There are no sufficient or convincing data
|
|
|
- Shanon Casey
- 8 years ago
- Views:
Transcription
1 35 Introduction There are no sufficient or convincing data in the literature about the algorithm to be followed against the failed original procedure in the spinal surgery. The issue is not homogeneous. The most frequent cause is erroneous selection of patients. The main principle in neck and low back surgery after correct patient selection must be to decompress the symptomatic area by avoiding the use of an insufficient technique that might require other operations following the original operation. The basic principle must be to leave the spine stable after complete neural decompression. Failure after the spinal surgery occurs mostly in the lumbar and cervical regions.²¹ Use of implants out of indication especially recently and erroneous design, using the radiologic studies including MRI (magnetic resonance imaging) and neglecting the classical examination methods, and omitting surgical principles can be listed among the main causes of failures. We know that the risk of failure is extremely low after decompression surgery in patients with significant neurologic compression is present if the clinical picture of the patient is suitable. However, we see failure in a small portion of the patients despite the correct decompression both in the cervical and lumbar regions. Failure in restoring the comfort of living of the patient after the decompression procedures applied, continuous need of analgesics, or any other failures causing re-operations bring these patients back to us with failed spinal surgery or failed neck and back syndrome. Although failure varies greatly Failures in Neck and Low-back Surgery: Causes and Outcomes when compared to the total number of cases, there are series with failure rates between 5-54% for the cervical region and with 7-70% for the lumbar region. 6 However, only 10% of these become symptomatic, thankfully. 21 The rates of the third operation for these patients can be given as 12%. This problem brings the psychosomatic complaints forth. It is very difficult to help a patient with an impaired quality of life. It is also seen as a problem with significant socio-economic dimension. Differential diagnosis of the pain can become difficult with this reason. Factors Causing Failure Include the Following: A- Insufficiency of diagnosis 1- Errors in the patient selection 2- Insufficient tests (occult brucellosis) 3- Sufficient tests with missed lack of clinical consistency (metastasis) 4- Tandem stenosis 5- Missed lesion (missed far-lateral disc) 6- Missed instability B- Incomplete decompression 1- Residual disc or presence of pathologic tissues 2- Reccurrence in the same level within the first 6 months 3- Appearing pathology in the adjacent level 4- Symptomatic massive granulation tissue 5- Failure in removal of the foraminal stenosis C- Lack of healing (Pseudoarthrosis) 1- Patinet-related factors 2- Surgery-related factors 221
2 222 D-Intra-operative errors 1- Wrong level 2- Wrong side 3- Neural damage related to over-manipulation 4- Creation of instability 5- Incompetence of the surgeon E-Epidural fibrosis 1- Symptomatic 2- Asymptomatic F-Araknoiditis 1- Primary 2- Secondary (iatrogenic) G-Infections 1- Superficial skin infections 2- Spondylodisciitis 3- Empyema 4- Cottonoma (foreign body) H- Postoperative muscular insufficiency I- Postoperative reflex sympathetic dystrophy İ- Postoperative epidural hemorrhage J- Complications related to position (brachial plexus, ulnar nerve) K- Neuropathic pain L- Missed psych-somatization In this section, the incomplete decompression and lack of healing, which are the most frequent causes of the failed neck and back surgery syndrome (FNBS) will be reviewed, and factors that are seen less will be mentioned briefly. Wrong Diagnosis that had tried all kinds of treatment modalities. The most frequent reason for the wrong diagnosis is the decision made without performing a neurological examination. For example, performing the cervical disc surgery in patients with trap neuropathy or fibromyalgia is the most frequent error². Lack of Healing (Pseudoarthrosis) The lack of healing after the osteosynthesis performed in the lumbar or cervical regions vary between 10 and 80%, whatever the known or performed surgical technique is; but thankfully, very few of them present themselves as low back or neck pain or become symptomatic. 19,22 In case the symptomatic cases have neurologic deficits with progression, the watchand-see algorithm must be abandoned and revision stage must be shifted to. For example, the condition causing the lack of healing resulting in axial neck or radicular pain after anterior cervical discectomy must be determined in the revision. In addition, an algorithm must be prepared to avoid recurrence after revision. If needed, anterior decompression can be reinforced with autograft with added posterior osteosynthesis. (Figure 1) The success of fusion in these cases reaches 90%. 3 It must be questioned if the additional measures (if taken) will be sufficient. If the endplates are not sufficiently curetted similarly in the cervical region, the graft placed in the mesh will be formed, but it will not be strong enough to bind to the body. (Figure 2) For example, in the ALIF (anterior lumbar interbody fusion) technique, the rate of pseudoarthrosis is Indications applied with a wide coverage with economic reasons are among the causes of FNBS. The advice you can be paralyzed if you do not undergo operation directs the patient to surgery; rate of cases operated this way because of low back and neck pain can be as high as 34%. 6 Another factor is the advice that there is no way other than surgery given to the patient without neural compression or instability Figure 1: (A) In the patient with unrelieved neck pain after the anterior cervical discectomy, lack of healing was considered, and (B) fusion was performed with anteroposterior autograft (C). The neck VAS score of the patient has been improved from 7 to 3.
3 Failures in Neck and Low-back Surgery: Causes and Outcomes There are articles reporting that adjacent segment disease is seen in more levels after very strong fusion particularly in the upper segment. 22 Meshes that can contain large volumes of graft must be used for the fusion. Implants occupying the bone graft cause incomplete healing. Surgeons that place only grafts between the bodies to eliminate this problem have reported fusion rate as Figure 2: See the allograft placed in mesh has been formed in the mesh, but has 95%. 9 It is recommended that not been bonded to the endplates. the surgeon should perform the technique s/he is familiar 38% event when structural tibia graft and bone morphogenic protein are used together %38 dır. 8 More For example, although PLIF (posterior lumbar inter- most with the least damage. than half of the grafts placed within the mesh in the body fusion) is a known technique, it is known that interbody fusion are resorbed. Therefore, graft must neural injuries with this technique are more frequent be placed in front of and behind the mesh. (Figure 3a) as compared to the TLIF technique. 8 Autograft application is the best technique for both ALIF and TLIF (transforaminal interbody fusion) and protects the patients against repeated revision procedures. In risky patients that fusion will develop late, performing posterior fusion in the same session against any anterior pseudoarthrosis is a protective approach against failure.²¹ (Figure 3b) 223 Figure 3a: The lack of interbody fusion is differentiated as the cause of the intractable low back pain in the preoperative period. Figure 3b: The failed anterior fusion after the spondylolisthesis surgery with ALIF technique can be recognized. Posterior fusion makes the system stronger, and the patient continues his/ her life without problems.
4 224 It is obvious that instrumentation on the area that fusion will not be applied will cause loosening and insufficiency. 5 Medical treatment with injections including transforaminal steroid, local anesthetics, or hyalurinidase must be applied in patients without neurologic deficits who are in the plateau period 7. Care must be given to the use of autografts in risky patients and factors that will prevent fusion like smoking must be prevented. Incomplete Decompression Incomplete decompression is most frequently seen in the foraminal level 4. For example, laminectomy in a very narrow channel can give the impression that decompression is complete. However, intraforaminal portion of the nerve can be missed. (Figure 4, 5) Exposure or decompression of the proximal of the nerve root will not relieve the extra-foraminal compression. Extra-foraminal decompression must be applied if needed where compressions extend outside the foramen. (Figure 4) The layout in the OR Figure 5: It is seen that the cause of incomplete decompression despite 3 operations lies in the foraminal level. is also very important. The surgeon must face the negatoscope particularly for the multiple pathologies and must frequently view the x-rays placed on the negatoscope with small spaces in-between. 4 Nine percent of the patients come back because of re-herniation after lumbar disc surgery. 14 In this context, timing of the pain is very important. While the cause of pain in the early period is wrong distance or residual disc, pain in later periods will be related to hematoma, fibrosis or instability. Figure 4: The curative surgery in the patient that was operated three times because of incomplete decompression was possible with extraforamial approach. Adjacent Segment Degeneration and Disease Is disease related to adjacent segment degeneration or is it related to natural ageing? Or, is it a strained joint disease? Is it an over-loading that developed after surgery? Full consensus appears to be difficult. Adjacent segment degeneration in the cervical and lumbar spine has been radiologically documented. Katsuura and colleagues 15 found significant degenerative changes in 21 patients out of 42 (50%) in radiologic examination, some of which were found in the adjacent levels, within a follow-up period of 9.8 years after anterior cervical fusion. Independent researchers examined patients clinically and radiologically. Deterioration was found in 92% of the cases in the adjacent levels. However, there was no correlation between the radiographic adjacent segment degeneration and clinical symptoms. Varying figures are reported for the incidence. However, incidence is in the range of 24-50% for
5 the cervical region, and for the lumbar region, fortunately only one-fourth being symptomatic 11. It is known that the frequency of hypermobility in the upper segment and narrowing is higher in the 5-year follow-up as compared to the lower segment. The rate of this problem being symptomatic is 5-12%. 11 Adjacent segment degeneration is a radiologic finding, and the point it will lead is suspicious. However, development of findings including scoliosis, sliding, narrow channel, Are-herniation and stress fractures can be possible years after the original operation. (Figure 6) The incidence of narrowing of the channel within 5 years is higher after strong fusion. However, it must be known that normal ageing, that is, the natural process can also contribute. Although the debate on whether or not the adjacent segment disease is related with long segment fusion, it is generally accepted that there is no relation. 18 It must be considered that especially kyphosis can develop after original operation performed without considering the sagittal balance. 1 To mention the recommendations on this issue: Absolute revision: where there is neurologic deficit consistent with the radiology Relative revision: This is recommended when there is pain, deformity in the adjacent vertebra, instability or lysthesis and narrowing of the channel. 23 It has been reported that approach must be more conservative in the lower adjacent segment disease, or the patient must be followed-up for a longer period. 23 Radical treatment must be performed after applying all kinds of pain treatment. Failures in Neck and Low-back Surgery: Causes and Outcomes Arachnoiditis It is known that arachnoiditis develops following multiple operations. Apart from this, it can develop after the intradural operations, use of contrast agent, after infections or pseudomeningocele. Causes of some of these are unknown. 3 ¹ Asymptomatic arachnoiditis can be present in the radiology. It has 3 types: 1- Those adhering to the medial dural wall of the nerve roots, which is the most frequent type (Figure 7) 2- Those adhering around the spinal cord 3- The inflammatory type called candle tripping. Since the nerve roots are edematous in this type, they appear as if adhered to each other, and give the pseudo tumor appearance radiologically. Patients have symptoms including, intermittent pain and cramps, paint in legs or hip. Such cases are mostly diagnosed after the further imaging studies and electrophysiological studies performed upon failure upon continuance of the pain in the postoperative period. Although treatment varies with the type; 10 a- Steroids b- Anti-epileptics c- Intrathecal hyaluronidase d- Surgical dissection of adhesions 225 Figure 6: The pars fracture is the cause of low back pain following the strong fixation at year 5. Figure 7: Being familiar with arachnoiditis cases will prevent failed spinal surgery. See the bunching of the cauda equina fibers in the periphery.
6 226 Scar Tissue The scar tissue seen in the studies made because of postoperative pain is mostly asymptomatic. Rate of the symptomatic cases is 10%. 2,3,7 Although they give the impression of nerve root or dural sac compression, these can only be accused in the presence of a related neurologic deficit, and operation or decompression can ne required as such. Cautery must not be used, and risk can be minimized through a tight hemostasis. Spinal chord stimulator must be applied in cases that pain cannot be relieved, and further surgical techniques must be applied as the last resort. 17 Wrong Distance Apart from the wrong patient, factors including wrong distance or wrong side are also among the factors that increase the number of operations. In the wrong distance, which is one of the causes of failure, the recent data continue to be disappointing, and incidence is as high as 15%. It is known that 99% of the lawsuits opened in the USA are related to wrong patient, wrong level and wrong procedure. 13 To prevent, the method ask the fluoroscopy image to everyone in the OR, ask yourself, suspect and ask again, if not sure, call the radiologist and ask him/her must be used. The congenital anatomy present in all the studies, advanced osteoporosis or obesity can prevent the peri-operative correct diagnosis of the distance during the fluoroscopy. With this reason, we must ask the question, am I in the correct location time and time again; even when we are most experienced and must be sure about the correctness of the distance and the side. The recommendation for this insufficiency is to suspect always in relation with surgery. In case there is no progressive neurologic deficit before the revision surgery, all kinds of medical treatments must be tried. Spinal chord stimulator must be considered at the last stage. There are articles reporting that this application gives good results. 5 Infections Infections are seen more frequently in the lumbar region, and rarely in the cervical region. Removal of the disc, which is an avascular structure, can eliminate the infection risk for the cervical region. Complete removal of the disc in risky patients like diabetics can prevent spondylodiscitis. The address of the severe pain developing in the lumbar region particularly between days 5 and 20 will be spondylodiscitis, while foreign materials most be considered for pain that develops months later. 9,10 Questions What type of surgery should I perform in the revision? From whom should I get help? Why did the inefficiency/failure happen? Will pain be relieved with revision? Should I take additional measures? (blood, Rbmp, TUR, etc.) A/P or combined surgery? Is the spinal chord stimulator a more correct choice? What are the Difficulties of the Revision? 1- Scar tissue barrier 2- Uncertainty of anatomy 3- Increase of bleeding 4- Reducing of the tissue strength and healing problems 5- Frequency of radiculitis or arachnoiditis 6- Complications related to the extended surgery Last Words Has the patient selection been performed correctly? Correct side and correct level? Is the decompression full? Are the nerve roots decompressed? Is there adjacent system disease? (add dynamic system?) Was a fusion-oriented surgery performed? Have the posterior tension band and facets been preserved? Is pseudoarthrosis is symptomatic or asymp- tomatic? The treatment of failed spinal surgery is to avoid it. It must be known that the highest success can be achieved with original operation, and success is gradually reduced with re-operations. FNBS is a syndrome that exhausts the patient, surgeon and society so that pull of is almost impossible with the severity increased in relation with socio-economical and psychosomatic problems, which two important results of FNBS syndrome.
7 References 1. Akamaru T, Kawahara N, Tim Yoon S, et al. Adjacent segment motion after a simulated lumbar fusion in different sagittal alignments: a biomechanical analysis. Spine 28(14): , Almeida DB, Prandini MN, Awamura Y, et al. Outcome following lumbar disc surgery: the role of fibrosis. Acta Neurochir (Wien) 150(11): , Auld AW. Chronic spinal arachnoiditis. A postoperative syndrome that may signal its onset. Spine 3(1): 88-91, Choi KC, Ahn Y, Kang BU, et al. Failed anterior lumbar interbody fusion due to incomplete foraminal decompression. Acta Neurochir (Wien) 153(3): , Choi J, Babu R, Bagley JH, et al. Utilization of 157 spinal cord stimulation in patients with failed back surgery syndrome. Neurosurgery 71(2): E562-3, Levin DA, Hale JJ, Bendo JA. Adjacent Segment Degeneration Following Spinal Fusion for Degenerative Disc Disease. Bulletin of the NYU Hospital for Joint Diseases 65(1): 29-36, Devulder J. Transforaminal nerve root sleeve injection with corticosteroids, hyaluronidase, and local anesthetic in the failed back surgery syndrome. J Spinal Disord 11(2):151-4, DiPaola CP, Molinari RW. Posterior lumbar interbody fusion. J Am Acad Orthop Surg 16(3): 130-9, Ekici MA, Ekici A, Per H, Tucer B, Kurtsoy A. Foreign body granuloma mimicking upper cervical spinal mass after dural repair with Tachocomb [correction of Tachocomp]: a case report. Pediatr Neurosurg 46(2): Gourie-Devi M, Satish P. Intrathecal hyaluronidase treatment of chronic spinal arachnoiditis of noninfective etiolog. Surg Neurol 22(3): , Hamburger C, Festenberg FV, Uhl E. Ventral discectomy with pmma interbody fusion for cervical disc disease: long-term results in 249 patients. Spine 26(3): , Hilibrand AS, Robbins M. Adjacent segment degeneration following spinal fusion for degenerative disc disease. Spine J 4(6 Suppl):190S-194S, 2004 Failures in Neck and Low-back Surgery: Causes and Outcomes 13. Hsiang J. Wrong-level surgery: A unique problem in spine surgery. Surg Neurol Int 2:47, Jönsson B, Strömqvist B. Repeat decompression of lumbar nerve roots. A prospective two-year evaluation. J Bone Joint Surg Br 75(6): 894-7, Katsuura A, Hukuda S, Saruhashi Y, Mori K. Kyphotic malalignment after anterior cervical fusion is one of the factors promoting the degenerative process in adjacent intervertebral levels. Eur Spine J10(4): 320-4, Kotil K, Akçetin M, Tari R, Ton T, Bilge T. Replacement of vertebral lamina (laminoplasty) in surgery for lumbar isthmic spondylolisthesis. A prospective clinical study. Turk Neurosurg 19(2): , Kumar K, Taylor RS, Jacques L, et al. Spinal cord stimulation versus conventional medical management for neuropathic pain: a multicentre randomised controlled trial in patients with failed back surgery syndrome. Pain 132(1-2): , Penta M, Sandhu A, Fraser RD. Magnetic resonance imaging assessment of disc degeneration 10 years after anterior lumbar interbody fusion. Spine 20(6):743-7, Pradhan BB, Bae HW, Dawson EG, Patel VV, Delamarter RB. Graft resorption with the use of bone morphogenetic protein: lessons from anterior lumbar interbody fusion using femoral ring allografts and recombinant human bone morphogenetic protein-2. Spine (Phila Pa 1976) 31(10): E277-84, Reinsel TE, Goldberg E, Granato DB, Wilkinson S, Penn R. Spinal subdural hematoma: a rare cause of recurrent postoperative radiculopathy. J Spinal Disord 6(1): 62-7, Sasani M, Ozer AF, Oktenoglu T, Cosar M, Karaarslan E, Sarioglu AC. Recurrent radiculopathy caused by epidural gas after spinal surgery: report of four cases and literature review. Spine 32(10): E320-5, Stoker GE. Cervical pseudarthrosis and lumbar fusion mass Spine J 12(3): 275, Theodosopoulos PV, Ringer AJ, McPherson CM, et al. Measuring surgical outcomes in neurosurgery: implementation, analysis, and auditing a prospective series of more than 5000 procedures. J Neurosurg 10,
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants
 White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
White Paper: Reducing Utilization Concerns Regarding Spinal Fusion and Artificial Disc Implants For Health Plans, Medical Management Organizations and TPAs Executive Summary Back pain is one of the most
ISPI Newsletter Archive Lumbar Spine Surgery
 ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
ISPI Newsletter Archive Lumbar Spine Surgery January 2005 Effects of Charite Artificial Disc on the Implanted and Adjacent Spinal Segments Mechanics Using a Hybrid Testing Protocol Spine. 30(24):2755-2764,
Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery
 Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery REVISION SPINE SURGERY Revision surgery is a very complex field which requires experience, training and evaluation in a very individual
Spine Clinic Neurospine Specialists, Orthopaedics and Neurosurgery REVISION SPINE SURGERY Revision surgery is a very complex field which requires experience, training and evaluation in a very individual
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
X Stop Spinal Stenosis Decompression
 X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
X Stop Spinal Stenosis Decompression Am I a candidate for X Stop spinal surgery? You may be a candidate for the X Stop spinal surgery if you have primarily leg pain rather than mostly back pain and your
Minimally Invasive Spine Surgery What is it and how will it benefit patients?
 Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
Minimally Invasive Spine Surgery What is it and how will it benefit patients? Dr Raoul Pope MBChB, FRACS, Neurosurgeon and Minimally Invasive Spine Surgeon Concord Hospital and Mater Private Hospital Sydney
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Advances In Spine Care. James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery
 Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Advances In Spine Care James D. Bruffey M.D. Scripps Clinic Division of Orthopaedic Surgery Section of Spinal Surgery Introduction The Spine - A common source of problems Back pain is the #2 presenting
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2015 5/2016 5/2015 Description of Procedure or Service Low back pain
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2015 5/2016 5/2015 Description of Procedure or Service Low back pain
Spinal Surgery 2. Teaching Aims. Common Spinal Pathologies. Disc Degeneration. Disc Degeneration. Causes of LBP 8/2/13. Common Spinal Conditions
 Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Patient Guide to Neck Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Anterior Cervical Fusion procedures. Patient Guide to Neck Surgery Anterior Cervical Fusion Trinica Select With the Trinica and
The following is a sampling of products offered by Zimmer Spine for use in Anterior Cervical Fusion procedures. Patient Guide to Neck Surgery Anterior Cervical Fusion Trinica Select With the Trinica and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
Cervical Spine Surgery. Orthopaedic Nursing Seminar. Dr Michelle Atkinson. Friday October 21 st 2011. Cervical Disc Herniation
 Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
Subject: BlueCross BlueShield of North Carolina Lumbar Spine Fusion Surgery Notification
 , 2010 Don W. Bradley, M.D. Senior Vice President, Healthcare & Chief Medical Officer Blue Cross and Blue Shield of North Carolina 5901 Chapel Hill Road Durham, NC 27707 Subject: BlueCross BlueShield of
, 2010 Don W. Bradley, M.D. Senior Vice President, Healthcare & Chief Medical Officer Blue Cross and Blue Shield of North Carolina 5901 Chapel Hill Road Durham, NC 27707 Subject: BlueCross BlueShield of
SPINAL FUSION. North American Spine Society Public Education Series
 SPINAL FUSION North American Spine Society Public Education Series WHAT IS SPINAL FUSION? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
SPINAL FUSION North American Spine Society Public Education Series WHAT IS SPINAL FUSION? The spine is made up of a series of bones called vertebrae ; between each vertebra are strong connective tissues
POST-OPERATIVE SPINE IMAGING M.Muto Chief Neuroradiology Dept Cardarelli Hospital Naples ITALY
 POST-OPERATIVE SPINE IMAGING M.Muto Chief Neuroradiology Dept Cardarelli Hospital Naples ITALY Postoperative spine imaging, either by surgery or by mini-invasive procedures, is a complex tool and depends
POST-OPERATIVE SPINE IMAGING M.Muto Chief Neuroradiology Dept Cardarelli Hospital Naples ITALY Postoperative spine imaging, either by surgery or by mini-invasive procedures, is a complex tool and depends
Patient Guide to Lower Back Surgery
 The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
The following is a sampling of products offered by Zimmer Spine for use in Open Lumbar Fusion procedures. Patient Guide to Lower Back Surgery Open Lumbar Fusion Dynesys The Dynesys Dynamic Stabilization
Update to the Treatment of Degenerative Cervical Disc Disease
 Update to the Treatment of Degenerative Cervical Disc Disease Michael Lynn, MD Neurosurgeon, Southeastern Neurosurgical & Spine Institute Adjunct Assistant Clinical Professor of Bioengineering, Clemson
Update to the Treatment of Degenerative Cervical Disc Disease Michael Lynn, MD Neurosurgeon, Southeastern Neurosurgical & Spine Institute Adjunct Assistant Clinical Professor of Bioengineering, Clemson
Lower Back Pain. Introduction. Anatomy
 Lower Back Pain Introduction Back pain is the number one problem facing the workforce in the United States today. To illustrate just how big a problem low back pain is, consider these facts: Low back pain
Lower Back Pain Introduction Back pain is the number one problem facing the workforce in the United States today. To illustrate just how big a problem low back pain is, consider these facts: Low back pain
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Balloon Kyphoplasty. Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures.
 Balloon Kyphoplasty Overview Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures. The technique is designed to: Reduce and stabilise the fracture in a controlled
Balloon Kyphoplasty Overview Balloon Kyphoplasty is a minimally invasive procedure to treat vertebral body compression fractures. The technique is designed to: Reduce and stabilise the fracture in a controlled
ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015
 Presented by: Teri Romano, RN, MBA, CPC, CMDP ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015 Source: http://journal.ahima.org/2015/02/04/us house committee to hold hearing on icd 10 implementation/ 2 2015 Web_Non
Presented by: Teri Romano, RN, MBA, CPC, CMDP ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015 Source: http://journal.ahima.org/2015/02/04/us house committee to hold hearing on icd 10 implementation/ 2 2015 Web_Non
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study
 Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF).
 Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Magnetic Resonance Imaging
 Magnetic Resonance Imaging North American Spine Society Public Education Series What Is Magnetic Resonance Imaging (MRI)? Magnetic resonance imaging (MRI) is a valuable diagnostic study that has been used
Magnetic Resonance Imaging North American Spine Society Public Education Series What Is Magnetic Resonance Imaging (MRI)? Magnetic resonance imaging (MRI) is a valuable diagnostic study that has been used
Treating Bulging Discs & Sciatica. Alexander Ching, MD
 Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
Treating Bulging Discs & Sciatica Alexander Ching, MD Disclosures Depuy Spine Teaching and courses K2 Spine Complex Spine Study Group Disclosures Take 2 I am a spine surgeon I like spine surgery I believe
Spinal Surgery Functional Status and Quality of Life Outcome Specifications 2015 (01/01/2013 to 12/31/2013 Dates of Procedure) September 2014
 Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Description Methodology For patients ages 18 years and older who undergo a lumbar discectomy/laminotomy or lumbar spinal fusion procedure during the measurement year, the following measures will be calculated:
Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, The Cervical Spine. What is the Cervical Spine?
 Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness in the neck, shoulders, arms, and even hands. This patient
Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness in the neck, shoulders, arms, and even hands. This patient
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
Contents. Introduction 1. Anatomy of the Spine 1. 2. Spinal Imaging 7. 3. Spinal Biomechanics 23. 4. History and Physical Examination of the Spine 33
 Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
CERVICAL PROCEDURES PHYSICIAN CODING
 CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
A Patient s Guide to the Disorders of the Cervical and Upper Thoracic Spine
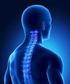 A Patient s Guide to the Disorders of the Cervical and Upper Thoracic Spine General Anatomy of the Spine The spine can be divided into four regions based on vertebral shape and sagittal plane curve.» CERVICAL:
A Patient s Guide to the Disorders of the Cervical and Upper Thoracic Spine General Anatomy of the Spine The spine can be divided into four regions based on vertebral shape and sagittal plane curve.» CERVICAL:
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Surgery for cervical disc prolapse or cervical osteophyte
 Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186 AH: 03 9483 4040 email: paul@pauldurso.com
Mr Paul S. D Urso MBBS(Hons), PhD, FRACS Neurosurgeon Provider Nº: 081161DY Epworth Centre Suite 6.1 32 Erin Street Richmond 3121 Tel: 03 9421 5844 Fax: 03 9421 4186 AH: 03 9483 4040 email: paul@pauldurso.com
How To Understand The Anatomy Of A Lumbar Spine
 Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
Sciatica: Low back and Leg Pain Diagnosis and Treatment Options Presented by Devesh Ramnath, MD Orthopaedic Associates Of Dallas Baylor Spine Center Sciatica Compression of the spinal nerves in the back
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 MEDICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: 2015T0004W Effective Date: December 1, 2015 Table of Contents BENEFIT CONSIDERATIONS COVERAGE RATIONALE APPLICABLE CODES..
MEDICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: 2015T0004W Effective Date: December 1, 2015 Table of Contents BENEFIT CONSIDERATIONS COVERAGE RATIONALE APPLICABLE CODES..
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE:
 James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF).
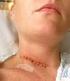 Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
ANTERIOR CERVICAL DISCECTOMY AND FUSION. Basic Anatomical Landmarks: Anterior Cervical Spine
 Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R.
 Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
Title: Interspinous Process Decompression with the X-Stop Device for Lumbar Spinal Stenosis: A Retrospective Review. Authors: Jennifer R. Madonia-Barr, MS, PA-C and David L. Kramer, MD Institution: Connecticut
A Patient s Guide to Artificial Cervical Disc Replacement
 A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA
 LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA Overview of Lumbar Spinal Stenosis Spine stabilization, which has equated
LUMBAR SPINAL STENOSIS OBSERVATIONS, EVIDENCE, AND TRENDS FULILLING THE UNMET CLINICAL NEED WRITTEN BY: HALLETT MATHEWS, MD, MBA Overview of Lumbar Spinal Stenosis Spine stabilization, which has equated
Cervical Spine Radiculopathy: Convervative Treatment. Christos K. Yiannakopoulos, MD Orthopaedic Surgeon
 Cervical Spine Radiculopathy: Convervative Treatment Christos K. Yiannakopoulos, MD Orthopaedic Surgeon Laboratory for the Research of the Musculoskeletal System, University of Athens & IASO General Hospital,
Cervical Spine Radiculopathy: Convervative Treatment Christos K. Yiannakopoulos, MD Orthopaedic Surgeon Laboratory for the Research of the Musculoskeletal System, University of Athens & IASO General Hospital,
OUTLINE. Anatomy Approach to LBP Discogenic LBP. Treatment. Herniated Nucleus Pulposus Annular Tear. Non-Surgical Surgical
 DISCOGENIC PAIN OUTLINE Anatomy Approach to LBP Discogenic LBP Herniated Nucleus Pulposus Annular Tear Treatment Non-Surgical Surgical Facet Joints: bear 20% of weight Discs bear 80% of weight Neural Foramen
DISCOGENIC PAIN OUTLINE Anatomy Approach to LBP Discogenic LBP Herniated Nucleus Pulposus Annular Tear Treatment Non-Surgical Surgical Facet Joints: bear 20% of weight Discs bear 80% of weight Neural Foramen
Anterior Approach Burn s Space Esophagus
 Cervical Complications Complications after Cervical Spine Surgery Dr. Rock Patel University of Michigan, Ann Arbor APPROACH RELATED Anterior Posterior PROCEDURE RELATED ACDF Disc Arthroplasty Laminectomy/Fusion
Cervical Complications Complications after Cervical Spine Surgery Dr. Rock Patel University of Michigan, Ann Arbor APPROACH RELATED Anterior Posterior PROCEDURE RELATED ACDF Disc Arthroplasty Laminectomy/Fusion
Management of spinal cord compression
 Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization
 APPROVED IRN10389-1.1-04 Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization Because it involves accessing the spine through the patient s side, the Direct Lateral approach
APPROVED IRN10389-1.1-04 Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization Because it involves accessing the spine through the patient s side, the Direct Lateral approach
Etiology of Long-term Failures of Lumbar Spine Surgery
 PAIN MEDICINE Volume 3 Number 1 2002 Etiology of Long-term Failures of Lumbar Spine Surgery Alexis Waguespack, MD, Jerome Schofferman, MD, Paul Slosar, MD, and James Reynolds, MD SpineCare Medical Group,
PAIN MEDICINE Volume 3 Number 1 2002 Etiology of Long-term Failures of Lumbar Spine Surgery Alexis Waguespack, MD, Jerome Schofferman, MD, Paul Slosar, MD, and James Reynolds, MD SpineCare Medical Group,
Herniated Cervical Disc
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis
 Bahrain Medical Bulletin, Vol.28, No.4, December 2006 The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis A.Aziz Mohammed, CABS, FRCS (Ortho, Tr)* Tariq El Kalifa,
Bahrain Medical Bulletin, Vol.28, No.4, December 2006 The outcome of Microscopic Selective Decompression of Degenerative Lumbar Spinal Stenosis A.Aziz Mohammed, CABS, FRCS (Ortho, Tr)* Tariq El Kalifa,
Risks of Spinal Surgery
 Risks of Spinal Surgery Infection One of the more common potential complications of any surgery is a wound infection. In spinal surgery this can be a very severe problem. It occurs in 1.5 percent to 3
Risks of Spinal Surgery Infection One of the more common potential complications of any surgery is a wound infection. In spinal surgery this can be a very severe problem. It occurs in 1.5 percent to 3
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 CLINICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAIN 019.16 T2 Effective Date: December 1, 2015 Table of Contents CONDITIONS OF COVERAGE... BENEFIT CONSIDERATIONS..
CLINICAL POLICY EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN Policy Number: PAIN 019.16 T2 Effective Date: December 1, 2015 Table of Contents CONDITIONS OF COVERAGE... BENEFIT CONSIDERATIONS..
Surgical Guideline for Lumbar Fusion (Arthrodesis)
 I. Introduction Surgical Guideline for Lumbar Fusion (Arthrodesis) The purpose of this guideline is: A. To provide utilization review staff with the information necessary to make recommendations about
I. Introduction Surgical Guideline for Lumbar Fusion (Arthrodesis) The purpose of this guideline is: A. To provide utilization review staff with the information necessary to make recommendations about
The Spine and Aging LOW BACK PAIN
 The Spine and Aging Disorders of the spine are extremely common as we age. Problems with the aging spine include spinal stenosis, disc herniation, spinal instability, fractures as a result of osteoporosis,
The Spine and Aging Disorders of the spine are extremely common as we age. Problems with the aging spine include spinal stenosis, disc herniation, spinal instability, fractures as a result of osteoporosis,
Surgical Procedures of the Spine
 Surgical Procedures of the Spine Jaideep Chunduri, M.D. Orthopaedic Spine Surgeon Beacon Orthopaedics and Sports Medicine Beacon Spine Center Objectives Discuss the 4 most common procedures performed in
Surgical Procedures of the Spine Jaideep Chunduri, M.D. Orthopaedic Spine Surgeon Beacon Orthopaedics and Sports Medicine Beacon Spine Center Objectives Discuss the 4 most common procedures performed in
A Patient's Guide to Neck Pain (Overview)
 Neck Pain Overview A Patient's Guide to Neck Pain (Overview) Introduction Over many years, our necks are subjected to repeated stress and minor injury. These injuries may not cause pain at the time of
Neck Pain Overview A Patient's Guide to Neck Pain (Overview) Introduction Over many years, our necks are subjected to repeated stress and minor injury. These injuries may not cause pain at the time of
Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization
 Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
ICD-10-PCS Documentation and Coding for Spinal Procedures October 22, 2015
 Questions and Answers 1. We have a question regarding a spinal surgical procedure. The diagnosis was bilateral lateral recess stenosis and central stenosis from L2-L5. The procedure was an open lumbar
Questions and Answers 1. We have a question regarding a spinal surgical procedure. The diagnosis was bilateral lateral recess stenosis and central stenosis from L2-L5. The procedure was an open lumbar
Degenerative Spine Solutions
 Degenerative Spine Solutions The Backbone for Your Surgical Needs Aesculap Spine Backbone for Your Degenerative Spine Needs Comprehensive operative solutions, unique product technology and world-class
Degenerative Spine Solutions The Backbone for Your Surgical Needs Aesculap Spine Backbone for Your Degenerative Spine Needs Comprehensive operative solutions, unique product technology and world-class
MINIMAL ACCESS SPINE SURGERY
 MINIMAL ACCESS SPINE SURGERY Spinal ailments are amongst the most common ailments that afflict mankind. Back pain, for example, has achieved epidemic proportions worldwide in the last two decades and is
MINIMAL ACCESS SPINE SURGERY Spinal ailments are amongst the most common ailments that afflict mankind. Back pain, for example, has achieved epidemic proportions worldwide in the last two decades and is
Aetna Injection Policy For Back Pain
 Aetna Injection Policy For Back Pain Number: 0016 Policy Aetna considers any of the following injections or procedures medically necessary for the treatment of back pain; provided, however, that only 1
Aetna Injection Policy For Back Pain Number: 0016 Policy Aetna considers any of the following injections or procedures medically necessary for the treatment of back pain; provided, however, that only 1
Consent for Lumbar Spine Surgery and Fusion at
 STEPHEN MARANO, M.D. JAMES COOK PA-C Consent for Lumbar Spine Surgery and Fusion at Patient Name: Patient Diagnosis: Lumbar Spinal Stenosis (Narrowing of the canal where the spinal cord and nerves are
STEPHEN MARANO, M.D. JAMES COOK PA-C Consent for Lumbar Spine Surgery and Fusion at Patient Name: Patient Diagnosis: Lumbar Spinal Stenosis (Narrowing of the canal where the spinal cord and nerves are
White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary?
 White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Cervical Disc Disease: An Overview The cervical
White Paper: Cervical Disc Replacement: When is the Mobi-C Cervical Disc Medically Necessary? For Health Plans, Medical Management Organizations and TPAs Cervical Disc Disease: An Overview The cervical
Spinal Surgery Clinical Coverage Policy No: 1A-30 Revised Date: DRAFT Table of Contents
 Clinical Coverage Policy No: 1A-30 Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligible Recipients... 2 2.1 General Provisions... 2 2.2 EPSDT Special
Clinical Coverage Policy No: 1A-30 Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1 Definitions... 1 2.0 Eligible Recipients... 2 2.1 General Provisions... 2 2.2 EPSDT Special
Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery
 Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery 221 Madison Ave Morristown, New Jersey 07960 (973) 538 4444 Fax (973) 538 0420 Patient
Marc A. Cohen, MD, FAAOS, FACS Diplomate American Board of Spinal Surgery Fellow American College of Spinal Surgery 221 Madison Ave Morristown, New Jersey 07960 (973) 538 4444 Fax (973) 538 0420 Patient
Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults
 Acta Orthop. Belg., 2005, 71, 83-87 ORIGINAL STUDY Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults Mohamed A. EL MASRY, Walaa I. EL ASSUITY, Youssry K. EL HAWARY,
Acta Orthop. Belg., 2005, 71, 83-87 ORIGINAL STUDY Instrumented in situ posterolateral fusion for low-grade lytic spondylolisthesis in adults Mohamed A. EL MASRY, Walaa I. EL ASSUITY, Youssry K. EL HAWARY,
Low Back Injury in the Industrial Athlete: An Anatomic Approach
 Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
SPINE AND NECK SURGERY: MAKING A DECISION THAT S RIGHT FOR YOU
 1. GET THE FACTS: Back and neck pain affects 8 out of 10 people at some point in their life. Acute back and neck pain comes on suddenly and usually lasts from a few days to a few weeks. Chronic back and
1. GET THE FACTS: Back and neck pain affects 8 out of 10 people at some point in their life. Acute back and neck pain comes on suddenly and usually lasts from a few days to a few weeks. Chronic back and
Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
 Page 42 / SA ORTHOPAEDIC JOURNAL Autumn 2008 CLINICAL ARTICLE C L I N I C A L A RT I C L E Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
Page 42 / SA ORTHOPAEDIC JOURNAL Autumn 2008 CLINICAL ARTICLE C L I N I C A L A RT I C L E Lumbar spinal stenosis JA Shipley MMed(Orth) Department Orthopaedic Surgery, University of the Free State, Bloemfontein
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Advanced Practice Provider Academy
 (+)Dean T. Harrison, MPAS,PA C,DFAAPA Director of Mid Level Practitioners; Assistant Medical Director Clinical Evaluation Unit, Division of Emergency Medicine, Department of Surgery, Duke University Medical
(+)Dean T. Harrison, MPAS,PA C,DFAAPA Director of Mid Level Practitioners; Assistant Medical Director Clinical Evaluation Unit, Division of Emergency Medicine, Department of Surgery, Duke University Medical
A review of spinal problems
 Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS
 ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS MPC 01414 ICD-9 756.12; 738.41; 756.11 DEFINITION Spondylolisthesis is generally defined as an anterior or posterior slipping or displacement
ENTITLEMENT ELIGIBILITY GUIDELINES SPONDYLOLISTHESIS AND SPONDYLOLYSIS MPC 01414 ICD-9 756.12; 738.41; 756.11 DEFINITION Spondylolisthesis is generally defined as an anterior or posterior slipping or displacement
Options for Cervical Disc Degeneration A Guide to the M6-C. clinical study
 Options for Cervical Disc Degeneration A Guide to the M6-C clinical study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause
Options for Cervical Disc Degeneration A Guide to the M6-C clinical study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause
Complications in Adult Deformity Surgery
 Complications in Adult Deformity Surgery Proximal Junctional Kyphosis: Thoracolumbar and Cervicothoracic Sigurd Berven, MD Professor in Residence UC San Francisco Disclosures Research/Institutional Support:
Complications in Adult Deformity Surgery Proximal Junctional Kyphosis: Thoracolumbar and Cervicothoracic Sigurd Berven, MD Professor in Residence UC San Francisco Disclosures Research/Institutional Support:
Patients with pain in the neck, arm, low back, or leg (sciatica) may benefit from ESI. Specifically, those with the following conditions:
 Overview An epidural steroid injection (ESI) is a minimally invasive procedure that can help relieve neck, arm, back, and leg pain caused by inflamed spinal nerves. ESI may be performed to relieve pain
Overview An epidural steroid injection (ESI) is a minimally invasive procedure that can help relieve neck, arm, back, and leg pain caused by inflamed spinal nerves. ESI may be performed to relieve pain
Clinical Policy Bulletin: Spinal Surgery: Laminectomy and Fusion
 Spinal Surgery: Laminectomy and Fusion Page 1 of 42 Clinical Policy Bulletin: Spinal Surgery: Laminectomy and Fusion Revised April 2014 Number: 0743 Policy I. Aetna considers cervical laminectomy (and/or
Spinal Surgery: Laminectomy and Fusion Page 1 of 42 Clinical Policy Bulletin: Spinal Surgery: Laminectomy and Fusion Revised April 2014 Number: 0743 Policy I. Aetna considers cervical laminectomy (and/or
Lumbar Decompression and Stabilisation for Degenerative Spondylolisthesis
 Lumbar Decompression and Stabilisation for Degenerative Spondylolisthesis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent investigations and consultation
Lumbar Decompression and Stabilisation for Degenerative Spondylolisthesis Spinal Unit Tel: 01473 702032 or 702097 Issue 5: August 2014 Review date: July 2017 Following your recent investigations and consultation
Low Back Pain (LBP) Prevalence. Low Back Pain (LBP) Prevalence. Lumbar Fusion: Where is the Evidence?
 15 th Annual Cleveland Clinic Pain Management Symposium Sarasota, Florida Lumbar Fusion: Where is the Evidence? Gordon R. Bell, M.D. Director, Cleveland Clinic Low Back Pain (LBP) Prevalence Lifetime prevalence:
15 th Annual Cleveland Clinic Pain Management Symposium Sarasota, Florida Lumbar Fusion: Where is the Evidence? Gordon R. Bell, M.D. Director, Cleveland Clinic Low Back Pain (LBP) Prevalence Lifetime prevalence:
The Surgical Spine. Sergio Rivero M.D.
 The Surgical Spine Sergio Rivero M.D. Goals: Review Current literature in spinal surgery. To utilize evidence based medicine to treat spinal pathology. It is much more important to know what sort of a
The Surgical Spine Sergio Rivero M.D. Goals: Review Current literature in spinal surgery. To utilize evidence based medicine to treat spinal pathology. It is much more important to know what sort of a
Spine and Femoral Head Instrumentation for the Radiologist. Mariam S. Aboian, Gillian Lieberman MBBS
 Spine and Femoral Head Instrumentation for the Radiologist Mariam S. Aboian, Gillian Lieberman MBBS Spine and Hip Instrumentation for the Radiologist Radiologists, Neurosurgeons, Orthopedic Surgeons =
Spine and Femoral Head Instrumentation for the Radiologist Mariam S. Aboian, Gillian Lieberman MBBS Spine and Hip Instrumentation for the Radiologist Radiologists, Neurosurgeons, Orthopedic Surgeons =
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis Introduction Lumbar spinal stenosis is defined as reduction in the diameter of the spinal canal, lateral nerve canals or neural foramina. The stenosis may involve multiple level
Lumbar Spinal Stenosis Introduction Lumbar spinal stenosis is defined as reduction in the diameter of the spinal canal, lateral nerve canals or neural foramina. The stenosis may involve multiple level
Spinal Cord Stimulation (SCS) Therapy: Fact Sheet
 Spinal Cord Stimulation (SCS) Therapy: Fact Sheet What is SCS Therapy? Spinal cord stimulation (SCS) may be a life-changing 1 surgical option for patients to control their chronic neuropathic pain and
Spinal Cord Stimulation (SCS) Therapy: Fact Sheet What is SCS Therapy? Spinal cord stimulation (SCS) may be a life-changing 1 surgical option for patients to control their chronic neuropathic pain and
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
IMPAIRMENT RATING 5 TH EDITION MODULE II
 IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
IMPAIRMENT RATING 5 TH EDITION MODULE II THE SPINE AND ALTERATION OF MOTION SEGMENT INTEGRITY (AOMSI) PRESENTED BY: RONALD J. WELLIKOFF, D.C., FACC, FICC In conjuction with: The chapter on the spine includes
Value Analysis Brief MIS Lateral Approach to Interbody Fusion
 Value Analysis Brief MIS Lateral Approach to Interbody Fusion Methods This value analysis brief presents information on the clinical and economic benefits of the minimally invasive lateral approach to
Value Analysis Brief MIS Lateral Approach to Interbody Fusion Methods This value analysis brief presents information on the clinical and economic benefits of the minimally invasive lateral approach to
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS
 SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
CONCOMITANT COMBINED DEGENERATIVE COMPRESSION OF THE SPINAL CORD AND CAUDA EQUINA: A REPORT ON THREE CASES
 CASE REPORT CONCOMITANT COMBINED DEGENERATIVE COMPRESSION OF THE SPINAL CORD AND CAUDA EQUINA: A REPORT ON THREE CASES Atanas Davarski 1, Ivo Kehayov 1, Tanya Kitova 2, Christo Zhelyazkov 1, Borislav Kitov
CASE REPORT CONCOMITANT COMBINED DEGENERATIVE COMPRESSION OF THE SPINAL CORD AND CAUDA EQUINA: A REPORT ON THREE CASES Atanas Davarski 1, Ivo Kehayov 1, Tanya Kitova 2, Christo Zhelyazkov 1, Borislav Kitov
Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011
 1 of 5 6/18/2012 11:08 AM Medical Policy Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011 Description/Scope
1 of 5 6/18/2012 11:08 AM Medical Policy Subject: Implanted Devices for Spinal Stenosis Policy #: SURG.00092 Current Effective Date: 07/13/2011 Status: Reviewed Last Review Date: 05/19/2011 Description/Scope
NON SURGICAL SPINAL DECOMPRESSION. Dr. Douglas A. VanderPloeg
 NON SURGICAL SPINAL DECOMPRESSION Dr. Douglas A. VanderPloeg CONTENTS I. Incidence of L.B.P. II. Anatomy Review III. IV. Disc Degeneration, Bulge, and Herniation Non-Surgical Spinal Decompression 1. History
NON SURGICAL SPINAL DECOMPRESSION Dr. Douglas A. VanderPloeg CONTENTS I. Incidence of L.B.P. II. Anatomy Review III. IV. Disc Degeneration, Bulge, and Herniation Non-Surgical Spinal Decompression 1. History
Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University
 Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University CanMEDS Roles / Competencies Name: PGY Rotation Dates: s s Exceeds N/A Attending Staff:
Adult Spine Rotation Specific Evaluation Orthopaedic Surgery Training Program School of Medicine, Queen s University CanMEDS Roles / Competencies Name: PGY Rotation Dates: s s Exceeds N/A Attending Staff:
