Aesculap Spine activ L
|
|
|
- Gervase Ferguson
- 10 years ago
- Views:
Transcription
1 Aesculap Spine activ L Lumbar intervertebral disc prosthesis Operating technique
2 2 activ L
3 Contents A) Pre-operative planning A.1 Size estimation 4 A.2 Patient positioning 4 B) Approach B.1 Marking the approach 5 B.2 Skin incision 5 B.3 Approach 6 B.4 Anatomical structures 7 C1) Instrumentation spike version C.1.1 Midline marking 10 C.1.2 Discectomy and segment mobilization 12 C.1.3 Parallel distraction, height measurement and size verification 14 C.1.4 En bloc implantation 17 C2) Instrumentation keel version C.2.1 Chisels for keel fixation 24 D) Revision and correction of implant position D.1 Inlay revision 26 D.2 Endplate revision 27 E1) Implant overview 30 E2) Instrument overview 31 3
4 A) Pre-operative planning A.1 Size estimation Measure the optimum or largest possible implant bed area using ct-scan diagnostics with x-ray templates, making sure that the template scale factor is correct. Assess the anatomy of the major vessels, especially the left common iliac vein. Can the vessels be mobilized sufficiently far away from the anterior of the spine? Would a pararectus approach be easier? NB: m Always use the largest possible endplate. Undersized endplates increase the risk of implant sinkage. m Select the correct inlay height to achieve height reconstruction whilst preserving adequate mobility in the joint. A.2 Patient positioning The operating table should permit image intensifier images in 2 planes in the operating zone. Place the patient in a supine position with slightly flexed hips to relieve tension from the major blood vessels. If the operating table permits a spread leg position, this fascilitates axially correct implantation of the prosthesis. Alternatively, the patient is positioned with both legs together. In this case the surgeon stands on the approach side of the patient. A right side approach is recommended for the L5/S1 level and a left side approach for higher levels. 4
5 B) Approach B.1 Marking the approach To mark the incision a lateral image is taken with a metal rod parallel to the defective disc compartment. The extension of this marking corresponds to the midpoint of the skin incision. The skin incision is marked under x-ray control so that the incision lies along the extended line of the intervertebral space. 5 8 cm is usually adequate for single level treatment. B.2 Skin incision The approach should be retroperitoneal. Transperitoneal approaches carry a considerably higher complication risk (ileus, lesion of the presacral plexus). Pararectus approach L2 - L5 Midline incision L2 - L5 Midline incision male L5 - S1 Midline incision female L5 - S1 5
6 B) Approach B.3 Approach Midline approach L5/S1 A midline approach is always used for the L5/S1 level. A Pfannenstiel s incision or a linear midline incision are possible. Both sides are possible for the approach. If no other level is to be operated on, the right side may be preferred. Pararectus approach L2/3, L3/4, L4/5 A midline approach or a pararectus approach (always left) are possible in the L2/3, L3/4 and L4/5 segments. Note: Advantages of the midline approach: m Considerably easier implant positioning, less retraction of the abdominal muscles required. Advantages of the pararectus approach: m Simpler retroperitoneal preparation, less manipulation of the vessels in L4/5. NB: m All approaches demand the greatest care in the preparation of the major vessels. m A vascular surgeon should be constantly available on call during this operation. 6
7 B.4 Anatomical structures Midline approach L5/S1 Pararectus approach Midline approach retroperitoneal Midline approach transperitoneal 7
8 B) Approach B.4 Anatomical structures Midline approach L5/S1 Pararectus approach L2/3, L3/4, L4/5 After the skin incision: linear incision of the anterior fascia of the rectus abdominis muscle a few millimeters paramedially. A blunt instrument is used to push the peritoneum away in a medial direction, first from the rear surface of the muscle and then from the lateral abdominal wall. Epigastric blood vessels must be coagulated and dissected if necessary. Midline approach: As described for ventral L5/S1. The essential difference from the L5/S1 level is that the rectus abdominis muscle in the central and upper abdomen also possesses a rear fascia which it does not have in the lower abdomen. Since this can only be removed from the peritoneum with great difficulty, it should be opened as far laterally as possible after retraction of the muscle. Pararectus approach: Considerably easier on the upper lumbar region of the spine, but only suitable for keelless implants. Higher risk of segmental denervation of the abdominal muscles. The muscle fascia are dissected longitudinally where they meet at the lateral margin of the rectus abdominis muscle. 8
9 Midline approach L5/S1 The ureter and the presacral plexus are carefully mobilized and retracted together with the peritoneum (coagulation should be avoided). The medial sacral vessels are ligated and dissected in the bifurcation of the major vessels. The vessels are mobilized as far to the left as is necessary (or possible) to facilitate implantation of the planned prosthesis size. NB: m The linea alba is not opened. The anterior fascia of the rectus is opened paramedially. Pararectus approach L2/3, L3/4, L4/5 A blunt instrument is used to push the peritoneum away from the abdominal wall whilst monitoring the epigastric vessels. The ureter is prepared away from the operating site together with the peritoneum. The ventrolateral spine is exposed at the anterior margin of the psoas muscle. The neighbouring segment vessels are ligated and dissected, including the ascending lumbar vein for the approach to the L4/5 segment, so that the major vessels can be mobilized to the opposite side. The sympathetic nerve is mobilized in a lateral direction. If possible the situs is fixed with self-retaining retractors. Note: m In the midline marking process, the lateral inclination of the operating table may have to be adjusted to compensate for any possible turning of the patient caused by retraction of the muscles and abdominal organs. m Small errors in the axial orientation of the control x-ray can lead to serious malpositioning of the implant. 9
10 C1) Instrumentation spike version C.1.1 Midline marking activ L spike version Midline approach L5/S1 Define the midline of the vertebral body under ap x-ray control. Pararectus approach* L2/3, L3/4, L4/5 The midline marker must be selected according to the preplanned implant size S, M, L or XL. ap projection Pararectus approach * The pararectus approach is only explicitly described when the instruments or technique differ from those of the mid line approach. Otherwise the midline approach is given as an example. 10
11 Midline approach L5/S1 The midline is marked with the pin in the disc compartment under image intensifier control. Alternatively, the marking can be set in the neighbouring vertebral body for the entire duration of the surgery (only sensible for the spike version). Pararectus approach L2/3, L3/4, L4/5 Define the 45 approach to the vertebral body with the help of the lateral midline marker under ap x-ray control. ap projection lateral projection First an ap x-ray is done to check the midline position of the marker. If the ap-midline is correct a lateral x-ray is done. Here too, the x-ray marker must represent the middle of the vertebra. If the size selected does not fit, choose a different sized marker. Mark the 45 position with the pin in the disc compartment. NB: m Make sure that the vertebrae are portrayed in an orthograde position on the x-ray. The pedicles and the spinous process serve as orientation aids for midline marking. m The exact position of the implant is of vital importance for correct function. 11
12 C1) Instrumentation spike version C.1.2 Discectomy and mobilization of the segment Discectomy A discectomy is performed and the endplates freed from disc residue with a curette. The cartilage is also removed to facilitate osteointegration into the Plasmapore µ-cap coating of the implant endplates. If necessary, wedges of the appropriate height or the angled distractor can be used to maintain the correct distance. The angled distractor provides a better view onto the operating site and makes simultaneous discectomy easier. NB: m The cartilage structures should be removed as completely as possible. Cartilage structures can impede osteointegration into the Plasmapore µ-cap coating of the implant endplates. m Overextensive preparation of the endplates could increase the risk of implant migration. m The anulus must only be resected laterally as far as is required by the implant size. If necessary measure the size of the incision using the parallel distractor with the appropriate trial implant. 12
13 Mobilization Mobilize the disc compartment with the distractor. Note: m Make sure that the instrument is advanced as far as possible dorsally into the disc compartment to avoid stress peaks on the endplates, and that distraction is as parallel as possible. m Wedge shaped intervertebral disc space distraction: The posterior intervertebral disc space must be adequately released so that here too a good possibility of distraction can be identified. If necessary the posterior longitudinal ligament must be moved away from the posterior margins of the vertebra. An angled raspatory can be used for this purpose. 13
14 C1) Instrumentation spike version C.1.3 Parallel distraction, height measurement and size verification Mount the trial implant of the defined angle and size onto the parallel distractor. Align the midline markings on the trial implant and the instrument. First verify the size of the trial implant in the disc compartment by x-ray. Expand the parallel distractor by turning the rear button until the resistance against distraction increases (sufficient distraction is achieved when the button can no longer be turned easily by hand). Check that the trial implant is sitting correctly by x-ray. If necessary mount a trial implant of a different size. NB: m If the forces in the intervertebral space are too extreme, they can cause the parallel distractor to bend. In this case the height shown on the scale would be too high. Always check on the x-ray that the instrument is still parallel. 14
15 Midline approach L5/S1 For the midline approach the trial implant is mounted centric. Pararectus approach L2/3, L3/4, L4/5 Align the side markings of the trial implant and the instrument. The angle of the parallel distractor (22.5 ) is half that of the inserter (45 ) in order to make it easier for frequent insertions. 15
16 C1) Instrumentation spike version Read the height on the scale. If the indicator lies between two numbers, choose the smaller height. Release and remove the parallel distractor. Position R for Release for disassembly. If necessary use the spacer of the appropriate height to maintain the correct distance after removal of the parallel distractor. Note: m The implants should cover most of the endplates. An undersized implant increases the risk of sinkage into the endplates. m An oversized inlay may lead to overdistraction, which can irritate the facets, (dura) or nerves. m An undersized inlay could mean that the implant sits too loosely in the degenerated disc compartment and that insufficient stability is achieved. 16
17 C.1.4 En bloc implantation Slide the inlay into the inferior plate with the notch towards the rear. Select the inserter that corresponds to the height of the inlay. The inserter spacers are colour coded: 8.5 mm: blue 10 mm: green 12 mm: black 14 mm: yellow Turn the rear button to move the spacer forward. The spacer ensures that the implant is introduced in a neutral position. spacer Turn the button to the right to move the spacer forward. Turn the button to the left to move the spacer backward. Turn lock to the right to mount the implant. Fork for neutral implant position. 17
18 C1) Instrumentation spike version Midline approach L5/S1 Mount the completely assembled implant onto the inserter, connecting the superior plate with the cranial marking on the inserter. Pararectus approach L2/3, L3/4, L4/5 For pararectus implantation the spacer must be slightly offset to the left. Turn the lock on the inserter to mount the implant securely. For the midline approach the implant is mounted symmetrically. For the pararectus approach the implant is mounted at an angle of 45. Note: m If possible do not touch the Plasmapore coating while mounting the implant onto the inserter. Hold on to the sides of endplates. 18
19 Keep checking the midline position during implantation. The marking on the inserter must be aligned with the midline marking. midline Hammer the implant in as far as possible under x-ray control to a maximum depth just in front of the posterior margin of the vertebra. Note: m Avoid tilting the implant sector caudally or cranially in order to advance both endplates evenly. m Use only the hammer with plastic end caps to implant the artificial disc. 19
20 C1) Instrumentation spike version Tips for correct lateral implantation Case 1: Ideal entry point for lateral implantation activ L is correctly positioned. Case 2: Entry point too far lateral: activ L is positioned too far laterally and can no longer be corrected, since no approach is possible from 90 laterally. lateral correction not possible 20
21 Tips for correct lateral implantation Case 3: Entry point too far anterior: activ L is too far anterior, but can still be corrected by pushing the implant further into the disc compartment with the impactor. Note: When in doubt, select a more anterior entry point, since in this case correction is still possible. Correction possible with the special impactor. Note: m Frequent x-ray checks in both planes are necessary. Aim first of all for a slightly anterior implant position, taking account of the 45 approach and an entry point located somewhat (1-2 mm) medially of the marking. (as described in case 3). When the correct midline position is achieved, exact posterior positioning can be achieved with the impactor. 21
22 C1) Instrumentation spike version C.1.4 En-Bloc-Implantation Before removing the insertion instrument turn the button on the instrument back to the left to remove the spacer. spacer button Release the lock and remove the inserter. 22
23 ap and lateral x-ray control of the inserted implant. Source: Dr. Sola, University Hospital of Rostock 23
24 C2) Instrumentation Keel version C.2.1 Chisels for keel fixation The surgery steps from discectomy to size verification are performed as for the standard version; please refer to pages Only the midline approach is possible with the keel version. For the keel version, the keel bed must be prepared using chisels. Depending on the implant version the double chisel or the single chisel has to be used. activ L keel version activ L combined version adjustment wheel for safety depth stop Chisels Mount the chisel guide of the desired implant height and angle onto the handle. Set the safety depth stop to the shortest chisel length by turning the wheel to the right. Introduce the chisel guide centrally into the disc compartment and set the safety stop to the desired depth under x-ray control. Note: m The adjustable stop defines the depth to which the chisel can be hammered into the disc space. 24
25 Remove the handle and introduce the single or double chisel through the chisel guide. Hammer the chisel into the vertebral body under x-ray control. The protection sleeve will retract automatically. The chisel guide must remain in the same position throughout the chiseling procedure. As soon as the safety stop is reached, do not hammer the chisel further in. Carefully withdraw the chisel using the slotted hammer. En bloc implantation Please refer to the spike version for this operating step, pages NB: m Inspect the disc compartment and the chisel slots for any bone residue before implanting the artificial disc. Note: m The chisels are very sharp instruments. They must be handled with extreme care to avoid injury to the vessels and nerve structures as well as to the surgical team. 25
26 D) Revision and correction of implant position D.1 Inlay revision Mittellinien-Zugang L5/S1 Special revision instruments for the endplates and the inlay are available for revision cases. Distract the endplates carefully with the revision distractor. Midline approach L5/S1 Pararectus approach L2/3, L3/4, L4/5 Clamp the inlay with the inlay revision instrument and remove it. If necessary, implant a new inlay using the same method. Note: m The inlay must be lifted over the edge of the inferior endplate. 26
27 D.2 Complete implant revision and correction of implant position Instrument for: revision correction of implant position intraoperative implant exchange For complete implant revision the endplates are removed separately. Revision instrument for endplates 27
28 D) Revision and correction of implant position Mittellinien-Zugang L5/S1 Thread the anchoring rods of the revision instrument into the cavity of the inferior or superior endplate. nose The noses on the instrument show the orientation of the anchoring rods. anchoring rods 90º Turn the anchoring rods through 90 clockwise or anticlockwise respectively. counter nut Lock the anchoring rods by turning the counternut anticlockwise. Note: Make sure the anchoring rods do not turn while fixing the counter nut. Otherwise the eyes are disconnected. 28
29 Mittellinien-Zugang L5/S1 Remove the endplate using the slotted hammer, alternately if necessary. The revision instrument can also be used to correct the implant position. Note: m Substantial integration of the endplates into the vertebral body may have occurred. This can make the revision procedure considerably more difficult. m Where such integration has developed over a long period, it may be necessary to free the endplate from the vertebral body using a chisel or elevator before the revision instrument is used. 29
30 E1) Implant overview Implants The implants are delivered sterile packed. PE inlay Height* 8, PE inlay SW965 SW966 SW967 SW968 *)The height given corresponds to the overall height of the implant measured at the posterior end. Endplates with spikes Größe Components S (26x31) M (28x34,5) L (30x39) XL (33x40) Superior plate Inferior plate Angle SW971K SW972K SW970K SW981K SW982K SW980K SW991K SW992K SW990K SW891K SW892K SW890K superior plate inferior plate Endplates with keel Size Components Superior plate Inferior plate Angle S (26x31) SW974K SW975K SW973K M (28x34,5) SW984K SW985K SW983K L (30x39) SW994K SW993K XL (33x40) SW894K SW995K SW895K SW893K superior plate inferior plate 30
31 E2) Instrument overview System overview Article no. FW931 Layer 1 Layer 2 Layer 3 Description Storage set for standard implantation Midline marking Distraction Insertion instruments FW933 Layer 1 Layer 2 Storage set for lumbar discectomy Rongeurs, punch Rongeurs, nerve hooks, scoops FW935 Layer 1 Layer 2 Layer 3 Storage set for keel preparation Chisel guides Double chisels Single chisels FW937 Layer 1 Storage set for revision Revision instrument for endplates and inlay 31
32 E2) Instrument overview System overview FW959 x-ray templates Standard Implantation Midline marking - Layer 1 FW955R Anterior midline marker FW956R Lateral midline marker Size S FW957R Lateral midline marker Size M FW958R Lateral midline marker Size L FW929R Lateral midline marker Size XL FW938SU Tip for anterior midline marker, single use FW939SU Tip for lateral midline marker, single use FW940R Shaft for wedge FW941R Wedge Height 6 mm FW942R Wedge Height 8 mm FW943R Wedge Height 10 mm FW944R Wedge Height 12 mm FW969R Impactor Distraction - Layer 2 FW960R Angled distractor FW951R Spacer Height 8.5 mm FW952R Spacer Height 10 mm FW953R Spacer Height 12 mm FW954R Spacer Height 14 mm FW970R Parallel distractor FW971R Trial implant inferior plate Size S 0 FW972R Trial implant inferior plate Size M 0 FW973R Trial implant inferior plate Size L 0 FW926R Trial implant inferior plate Size XL 0 FW974R Trial implant superior plate Size S 6 FW975R Trial implant superior plate Size S 11 FW976R Trial implant superior plate Size M 6 FW977R Trial implant superior plate Size M 11 FW978R Trial implant superior plate Size L 6 FW979R Trial implant superior plate Size L 11 FW927R Trial implant superior plate Size XL 6 FW928R Trial implant superior plate Size XL 11 32
33 Implantation instruments - Layer 3 FW961R Inserter 8.5 mm FW962R Inserter 10 mm FW963R Inserter 12 mm FW964R Inserter 14 mm FW945R Key for inserter FW946SU Spacer, single use, blue 8.5 mm FW947SU Spacer, single use, green 10 mm FW948SU Spacer, single use, black 12 mm FW949SU Spacer, single use, yellow 14 mm FL036R Hammer Lumbar discectomy Rongeurs, punch - Layer 1 FF839R Rongeur, straight 4 x 14 mm FF840R Rongeur, straight 6 x 16 mm FF850R Rongeur, angled 6 x 14 mm FF851R Rongeur, angled 4 x 14 mm FG894R Punch, 90 upward 2.5 mm 33
34 E2) Instrument overview Instrument overview Curettes, nerve hooks, scoops - Layer 2 FK826R Curette, round 6.4 mm FK822R Curette 7 x 5 mm FK780R Scoop, straight 4.4 x 6.2 mm FK781R Scoop, straight 5.2 x 7.3 mm FK791R Scoop, angled 5.2 x 7.3 mm FK392R Raspatory 8 mm BT070R Probe hook Keel preparation Chisel guides - Layer 1 FW980R Handle for chisel guide FW981R Chisel guide Height 8.5 mm, 6 FW982R Chisel guide Height 10 mm, 6 FW983R Chisel guide Height 12 mm, 6 FW984R Chisel guide Height 14 mm, 6 FW993R Chisel guide Height 8.5 mm,11 FW994R Chisel guide Height 10 mm,11 FW995R Chisel guide Height 12 mm,11 FW996R Chisel guide Height 14 mm,11 FW997R Osteotome FW579R Slotted hammer 34
35 Double chisels - Layer 2 FW985R Double chisel Height 8.5 mm FW986R Double chisel Height 10 mm FW987R Double chisel Height 12 mm FW988R Double chisel Height 14 mm Single chisel - Layer 3 FW989R Single chisel Height 8.5 mm FW990R Single chisel Height 10 mm FW991R Single chisel Height 12 mm FW992R Single chisel Height 14 mm Revision Revision instruments - Layer 1 FW965R Distractor for revision FW966R Revision instrument S, M FW967R Revision instrument L, XL FW968R Revision instrument for PE inlay For further information please refer to the instructions for use for the implants and instruments supplied with the original delivery: TA Implants TA Distraction instruments TA Insertion instruments 35
36 All rights reserved. Technical alterations are possible. This leaflet may be used for no other purposes than offering, buying and selling of our products. No part may be copied or reproduced in any form. In the case of misuse we retain the rights to recall our catalogues and pricelists and to take legal actions. Aesculap AG & Co. KG Am Aesculap-Platz Tuttlingen Phone Fax Brochure No. O /1/1
Aesculap Spine activ L
 Aesculap Spine activ L Lumbar Intervertebral Disc Prosthesis Operating technique 2 activ L Contents A) Product Information A.1 Product Features 4 A.2 Safety Information 5 A.3 Sterility 5 B) Pre-Operative
Aesculap Spine activ L Lumbar Intervertebral Disc Prosthesis Operating technique 2 activ L Contents A) Product Information A.1 Product Features 4 A.2 Safety Information 5 A.3 Sterility 5 B) Pre-Operative
Aesculap Spine activ L
 Aesculap Spine activ L Lumbar artificial disc Generation: activ Rotation + translation = mobilization Generation: activ Discover the innovative power of our latest development I N N O V Discover: Rotation
Aesculap Spine activ L Lumbar artificial disc Generation: activ Rotation + translation = mobilization Generation: activ Discover the innovative power of our latest development I N N O V Discover: Rotation
Aesculap Spine activ C
 Aesculap Spine activ C Cervical Disc Prosthesis Retain Mobility activ C Back to life enjoyed to the full I N N O V A Natural mobility Safety during surgery and in everyday life Stability in every situation
Aesculap Spine activ C Cervical Disc Prosthesis Retain Mobility activ C Back to life enjoyed to the full I N N O V A Natural mobility Safety during surgery and in everyday life Stability in every situation
CeSpace Titanium / PEEK
 Aesculap Anterior Cervical Interbody Fusion System CeSpace Titanium / PEEK Aesculap Spine CeSpace Content A Foreword 3 B Implant Material 4 C Implant Features 6 D Surgical Technique 8 E Ordering Information
Aesculap Anterior Cervical Interbody Fusion System CeSpace Titanium / PEEK Aesculap Spine CeSpace Content A Foreword 3 B Implant Material 4 C Implant Features 6 D Surgical Technique 8 E Ordering Information
ANTERIOR LUMBAR INTERBODY FUSION (ALIF) Basic Anatomical Landmarks: Anterior Lumbar Spine
 (ALIF) Anterior In human anatomy, referring to the front surface of the body or the position of one structure relative to another Lumbar Relating to the loins or the section of the back and sides between
(ALIF) Anterior In human anatomy, referring to the front surface of the body or the position of one structure relative to another Lumbar Relating to the loins or the section of the back and sides between
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach.
 Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
activ C Aesculap Cervical Disc Prosthesis Surgical Technique Aesculap Spine
 Aesculap Cervical Disc Prosthesis Surgical Technique activ C Aesculap Spine activ C Cervical Disc Prosthesis 2 Table of Contents General information activ C 4 A Approach A.1 Patient positioning 6 A.2 Approach
Aesculap Cervical Disc Prosthesis Surgical Technique activ C Aesculap Spine activ C Cervical Disc Prosthesis 2 Table of Contents General information activ C 4 A Approach A.1 Patient positioning 6 A.2 Approach
ANTERIOR CERVICAL DISCECTOMY AND FUSION. Basic Anatomical Landmarks: Anterior Cervical Spine
 Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
LUMBAR LAMINECTOMY AND DISCECTOMY. Basic Anatomical Landmarks: Posterior View Lumbar Spine
 Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Lumbar Relating to the loins or the section of the back and sides between the ribs and the pelvis. In the spinal column, the last five vertebrae (from superior to inferior, L1-L5) Laminectomy Surgical
Minimally Invasive Lumbar Fusion
 Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
Minimally Invasive Lumbar Fusion Biomechanical Evaluation (1) coflex-f screw Biomechanical Evaluation (1) coflex-f intact Primary Stability intact Primary Stability Extension Neutral Position Flexion Coflex
visualized. The correct level is then identified again. With the use of a microscope and
 SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
SURGERY FOR SPINAL STENOSIS Laminectomy A one inch (or longer for extensive stenosis) incision is made in the middle of the back over the effected region of the spine. The muscles over the bone are moved
Surgical Technique. coflex Surgical Technique
 Surgical Technique coflex Surgical Technique Interspinous Implant Overview I. Preparation II. Microsurgical Decompression III. Implant Site Preparation IV. Implant Insertion Preparation Patient Positioning
Surgical Technique coflex Surgical Technique Interspinous Implant Overview I. Preparation II. Microsurgical Decompression III. Implant Site Preparation IV. Implant Insertion Preparation Patient Positioning
Integra. Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE
 Integra Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE Table of contents Introduction Description... 2 Indications... 2 Contraindications... 2 Surgical Technique Step 1: Incision and Dissection...3
Integra Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE Table of contents Introduction Description... 2 Indications... 2 Contraindications... 2 Surgical Technique Step 1: Incision and Dissection...3
Aesculap Spine activ L
 Aesculap Spine activ L Training Concept Lumbar Artificial Disc Generation: activ Sharing Expertise in Non Fusion Technique Our goal is to acquire, preserve, and expand knowledge for the healthcare market.
Aesculap Spine activ L Training Concept Lumbar Artificial Disc Generation: activ Sharing Expertise in Non Fusion Technique Our goal is to acquire, preserve, and expand knowledge for the healthcare market.
A Patient s Guide to Artificial Cervical Disc Replacement
 A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
A Patient s Guide to Artificial Cervical Disc Replacement Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause pain and numbness
SPINAL SURGERY USING CHARITE ARTIFICIAL DISC MORRISTOWN MEMORIAL HOSPITAL, MORRISTOWN, NJ Broadcast June 24, 2005
 SPINAL SURGERY USING CHARITE ARTIFICIAL DISC MORRISTOWN MEMORIAL HOSPITAL, MORRISTOWN, NJ Broadcast June 24, 2005 NARRATOR 00:00:17:00 Today, orthopedic surgeons and spine specialists at Morristown Memorial
SPINAL SURGERY USING CHARITE ARTIFICIAL DISC MORRISTOWN MEMORIAL HOSPITAL, MORRISTOWN, NJ Broadcast June 24, 2005 NARRATOR 00:00:17:00 Today, orthopedic surgeons and spine specialists at Morristown Memorial
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
TABLE OF CONTENTS. Indications and Contraindications 3. Features and Benefits 4. Ease of connection 4 Stable fixation concept 5
 Surgical Technique TABLE OF CONTENTS Indications and Contraindications 3 Features and Benefits 4 Ease of connection 4 Stable fixation concept 5 Surgical Technique Steps 6 Identification and preparation
Surgical Technique TABLE OF CONTENTS Indications and Contraindications 3 Features and Benefits 4 Ease of connection 4 Stable fixation concept 5 Surgical Technique Steps 6 Identification and preparation
Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord.
 Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord. Normal List Kyphosis The human spine has 7 Cervical vertebra
Spine Anatomy and Spine General The purpose of the spine is to help us stand and sit straight, move, and provide protection to the spinal cord. Normal List Kyphosis The human spine has 7 Cervical vertebra
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery.
 Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by
Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL)
 Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Spine Surgery Coding
 Spine Surgery Coding Lynn M. Anderanin, CPC,CPC-I,COSC 1 Spine Anatomy 7 cervical (neck) vertebrae, 12 thoracic (chest) vertebrae, 5 lumbar (back) vertebrae, and 5 fused vertebra that make up the sacrum
Spine Surgery Coding Lynn M. Anderanin, CPC,CPC-I,COSC 1 Spine Anatomy 7 cervical (neck) vertebrae, 12 thoracic (chest) vertebrae, 5 lumbar (back) vertebrae, and 5 fused vertebra that make up the sacrum
The Abdominal Wall And Hernias. Stanley Kurek, DO, FACS Associate Professor of Surgery UTMCK
 The Abdominal Wall And Hernias Stanley Kurek, DO, FACS Associate Professor of Surgery UTMCK The Abdominal Wall The structure of the abdominal wall is similar in principle to the thoracic wall. There are
The Abdominal Wall And Hernias Stanley Kurek, DO, FACS Associate Professor of Surgery UTMCK The Abdominal Wall The structure of the abdominal wall is similar in principle to the thoracic wall. There are
Posterior Referencing. Surgical Technique
 Posterior Referencing Surgical Technique Posterior Referencing Surgical Technique INTRO Introduction Instrumentation Successful total knee arthroplasty depends in part on re-establishment of normal lower
Posterior Referencing Surgical Technique Posterior Referencing Surgical Technique INTRO Introduction Instrumentation Successful total knee arthroplasty depends in part on re-establishment of normal lower
DRAFT. Triathlon TS Knee System. Surgical Protocol. Version 1
 DRAFT Version 1 Triathlon TS Knee System Table of Contents Acknowledgments..........................................................2 Tibial Canal Preparation....................................................4
DRAFT Version 1 Triathlon TS Knee System Table of Contents Acknowledgments..........................................................2 Tibial Canal Preparation....................................................4
Zimmer FuZion Instruments. Surgical Technique (Beta Version)
 Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
Zimmer FuZion Surgical Technique (Beta Version) INTRO Surgical Technique Introduction Surgical goals during total knee arthroplasty (TKA) include establishment of normal leg alignment, secure implant fixation,
Options for Cervical Disc Degeneration A Guide to the M6-C. clinical study
 Options for Cervical Disc Degeneration A Guide to the M6-C clinical study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause
Options for Cervical Disc Degeneration A Guide to the M6-C clinical study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine condition that can cause
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF).
 Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Patient Information. Lateral Lumbar Interbody Fusion Surgery (LLIF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra, allows
Degenerative Spine Solutions
 Degenerative Spine Solutions The Backbone for Your Surgical Needs Aesculap Spine Backbone for Your Degenerative Spine Needs Comprehensive operative solutions, unique product technology and world-class
Degenerative Spine Solutions The Backbone for Your Surgical Needs Aesculap Spine Backbone for Your Degenerative Spine Needs Comprehensive operative solutions, unique product technology and world-class
X-Plain Neck Exercises Reference Summary
 X-Plain Neck Exercises Reference Summary Introduction Exercising your neck can make it stronger, more flexible and reduce neck pain that is caused by stress and fatigue. This reference summary describes
X-Plain Neck Exercises Reference Summary Introduction Exercising your neck can make it stronger, more flexible and reduce neck pain that is caused by stress and fatigue. This reference summary describes
TABLE OF CONTENTS. Surgical Technique 2. Indications 4. Product Information 5. 1. Patient Positioning and Approach 2
 Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
How To Fix A Radial Head Plate
 Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Lectures of Human Anatomy
 Lectures of Human Anatomy Vertebral Column-I By DR. ABDEL-MONEM AWAD HEGAZY M.B. with honor 1983, Dipl."Gynecology and Obstetrics "1989, Master "Anatomy and Embryology" 1994, M.D. "Anatomy and Embryology"
Lectures of Human Anatomy Vertebral Column-I By DR. ABDEL-MONEM AWAD HEGAZY M.B. with honor 1983, Dipl."Gynecology and Obstetrics "1989, Master "Anatomy and Embryology" 1994, M.D. "Anatomy and Embryology"
Malleolar fractures Anna Ekman, Lena Brauer
 Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
ZERO-P VA. Variable angle zero-profile anterior cervical interbody fusion (ACIF) device SURGICAL TECHNIQUE
 ZERO-P VA Variable angle zero-profile anterior cervical interbody fusion (ACIF) device SURGICAL TECHNIQUE Table of Contents Introduction Zero-P VA Instruments and Implants 2 AO Principles 4 Indications
ZERO-P VA Variable angle zero-profile anterior cervical interbody fusion (ACIF) device SURGICAL TECHNIQUE Table of Contents Introduction Zero-P VA Instruments and Implants 2 AO Principles 4 Indications
NETWORK FITNESS FACTS THE HIP
 NETWORK FITNESS FACTS THE HIP The Hip Joint ANATOMY OF THE HIP The hip bones are divided into 5 areas, which are: Image: www.health.com/health/static/hw/media/medical/hw/ hwkb17_042.jpg The hip joint is
NETWORK FITNESS FACTS THE HIP The Hip Joint ANATOMY OF THE HIP The hip bones are divided into 5 areas, which are: Image: www.health.com/health/static/hw/media/medical/hw/ hwkb17_042.jpg The hip joint is
MGB Chrome Bumper Conversion
 MGB Chrome Bumper Conversion Installation Instructions For 1974 1/2-1980 MGB This kit requires cutting, welding, and painting. Professional installation recommended. Note: Every MGB body is slightly different
MGB Chrome Bumper Conversion Installation Instructions For 1974 1/2-1980 MGB This kit requires cutting, welding, and painting. Professional installation recommended. Note: Every MGB body is slightly different
TransFx External Fixation System Large and Intermediate Surgical Technique
 TransFx External Fixation System Large and Intermediate Surgical Technique TransFx External Fixation System Large and Intermediate Surgical Technique 1 Surgical Technique For TransFx External Fixation
TransFx External Fixation System Large and Intermediate Surgical Technique TransFx External Fixation System Large and Intermediate Surgical Technique 1 Surgical Technique For TransFx External Fixation
Lower Body Exercise One: Glute Bridge
 Lower Body Exercise One: Glute Bridge Lying on your back hands by your side, head on the floor. Position your feet shoulder width apart close to your glutes, feet facing forwards. Place a theraband/mini
Lower Body Exercise One: Glute Bridge Lying on your back hands by your side, head on the floor. Position your feet shoulder width apart close to your glutes, feet facing forwards. Place a theraband/mini
MIS Direct Anterior Approach Surgical Protocol
 Joint Replacements MIS Direct Anterior Approach Surgical Protocol The Right Procedure and the Right Implant for the Right Patient Scientific advice and text: Franz Rachbauer, M.D., M.A.S., M.Sc. Associate
Joint Replacements MIS Direct Anterior Approach Surgical Protocol The Right Procedure and the Right Implant for the Right Patient Scientific advice and text: Franz Rachbauer, M.D., M.A.S., M.Sc. Associate
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
BONE PRESERVATION STEM
 TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
TRI-LOCK BONE PRESERVATION STEM Featuring GRIPTION Technology SURGICAL TECHNIQUE IMPLANT GEOMETRY Extending the TRI-LOCK Stem heritage The original TRI-LOCK Stem was introduced in 1981. This implant was
Spinal Arthrodesis Group Exercises
 Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
THE BENJAMIN INSTITUTE PRESENTS. Excerpt from Listen To Your Pain. Assessment & Treatment of. Low Back Pain. Ben E. Benjamin, Ph.D.
 THE BENJAMIN INSTITUTE PRESENTS Excerpt from Listen To Your Pain Assessment & Treatment of Low Back Pain A B E N J A M I N I N S T I T U T E E B O O K Ben E. Benjamin, Ph.D. 2 THERAPIST/CLIENT MANUAL The
THE BENJAMIN INSTITUTE PRESENTS Excerpt from Listen To Your Pain Assessment & Treatment of Low Back Pain A B E N J A M I N I N S T I T U T E E B O O K Ben E. Benjamin, Ph.D. 2 THERAPIST/CLIENT MANUAL The
Navico-Northstar 2kW JRC Radar Package, Scanner Cable Removal and Replacement
 Navico-Northstar 2kW JRC Radar Package, Scanner Cable Removal and Replacement This work instruction describes the methods and means for which to remove and reinstall optional scanner cable configurations
Navico-Northstar 2kW JRC Radar Package, Scanner Cable Removal and Replacement This work instruction describes the methods and means for which to remove and reinstall optional scanner cable configurations
C O N V E Y O R C O M P O N E N T S C H A I N S B E L T S B E A R I N G S
 C O N V E Y O R C O M P O N E N T S C H A I N S B E L T S B E A R I N G S January 2009 Issue 6 Valu Guide Brackets The Ultimate in Adjustability and Cost Savings Valu Guide brackets are part of a family
C O N V E Y O R C O M P O N E N T S C H A I N S B E L T S B E A R I N G S January 2009 Issue 6 Valu Guide Brackets The Ultimate in Adjustability and Cost Savings Valu Guide brackets are part of a family
Biomechanical Analysis of the Deadlift (aka Spinal Mechanics for Lifters) Tony Leyland
 Biomechanical Analysis of the Deadlift (aka Spinal Mechanics for Lifters) Tony Leyland Mechanical terminology The three directions in which forces are applied to human tissues are compression, tension,
Biomechanical Analysis of the Deadlift (aka Spinal Mechanics for Lifters) Tony Leyland Mechanical terminology The three directions in which forces are applied to human tissues are compression, tension,
NCB Distal Femur System. Surgical Technique
 NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
MIN Set. Instruments for Minimally Invasive Neurosurgery. Aesculap Neurosurgery
 MIN Set Instruments for Minimally Invasive Neurosurgery Aesculap Neurosurgery MIN Set Features Fine instrument tips Especially important when working in very narrow spaces and close to sensitive structures.
MIN Set Instruments for Minimally Invasive Neurosurgery Aesculap Neurosurgery MIN Set Features Fine instrument tips Especially important when working in very narrow spaces and close to sensitive structures.
Skeletal System. Axial Skeleton: Vertebral Column and Ribs
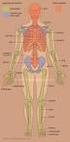 Skeletal System Axial Skeleton: Vertebral Column and Ribs Functions Regions Cervical Thoracic Lumbar Sacral Primary & secondary curvatures There are three major functions of the vertebral column. First,
Skeletal System Axial Skeleton: Vertebral Column and Ribs Functions Regions Cervical Thoracic Lumbar Sacral Primary & secondary curvatures There are three major functions of the vertebral column. First,
B. Braun Sutures Safil
 B. Braun Sutures Safil Strong, Safe and Soft Braided and coated synthetic mid-term absorbable suture material made of polyglycolic acid. Safil Strong, Safe and Soft The new Safil generation. What you most
B. Braun Sutures Safil Strong, Safe and Soft Braided and coated synthetic mid-term absorbable suture material made of polyglycolic acid. Safil Strong, Safe and Soft The new Safil generation. What you most
INSTRUCTIONS: LocknCharge Laptop Carts
 INSTRUCTIONS: LocknCharge Laptop Carts www.lockncharge.com Extra Tools required: Hammer, Philips head screwdriver, medium adjustable spanner. (Allen key supplied) (Panel colours for illustration purposes
INSTRUCTIONS: LocknCharge Laptop Carts www.lockncharge.com Extra Tools required: Hammer, Philips head screwdriver, medium adjustable spanner. (Allen key supplied) (Panel colours for illustration purposes
Aesculap Orthopaedics Metha
 Aesculap Orthopaedics Metha Short Hip Stem Evolving the State of Arthroplasty 2 Evolving the State of Arthroplasty Contents Short Hip Stem System 4 Short Stem Anchoring Concept 6 Variable Implant Options
Aesculap Orthopaedics Metha Short Hip Stem Evolving the State of Arthroplasty 2 Evolving the State of Arthroplasty Contents Short Hip Stem System 4 Short Stem Anchoring Concept 6 Variable Implant Options
Achilles Tendon Repair, Operative Technique
 *smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
*smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
Biomechanics of the Lumbar Spine
 Biomechanics of the Lumbar Spine Biomechanics of the Spine 6 degrees of freedom Extension & Flexion Translation Rotation Compression & Distraction The disc/annulus/all/pll complex is the major restraint
Biomechanics of the Lumbar Spine Biomechanics of the Spine 6 degrees of freedom Extension & Flexion Translation Rotation Compression & Distraction The disc/annulus/all/pll complex is the major restraint
VERSYS HERITAGE CDH HIP PROSTHESIS. Surgical Technique for CDH Hip Arthroplasty
 VERSYS HERITAGE CDH HIP PROSTHESIS Surgical Technique for CDH Hip Arthroplasty SURGICAL TECHNIQUE FOR VERSYS HERITAGE CDH HIP PROSTHESIS CONTENTS ANATOMICAL CONSIDERATIONS....... 2 PREOPERATIVE PLANNING............
VERSYS HERITAGE CDH HIP PROSTHESIS Surgical Technique for CDH Hip Arthroplasty SURGICAL TECHNIQUE FOR VERSYS HERITAGE CDH HIP PROSTHESIS CONTENTS ANATOMICAL CONSIDERATIONS....... 2 PREOPERATIVE PLANNING............
Lumbar Spine Anatomy. eorthopod.com 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.
 A Patient s Guide to Lumbar Spine Anatomy 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 [email protected] DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Lumbar Spine Anatomy 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 [email protected] DISCLAIMER: The information in this booklet is compiled
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
CSE511 Brain & Memory Modeling. Lect04: Brain & Spine Neuroanatomy
 CSE511 Brain & Memory Modeling CSE511 Brain & Memory Modeling Lect02: BOSS Discrete Event Simulator Lect04: Brain & Spine Neuroanatomy Appendix of Purves et al., 4e Larry Wittie Computer Science, StonyBrook
CSE511 Brain & Memory Modeling CSE511 Brain & Memory Modeling Lect02: BOSS Discrete Event Simulator Lect04: Brain & Spine Neuroanatomy Appendix of Purves et al., 4e Larry Wittie Computer Science, StonyBrook
POST SURGICAL RETURN OF RIGHT LEG PAIN. TREATED SUCCESSFULLY WITH COX FLEXION DISTRACTION DECOMPRESSION ADJUSTING
 POST SURGICAL RETURN OF RIGHT LEG PAIN. TREATED SUCCESSFULLY WITH COX FLEXION DISTRACTION DECOMPRESSION ADJUSTING A 47 year old white married female was seen for the chief complaint of low back and right
POST SURGICAL RETURN OF RIGHT LEG PAIN. TREATED SUCCESSFULLY WITH COX FLEXION DISTRACTION DECOMPRESSION ADJUSTING A 47 year old white married female was seen for the chief complaint of low back and right
ACL Reconstruction Physiotherapy advice for patients
 Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
TwinFix Cannulated Compression Screw
 TwinFix Cannulated Compression Screw Leibinger Solutions for Hand Surgery Procedural Guide TwinFix Sterilization, Organization, Storage 29-12020 Profyle MODULAR Sterilizing Container 29-40162 TwinFix Implant
TwinFix Cannulated Compression Screw Leibinger Solutions for Hand Surgery Procedural Guide TwinFix Sterilization, Organization, Storage 29-12020 Profyle MODULAR Sterilizing Container 29-40162 TwinFix Implant
Human Anatomy & Physiology
 PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 7 The Skeleton: Part B Annie Leibovitz/Contact Press Images Vertebral
PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 7 The Skeleton: Part B Annie Leibovitz/Contact Press Images Vertebral
Spinal Exercise Program/Core Stabilization Program Adapted from The Spine in Sports: Robert G. Watkins
 Spinal Exercise Program/Core Stabilization Program Adapted from The Spine in Sports: Robert G. Watkins Below is a description of a Core Stability Program, designed to improve the strength and coordination
Spinal Exercise Program/Core Stabilization Program Adapted from The Spine in Sports: Robert G. Watkins Below is a description of a Core Stability Program, designed to improve the strength and coordination
V-TEK IVP System 2.7 System 4.0
 V-TEK IVP System Ankle 2.7 Fix System 4.0 Surgical Technique Surgical Technique Titanium osteosynthesis system for tibio-talar and tibio-talo-calcaneal fusion SECTION 1 Ankle Fix System 4.0 Titanium osteosynthesis
V-TEK IVP System Ankle 2.7 Fix System 4.0 Surgical Technique Surgical Technique Titanium osteosynthesis system for tibio-talar and tibio-talo-calcaneal fusion SECTION 1 Ankle Fix System 4.0 Titanium osteosynthesis
Mechanics of the Human Spine Lifting and Spinal Compression
 Mechanics of the Human Spine Lifting and Spinal Compression Hamill and Knutzen: Chapter 7 Nordin and Frankel: Ch. 10 by Margareta Lindh Hall: Ch. 9 (more muscle anatomy detail than required) Low Back Pain
Mechanics of the Human Spine Lifting and Spinal Compression Hamill and Knutzen: Chapter 7 Nordin and Frankel: Ch. 10 by Margareta Lindh Hall: Ch. 9 (more muscle anatomy detail than required) Low Back Pain
Sheet 1A. Treating short/tight muscles using MET. Pectorals. Upper trapezius. Levator scapula
 Sheet 1A Treating short/tight muscles using MET Pectorals Once daily lie at edge of bed holding a half-kilo can, arm out sideways. Raise arm and hold for 10 seconds, then allow arm to hang down, stretching
Sheet 1A Treating short/tight muscles using MET Pectorals Once daily lie at edge of bed holding a half-kilo can, arm out sideways. Raise arm and hold for 10 seconds, then allow arm to hang down, stretching
This is how quickly your brain forgets things
 Brain gym starters This is how quickly your brain forgets things Your brain is a muscle Like every other muscle it needs exercise Brain gym is one way to exercise your mind so that you can learn better.
Brain gym starters This is how quickly your brain forgets things Your brain is a muscle Like every other muscle it needs exercise Brain gym is one way to exercise your mind so that you can learn better.
Removable Aluminium posts
 Post Solent Sail Shades Ltd 120 Billington Gardens Hedge End Southampton SO30 2RT Tel/Fax: 01489 788243 www.solentsailshades.co.uk Email: [email protected] Removable Aluminium posts Single Pole
Post Solent Sail Shades Ltd 120 Billington Gardens Hedge End Southampton SO30 2RT Tel/Fax: 01489 788243 www.solentsailshades.co.uk Email: [email protected] Removable Aluminium posts Single Pole
Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization
 APPROVED IRN10389-1.1-04 Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization Because it involves accessing the spine through the patient s side, the Direct Lateral approach
APPROVED IRN10389-1.1-04 Direct Lateral Interbody Fusion A Minimally Invasive Approach to Spinal Stabilization Because it involves accessing the spine through the patient s side, the Direct Lateral approach
ONSTEP Technique. Technique Guide * Anterior Approach to a Part Preperitoneal, Part Intramuscular Inguinal Hernia Repair
 ONSTEP Technique Technical Aspects of the ONSTEP Inguinal Hernia Repair Technique Using the PolySoft Hernia Patch with Interrupted Memory Recoil Ring Technique Guide * Anterior Approach to a Part Preperitoneal,
ONSTEP Technique Technical Aspects of the ONSTEP Inguinal Hernia Repair Technique Using the PolySoft Hernia Patch with Interrupted Memory Recoil Ring Technique Guide * Anterior Approach to a Part Preperitoneal,
Posttraumatic medial ankle instability
 Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Zimmer MOST Options System
 Zimmer MOST Options System Surgical Technique Modular Options for Severe Bone Loss and Trauma Zimmer MOST Options System Surgical Technique 1 MOST Options System Surgical Technique Table of Contents Introduction
Zimmer MOST Options System Surgical Technique Modular Options for Severe Bone Loss and Trauma Zimmer MOST Options System Surgical Technique 1 MOST Options System Surgical Technique Table of Contents Introduction
EQUIPMENT SET UP RECURVE BOW
 EQUIPMENT SET UP RECURVE BOW Archery Australia Inc Coaching and Standards Committee Proudly Sponsored By EQUIPMENT SET UP RECURVE BOW It is important that equipment to be used must be set up correctly
EQUIPMENT SET UP RECURVE BOW Archery Australia Inc Coaching and Standards Committee Proudly Sponsored By EQUIPMENT SET UP RECURVE BOW It is important that equipment to be used must be set up correctly
Thoracic Spine Anatomy
 A Patient s Guide to Thoracic Spine Anatomy 228 West Main, Suite C Missoula, MT 59802 Phone: [email protected] DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Thoracic Spine Anatomy 228 West Main, Suite C Missoula, MT 59802 Phone: [email protected] DISCLAIMER: The information in this booklet is compiled from a variety of sources.
Safe Lifting/Back Safety Training. Presented by Rita Gagnon Occupational Health Outreach Coordinator Benefis Health Systems 406-731-8328
 Safe Lifting/Back Safety Training Presented by Rita Gagnon Occupational Health Outreach Coordinator Benefis Health Systems 406-731-8328 Risk Factors Involved with Manual Handling Tasks: Bending at Trunk
Safe Lifting/Back Safety Training Presented by Rita Gagnon Occupational Health Outreach Coordinator Benefis Health Systems 406-731-8328 Risk Factors Involved with Manual Handling Tasks: Bending at Trunk
Drive shaft, servicing
 Volkswagen Passat B6 - Drive shaft, servicing Стр. 1 из 41 40-7 Drive shaft, servicing Drive shafts, overview I - Assembly overview: Drive axle with CV joint VL100 40-7, Drive axle with CV joint VL100,
Volkswagen Passat B6 - Drive shaft, servicing Стр. 1 из 41 40-7 Drive shaft, servicing Drive shafts, overview I - Assembly overview: Drive axle with CV joint VL100 40-7, Drive axle with CV joint VL100,
Technique Guide. DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation.
 Technique Guide DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation. Table of Contents Introduction Dynamic Hip Screw (DHS) 2 Dynamic Condylar Screw (DCS) 3 Indications
Technique Guide DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation. Table of Contents Introduction Dynamic Hip Screw (DHS) 2 Dynamic Condylar Screw (DCS) 3 Indications
Mike s Top Ten Tips for Reducing Back Pain
 Mike s Top Ten Tips for Reducing Back Pain The following article explains ways of preventing, reducing or eliminating back pain. I have found them to be very useful to myself, my clients and my patients.
Mike s Top Ten Tips for Reducing Back Pain The following article explains ways of preventing, reducing or eliminating back pain. I have found them to be very useful to myself, my clients and my patients.
Technique Guide. Screw Removal Set. Instruments for removing Synthes screws.
 Technique Guide Screw Removal Set. Instruments for removing Synthes screws. Table of Contents Introduction Screw Removal Set 2 Surgical Technique Preoperative Planning and Preparation 6 Removal of Intact
Technique Guide Screw Removal Set. Instruments for removing Synthes screws. Table of Contents Introduction Screw Removal Set 2 Surgical Technique Preoperative Planning and Preparation 6 Removal of Intact
4052 Slimplicity Tech final_layout 1 6/29/15 3:29 PM Page 2 Surgical Technique
 Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression
 Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Cervical Spondylotic Myelopathy Associated with Kyphosis or Sagittal Sigmoid Alignment: Outcome after Anterior or Posterior Decompression 1 Journal of Neurosurgery: Spine November 2009, Volume 11, pp.
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study
 Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Options for Cervical Disc Degeneration A Guide to the Fusion Arm of the M6 -C Artificial Disc Study Each year, hundreds of thousands of adults are diagnosed with Cervical Disc Degeneration, an upper spine
Clarification of Terms
 Shoulder Girdle Clarification of Terms Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus What is the purpose (or function) of the shoulder and entire upper
Shoulder Girdle Clarification of Terms Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus What is the purpose (or function) of the shoulder and entire upper
DIAMOND Retractable Rodding Robot Model SPRAYROD-R
 2004-12-21 2 1 (23) DIAMOND Retractable Rodding Robot Model SPRAYROD-R 2004-12-21 2 2 (23) Table of contents 1 TECHNICAL DESCRIPTION...4 1.1 MAIN DETAILS...5 1.2 COMPONENTS DESCRIPTION...5 1.2.1 Pneumatic
2004-12-21 2 1 (23) DIAMOND Retractable Rodding Robot Model SPRAYROD-R 2004-12-21 2 2 (23) Table of contents 1 TECHNICAL DESCRIPTION...4 1.1 MAIN DETAILS...5 1.2 COMPONENTS DESCRIPTION...5 1.2.1 Pneumatic
Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor
 Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Metasul LDH Large Diameter Head
 Metasul LDH Large Diameter Head Surgical Technique Metasul LDH Large Diameter Head Surgical Technique Enhancing Stability and Increasing Range of Motion Metasul LDH Large Diameter Head Surgical Technique
Metasul LDH Large Diameter Head Surgical Technique Metasul LDH Large Diameter Head Surgical Technique Enhancing Stability and Increasing Range of Motion Metasul LDH Large Diameter Head Surgical Technique
Zimmer Periarticular Proximal Tibial Locking Plate
 Zimmer Periarticular Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Tibial Locking Plate 1 Table of Contents Introduction 2 Locking Screw Technology
Zimmer Periarticular Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Tibial Locking Plate 1 Table of Contents Introduction 2 Locking Screw Technology
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF).
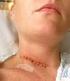 Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
Patient Information. Anterior Cervical Discectomy and Fusion Surgery (ACDF). Understanding your spine Disc Between each pair of vertebrae there is a disc that acts as a cushion to protect the vertebra,
Getting to the Backbone of Spinal Coding in ICD-10-PCS
 Getting to the Backbone of Spinal Coding in ICD-10-PCS Sponsored by 1915 N. Fine Ave #104 Fresno CA 93720-1565 Phone: (559) 251-5038 Fax: (559) 251-5836 www.californiahia.org Program Handouts Tuesday,
Getting to the Backbone of Spinal Coding in ICD-10-PCS Sponsored by 1915 N. Fine Ave #104 Fresno CA 93720-1565 Phone: (559) 251-5038 Fax: (559) 251-5836 www.californiahia.org Program Handouts Tuesday,
ACTIVE SEATING FOR PEOPLE WITH A KYPHOTIC SPINE. - backrest cushion for the kyphotic spine
 ACTIVE SEATING FOR PEOPLE WITH A KYPHOTIC SPINE - backrest cushion for the kyphotic spine Netti Kyphotic is designed for users who require optimum stabilization of their spinal curvature. The upholstery
ACTIVE SEATING FOR PEOPLE WITH A KYPHOTIC SPINE - backrest cushion for the kyphotic spine Netti Kyphotic is designed for users who require optimum stabilization of their spinal curvature. The upholstery
MINIMAL ACCESS SPINE SURGERY
 MINIMAL ACCESS SPINE SURGERY Spinal ailments are amongst the most common ailments that afflict mankind. Back pain, for example, has achieved epidemic proportions worldwide in the last two decades and is
MINIMAL ACCESS SPINE SURGERY Spinal ailments are amongst the most common ailments that afflict mankind. Back pain, for example, has achieved epidemic proportions worldwide in the last two decades and is
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
Expert LFN. Lateral Femoral Nail.
 Expert LFN. Lateral Femoral Nail. Surgical Technique EXPERT Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Expert LFN. Lateral Femoral Nail. Surgical Technique EXPERT Nailing System This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Femoral Nerve Block/3-in-1 Nerve Block
 Femoral Nerve Block/3-in-1 Nerve Block Femoral and/or 3-in-1 nerve blocks are used for surgical procedures on the front portion of the thigh down to the knee and postoperative analgesia. Both blocks are
Femoral Nerve Block/3-in-1 Nerve Block Femoral and/or 3-in-1 nerve blocks are used for surgical procedures on the front portion of the thigh down to the knee and postoperative analgesia. Both blocks are
Vertebral anatomy study guide. Human Structure Summer 2015. Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey.
 Vertebral anatomy study guide. Human Structure Summer 2015 Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey. 1. Plan of Action: In this guide you will learn to identify these structures: Cervical
Vertebral anatomy study guide. Human Structure Summer 2015 Prepared by Daniel Schmitt, Angel Zeininger, and Karyne Rabey. 1. Plan of Action: In this guide you will learn to identify these structures: Cervical
Placement of Epidural Catheter for Pain Management Shane Bateman DVM, DVSc, DACVECC
 Placement of Epidural Catheter for Pain Management Shane Bateman DVM, DVSc, DACVECC Indications: Patients with severe abdominal or pelvic origin pain that is poorly responsive to other analgesic modalities.
Placement of Epidural Catheter for Pain Management Shane Bateman DVM, DVSc, DACVECC Indications: Patients with severe abdominal or pelvic origin pain that is poorly responsive to other analgesic modalities.
HP Laser Jet 4200/4240/4250/4300/4350 Swing Plate
 HP Laser Jet 4200/4240/4250/4300/4350 Swing Plate 1 Swing Plate Assembly-RM1-0043 1 Swing Plate Kit-5851-2766 (RM1-0043 plus RM1-1091 gear) CAUTION: Fuser may be hot. Turn off printer, unplug it and allow
HP Laser Jet 4200/4240/4250/4300/4350 Swing Plate 1 Swing Plate Assembly-RM1-0043 1 Swing Plate Kit-5851-2766 (RM1-0043 plus RM1-1091 gear) CAUTION: Fuser may be hot. Turn off printer, unplug it and allow
