Diastolic Heart Failure: Restrictive Cardiomyopathy, Constrictive Pericarditis, and Cardiac Tamponade: Clinical and Echocardiographic Evaluation
|
|
|
- Brianne Poole
- 7 years ago
- Views:
Transcription
1 Cardiology in Review Volume 10, Number 4, pp Copyright 2002 Lippincott Williams & Wilkins Diastolic Heart Failure: Restrictive Cardiomyopathy, Constrictive Pericarditis, and Cardiac Tamponade: Clinical and Echocardiographic Evaluation CRAIG R. ASHER, MD, and ALLAN L. KLEIN, MD An understanding of the basic principles of diastolic function is important in order to recognize diseases that may result in diastolic dysfunction and diastolic heart failure. Although uncommon, restrictive cardiomyopathy, constrictive pericarditis, and cardiac tamponade are among the disorders that may affect primarily diastolic function with preservation of systolic function. Diastolic heart failure may manifest with chronic nonspecific symptoms or may present with acute hemodynamic compromise. Echocardiography plays a vital role in the diagnosis of diastolic dysfunction and differentiation of these disease processes. It also provides a basis for clinical decisions regarding management and surgical referral. This review summarizes the clinical features, pathophysiology, and hemodynamic and echocardiographic signs of restrictive cardiomyopathy, constrictive pericarditis, and cardiac tamponade. Key Words: Cardiac tamponade, Constrictive pericarditis, Diastolic dysfunction, Restrictive cardiomyopathy Department of Cardiovascular Medicine, Section of Cardiovascular Imaging, Cleveland Clinic Foundation, Cleveland, Ohio Address reprint requests to: Allan L. Klein, MD, Cleveland Clinic Foundation, Department of Cardiovascular Medicine, 9500 Euclid Avenue, Desk F15, Cleveland, OH Diastolic dysfunction is defined as the requirement for elevated filling pressures to maintain cardiac output. Augmented filling pressures may result in excessive cardiac volume and right-sided or leftsided congestion, the syndrome of diastolic heart failure (1). Although diastolic dysfunction contributes to heart failure in patients with abnormal systolic function, it may occur in patients with normal function (2). Numerous disease processes affecting the myocardium and pericardium are associated with diastolic dysfunction and heart failure. The clinical manifestations of these conditions are diverse, ranging from nonspecific, insidious symptoms such as exertional dyspnea to pulmonary edema or sudden hemodynamic collapse. The prevalence of diastolic heart failure is variably reported depending on the age, diagnostic criteria, and referral patterns of the populations studied (2). Hypertension, coronary artery disease, valvular heart disease, and hypertrophic cardiomyopathy are the predominant myocardial disorders that result in diastolic dysfunction with relatively preserved systolic function (3). Restrictive cardiomyopathies are less common causes of diastolic dysfunction because of myocardial storage or infiltration. All of these myocardial conditions cause diastolic dysfunction largely by their effect on ventricular relaxation and compliance (4). Constrictive pericarditis and cardiac tamponade are pericardial disorders that impede ventricular filling by extrinsic constraint or limitation of chamber loading. Pericardial disorders may result in a spectrum of acute and chronic hemodynamic disturbance. Distinguishing disorders that cause diastolic dysfunction is important so that management can be tailored to the specific disease. This review discusses the general principles of normal diastolic function and contrasts the abnormalities of diastolic dysfunction present with restrictive cardiomyopathy, constrictive pericarditis, and cardiac tamponade. The integral role of echocardiography in differentiating these diseases is highlighted. 218 CARDIOLOGY IN REVIEW
2 DIASTOLIC FUNCTION: PHYSIOLOGY Diastolic filling of the left ventricle (LV) encompasses the period of the cardiac cycle between aortic valve closure and mitral valve closure. Four distinct phases are distinguished: (1) isovolumic relaxation (between aortic valve closure and mitral valve opening), (2) rapid filling, (3) diastasis (slow filling), and (4) atrial contraction (5). There are multiple physiologic determinants of diastolic function. The major myocardial factors that affect diastolic function include LV myocardial relaxation, compliance, and left atrial function (5). Other parameters include heart rate, preload, afterload, atrioventricular conduction, right ventricular (RV) function, intrathoracic pressure, viscoelastic properties, coronary engorgement, neurohormonal activation, and pericardial constraint (6). RV diastolic function is concordant with LV diastolic function in healthy people, although discordant filling and differing external interactions may occur in some disease states. After LV contraction, diastole begins with the energy-dependent cellular process of ventricular relaxation, which extends into diastasis. LV relaxation is best characterized by the time constant of relaxation ( ), which describes the rate of LV pressure decay in an exponential equation. Until recently, only invasive methods were available to estimate ( )(7). Other, more dependent surrogate echocardiographic markers of relaxation include the isovolumic relaxation time (IVRT) and information obtained by color M-mode and Doppler tissue imaging. The IVRT characterizes the time when LV pressure declines and LV volume remains constant. When LV pressure drops below left atrial pressure, the mitral valve opens and the early rapid filling period begins. During the early filling period (mitral E wave), there is a rapid increase in the LV chamber volume, which contributes largely to the ventricular stroke volume (8). The amount of volume entering the LV cavity is influenced by many factors, including the pressure gradient between the pulmonary veins and LV, continued myocardial relaxation, elastic recoil (ventricular suction), and stiffness properties of the myocardium (5). LV stiffness (or its reciprocal, compliance) characterizes the change in pressure within the chamber with an increase in volume and is dependent on the many inherent properties of myocardial content, chamber dimension, and external constraints of the pericardium and thorax (5). The left atrial and LV pressures are equalized during diastasis, resulting in slow or minimal filling. Diastasis is followed by atrial contraction (mitral A wave), which contributes variably to LV enddiastolic volume. Aside from the left atrium s passive role as a conduit receptacle, it functions as a pump to regulate filling volume. When left atrial pressure is high at the end of diastole because of systolic heart disease, Frank-Starling mechanisms are activated (increased stretch, increased force of contraction), and atrial systole may contribute significantly to diastolic filling volume (9). DIASTOLIC FUNCTION: ECHOCARDIOGRAPHY The assessment of diastolic function has become an integral part of any echocardiographic study. Many causes of diastolic heart failure can be identified, including restrictive, hypertrophic, and ischemic cardiomyopathies and pericardial, valvular, and congenital heart disease. Diastolic filling patterns can be evaluated and stages of diastolic dysfunction determined that correlate with left-sided and right-sided filling pressures and disease-related prognosis (10 13). Other techniques such as radionuclide angiography, magnetic resonance imaging, and cardiac catheterization are more time consuming, invasive, and tedious, and are generally used only as adjuncts to echocardiography. Traditionally, the diastolic function exam focuses on pulsed Doppler recordings of left-sided mitral inflow E and A waves and pulmonary vein systolic (S), diastolic (D), and atrial reversal (AR) waves and the corresponding right-sided tricuspid inflow and hepatic vein flow waves (14). Measurements of deceleration and IVRT times and responses to physiologic maneuvers such as Valsalva provide more information. Using these parameters, 4 stages of diastolic dysfunction can be determined: (1) impaired relaxation, (2) pseudonormal stage, (3) restrictive, reversible stage, and (4) restrictive, irreversible function (15) (Fig. 1). Newer technologies have provided supplemental data to differentiate normal from pseudonormal patterns and to estimate left atrial and LV filling pressures more accurately (16) A color M- mode display shows a more precise spatial and temporal distribution of flow velocities propagating across the mitral valve into the LV. The flow propagation velocity (vp) provides a relatively preload-independent determination of relaxation in various disease states and can be used in a regression equation with the mitral inflow E wave Volume 10, Number 4, 2002 CARDIOLOGY IN REVIEW 219
3 Figure 1. Stages of diastolic function as assessed by Doppler echocardiography mitral inflow, pulmonary venous flow, tissue Doppler, and color M-mode. Using an integrated approach with these 4 modalities, the stages of diastolic dysfunction can be determined. A, mitral A-wave velocity; Am, tissue Doppler atrial contraction wave; CMM-vp, color M-mode flow propagation velocity; D, pulmonary venous diastolic wave; E, mitral E-wave velocity; Em, tissue Doppler early filling wave; PV, pulmonary vein; S, pulmonary venous systolic wave; Sm, tissue Doppler systolic wave; TDE, tissue Doppler echocardiography; vp, color M-mode flow propagation velocity. Reprinted with permission from Garcia MJ, Thomas JD, Klein AL: New Doppler echocardiographic applications for the study of diastolic function. J Am Coll Cardiol 1998;32: to estimate pulmonary capillary wedge pressure (17). Doppler tissue imaging obtains the low velocity and high amplitude signals of the myocardium rather than the high velocity and low amplitude blood signals (16). With this technique, spectral Doppler or color Doppler encoded velocities can be recorded. Spectral Doppler myocardial velocities of the mitral annulus provide systolic and diastolic velocities (Em, early filling; Ea or Am, atrial contraction) similar to the mitral inflow profiles. Studies have demonstrated that Em is relatively preload-independent in many disease states. As with vp, Em can be used to differentiate disease states such as restrictive cardiomyopathy and constrictive pericarditis and to assess LV filling pressures more accurately (18). Additionally, recent reports have emphasized the importance of assessing regional myocardial function by Doppler echocardiographic strain rate imaging (19). RESTRICTIVE CARDIOMYOPATHY As defined by the revised World Health Organization Task Force, restrictive cardiomyopathy is a disease characterized by restrictive filling and reduced diastolic volume of either or both ventricles with normal or near-normal systolic function. (20) Despite this rigid definition requiring that restrictive hemodynamics are present, several studies have demonstrated early forms of these disorders with earlier stages of diastolic impairment. These diseases may be idiopathic or associated with specific systemic conditions and may be further characterized as myocardial (noninfiltrative, infiltrative, and storage) or endomyocardial types (21). The prognosis of restrictive cardiomyopathies is generally poor, except for those with reversible causes such as hemochromatosis. Cardiac amyloidosis is the most prevalent restrictive cardiomyopathy, and the current literature addresses predominantly this specific disease (Fig. 2). Because of the resistance to biventricular filling, patients commonly develop a clinical profile related to congestive failure with fatigue, exercise intolerance, right-sided or left-sided heart failure, and atrial fibrillation (22,23). The clinical examination correlates with these symptoms. An elevated jugular venous pressure with an x and prominent y descent (early-stage, M wave), y descent only (late-stage), and Kussmaul s sign may be present, although pulsus paradoxus is always absent. Depending on the stage of disease, an S4 (early) or S3 (late) may be present (21). The electrocardiogram of amyloidosis typically shows a 220 CARDIOLOGY IN REVIEW Diastolic Heart Failure
4 Figure 2. Working classification of restrictive cardiomyopathy. Reprinted with permission from Leung D, Klein AL: Restrictive cardiomyopathy: diagnosis and prognostic implications. In Otto CM, ed: Practice of Clinical Echocardiography. Philadelphia, WB Saunders, 1997; large discordance between echocardiographic wall thickness and voltage (low voltage and increased wall thickness) (24). Pathophysiology As a result of myocardial or endocardial involvement such as amyloid infiltration, the ventricle is noncompliant or stiff and resists ventricular filling. Therefore, as the volume of the heart is increased, there is a steep rise in the pressure. Diastolic right-sided or left-sided heart failure may ensue (22). Hemodynamic Signs In the cardiac catheterization laboratory, invasive determination of operating stiffness may be demonstrated by pressure-volume curves, LV and RV hemodynamic tracings showing a dip and plateau or square root pattern (21). Other, less specific findings include a RV systolic pressure of greater than 50 mmhg with a RV end-diastolic pressure usually less than one third of the RV systolic pressure. Typically, the LV end-diastolic pressure is greater that the RV end-diastolic pressure (25). Echocardiographic signs Echocardiography is uniquely suited as a diagnostic modality to detect the anatomic and functional abnormalities associated with restrictive cardiomyopathies. A combination of 2-dimensional imaging, M-mode, and Doppler information is important to identifying specific features of restrictive cardiomyopathy. Amyloidosis is primarily discussed here because it is the prototype of this class of diseases, and although endomyocardial disorders have very distinct features, they are less commonly encountered in this country. Two-dimensional Imaging and M-mode Increased wall thickness of the LV and often the RV is a hallmark of amyloidosis and almost all the myocardial disorders (26). Both ventricular cavities are typically small with a decreased volume and large atria. The atrial septum and cardiac valves may also be thickened. A characteristic granular sparkling myocardial texture was described before harmonic and high frequency imaging, but this may be a less sensitive and specific finding with current imaging modalities. A pericardial effusion may be present. The inferior vena cava is usually dilated and does not collapse with inspiration (plethoric), reflecting increased right atrial pressure. Doppler Echocardiography Diastolic dysfunction is a requirement for a restrictive cardiomyopathy, although not all patients will have a restrictive diastolic filling pattern. In earlier stages of disease an impaired relaxation pattern may be present before the onset of abnormal compliance. Determination of the severity of diastolic impairment is important not only for diagnostic reasons; it has been demonstrated that the prognosis of patients with restrictive filling patterns have a nearly fivefold higher mortality than the nonrestrictive patterns (27). The classic Doppler pattern of advanced cardiac amyloidosis is as follows: (28) (1) Mitral inflow: large E wave and small A wave; E/A ratio greater than 2; short deceleration time (DT) less than 150 ms; short IVRT less than 60 ms; no significant change in mitral E wave, deceleration time, or IVRT with phases of respiration (2) Pulmonary veins: small S wave; large D wave; Volume 10, Number 4, 2002 CARDIOLOGY IN REVIEW 221
5 S/D ratio less than 0.5; prominent AR (except with atrial systolic failure) width greater than mitral A wave and high amplitude; no significant respiratory variation of D wave (3) Tricuspid inflow: similar to mitral inflow with an increased E/A ratio and short DT; with inspiration, there is further shortening of the DT and minimal change in E/A ratio (4) Hepatic veins: similar to pulmonary vein flow with S/D ratio less than 0.5 and prominent atrial and ventricular reversals; with inspiration and expiration, there is increased prominence of the reversal waves Superior vena cava flows are similar to hepatic vein flows, and right and left heart patterns are concordant in most patients. Other findings include the lack of respiratory variation of the tricuspid regurgitant jet with respiration and the presence of at least mild mitral and tricuspid regurgitation. Doppler tissue imaging and color M-mode flow propagation have provided invaluable information for the differentiation of restrictive cardiomyopathy and constrictive pericarditis. Patients with restrictive cardiomyopathy have an abnormality of both relaxation and compliance, whereas those with constrictive pericarditis generally have normal relaxation and impaired compliance because of pericardial impedance to filling. For this reason, patients with constrictive pericarditis generally have a normal or fast color M-mode vp and a normal or increased Em, differing from patients with restrictive cardiomyopathy (16,18,29). A recent case report demonstrated that an exception to the rule of higher Em velocities with constrictive pericarditis may occur when pericardial calcification and tethering involve the annulus (30). In these cases, Doppler imaging of the apex and strain rate imaging may help confirm constriction. Differential Diagnosis Differentiation of restrictive cardiomyopathy and constrictive pericarditis is essential because of the potential to relieve constrictive pericarditis effectively with surgical pericardial stripping (Table 1). It should be appreciated that certain conditions such as radiation of the heart may cause a mixed disease of constrictive pericarditis and restrictive physiology. Restrictive cardiomyopathy must also be distinguished from other pathologic conditions that cause an increase in wall thickness because of hypertrophy. These diseases are caused by either primary hypertrophy (hypertrophic cardiomyopathy) or secondary hypertrophy (ie, aortic valve disease, hypertension). CONSTRICTIVE PERICARDITIS The majority of contemporary cases of nonidiopathic constrictive pericarditis are caused by previous cardiac surgery, radiation exposure, and chronic pericarditis with a myriad of etiologies (31). With the increasing rates of patients undergoing cardiac surgery, the prevalence of constrictive pericarditis may be increasing. Constrictive pericarditis can be surgically cured with pericardial stripping, with acceptable surgical mortality rates and symptomatic benefits in most patients (31). Therefore, clinicians must consider the diagnosis among patients seeking treatment with symptoms that may be consistent with the condition. The clinical presentation of patients with constrictive pericarditis may be nonspecific and indolent in the early stages. Symptoms may include fatigue or decreased exercise tolerance. In more advanced stages, patients may develop both left and right heart failure, with the latter often predominating. Physical findings in advanced disease reflect the signs of cardiac congestion (32). The hallmarks of physical diagnosis include an elevated jugular venous pressure with a prominent y descent (Friedreich s sign) reflecting the predominance of filling in early diastole. Kussmaul s sign, an inspiratory increase in the jugular venous pressure, may be present but is not specific for constrictive pericarditis (32). Findings specific to constrictive pericarditis include a pericardial knock (occurs after an opening snap and before an S3 in timing) because of cessation in diastolic filling and retraction of the apical impulse in systole. In very advanced cases, patients develop severe right heart failure. In advanced cases, noninvasive diagnostic testing may be supportive of the diagnosis. The electrocardiogram may be low in voltage because of the pericardial encasement. The chest radiograph may show calcification of the pericardium and pleural effusions. Pathophysiology Most conditions that lead to constrictive pericarditis result in inflammation, fibrosis, adhesion, thickening, and calcification of the pericardium. Isolated constrictive pericarditis is characterized by an abnormality in compliance. Ventricular compli- 222 CARDIOLOGY IN REVIEW Diastolic Heart Failure
6 Table 1. Differentiation between restrictive cardiomyopathy and constrictive pericarditis. Evaluation Type Restrictive Cardiomyopathy Constrictive Pericarditis Physical Examination Kussmaul s sign may be present Kussmaul s sign usually present Apical impulse may be prominent Apical impulse usually not palpable S3 (advanced disease), S4 (early disease) Pericardial knock may be present Regurgitant murmurs common Regurgitant murmurs uncommon Parodoxical pulse absent Parodoxical pulse rare Electrocardiography Low voltage (especially in amyloidosis), Low voltage ( 50 percent) pseudoinfarction, left-axis deviation, atrial fibrillation, conduction disturbances common Chest x-ray Absent calcification Calcification sometimes Echocardiography Small LV cavity with large atria 1 wall thickness sometimes present Normal wall thickness (especially thickened interatrial septum in amyloidosis) Thickened cardiac valves (amyloidosis) Pericardial thickening seen Granular sparking texture (amyloidosis) Prominent early diastolic filling with abrupt displacement of interventricular septum Mitral inflow No resp variation of mitral inflow Inspiration 2 mitral inflow E wave, IVRT, E wave, prolonged IVRT E/A ratio 2 Expiration opposite changes Short DT Short DT Diastolic regurgitation Diastolic regurgitation Pulmonary vein Blunted S/D ratio (0.5), prominent & S/D ratio 1 prolonged AR No resp variation D wave Inspiration 2 PV, S and D waves, Expiration opposite changes Tricuspid inflow Mild resp variation of tricuspid inflow E wave Inspiration 1 tricuspid inflow E wave, 1 TR peak velocity E/A ratio 2 Expiration opposite changes TR peak velocity no significant resp change Short DT Short DT with inspiration Diastolic regurgitation Diastolic regurgitation Hepatic vein Blunted S/D ratio, inspiratory 1 reversals Inspiration Minimally 1 HV, S and D Expiration 2 diastolic flow & 1 reversals Inferior vena cava Plethoric Plethoric Color M-mode Slow flow propagation Rapid flow propagation ( 100 cm/s) Mitral annular motion Low velocity early filling ( 8 cm/s) High velocity early filling ( 8 cm/s) Cardiac catheterization Dip and plateau Dip and plateau LVEDP often 5 mmhg greater than RVEDP, RVEDP and LVEDP usually equal but may be identical RV systolic pressure 50 mmhg Inspiration 1 in RV systolic pressure 2 in LV systolic pressure RVEDP one-third of RV systolic pressure Expiration opposite changes Endomyocardial biopsy May reveal specific cause of restrictive cardiomyopathy May be normal or show nonspecific myocyte hypertrophy or myocardial fibrosis CT/MRT Pericardium usually normal Pericardium may be thickened Modified from Kushwaha SS, Fallon JT, Fuster V. N Engl J Med 1997; 336: , with permission in reference 43. ance is impaired because of external interference to diastolic filling from a rigid pericardium. The myocardium is unaffected in isolated constrictive pericarditis; therefore, systolic function and early diastolic filling are normal. Once ventricular diastolic filling reaches the limitations of the pericardial restraint, the pressure and volume in the cavity rise, filling ceases, and congestion occurs (33). Because of the isolated encasement of the pericardium and not the systemic veins or lungs, there is a dissociation between intrathoracic and intracardiac pressures with marked interventricular dependence, respiratory variation, and discordance in right and left heart filling (34). Volume 10, Number 4, 2002 CARDIOLOGY IN REVIEW 223
7 Figure 3. Example of the utility of transesophageal echocardiography and magnetic resonance imaging for demonstrating the location and extent of pericardial thickening and calcification with constrictive pericarditis. Reprinted with permission from Klein AL, et al: Am Heart J 1999;138: Hemodynamic Signs Cardiac catheterization is usually reserved for unclear cases of constrictive pericarditis in which the diagnosis is uncertain. The classic feature of constrictive pericarditis is near equalization of chamber pressures between the left atrium, right atrium, LV and RV in end-diastole (33). Other hemodynamic findings include an elevated right atrial pressure, a pulmonary artery pressure of less than 50 mmhg, and a RV diastolic pressure exceeding one third of the RV systolic pressure (25). Characteristic pressure tracings include the atrial waveform showing the W wave configuration with preserved x and prominent y descent and the simultaneous ventricular pressure waveform showing the dip and plateau configuration (33). Reciprocal changes with respiration can be observed, with the RV systolic pressure increasing with inspiration and the LV pressure decreasing. Echocardiographic Signs An integrated and dedicated echocardiographic examination including 2-dimensional imaging, M-mode, and Doppler are capable of diagnosing the anatomic and pathophysiologic features of constrictive pericarditis in most patients with suspected disease. Two-dimensional Imaging and M-mode The anatomic features of constrictive pericarditis may be recognized by 2-dimensional imaging (35). These include pericardial thickening, calcification, and localized tethering of the atrial or ventricular cavities (Fig. 3). A pericardial effusion may be present. The inferior vena cava is usually dilated (plethoric). The septal bounce is a classic feature of abnormal diastolic septal motion caused by abrupt termination of ventricular filling (35). LV and RV function are usually preserved in isolated cases. M-mode signs such as flattening of the LV free wall after early diastole are less well appreciated (36). Doppler Echocardiography Elucidation of the pathophysiologic features of constrictive pericarditis requires a comprehensive dedicated Doppler examination. The hallmark of the examination is reciprocal respiratory variation of right and left heart flows caused by interventricular dependence (37). Because the heart is encased in a rigid shell, when the right heart fills during inspiration, the left heart filling is restricted by the shift of the septum to the left. The opposite changes occur with expiration. The classic Doppler pattern of constrictive pericarditis is as follows (37 39) (Fig. 4): (1) Mitral inflow 224 CARDIOLOGY IN REVIEW Diastolic Heart Failure
8 Figure 4. Diagram of left (A) and right (B) ventricular inflow velocities and pulmonary (C) and hepatic (D) venous flows during different phases of respiration differentiating constrictive pericarditis and restrictive cardiomyopathy as assessed by echocardiography. Reprinted with permission from Klein AL, Cohen GI: Doppler echocardiographic assessment of constrictive pericarditis, cardiac amyloidosis, and cardiac tamponade. Cleve Clin J Med 1992;59: Inspiration: smaller E wave greater than A wave, longer IVRT and, usually shorter DT Expiration: larger E wave greater than A wave, shorter IVRT and usually longer DT; E wave is typically increased more than 25% with expiration, and the IVRT increased more than 50% with inspiration (2) Pulmonary veins Inspiration: S and D waves near equal in size Expiration: larger S and D waves (3) Tricuspid inflow: same pattern, with reciprocal changes compared with mitral inflow; tricuspid E wave increase is typically more than 40% with inspiration (4) Hepatic vein Inspiration: S greater than D wave, with small AR and ventricular reversals Expiration: S greater than D wave, with smaller or absent D wave and larger AR and ventricular reversals Also described in constrictive pericarditis is an inspiratory increase in the tricuspid regurgitant jet velocity and duration of the signal (40). Superior vena cava flow has been useful to distinguish respiratory changes caused by chronic obstructive lung disease from constrictive pericarditis, with the latter having less significant changes in systolic forward flow during inspiration (41). The Doppler findings of constrictive pericarditis with the hallmark of reciprocal respiratory variation contrast with the typical findings of restrictive cardiomyopathy. Doppler tissue imaging and color M-mode techniques provide more information for distinguishing these disorders. In addition, transesophageal echocardiography may be required for a more optimal Doppler examination and assessment of anatomic features of constriction. Differential Diagnosis There are limitations to the Doppler echocardiography differentiation of constrictive pericarditis and restrictive cardiomyopathy, and special clinical situations should be appreciated. Particular attention must be paid to the loading conditions and respiratory effort when performing a study. A respirometer is used to assess the timing of inspiration and expiration. The first beat after inspiration is measured because it is least likely to be affected by factors affecting the respiratory effort such as chronic obstructive lung disease (34). The optimal examination is performed during a period of euvolemia, possibly requiring saline loading for hypovolemic patients and maneuvers or diuresis for hypervolemic patients (42). Volume 10, Number 4, 2002 CARDIOLOGY IN REVIEW 225
9 The many special situations make interpretation particularly challenging (43). Patients with irregular heart rhythms like atrial fibrillation may require ventricular pacing to equalize the R-R intervals. Conditions such as mixed restriction and constriction and effusive and constrictive states have features of both diseases. Other diseases that exaggerate the rate or force of breathing such as pulmonary embolism, obesity, and chronic obstructive lung disease may cause reciprocal changes in right and left heart flows that must be differentiated from constrictive pericarditis. CARDIAC TAMPONADE Cardiac tamponade is a medical emergency caused by the inability of the heart to fill adequately to maintain cardiac output. Although the causes of pericardial effusions are numerous, in daily practice, most cases occur after cardiac surgery or with malignancy and any cause of acute or chronic pericarditis. Clinicians must be able to recognize and treat cardiac tamponade rapidly. Echocardiography is an essential modality to guide the choice of management. Patients may seek treatment with symptoms of low cardiac output or unheralded hemodynamic collapse. The medical or surgical history of the patient should provide ample clues to the potential for this event, because many events occur in patients after procedures or with known effusions. The bedside diagnosis of cardiac tamponade should be considered in a patient with elevated jugular veins, quiet heart sounds, tachycardia, and hypotension. The hallmark of the jugular venous waveform is the loss of the y descent with a maintained x descent (33). A pulsus paradoxus may be present but is not specific for cardiac tamponade and may be absent in many disorders in which the LV or RV diastolic pressure is high or there is decompression of respiratory changes in pressures, as with an atrial septal defect (44). Other supportive noninvasive tests include an electrocardiogram with low voltage and electrical alternans, and a chest radiograph with cardiomegaly. Pathophysiology A small volume of fluid is present in a normal pericardial sac. When fluid accumulates because of injury inflammation or hemorrhage, the intrapericardial volume and pressure rise proportionally with the compliance of the pericardial lining and the intracardiac pressures. When intrapericardial pressure exceeds intracardiac pressure, there is interference of diastolic filling and subsequent decreased cardiac output (44). With inspiration, intrathoracic pressure and pulmonary capillary wedge pressure decrease, whereas intracardiac pressure is unchanged because of the pericardial effusion. A decrease in gradient between the pulmonary veins and LV results in a decreased mitral inflow E wave with inspiration and an increase in tricuspid E-wave flow (45). Reciprocal changes occur during expiration. Because the cardiac chambers are in a finite space within the pericardium, there is equalization of pressures in all cardiac chambers. Hemodynamic Signs Right heart catheterization is an important tool to diagnose cardiac tamponade, particularly in patients in the intensive care unit setting, where physical diagnosis and echocardiography may have limitations. The typical hemodynamic signs include elevation of the central venous pressure with a prominent x descent and loss of the y descent and near equalization of right atrial, RV end-diastolic, pulmonary capillary wedge, and LV diastolic pressures (33). Tachycardia, a decreased stroke volume, cardiac output, and hypotension with a pulsus paradoxus may be present. Echocardiographic Signs In most patients with adequate image quality, echocardiography can rapidly and accurately make the diagnosis of cardiac tamponade. Causes of hemodynamic compromise other than cardiac tamponade may be excluded. The decision can also be made to evacuate the fluid via pericardiocentesis or surgery. An integrated echocardiographic study incorporating 2-dimensional imaging and Doppler must be performed to assess the presence of a pericardial effusion and the pathophysiologic consequences. In the intensive care unit setting, a transesophageal echocardiogram may be required if transthoracic imaging is suboptimal. Two-dimensional Imaging and M-mode A pericardial effusion is present in almost all cases of cardiac tamponade. Most pericardial effusions appear as an echocardiography-free space that is localized or circumferential, free-flowing or organized. Scanning in and out of the plane may be required to separate the visceral and parietal pericardium in order to distinguish a pericar- 226 CARDIOLOGY IN REVIEW Diastolic Heart Failure
10 dial effusion from a pleural effusion. Another clue is the presence of fluid anterior to the descending aorta in the parasternal view. Even small effusions can cause tamponade, depending on their location and rate of accumulation. Cardiac chamber collapse is a critical feature of cardiac tamponade. The chambers with the lowest intracardiac pressure are most likely to be compressed. Right atrial collapse is the earliest sign of tamponade, occurring toward the end of ventricular end-diastole and extending into ventricular systole. Because the right atrium may often invert even in normal hearts with low right atrial pressure, the specificity of right atrial collapse may be low (46). Extension of collapse greater than 1/3 of the cardiac cycle increases the sensitivity of this finding to more than 90% (46). Although RV diastolic collapse is generally a more specific indicator of tamponade, the sensitivity can be reduced because of conditions that increase RV pressure (47). Left atrial and LV collapse are unusual and are observed generally with massive effusions or, in the case of left atrial collapse, loculated effusions. A plethoric inferior vena cava (dilated with failure to collapse by more than 50%) is a highly sensitive sign of cardiac tamponade. This finding confirms high right atrial pressure, invariable with few exceptions in cardiac tamponade (48). Doppler Echocardiography The Doppler examination confirms the pathophysiologic hemodynamic aberrations that occur during cardiac tamponade. The classic Doppler pattern of cardiac tamponade is as follows: (37,45) (1) Mitral inflow: for inspiration, E wave decreases and IVRT increases by more than 30% compared with expiration (2) Tricuspid inflow: for inspiration, E wave increases more than 70% compared with expiration (3) Pulmonary vein: for inspiration, D wave decreases compared with expiration (4) Hepatic vein: for inspiration, S is greater than D; for expiration, an absent or very diminished D wave with prominent reversals Differential Diagnosis Aside from the differentiation of pericardial from pleural effusions, other echocardiographyfree spaces around the pericardium must be recognized. These include pericardial fat pads (more often anterior and echocardiography-dense), vascular structures (descending aorta, pseudoaneurysm, coronary sinus), other pericardial structures (cysts found in right cardiophrenic angle, hematoma, or tumor), and noncardiac structures (hiatal hernia) (49). In many situations, an incorrect diagnosis of cardiac tamponade is made based on the presence of confounding factors that affect respiratory variation or chamber collapse (50). Clinical history and other echocardiographic findings are important in differentiating these conditions. Conclusion The clinical presentation of restrictive cardiomyopathy, constrictive pericarditis, and cardiac tamponade may vary vastly from chronic nonspecific symptoms to acute hemodynamic deterioration. As diseases of diastolic dysfunction, there are common hemodynamic and echocardiographic features of these diseases. A comprehensive echocardiographic evaluation includes twodimensional imaging and pulsed Doppler with a respirometer. Color M-mode and Doppler tissue imaging should be performed. Volume loading maneuvers or transesophageal echocardiography may also be required. Together, these techniques help to distinguish anatomic and pathophysiologic findings specific to each process and provide the basis for clinical decisions regarding management. REFERENCES 1. European Study Group on Diastolic Heart Failure: How to diagnose diastolic heart failure. Eur Heart J 1998;19: A diagnostic criterion for diastolic heart failure is proposed. 2. Vasan RS, Benjamin EJ, Levy D: Prevalence, clinical features and prognosis of diastolic heart failure: An epidemiologic perspective. J Am Coll Cardiol 1995;26: Summary of studies of patients with congestive heart failure determining the prevalence of normal systolic function. 3. Grossman W: Diastolic dysfunction in congestive heart failure. N Engl J Med 1991;325: Review of conditions and mechanisms of diseases associated with diastolic heart failure. 4. Stauffer JC, Gaasch WH: Recognition and treatment of left ventricular diastolic dysfunction. Prog Cardiovasc Dis 1990;32: Description of pathophysiologic factors responsible for increased chamber stiffness and impaired relaxation leading to increased diastolic pressures and diastolic dysfunction. 5. Little WC, Downes TR: Clinical evaluation of left ventricular diastolic performance. Prog Cardiovasc Dis 1990;32: Review of the phases and determinants of diastolic function. Volume 10, Number 4, 2002 CARDIOLOGY IN REVIEW 227
11 6. Gaasch WH, Blaustein AS, LeWinter MM: Heart failure and clinical disorders of left ventricular diastolic function. In Gaasch W, LeWinter M, eds: Left Ventricular Diastolic Dysfunction and Heart Failure. Lea & Febiger, Philadelphia, 1994: Review of nonmyocardial determinants of diastolic dysfunction. 7. Scalia GM, Greenberg NL, McCarthy PM, et al: Noninvasive assessment of the ventricular relaxation time constant ( ) in humans by Doppler echocardiography. Circulation 1997;95: Validation of a noninvasive measurement of in humans as assessed by Doppler echocardiography. 8. Thomas JD, Weyman AE: Echocardiographic Doppler evaluation of left ventricular diastolic function: Physics and physiology. Circulation 1991;84: Detailed evaluation of the physical principles affecting diastolic function. 9. Matsuda Y, Toma Y, Ogawa H, et al: Importance of left atrial function in patients with myocardial infarction. Circulation 1983;67: Study of left atrial function after myocardial infarction using pressurevolume loops to show the correlation between left atrial work and LV ejection fraction. 10. Cohen GI, Pietrolungo JF, Thomas JD, et al: A practical guide to assessment of ventricular diastolic function using Doppler echocardiography. J Am Coll Cardiol 1996;27: Practical correlation among clinical examination, physiology, and Doppler study. 11. Appleton CP, Galloway JM, Gonzalez MS, et al: Estimation of left ventricular filling pressures using two-dimensional and Doppler echocardiography in adult patients with cardiac disease: Additional value of analyzing left atrial size, left atrial ejection fraction and the difference in duration of pulmonary venous and mitral flow velocity at atrial contraction. J Am Coll Cardiol 1993;22: Correlation of LV filling pressures with Doppler mitral and pulmonary vein patterns and left atrial size and volumes. 12. Rossvoll O, Hatle LK: Pulmonary venous flow velocities recorded by transthoracic Doppler ultrasound: Relation to left ventricular diastolic pressures. J Am Coll Cardiol 1993;21: Correlation of pulmonary venous flow reversal duration greater than mitral a wave duration with LV end-diastolic pressure greater than 15 mmhg. 13. Pozzoli M, Traversi E, Cioffi G, et al: Loading manipulations improve the prognostic value of Doppler evaluation of mitral flow in patients with chronic heart failure. Circulation 1997;95: Demonstration of the additive importance of determining reversibility of restrictive flow patterns in assessing prognosis. 14. Appleton CP, Jensen JL, Hatle LK, et al: Doppler evaluation of left and right ventricular diastolic function: A technical guide for obtaining optimal flow velocity recordings. J Am Soc Echocardiogr 1997;10: Technical guide reviewing performance and pitfalls of a comprehensive diastolic examination by Doppler echocardiography. 15. Nishimura RA, Tajik AJ: Evaluation of diastolic filling of left ventricle in health and disease: Doppler echocardiography is the clinician s Rosetta stone. J Am Coll Cardiol 1997;30:8 18. A grading system for diastolic dysfunction is proposed in this review. 16. Garcia MJ, Thomas JD, Klein AL: New Doppler echocardiographic applications for the study of diastolic function. J Am Coll Cardiol 1998;32: Review of the additive information to the diastolic function examination provided by color M-mode and Doppler tissue imaging. 17. Garcia MJ, Ares MA, Asher C, et al: An index of early left ventricular filling that combined with pulsed Doppler peak E velocity may estimate capillary wedge pressure. J Am Coll Cardiol 1997;29: Regression equation derived from color M-mode and mitral e-wave velocity that estimates pulmonary capillary wedge pressure. 18. Garcia MJ, Rodriguez L, Ares MA, et al: Differentiation of constrictive pericarditis from restrictive cardiomyopathy: Assessment of left ventricular diastolic velocities in longitudinal axis by Doppler tissue imaging. J Am Coll Cardiol 1996;27: Study illustrating the importance of E annular velocity to distinguish between constrictive pericarditis and restrictive cardiomyopathy. 19. Urheim S, Edvardsen T, Torp H, et al: Myocardial strain by Doppler echocardiography: Validation of a new method to quantify regional myocardial function. Circulation 2000; 102: Experimental study in dogs with hemodynamic validation of Doppler echocardiography determination of strain rate. 20. Richardson P, McKenna W, Bristow M, et al: Report of the 1995 World Health Organization/International Society and Federation of Cardiology Task Force on the Definition and Classification of Cardiomyopathies. Circulation 1996;93: Update of the 1980 report with revised definitions of cardiomyopathies. 21. Kushwaha SS, Fallon JT, Fuster V: Restrictive cardiomyopathy. N Engl J Med 1997;336: Review on restrictive cardiomyopathies with classification based on etiology. 22. Child JS, Perloff JK: The restrictive cardiomyopathies. Cardiol Clin 1988;6: Review of clinical manifestations of restrictive cardiomyopathies. 23. Benotti JR, Grossman W, Cohn PF: Clinical profile of restrictive cardiomyopathy. Circulation 1980;61: Early study reviewing the clinical manifestations of a small group of patients with restrictive cardiomyopathies. 24. Carroll JD, Gaasch WH, McAdam KP: Amyloid cardiomyopathy: Characterization by a distinctive voltage/mass relation. Am J Cardiol 1982;49:9 13. Demonstration of the low voltage/high mass relationship in amyloidosis. 25. Vaitkus PT, Kussmaul WG: Constrictive pericarditis versus restrictive cardiomyopathy: A reappraisal and update of diagnostic criteria. Am Heart J 1991;122: Review of the diagnostic accuracy of hemodynamic findings in the cardiac catheterization laboratory. 26. Klein AL, Oh JK, Miller FA, et al: Two-dimensional and Doppler echocardiographic assessment of infiltrative cardiomyopathy. J Am Soc Echocardiogr 1988;1: Description of the typical features of amyloidosis as seen on echocardiogram. 27. Klein AL, Hatle LK, Taliercio CP, et al: Prognostic significance of Doppler measures of diastolic function in cardiac amyloidosis: A Doppler echocardiography study. Circulation 1991;83: Patients with mitral E-wave deceleration time less than 150 msec had a significantly reduced survival compared with those with time greater than 150 msec. 28. Klein AL, Hatle LK, Burstow DJ, et al: Doppler characterization of left ventricular diastolic function in cardiac amyloidosis. J Am Coll Cardiol 1989;13: CARDIOLOGY IN REVIEW Diastolic Heart Failure
12 Spectrum of diastolic filling abnormalities associated with amyloidosis that include early forms without restrictive physiology. 29. Rajagopalan N, Garcia MJ, Rodriguez L, et al: Comparison of new Doppler echocardiographic methods to differentiate constrictive pericardial heart disease and restrictive cardiomyopathy. Am J Cardiol 2001;87: A color M-mode flow propagation slope greater than 100 cm/s was an accurate method for predicting constrictive pericarditis. 30. Arnold MF, Voight JU, Kukulski T, et al: Does atrioventricular ring motion always distinguish constriction from restriction? A Doppler myocardial imaging study. J Am Soc Echocardiogr 2001;14: Case report of 2 patients with constriction in whom Doppler tissue annular motion was inconsistent with the diagnosis. 31. Ling LH, Oh JK, Schaff HV, et al: Constrictive pericarditis in the modern era: Evolving clinical spectrum and impact on outcome after pericardiectomy. Circulation 1999;100: Contemporary evaluation of the causes and outcomes of patients undergoing pericardiectomy. 32. Myers RB, Spodick DH: Constrictive pericarditis: Clinical and pathophysiologic characteristics. Am Heart J 1999; 138: Comprehensive review of studies characterizing features and pathophysiology of constrictive pericarditis. 33. Shabetai R, Fowler NO, Guntheroth WG: The hemodynamics of cardiac tamponade and constrictive pericarditis. Am J Cardiol 1970;26: Review of the atrial and ventricular hemodynamic findings associated with pericardial diseases. 34. Hatle LK, Appleton CP, Popp RL: Differentiation of constrictive pericarditis and restrictive cardiomyopathy by Doppler echocardiography. Circulation 1989;79: Echocardiography study demonstrating the importance of respiratory variation as a pathophysiologic hallmark of constrictive pericarditis. 35. Himelman RB, Lee E, Schiller NB: Septal bounce, vena cava plethora, and pericardial adhesion: Informative twodimensional echocardiographic signs in the diagnosis of pericardial constriction. J Am Soc Echocardiogr 1988;1: Accuracy of 2-dimensional echocardiographic criteria for constrictive pericarditis is evaluated. 36. Voelkel AG, Pietro DA, Folland ED, et al: Echocardiographic features of constrictive pericarditis. Circulation 1978;58: Flattening of the LV endocardium was the most consistent M-mode finding of constrictive pericarditis. 37. Klein AL, Cohen GI: Doppler echocardiographic assessment of constrictive pericarditis, cardiac amyloidosis, and cardiac tamponade. Cleve Clin J Med 1992;59: Well illustrated review of the Doppler patterns characteristic of constrictive and restrictive cardiomyopathies. 38. Klein AL, Cohen GI, Pietrolungo JF, et al: Differentiation of constrictive pericarditis from restrictive cardiomyopathy by Doppler transesophageal echocardiographic measurements of respiratory variations in pulmonary venous flow. J Am Coll Cardiol 1993;22: Transesophageal echocardiography study determining the respiratory variation of mitral inflow and pulmonary venous flow consistent with constrictive pericarditis. 39. Oh JK, Hatle LK, Seward JB, et al: Diagnostic role of Doppler echocardiography in constrictive pericarditis. J Am Coll Cardiol 1994;23: Demonstration of the accuracy of a comprehensive diastology examination for diagnosis of constrictive pericarditis. 40. Klodas E, Nishimura RA, Appleton CP, et al: Doppler evaluation of patients with constrictive pericarditis: Use of tricuspid regurgitation velocity curves to determine enhanced ventricular interaction. J Am Coll Cardiol 1996;28: Description of another useful diagnostic criterion for constrictive pericarditis. 41. Boonyaratavej S, Oh JK, Tajik AJ, et al: Comparison of mitral inflow and superior vena cava Doppler velocities in chronic obstructive pulmonary disease and constrictive pericarditis. J Am Coll Cardiol 1998;32: Description of the marked inspiratory change in superior vena cava systolic flow velocity found with chronic obstructive lung disease but not with constrictive pericarditis. 42. Oh JK, Tajik AJ, Appleton CP, et al: Preload reduction to unmask the characteristic Doppler features of constrictive pericarditis: A new observation. Circulation 1997;95: Report of a group of patients with constrictive pericarditis who did not exhibit typical respiratory variation until maneuvers to reduce preload were performed. 43. Klein AL, Asher CR: Diseases of the pericardium, restrictive cardiomyopathy and diastolic dysfunction. In Topol EJ, ed: Textbook of Cardiovascular Medicine, edn 2. Lippincott-Raven Publishers, Philadelphia 2002, Comprehensive discussion of constrictive pericarditis with attention to difficult diagnostic situations. 44. Spodick DH: The normal and diseased pericardium: Current concepts of pericardial physiology, diagnosis and treatment. J Am Coll Cardiol 1983;1: Description of the normal physiology of the pericardium and pathogenesis of constrictive pericarditis and cardiac tamponade. 45. Appleton CP, Hatle LK, Popp RL: Cardiac tamponade and pericardial effusion: Respiratory variation in transvalvular flow velocities studied by Doppler echocardiography. J Am Coll Cardiol 1988;11: Study demonstrating the typical Doppler pattern of cardiac tamponade with reciprocal respiratory variation. 46. Gillam LA, Guyer DE, Gibson TC, et al: Hydrodynamic compression of the right atrium: A new echocardiographic sign of cardiac tamponade. Circulation 1983;68: Prolonged right atrial inversion greater than 0.34 of the cardiac cycle was a highly accurate diagnostic criterion for cardiac tamponade. 47. Singh S, Wann LS, Schuchard GH, et al: Right ventricular and right atrial collapse in patients with cardiac tamponade: A combined echocardiographic and hemodynamic study. Circulation 1984;70: Assessment of echocardiographic and hemodynamic findings related to chamber collapse with cardiac tamponade. 48. Himelman RB, Kircher B, Rockey DC, et al: Inferior vena cava plethora with blunted respiratory response: A sensitive echocardiographic sign of cardiac tamponade. J Am Coll Cardiol 1988;12: Dilated inferior vena cava with failure to collapse by more than 50% is found to be among the most sensitive findings of cardiac tamponade. 49. Spodick DH: Staying up-to-date on pericardial disease. Patient Care October 2000;15: Review of important pearls regarding the evaluation of pericardial disease. 50. Maxted WC, Segar DS: The utility of echocardiography in cardiac tamponade. ACC Curr J Rev 1997;6: Good comparative review of studies testing the utility of echocardiography for assessment of cardiac tamponade. Volume 10, Number 4, 2002 CARDIOLOGY IN REVIEW 229
Section Four: Pulmonary Artery Waveform Interpretation
 Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
Section Four: Pulmonary Artery Waveform Interpretation All hemodynamic pressures and waveforms are generated by pressure changes in the heart caused by myocardial contraction (systole) and relaxation/filling
RACE I Rapid Assessment by Cardiac Echo. Intensive Care Training Program Radboud University Medical Centre NIjmegen
 RACE I Rapid Assessment by Cardiac Echo Intensive Care Training Program Radboud University Medical Centre NIjmegen RACE Goal-directed study with specific questions Excludes Doppler ultrasound Perform 50
RACE I Rapid Assessment by Cardiac Echo Intensive Care Training Program Radboud University Medical Centre NIjmegen RACE Goal-directed study with specific questions Excludes Doppler ultrasound Perform 50
Traumatic Cardiac Tamponade. Shane KF Seal 19 November 2003 POS
 Traumatic Cardiac Tamponade Shane KF Seal 19 November 2003 POS Objectives Definition Pathophysiology Diagnosis Treatment Cardiac Tamponade The decompensated phase of cardiac compression resulting from
Traumatic Cardiac Tamponade Shane KF Seal 19 November 2003 POS Objectives Definition Pathophysiology Diagnosis Treatment Cardiac Tamponade The decompensated phase of cardiac compression resulting from
Exchange solutes and water with cells of the body
 Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
Chapter 8 Heart and Blood Vessels Three Types of Blood Vessels Transport Blood Arteries Carry blood away from the heart Transport blood under high pressure Capillaries Exchange solutes and water with cells
CONSTRICTIVE PERICARDITIS
 33 Profiles in Constrictive Pericarditis, Restrictive Cardiomyopathy, and Cardiac Tamponade Beverly H. Lorell and William Grossman BHL: Harvard Medical School, Hemodynamic and Molecular Physiology Research
33 Profiles in Constrictive Pericarditis, Restrictive Cardiomyopathy, and Cardiac Tamponade Beverly H. Lorell and William Grossman BHL: Harvard Medical School, Hemodynamic and Molecular Physiology Research
ECHOCARDIOGRAPHY PROPERTY OF ELSEVIER SAMPLE CONTENT - NOT FINAL CHAPTER 6. Hisham Dokainish, MD, FACC, FASE
 CHAPTER 6 ECHOCARDIOGRAPHY Hisham Dokainish, MD, FACC, FASE 1. How does echocardiography work? Echocardiography uses transthoracic and transesohageal probes that emit ultrasound directed at cardiac structures.
CHAPTER 6 ECHOCARDIOGRAPHY Hisham Dokainish, MD, FACC, FASE 1. How does echocardiography work? Echocardiography uses transthoracic and transesohageal probes that emit ultrasound directed at cardiac structures.
The pulse Tamás Fenyvesi
 The pulse Tamás Fenyvesi FT 3rd Dept.Med 1 The pulse has been studied for centuries Informations gained: 1. frequency, regularity 2. patency of peripheral arteries 3. characteristics of the arterial pressure
The pulse Tamás Fenyvesi FT 3rd Dept.Med 1 The pulse has been studied for centuries Informations gained: 1. frequency, regularity 2. patency of peripheral arteries 3. characteristics of the arterial pressure
Note: The left and right sides of the heart must pump exactly the same volume of blood when averaged over a period of time
 page 1 HEART AS A PUMP A. Functional Anatomy of the Heart 1. Two pumps, arranged in series a. right heart: receives blood from the systemic circulation (via the great veins and vena cava) and pumps blood
page 1 HEART AS A PUMP A. Functional Anatomy of the Heart 1. Two pumps, arranged in series a. right heart: receives blood from the systemic circulation (via the great veins and vena cava) and pumps blood
Practical class 3 THE HEART
 Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
Practical class 3 THE HEART OBJECTIVES By the time you have completed this assignment and any necessary further reading or study you should be able to:- 1. Describe the fibrous pericardium and serous pericardium,
Congestive heart failure (CHF) is a. Diastolic Heart Failure. By Michel D Astous, MD, FRCPC
 Diastolic Heart Failure The evaluation of both systolic and diastolic functions is of great importance among patients presenting with signs of CHF, as the treatment may be quite different depending on
Diastolic Heart Failure The evaluation of both systolic and diastolic functions is of great importance among patients presenting with signs of CHF, as the treatment may be quite different depending on
Auscultation of the Heart
 Review of Clinical Signs uscultation of the Heart Series Editor: Bernard Karnath, MD Bernard Karnath, MD William Thornton, MD uscultation of the heart can provide clues to the diagnosis of many cardiac
Review of Clinical Signs uscultation of the Heart Series Editor: Bernard Karnath, MD Bernard Karnath, MD William Thornton, MD uscultation of the heart can provide clues to the diagnosis of many cardiac
Cardiac Masses and Tumors
 Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
The P Wave: Indicator of Atrial Enlargement
 Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 8-12-2010 The P Wave: Indicator of Atrial Enlargement Patrick Loftis
Heart and Vascular System Practice Questions
 Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
Heart and Vascular System Practice Questions Student: 1. The pulmonary veins are unusual as veins because they are transporting. A. oxygenated blood B. de-oxygenated blood C. high fat blood D. nutrient-rich
FVMA 2015: Diagnosis and Management of Pericardial Disease PERICARDIAL EFFUSION Pathophysiology of Cardiac Tamponade
 FVMA 2015: Diagnosis and Management of Pericardial Disease Jonathan A. Abbott, DVM, Dipl. ACVIM (Cardiology) VA-MD College of Veterinary Medicine Virginia Tech, Blacksburg, Virginia Pericardial disease
FVMA 2015: Diagnosis and Management of Pericardial Disease Jonathan A. Abbott, DVM, Dipl. ACVIM (Cardiology) VA-MD College of Veterinary Medicine Virginia Tech, Blacksburg, Virginia Pericardial disease
Pericardium. Pericardial Diseases. Function of Pericardium 10/1/2012
 NO LASIX, PLEASE! PERICARDIAL DISEASE IN THE DOG Pericardium Michael Luethy, DVM Diplomate ACVIM Cardiology September 13 th, 2012 Tough, outer, parietal pericardium Delicate, serous, visceral pericardium
NO LASIX, PLEASE! PERICARDIAL DISEASE IN THE DOG Pericardium Michael Luethy, DVM Diplomate ACVIM Cardiology September 13 th, 2012 Tough, outer, parietal pericardium Delicate, serous, visceral pericardium
How To Understand What You Know
 Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Heart Disorders Glossary ABG (Arterial Blood Gas) Test: A test that measures how much oxygen and carbon dioxide are in the blood. Anemia: A condition in which there are low levels of red blood cells in
Normal & Abnormal Intracardiac. Lancashire & South Cumbria Cardiac Network
 Normal & Abnormal Intracardiac Pressures Lancashire & South Cumbria Cardiac Network Principle Pressures recorded from catheter tip Electrical transducer - wheatstone bridge mechanical to electrical waveform
Normal & Abnormal Intracardiac Pressures Lancashire & South Cumbria Cardiac Network Principle Pressures recorded from catheter tip Electrical transducer - wheatstone bridge mechanical to electrical waveform
Cardiovascular diseases. pathology
 Cardiovascular diseases pathology Atherosclerosis Vascular diseases A disease that results in arterial wall thickens as a result of build- up of fatty materials such cholesterol, resulting in acute and
Cardiovascular diseases pathology Atherosclerosis Vascular diseases A disease that results in arterial wall thickens as a result of build- up of fatty materials such cholesterol, resulting in acute and
Echocardiographic Evaluation of Pericardial Disease
 Echocardiographic Evaluation of Pericardial Disease Edwin G. Avery, IV, M.D. Chief, Division of Cardiac Anesthesia University Hospitals Case Medical Center Associate Professor of Anesthesiology Case Western
Echocardiographic Evaluation of Pericardial Disease Edwin G. Avery, IV, M.D. Chief, Division of Cardiac Anesthesia University Hospitals Case Medical Center Associate Professor of Anesthesiology Case Western
GERIATRYCZNE PROBLEMY KLINICZNE/GERIATRICS MEDICAL PROBLEMS
 65 G E R I A T R I A 2011; 5: 65-69 GERIATRYCZNE PROBLEMY KLINICZNE/GERIATRICS MEDICAL PROBLEMS Otrzymano/Submitted: 24.02.2011 Poprawiono/Corrected: 01.03.2011 Zaakceptowano/Accepted: 06.03.2011 Akademia
65 G E R I A T R I A 2011; 5: 65-69 GERIATRYCZNE PROBLEMY KLINICZNE/GERIATRICS MEDICAL PROBLEMS Otrzymano/Submitted: 24.02.2011 Poprawiono/Corrected: 01.03.2011 Zaakceptowano/Accepted: 06.03.2011 Akademia
HEART HEALTH WEEK 3 SUPPLEMENT. A Beginner s Guide to Cardiovascular Disease HEART FAILURE. Relatively mild, symptoms with intense exercise
 WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
WEEK 3 SUPPLEMENT HEART HEALTH A Beginner s Guide to Cardiovascular Disease HEART FAILURE Heart failure can be defined as the failing (insufficiency) of the heart as a mechanical pump due to either acute
Recommendations for the Evaluation of Left Ventricular Diastolic Function by Echocardiography
 GUIDELINES AND STANDARDS Recommendations for the Evaluation of Left Ventricular Diastolic Function by Echocardiography Sherif F. Nagueh, MD, Chair, Christopher P. Appleton, MD, Thierry C. Gillebert, MD,*
GUIDELINES AND STANDARDS Recommendations for the Evaluation of Left Ventricular Diastolic Function by Echocardiography Sherif F. Nagueh, MD, Chair, Christopher P. Appleton, MD, Thierry C. Gillebert, MD,*
Real-Time 3-Dimensional Transesophageal Echocardiography in the Evaluation of Post-Operative Mitral Annuloplasty Ring and Prosthetic Valve Dehiscence
 Journal of the American College of Cardiology Vol. 53, No. 17, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.12.059
Journal of the American College of Cardiology Vol. 53, No. 17, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.12.059
Introduction to CV Pathophysiology. Introduction to Cardiovascular Pathophysiology
 Introduction to CV Pathophysiology Munther K. Homoud, MD Tufts-New England Medical Center Spring 2008 Introduction to Cardiovascular Pathophysiology 1. Basic Anatomy 2. Excitation Contraction Coupling
Introduction to CV Pathophysiology Munther K. Homoud, MD Tufts-New England Medical Center Spring 2008 Introduction to Cardiovascular Pathophysiology 1. Basic Anatomy 2. Excitation Contraction Coupling
Normal Intracardiac Pressures. Lancashire & South Cumbria Cardiac Network
 Normal Intracardiac Pressures Lancashire & South Cumbria Cardiac Network Principle Pressures recorded from catheter tip Electrical transducer - wheatstone bridge mechanical to electrical waveform display
Normal Intracardiac Pressures Lancashire & South Cumbria Cardiac Network Principle Pressures recorded from catheter tip Electrical transducer - wheatstone bridge mechanical to electrical waveform display
CMEArticle ECGs with small QRS voltages
 Singapore Med J 2012; 53(5) : 299 CMEArticle ECGs with small QRS voltages Ting Ting Low 1, MBBS, MRCP, Voon Shiong Ronnie Tan 1, MBBS, Swee-Guan Teo 1, MBBS, MRCP, Kian-Keong Poh 1,2, FRCP, FACC Fig. 1
Singapore Med J 2012; 53(5) : 299 CMEArticle ECGs with small QRS voltages Ting Ting Low 1, MBBS, MRCP, Voon Shiong Ronnie Tan 1, MBBS, Swee-Guan Teo 1, MBBS, MRCP, Kian-Keong Poh 1,2, FRCP, FACC Fig. 1
Edwards FloTrac Sensor & Edwards Vigileo Monitor. Understanding Stroke Volume Variation and Its Clinical Application
 Edwards FloTrac Sensor & Edwards Vigileo Monitor Understanding Stroke Volume Variation and Its Clinical Application 1 Topics System Configuration Pulsus Paradoxes Reversed Pulsus Paradoxus What is Stroke
Edwards FloTrac Sensor & Edwards Vigileo Monitor Understanding Stroke Volume Variation and Its Clinical Application 1 Topics System Configuration Pulsus Paradoxes Reversed Pulsus Paradoxus What is Stroke
1 Congestive Heart Failure & its Pharmacological Management
 Harvard-MIT Division of Health Sciences and Technology HST.151: Principles of Pharmocology Instructor: Prof. Keith Baker 1 Congestive Heart Failure & its Pharmacological Management Keith Baker, M.D., Ph.D.
Harvard-MIT Division of Health Sciences and Technology HST.151: Principles of Pharmocology Instructor: Prof. Keith Baker 1 Congestive Heart Failure & its Pharmacological Management Keith Baker, M.D., Ph.D.
Cardiology Fellowship Manual. Goals & Objectives -Cardiac Imaging- 1 Page
 Cardiology Fellowship Manual Goals & Objectives -Cardiac Imaging- 1 Page 2015-2016 UNIV. OF NEBRASKA CHILDREN S HOSPITAL & MEDICAL CENTER DIVISION OF CARDIOLOGY FELLOWSHIP PROGRAM CARDIAC IMAGING ROTATION
Cardiology Fellowship Manual Goals & Objectives -Cardiac Imaging- 1 Page 2015-2016 UNIV. OF NEBRASKA CHILDREN S HOSPITAL & MEDICAL CENTER DIVISION OF CARDIOLOGY FELLOWSHIP PROGRAM CARDIAC IMAGING ROTATION
HYPERTROPHIC CARDIOMYOPATHY
 HYPERTROPHIC CARDIOMYOPATHY Most often diagnosed during infancy or adolescence, hypertrophic cardiomyopathy (HCM) is the second most common form of heart muscle disease, is usually genetically transmitted,
HYPERTROPHIC CARDIOMYOPATHY Most often diagnosed during infancy or adolescence, hypertrophic cardiomyopathy (HCM) is the second most common form of heart muscle disease, is usually genetically transmitted,
Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School
 Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School This guide is for middle and high school students participating in AIMS Anatomy of the Human Heart and
Distance Learning Program Anatomy of the Human Heart/Pig Heart Dissection Middle School/ High School This guide is for middle and high school students participating in AIMS Anatomy of the Human Heart and
Electrocardiography I Laboratory
 Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Heart Murmurs. Outline. Basic Pathophysiology
 Heart Murmurs David Leder Outline I. Basic Pathophysiology II. Describing murmurs III. Systolic murmurs IV. Diastolic murmurs V. Continuous murmurs VI. Summary Basic Pathophysiology Murmurs = Math Q =
Heart Murmurs David Leder Outline I. Basic Pathophysiology II. Describing murmurs III. Systolic murmurs IV. Diastolic murmurs V. Continuous murmurs VI. Summary Basic Pathophysiology Murmurs = Math Q =
Diagnostic and Therapeutic Procedures
 Diagnostic and Therapeutic Procedures Diagnostic and therapeutic cardiovascular s are central to the evaluation and management of patients with cardiovascular disease. Consistent with the other sections,
Diagnostic and Therapeutic Procedures Diagnostic and therapeutic cardiovascular s are central to the evaluation and management of patients with cardiovascular disease. Consistent with the other sections,
Chapter 20: The Cardiovascular System: The Heart
 Chapter 20: The Cardiovascular System: The Heart Chapter Objectives ANATOMY OF THE HEART 1. Describe the location and orientation of the heart within the thorax and mediastinal cavity. 2. Describe the
Chapter 20: The Cardiovascular System: The Heart Chapter Objectives ANATOMY OF THE HEART 1. Describe the location and orientation of the heart within the thorax and mediastinal cavity. 2. Describe the
The heart then repolarises (or refills) in time for the next stimulus and contraction.
 Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Atrial Fibrillation BRIEFLY, HOW DOES THE HEART PUMP? The heart has four chambers. The upper chambers are called atria. One chamber is called an atrium, and the lower chambers are called ventricles. In
Valve Disease and Diastology Summit
 Heart & Vascular Institute Valve Disease and Diastology Summit is offered in cooperation with the American Society of Echocardiography. Valve Disease and Diastology Summit March 4 6, 2016 Eden Roc Hotel
Heart & Vascular Institute Valve Disease and Diastology Summit is offered in cooperation with the American Society of Echocardiography. Valve Disease and Diastology Summit March 4 6, 2016 Eden Roc Hotel
Mr GH: Pericardial Window. Anaesthetic Management of Cardiac Tamponade
 Mr GH: Pericardial Window Anaesthetic Management of Cardiac Tamponade Mr GH 56 yo M HOPCx Asbestosis, adenoca R lung 8/52 6/52 cisplatin/ taxol chemo Weekly pleural taps for effusions Sent from Bendigo
Mr GH: Pericardial Window Anaesthetic Management of Cardiac Tamponade Mr GH 56 yo M HOPCx Asbestosis, adenoca R lung 8/52 6/52 cisplatin/ taxol chemo Weekly pleural taps for effusions Sent from Bendigo
Workshop B: Essentials of Neonatal Cardiology and CHD Anthony C. Chang, MD, MBA, MPH CARDIAC INTENSIVE CARE
 SHUNT LESIONS NEONATAL : CONGENITAL CARDIAC MALFORMATIONS AND CARDIAC SURGERY ANTHONY C. CHANG, MD, MBA, MPH CHILDREN S HOSPITAL OF ORANGE COUNTY ATRIAL SEPTAL DEFECT LEFT TO RIGHT SHUNT INCREASED PULMONARY
SHUNT LESIONS NEONATAL : CONGENITAL CARDIAC MALFORMATIONS AND CARDIAC SURGERY ANTHONY C. CHANG, MD, MBA, MPH CHILDREN S HOSPITAL OF ORANGE COUNTY ATRIAL SEPTAL DEFECT LEFT TO RIGHT SHUNT INCREASED PULMONARY
Fellow TEE Review Workshop Hemodynamic Calculations 2013. Director, Intraoperative TEE Program. Johns Hopkins School of Medicine
 Fellow TEE Review Workshop Hemodynamic Calculations 2013 Mary Beth Brady, MD, FASE Director, Intraoperative TEE Program Johns Hopkins School of Medicine At the conclusion of the workshop, the participants
Fellow TEE Review Workshop Hemodynamic Calculations 2013 Mary Beth Brady, MD, FASE Director, Intraoperative TEE Program Johns Hopkins School of Medicine At the conclusion of the workshop, the participants
5. Management of rheumatic heart disease
 5. Management of rheumatic heart disease The fundamental goal in the long-term management of RHD is to prevent ARF recurrences, and therefore, prevent the progression of RHD, and in many cases allow for
5. Management of rheumatic heart disease The fundamental goal in the long-term management of RHD is to prevent ARF recurrences, and therefore, prevent the progression of RHD, and in many cases allow for
Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity
 Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity Jean-Luc MONIN, MD, PhD Henri Mondor University Hospital Créteil, FRANCE Disclosures : None 77-year-old woman, mild dyspnea
Low-gradient severe aortic stenosis with normal LVEF: A disturbing clinical entity Jean-Luc MONIN, MD, PhD Henri Mondor University Hospital Créteil, FRANCE Disclosures : None 77-year-old woman, mild dyspnea
Adult Cardiac Surgery ICD9 to ICD10 Crosswalks
 164.1 Malignant neoplasm of heart C38.0 Malignant neoplasm of heart 164.1 Malignant neoplasm of heart C45.2 Mesothelioma of pericardium 198.89 Secondary malignant neoplasm of other specified sites C79.89
164.1 Malignant neoplasm of heart C38.0 Malignant neoplasm of heart 164.1 Malignant neoplasm of heart C45.2 Mesothelioma of pericardium 198.89 Secondary malignant neoplasm of other specified sites C79.89
New insights in the assessment of right ventricular function: an echocardiographic study. Avin Calcutteea
 New insights in the assessment of right ventricular function: an echocardiographic study Avin Calcutteea Department of Public Health and Clinical Medicine Umeå University, 2013 New insights in the assessment
New insights in the assessment of right ventricular function: an echocardiographic study Avin Calcutteea Department of Public Health and Clinical Medicine Umeå University, 2013 New insights in the assessment
Specific Basic Standards for Osteopathic Fellowship Training in Cardiology
 Specific Basic Standards for Osteopathic Fellowship Training in Cardiology American Osteopathic Association and American College of Osteopathic Internists BOT 07/2006 Rev. BOT 03/2009 Rev. BOT 07/2011
Specific Basic Standards for Osteopathic Fellowship Training in Cardiology American Osteopathic Association and American College of Osteopathic Internists BOT 07/2006 Rev. BOT 03/2009 Rev. BOT 07/2011
Starling s Law Regulation of Myocardial Performance Intrinsic Regulation of Myocardial Performance
 Regulation of Myocardial Performance Intrinsic Regulation of Myocardial Performance Just as the heart can initiate its own beat in the absence of any nervous or hormonal control, so also can the myocardium
Regulation of Myocardial Performance Intrinsic Regulation of Myocardial Performance Just as the heart can initiate its own beat in the absence of any nervous or hormonal control, so also can the myocardium
Potential Causes of Sudden Cardiac Arrest in Children
 Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Potential Causes of Sudden Cardiac Arrest in Children Project S.A.V.E. When sudden death occurs in children, adolescents and younger adults, heart abnormalities are likely causes. These conditions are
Educational Goals & Objectives
 Educational Goals & Objectives The Cardiology rotation will provide the resident with an understanding of cardiovascular physiology and its broad systemic manifestations. The resident will have the opportunity
Educational Goals & Objectives The Cardiology rotation will provide the resident with an understanding of cardiovascular physiology and its broad systemic manifestations. The resident will have the opportunity
Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery
 Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery Srinivasan Rajagopal M.D. Assistant Professor Division of Cardiothoracic Anesthesia Objectives Describe the pathophysiology
Management of the Patient with Aortic Stenosis undergoing Non-cardiac Surgery Srinivasan Rajagopal M.D. Assistant Professor Division of Cardiothoracic Anesthesia Objectives Describe the pathophysiology
What is echo? CHAPTER 1 1.1 BASIC NOTIONS. Ultrasound production and detection
 What is echo? CHAPTER 1 1.1 BASIC NOTIONS Echocardiography (echo) the use of ultrasound to examine the heart is a safe, powerful, non-invasive and painless technique. Echo is easy to understand as many
What is echo? CHAPTER 1 1.1 BASIC NOTIONS Echocardiography (echo) the use of ultrasound to examine the heart is a safe, powerful, non-invasive and painless technique. Echo is easy to understand as many
Common types of congenital heart defects
 Common types of congenital heart defects Congenital heart defects are abnormalities that develop before birth. They can occur in the heart's chambers, valves or blood vessels. A baby may be born with only
Common types of congenital heart defects Congenital heart defects are abnormalities that develop before birth. They can occur in the heart's chambers, valves or blood vessels. A baby may be born with only
Chapter 2 Cardiac Interpretation of Pediatric Chest X-Ray
 Chapter 2 Cardiac Interpretation of Pediatric Chest X-Ray Ra-id Abdulla and Douglas M. Luxenberg Key Facts The cardiac silhouette occupies 50 55% of the chest width on an anterior posterior chest X-ray
Chapter 2 Cardiac Interpretation of Pediatric Chest X-Ray Ra-id Abdulla and Douglas M. Luxenberg Key Facts The cardiac silhouette occupies 50 55% of the chest width on an anterior posterior chest X-ray
HISTORY. Questions: 1. What diagnosis is suggested by this history? 2. How do you explain her symptoms during pregnancy?
 HISTORY 33-year-old woman. CHIEF COMPLAINT: months duration. Dyspnea, fatigue and nocturnal wheezing of six PRESENT ILLNESS: At ages 5 and 9, she had migratory arthritis. At age 29, in the third trimester
HISTORY 33-year-old woman. CHIEF COMPLAINT: months duration. Dyspnea, fatigue and nocturnal wheezing of six PRESENT ILLNESS: At ages 5 and 9, she had migratory arthritis. At age 29, in the third trimester
Flash, Rocking on others Added value in DCM and CRT. C. Parsai Polyclinique des Fleurs France
 Flash, Rocking on others Added value in DCM and CRT C. Parsai Polyclinique des Fleurs France Cleland JGF et al. (2007) Nat Clin Pract Cardiovasc Med 4: 90 101 Predicting CRT Response Device Related Patient
Flash, Rocking on others Added value in DCM and CRT C. Parsai Polyclinique des Fleurs France Cleland JGF et al. (2007) Nat Clin Pract Cardiovasc Med 4: 90 101 Predicting CRT Response Device Related Patient
12-Lead EKG Interpretation. Judith M. Haluka BS, RCIS, EMT-P
 12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
12-Lead EKG Interpretation Judith M. Haluka BS, RCIS, EMT-P ECG Grid Left to Right = Time/duration Vertical measure of voltage (amplitude) Expressed in mm P-Wave Depolarization of atrial muscle Low voltage
Heart Sounds & Murmurs
 Cardiovascular Physiology Heart Sounds & Murmurs Dr. Abeer A. Al-Masri MBBS, MSc, PhD Associate Professor Consultant Cardiovascular Physiologist Faculty of Medicine, KSU Detected over anterior chest wall
Cardiovascular Physiology Heart Sounds & Murmurs Dr. Abeer A. Al-Masri MBBS, MSc, PhD Associate Professor Consultant Cardiovascular Physiologist Faculty of Medicine, KSU Detected over anterior chest wall
Anatomi & Fysiologi 060301. The cardiovascular system (chapter 20) The circulation system transports; What the heart can do;
 The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
The cardiovascular system consists of; The cardiovascular system (chapter 20) Principles of Anatomy & Physiology 2009 Blood 2 separate pumps (heart) Many blood vessels with varying diameter and elasticity
UNIVERSITA' DEGLI STUDI DI ROMA TOR VERGATA
 SYSTEMATIC PATHOLOGY I IIIYear Scientific Field DISCIPLINE TUTOR Systematic Pathology I MED/21 MED/10 Thoracic Surgery Respiratory Diseases Tommaso Claudio Mineo Paola Rogliani MED/10 Respiratory Diseases
SYSTEMATIC PATHOLOGY I IIIYear Scientific Field DISCIPLINE TUTOR Systematic Pathology I MED/21 MED/10 Thoracic Surgery Respiratory Diseases Tommaso Claudio Mineo Paola Rogliani MED/10 Respiratory Diseases
Non-Invasive Risk Predictors in (Children with) Pulmonary Hypertension
 Ideal risk prognosticator Easy to acquire Non-Invasive Risk Predictors in (Children with) Pulmonary Hypertension Safe -- Non-invasive Robust Gerhard-Paul Diller Astrid Lammers Division of Adult Congenital
Ideal risk prognosticator Easy to acquire Non-Invasive Risk Predictors in (Children with) Pulmonary Hypertension Safe -- Non-invasive Robust Gerhard-Paul Diller Astrid Lammers Division of Adult Congenital
Heart valve repair and replacement
 16 Heart valve repair and replacement 222 Valvular heart disease can be treated in a variety of ways: valve replacement, in which an artificial (prosthetic) heart valve is implanted surgically to replace
16 Heart valve repair and replacement 222 Valvular heart disease can be treated in a variety of ways: valve replacement, in which an artificial (prosthetic) heart valve is implanted surgically to replace
1p36 and the Heart. John Lynn Jefferies, MD, MPH, FACC, FAHA
 1p36 and the Heart John Lynn Jefferies, MD, MPH, FACC, FAHA Director, Advanced Heart Failure and Cardiomyopathy Services Associate Professor, Pediatric Cardiology and Adult Cardiovascular Diseases Associate
1p36 and the Heart John Lynn Jefferies, MD, MPH, FACC, FAHA Director, Advanced Heart Failure and Cardiomyopathy Services Associate Professor, Pediatric Cardiology and Adult Cardiovascular Diseases Associate
Diagnosis Code Crosswalk : ICD-9-CM to ICD-10-CM Cardiac Rhythm and Heart Failure Diagnoses
 Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Echocardiography can noninvasively
 Bedside echocardiography in the assessment of the critically ill Yanick Beaulieu, MD, FRCPC Advances in ultrasound technology continue to enhance its diagnostic applications in daily medical practice.
Bedside echocardiography in the assessment of the critically ill Yanick Beaulieu, MD, FRCPC Advances in ultrasound technology continue to enhance its diagnostic applications in daily medical practice.
Introduction to Electrocardiography. The Genesis and Conduction of Cardiac Rhythm
 Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
Example Theory Multiple Choice Questions
 Example Theory Multiple Choice Questions Q a). In an ultrasound imaging system: Sector width, sector depth and frame rate can all be controlled independently b) Frame rate falls as sector width increases
Example Theory Multiple Choice Questions Q a). In an ultrasound imaging system: Sector width, sector depth and frame rate can all be controlled independently b) Frame rate falls as sector width increases
Cardiovascular Physiology
 Cardiovascular Physiology Heart Physiology for the heart to work properly contraction and relaxation of chambers must be coordinated cardiac muscle tissue differs from smooth and skeletal muscle tissues
Cardiovascular Physiology Heart Physiology for the heart to work properly contraction and relaxation of chambers must be coordinated cardiac muscle tissue differs from smooth and skeletal muscle tissues
Pericardial Effusions Diagnosis and Treatment
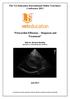 The Vet Education International Online Veterinary Conference 2013 Pericardial Effusions Diagnosis and Treatment With Dr Richard Woolley Specialist in Cardio-Respiratory Medicine July2013 Vet Education
The Vet Education International Online Veterinary Conference 2013 Pericardial Effusions Diagnosis and Treatment With Dr Richard Woolley Specialist in Cardio-Respiratory Medicine July2013 Vet Education
Disclosure. All the authors have no conflict of interest to disclose in this study.
 Assessment of Left Atrial Deformation and Dyssynchrony by Three-dimensional Speckle Tracking Imaging: Comparative Studies in Healthy Subjects and Patients with Atrial Fibrillation Atsushi Mochizuki, MD*;
Assessment of Left Atrial Deformation and Dyssynchrony by Three-dimensional Speckle Tracking Imaging: Comparative Studies in Healthy Subjects and Patients with Atrial Fibrillation Atsushi Mochizuki, MD*;
How To Treat Heart Valve Disease
 The Valve Clinic at Baptist Health Madisonville The Valve Clinic at Baptist Health Madisonville Welcome to the Baptist Health Madisonville Valve Clinic at the Jack L. Hamman Heart & Vascular Center. We
The Valve Clinic at Baptist Health Madisonville The Valve Clinic at Baptist Health Madisonville Welcome to the Baptist Health Madisonville Valve Clinic at the Jack L. Hamman Heart & Vascular Center. We
Type II Pulmonary Hypertension: Pulmonary Hypertension due to Left Heart Disease
 Heart Failure Center Hadassah University Hospital Type II Pulmonary Hypertension: Pulmonary Hypertension due to Left Heart Disease Israel Gotsman MD The Heart Failure Center, Heart Institute Hadassah University
Heart Failure Center Hadassah University Hospital Type II Pulmonary Hypertension: Pulmonary Hypertension due to Left Heart Disease Israel Gotsman MD The Heart Failure Center, Heart Institute Hadassah University
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES
 INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
INTRODUCTORY GUIDE TO IDENTIFYING ECG IRREGULARITIES NOTICE: This is an introductory guide for a user to understand basic ECG tracings and parameters. The guide will allow user to identify some of the
Resuscitation in congenital heart disease. Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto
 Resuscitation in congenital heart disease Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto Evolution of Congenital Heart Disease Extraordinary success: Overall
Resuscitation in congenital heart disease Peter C. Laussen MBBS FCICM Department Critical Care Medicine Hospital for Sick Children Toronto Evolution of Congenital Heart Disease Extraordinary success: Overall
Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular
 Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular Mitral Regurgitation Anatomy Mechanisms of MR Presentation Evaluation Management Repair Replace Clip
Managing Mitral Regurgitation: Repair, Replace, or Clip? Michael Howe, MD Traverse Heart & Vascular Mitral Regurgitation Anatomy Mechanisms of MR Presentation Evaluation Management Repair Replace Clip
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
Echocardiography has become the primary imaging
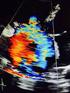 Guidelines and Standards for Performance of a Pediatric Echocardiogram: A Report from the Task Force of the Pediatric Council of the American Society of Echocardiography Wyman W. Lai, MD, MPH, FASE, Tal
Guidelines and Standards for Performance of a Pediatric Echocardiogram: A Report from the Task Force of the Pediatric Council of the American Society of Echocardiography Wyman W. Lai, MD, MPH, FASE, Tal
Carcinoid Hjärtsjukdom
 Carcinoid Hjärtsjukdom CARCINOID TUMORS 20/milj/år FORE-GUT 10% bronchial pancreatic gastric duodenal MID-GUT 70% 40% appendiceal jejunal 30% (6/m/år) ileal prox colonic HIND-GUT 20% distal colonic rectal
Carcinoid Hjärtsjukdom CARCINOID TUMORS 20/milj/år FORE-GUT 10% bronchial pancreatic gastric duodenal MID-GUT 70% 40% appendiceal jejunal 30% (6/m/år) ileal prox colonic HIND-GUT 20% distal colonic rectal
Treating AF: The Newest Recommendations. CardioCase presentation. Ethel s Case. Wayne Warnica, MD, FACC, FACP, FRCPC
 Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Treating AF: The Newest Recommendations Wayne Warnica, MD, FACC, FACP, FRCPC CardioCase presentation Ethel s Case Ethel, 73, presents with rapid heart beating and mild chest discomfort. In the ED, ECG
Teaching Med-5 Students Point-of-Care Transthoracic Echocardiography
 Teaching Med-5 Students Point-of-Care Transthoracic Echocardiography Anthony M.-H. Ho, Lester A. H. Critchley, Patricia Kan, Sylvia Au, Siu Keung Ng, Simon K. C. Chan, Philip Lam, Gordon Choi, Alex Lee,
Teaching Med-5 Students Point-of-Care Transthoracic Echocardiography Anthony M.-H. Ho, Lester A. H. Critchley, Patricia Kan, Sylvia Au, Siu Keung Ng, Simon K. C. Chan, Philip Lam, Gordon Choi, Alex Lee,
Signal-averaged electrocardiography late potentials
 SIGNAL AVERAGED ECG INTRODUCTION Signal-averaged electrocardiography (SAECG) is a special electrocardiographic technique, in which multiple electric signals from the heart are averaged to remove interference
SIGNAL AVERAGED ECG INTRODUCTION Signal-averaged electrocardiography (SAECG) is a special electrocardiographic technique, in which multiple electric signals from the heart are averaged to remove interference
Acute heart failure may be de novo or it may be a decompensation of chronic heart failure.
 Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Management of Acute Left Ventricular Failure Acute left ventricular failure presents as pulmonary oedema due to increased pressure in the pulmonary capillaries. It is important to realise though that left
Dynamic Auscultation of Heart Sounds and Murmurs. Acknowledgement. Disclosures Real or Potential Conflicts of Interest
 Dynamic Auscultation of Heart Sounds and Murmurs W. Lane Edwards, Jr., MSN, ARNP, ANP Hospitalist Group of Southwest Florida Affiliate Professor of Nursing, University of Alaska at Anchorage Acknowledgement
Dynamic Auscultation of Heart Sounds and Murmurs W. Lane Edwards, Jr., MSN, ARNP, ANP Hospitalist Group of Southwest Florida Affiliate Professor of Nursing, University of Alaska at Anchorage Acknowledgement
Questions FOETAL CIRCULATION ANAESTHESIA TUTORIAL OF THE WEEK 91 18 TH MAY 2008
 FOETAL CIRCULATION ANAESTHESIA TUTORIAL OF THE WEEK 91 18 TH MAY 2008 Dr. S. Mathieu, Specialist Registrar in Anaesthesia Dr. D. J. Dalgleish, Consultant Anaesthetist Royal Bournemouth and Christchurch
FOETAL CIRCULATION ANAESTHESIA TUTORIAL OF THE WEEK 91 18 TH MAY 2008 Dr. S. Mathieu, Specialist Registrar in Anaesthesia Dr. D. J. Dalgleish, Consultant Anaesthetist Royal Bournemouth and Christchurch
Heart Disease: Diagnosis & Treatment
 How I Treat Cardiology Peer Reviewed Heart Disease: Diagnosis & Treatment Amara Estrada, DVM, DACVIM (Cardiology) University of Florida Background Clinical heart disease is the stage of disease when a
How I Treat Cardiology Peer Reviewed Heart Disease: Diagnosis & Treatment Amara Estrada, DVM, DACVIM (Cardiology) University of Florida Background Clinical heart disease is the stage of disease when a
Atrial Septal Aneurysm: A Study in Five Hundred Adult Patients
 Premio al mejor Tema Libre Realizado por Médicos Residentes Atrial Septal Aneurysm: A Study in Five Hundred Adult Patients Olivares-Reyes Alexander; Al-Kamme Ahmad; Gonzalez Javier Cardiology Department
Premio al mejor Tema Libre Realizado por Médicos Residentes Atrial Septal Aneurysm: A Study in Five Hundred Adult Patients Olivares-Reyes Alexander; Al-Kamme Ahmad; Gonzalez Javier Cardiology Department
Electrodes placed on the body s surface can detect electrical activity, APPLIED ANATOMY AND PHYSIOLOGY. Circulatory system
 4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
4 READING AND INTERPRETING THE ELECTROCARDIOGRAM Electrodes placed on the body s surface can detect electrical activity, which occurs in the heart. The recording of these electrical events comprises an
NAME OF THE HOSPITAL: 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3
 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY
 BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY American Osteopathic Association and the American College of Osteopathic Internists Specific Requirements For Osteopathic Subspecialty Training In Cardiology
BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY American Osteopathic Association and the American College of Osteopathic Internists Specific Requirements For Osteopathic Subspecialty Training In Cardiology
Imaging. Impact of Progression of Diastolic Dysfunction on Mortality in Patients With Normal Ejection Fraction
 Imaging Impact of Progression of Diastolic Dysfunction on Mortality in Patients With Normal Ejection Fraction Wael AlJaroudi, MD; M. Chadi Alraies, MD; Carmel Halley, MD; Leonardo Rodriguez, MD; Richard
Imaging Impact of Progression of Diastolic Dysfunction on Mortality in Patients With Normal Ejection Fraction Wael AlJaroudi, MD; M. Chadi Alraies, MD; Carmel Halley, MD; Leonardo Rodriguez, MD; Richard
How To Teach An Integrated Ultrasound
 University of South Carolina School of Medicine Integrated Ultrasound Curriculum iusc Richard Hoppmann The Integrated Ultrasound Curriculum Initiated 2006 First (M1) and Second (M2) Year Medical Students
University of South Carolina School of Medicine Integrated Ultrasound Curriculum iusc Richard Hoppmann The Integrated Ultrasound Curriculum Initiated 2006 First (M1) and Second (M2) Year Medical Students
HEART FAILURE ROBERT SOUFER, M.D.
 CHAPTER 14 HEART FAILURE ROBERT SOUFER, M.D. The heart s primary function is to pump blood to all parts of the body, bringing nutrients and oxygen to the tissues and removing waste products. When the body
CHAPTER 14 HEART FAILURE ROBERT SOUFER, M.D. The heart s primary function is to pump blood to all parts of the body, bringing nutrients and oxygen to the tissues and removing waste products. When the body
Principles of Medical Ultrasound. Pai-Chi Li Department of Electrical Engineering National Taiwan University
 Principles of Medical Ultrasound Pai-Chi Li Department of Electrical Engineering National Taiwan University What is Medical Ultrasound? Prevention: actions taken to avoid diseases. Diagnosis: the process
Principles of Medical Ultrasound Pai-Chi Li Department of Electrical Engineering National Taiwan University What is Medical Ultrasound? Prevention: actions taken to avoid diseases. Diagnosis: the process
Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back
 Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back to the left atria from the left ventricle, blood is pumped
Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back to the left atria from the left ventricle, blood is pumped
Understanding your child s heart Atrial septal defect
 Understanding your child s heart Atrial septal defect About this factsheet This factsheet is for the parents of babies and children who have an atrial septal defect (ASD). It explains, what an atrial septal
Understanding your child s heart Atrial septal defect About this factsheet This factsheet is for the parents of babies and children who have an atrial septal defect (ASD). It explains, what an atrial septal
Chronic Postpericardiotomy Syndrome and Cardiac Tamponade Lasting for Two Years after Open Heart Surgery
 Case Reports Acta Cardiol Sin 2006;22:170 4 Chronic Postpericardiotomy Syndrome and Cardiac Tamponade Lasting for Two Years after Open Heart Surgery Nai-Chuan Chien and Ta-Chung Shen Postpericardiotomy
Case Reports Acta Cardiol Sin 2006;22:170 4 Chronic Postpericardiotomy Syndrome and Cardiac Tamponade Lasting for Two Years after Open Heart Surgery Nai-Chuan Chien and Ta-Chung Shen Postpericardiotomy
Atrial Fibrillation 2014 How to Treat How to Anticoagulate. Allan Anderson, MD, FACC, FAHA Division of Cardiology
 Atrial Fibrillation 2014 How to Treat How to Anticoagulate Allan Anderson, MD, FACC, FAHA Division of Cardiology Projection for Prevalence of Atrial Fibrillation: 5.6 Million by 2050 Projected number of
Atrial Fibrillation 2014 How to Treat How to Anticoagulate Allan Anderson, MD, FACC, FAHA Division of Cardiology Projection for Prevalence of Atrial Fibrillation: 5.6 Million by 2050 Projected number of
Atrial Fibrillation An update on diagnosis and management
 Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Dr Arvind Vasudeva Consultant Cardiologist Atrial Fibrillation An update on diagnosis and management Atrial fibrillation (AF) remains the commonest disturbance of cardiac rhythm seen in clinical practice.
Heart Failure EXERCISES. Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it.
 Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Heart Failure EXERCISES Ⅰ. True or false questions (mark for true question, mark for false question. If it is false, correct it. ) 1. Heart rate increase is a kind of economic compensation, which should
Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations.
 INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
2/20/2015. Cardiac Evaluation of Potential Solid Organ Transplant Recipients. Issues Specific to Transplantation. Kidney Transplantation.
 DISCLOSURES I have no relevant financial relationships to disclose. Cardiac Evaluation of Potential Solid Organ Transplant Recipients Michele Hamilton, MD Director, Heart Failure Program Cedars Sinai Heart
DISCLOSURES I have no relevant financial relationships to disclose. Cardiac Evaluation of Potential Solid Organ Transplant Recipients Michele Hamilton, MD Director, Heart Failure Program Cedars Sinai Heart
