Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique: initial evaluation of 42 cases
|
|
|
- Shon Russell
- 10 years ago
- Views:
Transcription
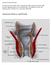
1 Original Article Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique: Carlos Mateus Rotta 1, Fernando Oriolli de Moraes 2, Araripe Fernandez Varella Neto 3, Thereza Cristina Ariza Rotta 4, João Vitor Antunes Marques Gregório 4, Alfredo Luiz Jacomo 6, Carlos Augusto Real Martinez 7 1 Professor Doctor of Coloproctology at the Surgical Clinic of the Medical School at Universidade de Mogi das Cruzes (UMC) Mogi das Cruzes (SP), Brazil. 2 Digestive Tract surgeon at Hospital e Maternidade Mogi D or Mogi das Cruzes (SP), Brazil. 3 Digestive Tract surgeon at Hospital Nove de Julho São Paulo (SP), Brazil. 4 Student at the 6th year of the Medical School of UMC Mogi das Cruzes (SP), Brazil. 5 Associate Professor by the Department of Surgery at Universidade de São Paulo (USP) São Paulo (SP), Brazil. 6 Associate Professor by the Department of Surgery at USP São Paulo (SP), Brazil; 7 Adjunct Professor of the Health Sciences Post-Graduation Program of Universidade São Francisco (USF) Bragança Paulista (SP), Brazil. Rotta CM, Moraes FO, Varella Neto AF, Rotta TCA, Gregório JVAM, Jacomo AL, Martinez CAR. Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique):. J Coloproct, 2012;32(4): ABSTRACT: The treatment of hemorrhoidal disease (HD) by conventional hemorrhoidectomy is associated with significant morbidity, mainly represented by the postoperative pain and the late return to daily activities. Doppler-guided hemorrhoid artery ligation (DGHAL) is a minimal-invasive surgical treatment for HD that has been used as an alternative method in order to reduce these inconveniences. Objective: To analyze the initial results of the DGHAL technique associated with rectal mucopexy in the treatment of HD. Methods: Forty-two patients with stage I, III and IV hemorrhoids who were submitted to DGHAL were analyzed from December 2010 to August Eleven patients (26%) were stage II; 21 (50%), stage III; and 10 (24%), stage IV HD. All patients were operated by the same surgeon under spinal anesthesia and using the same equipment and technique to perform the procedure. The 42 patients underwent ligation of six arterial branches followed by rectal mucopexia by uninterrupted suture. Nine patients needed concomitant removal of perianal skin tag. In the postoperative, the following parameters were evaluated: pain, tenesmus, bleeding, itching, prolapse, mucus discharge and recurrence. The mean postoperative follow-up lasted four months (one to nine months). Results: Tenesmus was the most common postoperative complaint for 85.7% of patients followed by pain, in 28.6%, perianal burning, in 12.3%, mucus discharge and perianal hematoma in 4.7%. Two patients had severe postoperative bleeding and required surgical haemostasis, one of which needed blood transfusion. Ninety-five percent of the patients declared to be satisfied with the method. Conclusion: Even though DGHAL has complications similar to those of other surgical methods, its results present less postoperative pain, allowing faster recovery and return to work. Studies with more cases and a longer follow-up are still necessary to assess the late recurrence. Keywords: hemorrhoids; hemorrhoids/surgery; ligation; ultrasonography, doppler. Resumo: O tratamento da doença hemorroidária (DH) pelas técnicas convencionais cursa com significante morbidade principalmente relacionada à dor pós-operatória e ao considerável tempo de afastamento do trabalho. A técnica de desarterialização hemorroidária transanal guiada por doppler (DHGD) associada à mucopexia retal é uma opção cirúrgica menos invasiva que vem sendo utilizada como método alternativo com objetivo de reduzir esses inconvenientes. Objetivo: Analisar os resultados iniciais com a técnica da DHGD associada à mucopexia retal no tratamento da DH. Método: Foram estudados 42 pacientes, portadores de DH de graus II, III e IV submetidos à técnica da DHGD, durante o período de dezembro de 2010 a agosto de Onze pacientes (26%) apresentavam DH do grau II, 21(50%) do III e 10 (24%) do IV. Todos os pacientes foram operados pelo mesmo cirurgião, sob anestesia raquidiana e sempre utilizando o mesmo equipamento e técnica para realização do procedimento. Os 42 pacientes foram submetidos à desarterialização de Study carried out at the Department of Surgery of the Medical School of Universidade de Mogi das Cruzes (UMC); Department of Surgery at Hospital e Maternidade Mogi-D or Mogi das Cruzes (SP), Brazil; Hospital Nove de Julho São Paulo (SP), Brazil; Health Sciences Post-Graduation Program of Universidade São Francisco (USP) Bragança Paulista (SP), Brazil. Financing source: none. Conflict of interest: nothing to declare. Submitted on: 03/06/2012 Approved on: 15/09/
2 Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique: 6 ramos arteriais seguida de mucopexia retal por sutura contínua. Nove necessitaram remoção concomitante de plicomas perianais. No pós-operatório, foram avaliados os parâmetros: dor, tenesmo, sangramento, prurido, prolapso, perda de muco e recidiva. O seguimento médio foi de quatro meses (um a nove meses). Resultados: O tenesmo foi a queixa pós-operatória referida por 85,7% dos pacientes, seguida da dor 28,6%, ardor perianal 12,3%, perda de muco e formação de hematoma perianal 4,7%. Dois pacientes apresentaram sangramento pós-operatório de maior intensidade necessitando hemostasia cirúrgica, sendo que em um houve necessidade de reposição sanguínea. Noventa e cinco por cento dos pacientes declararam-se satisfeitos com o método. Conclusão: A técnica da DHGD, apesar de apresentar complicações semelhantes a outros métodos cirúrgicos, apresenta bons resultados com pouca dor pós-operatória, possibilitando retorno rápido ao trabalho. Estudos com maior número de casos e tempo de seguimento mais prolongado ainda são necessários para avaliar a recidiva tardia. Palavras-chave: hemorroidas; hemorroidas/cirurgia; ligadura; ultrassonografia doppler. INTRODUCTION Hemorrhoidal disease (HD) is one of the most common illnesses in a specialized doctor s office.it is estimated that in industrialized countries, approximately 50% of the individuals aged more than 50 years develop some of its main symptoms throughout life 1,2. Even though people with HD in its early stage may temporarily benefit from conservative measures, most of the times, when the disease is at a more advanced stage, they need some sort of surgical treatment 3,4. The most frequent conventional surgical methods to treat for HD are Milligan-Morgan or Ferguson hemorrhoidectomy. In the hands of an expert, both present with few postoperative complications, excellent results in terms of healing the HD and acceptable recurrence rates. However, conventional hemorrhoidectomy (CD) presents some main limitations, such as severe postoperative pain and a prolonged period away from work because of the surgical anodermal wound, since this region has a lot of sensitive nervous terminations. The fear of postoperative pain leads many patients to avoid surgical treatment, choosing to live with the limiting symptoms of HD for the rest of their lives. With the objective to reduce the inconvenience of CD, from the 1990s on new methods have been proposed to treat HD. Among them, mechanical anorectopexy (MA) became the most diffuse surgical procedure as an alternative method to conventional techniques 5-7. In MA, the irrigation is interrupted and there is the fixation of the mucosa through the resection of mucosal and submucosal cuff in the lower rectum, above the pectineal line, reconstituting and fixating the borders of the remaining rectal mucosa by means of mechanical circular suture 6,7. Since no incisions are performed in the mucosa of the anal canal, patients evolved with few painful postoperative symptoms. The lower need to care for the surgical wounds enables the fast return to daily activities 7. However, despite these benefits, MA is not free of postoperative complications, and recent studies have shown higher recurrence rates at long term when compared to those of CH The presence of severe complications, such as major postoperative hemorrhage and perforation in the rectal wall, has also been described, and it was probably related to the impossibility to standardize the depth with which the purse-string suture was placed into the rectal wall before stapling 10. When it is too superficial, it might not comprehend the arterial branches present in the submucosa, thus increasing the chances of postoperative bleeding; when too deep, it might comprehend the whole rectal wall, causing the confection of low rectorectal anastomosis during stapling without the protection of a stoma 10. Aiming to interrupt the blood flow directly onto the branches of hemorrhoidal arteries and to avoid the deep penetration of the suture in the rectal wall, the technique of doppler-guided hemorrhoid artery ligation (DGHAL) 11 was proposed. With this method, it is possible to interrupt the blood flow onto the arterial branches, thus avoiding surgical incisions below the dentate line, which is the main cause of postoperative pain in CH 12,13. The DGHAL technique, when associated with rectal mucopexy, also enables the high fixation and, therefore, the correction of prolapsed internal hemorrhoids However, despite being used for years, especially in Europe, the DGHAL technique has been little diffused in Brazil. The objective of 373
3 Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique): this study is to present the initial experience with the DGHAL technique associated with rectal mucopexy in the surgical treatment of HD. METHODS Table 1 shows the characteristics of the studied patients. Fourty two of them (29 men), with mean age of 42.3 years (31 to 64) with HD were included in this study. Eleven (26%) presented with HD in stage II, refractory to conservative treatment, 21 (50%), stage III, and 10 (24%), stage IV. No patient had recurrence and nine of them presented with associated anal skin tags. Patients who were excluded presented with other associated anorectal disease, such as: anal fissure, perianal fistula, external hemorrhoid thrombosis, hidradenitis suppurativa, neoplastic disease of any origin or those who were on anticoagulants. All patients were enlightened as to the surgical procedure to which they would be submitted and, after agreeing to participate in the study, they signed an informed consent form. All surgeries were elective and performed by the same surgeon (CMR) from December 2010 to August Before the procedure, all volunteers were submitted to anamnesis with special focus on the time of evolution of the HD, frequency of bleeding, presence of pain, mucosal prolapsed, anal incontinence and history of prior hemorrhoid thrombosis. All of them were submitted to a full rectal examination with static and dynamic inspection, rectal touch and rigid proctosigmoidoscopy. No patient underwent anorectal manometry. Patients aged more than 50 years were submitted not only to rectal examination, but also to colonoscopy to track for colorectal cancer. All patients were followed-up for about four months (one to nine months). Equipment The system used was composed of a dopplerfluxometry unit associated with a cold light source (THD UK Ltd., Worcester, United Kingdom). The unit has two exits to which a transducer that captures sonic waves and an optical fiber cable are connected. An anoscope comes with the equipment, and it is especially confectioned for the procedure. It is comprised of a fixed part and a sliding bar to perform mucopexy, a central pivot at the extremity to couple the needle Table 1. Characteristic of the studied sample. Characteristic n % Gender Men Women Hemorrhoid stage II III IV Presence of associated skin tags Without skin tags With skin tags Mean age (years) 42.3 (31 64) Total of patients holder and the standardization of the stitch depth penetration performed through the lateral window. Suture thread with a knot threader and the optical fiber cable accompany the equipment. The double crystal transducer captures sonic waves emitted by the arterial branches located on the surface of the rectal wall. When connected to the unit, the sound is amplified. It is a sliding transducer, so it can be freely removed by the surgeon and addressed towards the operating window of the anoscope. Therefore, it is possible to identify the sound coming exclusively from the arterial branches. Doppler guided transanal hemorrhoidal dearterialization surgical technique All patients were admitted to the hospital in the morning and submitted to mechanical bowel preparation with enema containing 118 ml of dibasic sodium phosphate 0.06 g/ml and monobasic sodium phosphate 0.16 g/ml (Fleet-enema from Fleet Laboratories, Lynchburg, Virginia, USA), used three hours before the procedure. Surgeries were always performed with spinal anesthesia and all patients received antibiotic prophylaxis with metronidazole (Sanofi-Aventis Farmacêutica Ltda., Suzano, São Paulo, Brazil), 500 mg intravenously during anesthetic induction, repeated every 8 hours during the first 24 hours. All interventions were performed with patients in the lithotomy position. After rectal touch and gentle anal dilation, the anoscope was lubricated with gel and used to for ul- 374
4 Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique: trasound. The anoscope was previously coupled to the doppler equipment and introduced carefully, until it reached the lower portion of the rectum, approximately seven centimeters above the anal border. Afterwards, the set was moved to the craniocaudal and laterolateral direction until it was possible to hear the best intensity of the acoustic signal coming from the arterial branch identified in the upper lateral rectal wall. After identifying the cranial branch, the transducer was guided to the rectal direction identifying the segment of the rectal wall where there was no emission of sound waves (non-acoustic window). The traction progressed and was interrupted when finding a second point of sound emission located in the lower portion of the rectum. At this point, located above the dentate line, the mucosa was marked with an electric scalpel. Afterwards, the anoscope was repositioned in the cranial portion of the rectum and the needle-holder was introduced until its extremity was firmly coupled to the pivot, placed to the distal extremity of the anoscope. In its extremity, the needle-holder clenched a cylindrical curved needle with a 5/8 circumference, 2.65 of length, already coupled to the thread, monofilamental (2 0), absorbable and provided with the system. Dearterialization began at the cranial sound emission point by applying two transfixion X stitches manually tied. The depth of needle penetration in the rectal wall through the lateral window of the anoscope was limited by the pivot. After the ligation of the cranial branch, the mucosal prolapse was corrected by continuous suture (three to four) performed with straight vision from the rectum to the anal canal, going through the region without sound emission (non-acoustic window). The suture progressed to the place previously marked with the electric scalpel, where the second point of sound emission was located. Rectal mucopexy was concluded by tying the first to the last stitch. Dearteralization always began by the branch located at three hours clockwise. An identical procedure was repeated at 1, 5, 7, 8 and 11 hours, and six arterial branches were always dearterialized. After the procedure was finished, a healing patch was made by introducing a homeostatic sponge in the anal canal. At the postoperative period, patients were recommended to have a diet rich in fibers, liquids and Psyllium fiber twice a day. The recommendations for patients who were submitted to concomitant resection of skin tags were to have hip baths with warm water after evacuations. All patients were discharged on non-hormonal anti-inflammatories (Tenoxicam 60 mg/day) and tramadol chlorhydrate (200 mg/day) in case of severe pain. Postoperative follow-up took place in the first and fourth weeks and, afterwards, once a month, so there was no loss to follow-up in the considered period. After one month, all patients were interviewed in relation to the satisfaction with the method. RESULTS The main symptoms mentioned before surgery were: bleeding (97%), anal discomfort (95%), hemorrhoid prolapse (92%), anal pruritus (53%) and mucus discharge (23%). Mean surgery time was 35±10 minutes to perform dearterialization and mucopexy. All patients were submitted to rectal mucopexy and dearterialization of six arterial branches. In 9 of them (21.43%), besides dearterialization and mucopexy, there was the need to resect skin tags (one or more). Skin tag resection was performed by elliptical incision and afterwards it was sutured with absorbable monofilament thread (3 0). After dearterialization, there was the need for complementary haemostatic suture during surgery in five patients (8.4%). Figures 1 and 2 show the patients with HD before and after DGHAL with rectal mucopexy. Figure 3 represents the main complaints in the fourth week after surgery. Thirty six patients (85.71%) complained of tenesmus, 12 (28.6%), of anorectal pain, 8 (19.5%), of burning sensation, 6 (12.3%) of mucus discharge, 2 (4.76%), of anal pruritus. Two patients progressed with perianal hematoma (4.76%), and in one of them, full thrombus regression remained for 30 days. All patients who underwent skin tag resection complained of more frequent anal pain at the postoperative period. Twenty percent of patients developed urinary retention at the immediate postoperative period, requiring the use of probe. In one of them, who also evolved with concomitant external hematoma, the retention lasted for seven days requiring repeated bladder probes during this period. Two patients (4.76%) presented with postoperative bleeding, therefore needing surgical haemostasis, which was performed on the fifth and ninth postoperative days; one of them required blood replacement. One patient mentioned fecal incontinence for one day, and 375
5 Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique): A B Figure 1. (A) Preoperative aspecto f patient with hemorrhoid disease in stage III. (B) Immediate postoperative of the same patient submitted to the doppler-guided transanal hemorrhoidal dearterialization with mucopexy. A B Figure 2. (A) Preoperative aspect of patient with hemorrhoidal disease. (B) Immediate postoperative of the same patient submitted to the doppler-guided transanal hemorrhoidal dearterialization with mucopexy. two others (4.76%) developed anal fissure between the 7 th and 15 th postoperative days, which healed with clinical treatment. No recurrence was observed in the follow-up period. DISCUSSION The best surgical choice to treat symptomatic HD must consider the following: it should provide full remission of symptoms, be of simple technical execution and financially accessible, be well tolerated by the patients and progress with low rates of postoperative complications and recurrence 24,25. The great number of surgical procedures that are currently available to treat HD shows that until now none of the proposed techniques can gather all of these items. Nowadays, CH is still the most used surgical choice around the world for the treatment of HD. Despite being effective to control 376
6 Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique: Number of patients Tenesmus Pain Burning Mucus Pruritus Hematoma Hemorrhage discharge Figure 3. Main symptoms reported until the fourth week after the surgery. Fissure symptoms and evolving with low recurrence rates, its main limitations are the severe postoperative pain and the necessary care during convalescence, and because of that the patient is away from daily activities for a considerable amount of time 24,25. Aiming to come up with alternative methods that are able to minimize the inconvenient of CH, new surgical options have appeared to treat HD 6,11. In the modern group of therapies to treat HD, MA and DGHAL represent the most used alternatives 23,25. Despite the advantages of both methods concerning reduced postoperative pain and faster return to the patient s social daily life, the main limiting factors for the greater acceptance of such procedures are related to higher costs for the health systems (both public and private), which certainly do not cover all necessary expenses to perform these methods, thus condemning the patients to pay for part of them, and to the yet minor postoperative follow-up. The proposal of both techniques is to treat HD by the interruption of blood flow to the hemorrhoidal plexus and the reduction of mucosal prolapse with rectal mucopexy, thus restablishing the regular an rectal anatomy 6,11. Both procedures try to achieve these objectives by interrupting the blood flow to the hemorrhoidal plexux and by fixating the excess of rectal mucosal prolapse, resecting it and fixating it (MA), or just by fixating it inside the rectum (DGHAL) 14. The MA technique proposed by Longo 6, in 1998, interrupts the blood flow to the hemorrhoidal plexus and reduces prolapsed by the resection of a circular mucosal and submucosal segment above the dentate line, and fixating the remaining mucosa at a higher situation by means of mechanical circular suture 24. The resection of the excess of mucosa with posterior replacement inside the rectum, besides correcting hemorrhoidal prolapsed, also has the advantage to improve the mechanisms of continence since it normalizes the anal pressure at rest. Since there are no incisions below the dentate line, which is an anatomic region rich in sensitive terminations, the MA technique significantly reduces the intensity of postoperative pain when compared to conventional techniques 25. The absence of surgical wound in the anoderm decreases the need for frequent postoperative care and enables the patient to get back to daily activities faster 25. However, despite these undeniable advantages, recent sample reviews have shown that the MA technique evolves with long term recurrence rates up to 5.5 times higher than CH 8,25,26. The reduction of blood flow to the hemorrhoidal plexus, with the MA technique, is obtained by the 377
7 Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique): transaction of caudal branches of the upper rectal artery during the resection of the mucosal and submucosal cuff followed by mechanical stapling 23. However, a recent study evaluating arterial blood flow in the hemorrhoidal plexus, before and after the procedure, did not find significant differences, thus suggesting that the MA technique is not able to completely interrupt the blood flow by the intramural branches of the upper rectal artery, located below the point where the stapling was performed 27. It is possible that the height the rectum where the stapling is performed in the rectum may be involved in the lower dearterialization. The maintenance of blood supply by these caudal branches may be one of the factors responsible for higher rates of late recurrence when compared to CH 27. Concerning the complications of MA, major postoperative bleeding and pain resulting from the stapling being too close to the dentate line or because of the presence of the surgical staples are usually described 7,25. The urge to evacuate, tenesmus, sensation of a foreign body in the rectum, persisten proctalgia and incomplete evacuation have been increasingly described, while stenosis and lack of stapling are rarer complications 26,28. However, the most feared complication from MA is the risk of potential pelvic infections when the full resection of the whole rectal wall takes place during mechanical stapling The result of the complication is similar to performing an ultra low rectal anastomosis, in a rectum without mechanical preparation, and without the protection of a proximal stoma, which can evolve to severe abdominal and pelvic infections, mostly fatal Since this kind of complication can happen with surgeons at different stages in relation to learning the method, it is possible that it occurs due to the confection of suture in a purse string without the standardization of depth to penetrate the stitches into the rectal wall 10. In favor of this probability is the constant presence of segments of muscle layers from the rectal wall in the resected specimens, submitted to histopathological analysis 29. Changes in the initially designed equipment and new devices have been proposed in order to decrease the possibility of such a severe complication 11,30,31. As to the costs of MA, when compared to CH there is still controversy. Two studies demonstrated that MA costs more in relation to CH, while a third analysis showed the opposite With these considerations, despite the advantages in relation to CH concerning the less intense postoperative pain and the faster return to daily activities, the MA technique costs more and probably has higher recurrence rates at long term. The DGHAL technique, in theory, presents the same technical proposal of MA: the interruption of blood flow through the distal branches of the upper rectal artery by the application of transfixion stitches directly over these branches and posterior fixation of prolapsed hemorrhoids inside the rectum at a higher situation 11. Unlike MA, the use of a Doppler equipment associated with a light source attached to an anoscope, especially designed for the procedure, enables the precise location of the arterial branches that are present in the rectal wall 11,23. Therefore, these arteries are individually identified, which not only enables the employment of the transfixion stitch directly over these arteries, but also allows verifying if the blood flow has been completely stopped after the conclusion of the suture. The technological characteristics of the system is comprised of a double crystal echo acoustic transducer that can capture sonic waves emitted by the smallest branches located on the surface of the rectal wall, thus increasing the precision of the ligation of these vessels. The exact location through which an arterial branch passes enables the suture and the posterior mucopexy to be performed exactly onto the vessel throughout the longitudinal axis of the rectum, thus leaving free room between each stitch. This detail decreases the chance, at least in theory, as with MA, of the full blockage of the venous flow by the hemorrhoidal venous plexus, which is responsible for postoperative cases of external hemorrhoid thrombosis. The space between stitches also reduces the chance of the total obliteration of the rectal lumen, which is a complication described after the use of MA 28. Another advantage of DGHAL in relation to MA is that the provided anoscope already coupled to the transducer and cable light enables the application of transfixion stitches to be performed with straight view, and its depth is guided by the pivot placed in the equipment. Such details also help to decrease the chance of reaching the deeper layers of the rectal wall. Since the depth of the stitches becomes standardized, and there is no resection of the rectal mucosal and submucosal cuff, the possibility to completely cut the rectal wall, which is one of the main concerns with MA, is minor with DGHAL. However, 378
8 Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique: it is worth to mention that despite the greater risk of lesion in the rectal wall with MA, the possibility to resect and fixate a considerable segment of the prolapsed mucosa at a higher situation inside the rectum brings theoretical advantages to MA as to the lower chance of prolapsed recurrence at long term. The possibility to identify and perform the individual dearterialization of each arterial branch (5 9 branches) may explain the different number of ligations when comparing the DGHAL technique with other methods of elastic ligation of HD, in which it is not possible to identify exactly where the arterial branch passes 15,19-23,27, Because of the greater selectivity as to the location of arterial branches, the number of stitches (ligations) ranges from three to nine, according to different authors in most published articles In this study, six arterial branches were ligated and identified in positions 1, 3, 5, 7, 9 and 11 hours. The patient was in the lithotomy position. In this study, the DGHAL technique was indicated for patients with hemorrhoids in stage II, III and IV. Similarly to MA, the DGHAL technique was initially used with patients with stage II HD who were refractory to conservative treatment or those at the stage III of the disease 19,23,25,35. Afterwards, with the addition of mucopexy to surgical time, enabling the reduction and fixation of prolapsed hemorrhoids, it was possible to indicate the method for patients with stage IV HD Unlike what happens with MA, that is, the amount of resected tissue and the height of stapling range from case to case, with DGHAL it is possible to define the places where mucopexy will begin and end, as well as the amount of tissue involved, even for those with stage IV HD. A study assessed the DGHAL technique associated with rectal mucopexy in 35 patients with the objective to decrease the need to perform CH and, consequently, also decrease the intensity of postoperative pain in patients with non-fibrous stage IV HD 39. The authors dearterialized six arterial branches and average surgical time was of 33±12 minutes. They also checked that during postoperative follow-up, three patients (8.6%) presented with external hemorrhoid thrombosis; one of them needed additional surgical treatment and two (5.7%) evolved with postoperative bleeding. One of the latter needed haemostasis surgery. Five patients (14.3%) presented with urinary retention and required an intravesical probe, which was less than the findings in this study. At a mean postoperative follow-up of 10 months (2-28 months), there was a significant improvement of symptoms in 33 patients (94%). Nine patients (25.7%) evolved with irregular bleeding when evacuating in the first weeks they evacuated spontaneously, 3 (8.6%) had mild anal pain, 4 (11.4%) felt transitory anal burning, and 4 (11.4%) had tenesmus. Ten patients (28.6%) presented with some degree of residual prolapsed and only 2 (5.7%) had a more significant mucosal prolapse and needed surgery. Despite the short follow-up period, the authors could not find anal stenosis or incontinence. After applying a satisfaction questionnaire with the method, they noticed that after a ten-month follow-up, there was significant number of patients who were happy about it 39. However, even though some suggest the DGHAL technique can be used in patients with stage IV HD, the postoperative results, like with MA, do not present the same degree of satisfaction when compared to patients with less advanced stages of HD 39. A second multicenter study analyzing 507 patients with HD in stages II (28.4%), III (63%) and IV (8.6%), who were submitted to the DGHAL technique and followed-up for one year, found good results with the procedure with 69.2% of the patients, and acceptable in the remaining 4.8% 40. However, when gathering the patients according to the stage of HD, they observed that 92.4% of those with stage II hemorrhoids and 84% of patients with stage III were satisfied with the method, whilst only 41% of those with stage IV HD felt the same way 40. Studies have clearly shown the advantages of the MA technique in relation to CH, especially concerning the intensity of postoperative pain and the early return to daily activities 7, A review of 12 studies that compared CH with MA, with follow-up between 6 months to 4 years, showed that CH is more efficient to reduce long term recurrence (OR=3.85; 95%CI ; p<0.006) 43. CH also prevented the development of new hemorrhoids after 12 or more months of postoperative follow-up (OR=3.6; 95%CI ; p<0.02). CH was better in relation to preventing prolapsed (OR=2.96; 95%CI ; p<0.008), as well as to avoid the development of prolapse after one or more years of follow-up (OR=2.68; 95%CI ; p<0.05). There were no significant differences favoring CH when the following was analyzed: the proportion of 379
9 Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique): asymptomatic patients, presence of postoperative bleeding, mucus discharge, difficulties with hygiene and fecal incontinence, presence of perianal skin tags and need for future surgeries. As to MA, the authors could not find advantages concerning pain, anal pruritus, symptoms of obstructed evacuation or stenosis 43. However, few studies have compared the DGHAL technique with other surgical options to treat HD, which makes it difficult to conduct a more precise evaluation 44,45. Bursics et al. 14, in 2004, compared the DGHAL technique with CH after a one-year follow-up. They showed that the patients submitted to the DGHAL technique required less postoperative analgesia and less days to return to work faster 14. These results were confirmed by other authors 27,45. Avital et al. 46, in 2001, compared the MA and DGHAL techniques in 63 patients and found that those submitted to DGHAL presented less pain after evacuating (2.1±1.4 versus 5.5±1.9) and were on less painkillers. The length of hospital stay, the interval for the first evacuation and the complete functional recovery to evacuate were shorter for those submitted to DGHAL 46. However, 18% of patients treated with DGHAL remained with bleeding or hemorrhoidal prolapse and needed complementary surgical resection, compared to only 3% of those submitted to MA 46. When the questionnaire to assess the satisfaction of patients with the procedure was applied, it was observed that those submitted to MA were happier in relation to those who underwent DGHAL. As previously suggested it is likely that the higher incidence of prolapse after DGHAL is associated with the performance of a less effective rectal mucopexy. A recently published systematic literature review, whicht selected only randomized and controlled studies showed, in 150 patients (80 of them submitted to DGHAL and 70 to MA), that both procedures were similar in terms of satisfaction, length of operation, recurrence and postoperative complications 47. However, the DGHAL technique proved to be superior in relation to the intensity of postoperative pain 47. A double blind randomized study compared the simple elastic ligation from the hemorrhoidal plexus associated with mucopexy without using the DGHAL equipment with the conventional DGHAL method in patients with stage III HD 48. Results shows that the DGHAL technique presented longer surgical time, and patients presented more postoperative pan, thus needing to consume painkillers for longer 48. Probably, the most intense postoperative pain is related to the larger number of ligations performed with DGHAL and to the association of rectal mucopexy. One year after surgery, recurrence rates were similar 48. The authors concluded that the simple elastic ligation of HD is a simple and cost effective method to treat the disease in stage III, so there are no advantages to use the whole equipment of DGHAL to assist the ligation of hemorrhoidal vessels before mucopexy 48. Spyridakis et al. 49, in 2011, studied 90 patients who underwent the DGHAL technique and observed that the recurrence rate assessed by the presence of bleeding or mucosal prolapse was identified in 6.6% of patients, being more common in patients with stage IV hemorrhoids. The results found in this study showed that even though all patients were discharged still on anti-inflammatories, 85.71% of them complained of tenesmus at the postoperative period which regressed after the second week. Despite the use of anti-inflammatory, eight patients (19.5%) complained of anal pain, and six (12.30%) mentioned constant burning, which also regressed after the second and third weeks, respectively. In three patients, the pain was prolonged for one month and required the use of painkillers for longer. These results are different from those found by other authors, showing that 72% of patients submitted to DGHAL did not need postoperative analgesia 21,35. It is likely that these discomforts are owed to suture and fixation of the prolapsed hemorrhoid, which leads to ischemia, necrosis with a consequent inflammatory process at the site of mucopexy 21. That is why most of the patients followed-up in this study, as well as those described by other authors, presented with more intense pain and tenesmus in the first week after surgery, which disappeared as the days passed by 35. Most authors describe the occurrence of minor bleeding associated with evacuations in the first days after surgery, similarly to other techniques 35. Data from literature report that postoperative bleeding takes place in 1 to 20.9% of the patients submitted to DGHAL 12-15,17,18,34, A randomized study comparing patients submitted to MA and DGHAL report that 12% of those who underwent MA presented with more intense bleeding, thus requiring readmission to control the hemorrhage, compared to only 4% of the patients submitted to DGHAL 52. In this study, 380
10 Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique: in the first two weeks most patients (68%) presented with minor bleeding during evacuations. However, for two patients rectal bleeding was major and required reintervention for the hemostasis of the bleeding vessel. In one of them there was the need for blood replacement in order to control acute anemia. In one of the patients, bleeding came from one of the transfixion stitches, while in the second, with the major bleeding, it was originated from the site where pexy had been performed in one of the prolapsed hemorrhoids. It is probable that the hemorrhage is a result of necrosis, and consequent dehiscence of mucopexy, and that the continuous use of non-hormonal anti-inflammatory in the first week, since in interferes with the blood profile, may also have contributed for the bleeding. Other less frequent symptoms were mucus discharge in 6 (14.30%) patients, urinary retention in 8 (19.4%) and anal pruritus in 2 (4.76%). Two patients evolved with the formation of perianal hematoma at the postoperative period, and in one of them, with stage III HD, the perianal hematoma presented a larger proportion, lasting for 3 weeks and associated with prolonged urinary retention; however, it was healed after 30 days. These results are similar to those described by other authors who followed-up a larger sample 34. Even though DGHAL preserves the venous drainage between mucopexy sutures, which is not true for MA, it can also evolve with external hemorrhoid thrombosis associated with the difficulty of venous return. In this study, for 38 patients (90.5%) postoperative complaints did not prevent the return to regular activities one week after intervention. A systematic literature review considering all published DGHAL cases, and included 2,000 patients, showed recurrence rate of 10.8% for mucosal prolapse, 9.7% for postoperative bleeding and 8.7% for pain when evacuating 51. When considering only patients followed-up for more than one year, the recurrence of prolapse and bleeding increased to 10.8 and 9.7%, respectively 51. A recent randomized study that assessed patients submitted to CH, MA and DGHAL did not find differences between the techniques concerning the improvement of symptoms such as bleeding or pain 52. However, as to the healing of the prolapse, CH proved to be superior to MA and DGHAL 52. Another study comparing DGHAL associated with pexy and MA showed that 78% of the patients submitted to DGHAL and 83% of those submitted to MA presented with complete healing of symptoms 6 weeks after the intervention 52. In this study, the persistence of the mucosal prolapse was higher in patients who underwent DGHAL, however, most patients with stage IV hemorrhoids were placed in the DGHAL group, which may have influenced the results. In this study, it was observed that most patients who presented with postoperative discomfort had stage IV hemorrhoids or were submitted to skin tag resection. A recent study assessed 244 patients submitted to DGHAL and confirmed these observations 53. By using the multivariate logistic regression analysis, the authors concluded that the presence of mucosal prolapse is considered as a risk factor for the persistence of symptoms (OR=2.38; 95%CI ). They also observed that patients with HD in stages III and IV had higher risks of recurrence (OR=4.94; 95%CI ) and concluded that DGHAL should be carefully indicated for more advanced HD 53. In this study, it was noticed that the larger number of patients who referred being little satisfied with the technique also presented stage IV HD. They were submitted to concomitant perianal skin tag resection or presented with complications (hemorrhage, perianal hematoma or postoperative anal fissure). When considering the costs, one article comparing the conventional elastic ligation and DGHAL reports that even though the doppler-guided dearterialization is more efficient than elastic ligation to reduce postoperative pain, recurrence and also to improve the quality of life of patients with stage II and III hemorrhoids without mucosal prolapse, it costs more 54. Even with the reduced number of patients and the short follow-up at the postoperative period, the results of this study suggest that DGHAL can be considered as a valid choice to treat for HD. Despite the advantages in relation to the less intense postoperative pain and faster return to daily activities, the DGHAL technique may present the same postoperative complications described in other methods. As in other techniques, the postoperative results of DGHAL in stage IV HD seem to be worse, as well as when there is the need to perform procedures that include incisions in the perianal skin or the anal canal. Perianal incisions increase postoperative discomfort and decrease the degree of satisfaction with the method. The 381
11 Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique): results show that DGHAL is a simple surgical procedure to perform, with a small learning curve due to the possibility to repeat the procedure many times in the same patient. The technique provides the remission of symptoms, especially for those with HD in stages II and III, and is well tolerated. It evolves with acceptable short term recurrence rates. At the moment, the development of a multicenter national study is proposed in order to evaluate more patients with longer follow-up to confirm the validity of this new option of treatment for HD. Only this way it will be possible to verify if recurrence and satisfaction rates concerning the method remain stable throughout the years. CONCLUSION The DGHAL technique is a valid alternative to treat for HD in stages II and III, and its main benefits are to evolve with little postoperative pain and to enable the fast return of the patient to daily activities. Studies involving more cases and with longer followup are still necessary to assess late recurrence. REFERENCES 1. Kaidar-Person O, Person B, Wexner SD. Hemorrhoidal disease: a comprehensive review. J Am Coll Surg 2007;204(1): Johanson JF, Sonnenberg A. The prevalence of hemorrhoids and chronic constipation. An epidemiologic study. Gastroenterology 1990;98(2): Altomare DF, Roveran A, Pecorella G, Gaj F, Stortini E. The treatment of hemorrhoids: guidelines of the Italian Society of Colorectal Surgery. Tech Coloproctol 2006;10(3): Cataldo P, Ellis CN, Gregorcyk S, Hyman N, Buie WD, Church J, et al. Practice parameters for the management of hemorrhoids (revised). Dis Colon Rectum 2005;48(2): Sobrado CW, Cotti GCC, Coelho FF, Rocha JRM. Initial experience with stapled hemorrhoidopexy for treatment of hemorrhoids. Arq Gastroenterol 2006;43(3): Longo A. Treatment of haemorrhoids disease by reduction of mucosa and hemorrhoidal prolapse with circular suturing device: a new procedure. 6th World Congress of Endoscopic Surgery; Rome; 1998: Tjandra JJ, Chan MK. Systematic review on the procedure for prolapse and hemorrhoids (stapled hemorrhoidopexy). Dis Colon Rectum 2007;50(6): Kornaros S, Dalamangas K, Zisi-Sermpetzoglou A. Fulminant intra-abdominal sepsis after stapled hemorrhoidectomy. Surg Infect (Larchmt) 2011;12(2): Cirocco WC. Life threatening sepsis and mortality following stapled hemorrhoidopexy. Surgery 2008;143(6): Crepaldi Filho R, Martinez CAR, Palma RT, Priolli DG, Rezende Júnior HC, Waisberg J. Modificação do anuscópio auxiliar (PSA 33) do PPH para facilitar a realização da sutura em bolsa na hemorroidectomia por grampeamento. Rev Bras Colo-proct 2004;24(4): Morinaga K, Hasuda K, Ikeda T. A novel therapy for internal hemorrhoids: ligation of the hemorrhoidal artery with a newly devised instrument (Moricorn) in conjunction with a Doppler flowmeter. Am J Gastroenterol 1995;90(4): Sohn N, Aronoff JS, Cohen FS, Weinstein MA. Transanal hemorrhoidal dearterialization is an alternative to operative hemorrhoidectomy. Am J Surg 2001;182(5): Charúa Guindic L, Fonseca Muñoz E, García Pérez NJ, Osorio Hernández RM, Navarrete Cruces T, Avendaño Espinosa O, et al. Hemorrhoidal desarterialization guided by Doppler. A surgical alternative in hemorrhoidal disease management. Rev Gastroenterol Mex 2004;69(2):83-7. [Spanish]. 14. Bursics A, Morvay K, Kupcsulik P, Flautner L. Comparison of early and 1-year follow-up results of conventional hemorrhoidectomy and hemorrhoid artery ligation: a randomized study. Int J Colorectal Dis 2004;19(2): Ramirez JM, Gracia JA, Aguilella V, Elia M, Casamayor MC, Martinez M. Surgical management of symptomatic haemorrhoids: to cut, to hang or to strangle? A prospective randomized controlled trial. Colorectal Dis 2005;7: Felice G, Privitera A, Ellul E, Klaumann M. Dopplerguided hemorrhoidal artery ligation: an alternative to hemorrhoidectomy. Dis Colon Rectum 2005;48(11): Scheyer M, Antonietti E, Rollinger G, Mall H, Arnold S. Doppler-guided hemorrhoidal artery ligation. Am J Surg 2006;191(1): Greenberg R, Karin E, Avital S, Skornick Y, Werbin N. First 100 cases with Doppler-guided hemorrhoidal artery ligation. Dis Colon Rectum 2006;49(4): Wallis de Vries BM, van der Beek ES, de Wijkerslooth LR, van der Zwet WC, van der Hoeven JA, Eeftinck Shattenkerk M, et al. Treatment of grade 2 and 3 hemorrhoids with Doppler-guided hemorrhoidal artery ligation. Dig Surg 2007;24(6): Abdeldaim Y, Mabadeje O, Muhammad KM, Mc Avinchey D. Doppler-guided haemorrhoidal arteries ligation: preliminary clinical experience. Ir Med J 2007;100(7): Ratto C, Donisi L, Parello A, Litta F, Doglietto GB. Evaluation of transanal hemorrhoidal dearterialization as a minimally invasive therapeutic approach to hemorrhoids. Dis Colon Rectum 2010;53(5):
12 Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique: 22. Dal Monte PP, Tagariello C, Sarago M, Giordano P, Shafi A, Cudazzo E, et al. Transanal haemorrhoidal dearterialization: nonexcisional surgery for the treatment of haemorrhoidal disease. Tech Coloproctol 2007;11(4): Giordano P, Nastro P, Davies A, Gravante G. Prospective evaluation of stapled haemorrhoidopexy versus transanal haemorrhoidal dearterialisation for stage II and III haemorrhoids: three-year outcomes. Tech Coloproctol 2011;15(1): Lienert M, Ulrich B. Doppler-guided ligation of the hemorrhoidal arteries. Report of experiences with 248 patients. Dtsch Med Wochenschr 2004;129(17): [German]. 25. Giordano P, Gravante G, Sorge R, Ovens L, Nastro P. Longterm outcomes of stapled hemorrhoidopexy vs conventional hemorrhoidectomy: a meta-analysis of randomized controlled trials. Arch Surg 2009;144(3): Pescatori M, Gagliardi G. Postoperative complications after procedure for prolapsed hemorrhoids (PPH) and stapled transanal rectal resection (STARR) procedures. Tech Coloproctol 2008;12(1): Aigner F, Bodner G, Conrad F, Mbaka G, Kreczy A, Fritsch H. The superior rectal artery and its branching pattern with regard to its clinical influence on ligation techniques for internal hemorrhoids. Am J Surg 2004;187(1): Büyükaşik O, Hasdemir OA, Cöl C. Rectal lumen obliteration from stapled hemorrhoidopexy: can it be prevented? Tech Coloproctol 2009;13(4): Naldini G, Martellucci J, Moraldi L, Romano N, Rossi M. Is simple mucosal resection really possible? Considerations about histological findings after stapled hemorrhoidopexy. Int J Colorectal Dis 2009;24(5): Regadas FS, Regadas SM, Rodrigues LV, Misici R, Tramujas I, Barreto JB, et al. New devices for stapled rectal mucosectomy: a multicenter experience. Tech Coloproctol 2005;9(3): Rebuffat C, Porta MD, Ciccarese F, Rosati R. A new anoscope for transanal surgery. Am J Surg 2008;196(3):e Ho YH, Cheong WK, Tsang C, Ho J, Eu KW, Tang CL, et al. Stapled hemorrhoidectomy: cost and effectiveness. Randomized controlled trial including incontinence scoring, anorectal manometry, and endoanal ultrasound assessments at up three months. Dis Colon Rectum 2000;43(12): Kirsch JJ, Staude G, Herold A. The Longo and Milligan- Morgan hemorrhoidectomy. A prospective comparative study of 300 patients. Chirurg 2001;72(2): [German]. 34. Wilson MS, Pope V, Doran HE, Fearn SJ, Brough WA. Objective comparison of stapled anopexy and open hemorrhoidectomy: a randomized, controlled trial. Dis Colon Rectum 2002;45(11): Infantino A, Bellomo R, Dal Monte PP, Salafia C, Tagariello C, Tonizzo CA, et al. Transanal haemorrhoidal artery echodoppler ligation and anopexy (THD) is effective for II and III degree haemorrhoids: a prospective multicentric study. Colorectal Dis 2010;12(8): Theodoropoulos GE, Sevrisarianos N, Papaconstantinou J, Panoussopoulos SG, Dardamanis D, Stamopoulos P, et al. Doppler-guided haemorrhoidal artery ligation, rectoanal repair, sutured haemorrhoidopexy and minimal mucocutaneous excision for grades III-IV haemorrhoids: a multicenter prospective study of safety and efficacy. Colorectal Dis 2010;12(2): Satzinger U, Feil W, Glaser K. Recto Anal Repair (RAR): a viable new treatment option for high-grade hemorrhoids. One year results of a prospective study. Pelviperineology 2009;28(2): Zagriadskii EA. Trans-anal disarterization of internal hemorrhoids under Doppler control with mucopexy and lifting in treatment of stage III-IV hemorrhoids. Khirurgiia (Mosk) 2009;2:52-8. [Russian]. 39. Ratto C, Giordano P, Donisi L, Parello A, Litta F, Doglietto GB. Transanal haemorrhoidal dearterialization (THD) for selected fourth-degree haemorrhoids. Tech Coloproctol 2011;15(2): Wałega P, Scheyer M, Kenig J, Herman RM, Arnold S, Nowak M, et al. Two-center experience in the treatment of hemorrhoidal disease using Doppler-guided hemorrhoidal artery ligation: functional results after 1-year follow-up. Surg Endosc 2008;22(11): Shao WJ, Li GC, Zhang ZH, Yang BL, Sun GD, Chen YQ. Systematic review and meta-analysis of randomized controlled trials comparing stapled haemorrhoidopexy with conventional haemorrhoidectomy. Br J Surg 2008;95(2): Nisar PJ, Acheson AG, Neal KR, Scholefield JH. Stapled hemorrhoidopexy compared with conventional hemorrhoidectomy: systematic review of randomized, controlled trials. Dis Colon Rectum 2004;47(11): Jayaraman S, Colquhoun PH, Malthaner RA. Stapled hemorrhoidopexy is associated with a higher long-term recurrence rate of internal hemorrhoids compared with conventional excisional hemorrhoid surgery. Dis Colon Rectum 2007;50(9): Wałega P, Scheyer M, Kenig J, Herman RM, Arnold S, Nowak M, et al. Two-center experience in the treatment of hemorrhoidal disease using Doppler-guided hemorrhoidal artery ligation: functional results after 1-year follow-up. Surg Endosc 2008;22(11): Faucheron JL, Poncet G, Voirin D, Badic B, Gangner Y. Doppler-guided hemorrhoidal artery ligation and rectoanal repair (HAL-RAR) for the treatment of grade IV hemorrhoids: long-term results in 100 consecutive patients. Dis Colon Rectum 2011;54(2): Avital S, Itah R, Skornick Y, Greenberg R. Outcome of stapled hemorrhoidopexy versus doppler-guided hemorrhoidal artery ligation for grade III hemorrhoids. Tech Coloproctol 2011;15(3):
13 Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique): 47. Sajid MS, Parampalli U, Whitehouse P, Sains P, McFall MR, Baig MK. A systematic review comparing transanal haemorrhoidal de-arterialisation to stapled haemorrhoidopexy in the management of haemorrhoidal disease. Tech Coloproctol 2012;16(1): Gupta PJ, Kalaskar S, Taori S, Heda PS. Doppler-guided hemorrhoidal artery ligation does not offer any advantage over suture ligation of grade 3 symptomatic hemorrhoids. Tech Coloproctol 2011;15(4): Spyridakis M, Christodoulidis G, Symeonidis D, Dimas D, Diamantis A, Polychronopoulou E, et al. Outcomes of Dopplerguided hemorrhoid artery ligation: analysis of 90 consecutive patients. Tech Coloproctol 2011;15(Suppl 1):S Cantero R, Balibrea JM, Ferrigni C, Sanz M, García Pérez JC, Pérez R, et al. Doppler-guided transanal haemorrhoidal dearterialization: an alternative treatment for haemorrhoids. Cir Esp 2008;83(5): [Spanish]. 51. Giordano P, Overton J, Madeddu F, Zaman S, Gravante G. Transanal hemorrhoidal dearterialization: a systematic review. Dis Colon Rectum 2009;52(9): Festen S, van Hoogstraten MJ, van Geloven AA, Gerhards MF. Treatment of grade III and IV haemorrhoidal disease with PPH or THD. A randomized trial on postoperative complications and short-term results. Int J Colorectal Dis 2009;24(12): Pol RA, van der Zwet WC, Hoornenborg D, Makkinga B, Kaijser M, Eefitinck Schattenkerk M, et al. Results of 244 consecutive patients with hemorrhoids treated with Doppler-guided hemorrhoidal artery ligation. Dig Surg 2010;27(4): Giamundo P, Salfi R, Geraci M, Tibaldi L, Murru L, Valente M. The hemorrhoid laser procedure technique vs rubber band ligation: a randomized trial comparing 2 mini-invasive treatments for second- and third-degree hemorrhoids. Dis Colon Rectum 2011;54(6): Correspondence to: Carlos Mateus Rotta Rua Julio Prestes, 240 CEP: Mogi das Cruzes (SP), Brazil [email protected] 384
Recto Anal Repair (RAR): a viable new treatment option for high-grade hemorrhoids. One year results of a prospective study
 Original article Recto Anal Repair (RAR): a viable new treatment option for high-grade hemorrhoids. One year results of a prospective study ULRIKE SATZINGER (*) - WOLFGANG FEIL (**) - KARL GLASER (***)
Original article Recto Anal Repair (RAR): a viable new treatment option for high-grade hemorrhoids. One year results of a prospective study ULRIKE SATZINGER (*) - WOLFGANG FEIL (**) - KARL GLASER (***)
Treatment of grade III and IV haemorrhoidal disease with PPH or THD. A randomized trial on postoperative complications and short-term results
 Treatment of grade III and IV haemorrhoidal disease with PPH or THD. A randomized trial on postoperative complications and short-term results Authors: Sebastiaan Festen & M. J. Van Hoogstraten & A. A.
Treatment of grade III and IV haemorrhoidal disease with PPH or THD. A randomized trial on postoperative complications and short-term results Authors: Sebastiaan Festen & M. J. Van Hoogstraten & A. A.
UNDERSTANDING THE PROCEDURE FOR PROLAPSE AND HEMORRHOIDS
 UNDERSTANDING THE PROCEDURE FOR PROLAPSE AND HEMORRHOIDS AN ALTERNATIVE APPROACH TO THE SURGICAL TREATMENT OF HEMORRHOIDS pphinfo.com Identifying Patients for PPH Procedure for Prolapse and Hemorrhoids
UNDERSTANDING THE PROCEDURE FOR PROLAPSE AND HEMORRHOIDS AN ALTERNATIVE APPROACH TO THE SURGICAL TREATMENT OF HEMORRHOIDS pphinfo.com Identifying Patients for PPH Procedure for Prolapse and Hemorrhoids
Transanal Hemorrhoid Dearterialization and mucopexy: a minimal invasive approach for prolapsed hemorrhoids. Four cases report.
 Transanal Hemorrhoid Dearterialization and mucopexy: a minimal invasive approach for prolapsed hemorrhoids. Four cases report. Stefan Morarasu*,1, Emmanuel Eguare 2, Yasir Bashir 2, Qurat ul Ain 2, Anca
Transanal Hemorrhoid Dearterialization and mucopexy: a minimal invasive approach for prolapsed hemorrhoids. Four cases report. Stefan Morarasu*,1, Emmanuel Eguare 2, Yasir Bashir 2, Qurat ul Ain 2, Anca
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of haemorrhoidal artery ligation Haemorrhoids (also known as piles) are enlarged
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of haemorrhoidal artery ligation Haemorrhoids (also known as piles) are enlarged
Hemorrhoids Dearterialization Doppler. Keywords Laser
 DOI 10.1007/s00464-010-1370-x Doppler-guided hemorrhoidal laser procedure for the treatment of symptomatic hemorrhoids: experimental background and short-term clinical results of a new mini-invasive treatment
DOI 10.1007/s00464-010-1370-x Doppler-guided hemorrhoidal laser procedure for the treatment of symptomatic hemorrhoids: experimental background and short-term clinical results of a new mini-invasive treatment
Perianal Abscess and Fistula-in-ano. Background
 Perianal Abscess and Fistula-in-ano Background Anorectal abscesses are some of the more common anorectal conditions encountered, and they are potentially debilitating conditions. The current theory as
Perianal Abscess and Fistula-in-ano Background Anorectal abscesses are some of the more common anorectal conditions encountered, and they are potentially debilitating conditions. The current theory as
DG-RAR for the treatment of symptomatic grade III and grade IV haemorrhoids: a 12-month multi-centre, prospective observational study
 Eur Surg DOI 10.1007/s10353-012-0182-8 DG-RAR for the treatment of symptomatic grade III and grade IV haemorrhoids: a 12-month multi-centre, prospective observational study S. Roka, D. Gold, P. Walega,
Eur Surg DOI 10.1007/s10353-012-0182-8 DG-RAR for the treatment of symptomatic grade III and grade IV haemorrhoids: a 12-month multi-centre, prospective observational study S. Roka, D. Gold, P. Walega,
Peter C. Ambe 1,2* and Dirk R. Wassenberg 2
 Ambe and Wassenberg Patient Safety in Surgery (2015) 9:36 DOI 10.1186/s13037-015-0081-6 RESEARCH Proctitis after stapled hemorrhoidopexy is an underestimated complication of a widely used surgical procedure:
Ambe and Wassenberg Patient Safety in Surgery (2015) 9:36 DOI 10.1186/s13037-015-0081-6 RESEARCH Proctitis after stapled hemorrhoidopexy is an underestimated complication of a widely used surgical procedure:
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
WHAT ARE HEMORRHOIDS?
 Patient information regarding care and surgery associated with HEMORRHOIDS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia Stefanou, M.D. location: Michigan Heart & Vascular Institute, 5325
Patient information regarding care and surgery associated with HEMORRHOIDS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia Stefanou, M.D. location: Michigan Heart & Vascular Institute, 5325
Evidence of Crohn s Disease. Case Presentation
 Witt Wait to Treat tutiled Until Endoscopic Evidence of Crohn s Disease Raymond Cross, MD, MS, AGAF Associate Professor of Medicine Director, IBD Program University of Maryland School of Medicine Co-Director,
Witt Wait to Treat tutiled Until Endoscopic Evidence of Crohn s Disease Raymond Cross, MD, MS, AGAF Associate Professor of Medicine Director, IBD Program University of Maryland School of Medicine Co-Director,
The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence. Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center
 The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center Constipation Overview Constipation Normal Transit Constipation
The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center Constipation Overview Constipation Normal Transit Constipation
VAGINAL MESH FAQ. How do you decide who should get mesh as part of their repair?
 VAGINAL MESH FAQ How do you decide who should get mesh as part of their repair? Each patient with pelvic organ prolapse (POP) is considered individually. In younger women, women with an uncomplicated prolapse
VAGINAL MESH FAQ How do you decide who should get mesh as part of their repair? Each patient with pelvic organ prolapse (POP) is considered individually. In younger women, women with an uncomplicated prolapse
Prevention and Recognition of Obstetric Fistula Training Package. Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula
 Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Colocutaneous Fistula. Disclosures
 Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Colocutaneous Fistula Madhulika G. Varma MD Associate Professor Chief, Colorectal Surgery University of California, San Francisco Honoraria Applied Medical Covidien Disclosures 1 Colocutaneous Fistula
Anal Surgery. Colon and Rectal Surgery. Surgery of the Anus. Hemorrhoids Fistula Fissure Abscess
 Anal Surgery and Colon and Rectal Surgery Elizabeth J. McConnell MD FACS FASCRS Surgery of the Anus Hemorrhoids Fistula Fissure Abscess 1 Hemorrhoid Internal or External 1-3 columns Internal Band or Suture
Anal Surgery and Colon and Rectal Surgery Elizabeth J. McConnell MD FACS FASCRS Surgery of the Anus Hemorrhoids Fistula Fissure Abscess 1 Hemorrhoid Internal or External 1-3 columns Internal Band or Suture
Hemorrhoidectomy with LigaSure Small Jaw and Stapled Hemorrhoidopexy with EEA Hemorrhoid and Prolapse Stapler with DST
 Hemorrhoidectomy with LigaSure Small Jaw and Stapled Hemorrhoidopexy with EEA Hemorrhoid and Prolapse Stapler with DST Dr. Wong Kutt Sing MBBS (S pore), FRCS (Edin), FRCS (Glas), FAMS General Surgery Raffles
Hemorrhoidectomy with LigaSure Small Jaw and Stapled Hemorrhoidopexy with EEA Hemorrhoid and Prolapse Stapler with DST Dr. Wong Kutt Sing MBBS (S pore), FRCS (Edin), FRCS (Glas), FAMS General Surgery Raffles
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions
 Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Diagnosis and treatment of haemorrhoids
 CLINICAL GUIDELINES DANISH MEDICAL JOURNAL Diagnosis and treatment of haemorrhoids Steen Buntzen, Peter Christensen, Ali Khalid, Ken Ljungmann, Jan Lindholt, Lilli Lundby, Line Rossell Walker, Dennis Raahave
CLINICAL GUIDELINES DANISH MEDICAL JOURNAL Diagnosis and treatment of haemorrhoids Steen Buntzen, Peter Christensen, Ali Khalid, Ken Ljungmann, Jan Lindholt, Lilli Lundby, Line Rossell Walker, Dennis Raahave
ESD for colorectal lesions I am in favour. Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy
 ESD for colorectal lesions I am in favour Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Surgery for early colonic lesions 51 pts referred for lap colectomy
ESD for colorectal lesions I am in favour Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Surgery for early colonic lesions 51 pts referred for lap colectomy
Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606
 October 5, 2010 Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606 Dear Dr. Rosenberg, The American Gastroenterological
October 5, 2010 Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606 Dear Dr. Rosenberg, The American Gastroenterological
Transanal Radiofrequency Treatment of Fecal Incontinence
 Transanal Radiofrequency Treatment of Fecal Incontinence Policy Number: 2.01.58 Last Review: 12/2015 Origination: 1/2012 Next Review: 1/2016 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will
Transanal Radiofrequency Treatment of Fecal Incontinence Policy Number: 2.01.58 Last Review: 12/2015 Origination: 1/2012 Next Review: 1/2016 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will
Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients
 Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients What are Haemorrhoids? Haemorrhoids (piles) are enlarged blood vessels around the anus (back passage). There are two types of haemorrhoids:
Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients What are Haemorrhoids? Haemorrhoids (piles) are enlarged blood vessels around the anus (back passage). There are two types of haemorrhoids:
PREPARING FOR YOUR STOMA REVERSAL
 PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
Laparoscopic Repair of Incisional Hernia. Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds
 Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
NHS. Surgical repair of vaginal wall prolapse using mesh. National Institute for Health and Clinical Excellence. 1 Guidance.
 Issue date: June 2008 NHS National Institute for Health and Clinical Excellence Surgical repair of vaginal wall prolapse using mesh 1 Guidance 1.1 The evidence suggests that surgical repair of vaginal
Issue date: June 2008 NHS National Institute for Health and Clinical Excellence Surgical repair of vaginal wall prolapse using mesh 1 Guidance 1.1 The evidence suggests that surgical repair of vaginal
FAQ About Prostate Cancer Treatment and SpaceOAR System
 FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
Anorectal Abscess and Fistula
 Anorectal Abscess/Fistula by: Robert K Cleary MD, John C Eggenberger MD, Amalia J Stefanou, MD location: Michigan Heart & Vascular Institute, 5325 Elliott Dr, Suite 104 mailing address: PO Box 974, Ann
Anorectal Abscess/Fistula by: Robert K Cleary MD, John C Eggenberger MD, Amalia J Stefanou, MD location: Michigan Heart & Vascular Institute, 5325 Elliott Dr, Suite 104 mailing address: PO Box 974, Ann
Treatment of Fistula in Ano. Johanna Basa M.D. SUNY Downstate Medical Center August 2, 2012
 Treatment of Fistula in Ano Johanna Basa M.D. SUNY Downstate Medical Center August 2, 2012 Case Presentation HPI:54 yr old male with PMH of HTN, presented to clinic with complaints of 3rd perianal abscess
Treatment of Fistula in Ano Johanna Basa M.D. SUNY Downstate Medical Center August 2, 2012 Case Presentation HPI:54 yr old male with PMH of HTN, presented to clinic with complaints of 3rd perianal abscess
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Direct Current Therapy for Treatment of Hemorrhoids
 Direct Current Therapy for Treatment of Hemorrhoids [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr Go to Comunicados a Proveedores, and click Cartas
Direct Current Therapy for Treatment of Hemorrhoids [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr Go to Comunicados a Proveedores, and click Cartas
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Bowel Preparation for Colon Resection. Eric Klein, M.D. SUNY Downstate Department of Surgery
 Bowel Preparation for Colon Resection Eric Klein, M.D. SUNY Downstate Department of Surgery Historical Perspective During World War II, failure to treat penetrating colon injuries with diversion could
Bowel Preparation for Colon Resection Eric Klein, M.D. SUNY Downstate Department of Surgery Historical Perspective During World War II, failure to treat penetrating colon injuries with diversion could
Understanding Laparoscopic Colorectal Surgery
 Understanding Laparoscopic Colorectal Surgery University Colon & Rectal Surgery A Problem with Your Colon Your doctor has told you that you have a colon problem. Now you ve learned that surgery is needed
Understanding Laparoscopic Colorectal Surgery University Colon & Rectal Surgery A Problem with Your Colon Your doctor has told you that you have a colon problem. Now you ve learned that surgery is needed
Is co2 laser Hemorrhoidectomy superior to conventional open Hemorrhoidectomy?
 Is co2 laser Hemorrhoidectomy superior to conventional open Hemorrhoidectomy? *Sa`ad H Sultan M.B.Ch.B,D.S,CABS **Zuhair B Kamal M.B.Ch.B,CABS ***Mohammad A Al-Atroshi M.B.Ch.B,CABS ****Raysan Al-Fayadh
Is co2 laser Hemorrhoidectomy superior to conventional open Hemorrhoidectomy? *Sa`ad H Sultan M.B.Ch.B,D.S,CABS **Zuhair B Kamal M.B.Ch.B,CABS ***Mohammad A Al-Atroshi M.B.Ch.B,CABS ****Raysan Al-Fayadh
Bridging Techniques. What s between EMR and Traditional Surgery? Elisabeth C. McLemore, MD, FACS, FASCRS
 Bridging Techniques What s between EMR and Traditional Surgery? Elisabeth C. McLemore, MD, FACS, FASCRS Associate Professor of Surgery Assistant Program Director, General Surgery Residency Disclosures
Bridging Techniques What s between EMR and Traditional Surgery? Elisabeth C. McLemore, MD, FACS, FASCRS Associate Professor of Surgery Assistant Program Director, General Surgery Residency Disclosures
POEM Procedure for. Esophageal Achalasia
 POEM Procedure for Esophageal Achalasia POEM (Per-Oral endoscopic myotomy) is an incisionless procedure to treat esophageal achalasia, totally performed by endoscopy, without cutting the surface of the
POEM Procedure for Esophageal Achalasia POEM (Per-Oral endoscopic myotomy) is an incisionless procedure to treat esophageal achalasia, totally performed by endoscopy, without cutting the surface of the
The Smooth Tuck Procedure
 The Smooth Tuck Procedure plastic surgery AN ALTERNATIVE APPROACH TO ABDOMINAL CONTOURING FOR THE OVERWEIGHT PATIENT atnt By Matthew R. Schulman, M.D. Body fat on an adult tends to increase gradually over
The Smooth Tuck Procedure plastic surgery AN ALTERNATIVE APPROACH TO ABDOMINAL CONTOURING FOR THE OVERWEIGHT PATIENT atnt By Matthew R. Schulman, M.D. Body fat on an adult tends to increase gradually over
Patient. Frequently Asked Questions. Transvaginal Surgical Mesh for Pelvic Organ Prolapse
 Patient Frequently Asked Questions Transvaginal Surgical Mesh for Pelvic Organ Prolapse Frequently Asked Questions WHAT IS PELVIC ORGAN PROLAPSE AND HOW IS IT TREATED? Q: What is pelvic organ prolapse
Patient Frequently Asked Questions Transvaginal Surgical Mesh for Pelvic Organ Prolapse Frequently Asked Questions WHAT IS PELVIC ORGAN PROLAPSE AND HOW IS IT TREATED? Q: What is pelvic organ prolapse
HAVING AN ENDOSCOPIC MUCOSAL RESECTION (EMR)
 HAVING AN ENDOSCOPIC MUCOSAL RESECTION (EMR) Information Leaflet Your Health. Our Priority. Page 2 of 6 Having an EMR Previous tests have shown that you have a polyp in your large bowel (colon). Your doctor
HAVING AN ENDOSCOPIC MUCOSAL RESECTION (EMR) Information Leaflet Your Health. Our Priority. Page 2 of 6 Having an EMR Previous tests have shown that you have a polyp in your large bowel (colon). Your doctor
ARTHROSCOPIC HIP SURGERY
 ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
ARTHROSCOPIC HIP SURGERY Hip Arthroscopy is a relatively simple procedure whereby common disorders of the hip can be diagnosed and treated using keyhole surgery. Some conditions, which previously were
Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence (Adapted from the
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Minimally invasive techniques for the relief of stress urinary incontinence (Adapted from the
Minimally Invasive Mitral Valve Surgery
 Minimally Invasive Mitral Valve Surgery Stanford Health Care offers leading, superior options in cardiac surgery, including the latest techniques and research for Minimally Invasive Cardiac surgery. Advanced
Minimally Invasive Mitral Valve Surgery Stanford Health Care offers leading, superior options in cardiac surgery, including the latest techniques and research for Minimally Invasive Cardiac surgery. Advanced
Women s Health. The TVT procedure. Information for patients
 Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
INFORMATION FOR PATIENTS CONSIDERING LAPAROSCOPIC INGUINAL HERNIA REPAIR
 INFORMATION FOR PATIENTS CONSIDERING A LAPAROSCOPIC INGUINAL HERNIA REPAIR Prepared By Mr Peter Willson Consultant Surgeon Contents 1. Background... 3 2. What is an inguinal Hernia?... 3 3. What are the
INFORMATION FOR PATIENTS CONSIDERING A LAPAROSCOPIC INGUINAL HERNIA REPAIR Prepared By Mr Peter Willson Consultant Surgeon Contents 1. Background... 3 2. What is an inguinal Hernia?... 3 3. What are the
Considering a Hysterectomy?
 Considering a Hysterectomy? Learn more about virtually scarless surgery using da Vinci Single-Site technology { {Symptoms & Conditions: Chronic Pain, Heavy Bleeding, Fibroids, Endometriosis, Adenomyosis,
Considering a Hysterectomy? Learn more about virtually scarless surgery using da Vinci Single-Site technology { {Symptoms & Conditions: Chronic Pain, Heavy Bleeding, Fibroids, Endometriosis, Adenomyosis,
Navigating Anorectal Anatomy: Terms, Planes, Spaces, Structures
 Navigating Anorectal Anatomy: Terms, Planes, Spaces, Structures Lawrence M. Witmer, PhD Lawrence M. Witmer, PhD Department of Biomedical Sciences College of Osteopathic Medicine Ohio University Athens,
Navigating Anorectal Anatomy: Terms, Planes, Spaces, Structures Lawrence M. Witmer, PhD Lawrence M. Witmer, PhD Department of Biomedical Sciences College of Osteopathic Medicine Ohio University Athens,
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK)
 Lasik Center 2445 Broadway Quincy, IL 62301 217-222-8800 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information is being provided to you so that you can make an informed
Lasik Center 2445 Broadway Quincy, IL 62301 217-222-8800 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information is being provided to you so that you can make an informed
Guide to Abdominal or Gastroenterological Surgery Claims
 What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
Laparoscopic Repair of Hernias. A simple guide to help answer your questions
 Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Medicare C/D Medical Coverage Policy
 Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: September 16, 2015 Next Review: September, 2017 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Varicose Vein Treatment Medicare C/D Medical Coverage Policy Origination Date: June 1, 1993 Review Date: September 16, 2015 Next Review: September, 2017 DESCRIPTION OF PROCEDURE OR SERVICE Varicose veins
Having an Endoscopic Mucosal Resection (EMR)
 Having an Endoscopic Mucosal Resection (EMR) Patient Information Author ID: N Prasad Leaflet Number: End 011 Name of Leaflet: Having an Endoscopic Mucosal Resection (EMR) Date Produced: March 2014 Review
Having an Endoscopic Mucosal Resection (EMR) Patient Information Author ID: N Prasad Leaflet Number: End 011 Name of Leaflet: Having an Endoscopic Mucosal Resection (EMR) Date Produced: March 2014 Review
Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery
 Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
Surgery for Stress Incontinence
 Directorate of Women s Services Surgery for Stress Incontinence Tension Free Vaginal Tape Information for Patients Direct dial number Ward 40 0191 282 5640 Stress Incontinence Stress incontinence is a
Directorate of Women s Services Surgery for Stress Incontinence Tension Free Vaginal Tape Information for Patients Direct dial number Ward 40 0191 282 5640 Stress Incontinence Stress incontinence is a
C A R O L I N A S. Hernia Handbook ( C H A P T E R 2 ) B. Todd Heniford, MD
 C A R O L I N A S Hernia Handbook ( C H A P T E R 2 ) B. Todd Heniford, MD C H A P T E R 2 Umbilical Hernias C A R O L I N A S H E R N I A H A N D B O O K 17 Umbilical Hernias W H AT I S A N U M B I L
C A R O L I N A S Hernia Handbook ( C H A P T E R 2 ) B. Todd Heniford, MD C H A P T E R 2 Umbilical Hernias C A R O L I N A S H E R N I A H A N D B O O K 17 Umbilical Hernias W H AT I S A N U M B I L
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
X-Plain Varicose Veins Reference Summary
 X-Plain Varicose Veins Reference Summary Introduction Varicose veins are very common, in both women and men. Varicose veins can be painful and unattractive. Vein doctors use non-invasive ultrasound imaging
X-Plain Varicose Veins Reference Summary Introduction Varicose veins are very common, in both women and men. Varicose veins can be painful and unattractive. Vein doctors use non-invasive ultrasound imaging
Epi procolon The Blood Test for Colorectal Cancer Screening
 Epi procolon The Blood Test for Colorectal Cancer Screening Epi procolon is an approved blood test for colorectal cancer screening. The US Preventive Services Task Force, the American Cancer Society and
Epi procolon The Blood Test for Colorectal Cancer Screening Epi procolon is an approved blood test for colorectal cancer screening. The US Preventive Services Task Force, the American Cancer Society and
Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery
 Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Pancreatitis/Pancreatic Cancer The pancreas is an organ that produces enzymes and hormones to help your body digest
Facing Pancreatic Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Pancreatitis/Pancreatic Cancer The pancreas is an organ that produces enzymes and hormones to help your body digest
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
ALTERNATIVES TO LASIK
 EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
EYE PHYSICIANS OF NORTH HOUSTON 845 FM 1960 WEST, SUITE 101, Houston, TX 77090 Office: 281 893 1760 Fax: 281 893 4037 INFORMED CONSENT FOR LASER IN-SITU KERATOMILEUSIS (LASIK) INTRODUCTION This information
Hand-sewn Bowel Anastomosis: The Only Correct Choice. Ashok Babu, M.D. Department of Surgery University of Colorado
 Hand-sewn Bowel Anastomosis: The Only Correct Choice Ashok Babu, M.D. Department of Surgery University of Colorado Outline History Trial data in specific applications Colorectal Ileocolic Esophagogastric
Hand-sewn Bowel Anastomosis: The Only Correct Choice Ashok Babu, M.D. Department of Surgery University of Colorado Outline History Trial data in specific applications Colorectal Ileocolic Esophagogastric
The enigma of the transsphincteric anal fistula. Per-Olof Nyström, M.D., Ph.D. Karolinska University Hospital, Stockholm, Sweden
 The enigma of the transsphincteric anal fistula Per-Olof Nyström, M.D., Ph.D. Karolinska University Hospital, Stockholm, Sweden Four principles of treatment for anal fistula 1. Inactivate the fistula 2.
The enigma of the transsphincteric anal fistula Per-Olof Nyström, M.D., Ph.D. Karolinska University Hospital, Stockholm, Sweden Four principles of treatment for anal fistula 1. Inactivate the fistula 2.
UROLOGY GROUP of PRINCETON
 UROLOGY GROUP of PRINCETON 134 STANHOPE STREET, PRINCETON, NJ 08540 PHONE 609-924-6487 FAX 609-921-7020 BARRY ROSSMAN, M.D. ALEX VUKASIN, M.D. KAREN LATZKO, D.O. ALEXEI WEDMID, M.D. VASECTOMY, THE NO SCALPEL
UROLOGY GROUP of PRINCETON 134 STANHOPE STREET, PRINCETON, NJ 08540 PHONE 609-924-6487 FAX 609-921-7020 BARRY ROSSMAN, M.D. ALEX VUKASIN, M.D. KAREN LATZKO, D.O. ALEXEI WEDMID, M.D. VASECTOMY, THE NO SCALPEL
(Anorectum Anorectum)
 Surgical anatomy (Anorectum Anorectum) Surgery of the anorectum and the perianal region in small animals Dr. T. Németh, DVM, PhD Associate Professor Surgical anatomy (Anorectum Anorectum) Surgical anatomy
Surgical anatomy (Anorectum Anorectum) Surgery of the anorectum and the perianal region in small animals Dr. T. Németh, DVM, PhD Associate Professor Surgical anatomy (Anorectum Anorectum) Surgical anatomy
Patient information regarding care and surgery associated with ULCERATIVE COLITIS
 Patient information regarding care and surgery associated with ULCERATIVE COLITIS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou, M.D. location: Michigan Heart & Vascular Institute,
Patient information regarding care and surgery associated with ULCERATIVE COLITIS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou, M.D. location: Michigan Heart & Vascular Institute,
Spine University s Guide to Cauda Equina Syndrome
 Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Non-surgical treatment of severe varicose veins
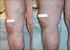 Non-surgical treatment of severe varicose veins Yasu Harasaki UCHSC Department of Surgery General Surgery Grand Rounds March 19, 2007 Definition Dilated, palpable, subcutaneous veins generally >3mm in
Non-surgical treatment of severe varicose veins Yasu Harasaki UCHSC Department of Surgery General Surgery Grand Rounds March 19, 2007 Definition Dilated, palpable, subcutaneous veins generally >3mm in
Prospective, Randomized Controlled Trial of Starion TM
 WANG./Dis Colon Rectum Page 1 Prospective, Randomized Controlled Trial of Starion TM versus Ligasure TM Hemorrhoidectomy for Prolapsed Hemorrhoids Jaw-Yuan Wang, M.D.,*, Hsiang-Lin Tsai M.D.,*, Fang-Ming
WANG./Dis Colon Rectum Page 1 Prospective, Randomized Controlled Trial of Starion TM versus Ligasure TM Hemorrhoidectomy for Prolapsed Hemorrhoids Jaw-Yuan Wang, M.D.,*, Hsiang-Lin Tsai M.D.,*, Fang-Ming
Laser Procedure Note
 Laser Procedure Note Patient Name Date 1. Pre procedure diagnosis 2. Procedure and Eye Eye: 3. Pre procedure topical medications administered (and time) 4. Vital signs BP / HR Acuity OD: OS: 5. IOP: OD
Laser Procedure Note Patient Name Date 1. Pre procedure diagnosis 2. Procedure and Eye Eye: 3. Pre procedure topical medications administered (and time) 4. Vital signs BP / HR Acuity OD: OS: 5. IOP: OD
CHOC CHILDREN SUROLOGY CENTER. Constipation
 Constipation What is constipation? Constipation is a condition in which a person has uncomfortable or infrequent bowel movements. Generally, a person is considered to be constipated when bowel movements
Constipation What is constipation? Constipation is a condition in which a person has uncomfortable or infrequent bowel movements. Generally, a person is considered to be constipated when bowel movements
Venous Reflux Disease and Current Treatments VN20-87-A 01/06
 Venous Reflux Disease and Current Treatments Leg Vein Anatomy Your legs are made up of a network of veins and vessels that carry blood back to the heart The venous system is comprised of: Deep veins Veins
Venous Reflux Disease and Current Treatments Leg Vein Anatomy Your legs are made up of a network of veins and vessels that carry blood back to the heart The venous system is comprised of: Deep veins Veins
Considering Endometriosis Surgery? Learn about minimally invasive da Vinci Surgery
 Considering Endometriosis Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Endometriosis Endometriosis is a condition in which the tissue that lines your uterus (the endometrium)
Considering Endometriosis Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Endometriosis Endometriosis is a condition in which the tissue that lines your uterus (the endometrium)
Study Design Of Medical Research
 Study Design Of Medical Research By Ahmed A.Shokeir, MD,PHD, FEBU Prof. Urology, Urology & Nephrology Center, Mansoura, Egypt Study Designs In Medical Research Topics Classification Case series studies
Study Design Of Medical Research By Ahmed A.Shokeir, MD,PHD, FEBU Prof. Urology, Urology & Nephrology Center, Mansoura, Egypt Study Designs In Medical Research Topics Classification Case series studies
Get the Facts, Be Informed, Make YOUR Best Decision. Pelvic Organ Prolapse
 Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
How To Perform Da Vinci Surgery
 Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
Hysterectomy. What is a hysterectomy? Why is hysterectomy done? Are there alternatives to hysterectomy?
 ROBERT LEVITT, MD JESSICA BERGER-WEISS, MD ADRIENNE POTTS, MD HARTAJ POWELL, MD, MPH COURTNEY LEVENSON, MD LAUREN BURNS, MSN, RN, WHNP OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is
ROBERT LEVITT, MD JESSICA BERGER-WEISS, MD ADRIENNE POTTS, MD HARTAJ POWELL, MD, MPH COURTNEY LEVENSON, MD LAUREN BURNS, MSN, RN, WHNP OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is
CONSENT FORM. Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK)
 CONSENT FORM Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) Surgeon: Jeffrey W. Liu, M.D. Peninsula Laser Eye Medical Group 1174 Castro Street, Ste. 100 Mountain View, CA 94040
CONSENT FORM Procedure: Descemet s Stripping Automated Endothelial Keratoplasty (DSAEK) Surgeon: Jeffrey W. Liu, M.D. Peninsula Laser Eye Medical Group 1174 Castro Street, Ste. 100 Mountain View, CA 94040
Considering a Hysterectomy?
 Considering a Hysterectomy? Learn more about virtually scarless surgery using da Vinci Single-Site technology { {Symptoms & Conditions: Chronic Pain, Heavy Bleeding, Fibroids, Endometriosis, Pelvic Prolapse
Considering a Hysterectomy? Learn more about virtually scarless surgery using da Vinci Single-Site technology { {Symptoms & Conditions: Chronic Pain, Heavy Bleeding, Fibroids, Endometriosis, Pelvic Prolapse
UNDERSTANDING & CODING WITH MODIFIERS
 UNDERSTANDING & CODING WITH MODIFIERS -21 Prolonged Evaluation and Management When the service provided is prolonged or otherwise greater than that usually required for the highest level of service in
UNDERSTANDING & CODING WITH MODIFIERS -21 Prolonged Evaluation and Management When the service provided is prolonged or otherwise greater than that usually required for the highest level of service in
Information for Patients having a Colonic Stent Placement
 Information for Patients having a Colonic Stent Placement Information for Patients having a Colonic Stent Placement The Digestive System To understand the procedure you are about to have, it helps to have
Information for Patients having a Colonic Stent Placement Information for Patients having a Colonic Stent Placement The Digestive System To understand the procedure you are about to have, it helps to have
INFORMED CONSENT FOR SLEEVE GASTRECTOMY
 INFORMED CONSENT FOR SLEEVE GASTRECTOMY This informed-consent document has been prepared to help inform you about your Sleeve Gastrectomy including the risks and benefits, as well as alternative treatments.
INFORMED CONSENT FOR SLEEVE GASTRECTOMY This informed-consent document has been prepared to help inform you about your Sleeve Gastrectomy including the risks and benefits, as well as alternative treatments.
Are any artificial parts used in the ACE Malone surgery?
 ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D.
 Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D. Professor of Medicine Germanis Kaufman Chair of Gastroenterology Director, Dept. of Gastroenterology Chaim Sheba Medical Center,
Early Colonoscopy in Patients with Acute Diverticulitis Simon Bar-Meir, M.D. Professor of Medicine Germanis Kaufman Chair of Gastroenterology Director, Dept. of Gastroenterology Chaim Sheba Medical Center,
Summa Health System. A Woman s Guide to Hysterectomy
 Summa Health System A Woman s Guide to Hysterectomy Hysterectomy A hysterectomy is a surgical procedure to remove a woman s uterus (womb). The uterus is the organ which shelters and nourishes a baby during
Summa Health System A Woman s Guide to Hysterectomy Hysterectomy A hysterectomy is a surgical procedure to remove a woman s uterus (womb). The uterus is the organ which shelters and nourishes a baby during
Billing Guideline. Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16
 Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
Vaginal prolapse repair surgery with mesh
 Vaginal prolapse repair surgery with mesh Your doctor has recommended a vaginal reconstructive procedure using mesh to treat your condition. The operation involves surgery to reattach the vagina to its
Vaginal prolapse repair surgery with mesh Your doctor has recommended a vaginal reconstructive procedure using mesh to treat your condition. The operation involves surgery to reattach the vagina to its
INTERVENTIONAL PROCEDURES PROGRAMME
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of radical laparoscopic hysterectomy for early stage cervical cancer Introduction This overview
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of radical laparoscopic hysterectomy for early stage cervical cancer Introduction This overview
VARICOSE VEINS. Information Leaflet. Your Health. Our Priority. VTE Ambulatory Clinic Stepping Hill Hospital
 VARICOSE VEINS Information Leaflet Your Health. Our Priority. Page 2 of 7 Varicose Veins There are no accurate figures for the number of people with varicose veins. Some studies suggest that 3 in 100 people
VARICOSE VEINS Information Leaflet Your Health. Our Priority. Page 2 of 7 Varicose Veins There are no accurate figures for the number of people with varicose veins. Some studies suggest that 3 in 100 people
Tucson Eye Care, PC. Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens
 Tucson Eye Care, PC Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is provided so that you may make an informed decision about having eye
Tucson Eye Care, PC Informed Consent for Cataract Surgery And/Or Implantation of an Intraocular Lens INTRODUCTION This information is provided so that you may make an informed decision about having eye
Beaumont Hospital. Varicose Veins. and their TREATMENT. Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM
 Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
Open Ventral Hernia Repair
 Ventral Hernias Open Ventral Hernia Repair UCSF Postgraduate Course in General Surgery Maui, HI March 21, 2011 Hobart W. Harris, MD, MPH Ventral Hernias: National Experience Occur following 11-23% of laparotomies,
Ventral Hernias Open Ventral Hernia Repair UCSF Postgraduate Course in General Surgery Maui, HI March 21, 2011 Hobart W. Harris, MD, MPH Ventral Hernias: National Experience Occur following 11-23% of laparotomies,
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
Facing a Hernia Repair? Learn about minimally invasive da Vinci Surgery
 Facing a Hernia Repair? Learn about minimally invasive da Vinci Surgery The Condition: Hernia A hernia happens when part of an internal organ or tissue bulges through a hole or weak area in the belly wall
Facing a Hernia Repair? Learn about minimally invasive da Vinci Surgery The Condition: Hernia A hernia happens when part of an internal organ or tissue bulges through a hole or weak area in the belly wall
