Principles of training in GI endoscopy
|
|
|
- Shauna Horn
- 9 years ago
- Views:
Transcription
1 Communication from the ASGE Training Committee REPORT ON TRAINING Principles of training in GI endoscopy This document, prepared by the American Society for Gastrointestinal Endoscopy Committee on Training, was undertaken to provide general guidelines for endoscopy training and written primarily for individuals involved in teaching endoscopic procedures to fellows/trainees. This updates the previous Principles of Training document. 1 Research in objective evaluation of procedural skills makes revision of the guidelines at this time highly appropriate. OBJECTIVES Upon completion of training in GI endoscopy, trainees should be prepared to (1) appropriately recommend endoscopic procedures as indicated by the findings of consultative evaluation, with explicit understanding of accepted specific indications, contraindications, and diagnostic/therapeutic alternatives; (2) perform procedures safely, completely, and expeditiously, including possessing a thorough understanding of the principles of conscious sedation/analgesia techniques, the use of anesthesia-assisted sedation where appropriate, and preprocedure clinical assessment and patient monitoring; (3) correctly interpret endoscopic findings and integrate them into medical or endoscopic therapy; (4) identify risk factors for each procedure, understand how to minimize each, and recognize and appropriately manage complications when they occur; (5) acknowledge the limitations of endoscopic procedures and personal skills and know when to request help; and (6) understand the principles of quality measurement and improvement. TRAINING PROGRAMS Copyright 2012 by the American Society for Gastrointestinal Endoscopy /$36.00 doi: /j.gie Institutions Training in GI endoscopy should take place within the context of a global clinical training program in the fields of adult or pediatric gastroenterology or general surgery. These training programs must be recognized by the Accreditation Council for Graduate Medical Education or the American Osteopathic Association and should exist within institutions where they are supported by the presence of accredited training programs in internal medicine, pediatrics, general surgery, radiology (including intervention training), and pathology. Supporting curriculum Competence in technical skills requires the foundation of didactic learning that occurs within the comprehensive training of a specialist in GI and liver disease. In particular, the endoscopic trainee must participate in a program of directed reading and teaching conferences that conveys the following: (1) the indications, limitations, and contraindications of endoscopic procedures; (2) procedure complications and their management; (3) the principles of safe sedation/analgesia techniques and patient monitoring and when to consider alternate forms of anesthesia; (4) medical, radiological, and surgical alternatives to endoscopic therapy; (5) issues of informed consent, advanced directives, and medical ethics as pertains to GI endoscopy (as in the evaluation of gastrostomy and cancer palliation candidates); (6) skills for critical assessment of new techniques and endoscopic scientific literature; (7) incorporating endoscopic findings into overall patient management; (8) preparation of endoscopy reports and communication with referring providers and other members of the care team; and (9) quality measurement and continuous quality improvement. The endoscopy training director Each training program should have an expert endoscopist and teacher who is designated as the endoscopy training director and will (1) monitor on a regular basis each trainee s acquisition of appropriate technical and cognitive skills, including maintenance of personal logs/ records documenting trainee s numerical procedural experience (including indications, findings, and complications) and success in achieving defined objective performance standards, as discussed in the following; (2) incorporate endoscopic teaching resources (textbooks, atlases, videotapes, electronic media) into the training program; (3) periodically review and update training methodology and quality of training within the program; (4) review evaluation forms from trainers with the trainee and allow for feedback from the trainee on the trainers and the program; and (5) review and update the training curriculum on an ongoing basis. Endoscopic faculty The endoscopic faculty should include experienced endoscopists and teachers with demonstrated expertise in Volume 75, No. 2 : 2012 GASTROINTESTINAL ENDOSCOPY 231
2 the procedures being taught. Faculty should (1) have time (and institutional financial support) dedicated to teaching; (2) be responsible for didactic instruction and supervision of trainees; (3) regularly attend GI continuing medical education sessions as well as interdisciplinary meetings with surgeons, radiologists, and pathologists; (4) be of adequate number the ratio of teachers to trainees should be approximately or greater than one; (5) communicate with the training director and/or each trainee should have a designated faculty supervisor; and (6) show active promotion of research or advancement of clinical practice that includes publications and participation in educational activities on local, regional, national, and international levels. The training process Successful trainees in GI endoscopy acquire their skills through a program of hands-on experiential training under the mentorship of expert endoscopic trainers that occurs over a prolonged period of time, such as that represented by a gastroenterology fellowship or surgical residency. Cognitive learning from outside reading, conferences, and instruction in the disciplines comprising the broad field of GI medicine is critical to this process and, through the efforts of both trainer and trainee, is intimately integrated with the technical aspects of procedural instruction and patient management. Training follows a natural progression as trainees accrue more technical expertise and confidence. Initially, a trainee may observe a procedure, followed by first attempting only the diagnostic or less technically demanding aspects of a procedure. At this stage, under constant supervision, trainees will learn key principles of anatomy and scope manipulation and practice basic techniques such as esophageal and pyloric intubation and retroflexion of the scope tip. They will also practice sedation techniques, begin to learn basic recognition of normal and abnormal endoscopic findings, learn integration of findings into a plan of treatment, and develop skills for writing and appropriate documentation of endoscopic findings. As experience grows, the trainee will progress to performing the entire procedure and attempting therapeutic interventions. Trainees must appreciate the seamless integration of diagnosis and therapy that is the hallmark of modern endoscopic practice. Examples include the delivery of hemostatic therapy during endoscopy in a bleeding patient and the performance of polypectomy during screening colonoscopy. The trainee is expected to progress through stages of decreasing supervision, extending from the initial phase of complete supervision through a period of partial supervision, in which the trainee is deemed competent to perform a procedure with reasonable safety and patient comfort. In the latter phase, the trainer is available to view pertinent findings and assist when problems arise. The rate of skill acquisition will vary among trainees and for a single trainee between different procedures, because of differences in manual dexterity, volume of procedures, trainee judgment, and quality of instruction. Ultimately, the trainee should reach a stage in which he or she is deemed competent by the endoscopic training director to perform a specific procedure without supervision. The current economic constraints placed on most academic training institutions will, however, likely mandate that supervision be maintained for most if not all procedures regardless of the trainee s proficiency. Standard procedures The amount of time and experience required to learn the effective and safe performance of endoscopic examinations varies considerably among trainees and from one procedure to another. Competence in one procedure does not equate to competence in other procedures. In most centers, training begins with procedures that are easier to master and progresses to more challenging procedures. ERCP and EUS training is expected to follow experience in less complex and technically demanding examinations. The American Society for Gastrointestinal Endoscopy thus upholds a distinction between two types of procedures, standard and advanced. Standard procedures are commonly performed and are readily available to most patients. These procedures are part of the core of diagnostic and therapeutic capability expected of physicians performing endoscopy. Most trainees can expect to master these procedures during a 3-year gastroenterology fellowship period (including a minimum core period of 18 months of clinical training). Standard procedures include EGD, flexible sigmoidoscopy, colonoscopy, capsule endoscopy, mucosal biopsy, polypectomy, dilation of peptic strictures of the esophagus, percutaneous liver biopsy, and PEG. Although the delivery of endoscopic hemostasis (injection and cautery techniques, esophageal variceal sclerotherapy, and band ligation) requires considerable endoscopic expertise, mastery of these techniques is essential for every endoscopist performing endoscopy in bleeding patients and are thus included among standard procedures. Advanced procedures Advanced procedures are more complex and technically demanding to perform and often carry a relatively higher risk of complications. These examinations, which often include complicated and high-risk diagnostic and therapeutic components, are required less frequently than standard procedures, and, thus, the number of individuals trained to perform them should be smaller than the number trained in standard procedures. Advanced procedures include ERCP and all associated interventions, EUS, pneumatic dilation for achalasia, dilation of complex esophageal strictures (eg, lye and radiation strictures), stent placement, Barrett s esophagus ablation therapies, EMR, deep enteroscopy, and endoscopic tumor ablation. 232 GASTROINTESTINAL ENDOSCOPY Volume 75, No. 2 :
3 The learning of advanced procedures is founded on a thorough mastery of standard procedures and often requires an additional year of training beyond the standard 3-year fellowship. Guidelines for training programs in advanced endoscopy were published by the American Society for Gastrointestinal Endoscopy in Not all trainees should pursue such advanced training because of variations in individual skill and the manpower needs of the health care system. Likewise, not all programs should offer advanced training; such training should be concentrated in those programs that have an adequate combination of patient volume and faculty expertise. In certain circumstances, select advanced procedures may be mastered during a standard 3-year training program when adequate patient volume and trainee aptitude are present. In general, however, good medical practice and the current health care climate both mandate the ideal of concentrating advancing techniques in a relatively small number of highly trained individuals. Training in advanced techniques should be undertaken only if there is a reasonable expectation that the trainee will be able to achieve proficiency in the procedure and be prepared for unsupervised function by the end of the training period. Providing brief exposure to an advanced procedure such as ERCP during standard fellowship with the expectation that the trainee will subsequently complete training in practice is no longer appropriate. Evaluation of trainee competence The evaluation of a trainee s progress in endoscopic skill acquisition continues throughout the duration of the training program. The endoscopy training director supervises the process, but all trainers must participate. In keeping with accreditation guidelines, there must be a written evaluation policy that is known by the trainee and includes provisions for frequent and regular structured feedback as well as evaluation of the program and trainers by the trainee. Ultimate assessment of trainee achievement rests with the expert opinion of the endoscopy training director, based on both subjective and objective measures. Components of trainee competence Evaluation encompasses both cognitive and technical abilities. In-service evaluations in both areas should be used. Trainee log books and records of procedural numbers should be provided by the trainee to the training director as a raw record of trainee experience. The utility of objective performance standards is discussed in the following. Careful subjective evaluation also must be made of trainees endoscopic interpretive skills, abilities to incorporate endoscopic findings into overall patient care, responses to incorporate endoscopic findings into overall patient care, responses to complications, adherence to safe patient monitoring and sedation practices, and the quality of their preprocedure and postprocedure patient teaching. Technical evaluation/performance standards The use of threshold procedure numbers at which competence may be globally assessed provides only a rough benchmark for guiding trainee evaluation. Few studies of the rate at which proficiency is attained have been performed, but available data suggest that at least 25 to 30 flexible sigmoidoscopies, upper endoscopies, and 200 colonoscopies are required at a minimum before the trainee can be assessed for competence. 4 Similarly, 180 to 200 ERCPs are needed before trainees can routinely achieve selective duct cannulation. 5 Available data on competency in EUS suggest that 100 examinations are needed for acceptable accuracy in the T-staging of esophageal carcinoma 6 ; most experts agree that pancreatobiliary EUS demands more experience than esophageal EUS, 7 whereas 40 to 50 cases may provide adequate preparation for the accurate evaluation of submucosal lesions. 8 It should be stressed that these minimal threshold numbers represent a benchmark before which a trainee s competency should not even be assessed. Most trainees will achieve competence much later. Training programs must be able to meet and exceed these procedural volumes for each trainee. For colonoscopy, 140 procedures had been previously cited as a minimum experience before competency could be assessed. This number was based on data limited to cecal intubation rates and based on expert opinion of competency thresholds ( 90%) for this metric. However, using these same limited metrics, Spier et al 9 found that even after 140 colonoscopies, no trainee exhibited procedural competency, yet by 500 procedures, all fellows had achieved procedural competency benchmarks. 10 To better define where within this range competency occurs, a more comprehensive definition of competency was required. A recently reported colonoscopy skills assessment form by Sedlack 11 provides a means to assess a broader range of both cognitive and motor skills for colonoscopy. With the use of this form, learning curves and competency thresholds for each of these core skills have been defined, and they suggest that competence is not achieved by the average trainee until she or he has performed roughly 275 colonoscopies. 4,12 Trainees, however, develop skills at widely varying rates. Data from studies by Sedlack 11 and Chung et al 12 show that a fraction of trainees can achieve competency as early as 175 to 200 procedures, whereas others achieve competency as late as 400 procedures. Absolute or threshold numbers may thus be misleading and should be used with caution in the evaluation of individual trainees. What this illustrates is that the recommended threshold numbers mentioned earlier for each type of procedure should be used only as a guide in curricula planning. The achievement of competence should be based on a separate assessment, either on a periodic or continuous basis, of a broad range of defined skills. It also should be stressed that the rate of skill Volume 75, No. 2 : 2012 GASTROINTESTINAL ENDOSCOPY 233
4 acquisition for a given trainee may vary among different procedures; hence, competence in one procedure does not imply competence in other procedures. 13 To enhance the quality of trainee evaluation and endoscopic training through the use of experience-based criteria, the American Society for Gastrointestinal Endoscopy recommends that program directors also incorporate the monitoring of specific technical skills (such as independent cecal intubation) and interpretive/diagnostic skill (polyp or adenoma detection) into the global assessment of trainees in a continuous manner or on a periodic basis at specified intervals of training. Such monitoring may be achieved through a variety of methods, including the following: (1) incorporating the reporting of performance data into electronic endoscopic report generation, (2) recording of performance data by supervising endoscopic trainers, (3) selective observation of trainees by a designated evaluator, and (4) self-reporting of performance parameters in trainee logs. Performance data for each trainee should be collected and tracked by the training director, who can then observe and document trends in each trainee s development. Programs may elect, for example, to monitor a few performance metrics on a continuous basis or multiple parameters intermittently. Although this monitoring effort entails an additional time investment by the faculty trainers, it will enhance the accurate measurement of each trainee s progress and readiness for successively more complex procedures and levels of training. Expert endoscopists are generally expected to perform at a 95% to 100% technical success level, and current research supports establishing a standard of 80% to 90% technical success before trainees are deemed competent in a specific skill In a given program, small variations in the standard of expected proficiency that is set from one procedure to the next may be appropriate, especially among procedures of varying complexity; however, the expected performance level should be uniform among all trainees. For any given procedure, training institutions should be able to provide trainees with a sufficient volume of procedures to achieve technical competence as defined by these standards. Adherence to objective assessment will help to guide programs in deciding which trainees are good candidates for advanced endoscopic training, how many trainees should be instructed in a given procedure, and for which procedures the program can provide a sufficient volume of cases to ensure adequate training. Ongoing competence, credentialing, and certification A certification of procedural competence will be provided by the endoscopy training director. Privileging to perform procedures in the clinical setting after training occurs falls under the purview of individual hospital credentialing committees. There are no established standards for monitoring ongoing procedural competence after the completion of training. Although most trainees will become more adept with additional experience after training, maintenance of expert performance cannot be assumed. The objective performance criteria applied here as minimum standards for trainees should serve as useful benchmarks for hospital credentialing authorities addressing this issue, in conjunction with evaluation of other factors such as case complexity, complications, and outcome. Acquisition and maintenance of documented levels of competency in the skills conveyed through a global training program in gastroenterology and GI endoscopy have important and positive implications for both the cost and quality of patient care. 18 Retraining and alternative pathway training As new technologies and techniques emerge, there is a natural desire among established practitioners to enhance and expand their own capabilities. It is rarely feasible for training programs to accommodate the retraining needs of past trainees. Such individuals may need to consider the option of pursuing advanced endoscopic training fellowship positions. Although most endoscopic training occurs in gastroenterology fellowships or surgical residency training programs, some practitioners may seek training in other settings. In previous position statements, the American Society for Gastrointestinal Endoscopy has defined the criteria that such alternative pathway endoscopic training programs must fulfill, emphasizing that training should be comprehensive and provide a working knowledge of the pathophysiology, diagnosis, and management of digestive diseases for which endoscopic procedures are indicated. 19 DISCLOSURE All authors disclosed no financial relationships relevant to this publication. REFERENCES 1. Principles of training in gastrointestinal endoscopy. Manchester (Mass): The American Society for Gastrointestinal Endoscopy; Guidelines for advanced endoscopic training. Manchester (Mass): The American Society for Gastrointestinal Endoscopy; Hawes R, Lehman GA, Hast J, et al. Training resident physicians in fiberoptic flexible sigmoidoscopy: How many supervised examinations are required to achieve competence? Am J Med 1986;80: Sedlack RE. Training to competency in colonoscopy: assessing and defining competency standards. Gastrointest Endosc 2011;74: Jowell PS, Baillie J, Branch MS, et al. Quantitative assessment of procedural competence: a prospective study of training in endoscopic retrograde cholangiopancreatography. Ann Intern Med 1996;125: Fockens P, Vanden Brande JH, Van Dullemen HM, et al. Endosonographic T-staging of esophageal carcinoma: a learning curve. Gastrointest Endosc 1996;44: Hoffman BJ, Hawes RH. Endoscopic ultrasound and clinical competence. Gastrointest Endosc Clin North Am 1995;5: GASTROINTESTINAL ENDOSCOPY Volume 75, No. 2 :
5 8. Van Dam J, Brady PG, Freeman M, et al. Guidelines for training in electronic ultrasound: guidelines for clinical application. Gastrointest Endosc 1999;49: Spier BJ, Benson M, Pfau PR, et al. Colonoscopy training in gastroenterology fellowships: determining competence. Gastrointest Endosc 2010; 71: Vargo JJ. North of 100 and south of 500: where does the sweet spot of colonoscopy competence lie? Gastrointest Endosc 2010;71: Sedlack RE. The Mayo Colonoscopy Skills Assessment Tool: validation of a unique instrument to assess colonoscopy skills in trainees. Gastrointest Endosc 2010;72: Chung JI, Kim N, Um MS, et al. Learning curves for colonoscopy: a prospective evaluation of gastroenterology fellows at a single center. Gut 2010;4: Wigton RS. Measuring procedural skills (editorial). Ann Intern Med 1996; 125: Cass OW, Freeman ML, Peine CJ, et al. Objective evaluation of endoscopy skills during training. Ann Intern Med 1993;118: Alternative pathways to training in gastrointestinal endoscopy. Manchester (Mass): The American Society for Gastrointestinal Endoscopy; Rex K, Cutler CS, Lemmel GT, et al. Colonoscopic miss rates of adenomas determined by back-to-back colonoscopies. Gastroenterology 1997; 112: Chak A, Cooper GS, Blades EW, et al. Prospective assessment of colonoscopic intubation skills in trainees. Gastrointest Endosc 1996;44: Zeroske JR, Wadsworth TM, Sargant M, et al. Comparison of GI hemorrhage (DRG 174) cost per case and length of stay when performed by gastroenterology vs. internal medicine departments. Am J Gastroenterol 1995;90:1669A. 19. Joint Statement. Principles of privileging and credentialing for endoscopy and colonoscopy. Gastrointest Endosc 2002;55: Prepared by: ASGE Training Committee Douglas G. Adler, MD Gennadiy Bakis, MD Walter J. Coyle, MD Barry DeGregorio, MD Kulwinder S. Dua, MD Linda S. Lee, MD Lee McHenry, Jr., MD Shireen A. Pais, MD Elizabeth Rajan, MD Robert E. Sedlack, MD Vanessa M. Shami, MD Ashley L. Faulx, MD, Chair This document was updated by the training committees 2010 to Volume 75, No. 2 : 2012 GASTROINTESTINAL ENDOSCOPY 235
CREDENTIALING FOR GASTROINTESTINAL ENDOSCOPY
 CREDENTIALING FOR GASTROINTESTINAL ENDOSCOPY A reference document for credentialing committees and physicians seeking hospital privileges to perform gastrointestinal endoscopy Produced in collaboration
CREDENTIALING FOR GASTROINTESTINAL ENDOSCOPY A reference document for credentialing committees and physicians seeking hospital privileges to perform gastrointestinal endoscopy Produced in collaboration
CPT COD1NG UPDATES Gastroenterology CPT Advisors
 2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
Center for Endoscopic Research & Therapeutics
 Center for Endoscopic Research & Therapeutics 5758 South Maryland Avenue (MC9028) Chicago, Illinois 60637 (773) 702-1459 www.uchospitals.edu Center for Endoscopic Research & Therapeutics To refer a patient
Center for Endoscopic Research & Therapeutics 5758 South Maryland Avenue (MC9028) Chicago, Illinois 60637 (773) 702-1459 www.uchospitals.edu Center for Endoscopic Research & Therapeutics To refer a patient
MU Inpatient Consult Rotation
 MU Inpatient Consult Rotation I. Description of Rotation and Educational Goal: This is a four-week rotation in which GI fellows gain exposure and acquire expertise in the evaluation and management of adult
MU Inpatient Consult Rotation I. Description of Rotation and Educational Goal: This is a four-week rotation in which GI fellows gain exposure and acquire expertise in the evaluation and management of adult
Endoscopic Mucosal Resection Perform with Confidence Expand your Practice. An Assessment-Based Curriculum
 Skills Training Assessment Reinforcement Endoscopic Mucosal Resection Perform with Confidence Expand your Practice Upper GI EMR An Assessment-Based Curriculum Earn 20 ABIM MOC Points! November 12-13, 2016
Skills Training Assessment Reinforcement Endoscopic Mucosal Resection Perform with Confidence Expand your Practice Upper GI EMR An Assessment-Based Curriculum Earn 20 ABIM MOC Points! November 12-13, 2016
Optimizing Endoscopy Center Efficiency Within the Safety-Net Hospital. Lukejohn W. Day MD
 Optimizing Endoscopy Center Efficiency Within the Safety-Net Hospital Lukejohn W. Day MD Webinar Goals Introduction and rationale California Healthcare Foundation (CHCF) planning grant Comprehensive literature
Optimizing Endoscopy Center Efficiency Within the Safety-Net Hospital Lukejohn W. Day MD Webinar Goals Introduction and rationale California Healthcare Foundation (CHCF) planning grant Comprehensive literature
The digestive system. Medicine and technology. Normal structure and function Diagnostic methods Example diseases and therapies
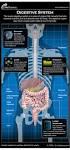 The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
The digestive system Medicine and technology Normal structure and function Diagnostic methods Example diseases and therapies The digestive system An overview (1) Oesophagus Liver (hepar) Biliary system
2016 Quick Reference Coding Chart
 43197 Trans nasal esophagoscopy 43198 Biospy Trans Nasal Esophagoscopy Esophagoscopy 43200 Esophagoscopy Includes collection of specimen(s) by brushing or washing, when performed. 43201 Submucosal injection
43197 Trans nasal esophagoscopy 43198 Biospy Trans Nasal Esophagoscopy Esophagoscopy 43200 Esophagoscopy Includes collection of specimen(s) by brushing or washing, when performed. 43201 Submucosal injection
How to Effectively Code for Endoscopic Procedures in Gastroenterology
 How to Effectively Code for Endoscopic Procedures in Gastroenterology Ariwan Rakvit, MD Associate Professor Interim Chief, Division of Gastroenterology Texas Tech University Health Science Center All rights
How to Effectively Code for Endoscopic Procedures in Gastroenterology Ariwan Rakvit, MD Associate Professor Interim Chief, Division of Gastroenterology Texas Tech University Health Science Center All rights
GASTROENTEROLOGY FELLOWSHIP PANCREATICOBILARY CONSULTATION SERVICE GOALS AND OBJECTIVES University of Toledo
 GASTROENTEROLOGY FELLOWSHIP PANCREATICOBILARY CONSULTATION SERVICE GOALS AND OBJECTIVES University of Toledo Educational Purpose: The Pancreaticobiliary Service at UTMC introduces the fellow to inpatient
GASTROENTEROLOGY FELLOWSHIP PANCREATICOBILARY CONSULTATION SERVICE GOALS AND OBJECTIVES University of Toledo Educational Purpose: The Pancreaticobiliary Service at UTMC introduces the fellow to inpatient
LOWER GI ENDOSCOPIES So why is CMS yanking our chain? General Concepts for all GI Endoscopy Procedures
 LOWER GI ENDOSCOPIES We have lots of changes to lower GI coding for 2015 to talk about. Code definitions have been revised and many new codes have been added to this chapter. First the good news: All these
LOWER GI ENDOSCOPIES We have lots of changes to lower GI coding for 2015 to talk about. Code definitions have been revised and many new codes have been added to this chapter. First the good news: All these
The Role of Industry Representatives in the Endoscopy Unit
 The Role of Industry Representatives in the Endoscopy Unit Vivek Kaul, MD 1 and Douglas Faigel, MD, FASGE 2 Introduction The modern endoscopy unit is a busy workplace environment. With the patient as the
The Role of Industry Representatives in the Endoscopy Unit Vivek Kaul, MD 1 and Douglas Faigel, MD, FASGE 2 Introduction The modern endoscopy unit is a busy workplace environment. With the patient as the
Captivator EMR Device
 Device Clinical Article and Abstract Summary Endoscopic Mucosal Bergman et al: EMR Training Tips Bergman et al: EMR Learning Curve ASGE: EMR & ESD Guidelines Bergman et al: Captivator EMR vs Cook Duette
Device Clinical Article and Abstract Summary Endoscopic Mucosal Bergman et al: EMR Training Tips Bergman et al: EMR Learning Curve ASGE: EMR & ESD Guidelines Bergman et al: Captivator EMR vs Cook Duette
GASTROENTEROLOGY FELLOWSHIP HEPATOLOGY ROTATION GOALS AND OBJECTIVES University of Toledo
 GASTROENTEROLOGY FELLOWSHIP HEPATOLOGY ROTATION GOALS AND OBJECTIVES University of Toledo Educational Purpose: The Hepatology Rotation introduces the fellow to the management of outpatients and inpatients
GASTROENTEROLOGY FELLOWSHIP HEPATOLOGY ROTATION GOALS AND OBJECTIVES University of Toledo Educational Purpose: The Hepatology Rotation introduces the fellow to the management of outpatients and inpatients
Evolution of Barrett s esophagus
 Endoscopic Treatment and Surveillance of Esophageal Cancer: GI Perspective Charles J. Lightdale, MD Columbia University New York, NY Evolution of Barrett s esophagus Squamous esophagus Chronic inflammation
Endoscopic Treatment and Surveillance of Esophageal Cancer: GI Perspective Charles J. Lightdale, MD Columbia University New York, NY Evolution of Barrett s esophagus Squamous esophagus Chronic inflammation
Endoscopic Resection for Barrett s Esophagus and Early Cancer 2014 Masters of Minimally Invasive Surgery
 Endoscopic Resection for Barrett s Esophagus and Early Cancer 2014 Masters of Minimally Invasive Surgery Matthew Hartwig, M.D. Duke Cancer Institute Case Presentation: Patient ER 51 y/o man with schizophrenia
Endoscopic Resection for Barrett s Esophagus and Early Cancer 2014 Masters of Minimally Invasive Surgery Matthew Hartwig, M.D. Duke Cancer Institute Case Presentation: Patient ER 51 y/o man with schizophrenia
GI Bleed. Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System. Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital
 October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
October 3, 2015 GI Bleed Steven Lichtenstein, D.O. Chief, Division of Gastroenterology Mercy Health System Director, Endoscopy/GI Lab Mercy Fitzgerald Hospital Clinical Associate Professor of Medicine
Core curriculum for EMR and ablative techniques
 Communication from the ASGE Training Committee CORE CURRICULUM Core curriculum for EMR and ablative techniques This document was prepared by the American Society for Gastrointestinal Endoscopy (ASGE) Training
Communication from the ASGE Training Committee CORE CURRICULUM Core curriculum for EMR and ablative techniques This document was prepared by the American Society for Gastrointestinal Endoscopy (ASGE) Training
Pediatric Gastroenterology Fellowship Pediatric Nutrition Rotation Goals and Objectives - 1 st Year
 Pediatric Nutrition Rotation Goals and Objectives - 1 st Year Goal 1: Gain experience and competency in managing common and rare gastrointestinal, liver and nutritional problems. (Competencies: patient
Pediatric Nutrition Rotation Goals and Objectives - 1 st Year Goal 1: Gain experience and competency in managing common and rare gastrointestinal, liver and nutritional problems. (Competencies: patient
This program is jointly provided by the New York Society for Gastrointestinal Endoscopy and Mount Sinai Beth Israel
 This program is jointly provided by the New York Society for Gastrointestinal Endoscopy and Mount Sinai Beth Israel Japan Society 333 East 47th Street (near First Avenue) 10017 COURSE DESCRIPTION The Spring
This program is jointly provided by the New York Society for Gastrointestinal Endoscopy and Mount Sinai Beth Israel Japan Society 333 East 47th Street (near First Avenue) 10017 COURSE DESCRIPTION The Spring
What is Barrett s esophagus? How does Barrett s esophagus develop?
 Barrett s Esophagus What is Barrett s esophagus? Barrett s esophagus is a pre-cancerous condition affecting the lining of the esophagus, the swallowing tube that carries foods and liquids from the mouth
Barrett s Esophagus What is Barrett s esophagus? Barrett s esophagus is a pre-cancerous condition affecting the lining of the esophagus, the swallowing tube that carries foods and liquids from the mouth
Specific Standards of Accreditation for Residency Programs in General Surgery
 Specific Standards of Accreditation for Residency Programs in General Surgery 2010 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation of the
Specific Standards of Accreditation for Residency Programs in General Surgery 2010 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation of the
Endoluminal stent placement core curriculum
 Communication from the ASGE Training Committee CORE CURRICULUM Endoluminal stent placement core curriculum This is one of a series of documents prepared by the American Society for Gastrointestinal Endoscopy
Communication from the ASGE Training Committee CORE CURRICULUM Endoluminal stent placement core curriculum This is one of a series of documents prepared by the American Society for Gastrointestinal Endoscopy
Learning Luncheon 7: Endoscopic Mucosal Resection: When, Where and How?
 Endoscopic Mucosal Resection (EMR): When, Where, and Charles J. Lightdale, MD Columbia University New York, NY Endoscopic Mucosal Resection (EMR) EMR developed for removal of sessile or flat neoplasms
Endoscopic Mucosal Resection (EMR): When, Where, and Charles J. Lightdale, MD Columbia University New York, NY Endoscopic Mucosal Resection (EMR) EMR developed for removal of sessile or flat neoplasms
Provincial Quality Management Programs for Mammography, Colonoscopy and Pathology in Ontario
 Provincial Quality Management Programs for Mammography, Colonoscopy and Pathology in Ontario Quality Management Partnership Consultation Materials: Heal th System Ad mi nistrato r s October 20, 2014 Table
Provincial Quality Management Programs for Mammography, Colonoscopy and Pathology in Ontario Quality Management Partnership Consultation Materials: Heal th System Ad mi nistrato r s October 20, 2014 Table
Colonoscopy Data Collection Form
 Identifier: Sociodemographic Information Type: Zip Code: Gender: Height: (inches) Race: Ethnicity Inpatient Outpatient Male Female Birth Date: Weight: (pounds) American Indian (Native American) or Alaska
Identifier: Sociodemographic Information Type: Zip Code: Gender: Height: (inches) Race: Ethnicity Inpatient Outpatient Male Female Birth Date: Weight: (pounds) American Indian (Native American) or Alaska
Professional Responsibilities in Undergraduate Medical Education
 COLLEGE OF PHYSICIANS AND SURGEONS OF ONTARIO P O L I C Y S TAT E M E N T # 1-1 2 Professional Responsibilities in Undergraduate Medical Education APPROVED BY COUNCIL: REVIEWED AND UPDATED: PUBLICATION
COLLEGE OF PHYSICIANS AND SURGEONS OF ONTARIO P O L I C Y S TAT E M E N T # 1-1 2 Professional Responsibilities in Undergraduate Medical Education APPROVED BY COUNCIL: REVIEWED AND UPDATED: PUBLICATION
Advances In Endoscopy for Everyday Practice. Friday, August 14 - Saturday, August 15
 Advances In Endoscopy for Everyday Practice Friday, August 14 - Saturday, August 15 Northwestern Memorial Hospital Chicago, Illinois Feinberg 3rd Floor Conference Room A http://chicagolive.nm.org/ Sponsored
Advances In Endoscopy for Everyday Practice Friday, August 14 - Saturday, August 15 Northwestern Memorial Hospital Chicago, Illinois Feinberg 3rd Floor Conference Room A http://chicagolive.nm.org/ Sponsored
CLINICAL GUIDELINE FOR MANAGEMENTS OF PATIENTS TAKING ANTICOAGULANTS IN ENDOSCOPY 1. Aim/Purpose of this Guideline
 CLINICAL GUIDELINE FOR MANAGEMENTS OF PATIENTS TAKING ANTICOAGULANTS IN ENDOSCOPY 1. Aim/Purpose of this Guideline 1.1. The purpose of this guideline is to assist decision making of whether anticoagulants
CLINICAL GUIDELINE FOR MANAGEMENTS OF PATIENTS TAKING ANTICOAGULANTS IN ENDOSCOPY 1. Aim/Purpose of this Guideline 1.1. The purpose of this guideline is to assist decision making of whether anticoagulants
Prepared by the ASGE Taskforce on Ensuring Competence in Endoscopy
 Prepared by the ASGE Taskforce on Ensuring Competence in Endoscopy Douglas O. Faigel MD, Chair Todd H. Baron, MD Blair Lewis, MD Bret Petersen, MD John Petrini, MD and American College of Gastroenterology
Prepared by the ASGE Taskforce on Ensuring Competence in Endoscopy Douglas O. Faigel MD, Chair Todd H. Baron, MD Blair Lewis, MD Bret Petersen, MD John Petrini, MD and American College of Gastroenterology
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy. M. Arvanitakis SRBG June 2009
 Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
Endoscopy and infection: Prevention of infection during endoscopy Treatment of infection by endoscopy M. Arvanitakis SRBG June 2009 Outline Antibiotic prophylaxis during endoscopy Upper GI endoscopy Lower
POSITION STATEMENT. Minimum Registered Nurse Staffing for Patient Care in the Gastrointestinal Endoscopy Unit
 POSITION STATEMENT Minimum Registered Nurse Staffing for Patient Care in the Gastrointestinal Endoscopy Unit Disclaimer The Society of Gastroenterology Nurses and Associates, Inc. (SGNA) assumes no responsibility
POSITION STATEMENT Minimum Registered Nurse Staffing for Patient Care in the Gastrointestinal Endoscopy Unit Disclaimer The Society of Gastroenterology Nurses and Associates, Inc. (SGNA) assumes no responsibility
2012 EDITORIAL REVISION NOVEMBER 2013 VERSION 3.1
 Specific Standards of Accreditation for Residency Programs in Orthopedic Surgery 2012 EDITORIAL REVISION NOVEMBER 2013 VERSION 3.1 INTRODUCTION A university wishing to have an accredited program in Orthopedic
Specific Standards of Accreditation for Residency Programs in Orthopedic Surgery 2012 EDITORIAL REVISION NOVEMBER 2013 VERSION 3.1 INTRODUCTION A university wishing to have an accredited program in Orthopedic
Complications of pediatric endoscopy and colonoscopy. Informed consent. Learning objectives. Complication types. Complications (adults) 10/3/2012
 Complications of pediatric endoscopy and colonoscopy I have no financial relationships with any commercial entity to disclose Petar Mamula, M.D. The Children s Hospital of Philadelphia University of Pennsylvania
Complications of pediatric endoscopy and colonoscopy I have no financial relationships with any commercial entity to disclose Petar Mamula, M.D. The Children s Hospital of Philadelphia University of Pennsylvania
Billing Guideline. Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16
 Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/2012 Last Update Effective: 4/16 Billing Guideline Background Health First administers benefit packages with full coverage
EMR Can anyone do this?
 EMR Can anyone do this? Norio Fukami, MD University of Colorado Piecemeal resection? 1 Endoscopic mucosal resection (EMR) and Endoscopic submucosal dissection (ESD) Endoscopic removal of premalignant or
EMR Can anyone do this? Norio Fukami, MD University of Colorado Piecemeal resection? 1 Endoscopic mucosal resection (EMR) and Endoscopic submucosal dissection (ESD) Endoscopic removal of premalignant or
Specific Standards of Accreditation for Residency Programs in Orthopedic Surgery
 Specific Standards of Accreditation for Residency Programs in Orthopedic Surgery 2012 INTRODUCTION A university wishing to have an accredited program in Orthopedic Surgery must also sponsor an accredited
Specific Standards of Accreditation for Residency Programs in Orthopedic Surgery 2012 INTRODUCTION A university wishing to have an accredited program in Orthopedic Surgery must also sponsor an accredited
Program Requirements for Fellowship Education in Neuro- Ophthalmology
 Program Requirements for Fellowship Education in Neuro- Ophthalmology [M] = Must have / required [S] = Should have I. Introduction A. Definition and Scope of Neuro ophthalmology Neuro ophthalmology is
Program Requirements for Fellowship Education in Neuro- Ophthalmology [M] = Must have / required [S] = Should have I. Introduction A. Definition and Scope of Neuro ophthalmology Neuro ophthalmology is
Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI)
 Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI) The American Society for Gastrointestinal Endoscopy PIVI on Endoscopic Bariatric Procedures (short form) Please see related White
Preservation and Incorporation of Valuable Endoscopic Innovations (PIVI) The American Society for Gastrointestinal Endoscopy PIVI on Endoscopic Bariatric Procedures (short form) Please see related White
Basic Standards for Fellowship Training in Primary Care Osteopathic Sports Medicine
 Basic Standards for Fellowship Training in Primary Care Osteopathic Sports Medicine American Osteopathic Association American Osteopathic Academy of Sports Medicine American College of Osteopathic Family
Basic Standards for Fellowship Training in Primary Care Osteopathic Sports Medicine American Osteopathic Association American Osteopathic Academy of Sports Medicine American College of Osteopathic Family
SAGES 2015 Flexible Endoscopy Course for Fellows
 Goals and Objectives: At the end of the course, the MIS fellow will be familiar with GI endoscopes, towers, and the instruments used for endoscopy and endoscopic surgery. The fellow will also be able to
Goals and Objectives: At the end of the course, the MIS fellow will be familiar with GI endoscopes, towers, and the instruments used for endoscopy and endoscopic surgery. The fellow will also be able to
Medicine in Osteopathic Family Practice and Manipulative Treatment
 0BBasic Standards for Fellowship Training in Addiction Medicine in Osteopathic Family Practice and Manipulative Treatment American Osteopathic Association and the American College of Osteopathic Family
0BBasic Standards for Fellowship Training in Addiction Medicine in Osteopathic Family Practice and Manipulative Treatment American Osteopathic Association and the American College of Osteopathic Family
STANDARDS FOR ACCREDITATION
 STANDARDS FOR ACCREDITATION OF POST-GRADUATE CRNA FELLOWSHIPS January 2014 Copyright 2014 by the Council on Accreditation of Nurse Anesthesia Educational Programs 222 S. Prospect Avenue, Park Ridge, Illinois,
STANDARDS FOR ACCREDITATION OF POST-GRADUATE CRNA FELLOWSHIPS January 2014 Copyright 2014 by the Council on Accreditation of Nurse Anesthesia Educational Programs 222 S. Prospect Avenue, Park Ridge, Illinois,
2015 Medicare Physician Fee Schedule Putting the Pieces Together for GI Colleen M. Schmitt, MD, MHA, FASGE ASGE President
 2015 Medicare Physician Fee Schedule Putting the Pieces Together for GI Colleen M. Schmitt, MD, MHA, FASGE ASGE President Glenn D. Littenberg, MD, MACP Chair, ASGE Practice Management Committee and CPT
2015 Medicare Physician Fee Schedule Putting the Pieces Together for GI Colleen M. Schmitt, MD, MHA, FASGE ASGE President Glenn D. Littenberg, MD, MACP Chair, ASGE Practice Management Committee and CPT
Australian and New Zealand College of Anaesthetists (ANZCA) Guidelines on Training and Practice of Perioperative Cardiac Ultrasound in Adults
 PS46 2014 Australian and New Zealand College of Anaesthetists (ANZCA) Guidelines on Training and Practice of Perioperative Cardiac Ultrasound in Adults 1. INTRODUCTION Ultrasound imaging of the heart is
PS46 2014 Australian and New Zealand College of Anaesthetists (ANZCA) Guidelines on Training and Practice of Perioperative Cardiac Ultrasound in Adults 1. INTRODUCTION Ultrasound imaging of the heart is
ERCP in Post Surgical Anatomy
 ERCP in Post Surgical Anatomy ACG Western Regional Course, 2013 John G. Lee, MD Division of Gastroenterology University of California, Irvine Medical Center Common surgical alterations Intact pancreaticobiliary
ERCP in Post Surgical Anatomy ACG Western Regional Course, 2013 John G. Lee, MD Division of Gastroenterology University of California, Irvine Medical Center Common surgical alterations Intact pancreaticobiliary
Lenox Hill Hospital Department of Surgery General Surgery Goals and Objectives
 Lenox Hill Hospital Department of Surgery General Surgery Goals and Objectives Medical Knowledge and Patient Care: Residents must demonstrate knowledge and application of the pathophysiology and epidemiology
Lenox Hill Hospital Department of Surgery General Surgery Goals and Objectives Medical Knowledge and Patient Care: Residents must demonstrate knowledge and application of the pathophysiology and epidemiology
Good Scientific Practice
 Section 1: The purpose of this document There are three key components to the Healthcare Science workforce in the UK: 1. Healthcare Science Associates and Assistants who perform a diverse range of task
Section 1: The purpose of this document There are three key components to the Healthcare Science workforce in the UK: 1. Healthcare Science Associates and Assistants who perform a diverse range of task
Captivator II. Single-Use Snares
 Captivator II Single-Use Snares Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication. The Captivator II Snare line
Captivator II Single-Use Snares Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication. The Captivator II Snare line
Billing Diagnosis & Billing in Endoscopy
 Billing Diagnosis & Billing in Endoscopy Luis S. Marsano,MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Louisville and Louisville VAMC 2014 Billing Diagnosis
Billing Diagnosis & Billing in Endoscopy Luis S. Marsano,MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Louisville and Louisville VAMC 2014 Billing Diagnosis
Post-DDW OAG Course - Therapeutic Endoscopy
 Post-DDW OAG Course - Therapeutic Endoscopy June 13, 2015 Jeffrey Mosko Division of Gastroenterology St. Michael's Hospital University of Toronto [email protected] Program Name: Post-DDW OAG course CanMEDS
Post-DDW OAG Course - Therapeutic Endoscopy June 13, 2015 Jeffrey Mosko Division of Gastroenterology St. Michael's Hospital University of Toronto [email protected] Program Name: Post-DDW OAG course CanMEDS
HEPATOLOGY CLERKSHIP
 College of Osteopathic Medicine HEPATOLOGY CLERKSHIP Office for Clinical Affairs 515-271-1629 FAX 515-271-1727 Elective Rotation General Description This elective rotation is a four (4) week introductory,
College of Osteopathic Medicine HEPATOLOGY CLERKSHIP Office for Clinical Affairs 515-271-1629 FAX 515-271-1727 Elective Rotation General Description This elective rotation is a four (4) week introductory,
9th Annual Rocky Mountain Interventional Endoscopy Course
 NON-PROFIT ORG. US POSTAGE PAID PERMIT NO 831 DENVER, CO Join us in Anschutz Medical Campus 9th Annual Rocky Mountain Interventional Endoscopy Course FEBRUARY 15-17, 2012 Photograph by Alice Chen Anschutz
NON-PROFIT ORG. US POSTAGE PAID PERMIT NO 831 DENVER, CO Join us in Anschutz Medical Campus 9th Annual Rocky Mountain Interventional Endoscopy Course FEBRUARY 15-17, 2012 Photograph by Alice Chen Anschutz
Department of Neurology and Neurosurgery Clinical and Clinical Research Fellowship Application Form
 Department of Neurology and Neurosurgery Clinical and Clinical Research Fellowship Application Form Fellowship in Multiple Sclerosis and Neuroinflammatory Disorders Type of Fellowship: Clinical Research
Department of Neurology and Neurosurgery Clinical and Clinical Research Fellowship Application Form Fellowship in Multiple Sclerosis and Neuroinflammatory Disorders Type of Fellowship: Clinical Research
The Practice Standards for Medical Imaging and Radiation Therapy. Sonography Practice Standards
 The Practice Standards for Medical Imaging and Radiation Therapy Sonography Practice Standards 2015 American Society of Radiologic Technologists. All rights reserved. Reprinting all or part of this document
The Practice Standards for Medical Imaging and Radiation Therapy Sonography Practice Standards 2015 American Society of Radiologic Technologists. All rights reserved. Reprinting all or part of this document
Basic Standards for Residency Training in Child and Adolescent Psychiatry
 Basic Standards for Residency Training in Child and Adolescent Psychiatry American Osteopathic Association and American College of Osteopathic Neurologists and Psychiatrists Adopted 1980 Revised, 1984
Basic Standards for Residency Training in Child and Adolescent Psychiatry American Osteopathic Association and American College of Osteopathic Neurologists and Psychiatrists Adopted 1980 Revised, 1984
2014 Procedural Reimbursement Guide for Endoscopy
 2014 Procedural Reimbursement Guide for Endoscopy 2014 Procedural Reimbursement Guide For THIS PROCEDURAL REIMBURSEMENT GUIDE, FOR SELECT ENDOSCOPY PROCEDURES, provides coding and reimbursement information
2014 Procedural Reimbursement Guide for Endoscopy 2014 Procedural Reimbursement Guide For THIS PROCEDURAL REIMBURSEMENT GUIDE, FOR SELECT ENDOSCOPY PROCEDURES, provides coding and reimbursement information
Liver Disease & Gastroenterology
 11 th UVa Annual Conference of Liver Disease & Gastroenterology COVERING ALL ASPECTS OF CARE FRIDAY AND SATURDAY, JUNE 10-11, 2016 DARDEN BUSINESS SCHOOL, CHARLOTTESVILLE, VA School of Medicine SPONSORED
11 th UVa Annual Conference of Liver Disease & Gastroenterology COVERING ALL ASPECTS OF CARE FRIDAY AND SATURDAY, JUNE 10-11, 2016 DARDEN BUSINESS SCHOOL, CHARLOTTESVILLE, VA School of Medicine SPONSORED
Use of stents in esophageal cancer" Hans Gerdes, M.D. Director, GI Endoscopy Unit Memorial Sloan-Kettering Cancer Center
 Use of stents in esophageal cancer" Hans Gerdes, M.D. Director, GI Endoscopy Unit Memorial Sloan-Kettering Cancer Center Features of esophageal cancer Esophageal cancer is an abnormal growth that arises
Use of stents in esophageal cancer" Hans Gerdes, M.D. Director, GI Endoscopy Unit Memorial Sloan-Kettering Cancer Center Features of esophageal cancer Esophageal cancer is an abnormal growth that arises
There must be an appropriate administrative structure for each residency program.
 Specific Standards of Accreditation for Residency Programs in Radiation Oncology 2015 VERSION 3.0 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation
Specific Standards of Accreditation for Residency Programs in Radiation Oncology 2015 VERSION 3.0 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation
Goals and Objectives for the General Surgery Rotation Resident PGY1 Hamilton Health Sciences or St. Joseph Healthcare (2 four-week rotational blocks)
 Goals and Objectives for the General Surgery Rotation Resident PGY1 Hamilton Health Sciences or St. Joseph Healthcare (2 four-week rotational blocks) Overview During the first year of their residency training
Goals and Objectives for the General Surgery Rotation Resident PGY1 Hamilton Health Sciences or St. Joseph Healthcare (2 four-week rotational blocks) Overview During the first year of their residency training
Training Requirements for the Specialty of Radiation Oncology
 Association internationale sans but lucratif AVENUE DE LA COURONNE, 20 BE- 1050 BRUSSELS www.uems.net International non-profit organisation T +32 2 649 51 64 F +32 2 640 37 30 [email protected] Training Requirements
Association internationale sans but lucratif AVENUE DE LA COURONNE, 20 BE- 1050 BRUSSELS www.uems.net International non-profit organisation T +32 2 649 51 64 F +32 2 640 37 30 [email protected] Training Requirements
European Academy of DentoMaxilloFacial Radiology
 European Academy of DentoMaxilloFacial Radiology Framework for Specialist Training in Dental and Maxillofacial Radiology Background The scope of DentoMaxilloFacial Radiology DMFR (Dental and Maxillofacial
European Academy of DentoMaxilloFacial Radiology Framework for Specialist Training in Dental and Maxillofacial Radiology Background The scope of DentoMaxilloFacial Radiology DMFR (Dental and Maxillofacial
Gary M. Annuniziata, D.O., F.A.C.P. Anh T. Duong, M.D. Jonathan C. Lin, M.D., MPH. Preparation for EGD, ERCP, Peg Placement.
 Gary M. Annuniziata, D.O., F.A.C.P. Anh T. Duong, M.D. Jonathan C. Lin, M.D., MPH Phone- (760) 321-2500 Fax- (760) 321-5720 Preparation for EGD, ERCP, Peg Placement Patient Name- Procedure Date and Time-
Gary M. Annuniziata, D.O., F.A.C.P. Anh T. Duong, M.D. Jonathan C. Lin, M.D., MPH Phone- (760) 321-2500 Fax- (760) 321-5720 Preparation for EGD, ERCP, Peg Placement Patient Name- Procedure Date and Time-
Exhibit 9 ADEA Competencies for Entry into the Allied Dental Professions (As approved by the 2010 ADEA House of Delegates)
 Exhibit 9 ADEA Competencies for Entry into the Allied Dental Professions (As approved by the 2010 ADEA House of Delegates) Introduction In 1998 99, the Section on Dental Hygiene of the American Association
Exhibit 9 ADEA Competencies for Entry into the Allied Dental Professions (As approved by the 2010 ADEA House of Delegates) Introduction In 1998 99, the Section on Dental Hygiene of the American Association
BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY
 BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY American Osteopathic Association and the American College of Osteopathic Internists Specific Requirements For Osteopathic Subspecialty Training In Cardiology
BASIC STANDARDS FOR RESIDENCY TRAINING IN CARDIOLOGY American Osteopathic Association and the American College of Osteopathic Internists Specific Requirements For Osteopathic Subspecialty Training In Cardiology
Standards for an Accredited Educational Program in Radiologic Sciences
 Standards for an Accredited Educational Program in Radiologic Sciences EFFECTIVE JANUARY 1, 2002 Adopted by: The Joint Review Committee on Education in Radiologic Technology: January 1996; Revised 2001
Standards for an Accredited Educational Program in Radiologic Sciences EFFECTIVE JANUARY 1, 2002 Adopted by: The Joint Review Committee on Education in Radiologic Technology: January 1996; Revised 2001
STANDARDS FOR ACCREDITATION
 STANDARDS FOR ACCREDITATION OF POST-GRADUATE FELLOWSHIPS The projected date for implementation of all standards, following further revision and approval, is January 2015. Draft 2 1 May 29, 2013 January
STANDARDS FOR ACCREDITATION OF POST-GRADUATE FELLOWSHIPS The projected date for implementation of all standards, following further revision and approval, is January 2015. Draft 2 1 May 29, 2013 January
The Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication.
 Captivator II Single-Use Snares The Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication. The Captivator II Snare
Captivator II Single-Use Snares The Captivator II Snares are the first line of stiff and rounded snares available in multiple sizes with both a hot and cold snaring indication. The Captivator II Snare
BSGIE national survey : The endoscopy unit
 BSGIE national survey : The endoscopy unit Dear Colleagues, The BSGIE organises a national survey on the organisation, equipment and activity of the endoscopic units in our hospitals. The results of this
BSGIE national survey : The endoscopy unit Dear Colleagues, The BSGIE organises a national survey on the organisation, equipment and activity of the endoscopic units in our hospitals. The results of this
Things your Alma Mater Never Taught You Craig Render
 Practice Management in Gastroenterology Things your Alma Mater Never Taught You Craig Render Lots of Decisions Academic vs. Private Hospital based vs. Office Endoscopy Group or Solo Full Time vs Part Time
Practice Management in Gastroenterology Things your Alma Mater Never Taught You Craig Render Lots of Decisions Academic vs. Private Hospital based vs. Office Endoscopy Group or Solo Full Time vs Part Time
2015 CPT coding changes will have mixed effects on payment for general surgeons
 CPT coding changes will have mixed effects on payment for general surgeons 17 by Linda Barney, MD, FACS, and Mark T. Savarise, MD, FACS JAN BULLETIN American College of Surgeons 18 Significant changes
CPT coding changes will have mixed effects on payment for general surgeons 17 by Linda Barney, MD, FACS, and Mark T. Savarise, MD, FACS JAN BULLETIN American College of Surgeons 18 Significant changes
The Practice Standards for Medical Imaging and Radiation Therapy. Radiography Practice Standards
 The Practice Standards for Medical Imaging and Radiation Therapy Radiography Practice Standards 2015 American Society of Radiologic Technologists. All rights reserved. Reprinting all or part of this document
The Practice Standards for Medical Imaging and Radiation Therapy Radiography Practice Standards 2015 American Society of Radiologic Technologists. All rights reserved. Reprinting all or part of this document
Management of Antithrombotic Therapy in the Peri-endoscopic Period: An Update
 Management of Antithrombotic Therapy in the Peri-endoscopic Period: An Update Nimeesh Shah, MD March 6, 2015 Santa Clara Valley Medical Center Stanford University School of Medicine None Financial Disclosures
Management of Antithrombotic Therapy in the Peri-endoscopic Period: An Update Nimeesh Shah, MD March 6, 2015 Santa Clara Valley Medical Center Stanford University School of Medicine None Financial Disclosures
Medical Coverage Policy Monitored Anesthesia Care (MAC)
 Medical Coverage Policy Monitored Anesthesia Care (MAC) Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2004 Policy Last Updated: 1/8/2013 Prospective review is recommended/required.
Medical Coverage Policy Monitored Anesthesia Care (MAC) Device/Equipment Drug Medical Surgery Test Other Effective Date: 9/1/2004 Policy Last Updated: 1/8/2013 Prospective review is recommended/required.
BASIC STANDARDS FOR TRAINING IN PRIMARY CARE OSTEOPATHIC SPORTS MEDICINE
 BASIC STANDARDS FOR TRAINING IN PRIMARY CARE OSTEOPATHIC SPORTS MEDICINE American Osteopathic Association American Osteopathic Academy of Sports Medicine American College of Osteopathic Family Physicians
BASIC STANDARDS FOR TRAINING IN PRIMARY CARE OSTEOPATHIC SPORTS MEDICINE American Osteopathic Association American Osteopathic Academy of Sports Medicine American College of Osteopathic Family Physicians
The Nurse Endoscopist SUMMARY. Conclusion
 The Nurse Endoscopist SUMMARY 1. There is increasing interest and demand from within both the medical and nursing professions for nurses to perform endoscopy. 2. Studies have shown that nurses can develop
The Nurse Endoscopist SUMMARY 1. There is increasing interest and demand from within both the medical and nursing professions for nurses to perform endoscopy. 2. Studies have shown that nurses can develop
A Guide for Patients Living with a Biliary Metal Stent
 A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
Endoscopic Submucosal Dissection (E.S.D.) vs. Endoscopic Mucosal Resection (E.M.R.) in Colombia. Advocating E.M.R.
 Controversies in Gastroenterology Endoscopic Submucosal Dissection (E.S.D.) vs. Endoscopic Mucosal Resection (E.M.R.) in Colombia. Advocating E.M.R. Raúl Cañadas Garrido, MD. 1 1 Internist-Gastroenterologist.
Controversies in Gastroenterology Endoscopic Submucosal Dissection (E.S.D.) vs. Endoscopic Mucosal Resection (E.M.R.) in Colombia. Advocating E.M.R. Raúl Cañadas Garrido, MD. 1 1 Internist-Gastroenterologist.
8th Annual Rocky Mountain Interventional Endoscopy Course
 NON-PROFIT ORG. US POSTAGE PAID PERMIT NO 2378 DENVER, CO Join us in Anschutz Medical Campus 8th Annual Rocky Mountain Interventional Endoscopy Course FEBRUARY 16-18, 2011 Photograph by Alice Chen Denver
NON-PROFIT ORG. US POSTAGE PAID PERMIT NO 2378 DENVER, CO Join us in Anschutz Medical Campus 8th Annual Rocky Mountain Interventional Endoscopy Course FEBRUARY 16-18, 2011 Photograph by Alice Chen Denver
These parameters cannot, at the present time, be determined by non-invasive imaging techniques.
 Endoscopic Mucosal Resection for Upper Gastrointestinal Lesions Kenneth K. Wang, M.D. Chairman, WEO Publication and Guidelines Committee Professor of Medicine, Mayo Clinic Rochester, Minnesota Upper gastrointestinal
Endoscopic Mucosal Resection for Upper Gastrointestinal Lesions Kenneth K. Wang, M.D. Chairman, WEO Publication and Guidelines Committee Professor of Medicine, Mayo Clinic Rochester, Minnesota Upper gastrointestinal
ESD for colorectal lesions I am in favour. Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy
 ESD for colorectal lesions I am in favour Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Surgery for early colonic lesions 51 pts referred for lap colectomy
ESD for colorectal lesions I am in favour Alessandro Repici, MD Digestive Endoscopy Unit IRCCS Istituto Clinico Humanitas Milano, Italy Surgery for early colonic lesions 51 pts referred for lap colectomy
By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA
 SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
SMALL BOWEL BLEEDING: CAUSES, DIAGNOSIS AND TREATMENT By Anne C. Travis, M.D., M.Sc. and John R. Saltzman, M.D., FACG Brigham and Women's Hospital Harvard Medical School Boston, MA 1. What is the small
How To Avoid Coding Errors. General Rules
 How To Avoid Coding Errors R. Bruce Cameron, M.D., FACG ACG Governors Best Practices Course Las Vegas January 24, 2014 General Rules Buy a current CPT book Buy a current ASGE coding book Send your office
How To Avoid Coding Errors R. Bruce Cameron, M.D., FACG ACG Governors Best Practices Course Las Vegas January 24, 2014 General Rules Buy a current CPT book Buy a current ASGE coding book Send your office
Guidance notes for commissioners implementing the policy on Complex endovascular stent grafts in the management of abdominal aortic aneurysm
 Guidance notes for commissioners implementing the policy on Complex endovascular stent grafts in the management of abdominal aortic aneurysm NHSCB/A04/P/a NHS England: Guidance notes for commissioners
Guidance notes for commissioners implementing the policy on Complex endovascular stent grafts in the management of abdominal aortic aneurysm NHSCB/A04/P/a NHS England: Guidance notes for commissioners
Post-Professional Athletic Training Residency Accreditation Standards & Guidelines. Version 1.2 August, 2010
 Post-Professional Athletic Training Residency Accreditation Standards & Guidelines Version 1.2 August, 2010 POST-PROFESSIONAL ATHLETIC TRAINING RESIDENCY STANDARDS & GUIDELINES Post-Professional Athletic
Post-Professional Athletic Training Residency Accreditation Standards & Guidelines Version 1.2 August, 2010 POST-PROFESSIONAL ATHLETIC TRAINING RESIDENCY STANDARDS & GUIDELINES Post-Professional Athletic
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
GASTROENTEROLOGY CPT ADVISORS
 GASTROENTEROLOGY CPT ADVISORS CHRISTOPHER Y. KIM, MD, MBA, ACG CPT ADVISOR JOEL V. BRILL, MD, AGA CPT ADVISOR GLENN D. LITTENBERG, MD, ASGE CPT ADVISOR 395-005PNQ_14-6 2015 CPT Coding Update The American
GASTROENTEROLOGY CPT ADVISORS CHRISTOPHER Y. KIM, MD, MBA, ACG CPT ADVISOR JOEL V. BRILL, MD, AGA CPT ADVISOR GLENN D. LITTENBERG, MD, ASGE CPT ADVISOR 395-005PNQ_14-6 2015 CPT Coding Update The American
