Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI)
|
|
|
- Aubrie Sutton
- 10 years ago
- Views:
Transcription
1 Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI) The American Society for Gastrointestinal Endoscopy PIVI on Endoscopic Bariatric Procedures (short form) Please see related White Paper: A Pathway to Endoscopic Bariatric Procedures, published in GIE:Gastrointestinal Endoscopy (Gastrointestinal Endoscopy Vol. 74, Issue 5, Pages ) The PIVI Initiative The PIVI initiative is an ASGE program that aims to identify important clinical questions related to endoscopy and to establish a priori diagnostic and/or therapeutic thresholds for endoscopic technologies designed to resolve these clinical questions. Additionally, PIVIs may also outline the data and or the research study design required for proving an established threshold is met. Once endoscopic technologies meet an established PIVI threshold, those technologies are appropriate to incorporate into clinical practice presuming the appropriate training in that endoscopic technology has been achieved. The ASGE encourages and supports the appropriate use of technologies that meet its established PIVI thresholds. The PIVI initiative was developed primarily to direct endoscopic technology development toward resolving important clinical issues in endoscopy. The PIVI initiative is also designed to minimize the possibility that potentially valuable innovations are prematurely abandoned due to lack of utilization and to avoid widespread use of an endoscopic technology before clinical studies documenting their effectiveness have been performed. The following document, or PIVI, is one of a series of statements defining the diagnostic or therapeutic threshold that must be met for a technique or device to become considered appropriate for incorporation into clinical practice. It is also meant to serve as a guide for researchers or those seeking to develop technologies that are designed to improve digestive health outcomes. An ad hoc committee under the auspices of the existing ASGE Technology and Standards of Practice Committees Chairs develops PIVIs. An expert in the subject area chairs the PIVI committee, with additional committee members chosen for their individual expertise. In preparing this document, evidence-based methodology was employed, using a MEDLINE and PubMed literature search to identify pertinent clinical studies on the topic. PIVIs are ultimately submitted to the ASGE Governing Board for approval, as is done for all Technology and Standards of Practice documents. This document is provided solely for educational and informational purposes and to support incorporating these endoscopic technologies into clinical practice. It should not be construed as establishing a legal standard of care. 1 P a g e
2 Endoscopic Bariatric Procedures PIVI (Short form) I. General clinical area of this PIVI: This PIVI is intended to establish thresholds for the adoption of endoscopic bariatric therapy (EBT) in the context of obesity class and comorbid disease. Obesity is a complex metabolic disease of excessive fat accumulation associated with a host of co-morbid conditions including heart disease, hypertension, dyslipidemia, type II diabetes, osteoarthritis, sleep apnea, certain malignancies, and all-cause mortality. Obesity is increasing worldwide. Medical treatment for obesity and associated metabolic comorbidities includes lifestyle modification, diet and pharmacologic agents. However, these approaches have limited effectiveness and limited durability, with high rates of attrition. Bariatric surgical interventions have been more effective, yielding significant and sustainable weight loss along with resolution of metabolic comorbidities in up to 80% of patients. While effective, these laparoscopic and open surgical bariatric procedures have morbidity rates of 3% to 20% and mortality rates of 0.1 to 0.5%. For these and other reasons, including limited access to care, only 1 in 400 morbidly obese individuals undergo bariatric surgery in the US. Given that all current surgical procedures require general anesthesia and have procedure specific complications, there is a need for less invasive weight loss interventions to potentially reduce morbidity and improve access. A range of novel endoscopic modalities may fit this profile. Any new endoscopic or nonsurgical weight loss intervention should include a defined threshold of efficacy, balanced with risks of the intervention. EBT, performed entirely through the gastrointestinal tract using flexible endoscopes, offers the potential for ambulatory weight loss procedures with a superior safety and cost profile compared to bariatric surgery. Such benefits would increase the appeal and acceptance of this therapy to patients. EBT shown to be feasible, safe, and effective may be appropriate intervention for individuals with lower classes of obesity. II. Threshold(s) recommended for this PIVI: Based on available evidence and expert opinion, the Taskforce recommends that an EBT intended as a primary obesity intervention in Class II/III obese individuals (Body Mass Index [BMI] > 35 kg/m 2 ) achieve a mean minimum threshold of 25% Excess Weight Loss (%EWL) measured at 12 months. This goal will vary depending on the category or intent of endoscopic bariatric procedure. EBT should be compared to a second treatment group, not sham. In addition to the absolute threshold of weight loss, the mean % EWL difference between a Primary EBT and control groups should be a minimum of 15% EWL, and be statistically significant. We advocate using 5% of total body weight (%TBW) lost as the absolute minimum threshold for any non-primary EBT (e.g., early intervention, bridging or metabolic therapy). The risk associated with EBP should equate to <5% incidence of serious adverse events. 2 P a g e
3 If a low risk EBT proves to have a significant impact on one or more obesity-related comorbidities, the threshold for intervention may extend to Class I obese individuals (BMI kg/m 2 ). III. Summary explanation of threshold recommended for this PIVI The weight loss threshold for the adoption of any new endoscopic procedures should be balanced against the risk of that procedure. Currently there are no thresholds established for endoscopic bariatric interventions. However, in general it is expected that endoscopic modalities should achieve weight loss superior to that anticipated with medical and intensive lifestyle interventions and approach that of operative therapies. Assessment of weight loss Weight loss after currently accepted interventions varies greatly. Comparison of nonsurgical and operative interventions is limited by differences in the primary outcome measure. The majority of medical therapy trials use the percent of total body weight lost (%TBW) to define efficacy. Weight loss after bariatric surgery is calculated as either changes in the baseline BMI or the percent of excess weight loss (%EWL). The %EWL is defined as: Amount of weight loss [Patient s initial weight Ideal body weight based on gender and height] x100 Ideal body weight is most commonly obtained from the Metropolitan Life Insurance table. Moreover, actual weight lost can be a deceiving outcome measure, particularly among class II and III obese individuals. But the overall magnitude of average weight loss attributed to operative interventions is significantly greater than that achieved with non-surgical therapies. In a meta-analysis published by Buchwald et al, Roux-en-Y-gastric-bypass (RYGB) achieves a mean excess weight loss of 68%, gastroplasty achieves 69%, and gastric banding 50% at varying follow-up time intervals. An EBT with a considerably lower risk profile compared to surgery may be held to a comparable reduction in expected weight loss for the surgical intervention but exceeding that for accepted non-surgical therapies. Intent of endoluminal therapies The primary goal of EBT is to induce enough weight loss to decrease obesity related metabolic co-morbidities and improve quality of life. Higher risk EBTs would be expected to yield substantial and sustainable positive outcomes to achieve a favorable risk/benefit profile; accordingly, a lower risk EBT would be afforded a comparable adjustment in efficacy threshold. With this concept in mind, EBT have many potential applications in obesity management. Primary Therapy The goal of primary EBT is to induce weight loss and improvement in medical co-morbidities, with a safety and efficacy profile similar to operative bariatric therapy. An EBT with a risk profile comparable to laparoscopic adjustable gastric banding should hold similar efficacy, with the potential to achieve approximately 40 % EWL. Alternatively, lower efficacy is acceptable for an EBT with a lower risk profile. Such a treatment would be for would patients with severe obesity (Class II, III), with or without obesity related co-morbidities. Therefore, based on 3 P a g e
4 available evidence and expert opinion, the Taskforce recommends that an EBT intended as a primary obesity intervention achieve a mean minimum threshold of 25% EWL measured at 12 months. EBT should be compared to a second treatment group, not sham. Sham groups in comparative trials evaluating the efficacy of bariatric therapies have shown considerable variability in weight loss (3-13%EWL). In addition to the absolute threshold of weight loss, the mean %EWL difference between a Primary EBT and control groups, should be a minimum of 15% EWL, and be statistically significant. Early Intervention / Preemptive Obesity Therapy Patients with Class I and II obesity are at risk for disease progression, have a higher cardiovascular risk profile, and have a substantially increased relative risk of all-cause mortality. There is evidence that patients with Class I obesity respond well to surgical intervention. As a result, the FDA has recently approved the use of gastric banding for patients with Class I obesity and at least one associated-comorbidity. Since the goal of Early Intervention/Preemptive Therapy is to achieve modest weight loss, the risk/benefit profile of gastric banding should serve as baseline for any EBT proposed for this indication. In this category, the durability or repeatability of an EBT would be important. Bridge Therapy The intent of Bridge Therapy is to promote weight loss specifically to reduce the risk from a subsequent intervention, including bariatric surgery. Patients with Class III (BMI>50) and those with metabolic comorbidities present greater technical challenges and surgical risk than less obese, healthier patients. Furthermore, these effects are more pronounced in patients with BMI>60 where there is a 2-3 times greater risk of morbidity or mortality. Examples of procedures which may benefit from preoperative weight loss include orthopedic, cardiovascular, organ transplant, and bariatric operations. Efficacy would be primarily measured by a reduction in post-operative morbidity and mortality following the intervention that required bridging. The magnitude of weight loss can be lower, since the primary objective is to significantly reduce the risk of a subsequent intervention. Similarly, durability is a less important feature. Metabolic Therapy EBT may be justified in patients with less severe obesity (Class I), where improvement in metabolic illness is the primary concern. In particular, comorbidities such as type II diabetes, hyperlipidemia, and hypertension, may improve or resolve with even modest weight loss. Procedures which aim to effect metabolic disease should have a lower risk profile and greater durability compared to therapies which specifically aim to induce massive weight loss. Substantial weight loss may not be necessary in order to achieve metabolic benefits in less severely obese individuals. Obese patients who lose 5% of their total body weight benefit from significant reductions in diabetes and cardiovascular risk factors including hypertension and dyslipidemia. Therefore, we advocate using 5% of total body weight lost as the absolute minimum threshold for any non-primary EBT (e.g., early intervention, bridging or metabolic therapy). IV. Areas for research 4 P a g e
5 As an EBT is developed and modified to address specific clinical needs various types of studies are required as to accommodate the regulatory process. Rigorous preclinical evaluation should be followed by feasibility studies in a limited number of human subjects as described in FDA guidance documents. With an emphasis on technical feasibility and safety, there are typically no efficacy targets and results are used to direct modification and to calculate sample size and establish parameters for a larger pivotal trial. The emphases of pivotal trial investigation are efficacy and safety. Pivotal trial design should vary depending on the category and intention of the specific EBT. Efficacy in terms of weight loss or resolution of comorbidities is most accurately assessed by comparison to a control group. Randomized controlled trials provide the highest level of evidence and are the preferred design. Importantly, EBT should be compared to a second treatment group, rather than a sham group. Sham groups in bariatric trials have proven to be unreliable with considerable variability in weight loss (3-13%EWL). Additionally, this type of design may put sham subjects at unnecessary risk. Studies must be designed to best evaluate the intended outcomes of the specific EBT, and the control group should be considered a reasonable alternative regarding potential risks and benefit. Primary EBT that might be considered an alternative to traditional surgery should have an absolute threshold of weight loss that is established based on its particular risk profile. Additionally, the mean %EWL difference between this type of EBT and a medical control group should be a minimum of 15% EWL, and should be statistically significant. If a surgical control group is thought to be more relevant, a non-inferiority trial design would be preferred. Similarly, for an early intervention EBT a non-inferiority design with randomization to a medical control group may be optimal. Intended duration of effect and study length will also depend on the category of EBT being evaluated. Bridge procedures should require a shorter interval (3-6 month) outcome assessment, since the objective is simply to reduce the risk of a downstream procedure. Similarly, some early interventions that are low risk and easily repeated may require shorter trial durations, however, long term studies would likely be necessary for primary EBT devices. For other devices, such as those in the metabolic EBT category, weight loss may only be a secondary endpoint. Control groups for these trials would be very different, and may involve medical treatment of DM, or other related conditions. Reduction in obesity-related co-morbidities Clinical studies have shown that sustained moderate weight loss achieved through dietary and lifestyle intervention lowers blood pressure, improves glucose control, prevents diabetes, and improves dyslipidemia, hemostatic and fibrinolytic factors. Obese patients who lose 5% of their total body weight benefit from significant reductions in diabetes and cardiovascular risk factors including hypertension and dyslipidemia. Therefore, we advocate using 5% of total body weight lost as the absolute minimum threshold for any non-primary EBT (e.g., early intervention, bridging or metabolic therapy). In light of this evidence, it is intuitive that EBT has the potential to induce significant metabolic effects; among them, an improvement in or resolution of obesityrelated co-morbidities such as diabetes mellitus, hypertension, obstructive sleep apnea and nonalcoholic fatty liver disease (NAFLD). If a low risk endoscopic intervention proves to have a significant impact on one or more of these co-morbidities, the threshold for intervention may extend to Class I obese individuals (BMI kg/m 2 ). 5 P a g e
6 In addition to lowering the prevalence of co-existent obesity-related metabolic illnesses, there is potential for an EBT to primarily prevent these comorbidities by promoting weight loss in mildly obese individuals. In this population, it is important that improvement/resolution of comorbidities be significantly better for endoscopic therapies compared to that of control groups, given the risks associated with any intervention despite how minimal they may be. Improvement and resolution of comorbidities should be defined using objective and standardized criteria. Changes in quality of life Weight loss can lead to a significant improvement in quality of life, anxiety and depression. Furthermore, the short-term improvements in body dissatisfaction and mood can positively affect long-term weight loss. Changes in quality of life, work productivity, and underlying psychological disorders represent important secondary endpoints in trials of EBT. V. Training issues/establishment of competency Weight loss interventions have been demonstrated to achieve superior outcomes when the intervention is performed as part of a comprehensive, multidisciplinary treatment program. EBT should also be performed in this context in order to achieve maximal benefit. Nutritional support, experienced nursing care, behavioral medicine specialists, and physicians experienced in the management of obese patients, are essential components of such programs. In addition, the ability and availability of physicians and surgeons willing and able to manage potential complications in obese patients is advised. Training and skill acquisition with EBT techniques and technologies are mandatory before clinical application is undertaken, and should include didactic as well as hands on practical education. Importantly, any practitioner who is interested in performing an EBT should also be educated in the clinical management of obese patients. The duration and type of training is likely to depend on the complexity of a particular EBT. For all EBTs, early studies should assess the learning curve in order to guide subsequent training and credentialing processes. VI. PIVI Committee ASGE/ASMBS Task Force on Endoscopic Bariatric Therapy Gregory G. Ginsberg, MD, Chair Bipan Chand, MD, Co-Chair Gregory A. Cote, MD Ramsey M. Dallal, MD Steven A. Edmundowicz, MD Ninh T. Nguyen, MD Aurora Pryor, MD Christopher C. Thompson, MD Please see related White Paper: A Pathway to Endoscopic Bariatric Procedures, published in GIE:Gastrointestinal Endoscopy (Gastrointestinal Endoscopy Vol. 74, Issue 5, Pages ) 6 P a g e
Bariatric Surgery. OHTAC Recommendation. Bariatric Surgery
 OHTAC Recommendation Bariatric Surgery January 21, 2005 1 The Ontario Health Technology Advisory Committee (OHTAC) met on January 21, 2005 and reviewed bariatric surgery for morbid obesity. Obesity is
OHTAC Recommendation Bariatric Surgery January 21, 2005 1 The Ontario Health Technology Advisory Committee (OHTAC) met on January 21, 2005 and reviewed bariatric surgery for morbid obesity. Obesity is
PREOPERATIVE MANAGEMENT FOR BARIATRIC PATIENTS. Adrienne R. Gomez, MD Bariatric Physician St. Vincent Bariatric Center of Excellence
 PREOPERATIVE MANAGEMENT FOR BARIATRIC PATIENTS Adrienne R. Gomez, MD Bariatric Physician St. Vincent Bariatric Center of Excellence BARIATRIC SURGERY Over 200,000 bariatric surgical procedures are performed
PREOPERATIVE MANAGEMENT FOR BARIATRIC PATIENTS Adrienne R. Gomez, MD Bariatric Physician St. Vincent Bariatric Center of Excellence BARIATRIC SURGERY Over 200,000 bariatric surgical procedures are performed
Bariatric Surgery. Beth A. Ryder, MD FACS. Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University
 Bariatric Surgery Beth A. Ryder, MD FACS Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University April 30, 2013 Why surgery? Eligibility criteria Most commonly
Bariatric Surgery Beth A. Ryder, MD FACS Assistant Professor of Surgery The Miriam Hospital Warren Alpert Medical School of Brown University April 30, 2013 Why surgery? Eligibility criteria Most commonly
Roux-en-Y Gastric Bypass
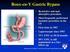 Roux-en-Y Gastric Bypass Restrictive and malabsorptive procedure Most frequently performed bariatric procedure in the US First done in 1967 Laparoscopic since 1993 75% EWL in 18-24 months 50% EWL is still
Roux-en-Y Gastric Bypass Restrictive and malabsorptive procedure Most frequently performed bariatric procedure in the US First done in 1967 Laparoscopic since 1993 75% EWL in 18-24 months 50% EWL is still
Catholic Medical Center & Androscoggin Valley Hospital. Surgical Weight Loss Options For a Healthier Tomorrow
 Catholic Medical Center & Androscoggin Valley Hospital Surgical Weight Loss Options For a Healthier Tomorrow Presentation Overview Obesity Health Related Risks Who Qualifies for Weight Loss Surgery? Gastric-bypass
Catholic Medical Center & Androscoggin Valley Hospital Surgical Weight Loss Options For a Healthier Tomorrow Presentation Overview Obesity Health Related Risks Who Qualifies for Weight Loss Surgery? Gastric-bypass
MEDICAL COVERAGE POLICY. SERVICE: Bariatric (Weight Loss) Surgery Policy Number: 053 Effective Date: 5/27/2014 Last Review: 4/24/2014
 Page 1 of 6 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms
Page 1 of 6 MEDICAL COVERAGE POLICY Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms
Obesity Affects Quality of Life
 Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16
 HEALTHSPAN BARIATRIC SURGERY Methodology: Expert Opinion Champion: Surgery Issue Date: Review Date: 12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16 RELEVANCE: The CPG for
HEALTHSPAN BARIATRIC SURGERY Methodology: Expert Opinion Champion: Surgery Issue Date: Review Date: 12-05 1-13, 4-14, 6-15 Key Stakeholders: Surgery, IM Depts. Next Update: 6-16 RELEVANCE: The CPG for
Treatment for Severely Obese Patients
 Treatment for Severely Obese Patients Associate Professor Jimmy So Senior Consultant Surgeon Director, Centre for Obesity Management and Surgery (COMS) National University Hospital Obesity Shortens Lives
Treatment for Severely Obese Patients Associate Professor Jimmy So Senior Consultant Surgeon Director, Centre for Obesity Management and Surgery (COMS) National University Hospital Obesity Shortens Lives
The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery
 Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Weight Loss Surgery Program
 Weight loss surgery helped me lose 112 pounds. Jennifer Weaver Weight Loss Surgery Program baylor university medical center at dallas Follow us on: Facebook.com/BaylorHealth YouTube.com/BaylorHealth When
Weight loss surgery helped me lose 112 pounds. Jennifer Weaver Weight Loss Surgery Program baylor university medical center at dallas Follow us on: Facebook.com/BaylorHealth YouTube.com/BaylorHealth When
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS
 BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
BARIATRIC SURGERY MAY CURE TYPE 2 DIABETES IN SOME PATIENTS Thomas Rogula MD, Stacy Brethauer MD, Bipand Chand MD, and Philip Schauer, MD. "Gastric bypass surgery has become a popular option for obese
Understanding Obesity
 Your Guide to Understanding Obesity As your partner in health for your life s journey, we want you to be as informed and confident as possible regarding the disease or medical issue you may be facing.
Your Guide to Understanding Obesity As your partner in health for your life s journey, we want you to be as informed and confident as possible regarding the disease or medical issue you may be facing.
The weight of the world.
 The weight of the world. SONY ANTHONY Obesity Derived from the Latin word obesus to devour Definition: having a very high amount of body fat in relation to lean body mass Classifications using Body Mass
The weight of the world. SONY ANTHONY Obesity Derived from the Latin word obesus to devour Definition: having a very high amount of body fat in relation to lean body mass Classifications using Body Mass
The Link Between Obesity and Diabetes The Rapid Evolution and Positive Results of Bariatric Surgery
 The Link Between Obesity and Diabetes The Rapid Evolution and Positive Results of Bariatric Surgery Michael E. Farkouh, MD, MSc Peter Munk Chair in Multinational Clinical Trials Director, Heart and Stroke
The Link Between Obesity and Diabetes The Rapid Evolution and Positive Results of Bariatric Surgery Michael E. Farkouh, MD, MSc Peter Munk Chair in Multinational Clinical Trials Director, Heart and Stroke
Sudbury Bariatric Regional Assessment & Treatment Centre
 Sudbury Bariatric Regional Assessment & Treatment Centre Outline Obesity as a Chronic Disease 5 A s of Obesity Management OBN & BRATC Referral Process Obesity Definition BMI Normal Weight 18.5-24.9 Overweight
Sudbury Bariatric Regional Assessment & Treatment Centre Outline Obesity as a Chronic Disease 5 A s of Obesity Management OBN & BRATC Referral Process Obesity Definition BMI Normal Weight 18.5-24.9 Overweight
Southcoast Center for Weight Loss
 Introduction Introducing the Southcoast Center for Weight Loss Left: Tobey Hospital, Wareham Right: Southcoast Health System at Rosebrook Business Park, Wareham The Southcoast Center for Weight Loss is
Introduction Introducing the Southcoast Center for Weight Loss Left: Tobey Hospital, Wareham Right: Southcoast Health System at Rosebrook Business Park, Wareham The Southcoast Center for Weight Loss is
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS
 GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS www.malleysurgical.com GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
Overview of Bariatric Surgery
 Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS. 201-795-8175 CarePointHealth.
 www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 201-795-8175 CarePointHealth.org 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
www.carepointhealth.org GASTRIC SLEEVE SURGERY FOR WEIGHT LOSS 201-795-8175 CarePointHealth.org 1 CONTENTS What is sleeve gastrectomy? Why choose sleeve gastrectomy? Health risks associated with excess
Weight Loss Surgery and Bariatric Nutrition. Jeanine Giordano, MS, RD, CDN
 Weight Loss urgery and Bariatric Nutrition Jeanine Giordano, M, RD, CDN UA: Mean BMI trends (age standardized) Prevalence of Obesity Among Adults United tates 68% Australia 59% Russia 54% United Kingdom
Weight Loss urgery and Bariatric Nutrition Jeanine Giordano, M, RD, CDN UA: Mean BMI trends (age standardized) Prevalence of Obesity Among Adults United tates 68% Australia 59% Russia 54% United Kingdom
SUMMA HEALTH SYSTEM BARIATRIC CARE CENTER. Laura Ilg RD, LD Adrian Dan MD, FACS
 SUMMA HEALTH SYSTEM BARIATRIC CARE CENTER Laura Ilg RD, LD Adrian Dan MD, FACS GOALS The Many Benefits of Bariatric surgery and Weight Reduction Bariatric Care Center Surgical Weight Loss Program Medical
SUMMA HEALTH SYSTEM BARIATRIC CARE CENTER Laura Ilg RD, LD Adrian Dan MD, FACS GOALS The Many Benefits of Bariatric surgery and Weight Reduction Bariatric Care Center Surgical Weight Loss Program Medical
Bariatric Surgery 101
 Bariatric Surgery 101 Dr. Brent Bell, MD Bariatric / General Surgeon Medical Conditions Caused By Morbid Obesity Type 2 DM Hypertension Cholesterol Sleep Apnea Fatty Liver Asthma Osteoarthritis Reduced
Bariatric Surgery 101 Dr. Brent Bell, MD Bariatric / General Surgeon Medical Conditions Caused By Morbid Obesity Type 2 DM Hypertension Cholesterol Sleep Apnea Fatty Liver Asthma Osteoarthritis Reduced
Bariatric Surgery. Overview of Procedural Options
 Bariatric Surgery Overview of Procedural Options The Obesity Epidemic In 1991, NO state had an obesity rate above 20% 1 As of 2010, more than two-thirds of states (38) now have adult obesity rates above
Bariatric Surgery Overview of Procedural Options The Obesity Epidemic In 1991, NO state had an obesity rate above 20% 1 As of 2010, more than two-thirds of states (38) now have adult obesity rates above
Medical Coverage Policy Bariatric Surgery
 Medical Coverage Policy Bariatric Surgery Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2011 Policy Last Updated: 11/01/2011 Prospective review is recommended/required. Please check
Medical Coverage Policy Bariatric Surgery Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2011 Policy Last Updated: 11/01/2011 Prospective review is recommended/required. Please check
Changes to Bariatric Surgery Prior Authorization Guidelines
 Update August 2011 No. 2011-44 Affected Programs: BadgerCare Plus, Medicaid To: Hospital Providers, Physician Assistants, Physician Clinics, Physicians, HMOs and Other Managed Care Programs Changes to
Update August 2011 No. 2011-44 Affected Programs: BadgerCare Plus, Medicaid To: Hospital Providers, Physician Assistants, Physician Clinics, Physicians, HMOs and Other Managed Care Programs Changes to
really help your physical, social and emotional wellbeing helping you do more of the things you want and feel more confident and relaxed.
 Weight loss surgery If you are seriously overweight, losing excess weight can transform your life. Find out how you can make that change with the help of Spire Healthcare. If you One are off seriously
Weight loss surgery If you are seriously overweight, losing excess weight can transform your life. Find out how you can make that change with the help of Spire Healthcare. If you One are off seriously
Bariatric Surgery. Required forms: (Forms are located at OHCA Forms ) Certification Criteria for Providers. Treatment for Obesity
 Bariatric Surgery Required forms: (Forms are located at OHCA Forms ) HCA-13A HCA-12A Certification Criteria for Providers To be eligible for reimbursement, bariatric surgery providers must be certified
Bariatric Surgery Required forms: (Forms are located at OHCA Forms ) HCA-13A HCA-12A Certification Criteria for Providers To be eligible for reimbursement, bariatric surgery providers must be certified
Weight Loss Surgery. Our Surgeons. A Patient s Guide
 Our Surgeons Our bariatric surgeons and support staff provide the information and support necessary to achieve substantial and sustainable weight loss. Our surgeons: Weight Loss Surgery A Patient s Guide
Our Surgeons Our bariatric surgeons and support staff provide the information and support necessary to achieve substantial and sustainable weight loss. Our surgeons: Weight Loss Surgery A Patient s Guide
HOUSTON METHODIST SURGICAL WEIGHT LOSS
 HOUSTON METHODIST SURGICAL WEIGHT LOSS Why choose surgical weight loss at Houston Methodist? Obesity causes many dangerous diseases and health conditions such as diabetes, high blood pressure, heart disease,
HOUSTON METHODIST SURGICAL WEIGHT LOSS Why choose surgical weight loss at Houston Methodist? Obesity causes many dangerous diseases and health conditions such as diabetes, high blood pressure, heart disease,
Some of the diseases and conditions associated with obesity include:
 WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
WEIGHT-LOSS SURGERY facts about obesity Obesity is rapidly becoming the nation s number-one health problem. Of the 97 million Americans who are overweight, 10 million are considered morbidly obese. Obesity
Treating Patients with PRE-DIABETES David Doriguzzi, PA-C First Valley Medical Group. Learning Objectives. Background. CAPA 2015 Annual Conference
 Treating Patients with PRE-DIABETES David Doriguzzi, PA-C First Valley Medical Group Learning Objectives To accurately make the diagnosis of pre-diabetes/metabolic syndrome To understand the prevalence
Treating Patients with PRE-DIABETES David Doriguzzi, PA-C First Valley Medical Group Learning Objectives To accurately make the diagnosis of pre-diabetes/metabolic syndrome To understand the prevalence
NHRMC General Surgery Specialists. Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303
 Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
Minimally Invasive Gastrointestinal Surgery Phone: 910-662-9300 Fax: 910-662-9303 W. Borden Hooks III, MD 1725 New Hanover Medical Park Drive Wilmington, NC 28403 Thank you for choosing NHRMC General Surgery
The Arguments: T2DM - tremendous economic burden globally Lifestyle / Pharm Rx:
 James Cromie The Arguments: T2DM - tremendous economic burden globally Lifestyle / Pharm Rx: INEFFECTIVE and UNSUSTAINED Bariatric surgery is an Effective and Durable treatment option Well established
James Cromie The Arguments: T2DM - tremendous economic burden globally Lifestyle / Pharm Rx: INEFFECTIVE and UNSUSTAINED Bariatric surgery is an Effective and Durable treatment option Well established
Weight Loss Surgery A Patient s Guide
 Our Surgeons Ibrahim M. Ibrahim, MD, FACS, BSCOE Medical Director of Bariatric Surgery at Englewood Hospital Weight Loss Surgery A Patient s Guide Jeffrey W. Strain, MD, FACS, BSCOE Celinés Morales-Ribeiro,
Our Surgeons Ibrahim M. Ibrahim, MD, FACS, BSCOE Medical Director of Bariatric Surgery at Englewood Hospital Weight Loss Surgery A Patient s Guide Jeffrey W. Strain, MD, FACS, BSCOE Celinés Morales-Ribeiro,
Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Abstract Background Methods:
 Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Mousa Khoursheed, Ibtisam Al-Bader, Ali Mouzannar, Abdulla Al-Haddad, Ali Sayed, Ali Mohammad,
Sleeve gastrectomy or gastric bypass as revisional bariatric procedures: retrospective evaluation of outcomes. Mousa Khoursheed, Ibtisam Al-Bader, Ali Mouzannar, Abdulla Al-Haddad, Ali Sayed, Ali Mohammad,
Surgical Weight Loss. Mission Bariatrics
 Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Bariatric Surgery Guide
 One Bariatric Surgery Guide Get back to enjoying the everyday moments. Obesity is one of the nation s leading health issues. More than half of Americans are overweight and roughly 12 million Americans
One Bariatric Surgery Guide Get back to enjoying the everyday moments. Obesity is one of the nation s leading health issues. More than half of Americans are overweight and roughly 12 million Americans
Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Laparoscopic adjustable gastric banding for the treatment of obesity (Update and re-appraisal)
Surgical Weight Loss Program for Teens
 Surgical Weight Loss Program for Teens Surgical Weight Loss Program for Teens The Surgical Weight Loss Program team understands the impact that being severely overweight can have on your life. Our guiding
Surgical Weight Loss Program for Teens Surgical Weight Loss Program for Teens The Surgical Weight Loss Program team understands the impact that being severely overweight can have on your life. Our guiding
abcdefghijklmnopqrstu
 The Quality Unit Planning and Quality Division E: [email protected] [email protected] T: 0131-244 2287 abcdefghijklmnopqrstu NHSScotland Board Chief Executives NHSScotland Board Medical
The Quality Unit Planning and Quality Division E: [email protected] [email protected] T: 0131-244 2287 abcdefghijklmnopqrstu NHSScotland Board Chief Executives NHSScotland Board Medical
American Society for Bariatric Surgery 100 SW 75th Street, Suite 201 Gainesville, FL 32607
 May 11, 2005 Steve E. Phurrough, MD, MPA Office of Clinical Standards & Quality Centers for Medicare and Medicaid Services 7500 Security Boulevard Mail Stop C1-09-06 Baltimore, MD 21244-1850 Re: Request
May 11, 2005 Steve E. Phurrough, MD, MPA Office of Clinical Standards & Quality Centers for Medicare and Medicaid Services 7500 Security Boulevard Mail Stop C1-09-06 Baltimore, MD 21244-1850 Re: Request
4/11/14. Medical Director, Bariatric Surgery Mountainview Regional Medical Center. ! None. ! Discuss the ongoing epidemic of obesity
 Medical Director, Bariatric Surgery Mountainview Regional Medical Center! None! Discuss the ongoing epidemic of obesity! Discuss current treatment options! Discuss the role of bariatric surgery! Review
Medical Director, Bariatric Surgery Mountainview Regional Medical Center! None! Discuss the ongoing epidemic of obesity! Discuss current treatment options! Discuss the role of bariatric surgery! Review
WEIGHT LOSS SURGERY. Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010
 WEIGHT LOSS SURGERY Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010 EDUCATIONAL OBJECTIVES: Discuss the available pharmaceutical options for weight loss and risks of these medications Explain the
WEIGHT LOSS SURGERY Pre-Clinic Conference Jennifer Kinley, MD 12/15/2010 EDUCATIONAL OBJECTIVES: Discuss the available pharmaceutical options for weight loss and risks of these medications Explain the
Weight-Loss Surgery. Regain your quality of life.
 Weight-Loss Surgery Regain your quality of life. If you are struggling with obesity consider weight-loss surgery at Aiken Regional. For the more than 10 million severely overweight people in the United
Weight-Loss Surgery Regain your quality of life. If you are struggling with obesity consider weight-loss surgery at Aiken Regional. For the more than 10 million severely overweight people in the United
Surgical Treatment of Obesity: A Surgeon s View
 Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
Surgical Treatment of Obesity: A Surgeon s View Jenny J. Choi, MD Director of Bariatrics Associate Director of Clinical Affairs Assistant Professor of Surgery Albert Einstein School of Medicine Montefiore
bariatric care center Surgical Weight Loss Management
 bariatric care center Surgical Weight Loss Management I chose Summa because of their reputation and the follow-up care. Diana Harper Watch Diana s story at summahealth.org/diana Contents 3 Program Overview
bariatric care center Surgical Weight Loss Management I chose Summa because of their reputation and the follow-up care. Diana Harper Watch Diana s story at summahealth.org/diana Contents 3 Program Overview
BARIATRIC SURGERY. Personalized Weight Loss Program
 BARIATRIC SURGERY Personalized Weight Loss Program Lafayette General Medical Center performs three major operations for weight loss surgery: Adjustable Gastric Band, Laparoscopic Sleeve Gastrectomy and
BARIATRIC SURGERY Personalized Weight Loss Program Lafayette General Medical Center performs three major operations for weight loss surgery: Adjustable Gastric Band, Laparoscopic Sleeve Gastrectomy and
Diabetes and Weight-Loss Surgery
 WHITE PAPER Diabetes and Weight-Loss Surgery Treat the cause. Cure the symptom. Center of Excellence BARIATRIC SURGERY Written July 2011 Bariatric Surgery: The Cure for Type II Diabetes? For most individuals
WHITE PAPER Diabetes and Weight-Loss Surgery Treat the cause. Cure the symptom. Center of Excellence BARIATRIC SURGERY Written July 2011 Bariatric Surgery: The Cure for Type II Diabetes? For most individuals
Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity
 Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity A Review of the Research for Adults With a BMI Between 30 and 35 Is This Information Right for Me? If
Weight-Loss Surgery for Adults With Diabetes or Prediabetes Who Are at the Lower Levels of Obesity A Review of the Research for Adults With a BMI Between 30 and 35 Is This Information Right for Me? If
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes
 Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes People with diabetes Losing excess weight will assist in the management of
Blue Distinction Centers for Bariatric Surgery Clinical Program Requirements for 2010 Mid-Point Designations
 Blue Distinction Centers for Bariatric Surgery Clinical Program Requirements for 2010 Mid-Point Designations Evaluation is based primarily on the facilities responses to the Blue Distinction Centers for
Blue Distinction Centers for Bariatric Surgery Clinical Program Requirements for 2010 Mid-Point Designations Evaluation is based primarily on the facilities responses to the Blue Distinction Centers for
Surgical Associates of Ithaca Guide to Weight-loss Surgery
 Surgical Associates of Ithaca Guide to Weight-loss Surgery Please read through this entire guide. Weight loss surgeons Dr. John Mecenas and Dr. Brian Bollo are bariatric trained surgeons affiliated with
Surgical Associates of Ithaca Guide to Weight-loss Surgery Please read through this entire guide. Weight loss surgeons Dr. John Mecenas and Dr. Brian Bollo are bariatric trained surgeons affiliated with
XXXXX Petitioner File No. 113467-001 v. Issued and entered this _12th_ day of October 2010 by Ken Ross Commissioner ORDER I PROCEDURAL BACKGROUND
 In the matter of STATE OF MICHIGAN DEPARTMENT OF ENERGY, LABOR & ECONOMIC GROWTH OFFICE OF FINANCIAL AND INSURANCE REGULATION Before the Commissioner of Financial and Insurance Regulation XXXXX Petitioner
In the matter of STATE OF MICHIGAN DEPARTMENT OF ENERGY, LABOR & ECONOMIC GROWTH OFFICE OF FINANCIAL AND INSURANCE REGULATION Before the Commissioner of Financial and Insurance Regulation XXXXX Petitioner
Section 2. Overview of Obesity, Weight Loss, and Bariatric Surgery
 Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
Section 2 Overview of Obesity, Weight Loss, and Bariatric Surgery What is Weight Loss? How does surgery help with weight loss? Short term versus long term weight loss? Conditions Improved with Weight Loss
BARIATRIC SURGERY. Prerequisites. Authorization, Notification and Referral
 BARIATRIC SURGERY Policy NHP reimburses participating providers for specific types of medically necessary bariatric surgery when needed to either alleviate or correct medical problems caused by severe
BARIATRIC SURGERY Policy NHP reimburses participating providers for specific types of medically necessary bariatric surgery when needed to either alleviate or correct medical problems caused by severe
ACS BSCN Accredita on. Program Manual. Version V4.03 01 11
 ACS BSCN Accredita on Program Manual Version V4.03 01 11 Table of Contents CHAPTER 1. INTRODUCTION... 3 1A. INTRODUCTION: BACKGROUND... 3 1B. INTRODUCTION: ACCREDITATION PROGRAM MANUAL... 4 CHAPTER 2.
ACS BSCN Accredita on Program Manual Version V4.03 01 11 Table of Contents CHAPTER 1. INTRODUCTION... 3 1A. INTRODUCTION: BACKGROUND... 3 1B. INTRODUCTION: ACCREDITATION PROGRAM MANUAL... 4 CHAPTER 2.
Weight Loss Surgery Information Session. WFBH Bariatric Surgery Program
 Weight Loss Surgery Information Session WFBH Bariatric Surgery Program What makes us different? Center of Excellence (COE) High volume center > 1000 procedures since 2003 Less complications than non-coe
Weight Loss Surgery Information Session WFBH Bariatric Surgery Program What makes us different? Center of Excellence (COE) High volume center > 1000 procedures since 2003 Less complications than non-coe
MORTALITY RISK FACTORS IN PATIENTS UNDERGOING GASTRIC BYPASS SURGERY
 Where Do We Stand? Alan M. Brader, MD Lancaster General Bariatrics Introduction The management of a patient with extreme obesity is a challenging task for most health care givers. Unfortunately, there
Where Do We Stand? Alan M. Brader, MD Lancaster General Bariatrics Introduction The management of a patient with extreme obesity is a challenging task for most health care givers. Unfortunately, there
Public Comments for State Plan Amendment (SPA) 16 001 Bariatric Surgery
 Public Comments for State Plan Amendment (SPA) 16 001 Bariatric Surgery Received: December 19, 2015 I have reviewed the Medicaid documents regarding Bariatric Coverage for the Medicaid Beneficiaries of
Public Comments for State Plan Amendment (SPA) 16 001 Bariatric Surgery Received: December 19, 2015 I have reviewed the Medicaid documents regarding Bariatric Coverage for the Medicaid Beneficiaries of
Advancing the Field of Bariatric Surgery at University Hospitals
 Advancing the Field of Bariatric Surgery at University Hospitals More Sharing ServicesShare Share on facebookshare on emailshare on favoritesshare on printrss Feed By: Alex Strauss Sunday, March 11, 2012
Advancing the Field of Bariatric Surgery at University Hospitals More Sharing ServicesShare Share on facebookshare on emailshare on favoritesshare on printrss Feed By: Alex Strauss Sunday, March 11, 2012
Emerging Concepts in Bariatric Surgery
 Emerging Concepts in Bariatric Surgery C Y N T H I A L. L O N G, M D, F A C S S I N A I H O S P I T A L O F B A L T I M O R E D E P A R T M E N T O F S U R G E R Y D I V I S I O N O F M I N I M A L L Y
Emerging Concepts in Bariatric Surgery C Y N T H I A L. L O N G, M D, F A C S S I N A I H O S P I T A L O F B A L T I M O R E D E P A R T M E N T O F S U R G E R Y D I V I S I O N O F M I N I M A L L Y
Weight Loss Surgery Info for Physicians
 Weight Loss Surgery Info for Physicians As physicians, we see it every day when we see our patients more and more people are obese, and it s affecting their health. It s estimated that at least 2/3 of
Weight Loss Surgery Info for Physicians As physicians, we see it every day when we see our patients more and more people are obese, and it s affecting their health. It s estimated that at least 2/3 of
Comprehensive Center for. Bariatric Surgery. Weight-Loss Counseling, Evaluation, & Surgery
 Comprehensive Center for Bariatric Surgery Weight-Loss Counseling, Evaluation, & Surgery Yes, there is a cure. Obesity is treatable. And solvable. It s dangerous and debilitating but fortunately medical
Comprehensive Center for Bariatric Surgery Weight-Loss Counseling, Evaluation, & Surgery Yes, there is a cure. Obesity is treatable. And solvable. It s dangerous and debilitating but fortunately medical
Dieting and Gallstones
 Dieting and Gallstones WIN Weight-control Information Network What are Gallstones are clusters of solid material that form in the gallbladder. The most common type is made mostly of cholesterol. Gallstones
Dieting and Gallstones WIN Weight-control Information Network What are Gallstones are clusters of solid material that form in the gallbladder. The most common type is made mostly of cholesterol. Gallstones
Insurance-mandated medical programs before bariatric surgery: do good things come to those who wait?
 Surgery for Obesity and Related Diseases 7 (2011) 526 530 Original article Insurance-mandated medical programs before bariatric surgery: do good things come to those who wait? Timothy S. Kuwada, M.D.*,
Surgery for Obesity and Related Diseases 7 (2011) 526 530 Original article Insurance-mandated medical programs before bariatric surgery: do good things come to those who wait? Timothy S. Kuwada, M.D.*,
Technical Aspects of Bariatric Surgical Procedures. Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital
 Technical Aspects of Bariatric Surgical Procedures Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital Disclosures Allergan, Inc. (Past) Faculty Member Educational
Technical Aspects of Bariatric Surgical Procedures Robert O. Carpenter, MD, MPH, FACS Department of Surgery Scott & White Memorial Hospital Disclosures Allergan, Inc. (Past) Faculty Member Educational
Adult Weight Management Training Summary
 Adult Weight Management Training Summary The Commission on Dietetic Registration, the credentialing agency for the Academy of Nutrition and Dietetics Marilyn Holmes, MS, RDN, LDN About This Presentation
Adult Weight Management Training Summary The Commission on Dietetic Registration, the credentialing agency for the Academy of Nutrition and Dietetics Marilyn Holmes, MS, RDN, LDN About This Presentation
Introduction to obesity surgery
 Introduction to obesity surgery Auckland weight loss Surgery Surgery ADDRESS Mercy Specialist Centre PHONE FAX EMAIL WEB 100 Mountain Road, Epsom, Auckland 09 623 2409 09 630 8589 [email protected] www.aucklandweightlosssurgery.co.nz
Introduction to obesity surgery Auckland weight loss Surgery Surgery ADDRESS Mercy Specialist Centre PHONE FAX EMAIL WEB 100 Mountain Road, Epsom, Auckland 09 623 2409 09 630 8589 [email protected] www.aucklandweightlosssurgery.co.nz
Obesity and Morbid Obesity Management
 Rule Category: Medical ` Ref: No: 2011-MN-0022 Version Control: Version No. 4.0 Effective Date: November 2011 Revision Date: August-2015 Obesity and Morbid Obesity Management Adjudication Rule Table of
Rule Category: Medical ` Ref: No: 2011-MN-0022 Version Control: Version No. 4.0 Effective Date: November 2011 Revision Date: August-2015 Obesity and Morbid Obesity Management Adjudication Rule Table of
Inova Weight Loss Services
 Inova Weight Loss Services Getting Started We encourage you to attend one of our free informational seminars where you can meet our expert team and learn more about our weight loss solutions. A referral
Inova Weight Loss Services Getting Started We encourage you to attend one of our free informational seminars where you can meet our expert team and learn more about our weight loss solutions. A referral
The first endoscopically-delivered device therapy for obese patients with type 2 diabetes
 DIABETES WEIGHT ENDOBARRIER THERAPY The first endoscopically-delivered device therapy for obese patients with type 2 diabetes Restore the metabolic health of your patients with EndoBarrier Therapy. Dual
DIABETES WEIGHT ENDOBARRIER THERAPY The first endoscopically-delivered device therapy for obese patients with type 2 diabetes Restore the metabolic health of your patients with EndoBarrier Therapy. Dual
SURGICAL PREAMBLE SPECIFIC ELEMENTS SURGICAL SERVICES WHICH ARE NOT LISTED AS A "Z" CODE
 Surgical PreambleApril 1, 2015 PREAMBLE SPECIFIC ELEMENTS In addition to the common elements, all surgical services include the following specific elements. A. Supervising the preparation of and/or preparing
Surgical PreambleApril 1, 2015 PREAMBLE SPECIFIC ELEMENTS In addition to the common elements, all surgical services include the following specific elements. A. Supervising the preparation of and/or preparing
Diabetes? Does Metabolic Surgery. Experts disagree about how surgery treats diabetes but agree more research needs to be done.
 Does Metabolic Surgery The combination of type 2 diabetes and being significantly overweight is a huge burden. Doctors tell you to lose weight, in essence, to save your life. Weight loss, in addition to
Does Metabolic Surgery The combination of type 2 diabetes and being significantly overweight is a huge burden. Doctors tell you to lose weight, in essence, to save your life. Weight loss, in addition to
TYPE 2 DIABETES MELLITUS: NEW HOPE FOR PREVENTION. Robert Dobbins, M.D. Ph.D.
 TYPE 2 DIABETES MELLITUS: NEW HOPE FOR PREVENTION Robert Dobbins, M.D. Ph.D. Learning Objectives Recognize current trends in the prevalence of type 2 diabetes. Learn differences between type 1 and type
TYPE 2 DIABETES MELLITUS: NEW HOPE FOR PREVENTION Robert Dobbins, M.D. Ph.D. Learning Objectives Recognize current trends in the prevalence of type 2 diabetes. Learn differences between type 1 and type
Medical Policy Bariatric Surgery
 Medical Policy Bariatric Surgery Document Number: 001 Commercial MassHealth and Qualified Health Plans Authorization required X X Notification within 24 hours of service or next business day No notification
Medical Policy Bariatric Surgery Document Number: 001 Commercial MassHealth and Qualified Health Plans Authorization required X X Notification within 24 hours of service or next business day No notification
NP/PA Clinical Hepatology Fellowship Summary of Year-Long Curriculum
 OVERVIEW OF THE FELLOWSHIP The goal of the AASLD NP/PA Fellowship is to provide a 1-year postgraduate hepatology training program for nurse practitioners and physician assistants in a clinical outpatient
OVERVIEW OF THE FELLOWSHIP The goal of the AASLD NP/PA Fellowship is to provide a 1-year postgraduate hepatology training program for nurse practitioners and physician assistants in a clinical outpatient
Trends in Bariatric Surgery for Morbid Obesity. in Wisconsin
 Trends in Bariatric Surgery for Morbid Obesity in Wisconsin Jennifer L. Erickson, B.A. Patrick L. Remington, M.D., M.P.H. Paul E. Peppard, PhD A Working Paper of the Wisconsin Public Health and Health
Trends in Bariatric Surgery for Morbid Obesity in Wisconsin Jennifer L. Erickson, B.A. Patrick L. Remington, M.D., M.P.H. Paul E. Peppard, PhD A Working Paper of the Wisconsin Public Health and Health
Gastric Surgery for Clinically Severe (Morbid) Obesity
 Origination: 03/28/01 Revised: 01/16/15 Annual Review: 11/12/15 Purpose: The Medical Technology Assessment Committee will review published scientific literature and information from appropriate government
Origination: 03/28/01 Revised: 01/16/15 Annual Review: 11/12/15 Purpose: The Medical Technology Assessment Committee will review published scientific literature and information from appropriate government
How to Avoid Malpractice Suits in Bariatric Surgery
 How to Avoid Malpractice Suits in Bariatric Surgery Robin Blackstone, MD, FACS Masters of Minimally Invasive Bariatric Surgery April 5, 2013 Orlando, Florida ACS Claims Study 2003-2004 Charge of negligence
How to Avoid Malpractice Suits in Bariatric Surgery Robin Blackstone, MD, FACS Masters of Minimally Invasive Bariatric Surgery April 5, 2013 Orlando, Florida ACS Claims Study 2003-2004 Charge of negligence
INFORMED CONSENT FOR SLEEVE GASTRECTOMY
 INFORMED CONSENT FOR SLEEVE GASTRECTOMY This informed-consent document has been prepared to help inform you about your Sleeve Gastrectomy including the risks and benefits, as well as alternative treatments.
INFORMED CONSENT FOR SLEEVE GASTRECTOMY This informed-consent document has been prepared to help inform you about your Sleeve Gastrectomy including the risks and benefits, as well as alternative treatments.
U.S. Food and Drug Administration
 U.S. Food and Drug Administration Notice: Archived Document The content in this document is provided on the FDA s website for reference purposes only. It was current when produced, but is no longer maintained
U.S. Food and Drug Administration Notice: Archived Document The content in this document is provided on the FDA s website for reference purposes only. It was current when produced, but is no longer maintained
Karen Kovach M.S, R.D Chief Scientific Officer Weight Watchers International Inc.
 Waking up to real solutions to Chronic Disease: Tackling obesity can reduce the burden of chronic disease and deliver substantial cost savings to struggling European healthcare systems Karen Kovach M.S,
Waking up to real solutions to Chronic Disease: Tackling obesity can reduce the burden of chronic disease and deliver substantial cost savings to struggling European healthcare systems Karen Kovach M.S,
