NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
|
|
|
- Darrell Edwards
- 9 years ago
- Views:
Transcription
1 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of haemorrhoidal artery ligation Haemorrhoids (also known as piles) are enlarged blood vessels in or around the lower part of the bowel. They can cause itching, bleeding or pain, and may protrude outside the anus. This procedure is carried out on an area of the lower part of the bowel that is relatively less sensitive to pain. It does not involve tissue removal. Blood vessels are stitched to reduce the blood supply to the haemorrhoids, which relieves symptoms of bleeding and discomfort, and can help them to shrink. If they are large, the tissue overlying the haemorrhoids may also be folded up and stitched. Introduction The National Institute for Health and Clinical Excellence (NICE) has prepared this overview to help members of the Interventional Procedures Advisory Committee (IPAC) make recommendations about the safety and efficacy of an interventional procedure. It is based on a rapid review of the medical literature and specialist opinion. It should not be regarded as a definitive assessment of the procedure. Date prepared This overview was prepared in September Procedure name Haemorrhoidal artery ligation Transanal haemorrhoidal dearterialisation Specialty societies Association of Coloproctology of Great Britain and Ireland. IP overview: Haemorrhoidal artery ligation Page 1 of 34
2 Description Indications and current treatment Haemorrhoids (also known as piles) occur when the vascular anal cushions become enlarged. Some patients may be asymptomatic, but others have symptoms of bleeding, itching or discomfort (grade I). If the haemorrhoids are large, they may prolapse out of the rectum. Haemorrhoids that prolapse may reduce (return into the anal canal) spontaneously after defaecation (grade II); they may need to be reduced digitally (grade III); or they may not be reducible, remaining continually prolapsed (grade IV). Grade I or II haemorrhoids may be managed by diet modification or treated by topical applications. Interventional treatments include rubber band ligation and scleroscant injections. Treatments for Grade III and IV haemorrhoids include surgical excision of the haemorrhoids (haemorrhoidectomy) or stapled haemorrhoidopexy. What the procedure involves Haemorrhoidal artery ligation is a non-excisional procedure that aims to reduce symptoms of discomfort and bleeding by removing the blood flow to the haemorrhoids. The procedure is usually performed with the patient under general anaesthesia and is usually carried out after an enema. Using a proctoscope, the haemorrhoidal arteries are ligated with sutures (above the dentate line) to remove the flow of blood to the haemorrhoids. A Doppler probe may be used to help locate the haemorrhoidal arteries. For larger prolapsing haemorrhoids, an adjunctive mucosal plication procedure is done. The prolapsing mucosa is plicated up to the level of the dentate line where it is fixed by ligation of the plicating sutures (haemorrhoidopexy). Literature review Rapid review of literature The medical literature was searched to identify studies and reviews relevant to haemorrhoidal artery ligation. Searches were conducted of the following databases, covering the period from their commencement to 11 January 2010: MEDLINE, PREMEDLINE, EMBASE, Cochrane Library and other databases. Trial registries and the Internet were also searched. No language restriction was applied to the searches (see appendix C for details of search strategy). Relevant published studies identified during consultation or resolution that are published after this date may also be considered for inclusion. IP overview: Haemorrhoidal artery ligation Page 2 of 34
3 The following selection criteria (table 1) were applied to the abstracts identified by the literature search. Where selection criteria could not be determined from the abstracts the full paper was retrieved. Table 1 Inclusion criteria for identification of relevant studies Characteristic Publication type Patient Intervention/test Outcome Language Criteria Clinical studies were included. Emphasis was placed on identifying good quality studies. Abstracts were excluded where no clinical outcomes were reported, or where the paper was a review, editorial, or a laboratory or animal study. Conference abstracts were also excluded because of the difficulty of appraising study methodology, unless they reported specific adverse events that were not available in the published literature. Patients with grades II to IV haemorrhoids. Haemorrhoidal artery ligation. Articles were retrieved if the abstract contained information relevant to the safety and/or efficacy. Non-English-language articles were excluded unless they were thought to add substantively to the English-language evidence base. List of studies included in the overview This overview is based on approximately 3061 patients from 1 systematic review, 3 randomised controlled trials (RCTs), 1 non-randomised trial and 4 case series. Other studies that were considered to be relevant to the procedure but were not included in the main extraction table (table 2) have been listed in appendix A. IP overview: Haemorrhoidal artery ligation Page 3 of 34
4 Table 2 Summary of key efficacy and safety findings on haemorrhoidal artery ligation Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments Giordano P (2009) 1 Number of patients analysed: 1996 with an average of 6 Follow-up issues: arteries ligated Systematic review UK Recruitment period: literature search from 1995 onwards Study population: patients with haemorrhoids: 2% GI (6/305), 36.3% GII (482/1329), 57.4% GIII (912/1589), and 14.6% GIV (189/1295). n = 1996 (from 16 case series and 1 RCT) Age: 21 to 93 years Sex: 58.4% male Patient selection criteria: not stated Technique: THD with or without mucosopexy; various forms of anaesthesia used (general, local, general and local). Morinaga 1995 Sohn 2001 Arnold 2002 Shelygin 2003 Charύa Guindic 2004 Bursics 2004 Lienert and Ulrich 2004 Narro 2004 Vavra 2004 Ramirez 2005 Felice 2005 Scheyer 2006 Greenberg 2006 Wallis de Vries 2007 Abdeldaim 2007 Dal Monte 2007 Results overall Outcome % of patients Itching 10.6 (27/254) Prolapse 9.0 (96/1065) Bleeding 7.8 (89/1145) Pain on 4.7 (53/1123) defaecation In the 6 studies with 1-year follow-up: Outcome % of patients Prolapse 10.8 (46/427) Bleeding 9.7 (49/507) Pain on 8.7 (18/206) defaecation Recurrence: 27 patients required a second procedure for recurrent haemorrhoidal prolapse. Return to normal activity: this occurred between 2 and 3 days after the procedure for most studies (but at a mean of 3.5 days in Dal Monte 6 ). Comparison of studies with 1-year (n = 6) and < 1-year (n = 9) follow-up* Outcome < 1-year follow-up 1-year follow-up p value 3 patients developed significant haemorrhage requiring blood transfusion: 1 patient lost 1.3 litres postoperatively requiring transfusion and surgical intervention. 1 patient bled on the 8th day postoperatively and required 2 transfusions. 1 patient who had coagulopathy (no more details given) Early postoperative events % of patients Fever 3.9 (15/383) Thrombosed 1.8 (25/1386) haemorrhoids Anal fissure* 0.8 (14/1695) Urinary 0.7 (10/1468) retention Incontinence 0.4 (3/693) Anal fistulas 0.4 (3/815) Proctitis 0.2 (2/909) Stool retention 0.1 (1/711) * The study later states that anal fissure occurred in 2.3% (4/177) of patients overall. It is unclear why this figure is less than the early postoperative occurrence of this event patients completed follow-up (average followup of patients not given). Study design issues: Data collection and analysis was performed by two researchers independently of each other. Included non-english articles; excluded abstracts, studies without the use of a Doppler and any studies reporting on patients already reported on. Study population issues: Some of the patients (563) had undergone previous procedures (rubber-band ligation, 223; sclerotherapy, 322; stapled haemorrhoidopexy, 2; open haemorrhoidopexy, 3). 23 patients had concurrent procedures (such as fissurectomy, skin tag resection, herniorrhaphy). The study stated that results by grade of haemorrhoids were given IP overview: Haemorrhoidal artery ligation Page 4 of 34
5 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments Cantero 2008 Bleeding 6.3% 9.7% < 0.05 (40/638) (49/507) Follow-up: mean follow-up not stated (range 1 to 79 months) Conflict of interest/source of funding: not reported Pain on defaecation 3.8% (35/917) Prolapse 7.8% (50/638) * 1 study did not report follow-up. 8.7% (18/206) 10.8% (46/427) < 0.01 Not significan t Pre-operative outcomes The pre-operative proportion of patients with bleeding, pain and prolapse ranged from 45%-100%, 12%-83% and 12%-100% respectively across the studies. by 2 studies. These 2 studies are included in this table so this detail is not included here 5,6. Other issues: Type of anaesthesia was not described in 10 studies. The others used general (1), local (5) or both general and local anaesthesia (1). It appears that only one study performed mucosopexy after dearterialisation 6. IP overview: Haemorrhoidal artery ligation Page 5 of 34
6 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments Bursics A (2004) 2 Number of patients analysed: 60 (30 vs 30) with an Postoperative complications Follow-up issues: average of 6 arteries ligated Outcome Group Group RCT Early postoperative period A B Hungary Group A Group B p- Fever a 9 0 value Recruitment period: not stated Nausea b 6 2 Doses of < Study population: patients with haemorrhoids Urinary 1 0 minor (GI 1, GII 13, GIII 19, GIV 27); presenting with retention analgesics bleeding (49), pain (26), prolapse (3) and requiring discharge (2) (some presented with more than Patients 9 0 NS catheterisa one symptom). requiring tion opioid n = 60 (30 closed scissor Anal 0 3 analgesics haemorrhoidectomy [group A] vs 30 fissure c DGHAL [group B]) 2 23 NS Mean age: 47.5 years Sex: 45% male Patient selection criteria: patients underwent clinical exam, rigid sigmoidoscopy and anoscopy for diagnosis and staging; those with underlying pathologies were excluded by barium enema or colonoscopy, if necessary. Technique: DGHAL; mode of anaesthetic varied (see comments section). Mean follow-up: 11.7 months Conflict of interest/source of funding: not reported Patients not requiring pain relief Return to normal activities* 24.9 days 3 days < * Defined as return to job or no longer needing help taking care of themselves Longer term symptom status Group A Group B Symptoms at 6 weeks 5/26 a 5/26 b Symptoms during 5/26 c 3/26 d remaining follow-up a 1 patient had bleeding diverticulosis but this resolved with conservative treatment; 1 had symptoms which resolved after 3 sessions of rubber band ligation; 2 did not have further therapies; 1 patient with no problems had prolapsing secondary haemorrhoid in one direction. b 3 patients had perianal fullness and/or pain and had Overall d 14 2 a These occurred during the first postoperative week; 2 were given antibiotics and the others resolved spontaneously. b All cases required intravenous fluid replacement. c These occurred during the follow-up of 11.5 months; 1 healed with conservative therapy, and the other 2 healed after fissurectomy or lateral sphincterotomy before the end of the follow-up period. d The difference in complications between the groups was statistically significant (p < 0.05) (except for anal fissure for which the significance was not reported). Late complications There were no reports of stricture formation, incontinence or evacuation Follow-up occurred 6 weeks after the operation and then every 3 months afterwards. It involved a rectal digital examination and also rigid sigmoidoscopy if the patient had complaints. 3 patients in group A and 1 in group B were lost to follow-up after 3 months (it is not stated whether or not these were the patients who presented with symptoms at 6 weeks). These patients were contacted by letter and by phone. Study design issues: Inadequate randomisation (completed based on the date the patients attended the outpatient clinic). Methods used to recruit patients and whether or not blinding was attempted was not stated. Intention to treat analysis not described. The study did not state which underlying pathologies were excluded. IP overview: Haemorrhoidal artery ligation Page 6 of 34
7 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments prolapse on straining but bleeding stopped and no further problems at 1 year follow-up. Study population issues: therapy was required; 2 (with bleeding and pain, not There were no statistically prolapse) were successfully treated with suppositories. significant differences c 2 were patients with problems at 6 weeks; 3 were between the groups in patients with newly reported recurrences (the study reported that these were bleeding in 3 instances, pain in grades of the disease, sex, age and length of follow-up. 4, discharge in 1 and prolapse in 1, but it is not clear if these are for all 5 patients or just those with new symptoms). Other issues: d 2 were patients with problems at 6 weeks; 1 reported recurrent bleeding requiring a second DGHAL which was successful. At the end of the follow-up period 28 patients treated by DGHAL were complaint free and 25 patients in the haemorroidectomy group were complaint free (not significant). This is included in the systematic review 1. The authors state that the first 10 patients treated by DGHAL had a general anaesthetic and the remaining 20 were treated under local anaesthetic after the surgeons had more experience (15 of these had infiltration and the last 5 had surface anaesthesia). All patients in group A (except 3) were treated under general anaesthesia. IP overview: Haemorrhoidal artery ligation Page 7 of 34
8 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments Khafagy W (2009) 3 Number of patients analysed: 45 (15 vs 15 vs 15) with 5 Early postoperative complications Follow-up issues: to 6 arteries ligated for each patient. Bleeding Urine RCT Egypt Pain Determined on 10-cm VAS score Staple 1 (6.7%) retention 1 (6.7%) Recruitment period: 2002 to 2004 Followup A p C (betwe Group Group B Grou p value Open 0 5 (33.3%) Study population: patients with GIII or GIV DGHAL 0 0 en haemorrhoids presenting with anal discomfort groups (There was no significant difference (all), post-defaecation bleeding (41) and A and between groups.) prolapse (26). C) n = 45 (15 each treated by stapled Study design issues: 1st NS haemorrhoidectomy [group A], open hours haemorrhoidectomy [group B] and DGHAL [group C]) NS Age: 21 to 61 years Sex: 71% male Patient selection criteria: patients with thrombosis, acute irreducible prolapse, coexisting anorectal disease (such as anal fissure, faecal incontinence or perianal fissure) or pregnancy were excluded. Technique: DGHAL (each procedure was carried out with spinal or general anaesthesia). Follow-up: not reported Conflict of interest/source of funding: not reported At 1st motion range 1 week NS (The difference between group B and groups A and C was significant at each period; p < 0.01.) (the study authors appear to have made an error and reported p > 0.01) Improvement of symptoms Group A Group B Group C p val ue Bleeding 60.0% 73.0% 53.0% NS Prolapse 66.7% 100.0% 60.0% < 0.01 Pain 33.3% 46.7% 53.0% NS Pruritus 20.0% 33.3% 46.7% NS Incontine 100.0% NS nce (Follow-up for these outcomes not stated.) All patients were assessed 12 weeks postoperatively (included symptom questionnaire, measurement of postoperative stenosis and postoperative incontinence, anorectal manometry). Randomisation was through a computergenerated table and put into an envelope for patient selection. Patients were blinded. Patient recruitment not described. Study population issues: There was no significant difference between groups for age, sex or presenting symptoms. Other issues: The authors state that grade IV patients were included in the study but then state that those with irreducible prolapsed haemorrhoids were excluded. It is uncertain IP overview: Haemorrhoidal artery ligation Page 8 of 34
9 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments Functional outcomes (from anorectal manometry) There was no significant difference between anal pressure and rectal volumes between the 3 groups. which criteria they used for staging since irreducible prolapse is a criterion for grade IV according to the Goligher scale. IP overview: Haemorrhoidal artery ligation Page 9 of 34
10 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments Festen S (2009) 9 Number of patients analysed: 41 (23 vs 18) Complications Follow-up issues: Pain Stapled THD RCT This was assessed 1 day and 1 and 3 weeks after the haemorrh The Netherlands procedure on a VAS. oidopexy Bleeding 11% (2)* 4.3% Recruitment period: 2006 to 2007 (1)** Study population: patients with GIII or GIV Stapled THD Difference p haemorrhoids with a history of rubber band haemorr (95% CI) value 5.6% (1) ligation hoidope xy n = 41 (23 THD vs 18 stapled haemorrhoidopexy) VAS (range) Study design issues: Mean age: 50 years Sex: 75% male Patient selection criteria: patients below 18 years, unavailable for follow-up (because of language or residence), inflammatory bowel disease and history of haemorrhoidal or anal surgery were excluded. Technique: THD under general or spinal anaesthesia including additional reefing of mucosa with same suture used for ligation. Follow-up: 6 weeks Conflict of interest/source of funding: not reported Day ( to 2.94) Day ( to 2.62) Day ( to 1.74) (The scale and direction of VAS was not described. According to the discussion, a higher score meant higher pain.) Resolution of symptoms after 6 weeks. Stapled haemorrhoidopexy 83% (15) THD 78.3% (18) (p = 0.648) Of those with continuing symptoms in the stapled haemorrhoidopexy: 1 had persistent anal blood loss treated by haemorrhoidectomy, 2 had persistent prolapse. The 5 patients with persistent problems in the THD group had persistent prolapse. Postop mild bladder dysfunction resolving spontaneous ly in 6 weeks. Soiling 4.3% (1)*** * both patients were treated by intraanal application of a gauze soaked in lidocaine and adrenaline ** treated with haemostatic stitch to control bleeding *** treatment with fibre supplements Patients were assessed for postoperative pain at 1 day and 1, 3 and 6 weeks after the procedure. This was a pilot study. Patient recruitment not described. Randomisation was completed with the use of opaque envelopes (not otherwise described). Blinding not described. Study was performed by 2 experienced surgeons. The size and scale of the VAS was not described. Study population issues: All patients had a history of rubber band ligation. There was no significant difference between groups for age, sex, grade of haemorrhoids, or number of previous rubber band ligations. Other issues: The authors stated that the persistence of prolapse in those treated with the IP overview: Haemorrhoidal artery ligation Page 10 of 34
11 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments stapled procedure is higher than previous reported. They propose that the stapler may have been positioned too high. The authors also suggest the high rate of persistent prolapse (in relation to previous literature) may be due to the high grade of haemorrhoids in study patients. IP overview: Haemorrhoidal artery ligation Page 11 of 34
12 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments Hajdarevic B (2009) 4 Number of patients analysed: 70 (35 vs 35) with 6 arteries Complications Follow-up issues: ligated for each patient on average. Non-randomised trial Bosnia and Herzegovina Recruitment period: not reported Study population: patients who presented at a hospital or private specialists who had confirmed grade II or III haemorrhoids. n = 70 (35 treated by DGHAL [group A] vs 35 control [group B]) Age: not stated Sex: not stated Patient selection criteria: patients with frequent heavy bleeding in at least 4 of the last 12 months, verification with secondary anaemia and previous treatment were included. Technique: DGHAL with the use of a sedative and local anaesthesia. Follow-up: 12 to 13 months Conflict of interest/source of funding: not reported Treatment success This was determined to be successful based on no recurrence of bleeding or prolapse at 12 to 13 months follow-up. % of patients Group A 91.4 (32)* Group B 22.9 (8) * The 3 patients without success had recurrence of bleeding but there was no further description of these patients. Patients deemed to be unsuccessful in the control group were not described. Group A Group B % at 8 days after treatment % at 25 days after treatment 11.4 (4) 2.8 (1) 74.2 (26) 11.4 (4) It is not stated what the complications were, though the authors state that complications usually arose after thrombosis of external haemorrhoids. Postoperative complications were detected at 15-day follow-up examinations. The difference between occurrence of complications 8 days after treatment was statistically significant between the groups (p < 0.01), but the difference after 25 days was not significant. The study stated that patients were examined after 12 to 13 months but did not state if any patients were lost to follow-up. Study design issues: The study was described to be retrospectiveprospective but it was not explicitly explained what this meant. Questionnaires appear to have been sent to patients, but how many questionnaires were sent out or the response rate was not described. The follow-up exam at 12 to 13 months appeared to be performed (including anorectal pressure measurement and an overview of HAL proctoscopy). The comparator procedure was not well described so it is not clear what procedure was performed on these patients. Study population issues: The authors stated that there was no significant difference between age and IP overview: Haemorrhoidal artery ligation Page 12 of 34
13 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments gender between groups but these were not reported. Other issues: This study was not written clearly so was difficult to read. IP overview: Haemorrhoidal artery ligation Page 13 of 34
14 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments Gupta (2008) 8 Number of patients analysed: 616 (4 weeks), 523 (12 Complications Follow-up issues: months) with average 3.12 haemorrhoids ligated for each Complications occurred in 9% (56/616) patient. of patients Case series India Recruitment period: 1997 to 2007 Study population: patients with symptomatic, prolapsing haemorrhoids for mean 6.3 years; GII 76, GIII 441, GIV 99 n = 616 Mean age: Sex: 58.6% male Patient selection criteria: patients with acute thrombosed piles or concurrent anal pathology (such as fistula or fissures) were excluded (some patients with GII were included if they had severe refractory symptoms). Technique: ligation and mucosopexy (no Doppler guidance see comments section); use of general, spinal or local anaesthesia based on decision of anaesthetist Mean follow-up: not stated Conflict of interest/source of funding: no competing interests declared Postoperative pain Mean analgesics required: 14 ± 4 tablets over mean 9 ± 3 days Symptomatic resolution at 4 weeks % with resolution (no.) Bleeding 95.6 (589) Prolapse 98 Pain on 96 defaecation *patient numbers not reported Of the 93% of patients who completed 1-year follow-up, 89 were asymptomatic at 1-year follow-up (total figure of those who completed 1-year follow-up was not reported; 93% of patients is around 523 patients so patients with no symptoms at 1-year follow-up was around 17% [89/523]). Patient satisfaction (n = 523) This was assessed on a 10-cm VAS (10 being most satisfied) at a visit at 12-month follow-up. The mean patient score was 8.2 (based on 93% [probably 523] patients). (the paper this was written as 8.2% which is presumably incorrectly written). Inquiry in 2007 (n = 307) The following results were based on 307 patients treated by May 2006 (485 had been treated by this date but only Perianal thrombosis Bleeding* 4 Pain* 2 Urinary 9 retention Pruritus ani 2 Mucosal 6 prolapse Skin tag 13 Constipation 4 Tenesmus 4 * requiring readmission No. patients 12 93% completed 1-year follow-up (number of patients not reported and reason for loss of follow-up not reported) Postoperative pain was assessed on a VAS by patients at home and they also recorded analgesics used each day for the first 14 days after surgery. Patients were then followed up at 4 weeks, 6 months and 1 year and later if they had complaints. Patients in the study were recruited up until the end of 2007, however, the authors completed an inquiry at the beginning of 2007 which included 485 patients who were treated up until May It was not stated how these patients were contacted. Only 63% (307) of these patients responded. Study design issues: Unlike the other studies in this table, this study did not use Doppler-guidance. The study described the use of artery forceps to retract the haemorrhoidal cushions and visualise the IP overview: Haemorrhoidal artery ligation Page 14 of 34
15 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments 63% [307] responded). haemorrhoids. % with resolution Bleeding and pain during defaecation 94* Prolapse 89** (total number and mean follow-up not reported) *Those who still had bleeding were treated conservatively but some not responding to these measures were treated with band ligation or infrared coagulation (number of patients treated by this means not stated) ** The remaining 11% completed rectal examination. 4% of these had skin tags which the patients considered to be prolapse; all patients were offered a redo procedure (it was not reported how many had another procedure) IP overview: Haemorrhoidal artery ligation Page 15 of 34
16 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments Walega P (2008) 5 Number of patients analysed: 507 with 3 to 7 arteries Follow-up issues: ligated for each patient. Case series Poland and Austria Recruitment period: 2000 to 2006 Study population: patients treated at 2 centres with grades II to IV haemorrhoids (GII 144, GIII 319, GIV 44). n = 507 (308 phase 1 in Austria, 199 phase 2 in Poland) Mean age: 50.1 years (Austria) and 41 years (Poland) Sex: 61% male (Austria) and 65% male (Poland) Patient selection criteria: physical examination confirming stage and medical history which included stinging in anal canal, pruritus, pain and bleeding; those with neoplastic changes in the anal canal were excluded. Technique: DGHAL; first group had sedation and the second group a local anaesthetic with sedation. Follow-up: 1 year Conflict of interest/source of funding: not reported Patient-reported success The following was given by patients at 1-year follow-up: 69.2% (351) had good results (significant symptom relief). 14.8% (75) had acceptable results (the reported success by the other 81 patients was not reported). By grade status group: 92.4% (133/144) of patients with grade II and 84.0% (272/324) of patients with grade III had very good or good results ( very good free of the disease, good when patients had significant symptom relief). Of those with grade IV disease, only 40.9% (18/44) of patients were satisfied with the operation. Effects on symptoms Phase 1 group Phase 2 group Recurrence 15.6% (48) 20.6% (41) Pain on 0.97% (3) 1.0% (2) defaecation Bleeding 5.2% (16) 7.5% (15) The number of patients with each outcome by grade were: Outcome Grade 2 Grade 3 Grade 4 Recurrence Pain on defaecation Bleeding There were no intraoperative or immediate postoperative complications. 18.1% of patients needed analgesics for 1 to 2 days (number of patients not reported) Postoperative complications Compli cation Throm bosis Phase 1 group Phase 2 group 2.9% (9) 4.5% (9) Fistula 0.3% (1) 0% (0) Fissure 1.3% (4) 3.5% (7) Anorectal manometry tests were performed before treatment and at 1, 3 and 12 months after treatment. Completeness of follow-up not reported. Study design issues: This study was complete in two phases: the first in Austria and the second in Poland. The purpose of the study was to determine clinical effectiveness and functional results by anorectal manometry. Study population issues: Some patients may have been included in Scheyer which is in the systematic review 1. In the first group, 23 patients also had fissurectomy, resection of skin tags, and herniorraphies; in the second group, 32 patients also had anorectal folds excised and 4 patients had anal polyp excision. IP overview: Haemorrhoidal artery ligation Page 16 of 34
17 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments Functional outcomes There were no significant differences in basal anal pressure, squeeze pressure or vector volume after the procedure. In 5 patients, a recto-anal inhibitory reflex was observed 1 month after DGHAL. IP overview: Haemorrhoidal artery ligation Page 17 of 34
18 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments Dal Monte PP (2007) 6 Number of patients analysed: 330 There were 23 postoperative Follow-up issues: complications (6.9% complication rate). Case series Italy and UK Recruitment period: 2000 to 2006 Study population: patients with symptomatic grades II, III or IV haemorrhoids (GII 138, GIII 162, GIV 30) presenting with bleeding (212) or prolapse (192). n = 330 Mean age: 52.4 years Sex: 55% male Patient selection criteria: not reported Technique: THD with general anaesthesia in the first patients and spinal anaesthesia (or perineal block) in later patients, depending on patient preference followed by mucosopexy or figure-of-8 stitch. Follow-up: not reported Conflict of interest/source of funding: not reported Return to normal activities In 276 patients, this was 3.5 days on average. Postoperative pain (on VAS 0 being no pain) This was not reported by 150 patients. Of those who reported pain, mean VAS score was 1.32: % of patients Mild pain (VAS < 2) 35.5% (117) Moderate pain (2 < 16.% (54) VAS < 8) Severe pain (VAS > 8) 2.7% (9) Analgesia was not required in 56.4% (186) of patients, needed for no more than 2 days in 38.8% (128) and for up to 7 days in 4.9% (16) of patients. Short-term resolution of symptoms (n = 330, 1 month) Outcome % of patients with resolution Bleeding 91.9% (204/222)* Prolapse 95.8% (184/192)** * Of those who did not respond, 4 were GII, 3 GIII, and 1 GIV; minor oozing was observed from ligation sites in some patients but this stopped once the sutures were absorbed. ** 111 of these patients were treated with anopexy; of those who did not respond, 3 were GIII and 5 GIV. Number of patients Fissure 2 Thrombosis 5 Urinary 2 retention needing catheterisation Submucosal 4 haematoma Haematuria 1 Immediate 4 bleeding* Delayed 3 bleeding** Needle 2 rupture*** * 1 was due to laceration of a rectal polyp when the device was introduced (the patient had refused preoperative colonoscopy). ** 1 required an operation to stop the bleeding. *** needle tip chipped and was left in the submucosa with no consequence Patients were followed up at 1 week, 1 month and 6 months (this involved an interview, physical exam and anoscopy or rectosignoidoscopy). Only 219 patients were followed up for 46 months. Further details were not given. Study population issues: Of the patients treated, 177 had already undergone rubber band ligation (96), sclerotherapy (64), cryotherapy (13), stapled haemorrhoidopexy (2) or open haemorrhoidectomy (2). Other issues: This study is included in the systematic review 1. Use of anaesthetic was general for the first patients. Spinal anaesthesia was also offered to patients later in the series if they preferred it (numbers of patients treated by each not reported). IP overview: Haemorrhoidal artery ligation Page 18 of 34
19 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments Long-term resolution of symptoms (n = 219, 46 months) Of these 100 were GII, 104 were GIII and 15 were GIV. Outcome % of patients with resolution Bleeding 92.9 (132/142)* Prolapse 92.4 (110/119)** * Of those with recurrence of bleeding, 7 patients were GII, 2 were GIII and 1 was GIV. ** Recurrence occurred in 5 patients with GIII and 4 with GIV. Patients also treated with anopexy Of the 219 patients, 63 were treated with running suture anopexy and 56 with a figure-of-8 stitch. Only prolapsed haemorrhoids were treated with anopexy. The relapse rate of those treated with anopexy by grade was: % of patients with running suture (n = 63) % of patients with figure-of-8 stitch (n = 56) GIII 6 (3/50) 3.7 (2/54) GIV 50 (3/6) 11.1 (1/9) (These figures were not statistically significant.) IP overview: Haemorrhoidal artery ligation Page 19 of 34
20 Abbreviations used: CI, confidence interval; DGHAL, Doppler-guided haemorrhoidal artery ligation; GI, grade I; GII, grade II; GIII, grade III; GIV, grade IV; HAL, haemorrhoidal artery ligation; NS, not significant; RCT, randomised controlled trial; THD, transanal haemorrhoidal dearterialisation; VAS, visual analogue scale Study details Key efficacy findings Key safety findings Comments Faucheron J-L (2008) 7 Number of patients analysed: 100 with an average of 8.4 There were 6 early and 6 late Follow-up issues: ligatures placed in each patient. complications (12%). Case series France Recruitment period: 2002 to 2004 Study population: patients with grades II to IV haemorrhoids (GII 1, GIII 78, GIV 21) presenting with bleeding (87) and pain (77) (58 also had skin tags). n = 100 Mean age: 45 years Sex: 46% male Patient selection criteria: patients with thrombosis, uncertain diagnosis, associated infections, anal fissure, pregnancy and less than 18 years old were excluded. Technique: DGHAL with local or spinal anaesthesia. Mean follow-up: 3 years Conflict of interest/source of funding: not reported Return to normal activities 79 patients were discharged and returned to normal activities on the same day as surgery. Recurrence There were 12 recurrences at mean 12.6-month follow-up (7 GIII, 5 GIV). These were treated by DGHAL (1), stapled haemorrhoidopexy (7) or haemorrhoidectomy (4) (recurrence not defined). Early complications Acute fissure (day 9, 10, 15) No. of patient s 3 Bleeding (day 11) 1* Dyschezia (painful 1 (GIV) defaecation) lasting 6 days but not requiring treatment Requirement of 1 analgesia for 4 days * This patient later presented with anal fissure at 11-month follow-up. Late complications No. of patients Anal pain 1 Anal fissure (at 2 8, 11 months) Thrombosis (at 3* 4, 7, 17 months) * These patients were treated with thrombectomy (2) or haemorrhoidectomy (1); all had GIII haemorrhoids and one also had skin tag resection. This was completed at 1 month and 3 years; there was no reported loss to follow-up. Study population issues: 18 had previous surgery (12 sclerosis or rubber band ligation, 4 stapled anopexy, 2 haemorrhoidectomy). 19 patients had simultaneous procedures: fissurectomy (7), skin tags (12). Other issues: The mode of anaesthetic used depended on patient preference (47 pudental block, 47 spinal anaesthesia, 6 general anaesthesia). IP overview: Haemorrhoidal artery ligation Page 20 of 34
21 Efficacy Symptom resolution A systematic review of 17 studies including 1996 patients reported recurrence of bleeding, pain on defaecation and prolapse in 6% (40/638), 4% (35/917) and 8% (50/638) of patients respectively in 9 studies with follow-up of less than 1 year; these figures were 10% (49/507), 9% (18/206) and 11% (46/427) respectively in the 6 studies with follow-up of 1 year or more 1. In general the proportion of patients with preoperative bleeding, pain and prolapse ranged from 45% to 100%, 12% to 83% and 12% to 100% respectively across the studies 1. A case series of 100 patients reported that in the 3 years of follow-up, there were 12 recurrences (7 grade III, 5 grade IV) of haemorrhoids which occurred at a mean of 12.6 months of follow-up 7. A randomised controlled trial (RCT) of 45 patients reported that significantly more patients treated with open haemorroidectomy had an improvement in prolapse symptoms than those treated by staple haemorrhoidectomy and artery ligation (100% vs 67% and 60% respectively; p < 0.01; follow-up not stated) 3. An RCT of 41 patients reported resolution of symptoms in 78% (18/23) of the 23 patients treated with haemorrhoidal ligation and 83% (15/18) of the 18 patients treated with stapled haemorrhoidopexy, but this difference was not significant 9. A non-randomised trial of 70 patients reported that 91% (32/35) of patients treated with Doppler-guided artery ligation had treatment success (with no recurrence of bleeding or prolapse) compared with 23% (8/35) of patients treated with the comparator (not described) at 12 to 13 months of follow-up 4. A case series of 616 patients treated with the procedure without the use of Doppler guidance reported symptom resolution in 96%, 98%, and 96% of patients who presented with bleeding, prolapse, and pain on defaecation, respectively, at 4-week follow-up. A study of the 485 patients treated from 1997 until early 2007 reported that among the 307 patients who responded (63%), 94% had resolution of bleeding or pain on defaecation and 89% had resolution of prolapse (mean follow-up of these patients not reported) 8. A case series of 330 patients reported 93% (132/142) of patients who presented with bleeding and 92% (110/119) of patients who presented with prolapse had a resolution of symptoms at mean 46-month follow-up (80 and 73 patients respectively were lost to follow-up; no reason given). Of those with recurrence of bleeding, 7 patients had grade II, 2 had grade III and 1 had grade IV haemorrhoids. Of those with recurrence of prolapse, 5 patients had grade III and 4 had grade IV haemorrhoids 6. Postoperative pain and recovery period IP overview: Haemorrhoidal artery ligation Page 21 of 34
22 An RCT of 60 patients reported significantly less requirement for analgesics (3 compared with 12 doses) and a faster return to normal activities (no longer requiring help to care for themselves; from 3 to 25 days) in the 30 patients treated with haemorrhoidal artery ligation compared with the 30 patients treated by closed haemorrhoidectomy (p < for both) 2. The RCT of 45 patients reported that the 15 patients treated by artery ligation and the 15 patients treated by stapled haemorrhoidectomy had a significantly better improvement in pain than the 15 patients treated by open haemorrhoidectomy during the first 24 hours after the procedure (measured on a 10-cm visual analogue scale [VAS] with 10 as worst pain; less than 3 in the first 2 groups and 8 in the open group; p > 0.01) 3. The RCT of 41 patients reported lower postoperative pain in the 23 patients treated with haemorrhoidal ligation than the 19 patients treated with stapled haemorrhoidopexy at 3-week follow-up (3.1 versus 5.1 at 1 day and 1.6 to 3.2 at 7 days; a higher number referred to higher pain but the VAS scale was not described). This difference was no longer significant at 6-week follow-up 9. Patient satisfaction The case series of 616 patients reported a mean score of 8.2 (10-cm VAS from 1 to 10; 10 being most satisfied) among the 523 patients who were reported on at 1-year follow-up (reason for loss to follow-up not reported) 8. Of the 507 patients in the case series, 69% (351) considered that they had good results (good symptom relief) and 15% (75) had results they felt were acceptable (remaining 81 patients not reported). Very good (free of disease) or good results were reported in 92% (133/144) and 84% (272/324) of patients with grades II and III haemorrhoids respectively. Only 41% (18/44) of patients with grade IV haemorrhoids were satisfied with the operation 5. Safety The systematic review reported 3 cases of significant postoperative haemorrhaging requiring blood transfusion in 2 patients (the other patient developed coagulopathy and treatment was not further described) 1. An RCT reported significantly more complications in the 30 patients treated with closed scissor haemorrhoidectomy than the 30 treated by artery ligation (p < 0.05). In the closed scissor haemorrhoidectomy group fever, nausea and urinary retention requiring catheterisation were reported in 9, 6 and 1 patient respectively while only 2 patients developed nausea among those treated with artery ligation (all patients with nausea required intravenous fluid replacement) 2. The non-randomised trial of 70 patients reported significantly more complications in those in the control group (not clearly described) than in those treated with artery ligation 8 days after treatment (74% [26/35] versus 11% [4/35]; p < 0.01; IP overview: Haemorrhoidal artery ligation Page 22 of 34
23 complications not described) 4. The difference in complications was no longer significant 25 days after the procedure (11% [4/35] versus 2.8% [1/35]). The case series of 616 patients reported complications in 9% (56/616) of patients including perianal thrombosis (12), bleeding requiring readmission (4), pain requiring readmission (2), urinary retention (9), pruritus ani (or itchiness; 2), mucosal prolapse (6), skin tag (13), constipation (4) and tenesmus (or feeling of incomplete defaecation; 4) 8. The case series of 507 patients reported haemorrhoidal thrombosis (very painful haemorrhoids which may require hospitalisation to manage the pain) (18), fistula (1) and fissure (11) which occurred postoperatively (time of occurrence not reported) 5. The case series of 330 patients reported a 7% (23/330) complication rate (fissure 2, haemorrhoidal thrombosis 5, urinary retention requiring catheterisation 2, submucosal haematoma 4, haematuria 1, immediate bleeding 4 and delayed bleeding 3; time of occurrence not reported) 6. The case series of 100 patients reported 6 early and 6 late complications. 7 The early complications included 3 cases of acute fissure at 9, 10 and 15 days postoperatively, 1 case of bleeding 11 days postoperatively, and 1 case of dyschezia (painful defaecation) lasting 6 days (not requiring treatment). Late complications included 1 case of anal pain, 2 cases of anal fissure at 8 and 11 months postoperatively, and 3 cases of thrombosis 4, 7 and 17 months postoperatively. The patients with thrombosis had grade III haemorrhoids and were treated with thrombectomy (2) or haemorrhoidectomy (1). Validity and generalisability of the studies There were 3 randomised studies (one included in the systematic review). One compared the procedure with closed scissor haemorrhoidectomy, another compared the procedure with both stapled haemorrhoidopexy and open haemorrhoidectomy, and a third compared it with stapled haemorrhoidopexy 2,3,9. A non-randomised trial compared the procedure with a control group but the control treatment was not well defined 4. The remaining studies were case series. The longest follow-up reported in the studies was on 219 patients at 46 months 6 ; another study reported on 100 patients at 36 months (3 years) 7. Most studies include patients with grade II to IV haemorrhoids. Very few patients with grade I haemorrhoids were included. IP overview: Haemorrhoidal artery ligation Page 23 of 34
24 There were a number of non-english publications on the use of this procedure which were identified in the literature but were not included; the conditions that would have required recourse to non-english literature as set out in the Programme s guides were not met. The notifier of the procedure (also the manufacturer) had stated that the procedure is used with general anaesthetic in the UK, but local anaesthetic or sedation is sometimes used for early grades of haemorrhoids in other countries. The variation in the use of anaesthetic in the evidence reflects this. Only 3 studies in table 2 of this overview completed plication or mucopexy after artery ligation 6, 8, 9. A similar procedure, recto-anal repair (RAR ) is also reported in four of the studies in the appendix (Conaghan 2009, Theodoropoulos 2008, Satzinger 2009, and Zagryadskiy 2008). Existing assessments of this procedure There were no published assessments from other organisations identified at the time of the literature search. Related NICE guidance Below is a list of NICE guidance related to this procedure. Appendix B gives details of the recommendations made in each piece of guidance listed. Interventional procedures Circular stapled haemorrhoidectomy. NICE interventional procedures guidance 34 (2003). Available from Technology appraisals Stapled haemorrhoidopexy for the treatment of haemorrhoids. NICE technology appraisal 128 (2007). Available from Specialist Advisers opinions Specialist advice was sought from consultants who have been nominated or ratified by their Specialist Society or Royal College. The advice received is their individual opinion and does not represent the view of the society. IP overview: Haemorrhoidal artery ligation Page 24 of 34
25 Mr Steve Brown, Mr Simon Middleton, Miss Karen Nugent, Mr Graham Williams (Association of Coloproctology of Great Britain and Ireland). Less than 10% of specialists are engaged in this area of work. Surgeons should be trained and mentored by an experienced surgeon. Training should include observation, and, if possible, practice on a bowel or anal model. Comparator procedures include mucosal banding, conventional haemorrhoidectomy or stapled anopexy. Efficacy Key efficacy outcomes include reduction in postoperative pain compared with other treatments, resolution of haemorrhoids, and resolution of symptoms such as bleeding, prolapse, swelling, pain, soreness, itching in the short and long term. One Adviser states that while surgeons have been performing the procedure for up to 5 years, the efficacy is uncertain, particularly in the long term. There are no randomised trials that show that short-term results are maintained in the long term. The published evidence only includes lesser-grade piles and does not compare the procedure with alternatives which would be considered lesser means (such as banding). Safety It appears to be as safe as conventional surgery and potentially has fewer risks than banding or haemorrhoidectomy. Anal fissure, external anal thrombosis, pain and bleeding were reported as anecdotal adverse events. Theoretical adverse events include rectal perforation, pelvic abscess, stenosis, haemorrhage, infection, acute and chronic pain, urinary retention, faecal incontinence, and complications associated with general anaesthesia. Patient Commentators opinions NICE s Patient and Public Involvement Programme was unable to obtain patient commentary for this procedure. IP overview: Haemorrhoidal artery ligation Page 25 of 34
26 Issues for consideration by IPAC A publication on the use of stapled haemorrhoidopexy (the other minimally invasive technique for this condition) reported a broken condom in a homosexual patient. Since THD does not involve the use of staples, it may be of significant benefit and of less risk of a safety event than stapled haemorrhoidopexy. IP overview: Haemorrhoidal artery ligation Page 26 of 34
27 References 1. Giordano P, Overton J, Madeddu F et al. (2009) Transanal hemorrhoidal dearterialization: a systematic review. Diseases of the Colon and Rectum 52: Bursics A, Morvay K, Kupcsulik P et al. (2004) Comparison of early and 1- year follow-up results of conventional hemorrhoidectomy and hemorrhoid artery ligation: a randomized study. International Journal of Colorectal Disease 19: Khafagy W, El NA, Fouda E et al. (2009) Conventional haemorrhoidectomy, stapled haemorrhoidectomy, Doppler guided haemorrhoidectomy artery ligation; post operative pain and anorectal manometric assessment. Hepato-Gastroenterology 56: Hajdarevic B, Slaku J, Pandza H et al. (2009) Application of simple digital methods in the treatment of hemorrhoid disease. Studies in Health Technology and Informatics 150: Walega P, Scheyer M, Kenig J et al. (2008) Two-center experience in the treatment of hemorrhoidal disease using Doppler-guided hemorrhoidal artery ligation: functional results after 1-year follow-up. Surgical Endoscopy 22: Dal Monte PP, Tagariello C, Giordano P et al. (2007) Transanal haemorrhoidal dearterialisation: nonexcisional surgery for the treatment of haemorrhoidal disease. Techniques in Coloproctology 11: Faucheron J-L, Gangner Y. (2008) Doppler-guided hemorrhoidal artery ligation for the treatment of symptomatic hemorrhoids: Early and threeyear follow-up results in 100 consecutive patients. Diseases of the Colon and Rectum 51: Gupta PJ, Kalaskar S. (2008) Ligation and mucosopexy for prolapsing haemorrhoids a ten year experience. Annals of Surgical Innovation and Research 2: Festen S, van Hoogstraten MJ, van Geloven AAW et al. (2009) Treatment of grade III and IV haemorrhoidal disease with PPH or THD. A randomised trial on postoperative complication and short-term results. International journal of colorectal disease 24: IP overview: Haemorrhoidal artery ligation Page 27 of 34
28 Appendix A: Additional papers on haemorrhoidal artery ligation The following table outlines the studies that are considered potentially relevant to the overview but were not included in the main data extraction table (table 2). It is by no means an exhaustive list of potentially relevant studies. IP overview: Haemorrhoidal artery ligation Page 28 of 34
29 Article Number of patients/follow-up Case series n = 35 Follow-up = 18 months Direction of conclusions 91.5% (11/12) success in those with pain, 85% (28/33) in those with bleeding, 93% (14/15) in those with pruritis, 92% (12/13) in those with discharge and 81% (17/21) in those with prolapse. 12 had recurrence (6 with prolapsed and 6 with bleeding) and were subsequently treated with haemorrhoidectomy (1) or the same procedure with rectoanal repair (11). Reasons for noninclusion in table 2 Studies with more patients and longer follow-up in table 2. Abdeldaim Y, Mabadeje O, Muhammad KM et al. (2007) Doppler-guided haemorrhoidal arteries ligation: preliminary clinical experience. Irish Medical Journal 100: Conaghan P, Farouk R. (2009) Doppler-guided hemorrhoid artery ligation reduces the need for conventional hemorrhoid surgery in patients who fail rubber band ligation treatment. Diseases of the Colon and Rectum 52: Felice G, Privitera A, Ellul E et al. (2005) Doppler-guided hemorrhoidal artery ligation: an alternative to hemorrhoidectomy. Diseases of the Colon and Rectum 48: Gehlen JMLG, van Gemert WG, de Haan MW et al. (2007) Severe anal bleeding in Proteus syndrome: A case report. Techniques in Coloproctology 11: Greenberg R, Karin E, Avital S et al. (2006) First 100 cases with Doppler-guided hemorrhoidal artery ligation. Diseases of the Colon and Rectum 49: Case series n = 52 Follow-up = 18 months Studies with more patients and longer follow-up in table 2. Case series n = 68 Follow-up = 11 months Resolution of bleeding in 91%, of pain in 73% and of prolapse in 94%. Studies with more patients and longer follow-up in table 2. Case report n = 1 Description of a patient with proteus syndrome treated with this procedure. Studies with more patients and longer follow-up in table 2. Case series n = 100 Follow-up = 12 months Mean pain decreased from 2.1 postoperatively to 1.3 one day later. 94 patients remained asymptomatic at 6 months (4 required additional surgical excision and 2 required rubber band ligation). 78% (50/64) of patients with prolapse successfully treated (96% [50/52] and 96% [92/96] of patients with pain and bleeding were successfully treated). Studies with more patients and longer follow-up in table 2. Morinaga K, Hasuda K, Ikeda T. (1995) A novel therapy for internal hemorrhoids: ligation of the hemorrhoidal artery with a newly devised instrument (Moricorn) in conjunction with a Doppler flowmeter. American Journal of Gastroenterology 90: Case series n = 116 Follow-up = not stated (presumably postoperative) Studies with more patients and longer follow-up in table 2. IP overview: Haemorrhoidal artery ligation Page 29 of 34
30 Ramirez JM, Aguilella V, Elia M et al. (2005) Doppler-guided hemorrhoidal artery ligation in the management of symptomatic hemorrhoids. Revista Espanola de Enfermedades Digestivas 97: Satzinger U, Feil W, Glaser K. (2009) Recto anal repair (RAR): a viable new treatment option for high-grade hemorrhoids. One year results of a prospective study. Pelviperineology 28: Case series n = 32 Follow-up = 1 year 19 patients free from symptoms at 1 year and 6 with significant symptom relief (failed in patients with grades III or IV). Studies with more patients and longer follow-up in table 2. Case series n = 83 with grade III and IV haemorrhoids Follow-up = up to 12 months Bleeding resolved in 89%, itching in 95%, burning sensation in 100% and soiling in 100%. No prolapse at 12 months in 89%; 5 had recurrent prolapse 3 were considered de novo prolapse. Patient satisfaction >90% at all points of follow-up. Average of 6 ligatures placed; recurrence in 15.6 % (48/308) of patients: fissure in 1.3% (4), thrombosis in 2.9% (9), and fistula, proctitis and stool retention in 1 patient each (0.3%). Resolution of bleeding in 88%, of protrusion in 92% and of pain in 71%. Unsuccessful in 2 (3%). Studies with more patients and longer follow-up in table 2. Scheyer M, Antonietti E, Rollinger G et al. (2006) Doppler-guided hemorrhoidal artery ligation. American Journal of Surgery 191: Case series n = 308 Follow-up = 18 months Same patients as reported in Walega (2008). Sohn N, Aronoff JS, Cohen FS et al. (2001) Transanal hemorrhoidal dearterialization is an alternative to operative hemorrhoidectomy. American Journal of Surgery 182: Theodoroupoulos G, Sevrisarianos N, Papaconstantinou J et al. (2008) Dopplerguided haemorrhoidal artery ligation (DGHAL), rectoanal repair (RAR), sutured haemorrhoidopexy (SHP) and minimal mucocutaneous excision (MMCE) for grade III-IV haemorrhoids: A multicentre prospective study of safety and efficacy. Colorectal disease. Nov 14 pub ahead of print. Case series n = 60 Follow-up = 5 to 12 months Studies with more patients and longer follow-up in table 2. Case series n = 147 Follow-up = 15 months More ligations required for patients with grade IV (52) than III (95), 43 patients required sutured haemorrhoidopexy and rectoanal repair; 23 had mucocutaneous excision 96% asymptomatic at follow-up and 95% satisfied. No analgesia required by 30%, 31%, 16%, and 14% of patients on day 1-3, 4-7, and > 7, respectively. Complications: residual prolapse (10), bleeding (15), thrombosis (4), fissure (3), fistula (1). Studies with more patients and longer follow-up in table 2. IP overview: Haemorrhoidal artery ligation Page 30 of 34
31 Wallis de Vries BM, van der Beek ES, de Wijkerslooth LR et al. (2007) Treatment of grade 2 and 3 hemorrhoids with Doppler-guided hemorrhoidal artery ligation. Digestive Surgery 24: Wilkerson PM, Strbac M, Reece-Smith H et al. (2009) Doppler-guided haemorrhoidal artery ligation: long-term outcome and patient satisfaction. Colorectal Disease 11: Zagryadskiy EA, Gorelov SI. (2008) Transanal doppler-guided hemorrhoidal artery ligation/recto anal repair (HAL-RAR ) for treatment of Grade 3-4 hemorrhoids: a new mini-invasive technology. Pelviperineology 27: Case series n = 110 Follow-up = 37 weeks 88% (97/110) had significant improvement at 6 weeks, 84.5% (93/110) were satisfied at 37 weeks. Studies with more patients and longer follow-up in table 2. Case series n = 113 Follow-up = 30 months 90% (93/103) had complete or significant relief at 6 weeks and 86% (77/90) at 30 months. Studies with more patients and longer follow-up in table 2. Case series n = 85 with grade III-IV symptomatic haemorrhoids (treated with both haemorrhoidal arterial ligation and recto-anal repair) Mean follow-up = 10 months Postoperative discomfort on a VAS was 33.2 mm on the first day, and 16.5 mm after 5 days (preoperative value not given). Bleeding resolved in 96.5% (82), prolapse resolved in 91.8% (78). Thrombosis in 7 patients and fever in 3. Studies with more patients and longer follow-up in table 2. IP overview: Haemorrhoidal artery ligation Page 31 of 34
32 Appendix B: Related NICE guidance for haemorrhoidal artery ligation Guidance Interventional procedures Technology appraisals Recommendations Circular stapled haemorrhoidectomy. NICE interventional procedures guidance 34 (2003) 1.1 Current evidence on the safety and efficacy of circular stapled haemorrhoidectomy appears adequate to support the use of the procedure, provided that normal arrangements are in place for consent, audit and clinical governance. 1.2 Clinicians wishing to learn circular stapled haemorrhoidectomy should be trained, mentored and monitored, as described in the Association of Coloproctology s consensus document on the procedure (see the Association s website: Stapled haemorrhoidopexy for the treatment of haemorrhoids. NICE technology appraisal 128 (2007) This technology appraisal examined the currently available devices for stapled haemorrhoidopexy. The evidence considered refers to the HCS33 circular stapler (models PPH01 and PPH03, Ethicon Endo-Surgery). At the time of the technology appraisal, there was no evidence to make recommendations for the Autosuture stapler with the STRAM kit adaptor. 1.1 Stapled haemorrhoidopexy, using a circular stapler specifically developed for haemorrhoidopexy, is recommended as an option for people in whom surgical intervention is considered appropriate for the treatment of prolapsed internal haemorrhoids. IP overview: Haemorrhoidal artery ligation Page 32 of 34
33 Appendix C: Literature search for haemorrhoidal artery ligation Database Date searched Version/files Cochrane Database of 11/02/2010 Issue 4, 2009 Systematic Reviews CDSR (Cochrane Library) Database of Abstracts of 11/02/ Reviews of Effects DARE (CRD website) HTA database (CRD website) 11/02/ Cochrane Central Database of 11/02/2010 Issue 4, 2009 Controlled Trials CENTRAL (Cochrane Library) MEDLINE (Ovid) 11/02/ to December Week MEDLINE In-Process (Ovid) 11/02/2010 January 8, 2010 EMBASE (Ovid) 11/02/ to 2010 Week 01 CINAHL (NLH Search 11/02/ present 2.0/EBSCOhost) Zetoc 13/01/ The following search strategy was used to identify papers in MEDLINE. A similar strategy was used to identify papers in other databases. 1 exp Hemorrhoids/ 2 Hemorrhoid*.tw. 3 Haemorrhoid*.tw. 4 ((Intern* or Extern* or prolaps*) adj3 (hemorrhoid* or haemorrhoid* or pile*)).tw. 5 pile*.tw. 6 or/1-5 7 Dearteriali?at*.tw. 8 THD.tw. 9 Transan* Haemorrhoid* dearterialis*.tw. 10 Transan* Hemorrhoid* dearterialis*.tw. 11 Transan* Hemorrhoid* dearterializ*.tw. 12 Transan* Haemorrhoid* dearterializ*.tw. 13 (THD adj3 Doppler*).tw. 14 (transanal* adj5 (hemmor* or haemorrhoid*)).tw. 15 (transan* adj3 doppler*).tw. 16 (Transan* adj3 doppler* Guid*).tw. 17 (Doppler*- Guid* adj3 Transan*).tw. 18 Ligation/ 19 ligatio*.tw. 20 Ultrasonography, Doppler/ 21 (Ultrasonograp* adj3 Doppler*).tw. IP overview: Haemorrhoidal artery ligation Page 33 of 34
34 22 or/ and 6 24 Animals/ not Humans/ not from 25 keep IP overview: Haemorrhoidal artery ligation Page 34 of 34
Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients
 Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients What are Haemorrhoids? Haemorrhoids (piles) are enlarged blood vessels around the anus (back passage). There are two types of haemorrhoids:
Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients What are Haemorrhoids? Haemorrhoids (piles) are enlarged blood vessels around the anus (back passage). There are two types of haemorrhoids:
NHS. Surgical repair of vaginal wall prolapse using mesh. National Institute for Health and Clinical Excellence. 1 Guidance.
 Issue date: June 2008 NHS National Institute for Health and Clinical Excellence Surgical repair of vaginal wall prolapse using mesh 1 Guidance 1.1 The evidence suggests that surgical repair of vaginal
Issue date: June 2008 NHS National Institute for Health and Clinical Excellence Surgical repair of vaginal wall prolapse using mesh 1 Guidance 1.1 The evidence suggests that surgical repair of vaginal
DG-RAR for the treatment of symptomatic grade III and grade IV haemorrhoids: a 12-month multi-centre, prospective observational study
 Eur Surg DOI 10.1007/s10353-012-0182-8 DG-RAR for the treatment of symptomatic grade III and grade IV haemorrhoids: a 12-month multi-centre, prospective observational study S. Roka, D. Gold, P. Walega,
Eur Surg DOI 10.1007/s10353-012-0182-8 DG-RAR for the treatment of symptomatic grade III and grade IV haemorrhoids: a 12-month multi-centre, prospective observational study S. Roka, D. Gold, P. Walega,
WHAT ARE HEMORRHOIDS?
 Patient information regarding care and surgery associated with HEMORRHOIDS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia Stefanou, M.D. location: Michigan Heart & Vascular Institute, 5325
Patient information regarding care and surgery associated with HEMORRHOIDS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia Stefanou, M.D. location: Michigan Heart & Vascular Institute, 5325
Prevention and Recognition of Obstetric Fistula Training Package. Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula
 Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Perianal Abscess and Fistula-in-ano. Background
 Perianal Abscess and Fistula-in-ano Background Anorectal abscesses are some of the more common anorectal conditions encountered, and they are potentially debilitating conditions. The current theory as
Perianal Abscess and Fistula-in-ano Background Anorectal abscesses are some of the more common anorectal conditions encountered, and they are potentially debilitating conditions. The current theory as
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE
 279 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of division of ankyloglossia (tongue-tie) in babies with difficulty breastfeeding Introduction
279 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of division of ankyloglossia (tongue-tie) in babies with difficulty breastfeeding Introduction
PREPARING FOR YOUR STOMA REVERSAL
 PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
Women s Health. The TVT procedure. Information for patients
 Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
Women s Health The TVT procedure Information for patients What is a TVT procedure? A TVT (Tension-free Vaginal Tape) procedure is an operation to help women with stress incontinence the leakage of urine
UNDERSTANDING THE PROCEDURE FOR PROLAPSE AND HEMORRHOIDS
 UNDERSTANDING THE PROCEDURE FOR PROLAPSE AND HEMORRHOIDS AN ALTERNATIVE APPROACH TO THE SURGICAL TREATMENT OF HEMORRHOIDS pphinfo.com Identifying Patients for PPH Procedure for Prolapse and Hemorrhoids
UNDERSTANDING THE PROCEDURE FOR PROLAPSE AND HEMORRHOIDS AN ALTERNATIVE APPROACH TO THE SURGICAL TREATMENT OF HEMORRHOIDS pphinfo.com Identifying Patients for PPH Procedure for Prolapse and Hemorrhoids
Direct Current Therapy for Treatment of Hemorrhoids
 Direct Current Therapy for Treatment of Hemorrhoids [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr Go to Comunicados a Proveedores, and click Cartas
Direct Current Therapy for Treatment of Hemorrhoids [For the list of services and procedures that need preauthorization, please refer to www.mcs.com.pr Go to Comunicados a Proveedores, and click Cartas
Recto Anal Repair (RAR): a viable new treatment option for high-grade hemorrhoids. One year results of a prospective study
 Original article Recto Anal Repair (RAR): a viable new treatment option for high-grade hemorrhoids. One year results of a prospective study ULRIKE SATZINGER (*) - WOLFGANG FEIL (**) - KARL GLASER (***)
Original article Recto Anal Repair (RAR): a viable new treatment option for high-grade hemorrhoids. One year results of a prospective study ULRIKE SATZINGER (*) - WOLFGANG FEIL (**) - KARL GLASER (***)
TRANSVAGINAL MESH IN PELVIC ORGAN PROLAPSE REPAIR.
 TRANSVAGINAL MESH IN PELVIC ORGAN PROLAPSE REPAIR. Spanish full text SUMMARY Introduction: Pelvic organ prolapse (POP) is characterised by the descent or herniation of the uterus, vaginal vault, bladder
TRANSVAGINAL MESH IN PELVIC ORGAN PROLAPSE REPAIR. Spanish full text SUMMARY Introduction: Pelvic organ prolapse (POP) is characterised by the descent or herniation of the uterus, vaginal vault, bladder
Treatment of grade III and IV haemorrhoidal disease with PPH or THD. A randomized trial on postoperative complications and short-term results
 Treatment of grade III and IV haemorrhoidal disease with PPH or THD. A randomized trial on postoperative complications and short-term results Authors: Sebastiaan Festen & M. J. Van Hoogstraten & A. A.
Treatment of grade III and IV haemorrhoidal disease with PPH or THD. A randomized trial on postoperative complications and short-term results Authors: Sebastiaan Festen & M. J. Van Hoogstraten & A. A.
VAGINAL MESH FAQ. How do you decide who should get mesh as part of their repair?
 VAGINAL MESH FAQ How do you decide who should get mesh as part of their repair? Each patient with pelvic organ prolapse (POP) is considered individually. In younger women, women with an uncomplicated prolapse
VAGINAL MESH FAQ How do you decide who should get mesh as part of their repair? Each patient with pelvic organ prolapse (POP) is considered individually. In younger women, women with an uncomplicated prolapse
Hemorrhoids and Varicose Veins: A Review of Treatment Options Alternative Medicine Review, April, 2001 by Douglas MacKay
 Hemorrhoids and Varicose Veins: A Review of Treatment Options Alternative Medicine Review, April, 2001 by Douglas MacKay Abstract Hemorrhoids and varicose veins are common conditions seen by general practitioners.
Hemorrhoids and Varicose Veins: A Review of Treatment Options Alternative Medicine Review, April, 2001 by Douglas MacKay Abstract Hemorrhoids and varicose veins are common conditions seen by general practitioners.
HAVING AN ENDOSCOPIC MUCOSAL RESECTION (EMR)
 HAVING AN ENDOSCOPIC MUCOSAL RESECTION (EMR) Information Leaflet Your Health. Our Priority. Page 2 of 6 Having an EMR Previous tests have shown that you have a polyp in your large bowel (colon). Your doctor
HAVING AN ENDOSCOPIC MUCOSAL RESECTION (EMR) Information Leaflet Your Health. Our Priority. Page 2 of 6 Having an EMR Previous tests have shown that you have a polyp in your large bowel (colon). Your doctor
Hemorrhoids Dearterialization Doppler. Keywords Laser
 DOI 10.1007/s00464-010-1370-x Doppler-guided hemorrhoidal laser procedure for the treatment of symptomatic hemorrhoids: experimental background and short-term clinical results of a new mini-invasive treatment
DOI 10.1007/s00464-010-1370-x Doppler-guided hemorrhoidal laser procedure for the treatment of symptomatic hemorrhoids: experimental background and short-term clinical results of a new mini-invasive treatment
Chief Investigator: Steven Brown, Sheffield Teaching Hospitals NHS Foundation Trust
 A multi-centre randomised controlled trial comparing rubber band ligation with haemorrhoidal artery ligation in the management of symptomatic second and third degree haemorrhoids. Version 8.0; 4 th June
A multi-centre randomised controlled trial comparing rubber band ligation with haemorrhoidal artery ligation in the management of symptomatic second and third degree haemorrhoids. Version 8.0; 4 th June
Anal Surgery. Colon and Rectal Surgery. Surgery of the Anus. Hemorrhoids Fistula Fissure Abscess
 Anal Surgery and Colon and Rectal Surgery Elizabeth J. McConnell MD FACS FASCRS Surgery of the Anus Hemorrhoids Fistula Fissure Abscess 1 Hemorrhoid Internal or External 1-3 columns Internal Band or Suture
Anal Surgery and Colon and Rectal Surgery Elizabeth J. McConnell MD FACS FASCRS Surgery of the Anus Hemorrhoids Fistula Fissure Abscess 1 Hemorrhoid Internal or External 1-3 columns Internal Band or Suture
Information for patients having Total Laparoscopic Hysterectomy (TLH)
 1 TOTAL LAPAROSCOPIC HYSTERECTOMY LEAFLET (For patients, relatives and hospital personnel) Information for patients having Total Laparoscopic Hysterectomy (TLH) You have been given this information sheet
1 TOTAL LAPAROSCOPIC HYSTERECTOMY LEAFLET (For patients, relatives and hospital personnel) Information for patients having Total Laparoscopic Hysterectomy (TLH) You have been given this information sheet
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence. Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center
 The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center Constipation Overview Constipation Normal Transit Constipation
The Work Up of Pelvic Floor Dyssynergia and Fecal Incontinence Gina R. Sam, MD/MPH Director, Mount Sinai Gastrointestinal Motility Center Constipation Overview Constipation Normal Transit Constipation
Colonoscopy Data Collection Form
 Identifier: Sociodemographic Information Type: Zip Code: Gender: Height: (inches) Race: Ethnicity Inpatient Outpatient Male Female Birth Date: Weight: (pounds) American Indian (Native American) or Alaska
Identifier: Sociodemographic Information Type: Zip Code: Gender: Height: (inches) Race: Ethnicity Inpatient Outpatient Male Female Birth Date: Weight: (pounds) American Indian (Native American) or Alaska
Uterine Fibroid Symptoms, Diagnosis and Treatment
 Fibroids and IR Uterine Fibroid Symptoms, Diagnosis and Treatment Interventional radiologists use MRIs to determine if fibroids can be embolised, detect alternate causes for the symptoms and rule out misdiagnosis,
Fibroids and IR Uterine Fibroid Symptoms, Diagnosis and Treatment Interventional radiologists use MRIs to determine if fibroids can be embolised, detect alternate causes for the symptoms and rule out misdiagnosis,
Femoral Hernia Repair
 Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Varicose Veins Operation. Patient information Leaflet
 Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
Varicose Veins Operation Patient information Leaflet 22 nd August 2014 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the
YALE UNIVERSITY SCHOOL OF MEDICINE: SECTION OF OTOLARYNGOLOGY PATIENT INFORMATION FUNCTIONAL ENDOSCOPIC SINUS SURGERY
 YALE UNIVERSITY SCHOOL OF MEDICINE: SECTION OF OTOLARYNGOLOGY PATIENT INFORMATION FUNCTIONAL ENDOSCOPIC SINUS SURGERY What is functional endoscopic sinus surgery (FESS)? Functional endoscopic sinus surgery
YALE UNIVERSITY SCHOOL OF MEDICINE: SECTION OF OTOLARYNGOLOGY PATIENT INFORMATION FUNCTIONAL ENDOSCOPIC SINUS SURGERY What is functional endoscopic sinus surgery (FESS)? Functional endoscopic sinus surgery
Anorectal Abscess and Fistula
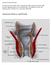 Anorectal Abscess/Fistula by: Robert K Cleary MD, John C Eggenberger MD, Amalia J Stefanou, MD location: Michigan Heart & Vascular Institute, 5325 Elliott Dr, Suite 104 mailing address: PO Box 974, Ann
Anorectal Abscess/Fistula by: Robert K Cleary MD, John C Eggenberger MD, Amalia J Stefanou, MD location: Michigan Heart & Vascular Institute, 5325 Elliott Dr, Suite 104 mailing address: PO Box 974, Ann
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions
 Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Inguinal Hernia (Female)
 Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Guide to Abdominal or Gastroenterological Surgery Claims
 What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
How common is bowel cancer?
 information Primary Care Society for Gastroenterology Bowel Cancer (1 of 6) How common is bowel cancer? Each year 35,000 people in Britain are diagnosed with cancer of the bowel, that is to say cancer
information Primary Care Society for Gastroenterology Bowel Cancer (1 of 6) How common is bowel cancer? Each year 35,000 people in Britain are diagnosed with cancer of the bowel, that is to say cancer
Excision or Open Biopsy of a Breast Lump Your Operation Explained
 Excision or Open Biopsy of a Breast Lump Your Operation Explained Patient Information Introduction This leaflet tells you about the procedure known as excision or open biopsy of a breast lump. It explains
Excision or Open Biopsy of a Breast Lump Your Operation Explained Patient Information Introduction This leaflet tells you about the procedure known as excision or open biopsy of a breast lump. It explains
Beaumont Hospital. Varicose Veins. and their TREATMENT. Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM
 Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
Beaumont Hospital Varicose Veins and their TREATMENT Professor Austin Leahy, MCh, FRCS, FRCSI WWW.VEINCLINICSOFIRELAND.COM Department of Surgery Beaumont Hospital and Royal College of Surgeons in Ireland
1.6 Spider naevi These are skin blood vessels which have become enlarged to form spidery red blobs in the skin. They can be cauterised away.
 MINOR SURGERY 1 MINOR SKIN CONDITIONS...1 1.1 Skin tags...1 1.2 Moles...2 1.3 Warts...2 1.4 Sebaceous cysts...3 1.5 Lipomas...4 1.6 Spider naevi...4 1.7 Basal Cell Carcinomas (rodent ulcers or BCCs)...4
MINOR SURGERY 1 MINOR SKIN CONDITIONS...1 1.1 Skin tags...1 1.2 Moles...2 1.3 Warts...2 1.4 Sebaceous cysts...3 1.5 Lipomas...4 1.6 Spider naevi...4 1.7 Basal Cell Carcinomas (rodent ulcers or BCCs)...4
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Epidurals for pain relief after surgery
 Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
Epidurals for pain relief after surgery This information leaflet is for anyone who may benefit from an epidural for pain relief after surgery. We hope it will help you to ask questions and direct you to
An operation for stress incontinence Tension-free Vaginal Tape (TVT)
 Saint Mary s Hospital The Warrell Unit An operation for stress incontinence Tension-free Vaginal Tape (TVT) Information for Patients 1 Stress Incontinence Stress incontinence is a leakage of urine occurring
Saint Mary s Hospital The Warrell Unit An operation for stress incontinence Tension-free Vaginal Tape (TVT) Information for Patients 1 Stress Incontinence Stress incontinence is a leakage of urine occurring
Billing Guideline. Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16
 Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
An operation for prolapse Sacrospinous Fixation Sacrospinous Hysteropexy
 Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Sacrospinous Fixation Sacrospinous Hysteropexy Information For Patients 1 What is a prolapse? Prolapse is a bulge or lump
Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Sacrospinous Fixation Sacrospinous Hysteropexy Information For Patients 1 What is a prolapse? Prolapse is a bulge or lump
SUPRAPUBIC CATHETER INSERTION INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] INFORMATION
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] INFORMATION
Vaginal prolapse repair surgery with mesh
 Vaginal prolapse repair surgery with mesh Your doctor has recommended a vaginal reconstructive procedure using mesh to treat your condition. The operation involves surgery to reattach the vagina to its
Vaginal prolapse repair surgery with mesh Your doctor has recommended a vaginal reconstructive procedure using mesh to treat your condition. The operation involves surgery to reattach the vagina to its
What is an Anal Fissure?
 Patient information regarding care and surgery associated with ANAL FISSURE by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Patient information regarding care and surgery associated with ANAL FISSURE by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Surgery for Stress Incontinence
 Directorate of Women s Services Surgery for Stress Incontinence Tension Free Vaginal Tape Information for Patients Direct dial number Ward 40 0191 282 5640 Stress Incontinence Stress incontinence is a
Directorate of Women s Services Surgery for Stress Incontinence Tension Free Vaginal Tape Information for Patients Direct dial number Ward 40 0191 282 5640 Stress Incontinence Stress incontinence is a
NHS Greater Glasgow and Clyde Yorkhill Hospital CONSTIPATION IN CHILDREN
 NHS Greater Glasgow and Clyde Yorkhill Hospital CONSTIPATION IN CHILDREN Constipation in Children Version: 1 Page 1 of 8 Background Constipation is a common complaint in infants and children. The aetiology
NHS Greater Glasgow and Clyde Yorkhill Hospital CONSTIPATION IN CHILDREN Constipation in Children Version: 1 Page 1 of 8 Background Constipation is a common complaint in infants and children. The aetiology
Periurethral bulking agent for stress urinary incontinence (macroplastique)
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Who is this leaflet for? This leaflet provides information about having an injection
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label Who is this leaflet for? This leaflet provides information about having an injection
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
However, each person may be managed in a different way as bowel pattern is different in each person.
 Department of colorectal surgery Reversal of ileostomy A guide for patients Introduction This booklet is designed to tell you about your reversal of ileostomy operation and how your bowels might work after
Department of colorectal surgery Reversal of ileostomy A guide for patients Introduction This booklet is designed to tell you about your reversal of ileostomy operation and how your bowels might work after
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
Laparoscopic Surgery for Inguinal Hernia Repair
 Laparoscopic Surgery for Inguinal Hernia Repair What is an Inguinal Hernia Repair? 2 What is a Laparoscopic Inguinal Hernia Repair? 2 Are there any alternatives to Laparoscopic Hernia Repair? 3 Am I a
Laparoscopic Surgery for Inguinal Hernia Repair What is an Inguinal Hernia Repair? 2 What is a Laparoscopic Inguinal Hernia Repair? 2 Are there any alternatives to Laparoscopic Hernia Repair? 3 Am I a
Treating your enlarged prostate gland HoLEP (holmium laser enucleation of the prostate)
 Treating your enlarged prostate gland HoLEP (holmium laser enucleation of the prostate) This leaflet is designed to answer any questions you may have about having holmium laser treatment for your enlarged
Treating your enlarged prostate gland HoLEP (holmium laser enucleation of the prostate) This leaflet is designed to answer any questions you may have about having holmium laser treatment for your enlarged
Information and advice following placement of seton for anal fistula
 Oxford University Hospitals NHS Trust Information and advice following placement of seton for anal fistula page 2 What is a fistula? You can get an anal fistula as a result of an infection or a collection
Oxford University Hospitals NHS Trust Information and advice following placement of seton for anal fistula page 2 What is a fistula? You can get an anal fistula as a result of an infection or a collection
Spigelian Hernia Repair
 Spigelian Hernia Repair WHAT IS A SPIGELIAN HERNIA? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 2 SPIGELIAN HERNIA REPAIR 3 WHAT ARE
Spigelian Hernia Repair WHAT IS A SPIGELIAN HERNIA? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 2 SPIGELIAN HERNIA REPAIR 3 WHAT ARE
Vaginal Repair- with Mesh A. Interpreter / cultural needs B. Condition and treatment C. Risks of a vaginal repair- with mesh
 The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from [email protected] DO NOT WRITE IN THIS BINDING MARGIN v2.00-03/2011 SW9226 Facility: A. Interpreter
The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from [email protected] DO NOT WRITE IN THIS BINDING MARGIN v2.00-03/2011 SW9226 Facility: A. Interpreter
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
2.0 Synopsis. Vicodin CR (ABT-712) M05-765 Clinical Study Report R&D/07/095. (For National Authority Use Only) to Part of Dossier: Volume:
 2.0 Synopsis Abbott Laboratories Name of Study Drug: Vicodin CR Name of Active Ingredient: Hydrocodone/Acetaminophen Extended Release (ABT-712) Individual Study Table Referring to Part of Dossier: Volume:
2.0 Synopsis Abbott Laboratories Name of Study Drug: Vicodin CR Name of Active Ingredient: Hydrocodone/Acetaminophen Extended Release (ABT-712) Individual Study Table Referring to Part of Dossier: Volume:
There are many different types of cancer and sometimes cancer is diagnosed when in fact you are not suffering from the disease at all.
 About Cancer Cancer is a disease where there is a disturbance in the normal pattern of cell replacement. The cells mutate and become abnormal or grow uncontrollably. Not all tumours are cancerous (i.e.
About Cancer Cancer is a disease where there is a disturbance in the normal pattern of cell replacement. The cells mutate and become abnormal or grow uncontrollably. Not all tumours are cancerous (i.e.
Patient Information. Lumbar Spine Segmental Decompression. Royal Devon and Exeter NHS Foundation Trust
 Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
Lumbar Spine Segmental Decompression Royal Devon and Exeter NHS Foundation Trust Patient Information Lumbar Spine Segmental Decompression Reference Number: TO 05 004 004 (version date: June 2015) Introduction
Having an Endoscopic Mucosal Resection (EMR)
 Having an Endoscopic Mucosal Resection (EMR) Patient Information Author ID: N Prasad Leaflet Number: End 011 Name of Leaflet: Having an Endoscopic Mucosal Resection (EMR) Date Produced: March 2014 Review
Having an Endoscopic Mucosal Resection (EMR) Patient Information Author ID: N Prasad Leaflet Number: End 011 Name of Leaflet: Having an Endoscopic Mucosal Resection (EMR) Date Produced: March 2014 Review
QS114. NICE quality standard for irritable bowel syndrome in adults (QS114)
 NICE quality standard for irritable bowel syndrome in adults (QS114) QS114 NICE approved the reproduction of its content for this booklet. The production of this booklet is sponsored by Thermo Fisher Scientific,
NICE quality standard for irritable bowel syndrome in adults (QS114) QS114 NICE approved the reproduction of its content for this booklet. The production of this booklet is sponsored by Thermo Fisher Scientific,
Epigastric Hernia Repair
 Epigastric Hernia Repair WHAT IS EPIGASTRIC HERNIA REPAIR? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 3 EPIGASTRIC HERNIA REPAIR 3 WHAT
Epigastric Hernia Repair WHAT IS EPIGASTRIC HERNIA REPAIR? 2 WHAT CAUSES IT? 2 WHAT DOES TREATMENT/MANAGEMENT INVOLVE? 2 WHAT WOULD HAPPEN IF THE HERNIA WAS NOT TREATED? 3 EPIGASTRIC HERNIA REPAIR 3 WHAT
Lymph Node Dissection for Penile Cancer
 Lymph Node Dissection for Penile Cancer Exceptional healthcare, personally delivered Removal of Lymph Nodes Why are the Lymph Nodes so important when I have penile cancer? Lymph nodes are small bean shaped
Lymph Node Dissection for Penile Cancer Exceptional healthcare, personally delivered Removal of Lymph Nodes Why are the Lymph Nodes so important when I have penile cancer? Lymph nodes are small bean shaped
X-Plain Abdominal Aortic Aneurysm Vascular Surgery Reference Summary
 X-Plain Abdominal Aortic Aneurysm Vascular Surgery Reference Summary Ballooning of the aorta, also known as an "abdominal aortic aneurysm," can lead to life threatening bleeding. Doctors may recommend
X-Plain Abdominal Aortic Aneurysm Vascular Surgery Reference Summary Ballooning of the aorta, also known as an "abdominal aortic aneurysm," can lead to life threatening bleeding. Doctors may recommend
Fissure-in-Ano and Treatment
 FISSURE PHYSIOLOGY: Fissure-in-Ano and Treatment Written By: David B. Rosenfeld, M.D., F.A.C.S., F.A.S.C.R.S. 2650 Jones Way #25 Simi Valley, CA 93065 Office (805) 579-8972 Fax (805) 579-9784 A fissure
FISSURE PHYSIOLOGY: Fissure-in-Ano and Treatment Written By: David B. Rosenfeld, M.D., F.A.C.S., F.A.S.C.R.S. 2650 Jones Way #25 Simi Valley, CA 93065 Office (805) 579-8972 Fax (805) 579-9784 A fissure
GUIDELINE Sinusitis. David M. Poetker MD, MA Associate Professor. Division of Rhinology and Sinus Surgery
 GUIDELINE Sinusitis David M. Poetker MD, MA Associate Professor Division of Rhinology and Sinus Surgery Guideline Fokkens et al. The European Position Paper on Rhinosinusitis and Nasal Polyps 2012. Rhinology.
GUIDELINE Sinusitis David M. Poetker MD, MA Associate Professor Division of Rhinology and Sinus Surgery Guideline Fokkens et al. The European Position Paper on Rhinosinusitis and Nasal Polyps 2012. Rhinology.
PROCEDURE- SPECIFIC INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
Your spinal Anaesthetic
 Your spinal Anaesthetic Information for patients Your spinal anaesthetic This information leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients,
Your spinal Anaesthetic Information for patients Your spinal anaesthetic This information leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients,
Laparoscopic Repair of Hernias. A simple guide to help answer your questions
 Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Catheter insertion of a new aortic valve to treat aortic stenosis
 Issue date March 2012 Understanding NICE guidance Information for people who use NHS services NICE interventional procedures guidance advises the NHS on when and how new procedures can be used in clinical
Issue date March 2012 Understanding NICE guidance Information for people who use NHS services NICE interventional procedures guidance advises the NHS on when and how new procedures can be used in clinical
Peter C. Ambe 1,2* and Dirk R. Wassenberg 2
 Ambe and Wassenberg Patient Safety in Surgery (2015) 9:36 DOI 10.1186/s13037-015-0081-6 RESEARCH Proctitis after stapled hemorrhoidopexy is an underestimated complication of a widely used surgical procedure:
Ambe and Wassenberg Patient Safety in Surgery (2015) 9:36 DOI 10.1186/s13037-015-0081-6 RESEARCH Proctitis after stapled hemorrhoidopexy is an underestimated complication of a widely used surgical procedure:
An operation for prolapse Colpocleisis
 Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Colpocleisis Information for Patients What is a prolapse? A prolapse is a bulge or lump in the vagina caused by sagging
Saint Mary s Hospital Gynaecology Service Warrell Unit An operation for prolapse Colpocleisis Information for Patients What is a prolapse? A prolapse is a bulge or lump in the vagina caused by sagging
Transanal Hemorrhoid Dearterialization and mucopexy: a minimal invasive approach for prolapsed hemorrhoids. Four cases report.
 Transanal Hemorrhoid Dearterialization and mucopexy: a minimal invasive approach for prolapsed hemorrhoids. Four cases report. Stefan Morarasu*,1, Emmanuel Eguare 2, Yasir Bashir 2, Qurat ul Ain 2, Anca
Transanal Hemorrhoid Dearterialization and mucopexy: a minimal invasive approach for prolapsed hemorrhoids. Four cases report. Stefan Morarasu*,1, Emmanuel Eguare 2, Yasir Bashir 2, Qurat ul Ain 2, Anca
Hemorrhoidectomy with LigaSure Small Jaw and Stapled Hemorrhoidopexy with EEA Hemorrhoid and Prolapse Stapler with DST
 Hemorrhoidectomy with LigaSure Small Jaw and Stapled Hemorrhoidopexy with EEA Hemorrhoid and Prolapse Stapler with DST Dr. Wong Kutt Sing MBBS (S pore), FRCS (Edin), FRCS (Glas), FAMS General Surgery Raffles
Hemorrhoidectomy with LigaSure Small Jaw and Stapled Hemorrhoidopexy with EEA Hemorrhoid and Prolapse Stapler with DST Dr. Wong Kutt Sing MBBS (S pore), FRCS (Edin), FRCS (Glas), FAMS General Surgery Raffles
Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence
 Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence This leaflet explains more about tension-free vaginal tape (TVT) including the benefits, risks and any alternatives, and
Having a tension-free vaginal tape (TVT) operation for stress urinary incontinence This leaflet explains more about tension-free vaginal tape (TVT) including the benefits, risks and any alternatives, and
Promoting recovery after sustaining a third and fourth degree tear
 Promoting recovery after sustaining a third and fourth degree tear Women s Health Physiotherapy Patient Information Page 2 Promoting recovery after sustaining a third and fourth degree tears What has happened?
Promoting recovery after sustaining a third and fourth degree tear Women s Health Physiotherapy Patient Information Page 2 Promoting recovery after sustaining a third and fourth degree tears What has happened?
Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology
 Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind
Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind
Post-operative Pain Management
 Post-operative Pain Management Total Hip Replacement www.ormc.org A member of the Greater Hudson Valley Health System Post-operative Pain MANAGEMENT Post-operative pain management after total joint replacement
Post-operative Pain Management Total Hip Replacement www.ormc.org A member of the Greater Hudson Valley Health System Post-operative Pain MANAGEMENT Post-operative pain management after total joint replacement
Get the Facts, Be Informed, Make YOUR Best Decision. Pelvic Organ Prolapse
 Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
LOWER GASTROINTESTINAL BLEEDING GED/05/08
 LOWER GASTROINTESTINAL BLEEDING GED/05/08 LOWER GI-BLEEDING SEARCH FOR SOURCES Epidemiological prerequisites and differential diagnosis Techniques for detection of bleeding sources Practical approach GED/05/44
LOWER GASTROINTESTINAL BLEEDING GED/05/08 LOWER GI-BLEEDING SEARCH FOR SOURCES Epidemiological prerequisites and differential diagnosis Techniques for detection of bleeding sources Practical approach GED/05/44
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
INTERVENTIONAL PROCEDURES PROGRAMME
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of radical laparoscopic hysterectomy for early stage cervical cancer Introduction This overview
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of radical laparoscopic hysterectomy for early stage cervical cancer Introduction This overview
SACROSPINOUS FIXATION
 SACROSPINOUS FIXATION Information Leaflet Your Health. Our Priority. Page 2 of 9 What is a vaginal vault prolapse? The vagina is held in position by the body's natural supporting structures. A vaginal
SACROSPINOUS FIXATION Information Leaflet Your Health. Our Priority. Page 2 of 9 What is a vaginal vault prolapse? The vagina is held in position by the body's natural supporting structures. A vaginal
Is co2 laser Hemorrhoidectomy superior to conventional open Hemorrhoidectomy?
 Is co2 laser Hemorrhoidectomy superior to conventional open Hemorrhoidectomy? *Sa`ad H Sultan M.B.Ch.B,D.S,CABS **Zuhair B Kamal M.B.Ch.B,CABS ***Mohammad A Al-Atroshi M.B.Ch.B,CABS ****Raysan Al-Fayadh
Is co2 laser Hemorrhoidectomy superior to conventional open Hemorrhoidectomy? *Sa`ad H Sultan M.B.Ch.B,D.S,CABS **Zuhair B Kamal M.B.Ch.B,CABS ***Mohammad A Al-Atroshi M.B.Ch.B,CABS ****Raysan Al-Fayadh
Fistulectomy versus fistulotomy with marsupialisation in the treatment of low fistula-inano: a prospective randomized controlled trial
 Fistulectomy versus fistulotomy with marsupialisation in the treatment of low fistula-inano: a prospective randomized controlled trial PHILLIPO L. CHALYA * and JOSEPH B. MABULA Department of Surgery, Catholic
Fistulectomy versus fistulotomy with marsupialisation in the treatment of low fistula-inano: a prospective randomized controlled trial PHILLIPO L. CHALYA * and JOSEPH B. MABULA Department of Surgery, Catholic
What should I expect before the procedure?
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E- mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk [email protected] PROCEDURE-
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND
 RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
Chapter 6 Gastrointestinal Impairment
 Chapter 6 Gastrointestinal This chapter consists of 2 parts: Part 6.1 Diseases of the digestive system Part 6.2 Abdominal wall hernias and obesity PART 6.1: DISEASES OF THE DIGESTIVE SYSTEM Diseases of
Chapter 6 Gastrointestinal This chapter consists of 2 parts: Part 6.1 Diseases of the digestive system Part 6.2 Abdominal wall hernias and obesity PART 6.1: DISEASES OF THE DIGESTIVE SYSTEM Diseases of
Information for you Abortion care
 Information for you Abortion care Published in February 2012 This information is for you if you are considering having an abortion. It tells you: how you can access abortion services the care you can expect
Information for you Abortion care Published in February 2012 This information is for you if you are considering having an abortion. It tells you: how you can access abortion services the care you can expect
Endoscopic Plantar Fasciotomy
 Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Laparoscopic Hysterectomy
 Any further questions? Please contact the matron for Women s Health on 020 7288 5161 (answerphone) Monday - Thursday 9am - 5pm. For more information: Royal College of Obstetrics and Gynaecology Recovering
Any further questions? Please contact the matron for Women s Health on 020 7288 5161 (answerphone) Monday - Thursday 9am - 5pm. For more information: Royal College of Obstetrics and Gynaecology Recovering
Acute pelvic inflammatory disease: tests and treatment
 Acute pelvic inflammatory disease: tests and treatment Information for you Information for you Published August 2010 Published in August 2010 (next review date: 2014) Acute What is pelvic inflammatory
Acute pelvic inflammatory disease: tests and treatment Information for you Information for you Published August 2010 Published in August 2010 (next review date: 2014) Acute What is pelvic inflammatory
