Hospice Austin s Caregiver Guide
|
|
|
- Jocelyn Cannon
- 8 years ago
- Views:
Transcription
1 Hospice Austin s Caregiver Guide The more you understand about how you can best care for your loved one, the richer and more meaningful your time together will be. The information that we provide should help you recognize changes, what the changes mean, and how to provide care as these changes occur. It is our hope that this guide, along with all of the other support Hospice Austin provides, will help you through this emotional time. Caregiving advice is also available by visiting HospiceAustin.org/caregiving. Please call us any time you have a question or concern. Nutrition We connect food with life. When a person doesn t eat, not only are the comforting routines of meal times lost, but fears about survival are common. Family members work hard to prepare foods that might be appealing, only to have the person take a few bites and report feeling full or that the food doesn t taste good. Family members feel frustrated, helpless and afraid of what will happen if the patient doesn't eat. The patient can sense the frustration and feel pressured to eat to please loved ones. Why do patients have a loss of appetite or the ability to eat? A change in the ability to eat is a natural consequence of an advanced disease process. As the body slows down, the digestive process slows as well. This change usually begins as mild distaste for certain foods, progresses to a desire for only a few foods and finally results in an almost complete lack of ability to eat. Your loved one may experience feelings of sadness or depression; however, the lack of appetite is directly related to the disease process and the body's deterioration. What strategies are most effective? Accept the loss of appetite as an expected and normal part of the disease. Allow your loved one to select food and drinks. Offer different choice but don't push! Find other ways of showing love and concern such as giving a foot massage, reading aloud or playing cards. Recognize that this is a loss, and like all losses that are part of this illness, talking about it may make it less burdensome. Know that prolonged use of intravenous fluids and artificial nutrition usually are not effective for people with advanced disease. This can actually omplicate care and physical well-being. As the ability to digest decreases, the food or supplements can accumulate and cause increased pain, nausea and suffering.
2 At mealtime, try the following suggestions: Offer medication for pain or nausea one hour before eating. Serve food in a pleasant environment, preferably at the table if it s comfortable for the patient. Ask what tastes best. Many people do not tolerate red meat, fried, or spicy foods. Cool, bland and soft foods are often the most appealing. Experiment with supplements and powdered breakfast drinks. People at the end of life have stated that dehydration is not painful, but the mouth does get dry. You can use ice chips, artificial saliva and lip moisturizers. Flavored ice cubes (made from fruit juice) crushed into ice chips can be enjoyable. Basic Hygiene Mouth Care Your loved one may develop a dry mouth. Relief can be provided by following these steps: Moisten mouth swab with baking soda mouthwash (1 teaspoon salt and 1 teaspoon baking soda in 1 quart of water). Clean inside the mouth and around teeth. Clean the roof of the mouth. Repeat this process every 30 minutes to 1 hour, depending on comfort needs. To prevent dry lips, try applying a thin layer of petroleum jelly. If your loved one is using oxygen, use a non-petroleum-based lubricant (Aloe Vera, Beeswax products). Perfumed lip balms and lemon-glycerin swabs can be drying and irritating. If your loved one is unable to brush teeth, you can provide mouth care at least twice a day. Gently brush natural teeth or remove dentures and clean them. If your loved one is unresponsive, a mouth swab should be used in the mouth. Either a swab or a 4"x4" gauze pad squeezed almost dry with mouth wash can be used to clean and refresh the mouth (your nurse will supply mouth swabs). Remember, your loved one may not be able to swallow, so use only a small amount of liquid. Bathing When providing help with bathing: Gather wash basin, towel, and wash cloth or sponge. Frequently change water. Water should be warm rather than hot. Use mild soap. Wash, rinse and completely dry separate areas. Wash the face and neck first, then the trunk and arms, legs and feet and lastly, the private areas. Always dry each area completely. Add a little powder or deodorant. Look for any reddened areas, especially the bony parts or pressure areas (elbows, heels, upper buttocks,shoulders, even ears). Apply lotion to reddened areas. 2
3 Skin Care Keeping the skin in good condition is very important, especially if your loved one is bed-bound or is not able to change position often. A good time to check the skin is during the bath. Dry skin may look flaky and white, may itch, or be red and look like a rash. This may be the beginning of a bedsore. Although it is up to the nurse and doctor to decide what treatment will help the area heal, there are several things you can do to lessen the risk of bedsores: Change your loved one s position frequently in bed or help shift him or her from side to side in a wheelchair. Apply lotion gently to the bony areas. Make sure pain medication is given to a person who has pain. This will make your loved one more willing to move and make it easier to do so. Keep skin clean and dry. Keep the sheets dry, and smooth out any wrinkles. Do not use extra cushioning or donut pillows around the boney areas as this actually increases the pressure. Your Hospice Austin team can provide a special mattress that can help make your loved one more comfortable. Getting Someone Out of Bed Nurses can demonstrate the correct way to perform this procedure. Roll the person on his or her side facing the caregiver. If using a hospital bed, raise the bed. If not, place your arms under your loved one s underarms and gently pull to a sitting position. Bring his or her legs around to dangle from the bed. If your loved one is unable to sit up, you can support the head and trunk to move him or her to a sitting position. Reposition yourself to ensure a stable balance. Place your hands in a hugging position under the person s arms. Brace the knee against your loved one s knee by placing one leg between the person s legs and gently lift up. When both parties are standing, pivot towards a chair and gently let the person sit. Remember to have the chair in a nearby position to make moving easier. Also, if lifting to a wheelchair, be sure it is in a locked position. Getting On and Off the Bedpan If your loved one is not able to get out of bed or if it is easier to use a bedpan at night, use these steps: Wear protective gloves (Your Hospice Austin team can provide gloves). When lying on his or her back, begin by crossing your loved one s legs. If you will be rolling to the left, place your loved one s right leg over the left, and cross their right arm over the chest (do this with the opposite side if turning to the right). Your loved one may be able to grab the side rail to help roll onto the side. Place the bedpan as close to the buttocks as possible and then roll the person onto the pan. If using a fracture pan, place the handle to the front and the flat part against your loved one s back. When finished, you will repeat these steps above to remove the pan. 3
4 When the pan is removed, keep your loved one on his/her side to wash and dry the area. It is easier to clean the private area while the person is still on his or her side. To finish, roll into a comfortable position. Positioning a Patient in Bed Use pillows to place behind your loved one s back to prevent rolling. Use small pillows or soft thin blankets to place between the legs and arms to prevent pressure. Remember, it is very important to change position often for a person who is lying in bed. After positioning, always look and see if your loved one is comfortable. If the position seems comfortable, it most likely is. It is also okay to ask. Using a Draw Sheet If your loved one is unable to move, draw sheets can be very helpful. Draw sheets usually consist of a soft blanket or folded sheet, large enough to reach from shoulders to mid-thigh, with six inches or more on either side in order for the caregiver to grab hold of it. Place the sheet under your loved one using the same technique of rolling from side to side (see bedpan placement). Keep the draw sheet wrinkle-free underneath to prevent pressure sores. When the draw sheet is underneath, your loved can then be scooted higher or lower in the bed or rolled from side to side using the draw sheet. Use two people to hold either side of the draw sheet. Roll the draw sheet up to your loved one on both sides. On the count of three, move the person in unison. Elimination When a person becomes very ill, he or she may have problems controlling urine and stool. This can be upsetting and embarrassing to both of you, but is a normal bodily function. Remember that urine output will lessen due to the decreased fluid intake and decreased circulation. Urine and stool incontinence Use adult briefs or place a disposable underpad under a person with loss of bladder and bowel control. Wearing protective gloves, change your loved one when he or she is soiled with either urine or stool. Wash the area with warm soapy water, rinse and completely dry. Apply lotion to reddened areas. Use the technique of rolling from side to side (see getting off of bedpan above) to change the underpad or briefs. Foley Care Many people come home from the hospital with a Foley catheter. This is a small, flexible rubber-like tube anchored with a balloon inserted into the bladder, which allows urine to flow through to a large collection bag. This enables a person to remain dry and comfortable without having to get out of bed. 4
5 If your loved one has a catheter, here are some tips to help you keep it clean: Put on protective gloves Wash the area where the tube enters the body with warm soapy water, washing and rinsing away from the body. Rinse well and completely dry. This should be done at least once a day. Make sure that the tubing from the bladder to the collection bag is without kinks or folds. Always place the collection bag below your loved one s bladder. This is so gravity will draw urine into the bag. Sometimes a catheter will leak. If that happens, place an absorbent disposable pad under the person. Call your Hospice Austin team so that they can evaluate the problem. Empty the collection bag twice a day. There is a special spout at the bottom of the bag. The nurse or home health aide will demonstrate how this is done. Constipation Your loved one may experience constipation due to decreased physical activity, changes in diet, and some medications. Here are some suggestions that may help: Increase activity, if possible. Increase fluids and fiber in the diet, if tolerated, such as water, juices, fruits, bran, and vegetables. Provide stool softeners and laxatives as instructed. Diarrhea Poor digestion and absorption along with certain treatments and medications may cause your loved one to experience diarrhea. Here are some guidelines to follow: Review the person s dietary intake for the past 24 hours. Increase fluid intake. Encourage eating small amounts frequently. Provide foods that are mild and tend not to cause diarrhea, e.g. rice, bananas, applesauce (no skins) or toast. Fatigue Fatigue (generalized weakness) will increase. As it does, it will become more difficult for your loved one to move around in bed. Being unable to move can be uncomfortable. To decrease discomfort, you can help by performing gentle guided movement of your loved one s extremities, and this can be done throughout the day. These are called Passive Range of Motion Exercises. Your Hospice Austin nurse can show you how to perform them. There may come a time when your loved one will need help to change positions in bed. If turning is tolerated, try doing this as frequently as every two hours. Your Hospice Austin nurse will teach which positions are best and how to use a draw sheet to help this process. 5
6 Pain Management Our primary objective is to keep your loved one in his or her chosen place of residence and free from pain. Here are a few guidelines to follow to keep pain under control: Give oral pain medication at the prescribed times, even if pain is not currently present. This maintains a level of pain medication and will help keep your loved one comfortable. When awake and alert, your loved one can say when pain occurs. When unresponsive, look for signs of restlessness, moaning or wincing. Continue to give medication as prescribed and change the patient's position for comfort. If your loved one is having difficulty swallowing a pill, call your nurse. Pain medication can be prescribed in a different form or prepared in a different manner. Some medications are given as a suppository. The Hospice Austin nurse can teach you how to administer a dosage. Pain does not normally increase as a person approaches death. However, if it does, your Hospice Austin team will be able to help manage that pain with appropriate medications and, if possible, other comfort measures. Shortness of Breath Sometimes people can experience trouble breathing and shortness of breath. Signs include restlessness, rapid, short, shallow breaths and anxiety. If this happens to your loved one, this can be very frightening to both of you. However, there are some steps you can take: Keep the room cool and well-ventilated. Allow for adequate rest between meals and after a bath. Raise the head of the bed or have your loved one sit up. Put pillows behind the head to ensure good support. Have the person lean forward and encircle his or her arms around a pillow or over an over-the-bed table. Place your loved one in the position identified as most comfortable. Stay calm and reassure him or her. Place a small oscillating fan at the bedside to help the person feel as if he or she is receiving more air. Check the person s temperature and notice any changes in mucous (especially thickness). Offer warm fluids and a room humidifier if mucous is thick. Remove all highly scented items from the area. Ensure that no one is smoking in the immediate area. If oxygen is in the home, administer it until shortness of breath subsides. Minimize visitors at the bedside to one at a time. One-to-one support is best. Take turns if necessary. Have the person do deep breathing exercises (this helps to slow breathing and increase oxygen flow): o Breathe in and out slowly through the nose, using the stomach muscles. o Feel the abdomen rise and fall with each inhalation and exhalation. Try pursed-lip breathing. Breathe in slowly through the nose. Hold this breath and count to three. Purse the lips as if to whistle. Breathe out slowly through pursed lips, to the count of six. 6
7 Agitation The last days and hours of life can be a time of peace and comfort. However, some patients may experience restlessness. Restlessness is when the patient experiences agitation in the days or hours prior to death. Signs of Restlessness Prior to death, the patient may become agitated, confused, and very restless. Some signs of this restlessness may include: Making faces, clenching teeth. Pulling or picking at bed linens. Attempting to remove clothing. Constantly moving in bed, trying to get out of bed, or sleeping very little. Crying out, moaning. It is not always possible to determine why restlessness occurs. Your Hospice Austin team will look for these and other possible causes so that the symptoms can be managed: pain, constipation, inability to urinate, lack of oxygen, fear. What You Can Do Caring for a patient with restlessness can make you feel tired, overwhelmed, and frustrated. Call your Hospice Austin team immediately if the patient shows any signs of restlessness. They can work with you and your doctor to find treatments to help decrease the restlessness. Some things you can do to help the patient are: Keep the patient safe by padding the sides of the patient with pillows or placing pillows against the bed s side rails. Provide constant supervision. Ask family members, friends, and your Hospice Austin team to help. Keep the room as peaceful and quiet as possible. Keep noise levels low. Gently reassure the patient and give the patient time to talk about any worries. Turn down bright lights. Try playing soft, soothing music. Explain to visitors the need for quiet, soothing surroundings. Talk to the patient in a calm, quiet voice. When giving care, softly explain what you are doing. Take time for yourself. Ask someone to stay with the patient while you rest, go for a walk, run an errand, or do an activity you enjoy. Talk to your Hospice Austin team about any concerns you may have. Please feel free to call your Hospice Austin team at (512) any time for questions or concerns about restlessness. They will help you draw from your own resources and those available to you through Hospice Austin to ease this difficult time. You are not alone. 7
8 Emotional Care Emotional care is every bit as important as the relief of physical pain. Many people feel anger or depression at the thought of dying; feelings of guilt or regret over the past are also common. Ultimately, with loving, caring support from family, friends and Hospice Austin staff, most terminally ill people come to terms with the thought of death. A great cause of anxiety may be fear of a painful end. You can reassure your loved one that adequate pain relief will be maintained at all times, and that even when death is near, there is no need to fear suffering. Most people drift into unconsciousness just before the end, and die in their sleep. Many people are concerned that they will die alone. Hospice Austin has a special volunteer program to help ensure that the person and/or family has a supportive presence there with them if they so wish. Preparing for death may include practical matters such as writing a will or planning funeral arrangements. It may include less tangible things such as saying "I'm sorry," "thank you," or "goodbye." Speaking with a clergy member is also important for some people. Perhaps the most pressing need for the terminally ill person is open, honest communication. Relatives, friends and caregivers must be willing to share the dying person's concerns. Family, friends, and caregivers should be sensitive to the following needs of their loved one: The need for open, honest communication. The need for emotional stability. The need to talk and share feelings. The need to be included. The need for someone to listen. The need for unconditional love, time and patience. The need for intimacy through human touch. The need for laughter and pleasure. Taking Care of Yourself Taking care of a loved one at home can be very rewarding. It can also be physically and emotionally draining to you. Sometimes you will feel like you have no time for yourself and that responsibilities are overwhelming. Emotionally, you may be trying to deal with the impending loss of your family member and at the same time feel like you have to hold your entire family together. Many times you may think that you have no one to talk to about your own personal problems. Physically, caring for the needs of the patient, a home and a family can be difficult as well. When doing all of these things, remember to not neglect a very valuable piece of the puzzle... yourself. If you don t take care of yourself, you won t be able to take the best care of your loved one. Some of the things you can do to perform self-care are: Get enough rest. Your outlook and ability to deal with things are greatly improved with adequate rest. Try to get at least six hours of sleep a night, and nap during the day while your loved one is sleeping. Sometimes it is difficult to wind down, so try deep breathing exercises, listen to music, or take a warm bath. If you are having trouble falling asleep, try some warm milk, or read for a while. 8
9 Eat well. You will be able to resist colds and other common sicknesses much better if you eat a balanced diet at regular times. Eating well will save energy. It s not advisable to diet during this stressful time. Watch your caffeine intake to help manage your stress. Delegate. Ask your family members to share in the care of your loved one. You can also ask your friends or neighbors to take over to allow for a few hours by yourself. If you or your loved one attend church, ask if there are members willing to help with things like meals, shopping, cleaning or respite. Take people up on their offers of help. Request a Hospice Austin volunteer. Volunteers can provide a calm, listening presence for every member of the family and can provide respite for up to four hours a week. Talk to someone. Find a person to confide in or talk to the Hospice Austin social worker, nurse, spiritual care advisor or volunteer. They are experts in communication. Take time for yourself. Schedule time off to do things that you enjoy. If you are taking a leave of absence from work, arrange to have lunch with a friend or coworker. Sometimes asking people to come over can help and they can bring something such as food, as well. Remember that taking time out for yourself is not selfish, and don't be afraid to find humor in everyday life. Laughing has healing powers. Ask your nurse or social worker if you need additional support from a nurse, nurse aide, or volunteer. You do not have to do this alone
Caregiver Guide. HOSPICE of Orange & Sullivan Counties, Inc. In your home or in ours it s about how you live.
 Caregiver Guide HOSPICE of Orange & Sullivan Counties, Inc. In your home or in ours it s about how you live. 1 INDEX An Instructional Guide for Caregivers 3 Activities of Daily Care 4 Pain Management.
Caregiver Guide HOSPICE of Orange & Sullivan Counties, Inc. In your home or in ours it s about how you live. 1 INDEX An Instructional Guide for Caregivers 3 Activities of Daily Care 4 Pain Management.
Approaching the End of Life. A Guide for Family & Friends
 Approaching the End of Life A Guide for Family & Friends Approaching the End of Life A Guide for Family & Friends Patrice Villars, MS, GNP and Eric Widera, MD Introduction In this booklet you will find
Approaching the End of Life A Guide for Family & Friends Approaching the End of Life A Guide for Family & Friends Patrice Villars, MS, GNP and Eric Widera, MD Introduction In this booklet you will find
Please Do Not Call 911
 The Last Hours of Life - What to Expect Names and Phone Numbers You May Need Name Phone Family Dr. Palliative Dr. After Hours Access Centre Visiting Nurse Hospice Clergy Funeral Contact Please Do Not Call
The Last Hours of Life - What to Expect Names and Phone Numbers You May Need Name Phone Family Dr. Palliative Dr. After Hours Access Centre Visiting Nurse Hospice Clergy Funeral Contact Please Do Not Call
You will be having surgery to remove a tumour(s) from your liver.
 Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Liver surgery You will be having surgery to remove a tumour(s) from your liver. This handout will help you learn about the surgery, how to prepare for surgery and your care after surgery. Surgery can be
Controlling Your Pain Without Medicine
 Controlling Your Pain Without Medicine The following information is based on the general experiences of many prostate cancer patients. Your experience may be different. If you have any questions about
Controlling Your Pain Without Medicine The following information is based on the general experiences of many prostate cancer patients. Your experience may be different. If you have any questions about
Urinary Indwelling Catheter. The Urinary System
 Patient Education CARE AND TREATMENT Urinary Indwelling Catheter This information will help you care for a urinary indwelling catheter at home. It will answer many of your questions. Please ask your doctor
Patient Education CARE AND TREATMENT Urinary Indwelling Catheter This information will help you care for a urinary indwelling catheter at home. It will answer many of your questions. Please ask your doctor
Living With Chronic Obstructive Pulmonary Disease (COPD) * Managing Your Diet, Fitness, and Moods. *Includes chronic bronchitis, emphysema, or both.
 DISEASE MANAGEMENT Living With Chronic Obstructive Pulmonary Disease (COPD) * Managing Your Diet, Fitness, and Moods *Includes chronic bronchitis, emphysema, or both. Learning to Live Well With COPD To
DISEASE MANAGEMENT Living With Chronic Obstructive Pulmonary Disease (COPD) * Managing Your Diet, Fitness, and Moods *Includes chronic bronchitis, emphysema, or both. Learning to Live Well With COPD To
X-Plain Foley Catheter Male Reference Summary
 X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
Date Problem Goal Interventions Discipline Review 12/30/ Worried and scared since readmission Crying more frequently
 Mrs. M. Care Plan (Post Significant Change) Mrs. Cynthia M is a 90-year-old, Caucasian female, born June 22, 1920 in Germany and immigrated to the United States when she was seven years old. Mrs. M speaks
Mrs. M. Care Plan (Post Significant Change) Mrs. Cynthia M is a 90-year-old, Caucasian female, born June 22, 1920 in Germany and immigrated to the United States when she was seven years old. Mrs. M speaks
Urine Leaks After Prostate Cancer Treatment
 Managing Symptoms After Prostate Cancer Urine Leaks After Prostate Cancer Treatment Urine leaks after surgery or radiation for prostate cancer are common. The medical term for this is incontinence (say:
Managing Symptoms After Prostate Cancer Urine Leaks After Prostate Cancer Treatment Urine leaks after surgery or radiation for prostate cancer are common. The medical term for this is incontinence (say:
FIM ITEM SCORING EXERCISE SHEETS 2015
 FIM EXERCISE - EATING The helper applies the universal cuff on to the patient s hand before she eats. The patient then brings food to her mouth, chews & swallows by herself. The helper scoops all food
FIM EXERCISE - EATING The helper applies the universal cuff on to the patient s hand before she eats. The patient then brings food to her mouth, chews & swallows by herself. The helper scoops all food
Understand nurse aide skills needed to promote skin integrity.
 Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Unit B Resident Care Skills Essential Standard NA5.00 Understand nurse aide s role in providing residents hygiene, grooming, and skin care. Indicator Understand nurse aide skills needed to promote skin
Manage cancer related fatigue:
 Manage cancer related fatigue: For People Affected by Cancer In this pamphlet: What can I do to manage fatigue? What is cancer related fatigue? What causes cancer related fatigue? How can my health care
Manage cancer related fatigue: For People Affected by Cancer In this pamphlet: What can I do to manage fatigue? What is cancer related fatigue? What causes cancer related fatigue? How can my health care
Preparing for Death. The Body Begins to Shut Down. Emotional, Spiritual and Mental Release. Unresolved Issues and Physical Shut Down
 Preparing for Death The patient in the final stages of a terminal illness will exhibit many outward physical signs that may indicate he or she is near death. These signs are normal and do not need to be
Preparing for Death The patient in the final stages of a terminal illness will exhibit many outward physical signs that may indicate he or she is near death. These signs are normal and do not need to be
NURSING ASSISTANT/NURSE AIDE Knowledge Competency Examination PRACTICE TEST. 2 Hours
 - 1 - NURSING ASSISTANT/NURSE AIDE Knowledge Competency Examination PRACTICE TEST 2 Hours Directions: This test contains 50 questions. Each question has four suggested answers, (A), (B), (C), and (D).
- 1 - NURSING ASSISTANT/NURSE AIDE Knowledge Competency Examination PRACTICE TEST 2 Hours Directions: This test contains 50 questions. Each question has four suggested answers, (A), (B), (C), and (D).
Pressure Ulcers. Occupational Therapy. This leaflet is for both yourself and Carers
 Pressure Ulcers Occupational Therapy This leaflet is for both yourself and Carers Contents What is a pressure ulcer? 3 Who is at risk of developing a pressure ulcer? 4 How can I avoid developing a pressure
Pressure Ulcers Occupational Therapy This leaflet is for both yourself and Carers Contents What is a pressure ulcer? 3 Who is at risk of developing a pressure ulcer? 4 How can I avoid developing a pressure
Living With Chronic Obstructive Pulmonary Disease (COPD) * Managing Your Diet, Fitness, and Moods. *Includes chronic bronchitis, emphysema, or both.
 DISEASE MANAGEMENT Living With Chronic Obstructive Pulmonary Disease (COPD) * Managing Your Diet, Fitness, and Moods *Includes chronic bronchitis, emphysema, or both. Learning to Live Well With COPD To
DISEASE MANAGEMENT Living With Chronic Obstructive Pulmonary Disease (COPD) * Managing Your Diet, Fitness, and Moods *Includes chronic bronchitis, emphysema, or both. Learning to Live Well With COPD To
LIVING WITH CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD)*: MANAGING YOUR DIET, FITNESS, AND MOODS
 LIVING WITH CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD)*: MANAGING YOUR DIET, FITNESS, AND MOODS Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises
LIVING WITH CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD)*: MANAGING YOUR DIET, FITNESS, AND MOODS Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises
Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased.
 Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased. This graph shows the percent of residents whose need for help doing basic daily tasks
Quality Measures for Long-stay Residents Percent of residents whose need for help with daily activities has increased. This graph shows the percent of residents whose need for help doing basic daily tasks
Heat Illnesses. Common Heat Rash Sites
 Heat Illnesses Introduction Heat illnesses happen when the body becomes too hot and cannot cool itself. There are several different types of heat-related illnesses. This includes heat cramps, heat exhaustion,
Heat Illnesses Introduction Heat illnesses happen when the body becomes too hot and cannot cool itself. There are several different types of heat-related illnesses. This includes heat cramps, heat exhaustion,
Geriatric Medicine. Advice on. Constipation and Laxatives
 Geriatric Medicine Advice on Constipation and Laxatives 1 Constipation Constipation is defined as having bowel movements less than three times a week. Stools are usually hard, dry, small in size and difficult
Geriatric Medicine Advice on Constipation and Laxatives 1 Constipation Constipation is defined as having bowel movements less than three times a week. Stools are usually hard, dry, small in size and difficult
FOLFOX Chemotherapy. This handout provides information about FOLFOX chemotherapy. It is sometimes called as FLOX chemotherapy.
 FOLFOX Chemotherapy This handout provides information about FOLFOX chemotherapy. It is sometimes called as FLOX chemotherapy. What is chemotherapy? Chemotherapy is a method of treating cancer by using
FOLFOX Chemotherapy This handout provides information about FOLFOX chemotherapy. It is sometimes called as FLOX chemotherapy. What is chemotherapy? Chemotherapy is a method of treating cancer by using
A Guide to Help You Manage Your Catheter and Drainage Bags
 A Guide to Help You Manage Your Catheter and Drainage Bags A catheter can make a difference to your health and quality of life. We understand that it can be a big adjustment for you. This information will
A Guide to Help You Manage Your Catheter and Drainage Bags A catheter can make a difference to your health and quality of life. We understand that it can be a big adjustment for you. This information will
INTRODUCTION TO POSITIONING. MODULE 3: Positioning and Carrying
 MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
How To Care For A Sick Person
 39 How to Take Care of a Sick Person Sickness weakens the body. To gain strength and get well quickly, special care is needed. Medicines are often not necessary. But good care is always important. The
39 How to Take Care of a Sick Person Sickness weakens the body. To gain strength and get well quickly, special care is needed. Medicines are often not necessary. But good care is always important. The
Faecal Incontinence Patient advice and information leaflet on the management of faecal incontinence
 Oxford University Hospitals NHS Trust Oxford Pelvic Floor Service Faecal Incontinence Patient advice and information leaflet on the management of faecal incontinence What is faecal incontinence? Faecal
Oxford University Hospitals NHS Trust Oxford Pelvic Floor Service Faecal Incontinence Patient advice and information leaflet on the management of faecal incontinence What is faecal incontinence? Faecal
PAIN MANAGEMENT During Your Hospital Stay
 PAIN MANAGEMENT During Your Hospital Stay TABLE OF CONTENTS Understanding Pain...2 Pain Assessment...2 Describing Your Pain...5 Pain Treatment...5 Comfort Measures...6 Medication...7 Specialty Procedures...8
PAIN MANAGEMENT During Your Hospital Stay TABLE OF CONTENTS Understanding Pain...2 Pain Assessment...2 Describing Your Pain...5 Pain Treatment...5 Comfort Measures...6 Medication...7 Specialty Procedures...8
The Last Hours of Living
 The Last Hours of Living Ian Anderson Continuing Education Program in End-of of-life Care The Last Hours of Living! Over 90% of us will die after long illness! Last hours can be some of most significant
The Last Hours of Living Ian Anderson Continuing Education Program in End-of of-life Care The Last Hours of Living! Over 90% of us will die after long illness! Last hours can be some of most significant
Better Breathing with COPD
 Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
MANAGING BREATHLESSNESS
 12 Leaflet issued by: Pulmonary Rehabilitation Service Anglian Community Enterprise (CIC) Kennedy House Kennedy Way, Clacton-on-sea Essex CO15 4AB Tel: 01255 206263 MANAGING BREATHLESSNESS On request,
12 Leaflet issued by: Pulmonary Rehabilitation Service Anglian Community Enterprise (CIC) Kennedy House Kennedy Way, Clacton-on-sea Essex CO15 4AB Tel: 01255 206263 MANAGING BREATHLESSNESS On request,
Your Recovery After a Cesarean Delivery
 Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Controlling Pain Part 2: Types of Pain Medicines for Your Prostate Cancer
 Controlling Pain Part 2: Types of Pain Medicines for Your Prostate Cancer The following information is based on the general experiences of many prostate cancer patients. Your experience may be different.
Controlling Pain Part 2: Types of Pain Medicines for Your Prostate Cancer The following information is based on the general experiences of many prostate cancer patients. Your experience may be different.
Functional rehab after breast reconstruction surgery
 Functional rehab after breast reconstruction surgery UHN A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read
Functional rehab after breast reconstruction surgery UHN A guide for women who had DIEP, latissimus dorsi with a tissue expander or implant, or two-stage implant based breast reconstruction surgery Read
Endovascular Abdominal Aortic Aneurysm Repair Surgery
 Endovascular Abdominal Aortic Aneurysm Repair Surgery You are scheduled for an admission to Cooper University Hospital for Endovascular Abdominal Aortic Aneurysm surgery (EVAR). Please read this handout,
Endovascular Abdominal Aortic Aneurysm Repair Surgery You are scheduled for an admission to Cooper University Hospital for Endovascular Abdominal Aortic Aneurysm surgery (EVAR). Please read this handout,
Preventing pressure ulcers
 Golden Jubilee National Hospital NHS National Waiting Times Centre Preventing pressure ulcers Patient information guide for adults at risk of pressure ulcers Agamemnon Street Clydebank, G81 4DY (: 0141
Golden Jubilee National Hospital NHS National Waiting Times Centre Preventing pressure ulcers Patient information guide for adults at risk of pressure ulcers Agamemnon Street Clydebank, G81 4DY (: 0141
Care of a Foley Catheter
 Care of a Foley Catheter A Foley catheter is a tube that is put into the bladder to drain urine out of the body. A Foley catheter can stay in the bladder for hours or weeks. Having the catheter put in
Care of a Foley Catheter A Foley catheter is a tube that is put into the bladder to drain urine out of the body. A Foley catheter can stay in the bladder for hours or weeks. Having the catheter put in
Recovery After Stroke: Bladder & Bowel Function
 Recovery After Stroke: Bladder & Bowel Function Problems with bladder and bowel function are common but distressing for stroke survivors. Going to the bathroom after suffering a stroke may be complicated
Recovery After Stroke: Bladder & Bowel Function Problems with bladder and bowel function are common but distressing for stroke survivors. Going to the bathroom after suffering a stroke may be complicated
Falling Asleep & Staying Asleep Handout
 Falling Asleep & Staying Asleep Handout This handout contains information that may help if you have difficulty falling asleep or staying asleep. In the pages that follow, you will learn about sleep disorders
Falling Asleep & Staying Asleep Handout This handout contains information that may help if you have difficulty falling asleep or staying asleep. In the pages that follow, you will learn about sleep disorders
Gallbladder Surgery with an Incision (Cholecystectomy)
 Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY
 PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
HOSPICE ORIENTATION FOR SKILLED NURSING FACILITIES
 HOSPICE ORIENTATION FOR SKILLED NURSING FACILITIES (2008 Medicare Conditions of Participation for Hospice Care 418.122 (f)) Hospice Philosophy Hospice is a unique concept of care designed to provide comfort
HOSPICE ORIENTATION FOR SKILLED NURSING FACILITIES (2008 Medicare Conditions of Participation for Hospice Care 418.122 (f)) Hospice Philosophy Hospice is a unique concept of care designed to provide comfort
Colon Cancer Surgery and Recovery. A Guide for Patients and Families
 Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
Colon Cancer Surgery and Recovery A Guide for Patients and Families This Booklet You are receiving this booklet because you will be having surgery shortly. This booklet tells you what to do before, during,
What to expect when someone important to you is dying. A guide for carers, families and friends of dying people
 What to expect when someone important to you is dying A guide for carers, families and friends of dying people About this booklet If you are caring for someone who is in the last stages of life, or who
What to expect when someone important to you is dying A guide for carers, families and friends of dying people About this booklet If you are caring for someone who is in the last stages of life, or who
Radiation Therapy To the Arms or Legs
 Radiation Therapy To the Arms or Legs You will be receiving two to six weeks of radiation to the arms or legs. It will describe how your treatments are given. It will also describe how to take care of
Radiation Therapy To the Arms or Legs You will be receiving two to six weeks of radiation to the arms or legs. It will describe how your treatments are given. It will also describe how to take care of
Progression END OF LIFE. What is Alzheimer s disease? End of life what to expect
 Progression END OF LIFE This document is one in a five-part series on the stages of Alzheimer s disease and is written for the person with the disease, their family and caregivers. The end of life stage
Progression END OF LIFE This document is one in a five-part series on the stages of Alzheimer s disease and is written for the person with the disease, their family and caregivers. The end of life stage
Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions
 Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions No lifting greater than 10 15 lbs for the first three weeks following your surgery. Walking around the house, office
Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions No lifting greater than 10 15 lbs for the first three weeks following your surgery. Walking around the house, office
However, if your child is learning how to use the toilet without problems, there is no need to stop because of these situations.
 Toilet Training Readiness When do I start? Bowel and bladder control is a necessary skill. Teaching your child to use the toilet takes time, understanding, and patience. The important thing to remember
Toilet Training Readiness When do I start? Bowel and bladder control is a necessary skill. Teaching your child to use the toilet takes time, understanding, and patience. The important thing to remember
Home Care Of The Hospice Patient. An Information/Instructional Booklet for Caregivers in the Home
 Home Care Of The Hospice Patient An Information/Instructional Booklet for Caregivers in the Home Provided by Purdue Pharma L.P. Sponsors of Partners Against Pain partnersagainstpain.com In our society,
Home Care Of The Hospice Patient An Information/Instructional Booklet for Caregivers in the Home Provided by Purdue Pharma L.P. Sponsors of Partners Against Pain partnersagainstpain.com In our society,
Opioid Analgesic Medication Information
 Opioid Analgesic Medication Information This handout provides information about treating pain with opioid analgesics or narcotics. Please read this entire handout. We want to be sure that you understand
Opioid Analgesic Medication Information This handout provides information about treating pain with opioid analgesics or narcotics. Please read this entire handout. We want to be sure that you understand
Knowledge Brochure Series MS & SYMPTOM MANAGEMENT
 Knowledge Brochure Series MS & SYMPTOM MANAGEMENT Identifying your multiple sclerosis (MS) symptoms 1 A chronic disease like MS can cause a number of different symptoms and spotting yours is the first
Knowledge Brochure Series MS & SYMPTOM MANAGEMENT Identifying your multiple sclerosis (MS) symptoms 1 A chronic disease like MS can cause a number of different symptoms and spotting yours is the first
Chapter. Some days I m so stiff. But even then, your firm yet gentle guidance always helps me move more easily. MOVING AND POSITIONING
 15 MOVING AND POSITIONING Chapter Helping a resident move and be comfortably positioned is one of the most important things you do as a nurse assistant. Remember that CMS Guidelines say that all long term
15 MOVING AND POSITIONING Chapter Helping a resident move and be comfortably positioned is one of the most important things you do as a nurse assistant. Remember that CMS Guidelines say that all long term
Living With Congestive Heart Failure
 Living With Congestive Heart Failure Information for patients and their families Patient information developed by EPICORE Centre, Division of Cardiology, University of Alberta The REACT study: supported
Living With Congestive Heart Failure Information for patients and their families Patient information developed by EPICORE Centre, Division of Cardiology, University of Alberta The REACT study: supported
There is no cure for COPD Chronic Bronchitis Emphysema
 Live Well With COPD Chronic Obstructive Pulmonary Disease, or COPD is a lung disease. People with COPD have a hard time getting air in and out of their lungs. There is no cure for COPD. COPD is also commonly
Live Well With COPD Chronic Obstructive Pulmonary Disease, or COPD is a lung disease. People with COPD have a hard time getting air in and out of their lungs. There is no cure for COPD. COPD is also commonly
Intermittent Self-Catheterization. A Step by Step Guide for Men and Women
 Inside this book Intermittent Self-Catheterization A Step by Step Guide for Men and Women 1986 2005 St. Joseph s Healthcare Hamilton Hamilton, Ontario Contributors: Jennifer Skelly Paula Eyles Linda Hilts
Inside this book Intermittent Self-Catheterization A Step by Step Guide for Men and Women 1986 2005 St. Joseph s Healthcare Hamilton Hamilton, Ontario Contributors: Jennifer Skelly Paula Eyles Linda Hilts
Clinical Skills Test Checklist
 Clinical Skills Test Checklist During training, you learn many skills that are important in caring for residents. There are 22 skills that are part of the Clinical Skills Test and ONLY in Nevada are there
Clinical Skills Test Checklist During training, you learn many skills that are important in caring for residents. There are 22 skills that are part of the Clinical Skills Test and ONLY in Nevada are there
Controlling symptoms of mesothelioma
 Controlling symptoms of mesothelioma This information is an extract from the booklet Understanding mesothelioma. You may find the full booklet helpful. We can send you a free copy see page 9. Contents
Controlling symptoms of mesothelioma This information is an extract from the booklet Understanding mesothelioma. You may find the full booklet helpful. We can send you a free copy see page 9. Contents
HOW WOULD I KNOW? WHAT CAN I DO?
 HOW WOULD I KNOW? WHAT CAN I DO? How to help someone with dementia who is in pain or distress Help! 1 Unusual behaviour may be a sign of pain or distress If you are giving care or support to somebody with
HOW WOULD I KNOW? WHAT CAN I DO? How to help someone with dementia who is in pain or distress Help! 1 Unusual behaviour may be a sign of pain or distress If you are giving care or support to somebody with
Excision of Vaginal Mesh
 What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
What is excision of vaginal mesh? This procedure is done to remove mesh from the vagina. When is this surgery used? If mesh has eroded into the vagina, bladder, urethra, or bowel If there is pain associated
Pain Management for Labour & Delivery
 Pain Management for Labour & Delivery Departments of Anesthesia, Obstetrics, and Obstetrical Nursing December 2008 This pamphlet has been prepared to provide you, members of your family, and others who
Pain Management for Labour & Delivery Departments of Anesthesia, Obstetrics, and Obstetrical Nursing December 2008 This pamphlet has been prepared to provide you, members of your family, and others who
Anxiety and breathing difficulties
 Patient information factsheet Anxiety and breathing difficulties Breathing is something that we all automatically do and we often take this for granted. Some chronic health conditions, for example asthma
Patient information factsheet Anxiety and breathing difficulties Breathing is something that we all automatically do and we often take this for granted. Some chronic health conditions, for example asthma
CHOP Chemotherapy Regimen for Lymphoma Information for Patients
 CHOP Chemotherapy Regimen for Lymphoma Information for Patients The Regimen Contains: C: Cytoxan (cyclophosphamide) H: Adriamycin (hydroxy doxorubicin) O: vincristine (Oncovin ) P: Prednisone How Is This
CHOP Chemotherapy Regimen for Lymphoma Information for Patients The Regimen Contains: C: Cytoxan (cyclophosphamide) H: Adriamycin (hydroxy doxorubicin) O: vincristine (Oncovin ) P: Prednisone How Is This
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY
 CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
CORONARY ARTERY BYPASS GRAFT & HEART VALVE SURGERY www.cpmc.org/learning i learning about your health What to Expect During Your Hospital Stay 1 Our Team: Our cardiac surgery specialty team includes nurses,
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Range of Motion. A guide for you after spinal cord injury. Spinal Cord Injury Rehabilitation Program
 Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Activities for the Young Baby
 31 Chapter 5 Activities for the Young Baby (Birth to 6 Months) A new baby does not usually look as though she is doing very much. She spends most of her time eating, sleeping, and resting. But even though
31 Chapter 5 Activities for the Young Baby (Birth to 6 Months) A new baby does not usually look as though she is doing very much. She spends most of her time eating, sleeping, and resting. But even though
Pelvic Girdle Pain (PGP) Fact Sheet
 Pelvic Girdle Pain (PGP) Fact Sheet Physiotherapy PGP describes pain that is experienced in the front (symphysis pubis joint) and/or back (sacroiliac joints) of your pelvis. This is a common problem, affecting
Pelvic Girdle Pain (PGP) Fact Sheet Physiotherapy PGP describes pain that is experienced in the front (symphysis pubis joint) and/or back (sacroiliac joints) of your pelvis. This is a common problem, affecting
Clinical Skills Test Checklist
 Clinical Skills Test Checklist During training, you learn many skills that are important in caring for residents. There are 22 skills that are part of the Clinical Skills Test. When you are registered
Clinical Skills Test Checklist During training, you learn many skills that are important in caring for residents. There are 22 skills that are part of the Clinical Skills Test. When you are registered
Medications to help you quit smoking
 Medications to help you quit smoking How can medication help me quit smoking? Using medications can increase your chances of quitting smoking 2 to 3 times more than quitting without using medications.
Medications to help you quit smoking How can medication help me quit smoking? Using medications can increase your chances of quitting smoking 2 to 3 times more than quitting without using medications.
Assisting Patients who are Short of Breath
 TIPS for Assisting Patients who are Short of Breath Shortness of breath or shortness of air is called dyspnea. This is a common symptom in patients with advanced disease. Dyspnea is similar to pain in
TIPS for Assisting Patients who are Short of Breath Shortness of breath or shortness of air is called dyspnea. This is a common symptom in patients with advanced disease. Dyspnea is similar to pain in
Tube Feeding at Home Gravity or Syringe Feeding
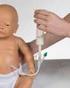 Tube Feeding at Home Gravity or Syringe Feeding Adapted from the former Taming the Feeding Tube, North Shore Hospital. 1 Where do I find information in this booklet? Subject Page How do I contact my health
Tube Feeding at Home Gravity or Syringe Feeding Adapted from the former Taming the Feeding Tube, North Shore Hospital. 1 Where do I find information in this booklet? Subject Page How do I contact my health
Potty Training. When are children ready to potty train?
 Potty Training It can be messy! There will be accidents! Potty training is an important milestone for your child, but learning to gain control of the bowel and bladder can be a complicated process and
Potty Training It can be messy! There will be accidents! Potty training is an important milestone for your child, but learning to gain control of the bowel and bladder can be a complicated process and
Incontinence. in con ti nent. adjective. 1. unable to restrain natural discharges or evacuations of urine or faeces.
 PBO 930022142 NPO 049-191 Incontinence Incontinence can be upsetting and humiliating for the person with dementia as well as stressful for the carer. However, there are many ways in which the situation
PBO 930022142 NPO 049-191 Incontinence Incontinence can be upsetting and humiliating for the person with dementia as well as stressful for the carer. However, there are many ways in which the situation
Radiation Therapy for Breast Cancer
 Radiation Therapy for Breast Cancer www.cpmc.org/learning i learning about your health What Is? Radiation therapy is a treatment for cancer that uses high-energy x-rays to destroy cancer cells. (Radiation
Radiation Therapy for Breast Cancer www.cpmc.org/learning i learning about your health What Is? Radiation therapy is a treatment for cancer that uses high-energy x-rays to destroy cancer cells. (Radiation
Brain Injury: Stages of Recovery
 Brain Injury: Stages of Recovery Recovery after brain injury is a process that occurs in stages. Some people move quickly through the stages, while others make slow, but steady gains. The Rancho Los Amigos'
Brain Injury: Stages of Recovery Recovery after brain injury is a process that occurs in stages. Some people move quickly through the stages, while others make slow, but steady gains. The Rancho Los Amigos'
Caring for the Client with Heart Failure
 Peak Development Resources, LLC P.O. Box 13267 Richmond, VA 23225 Phone: (804) 233-3707 Fax: (804) 233-3705 After reading the newsletter, the home health aide should be able to: 1. Define heart failure.
Peak Development Resources, LLC P.O. Box 13267 Richmond, VA 23225 Phone: (804) 233-3707 Fax: (804) 233-3705 After reading the newsletter, the home health aide should be able to: 1. Define heart failure.
In-Patient Radioactive Iodine ( 131 I) Treatment
 In-Patient Radioactive Iodine ( 131 I) Treatment Information for patients and families Princess Margaret Read this booklet to learn: what radioactive iodine treatment is what to expect instructions to
In-Patient Radioactive Iodine ( 131 I) Treatment Information for patients and families Princess Margaret Read this booklet to learn: what radioactive iodine treatment is what to expect instructions to
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
online version Understanding Indwelling Urinary Catheters and Drainage Systems Useful information When to call for help
 When to call for help This will depend on the individual situation, but usually help should be sought if any of the following occurs: 1. The catheter does not start to drain, despite trying the problem
When to call for help This will depend on the individual situation, but usually help should be sought if any of the following occurs: 1. The catheter does not start to drain, despite trying the problem
For the Patient: GDP Other names: LYGDP
 1 For the Patient: GDP Other names: LYGDP G D P Gemcitabine Dexamethasone (taken by mouth) CISPlatin Uses: GDP is a drug treatment given for Non-Hodgkins and Hodgkin Lymphoma with the expectation of destroying
1 For the Patient: GDP Other names: LYGDP G D P Gemcitabine Dexamethasone (taken by mouth) CISPlatin Uses: GDP is a drug treatment given for Non-Hodgkins and Hodgkin Lymphoma with the expectation of destroying
Information for patients receiving short-term hormone treatment and radiotherapy for prostate cancer
 Information for patients receiving short-term hormone treatment and radiotherapy for prostate cancer Northern Centre for Cancer Care (NCCC) Freeman Hospital Introduction This leaflet has been written to
Information for patients receiving short-term hormone treatment and radiotherapy for prostate cancer Northern Centre for Cancer Care (NCCC) Freeman Hospital Introduction This leaflet has been written to
How To Plan For A Hospital Discharge
 Family Caregiver Guide Rehab-to-Home Discharge Guide In Rehab: Planning for Discharge The best time to start planning for discharge is just after your family member is admitted. While it may seem too soon
Family Caregiver Guide Rehab-to-Home Discharge Guide In Rehab: Planning for Discharge The best time to start planning for discharge is just after your family member is admitted. While it may seem too soon
Side Effects of Chemotherapy Treatment
 Side Effects of Chemotherapy Treatment Chemotherapy drugs affect all body cells. They affect cancer cells and also normal cells. That's the reason for some of the side effects. Chemotherapy drugs especially
Side Effects of Chemotherapy Treatment Chemotherapy drugs affect all body cells. They affect cancer cells and also normal cells. That's the reason for some of the side effects. Chemotherapy drugs especially
Welcome to your LOW BACK PAIN treatment guide
 Welcome to your LOW BACK PAIN treatment guide You are receiving this guide because you have recently experienced low back pain. Back pain is one of the most common musculoskeletal problems treated in medicine
Welcome to your LOW BACK PAIN treatment guide You are receiving this guide because you have recently experienced low back pain. Back pain is one of the most common musculoskeletal problems treated in medicine
HEAT ILLNESS PREVENTION PLAN FOR SUTTER COUNTY SUPERINTENDENT OF SCHOOLS
 HEAT ILLNESS PREVENTION PLAN FOR SUTTER COUNTY SUPERINTENDENT OF SCHOOLS TABLE OF CONTENTS 1.0 Purpose... 1 2.0 Heat Illness Prevention... 2 2.1 Heat Stroke... 2 2.2 Heat Exhaustion... 2 2.3 Heat Cramps...
HEAT ILLNESS PREVENTION PLAN FOR SUTTER COUNTY SUPERINTENDENT OF SCHOOLS TABLE OF CONTENTS 1.0 Purpose... 1 2.0 Heat Illness Prevention... 2 2.1 Heat Stroke... 2 2.2 Heat Exhaustion... 2 2.3 Heat Cramps...
Depression: What You Need to Know
 Depression: What You Need to Know What is a Depressive Illness? A depressive illness is a whole-body illness, involving your body, mood, thoughts, and behavior. It affects the way you eat and sleep, the
Depression: What You Need to Know What is a Depressive Illness? A depressive illness is a whole-body illness, involving your body, mood, thoughts, and behavior. It affects the way you eat and sleep, the
STROKE CARE PLAN: BLADDER & BOWEL CONTINENCE
 Urinary incontinence related to loss of ability to identify and respond to need to urinate; involuntary bladder contractions, increased nightly urine production, difficulty communication need to urinate
Urinary incontinence related to loss of ability to identify and respond to need to urinate; involuntary bladder contractions, increased nightly urine production, difficulty communication need to urinate
A GUIDE TO SPICA CAST CARE
 A GUIDE TO SPICA CAST CARE KAPI'OLANI ORTHOPAEDIC ASSOCIATES Pediatric Orthopaedics Spine Deformity Sports & Dance Medicine Young Adult Hip Preservation 1319 Punahou Street Suite #630 Honolulu, Hawaii
A GUIDE TO SPICA CAST CARE KAPI'OLANI ORTHOPAEDIC ASSOCIATES Pediatric Orthopaedics Spine Deformity Sports & Dance Medicine Young Adult Hip Preservation 1319 Punahou Street Suite #630 Honolulu, Hawaii
CARING FOR YOUR URINARY CATHETER GRAMPIANS REGIONAL CONTINENCE SERVICE. Author: GRCS Date: 20/06/09 Catalogue No: 712438
 CARING FOR YOUR URINARY CATHETER GRAMPIANS REGIONAL CONTINENCE SERVICE Author: GRCS Date: 20/06/09 Catalogue No: 712438 What is a urinary catheter? A urinary catheter is a hollow tube which drains urine
CARING FOR YOUR URINARY CATHETER GRAMPIANS REGIONAL CONTINENCE SERVICE Author: GRCS Date: 20/06/09 Catalogue No: 712438 What is a urinary catheter? A urinary catheter is a hollow tube which drains urine
Total Abdominal Hysterectomy
 What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
What is a total abdominal hysterectomy? Is the removal of the uterus and cervix through an abdominal incision (either an up and down or bikini cut). Removal of the ovaries and tubes depends on the patient.
Promoting recovery after sustaining a third and fourth degree tear
 Promoting recovery after sustaining a third and fourth degree tear Women s Health Physiotherapy Patient Information Page 2 Promoting recovery after sustaining a third and fourth degree tears What has happened?
Promoting recovery after sustaining a third and fourth degree tear Women s Health Physiotherapy Patient Information Page 2 Promoting recovery after sustaining a third and fourth degree tears What has happened?
BLADDER CONTROL DURING PREGNANCY AND AFTER THE BIRTH OF YOUR BABY
 BLADDER CONTROL DURING PREGNANCY AND AFTER THE BIRTH OF YOUR BABY Information Leaflet Your Health. Our Priority. Page 2 of 8 Contents Stress incontinence... 3 Pelvic floor exercises... 3 Urgency and frequency...
BLADDER CONTROL DURING PREGNANCY AND AFTER THE BIRTH OF YOUR BABY Information Leaflet Your Health. Our Priority. Page 2 of 8 Contents Stress incontinence... 3 Pelvic floor exercises... 3 Urgency and frequency...
The following document includes information about:
 Patient information WHAT TO EXPECT WHILE RECEIVING RADIATION THERAPY FOR PROSTATE CANCER Oncology Vitalité Zone : 1B 4 5 6 Facility : Dr. Léon-Richard Oncology Centre The following document includes information
Patient information WHAT TO EXPECT WHILE RECEIVING RADIATION THERAPY FOR PROSTATE CANCER Oncology Vitalité Zone : 1B 4 5 6 Facility : Dr. Léon-Richard Oncology Centre The following document includes information
Long Term Tube Feeding. Sunnybrook. A Guide for Patients and Substitute Decision Makers VETERANS & COMMUNITY
 Long Term Tube Feeding A Guide for Patients and Substitute Decision Makers Sunnybrook VETERANS & COMMUNITY Sunnybrook VETERANS & COMMUNITY This brochure has been produced by: Sunnybrook Health Sciences
Long Term Tube Feeding A Guide for Patients and Substitute Decision Makers Sunnybrook VETERANS & COMMUNITY Sunnybrook VETERANS & COMMUNITY This brochure has been produced by: Sunnybrook Health Sciences
Coping with Multiple Sclerosis Strategies for you and your family
 Patient Education Coping with Multiple Sclerosis Strategies for you and your family Most people are not prepared to deal with the changes in routine and lifestyle that MS may require. Coping with MS can
Patient Education Coping with Multiple Sclerosis Strategies for you and your family Most people are not prepared to deal with the changes in routine and lifestyle that MS may require. Coping with MS can
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
Managing Acute Side Effects of Pelvic Radiation for Gynaecological Cancers
 RADIATION THERAPY SYMPTOM MANAGEMENT Managing Acute Side Effects of Pelvic Radiation for Gynaecological Cancers In this booklet you will learn about: Common side effects when you receive radiation therapy
RADIATION THERAPY SYMPTOM MANAGEMENT Managing Acute Side Effects of Pelvic Radiation for Gynaecological Cancers In this booklet you will learn about: Common side effects when you receive radiation therapy
Potty/toilet training
 Behaviour Potty/toilet training Information for parents of disabled children in England, Northern Ireland, Scotland and Wales Contents Introduction 3 What do we mean by toilet training 4 When should you
Behaviour Potty/toilet training Information for parents of disabled children in England, Northern Ireland, Scotland and Wales Contents Introduction 3 What do we mean by toilet training 4 When should you
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Kids Have Stress Too! Especially at Back to School Time As a Parent, You Can Help!
 1 Kids Have Stress Too! Especially at Back to School Time As a Parent, You Can Help! Stress can infect and affect the physical, emotional, intellectual and academic well being of children. It can interfere
1 Kids Have Stress Too! Especially at Back to School Time As a Parent, You Can Help! Stress can infect and affect the physical, emotional, intellectual and academic well being of children. It can interfere
What Is. Norovirus? Learning how to control the spread of norovirus. Web Sites
 Web Sites Centers for Disease Control and Prevention (CDC) http://www.cdc.gov/norovirus/index.html Your Local Health Department http://www.azdhs.gov/diro/lhliaison/countymap.htm What Is Ocument dn Norovirus?
Web Sites Centers for Disease Control and Prevention (CDC) http://www.cdc.gov/norovirus/index.html Your Local Health Department http://www.azdhs.gov/diro/lhliaison/countymap.htm What Is Ocument dn Norovirus?
