Diagnosis and Management of Acute Pyelonephritis in Adults
|
|
|
- Joseph Harrison
- 9 years ago
- Views:
Transcription
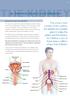
1 This is a corrected version of the article that appeared in print. Diagnosis and Management of Acute Pyelonephritis in Adults KALYANAKRISHNAN RAMAKRISHNAN, M.D., and DEWEY C. SCHEID, M.D., M.P.H. University of Oklahoma Health Sciences Center, Oklahoma City, Oklahoma There are approximately 250,000 cases of acute pyelonephritis each year, resulting in more than 100,000 hospitalizations. The most common etiologic cause is infection with Escherichia coli. The combination of the leukocyte esterase test and the nitrite test (with either test proving positive) has a sensitivity of 75 to 84 percent and a specificity of 82 to 98 percent for urinary tract infection. Urine cultures are positive in 90 percent of patients with acute pyelonephritis, and cultures should be obtained before antibiotic therapy is initiated. The use of blood cultures should be reserved for patients with an uncertain diagnosis, those who are immunocompromised, and those who are suspected of having hematogenous infections. Outpatient oral antibiotic therapy with a fluoroquinolone is successful in most patients with mild uncomplicated pyelonephritis. Other effective alternatives include extended-spectrum penicillins, amoxicillin-clavulanate potassium, cephalosporins, and trimethoprim-sulfamethoxazole. Indications for inpatient treatment include complicated infections, sepsis, persistent vomiting, failed outpatient treatment, or extremes of age. In hospitalized patients, intravenous treatment is recommended with a fluoroquinolone, aminoglycoside with or without ampicillin, or a third-generation cephalosporin. The standard duration of therapy is seven to 14 days. Urine culture should be repeated one to two weeks after completion of antibiotic therapy. Treatment failure may be caused by resistant organisms, underlying anatomic/functional abnormalities, or immunosuppressed states. Lack of response should prompt repeat blood and urine cultures and, possibly, imaging studies. A change in antibiotics or surgical intervention may be required. (Am Fam Physician 2005;71: Copyright 2005 American Academy of Family Physicians.) See page 835 for strengthof-recommendation labels. In more than 80 percent of cases of acute pyelonephritis, the etiologic agent is Escherichia coli. Acute pyelonephritis is an infection of the upper urinary tract, specifically the renal parenchyma and renal pelvis (Figure 1). Acute pyelonephritis is considered uncomplicated if the infection is caused by a typical pathogen in an immunocompetent patient who has normal urinary tract anatomy and renal function. Misdiagnosis can lead to sepsis, renal abscesses, and chronic pyelonephritis that may cause secondary hypertension and renal failure. Risk factors for complicated acute pyelonephritis are those that increase susceptibility or reduce host response to infections (Table 1). 1,2 Approximately 250,000 cases of acute pyelonephritis occur each year, resulting in more than 100,000 hospitalizations. 3 Women are approximately five times more likely than men to be hospitalized with this condition (11.7 versus 2.4 hospitalizations per 10,000 cases, respectively); however, women have a lower mortality rate than men (7.3 versus 16.5 deaths per 1,000 cases, respectively). 4 Acute pyelonephritis occurs in 1 to 2 percent of pregnant women, increasing the risk for premature labor and low-birth-weight infants. 5 Pathogenesis Most renal parenchymal infections occur secondary to bacterial ascent through the urethra and urinary bladder. In men, prostatitis and prostatic hypertrophy causing urethral obstruction predispose to bacteriuria. 6 Hematogenous acute pyelonephritis occurs most often in debilitated, chronically ill patients and those receiving immunosuppressive therapy. Metastatic staphylococcal or fungal infections may spread to the kidney from distant foci in the bone or skin. In more than 80 percent of cases of acute pyelonephritis, the etiologic agent is Escherichia coli. 7 Other etiologic causes include aerobic gram-negative bacteria, Staphylococcus saprophyticus, and enterococci. The microbial spectrum associated with different types of urinary tract infections (UTIs) is Downloaded from the American Family Physician Web site at Copyright 2005 American Academy of Family Physicians. For the private, noncommercial 1, 2005 use of Volume one individual 71, Number user of the 5 Web site. All other rights reserved. Contact [email protected] for copyright American questions and/or Family permission Physician requests. March 933
2 Strength of Recommendations Key clinical recommendation Label References Blood cultures should be obtained in patients with acute pyelonephritis only if there is diagnostic uncertainty, the patient is immunosuppressed, or a hematogenous source is suspected. Outpatient oral therapy is successful in 90 percent of selected patients with uncomplicated acute pyelonephritis who can tolerate oral intake, will be compliant with the treatment regimen, will return for early follow-up, and have adequate social support. Patients hospitalized with acute pyelonephritis should be treated with one of three initial intravenous therapies: a fluoroquinolone; an aminoglycoside with or without ampicillin; or an extended-spectrum cephalosporin with or without an aminoglycoside. C 24, 25 B 27, 28 B 29 A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, opinion, or case series. See page 835 for more information. ILLUSTRATION BY DAVID KLEMM Renal pyramids Capsule Figure 1. Anatomy of the kidney. wide (Table 2). 8,9 In elderly patients, E. coli is a less common (60 percent) cause of acute pyelonephritis. The increased use of catheters and instruments among these patients predisposes them to infections with other gram-negative organisms such as Proteus, Klebsiella, Serratia, or Pseudomonas. Renal cortex Renal medulla Renal pelvis Ureter Patients who have diabetes mellitus tend to have infections caused by Klebsiella, Enterobacter, Clostridium, or Candida. They also are at an increased risk of developing emphysematous pyelonephritis and papillary necrosis, leading to shock and renal failure. 1,10 Bacteriuria, which frequently is polymicrobial, develops in more than 50 percent of patients who require catheterization for more than five days, and in virtually all patients who have indwelling urinary catheters for more than one month. 1 Immunosuppression favors the development of subclinical (silent) pyelonephritis and infections caused by nonenteric, aerobic, gram-negative rods and Candida. Acute pyelonephritis occurs within two months following renal transplant in 30 to 50 percent of patients because of concomitant immunosuppression and postsurgical vesicoureteric reflux. 2 Acute pyelonephritis is considered complicated in men because they have a higher probability of urinary tract abnormalities, prostatic enlargement causing urethral obstruction with incomplete voiding, or an age-related decrease of antibacterial activity in prostatic secretions. Clinical Presentation The spectrum of acute pyelonephritis is wide, ranging from a mild illness to sepsis syndrome. 1 To diagnose acute pyelonephri- 934 American Family Physician Volume 71, Number 5 March 1, 2005
3 Pyelonephritis TABLE 1 Risk Factors for Complicated Acute Pyelonephritis Age Immunosuppressed state Obstruction Infants Diabetes mellitus Foreign body Elderly (> 60 years of age) Sickle cell disease Calculi Anatomic/functional abnormality Transplantation Bladder neck obstruction Polycystic kidney disease Malignancy Posterior urethral valve Horseshoe kidney Chemoradiation Benign prostatic hypertrophy Double ureter HIV infections Neurogenic bladder Ureterocele Corticosteroid use Pregnancy Vesicoureteric reflux Male sex Miscellaneous Foreign body Anatomic abnormalities Inappropriate antibiotics Urinary, ureteric, or nephrostomy catheters Calculus Prostatic obstruction Resistant organisms Instrumentation HIV = human immunodeficiency virus. Information from references 1 and 2. tis, physicians must rely on evidence of UTI from urinalysis or culture, along with signs and symptoms suggesting upper UTI (fever, chills, flank pain, nausea, vomiting, costovertebral angle tenderness). Symptoms that are suggestive of cystitis (dysuria, urinary bladder frequency and urgency, and suprapubic pain) also may be present. In a study 11 of young and middle-aged women presenting to an emergency depart- TABLE 2 Microbial Organisms Causing Specific Types of Urinary Tract Infections Microbial organism Acute uncomplicated cystitis (%)* Acute uncomplicated pyelonephritis (%) Complicated UTI (%) Catheter-associated UTI (%) Escherichia coli Staphylococcus saprophyticus Proteus Klebsiella Enterococci Pseudomonas Mixed Yeast UTI = urinary tract infection. * One study 9 showed that 25 percent of E. coli isolates were resistant to ampicillin, 24 percent to tetracyclines, and 11 percent to trimethoprim-sulfamethoxazole (TMP-SMX; Bactrim, Septra). Adapted with permission from The Johns Hopkins Ambulatory Clerkship in Medicine. Dysuria. Accessed online December 5, 2004, at: with additional information from reference 9. March 1, 2005 Volume 71, Number 5 American Family Physician 935
4 ment with fever, pyuria, and other features of upper UTI, 98 percent had acute pyelonephritis. In the absence of fever, 16 percent were given alternative diagnoses. 11 However, up to one third of elderly patients with acute pyelonephritis have no fever; in 20 percent of elderly patients, the predominant symptoms are gastrointestinal or pulmonary. 1 Fever and leukocytosis are of little value in diagnosing acute pyelonephritis in patients who have indwelling bladder catheters, especially when infections are caused by gram-positive cocci or Candida. 12 The differential diagnosis of acute pyelonephritis includes pelvic inflammatory disease, cholecystitis, appendicitis, lower lobe pneumonia, perforated viscus, and the prodrome of herpes zoster. Up to 30 percent of women presenting with cystitis-like symptoms have upper urinary tract involvement (subclinical pyelonephritis), but these infections rarely cause any cortical Fever and leukocytosis are of little value in diagnosing acute pyelonephritis in damage. This situation is more common in pregnant women patients who have indwelling bladder catheters. diabetes, immunosuppression, and patients with recurrent UTI, renal tract pathology, or previous UTI occurring before 12 years of age. 2 In the presence of obstruction (stone, tumor, bladder neck obstruction, enlarged prostate), acute pyelonephritis can be extremely severe and recalcitrant to treatment, and may progress to renal abscess. The Authors KALYANAKRISHNAN RAMAKRISHNAN, M.D., is associate professor in the Department of Family and Preventive Medicine at the University of Oklahoma Health Sciences Center, Oklahoma City. Dr. Ramakrishnan received his medical degree from the Jawaharlal Institute, Pondicherry, India. He completed a family practice residency at the University of Oklahoma Health Sciences Center. DEWEY C. SCHEID, M.D., M.P.H., is associate professor in the Department of Family and Preventive Medicine at the University of Oklahoma Health Sciences Center. Dr. Scheid received his medical degree from the University of Cincinnati (Ohio) College of Medicine. He completed a family practice residency at Memorial Medical Center in Corpus Christi, Tex., and a master of public health degree at the Johns Hopkins Bloomberg School of Public Health. Address correspondence to Kalyanakrishnan Ramakrishnan, M.D., University of Oklahoma Health Sciences Center, Dept. of Family and Preventive Medicine, Residency Division, 900 N.E. 10th St., Room 2614, Oklahoma City, OK ( [email protected]). Reprints are not available from the authors. Diagnostic Testing Urinalysis and urine culture confirm the diagnosis of acute pyelonephritis. The consensus definition of pyelonephritis established by the Infectious Diseases Society of America (IDSA) is a urine culture showing at least 10,000 colony-forming units (CFU) per mm 3 and symptoms compatible with the diagnosis. 13 Lower counts (1,000 to 9,999 CFU per mm 3 ) are of concern in men and pregnant women. Urine specimens generally are obtained by a midstream cleancatch technique, and one study 14 showed that cleansing does not decrease contamination rates in adults. Pyuria is present in almost all patients with acute pyelonephritis and can be detected rapidly with the leukocyte esterase test or the nitrite test. The combination of the leukocyte esterase and nitrite tests (with a positive result on either) for UTI is more specific but less sensitive than either test alone 15 (Table 3). 3,15-21 Although white cell casts may be observed in other conditions, they are, along with other features of UTI, specific for acute pyelonephritis. Hematuria may be present in patients with cystitis and pyelonephritis. 3 In some complicated cases, Gram stain analysis of urine can aid in the choice of initial antibiotic therapy. 22 Another option is the use of the antibody-coated bacteria assay, which may be helpful in localizing subclinical upper UTIs. 23 Urine cultures are positive in 90 percent of patients with acute pyelonephritis, and culture specimens should be obtained before initiation of antibiotic therapy. Blood cultures have been recommended for hospitalized patients; up to 20 percent of these patients have positive cultures. 1 In two studies, 24,25 however, completion of blood cultures did not result in changes in management strategies in patients with acute pyelonephritis. There is no evidence that positive blood cultures indicate a more complicated course in otherwise healthy persons with pyelonephritis. 26 Therefore, blood cultures are indicated only if there is diagnostic uncertainty, the patient is immunosuppressed, or a hematogenous source is suspected. 24, American Family Physician Volume 71, Number 5 March 1, 2005
5 Pyelonephritis TABLE 3 Laboratory Diagnosis of Urinary Tract Infection Test Finding Sensitivity (%)* Specificity (%)* Urinalysis 16,17 > 5 WBCs/HPF 72 to to 82 > 10 WBCs/HPF 58 to to 86 Leukocyte esterase test 3 Positive 74 to to 98 Nitrite test 18 Positive 35 to to 100 Leukocyte esterase and Either test positive 75 to to 98 nitrite tests 15,19 Dipstick hematuria 20 Positive Gram stain of uncentrifuged > 1 bacterium per HPF urine 21 WBCs/HPF = white blood cells per high-power field. * For identification of > 100,000 colony-forming units per mm 3. Information from references 3 and 15 through 21. Treatment Although patients with acute pyelonephritis traditionally have been hospitalized and treated with intravenous antibiotics, outpatient oral therapy is successful in 90 percent of selected patients with uncomplicated acute pyelonephritis who can tolerate oral intake, will be compliant with the treatment regimen, TABLE 4 Indications for Hospitalization in Patients with Acute Pyelonephritis Absolute indications Persistent vomiting Progression of uncomplicated UTI Suspected sepsis Uncertain diagnosis Urinary tract obstruction Relative indications Age > 60 years Anatomic urinary tract abnormality Immunocompromised (diabetes mellitus, cancer, sickle cell disease, organ transplant) Inadequate access to follow-up Frailty, poor social support UTI = urinary tract infection. Information from reference 1. will return for early follow-up, and have adequate social support 27,28 (Figure 2). Patients with complicated acute pyelonephritis who are more ill or have not responded to outpatient therapy should be hospitalized. Using specific hospitalization criteria (Table 4), 1 up to 70 percent of patients can be selected for outpatient management. Another option is initial therapy with parenteral antibiotics in an inpatient observation unit, followed by oral therapy as an outpatient. 26,29 Of the common uropathogens, resistance to fluoroquinolones remains very low (1 to 3 percent). 30 Fluoroquinolones are absorbed well from the gastrointestinal tract and have excellent kidney penetration. In selected patients with moderate Urine cultures should be or severe acute pyelonephritis, obtained before initiation clinical outcomes are equivalent with intravenous and oral of antibiotic therapy. ciprofloxacin (Cipro) therapy. 31 Therefore, for empiric therapy in uncomplicated acute pyelonephritis, the IDSA recommends the use of an oral fluoroquinolone 29 (Table 5). Oral amoxicillin-clavulanate potassium (Augmentin), a cephalosporin, and trimethoprim-sulfamethoxazole (TMP- SMX; Bactrim, Septra) provide acceptable alternatives for susceptible organisms. 29 The U.S. Food and Drug Administration has classified fluoroquinolones as pregnancy March 1, 2005 Volume 71, Number 5 American Family Physician 937
6 Evaluation and Management of Acute Pyelonephritis Patient with UTI and signs and symptoms of acute pyelonephritis Fever/chills Flank pain Nausea/vomiting Costovertebral angle tenderness Specific management depends on risk factors (see text) Yes High risk for complications? Anatomic/functional abnormality Foreign body Immunosuppressed state Obstruction Pregnancy Inappropriate antibiotics Failure to respond Instrumentation No Hospitalization indicated? Anatomic urinary tract abnormality Immunocompromised state Urinary tract obstruction Outpatient treatment failure Uncomplicated UTI progression Persistent nausea/vomiting Suspected sepsis Age > 60 years Poor social support Inadequate access to follow-up care Uncertain diagnosis Yes No Urine culture and sensitivity IV antibiotics Fluoroquinolone Aminoglycoside with or without ampicillin, or Extended-spectrum cephalosporin with or without an aminoglycoside Ampicillin-sulbactam (Unasyn) with or without an aminoglycoside (gram-positive cocci) Hydration Fever control Pain management Urine culture and sensitivity Oral antibiotics Fluoroquinolone Improvement in 72 hours? Afebrile Tolerates fluids, foods, and oral medications Decreased pain Yes No Oral antibiotics for a total of 14 days Test for cure one week after completion of antibiotics Hospitalization if ambulatory Check sensitivities Check obstruction (ultrasonography) Consider other causes Figure 2. Algorithm for the evaluation and management of acute pyelonephritis (UTI = urinary tract infection; IV = intravenous). category C drugs, and their use should be avoided in pregnant women. Amoxicillin or amoxicillin-clavulanate potassium is preferred during pregnancy and in the treatment of infections caused by gram-positive organisms. Some physicians administer a single parenteral dose of an antibiotic (ceftriaxone [Rocephin], gentamicin [Garamy- 938 American Family Physician Volume 71, Number 5 March 1, 2005
7 Pyelonephritis cin], or a fluoroquinolone) before initiating oral therapy, 29 but there is little evidence that this step improves outcomes. 1 Table 5 reviews antimicrobial agents used in the treatment of acute pyelonephritis. If the patient requires hospitalization, the IDSA guidelines 29 recommend one of three initial intravenous therapies: (1) a fluoroquinolone; (2) an aminoglycoside with or without ampicillin; or (3) an extended-spectrum TABLE 5 Antimicrobial Agents Used in the Treatment of Acute Pyelonephritis Agent Dosing schedule Oral dose (mg) IV dose Comments Penicillins Amoxicillin Every 8 to 12 hours 500 None Amoxicillin- clavulanate potassium (Augmentin) Ampicillin-sulbactam (Unasyn) Every 8 to 12 hours 500/125 GI side effects* Every 4 to 6 hours 150 to 200 mg per kg per day GI side effects* Aztreonam (Azactam) Every 6 to 8 hours 1 to 2 g Phlebitis; GI side effects* Imipenem (Primaxin I.V.) Every 6 hours 0.5 g None Piperacillin (Pipracil) Every 6 hours 3 g GI side effects*; phlebitis Piperacillin-tazobactam (Zosyn) Ticarcillin-clavulanate (Timentin) Cephalosporins Every 6 to 8 hours g/4.5 g GI side effects*; rash; headaches; insomnia Every 4 to 6 hours 3.1 g GI side effects*; rash; phlebitis Cefotaxime (Claforan) Every 8 to 12 hours 1 to 2 g Thrombophlebitis Ceftriaxone (Rocephin) Once in 24 hours 1 to 2 g Leukopenia; elevated BUN and liver enzyme levels Cephalexin (Keflex) Every 6 hours 500 GI side effects* Fluoroquinolones Ciprofloxacin (Cipro) Every 12 hours mg Nausea; headache; photosensitivity; pregnancy category C Enoxacin (Penetrex) Every 24 hours 400 Pregnancy category C Gatifloxacin (Tequin) Every 24 hours 400 mg Pregnancy category C Levofloxacin (Levaquin) Every 24 hours 250 to to 750 mg ECG QT prolongation; pregnancy category C Lomefloxacin (Maxaquin) Every 24 hours 400 Pregnancy category C Norfloxacin (Noroxin) Every 12 hours 400 Pregnancy category C Ofloxacin (Floxin) Every 12 hours 200 to mg Pregnancy category C Aminoglycosides Amikacin (Amikin) Every 12 hours 7.5 mg per kg Ototoxicity; nephrotoxicity Gentamicin (Garamycin) Every 24 hours 5 to 7 mg per kg Ototoxicity; nephrotoxicity Tobramycin (Nebcin) Every 24 hours 5 to 7 mg per kg Ototoxicity; nephrotoxicity Other antibiotics TMP-SMX (Bactrim; Septra) Every 12 hours 160/800 8 to 10 mg per kg (TMP) G6PD deficiency; sulfa allergy; do not use in third trimester IV = intravenous; GI = gastrointestinal; BUN = blood urea nitrogen; ECG = electrocardiogram; TMP-SMX = trimethoprim-sulfamethoxazole; G6PD = glucose-6-phosphate dehydrogenase. * GI side effects include nausea, vomiting, and diarrhea. March 1, 2005 Volume 71, Number 5 American Family Physician 939
8 cephalosporin with or without an aminoglycoside. With gram-positive cocci, ampicillin-sulbactam (Unasyn) with or without an aminoglycoside is recommended. Aminoglycosides should be avoided in patients with pre-existing renal disease. Oral treatment is feasible as soon as the patient becomes afebrile, has improved clinically, and can tolerate oral hydration and medications. It is not necessary to use the same agent for both parenteral and oral therapy. 26 There is no benefit from additional hospital observation to determine the success of switching to an oral antibiotic. 32 A seven- to 14-day course of antibiotics is effective in women who are immunocompetent and do not have underlying illness. 1,27,30 Studies 29,33,34 suggest that therapy lasting only five to seven days is comparable Short-term antibiotic to seven to 14 days in terms therapy (three days), which of clinical and bacteriologic outcome in patients with mild is appropriate in the treatment of cystitis, results in pyelonephritis and in those having a dramatic initial response a 50 percent relapse rate in to therapy. Acute pyelonephritis patients who have subclinical acute pyelonephritis. associated with immunosuppressive states responds well to a 14- to 21-day course of a fluoroquinolone or TMP-SMX. 2 Post-treatment urine cultures are recommended in all patients at the follow-up visit, one to two weeks after completion of antibiotic therapy. 35 Fever generally resolves within 72 hours of starting antibiotic therapy. In a study 36 of hospitalized patients who had no complications, however, 26 percent remained febrile at 48 hours, and 13 percent were febrile at 72 hours. Thus, persistence of fever after 72 hours in an otherwise stable and improving patient may not necessarily warrant a change in therapy or further investigation. The two most common causes of initial treatment failure are resistant organisms and nephrolithiasis. In the absence of clinical response, many physicians obtain a blood count, urinalysis, and blood and urine cultures, seeking an indication of persisting infection and antibiotic resistance; however, there is little evidence to support the routine use of these tests. A rectal or vaginal examination should be performed. Imaging studies may identify complicating factors such as anatomic abnormalities, obstruction, acute bacterial nephritis (localized, nonliquified interstitial inflammation), or subjacent infections such as appendicitis, cholecystitis, or perinephric abscess (Figure 2). Options include plain radiography of the kidneys, ureter, and bladder; renal ultrasonography; computed tomographic (CT) scan; magnetic resonance imaging; and intravenous pyelography. In most patients, ultrasound examination identifies acute bacterial nephritis, abscesses, ureteral obstruction, and hydronephrosis. 37 Acute bacterial nephritis may progress to frank abscess and requires a protracted course of antibiotics. If renal ultrasonography fails to define a lesion but shows marked renal enlargement, or if invasive intervention is being considered, a CT scan can exclude renal and perinephric abscesses. Differences between UTI in men and women support the classification of male acute pyelonephritis as complicated. Men younger than 60 years without obstruction, renal abnormalities, or prostatitis respond well to 14 days of antibiotic therapy. 2 Men who have recurrent UTIs require a six-week regimen. Men with acute prostatitis require four weeks of treatment with an antibiotic that has high penetration into prostatic tissue, such as doxycycline (Vibramycin), TMP-SMX, or a fluoroquinolone; men with chronic prostatitis require six to 12 weeks of such therapy. 2,38 The optimal duration of treatment for hospitalized patients is 14 days. Short-term antibiotic therapy (three days), which is appropriate in the treatment of cystitis, results in a 50 percent relapse rate in patients with subclinical acute pyelonephritis. The most reliable indicator of treatment failure is a positive follow-up culture in patients with presumed cystitis. 2 If relapse is noted after a two-week course of antibiotics, and no urologic abnormality is found on imaging, the uropathogen and sensitivities should be confirmed and treatment extended to six weeks. If the pathogen causing reinfection is different from the original pathogen, two weeks of treatment are sufficient. Immedi- 940 American Family Physician Volume 71, Number 5 March 1, 2005
9 Pyelonephritis ate release of any existing obstruction combined with a 14-day course of appropriate antibiotics minimizes failure and recurrence. 2 Relief of obstruction and antibiotic therapy may be successful in emphysematous pyelonephritis, but nephrectomy must be strongly considered in patients with unresponsive infections. 1 If parenchymal involvement including abscesses is observed, longer courses of antibiotics (intravenous or oral) or sequential therapy may be necessary. Pregnant women with pyelonephritis require hospitalization (for at least a short observation period) for aggressive hydration and parenteral antibiotics. Antibiotic treatment is similar to the treatments of other adult regimens. During pregnancy, 86 percent of women have uterine contractions in the first hour after initiation of antimicrobial therapy, and 50 percent continue to have contractions after five hours of therapy. 39 One study 40 found no difference in clinical responses among pregnant women treated with ampicillin and gentamicin, cefazolin (Ancef), or ceftriaxone. Fluoroquinolones should be avoided because of concerns about their teratogenic effects on the fetus. 1 Most patients with mild acute pyelonephritis who are pregnant (90 percent) can be treated successfully with parenteral antibiotics under brief (two to 24 hours) observation, followed by outpatient oral therapy. 41,42 Although some experts state that selected patients may be treated safely with oral antibiotics, there have been no outpatient trials in which oral therapy alone was used. 43 Because 25 percent of patients with mild acute pyelonephritis who are pregnant have a recurrence, these patients should have monthly urine cultures or antimicrobial suppression with oral nitrofurantoin (Macrodantin), 100 mg daily, until four to six weeks postpartum. 43 All pregnant women, especially those who have diabetes and had a previous UTI, should be screened for asymptomatic bacteriuria during the first prenatal visit. No antibiotic prophylaxis is effective in reducing complications associated with indwelling catheters. Sterile insertion and care of the catheter, minimizing the duration of catheterization, intermittent catheterization, closed drainage systems, and silver-alloy coated catheters may reduce the risk of symptomatic infection. 1,44 Members of various medical faculties develop articles for Practical Therapeutics. This article is one in a series coordinated by the Department of Family and Preventive Medicine at the University of Oklahoma Health Sciences Center, Tulsa, Okla. Coordinator of the series is John Tipton, M.D. The authors indicate that they do not have any conflicts of interest. Sources of funding: none reported. REFERENCES 1. Bass PF 3d, Jarvis JA, Mitchell CK. Urinary tract infections. Prim Care 2003;30: Bergeron MG. Treatment of pyelonephritis in adults. Med Clin North Am 1995;79: Hooton TM, Stamm WE. Diagnosis and treatment of uncomplicated urinary tract infection. Infect Dis Clin North Am 1997;11: Foxman B, Klemstine KL, Brown PD. Acute pyelonephritis in US hospitals in 1997: hospitalization and in-hospital mortality. Ann Epidemiol 2003;13: Gilstrap LC 3d, Ramin SM. Urinary tract infections during pregnancy. Obstet Gynecol Clin North Am 2001;28: Stamm WE. Urinary tract infections and pyelonephritis. In: Harrison TR, Braunwald E, eds. Harrison s Principles of internal medicine. 15th ed. New York: McGraw-Hill, 2001: Stamm WE, Hooton TM. Management of urinary tract infections in adults. N Engl J Med 1993;329: The Johns Hopkins Ambulatory Clerkship in Medicine. Dysuria. Accessed online December 5, 2004, at: deptmed.med.som.jhmi.edu/ambclerk/dysuria.html. 9. Gupta K, Hooten TM, Wobbe CL, Stamm WE. The prevalence of antimicrobial resistance among uropathogens causing acute uncomplicated cystitis in young women. Int J Antimicrob Agents 1999;11: Roberts JA. Management of pyelonephritis and upper urinary tract infections. Urol Clin North Am 1999;26: Pinson AG, Philbrick JT, Lindbeck GH, Schorling JB. Fever in the clinical diagnosis of acute pyelonephritis. Am J Emerg Med 1997;15: Tambyah PA, Maki DG. Catheter-associated urinary tract infection is rarely symptomatic: a prospective study of 1,497 catheterized patients. Arch Intern Med 2000;160: Rubin RH, Shapiro ED, Andriole VT, Davis RJ, Stamm WE. Evaluation of new anti-infective drugs for the treatment of urinary tract infection. Infectious Diseases Society of America and the Food and Drug Administration. Clin Infect Dis 1992;15(suppl 1):S Lifshitz E, Kramer L. Outpatient urine culture: does collection technique matter? Arch Intern Med 2000;160: March 1, 2005 Volume 71, Number 5 American Family Physician 941
10 Pyelonephritis 15. Semeniuk H, Church D. Evaluation of the leukocyte esterase and nitrite urine dipstick screening tests for detection of bacteriuria in women with suspected uncomplicated urinary tract infections. J Clin Microbiol 1999;37: Bailey BL Jr. Urinalysis predictive of urine culture results. J Fam Pract 1995;40: Ferry S, Andersson SO, Burman LG, Westman G. Optimized urinary microscopy for assessment of bacteriuria in primary care. J Fam Pract 1990;31: Pollock HM. Laboratory techniques for detection of urinary tract infection and assessment of value. Am J Med 1983;75: Pfaller MA, Koontz FP. Laboratory evaluation of leukocyte esterase and nitrite tests for the detection of bacteriuria. J Clin Microbiol 1985;21: Blum RN, Wright RA. Detection of pyuria and bacteriuria in symptomatic ambulatory women. J Gen Intern Med 1992;7: Moyer VA, Elliott EJ, eds. Evidence based pediatrics and child health. 2d ed. London: BMJ Books, Gorelick MH, Shaw KN. Screening tests for urinary tract infection in children: a meta-analysis. Pediatrics 1999;104:e McCue JD. The management of complicated urinary tract infections. Accessed online December 5, 2004, at: McMurray BR, Wrenn KD, Wright SW. Usefulness of blood cultures in pyelonephritis. Am J Emerg Med 1997;15: Velasco M, Martinez JA, Moreno-Martinez A, Horcajada JP, Ruiz J, Barranco M, et al. Blood cultures for women with uncomplicated acute pyelonephritis: are they necessary? Clin Infect Dis 2003;37: Miller O 2d, Hemphill RR. Urinary tract infection and pyelonephritis. Emerg Med Clin North Am 2001;19: Safrin S, Siegel D, Black D. Pyelonephritis in adult women: inpatient versus outpatient therapy. Am J Med 1988;85: Bach D, van den Berg-Segers A, Hubner A, van Breukelen G, Cesana M, Pletan Y. Rufloxacin once daily versus ciprofloxacin twice daily in the treatment of patients with acute uncomplicated pyelonephritis. J Urol 1995;154: Warren JW, Abrutyn E, Hebel JR, Johnson JR, Schaeffer AJ, Stamm WE. Guidelines for antimicrobial treatment of uncomplicated acute bacterial cystitis and acute pyelonephritis in women. Infectious Diseases Society of America (IDSA). Clin Infect Dis 1999;29: Nicolle LE. Urinary tract infection: traditional pharmacologic therapies. Am J Med 2002;113(suppl 1A): 35S-44S. 31. Mombelli G, Pezzoli R, Pinoja-Lutz G, Monotti R, Marone C, Franciolli M. Oral vs intravenous ciprofloxacin in the initial empirical management of severe pyelonephritis or complicated urinary tract infections: a prospective randomized clinical trial. Arch Intern Med 1999;159: Caceres VM, Stange KC, Kikano GE, Zyzanski SJ. The clinical utility of a day of hospital observation after switching from intravenous to oral antibiotic therapy in the treatment of pyelonephritis. J Fam Pract 1994;39: Talen D, Stamm WE, Reuning-Scherer J, Church D. Ciprofloxacin (CIP) 7-day vs. TMP/SMX 14-day 1/2 ceftriaxone (CRO) for acute uncomplicated pyelonephritis: a randomized, double-blind trial. Boston: International Congress of Infectious Diseases, Bailey RR. Duration of antimicrobial treatment and the use of drug combinations for the treatment of uncomplicated acute pyelonephritis. Infection 1994;22(suppl 1):S Delzell JE JR, Fitzsimmons A. Urinary tract infection. The American Board of Family Practice. Reference Guide. 7th ed. American Board of Family Practice, Accessed online December 5, 2004, at: Behr MA, Drummond R, Libman MD, Delaney JS, Dylewski JS. Fever duration in hospitalized acute pyelonephritis patients. Am J Med 1996;101: Huang JJ, Sung JM, Chen KW, Ruaan MK, Shu GH, Chuang YC. Acute bacterial nephritis: a clinicoradiologic correlation based on computed tomography. Am J Med 1992;93: Lipsky BA. Prostatitis and urinary tract infection in men: what s new; what s true? Am J Med 1999;106: Graham JM, Oshiro BT, Blanco JD, Magee KP. Uterine contractions after antibiotic therapy for pyelonephritis in pregnancy. Am J Obstet Gynecol 1993;168: Wing DA, Hendershott CM, Debuque L, Millar LK. A randomized trial of three antibiotic regimens for the treatment of pyelonephritis in pregnancy. Obstet Gynecol 1998;92: Millar LK, Wing DA, Paul RH, Grimes DA. Outpatient treatment of pyelonephritis in pregnancy: a randomized controlled trial. Obstet Gynecol 1995;86(4 pt 1): Wing DA, Hendershott CM, Debuque L, Millar LK. Outpatient treatment of acute pyelonephritis in pregnancy after 24 weeks. Obstet Gynecol 1999;94(5 pt 1): Wing DA. Pyelonephritis. Clin Obstet Gynecol 1998; 41: Christensen M, Jepsen OB. Reduced rates of hospitalacquired UTI in medical patients. Prevalence surveys indicate effect of active infection control programmes. J Hosp Infect 2001;47: American Family Physician Volume 71, Number 5 March 1, 2005
Urinary Tract Infections
 Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections
 A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections By Gary R. Skankey, MD, FACP, Infectious Disease, Las Vegas, NV Sponsored
A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections By Gary R. Skankey, MD, FACP, Infectious Disease, Las Vegas, NV Sponsored
A Summary of the Guideline for the Diagnosis and Management of. Urinary Tract Infections in Long Term Care
 A Summary of the Guideline for the Diagnosis and Management of Urinary Tract Infections in Long Term Care Exclusions Community acquired UTIs UTIs in acute care Prevention Limit use of catheters Ensure
A Summary of the Guideline for the Diagnosis and Management of Urinary Tract Infections in Long Term Care Exclusions Community acquired UTIs UTIs in acute care Prevention Limit use of catheters Ensure
Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD
 82 Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD Abstract Urinary tract infections are commonly treated in urgent care practice. Clinicians need to be aware of the advantages and limitations
82 Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD Abstract Urinary tract infections are commonly treated in urgent care practice. Clinicians need to be aware of the advantages and limitations
Urinary Tract Infections. Clinical Scenario #1. Urinary Tract Infections. Clinical Scenario #1 : Labs
 Clinical Scenario #1 : Labs Urinary Tract Infections Magdalena Sobieszczyk, MD Urinalysis: pyuria (WBC too numerous to count), RBC and bacteria present Urine dipstick: positive leukocyte esterase and nitrite
Clinical Scenario #1 : Labs Urinary Tract Infections Magdalena Sobieszczyk, MD Urinalysis: pyuria (WBC too numerous to count), RBC and bacteria present Urine dipstick: positive leukocyte esterase and nitrite
Urinary Tract Infections
 Urinary Tract Infections Magdalena Sobieszczyk, MD MPH Division of Infectious Diseases Columbia University Clinical Scenario #1 23 y.o woman presents to her doctor complaining of 1 day of increased urinary
Urinary Tract Infections Magdalena Sobieszczyk, MD MPH Division of Infectious Diseases Columbia University Clinical Scenario #1 23 y.o woman presents to her doctor complaining of 1 day of increased urinary
POAC CLINICAL GUIDELINE
 POAC CLINICAL GUIDELINE Acute Pylonephritis DIAGNOSIS COMPLICATED PYELONEPHRITIS EXCLUSION CRITERIA: Male Known or suspected renal impairment (egfr < 60) Abnormality of renal tract Known or suspected renal
POAC CLINICAL GUIDELINE Acute Pylonephritis DIAGNOSIS COMPLICATED PYELONEPHRITIS EXCLUSION CRITERIA: Male Known or suspected renal impairment (egfr < 60) Abnormality of renal tract Known or suspected renal
Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults. A Systematic Review (Cochrane database August 2013)
 Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults A Systematic Review (Cochrane database August 2013) Gail Lusardi, Senior Lecturer Dr Allyson Lipp, Principal Lecturer, Dr Chris
Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults A Systematic Review (Cochrane database August 2013) Gail Lusardi, Senior Lecturer Dr Allyson Lipp, Principal Lecturer, Dr Chris
Open the Flood Gates Urinary Obstruction and Kidney Stones. Dr. Jeffrey Rosenberg Dr. Emilio Lastarria Dr. Richard Kasulke
 Open the Flood Gates Urinary Obstruction and Kidney Stones Dr. Jeffrey Rosenberg Dr. Emilio Lastarria Dr. Richard Kasulke Nephrology vs. Urology Nephrologist a physician who has been trained in the diagnosis
Open the Flood Gates Urinary Obstruction and Kidney Stones Dr. Jeffrey Rosenberg Dr. Emilio Lastarria Dr. Richard Kasulke Nephrology vs. Urology Nephrologist a physician who has been trained in the diagnosis
Urinary Tract Infection and Asymptomatic Bacteriuria Guidance
 Urinary Tract Infection and Asymptomatic Bacteriuria Guidance Urinary tract infection (UTI) is the most common indication for antimicrobial use in hospitals and a significant proportion of this use is
Urinary Tract Infection and Asymptomatic Bacteriuria Guidance Urinary tract infection (UTI) is the most common indication for antimicrobial use in hospitals and a significant proportion of this use is
UTI in children. Quick reference guide. Issue date: August 2007. Urinary tract infection in children: diagnosis, treatment and long-term management
 Issue date: August 2007 UTI in children Urinary tract infection in children: diagnosis, treatment and long-term management Developed by the National Collaborating Centre for Women s and Children s Health
Issue date: August 2007 UTI in children Urinary tract infection in children: diagnosis, treatment and long-term management Developed by the National Collaborating Centre for Women s and Children s Health
Intra-abdominal abdominal Infections
 Intra-abdominal abdominal Infections Marnie Peterson, Pharm.D., BCPS Dept. of Pediatric Infectious Diseases Medical School University of Minnesota Intra-abdominal abdominal Infections Intra-abdominal abdominal
Intra-abdominal abdominal Infections Marnie Peterson, Pharm.D., BCPS Dept. of Pediatric Infectious Diseases Medical School University of Minnesota Intra-abdominal abdominal Infections Intra-abdominal abdominal
The American Academy of Pediatrics
 Revised AAP Guideline on UTI in Febrile Infants and Young Children KENNETH B. ROBERTS, MD, University of rth Carolina School of Medicine, Chapel Hill, rth Carolina In 2011, the American Academy of Pediatrics
Revised AAP Guideline on UTI in Febrile Infants and Young Children KENNETH B. ROBERTS, MD, University of rth Carolina School of Medicine, Chapel Hill, rth Carolina In 2011, the American Academy of Pediatrics
Protocol for Macroscopic and Microscopic Urinalysis and Investigation of Urinary Tract Infections
 Protocol for Macroscopic and Microscopic Urinalysis and Investigation of Urinary Tract Infections Reprinted 2004 Scope The purpose of this protocol is to avoid unnecessary testing in routine cases while
Protocol for Macroscopic and Microscopic Urinalysis and Investigation of Urinary Tract Infections Reprinted 2004 Scope The purpose of this protocol is to avoid unnecessary testing in routine cases while
GUIDELINES ON UROLOGICAL INFECTIONS
 GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2010) M. Grabe (chairman), T.E. Bjerklund-Johansen, H. Botto, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction Infections
GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2010) M. Grabe (chairman), T.E. Bjerklund-Johansen, H. Botto, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction Infections
Pyelonephritis: Kidney Infection
 Pyelonephritis: Kidney Infection National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is pyelonephritis? Pyelonephritis
Pyelonephritis: Kidney Infection National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is pyelonephritis? Pyelonephritis
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page
 A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Etiology and treatment of chronic bacterial prostatitis the Croatian experience
 Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 Catheter-Associated Urinary Tract Infection () Event Introduction: Urinary tract infections (UTIs) are tied with pneumonia as the second most common type of healthcare-associated infection, second only
Catheter-Associated Urinary Tract Infection () Event Introduction: Urinary tract infections (UTIs) are tied with pneumonia as the second most common type of healthcare-associated infection, second only
GUIDELINES ON UROLOGICAL INFECTIONS
 GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2014) M. Grabe (chair), R. Bartoletti, T.E. Bjerklund-Johansen, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction
GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2014) M. Grabe (chair), R. Bartoletti, T.E. Bjerklund-Johansen, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction
Urinary Tract Infections
 1 Infections in the urinary tract are relatively common. These infections are often referred to as bladder infections. They are also known as UTI s or urinary tract infections. When an infection is confined
1 Infections in the urinary tract are relatively common. These infections are often referred to as bladder infections. They are also known as UTI s or urinary tract infections. When an infection is confined
190.12 - Urine Culture, Bacterial Summary Information Highlighted items indicate most frequently used codes.
 Medicare National Coverage Determination (NCD) (Jan 2011) Source: CMS: Centers for Medicare & Medicaid Services To view full document: www.cms.gov/coveragegeninfo. Select Lab NCDs, then select NCD Coding
Medicare National Coverage Determination (NCD) (Jan 2011) Source: CMS: Centers for Medicare & Medicaid Services To view full document: www.cms.gov/coveragegeninfo. Select Lab NCDs, then select NCD Coding
Urinary Tract Infections
 Urinary Tract Infections Leading cause of morbidity and health care expenditures in persons of all ages. An estimated 50 % of women report having had a UTI at some point in their lives. 8.3 million office
Urinary Tract Infections Leading cause of morbidity and health care expenditures in persons of all ages. An estimated 50 % of women report having had a UTI at some point in their lives. 8.3 million office
URINARY TRACT INFECTION IN CHILDREN. Yap Hui Kim, Belinda Murugasu
 URINARY TRACT INFECTION IN CHILDREN Yap Hui Kim, Belinda Murugasu Urinary tract infection (UTI) is a common problem in childhood and the primary health care practitioner is usually the frontline in diagnosis
URINARY TRACT INFECTION IN CHILDREN Yap Hui Kim, Belinda Murugasu Urinary tract infection (UTI) is a common problem in childhood and the primary health care practitioner is usually the frontline in diagnosis
Beryl Navti SEPT Pharmacy Department. 24/06/2013 Beryl Navti, Clinical Pharmacist, SEPT
 URINARY TRACT INFECTIONS Beryl Navti SEPT Pharmacy Department The Genitourinary System The organs system of the reproductive organs and urinary system Grouped dtogether th because of their proximity it
URINARY TRACT INFECTIONS Beryl Navti SEPT Pharmacy Department The Genitourinary System The organs system of the reproductive organs and urinary system Grouped dtogether th because of their proximity it
Diagnosis and Treatment of Acute Uncomplicated Cystitis
 Diagnosis and Treatment of Acute Uncomplicated Cystitis RICHARD COLGAN, MD, and MOZELLA WILLIAMS, MD University of Maryland School of Medicine, Baltime, Maryland Urinary tract infections are the most common
Diagnosis and Treatment of Acute Uncomplicated Cystitis RICHARD COLGAN, MD, and MOZELLA WILLIAMS, MD University of Maryland School of Medicine, Baltime, Maryland Urinary tract infections are the most common
THE KIDNEY. Bulb of penis Abdominal aorta Scrotum Adrenal gland Inferior vena cava Urethra Corona glandis. Kidney. Glans penis Testicular vein
 29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
2015 RN.ORG, S.A., RN.ORG, LLC
 Upper Urinary Tract Infections WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG,
Upper Urinary Tract Infections WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG,
Diagnosis and Treatment of Urinary Tract Infections in Children
 Diagnosis and Treatment of Urinary Tract Infections in Children BRETT WHITE, MD, Oregon Health and Science University, Portland, Oregon Acute urinary tract infections are relatively common in children,
Diagnosis and Treatment of Urinary Tract Infections in Children BRETT WHITE, MD, Oregon Health and Science University, Portland, Oregon Acute urinary tract infections are relatively common in children,
CARE PROCESS STEP EXPECTATIONS RATIONALE
 URINARY INCONTINENCE CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for urinary incontinence and any history of urinary
URINARY INCONTINENCE CARE PROCESS STEP EXPECTATIONS RATIONALE ASSESSMENT/PROBLEM RECOGNITION 1. Did the staff and physician seek and document risk factors for urinary incontinence and any history of urinary
ANTIBIOTICS IN SEPSIS
 ANTIBIOTICS IN SEPSIS Jennifer Curello, PharmD, BCPS Clinical Pharmacist, Infectious Diseases Antimicrobial Stewardship Program Ronald Reagan UCLA Medical Center October 27, 2014 The power of antibiotics
ANTIBIOTICS IN SEPSIS Jennifer Curello, PharmD, BCPS Clinical Pharmacist, Infectious Diseases Antimicrobial Stewardship Program Ronald Reagan UCLA Medical Center October 27, 2014 The power of antibiotics
Practice Guidelines. Updated Guideline on Diagnosis and Treatment of Intra-abdominal Infections
 Updated Guideline on Diagnosis and Treatment of Intra-abdominal Infections CARRIE ARMSTRONG Guideline source: Surgical Infection Society, Infectious Diseases Society of America Literature search described?
Updated Guideline on Diagnosis and Treatment of Intra-abdominal Infections CARRIE ARMSTRONG Guideline source: Surgical Infection Society, Infectious Diseases Society of America Literature search described?
Kalpana Gupta, M.D. Associate Professor Department of Medicine Section of Infectious Diseases Boston University School of Medicine
 2010 Clinical Practice Guidelines by the Infectious Diseases Society of America and the European Society for Clinical Microbiology and Infectious Diseases Kalpana Gupta, M.D. Associate Professor Department
2010 Clinical Practice Guidelines by the Infectious Diseases Society of America and the European Society for Clinical Microbiology and Infectious Diseases Kalpana Gupta, M.D. Associate Professor Department
Case Studies in Urinary Tract Infections
 Case Studies in Urinary Tract Infections Robert L. Holley, MSc, MD Professor of Obstetrics and Gynecology Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology
Case Studies in Urinary Tract Infections Robert L. Holley, MSc, MD Professor of Obstetrics and Gynecology Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology
Urinary Tract Infection
 Guidelines for Clinical Care Ambulatory Urinary Tract Infection Guideline Team Team Leader Steven E Gradwohl, MD General Medicine Team Members Catherine M Bettcher, MD Family Medicine Carol E Chenoweth,
Guidelines for Clinical Care Ambulatory Urinary Tract Infection Guideline Team Team Leader Steven E Gradwohl, MD General Medicine Team Members Catherine M Bettcher, MD Family Medicine Carol E Chenoweth,
Urinary tract infections (UTIs)
 in Adults RICHARD COLGAN, M.D, University of Maryland School of Medicine, Baltimore, Maryland LINDSAY E. NICOLLE, M.D., University of Manitoba, Winnipeg, Canada ANDREW McGLONE, M.D., University of Maryland
in Adults RICHARD COLGAN, M.D, University of Maryland School of Medicine, Baltimore, Maryland LINDSAY E. NICOLLE, M.D., University of Manitoba, Winnipeg, Canada ANDREW McGLONE, M.D., University of Maryland
Management of Urinary Tract Infections in Patients with Urinary Catheters
 Clinical Review Article Management of Urinary Tract Infections in Patients with Urinary Catheters Maria L. Alcaide, MD Daniel M. Lichtstein, MD Urinary tract infections (UTIs) in patients with urinary
Clinical Review Article Management of Urinary Tract Infections in Patients with Urinary Catheters Maria L. Alcaide, MD Daniel M. Lichtstein, MD Urinary tract infections (UTIs) in patients with urinary
ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS LAUREN HYNICKA, PHARM.D.
 ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS LAUREN HYNICKA, PHARM.D. ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS ACTIVITY DESCRIPTION Antibiotic use in the safest
ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS LAUREN HYNICKA, PHARM.D. ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS ACTIVITY DESCRIPTION Antibiotic use in the safest
C-Difficile Infection Control and Prevention Strategies
 C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer [email protected] 1/18/2016 1 Disclosure This educational activity does not have commercial
C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer [email protected] 1/18/2016 1 Disclosure This educational activity does not have commercial
URINARY TRACT INFECTIONS IN YOUNG WOMEN
 URINARY TRACT INFECTIONS IN YOUNG WOMEN Reviewed by Finnish Centre for Health Promotion Publisher: Ylioppilaiden terveydenhoitosäätiö Töölönkatu 37 A 00260 Helsinki Orders: [email protected] Author:
URINARY TRACT INFECTIONS IN YOUNG WOMEN Reviewed by Finnish Centre for Health Promotion Publisher: Ylioppilaiden terveydenhoitosäätiö Töölönkatu 37 A 00260 Helsinki Orders: [email protected] Author:
MODULE 2: ADULT URINARY TRACT INFECTIONS
 MODULE 2: ADULT URINARY TRACT INFECTIONS KEYWORDS: Urinary tract infection (UTI); cystitis; pyelonephritis; uropathogens; antibiotics LEARNING OBJECTIVES At the end of this clerkship, the learner will
MODULE 2: ADULT URINARY TRACT INFECTIONS KEYWORDS: Urinary tract infection (UTI); cystitis; pyelonephritis; uropathogens; antibiotics LEARNING OBJECTIVES At the end of this clerkship, the learner will
Riesa Gusewelle, MNSc, RN, APRN, GNP-BC. OBJECTIVES Identify early warning signs of urinary tract
 Detection, Early Management & Prevention, of Urinary Tract Infections in Older Adults Riesa Gusewelle, MNSc, RN, APRN, GNP-BC OBJECTIVES Identify early warning signs of urinary tract infections (UTIs)
Detection, Early Management & Prevention, of Urinary Tract Infections in Older Adults Riesa Gusewelle, MNSc, RN, APRN, GNP-BC OBJECTIVES Identify early warning signs of urinary tract infections (UTIs)
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention. Basics of Infection Prevention 2 Day Mini-Course 2013
 Catheter-Associated Urinary Tract Infection (CAUTI) Prevention Basics of Infection Prevention 2 Day Mini-Course 2013 2 Objectives Define the scope of healthcare-associated urinary tract infections (UTI)
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention Basics of Infection Prevention 2 Day Mini-Course 2013 2 Objectives Define the scope of healthcare-associated urinary tract infections (UTI)
COMPASS Therapeutic Notes on the Management of Bacterial Urinary Tract Infections in Primary Care
 COMPASS Therapeutic Notes on the Management of Bacterial Urinary Tract Infections in Primary Care In this issue: Page Introduction, Background & Diagnostic Tests 1 UTI in non-pregnant women 3 UTI in pregnant
COMPASS Therapeutic Notes on the Management of Bacterial Urinary Tract Infections in Primary Care In this issue: Page Introduction, Background & Diagnostic Tests 1 UTI in non-pregnant women 3 UTI in pregnant
Don t Go With The Flow! Control and Management of UTIs in the Elderly
 Don t Go With The Flow! Control and Management of UTIs in the Elderly Acknowledgements Central West Infection Control Network Toronto Central Infection Control Network Erie St Clair Infection Control Network
Don t Go With The Flow! Control and Management of UTIs in the Elderly Acknowledgements Central West Infection Control Network Toronto Central Infection Control Network Erie St Clair Infection Control Network
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis
 Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
Palm Beach Obstetrics & Gynecology, PA
 Palm Beach Obstetrics & Gynecology, PA 4671 S. Congress Avenue, Lake Worth, FL 33461 561.434.0111 4631 N. Congress Avenue, Suite 102, West Palm Beach, FL 33407 Urinary Tract Infection About one of every
Palm Beach Obstetrics & Gynecology, PA 4671 S. Congress Avenue, Lake Worth, FL 33461 561.434.0111 4631 N. Congress Avenue, Suite 102, West Palm Beach, FL 33407 Urinary Tract Infection About one of every
Blood in the urine (hematuria)
 Blood in the urine (hematuria) Hematuria refers to the presence of blood in the urine. It is important to investigate the cause of hematuria because rarely, it is caused by a serious condition, such as
Blood in the urine (hematuria) Hematuria refers to the presence of blood in the urine. It is important to investigate the cause of hematuria because rarely, it is caused by a serious condition, such as
Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection
 Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection Emi Minejima, PharmD Assistant Professor of Clinical Pharmacy USC School of Pharmacy [email protected]
Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection Emi Minejima, PharmD Assistant Professor of Clinical Pharmacy USC School of Pharmacy [email protected]
Prevention of CAUTI is discussed in the CDC/HICPAC document, Guideline for Prevention of Catheter-associated Urinary Tract Infection 4.
 Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [] and Non-Catheter-Associated Urinary Tract Infection [UTI]) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [] and Non-Catheter-Associated Urinary Tract Infection [UTI]) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Why Do Some Antibiotics Fail?
 Why Do Some Antibiotics Fail? Patty W. Wright, M.D. April 2010 Objective To outline common reasons why antibiotic therapy is not successful and how this can be avoided. And to teach you a little bit about
Why Do Some Antibiotics Fail? Patty W. Wright, M.D. April 2010 Objective To outline common reasons why antibiotic therapy is not successful and how this can be avoided. And to teach you a little bit about
Prevention of catheter associated urinary tract infections
 Prevention of catheter associated urinary tract infections Dr. Suzan Sanavi, Nephrologist, M.D University of Social Welfare and Rehabilitation Akhavan Physical Spine Center INTRODUCTION Urinary bladder
Prevention of catheter associated urinary tract infections Dr. Suzan Sanavi, Nephrologist, M.D University of Social Welfare and Rehabilitation Akhavan Physical Spine Center INTRODUCTION Urinary bladder
IDSA GUIDELINES EXECUTIVE SUMMARY
 IDSA GUIDELINES International Clinical Practice Guidelines for the Treatment of Acute Uncomplicated Cystitis and Pyelonephritis in Women: A 2010 Update by the Infectious Diseases Society of America and
IDSA GUIDELINES International Clinical Practice Guidelines for the Treatment of Acute Uncomplicated Cystitis and Pyelonephritis in Women: A 2010 Update by the Infectious Diseases Society of America and
10. Treatment of peritoneal dialysis associated fungal peritonitis
 10. Treatment of peritoneal dialysis associated fungal peritonitis Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) The use of
10. Treatment of peritoneal dialysis associated fungal peritonitis Date written: February 2003 Final submission: July 2004 Guidelines (Include recommendations based on level I or II evidence) The use of
NewYork-Presbyterian Hospital Sites: Columbia University Medical Center Guideline: Medication Use Manual Page 1 of 12
 Page 1 of 12 TITLE: ANTIBIOTICS IN ADULT PATIENTS EMPIRIC USE GUIDELINES, COLUMBIA UNIVERSITY MEDICAL CENTER MEDICATION GUIDELINE PURPOSE: These are the 2011 guidelines for the empiric use of antibiotics
Page 1 of 12 TITLE: ANTIBIOTICS IN ADULT PATIENTS EMPIRIC USE GUIDELINES, COLUMBIA UNIVERSITY MEDICAL CENTER MEDICATION GUIDELINE PURPOSE: These are the 2011 guidelines for the empiric use of antibiotics
Welcome and Instructions
 Welcome and Instructions For audio, join by telephone at 877-594-8353, participant code: 56350822 Your line is OPEN. Please do not use the hold feature on your phone but do mute your line by dialing *6.
Welcome and Instructions For audio, join by telephone at 877-594-8353, participant code: 56350822 Your line is OPEN. Please do not use the hold feature on your phone but do mute your line by dialing *6.
How To Find Out If A Diabetic Woman Has A Urinary Tract Infection
 Mindanao Journal of Science and Technology Vol. 12 (2014) 171-178 Difference on the Incidence of Urinary Tract Infection (UTI) between Diabetic and Non-diabetic Women Admitted in Metro Cebu, Philippines
Mindanao Journal of Science and Technology Vol. 12 (2014) 171-178 Difference on the Incidence of Urinary Tract Infection (UTI) between Diabetic and Non-diabetic Women Admitted in Metro Cebu, Philippines
Study of bacteria isolated from urinary tract infections and determination of their susceptibility to antibiotics
 Jundishapur Journal of Microbiology (2009); 2(3): 118-123 118 Original article Study of bacteria isolated from urinary tract infections and determination of their susceptibility to antibiotics Mansour
Jundishapur Journal of Microbiology (2009); 2(3): 118-123 118 Original article Study of bacteria isolated from urinary tract infections and determination of their susceptibility to antibiotics Mansour
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Contents
 Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 Initial assessment and investigation of urinary incontinence bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used
Initial assessment and investigation of urinary incontinence bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used
Urinary Tract Infections
 Urinary Tract Infections www.kidney.org Did you know that... n Urinary tract infections (UTIs) are responsible for nearly 10 million doctor visits each year. n One in five women will have at least one
Urinary Tract Infections www.kidney.org Did you know that... n Urinary tract infections (UTIs) are responsible for nearly 10 million doctor visits each year. n One in five women will have at least one
Understanding and Preventing Bladder Infections in Women
 Understanding and Preventing Bladder Infections in Women Understanding and Preventing Bladder Infections in Women Recurrent bladder or urinary tract infections (UTI s) are a very common diagnosis. In fact,
Understanding and Preventing Bladder Infections in Women Understanding and Preventing Bladder Infections in Women Recurrent bladder or urinary tract infections (UTI s) are a very common diagnosis. In fact,
Urinary Tract Infection in Stone Patients and in Patients with Indwelling Urethral Catheters
 Urinary Tract Infection in Stone Patients and in Patients with Indwelling Urethral Catheters Pages with reference to book, From 254 To 258 Farakh A. Khan, Salman H. Siddiqui, Nasreen Akhtar ( Department
Urinary Tract Infection in Stone Patients and in Patients with Indwelling Urethral Catheters Pages with reference to book, From 254 To 258 Farakh A. Khan, Salman H. Siddiqui, Nasreen Akhtar ( Department
GUIDELINES ON UROLOGICAL INFECTIONS
 GUIDELINES ON UROLOGICAL INFECTIONS (Limited text update March 2015) M. Grabe (Chair), R. Bartoletti, T.E. Bjerklund Johansen, M. Çek, B. Köves (Guidelines Associate), K.G. Naber, R.S. Pickard, P. Tenke,
GUIDELINES ON UROLOGICAL INFECTIONS (Limited text update March 2015) M. Grabe (Chair), R. Bartoletti, T.E. Bjerklund Johansen, M. Çek, B. Köves (Guidelines Associate), K.G. Naber, R.S. Pickard, P. Tenke,
PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS. (CAUTIs)
 PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS (CAUTIs) CAUTIs A UTI where an indwelling urinary catheter was in place for >2 calendar days on the date of event. OR If an indwelling urinary
PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS (CAUTIs) CAUTIs A UTI where an indwelling urinary catheter was in place for >2 calendar days on the date of event. OR If an indwelling urinary
A THREE YEAR REVIEW OF CATHETER-ASSOCIATED URINARY TRACT INFECTIONS REPORTED TO THE NATIONAL HEALTHCARE SAFETY NETWORK AT A TERTIARY CARE HOSPITAL
 A THREE YEAR REVIEW OF CATHETER-ASSOCIATED URINARY TRACT INFECTIONS REPORTED TO THE NATIONAL HEALTHCARE SAFETY NETWORK AT A TERTIARY CARE HOSPITAL by Jessi Marie Bond BS, Clinical Laboratory Science, Idaho
A THREE YEAR REVIEW OF CATHETER-ASSOCIATED URINARY TRACT INFECTIONS REPORTED TO THE NATIONAL HEALTHCARE SAFETY NETWORK AT A TERTIARY CARE HOSPITAL by Jessi Marie Bond BS, Clinical Laboratory Science, Idaho
ECG may be indicated for patients with cardiovascular risk factors
 eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
eappendix A. Summary for Preoperative ECG American College of Cardiology/ American Heart Association, 2007 A1 2002 A2 European Society of Cardiology and European Society of Anaesthesiology, 2009 A3 Improvement,
Staphylococcus aureus Bloodstream Infection Treatment Guideline
 Staphylococcus aureus Bloodstream Infection Treatment Guideline Purpose: To provide a framework for the evaluation and management patients with Methicillin- Susceptible (MSSA) and Methicillin-Resistant
Staphylococcus aureus Bloodstream Infection Treatment Guideline Purpose: To provide a framework for the evaluation and management patients with Methicillin- Susceptible (MSSA) and Methicillin-Resistant
Bard: Intermittent Catheters. A guide to. Bard: Pelvic Organ Prolapse. An REIMBURSEMENT. overview of OF INTERMITTENT. Prolapse CATHETERS
 Bard: Intermittent Catheters A guide to Bard: Pelvic Organ Prolapse An REIMBURSEMENT overview of Pelvic OF INTERMITTENT Organ Prolapse CATHETERS 1 Intermittent catheterization is a covered Medicare benefit
Bard: Intermittent Catheters A guide to Bard: Pelvic Organ Prolapse An REIMBURSEMENT overview of Pelvic OF INTERMITTENT Organ Prolapse CATHETERS 1 Intermittent catheterization is a covered Medicare benefit
Ceftriaxone Therapy Vs. Ciprofloxacin In Treatment Of Typhoid Fever In Adult Patients.
 Dec QMJ VOL.5 No.8 Ceftriaxone Therapy Vs. Ciprofloxacin In Treatment Of Typhoid Fever In Adult Patients. Radhi F.Alshaibani* الخلاصھ لا زالت حمى التایفوید سببا مھما من اسباب الامراض وفقدان ساعات العمل
Dec QMJ VOL.5 No.8 Ceftriaxone Therapy Vs. Ciprofloxacin In Treatment Of Typhoid Fever In Adult Patients. Radhi F.Alshaibani* الخلاصھ لا زالت حمى التایفوید سببا مھما من اسباب الامراض وفقدان ساعات العمل
PREVENTION OF CATHETER-ASSOCIATED URINARY TRACT INFECTION FOLLOWING GYNAECOLOGIC SURGERY: A SYSTEMATIC REVIEW
 PREVENTION OF CATHETER-ASSOCIATED URINARY TRACT INFECTION FOLLOWING GYNAECOLOGIC SURGERY: A SYSTEMATIC REVIEW *Christine M. Chu, Lily A. Arya Division of Urogynecology, Department of Obstetrics and Gynecology,
PREVENTION OF CATHETER-ASSOCIATED URINARY TRACT INFECTION FOLLOWING GYNAECOLOGIC SURGERY: A SYSTEMATIC REVIEW *Christine M. Chu, Lily A. Arya Division of Urogynecology, Department of Obstetrics and Gynecology,
SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS
 Page 1 of 8 TITLE: SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS GUIDELINE: Antibiotics are administered prior to surgical procedures to prevent surgical site infections. PURPOSE:
Page 1 of 8 TITLE: SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS GUIDELINE: Antibiotics are administered prior to surgical procedures to prevent surgical site infections. PURPOSE:
Other Causes of Fever
 T e c h n i c a l S e m i n a r s Other Causes of Fever Febrile Illness Causes Fever After Seven Days Referral Relapsing Fever - Borreliosis Overview JHR Adaptation Sore Throat Overview Prevention Management
T e c h n i c a l S e m i n a r s Other Causes of Fever Febrile Illness Causes Fever After Seven Days Referral Relapsing Fever - Borreliosis Overview JHR Adaptation Sore Throat Overview Prevention Management
CDC 2015 STD Treatment Guidelines: Update for IHS Providers Sharon Adler M.D., M.P.H.
 CDC 2015 STD Treatment Guidelines: Update for IHS Providers Sharon Adler M.D., M.P.H. Clinical Faculty, CA Prevention Training Center Disclosure Information Sharon Adler MD, MPH I have no financial relationships
CDC 2015 STD Treatment Guidelines: Update for IHS Providers Sharon Adler M.D., M.P.H. Clinical Faculty, CA Prevention Training Center Disclosure Information Sharon Adler MD, MPH I have no financial relationships
Prevention and Recognition of Obstetric Fistula Training Package. Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula
 Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
TREATMENT OF PERITONEAL DIALYSIS (PD) RELATED PERITONITIS. General Principles
 WA HOME DIALYSIS PROGRAM (WAHDIP) GUIDELINES General Principles 1. PD related peritonitis is an EMERGENCY early empiric treatment followed by close review is essential 2. When culture results and sensitivities
WA HOME DIALYSIS PROGRAM (WAHDIP) GUIDELINES General Principles 1. PD related peritonitis is an EMERGENCY early empiric treatment followed by close review is essential 2. When culture results and sensitivities
Blue Team Teaching Module: Periorbital/Orbital Infections
 Blue Team Teaching Module: Periorbital/Orbital Infections Format: 1. Case 2. Topic Summary 3. Questions 4. References Case: A 3-year-old boy presents with 2 days of increasing redness, swelling, and pain
Blue Team Teaching Module: Periorbital/Orbital Infections Format: 1. Case 2. Topic Summary 3. Questions 4. References Case: A 3-year-old boy presents with 2 days of increasing redness, swelling, and pain
Evaluation and Follow-up of Fetal Hydronephrosis
 Evaluation and Follow-up of Fetal Hydronephrosis Deborah M. Feldman, MD, Marvalyn DeCambre, MD, Erin Kong, Adam Borgida, MD, Mujgan Jamil, MBBS, Patrick McKenna, MD, James F. X. Egan, MD Objective. To
Evaluation and Follow-up of Fetal Hydronephrosis Deborah M. Feldman, MD, Marvalyn DeCambre, MD, Erin Kong, Adam Borgida, MD, Mujgan Jamil, MBBS, Patrick McKenna, MD, James F. X. Egan, MD Objective. To
Prevention of CAUTI is discussed in the CDC/HICPAC document, Guideline for Prevention of Catheter-associated Urinary Tract Infection 4.
 Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [CA] and Non-Catheter-Associated Urinary Tract Infection []) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [CA] and Non-Catheter-Associated Urinary Tract Infection []) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Childhood Urinary Tract Infections
 Childhood Urinary Tract Infections What is a UTI? Urinary tract infection (UTI) is one of the most common infections in childhood. It can cause distress to the child, concerns to the parents, and may
Childhood Urinary Tract Infections What is a UTI? Urinary tract infection (UTI) is one of the most common infections in childhood. It can cause distress to the child, concerns to the parents, and may
Urinary Tract Infection among Clean-Room Workers
 J Occup Health 2002; 44: 329 333 Journal of Occupational Health Urinary Tract Infection among Clean-Room Workers Jian-Nan WANG 1, Shih-Bin SU 2, 3 and How-Ran GUO 3 1 Department of Family Medicine, Chie-Mei
J Occup Health 2002; 44: 329 333 Journal of Occupational Health Urinary Tract Infection among Clean-Room Workers Jian-Nan WANG 1, Shih-Bin SU 2, 3 and How-Ran GUO 3 1 Department of Family Medicine, Chie-Mei
Urinary Tract Infections - How to Identify, Treat and Prevent Them
 1 of 12 4/29/2016 1:49 PM Library Home Find A Physician Find A Practice Request An Appointment Search Clinical Studies Classes and Support Groups Ask A Health Librarian Subscribe to enewsletters Bone and
1 of 12 4/29/2016 1:49 PM Library Home Find A Physician Find A Practice Request An Appointment Search Clinical Studies Classes and Support Groups Ask A Health Librarian Subscribe to enewsletters Bone and
Hemodialysis catheter infection
 Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Catheter-Associated Urinary Tract Infection (CAUTI) Definitions and Reporting
 AHRQ Safety Program for Long-term Care: HAIs/CAUTI Learning Objectives Upon completion of the webinar, core team members will be able to: Catheter-Associated Urinary Tract Infection (CAUTI) Definitions
AHRQ Safety Program for Long-term Care: HAIs/CAUTI Learning Objectives Upon completion of the webinar, core team members will be able to: Catheter-Associated Urinary Tract Infection (CAUTI) Definitions
Catheter-Associated Urinary Tract Infections Lauren Tew, Bard Ltd, UK A Webber Training Teleclass Catheter-Associated Urinary Tract Infection
 Catheter-Associated Urinary Tract Infection Lauren Tew Infection Control Nurse and Clinical Consultant Hosted by Debbie King [email protected] www.webbertraining.com Tew L, Pomfret I & King D (2005)
Catheter-Associated Urinary Tract Infection Lauren Tew Infection Control Nurse and Clinical Consultant Hosted by Debbie King [email protected] www.webbertraining.com Tew L, Pomfret I & King D (2005)
Managing the E coli UTI
 C o n s u l t a n t o n C a l l I N F E C T I O U S / Z O O N O T I C D I S E A S E Peer Reviewed Kate S. KuKanich, DVM, PhD, Diplomate ACVIM Kansas State University Managing the E coli UTI PROFILE Definition
C o n s u l t a n t o n C a l l I N F E C T I O U S / Z O O N O T I C D I S E A S E Peer Reviewed Kate S. KuKanich, DVM, PhD, Diplomate ACVIM Kansas State University Managing the E coli UTI PROFILE Definition
Have a shower, rather than a bath to avoid exposing your genitals to the chemicals in your cleaning products for too long. Always empty your bladder
 Cystitis, Avenue Medical Practice Neat Guideline Introduction Cystitis means 'inflammation of the bladder'. It causes: an urgent and frequent need to urinate, and Pain, or stinging, when passing urine.
Cystitis, Avenue Medical Practice Neat Guideline Introduction Cystitis means 'inflammation of the bladder'. It causes: an urgent and frequent need to urinate, and Pain, or stinging, when passing urine.
RECOMMENDATIONS. MULTIPLE SCLEROSIS AND MANAGEMENT OF URINARY TRACT INFECTION Clinical Practice Guideline November 2013 PRACTICE POINT
 MULTIPLE SCLEROSIS AND MANAGEMENT OF URINARY TRACT INFECTION Clinical Practice Guideline November 2013 GOALS Urgent primary care assessment and management of urinary tract infections (UTIs) in patients
MULTIPLE SCLEROSIS AND MANAGEMENT OF URINARY TRACT INFECTION Clinical Practice Guideline November 2013 GOALS Urgent primary care assessment and management of urinary tract infections (UTIs) in patients
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Nosocomial Bloodstream infection. Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
 Nosocomial Bloodstream infection Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand. Nosocomial UTI Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
Nosocomial Bloodstream infection Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand. Nosocomial UTI Khachornsakdi Silpapojakul MD Prince of Songkla University Hat yai, Thailand.
Appropriate Treatment for Children with Upper Respiratory Infection
 BCBS ACO Measure Appropriate Treatment for Children with Upper Respiratory Infection HEDIS Measure CPT II coding required: YES Click here to go to Table of Contents BCBS Measure: Page 50 of 234 Dated:
BCBS ACO Measure Appropriate Treatment for Children with Upper Respiratory Infection HEDIS Measure CPT II coding required: YES Click here to go to Table of Contents BCBS Measure: Page 50 of 234 Dated:
