Received 4 July 2010; returned 10 August 2010; revised 27 September 2010; accepted 30 September 2010
|
|
|
- Duane Patterson
- 8 years ago
- Views:
Transcription
1 J Antimicrob Chemother 2011; 66: doi: /jac/dkq404 Advance Access publication 8 November 2010 Sustained reduction in antimicrobial use and decrease in methicillin-resistant Staphylococcus aureus and Clostridium difficile infections following implementation of an electronic medical record at a tertiary-care teaching hospital Paul P. Cook 1 *, Shemra Rizzo 2, Michael Gooch 3, Michelle Jordan 3, Xiangming Fang 4 and Suzanne Hudson 4 1 Division of Infectious Diseases, Department of Medicine, Brody School of Medicine at East Carolina University, Greenville, NC, USA; 2 Department of Biostatistics, University of California at Los Angeles, Los Angeles, CA, USA; 3 Pitt County Memorial Hospital, Greenville, NC, USA; 4 Department of Biostatistics, East Carolina University, Greenville, NC, USA *Corresponding author. Tel: ; Fax: ; cookp@ecu.edu Received 4 July 2010; returned 10 August 2010; revised 27 September 2010; accepted 30 September 2010 Objectives: We evaluated the effect of implementation of an electronic medical record (EMR) on the use of antimicrobial agents and on the rates of infections with Clostridium difficile and methicillin-resistant Staphylococcus aureus (MRSA). Methods: This was a retrospective, observational study conducted between 1 January 2005 and 31 December Antimicrobial drug use, rates of nosocomial C. difficile infection (CDI) and MRSA infection, the number of medical charts reviewed and number of antimicrobial recommendations made and accepted were compared before and after implementing the EMR utilizing interrupted time-series analysis. Results: Compared with the 10 quarters prior to implementing the EMR, there was a 36.6% increase in the number of charts reviewed (P, ), a 98.1% increase in the number of antimicrobial recommendations made (P, ) and a 124% increase in the number of recommendations accepted (P, ). There was a 28.8% decrease in the use of 41 commonly used antibacterial agents (P, ). Nosocomial CDI decreased by 18.7% (P¼0.07) and nosocomial MRSA infections decreased by 45.2% (P, ) following implementation of the EMR. Conclusions: Adoption of an EMR facilitated a significant increase in chart reviews and antimicrobial recommendations, which resulted in a sustained decrease in antimicrobial use. There were decreased nosocomial infections with MRSA and a trend towards decreasing CDIs following implementation of the EMR. Keywords: antibiotic management, antibiotic resistance, nosocomial infections Introduction The use and overuse of antimicrobial agents has led to the development of antibiotic resistance in both the community and the hospital setting. Recommendations from various experts and organizations have promoted the prudent use of antimicrobial agents as a means of controlling resistance. 1 3 Recent guidelines from the Infectious Diseases Society of America (IDSA) promote the concept of an electronic medical record (EMR) with computerized physician order entry (CPOE) as a means of facilitating the goals of an antimicrobial stewardship programme (ASP). 3 Our hospital adopted an EMR with CPOE in July We examined the hospital use of antimicrobial agents before and after implementation of the EMR at our institution. We also determined the incidence of nosocomial infections with Clostridium difficile and methicillin-resistant Staphylococcus aureus (MRSA) during the same time period, as these infections are associated with antimicrobial use. 2,4 8 Methods Pitt County Memorial Hospital is an 861-bed, tertiary-care, teaching hospital affiliated with The Brody School of Medicine at East Carolina University. The hospital has a busy trauma unit, cardiothoracic surgery service, orthopaedic service, paediatric unit, oncology service and dialysis unit. Renal transplantations are performed at the hospital, but there are no bone marrow transplantation or burn units. Ethics approval was not required for this study because we used only routine data collected on # The Author Published by Oxford University Press on behalf of the British Society for Antimicrobial Chemotherapy. All rights reserved. For Permissions, please journals.permissions@oxfordjournals.org 205
2 Cook et al. hospital wards. This was an observational study from 1 January 2005 until 31 December Our ASP was established in 2001 and has been described previously. 9 Antimicrobial drug use was measured in defined daily doses per 1000 patient days (DDDs/1000 PDs) using the standards of the WHO ( Beginning in July 2007, Pitt County Memorial Hospital implemented an EMR (EPIC, Madison, WI, USA) with CPOE. Recommended dosing was built into the order screens for antibiotics following national guidelines. Reports for the ASP pharmacists were built into the EMR and were reviewed daily. The programme operated 5 days a week. The report listed all patients receiving antimicrobial agents continuously for at least 48 h. Information in the report included patient location, patient weight, allergies and ordering physician. The EMR allowed the ASP pharmacists to open an intervention on a patient and allowed documentation within the report on what recommendation was made. If a patient had cultures that had not been finalized, the intervention could be left open and a report run later listing the open interventions for follow-up. If a patient s initial antibiotic regimen was deemed appropriate, but follow-up was desired to ensure the patient received the recommended time course of therapy, the intervention could also be left open for that purpose. Information entered into the interventional database stayed with the patient s intervention record and could be seen if that patient came up for review at a later date. Reports were also available to calculate antibiotic usage overall, by unit and by service, allowing targeted education efforts. The ASP pharmacists entered their recommendations as a progress note and then entered an order for antimicrobial monitoring. This triggered a pop-up screen whenever a physician, nurse practitioner or physician s assistant entered that particular patient s record, directing them to the recommendation in the progress note. The physician had to acknowledge seeing the record at the time. It was possible for the pharmacists to determine whether the pop-up had been triggered and who had seen it. The antimicrobial management programme reviewed 49 antimicrobial agents used at the hospital (Table 1). Broad-spectrum antibiotics were divided into seven classes. Extended-spectrum penicillins included ampicillin, amoxicillin, ampicillin/sulbactam, piperacillin and piperacillin/ tazobactam. Cephalosporins included cefazolin, cefadroxil, cefalexin, cefuroxime, cefotetan, ceftriaxone, ceftazidime, cefotaxime and cefepime. The quinolone class included moxifloxacin and ciprofloxacin. Table 1. List of antibacterial and antifungal agents that were monitored as part of the ASP Antibacterial agents amikacin, amoxicillin, amoxicillin/clavulanate, ampicillin, ampicillin/sulbactam, azithromycin, aztreonam, cefaclor, cefadroxil, cefazolin, cefepime, cefotaxime, cefoxitin, cefotetan, ceftazidime, ceftriaxone, cefuroxime, cefalexin, ciprofloxacin, clarithromycin, clindamycin, daptomycin, doripenem, doxycycline, ertapenem, erythromycin, gentamicin, imipenem, linezolid, meropenem, metronidazole, moxifloxacin, nafcillin, piperacillin, piperacillin/tazobactam, sulfamethoxazole/trimethoprim, telithromycin, tetracycline, tigecycline, tobramycin, vancomycin Antifungal agents amphotericin B, anidulafungin, caspofungin, fluconazole, itraconazole, micafungin, posaconazole, voriconazole Imipenem was replaced by meropenem in the hospital formulary in 2006; meropenem was replaced by doripenem in Carbapenems included ertapenem, doripenem, imipenem and meropenem. Macrolides included azithromycin, erythromycin, clarithromycin and telithromycin. Aminoglycosides included amikacin, gentamicin and tobramycin. Tetracyclines/glycylcyclines included tetracycline, doxycycline and tigecycline. Clindamycin, aztreonam, vancomycin, nafcillin, linezolid, daptomycin, metronidazole and trimethoprim/sulfamethoxazole were examined separately. Stool samples were tested for the presence of C. difficile toxin using a standard cell culture cytotoxicity assay with MRC-5 lung fibroblast cells and antitoxin from TechLab (Blacksburg, VA, USA). Clinical cultures for S. aureus included blood, CSF, wounds, respiratory specimens, pleural fluid, tissue specimens and urine. Surveillance cultures were not included. In vitro bacterial susceptibilities were determined using the MicroScan system (Dade Behring). The nosocomial C. difficile and MRSA datasets were created by querying MedMined (CareFusion, Birmingham, AL, USA). In an effort to limit the analysis to nosocomial infections, only cultures or stool specimens from patients who were in hospital more than 3 days following admission were included for evaluation. Duplicate positive test results from the same patient within a 3 month period were counted only once. Rates of nosocomial C. difficile and MRSA infections were expressed as cases per patient hospital days. In evaluating the effect of implementation of EMR on the use of antibiotic agents and on the rates of infections with C. difficile and MRSA, we adopted interrupted time-series models to control for the serial correlation among the data. It turned out that an interrupted AR(1) model (where AR stands for autoregressive) was able to sufficiently account for the autocorrelation and thus was selected for our final analysis. The model can be formulated as follows: Y t O/ Y t 1 = b 0 + b 1 Intervention + e t where Y t is the response value at time t, Ø is the lag 1 coefficient of the AR(1) model, e t is the measurement error and Intervention is an indicator variable whose value is 0 for timepoints before EMR was implemented and 1 for timepoints after EMR was implemented. Due to the fact that our time-series data are fairly stationary both before and after the introduction of EMR, we did not include a linear trend in the model above. Thus b 0 is (12Ø) times the mean response before EMR was implemented and b 1 is the change in (12Ø) times the mean response due to the implementation of EMR. As a result, testing on the effect of EMR is equivalent to testing on the significance of b 1. This interrupted AR(1) model was fitted using the ARIMA procedure in SAS 9.2. This statistical method was used to compare antibiotic use, number of charts reviewed, number of recommendations made, number of recommendations accepted, demographic data and rates of C. difficile infection (CDI) and MRSA infection with P,0.05 as the level of significance. Linear regression was used to assess hand washing compliance rates over the 5 year period of the study. Spearman s rank correlation coefficient was used to correlate antimicrobial use with rates of CDI and MRSA infection. Results Effect of EMR on chart reviews There were statistically significant increases in the number of charts reviewed, number of antimicrobial recommendations made and number of accepted recommendations following implementation of the EMR (Table 2). Compared with the 10 quarters prior to implementing the EMR, there was a 36.6% increase in the number of charts reviewed (P, ), a 98.1% increase in the number of antimicrobial recommendations made (P,0.0001) and a 124% increase in the number of recommendations accepted (P, ). Recommendations for antimicrobial changes were made on 23.6% of the charts 206
3 Effect of EMR on antimicrobial use, MRSA infections and CDIs JAC reviewed prior to implementation of the EMR; this number increased to 34.3% following implementation of the EMR. The percentage of recommendations that were accepted increased from 81.2% prior to implementation of the EMR to 91.7% following implementation of the EMR. The time to implementation of ASP recommendations decreased from 23 h prior to the EMR to 8 h after the EMR was implemented (P¼0.0001). Antibacterial drug use For the 41 antibacterial drugs monitored, there was a 28.8% decrease in use following implementation of the EMR (Figure 1 and Table 3). There were significant decreases in use of Table 2. Mean number of charts reviewed, number of recommendations made and number of recommendations accepted per quarter before and after implementation of the EMR No. of charts reviewed/ quarter No. of charts recommendations/ quarter No. of charts recommendations accepted/quarter #/ PDs Pre-EMR Post-EMR Percentage change MRSA infections/ PDs CDIs/ PDs DDDs/1000 PDs st nd rd th st nd rd th st nd rd th st nd rd th st nd rd th Figure 1. Antibacterial drug use, nosocomial MRSA infection rate and nosocomial CDI rate plotted over the study time period. The time units are quarters. The EMR with CPOE was implemented at the beginning of the third quarter of Antibacterial drug use is measured in DDDs/ 1000 PDs. The rates of MRSA infection and CDI are expressed as the number of cases per patient days (#/ PDs). 0.0 P value , , , P values are based on interrupted time-series analysis. DDDs/1000 PDs Table 3. Antibacterial agent use before and after implementing the EMR Antimicrobial agent(s) extended-spectrum penicillins, cephalosporins, clindamycin, quinolones, macrolides, metronidazole, vancomycin and aminoglycosides. The use of cefazolin, the drug of choice for surgical prophylaxis, decreased by 53% (81 DDDs/1000 PDs to 38 DDDs/ 1000 PDs) following implementation of the EMR (P,0.0001). There were no significant changes in use of nafcillin, daptomycin, tetracyclines/glycylcyclines, trimethoprim/sulfamethoxazole or linezolid. Carbapenem use increased by 51.3% (P, ). Antifungal drug use Pre-EMR, DDDs/ 1000 PDs Post-EMR, DDDs/ 1000 PDs Percentage change P value Extended-spectrum penicillins Cephalosporins , Quinolones , Clindamycin Tetracyclines/ glycylcyclines Carbapenems Macrolides Daptomycin Linezolid Nafcillin Vancomycin , Metronidazole , Trimethoprim/ sulfamethoxazole Aminoglycosides , All antibacterial agents , Usage is expressed in DDDs/1000 PDs. Values are means. Pre-EMR and post-emr represent drug use for the 10 quarters prior to and the 10 quarters following implementation of the EMR, respectively. P values are based on interrupted time-series analysis. Total antifungal use decreased by 17.8% (P¼0.01) following implementation of the EMR. MRSA rate There were 807 nosocomial MRSA infections during the study period. Nosocomial MRSA infections decreased by 45.2% (P, ) following implementation of the EMR (Figure 1). There was a correlation of MRSA infection with total antibacterial agent use; the correlation was strongest with use of quinolones, followed by cephalosporins, then extended-spectrum penicillins (Table 4). Because of the known association of MRSA infections with poor hand hygiene, we examined hand hygiene compliance rates over the 5 year period of the study. The monthly mean compliance rate was 83.7%. Over the course of the study 207
4 Cook et al. Table 4. Correlation of antibacterial class use with MRSA infections (r MRSA) and CDIs (r CDI) Antimicrobial agents r MRSA r CDI Extended-spectrum penicillins 0.65 (P¼0.002) 0.35 (P¼0.13) Cephalosporins 0.66 (P¼0.001) 0.61 (P¼0.004) Quinolones 0.70 (P¼0.0006) 0.43 (P¼0.055) Total antibacterial agents 0.62 (P¼0.003) 0.38 (P¼0.10) For MRSA infections, the correlation was highest with quinolone use. For CDIs, the correlation was highest with cephalosporin use. period, linear regression analysis revealed a slight, but statistically significant (P¼0.02), decrease in hand hygiene compliance hospital-wide. CDI rate There were a total of 394 nosocomial C. difficile toxin-positive cases during the study period. There were no significant differences in the average length of stay of all patients before and after implementation of the EMR and there were no significant differences in the ages of patients with CDI in the period before and after implementation of the EMR (data not shown). Similarly, there were no differences in the two groups with regard to time in hospital prior to the first positive C. difficile toxin-positive stool (data not shown). The hospital rates for CDI per quarter are shown in Figure 1. There was an 18.7% decrease in the rate of CDI following implementation of the EMR (P¼0.07). The mean rate of nosocomial CDI prior to implementation of the EMR was 3.9 cases/10000 PDs; after the EMR was implemented, the mean rate of nosocomial CDI was 3.2 cases/10000 PDs. The rate of nosocomial CDI correlated best with the use of cephalosporins and, to a lesser extent, quinolones (Table 4). Discussion The IDSA has recommended that hospitals adopt an ASP as a means of controlling unnecessary and inappropriate antibiotic use within hospitals. 3 That same organization has recommended that an EMR be adopted by institutions to facilitate the process of antimicrobial stewardship. 3 There are very few data regarding the effect of computerized programmes on antibiotic use and outcomes. 10,11 Our hospital instituted an ASP in January 2001 and we previously reported significant reductions in antimicrobial use following implementation of that programme. 9 In July 2007 our institution implemented an EMR with CPOE. Our programme involved feedback to the provider once microbiology cultures and susceptibility data were available. The present study demonstrates significant reductions in antimicrobial use following the implementation of this programme. Our data show that the EMR was a tool that allowed our pharmacists (M. G. and M. J.) to review more charts and to make more recommendations. Following implementation of the EMR, the majority of ASP recommendations were accepted within a few hours. Also, the antibiotic order sets that were built into the EMR did not allow inappropriately high doses of antimicrobial agents, as sometimes occurred before the EMR was implemented. By reviewing more charts and having their recommendations accepted sooner, the pharmacists were able to discontinue unnecessary antimicrobial agents in more patients, thus accounting for the large decrease in antimicrobial use. There were large decreases in the use of cephalosporins, extended-spectrum penicillins and quinolones, agents that are 7,8,12 16 highly associated with both MRSA infections and CDIs. Use of cefazolin, the drug of choice for surgical prophylaxis, decreased by 53% following implementation of the EMR. We suspect that the EMR facilitated the appropriate dose and duration of antibiotic use for surgical cases, and eliminated prolonged courses of unnecessary antibiotic prophylaxis in this patient population. With regard to quinolones, ciprofloxacin use was restricted at our institution beginning in July Quinolones accounted for approximately 15% of the total antibacterial agent use prior to the implementation of the EMR, but that use decreased to 6.5% following implementation of the programme. Our data show a high correlation of quinolone use with MRSA infection, and, to a lesser extent, CDI. Furthermore, our results demonstrate a high correlation of cephalosporin use with both C. difficile and MRSA infections. We speculate that reduced cephalosporin and quinolone use contributed to the decreased nosocomial infection rates of both C. difficile and MRSA. We suspect that the increase in carbapenem use following implementation of the EMR was a result of our efforts to reduce the use of both quinolones and antipseudomonal penicillins (primarily piperacillin/tazobactam) at the hospital. In other words, carbapenems became an alternative agent to quinolones and piperacillin/tazobactam. Despite the large increase in carbapenem use, the total use of these drugs remained less than the use of both the extended-spectrum penicillins and the quinolones (Table 3). There are several limitations associated with an aggregate data study such as this. The duration of antibiotic use for individual patients was not assessed. Also, it is not clear whether all of the C. difficile or MRSA infections began in hospital or prior to hospital admission. We tried to account for this possibility by only including specimens positive for C. difficile toxin or MRSA from patients who had been in hospital for more than 3 days. Antibiotics are only one of many risk factors for the development of CDI or MRSA infection Factors such as renal insufficiency, malignancy, gastrointestinal surgery, use of proton pump inhibitors, previous antibiotic exposures and enteral feeding were not evaluated in this study. Also, nosocomial spread of C. difficile or MRSA was not assessed. Nevertheless, our assessment of compliance with hand washing demonstrated a slight decrease in hand hygiene compliance over the course of the study period, suggesting that the improvements in CDI and MRSA rates were not completely related to improvements in infection control policies. Finally, our hospital began a programme to identify all incoming patients with MRSA colonization of the nares in February As part of this programme, all patients who screened positive for MRSA were placed in private rooms with strict contact isolation infection control measures. There is no question that infection control policies play a major role in the rates of nosocomial MRSA as well as CDIs. Our data support the concept that programmes that promote both infection control surveillance and antimicrobial stewardship are more likely to be effective than either measure alone
5 Effect of EMR on antimicrobial use, MRSA infections and CDIs JAC Infections with MRSA and C. difficile are associated with an increase in hospital length of stay, high mortality and increased hospital costs Our data support the use of an EMR with CPOE as a means of reducing unnecessary antimicrobial use. Reduction in antimicrobial drug use facilitated by the EMR can indirectly lead to decreased rates of infection with both MRSA and C. difficile. Acknowledgements Portions of this work were presented at the IDSA Meeting, Philadelphia, PA, We thank Delores Nobles and Kathy Cochran for help with the MedMined queries and hand hygiene data and Joy Barwick for her assistance with the C. difficile data. Funding No specific funding. Data for this manuscript were collected as part of routine surveillance of the hospital antibiotic management programme. Transparency declarations P. P. C. is a member of the speakers bureau of Pfizer, Astellas and Merck. P. P. C. has received research funding from GlaxoSmithKline, Merck, Gilead, Pfizer and Bristol-Myers Squibb. All other authors: none to declare. References 1 MacDougall C, Polk RE. Antimicrobial stewardship programs in healthcare systems. Clin Microbiol Rev 2005; 18: Gould IM. Antibiotic policies to control hospital-acquired infection. J Antimicrob Chemother 2008; 61: Dellit TH, Owens RC, McGowan JE Jr et al. Infectious Diseases Society of America and the Society for Healthcare Epidemiology of America guidelines for developing an institutional program to enhance antimicrobial stewardship. Clin Infect Dis 2007; 44: Aldeyab MA, Monnet DL, Lopez-Lozano JM et al. Modelling the impact of antibiotic use and infection control practices on the incidence of hospital-acquired methicillin-resistant Staphylococcus aureus: a time-series analysis. J Antimicrob Chemother 2008; 62: Vernaz N, Sax H, Pittet D et al. Temporal effects of antibiotic use and hand rub consumption on the incidence of MRSA and Clostridium difficile. J Antimicrob Chemother 2008; 62: Muller A, Mauny F, Talon D et al. Effect of individual- and group-level antibiotic exposure on MRSA isolation: a multilevel analysis. J Antimicrob Chemother 2006; 58: Dancer SJ. The effect of antibiotics on methicillin-resistant Staphylococcus aureus. J Antimicrob Chemother 2008; 61: Owens RC, Donskey CJ, Gaynes RP et al. Antimicrobial-associated risk factors for Clostridium difficile infection. Clin Infect Dis 2008; 46 Suppl 1: S Cook PP, Catrou PG, Christie JD et al. Reduction in broad-spectrum antimicrobial use associated with no improvement in hospital antibiogram. J Antimicrob Chemother 2004; 53: Buising KL, Thursky KA, Robertson MB et al. Electronic antibiotic stewardship reduced consumption of broad-spectrum antibiotics using a computerized antimicrobial approval system in a hospital setting. J Antimicrob Chemother 2008; 62: Lesprit P, Duong T, Girou E et al. Impact of a computer-generated alert system prompting review of antibiotic use in hospitals. J Antimicrob Chemother 2009; 63: Weber SG, Gold HS, Hooper DC et al. Fluoroquinolones and the risk for methicillin-resistant Staphylococcus aureus in hospitalized patients. Emerg Infect Dis 2003; 9: Charbonneau P, Parienti J, Thibon P et al. Fluoroquinolone use and methicillin-resistant Staphylococcus aureus isolation rates in hospitalized patients: a quasi experimental study. Clin Infect Dis 2006; 42: Pepin J, Saheb N, Coulombe MA et al. Emergence of fluoroquinolones as the predominant risk factor for Clostridium difficile-associated diarrhea: a cohort study during an epidemic in Quebec. Clin Infect Dis 2005; 41: Cook PP, Catrou P, Gooch M et al. Effect of reduction in ciprofloxacin use on prevalence of methicillin-resistant Staphylococcus aureus rates within individual units of a tertiary care hospital. J Hosp Infect 2006; 64: Muto CA, Pokrywka M, Shutt K et al. A large outbreak of Clostridium difficile-associated disease with an unexpected proportion of deaths and colectomies at a teaching hospital following increased fluoroquinolone use. Infect Control Hosp Epidemiol 2005; 26: Dial S, Alrasadi K, Manoukian C et al. Risk of Clostridium difficile diarrhea among hospital inpatients prescribed proton pump inhibitors: cohort and case-control studies. CMAJ 2004; 171: Bartlett JG. Antibiotic-associated diarrhea. N Engl J Med 2002; 346: Kyne L, Sougioultzis S, McFarland LV et al. Underlying disease severity as a major risk factor for nosocomial Clostridium difficile diarrhea. Infect Control Hosp Epidemiol 2002; 23: Cunningham R, Dale B, Undy B et al. Proton pump inhibitors as a risk factor for Clostridium difficile diarrhoea. J Hosp Infect 2003; 54: Merrer J, Santoli F, Appere de Vecchi C et al. Colonization pressure and risk of acquisition of methicillin-resistant Staphylococcus aureus in a medical intensive care unit. Infect Control Hosp Epidemiol 2000; 21: Muto CA, Jernigan JA, Ostrowsky BE et al. SHEA guideline for preventing nosocomial transmission of multidrug-resistant strains of Staphylococcus aureus and Enterococcus. Infect Control Hosp Epidemiol 2003; 24: Kyne L, Hamel MB, Polavaram R et al. Health care costs and mortality associated with nosocomial diarrhea due to Clostridium difficile. Clin Infect Dis 2002; 34: O Brien JA, Lahue BJ, Caro JJ et al. The emerging infectious challenge of Clostridium difficile-associated disease in Massachusetts hospitals: clinical and economic consequences. Infect Control Hosp Epidemiol 2007; 28: Dubberke ER, Reske KA, Olsen MA et al. Short and long term attributable cost of Clostridium difficile-associated disease in non-surgical patients. Clin Infect Dis 2008; 46:
Date: November 30, 2010
 Department of Health and Human Services Public Health Service Food and Drug Administration Center for Drug Evaluation and Research Date: November 30, 2010 To: Through: From: Subject: Drug Name(s): Application
Department of Health and Human Services Public Health Service Food and Drug Administration Center for Drug Evaluation and Research Date: November 30, 2010 To: Through: From: Subject: Drug Name(s): Application
Drug Use Review. Edward Cox, M.D. Director Office of Antimicrobial Products
 Department of Health and Human Services Public Health Service Food and Drug Administration Center for Drug Evaluation and Research Drug Use Review Date: April 5, 2012 To: Through: Edward Cox, M.D. Director
Department of Health and Human Services Public Health Service Food and Drug Administration Center for Drug Evaluation and Research Drug Use Review Date: April 5, 2012 To: Through: Edward Cox, M.D. Director
Urinary Tract Infections
 Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
ANTIBIOTICS IN SEPSIS
 ANTIBIOTICS IN SEPSIS Jennifer Curello, PharmD, BCPS Clinical Pharmacist, Infectious Diseases Antimicrobial Stewardship Program Ronald Reagan UCLA Medical Center October 27, 2014 The power of antibiotics
ANTIBIOTICS IN SEPSIS Jennifer Curello, PharmD, BCPS Clinical Pharmacist, Infectious Diseases Antimicrobial Stewardship Program Ronald Reagan UCLA Medical Center October 27, 2014 The power of antibiotics
ANTIMICROBIAL AGENT CLASSES AND SUBCLASSES
 ANTIMICROBIAL AGENT CLASSES AND SUBCLASSES FOR USE WITH CLSI DOCUMENTS M2 AND M7 Beta-lactams: penicillins e penicillin a penicillin beta-lactam/beta-lactamase inhibitor combinations aminopenicillin a
ANTIMICROBIAL AGENT CLASSES AND SUBCLASSES FOR USE WITH CLSI DOCUMENTS M2 AND M7 Beta-lactams: penicillins e penicillin a penicillin beta-lactam/beta-lactamase inhibitor combinations aminopenicillin a
2013 Indiana Healthcare Provider and Hospital Administrator Multi-Drug Resistant Organism Survey
 2013 Indiana Healthcare Provider and Hospital Administrator Multi-Drug Resistant Organism Survey Antibiotic resistance is a global issue that has significant impact in the field of infectious diseases.
2013 Indiana Healthcare Provider and Hospital Administrator Multi-Drug Resistant Organism Survey Antibiotic resistance is a global issue that has significant impact in the field of infectious diseases.
Develop an understanding of the differential diagnosis of pseudomembranous colitis
 Update on Clostridium difficile Colitis Clostridium difficile infection has recently emerged in populations without any known risk factors. This presentation will focus on the historical background, diagnosis,
Update on Clostridium difficile Colitis Clostridium difficile infection has recently emerged in populations without any known risk factors. This presentation will focus on the historical background, diagnosis,
Liofilchem - Antibiotic Disk Interpretative Criteria and Quality Control - F14013 - Rev.7 / 20.02.2013
 Liofilchem Antibiotic Disk Interpretative Criteria and Quality Control F0 Rev.7 /.02. Amikacin AK Amoxicillin + Clavulanic acid AUG (+) ATCC 352 Coagulasenegative staphylococci Amoxicillin + Clavulanic
Liofilchem Antibiotic Disk Interpretative Criteria and Quality Control F0 Rev.7 /.02. Amikacin AK Amoxicillin + Clavulanic acid AUG (+) ATCC 352 Coagulasenegative staphylococci Amoxicillin + Clavulanic
Outpatient Parenteral Antimicrobial Therapy
 Outpatient Parenteral Antimicrobial Therapy Jason E. Bowling, MD a,b, *, James S. Lewis II, PharmD c,d, Aaron D. Owens, MD a,e KEYWORDS Outpatient parenteral antimicrobial therapy Antibiotics Adverse events
Outpatient Parenteral Antimicrobial Therapy Jason E. Bowling, MD a,b, *, James S. Lewis II, PharmD c,d, Aaron D. Owens, MD a,e KEYWORDS Outpatient parenteral antimicrobial therapy Antibiotics Adverse events
Practice Guidelines. Updated Guideline on Diagnosis and Treatment of Intra-abdominal Infections
 Updated Guideline on Diagnosis and Treatment of Intra-abdominal Infections CARRIE ARMSTRONG Guideline source: Surgical Infection Society, Infectious Diseases Society of America Literature search described?
Updated Guideline on Diagnosis and Treatment of Intra-abdominal Infections CARRIE ARMSTRONG Guideline source: Surgical Infection Society, Infectious Diseases Society of America Literature search described?
Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection
 Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection Emi Minejima, PharmD Assistant Professor of Clinical Pharmacy USC School of Pharmacy minejima@usc.edu
Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection Emi Minejima, PharmD Assistant Professor of Clinical Pharmacy USC School of Pharmacy minejima@usc.edu
5 Measuring the performance
 5 Measuring the performance of antimicrobial stewardship programs Authors: David Looke and Margaret Duguid 5.1 Key points Part I Measuring the performance of antimicrobial stewardship programs Monitoring
5 Measuring the performance of antimicrobial stewardship programs Authors: David Looke and Margaret Duguid 5.1 Key points Part I Measuring the performance of antimicrobial stewardship programs Monitoring
GUIDELINES EXECUTIVE SUMMARY
 GUIDELINES Infectious Diseases Society of America and the Society for Healthcare Epidemiology of America Guidelines for Developing an Institutional Program to Enhance Antimicrobial Stewardship Timothy
GUIDELINES Infectious Diseases Society of America and the Society for Healthcare Epidemiology of America Guidelines for Developing an Institutional Program to Enhance Antimicrobial Stewardship Timothy
growing problem By: Jena Cummins, Doctor of Pharmacy Candidate
 Clostridium difficile: A growing problem By: Jena Cummins, Doctor of Pharmacy Candidate Introduction The word difficile il is Latin for the word difficult. Clostridium difficile, affectionately known as
Clostridium difficile: A growing problem By: Jena Cummins, Doctor of Pharmacy Candidate Introduction The word difficile il is Latin for the word difficult. Clostridium difficile, affectionately known as
Dosing information in renal impairment
 No. Drug name Usual dose Adjustment for Renal failure estimated CrCl (ml/min) Aminoglycoside antibiotics 1 Amikacin 2 Gentamicin 7.5 mg /kg q 12 hr > 50-90 7.5 mg/kg q 12 hr 10-50 7.5 mg/kg q 24 hr < 10
No. Drug name Usual dose Adjustment for Renal failure estimated CrCl (ml/min) Aminoglycoside antibiotics 1 Amikacin 2 Gentamicin 7.5 mg /kg q 12 hr > 50-90 7.5 mg/kg q 12 hr 10-50 7.5 mg/kg q 24 hr < 10
Antimicrobial Stewardship:
 Antimicrobial Stewardship: Arizona Partnerships Working to Improve the Use of Antimicrobials in the Hospital and Community Part 4 Antibacterials indeed, anti-infectives as a whole are unique in that misuse
Antimicrobial Stewardship: Arizona Partnerships Working to Improve the Use of Antimicrobials in the Hospital and Community Part 4 Antibacterials indeed, anti-infectives as a whole are unique in that misuse
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis
 Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
Clostridium difficile Infection (CDI) Gail Bennett, RN, MSN, CIC
 Clostridium difficile Infection (CDI) Gail Bennett, RN, MSN, CIC 1 Clostridium difficile (C.difficile) Antibiotic induced diarrhea Can cause pseudomembranous colitis Most common cause of acute infectious
Clostridium difficile Infection (CDI) Gail Bennett, RN, MSN, CIC 1 Clostridium difficile (C.difficile) Antibiotic induced diarrhea Can cause pseudomembranous colitis Most common cause of acute infectious
ORIGINAL ARTICLE. 10.1111/j.1469-0691.2006.01613.x
 ORIGINAL ARTICLE 10.1111/j.1469-0691.2006.01613.x Benchmarking antimicrobial drug use at university hospitals in five European countries V. Vlahović-Palc evski 1, U. Dumpis 2, P. Mitt 3, J. Gulbinovic
ORIGINAL ARTICLE 10.1111/j.1469-0691.2006.01613.x Benchmarking antimicrobial drug use at university hospitals in five European countries V. Vlahović-Palc evski 1, U. Dumpis 2, P. Mitt 3, J. Gulbinovic
Guidelines for Antimicrobial Stewardship in Hospitals in Ireland. A Strategy for the Control of Antimicrobial Resistance in Ireland
 A Strategy for the Control of Antimicrobial Resistance in Ireland Guidelines for Antimicrobial Stewardship in Hospitals in Ireland Hospital Antimicrobial Stewardship Working Group Guidelines for Antimicrobial
A Strategy for the Control of Antimicrobial Resistance in Ireland Guidelines for Antimicrobial Stewardship in Hospitals in Ireland Hospital Antimicrobial Stewardship Working Group Guidelines for Antimicrobial
HSE Health Protection Surveillance Centre. Sample Root Cause Analysis Tool of Hospital-acquired Clostridium difficile Infection
 Clostridium difficile Sub-Committee Health Protection Surveillance Centre Sample Root Cause Analysis Tool of Hospital-acquired Clostridium difficile Infection Version 3, January 2016 This document has
Clostridium difficile Sub-Committee Health Protection Surveillance Centre Sample Root Cause Analysis Tool of Hospital-acquired Clostridium difficile Infection Version 3, January 2016 This document has
Bringing the Power to Cerner s PowerChart for Antimicrobial Stewardship
 Clinical Infectious Diseases Advance Access published May 22, 2014 INVITED ARTICLE CLINICAL PRACTICE Ellie J. C. Goldstein, Section Editor Bringing the Power to Cerner s PowerChart for Antimicrobial Stewardship
Clinical Infectious Diseases Advance Access published May 22, 2014 INVITED ARTICLE CLINICAL PRACTICE Ellie J. C. Goldstein, Section Editor Bringing the Power to Cerner s PowerChart for Antimicrobial Stewardship
Treatment of skin and soft tissue infections due to methicillin-resistant Staphylococcus aureus in adults
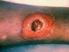 1 of 6 9/24/2010 11:16 AM Official reprint from UpToDate www.uptodate.com 2010 UpToDate Treatment of skin and soft tissue infections due to methicillin-resistant Staphylococcus aureus in adults Author
1 of 6 9/24/2010 11:16 AM Official reprint from UpToDate www.uptodate.com 2010 UpToDate Treatment of skin and soft tissue infections due to methicillin-resistant Staphylococcus aureus in adults Author
Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings
 Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings Dr. Mary Vearncombe PIDAC-IPC February 2012 Objectives: To provide an overview of the RP/AP Annex
Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings Dr. Mary Vearncombe PIDAC-IPC February 2012 Objectives: To provide an overview of the RP/AP Annex
4.06. Infection Prevention and Control at Long-term-care Homes. Chapter 4 Section. Background. Follow-up on VFM Section 3.06, 2009 Annual Report
 Chapter 4 Section 4.06 Infection Prevention and Control at Long-term-care Homes Follow-up on VFM Section 3.06, 2009 Annual Report Background Long-term-care nursing homes and homes for the aged (now collectively
Chapter 4 Section 4.06 Infection Prevention and Control at Long-term-care Homes Follow-up on VFM Section 3.06, 2009 Annual Report Background Long-term-care nursing homes and homes for the aged (now collectively
SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS
 Page 1 of 8 TITLE: SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS GUIDELINE: Antibiotics are administered prior to surgical procedures to prevent surgical site infections. PURPOSE:
Page 1 of 8 TITLE: SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS GUIDELINE: Antibiotics are administered prior to surgical procedures to prevent surgical site infections. PURPOSE:
MAKING THE BUSINESS CASE FOR ASP: TAKING IT TO THE C-SUITE
 MAKING THE BUSINESS CASE FOR ASP: TAKING IT TO THE C-SUITE Gary R Kravitz MD FACP FIDSA FSHEA St. Paul Infectious Disease Associates Hospital Epidemiologist/ Director ASP United Hospital, St. Paul, MN
MAKING THE BUSINESS CASE FOR ASP: TAKING IT TO THE C-SUITE Gary R Kravitz MD FACP FIDSA FSHEA St. Paul Infectious Disease Associates Hospital Epidemiologist/ Director ASP United Hospital, St. Paul, MN
healthcare associated infection 1.2
 healthcare associated infection A C T I O N G U I D E 1.2 AUSTRALIAN SAFETY AND QUALITY GOALS FOR HEALTH CARE What are the goals? The Australian Safety and Quality Goals for Health Care set out some important
healthcare associated infection A C T I O N G U I D E 1.2 AUSTRALIAN SAFETY AND QUALITY GOALS FOR HEALTH CARE What are the goals? The Australian Safety and Quality Goals for Health Care set out some important
Drug Utilization and Evaluation of Cephalosporin s At Tertiary Care Teaching Hospital, Bangalore
 Research Article Drug Utilization and Evaluation of Cephalosporin s At Tertiary Care Teaching Hospital, Bangalore HS. Shekar 1*, HR. Chandrashekhar 2, M. Govindaraju 3, P. Venugopalreddy 1, Chikkalingiah
Research Article Drug Utilization and Evaluation of Cephalosporin s At Tertiary Care Teaching Hospital, Bangalore HS. Shekar 1*, HR. Chandrashekhar 2, M. Govindaraju 3, P. Venugopalreddy 1, Chikkalingiah
Staphyloccus aureus sepsis: follow- up practice guidelines
 Staphyloccus aureus sepsis: follow- up practice guidelines March 17, 2012 National Study Day Hospital Antibiotic Stewardship prof. dr. Dirk Vogelaers, Ghent University Hospital apr. Franky Buyle, Ghent
Staphyloccus aureus sepsis: follow- up practice guidelines March 17, 2012 National Study Day Hospital Antibiotic Stewardship prof. dr. Dirk Vogelaers, Ghent University Hospital apr. Franky Buyle, Ghent
Antimicrobial Stewardship Programs
 A Hospital Pharmacist s Guide to Antimicrobial Stewardship Programs For more information on antimicrobial stewardship, please visit this initiative s website at www.ashpadvantage.com/stewardship Developed
A Hospital Pharmacist s Guide to Antimicrobial Stewardship Programs For more information on antimicrobial stewardship, please visit this initiative s website at www.ashpadvantage.com/stewardship Developed
Antibacterial Drug Shortages From 2001 to 2013: Implications for Clinical Practice
 MAJOR ARTICLE EMBARGOED UNTIL 12:01 A.M. EDT ON THURSDAY, APRIL 23, 2015 Antibacterial Drug Shortages From 2001 to 2013: Implications for Clinical Practice Farha Quadri, 1 Maryann Mazer-Amirshahi, 2 Erin
MAJOR ARTICLE EMBARGOED UNTIL 12:01 A.M. EDT ON THURSDAY, APRIL 23, 2015 Antibacterial Drug Shortages From 2001 to 2013: Implications for Clinical Practice Farha Quadri, 1 Maryann Mazer-Amirshahi, 2 Erin
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Optimizing Antimicrobial Susceptibility Test Reporting
 JOURNAL OF CLINICAL MICROBIOLOGY, Sept. 2011, p. S15 S19 0095-1137/11/$12.00 doi:10.1128/jcm.00712-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. VOL. 49, NO. 9 SUPPL. Optimizing
JOURNAL OF CLINICAL MICROBIOLOGY, Sept. 2011, p. S15 S19 0095-1137/11/$12.00 doi:10.1128/jcm.00712-11 Copyright 2011, American Society for Microbiology. All Rights Reserved. VOL. 49, NO. 9 SUPPL. Optimizing
Appropriate Treatment for Children with Upper Respiratory Infection
 BCBS ACO Measure Appropriate Treatment for Children with Upper Respiratory Infection HEDIS Measure CPT II coding required: YES Click here to go to Table of Contents BCBS Measure: Page 50 of 234 Dated:
BCBS ACO Measure Appropriate Treatment for Children with Upper Respiratory Infection HEDIS Measure CPT II coding required: YES Click here to go to Table of Contents BCBS Measure: Page 50 of 234 Dated:
ANTIBIOTIC RESISTANCE THREATS. in the United States, 2013
 ANTIBIOTIC RESISTANCE THREATS in the United States, 2013 TABLE OF CONTENTS Foreword... 5 Executive Summary.... 6 Section 1: The Threat of Antibiotic Resistance... 11 Introduction.... 11 National Summary
ANTIBIOTIC RESISTANCE THREATS in the United States, 2013 TABLE OF CONTENTS Foreword... 5 Executive Summary.... 6 Section 1: The Threat of Antibiotic Resistance... 11 Introduction.... 11 National Summary
Appendix M: Guidelines for the Prophylaxis and Management of Intraabdominal, Biliary, and Appendiceal Infections
 Appendix M: Guidelines for the Prophylaxis and Management of Intraabdominal, Biliary, and Appendiceal Infections University of Wisconsin Hospital and Clinics Intraabdominal Infections Prophylaxis and Management
Appendix M: Guidelines for the Prophylaxis and Management of Intraabdominal, Biliary, and Appendiceal Infections University of Wisconsin Hospital and Clinics Intraabdominal Infections Prophylaxis and Management
C-Difficile Infection Control and Prevention Strategies
 C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer Adrienne.Mims@AlliantQuality.org 1/18/2016 1 Disclosure This educational activity does not have commercial
C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer Adrienne.Mims@AlliantQuality.org 1/18/2016 1 Disclosure This educational activity does not have commercial
CONSUMERS UNION POLICY BRIEF HOSPITAL-ACQUIRED C. DIFFICILE INFECTIONS (CDI) 11-08
 CONSUMERS UNION POLICY BRIEF HOSPITAL-ACQUIRED C. DIFFICILE INFECTIONS (CDI) 11-08 The growth of infections caused by Clostridium difficile (C.diff) is a highly alarming trend in hospitals today. In 1993
CONSUMERS UNION POLICY BRIEF HOSPITAL-ACQUIRED C. DIFFICILE INFECTIONS (CDI) 11-08 The growth of infections caused by Clostridium difficile (C.diff) is a highly alarming trend in hospitals today. In 1993
How To Treat Mrsa From A Dead Body
 HUSRES Annual Report 2012 Martti Vaara www.huslab.fi www.intra.hus.fi Martti Vaara 2013 1 The basis of this HUSRES 2012 report is the HUSLAB/Whonet database 2012, which contains susceptibility data on
HUSRES Annual Report 2012 Martti Vaara www.huslab.fi www.intra.hus.fi Martti Vaara 2013 1 The basis of this HUSRES 2012 report is the HUSLAB/Whonet database 2012, which contains susceptibility data on
NewYork-Presbyterian Hospital Sites: Columbia University Medical Center Guideline: Medication Use Manual Page 1 of 12
 Page 1 of 12 TITLE: ANTIBIOTICS IN ADULT PATIENTS EMPIRIC USE GUIDELINES, COLUMBIA UNIVERSITY MEDICAL CENTER MEDICATION GUIDELINE PURPOSE: These are the 2011 guidelines for the empiric use of antibiotics
Page 1 of 12 TITLE: ANTIBIOTICS IN ADULT PATIENTS EMPIRIC USE GUIDELINES, COLUMBIA UNIVERSITY MEDICAL CENTER MEDICATION GUIDELINE PURPOSE: These are the 2011 guidelines for the empiric use of antibiotics
Treating Clostridium difficile infection (CDI) the second time around
 Treating Clostridium difficile infection (CDI) the second time around Ciarán P. Kelly, MD Professor of Medicine Harvard Medical School. Beth Israel Deaconess Medical Center, Boston The difficult Clostridium
Treating Clostridium difficile infection (CDI) the second time around Ciarán P. Kelly, MD Professor of Medicine Harvard Medical School. Beth Israel Deaconess Medical Center, Boston The difficult Clostridium
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #65 (NQF 0069): Appropriate Treatment for Children with Upper Respiratory Infection (URI) National Quality Strategy Domain: Efficiency and Cost Reduction 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES:
Measure #65 (NQF 0069): Appropriate Treatment for Children with Upper Respiratory Infection (URI) National Quality Strategy Domain: Efficiency and Cost Reduction 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES:
Recommendations for Metrics for Multidrug-Resistant Organisms in Healthcare Settings: SHEA/HICPAC Position Paper
 infection control and hospital epidemiology october 2008, vol. 29, no. 10 shea/hicpac position paper Recommendations for Metrics for Multidrug-Resistant Organisms in Healthcare Settings: SHEA/HICPAC Position
infection control and hospital epidemiology october 2008, vol. 29, no. 10 shea/hicpac position paper Recommendations for Metrics for Multidrug-Resistant Organisms in Healthcare Settings: SHEA/HICPAC Position
Why Do Some Antibiotics Fail?
 Why Do Some Antibiotics Fail? Patty W. Wright, M.D. April 2010 Objective To outline common reasons why antibiotic therapy is not successful and how this can be avoided. And to teach you a little bit about
Why Do Some Antibiotics Fail? Patty W. Wright, M.D. April 2010 Objective To outline common reasons why antibiotic therapy is not successful and how this can be avoided. And to teach you a little bit about
SAMPLE ANTIMICROBIAL STEWARDSHIP POLICY
 SAMPLE ANTIMICROBIAL STEWARDSHIP POLICY FOR A LOCAL HEALTH DISTRICT OR NETWORK Purpose of this document The development of an official policy for Antimicrobial Stewardship (AMS) is a fundamental step towards
SAMPLE ANTIMICROBIAL STEWARDSHIP POLICY FOR A LOCAL HEALTH DISTRICT OR NETWORK Purpose of this document The development of an official policy for Antimicrobial Stewardship (AMS) is a fundamental step towards
Vancomycin. Beta-lactams. Beta-lactams. Vancomycin (Glycopeptide) Rifamycins (rifampin) MID 4
 Antibiotic Classes Introduction to Antimicrobials Rachel J. Gordon, MD, MPH Assistant Professor of Clinical Medicine and Epidemiology Beta-lactams Inhibit cell wall synthesis Penicillins Cephalosporins
Antibiotic Classes Introduction to Antimicrobials Rachel J. Gordon, MD, MPH Assistant Professor of Clinical Medicine and Epidemiology Beta-lactams Inhibit cell wall synthesis Penicillins Cephalosporins
British Society for Antimicrobial Chemotherapy
 British Society for Antimicrobial Chemotherapy BSAC to actively support the EUCAST Disc Diffusion Method for Antimicrobial Susceptibility Testing in preference to the current BSAC Disc Diffusion Method
British Society for Antimicrobial Chemotherapy BSAC to actively support the EUCAST Disc Diffusion Method for Antimicrobial Susceptibility Testing in preference to the current BSAC Disc Diffusion Method
Antimicrobial Stewardship in Australian Hospitals. Editors: Margaret Duguid and Marilyn Cruickshank
 Antimicrobial Stewardship in Australian Hospitals 2011 Editors: Margaret Duguid and Marilyn Cruickshank Antimicrobial stewardship in Australian hospitals Editors: Margaret Duguid and Marilyn Cruickshank
Antimicrobial Stewardship in Australian Hospitals 2011 Editors: Margaret Duguid and Marilyn Cruickshank Antimicrobial stewardship in Australian hospitals Editors: Margaret Duguid and Marilyn Cruickshank
Antibiotic Prophylaxis for the Prevention of Infective Endocarditis and Prosthetic Joint Infections for Dentists
 PRACTICE ADVISORY SERVICE FAQ 6 Crescent Road, Toronto, ON Canada M4W 1T1 T: 416.961.6555 F: 416.961.5814 Toll Free: 1.800.565.4591 www.rcdso.org Antibiotic Prophylaxis for the Prevention of Infective
PRACTICE ADVISORY SERVICE FAQ 6 Crescent Road, Toronto, ON Canada M4W 1T1 T: 416.961.6555 F: 416.961.5814 Toll Free: 1.800.565.4591 www.rcdso.org Antibiotic Prophylaxis for the Prevention of Infective
Intra-abdominal abdominal Infections
 Intra-abdominal abdominal Infections Marnie Peterson, Pharm.D., BCPS Dept. of Pediatric Infectious Diseases Medical School University of Minnesota Intra-abdominal abdominal Infections Intra-abdominal abdominal
Intra-abdominal abdominal Infections Marnie Peterson, Pharm.D., BCPS Dept. of Pediatric Infectious Diseases Medical School University of Minnesota Intra-abdominal abdominal Infections Intra-abdominal abdominal
APPENDIX B: UWHC SURGICAL ANTIMICROBIAL PROPHYLAXIS GUIDELINES
 APPENDIX B: UWHC SURGICAL ANTIMICROBIAL PROPHYLAXIS GUIDELINES Principles of prophylaxis 1) Use antimicrobials for surgical procedures where prophylactic antimicrobials have been found to be beneficial.
APPENDIX B: UWHC SURGICAL ANTIMICROBIAL PROPHYLAXIS GUIDELINES Principles of prophylaxis 1) Use antimicrobials for surgical procedures where prophylactic antimicrobials have been found to be beneficial.
Product Catalogue 2015 Clinical and Industrial Microbiology
 Product Catalogue 201 Antibiotic discs in cartridge µg CLSI 1,2 EUCAST 3,4 BSAC Packaging * Amikacin AK x0 Discs 9004 Amoxicillin AML 2 x0 Discs 911 Amoxicillin AML x0 Discs 9133 Amoxicillin AML 2 x0 Discs
Product Catalogue 201 Antibiotic discs in cartridge µg CLSI 1,2 EUCAST 3,4 BSAC Packaging * Amikacin AK x0 Discs 9004 Amoxicillin AML 2 x0 Discs 911 Amoxicillin AML x0 Discs 9133 Amoxicillin AML 2 x0 Discs
HUSRES Annual Report 2008 Martti Vaara. www.huslab.fi www.intra.hus.fi
 HUSRES Annual Report 2008 Martti Vaara www.huslab.fi www.intra.hus.fi The basis of this HUSRES 2008 report is the HUSLAB/Whonet database 2008, which contains susceptibility data on about 180.000 bacteria
HUSRES Annual Report 2008 Martti Vaara www.huslab.fi www.intra.hus.fi The basis of this HUSRES 2008 report is the HUSLAB/Whonet database 2008, which contains susceptibility data on about 180.000 bacteria
PRMCE ANTI-INFECTIVES SELECTION GUIDELINE FOR ADULTS
 PRMCE ANTI-INFECTIVES SELECTION GUIDELINE FOR ADULTS SKIN AND SOFT TISSUE INFECTIONS: Mild A. Cellulitis: MRSA uncommonly causes cellulitis in the absence of a wound abscess. Add empiric anti-mrsa therapy
PRMCE ANTI-INFECTIVES SELECTION GUIDELINE FOR ADULTS SKIN AND SOFT TISSUE INFECTIONS: Mild A. Cellulitis: MRSA uncommonly causes cellulitis in the absence of a wound abscess. Add empiric anti-mrsa therapy
Massachusetts Department of Developmental Services MRSA, VRE, and C. Diff Management Protocol
 Massachusetts Department of Developmental Services MRSA, VRE, and C. Diff Management Protocol PURPOSE: To provide guidance for personnel in order to prevent the spread of Antibiotic Resistant Microorganisms
Massachusetts Department of Developmental Services MRSA, VRE, and C. Diff Management Protocol PURPOSE: To provide guidance for personnel in order to prevent the spread of Antibiotic Resistant Microorganisms
IDSA GUIDELINES EXECUTIVE SUMMARY
 IDSA GUIDELINES Diagnosis and Management of Complicated Intra-abdominal Infection in Adults and Children: Guidelines by the Surgical Infection Society and the Infectious Diseases Society of America Joseph
IDSA GUIDELINES Diagnosis and Management of Complicated Intra-abdominal Infection in Adults and Children: Guidelines by the Surgical Infection Society and the Infectious Diseases Society of America Joseph
California Antimicrobial Stewardship Program Initiative & Clostridium difficile Infection (CDI) Project
 1 California Antimicrobial Stewardship Program Initiative & Clostridium difficile Infection (CDI) Project Hospital Association of Southern California Conference February 26, 2015 Vicki Keller, RN,MSN,CIC
1 California Antimicrobial Stewardship Program Initiative & Clostridium difficile Infection (CDI) Project Hospital Association of Southern California Conference February 26, 2015 Vicki Keller, RN,MSN,CIC
Clinical Practice Guidelines for Antimicrobial Prophylaxis in Surgery
 600 ASHP Therapeutic Guidelines Clinical Practice Guidelines for Antimicrobial Prophylaxis in Surgery These guidelines were developed jointly by the American Society of Health-System Pharmacists (ASHP),
600 ASHP Therapeutic Guidelines Clinical Practice Guidelines for Antimicrobial Prophylaxis in Surgery These guidelines were developed jointly by the American Society of Health-System Pharmacists (ASHP),
Inhibit terminal acid secretion from parietal cells by blocking H + /K + - ATPase pump
 Chris J. Taylor, Pharm.D., BCPS Clinical Pharmacist Phoenix VA Health Care System Review pharmacology of PPIs Discuss possible association between PPI use and development of the following: Pneumonia (community-acquired
Chris J. Taylor, Pharm.D., BCPS Clinical Pharmacist Phoenix VA Health Care System Review pharmacology of PPIs Discuss possible association between PPI use and development of the following: Pneumonia (community-acquired
Disease Site Breast. Less than 120 kg: Cefazolin 2 grams IV Greater than or equal to 120 kg: Cefazolin 3 grams IV. Head & Neck
 Patients scheduled for surgery should have the following antibiotics administered prior to their procedure Vancomycin and Ciprofloxacin are to be initiated 60 to 120 minutes prior to incision and all other
Patients scheduled for surgery should have the following antibiotics administered prior to their procedure Vancomycin and Ciprofloxacin are to be initiated 60 to 120 minutes prior to incision and all other
Treatment of Fever and Infection in Children with Transfusion Dependent Thalassaemia
 Treatment of Fever and Infection in Children with Transfusion Dependent Thalassaemia Document Information Version: 2 Date: June 2014 Authors (incl. job title): Professor David Rees, Sue Height (consultant
Treatment of Fever and Infection in Children with Transfusion Dependent Thalassaemia Document Information Version: 2 Date: June 2014 Authors (incl. job title): Professor David Rees, Sue Height (consultant
ANTIMICROBIAL STEWARDSHIP TOOLKIT BEST PRACTICES FROM THE GNYHA/UHF ANTIMICROBIAL STEWARDSHIP COLLABORATIVE
 Greater New York Hospital Association United Hospital Fund ANTIMICROBIAL STEWARDSHIP TOOLKIT BEST PRACTICES FROM THE GNYHA/UHF ANTIMICROBIAL STEWARDSHIP COLLABORATIVE ANTIMICROBIAL STEWARDSHIP PROJECT
Greater New York Hospital Association United Hospital Fund ANTIMICROBIAL STEWARDSHIP TOOLKIT BEST PRACTICES FROM THE GNYHA/UHF ANTIMICROBIAL STEWARDSHIP COLLABORATIVE ANTIMICROBIAL STEWARDSHIP PROJECT
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Contents
 Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
HUSRES Annual Report 2010 Martti Vaara www.huslab.fi www.intra.hus.fi
 HUSRES Annual Report 2010 Martti Vaara www.huslab.fi www.intra.hus.fi Martti Vaara, 2/2011 1 The basis of this HUSRES 2010 report is the HUSLAB/Whonet database 2010, which contains susceptibility data
HUSRES Annual Report 2010 Martti Vaara www.huslab.fi www.intra.hus.fi Martti Vaara, 2/2011 1 The basis of this HUSRES 2010 report is the HUSLAB/Whonet database 2010, which contains susceptibility data
Urinary Tract Infection and Asymptomatic Bacteriuria Guidance
 Urinary Tract Infection and Asymptomatic Bacteriuria Guidance Urinary tract infection (UTI) is the most common indication for antimicrobial use in hospitals and a significant proportion of this use is
Urinary Tract Infection and Asymptomatic Bacteriuria Guidance Urinary tract infection (UTI) is the most common indication for antimicrobial use in hospitals and a significant proportion of this use is
for Extended Stability Parenteral Drugs Third Edition Caryn M. Bing, R.Ph., M.S., FASHP Editor
 Extended Stability for Parenteral Drugs Third Edition Editor Caryn M. Bing, R.Ph., M.S., FASHP 1 American Society of Health-System Pharmacists Bethesda, Maryland Contents Preface Acknowledgments x/ Dedication
Extended Stability for Parenteral Drugs Third Edition Editor Caryn M. Bing, R.Ph., M.S., FASHP 1 American Society of Health-System Pharmacists Bethesda, Maryland Contents Preface Acknowledgments x/ Dedication
THIS IS AN OFFICIAL NH DHHS HEALTH ALERT
 THIS IS AN OFFICIAL NH DHHS HEALTH ALERT Distributed by the NH Health Alert Network Health.Alert@nh.gov August 13, 2015 1400 EDT (2:00 PM EDT) NH-HAN 20150813 Updated Centers for Disease Control (CDC)
THIS IS AN OFFICIAL NH DHHS HEALTH ALERT Distributed by the NH Health Alert Network Health.Alert@nh.gov August 13, 2015 1400 EDT (2:00 PM EDT) NH-HAN 20150813 Updated Centers for Disease Control (CDC)
Improving Timely Surgical Antibiotic Prophylaxis Redosing Administration Using Computerized Record Prompts ABSTRACT
 SURGICAL INFECTIONS Volume 6, Number 2, 2005 Mary Ann Liebert, Inc. Improving Timely Surgical Antibiotic Prophylaxis Redosing Administration Using Computerized Record Prompts PAUL ST. JACQUES, 1 NEAL SANDERS,
SURGICAL INFECTIONS Volume 6, Number 2, 2005 Mary Ann Liebert, Inc. Improving Timely Surgical Antibiotic Prophylaxis Redosing Administration Using Computerized Record Prompts PAUL ST. JACQUES, 1 NEAL SANDERS,
The US health care system faces numerous challenges,
 Hosp Pharm 2013;48(9):1 9 2013 Ó Thomas Land Publishers, Inc. www.hospital-pharmacy.com doi: 10.1310/hpj4809-nnn Original Article Impact of a Clinical Decision Support System on Pharmacy Clinical Interventions,
Hosp Pharm 2013;48(9):1 9 2013 Ó Thomas Land Publishers, Inc. www.hospital-pharmacy.com doi: 10.1310/hpj4809-nnn Original Article Impact of a Clinical Decision Support System on Pharmacy Clinical Interventions,
Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations. J. Stuart Wolf, Jr., M.D.
 Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations J. Stuart Wolf, Jr., M.D. Department of Urology University of Michigan Ann Arbor, MI Official Recommendations for
Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations J. Stuart Wolf, Jr., M.D. Department of Urology University of Michigan Ann Arbor, MI Official Recommendations for
PERTUSSIS SURVEILLANCE AND RESPONSE PROTOCOL
 PERTUSSIS SURVEILLANCE AND RESPONSE PROTOCOL Public Health Action 1. Educate the public, particularly parents of infants, about the dangers of whooping cough and the advantages of initiating immunization
PERTUSSIS SURVEILLANCE AND RESPONSE PROTOCOL Public Health Action 1. Educate the public, particularly parents of infants, about the dangers of whooping cough and the advantages of initiating immunization
Hialeah Nursing and Rehabilitation Center Combines Technology and Best Practices to Improve Infection Control Specific to C.diff
 RESEARCH ARTICLE Page 1 of 5 Hialeah Nursing and Rehabilitation Center Combines Technology and Best Practices to Improve Infection Control Specific to C.diff ABSTRACT RB Health Partners, Inc., June 24,
RESEARCH ARTICLE Page 1 of 5 Hialeah Nursing and Rehabilitation Center Combines Technology and Best Practices to Improve Infection Control Specific to C.diff ABSTRACT RB Health Partners, Inc., June 24,
Antimicrobial Stewardship:
 Antimicrobial Stewardship: Arizona Partnerships Working to Improve the Use of Antimicrobials in the Hospital and Community Part 7 Antibacterials indeed, anti-infectives as a whole are unique in that misuse
Antimicrobial Stewardship: Arizona Partnerships Working to Improve the Use of Antimicrobials in the Hospital and Community Part 7 Antibacterials indeed, anti-infectives as a whole are unique in that misuse
Bachir K. Younes, M.D., M.P.H.
 Work: 36923 Cook St. # 103 Palm Desert, CA 92211 Phone (760) 636-1336 Fax (760) 636-1335 Bachir K. Younes, M.D., M.P.H. Personal Born: Jan. 1 st, 1971 in Lebanon Marital Status: Married to Roula Sleilati
Work: 36923 Cook St. # 103 Palm Desert, CA 92211 Phone (760) 636-1336 Fax (760) 636-1335 Bachir K. Younes, M.D., M.P.H. Personal Born: Jan. 1 st, 1971 in Lebanon Marital Status: Married to Roula Sleilati
Solid Organ Transplantation
 Solid Organ Transplantation Infection Prevention And Control Transplant Atlantic 2011 October 13/2011 Kathy Hart Introduction In the past several years, the drugs that we use, the surgeries themselves,
Solid Organ Transplantation Infection Prevention And Control Transplant Atlantic 2011 October 13/2011 Kathy Hart Introduction In the past several years, the drugs that we use, the surgeries themselves,
ANTIMICROBIAL USE GUIDELINES
 ANTIMICROBIAL USE GUIDELINES University of Wisconsin Hospital and Clinics Pharmacy and Therapeutics Committee Department of Pharmacy Drug Policy Program July 2011 to June 2012 Twenty-First Edition PREFACE
ANTIMICROBIAL USE GUIDELINES University of Wisconsin Hospital and Clinics Pharmacy and Therapeutics Committee Department of Pharmacy Drug Policy Program July 2011 to June 2012 Twenty-First Edition PREFACE
Oscar E. Guzman, PharmD, BCPS
 P Chapter 32 Antibiotic Streamlining Oscar E. Guzman, PharmD, BCPS Introduction Antibiotic streamlining is one of the most important methods pharmacists can use to encourage appropriate antibiotic use,
P Chapter 32 Antibiotic Streamlining Oscar E. Guzman, PharmD, BCPS Introduction Antibiotic streamlining is one of the most important methods pharmacists can use to encourage appropriate antibiotic use,
GLOBAL OVERVIEW OF ANTIMICROBIAL RESISTANCE STD AGENTS
 GLOBAL OVERVIEW OF ANTIMICROBIAL RESISTANCE STD AGENTS IN Dr.P.Bhalla Director Professor and Head Dept. of Microbiology Maulana Azad Medical College New Delhi, INDIA STDs & RTIs l HIV l Gonococcal infections/
GLOBAL OVERVIEW OF ANTIMICROBIAL RESISTANCE STD AGENTS IN Dr.P.Bhalla Director Professor and Head Dept. of Microbiology Maulana Azad Medical College New Delhi, INDIA STDs & RTIs l HIV l Gonococcal infections/
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention. Basics of Infection Prevention 2 Day Mini-Course 2013
 Catheter-Associated Urinary Tract Infection (CAUTI) Prevention Basics of Infection Prevention 2 Day Mini-Course 2013 2 Objectives Define the scope of healthcare-associated urinary tract infections (UTI)
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention Basics of Infection Prevention 2 Day Mini-Course 2013 2 Objectives Define the scope of healthcare-associated urinary tract infections (UTI)
Antibiotic resistance does it matter in paediatric clinical practice? Jette Bangsborg Department of Clinical Microbiology Herlev Hospital
 Antibiotic resistance does it matter in paediatric clinical practice? Jette Bangsborg Department of Clinical Microbiology Herlev Hospital Background The Department of Clinical Microbiology at Herlev Hospital
Antibiotic resistance does it matter in paediatric clinical practice? Jette Bangsborg Department of Clinical Microbiology Herlev Hospital Background The Department of Clinical Microbiology at Herlev Hospital
How To Treat Mrsa In Finnish
 HUSRES Annual Report 2013 Martti Vaara www.huslab.fi www.intra.hus.fi Martti Vaara 2014 1 The basis of this HUSRES 2013 report is the HUSLAB/Whonet database 2013, which contains susceptibility data on
HUSRES Annual Report 2013 Martti Vaara www.huslab.fi www.intra.hus.fi Martti Vaara 2014 1 The basis of this HUSRES 2013 report is the HUSLAB/Whonet database 2013, which contains susceptibility data on
Changes in the use of broad-spectrum antibiotics after cefepime shortage: a time
 AAC Accepts, published online ahead of print on 28 November 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.05560-11 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
AAC Accepts, published online ahead of print on 28 November 2011 Antimicrob. Agents Chemother. doi:10.1128/aac.05560-11 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions.
ASP 101. What is Antimicrobial Stewardship?
 ASP 101 What is Antimicrobial Stewardship? Objectives To describe the rationale for antimicrobial stewardship; To state the definition and goals of antimicrobial stewardship; To identify the important
ASP 101 What is Antimicrobial Stewardship? Objectives To describe the rationale for antimicrobial stewardship; To state the definition and goals of antimicrobial stewardship; To identify the important
Introduction to Antimicrobial Therapy
 Introduction to Antimicrobial Therapy Christine Kubin, Pharm.D., BCPS Clinical Pharmacist, Infectious Diseases Case #1 L.G. is a 78 yo woman admitted for cardiac cath. 3-vessel disease was identified and
Introduction to Antimicrobial Therapy Christine Kubin, Pharm.D., BCPS Clinical Pharmacist, Infectious Diseases Case #1 L.G. is a 78 yo woman admitted for cardiac cath. 3-vessel disease was identified and
Adjustment of antibiotic treatment according to the results of blood cultures leads to decreased antibiotic use and costs
 Journal of Antimicrobial Chemotherapy (2006) 57, 326 330 doi:10.1093/jac/dki463 Advance Access publication 29 December 2005 Adjustment of antibiotic treatment according to the results of blood cultures
Journal of Antimicrobial Chemotherapy (2006) 57, 326 330 doi:10.1093/jac/dki463 Advance Access publication 29 December 2005 Adjustment of antibiotic treatment according to the results of blood cultures
How To Diagnose And Treat Community Acquired Pneumonia
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Prina E, Ranzani OT, Torres A. Community-acquired
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Prina E, Ranzani OT, Torres A. Community-acquired
Streptococcus pneumoniae IgG AB (13 Serotypes), MAID... 7
 Volume 12 December 2011 Table of Contents Summary of Test Changes... 3 Test Changes... 6 Human Anti-Mouse AB (HAMA), ELISA... 6 Hepatitis E Antibody (IgG, IgM)... 6 Hepatitis E Antibody (IgG)... 6 Hepatitis
Volume 12 December 2011 Table of Contents Summary of Test Changes... 3 Test Changes... 6 Human Anti-Mouse AB (HAMA), ELISA... 6 Hepatitis E Antibody (IgG, IgM)... 6 Hepatitis E Antibody (IgG)... 6 Hepatitis
2015/2016 Schedule of Home Medical Services and Fees for Approved Agencies
 2015/2016 Schedule of Home Medical Services and Fees for Approved Agencies Legislative Authority: Health Insurance Act (Standard Hospital Benefit) Regulations 1971- Section 3(xv) This schedule lists the
2015/2016 Schedule of Home Medical Services and Fees for Approved Agencies Legislative Authority: Health Insurance Act (Standard Hospital Benefit) Regulations 1971- Section 3(xv) This schedule lists the
Antimicrobial Activity and Spectrum of PPI-0903M (T-91825), a Novel Cephalosporin, Tested against a Worldwide Collection of Clinical Strains
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Aug. 2005, p. 3501 3512 Vol. 49, No. 8 0066-4804/05/$08.00 0 doi:10.1128/aac.49.8.3501 3512.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved.
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Aug. 2005, p. 3501 3512 Vol. 49, No. 8 0066-4804/05/$08.00 0 doi:10.1128/aac.49.8.3501 3512.2005 Copyright 2005, American Society for Microbiology. All Rights Reserved.
SHEA Position Paper. Vol. 18 No. 4 INFECTION CONTROL AND HOSPITAL EPIDEMIOLOGY 275
 Vol. 18 No. 4 INFECTION CONTROL AND HOSPITAL EPIDEMIOLOGY 275 SHEA Position Paper Society for Healthcare Epidemiology of America and Infectious Diseases Society of America Joint Committee on the Prevention
Vol. 18 No. 4 INFECTION CONTROL AND HOSPITAL EPIDEMIOLOGY 275 SHEA Position Paper Society for Healthcare Epidemiology of America and Infectious Diseases Society of America Joint Committee on the Prevention
Methicillin-resistant S taphylococcus
 Nevio Cimolai, MD, FRCPC Community-acquired MRSA infection: An emerging trend The use of culture as backup to empiric treatment of staphylococcal infection can help deal with widespread antibiotic resistance.
Nevio Cimolai, MD, FRCPC Community-acquired MRSA infection: An emerging trend The use of culture as backup to empiric treatment of staphylococcal infection can help deal with widespread antibiotic resistance.
Fungal Infection in Total Joint Arthroplasty. Dr.Wismer Dr.Al-Sahan
 Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
Controversies in Hospital Medicine: Antifungal Therapy. Empiric Therapy, Combination Therapy, and the Question of Central Venous Catheters
 Controversies in Hospital Medicine: Antifungal Therapy Empiric Therapy, Combination Therapy, and the Question of Central Venous Catheters Douglas Fish, Pharm.D. Professor of Pharmacy, University of Colorado
Controversies in Hospital Medicine: Antifungal Therapy Empiric Therapy, Combination Therapy, and the Question of Central Venous Catheters Douglas Fish, Pharm.D. Professor of Pharmacy, University of Colorado
Practice Guidelines for Outpatient Parenteral Antimicrobial Therapy
 IDSA GUIDELINES Practice Guidelines for Outpatient Parenteral Antimicrobial Therapy Alan D. Tice, 1 Susan J. Rehm, 2 Joseph R. Dalovisio, 3 John S. Bradley, 4 Lawrence P. Martinelli, 5 Donald R. Graham,
IDSA GUIDELINES Practice Guidelines for Outpatient Parenteral Antimicrobial Therapy Alan D. Tice, 1 Susan J. Rehm, 2 Joseph R. Dalovisio, 3 John S. Bradley, 4 Lawrence P. Martinelli, 5 Donald R. Graham,
Learning Data-Driven Patient Risk Stratification Models for Clostridium difficile
 MAJOR ARTICLE Learning Data-Driven Patient Risk Stratification Models for Clostridium difficile Jenna Wiens, 1 Wayne N. Campbell, 2 Ella S. Franklin, 3 John V. Guttag, 1 and Eric Horvitz 4 1 Department
MAJOR ARTICLE Learning Data-Driven Patient Risk Stratification Models for Clostridium difficile Jenna Wiens, 1 Wayne N. Campbell, 2 Ella S. Franklin, 3 John V. Guttag, 1 and Eric Horvitz 4 1 Department
C. difficile Infections
 C. difficile Infections Introduction C. difficile is a type of bacteria that can cause diarrhea and infection of the colon. This bacterium is more likely to infect patients at hospitals and other healthcare
C. difficile Infections Introduction C. difficile is a type of bacteria that can cause diarrhea and infection of the colon. This bacterium is more likely to infect patients at hospitals and other healthcare
Showcase Hospitals Local Technology Review Report number 6. Smartphone application for antibiotic prescribing
 Showcase Hospitals Local Technology Review Report number 6 Smartphone application for antibiotic prescribing The Healthcare Associated Infections (HCAI) Technology Innovation Programme The basic ways of
Showcase Hospitals Local Technology Review Report number 6 Smartphone application for antibiotic prescribing The Healthcare Associated Infections (HCAI) Technology Innovation Programme The basic ways of
ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM
 ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 77th Annual Meeting March 9-12, 2010 New Orleans, Louisiana COMMITTEE ON PATIENT SAFETY PREPARED
ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 77th Annual Meeting March 9-12, 2010 New Orleans, Louisiana COMMITTEE ON PATIENT SAFETY PREPARED
