Scandinavian Journal of Surgery 103: , 2014
|
|
|
- Martin Holland
- 9 years ago
- Views:
Transcription
1 509984SJS / Six-month results of RCT on SG vs RYGBM. Helmiö, et al. research-article2014 Original Article Scandinavian Journal of Surgery 103: , 2014 Comparison of short-term outcome of laparoscopic sleeve gastrectomy and gastric bypass in the treatment of morbid obesity: A Prospective Randomized Controlled Multicenter Sleevepass Study With 6-Month Follow-Up M. Helmiö 1, M. Victorzon 2, J. Ovaska 1, M. Leivonen 3, A. Juuti 3, P. Peromaa- Haavisto 2,4, P. Nuutila 5,6, T. Vahlberg 7, P. Salminen 1 1 Division of Digestive Surgery and Urology, Turku University Hospital, Turku, Finland 2 Department of Surgery, Vaasa Central Hospital, Vaasa, Finland 3 Department of Surgery, Helsinki University Central Hospital, Vantaa, Finland 4 Department of Surgery, Hatanpää Hospital, Tampere, Finland 5 Turku PET Centre, University of Turku, Turku, Finland 6 Department of Medicine, Turku University Hospital, Turku, Finland 7 Department of Biostatistics, University of Turku, Turku, Finland Abstract Background and Aims: The long-term efficacy of laparoscopic Roux-en-Y gastric bypass in the treatment of morbid obesity has already been demonstrated. Laparoscopic sleeve gastrectomy has shown promising short-term results, but the long-term efficacy is still unclear. The aim of this prospective randomized multicenter study is to compare the results of Roux-en-Y gastric bypass and sleeve gastrectomy. Material and Methods: A total of 240 morbidly obese patients were randomized to undergo either Roux-en-Y gastric bypass or sleeve gastrectomy. The primary end point of study was weight loss, and the secondary end points were resolution of comorbidities and morbidity. The short-term results at 6 months were analyzed. Results: The mean excess weight loss at 6 months was 49.2% in the sleeve gastrectomy group and 52.9% in the Roux-en-Y gastric bypass group (p = 0.086). Type 2 diabetes was resolved or improved in 84.3% of patients in the sleeve gastrectomy group and 93.3% in the Roux-en-Y gastric bypass group (p = 0.585). The corresponding results for arterial hypertension were 76.8% and 81.9% (p = 0.707) and for hypercholesterolemia 64.1% and 69.0% (p = 0.485). There was no mortality at 6 months. There was one major complication following sleeve gastrectomy and two after Roux-en-Y gastric bypass (p = 0.531). Eight sleeve gastrectomy patients and 11 Roux-en-Y gastric bypass patients had minor complications (p = 0.403). Correspondence: Mika Helmiö, M.D. Division of Digestive Surgery and Urology Turku University Hospital PL 52 FIN Turku Finland [email protected]
2 176 M. Helmiö, et al. Conclusion: The short-term results of sleeve gastrectomy and Roux-en-Y gastric bypass regarding weight loss, resolution of obesity-related comorbidities and complications were not different at 6 months. Key words: Bariatric surgery; morbid obesity; sleeve gastrectomy; gastric bypass; randomized study Introduction Bariatric surgery is the most effective treatment for morbid obesity and the long-term results regarding weight loss and improvement of obesity-related comorbidities have been well established (1, 2). Laparoscopic Roux-en-Y gastric bypass (RYGB) is considered the gold standard in bariatric surgery providing significant and sustained weight loss resulting in resolution or improvement of obesity-related comorbidities at long-term follow-up (3, 4). However, during the last few years, laparoscopic sleeve gastrectomy (SG) has increasingly been performed as a primary procedure. SG was first described in the 1990s by Marceau et al. (5) and Hess and Hess (6) as part of the duodenal switch operation, then introduced as a first step of a two-stage operation for high-risk super obese patients (7). The promising short-term results of SG have somewhat altered the paradigm for SG from a two-stage procedure to a stand-alone definitive bariatric procedure (8 12). As RYGB is the gold standard in bariatric surgery, all other procedures should be compared with RYGB. However, to our knowledge, there are only few reports of randomized prospective studies comparing RYGB and SG with a small number of patients and a short follow-up (13 16). The available long-term results of SG are also scarce (9, 11, 17 19). SG is perceived less invasive, technically simpler and easier to perform compared with RYGB. The possible long-term benefits of SG include an intact gastrointestinal tract, the absence of internal hernias, and the lack of malabsorption requiring lifelong follow-up of nutritional status. SG could thus become the procedure of choice in treating morbid obesity provided that the long-term results of SG are comparable with RYGB regarding weight loss, the resolution of comorbidities, and improvement in the quality of life. The aim of this prospective randomized multicenter SLEEVEPASS study is to compare RYGB and SG in the treatment of morbid obesity and to report our shortterm outcome at 6 months regarding weight loss, resolution of obesity associated comorbidities, and overall morbidity. Material And Methods SLEEVEPASS study was carried out at three tertiary referral hospitals in Finland. Between April 2008 and June 2010, a total of 240 patients assigned for surgical treatment for morbid obesity were randomized to undergo either laparoscopic SG or RYGB. The randomization was done by a closed envelope method at the preoperative visit. The study was approved by the Ethics Committee of Turku University Hospital, and a written informed consent was obtained from all patients. The inclusion criteria for the study were (1) body mass index (BMI) 40 or BMI 35 with a significant comorbidity associated with morbid obesity (type 2 diabetes, hypertension, obstructive sleep apnea, dyslipidemia, and arthrosis), (2) age years, and (3) previous successfully instituted and supervised but failed adequate diet and exercise program. The exclusion criteria included BMI > 60, significant psychiatric disorder, severe eating disorder (binge eating), active alcohol or substance abuse, active gastric ulcer disease, difficult gastroesophageal reflux disease (GERD) with a large hiatal hernia, and previous bariatric surgery. Both study groups were similar regarding age, gender, BMI, and comorbidities. The preoperative evaluation and surgical techniques have been described in detail together with the 30-day preliminary results (20). The primary end point of the SLEEVEPASS trial is weight loss. The secondary end points assess the associated resolution of obesity-related comorbidities, the improvement of quality of life, and the overall morbidity and mortality of the procedures. According to our study protocol, the patients came to postoperative outpatient control visits at 3 and 6 months. All the data concerning weight loss, state of obesity-related comorbidities, and possible complications were thoroughly recorded. Postoperatively obesity-related comorbidities were classified as persisting (medication same as preoperatively), improved (reduction in medication), or resolved (no more need for medication) after a consulting endocrinologist visit. Postoperative complications were classified as major or minor; morbidity resulting in death or a reoperation, a hospital stay exceeding 7 days, or a need for blood transfusions of four or more units constituted a major complication. All other postoperative problems were evaluated as minor complications. Statistical Analyses Sample size calculations were based on a test of mean difference between bypass and sleeve procedures in excessive weight loss (EWL) in 1 year. A mean of 60 and standard deviation (SD) of 20 in the bypass group were assumed and α-level of 0.05 was used in calculations. By using an equivalence design with a margin of equivalence of 15% ( 9 to 9), a sample size of 108 patients per group is needed for 90% power. When a 10% dropout is taken into account, 120 patients per group were enrolled in the study. Categorical variables were characterized using frequencies and percents. For normally distributed continuous variables mean, range, and SD and for non-normally distributed continuous variables median and range were used. Associations between
3 Six-month results of RCT on SG vs RYGB 177 Fig. 1. CONSORT flowchart for the trial. categorical variables were statistically tested using Pearson s χ 2 test, and for small frequencies, Fisher s exact test was used. Differences between groups in normally distributed continuous variables were tested using independent samples t test, and for non-normally distributed variables, the Mann Whitney U test was used. The p-values < 0.05 were considered statistically significant. Statistical analyses were performed using SAS System for Windows ver. 9.2 (SAS Institute, Cary, NC, USA). Results Altogether 121 patients were operated in the SG group and 117 in the RYGB group. The follow-up results at 6 months were obtained from 119 patients in the SG group (98.3% follow-up rate) and 111 patients in the RYGB group (93.3% follow-up rate). The CONSORT 6-month flowchart is presented in Fig. 1. The mean excess weight loss (EWL) at 6 months was 51.0% (range: 10.7% 94.8%, SD: 16.4%), and there was no statistical difference between the study groups (p = 0.086). The mean postoperative EWL and median postoperative BMI at 3 and 6 months are presented in detail in Figs 2 and 3. Type 2 diabetes was resolved or improved in 84.3% of patients in the SG group and 93.3% in the RYGB group (p = 0.585). The corresponding results for arterial hypertension were 76.8% and 81.9% (p = 0.707) and for hypercholesterolemia 64.1% and 69.0% (p = 0.485). The detailed data on comorbidity resolution are presented in Figs 4 to 6. There was no mortality at 6 months. All the major and minor postoperative complications between 30 days and 6 months are presented in detail in Table 1. There was one (0.8%) major complication following SG and two (1.8%) after RYGB (p = 0.531). Eight (6.7%) SG patients and 11 (9.9%) RYGB patients had minor complications (p = 0.403). The readmission rate was 4.2% for SG and 2.7% for RYGB. There was one reoperation in the RYGB group between 1 and 6 months postoperatively due to incarcerated incisional hernia at the trocar site successfully treated by relaparoscopy. Discussion RYGB is a safe and effective bariatric procedure with excellent long-term results regarding weight loss and resolution of obesity-related comorbidities (3, 21). However, in recent years, SG has attracted vast surgical interest because of its perceived technical simplicity and feasibility compared with RYGB. In addition to this, SG also has possible long-term advantages over RYGB such as preservation of endoscopic access to the upper gastrointestinal tract, prevention of the dumping syndrome by pylorus preservation, normal
4 178 M. Helmiö, et al. Fig. 2. Mean percent EWL at 3 and 6 months. Values are mean (minimum maximum; SD). EWL: excess weight loss; SD: standard deviation. Fig. 3. Median BMI at baseline and 3 and 6 months. Values are median (minimum maximum). BMI: body mass index. Fig. 5. Percent resolution of arterial hypertension at 3 and 6 months. Fig. 4. Percent resolution of DM2 at 3 and 6 months. DM2: type 2 diabetes mellitus. Fig. 6. Percent resolution of hypercholesterolemia at 3 and 6 months. intestinal absorption, and avoiding the risk of internal herniation associated with RYGB anastomosis. Most of the weight loss after bariatric surgery takes place during the first 6 months after the operation.
5 Six-month results of RCT on SG vs RYGB 179 Table 1 Detailed comparison of major and minor postoperative complications after laparoscopic SG and RYGB between 30 days and 6 months. Complication SG minor RYGB minor SG major RYGB major Intra-abdominal infection/ 2 infection of unknown origin Pneumonia 1 1 Reflux esophagitis 1 Stricture at GEJ 1 Ketoacidosis 1 Persistent difficulties in eating 1 Dumping 1 3 Ulcer/stricture at GJA 4 Persisting trocar site pain 1 Diarrhea 1 Dehydration 1 1 Recurrent aspirational pneumonia 1 Incarcerated incisional hernia 1 Total 8 (6.7%) 11 (9.9%) 1 (0.8%) 2 (1.8%) SG: sleeve gastrectomy; RYGB: Roux-en-Y gastric bypass; GEJ: gastroesophageal junction; GJA: gastojejunal anastomosis. Values are n (%). After this, the weight loss gradually slows down continuing up to 2 years postoperatively often followed by a slight regain in weight in the next few years. The short-term follow-up of 6 months may be assessed as a weak point of our study. However, considering this paradigm and schedule of postoperative weight loss, we evaluated the weight loss results and resolution of comorbidities between the study groups to be of importance already at this short-term follow-up especially as randomized studies comparing these bariatric procedures are so scarce. This weight loss tendency can be identified after all bariatric procedures, and despite this slight postoperative weight regain, the long-term weight loss results of bariatric surgery are clearly superior compared to conservative treatment as demonstrated by Sjöström et al. (4) in the Swedish obese subject (SOS) study. In this prospective randomized study, we have demonstrated that at 6 months postoperatively, the EWL of SG and RYGB is similar. There are reports from nonrandomized trials on tendency for weight regain after SG at 3 5 years following surgery (9, 11). However, this is a general phenomenon following bariatric surgery, and it is not specifically related only to SG. On the contrary, Boza et al. (12) have recently reported excellent results of 1000 consecutive SG procedures with a mean EWL of 84.5% at 3-year follow-up and with minimal weight regain after the first postoperative year. The available data on EWL following SG are largely based on follow-up of only up to 2 years. In a recent systematic review by Fischer et al., a total of 12,129 SG patients were analyzed and 3-year follow-up data were available in only eight studies resulting in a total of 363 patients (3.0%), and 5-year follow-up results were available from only 64 patients (0.5%). The mean EWL of 49.2% in our SG study group at 6 months is comparable with the corresponding 45.2% from 42 articles included in this review article (17). The technical aspects of SG somewhat lack standardization. The use of a smaller bougie size as calibration during the operation has been reported to associate with a better weight loss and resolution of comorbidities, but on the contrary also with a higher leak rate (22 24). Similarly, the preservation of the antrum and the use of reinforced staple lines have been controversial issues. Recently, an expert panel consensus statement on best practice guidelines for SG was published addressing several of these technical issues as well as indications and contraindications for SG and also evaluating both management and prevention of complications (25). As there is variety in the published data regarding these technical details of SG, we aimed to standardize our procedures, and all the sleeves were created narrow using Fr bougie, the distal resection was started 4 6 cm proximal to the pylorus, and all the staple lines were reinforced (20). From the obesity-related comorbidities type 2 diabetes, arterial hypertension and hypercholesterolemia were analyzed. The state of these comorbid conditions was easy to evaluate in our study as all of the patients underwent regular postoperative endocrinologist evaluation. In this prospective randomized study, we have demonstrated that at 6-month follow-up, the improvement or resolution of these obesity-related comorbidities is equally good between SG and RYGB. Similar results have also been shown in previous randomized or prospective studies only with a smaller number of patients (13, 15, 26). In Finland as a whole, bariatric surgery has only been performed on a larger scale for the last few years. When our SLEEVEPASS study was initiated in 2008, there were only 430 bariatric procedures performed that year in the whole country, but the number of operations has since been steadily growing. There are no hospitals specialized only in bariatric surgery in Finland, and none of the hospitals performing bariatric surgery can be considered a high-volume center. All of the surgeons performing the procedures were experienced laparoscopists with relative personal experience on bariatric surgery. These factors present
6 180 M. Helmiö, et al. a weakness in our study as both the individual and the institutional learning curve effect may have a role in the relatively high complication rates when compared with some previous studies (27 29). For example, the overall morbidity in our SG study group is 20.7% when the early 30-day results (20) are also taken into account, and this is somewhat higher than the 0.0% 17.7% morbidity rates presented in the studies included in the review article by Fischer et al. (17). However, the direct and valid comparison of complication rates in different studies is difficult as the definition and reporting of complications varies significantly emphasizing the need for standardized and concise international criteria for grading postoperative complications after bariatric surgery. On the contrary, the reported complication rates in this study also present a strong element of our trial as special emphasis was focused on the thorough prospective recording of all major and minor complications. A strong advantage of this study is the randomized prospective multicenter setting. The group of patients in our study can be considered to represent average candidates for bariatric surgery and the patient selection was done according to generally accepted international guidelines (30). Due to the multicenter nature, the results may be applied on a larger scale, compared with specialized high-volume bariatric centers. In conclusion, at 6-month analysis, there were no statistical differences between SG and RYGB regarding weight loss, resolution of obesity-related comorbidities or overall morbidity. Long-term follow-up from prospective randomized trials comparing SG with RYGB is needed to elucidate the status of SG among the surgical treatment options for morbid obesity. Acknowledgements The trial was registered at clinicaltrials.gov NCT The trial was approved by the Ethics Committee of Turku University Hospital DNRO 6/ Declaration Of Conflicting Interests None declared. Funding Mika Helmiö received grants from Turku University research grant and The Finnish Medical Society Duodecim research grant. Paulina Salminen received a grant from The Mary and Georg C. Ehrnrooth Foundation. References 1. Buchwald H, Panel CC: Consensus conference statement bariatric surgery for morbid obesity: Health implications for patients, health professionals, and third-party payers. Surg Obes Relat Dis 2005;1: Maggard MA, Shugarman LR, Suttorp M et al: Meta-analysis: Surgical treatment of obesity. Ann Intern Med 2005; 142: Buchwald H, Estok R, Fahrbach K et al: Weight and type 2 diabetes after bariatric surgery: Systematic review and metaanalysis. Am J Med 2009;122: e5. 4. Sjöström L, Narbro K, Sjöström CD et al: Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med 2007; 357: Marceau P, Biron S, Bourque RA et al: Biliopancreatic diversion with a new type of gastrectomy. Obes Surg 1993;3: Hess DS, Hess DW: Biliopancreatic diversion with a duodenal switch. Obes Surg 1998; 8: Regan JP, Inabnet WB, Gagner M et al: Early experience with two-stage laparoscopic Roux-en-Y gastric bypass as an alternative in the super-super obese patient. Obes Surg 2003;13: Bohdjalian A, Langer FB, Shakeri-Leidenmühler S et al: Sleeve gastrectomy as sole and definitive bariatric procedure: 5-year results for weight loss and ghrelin. Obes Surg 2010; 20: D Hondt M, Vanneste S, Pottel H et al: Laparoscopic sleeve gastrectomy as a single-stage procedure for the treatment of morbid obesity and the resulting quality of life, resolution of comorbidities, food tolerance, and 6-year weight loss. Surg Endosc 2011;25: Chopra A, Chao E, Etkin Y et al: Laparoscopic sleeve gastrectomy for obesity: Can it be considered a definitive procedure? Surg Endosc 2012; 26: Himpens J, Dobbeleir J, Peeters G: Long-term results of laparoscopic sleeve gastrectomy for obesity. Ann Surg 2010;252: Boza C, Salinas J, Salgado N et al: Laparoscopic sleeve gastrectomy as a stand-alone procedure for morbid obesity: Report of 1,000 cases and 3-year follow-up. Obes Surg 2012; 22: Kehagias I, Karamanakos SN, Argentou M et al: Randomized clinical trial of laparoscopic Roux-en-Y gastric bypass versus laparoscopic sleeve gastrectomy for the management of patients with BMI < 50 kg/m 2. Obes Surg 2011;21: Peterli R, Steinert RE, Woelnerhanssen B et al: Metabolic and hormonal changes after laparoscopic Roux-en-Y gastric bypass and sleeve gastrectomy: A randomized, prospective trial. Obes Surg 2012; 22: Woelnerhanssen B, Peterli R, Steinert RE et al: Effects of postbariatric surgery weight loss on adipokines and metabolic parameters: Comparison of laparoscopic Roux-en-Y gastric bypass and laparoscopic sleeve gastrectomy A prospective randomized trial. Surg Obes Relat Dis 2011;7: Karamanakos SN, Vagenas K, Kalfarentzos F et al: Weight loss, appetite suppression, and changes in fasting and postprandial ghrelin and peptide-yy levels after Roux-en-Y gastric bypass and sleeve gastrectomy: A prospective, double blind study. Ann Surg 2008; 247: Fischer L, Hildebrandt C, Bruckner T et al: Excessive weight loss after sleeve gastrectomy: A systematic review. Obes Surg 2012;22: Victorzon M. An update on sleeve gastrectomy. Minerva Chir 2012; 67: Sarela AI, Dexter SP, O Kane M et al: Long-term follow-up after laparoscopic sleeve gastrectomy: 8-9-year results. Surg Obes Relat Dis 2011;8: Helmiö M, Victorzon M, Ovaska J et al: SLEEVEPASS: A randomized prospective multicenter study comparing laparoscopic sleeve gastrectomy and gastric bypass in the treatment of morbid obesity: Preliminary results. Surg Endosc 2012; 26: Garb J, Welch G, Zagarins S et al: Bariatric surgery for the treatment of morbid obesity: A meta-analysis of weight loss outcomes for laparoscopic adjustable gastric banding and laparoscopic gastric bypass. Obes Surg 2009;19: Gagner M. Leaks after sleeve gastrectomy are associated with smaller bougies: Prevention and treatment strategies. Surg Laparosc Endosc Percutan Tech 2010; 20:
7 Six-month results of RCT on SG vs RYGB Atkins ER, Preen DB, Jarman C et al: Improved obesity reduction and co-morbidity resolution in patients treated with 40-French bougie versus 50-French bougie four years after laparoscopic sleeve gastrectomy. Analysis of 294 patients. Obes Surg 2012;22: Aurora AR, Khaitan L, Saber AA: Sleeve gastrectomy and the risk of leak: A systematic analysis of 4,888 patients. Surg Endosc 2012; 26: Rosenthal RJ, Diaz AA, Arvidsson D et al: International sleeve gastrectomy expert panel consensus statement: Best practice guidelines based on experience of >12,000 cases. Surg Obes Relat Dis 2012;8: Nocca D, Guillaume F, Noel P et al: Impact of laparoscopic sleeve gastrectomy and laparoscopic gastric bypass on HbA1c blood level and pharmacological treatment of type 2 diabetes mellitus in severe or morbidly obese patients. Results of a multicenter prospective study at 1 year. Obes Surg 2011; 21: Fuks D, Verhaeghe P, Brehant O et al: Results of laparoscopic sleeve gastrectomy: A prospective study in 135 patients with morbid obesity. Surgery 2009;145: Leyba JL, Aulestia SN, Llopis SN: Laparoscopic Roux-en-Y gastric bypass versus laparoscopic sleeve gastrectomy for the treatment of morbid obesity. A prospective study of 117 patients. Obes Surg 2011; 21: Basso N, Casella G, Rizzello M et al: Laparoscopic sleeve gastrectomy as first stage or definitive intent in 300 consecutive cases. Surg Endosc 2011;25: NIH Conference: Gastrointestinal surgery for severe obesity. Consensus Development Conference Panel. Ann Intern Med 1991;115: Received: July 8, 2013 Accepted: September 25, 2013
Overview of Bariatric Surgery
 Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Medical Coverage Policy Bariatric Surgery
 Medical Coverage Policy Bariatric Surgery Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2011 Policy Last Updated: 11/01/2011 Prospective review is recommended/required. Please check
Medical Coverage Policy Bariatric Surgery Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2011 Policy Last Updated: 11/01/2011 Prospective review is recommended/required. Please check
Advancing the Field of Bariatric Surgery at University Hospitals
 Advancing the Field of Bariatric Surgery at University Hospitals More Sharing ServicesShare Share on facebookshare on emailshare on favoritesshare on printrss Feed By: Alex Strauss Sunday, March 11, 2012
Advancing the Field of Bariatric Surgery at University Hospitals More Sharing ServicesShare Share on facebookshare on emailshare on favoritesshare on printrss Feed By: Alex Strauss Sunday, March 11, 2012
Roux-en-Y Gastric Bypass
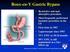 Roux-en-Y Gastric Bypass Restrictive and malabsorptive procedure Most frequently performed bariatric procedure in the US First done in 1967 Laparoscopic since 1993 75% EWL in 18-24 months 50% EWL is still
Roux-en-Y Gastric Bypass Restrictive and malabsorptive procedure Most frequently performed bariatric procedure in the US First done in 1967 Laparoscopic since 1993 75% EWL in 18-24 months 50% EWL is still
The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery
 Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS
 BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
Bariatric Surgery. Beth A. Ryder, MD FACS. Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University
 Bariatric Surgery Beth A. Ryder, MD FACS Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University April 30, 2013 Why surgery? Eligibility criteria Most commonly
Bariatric Surgery Beth A. Ryder, MD FACS Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University April 30, 2013 Why surgery? Eligibility criteria Most commonly
Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Abstract Background Methods:
 Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Mousa Khoursheed, Ibtisam Al-Bader, Ali Mouzannar, Abdulla Al-Haddad, Ali Sayed, Ali Mohammad,
Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Mousa Khoursheed, Ibtisam Al-Bader, Ali Mouzannar, Abdulla Al-Haddad, Ali Sayed, Ali Mohammad,
Treatment for Severely Obese Patients
 Treatment for Severely Obese Patients Associate Professor Jimmy So Senior Consultant Surgeon Director, Centre for Obesity Management and Surgery (COMS) National University Hospital Obesity Shortens Lives
Treatment for Severely Obese Patients Associate Professor Jimmy So Senior Consultant Surgeon Director, Centre for Obesity Management and Surgery (COMS) National University Hospital Obesity Shortens Lives
Technical Aspects of Bariatric Surgical Procedures. Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital
 Technical Aspects of Bariatric Surgical Procedures Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital Disclosures Allergan, Inc. (Past) Faculty Member Educational
Technical Aspects of Bariatric Surgical Procedures Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital Disclosures Allergan, Inc. (Past) Faculty Member Educational
Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI)
 Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI) The American Society for Gastrointestinal Endoscopy PIVI on Endoscopic Bariatric Procedures (short form) Please see related White
Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI) The American Society for Gastrointestinal Endoscopy PIVI on Endoscopic Bariatric Procedures (short form) Please see related White
Gastric Bypass and Other Bariatric Surgical Procedures*
 Subject: Gastric Bypass and Other Bariatric Surgical Procedures* Updated: February 24, 2009 Department(s): Policy: Objective: Utilization Management Medically necessary bariatric surgical procedures are
Subject: Gastric Bypass and Other Bariatric Surgical Procedures* Updated: February 24, 2009 Department(s): Policy: Objective: Utilization Management Medically necessary bariatric surgical procedures are
WEIGHT LOSS SURGERY. Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010
 WEIGHT LOSS SURGERY Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010 EDUCATIONAL OBJECTIVES: Discuss the available pharmaceutical options for weight loss and risks of these medications Explain the
WEIGHT LOSS SURGERY Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010 EDUCATIONAL OBJECTIVES: Discuss the available pharmaceutical options for weight loss and risks of these medications Explain the
Why a loop and new approach makes sense!
 IP: tomach Intestinal Pylorus paring urgery Why a loop and new approach makes sense! Mitchell Roslin, MD, FAC Chief of Bariatric and Metabolic urgery Lenox Hill Hospital Northern Westchester Hospital Center
IP: tomach Intestinal Pylorus paring urgery Why a loop and new approach makes sense! Mitchell Roslin, MD, FAC Chief of Bariatric and Metabolic urgery Lenox Hill Hospital Northern Westchester Hospital Center
Obesity Affects Quality of Life
 Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Bariatric Surgery. OHTAC Recommendation. Bariatric Surgery
 OHTAC Recommendation Bariatric Surgery January 21, 2005 1 The Ontario Health Technology Advisory Committee (OHTAC) met on January 21, 2005 and reviewed bariatric surgery for morbid obesity. Obesity is
OHTAC Recommendation Bariatric Surgery January 21, 2005 1 The Ontario Health Technology Advisory Committee (OHTAC) met on January 21, 2005 and reviewed bariatric surgery for morbid obesity. Obesity is
Laparoscopic One Anastomosis Gastric Bypass (LOAGB) How I do it
 CENTER OF EXCELLENCE FOR THE STUDY AND OBESITY TREATMENT Laparoscopic One Anastomosis Gastric Bypass (LOAGB) How I do it Concepts and Results in a series of 11-years experience with 2,200 patients Miguel-A.
CENTER OF EXCELLENCE FOR THE STUDY AND OBESITY TREATMENT Laparoscopic One Anastomosis Gastric Bypass (LOAGB) How I do it Concepts and Results in a series of 11-years experience with 2,200 patients Miguel-A.
The Arguments: T2DM - tremendous economic burden globally Lifestyle / Pharm Rx:
 James Cromie The Arguments: T2DM - tremendous economic burden globally Lifestyle / Pharm Rx: INEFFECTIVE and UNSUSTAINED Bariatric surgery is an Effective and Durable treatment option Well established
James Cromie The Arguments: T2DM - tremendous economic burden globally Lifestyle / Pharm Rx: INEFFECTIVE and UNSUSTAINED Bariatric surgery is an Effective and Durable treatment option Well established
Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy
 Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy The Vertical Sleeve Gastrectomy procedure (also called Sleeve Gastrectomy, Vertical Gastrectomy, Greater Curvature
Vertical Sleeve Gastrectomy (VSG) - Also known as Sleeve Gastrectomy, Vertical Gastrectomy The Vertical Sleeve Gastrectomy procedure (also called Sleeve Gastrectomy, Vertical Gastrectomy, Greater Curvature
Some of the diseases and conditions associated with obesity include:
 WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
MEDICAL COVERAGE POLICY. SERVICE: Bariatric (Weight Loss) Surgery Policy Number: 053 Effective Date: 5/27/2014 Last Review: 4/24/2014
 Page 1 of 6 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms
Page 1 of 6 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms
When, Why, and How to Revise a Failed Sleeve Gastrectomy
 When, Why, and How to Revise a Failed Sleeve Gastrectomy Jin S. Yoo M.D. Assistant Professor of Surgery Duke University Medical Center April 6, 2013 When and Why Already Covered Let s Talk About How Overview
When, Why, and How to Revise a Failed Sleeve Gastrectomy Jin S. Yoo M.D. Assistant Professor of Surgery Duke University Medical Center April 6, 2013 When and Why Already Covered Let s Talk About How Overview
Teresa LaMasters MD, FACS Minimally Invasive Bariatric Surgeon Iowa Health Weight Loss Specialists Throckmorton Surgical Society May 4, 2012
 Laparoscopic Sleeve Gastrectomy Teresa LaMasters MD, FACS Minimally Invasive Bariatric Surgeon Iowa Health Weight Loss Specialists Throckmorton Surgical Society May 4, 2012 Objectives Understand the anatomy
Laparoscopic Sleeve Gastrectomy Teresa LaMasters MD, FACS Minimally Invasive Bariatric Surgeon Iowa Health Weight Loss Specialists Throckmorton Surgical Society May 4, 2012 Objectives Understand the anatomy
Surgical Treatment of Obesity: A Surgeon s View
 Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
The Link Between Obesity and Diabetes The Rapid Evolution and Positive Results of Bariatric Surgery
 The Link Between Obesity and Diabetes The Rapid Evolution and Positive Results of Bariatric Surgery Michael E. Farkouh, MD, MSc Peter Munk Chair in Multinational Clinical Trials Director, Heart and Stroke
The Link Between Obesity and Diabetes The Rapid Evolution and Positive Results of Bariatric Surgery Michael E. Farkouh, MD, MSc Peter Munk Chair in Multinational Clinical Trials Director, Heart and Stroke
12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16
 HEALTHSPAN BARIATRIC SURGERY Methodology: Expert Opinion Champion: Surgery Issue Date: Review Date: 12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16 RELEVANCE: The CPG for
HEALTHSPAN BARIATRIC SURGERY Methodology: Expert Opinion Champion: Surgery Issue Date: Review Date: 12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16 RELEVANCE: The CPG for
NHRMC General Surgery Specialists. Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303
 Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
BARIATRIC SURGERY. Prerequisites. Authorization, Notification and Referral
 BARIATRIC SURGERY Policy NHP reimburses participating providers for specific types of medically necessary bariatric surgery when needed to either alleviate or correct medical problems caused by severe
BARIATRIC SURGERY Policy NHP reimburses participating providers for specific types of medically necessary bariatric surgery when needed to either alleviate or correct medical problems caused by severe
Catholic Medical Center & Androscoggin Valley Hospital. Surgical Weight Loss Options For a Healthier Tomorrow
 Catholic Medical Center & Androscoggin Valley Hospital Surgical Weight Loss Options For a Healthier Tomorrow Presentation Overview Obesity Health Related Risks Who Qualifies for Weight Loss Surgery? Gastric-bypass
Catholic Medical Center & Androscoggin Valley Hospital Surgical Weight Loss Options For a Healthier Tomorrow Presentation Overview Obesity Health Related Risks Who Qualifies for Weight Loss Surgery? Gastric-bypass
PREOPERATIVE MANAGEMENT FOR BARIATRIC PATIENTS. Adrienne R. Gomez, MD Bariatric Physician St. Vincent Bariatric Center of Excellence
 PREOPERATIVE MANAGEMENT FOR BARIATRIC PATIENTS Adrienne R. Gomez, MD Bariatric Physician St. Vincent Bariatric Center of Excellence BARIATRIC SURGERY Over 200,000 bariatric surgical procedures are performed
PREOPERATIVE MANAGEMENT FOR BARIATRIC PATIENTS Adrienne R. Gomez, MD Bariatric Physician St. Vincent Bariatric Center of Excellence BARIATRIC SURGERY Over 200,000 bariatric surgical procedures are performed
Diabetes and Weight-Loss Surgery
 WHITE PAPER Diabetes and Weight-Loss Surgery Treat the cause. Cure the symptom. Center of Excellence BARIATRIC SURGERY Written July 2011 Bariatric Surgery: The Cure for Type II Diabetes? For most individuals
WHITE PAPER Diabetes and Weight-Loss Surgery Treat the cause. Cure the symptom. Center of Excellence BARIATRIC SURGERY Written July 2011 Bariatric Surgery: The Cure for Type II Diabetes? For most individuals
Obesity When to Recommend Surgery. Lily Chang, MD September 27, 2013
 Obesity When to Recommend Surgery Lily Chang, MD September 27, 2013 Obesity BMI >30 Trends Among U.S. Adults Source: Behavioral Risk Factor Surveillance System, CDC, 2012 Obesity Related Co-Morbidities
Obesity When to Recommend Surgery Lily Chang, MD September 27, 2013 Obesity BMI >30 Trends Among U.S. Adults Source: Behavioral Risk Factor Surveillance System, CDC, 2012 Obesity Related Co-Morbidities
Surgical Weight Loss. Mission Bariatrics
 Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Comparative Studies and Metabolic Effects of Sleeve Gastrectomy
 Comparative Studies and Metabolic Effects of Sleeve Gastrectomy Alfonso Torquati MD, MSCI Associate Professor of Surgery Discosures NIH-NIDDK: grant support Covidien: consulting agreement, grant support
Comparative Studies and Metabolic Effects of Sleeve Gastrectomy Alfonso Torquati MD, MSCI Associate Professor of Surgery Discosures NIH-NIDDK: grant support Covidien: consulting agreement, grant support
Weight Loss Surgery Info for Physicians
 Weight Loss Surgery Info for Physicians As physicians, we see it every day when we see our patients more and more people are obese, and it s affecting their health. It s estimated that at least 2/3 of
Weight Loss Surgery Info for Physicians As physicians, we see it every day when we see our patients more and more people are obese, and it s affecting their health. It s estimated that at least 2/3 of
Intraoperative Prevention of Stenosis for Laparoscopic Sleeve Gastrectomy
 CASE REPORT Intraoperative Prevention of Stenosis for Laparoscopic Sleeve Gastrectomy Ramon Vilallonga, MD, PhD, Jacques Himpens, MD Division of Bariatric Surgery, AZ St. Blasius, Dendermonde, Belgium
CASE REPORT Intraoperative Prevention of Stenosis for Laparoscopic Sleeve Gastrectomy Ramon Vilallonga, MD, PhD, Jacques Himpens, MD Division of Bariatric Surgery, AZ St. Blasius, Dendermonde, Belgium
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Weight Loss Surgery Information Session. WFBH Bariatric Surgery Program
 Weight Loss Surgery Information Session WFBH Bariatric Surgery Program What makes us different? Center of Excellence (COE) High volume center > 1000 procedures since 2003 Less complications than non-coe
Weight Loss Surgery Information Session WFBH Bariatric Surgery Program What makes us different? Center of Excellence (COE) High volume center > 1000 procedures since 2003 Less complications than non-coe
The hidden endoscopic burden of sleeve gastrectomy and its comparison with Roux-en-Y gastric bypass
 ORIGINAL ARTICLE Annals of Gastroenterology (2015) 28, 1-6 The hidden endoscopic burden of sleeve gastrectomy and its comparison with Roux-en-Y gastric bypass Katherine Arndtz a, Helen Steed b, James Hodson
ORIGINAL ARTICLE Annals of Gastroenterology (2015) 28, 1-6 The hidden endoscopic burden of sleeve gastrectomy and its comparison with Roux-en-Y gastric bypass Katherine Arndtz a, Helen Steed b, James Hodson
Types of Bariatric Procedures. Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012
 Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
If you are morbidly obese, you should remember these important points:
 What is Morbid Obesity? Morbid obesity is a serious medical condition. If you are morbidly obese, it means that you are severely overweight, usually by at least 100 pounds. It also means that you have
What is Morbid Obesity? Morbid obesity is a serious medical condition. If you are morbidly obese, it means that you are severely overweight, usually by at least 100 pounds. It also means that you have
Bariatric Surgery. Overview of Procedural Options
 Bariatric Surgery Overview of Procedural Options The Obesity Epidemic In 1991, NO state had an obesity rate above 20% 1 As of 2010, more than two-thirds of states (38) now have adult obesity rates above
Bariatric Surgery Overview of Procedural Options The Obesity Epidemic In 1991, NO state had an obesity rate above 20% 1 As of 2010, more than two-thirds of states (38) now have adult obesity rates above
Top Ten Things You Need to Know About Bariatric Surgery Patients. Laura Dyck, M.S., R.D., LDN Comprehensive Weight Management Center, Kingsport, TN
 Top Ten Things You Need to Know About Bariatric Surgery Patients Laura Dyck, M.S., R.D., LDN Comprehensive Weight Management Center, Kingsport, TN Top Ten Things You Need to Know About Bariatric Surgery
Top Ten Things You Need to Know About Bariatric Surgery Patients Laura Dyck, M.S., R.D., LDN Comprehensive Weight Management Center, Kingsport, TN Top Ten Things You Need to Know About Bariatric Surgery
5/9/2012. What is Morbid Obesity? Obesity Trends* Among U.S. Adults BRFSS, 1990, 1998, 2007 (*BMI 30, or about 30 lbs. overweight for 5 4 person)
 Obesity Trends* Among U.S. Adults BRFSS, 1990, 1998, 2007 (*BMI 30, or about 30 lbs. overweight for 5 4 person) 1990 1998 The Bariatric and Metabolic Center of Colorado Bariatric Surgery: Options, Care
Obesity Trends* Among U.S. Adults BRFSS, 1990, 1998, 2007 (*BMI 30, or about 30 lbs. overweight for 5 4 person) 1990 1998 The Bariatric and Metabolic Center of Colorado Bariatric Surgery: Options, Care
Considering Bariatric Surgery? Learn about minimally invasive da Vinci Surgery
 Considering Bariatric Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Obesity Obesity is defined as having a body mass index (BMI) of 30 or greater. Obesity is a serious medical
Considering Bariatric Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Obesity Obesity is defined as having a body mass index (BMI) of 30 or greater. Obesity is a serious medical
Lose the Weight, Find your Life
 Bariatric Surgery: University of Iowa Lose the Weight, Find your Life Isaac Samuel, MD, FRCS, FACS Professor of Surgery Director, Bariatric Surgery 1 Present UI Bariatric Surgeons Jessica Smith, MD Peter
Bariatric Surgery: University of Iowa Lose the Weight, Find your Life Isaac Samuel, MD, FRCS, FACS Professor of Surgery Director, Bariatric Surgery 1 Present UI Bariatric Surgeons Jessica Smith, MD Peter
BARIATRIC SURGERY. Personalized Weight Loss Program
 BARIATRIC SURGERY Personalized Weight Loss Program Lafayette General Medical Center performs three major operations for weight loss surgery: Adjustable Gastric Band, Laparoscopic Sleeve Gastrectomy and
BARIATRIC SURGERY Personalized Weight Loss Program Lafayette General Medical Center performs three major operations for weight loss surgery: Adjustable Gastric Band, Laparoscopic Sleeve Gastrectomy and
What is the Sleeve Gastrectomy?
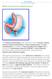 What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
What is the Sleeve Gastrectomy? The Sleeve Gastrectomy (also referred to as the Gastric Sleeve, Vertical Sleeve Gastrectomy, Partial Gastrectomy, or Tube Gastrectomy) is a relatively new procedure for
UW MEDICINE PATIENT EDUCATION. Weight Loss Surgery. What is bariatric surgery?
 UW MEDICINE PATIENT EDUCATION Weight Loss Surgery Divided proximal roux-y-gastric bypass, laparoscopic adjustable gastric banding, and laparoscopic sleeve gastrectomy. This section of the Guide to Your
UW MEDICINE PATIENT EDUCATION Weight Loss Surgery Divided proximal roux-y-gastric bypass, laparoscopic adjustable gastric banding, and laparoscopic sleeve gastrectomy. This section of the Guide to Your
Surgical Weight Loss Program for Teens
 Surgical Weight Loss Program for Teens Surgical Weight Loss Program for Teens The Surgical Weight Loss Program team understands the impact that being severely overweight can have on your life. Our guiding
Surgical Weight Loss Program for Teens Surgical Weight Loss Program for Teens The Surgical Weight Loss Program team understands the impact that being severely overweight can have on your life. Our guiding
Treatment for severe GERD after Sleeve Gastrectomy: conversion to gastric bypass or endoluminal radiofrequency. Alfonso Torquati, MD, MSCI, FACS
 Treatment for severe GERD after Sleeve Gastrectomy: conversion to gastric bypass or endoluminal radiofrequency. Alfonso Torquati, MD, MSCI, FACS Associate Professor and Chief Division of Metabolic and
Treatment for severe GERD after Sleeve Gastrectomy: conversion to gastric bypass or endoluminal radiofrequency. Alfonso Torquati, MD, MSCI, FACS Associate Professor and Chief Division of Metabolic and
The Evolution of Bariatric Surgery. History of the Development of a Successful Bariatric Program at the University of Iowa Hospitals & Clinics
 The Evolution of Bariatric Surgery History of the Development of a Successful Bariatric Program at the University of Iowa Hospitals & Clinics It s a BIG Problem & it s Getting Worse Obesity is now a disease
The Evolution of Bariatric Surgery History of the Development of a Successful Bariatric Program at the University of Iowa Hospitals & Clinics It s a BIG Problem & it s Getting Worse Obesity is now a disease
Changes to Bariatric Surgery Prior Authorization Guidelines
 Update August 2011 No. 2011-44 Affected Programs: BadgerCare Plus, Medicaid To: Hospital Providers, Physician Assistants, Physician Clinics, Physicians, HMOs and Other Managed Care Programs Changes to
Update August 2011 No. 2011-44 Affected Programs: BadgerCare Plus, Medicaid To: Hospital Providers, Physician Assistants, Physician Clinics, Physicians, HMOs and Other Managed Care Programs Changes to
at Putnam Hospital Center A Partnership for Lifelong Weight Loss Begins Mid Hudson
 Mid Hudson A BUSINESS & PRACTICE MANAGEMENT MAGAZINE ABOUT PHYSICIANS FROM PHYSICIANS FOR PHYSICIANS A Partnership for Lifelong Weight Loss Begins at Putnam Hospital Center Ashutosh Kaul, MD, FRCS, FACS,
Mid Hudson A BUSINESS & PRACTICE MANAGEMENT MAGAZINE ABOUT PHYSICIANS FROM PHYSICIANS FOR PHYSICIANS A Partnership for Lifelong Weight Loss Begins at Putnam Hospital Center Ashutosh Kaul, MD, FRCS, FACS,
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes
 Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Weight Loss Surgery Program
 Weight loss surgery helped me lose 112 pounds. Jennifer Weaver Weight Loss Surgery Program baylor university medical center at dallas Follow us on: Facebook.com/BaylorHealth YouTube.com/BaylorHealth When
Weight loss surgery helped me lose 112 pounds. Jennifer Weaver Weight Loss Surgery Program baylor university medical center at dallas Follow us on: Facebook.com/BaylorHealth YouTube.com/BaylorHealth When
American Society for Bariatric Surgery 100 SW 75th Street, Suite 201 Gainesville, FL 32607
 May 11, 2005 Steve E. Phurrough, MD, MPA Office of Clinical Standards & Quality Centers for Medicare and Medicaid Services 7500 Security Boulevard Mail Stop C1-09-06 Baltimore, MD 21244-1850 Re: Request
May 11, 2005 Steve E. Phurrough, MD, MPA Office of Clinical Standards & Quality Centers for Medicare and Medicaid Services 7500 Security Boulevard Mail Stop C1-09-06 Baltimore, MD 21244-1850 Re: Request
Bariatric Surgery 101
 Bariatric Surgery 101 Dr. Brent Bell, MD Bariatric / General Surgeon Medical Conditions Caused By Morbid Obesity Type 2 DM Hypertension Cholesterol Sleep Apnea Fatty Liver Asthma Osteoarthritis Reduced
Bariatric Surgery 101 Dr. Brent Bell, MD Bariatric / General Surgeon Medical Conditions Caused By Morbid Obesity Type 2 DM Hypertension Cholesterol Sleep Apnea Fatty Liver Asthma Osteoarthritis Reduced
Medical Policy Bariatric Surgery
 Medical Policy Bariatric Surgery Document Number: 001 Commercial MassHealth and Qualified Health Plans Authorization required X X Notification within 24 hours of service or next business day No notification
Medical Policy Bariatric Surgery Document Number: 001 Commercial MassHealth and Qualified Health Plans Authorization required X X Notification within 24 hours of service or next business day No notification
Morbid obesity is defined as a body mass index (BMI) >40 kg/m2 (normal BMI range: 19-25 kg/m2)
 Medical Policy Manual Topic: Bariatric Surgery Date of Origin: January 1996 Section: Surgery Last Reviewed Date: August 2015 Policy No: 58 Effective Date: September 1, 2015 IMPORTANT REMINDER Medical Policies
Medical Policy Manual Topic: Bariatric Surgery Date of Origin: January 1996 Section: Surgery Last Reviewed Date: August 2015 Policy No: 58 Effective Date: September 1, 2015 IMPORTANT REMINDER Medical Policies
Gastric Surgery for Clinically Severe (Morbid) Obesity
 Origination: 03/28/01 Revised: 01/16/15 Annual Review: 11/12/15 Purpose: The Medical Technology Assessment Committee will review published scientific literature and information from appropriate government
Origination: 03/28/01 Revised: 01/16/15 Annual Review: 11/12/15 Purpose: The Medical Technology Assessment Committee will review published scientific literature and information from appropriate government
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
Southcoast Center for Weight Loss
 Introduction Introducing the Southcoast Center for Weight Loss Left: Tobey Hospital, Wareham Right: Southcoast Health System at Rosebrook Business Park, Wareham The Southcoast Center for Weight Loss is
Introduction Introducing the Southcoast Center for Weight Loss Left: Tobey Hospital, Wareham Right: Southcoast Health System at Rosebrook Business Park, Wareham The Southcoast Center for Weight Loss is
The weight of the world.
 The weight of the world. SONY ANTHONY Obesity Derived from the Latin word obesus to devour Definition: having a very high amount of body fat in relation to lean body mass Classifications using Body Mass
The weight of the world. SONY ANTHONY Obesity Derived from the Latin word obesus to devour Definition: having a very high amount of body fat in relation to lean body mass Classifications using Body Mass
Bariatric Weight Loss Surgery
 BARIATRIC SURGERY Bariatric Weight Loss Surgery The heart and science of medicine. Weight loss surgery, also known as bariatric surgery, was developed as a tool to help people with morbid obesity reduce
BARIATRIC SURGERY Bariatric Weight Loss Surgery The heart and science of medicine. Weight loss surgery, also known as bariatric surgery, was developed as a tool to help people with morbid obesity reduce
Sudbury Bariatric Regional Assessment & Treatment Centre
 Sudbury Bariatric Regional Assessment & Treatment Centre Outline Obesity as a Chronic Disease 5 A s of Obesity Management OBN & BRATC Referral Process Obesity Definition BMI Normal Weight 18.5-24.9 Overweight
Sudbury Bariatric Regional Assessment & Treatment Centre Outline Obesity as a Chronic Disease 5 A s of Obesity Management OBN & BRATC Referral Process Obesity Definition BMI Normal Weight 18.5-24.9 Overweight
5. Conversion Procedures that change from an index procedure to a different type of procedure.
 Benefit Coverage Covered Benefit for lines of business including Health Benefits Exchange (HBE), Rite Care (MED), Children with Special Needs (CSN), Substitute Care (SUB), Rhody Health Partners (RHP),
Benefit Coverage Covered Benefit for lines of business including Health Benefits Exchange (HBE), Rite Care (MED), Children with Special Needs (CSN), Substitute Care (SUB), Rhody Health Partners (RHP),
Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery
 Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery Authors: Chiranjiv S Virk, I Michael Leitman and Elliot R Goodman. Location: Beth Israel
Endoscopic gastric pouch plication - a novel endoluminal incision free approach to revisional bariatric surgery Authors: Chiranjiv S Virk, I Michael Leitman and Elliot R Goodman. Location: Beth Israel
Bariatric Surgery. Required forms: (Forms are located at OHCA Forms ) Certification Criteria for Providers. Treatment for Obesity
 Bariatric Surgery Required forms: (Forms are located at OHCA Forms ) HCA-13A HCA-12A Certification Criteria for Providers To be eligible for reimbursement, bariatric surgery providers must be certified
Bariatric Surgery Required forms: (Forms are located at OHCA Forms ) HCA-13A HCA-12A Certification Criteria for Providers To be eligible for reimbursement, bariatric surgery providers must be certified
HOUSTON METHODIST SURGICAL WEIGHT LOSS
 HOUSTON METHODIST SURGICAL WEIGHT LOSS Why choose surgical weight loss at Houston Methodist? Obesity causes many dangerous diseases and health conditions such as diabetes, high blood pressure, heart disease,
HOUSTON METHODIST SURGICAL WEIGHT LOSS Why choose surgical weight loss at Houston Methodist? Obesity causes many dangerous diseases and health conditions such as diabetes, high blood pressure, heart disease,
Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of
 Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of Surgery & Associate Residency Program Director UC Irvine
Surgical & Nutritional Complications of Bariatric Surgery: What Every GI Doc Needs to Know Brian R. Smith, MD, FACS Associate Clinical Professor of Surgery & Associate Residency Program Director UC Irvine
Weight Loss Surgery and Bariatric Nutrition. Jeanine Giordano, MS, RD, CDN
 Weight Loss urgery and Bariatric Nutrition Jeanine Giordano, M, RD, CDN UA: Mean BMI trends (age standardized) Prevalence of Obesity Among Adults United tates 68% Australia 59% Russia 54% United Kingdom
Weight Loss urgery and Bariatric Nutrition Jeanine Giordano, M, RD, CDN UA: Mean BMI trends (age standardized) Prevalence of Obesity Among Adults United tates 68% Australia 59% Russia 54% United Kingdom
Weight Loss Surgery: Pre- and Post-Operative Care
 Weight Loss Surgery: Pre- and Post-Operative Care Dan Bessesen, MD Chief of Endocrinology; Denver Health Medical Center Professor of Medicine, University of Colorado School of Medicine [email protected]
Weight Loss Surgery: Pre- and Post-Operative Care Dan Bessesen, MD Chief of Endocrinology; Denver Health Medical Center Professor of Medicine, University of Colorado School of Medicine [email protected]
Roux-en-y gastric bypass - clinical perspectives
 Roux-en-y gastric bypass - clinical perspectives Tom Mala Consultant surgeon Department of Gastroenterologic Surgery Oslo University Hospital Bariatric surgery weight loss Sjøstrøm L, JAMA 2012 Five-year
Roux-en-y gastric bypass - clinical perspectives Tom Mala Consultant surgeon Department of Gastroenterologic Surgery Oslo University Hospital Bariatric surgery weight loss Sjøstrøm L, JAMA 2012 Five-year
Bariatric i Surgery: Optimalizing Outcome Results. Dr. B. Dillemans AZ Sint-Jan AV Brugge-Oostende BARIATRIC SURGERY
 Bariatric i Surgery: Optimalizing i Outcome Results Dr. B. Dillemans AZ Sint-Jan AV Brugge-Oostende THE OBESE PATIENT : A CHALLENGE FOR ANAESTHESIA, Ostend,14/11/09 BARIATRIC SURGERY 50 s : First Reported
Bariatric i Surgery: Optimalizing i Outcome Results Dr. B. Dillemans AZ Sint-Jan AV Brugge-Oostende THE OBESE PATIENT : A CHALLENGE FOR ANAESTHESIA, Ostend,14/11/09 BARIATRIC SURGERY 50 s : First Reported
