Transanal Hemorrhoid Dearterialization and mucopexy: a minimal invasive approach for prolapsed hemorrhoids. Four cases report.
|
|
|
- Prosper Curtis
- 9 years ago
- Views:
Transcription
1 Transanal Hemorrhoid Dearterialization and mucopexy: a minimal invasive approach for prolapsed hemorrhoids. Four cases report. Stefan Morarasu*,1, Emmanuel Eguare 2, Yasir Bashir 2, Qurat ul Ain 2, Anca Bradu 1 1 Gr. T. Popa University of Medicine and Pharmacy, Iasi, Romania, 2 Allen Ward, Naas General Hospital, Naas, Co. Kildare, Ireland Abstract Hemorrhoidal disease is one of the most frequent causes of anal pathology. Surgical therapy is reserved for patients who do not respond to non-operative management and for advanced third and fourth degree hemorrhoids. Milligan-Morgan and Ferguson hemorrhoidectomies are considered the first-choice therapy, but these procedures are associated with postoperative complications including infection, stenosis, pelvic floor dysfunction, rectal bleeding and postoperative pain. In order to minimize postoperative complications, less invasive procedures have been described and two of them are reported with promising results: Stapled hemorrhoidopexy (PPH) and Transanal Hemorrhoid Dearterialization (THD). THD involves ligation of the hemorrhoidal arteries under Doppler guidance resulting reduced inflow that facilitates reduction in size of hemorrhoids, while suture mucopexy addresses the prolapsed mucosa. THD is proven as a reliable technique for third degree hemorrhoids, but its role in fourth degree hemorrhoids is not generally accepted. Herein we report four cases of prolapsed hemorrhoids which were treated with THD and mucopexy. The procedure was successful in all patients. Photographs taken, before and after the procedure, show an impressive reduction of the prolapsed hemorrhoids. THD and mucopexy appears to be an effective technique with the potential of treating not only third degree, but advanced hemorrhoids as a safe one-day procedure with immediate visible results. Keywords: THD, Transanal hemorrhoidal dearterialization, hemorrhoids, hemorrhoidectomy Introduction Hemorrhoids are cushions of submucosal tissue containing venules, arterioles and smooth-muscle fibers that are normally located in the anal canal and contribute toward maintaining fecal continence and the entire continence mechanism [1]. When hemorrhoids are associated with bleeding, pruritus, mucous discharge per rectum or prolapse, they are referred as symptomatic and in the presence Received: September 2015; Accepted after review: March 2016; Published: March *Corresponding author: Stefan Morarasu, MD, Gr. T. Popa University of Medicine and Pharmacy, Iasi, Romania. [email protected] of symptom associations they are referred to as hemorrhoidal disease [2-4]. Even though they are probably one of the most common causes of anal pathology, the true prevalence of hemorrhoids is difficult to establish, because many patients don t seek medical care. Increased abdominal pressure (obesity, pregnancy), constipation and prolonged straining are believed to be the main causes for prolapse of hemorrhoidal tissue [5]. There are mainly three therapy choices for hemorrhoidal disease: (1) medical management and diet, (2) office-based procedures and (3) surgical therapy [6]. Symptomatic first and second degree hemorrhoids are best managed with diet and decrease in straining (high-fiber diet, regular exercise, stool softeners) and with medical 10 Arch Clin Cases 2016; 3(1):10-17
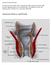
2 therapy (topical ointments, creams, suppositories) [7, 8]. Office-based procedures (rubber band ligation, sclerotherapy, infrared photocoagulation, and cryotherapy) are a suitable tool for persistent first and second degree hemorrhoids and for selected third degree cases [1, 2, 8, 9]. Surgical therapy is reserved for patients who fail non-operative management techniques and for advanced prolapsed third and fourth degree hemorrhoids [10, 11]. Transanal Hemorrhoid Dearterialization (THD) and mucopexy is the newest addition to a surgeon s repertoire. It was first described by Morinaga et al. [12] and since then the technique and the operative equipment have been improved. THD procedure involves ligation of the hemorrhoidal arteries under Doppler guidance resulting in reduced inflow that facilitates reduction in size of hemorrhoids, while suture mucopexy addresses the prolapsed mucosa [4]. Kjaer et al. [13] reported a low success rate (64%) after a median follow-up periods of nine months in patients with three and fourth degree hemorrhoids who underwent THD and mucopexy, while other authors described THD as a safe one-day procedure for patients with hemorrhoids [14 16]. Herein we report four cases of advanced prolapsed hemorrhoids, which were treated with THD and mucopexy. We emphasize that THD is an effective procedure with minimal postoperative pain and early return to normal activity. Cases report Four patients (three male, one female) diagnosed with 4 th degree hemorrhoids underwent operative management using THD and mucopexy procedure at Naas General Hospital, Naas, Co. Kildare, Ireland. Main complaints were pruritus ani and long standing rectal bleeding. These patients underwent colonoscopy as part of their pre-operative work-up. Preoperatively phosphate enema was prescribed and Digital Rectal Examination was performed to assess any other concomitant anal or/and rectal pathologies. Procedures were performed under general anesthesia and patients were placed into lithotomy position. THD device consists of an anoscope equipped on the superior surface with a Doppler sensor and a light source. After digital examination with lubricant, the anoscope was inserted with the Doppler sensor placed at different clock positions (1, 3, 5, 7, 9, 11) (Figure1) and at each position the Doppler value was noted in order to localize the hemorrhoidal arteries. Once identified, all six arteries were ligated with a 2-0 absorbable suture (Figures 2 and 3). The suturing equipment is also specially designed: the needle holder is longer and has a marked line at the tip where the needle should be placed; the needle is 5/8 of a circle, so that it perfectly fits in the suturing groove. When the artery was identified, the needle holder was inserted inside the anoscope with the tip placed into groove at the end of the inside surface of the anoscope and with circular motions of the needle-holder an 8-figure suture was placed to ligate each artery. All arteries were ligated. Fig. 1. Anoscope inserted at 1 o clock in order to assess Doppler signal from the artery. Fig. 2. Hemorrhoidal artery ligated at 1 o clock position Arch Clin Cases 2016; 3(1):10-17
3 THD procedure ligates the arteries and decreases the arterial blood flow. In order to lift the prolapsed mucosa, mucopexy was necessary. With the anoscope inserted, using the technique described above, multiple running sutures were placed above the dentate line, in order to avoid the anoderm and tied at the proximal end of the hemorrhoid (Figure 4). Fig. 3. Hemorrhoidal artery ligated at 5 o clock position. Fig. 4. THD and mucopexy illustration. The hemorrhoidal artery is ligated with an 8 figure suture and multiple running sutures are used to lift the prolapsed mucosa (left of the image). Notice that all sutures are placed above the dentate line. Once the final knot is tied between the distal and the proximal end, the mucosa is shrunk and fixed, thus the mucopexy is done, as seen on the right of the image. Anal packing was done using a cylindrical sponge soaked in anesthetic and antiseptic gel (Figure 5). Fig. 5. Anal packing with cylindrical sponge soaked in anesthetic and antiseptic gel. The mean operative time was approx. 45 min. The procedure was successful in all patients without any intra-operative and postoperative complications. Photographs taken, before and after the procedure, show an impressive reduction of the prolapsed hemorrhoids (Figures 6-13). On ward follow-up patients did not have major symptomatic complaints, except mild nausea, presumably anesthetic related. All patients were discharged in the same day and were prescribed Lactulose 15mg/twice daily, Flagyl (metronidazole) 400mg/three times daily, Acetaminophen 1g/three times daily and Difene (diclofenac) 50mg/twice daily (each for 5 days) Arch Clin Cases 2016; 3(1):10-17
4 Patients were referred back to their general practitioners and were scheduled in the outpatient department for reassessment. Fig. 6. Patient 1 with prolapsed fourth degree hemorrhoids before the procedure. Fig. 7. Patient 1 after the procedure. Prolapsed mucosa is effectively reduced. Fig. 8. Patient 2 with fourth degree hemorrhoids before the procedure. Fig. 9. Patient 2 after the procedure. Hemorrhoids are reduced. Fig. 10. Patient 3 with advanced fourth degree hemorrhoids before the procedure. Notice the severe mucosal prolapse. Fig. 11. Patient 3 after the procedure. Prolapsed mucosa is significantly reduced Arch Clin Cases 2016; 3(1):10-17
5 Fig. 12. Patient 4 with fourth degree hemorrhoids before the procedure. Fig. 13. Patient 4 after the procedure. Hemorrhoidal tissue is effectively reduced. Discussions The purpose of this article is to prove the effectiveness of THD in reducing 4 th degree prolapsed hemorrhoids as a safe one-day procedure with minimal-to-none pain and other early, hemorrhoidectomy associated, postoperative symptoms. While the results presented herein prove better outcomes for THD in the first 24 h post-op, further research is needed to assess the feasibility of this procedure in the long-run. In this case report, there is no data regarding long-term follow up, therefore it is early and beyond this article s reach to say that THD has superior long-term outcomes when compared to other surgical alternatives for 4 th degree hemorrhoids. For patients with second and third degree hemorrhoids, Giordano et al. [17] thoroughly evaluated, in a prospective study, the three years outcomes of THD in comparison with stapled hemorrhoidopexy and their results show higher patient satisfaction rates and promising complication rates for THD. Milligan-Morgan (open) and Ferguson (closed) hemorrhoidectomy techniques are still considered the gold-standard for the operative management of advanced hemorrhoids [4]. However, these procedures are associated with postoperative complications including infection, ano-rectal stenosis, incontinence, urinary retention, severe rectal bleeding and postoperative pain [4, 6, 18]. Firstly described by Milligan and Morgan in 1937 [19], the open hemorrhoidectomy involves a full-thickness excision of the affected mucosa and submucosa: the hemorrhoid is grasped using a forceps and an ellipsoidal incision is made at its base; scissors are used to dissect the remaining hemorrhoid. At the end of the procedure the wound is left open, hence the name open hemorrhoidectomy. If the mucosa is closed with an absorbable running suture, the procedure is named Ferguson s closed hemorrhoidectomy [10] (Figure 14). Fig. 14. Ferguson s closed hemorrhoidectomy. The hemorrhoid is grasped using a forceps and incised at its base (right). After the entire hemorrhoid is dissected, the mucosa is closed using an absorbable running suture (left). Note that the incision is made in the anoderm bellow the dentate line, where the skin is highly sensitive to pain Arch Clin Cases 2016; 3(1):10-17
6 In order to minimize complications and postoperative pain, several less invasive procedures have been described and two of them are reported with promising results: PPH/stapled hemorrhoidopexy and Transanal Hemorrhoid Dearterialization (THD)/Doplerguided hemorrhoidal artery ligation (DGHAL). In the past years, stapled hemorrhoidopexy became less popular even though early postoperative pain is not as severe as after hemorrhoidectomy [20]. Various studies have shown that PPH is associated with a greater recurrence rate [21], higher stenosis rate [15] when compared with the standard hemorrhoidectomy and it is related with other unusual complications (chronic proctalgia, bleeding granulomatous polyps due to retained staples, rectovaginal fistulae etc.) which are not described after Ferguson or Milligan-Morgan approach [18]. Associated with mucopexy, THD appears to be an effective technique for the management of advanced fourth degree hemorrhoids and offers immediate results as seen in the cases presented above. It is a relatively new procedure developed as an alternative to excisional hemorrhoidectomy and it is increasingly being embraced by surgeons for its better outcomes, higher patient satisfaction and fewer postoperative complications [23 26]. For II and III degree hemorrhoids, THD is a widely accepted therapeutic choice, but there is little information of the results of THD for grade IV hemorrhoids [14]. Table. 1. Comparison between open and closed hemorrhoidectomies and THD. THD is associated with a significant shorter hospital stay. Open Hemorrhoidectomy [27] Closed hemorrhoidectomy [27] THD and mucopexy Mean operative time approx. 25 min. approx. 31 min. approx. 45 min. Hospital days 3-5 days 2-4 days one-day case Milligan-Morgan (open)/ferguson (closed) hemorrhoidectomy techniques withstood over the years because of their efficacy, but the notorious postoperative pain pushed researchers in developing less invasive treatments. THD is a non-excisional operative technique that spares the anoderm; therefore it is associated with less postoperative pain when compared to the excisional approaches. Popo et al. [28] published a comparison between THD and two excisional procedures: Milligan-Morgan and Whitehead hemorrhoidectomy; they found that THD is linked with shorter hospital stay, less discomfort in postoperative period and an excellent aesthetic effect. Another famous less invasive treatment for hemorrhoidal disease that offers superior results to the classic procedures is stapled hemorrhoidopexy (PPH). Several studies comparing THD and PPH [29, 30] described that both procedures seem an effective and safe treatment for hemorrhoids, but THD seems to be superior when it comes to pain score and return to normal daily activities. Verre et al. [31] report better results in terms of pain and postoperative complications after THD surgery, while Lucarelli et al. [32] describe a higher recurrence rate after THD and similar long-term follow-up results regarding symptom control and patient satisfaction. The approach and equipment used in the cases presented above are relatively new, being described by Ratto in 2014 [33]. Conclusions Since its first report, the THD procedure has been constantly modified and improved. THD is a promising minimal invasive technique and it offers major advantages such as higher patient satisfaction, fewer complications, less pain and earlier return to normal daily 15 Arch Clin Cases 2016; 3(1):10-17
7 activities. Even so, many surgeons do not embrace this procedure as the standard of care for grade III-IV hemorrhoids mainly because of high recurrence rate, expensive equipment and lack of success in reducing severe prolapsed mucosa. These patients had severe mucosal prolapse and, as seen in pictures, ligation of all arteries accompanied by a continuous suture placed above the dentate line can effectively reduce and fix even prolapsed hemorrhoids. We believe that THD with mucopexy can be safely used in advanced fourth degree hemorrhoids as a safe one-day procedure with immediate visible results. Without proper equipment, finding and ligating the arteries is technically demanding and can lead to poor results. Even though it is expensive, this new THD equipment provides standardization, reduces recurrence rate and it may become cost-effective, because postoperative hospitalization costs are kept at a minimum. Further research is needed to establish which of the two well-known less invasive procedures (PPH and THD) is the treatment of choice for IV degree hemorrhoids. Acknowledgements This article was designed and written with special contributions from Mr. Emmanuel Eguare and his operative team. The cases presented in this manuscript are patients treated by Mr. Emmanuel Eguare at Naas General Hospital and the paper was conducted during my (S. Morarasu) summer elective clinical clerkship in Mr. Eguare s clinic. The corresponding author would like to express his deepest gratitude to all the staff at Naas General Hospital, Naas, Co. Kildare, Ireland. References 1. Brunicardi FC, Andersen DK, Billiar TR, et al. Schwartz s Principles of Surgery, 9e: The McGraw-Hill Companies, Inc Kaidar-Person O, Person B, Wexner SD. Hemorrhoidal disease: a comprehensive review. J Am Coll Surg 2007; 204: Jacobs D. Hemorrhoids. N Engl J Med 2014; 371: LaBella GD, Main WPL, Hussain LR. Evaluation of transanal hemorrhoidal dearterialization: a single surgeon experience. Tech Coloproctol 2015; 19: Lohsiriwat V. Hemorrhoids: From basic pathophysiology to clinical management. World J Gastroenterol 2012; 18(Suppl 17): Beck DE, Roberts PL, Saclarides TJ, et al. The ASCRS Textbook of Colon and Rectal Surgery, second Edition. Springer Science + Business Media, 2011: MacKay D. Hemorrhoids and varicose veins: a review of treatment options. Altern Med Rev 2001; 6(Suppl 2): Mounsey AL, Halladay J, Sadiq TS. Hemorrhoids. Am Fam Physician 2011; 84(Suppl 2): Brill AL, Fleshman JW, Ramshaw BJ, et al. Minimally invasive procedures: What family physicians need to know? J Fam Pract 2005; 54(Suppl 1): Tsikitis VL. Anal surgery for hemorrhoids [ 8-overview available at ]. 11. Cerato MM, Cerato NL, Passos P et al. Surgical treatment of hemorrhoids: a critical appraisal of the current options. ABCD Arq Bras Cir Dig 2014; 27(Suppl 1): Morinaga K, Hasuda K, Ikeda T. A novel therapy for internal hemorrhoids: ligation of the hemorrhoidal artery with a newly devised instrument (Moricorn) in conjunction with a Doppler flowmeter. Am J Gastroenterol 1995; 90(Suppl 4): Kjaer S, Lund HK, Schulze S, Bisgaard T. Limited success in patients treated with transanal hemorrhoidal dearterialisation. Dan Med J 2014; 61(Suppl 12):A Giordano P, Tomasi I, Pascariello A, Mills E, Elahi S. Transanal dearterialization with targeted mucopexy is effective for advanced hemorrhoids. Colorectal Disease 2014; 16: Noguerales F, Diaz R, Salim B et al. Treatment of hemorrhoids by transanal hemorrhoidal dearterialisation. Experience of Several Specialized Units. Cir Esp 2015; 93(Suppl 4): Ratto C, Giordano P, Donisi L et al. Transanal Hemorrhoid Dearterialization (THD) for selected four-degree hemorrhoids. Tech Coloproctol 2011; 15(Suppl 2): Giordano P, Nastro P, Davies A, Gravante G. Prospective evaluation of stapled hemorrhoidopexy versus transanal haemorrhoidal dearterialisation for stage II and 16 Arch Clin Cases 2016; 3(1):10-17
8 III haemorrhoids: three-year outcomes. Tech Coloproctol 2011; 15(Suppl 1): Pescatori M. Prevention and Treatment of Complications in Proctological Surgery. Springer Verlang Italia, Agbo SP. Surgical Management of Hemorrhoids. J Surg Tech Case Rep. 2011; 3(Suppl 2): Tjandra JJ, Chan MK. Systematic review on the procedure for prolapse and hemorrhoids (stapled hemorrhoidopexy). Dis Colon Rectum 2007; 50(Suppl 6): Rahman ASMT, Rahman ASMZ, Biswas SK et al. Stapled hemorrhoidopexy compared with conventional hemorrhoidectomy A systematic review. Faridpur Med. Coll. J. 2012; 7(Suppl 1): Senagore AJ, Singer M, Abcarian H et al. Procedure for Prolapse and Hemorrhoids (PPH) Multicenter Study Group. A prospective, randomized, controlled multicenter trial comparing stapled hemorrhoidopexy and Ferguson hemorrhoidectomy: perioperative and one-year results. Dis Colon Rectum 2004; 47(Suppl 11): Ratto C, Parello A, Veronese E et al. Dopplerguided transanal haemorrhoidal dearterialization for haemorrhoids: results from a multicentre trial. Colorectal Disease 2015; 17: Loganathan A, Das A, Luck A, Hewett P. Transanal haemorrhoidal dearterialization for the treatment of grade III and IV haemorrhoids: a 3-year experience. Anz J Surg 2016; 86(1-2): Tempel MB, Pearson EG, Page M, et al. Survey of patient satisfaction after Dopplerguided transanal haemorrhoidal dearterialization performed in ambulatory settings. Tech Coloproctol 2014; 18: Talha S, Burke JP, Waldron D, Coffey JC, Condon E. Early quality of life outcomes following Doppler guided transanal hemorrhoidal dearterialisation: a prospective observational study. Acta Gastroenterol Belg 2013; 76(Suppl 2): Shaikh AR, Dalwani AG, Soomro N. An evaluation of Milligan-Morgan And Ferguson procedures for haemorrhoidectomy at Liaquat University Hospital Jamshoro, Hyderabad, Pakistan. Pak J Med Sci 2013; 29(Suppl 1): Popov V, Zhivkov E, Tokov P, et al. Advantages of transanal hemorrhoidal dearterialisation as compared to other surgical techniques for the treatment of hemorrhoidal disease. Khirurgiia 2013; 3: Infantino A, Altomare DF, Bottini C, et al. Prospective randomized multicenter study comparing stapler hemorrhoidopexy with doppler-guided transanal hemorrhoids dearterialization for third degree hemorrhoids. Colorectal Disease 2011; 14(Suppl 2): Tsang YP, Fok KL, Cheung YS, LI KW, Tang CN. Comparison of transanal haemorrhoidal dearterialisation and stapled hemorrhoidopexy in management of hemorrhoidal disease: a retrospective study and literature review. Tech Coloproctol 2014; 18(Suppl 11): Verre L, Rossi R, Gaggelli I, et al. PPH versus THD: a comparison of two techniques for III and IV degree hemorrhoids. Personal experience. Minerva Chir 2013; 68(Suppl6): Lucarelli P, Picchio M, Caporossi M, et al. Transanal haemorrhoidal dearterialisation with mucopexy versus stapler haemorrhoidopexy: a randomized trial with long-term follow-up. Ann R Coll Surg Engl 2013; 95(Suppl 4): Ratto C. THD Doppler procedure for hemorrhoids: the surgical technique. Tech Coloproctol 2014; 18: Arch Clin Cases 2016; 3(1):10-17
UNDERSTANDING THE PROCEDURE FOR PROLAPSE AND HEMORRHOIDS
 UNDERSTANDING THE PROCEDURE FOR PROLAPSE AND HEMORRHOIDS AN ALTERNATIVE APPROACH TO THE SURGICAL TREATMENT OF HEMORRHOIDS pphinfo.com Identifying Patients for PPH Procedure for Prolapse and Hemorrhoids
UNDERSTANDING THE PROCEDURE FOR PROLAPSE AND HEMORRHOIDS AN ALTERNATIVE APPROACH TO THE SURGICAL TREATMENT OF HEMORRHOIDS pphinfo.com Identifying Patients for PPH Procedure for Prolapse and Hemorrhoids
Hemorrhoids Dearterialization Doppler. Keywords Laser
 DOI 10.1007/s00464-010-1370-x Doppler-guided hemorrhoidal laser procedure for the treatment of symptomatic hemorrhoids: experimental background and short-term clinical results of a new mini-invasive treatment
DOI 10.1007/s00464-010-1370-x Doppler-guided hemorrhoidal laser procedure for the treatment of symptomatic hemorrhoids: experimental background and short-term clinical results of a new mini-invasive treatment
Treatment of grade III and IV haemorrhoidal disease with PPH or THD. A randomized trial on postoperative complications and short-term results
 Treatment of grade III and IV haemorrhoidal disease with PPH or THD. A randomized trial on postoperative complications and short-term results Authors: Sebastiaan Festen & M. J. Van Hoogstraten & A. A.
Treatment of grade III and IV haemorrhoidal disease with PPH or THD. A randomized trial on postoperative complications and short-term results Authors: Sebastiaan Festen & M. J. Van Hoogstraten & A. A.
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of haemorrhoidal artery ligation Haemorrhoids (also known as piles) are enlarged
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of haemorrhoidal artery ligation Haemorrhoids (also known as piles) are enlarged
WHAT ARE HEMORRHOIDS?
 Patient information regarding care and surgery associated with HEMORRHOIDS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia Stefanou, M.D. location: Michigan Heart & Vascular Institute, 5325
Patient information regarding care and surgery associated with HEMORRHOIDS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia Stefanou, M.D. location: Michigan Heart & Vascular Institute, 5325
DG-RAR for the treatment of symptomatic grade III and grade IV haemorrhoids: a 12-month multi-centre, prospective observational study
 Eur Surg DOI 10.1007/s10353-012-0182-8 DG-RAR for the treatment of symptomatic grade III and grade IV haemorrhoids: a 12-month multi-centre, prospective observational study S. Roka, D. Gold, P. Walega,
Eur Surg DOI 10.1007/s10353-012-0182-8 DG-RAR for the treatment of symptomatic grade III and grade IV haemorrhoids: a 12-month multi-centre, prospective observational study S. Roka, D. Gold, P. Walega,
Peter C. Ambe 1,2* and Dirk R. Wassenberg 2
 Ambe and Wassenberg Patient Safety in Surgery (2015) 9:36 DOI 10.1186/s13037-015-0081-6 RESEARCH Proctitis after stapled hemorrhoidopexy is an underestimated complication of a widely used surgical procedure:
Ambe and Wassenberg Patient Safety in Surgery (2015) 9:36 DOI 10.1186/s13037-015-0081-6 RESEARCH Proctitis after stapled hemorrhoidopexy is an underestimated complication of a widely used surgical procedure:
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Hemorrhoidectomy with LigaSure Small Jaw and Stapled Hemorrhoidopexy with EEA Hemorrhoid and Prolapse Stapler with DST
 Hemorrhoidectomy with LigaSure Small Jaw and Stapled Hemorrhoidopexy with EEA Hemorrhoid and Prolapse Stapler with DST Dr. Wong Kutt Sing MBBS (S pore), FRCS (Edin), FRCS (Glas), FAMS General Surgery Raffles
Hemorrhoidectomy with LigaSure Small Jaw and Stapled Hemorrhoidopexy with EEA Hemorrhoid and Prolapse Stapler with DST Dr. Wong Kutt Sing MBBS (S pore), FRCS (Edin), FRCS (Glas), FAMS General Surgery Raffles
Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients
 Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients What are Haemorrhoids? Haemorrhoids (piles) are enlarged blood vessels around the anus (back passage). There are two types of haemorrhoids:
Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients What are Haemorrhoids? Haemorrhoids (piles) are enlarged blood vessels around the anus (back passage). There are two types of haemorrhoids:
Recto Anal Repair (RAR): a viable new treatment option for high-grade hemorrhoids. One year results of a prospective study
 Original article Recto Anal Repair (RAR): a viable new treatment option for high-grade hemorrhoids. One year results of a prospective study ULRIKE SATZINGER (*) - WOLFGANG FEIL (**) - KARL GLASER (***)
Original article Recto Anal Repair (RAR): a viable new treatment option for high-grade hemorrhoids. One year results of a prospective study ULRIKE SATZINGER (*) - WOLFGANG FEIL (**) - KARL GLASER (***)
Direct Current Therapy for Treatment of Hemorrhoids
 Direct Current Therapy for Treatment of Hemorrhoids [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr Go to Comunicados a Proveedores, and click Cartas
Direct Current Therapy for Treatment of Hemorrhoids [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr Go to Comunicados a Proveedores, and click Cartas
Is co2 laser Hemorrhoidectomy superior to conventional open Hemorrhoidectomy?
 Is co2 laser Hemorrhoidectomy superior to conventional open Hemorrhoidectomy? *Sa`ad H Sultan M.B.Ch.B,D.S,CABS **Zuhair B Kamal M.B.Ch.B,CABS ***Mohammad A Al-Atroshi M.B.Ch.B,CABS ****Raysan Al-Fayadh
Is co2 laser Hemorrhoidectomy superior to conventional open Hemorrhoidectomy? *Sa`ad H Sultan M.B.Ch.B,D.S,CABS **Zuhair B Kamal M.B.Ch.B,CABS ***Mohammad A Al-Atroshi M.B.Ch.B,CABS ****Raysan Al-Fayadh
Anorectal Abscess and Fistula
 Anorectal Abscess/Fistula by: Robert K Cleary MD, John C Eggenberger MD, Amalia J Stefanou, MD location: Michigan Heart & Vascular Institute, 5325 Elliott Dr, Suite 104 mailing address: PO Box 974, Ann
Anorectal Abscess/Fistula by: Robert K Cleary MD, John C Eggenberger MD, Amalia J Stefanou, MD location: Michigan Heart & Vascular Institute, 5325 Elliott Dr, Suite 104 mailing address: PO Box 974, Ann
Prospective, Randomized Controlled Trial of Starion TM
 WANG./Dis Colon Rectum Page 1 Prospective, Randomized Controlled Trial of Starion TM versus Ligasure TM Hemorrhoidectomy for Prolapsed Hemorrhoids Jaw-Yuan Wang, M.D.,*, Hsiang-Lin Tsai M.D.,*, Fang-Ming
WANG./Dis Colon Rectum Page 1 Prospective, Randomized Controlled Trial of Starion TM versus Ligasure TM Hemorrhoidectomy for Prolapsed Hemorrhoids Jaw-Yuan Wang, M.D.,*, Hsiang-Lin Tsai M.D.,*, Fang-Ming
Anal Surgery. Colon and Rectal Surgery. Surgery of the Anus. Hemorrhoids Fistula Fissure Abscess
 Anal Surgery and Colon and Rectal Surgery Elizabeth J. McConnell MD FACS FASCRS Surgery of the Anus Hemorrhoids Fistula Fissure Abscess 1 Hemorrhoid Internal or External 1-3 columns Internal Band or Suture
Anal Surgery and Colon and Rectal Surgery Elizabeth J. McConnell MD FACS FASCRS Surgery of the Anus Hemorrhoids Fistula Fissure Abscess 1 Hemorrhoid Internal or External 1-3 columns Internal Band or Suture
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions
 Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Prevention and Recognition of Obstetric Fistula Training Package. Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula
 Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
CHOC CHILDREN SUROLOGY CENTER. Constipation
 Constipation What is constipation? Constipation is a condition in which a person has uncomfortable or infrequent bowel movements. Generally, a person is considered to be constipated when bowel movements
Constipation What is constipation? Constipation is a condition in which a person has uncomfortable or infrequent bowel movements. Generally, a person is considered to be constipated when bowel movements
Transanal Radiofrequency Treatment of Fecal Incontinence
 Transanal Radiofrequency Treatment of Fecal Incontinence Policy Number: 2.01.58 Last Review: 12/2015 Origination: 1/2012 Next Review: 1/2016 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will
Transanal Radiofrequency Treatment of Fecal Incontinence Policy Number: 2.01.58 Last Review: 12/2015 Origination: 1/2012 Next Review: 1/2016 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will
Perianal Abscess and Fistula-in-ano. Background
 Perianal Abscess and Fistula-in-ano Background Anorectal abscesses are some of the more common anorectal conditions encountered, and they are potentially debilitating conditions. The current theory as
Perianal Abscess and Fistula-in-ano Background Anorectal abscesses are some of the more common anorectal conditions encountered, and they are potentially debilitating conditions. The current theory as
The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence. Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center
 The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center Constipation Overview Constipation Normal Transit Constipation
The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center Constipation Overview Constipation Normal Transit Constipation
Diagnosis and treatment of haemorrhoids
 CLINICAL GUIDELINES DANISH MEDICAL JOURNAL Diagnosis and treatment of haemorrhoids Steen Buntzen, Peter Christensen, Ali Khalid, Ken Ljungmann, Jan Lindholt, Lilli Lundby, Line Rossell Walker, Dennis Raahave
CLINICAL GUIDELINES DANISH MEDICAL JOURNAL Diagnosis and treatment of haemorrhoids Steen Buntzen, Peter Christensen, Ali Khalid, Ken Ljungmann, Jan Lindholt, Lilli Lundby, Line Rossell Walker, Dennis Raahave
Treatment of hemorrhoids: A coloproctologist s view
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v21.i31.9245 World J Gastroenterol 2015 August 21; 21(31): 9245-9252 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v21.i31.9245 World J Gastroenterol 2015 August 21; 21(31): 9245-9252 ISSN 1007-9327
Hemorrhoid Embolization Results: 15 years Experince
 Krasnoyarsk State Medical University named after prof. Voyno-Yasenetsky Russia A. Zakharchenko E. Galkin Hemorrhoid Embolization Results: 5 years Experince Alexander Zakharchenko, MD No relevant financial
Krasnoyarsk State Medical University named after prof. Voyno-Yasenetsky Russia A. Zakharchenko E. Galkin Hemorrhoid Embolization Results: 5 years Experince Alexander Zakharchenko, MD No relevant financial
Laparoscopic Repair of Incisional Hernia. Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds
 Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
Laparoscopic Repair of Incisional Hernia Maria B. ALBUJA-CRUZ, MD University of Colorado Department of Surgery-Grand Rounds Overview Definition Advantages of Laparoscopic Repair Disadvantages of Open Repair
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Hemorrhoids and Varicose Veins: A Review of Treatment Options Alternative Medicine Review, April, 2001 by Douglas MacKay
 Hemorrhoids and Varicose Veins: A Review of Treatment Options Alternative Medicine Review, April, 2001 by Douglas MacKay Abstract Hemorrhoids and varicose veins are common conditions seen by general practitioners.
Hemorrhoids and Varicose Veins: A Review of Treatment Options Alternative Medicine Review, April, 2001 by Douglas MacKay Abstract Hemorrhoids and varicose veins are common conditions seen by general practitioners.
LIFT : A New approach to anal fistula Ligation of Intersphincteric FistulaTract
 LIFT : A New approach to anal fistula Ligation of Intersphincteric FistulaTract Charles TSANG Division of Colorectal Surgery, National University Health System [email protected] Evolution in the
LIFT : A New approach to anal fistula Ligation of Intersphincteric FistulaTract Charles TSANG Division of Colorectal Surgery, National University Health System [email protected] Evolution in the
Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606
 October 5, 2010 Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606 Dear Dr. Rosenberg, The American Gastroenterological
October 5, 2010 Alan Rosenberg, MD VP Medical Policy, Technology Assessment and Credentialing WellPoint, Inc. 233 S. Wacker Drive, Suite 3900 Chicago, IL 60606 Dear Dr. Rosenberg, The American Gastroenterological
VAGINAL MESH FAQ. How do you decide who should get mesh as part of their repair?
 VAGINAL MESH FAQ How do you decide who should get mesh as part of their repair? Each patient with pelvic organ prolapse (POP) is considered individually. In younger women, women with an uncomplicated prolapse
VAGINAL MESH FAQ How do you decide who should get mesh as part of their repair? Each patient with pelvic organ prolapse (POP) is considered individually. In younger women, women with an uncomplicated prolapse
NHS. Surgical repair of vaginal wall prolapse using mesh. National Institute for Health and Clinical Excellence. 1 Guidance.
 Issue date: June 2008 NHS National Institute for Health and Clinical Excellence Surgical repair of vaginal wall prolapse using mesh 1 Guidance 1.1 The evidence suggests that surgical repair of vaginal
Issue date: June 2008 NHS National Institute for Health and Clinical Excellence Surgical repair of vaginal wall prolapse using mesh 1 Guidance 1.1 The evidence suggests that surgical repair of vaginal
Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique: initial evaluation of 42 cases
 Original Article Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique: Carlos Mateus Rotta 1, Fernando Oriolli de Moraes 2, Araripe Fernandez Varella Neto 3, Thereza Cristina Ariza
Original Article Doppler-guided hemorrhoidal artery ligation with rectal mucopexy technique: Carlos Mateus Rotta 1, Fernando Oriolli de Moraes 2, Araripe Fernandez Varella Neto 3, Thereza Cristina Ariza
Effectiveness of Day-case Surgery in Urology: Single Surgeon Experience
 Bahrain Medical Bulletin 29, No. 3, September 2007 Effectiveness of Day-case Surgery in Urology: Single Surgeon Experience Mohamed H. Durazi, FRCS ED, FRCSI* Reem Al-Bareeq, MRCSI, CAB(Urol)** Mohamed
Bahrain Medical Bulletin 29, No. 3, September 2007 Effectiveness of Day-case Surgery in Urology: Single Surgeon Experience Mohamed H. Durazi, FRCS ED, FRCSI* Reem Al-Bareeq, MRCSI, CAB(Urol)** Mohamed
The enigma of the transsphincteric anal fistula. Per-Olof Nyström, M.D., Ph.D. Karolinska University Hospital, Stockholm, Sweden
 The enigma of the transsphincteric anal fistula Per-Olof Nyström, M.D., Ph.D. Karolinska University Hospital, Stockholm, Sweden Four principles of treatment for anal fistula 1. Inactivate the fistula 2.
The enigma of the transsphincteric anal fistula Per-Olof Nyström, M.D., Ph.D. Karolinska University Hospital, Stockholm, Sweden Four principles of treatment for anal fistula 1. Inactivate the fistula 2.
Bridging Techniques. What s between EMR and Traditional Surgery? Elisabeth C. McLemore, MD, FACS, FASCRS
 Bridging Techniques What s between EMR and Traditional Surgery? Elisabeth C. McLemore, MD, FACS, FASCRS Associate Professor of Surgery Assistant Program Director, General Surgery Residency Disclosures
Bridging Techniques What s between EMR and Traditional Surgery? Elisabeth C. McLemore, MD, FACS, FASCRS Associate Professor of Surgery Assistant Program Director, General Surgery Residency Disclosures
Get the Facts, Be Informed, Make YOUR Best Decision. Pelvic Organ Prolapse
 Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
What is an Anal Fissure?
 Patient information regarding care and surgery associated with ANAL FISSURE by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Patient information regarding care and surgery associated with ANAL FISSURE by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Treatment of Fistula in Ano. Johanna Basa M.D. SUNY Downstate Medical Center August 2, 2012
 Treatment of Fistula in Ano Johanna Basa M.D. SUNY Downstate Medical Center August 2, 2012 Case Presentation HPI:54 yr old male with PMH of HTN, presented to clinic with complaints of 3rd perianal abscess
Treatment of Fistula in Ano Johanna Basa M.D. SUNY Downstate Medical Center August 2, 2012 Case Presentation HPI:54 yr old male with PMH of HTN, presented to clinic with complaints of 3rd perianal abscess
How common is bowel cancer?
 information Primary Care Society for Gastroenterology Bowel Cancer (1 of 6) How common is bowel cancer? Each year 35,000 people in Britain are diagnosed with cancer of the bowel, that is to say cancer
information Primary Care Society for Gastroenterology Bowel Cancer (1 of 6) How common is bowel cancer? Each year 35,000 people in Britain are diagnosed with cancer of the bowel, that is to say cancer
Navigating Anorectal Anatomy: Terms, Planes, Spaces, Structures
 Navigating Anorectal Anatomy: Terms, Planes, Spaces, Structures Lawrence M. Witmer, PhD Lawrence M. Witmer, PhD Department of Biomedical Sciences College of Osteopathic Medicine Ohio University Athens,
Navigating Anorectal Anatomy: Terms, Planes, Spaces, Structures Lawrence M. Witmer, PhD Lawrence M. Witmer, PhD Department of Biomedical Sciences College of Osteopathic Medicine Ohio University Athens,
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
PREPARING FOR YOUR STOMA REVERSAL
 PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
Bowel Preparation for Colon Resection. Eric Klein, M.D. SUNY Downstate Department of Surgery
 Bowel Preparation for Colon Resection Eric Klein, M.D. SUNY Downstate Department of Surgery Historical Perspective During World War II, failure to treat penetrating colon injuries with diversion could
Bowel Preparation for Colon Resection Eric Klein, M.D. SUNY Downstate Department of Surgery Historical Perspective During World War II, failure to treat penetrating colon injuries with diversion could
YALE UNIVERSITY SCHOOL OF MEDICINE: SECTION OF OTOLARYNGOLOGY PATIENT INFORMATION FUNCTIONAL ENDOSCOPIC SINUS SURGERY
 YALE UNIVERSITY SCHOOL OF MEDICINE: SECTION OF OTOLARYNGOLOGY PATIENT INFORMATION FUNCTIONAL ENDOSCOPIC SINUS SURGERY What is functional endoscopic sinus surgery (FESS)? Functional endoscopic sinus surgery
YALE UNIVERSITY SCHOOL OF MEDICINE: SECTION OF OTOLARYNGOLOGY PATIENT INFORMATION FUNCTIONAL ENDOSCOPIC SINUS SURGERY What is functional endoscopic sinus surgery (FESS)? Functional endoscopic sinus surgery
Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place.
 What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
Total Abdominal Hysterectomy
 What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
Information for men considering a male sling procedure
 Information for men considering a male sling procedure Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Information for men considering a male sling procedure Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Fistula-tract Laser Closure (FiLaC TM ): long-term results and new operative strategies
 DOI 10.1007/s10151-015-1282-9 ORIGINAL ARTICLE Fistula-tract Laser Closure (FiLaC TM ): long-term results and new operative strategies P. Giamundo L. Esercizio M. Geraci L. Tibaldi M. Valente Received:
DOI 10.1007/s10151-015-1282-9 ORIGINAL ARTICLE Fistula-tract Laser Closure (FiLaC TM ): long-term results and new operative strategies P. Giamundo L. Esercizio M. Geraci L. Tibaldi M. Valente Received:
Understanding Laparoscopic Colorectal Surgery
 Understanding Laparoscopic Colorectal Surgery University Colon & Rectal Surgery A Problem with Your Colon Your doctor has told you that you have a colon problem. Now you ve learned that surgery is needed
Understanding Laparoscopic Colorectal Surgery University Colon & Rectal Surgery A Problem with Your Colon Your doctor has told you that you have a colon problem. Now you ve learned that surgery is needed
Beaumont Hospital. Varicose Veins. and their TREATMENT. Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM
 Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions
 Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions No lifting greater than 10 15 lbs for the first three weeks following your surgery. Walking around the house, office
Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions No lifting greater than 10 15 lbs for the first three weeks following your surgery. Walking around the house, office
Total Vaginal Hysterectomy with an Anterior and Posterior Repair
 Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
41 Assisting with Minor Surgery
 Learning Outcomes 41.1 Define the medical assistant s role in minor surgical procedures. 41-2 CHAPTER 41 Assisting with Minor Surgery 41.2 Describe types of wounds and explain how they heal. 41.3 Describe
Learning Outcomes 41.1 Define the medical assistant s role in minor surgical procedures. 41-2 CHAPTER 41 Assisting with Minor Surgery 41.2 Describe types of wounds and explain how they heal. 41.3 Describe
C A R O L I N A S. Hernia Handbook ( C H A P T E R 2 ) B. Todd Heniford, MD
 C A R O L I N A S Hernia Handbook ( C H A P T E R 2 ) B. Todd Heniford, MD C H A P T E R 2 Umbilical Hernias C A R O L I N A S H E R N I A H A N D B O O K 17 Umbilical Hernias W H AT I S A N U M B I L
C A R O L I N A S Hernia Handbook ( C H A P T E R 2 ) B. Todd Heniford, MD C H A P T E R 2 Umbilical Hernias C A R O L I N A S H E R N I A H A N D B O O K 17 Umbilical Hernias W H AT I S A N U M B I L
Total Vaginal Hysterectomy
 What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
Patient information regarding care and surgery associated with ULCERATIVE COLITIS
 Patient information regarding care and surgery associated with ULCERATIVE COLITIS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou, M.D. location: Michigan Heart & Vascular Institute,
Patient information regarding care and surgery associated with ULCERATIVE COLITIS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou, M.D. location: Michigan Heart & Vascular Institute,
ESD for colorectal lesions I am in favour. Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy
 ESD for colorectal lesions I am in favour Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Surgery for early colonic lesions 51 pts referred for lap colectomy
ESD for colorectal lesions I am in favour Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Surgery for early colonic lesions 51 pts referred for lap colectomy
Recto-vaginal Fistula Repair
 What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
Laparoscopic Repair of Hernias. A simple guide to help answer your questions
 Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Patient. Frequently Asked Questions. Transvaginal Surgical Mesh for Pelvic Organ Prolapse
 Patient Frequently Asked Questions Transvaginal Surgical Mesh for Pelvic Organ Prolapse Frequently Asked Questions WHAT IS PELVIC ORGAN PROLAPSE AND HOW IS IT TREATED? Q: What is pelvic organ prolapse
Patient Frequently Asked Questions Transvaginal Surgical Mesh for Pelvic Organ Prolapse Frequently Asked Questions WHAT IS PELVIC ORGAN PROLAPSE AND HOW IS IT TREATED? Q: What is pelvic organ prolapse
Example 1 is the Chart Audit Form. A few comments about the items are:
 Dear Colleague: We appreciate your interest in the Pain Audit Tools developed and used at the City of Hope Medical Center. Attached for your information and use are three examples. Example 1 is the Chart
Dear Colleague: We appreciate your interest in the Pain Audit Tools developed and used at the City of Hope Medical Center. Attached for your information and use are three examples. Example 1 is the Chart
FAQ About Prostate Cancer Treatment and SpaceOAR System
 FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
UCHSC Grand Rounds 5-16-11
 UCHSC Grand Rounds 5-16-11 Common disorders Hemorrhoids Anal Fissure Pilonidal Disease Fistula in Ano Anorectal evaluation (never forget!) COMPLETE History You NEED to ask every patient about continence
UCHSC Grand Rounds 5-16-11 Common disorders Hemorrhoids Anal Fissure Pilonidal Disease Fistula in Ano Anorectal evaluation (never forget!) COMPLETE History You NEED to ask every patient about continence
Billing Guideline. Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16
 Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
By James D. Gould, MD FACS
 By James D. Gould, MD FACS BACKGROUND Balloon devices enlarge narrowed sinus ostia and outflow tracts by remodeling the surrounding bone and paranasal sinus structures. Multiple studies have demonstrated
By James D. Gould, MD FACS BACKGROUND Balloon devices enlarge narrowed sinus ostia and outflow tracts by remodeling the surrounding bone and paranasal sinus structures. Multiple studies have demonstrated
Colon Cancer. What Is Colon Cancer? What Are the Screening Methods?
 Cancer of the colon or rectum (colorectal cancer) is the second most common cancer in the U.S. In fact, of all people born, 1 in 40 will die of the disease. What Is Colon Cancer? Colon cancer begins with
Cancer of the colon or rectum (colorectal cancer) is the second most common cancer in the U.S. In fact, of all people born, 1 in 40 will die of the disease. What Is Colon Cancer? Colon cancer begins with
Fistulectomy versus fistulotomy with marsupialisation in the treatment of low fistula-inano: a prospective randomized controlled trial
 Fistulectomy versus fistulotomy with marsupialisation in the treatment of low fistula-inano: a prospective randomized controlled trial PHILLIPO L. CHALYA * and JOSEPH B. MABULA Department of Surgery, Catholic
Fistulectomy versus fistulotomy with marsupialisation in the treatment of low fistula-inano: a prospective randomized controlled trial PHILLIPO L. CHALYA * and JOSEPH B. MABULA Department of Surgery, Catholic
TRANSVAGINAL MESH IN PELVIC ORGAN PROLAPSE REPAIR.
 TRANSVAGINAL MESH IN PELVIC ORGAN PROLAPSE REPAIR. Spanish full text SUMMARY Introduction: Pelvic organ prolapse (POP) is characterised by the descent or herniation of the uterus, vaginal vault, bladder
TRANSVAGINAL MESH IN PELVIC ORGAN PROLAPSE REPAIR. Spanish full text SUMMARY Introduction: Pelvic organ prolapse (POP) is characterised by the descent or herniation of the uterus, vaginal vault, bladder
Inguinal Hernia (Female)
 Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Dacryocystorhinostomy (DCR)
 Patient information Adnexal Dacryocystorhinostomy (DCR) Patient information about an operation to form a new tear drain between the eye and the nose when there has been a blockage What is dacryocystorhinostomy
Patient information Adnexal Dacryocystorhinostomy (DCR) Patient information about an operation to form a new tear drain between the eye and the nose when there has been a blockage What is dacryocystorhinostomy
INFORMED CONSENT FOR SLEEVE GASTRECTOMY
 INFORMED CONSENT FOR SLEEVE GASTRECTOMY This informed-consent document has been prepared to help inform you about your Sleeve Gastrectomy including the risks and benefits, as well as alternative treatments.
INFORMED CONSENT FOR SLEEVE GASTRECTOMY This informed-consent document has been prepared to help inform you about your Sleeve Gastrectomy including the risks and benefits, as well as alternative treatments.
Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization
 Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Hysterectomy. What is a hysterectomy? Why is hysterectomy done? Are there alternatives to hysterectomy?
 ROBERT LEVITT, MD JESSICA BERGER-WEISS, MD ADRIENNE POTTS, MD HARTAJ POWELL, MD, MPH COURTNEY LEVENSON, MD LAUREN BURNS, MSN, RN, WHNP OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is
ROBERT LEVITT, MD JESSICA BERGER-WEISS, MD ADRIENNE POTTS, MD HARTAJ POWELL, MD, MPH COURTNEY LEVENSON, MD LAUREN BURNS, MSN, RN, WHNP OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is
Patient Information Leaflet Anal Fistula operation
 Patient Information Leaflet Anal Fistula operation SM07/04 Anal Fistula operation What is a fistula? An anal fistula is a track between the skin on the outside of the buttock/anal area and the anal canal
Patient Information Leaflet Anal Fistula operation SM07/04 Anal Fistula operation What is a fistula? An anal fistula is a track between the skin on the outside of the buttock/anal area and the anal canal
Back & Neck Pain Survival Guide
 Back & Neck Pain Survival Guide www.kleinpeterpt.com Zachary - 225-658-7751 Baton Rouge - 225-768-7676 Kleinpeter Physical Therapy - Spine Care Program Finally! A Proven Assessment & Treatment Program
Back & Neck Pain Survival Guide www.kleinpeterpt.com Zachary - 225-658-7751 Baton Rouge - 225-768-7676 Kleinpeter Physical Therapy - Spine Care Program Finally! A Proven Assessment & Treatment Program
Colorectal Cancer Care A Cancer Care Map for Patients
 Colorectal Cancer Care A Cancer Care Map for Patients Understanding the process of care that a patient goes through in the diagnosis and treatment of colorectal cancer in BC. Colorectal Cancer Care Map
Colorectal Cancer Care A Cancer Care Map for Patients Understanding the process of care that a patient goes through in the diagnosis and treatment of colorectal cancer in BC. Colorectal Cancer Care Map
Tone Up Your Pelvic Floor. A regular pelvic floor exercise ( Kegel ) routine can prevent symptoms before, during, and after childbirth.
 Will Breastfeeding Affect Incontinence and Pelvic Symptoms? Yes, often for as long as you re nursing. Many breastfeeding women are unaware that a natural drop in estrogen which persists for as long as
Will Breastfeeding Affect Incontinence and Pelvic Symptoms? Yes, often for as long as you re nursing. Many breastfeeding women are unaware that a natural drop in estrogen which persists for as long as
Breast Reduction Post-Operative Instructions
 Breast Reduction Post-Operative Instructions What are my post-operative instructions? Have someone drive you home after surgery and help you at home for 1-2 days. Get plenty of rest and follow a balanced
Breast Reduction Post-Operative Instructions What are my post-operative instructions? Have someone drive you home after surgery and help you at home for 1-2 days. Get plenty of rest and follow a balanced
Radiation Therapy for Prostate Cancer
 Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Endoscopic therapy for obesity and complications of bariatric surgery
 Endoscopic therapy for obesity and complications of bariatric surgery Jacques Devière, MD, PhD Erasme University Hospital Brussels Belgium [email protected] Obesity Affects 300 millions
Endoscopic therapy for obesity and complications of bariatric surgery Jacques Devière, MD, PhD Erasme University Hospital Brussels Belgium [email protected] Obesity Affects 300 millions
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
M O V I N G F R E E LY. HerniaCenter. The Columbia Hernia Center at ColumbiaDoctors Midtown
 M O V I N G F R E E LY HerniaCenter The Columbia Hernia Center at ColumbiaDoctors Midtown Director, Dr. Peter L. Geller The Columbia Hernia Center brings together a group of surgeons adept in using the
M O V I N G F R E E LY HerniaCenter The Columbia Hernia Center at ColumbiaDoctors Midtown Director, Dr. Peter L. Geller The Columbia Hernia Center brings together a group of surgeons adept in using the
Transobturator tape sling Female sling system
 Transobturator tape sling Female sling system Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Transobturator tape sling Female sling system Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
MANAGEMENT OF SLING COMPLICATIONS IN FEMALES. Jorge L. Lockhart M.D. Program Director Division of Urology University of South Florida
 MANAGEMENT OF SLING COMPLICATIONS IN FEMALES Jorge L. Lockhart M.D. Program Director Division of Urology University of South Florida INTRODUCTION The traditional gold standard treatments for stress urinary
MANAGEMENT OF SLING COMPLICATIONS IN FEMALES Jorge L. Lockhart M.D. Program Director Division of Urology University of South Florida INTRODUCTION The traditional gold standard treatments for stress urinary
Information and advice following placement of seton for anal fistula
 Oxford University Hospitals NHS Trust Information and advice following placement of seton for anal fistula page 2 What is a fistula? You can get an anal fistula as a result of an infection or a collection
Oxford University Hospitals NHS Trust Information and advice following placement of seton for anal fistula page 2 What is a fistula? You can get an anal fistula as a result of an infection or a collection
Original Policy Date
 MP 7.01.103 Plugs for Fistula Repair Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
MP 7.01.103 Plugs for Fistula Repair Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
COLORECTAL CANCER SCREENING
 COLORECTAL CANCER SCREENING By Douglas K. Rex, M.D., FACG & Suthat Liangpunsakul, M.D. Division of Gastroenterology and Hepatology, Department of Medicine Indiana University School of Medicine Indianapolis,
COLORECTAL CANCER SCREENING By Douglas K. Rex, M.D., FACG & Suthat Liangpunsakul, M.D. Division of Gastroenterology and Hepatology, Department of Medicine Indiana University School of Medicine Indianapolis,
Uterine Fibroid Symptoms, Diagnosis and Treatment
 Fibroids and IR Uterine Fibroid Symptoms, Diagnosis and Treatment Interventional radiologists use MRIs to determine if fibroids can be embolised, detect alternate causes for the symptoms and rule out misdiagnosis,
Fibroids and IR Uterine Fibroid Symptoms, Diagnosis and Treatment Interventional radiologists use MRIs to determine if fibroids can be embolised, detect alternate causes for the symptoms and rule out misdiagnosis,
Are any artificial parts used in the ACE Malone surgery?
 ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
Femoral Hernia Repair
 Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Laparoscopic Ventral Rectopexy
 Laparoscopic Ventral Rectopexy Patient information leaflet What is a laparoscopic ventral rectopexy? It is a keyhole operation, performed whilst you are asleep; the rectum is suspended back into its normal
Laparoscopic Ventral Rectopexy Patient information leaflet What is a laparoscopic ventral rectopexy? It is a keyhole operation, performed whilst you are asleep; the rectum is suspended back into its normal
Considering a Hysterectomy?
 Considering a Hysterectomy? Learn more about virtually scarless surgery using da Vinci Single-Site technology { {Symptoms & Conditions: Chronic Pain, Heavy Bleeding, Fibroids, Endometriosis, Adenomyosis,
Considering a Hysterectomy? Learn more about virtually scarless surgery using da Vinci Single-Site technology { {Symptoms & Conditions: Chronic Pain, Heavy Bleeding, Fibroids, Endometriosis, Adenomyosis,
Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery
 Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
Facing a Hysterectomy? If you ve been diagnosed with early stage gynecologic cancer, learn about minimally invasive da Vinci Surgery The Condition: Early Stage Gynecologic Cancer A variety of gynecologic
