Plantar Fasciitis (Heel Pain)
|
|
|
- Sandra Phelps
- 7 years ago
- Views:
Transcription
1 Discussion paper prepared for The Workplace Safety and Insurance Appeals Tribunal March 2003 Prepared by: Timothy Daniels, MD, FRCSC Division of Orthopaedic Surgery, St. Michael s Hospital, Toronto, Ontario Assistant Professor, Department of Surgery University of Toronto Dr. Timothy R. Daniels graduated from the University of Saskatchewan in He did post-graduate training in orthopaedics at the Royal University Hospital in Saskatoon from 1987 to He became a Fellow in orthopaedics in He went on to do a foot and ankle fellowship at the Emory University School of Medicine in Atlanta, Georgia, from 1992 to 1993 and a research fellowship at Milwaukee County Medical Complex, Wisconsin, in He was an Associate Professor at Emory University School of Medicine from 1992 to 1993 and joined the faculty at the University of Toronto in He currently holds the rank of Associate Professor in the Department of Surgery. He is a Reviewer for the Journal of Rheumatology, the Canadian Journal of Surgery and the Canadian Medical Association Journal (CMAJ) and an Associate Editor for Foot & Ankle International. His clinical and research interests are in orthopaedics and foot/ankle conditions. He has published extensively on these subjects. This medical discussion paper will be useful to those seeking general information about the medical issue involved. It is intended to provide a broad and general overview of a medical topic that is frequently considered in Tribunal appeals. Each medical discussion paper is written by a recognized expert in the field, who has been recommended by the Tribunal s medical counsellors. Each author is asked to present a balanced view of the current medical knowledge on the topic. Discussion papers are not peer reviewed. They are written to be understood by lay individuals. Discussion papers do not necessarily represent the views of the Tribunal. A vice-chair or panel may consider and rely on the medical information provided in the discussion paper, but the Tribunal is not bound by an opinion expressed in a discussion paper in any particular case. Every Tribunal decision must be based on the facts of the particular appeal. Tribunal adjudicators recognize that it is always open to the parties to an appeal to rely on or to distinguish a medical discussion paper, and to challenge it with alternative evidence: see Kamara v. Ontario (Workplace Safety and Insurance Appeals Tribunal) [2009] O.J. No (Ont Div Court).
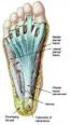
2 PLANTAR FASCIITIS (HEEL PAIN) Mechanics: The plantar fascia is a multilayered inelastic fibrous sheet (aponeurosis) composed primarily of Type I collagen. It originates from a bony prominence on the bottom of the heel bone (the medial calcaneal tuberosity) and inserts through several fibrous bands into the plantar plate of the metatarsophalangeal joints, flexor tendon sheaths and the base of the proximal phalanges of the toes. The distal insertion site of the Achilles tendon (heel cord) and the origin of the plantar fascia are close in proximity and the outer layer of the two structures is continuous. Since the plantar fascia originates proximally and inserts distally to the subtalar and midtarsal joints, any functional change in its length can alter the position of the said joints. The plantar fascia is the most important static soft tissue supporter of the medial arch; transecting it in loaded Cadaveric specimens results in a 21% loss of the height of the medial arch [1]. The plantar fascia has an important functional role in the normal gait cycle. In the latter part of the stance phase, the toes dorsiflex. This functionally shortens the plantar fascia causing the calcaneus to rotate inwards (into varus) and the medial arch to elevate (windlass mechanism). The internal rotation of the calcaneus causes a divergence in the joint axis of two of the mid-foot joints (the talonavicular and calcaneocuboid joints), thereby locking the joint complex. The now stable midfoot allows for the smooth transition of forces to occur from the hindfoot to the forefoot. In this manner, the plantar fascia is an important soft tissue stabilizer of the foot with an essential functional role during gait. Pathophysiology: The bottom surface of the heel (calcaneal fat pad) is made up of elastic adipose-tissue-supported spiral fibrous bands (septa) and is the primary structure that cushions the heel from compressive forces at heel strike [2]. The plantar fascia acts as a tie-rod in the foot truss. The primary forces it is subjected to are tensile. The tension is (greatest) at the origin of the plantar fascia near its insertion at the medial calcaneal tuberosity [3]. This is also the location where the plantar fascia commonly becomes swollen and inflamed. It is theorized that the repetitive tensile forces created by walking or standing cause micro-tears in the fascia, leading to acute and eventual chronic inflammation. If the inflammation affects the entire plantar fascia, it is referred to as a plantar fasciitis; however, if it is isolated to the insertion site of the heel, it is called a heel pain (the more common of the two.) MRI studies have demonstrated an increased thickness of the plantar fascia from 3 mm in a normal heel to 7.4 mm in patients with a chronic heel pain [4]. Biopsies of the inflamed area have revealed collagen necrosis (death of some of the fibrous tissue), angiofibroblastic hyperplasia (overgrowth of fibrous tissue and tiny blood vessels), chondroid metaplasia (formation of cartilage tissue) and matrix 1
3 calcification -all microscopic changes typically seen in areas with chronic inflammation and deficient blood flow. On physical examination, the patient often has tightness of the Achilles tendon - this is consistent with the close anatomical relationship of the heel cord with the plantar fascia [5]. It is unclear whether a tight heel cord is a precipitating factor or simply associated with the heel pain [6-9]. In a small percentage of patients, the heel pain is the result of both inflammation of the plantar fascia and entrapment of the nerves in the distal tarsal tunnel. The most common nerve involved in this process is the first branch of the lateral plantar nerve sometimes referred to as Baxter s nerve. This is a motor sensory branch which supplies sensory nerves to the periosteum of the calcaneus and motor nerves to the abductor digiti minimi muscle. Etiology: Heel pain may be caused by plantar fascia rupture, fat pad atrophy, stress fractures of the calcaneus, proximal plantar fasciitis, distal plantar fasciitis, plantar fibromatosis, tendonitis of the flexor hallucis longus, tumor of the calcaneus and nerve entrapment, or injury [5]. The most common cause is inflammation of the proximal portion of the plantar fascia. There is no consensus regarding etiology. Snook and Christman wrote, it is reasonably certain that a condition which has so many different theories of etiology and treatment does not have valid proof of any one cause [10]. Factors associated with or aggravating this condition are better defined: age, sex, obesity, seronegative inflammatory disorders and activity levels. The average age is 45 years. Prevalence is twice in females vs. males [5]. There may be a history of elevated stress to the foot as a result of increased activities, prolonged standing or weight gain. Physical activity certainly aggravates and can sometimes precipitate the heel pain [11-14]. A retrospective review of injuries among runners cited plantar fasciitis as one of the five most common injuries [14]. Numerous studies have assessed whether or not abnormal foot mechanics predispose an individual to heel pain [5, 7, 9, 12, 13, 15]. Pes planus [16] and pes cavus were the most common foot deformities assessed. A predominance of either deformity has not been identified. Theoretically, both deformities can cause abnormal stresses on the plantar fascia [3, 16-21] and clinical correlations have been suggested [12]. However, a consistent correlation has not been evidenced by retrospective clinical reviews. Several studies have implicated body weight as a causative factor [8, 10, 22, 23]. Furey [22] identified an increased prevalence of heel pain among obese patients, and Snook and Chrisman [10] noted half of their patients with heel pain were overweight. This makes intuitive sense given that heel pain is 2
4 considered an over-use syndrome associated with advancing in age. Increased body mass elevates the forces on the aging soft tissues that are less capable of tolerating the stresses. Weight loss in such patients is often impossible since the painful heel limits their activities. Factors such as acute injury, the presence of a heel spur, the type of footwear, the walking surface and employment or chronic repetitive activity (other than athletics) have been proposed, but they have not been established as causative [24]. A correlation between prolonged standing or walking has been suggested [8, 9, 25, 26], but direct causation is unsubstantiated since heel pain can occur in all types of patients with varying levels of recreational activities and job requirements. The consistency of the surface on which one walks has not been established as a causative or aggravating factor. This is likely because tension, rather than compression, is the primary force which precipitates injury and inflammation of the plantar fascia. The magnitude of the tensile forces placed through the plantar fascia is related more to the activity level, types of activities, body weight and stability of the medial arch [3, 17-21] rather than the consistency of the walking surface. Although many patients are concerned with the presence of a heel spur, it is not recognized as an etiologic factor. Approximately 50% of patients with a heel pain and 16% without have a heel spur [27]. Anatomically, the heel spur is located at the origin of the flexor digitorum brevis muscle, not at the origin of the plantar fascia. Presumably, the same process occurring at the plantar fascia can occur at the origin of the intrinsic muscles of the foot leading to periostitis and new bone formation. Lapidus et al have demonstrated that successful treatment of heel pain is not contingent with excision of the heel spur [8]. Pain at the sites of tendon or ligament insertion (enthesiopathy) is often observed in patients with seronegative arthropathies [5]. Clinical syndromes such as ankylosing spondylitis, psoriatic arthritis, Reiter s syndrome, inflammatory bowel disease and Behcet s syndrome must be ruled out. Associated complaints such as skin lesions, conjunctivitis, arthritis, back pain or abdominal complaints should prompt a referral to a rheumatologist. Screening tests include antigen-b27 (HLA-B27) and sedimentation rate (ESR) can aid in the diagnosis. Conclusion: The plantar fascia is an inelastic structure that plays an important role in maintaining the stability of the medial arch and midtarsal joints. The primary force placed through the plantar fascia is tension, not compression. It functions as a tie-rod in the foot truss and, during the gait cycle, is under maximal tension in the mid-portion and terminal portions of the stance phase. It is generally accepted that the primary etiology of heel 3
5 pain is the result of repetitive tensile forces placed through aging tissue that is no longer capable of tolerating the stresses. While associated factors for this condition have been identified, no one activity is known to be the cause of heel pain. Figure 1 - The plantar fascia is a multilayered fibrous aponeurosis 4
6 Figure 2 - The windlass mechanism puts tension on the plantar fascia and raises the arch passively References 1. Huang, C.K., H.B. Kitaoka, K.N. An, and E.Y. Chao, Biomechanical evaluation of longitudinal arch stability. Foot Ankle, (6): p Miller, W.E., The heel pad. Am J Sports Med, : p Kitaoka, H.B., Z.P. Luo, E.S. Growney, L.J. Berglund, and K.N. An, Material properties of the plantar aponeurosis. Foot Ankle Int, (10): p
7 4. Berkowitz, J.F. and S. Rudicel, Plantar Fascia: MR Imaging. Radiology, : p Pfeffer, G.B., ed. Plantar Heel Pain. first ed. Foot and Ankle Disorders, ed. S.M. Myerson. Vol , W.B. Saunders Co.: Philadelphia Sellman, J., Plantar fascia rupture associated with corticosteroid injection. Foot & Ankle Int., : p Davis, P., E. Severud, and D. Baxter, Painful heel syndrome: Results lf nonoperative treatment. Foot & Ankle Int., : p Lapidus, P.W. and F.P. Guidotti, Painful Heel: Report of three hundred twenty-three patients with three hundred sixty-four painful heels. Clin Orthop, : p Karr, S., Subcalcaneal heel pain. Orthop Clin North Am, : p Snook, G.A. and O.D. Chrisman, The management of subcalcaneal pain. Clin. Orthop., : p Leach, R. and A. Schepsos, Hindfoot pain in athletes: Why, and what can be done? J Musculoskel Med, : p Baxter, D. and C. Thigpen, Heel pain: Operative results. Foot Ankle, : p McBryde, A.J., Plantar Fasciitis. Instr Course Lect, : p Taunton JE, Ryan MB, Clement DB, McKenzie DC, Lloyd-Smith DR, and Z. BD, A retrospective case-control analysis of 2002 running injuries. Br J Sports Med, (2): p Williams, P., The painful heel. Br J Hosp Med, : p Labib, S.A., J.S. Gould, F.A. Rodriguez-del-Rio, and S. Lyman, Heel pain triad (HPT): the combination of plantar fasciitis, posterior tibial tendon dysfunction and tarsal tunnel syndrome. Foot Ankle Int, (3): p Kitaoka, H.B., A. Lundberg, Z.P. Luo, and K.N. An, Kinematics of the normal arch of the foot and ankle under physiologic loading. Foot Ankle Int, (8): p Kitaoka, H.B., Z.P. Luo, and K.N. An, Effect of plantar fasciotomy on stability of arch of foot. Clin Orthop, 1997(344): p Kitaoka, H.B., T.K. Ahn, Z.P. Luo, and K.N. An, Stability of the arch of the foot. Foot Ankle Int, (10): p Kitaoka, H.B., Z.P. Luo, and K.N. An, Analysis of longitudinal arch supports in stabilizing the arch of the foot. Clin Orthop, 1997(341): p Kitaoka, H.B., Z.P. Luo, and K.N. An, Mechanical behavior of the foot and ankle after plantar fascia release in the unstable foot. Foot Ankle Int, (1): p
8 22. Furey, J., Plantar fasciitis: The painful heel syndrome. J Bone Joint Surg Am, : p Hill, J.J. and P. Cutting, Heel pain and body weight. Foot Ankle, : p Gill, L., Plantar Fasciitis: Diagnosis and Conservative Management. J of the Am Academy of Ortho Surgeons, (2): p Blockey, N., The painful heel: A controlled trial of the value of hydrocortisone. BMJ, : p Gill, L. and G. Kiebzak, Outcome of Nonsurgical Treatment for Plantar Fasciitis. Foot & Ankle Int., (9): p Tanz, S.S., Heel pain. Clin Orthop, : p
Common Foot & Ankle Sports Injuries
 Common Foot & Ankle Sports Injuries Symptoms Related to Abnormal Foot Biomechanics & their Differential Diagnosis Daniel Pang BSc (Hon) P&O, Cped Certified Pedorthist (USA) Only 10% of foot having structure
Common Foot & Ankle Sports Injuries Symptoms Related to Abnormal Foot Biomechanics & their Differential Diagnosis Daniel Pang BSc (Hon) P&O, Cped Certified Pedorthist (USA) Only 10% of foot having structure
Chapter 140 Heel Pain
 Chapter 140 Heel Pain David R. Richardson, MD E. Greer Richardson, MD I. Overview and Epidemiology A. General characteristics Heel pain (subcalcaneal pain syndrome) is the most common foot-related symptom
Chapter 140 Heel Pain David R. Richardson, MD E. Greer Richardson, MD I. Overview and Epidemiology A. General characteristics Heel pain (subcalcaneal pain syndrome) is the most common foot-related symptom
The role of bone scintigraphy in determining the etiology of heel pain
 ORIGINAL ARTICLE Annals of Nuclear Medicine Vol. 16, No. 6, 395 401, 2002 The role of bone scintigraphy in determining the etiology of heel pain Hakan ÖZDEMI%R,* Aysun ÖZDEMI%R,** Yetkin SOYUNCU* and Mustafa
ORIGINAL ARTICLE Annals of Nuclear Medicine Vol. 16, No. 6, 395 401, 2002 The role of bone scintigraphy in determining the etiology of heel pain Hakan ÖZDEMI%R,* Aysun ÖZDEMI%R,** Yetkin SOYUNCU* and Mustafa
Plantar fascia. Plantar Fasciitis (pain in the heel of the foot)
 ! Plantar fascia Plantar Fasciitis (pain in the heel of the foot) Plantar Fasciitis is the most common foot problem seen in runners and is often associated with an increase in running mileage. Typically
! Plantar fascia Plantar Fasciitis (pain in the heel of the foot) Plantar Fasciitis is the most common foot problem seen in runners and is often associated with an increase in running mileage. Typically
Page 2 of 6 plantar fascia. This is called the windlass mechanism. Later, we'll discuss how this mechanism is used to treat plantar fasciitis with str
 Page 1 of 6 Plantar Fasciitis (Heel Pain) Plantar fasciitis is a painful condition affecting the bottom of the foot. It is a common cause of heel pain and is sometimes called a heel spur. Plantar fasciitis
Page 1 of 6 Plantar Fasciitis (Heel Pain) Plantar fasciitis is a painful condition affecting the bottom of the foot. It is a common cause of heel pain and is sometimes called a heel spur. Plantar fasciitis
Clinical outcome of surgical intervention for recalcitrant infero-medial heel pain
 Acta Orthop. Belg., 2008, 74, 483-488 ORIGINAL STUDY Clinical outcome of surgical intervention for recalcitrant infero-medial heel pain Friedl SINNAEVE, Geoffroy VANDEPUTTE From the Heilig Hartziekenhuis
Acta Orthop. Belg., 2008, 74, 483-488 ORIGINAL STUDY Clinical outcome of surgical intervention for recalcitrant infero-medial heel pain Friedl SINNAEVE, Geoffroy VANDEPUTTE From the Heilig Hartziekenhuis
Heel pain and Plantar fasciitis
 A patient s guide Heel pain and Plantar fasciitis Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon Alex Wee BSc FRCS(orth) Consultant Trauma & Orthopaedic Surgeon. What causes
A patient s guide Heel pain and Plantar fasciitis Fred Robinson BSc FRCS FRCS(orth) Consultant Trauma & Orthopaedic Surgeon Alex Wee BSc FRCS(orth) Consultant Trauma & Orthopaedic Surgeon. What causes
PHYSICAL EXAMINATION OF THE FOOT AND ANKLE
 PHYSICAL EXAMINATION OF THE FOOT AND ANKLE Presenter Dr. Richard Coughlin AOFAS Lecture Series OBJECTIVES 1. ASSESS 2. DIAGNOSE 3. TREAT HISTORY TAKING Take a HISTORY What is the patient s chief complaint?
PHYSICAL EXAMINATION OF THE FOOT AND ANKLE Presenter Dr. Richard Coughlin AOFAS Lecture Series OBJECTIVES 1. ASSESS 2. DIAGNOSE 3. TREAT HISTORY TAKING Take a HISTORY What is the patient s chief complaint?
Clinical Analysis of Foot Problems
 Clinical Analysis of Foot Problems by Karen S. Seale, M.D. Introduction Orthotists are vital members of the foot care team. Their expertise and special interests in materials and biomechanics add a unique
Clinical Analysis of Foot Problems by Karen S. Seale, M.D. Introduction Orthotists are vital members of the foot care team. Their expertise and special interests in materials and biomechanics add a unique
Plantar Fasciitis - Ayurvedic Strain
 BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Physical Therapy Case Type / Diagnosis: (diagnosis specific, impairment/ dysfunction specific) ICD9-728.71 plantar fibromatosis Plantar
BRIGHAM AND WOMEN S HOSPITAL Department of Rehabilitation Services Physical Therapy Case Type / Diagnosis: (diagnosis specific, impairment/ dysfunction specific) ICD9-728.71 plantar fibromatosis Plantar
A Patient s Guide to Plantar Fasciitis. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Plantar Fasciitis Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
A Patient s Guide to Plantar Fasciitis Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
Plantar Heel Pain. By: Kevin Kleiner, M.B.S. New York College of Podiatric Medicine
 Plantar Heel Pain By: Kevin Kleiner, M.B.S. New York College of Podiatric Medicine Plantar Heel Pain: - Many Etiologies but few solutions Plantar heel pain more specifically: Heel pain felt in ones rear-foot
Plantar Heel Pain By: Kevin Kleiner, M.B.S. New York College of Podiatric Medicine Plantar Heel Pain: - Many Etiologies but few solutions Plantar heel pain more specifically: Heel pain felt in ones rear-foot
A Guide to Heel Pain
 The Society of Chiropodists and Podiatrists A Guide to Heel Pain The Society of Chiropodists and Podiatrists Heel pain may be caused by a number of different problems; for effective treatment you need
The Society of Chiropodists and Podiatrists A Guide to Heel Pain The Society of Chiropodists and Podiatrists Heel pain may be caused by a number of different problems; for effective treatment you need
PLANTAR FASCIITIS. Plantar Fasciitis. Plantar Fasciitis. Heel Pain - common causes. Plantar Fasciitis 1/16/2012. Robert A Erdin III, MD
 PLANTAR FASCIITIS Robert A Erdin III, MD Special thanks to the AOFAS and David Richardson MD for slide reproductions Most common symptom related to the foot leading a patient to seek professional care
PLANTAR FASCIITIS Robert A Erdin III, MD Special thanks to the AOFAS and David Richardson MD for slide reproductions Most common symptom related to the foot leading a patient to seek professional care
Plantar Fasciitis. Plantar Fascia
 Plantar Fasciitis Introduction Plantar fasciitis is an inflammation of the thick band of tissue that connects your heel bone to your toes. This thick band of tissue is called the plantar fascia. Plantar
Plantar Fasciitis Introduction Plantar fasciitis is an inflammation of the thick band of tissue that connects your heel bone to your toes. This thick band of tissue is called the plantar fascia. Plantar
.org. Plantar Fasciitis and Bone Spurs. Anatomy. Cause
 Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
The Diagnosis and Management of Heel Pain in Active People
 The Diagnosis and Management of Heel Pain in Active People Perry Julien, D.P.M. Past President, American Academy of Podiatric Sports Medicine Podiatry Coordinator, 1996 Summer Olympic Games Atlanta Georgia
The Diagnosis and Management of Heel Pain in Active People Perry Julien, D.P.M. Past President, American Academy of Podiatric Sports Medicine Podiatry Coordinator, 1996 Summer Olympic Games Atlanta Georgia
HEEL PAIN. Differential diagnosis. 1. Insertional Plantar fascitis. 2. Enthesis. 3. Heel pad atrophy. 4. Tarsal tunnel syndrome
 HEEL PAIN Differential diagnosis 1. Insertional Plantar fascitis 2. Enthesis 3. Heel pad atrophy 4. Tarsal tunnel syndrome 5. Calcaneal stress fracture 6. Haglund s syndrome 7. Posterior ankle impingement
HEEL PAIN Differential diagnosis 1. Insertional Plantar fascitis 2. Enthesis 3. Heel pad atrophy 4. Tarsal tunnel syndrome 5. Calcaneal stress fracture 6. Haglund s syndrome 7. Posterior ankle impingement
Plantar fasciitis is a common foot problem that occurs in 10%
 Review Article Plantar Fasciitis Heel Pain: Part 1 a Practical Management Plantar fasciitis is a common foot problem that occurs in 10% of the population. 1,2 The most involved age group is 40-50 3,4 Actually,
Review Article Plantar Fasciitis Heel Pain: Part 1 a Practical Management Plantar fasciitis is a common foot problem that occurs in 10% of the population. 1,2 The most involved age group is 40-50 3,4 Actually,
Using Might Splints in the Treatment
 Journal of Sport Rehabilitation, 1993, 2, 287-297 @ 1993 Human Kinetics Publishers, Inc. Using Might Splints in the Treatment of Plantar Fasciitis in the Athlete David J. Pezzullo Plantar fasciitis is
Journal of Sport Rehabilitation, 1993, 2, 287-297 @ 1993 Human Kinetics Publishers, Inc. Using Might Splints in the Treatment of Plantar Fasciitis in the Athlete David J. Pezzullo Plantar fasciitis is
49 Plantar fasciitis. 49.1 Introduction. 49.2 Anatomy. OrthopaedicsOne Articles. Contents
 49 Plantar fasciitis Contents Introduction Anatomy Clinical Presentation Pathogenesis Physical Examination Imaging Conservative Treatment Operative Treatment Controversy References 49.1 Introduction Plantar
49 Plantar fasciitis Contents Introduction Anatomy Clinical Presentation Pathogenesis Physical Examination Imaging Conservative Treatment Operative Treatment Controversy References 49.1 Introduction Plantar
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
By: Jerry Ryan, M.D., University of Wisconsin Medical School, Madison, Wisconsin
 UAmerican Family PhysicianU September 1995 Use of Posterior Night Splints in the Treatment of Plantar Fasciitis Plantar fasciitis is a frequent cause of heel pain in athletes, as well as in persons who
UAmerican Family PhysicianU September 1995 Use of Posterior Night Splints in the Treatment of Plantar Fasciitis Plantar fasciitis is a frequent cause of heel pain in athletes, as well as in persons who
Heel Pain: Heal! Amie C. Scantlin, DPM, MS, FACFAS Glencoe Regional Health Services (320) 864-3121 ext. 1933
 Heel Pain: Heal! Amie C. Scantlin, DPM, MS, FACFAS Glencoe Regional Health Services (320) 864-3121 ext. 1933 www.grhsonline.org Important Notice The information contained in this document is for informational
Heel Pain: Heal! Amie C. Scantlin, DPM, MS, FACFAS Glencoe Regional Health Services (320) 864-3121 ext. 1933 www.grhsonline.org Important Notice The information contained in this document is for informational
Heel Pain Syndromes DELLON INSTITUTES FOR PERIPHERAL NERVE SURGERY
 Heel Pain s 5 3333 N CALVERT ST, SUITE 370, BALTIMORE, MD 21218 T410 467 5400 F410 366 9826 delloninstitutes.com your complaints are Pain, numbness or burning in your heel. The timing of this pain and
Heel Pain s 5 3333 N CALVERT ST, SUITE 370, BALTIMORE, MD 21218 T410 467 5400 F410 366 9826 delloninstitutes.com your complaints are Pain, numbness or burning in your heel. The timing of this pain and
Objectives Learn the anatomy of the foot. Identify key terms associated with plantar fasciitis. Determine the causes of plantar fasciitis and understa
 Plantar Fasciitis Objectives Learn the anatomy of the foot. Identify key terms associated with plantar fasciitis. Determine the causes of plantar fasciitis and understand why it occurs. Recognize the injury
Plantar Fasciitis Objectives Learn the anatomy of the foot. Identify key terms associated with plantar fasciitis. Determine the causes of plantar fasciitis and understand why it occurs. Recognize the injury
Osteoarthritis progresses slowly and the pain and stiffness it causes worsens over time.
 Arthritis of the Foot and Ankle Arthritis is the leading cause of disability in the United States. It can occur at any age, and literally means "pain within a joint." As a result, arthritis is a term used
Arthritis of the Foot and Ankle Arthritis is the leading cause of disability in the United States. It can occur at any age, and literally means "pain within a joint." As a result, arthritis is a term used
COMPLICATIONS OF PLANTAR FASCIA RELEASE
 C H A P T E R 8 COMPLICATIONS OF PLANTAR FASCIA RELEASE Michelle L. Butterworth, DPM INTRODUCTION Heel pain is one of the most common disorders that foot and ankle surgeons treat. Investigators have stated
C H A P T E R 8 COMPLICATIONS OF PLANTAR FASCIA RELEASE Michelle L. Butterworth, DPM INTRODUCTION Heel pain is one of the most common disorders that foot and ankle surgeons treat. Investigators have stated
Outline. The Agony of the Foot: Disclosure. Plantar Fasciitis. Top 5 Foot and Ankle Problems in Primary Care. Daniel Thuillier, M.D.
 The Agony of the Foot: Top 5 Foot and Ankle Problems in Primary Care Daniel Thuillier, M.D. Assistant Professor of Clinical Orthopaedics University of California San Francisco Plantar Fasciitis Achilles
The Agony of the Foot: Top 5 Foot and Ankle Problems in Primary Care Daniel Thuillier, M.D. Assistant Professor of Clinical Orthopaedics University of California San Francisco Plantar Fasciitis Achilles
Structure & Function of the Ankle and Foot. A complicated model of simplicity that you really think little about until you have a problem with one.
 Structure & Function of the Ankle and Foot A complicated model of simplicity that you really think little about until you have a problem with one. The Foot and Ankle Terminology Plantar flexion Dorsi flexion
Structure & Function of the Ankle and Foot A complicated model of simplicity that you really think little about until you have a problem with one. The Foot and Ankle Terminology Plantar flexion Dorsi flexion
RUNNING INJURIES: PREVENTION AND REHABILITATION
 RUNNING INJURIES: PREVENTION AND REHABILITATION Topics of Tonight s s Lecture Common Injuries and Treatments Causes of Common Injuries Measures to Avoid Injury Most Common Running Injuries Plantar Fascitis
RUNNING INJURIES: PREVENTION AND REHABILITATION Topics of Tonight s s Lecture Common Injuries and Treatments Causes of Common Injuries Measures to Avoid Injury Most Common Running Injuries Plantar Fascitis
Title Diagnosing Heel Pain in Adults
 Title Diagnosing Heel Pain in Adults AUTHOR TRACY ALDRIDGE, NAME, Location M.D., Southern Illinois University School of Medicine, Springfield, Illinois Heel pain is a common condition in adults that may
Title Diagnosing Heel Pain in Adults AUTHOR TRACY ALDRIDGE, NAME, Location M.D., Southern Illinois University School of Medicine, Springfield, Illinois Heel pain is a common condition in adults that may
PLANTAR FASCITIS (Heel Spur Syndrome)
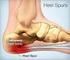 PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
PODIATRIC SURGERY INFORMATION GUIDE: MANAGEMENT OF PLANTAR FASCIITIS/HEEL PAIN
 PODIATRIC SURGERY INFORMATION GUIDE: MANAGEMENT OF PLANTAR FASCIITIS/HEEL PAIN What is Plantar Fasciitis? Plantar fasciitis is pain in the heel and arch area of the foot. The plantar fascia is a strong
PODIATRIC SURGERY INFORMATION GUIDE: MANAGEMENT OF PLANTAR FASCIITIS/HEEL PAIN What is Plantar Fasciitis? Plantar fasciitis is pain in the heel and arch area of the foot. The plantar fascia is a strong
Podo Pediatrics Identifying Biomechanical Pathologies
 Podo Pediatrics Identifying Biomechanical Pathologies David Lee, D.P.M., D. A.B.P.S. Purpose Identification of mechanical foot and ankle conditions Base treatments Knowing when to refer to a podiatrist
Podo Pediatrics Identifying Biomechanical Pathologies David Lee, D.P.M., D. A.B.P.S. Purpose Identification of mechanical foot and ankle conditions Base treatments Knowing when to refer to a podiatrist
Endoscopic Plantar Fasciotomy
 Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Lower Back Spinal Fusion & Exercise
 & Exercise with Rick Kaselj, MS More FREE Information on Exercise & Injuries $299 Fitness Education Returning the Shoulder Back to Optimal Function Seminar Exercise Modification for the Sensitive Shoulder
& Exercise with Rick Kaselj, MS More FREE Information on Exercise & Injuries $299 Fitness Education Returning the Shoulder Back to Optimal Function Seminar Exercise Modification for the Sensitive Shoulder
Plantar Fascia Release
 Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Plantar fasciitis - suspected
 Proximal plantar fasciitis suspected Clinical presentation History Examination Consider alternative causes of plantar heel pain Heel pad pain Neurologic plantar heel pain Arthritic plantar heel pain Traumatic
Proximal plantar fasciitis suspected Clinical presentation History Examination Consider alternative causes of plantar heel pain Heel pad pain Neurologic plantar heel pain Arthritic plantar heel pain Traumatic
GET A HANDLE ON YOUR HEEL PAIN GUIDE
 GET A HANDLE ON YOUR HEEL PAIN GUIDE American Podiatric Medical Association www.apma.org/heelpain Take a Moment to Focus in on Your Feet. Does one (or even both) of your heels hurt? If so, you aren t alone.
GET A HANDLE ON YOUR HEEL PAIN GUIDE American Podiatric Medical Association www.apma.org/heelpain Take a Moment to Focus in on Your Feet. Does one (or even both) of your heels hurt? If so, you aren t alone.
Predislocation syndrome
 Predislocation syndrome Sky Ridge Medical Center, Aspen Building Pre-dislocation syndrome, capsulitis, and metatarsalgia are all similar problems usually at the ball of the foot near the second and third
Predislocation syndrome Sky Ridge Medical Center, Aspen Building Pre-dislocation syndrome, capsulitis, and metatarsalgia are all similar problems usually at the ball of the foot near the second and third
Plantar Fasciitis Information Leaflet. Maneesh Bhatia. Consultant Orthopaedic Surgeon
 Plantar Fasciitis Information Leaflet Maneesh Bhatia Consultant Orthopaedic Surgeon What is plantar fasciitis? The plantar fascia is a strong band of tissue that stretches from the heel to the toes. It
Plantar Fasciitis Information Leaflet Maneesh Bhatia Consultant Orthopaedic Surgeon What is plantar fasciitis? The plantar fascia is a strong band of tissue that stretches from the heel to the toes. It
The Five Most Common Pathomechanical Foot Types (Rearfoot varus, forefoot varus, equinus, plantarflexed first ray, forefoot valgus)
 The Five Most Common Pathomechanical Foot Types (Rearfoot varus, forefoot varus, equinus, plantarflexed first ray, forefoot valgus) Pathomechanical foot types usually refer to structural deformities that
The Five Most Common Pathomechanical Foot Types (Rearfoot varus, forefoot varus, equinus, plantarflexed first ray, forefoot valgus) Pathomechanical foot types usually refer to structural deformities that
Hyperpronation and Foot Pain
 Hyperpronation and Foot Pain Steps Toward Pain-Free Feet Steven D. Stovitz, MD; J. Chris Coetzee, MD THE PHYSICIAN AND SPORTSMEDICINE - VOL 32 - NO. 8 - AUGUST 2004 For CME accreditation information, instructions
Hyperpronation and Foot Pain Steps Toward Pain-Free Feet Steven D. Stovitz, MD; J. Chris Coetzee, MD THE PHYSICIAN AND SPORTSMEDICINE - VOL 32 - NO. 8 - AUGUST 2004 For CME accreditation information, instructions
Posttraumatic medial ankle instability
 Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Calcaneus (Heel Bone) Fractures
 Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
Copyright 2010 American Academy of Orthopaedic Surgeons Calcaneus (Heel Bone) Fractures Fractures of the heel bone, or calcaneus, can be disabling injuries. They most often occur during high-energy collisions
The Land of Os: Accessory Ossicles of the Foot
 The Land of Os: Accessory Ossicles of the Foot Susan Cross, Anshul Rastogi, Rosy Jalan; Dept of Radiology, Barts Health NHS Trust, London, UK Contact: susan.cross@bartshealth.nhs.uk Pictorial review Abstract
The Land of Os: Accessory Ossicles of the Foot Susan Cross, Anshul Rastogi, Rosy Jalan; Dept of Radiology, Barts Health NHS Trust, London, UK Contact: susan.cross@bartshealth.nhs.uk Pictorial review Abstract
The Best Treatments for Plantar Heel Pain
 CLINICAL PODIATRY The Best Treatments for Plantar Heel Pain Objectives 1) Understand the pathway to wound healing through the three phases of inflammatory, proliferative, and remodeling. 2) Introduce the
CLINICAL PODIATRY The Best Treatments for Plantar Heel Pain Objectives 1) Understand the pathway to wound healing through the three phases of inflammatory, proliferative, and remodeling. 2) Introduce the
Common Foot Pathologies
 Common Foot Pathologies Chondromalacia Patella (patellofemoral pain syndrome) Chondromalacia Patella (patellofemoral pain syndrome) What is it? Chondromalacia (of Greek origin meaning softening of the
Common Foot Pathologies Chondromalacia Patella (patellofemoral pain syndrome) Chondromalacia Patella (patellofemoral pain syndrome) What is it? Chondromalacia (of Greek origin meaning softening of the
FORGET ME NOT: The Triple Arthrodesis
 C H A P T E R 1 5 FORGET ME NOT: The Triple Arthrodesis Andrea D. Cass, DPM INTRODUCTION The triple arthrodesis is a procedure that is performed much less commonly for the same conditions as it was 20
C H A P T E R 1 5 FORGET ME NOT: The Triple Arthrodesis Andrea D. Cass, DPM INTRODUCTION The triple arthrodesis is a procedure that is performed much less commonly for the same conditions as it was 20
CPME Memorandum Proper Logging of Surgical Procedures November 15, 2012
 For the procedure codes listed below, the program director must review each entry to determine proper usage. 1.13 other osseous digital procedure not listed above 2.3.10 other first ray procedure not listed
For the procedure codes listed below, the program director must review each entry to determine proper usage. 1.13 other osseous digital procedure not listed above 2.3.10 other first ray procedure not listed
Rheumatoid Arthritis of the Foot and Ankle
 Copyright 2011 American Academy of Orthopaedic Surgeons Rheumatoid Arthritis of the Foot and Ankle Rheumatoid arthritis is a chronic disease that attacks multiple joints throughout the body. It most often
Copyright 2011 American Academy of Orthopaedic Surgeons Rheumatoid Arthritis of the Foot and Ankle Rheumatoid arthritis is a chronic disease that attacks multiple joints throughout the body. It most often
How To Treat Heel Pain
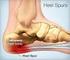 Plantar Fasciitis, Heel Spurs, Heel Pain The Plantar Fasciitis Organization is dedicated to the understanding of Plantar Fasciitis, Heel Spurs, and all other forms of Heel Pain. Welcome to the Plantar
Plantar Fasciitis, Heel Spurs, Heel Pain The Plantar Fasciitis Organization is dedicated to the understanding of Plantar Fasciitis, Heel Spurs, and all other forms of Heel Pain. Welcome to the Plantar
Foot Pain. Aching in arch of foot - worse after prolonged weight bearing
 1 Foot Pain "Pronatory Disorder" ICD-9-CM: 734 Flat foot (pes planus-acquired) Diagnostic Criteria History: Physical Exam: Aching in arch of foot - worse after prolonged weight bearing Excessive pronation
1 Foot Pain "Pronatory Disorder" ICD-9-CM: 734 Flat foot (pes planus-acquired) Diagnostic Criteria History: Physical Exam: Aching in arch of foot - worse after prolonged weight bearing Excessive pronation
.org. Lisfranc (Midfoot) Injury. Anatomy. Description
 Lisfranc (Midfoot) Injury Page ( 1 ) Lisfranc (midfoot) injuries result if bones in the midfoot are broken or ligaments that support the midfoot are torn. The severity of the injury can vary from simple
Lisfranc (Midfoot) Injury Page ( 1 ) Lisfranc (midfoot) injuries result if bones in the midfoot are broken or ligaments that support the midfoot are torn. The severity of the injury can vary from simple
Council on Podiatric Medical Education
 CPME MEMORANDUM November 15, 2012 TO: Program Directors and Residents FROM: Council on Podiatric Medical Education SUBJECT: By conference call in October 2012, members of the Council's Residency Review
CPME MEMORANDUM November 15, 2012 TO: Program Directors and Residents FROM: Council on Podiatric Medical Education SUBJECT: By conference call in October 2012, members of the Council's Residency Review
ADVANCEMENTS IN PLANTAR FASCIA SURGERY
 C H A P T E R 3 3 ADVANCEMENTS IN PLANTAR FASCIA SURGERY James L. Bouchard, DPM Andrea Cass, DPM INTRODUCTION It has been estimated that 90% of patients with plantar fasciitis and heel spur syndrome get
C H A P T E R 3 3 ADVANCEMENTS IN PLANTAR FASCIA SURGERY James L. Bouchard, DPM Andrea Cass, DPM INTRODUCTION It has been estimated that 90% of patients with plantar fasciitis and heel spur syndrome get
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
CAPPAGH NATIONAL ORTHOPAEDIC HOSPITAL, FINGLAS, DUBLIN 11. The Sisters of Mercy. Plantar Fascitis
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 2 7.0 Guideline... 3 7.1 Assessment... 3 7.2 Treatment...
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 2 7.0 Guideline... 3 7.1 Assessment... 3 7.2 Treatment...
Sports Injuries of the Foot and Ankle. Dr. Travis Kieckbusch August 7, 2014
 Sports Injuries of the Foot and Ankle Dr. Travis Kieckbusch August 7, 2014 Foot and Ankle Injuries in Athletes Lateral ankle sprains Syndesmosis sprains high ankle sprain Achilles tendon injuries Lisfranc
Sports Injuries of the Foot and Ankle Dr. Travis Kieckbusch August 7, 2014 Foot and Ankle Injuries in Athletes Lateral ankle sprains Syndesmosis sprains high ankle sprain Achilles tendon injuries Lisfranc
.org. Shoulder Pain and Common Shoulder Problems. Anatomy. Cause
 Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Plantar Fasciitis: Nonsurgical & Surgical Options for Chronic Heel Pain. Mathew M. John, DPM, FACFAS Atlanta, GA
 Plantar Fasciitis: Nonsurgical & Surgical Options for Chronic Heel Pain Mathew M. John, DPM, FACFAS Atlanta, GA Heel Pain:Plantar fasciitis Over 2 million Americans suffer from heel pain Most common cause
Plantar Fasciitis: Nonsurgical & Surgical Options for Chronic Heel Pain Mathew M. John, DPM, FACFAS Atlanta, GA Heel Pain:Plantar fasciitis Over 2 million Americans suffer from heel pain Most common cause
INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D.
 05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
By Agnes Tan (PT) I-Sports Rehab Centre Island Hospital
 By Agnes Tan (PT) I-Sports Rehab Centre Island Hospital Physiotherapy Provides aids to people Deals with abrasion and dysfunction (muscles, joints, bones) To control and repair maximum movement potentials
By Agnes Tan (PT) I-Sports Rehab Centre Island Hospital Physiotherapy Provides aids to people Deals with abrasion and dysfunction (muscles, joints, bones) To control and repair maximum movement potentials
Arches. Foot Injuries. Medial Longitudinal Arch. Lateral Longitudinal Arch. Transverse Arch. Arch Strains
 Arches Foot Injuries Three arches in the foot: 1) Lateral longitudinal arch 2) Medial longitudinal arch 3) Transverse arch These arches are maintained and supported by the wedging of the interlocking tarsal
Arches Foot Injuries Three arches in the foot: 1) Lateral longitudinal arch 2) Medial longitudinal arch 3) Transverse arch These arches are maintained and supported by the wedging of the interlocking tarsal
Plantar Heel Pain. Papers. Shazia Ali, FY2 Davinder Paul Singh Baghla
 Shazia Ali, FY2 Davinder Paul Singh Baghla Abstract Plantar Heel pain is one of the most commonly encountered problems of foot pain in active adults over the age of 40. One in ten people will experience
Shazia Ali, FY2 Davinder Paul Singh Baghla Abstract Plantar Heel pain is one of the most commonly encountered problems of foot pain in active adults over the age of 40. One in ten people will experience
Deformities. Assessment of Foot. The majority of foot deformities occur in otherwise healthy infants. However most generalized.
 Assessment of Foot Deformities in the Infant By Maureen Baxter, MDCM, FRCS The majority of foot deformities occur in otherwise healthy infants. However most generalized neurologic disorders (spina bifida,
Assessment of Foot Deformities in the Infant By Maureen Baxter, MDCM, FRCS The majority of foot deformities occur in otherwise healthy infants. However most generalized neurologic disorders (spina bifida,
Physician Assistant Post Graduate Orthopaedic Surgery Fellowship Program. Watauga Orthopaedics
 Physician Assistant Post Graduate Orthopaedic Surgery Fellowship Program Watauga Orthopaedics Physician Assistant Post-Graduate Fellowship Program in Orthopaedic Surgery Required Texts: 1. Backache Macnab,
Physician Assistant Post Graduate Orthopaedic Surgery Fellowship Program Watauga Orthopaedics Physician Assistant Post-Graduate Fellowship Program in Orthopaedic Surgery Required Texts: 1. Backache Macnab,
Understanding. Heel Pain
 Understanding Heel Pain What Causes Heel Pain? Heel pain is a common problem that occurs when the heel is placed under too much stress. Heel pain is most often caused by walking in ways that irritate tissues
Understanding Heel Pain What Causes Heel Pain? Heel pain is a common problem that occurs when the heel is placed under too much stress. Heel pain is most often caused by walking in ways that irritate tissues
Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma. Magee, 2008. pg.
 PTA 216 Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma Magee, 2008. pg. 396 28 bones Numerous articulations 19 intrinsic muscles
PTA 216 Most active and intricate part of the upper extremity Especially vulnerable to injury Do not respond well to serious trauma Magee, 2008. pg. 396 28 bones Numerous articulations 19 intrinsic muscles
LATERAL PAIN SYNDROMES OF THE FOOT AND ANKLE
 C H A P T E R 3 LATERAL PAIN SYNDROMES OF THE FOOT AND ANKLE William D. Fishco, DPM The majority of patient encounters with the podiatrist are secondary to pain in the foot and/or ankle. If we draw an
C H A P T E R 3 LATERAL PAIN SYNDROMES OF THE FOOT AND ANKLE William D. Fishco, DPM The majority of patient encounters with the podiatrist are secondary to pain in the foot and/or ankle. If we draw an
Pilates for Plantar Fasciitis
 Pilates for Plantar Fasciitis Written by: Heather Light Date: August, 2011 This is a student paper, submitted to BASI Pilates by the writer as a requirement for completion of the BASI Pilates Comprehensive
Pilates for Plantar Fasciitis Written by: Heather Light Date: August, 2011 This is a student paper, submitted to BASI Pilates by the writer as a requirement for completion of the BASI Pilates Comprehensive
Glossary of Foot & Ankle Terminology
 Glossary of Foot & Ankle Terminology Achilles Tendon One of the longer tendons in the body, stretching from the bones of the heel to the calf muscles. Abrasion An injury in which superficial layers of
Glossary of Foot & Ankle Terminology Achilles Tendon One of the longer tendons in the body, stretching from the bones of the heel to the calf muscles. Abrasion An injury in which superficial layers of
November 2012 Case Study. Authors: Kyle Nagle, MD, MPH; Karl Fry, PT, DPT, OCS; David Bernhardt, MD
 CC: Right foot pain November 2012 Case Study Authors: Kyle Nagle, MD, MPH; Karl Fry, PT, DPT, OCS; David Bernhardt, MD HPI: A 17 year old female cross country runner presents with right foot pain. At a
CC: Right foot pain November 2012 Case Study Authors: Kyle Nagle, MD, MPH; Karl Fry, PT, DPT, OCS; David Bernhardt, MD HPI: A 17 year old female cross country runner presents with right foot pain. At a
Hip Bursitis/Tendinitis
 Hip Bursitis/Tendinitis Anatomy and Biomechanics The hip is a ball and socket joint that occurs between the head of the femur (ball) and the acetabulum of the pelvis (socket). It is protected by several
Hip Bursitis/Tendinitis Anatomy and Biomechanics The hip is a ball and socket joint that occurs between the head of the femur (ball) and the acetabulum of the pelvis (socket). It is protected by several
Foot and Ankle Complaints
 Foot and Ankle Complaints INTRODUCTION Anatomy and Function Foot Ankle Common complaints Common diagnoses FOOT AND ANKLE ANATOMY 26 bones and 2 sesamoids Forefoot Metatarsals phalanges Midfoot 5 tarsals
Foot and Ankle Complaints INTRODUCTION Anatomy and Function Foot Ankle Common complaints Common diagnoses FOOT AND ANKLE ANATOMY 26 bones and 2 sesamoids Forefoot Metatarsals phalanges Midfoot 5 tarsals
How To Treat Turf Toe Injuries
 How To Treat Turf Toe Injuries Turf toe injuries can have a significant impact upon the playing time of professional athletes. Accordingly, this author reviews the etiology of these injuries and assesses
How To Treat Turf Toe Injuries Turf toe injuries can have a significant impact upon the playing time of professional athletes. Accordingly, this author reviews the etiology of these injuries and assesses
Rehabilitation Guidelines for Lateral Ankle Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Lateral Ankle Reconstruction The ankle is a very complex joint. There are actually three joints that make up the ankle complex: the tibiotalar
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Lateral Ankle Reconstruction The ankle is a very complex joint. There are actually three joints that make up the ankle complex: the tibiotalar
Field Evaluation and Management of Non-Battle Related Knee and Ankle Injuries by the ATP in the
 Field Evaluation and Management of Non-Battle Related Knee and Ankle Injuries by the ATP in the JF Rick Hammesfahr, MD Editor s Note: Part Three consists of ankle injury evaluation and taping. Part Two
Field Evaluation and Management of Non-Battle Related Knee and Ankle Injuries by the ATP in the JF Rick Hammesfahr, MD Editor s Note: Part Three consists of ankle injury evaluation and taping. Part Two
Pathomechanics, Gait Deviations, and Treatment of the Rheumatoid Foot
 Pathomechanics, Gait Deviations, and Treatment of the Rheumatoid Foot A Clinical Report PHYLLIS DIMONTE and HOLLIS LIGHT This article describes the five major foot deformities or problems often seen in
Pathomechanics, Gait Deviations, and Treatment of the Rheumatoid Foot A Clinical Report PHYLLIS DIMONTE and HOLLIS LIGHT This article describes the five major foot deformities or problems often seen in
Do I need a physician referral? Yes, we see patients on referral from a health care provider.
 FAQS FOR OFFICE POLICIES How do I get an appointment? New appointments are made by physician referral only. Your referring health care provided will call for the appointment for you. What do I need to
FAQS FOR OFFICE POLICIES How do I get an appointment? New appointments are made by physician referral only. Your referring health care provided will call for the appointment for you. What do I need to
The plantar fascia as a source of painfbiomechanics, presentation and treatment
 Journal of Bodywork and Movement Therapies (2004) 8, 214 226 ARTICLE IN PRESS Journal of Bodywork and Movement Therapies www.intl.elsevierhealth.com/journals/jbmt PLANTAR HEEL PAIN SYNDROME: OVERVIEW AND
Journal of Bodywork and Movement Therapies (2004) 8, 214 226 ARTICLE IN PRESS Journal of Bodywork and Movement Therapies www.intl.elsevierhealth.com/journals/jbmt PLANTAR HEEL PAIN SYNDROME: OVERVIEW AND
Synopsis of Causation. Pes Planus
 Ministry of Defence Synopsis of Causation Pes Planus Author: Mr Matthew J Wilson, Ninewells Hospital and Medical School, Dundee Validator: Mr William Body, The Hillingdon Hospital, Uxbridge September 2008
Ministry of Defence Synopsis of Causation Pes Planus Author: Mr Matthew J Wilson, Ninewells Hospital and Medical School, Dundee Validator: Mr William Body, The Hillingdon Hospital, Uxbridge September 2008
Runner's Injury Prevention
 JEN DAVIS DPT Runner's Injury Prevention Jen Davis DPT Orthopedic Physical Therapy Foot Traffic 7718 SE 13th Ave Portland, OR 97202 (503) 482-7232 Jen@runfastpt.com www.runfastpt.com!1 THE AMAZING RUNNER
JEN DAVIS DPT Runner's Injury Prevention Jen Davis DPT Orthopedic Physical Therapy Foot Traffic 7718 SE 13th Ave Portland, OR 97202 (503) 482-7232 Jen@runfastpt.com www.runfastpt.com!1 THE AMAZING RUNNER
Most Common Running Injuries
 Most Common Running Injuries 1. Achilles Tendonitis 2. Chrondomalacia Runner s Knee 3. Iliotibial Band (ITB) syndrome 4. Plantar Fasciitis 5. Shin Splints Achilles Tendonitis inflammation of the Achilles
Most Common Running Injuries 1. Achilles Tendonitis 2. Chrondomalacia Runner s Knee 3. Iliotibial Band (ITB) syndrome 4. Plantar Fasciitis 5. Shin Splints Achilles Tendonitis inflammation of the Achilles
This is caused by muscle strain to the Achilles tendon in the heel of the foot.
 Foot Facts Our feet were designed to move across uneven earthy surfaces. The hard, inflexible surfaces that we regularly walk on today, such as concrete, tile or wood, leave our feet wanting in terms of
Foot Facts Our feet were designed to move across uneven earthy surfaces. The hard, inflexible surfaces that we regularly walk on today, such as concrete, tile or wood, leave our feet wanting in terms of
Plantar Fascia: Imaging Diagnosis and Guided Treatment
 Plantar Fascia: Imaging Diagnosis and Guided Treatment Eugene G. McNally, F.R.C.P.I., F.R.C.R. 1 and Shilpa Shetty, F.R.C.R. 1 ABSTRACT Plantar fasciopathy is a common cause of heel pain. This article
Plantar Fascia: Imaging Diagnosis and Guided Treatment Eugene G. McNally, F.R.C.P.I., F.R.C.R. 1 and Shilpa Shetty, F.R.C.R. 1 ABSTRACT Plantar fasciopathy is a common cause of heel pain. This article
JOINT PAIN IN THE ADOLESCENT
 JOINT PAIN IN THE ADOLESCENT HOW SERIOUS CAN THAT BE? ROBERT A. KELLY, M.D. RESURGENS ORTHOPAEDICS JOINT PAIN IN THE ADOLESCENT INJURIES ABOUT JOINTS CAN BE CLASSIFIED AS EITHER: ACUTE/TRAUMATIC OR REPETITIVE/OVERUSE
JOINT PAIN IN THE ADOLESCENT HOW SERIOUS CAN THAT BE? ROBERT A. KELLY, M.D. RESURGENS ORTHOPAEDICS JOINT PAIN IN THE ADOLESCENT INJURIES ABOUT JOINTS CAN BE CLASSIFIED AS EITHER: ACUTE/TRAUMATIC OR REPETITIVE/OVERUSE
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Spinal Anatomy. * MedX research contends that the lumbar region really starts at T-11, based upon the attributes of the vertebra.
 Spinal Anatomy Overview Neck and back pain, especially pain in the lower back, is one of the most common health problems in adults. Fortunately, most back and neck pain is temporary, resulting from short-term
Spinal Anatomy Overview Neck and back pain, especially pain in the lower back, is one of the most common health problems in adults. Fortunately, most back and neck pain is temporary, resulting from short-term
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
Commonly Missed Fractures in the Emergency Department
 Commonly Missed Fractures in the Emergency Department Taylor Sittler MS IV - UMASS Images courtesy of Jim Wu, MD, Sanjay Shetty, MD and Mary Hochman, MD Diagnostic Errors in the ED Taylor Sittler, MS IV
Commonly Missed Fractures in the Emergency Department Taylor Sittler MS IV - UMASS Images courtesy of Jim Wu, MD, Sanjay Shetty, MD and Mary Hochman, MD Diagnostic Errors in the ED Taylor Sittler, MS IV
What is petellofemoral Pain syndrome?
 Jackie Davis What is petellofemoral Pain syndrome? Patellofemoral Syndrome can be defined as retropatellar or peripatellar pain resulting from physical and biochemical changes in the patellofemoral joint.
Jackie Davis What is petellofemoral Pain syndrome? Patellofemoral Syndrome can be defined as retropatellar or peripatellar pain resulting from physical and biochemical changes in the patellofemoral joint.
OS TRIGONUM SYNDROME. Incidence: 10% unilateral and 2% bilateral in general population 1. Bilateral occurs in 50% of os trigonum population 4.
 OS TRIGONUM SYNDROME Incidence: 10% unilateral and 2% bilateral in general population 1. Bilateral occurs in 50% of os trigonum population 4. Mechanism of Injury: Os trigonum syndrome occurs due to repetitive,
OS TRIGONUM SYNDROME Incidence: 10% unilateral and 2% bilateral in general population 1. Bilateral occurs in 50% of os trigonum population 4. Mechanism of Injury: Os trigonum syndrome occurs due to repetitive,
Plantar fasciitis in a Professional Boxer:
 Plantar fasciitis in a Professional Boxer: Clinical Case Report for The Trevor Silver Memorial Essay Prize Gurjit Bhogal MBChB (Hons) MSc MRCGP July 2012 Total Word Count (excluding References) 2976 words
Plantar fasciitis in a Professional Boxer: Clinical Case Report for The Trevor Silver Memorial Essay Prize Gurjit Bhogal MBChB (Hons) MSc MRCGP July 2012 Total Word Count (excluding References) 2976 words
Acute Ankle Injuries, Part 1: Office Evaluation and Management
 t June 08, 2009 Each acute ankle injury commonly seen in the office has associated with it a mechanism by which it can be injured, trademark symptoms that the patient experiences during the injury, and
t June 08, 2009 Each acute ankle injury commonly seen in the office has associated with it a mechanism by which it can be injured, trademark symptoms that the patient experiences during the injury, and
Biomechanical Explanations for Selective Sport Injuries of the Lower Extremity
 Biomechanical Explanations for Selective Sport Injuries of the Lower Extremity DR. LEE S. COHEN Podiatric Consultant: Philadelphia Eagles Philadelphia 76ers Philadelphia Wings Understanding Normalcy What
Biomechanical Explanations for Selective Sport Injuries of the Lower Extremity DR. LEE S. COHEN Podiatric Consultant: Philadelphia Eagles Philadelphia 76ers Philadelphia Wings Understanding Normalcy What
Imaging of Lisfranc Injury
 November 2011 Imaging of Lisfranc Injury Greg Cvetanovich, Harvard Medical School Year IV Agenda Case Presentation Introduction Anatomy Lisfranc Injury Classification Imaging Treatment 2 Case Presentation
November 2011 Imaging of Lisfranc Injury Greg Cvetanovich, Harvard Medical School Year IV Agenda Case Presentation Introduction Anatomy Lisfranc Injury Classification Imaging Treatment 2 Case Presentation
For lecture notes: Allied OSI Orthotic Lab. Demographics. www.richiebrace.com/handouts.htm. Lecture Handout Courtesy Of:
 New Thoughts and Orthotic Strategies in the Treatment of Plantar Heel Pain Syndrome Lecture Handout Courtesy Of: Allied OSI Orthotic Lab Douglas H. Richie Jr., DPM Adjunct Associate Clinical Professor-Department
New Thoughts and Orthotic Strategies in the Treatment of Plantar Heel Pain Syndrome Lecture Handout Courtesy Of: Allied OSI Orthotic Lab Douglas H. Richie Jr., DPM Adjunct Associate Clinical Professor-Department
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY.
 QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
