Vestibular Rehabilitation Therapy for the Dizzy Patient
|
|
|
- Corey Bailey
- 9 years ago
- Views:
Transcription
1 Review Article 289 Vestibular Rehabilitation Therapy for the Dizzy Patient LH Tee, 1 Bphty, Mphty (Neurology), NWC Chee, 2 MBBS, FRCS (Edin & Glasg), FAMS (ORL) Abstract A customised vestibular rehabilitation therapy (VRT) programme is an important treatment modality in patients with vestibular dysfunction resulting in motion-provoked vertigo, oscillopsia (gaze instability), disequilibrium and gait disturbances. We discuss in this paper the patient selection criteria for VRT, rehabilitation strategies for unilateral and bilateral vestibular deficits, and some of the compelling evidence to support the use of VRT in treating such patients. Ann Acad Med Singapore 2005;34: Key words: Disequilibrium, Gaze stability, Oscillopsia, Vertigo, Vestibular exercises Introduction The use of vestibular exercises to treat patients with persistent symptoms of positional vertigo and disequilibrium has been around for many years. The Cawthorne and Cooksey exercises, developed in the 1940s, consist of a series of eye, head and body movements aimed at treating patients with unilateral vestibular paresis and postconcussion syndrome. The rationale for the exercises, which originated from the observation that patients who were active recovered faster, was based on the supposition that the head movements that provoke the patient s dizziness play an important role in hastening the recovery process. With a better understanding of the function and adaptation of the vestibular system, a customised vestibular rehabilitation therapy (VRT) programme adapted to suit the specific needs of the individual became widely accepted in the 1990s and has become the primary modality of treatment for a large number of patients with dizziness. VRT involves the active participation of the patient. A trained vestibular therapist would initially assess the patient to establish the individual s main impairments and problems. Realistic treatment goals will be set with the patient. Treatment can be delivered in the form of supervised outpatient exercises or home exercise programmes. Vestibular exercises are supervised and progressed by the therapist. Appropriate outcome measures to measure dynamic visual acuity (DVA), balance and gait are adopted to measure the patient s progression. The average duration of a VRT programme ranges from 4 to 10 weeks. 1-8 Which Types of Patients are Suitable for Vestibular Rehabilitation Therapy? VRT is most effective in individuals with a stable unilateral peripheral vestibular deficit with incomplete central compensation. Following an acute vestibular dysfunction such as in vestibular neuritis, sign and symptoms of skew deviation, nystagmus, vertigo, oscillopsia, disequilibrium, nausea and vomiting will typically resolve when acute compensation of the central nervous system (CNS) is achieved within the first 24 to 72 hours. Acute compensation occurs at the level of the vestibular nuclei under the influence of the cerebellum. 2 The system has to release the cerebellar inhibition to establish symmetrical tonic firing rates in the second-order neurons originating in the vestibular nuclei. Dynamic compensation to enable accurate vestibular responses to head movement is a slower process that takes several weeks and occurs by reorganisation of the brainstem and cerebellar pathways. While some patients may recover rapidly and spontaneously, patients who have an incomplete compensation or decompensation of the CNS to the vestibular system after the acute lesion will complain of residual motionprovoked vertigo, oscillopsia and disequilibrium. Such patients are good candidates for VRT and will benefit from a period of customised VRT supervised by a trained vestibular therapist. VRT is also indicated in patients with stable bilateral vestibular deficits. The treatment strategies differ for 1 Department of Physiotherapy 2 Department of Otorhinolaryngology Tan Tock Seng Hospital, Singapore Address for Reprints: Dr Nelson Chee, Department of Otorhinolaryngology, Tan Tock Seng Hospital, 11 Jalan Tan Tock Seng, Singapore May 2005, Vol. 34 No. 4
2 290 unilateral and bilateral vestibular dysfunction and will be discussed in more detail below. VRT is not suitable for patients whose symptoms occur in spontaneous episodes, such as in Meniere s disease, and when postural changes or body movements do not reliably provoke the sensation of dizziness. Alternative medical or surgical treatment strategies should be considered in such cases. Unilateral Vestibular Lesion (UVL) Patients with UVL will present with one or more of the following physical impairments: 1. Gaze instability or oscillopsia i.e, blurring of vision associated with head movements due to decreased vestibular-ocular reflex (VOR) gain (ideal VOR gain = 1). 4 Individuals will complain of gaze instability with head movements or disequilibrium. They often have difficulties watching television or reading due to blurring of vision. Road signs become blurred when these individuals try to read as they walk down the streets. 2. Motion-provoked vertigo is dizziness induced by specific head movements or activities/positions. Individuals tend to avoid head movements or certain activities due to hypersensitivity to movements. 3. Postural instability: Patients with UVL may present with disequilibrium either during static or dynamic activities. Disequilibrium increases when the individual is required to incorporate head movements or perform the task at a faster speed. Take for instance, crossing a busy street while turning the head sideways to look out for oncoming vehicles or running after a bus. 4. Sensitivity to motion in their environment: Individuals may complain of disequilibrium or dizziness induced by movement in their environment. This is due to a failure to differentiate between exocentric and egocentric motion. Individuals may experience imbalance or dizziness when standing or walking through crowds or visually busy environments, which worsens when they walk against the crowds. Challenging environments may include places such as supermarkets, shopping malls and train stations. 5: Physical de-conditioning: With prolonged avoidance of activities in the fear of reproducing symptoms and falls, individuals with UVL tend to develop physical deconditioning. Treatment for Patients with UVL The main aims of VRT are to: 1) Increase gaze stability i.e., DVA during both static and dynamic activities of daily living (ADLs). ADLs, such as engaging in a conversation, nodding one s head, and walking along the street, require the individual to move his head. 2) Reduce the symptoms of dizziness. 3) Improve postural and gait stability. 4) Improve independence in ADLs. 5) Increase cardiovascular conditioning. 1. Treatment for Gaze Stability The best stimulus for vestibular adaptation is by inducing a movement of the visual image across the retina known as a retinal slip during head movement. This retinal slip generates an error signal, and the CNS compensates to decrease the error signal by increasing the VOR gain. 9 VOR X1 and X2 viewing exercises as described by Herdman 10,11 enhance vestibular adaptation by improving VOR gain and thus improve gaze stabilisation. In the VOR X1 viewing exercise, the patient views a stationary object while turning his head back and forth to the point where oscillopsia is induced. In the VOR X2 viewing exercise, the target moves in the opposite direction to the head rotation, again to the point where oscillopsia occurs. Both horizontal and vertical head rotations and target movements are performed. Adaptation exercises need to be context- and environmentspecific. The exercises should be designed such that they reflect the various environments in which the individual performs his or her normal ADLs. In addition, the exercise programme can be designed to be performed at different head positions or frequencies for optimal effects (Fig. 1). This is because the VOR, adapted at a single frequency of head rotation, will only have the greatest VOR gain at that particular frequency and less gain at other frequencies. 12 VOR exercises are often incorporated with other balance exercises as appropriate. 1. Duration Begin with 1 min (if tolerated) Progress to 2 min Primary variable 4. Speed Begin slowly Progress to faster speed while maintaining target focus and stability VOR function at 2 Hz and faster 2. Background and Distraction Begin with 1 min background Progress to conflicting full field background (e.g., checkerboard) Progress outdoors Gaze Stabilisation Exercise X1 and X2 Horizontal and Vertical 5. Frequency Begin twice a day Progress to maximum of 5 times a day 3. Position Begin in standing position (if tolerated), otherwise start in sitting position Progress to walking forward/backward, step up and down 6. Distance Start with near target (3 feet) Progress to far target (8 to 10 feet) Fig. 1. Treatment progression for gaze stabilisation exercises (X1 and X2 viewing). Annals Academy of Medicine
3 Treatment for Motion-provoked Vertigo Habituation exercise reduces the symptoms of dizziness by repetitive exposure to the specific movement that provokes dizziness. It is the learned suppression of vertigo via repetitive exposure to movements. During habituation, there is a reduction in the amplitude of synaptic potentials (excitatory postsynaptic potential/epsp) produced by the sensory neuron on the interneuron and motor neuron. The short-term changes of decreased ESPS amplitude during habituation exercises result in initial temporary reduction of vertigo. With persistent exposure to the provoking movements, the individual will experience gradual and permanent decline in dizziness across sessions. Reduction of dizziness is due to the long-term structural changes in the sensory cells, resulting in a decrease in the number of synaptic connections between the sensory neuron, interneurons and motor neurons. In addition, the number of active transmitting zones within the existing connections decreases. Habituation needs to persist for weeks to months to allow the structural changes of the sensory cells to take place so that the individual can experience permanent decline in the intensity of dizziness. 13 The vestibular therapist will first identify specific positions or movements that provoked the patient s vertigo. The Motion Sensitivity Quotient Test developed by Shepard and Telian 14 can be used as a reference to assess and establish an individualised habituation exercise programme for patients with chronic UVL. The therapist needs to be creative in assessing provoking movements that may be experienced by the patients. The therapist can choose up to 4 movements that produce mild to moderate dizziness for the individual to practise repeatedly. Each movement is performed as quickly as possible to produce mild to moderate symptoms, with rest between each movement to allow symptoms to subside and an additional 30-second wait before the next repetition. Three to 5 sets of exercises are performed once or twice daily. As habituation sets in, movements can be performed more rapidly in different positions or activities. 3. Treatment for Postural Instability Treatment of postural instability for an individual with vestibular dysfunction requires an exercise programme that includes a variety of sensory environments involving alteration of the visual, somatosensory and vestibular inputs. Treatment aims to force-use the remaining vestibular inputs and recruiting substitution of the somatosensory and visual inputs to maintain postural control. Alteration of visual inputs can include keeping the eyes closed, introducing a full visual field background (e.g., conflicting checkerboard), incorporating head movement, decreasing the lighting, and introducing a busy, conflicting visual environment or moving stimuli (e.g., a train moving pass the train platform). Some ways to alter the somatosensory inputs involve varying the supporting surfaces i.e., introducing conforming, uneven or moving surfaces or by decreasing the base of support. Balance can be challenged by standing or balancing on conforming surfaces (e.g., foam, wobble board, trampoline or balance beam) and walking on uneven surfaces (e.g., grass, ramps or treadmill). Incorporating head movement in various orientations during exercises can alter vestibular inputs. Take for instance, moving the head sideways, vertically and diagonally while standing, and subsequently, while walking; tossing a tennis ball sideways, up and down while standing, and subsequently, while walking, will also incorporate head movement. Habituation is facilitated if the individual also has motion-provoked dizziness induced by head movement. Eye tracking of the tennis ball as it is being tossed sideways or up and down also helps to train the smooth pursuit of the eyes. Postural stability training involves the alteration of one or both of the visual, and somatosensory and vestibular environments. Balance training should begin with altering a single sensory modality, followed by involving multiple sensory modalities as the individual s balance improves. 9 Both the visual and somatosensory inputs can be altered as one s balance improves by practicing standing on conforming support surfaces (foam, wobble board, grass, mat) with the eyes closed or with head movement incorporated. More challenges can be introduced by tossing a tennis ball or bean bags while walking or doing a tandem walk on a thick carpet, a mat or grass, or walking on a treadmill and performing head movements. Subsequently, patients are encouraged to do these exercises outdoors (e.g., in the garden or a park). 4. Treatment to Decrease Sensitivity to Motion in the Environment Individuals with increased sensitivity to motion in the environment can be gradually trained to become less sensitive by initially getting them to sit in a visually busy environment such as a shopping mall or supermarket. Subsequently, the individual may first push a trolley in the supermarket or shopping mall and then progress to walking independently, initially with the crowd, then against it. Head movements (horizontal, vertical or diagonal) can be incorporated as appropriate to increase the difficulty of the exercise. 5. Treatment for Physical Conditioning A physical conditioning programme consisting of thrice weekly, 15- to 20-minute sessions should be included in a vestibular rehabilitation programme as appropriate to prevent or maintain cardiovascular endurance. These May 2005, Vol. 34 No. 4
4 292 exercises can include brisk walking, stair climbing, walking on the treadmill, riding a stationary bicycle or swimming. Bilateral Vestibular Lesion (BVL) Patients with BVL will present with one or more of the following physical impairments, which are quite similar to that for UVL: 1. Gaze instability or oscillopsia associated with head movements is recognised as a hallmark of BVL. 15 Approximately one-third of the patients with BVL reported oscillopsia. The oscillopsia is worse when patients walk in dim light. 2. Postural instability and gait disturbances: Disequilibrium and gait disturbances are common problems in patients with BVL. Symptoms manifest most clearly in the dark. This is because individuals with BVL tend to rely on visual cues for maintaining balance. Difficulty with balance increases when either visual or somatosensory input is decreased. Individuals with BVL also tend to ambulate with a big base of support to compensate for postural instability. They have difficulty changing directions while walking as turning often results in disequilibrium. Herdman et al 16 reported that the incidence of falls in subjects with BVL was significantly higher compared to subjects with UVL. The study suggested that the increased risk for falling in patients with vestibular loss is related to the degree of vestibular impairment as well as increasing age. 3. Physical de-conditioning: With gaze instability associated with head movements and the increased risk for falling, individuals with BVL tend to decrease their level of activity and mobility. With time, decreased activity can lead to cardiovascular de-conditioning. Treatment for Patients with BVL Rehabilitation for individuals with BVL would involve exercises to enhance remaining vestibular function, as well as substitution strategies to replace the lost vestibular function and to improve gaze stability and postural stability. 1. Treatment for Gaze Stability Strategies to improve gaze stability include: (i) Potentiation of the cervical-ocular reflex (COR), where receptors in the muscles and joint facets in the upper cervical spine region project to the contralateral vestibular nucleus, producing a compensatory slow phase eye movement. This compensatory eye movement is opposite to the direction of head movement during low-frequency, brief head movements and complements the VOR. (ii) Modification of saccades either by decreasing the amplitude of saccades or the use of corrective saccades during combined eye and head movement to maintain gaze stability on a visual target. (iii) Increased smooth pursuit eye movement. (iv) Central preprogramming of eye movement. This is an effective compensatory eye movement strategy to maintain gaze stability if the task is predictable. 12 Central programming of eye movements is based on the prediction or anticipation of intended motor behaviour. Herdman et al, 17 in their study to determine the role of central preprogramming in dynamic visual acuity with vestibular loss, suggested that both healthy subjects and subjects with UVL and BVL used central preprogramming to maintain gaze stability during predictable head movements. All the above substitution strategies are, however, only effective for lowfrequency head movement (<1 Hz). (v) Restriction of head movements to fixate gaze. Some exercises that can be performed to improve gaze stability are as follows: (i) VOR X1 and X2 viewing exercises to improve the remaining vestibular function and central preprogramming of eye movements. (ii) The exercise involving active eye-head movements between 2 targets, as described by Herdman, 11 helps to facilitate the use of saccadic or smooth pursuit strategies and central pre-programming. (iii) Imaginary target exercise helps to facilitate the central preprogramming of eye movements Treatment for Postural Instability and Gait Disturbances To improve postural stability, substitution strategies include: (i) the utilisation of visual and somatosensory cues; and (ii) central preprogramming of movement, which is also an effective compensatory strategy for postural stability when making an anticipated movement. 12 Treatment progression for postural imbalance is similar to that of UVL. In patients with BVL, the focus is on training with a decreased step width to tandem ambulation, i.e., gradually decreasing the base of support as tolerated. Balance training could also include an obstacle course or functional tasks that require positional changes or head movements. Behavioural and environmental modifications should also be considered, such as ensuring adequate lighting, non-skid floors, non-obstructed walkways, avoiding rushed movements, planning of movement before moving in crowded places and working in a sitting position to reduce the risk of falls. The therapist may need to consider prescribing walking assistive aids for individuals who cannot safely walk independently. Annals Academy of Medicine
5 Treatment for Physical De-conditioning The treatment for physical de-conditioning for BVL is similar to that for UVL. Effectiveness of Vestibular Rehabilitation VRT has become one of the main treatment modalities for patients suffering from vestibular dysfunctions. Patients are referred for VRT with the aim of helping to relieve them of symptoms of dizziness, gaze instability, disequilibrium and to improve their functional status. Studies have been done to evaluate the efficacy of VRT. To date, there have been a few randomised controlled studies conducted. One early study by Horak et al 3 aimed to investigate the effectiveness of an individualised VRT programme compared with general conditioning exercise and vestibular suppressant medication in reducing dizziness and imbalance in patients with chronic UVL. Twenty-five subjects were randomly allocated to 1 of 3 treatment groups (VRT, general conditioning exercise and medication). The customised VRT programme consisted of habituation, gaze stability, eye-head coordination, balance and general conditioning exercises. A computerised dynamic posturography test was used to measure static balance function. The subject s self-rating of the intensity of dizziness and a dizziness questionnaire was used to document changes in self-perceived dizziness. The researchers demonstrated that after 6 weeks of treatment, all 3 treatment approaches reduced the symptom of dizziness, but only VRT improved balance. Another study by Herdman et al 18 aimed to determine whether VRT facilitated the onset and rate of recovery of patients with UVL post-acoustic neuroma resection. Twenty-one subjects were randomised into experimental and control groups. The experimental group performed gaze stability exercises to improve vestibular gain and ambulation on postoperative day 3. Subjects in the control group did only smooth pursuit eye movement exercises and ambulation, also starting on postoperative day 3. Posturography test was used to evaluate the balance function. Patient s self-perceived vertigo and disequilibrium were reported on a visual analogue scale of 0 to10. The authors reported greater improvement in postural stability and selfperceived disequilibrium with the subjects in the experimental group. A third experimental study by Krebs et al 4 evaluated the effects of VRT in 8 subjects with BVL. The subjects were randomly assigned to 2 groups. The experimental group received 8 weeks of outpatient VRT and 8 weeks of home VRT exercises. The control group received 8 weeks of control treatment (isometric strengthening exercises) followed by 8 weeks of outpatient VRT exercises. The VRT programme consisted of a combination of vestibular adaptation and substitution exercises, depending on the subject s rate of progress. Unlike the previous 2 studies mentioned earlier, gait and stairs locomotion were used as outcome measures to determine the effectiveness of intervention. In addition, the Dizziness Handicap Inventory was used to document the subject s self-perceived dizziness in the psychosocial and functional aspects. The results indicated that at the end of 8 weeks, subjects who underwent VRT walked faster and had better stability during walking and stair climbing compared to the control group during control treatment, even though there was no significant difference in their self-reported Dizziness Handicap Inventory scores. At the end of 16 weeks, both groups showed improvement in their functional testing and selfreported symptom scores. The sample size for the study, however, was too small to permit the generalisation of results. In a recent larger scale experimental study by Krebs et al, 7 the authors sought to determine whether VRT improves gait stability (i.e., increased speed of walking and decreased base of support). One hundred and twenty-four subjects with both UVL and BVL were recruited for the study. Eighty-six subjects completed the 12-week intervention. Subjects were randomly assigned to 2 groups. The experimental group received 6 weeks of outpatient VRT (one session a week), followed by 6 weeks of home VRT. The control group received 6 weeks of placebo treatment (i.e., isometric strengthening exercise), followed by 6 weeks of outpatient VRT (one session a week). The VRT programme consisted of both adaptation and substitution exercises for gaze stability training and balance training, according to the individual s rate of progression. Gait-dependent variables were assessed at preferred speed using the 10-metre walk test and at a paced gait of 120 steps/min. The experimental group demonstrated greater improvement in gait velocity and stability at 6 weeks post- VRT treatment. At 12 weeks (after both groups had had VRT), both groups showed improvement in gait, with the experimental group demonstrating slightly more significant improvement. Most of the above studies included training for gaze stability but did not include outcome measures to assess this variable. A recent study by Herdman et al 19 evaluated the effect of a VRT intervention on visual acuity during head movement in patients with UVL. This study is to date the only research that has used a dynamic visual acuity (DVA) test to assess improvement in gaze stability postintervention. In this study, 21 subjects were randomly allocated into the experimental group and control group. The experimental group received a progressive home exercise programme that included adaptation, eye-head coordination and substitution exercises to improve gaze May 2005, Vol. 34 No. 4
6 294 stability, and also performed balance and gait training exercises. The control group did placebo home exercises that consisted of saccadic eye movement with the head stationary, and balance and gait exercises without head movement. Both the experimental and control groups underwent 4 to 5 weeks of the home exercise programme at a frequency of 4 to 5 times daily (approximately 40 minutes of exercises daily, including 20 minutes of balance and gait exercises). DVA during predictable and unpredictable head movements were used to evaluate changes in the subject s DVA. The subject s symptom of oscillopsia was measured on a visual analogue scale of 0 to 10. The authors demonstrated that there was significant improvement of DVA during predictable head movements in the experimental group after less than 5 weeks of treatment. Both the experimental and control groups reported a significant decrease in self-perceived oscillopsia. There was no correlation between improvement in oscillopsia and improvement in DVA during predictable or unpredictable head movements. In addition, age and time from onset did not contribute to the recovery of DVA, suggesting that the elderly or individuals with chronic vestibular hypofunction may benefit from VRT. The results suggested that the use of vestibular exercises fostered the recovery of DVA during predictable head movements. Conclusion VRT has been shown to improve vestibular function in patients with both UVL and BVL. VRT facilitates the reduction of self-perceived dizziness provoked by head movement or movement in a busy visual environment, improves mobility and balance function, and improves gaze stability associated with head movement. VRT needs to be customised to the individual s impairments and the exercises should be tailored according to each patient s rate of progression. REFERENCES 1. Horak FB, Nasher LM, Diener HC. Postural strategies associated with somatosensory and vestibular loss. Exp Brain Res 1990;82: Smith PF, Darlington CL. Neuromechemical mechanisms of recovery from peripheral vestibular lesions. Brain Res Brain Res Rev 1991;16: Erratum in: Brain Res Brain Res Rev 1992;17: Horak FB, Jones-Rycewicz C, Black FO, Shumway-Cook A. Effects of vestibular rehabilitation on dizziness and imbalance. Otolaryngol Head Neck Surg 1992;106: Krebs DE, Gill-Body KM, Riley PO, Parker SW. Double-blind, placebocontrolled trial of rehabilitation for bilateral vestibular hypofunction: preliminary report. Otolaryngol Head Neck Surg 1993;109: Shepard NT, Telian SA, Smith-Wheelock M, Raj A. Vestibular and balance rehabilitation therapy. Ann Otol Rhinol Laryngol 1993;102: Black FO, Angel CR, Pesznecker SC, Gianna C. Outcome analysis of individualized vestibular rehabilitation protocols. Am J Otol 2000;21: Krebs DE, Gill-Body KM, Parker SW, Ramirez JV, Wernick-Robinson M. Vestibular rehabilitation: useful but not universally so. Otolaryngol Head Neck Surg 2003;128: Cohen HS, Kimball KT. Increased independence and decreased vertigo after vestibular rehabilitation. Otolaryngol Head Neck Surg 2003;128: Clendaniel RA, Helminaski JO. Rehabilitation strategies for patients with vestibular deficits. In: Arenberg LK, editor. Dizziness and Balance Disorders. New York: Kugler Publications, 1993: Herdman, SJ, Whitney SL. Treatment of vestibular hypofunction. In: Herdman SJ, editor. Vestibular Rehabilitation (Contemporary Perspectives in Rehabilitation). 2nd ed. USA: F A Davis, 2000: Herdman SJ. Assessment and treatment of balance disorders in vestibular deficient patient. In: Duncan P, editor. Balance Proceedings of the APTA Forum. Nashville, TN; 1990: Herdman SJ. Role of vestibular adaptation in vestibular rehabilitation. Otolaryngol Head Neck Surg 1998;119: Shumway-Cook A, Woollacott MH. Motor Control. Theory and Practical Applications. 2nd ed. USA: Lippincott Williams & Wilkins, 2001: Shepard NT, Telian SA. Programmatic vestibular rehabilitation. Otolaryngol Head Neck Surg 1995;112: Bhansali SA, Stockwell CW, Borjrab DI. Oscillopsia in patients with loss of vestibular function. Otolaryngol Head Neck Surg 1993;109: Herdman SJ, Blatt P, Schubert MC, Tusa RJ. Falls in patients with vestibular deficits. Am J Otol 2000: Herdman SJ, Schubert MC, Tusa RJ. Role of central preprogramming in dynamic visual acuity with vestibular loss. Arch Otolaryngol Head Neck Surg 2001;127: Herdman SJ, Clendaniel RA, Mattox DE, Holiday MJ, Niparko JK. Vestibular adaptation exercises and recovery: acute stage after acoustic neuroma resection. Otolaryngol Head Neck Surg 1995;113: Herdman SJ, Schubert MC, Das VE, Tusa RJ. Recovery of dynamic visual acuity in unilateral vestibular hypofunction. Arch Otolaryngol Head Neck Surgery 2003;129: Annals Academy of Medicine
A STUDY OF THE EFFECTS OF A VESTIBULAR REHABILITATION PROGRAM ON PATIENTS WITH PERIPHERAL VESTIBULAR DYSFUNCTIONS
 The Indian Journal of Occupational Therapy : Vol. XXXVI : No. 1 (April - July 04) A STUDY OF THE EFFECTS OF A VESTIBULAR REHABILITATION PROGRAM ON PATIENTS WITH PERIPHERAL VESTIBULAR DYSFUNCTIONS * Pina
The Indian Journal of Occupational Therapy : Vol. XXXVI : No. 1 (April - July 04) A STUDY OF THE EFFECTS OF A VESTIBULAR REHABILITATION PROGRAM ON PATIENTS WITH PERIPHERAL VESTIBULAR DYSFUNCTIONS * Pina
The Human Balance System
 PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 [email protected] WWW.VESTIBULAR.ORG The Human Balance System A Complex Coordination of Central and Peripheral Systems By the Vestibular
PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 [email protected] WWW.VESTIBULAR.ORG The Human Balance System A Complex Coordination of Central and Peripheral Systems By the Vestibular
Vestibular Injury. Vestibular Disorders Association www.vestibular.org Page 1 of 5
 PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 [email protected] WWW.VESTIBULAR.ORG Vestibular Injury Compensation, De-compensation, and Failure to Compensate By Thomas E. Boismier,
PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 [email protected] WWW.VESTIBULAR.ORG Vestibular Injury Compensation, De-compensation, and Failure to Compensate By Thomas E. Boismier,
The Human Balance System
 5018 NE 15 TH AVE PORTLAND, OR 97211 FAX: (503) 229-8064 (800) 837-8428 [email protected] VESTIBULAR.ORG The Human Balance System A Complex Coordination of Central and Peripheral Systems By the Vestibular
5018 NE 15 TH AVE PORTLAND, OR 97211 FAX: (503) 229-8064 (800) 837-8428 [email protected] VESTIBULAR.ORG The Human Balance System A Complex Coordination of Central and Peripheral Systems By the Vestibular
Vestibular Injury: Compensation, Decompensation, and Failure to Compensate
 VESTIBULAR DISORDERS ASSOCIATION PO Box 13305 Portland, OR 97213 fax: (503) 229-8064 toll-free voice-mail: (800) 837-8428 [email protected] http://www.vestibular.org/ VEDA Publication No. F-26 Vestibular
VESTIBULAR DISORDERS ASSOCIATION PO Box 13305 Portland, OR 97213 fax: (503) 229-8064 toll-free voice-mail: (800) 837-8428 [email protected] http://www.vestibular.org/ VEDA Publication No. F-26 Vestibular
Using the Balance Board in Therapy
 Using the Balance Board in Therapy Practical applications for linking somato-sensory and vestibular systems to the collaboration between the eyes and brain. Vision Therapy establishes and supports visual
Using the Balance Board in Therapy Practical applications for linking somato-sensory and vestibular systems to the collaboration between the eyes and brain. Vision Therapy establishes and supports visual
Speaker: Shayla Moore, BMR(PT) Relationship with commercial interests: Employee at Creekside Physiotherapy Clinic
 Speaker: Shayla Moore, BMR(PT) Relationship with commercial interests: Employee at Creekside Physiotherapy Clinic 1 Vestibular Rehabilitation Managing dizziness to maintain mobility in the elderly" Dizziness:
Speaker: Shayla Moore, BMR(PT) Relationship with commercial interests: Employee at Creekside Physiotherapy Clinic 1 Vestibular Rehabilitation Managing dizziness to maintain mobility in the elderly" Dizziness:
Vestibular Rehabilitation
 PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 [email protected] WWW.VESTIBULAR.ORG Vestibular Rehabilitation An Effective, Evidence-Based Treatment By Anne Shumway-Cook, PT, PhD;
PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 [email protected] WWW.VESTIBULAR.ORG Vestibular Rehabilitation An Effective, Evidence-Based Treatment By Anne Shumway-Cook, PT, PhD;
Vestibular Assessment
 Oculomotor Examination A. Tests performed in room light Vestibular Assessment 1. Spontaneous nystagmus 2. Gaze holding nystagmus 3. Skew deviation 4. Vergence 5. Decreased vestibular ocular reflex i. Head
Oculomotor Examination A. Tests performed in room light Vestibular Assessment 1. Spontaneous nystagmus 2. Gaze holding nystagmus 3. Skew deviation 4. Vergence 5. Decreased vestibular ocular reflex i. Head
Vestibular Rehabilitation What s the Spin?
 Vestibular Rehabilitation What s the Spin? Carolyn Tassini, PT, DPT, NCS Vestibular Certified Rehabilitation Supervisor Bancroft NeuroRehab Objectives Attendees demonstrate a basic understanding of the
Vestibular Rehabilitation What s the Spin? Carolyn Tassini, PT, DPT, NCS Vestibular Certified Rehabilitation Supervisor Bancroft NeuroRehab Objectives Attendees demonstrate a basic understanding of the
ARE THE USE OF MEDICARE G CODES MAKING YOU SPIN?
 1 2 3 4 5 6 7 8 ARE THE USE F MEDICARE G CDES MAKING YU SPIN? HERE ARE SME ANSWERS: VESTIBULAR REHABILITATIN SPECIAL INTEREST GRUP Functional Limitation Reporting Kenda Fuller, PT South Valley Physical
1 2 3 4 5 6 7 8 ARE THE USE F MEDICARE G CDES MAKING YU SPIN? HERE ARE SME ANSWERS: VESTIBULAR REHABILITATIN SPECIAL INTEREST GRUP Functional Limitation Reporting Kenda Fuller, PT South Valley Physical
Balance and Vestibular Center Programs to treat dizziness and reduce your risk of falling
 Balance and Vestibular Center Programs to treat dizziness and reduce your risk of falling Helping you overcome dizziness and vertigo Most people will experience dizziness at some point in their lives.
Balance and Vestibular Center Programs to treat dizziness and reduce your risk of falling Helping you overcome dizziness and vertigo Most people will experience dizziness at some point in their lives.
BALANCE AND VESTIBULAR REHABILITATION THERAPY MANUAL
 BALANCE AND VESTIBULAR REHABILITATION THERAPY MANUAL Copyright AMERICAN HEARING & BALANCE CENTERS, INC., 2010 2010 Revision 3.01 TABLE OF CONTENTS Description Page Five Indications For Therapy... 1 Treatments
BALANCE AND VESTIBULAR REHABILITATION THERAPY MANUAL Copyright AMERICAN HEARING & BALANCE CENTERS, INC., 2010 2010 Revision 3.01 TABLE OF CONTENTS Description Page Five Indications For Therapy... 1 Treatments
GAZE STABILIZATION SYSTEMS Vestibular Ocular Reflex (VOR) Purpose of VOR Chief function is to stabilize gaze during locomotion. Acuity declines if
 GAZE STABILIZATION SYSTEMS Vestibular Ocular Reflex (VOR) Purpose of VOR Chief function is to stabilize gaze during locomotion. Acuity declines if slip exceeds 3-5 deg/sec. Ex: Head bobbing and heel strike
GAZE STABILIZATION SYSTEMS Vestibular Ocular Reflex (VOR) Purpose of VOR Chief function is to stabilize gaze during locomotion. Acuity declines if slip exceeds 3-5 deg/sec. Ex: Head bobbing and heel strike
Outcomes After Rehabilitation for Adults With Balance Dysfunction
 227 Outcomes After Rehabilitation for Adults With Balance Dysfunction Mary Beth Badke, PhD, PT, Terry A. Shea, BSc, PT, James A. Miedaner, MS, PT, Colin R. Grove, BSc, PT ABSTRACT. Badke MB, Shea TA, Miedaner
227 Outcomes After Rehabilitation for Adults With Balance Dysfunction Mary Beth Badke, PhD, PT, Terry A. Shea, BSc, PT, James A. Miedaner, MS, PT, Colin R. Grove, BSc, PT ABSTRACT. Badke MB, Shea TA, Miedaner
Proposed Treatment for Vestibular Dysfunction in Dogs By Margaret Kraeling, DPT, CCRT
 Proposed Treatment for Vestibular Dysfunction in Dogs By Margaret Kraeling, DPT, CCRT Vestibular dysfunction in the dog can be a disturbing condition for owners, as well as somewhat confounding for the
Proposed Treatment for Vestibular Dysfunction in Dogs By Margaret Kraeling, DPT, CCRT Vestibular dysfunction in the dog can be a disturbing condition for owners, as well as somewhat confounding for the
Recovering from a Mild Traumatic Brain Injury (MTBI)
 Recovering from a Mild Traumatic Brain Injury (MTBI) What happened? You have a Mild Traumatic Brain Injury (MTBI), which is a very common injury. Some common ways people acquire this type of injury are
Recovering from a Mild Traumatic Brain Injury (MTBI) What happened? You have a Mild Traumatic Brain Injury (MTBI), which is a very common injury. Some common ways people acquire this type of injury are
Cerebellum and Basal Ganglia
 Cerebellum and Basal Ganglia 1 Contents Cerebellum and Basal Ganglia... 1 Introduction... 3 A brief review of cerebellar anatomy... 4 Basic Circuit... 4 Parallel and climbing fiber input has a very different
Cerebellum and Basal Ganglia 1 Contents Cerebellum and Basal Ganglia... 1 Introduction... 3 A brief review of cerebellar anatomy... 4 Basic Circuit... 4 Parallel and climbing fiber input has a very different
Post-Concussion Syndrome
 Post-Concussion Syndrome Anatomy of the injury: The brain is a soft delicate structure encased in our skull, which protects it from external damage. It is suspended within the skull in a liquid called
Post-Concussion Syndrome Anatomy of the injury: The brain is a soft delicate structure encased in our skull, which protects it from external damage. It is suspended within the skull in a liquid called
Presented by: Paul G. Vidal, PT, MHSc, DPT, OCS, FAAOMPT Specialized Physical Therapy, LLC 2015 AOASM Annual Clinical Conference Philadelphia, PA
 Presented by: Paul G. Vidal, PT, MHSc, DPT, OCS, FAAOMPT Specialized Physical Therapy, LLC 2015 AOASM Annual Clinical Conference Philadelphia, PA Concussion The Role of the Physical Therapist Valuable
Presented by: Paul G. Vidal, PT, MHSc, DPT, OCS, FAAOMPT Specialized Physical Therapy, LLC 2015 AOASM Annual Clinical Conference Philadelphia, PA Concussion The Role of the Physical Therapist Valuable
Concussions and Mild Head Injury. Post Concussion Syndrome. Whiplash Injuries
 Concussions and Mild Head Injury Post Concussion Syndrome Whiplash Injuries Treat the cause, not just the symptoms NeuroSensory Center of Eastern Pennsylvania 250 Pierce Street, Suite 317 Kingston, PA
Concussions and Mild Head Injury Post Concussion Syndrome Whiplash Injuries Treat the cause, not just the symptoms NeuroSensory Center of Eastern Pennsylvania 250 Pierce Street, Suite 317 Kingston, PA
2014 Neurologic Physical Therapy Professional Education Consortium Webinar Course Descriptions and Objectives
 Descriptions and Neuroplasticity Health care providers are facing greater time restrictions to render services to the individual with neurological dysfunction. However, the scientific community has recognized
Descriptions and Neuroplasticity Health care providers are facing greater time restrictions to render services to the individual with neurological dysfunction. However, the scientific community has recognized
Concussion/MTBI Certification Series. Featuring: Frederick R Carrick, DC, PhD Distinguished Professor of Neurology, Life University
 Concussion/MTBI Certification Series Featuring: Frederick R Carrick, DC, PhD Distinguished Professor of Neurology, Life University Please note that spaces are limited for this specialty certification program.
Concussion/MTBI Certification Series Featuring: Frederick R Carrick, DC, PhD Distinguished Professor of Neurology, Life University Please note that spaces are limited for this specialty certification program.
How To Cover Occupational Therapy
 Guidelines for Medical Necessity Determination for Occupational Therapy These Guidelines for Medical Necessity Determination (Guidelines) identify the clinical information MassHealth needs to determine
Guidelines for Medical Necessity Determination for Occupational Therapy These Guidelines for Medical Necessity Determination (Guidelines) identify the clinical information MassHealth needs to determine
BESTest Balance Evaluation Systems Test Fay Horak PhD Copyright 2008
 BESTest Balance Evaluation Systems Test Fay Horak PhD Copyright 2008 TEST NUMBER/SUBJECT CODE DATE EXAMINER NAME EXAMINER Instructions for BESTest 1. Subjects should be tested with flat heeled shoes or
BESTest Balance Evaluation Systems Test Fay Horak PhD Copyright 2008 TEST NUMBER/SUBJECT CODE DATE EXAMINER NAME EXAMINER Instructions for BESTest 1. Subjects should be tested with flat heeled shoes or
How to test ocular movements in PSP Jan Kassubek
 How to test ocular movements in PSP Jan Kassubek Universitätsklinik für Neurologie, Ulm Bedside Screening: PSP initially slowing of vertical saccades slowing of downward saccades is considered the hallmark
How to test ocular movements in PSP Jan Kassubek Universitätsklinik für Neurologie, Ulm Bedside Screening: PSP initially slowing of vertical saccades slowing of downward saccades is considered the hallmark
Vestibular Rehabilitation Therapy (Rationale) Adaptation Guidelines. Substitution guidelines. Habituation exercise guidelines. Substitution guidelines
 Vestibular Rehabilitation Therapy Outline: Rationale for the effect of exercises Framework for exercise prescription Exercise progression Preferred prescription patterns Case study General treatment guidelines
Vestibular Rehabilitation Therapy Outline: Rationale for the effect of exercises Framework for exercise prescription Exercise progression Preferred prescription patterns Case study General treatment guidelines
Dizziness and Vertigo
 Dizziness and Vertigo Introduction When you are dizzy, you may feel lightheaded or lose your balance. If you also feel that the room is spinning, you may have vertigo. Vertigo is a type of severe dizziness.
Dizziness and Vertigo Introduction When you are dizzy, you may feel lightheaded or lose your balance. If you also feel that the room is spinning, you may have vertigo. Vertigo is a type of severe dizziness.
V~stibular Rehabilitation: Critical Decision Analysis
 V~stibular Rehabilitation: Critical Decision Analysis Richard E. Gans, Ph.D., FAAA, ABSTRACT Vestibular Rehabilitation Therapy (VRT) is used by audiologists, physical and occupational therapists, and physicians
V~stibular Rehabilitation: Critical Decision Analysis Richard E. Gans, Ph.D., FAAA, ABSTRACT Vestibular Rehabilitation Therapy (VRT) is used by audiologists, physical and occupational therapists, and physicians
Vestibular Rehabilitation
 5018 NE 15 TH AVE PORTLAND, OR 97211 FAX: (503) 229-8064 (800) 837-8428 [email protected] VESTIBULAR.ORG Vestibular Rehabilitation An Effective, Evidence-Based Treatment By Lisa Farrell, PT, PhD, AT,C;
5018 NE 15 TH AVE PORTLAND, OR 97211 FAX: (503) 229-8064 (800) 837-8428 [email protected] VESTIBULAR.ORG Vestibular Rehabilitation An Effective, Evidence-Based Treatment By Lisa Farrell, PT, PhD, AT,C;
Vestibular Rehabilitation Therapy. Melissa Nelson
 Vestibular Rehabilitation Therapy Melissa Nelson What is Vestibular Rehabilitation Therapy (VRT)? VRT is an exercise-based program designed to promote CNS compensation for inner ear deficits. The goal
Vestibular Rehabilitation Therapy Melissa Nelson What is Vestibular Rehabilitation Therapy (VRT)? VRT is an exercise-based program designed to promote CNS compensation for inner ear deficits. The goal
2016 VISION REHABILITATION SERVICES PROGRAM DESCRIPTIONS
 2016 VISION REHABILITATION SERVICES PROGRAM DESCRIPTIONS Contents Comprehensive Blind Rehabilitation Services (CBRS)... 2 Outpatient Low Vision and Blind Rehabilitation Services for Veterans and Active
2016 VISION REHABILITATION SERVICES PROGRAM DESCRIPTIONS Contents Comprehensive Blind Rehabilitation Services (CBRS)... 2 Outpatient Low Vision and Blind Rehabilitation Services for Veterans and Active
National Hospital for Neurology and Neurosurgery. Inner ear balance problems. Department of Neuro-otology
 National Hospital for Neurology and Neurosurgery Inner ear balance problems Department of Neuro-otology If you would like this document in another language or format or if you require the services of an
National Hospital for Neurology and Neurosurgery Inner ear balance problems Department of Neuro-otology If you would like this document in another language or format or if you require the services of an
The Role of Physical Therapy in Post Concussion Management. Non Disclosure
 The Role of Physical Therapy in Post Concussion Management. Cook Children s Sports Medicine Symposium Ryan Blankenship, PT, SCS Non Disclosure No conflicts of interest. 1 Course Objectives Participants
The Role of Physical Therapy in Post Concussion Management. Cook Children s Sports Medicine Symposium Ryan Blankenship, PT, SCS Non Disclosure No conflicts of interest. 1 Course Objectives Participants
PEOPLE WITH DYSFUNCTION within the vestibular system
 ORIGINAL ARTICLE Short-Term Effects of Vestibular Rehabilitation in Patients With Chronic Unilateral Vestibular Dysfunction: A Randomized Controlled Study Murat Giray, MD, Yesim Kirazli, MD, Hale Karapolat,
ORIGINAL ARTICLE Short-Term Effects of Vestibular Rehabilitation in Patients With Chronic Unilateral Vestibular Dysfunction: A Randomized Controlled Study Murat Giray, MD, Yesim Kirazli, MD, Hale Karapolat,
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery
 RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital we recognise that our broad and often complex patient
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital we recognise that our broad and often complex patient
Handicap after acute whiplash injury A 1-year prospective study of risk factors
 1 Handicap after acute whiplash injury A 1-year prospective study of risk factors Neurology 2001;56:1637-1643 (June 26, 2001) Helge Kasch, MD, PhD; Flemming W Bach, MD, PhD; Troels S Jensen, MD, PhD From
1 Handicap after acute whiplash injury A 1-year prospective study of risk factors Neurology 2001;56:1637-1643 (June 26, 2001) Helge Kasch, MD, PhD; Flemming W Bach, MD, PhD; Troels S Jensen, MD, PhD From
OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES
 OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES General Therapy Guidelines 1. Therapy evaluations must be provided by licensed physical and/or occupational therapists. Therapy evaluations
OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES General Therapy Guidelines 1. Therapy evaluations must be provided by licensed physical and/or occupational therapists. Therapy evaluations
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery
 RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital, we recognise that our broad and often complex patient
RNOH Physiotherapy Department (020 8909 5820) Rehabilitation guidelines for patients undergoing spinal surgery As a specialist orthopaedic hospital, we recognise that our broad and often complex patient
IF IN DOUBT, SIT THEM OUT.
 IF IN DOUBT, SIT THEM OUT. Scottish Sports Concussion Guidance: Grassroots sport and general public Modified from World Rugby s Guidelines on Concussion Management for the General Public Introduction The
IF IN DOUBT, SIT THEM OUT. Scottish Sports Concussion Guidance: Grassroots sport and general public Modified from World Rugby s Guidelines on Concussion Management for the General Public Introduction The
Less common vestibular disorders presenting with funny turns
 Less common vestibular disorders presenting with funny turns Charlotte Agrup, Department of Neuro-otology, The National Hospital for Neurology and Neurosurgery, London Making the diagnosis Making the diagnosis
Less common vestibular disorders presenting with funny turns Charlotte Agrup, Department of Neuro-otology, The National Hospital for Neurology and Neurosurgery, London Making the diagnosis Making the diagnosis
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
New York State Workers' Comp Board. Mid and Lower Back Treatment Guidelines. Summary From 1st Edition, June 30, 2010. Effective December 1, 2010
 New York State Workers' Comp Board Mid and Lower Back Treatment Guidelines Summary From 1st Edition, June 30, 2010 Effective December 1, 2010 General Principles Treatment should be focused on restoring
New York State Workers' Comp Board Mid and Lower Back Treatment Guidelines Summary From 1st Edition, June 30, 2010 Effective December 1, 2010 General Principles Treatment should be focused on restoring
Cervical Whiplash: Considerations in the Rehabilitation of Cervical Myofascial Injury. Canadian Family Physician
 Cervical Whiplash: Considerations in the Rehabilitation of Cervical Myofascial Injury 1 Canadian Family Physician Volume 32, September 1986 Arthur Ameis, MD Dr. Ames practices physical medicine and rehabilitation,
Cervical Whiplash: Considerations in the Rehabilitation of Cervical Myofascial Injury 1 Canadian Family Physician Volume 32, September 1986 Arthur Ameis, MD Dr. Ames practices physical medicine and rehabilitation,
Clinical Medical Policy Outpatient Rehab Therapies (PT & OT) for Members With Special Needs
 Benefit Coverage Rehabilitative services, (PT, OT,) are covered for members with neurodevelopmental disorders when recommended by a medical provider to address a specific condition, deficit, or dysfunction,
Benefit Coverage Rehabilitative services, (PT, OT,) are covered for members with neurodevelopmental disorders when recommended by a medical provider to address a specific condition, deficit, or dysfunction,
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Lumbar Spinal Stenosis North American Spine Society Public Education Series What Is Lumbar Spinal Stenosis? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Vestibular Rehabilitation: A Competency-Based Course
 Vestibular Rehabilitation: A Competency-Based Course Emory Conference Center and Hotel 1615 Clifton Road, NE Atlanta, Georgia 30329 Course Description This intense, evidence- based, six- day course is
Vestibular Rehabilitation: A Competency-Based Course Emory Conference Center and Hotel 1615 Clifton Road, NE Atlanta, Georgia 30329 Course Description This intense, evidence- based, six- day course is
Benign Paroxysmal Positional Vertigo. By Mick Benson
 Benign Paroxysmal Positional Vertigo By Mick Benson Definition Benign - not life-threatening Paroxysmal - a sudden onset Positional - response provoked by change in head position Vertigo - sensation of
Benign Paroxysmal Positional Vertigo By Mick Benson Definition Benign - not life-threatening Paroxysmal - a sudden onset Positional - response provoked by change in head position Vertigo - sensation of
Vestibular Rehabilitation: A Competency-Based Course
 Vestibular Rehabilitation: A Competency-Based Course Emory Conference Center and Hotel 1615 Clifton Road, NE Atlanta, Georgia 30329 Course Description This intense, evidence- based, six- day course is
Vestibular Rehabilitation: A Competency-Based Course Emory Conference Center and Hotel 1615 Clifton Road, NE Atlanta, Georgia 30329 Course Description This intense, evidence- based, six- day course is
Functions of the Brain
 Objectives 0 Participants will be able to identify 4 characteristics of a healthy brain. 0 Participants will be able to state the functions of the brain. 0 Participants will be able to identify 3 types
Objectives 0 Participants will be able to identify 4 characteristics of a healthy brain. 0 Participants will be able to state the functions of the brain. 0 Participants will be able to identify 3 types
Case Studies Updated 10.24.11
 S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
S O L U T I O N S Case Studies Updated 10.24.11 Hill DT Solutions Cervical Decompression Case Study An 18-year-old male involved in a motor vehicle accident in which his SUV was totaled suffering from
Clinically isolated syndrome (CIS)
 Clinically isolated syndrome (CIS) Spirella Building, Letchworth, SG6 4ET 01462 476700 www.mstrust.org.uk reg charity no. 1088353 We hope you find the information in this factsheet helpful. If you would
Clinically isolated syndrome (CIS) Spirella Building, Letchworth, SG6 4ET 01462 476700 www.mstrust.org.uk reg charity no. 1088353 We hope you find the information in this factsheet helpful. If you would
Integrated Neuropsychological Assessment
 Integrated Neuropsychological Assessment Dr. Diana Velikonja C.Psych Neuropsychology, Hamilton Health Sciences, ABI Program Assistant Professor, Psychiatry and Behavioural Neurosciences Faculty of Health
Integrated Neuropsychological Assessment Dr. Diana Velikonja C.Psych Neuropsychology, Hamilton Health Sciences, ABI Program Assistant Professor, Psychiatry and Behavioural Neurosciences Faculty of Health
CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery
 CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery For patients of Jeffrey Kramer, MD As you re discharged from the hospital, you may have questions about your continuing
CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery For patients of Jeffrey Kramer, MD As you re discharged from the hospital, you may have questions about your continuing
The Taxi Program provides services only to residents of the City of Napa.
 The NCTPA Taxi Program is a valuable taxpayer funded component of our agency s transportation services. While not intended as a primary means of transportation, this program was created to provide a lifeline
The NCTPA Taxi Program is a valuable taxpayer funded component of our agency s transportation services. While not intended as a primary means of transportation, this program was created to provide a lifeline
Physiotherapy in Rheumatoid Arthritis. Information for patients Gina Wall Senior Physiotherapist
 Physiotherapy in Rheumatoid Arthritis Information for patients Gina Wall Senior Physiotherapist What do Physiotherapists do? We conduct assessments by asking detailed questions about your symptoms, medical
Physiotherapy in Rheumatoid Arthritis Information for patients Gina Wall Senior Physiotherapist What do Physiotherapists do? We conduct assessments by asking detailed questions about your symptoms, medical
Whiplash injuries can be visible by functional magnetic resonance imaging. Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp.
 Whiplash injuries can be visible by functional magnetic resonance imaging 1 Bengt H Johansson, MD FROM ABSTRACT: Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp. 197-199 Whiplash trauma can
Whiplash injuries can be visible by functional magnetic resonance imaging 1 Bengt H Johansson, MD FROM ABSTRACT: Pain Research and Management Autumn 2006; Vol. 11, No. 3, pp. 197-199 Whiplash trauma can
Balance and Aging By Charlotte Shupert, PhD, with contributions by Fay Horak, PhD, PT Oregon Health & Science University, Portland, Oregon
 PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 [email protected] WWW.VESTIBULAR.ORG Balance and Aging By Charlotte Shupert, PhD, with contributions by Fay Horak, PhD, PT Oregon Health
PO BOX 13305 PORTLAND, OR 97213 FAX: (503) 229-8064 (800) 837-8428 [email protected] WWW.VESTIBULAR.ORG Balance and Aging By Charlotte Shupert, PhD, with contributions by Fay Horak, PhD, PT Oregon Health
Outpatient Neurological Rehabilitation Victoria General Hospital. Pam Loadman BSC.P.T., MSc. Physiotherapist
 Outpatient Neurological Rehabilitation Victoria General Hospital Pam Loadman BSC.P.T., MSc. Physiotherapist OPN - overview Who we see: Inclusion criteria Diagnoses Who we are: Clinicians involved What
Outpatient Neurological Rehabilitation Victoria General Hospital Pam Loadman BSC.P.T., MSc. Physiotherapist OPN - overview Who we see: Inclusion criteria Diagnoses Who we are: Clinicians involved What
Back & Neck Pain Survival Guide
 Back & Neck Pain Survival Guide www.kleinpeterpt.com Zachary - 225-658-7751 Baton Rouge - 225-768-7676 Kleinpeter Physical Therapy - Spine Care Program Finally! A Proven Assessment & Treatment Program
Back & Neck Pain Survival Guide www.kleinpeterpt.com Zachary - 225-658-7751 Baton Rouge - 225-768-7676 Kleinpeter Physical Therapy - Spine Care Program Finally! A Proven Assessment & Treatment Program
Dizziness and balance problems
 Dizziness and balance problems Dizziness and balance problems, Action on Hearing Loss Information, May 2011 1 Dizziness and balance problems This factsheet is part of our Ears and ear problems range. It
Dizziness and balance problems Dizziness and balance problems, Action on Hearing Loss Information, May 2011 1 Dizziness and balance problems This factsheet is part of our Ears and ear problems range. It
Transmittal 55 Date: MAY 5, 2006. SUBJECT: Changes Conforming to CR3648 for Therapy Services
 CMS Manual System Pub 100-03 Medicare National Coverage Determinations Department of Health & Human Services (DHHS) Centers for Medicare & Medicaid Services (CMS) Transmittal 55 Date: MAY 5, 2006 Change
CMS Manual System Pub 100-03 Medicare National Coverage Determinations Department of Health & Human Services (DHHS) Centers for Medicare & Medicaid Services (CMS) Transmittal 55 Date: MAY 5, 2006 Change
Cervical Exercise: How important is it? What can be done? The Backbone of Spine Treatment. North American Spine Society Public Education Series
 Cervical Exercise: The Backbone of Spine Treatment How important is it? What can be done? North American Spine Society Public Education Series Important: If you have had an accident that started your neck
Cervical Exercise: The Backbone of Spine Treatment How important is it? What can be done? North American Spine Society Public Education Series Important: If you have had an accident that started your neck
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
Rehabilitation of Sports Hernia
 Rehabilitation of Sports Hernia (Involving Adductor Tenotomy, Ilioinguinal Neurectomy and Osteitis Pubis) An appendix follows this protocol for examples of exercises in each phase of rehabilitation. There
Rehabilitation of Sports Hernia (Involving Adductor Tenotomy, Ilioinguinal Neurectomy and Osteitis Pubis) An appendix follows this protocol for examples of exercises in each phase of rehabilitation. There
REHABILITATION SERVICES
 REHABILITATION SERVICES S O U T H A M P T O N H O S P I T A L C o m m i t t e d to E xc e l l e n c e, to C o m m u n i t y, a n d to Yo u. A c ute C a r e R e h a b i l itati o n C a r d i o p u l m o
REHABILITATION SERVICES S O U T H A M P T O N H O S P I T A L C o m m i t t e d to E xc e l l e n c e, to C o m m u n i t y, a n d to Yo u. A c ute C a r e R e h a b i l itati o n C a r d i o p u l m o
Whiplash and Whiplash- Associated Disorders
 Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
NFL Head, Neck and Spine Committee s Protocols Regarding Diagnosis and Management of Concussion
 NFL Head, Neck and Spine Committee s Protocols Regarding Diagnosis and Management of Concussion Introduction Concussion is an important injury for the professional football player, and the diagnosis, prevention,
NFL Head, Neck and Spine Committee s Protocols Regarding Diagnosis and Management of Concussion Introduction Concussion is an important injury for the professional football player, and the diagnosis, prevention,
adj., departing from the norm, not concentric, utilizing negative resistance for better client outcomes
 Why Eccentrics? What is it? Eccentric adj., departing from the norm, not concentric, utilizing negative resistance for better client outcomes Eccentrics is a type of muscle contraction that occurs as the
Why Eccentrics? What is it? Eccentric adj., departing from the norm, not concentric, utilizing negative resistance for better client outcomes Eccentrics is a type of muscle contraction that occurs as the
RIABILITAZIONE VESTIBOLARE
 Fiuggi 2013 LA RIABILITAZIONE VESTIBOLARE Università degli studi di Perugia Dott. MARIO FARALLI Responsabile del Servizio di Vestibologia della Clinica Otorinolaringoiatrica di Perugia VESTIBULAR REHABILITATION
Fiuggi 2013 LA RIABILITAZIONE VESTIBOLARE Università degli studi di Perugia Dott. MARIO FARALLI Responsabile del Servizio di Vestibologia della Clinica Otorinolaringoiatrica di Perugia VESTIBULAR REHABILITATION
Rehabilitation Documentation and Proper Coding Guidelines
 Rehabilitation Documentation and Proper Coding Guidelines Purpose: 1) Develop a guide for doctors in South Dakota to follow when performing reviews on rehabilitation cases. 2) Provide doctors in South
Rehabilitation Documentation and Proper Coding Guidelines Purpose: 1) Develop a guide for doctors in South Dakota to follow when performing reviews on rehabilitation cases. 2) Provide doctors in South
by Argyrios Stampas, MD, Carolin Dohle, MD, and Elizabeth Dominick, PT, DPT, NCS
 by Argyrios Stampas, MD, Carolin Dohle, MD, and Elizabeth Dominick, PT, DPT, NCS Therapist Jennifer Metz (right) helps a patient use a body-weight support treadmill system. Up and Moving Blending dedication
by Argyrios Stampas, MD, Carolin Dohle, MD, and Elizabeth Dominick, PT, DPT, NCS Therapist Jennifer Metz (right) helps a patient use a body-weight support treadmill system. Up and Moving Blending dedication
A Flow Chart For Classification Of Nystagmus
 A Flow Chart For Classification Of Nystagmus Is fixation impaired because of a slow drift, or an intrusive saccade, away from the target? If a slow drift is culprit Jerk Pendular Unidrectional (constant
A Flow Chart For Classification Of Nystagmus Is fixation impaired because of a slow drift, or an intrusive saccade, away from the target? If a slow drift is culprit Jerk Pendular Unidrectional (constant
STROKE CARE NOW NETWORK CONFERENCE MAY 22, 2014
 STROKE CARE NOW NETWORK CONFERENCE MAY 22, 2014 Rehabilitation Innovations in Post- Stroke Recovery Madhav Bhat, MD Fort Wayne Neurological Center DISCLOSURE Paid speaker for TEVA Neuroscience Program.
STROKE CARE NOW NETWORK CONFERENCE MAY 22, 2014 Rehabilitation Innovations in Post- Stroke Recovery Madhav Bhat, MD Fort Wayne Neurological Center DISCLOSURE Paid speaker for TEVA Neuroscience Program.
Spine Vol. 30 No. 16; August 15, 2005, pp 1799-1807
 A Randomized Controlled Trial of an Educational Intervention to Prevent the Chronic Pain of Whiplash Associated Disorders Following Rear-End Motor Vehicle Collisions 1 Spine Vol. 30 No. 16; August 15,
A Randomized Controlled Trial of an Educational Intervention to Prevent the Chronic Pain of Whiplash Associated Disorders Following Rear-End Motor Vehicle Collisions 1 Spine Vol. 30 No. 16; August 15,
Pulmonary Rehabilitation Program - Home Exercise Program
 Pulmonary Rehabilitation Program - Home Exercise Program Getting Started Regular exercise should be a part of life for everyone. Exercise improves the body's tolerance to activity and work, and strengthens
Pulmonary Rehabilitation Program - Home Exercise Program Getting Started Regular exercise should be a part of life for everyone. Exercise improves the body's tolerance to activity and work, and strengthens
INTERNATIONAL RUGBY BOARD Putting players first
 Summary Principles Concussion must be taken extremely seriously to safeguard the long term welfare of Players. Players suspected of having concussion must be removed from play and must not resume play
Summary Principles Concussion must be taken extremely seriously to safeguard the long term welfare of Players. Players suspected of having concussion must be removed from play and must not resume play
NEUROLOCALIZATION MADE EASY
 NEUROLOCALIZATION MADE EASY Jared B. Galle, DVM, Diplomate ACVIM (Neurology) Dogwood Veterinary Referral Center 4920 Ann Arbor-Saline Road Ann Arbor, MI 48103 Localizing a neurologic problem to an anatomical
NEUROLOCALIZATION MADE EASY Jared B. Galle, DVM, Diplomate ACVIM (Neurology) Dogwood Veterinary Referral Center 4920 Ann Arbor-Saline Road Ann Arbor, MI 48103 Localizing a neurologic problem to an anatomical
Falls and falls injury prevention activity audit for residential aged care facilities
 Falls and falls injury prevention activity audit for residential aged care facilities National Ageing Research Institute October 2009 www.nari.unimelb.edu.au This tool is based on a tool that was originally
Falls and falls injury prevention activity audit for residential aged care facilities National Ageing Research Institute October 2009 www.nari.unimelb.edu.au This tool is based on a tool that was originally
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Instructions & Forms for Submitting Claims to Medicare
 Instructions & Forms for Submitting Claims to Medicare The Centers for Medicare and Medicaid services have issued a national coverage policy for the WalkAide. CMS will cover patients who have a diagnosis
Instructions & Forms for Submitting Claims to Medicare The Centers for Medicare and Medicaid services have issued a national coverage policy for the WalkAide. CMS will cover patients who have a diagnosis
Hip Arthroscopy Post-operative Rehabilitation Protocol
 Hip Arthroscopy Post-operative Rehabilitation Protocol Introduction Since the early 20 th century, when hip arthroscopy was regarded as being almost impossible to undertake, the procedure has developed
Hip Arthroscopy Post-operative Rehabilitation Protocol Introduction Since the early 20 th century, when hip arthroscopy was regarded as being almost impossible to undertake, the procedure has developed
PATIENT INFORMATION BOOKLET
 (060110) VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE ( BY DR. ISAAC LIPSHITZ ) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL END-STAGE AGE-RELATED MACULAR
(060110) VISIONCARE S IMPLANTABLE MINIATURE TELESCOPE ( BY DR. ISAAC LIPSHITZ ) AN INTRAOCULAR TELESCOPE FOR TREATING SEVERE TO PROFOUND VISION IMPAIRMENT DUE TO BILATERAL END-STAGE AGE-RELATED MACULAR
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com
 Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Knee Replacement Protocol Brian White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Trunk Strengthening and Muscle and Coordination Exercises for Lower Limb Amputees
 Trunk Strengthening and Muscle and Coordination Exercises for Lower Limb Amputees Part One: Trunk Strengthening Trunk Extension Needed: Sturdy chair or stool, Theraband, and a Theraball if necessary. Sit
Trunk Strengthening and Muscle and Coordination Exercises for Lower Limb Amputees Part One: Trunk Strengthening Trunk Extension Needed: Sturdy chair or stool, Theraband, and a Theraball if necessary. Sit
Audit on treatment and recovery of ankle sprain
 Hong Kong Journal of Emergency Medicine Audit on treatment and recovery of ankle sprain WY Lee Study Objectives: The object of this study is to audit the care of ankle sprain of different severity and
Hong Kong Journal of Emergency Medicine Audit on treatment and recovery of ankle sprain WY Lee Study Objectives: The object of this study is to audit the care of ankle sprain of different severity and
Standard of Care: Cervical Radiculopathy
 Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
Primary Motor Pathway
 Understanding Eye Movements Abdullah Moh. El-Menaisy, MD, FRCS Chief, Neuro-ophthalmology ophthalmology & Investigation Units, Dhahran Eye Specialist Hospital, Dhahran, Saudi Arabia Primary Motor Pathway
Understanding Eye Movements Abdullah Moh. El-Menaisy, MD, FRCS Chief, Neuro-ophthalmology ophthalmology & Investigation Units, Dhahran Eye Specialist Hospital, Dhahran, Saudi Arabia Primary Motor Pathway
PLANTAR FASCITIS (Heel Spur Syndrome)
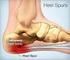 PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
THE MANAGEMENT OF CONCUSSION IN AUSTRALIAN FOOTBALL
 THE MANAGEMENT OF CONCUSSION IN AUSTRALIAN FOOTBALL AFL Research board AFL MEDICAL OFFICERS' ASSOCIATION THE MANAGEMENT OF CONCUSSION IN AUSTRALIAN FOOTBALL This document has been published by the AFL
THE MANAGEMENT OF CONCUSSION IN AUSTRALIAN FOOTBALL AFL Research board AFL MEDICAL OFFICERS' ASSOCIATION THE MANAGEMENT OF CONCUSSION IN AUSTRALIAN FOOTBALL This document has been published by the AFL
Concussion Guidance for the General Public
 CONCUSSION FACTS A concussion is a brain injury. All concussions are serious. Concussions can occur without loss of consciousness. All athletes with any symptoms following a head injury must be removed
CONCUSSION FACTS A concussion is a brain injury. All concussions are serious. Concussions can occur without loss of consciousness. All athletes with any symptoms following a head injury must be removed
12-week Half Marathon Training Program By Ben Wisbey
 12-week Half Marathon Training Program By Ben Wisbey Introduction The half marathon is often the intermediate goal for those runners looking at doing their first marathon. It is also the longest distance
12-week Half Marathon Training Program By Ben Wisbey Introduction The half marathon is often the intermediate goal for those runners looking at doing their first marathon. It is also the longest distance
