Relax and Learn at the FARM History of Cardiac Monitoring. History of Cardiac Monitoring 10/17/2012
|
|
|
- Eustace Wilkerson
- 7 years ago
- Views:
Transcription
1 Relax and Learn at the FARM 2012 Session 3: Bedside Cardiac Monitoring: Arrhythmias, ST Segments, and QT Interval Karen MarzlinDNP, RN, CCNS, CCRN-CMC, CHFN Cardiovascular Nursing Education Associates 1 Professional nursing practice can only advance as much as individual nurses are aware that a knowledge gap exists in their practice, feel empowered to access further learning, and integrate evidence based competencies into their professional practice to provide safe, effective, efficient, patient centered, equitable care. 2 History of Cardiac Monitoring st monitoring begins in Sydney Australia by Dr. Desmond Julian who noted: All wards admitting patients with acute myocardial infarction should have a system capable of sounding an alarm at the onset of an important rhythm change and recording the rhythm automatically on an ECG.the provision of the appropriate apparatus would not be prohibitively expensive if these patients were admitted to special intensive care units. Such units should be staffed by suitably experienced people throughout the 24 hours. History of Cardiac Monitoring Later that year the 1 st CCU in the US opened in Kansas City by Dr. Hugh Day Early cardiac monitoring focused on observing heart rates and monitoring for life threatening arrhythmias Monitoring equipment has changed greatly over the past 40+ years Despite advances in technology, the need for human over site in the interpretation of the ECG is as important as it was 40 ago for the following reasons: With the high sensitivity capabilities of the current monitors numerous alarms must be evaluated to prevent over treatment More aggressive approaches to treatment of myocardial ischemia improves outcomes requiring ongoing surveillance Complex device technology requires expert analysis of ECG monitoring data Many more drugs have been that prolong QT intervals failure to identify patients at risk increases the incidence of sudden cardiac death Only humans not monitors can determine the goals of monitoring for individual patients 6 1
2 Short supply of skilled healthcare professionals with expertise in electrocardiography and cardiac monitoring for the following reasons: Multipurpose ICUs have replaced pure CCUs Shortage of critical care nurses results in under trained nurses working in the ICU Medical students, residents, and cardiology trainees are often inadequately trained in ECG interpretation and learn even less about cardiac monitoring leads, technology, and interpretation Staff Qualifications Dedicated monitor watcher Pros and cons Investing in advanced monitoring technology may be more cost effective than dedicated watchers Combination of monitors from several units at a remote site by a dedicated watcher Not recommended UNLESS expertise of the remote monitor watcher is superior and training cannot be provided to nurses on each monitored unit. Pagers that signal the nurse with monitor alarms that displays arrhythmia is helpful 7 8 Staff Qualifications Monitoring needs are different for each unit requiring different training for each unit Staff proficiencies should be determined based on unit population and purpose of monitoring Formal orientation to include both didactic and hands on practice with return demonstration Accurate electrode placement is an essential part of the orientation process 9 Understanding Specific ECG Abnormalities Normal Rhythms Intraventricular conduction defects Bundle branch blocks Aberrant conduction Tachyarrhythmias Supraventricular AV reentrant AV nodal reentrant A fib / flutter Multifocalatrial tachycardia Atrial tachycardia Junctional ectopic tachycardia Ventricular Accelerated V arrhythmias Nonsustainded/ sustainted polymorphic VT Prolonged QT interval associated VT VF Bradyarrhythmias Premature complexes Supraventricular Ventricular Pacemaker Electrocardiology Failure to capture, pace, or sense Failure to capture both ventricles in biventricularpacing ECG abnormalities in acute myocardial infarction ST segment elevation or depression T Wave inversion Muscle or other artifacts 10 Understand General Electrophysiology Concepts Automaticity Excitation Conduction Sinus node physiology AV node physioloyg Wide and narrow QRS complexes Observation with arrhythmias Sustained vs nonsustained Monomorphicvs polymorohic Stable vs nonstable Symptomatic vs asymptomatic Association with heart disease vs no heart disease Syncope Hemodynamic effects of arrhythmias Influence of rate Influence of heart disease Influence of A-V synchrony Influence of LV synchrony Function of Implantable devices Acute myocardial ischemia STEMI ST recovery of successful reperfusion Reperfusion arrhythmias NonSTEMI Transient ischemia Effects of common antiarrhythmic drugs, rate control vsrhythm control 11 Specific Monitoring Skills Operation of monitoring system Recognition of limitations of computerized algorhithms Proper skin prep Accurate lead placement Setting heart rate, ST alarm parameters Measurement of HR Measurement of intervals (with calipers) Recognition of atrial activity Evaluating pauses Diagnosis of specific rhythms Recording from postoperative epicardial wires Ability to intervene (unit protocols for responding, reporting, and documenting) in patients with: Bradycardia Tachycardia Syncope Cardiorespiratoryarrest Implantable devices Temporary pacemakers Transcutaneous pacemakers 12 2
3 Electrical Conduction Pathway SA Node AV Node Bundle of His AV Junction Right and Left Bundle Branches Anterior and Posterior Fascicles PurkingeFibers WAVES and COMPLEXES QRS P PR Interval QRS P wave: atrial depolarization QRS: ventricular depolarization T wave: ventricular repolarization PR interval: AV conduction time QRS width: intraventricular conduction time ST Segment: entire ventricular depolarization QT interval: used to reflect ventricular repolarization time QT Interval ST Segment T QRS Complex Not every QRS complex contains a Q wave, R wave and S wave!! Q always negative (below baseline) R first positive above the baseline R second positive above the baseline S negative deflection following R wave or second component to entirely complex S second negative deflection ECG Paper Horizontal Axis Normal speed 25 mm/ sec Smallest box 1mm x 1mm 1 small box 0.04 sec 1 large box 0.20 sec 5 large boxes 1.0 sec Measuring Rate on Irregular Rhythms Irregular rhythms Count number of R-R intervals in a 6 second strip and multiply by 10 Measuring Rate on Regular Rhythms Regular rhythms Count number of large boxes between R waves and divide into 300: 1 = = 50 2 = = 43 3 = = 37 4 = 75 9 = 33 5 = = X 10 = =
4 Calculating Rate Utilizing the Bedside Monitor to Provide 12 Lead ECG Information Many Options 3 lead 5 lead 6 lead Hard Wired Telemetry Derived ECG Standard Lead Placement 6 Lead System Modified 5 Lead System Standard 6 Lead Placement 21 Standard 6 Lead Placement 5 Lead Placement (No C6) Modified 5 lead Placement- MCL6 22 Standard 3 Lead Electrode Placement 3 Lead Placement for Modified Chest Lead 1 (MCL1) Lead 3 (MCL6) Importance of the Positive Electrode Consider the positive electrode the the camera (exploring electrode) RA LA + RV L V 23 4
5 Comparing Bedside Monitoring to the 12 Lead ECG Remember View of Positive Electrode (Camera) Importance of Lead Placement Identify Correct Lead on Rhythm Strip 25 E: Lower extreme of the sternum (Brown +) A: Left mid-axillary line, same transverse line as E (Black +) S: Sternal manubrium (Red -) I: Right mid-axillary line, same transverse line as E (White -) G: Fifth electrode is the ground and can be placed anywhere on the torso (Green no polarity) Derived ECG 26 Rating System for Recommendations Circulation. 2004;110: doi: /01.CIR Class I Recommendations Cardiac monitoring indicated in most, if not all, patients in this group. Class II Recommendations Cardiac monitoring may be of benefit in some patients but is not considered essential for all patients. Class III Recommendations Cardiac monitoring is not indicated because a patient s risk of a serious event is so low that monitoring has no 28 therapeutic benefit. Three Reasons for Bedside Cardiac Monitoring Arrhythmia Detection Ischemia Monitoring QT Interval Monitoring 29 Class I Arrhythmia Monitoring Recommendations Patients resuscitated from cardiac arrest Patients in early phase of Acute Coronary Syndromes (including Rule Outs ) Patients with unstable coronary syndromes and newly diagnosed high-risk coronary lesions Adults and children who have undergone cardiac surgery Patients after nonurgent percutaneous coronary interventions with complications Patients after ICD implant or pacer lead placement if pacer dependent Patients with temporary pacemaker or transcutaneous pacing pads Patients with AV block 30 5
6 Class I Arrhythmia Monitoring Recommendations Patients with Arrhythmias complicating Wolff-Parkinson- White Syndrome with rapid anterogradeconduction over an accessory pathway Patients with Long-QT Syndrome and associated ventricular arrhythmias Patients with intraaortic balloon pump Patients with acute heart failure/ pulmonary edema Patients with indications for intensive care Patient under going diagnostic / therapeutic procedures requiring conscious sedation or anesthesia Patients with any other hemodynamicallyunstable arrhythmias Diagnosis of arrhythmias in pediatric patients 31 Arrhythmia Monitoring Candidates Primary purpose for all patients on cardiac monitor Purpose Detection of and prompt interventionfor life threatening arrhythmias Leads of Choice V1 V6 (or MCL6) 32 Acute Management of Ventricular Arrhythmias Wide complex tachycardia presumed to be VT if diagnosis is unclear DC cardioversion with sedation if hemodynamically unstable Don t assume VT cannot be well tolerated! The rate, size of the heart and presence of additional complications are often more important than the source of the tachycardia Check the patient (need for defibrilllation?) Check the blood pressure (need for cardioversion?) Check the ECG (determine the rhythm) Ectopy Versus Aberrancy Ectopy: Ventricular Tachycardia Aberrancy: SVT conducted aberrantly (with a bundle branch block) Criteria for Differentiating Ectopy from Aberrancy Patient history / assessment QRS Width Concordance AV Dissociation Axis Morphology Note: VT is much more common than supraventriculartachycardia with bundle branch aberration. In wide QRS tachycardiasvt is the right answer up to 80% of the time. A wide complex tachycardia is always considered ventricular in origin if the diagnosis is uncertain 35 Patient History Acute ischemia / injury (Abnormal automaticity) Post myocardial infarction / ischemic cardiomyopathy (Reentrant circuit within myocardium) Non ischemic dilated cardiomyopathy (Bundle branch reentrant VT) QRS Width The wider the QRS VT is favored However: SVT with LBBB will have a wider QRS than SVT with RBBB Other causes of SVT with wider than expected QRS: antidromic tachycardia and patients on Class I antiarrhythmics or amiodarone Not all VT is significantly wide VT originating from septum more narrow than VT from free wall If QRS more narrow than sinus rhythm = VT 36 6
7 Negative Concordance AV Dissociation SVTs with aberration : 1 st complex preceded by atrial activity Only seen in 30% VTs Independent atrial and ventricular activity (AV dissociation) is diagnostic for ventricular ectopy Positive Concordance: Cannot rule out antidromictachycardia in WPW 37 Ventricular tachycardia may also have retrograde P waves (retrograde P waves do not confirm VT) 38 Sinus Capture Beat: Another Way to Prove AV Dissociation Axis Axis Extreme axis is strong indicator of ventricular ectopy Right axis deviation confirms ventricular ectopy with LBBB pattern Ventricular tachycardia rarelyoccurs with normal axis Axis Practice Morphology (Shape) Ventricular Ectopycompared to Aberrancy (BBB) 41 Morphology Challenges: BBB Reentrant VT Idiopathic RVOT Antidromictachycardia 42 7
8 Bedside Cardiac Monitoring LBBB RBBB LVT RVT RBBB Comparison of Morphology in Lead V1 LBBB V1 and V6 are gold standard monitoring leads for ectopy versus aberrancy Bundle branch block patterns and ventricle ectopycan be differentiated by using the morphology of these leads. VT from Left Ventricle VT from Right Ventricle DON T rely on Lead II!! Physiological Critical Thinking Questions? In a right BBB which ventricle depolarizes first? In a left BBB which ventricle depolarizes first? RBBB Comparison of Morphology in Lead V1 Left ventricle first LBBB Right ventricle first If VT starts in the left ventricle which ventricle depolarizes first? If VT starts in the right ventricle which ventricle depolarizes first? VT from Left Ventricle Left ventricle first VT from Right Ventricle Right ventricle first Lead V1 (VT Patterns) RBBB Comparison of Morphology in Lead V1 LBBB VT from Left Ventricle VT from Right Ventricle VT with RBBB pattern or LVT VT with LBBB pattern or RVT
9 Bundle Branch Block Morphology in Lead V6 Practice EKGs RBBB LBBB It is important to recognize RBBB and LBBB morphology in lead V1 (and document) when patients are in SR. This skill allows you to better differentiate between VT and SVT with BBB (aberrancy) when the patient is in a wide complex tachycardia. RBBB Above are two examples of RBBB morphology in lead V1. The first strip shows the classic rsr pattern. The second strip shows a qr pattern. Patients who have infarcted their septum lose the first r wave and will typically demonstrate a qr pattern. In the examples above the patient is in an atrial flutter. In the first strip the patient is conducting with a normal QRS width. The second strip the patient is now in a 2:1 atrial flutter with an increased ventricular rate resulting in the right bundle becoming refractory. Therefore the patient conducts with a RBBB
10
11 These strips are all from the same patient. None of these episodes of non sustained VT were documented. Nor, was there any documentation of provider notification. These arrhythmias were discovered while preparing for discharge. EP was consulted at that time which resulted in a delay in treatment and subsequent discharge
12 Case Study Case Study Case Study I avr V1 V4 Clinical Pearls for Ventricular Arrhythmias V-fib seldom is seldom preceded by warning arrhythmias Prophylactic lidocainenot indicated R on T PVCs are typically only important first 24 hours of myocardial infarction Bigeminy may need treated if cardiac output effected Ventricular ectopy (as infrequent as 15% burden) can result in heart failure Clinical Pearls for Ventricular Arrhythmias Potential reversible causes Hypokalemia: K < 3.2 meq/l (cause or result) Magnesium < 1.5 meq/dl Ischemia Use of inotropic agents Three Reasons for Bedside Cardiac Monitoring Arrhythmia Detection Ischemia Monitoring QT Interval Monitoring
13 Ischemia (ST) Monitoring Purpose To monitor changes in ST segments (compared to baseline) in select leads Leads of Choice Based on area of known or potential ischemia Anterior wall / Left anterior descending coronary Lead V3 Inferior wall / Right Coronary artery Lead III Lateral wall / Circumflex coronary artery Lead V6 Class I ST Segment Monitoring Recommendations Patients in early phase of Acute Coronary Syndromes (including Rule Out ) Patients who present to ED with chest pain or anginal equivalent symptoms Patients who have had nonurgent percutaneous coronary interventions with suboptimal results Patients with possible variant angina resulting from coronary vasospasm Class II ST Segment Monitoring Recommendations Patients postacute MI Patients after nonurgent uncomplicated percutaneous coronary intervention Patients at high risk for ischemia after cardiac or noncardiac surgery Pediatric patients at risk of ischemia or infarction resulting from congenital or acquired conditions 75 Class III ST Segment Monitoring Recommendations Patients with left bundle branch block Patients with ventricular paced rhythms Patients with other confounding arrhythmias that obscure the ST Segment Patients who are agitated 76 Methods To Improve ST Segment Monitoring Identification of body position changes Careful skin preparation Consistent lead placement Tailoring alarm parameters to patients baseline ST level Understand goals of monitoring in the individual patient Analyze ECG print out rather than just graphic trends 77 Body Position STsmay fluctuate with body position changes May cause false alarms ST should be evaluated with patient in the supine position Careful Prep ECG noise impedes accurate diagnosis Skin prep essential to good tracing Clipping to remove hair Remove skin oils with abrasion (dry 4x4) Keep electrodes in original package start to dry 20 minutes after opening Lead Placement Mark electrode placement Waveform changes may occur with as little as 1cm change in location Assess change in ST for true change or change lead location 78 13
14 Tailor Alarms Alarms must be set to reflect each individual patient s baseline 1mm above and below for precordial leads 0.5 mm for limb leads 2mm reasonable in the more stable patient (helps eliminate false alarms) Understand Goals of Monitoring Monitor for silent ischemia Monitor for recurrent ischemia Bad Alarm Monitor for ST recovery after intervention with fibrinolytic or PCI Good Alarm Analyze ECG Printout Graphic trends are capable on most monitors with ST segment monitoring Convenient for quick identification of ischemia Should never replace evaluation of rhythm strips When in doubt always verify with a 12 lead ECG 79 ST Segment In limb leads the ST segment is normally isoelectric but may be slightly elevated or depressed by less than 1mm In precordial leads ST segment elevation is normally not more than 1 to 2 mm (small elevation normal in many people) Clinical Application: 1) Do not accept any ST elevation in limb leads 2) Do not accept any ST depression in chest leads 80 The J Point ST Depression from Atrial Repolarization Point where the QRS complex and the ST segment meet. Clinical Application: There can be ST segment elevation with no J point elevation. 81 ST segments are measured 60 to 80 msec from J point. 82 T Waves Represents ventricular repolarization Slightly asymmetrical Usually oriented in the same direction as the previous QRS Not normally > than 5mm (limb leads) to 10 mm (precordial) high T Waves Too Big????? Clinical Application: Do not accept any T wave that is too big in any lead
15 Answer: YES (same patient 2 hours later) ECG Assessment Priorities 1) Assess for ST segment elevation first ST elevation and need for reperfusion 2) Assess for T wave inversion next Non STEMI or Unstable angina (ischemia) 85 3) Assess for ST segment depression third Ischemia 86 Patterns of ST Elevation Injury Hyperacute T Wave As early as 2 minutes after occlusion J Point Elevation Hyper Acute T Wave with J Point Depression Post Hyper Acute T Waves Patterns of ST Elevation Injury Subtle ST Elevation Forming Broad T Wave
16 Subtle Inferior Elevation Most Obvious J Point Elevation T Wave Inversion: Key Points T wave should be positive in lead I and II Normal inversion is rare in V2 V6 Inversion in lead III, avl and avfmay be normal Inversion in V1 is common -always compare to previous ECG T Wave Inversion Associated With Ischemia /Infarction Deep T wave Inversion Disproportionate T wave Inversion (in relation to QRS voltage) New or changing T wave Inversion QTc usually increased Terminal T wave inversion 2 Types of T Wave Inversion: NSTEMI or Ischemia Symmetrical T wave inversion More on T Wave Inversion ECG Changes After STEMI T wave inversion is a warning (for ischemia or injury) unless The T wave inversion is after a STEMI After a STEMI T wave inversion is expected Terminal T wave inversion is a sign of reperfusion after a STEMI Symmetrical T wave inversion will develop after terminal T inversion 95 Non Reperfused T wave enlargement ST elevation Q wave formation or loss of R wave amplitude ST stabilization T wave inversion(within hours)before ST resolution ST resolution T waves stays inverted for period of time (takes weeks to months) Possible disappearance of Q waves Reperfused Earlier ST normalization and stabilization T wave inversion may accelerate Terminal T wave inversion initially T waves deepen symmetrically over time Q wave development is less pronounced or even absent 96 16
17 ST Evolution: Pseudo Normalization Right Sided and Posterior Quick Look with V1 Lead on Bedside Monitor Right Sided Lead Place electrode in V4R Position 5 th ICS RMCL Attach V monitoring lead (Brown Lead) to electrode Assure monitor lead selector is on V If ST elevation noted RV Infarct Run strip and clearly mark V4 Right Lead Posterior Lead Place electrode in V8 position Under tip of left scapula same level as V6 Attach V monitoring lead (Brown Lead) to electrode Assure monitor lead selector is on V If ST elevation noted Posterior Infarct Run strip and clearly mark V8 Posterior Lead ECG showing ST segment elevation in the inferior Leads (II, III, and avf) with reciprocal depression in Leads I and avl. There is also depression in V2 and V3 most likely representing reciprocal changes from ST elevation in the posterior leads. This is an ideal patient for a 16 lead ECG to assess for injury to the right ventricle and posterior wall of the left ventricle. V3 V Same Patient as Previous 12 Lead: Do to hypotension the point of care nurse used the V lead from bedside monitoring to record a V4R lead. This recording confirms RV injury and this knowledge was used to guide treatment. ST Segment Monitoring A SUCCESS Story!! The next 2 slides show the following: 1. Admission ECG for a patient with an anteroseptal / lateral wall STEMI. 2. ECG post intervention for same patient. 1. Note: The T waves have not yet inverted post intervention. Ideally T waves will begin to invert after an intervention showing evidence of reperfusion. REMEMBER: T wave must invert within hours after a STEMI (the sooner the better). Failure of T waves to invert after a STEMI is indicative of post infarction regional pericarditis and the patient is at higher risk for myocardial rupture
18 The strip below assessing ST segments in V3 was done 48 hours post STEMI (same patient as previous 2 ECGs.). The failure of the T waves to invert is indicative of post infarction regional pericarditis with increased risk of myocardial rupture. The patient was hypotensive, which raises the concern for cardiac tamponade as the etiology of the hypotension. This assessment finding was communicated to the cardiologist. The patient s echocardiogram showed a large pericardial effusion and the patient subsequently underwent a surgical pericardial window. ST Segment Monitoring An Example to Improve Practice Please review the ECG on the next slide demonstrating ST segment elevation in leads II, III, avf, and V4, V5, and V6. The patient was admitted to CCU from Woodlawn post CABG. The ECG on the next slide was approximately 5 weeks post CABG. The ECG changes on the next slide occurred with a hemoglobin < 8.0. The patient continued to have a hemoglobin level below normal for the remainder of the hospital stay. However, 5 days later it was charted that the patient met exclusion for ST segment monitoring. Important points: Graft occlusion is a potential complication post CABG. Anemia decreases myocardial oxygen supply and contribute to an acute coronary event ST Segment Monitoring Just 5 days after this ECG with ongoing anemia. An Example to Improve Practice This patient received ST segment monitoring on admission to the hospital due to admitting diagnosis of chest pain. Please read the results on the next slide of the patient s stress test (first report) and cardiac catheterization results (second report)
19 ST Segment Monitoring An Example to Improve Practice Although the patient needed further revascularization, it was unable to be performed because the patient required an urgent surgery, resulting in the inability to continue clopidogrel or prasugrel after the placement of an intracoronary stent. The decision was made to proceed with the high risk urgent surgery (due to inability to revascularize an ischemic patient) and later proceed with coronary intervention pending post op recovery and results of urgent surgery ST Segment Monitoring An Example to Improve Practice The patient received ST segment monitoring pre operatively. The patient returned to CCU post operatively but did not receive post operative ST segment monitoring. Note: There is high risk for perioperative ischemia and infarction in high risk surgical patients and therefore ST segment monitoring should have been continued. Three Reasons for Bedside Cardiac Monitoring Arrhythmia Detection Ischemia Monitoring QT Interval Monitoring QT Interval Monitoring Purpose To monitor for increase in QT interval to identify and intervene in patients at high risk for Torsadesde Pointes Leads of Choice Lead where an accurate QT Interval can be measured Patient can be changed to another lead to run a strip to measure QT or 12 lead can be done if QT not easily measured in V1 or V 6 Notes: QT interval needs to be adjusted for HR V2 and V3 usually have the longest QT Dynamic changes are most important Abnormal findings are uncovered during abrupt changes in the R to R
20 The Electronics Action Potential of Cardiac Cells Phase 0: Rapid depolarization Sodium Influx (beginning of QRS complex) Phase 1: Brief, rapid initiation of repolarization The Electronics Phase 2: Plateau phase Calcium Influx (greater than potassium efflux) correlates with ST segment Phase 3: Sudden acceleration in the rate of repolarization -Potassium Efflux Correlates with T wave Phase 4: Resting membrane potential QT represents both depolarization and repolarization Measurements are using seconds. Bazett Formula Formula not reliable at slow rates (under estimates); over estimates QT interval at fast HRs QT Dynamics Linear regression analysis
21 Expected QTcIntervals 1 to 15 Years Adult Males Adult Females Normal <.44 seconds <.43 seconds <.45 seconds Borderline.44 to.46 seconds.43 to.45 seconds.45 to.47 seconds Prolonged >.46 seconds >.45 seconds >.47 seconds Source: Moss AJ, Robinson JL. Long QT Syndromes. Heart Dis Stroke. 1992; Assessing for Risk of Torsades de Pointes in Atrial Fibrillation Print a long rhythm strip to assess over the course of the strip if the interval from the R wave to the peak of the following T wave is more than 50% of the proceeding RR interval. If so this is considered too long a QT interval and the risk for Torsades de Pointes is increased. QTc.50 sec (500 msecor more is dangerous and should be considered an ominous sign of impending Torsade's de Pointes. 121 Source: Sommargren& Drew, Class I QT Interval Monitoring Recommendations Patients administered an antiarrhythmic drug know to cause Torsades de Pointes Patients who overdose from a potentially proarrhythmic agent Patients with new onset bradyarrhythmias Patients with severe hypokalemiaor hypomagnesemia Class II QT Interval Monitoring Recommendations Patients who require treatment with antipsychoticsor other drugs with possible risk of Torsades de Pointes Patients with acute neurologic events Class III Healthy patients administered drugs that pose little risk for Torsades de Pointes Cardiac Ion Channel Abnormalities Long QT Syndrome (LQTS) Brugadadisease Idiopathic short QT < 300 to 340 msec Diagnosed by family history and ECG Note: Patients with heart failure can develop channelopathies Torsade's De Pointes Recognition of this life-threatening arrhythmia is important because it is not treated like other VTs Two groups: Acquired and congenital Acquired Drugs prolonging repolarization Most often as a result of blocking the potassium channel Electrolyte abnormalities Low potassium Low magnesium Severe bradycardias/ pauses
22 More on Drugs that Prolong Repolarization (blocking of potassium channel efflux) Class Ia and Class III antiarrhythmics Some antihistamines Some antibiotics Some antipsychotics Some antidepressants Some sedatives Some gastric motility agents Other Risk Factors for Torsade's de Pointes Rapid (IV) administration of QT prolonging agent Renal or hepatic dysfunction Female gender (particularly for drug induced) Advanced age Anorexia Heart disease Poly pharmacy Acquired Torsade's De Pointes Warning Signs: QTc prolongation Usually greater than 0.5 sec T Wave aberration or T wave alternans Prominent U waves Couplet of PVCsand couplets Initiated by short long RR interval (Pause dependent) Short bursts: QRS peaks first appear to be up and then to be down (Can degenerate into V fib) Torsade's de Pointes Class I Discontinue offending drugs Note: Class IA drug induced TdPusually appears soon after the initial administration of the drug Correct electrolytes Magnesium Magnesium is Potassium considered treatment Increase HR of choice. Isoproteronol 2 mcg/min then titrate to HR of 100 beats per minute Temporary pacing at rate of 100 to 110 Permanent pacing if bradycardiaor CHB cannot be resolved. Defibrillation if sustained However, continue to assess for and treat cause More on Magnesium in Torsade's de Pointes 2 GmIV bolus over 1-2 minutes Followed in 15 minutes by another bolus if necessary May start continuous infusion at rate of 3-20 mg/min Benefit occurs without shortening of QT interval and in presence of normal Magnesium level
23 QT Interval Monitoring Patient admitted for syncope after having motor vehicle crash while driving. Long standing history of paroxysmal atrial fibrillation on dofetilide(tykosin) for several years. Recent chemotherapy for breast CA resulting in a reduction of EF. Recent increase in carvediloland lisinoprilper general cardiology to improve EF. Next slide is admission ECG. Note the QTcinterval Same patient with sustained Torsades de Pointes. Treated effectively with 2 grams IV Magnesium (magnesium level was normal at baseline). Magnesium is the drug of choice to stabilize the cardiac membrane. Dofetilide (Tikosyn) was also discontinued. 1. Strip 1: QTc consistent with admission ECG. 2. Strip 2: Marked QTc prolongation when patient asleep. 3. Initial run of ventricular tachycardia initiated by PVC firing at end of T wave, Note: Although the patient had been on dofetilide (Tikosyn) for several years, the recent change in ejection fraction and increase in beta blocker therapy increased her risk for Torsades de Pointes Polymorphic VT with normal QT: Seen frequently in ischemic conditions role of beta blockers) Special Considerations: Polymorphic VT (normal QT) DC cardioversionwith sedation when unstable IV beta-blockers if ischemia suspected Improve mortality IV amiodaronein absence of abnormal repolarization Amiodarone better than placebo Magnesium not better than placebo Urgent angiography to exclude ischemia Lidocainemay be reasonable if ischemia suspected Check electrolytes Consider any other potential reversible cause
24 Special Considerations in Atrial Arrhythmias: Lewis Lead Bedside Monitoring ADDITIONAL CLINICAL APPLICATIONS The Lewis Lead When P waves are not clearly seen in a rhythm strip (see lead 3 above), the Lewis lead can be very helpful in assessing for the presence of atrial activity. As seen in the Lewis lead above this patient is clearly in an atrial flutter. The atrial flutter is not as obvious in the lead III rhythm strip Lewis Lead Atrial Lead: Atrial Pacing Wire Telemetry Pack R A Lead 1 L A
25 General Principles for Atrial Arrhythmias Atrial Fibrillation Rate control is first priority Optimize rate control based on clinical assessment of perfusion Hemodynamic instability BP < 90 systolic or HR > 150 BPM Anticipate need for rhythm control with atrial flutter Critical care setting associated with increased catecholamine levels Treat infection Treat inflammation Correct electrolytes Class Class I A Class I B Class I C Antiarrhythmics in Atrial Fibrillation Specific Medications Disopyramide Procainamide Quinidine Not used in atrial fibrillation Flecainide Propofenone Purpose of Medication Rhythm Control Rhythm Control Rhythm Control Rhythm Control Rhythm Control Class II Beta Blockers Rate Control Class III Amiodarone Dofetilide Ibutilide Sotalol (also contains beta blocker) Rhythm / Rate Control Rhythm Control Rhythm Control Rhythm Control (also controls rate) Major Cardiac Side Effects Torsade de pointes, HF Torsade de pointes Torsade de pointes Ventricular tachycardia, HF, Atrial Flutter Ventricular tachycardia, HF, Atrial Flutter Torsade de pointes (rare) * Organ toxicity Torsade de pointes Torsade de pointes Torsade de pointes, HF, Beta blocker side effects Class IV Calcium Channel Rate Control Blockers Delta Wave of Pre-excitation Syndrome 60 to 70% of WPW shows evidence in SR Left sided accessory pathway: Positive delta wave in V1 Arrhythmias of WPW (AVRT or CMT) Right sided accessory pathway: Negative delta wave in V Patient Characteristics Ejection fraction < 30% Implantable cardioverter defibrillator Non ischemic cardiomyopathy Syncope as reason for admission Current frequent premature beats or short runs of tachycardias Critical Thinking Guideline for Cardiac Monitoring NEEDS OF THE PATIENT DRIVE THE DECISIONS Monitoring Priorities Arrhythmia monitoring: Use V1 and V6 (or MCL6) as primary monitoring leads
26 Patient Characteristics New administration of class I or class III antiarrhythmics Electrolyte abnormalities (hypokalemia, hypomagnesemia, hypocalcemia) QTc >.45 seconds Receiving Haldol or other high risk medications Patient Characteristics Stable acute coronary syndrome (ACS) or rule out ACS as reason for admission Admission symptoms suspicious for ischemia (shortness of breath, nausea, fatigue, etc) Admission with heart failure with history of recent revascularization Monitoring Priorities Use arrhythmia monitoring leads as baseline monitoring leads. Measure QTc interval q 4 hours with rhythm interpretation in lead where QT interval can be clearly defined. Document and record lead used for measurement. Use consistent lead in the measuring of QTc. Ischemic monitoring: Use V3 and lead III are primary ischemia detection leads if area of ischemia or culprit vessel is unknown If known choose ischemia monitoring leads based on ECG footprint during active ischemia document reason for use of chosen leads Perform ECG with posterior leads during symptomatic episodes with non Monitoring diagnostic standard 12 Lead Priorities Simultaneously monitor in V1 for arrhythmia detection for patients admitted to ICU or step down level of care Note: Whenever possible in ICU and step down level patients a 6 lead telemetry system should be used in order to monitor V1 for arrhythmia detection and the second V lead for ischemia monitoring Patient Characteristics High risk (hemodynamic or electrical instability) ACS Moral of today s class: Treat the patient and not the ECG. Monitoring Priorities Patients will typically be monitored with 5 lead hardwire due to other monitoring needs V1 must be used as primary monitoring lead in any unstable patient Secondary monitoring can be a limb lead or modified chest lead to aid in either arrhythmia interpretation or ischemia detection A Final Thought: We must not, in trying to think about how we can make a big difference, ignore the small daily differences we can make which, overtime, add up to big differences that we often cannot foresee. -Marian Wright Edelman
12-Lead EKG Interpretation. Judith M. Haluka BS, RCIS, EMT-P
 12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
NEONATAL & PEDIATRIC ECG BASICS RHYTHM INTERPRETATION
 NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
Introduction to Electrocardiography. The Genesis and Conduction of Cardiac Rhythm
 Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
BIPOLAR LIMB LEADS UNIPOLAR LIMB LEADS PRECORDIAL (UNIPOLAR) LEADS VIEW OF EACH LEAD INDICATIVE ECG CHANGES
 BIPOLAR LIMB LEADS Have both a distinctive positive and negative pole. Lead I LA (positive) RA (negative) Lead II LL (positive) RA (negative) Lead III LL (positive) LA (negative) UNIPOLAR LIMB LEADS Have
BIPOLAR LIMB LEADS Have both a distinctive positive and negative pole. Lead I LA (positive) RA (negative) Lead II LL (positive) RA (negative) Lead III LL (positive) LA (negative) UNIPOLAR LIMB LEADS Have
Systematic Approach to 12 Lead EKG Interpretation
 Systematic Approach to 12 Lead EKG Interpretation Maureen Knechtel MPAS, PA-C Wellmont CVA Heart Institute Disclosure Statement of Financial Interest I, Maureen Knechtel, do not have a financial interest/arrangement
Systematic Approach to 12 Lead EKG Interpretation Maureen Knechtel MPAS, PA-C Wellmont CVA Heart Institute Disclosure Statement of Financial Interest I, Maureen Knechtel, do not have a financial interest/arrangement
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Understanding the Electrocardiogram. David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem
 Understanding the Electrocardiogram David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem Overview 1. History 2. Review of the conduction system 3. EKG: Electrodes and Leads 4. EKG: Waves and Intervals
Understanding the Electrocardiogram David C. Kasarda M.D. FAAEM St. Luke s Hospital, Bethlehem Overview 1. History 2. Review of the conduction system 3. EKG: Electrodes and Leads 4. EKG: Waves and Intervals
NAME OF THE HOSPITAL: 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3
 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
Diagnosis Code Crosswalk : ICD-9-CM to ICD-10-CM Cardiac Rhythm and Heart Failure Diagnoses
 Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
ST Segment Elevation Nothing is ever as hard (or easy) as it looks
 ST Segment Elevation Nothing is ever as hard (or easy) as it looks Cameron Guild, MD Division of Cardiology University of Mississippi Medical Center February 17, 2012 Objectives 1. Describe the electrical
ST Segment Elevation Nothing is ever as hard (or easy) as it looks Cameron Guild, MD Division of Cardiology University of Mississippi Medical Center February 17, 2012 Objectives 1. Describe the electrical
the basics Perfect Heart Institue, Piyavate Hospital
 ECG INTERPRETATION: the basics Damrong Sukitpunyaroj MD Damrong Sukitpunyaroj, MD Perfect Heart Institue, Piyavate Hospital Overview Conduction Pathways Systematic Interpretation Common abnormalities in
ECG INTERPRETATION: the basics Damrong Sukitpunyaroj MD Damrong Sukitpunyaroj, MD Perfect Heart Institue, Piyavate Hospital Overview Conduction Pathways Systematic Interpretation Common abnormalities in
QRS Complexes. Fast & Easy ECGs A Self-Paced Learning Program
 6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
6 QRS Complexes Fast & Easy ECGs A Self-Paced Learning Program Q I A ECG Waveforms Normally the heart beats in a regular, rhythmic fashion producing a P wave, QRS complex and T wave I Step 4 of ECG Analysis
By the end of this continuing education module the clinician will be able to:
 EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
Automatic External Defibrillators
 Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES
 INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
Scott Hubbell, MHSc, RRT-NPS, C-NPT, CCT Clinical Education Coordinator/Flight RRT EagleMed
 Scott Hubbell, MHSc, RRT-NPS, C-NPT, CCT Clinical Education Coordinator/Flight RRT EagleMed Identify the 12-Lead Views Explain the vessels of occlusion Describe the three I s Basic Interpretation of 12-Lead
Scott Hubbell, MHSc, RRT-NPS, C-NPT, CCT Clinical Education Coordinator/Flight RRT EagleMed Identify the 12-Lead Views Explain the vessels of occlusion Describe the three I s Basic Interpretation of 12-Lead
ACLS Chapter 3 Rhythm Review Instructor Lesson Plan to Accompany ACLS Study Guide 3e
 ACLS Chapter 3 Rhythm Review Lesson Plan Required reading before this lesson: ACLS Study Guide 3e Textbook Chapter 3 Materials needed: Multimedia projector, computer, ACLS Chapter 3 Recommended minimum
ACLS Chapter 3 Rhythm Review Lesson Plan Required reading before this lesson: ACLS Study Guide 3e Textbook Chapter 3 Materials needed: Multimedia projector, computer, ACLS Chapter 3 Recommended minimum
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
Normal Sinus Rhythm. Sinus Bradycardia. Sinus Tachycardia. Rhythm ECG Characteristics Example (NSR) & consistent. & consistent.
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Interpreting a rhythm strip
 3 Interpreting a rhythm strip Just the facts In this chapter, you ll learn: the components of an ECG complex and their significance and variations techniques for calculating the rate and rhythm of an ECG
3 Interpreting a rhythm strip Just the facts In this chapter, you ll learn: the components of an ECG complex and their significance and variations techniques for calculating the rate and rhythm of an ECG
RAPID INTERPRETATION OF. EKG s
 Personal Quick Reference Sheets 333 (pages 333 to 346) There is no need to remove these reference pages from your book. To download and print them in full color, go to: www.themdsite.com Reference Sheets
Personal Quick Reference Sheets 333 (pages 333 to 346) There is no need to remove these reference pages from your book. To download and print them in full color, go to: www.themdsite.com Reference Sheets
Electrophysiology Introduction, Basics. The Myocardial Cell. Chapter 1- Thaler
 Electrophysiology Introduction, Basics Chapter 1- Thaler The Myocardial Cell Syncytium Resting state Polarized negative Membrane pump Depolarization fundamental electrical event of the heart Repolarization
Electrophysiology Introduction, Basics Chapter 1- Thaler The Myocardial Cell Syncytium Resting state Polarized negative Membrane pump Depolarization fundamental electrical event of the heart Repolarization
PRO-CPR. 2015 Guidelines: PALS Algorithm Overview. (Non-AHA supplementary precourse material)
 PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
Acquired, Drug-Induced Long QT Syndrome
 Acquired, Drug-Induced Long QT Syndrome A Guide for Patients and Health Care Providers Sudden Arrhythmia Death Syndromes (SADS) Foundation 508 E. South Temple, Suite 202 Salt Lake City, Utah 84102 800-STOP
Acquired, Drug-Induced Long QT Syndrome A Guide for Patients and Health Care Providers Sudden Arrhythmia Death Syndromes (SADS) Foundation 508 E. South Temple, Suite 202 Salt Lake City, Utah 84102 800-STOP
An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams
 Arrhythmias 1 An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams Things to keep in mind when analyzing arrhythmias: Electrical activity recorded in 12 and 15 leads Examine
Arrhythmias 1 An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams Things to keep in mind when analyzing arrhythmias: Electrical activity recorded in 12 and 15 leads Examine
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
Introduction to Electrophysiology. Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center
 Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
Introduction to Electrophysiology Wm. W. Barrington, MD, FACC University of Pittsburgh Medical Center Objectives Indications for EP Study How do we do the study Normal recordings Abnormal Recordings Limitations
Atrial Fibrillation Management Across the Spectrum of Illness
 Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
The new generation in ECG interpretation
 The new generation in ECG interpretation Philips DXL ECG Algorithm, Release PH100B The Philips DXL ECG Algorithm, developed by the Advanced Algorithm Research Center, uses sophisticated analytical methods
The new generation in ECG interpretation Philips DXL ECG Algorithm, Release PH100B The Philips DXL ECG Algorithm, developed by the Advanced Algorithm Research Center, uses sophisticated analytical methods
Atrial Fibrillation Peter Santucci, MD Revised May, 2008
 Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Electrocardiography Review and the Normal EKG Response to Exercise
 Electrocardiography Review and the Normal EKG Response to Exercise Cardiac Anatomy Electrical Pathways in the Heart Which valves are the a-v valves? Closure of the a-v valves is associated with which heart
Electrocardiography Review and the Normal EKG Response to Exercise Cardiac Anatomy Electrical Pathways in the Heart Which valves are the a-v valves? Closure of the a-v valves is associated with which heart
Wide-Complex Tachycardias in the ED: Myths and Pitfalls
 Wide-Complex Tachycardias in the ED: Myths and Pitfalls, FACEP, FAAEM Professor and Vice Chair Director, Emergency Cardiology Fellowship Department of Emergency Medicine University of Maryland School of
Wide-Complex Tachycardias in the ED: Myths and Pitfalls, FACEP, FAAEM Professor and Vice Chair Director, Emergency Cardiology Fellowship Department of Emergency Medicine University of Maryland School of
Tips and Tricks to Demystify 12 Lead ECG Interpretation
 Tips and Tricks to Demystify 12 Lead ECG Interpretation Mission: Lifeline North Dakota Regional EMS and Hospital Conference Samantha Kapphahn, DO Essentia Health- Interventional Cardiology June 5th, 2014
Tips and Tricks to Demystify 12 Lead ECG Interpretation Mission: Lifeline North Dakota Regional EMS and Hospital Conference Samantha Kapphahn, DO Essentia Health- Interventional Cardiology June 5th, 2014
Perioperative Cardiac Evaluation
 Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
Perioperative Cardiac Evaluation Caroline McKillop Advisor: Dr. Tam Psenka 10-3-2007 Importance of Cardiac Guidelines -Used multiple times every day -Patient Safety -Part of Surgical Care Improvement Project
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001
 BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
ECG Findings. IV Access. 12 Lead Interpretation: STEMI and NSTEMI. ACLS Acute Coronary Syndrome Chest Pain Suggestive of Ischemia.
 12 Lead Interpretation: STEMI and NSTEMI Presented by Annmarie Keck, RN, BSN, CEN Northwest MedStar Clinical Outreach Educator ACLS Acute Coronary Syndrome Chest Pain Suggestive of Ischemia Immediate Assessment
12 Lead Interpretation: STEMI and NSTEMI Presented by Annmarie Keck, RN, BSN, CEN Northwest MedStar Clinical Outreach Educator ACLS Acute Coronary Syndrome Chest Pain Suggestive of Ischemia Immediate Assessment
Current Management of Atrial Fibrillation DISCLOSURES. Heart Beat Anatomy. I have no financial conflicts to disclose
 Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Atrial Fibrillation The Basics
 Atrial Fibrillation The Basics Family Practice Symposium Tim McAveney, M.D. 10/23/09 Objectives Review the fundamentals of managing afib Discuss the risks for stroke and the indications for anticoagulation
Atrial Fibrillation The Basics Family Practice Symposium Tim McAveney, M.D. 10/23/09 Objectives Review the fundamentals of managing afib Discuss the risks for stroke and the indications for anticoagulation
EKG Abnormalities. I. Early repolarization abnormality:
 I. Early repolarization abnormality: EKG Abnormalities A. A normal variant. Early repolarization is most often seen in healthy young adults. Look for ST elevation, tall QRS voltage, "fishhook" deformity
I. Early repolarization abnormality: EKG Abnormalities A. A normal variant. Early repolarization is most often seen in healthy young adults. Look for ST elevation, tall QRS voltage, "fishhook" deformity
Management of Pacing Wires After Cardiac Surgery
 Management of Pacing Wires After Cardiac Surgery David E. Lizotte, Jr. PA C, MPAS, FAPACVS President, Association of Physician Assistants in Cardiovascular Surgery Conflicts: None Indications 2008 Journal
Management of Pacing Wires After Cardiac Surgery David E. Lizotte, Jr. PA C, MPAS, FAPACVS President, Association of Physician Assistants in Cardiovascular Surgery Conflicts: None Indications 2008 Journal
The abbreviation EKG, for electrocardiogram,
 CLIN PEDIATR OnlineFirst, published on January 28, 2010 as doi:10.1177/0009922809336206 Simplified Pediatric Electrocardiogram Interpretation Clinical Pediatrics Volume XX Number X Month XXXX xx-xx 2009
CLIN PEDIATR OnlineFirst, published on January 28, 2010 as doi:10.1177/0009922809336206 Simplified Pediatric Electrocardiogram Interpretation Clinical Pediatrics Volume XX Number X Month XXXX xx-xx 2009
Electrolyte Physiology. Something in the way she moves
 Electrolyte Physiology Something in the way she moves me Electrolyte Movement CONCENTRATION GRADIENT ELECTRICAL GRADIENT DRIVING FORCE NERNST NUMBER (E-ion) CONDUCTANCE (G-ion) PERMEABILITY CHANNELS: small
Electrolyte Physiology Something in the way she moves me Electrolyte Movement CONCENTRATION GRADIENT ELECTRICAL GRADIENT DRIVING FORCE NERNST NUMBER (E-ion) CONDUCTANCE (G-ion) PERMEABILITY CHANNELS: small
Sleep Heart Health Study (SHHS) ECG Protocol
 Sleep Heart Health Study (SHHS) ECG Protocol SHHS 1 Electrocardiography (ECG) Baseline ECG is performed in all parent study clinic visits preceding the PSG. All sites perform a standard resting 12-lead
Sleep Heart Health Study (SHHS) ECG Protocol SHHS 1 Electrocardiography (ECG) Baseline ECG is performed in all parent study clinic visits preceding the PSG. All sites perform a standard resting 12-lead
ECG made extra easy. medics.cc
 ElectroCardioGraphyraphy ECG made extra easy Overview Objectives for this tutorial What is an ECG? Overview of performing electrocardiography on a patient Simple physiology Interpreting the ECG Objectives
ElectroCardioGraphyraphy ECG made extra easy Overview Objectives for this tutorial What is an ECG? Overview of performing electrocardiography on a patient Simple physiology Interpreting the ECG Objectives
GENERAL HEART DISEASE KNOW THE FACTS
 GENERAL HEART DISEASE KNOW THE FACTS WHAT IS Heart disease is a broad term meaning any disease affecting the heart. It is commonly used to refer to coronary heart disease (CHD), a more specific term to
GENERAL HEART DISEASE KNOW THE FACTS WHAT IS Heart disease is a broad term meaning any disease affecting the heart. It is commonly used to refer to coronary heart disease (CHD), a more specific term to
GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS. (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support)
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI)
 Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Review of Important ECG Findings in Patients with Syncope Joseph Toscano, MD
 92 Review of Important ECG Findings in Patients with Syncope Joseph Toscano, MD Abstract Guidelines recommend 12-lead ECG as an important test to perform in patients with syncope. Though the incidence
92 Review of Important ECG Findings in Patients with Syncope Joseph Toscano, MD Abstract Guidelines recommend 12-lead ECG as an important test to perform in patients with syncope. Though the incidence
ACLS RHYTHM TEST. 2. A 74-year-old woman with chest pain. Blood pressure 192/90 and rates her pain 9/10.
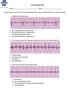 ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations.
 INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It?
 The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It? Indiana Chapter-ACC 17 th Annual Meeting Indianapolis, Indiana October 19, 2013 Deepak Bhakta MD FACC FACP FAHA FHRS CCDS Associate
The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It? Indiana Chapter-ACC 17 th Annual Meeting Indianapolis, Indiana October 19, 2013 Deepak Bhakta MD FACC FACP FAHA FHRS CCDS Associate
Cardiovascular Guidelines for DOT Physical Exams By Maureen Collins MSN, APRN, BC
 Cardiovascular Guidelines for DOT Physical Exams By Maureen Collins MSN, APRN, BC The Federal Motor Carrier Safety Administration (FMCSA) administers the Federal Motor Carrier Safety Regulations (FMCSRs)
Cardiovascular Guidelines for DOT Physical Exams By Maureen Collins MSN, APRN, BC The Federal Motor Carrier Safety Administration (FMCSA) administers the Federal Motor Carrier Safety Regulations (FMCSRs)
Recurrent AF: Choosing the Right Medication.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
Policy & Procedures. I.D. Number: 1142
 Policy & Procedures Title: CARDIAC (ECG) MONITORING I.D. Number: 1142 Authorization: [X] SHR Nursing Practice Committee Source: Date Revised: November 2012 Date Effective: October 2004 Scope: SHR - Acute
Policy & Procedures Title: CARDIAC (ECG) MONITORING I.D. Number: 1142 Authorization: [X] SHR Nursing Practice Committee Source: Date Revised: November 2012 Date Effective: October 2004 Scope: SHR - Acute
ST Segment Monitoring. IntelliVue Patient Monitor and Information Center, Application Note
 ST Segment Monitoring ST/AR Algorithm IntelliVue Patient Monitor and Information Center, Application Note This application note describes principles and uses for continuous ST segment monitoring. It also
ST Segment Monitoring ST/AR Algorithm IntelliVue Patient Monitor and Information Center, Application Note This application note describes principles and uses for continuous ST segment monitoring. It also
Electrophysiology Daymar College. Lisa H. Young, RN, BSN, MAE 2011
 Electrophysiology Daymar College Lisa H. Young, RN, BSN, MAE 2011 Electrical Conduction Pathway Chemical Basis for Impulse Formation Cardiac Action Potential Phases http://www.youtube.com/watch?v=oqpffilde0e
Electrophysiology Daymar College Lisa H. Young, RN, BSN, MAE 2011 Electrical Conduction Pathway Chemical Basis for Impulse Formation Cardiac Action Potential Phases http://www.youtube.com/watch?v=oqpffilde0e
An ECG Primer. Quick Look. I saw it, but I did not realize it. Elizabeth Peabody
 4 An ECG Primer Quick Look Cardiac Monitoring System - p. 64 ECG Paper - p. 73 Lead Polarity and Vectors - p. 77 Basic ECG Components - p. 79 Heart Rate and Pulse Rate - p. 91 Summary - p. 94 Chapter Quiz
4 An ECG Primer Quick Look Cardiac Monitoring System - p. 64 ECG Paper - p. 73 Lead Polarity and Vectors - p. 77 Basic ECG Components - p. 79 Heart Rate and Pulse Rate - p. 91 Summary - p. 94 Chapter Quiz
Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians
 Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians May 19, 2015 Disclaimer This presentation is intended for educational use. Any duplication is prohibited without written consent
Medtronic Cardiac Rhythm and Heart Failure ICD-10 Coding for Physicians May 19, 2015 Disclaimer This presentation is intended for educational use. Any duplication is prohibited without written consent
Palpitations & AF. Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust
 Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
CLINICAL PRACTICE GUIDELINE - Telemetry
 Introduction CLINICAL PRACTICE GUIDELINE - Telemetry The purpose of the guideline is to establish evidence-informed criteria for telemetry monitoring, outline nursing assessment parameters and provide
Introduction CLINICAL PRACTICE GUIDELINE - Telemetry The purpose of the guideline is to establish evidence-informed criteria for telemetry monitoring, outline nursing assessment parameters and provide
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY. Guidelines for Use of Intravenous Isoproterenol
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
 ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
Premature Ventricular Contractions. Ralph Augostini, MD FACC FHRS
 Premature Ventricular Contractions Ralph Augostini, MD FACC FHRS Orlando, Florida October 7-9, 2011 Premature Ventricular Contractions: ACC/AHA/ESC 2006 Guidelines for Management of Patients With Ventricular
Premature Ventricular Contractions Ralph Augostini, MD FACC FHRS Orlando, Florida October 7-9, 2011 Premature Ventricular Contractions: ACC/AHA/ESC 2006 Guidelines for Management of Patients With Ventricular
8 Peri-arrest arrhythmias
 8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
Medical management of CHF: A New Class of Medication. Al Timothy, M.D. Cardiovascular Institute of the South
 Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Electrophysiology Heart Study - EPS -
 Electrophysiology Heart Study - EPS - What is an EPS? EPS is short for ElectroPhysiology heart Study. This procedure looks at the electrical system of your heart. An EPS will show if you have a heart rhythm
Electrophysiology Heart Study - EPS - What is an EPS? EPS is short for ElectroPhysiology heart Study. This procedure looks at the electrical system of your heart. An EPS will show if you have a heart rhythm
12 Lead ECGs: Ischemia, Injury & Infarction Part 2
 12 Lead ECGs: Ischemia, Injury & Infarction Part 2 McHenry Western Lake County EMS Localization: Left Coronary Artery Right Coronary Artery Right Ventricle Septal Wall Anterior Descending Artery Left Main
12 Lead ECGs: Ischemia, Injury & Infarction Part 2 McHenry Western Lake County EMS Localization: Left Coronary Artery Right Coronary Artery Right Ventricle Septal Wall Anterior Descending Artery Left Main
Catheter Ablation. A Guided Approach for Treating Atrial Arrhythmias
 Catheter Ablation A Guided Approach for Treating Atrial Arrhythmias A P A T I E N T H A N D B O O K This brochure will provide an overview of atrial arrhythmias (heart rhythm problems affecting the upper
Catheter Ablation A Guided Approach for Treating Atrial Arrhythmias A P A T I E N T H A N D B O O K This brochure will provide an overview of atrial arrhythmias (heart rhythm problems affecting the upper
Potential Causes of Sudden Cardiac Arrest in Children
 Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL)
 ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
Presenter Disclosure Information
 2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
Section Four: Pulmonary Artery Waveform Interpretation
 Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
How to read the ECG in athletes: distinguishing normal form abnormal
 How to read the ECG in athletes: distinguishing normal form abnormal Antonio Pelliccia, MD Institute of Sport Medicine and Science www.antoniopelliccia.it Cardiac adaptations to Rowing Vagotonia Sinus
How to read the ECG in athletes: distinguishing normal form abnormal Antonio Pelliccia, MD Institute of Sport Medicine and Science www.antoniopelliccia.it Cardiac adaptations to Rowing Vagotonia Sinus
Atrial Fibrillation The High Risk Obese Patient
 Atrial Fibrillation The High Risk Obese Patient Frederick Schaller, D.O.,F.A.C.O.I. Professor and Vice Dean Touro University Nevada A 56 year old male with a history of hypertension and chronic stable
Atrial Fibrillation The High Risk Obese Patient Frederick Schaller, D.O.,F.A.C.O.I. Professor and Vice Dean Touro University Nevada A 56 year old male with a history of hypertension and chronic stable
How To Understand What You Know
 Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Electrodes placed on the body s surface can detect electrical activity, APPLIED ANATOMY AND PHYSIOLOGY. Circulatory system
 4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
JAPI VOL. 52 NOVEMBER 2004 www.japi.org 883
 Review Article Wide Complex Tachycardia : Recognition and Management in the Emergency Room IB Ray Abstract Cardiac arrhythmias often present as urgent medical conditions requiring immediate care. Patient
Review Article Wide Complex Tachycardia : Recognition and Management in the Emergency Room IB Ray Abstract Cardiac arrhythmias often present as urgent medical conditions requiring immediate care. Patient
Cardioversion for. Atrial Fibrillation. Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation
 Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
Bradycardia CHAPTER 12 CODE SCENARIO
 Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
ACLS PRE-TEST ANNOTATED ANSWER KEY
 ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
Atrial fibrillation (AF) care pathways. for the primary care physicians
 Atrial fibrillation (AF) care pathways for the primary care physicians by University of Minnesota Physicians Heart, October, 2011 Evaluation by the primary care physician: 1. Comprehensive history and
Atrial fibrillation (AF) care pathways for the primary care physicians by University of Minnesota Physicians Heart, October, 2011 Evaluation by the primary care physician: 1. Comprehensive history and
Evaluation copy. Analyzing the Heart with EKG. Computer
 Analyzing the Heart with EKG Computer An electrocardiogram (ECG or EKG) is a graphical recording of the electrical events occurring within the heart. In a healthy heart there is a natural pacemaker in
Analyzing the Heart with EKG Computer An electrocardiogram (ECG or EKG) is a graphical recording of the electrical events occurring within the heart. In a healthy heart there is a natural pacemaker in
Provider Checklist-Outpatient Imaging. Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469)
 Provider Checklist-Outpatient Imaging Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469) Medical Review Note: Per InterQual, if any of the following are present,
Provider Checklist-Outpatient Imaging Checklist: Nuclear Stress Test, Thallium/Technetium/Sestamibi (CPT Code 78451-78454 78469) Medical Review Note: Per InterQual, if any of the following are present,
2/20/2015. Cardiac Evaluation of Potential Solid Organ Transplant Recipients. Issues Specific to Transplantation. Kidney Transplantation.
 DISCLOSURES I have no relevant financial relationships to disclose. Cardiac Evaluation of Potential Solid Organ Transplant Recipients Michele Hamilton, MD Director, Heart Failure Program Cedars Sinai Heart
DISCLOSURES I have no relevant financial relationships to disclose. Cardiac Evaluation of Potential Solid Organ Transplant Recipients Michele Hamilton, MD Director, Heart Failure Program Cedars Sinai Heart
Life Threatening EKG s In The Office. Joseph A Manfredi, MD, FACC, FHRS GHS Cardiovascular Symposium
 Life Threatening EKG s In The Office Joseph A Manfredi, MD, FACC, FHRS GHS Cardiovascular Symposium January 24 th, 2015 Disclosures Speaker Honorariums: STJM, Boston Scientific Advisory role: Medtronic
Life Threatening EKG s In The Office Joseph A Manfredi, MD, FACC, FHRS GHS Cardiovascular Symposium January 24 th, 2015 Disclosures Speaker Honorariums: STJM, Boston Scientific Advisory role: Medtronic
Interpreting AV (Heart) Blocks: Breaking Down the Mystery
 Interpreting AV (Heart) Blocks: Breaking Down the Mystery 2 Contact Hours Copyright 2012 by RN.com. All Rights Reserved. Reproduction and distribution of these materials is prohibited without the express
Interpreting AV (Heart) Blocks: Breaking Down the Mystery 2 Contact Hours Copyright 2012 by RN.com. All Rights Reserved. Reproduction and distribution of these materials is prohibited without the express
6/5/2014. Objectives. Acute Coronary Syndromes. Epidemiology. Epidemiology. Epidemiology and Health Care Impact Pathophysiology
 Objectives Acute Coronary Syndromes Epidemiology and Health Care Impact Pathophysiology Unstable Angina NSTEMI STEMI Clinical Clues Pre-hospital Spokane County EMS Epidemiology About 600,000 people die
Objectives Acute Coronary Syndromes Epidemiology and Health Care Impact Pathophysiology Unstable Angina NSTEMI STEMI Clinical Clues Pre-hospital Spokane County EMS Epidemiology About 600,000 people die
Activity 4.2.3: EKG. Introduction. Equipment. Procedure
 Activity 4.2.3: EKG The following is used with permission of Vernier Software and Technology. This activity is based on the experiment Analyzing the Heart with EKG from the book Human Physiology with Vernier,
Activity 4.2.3: EKG The following is used with permission of Vernier Software and Technology. This activity is based on the experiment Analyzing the Heart with EKG from the book Human Physiology with Vernier,
What Are Arrhythmias?
 What Are Arrhythmias? Many people have questions about what the word arrhythmia means, and arrhythmias can be a difficult subject to understand. The text below should give you a better understanding of
What Are Arrhythmias? Many people have questions about what the word arrhythmia means, and arrhythmias can be a difficult subject to understand. The text below should give you a better understanding of
ECG Measurments and Interpretation Programs
 ECG Measurments and Interpretation Programs Physician s Guide Distributed by Welch Allyn 4341 State Street Road, PO Box 220 Skaneateles Falls, NY 13153-0220 www.welchallyn.com Sales and Service information:
ECG Measurments and Interpretation Programs Physician s Guide Distributed by Welch Allyn 4341 State Street Road, PO Box 220 Skaneateles Falls, NY 13153-0220 www.welchallyn.com Sales and Service information:
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION
 COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
COVERAGE GUIDANCE: ABLATION FOR ATRIAL FIBRILLATION Question: How should the EGBS Coverage Guidance regarding ablation for atrial fibrillation be applied to the Prioritized List? Question source: Evidence
Patient Information Sheet Electrophysiological study
 Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
Patient Information Sheet Electrophysiological study Your doctor has recommended performing an electrophysiological study (also called EPS). EPS is a diagnostic procedure designed to test and evaluate
The Basics of 12 Lead EKG s
 EMS Solutions Presents The Basics of 12 Lead EKG s NOTICE: You DO NOT Have the Right to Reprint or Resell this Publication. However, you MAY give this report away, provided you do not change or alter the
EMS Solutions Presents The Basics of 12 Lead EKG s NOTICE: You DO NOT Have the Right to Reprint or Resell this Publication. However, you MAY give this report away, provided you do not change or alter the
PRACTICAL APPROACH TO SVT. Graham C. Wong MD MPH Division of Cardiology Vancouver General Hospital University of British Columbia
 PRACTICAL APPROACH TO SVT Graham C. Wong MD MPH Division of Cardiology Vancouver General Hospital University of British Columbia CONDUCTION SYSTEM OF THE HEART SA node His bundle Left bundle AV node Right
PRACTICAL APPROACH TO SVT Graham C. Wong MD MPH Division of Cardiology Vancouver General Hospital University of British Columbia CONDUCTION SYSTEM OF THE HEART SA node His bundle Left bundle AV node Right
Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements
 Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements Salmaan Kanji, Pharm.D. The Ottawa Hospital The Ottawa Hospital Research Institute Conflict of Interest No financial, proprietary
Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements Salmaan Kanji, Pharm.D. The Ottawa Hospital The Ottawa Hospital Research Institute Conflict of Interest No financial, proprietary
The P Wave: Indicator of Atrial Enlargement
 Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
