Practice Guidelines. Updated Guideline on Diagnosis and Treatment of Intra-abdominal Infections
|
|
|
- Silvester Hood
- 7 years ago
- Views:
Transcription
1 Updated Guideline on Diagnosis and Treatment of Intra-abdominal Infections CARRIE ARMSTRONG Guideline source: Surgical Infection Society, Infectious Diseases Society of America Literature search described? Yes Evidence rating system used? Yes Published source: Clinical Infectious Diseases, January 15, 2010 Available at: full/ / Coverage of guidelines from other organizations does not imply endorsement by AFP or the AAFP. Intra-abdominal infections are the second most common cause of infectious mortality in intensive care units. Complicated intra-abdominal infection, which extends into the peritoneal space, is associated with abscess formation and peritonitis. Uncomplicated infection, which involves intramural inflammation of the gastrointestinal tract, may progress to complicated infection if left untreated. Treatment of intra-abdominal infections has evolved in recent years because of advances in supportive care, diagnostic imaging, minimally invasive intervention, and antimicrobial therapy. Based on this new evidence, the Surgical Infection Society and the Infectious Diseases Society of America recently updated recommendations for diagnosis and treatment of these infections. The new guideline includes recommendations for treatment of intra-abdominal infections in children, management of appendicitis, and treatment of necrotizing enterocolitis in newborns. Initial Evaluation Routine history, physical examination, and laboratory studies will identify most patients who require further evaluation. Intra-abdominal infection should be considered in patients with unreliable physical examination findings (e.g., those with impaired mental status or spinal cord injury) who present with evidence of infection from an undetermined source. Further diagnostic imaging is not necessary in patients with obvious signs of diffuse peritonitis and in whom immediate surgical intervention is required. Computed tomography (CT) should be performed to determine whether an intra-abdominal infection is present in adults who are not undergoing immediate laparotomy. Fluid Resuscitation Rapid restoration of intravascular volume should be undertaken, as should any additional measures necessary to promote physiologic stability. In patients with septic shock, resuscitation should begin immediately after hypotension is identified. In patients with no evidence of volume depletion, intravenous fluid therapy should begin as soon as intra-abdominal infection is suspected. Interventions A source control procedure to drain infected foci, control ongoing peritoneal contamination, and restore anatomic and physiologic function is in virtually all patients with intra-abdominal infection. Emergency surgery should be performed in patients with diffuse peritonitis, even if measures to restore physiologic stability must be continued during the procedure. An urgent approach also should be taken in hemodynamically stable patients without evidence of acute organ failure. However, intervention may be delayed for up to 24 hours in closely monitored patients who have started antimicrobial therapy. Select patients with minimal physiologic derangement and a well-circumscribed focus of infection can be treated with antimicrobial therapy without a source control procedure if close clinical follow-up is possible. In patients with severe peritonitis, relaparotomy is not in the absence of intestinal discontinuity, abdominal fascial loss that prevents abdominal wall closure, or intra-abdominal hypertension. Laboratory Evaluation Routine blood cultures and Gram stains are not in patients with community-acquired intra-abdominal infection. Anaerobic cultures are not Downloaded from the American Family Physician Web site at Copyright 2010 American Academy of Family Physicians. For the private, noncommercial use of 694 American one Family individual Physician user of the Web site. All other rights reserved. Contact copyrights@aafp.org for copyright questions Volume and/or 82, Number permission 6 requests. September 15, 2010
2 necessary in these patients if empiric antimicrobial therapy is provided. However, routine aerobic and anaerobic cultures may be of value in determining resistance patterns and follow-up oral therapy in lower-risk patients with community-acquired infection. In higher-risk patients, cultures should be obtained from the infection site, particularly in those with previous antibiotic exposure. The specimen should be representative of the material associated with the infection and should be of sufficient volume (at least 1 ml). For optimal recovery of aerobic bacteria, 1 to 10 ml of fluid should be inoculated directly into an aerobic blood culture bottle. In addition, 0.5 ml of fluid should be sent to the laboratory for Gram stain testing and, if indicated, fungal cultures. If anaerobic cultures are requested, at least 0.5 ml of fluid or 0.5 g of tissue should be placed in an anaerobic transport tube. Alternately, 1 to 10 ml of fluid can be inoculated directly into an anaerobic blood culture bottle. Routine culture and susceptibility studies should be performed in patients with perforated appendicitis or other community-acquired intra-abdominal infection if a common community isolate (e.g., Escherichia coli) is resistant to antimicrobials in widespread local use. Susceptibility testing should be performed for Pseudomonas, Proteus, Acinetobacter, Staphylococcus aureus, and predominant Enterobacteriaceae (as determined by moderate-to-heavy growth), because resistance is more likely in these organisms. Antimicrobial Therapy Antimicrobial therapy should be started as soon as intraabdominal infection is diagnosed or suspected. Antibiotics should be administered as soon as possible in patients with septic shock. Those who do not have septic shock should begin antimicrobial therapy in the emergency department. Adequate drug levels should be maintained during the source control procedure, which may necessitate additional administration of antimicrobials. MILD TO MODERATE COMMUNITY-ACQUIRED INFECTION IN ADULTS Antibiotics used for empiric treatment of communityacquired intra-abdominal infection should be active against enteric gram-negative aerobic and facultative bacilli and enteric gram-positive streptococci. Coverage for obligate anaerobic bacilli should be provided for distal small bowel, appendiceal, and colon-derived infection and for more proximal gastrointestinal perforations in the presence of obstruction or paralytic ileus. In adults with mild-to-moderate community-acquired infection, the use of ticarcillin/clavulanate (Timentin), cefoxitin, ertapenem (Invanz), moxifloxacin (Avelox), or tigecycline (Tygacil) as a single-agent therapy, or a combination of metronidazole (Flagyl) with cefazolin, cefuroxime, ceftriaxone (Rocephin), cefotaxime (Claforan), levofloxacin (Levaquin), or ciprofloxacin (Cipro) is preferable to regimens with substantial antipseudomonal activity (Table 1). Ampicillin/sulbactam (Unasyn) is not because of high resistance rates in community-acquired E. coli. Cefotetan and clindamycin (Cleocin) are not because of increasing resistance among the Bacteroides fragilis group. Aminoglycosides are not for routine use in adults with communityacquired intra-abdominal infection because less toxic agents are available that are equally effective. HIGH-RISK COMMUNITY-ACQUIRED INFECTION IN ADULTS Patients with severe community-acquired intra-abdominal infection should be treated empirically with antimicrobial regimens that have broad-spectrum activity against gram-negative organisms, such as meropenem (Merrem), imipenem/cilastatin (Primaxin), doripenem (Doribax), or piperacillin/tazobactam (Zosyn) as single agents, or a combination of metronidazole with ciprofloxacin, levofloxacin, ceftazidime (Fortaz), or cefepime (Maxipime; Table 1). A combination of aztreonam (Azactam) and metronidazole is an alternative, but the addition of an agent effective against gram-positive cocci is. The routine use of aminoglycosides is not unless there is evidence that the patient harbors resistant organisms. The use of agents effective against methicillin-resistant S. aureus (MRSA) or yeast is not unless there is evidence of infection with these organisms. Quinolone-resistant strains of E. coli are common in some communities; therefore, quinolones should not be used unless hospital surveys indicate more than 90 percent susceptibility of E. coli to these agents. HEALTH CARE ASSOCIATED INFECTION IN ADULTS Empiric antibiotic therapy for health care associated intra-abdominal infection should be driven by local microbiologic results. To achieve empiric coverage of likely pathogens, multidrug regimens that include agents with expanded activity against gram-negative aerobic and facultative bacilli may be necessary (Table 2). Broadspectrum antimicrobial therapy should be tailored when culture and susceptibility reports become available. CHOLECYSTITIS AND CHOLANGITIS IN ADULTS Antimicrobial therapy should be initiated in patients with suspected infection and acute cholecystitis or cholangitis (Table 3). However, anaerobic therapy is not indicated unless a biliary-enteric anastomosis is present. 698 American Family Physician Volume 82, Number 6 September 15, 2010
3 Table 1. Pharmacologic Options for Initial Empiric Treatment of Extrabiliary Complicated Intra-abdominal Infection Community-acquired infection in children Community-acquired infection in adults Mild to moderate infection* Severe infection or high-risk patient Single agent Combination therapy Ertapenem (Invanz) Imipenem/cilastatin (Primaxin) Meropenem (Merrem) Piperacillin/tazobactam (Zosyn) Ticarcillin/clavulanate (Timentin) Cefepime (Maxipime) Cefotaxime (Claforan) Ceftazidime (Fortaz) Ceftriaxone (Rocephin) Plus metronidazole (Flagyl) or Gentamicin Tobramycin Plus clindamycin (Cleocin) or metronidazole With or without ampicillin Cefoxitin Ertapenem Moxifloxacin (Avelox) Ticarcillin/clavulanate Tigecycline (Tygacil) Cefazolin Cefotaxime Ceftriaxone Cefuroxime Ciprofloxacin (Cipro) Levofloxacin (Levaquin) Plus metronidazole Doripenem (Doribax) Imipenem/cilastatin Meropenem Piperacillin/tazobactam Cefepime Ceftazidime Ciprofloxacin Levofloxacin Plus metronidazole * Includes perforated appendicitis, abscessed appendix, and other infections of mild to moderate severity. Includes severe physiologic disturbance and older or immunocompromised patients. Because of increasing resistance of Escherichia coli to fluoroquinolones, local population susceptibility profiles and isolate susceptibility should be reviewed. Adapted with permission from Solomkin JS, Mazuski JE, Bradley JS, et al.; Surgical Infection Society; Infectious Diseases Society of America. Diagnosis and management of complicated intra-abdominal infection in adults and children: guidelines by the Surgical Infection Society and the Infectious Diseases Society of America. Clin Infect Dis. 2010;50(2):135. If the patient is undergoing cholecystectomy for acute cholecystitis, antimicrobial therapy should be discontinued within 24 hours unless there is evidence of infection outside the wall of the gallbladder. INFECTION IN CHILDREN Routine use of broad-spectrum antimicrobial agents is not indicated in children with fever and abdominal pain unless complicated appendicitis or other acute intraabdominal infection is suspected. Selection of antimicrobial regimens should be based on the origin of infection (community versus health care), severity of the illness, and safety profiles of the antimicrobial agents in children. Acceptable broad-spectrum antimicrobial regimens for children with complicated intra-abdominal infection include aminoglycosides, carbapenems (imipenem/ cilastatin, meropenem, or ertapenem), combined betalactam antibiotics or beta-lactamase inhibitors (piperacillin/tazobactam or ticarcillin/clavulanate), and advanced-generation cephalosporins (cefotaxime, ceftriaxone, ceftazidime, or cefepime) with metronidazole (Table 1). For children with severe reactions to beta-lactam antibiotics, a combination of ciprofloxacin and metronidazole or an aminoglycoside-based regimen is. Necrotizing enterocolitis in newborns is managed with fluid resuscitation, intravenous broad-spectrum antibiotics (possibly including antifungal agents), and bowel decompression. Broad-spectrum antibiotic therapies that may be useful in such cases include ampicillin, gentamicin, and metronidazole; ampicillin, cefotaxime, and metronidazole; or meropenem. Vancomycin may be used instead of ampicillin when MRSA or ampicillinresistant enterococcal infection is suspected. ANTIFUNGAL THERAPY Antifungal therapy for patients with severe communityacquired or health care associated infection is if Candida is isolated from intra-abdominal cultures. If Candida albicans is isolated, fluconazole September 15, 2010 Volume 82, Number 6 American Family Physician 699
4 Table 2. Recommendations for Empiric Antimicrobial Therapy for Health Care Associated Complicated Intra-abdominal Infection Organism Carbapenem* Piperacillin/ tazobactam (Zosyn) Cefepime (Maxipime) or ceftazidime (Fortaz), plus metronidazole (Flagyl) Aminoglycoside Vancomycin < 20% resistant Pseudomonas aeruginosa, ESBL-producing Enterobacteriaceae, Acinetobacter, or other multidrug-resistant gramnegative bacilli ESBL-producing Enterobacteriaceae P. aeruginosa > 20% resistant to ceftazidime Methicillin-resistant Staphylococcus aureus Recommended Recommended Recommended Recommended Recommended Recommended Recommended Recommended Recommended Recommended NOTE: Recommended indicates that the agent or drug class is for empiric use, before culture and susceptibility data are available, at institutions that encounter these isolates from other health care associated infections. These may be unit- or hospital-specific. ESBL = extended-spectrum beta-lactamase. * Drug class includes doripenem (Doribax), imipenem/cilastatin (Primaxin), and meropenem (Merrem). Adapted with permission from Solomkin JS, Mazuski JE, Bradley JS, et al.; Surgical Infection Society; Infectious Diseases Society of America. Diagnosis and management of complicated intra-abdominal infection in adults and children: guidelines by the Surgical Infection Society and the Infectious Diseases Society of America. Clin Infect Dis. 2010;50(2):136. (Diflucan) is an appropriate treatment option. For fluconazole-resistant Candida species, an echinocandin (e.g., caspofungin [Cancidas], micafungin [Mycamine], or anidulafungin [Eraxis]) is appropriate. In newborns, empiric antifungal therapy should be initiated if Candida is suspected. An echinocandin should be the initial treatment in critically ill patients. Amphotericin B is not as initial therapy because of its toxicity. ANTI-ENTEROCOCCAL THERAPY Antimicrobial therapy for enterococci should be given when enterococci are recovered from patients with health care associated infection. Empiric anti-enterococcal therapy is in patients with health care associated intra-abdominal infection, particularly those with postoperative infection; in patients who have previously taken cephalosporins or other antimicrobial agents selecting for Enterococcus species; in immunocompromised patients; and in those with valvular heart disease or prosthetic intravascular materials. Initial empiric anti-enterococcal therapy should be directed against Enterococcus Table 3. Pharmacologic Options for Initial Empiric Treatment of Biliary Infection in Adults Infection Community-acquired acute cholecystitis (mild to moderate) Community-acquired acute cholecystitis of severe physiologic disturbance, advanced age, or immunocompromised state Acute cholangitis after biliary-enteric anastomosis (any severity) Health care associated biliary infection (any severity) Cefazolin, ceftriaxone (Rocephin), or cefuroxime cefepime (Maxipime), ciprofloxacin (Cipro), doripenem (Doribax), imipenem/cilastatin (Primaxin), levofloxacin (Levaquin), meropenem (Merrem), or piperacillin/tazobactam (Zosyn) Plus metronidazole (Flagyl)* cefepime, ciprofloxacin, doripenem, imipenem/cilastatin, levofloxacin, meropenem, or piperacillin/tazobactam Plus metronidazole* cefepime, ciprofloxacin, doripenem, imipenem/cilastatin, levofloxacin, meropenem, or piperacillin/tazobactam Plus metronidazole and vancomycin* * Because of increasing resistance of Escherichia coli to fluoroquinolones, local population susceptibility profiles and isolate susceptibility should be reviewed. Adapted with permission from Solomkin JS, Mazuski JE, Bradley JS, et al.; Surgical Infection Society; Infectious Diseases Society of America. Diagnosis and management of complicated intra-abdominal infection in adults and children: guidelines by the Surgical Infection Society and the Infectious Diseases Society of America. Clin Infect Dis. 2010;50(2):137. September 15, 2010 Volume 82, Number 6 American Family Physician 703
5 faecalis. Antibiotics that can be used against this organism include ampicillin, piperacillin/tazobactam, and vancomycin. Empiric therapy for vancomycinresistant Enterococcus faecium is not unless the patient is at high risk of infection. ANTI-MRSA THERAPY Empiric antimicrobial coverage against MRSA should be provided to patients with health care associated intraabdominal infection who are colonized with the organism or who are at risk of infection because of previous treatment failure and antibiotic exposure. Vancomycin is for treatment of suspected or proven MRSA intra-abdominal infection. Diagnosis and Management of Patients with Suspected Acute Appendicitis A constellation of findings, including characteristic abdominal pain, localized abdominal tenderness, and laboratory evidence of acute inflammation, identifies most patients with suspected appendicitis. Helical CT of the abdomen and pelvis with intravenous but not oral or rectal contrast dye is in patients with suspected appendicitis. A pregnancy test should be performed in women of childbearing age before they undergo imaging; if they are in the first trimester of pregnancy, ultrasonography or magnetic resonance imaging should be used instead of CT. Imaging should be performed in all children in whom the diagnosis of appendicitis is uncertain, particularly in those younger than three years. CT is preferred, but ultrasonography is an alternative if exposure to ionizing radiation is a concern. For patients in whom imaging does not detect appendicitis, followup at 24 hours is to ensure resolution of signs and symptoms. Antimicrobial therapy with agents effective against facultative and aerobic gram-negative organisms and anaerobic organisms should be initiated in all patients diagnosed with appendicitis. In patients with suspected appendicitis who have equivocal imaging findings, antimicrobial therapy should be initiated in combination with pain medication and antipyretics, if indicated. Antimicrobial therapy should continue for at least three days in adults, until clinical symptoms and signs of infection resolve or a definitive diagnosis is made. Laparoscopy or open appendectomy should be performed as soon as possible in patients with acute, nonperforated appendicitis. Nonsurgical treatment can be considered in select patients with acute, nonperforated appendicitis if there is a marked improvement in the patient s condition before surgery. Patients with perforated appendicitis should undergo urgent intervention for source control. Percutaneous or operative drainage can be performed, if necessary, in patients with a well-circumscribed periappendiceal abscess. Appendectomy is generally deferred in these patients. September 15, 2010 Volume 82, Number 6 American Family Physician 709
IDSA GUIDELINES EXECUTIVE SUMMARY
 IDSA GUIDELINES Diagnosis and Management of Complicated Intra-abdominal Infection in Adults and Children: Guidelines by the Surgical Infection Society and the Infectious Diseases Society of America Joseph
IDSA GUIDELINES Diagnosis and Management of Complicated Intra-abdominal Infection in Adults and Children: Guidelines by the Surgical Infection Society and the Infectious Diseases Society of America Joseph
Appendix M: Guidelines for the Prophylaxis and Management of Intraabdominal, Biliary, and Appendiceal Infections
 Appendix M: Guidelines for the Prophylaxis and Management of Intraabdominal, Biliary, and Appendiceal Infections University of Wisconsin Hospital and Clinics Intraabdominal Infections Prophylaxis and Management
Appendix M: Guidelines for the Prophylaxis and Management of Intraabdominal, Biliary, and Appendiceal Infections University of Wisconsin Hospital and Clinics Intraabdominal Infections Prophylaxis and Management
Intra-abdominal abdominal Infections
 Intra-abdominal abdominal Infections Marnie Peterson, Pharm.D., BCPS Dept. of Pediatric Infectious Diseases Medical School University of Minnesota Intra-abdominal abdominal Infections Intra-abdominal abdominal
Intra-abdominal abdominal Infections Marnie Peterson, Pharm.D., BCPS Dept. of Pediatric Infectious Diseases Medical School University of Minnesota Intra-abdominal abdominal Infections Intra-abdominal abdominal
Urinary Tract Infections
 Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
ANTIBIOTICS IN SEPSIS
 ANTIBIOTICS IN SEPSIS Jennifer Curello, PharmD, BCPS Clinical Pharmacist, Infectious Diseases Antimicrobial Stewardship Program Ronald Reagan UCLA Medical Center October 27, 2014 The power of antibiotics
ANTIBIOTICS IN SEPSIS Jennifer Curello, PharmD, BCPS Clinical Pharmacist, Infectious Diseases Antimicrobial Stewardship Program Ronald Reagan UCLA Medical Center October 27, 2014 The power of antibiotics
APPENDIX B: UWHC SURGICAL ANTIMICROBIAL PROPHYLAXIS GUIDELINES
 APPENDIX B: UWHC SURGICAL ANTIMICROBIAL PROPHYLAXIS GUIDELINES Principles of prophylaxis 1) Use antimicrobials for surgical procedures where prophylactic antimicrobials have been found to be beneficial.
APPENDIX B: UWHC SURGICAL ANTIMICROBIAL PROPHYLAXIS GUIDELINES Principles of prophylaxis 1) Use antimicrobials for surgical procedures where prophylactic antimicrobials have been found to be beneficial.
Acute abdominal conditions Key Points
 7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
NewYork-Presbyterian Hospital Sites: Columbia University Medical Center Guideline: Medication Use Manual Page 1 of 12
 Page 1 of 12 TITLE: ANTIBIOTICS IN ADULT PATIENTS EMPIRIC USE GUIDELINES, COLUMBIA UNIVERSITY MEDICAL CENTER MEDICATION GUIDELINE PURPOSE: These are the 2011 guidelines for the empiric use of antibiotics
Page 1 of 12 TITLE: ANTIBIOTICS IN ADULT PATIENTS EMPIRIC USE GUIDELINES, COLUMBIA UNIVERSITY MEDICAL CENTER MEDICATION GUIDELINE PURPOSE: These are the 2011 guidelines for the empiric use of antibiotics
THERAPY OF ANAEROBIC INFECTIONS LUNG ABSCESS BRAIN ABSCESS
 THERAPY OF ANAEROBIC INFECTIONS Douglas Black, Pharm.D. Associate Professor School of Pharmacy University of Washington dblack@u.washington.edu LUNG ABSCESS A lung abscess is a localized pus cavity in
THERAPY OF ANAEROBIC INFECTIONS Douglas Black, Pharm.D. Associate Professor School of Pharmacy University of Washington dblack@u.washington.edu LUNG ABSCESS A lung abscess is a localized pus cavity in
TREATMENT OF PERITONEAL DIALYSIS (PD) RELATED PERITONITIS. General Principles
 WA HOME DIALYSIS PROGRAM (WAHDIP) GUIDELINES General Principles 1. PD related peritonitis is an EMERGENCY early empiric treatment followed by close review is essential 2. When culture results and sensitivities
WA HOME DIALYSIS PROGRAM (WAHDIP) GUIDELINES General Principles 1. PD related peritonitis is an EMERGENCY early empiric treatment followed by close review is essential 2. When culture results and sensitivities
SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS
 Page 1 of 8 TITLE: SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS GUIDELINE: Antibiotics are administered prior to surgical procedures to prevent surgical site infections. PURPOSE:
Page 1 of 8 TITLE: SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS GUIDELINE: Antibiotics are administered prior to surgical procedures to prevent surgical site infections. PURPOSE:
Oscar E. Guzman, PharmD, BCPS
 P Chapter 32 Antibiotic Streamlining Oscar E. Guzman, PharmD, BCPS Introduction Antibiotic streamlining is one of the most important methods pharmacists can use to encourage appropriate antibiotic use,
P Chapter 32 Antibiotic Streamlining Oscar E. Guzman, PharmD, BCPS Introduction Antibiotic streamlining is one of the most important methods pharmacists can use to encourage appropriate antibiotic use,
Appendicitis v.1.2. Inclusion Criteria Age > 3 months with confirmed appendicitis by the surgical team requiring acute or delayed appendectomy
 Appendicitis v.1.2 Executive Summary Citation Information Inclusion Criteria Age > 3 months with confirmed appendicitis by the surgical team requiring acute or delayed appendectomy Exclusion Criteria Age
Appendicitis v.1.2 Executive Summary Citation Information Inclusion Criteria Age > 3 months with confirmed appendicitis by the surgical team requiring acute or delayed appendectomy Exclusion Criteria Age
Drug Use Review. Edward Cox, M.D. Director Office of Antimicrobial Products
 Department of Health and Human Services Public Health Service Food and Drug Administration Center for Drug Evaluation and Research Drug Use Review Date: April 5, 2012 To: Through: Edward Cox, M.D. Director
Department of Health and Human Services Public Health Service Food and Drug Administration Center for Drug Evaluation and Research Drug Use Review Date: April 5, 2012 To: Through: Edward Cox, M.D. Director
Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings
 Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings Dr. Mary Vearncombe PIDAC-IPC February 2012 Objectives: To provide an overview of the RP/AP Annex
Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings Dr. Mary Vearncombe PIDAC-IPC February 2012 Objectives: To provide an overview of the RP/AP Annex
SURGICAL ANTIBIOTIC PROPHYLAXIS. Steve Johnson, PharmD, BCPS Prime Therapeutics, Inc
 SURGICAL ANTIBIOTIC PROPHYLAXIS Steve Johnson, PharmD, BCPS Prime Therapeutics, Inc OBJECTIVES Discuss antibiotic use as prophylaxis vs presumptive therapy vs treatment of infections. Discuss risk factors
SURGICAL ANTIBIOTIC PROPHYLAXIS Steve Johnson, PharmD, BCPS Prime Therapeutics, Inc OBJECTIVES Discuss antibiotic use as prophylaxis vs presumptive therapy vs treatment of infections. Discuss risk factors
Date: November 30, 2010
 Department of Health and Human Services Public Health Service Food and Drug Administration Center for Drug Evaluation and Research Date: November 30, 2010 To: Through: From: Subject: Drug Name(s): Application
Department of Health and Human Services Public Health Service Food and Drug Administration Center for Drug Evaluation and Research Date: November 30, 2010 To: Through: From: Subject: Drug Name(s): Application
Antibiotic resistance does it matter in paediatric clinical practice? Jette Bangsborg Department of Clinical Microbiology Herlev Hospital
 Antibiotic resistance does it matter in paediatric clinical practice? Jette Bangsborg Department of Clinical Microbiology Herlev Hospital Background The Department of Clinical Microbiology at Herlev Hospital
Antibiotic resistance does it matter in paediatric clinical practice? Jette Bangsborg Department of Clinical Microbiology Herlev Hospital Background The Department of Clinical Microbiology at Herlev Hospital
PRMCE ANTI-INFECTIVES SELECTION GUIDELINE FOR ADULTS
 PRMCE ANTI-INFECTIVES SELECTION GUIDELINE FOR ADULTS SKIN AND SOFT TISSUE INFECTIONS: Mild A. Cellulitis: MRSA uncommonly causes cellulitis in the absence of a wound abscess. Add empiric anti-mrsa therapy
PRMCE ANTI-INFECTIVES SELECTION GUIDELINE FOR ADULTS SKIN AND SOFT TISSUE INFECTIONS: Mild A. Cellulitis: MRSA uncommonly causes cellulitis in the absence of a wound abscess. Add empiric anti-mrsa therapy
ANTIMICROBIAL AGENT CLASSES AND SUBCLASSES
 ANTIMICROBIAL AGENT CLASSES AND SUBCLASSES FOR USE WITH CLSI DOCUMENTS M2 AND M7 Beta-lactams: penicillins e penicillin a penicillin beta-lactam/beta-lactamase inhibitor combinations aminopenicillin a
ANTIMICROBIAL AGENT CLASSES AND SUBCLASSES FOR USE WITH CLSI DOCUMENTS M2 AND M7 Beta-lactams: penicillins e penicillin a penicillin beta-lactam/beta-lactamase inhibitor combinations aminopenicillin a
growing problem By: Jena Cummins, Doctor of Pharmacy Candidate
 Clostridium difficile: A growing problem By: Jena Cummins, Doctor of Pharmacy Candidate Introduction The word difficile il is Latin for the word difficult. Clostridium difficile, affectionately known as
Clostridium difficile: A growing problem By: Jena Cummins, Doctor of Pharmacy Candidate Introduction The word difficile il is Latin for the word difficult. Clostridium difficile, affectionately known as
Appendicitis National Digestive Diseases Information Clearinghouse
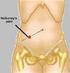 Appendicitis National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH The appendix is a small, tube-like structure
Appendicitis National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH The appendix is a small, tube-like structure
Treatment of Fever and Infection in Children with Transfusion Dependent Thalassaemia
 Treatment of Fever and Infection in Children with Transfusion Dependent Thalassaemia Document Information Version: 2 Date: June 2014 Authors (incl. job title): Professor David Rees, Sue Height (consultant
Treatment of Fever and Infection in Children with Transfusion Dependent Thalassaemia Document Information Version: 2 Date: June 2014 Authors (incl. job title): Professor David Rees, Sue Height (consultant
POAC CLINICAL GUIDELINE
 POAC CLINICAL GUIDELINE Acute Pylonephritis DIAGNOSIS COMPLICATED PYELONEPHRITIS EXCLUSION CRITERIA: Male Known or suspected renal impairment (egfr < 60) Abnormality of renal tract Known or suspected renal
POAC CLINICAL GUIDELINE Acute Pylonephritis DIAGNOSIS COMPLICATED PYELONEPHRITIS EXCLUSION CRITERIA: Male Known or suspected renal impairment (egfr < 60) Abnormality of renal tract Known or suspected renal
Streptococcus pneumoniae IgG AB (13 Serotypes), MAID... 7
 Volume 12 December 2011 Table of Contents Summary of Test Changes... 3 Test Changes... 6 Human Anti-Mouse AB (HAMA), ELISA... 6 Hepatitis E Antibody (IgG, IgM)... 6 Hepatitis E Antibody (IgG)... 6 Hepatitis
Volume 12 December 2011 Table of Contents Summary of Test Changes... 3 Test Changes... 6 Human Anti-Mouse AB (HAMA), ELISA... 6 Hepatitis E Antibody (IgG, IgM)... 6 Hepatitis E Antibody (IgG)... 6 Hepatitis
Received 4 July 2010; returned 10 August 2010; revised 27 September 2010; accepted 30 September 2010
 J Antimicrob Chemother 2011; 66: 205 209 doi:10.1093/jac/dkq404 Advance Access publication 8 November 2010 Sustained reduction in antimicrobial use and decrease in methicillin-resistant Staphylococcus
J Antimicrob Chemother 2011; 66: 205 209 doi:10.1093/jac/dkq404 Advance Access publication 8 November 2010 Sustained reduction in antimicrobial use and decrease in methicillin-resistant Staphylococcus
How To Treat Mrsa From A Dead Body
 HUSRES Annual Report 2012 Martti Vaara www.huslab.fi www.intra.hus.fi Martti Vaara 2013 1 The basis of this HUSRES 2012 report is the HUSLAB/Whonet database 2012, which contains susceptibility data on
HUSRES Annual Report 2012 Martti Vaara www.huslab.fi www.intra.hus.fi Martti Vaara 2013 1 The basis of this HUSRES 2012 report is the HUSLAB/Whonet database 2012, which contains susceptibility data on
Colocutaneous Fistula. Disclosures
 Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
HUSRES Annual Report 2010 Martti Vaara www.huslab.fi www.intra.hus.fi
 HUSRES Annual Report 2010 Martti Vaara www.huslab.fi www.intra.hus.fi Martti Vaara, 2/2011 1 The basis of this HUSRES 2010 report is the HUSLAB/Whonet database 2010, which contains susceptibility data
HUSRES Annual Report 2010 Martti Vaara www.huslab.fi www.intra.hus.fi Martti Vaara, 2/2011 1 The basis of this HUSRES 2010 report is the HUSLAB/Whonet database 2010, which contains susceptibility data
Why Do Some Antibiotics Fail?
 Why Do Some Antibiotics Fail? Patty W. Wright, M.D. April 2010 Objective To outline common reasons why antibiotic therapy is not successful and how this can be avoided. And to teach you a little bit about
Why Do Some Antibiotics Fail? Patty W. Wright, M.D. April 2010 Objective To outline common reasons why antibiotic therapy is not successful and how this can be avoided. And to teach you a little bit about
HUSRES Annual Report 2008 Martti Vaara. www.huslab.fi www.intra.hus.fi
 HUSRES Annual Report 2008 Martti Vaara www.huslab.fi www.intra.hus.fi The basis of this HUSRES 2008 report is the HUSLAB/Whonet database 2008, which contains susceptibility data on about 180.000 bacteria
HUSRES Annual Report 2008 Martti Vaara www.huslab.fi www.intra.hus.fi The basis of this HUSRES 2008 report is the HUSLAB/Whonet database 2008, which contains susceptibility data on about 180.000 bacteria
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis
 Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
Objectives. Fluids. Sterile IV Techniques. How many of you have sterile compounding technique procedures at your institution?
 Objectives Intravenous Medications in the Intensive Care Unit Paul Juang, Pharm.D., BCPS Assistant Professor of Pharmacy Practice St. Louis College of Pharmacy April 16, 2011 The speaker has no conflict
Objectives Intravenous Medications in the Intensive Care Unit Paul Juang, Pharm.D., BCPS Assistant Professor of Pharmacy Practice St. Louis College of Pharmacy April 16, 2011 The speaker has no conflict
Staphylococcus aureus Bloodstream Infection Treatment Guideline
 Staphylococcus aureus Bloodstream Infection Treatment Guideline Purpose: To provide a framework for the evaluation and management patients with Methicillin- Susceptible (MSSA) and Methicillin-Resistant
Staphylococcus aureus Bloodstream Infection Treatment Guideline Purpose: To provide a framework for the evaluation and management patients with Methicillin- Susceptible (MSSA) and Methicillin-Resistant
Therapeutic protocoles for adults concerning ESBL Enterobacteria infections in health care institutions
 Therapeutic protocoles for adults concerning ESBL Enterobacteria infections in health care institutions CYSTITIS The growing importance of resistance to quinolones, their environmental impact and reduced
Therapeutic protocoles for adults concerning ESBL Enterobacteria infections in health care institutions CYSTITIS The growing importance of resistance to quinolones, their environmental impact and reduced
Develop an understanding of the differential diagnosis of pseudomembranous colitis
 Update on Clostridium difficile Colitis Clostridium difficile infection has recently emerged in populations without any known risk factors. This presentation will focus on the historical background, diagnosis,
Update on Clostridium difficile Colitis Clostridium difficile infection has recently emerged in populations without any known risk factors. This presentation will focus on the historical background, diagnosis,
Outpatient Parenteral Antimicrobial Therapy
 Outpatient Parenteral Antimicrobial Therapy Jason E. Bowling, MD a,b, *, James S. Lewis II, PharmD c,d, Aaron D. Owens, MD a,e KEYWORDS Outpatient parenteral antimicrobial therapy Antibiotics Adverse events
Outpatient Parenteral Antimicrobial Therapy Jason E. Bowling, MD a,b, *, James S. Lewis II, PharmD c,d, Aaron D. Owens, MD a,e KEYWORDS Outpatient parenteral antimicrobial therapy Antibiotics Adverse events
The Five Intravenous Antibiotics You Need to Know
 The Five Intravenous Antibiotics You Need to Know Ray Geyer, DO Infectious Disease Specialist Medical Director, Benefis Infection Prevention Empirical Antimicrobial Prescribing: Save the Patient and Kill
The Five Intravenous Antibiotics You Need to Know Ray Geyer, DO Infectious Disease Specialist Medical Director, Benefis Infection Prevention Empirical Antimicrobial Prescribing: Save the Patient and Kill
Fungal Infection in Total Joint Arthroplasty. Dr.Wismer Dr.Al-Sahan
 Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
British Society for Antimicrobial Chemotherapy
 British Society for Antimicrobial Chemotherapy BSAC to actively support the EUCAST Disc Diffusion Method for Antimicrobial Susceptibility Testing in preference to the current BSAC Disc Diffusion Method
British Society for Antimicrobial Chemotherapy BSAC to actively support the EUCAST Disc Diffusion Method for Antimicrobial Susceptibility Testing in preference to the current BSAC Disc Diffusion Method
How To Treat Mrsa In Finnish
 HUSRES Annual Report 2013 Martti Vaara www.huslab.fi www.intra.hus.fi Martti Vaara 2014 1 The basis of this HUSRES 2013 report is the HUSLAB/Whonet database 2013, which contains susceptibility data on
HUSRES Annual Report 2013 Martti Vaara www.huslab.fi www.intra.hus.fi Martti Vaara 2014 1 The basis of this HUSRES 2013 report is the HUSLAB/Whonet database 2013, which contains susceptibility data on
GUIDELINES EXECUTIVE SUMMARY
 GUIDELINES Infectious Diseases Society of America and the Society for Healthcare Epidemiology of America Guidelines for Developing an Institutional Program to Enhance Antimicrobial Stewardship Timothy
GUIDELINES Infectious Diseases Society of America and the Society for Healthcare Epidemiology of America Guidelines for Developing an Institutional Program to Enhance Antimicrobial Stewardship Timothy
Beta-lactam antibiotics - Cephalosporins
 Beta-lactam antibiotics - Cephalosporins Targets - PBP s Activity - Cidal - growing organisms (like the penicillins) Principles of action - Affinity for PBP s Permeability ypropertiesp Stability to bacterial
Beta-lactam antibiotics - Cephalosporins Targets - PBP s Activity - Cidal - growing organisms (like the penicillins) Principles of action - Affinity for PBP s Permeability ypropertiesp Stability to bacterial
ANTIMICROBIAL USE GUIDELINES
 ANTIMICROBIAL USE GUIDELINES University of Wisconsin Hospital and Clinics Pharmacy and Therapeutics Committee Department of Pharmacy Drug Policy Program July 2011 to June 2012 Twenty-First Edition PREFACE
ANTIMICROBIAL USE GUIDELINES University of Wisconsin Hospital and Clinics Pharmacy and Therapeutics Committee Department of Pharmacy Drug Policy Program July 2011 to June 2012 Twenty-First Edition PREFACE
PACKAGE LEAFLET. CLINDAMYCIN capsules Clidamycin. One capsule of 75 mg contains 75 mg Clindamycin (as hydrochloride).
 PACKAGE LEAFLET CLINDAMYCIN capsules Clidamycin COMPOSITION One capsule of 75 mg contains 75 mg Clindamycin (as hydrochloride). One capsule of 150 mg contains 150 mg Clindamycin (as hydrochloride). PROPERTIES
PACKAGE LEAFLET CLINDAMYCIN capsules Clidamycin COMPOSITION One capsule of 75 mg contains 75 mg Clindamycin (as hydrochloride). One capsule of 150 mg contains 150 mg Clindamycin (as hydrochloride). PROPERTIES
ANTIBIOTIC RESISTANCE THREATS. in the United States, 2013
 ANTIBIOTIC RESISTANCE THREATS in the United States, 2013 TABLE OF CONTENTS Foreword... 5 Executive Summary.... 6 Section 1: The Threat of Antibiotic Resistance... 11 Introduction.... 11 National Summary
ANTIBIOTIC RESISTANCE THREATS in the United States, 2013 TABLE OF CONTENTS Foreword... 5 Executive Summary.... 6 Section 1: The Threat of Antibiotic Resistance... 11 Introduction.... 11 National Summary
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Clinical Practice Guidelines for Antimicrobial Prophylaxis in Surgery
 600 ASHP Therapeutic Guidelines Clinical Practice Guidelines for Antimicrobial Prophylaxis in Surgery These guidelines were developed jointly by the American Society of Health-System Pharmacists (ASHP),
600 ASHP Therapeutic Guidelines Clinical Practice Guidelines for Antimicrobial Prophylaxis in Surgery These guidelines were developed jointly by the American Society of Health-System Pharmacists (ASHP),
Adjustment of antibiotic treatment according to the results of blood cultures leads to decreased antibiotic use and costs
 Journal of Antimicrobial Chemotherapy (2006) 57, 326 330 doi:10.1093/jac/dki463 Advance Access publication 29 December 2005 Adjustment of antibiotic treatment according to the results of blood cultures
Journal of Antimicrobial Chemotherapy (2006) 57, 326 330 doi:10.1093/jac/dki463 Advance Access publication 29 December 2005 Adjustment of antibiotic treatment according to the results of blood cultures
Guidelines for Antimicrobial Stewardship in Hospitals in Ireland. A Strategy for the Control of Antimicrobial Resistance in Ireland
 A Strategy for the Control of Antimicrobial Resistance in Ireland Guidelines for Antimicrobial Stewardship in Hospitals in Ireland Hospital Antimicrobial Stewardship Working Group Guidelines for Antimicrobial
A Strategy for the Control of Antimicrobial Resistance in Ireland Guidelines for Antimicrobial Stewardship in Hospitals in Ireland Hospital Antimicrobial Stewardship Working Group Guidelines for Antimicrobial
A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections
 A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections By Gary R. Skankey, MD, FACP, Infectious Disease, Las Vegas, NV Sponsored
A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections By Gary R. Skankey, MD, FACP, Infectious Disease, Las Vegas, NV Sponsored
Nosocomial Antibiotic Resistance in Multiple Gram-Negative Species: Experience at One Hospital with Squeezing the Resistance Balloon at Multiple Sites
 INVITED ARTICLE HEALTHCARE EPIDEMIOLOGY Robert A. Weinstein, Section Editor Nosocomial Antibiotic Resistance in Multiple Gram-Negative Species: Experience at One Hospital with Squeezing the Resistance
INVITED ARTICLE HEALTHCARE EPIDEMIOLOGY Robert A. Weinstein, Section Editor Nosocomial Antibiotic Resistance in Multiple Gram-Negative Species: Experience at One Hospital with Squeezing the Resistance
State of Kuwait Ministry of Health Infection Control Directorate. Guidelines for Prevention of Surgical Site Infection (SSI)
 State of Kuwait Ministry of Health Infection Control Directorate Guidelines for Prevention of Surgical Site Infection (SSI) September 1999 Updated 2007 Surgical Wound: According to 1998 Kuwait National
State of Kuwait Ministry of Health Infection Control Directorate Guidelines for Prevention of Surgical Site Infection (SSI) September 1999 Updated 2007 Surgical Wound: According to 1998 Kuwait National
Controversies in Hospital Medicine: Antifungal Therapy. Empiric Therapy, Combination Therapy, and the Question of Central Venous Catheters
 Controversies in Hospital Medicine: Antifungal Therapy Empiric Therapy, Combination Therapy, and the Question of Central Venous Catheters Douglas Fish, Pharm.D. Professor of Pharmacy, University of Colorado
Controversies in Hospital Medicine: Antifungal Therapy Empiric Therapy, Combination Therapy, and the Question of Central Venous Catheters Douglas Fish, Pharm.D. Professor of Pharmacy, University of Colorado
Urinary Tract Infection and Asymptomatic Bacteriuria Guidance
 Urinary Tract Infection and Asymptomatic Bacteriuria Guidance Urinary tract infection (UTI) is the most common indication for antimicrobial use in hospitals and a significant proportion of this use is
Urinary Tract Infection and Asymptomatic Bacteriuria Guidance Urinary tract infection (UTI) is the most common indication for antimicrobial use in hospitals and a significant proportion of this use is
Pennsylvania Statewide Critical Care Transport Protocols
 Pennsylvania Statewide Critical Care Transport Protocols Pennsylvania Department of Health Bureau of Emergency Medical Services Effective April 2, 2015 (717) 787-8740 April 2, 2015 Dear EMS Provider: The
Pennsylvania Statewide Critical Care Transport Protocols Pennsylvania Department of Health Bureau of Emergency Medical Services Effective April 2, 2015 (717) 787-8740 April 2, 2015 Dear EMS Provider: The
Pneumonia is the second most common
 Treatment of Nursing Home Acquired Pneumonia KYLE MILLS, PharmD, BCPS, and A. CHRISTIE NELSON, PharmD University of Wyoming School of Pharmacy, Laramie, Wyoming BRADFORD T. WINSLOW, MD, FAAFP, Swedish
Treatment of Nursing Home Acquired Pneumonia KYLE MILLS, PharmD, BCPS, and A. CHRISTIE NELSON, PharmD University of Wyoming School of Pharmacy, Laramie, Wyoming BRADFORD T. WINSLOW, MD, FAAFP, Swedish
Title: Antibiotic Guideline for Acute Pelvic Inflammatory Disease
 Title: Antibiotic Guideline for Acute Pelvic Inflammatory Disease Version 3 Date ratified December 2007 Review date December 2009 Ratified by NUH Antimicrobial Guidelines Committee Gynaecology Directorate
Title: Antibiotic Guideline for Acute Pelvic Inflammatory Disease Version 3 Date ratified December 2007 Review date December 2009 Ratified by NUH Antimicrobial Guidelines Committee Gynaecology Directorate
James T. Dwyer DO, FACOI
 Antibiotics in the Surgical Patient James T. Dwyer DO, FACOI Objectives Define current prophylactic recommendations for the use of antibiotics in the surgical patient List current antibiotics available
Antibiotics in the Surgical Patient James T. Dwyer DO, FACOI Objectives Define current prophylactic recommendations for the use of antibiotics in the surgical patient List current antibiotics available
HUSRES Annual Report 2015
 HUSRES Annual Report 2015 1 This report is based on the HUSLAB/Whonet database 2015, which contains data on more than 190.000 microbes. EUCAST 2015 clinical breakpoints have mainly been used. The doses
HUSRES Annual Report 2015 1 This report is based on the HUSLAB/Whonet database 2015, which contains data on more than 190.000 microbes. EUCAST 2015 clinical breakpoints have mainly been used. The doses
Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations. J. Stuart Wolf, Jr., M.D.
 Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations J. Stuart Wolf, Jr., M.D. Department of Urology University of Michigan Ann Arbor, MI Official Recommendations for
Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations J. Stuart Wolf, Jr., M.D. Department of Urology University of Michigan Ann Arbor, MI Official Recommendations for
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Contents
 Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
Surgical Site Infection. Kings County Hospital Center Audrey C. Durrant 6/10/2005
 Surgical Site Infection Kings County Hospital Center Audrey C. Durrant 6/10/2005 Case Presentation HPI patient xx year old presented with approximately xx days periumbillical pain 10/10 on pain scale,
Surgical Site Infection Kings County Hospital Center Audrey C. Durrant 6/10/2005 Case Presentation HPI patient xx year old presented with approximately xx days periumbillical pain 10/10 on pain scale,
Blue Team Teaching Module: Periorbital/Orbital Infections
 Blue Team Teaching Module: Periorbital/Orbital Infections Format: 1. Case 2. Topic Summary 3. Questions 4. References Case: A 3-year-old boy presents with 2 days of increasing redness, swelling, and pain
Blue Team Teaching Module: Periorbital/Orbital Infections Format: 1. Case 2. Topic Summary 3. Questions 4. References Case: A 3-year-old boy presents with 2 days of increasing redness, swelling, and pain
10. Treatment of peritoneal dialysis associated fungal peritonitis
 10. Treatment of peritoneal dialysis associated fungal peritonitis Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) The use of
10. Treatment of peritoneal dialysis associated fungal peritonitis Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) The use of
Dosing information in renal impairment
 No. Drug name Usual dose Adjustment for Renal failure estimated CrCl (ml/min) Aminoglycoside antibiotics 1 Amikacin 2 Gentamicin 7.5 mg /kg q 12 hr > 50-90 7.5 mg/kg q 12 hr 10-50 7.5 mg/kg q 24 hr < 10
No. Drug name Usual dose Adjustment for Renal failure estimated CrCl (ml/min) Aminoglycoside antibiotics 1 Amikacin 2 Gentamicin 7.5 mg /kg q 12 hr > 50-90 7.5 mg/kg q 12 hr 10-50 7.5 mg/kg q 24 hr < 10
DRG 416 Septicemia. ICD-9-CM Coding Guidelines
 oding uidelines Septicemia ICD-9-CM Coding Guidelines The below listed septicemia guidelines are not inclusive. The coder should refer to the applicable Coding Clinic guidelines for additional information.
oding uidelines Septicemia ICD-9-CM Coding Guidelines The below listed septicemia guidelines are not inclusive. The coder should refer to the applicable Coding Clinic guidelines for additional information.
Disease Site Breast. Less than 120 kg: Cefazolin 2 grams IV Greater than or equal to 120 kg: Cefazolin 3 grams IV. Head & Neck
 Patients scheduled for surgery should have the following antibiotics administered prior to their procedure Vancomycin and Ciprofloxacin are to be initiated 60 to 120 minutes prior to incision and all other
Patients scheduled for surgery should have the following antibiotics administered prior to their procedure Vancomycin and Ciprofloxacin are to be initiated 60 to 120 minutes prior to incision and all other
Medical Microbiology Microscopic slides and media
 Medical Microbiology Microscopic slides and media Head of Microbiology Department and Laboratory Medical Immunology : Janina Grzegorczyk MD, PhD, professor Implementators: Małgorzata Brauncajs MD Zbigniew
Medical Microbiology Microscopic slides and media Head of Microbiology Department and Laboratory Medical Immunology : Janina Grzegorczyk MD, PhD, professor Implementators: Małgorzata Brauncajs MD Zbigniew
Version 11.1 May 2012
 BSAC Methods for Antimicrobial Susceptibility Testing Version 11.1 May 2012 All enquiries to: Jenny Andrews at: + 44 (0) 121 507 5693 Email: jenny.andrews1@nhs.net Contents Page Working Party members 5
BSAC Methods for Antimicrobial Susceptibility Testing Version 11.1 May 2012 All enquiries to: Jenny Andrews at: + 44 (0) 121 507 5693 Email: jenny.andrews1@nhs.net Contents Page Working Party members 5
Hemodialysis catheter infection
 Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection
 Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection Emi Minejima, PharmD Assistant Professor of Clinical Pharmacy USC School of Pharmacy minejima@usc.edu
Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection Emi Minejima, PharmD Assistant Professor of Clinical Pharmacy USC School of Pharmacy minejima@usc.edu
Antimicrobial Activity and Spectrum of PPI-0903M (T-91825), a Novel Cephalosporin, Tested against a Worldwide Collection of Clinical Strains
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Aug. 2005, p. 3501 3512 Vol. 49, No. 8 0066-4804/05/$08.00 0 doi:10.1128/aac.49.8.3501 3512.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved.
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Aug. 2005, p. 3501 3512 Vol. 49, No. 8 0066-4804/05/$08.00 0 doi:10.1128/aac.49.8.3501 3512.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved.
Introduction to Antimicrobial Therapy
 Introduction to Antimicrobial Therapy Christine Kubin, Pharm.D., BCPS Clinical Pharmacist, Infectious Diseases Case #1 L.G. is a 78 yo woman admitted for cardiac cath. 3-vessel disease was identified and
Introduction to Antimicrobial Therapy Christine Kubin, Pharm.D., BCPS Clinical Pharmacist, Infectious Diseases Case #1 L.G. is a 78 yo woman admitted for cardiac cath. 3-vessel disease was identified and
C-Difficile Infection Control and Prevention Strategies
 C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer Adrienne.Mims@AlliantQuality.org 1/18/2016 1 Disclosure This educational activity does not have commercial
C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer Adrienne.Mims@AlliantQuality.org 1/18/2016 1 Disclosure This educational activity does not have commercial
Bile Leaks After Laparoscopic Cholecystectomy. Kings County Hospital Center Eliana A. Soto, MD
 Bile Leaks After Laparoscopic Cholecystectomy Kings County Hospital Center Eliana A. Soto, MD Biliary Injuries during Cholecystectomy In the 1990s, high rate of biliary injury was due in part to learning
Bile Leaks After Laparoscopic Cholecystectomy Kings County Hospital Center Eliana A. Soto, MD Biliary Injuries during Cholecystectomy In the 1990s, high rate of biliary injury was due in part to learning
IDSA GUIDELINES EXECUTIVE SUMMARY
 IDSA GUIDELINES Clinical Practice Guidelines for the Diagnosis and Management of Intravascular Catheter-Related Infection: 2009 Update by the Infectious Diseases Society of America Leonard A. Mermel, 1
IDSA GUIDELINES Clinical Practice Guidelines for the Diagnosis and Management of Intravascular Catheter-Related Infection: 2009 Update by the Infectious Diseases Society of America Leonard A. Mermel, 1
Tuberculosis Exposure Control Plan for Low Risk Dental Offices
 Tuberculosis Exposure Control Plan for Low Risk Dental Offices A. BACKGROUND According to the CDC, approximately one-third of the world s population, almost two billion people, are infected with tuberculosis.
Tuberculosis Exposure Control Plan for Low Risk Dental Offices A. BACKGROUND According to the CDC, approximately one-third of the world s population, almost two billion people, are infected with tuberculosis.
Lab ID Events MRSA Bloodstream Infection and C. difficile
 Lab ID Events MRSA Bloodstream Infection and C. difficile MDRO and CDI Module Methicillin-resistant Staphylococcus (MRSA), Vancomycinresistant Enterococcus(VRE), certain gram negative bacilli, Clostridium
Lab ID Events MRSA Bloodstream Infection and C. difficile MDRO and CDI Module Methicillin-resistant Staphylococcus (MRSA), Vancomycinresistant Enterococcus(VRE), certain gram negative bacilli, Clostridium
Antibacterial Drug Shortages From 2001 to 2013: Implications for Clinical Practice
 MAJOR ARTICLE EMBARGOED UNTIL 12:01 A.M. EDT ON THURSDAY, APRIL 23, 2015 Antibacterial Drug Shortages From 2001 to 2013: Implications for Clinical Practice Farha Quadri, 1 Maryann Mazer-Amirshahi, 2 Erin
MAJOR ARTICLE EMBARGOED UNTIL 12:01 A.M. EDT ON THURSDAY, APRIL 23, 2015 Antibacterial Drug Shortages From 2001 to 2013: Implications for Clinical Practice Farha Quadri, 1 Maryann Mazer-Amirshahi, 2 Erin
Helsingin ja Uudenmaan alueen herkkyystilastoja 2003. www.infektiofoorumi.fi www.huslab.fi www.intra.hus.fi
 Helsingin ja Uudenmaan alueen herkkyystilastoja 2003 www.infektiofoorumi.fi www.huslab.fi www.intra.hus.fi 12 10 Staph. aureus Pus and blood isolates % R+I, at HUCH (7 hospitals) [one isolate/patient (the
Helsingin ja Uudenmaan alueen herkkyystilastoja 2003 www.infektiofoorumi.fi www.huslab.fi www.intra.hus.fi 12 10 Staph. aureus Pus and blood isolates % R+I, at HUCH (7 hospitals) [one isolate/patient (the
Percutaneous Abscess Drainage
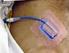 Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
Antimicrobial Therapy. Otolaryngology Head and Neck Surgery
 Pocket Guide to Antimicrobial Therapy in Otolaryngology Head and Neck Surgery 13th Edition DAVID N.F. FAIRBANKS, M.D. The American Academy of Otolaryngology Head and Neck Surgery Foundation EMPIRIC DRUG
Pocket Guide to Antimicrobial Therapy in Otolaryngology Head and Neck Surgery 13th Edition DAVID N.F. FAIRBANKS, M.D. The American Academy of Otolaryngology Head and Neck Surgery Foundation EMPIRIC DRUG
ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy. Case Series
 ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy Case Series Summary of Cases: USER EXPERIENCE The ABThera OA NPT system was found by surgeons to be a convenient and effective
ABThera Open Abdomen Negative Pressure Therapy for Active Abdominal Therapy Case Series Summary of Cases: USER EXPERIENCE The ABThera OA NPT system was found by surgeons to be a convenient and effective
Achaogen, Inc. (AKAO)
 Americas/United States Equity Research Biotechnology Achaogen, Inc. (AKAO) SMALL & MID CAP RESEARCH Focus on Killer Bacteria; Aiming for Superiority in Phase III We are initiating coverage of Achaogen
Americas/United States Equity Research Biotechnology Achaogen, Inc. (AKAO) SMALL & MID CAP RESEARCH Focus on Killer Bacteria; Aiming for Superiority in Phase III We are initiating coverage of Achaogen
URINE CULTURES GENERAL PROCEDURE
 University of Nebraska Medical Center Division of Laboratory Science Clinical Laboratory Science Program CLS 418/CLS 419 URINE CULTURES GENERAL PROCEDURE I. Principle Urine cultures are performed to detect
University of Nebraska Medical Center Division of Laboratory Science Clinical Laboratory Science Program CLS 418/CLS 419 URINE CULTURES GENERAL PROCEDURE I. Principle Urine cultures are performed to detect
Version 12 May 2013. BSAC Methods for Antimicrobial Susceptibility Testing. All enquiries to: Mandy Wootton. Email: Mandy.Wootton@wales.nhs.
 BSAC Methods for Antimicrobial Susceptibility Testing Version 12 May 2013 All enquiries to: Mandy Wootton Email: Mandy.Wootton@wales.nhs.uk Telephone: +44 (0) 2920 746581 Contents Page Working Party members
BSAC Methods for Antimicrobial Susceptibility Testing Version 12 May 2013 All enquiries to: Mandy Wootton Email: Mandy.Wootton@wales.nhs.uk Telephone: +44 (0) 2920 746581 Contents Page Working Party members
Helsingin ja Uudenmaan alueen herkkyystilastoja 2004. www.huslab.fi www.intra.hus.fi
 Helsingin ja Uudenmaan alueen herkkyystilastoja 2004 www.huslab.fi www.intra.hus.fi Staph. aureus 2004 (%R+I) Pus and blood isolates at six hospitals (M,T,L,K,N,Ma) in Helsinki University Central Hospital,
Helsingin ja Uudenmaan alueen herkkyystilastoja 2004 www.huslab.fi www.intra.hus.fi Staph. aureus 2004 (%R+I) Pus and blood isolates at six hospitals (M,T,L,K,N,Ma) in Helsinki University Central Hospital,
Management of Hospital-Acquired Pneumonia at a Tertiary-Care Teaching Hospital
 ARTICLE Management of Hospital-Acquired Pneumonia at a Tertiary-Care Teaching Hospital Ada Seto, Sandra Walker, and Anita Rachlis ABSTRACT Background: The rising resistance of pathogens commonly implicated
ARTICLE Management of Hospital-Acquired Pneumonia at a Tertiary-Care Teaching Hospital Ada Seto, Sandra Walker, and Anita Rachlis ABSTRACT Background: The rising resistance of pathogens commonly implicated
Liofilchem - Antibiotic Disk Interpretative Criteria and Quality Control - F14013 - Rev.7 / 20.02.2013
 Liofilchem Antibiotic Disk Interpretative Criteria and Quality Control F0 Rev.7 /.02. Amikacin AK Amoxicillin + Clavulanic acid AUG (+) ATCC 352 Coagulasenegative staphylococci Amoxicillin + Clavulanic
Liofilchem Antibiotic Disk Interpretative Criteria and Quality Control F0 Rev.7 /.02. Amikacin AK Amoxicillin + Clavulanic acid AUG (+) ATCC 352 Coagulasenegative staphylococci Amoxicillin + Clavulanic
Antibiotic Lock Therapy Guideline
 Antibiotic Lock Therapy Guideline I. PURPOSE Central venous catheters are an integral part in medical management for patients requiring long-term total parenteral nutrition, chemotherapy, or hemodialysis,
Antibiotic Lock Therapy Guideline I. PURPOSE Central venous catheters are an integral part in medical management for patients requiring long-term total parenteral nutrition, chemotherapy, or hemodialysis,
National Quality Forum (NQF) Endorsed Set of 34 Safe Practices*
 NQF Endorsed Set of Safe Practices (released 2009) 1. Leadership Structures and Systems Leadership structures and systems must be established to ensure that there is organization-wide awareness of patient
NQF Endorsed Set of Safe Practices (released 2009) 1. Leadership Structures and Systems Leadership structures and systems must be established to ensure that there is organization-wide awareness of patient
World Health Organization Department of Communicable Disease Surveillance and Response
 WHO/CDS/CSR/DRS/2001.7 Infection control programmes to contain antimicrobial resistance Lindsay E. Nicolle World Health Organization Department of Communicable Disease Surveillance and Response This document
WHO/CDS/CSR/DRS/2001.7 Infection control programmes to contain antimicrobial resistance Lindsay E. Nicolle World Health Organization Department of Communicable Disease Surveillance and Response This document
IDSA GUIDELINES EXECUTIVE SUMMARY
 IDSA GUIDELINES Clinical Practice Guideline for the Use of Antimicrobial Agents in Neutropenic Patients with Cancer: 2010 Update by the Infectious Diseases Society of America Alison G. Freifeld, 1 Eric
IDSA GUIDELINES Clinical Practice Guideline for the Use of Antimicrobial Agents in Neutropenic Patients with Cancer: 2010 Update by the Infectious Diseases Society of America Alison G. Freifeld, 1 Eric
Pathway for the Management of Acute Gallstone Diseases
 Pathway for the Management of Acute Gallstone Diseases What s in this document? Pathways to encourage safer, faster and more cost effective management of acute gallstone (GS) disease by stratification
Pathway for the Management of Acute Gallstone Diseases What s in this document? Pathways to encourage safer, faster and more cost effective management of acute gallstone (GS) disease by stratification
The 14th EURL-AR Proficiency Test - enterococci, staphylococci and E. coli 2013. Lina Cavaco Susanne Karlsmose Rene S. Hendriksen Frank M.
 The 14th EURL-AR Proficiency Test - enterococci, staphylococci and E. coli 2013 Lina Cavaco Susanne Karlsmose Rene S. Hendriksen Frank M. Aarestrup The 14TH EURL-AR Proficiency Test Enterococci, Staphylococci
The 14th EURL-AR Proficiency Test - enterococci, staphylococci and E. coli 2013 Lina Cavaco Susanne Karlsmose Rene S. Hendriksen Frank M. Aarestrup The 14TH EURL-AR Proficiency Test Enterococci, Staphylococci
Urinary tract infections caused by extended spectrum β-lactamase (ESBL) producing Escherichia coli and Klebsiella pneumoniae
 African Journal of Biotechnology Vol. 10(73), pp. 16661-16666, 21 November, 2011 Available online at http://www.academicjournals.org/ajb DOI: 10.5897/AJB11.2449 ISSN 1684 5315 2011 Academic Journals Full
African Journal of Biotechnology Vol. 10(73), pp. 16661-16666, 21 November, 2011 Available online at http://www.academicjournals.org/ajb DOI: 10.5897/AJB11.2449 ISSN 1684 5315 2011 Academic Journals Full
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #65 (NQF 0069): Appropriate Treatment for Children with Upper Respiratory Infection (URI) National Quality Strategy Domain: Efficiency and Cost Reduction 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES:
Measure #65 (NQF 0069): Appropriate Treatment for Children with Upper Respiratory Infection (URI) National Quality Strategy Domain: Efficiency and Cost Reduction 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES:
CANDIDA INFECTIONS - TREATMENT GUIDELINES IN ADULT
 Page 1 of 6 TITLE: PATIENTS CANDIDA INFECTIONS - TREATMENT GUIDELINES IN ADULT GUIDELINES: These are the 2011 Guidelines for the Treatment of Candida species infections in adult patients. These recommendations
Page 1 of 6 TITLE: PATIENTS CANDIDA INFECTIONS - TREATMENT GUIDELINES IN ADULT GUIDELINES: These are the 2011 Guidelines for the Treatment of Candida species infections in adult patients. These recommendations
