REFERRALS CPT CODES COMMENTS
|
|
|
- William Fowler
- 9 years ago
- Views:
Transcription
1 Gundersen Health Plan (GHP) Procedures & Services Requiring Prior Authorization Benefits and eligibility must be verified with the Health Plan Customer Service. Self-funded and Fully Insured Employer Group Plans: or Senior Preferred: or BadgerCare Plus: or GundersenOne: or This grid applies to all GHP members; it is intended to be a guide and does not guarantee coverage. Medical benefit plan language supersedes the general information provided on this grid. The presence or absence of an item on this list does not define whether or not coverage or benefits exist for the service or procedure and/or CPT code. Failure to prior authorize procedures or services on this grid may result in denial of coverage; as a result financial responsibility may be yours. Senior Preferred members may see Evidence of Coverage for complete benefit information. REFERRALS CPT CODES COMMENTS Any referral to a non-participating provider/facility for non-emergent services A signed written referral from the Health Plan is required prior to receiving services from a non participating provider/facility Initial Low Back Pain Consults with Orthopedic or Neurosurgery departments (follow up visits do not require prior authorization) For State of Wisconsin ETF members. Submit supporting medical documentation. Effective 1/01/2013 EXPERIMENTAL Experimental/Investigational Considered provider responsibility when the member would not be reasonably expected to know that the service is experimental. The Health Plan utilizes Hayes Medical Technology Directory to determine if services are experimental/ investigational. In addition to Hayes, other sources may be reviewed which include but are not limited to the evidence based medical literature, specialty Medical Advisory Panel, and other technology review resources.
2 MEDICAL SERVICES CPT CODES COMMENTS Autism Spectrum Disorders Continuous Passive Motion (CPM) E0935 (Coverage limited to knee only) Prior authorization required for CPM usage beyond 21 days post op. Submit supporting medical documentation Cranial Remolding Orthotic S1040 Durable Medical Equipment (DME) Senior Preferred All DME purchases, rentals and repairs (no dollar threshold) Senior Preferred Call Customer Service to verify eligibility of member Review Medicare criteria: - If item is statutorily excluded by Medicare, notify member item is not covered by Senior Preferred; if member wants to purchase item, obtain signature on NDMC (available on website) - If item meets Medicare criteria, dispense and bill Health Plan - If item does not meet Medicare medical necessity criteria, submit PA to Health Plan for organizational determination Commercial/BadgerCare Plus/ GundersenOne DME purchases exceeding dollar threshold (varies by group) and all rentals and repairs Commercial/BadgerCare Plus/GundersenOne Call Customer Service to verify eligibility of member and prior authorization requirements (please provide HCPCS code) Enteral Therapy B4034-B9999 Genetic Testing Home Health Member must be homebound and meet criteria for home health. Home Prothrombin Time Monitoring G0249, G0248 Home Sleep Studies (under C-PAP policy) Prior authorization required from a sleep disorder physician specialist or provider practicing under the supervision of a sleep disorder specialist. Submit supporting medical documentation Hyperbaric Oxygen Therapy (HBOT) Prior authorization is required. Submit supporting medical documentation.
3 Insulin pumps /Continuous glucose monitors/receivers and supplies IV Drugs outpatient hospital and clinic (except EPO) IV Infusions Mental Health, Alcohol and other drug addictions (M.H./A.O.D.A), Transitional Treatment (includes Partial Hospitalization services), Day Treatment BadgerCare Therapies E0784/S1030, S1031, A9276-A9278, E0607, E2100, E2101 Home IV Therapy requires prior authorization. Request to be received from supplier. Prior authorizations required after 35 visits per therapy discipline; however, some services always require prior authorization per ForwardHealth Guidelines. Please refer to the ForwardHealth portal. Providers must use the PA forms available via the portal. Senior Preferred Part B Therapies. All Part B therapies require prior authorization. Refer the Health Plan website for detailed instructions. Skilled Nursing Facility Prior authorization required from facility. Swing Bed Prior authorization required prior to admission. TheraSphere/Sir-Spheres Treatment CPT: 77790, 36245, 75726, 77778, HCPCS: C2616, Q3001, S2095 Submit supporting medical documentation and appropriate codes. PROCEDURES\SURGICAL CPT CODES COMMENTS TREATMENTS Abortions Only if medically necessary as determined by the Health Plan. Artificial Intervertebral Disc Replacement for Cervical and Lumbar Degenerative Disc Disease 0092T, 0095T, 0098T, 0163T, 0164T, 0165T, Member must be 18 or over. Medicare does not provide coverage for patients over age 60. Coverage will be limited to the cost of the procedure and the cost of one artificial intervertebral disc. Bone Anchored Hearing Aide (BAHA) Bariatric surgical treatment for Severe Obesity , , , S2083, 43886,43888 Blepharoplasty Upper and lower lid blepharoplasty will be subject to prior authorization. Photos and visual fields will be required.
4 CardioMems C97412, C2624 Chorionic Villus Sampling (CVS) Cochlear Implants 69930, Required for members age 18 and over LINX Reflux Management System Submit supporting medical documentation PROCEDURES/SURGICAL CPT CODES TREATMENTS CONTINUED Deep Brain Stimulation , L8680-L8689 High Tech Radiology Tests CT & CTA: 70450,70460,70470, , , , 70496, 70498, 71250, 71260, 71270, 71275, , , , 73206,73700, 73702, , 74150, 74160, 74170, , , , 75635, 76380, 77078,77079,S8092 COMMENTS For State of Wisconsin ETF members. Submit supporting medical documentation. Effective 1/01/2013. MRI & MRA: 70336, 70540, , ,71555, 72141, 72142, , , , ,73225, ,73725, , 74185, 75557, 75559, 75561, 75563, 75565, 77058, 77059, 77084, S8037, PET: 78608, 78609, , G0235, 0159T, S8037, , Nuclear Stress Test: , 78481, 78483, 78499, Hyperhidrosis, Surgical Treatment Reduction Mammoplasty Refractive Surgery 65765, S0800, S0810, S0812 Rhinoplasty or Rhino portion of Septorhinoplasty Surgical Removal of Redundant Skin , Surgical Treatment of Obstructive Sleep Apnea(OSA) Pillar Implants are not covered for Commercial or GundersenOne members.
5 Surgical Treatment of Pectus Excavatum and Carinatum Syndrome Transmyocardial Revascularization (TMR) Transplants (excluding corneal A referral request is required for all members. transplants) Surgical/Laser Treatment of Scars Vagus Nerve Stimulation , Varicose Vein Treatment (excludes vein stripping) 36468, 36469, , 37766
Advance Notification Requirements for New York Effective June 1, 2015
 Advance Notification Requirements for New York Effective June 1, 2015 General Information This list represents our prior authorization review requirements for UnitedHealthcare Community Plan of New York.
Advance Notification Requirements for New York Effective June 1, 2015 General Information This list represents our prior authorization review requirements for UnitedHealthcare Community Plan of New York.
The Deductible is applicable to all covered services except for flat dollar Copayment services.
 PRIORITY HEALTH www.priorityhealth.com/mpsers PRIORITYHMO SM PLUS PLAN MICHIGAN PUBLIC SCHOOL EMPLOYEES RETIREMENT SYSTEM (MPSERS) Effective January 1, 2016 through December 31, 2016 The HMO Plus plan
PRIORITY HEALTH www.priorityhealth.com/mpsers PRIORITYHMO SM PLUS PLAN MICHIGAN PUBLIC SCHOOL EMPLOYEES RETIREMENT SYSTEM (MPSERS) Effective January 1, 2016 through December 31, 2016 The HMO Plus plan
Prior Authorization Requirements for Florida Effective March 1, 2015
 for Florida Effective March 1, 215 General Information The following list represents our prior authorization requirements for UnitedHealthcare in Florida. All services rendered by a non-contracted physician,
for Florida Effective March 1, 215 General Information The following list represents our prior authorization requirements for UnitedHealthcare in Florida. All services rendered by a non-contracted physician,
COMPREHENSIVE PRIOR AUTHORIZATION LISTS NJ FAMILYCARE/MEDICAID & DUAL COMPLETE HMO SNP PRODUCTS EFFECTIVE 7/1/13
 TO ALL HEALTHCARE PROFESSIONALS: COMPREHENSIVE PRIOR AUTHORIZATION LISTS NJ FAMILYCARE/MEDICAID & DUAL COMPLETE HMO SNP PRODUCTS EFFECTIVE 7/1/13 BEFORE SEEKING PRIOR AUTHORIZATION, PLEASE VERIFY MEMBER
TO ALL HEALTHCARE PROFESSIONALS: COMPREHENSIVE PRIOR AUTHORIZATION LISTS NJ FAMILYCARE/MEDICAID & DUAL COMPLETE HMO SNP PRODUCTS EFFECTIVE 7/1/13 BEFORE SEEKING PRIOR AUTHORIZATION, PLEASE VERIFY MEMBER
Prior Authorization List Adults, FHP, CHP
 Please verify the member s benefits before requesting prior authorization (PA). Services vary within plans. To check member eligibility, please call Provider Services at 888-362-3368 or visit UnitedHealthcareOnline.com.
Please verify the member s benefits before requesting prior authorization (PA). Services vary within plans. To check member eligibility, please call Provider Services at 888-362-3368 or visit UnitedHealthcareOnline.com.
Anthem Blue Cross and Blue Shield in New Hampshire Precertification Guidelines
 Anthem Blue Cross and Blue Shield in New Hampshire Precertification Guidelines The following guidelines apply to Anthem Blue Cross and Blue Shield ( Anthem ) products issued and delivered by Anthem in
Anthem Blue Cross and Blue Shield in New Hampshire Precertification Guidelines The following guidelines apply to Anthem Blue Cross and Blue Shield ( Anthem ) products issued and delivered by Anthem in
PRIORITY HEALTH priorityhealth.com HealthbyChoice Incentives Summary of Benefits TRINITY HEALTH -HbCI 2 1/1/13 12/31/13
 PRIORITY HEALTH priorityhealth.com Healthby Incentives Summary of Benefits TRINITY HEALTH -HbCI 2 1/1/13 12/31/13 The Healthby Incentives HMO plan is a Consumer Engaged Health plan that offers a choice
PRIORITY HEALTH priorityhealth.com Healthby Incentives Summary of Benefits TRINITY HEALTH -HbCI 2 1/1/13 12/31/13 The Healthby Incentives HMO plan is a Consumer Engaged Health plan that offers a choice
Anthem Blue Cross and Blue Shield in Connecticut Precertification Guidelines
 Anthem Blue Cross and Blue Shield in Connecticut Precertification Guidelines The following guidelines apply to Anthem Blue Cross and Blue Shield ( Anthem ) products issued and delivered by Anthem in Connecticut.
Anthem Blue Cross and Blue Shield in Connecticut Precertification Guidelines The following guidelines apply to Anthem Blue Cross and Blue Shield ( Anthem ) products issued and delivered by Anthem in Connecticut.
UnitedHealthcare Medicare Solutions Notification/Prior Authorization Requirements Effective Jan. 1, 2016
 This list represents our advance notification/prior authorization review requirements as referenced in the UnitedHealthcare Physician, Health Care Professional, Facility and Ancillary Provider 2016 Administrative
This list represents our advance notification/prior authorization review requirements as referenced in the UnitedHealthcare Physician, Health Care Professional, Facility and Ancillary Provider 2016 Administrative
Provider Information Guide 2014
 MDwise Eskenazi Health Hoosier Healthwise Provider Information Guide 2014 MDwise Eskenazi Health Hoosier Healthwise All members will have an ID card. The Hoosier Healthwise ID card is the standard, state
MDwise Eskenazi Health Hoosier Healthwise Provider Information Guide 2014 MDwise Eskenazi Health Hoosier Healthwise All members will have an ID card. The Hoosier Healthwise ID card is the standard, state
(FIDA) FIDELIS CARE AUTHORIZATION REQUIREMENTS
 Fully Integrated Duals Advantage (FIDA) FIDELIS CARE AUTHORIZATION REQUIREMENTS Benefit/Service Detail SERVICES AND PROCEDURES WHICH REQUIRE AUTHORIZATION 7/1/2016 I. Inpatient Admissions-All inpatient
Fully Integrated Duals Advantage (FIDA) FIDELIS CARE AUTHORIZATION REQUIREMENTS Benefit/Service Detail SERVICES AND PROCEDURES WHICH REQUIRE AUTHORIZATION 7/1/2016 I. Inpatient Admissions-All inpatient
Medical Management Requirements Effective January 1, 2008
 December 1, 2007 Dear Provider and Colleague: Please be advised that effective January 1, 2008, Health Plan will change its Medical Management Policies to include new requirements for prior authorizations
December 1, 2007 Dear Provider and Colleague: Please be advised that effective January 1, 2008, Health Plan will change its Medical Management Policies to include new requirements for prior authorizations
I. Out of Network: There are no OON benefits. However for any medically necessary service not available in network, authorization will be provided
 The New York State of Health Authorization Grid FIDELIS CARE AUTHORIZATION REQUIREMENTS Benefit/Service Detail SERVICES AND PROCEDURES WHICH REQUIRE AUTHORIZATION EFFECTIVE 7/1/2016 I. Out of Network:
The New York State of Health Authorization Grid FIDELIS CARE AUTHORIZATION REQUIREMENTS Benefit/Service Detail SERVICES AND PROCEDURES WHICH REQUIRE AUTHORIZATION EFFECTIVE 7/1/2016 I. Out of Network:
PREVENTIVE CARE See the REHP Benefits Handbook for a list of preventive benefits* MATERNITY SERVICES Office visits Covered in full including first
 Network Providers Non Network Providers** DEDUCTIBLE (Per Calendar Year) None $250 per person $500 per family OUT-OF-POCKET MAXIMUM (When the out-of-pocket maximum is reached, benefits are paid at 100%
Network Providers Non Network Providers** DEDUCTIBLE (Per Calendar Year) None $250 per person $500 per family OUT-OF-POCKET MAXIMUM (When the out-of-pocket maximum is reached, benefits are paid at 100%
Schedule of Benefits HARVARD PILGRIM LAHEY HEALTH VALUE HMO MASSACHUSETTS MEMBER COST SHARING
 Schedule of s HARVARD PILGRIM LAHEY HEALTH VALUE HMO MASSACHUSETTS ID: MD0000003378_ X Please Note: In this plan, Members have access to network benefits only from the providers in the Harvard Pilgrim-Lahey
Schedule of s HARVARD PILGRIM LAHEY HEALTH VALUE HMO MASSACHUSETTS ID: MD0000003378_ X Please Note: In this plan, Members have access to network benefits only from the providers in the Harvard Pilgrim-Lahey
Preauthorization Requirements * (as of January 1, 2016)
 OFFICE VISITS Primary Care Office Visits Primary Care Home Visits Specialist Office Visits No Specialist Home Visits PREVENTIVE CARE Well Child Visits and Immunizations Adult Annual Physical Examinations
OFFICE VISITS Primary Care Office Visits Primary Care Home Visits Specialist Office Visits No Specialist Home Visits PREVENTIVE CARE Well Child Visits and Immunizations Adult Annual Physical Examinations
AVMED POS PLAN. Allergy Injections No charge 30% co-insurance after deductible Allergy Skin Testing $30 per visit 30% co-insurance after deductible
 AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copays for 2015. This is not a contract, it s a summary of the plan highlights and is subject to change. For specific
AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copays for 2015. This is not a contract, it s a summary of the plan highlights and is subject to change. For specific
2015 Medical Plan Summary
 2015 Medical Plan Summary AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copayments for 2015. This is not a contract, it s a summary of the plan highlights and is
2015 Medical Plan Summary AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copayments for 2015. This is not a contract, it s a summary of the plan highlights and is
HUSKY Health Benefits and Prior Authorization Requirements Grid* Hospital Outpatient Effective: January 1, 2012
 Cardiac Rehab 100% covered 100% covered 100% covered Dialysis 100% covered 100% covered 100% covered Emergency Care Covered no co- pays for Emergency Room visits Covered no co- pays for Emergency Room
Cardiac Rehab 100% covered 100% covered 100% covered Dialysis 100% covered 100% covered 100% covered Emergency Care Covered no co- pays for Emergency Room visits Covered no co- pays for Emergency Room
OFFICE OF GROUP BENEFITS 2014 OFFICE OF GROUP BENEFITS CDHP PLAN FOR STATE OF LOUISIANA EMPLOYEES AND RETIREES PLAN AMENDMENT
 OFFICE OF GROUP BENEFITS 2014 OFFICE OF GROUP BENEFITS CDHP PLAN FOR STATE OF LOUISIANA EMPLOYEES AND RETIREES PLAN AMENDMENT This Amendment is issued by the Plan Administrator for the Plan documents listed
OFFICE OF GROUP BENEFITS 2014 OFFICE OF GROUP BENEFITS CDHP PLAN FOR STATE OF LOUISIANA EMPLOYEES AND RETIREES PLAN AMENDMENT This Amendment is issued by the Plan Administrator for the Plan documents listed
Harvard Pilgrim Health Care of New England, Inc. THE HARVARD PILGRIM BEST BUY TIERED COPAYMENT HMO - LP NEW HAMPSHIRE
 ID: MD0000003228_B3 X Schedule of s Harvard Pilgrim Health Care of New England, Inc. THE HARVARD PILGRIM BEST BUY TIERED COPAYMENT HMO - LP NEW HAMPSHIRE Coverage under this Plan is under the jurisdiction
ID: MD0000003228_B3 X Schedule of s Harvard Pilgrim Health Care of New England, Inc. THE HARVARD PILGRIM BEST BUY TIERED COPAYMENT HMO - LP NEW HAMPSHIRE Coverage under this Plan is under the jurisdiction
Blue Cross Premier Bronze Extra
 An individual PPO health plan from Blue Cross Blue Shield of Michigan. You will have a broad choice of doctors and hospitals within Blue Cross Blue Shield of Michigan s unsurpassed statewide PPO network
An individual PPO health plan from Blue Cross Blue Shield of Michigan. You will have a broad choice of doctors and hospitals within Blue Cross Blue Shield of Michigan s unsurpassed statewide PPO network
Benefit Summary - A, G, C, E, Y, J and M
 Benefit Summary - A, G, C, E, Y, J and M Benefit Year: Calendar Year Payment for Services Deductible Individual $600 $1,200 Family (Embedded*) $1,200 $2,400 Coinsurance (the percentage amount the Covered
Benefit Summary - A, G, C, E, Y, J and M Benefit Year: Calendar Year Payment for Services Deductible Individual $600 $1,200 Family (Embedded*) $1,200 $2,400 Coinsurance (the percentage amount the Covered
Chapter 2. Medical Management and Quality Improvement
 Medical Management Overview...3 Introduction...3 Objectives...3 Important Program Points...3 Prior Authorization...4 Overview...4 MedicareBlue PPO Covered Items and Services...4 Medical Policy...5 Prior
Medical Management Overview...3 Introduction...3 Objectives...3 Important Program Points...3 Prior Authorization...4 Overview...4 MedicareBlue PPO Covered Items and Services...4 Medical Policy...5 Prior
What is the overall deductible? Are there other deductibles for specific services?
 : MyPriority POS RxPlus Silver 1800 Coverage Period: Beginning on or after 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Subscriber/Dependent Plan Type:
: MyPriority POS RxPlus Silver 1800 Coverage Period: Beginning on or after 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Subscriber/Dependent Plan Type:
BENEFIT PLAN. What Your Plan Covers and How Benefits are Paid. Appendix A. Prepared Exclusively for The Dow Chemical Company
 Appendix A BENEFIT PLAN Prepared Exclusively for The Dow Chemical Company What Your Plan Covers and How Benefits are Paid Choice POS II (MAP Plus Option 2 - High Deductible Health Plan (HDHP) with Prescription
Appendix A BENEFIT PLAN Prepared Exclusively for The Dow Chemical Company What Your Plan Covers and How Benefits are Paid Choice POS II (MAP Plus Option 2 - High Deductible Health Plan (HDHP) with Prescription
Oregon CPT Preapproval Grid
 * The following grid only identifies items that require preapproval from. Breast Pumps Notes: No preapproval required for 1st month rental; beyond one month rental requires preapproval Genetic Testing
* The following grid only identifies items that require preapproval from. Breast Pumps Notes: No preapproval required for 1st month rental; beyond one month rental requires preapproval Genetic Testing
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.pplusic.com or by calling 608-282-8900 (1-800-545-5015).
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.pplusic.com or by calling 608-282-8900 (1-800-545-5015).
Physicians Plus Insurance Corporation Coverage Period: 01/01/2016 12/31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.pplusic.com or by calling 1-800-545-5015. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.pplusic.com or by calling 1-800-545-5015. Important Questions
NJ FamilyCare D. Medicaid, NJ FamilyCare A and Alternative Benefit Plan (ABP) NJ FamilyCare B NJ FamilyCare C
 Service Medicaid, NJ FamilyCare A and Alternative Benefit Plan (ABP) NJ Division of Developmental Disabilities (DDD) NJ FamilyCare B NJ FamilyCare C NJ FamilyCare D Abortions and related services (covered
Service Medicaid, NJ FamilyCare A and Alternative Benefit Plan (ABP) NJ Division of Developmental Disabilities (DDD) NJ FamilyCare B NJ FamilyCare C NJ FamilyCare D Abortions and related services (covered
SUMMARY OF BENEFITS. Cigna Health and Life Insurance Co. Laramie County School District 2 Open Access Plus Base - Effective 7/1/2015
 SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Laramie County School District 2 Open Access Plus Base - Effective General Services In-Network Out-of-Network Physician office visit Urgent care
SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Laramie County School District 2 Open Access Plus Base - Effective General Services In-Network Out-of-Network Physician office visit Urgent care
BadgerCare Plus and Wisconsin Medicaid Covered Services Comparison Chart
 and Wisconsin Covered Services Comparison Chart The covered services information in the following chart is provided as general information. Providers should refer to their service-specific publications
and Wisconsin Covered Services Comparison Chart The covered services information in the following chart is provided as general information. Providers should refer to their service-specific publications
Plans. Who is eligible to enroll in the Plan? Blue Care Network (BCN) Health Alliance Plan (HAP) Health Plus. McLaren Health Plan
 Who is eligible to enroll in the Plan? All State of Michigan Employees who reside in the coverage area determined by zip code. All State of Michigan Employees who reside in the coverage area determined
Who is eligible to enroll in the Plan? All State of Michigan Employees who reside in the coverage area determined by zip code. All State of Michigan Employees who reside in the coverage area determined
Covered Benefits. Covered. Must meet current federal and state guidelines. Abortions. Covered. Allergy Testing. Covered. Audiology. Covered.
 Covered Benefits Services Abortions Allergy Testing Audiology Birth Control Services Blood & Blood Plasma Bone Mass Measurement (bone density) Case Management Chemotherapy Chiropractor Services (manipulation/subluxation)
Covered Benefits Services Abortions Allergy Testing Audiology Birth Control Services Blood & Blood Plasma Bone Mass Measurement (bone density) Case Management Chemotherapy Chiropractor Services (manipulation/subluxation)
Medical Benefits. The Regional Health Plan is a self insured plan. The claims administrator is NGS CoreSource.
 The Regional Health Plan is a self insured plan. The claims administrator is NGS CoreSource. For a complete outline of your benefits, please refer to the Regional Health INTRANET site Employee Hub/Summary
The Regional Health Plan is a self insured plan. The claims administrator is NGS CoreSource. For a complete outline of your benefits, please refer to the Regional Health INTRANET site Employee Hub/Summary
National PPO 1000. PPO Schedule of Payments (Maryland Small Group)
 PPO Schedule of Payments (Maryland Small Group) National PPO 1000 The benefits outlined in this Schedule are in addition to the benefits offered under Coventry Health & Life Insurance Company Small Employer
PPO Schedule of Payments (Maryland Small Group) National PPO 1000 The benefits outlined in this Schedule are in addition to the benefits offered under Coventry Health & Life Insurance Company Small Employer
New York. UnitedHealthcare Community Plan Claims System Migration Provider Quick Reference Guide. Complete Claims. Our Claims Process
 Our Claims Process Here are a few steps to ensure you receive prompt payment: 1 Review and copy both sides of the member s ID card. members receive an ID card containing information that helps you process
Our Claims Process Here are a few steps to ensure you receive prompt payment: 1 Review and copy both sides of the member s ID card. members receive an ID card containing information that helps you process
UnitedHealthcare Choice Plus. UnitedHealthcare Insurance Company. Certificate of Coverage
 UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Health Savings Account (HSA) Plan 4X8 of Southern State Community College Enrolling Group Number: 755032
UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Health Savings Account (HSA) Plan 4X8 of Southern State Community College Enrolling Group Number: 755032
HUSKY Health Benefits and Prior Authorization Requirements Grid* Hospital Outpatient Effective: January 1, 2012
 Cardiac Rehab 100% covered 100% covered 100% covered Dialysis 100% covered 100% covered 100% covered Emergency Care Covered no co-pays for Emergency Room visits Covered no co-pays for Emergency Room visits.
Cardiac Rehab 100% covered 100% covered 100% covered Dialysis 100% covered 100% covered 100% covered Emergency Care Covered no co-pays for Emergency Room visits Covered no co-pays for Emergency Room visits.
SUMMARY OF BENEFITS. Cigna Health and Life Insurance Co. Grand County Open Access Plus Effective 1/1/2015
 SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Grand County Open Access Plus Effective General Services In-Network Out-of-Network Primary care physician You pay $25 copay per visit Physician office
SUMMARY OF BENEFITS Cigna Health and Life Insurance Co. Grand County Open Access Plus Effective General Services In-Network Out-of-Network Primary care physician You pay $25 copay per visit Physician office
California Small Group MC Aetna Life Insurance Company
 PLAN FEATURES Deductible (per calendar year) $1,000 per member $1,000 per member Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate
PLAN FEATURES Deductible (per calendar year) $1,000 per member $1,000 per member Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate
American Maritime Officers Medical Plan Employer Identification Number: 13-5600786 Plan Number: 501 Group Number: 0081717
 AMENDMENT #4 American Maritime Officers Medical Plan Employer Identification Number: 13-5600786 Plan Number: 501 Group Number: 0081717 This Amendment is duly adopted and effective as of October 1, 2014.
AMENDMENT #4 American Maritime Officers Medical Plan Employer Identification Number: 13-5600786 Plan Number: 501 Group Number: 0081717 This Amendment is duly adopted and effective as of October 1, 2014.
CHAPTER 7: UTILIZATION MANAGEMENT
 OVERVIEW The Plan s Utilization Management (UM) program is collaboration with providers to promote and document the appropriate use of health care resources. The program reflects the most current utilization
OVERVIEW The Plan s Utilization Management (UM) program is collaboration with providers to promote and document the appropriate use of health care resources. The program reflects the most current utilization
PPO Schedule of Payments (Maryland Large Group) Qualified High Deductible Health Plan National QA2000-20
 PPO Schedule of Payments (Maryland Large Group) Qualified High Health Plan National QA2000-20 Benefit Year Individual Family (Amounts for Participating and s services are separated in calculating when
PPO Schedule of Payments (Maryland Large Group) Qualified High Health Plan National QA2000-20 Benefit Year Individual Family (Amounts for Participating and s services are separated in calculating when
GLANCE GATEWAY. Providers AT A. for Medicare Assured SM. Gateway Health Medicare Assured SM 444 Liberty Avenue, Suite 2100 Pittsburgh, PA 15222-1222
 GATEWAY AT A GLANCE for Medicare Assured SM Providers Gateway Health Medicare Assured SM 444 Liberty Avenue, Suite 2100 Pittsburgh, PA 15222-1222 YOUR PROVIDER NUMBERS: Group Provider Number : Individual
GATEWAY AT A GLANCE for Medicare Assured SM Providers Gateway Health Medicare Assured SM 444 Liberty Avenue, Suite 2100 Pittsburgh, PA 15222-1222 YOUR PROVIDER NUMBERS: Group Provider Number : Individual
I. Out of Network: Any Medicaid, CHP and HealthierLife service provided by a nonparticipating provider/facility/physician requires authorization.
 Medicaid, Child Health and HealthierLife (HARP) Plus Authorization Grid FIDELIS CARE AUTHORIZATION REQUIREMENTS Benefit/Service Detail SERVICES AND PROCEDURES WHICH REQUIRE AUTHORIZATION REVISED 1/1/2016
Medicaid, Child Health and HealthierLife (HARP) Plus Authorization Grid FIDELIS CARE AUTHORIZATION REQUIREMENTS Benefit/Service Detail SERVICES AND PROCEDURES WHICH REQUIRE AUTHORIZATION REVISED 1/1/2016
Iowa Wellness Plan Benefits Coverage List
 Iowa Wellness Plan Benefits Coverage List Service Category Covered Duration, Scope, exclusions, and Limitations Excluded Coding 1. Ambulatory Services Primary Care Illness/injury Physician Services Should
Iowa Wellness Plan Benefits Coverage List Service Category Covered Duration, Scope, exclusions, and Limitations Excluded Coding 1. Ambulatory Services Primary Care Illness/injury Physician Services Should
Miscellaneous Services
 Miscellaneous Services Acute Physical Medicine and Rehabilitation (Acute PM&R) Inpatient PM&R is limited to Department-contracted facilities. Please see the Department s Acute PM&R Billing Instructions
Miscellaneous Services Acute Physical Medicine and Rehabilitation (Acute PM&R) Inpatient PM&R is limited to Department-contracted facilities. Please see the Department s Acute PM&R Billing Instructions
Summary of Services and Cost Shares
 Summary of Services and Cost Shares This summary does not describe benefits. For the description of a benefit, including any limitations or exclusions, please refer to the identical heading in the Benefits
Summary of Services and Cost Shares This summary does not describe benefits. For the description of a benefit, including any limitations or exclusions, please refer to the identical heading in the Benefits
Service Name Prior Auth Reqd? PA Form Notification Reqd? Notify. Form Threshold Product List. Yes, notification within 24 hours.
 *Prior authorization confirms medical necessity only and does not guarantee payment. *Payment is determined at the time the claim is received and is subject to health plan exclusions and out-of-network
*Prior authorization confirms medical necessity only and does not guarantee payment. *Payment is determined at the time the claim is received and is subject to health plan exclusions and out-of-network
Health Plan of Nevada, Inc. ( HPN ) Small Business Point-Of-Service ( POS ) Rider to the Small Business Evidence of Coverage ( EOC )
 Health Plan of Nevada, Inc. ( HPN ) Small Business Point-Of-Service ( POS ) Rider to the Small Business Evidence of Coverage ( EOC ) This Rider is a supplement to your EOC issued by HPN. Subject to the
Health Plan of Nevada, Inc. ( HPN ) Small Business Point-Of-Service ( POS ) Rider to the Small Business Evidence of Coverage ( EOC ) This Rider is a supplement to your EOC issued by HPN. Subject to the
MyHPN Solutions HMO Silver 4
 MyHPN Solutions HMO Silver 4 Attachment A Schedule Calendar Year Deductible (CYD): $2,250 of EME per Member and $4,500 of EME per family. The Calendar Year Out of Pocket Maximum includes the CYD and is
MyHPN Solutions HMO Silver 4 Attachment A Schedule Calendar Year Deductible (CYD): $2,250 of EME per Member and $4,500 of EME per family. The Calendar Year Out of Pocket Maximum includes the CYD and is
UnitedHealthcare Choice Plus. UnitedHealthcare Insurance Company. Certificate of Coverage
 UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Plan 7EG of Educators Benefit Services, Inc. Enrolling Group Number: 717578 Effective Date: January 1, 2012
UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Plan 7EG of Educators Benefit Services, Inc. Enrolling Group Number: 717578 Effective Date: January 1, 2012
UnitedHealthcare Choice Plus. UnitedHealthcare Insurance Company. Certificate of Coverage
 UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Health Savings Account (HSA) Plan 7PD of Educators Benefit Services, Inc. Enrolling Group Number: 717578
UnitedHealthcare Choice Plus UnitedHealthcare Insurance Company Certificate of Coverage For the Health Savings Account (HSA) Plan 7PD of Educators Benefit Services, Inc. Enrolling Group Number: 717578
Corporate Medical Policy Durable Medical Equipment (DME)
 Corporate Medical Policy Durable Medical Equipment (DME) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: durable_medical_equipment_(dme) 1/2000 9/2015 9/2016 9/2015 Description of
Corporate Medical Policy Durable Medical Equipment (DME) File Name: Origination: Last CAP Review: Next CAP Review: Last Review: durable_medical_equipment_(dme) 1/2000 9/2015 9/2016 9/2015 Description of
Section IV - Information for People with Medicare and Medicaid
 TM Section IV - Information for People with Medicare and People who qualify for Medicare and are known as dual eligibles. As a dual eligible, you are eligible for benefits under both the federal Medicare
TM Section IV - Information for People with Medicare and People who qualify for Medicare and are known as dual eligibles. As a dual eligible, you are eligible for benefits under both the federal Medicare
COVERAGE SCHEDULE. The following symbols are used to identify Maximum Benefit Levels, Limitations, and Exclusions:
 Exhibit D-3 HMO 1000 Coverage Schedule ROCKY MOUNTAIN HEALTH PLANS GOOD HEALTH HMO $1000 DEDUCTIBLE / 75 PLAN EVIDENCE OF COVERAGE LARGE GROUP Underwritten by Rocky Mountain Health Maintenance Organization,
Exhibit D-3 HMO 1000 Coverage Schedule ROCKY MOUNTAIN HEALTH PLANS GOOD HEALTH HMO $1000 DEDUCTIBLE / 75 PLAN EVIDENCE OF COVERAGE LARGE GROUP Underwritten by Rocky Mountain Health Maintenance Organization,
NATIONWIDE INSURANCE $20-40 / 250A NATIONAL MANAGED CARE SCHEDULE OF BENEFITS
 WASHINGTON NATIONWIDE INSURANCE $20-40 / 250A NATIONAL MANAGED CARE SCHEDULE OF BENEFITS General Features Calendar Year Deductible Lifetime Benefit Maximum (Does not apply to Chemical Dependency) ($5,000.00
WASHINGTON NATIONWIDE INSURANCE $20-40 / 250A NATIONAL MANAGED CARE SCHEDULE OF BENEFITS General Features Calendar Year Deductible Lifetime Benefit Maximum (Does not apply to Chemical Dependency) ($5,000.00
27. Will the plan pay for radiology done in the provider s office?... 10 28. How do providers request assistance with care management issues?...
 Provider Q&A Contents 1. Who is Florida True Health?... 3 2. What is the new product name?... 3 3. Does the plan have a website?... 3 4. How will physicians be paid? (FFS or capitation)... 3 5. What clearing
Provider Q&A Contents 1. Who is Florida True Health?... 3 2. What is the new product name?... 3 3. Does the plan have a website?... 3 4. How will physicians be paid? (FFS or capitation)... 3 5. What clearing
CU Care Management Matrix
 CU Care Matrix Group Name(s) Exclusive Exclusive Exclusive High Deductible HSA Compatible and Extended Capitated/FFS Facilities Capitated for physician only UCH Childrens FFS FFS FFS Poudre Valley Center
CU Care Matrix Group Name(s) Exclusive Exclusive Exclusive High Deductible HSA Compatible and Extended Capitated/FFS Facilities Capitated for physician only UCH Childrens FFS FFS FFS Poudre Valley Center
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 Gold 80 PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type:
Gold 80 PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type:
SUMMARY OF BADGERCARE PLUS BENEFITS
 SUMMARY OF BADGERCARE PLUS BENEFITS Medical, mental health and substance abuse services Dental emergency NOT Pharmacy, chiropractic and dental services NOT 13 Ambulatory surgery centers Coverage of certain
SUMMARY OF BADGERCARE PLUS BENEFITS Medical, mental health and substance abuse services Dental emergency NOT Pharmacy, chiropractic and dental services NOT 13 Ambulatory surgery centers Coverage of certain
KAISER PERMANENTE PLAN (Non-Medicare Eligible)
 CEMENT MASONS HEALTH AND WELFARE TRUST FUND FOR NORTHERN CALIFORNIA RETIRED CEMENT MASONS AND THEIR ELIGIBLE DEPENDENTS EFFECTIVE JANUARY 1, 2015 GENERAL When You Can Change Plans Type of Plan, Service
CEMENT MASONS HEALTH AND WELFARE TRUST FUND FOR NORTHERN CALIFORNIA RETIRED CEMENT MASONS AND THEIR ELIGIBLE DEPENDENTS EFFECTIVE JANUARY 1, 2015 GENERAL When You Can Change Plans Type of Plan, Service
OGB MAGNOLIA LOCAL COMPREHENSIVE MEDICAL BENEFIT PLAN SCHEDULE OF BENEFITS
 OGB MAGNOLIA LOCAL COMPREHENSIVE MEDICAL BENEFIT PLAN SCHEDULE OF BENEFITS Network coverage available only in Baton Rouge, New Orleans, Shreveport and St. Tammany Blue Connect and Community Blue BENEFIT
OGB MAGNOLIA LOCAL COMPREHENSIVE MEDICAL BENEFIT PLAN SCHEDULE OF BENEFITS Network coverage available only in Baton Rouge, New Orleans, Shreveport and St. Tammany Blue Connect and Community Blue BENEFIT
Gundersen Health Plan: MN NJ Silver $2000-0% Coverage Period: 01/01/2015-12/31/2015
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gundersenhealthplan.org or by calling 1-800-897-1923.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.gundersenhealthplan.org or by calling 1-800-897-1923.
UnitedHealthcare Choice. UnitedHealthcare Insurance Company. Certificate of Coverage
 UnitedHealthcare Choice UnitedHealthcare Insurance Company Certificate of Coverage For the Plan 9DF of District of Columbia Government Enrolling Group Number: 712971 Effective Date: January 1, 2013 Offered
UnitedHealthcare Choice UnitedHealthcare Insurance Company Certificate of Coverage For the Plan 9DF of District of Columbia Government Enrolling Group Number: 712971 Effective Date: January 1, 2013 Offered
UnitedHealthcare Choice Plus. United HealthCare Insurance Company. Certificate of Coverage
 UnitedHealthcare Choice Plus United HealthCare Insurance Company Certificate of Coverage For Westminster College Enrolling Group Number: 715916 Effective Date: January 1, 2009 Offered and Underwritten
UnitedHealthcare Choice Plus United HealthCare Insurance Company Certificate of Coverage For Westminster College Enrolling Group Number: 715916 Effective Date: January 1, 2009 Offered and Underwritten
Important Questions Answers Why this Matters:
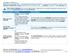 Minimum Coverage PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan
Minimum Coverage PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 : VIVA HEALTH Access Plan Coverage Period: 01/01/2015 12/31/2015 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document
: VIVA HEALTH Access Plan Coverage Period: 01/01/2015 12/31/2015 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document
You don't have to meet deductibles for specific services, but see the chart starting on page 2 for other costs for services this plan covers.
 Blue Cross Blue Shield Solution 102, a Multi-State Plan SM Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family
Blue Cross Blue Shield Solution 102, a Multi-State Plan SM Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family
Active and Retiree Health Benefit Summary Plan Description And Plan Document 7670-00-411309/7670-03-411309
 Active and Retiree Health Benefit Summary Plan Description And Plan Document 7670-00-411309/7670-03-411309 BENEFITS ADMINISTERED BY Table of Contents INTRODUCTION... 1 PLAN INFORMATION... 2 BENEFIT CLASS
Active and Retiree Health Benefit Summary Plan Description And Plan Document 7670-00-411309/7670-03-411309 BENEFITS ADMINISTERED BY Table of Contents INTRODUCTION... 1 PLAN INFORMATION... 2 BENEFIT CLASS
United HealthCare Choice Plus. Plan 7EH. United HealthCare Insurance Company. Certificate of Coverage
 United HealthCare Choice Plus Plan 7EH United HealthCare Insurance Company Certificate of Coverage For SCSVEBA (Southern California Schools VEBA) Enrolling Group Number: 714846 Effective Date: January
United HealthCare Choice Plus Plan 7EH United HealthCare Insurance Company Certificate of Coverage For SCSVEBA (Southern California Schools VEBA) Enrolling Group Number: 714846 Effective Date: January
BlueCare Direct Gold SM HMO 101 BlueCare Direct SM HMO Network
 BlueCare Direct Gold SM HMO 101 BlueCare Direct SM HMO Network OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your
BlueCare Direct Gold SM HMO 101 BlueCare Direct SM HMO Network OUTLINE OF COVERAGE 1. READ YOUR POLICY CAREFULLY. This outline of coverage provides a brief description of the important features of your
SECTION 5 1 REFERRAL AND AUTHORIZATION PROCESS
 SECTION 5 1 REFERRAL AND AUTHORIZATION PROCESS Primary Care Physician Referral Process 1 Referral from PCP to Participating Specialists 1 Referral from Participating Specialist to Participating Specialists
SECTION 5 1 REFERRAL AND AUTHORIZATION PROCESS Primary Care Physician Referral Process 1 Referral from PCP to Participating Specialists 1 Referral from Participating Specialist to Participating Specialists
American Commerce Insurance Company
 American Commerce Insurance Company INITIAL INFORMATION LETTER TO INSURED/CLAIMANT/PROVIDERS Dear Insured and/or /Eligible Injured Person/Medical Provider: Please read this letter carefully because it
American Commerce Insurance Company INITIAL INFORMATION LETTER TO INSURED/CLAIMANT/PROVIDERS Dear Insured and/or /Eligible Injured Person/Medical Provider: Please read this letter carefully because it
PLAN DESIGN AND BENEFITS - Tx OAMC 1500-10 PREFERRED CARE
 PLAN FEATURES Deductible (per calendar year) $1,500 Individual $3,000 Individual $4,500 Family $9,000 Family 3 Individuals per Family 3 Individuals per Family Unless otherwise indicated, the Deductible
PLAN FEATURES Deductible (per calendar year) $1,500 Individual $3,000 Individual $4,500 Family $9,000 Family 3 Individuals per Family 3 Individuals per Family Unless otherwise indicated, the Deductible
HPN Solutions HMO 15 V2 $7/35/55
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.myhpnonline.com or by calling (702) 242-7300 or 1-800-777-1840.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.myhpnonline.com or by calling (702) 242-7300 or 1-800-777-1840.
SECTION A. Summary of Benefits LW-V, 10/09
 SECTION A. Summary of Benefits LW-V, 10/09 This Summary is part of your Benefit Handbook. It states the Cost Sharing amounts that you must pay for Covered Benefits and some important limitations on your
SECTION A. Summary of Benefits LW-V, 10/09 This Summary is part of your Benefit Handbook. It states the Cost Sharing amounts that you must pay for Covered Benefits and some important limitations on your
How To Get Health Net From Health Net
 INDIVIDUAL & FAMILY PLANS QUICK NET SHORT-TERM COVERAGE BY THE DAY OR MONTH Health coverage made easy. Effective April 15, 2007 IT S A FAST-MOVING WORLD. Keep up with Quick Net from Health Net. TWO KINDS
INDIVIDUAL & FAMILY PLANS QUICK NET SHORT-TERM COVERAGE BY THE DAY OR MONTH Health coverage made easy. Effective April 15, 2007 IT S A FAST-MOVING WORLD. Keep up with Quick Net from Health Net. TWO KINDS
Perioperative Charge Process
 There are eight components to the charge process for surgical services: 1. Pre op prep and care 2. Anesthesia 3. Operating room time charges 4. Equipment charges 5. Recovery / Post Anesthesia Care Unit
There are eight components to the charge process for surgical services: 1. Pre op prep and care 2. Anesthesia 3. Operating room time charges 4. Equipment charges 5. Recovery / Post Anesthesia Care Unit
PLAN DESIGN AND BENEFITS - Tx OAMC 2500 08 PREFERRED CARE
 PLAN FEATURES Deductible (per calendar year) $2,500 Individual $5,000 Individual $7,500 3 Individuals per $15,000 3 Individuals per Unless otherwise indicated, the Deductible must be met prior to benefits
PLAN FEATURES Deductible (per calendar year) $2,500 Individual $5,000 Individual $7,500 3 Individuals per $15,000 3 Individuals per Unless otherwise indicated, the Deductible must be met prior to benefits
Quick Guide 2016. Peoples Health Choices 65 #14 (HMO) Jefferson, Orleans and Plaquemines parishes
 Quick Guide 2016 $0 mium* Plan Pre Peoples Health Choices 65 #14 (HMO) Jefferson, Orleans and Plaquemines parishes *You must continue to pay your Medicare Part B premium. H1961_PH16C65S1QG Accepted Thank
Quick Guide 2016 $0 mium* Plan Pre Peoples Health Choices 65 #14 (HMO) Jefferson, Orleans and Plaquemines parishes *You must continue to pay your Medicare Part B premium. H1961_PH16C65S1QG Accepted Thank
PPO product with drug plan being offered for January 1, 2013
 PPO product with drug plan being offered for January 1, 2013 Austin area: 8 counties Dallas/Fort Worth area: 4 counties Houston area: 3 counties Austin Area Counties (8) Bastrop Burnet Caldwell Fayette
PPO product with drug plan being offered for January 1, 2013 Austin area: 8 counties Dallas/Fort Worth area: 4 counties Houston area: 3 counties Austin Area Counties (8) Bastrop Burnet Caldwell Fayette
FEATURES NETWORK OUT-OF-NETWORK
 Schedule of Benefits Employer: The Vanguard Group, Inc. ASA: 697478-A Issue Date: January 1, 2014 Effective Date: January 1, 2014 Schedule: 3B Booklet Base: 3 For: Choice POS II - 950 Option - Retirees
Schedule of Benefits Employer: The Vanguard Group, Inc. ASA: 697478-A Issue Date: January 1, 2014 Effective Date: January 1, 2014 Schedule: 3B Booklet Base: 3 For: Choice POS II - 950 Option - Retirees
GATEWAY AT A GLANCE for Medicare Assured SM Providers
 GATEWAY AT A GLANCE for Medicare Assured SM Providers Gateway Health Medicare Assured SM offers options designed to provide more than healthcare for those who qualify. Medicare Assured SM offers medical
GATEWAY AT A GLANCE for Medicare Assured SM Providers Gateway Health Medicare Assured SM offers options designed to provide more than healthcare for those who qualify. Medicare Assured SM offers medical
Covered 100% No deductible Not Applicable (exam, related tests and x-rays, immunizations, pap smears, mammography and screening tests)
 A AmeriHealth EPO Individual Summary of Benefits Value Network IHC EPO $30/50% Benefit Network Non network Benefit Period+ Calendar year Individual deductible $2,500 Family deductible $5,000 50% Individual
A AmeriHealth EPO Individual Summary of Benefits Value Network IHC EPO $30/50% Benefit Network Non network Benefit Period+ Calendar year Individual deductible $2,500 Family deductible $5,000 50% Individual
STATE OF NEVADA DEPARTMENT OF BUSINESS & INDUSTRY DIVISION OF INDUSTRIAL RELATIONS WORKERS COMPENSATION SECTION
 STATE OF NEVADA DEPARTMENT OF BUSINESS & INDUSTRY DIVISION OF INDUSTRIAL RELATIONS WORKERS COMPENSATION SECTION NEVADA MEDICAL FEE SCHEDULE MAXIMUM ALLOWABLE PROVIDER PAYMENT February 1, 2012 through January
STATE OF NEVADA DEPARTMENT OF BUSINESS & INDUSTRY DIVISION OF INDUSTRIAL RELATIONS WORKERS COMPENSATION SECTION NEVADA MEDICAL FEE SCHEDULE MAXIMUM ALLOWABLE PROVIDER PAYMENT February 1, 2012 through January
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at http://www.whyviva.com/memberaccess.aspx or by calling 1-800-294-7780.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at http://www.whyviva.com/memberaccess.aspx or by calling 1-800-294-7780.
2015 EMPIRE PLAN BENEFIT SUMMARY For Active Employees and Retirees
 PRE-ADMISSION CERTIFICATION 2015 EMPIRE PLAN BENEFIT SUMMARY For Active Employees and Retirees Prior authorization of inpatient hospitalization charges required. $200 penalty for failure to precertify.
PRE-ADMISSION CERTIFICATION 2015 EMPIRE PLAN BENEFIT SUMMARY For Active Employees and Retirees Prior authorization of inpatient hospitalization charges required. $200 penalty for failure to precertify.
We know that you value your employees. Thank you for considering Optima Health to meet your employees healthcare needs.
 We know that you value your employees. Thank you for considering Optima Health to meet your employees healthcare needs. Optima Health Products and Services Our Value Statement 1 TABLE OF CONTENTS 2 CONSUMER-DIRECTED
We know that you value your employees. Thank you for considering Optima Health to meet your employees healthcare needs. Optima Health Products and Services Our Value Statement 1 TABLE OF CONTENTS 2 CONSUMER-DIRECTED
(HSA) 1500/3000 10/30 (LHSA497)
 Lumenos Health Savings Account (HSA) 1500/3000 10/30 (LHSA497) 1/1/2016 This Summary of Benefits is a brief overview of your plan's benefits only. The benefits listed are for both in state and out of state
Lumenos Health Savings Account (HSA) 1500/3000 10/30 (LHSA497) 1/1/2016 This Summary of Benefits is a brief overview of your plan's benefits only. The benefits listed are for both in state and out of state
Medicare Drug Coverage Under Part A, Part B, and Part D
 Medicare Drug Coverage Under Part A, Part B, and Part D Medicare Part A and Part B generally do not cover outpatient prescription drugs, most of which are now covered under Part D. This document and the
Medicare Drug Coverage Under Part A, Part B, and Part D Medicare Part A and Part B generally do not cover outpatient prescription drugs, most of which are now covered under Part D. This document and the
please refer to our internet site, www.harvardpilgrim.org, or contact the Member Services
 Schedule of s HPHC Insurance Company, Inc. THE HPHC INSURANCE COMPANY PPO PLAN MAINE ID: MD0000000750_F2 X This Schedule of s summarizes your benefits under The HPHC Insurance Company PPO Plan (the Plan)
Schedule of s HPHC Insurance Company, Inc. THE HPHC INSURANCE COMPANY PPO PLAN MAINE ID: MD0000000750_F2 X This Schedule of s summarizes your benefits under The HPHC Insurance Company PPO Plan (the Plan)
