Atrial Fibrillation The High Risk Obese Patient
|
|
|
- Berniece Dennis
- 7 years ago
- Views:
Transcription
1 Atrial Fibrillation The High Risk Obese Patient Frederick Schaller, D.O.,F.A.C.O.I. Professor and Vice Dean Touro University Nevada
2 A 56 year old male with a history of hypertension and chronic stable angina presents to the clinic with sudden onset of dizzyness and dyspnea. This occurred several hours prior with no change in medications, physical stress or any other factors. He has been well and active, functioning at NYHA Class 1. He leads a sedentary life and notes more fatigue recently than usual. His angina has been minimal and not active for the past three months. Medications are enalapril 10mg BID, ASA 325 daily, and NTG sublinqual prn. On examination, BP 148/78, pulse 138 and irregular. His weight is 320# and height 70. He has a soft right carotid bruit, no JVD, and clear lungs. Heart is rapid and irregular with a soft systolic outflow murmur in the second interspace right. Abdomen is obese. There are good peripheral pulses and no edema.
3 Questions: 1. What is the likely l cause of his presentation? ti 2. What testing should be performed at this time? 3. Is emergent therapy indicated? 4. Does he warrant hospitalization? 5. Is long term therapy indicated? 6. Should anticoagulation be initiated?
4 Objectives Describe the common etiologies of Atrial Fibrillation and association with Obesity Identify the appropriate evaluation Discuss authoritative guidelines for evaluation and therapeutic intervention Describe current and evolving invasive i management options
5 Definition An irregularly irregular rhythm with no discernable P waves Small irregular deviations of the baseline are called f waves these may be coarse or fine The conduction to the ventricle may range The conduction to the ventricle may range from bradycardia to severe tachycardia
6 Definition cont. Types Recurrent: more than two episodes Paroxysmal: spontaneous conversion to sinus Persistent: lasting greater than 7 days Permanent: lasting 1 year or more with failed attempts at cardioversion Lone : no underlying heart dysfunction or risk factors, under age 60
7 Epidemiology Found in 1% of population over 60, and 6% in population p over 70 Over 2 million persons in the USA have AF Somewhat more common in men than women With coronary disease in age group>70, incidence is 10% Morbid Obesity increases risk 50%
8 Etiology Ischemic Heart Disease Hypertension Morbid Obesity/ Sleep apnea Acute inflammation i pericarditis pneumonia/pleuritis
9 Etiology cont. Chronic Inflammation Connective tissue disorders Valvular heart disease Cardiotoxinsins Chemotherapeutics Alcohol l Stimulant drugs
10 Etiology cont. Thyrotoxicosis and hyperthyroidism Cardiomyopathy Lone no discernable etiology Age less than 60 years
11 Evaluation Physical findings irregular rhythm varying intensity of first heart sound occasional pulse deficit compared to ascultated rate other findings associated with etiology
12 Evaluation Screen for etiology echocardiogram for valve disorder, cardiomyopathy, and pericardial effusion stress testing for ischemia laboratory evaluation for thyroid function, glucose, and inflammatory markers if indicated Sleep study in obese patients suspected of apnea
13 Evaluation Methods to identify the occurrence of fibrillation if not present at time of examination 24 hour Holter monitoring 30 day Event recorder Continuous loop recorder Implanted continuous recorder
14 Therapeutic Approach Reverse reversables Control hypertension Revascularize if needed Weight loss and CPAP if indicated Control inflammation Normalize thyroid function
15 Therapeutic Approach Three major objectives Control rate while patient remains in fibrillation Convert rhythm to sinus Prevent thromboembolism
16 Rate Control Any agent that reduces AV node conduction will slow the ventricular response Digoxin Beta Blocker Verapamil Diltiazem Amiodarone
17 Rate Control This option is selected when underlying etiology cannot be reversed Also appropriate when patient has been in persistent fibrillation for more than 3 months rate of recurrence >50% at one year and 80%at rate of recurrence >50% at one year and 80% at three years if cardioversion attempted
18 Rate Control Therapeutic options: acute IV beta blocker propranol, metoprolol, atenolol, esmolol IV diltiazem IV verapamil IV digoxin Adenosine of little use due to short duration of effect
19 Rate Control Therapeutic options: chronic Oral beta blocker. NOT carvedolol Oral digoxin: must evaluate heart rate in exercise if used alone. Likely will not be adequate Oral diltiazem Oral verapamil Oral Amiodarone
20 Conversion to Sinus If patient hemodynamically unstable, immediate conversion required Electrical preferred Medical options Address and stabilize causational factors Success less with significant enlargement of LV, LA or RA, or with significant valve disease
21 Conversion cont. Electrical Bipolar countershock most effective at lower energy Sedation required Rare serious complication Ventricular fibrillation Cardiac standstill Embolization
22 Conversion cont. Electrical, cont 85% successful initially Reversion to fibrillation most frequent within 24 hours Patient may develop first or second degree burn at pad sites If unsuccessful or if recurs, may repeat with pretreatment with antiarrhythmic
23 Conversion cont. Medical Intravenous Ibutilide bolus X2 Dofetilide Amiodarone Oral Dofetilide Flecainide Propafenone
24 Conversion cont. Cautions with medical conversion All agents except amiodarone increase risk of vetricular proarrhythmia in patients with reduced LV function or chamber dilation Sotolol and amiodarone may be used safely as outpatient therapy, but all others must be used in hospital with telemetry monitoring All agents may prolong QTc, so screen for other agents that may worsen this (H2 blockers, tricyclics, etc)
25 Maintenance of Sinus Long term success of conversion varies depending on etiology and duration of fibrillation Low risk patients: (one or no risk factors) No antiarrhythmic indicated Higher risk patients: (more than one risk factor or prior episode) Antiarrhythmic indicated Recurrence rate still approaches 50% at one year With advanced AV node disease, antiarrhythmics should not be used without permanent pacemaker
26 Maintenance of Sinus, cont Medical options Verapamil/diltiazem: low and moderate risk patients with normal LV function Amiodarone: statistically best for maintenance in all risk groups Sotolol: nearly as effective as amiodarone, but cannot be used in patients with heart failure Dofetilide, Dronedarone, Propaphenone in patients with no LV dysfunction
27 Prevention of Thrombosis Clinically most important risk of atrial fibrillation is thrombosis and embolus, especially cerebral Highest risk Rheumatic or other significant valvular disease Dilated LA or LV with cardiomyopathy Prior embolic event
28 Thrombosis Risk Risk of embolus 14% annual risk in highest group 7% annual risk in general group <1%riskinLoneA-Fib in
29 Thrombus Prevention Multiple randomized trials over the past ten years clearly indicate the benefit of anticoagulation. Risk reduction by 60% Requires warfarin anticoagulation to an INR level of 2.0 to attain best reduction Risk of bleed when carefully monitored is less than 3% per year in patients under 70years of age
30 Thrombus Prevention Anticoagulation not indicated: bleeding disorder history of hemorrhage compliance problems CNS tumor Alternative in these cases is Aspirin therapy Alternative in these cases is Aspirin therapy at mg daily. Risk reduction 30%
31 Thrombosis Prevention In chronic afib, coumadin may be held for up to 1 week for procedures If anticoagulation must be held for more than one week, heparin should be initiated ASA, if required for other reasons, may be combined with warfarin with small increase bleeding risk Clopidogrel or Prasugrel, if required, may be used in combination but the risk of bleeding is significantly increased.
32 Thrombosis Prevention If thromboembolic event occurs with INR at target, new target INR of should be established before adding platelet inhibitors Use of Dabigatran approved in nonvalvular atrial fibrillation, but recommendations on dose adjustments with concomitant use of platelet agents are not well defined
33 Interventional Therapy AV Node ablation with permanent pacemaker Indicated for refractory afib with uncontrollable rapid rate response Catheter Ablation Newer techniques enable success at 60-70% Still requires anticoagulation
34 Interventional Therapy Surgical occlusion of atrial appendage at time of valve or bypass surgery Transcatheter occlusion of atrial appendage with mesh device Surgical atrial ablation: Maze procedure Effective at time of valvular l surgery
35 A 56 year old male with a history of hypertension and chronic stable angina presents to the clinic with sudden onset of dizzyness and dyspnea. This occurred several hours prior with no change in medications, physical stress or any other factors. He has been well and active, functioning at NYHA Class 1. He is sedentary but has experienced more fatigue recently than usual. His angina has been minimal and not active for the past three months. Medications are enalapril 10mg BID, ASA 325 dil daily, and NTG sublinqual lprn. On examination, BP 148/78, pulse 138 and irregular. Height 70 and weight 320#. He has a soft right carotid bruit, no JVD, and clear lungs. Heart is rapid and irregular with a soft systolic outflow murmur in the second interspace right. Abdomen is obese. There are good peripheral pulses and no edema.
36 Questions: 1. What is the likely l cause of his presentation? ti 2. What testing should be performed at this time? 3. Is emergent therapy indicated? 4. Does he warrant hospitalization? 5. Is long term therapy indicated? 6. Should anticoagulation be initiated?
Atrial Fibrillation 2012: Latest Approaches to Diagnosis, Treatment, and Stroke Prevention
 Atrial Fibrillation 2012: Latest Approaches to Diagnosis, Treatment, and Stroke Prevention Michael G. Clark, PA-C, MPAS, Ph.D., AACC Fisher Cardiology and Electrophysiology Bedford, Texas Disclosures Speakers
Atrial Fibrillation 2012: Latest Approaches to Diagnosis, Treatment, and Stroke Prevention Michael G. Clark, PA-C, MPAS, Ph.D., AACC Fisher Cardiology and Electrophysiology Bedford, Texas Disclosures Speakers
Atrial Fibrillation Peter Santucci, MD Revised May, 2008
 Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Atrial Fibrillation Management Across the Spectrum of Illness
 Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Recurrent AF: Choosing the Right Medication.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Atrial Fibrillation The Basics
 Atrial Fibrillation The Basics Family Practice Symposium Tim McAveney, M.D. 10/23/09 Objectives Review the fundamentals of managing afib Discuss the risks for stroke and the indications for anticoagulation
Atrial Fibrillation The Basics Family Practice Symposium Tim McAveney, M.D. 10/23/09 Objectives Review the fundamentals of managing afib Discuss the risks for stroke and the indications for anticoagulation
Atrial Fibrillation: Drugs, Ablation, or Benign Neglect. Robert Kennedy, MD October 10, 2015
 Atrial Fibrillation: Drugs, Ablation, or Benign Neglect Robert Kennedy, MD October 10, 2015 Definitions 2014 AHA/ACC/HRS Guideline for the Management of Patients With Atrial Fibrillation: Executive Summary.
Atrial Fibrillation: Drugs, Ablation, or Benign Neglect Robert Kennedy, MD October 10, 2015 Definitions 2014 AHA/ACC/HRS Guideline for the Management of Patients With Atrial Fibrillation: Executive Summary.
Cardioversion for. Atrial Fibrillation. Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation
 Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
Atrial fibrillation (AF) care pathways. for the primary care physicians
 Atrial fibrillation (AF) care pathways for the primary care physicians by University of Minnesota Physicians Heart, October, 2011 Evaluation by the primary care physician: 1. Comprehensive history and
Atrial fibrillation (AF) care pathways for the primary care physicians by University of Minnesota Physicians Heart, October, 2011 Evaluation by the primary care physician: 1. Comprehensive history and
ATRIAL FIBRILLATION IN THE 21 ST CENTURY TIMOTHY DOWLING, D.O. FAMILY PHYSICIAN
 ATRIAL FIBRILLATION IN THE 21 ST CENTURY TIMOTHY DOWLING, D.O. FAMILY PHYSICIAN GOALS AND OBJECTIVES At The end of this talk you should understand: What is Atrial Fibrillation Causes of Atrial Fibrillation
ATRIAL FIBRILLATION IN THE 21 ST CENTURY TIMOTHY DOWLING, D.O. FAMILY PHYSICIAN GOALS AND OBJECTIVES At The end of this talk you should understand: What is Atrial Fibrillation Causes of Atrial Fibrillation
Managing the Patient with Atrial Fibrillation
 Pocket Guide Managing the Patient with Atrial Fibrillation Updated April 2012 Editor Stephen R. Shorofsky, MD, Ph.D. Assistant Editors Anastasios Saliaris, MD Shawn Robinson, MD www.hrsonline.org DEFINITION
Pocket Guide Managing the Patient with Atrial Fibrillation Updated April 2012 Editor Stephen R. Shorofsky, MD, Ph.D. Assistant Editors Anastasios Saliaris, MD Shawn Robinson, MD www.hrsonline.org DEFINITION
Current Management of Atrial Fibrillation DISCLOSURES. Heart Beat Anatomy. I have no financial conflicts to disclose
 Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Presenter Disclosure Information
 2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
2:15 3 pm Managing Arrhythmias in Primary Care Presenter Disclosure Information The following relationships exist related to this presentation: Raul Mitrani, MD, FACC, FHRS: Speakers Bureau for Medtronic.
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL)
 ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
ATRIAL FIBRILLATION (RATE VS RHYTHM CONTROL) By Prof. Dr. Helmy A. Bakr Mansoura Universirty 2014 AF Classification: Mechanisms of AF : Selected Risk Factors and Biomarkers for AF: WHY AF? 1. Atrial fibrillation
Atrial fibrillation. Quick reference guide. Issue date: June 2006. The management of atrial fibrillation
 Quick reference guide Issue date: June 2006 Atrial fibrillation The management of atrial fibrillation Developed by the National Collaborating Centre for Chronic Conditions Contents Contents Patient-centred
Quick reference guide Issue date: June 2006 Atrial fibrillation The management of atrial fibrillation Developed by the National Collaborating Centre for Chronic Conditions Contents Contents Patient-centred
INFORMATION FOR PATIENTS AND FAMILIES A Patient s Guide to Living with Atrial Fibrillation
 INFORMATION FOR PATIENTS AND FAMILIES A Patient s Guide to Living with Atrial Fibrillation 30 Bond Street, Toronto, ON M5B 1W8 Canada 416.864.6060 stmichaelshospital.com Form No. XXXXX Dev. XX/XXXX GOALS
INFORMATION FOR PATIENTS AND FAMILIES A Patient s Guide to Living with Atrial Fibrillation 30 Bond Street, Toronto, ON M5B 1W8 Canada 416.864.6060 stmichaelshospital.com Form No. XXXXX Dev. XX/XXXX GOALS
Atrial Fibrillation An update on diagnosis and management
 Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier
 Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier Most common dysrhythmia seen in ED, and incidence increasing with ageing population Presentation Common presentations: younger patients often
Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier Most common dysrhythmia seen in ED, and incidence increasing with ageing population Presentation Common presentations: younger patients often
Management of ATRIAL FIBRILLATION. in general practice. 22 BPJ Issue 39
 Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Atrial Fibrillation: Do We Have A Cure? Raymond Kawasaki, MD AMG Electrophysiology February 21, 2015
 Atrial Fibrillation: Do We Have A Cure? Raymond Kawasaki, MD AMG Electrophysiology February 21, 2015 Disclaimer I have no relationships to disclose Do we have a cure for Atrial Fibrillation? The short
Atrial Fibrillation: Do We Have A Cure? Raymond Kawasaki, MD AMG Electrophysiology February 21, 2015 Disclaimer I have no relationships to disclose Do we have a cure for Atrial Fibrillation? The short
The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It?
 The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It? Indiana Chapter-ACC 17 th Annual Meeting Indianapolis, Indiana October 19, 2013 Deepak Bhakta MD FACC FACP FAHA FHRS CCDS Associate
The Emerging Atrial Fibrillation Epidemic: Treat It, Leave It or Burn It? Indiana Chapter-ACC 17 th Annual Meeting Indianapolis, Indiana October 19, 2013 Deepak Bhakta MD FACC FACP FAHA FHRS CCDS Associate
New Treatments for Stroke Prevention in Atrial Fibrillation. John C. Andrefsky, MD, FAHA NEOMED Internal Medicine Review course May 5 th, 2013
 New Treatments for Stroke Prevention in Atrial Fibrillation John C. Andrefsky, MD, FAHA NEOMED Internal Medicine Review course May 5 th, 2013 Classification Paroxysmal atrial fibrillation (AF) Last < 7
New Treatments for Stroke Prevention in Atrial Fibrillation John C. Andrefsky, MD, FAHA NEOMED Internal Medicine Review course May 5 th, 2013 Classification Paroxysmal atrial fibrillation (AF) Last < 7
Ngaire has Palpitations
 Ngaire has Palpitations David Heaven Cardiac Electrophysiologist/Heart Rhythm Specialist Middlemore, Auckland City and Mercy Hospitals Auckland Heart Group MCQ Ms A is 45, and a healthy marathon runner.
Ngaire has Palpitations David Heaven Cardiac Electrophysiologist/Heart Rhythm Specialist Middlemore, Auckland City and Mercy Hospitals Auckland Heart Group MCQ Ms A is 45, and a healthy marathon runner.
Atrial Fibrillation Centre
 About this guide We have prepared this guide to help you to: learn about atrial fibrillation manage atrial fibrillation and reduce the risk of stroke find out about medicines and other treatment options
About this guide We have prepared this guide to help you to: learn about atrial fibrillation manage atrial fibrillation and reduce the risk of stroke find out about medicines and other treatment options
Atrial Fibrillation (AF) March, 2013
 Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
Atrial Fibrillation (AF) March, 2013 This handout is meant to help with discussions about the condition, and it is not a complete discussion of AF. We hope it will complement your appointment with one
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT of Atrial Fibrillation (AF) Key priorities Identification and diagnosis Treatment for persistent AF Treatment for permanent AF Antithrombotic
Atrial Fibrillation and Ablation Therapy: A Patient s Guide
 Atrial Fibrillation and Ablation Therapy: A Patient s Guide ATRIAL FIBRILLATION CENTER AT UNIVERSITY OF ROCHESTER MEDICAL CENTER www.heart.urmc.edu 585-275-4775 INTRODUCTION Our goal at the Atrial Fibrillation
Atrial Fibrillation and Ablation Therapy: A Patient s Guide ATRIAL FIBRILLATION CENTER AT UNIVERSITY OF ROCHESTER MEDICAL CENTER www.heart.urmc.edu 585-275-4775 INTRODUCTION Our goal at the Atrial Fibrillation
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
Protocol for the management of atrial fibrillation in primary care
 Protocol for the management of atrial fibrillation in primary care Protocol for the management of atrial fibrillation in primary care Contents Page no Definition 2 Classification of AF 2 3 Identification
Protocol for the management of atrial fibrillation in primary care Protocol for the management of atrial fibrillation in primary care Contents Page no Definition 2 Classification of AF 2 3 Identification
Palpitations & AF. Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust
 Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
Palpitations & AF Richard Grocott Mason Consultant Cardiologist THH NHS Foundation Trust & Royal Brompton & Harefield NHS Foundation Trust Palpitations Frequent symptom Less than 50% associated with arrhythmia
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Visited 9/14/2011. What is Atrial Fibrillation? What you need to know about Atrial Fibrillation. The Normal Heart Rhythm. 1 of 7 9/14/2011 10:50 AM
 1 of 7 9/14/2011 10:50 AM Current URL: What you need to know about Atrial Fibrillation What is atrial fibrillation? What causes atrial fibrillation? How is atrial fibrillation diagnosed? What are the dangers
1 of 7 9/14/2011 10:50 AM Current URL: What you need to know about Atrial Fibrillation What is atrial fibrillation? What causes atrial fibrillation? How is atrial fibrillation diagnosed? What are the dangers
New in Atrial Fibrillation
 New in Atrial Fibrillation September 2011 Stroke prevention more options Rhythm Control -drugs - alternatives to drugs; ablation Rate Control - pace + ablate A-FIB Dell Stroke Risk AFib Two Principles
New in Atrial Fibrillation September 2011 Stroke prevention more options Rhythm Control -drugs - alternatives to drugs; ablation Rate Control - pace + ablate A-FIB Dell Stroke Risk AFib Two Principles
Atrial Fibrillation Based on ESC Guidelines. Moshe Swissa MD Kaplan Medical Center
 Atrial Fibrillation Based on ESC Guidelines Moshe Swissa MD Kaplan Medical Center Epidemiology AF affects 1 2% of the population, and this figure is likely to increase in the next 50 years. AF may long
Atrial Fibrillation Based on ESC Guidelines Moshe Swissa MD Kaplan Medical Center Epidemiology AF affects 1 2% of the population, and this figure is likely to increase in the next 50 years. AF may long
PRACTICAL APPROACH TO SVT. Graham C. Wong MD MPH Division of Cardiology Vancouver General Hospital University of British Columbia
 PRACTICAL APPROACH TO SVT Graham C. Wong MD MPH Division of Cardiology Vancouver General Hospital University of British Columbia CONDUCTION SYSTEM OF THE HEART SA node His bundle Left bundle AV node Right
PRACTICAL APPROACH TO SVT Graham C. Wong MD MPH Division of Cardiology Vancouver General Hospital University of British Columbia CONDUCTION SYSTEM OF THE HEART SA node His bundle Left bundle AV node Right
ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY
 Care Pathway Triage category ATRIAL FIBRILLATION PATHWAY ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY AF/ FLUTTER IS PRIMARY REASON FOR PRESENTATION YES NO ONSET SYMPTOMS OF AF./../ TIME DURATION OF AF
Care Pathway Triage category ATRIAL FIBRILLATION PATHWAY ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY AF/ FLUTTER IS PRIMARY REASON FOR PRESENTATION YES NO ONSET SYMPTOMS OF AF./../ TIME DURATION OF AF
Treatments to Restore Normal Rhythm
 Treatments to Restore Normal Rhythm In many instances when AF causes significant symptoms or is negatively impacting a patient's health, the major goal of treatment is to restore normal rhythm and prevent
Treatments to Restore Normal Rhythm In many instances when AF causes significant symptoms or is negatively impacting a patient's health, the major goal of treatment is to restore normal rhythm and prevent
Quiz 4 Arrhythmias summary statistics and question answers
 1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
Atrial fibrillation (AF) patient information
 AF A Atrial fibrillation (AF) patient information Providing information, support and access to established, new or innovative treatments for Atrial Fibrillation www.atrialfibrillation-au.org Glossary Antiarrhythmic
AF A Atrial fibrillation (AF) patient information Providing information, support and access to established, new or innovative treatments for Atrial Fibrillation www.atrialfibrillation-au.org Glossary Antiarrhythmic
Treatment Options for Atrial Fibrillation Patient Information
 Patient Information Treatment Options for Atrial Fibrillation Page 1 of 8 Treatment Options for Atrial Fibrillation Patient Information Emory University Hospital Midtown Cardiac Electrophysiology Service
Patient Information Treatment Options for Atrial Fibrillation Page 1 of 8 Treatment Options for Atrial Fibrillation Patient Information Emory University Hospital Midtown Cardiac Electrophysiology Service
Anticoagulation: How Do I Pick From All the Choices? Jeffrey H. Neuhauser, DO, FACC BHHI Primary Care Symposium February 28, 2014
 Anticoagulation: How Do I Pick From All the Choices? Jeffrey H. Neuhauser, DO, FACC BHHI Primary Care Symposium February 28, 2014 Atrial Fibrillation 2 Atrial Fibrillation The most common arrhythmia encountered
Anticoagulation: How Do I Pick From All the Choices? Jeffrey H. Neuhauser, DO, FACC BHHI Primary Care Symposium February 28, 2014 Atrial Fibrillation 2 Atrial Fibrillation The most common arrhythmia encountered
Introduction to Atrial Fibrillation (AFib)
 Introduction to Atrial Fibrillation (AFib) Learn About: 1. What is atrial fibrillation? 2. How will I feel? 3. Who gets AFib? 4. Risk of stroke 5. AFib treatment 6. How to live well with AFib 1. What is
Introduction to Atrial Fibrillation (AFib) Learn About: 1. What is atrial fibrillation? 2. How will I feel? 3. Who gets AFib? 4. Risk of stroke 5. AFib treatment 6. How to live well with AFib 1. What is
TABLE 1 Clinical Classification of AF. New onset AF (first detected) Paroxysmal (<7 days, mostly < 24 hours)
 Clinical Practice Guidelines for the Management of Patients With Atrial Fibrillation Deborah Ritchie RN, MN, Robert S Sheldon MD, PhD Cardiovascular Research Group, University of Calgary, Alberta Partly
Clinical Practice Guidelines for the Management of Patients With Atrial Fibrillation Deborah Ritchie RN, MN, Robert S Sheldon MD, PhD Cardiovascular Research Group, University of Calgary, Alberta Partly
These guidelines have been withdrawn
 These guidelines have been withdrawn MOH clinical practice guidelines are considered withdrawn five years after publication unless otherwise specified in individual guidelines. Users should keep in mind
These guidelines have been withdrawn MOH clinical practice guidelines are considered withdrawn five years after publication unless otherwise specified in individual guidelines. Users should keep in mind
A 35 yo female presents increasing fatigue and shortness of breath for several days. She is found to be in atrial fibrillation.
 Ryan G. Aleong Cardiology Department University of Colorado A 35 yo female presents increasing fatigue and shortness of breath for several days. She is found to be in atrial fibrillation. 1. Initiation
Ryan G. Aleong Cardiology Department University of Colorado A 35 yo female presents increasing fatigue and shortness of breath for several days. She is found to be in atrial fibrillation. 1. Initiation
Classification (ACC/AHA/ESC 2006)
 ATRIAL FIBRILLATION Atrial Fibrillation Atrial fibrillation is a common disorder which affects 0.4% of the general population. The risk increases sharply with age so that the lifetime prevalence of AF
ATRIAL FIBRILLATION Atrial Fibrillation Atrial fibrillation is a common disorder which affects 0.4% of the general population. The risk increases sharply with age so that the lifetime prevalence of AF
NORTHERN NETWORK OF CARDIAC CARE GUIDELINES FOR THE DETECTION AND MANAGEMENT OF ATRIAL FIBRILLATION (AF)
 NORTHERN NETWORK OF CARDIAC CARE GUIDELINES FOR THE DETECTION AND MANAGEMENT OF ATRIAL FIBRILLATION (AF) These notes should be read in conjunction with the summary algorithms July 2007 CONTENTS 1. Introduction
NORTHERN NETWORK OF CARDIAC CARE GUIDELINES FOR THE DETECTION AND MANAGEMENT OF ATRIAL FIBRILLATION (AF) These notes should be read in conjunction with the summary algorithms July 2007 CONTENTS 1. Introduction
Atrial Fibrillation. Patient Information. 828361 Dec 19-12
 Atrial Fibrillation Patient Information 828361 Dec 19-12 Contents Introduction 1 Treatment & decrease stroke options 2 Information for people who are taking warfarin (Coumadin ) 5 Information for people
Atrial Fibrillation Patient Information 828361 Dec 19-12 Contents Introduction 1 Treatment & decrease stroke options 2 Information for people who are taking warfarin (Coumadin ) 5 Information for people
Anticoagulants in Atrial Fibrillation
 Anticoagulants in Atrial Fibrillation Starting and Stopping Them Safely Carmine D Amico, D.O. Overview Learning objectives Introduction Basic concepts Treatment strategy & options Summary 1 Learning objectives
Anticoagulants in Atrial Fibrillation Starting and Stopping Them Safely Carmine D Amico, D.O. Overview Learning objectives Introduction Basic concepts Treatment strategy & options Summary 1 Learning objectives
Atrial Fibrillation. Management Strategies Marc D. Schrode, D.O., F.A.C.C.,F.A.C.O.I.
 Atrial Fibrillation Management Strategies Marc D. Schrode, D.O., F.A.C.C.,F.A.C.O.I. Atrial Fibrillation Estimated that 2.6 to 6.1 million people in the U.S. with Afib as of 2010 By 2050 it is expected
Atrial Fibrillation Management Strategies Marc D. Schrode, D.O., F.A.C.C.,F.A.C.O.I. Atrial Fibrillation Estimated that 2.6 to 6.1 million people in the U.S. with Afib as of 2010 By 2050 it is expected
Atrial Fibrillation. Information for you, and your family, whänau and friends. Published by the New Zealand Guidelines Group
 Atrial Fibrillation Information for you, and your family, whänau and friends Published by the New Zealand Guidelines Group CONTENTS Introduction 1 The heart 2 What is atrial fibrillation? 3 How common
Atrial Fibrillation Information for you, and your family, whänau and friends Published by the New Zealand Guidelines Group CONTENTS Introduction 1 The heart 2 What is atrial fibrillation? 3 How common
Nursing Care and Considerations for Patients with Atrial Fibrillation. Kris Kinghorn RN, MSN, ANP-BC
 Nursing Care and Considerations for Patients with Atrial Fibrillation Kris Kinghorn RN, MSN, ANP-BC Case Study 66 y/o female (Mrs. Olus A. Blader) Admitted with c/o palpitations and lightheadedness PMH:
Nursing Care and Considerations for Patients with Atrial Fibrillation Kris Kinghorn RN, MSN, ANP-BC Case Study 66 y/o female (Mrs. Olus A. Blader) Admitted with c/o palpitations and lightheadedness PMH:
Introduction 2/9/2015
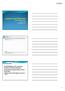 Thomas Haffey, D.O. FACC, FACOI, FNLA, CSOM February, 2015 Atrial Tachycardias Diagram summarizing types of atrial tachycardias often encountered in patients with a history of AF, including those seen
Thomas Haffey, D.O. FACC, FACOI, FNLA, CSOM February, 2015 Atrial Tachycardias Diagram summarizing types of atrial tachycardias often encountered in patients with a history of AF, including those seen
Atrial Fibrillation Cardiac rate control or rhythm control could be the key to AF therapy
 Cardiac rate control or rhythm control could be the key to AF therapy Recent studies have proven that an option of pharmacologic and non-pharmacologic therapy is available to patients who suffer from AF.
Cardiac rate control or rhythm control could be the key to AF therapy Recent studies have proven that an option of pharmacologic and non-pharmacologic therapy is available to patients who suffer from AF.
Practical Rate and Rhythm Management of Atrial Fibrillation
 Practical Rate and Rhythm Management of Atrial Fibrillation pocket guide UPDATED FEBRUARY 2013 Adapted from the ACCF/AHA/HRS 2011 Focused Updates Incorporated into the ACC/AHA/ESC Guidelines for the Management
Practical Rate and Rhythm Management of Atrial Fibrillation pocket guide UPDATED FEBRUARY 2013 Adapted from the ACCF/AHA/HRS 2011 Focused Updates Incorporated into the ACC/AHA/ESC Guidelines for the Management
Survey of Canadian Physicians Use of anti-thrombotic therapy for Atrial Fibrillation
 Survey of Canadian Physicians Use of anti-thrombotic therapy for Atrial Fibrillation On the following pages are a number of questions asking about the conditions under which you would prescribe anticoagulation
Survey of Canadian Physicians Use of anti-thrombotic therapy for Atrial Fibrillation On the following pages are a number of questions asking about the conditions under which you would prescribe anticoagulation
Atrial Fibrillation (AF) Explained
 James Paget University Hospitals NHS Foundation Trust Atrial Fibrillation (AF) Explained Patient Information Contents What are the symptoms of atrial fibrillation (AF)? 3 Normal heartbeat 4 How common
James Paget University Hospitals NHS Foundation Trust Atrial Fibrillation (AF) Explained Patient Information Contents What are the symptoms of atrial fibrillation (AF)? 3 Normal heartbeat 4 How common
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT
 THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
THE INTERNET STROKE CENTER PRESENTATIONS AND DISCUSSIONS ON STROKE MANAGEMENT Stroke Prevention in Atrial Fibrillation Gregory Albers, M.D. Director Stanford Stroke Center Professor of Neurology and Neurological
Management of Atrial Fibrillation in the Emergency Department
 Management of Atrial Fibrillation in the Emergency Department Ref: Emergency Medicine Clinics of North America, 2005 Introduction AfAf is most common cardiac arrhythmia Sequelae: : range from none to devastating:
Management of Atrial Fibrillation in the Emergency Department Ref: Emergency Medicine Clinics of North America, 2005 Introduction AfAf is most common cardiac arrhythmia Sequelae: : range from none to devastating:
Management of Atrial Fibrillation in Heart Failure
 Disadvantages of AV Junction Ablation Persistent AFib- no AV synchrony Ongoing risk of thromboembolism Life-long dependency on pacemaker Comparison of LA Ablation vs. AVN Ablation LA Ablation AVN Ablation
Disadvantages of AV Junction Ablation Persistent AFib- no AV synchrony Ongoing risk of thromboembolism Life-long dependency on pacemaker Comparison of LA Ablation vs. AVN Ablation LA Ablation AVN Ablation
ATRIAL FIBRILLATION: Scope of the Problem. October 2015
 ATRIAL FIBRILLATION: Scope of the Problem October 2015 Purpose of the Presentation Review the worldwide incidence and prognosis associated with atrial fibrillation (AF) Identify the types of AF, clinical
ATRIAL FIBRILLATION: Scope of the Problem October 2015 Purpose of the Presentation Review the worldwide incidence and prognosis associated with atrial fibrillation (AF) Identify the types of AF, clinical
ATRIAL FIBRILLATION. What you need to know
 ATRIAL FIBRILLATION What you need to know Table of contents Atrial fibrillation overview... 1 What is a-fib?.... 2 Risk factors for a-fib... 3 Symptoms of a-fib.... 4 Complications from a-fib... 4 How
ATRIAL FIBRILLATION What you need to know Table of contents Atrial fibrillation overview... 1 What is a-fib?.... 2 Risk factors for a-fib... 3 Symptoms of a-fib.... 4 Complications from a-fib... 4 How
Atrial Fibrillation: Manual of Clinical Guidelines
 Atrial Fibrillation: Manual of Clinical Guidelines Table of Contents Table of Contents...1 Introduction...2 How to Use this Manual...3 Atrial Fibrillation: COMMON ELEMENTS OF CARE...4 Definitions...4 Controlling
Atrial Fibrillation: Manual of Clinical Guidelines Table of Contents Table of Contents...1 Introduction...2 How to Use this Manual...3 Atrial Fibrillation: COMMON ELEMENTS OF CARE...4 Definitions...4 Controlling
ACUTE ATRIAL FIBRILLATION TREATMENT IN THE SURGICAL PATIENT
 DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
DISCLAIMER: These guidelines were prepared by the Department of Surgical Education, Orlando Regional Medical Center. They are intended to serve as a general statement regarding appropriate patient care
DISCLOSURE. Atrial Fibrillation Management An Evidence-based Approach OBJECTIVES BACKGROUND AFFIRM 9/16/2015
 Death (%) Mortality (%) 9/16/2015 DISCLOSURE Atrial Fibrillation Management An Evidence-based Approach Jonathon Adams, MD, FHRS Relevant Financial Relationship(s) None Off Label Usage None OBJECTIVES What
Death (%) Mortality (%) 9/16/2015 DISCLOSURE Atrial Fibrillation Management An Evidence-based Approach Jonathon Adams, MD, FHRS Relevant Financial Relationship(s) None Off Label Usage None OBJECTIVES What
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY
 Measure #326 (NQF 1525): Atrial Fibrillation and Atrial Flutter: Chronic Anticoagulation Therapy National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS,
Measure #326 (NQF 1525): Atrial Fibrillation and Atrial Flutter: Chronic Anticoagulation Therapy National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS,
A CAREGIVER s Guide to. Complicated Atrial Fibrillation
 A CAREGIVER s Guide to Complicated Atrial Fibrillation Introduction Atrial fibrillation (also known as AFib or AF) is a common heart condition, particularly among older people. It s estimated that AF affects
A CAREGIVER s Guide to Complicated Atrial Fibrillation Introduction Atrial fibrillation (also known as AFib or AF) is a common heart condition, particularly among older people. It s estimated that AF affects
Atrial Fibrillation. Management of Patients With. ACCF/AHA Pocket Guideline
 ACCF/AHA Pocket Guideline Management of Patients With Atrial Fibrillation (Adapted from the 2006 ACC/AHA/ESC Guideline and the 2011 ACCF/AHA/HRS Focused Updates) 2011 American College of Cardiology Foundation
ACCF/AHA Pocket Guideline Management of Patients With Atrial Fibrillation (Adapted from the 2006 ACC/AHA/ESC Guideline and the 2011 ACCF/AHA/HRS Focused Updates) 2011 American College of Cardiology Foundation
Atrial fibrillation. Treatment Guide
 Treatment Guide Atrial fibrillation Atrial fibrillation (AF or AFib) is the most common irregular or abnormal heart rhythm disorder, affecting more than 3 million Americans today. Thankfully, more options
Treatment Guide Atrial fibrillation Atrial fibrillation (AF or AFib) is the most common irregular or abnormal heart rhythm disorder, affecting more than 3 million Americans today. Thankfully, more options
Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter
 22 July 2010 EMA/CHMP/EWP/213056/2010 Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter Draft Agreed by Efficacy Working Party July 2008 Adoption by CHMP for release
22 July 2010 EMA/CHMP/EWP/213056/2010 Addendum to the Guideline on antiarrhythmics on atrial fibrillation and atrial flutter Draft Agreed by Efficacy Working Party July 2008 Adoption by CHMP for release
National Medicines Information Centre
 National Medicines Information Centre ST. JAMES S HOSPITAL DUBLIN 8 TEL 01-4730589 or 1850-727-727 FAX 01-4730596 www.nmic.ie THE CONTEMPORARY MANAGEMENT OF ATRIAL FIBRILLATION VOLUME 12 NUMBER 3 2006
National Medicines Information Centre ST. JAMES S HOSPITAL DUBLIN 8 TEL 01-4730589 or 1850-727-727 FAX 01-4730596 www.nmic.ie THE CONTEMPORARY MANAGEMENT OF ATRIAL FIBRILLATION VOLUME 12 NUMBER 3 2006
ATRIAL FIBRILLATION RATE VS RHYTHM CONTROL NCVH BIRMINGHAM 2014
 ATRIAL FIBRILLATION RATE VS RHYTHM CONTROL NCVH BIRMINGHAM 2014 Facts 4 million or so people have atrial fibrillation 16 billion dollars spent yearly in USA 30% of strokes attributable to AF and AFL 3-5
ATRIAL FIBRILLATION RATE VS RHYTHM CONTROL NCVH BIRMINGHAM 2014 Facts 4 million or so people have atrial fibrillation 16 billion dollars spent yearly in USA 30% of strokes attributable to AF and AFL 3-5
Antiplatelet and Antithrombotic Therapy. Dr Curry Grant Stroke Prevention Clinic Quinte Health Care
 Antiplatelet and Antithrombotic Therapy Dr Curry Grant Stroke Prevention Clinic Quinte Health Care Disclosure of Potential for Conflict of Interest Dr. F.C. Grant Atrial Fibrillation FINANCIAL DISCLOSURE:
Antiplatelet and Antithrombotic Therapy Dr Curry Grant Stroke Prevention Clinic Quinte Health Care Disclosure of Potential for Conflict of Interest Dr. F.C. Grant Atrial Fibrillation FINANCIAL DISCLOSURE:
RUSSELLS HALL HOSPITAL EMERGENCY DEPARTMENT
 RUSSELLS HALL HOSPITAL EMERGENCY DEPARTMENT CLINICAL GUIDELINE ATRIAL FIBRILLATION March 2011 For quick links to AF algorithms: UNSTABLE PATIENT STABLE PATIENT - 1 - Introduction Atrial fibrillation is
RUSSELLS HALL HOSPITAL EMERGENCY DEPARTMENT CLINICAL GUIDELINE ATRIAL FIBRILLATION March 2011 For quick links to AF algorithms: UNSTABLE PATIENT STABLE PATIENT - 1 - Introduction Atrial fibrillation is
Practical Management of Atrial Fibrillation
 Practical Management of Atrial Fibrillation UPDATED JULY 2014 Adapted from the AHA/ACC/HRS 2014 Guideline for the Management of Patients with Atrial Fibrillation Editor: Bradley P. Knight, MD, FACC, FHRS
Practical Management of Atrial Fibrillation UPDATED JULY 2014 Adapted from the AHA/ACC/HRS 2014 Guideline for the Management of Patients with Atrial Fibrillation Editor: Bradley P. Knight, MD, FACC, FHRS
PATIENT INFORMATION BOOKLET FOR ATRIAL FIBRILLATION
 PATIENT INFORMATION BOOKLET FOR ATRIAL FIBRILLATION Prepared by Karen Jones MBA and Nancy Marco NP for the Complex Arrhythmia Clinic Toronto General Hospital Peter Munk Cardiac Centre University Health
PATIENT INFORMATION BOOKLET FOR ATRIAL FIBRILLATION Prepared by Karen Jones MBA and Nancy Marco NP for the Complex Arrhythmia Clinic Toronto General Hospital Peter Munk Cardiac Centre University Health
Medical management of CHF: A New Class of Medication. Al Timothy, M.D. Cardiovascular Institute of the South
 Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Medical management of CHF: A New Class of Medication Al Timothy, M.D. Cardiovascular Institute of the South Disclosures Speakers Bureau for Amgen Background Chronic systolic congestive heart failure remains
Sign up to receive ATOTW weekly - email wfsahq@anaesthesiologists.org
 ATRIAL FIBRILLATION (AF). PERI-OPERATIVE MANAGEMENT FOR NON-CARDIAC SURGERY ANAESTHESIA TUTORIAL OF THE WEEK 307 28 th APRIL 2014 Dr J Sokhi Southend University Hospital, UK Professor J Kinnear Southend
ATRIAL FIBRILLATION (AF). PERI-OPERATIVE MANAGEMENT FOR NON-CARDIAC SURGERY ANAESTHESIA TUTORIAL OF THE WEEK 307 28 th APRIL 2014 Dr J Sokhi Southend University Hospital, UK Professor J Kinnear Southend
Difficult Cases in Atrial Fibrillation. Ascot Cardiology GP Symposium April 2014
 Difficult Cases in Atrial Fibrillation Ascot Cardiology GP Symposium April 2014 Atrial Fibrillation 1-2% general population 40-50yrs
Difficult Cases in Atrial Fibrillation Ascot Cardiology GP Symposium April 2014 Atrial Fibrillation 1-2% general population 40-50yrs
Secondary Stroke Prevention Luke Bradbury, MD 10/4/14 Fall WAPA Conferfence
 Guidelines Secondary Stroke Prevention Luke Bradbury, MD 10/4/14 Fall WAPA Conferfence Stroke/TIA Nearly 700,000 ischemic strokes and 240,000 TIAs every year in the United States Currently, the risk for
Guidelines Secondary Stroke Prevention Luke Bradbury, MD 10/4/14 Fall WAPA Conferfence Stroke/TIA Nearly 700,000 ischemic strokes and 240,000 TIAs every year in the United States Currently, the risk for
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION A Comprehensive Resource from the Heart Rhythm Society AF 360 provides a single, trusted resource for the most comprehensive and relevant information and
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION A Comprehensive Resource from the Heart Rhythm Society AF 360 provides a single, trusted resource for the most comprehensive and relevant information and
GUIDE TO ATRIAL FIBRILLATION
 PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
PATIENT INFORMATION GUIDE TO ATRIAL FIBRILLATION Atrial Fibrillation (AF) Atrial Flutter (AFL) Rate and Rhythm Control Stroke Prevention This document is endorsed by: A Comprehensive Resource from the
Atrial Fibrillation. By Danielle Flint
 Atrial Fibrillation By Danielle Flint Outline Definition Epidemiology Clinical Aspects Treatment Effects of Exercise Exercise Testing Exercise Prescription Summary References Definition: What is Atrial
Atrial Fibrillation By Danielle Flint Outline Definition Epidemiology Clinical Aspects Treatment Effects of Exercise Exercise Testing Exercise Prescription Summary References Definition: What is Atrial
ATRIAL FIBRILLATION. Michael Diamant and Luke Rannelli Internal Medicine PGY-3
 ATRIAL FIBRILLATION Michael Diamant and Luke Rannelli Internal Medicine PGY-3 OBJECTIVES Guidelines-based approach to the following: Initial diagnosis and work-up Management as an outpatient Rate control
ATRIAL FIBRILLATION Michael Diamant and Luke Rannelli Internal Medicine PGY-3 OBJECTIVES Guidelines-based approach to the following: Initial diagnosis and work-up Management as an outpatient Rate control
About the British Heart Foundation
 Atrial fibrillation About the British Heart Foundation The British Heart Foundation (BHF) is the nation s heart charity, saving lives through pioneering research, patient care and vital information. What
Atrial fibrillation About the British Heart Foundation The British Heart Foundation (BHF) is the nation s heart charity, saving lives through pioneering research, patient care and vital information. What
Antiplatelet and Antithrombotics From clinical trials to guidelines
 Antiplatelet and Antithrombotics From clinical trials to guidelines Ashraf Reda, MD, FESC Prof and head of Cardiology Dep. Menofiya University Preisedent of EGYBAC Chairman of WGLVR One of the big stories
Antiplatelet and Antithrombotics From clinical trials to guidelines Ashraf Reda, MD, FESC Prof and head of Cardiology Dep. Menofiya University Preisedent of EGYBAC Chairman of WGLVR One of the big stories
Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements
 Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements Salmaan Kanji, Pharm.D. The Ottawa Hospital The Ottawa Hospital Research Institute Conflict of Interest No financial, proprietary
Atrial Fibrillation in the ICU: Attempting to defend 4 controversial statements Salmaan Kanji, Pharm.D. The Ottawa Hospital The Ottawa Hospital Research Institute Conflict of Interest No financial, proprietary
A randomized, controlled trial comparing the efficacy of carvedilol vs. metoprolol in the treatment of atrial fibrillation
 A randomized, controlled trial comparing the efficacy of carvedilol vs. metoprolol in the treatment of atrial fibrillation Gabriel Sayer Lay Abstract: Atrial fibrillation is a common form of irregular,
A randomized, controlled trial comparing the efficacy of carvedilol vs. metoprolol in the treatment of atrial fibrillation Gabriel Sayer Lay Abstract: Atrial fibrillation is a common form of irregular,
Radiofrequency Ablation for Atrial Fibrillation. A Guide for Adults
 Radiofrequency Ablation for Atrial Fibrillation A Guide for Adults Fast Facts n There are different ways to treat atrial fibrillation (A-fib). One kind of treatment involves putting the heart back into
Radiofrequency Ablation for Atrial Fibrillation A Guide for Adults Fast Facts n There are different ways to treat atrial fibrillation (A-fib). One kind of treatment involves putting the heart back into
Unrestricted grant Boehringer Ingelheim
 ED Management of Recent Onset tat Atrial Fibrillation and Flutter (RAFF) Canadian Cardiovascular Society Guidelines 2010 CAEP St John s 2011 Ian Stiell MD MSc FRCPC Professor and Chair, Dept of Emergency
ED Management of Recent Onset tat Atrial Fibrillation and Flutter (RAFF) Canadian Cardiovascular Society Guidelines 2010 CAEP St John s 2011 Ian Stiell MD MSc FRCPC Professor and Chair, Dept of Emergency
New Approaches to Anticoagulation in Atrial Fibrillation
 New Approaches to Anticoagulation in Atrial Fibrillation Hugh Calkins M.D. Nicholas J. Fortuin Professor of Cardiology Professor of Medicine Director of Electrophysiology Johns Hopkins Medical Institutions
New Approaches to Anticoagulation in Atrial Fibrillation Hugh Calkins M.D. Nicholas J. Fortuin Professor of Cardiology Professor of Medicine Director of Electrophysiology Johns Hopkins Medical Institutions
Atrial Fibrillation New Treatment, New Hope. Atrial Fibrillation It Just Sucks. Atrial Fibrillation Disclosure Information 1/30/2014
 New Treatment, New Hope Emerging Concepts And Novel Management Strategies James J. Merrill, MD February 1, 2014 Wellmont CVA Heart Institute Kingsport, TN It Just Sucks We Don t Know What Causes It Or
New Treatment, New Hope Emerging Concepts And Novel Management Strategies James J. Merrill, MD February 1, 2014 Wellmont CVA Heart Institute Kingsport, TN It Just Sucks We Don t Know What Causes It Or
Atrial Fibrillation, Chronic - Antithrombotic Treatment - OBSOLETE
 Atrial Fibrillation, Chronic - Antithrombotic Treatment - OBSOLETE Clinical practice guidelines serve as an educational reference, and do not supersede the clinical judgment of the treating physician with
Atrial Fibrillation, Chronic - Antithrombotic Treatment - OBSOLETE Clinical practice guidelines serve as an educational reference, and do not supersede the clinical judgment of the treating physician with
9/5/14. Objectives. Atrial Fibrillation (AF)
 Novel Anticoagulation for Prevention of Stroke in Patients with Atrial Fibrillation Objectives 1. Review current evidence on use of warfarin in individuals with atrial fibrillation 2. Compare the three
Novel Anticoagulation for Prevention of Stroke in Patients with Atrial Fibrillation Objectives 1. Review current evidence on use of warfarin in individuals with atrial fibrillation 2. Compare the three
Traditionally, the goal of atrial fibrillation (AF)
 358 Clinical Pharmacist November 2010 Vol 2 Treatment of atrial fibrillation usually involves controlling ventricular rate or restoring sinus rhythm. Equally important is thromboembolic risk assessment
358 Clinical Pharmacist November 2010 Vol 2 Treatment of atrial fibrillation usually involves controlling ventricular rate or restoring sinus rhythm. Equally important is thromboembolic risk assessment
New Anticoagulants and GI bleeding
 New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
New Anticoagulants and GI bleeding DR DANNY MYERS MD FRCP(C) CLINICAL ASSISTANT PROFESSOR OF MEDICINE, UBC Conflicts of Interest None I am unbiased in the use of NOAC s vs Warfarin based on risk benefit
I know my value. Be an active part of your anticoagulation therapy with INR self-monitoring
 I know my value Be an active part of your anticoagulation therapy with INR self-monitoring INR* self-monitoring needs only a drop of blood, is easy, fast and decreases the possibility Be involved in your
I know my value Be an active part of your anticoagulation therapy with INR self-monitoring INR* self-monitoring needs only a drop of blood, is easy, fast and decreases the possibility Be involved in your
written by Harvard Medical School Atrial Fibrillation Coping With a Chaotic Heartbeat www.patientedu.org
 written by Harvard Medical School Atrial Fibrillation Coping With a Chaotic Heartbeat www.patientedu.org What Is Atrial Fibrillation? Atrial fibrillation is a fast and irregular heartbeat. It occurs in
written by Harvard Medical School Atrial Fibrillation Coping With a Chaotic Heartbeat www.patientedu.org What Is Atrial Fibrillation? Atrial fibrillation is a fast and irregular heartbeat. It occurs in
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Projected Number of Adults With AF in the US. Review the growing incidence and importance of AF in the population
 Atrial Fibrillation Troy E. Rhodes, MD, PhD Division of Cardiovascular Medicine, Electrophysiology Ohio State University Medical Center Learning Objectives Review the growing incidence and importance of
Atrial Fibrillation Troy E. Rhodes, MD, PhD Division of Cardiovascular Medicine, Electrophysiology Ohio State University Medical Center Learning Objectives Review the growing incidence and importance of
