MALE GENITOURINARY EMERGENCIES
|
|
|
- Allen Holt
- 10 years ago
- Views:
Transcription
1 MALE GENITOURINARY EMERGENCIES Objectives: 1. Distinguish between testicular torsion and epididymitis regarding the history and physical findings 2. Describe Prehn s sign and the cremasteric reflex and their utility in the diagnosis of testicular torsion 3. Discuss the meaning of the following: In the patient with suspected renal colic, the physical exam should be remarkably unremarkable 4. List the indications for hospitalization and/or urology consultation in a patient with renal colic Copyright UC Regents 1
2 MALE GENITOURINARY EMERGENCIES Anatomy a. penis 1. composed of three cylindrical bodies: two corpora cavernosa (erectile bodies) which are surrounded by tunica albuginea (connective tissue) and corpus spongiosum which surrounds the urethra. All three covered by Buck's fascia 2. blood supply is from internal pudendal artery 3. lymphatics drain into deep and superficial inguinal nodes b. scrotum & testis 1. testes lie vertically, are encased in tunica albuginea except posterolaterally where epididymis lies, average size 4X3 cm 2. tunica vaginalis anchors testis and epididymis to posterior scrotal wall 3. inferiorly testis anchored to scrotum by the scrotal ligament (gubernaculum) 4. posteriorly the tunica vaginalis and tunica albuginea are contiguous. 5. blood supply via the spermatic arteries in the spermatic cord 6. epididymis -a tubular structure that promotes sperm maturation and motility a. lies posterolaterally on the testis b. vestigial embryonic structures located here include the appendix epididymis and the appendix testis 7. vas deferens easily palpable within the adnexa of scrotal sac. It extends in the spermatic cord from the tail of the epididymis through the inguinal canal, behind the bladder, over the ureters, and joins the seminal vesicles to form the ejaculatory ducts in the prostatic urethra c. prostate 1. heart shaped structure 4x3x2 cm at base of bladder, surrounding urethra 2. two lateral lobes separated by median sulcus 3. when enlarges with age or with hyperplastic adenoma, may envelop the urethra between the bladder neck and the urogenital diaphragm causing bladder outlet obstruction PHYSICAL EXAMINATION a. **male abdominal exam not complete until GU exam done b. **male GU exam not complete until rectal done c. visual inspection, palpation d. includes exam of prostate, inguinal canals e. in trauma patient 1. inspect perineum for blood, echymosis, blood at urethral meatus 2. rectal exam for boggy, or high riding prostate, for sphincter tone, blood 3. inspect/palpate scrotum/testis for blood, testis disruption Copyright UC Regents 2
3 PENIS a. balanitis 1. inflammation of glans/foreskin 2. glans purulent, excoriated, tender, malodorous 3. often in children 2-5 yr. caused by irritant, infection, or poor hygiene 4. in adults may be presenting sign of diabetes 5. treatment, antibiotics for gram positive organisms, cleaning, drying, antifungal creams, sometimes circumcision b. phimosis- can t pull foreskin backwards 1. opening of foreskin so small that foreskin can't be retracted behind the glans 2. normal at birth, but 90% boys can retract foreskin by school age; don t forcibly retract 3. etiologies - poor hygiene, infection, scar tissue from prior injury 4. signs- redness, swelling of foreskin, purulent discharge, pain 5. treatment- 0.1% TAC, hot soaks, sitz baths, rarely may need dorsal incision or hemostat dilation of opening of foreskin 6. later, circumcision 7. Urology consultation if urinary retention or cellulites in diabetic 8. Don t blindly catheterize c. paraphimosis- can t bring foreskin forward 1. tight foreskin is retracted, becomes edematous, and can't be pulled back over the glans. Edema impedes circulation of the glans, and distal penis swells 2. causes- balanitis with contracture of foreskin, from hair wound around penis, cock ring 3. to prevent paraphimosis, after urinary catheterization, always pull the foreskin back over the glans, tape penis in upward position so catheter doesn t pull on urinary meatus and cause urethral injury 4. treatment- must reduce foreskin a. manual compression of glans for 5 minutes, or 2X2 gauze bandage wrapped around glans b. may need dorsal nerve block, or procedural sedation 1. circumcision to avoid recurrence d. Peyronie's Disease 1. patient complains of lump on dorsum of penis and painful penile curvature with erection 2. plaque involving the tunica albuginea of the corpora without urethra involvement 3. etiology unknown 4. on exam, palpate hard plaque, not movable, on dorsal surface of penis a. may be associated with Dupuytren's contracture of the hand b. non-emergent urology referral. Up to 50% regress spontaneously within 1 yr. Copyright UC Regents 3
4 e. priapism- Urologic Emergency 1. prolonged, involuntary erection, painful, not associated with sexual arousal 2. thought to be due to imbalance between neural stimuli, and/or from mechanical interference of venous outflow from penis 3. corpora cavernosa becomes engorged with stagnant blood, corpus spongiosum is flaccid and patient can void 4. intracavernosal pressures may exceed arterial systolic pressures resulting in ischemia, therefore is a urologic emergency requiring consultation. Rapid treatment needed to prevent corporal fibrosis and erectile dysfunction 5. morbidity is time dependent a. 6 hr. may be OK b. 24 hr. probably too late 6. types a. low flow or ischemic (from decreased penile venous outflow, sludging, blood stasis) 1. etiologies a) sickle cell, thalassemia b) leukemic infiltration causing sludging c) drugs- trazadone, cocaine, alcohol, marijuana, antihypertensives injections of papaverine, phentolamine, or prostaglandin E1for erectile dysfunction 2. on exam, corpus cavernosum is involved (penile shaft is hard) and spongeosum is spared (glans is soft) 3. diagnosis of type is made with blood gas on blood from corpora with low O 2 and high CO 2 4. treatment a) emergent Urology consultation b) pain relief c) oxygen, hydration d) if sickle cell- transfusion to hemoglobin>10g/d e) corporal aspiration of blood 1) 21 gauge butterfly, aspirate 60 cc from corporus, close to glans 2) irrigate with 10 cc normal saline to stir up sludge, then withdraw and instill phenylephrine 100μg or epi 1:100,000 (1 mg in 10 cc NS), inject 2-3 cc to maximum of 10 cc. 3) monitor, if no improvement need surgical shunt 5. complications- time dependent a) resulting impotence not in future treatable with viagra, only penile prosthesis b) fibrosis, gangrene Copyright UC Regents 4
5 b. highflow (from increased arterial blood flow that overwhelms venous system of penis) 1. from arterial-cavernosal shunt from groin/straddle injury 2. doesn t cause ischemia, not true emergency 3. treatment is conservative vs embolization 4. priapism from spinal cord trauma has similar physiology SCROTAL DISEASE a. soft tissue 1. sebaceous cysts, superficial abscesses 2. look for deeper involvement of bulbous urethra, testis, epididymis 3. if deeper involvement, evaluate by ultrasound b. scrotal (Fournier's) gangrene- necrotizing fasciitis of perineum 1. Urologic Emergency 2. life threatening 3. polymicrobial infection of subcutaneous tissues that originates from perineal, perirectal site 4. surgical emergency requiring extensive debridement 5. peak incidence years 6. rapidly progressive, in hours, preceded by genital discomfort, sweats, fever, chills 7. may be toxic appearing 8. risk factors a) 2/3 have diabetes b) immunocompromised c) alcoholic, wheelchair bound, poor hygeine d) local trauma, surgery e) think about entity in immunocompromised men with scrotal, rectal, genital complaints out of proportion to physical findings 9. infection is foul smelling (anaerobes), may have evidence of gangrene, gas in soft tissues. Early on may only be scrotal edema, blotchy erythema 10. multiple organisms involved including gram negatives, bacteroides, clostridia 11. treatment - antibiotic coverage for gram +, gram -, and anaerobes (amp/genta/flagyl) AND wide, aggressive debridement, ICU care 12. mortality 13% c. hydrocele 1. fluid collection within tunica vaginalis 2. if from infection (epididymitis/orchitis), develops over days 3. if from tumor, accumulates more slowly 4. if idiopathic, is chronic 5. transilluminate the scrotum. If it doesn't transilluminate or testicle can't be palpated adequately, may need ultrasound and urologic referral to establish if idiopathic etiology Copyright UC Regents 5
6 d. paratesticular masses- cancer 1. all testicular masses should be seen by Urology within 1 week 2. gradual, painless enlargement testicle 3. 10% acute testicular pain 4. 10% present with metastasis a) back pain from retroperitoneal mets to nerve roots b) cough, SOB from pulmonary mets c) bone pain from skeletal mets d) extremity swelling from vena caval obstruction 5. physical exam a) firm, nontender mass separate from epididymis b) initial misdiagnosis- epididymitis or hydrocele e. orchitis (isolated), rare 1. usually mumps (in post pubertal boys) and preceded by parotiditis 2. may have severe pain and swelling, nausea, vomiting, fever, chills 3. unilateral in 70% cases 4. usually resolves in 5-10 days 5. treatment is supportive with bedrest, analgesics, scrotal support 6. seldom results in infertility 7. other viruses including dengue, influenza, mononucleosis, varicella, echovirus, coxsackie ACUTE SCROTAL PAIN Differential diagnosis includes orchitis, trauma, hernia, renal colic, abscess, varicocele, neoplasm, leukemia, Henoch-Schonlein purpura, hydrocele, torsion, and epididymitis. Most important to differentiate are torsion and epididymitis. TESTICULAR TORSION Urologic Emergency where Time is of the Essence a. introduction 1. annual incidence 1/4000 males under age of 25; about 3-4 patients/yr. in large hospital 2. age a) can occur at any age, reported in utero to 90 years b) neonatal- from twisting before complete testicular descent and fusion toscrotal wall c) most common at puberty, but % occur after adolescence b. pathophysiology 1. predisposed in testes with an abnormally high attachment of the tunica vaginalis. If the tunica attaches not on the posterolateral surface, but above the epididymis, the testes can rotate within the tunica, testis and spermatic cord twists, occluding venous return, leads to edema, and decreased arterial flow, infarction, necrosis 2. spermatogenesis on unaffected side may decrease 3. salvageability is time dependent and dependent on # of rotations of cord Copyright UC Regents 6
7 a) 3 hr., 5 hr., 8 hr. b) 10 hr., 24hr. c) testicles can torse and detorse, so diagnose even if many hours have passed c. symptoms 1. sudden onset pain in scrotum, but may complain of groin, abdomen, flank pain 2. 50% occur in sleep 3. 42% have nausea, vomiting 4. urinary voiding symptoms are rare 5. because may only have abdominal pain, all males with abdominal pain should have a careful genital exam d. physical findings 1. rare to have significant fever 2. extreme pain and swelling typically results in sub-optimal exam and difficulty differentiating scrotal contents 3. twists in the cord my lead testicle to have "horizontal lie", or be "highriding" because of spermatic cord shortening 4. epididymis may be rotated anteriorally 5. testicle may be larger secondary to venous congestion 6. elevation of the testicle (Prehn's sign) does not give relief, but is a very unreliable diagnostic maneuver 7. cremasteric reflex usually is absent in torsion (stroking inner thigh normally elicits retraction of the ipsilateral testicle moving upward at least.5cm) e. history of spontaneous resolution, and previous episodes in only 11-50% f. laboratory findings 1. urinalysis is normal in 90% 2. 1/3 patients may have leukocytosis 3. ancillary studies looking for decreased blood flow (shouldn t delay surgery) a) ultrasonography may be helpful, but is operator dependent 1) if pulses are not preset, is very predictive of torsion 2) if pulse is found, may be false negative, doesn't rule out torsion b) technetium-99m pertechnetate scans show "cold", hypoperfused area with torsion, not always available, may be time delay c) "ultimate" ancillary study is surgical exploration g. treatment 1. surgery 2. temporizing measure is to detorse testicle manually. Testes twist medially, treat by opening the book, hard to do because very painful a) should give relief of pain (over hours) b) but maneuver may only detorse partially, if testicle is twisted many times h. torsed testicular appendages (appendix testis, or appendix epididymis) 1. are vestigial tissues with no known function Copyright UC Regents 7
8 2. less marked pain than testicular torsion 3. see pathognomonic "blue dot" through scrotal skin, or palpable tender nodule at superior aspect of testicle next to epididymis 4. consult Urology, but can treat this conservatively if can exclude testicular torsion by ultrasound EPIDIDYMITIS a. introduction 1. most common cause of acute scrotal pain/mass 2. incidence is 1/1000 men/year 3. disease of adult men, rarely occurs at puberty, and even more rarely in prepubertal boys 4. rarely is there isolated epdidymitis, usually epididymo-orchitis 5. complications are abscess, chronic pain b. etiology 1. from retrograde spread of organism from vas deferens from infected urine in bladder, urethra, prostate. 10% time is bilateral 2. organisms in younger (<40 yr) men- chlamydia, gonorrhea 3. in "older" men- coliforms as E.Coli, Pseudomonas, Proteus more common 4. in immunocompromised- TB, cryptococcus, fungal c. symptoms 1. pain begins gradually, peaking over many hours, sometimes described as "sudden onset" 2. pain may be sharp and radiate to groin, or dull, aching, scrotal discomfort % have urinary frequency, urgency, dysuria 4. may begin after straining, GU surgery, instrumentation, sexual contact d. physical findings 1. may have low grade fever, sepsis is rare 2. early on is localized, indurated, tender epididymis 3. scrotum may be erythematous, edematous 4. scrotal elevation/support may give relief (positive Prehn's sign) e. laboratory findings 1. urinalysis- 90% have pyruia/bacteruria (>10 WBC/hpf) 2. WBC may be 10-30,000 f. treatment 1. strict bed rest with scrotal elevation 2. analgesics, ice pack or heat 3. antibiotics a) <35 yr- ceftriaxone 125 mg IM and doxycycline 100mg bid for 7 days b) in older men, consider treatment for gram negatives, i.e. fluroquinolone Copyright UC Regents 8
9 4. **urology follow-up, testicular cancer may initially be misdiagnosed as epdidymitis, pain is due to acute hemorrhage in the tumor 5. indications for hospitalization/urology consultation a) intractable pain, nausea, vomiting b) sepsis with high fever, rigors c) all pediatric cases (rare, diagnosis more likely torsion) PROSTATITIS a. most misdiagnosed disorder in male urology b. acute bacterial prostatitis 1. significant dysuria, frequency, urgency, back or perineal pain, fever, chills, dehydration 2. prostatic tenderness, swelling, hard or boggy 3. organisms include coliforms, gc, chlamydia 4. hospitalize and treat with quinolone for 4-6 weeks 5. avoid foley catheterization which can obstruct prostatic drainage, may need suprapubic catheter if can t void 6. don t massage the prostate 7. bed rest, analgesics, stool softeners, antipyretics c. chronic bacterial prostatitis 1. variable symptoms of dysuria, urgency, frequency, nocturia, pain; rectal exam not helpful 2. diagnosis based on recurrent positive cultures after prostate massage 3. usually gram negatives, treat with antibiotics for 4-6 weeks d. nonbacterial prostatitis 1. like chronic prostatitis, but cultures negative 2. treat like chronic prostatitis plus NSAIDs, sitz bath ACUTE URINARY RETENTION & OVERFLOW INCONTINENCE a. etiologies (really two types: detrusor failure, e.g. pump failure, and outflow obstruction) 1. neurogenic (spinal cord compression below L4/5) 2. trauma- urethral disruption, penile strangulation 3. obstructive most common etiology (BPH, prostate or bladder cancer, urethral stricture) 4. degenerative (diabetes, multiple sclerosis, Parkinson's) 5. pharmacologic- anticholinergics, sympathomimetics acting that inhibit bladder emptying b. history 1. obtain history of medications 2. obtain history for obstruction, i.e. nocturia, hesitancy, diminished force of voiding, poor urinary stream, urethritis, stricture history, low abdominal pain inability to void, urgency Copyright UC Regents 9
10 c. exam 1. perform good neuro exam, especially of lower extremities because of similar neurovascular innervation 2. good GU/rectal exam for meatus stenosis, masses, abscesses, prostate size 3. percuss/palpate for bladder distention d. treatment- catheterization 1. lubrication of catheter (lidocaine jelly into the urethra first), 16F-18F foley or Coude catheter which has a firm, angulated tip 2. hold penis straight up when passing catheter 3. don't inflate balloon until catheter fully inserted 4. if no urine, before inflate balloon, irrigate the foley with 60 cc NS, then will typically get drainage 5. don't have to drain bladder in stages 6. occasionally if chronic distention, may have bladder mucosal edema and rapid decompression will result in transient gross hematuria (2-16%) not clinically significant 7. treat with antibiotics if urine is infected or catheter will be in place for more than 5 days 8. watch for post obstructive diuresis. If urinary retention has been chronic, should observe for several hours to assess for this. More likely if patient has an elevated BUN/creatinine > 4.0 or if urine output>200cc/hr for more than 4 hr. Therefore should observe for several hours 9. Urology follow-up GU EVALUATION IN MULTIPLE TRAUMA a. life threatening injuries take precedence over diagnostic evaluation of GU tract b. GU evaluation during secondary survey c. Suspect GU injury if: 1. blood at meatus 2. gross hematuria or microscopic hematuria in setting of hypotension 3. abnormal prostate exam a) high riding, boggy b) prostate sheared from pelvis and migrates up, and hematoma fills normal position of prostate 4. flank, abdominal, perineal hematoma/eccymosis 5. fractures of the pelvis, lower ribs, lumbar spine d. penile injuries 1. penile fracture a) from sudden flexion of erect penis (i.e. penis slips out of vagina and thrust against perineum) b) from linear tear in tunica albuginea with injury to corporal body due to trauma to erect penis Copyright UC Regents 10
11 c) complain of sudden, severe pain, snapping sound, loss of erection d) physical- tender, swelling, eccymosis of penile shaft e) treatment- may have associated urethral disruption (consider if blood at meatus or hematuria), need retrograde urethrogram to evaluate f) consult Urology, surgery usually necessary to correct or prevent sequelae 2. entrapment a) from objects around penis (string, metal rings, wire, etc.) occluding venous, then arterial blood supply may result in severe edema, urinary retention, gangrene of skin, fistulas b) in young boys, entrapped hair is often cause of glans swelling after careful removal, need to ensure urethra and blood supply are intact c) zipper entrapment- cut median bar of zipper or cut across zipper transversely below entrapment and zipper pulls apart 3. penile amputation a) high success rate of reimplantation, with good urinary and erectile function b) penis should be placed in bag, and bag on ice in a cooler e. urethral injury 1. may manifest as blood at urethral meatus, inability to void, difficulty in catheter insertion, perineal ecchymosis, high riding prostate on exam 2. if is blood at meatus, etc. need retrograde urethrogram before instrumentation to prevent partial urethral laceration from becoming complete, or false passage 3. alternative is suprapubic cystostomy 4. anterior urethral injury (distal to urogenital diaphragm) a) straddle injuries, fractured pelvis, foreign body b) signs- hematuria, pain, butterfly hematoma of perineum (blood through Buck s fascia to Colles fascia), abdominal wall c) rarely an isolated injury, complications of stricture, fistula, incontinence, impotence d) evaluation is retrograde urethrogram (RUG) 1) Foley cath tip into urethra, occlude urethra gently with pressure around glans 2) gently insert cc water soluble contrast (renografin) with Toomey syringe 3) get oblique x-ray to visualize best urethral disruption 5. posterior urethral injury (membranous/prostatic urethra) a) most associated with pelvic fracture; 35% have associated bladder injury b) signs include distended bladder, can't urinate, blood at meatus, gross hematuria, low abdominal pain c) high riding or boggy prostate d) diagnosis with retrograde urethrogram e) treatment is suprapubic drainage, delayed repair Copyright UC Regents 11
12 f) complications are stricture, incontinence, impotence f. bladder injury 1. associated with other injuries, 2/3 with pelvic fractures, or with steering wheel injury 2. severe abdominal pain, tender abdomen, shock, can't urinate, no urine with Foley, blood at meatus 3. gross hematuria (10% have no hematuria) 4. diagnosis by CT cystogram 5. treatment is foley catheter if rupture is extraperitoneal, surgery if intraperitoneal g. ureter injury 1. 90% are from penetrating or iatrogenic (post hystererctomy) 2. asymptomatic and often missed and found during surgery 3. U/A doesn t predict/exclude injury 4. IVP sensitive, CT is poor at diagnosing 5. complications include abscess, urinoma, hydronephrosis 6. repair surgically h. renal injury- Grades % from blunt trauma 2. usually associated with injury to other organs 3. suspect if gross hematuria, or microscopic with hypotension 4. diagnosis by CT scan 5. treatment a) increasingly conservative, non-operative for Grades 1-3 b) Grade 3- through medulla, not into collecting system c) Grade 4- through collecting system d) Grade 5- shattered kidney, avulsed from pedicle treat with nephrectomy i. renal vascular injury 1. think about with lower rib fracture, transverse process fracture of L in children think when is mechcanism of deceleration (injury typically of left kidney) 3. think if have previously abnormal kidney 4. 30% have no hematuria Copyright UC Regents 12
13 MALE GENITOURINARY EMERGENCIES Case 1 A 16 year old adolescent male comes to the ED complaining of severe right flank and scrotal pain beginning several hours ago, awakening him from sleep. He denies GU trauma, fever, chills, sexual activity, dysuria, hematuria, urinary discharge, frequency, nocturia. On physical examination he appears in moderate pain. His BP =130/88, P=100 R=20, T=37 C. 1. What is your differential diagnosis for acute scrotal pain, and what is this patient s worst possible diagnosis? 2. What should you look for in the GU exam? 3. What laboratory studies should be sent? Why? Any ancillary studies? Case 2 A 35 year old man presents to the ED with the sudden onset of severe LLQ abdominal pain radiating to his left groin. He notes urinary urgency, and frequency, but denies fever, chills, hematuria. He states he had a kidney stone 5 years ago and his current symptoms are identical. 1. Is the physical examination helpful in diagnosing kidney stones? 2. What laboratory or ancillary tests should be ordered in patients suspected of having renal colic? What is the best way to diagnose a kidney stone? 3. How is renal colic treated in the ED? 4. What are the indications for admitting a patient with renal colic to the hospital? Copyright UC Regents 13
14 ANSWERS Case 1 1) The major entities to be distinguished in acute non-traumatic scrotal pain are testicular torsion and epididymitis. Of these two, torsion is the worst, as untreated torsion will result within hours in testicular ischemia, possible necrosis, and possible resulting infertility. 2) The GU exam in patients with acute scrotal pain can be difficult. Patients with epididymitis typically have associated orchitis and severe tenderness. It is frequently very difficult to delineate the epididymitis. Patients with torsion may have a horizontal orientation of the torsed testicle. They may have increased pain on elevation of the scrotum (i.e. Prehn s sign, a test which is insensitive and nonspecific for torsion). The presence of a cremasteric reflex makes torsion unlikely, but if missing does not rule out (or in) torsion. 3) A urinalysis (looking for pyruia0 is the best quick ED test for epididymitis, although up to 15% of patients with epididymitis may not have pyuria. A CBC is unhelpful as patients with both epididymitis and torsion may have elevated white blood cell counts (why?). The best ancillary test to diagnose torsion is a testicular ultrasound, although surgery is the gold standard. Case 2 1) The physical examination in a patient with kidney stones should be remarkably unremarkable. This means that any significant findings suggest that the patient does NOT have renal colic. Peritoneal findings on the abdominal exam are NOT found in renal colic, and other diagnoses must be entertained. Similarly, women with an abnormal pelvic exam, and men with abnormal GU/rectal exams, probably do not have renal colic. 2) Urinalysis (looking for microscopic hematuria) should be obtained. Electrolytes and renal function tests are also appropriate. CBC should be sent if other abdominal/gu pathology or infection is being considered. Other tests such as calcium and uric acid will not typically change ED management of renal colic, but may be helpful to the physician providing follow-up. 3) Pain management is of foremost importance in patients with renal colic. Ketorolac (30 mg IV) may be tried. If this does not relieve their pain within 20 minutes, morphine, the gold standard, should be titrated to effect. Patients should be given enough IV fluids to make them euvolemic, but should not be flooded with fluids, as there is no evidence large amounts of fluid facilitates passage of the stone, and may cause increased pain. Copyright UC Regents 14
15 4) Indications for hospitalization or Urology consultation for patients with kidney stones include: a. fever b. intractable pain c. intractable nausea and vomiting d. renal insufficiency, one kidney e. kidney stones >5mm size f.?immunocompromise Copyright UC Regents 15
16 MALE GENITOURINARY EMERGENCIES Bibliography 1. Bakht FR, Guerriero WG. Genitourinary emergencies. Prim Care Dec;16(4): Rosenstein D, McAninch JW. Urologic emergencies. Med Clin North Am Mar;88(2): Marcozzi D, Suner S. The nontraumatic, acute scrotum. Emerg Med Clin North Am Aug;19(3): Galejs LE. Diagnosis and treatment of the acute scrotum. Am Fam Physician Feb 15;59(4): Hanno PM, Wein AJ. UrologicTrauma. Emerg Med Clin North Am Nov;2(4): Copyright UC Regents 16
Urinary tract and perineum
 9 Urinary tract and perineum Key Points 9.1 9.1 THE URINARY BLADDER URINARY RETENTION Acute retention of urine is an indication for emergency drainage of the bladder The common causes of acute retention
9 Urinary tract and perineum Key Points 9.1 9.1 THE URINARY BLADDER URINARY RETENTION Acute retention of urine is an indication for emergency drainage of the bladder The common causes of acute retention
Penile pain- What s wrong, doc? Lincoln Tan Registrar
 Penile pain- What s wrong, doc? Lincoln Tan Registrar The Good Penile pain associated with symptoms or signs consistent with common causes e.g STDs, UTIs The Bad Chronic penile pain without other features
Penile pain- What s wrong, doc? Lincoln Tan Registrar The Good Penile pain associated with symptoms or signs consistent with common causes e.g STDs, UTIs The Bad Chronic penile pain without other features
2. Does the patient have one of the following appropriate indications for placing indwelling urinary catheters?
 A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
Spine University s Guide to Cauda Equina Syndrome
 Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
Spine University s Guide to Cauda Equina Syndrome 2 Introduction Your spine is a very complicated part of your body. It s made up of the bones (vertebrae) that keep it aligned, nerves that channel down
THE KIDNEY. Bulb of penis Abdominal aorta Scrotum Adrenal gland Inferior vena cava Urethra Corona glandis. Kidney. Glans penis Testicular vein
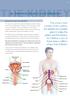 29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page
 A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
Foley Catheter Placement
 Foley Catheter Placement Indications for a Foley Catheter Retention of urine leading to urinary hesitancy, straining to urinate, decrease in size and force of the urinary stream, interruption of urinary
Foley Catheter Placement Indications for a Foley Catheter Retention of urine leading to urinary hesitancy, straining to urinate, decrease in size and force of the urinary stream, interruption of urinary
URINARY CATHETER CARE
 URINARY CATHETER CARE INTRODUCTION Urinary catheter care is a very important skill, and it is a skill that many certified nursing assistants (CNAs) must know. Competence at providing urinary catheter care
URINARY CATHETER CARE INTRODUCTION Urinary catheter care is a very important skill, and it is a skill that many certified nursing assistants (CNAs) must know. Competence at providing urinary catheter care
150640_Brochure_B 4/12/07 2:58 PM Page 2. Patient Information. Freedom From an Enlarged Prostate
 150640_Brochure_B 4/12/07 2:58 PM Page 2 Patient Information Freedom From an Enlarged Prostate 150640_Brochure_B 4/12/07 2:58 PM Page 3 GreenLight Laser Therapy 1 150640_Brochure_B 4/12/07 2:58 PM Page
150640_Brochure_B 4/12/07 2:58 PM Page 2 Patient Information Freedom From an Enlarged Prostate 150640_Brochure_B 4/12/07 2:58 PM Page 3 GreenLight Laser Therapy 1 150640_Brochure_B 4/12/07 2:58 PM Page
BERGEN COMMUNITY COLLEGE DIAGNOSTIC MEDICAL SONOGRAPHY PROGRAM Division of Health Professions DMS 213 SYLLABUS
 BERGEN COMMUNITY COLLEGE DIAGNOSTIC MEDICAL SONOGRAPHY PROGRAM Division of Health Professions DMS 213 SYLLABUS Course Title: DMS 213 - Abdominal Sonography 2 2 lec. 3 lab. 3 credits (5 hours) Required
BERGEN COMMUNITY COLLEGE DIAGNOSTIC MEDICAL SONOGRAPHY PROGRAM Division of Health Professions DMS 213 SYLLABUS Course Title: DMS 213 - Abdominal Sonography 2 2 lec. 3 lab. 3 credits (5 hours) Required
Open the Flood Gates Urinary Obstruction and Kidney Stones. Dr. Jeffrey Rosenberg Dr. Emilio Lastarria Dr. Richard Kasulke
 Open the Flood Gates Urinary Obstruction and Kidney Stones Dr. Jeffrey Rosenberg Dr. Emilio Lastarria Dr. Richard Kasulke Nephrology vs. Urology Nephrologist a physician who has been trained in the diagnosis
Open the Flood Gates Urinary Obstruction and Kidney Stones Dr. Jeffrey Rosenberg Dr. Emilio Lastarria Dr. Richard Kasulke Nephrology vs. Urology Nephrologist a physician who has been trained in the diagnosis
Advanced Practice Provider Academy
 (+)Dean T. Harrison, MPAS,PA C,DFAAPA Director of Mid Level Practitioners; Assistant Medical Director Clinical Evaluation Unit, Division of Emergency Medicine, Department of Surgery, Duke University Medical
(+)Dean T. Harrison, MPAS,PA C,DFAAPA Director of Mid Level Practitioners; Assistant Medical Director Clinical Evaluation Unit, Division of Emergency Medicine, Department of Surgery, Duke University Medical
CHAPTER 5 PELVIC FRACTURES AND CRUSH INJURIES OF THE BLADDER 113
 PELVIC FRACTURES AND CRUSH INJURIES OF THE BLADDER 113 CHAPTER 5 PELVIC FRACTURES AND CRUSH INJURIES OF THE BLADDER GU Tract Ch 2 Ch 3 Ch 4,5 Ch 6,7,8,11 Ch 8,9 Ch 8,9 Ch 8,10 Structure Kidney Ureter Bladder
PELVIC FRACTURES AND CRUSH INJURIES OF THE BLADDER 113 CHAPTER 5 PELVIC FRACTURES AND CRUSH INJURIES OF THE BLADDER GU Tract Ch 2 Ch 3 Ch 4,5 Ch 6,7,8,11 Ch 8,9 Ch 8,9 Ch 8,10 Structure Kidney Ureter Bladder
Anatomy of Male Reproductive System
 Anatomy of Male Reproductive System A. Reproductive Systems 1. Gonads: primary sex organs a. Produce gametes b. Produce hormones c. Male Gonads: testes d. Female Gonads: ovaries 2. Gametes: sex cells a.
Anatomy of Male Reproductive System A. Reproductive Systems 1. Gonads: primary sex organs a. Produce gametes b. Produce hormones c. Male Gonads: testes d. Female Gonads: ovaries 2. Gametes: sex cells a.
Male Infertility. Penis. Epididymis
 Male Infertility Introduction Infertility is a term used when a man is unable to get a woman pregnant. But the term is only used after at least one year of trying. Infertility is a common problem. About
Male Infertility Introduction Infertility is a term used when a man is unable to get a woman pregnant. But the term is only used after at least one year of trying. Infertility is a common problem. About
Spinal Cord and Bladder Management Male: Intermittent Catheter
 Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Men s Health: Testicular & Breast. September 2012
 Men s Health: Testicular & Breast September 2012 Objectives: You will learn: How to perform a testicular self-exam and breast self-exam. You will know when to perform testicular and breast self-exams.
Men s Health: Testicular & Breast September 2012 Objectives: You will learn: How to perform a testicular self-exam and breast self-exam. You will know when to perform testicular and breast self-exams.
LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE
 LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE TALKING ABOUT STRESS INCONTINENCE (SUI) Millions of women suffer from stress incontinence (SUI). This condition results in accidental
LOSS OF BLADDER CONTROL IS TREATABLE TAKE CONTROL AND RESTORE YOUR LIFESTYLE TALKING ABOUT STRESS INCONTINENCE (SUI) Millions of women suffer from stress incontinence (SUI). This condition results in accidental
Urinary Tract Infections
 1 Infections in the urinary tract are relatively common. These infections are often referred to as bladder infections. They are also known as UTI s or urinary tract infections. When an infection is confined
1 Infections in the urinary tract are relatively common. These infections are often referred to as bladder infections. They are also known as UTI s or urinary tract infections. When an infection is confined
Bladder Health Promotion
 Bladder Health Promotion Community Awareness Presentation Content contributions provided by the Society of Urologic Nurses (SUNA) National Association for Continence (NAFC) Simon Foundation for Continence
Bladder Health Promotion Community Awareness Presentation Content contributions provided by the Society of Urologic Nurses (SUNA) National Association for Continence (NAFC) Simon Foundation for Continence
BLUNT TORSO INJURY FROM IMPACT OR DECELERATION HAS ABDOMINAL SOLID ORGAN TRAUMA UNTIL PROVEN OTHERWISE
 Abdominal and Pelvic Trauma In the primary survey, the circulation part includes thinking about the abdomen as a source of occult hemorrhage The OBVIOUS THING is a penetrating abdominal injury Generally
Abdominal and Pelvic Trauma In the primary survey, the circulation part includes thinking about the abdomen as a source of occult hemorrhage The OBVIOUS THING is a penetrating abdominal injury Generally
Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly. Prapa Pattrapornpisut 7 June 2012
 1 Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly Prapa Pattrapornpisut 7 June 2012 2 Urinary incontinence Definition the complaint of any involuntary leakage of
1 Topic review: Clinical presentation and diagnosis of urinary incontinence in the elderly Prapa Pattrapornpisut 7 June 2012 2 Urinary incontinence Definition the complaint of any involuntary leakage of
symptoms of Incontinence
 Types, causes and symptoms of Urinary Incontinence Aims and Objectives Aim: To have an understanding of the types and causes of urinary incontinence. Objectives: To be aware of the incidence and prevalence
Types, causes and symptoms of Urinary Incontinence Aims and Objectives Aim: To have an understanding of the types and causes of urinary incontinence. Objectives: To be aware of the incidence and prevalence
Bladder Health Promotion
 Bladder Health Promotion Community Awareness Presentation endorsed by the Society of Urologic Nurses (SUNA) National Association for Continence( NAFC) Simon Foundation for Continence This presentation
Bladder Health Promotion Community Awareness Presentation endorsed by the Society of Urologic Nurses (SUNA) National Association for Continence( NAFC) Simon Foundation for Continence This presentation
GU Assessment, Diagnosis and Case Studies. Jami Windhorn, RN BSN SOAR Session #7
 GU Assessment, Diagnosis and Case Studies Jami Windhorn, RN BSN SOAR Session #7 GU System Kidneys: Ultrafiltration of the blood, maintain water and electrolyte homeostasis Pelvicalyceal systems: urine
GU Assessment, Diagnosis and Case Studies Jami Windhorn, RN BSN SOAR Session #7 GU System Kidneys: Ultrafiltration of the blood, maintain water and electrolyte homeostasis Pelvicalyceal systems: urine
Vasectomy What happens under normal conditions? What is a vasectomy? How is a vasectomy performed?
 Vasectomy The decision to proceed with a vasectomy is a very personal one. It is important that you have a clear understanding of what a vasectomy is and what it is not. Most patients can expect to recover
Vasectomy The decision to proceed with a vasectomy is a very personal one. It is important that you have a clear understanding of what a vasectomy is and what it is not. Most patients can expect to recover
X-Plain Low Testosterone Reference Summary
 X-Plain Low Testosterone Reference Summary Introduction Testosterone is the most important male sex hormone. It helps the body produce and maintain adult male features. Low levels of testosterone affect
X-Plain Low Testosterone Reference Summary Introduction Testosterone is the most important male sex hormone. It helps the body produce and maintain adult male features. Low levels of testosterone affect
Radiation Therapy for Prostate Cancer
 Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Overactive Bladder (OAB)
 Overactive Bladder (OAB) Overactive bladder is a problem with bladder storage function that causes a sudden urge to urinate. The urge may be difficult to suppress, and overactive bladder can lead to the
Overactive Bladder (OAB) Overactive bladder is a problem with bladder storage function that causes a sudden urge to urinate. The urge may be difficult to suppress, and overactive bladder can lead to the
X-Plain Inguinal Hernia Repair Reference Summary
 X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
X-Plain Inguinal Hernia Repair Reference Summary Introduction Hernias are common conditions that affect men and women of all ages. Your doctor may recommend a hernia operation. The decision whether or
PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS. (CAUTIs)
 PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS (CAUTIs) CAUTIs A UTI where an indwelling urinary catheter was in place for >2 calendar days on the date of event. OR If an indwelling urinary
PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS (CAUTIs) CAUTIs A UTI where an indwelling urinary catheter was in place for >2 calendar days on the date of event. OR If an indwelling urinary
Prostate Cancer. There is no known association with an enlarged prostate or benign prostatic hyperplasia (BPH).
 Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Prevention and Recognition of Obstetric Fistula Training Package. Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula
 Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Urinary Incontinence. Anatomy and Terminology Overview. Moeen Abu-Sitta, MD, FACOG, FACS
 Urinary Incontinence Anatomy and Terminology Overview Moeen Abu-Sitta, MD, FACOG, FACS Purpose Locate and describe the anatomy of the Female Urinary System Define terminology related to Incontinence Describe
Urinary Incontinence Anatomy and Terminology Overview Moeen Abu-Sitta, MD, FACOG, FACS Purpose Locate and describe the anatomy of the Female Urinary System Define terminology related to Incontinence Describe
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
These rare variants often act aggressively and may respond differently to therapy than the more common prostate adenocarcinoma.
 Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
FEMALE INCONTINENCE REVIEW
 200 S. Wenona Suite 298 Steven L. Jensen, M.D. 5400 Mackinaw, Suite 4302 Bay City, MI 48706 Frank H. Kim, M.D. Saginaw, MI 48604 Telephone (989) 895-2634 Adult & Pediatric Urologists (989) 791-4020 Fax
200 S. Wenona Suite 298 Steven L. Jensen, M.D. 5400 Mackinaw, Suite 4302 Bay City, MI 48706 Frank H. Kim, M.D. Saginaw, MI 48604 Telephone (989) 895-2634 Adult & Pediatric Urologists (989) 791-4020 Fax
A912: Kidney, Renal cell carcinoma
 A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
A912: Kidney, Renal cell carcinoma General facts of kidney cancer Renal cell carcinoma, a form of kidney cancer that involves cancerous changes in the cells of the renal tubule, is the most common type
Riesa Gusewelle, MNSc, RN, APRN, GNP-BC. OBJECTIVES Identify early warning signs of urinary tract
 Detection, Early Management & Prevention, of Urinary Tract Infections in Older Adults Riesa Gusewelle, MNSc, RN, APRN, GNP-BC OBJECTIVES Identify early warning signs of urinary tract infections (UTIs)
Detection, Early Management & Prevention, of Urinary Tract Infections in Older Adults Riesa Gusewelle, MNSc, RN, APRN, GNP-BC OBJECTIVES Identify early warning signs of urinary tract infections (UTIs)
Kaiser Oakland Urology
 Kaiser Oakland Urology The Main Purpose of Bladder Catheterization Complete Bladder Emptying! Help maintain a healthy bladder Help maintain healthy kidneys Reduce the chances of significant urinary tract
Kaiser Oakland Urology The Main Purpose of Bladder Catheterization Complete Bladder Emptying! Help maintain a healthy bladder Help maintain healthy kidneys Reduce the chances of significant urinary tract
Pyelonephritis: Kidney Infection
 Pyelonephritis: Kidney Infection National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is pyelonephritis? Pyelonephritis
Pyelonephritis: Kidney Infection National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is pyelonephritis? Pyelonephritis
Lymph Node Dissection for Penile Cancer
 Lymph Node Dissection for Penile Cancer Exceptional healthcare, personally delivered Removal of Lymph Nodes Why are the Lymph Nodes so important when I have penile cancer? Lymph nodes are small bean shaped
Lymph Node Dissection for Penile Cancer Exceptional healthcare, personally delivered Removal of Lymph Nodes Why are the Lymph Nodes so important when I have penile cancer? Lymph nodes are small bean shaped
Location: Clinical Practice Manual
 Subject: Area: Classification: Relevant to: Bladder Management Clinical Practice All Clinical Staff Implementation Date: March 2001 Review Date: March 2004 Responsible for Review: Approved by: Distribution:
Subject: Area: Classification: Relevant to: Bladder Management Clinical Practice All Clinical Staff Implementation Date: March 2001 Review Date: March 2004 Responsible for Review: Approved by: Distribution:
Erectile Dysfunction (ED)
 Information from your Patient Aligned Care Team What is Erectile Dysfunction or ED? Erectile dysfunction (also known as impotence) is the inability to get and keep an erection firm enough for sex. Having
Information from your Patient Aligned Care Team What is Erectile Dysfunction or ED? Erectile dysfunction (also known as impotence) is the inability to get and keep an erection firm enough for sex. Having
male sexual dysfunction
 male sexual dysfunction lack of desire Both men and women often lose interest in sex during cancer treatment, at least for a time. At first, concern for survival is so overwhelming that sex is far down
male sexual dysfunction lack of desire Both men and women often lose interest in sex during cancer treatment, at least for a time. At first, concern for survival is so overwhelming that sex is far down
Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide
 Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide Urinary Incontinence (Urine Loss) This booklet is intended to give you some facts on urinary incontinence - what it is, and is not, and
Urinary Incontinence (Involuntary Loss of Urine) A Patient Guide Urinary Incontinence (Urine Loss) This booklet is intended to give you some facts on urinary incontinence - what it is, and is not, and
INFORMATION FOR PATIENTS CONSIDERING LAPAROSCOPIC INGUINAL HERNIA REPAIR
 INFORMATION FOR PATIENTS CONSIDERING A LAPAROSCOPIC INGUINAL HERNIA REPAIR Prepared By Mr Peter Willson Consultant Surgeon Contents 1. Background... 3 2. What is an inguinal Hernia?... 3 3. What are the
INFORMATION FOR PATIENTS CONSIDERING A LAPAROSCOPIC INGUINAL HERNIA REPAIR Prepared By Mr Peter Willson Consultant Surgeon Contents 1. Background... 3 2. What is an inguinal Hernia?... 3 3. What are the
Prevention of catheter associated urinary tract infections
 Prevention of catheter associated urinary tract infections Dr. Suzan Sanavi, Nephrologist, M.D University of Social Welfare and Rehabilitation Akhavan Physical Spine Center INTRODUCTION Urinary bladder
Prevention of catheter associated urinary tract infections Dr. Suzan Sanavi, Nephrologist, M.D University of Social Welfare and Rehabilitation Akhavan Physical Spine Center INTRODUCTION Urinary bladder
RENAL ANGIOMYOLIPOMA EMBOLIZATION
 RENAL ANGIOMYOLIPOMA EMBOLIZATION The information about renal angiomyolipomas on the next several pages includes questions commonly asked about the embolization procedure. Please take a few moments to
RENAL ANGIOMYOLIPOMA EMBOLIZATION The information about renal angiomyolipomas on the next several pages includes questions commonly asked about the embolization procedure. Please take a few moments to
Medical Tests for Prostate Problems
 Medical Tests for Prostate Problems National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is the prostate? The
Medical Tests for Prostate Problems National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is the prostate? The
Preparation for your vasectomy
 Preparation for your vasectomy You have been scheduled for a vasectomy with the SIU Division of Urology. Please read through this information carefully. Vasectomies are performed in the REI clinic, 751
Preparation for your vasectomy You have been scheduled for a vasectomy with the SIU Division of Urology. Please read through this information carefully. Vasectomies are performed in the REI clinic, 751
Prostate Cancer Action Plan: Choosing the treatment that s right for you
 Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
Hernia- Open Inguinal Hernia Repair PROCEDURAL CONSENT FORM. A. Interpreter / cultural needs. B. Condition and treatment
 DO NOT WRITE IN THIS BINDING MARGIN v5.00-04/2011 SW9317 Hernia- Open Inguinal Hernia Repair Facility: A. Interpreter / cultural needs An Interpreter Service is required? Yes No If Yes, is a qualified
DO NOT WRITE IN THIS BINDING MARGIN v5.00-04/2011 SW9317 Hernia- Open Inguinal Hernia Repair Facility: A. Interpreter / cultural needs An Interpreter Service is required? Yes No If Yes, is a qualified
AMS Sphincter 800 Urinary Prosthesis
 AMS Sphincter 800 Urinary Prosthesis AMS Sphincter 800 AMS Sphincter 800 AMS Sphincter 800 The device is implanted in the body and cannot be seen. The cuff can be placed at the bulbous urethra or at the
AMS Sphincter 800 Urinary Prosthesis AMS Sphincter 800 AMS Sphincter 800 AMS Sphincter 800 The device is implanted in the body and cannot be seen. The cuff can be placed at the bulbous urethra or at the
Get the Facts, Be Informed, Make YOUR Best Decision. Pelvic Organ Prolapse
 Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Pelvic Organ Prolapse ETHICON Women s Health & Urology, a division of ETHICON, INC., a Johnson & Johnson company, is dedicated to providing innovative solutions for common women s health problems and to
Appropriate Urinary Catheter Use and Management
 Appropriate Urinary Catheter Use and Management Nursing Education Material Mohamad Fakih, MD, MPH 1 This presentation This presentation targets all nurses with patient care responsibilities including the
Appropriate Urinary Catheter Use and Management Nursing Education Material Mohamad Fakih, MD, MPH 1 This presentation This presentation targets all nurses with patient care responsibilities including the
Palm Beach Obstetrics & Gynecology, PA
 Palm Beach Obstetrics & Gynecology, PA 4671 S. Congress Avenue, Lake Worth, FL 33461 561.434.0111 4631 N. Congress Avenue, Suite 102, West Palm Beach, FL 33407 Urinary Tract Infection About one of every
Palm Beach Obstetrics & Gynecology, PA 4671 S. Congress Avenue, Lake Worth, FL 33461 561.434.0111 4631 N. Congress Avenue, Suite 102, West Palm Beach, FL 33407 Urinary Tract Infection About one of every
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
URINARY CATHETER INSERTION - STRAIGHT OR INDWELLING CATHETER
 URINARY CATHETER INSERTION - STRAIGHT OR INDWELLING CATHETER PURPOSE To obtain a sterile urine specimen. To facilitate emptying bladder. To relieve bladder distention. To irrigate bladder. To measure residual
URINARY CATHETER INSERTION - STRAIGHT OR INDWELLING CATHETER PURPOSE To obtain a sterile urine specimen. To facilitate emptying bladder. To relieve bladder distention. To irrigate bladder. To measure residual
surg urin Surgery: Urinary System 1
 Surgery: Urinary System 1 This section contains information to assist providers in billing for surgical procedures related to the urinary system. Extracorporeal Shock Wave Lithotripsy Medi-Cal covers Extracorporeal
Surgery: Urinary System 1 This section contains information to assist providers in billing for surgical procedures related to the urinary system. Extracorporeal Shock Wave Lithotripsy Medi-Cal covers Extracorporeal
Normal bladder function requires a coordinated effort between the brain, spinal cord, and the bladder.
 .. Urinary Incontinence Urinary incontinence is not an inevitable part of aging, and it is not a disease. The loss of bladder control - called urinary incontinence - affects between 13 and 17 million adult
.. Urinary Incontinence Urinary incontinence is not an inevitable part of aging, and it is not a disease. The loss of bladder control - called urinary incontinence - affects between 13 and 17 million adult
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 21 CBULP 2011 068 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 21 CBULP 2011 068 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Urinary Incontinence in Women. Susan Hingle, M.D. Department of Medicine
 Urinary Incontinence in Women Susan Hingle, M.D. Department of Medicine Background Estimated 13 million Americans with urinary incontinence Women are affected twice as frequently as men Only 25% will seek
Urinary Incontinence in Women Susan Hingle, M.D. Department of Medicine Background Estimated 13 million Americans with urinary incontinence Women are affected twice as frequently as men Only 25% will seek
NUR 111 Anne Marie Holler RN MSN(c)
 NUR 111 Anne Marie Holler RN MSN(c) Assignments Required Readings: Potter & Perry: pp. 1042-1085 Skills book: 809-840 Knowledge Base Anatomy Control Mechanisms Factors that inhibit micturation (voiding)
NUR 111 Anne Marie Holler RN MSN(c) Assignments Required Readings: Potter & Perry: pp. 1042-1085 Skills book: 809-840 Knowledge Base Anatomy Control Mechanisms Factors that inhibit micturation (voiding)
Sonography of Hernias
 Sonography of Hernias Cindy Rapp BS, RDMS, FAIUM, FSDMS Sr. Clinical Marketing Manager Toshiba America Medical Systems Tustin, California What is a hernia? A hernia is a protrusion of an organ or tissue
Sonography of Hernias Cindy Rapp BS, RDMS, FAIUM, FSDMS Sr. Clinical Marketing Manager Toshiba America Medical Systems Tustin, California What is a hernia? A hernia is a protrusion of an organ or tissue
95% of childhood kidney cancer cases are Wilms tumours. Childhood kidney cancer is extremely rare, with only 90 cases a year in
 James Whale Fund for Kidney Cancer Childhood kidney cancer factsheet Kidney cancer rarely afflicts children and about 90 paediatric cases are diagnosed in the UK each year. About 75% of childhood kidney
James Whale Fund for Kidney Cancer Childhood kidney cancer factsheet Kidney cancer rarely afflicts children and about 90 paediatric cases are diagnosed in the UK each year. About 75% of childhood kidney
PATIENT GUIDE. Localized Prostate Cancer
 PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma
 Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma Chapter 50 Abdominal Trauma 1 Describe the epidemiology, including morbidity, mortality rates, and prevention strategies,
Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma Chapter 50 Abdominal Trauma 1 Describe the epidemiology, including morbidity, mortality rates, and prevention strategies,
Inguinal (Groin) Hernia Repair
 Information for patients Inguinal (Groin) Hernia Repair General Surgery Tel: 01473 712233 DMI ref: 11582-09.indd(RP) Issue 1: February 2010 The Ipswich Hospital NHS Trust, 2010. All rights reserved. Not
Information for patients Inguinal (Groin) Hernia Repair General Surgery Tel: 01473 712233 DMI ref: 11582-09.indd(RP) Issue 1: February 2010 The Ipswich Hospital NHS Trust, 2010. All rights reserved. Not
Coding Companion for Urology/Nephrology. A comprehensive illustrated guide to coding and reimbursement
 Coding Companion for Urology/Nephrology A comprehensive illustrated guide to coding and reimbursement 2013 Contents Getting Started with Coding Companion...i Integumentary...1 Arteries and Veins...15 Lymph
Coding Companion for Urology/Nephrology A comprehensive illustrated guide to coding and reimbursement 2013 Contents Getting Started with Coding Companion...i Integumentary...1 Arteries and Veins...15 Lymph
Self Catheterization Guide
 Self Catheterization Guide An introduction to intermittent self-catheterization Medical professionals have recommended that you selfcatheterize in order to completely empty your bladder. This prevents
Self Catheterization Guide An introduction to intermittent self-catheterization Medical professionals have recommended that you selfcatheterize in order to completely empty your bladder. This prevents
Bowel and Bladder Dysfunction in MS. Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center. Bladder Dysfunction
 Bowel and Bladder Dysfunction in MS Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center Bladder Dysfunction Approximately 75% of people with MS experience bladder problems
Bowel and Bladder Dysfunction in MS Tracy Walker, WOCN, MSCN, FNP C Nurse Practitioner MS Institute at Shepherd Center Bladder Dysfunction Approximately 75% of people with MS experience bladder problems
Going Home with a Urinary Catheter
 Going Home with a Urinary Catheter Doctor: Phone Number: About Your Catheter A urinary catheter is a small tube that goes through your urethra and into your bladder. This tube then drains the urine made
Going Home with a Urinary Catheter Doctor: Phone Number: About Your Catheter A urinary catheter is a small tube that goes through your urethra and into your bladder. This tube then drains the urine made
Blood in the urine (hematuria)
 Blood in the urine (hematuria) Hematuria refers to the presence of blood in the urine. It is important to investigate the cause of hematuria because rarely, it is caused by a serious condition, such as
Blood in the urine (hematuria) Hematuria refers to the presence of blood in the urine. It is important to investigate the cause of hematuria because rarely, it is caused by a serious condition, such as
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options
 AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
Ovarian Cyst. Homoeopathy Clinic. Introduction. Types of Ovarian Cysts. Contents. Case Reports. 21 August 2002
 Case Reports 21 August 2002 Ovarian Cyst Homoeopathy Clinic Check Yourself If you have any of the following symptoms call your doctor. Sense of fullness or pressure or a dull ache in the abdomen Pain during
Case Reports 21 August 2002 Ovarian Cyst Homoeopathy Clinic Check Yourself If you have any of the following symptoms call your doctor. Sense of fullness or pressure or a dull ache in the abdomen Pain during
HEALTH NEWS PROSTATE CANCER THE PROSTATE
 HEALTH NEWS PROSTATE CANCER THE PROSTATE Prostate comes from the Greek meaning to stand in front of ; this is very different than prostrate which means to lie down flat. The prostate is a walnut-sized
HEALTH NEWS PROSTATE CANCER THE PROSTATE Prostate comes from the Greek meaning to stand in front of ; this is very different than prostrate which means to lie down flat. The prostate is a walnut-sized
Female Urinary Disorders and Pelvic Organ Prolapse
 Female Urinary Disorders and Pelvic Organ Prolapse Richard S. Bercik, M.D. Director, Division of Urogynecology & Reconstruction Pelvic Surgery Department of Obstetrics, Gynecology & Reproductive Sciences
Female Urinary Disorders and Pelvic Organ Prolapse Richard S. Bercik, M.D. Director, Division of Urogynecology & Reconstruction Pelvic Surgery Department of Obstetrics, Gynecology & Reproductive Sciences
Urinary Incontinence FAQ Sheet
 Urinary Incontinence FAQ Sheet Are you reluctant to talk to your doctor about your bladder control problem? Don t be. There is help. Loss of bladder control is called urinary incontinence. It can happen
Urinary Incontinence FAQ Sheet Are you reluctant to talk to your doctor about your bladder control problem? Don t be. There is help. Loss of bladder control is called urinary incontinence. It can happen
Simple Urinary Techniques to Diagnose and Treat Complex Urinary Conditions
 Simple Urinary Techniques to Diagnose and Treat Complex Urinary Conditions Jody P. Lulich, DVM,PhD, The Minnesota Urolith Center, St Paul MN 55108 USA NONSURGICAL STONE REMOVAL: VOIDING UROHYDROPROPULSION
Simple Urinary Techniques to Diagnose and Treat Complex Urinary Conditions Jody P. Lulich, DVM,PhD, The Minnesota Urolith Center, St Paul MN 55108 USA NONSURGICAL STONE REMOVAL: VOIDING UROHYDROPROPULSION
KEYHOLE HERNIA SURGERY
 Disclaimer This movie is an educational resource only and should not be used to manage a hernia or abdominal pain. All decisions about the management of a hernia must be made in conjunction with your Physician
Disclaimer This movie is an educational resource only and should not be used to manage a hernia or abdominal pain. All decisions about the management of a hernia must be made in conjunction with your Physician
Vasectomy Services Patient Information
 Vasectomy Services Patient Information Vasectomy Vasectomy Please read this information leaflet and consent form carefully, and bring it with you to your appointment. Please ask the doctor any questions
Vasectomy Services Patient Information Vasectomy Vasectomy Please read this information leaflet and consent form carefully, and bring it with you to your appointment. Please ask the doctor any questions
Bladder Catheterization
 Approved by: Bladder Catheterization Gail Cameron Senior Director, Operations, Maternal, Neonatal & Child Health Programs Dr. Ensenat Medical Director, Neonatology Neonatal Nursery Policy & Procedures
Approved by: Bladder Catheterization Gail Cameron Senior Director, Operations, Maternal, Neonatal & Child Health Programs Dr. Ensenat Medical Director, Neonatology Neonatal Nursery Policy & Procedures
1. What is the prostate-specific antigen (PSA) test?
 1. What is the prostate-specific antigen (PSA) test? Prostate-specific antigen (PSA) is a protein produced by the cells of the prostate gland. The PSA test measures the level of PSA in the blood. The doctor
1. What is the prostate-specific antigen (PSA) test? Prostate-specific antigen (PSA) is a protein produced by the cells of the prostate gland. The PSA test measures the level of PSA in the blood. The doctor
International Journal of Case Reports in Medicine
 International Journal of Case Reports in Medicine Vol. 2013 (2013), Article ID 340925, 18 minipages. DOI:10.5171/2013.340925 www.ibimapublishing.com Copyright 2013. Massinde Anthony. Distributed under
International Journal of Case Reports in Medicine Vol. 2013 (2013), Article ID 340925, 18 minipages. DOI:10.5171/2013.340925 www.ibimapublishing.com Copyright 2013. Massinde Anthony. Distributed under
United States Department of Transportation National Highway Traffic Safety Administration Paramedic: National Standard Curriculum 1
 UNIT TERMINAL OBJECTIVE 4-8 At the completion of this unit, the paramedic student will be able to integrate pathophysiologic principles and the assessment findings to formulate a field impression and implement
UNIT TERMINAL OBJECTIVE 4-8 At the completion of this unit, the paramedic student will be able to integrate pathophysiologic principles and the assessment findings to formulate a field impression and implement
Urinary Tract Infections in Children
 Urinary Tract Infections in Children National Kidney and Urologic Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH Urinary
Urinary Tract Infections in Children National Kidney and Urologic Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH Urinary
CARE PROCESS STEP EXPECTATIONS RATIONALE
 URINARY INCONTINENCE CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for urinary incontinence and any history of urinary
URINARY INCONTINENCE CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for urinary incontinence and any history of urinary
Incontinence. What is incontinence?
 Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
Incontinence What is incontinence? Broadly speaking, the medical term incontinence refers to any involuntary release of bodily fluids, but many people associate it strongly with the inability to control
The main surgical options for treating early stage cervical cancer are:
 INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
INFORMATION LEAFLET ON TOTAL LAPAROSCOPIC RADICAL HYSTERECTOMY (TLRH) FOR EARLY STAGE CERVICAL CANCER (TREATING EARLY STAGE CERVICAL CANCER BY RADICAL HYSTERECTOMY THROUGH KEYHOLE SURGERY) Aim of the leaflet
Acute abdominal conditions Key Points
 7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
190.12 - Urine Culture, Bacterial Summary Information Highlighted items indicate most frequently used codes.
 Medicare National Coverage Determination (NCD) (Jan 2011) Source: CMS: Centers for Medicare & Medicaid Services To view full document: www.cms.gov/coveragegeninfo. Select Lab NCDs, then select NCD Coding
Medicare National Coverage Determination (NCD) (Jan 2011) Source: CMS: Centers for Medicare & Medicaid Services To view full document: www.cms.gov/coveragegeninfo. Select Lab NCDs, then select NCD Coding
URINARY INCONTINENCE IN WOMEN
 URINARY INCONTINENCE IN WOMEN Definition Urinary incontinence (UI) is defined as involuntary loss of urine that is a social or hygienic problem (International Continence Society, 1973) Magnitude of the
URINARY INCONTINENCE IN WOMEN Definition Urinary incontinence (UI) is defined as involuntary loss of urine that is a social or hygienic problem (International Continence Society, 1973) Magnitude of the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
Laparoscopic Repair of Hernias. A simple guide to help answer your questions
 Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Laparoscopic Repair of Hernias A simple guide to help answer your questions What is a hernia? A hernia is defined as a hole or defect in the abdominal (belly) wall. A hernia can either be congenital (a
Long-term result of Memokath urethral sphincter stent in. spinal cord injury patients
 1 Long-term result of Memokath urethral sphincter stent in spinal cord injury patients Subramanian Vaidyanathan 1 E-mail: [email protected] Bakul M Soni 1 E-mail: [email protected]
1 Long-term result of Memokath urethral sphincter stent in spinal cord injury patients Subramanian Vaidyanathan 1 E-mail: [email protected] Bakul M Soni 1 E-mail: [email protected]
