Psoriasis takes center stage in immune-mediated diseases
|
|
|
- Roger Anderson
- 8 years ago
- Views:
Transcription
1 BUMC Proceedings 1998;11: Psoriasis takes center stage in immune-mediated diseases SARAH RODMAN 4TH YR STUDENT The University of Texas Southwestern Medical School ALAN MENTER, MD Medical Director, Psoriasis Research Center, BUMC soriasis has long been considered a banal disease confined to the skin. Early researchers focused on the impressive epidermal proliferation seen in this disease, believing that the root cause was a defect in the epidermis. However, in the past 20 years, the focus has shifted dramatically away from the epidermal surface toward the immune system s role in psoriasis. This change was sparked by the 1979 discovery that cyclosporine, a drug that inhibits T-cell activation and cytokine release, cleared concurrent psoriasis in a patient with rheumatoid arthritis (1). Additional strong evidence linking the immune system to psoriasis comes from the fact that psoriasis is associated with the inheritance of certain major histocompatibility complex (MHC) antigens. Furthermore, immunohistochemical analysis of psoriatic lesions has isolated activated T cells within the lesions. This evidence has led current investigators to believe that immune abnormalities are at the heart of this disease and to aim toward defining them. Psoriasis is now considered to be a systemic disease of immune dysfunction that just happens to be visible on the skin, much like the immune abnormalities of rheumatoid arthritis (RA) that show up in joints, and those of Crohn s disease, in the bowel. Evidence supports the central role that psoriasis plays in diseases of the immune system and that drugs currently used for psoriasis and those under development may have a role in the treatment of other immune-mediated diseases, including cancers and graft-versus-host disease (GVHD) after bone marrow transplantation. EPIDEMIOLOGIC AND CLINICAL FINDINGS Psoriasis is a common disease that affects up to 2% of the population in Western countries (2). Based on epidemiologic and clinical studies, the peak onset of psoriasis is between 20 and 35 years of age, and 70% to 90% of patients manifest the disease before reaching 40 years of age. However, <10% of patients present with lesions during childhood. Psoriasis has been divided into 2 subtypes, much like diabetes mellitus, based on the age of onset: type I psoriasis, which typically presents prior to age 40, and type II psoriasis, which occurs after age 50. Immunogenetic distinctions between the 2 types will be discussed later. The 3 cardinal features of psoriasis are scaling, erythema, and induration. The characteristic silvery scale reflects the increased proliferation and turnover of keratinocytes and is the pathogenic process that differentiates psoriasis from other common inflammatory skin diseases such as eczema. Erythema and induration reflect the inflammatory infiltrate of T lymphocytes, monocytes, and neutrophils in psoriatic lesions (3). A classic feature of psoriasis is demonstrated by scratching the lesion surface lightly with a fingernail or tongue depressor to elicit fine pinpoint bleeding within seconds. This is the Auspitz sign, which is due to enlarged and tortuous capillaries close to the skin surface. These capillaries not only reflect the inflammation going on within the plaque, but also impart the characteristic red hue to the lesions.
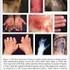
2 Although these features comprise the cutaneous manifestations of psoriasis, the disease can present in a number of phenotypically distinct ways (4, 5). Morphological variants include discoid plaque psoriasis, elephantine psoriasis, erythrodermic psoriasis, flexural psoriasis, guttate psoriasis, palmar-plantar psoriasis, and pustular psoriasis. Chronic plaque psoriasis accounts for 90% of the cases and consists of localized disk-shaped plaques, usually on the elbows, knees, and scalp, that remain stable throughout the history of the disease (Figure 1). Other classic areas of involvement include the face, genital regions, and intertriginous folds. In most cases, the distribution of lesions is highly symmetrical, although trauma or scratching can modify the symmetry. Flexural psoriasis is characterized by plaques in body folds, including the buttocks, axillae, groin, breasts, ears, and glans penis. It is seen most in the skin folds of obese patients, frequently in association with candidiasis. Elephantine psoriasis describes the variant of large, thick plaques >15 cm in diameter that may be found on the lumbosacral regions and legs of patients with long-standing disease. Guttate psoriasis is characterized by guttate lesions, or papules, between 0.1 cm and 1.0 cm in diameter, commonly seen after streptococcal infections in young patients. In palmar-plantar psoriasis, the palms and soles may be involved as part of a generalized eruption, or they may be the only manifestation of the disease (Figure 2). Generalized pustular psoriasis is a rare but serious and sometimes fatal disease. Numerous tiny, sterile pustules evolve from an erythematous base and coalesce into lakes of pus. Erythrodermic psoriasis is a severe and highly unstable disease (Figure 3) that usually covers the entire body surface and is triggered by infections, inappropriate systemic glucocorticoid use, burns incurred during phototherapy, or by abrupt discontinuation of methotrexate therapy. Psoriasis also manifests itself in the nails and in the joints (Figure 4). Pitting is the best known and probably most frequent nail abnormality. Others include separation of the nail from the nail bed (onycholysis), subungual crusting from hyperkeratosis, and nail fragmentation and crumbling. Psoriatic arthritis is a distinct form of arthritis that is rheumatoid factor negative. It affects 5% to 8% of psoriatics. The prevalence is higher among patients with more severe cutaneous disease. Psoriasis is a disease of wide clinical variability. With the new understanding that it is a systemic, immune-mediated disease, psoriasis needs to be recognized as a spectrum of diseases, in the same light as lupus erythematosus (LE), another immune-mediated disease. Lupus erythematosus can range from mild-to-moderate disease confined to the skin, to a devastating systemic disease involving the heart, kidneys, and central nervous system. Similarly, psoriasis can range from well-controlled, stable plaques involving <10% of the body surface, to erythrodermic and pustular forms with joint and nail deformities that can cause significant morbidity and even death. IMMUNOPATHOLOGY Systemic immunological abnormalities Early clues that psoriasis is a disease of the immune system came from the observance of systemic alterations. Raised serum levels of immunoglobulin A, E, and G have been demonstrated, as well as circulating immune complexes (6). Psoriasis patients have variations in suppressor-helper T-cell ratios and in granulocyte and monocyte function (7). Elevated circulating soluble interleukin (IL)-2 receptor, neopterin, and soluble adhesion molecules (intercellular adhesion molecule [ICAM-1], vascular cell adhesion molecule [VCAM-1], and E-selectin) also have been observed (8) (Groves RW, Barker JN, Haskard
3 DO, Bird C, MacDonald DM: Circulating cytokines and soluble adhesion molecules in widespread inflammatory skin disease. Brit J Derm 1992;127:428 [abstract]). Whether these abnormalities are secondary to the process occurring within psoriatic plaques or are more central to the pathogenic process is unknown. Local immunological abnormalities Current theory on the immunopathogenesis of psoriasis has at its center an interaction between antigen-presenting cells (APCs) and T lymphocytes (9). Lesional APCs process an antigen and present it on their surface through MHC class I or II molecules. This antigen causes the T cell to interact with the APC, and the interaction triggers an immune response through the activation of T cells and subsequent release of lymphokines. This immunologic activation injures the epidermis, leading to hyperproliferation and disordered differentiation. It also activates the keratinocytes themselves, causing them to release cytokines that perpetuate the inflammation and the cell-mediated immune response. Thus, the current model no longer considers the epidermal changes themselves to be primary causative factors of psoriasis, but instead to be a response to underlying immunologic injury. Although the antigen triggering the APC T cell interaction in psoriasis has not been identified, there are several current theories. One thought is that streptococcal proteins or toxins may be the trigger, because a sizable fraction of adolescent patients with acute guttate psoriasis have as a precipitating factor an antecedent streptococcal infection (10). Crossreactivity exists between streptococcal antigens and antigens present in the skin (11), and monoclonal antibodies raised to group A streptococci cross-react with various keratinocyte proteins (12). This leads to the molecular mimicry theory of autoimmunity in psoriasis, where T lymphocytes responding to a peptide fragment of an infectious agent in the skin see a host protein as homologous and react to self as well as to the infectious agent. The fact that most patients have no preceding streptococcal infection lends more weight to the theory that autoantigens alone are triggering the APC T cell interaction in genetically susceptible patients. Another theory is that in patients with explosive acute guttate psoriasis, streptococcal superantigens stimulate a polyclonal T-cell response (13). Superantigens stimulate T cells by binding to distinct V? regions of the T-cell receptor. However, another study found that single T-cell receptor sequences from lesional skin accounted for up to 56% of a T-cell receptor family, and these were absent in V? T-cell receptors amplified from normal skin (14). These results are evidence against a superantigen-driven T-cell stimulation and suggest instead an antigen-specific immune response. Although the antigen triggering the immune response in psoriasis is unclear, there are data to support the APC T cell interaction as instigating the immune response in psoriatic lesions. In normal human skin, APCs are represented by Langerhans cells that are MHC II positive (HLA-DR + ). Baadsgaard et al have shown that the activated APCs driving T cells are actually non-langerhans cell CD1a DR + macrophage-like cells (15). The APCs have been shown to induce T lymphocytes to produce a range of cytokines that may modulate the psoriatic process (7). Morganroth et al have shown that a second type of APC is present within the lesional dermis (16). These activated APCs, termed dermal dendrocytes, are located high in the papillary dermis around blood vessels and are factor XIIIA positive. These 2 types of activated APCs are responsible for the heightened APC activity found in the lesions and support the role of the APC presenting lesional T cells with an antigen to cause T-cell activation.
4 Further data support the role of T cells in psoriasis. Histologic studies of skin biopsies of early psoriatic skin lesions demonstrate CD4 + and CD8 + T lymphocytes in both the dermis and the epidermis (17). Their influx precedes that of neutrophils and precedes the epidermal hyperproliferation characteristic of psoriasis (18). Interleukin-2 receptor positivity on lesional T cells is evidence that these T cells are activated and proliferating and thus have the potential to cause disease (9). Lesional T cells also have been shown to produce the lymphokines of activated T-1 cells: IL-2 and interferon (IFN)- (19).The injection of IL-2 or IFN- into psoriasis patients has resulted in disease flares in significant numbers of patients (20). In addition, lymphokine-containing supernatants prepared from T cells cloned from psoriatic lesions caused the proliferation of uninvolved psoriatic keratinocytes when they were added to the keratinocytes in vitro. This keratinocyte growth was inhibited by adding antibodies to IFN- to the supernatants prior to adding to the keratinocyte cultures (21). These data implicate IFN- release from T-1 type T cells within the lesions as a critical factor in the disease pathogenesis. They also link immune system activation to the epidermal hyperproliferation seen in psoriasis. Current research aims to more precisely define the role of CD4 + and CD8 + T lymphocytes. Other goals include finding therapies targeted at inhibiting cytokine release and reducing the activity of the infiltrating lymphocytic cells. IMMUNOTHERAPY Since the serendipitous finding of Mueller and Hermann that cyclosporine cleared psoriasis (1), immunosuppressive drugs have been studied for, and used to treat, psoriasis. Based on the above discussion of the activated APC T cell complex in psoriatic lesions, drugs that suppress any part of this complex and its subsequent release of lymphokines should clear psoriatic lesions. Cyclosporine impairs the signal transduction mechanism within T cells and thereby blocks T-cell growth and IFN- release. Ellis et al have shown that cyclosporine produces rapid resolution of psoriatic lesions when given systemically (22). It is also effective intralesionally, but not topically, most likely because of lack of penetration through epidermal structures (23). Tacrolimus, ascomycin, and rapamycin have the same mechanism of action as cyclosporine and also have shown to be beneficial in psoriasis. Methotrexate currently is the gold standard systemic therapy for psoriasis, having been used for over 30 years. It was originally thought to work in psoriasis through inhibiting DNA synthesis in the rapidly dividing cells of the hyperproliferating epidermis. Now that immunologic activation is believed to cause psoriasis, methotrexate is thought to clear the lesions through its immunosuppressive effects. Methotrexate promotes the accumulation of extracellular adenosine, which, via A2 receptors, causes immunosuppression (24). Sulfasalazine appears to act via a similar mechanism (25). Other agents commonly used to treat psoriasis, such as steroids, retinoids, and vitamin D 3 derivatives, block T-cell transcription of lymphokine genes (26, 27). Ultraviolet radiation works by inducing the formation of IL-10 which is believed to be a natural suppressant of the cutaneous inflammatory response (28). Current research in psoriasis immunotherapy is testing antibodies to various lymphokines and CD4 + cell receptors, as well as peptide vaccines. Multiple clinical studies using immune-modulating drugs, including CTLA4IG, fusion protein LFA-3/IgG 1, anti IL-8, and IL-10, are currently under way at the Baylor Psoriasis Research Unit. The common mechanism to all these therapeutic approaches is immunosuppression, which may have important applications for other immune-mediated diseases. Because psoriasis manifests so
5 visibly on the skin, the therapeutic response can be monitored easily. In addition, as most psoriasis subjects are relatively healthy, they represent a good model in which to study the effects of immunosuppressive therapy. OTHER IMMUNE-MEDIATED DISEASES WITH CUTANEOUS MANIFESTATIONS Lupus erythematosus Psoriasis is one of several immune-mediated diseases that affect the skin (29, 30). Lupus erythematosus is a systemic disease that, like psoriasis, has a spectrum of disease manifestations. Discoid LE consists primarily of lesions localized to the skin, with systemic involvement in only 5% to 10% of patients. The lesions are most often on the face, scalp, or external ears and consist of erythematous papules or plaques with a thick adherent scale that occludes hair follicles. Long-standing lesions develop atrophy, scarring, and hypopigmentation with erythematous raised borders at the periphery. Subacute cutaneous LE is a more serious form of cutaneous LE, characterized by a widespread photosensitive nonscarring eruption. It is often papulosquamous and closely resembles psoriasis (Figure 5). About half of these patients have systemic LE, but severe renal or central nervous system involvement is uncommon. Acute cutaneous LE often occurs with multisystem disease and is characterized by erythema of the nose and malar eminencies in a butterfly distribution. It can also show widespread indurated erythema, especially on the extensor surfaces of the extremities and upper chest. The tissue damage of LE is caused by production of numerous diverse autoantibodies to nuclear and cytoplasmic cell components and by immune complexes. Immunofluorescent microscopy of the skin lesions shows deposition of immunoglobulin and complement along the dermal-epidermal junction. In subacute cutaneous LE, antibodies to Ro/SSA antigens have been found. There is thought to be a clonal selection of B cells secreting antibodies to autoantigens. In most murine lupus models, T-cell help is critical to the development of fullblown disease. CD4 +, CD8 +, and CD4 CD8 T cells all help autoantibody production in murine and human LE. Rheumatoid arthritis Rheumatoid arthritis is characterized by a persistent inflammatory synovitis, usually involving peripheral joints in a symmetric distribution. The synovial inflammation causes cartilage destruction and bone erosions with subsequent changes in joint integrity. Rheumatoid factor is positive in 90% of cases. Rheumatoid arthritis is identical to 1 of the 5 forms of psoriatic arthritis, except for rheumatoid factor being negative in psoriatic joint disease. Proximal interphalangeal and metacarpophalangeal joints of the hands, wrists, ankles, and knees are commonly involved in a symmetric fashion in RA. The distal interphalangeal joints are rarely involved. Joints are red, swollen, tender, and limited in motion. Characteristic deformities of the hands include ulnar deviation of the digits and swan-neck and boutonni?re deformities. Extra-articular manifestations include rheumatoid nodules, weakness and atrophy of skeletal muscle, pleuropulmonary manifestations, splenomegaly, neutropenia, osteoporosis, and rheumatoid vasculitis. When rheumatoid vasculitis affects the skin, it presents as crops of small brown spots in the nail beds, nail folds, and digital pulp. Larger ischemic skin ulcers also may develop, especially in the
6 lower extremities. Rheumatoid arthritis is an immune disease of both activated T cells and B cells. The earliest event in the synovitis appears to be a nonspecific inflammatory response initiated by an unknown stimulus. Subsequently, a response of CD4 + T cells is induced that amplifies and perpetuates the inflammation. The presence of activated T cells is thought to induce polyclonal B-cell stimulation and the local production of rheumatoid factor. The activity of cytokines produced from active lymphocytes, macrophages, and fibroblasts causes synovial tissue inflammation, synovial fluid inflammation, synovial proliferation, cartilage and bone damage, and even the systemic manifestations of RA. Thus, the inflammatory cascade in RA is similar to that of psoriasis, with the synovium substituted for the skin. As tissue damage in RA occurs, additional autoantigens are revealed, and further clones of CD4 + T cells are recruited to the inflammatory site. As a result of persistent exposure to the inflammatory milieu, the function of synovial fibroblasts is altered so that they acquire destructive potential that no longer requires stimulation from T cells or macrophages, and damage progresses without control. Drugs used in therapy for RA, as well as for LE, include steroids, azathioprine, sulfasalazine, and cyclosporine. These are often first-line drugs for patients with psoriasis. Graft-versus-host disease In GVHD, the histoincompatible, immunocompetent donor bone marrow cells attack the tissues of the host. Even when the donor and host are completely matched at the HLA loci, there are differences at minor histocompatibility loci. Donor CD4 + and CD8 + and natural killer cells participate in the immune response against host antigens. The activated T cells and natural killer cells produce IFN- and tumor necrosis factor (TNF)-, which are thought to mediate the tissue destruction in acute GVHD that occurs within 3 months of transplantation. Interleukin-4 from activated T cells has been suggested as the primary mediator of chronic GVHD, which can evolve from acute GVHD or can arise de novo. Graft-versus-host disease is characterized by acute cutaneous changes ranging from maculopapular eruption to toxic epidermal necrolysis. Diarrhea and liver dysfunction also occur acutely. Chronic skin changes include lichenoid eruptions and changes identical to scleroderma. Psoralen plus ultraviolet A therapy, commonly used to treat psoriasis, frequently is of great value in treating patients with GVHD. Cutaneous T-cell lymphoma As the name implies, cutaneous T-cell lymphoma (CTCL) is a malignancy of helper T cells (CD4 + ) that first manifests in the skin.however, because the neoplastic process involves the entire lymphoreticular system, the lymph nodes and internal organs become involved in the course of the disease. Skin findings in mycosis fungoides, the primary form of CTCL, progress through various stages. Initially, lesions can vary from a nonspecific pruritic eruption or pruritus alone, to eczematous patches, psoriasis-like plaques, and cigarettepaper atrophic skin lesions with telangiectasia and mottled pigmentation (Figure 6). A number of patients have been referred to the Psoriasis Treatment Center at Baylor with a working diagnosis of psoriasis and have been shown on further evaluation to have CTCL. The disease then progresses through a patch stage, a plaque stage, and finally a tumor stage. In the early stages, the disease remains confined to the skin. Superficial lymphadenopathy may be detected in the plaque stage, and deep lymphadenopathy with visceral metastases to
7 the spleen, lungs, or gastrointestinal tract may occur during the tumor stage. Cutaneous T-cell lymphoma is a malignancy of a single clone of CD4 + T cells that may originate from stimulation by an antigen, possibly from a mutation or a virus. The malignant cells express mature, activated T helper cell markers: CD2, CD3, CD4, CD5, CD7, IL-2 receptor, and transferrin receptor. Initially, Langerhans cells carry antigens from the skin to peripheral lymph nodes. There they present the antigens to CD4 + T cells and convert them to cutaneous T cell lymphoma cells. These cells acquire cutaneous lymphoid antigen on their surface, which acts as a homing receptor directing them to the skin. The cellular growth environment of the epidermis is conducive to the malignant cells proliferation. Agents currently used to treat CTCL include systemic retinoids and psoralen plus ultraviolet A therapy, which are both used as well for psoriasis patients. Acquired immunodeficiency syndrome Psoriasis can be the initial sign or one of the first signs of acquired immunodeficiency syndrome (AIDS). An explosive onset of psoriasis with erythroderma or pustular lesions should lead to the suspicion of AIDS. This association with the human immunodeficiency virus (HIV), one that dysregulates and destroys the human immune system, supports the hypothesis that psoriasis is an immune-mediated disease. Duvic suggests several hypotheses regarding HIV-associated psoriasis (31). One is that the immunodysregulation resulting from HIV infection may trigger psoriasis, especially if psoriasis is an autoimmune disease. Another is that the decreased cellular immunity may allow the emergence of opportunistic infectious organisms that could act as the antigens triggering psoriasis or could activate a latent retrovirus. Because HIV has been shown to infect the cutaneous Langerhans cells, Duvic also proposes that HIV may have a more direct causative role in psoriasis. The fact that zidovudine, a drug that reduces viral replication, is associated with a dramatic remission when given to patients with HIV-associated psoriasis supports the role of the virus in causing psoriasis (32). Acquired immunodeficiency syndrome provides an interesting model in which to study the role of the immune system and specific gene products in the pathogenesis of psoriasis and other immune diseases. IMMUNOGENETICS There is overwhelming evidence that psoriasis is a genetic disease. Family studies have shown that up to 30% of patients have an affected first-degree relative, and monozygotic twins show a 72% concordance rate (33). Disease association studies link psoriasis to a number of HLA antigens, which not only suggests immune system involvement in the pathogenesis, but makes a case for autoimmunity. The strongest association appears to be with HLA-Cw6. Patients with type I psoriasis are much more likely to possess the Cw6 antigen and have a first-degree relative with the disease than are patients with type II. The 70% concordance rate for monozygotic twins is evidence that environmental factors also play a role in triggering the disease. A consensus on the genetic locus for psoriasis susceptibility has yet to be determined. The National Psoriasis Gene Tissue Bank (NPGTB) at Baylor was created to help find the genes involved in psoriasis. It provides a tissue bank resource of immortalized cells derived from hundreds of members of psoriatic families for gene study by all interested geneticists. Initial families enrolled in the NPGTB were required to have had at least 3 generations of living
8 family members with psoriasis, of which at least a pair of siblings was affected and at least 2 living members were unaffected. Current studies are enrolling 250 sibling pairs with psoriasis and 1 living parent. Using genetic linkage analysis strategy in conjunction with The University of Texas Southwestern Medical School, analysis of 8 of our original families in the NPGTB revealed the first published psoriasis locus, at the distal end of chromosome 17q (34). Evaluation of 7 Irish families revealed another genetic linkage was found at 4q (35). Subsequently, another study failed to find association between the disease and chromosomes 17q or 4q (36). Most recently, family studies have produced evidence for linkage to 2 new foci, 16q and 20p, as well as confirmed the previous findings of 17q and HLAB and C linkages (37). The newly discovered gene locus associated with Crohn s disease, a disease also thought to have an immune basis, is on 16q, very close to the one for psoriasis, thus implying that the immune abnormalities in these 2 diseases may have a common genetic basis. The ultimate treatment for psoriasis and other autoimmune and inflammatory diseases is gene-based therapy. Treatment of RA using local gene transfer to joints is being studied. Systemic delivery of proteins therapeutic for RA, such as inhibitors of TNF- and IL-1, also are being considered using genetically modified cells. As vectors to transfer the genes improve and identification of appropriate therapeutic proteins progresses, the prospects for gene therapy for psoriasis become more promising, making a gene patch for psoriasis a fascinating therapeutic possibility. SUMMARY Now considered to be a systemic, immune-mediated condition, psoriasis represents a spectrum of diseases that have their primary manifestations on the skin. Systemic immunological abnormalities in psoriasis are important clues, but studies of the local inflammatory milieu provide ample evidence to support the APC T cell interaction as the backbone of the immune response. Activated APCs have been characterized in the lesions, as have activated CD4 + and CD8 + lymphocytes. The antigen triggering the immune response remains unclear, but cross-reactivity between streptococcal antigens and skin antigens may play a role, or streptococcal antigens may be acting as superantigens to trigger the response. The mainstay of psoriasis treatment is immunosuppressive therapy. Current research in psoriasis immunotherapy involves testing the efficacy of antibodies to lymphokines and T- lymphocyte receptors, as well as peptide vaccines. Because psoriasis has visible manifestations of disease, it provides an excellent model in which to study various advances in immunotherapy. Interaction with our colleagues at BUMC in gastroenterology, rheumatology, transplantation, oncology, and the newly established Baylor Institute for Immunology Research will enable us to further define new immunotherapeutic agents of potential benefit not only to psoriasis, but to other disorders of the immune system, such as LE, RA, GVHD, CTCL, and cancer. Finally, the results of our NPGTB endeavors continue to further establish the genetic loci involved in psoriasis. Ultimately, this may lead to gene therapy, not only for psoriasis, but also for other diseases associated with dysfunction of the immune system.
9 References 1 Mueller W, Herrmann B: Cyclosporin A for psoriasis. N Engl J Med 1979;301: Christophers E: The immunopathology of psoriasis. Int Arch Allergy Immunol 1996;110: Menter A: Pathogenesis and genetics of psoriasis. Cutis 1998;61: Menter A: Psoriasis in primary care: diagnosis and management. Family Practice Recertification 1997;19(5): Menter A, Barker JN: Psoriasis in practice. Lancet 1991;338: Hall RP, Peck GL, Lawley TJ: Circulating IgA immune complexes in patients with psoriasis. J Invest Dermatol 1983;80: Barker JN: The immunopathology of psoriasis. Baillieres Clin Rheumatol 1994;8: Harland CC, Whitaker RP, Barron JL, Holden CA: Increased urine neopterin levels in psoriasis. Br J Dermatol 1992;127: Voorhees JJ: Dohi Memorial Lecture. Psoriasis: an immunological disease. J Dermatol 1996;23: Valdimarsson H, Baker BS, Jonsdottir I, Powles A, Fry L: Psoriasis: a T-cell mediated autoimmune disease induced by streptococcal superantigens? Immunol Today 1995;16: Fry L: Psoriasis. Br J Dermatol 1988;199: Swerlick RA, Cunningham MW, Hall NK: Monoclonal antibodies cross-reactive with group A streptococci and normal and psoriatic human skin. J Invest Dermatol 1986;87: Leung DY, Travers JB, Giorno R, Norris DA, Skinner R, Aelion J, Kazemi LV, Kim MH, Trumble AE, Kotb M, Schlievert PM: Evidence for a streptococcal superantigen-driven process in acute guttate psoriasis. J Clin Invest 1995;96: Menssen A, Trommler P, Vollmer S, Schendel D, Albert E, Gurtler L, Riethmuller G, Prinz JC: Evidence for an antigen-specific cellular immune response in skin lesions of patients with psoriasis vulgaris. J Immunol 1995;155: Baadsgaard O, Gupta AK, Taylor RS, Ellis CN, Voorhees JJ, Cooper KD: Psoriatic epidermal cells demonstrate increased numbers and function of non-langerhans antigenpresenting cells. J Invest Dermatol 1989;92: Morganroth GS, Chan LS, Weinstein GD, Voorhees JJ, Cooper KD: Proliferating cells in psoriatic dermis are comprised primarily of T cells, endothelial cells, and factor XIIIa + perivascular dendritic cells. J Invest Dermatol 1991;96: Griffiths CE, Voorhees JJ: Psoriasis, T cells and autoimmunity. J R Soc Med 1996;89: Bjerke JR, Krogh HK, Matre R: Characterization of mononuclear cell infiltrates in psoriatic lesions. J Invest Dermatol 1978;71: Uyemura K, Yamamura M, Fivenson DF, Modlin RL, Nickoloff BJ: The cytokine network in lesional and lesion-free psoriatic skin is characterized by a T-helper type 1 cell-mediated response. J Invest Dermatol 1993;101: Griffiths CE, Voorhees JJ: Immunological mechanisms involved in psoriasis. Springer Semin Immunopathol 1992;13: Bata-Csorgo Z, Hammerberg C, Voorhees JJ, Cooper KD: Intralesional T-lymphocyte activation as a mediator of psoriatic epidermal hyperplasia. J Invest Dermatol 1995;105(1 Suppl):89s 94s. 22 Ellis CN, Fradin MS, Messana JM, Brown MD, Siegel MT, Hartley AH, Rocher LL, Wheeler S, Hamilton TA, Parish TG, Ellis-Madu M, Duell E, Annesley TM, Cooper KD, Voorhees JJ: Cyclosporine for plaque-type psoriasis: results of a multidose, double-blind trial. N Engl J Med 1991;324: Ho VC, Griffiths CEM, Ellis CN, Gupta AK, McCuaig CC, Nickoloff BJ, Cooper KD, Hamilton TA, Voorhees JJ: Intralesional cyclosporine A in the treatment of psoriasis: a
10 clinical immunologic and pharmacokinetic study. J Am Acad Dermatol 1990;22: Cronstein BN: A novel approach to the development of anti-inflammatory agents: adenosine release at inflamed sites. J Investig Med 1995;43: Gandangi P, Longaker M, Naime D, Levin RI, Recht PA, Montesinos MC, Buckley MT, Carlin G, Cronstein BN: The anti-inflammatory mechanism of sulfasalazine is related to adenosine release at inflamed sites. J Immunol 1996;156: Scheinman RI, Cogswell PC, Lofquist AK, Baldwin Jr AS: Role of transcriptional activation of IkBa in mediation of immunosuppression by glucocorticoids. Science 1995;270: Alroy I, Towers TL, Freedman LP: Transcriptional repression of the interleukin-2 gene by vitamin D3: direct inhibition of NFATp/AP-1 complex formation by a nuclear hormone receptor. Mol Cell Biol 1995;15: Berg DJ, Leach MW, Kuhn R, Rajewsky K, Muller W, Davidson NJ, Rennick D: Interleukin 10 but not interleukin 4 is a natural suppressant of cutaneous inflammatory responses. J Exp Med 1995;182: Fauci AS, Braunwald E, Isselbacher KJ, Wilson JD, Martin JB, Kasper DL, Hauser SL, and Longo DL, eds: Harrison s Principles of Internal Medicine, 14th ed. New York: McGraw- Hill, Inc., Habif TP: Clinical Dermatology: A Color Guide to Diagnosis and Therapy, 3rd ed. St. Louis: Mosby-Year Book, Inc., Duvic M: Immunology of AIDS related to psoriasis. J Invest Dermatol 1990;95:38s 40s. 32 Duvic M, Rios A, Brewton GW: Remission of AIDS-associated psoriasis with zidovudine. Lancet 1987;2: Brandrup F, Hauge M, Henningsen K, Eriksen B: Psoriasis in an unselected series of twins. Arch Dermatol 1978;114: Tomfohrde J, Silverman A, Barnes R, Fernandez-Vina MA, Young M, Lory D, Morris L, Wuepper KD, Stastny P, Menter A, Bowcock A: Gene for familial psoriasis susceptibility mapped to the distal end of human chromosome 17q. Science 1994;264: Matthews D, Fry L, Powles A, Weissenbach J, Williamson R: Confirmation of genetic heterogenicity in familial psoriasis. J Med Genet 1995;32: Trembath RC, Clough RL, Rosbotham JL, Jones AB, Camp RD, Frodsham A, Browne J, Barber R, Terwilliger J, Lathrop GM, Barker JN: Identification of a major susceptibility locus on chromosome 6p and evidence for further disease loci revealed by a two stage genome-wide search in psoriasis. Hum Mol Genet 1997;6: Nair RP, Henseler T, Jenisch S, Stuart P, Bichakjian CK, Lenk W, Westphal E, Guo SW, Christophers E, Voorhees JJ, Elder JT: Evidence for two psoriasis susceptibility loci (HLA and 17q) and two novel candidate regions (16q and 20p) by genome-wide scan. Hum Mol Genet 1997;6:
11 Figure 1 Figure 2 Figure 3
12 Figure 4 Figure 5 Figure 6
Psoriasis. Student's Name. Institution. Date of Submission
 Running head: PSORIASIS Psoriasis Student's Name Institution Date of Submission PSORIASIS 1 Abstract Psoriasis is a non-contagious chronic skin disease that is characterized by inflammatory and multiplying
Running head: PSORIASIS Psoriasis Student's Name Institution Date of Submission PSORIASIS 1 Abstract Psoriasis is a non-contagious chronic skin disease that is characterized by inflammatory and multiplying
specific B cells Humoral immunity lymphocytes antibodies B cells bone marrow Cell-mediated immunity: T cells antibodies proteins
 Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
Adaptive Immunity Chapter 17: Adaptive (specific) Immunity Bio 139 Dr. Amy Rogers Host defenses that are specific to a particular infectious agent Can be innate or genetic for humans as a group: most microbes
X-Plain Psoriasis Reference Summary
 X-Plain Psoriasis Reference Summary Introduction Psoriasis is a long-lasting skin disease that causes the skin to become inflamed. Patches of thick, red skin are covered with silvery scales. It affects
X-Plain Psoriasis Reference Summary Introduction Psoriasis is a long-lasting skin disease that causes the skin to become inflamed. Patches of thick, red skin are covered with silvery scales. It affects
Psoriasis. Psoriasis. Mark A. Bechtel, M.D. Director of Dermatology The Ohio State University College of Medicine
 Psoriasis Mark A. Bechtel, M.D. Director of Dermatology The Ohio State University College of Medicine Psoriasis Psoriasis is a chronic skin disorder resulting from a polygenic predisposition combined with
Psoriasis Mark A. Bechtel, M.D. Director of Dermatology The Ohio State University College of Medicine Psoriasis Psoriasis is a chronic skin disorder resulting from a polygenic predisposition combined with
Autoimmunity and immunemediated. FOCiS. Lecture outline
 1 Autoimmunity and immunemediated inflammatory diseases Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline Pathogenesis of autoimmunity: why selftolerance fails Genetics of autoimmune diseases Therapeutic
1 Autoimmunity and immunemediated inflammatory diseases Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline Pathogenesis of autoimmunity: why selftolerance fails Genetics of autoimmune diseases Therapeutic
A Genetic Analysis of Rheumatoid Arthritis
 A Genetic Analysis of Rheumatoid Arthritis Introduction to Rheumatoid Arthritis: Classification and Diagnosis Rheumatoid arthritis is a chronic inflammatory disorder that affects mainly synovial joints.
A Genetic Analysis of Rheumatoid Arthritis Introduction to Rheumatoid Arthritis: Classification and Diagnosis Rheumatoid arthritis is a chronic inflammatory disorder that affects mainly synovial joints.
The Immune System: A Tutorial
 The Immune System: A Tutorial Modeling and Simulation of Biological Systems 21-366B Shlomo Ta asan Images taken from http://rex.nci.nih.gov/behindthenews/uis/uisframe.htm http://copewithcytokines.de/ The
The Immune System: A Tutorial Modeling and Simulation of Biological Systems 21-366B Shlomo Ta asan Images taken from http://rex.nci.nih.gov/behindthenews/uis/uisframe.htm http://copewithcytokines.de/ The
Chapter 43: The Immune System
 Name Period Our students consider this chapter to be a particularly challenging and important one. Expect to work your way slowly through the first three concepts. Take particular care with Concepts 43.2
Name Period Our students consider this chapter to be a particularly challenging and important one. Expect to work your way slowly through the first three concepts. Take particular care with Concepts 43.2
The Most Common Autoimmune Disease: Rheumatoid Arthritis. Bonita S. Libman, M.D.
 The Most Common Autoimmune Disease: Rheumatoid Arthritis Bonita S. Libman, M.D. Disclosures Two googled comics The Normal Immune System Network of cells and proteins that work together Goal: protect against
The Most Common Autoimmune Disease: Rheumatoid Arthritis Bonita S. Libman, M.D. Disclosures Two googled comics The Normal Immune System Network of cells and proteins that work together Goal: protect against
Rheumatoid arthritis: an overview. Christine Pham MD
 Rheumatoid arthritis: an overview Christine Pham MD RA prevalence Chronic inflammatory disease affecting approximately 0.5 1% of the general population Prevalence is higher in North America (approaching
Rheumatoid arthritis: an overview Christine Pham MD RA prevalence Chronic inflammatory disease affecting approximately 0.5 1% of the general population Prevalence is higher in North America (approaching
Is Monotherapy Treatment of Etanercept Effective Against Plaque Psoriasis?
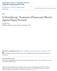 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2011 Is Monotherapy Treatment of Etanercept
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2011 Is Monotherapy Treatment of Etanercept
FastTest. You ve read the book... ... now test yourself
 FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
Natalia Taborda Vanegas. Doc. Sci. Student Immunovirology Group Universidad de Antioquia
 Pathogenesis of Dengue Natalia Taborda Vanegas Doc. Sci. Student Immunovirology Group Universidad de Antioquia Infection process Epidermis keratinocytes Dermis Archives of Medical Research 36 (2005) 425
Pathogenesis of Dengue Natalia Taborda Vanegas Doc. Sci. Student Immunovirology Group Universidad de Antioquia Infection process Epidermis keratinocytes Dermis Archives of Medical Research 36 (2005) 425
Cutaneous Lymphoma FAST FACTS
 Cutaneous Lymphoma FAST FACTS What is Cutaneous Lymphoma? Cutaneous lymphomas are types of non-hodgkin s lymphomas (NHL) that originate in the lymphocytes (white blood cells). Unlike most other types of
Cutaneous Lymphoma FAST FACTS What is Cutaneous Lymphoma? Cutaneous lymphomas are types of non-hodgkin s lymphomas (NHL) that originate in the lymphocytes (white blood cells). Unlike most other types of
ANIMALS FORM & FUNCTION BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES. Animals Form & Function Activity #4 page 1
 AP BIOLOGY ANIMALS FORM & FUNCTION ACTIVITY #4 NAME DATE HOUR BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES Animals Form & Function Activity #4 page 1 INFLAMMATORY RESPONSE ANTIMICROBIAL
AP BIOLOGY ANIMALS FORM & FUNCTION ACTIVITY #4 NAME DATE HOUR BODY DEFENSES NONSPECIFIC DEFENSES PHYSICAL BARRIERS PHAGOCYTES Animals Form & Function Activity #4 page 1 INFLAMMATORY RESPONSE ANTIMICROBIAL
Rheumatoid arthritis
 Rheumatoid arthritis Rheumatoid arthritis Chronic multisystem disease Unknown cause Characteristic feature persistent inflammation of synovia in symmetric peripheral joints Synovial inflammation cartilage
Rheumatoid arthritis Rheumatoid arthritis Chronic multisystem disease Unknown cause Characteristic feature persistent inflammation of synovia in symmetric peripheral joints Synovial inflammation cartilage
PSORIASIS. -Multi factorial. -Papulosquamous disorder. -Genetically determined (few) -Chronic Scaly lesions. -Seasonal variations
 PSORIASIS -Multi factorial -Papulosquamous disorder -Genetically determined (few) -Chronic Scaly lesions -Seasonal variations -Recurrences & remissions Etiology & Pathogenesis T-cell mediated autoimmune
PSORIASIS -Multi factorial -Papulosquamous disorder -Genetically determined (few) -Chronic Scaly lesions -Seasonal variations -Recurrences & remissions Etiology & Pathogenesis T-cell mediated autoimmune
Collaborative Association Study of Psoriasis. Gonçalo Abecasis, Anne Bowcock, James Elder, Jerry Krueger
 Collaborative Association Study of Psoriasis Gonçalo Abecasis, Anne Bowcock, James Elder, Jerry Krueger Psoriasis Chronic, inflammatory skin condition Characteristic lesions, can affect substantial proportion
Collaborative Association Study of Psoriasis Gonçalo Abecasis, Anne Bowcock, James Elder, Jerry Krueger Psoriasis Chronic, inflammatory skin condition Characteristic lesions, can affect substantial proportion
Phenotypes and Classification of Psoriasis
 Rheumatology 2010 Birmingham 21 April 2010 Phenotypes and Classification of Psoriasis Christopher E.M. Griffiths Abbott Centocor Incyte Galderma Janssen-Cilag Leo Pharma Lynxx Novartis Pfizer Schering-Plough
Rheumatology 2010 Birmingham 21 April 2010 Phenotypes and Classification of Psoriasis Christopher E.M. Griffiths Abbott Centocor Incyte Galderma Janssen-Cilag Leo Pharma Lynxx Novartis Pfizer Schering-Plough
Microbiology AN INTRODUCTION EIGHTH EDITION
 TORTORA FUNKE CASE Microbiology AN INTRODUCTION EIGHTH EDITION Differentiate between innate and acquired immunity. Chapter 17 Specific Defenses of the Host: The Immune Response B.E Pruitt & Jane J. Stein
TORTORA FUNKE CASE Microbiology AN INTRODUCTION EIGHTH EDITION Differentiate between innate and acquired immunity. Chapter 17 Specific Defenses of the Host: The Immune Response B.E Pruitt & Jane J. Stein
NURS 821 Alterations in the Musculoskeletal System. Rheumatoid Arthritis. Type III Hypersensitivity Response
 NURS 821 Alterations in the Musculoskeletal System Margaret H. Birney PhD, RN Lecture 12 Part 2 Joint Disorders (cont d) Rheumatoid Arthritis Definition: Autoimmune disorder occurring in genetically sensitive
NURS 821 Alterations in the Musculoskeletal System Margaret H. Birney PhD, RN Lecture 12 Part 2 Joint Disorders (cont d) Rheumatoid Arthritis Definition: Autoimmune disorder occurring in genetically sensitive
HLA-Cw*0602 associates with a twofold higher prevalence. of positive streptococcal throat swab at the onset of
 1 HLA-Cw*0602 associates with a twofold higher prevalence of positive streptococcal throat swab at the onset of psoriasis: a case control study Lotus Mallbris, MD, PhD, Katarina Wolk, MD, Fabio Sánchez
1 HLA-Cw*0602 associates with a twofold higher prevalence of positive streptococcal throat swab at the onset of psoriasis: a case control study Lotus Mallbris, MD, PhD, Katarina Wolk, MD, Fabio Sánchez
Rheumatoid Arthritis. Nicole Klett,, M.D.
 Rheumatoid Arthritis Nicole Klett,, M.D. Rheumatoid Arthritis Systemic Chronic Inflammatory Primarily targets the synovium of diarthrodial joints Etiology likely combination genetic and environmental Diarthrodial
Rheumatoid Arthritis Nicole Klett,, M.D. Rheumatoid Arthritis Systemic Chronic Inflammatory Primarily targets the synovium of diarthrodial joints Etiology likely combination genetic and environmental Diarthrodial
Name (print) Name (signature) Period. (Total 30 points)
 AP Biology Worksheet Chapter 43 The Immune System Lambdin April 4, 2011 Due Date: Thurs. April 7, 2011 You may use the following: Text Notes Power point Internet One other person in class "On my honor,
AP Biology Worksheet Chapter 43 The Immune System Lambdin April 4, 2011 Due Date: Thurs. April 7, 2011 You may use the following: Text Notes Power point Internet One other person in class "On my honor,
The Body s Defenses CHAPTER 24
 CHAPTER 24 The Body s Defenses PowerPoint Lectures for Essential Biology, Third Edition Neil Campbell, Jane Reece, and Eric Simon Essential Biology with Physiology, Second Edition Neil Campbell, Jane Reece,
CHAPTER 24 The Body s Defenses PowerPoint Lectures for Essential Biology, Third Edition Neil Campbell, Jane Reece, and Eric Simon Essential Biology with Physiology, Second Edition Neil Campbell, Jane Reece,
Immuno-Oncology Therapies to Treat Lung Cancer
 Immuno-Oncology Therapies to Treat Lung Cancer What you need to know ONCHQ14NP07519 Introduction: Immuno-oncology represents an innovative approach to cancer research that seeks to harness the body s own
Immuno-Oncology Therapies to Treat Lung Cancer What you need to know ONCHQ14NP07519 Introduction: Immuno-oncology represents an innovative approach to cancer research that seeks to harness the body s own
chronic leukemia lymphoma myeloma differentiated 14 September 1999 Pre- Transformed Ig Surface Surface Secreted Myeloma Major malignant counterpart
 Disease Usual phenotype acute leukemia precursor chronic leukemia lymphoma myeloma differentiated Pre- B-cell B-cell Transformed B-cell Plasma cell Ig Surface Surface Secreted Major malignant counterpart
Disease Usual phenotype acute leukemia precursor chronic leukemia lymphoma myeloma differentiated Pre- B-cell B-cell Transformed B-cell Plasma cell Ig Surface Surface Secreted Major malignant counterpart
Arthritis and Rheumatology Clinics of Kansas Patient Education. Reactive Arthritis (ReA) / Inflammatory Bowel Disease (IBD) Arthritis
 Arthritis and Rheumatology Clinics of Kansas Patient Education Reactive Arthritis (ReA) / Inflammatory Bowel Disease (IBD) Arthritis Introduction: For as long as scientists have studied rheumatic disease,
Arthritis and Rheumatology Clinics of Kansas Patient Education Reactive Arthritis (ReA) / Inflammatory Bowel Disease (IBD) Arthritis Introduction: For as long as scientists have studied rheumatic disease,
Mosby s PATHOLOGY for Massage Therapists. Lesson 9.1 Objectives. Chapter 9 Lymphatic and Immune Pathologies. Lymphatic System Overview
 Mosby s PATHOLOGY for Massage Therapists Chapter 9 Lymphatic and Immune Pathologies Lesson 9.1 Objectives Discuss anatomic structures and physiologic processes related to the lymphatic system. Describe
Mosby s PATHOLOGY for Massage Therapists Chapter 9 Lymphatic and Immune Pathologies Lesson 9.1 Objectives Discuss anatomic structures and physiologic processes related to the lymphatic system. Describe
T Cell Maturation,Activation and Differentiation
 T Cell Maturation,Activation and Differentiation Positive Selection- In thymus, permits survival of only those T cells whose TCRs recognize self- MHC molecules (self-mhc restriction) Negative Selection-
T Cell Maturation,Activation and Differentiation Positive Selection- In thymus, permits survival of only those T cells whose TCRs recognize self- MHC molecules (self-mhc restriction) Negative Selection-
Activation and effector functions of HMI
 Activation and effector functions of HMI Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 August 2015 ว ตถ ประสงค หล งจากช วโมงบรรยายน แล วน กศ กษาสามารถ
Activation and effector functions of HMI Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 August 2015 ว ตถ ประสงค หล งจากช วโมงบรรยายน แล วน กศ กษาสามารถ
Once the immune system is triggered, cells migrate from the blood into the joints and produce substances that cause inflammation.
 HealthExchange Points For Your Joints An Arthritis Talk Howard Epstein, MD Orthopaedic & Rheumatologic Institute Rheumatic & Immunologic Disease Cleveland Clinic Beachwood Family Health & Surgery Center
HealthExchange Points For Your Joints An Arthritis Talk Howard Epstein, MD Orthopaedic & Rheumatologic Institute Rheumatic & Immunologic Disease Cleveland Clinic Beachwood Family Health & Surgery Center
B Cells and Antibodies
 B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
B Cells and Antibodies Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School Lecture outline Functions of antibodies B cell activation; the role of helper T cells in antibody production
Understanding Rheumatoid Arthritis
 Understanding Rheumatoid Arthritis Understanding Rheumatoid Arthritis What Is Rheumatoid Arthritis? 1,2 Rheumatoid arthritis (RA) is a chronic autoimmune disease. It causes joints to swell and can result
Understanding Rheumatoid Arthritis Understanding Rheumatoid Arthritis What Is Rheumatoid Arthritis? 1,2 Rheumatoid arthritis (RA) is a chronic autoimmune disease. It causes joints to swell and can result
A LTCI Approach to Managing Rheumatoid Arthritis
 A LTCI Approach to Managing Rheumatoid Arthritis A bit of Science, a bit of Art, a lot of Perseverance... Stephen K. Holland, MD Senior Vice President & Medical Director Long Term Care Group, Inc. Long
A LTCI Approach to Managing Rheumatoid Arthritis A bit of Science, a bit of Art, a lot of Perseverance... Stephen K. Holland, MD Senior Vice President & Medical Director Long Term Care Group, Inc. Long
Efficacy and Safety of Calcipotriol Ointment in Psoriasis Vulgaris - Experiences in Hong Kong
 ORIGINAL ARTICLES Efficacy and Safety of Calcipotriol Ointment in Psoriasis Vulgaris - Experiences in Hong Kong Drs. C. W. Fung, L.Y. Chong, C.Y. Leung, C. N. Look, K.K. Lo, K. M. Ho Social Hygiene Service
ORIGINAL ARTICLES Efficacy and Safety of Calcipotriol Ointment in Psoriasis Vulgaris - Experiences in Hong Kong Drs. C. W. Fung, L.Y. Chong, C.Y. Leung, C. N. Look, K.K. Lo, K. M. Ho Social Hygiene Service
Juvenile Dermatomyositis Joseph Junewick, MD FACR
 Juvenile Dermatomyositis Joseph Junewick, MD FACR 10/11/2015 History Child with several month history of weakness, arthralgias and palpable abnormalities at the knee Diagnosis Juvenile Dermatomyositis
Juvenile Dermatomyositis Joseph Junewick, MD FACR 10/11/2015 History Child with several month history of weakness, arthralgias and palpable abnormalities at the knee Diagnosis Juvenile Dermatomyositis
Summary of the risk management plan (RMP) for Accofil (filgrastim)
 EMA/475472/2014 Summary of the risk management plan (RMP) for Accofil (filgrastim) This is a summary of the risk management plan (RMP) for Accofil, which details the measures to be taken in order to ensure
EMA/475472/2014 Summary of the risk management plan (RMP) for Accofil (filgrastim) This is a summary of the risk management plan (RMP) for Accofil, which details the measures to be taken in order to ensure
Autoimmunity. Autoimmunity. Genetic Contributions to Autoimmunity. Targets of Autoimmunity
 Autoimmunity Factors predisposing an individual to autoimmune disease Mechanisms of initiation of autoimmunity Pathogenesis of particular autoimmune disease Animal models of autoimmune disease Treatment
Autoimmunity Factors predisposing an individual to autoimmune disease Mechanisms of initiation of autoimmunity Pathogenesis of particular autoimmune disease Animal models of autoimmune disease Treatment
1) Siderophores are bacterial proteins that compete with animal A) Antibodies. B) Red blood cells. C) Transferrin. D) White blood cells. E) Receptors.
 Prof. Lester s BIOL 210 Practice Exam 4 (There is no answer key. Please do not email or ask me for answers.) Chapters 15, 16, 17, 19, HIV/AIDS, TB, Quorum Sensing 1) Siderophores are bacterial proteins
Prof. Lester s BIOL 210 Practice Exam 4 (There is no answer key. Please do not email or ask me for answers.) Chapters 15, 16, 17, 19, HIV/AIDS, TB, Quorum Sensing 1) Siderophores are bacterial proteins
Genetics of Rheumatoid Arthritis Markey Lecture Series
 Genetics of Rheumatoid Arthritis Markey Lecture Series Al Kim akim@dom.wustl.edu 2012.09.06 Overview of Rheumatoid Arthritis Rheumatoid Arthritis (RA) Autoimmune disease primarily targeting the synovium
Genetics of Rheumatoid Arthritis Markey Lecture Series Al Kim akim@dom.wustl.edu 2012.09.06 Overview of Rheumatoid Arthritis Rheumatoid Arthritis (RA) Autoimmune disease primarily targeting the synovium
Synopsis of Causation
 Ministry of Defence Synopsis of Causation Psoriasis Author: Dr Tony Fisher, Medical Author, Medical Text, Edinburgh Validator: Dr Cameron Kennedy, Bristol Royal Infirmary, Bristol September 2008 Disclaimer
Ministry of Defence Synopsis of Causation Psoriasis Author: Dr Tony Fisher, Medical Author, Medical Text, Edinburgh Validator: Dr Cameron Kennedy, Bristol Royal Infirmary, Bristol September 2008 Disclaimer
Adult Medical-Surgical Nursing H A E M A T O L O G Y M O D U L E : L E U K A E M I A 2
 Adult Medical-Surgical Nursing H A E M A T O L O G Y M O D U L E : L E U K A E M I A 2 Leukaemia: Description A group of malignant disorders affecting: White blood cells (lymphocytes or leucocytes) Bone
Adult Medical-Surgical Nursing H A E M A T O L O G Y M O D U L E : L E U K A E M I A 2 Leukaemia: Description A group of malignant disorders affecting: White blood cells (lymphocytes or leucocytes) Bone
Do I need a physician referral? Yes, we see patients on referral from a health care provider.
 FAQS FOR OFFICE POLICIES How do I get an appointment? New appointments are made by physician referral only. Your referring health care provided will call for the appointment for you. What do I need to
FAQS FOR OFFICE POLICIES How do I get an appointment? New appointments are made by physician referral only. Your referring health care provided will call for the appointment for you. What do I need to
Rheumatoid Arthritis
 Rheumatoid Arthritis Rheumatoid arthritis (RA) is an autoimmune disease that causes chronic inflammation of the joints. Autoimmune diseases are illnesses that occur when the body's tissues are mistakenly
Rheumatoid Arthritis Rheumatoid arthritis (RA) is an autoimmune disease that causes chronic inflammation of the joints. Autoimmune diseases are illnesses that occur when the body's tissues are mistakenly
Welcome to Mini Med School at the Child & Family Research Institute
 Glossary Welcome to Mini Med School at the Child & Family Research Institute On behalf of the Faculty and Staff at the Child & Family Research Institute (CFRI), we would like to welcome you to CFRI s
Glossary Welcome to Mini Med School at the Child & Family Research Institute On behalf of the Faculty and Staff at the Child & Family Research Institute (CFRI), we would like to welcome you to CFRI s
TREATING AUTOIMMUNE DISEASES WITH HOMEOPATHY. Dr. Stephen A. Messer, MSEd, ND, DHANP Professor and Chair of Homeopathic Medicine
 TREATING AUTOIMMUNE DISEASES WITH HOMEOPATHY Dr. Stephen A. Messer, MSEd, ND, DHANP Professor and Chair of Homeopathic Medicine AUTOIMMUNE DISEASES An autoimmune disorder occurs when the body s immune
TREATING AUTOIMMUNE DISEASES WITH HOMEOPATHY Dr. Stephen A. Messer, MSEd, ND, DHANP Professor and Chair of Homeopathic Medicine AUTOIMMUNE DISEASES An autoimmune disorder occurs when the body s immune
One of the more complex systems we re looking at. An immune response (a response to a pathogen) can be of two types:
 Immune system. One of the more complex systems we re looking at. An immune response (a response to a pathogen) can be of two types: (pathogen - disease causing organism) 1) Non specific. Anything foreign
Immune system. One of the more complex systems we re looking at. An immune response (a response to a pathogen) can be of two types: (pathogen - disease causing organism) 1) Non specific. Anything foreign
Nutrition and Toxicants in Autoimmune Disease: Implications for Prevention and Treatment
 Nutrition and Toxicants in Autoimmune Disease: Implications for Prevention and Treatment Collaborative on Health and the Environment June 17, 2014 Ted Schettler MD, MPH 1 Autoimmune diseases Autoimmunity
Nutrition and Toxicants in Autoimmune Disease: Implications for Prevention and Treatment Collaborative on Health and the Environment June 17, 2014 Ted Schettler MD, MPH 1 Autoimmune diseases Autoimmunity
How To Understand The Cause Of Psoriasis
 CONTINUING MEDICAL EDUCATION The immunologic basis for the treatment of psoriasis with new biologic agents James G. Krueger, MD, PhD New York, New York Psoriasis vulgaris is the most prevalent T-cell mediated
CONTINUING MEDICAL EDUCATION The immunologic basis for the treatment of psoriasis with new biologic agents James G. Krueger, MD, PhD New York, New York Psoriasis vulgaris is the most prevalent T-cell mediated
The Immune System. 2 Types of Defense Mechanisms. Lines of Defense. Line of Defense. Lines of Defense
 The Immune System 2 Types of Defense Mechanisms Immune System the system that fights infection by producing cells to inactivate foreign substances to avoid infection and disease. Immunity the body s ability
The Immune System 2 Types of Defense Mechanisms Immune System the system that fights infection by producing cells to inactivate foreign substances to avoid infection and disease. Immunity the body s ability
Blood & Marrow Transplant Glossary. Pediatric Blood and Marrow Transplant Program Patient Guide
 Blood & Marrow Transplant Glossary Pediatric Blood and Marrow Transplant Program Patient Guide Glossary Absolute Neutrophil Count (ANC) -- Also called "absolute granulocyte count" amount of white blood
Blood & Marrow Transplant Glossary Pediatric Blood and Marrow Transplant Program Patient Guide Glossary Absolute Neutrophil Count (ANC) -- Also called "absolute granulocyte count" amount of white blood
Etanercept in childhood psoriasis: An experience from Kuwait
 ORIGINAL ARTICLE Etanercept in childhood psoriasis: An experience from Kuwait Nawaf Al-Mutairi, MD, FRCP, Azari Al-Dhouki, MD, Mazen Al-Shiltawi, MD Department of Dermatology, Farwaniya Hospital, Kuwait
ORIGINAL ARTICLE Etanercept in childhood psoriasis: An experience from Kuwait Nawaf Al-Mutairi, MD, FRCP, Azari Al-Dhouki, MD, Mazen Al-Shiltawi, MD Department of Dermatology, Farwaniya Hospital, Kuwait
Selective IgA deficiency (slgad) hello@piduk.org 0800 987 8986 www.piduk.org
 Selective IgA deficiency (slgad) hello@piduk.org 0800 987 8986 www.piduk.org About this booklet This booklet provides information on selective IgA deficiency (sigad). It has been produced by the PID UK
Selective IgA deficiency (slgad) hello@piduk.org 0800 987 8986 www.piduk.org About this booklet This booklet provides information on selective IgA deficiency (sigad). It has been produced by the PID UK
ALLIANCE FOR LUPUS RESEARCH AND PFIZER S CENTERS FOR THERAPEUTIC INNOVATION CHALLENGE GRANT PROGRAM PROGRAM GUIDELINES
 ALLIANCE FOR LUPUS RESEARCH AND PFIZER S CENTERS FOR THERAPEUTIC INNOVATION CHALLENGE GRANT PROGRAM PROGRAM GUIDELINES DESCRIPTION OF GRANT MECHANISM The Alliance for Lupus Research (ALR) is an independent,
ALLIANCE FOR LUPUS RESEARCH AND PFIZER S CENTERS FOR THERAPEUTIC INNOVATION CHALLENGE GRANT PROGRAM PROGRAM GUIDELINES DESCRIPTION OF GRANT MECHANISM The Alliance for Lupus Research (ALR) is an independent,
PSORIATIC ARTHRITIS. Chryssanthie Kafkala, M.D. INTRODUCTION:
 PSORIATIC ARTHRITIS Chryssanthie Kafkala, M.D. INTRODUCTION: Psoriatic arthritis is a disease with generally good prognosis. Both ocular and systemic involvement is usually benign, however, the following
PSORIATIC ARTHRITIS Chryssanthie Kafkala, M.D. INTRODUCTION: Psoriatic arthritis is a disease with generally good prognosis. Both ocular and systemic involvement is usually benign, however, the following
Psoriasis Treatment Transition Pathway
 Psoriasis Treatment Transition Pathway A Treatment Support Tool Adapted from Circle Nottingham NHS Treatment Centre Psoriasis Pathway (under consultation) with support from Abbvie Ltd Treatment Pathways
Psoriasis Treatment Transition Pathway A Treatment Support Tool Adapted from Circle Nottingham NHS Treatment Centre Psoriasis Pathway (under consultation) with support from Abbvie Ltd Treatment Pathways
2) Macrophages function to engulf and present antigen to other immune cells.
 Immunology The immune system has specificity and memory. It specifically recognizes different antigens and has memory for these same antigens the next time they are encountered. The Cellular Components
Immunology The immune system has specificity and memory. It specifically recognizes different antigens and has memory for these same antigens the next time they are encountered. The Cellular Components
Biologic Treatments for Rheumatoid Arthritis
 Biologic Treatments Rheumatoid Arthritis (also known as cytokine inhibitors, TNF inhibitors, IL 1 inhibitor, or Biologic Response Modifiers) Description Biologics are new class of drugs that have been
Biologic Treatments Rheumatoid Arthritis (also known as cytokine inhibitors, TNF inhibitors, IL 1 inhibitor, or Biologic Response Modifiers) Description Biologics are new class of drugs that have been
Gene Therapy. The use of DNA as a drug. Edited by Gavin Brooks. BPharm, PhD, MRPharmS (PP) Pharmaceutical Press
 Gene Therapy The use of DNA as a drug Edited by Gavin Brooks BPharm, PhD, MRPharmS (PP) Pharmaceutical Press Contents Preface xiii Acknowledgements xv About the editor xvi Contributors xvii An introduction
Gene Therapy The use of DNA as a drug Edited by Gavin Brooks BPharm, PhD, MRPharmS (PP) Pharmaceutical Press Contents Preface xiii Acknowledgements xv About the editor xvi Contributors xvii An introduction
Systemic Lupus Erythematosus
 Harvard-MIT Division of Health Sciences and Technology HST.021: Musculoskeletal Pathophysiology, IAP 2006 Course Director: Dr. Dwight R. Robinson Systemic Lupus Erythematosus A multi-system autoimmune
Harvard-MIT Division of Health Sciences and Technology HST.021: Musculoskeletal Pathophysiology, IAP 2006 Course Director: Dr. Dwight R. Robinson Systemic Lupus Erythematosus A multi-system autoimmune
Medical Results of Propylthiouracil in Psoriasis
 Serum TNF- in psoriasis after treatment with propylthiouracil, an antithyroid thioureylene Alan N. Elias 1, Vanda S. Nanda 2, and Raj Pandian 3 1 Department of Medicine, Division of Endocrinology and Metabolism,
Serum TNF- in psoriasis after treatment with propylthiouracil, an antithyroid thioureylene Alan N. Elias 1, Vanda S. Nanda 2, and Raj Pandian 3 1 Department of Medicine, Division of Endocrinology and Metabolism,
Thymus Cancer. This reference summary will help you better understand what thymus cancer is and what treatment options are available.
 Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT
 1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT Learning that your pet has a diagnosis of cancer can be overwhelming. We realize that your pet
1400 Telegraph Bloomfield Hills, MI 48302 248-334-6877-Phone number/248-334-6877-fax Number CANCER TREATMENT Learning that your pet has a diagnosis of cancer can be overwhelming. We realize that your pet
Corporate Medical Policy
 Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplantation_for_cll_and_sll
Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplantation_for_cll_and_sll
PATIENT RESOURCES: PSORIASIS
 PATIENT RESOURCES: PSORIASIS Psoriasis is a persistent skin disorder in which there are red, thickened areas with silvery scales, most often on the scalp, elbows, knees, and lower back. Some cases, of
PATIENT RESOURCES: PSORIASIS Psoriasis is a persistent skin disorder in which there are red, thickened areas with silvery scales, most often on the scalp, elbows, knees, and lower back. Some cases, of
An overview of CLL care and treatment. Dr Dean Smith Haematology Consultant City Hospital Nottingham
 An overview of CLL care and treatment Dr Dean Smith Haematology Consultant City Hospital Nottingham What is CLL? CLL (Chronic Lymphocytic Leukaemia) is a type of cancer in which the bone marrow makes too
An overview of CLL care and treatment Dr Dean Smith Haematology Consultant City Hospital Nottingham What is CLL? CLL (Chronic Lymphocytic Leukaemia) is a type of cancer in which the bone marrow makes too
A disease and antibody biology approach to antibody drug discovery
 A disease and antibody biology approach to antibody drug discovery Björn Frendéus, PhD VP, Preclinical research Presenter: Björn Frendéus Date: 2011-11-08 1 Antibodies have revolutionized Cancer Treatment!
A disease and antibody biology approach to antibody drug discovery Björn Frendéus, PhD VP, Preclinical research Presenter: Björn Frendéus Date: 2011-11-08 1 Antibodies have revolutionized Cancer Treatment!
Things You Don t Want to Miss in Multiple Myeloma
 Things You Don t Want to Miss in Multiple Myeloma Sreenivasa Chandana, MD, PhD Attending Hematologist and Medical Oncologist West Michigan Cancer Center Assistant Professor, Western Michigan University
Things You Don t Want to Miss in Multiple Myeloma Sreenivasa Chandana, MD, PhD Attending Hematologist and Medical Oncologist West Michigan Cancer Center Assistant Professor, Western Michigan University
MULTIPLE MYELOMA. Dr Malkit S Riyat. MBChB, FRCPath(UK) Consultant Haematologist
 MULTIPLE MYELOMA Dr Malkit S Riyat MBChB, FRCPath(UK) Consultant Haematologist Multiple myeloma is an incurable malignancy that arises from postgerminal centre, somatically hypermutated B cells.
MULTIPLE MYELOMA Dr Malkit S Riyat MBChB, FRCPath(UK) Consultant Haematologist Multiple myeloma is an incurable malignancy that arises from postgerminal centre, somatically hypermutated B cells.
The immune system. Bone marrow. Thymus. Spleen. Bone marrow. NK cell. B-cell. T-cell. Basophil Neutrophil. Eosinophil. Myeloid progenitor
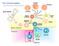 The immune system Basophil Neutrophil Bone marrow Eosinophil Myeloid progenitor Dendritic cell Pluripotent Stem cell Lymphoid progenitor Platelets Bone marrow Thymus NK cell T-cell B-cell Spleen Cancer
The immune system Basophil Neutrophil Bone marrow Eosinophil Myeloid progenitor Dendritic cell Pluripotent Stem cell Lymphoid progenitor Platelets Bone marrow Thymus NK cell T-cell B-cell Spleen Cancer
The role of IBV proteins in protection: cellular immune responses. COST meeting WG2 + WG3 Budapest, Hungary, 2015
 The role of IBV proteins in protection: cellular immune responses COST meeting WG2 + WG3 Budapest, Hungary, 2015 1 Presentation include: Laboratory results Literature summary Role of T cells in response
The role of IBV proteins in protection: cellular immune responses COST meeting WG2 + WG3 Budapest, Hungary, 2015 1 Presentation include: Laboratory results Literature summary Role of T cells in response
2-5 % Europeans A distressing, life-long, inflammatory disease Impairs patients Quality of Life
 Psoriasis: 2-5 % Europeans A distressing, life-long, inflammatory disease Impairs patients Quality of Life 15-25%: moderate-to-severe disease - candidates for systemic therapies - often difficult to manage
Psoriasis: 2-5 % Europeans A distressing, life-long, inflammatory disease Impairs patients Quality of Life 15-25%: moderate-to-severe disease - candidates for systemic therapies - often difficult to manage
Disclosures. Consultant and Speaker for Biogen Idec, TEVA Neuroscience, EMD Serrono, Mallinckrodt, Novartis, Genzyme, Accorda Therapeutics
 Mitzi Joi Williams, MD Neurologist MS Center of Atlanta, Atlanta, GA Disclosures Consultant and Speaker for Biogen Idec, TEVA Neuroscience, EMD Serrono, Mallinckrodt, Novartis, Genzyme, Accorda Therapeutics
Mitzi Joi Williams, MD Neurologist MS Center of Atlanta, Atlanta, GA Disclosures Consultant and Speaker for Biogen Idec, TEVA Neuroscience, EMD Serrono, Mallinckrodt, Novartis, Genzyme, Accorda Therapeutics
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Adalimumab, etanercept, infliximab, rituximab and abatacept for the treatment of rheumatoid arthritis after the failure
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Adalimumab, etanercept, infliximab, rituximab and abatacept for the treatment of rheumatoid arthritis after the failure
Malignant Lymphomas and Plasma Cell Myeloma
 Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
High Impact Rheumatology
 High Impact Rheumatology Rheumatology at a Glance Osteoarthritis: Typical hand Hard boney enlargements Heberden s nodes at the DIP joints Bouchard s nodes at the PIP joints Often have squared first CMC
High Impact Rheumatology Rheumatology at a Glance Osteoarthritis: Typical hand Hard boney enlargements Heberden s nodes at the DIP joints Bouchard s nodes at the PIP joints Often have squared first CMC
Psoriatic Arthritis. having psoriatic arthritis.
 Psoriatic Arthritis having psoriatic arthritis. Psoriatic arthritis is a chronic disease characterized by a form of inflammation of the skin (psoriasis) and joints (inflammatory arthritis). Psoriasis is
Psoriatic Arthritis having psoriatic arthritis. Psoriatic arthritis is a chronic disease characterized by a form of inflammation of the skin (psoriasis) and joints (inflammatory arthritis). Psoriasis is
Understanding How Existing and Emerging MS Therapies Work
 Understanding How Existing and Emerging MS Therapies Work This is a promising and hopeful time in the field of multiple sclerosis (MS). Many new and different therapies are nearing the final stages of
Understanding How Existing and Emerging MS Therapies Work This is a promising and hopeful time in the field of multiple sclerosis (MS). Many new and different therapies are nearing the final stages of
Recognition of T cell epitopes (Abbas Chapter 6)
 Recognition of T cell epitopes (Abbas Chapter 6) Functions of different APCs (Abbas Chapter 6)!!! Directon Routes of antigen entry (Abbas Chapter 6) Flow of Information Barrier APCs LNs Sequence of Events
Recognition of T cell epitopes (Abbas Chapter 6) Functions of different APCs (Abbas Chapter 6)!!! Directon Routes of antigen entry (Abbas Chapter 6) Flow of Information Barrier APCs LNs Sequence of Events
FastTest. You ve read the book... ... now test yourself
 FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
Immune modulation in rheumatology. Geoff McColl University of Melbourne/Australian Rheumatology Association
 Immune modulation in rheumatology Geoff McColl University of Melbourne/Australian Rheumatology Association A traditional start to a presentation on biological agents in rheumatic disease is Plasma cell
Immune modulation in rheumatology Geoff McColl University of Melbourne/Australian Rheumatology Association A traditional start to a presentation on biological agents in rheumatic disease is Plasma cell
Bio 20 Chapter 11 Workbook Blood and the Immune System Ms. Nyboer
 Bio 20 Chapter 11 Workbook Blood and the Immune System Ms. Nyboer Name: Part A: Components of Blood 1. List the 3 plasma proteins and describe the function of each Albumins osmotic balance Globulins antibodies,
Bio 20 Chapter 11 Workbook Blood and the Immune System Ms. Nyboer Name: Part A: Components of Blood 1. List the 3 plasma proteins and describe the function of each Albumins osmotic balance Globulins antibodies,
Rheumatology Labs for Primary Care Providers. Robert Monger, M.D., F.A.C.P. 2015 Frontiers in Medicine
 Rheumatology Labs for Primary Care Providers Robert Monger, M.D., F.A.C.P. 2015 Frontiers in Medicine Objectives Review the Indications for and Interpretation of lab testing for the following diseases:
Rheumatology Labs for Primary Care Providers Robert Monger, M.D., F.A.C.P. 2015 Frontiers in Medicine Objectives Review the Indications for and Interpretation of lab testing for the following diseases:
Psoriasis. Background
 Psoriasis Plaque psoriasis is a chronic inflammatory disease with an unknown cause and no cure. Much research is based on the theory that psoriasis is a T cell mediated disorder. This review suggests that
Psoriasis Plaque psoriasis is a chronic inflammatory disease with an unknown cause and no cure. Much research is based on the theory that psoriasis is a T cell mediated disorder. This review suggests that
LYMPHOMA. BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons
 LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
Lymph capillaries, Lymphatic collecting vessels, Valves, Lymph Duct, Lymph node, Vein
 WLHS/A&P/Oppelt Name Lymphatic System Practice 1. Figure 12-1 provides an overview of the lymphatic vessels. First color code the following structures. Color code in Figure 12-1 Heart Veins Lymphatic vessels/lymph
WLHS/A&P/Oppelt Name Lymphatic System Practice 1. Figure 12-1 provides an overview of the lymphatic vessels. First color code the following structures. Color code in Figure 12-1 Heart Veins Lymphatic vessels/lymph
Rheumatoid Arthritis Information
 Rheumatoid Arthritis Information Definition Rheumatoid arthritis (RA) is a long-term disease that leads to inflammation of the joints and surrounding tissues. It can also affect other organs. Alternative
Rheumatoid Arthritis Information Definition Rheumatoid arthritis (RA) is a long-term disease that leads to inflammation of the joints and surrounding tissues. It can also affect other organs. Alternative
Autoimmune Diseases More common than you think Randall Stevens, MD
 Autoimmune Diseases More common than you think Randall Stevens, MD picture placeholder Autoimmune Diseases More than 60 different disorders Autoimmune disorders (AID) diseases caused by the immune system
Autoimmune Diseases More common than you think Randall Stevens, MD picture placeholder Autoimmune Diseases More than 60 different disorders Autoimmune disorders (AID) diseases caused by the immune system
A Psoriasis. Clinical Presentation. 2 Types of Psoriasis. Plaque Psoriasis. 1 Introduction
 Clinical Presentation A Psoriasis Jennifer Soung, Mark Lebwohl Contents 1 Introduction 67 2 Types of Psoriasis 67 Plaque Psoriasis 67 Guttate Psoriasis 68 Pustular Psoriasis 69 Inverse Psoriasis 70 Erythrodermic
Clinical Presentation A Psoriasis Jennifer Soung, Mark Lebwohl Contents 1 Introduction 67 2 Types of Psoriasis 67 Plaque Psoriasis 67 Guttate Psoriasis 68 Pustular Psoriasis 69 Inverse Psoriasis 70 Erythrodermic
Overview of the Cattle Immune System 1
 Oregon State University BEEF043 Beef Cattle Library Beef Cattle Sciences Overview of the Cattle Immune System 1 Reinaldo F. Cooke 2 Introduction On average, the U.S. cattle industry loses more than $1
Oregon State University BEEF043 Beef Cattle Library Beef Cattle Sciences Overview of the Cattle Immune System 1 Reinaldo F. Cooke 2 Introduction On average, the U.S. cattle industry loses more than $1
Highlights on Clinical Picture of Psoriasis
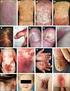 Highlights on Clinical Picture of Psoriasis PROF DR DOAA MAHGOUB CAIRO UNIVERSITY 1 Chronic Plaque Psoriasis Symmetric distribution of sharply defined, erythematous, scaly plaques. The scalp, elbows, knees
Highlights on Clinical Picture of Psoriasis PROF DR DOAA MAHGOUB CAIRO UNIVERSITY 1 Chronic Plaque Psoriasis Symmetric distribution of sharply defined, erythematous, scaly plaques. The scalp, elbows, knees
STEM CELL FELLOWSHIP
 Module I: The Basic Principles of Stem Cells 1. Basics of Stem Cells a. Understanding the development of embryonic stem cells i. Embryonic stem cells ii. Embryonic germ cells iii. Differentiated stem cell
Module I: The Basic Principles of Stem Cells 1. Basics of Stem Cells a. Understanding the development of embryonic stem cells i. Embryonic stem cells ii. Embryonic germ cells iii. Differentiated stem cell
BIOM 255 - Firestein, Winter 2009. Rheumatoid arthritis. Page 1
 Rheumatoid arthritis Page 1 Vascular events in RA Synovium in rheumatoid arthritis Non-extra articular RA Extra articular RA Turesson, et al. Ann Rheum Dis. 2007;66:60 Normal Rheumatoid Arthritis Major
Rheumatoid arthritis Page 1 Vascular events in RA Synovium in rheumatoid arthritis Non-extra articular RA Extra articular RA Turesson, et al. Ann Rheum Dis. 2007;66:60 Normal Rheumatoid Arthritis Major
Analysis of Factors Influencing Clinical Types of Psoriasis Vulgaris
 대 한 건 선 학 회 지 제 5 권, 제 1 호 Journal of the Korean Society for Psoriasis Vol. 5, No. 1, 43-47, 2008 Analysis of Factors Influencing Clinical Types of Psoriasis Vulgaris Sang Eun Lee, M.D., Jung Eun Lee,
대 한 건 선 학 회 지 제 5 권, 제 1 호 Journal of the Korean Society for Psoriasis Vol. 5, No. 1, 43-47, 2008 Analysis of Factors Influencing Clinical Types of Psoriasis Vulgaris Sang Eun Lee, M.D., Jung Eun Lee,
treatments) worked by killing cancerous cells using chemo or radiotherapy. While these techniques can
 Shristi Pandey Genomics and Medicine Winter 2011 Prof. Doug Brutlag Chronic Myeloid Leukemia: A look into how genomics is changing the way we treat Cancer. Until the late 1990s, nearly all treatment methods
Shristi Pandey Genomics and Medicine Winter 2011 Prof. Doug Brutlag Chronic Myeloid Leukemia: A look into how genomics is changing the way we treat Cancer. Until the late 1990s, nearly all treatment methods
Cancer Immunotherapy: Can Your Immune System Cure Cancer? Steve Emerson, MD, PhD Herbert Irving Comprehensive Cancer Center
 Cancer Immunotherapy: Can Your Immune System Cure Cancer? Steve Emerson, MD, PhD Herbert Irving Comprehensive Cancer Center Bodnar s Law Simple Things are Important Very Simple Things are Very Important
Cancer Immunotherapy: Can Your Immune System Cure Cancer? Steve Emerson, MD, PhD Herbert Irving Comprehensive Cancer Center Bodnar s Law Simple Things are Important Very Simple Things are Very Important
Spongiotic reaction pattern Spongiosis = Intercellular edema Elongation of bridges vesiculation, bullae?mechanism unclear Fluid comes from dermis Impo
 Spongiotic Reaction Pattern and review Nathan C. Walk, M.D. Spongiotic reaction pattern Spongiosis = Intercellular edema Elongation of bridges vesiculation, bullae?mechanism unclear Fluid comes from dermis
Spongiotic Reaction Pattern and review Nathan C. Walk, M.D. Spongiotic reaction pattern Spongiosis = Intercellular edema Elongation of bridges vesiculation, bullae?mechanism unclear Fluid comes from dermis
Figure 14.2 Overview of Innate and Adaptive Immunity
 I M M U N I T Y Innate (inborn) Immunity does not distinguish one pathogen from another Figure 14.2 Overview of Innate and Adaptive Immunity Our first line of defense includes physical and chemical barriers
I M M U N I T Y Innate (inborn) Immunity does not distinguish one pathogen from another Figure 14.2 Overview of Innate and Adaptive Immunity Our first line of defense includes physical and chemical barriers
(Intro to Arthritis with a. Arthritis) Manager of Education & Services for the Vancouver Island Region of The Arthritis Society
 Arthritis 101 (Intro to Arthritis with a Focus on Rheumatoid Arthritis) by Cari Taylor by Cari Taylor Manager of Education & Services for the Vancouver Island Region of The Arthritis Society What You Will
Arthritis 101 (Intro to Arthritis with a Focus on Rheumatoid Arthritis) by Cari Taylor by Cari Taylor Manager of Education & Services for the Vancouver Island Region of The Arthritis Society What You Will
