MONITORING THE ANESTHETIZED PATIENT
|
|
|
- Jocelin Willis
- 8 years ago
- Views:
Transcription
1 MONITORING THE ANESTHETIZED PATIENT The administration and monitoring of anesthesia for surgical procedures is a complex and multifaceted skill that requires both knowledge and practice. The safety of your patient is dependent on your awareness and response to potential problems. A thorough understanding of the principles of anesthetic monitoring and awareness of normal and abnormal patient parameters is crucial to providing safe anesthesia. The most important thing to remember is to ASK QUESTIONS-anytime you have a question or concern about a patient's status. Don t ever hesitate to ask for help. It is the anesthetist's sole responsibility to monitor the safety of his/her patient at all times. An anesthetized animal should NEVER be left unattended for any reason. Monitoring of the anesthetized patient is a continual process throughout the anesthetic event from pre-medication to full recovery. Vital signs and other monitoring parameters are recorded to the surgery record every 5 minutes throughout the procedure, but patient monitoring should be continuous. The anesthetist should be aware of subtle changes in parameters and prepared to address any issues immediately as they arise. Remember when assessing the anesthetized patient that, while absolute numbers are obviously important, subtle change and trends are often an early indicator that the patient is beginning to decompensate. Do not wait until a patient's monitoring parameters are in the critical range to act or to ask for assistance. These training materials are intended as a basic review of these important topics. For more information please refer to one of the numerous texts available. As you review these materials, keep in mind that anesthesia and surgery are clinical skills, not just academic pursuits. You are going to be DOING these things, not just passing an exam. If you have questions about any of this information you are welcome to contact us prior to your trip. PARAMETERS TO BE ASSESSED CONTINOUSLY THROUGHOUT ANESTHETIC PERIOD (RECORDED EVERY 5 MINUTES): Respiratory Airway Respiratory rate, depth and character Oxygen saturation (SpO 2 ) Cardiovascular Heart rate and rhythm Pulse rate and strength Mucous membrane color and capillary refill time Arterial blood pressure Body Temperature Anesthetic depth/patient status Reflexes and muscle tone Eye position and pupillary reflex activity Heart and respiratory rates Status of surgical procedure Equipment function Anesthetic level, Vaporizer and oxygen flowmeter settings Pressure relief (pop-off) valve 1
2 Respiratory ASSESSING MONITORING PARAMETERS Airway Check regularly that the endotracheal tube has not kinked, slipped out or been placed too deeply. Listen for accumulation of moisture in the endotracheal tube. In recovery, animals should be placed with the neck extended so the ET tube is not bent or kinked. Recovering animals should be placed facing forward in their cages with the tongue protruding to allow easy visualization of the animal's mucous membrane color. Respiratory rate (RR), depth and character Normal RR: breaths/minute (rates up to 40 may be seen occasionally) Normal inspiration lasts seconds and expiration lasts 2-3 seconds Basic respiratory monitoring is based on clinical observations. The rate and depth can be assessed by observing movement of the chest or reservoir bag. Chest excursions should be assessed with both spontaneous respiration and assisted ventilation. Respiratory rate and character can be evaluated via esophageal stethoscope. The degree of compliance felt when manually ventilating the animal can provide important information about potential respiratory or mechanical dysfunction. With increasing depth of anesthesia there is a decrease in both the rate and tidal volume (volume of air taken in with each breath). When the animal hypoventilates, some alveoli may not adequately inflate. These alveoli partially collapse, leading to atelectasis. Periodic 'bagging' (every 5 minutes) throughout the procedure can prevent this. To bag a patient, partially close pop-off valve and gently squeeze the reservoir bag just enough to cause a slight rise in the chest. Be sure to re-open the pop-off valve to avoid the buildup of pressure in the anesthetic circuit. An abnormally low respiratory rate (<8-10 bpm) is cause for concern and should be reported to a supervising veterinarian or technician immediately. Apneic animals who are otherwise maintained at an appropriate anesthetic level may need to be manually ventilated throughout the procedure at a rate of 8-12 bpm. The anesthetist may occasionally note an increase in respiratory rate (tachypnea) and depth (hyperventilation). True hyperventilation and tachypnea (as opposed to panting) are the body's response to increased carbon dioxide in the blood or metabolic acidosis. Hyperventilation may indicate that the CO 2 is not being adequately removed from the breathing circuit by the CO 2 absorber. Hyperventilation is also seen as a response to mild surgical stimulus (e.g. when surgeon pulls on suspensory ligament during OVH). An elevated respiratory rate may indicate a progression from moderate to light anesthesia and is often one of the first signs of arousal from anesthesia. Breathing should be smooth and regular, with thoracic and diaphragmatic components. Difficult or labored breathing may indicate the presence of an airway obstruction. Animals anesthetized with ketamine may exhibit an apneustic respiratory pattern, in which inspiration is followed by a prolonged pause before expiration. Normal respiratory sounds are almost inaudible. Harsh noises, whistles or squeaks may indicate narrow or obstructed airways or the presence of fluid in the airways. Oxygen saturation (SpO 2 ) - (see 'Monitoring Equipment' for more information) Normal SpO 2 : % The patient's SpO 2 is the percentage of oxygen-saturated hemoglobin, and indicates how well the lungs are delivering oxygen to the blood. The pulse oximeter measures both SpO 2 and heart rate and is monitored continuously. 2
3 Cardiovascular A pulse ox reading of 90-95% indicates that the patient's hemoglobin is not fully saturated and a respiratory or cardiovascular problem may be present. The patient will not become hypoxic until the reading falls to 90% or less. It is hoped that the anesthetist will be able to correct the problem before this occurs. Without pulse oximetry, early hypoxia can be difficult to assess as cyanosis only becomes apparent if values fall below 85% saturation. As with any monitoring device, the pulse oximeter can sometimes fail or provide an inaccurate reading. Anytime the reading changes significantly, evaluate the clinical status of your patient before assuming that the reading is accurate. However, do not assume that a low reading is a malfunction. Again, EVALUATE YOUR PATIENT before making any decisions. Heart rate (HR) and rhythm Normal HR: Canine: bpm; Feline: bpm Assess via auscultation. Bradycardia may indicate excessive anesthetic depth, a response to vagal stimulation or other causes. Heart rates less than 80 bpm in dogs and 100 bpm in cats should be reported to a supervising veterinarian or technician for evaluation. Tachycardia may be a response to surgical stimulation and, in combination with other factors may indicate an inadequate anesthetic level. However, some response to surgical stimulation is normal. The presence of a beating heart does not necessarily mean that circulation is adequate. Heartbeat should always be assessed in conjunction with pulse strength and quality. Pulse rate and strength/quality The pulse can be detected at several locations, including the lingual, femoral, carotid and dorsal pedal arteries. You should know a least 3 different places to evaluate a pulse. The pulse should be strong and synchronized with the heartbeat. Mucous membrane (MM) color and capillary refill time (CRT) Normal: mm pink, CRT < 2 sec Mucous membrane color is usually most easily assessed at the gingiva. Pale mucous membranes may indicate blood loss or anemia or may result from poor perfusion. Purple or blue mucous membranes indicate cyanosis, a shortage of oxygen in the tissues. Cyanosis during anesthesia is usually the result of respiratory failure or upper airway obstruction and must be addressed immediately. Capillary refill time is the rate of color return to a mucous membrane after the application of gentle pressure and reflects tissue perfusion. Pressure on the mucous membranes compressed the small capillaries and blocks blood flow to that area. When the pressure is released, the capillaries rapidly refill with blood and the color returns, provided the heart is able to generate sufficient blood pressure. However, a short CRT is not an infallible indication that circulation is adequate. A prolonged CRT (> 2 sec) may indicate hypotension resulting from excessive anesthetic depth or circulatory shock. CRT is usually prolonged in patients in whom the systolic blood pressure is less than 80 mm Hg. Animals suffering from this degree of hypotension will usually feel cold and have pale mucous membranes. Other factors that may cause prolonged CRT or poor perfusion include hypothermia, vasodilation and cardiac failure. 3
4 Arterial Blood Pressure (see 'Monitoring Equipment' for more information) Normal BP: 120/80 mm Hg ( mmhg systolic, mmhg diastolic). Normal Mean Arterial Pressure between mmhg Measurement of arterial blood pressure provides information regarding the adequacy of blood flow to the patient's tissue. Arterial blood pressure may be monitored using various methods such as a Doppler ultrasound probe coupled with a pressure cuff and sphygmomanometer or an automated oscillometric device (e.g., Dinamap), which are most commonly used in RAVS clinics. The disadvantage of oscillometric detector is decreased accuracy and efficiency when used on hypotensive or small patients (less than 5 kg body weight). The minimum acceptable BP is 80/40. If the mean arterial blood pressure (MAP) is below 60 mmhg, organ and tissue perfusion is inadequate. The most common cause of hypotension is excessive anesthetic depth. Other causes include hypovolemia due to intra-operative bleeding or pre-operative dehydration, hypothermia or hypoxia. Body Temperature Anesthesia will typically lower the body temperature and can lead to hypothermia, which can result in prolonged recovery from anesthesia as well as other complications. Small puppies and kittens are especially vulnerable. The greatest loss in body heat occurs within the first 20 minutes of anesthesia. Cold surfaces and excessive use of cold scrub solutions should be avoided. During surgery, Snuggle Safe warming disks should be placed under a towel between the patient and surgery table to help the animal conserve body heat. Animals in recovery can be placed on a covered heating pad and covered with a blanket until the body temperature is normalized. Care should always be taken with any supplemental heat source to avoid burns or hyperthermia. Heating pads should ALWAYS be set at the LOW setting. Warming devices and hot water bottles should be wrapped in a towel or other barrier. Body temperature should be monitored frequently and supplemental heat should be discontinued when the patient's temperature is o F. Anesthetic Depth/Patient Status - (For more information see 'Assessing Anesthetic Depth') During the course of anesthesia, the anesthetist should monitor as many parameters as possible and weigh all available evidence before judging the anesthetic depth of the patient. No one piece of information is unfailingly reliable and each animal has a unique individual response to any given anesthetic protocol. Although anesthetic stages and planes may appear easy to differentiate on paper, they are not well defined in every animal. The anesthetist must assess as many parameters as possible to come to a conclusion regarding the patient's depth of anesthesia. The basic rule is that if there is any doubt about the level of anesthesia, one should decrease the vaporizer setting and monitor the animal until the anesthetic depth can be determined. Classic Stages of Anesthesia Stage I - Not anesthetized Stage II - Excitatory phase, not anesthetized Stage III Plane 1 - light anesthesia Plane 2 - moderate anesthesia (surgical plane) Plane 3 - deep anesthesia Stage IV - Overdose Stage V - Death 4
5 Reflexes Normal, conscious animals demonstrate predictable protective reflex responses to certain stimuli. These protective reflexes are progressively depressed at increasing depths of anesthesia. Progressive return of reflexes indicates imminent arousal from anesthesia. Palpebral (blink) - tested by lightly tapping the medial or lateral canthus of the eye and observing whether the animal blinks in response. Generally present throughout stages I and II, diminished in Stage III and lost in Stage IV. Swallowing - Occurs spontaneously in awake animals. Usually stimulated by the presence of saliva or food in the pharynx. Monitored by observing movement in the ventral neck area. The swallowing reflex is lost at a medium depth of anesthesia and usually regained just before the patient recovers consciousness. The return of the swallow reflex during recovery indicates that it is safe to remove the endotracheal tube. Pedal - Elicited by pinching a digit and observing whether animal flexes the leg, withdrawing the paw. With inhalants, the pedal reflex is normally lost during induction. Corneal - Tested by touching the cornea with a sterile object (a drop of water or saline can be used) and noting whether the animal blinks and withdraws the eye into the orbit. This reflex is not commonly tested unless it is necessary to determine if the patient is too deeply anesthetized. Usually present until stage III, plane 4 anesthesia. Laryngeal - Stimulated when the larynx is touched by an object. The response is an immediate closure of the epiglottis and vocal cords. May be observed during intubation if the animal is not sufficiently anesthetized to allow the tube to be passed. Jaw tone - With increasing anesthetic depth, skeletal muscles become more relaxed and offer little resistance to movement. Jaw tone is one of the easiest ways to evaluate muscle tone. Jaw tone is assessed by attempting to open the jaws wide and estimating the amount of passive resistance. During anesthesia, it should be decreased but always present to some extent. Extreme laxity of the jaw suggests excessive anesthetic depth. The degree of muscle relaxation is dependent not only on the depth but also on the particular drugs administered to the animal and the animal s normal muscle tone. Eye position, pupil size and pupillary light response - (See 'Assessing Anesthetic Depth') In combination with other factors, the position of the eyeball and size of pupils may provide information regarding anesthetic depth. However, there is considerable variation among individual animals and anesthetic protocols. Heart and respiratory rates As indicators of anesthetic depth, the patient's heart and respiratory rates are only valuable in combination with assessment of other factors (reflexes, muscle tone, etc). In general, an abnormally low HR or RR may be associated with excessive anesthetic depth. Increased HR or RR may be the result of surgical stimulation or arousal. Response to surgical stimuli Minor changes in heart rate during surgery are considered normal. The absence of such a response may indicate an unnecessarily deep level of anesthesia. Animals perceiving surgical stimulation may show an increase in heart rate. This does not necessarily indicate that the anesthetic depth is inadequate unless the increase in heart rate is considerable and/or other changes in other parameters are noted. Surgical stimulation may also induce a decrease in heart rate due to increased vagal tone. Increased respiratory rate and signs of voluntary movement by the patient, however, do indicate insufficient anesthetic depth and perception of pain. Increased tear production, salivation and sweating (observed on the foot pads) also indicate that the patient maybe perceiving painful stimuli and that the depth is inadequate. 5
6 Status of surgical procedure The anesthetist should maintain communication with the surgical team regarding progress of the procedure and any problems or abnormalities that may occur. Familiarity with the procedure being performed allows the anesthetist to foresee changes in anesthetic requirements and adjust accordingly. Equipment function Regular evaluation of the anesthetic machine should become part of your standard monitoring routine. Equipment problems, either as a result of malfunction or human error are the cause of many common anesthetic complications. It is crucial that you are thoroughly comfortable with the setup and operation of the machine you will be using before you anesthetize a patient. Vaporizer setting and anesthetic level Observation of the vaporizer setting does not in itself indicate the patient's anesthetic depth as there is a tremendous variation in patient response. The concentration of anesthetic gas received by the animal will vary with the oxygen flow rate and quality of ventilation received by the patient. The vaporizer setting should be continually adjusted according to the depth of anesthesia and status of procedure. In general, a relatively high anesthetic dose (2.5-3%) will be required for the first several minutes after induction. When a stable anesthetic plane has been reached, the vaporizer setting is lowered and adjusted to maintain an appropriate depth. Once the most stimulating part of procedure is complete, it is usually possible to decrease the vaporizer setting gradually lowering the dose as the procedure nears completion. As a safety precaution, it is our policy that the isoflurane vaporizer is never set higher than 3%. If the patient needs to be more deeply anesthetized, increasing the oxygen flow rate and manually ventilating will increase the uptake of isoflurane. Periodically monitor the level of isoflurane in the machine. This should be done as part of your pre-anesthetic machine check, several times throughout the procedure and again at the completion of the procedure. If the isoflurane setting is below the half-way mark, be sure to fill the reservoir prior to beginning the procedure. Oxygen flow meter setting In general, an oxygen flow rate of L/min is appropriate for most patients. If the reservoir bag is overfilling and the animal is breathing normally, check that the popoff valve is open then reduce oxygen flow to maintain an appropriate volume in the bag. Pressure relief (pop-off) valve The pop-off valve should be in the OPEN (or mostly open) position except when manually ventilating (bagging) the patient. The pop-off valve prevents the build-up of excessive pressure or volume of gases in the circuit. If allowed to occur (as when the valve is left in the closed position), this pressure can reach the animals lungs, causing the alveoli to distend and eventually rupture. 6
Reading Assignment: Tasks for the Veterinary Assistant, pages 467-473, Appendix L, O and P
 Patient Monitoring Reading Assignment: Tasks for the Veterinary Assistant, pages 467-473, Appendix L, O and P Patient monitoring during surgery is an extremely important task that is commonly the responsibility
Patient Monitoring Reading Assignment: Tasks for the Veterinary Assistant, pages 467-473, Appendix L, O and P Patient monitoring during surgery is an extremely important task that is commonly the responsibility
RESPONDING TO ANESTHETIC COMPLICATIONS
 RESPONDING TO ANESTHETIC COMPLICATIONS General anesthesia poses minimal risk to most patients when performed by a capable anesthetist using appropriate protocols and proper monitoring. However, it is vitally
RESPONDING TO ANESTHETIC COMPLICATIONS General anesthesia poses minimal risk to most patients when performed by a capable anesthetist using appropriate protocols and proper monitoring. However, it is vitally
GENERAL ANESTHESIA BASICS
 GENERAL ANESTHESIA BASICS INTRODUCTION The goal in the administration of general anesthesia is to provide a stage of reversible unconsciousness with adequate analgesia and muscle relaxation for surgical
GENERAL ANESTHESIA BASICS INTRODUCTION The goal in the administration of general anesthesia is to provide a stage of reversible unconsciousness with adequate analgesia and muscle relaxation for surgical
Oxygenation. Chapter 21. Anatomy and Physiology of Breathing. Anatomy and Physiology of Breathing*
 Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Understanding Anesthetic Delivery Systems Dean Knoll, CVT, VTS (Anes.) Anesthesia Technician Supervisor University of Wisconsin Madison, WI May 2003
 Understanding Anesthetic Delivery Systems Dean Knoll, CVT, VTS (Anes.) Anesthesia Technician Supervisor University of Wisconsin Madison, WI May 2003 Knowing the functions of the anesthetic delivery system
Understanding Anesthetic Delivery Systems Dean Knoll, CVT, VTS (Anes.) Anesthesia Technician Supervisor University of Wisconsin Madison, WI May 2003 Knowing the functions of the anesthetic delivery system
Obstetrical Emergencies
 Date: July 18, 2014 Page 1 of 5 Obstetrical Emergencies Purpose: To provide the process for the assessment and management of the patient with an obstetrical related emergency. Pre-Medical Control 1. Follow
Date: July 18, 2014 Page 1 of 5 Obstetrical Emergencies Purpose: To provide the process for the assessment and management of the patient with an obstetrical related emergency. Pre-Medical Control 1. Follow
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
*Reflex withdrawal from a painful stimulus is NOT considered a purposeful response.
 Analgesia and Moderate Sedation This Nebraska Board of Nursing advisory opinion is issued in accordance with Nebraska Revised Statute (NRS) 71-1,132.11(2). As such, this advisory opinion is for informational
Analgesia and Moderate Sedation This Nebraska Board of Nursing advisory opinion is issued in accordance with Nebraska Revised Statute (NRS) 71-1,132.11(2). As such, this advisory opinion is for informational
DISCHARGE CRITERIA FOR PHASE I & II- POST ANESTHESIA CARE
 REFERENCES: The Joint Commission Accreditation Manual for Hospitals American Society of Post Anesthesia Nurses: Standards of Post Anesthesia Nursing Practice (1991, 2002). RELATED DOCUMENTS: SHC Administrative
REFERENCES: The Joint Commission Accreditation Manual for Hospitals American Society of Post Anesthesia Nurses: Standards of Post Anesthesia Nursing Practice (1991, 2002). RELATED DOCUMENTS: SHC Administrative
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Vtial sign #1: PULSE. Vital Signs: Assessment and Interpretation. Factors that influence pulse rate: Importance of Vital Signs
 Vital Signs: Assessment and Interpretation Elma I. LeDoux, MD, FACP, FACC Associate Professor of Medicine Vtial sign #1: PULSE Reflects heart rate (resting 60-90/min) Should be strong and regular Use 2
Vital Signs: Assessment and Interpretation Elma I. LeDoux, MD, FACP, FACC Associate Professor of Medicine Vtial sign #1: PULSE Reflects heart rate (resting 60-90/min) Should be strong and regular Use 2
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
Section Two: Arterial Pressure Monitoring
 Section Two: Arterial Pressure Monitoring Indications An arterial line is indicated for blood pressure monitoring for the patient with any medical or surgical condition that compromises cardiac output,
Section Two: Arterial Pressure Monitoring Indications An arterial line is indicated for blood pressure monitoring for the patient with any medical or surgical condition that compromises cardiac output,
Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
 Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
STANDARD OPERATING PROCEDURE #201 RODENT SURGERY
 STANDARD OPERATING PROCEDURE #201 RODENT SURGERY 1. PURPOSE The intent of this Standard Operating Procedure (SOP) is to describe procedures for survival rodent surgery. 2. RESPONSIBILITY Principal investigators
STANDARD OPERATING PROCEDURE #201 RODENT SURGERY 1. PURPOSE The intent of this Standard Operating Procedure (SOP) is to describe procedures for survival rodent surgery. 2. RESPONSIBILITY Principal investigators
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
Chapter 26. Assisting With Oxygen Needs. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 26 Assisting With Oxygen Needs Oxygen (O 2 ) is a gas. Oxygen It has no taste, odor, or color. It is a basic need required for life. Death occurs within minutes if breathing stops. Brain damage
Chapter 26 Assisting With Oxygen Needs Oxygen (O 2 ) is a gas. Oxygen It has no taste, odor, or color. It is a basic need required for life. Death occurs within minutes if breathing stops. Brain damage
NRP 2012 Putting New Resuscitation Guidelines into Practice
 Outreach Education Online Video Library for Healthcare Professionals NRP 2012 Putting New Resuscitation Guidelines into Practice. Jeanette Zaichkin, RN, MN, NNP-BC December 2, 2010 Program Handouts This
Outreach Education Online Video Library for Healthcare Professionals NRP 2012 Putting New Resuscitation Guidelines into Practice. Jeanette Zaichkin, RN, MN, NNP-BC December 2, 2010 Program Handouts This
How To Treat A Heart Attack
 13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
CH CONSCIOUS SEDATION
 Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Summary: CH CONSCIOUS SEDATION It is the policy of Carondelet Health that moderate conscious sedation of patients will be undertaken with appropriate evaluation and monitoring. Effective Date: 9/4/04 Revision
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice
 PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice P.O. BOX 2129 Raleigh, NC 27602 (919) 782-3211 FAX (919) 781-9461 Nurse Aide II Registry (919) 782-7499 www.ncbon.com Issue: Administration
PROCEDURAL SEDATION/ANALGESIA NCBON Position Statement for RN Practice P.O. BOX 2129 Raleigh, NC 27602 (919) 782-3211 FAX (919) 781-9461 Nurse Aide II Registry (919) 782-7499 www.ncbon.com Issue: Administration
Scope and Standards for Nurse Anesthesia Practice
 Scope and Standards for Nurse Anesthesia Practice Copyright 2013 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Scope and Standards for Nurse Anesthesia Practice Copyright 2013 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider. www.umke.org
 Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider Objectives: Identify the indications, contraindications and side effects of LMA use. Identify the equipment necessary for
Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider Objectives: Identify the indications, contraindications and side effects of LMA use. Identify the equipment necessary for
Mississippi Board of Nursing
 Mississippi Board of Nursing Regulating Nursing Practice www.msbn.state.ms.us 713 Pear Orchard Road, Suite 300 Ridgeland, MS 39157 Administration and Management of Intravenous (IV) Moderate Sedation POSITION
Mississippi Board of Nursing Regulating Nursing Practice www.msbn.state.ms.us 713 Pear Orchard Road, Suite 300 Ridgeland, MS 39157 Administration and Management of Intravenous (IV) Moderate Sedation POSITION
Oxygenation and Oxygen Therapy Michael Billow, D.O.
 Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
CRITICAL CARE MONITORING: WHAT, WHEN, AND HOW? Susan G. Hackner, BVSc.MRCVS.DACVIM.DACVECC.
 CRITICAL CARE MONITORING: WHAT, WHEN, AND HOW? Susan G. Hackner, BVSc.MRCVS.DACVIM.DACVECC. A crucial goal in the critical patient is the maintenance and optimization of cellular (and organ) health. Cellular
CRITICAL CARE MONITORING: WHAT, WHEN, AND HOW? Susan G. Hackner, BVSc.MRCVS.DACVIM.DACVECC. A crucial goal in the critical patient is the maintenance and optimization of cellular (and organ) health. Cellular
PEDIATRIC TREATMENT GUIDELINES
 P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
MEASURING AND RECORDING BLOOD PRESSURE
 MEASURING AND RECORDING BLOOD PRESSURE INTRODUCTION The blood pressure, along with the body temperature, pulse, and respirations, is one of the vital signs. These measurements are used to quickly, easily,
MEASURING AND RECORDING BLOOD PRESSURE INTRODUCTION The blood pressure, along with the body temperature, pulse, and respirations, is one of the vital signs. These measurements are used to quickly, easily,
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
Corporate Medical Policy
 File Name: anesthesia_services Origination: 8/2007 Last CAP Review: 1/2016 Next CAP Review: 1/2017 Last Review: 1/2016 Corporate Medical Policy Description of Procedure or Service There are three main
File Name: anesthesia_services Origination: 8/2007 Last CAP Review: 1/2016 Next CAP Review: 1/2017 Last Review: 1/2016 Corporate Medical Policy Description of Procedure or Service There are three main
AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 RECOMMENDATIONS FOR THE POST-ANAESTHESIA RECOVERY ROOM
 Review PS4 (2006) AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 RECOMMENDATIONS FOR THE POST-ANAESTHESIA RECOVERY ROOM 1. INTRODUCTION A well-planned, well-equipped, well-staffed
Review PS4 (2006) AUSTRALIAN AND NEW ZEALAND COLLEGE OF ANAESTHETISTS ABN 82 055 042 852 RECOMMENDATIONS FOR THE POST-ANAESTHESIA RECOVERY ROOM 1. INTRODUCTION A well-planned, well-equipped, well-staffed
Surgical procedures conducted at field sites need not be performed in dedicated facilities, but must be performed using aseptic procedures.
 UNMC/UNO ANIMAL CARE AND USE PROGRAM POLICIES AND PROCEDURES APPROVAL DATE: 10/16/2013 TITLE: Policy for Surgery PAGE 1 OF 5 POLICY Successful surgical outcomes depend on appropriate pre-surgical planning,
UNMC/UNO ANIMAL CARE AND USE PROGRAM POLICIES AND PROCEDURES APPROVAL DATE: 10/16/2013 TITLE: Policy for Surgery PAGE 1 OF 5 POLICY Successful surgical outcomes depend on appropriate pre-surgical planning,
ADMINISTERING EMERGENCY OXYGEN
 FACT SHEET ADMINISTERING EMERGENCY OXYGEN Emergency oxygen can be given for many breathing and cardiac emergencies. It can help improve hypoxia (insufficient oxygen reaching the cells) and reduce pain
FACT SHEET ADMINISTERING EMERGENCY OXYGEN Emergency oxygen can be given for many breathing and cardiac emergencies. It can help improve hypoxia (insufficient oxygen reaching the cells) and reduce pain
Pulmonary Diseases. Lung Disease: Pathophysiology, Medical and Exercise Programming. Overview of Pathophysiology
 Lung Disease: Pathophysiology, Medical and Exercise Programming Overview of Pathophysiology Ventilatory Impairments Increased airway resistance Reduced compliance Increased work of breathing Ventilatory
Lung Disease: Pathophysiology, Medical and Exercise Programming Overview of Pathophysiology Ventilatory Impairments Increased airway resistance Reduced compliance Increased work of breathing Ventilatory
Fainting - Syncope. This reference summary explains fainting. It discusses the causes and treatment options for the condition.
 Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Surgery Health Care Aide
 Surgery Health Care Aide Buddy Center Volunteer Training Manual 1 Surgery Health-Care Aide Thank you for volunteering in the Surgery department as a health-care aide. This packet includes information to
Surgery Health Care Aide Buddy Center Volunteer Training Manual 1 Surgery Health-Care Aide Thank you for volunteering in the Surgery department as a health-care aide. This packet includes information to
Guidelines for Spay/Neuter
 Guidelines for Standards of Care in Animal Shelters Guidelines for Spay/Neuter Cynthia Barker Cox, DVM MSPCA Boston, MA Natalie Isaza, DVM College of Veterinary Medicine University of Florida Guidelines
Guidelines for Standards of Care in Animal Shelters Guidelines for Spay/Neuter Cynthia Barker Cox, DVM MSPCA Boston, MA Natalie Isaza, DVM College of Veterinary Medicine University of Florida Guidelines
PULMONARY PHYSIOLOGY
 I. Lung volumes PULMONARY PHYSIOLOGY American College of Surgeons SCC Review Course Christopher P. Michetti, MD, FACS and Forrest O. Moore, MD, FACS A. Tidal volume (TV) is the volume of air entering and
I. Lung volumes PULMONARY PHYSIOLOGY American College of Surgeons SCC Review Course Christopher P. Michetti, MD, FACS and Forrest O. Moore, MD, FACS A. Tidal volume (TV) is the volume of air entering and
NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS
 NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION 4 TEMPERATURE CONTROL.4 CLEARING THE AIRWAY OF MECONIUM 5
NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION 4 TEMPERATURE CONTROL.4 CLEARING THE AIRWAY OF MECONIUM 5
(C) AMBULANCE VICTORIA
 The Newborn Baby: Definitions and Contacts Newborn definition 'Newborn' refers to the first min to hours post birth. For the purpose of resuscitation, AV accepts up to the first 24 hours from birth in
The Newborn Baby: Definitions and Contacts Newborn definition 'Newborn' refers to the first min to hours post birth. For the purpose of resuscitation, AV accepts up to the first 24 hours from birth in
Cardiac Arrest VF/Pulseless VT Learning Station Checklist
 Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Heat Production and Loss. Environmental Emergencies. Heat Regulation. Body Temperature Ranges. Focused Assessment: Your Patient: Heat Production
 Heat Production and Loss Environmental Emergencies Messing with Mother Nature Heat Production Basal Metabolism processes in the body that generate heat through nominal functions Activity, fever, metabolic
Heat Production and Loss Environmental Emergencies Messing with Mother Nature Heat Production Basal Metabolism processes in the body that generate heat through nominal functions Activity, fever, metabolic
Scope and Standards for Nurse Anesthesia Practice
 Scope and Standards for Nurse Anesthesia Practice Copyright 2010 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
Scope and Standards for Nurse Anesthesia Practice Copyright 2010 222 South Prospect Ave. Park Ridge, IL 60068 www.aana.com Scope and Standards for Nurse Anesthesia Practice The AANA Scope and Standards
PTA 210 PTA Technique. Vital Signs
 PTA 210 PTA Technique Vital Signs Review Last Lecture Why learn aseptic technique? 3 modes of infection transmission 3 levels of cleanliness Standard precautions (hand hygiene, PPE, respiratory hygiene,
PTA 210 PTA Technique Vital Signs Review Last Lecture Why learn aseptic technique? 3 modes of infection transmission 3 levels of cleanliness Standard precautions (hand hygiene, PPE, respiratory hygiene,
Bier Block (Intravenous Regional Anesthesia)
 Bier Block (Intravenous Regional Anesthesia) History August Bier introduced this block in 1908. Early methods included the use of two separate tourniquets and procaine was the local anesthetic of choice.
Bier Block (Intravenous Regional Anesthesia) History August Bier introduced this block in 1908. Early methods included the use of two separate tourniquets and procaine was the local anesthetic of choice.
MECHINICAL VENTILATION S. Kache, MD
 MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
Veterinary Clinics and Hospitals
 Anesthetic Gases: Guidelines for Workplace Exposure Veterinary Clinics and Hospitals Inhalation anesthesia in veterinary hospitals is practiced in a manner similar to that in human hospitals. Generally,
Anesthetic Gases: Guidelines for Workplace Exposure Veterinary Clinics and Hospitals Inhalation anesthesia in veterinary hospitals is practiced in a manner similar to that in human hospitals. Generally,
Introduction to Cardiopulmonary Exercise Testing
 Introduction to Cardiopulmonary Exercise Testing 2 nd Edition Andrew M. Luks, MD Robb Glenny, MD H. Thomas Robertson, MD Division of Pulmonary and Critical Care Medicine University of Washington Section
Introduction to Cardiopulmonary Exercise Testing 2 nd Edition Andrew M. Luks, MD Robb Glenny, MD H. Thomas Robertson, MD Division of Pulmonary and Critical Care Medicine University of Washington Section
Body cavities. Body Planes
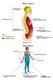 Body cavities Body Planes Directional terms http://homepage.smc.edu/wissmann_paul/anatomy1textbook/1anatomytextch1.html abdomen abdominal front of elbow antecubital arm brachial groin inguinal armpit axillary
Body cavities Body Planes Directional terms http://homepage.smc.edu/wissmann_paul/anatomy1textbook/1anatomytextch1.html abdomen abdominal front of elbow antecubital arm brachial groin inguinal armpit axillary
Neonatal Emergencies. Care of the Neonate. Care of the Neonate. Care of the Neonate. Student Objectives. Student Objectives continued.
 Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
Patient Care Services Policy & Procedure Title: No. 8720-0059
 Page: 1 of 8 I. SCOPE: This policy applies to Saint Francis Hospital, its employees, medical staff, contractors, patients and visitors regardless of service location or category of patient. This policy
Page: 1 of 8 I. SCOPE: This policy applies to Saint Francis Hospital, its employees, medical staff, contractors, patients and visitors regardless of service location or category of patient. This policy
Types of electrical injuries
 Types of electrical injuries Electrical injury is a term for all injuries caused by contact with electrical energy. Electrical contact can cause a wide variety of injuries involving most organ systems.
Types of electrical injuries Electrical injury is a term for all injuries caused by contact with electrical energy. Electrical contact can cause a wide variety of injuries involving most organ systems.
GRADE 11F: Biology 3. UNIT 11FB.3 9 hours. Human gas exchange system and health. Resources. About this unit. Previous learning.
 GRADE 11F: Biology 3 Human gas exchange system and health UNIT 11FB.3 9 hours About this unit This unit is the third of six units on biology for Grade 11 foundation. The unit is designed to guide your
GRADE 11F: Biology 3 Human gas exchange system and health UNIT 11FB.3 9 hours About this unit This unit is the third of six units on biology for Grade 11 foundation. The unit is designed to guide your
Southern Stone County Fire Protection District Emergency Medical Protocols
 TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
The EMT Instructional Guidelines in this section include all the topics and material at the EMR level PLUS the following material:
 Airway Management, Respiration and Artificial Ventilation EMR Applies knowledge (fundamental depth, foundational breadth) of general anatomy and physiology to assure a patent airway, adequate mechanical
Airway Management, Respiration and Artificial Ventilation EMR Applies knowledge (fundamental depth, foundational breadth) of general anatomy and physiology to assure a patent airway, adequate mechanical
Guidelines for the Use of Sedation and General Anesthesia by Dentists
 Guidelines for the Use of Sedation and General Anesthesia by Dentists I. Introduction The administration of local anesthesia, sedation and general anesthesia is an integral part of dental practice. The
Guidelines for the Use of Sedation and General Anesthesia by Dentists I. Introduction The administration of local anesthesia, sedation and general anesthesia is an integral part of dental practice. The
Understanding Hypoventilation and Its Treatment by Susan Agrawal
 www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
Early Warning Scores (EWS) Clinical Sessions 2011 By Bhavin Doshi
 Early Warning Scores (EWS) Clinical Sessions 2011 By Bhavin Doshi What is EWS? After qualifying, junior doctors are expected to distinguish between the moderately sick patients who can be managed in the
Early Warning Scores (EWS) Clinical Sessions 2011 By Bhavin Doshi What is EWS? After qualifying, junior doctors are expected to distinguish between the moderately sick patients who can be managed in the
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course
 Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
3100B Clinical Training Program. 3100B HFOV VIASYS Healthcare
 3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
Hypoxia and Oxygenation Hypoxia is a serious threat to patients and escorts alike when
 Chapter 4 2 71 Hypoxia and Oxygenation Hypoxia is a serious threat to patients and escorts alike when they fly. Air medical escorts need to understand what causes hypoxia, why some people are more likely
Chapter 4 2 71 Hypoxia and Oxygenation Hypoxia is a serious threat to patients and escorts alike when they fly. Air medical escorts need to understand what causes hypoxia, why some people are more likely
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings
 AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
TABLE 2 ASA Physical Status Classification
 TABLE 2 ASA Physical Status Classification ASA Class I II III IV V Description A normal, healthy patient, without organic, physiologic, or psychiatric disturbances A patient with controlled medical conditions
TABLE 2 ASA Physical Status Classification ASA Class I II III IV V Description A normal, healthy patient, without organic, physiologic, or psychiatric disturbances A patient with controlled medical conditions
TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING
 TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING PROGRAM: School Health APPROVED BY: Board of Health School Medical Advisor POLICY: With Portable Suction Machine DATE: March 14, 1994 POLICY DEFINITION:
TOWN OF FAIRFIELD HEALTH DEPARTMENT PUBLIC HEALTH NURSING PROGRAM: School Health APPROVED BY: Board of Health School Medical Advisor POLICY: With Portable Suction Machine DATE: March 14, 1994 POLICY DEFINITION:
Community Ambulance Service of Minot ALS Standing Orders Legend
 Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Michigan Adult Cardiac Protocols CARDIAC ARREST GENERAL. Date: May 31, 2012 Page 1 of 5
 Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log
 First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
Circulatory System Review
 Circulatory System Review 1. Draw a table to describe the similarities and differences between arteries and veins? Anatomy Direction of blood flow: Oxygen concentration: Arteries Thick, elastic smooth
Circulatory System Review 1. Draw a table to describe the similarities and differences between arteries and veins? Anatomy Direction of blood flow: Oxygen concentration: Arteries Thick, elastic smooth
8/6/2010. Name of medication Concentration (1:1,000 or 1mg/1ml) Expiration date
 Learning Objectives: Anaphylaxis & Epinephrine Administration by the EMT Adapted with permission from the Pilot Project for the Administration of Epinephrine by Washington EMTs With successful completion
Learning Objectives: Anaphylaxis & Epinephrine Administration by the EMT Adapted with permission from the Pilot Project for the Administration of Epinephrine by Washington EMTs With successful completion
Principles of the Anesthetic Machine
 Principles of the Anesthetic Machine This training pamphlet was a result of a collaborative effort with Marcelo Couto, DVM, The Scripps Research Institute, La Jolla, California and Jim Houts, OmniMed Inc.,
Principles of the Anesthetic Machine This training pamphlet was a result of a collaborative effort with Marcelo Couto, DVM, The Scripps Research Institute, La Jolla, California and Jim Houts, OmniMed Inc.,
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive.
 It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
Fall Arrest System: A series of equipment components designed to stop the fall of individuals working at heights should they fall.
 Blog Back to Blog Listings Suspension Trauma 101 March 18, 2016 @ 10:37am Why are rescue at height plans so important? Why do we talk so much about knowing what to do when sh!t hits the fan? One of the
Blog Back to Blog Listings Suspension Trauma 101 March 18, 2016 @ 10:37am Why are rescue at height plans so important? Why do we talk so much about knowing what to do when sh!t hits the fan? One of the
PHSW Procedural Sedation Post-Test Answer Key. For the following questions, circle the letter of the correct answer(s) or the word true or false.
 PHSW Procedural Sedation Post-Test Answer Key 1 1. Define Procedural (Conscious) Sedation: A medically controlled state of depressed consciousness where the patient retains the ability to continuously
PHSW Procedural Sedation Post-Test Answer Key 1 1. Define Procedural (Conscious) Sedation: A medically controlled state of depressed consciousness where the patient retains the ability to continuously
RODENT SURVIVAL SURGERY
 Institutional Animal Care Program Title: RODENT SURVIVAL SURGERY Policy#: IACP 004 Date in Effect: 12/14/07 Rev #: 04 Rev Date: 12/13/13 In Effect Rescinded Date Rescinded: A) PURPOSE In accordance with
Institutional Animal Care Program Title: RODENT SURVIVAL SURGERY Policy#: IACP 004 Date in Effect: 12/14/07 Rev #: 04 Rev Date: 12/13/13 In Effect Rescinded Date Rescinded: A) PURPOSE In accordance with
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT What to wear STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT ITLS is a practical course that stresses hands-on teaching. You should wear comfortable clothes that you
INTERNATIONAL TRAUMA LIFE SUPPORT What to wear STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT ITLS is a practical course that stresses hands-on teaching. You should wear comfortable clothes that you
National Registry of Emergency Medical Technicians Emergency Medical Technician Psychomotor Examination BLEEDING CONTROL/SHOCK MANAGEMENT
 BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
5/30/2014 OBJECTIVES THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM. Disclosure
 THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
Vital and Diagnostic Signs
 GENERAL The four vital signs and the five diagnostic signs evaluated during patient assessment provide valuable information to the care provider, and when recorded properly, to the receiving facility/personnel.
GENERAL The four vital signs and the five diagnostic signs evaluated during patient assessment provide valuable information to the care provider, and when recorded properly, to the receiving facility/personnel.
What You Need to know about Your Pet s Upcoming Dentistry and Periodontal Treatment
 What You Need to know about Your Pet s Upcoming Dentistry and Periodontal Treatment We are sending this packet of information in anticipation of your pet s upcoming dental procedure. Many people have questions
What You Need to know about Your Pet s Upcoming Dentistry and Periodontal Treatment We are sending this packet of information in anticipation of your pet s upcoming dental procedure. Many people have questions
STAGES OF SHOCK. IRREVERSIBLE SHOCK Heart deteriorates until it can no longer pump and death occurs.
 STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
STAGES OF SHOCK SHOCK : A profound disturbance of circulation and metabolism, which leads to inadequate perfusion of all organs which are needed to maintain life. COMPENSATED NONPROGRESSIVE SHOCK 30 sec
POLICIES AND PROCEDURES
 July 1, 2011 Approved by R. Dale Horne Fire Chief Page 1 of 5 PURPOSE: A primary mission for Anderson City Fire IC is to identify, examine and evaluate the physical and mental status of fire-rescue personnel
July 1, 2011 Approved by R. Dale Horne Fire Chief Page 1 of 5 PURPOSE: A primary mission for Anderson City Fire IC is to identify, examine and evaluate the physical and mental status of fire-rescue personnel
Cardiac Catheterization
 Page 1 Cardiac Catheterization What Other Terms Are Used To Describe Cardiac Catheterization? Heart Cath (catheter) Angiogram What Is Cardiac Catheterization? This procedure is nonsurgical and is performed
Page 1 Cardiac Catheterization What Other Terms Are Used To Describe Cardiac Catheterization? Heart Cath (catheter) Angiogram What Is Cardiac Catheterization? This procedure is nonsurgical and is performed
Hyperbaric Oxygen Therapy WWW.RN.ORG
 Hyperbaric Oxygen Therapy WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A.,
Hyperbaric Oxygen Therapy WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A.,
240- PROBLEM SET INSERTION OF SWAN-GANZ SYSTEMIC VASCULAR RESISTANCE. Blood pressure = f(cardiac output and peripheral resistance)
 240- PROBLEM SET INSERTION OF SWAN-GANZ 50 kg Pig Rt Jugular 0 cm Rt Atrium 10 cm Rt ventricle 15 cm Wedge 20-25 cm SYSTEMIC VASCULAR RESISTANCE Blood pressure = f(cardiac output and peripheral resistance)
240- PROBLEM SET INSERTION OF SWAN-GANZ 50 kg Pig Rt Jugular 0 cm Rt Atrium 10 cm Rt ventricle 15 cm Wedge 20-25 cm SYSTEMIC VASCULAR RESISTANCE Blood pressure = f(cardiac output and peripheral resistance)
Ventilation Perfusion Relationships
 Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
ANESTHESIA - Medicare
 ANESTHESIA - Medicare Policy Number: UM14P0008A2 Effective Date: August 19, 2014 Last Reviewed: January 1, 2016 PAYMENT POLICY HISTORY Version DATE ACTION / DESCRIPTION Version 2 January 1, 2016 Under
ANESTHESIA - Medicare Policy Number: UM14P0008A2 Effective Date: August 19, 2014 Last Reviewed: January 1, 2016 PAYMENT POLICY HISTORY Version DATE ACTION / DESCRIPTION Version 2 January 1, 2016 Under
Surgery: Setup and Supplies
 THE SURGERY SUITE Surgeries other than routine neuters and treatment of abscesses are performed in the surgery suite. We keep a chart with the preferences of our various surgeons, including which side
THE SURGERY SUITE Surgeries other than routine neuters and treatment of abscesses are performed in the surgery suite. We keep a chart with the preferences of our various surgeons, including which side
Breathing and Holding Your Breath copyright, 2005, Dr. Ingrid Waldron and Jennifer Doherty, Department of Biology, University of Pennsylvania 1
 Breathing and Holding Your Breath copyright, 2005, Dr. Ingrid Waldron and Jennifer Doherty, Department of Biology, University of Pennsylvania 1 Introduction Everybody breathes all day, every day. Why?
Breathing and Holding Your Breath copyright, 2005, Dr. Ingrid Waldron and Jennifer Doherty, Department of Biology, University of Pennsylvania 1 Introduction Everybody breathes all day, every day. Why?
Cardiovascular Physiology
 Cardiovascular Physiology Heart Physiology for the heart to work properly contraction and relaxation of chambers must be coordinated cardiac muscle tissue differs from smooth and skeletal muscle tissues
Cardiovascular Physiology Heart Physiology for the heart to work properly contraction and relaxation of chambers must be coordinated cardiac muscle tissue differs from smooth and skeletal muscle tissues
Objectives. Burn Assessment and Management. Questions Regarding the Case Study. Case Study. Patient Assessment. Patient Assessment
 Objectives Burn Assessment and Management Discuss the mechanisms and complications of a thermal burn, electrical burn and an inhalation burn Explain the factors to consider when determining the severity
Objectives Burn Assessment and Management Discuss the mechanisms and complications of a thermal burn, electrical burn and an inhalation burn Explain the factors to consider when determining the severity
What, roughly, is the dividing line between the upper and lower respiratory tract? The larynx. What s the difference between the conducting zone and
 What, roughly, is the dividing line between the upper and lower respiratory tract? The larynx. What s the difference between the conducting zone and the respiratory zone? Conducting zone is passageways
What, roughly, is the dividing line between the upper and lower respiratory tract? The larynx. What s the difference between the conducting zone and the respiratory zone? Conducting zone is passageways
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination PATIENT ASSESSMENT/MANAGEMENT TRAUMA
 PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
11 Newborn Life Support
 11 Newborn Life Support Introduction Passage through the birth canal is a hypoxic experience for the fetus, since significant respiratory exchange at the placenta is prevented for the 50-75 s duration
11 Newborn Life Support Introduction Passage through the birth canal is a hypoxic experience for the fetus, since significant respiratory exchange at the placenta is prevented for the 50-75 s duration
Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back
 Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back to the left atria from the left ventricle, blood is pumped
Vascular System The heart can be thought of 2 separate pumps from the right ventricle, blood is pumped at a low pressure to the lungs and then back to the left atria from the left ventricle, blood is pumped
81 First Responder Respiratory
 81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
TRANSPORT OF CRITICALLY ILL PATIENTS
 TRANSPORT OF CRITICALLY ILL PATIENTS Introduction Inter-hospital and intra-hospital transport of critically ill patients places the patient at risk of adverse events and increased morbidity and mortality.
TRANSPORT OF CRITICALLY ILL PATIENTS Introduction Inter-hospital and intra-hospital transport of critically ill patients places the patient at risk of adverse events and increased morbidity and mortality.
Title 10 DEPARTMENT OF HEALTH AND MENTAL HYGIENE
 Title 10 DEPARTMENT OF HEALTH AND MENTAL HYGIENE Subtitle 44 BOARD OF DENTAL EXAMINERS Chapter 12 Anesthesia and Sedation Authority: Health Occupations Article, 4-205 Annotated Code of Maryland.01 Scope.
Title 10 DEPARTMENT OF HEALTH AND MENTAL HYGIENE Subtitle 44 BOARD OF DENTAL EXAMINERS Chapter 12 Anesthesia and Sedation Authority: Health Occupations Article, 4-205 Annotated Code of Maryland.01 Scope.
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination BVM VENTILATION OF AN APNEIC ADULT PATIENT
 BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
