GUIDELINES ON UROLOGICAL INFECTIONS
|
|
|
- Emory Harmon
- 9 years ago
- Views:
Transcription
1 GUIDELINES ON UROLOGICAL INFECTIONS (Limited text update March 2015) M. Grabe (Chair), R. Bartoletti, T.E. Bjerklund Johansen, M. Çek, B. Köves (Guidelines Associate), K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction Urinary tract infections (UTIs) pose a serious health problem for patients with high cost to society. UTIs are also the most frequent healthcare associated infections. E. coli is the predominant pathogen in uncomplicated UTIs. Besides E. coli, other Enterobacteriaceae, Enterococcus spp, and Pseudomonas aeruginosa are also cultured in patients with urological diseases. Microbial resistance is developing at an alarming rate with country-specific resistance rates related to the amount of antibiotics used. Particularly of concern is the increasing resistance to broad spectrum antibiotics. It is thus essential to limit the use of antibiotics in general and fluoroquinolones and cephalosporins in particular, especially in uncomplicated infections and asymptomatic bacteriuria. Classification and definitions For practical clinical reasons, UTIs and male genital tract infections are classified into entities defined by the predominant location of clinical symptoms and underlying risk factors (Table 1). Urological Infections 237
2 Table 1: Classification of urinary tract and male genital infections Uncomplicated lower UTI: cystitis (acute, sporadic or recurrent) Uncomplicated upper UTI: Pyelonephritis (acute, sporadic, no risk factor identified) Complicated UTI with or without pyelonephritis (underlying urological, nephrological or other medical risk factors) Urosepsis Urethritis MAGI: Prostatitis, epididymitis, orchitis MAGI: male accessory gland infection. The definitions of bacteriuria are listed in Table 2. Table 2: Relevant bacterial growth in adults uropathogens/ml in midstream urine in acute uncomplicated cystitis in women uropathogens/ml in midstream urine in acute uncomplicated pyelonephritis in women uropathogens/ml in midstream urine in women or 10 4 uropathogens/ml in midstream urine in men (or in straight catheter urine in women) with complicated UTI. 4. In a suprapubic bladder puncture specimen, any count of bacteria is relevant. Asymptomatic bacteriuria (ABU) Asymptomatic bacteriuria is defined as two positive urine cultures taken more than 24 hours apart containing 10 5 uropathogens/ml of the same bacterial strain (in a patient without any clinical symptoms), irrespective of an accompanying pyuria. ABU is not considered an infection but rather a commensal colonisation, and in some clinical 238 Urological Infections
3 situations a risk factor. Therefore ABU should not be treated and not screened for. There is some evidence that ABU in recurrent UTI could even be protective. Pyuria The diagnostic requirement for pyuria is 10 white blood cells per high-power field (HPF) (x400) in the re-suspended sediment of a centrifuged aliquot of urine or per mm 3 in unspun urine. For routine investigation, a dipstick method can also be used, including a leukocyte esterase test and assessment of haemoglobin and nitrites. Classification of prostatitis/chronic pelvic pain syndrome It is recommended to use the classification according to NIDDK/NIH (Table 3). Only acute and chronic bacterial prostatitis are covered in these Guidelines. Table 3: Classification of prostatitis according to NIDDK/ NIH I Acute bacterial prostatitis (ABP) II Chronic bacterial prostatitis (CBP) III Chronic pelvic pain syndrome (CPPS) IIIA Inflammatory CPPS: WBC in EPS/voided bladder urine-3 (VB3)/semen IIIB Non-inflammatory CPPS: no WBC/EPS/VB3/semen IV Asymptomatic inflammatory prostatitis (histological prostatitis) Epididymitis, orchitis Most cases of epididymitis, with or without orchitis, are caused by common urinary pathogens. Bladder outlet obstruction and urogenital malformations are risk factors. Consider Chlamydia trachomatis infection in the younger male population. Urological Infections 239
4 Diagnosis UTI (general) A disease history, assessment of symptoms, physical examination and dipstick urine analysis, including white and red blood cells and nitrite reaction, is recommended for routine diagnosis. A urine culture is recommended in all types of UTI before treatment, except for sporadic episodes of uncomplicated cystitis in premenopausal women, in order to adjust antimicrobial therapy if necessary. Pyelonephritis Acute Pyelonephritis is suggested by flank pain, nausea and vomiting, fever (>38 C), costovertebral angle tenderness, and it can occur both with and without symptoms of cystitis. It may be necessary to evaluate the urinary tract to rule out upper urinary tract obstruction or stone disease. Urethritis Symptomatic urethritis is characterised by alguria and purulent discharge. Pyogenic urethritis is indicated by a Gram stain of secretion or urethral smear that shows more than five leukocytes per HPF (x1,000) and in case of gonorrhoea, gonococci are located intracellularly as Gram-negative diplococci. A positive leukocyte esterase test or more than 10 leukocytes per HPF (x400) in the first voiding urine specimen is diagnostic. Bacterial Prostatitis Acute bacterial prostatitis is a usually febrile infection of the prostate that can be severe and the diagnosis is based on the clinical symptoms and signs and positive urine culture. Chronic bacterial prostatitis is usually characterised by recurrent symptoms and UTI. In patients with prostatitis-like symptoms, an attempt should be made to differentiate between bacterial prostatitis and CPPS. This 240 Urological Infections
5 is best done by the four glass test according to Meares & Stamey, if acute UTI and STD can be ruled out. Treatment Treatment of UTI depends on a variety of factors. Table 4 provides an overview of the most common pathogens, antimicrobial agents and duration of treatment for different conditions. Urological Infections 241
6 Table 4: Recommendations for antimicrobial therapy in urology Diagnosis Most frequent pathogen/species Asymptomatic bacteriuria E. coli (usually low virulent) Other species can also be found Cystitis acute, sporadic and uncomplicated in otherwise healthy women E. coli Klebsiella sp. Proteus sp. Staphylococci Pyelonephritis, acute, sporadic, usually febrile (Uncomplicated) E. coli Proteus sp. Klebsiella sp. Other enterobacteriaceae (Febrile) UTI with urological complicating factors E. coli Klebsiella sp. 242 Urological Infections
7 Initial, empirical antimicrobial therapy No treatment Exception: before urological surgery entering the urinary tract and during pregnancy (low evidence) Fosfomycin trometamol Nitrofurantoin macrocrystal Pivmecillinam Alternative: Cephalosporin (group 1, 2) TMP-SMX 1 Fluoroquinolone 2,3 Fluoroquinolone 2 Cephalosporin (group 3a) Alternatives: Aminopenicillin/BLI Aminoglycoside TMP-SMX 1 Fluoroquinolone 2 Aminopenicillin/BLI Cephalosporin (group 3a) Aminoglycoside TMP-SMX 1 Therapy duration 3-5 days treatment of bacteriuria prior to urological surgery according to sensitivity testing 4 For pregnancy: refer to national recommendation if available 1 dose 5 days 3 days 3 days 3 days (1-)3 days 7-10 days After improvement, switch to oral therapy according to sensitivity testing 7-14 days As for pyelonephritis consider combination of two antibiotics in severe infections Urological Infections 243
8 Pyelonephritis, acute, febrile, severe with complicating factors Healthcare associated (Nosocomial) UTI Catheter-associated febrile UTI Proteus sp. Enterobacter sp. Serratia Other enterobacteriaceae Pseudomonas Enterococci Staphylococci High risk of multi-resistant strains In case of Candida sp. Urosepsis Pathogen as above 1 Only in areas with resistance rate < 20% (for E. coli). 2 Fluoroquinolone with mainly renal excretion (see text). 3 Avoid Fluoroquinolones in uncomplicated cystitis whenever possible. 4 Bacteriuria is a risk factor, though no clear regimen has been defined in available literature. The given recommendation is based on a reasonable expert opinion. BLI = beta-lactamase inhibitor; UTI = urinary tract infection. 244 Urological Infections
9 In case of failure of initial therapy within 1-3 days or in clinical cases: Anti-Pseudomonas active: Fluoroquinolone, if not used initially Piperacillin/tazobactam Cephalosporin (group 3b) Carbapenem ± Aminoglycoside 3-5 days after defervescence or control/ elimination of complicating factor (drainage, surgery as required) Fluconazole Amphotericin B Cephalosporin (group 3a/b) Fluoroquinolone 2 Anti-Pseudomonas active acylaminopenicillin/bli Carbapenem ± Aminoglycoside As above Consider combination of two antibiotics in severe infection Urological Infections 245
10 Table 5: Summary of male accessory gland infections Diagnosis Most frequent pathogen/species Prostatitis, acute bacterial (febrile) NIH type I Acute febrile Epididymitis E. coli Other enterobacteriaceae Pseudomonas Enterococcus feacalis Staphylococci Prostatitis, chronic bacterial NIH type II As above Prostatitis, acute or chronic Epididymitis Urethritis, caused by Chlamydia sp Ureaplasma sp Special situations UTI in pregnancy A urine culture is recommended. Only antimicrobials considered safe in pregnancy should be used, e.g. penicillins, cephalosporins, fosfomycin; trimethoprim not in the first and sulphonamides not in the third trimenon; nitrofuantoin not in the last weeks of pregnancy to avoid glucose-6-phosphate deficiency of the embryo. 246 Urological Infections
11 (MAGI) management Initial, empirical antimicrobial therapy Fluoroquinolone Cephalosporin (group 3a or b) Aminoglycoside TMP-SMX Fluoroquinolone Alternative to consider based on isolated pathogen TMP-SMX Doxycycline Macrolide Doxycycline Fluoroquinolone active on species (e.g. ofloxacin, levofloxacin) Macrolide Therapy duration Initial parenteral Consider combination of two antibiotics in severe infections After improvement, switch to oral therapy according to sensitivity test for 2 (-4) weeks Oral 4-6 weeks 7 (-14) days (Follow national guidelines if available) UTI in children Treatment periods should be extended to 7-10 days. Tetracyclines and fluoroquinolones should not be used because of adverse effects on teeth and cartilage. Acute uncomplicated UTI in young men A urine culture is recommended. Treatment should last at least 7 days for uncomplicated UTI. Consider the option of a bacterial prostatitis that requires a longer treatment. Urological Infections 247
12 Complicated UTI due to urological disorders The underlying disorder must be managed if a permanent cure is to be achieved. Whenever possible, treatment should be guided by urine culture to avoid missing and/or inducing resistant strains. Sepsis in urology (urosepsis) Patients with complicated UTI may develop sepsis. Early signs of systemic inflammatory response (fever or hypothermia, tachycardia, tachypnoea, hypotension, oliguria, leukopenia) should be recognised as the first signs of possible multi-organ failure. As well as appropriate antibiotic therapy, life-support therapy in collaboration with an intensive care specialist may be necessary. Any obstruction in the urinary tract must be drained. Follow-up of patients with UTI For routine follow-up after uncomplicated UTI and pyelonephritis in women, assessment of symptoms and dipstick urine analysis is sufficient. In women with a recurrence of UTI within 2 weeks, repeated urinary culture with antimicrobial testing and urinary tract evaluation is recommended. In the elderly, newly developed recurrent UTI may warrant a full evaluation of the urinary tract. In men with UTI, a urological evaluation should be performed in adolescent patients, cases of recurrent infection and all cases of pyelonephritis. This recommendation should also be followed in patients with prostatitis, epididymitis and orchitis. In children, urological investigations are recommended after two episodes of UTI in girls and one episode in boys. Recommended investigations are ultrasound of the urinary tract supplemented by voiding cystourethrography. 248 Urological Infections
13 Prevention of recurrent UTI (ruti) Prevention of ruti includes i) counselling and behavioural modifications, i.e. avoidance of risk factors, ii) non-antimicrobial measures and iii) antimicrobial prophylaxis, which should be attempted also in this order. Urological risk factors need to be looked for and eliminated as far as possible. Significant residual urine should be treated optimally, which also includes clean intermittent catheterisation (CIC) when valued necessary. Non-antimicrobial prophylaxis Hormonal replacement Local oestriol replacement, especially in postmenopausal women (GR: C) Immunoactive prophylaxis OM-89 (Urovaxom ) is documented with several placebo-controlled studies and useful in clinical practice (GR: B). The vaginal vaccine (Urovac ) and the parenteral products (StroVac and SolcoUrovac ) demonstrated efficacy in only smaller controlled studies (GR: C). Probiotics Only in clinically proven studies are probiotics recommended (GR: C). D-Mannose To be used only in clinical trials for further evaluation. Cannot be recommended presently. Endovesical instillation Glycosaminoglycan (GAG) layer replenishement is used but recent review shows insufficient background for any recommendation. Antimicrobial prophylaxis of ruti Antimicrobial prophylaxis can be given continuously (daily, weekly) for longer periods of time (3-6 months), as short courses after self-diagnosis in cooperative women or as a Urological Infections 249
14 single post-coital dose. It should be considered only after counselling and behavioural modification has been attempted, and when non-antimicrobial measures have been unsuccessful (GR: B). Regimens for women with rutis include e.g. cotrimoxazole (TMP/SMX) 40/200 mg once daily or thrice weekly, nitrofurantoin 50 mg or 100 mg once daily, fosfomycin trometamol 3 g every 10 days, and during pregnancy e.g. cephalexin 125 mg or 250 mg or cefaclor 250 mg once daily. Urethritis The following guidelines for therapy comply with the recommendations of the Center for Disease Control and Prevention (2010 and later update). For the treatment of gonorrhoea, the following antimicrobials can be recommended (Table 6): Table 6: Antibiotic therapy for treatment of gonorrhoea 1 First choice Second choice 2 Ceftriaxone g iv/im Cefixime 400 mg p.o. SD (with local anaesthesia) Azithromycin 1.5 g p.o. SD plus Cefuroxime 400 mg p.o. SD Azithromycin g p.o. Ciprofloxacin 500 mg p.o. SD as SD Levofloxacin 250 mg p.o. SD 1 always culture and susceptibility testing before therapy and PCR 2 weeks after therapy 2 only if susceptibility is shown by culture 3 if i.m. injection contraindicated and i.v. administration not possible: cefixime 800 mg p.o. As gonorrhoea is often accompanied by chlamydial infection, an anti-chlamydial active therapy should be added. The following treatment has been successfully applied in Chlamydia trachomatis infections (Table 7): 250 Urological Infections
15 Table 7: Antibiotic therapy for Chlamydia trachomatis infections First choice Second choice Azithromycin Erythromycin 1.5 g (= mg) 4 times daily 500 mg orally as single dose orally for 7 days Doxycycline 1 Ofloxacin 2 times daily 2 times daily 100 mg orally 300 mg orally or for 7 (-14) days Levofloxacin once daily 500 mg orally for 7 days 1 contraindicated in children less than 8 years, in pregnant breast feeding women. If therapy fails, infections with Trichomonas vaginalis and/or Mycoplasma spp. should be considered. These can be treated with a combination of metronidazole (2 g orally as a single dose) and erythromycin (500 mg orally, 4 times daily, for 7 days). Bacterial Prostatitis Acute bacterial prostatitis has increased as a result of diagnostic trans-rectal prostate biopsy and can be a serious infection. The parenteral administration of high doses of bactericidal antibiotics, such as an aminoglycoside and a penicillin derivative or a third-generation cephalosporin, is required until defervescence occurs and infection parameters return to normal. In less severe cases, a fluoroquinolone may be given orally for at least days. In chronic bacterial prostatitis and inflammatory CPPS, a fluoroquinolone or trimethoprim should be given orally for 2 weeks after the initial diagnosis. The patient should then be reassessed and antibiotics only continued if the pre-treatment cultures were positive or if the patient has reported positive Urological Infections 251
16 effects from the treatment. A total treatment period of 4-6 weeks is recommended. Drainage/Surgery Bladder catheter drainage might be needed in case of residual urine. Abscess of the prostate may develop in rare situations and require drainage. Epididymitis, orchitis Prior to antimicrobial therapy, a urethral swab and midstream urine sample should be obtained for microbiological investigation. The first choice of drug therapy should be fluoroquinolones, preferably those agents that react well against C. trachomatis (e.g. ofloxacin, levofloxacin), because of their broad antibacterial spectra and favourable penetration into urogenital tract tissues. In cases caused by C. trachomatis, treatment may also be continued with doxycycline, 200 mg/day, for a total treatment period of at least 2 weeks. Macrolides are alternative agents. In cases of C. trachomatis infection, the sexual partner should also be treated. Perioperative antibacterial prophylaxis in urological surgery The aim of antimicrobial prophylaxis in urological surgery is to reduce the load of bacteria at the site of surgery and thus to prevent symptomatic or febrile urogenital infections, such as acute pyelonephritis, prostatitis, epididymitis and urosepsis, as well as serious wound infections in conjunction with surgery. In recent years increased resistance of the faecal flora, especially against fluoroquinolones, has been reported which may impact on prophylaxis mode. It is recommended to assess the risk, e.g. prior to prostate biopsy. A urine culture is recommended prior to urological surgery when the urinary tract is entered both to identify ABU and any resistant strain. 252 Urological Infections
17 The basic recommendations for short-term peri-operative antibacterial prophylaxis in standard urological interventions are listed in Table 8. This short booklet text is based on the more comprehensive EAU Guidelines (ISBN ), available to all members of the European Association of Urology at their website, Urological Infections 253
18 Table 8: Basic recommendations for peri-operative text Guidelines (Tables 19-24) Procedure Pathogens Prophylaxis (expected) (standard) Diagnostic procedures Transrectal biopsy of the Enterobacteriaceae All patients prostate 1 (Anaerobes?) Cystoscopy Enterobacteriaceae No Urodynamic study Enterococci Staphylococci Ureteroscopy Enterobacteriaceae No Enterococci Staphylococci Endourological surgery and SWL SWL Enterobacteriaceae No Enterococci Ureteroscopy for Enterobacteriaceae No uncomplicated distal stone Enterococci Staphylococci Ureteroscopy of proximal Enterobacteriaceae All patients or impacted stone and Enterococci percutaneous stone Staphylococci extraction TUR of the prostate Enterobacteriaceae All patients Enterococci 254 Urological Infections
19 antibacterial prophylaxis in urology. For details, see full Antibiotics Remarks Fluoroquinolones 1 TMP ± SMX Metronidazole 2 TMP ± SMX Cephalosporin TMP ± SMX Cephalosporin Single dose effective in low risk. Consider prolonged course in risk patients Consider in risk patients Consider in risk patients TMP ± SMX Cephalosporin Aminopenicillin/BLI 3 TMP ± SMX Cephalosporin Aminopenicillin/BLI TMP ± SMX Cephalosporin Aminopenicillin/BLI (Fluoroquinolones) TMP ± SMX Cephalosporin Aminopenicillin/BLI In patients with stent or nephrostomy tube or other known risk factor Consider in risk patients Single dose or short course Low-risk patients and small-size prostate require no prophylaxis Urological Infections 255
20 TUR of bladder tumour Enterobacteriaceae No (see Enterococci remarks) Open or laparoscopic urological surgery 4 Clean operations Skin-related No pathogens, e.g. staphylococci Catheterassociated uropathogens Clean-contaminated Enterobacteriaceae Recommended (opening of urinary tract) Enterococci Staphylococci Clean-contaminated/ Enterobacteriaceae All patients contaminated (use of bowel Enterococci segments) Anaerobes Skin-related bacteria Implant of prosthetic Skin-related All patients devices bacteria, e.g. staphylococci BLI = beta-lactamase inhibitor; TMP ± SMX = trimethoprim with thral resection. 1 Increased resistance of faecal flora recorded (see text). 2 No evidence for the use of metronidazole in prostate core biopsies. 3 Gram-negative bacteria excluding Pseudomonas aeruginosa. 4 Classifications of surgical field contamination (CDC). 256 Urological Infections
21 TMP ± SMX Cephalosporin Aminopenicillin/BLI Consider in risk patients and large resections tumours and necrotic tumours Consider in high-risk patients. Short post-operative catheter requires no treatment TMP ± SMX Cephalosporin Aminopenicillin/BLI Cephalosporin Metronidazole Single peri-operative course As for colonic surgery Cephalosporin Penicillin (penicillinase stable) or without sulphamethoxale (co-trimoxazole); TUR = transure- Urological Infections 257
GUIDELINES ON UROLOGICAL INFECTIONS
 GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2014) M. Grabe (chair), R. Bartoletti, T.E. Bjerklund-Johansen, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction
GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2014) M. Grabe (chair), R. Bartoletti, T.E. Bjerklund-Johansen, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction
GUIDELINES ON UROLOGICAL INFECTIONS
 GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2010) M. Grabe (chairman), T.E. Bjerklund-Johansen, H. Botto, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction Infections
GUIDELINES ON UROLOGICAL INFECTIONS (Text update April 2010) M. Grabe (chairman), T.E. Bjerklund-Johansen, H. Botto, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt Introduction Infections
Urinary Tract Infections
 Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections
 A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections By Gary R. Skankey, MD, FACP, Infectious Disease, Las Vegas, NV Sponsored
A Practical Guide to Diagnosis and Treatment of Infection in the Outpatient Setting Diagnosis and Treatment of Urinary Tract Infections By Gary R. Skankey, MD, FACP, Infectious Disease, Las Vegas, NV Sponsored
Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults. A Systematic Review (Cochrane database August 2013)
 Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults A Systematic Review (Cochrane database August 2013) Gail Lusardi, Senior Lecturer Dr Allyson Lipp, Principal Lecturer, Dr Chris
Antibiotic Prophylaxis for Short-term Catheter Bladder Drainage in adults A Systematic Review (Cochrane database August 2013) Gail Lusardi, Senior Lecturer Dr Allyson Lipp, Principal Lecturer, Dr Chris
Guidelines on Urological Infections
 Guidelines on Urological Infections M. Grabe (Chair), R. Bartoletti, T.E. Bjerklund Johansen, T. Cai (Guidelines Associate), M. Çek, B. Köves (Guidelines Associate), K.G. Naber, R.S. Pickard, P. Tenke,
Guidelines on Urological Infections M. Grabe (Chair), R. Bartoletti, T.E. Bjerklund Johansen, T. Cai (Guidelines Associate), M. Çek, B. Köves (Guidelines Associate), K.G. Naber, R.S. Pickard, P. Tenke,
Etiology and treatment of chronic bacterial prostatitis the Croatian experience
 Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
A Summary of the Guideline for the Diagnosis and Management of. Urinary Tract Infections in Long Term Care
 A Summary of the Guideline for the Diagnosis and Management of Urinary Tract Infections in Long Term Care Exclusions Community acquired UTIs UTIs in acute care Prevention Limit use of catheters Ensure
A Summary of the Guideline for the Diagnosis and Management of Urinary Tract Infections in Long Term Care Exclusions Community acquired UTIs UTIs in acute care Prevention Limit use of catheters Ensure
Title: Antibiotic Guideline for Acute Pelvic Inflammatory Disease
 Title: Antibiotic Guideline for Acute Pelvic Inflammatory Disease Version 3 Date ratified December 2007 Review date December 2009 Ratified by NUH Antimicrobial Guidelines Committee Gynaecology Directorate
Title: Antibiotic Guideline for Acute Pelvic Inflammatory Disease Version 3 Date ratified December 2007 Review date December 2009 Ratified by NUH Antimicrobial Guidelines Committee Gynaecology Directorate
Urinary Tract Infections. Clinical Scenario #1. Urinary Tract Infections. Clinical Scenario #1 : Labs
 Clinical Scenario #1 : Labs Urinary Tract Infections Magdalena Sobieszczyk, MD Urinalysis: pyuria (WBC too numerous to count), RBC and bacteria present Urine dipstick: positive leukocyte esterase and nitrite
Clinical Scenario #1 : Labs Urinary Tract Infections Magdalena Sobieszczyk, MD Urinalysis: pyuria (WBC too numerous to count), RBC and bacteria present Urine dipstick: positive leukocyte esterase and nitrite
Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD
 82 Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD Abstract Urinary tract infections are commonly treated in urgent care practice. Clinicians need to be aware of the advantages and limitations
82 Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD Abstract Urinary tract infections are commonly treated in urgent care practice. Clinicians need to be aware of the advantages and limitations
Urinary Tract Infections
 Urinary Tract Infections Magdalena Sobieszczyk, MD MPH Division of Infectious Diseases Columbia University Clinical Scenario #1 23 y.o woman presents to her doctor complaining of 1 day of increased urinary
Urinary Tract Infections Magdalena Sobieszczyk, MD MPH Division of Infectious Diseases Columbia University Clinical Scenario #1 23 y.o woman presents to her doctor complaining of 1 day of increased urinary
Guidelines on Urological Infections
 Guidelines on Urological Infections M. Grabe (chairman), T.E. Bjerklund-Johansen, H. Botto, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt European Association of Urology 2013 TABLE
Guidelines on Urological Infections M. Grabe (chairman), T.E. Bjerklund-Johansen, H. Botto, M. Çek, K.G. Naber, R.S. Pickard, P. Tenke, F. Wagenlehner, B. Wullt European Association of Urology 2013 TABLE
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page
 A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
A PRINTED copy of this guideline may not be the most recent version. The OFFICIAL version is located on IHNET at the Policies & Procedures Home Page IX0200: Prevention & Control of Catheter Associated
UTI in children. Quick reference guide. Issue date: August 2007. Urinary tract infection in children: diagnosis, treatment and long-term management
 Issue date: August 2007 UTI in children Urinary tract infection in children: diagnosis, treatment and long-term management Developed by the National Collaborating Centre for Women s and Children s Health
Issue date: August 2007 UTI in children Urinary tract infection in children: diagnosis, treatment and long-term management Developed by the National Collaborating Centre for Women s and Children s Health
Catheter-Associated Urinary Tract Infection (CAUTI) Event
 Catheter-Associated Urinary Tract Infection () Event Introduction: Urinary tract infections (UTIs) are tied with pneumonia as the second most common type of healthcare-associated infection, second only
Catheter-Associated Urinary Tract Infection () Event Introduction: Urinary tract infections (UTIs) are tied with pneumonia as the second most common type of healthcare-associated infection, second only
Urinary Tract Infection and Asymptomatic Bacteriuria Guidance
 Urinary Tract Infection and Asymptomatic Bacteriuria Guidance Urinary tract infection (UTI) is the most common indication for antimicrobial use in hospitals and a significant proportion of this use is
Urinary Tract Infection and Asymptomatic Bacteriuria Guidance Urinary tract infection (UTI) is the most common indication for antimicrobial use in hospitals and a significant proportion of this use is
Case Studies in Urinary Tract Infections
 Case Studies in Urinary Tract Infections Robert L. Holley, MSc, MD Professor of Obstetrics and Gynecology Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology
Case Studies in Urinary Tract Infections Robert L. Holley, MSc, MD Professor of Obstetrics and Gynecology Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology
POAC CLINICAL GUIDELINE
 POAC CLINICAL GUIDELINE Acute Pylonephritis DIAGNOSIS COMPLICATED PYELONEPHRITIS EXCLUSION CRITERIA: Male Known or suspected renal impairment (egfr < 60) Abnormality of renal tract Known or suspected renal
POAC CLINICAL GUIDELINE Acute Pylonephritis DIAGNOSIS COMPLICATED PYELONEPHRITIS EXCLUSION CRITERIA: Male Known or suspected renal impairment (egfr < 60) Abnormality of renal tract Known or suspected renal
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations. J. Stuart Wolf, Jr., M.D.
 Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations J. Stuart Wolf, Jr., M.D. Department of Urology University of Michigan Ann Arbor, MI Official Recommendations for
Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations J. Stuart Wolf, Jr., M.D. Department of Urology University of Michigan Ann Arbor, MI Official Recommendations for
THIS IS AN OFFICIAL NH DHHS HEALTH ALERT
 THIS IS AN OFFICIAL NH DHHS HEALTH ALERT Distributed by the NH Health Alert Network [email protected] August 13, 2015 1400 EDT (2:00 PM EDT) NH-HAN 20150813 Updated Centers for Disease Control (CDC)
THIS IS AN OFFICIAL NH DHHS HEALTH ALERT Distributed by the NH Health Alert Network [email protected] August 13, 2015 1400 EDT (2:00 PM EDT) NH-HAN 20150813 Updated Centers for Disease Control (CDC)
SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS
 Page 1 of 8 TITLE: SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS GUIDELINE: Antibiotics are administered prior to surgical procedures to prevent surgical site infections. PURPOSE:
Page 1 of 8 TITLE: SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS GUIDELINE: Antibiotics are administered prior to surgical procedures to prevent surgical site infections. PURPOSE:
URINARY TRACT INFECTION IN CHILDREN. Yap Hui Kim, Belinda Murugasu
 URINARY TRACT INFECTION IN CHILDREN Yap Hui Kim, Belinda Murugasu Urinary tract infection (UTI) is a common problem in childhood and the primary health care practitioner is usually the frontline in diagnosis
URINARY TRACT INFECTION IN CHILDREN Yap Hui Kim, Belinda Murugasu Urinary tract infection (UTI) is a common problem in childhood and the primary health care practitioner is usually the frontline in diagnosis
CDC 2015 STD Treatment Guidelines: Update for IHS Providers Sharon Adler M.D., M.P.H.
 CDC 2015 STD Treatment Guidelines: Update for IHS Providers Sharon Adler M.D., M.P.H. Clinical Faculty, CA Prevention Training Center Disclosure Information Sharon Adler MD, MPH I have no financial relationships
CDC 2015 STD Treatment Guidelines: Update for IHS Providers Sharon Adler M.D., M.P.H. Clinical Faculty, CA Prevention Training Center Disclosure Information Sharon Adler MD, MPH I have no financial relationships
Treatment of sexually transmitted and other genital infections
 www.bpac.org.nz keyword: sti Treatment of sexually transmitted and other genital infections Key reviewer: Dr Murray Reid, Sexual Health Physician, Auckland Sexual Health Service General points: If one
www.bpac.org.nz keyword: sti Treatment of sexually transmitted and other genital infections Key reviewer: Dr Murray Reid, Sexual Health Physician, Auckland Sexual Health Service General points: If one
Frequently Asked Questions
 Guidelines for Testing and Treatment of Gonorrhea in Ontario, 2013 Frequently Asked Questions Table of Contents Background... 1 Treatment Recommendations... 2 Treatment of Contacts... 4 Administration
Guidelines for Testing and Treatment of Gonorrhea in Ontario, 2013 Frequently Asked Questions Table of Contents Background... 1 Treatment Recommendations... 2 Treatment of Contacts... 4 Administration
190.12 - Urine Culture, Bacterial Summary Information Highlighted items indicate most frequently used codes.
 Medicare National Coverage Determination (NCD) (Jan 2011) Source: CMS: Centers for Medicare & Medicaid Services To view full document: www.cms.gov/coveragegeninfo. Select Lab NCDs, then select NCD Coding
Medicare National Coverage Determination (NCD) (Jan 2011) Source: CMS: Centers for Medicare & Medicaid Services To view full document: www.cms.gov/coveragegeninfo. Select Lab NCDs, then select NCD Coding
Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings
 Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings Dr. Mary Vearncombe PIDAC-IPC February 2012 Objectives: To provide an overview of the RP/AP Annex
Management of Extended Spectrum Beta- Lactamase (ESBL) Producing Enterobacteriaceae in health care settings Dr. Mary Vearncombe PIDAC-IPC February 2012 Objectives: To provide an overview of the RP/AP Annex
URINARY TRACT INFECTIONS IN YOUNG WOMEN
 URINARY TRACT INFECTIONS IN YOUNG WOMEN Reviewed by Finnish Centre for Health Promotion Publisher: Ylioppilaiden terveydenhoitosäätiö Töölönkatu 37 A 00260 Helsinki Orders: [email protected] Author:
URINARY TRACT INFECTIONS IN YOUNG WOMEN Reviewed by Finnish Centre for Health Promotion Publisher: Ylioppilaiden terveydenhoitosäätiö Töölönkatu 37 A 00260 Helsinki Orders: [email protected] Author:
GONORRHOEA. Use of lidocaine as a diluent when using ceftriaxone (see Appendix 1)
 Key practice notes: 1 st line therapy GONORRHOEA Decreasing sensitivity of gonorrhoea to cephalosporins is now a real threat: CEFTRIAXONE 500mg IM stat first-line for all gonococcal infections AZITHROMYCIN
Key practice notes: 1 st line therapy GONORRHOEA Decreasing sensitivity of gonorrhoea to cephalosporins is now a real threat: CEFTRIAXONE 500mg IM stat first-line for all gonococcal infections AZITHROMYCIN
IDSA GUIDELINES EXECUTIVE SUMMARY
 IDSA GUIDELINES International Clinical Practice Guidelines for the Treatment of Acute Uncomplicated Cystitis and Pyelonephritis in Women: A 2010 Update by the Infectious Diseases Society of America and
IDSA GUIDELINES International Clinical Practice Guidelines for the Treatment of Acute Uncomplicated Cystitis and Pyelonephritis in Women: A 2010 Update by the Infectious Diseases Society of America and
APPENDIX B: UWHC SURGICAL ANTIMICROBIAL PROPHYLAXIS GUIDELINES
 APPENDIX B: UWHC SURGICAL ANTIMICROBIAL PROPHYLAXIS GUIDELINES Principles of prophylaxis 1) Use antimicrobials for surgical procedures where prophylactic antimicrobials have been found to be beneficial.
APPENDIX B: UWHC SURGICAL ANTIMICROBIAL PROPHYLAXIS GUIDELINES Principles of prophylaxis 1) Use antimicrobials for surgical procedures where prophylactic antimicrobials have been found to be beneficial.
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis
 Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
GLOBAL OVERVIEW OF ANTIMICROBIAL RESISTANCE STD AGENTS
 GLOBAL OVERVIEW OF ANTIMICROBIAL RESISTANCE STD AGENTS IN Dr.P.Bhalla Director Professor and Head Dept. of Microbiology Maulana Azad Medical College New Delhi, INDIA STDs & RTIs l HIV l Gonococcal infections/
GLOBAL OVERVIEW OF ANTIMICROBIAL RESISTANCE STD AGENTS IN Dr.P.Bhalla Director Professor and Head Dept. of Microbiology Maulana Azad Medical College New Delhi, INDIA STDs & RTIs l HIV l Gonococcal infections/
Urinary Tract Infections
 Urinary Tract Infections www.kidney.org Did you know that... n Urinary tract infections (UTIs) are responsible for nearly 10 million doctor visits each year. n One in five women will have at least one
Urinary Tract Infections www.kidney.org Did you know that... n Urinary tract infections (UTIs) are responsible for nearly 10 million doctor visits each year. n One in five women will have at least one
Have a shower, rather than a bath to avoid exposing your genitals to the chemicals in your cleaning products for too long. Always empty your bladder
 Cystitis, Avenue Medical Practice Neat Guideline Introduction Cystitis means 'inflammation of the bladder'. It causes: an urgent and frequent need to urinate, and Pain, or stinging, when passing urine.
Cystitis, Avenue Medical Practice Neat Guideline Introduction Cystitis means 'inflammation of the bladder'. It causes: an urgent and frequent need to urinate, and Pain, or stinging, when passing urine.
Understanding and Preventing Bladder Infections in Women
 Understanding and Preventing Bladder Infections in Women Understanding and Preventing Bladder Infections in Women Recurrent bladder or urinary tract infections (UTI s) are a very common diagnosis. In fact,
Understanding and Preventing Bladder Infections in Women Understanding and Preventing Bladder Infections in Women Recurrent bladder or urinary tract infections (UTI s) are a very common diagnosis. In fact,
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 Initial assessment and investigation of urinary incontinence bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used
Initial assessment and investigation of urinary incontinence bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used
Frequently Asked Questions
 Frequently Asked Questions Testing for Gonorrhea Q1: What test should be completed for accurately diagnosing gonorrhea? A1: Testing is done with either a culture or a NAAT (nucleic acid amplification test).
Frequently Asked Questions Testing for Gonorrhea Q1: What test should be completed for accurately diagnosing gonorrhea? A1: Testing is done with either a culture or a NAAT (nucleic acid amplification test).
SYNDROMIC CASE MANAGEMENT OF RTIs Advantages, Limitations, Optimization
 WHO COLLABORATING CENTRE FOR RESEARCH IN HUMAN REPRODUCTION Hôpitaux Universitaires de Genève SYNDROMIC CASE MANAGEMENT OF RTIs Advantages, Limitations, Optimization Dr SALONEY NAZEER Department of Gynaecology
WHO COLLABORATING CENTRE FOR RESEARCH IN HUMAN REPRODUCTION Hôpitaux Universitaires de Genève SYNDROMIC CASE MANAGEMENT OF RTIs Advantages, Limitations, Optimization Dr SALONEY NAZEER Department of Gynaecology
Prevention of CAUTI is discussed in the CDC/HICPAC document, Guideline for Prevention of Catheter-associated Urinary Tract Infection 4.
 Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [] and Non-Catheter-Associated Urinary Tract Infection [UTI]) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [] and Non-Catheter-Associated Urinary Tract Infection [UTI]) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention. Basics of Infection Prevention 2 Day Mini-Course 2013
 Catheter-Associated Urinary Tract Infection (CAUTI) Prevention Basics of Infection Prevention 2 Day Mini-Course 2013 2 Objectives Define the scope of healthcare-associated urinary tract infections (UTI)
Catheter-Associated Urinary Tract Infection (CAUTI) Prevention Basics of Infection Prevention 2 Day Mini-Course 2013 2 Objectives Define the scope of healthcare-associated urinary tract infections (UTI)
Urinary Tract Infections
 1 Infections in the urinary tract are relatively common. These infections are often referred to as bladder infections. They are also known as UTI s or urinary tract infections. When an infection is confined
1 Infections in the urinary tract are relatively common. These infections are often referred to as bladder infections. They are also known as UTI s or urinary tract infections. When an infection is confined
Beryl Navti SEPT Pharmacy Department. 24/06/2013 Beryl Navti, Clinical Pharmacist, SEPT
 URINARY TRACT INFECTIONS Beryl Navti SEPT Pharmacy Department The Genitourinary System The organs system of the reproductive organs and urinary system Grouped dtogether th because of their proximity it
URINARY TRACT INFECTIONS Beryl Navti SEPT Pharmacy Department The Genitourinary System The organs system of the reproductive organs and urinary system Grouped dtogether th because of their proximity it
PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS. (CAUTIs)
 PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS (CAUTIs) CAUTIs A UTI where an indwelling urinary catheter was in place for >2 calendar days on the date of event. OR If an indwelling urinary
PREVENTION OF CATHETER ASSOCIATED URINARY TRACT INFECTIONS (CAUTIs) CAUTIs A UTI where an indwelling urinary catheter was in place for >2 calendar days on the date of event. OR If an indwelling urinary
Urinary Tract Infections
 Urinary Tract Infections Leading cause of morbidity and health care expenditures in persons of all ages. An estimated 50 % of women report having had a UTI at some point in their lives. 8.3 million office
Urinary Tract Infections Leading cause of morbidity and health care expenditures in persons of all ages. An estimated 50 % of women report having had a UTI at some point in their lives. 8.3 million office
Fungal Infection in Total Joint Arthroplasty. Dr.Wismer Dr.Al-Sahan
 Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
COMPASS Therapeutic Notes on the Management of Bacterial Urinary Tract Infections in Primary Care
 COMPASS Therapeutic Notes on the Management of Bacterial Urinary Tract Infections in Primary Care In this issue: Page Introduction, Background & Diagnostic Tests 1 UTI in non-pregnant women 3 UTI in pregnant
COMPASS Therapeutic Notes on the Management of Bacterial Urinary Tract Infections in Primary Care In this issue: Page Introduction, Background & Diagnostic Tests 1 UTI in non-pregnant women 3 UTI in pregnant
Expedited Partner Therapy (EPT) for Sexually Transmitted Diseases Protocol for Health Care Providers in Oregon
 Expedited Partner Therapy (EPT) for Sexually Transmitted Diseases Protocol for Health Care Providers in Oregon Oregon Health Authority Center for Public Health Practice HIV/STD/TB Section Principles of
Expedited Partner Therapy (EPT) for Sexually Transmitted Diseases Protocol for Health Care Providers in Oregon Oregon Health Authority Center for Public Health Practice HIV/STD/TB Section Principles of
State of Kuwait Ministry of Health Infection Control Directorate. Guidelines for Prevention of Surgical Site Infection (SSI)
 State of Kuwait Ministry of Health Infection Control Directorate Guidelines for Prevention of Surgical Site Infection (SSI) September 1999 Updated 2007 Surgical Wound: According to 1998 Kuwait National
State of Kuwait Ministry of Health Infection Control Directorate Guidelines for Prevention of Surgical Site Infection (SSI) September 1999 Updated 2007 Surgical Wound: According to 1998 Kuwait National
TREATMENT OF STI CONTACTS
 This decision support tool is effective as of October 2014. For more information or to provide feedback on this or any other decision support tool, email [email protected] TREATMENT OF STI CONTACTS
This decision support tool is effective as of October 2014. For more information or to provide feedback on this or any other decision support tool, email [email protected] TREATMENT OF STI CONTACTS
Catheter-Associated Urinary Tract Infections Lauren Tew, Bard Ltd, UK A Webber Training Teleclass Catheter-Associated Urinary Tract Infection
 Catheter-Associated Urinary Tract Infection Lauren Tew Infection Control Nurse and Clinical Consultant Hosted by Debbie King [email protected] www.webbertraining.com Tew L, Pomfret I & King D (2005)
Catheter-Associated Urinary Tract Infection Lauren Tew Infection Control Nurse and Clinical Consultant Hosted by Debbie King [email protected] www.webbertraining.com Tew L, Pomfret I & King D (2005)
Prevention of catheter associated urinary tract infections
 Prevention of catheter associated urinary tract infections Dr. Suzan Sanavi, Nephrologist, M.D University of Social Welfare and Rehabilitation Akhavan Physical Spine Center INTRODUCTION Urinary bladder
Prevention of catheter associated urinary tract infections Dr. Suzan Sanavi, Nephrologist, M.D University of Social Welfare and Rehabilitation Akhavan Physical Spine Center INTRODUCTION Urinary bladder
NewYork-Presbyterian Hospital Sites: Columbia University Medical Center Guideline: Medication Use Manual Page 1 of 12
 Page 1 of 12 TITLE: ANTIBIOTICS IN ADULT PATIENTS EMPIRIC USE GUIDELINES, COLUMBIA UNIVERSITY MEDICAL CENTER MEDICATION GUIDELINE PURPOSE: These are the 2011 guidelines for the empiric use of antibiotics
Page 1 of 12 TITLE: ANTIBIOTICS IN ADULT PATIENTS EMPIRIC USE GUIDELINES, COLUMBIA UNIVERSITY MEDICAL CENTER MEDICATION GUIDELINE PURPOSE: These are the 2011 guidelines for the empiric use of antibiotics
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
SURGICAL ANTIBIOTIC PROPHYLAXIS. Steve Johnson, PharmD, BCPS Prime Therapeutics, Inc
 SURGICAL ANTIBIOTIC PROPHYLAXIS Steve Johnson, PharmD, BCPS Prime Therapeutics, Inc OBJECTIVES Discuss antibiotic use as prophylaxis vs presumptive therapy vs treatment of infections. Discuss risk factors
SURGICAL ANTIBIOTIC PROPHYLAXIS Steve Johnson, PharmD, BCPS Prime Therapeutics, Inc OBJECTIVES Discuss antibiotic use as prophylaxis vs presumptive therapy vs treatment of infections. Discuss risk factors
Urinary Tract Infection
 Guidelines for Clinical Care Ambulatory Urinary Tract Infection Guideline Team Team Leader Steven E Gradwohl, MD General Medicine Team Members Catherine M Bettcher, MD Family Medicine Carol E Chenoweth,
Guidelines for Clinical Care Ambulatory Urinary Tract Infection Guideline Team Team Leader Steven E Gradwohl, MD General Medicine Team Members Catherine M Bettcher, MD Family Medicine Carol E Chenoweth,
STD Treatment Chart Nancy Harris, N.P. Women s Health Coordinator August 2003 Disease Treatment Alternative treatment
 STD Treatment Chart Nancy Harris, N.P. Women s Health Coordinator August 2003 Disease Treatment Alternative Pregnancy Chlamydia Chancroid Epdidymitis Gonorrhea: Uncomplicated (cx, urethra, and rectum):
STD Treatment Chart Nancy Harris, N.P. Women s Health Coordinator August 2003 Disease Treatment Alternative Pregnancy Chlamydia Chancroid Epdidymitis Gonorrhea: Uncomplicated (cx, urethra, and rectum):
Guideline for Preventing Catheter- Associated Urinary Tract Infections
 Guideline for Preventing Catheter- Associated Urinary Tract Infections Craig Umscheid, MD, MSCE Carolyn Gould, MD, MSCR and David A. Pegues, MD HICPAC Meeting November 13, 2008 Washington, DC Outline Progress
Guideline for Preventing Catheter- Associated Urinary Tract Infections Craig Umscheid, MD, MSCE Carolyn Gould, MD, MSCR and David A. Pegues, MD HICPAC Meeting November 13, 2008 Washington, DC Outline Progress
A THREE YEAR REVIEW OF CATHETER-ASSOCIATED URINARY TRACT INFECTIONS REPORTED TO THE NATIONAL HEALTHCARE SAFETY NETWORK AT A TERTIARY CARE HOSPITAL
 A THREE YEAR REVIEW OF CATHETER-ASSOCIATED URINARY TRACT INFECTIONS REPORTED TO THE NATIONAL HEALTHCARE SAFETY NETWORK AT A TERTIARY CARE HOSPITAL by Jessi Marie Bond BS, Clinical Laboratory Science, Idaho
A THREE YEAR REVIEW OF CATHETER-ASSOCIATED URINARY TRACT INFECTIONS REPORTED TO THE NATIONAL HEALTHCARE SAFETY NETWORK AT A TERTIARY CARE HOSPITAL by Jessi Marie Bond BS, Clinical Laboratory Science, Idaho
signs suggesting chlamydia:
 Chlamydia - uncomplicated genital - Management View full scenario When should I suspect and test for chlamydia? Women: o Test for chlamydia if they are sexually active with symptoms and signs suggesting
Chlamydia - uncomplicated genital - Management View full scenario When should I suspect and test for chlamydia? Women: o Test for chlamydia if they are sexually active with symptoms and signs suggesting
Blood in the urine (hematuria)
 Blood in the urine (hematuria) Hematuria refers to the presence of blood in the urine. It is important to investigate the cause of hematuria because rarely, it is caused by a serious condition, such as
Blood in the urine (hematuria) Hematuria refers to the presence of blood in the urine. It is important to investigate the cause of hematuria because rarely, it is caused by a serious condition, such as
THE KIDNEY. Bulb of penis Abdominal aorta Scrotum Adrenal gland Inferior vena cava Urethra Corona glandis. Kidney. Glans penis Testicular vein
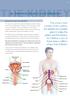 29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
29 THE KIDNEY 9. Recurrent urinary tract infections Recurrent urinary tract infections The urinary tract consists of the urethra, the bladder, the ureters, the kidneys and in men the prostate gland. An
ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS LAUREN HYNICKA, PHARM.D.
 ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS LAUREN HYNICKA, PHARM.D. ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS ACTIVITY DESCRIPTION Antibiotic use in the safest
ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS LAUREN HYNICKA, PHARM.D. ANTIBIOTICS FROM HEAD TO TOE: PART 5 - URINARY TRACT INFECTIONS ACTIVITY DESCRIPTION Antibiotic use in the safest
MANAGEMENT OF PROSTATE ENLARGEMENT/BPH
 MANAGEMENT OF PROSTATE ENLARGEMENT/BPH J E S S I C A E. P A O N E S S A, M. D. A S S I S T A N T P R O F E S S O R D E P A R T M E N T O F U R O L O G Y S U N Y U P S T A T E M E D I C A L U N I V E R
MANAGEMENT OF PROSTATE ENLARGEMENT/BPH J E S S I C A E. P A O N E S S A, M. D. A S S I S T A N T P R O F E S S O R D E P A R T M E N T O F U R O L O G Y S U N Y U P S T A T E M E D I C A L U N I V E R
Prevention of CAUTI is discussed in the CDC/HICPAC document, Guideline for Prevention of Catheter-associated Urinary Tract Infection 4.
 Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [CA] and Non-Catheter-Associated Urinary Tract Infection []) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Urinary Tract Infection (Catheter-Associated Urinary Tract Infection [CA] and Non-Catheter-Associated Urinary Tract Infection []) and Other Urinary System Infection [USI]) Events Introduction: Urinary
Intra-abdominal abdominal Infections
 Intra-abdominal abdominal Infections Marnie Peterson, Pharm.D., BCPS Dept. of Pediatric Infectious Diseases Medical School University of Minnesota Intra-abdominal abdominal Infections Intra-abdominal abdominal
Intra-abdominal abdominal Infections Marnie Peterson, Pharm.D., BCPS Dept. of Pediatric Infectious Diseases Medical School University of Minnesota Intra-abdominal abdominal Infections Intra-abdominal abdominal
URINE CULTURES GENERAL PROCEDURE
 University of Nebraska Medical Center Division of Laboratory Science Clinical Laboratory Science Program CLS 418/CLS 419 URINE CULTURES GENERAL PROCEDURE I. Principle Urine cultures are performed to detect
University of Nebraska Medical Center Division of Laboratory Science Clinical Laboratory Science Program CLS 418/CLS 419 URINE CULTURES GENERAL PROCEDURE I. Principle Urine cultures are performed to detect
Pyelonephritis: Kidney Infection
 Pyelonephritis: Kidney Infection National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is pyelonephritis? Pyelonephritis
Pyelonephritis: Kidney Infection National Kidney and Urologic Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is pyelonephritis? Pyelonephritis
Rhode Island Department of Health Division of Infectious Diseases and Epidemiology
 Rhode Island Department of Health Division of Infectious Diseases and Epidemiology STD (Sexually Transmitted Disease) PROGRAM Expedited Partner Therapy (EPT) for STDs Guidance for Medical Providers in
Rhode Island Department of Health Division of Infectious Diseases and Epidemiology STD (Sexually Transmitted Disease) PROGRAM Expedited Partner Therapy (EPT) for STDs Guidance for Medical Providers in
Management of Urinary Tract Infections in Patients with Urinary Catheters
 Clinical Review Article Management of Urinary Tract Infections in Patients with Urinary Catheters Maria L. Alcaide, MD Daniel M. Lichtstein, MD Urinary tract infections (UTIs) in patients with urinary
Clinical Review Article Management of Urinary Tract Infections in Patients with Urinary Catheters Maria L. Alcaide, MD Daniel M. Lichtstein, MD Urinary tract infections (UTIs) in patients with urinary
Catheter-Associated Urinary Tract Infection (CAUTI) Definitions and Reporting
 AHRQ Safety Program for Long-term Care: HAIs/CAUTI Learning Objectives Upon completion of the webinar, core team members will be able to: Catheter-Associated Urinary Tract Infection (CAUTI) Definitions
AHRQ Safety Program for Long-term Care: HAIs/CAUTI Learning Objectives Upon completion of the webinar, core team members will be able to: Catheter-Associated Urinary Tract Infection (CAUTI) Definitions
Kalpana Gupta, M.D. Associate Professor Department of Medicine Section of Infectious Diseases Boston University School of Medicine
 2010 Clinical Practice Guidelines by the Infectious Diseases Society of America and the European Society for Clinical Microbiology and Infectious Diseases Kalpana Gupta, M.D. Associate Professor Department
2010 Clinical Practice Guidelines by the Infectious Diseases Society of America and the European Society for Clinical Microbiology and Infectious Diseases Kalpana Gupta, M.D. Associate Professor Department
Riesa Gusewelle, MNSc, RN, APRN, GNP-BC. OBJECTIVES Identify early warning signs of urinary tract
 Detection, Early Management & Prevention, of Urinary Tract Infections in Older Adults Riesa Gusewelle, MNSc, RN, APRN, GNP-BC OBJECTIVES Identify early warning signs of urinary tract infections (UTIs)
Detection, Early Management & Prevention, of Urinary Tract Infections in Older Adults Riesa Gusewelle, MNSc, RN, APRN, GNP-BC OBJECTIVES Identify early warning signs of urinary tract infections (UTIs)
Welcome and Instructions
 Welcome and Instructions For audio, join by telephone at 877-594-8353, participant code: 56350822 Your line is OPEN. Please do not use the hold feature on your phone but do mute your line by dialing *6.
Welcome and Instructions For audio, join by telephone at 877-594-8353, participant code: 56350822 Your line is OPEN. Please do not use the hold feature on your phone but do mute your line by dialing *6.
PREVENTION OF CATHETER-ASSOCIATED URINARY TRACT INFECTION FOLLOWING GYNAECOLOGIC SURGERY: A SYSTEMATIC REVIEW
 PREVENTION OF CATHETER-ASSOCIATED URINARY TRACT INFECTION FOLLOWING GYNAECOLOGIC SURGERY: A SYSTEMATIC REVIEW *Christine M. Chu, Lily A. Arya Division of Urogynecology, Department of Obstetrics and Gynecology,
PREVENTION OF CATHETER-ASSOCIATED URINARY TRACT INFECTION FOLLOWING GYNAECOLOGIC SURGERY: A SYSTEMATIC REVIEW *Christine M. Chu, Lily A. Arya Division of Urogynecology, Department of Obstetrics and Gynecology,
California Guidelines for STD Screening and Treatment in Pregnancy
 California Guidelines for STD Screening and Treatment in Pregnancy These guidelines were developed by the California Department of Public Health (CDPH) Sexually Transmitted Diseases (STD) Control Branch
California Guidelines for STD Screening and Treatment in Pregnancy These guidelines were developed by the California Department of Public Health (CDPH) Sexually Transmitted Diseases (STD) Control Branch
Why Do Some Antibiotics Fail?
 Why Do Some Antibiotics Fail? Patty W. Wright, M.D. April 2010 Objective To outline common reasons why antibiotic therapy is not successful and how this can be avoided. And to teach you a little bit about
Why Do Some Antibiotics Fail? Patty W. Wright, M.D. April 2010 Objective To outline common reasons why antibiotic therapy is not successful and how this can be avoided. And to teach you a little bit about
The Minnesota Chlamydia Strategy: Action Plan to Reduce and Prevent Chlamydia in Minnesota Minnesota Chlamydia Partnership, April 2011
 The Minnesota Chlamydia Strategy: Action Plan to Reduce and Prevent Chlamydia in Minnesota Minnesota Chlamydia Partnership, April 2011 Section 5: Screening, Treating and Reporting Chlamydia While the information
The Minnesota Chlamydia Strategy: Action Plan to Reduce and Prevent Chlamydia in Minnesota Minnesota Chlamydia Partnership, April 2011 Section 5: Screening, Treating and Reporting Chlamydia While the information
STANDARD PROTOCOL STD AND HIV SCREENING AND EPIDEMIOLOGIC STD TREATMENT
 STANDARD PROTOCOL STD AND HIV SCREENING AND EPIDEMIOLOGIC STD TREATMENT RELEASE DATE: REVIEW INTERVAL: YEARLY REVIEW DATE: SITE/SERVICE UNIT: IMPLEMENTATION DATE: REVIEWED BY: CONTACT: APPROVED BY: CONTENTS
STANDARD PROTOCOL STD AND HIV SCREENING AND EPIDEMIOLOGIC STD TREATMENT RELEASE DATE: REVIEW INTERVAL: YEARLY REVIEW DATE: SITE/SERVICE UNIT: IMPLEMENTATION DATE: REVIEWED BY: CONTACT: APPROVED BY: CONTENTS
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Contents
 Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
Acute pelvic inflammatory disease: tests and treatment
 Acute pelvic inflammatory disease: tests and treatment Information for you Information for you Published August 2010 Published in August 2010 (next review date: 2014) Acute What is pelvic inflammatory
Acute pelvic inflammatory disease: tests and treatment Information for you Information for you Published August 2010 Published in August 2010 (next review date: 2014) Acute What is pelvic inflammatory
Prevention and Recognition of Obstetric Fistula Training Package. Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula
 Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
Prevention and Recognition of Obstetric Fistula Training Package Module 8: Pre-repair Care and Referral for Women with Obstetric Fistula Early detection and treatment If a woman has recently survived a
2014 CDC Treatment Guidelines for STDs What s New, What s Important, What s Essential. STD Treatment Guidelines. How are the guidelines prepared?
 2014 CDC Treatment Guidelines for STDs What s New, What s Important, What s Essential Bradley Stoner, MD, PhD Associate Professor, Washington University School of Medicine Medical Director, St. Louis STD/HIV
2014 CDC Treatment Guidelines for STDs What s New, What s Important, What s Essential Bradley Stoner, MD, PhD Associate Professor, Washington University School of Medicine Medical Director, St. Louis STD/HIV
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #65 (NQF 0069): Appropriate Treatment for Children with Upper Respiratory Infection (URI) National Quality Strategy Domain: Efficiency and Cost Reduction 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES:
Measure #65 (NQF 0069): Appropriate Treatment for Children with Upper Respiratory Infection (URI) National Quality Strategy Domain: Efficiency and Cost Reduction 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES:
STI case management. Francis Ndowa - GFMER Theodora Wi - WHO
 Training Course in Sexual and Reproductive Health Research 2014 Module: Principles and Practice of Sexually Transmitted Infections Prevention and Care STI case management Francis Ndowa - GFMER Theodora
Training Course in Sexual and Reproductive Health Research 2014 Module: Principles and Practice of Sexually Transmitted Infections Prevention and Care STI case management Francis Ndowa - GFMER Theodora
MODULE 2: ADULT URINARY TRACT INFECTIONS
 MODULE 2: ADULT URINARY TRACT INFECTIONS KEYWORDS: Urinary tract infection (UTI); cystitis; pyelonephritis; uropathogens; antibiotics LEARNING OBJECTIVES At the end of this clerkship, the learner will
MODULE 2: ADULT URINARY TRACT INFECTIONS KEYWORDS: Urinary tract infection (UTI); cystitis; pyelonephritis; uropathogens; antibiotics LEARNING OBJECTIVES At the end of this clerkship, the learner will
PRIORITY RESEARCH TOPICS
 PRIORITY RESEARCH TOPICS Understanding all the issues associated with antimicrobial resistance is probably impossible, but it is clear that there are a number of key issues about which we need more information.
PRIORITY RESEARCH TOPICS Understanding all the issues associated with antimicrobial resistance is probably impossible, but it is clear that there are a number of key issues about which we need more information.
Don t Go With The Flow! Control and Management of UTIs in the Elderly
 Don t Go With The Flow! Control and Management of UTIs in the Elderly Acknowledgements Central West Infection Control Network Toronto Central Infection Control Network Erie St Clair Infection Control Network
Don t Go With The Flow! Control and Management of UTIs in the Elderly Acknowledgements Central West Infection Control Network Toronto Central Infection Control Network Erie St Clair Infection Control Network
SECTION 12.1 URINARY CATHETERS
 SECTION 12.1 URINARY CATHETERS Introduction Summary of Recommendations taken from Guidelines for the Prevention of Catheter-associated Urinary Tract Infection, Published on behalf of SARI by HSE Health
SECTION 12.1 URINARY CATHETERS Introduction Summary of Recommendations taken from Guidelines for the Prevention of Catheter-associated Urinary Tract Infection, Published on behalf of SARI by HSE Health
