Patient information regarding care and surgery associated with ULCERATIVE COLITIS
|
|
|
- Kristina Brown
- 7 years ago
- Views:
Transcription
1 Patient information regarding care and surgery associated with ULCERATIVE COLITIS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou, M.D. location: Michigan Heart & Vascular Institute, 5325 Elliott Dr., Suite 104 mailing address: P.O. Box 974, Ann Arbor, MI Ulcerative Colitis Ulcerative colitis is an inflammation of the lining of the colon of unknown etiology. It always involves the rectum and often involves the colon to a variable degree. It almost never involves the small bowel and stomach which makes ulcerative colitis different than Crohn s disease. Some patients have minimal symptoms and are well controlled with medications. At least 1/3 of patients with ulcerative colitis develop severe symptoms that may ultimately require surgery. Ulcerative colitis can cause colon cancer in those who have had the disease for longer than 7-10 years. Therefore, surveillance with colonoscopy is indicated for patients with this disease. About the Colon and Rectum The colon and rectum is about 5 feet long. Food passes through the stomach, then the small bowel, then the colon, and finally the rectum and anus. The small bowel is feet and is largely responsible for absorption of nutrients and vitamins in food. The colon absorbs water but the small bowel can assume this function in the absence of the colon. In fact, there are several diseases that require removal of the entire colon and rectum (like Ulcerative Colitis). These patients generally lead normal lives and do not develop malnutrition because their small bowel is intact. Removing a portion or all of the colon and rectum may result in diarrhea, urgency, or gas/stool leakage but usually not.
2 Symptoms Symptoms of ulcerative colitis include rectal bleeding, bloody diarrhea, and abdominal cramps. Patients may also have weight loss, fever, and other symptoms. Many patients have mild or moderate forms of the disease which may be readily controlled with medications. Others have more severe symptoms that warrant admission to the hospital. Surgery may be necessary if the disease is not able to be controlled with medication. About 40% of patients have disease limited to the rectum and left colon. Another 40% have disease of the entire colon and rectum. Other diseases result in symptoms that may mimic ulcerative colitis and include irritable bowel syndrome (IBS), ischemic colitis, infectious colitis, Crohn s disease, antibiotic-associated (C difficile) colitis, and others. Medical Treatment Ulcerative colitis is usually treated with medicines initially. These medications include azulfidine, cipro, metronidazole, mesalamine, prednisone, imuran, cyclosporine, infliximab, and others. Patients on these medications are usually managed by an internist or
3 gastroenterologist. These medications may be required for a long period of time. Steroids, including prednisone, have significant side effects, would may preclude long term use. Surgery may be indicated for patients who have life threatening complications of ulcerative colitis like excessive bleeding, perforation (rare), or fulminant colitis causing fever, decrease in blood pressure, high heart rate, dehydration, or other more urgent symptoms. Surgery may also be indicated in patients with ulcerative colitis not responsive to medical management, intractable symptoms, or biopsies at colonoscopy suggesting a premalignant or malignant condition. At the Time of Your Visit When you are seen by the colorectal specialist, you will be asked several questions with respect to your history. If you have had blood tests, x-rays, colonoscopy, ultrasound, and CT scans, make sure these are made available to your colorectal specialist prior to your visit. Some of these tests may be ordered by the colorectal specialist if they have not already been done. A general examination to include heart, lungs, and abdomen will likely be performed. Following this examination, if enough information is available, a detailed discussion with your colorectal specialist regarding treatment options will follow. If your operation involves the possibility of a colostomy or ileostomy, you should have an appointment with the enterostomal nurse prior to surgery. She will provide important information regarding life with a stoma, educate you regarding any nuances, and may mark an optimum site on your abdominal skin. At the time your surgery is scheduled, you may be asked to have preprocedure testing which may include blood tests, a chest xray, and an EKG. You may also be instructed in a mechanical bowel prep which will clean out your colon in preparation for surgery and is described below. Surgical Treatment Options 1) Proctocolectomy and Ileostomy This operation involves removing the entire colon, rectum, and anus. It requires a midline abdominal incision to remove the colon and a separate incision at the anus to remove the rectum and anus. This operation also requires a permanent ileostomy (bag constructed from small bowel). This operation was, at one time, the most common operation performed for ulcerative colitis. It cures the intestinal phase of the disease because ulcerative colitis does not occur in the small bowel and stomach. Because all nutrients are absorbed in the small bowel, patients can lead normal lives after the removal of the entire colon and rectum with intact nutrition. Because of the advent of the pelvic pouch procedure (see below), this operation is not as commonly performed for this disease today. The most common indications for this operation today are:
4 1) poor sphincter muscles or nerves with inability to control bowel movements 2) concomitant rectal cancer 3) patient preference This operation can sometimes be done while sparing the anal sphincter muscles and lowermost rectum in patients who want to be considered for a pelvic pouch in the future. However, if the pelvic pouch is not ultimately performed in this circumstance, a second operation to remove the remaining rectum and anus may be necessary. 2) Subtotal Colectomy This operation is performed by removing the colon and connecting the small bowel to the rectum. Since ulcerative colitis almost always involves the rectum, this operation is rarely used for this disease. The advantage is that the rectum remains and there is no colostomy but the disadvantage is that the remaining rectum is at risk for persistent ulcerative colitis and cancer. A significant percentage of patients with this operation subsequently need another operation to remove the rectum due to poor functional results (stool urgency and leakage), persistent ulcerative colitis, or the development of cancer in the rectum. 3) Restorative Proctocolectomy with Ileoanal J Pouch (Pelvic Pouch) The ileoanal J pouch is the most commonly utilized operation for ulcerative colitis today. It involves the removal of the entire colon and most of the rectum. The anal canal and, sometimes, the lowermost rectum are preserved. A new rectum is constructed from the end of the small bowel and stapled or sutured to the lowermost rectum or top of the anal canal. Therefore intestinal continuity is preserved without the need for a permanent ileostomy. However, the vast majority of the time, a temporary loop ileostomy is constructed to divert
5 the fecal stream for 3 months allowing the new rectum (ileoanal pouch) to heal without the fecal stream going by it. Should the pouch develop a leak, the temporary ileostomy prevents the fecal stream from contaminating the leak and, therefore, decreases the risk for sepsis. The temporary ileostomy also allows the patient to recover from a major abdominal operation without having to deal with frequent bowel movements immediately after surgery. This temporary ileostomy is then returned to the abdomen 3 months after surgery. This is another operation that requires another anesthetic but can almost always be done through a smaller incision around the ileostomy (rather than through the midline incision), and is associated with a quicker recovery time. Time may be needed to adjust to bowel movement frequency after ileostomy takedown. Most patients have 5-7 BMs per 24 hours. About 25-50% require slowing medications (Imodium or Lomotil) to have acceptable bowel movement frequencies. About 10-20% have some leakage at night during sleep requiring the use of a perineal pad. A small number of patients develop inflammation of the lowermost rectum after this operation requiring topical medications. Up to 10% of patients ultimately require pouch excision due to septic complications or poor functional results in which case a permanent ileostomy will be necessary. Therefore, at least 90% of patients go back to school or work and have normal or near normal lifestyles without a permanent ileostomy. 4) Subtotal Colectomy and Ileostomy Some patients with ulcerative colitis present quite ill, are hospitalized, and do not respond to medical treatment. Those patients who are operated on under more urgent conditions may not be candidates for a definitive operation at that time. Often, under these circumstances, the patient will be taken to the operating room at which time the entire colon will be removed, an ileostomy constructed, and the remaining rectum is closed and left in the pelvis. This allows the patient time to recover from the systemic and sometimes life threatening effects of fulminant colitis. Once the patient has recovered, he or she may then be a candidate for a pelvic pouch procedure several months later under healthier circumstances. 5) Continent Ileostomy A continent ileostomy is essentially a pouch placed on the abdominal wall instead of the pelvis. Because the abdominal wall does not have sphincter muscles to control bowel movements, the operation also involves creating a nipple valve and collar to provide this control. This operation is an option for patients who have had a proctocolectomy and permanent ileostomy or have poor anal sphincter muscle function but want to control their bowel movements. The operation is much more complicated than the pelvic pouch and requires more staple and suture lines, which along with the nuances of the nipple valve and collar, make it an operation at increased risk for complications and need for reoperation. Perhaps for these reasons, the operation is not performed as often as in the past, especially with the advent of the pelvic pouch.
6 Preparation for Operation Those patients who are not operated on emergently may be asked to drink a solution that clears the colon and rectum of stool. This preparation is usually done at home the day prior to surgery. You may be asked to take antibiotics by mouth every hour for 3 doses after completing the mechanical bowel preparation. You will be asked not to eat or drink anything after midnight prior to surgery but you may take your medications with a sip of water. You will be asked to arrive at the hospital several hours prior to the scheduled surgery time. Upon arrival you will meet the nursing staff who will ask you historical questions and prepare you. You will meet the anesthesiologist who will explain anesthetic options. The vast majority of our patients have an epidural or abdominal wall anesthetic in addition to a general anesthetic. The epidural catheter is left in your back (well secured) for about 4 days after surgery as it is the best method to obtain pain control without many of the mental cloudy side effects. You will be expected to walk with or without assistance the day after surgery. We expect you to feel comfortable especially if you have an epidural or abdominal wall catheter in place. You will likely start on liquids within 2-3 days after surgery and will be eating regular food prior to discharge from the hospital. If you have an ileostomy or colostomy, an enterostomal nurse will visit you and educate and instruct you with regard to care of the stoma. The most suitable operations will be discussed with you in detail at the time of your office visit. The operation is typically done through a midline (up and down) incision. If you are a candidate for a minimally invasive procedure (laparoscopic or robot), you should read our Minimally Invasive Surgery handout. You will likely have a catheter in your bladder placed at the time of surgery. You may or may not have a tube placed in your nose to your stomach at the time of surgery. Options and risks will be discussed at length at the time of your office visit. If anything is not clear or if you have questions, you should ask your colorectal specialist during this office visit. Risks of Surgery Our hope and expectation is that you have uncomplicated surgery and a successful outcome. This is not always predictable, however, and something that cannot be guaranteed. The risks of surgery for ulcerative colitis include 1) bleeding 2) infection a. abdominal wound or intra-abdominal infection or abscess 3) *anastomotic leak (suture or staple line leak)
7 a. may require antibiotics, longer hospitalization, drainage with CT scan guidance, or another surgery to resolve b. may require temporary or permanent colostomy or ileostomy c. may result in death from sepsis (rare) 4) abscess a. may require antibiotics, longer hospitalization, drainage with CT scan guidance, or another surgery to resolve 5) increased bowel movement frequency 6) *bowel movement leakage 7) *bowel movement urgency 8) injury to ureter a. structure than carries urine from kidneys to bladder 9) injury to other bowel, spleen, or blood vessels injury to spleen may require removal and lead to increased risk for infection 10) injury to or dysfunction of urinary bladder 11) bowel obstruction a. usually from adhesions from surgery b. can occur in 10-20% of patients c. may require another operation 12) ileus a. the bowels normally stop working for a few days after surgery. If the bowels continue not to function after this, it is referred to as an ileus 13) sexual dysfunction a. impotence or retrograde ejaculation in men (rare) b. depends on age and level of rectal dissection c. pain with intercourse in women 14) possible temporary or permanent colostomy (bag) or ileostomy a. implies use of appliance on abdominal wall to collect stool from the bowel 15) stoma complications a. those patients with ileostomy or colostomy b. retraction, ischemia (poor blood supply), hernia, prolapse 16) possible need to abandon pouch intraoperative findings may require that pouch be abandoned a) pouch may not reach lower rectum (4-6%)
8 b) possible discovery of Crohn s disease c) other findings 17) general operative complications a. heart attack : especially those with heart history b. pneumonia c. sepsis d. blood clot in leg e. blood clot from leg to lung (can be life threatening) f. urinary tract infection g. leg nerve injuries (result of retractors or leg stirrups: rare) 18) incisional hernia a. may require operation to repair 19) *anastomotic stricture a. may result in constipation (unusual) b. may require dilation through scope to repair c. may require operation to repair 20) nonhealing perineal wounds and persistent sinuses a. some patients who require removal of the anus may have a wound that takes a long time to heal or never heals (rare) 21) possible death * does not apply to patients with proctocolectomy and ileostomy because there is no anastomosis (staple or suture line connection) and the stool is completely diverted In addition to the above risks, those patients who have a pelvic pouch procedure are at risk for 1) pouch sinuses and fistulas may sometimes result in loss of the pouch 2) pouch fistula to vagina may sometimes result in loss of the pouch 3) pouchitis inflammation of pouch that often resolves with antibiotics but rarely may result in loss of the pouch 4) dehydration any patient with an ileostomy may develop dehydration or need medications to slow down the gastrointestinal tract
9 5) short bowel syndrome very rarely, a patient who has a failed pouch resulting in its removal may develop nutritional depletion to the point of requiring intravenous nutrition 6) pouch ischemia poor blood supply to pouch 7) Crohn s disease Some patients who are thought to have ulcerative colitis subsequently are found to have Crohn s disease. These patients are at increased risk for pouch inflammation, pouch complications, loss of the pouch, and short bowel syndrome 8) pouch prolapse rare complication that may be difficult to treat without loss of pouch 9) pouch excision may occur in up to 10% of patients who have pelvic pouch usually due to infectious complications like leaks and fistulas described above, but may also be due to poor functional results with frequent bowel movements and incontinence (stool leakage) After Surgery After major abdominal surgery, expect to be in the hospital 4-8 days. Some patients are ready for discharge as early as 4 days after surgery. Some may remain longer than 8 days if the bowels are slow to recover or if a complication develops. The specimen removed at the time of surgery is sent to the pathologist who examines it. About 4 working days (not including Saturday and Sunday) after surgery, a pathology report will be generated. Your colorectal surgeon will review this report with you and discuss its implications. After Discharge Prior to discharge from the hospital, you will receive oral and typewritten discharge instructions. If you have an abdominal incision you should not lift anything greater than 10 pounds for 6 weeks from your surgery date. Unless otherwise instructed, you may eat a regular diet, walk, and climb stairs. You should not drive until at least your first office visit at which time you will be further instructed. You may ride in a car. You should call our office
10 ( ) if you develop a fever > degrees and should take your temperature at least 4 times a day. You should also call for nausea, vomiting, problems with the incision including unusual pain, redness, warmth, swelling, separation of skin or underlying tissues, constipation or diarrhea, or other problems that you feel need to be addressed. If you develop chest pain or shortness of breath or leg swelling, you should call your primary physician or our office or come to the emergency room. If you feel it is an emergency, call 911. Most patients take 6 weeks off from work after having abdominal surgery. You may feel more tired than usual. You may take naps more frequently than usual. Do not be alarmed if you feel fatigued and are not your old self for about 6 weeks after surgery. Colorectal Cancer Screening Those individuals without risk factors for colorectal cancer (rectal bleeding, positive family history of colon cancer) should be screened for colon cancer starting at age 50 years. There are several options which include testing stool for blood, flexible sigmoidoscopy, and colonoscopy. You should discuss the most appropriate option with your primary care physician or colorectal specialist. If you have rectal bleeding, colorectal cancer screening may be warranted at an earlier age depending on other factors involved. If you have a first degree relative with colorectal cancer, you should have colonoscopy starting at age 40 years or 10 years prior to the age of the youngest relative with colorectal cancer. The test should be repeated every 3 to 5 years if normal and possibly sooner if polyps are found. Others at risk for colorectal cancer that warrant further investigation are those with a history of inflammatory bowel disease (ulcerative colitis and Crohn s disease) and possibly those with other cancers (breast, uterus, ovary). At this time, many colorectal specialists advocate 2 colonoscopies 10 years apart starting at age 50 for those without other risk factors. Again, you should discuss these options with your colorectal specialist. Websites For additional information try the American Society of Colon and Rectal Surgeons at and
Colon Cancer. About the Colon and Rectum. Symptoms. Colorectal Cancer Screening
 Patient information regarding care and surgery associated with COLON CANCER by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Patient information regarding care and surgery associated with COLON CANCER by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Understanding Laparoscopic Colorectal Surgery
 Understanding Laparoscopic Colorectal Surgery University Colon & Rectal Surgery A Problem with Your Colon Your doctor has told you that you have a colon problem. Now you ve learned that surgery is needed
Understanding Laparoscopic Colorectal Surgery University Colon & Rectal Surgery A Problem with Your Colon Your doctor has told you that you have a colon problem. Now you ve learned that surgery is needed
Total Abdominal Hysterectomy
 What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Total Vaginal Hysterectomy
 What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
What is a total vaginal hysterectomy? Is the removal of the uterus and cervix through the vagina. Removal of the ovaries and tubes depends on the patient. Why is this surgery used? To treat disease of
Total Vaginal Hysterectomy with an Anterior and Posterior Repair
 Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions
 Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place.
 What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
What is an abdominal myomectomy? Surgical removal of fibroids through an abdominal incision-either up and down or bikini cut. The uterus and cervix are left in place. When is this surgery used? Treatment
Complications that may occur with ulcerative colitis:
 Ulcerative Colitis What is ulcerative colitis? Ulcerative colitis is one of the major forms of inflammatory bowel disease. The other major form is Crohn s disease. Ulcerative colitis is felt to be due
Ulcerative Colitis What is ulcerative colitis? Ulcerative colitis is one of the major forms of inflammatory bowel disease. The other major form is Crohn s disease. Ulcerative colitis is felt to be due
Recto-vaginal Fistula Repair
 What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
What is a recto-vaginal fistula repair? Rectovaginal fistula repair is a procedure in which the healthy tissue between the rectum and vagina is closed in multiple tissue layers. An incision is made either
PREPARING FOR YOUR STOMA REVERSAL
 PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
PREPARING FOR YOUR STOMA REVERSAL Information Leaflet Your Health. Our Priority. Page 2 of 6 Introduction- What you need to know As part of your bowel operation you may have had a temporary stoma formed.
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
Bowel Control Problems
 Bowel Control Problems WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Bowel control problems affect at least 1 million people in the United States. Loss of normal control of the bowels is
Bowel Control Problems WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Bowel control problems affect at least 1 million people in the United States. Loss of normal control of the bowels is
Subtotal Colectomy. Delivering the best in care. UHB is a no smoking Trust
 Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
Subtotal Colectomy Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm This leaflet
Hysteroscopy. What is a hysteroscopy? When is this surgery used? How do I prepare for surgery?
 What is a hysteroscopy? This is a procedure where a doctor uses a thin tube with a tiny camera to look inside the uterus. There are no incisions. Saline solution is used to expand the uterus in order to
What is a hysteroscopy? This is a procedure where a doctor uses a thin tube with a tiny camera to look inside the uterus. There are no incisions. Saline solution is used to expand the uterus in order to
Guide to Abdominal or Gastroenterological Surgery Claims
 What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
What are the steps towards abdominal surgery? Investigation and Diagnosis It is very important that all necessary tests are undertaken to investigate the patient s symptoms appropriately and an accurate
Colorectal Cancer Care A Cancer Care Map for Patients
 Colorectal Cancer Care A Cancer Care Map for Patients Understanding the process of care that a patient goes through in the diagnosis and treatment of colorectal cancer in BC. Colorectal Cancer Care Map
Colorectal Cancer Care A Cancer Care Map for Patients Understanding the process of care that a patient goes through in the diagnosis and treatment of colorectal cancer in BC. Colorectal Cancer Care Map
X-Plain Inguinal Hernia Repair Reference Summary
 X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
Laparoscopic Bilateral Salpingo-Oophorectomy
 Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
Laparoscopic Bilateral Salpingo-Oophorectomy What is a? This is a surgery where your doctor uses a thin, lighted camera and small surgical tool placed through a small (1/2 inch) incision usually in the
X-Plain Abdominal Aortic Aneurysm Vascular Surgery Reference Summary
 X-Plain Abdominal Aortic Aneurysm Vascular Surgery Reference Summary Ballooning of the aorta, also known as an "abdominal aortic aneurysm," can lead to life threatening bleeding. Doctors may recommend
X-Plain Abdominal Aortic Aneurysm Vascular Surgery Reference Summary Ballooning of the aorta, also known as an "abdominal aortic aneurysm," can lead to life threatening bleeding. Doctors may recommend
PREOPERATIVE INSTRUCTIONS FOR COLON AND RECTAL SURGERY
 PREOPERATIVE INSTRUCTIONS FOR COLON AND RECTAL SURGERY University Colon & Rectal Surgery Removal of a portion of the small bowel, colon, or rectum is a major operation. After a period of hospitalization
PREOPERATIVE INSTRUCTIONS FOR COLON AND RECTAL SURGERY University Colon & Rectal Surgery Removal of a portion of the small bowel, colon, or rectum is a major operation. After a period of hospitalization
Colon and Rectal Cancer
 Colon and Rectal Cancer What is colon or rectal cancer? Colon or rectal cancer is the growth of abnormal cells in your large intestine, which is also called the large bowel. The colon is the last 5 feet
Colon and Rectal Cancer What is colon or rectal cancer? Colon or rectal cancer is the growth of abnormal cells in your large intestine, which is also called the large bowel. The colon is the last 5 feet
ANTERIOR RESECTION YOUR OPERATION EXPLAINED
 ANTERIOR RESECTION YOUR OPERATION EXPLAINED Information Leaflet Your Health. Our Priority. Page 2 of 10 Introduction This leaflet explains the procedure known as an Anterior Resection. It includes what
ANTERIOR RESECTION YOUR OPERATION EXPLAINED Information Leaflet Your Health. Our Priority. Page 2 of 10 Introduction This leaflet explains the procedure known as an Anterior Resection. It includes what
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES
 Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
Anorectal Abscess and Fistula
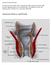 Anorectal Abscess/Fistula by: Robert K Cleary MD, John C Eggenberger MD, Amalia J Stefanou, MD location: Michigan Heart & Vascular Institute, 5325 Elliott Dr, Suite 104 mailing address: PO Box 974, Ann
Anorectal Abscess/Fistula by: Robert K Cleary MD, John C Eggenberger MD, Amalia J Stefanou, MD location: Michigan Heart & Vascular Institute, 5325 Elliott Dr, Suite 104 mailing address: PO Box 974, Ann
Vaginal Repair- with Mesh A. Interpreter / cultural needs B. Condition and treatment C. Risks of a vaginal repair- with mesh
 The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v2.00-03/2011 SW9226 Facility: A. Interpreter
The State of Queensland (Queensland Health), 2011 Permission to reproduce should be sought from ip_officer@health.qld.gov.au DO NOT WRITE IN THIS BINDING MARGIN v2.00-03/2011 SW9226 Facility: A. Interpreter
What is an Anal Fissure?
 Patient information regarding care and surgery associated with ANAL FISSURE by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Patient information regarding care and surgery associated with ANAL FISSURE by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Hysterectomy. What is a hysterectomy? Why is hysterectomy done? Are there alternatives to hysterectomy?
 ROBERT LEVITT, MD JESSICA BERGER-WEISS, MD ADRIENNE POTTS, MD HARTAJ POWELL, MD, MPH COURTNEY LEVENSON, MD LAUREN BURNS, MSN, RN, WHNP OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is
ROBERT LEVITT, MD JESSICA BERGER-WEISS, MD ADRIENNE POTTS, MD HARTAJ POWELL, MD, MPH COURTNEY LEVENSON, MD LAUREN BURNS, MSN, RN, WHNP OBGYNCWC.COM What is a hysterectomy? Hysterectomy Hysterectomy is
Sleeve Gastrectomy Surgery & Follow Up Care
 Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Are any artificial parts used in the ACE Malone surgery?
 ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
Prevention and Recognition of Obstetric Fistula Training Package. Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula
 Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Crohn s Disease. What I need to know about. U.S. Department of Health and Human Services
 What I need to know about Crohn s Disease NATIONAL INSTITUTES OF HEALTH National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services What I need to know about Crohn
What I need to know about Crohn s Disease NATIONAL INSTITUTES OF HEALTH National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services What I need to know about Crohn
WHAT ARE HEMORRHOIDS?
 Patient information regarding care and surgery associated with HEMORRHOIDS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia Stefanou, M.D. location: Michigan Heart & Vascular Institute, 5325
Patient information regarding care and surgery associated with HEMORRHOIDS by: Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia Stefanou, M.D. location: Michigan Heart & Vascular Institute, 5325
GASTRIC BYPASS SURGERY CONSENT FORM
 Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
Colon Cancer Surgery and Recovery. A Guide for Patients and Families
 Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Transobturator tape sling Female sling system
 Transobturator tape sling Female sling system Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Transobturator tape sling Female sling system Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Laparoscopic Adrenal Gland Removal (Adrenalectomy) Patient Information from SAGES
 Laparoscopic Adrenal Gland Removal (Adrenalectomy) Patient Information from SAGES What are the Adrenal Glands? The adrenal glands are two small organs, one located above each kidney. They are triangular
Laparoscopic Adrenal Gland Removal (Adrenalectomy) Patient Information from SAGES What are the Adrenal Glands? The adrenal glands are two small organs, one located above each kidney. They are triangular
Anterior Resection Your Operation Explained
 Anterior Resection Your Operation Explained Patient Information Introduction This leaflet tells you about the procedure known as an anterior resection. It explains what is involved, and some of the common
Anterior Resection Your Operation Explained Patient Information Introduction This leaflet tells you about the procedure known as an anterior resection. It explains what is involved, and some of the common
Informed Consent for Laparoscopic Roux en Y Gastric Bypass. Patient Name
 Informed Consent for Laparoscopic Roux en Y Gastric Bypass Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Roux en Y Gastric
Informed Consent for Laparoscopic Roux en Y Gastric Bypass Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Roux en Y Gastric
Femoral Hernia Repair
 Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Femoral Hernia Repair WHAT IS A FEMORAL HERNIA REPAIR? 2 WHAT CAUSES A FEMORAL HERNIA? 2 WHAT DOES TREATMENT/ MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
Laparoscopic Cholecystectomy Gallbladder removal is one of the most commonly performed surgical procedures in the United States. Today,gallbladder surgery is performed laparoscopically. The medical name
Inguinal Hernia (Female)
 Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Inguinal Hernia (Female) WHAT IS AN INGUINAL HERNIA? 2 WHAT CAUSES AN INGUINAL HERNIA? 2 WHAT DOES TREATMENT / MANAGEMENT INVOLVE? 3 DAY SURGERY MANAGEMENT 3 SURGICAL REPAIR 4 WHAT ARE THE RISKS/COMPLICATIONS
Surgery. for Crohn s Disease and Ulcerative Colitis
 Surgery for Crohn s Disease and Ulcerative Colitis What s Inside? About Crohn s disease and 2 ulcerative colitis When is surgery necessary? 3 Reasons for elective surgery 3 Conditions that require 5 immediate
Surgery for Crohn s Disease and Ulcerative Colitis What s Inside? About Crohn s disease and 2 ulcerative colitis When is surgery necessary? 3 Reasons for elective surgery 3 Conditions that require 5 immediate
I can t empty my rectum without pressing my fingers in or near my vagina
 Since the birth of my baby, I can t control my bowel movements Normally bowel movements (stools) are stored in the rectum until the bowel sends a message to the brain that it is full, and the person finds
Since the birth of my baby, I can t control my bowel movements Normally bowel movements (stools) are stored in the rectum until the bowel sends a message to the brain that it is full, and the person finds
Radical Hysterectomy and Pelvic Lymph Node Dissection
 Radical Hysterectomy and Pelvic Lymph Node Dissection Tena koutou katoa, Kia orana, Talofa lava, Malo e lelei, Fakaalofa lahi atu, Taloha Ni, Ni Sa Bula Vinaka, Greetings and Welcome to National Women's
Radical Hysterectomy and Pelvic Lymph Node Dissection Tena koutou katoa, Kia orana, Talofa lava, Malo e lelei, Fakaalofa lahi atu, Taloha Ni, Ni Sa Bula Vinaka, Greetings and Welcome to National Women's
Sigmoid Colectomy Your Operation Explained
 Sigmoid Colectomy Your Operation Explained Patient Information Information for patients This leaflet tells you about the procedure known as a sigmoid colectomy. It explains what is involved, and some of
Sigmoid Colectomy Your Operation Explained Patient Information Information for patients This leaflet tells you about the procedure known as a sigmoid colectomy. It explains what is involved, and some of
Information for men considering a male sling procedure
 Information for men considering a male sling procedure Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Information for men considering a male sling procedure Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
CHOC CHILDREN SUROLOGY CENTER. Constipation
 Constipation What is constipation? Constipation is a condition in which a person has uncomfortable or infrequent bowel movements. Generally, a person is considered to be constipated when bowel movements
Constipation What is constipation? Constipation is a condition in which a person has uncomfortable or infrequent bowel movements. Generally, a person is considered to be constipated when bowel movements
Surgery for rectal cancer
 This information is an extract from the booklet Understanding rectal cancer. You may find the full booklet helpful. We can send you a free copy see page 12. Contents Enhanced recovery programme (ERP) Before
This information is an extract from the booklet Understanding rectal cancer. You may find the full booklet helpful. We can send you a free copy see page 12. Contents Enhanced recovery programme (ERP) Before
Consent for Treatment/Procedure Laparoscopic Sleeve Gastrectomy
 Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Patient's Name: Today's Date: / / The purpose of this document is to confirm, in the presence of witnesses, your informed request to have Surgery for obesity. You are asked to read the following document
Problems of the Digestive System
 The American College of Obstetricians and Gynecologists f AQ FREQUENTLY ASKED QUESTIONS FAQ120 WOMEN S HEALTH Problems of the Digestive System What are some common digestive problems? What is constipation?
The American College of Obstetricians and Gynecologists f AQ FREQUENTLY ASKED QUESTIONS FAQ120 WOMEN S HEALTH Problems of the Digestive System What are some common digestive problems? What is constipation?
Weight Loss before Hernia Repair Surgery
 Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
Weight Loss before Hernia Repair Surgery What is an abdominal wall hernia? The abdomen (commonly called the belly) holds many of your internal organs. In the front, the abdomen is protected by a tough
What is the Sleeve Gastrectomy?
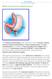 What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
Hysterectomy Vaginal hysterectomy Abdominal hysterectomy
 Hysterectomy A hysterectomy is a surgery to remove a woman s uterus. The uterus is one of the organs of the female reproductive system and is about the size of a closed hand. You can no longer have children
Hysterectomy A hysterectomy is a surgery to remove a woman s uterus. The uterus is one of the organs of the female reproductive system and is about the size of a closed hand. You can no longer have children
Preparing for your Surgery:
 Preparing for your Surgery: Information for Patients Undergoing a: UHN Minimally Invasive Radical Hysterectomy Possible removal of one or both ovaries and tubes Possible removal of pelvic lymph nodes Patient
Preparing for your Surgery: Information for Patients Undergoing a: UHN Minimally Invasive Radical Hysterectomy Possible removal of one or both ovaries and tubes Possible removal of pelvic lymph nodes Patient
Colon Cancer vs. Rectal Cancer: What is the Difference? Webcast March 31, 2010 Karen Horvath, M.D., F.A.C.S. Introduction
 Colon Cancer vs. Rectal Cancer: What is the Difference? Webcast March 31, 2010 Karen Horvath, M.D., F.A.C.S. Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle
Colon Cancer vs. Rectal Cancer: What is the Difference? Webcast March 31, 2010 Karen Horvath, M.D., F.A.C.S. Please remember the opinions expressed on Patient Power are not necessarily the views of Seattle
Laparoscopic Cholecystectomy
 Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Laparoscopic Cholecystectomy Removal of Gall Bladder Page 12 Patient Information Further Information We endeavour to provide an excellent service at all times, but should you have any concerns please,
Information and advice following placement of seton for anal fistula
 Oxford University Hospitals NHS Trust Information and advice following placement of seton for anal fistula page 2 What is a fistula? You can get an anal fistula as a result of an infection or a collection
Oxford University Hospitals NHS Trust Information and advice following placement of seton for anal fistula page 2 What is a fistula? You can get an anal fistula as a result of an infection or a collection
Gastric Sleeve Surgery
 Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Gastric Sleeve Surgery Introduction Obesity is associated with many diseases such as diabetes, high blood pressure, heart problems, and degeneration of the joints. These diseases and the obesity itself
Ulcerative Colitis. National Digestive Diseases Information Clearinghouse. What is ulcerative colitis (UC)?
 Ulcerative Colitis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is ulcerative colitis (UC)? Ulcerative colitis is
Ulcerative Colitis National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is ulcerative colitis (UC)? Ulcerative colitis is
Laser of the Vulva. This is a surgery where your doctor will use a laser light to remove unhealthy tissue.
 What is laser of the vulva? This is a surgery where your doctor will use a laser light to remove unhealthy tissue. Why is this surgery used? To treat diseases of the vulva Vulvar Intraepithelial Neoplasia
What is laser of the vulva? This is a surgery where your doctor will use a laser light to remove unhealthy tissue. Why is this surgery used? To treat diseases of the vulva Vulvar Intraepithelial Neoplasia
Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions
 Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions No lifting greater than 10 15 lbs for the first three weeks following your surgery. Walking around the house, office
Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions No lifting greater than 10 15 lbs for the first three weeks following your surgery. Walking around the house, office
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Laparoscopic Nephrectomy Information for Patients This leaflet explains: What is a Nephrectomy?... 2 Why do I need a nephrectomy?... 3 What are the risks and side effects of laparoscopic nephrectomy?...
Surgical Weight Loss. Mission Bariatrics
 Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
AMERICAN COLLEGE OF SURGEONS DIVISION OF EDUCATION. The Condition
 AMERICAN COLLEGE OF SURGEONS DIVISION OF EDUCATION Surgical Removal of the Ascending Digestive System Rectum Anus Transverse Patient Education This educational information is to help you be better informed
AMERICAN COLLEGE OF SURGEONS DIVISION OF EDUCATION Surgical Removal of the Ascending Digestive System Rectum Anus Transverse Patient Education This educational information is to help you be better informed
VAGINAL MESH FAQ. How do you decide who should get mesh as part of their repair?
 VAGINAL MESH FAQ How do you decide who should get mesh as part of their repair? Each patient with pelvic organ prolapse (POP) is considered individually. In younger women, women with an uncomplicated prolapse
VAGINAL MESH FAQ How do you decide who should get mesh as part of their repair? Each patient with pelvic organ prolapse (POP) is considered individually. In younger women, women with an uncomplicated prolapse
Bladder reconstruction (neo-bladder)
 Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
Bladder reconstruction (neo-bladder) We have written this leaflet to help you understand about your operation. It is designed to help you answer any questions you may have. The leaflet contains the following
Your Recovery After a Cesarean Delivery
 Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES
 Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Surgery for "Heartburn" If you suffer from moderate to severe "heartburn" your surgeon may have recommended Laparoscopic Antireflux
Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Surgery for "Heartburn" If you suffer from moderate to severe "heartburn" your surgeon may have recommended Laparoscopic Antireflux
Summa Health System. A Woman s Guide to Hysterectomy
 Summa Health System A Woman s Guide to Hysterectomy Hysterectomy A hysterectomy is a surgical procedure to remove a woman s uterus (womb). The uterus is the organ which shelters and nourishes a baby during
Summa Health System A Woman s Guide to Hysterectomy Hysterectomy A hysterectomy is a surgical procedure to remove a woman s uterus (womb). The uterus is the organ which shelters and nourishes a baby during
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS
 INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
INTRAPERITONEAL HYPERTHERMIC CHEMOTHERAPY (IPHC) FOR PERITONEAL CARCINOMATOSIS AND MALIGNANT ASCITES. INFORMATION FOR PATIENTS AND FAMILY MEMBERS Description of Treatment A major difficulty in treating
About the Uterus. Hysterectomy may be done to treat conditions that affect the uterus. Some reasons a hysterectomy may be needed include:
 Hysterectomy removal of the uterus is a way of treating problems that affect the uterus. Many conditions can be cured with hysterectomy. Because it is major surgery, your doctor may suggest trying other
Hysterectomy removal of the uterus is a way of treating problems that affect the uterus. Many conditions can be cured with hysterectomy. Because it is major surgery, your doctor may suggest trying other
Crohn's disease and ulcerative colitis
 Crohn's disease and ulcerative colitis Summary Crohn s disease and ulcerative colitis are collectively known as inflammatory bowel disease (IBD). Crohn s disease can appear in any part of a person s digestive
Crohn's disease and ulcerative colitis Summary Crohn s disease and ulcerative colitis are collectively known as inflammatory bowel disease (IBD). Crohn s disease can appear in any part of a person s digestive
The degree of liver inflammation or damage (grade) Presence and extent of fatty liver or other metabolic liver diseases
 ilearning about your health Liver Biopsy www.cpmc.org/learning What is a Liver Biopsy? A liver biopsy is a procedure where a specially trained doctor (typically a hepatologist, radiologist, or gastroenterologist)
ilearning about your health Liver Biopsy www.cpmc.org/learning What is a Liver Biopsy? A liver biopsy is a procedure where a specially trained doctor (typically a hepatologist, radiologist, or gastroenterologist)
You will be having surgery to remove a tumour(s) from your liver.
 Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Incontinence. What is incontinence?
 Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Laparoscopic Repair of Hernias. A simple guide to help answer your questions
 Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
How common is bowel cancer?
 information Primary Care Society for Gastroenterology Bowel Cancer (1 of 6) How common is bowel cancer? Each year 35,000 people in Britain are diagnosed with cancer of the bowel, that is to say cancer
information Primary Care Society for Gastroenterology Bowel Cancer (1 of 6) How common is bowel cancer? Each year 35,000 people in Britain are diagnosed with cancer of the bowel, that is to say cancer
Hartmann s Procedure Your operation explained
 Hartmann s Procedure Your operation explained Patient Information Introduction This leaflet tells you about the operation known as Hartmann s procedure. It explains what is involved and some of the common
Hartmann s Procedure Your operation explained Patient Information Introduction This leaflet tells you about the operation known as Hartmann s procedure. It explains what is involved and some of the common
Spinal Cord and Bladder Management Male: Intermittent Catheter
 Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Colorectal Cancer: Preventable, Beatable, Treatable. American Cancer Society
 Colorectal Cancer: Preventable, Beatable, Treatable American Cancer Society Reviewed January 2013 What we ll be talking about How common is colorectal cancer? What is colorectal cancer? What causes it?
Colorectal Cancer: Preventable, Beatable, Treatable American Cancer Society Reviewed January 2013 What we ll be talking about How common is colorectal cancer? What is colorectal cancer? What causes it?
Appendicitis National Digestive Diseases Information Clearinghouse
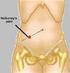 Appendicitis National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH The appendix is a small, tube-like structure
Appendicitis National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH The appendix is a small, tube-like structure
Preparing for your laparoscopic pyeloplasty
 Preparing for your laparoscopic pyeloplasty Welcome We look forward to welcoming you to The Royal London Hospital. You have been referred to us for a laparoscopic pyeloplasty, which is an operation using
Preparing for your laparoscopic pyeloplasty Welcome We look forward to welcoming you to The Royal London Hospital. You have been referred to us for a laparoscopic pyeloplasty, which is an operation using
The Hereditary Colorectal Cancer Website has been sponsored by the Robert Rauschenberg Foundation
 Introduction The Hereditary Colorectal Cancer Website has been sponsored by the Robert Rauschenberg Foundation Hereditary nonpolyposis colorectal cancer (HNPCC) syndrome was first described over 100 years
Introduction The Hereditary Colorectal Cancer Website has been sponsored by the Robert Rauschenberg Foundation Hereditary nonpolyposis colorectal cancer (HNPCC) syndrome was first described over 100 years
Enhanced recovery programme (ERP) for patients undergoing bowel surgery
 Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
Enhanced recovery programme (ERP) for patients undergoing bowel surgery Information for patients, relatives and carers An enhanced recovery programme (ERP) has been established at Imperial College Healthcare
Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients
 Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients What are Haemorrhoids? Haemorrhoids (piles) are enlarged blood vessels around the anus (back passage). There are two types of haemorrhoids:
Removal of Haemorrhoids (Haemorrhoidectomy) Information for patients What are Haemorrhoids? Haemorrhoids (piles) are enlarged blood vessels around the anus (back passage). There are two types of haemorrhoids:
Ulcerative Colitis & Proctitis. About Ulcerative Colitis & Proctitis
 Ulcerative Colitis & Proctitis About Ulcerative Colitis & Proctitis When you first learn that you have ulcerative colitis, you will probably feel overwhelmed. You may not even have heard of ulcerative
Ulcerative Colitis & Proctitis About Ulcerative Colitis & Proctitis When you first learn that you have ulcerative colitis, you will probably feel overwhelmed. You may not even have heard of ulcerative
WHAT IS INCONTINENCE?
 CNA Workbook WHAT IS INCONTINENCE? Incontinence is the inability to control the flow of urine or feces from your body. Approximately 26 million Americans are incontinent. Many people don t report it because
CNA Workbook WHAT IS INCONTINENCE? Incontinence is the inability to control the flow of urine or feces from your body. Approximately 26 million Americans are incontinent. Many people don t report it because
LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE
 LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE TALKING ABOUT STRESS INCONTINENCE (SUI) Millions of women suffer from stress incontinence (SUI). This condition results in accidental
LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE TALKING ABOUT STRESS INCONTINENCE (SUI) Millions of women suffer from stress incontinence (SUI). This condition results in accidental
Surgery for Stress Incontinence
 Directorate of Women s Services Surgery for Stress Incontinence Tension Free Vaginal Tape Information for Patients Direct dial number Ward 40 0191 282 5640 Stress Incontinence Stress incontinence is a
Directorate of Women s Services Surgery for Stress Incontinence Tension Free Vaginal Tape Information for Patients Direct dial number Ward 40 0191 282 5640 Stress Incontinence Stress incontinence is a
Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology
 Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind
Trans Urethral Resection of the Prostate (TURP) Trans Urethral Incision of the Prostate (TUIP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind
Considering a Hysterectomy?
 Considering a Hysterectomy? Learn more about virtually scarless surgery using da Vinci Single-Site technology { {Symptoms & Conditions: Chronic Pain, Heavy Bleeding, Fibroids, Endometriosis, Pelvic Prolapse
Considering a Hysterectomy? Learn more about virtually scarless surgery using da Vinci Single-Site technology { {Symptoms & Conditions: Chronic Pain, Heavy Bleeding, Fibroids, Endometriosis, Pelvic Prolapse
The following document includes information about:
 Patient information WHAT TO EXPECT WHILE RECEIVING RADIATION THERAPY FOR PROSTATE CANCER Oncology Vitalité Zone : 1B 4 5 6 Facility : Dr. Léon-Richard Oncology Centre The following document includes information
Patient information WHAT TO EXPECT WHILE RECEIVING RADIATION THERAPY FOR PROSTATE CANCER Oncology Vitalité Zone : 1B 4 5 6 Facility : Dr. Léon-Richard Oncology Centre The following document includes information
Femoral artery bypass graft (Including femoral crossover graft)
 Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
Femoral artery bypass graft (Including femoral crossover graft) Why do I need the operation? You have a blockage or narrowing of the arteries supplying blood to your leg. This reduces the blood flow to
After Your Gastrectomy
 After Your Gastrectomy UHN Information for patients and families Read this information to learn: what a gastrectomy is how to care for yourself what problems to look out for who to call if you have any
After Your Gastrectomy UHN Information for patients and families Read this information to learn: what a gastrectomy is how to care for yourself what problems to look out for who to call if you have any
