About 23 million persons, or 10
|
|
|
- Collin Hunt
- 9 years ago
- Views:
Transcription
1 PRACTICAL THERAPEUTICS Trigger Points: Diagnosis and Management DAVID J. ALVAREZ, D.O., and PAMELA G. ROCKWELL, D.O., University of Michigan Medical School, Ann Arbor, Michigan Trigger points are discrete, focal, hyperirritable spots located in a taut band of skeletal muscle. They produce pain locally and in a referred pattern and often accompany chronic musculoskeletal disorders. Acute trauma or repetitive microtrauma may lead to the development of stress on muscle fibers and the formation of trigger points. Patients may have regional, persistent pain resulting in a decreased range of motion in the affected muscles. These include muscles used to maintain body posture, such as those in the neck, shoulders, and pelvic girdle. Trigger points may also manifest as tension headache, tinnitus, temporomandibular joint pain, decreased range of motion in the legs, and low back pain. Palpation of a hypersensitive bundle or nodule of muscle fiber of harder than normal consistency is the physical finding typically associated with a trigger point. Palpation of the trigger point will elicit pain directly over the affected area and/or cause radiation of pain toward a zone of reference and a local twitch response. Various modalities, such as the Spray and Stretch technique, ultrasonography, manipulative therapy and injection, are used to inactivate trigger points. Trigger-point injection has been shown to be one of the most effective treatment modalities to inactivate trigger points and provide prompt relief of symptoms. (Am Fam Physician 2002;65: Copyright 2002 American Academy of Family Physicians.) Members of various medical faculties develop articles for Practical Therapeutics. This article is one in a series coordinated by the Department of Family Medicine at the University of Michigan Medical School, Ann Arbor. Guest editor of the series is Barbara S. Apgar, M.D., M.S., who is also an associate editor of AFP. TABLE 1 Trigger Points vs. Tender Points Trigger points About 23 million persons, or 10 percent of the U.S. population, have one or more chronic disorders of the musculoskeletal system. 1 Musculoskeletal disorders are the main cause of disability in the working-age population and are among the leading causes of disability in other age groups. 2 Myofascial pain syndrome is a common painful muscle disorder caused by myofascial trigger points. 3 This must be differentiated from fibromyalgia syndrome, which involves multiple tender spots or tender points. 3 These pain syndromes are often concomitant and may interact with one another. Trigger points are discrete, focal, hyperirri- Tender points Local tenderness, taut band, local Local tenderness twitch response, jump sign Singular or multiple Multiple May occur in any skeletal muscle Occur in specific locations that are symmetrically located May cause a specific referred Do not cause referred pain, but often cause pain pattern a total body increase in pain sensitivity table spots located in a taut band of skeletal muscle. The spots are painful on compression and can produce referred pain, referred tenderness, motor dysfunction, and autonomic phenomena. 4 Trigger points are classified as being active or latent, depending on their clinical characteristics. 5 An active trigger point causes pain at rest. It is tender to palpation with a referred pain pattern that is similar to the patient s pain complaint. 3,5,6 This referred pain is felt not at the site of the trigger-point origin, but remote from it. The pain is often described as spreading or radiating. 7 Referred pain is an important characteristic of a trigger point. It differentiates a trigger point from a tender point, which is associated with pain at the site of palpation only (Table 1). 8 A latent trigger point does not cause spontaneous pain, but may restrict movement or cause muscle weakness. 6 The patient presenting with muscle restrictions or weakness may become aware of pain originating from a latent trigger point only when pressure is applied directly over the point. 9 Moreover, when firm pressure is applied over the trigger point in a snapping fashion perpendicular to the muscle, a local twitch response is often elicited. 10 A local twitch response is defined as a transient visible or palpable contraction or dimpling of the mus- FEBRUARY 15, 2002 / VOLUME 65, NUMBER 4 AMERICAN FAMILY PHYSICIAN 653
2 ILLUSTRATIONS BY RENEE L. CANNON cle and skin as the tense muscle fibers (taut band) of the trigger point contract when pressure is applied. This response is elicited by a sudden change of pressure on the trigger point by needle penetration into the trigger point or by transverse snapping palpation of the trigger point across the direction of the taut band of muscle fibers. Thus, a classic trigger point is defined as the presence of discrete focal tenderness located in a palpable taut band of skeletal muscle, which produces both referred regional pain (zone of reference) and a local twitch response. Trigger points help define myofascial pain syndromes. Tender points, by comparison, are associated with pain at the site of palpation only, are FIGURE 1. Most frequent locations of myofascial trigger points. not associated with referred pain, and occur in the insertion zone of muscles, not in taut bands in the muscle belly. 8 Patients with fibromyalgia have tender points by definition. Concomitantly, patients may also have trigger points with myofascial pain syndrome. Thus, these two pain syndromes may overlap in symptoms and be difficult to differentiate without a thorough examination by a skilled physician. Pathogenesis There are several proposed histopathologic mechanisms to account for the development of trigger points and subsequent pain patterns, but scientific evidence is lacking. Many researchers agree that acute trauma or repetitive microtrauma may lead to the development of a trigger point. Lack of exercise, prolonged poor posture, vitamin deficiencies, sleep disturbances, and joint problems may all predispose to the development of microtrauma. 5 Occupational or recreational activities that produce repetitive stress on a specific muscle or muscle group commonly cause chronic stress in muscle fibers, leading to trigger points. Examples of predisposing activities include holding a telephone receiver between the ear and shoulder to free arms; prolonged bending over a table; sitting in chairs with poor back support, improper height of arm rests or none at all; and moving boxes using improper body mechanics. 11 Acute sports injuries caused by acute sprain or repetitive stress (e.g., pitcher s or tennis elbow, golf shoulder), surgical scars, and tissues under tension frequently found after spinal surgery and hip replacement may also predispose a patient to the development of trigger points. 12 Clinical Presentation Patients who have trigger points often report regional, persistent pain that usually results in a decreased range of motion of the muscle in question. Often, the muscles used to maintain body posture are affected, namely 654 AMERICAN FAMILY PHYSICIAN VOLUME 65, NUMBER 4 / FEBRUARY 15, 2002
3 Trigger Points the muscles in the neck, shoulders, and pelvic girdle, including the upper trapezius, scalene, sternocleidomastoid, levator scapulae, and quadratus lumborum. 13 Although the pain is usually related to muscle activity, it may be constant. It is reproducible and does not follow a dermatomal or nerve root distribution. Patients report few systemic symptoms, and associated signs such as joint swelling and neurologic deficits are generally absent on physical examination. 14 In the head and neck region, myofascial pain syndrome with trigger points can manifest as tension headache, tinnitus, temporomandibular joint pain, eye symptoms, and torticollis. 15 Upper limb pain is often referred and pain in the shoulders may resemble visceral pain or mimic tendonitis and bursitis. 5,16 In the lower extremities, trigger points may involve pain in the quadriceps and calf muscles and may lead to a limited range of motion in the knee and ankle. Trigger-point hypersensitivity in the gluteus maximus and gluteus medius often produces intense pain in the low back region. 15 Examples of triggerpoint locations are illustrated in Figure Evaluation Palpation of a hypersensitive bundle or nodule of muscle fiber of harder than normal consistency is the physical finding most often associated with a trigger point. 10 Localization of a trigger point is based on the physician s sense of feel, assisted by patient expressions of pain and by visual and palpable observations of local twitch response. 10 This palpation will elicit pain over the palpated muscle and/or cause radiation of pain toward the zone of reference in addition to a twitch response. The commonly encountered locations of trigger points and their pain reference zones are consistent. 8 Many of these sites and zones of referred pain have been illustrated in Figure A. Peripheral B. Mostly central C. Local FIGURE 2. Examples of the three directions in which trigger points (Xs) may refer pain (red). (A) Peripheral projection of pain from suboccipital and infraspinatus trigger points. (B) Mostly central projection of pain from biceps brachii trigger points with some pain in the region of the distal tendinous attachment of the muscle. (C) Local pain from a trigger point in the serratus posterior inferior muscle. FEBRUARY 15, 2002 / VOLUME 65, NUMBER 4 AMERICAN FAMILY PHYSICIAN 655
4 No specific laboratory test, imaging study, or interventional modality such as electromyography or muscle biopsy has been established for diagnosing trigger points. No laboratory test or imaging technique has been established for diagnosing trigger points. 9 However, the use of ultrasonography, electromyography, thermography, and muscle biopsy has been studied. Management Predisposing and perpetuating factors in chronic overuse or stress injury on muscles must be eliminated, if possible. Pharmacologic treatment of patients with chronic musculoskeletal pain includes analgesics and medications to induce sleep and relax muscles. Antidepressants, neuroleptics, or nonsteroidal anti-inflammatory drugs are often prescribed for these patients. 1 Nonpharmacologic treatment modalities include acupuncture, osteopathic manual medicine techniques, massage, acupressure, ultrasonography, application of heat or ice, diathermy, transcutaneous electrical nerve stimulation, ethyl chloride Spray and Stretch technique, dry needling, and trigger-point injections with local anesthetic, saline, or steroid. The long-term clinical efficacy of various therapies is not clear, because data that incorporate pre- and post-treatment assessments with control groups are not available. The Spray and Stretch technique involves passively stretching the target muscle while simultaneously applying dichlorodifluoromethane-trichloromonofluoromethane (Fluori-Methane) or ethyl chloride spray topically. 5 The sudden drop in skin temperature is thought to produce temporary anesthesia by blocking the spinal stretch reflex and the sensation of pain at a higher center. 5,10 The decreased pain sensation allows the muscle to be passively stretched toward normal length, which then helps to inactivate trigger points, relieve muscle spasm, and reduce referred pain. 5 Dichlorodifluoromethane-trichloromonofluoromethane is a nontoxic, nonflammable vapor coolant spray that does not irritate the skin but is no longer commercially available for other purposes because of its effect in reducing the ozone layer. However, its use is safer for both patient and physician than the original volatile vapor coolant, ethyl chloride. Ethyl chloride is a rapid-acting general anesthetic that becomes flammable and explosive when 4 to 15 percent of the vapor is mixed with air. 10 Nevertheless, ethyl chloride remains a popular agent because of its local anesthetic action and its greater cooling effect than that of dichlorodifluoromethanetrichloromonofluoromethane. 5 The decision to treat trigger points by manual methods or by injection depends strongly on the training and skill of the physician as well as the nature of the trigger point itself. 10 For trigger points in the acute stage of formation (before additional pathologic changes develop), effective treatment may be delivered through physical therapy. Furthermore, manual methods are indicated for patients who have an extreme fear of needles or when the trigger point is in the middle of a muscle belly TABLE 2 Equipment Needed for Trigger-Point Injection Rubber gloves Gauze pads Alcohol pads for cleansing skin 3- or 5-mL syringe Lidocaine (Xylocaine, 1 percent, without epinephrine) or procaine (Novocain, 1 percent) 22-, 25-, or 27-gauge needles of varying lengths, depending on the site to be injected Adhesive bandage Information from references 10 and AMERICAN FAMILY PHYSICIAN VOLUME 65, NUMBER 4 / FEBRUARY 15, 2002
5 Trigger Points TABLE 3 Contraindications to Trigger-Point Injection Anticoagulation or bleeding disorders Aspirin ingestion within three days of injection The presence of local or systemic infection Allergy to anesthetic agents Acute muscle trauma Extreme fear of needles Information from references 10 and 18. Injection with lidocaine has been shown to be effective in patients who have symptomatic active trigger points that produce a twitch response to pressure and create a pattern of referred pain. not easily accessible by injection (i.e., psoas and iliacus muscles). 10 The goal of manual therapy is to train the patient to effectively self-manage the pain and dysfunction. However, manual methods are more likely to require several treatments and the benefits may not be as fully apparent for a day or two when compared with injection. 10 While relatively few controlled studies on trigger-point injection have been conducted, trigger-point injection and dry needling of trigger points have become widely accepted. This therapeutic approach is one of the most effective treatment options available and is cited repeatedly as a way to achieve the best results. 5 Trigger-point injection is indicated for patients who have symptomatic active trigger points that produce a twitch response to pressure and create a pattern of referred pain. In comparative studies, 17 dry needling was found to be as effective as injecting an anesthetic solution such as procaine (Novocain) or lidocaine (Xylocaine). 10 However, postinjection soreness resulting from dry needling was found to be more intense and of longer duration than the soreness experienced by patients injected with lidocaine. 10 One noncontrolled study 17 comparing the use of dry needling versus injection of lidocaine to treat trigger points showed that 58 percent of patients reported complete relief of pain immediately after triggerpoint injection and the remaining 42 percent of patients claimed that their pain was minimal (1-2/10) on the pain scale. Both dry needling and injection with 0.5 percent lidocaine were equally successful in reducing myofascial pain. Postinjection soreness, a different entity than myofascial pain, often developed, especially after use of the dry needling technique. 17 These results support the opinion of most researchers that the critical therapeutic factor in both dry needling and injection is mechanical disruption by the needle. 1,10 TECHNIQUE OF TRIGGER-POINT INJECTION Trigger-point injection can effectively inactivate trigger points and provide prompt, symptomatic relief. Table 2 10,18 outlines the necessary equipment for trigger-point injection. Contraindications to trigger-point injection are listed in Table 3 10,18 and possible complications are outlined in Table 4. Preinjection. Increased bleeding tendencies should be explored before injection. Capillary hemorrhage augments postinjection soreness and leads to unsightly ecchymosis. 10 Patients TABLE 4 Complications of Trigger-Point Injections Vasovagal syncope Skin infection Pneumothorax; avoid pneumothorax complications by never aiming a needle at an intercostal space. Needle breakage; avoid by never inserting the needle to its hub. Hematoma formation; avoid by applying direct pressure for at least two minutes after injection. FEBRUARY 15, 2002 / VOLUME 65, NUMBER 4 AMERICAN FAMILY PHYSICIAN 657
6 The Authors should refrain from daily aspirin dosing for at least three days before injection to avoid increased bleeding. The patient should be placed in a comfortable or recumbent position to produce muscle relaxation. This is best achieved by positioning the patient in the prone or supine position. This positioning may also help the patient to avoid injury if he or she has a vasovagal reaction. 18 Needle Selection. The choice of needle size depends on the location of the muscle being injected. The needle must be long enough to reach the contraction knots in the trigger point to disrupt them. A 22-gauge, 1.5-inch needle is usually adequate to reach most superficial muscles. For thick subcutaneous muscles such as the gluteus maximus or paraspinal muscles in persons who are not obese, a 21-gauge, 2.0-inch needle is usually necessary. 10 A 21-gauge, 2.5-inch needle is required to reach the deepest muscles, such as the gluteus minimus and quadratus lumborum, and is available as a hypodermic needle. Using a needle with a smaller diameter may cause less discomfort; however, it may provide neither the required mechanical disruption of the trigger point nor adequate sensitivity to the physician when penetrating the overlying skin and subcutaneous tissue. A needle with a smaller gauge may also be DAVID J. ALVAREZ, D.O., is a clinical instructor in the Department of Family Medicine at the University of Michigan Medical School, Ann Arbor, where he completed a fellowship in sports medicine. Dr. Alvarez received his medical degree from Michigan State University College of Osteopathic Medicine, East Lansing, and completed a transitional internship at Naval Medical Center, San Diego, and a family practice residency at the University of Michigan Medical School. PAMELA G. ROCKWELL, D.O., is a clinical assistant professor in the Department of Family Medicine at the University of Michigan Medical School. Dr. Rockwell also serves as the medical director of the Family Practice Clinic at East Ann Arbor Health Center, which is affiliated with the University of Michigan Medical School. She received her medical degree from Michigan State University College of Osteopathic Medicine and completed a family practice residency at Eastern Virginia Medical School in Norfolk. Address correspondence to David J. Alvarez, D.O., East Ann Arbor Health Center, 4260 Plymouth Rd., Ann Arbor, MI ( [email protected]). Reprints are not available from the authors. deflected away from a very taut muscular band, thus preventing penetration of the trigger point. The needle should be long enough so that it never has to be inserted all the way to its hub, because the hub is the weakest part of the needle and breakage beneath the skin could occur. 6 Injection Solutions. An injectable solution of 1 percent lidocaine or 1 percent procaine is usually used. Several other substances, including diclofenac (Voltaren), botulinum toxin type A (Botox), and corticosteroids, have been used in trigger-point injections. However, these substances have been associated with significant myotoxicity. 10,19 Procaine has the distinction of being the least myotoxic of all local injectable anesthetics. 10 Injection Technique. Once a trigger point has been located and the overlying skin has been cleansed with alcohol, the clinician isolates that point with a pinch between the thumb and index finger or between the index and middle finger, whichever is most comfortable (Figures 3a and 3b). Using sterile technique, the needle is then inserted 1 to 2 cm away from the trigger point so that the needle may be advanced into the trigger point at an acute angle of 30 degrees to the skin. The stabilizing fingers apply pressure on either side of the injection site, ensuring adequate tension of the muscle fibers to allow penetration of the trigger point but preventing it from rolling away from the advancing needle. 10 The application of pressure also helps to prevent bleeding within the subcutaneous tissues and the subsequent irritation to the muscle that the bleeding may produce. The serious complication of pneumothorax can be avoided by refraining from aiming the needle at an intercostal space. Before advancing the needle into the trigger point, the physician should warn the patient of the possibility of sharp pain, muscle twitching, or an unpleasant sensation as the needle contacts the taut muscular band. 17 To ensure that the needle is not within a blood vessel, the plunger should be withdrawn before 658 AMERICAN FAMILY PHYSICIAN VOLUME 65, NUMBER 4 / FEBRUARY 15, 2002
7 Trigger Points The needle should be inserted 1 to 2 cm away from the trigger point and slowly advanced at a 30-degree angle to the skin into the area of pain. A B C FIGURE 3. Cross-sectional schematic drawing of flat palpation to localize and hold the trigger point (dark red spot) for injection. (A, B) Use of alternating pressure between two fingers to confirm the location of the palpable nodule of the trigger point. (C) Positioning of the trigger point halfway between the fingers to keep it from sliding to one side during the injection. Injection is away from fingers, which have pinned down the trigger point so that it cannot slide away from the needle. Dotted outline indicates additional probing to explore for additional adjacent trigger points. The fingers are pressing downward and apart to maintain pressure for hemostasis. injection. A small amount (0.2 ml) of anesthetic should be injected once the needle is inside the trigger point. The needle is then withdrawn to the level of the subcutaneous tissue, then redirected superiorly, inferiorly, laterally and medially, repeating the needling and injection process in each direction until the local twitch response is no longer elicited or resisting muscle tautness is no longer perceived (Figure 3c). 10 Post-injection Management. After injection, the area should be palpated to ensure that no other tender points exist. If additional tender points are palpable, they should be isolated, needled and injected. Pressure is then applied to the injected area for two minutes to promote hemostasis. 10 A simple adhesive bandage is usually adequate for skin coverage. One study 20 emphasizes that stretching the affected muscle group immediately after injection further increases the efficacy of trigger point therapy. Travell recommends that this is best performed by immediately having the patient actively move each injected muscle through its full range of motion three times, reaching its fully shortened and its fully lengthened position during each cycle. 10 Postinjection soreness is to be expected in most cases, and the patient s stated relief of the referred pain pattern notes the success of the injection. Re-evaluation of the injected areas may be necessary, but reinjection of the trigger points is not recommended until the postinjection soreness resolves, usually after three to four days. Repeated injections in a particular muscle are not recommended if two or three previous attempts have been unsuccessful. Patients are encouraged to remain active, putting muscles through their full range of motion in the week following FEBRUARY 15, 2002 / VOLUME 65, NUMBER 4 AMERICAN FAMILY PHYSICIAN 659
8 Trigger Points trigger-point injections, but are advised to avoid strenuous activity, especially in the first three to four days after injection. 10 The authors indicate that they do not have any conflicts of interest. Sources of funding: none reported. REFERENCES 1. Imamura ST, Fischer AA, Imamura M, Teixeira MJ, Tchia Yeng Lin, Kaziyama HS, et al. Pain management using myofascial approach when other treatment failed. Phys Med Rehabil Clin North Am 1997;8: Cole TM, Edgerton VR. Musculoskeletal disorders. In: Cole TM, Edgerton VR, eds. Report of the Task Force on Medical Rehabilitation Research: June 28-29, 1990, Hunt Valley Inn, Hunt Valley, Md. Bethesda: National Institutes of Health, 1990: Hong CZ, Hsueh TC. Difference in pain relief after trigger point injections in myofascial pain patients with and without fibromyalgia. Arch Phys Med Rehabil 1996;77: Simons DG, Travell JG, Simons LS. Travell & Simons Myofascial pain and dysfunction: the trigger point manual. 2d ed. Baltimore: Williams & Wilkins, 1999:5. 5. Han SC, Harrison P. Myofascial pain syndrome and trigger-point management. Reg Anesth 1997;22: Ling FW, Slocumb JC. Use of trigger point injections in chronic pelvic pain. Obstet Gynecol Clin North Am 1993;20: Mense S, Schmit RF. Muscle pain: which receptors are responsible for the transmission of noxious stimuli? In: Rose FC, ed. Physiological aspects of clinical neurology. Oxford: Blackwell Scientific Publications, 1977: Hopwood MB, Abram SE. Factors associated with failure of trigger point injections. Clin J Pain 1994;10: Fricton JR, Kroening R, Haley D, Siegert R. Myofascial pain syndrome of the head and neck: a review of clinical characteristics of 164 patients. Oral Surg Oral Med Oral Pathol 1985;60: Simons DG, Travell JG, Simons LS. Travell & Simons Myofascial pain and dysfunction: the trigger point manual. 2d ed. Baltimore: Williams & Wilkins, 1999: Rachlin ES. Trigger points. In: Rachlin ES, ed. Myofascial pain and fibromyalgia: trigger point management. St. Louis: Mosby, 1994: Fischer AA. Injection techniques in the management of local pain. J Back Musculoskeletal Rehabil 1996;7: Simons DG, Travell JG, Simons LS. Travell & Simons Myofascial pain and dysfunction: the trigger point manual. 2d ed. Baltimore: Williams & Wilkins, 1999: Yunus MB. Fibromyalgia syndrome and myofascial pain syndrome: clinical features, laboratory tests, diagnosis, and pathophysiologic mechanisms. In: Rachlin ES, ed. Myofascial pain and fibromyalgia: trigger point management. St. Louis: Mosby, 1994: Sola AE, Bonica JJ. Myofascial pain syndromes. In: Bonica JJ, ed. The management of pain. 2d ed. Philadelphia: Lea & Febiger, 1990: Rachlin ES. History and physical examination for regional myofascial pain syndrome. In: Rachlin ES, ed. Myofascial pain and fibromyalgia: trigger point management. St. Louis: Mosby, 1994: Hong CZ. Lidocaine injection versus dry needling to myofascial trigger point. The importance of the local twitch response. Am J Phys Med Rehabil 1994;73: Ruoff GE. Technique of trigger point injection. In: Pfenninger JL, Fowler GC, eds. Procedures for primary care physicians. St. Louis: Mosby, 1994: Fischer AA. New approaches in treatment of myofascial pain. Phys Med Rehabil Clin North Am 1997;8: Zohn DA, Mennell JM. Musculoskeletal pain: diagnosis and physical treatment. Boston: Little, Brown, 1976:126-9, AMERICAN FAMILY PHYSICIAN VOLUME 65, NUMBER 4 / FEBRUARY 15, 2002
Trigger Point Workshop: A Practical OMT Approach Only the Stuff that s Useful
 Trigger Point Workshop: A Practical OMT Approach Only the Stuff that s Useful Sam Detwiler, DO Butler Health System FastERcare Clinical Associate Professor of Family Medicine, OUCOM Why Care About a Trigger
Trigger Point Workshop: A Practical OMT Approach Only the Stuff that s Useful Sam Detwiler, DO Butler Health System FastERcare Clinical Associate Professor of Family Medicine, OUCOM Why Care About a Trigger
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
.org. Cervical Spondylosis (Arthritis of the Neck) Anatomy. Cause
 Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
PLANTAR FASCITIS (Heel Spur Syndrome)
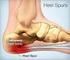 PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
Local Coverage Determination (LCD) for Trigger Point Injections (L28310)
 Page 1 of 8 Search Home Medicare Medicaid CHIP About CMS Regulations & Guidance Research, Statistics, Data & Systems Outreach & Education People with Medicare & Medicaid Questions Careers Newsroom Contact
Page 1 of 8 Search Home Medicare Medicaid CHIP About CMS Regulations & Guidance Research, Statistics, Data & Systems Outreach & Education People with Medicare & Medicaid Questions Careers Newsroom Contact
Neck Pain Overview Causes, Diagnosis and Treatment Options
 Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
For Deep Pressure Massage
 T H E R A C A N E O W N E R S M A N U A L For Deep Pressure Massage Thera Cane is a self massager used to apply pressure to sore muscles. The unique design of the Thera Cane lets you apply deep pressure
T H E R A C A N E O W N E R S M A N U A L For Deep Pressure Massage Thera Cane is a self massager used to apply pressure to sore muscles. The unique design of the Thera Cane lets you apply deep pressure
Rotator Cuff Pathophysiology. treatment program that will effectively treat it. The tricky part about the shoulder is that it is a ball and
 Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Cervical Spondylosis (Arthritis of the Neck)
 Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
It is a syndrome characterized by chronic pain caused by multiple trigger points and
 1 WHAT IS MYOFASCIAL PAIN SYNDROME? It is a syndrome characterized by chronic pain caused by multiple trigger points and myofascial tightening. The term fascial pertains to the muscle, and it is a lining
1 WHAT IS MYOFASCIAL PAIN SYNDROME? It is a syndrome characterized by chronic pain caused by multiple trigger points and myofascial tightening. The term fascial pertains to the muscle, and it is a lining
.org. Cervical Radiculopathy (Pinched Nerve) Anatomy. Cause
 Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
Cervical Radiculopathy (Pinched Nerve) Page ( 1 ) Cervical radiculopathy, commonly called a pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal
Shoulder Tendonitis. Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696
 Shoulder Tendonitis Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Shoulder tendinitis is a common overuse injury in sports (such as swimming,
Shoulder Tendonitis Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Shoulder tendinitis is a common overuse injury in sports (such as swimming,
ALL ABOUT SPASTICITY. www.almirall.com. Solutions with you in mind
 ALL ABOUT SPASTICITY www.almirall.com Solutions with you in mind WHAT IS SPASTICITY? The muscles of the body maintain what is called normal muscle tone, a level of muscle tension that allows us to hold
ALL ABOUT SPASTICITY www.almirall.com Solutions with you in mind WHAT IS SPASTICITY? The muscles of the body maintain what is called normal muscle tone, a level of muscle tension that allows us to hold
.org. Plantar Fasciitis and Bone Spurs. Anatomy. Cause
 Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Integrated Manual Therapy & Orthopedic Massage For Low Back Pain, Hip Pain, and Sciatica
 Integrated Manual Therapy & Orthopedic Massage For Low Back Pain, Hip Pain, and Sciatica Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises By Author & International Lecturer
Integrated Manual Therapy & Orthopedic Massage For Low Back Pain, Hip Pain, and Sciatica Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises By Author & International Lecturer
THE BENJAMIN INSTITUTE PRESENTS. Excerpt from Listen To Your Pain. Assessment & Treatment of. Low Back Pain. Ben E. Benjamin, Ph.D.
 THE BENJAMIN INSTITUTE PRESENTS Excerpt from Listen To Your Pain Assessment & Treatment of Low Back Pain A B E N J A M I N I N S T I T U T E E B O O K Ben E. Benjamin, Ph.D. 2 THERAPIST/CLIENT MANUAL The
THE BENJAMIN INSTITUTE PRESENTS Excerpt from Listen To Your Pain Assessment & Treatment of Low Back Pain A B E N J A M I N I N S T I T U T E E B O O K Ben E. Benjamin, Ph.D. 2 THERAPIST/CLIENT MANUAL The
WHIPLASH! Therapeutic Massage by Lucy Lucy Dean, LMT, NMT, MMT. Helpful and effective treatment with Neuromuscular Therapy. What does Whiplash mean?
 WHIPLASH! Helpful and effective treatment with Neuromuscular Therapy Therapeutic Massage by Lucy Lucy Dean, LMT, NMT, MMT What does Whiplash mean? Whiplash is a non-medical term used to describe neck pain
WHIPLASH! Helpful and effective treatment with Neuromuscular Therapy Therapeutic Massage by Lucy Lucy Dean, LMT, NMT, MMT What does Whiplash mean? Whiplash is a non-medical term used to describe neck pain
What Are Bursitis and Tendinitis?
 Bursitis and tendinitis are both common conditions that cause swelling around muscles and bones. They occur most often in the shoulder, elbow, wrist, hip, knee, or ankle. A bursa is a small, fluid-filled
Bursitis and tendinitis are both common conditions that cause swelling around muscles and bones. They occur most often in the shoulder, elbow, wrist, hip, knee, or ankle. A bursa is a small, fluid-filled
THE LUMBAR SPINE (BACK)
 THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
TheraCane. Owner's Manual
 TheraCane Owner's Manual THERA CANE 411 Thera Cane is a therapeutic massager that allows you to apply pressure to treat muscle dysfunction. Benefits of using the Thera Cane Eliminate painful knots in your
TheraCane Owner's Manual THERA CANE 411 Thera Cane is a therapeutic massager that allows you to apply pressure to treat muscle dysfunction. Benefits of using the Thera Cane Eliminate painful knots in your
.org. Rotator Cuff Tears. Anatomy. Description
 Rotator Cuff Tears Page ( 1 ) A rotator cuff tear is a common cause of pain and disability among adults. In 2008, close to 2 million people in the United States went to their doctors because of a rotator
Rotator Cuff Tears Page ( 1 ) A rotator cuff tear is a common cause of pain and disability among adults. In 2008, close to 2 million people in the United States went to their doctors because of a rotator
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
.org. Shoulder Pain and Common Shoulder Problems. Anatomy. Cause
 Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons
 Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons Informed Patient - Carpal Tunnel Release Surgery Introduction Welcome to the American Academy of Orthopaedic Surgeons'
Informed Patient Tutorial Copyright 2012 by the American Academy of Orthopaedic Surgeons Informed Patient - Carpal Tunnel Release Surgery Introduction Welcome to the American Academy of Orthopaedic Surgeons'
MUSCLE PAIN RELIEF CLINIC
 MUSCLE PAIN RELIEF CLINIC LONG GRAIGUE Revolutionary Muscle Pain Relief Clinic All Injuries Treated Including Back Pain Shoulders Necks Hips Knees Ankles Complete Evaluation Postural Alignment Sports Injuries
MUSCLE PAIN RELIEF CLINIC LONG GRAIGUE Revolutionary Muscle Pain Relief Clinic All Injuries Treated Including Back Pain Shoulders Necks Hips Knees Ankles Complete Evaluation Postural Alignment Sports Injuries
Acute Low Back Pain. North American Spine Society Public Education Series
 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
.org. Tennis Elbow (Lateral Epicondylitis) Anatomy. Cause
 Tennis Elbow (Lateral Epicondylitis) Page ( 1 ) Tennis elbow, or lateral epicondylitis, is a painful condition of the elbow caused by overuse. Not surprisingly, playing tennis or other racquet sports can
Tennis Elbow (Lateral Epicondylitis) Page ( 1 ) Tennis elbow, or lateral epicondylitis, is a painful condition of the elbow caused by overuse. Not surprisingly, playing tennis or other racquet sports can
1st Edition 2015. Quick reference guide for the management of acute whiplash. associated disorders
 1 1st Edition 2015 Quick reference guide for the management of acute whiplash associated disorders 2 Quick reference guide for the management of acute whiplash associated disorders, 2015. This quick reference
1 1st Edition 2015 Quick reference guide for the management of acute whiplash associated disorders 2 Quick reference guide for the management of acute whiplash associated disorders, 2015. This quick reference
CONSENT FOR STEROID INJECTION
 CONSENT FOR STEROID INJECTION What is Cortisone? Cortisone is the name used to describe a group of drugs correctly known as corticosteroids. Cortisone is used to treat pain in various parts of the body
CONSENT FOR STEROID INJECTION What is Cortisone? Cortisone is the name used to describe a group of drugs correctly known as corticosteroids. Cortisone is used to treat pain in various parts of the body
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Athletic/Sports Massage
 CHAPTER18 Athletic/Sports Massage COMPLETION: In the space(s) provided, write the word(s) that correctly complete(s) each statement. 1. The 1972 Olympic gold medalist who was known as the flying Finn and
CHAPTER18 Athletic/Sports Massage COMPLETION: In the space(s) provided, write the word(s) that correctly complete(s) each statement. 1. The 1972 Olympic gold medalist who was known as the flying Finn and
Chapter 11. Everting skin edges
 Chapter 11 PRIMARY WOUND CLOSURE KEY FIGURE: Everting skin edges In primary wound closure, the skin edges of the wound are sutured together to close the defect. Whenever possible and practical, primary
Chapter 11 PRIMARY WOUND CLOSURE KEY FIGURE: Everting skin edges In primary wound closure, the skin edges of the wound are sutured together to close the defect. Whenever possible and practical, primary
Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario
 Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Sports Injury Treatment
 Sports Injury Treatment Participating in a variety of sports is fun and healthy for children and adults. However, it's critical that before you participate in any sport, you are aware of the precautions
Sports Injury Treatment Participating in a variety of sports is fun and healthy for children and adults. However, it's critical that before you participate in any sport, you are aware of the precautions
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
.org. Achilles Tendinitis. Description. Cause. Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel.
 Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Lateral pterygoid muscle Medial pterygoid muscle
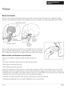 PATIENT INFORMATION BOOKLET Trismus Normal Jaw Function The jaw is a pair of bones that form the framework of the mouth and teeth. The upper jaw is called the maxilla. The lower jaw is called the mandible.
PATIENT INFORMATION BOOKLET Trismus Normal Jaw Function The jaw is a pair of bones that form the framework of the mouth and teeth. The upper jaw is called the maxilla. The lower jaw is called the mandible.
A Syndrome (Pattern) Approach to Low Back Pain. History
 A Syndrome (Pattern) Approach to Low Back Pain Hamilton Hall MD FRCSC Professor, Department of Surgery, University of Toronto Medical Director, CBI Health Group Executive Director, Canadian Spine Society
A Syndrome (Pattern) Approach to Low Back Pain Hamilton Hall MD FRCSC Professor, Department of Surgery, University of Toronto Medical Director, CBI Health Group Executive Director, Canadian Spine Society
THORACIC OUTLET SYNDROME
 THORACIC OUTLET SYNDROME The Problem The term thoracic outlet syndrome is used to describe a condition of compression of the nerves and/or blood vessels in the region around the neck and collarbone, called
THORACIC OUTLET SYNDROME The Problem The term thoracic outlet syndrome is used to describe a condition of compression of the nerves and/or blood vessels in the region around the neck and collarbone, called
A Patient s Guide to Rib Joint Pain
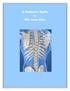 A Patient s Guide to Rib Joint Pain Anatomy Where are the rib joints? Your rib cage is made up of twelve pairs of ribs. The ribs attach to the spine in the back, and to the breastbone in the front. The
A Patient s Guide to Rib Joint Pain Anatomy Where are the rib joints? Your rib cage is made up of twelve pairs of ribs. The ribs attach to the spine in the back, and to the breastbone in the front. The
NIH Clinical Center Patient Education Materials Giving a subcutaneous injection
 NIH Clinical Center Patient Education Materials What is a subcutaenous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous injection into the fatty
NIH Clinical Center Patient Education Materials What is a subcutaenous injection? A subcutaneous injection is given in the fatty layer of tissue just under the skin. A subcutaneous injection into the fatty
Shoulder Impingement/Rotator Cuff Tendinitis
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Impingement/Rotator Cuff Tendinitis One of the most common physical complaints is shoulder pain. Your shoulder is made up of several joints
Herniated Lumbar Disc
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
X-Plain Trigeminal Neuralgia Reference Summary
 X-Plain Trigeminal Neuralgia Reference Summary Introduction Trigeminal neuralgia is a condition that affects about 40,000 patients in the US every year. Its treatment mostly involves the usage of oral
X-Plain Trigeminal Neuralgia Reference Summary Introduction Trigeminal neuralgia is a condition that affects about 40,000 patients in the US every year. Its treatment mostly involves the usage of oral
Arthritis www.patientedu.org
 written by Harvard Medical School Arthritis www.patientedu.org Arthritis is the most common chronic disease in the world, and it s the leading cause of disability in the United States. There are more than
written by Harvard Medical School Arthritis www.patientedu.org Arthritis is the most common chronic disease in the world, and it s the leading cause of disability in the United States. There are more than
EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella)
 EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella) Description Maintain appropriate conditioning: Excessive lateral patellar compression syndrome is characterized by pain in the knee
EXCESSIVE LATERAL PATELLAR COMPRESSION SYNDROME (Chondromalacia Patella) Description Maintain appropriate conditioning: Excessive lateral patellar compression syndrome is characterized by pain in the knee
A Patient s Guide to Guyon s Canal Syndrome
 A Patient s Guide to DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete or timely. It does not cover all diseases, physical conditions, ailments or
A Patient s Guide to DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete or timely. It does not cover all diseases, physical conditions, ailments or
Herniated Cervical Disc
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Evaluating muscle injuries and residuals of shell fragment and gunshot wounds
 Evaluating muscle injuries and residuals of shell fragment and gunshot wounds Training conducted by: Michael Fishman and Sandrine Fisher 1 Objectives To become familiar with the application of the rating
Evaluating muscle injuries and residuals of shell fragment and gunshot wounds Training conducted by: Michael Fishman and Sandrine Fisher 1 Objectives To become familiar with the application of the rating
Page 2 of 6 plantar fascia. This is called the windlass mechanism. Later, we'll discuss how this mechanism is used to treat plantar fasciitis with str
 Page 1 of 6 Plantar Fasciitis (Heel Pain) Plantar fasciitis is a painful condition affecting the bottom of the foot. It is a common cause of heel pain and is sometimes called a heel spur. Plantar fasciitis
Page 1 of 6 Plantar Fasciitis (Heel Pain) Plantar fasciitis is a painful condition affecting the bottom of the foot. It is a common cause of heel pain and is sometimes called a heel spur. Plantar fasciitis
UNDERSTANDING STRESS AND YOUR BODY
 UNDERSTANDING STRESS AND YOUR BODY Life s demands create stress and although some stress may be good, too much can cause health problems. Most people equate stress with high blood pressure, a heart attack
UNDERSTANDING STRESS AND YOUR BODY Life s demands create stress and although some stress may be good, too much can cause health problems. Most people equate stress with high blood pressure, a heart attack
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Ankle Block. Indications The ankle block is suitable for the following: Orthopedic and podiatry surgical procedures of the distal foot.
 Ankle Block The ankle block is a common peripheral nerve block. It is useful for procedures of the foot and toes, as long as a tourniquet is not required above the ankle. It is a safe and effective technique.
Ankle Block The ankle block is a common peripheral nerve block. It is useful for procedures of the foot and toes, as long as a tourniquet is not required above the ankle. It is a safe and effective technique.
PERFORMANCE RUNNING. Piriformis Syndrome
 Piriformis Syndrome Have you started to experience pain in your hip or down your leg while beginning or advancing your fitness program? This pain may be stemming from the piriformis muscle in your hip.
Piriformis Syndrome Have you started to experience pain in your hip or down your leg while beginning or advancing your fitness program? This pain may be stemming from the piriformis muscle in your hip.
Imagine LIFE WITHOUT PAIN
 Imagine LIFE WITHOUT PAIN High Dosage Laser Therapy (HDLT) What does it do? High Dosage Laser Therapy (HDLT) from Diowave offers a powerful new solution for numerous painful conditions previously refractive
Imagine LIFE WITHOUT PAIN High Dosage Laser Therapy (HDLT) What does it do? High Dosage Laser Therapy (HDLT) from Diowave offers a powerful new solution for numerous painful conditions previously refractive
CONSTRUCTION WORK and CUMULATIVE TRAUMA DISORDERS
 Connecticut Department of Public Health Environmental and Occupational Health Assessment Program 410 Capitol Avenue MS # 11OSP, PO Box 340308 Hartford, CT 06134-0308 (860) 509-7740 http://www.ct.gov/dph
Connecticut Department of Public Health Environmental and Occupational Health Assessment Program 410 Capitol Avenue MS # 11OSP, PO Box 340308 Hartford, CT 06134-0308 (860) 509-7740 http://www.ct.gov/dph
Musculoskeletal System
 CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Offering Solutions for The Management of Pain
 Integrative Pain Treatment Center Integrative Pain Treatment Center Offering Solutions for The Management of Pain ADACHES BACK AND NECK PAIN FIBROMYALGIA MYOFASCIAL PAIN ARTHRITIS SPINAL STENOSIS JOINT
Integrative Pain Treatment Center Integrative Pain Treatment Center Offering Solutions for The Management of Pain ADACHES BACK AND NECK PAIN FIBROMYALGIA MYOFASCIAL PAIN ARTHRITIS SPINAL STENOSIS JOINT
What is the Spasticity Clinic?
 The Spasticity Clinic This booklet can help you learn about: the Spasticity Clinic at McMaster Children s Hospital spasticity and how it may be treated Your therapist will give you more information and
The Spasticity Clinic This booklet can help you learn about: the Spasticity Clinic at McMaster Children s Hospital spasticity and how it may be treated Your therapist will give you more information and
Elbow Examination. Haroon Majeed
 Elbow Examination Haroon Majeed Key Points Inspection Palpation Movements Neurological Examination Special tests Joints above and below Before Starting Introduce yourself Explain to the patient what the
Elbow Examination Haroon Majeed Key Points Inspection Palpation Movements Neurological Examination Special tests Joints above and below Before Starting Introduce yourself Explain to the patient what the
The Neck: Whiplash & Central Ligament Sprains. Presented by Dr. Ben Benjamin
 Debilitating Orthopedic Injury Sampler #1 The Neck: Whiplash & Central Ligament Sprains Presented by Dr. Ben Benjamin Instructor: Ben Benjamin, Ph.D. 2 1 Instructor: Ben Benjamin, Ph.D. [email protected]
Debilitating Orthopedic Injury Sampler #1 The Neck: Whiplash & Central Ligament Sprains Presented by Dr. Ben Benjamin Instructor: Ben Benjamin, Ph.D. 2 1 Instructor: Ben Benjamin, Ph.D. [email protected]
*A discrete, hypersensitive nodule within tight band of muscle or fascia that present with classic pattern of pain referral that does not follow
 A patient presents with c/o cervical spine pain and chronic headaches that radiates across the top of his head. He also experiences frequent bouts of nausea, dizziness and indigestion. The patient also
A patient presents with c/o cervical spine pain and chronic headaches that radiates across the top of his head. He also experiences frequent bouts of nausea, dizziness and indigestion. The patient also
Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions
 Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises Artwork and slides taken from the book Clinical
Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises Artwork and slides taken from the book Clinical
COMPUTER-RELATED MUSCLE, TENDON, AND JOINT INJURIES
 CHAPTER ELEVEN COMPUTER-RELATED MUSCLE, TENDON, AND JOINT INJURIES To reduce the risk of pain in your neck and shoulders, stay within these recommended ranges of movement: Neck Flexion: 0 o -15 o (bending
CHAPTER ELEVEN COMPUTER-RELATED MUSCLE, TENDON, AND JOINT INJURIES To reduce the risk of pain in your neck and shoulders, stay within these recommended ranges of movement: Neck Flexion: 0 o -15 o (bending
Psoas Syndrome. The pain is worse from continued standing and from twisting at the waist without moving the feet.
 Psoas Syndrome The iliopsoas muscle is a major body mover but seldom considered as a source of pain. Chronic lower back pain involving the hips, legs, or thoracic regions can often be traced to an iliopsoas
Psoas Syndrome The iliopsoas muscle is a major body mover but seldom considered as a source of pain. Chronic lower back pain involving the hips, legs, or thoracic regions can often be traced to an iliopsoas
Arthritis of the Shoulder
 Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Arthritis of the Shoulder In 2011, more than 50 million people in the United States reported that they had been diagnosed with some form of arthritis, according to the National Health Interview Survey.
Rehabilitation Documentation and Proper Coding Guidelines
 Rehabilitation Documentation and Proper Coding Guidelines Purpose: 1) Develop a guide for doctors in South Dakota to follow when performing reviews on rehabilitation cases. 2) Provide doctors in South
Rehabilitation Documentation and Proper Coding Guidelines Purpose: 1) Develop a guide for doctors in South Dakota to follow when performing reviews on rehabilitation cases. 2) Provide doctors in South
Hand & Plastics Physiotherapy Department Carpal Tunnel Syndrome Information for patients
 Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Carpal Tunnel Syndrome Information for patients page 2 What is the Carpal Tunnel? The carpal tunnel is made up of the bones
Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Carpal Tunnel Syndrome Information for patients page 2 What is the Carpal Tunnel? The carpal tunnel is made up of the bones
Hand Injuries and Disorders
 Hand Injuries and Disorders Introduction Each of your hands has 27 bones, 15 joints and approximately 20 muscles. There are many common problems that can affect your hands. Hand problems can be caused
Hand Injuries and Disorders Introduction Each of your hands has 27 bones, 15 joints and approximately 20 muscles. There are many common problems that can affect your hands. Hand problems can be caused
Standard of Care: Cervical Radiculopathy
 Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
Lower Back Pain An Educational Guide
 Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
1 of 6 1/22/2015 10:06 AM
 1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
Interscalene Block. Nancy A. Brown, MD
 Interscalene Block Nancy A. Brown, MD What is an Interscalene Block? An Interscalene block is a form of regional anesthesia used in conjunction with general anesthesia for surgeries of the shoulder and
Interscalene Block Nancy A. Brown, MD What is an Interscalene Block? An Interscalene block is a form of regional anesthesia used in conjunction with general anesthesia for surgeries of the shoulder and
STANDARD OPERATING PROCEDURE. Administration of High Dose Muscular Vitamin Supplements for Undergoing Alcohol
 STANDARD OPERATING PROCEDURE Administration of High Dose Muscular Vitamin Supplements for Undergoing Alcohol DOCUMENT CONTROL: Version: 2 Ratified by: Clinical Effectiveness Committee Date ratified: 03
STANDARD OPERATING PROCEDURE Administration of High Dose Muscular Vitamin Supplements for Undergoing Alcohol DOCUMENT CONTROL: Version: 2 Ratified by: Clinical Effectiveness Committee Date ratified: 03
INFORMATION FOR YOU. Lower Back Pain
 INFORMATION FOR YOU Lower Back Pain WHAT IS ACUTE LOWER BACK PAIN? Acute lower back pain is defined as low back pain present for up to six weeks. It may be experienced as aching, burning, stabbing, sharp
INFORMATION FOR YOU Lower Back Pain WHAT IS ACUTE LOWER BACK PAIN? Acute lower back pain is defined as low back pain present for up to six weeks. It may be experienced as aching, burning, stabbing, sharp
Diagnosis of Acromioclavicular Joint Injuries
 PO Box 15 Rocky Hill, CT 06067 (860) 463-9003 [email protected] www.chirocredit.com ChiroCredit.com is proud to present a section from one of our continuing education programs: Physical Diagnosis
PO Box 15 Rocky Hill, CT 06067 (860) 463-9003 [email protected] www.chirocredit.com ChiroCredit.com is proud to present a section from one of our continuing education programs: Physical Diagnosis
Stretching the Major Muscle Groups of the Lower Limb
 2 Stretching the Major Muscle Groups of the Lower Limb In this chapter, we present appropriate stretching exercises for the major muscle groups of the lower limb. All four methods (3S, yoga, slow/static,
2 Stretching the Major Muscle Groups of the Lower Limb In this chapter, we present appropriate stretching exercises for the major muscle groups of the lower limb. All four methods (3S, yoga, slow/static,
Dr. Enas Elsayed. Brunnstrom Approach
 Brunnstrom Approach Learning Objectives: By the end of this lab, the student will be able to: 1. Demonstrate different reflexes including stimulus and muscle tone response. 2. Demonstrate how to evoke
Brunnstrom Approach Learning Objectives: By the end of this lab, the student will be able to: 1. Demonstrate different reflexes including stimulus and muscle tone response. 2. Demonstrate how to evoke
Natural Modality in the Treatment of Primary Headaches. William S. Mihin, D.C. Catharine Helms, M.S. Michelle M. Anderson, M.S.N., F.N.P.
 Natural Modality in the Treatment of Primary Headaches William S. Mihin, D.C. Catharine Helms, M.S. Michelle M. Anderson, M.S.N., F.N.P. Abstract Headaches are both a prevalent and disabling condition.
Natural Modality in the Treatment of Primary Headaches William S. Mihin, D.C. Catharine Helms, M.S. Michelle M. Anderson, M.S.N., F.N.P. Abstract Headaches are both a prevalent and disabling condition.
Muscular System. Principles of Health Science Dr. Wood
 Muscular System Principles of Health Science Dr. Wood Characteristics of muscles Excitability: : irritability or ability to respond to stimulus Contractibility: : ability to contract (become short and
Muscular System Principles of Health Science Dr. Wood Characteristics of muscles Excitability: : irritability or ability to respond to stimulus Contractibility: : ability to contract (become short and
Fact Sheet: Occupational Overuse Syndrome (OOS)
 Fact Sheet: Occupational Overuse Syndrome (OOS) What is OOS? Occupational Overuse Syndrome (OOS) is the term given to a range of conditions characterised by discomfort or persistent pain in muscles, tendons
Fact Sheet: Occupational Overuse Syndrome (OOS) What is OOS? Occupational Overuse Syndrome (OOS) is the term given to a range of conditions characterised by discomfort or persistent pain in muscles, tendons
National Hospital for Neurology and Neurosurgery. Managing Spasticity. Spasticity Service
 National Hospital for Neurology and Neurosurgery Managing Spasticity Spasticity Service If you would like this document in another language or format, or require the services of an interpreter please contact
National Hospital for Neurology and Neurosurgery Managing Spasticity Spasticity Service If you would like this document in another language or format, or require the services of an interpreter please contact
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
THE WRIST. At a glance. 1. Introduction
 THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
Oh, 14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8
 14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8 Oh, my aching head NEW DOCTOR TEAM ADDRESSES CHRONIC HEADACHE PROBLEMS SEVERE HEADACHES IN THIS COUNTRY ARE A LEADING CAUSE OF DISRUP- TION
14 C O M M U N I T Y M A G A Z I N E S M A Y / J U N E 2 0 0 8 Oh, my aching head NEW DOCTOR TEAM ADDRESSES CHRONIC HEADACHE PROBLEMS SEVERE HEADACHES IN THIS COUNTRY ARE A LEADING CAUSE OF DISRUP- TION
Whiplash and Cervical Spine Disorders: Evaluation and Management
 Whiplash and Cervical Spine Disorders: Evaluation and Management Dr. Corrie Graboski Definition by Quebec Task Force Pain Generators an acceleration-deceleration mechanism of energy transfer to the neck
Whiplash and Cervical Spine Disorders: Evaluation and Management Dr. Corrie Graboski Definition by Quebec Task Force Pain Generators an acceleration-deceleration mechanism of energy transfer to the neck
Lumbar Disc Herniation/Bulge Protocol
 Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE
 TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE The temporomandibular joint is the point at which the mandible (lower jaw) hinges on the skull. Frequently, the pain experienced is ear pain, s o patients are
TMJ DISEASE TEMPOROMANDIBULAR JOINT DISEASE The temporomandibular joint is the point at which the mandible (lower jaw) hinges on the skull. Frequently, the pain experienced is ear pain, s o patients are
Medical Treatment Guidelines Washington State Department of Labor and Industries
 Complex regional pain syndrome (CRPS) Formerly known as reflex sympathetic dystrophy 1. Introduction This bulletin outlines the Department of Labor and Industries guidelines for diagnosing and treating
Complex regional pain syndrome (CRPS) Formerly known as reflex sympathetic dystrophy 1. Introduction This bulletin outlines the Department of Labor and Industries guidelines for diagnosing and treating
Treatment of Spastic Foot Deformities
 Penn Comprehensive Neuroscience Center Treatment of Spastic Foot Deformities Penn Neuro-Orthopaedics Service 1 Table of Contents Overview Overview 1 Treatment 2 Procedures 4 Achilles Tendon Lengthening
Penn Comprehensive Neuroscience Center Treatment of Spastic Foot Deformities Penn Neuro-Orthopaedics Service 1 Table of Contents Overview Overview 1 Treatment 2 Procedures 4 Achilles Tendon Lengthening
Flexibility Assessment and Improvement Compiled and Adapted by Josh Thompson
 Flexibility Assessment and Improvement Compiled and Adapted by Josh Thompson Muscles must have a full and normal range of motion in order for joints and skeletal structure to function properly. Flexibility
Flexibility Assessment and Improvement Compiled and Adapted by Josh Thompson Muscles must have a full and normal range of motion in order for joints and skeletal structure to function properly. Flexibility
Abdominal Wall Pain. What is Abdominal Wall Pain?
 Abdominal Wall Pain What is Abdominal Wall Pain? Abdominal Wall Pain is a syndrome (an experience) of abdominal pain that can occur at any time of life and is not unique to children. It is diagnosed by
Abdominal Wall Pain What is Abdominal Wall Pain? Abdominal Wall Pain is a syndrome (an experience) of abdominal pain that can occur at any time of life and is not unique to children. It is diagnosed by
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN
 CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
Westmount UCC 751 Victoria Street South, Kitchener, ON N2M 5N4 519-745-2273 Fairway UCC 385 Fairway Road South, Kitchener, ON N2C 2N9 519-748-2327
 K-W URGENT CARE CLINICS INC. Westmount UCC 751 Victoria Street South, Kitchener, ON N2M 5N4 519-745-2273 Fairway UCC 385 Fairway Road South, Kitchener, ON N2C 2N9 519-748-2327 OPEN Mon-Fri 8am-5pm, Sa
K-W URGENT CARE CLINICS INC. Westmount UCC 751 Victoria Street South, Kitchener, ON N2M 5N4 519-745-2273 Fairway UCC 385 Fairway Road South, Kitchener, ON N2C 2N9 519-748-2327 OPEN Mon-Fri 8am-5pm, Sa
Overuse injuries. 1. Main types of injuries
 OVERUSE INJURIES Mr. Sansouci is an ardent runner and swimmer. To train for an upcoming 10-km race, he has decided to increase the intensity of his training. Lately, however, his shoulder and Achilles
OVERUSE INJURIES Mr. Sansouci is an ardent runner and swimmer. To train for an upcoming 10-km race, he has decided to increase the intensity of his training. Lately, however, his shoulder and Achilles

 Full version is >>> HERE
Full version is >>> HERE