting. This commonly takes four to eight weeks. Daily observation of the surgical site by health-care providers. Range of motion exercises for your hips and knees to get you are ready to begin sitting. The timing of this is determined by the surgeon. Progressive sitting program to build up tolerance on the surgical site. Assessment of relevant equipment for repair or replacement (wheelchair, cushion(s), etc.). Full recovery may take 8 weeks or longer. Some people who have had pressure ulcer surgery will stay in the hospital
33 A Guide for People with Spinal Cord Injury 31 throughout the entire course of treatment and recovery. Others will leave the hospital for part of the post-surgery time and return for a sitting program and equipment assessment and fitting. This will vary depending on where you had your surgery and your financial and social resources. The timeframes described are general. Be sure to ask your health-care provider what you should expect, so that you can make plans for your recovery. Also, remember that your health-care provider can do only so much. It is up to you to stick with your recovery plan and let your health-care provider know if you have any problems or if there are obstacles (barriers) to your complying with the instructions. Can Pressure Ulcers Come Back After They Heal? The recurrence of pressure ulcers is very common among people with spinal cord injury. However, the type of treatment you receive for your pressure ulcer nonsurgical or surgical does not affect how many times you get pressure ulcers, either at the same site as an earlier ulcer or another area of your body. There are a number of factors that put a person at higher risk that pressure ulcers will recur. Some examples include (see Table 1 page 10): Smoking Diabetes Heart disease Previous pressure ulcers and or surgery People with any of the above risk factors need to examine their skin regularly to detect the early warning signs of pressure ulcers. Other factors that may contribute to recurrence include: Poor nutrition Worn-out or inadequate cushions Poor personal hygiene Incontinence Sitting or lying in one place too long
34 32 PRESSURE ULCERS: What You Should Know What Are Some of the Complications of Pressure Ulcers? Pressure ulcers can contribute to other health problems, and other health problems can make pressure ulcers more likely. Common causes and complications are described below. Infection Infections can affect the skin, tissue, or bones. Whether your treatment involved surgery or not, infections can delay healing. They also increase the odds that a healed ulcer will come back. Be alert to signs of infection, which include: Skin redness (erythema) or any other change in skin color. Hardness, like a knot or lump under the skin (induration). Pus in the infected area or oozing from it (purulence). A bad odor coming from the affected area. Your health-care provider will use specific laboratory tests to confirm the presence of an infection and identify what type it is. It may be necessary to do a biopsy, which is to remove tissue and/or bone and test them for infection. Once the infection type is known, your health-care provider can prescribe the right medication. Poor nutrition Pressure ulcers can deplete your body of the protein and fluids that it needs. Pressure ulcers also can trigger changes in your body s metabolism that can cause you to lose weight and lean body tissue (not just fat). A special eating plan and vitamins can help. Your health-care provider may recommend that you consult a nutritionist for the best combination of foods and vitamins for healthy skin. Deconditioning While you are being treated for a pressure ulcer, your mobility will be significantly reduced, at least for a while. Weeks of bedrest are a possibility. As a result, you may become deconditioned. This will affect all major aspects of your fitness, including your flexibility, strength, and heart and lung (cardiovascular) endurance. During your recovery, ask your health-care provider about getting back to a progressive
35 A Guide for People with Spinal Cord Injury 33 exercise program in which you start slowly and build your fitness and activities back to previous levels. As you make progress, you can revise your exercise program to fit your needs. The wound Surgery is performed to close a pressure ulcer. However, occasionally the surgical site can separate or split open again before it has had time to completely heal. Infection or trauma to the area are two of the things that can cause the site to open. If this happens to you, your health-care provider will try to determine the cause, so that it will not happen again. Surgery may be needed to re-close the wound. Depression Pressure ulcers are a very serious problem for people with spinal cord injury. They can interfere with and limit every aspect of your life your mobility, pursuit of educational and/or vocational goals, functional independence, and social /leisure activities. They are also very expensive to treat and may result in a drain on your financial resources. They may also affect the way you look at yourself pressure ulcers have been reported to lower self-esteem and diminish already achieved levels of functional independence. Any one of these factors can lead to depression. If you develop a pressure ulcer and you feel frustrated or depressed, consider the following: Use the recovery time to learn more about preventing pressure ulcers. Ask the hospital-based social worker, case manager, doctor, or therapist who works on the SCI unit about support groups for people with SCI (see Appendix A page 38). Order a copy of Depression: What You Should Know by calling toll-free (888) or download a free copy by visiting the Consortium for Spinal Cord Medicine s web site Tell your healthcare provider about the professional guideline that is available and where to download a free copy.
36 34 PRESSURE ULCERS: What You Should Know Ask your health-care provider for a referral to a mental health provider. Depression is a medical problem that can be treated effectively. Important: Your body changes over time, and so do your health care needs. As an individual with an SCI, you should be re-evaluated at least once each year to monitor those changes that might have an effect on your general health and skin status. A Final Note Pressure ulcers are a life long threat to people with SCI. In general, however, they are preventable. This requires your active participation by regularly examining your skin, keeping it clean and dry, eating properly, performing weight shifts, and monitoring the condition of your equipment. If you are unable to do these things independently, ask someone to help you. If you depend on others to help you, provide them with the information and direction essential to maintaining healthy skin. If you are experiencing problems with your skin or equipment, consult your health-care provider for direction to alleviate the problem as soon as you can. Pressure ulcer prevention must be a team effort. However, you, the person with a SCI, are the team leader. Take the responsibility; ensure that you are able to enjoy a long and happy life.
37 A Guide for People with Spinal Cord Injury 35 Glossary adherence (ad-hear-enss) Following a health plan or instructions. This includes everything from taking medicines on time and as prescribed to keeping a health-care provider s appointment. alginates Soft, absorbent, nonwoven dressings derived from seaweed that have a fluffy cotton-like appearance. autonomic dysreflexia (AUT-oh- NOME-ic diss-ree-flex-ee-uh) An abnormal response to a problem in the body, below an SCI, that causes high blood pressure. It s most likely to happen if the SCI is at or above T6. bony prominences (PRAHM-in-unsuz) Parts of the skeleton over which skin is especially at risk for pressure ulcers, e.g., ischium, trochanters, sacrum, coccyx, ankles, and knees bottoming out What happens to a mattress overlay or seat cushion when it has been flattened by pressure over time and no longer provides enough support. A surface is said to have bottomed out when a hand check (upturned palm under the surface) finds less than an inch of support material where vulnerable parts of the body or an existing pressure ulcer would rest. coccyx (COCK-six) A small bone at the base of the spine (tailbone). comorbid (koh-more-bid) conditions Several health problems that exist in the same person, for example, SCI and heart disease. deconditioned Changes in the way the body functions as a result of physical inactivity. Changes include decreased maximum oxygen uptake, shortened time to fatigue during submaximal work, decreased muscle strength, and decreases in reaction time, balance, and flexibility. dermis (DER-miss) The second layer of skin, beneath the epidermis. dynamic support surface A pressure-reducing device that changes its support features in timed cycles, for example, alternating-air mattresses and shape-changing seats. edema (eh-dee-muh) Excessive amounts of fluid in the tissues. epidermis (eh-pih-der-miss) The outermost layer of skin. erythema (ur-uh-theme-uh) Skin redness, for example, caused by sunburn or infection. eschar (ESS-kar) Thick, leathery, dead tissue. exudate (ECKS-yoo-date) Fluids caused by injury or swelling. For a pressure ulcer, the health-care provider will describe exudate by the amount, smell, consistency (e.g., thin and runny or thick and jelly-like), and color. fascia (FASH-ee-uh) A band of fibrous tissue deep below the skin. Fascia also surrounds muscles and some organs of the body.
38 36 PRESSURE ULCERS: What You Should Know friction The mechanical force that occurs when skin is dragged across a coarse surface, like bed linens. health-care provider A person who plans and implements various aspects of your care. This person may be at any given time, a doctor, nurse, therapist, social worker, or psychologist. hydrocolloids A wound dressing containing absorbant gel surrounded by a flexible polyurethane foam of film baking. Available in paste form or adhesive wafers. hydrogels Water or glycerin-based gels. Insoluble in water. Available in solid sheets, amorphous gels, or impregnated gauze. incontinence Inability to control bowel or bladder function. induration (in-der-a-shun) Hardness, for example, a hard lump of tissue under the skin. ischia (ISS-kee-uh) The lowest of the three major bones that make up each half of the pelvis ( seat bones ). ischial tuberosities Plural of ischium. These are the bones of the lower pelvis and are often called seat bones. ischium One ischial tuberosity (see ischial tuberosities). maceration (mass-er-a-shun) Skin damage that occurs when skin has been kept too moist. perineum (pair-ih-nee-uhm) The lower part of the pelvis, from the bony pubic arch in front to the coccyx in the back. personal care attendant A person such as a family member, friend, or hired helper who assists with personal care or household tasks on a routine basis. primary care physician The physician who is responsible for managing your health needs and referring you to medical specialists as indicated. purulence (PURE-uh-lunce) Containing or oozing pus. range of motion The amount (range) or scope of movement at a specific joint. recurrence Formation of a pressure ulcer elsewhere subsequent to another ulcer or formation of a new ulcer at the site of a previous ulcer. reflex sweating An abnormal reflexive response to physical stimuli such as change in position, noxious stimuli, etc. that produces uncontrollable episodes of sweating below the level of injury. sacrum (SAY-krum) A triangleshaped bone made up of five fused vertebrae that forms the back section of the pelvis. scapulae (SKAP-yoo-lee) The large, flat bones that form the back of the shoulder (the shoulder blade). necrosis (neh-crow-sis) Tissue death.
39 A Guide for People with Spinal Cord Injury 37 shear A mechanical force that causes an opposite but parallel sliding motion of the body and the skin when they come in contact with different materials, like a support surface. static support surface A device that is placed on a bed or in a wheelchair and either because of the material(s) of which it is made or its design can reduce pressure. Examples are foam blocks, gels, and water-filled devices. transparent films A transparent, waterproof adhesive film that is moisture-vapor permeable and comfortable and that provides a moist, wound-healing environment. trochanters (troe-kant-ers) The bumps on the neck of the thigh bone (femur). subcutaneous tissue The area beneath the skin (often called superficial fascia) that is composed of connective tissue, which provides strength and support, and fat tissue, which provides some padding.
40 38 PRESSURE ULCERS: What You Should Know Appendix A Resources for People with SCI Look in your local phone book to find federal, state, county, and local government agencies. For information on local resources, call the National Council on Independent Living at (703) ; or check the Internet at Housing Assisted living; personal care homes; return to own home; independent living centers; state veterans homes; nursing home placement; housing authority for subsidized housing and rental aid programs; local realtor; U.S. Department of Housing and Urban Development. Finances Supplement Security Income (SSI); Social Security Disability Income (SSDI); VA* for veterans who served in wartime or are connected to a branch of military service; workers compensation; food stamps; Aid to Families with Dependent Children (AFDC); State department of rehabilitation services. Transportation Local public transit authority; area agency on aging; state division of rehabilitation services; Medicaid taxi services; VA*; independent living centers; places of worship (churches, synagogues, mosques); rental van services. Caregiver support VA* for respite for veterans; respite care through local hospitals and nursing homes; homemaker services through VA or state funding; local support groups; the National Caregivers Association; mental health center or professional. Personal care assistance Home health agencies; independent living centers; family members; training of people who can hire and manage their own employees; Medicaid waiver programs; state funding options; VA*. Peer support Independent living centers; local rehabilitation hospitals; PVA*; National Spinal Cord Injury Association; local SCI or PVA* chapters; disabilityspecific support groups. Home access Independent living centers; civic groups; houses of worship; state department rehabilitation services; Medicaid waiver programs; VA*; PVA* Architecture; workers compensation. Adaptive equipment VA*; independent living centers; PVA*; National Spinal Cord Injury Association; Medicare; private insurance.
41 A Guide for People with Spinal Cord Injury 39 Leisure, sports, and recreation Independent living centers; PVA*; National Spinal Cord Injury Association; houses of worship; YMCA/ YWCA; local fitness centers; county parks and recreation service; Chamber of Commerce; state sports associations; senior citizen centers. Individual, family, and caregiver support Independent living centers; local rehabilitation hospitals; mental health center or professional; local SCI or PVA* chapters; disability-specific support groups. Jobs, vocational help State employment agency; independent living centers; state department of vocational rehabilitation; VA*. *VA = Department of Veterans Affairs; PVA = Paralyzed Veterans of America. References to VA are appropriate for veterans only.
42 40 PRESSURE ULCERS: What You Should Know Medical History Name Date of birth: / / Sex: M or F Date of spinal cord injury: / / Level of injury: Complete Incomplete Allergies, including medications: List medications taken regularly (prescription and over-the-counter): List medications taken as needed (prescription and over-the-counter):
43 A Guide for People with Spinal Cord Injury 41 Description of pressure ulcer(s): (include location, grade, duration, treatment plan, outcome, etc.): Date: / / Location: Grade: Date resolved: / / Date: / / Location: Grade: Date resolved: / / Date: / / Location: Grade: Date resolved: / / Date: / / Location: Grade: Date resolved: / / Date: / / Location: Grade: Date resolved: / / Date: / / Location: Grade: Date resolved: / /
44 42 PRESSURE ULCERS: What You Should Know Equipment Diary (e.g., wheelchair, bed, cushion(s), mattress/overlay, shower chair/commode) Item Type Size Serial Vendor/ Date Warranty Number Manufacturer received Expiration
45 A Guide for People with Spinal Cord Injury 43 Emergency Information In Case of Emergency, Call: Relationship: Phone Number: ( ) Alternative Phone Number: ( ) Insurance Information Name of Insurance Company: Identification Number: Group Number: Phone Number: ( ) Attendant/Caregiver Information Name: Date Hired: Address: City: State: Zip: Home Phone: ( ) Cell Phone: ( ) Pager Number: ( ) Address: ( )
46 44 PRESSURE ULCERS: What You Should Know Acknowledgements The Consortium for Spinal Cord Medicine Clinical Practice Guidelines is composed of 19 organizations committed to improving spinal cord injury (SCI) care and treatment. The Consortium Steering Committee established a guideline development panel to make recommendations on the prevention and treatment of pressure ulcers following SCI. The recommendations within this consumer guide are based on scientific research compiled from 1966 to 2000 and used in the Consortium s clinical practice guideline (CPG) Prevention and Treatment of Pressure Ulcers Following Spinal Cord Injury: A Clinical Practice Guideline for Health-Care Professionals. The CPG development panel was assisted by an expert team from the University of North Carolina at Chapel Hill who reviewed the literature and determined the quality of the research. The Paralyzed Veterans of America provided financial support and administrative resources for all aspects of guideline and consumer guide development. The consumer panel chairperson was Susan L. Garber, MA, OTR, FAOTA. The panel consisted of five members with experience in the management and treatment of the pressure ulcers in SCI individuals. For many with SCI, pressure ulcers are a major life-limiting problem. Creation of a consumer guide that addresses the problems of and the many solutions to the prevention and treatment of pressure ulcers required a diverse, experienced, and sensitive panel. The Consortium would like to thank all members of the consumer guide panel for providing the essential ingredients of knowledge, experience, empathy, and practicality. The Consortium is also appreciative of the outstanding work of the entire PVA publications support staff. In particular, the Consortium would like to recognize the professional writer Barbara Shapiro, the graphic designer Sarah Ornstein, PVA Senior Editor Patricia E. Scully, PVA Project Administrator Dawn M. Sexton, and Consortium Coordinator J. Paul Thomas. In the end, it is those with SCI who are continually living with and learning about pressure ulcers that are the best evaluators of a teaching tool such as this consumer guide. The Consortium would like to thank the consumer focus group for their critical review and comments on the manuscript, including Chairman Fred Cowell, Ronald P. Amador, Dr. Craig Bash, Robert Herman, Ronald Hoskins, Kenneth Huber, and John Jackson. Their varied life experiences with SCI provided wise perspectives that refined and improved the consumer guide. Finally, it is essential to recognize all investigators studying the effects
47 A Guide for People with Spinal Cord Injury 45 of pressure ulcers following SCI. Research is the source of solutions; there is still much to be done in the future. Pressure ulcers continue to be a fertile area for research! The Consortium will continue to develop clinical practice guidelines and consumer guides on topics in spinal cord injury care. Look for consumer guides on other topics in spinal cord injury at
48 Administrative and financial support provided by PARALYZED VETERANS OF AMERICA 801 Eighteenth Street, NW Washington, DC (800) (800) tty March 2002 (888) (toll-free distribution center) (Consortium for Spinal Cord Medicine web site)
Pressure Ulcers. Occupational Therapy. This leaflet is for both yourself and Carers
 Pressure Ulcers Occupational Therapy This leaflet is for both yourself and Carers Contents What is a pressure ulcer? 3 Who is at risk of developing a pressure ulcer? 4 How can I avoid developing a pressure
Pressure Ulcers Occupational Therapy This leaflet is for both yourself and Carers Contents What is a pressure ulcer? 3 Who is at risk of developing a pressure ulcer? 4 How can I avoid developing a pressure
Preventing pressure ulcers
 Golden Jubilee National Hospital NHS National Waiting Times Centre Preventing pressure ulcers Patient information guide for adults at risk of pressure ulcers Agamemnon Street Clydebank, G81 4DY (: 0141
Golden Jubilee National Hospital NHS National Waiting Times Centre Preventing pressure ulcers Patient information guide for adults at risk of pressure ulcers Agamemnon Street Clydebank, G81 4DY (: 0141
Understand nurse aide skills needed to promote skin integrity.
 Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
APPLICATION OF DRY DRESSING
 G-100 APPLICATION OF DRY DRESSING PURPOSE To aid in the management of a wound with minimal drainage. To protect the wound from injury, prevent introduction of bacteria, reduce discomfort, and assist with
G-100 APPLICATION OF DRY DRESSING PURPOSE To aid in the management of a wound with minimal drainage. To protect the wound from injury, prevent introduction of bacteria, reduce discomfort, and assist with
Working together to prevent pressure ulcers (prevention and pressure-relieving devices)
 Working together to prevent pressure ulcers (prevention and pressure-relieving devices) Understanding NICE guidance information for people at risk of pressure ulcers, their carers, and the public Draft
Working together to prevent pressure ulcers (prevention and pressure-relieving devices) Understanding NICE guidance information for people at risk of pressure ulcers, their carers, and the public Draft
Anyone who has difficulty moving can get a pressure sore. But you are more likely to get one if you:
 Patient information from the BMJ Group Pressure sores Anyone can get a pressure sore if they sit or lie still for too long without moving. People who are old or very ill are most likely to get them. Careful
Patient information from the BMJ Group Pressure sores Anyone can get a pressure sore if they sit or lie still for too long without moving. People who are old or very ill are most likely to get them. Careful
How To Recover From A Surgical Wound From A Cast
 Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
Wound Care: The Basics
 Wound Care: The Basics Suzann Williams-Rosenthal, RN, MSN, WOC, GNP Norma Branham, RN, MSN, WOC, GNP University of Virginia May, 2010 What Type of Wound is it? How long has it been there? Acute-generally
Wound Care: The Basics Suzann Williams-Rosenthal, RN, MSN, WOC, GNP Norma Branham, RN, MSN, WOC, GNP University of Virginia May, 2010 What Type of Wound is it? How long has it been there? Acute-generally
Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased.
 Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased. This graph shows the percent of residents whose need for help doing basic daily tasks
Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased. This graph shows the percent of residents whose need for help doing basic daily tasks
Spinal Cord Injury Education. Common Medical Problems Following Spinal Cord Injury
 Spinal Cord Injury Education Common Medical Problems Following Spinal Cord Injury Common Medical Complications After SCI, your body is vulnerable to various complications This presentation gives a brief
Spinal Cord Injury Education Common Medical Problems Following Spinal Cord Injury Common Medical Complications After SCI, your body is vulnerable to various complications This presentation gives a brief
Spinal Cord Injury Rehabilitation Program
 Workbook Spinal Cord Injury Rehabilitation Program Table of Contents Page Before coming to Rehab... 1 Tests before starting your Rehabilitation Program... 2 SCI Personal Goal Tracking Tool... 3 To do
Workbook Spinal Cord Injury Rehabilitation Program Table of Contents Page Before coming to Rehab... 1 Tests before starting your Rehabilitation Program... 2 SCI Personal Goal Tracking Tool... 3 To do
Pressure Ulcers Assessing and Staging. Anne Pirzadeh RN CWOCN University of Colorado Hospital June 2010
 Pressure Ulcers Assessing and Staging Anne Pirzadeh RN CWOCN University of Colorado Hospital June 2010 Never Events: Pressure Ulcers Pressure Ulcer Codes: MD documentation of pressure ulcers determines
Pressure Ulcers Assessing and Staging Anne Pirzadeh RN CWOCN University of Colorado Hospital June 2010 Never Events: Pressure Ulcers Pressure Ulcer Codes: MD documentation of pressure ulcers determines
PATIENT HANDBOOK AND JOURNAL POST SURGERY
 PATIENT HANDBOOK AND JOURNAL POST SURGERY POST ANESTHESIA CARE UNIT (PACU) After surgery you will be moved from the Operating Room directly to a special recovery room, called the Post Anesthesia Care Unit
PATIENT HANDBOOK AND JOURNAL POST SURGERY POST ANESTHESIA CARE UNIT (PACU) After surgery you will be moved from the Operating Room directly to a special recovery room, called the Post Anesthesia Care Unit
7/11/2011. Pressure Ulcers. Moisture-NOT Pressure. Wounds NOT Caused by Pressure
 Assessment and Documentation of Pressure Ulcers Jeri Ann Lundgren, RN, BSN, PHN, CWS, CWCN Pathway Health Services July 19, 2011 Training Objectives Describe etiologies of pressure ulcers Discuss how to
Assessment and Documentation of Pressure Ulcers Jeri Ann Lundgren, RN, BSN, PHN, CWS, CWCN Pathway Health Services July 19, 2011 Training Objectives Describe etiologies of pressure ulcers Discuss how to
Recovery After Stroke: Bladder & Bowel Function
 Recovery After Stroke: Bladder & Bowel Function Problems with bladder and bowel function are common but distressing for stroke survivors. Going to the bathroom after suffering a stroke may be complicated
Recovery After Stroke: Bladder & Bowel Function Problems with bladder and bowel function are common but distressing for stroke survivors. Going to the bathroom after suffering a stroke may be complicated
Pressure Sores (Decubitus Ulcers)
 Pressure Sores (Decubitus Ulcers) Judith Stevens, M.Ed. With thanks to Dr. Toni Benton, Jennifer Thorne-Lehman, Araceli Domingo for contributing resource information. Thanks to Ann Chase Stevens for sharing
Pressure Sores (Decubitus Ulcers) Judith Stevens, M.Ed. With thanks to Dr. Toni Benton, Jennifer Thorne-Lehman, Araceli Domingo for contributing resource information. Thanks to Ann Chase Stevens for sharing
call 811 to get advice from a nurse, or have someone drive the patient to a hospital Emergency Department. Patients should NOT drive themselves.
 Taking Care at Home After Surgery This checklist is to help you and your support person know what to do after you go home following your surgery. If you are given instructions verbally or in writing by
Taking Care at Home After Surgery This checklist is to help you and your support person know what to do after you go home following your surgery. If you are given instructions verbally or in writing by
Spinal Cord and Bladder Management Male: Intermittent Catheter
 Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
FUNCTIONS OF THE SKIN
 FUNCTIONS OF THE SKIN Skin is the largest organ of the body. The average adult has 18 square feet of skin which account for 16% of the total body weight. Skin acts as a physical barrier for you to the
FUNCTIONS OF THE SKIN Skin is the largest organ of the body. The average adult has 18 square feet of skin which account for 16% of the total body weight. Skin acts as a physical barrier for you to the
How does Diabetes Effect the Feet
 How does Diabetes Effect the Feet What Skin Changes May Occur? Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. The problem is that
How does Diabetes Effect the Feet What Skin Changes May Occur? Diabetes can cause changes in the skin of your foot. At times your foot may become very dry. The skin may peel and crack. The problem is that
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Skin & Wound Care Prevention & Treatment. By Candy Houk, RN Skin & Wound Program Manager
 Skin & Wound Care Prevention & Treatment By Candy Houk, RN Skin & Wound Program Manager OBJECTIVES Classify Stage 1 and 2 pressure ulcers Recognize suspected Stage 3, 4, DTI, and unstageable pressure ulcers
Skin & Wound Care Prevention & Treatment By Candy Houk, RN Skin & Wound Program Manager OBJECTIVES Classify Stage 1 and 2 pressure ulcers Recognize suspected Stage 3, 4, DTI, and unstageable pressure ulcers
We ve got your back. Physical Therapy After Lumbar Fusion Surgery
 We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
PATIENT TEACHING GUIDE: Wound Care Handbook
 PATIENT TEACHING GUIDE: Wound Care Handbook PATIENT TEACHING GUIDE: WOUND CARE Design by Mariscal Design, Illustrations by Lysa Hawke. The Wound Care Self Care Guide was written and prepared by: Barbara
PATIENT TEACHING GUIDE: Wound Care Handbook PATIENT TEACHING GUIDE: WOUND CARE Design by Mariscal Design, Illustrations by Lysa Hawke. The Wound Care Self Care Guide was written and prepared by: Barbara
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Safety FIRST: Infection Prevention Tips
 Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
Reading Hospital Safety FIRST: Infection Prevention Tips Reading Hospital is committed to providing high quality care to our patients. Your healthcare team does many things to help prevent infections.
SCI Rehab. Stages of Pressure Sores. Prevention of Pressure Sores Develop due to pressure on skin, lack of blood supply, tissue death.
 SCI Rehab Basics of Bowel and Bladder Management, Skin Protection, Bathroom DME, Positioning, and Transfers SCI Rehab 101 Rehab Education Basics Skin, Bladder, Bowel Skin Protection and Pressure Sore Prevention!
SCI Rehab Basics of Bowel and Bladder Management, Skin Protection, Bathroom DME, Positioning, and Transfers SCI Rehab 101 Rehab Education Basics Skin, Bladder, Bowel Skin Protection and Pressure Sore Prevention!
Pressure Ulcers: Facility Assessment Checklists
 Pressure Ulcers: Facility Assessment Checklists This is a series of self-assessment checklists for nursing home staff to use to assess processes related to managing pressure ulcers in the facility, in
Pressure Ulcers: Facility Assessment Checklists This is a series of self-assessment checklists for nursing home staff to use to assess processes related to managing pressure ulcers in the facility, in
Multiple Sclerosis (MS)
 Multiple Sclerosis (MS) Purpose/Goal: Care partners will have an understanding of Multiple Sclerosis and will demonstrate safety and promote independence while providing care to the client with MS. Introduction
Multiple Sclerosis (MS) Purpose/Goal: Care partners will have an understanding of Multiple Sclerosis and will demonstrate safety and promote independence while providing care to the client with MS. Introduction
Going Home after Replantation Surgery
 Going Home after Replantation Surgery TWH Information for patients and families Read this booklet to learn: how to care for yourself what problems to look out for how to take care of your wound sites who
Going Home after Replantation Surgery TWH Information for patients and families Read this booklet to learn: how to care for yourself what problems to look out for how to take care of your wound sites who
Heat Illnesses. Common Heat Rash Sites
 Heat Illnesses Introduction Heat illnesses happen when the body becomes too hot and cannot cool itself. There are several different types of heat-related illnesses. This includes heat cramps, heat exhaustion,
Heat Illnesses Introduction Heat illnesses happen when the body becomes too hot and cannot cool itself. There are several different types of heat-related illnesses. This includes heat cramps, heat exhaustion,
Inservice: Wound Care and Dressings. Friday, June 26, 2009. A. Closed Wounds tissue is injured but skin is not BROKEN
 f Inservice: Wound Care and Dressings Friday, June 26, 2009 WOUNDS: Are injuries of the skin and underlying subcutaneous tissues and muscles (Nursing Manual by Lippincott) Are disruptions in the integrity
f Inservice: Wound Care and Dressings Friday, June 26, 2009 WOUNDS: Are injuries of the skin and underlying subcutaneous tissues and muscles (Nursing Manual by Lippincott) Are disruptions in the integrity
X-Plain Foley Catheter Male Reference Summary
 X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
INTRODUCTION TO POSITIONING. MODULE 3: Positioning and Carrying
 MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
Illinois Department of Public Health STATEMENT OF DEFICIENCIES AND PLAN OF CORRECTION. Statement of LICENSURE Violations
 (X1) PROVER/SUPPLIER/CLIA ENTIFICATION NUMBER: (X3) SURVEY D NAME OF PROVER OR SUPPLIER (X4) SUMMARY REGULATORY OR LSC ENTIFYING INFORMATION) PROVER'S PLAN OF CORRECTION Final Observations Statement of
(X1) PROVER/SUPPLIER/CLIA ENTIFICATION NUMBER: (X3) SURVEY D NAME OF PROVER OR SUPPLIER (X4) SUMMARY REGULATORY OR LSC ENTIFYING INFORMATION) PROVER'S PLAN OF CORRECTION Final Observations Statement of
Mobility After Stroke
 Mobility After Stroke Issues facing stroke survivors and their families Regaining Mobility Moving around safely and easily is not something you may think about, until you have had a stroke. Each year more
Mobility After Stroke Issues facing stroke survivors and their families Regaining Mobility Moving around safely and easily is not something you may think about, until you have had a stroke. Each year more
Herniated Lumbar Disc
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
OASIS-C Integument Assessment: Not for Wimps! Part I: Pressure Ulcers
 OASIS-C Integument Assessment: Not for Wimps! Part I: Pressure Ulcers Presented by: Rhonda Will, RN, BS, COS-C, HCS-D Assistant Director, OASIS Competency Institute 243 King Street, Suite 246 Northampton,
OASIS-C Integument Assessment: Not for Wimps! Part I: Pressure Ulcers Presented by: Rhonda Will, RN, BS, COS-C, HCS-D Assistant Director, OASIS Competency Institute 243 King Street, Suite 246 Northampton,
Exercise After Breast Surgery. Post Mastectomy Therapy
 Exercise After Breast Surgery Post Mastectomy Therapy Dear Patient, Breast cancer is a journey and you have made it this far successfully. This booklet will help you continue your journey to recovery.
Exercise After Breast Surgery Post Mastectomy Therapy Dear Patient, Breast cancer is a journey and you have made it this far successfully. This booklet will help you continue your journey to recovery.
Position Statement: Pressure Ulcer Staging
 Position Statement: Pressure Ulcer Staging Statement of Position The Wound, Ostomy and Continence Nurses (WOCN) Society supports the use of the National Pressure Ulcer Advisory Panel Staging System (NPUAP).
Position Statement: Pressure Ulcer Staging Statement of Position The Wound, Ostomy and Continence Nurses (WOCN) Society supports the use of the National Pressure Ulcer Advisory Panel Staging System (NPUAP).
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Preventing Pressure Ulcers and Assisting With Wound Care
 Preventing Pressure Ulcers and Assisting With Wound Care C H A P T E R 19 A nursing assistant makes an occupied bed. Providing clean, wrinkle-free linens is just one way that nursing assistants help to
Preventing Pressure Ulcers and Assisting With Wound Care C H A P T E R 19 A nursing assistant makes an occupied bed. Providing clean, wrinkle-free linens is just one way that nursing assistants help to
Cast removal what to expect #3 Patient Information Leaflet
 Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Patient s Handbook. Provincial Rehabilitation Unit ONE ISLAND HEALTH SYSTEM ONE ISLAND FUTURE 11HPE41-30364
 Patient s Handbook Provincial Rehabilitation Unit ONE ISLAND FUTURE ONE ISLAND HEALTH SYSTEM 11HPE41-30364 REHABILITATION EQUIPMENT USED ON UNIT 7 During a patient s stay on Unit 7, various pieces of
Patient s Handbook Provincial Rehabilitation Unit ONE ISLAND FUTURE ONE ISLAND HEALTH SYSTEM 11HPE41-30364 REHABILITATION EQUIPMENT USED ON UNIT 7 During a patient s stay on Unit 7, various pieces of
Expected Outcomes: What You Should Know
 C6 CONSUMER GUIDE: EXPECTED OUTCOMES SPINAL CORD MEDICINE Expected Outcomes: What You Should Know A Guide for People with C6 Spinal Cord Injury Administrative and financial support provided by Paralyzed
C6 CONSUMER GUIDE: EXPECTED OUTCOMES SPINAL CORD MEDICINE Expected Outcomes: What You Should Know A Guide for People with C6 Spinal Cord Injury Administrative and financial support provided by Paralyzed
How To Stage A Pressure Ulcer
 WOCN Society Position Statement: Pressure Ulcer Staging Originated By: Wound Committee Date Completed: 1996 Reviewed/Revised: July 2006 Revised: August 2007 Reviewed/Revised: April 2011 Definition of Pressure
WOCN Society Position Statement: Pressure Ulcer Staging Originated By: Wound Committee Date Completed: 1996 Reviewed/Revised: July 2006 Revised: August 2007 Reviewed/Revised: April 2011 Definition of Pressure
Total Hip Replacement Surgery Home Care Instructions
 Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Total Hip Replacement Surgery Home Care Instructions Surgery: Date: Doctor: This handout will review the care you need to follow once you are home. If you have any questions or concerns, please ask your
Individualized Care Plans Fully Developed
 Appendix Individualized Care Plans Fully Developed A Refer to Chapter 1 The Nursing Process: A Synopsis, p. 32: Two Individualized Care Plans Fully Developed; Care Plan 1 for Mr. John Walters, Care Plan
Appendix Individualized Care Plans Fully Developed A Refer to Chapter 1 The Nursing Process: A Synopsis, p. 32: Two Individualized Care Plans Fully Developed; Care Plan 1 for Mr. John Walters, Care Plan
ROTATOR CUFF HOME EXERCISE PROGRAM
 ROTATOR CUFF HOME EXERCISE PROGRAM Contact us! Vanderbilt Sports Medicine Medical Center East, South Tower, Suite 3200 1215 21st Avenue South Nashville, TN 37232-8828 For more information on this and other
ROTATOR CUFF HOME EXERCISE PROGRAM Contact us! Vanderbilt Sports Medicine Medical Center East, South Tower, Suite 3200 1215 21st Avenue South Nashville, TN 37232-8828 For more information on this and other
What is the Spasticity Clinic?
 The Spasticity Clinic This booklet can help you learn about: the Spasticity Clinic at McMaster Children s Hospital spasticity and how it may be treated Your therapist will give you more information and
The Spasticity Clinic This booklet can help you learn about: the Spasticity Clinic at McMaster Children s Hospital spasticity and how it may be treated Your therapist will give you more information and
Total Hip Replacement
 NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
NOTES Total Hip Replacement QUESTIONS DATES PHONE NOS. Compiled by Mr John F Nolan FRCS for The British Hip Society 2009. A patient s information booklet 16 1 Introduction This booklet has been produced
What are Core Muscles?... 2. A Healthy Lumbar Spine...3. What is Low Back Pain?...4. Rehabilitation...6. Stages of Rehabilitation...
 Table of Contents What are Core Muscles?... 2 A Healthy Lumbar Spine...3 What is Low Back Pain?...4 Rehabilitation...6 Stages of Rehabilitation...7 Pain Management....................... 8 Heat/Ice What
Table of Contents What are Core Muscles?... 2 A Healthy Lumbar Spine...3 What is Low Back Pain?...4 Rehabilitation...6 Stages of Rehabilitation...7 Pain Management....................... 8 Heat/Ice What
TOWN CENTER ORTHOPAEDIC ASSOCIATES P.C. Labral Tears
 Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Cervical Spondylosis (Arthritis of the Neck)
 Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Be Safe! Manage Heat Stress. Be Safe! Manage Heat Stress.
 Be Safe! Manage Heat Stress. Be Safe! Manage Heat Stress. Overview Workers who are exposed to extreme heat or work in hot environments may be at risk of heat stress. Exposure to extreme heat can result
Be Safe! Manage Heat Stress. Be Safe! Manage Heat Stress. Overview Workers who are exposed to extreme heat or work in hot environments may be at risk of heat stress. Exposure to extreme heat can result
Radiation Therapy To the Arms or Legs
 Radiation Therapy To the Arms or Legs You will be receiving two to six weeks of radiation to the arms or legs. It will describe how your treatments are given. It will also describe how to take care of
Radiation Therapy To the Arms or Legs You will be receiving two to six weeks of radiation to the arms or legs. It will describe how your treatments are given. It will also describe how to take care of
Preventing & Treating Low Back Pain
 Preventing & Treating Low Back Pain An Introduction to Low Back Pain Low back pain is the number two reason that Americans see a health care practitioner second only to colds and flu. While most people
Preventing & Treating Low Back Pain An Introduction to Low Back Pain Low back pain is the number two reason that Americans see a health care practitioner second only to colds and flu. While most people
HOPE EXERCISE RECOVERY RESOURCES RELATIONSHIPS INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RELATIONSHIPS MOVEMENT. A Stroke Recovery Guide
 INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RECOVERY HOPE A Stroke Recovery Guide RELATIONSHIPS MOVEMENT RESOURCES RELATIONSHIPS EXERCISE www.stroke.org CHAPTER FOUR Movement and Exercise Moving
INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RECOVERY HOPE A Stroke Recovery Guide RELATIONSHIPS MOVEMENT RESOURCES RELATIONSHIPS EXERCISE www.stroke.org CHAPTER FOUR Movement and Exercise Moving
Urine Leaks After Prostate Cancer Treatment
 Managing Symptoms After Prostate Cancer Urine Leaks After Prostate Cancer Treatment Urine leaks after surgery or radiation for prostate cancer are common. The medical term for this is incontinence (say:
Managing Symptoms After Prostate Cancer Urine Leaks After Prostate Cancer Treatment Urine leaks after surgery or radiation for prostate cancer are common. The medical term for this is incontinence (say:
INSULIN INJECTION KNOW-HOW
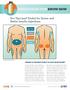 0-0- 0 INSULIN INJECTION KNOW-HOW pro tips (and tricks) for easier and better Insulin Injections ABDOMEN THIGHS BUTTOCKS ARMS recommended injection sites WHERE IS THE BEST PLACE TO GIVE INJECTIONS? 0-
0-0- 0 INSULIN INJECTION KNOW-HOW pro tips (and tricks) for easier and better Insulin Injections ABDOMEN THIGHS BUTTOCKS ARMS recommended injection sites WHERE IS THE BEST PLACE TO GIVE INJECTIONS? 0-
Pressure Ulcer Passport
 Pressure Ulcer Passport Information for patients This is a record of the treatment you are receiving for your pressure ulcer injury. Please bring it with you to all your healthcare appointments. This will
Pressure Ulcer Passport Information for patients This is a record of the treatment you are receiving for your pressure ulcer injury. Please bring it with you to all your healthcare appointments. This will
Management of Burns. The burns patient has the same priorities as all other trauma patients.
 Management of Burns The burns patient has the same priorities as all other trauma patients. Assess: - Airway - Breathing: beware of inhalation and rapid airway compromise - Circulation: fluid replacement
Management of Burns The burns patient has the same priorities as all other trauma patients. Assess: - Airway - Breathing: beware of inhalation and rapid airway compromise - Circulation: fluid replacement
Obesity Affects Quality of Life
 Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Musculoskeletal System
 CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
Community home-based prevention of disability due to lymphatic filariasis
 Community home-based prevention of disability due to lymphatic filariasis World Health Organization Geneva WHO/CDS/CPE/CEE/2003.35 Part 3 Figure 1 Wash your leg, or other part of the body affected by lymphoedema,
Community home-based prevention of disability due to lymphatic filariasis World Health Organization Geneva WHO/CDS/CPE/CEE/2003.35 Part 3 Figure 1 Wash your leg, or other part of the body affected by lymphoedema,
Lumbar or Thoracic Decompression and Fusion
 Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Lumbar or Thoracic Decompression and Fusion DO NOT TAKE ANY ASPIRIN PRODUCTS OR NON-STEROIDAL ANTI- INFLAMMATORY DRUGS (ie NSAIDs, Advil, Celebrex, Ibuprofen, Motrin, Naprosyn, Aleve, etc) FOR 2 WEEKS
Diabetic Foot Ulcers and Pressure Ulcers. Laurie Duckett D.O. Plastic and Reconstructive Surgeon Oklahoma State University Center for Health Sciences
 Diabetic Foot Ulcers and Pressure Ulcers Laurie Duckett D.O. Plastic and Reconstructive Surgeon Oklahoma State University Center for Health Sciences Lecture Objectives Identify risk factors Initiate appropriate
Diabetic Foot Ulcers and Pressure Ulcers Laurie Duckett D.O. Plastic and Reconstructive Surgeon Oklahoma State University Center for Health Sciences Lecture Objectives Identify risk factors Initiate appropriate
CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery
 CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery For patients of Jeffrey Kramer, MD As you re discharged from the hospital, you may have questions about your continuing
CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery For patients of Jeffrey Kramer, MD As you re discharged from the hospital, you may have questions about your continuing
Lower Back Pain An Educational Guide
 Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
Spinal Cord Injury Education. An Overview for Patients, Families, and Caregivers
 Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
Calcaneus (Heel Bone) Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Extreme Heat: A Prevention Guide to Promote Your Personal Health and Safety
 Extreme Heat: A Prevention Guide to Promote Your Personal Health and Safety Heat-related deaths and illness are preventable yet annually many people succumb to extreme heat. Historically, from 1979-2003,
Extreme Heat: A Prevention Guide to Promote Your Personal Health and Safety Heat-related deaths and illness are preventable yet annually many people succumb to extreme heat. Historically, from 1979-2003,
HOW TO CARE FOR A PATIENT WITH DIABETES
 HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
HOW TO CARE FOR A PATIENT WITH DIABETES INTRODUCTION Diabetes is one of the most common diseases in the United States, and diabetes is a disease that affects the way the body handles blood sugar. Approximately
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Home Care for Your Nephrostomy Catheter
 Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
2. When temperature and wind chill falls below 35 degrees including the wind chill, students, are kept indoors.
 Weather /Environmental Guidelines Time spent outdoors is an important part of the school day. It is difficult to set guidelines that fit every circumstance and condition in regards to outside activities.
Weather /Environmental Guidelines Time spent outdoors is an important part of the school day. It is difficult to set guidelines that fit every circumstance and condition in regards to outside activities.
YOUR GUIDE TO TOTAL HIP REPLACEMENT
 A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
Range of Motion. A guide for you after spinal cord injury. Spinal Cord Injury Rehabilitation Program
 Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
The road to recovery. The support available to help you with your recovery after stroke
 The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Introduction Need to talk? Call our confidential Stroke Helpline
The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Introduction Need to talk? Call our confidential Stroke Helpline
THERAPEUTIC USE OF HEAT AND COLD
 THERAPEUTIC USE OF HEAT AND COLD INTRODUCTION Heat and cold are simple and very effective therapeutic tools. They can be used locally or over the whole body, and the proper application of heat and cold
THERAPEUTIC USE OF HEAT AND COLD INTRODUCTION Heat and cold are simple and very effective therapeutic tools. They can be used locally or over the whole body, and the proper application of heat and cold
PRESSURE ULCER GUIDELINES FOR TOPICAL TREATMENT
 PRESSURE ULCER GUIDELINES FOR TOPICAL TREATMENT The following are suggested guidelines for treatment of pressure ulcers using products from Swiss-American Products, Inc. and are intended to supplement
PRESSURE ULCER GUIDELINES FOR TOPICAL TREATMENT The following are suggested guidelines for treatment of pressure ulcers using products from Swiss-American Products, Inc. and are intended to supplement
CHAPTER V CONCLUSION AND RECOMMENDATIONS. findings are presented, implications for nursing practice and education are discussed,
 CHAPTER V CONCLUSION AND RECOMMENDATIONS In this chapter, a summary of the findings and conclusion drawn from the findings are presented, implications for nursing practice and education are discussed,
CHAPTER V CONCLUSION AND RECOMMENDATIONS In this chapter, a summary of the findings and conclusion drawn from the findings are presented, implications for nursing practice and education are discussed,
Department of Surgery
 Thoracic Surgery After Your Lung Surgery Patient Education Discharge Information You have just had lung surgery. The following are definitions of terms you may hear in connection with your surgery: THORACOTOMY
Thoracic Surgery After Your Lung Surgery Patient Education Discharge Information You have just had lung surgery. The following are definitions of terms you may hear in connection with your surgery: THORACOTOMY
Herniated Disk in the Lower Back
 Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological Institute Al Maryah Island
Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological Institute Al Maryah Island
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Pulmonary Rehabilitation Program - Home Exercise Program
 Pulmonary Rehabilitation Program - Home Exercise Program Getting Started Regular exercise should be a part of life for everyone. Exercise improves the body's tolerance to activity and work, and strengthens
Pulmonary Rehabilitation Program - Home Exercise Program Getting Started Regular exercise should be a part of life for everyone. Exercise improves the body's tolerance to activity and work, and strengthens
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY
 CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
Helping you manage symptoms and side effects associated with metastatic breast cancer treatment
 Helping you manage symptoms and side effects associated with metastatic breast cancer treatment 2015 AstraZeneca. All rights reserved. 3156710 Last Updated 9/15 with metastatic breast cancer treatment
Helping you manage symptoms and side effects associated with metastatic breast cancer treatment 2015 AstraZeneca. All rights reserved. 3156710 Last Updated 9/15 with metastatic breast cancer treatment
Wound and Skin Assessment. Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center
 Wound and Skin Assessment Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center Skin The largest Organ Weighs between 6 and 8 pounds Covers over 20 square feet Thickness
Wound and Skin Assessment Mary Carvalho RN, BSN, MBA Clinical Coordinator Johnson Creek Wound and Edema Center Skin The largest Organ Weighs between 6 and 8 pounds Covers over 20 square feet Thickness
Throughout this reference summary, you will find out what massage therapy is, its benefits, risks, and what to expect during and after a massage.
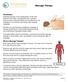 Massage Therapy Introduction Massage therapy is the manipulation of the soft tissues of the body, including the skin, tendons, muscles and connective tissue by a professional, for relaxation or to enhance
Massage Therapy Introduction Massage therapy is the manipulation of the soft tissues of the body, including the skin, tendons, muscles and connective tissue by a professional, for relaxation or to enhance
Colon Cancer Surgery and Recovery. A Guide for Patients and Families
 Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
