Treatment of pneumothorax, the abnormal collection
|
|
|
- Evan Benson
- 10 years ago
- Views:
Transcription
1 Detection of Pneumothorax with Ultrasound Jonathan P. Kline, CRNA, MSNA David Dionisio, CRNA Kevin Sullivan, CRNA Trey Early, CRNA Joshua Wolf, CRNA Deanna Kline, CRNA, DNP Diagnosis of a pneumothorax in the perioperative area can be difficult. Traditional gold-standard modalities may not be available or feasible to institute. Ultrasound guidance allows the anesthesia provider a method of quickly ruling out this potentially life-threatening complication. In this article we detail the use of sonography for fast and accurate diagnosis of pneumothorax. The essential terms relative to the use of ultrasonography to detect pneumothorax are also defined. Keywords: Bat sign, lung sliding, pleural line, pneumothorax, seashore sign, ultrasound. Treatment of pneumothorax, the abnormal collection of air between the visceral and parietal pleural layers of the lung, was first detected and treated by a 15th century physician from Anatolia named Serefeddin Sabuncuoglu. His illustrated surgical text written in 1465 first described this phenomenon as a result of trauma to the chest. He first correlated that shortness of breath, cough, and hemoptysis may signal a puncture in the pleura. Treatment of a pneumothorax in the 15th century was called mihceme, also known as cupping therapy. The skin over the traumatic area was incised by the physician, and a device was placed over the area to cause aspiration of the abnormal air collection. A flame was placed into the glass tool to burn oxygen and create a vacuum. 1 This negative pressure would then relieve the pneumothorax. Treatment of a pneumothorax was not a standard procedure until World War II. Today, modern technology indicates that the use of ultrasonography is safe, fast, and effective for detecting this complication. Diagnosis of a pneumothorax has traditionally been obtained through a variety of ways such as patient history, clinical examination, chest radiography, and computed tomography (CT) scanning. During the history, examination, or report, the anesthesia provider should be made aware of any precipitating factors that may put a patient at risk of a pneumothorax. These factors include any instrumentation or needles near the neck, chest wall, or trachea; fractured ribs or crush injury to the chest; blunt trauma to the chest; increased pressure to the airway or bullous lung disease; and nitrous oxide administration. Many of the mentioned modalities for pneumothorax detection are not readily available while patients are under general anesthesia. The signs of a pneumothorax while a patient is under anesthesia can be nonspecific and difficult to decipher. They may include difficulty maintaining adequate ventilation, hypotension, heart rate changes, distended neck veins, abdominal distention, altered breath sounds on the side of the pneumothorax, and possibly unilateral chest expansion with tracheal deviation. 2 The application of positive pressure ventilation to even a small, asymptomatic pneumothorax can cause progression to a life-threatening tension pneumothorax. Computed tomography is considered to be the gold standard for detecting pneumothoraces 3 ; however, it does have drawbacks. Some of these include patient transport to the scanner, the need for a radiation technologist to perform the scan, the need for physician interpretation, and the greatest radiation exposure to the patient of all detection methods. It is also not feasible to obtain a CT scan during a general anesthetic in the operating suite. Traditionally, when a clinician suspects a pneumothorax, a chest radiograph is obtained. This presents problems for the patient under anesthesia. Chest radiographs are best at detecting a pneumothorax if obtained with the patient in the upright position. 4 The radiographic appearance of a pneumothorax is dependent on gravity, and studies have shown that anteroposterior supine radiographs may detect only a large pneumothorax. 4 One study showed more than half of the traumatic pneumothoraces that were detected by CT were missed by supine chest radiographs. 5 Obtaining upright inspiratory and expiratory anterior/posterior and lateral chest radiographs while the patient is under anesthesia would be problematic at best. Portable ultrasonography has recently been studied for use in the detection of a pneumothorax. 3 An evidence-based review of the literature was done to evaluate ultrasonography vs chest radiography to detect traumatic pneumothoraces. This review found that bedside ultrasonography was a much more sensitive screening test for detection of pneumothorax than supine chest radiography in the trauma patient. 1 Another recent study that AANA Journal August 2013 Vol. 81, No
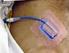
2 compared ultrasonographic detection of pneumothoraces vs chest radiography found that not only was ultrasonography superior to chest radiography in detection, ultrasonography was able to differentiate between different sizes of pneumothoraces and its diagnostic value rivaled that of the CT scan. 6 Ultrasonographic equipment is now easily portable and quickly produces high-quality images. Sonography is a highly effective diagnostic tool that can lead to prompt intervention when life-threatening situations arise in the operating room, whereas CT scanning may not be available to the anesthesia provider. Ultrasonography has assisted providers in the detection of pneumothorax for nearly 2 decades. Nearly all early published work originated from the emergency medicine and intensive care medicine journals. Only recently has this interesting topic been adopted by the anesthesia literature. Although chest CT remains the gold standard and many articles still use chest radiography for comparison, the use of ultrasonography to diagnose pneumothorax has numerous advantages. The most important advantage is a dramatic decrease in the time it takes to make a diagnosis. One article claimed that the time to diagnose pneumothorax was about 7 minutes for ultrasonography vs 80 minutes in the x-ray group. They also pointed out the degree of deviation in the x-ray group was ± 66 minutes, meaning it could have been as long as 140 minutes to diagnose this potentially life-threatening complication. 1 Ultrasonography has been demonstrated to be more accurate than chest CT to diagnose a pneumothorax. 6 One recent article demonstrated impressive success rates of prehospital medical personnel being trained quickly to identify a pneumothorax on ultrasound. This suggests that other providers can be trained to quickly perform ultrasonographic scanning and to recognize a suspected pneumothorax with sonography. 7 Other advantages include omission of radiation exposure to the staff and patient, reduction in cost, completion of diagnosis without the need for a radiologist (eg, late-night care in tertiary facilities), and ease of use. There are several drawbacks to the use of ultrasonography in this clinical situation. The first drawback is that bullous lesions and severe chronic obstructive pulmonary disease (COPD) can mimic pneumothorax on ultrasonography. This could lead to a false-positive diagnosis of pneumothorax using ultrasonography compared with the same patient evaluated by chest radiography. The second drawback is that the overall sensitivity and specificity for ultrasonography to diagnose pneumothorax seems to decrease after the first 24 hours, meaning that the same patient with the same symptoms would be less likely to display the necessary ultrasonographic findings after a 24-hour period. Lastly, these scans are also complicated by morbid obesity, as resolution is lost at deeper measurements. 3 Performing Lung Scans Performing and interpreting lung ultrasound scans revolve around understanding the ultrasound principle that dense material, such as bone, prevents sound waves from penetrating through it. Therefore, chest scanning with ultrasound must be performed at each intercostal space of interest. The intercostal spaces are bordered by a superior and inferior rib. Between them lies the intercostal space. This space will provide an adequate window to the lung below and can reveal a variety of pulmonary illnesses. Ultrasonography to rule out pneumothorax is a relatively simple and rapid technique to perform. Early literature advocated curvilinear probe use; the current literature routinely uses high-frequency linear probes with initial frequencies around 5 MHz. 3 This disparity may reflect increases in linear imaging technology and the current flexibility of many machine settings. It is important to consider that pneumothorax air will rise to the highest point. If the patient is in the supine position, the anterior aspect of the chest is the most likely point to make the diagnosis and should therefore be scanned first. Patients who arrive with penetrating injuries to the lateral aspect of the chest should ideally be scanned in the lateral position with the area of injury at the highest position. The chest is divided into sections, and each section is scanned separately. Supine patients should have their scans initiated by placing the ultrasonic probe near the sternal border of the anterior section of the chest. The intercostal spaces of interest are then identified, and the ultrasound beam is placed between the ribs. The posterior section of the chest is best scanned with the patient in the lateral decubitus position. The posterior lung bases, which are protected by the scapulae, cannot be scanned. Imaging the posterior lung bases must therefore be done around the scapulae. This does limit sonographic access to this region; however, in the case of the supine patient, it is of little value. Some authors have described the ultrasonographic chest scan sectioning as similar to lung sound assessment with a stethoscope. The images should be compared with images of the opposite side for symmetry. Once the presence of lung sliding (the movement of parietal pleura as it joins with the visceral pleura, as described later) has been confirmed in all lung sections, the suspicion for pneumothorax is greatly reduced (Figure 1). Ultrasonographic Terms Each pulmonary abnormality has a unique sonographic presentation, and there are a few terms that specifically relate to this diagnostic scan. The lung sonogram produces waves that are named like the electrocardiography (ECG) nomenclature. Instead of starting at P for P wave, it begins with A for A-line. To interpret these scans, each provider must be familiar with the characteristic signs produced by ultrasonography. The 266 AANA Journal August 2013 Vol. 81, No. 4
3 Figure 1. Proper Placement of Ultrasonic Probe for Imaging Left Anterior Aspect of Chest Figure 2. Normal Lung Image That Shows Bat Sign Note thick, white pleural line (middle) and the 2 ribs in short axis (right and left). Term Definition Ultrasound mode Pleural line Hyperechoic horizontal line indicating the pleural layers B- and M-mode Lung sliding Dynamic horizontal movement of the pleural line during respiration B-mode Lung point Precise area of chest wall where lung sliding stops and is replaced B- and M-mode by pneumothorax Z-lines/comet Small, vertical tapering hyperechoic lines that diminish distally, B-mode tails/rockets caused by air-fluid interface at the pleural line Seashore sign Ground-glass or sandy appearance under the pleural line indicating M-mode normal lung tissue Stratosphere/ Absence of normal seashore sign below the pleural line; replaced M-mode barcode sign with multiple small horizontal lines indicating pneumothorax A-lines Horizontal, hyperechoic lines indicating normal lung surface B-mode B-lines Larger, hyperechoic vertical lines that diminish toward the B-mode bottom of the image Bat sign Basic sign indicating 2 ribs and the pleural line in short axis B-mode Table. Terms and Definitions Associated With Ultrasonographic Detection of Pneumothorax essential terms include lung sliding, bat sign, pleural lines, A-lines, B-lines, and the lung point. The use of M-mode and B-mode is also briefly discussed as it specifically relates to this topic. The Table summarizes the terms and definitions. B-Mode. B-mode, or brightness mode, is the ultrasound mode most commonly used by anesthesia providers. The brightness corresponds to the amplitude of reflected sound. B-mode provides real-time imaging of structures that are clearly discernible and is most often used to obtain vascular access or administer regional anesthetics. Traditionally, anesthesia providers use ultrasonographic images in B-mode or brightness mode. Bat Sign. The bat sign is a basic sonographic landmark that describes a particular pattern seen on the lung scan. This simple sign can be noticed quickly, even AANA Journal August 2013 Vol. 81, No
4 by novices, and represents normal chest anatomy. It is termed bat sign due to its likeness to a bat flying with its wings up, toward the viewer. It consists of an upper rib, a lower rib, and the pleural line. The outer portion of the parietal pleura forms the body of the bat sign. The superficial hyperechoic ribs become the bat s wings, raised above it, and the body is made up of the pleural line underneath and between the wings (Figure 2). 3 M-Mode. M-mode, or motion mode, does not have a great deal of utility for anesthesia providers except as an application for diagnosing a pneumothorax. M-mode uses acoustic waves to determine a structure s movement over time. It is a layering of returned ultrasound waves stacked next to each other. Looking at M-mode processing is much like reading an ECG strip, and it reflects activity over time. An important term relating to M-mode use when diagnosing a pneumothorax is the seashore sign. Normal lung scans produce this characteristic seashore sign. 8 These normal images are viewed as hyperechoic, horizontal lines that run the entire distance from the left side to the right side of the image. Near the top of the image, the bright-white pleural line will be visible. Below the pleural line, the landscape will change to become granular appearing, like ground glass. The image has been described as one of standing on the beach viewing the sea in the distance. The water appears as thin, horizontal lines that traverse the entire top portion of the screen. The sign associated with air in the pleural layer is the barcode sign or stratosphere sign. The stratosphere sign is present with a pneumothorax, and the air will produce only the horizontal lines throughout the image (Figures 3 and 4). Pleural Line. Identification of the pleural line is important in B-mode and M-mode. The pleural line is a hyperechoic (bright-white), horizontal line indicating the superficial surface of the parietal pleura. Normal pleural lines are thick, horizontal, hyperechoic lines that provide the location for the lung sliding described in the next paragraph. Pleural lines are generally seen lying about 0.5 to 2 cm below the upper portion of the ribs. The pleural line exists below each of the ribs, but ultrasound waves are unable to image below the ribs because of the acoustic shadow that the ribs produce. Essentially, the pleural line can be viewed only at the intercostal space. Lung Sliding. Lung sliding is the term describing the movement of parietal pleura as it joins with the visceral pleura. This is a normal finding on healthy patients and is easily identified during respiration. This sign is best seen with the patient breathing spontaneously, 9 but can be easily seen in mechanically ventilated patients as well. The pneumothorax air separates the 2 pleural layers, preventing imaging of normal lung sliding. This is the first important dynamic sign to be viewed after normal anatomical findings such as the bat sign and pleural line have been identified. Normal sonograms do not distinguish between the 2 pleural layers, but they do indicate presence of the visceral pleura near the parietal pleura. 4 Therefore, the presence of lung sliding rules out pneumothorax at the location of the probe. The scan should reveal this finding about 0.5 to 1 cm below the ribs. 3 If air is seen instead of lung sliding, or if lung sliding is absent, pneumothorax is highly suspected. Severe COPD and bullous lesions can abolish normal lung sliding in certain areas and appear to mimic a pneumothorax on ultrasonography. Other factors that confound ultrasonographic diagnosis of pneumothorax are previous pneumonectomy, pulmonary fibrosis, high-frequency ventilation, and adult respiratory distress syndrome. 10 In the absence of normal lung sliding, the lung point (discussed below) should be identified both on B-mode and M-mode, to distinguish the borders of a suspected pneumothorax. Lines. The early ultrasonographic literature has described as many as 26 different lines; however, only the basics are covered here. Identification of A-lines and B-lines as well as Z-lines in lung ultrasonography as a bedside tool are described by Lichtenstein et al. 3 These lines are all described in B-mode. A-Lines. A-lines are hyperechoic, repeated, horizontal lines that indicate normal lung surfaces with ultrasonography viewed in B-mode. 8 The A-line is essentially a repetition or echo of the pleural line. A-lines will often appear at repeated intervals. These intervals are the same distance from one to another, as the distance found from the skin to the pleural line. If the distance from the skin to the pleural line is 1 cm, the first A-line may appear at 2 cm and may repeat this pattern until the beam is exhausted, or the anatomy changes. A-lines normally indicate subpleural air. The length of an A-line is essentially the same as the pleural line; however, it may appear shorter, and sometimes is not visible. B-Lines. There are a variety of B-lines described in the literature. Each one is viewed in B-mode and has unique characteristics and its own significance. The B-line generally appears as a vertical shard of light or comet-tail artifact. A single vertical B-line that extends the entire depth of the scan may be a normal variant representing a lung fissure and may extend the entire distance between the pleural line and the deep portion of the image. These lines may or may not move with respiration and have also been described as lung rockets or laser beams. Multiple B-lines appear as sunlight penetrating the deep-water view of an undersea diver. The number of B-lines increases when there is an increase in interstitial edema and diseased lungs. 4 B-lines or lung rockets are not only a strong indicator to rule out pneumothorax, but they also have been described as an indicator for elevated pulmonary artery occlusive pressure and pulmonary edema. 8 These B-lines 268 AANA Journal August 2013 Vol. 81, No. 4
5 Figure 3. Normal Lung Ultrasound and Characteristic Seashore Sign Viewed Between the 2nd and 3rd Ribs This is in B-mode (upper image), and M-mode (larger, horizontal, lower image). The pleural line appears as a thick, hyperechoic, horizontal line crossing the arrow s tip. (Image by Jonathan Kline, CRNA.) may appear in about 27% of healthy patients, but they have also been associated with the presence of subpleural interstitial edema. 8 The B-line is generated by a combination of fluid and air. This occurs when the alveoli become edematous. It is thought that the B-line is created by the ultrasound beam reverberating from the probe to the liquid dense alveoli multiple times. The B-lines appear in B-mode ultrasonography as thin, vertical beams; however, they are really tiny horizontal lines tightly stacked on top of each other at increasing depth. B-lines that occur in a series of 3 or more have been termed B+ lines. 4 The presence of B-lines is especially important to rule out pneumothorax. One B-line indicates contact of the visceral pleura with the parietal pleura. This represents a normal lung surface. However, multiple lung rockets have a high degree of sensitivity and specificity for diagnosing lung interstitial edema. In summary, A-lines are horizontal items, and B-Lines are vertical items. They are not generally seen together. Z-Lines. The last in this series of lung ultrasound lines are the Z-lines. Z-lines or, comet tails, are viewed in B-mode, and their presence is useful in ruling out pneumothorax. Z-lines differ from B-lines in that Z-lines are small, tapering, hyperechoic lines that diminish distally from the visceral pleura. They occur as reverberation artifacts created by an air-fluid interface. Z-lines can be Figure 4. Ultrasound of Pneumothorax Note the characteristic streaking of the stratosphere or barcode sign. (Image by Kevin Sullivan, CRNA, of a patient with a diagnosed pneumothorax.) more confusing. They can occur in normal lung surface, and they have been described as being devoid of meaning. However, they can also be present with a pneumothorax. 4 Lung Point. The term lung point represents a precise border of a pneumothorax. This is the area where lung sliding and motionless pleura can be viewed in the same screen. The lung point is the border at which normal parietal and visceral pleural separate to become the pneumothorax. This point is where the absence of lung sliding begins or ends. Identification of the lung point is also a positive sign for pneumothorax, and visualization of it is 100% specific for ruling in pneumothorax. 11 However, lung point loses sensitivity when the lung is completely collapsed and no lung point can be visualized. 4 Lung point can be seen in either B- mode or M-mode and will demonstrate the contrast between the normal and abnormal signs described earlier (Figure 5). Suggested Method for Lung Scanning Lung scanning should be logical and methodical. The first thing to consider is the position of the patient. Consider also the patient s history such as recent blunt or penetrating trauma. The patient s position for scanning should represent the position most reasonable to diagnose the pneumothorax as described earlier. Select a high-frequency linear probe and set the depth to allow viewing of the deep lung area; on most adults this should be at least 4 cm. Begin by scanning the area most likely to show the pneumothorax. For the typical supine patient this would AANA Journal August 2013 Vol. 81, No
6 Figure 6. Decision Algorithm for Ultrasonographic Detection of Pneumothorax Figure 5. Arrow Indicates the Lung Point in M-mode This is the region where the intra-pleural air (pneumothorax) ends and normal pleural connection (seashore sign) begins. Note the characteristic streaking of the barcode/stratosphere sign on the lower indicating pneumothorax. The B-mode image (upper portion of image) will reveal the absence of lung sliding on a dynamic ultrasound scan. (Image by Jonathan Kline, CRNA.) be the anterior section of the chest. Select B-mode and place the probe on the anterior part of the chest. Obtain the bat sign showing 2 ribs in short axis and identify the pleural line. Check for lung sliding during any respiration. If absence of lung sliding is seen, switch the ultrasound to M-mode and check for the seashore sign. If a seashore sign cannot be seen, and instead a barcode sign is viewed in the same location as the absence of lung sliding, pneumothorax can be ruled in with high probability. If the pneumothorax is ruled in, scan the lateral section of the chest and identify the lung point. The presence of a lung point is highly indicative of a pneumothorax. If no abnormalities are seen, move the probe to several intercostal locations covering the anterior aspect of the chest and repeat the process of checking for lung sliding. Compare these images to those from the anterior contralateral side of the chest. After the anterior chest site has been scanned in several locations, begin scanning the lateral aspect of the chest on the contralateral side. Each time an anomaly is seen, the image should be viewed in M-mode to check for the seashore, or barcode signs. Suggested Systematic Approach for Lung Scanning A systematic approach for ultrasonographic lung scanning is described here and is depicted in Figure Lung scanning should be logical and methodical. Consider the patient s history and general physical condition, including lung pathologies, lung surgeries, or recent blunt or penetrating chest trauma. 2. Consider the position of the patient. The patient s position for scanning should represent the position most reasonable in which to diagnose the pneumothorax, or the suspected lung region affected. Begin by scanning the area most likely to show the pneumothorax. For the typical supine patient this would be the anterior chest area. 3. Select a high-frequency linear probe and set the depth to allow viewing of the deep lung area; on most adults this should be at least 4 cm. 4. Begin by selecting B-mode and place the probe on the anterior part of the chest. 5. Obtain the bat sign showing 2 ribs in short axis and identify the pleural line. Check for lung sliding during any respiration. 6. Each time an anomaly is seen, the image should be viewed in M-mode to check for the seashore or barcode sign. 7. If a seashore sign cannot be seen, and instead a barcode sign is viewed in the same location as the absence of lung sliding, pneumothorax can be ruled in with high probability. If the pneumothorax is ruled in, continue laterally scanning the lateral part of the chest and identify 270 AANA Journal August 2013 Vol. 81, No. 4
7 the lung point. The presence of a lung point is highly indicative of a pneumothorax. 8. If no abnormalities are seen, systematically move the probe to the next several intercostal locations covering the anterior aspect of the chest and repeat the process of checking for lung sliding. Use a method similar to a lung sound assessment. 9. Compare these images to the anterior contralateral side of the chest. After the anterior chest area has been scanned in several locations, begin scanning the lateral aspect of the chest on the contralateral side. Conclusion Sonographic diagnosis of pneumothorax is rapid, accurate, and easily deployed and can be lifesaving when appropriate interventions are initiated to treat the discovered pneumothorax. The efficacy of ultrasonography as a tool for assessing and diagnosing abnormalities in the chest, including pneumothorax, has been demonstrated and has been adopted by our emergency medicine, critical care, pulmonary, trauma, and radiology colleagues. Ultrasonography technology is being rapidly adopted in anesthesia care for accurate and successful placement of regional anesthesia, central and peripheral venous access, and arterial cannulation. 12 It also avoids concerns with use of CT about radiation exposure, the need for trained radiology technologists to perform CT scans, and the demand for formal training to interpret the CT scans. The international literature, across multiple disciplines, clearly demonstrates the efficacy of ultrasonography utilization in the diagnosis of pneumothorax. The advantages of ultrasonography in diagnosing pneumothorax show tremendous value to anesthesia providers for use in the operating room and outweigh its few limitations. Incorporating it into anesthesia practice seems prudent and beneficial. REFERENCES 1. Kaya SO, Karatepe M, Tok T, Onem G, Dursunoglu N, Goksin I. Were pneumothorax and its management known in 15th-century anatolia? Tex Heart Inst J. 2009; 36(2): Bacon AK, Paix AD, Williamson JA, Webb RK, Chapman MJ. Crisis management during anaesthesia: pneumothorax. Qual Saf Health Care. 2005;14(3):e18. doi: /qshc Lichtenstein DA, Mezière G, Lascols N, et al. Ultrasound diagnosis of occult pneumothorax. Crit Care Med. 2005;33(6): doi: /01.ccm b4. 4. Volpicelli G. Sonographic diagnosis of pneumothorax. Intensive Care Med. 2011;37(2): doi: /s y. 5. Rowan KR, Kirkpatrick AW, Liu D, Forkheim KE, Mayo JR, Nicolaou S. Traumatic pneumothorax detection with thoracic US: correlation with chest radiography and CT initial experience. Radiology. 2002;225(1): doi: /radiol Blaivas M, Lyon M, Duggal S. A prospective comparison of supine chest radiography and bedside ultrasound for the diagnosis of traumatic pneumothorax. Acad Emerg Med. 2005;12(9): doi: /j tb00960.x. 7. Chin EJ, Chan CH, Mortazavi R, et al. A pilot study examining the viability of a Prehospital Assessment with UltraSound for Emergencies (PAUSE) protocol [published online May 15, 2012]. J Emerg Med. 2013;44(1) Lichtenstein DA, Meziere GA, Lagoueyte JF, Biderman P, Goldstein I, Gepner A. A-lines and B-lines: lung ultrasound as a bedside tool for predicting pulmonary artery occlusion pressure in the critically ill. Chest. 2009;136(4): Razzaq QM. Use of the sliding lung sign in emergency bedside ultrasound. Eur J Emerg Med. 2008;15(4): doi: /mej.0b01 3e3282f4d15b. 10. Gardelli G, Feletti F, Nanni A, Mughetti M, Piraccini A, Zompatori M. Chest ultrasonography in the ICU. Respir Care. 2012;57(5): doi: /respcare Lichtenstein D, Mezière G, Biderman P, Gepner A. The lung point : an ultrasound sign specific to pneumothorax. Intensive Care Med. 2000;26(10): doi: /s Kline JP. Ultrasound guidance in anesthesia [published correction appears in AANA J 2011;79(6):455]. AANA J. 2011;79(3): AUTHORS Jonathan P. Kline, CRNA, MSNA, is the director of education for Twin Oaks Anesthesia Services, Wesley Chapel, Florida. He is currently actively involved with instruction of anesthesia providers in the speciality of ultrasound guidance and peripheral nerve blocks. nerveblocker@ gmail.com. David Dionisio, CRNA, is a full-time clinician at Blake Medical Center in Bradenton, Florida, and a station instructor for Twin Oaks Anesthesia Services. [email protected]. Kevin Sullivan, CRNA, is a full-time clinician at Bayfront Medical Center in St Petersburg, Florida, and a station instructor for Twin Oaks Anesthesia Services. [email protected]. Trey Early, CRNA, is a full-time clinician at Citrus Memorial Hospital in Inverness, Florida, and a station instructor for Twin Oaks Anesthesia Services. [email protected]. Joshua Wolf, CRNA, is a full-time clinician at St Joseph s Hospital in Tampa, Florida, and a station instructor for Twin Oaks Anesthesia Services. [email protected]. Deanna Kline, CRNA, DNP, is a part-time clinician through Twin Oaks Anesthesia Services at Florida Hospital Tampa, Tampa, Florida. She is also the president of and a station instructor for Twin Oaks Anesthesia Services. [email protected]. ACKNOWLEDGMENT I would like to formally thank Barbara Verhoff, CRNA, for her editorial contributions to this article. AANA Journal August 2013 Vol. 81, No
FALLS-protocol: lung ultrasound in hemodynamic assessment of shock
 Review article Heart, Lung and Vessels. 2013; 5(3): 142-147 142 FALLS-protocol: lung ultrasound in hemodynamic assessment of shock D. Lichtenstein Service de Réanimation Médicale, Hôpital Ambroise-Paré,
Review article Heart, Lung and Vessels. 2013; 5(3): 142-147 142 FALLS-protocol: lung ultrasound in hemodynamic assessment of shock D. Lichtenstein Service de Réanimation Médicale, Hôpital Ambroise-Paré,
NEEDLE THORACENTESIS Pneumothorax / Hemothorax
 NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
NEEDLE THORACENTESIS Pneumothorax / Hemothorax By: Steven Jones, NREMT-P Pneumothorax Pneumothorax is a collection of air or gas in the pleural space of the lung, causing the lung to collapse. Pneumothorax
N26 Chest Tubes 5/9/2012
 Thoracic cavity, pleural space 1 Conditions requiring chest drainage_1 Air between the pleurae is a pneumothorax Occurs when there is an opening on the surface of the lung or in the airways, y, in the
Thoracic cavity, pleural space 1 Conditions requiring chest drainage_1 Air between the pleurae is a pneumothorax Occurs when there is an opening on the surface of the lung or in the airways, y, in the
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT NEEDLE DECOMPRESSION OF TENSION PNEUMOTHORAX Roy Alson, MD, PhD, FACEP, FAAEM and Sabina Braithwaite, MD, MPH, FACEP INTRODUCTION The purpose of this document is to update
INTERNATIONAL TRAUMA LIFE SUPPORT NEEDLE DECOMPRESSION OF TENSION PNEUMOTHORAX Roy Alson, MD, PhD, FACEP, FAAEM and Sabina Braithwaite, MD, MPH, FACEP INTRODUCTION The purpose of this document is to update
Bedside Lung Ultrasound in Critical Care Units
 Med. J. Cairo Univ., Vol. 78, No. 2, September: 197-203, 2010 www.medicaljournalofcairouniversity.com Bedside Lung Ultrasound in Critical Care Units MOHAMED TALAAT ELKHOLY, M.D. *; HATEM S. ABDELHAMID,
Med. J. Cairo Univ., Vol. 78, No. 2, September: 197-203, 2010 www.medicaljournalofcairouniversity.com Bedside Lung Ultrasound in Critical Care Units MOHAMED TALAAT ELKHOLY, M.D. *; HATEM S. ABDELHAMID,
Basic techniques of pulmonary physical therapy (I) 100/04/24
 Basic techniques of pulmonary physical therapy (I) 100/04/24 Evaluation of breathing function Chart review History Chest X ray Blood test Observation/palpation Chest mobility Shape of chest wall Accessory
Basic techniques of pulmonary physical therapy (I) 100/04/24 Evaluation of breathing function Chart review History Chest X ray Blood test Observation/palpation Chest mobility Shape of chest wall Accessory
X-ray (Radiography), Chest
 X-ray (Radiography), Chest What is a Chest X-ray (Chest Radiography)? The chest x-ray is the most commonly performed diagnostic x-ray examination. A chest x-ray makes images of the heart, lungs, airways,
X-ray (Radiography), Chest What is a Chest X-ray (Chest Radiography)? The chest x-ray is the most commonly performed diagnostic x-ray examination. A chest x-ray makes images of the heart, lungs, airways,
X-ray (Radiography) - Chest
 Scan for mobile link. X-ray (Radiography) - Chest What is a Chest X-ray (Chest Radiography)? The chest x-ray is the most commonly performed diagnostic x-ray examination. A chest x-ray produces images of
Scan for mobile link. X-ray (Radiography) - Chest What is a Chest X-ray (Chest Radiography)? The chest x-ray is the most commonly performed diagnostic x-ray examination. A chest x-ray produces images of
Lung Sonography. Rahul Khosla Pulmonary & Critical Care Medicine Veterans Affairs Medical Center, Washington DC USA. 1.
 6 Lung Sonography Rahul Khosla Pulmonary & Critical Care Medicine Veterans Affairs Medical Center, Washington DC USA 1. Introduction Lung ultrasonography has come of age and is a well established technique
6 Lung Sonography Rahul Khosla Pulmonary & Critical Care Medicine Veterans Affairs Medical Center, Washington DC USA 1. Introduction Lung ultrasonography has come of age and is a well established technique
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
General Information About Non-Small Cell Lung Cancer
 General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
General Information About Non-Small Cell Lung Cancer Non-small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing
The lung has, step by step,
 Ultrasound in the management of thoracic disease Daniel A. Lichtenstein, MD Using simple and standardized semiology, the lung appears accessible to ultrasound, despite previous opinions otherwise. Lung
Ultrasound in the management of thoracic disease Daniel A. Lichtenstein, MD Using simple and standardized semiology, the lung appears accessible to ultrasound, despite previous opinions otherwise. Lung
Sonography for Trauma
 Sonography for Trauma Christine Butts and Justin Cook 9 KEY POINTS Focused abdominal sonography for trauma (FAST) is sensitive and specific for the detection of intraperitoneal free fluid, but it has poor
Sonography for Trauma Christine Butts and Justin Cook 9 KEY POINTS Focused abdominal sonography for trauma (FAST) is sensitive and specific for the detection of intraperitoneal free fluid, but it has poor
Understanding Pleural Mesothelioma
 Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
Understanding Pleural Mesothelioma UHN Information for patients and families Read this booklet to learn about: What is pleural mesothelioma? What causes it? What are the symptoms? What tests are done to
How To Learn To Perform An Ultrasound
 CAE ICCU E-Learning CAE VIMEDIX Ultrasound Simulator Master Ultrasonography of the Thoracic, Abdominal and Pelvic Cavities An Engaging Learning Solution for Ultrasound Hands-on Simulation, Multimedia Content,
CAE ICCU E-Learning CAE VIMEDIX Ultrasound Simulator Master Ultrasonography of the Thoracic, Abdominal and Pelvic Cavities An Engaging Learning Solution for Ultrasound Hands-on Simulation, Multimedia Content,
Small cell lung cancer
 Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
Congestive Heart Failure
 William Herring, M.D. 2002 Congestive Heart Failure In Slide Show mode, to advance slides, press spacebar or click left mouse button Congestive Heart Failure Causes of Coronary artery disease Hypertension
William Herring, M.D. 2002 Congestive Heart Failure In Slide Show mode, to advance slides, press spacebar or click left mouse button Congestive Heart Failure Causes of Coronary artery disease Hypertension
Ultrasound - Vascular
 Scan for mobile link. Ultrasound - Vascular Vascular ultrasound uses sound waves to evaluate the body s circulatory system and help identify blockages and detect blood clots. A Doppler ultrasound study
Scan for mobile link. Ultrasound - Vascular Vascular ultrasound uses sound waves to evaluate the body s circulatory system and help identify blockages and detect blood clots. A Doppler ultrasound study
An abdominal ultrasound produces a picture of the organs and other structures in the upper abdomen.
 Scan for mobile link. Ultrasound - Abdomen Ultrasound imaging of the abdomen uses sound waves to produce pictures of the structures within the upper abdomen. It is used to help diagnose pain or distention
Scan for mobile link. Ultrasound - Abdomen Ultrasound imaging of the abdomen uses sound waves to produce pictures of the structures within the upper abdomen. It is used to help diagnose pain or distention
Principles of Medical Ultrasound. Pai-Chi Li Department of Electrical Engineering National Taiwan University
 Principles of Medical Ultrasound Pai-Chi Li Department of Electrical Engineering National Taiwan University What is Medical Ultrasound? Prevention: actions taken to avoid diseases. Diagnosis: the process
Principles of Medical Ultrasound Pai-Chi Li Department of Electrical Engineering National Taiwan University What is Medical Ultrasound? Prevention: actions taken to avoid diseases. Diagnosis: the process
R/F. Efforts to Reduce Exposure Dose in Chest Tomosynthesis Targeting Lung Cancer Screening. 3. Utility of Chest Tomosynthesis. 1.
 R/F Efforts to Reduce Exposure Dose in Chest Tomosynthesis Targeting Lung Cancer Screening Department of Radiology, National Cancer Center Hospital East Kaoru Shimizu Ms. Kaoru Shimizu 1. Introduction
R/F Efforts to Reduce Exposure Dose in Chest Tomosynthesis Targeting Lung Cancer Screening Department of Radiology, National Cancer Center Hospital East Kaoru Shimizu Ms. Kaoru Shimizu 1. Introduction
Percutaneous Abscess Drainage
 Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
Scan for mobile link. Percutaneous Abscess Drainage An abscess is an infected fluid collection within the body. Percutaneous abscess drainage uses imaging guidance to place a thin needle through the skin
Defending the Rest Basics on Lung Cancer, Other Cancers and Asbestosis: Review of the B-Read and Pulmonary Function Testing
 Defending the Rest Basics on Lung Cancer, Other Cancers and Asbestosis: Review of the B-Read and Pulmonary Function Testing ASBESTOSIS November 2013 Bruce T. Bishop Lucy L. Brandon Willcox & Savage 440
Defending the Rest Basics on Lung Cancer, Other Cancers and Asbestosis: Review of the B-Read and Pulmonary Function Testing ASBESTOSIS November 2013 Bruce T. Bishop Lucy L. Brandon Willcox & Savage 440
Mesothelioma. 1995-2013, The Patient Education Institute, Inc. www.x-plain.com ocft0101 Last reviewed: 03/21/2013 1
 Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
CHEST TUBES AND CHEST DRAINAGE SYSTEMS
 CHEST TUBES AND CHEST DRAINAGE SYSTEMS Central Nursing Orientation April 2008 Revised September 2011 OBJECTIVES Describe common tubes and indications for use at LHSC Review indications and contraindications,
CHEST TUBES AND CHEST DRAINAGE SYSTEMS Central Nursing Orientation April 2008 Revised September 2011 OBJECTIVES Describe common tubes and indications for use at LHSC Review indications and contraindications,
Autonomous Diagnostic Imaging Performed by Untrained Operators using Augmented Reality as a Form of Just in Time Training
 Autonomous Diagnostic Imaging Performed by Untrained Operators using Augmented Reality as a Form of Just in Time Training PROPOSAL TEAM PI: David S. Martin, MS, Wyle Science, Technology, and Engineering
Autonomous Diagnostic Imaging Performed by Untrained Operators using Augmented Reality as a Form of Just in Time Training PROPOSAL TEAM PI: David S. Martin, MS, Wyle Science, Technology, and Engineering
Patient Prep Information
 Stereotactic Breast Biopsy Patient Prep Information Imaging Services Cannon Memorial Hospital Watauga Medical Center Table Weight Limits for each facility Cannon Memorial Hospital Watauga Medical Center
Stereotactic Breast Biopsy Patient Prep Information Imaging Services Cannon Memorial Hospital Watauga Medical Center Table Weight Limits for each facility Cannon Memorial Hospital Watauga Medical Center
Lung Cancer: Diagnosis, Staging and Treatment
 PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
PATIENT EDUCATION patienteducation.osumc.edu Lung Cancer: Diagnosis, Staging and Treatment Cancer begins in our cells. Cells are the building blocks of our tissues. Tissues make up the organs of the body.
Ultrasound Billing CPT Codes Summary and Notes
 Ultrasound Billing CPT Codes Summary and Notes CPT codes for ultrasound examinations are considered to be complete studies unless specified as limited studies in their code definitions. A limited study
Ultrasound Billing CPT Codes Summary and Notes CPT codes for ultrasound examinations are considered to be complete studies unless specified as limited studies in their code definitions. A limited study
Thoracic Ultrasound. Joel P. Turner, MD, MSc, FRCP a,b,c,d, *, Jerrald Dankoff, MDCM, CSPQ e
 Thoracic Ultrasound Joel P. Turner, MD, MSc, FRCP a,b,c,d, *, Jerrald Dankoff, MDCM, CSPQ e KEYWORDS Ultrasound Thoracic Pneumothorax Pleural effusion Pneumonia Blue B-lines Pleural line Patients with
Thoracic Ultrasound Joel P. Turner, MD, MSc, FRCP a,b,c,d, *, Jerrald Dankoff, MDCM, CSPQ e KEYWORDS Ultrasound Thoracic Pneumothorax Pleural effusion Pneumonia Blue B-lines Pleural line Patients with
UW MEDICINE PATIENT EDUCATION. Aortic Stenosis. What is heart valve disease? What is aortic stenosis?
 UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
UW MEDICINE PATIENT EDUCATION Aortic Stenosis Causes, symptoms, diagnosis, and treatment This handout describes aortic stenosis, a narrowing of the aortic valve in your heart. It also explains how this
Pleural Ultrasonography
 Clin Chest Med 27 (2006) 215 227 Pleural Ultrasonography Paul H. Mayo, MD a, T, Peter Doelken, MD b a Albert Einstein College of Medicine, Bronx, NY, USA b Division of Pulmonary, Critical Care, Allergy,
Clin Chest Med 27 (2006) 215 227 Pleural Ultrasonography Paul H. Mayo, MD a, T, Peter Doelken, MD b a Albert Einstein College of Medicine, Bronx, NY, USA b Division of Pulmonary, Critical Care, Allergy,
First floor, Main Hospital North Services provided 24/7 365 days per year
 First floor, Main Hospital North Services provided 24/7 365 days per year General Radiology (X-ray) Fluoroscopy Ultrasound (Sonography) Nuclear Medicine P.E.T. imaging Computed Tomography (CT scan) Magnetic
First floor, Main Hospital North Services provided 24/7 365 days per year General Radiology (X-ray) Fluoroscopy Ultrasound (Sonography) Nuclear Medicine P.E.T. imaging Computed Tomography (CT scan) Magnetic
Inferior Vena Cava filter and removal
 Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Inferior Vena Cava filter and removal What is Inferior Vena Cava Filter Placement and Removal? An inferior vena cava filter placement procedure involves an interventional radiologist (a specialist doctor)
Health Science Career Field Allied Health and Nursing Pathway (JM)
 Health Science Career Field Allied Health and Nursing Pathway (JM) ODE Courses Possible Sinclair Courses CTAG Courses for approved programs Health Science and Technology 1 st course in the Career Field
Health Science Career Field Allied Health and Nursing Pathway (JM) ODE Courses Possible Sinclair Courses CTAG Courses for approved programs Health Science and Technology 1 st course in the Career Field
The degree of liver inflammation or damage (grade) Presence and extent of fatty liver or other metabolic liver diseases
 ilearning about your health Liver Biopsy www.cpmc.org/learning What is a Liver Biopsy? A liver biopsy is a procedure where a specially trained doctor (typically a hepatologist, radiologist, or gastroenterologist)
ilearning about your health Liver Biopsy www.cpmc.org/learning What is a Liver Biopsy? A liver biopsy is a procedure where a specially trained doctor (typically a hepatologist, radiologist, or gastroenterologist)
Emergency Ultrasound Course
 Emergency Ultrasound Course Dr Justin Bowra ED Course Manual 2: EFAST Extended Focused Assessment with Sonography in Trauma JUSTIN BOWRA 1 The Questions: 1. Is there free fluid (FF) a. In the pleural space?
Emergency Ultrasound Course Dr Justin Bowra ED Course Manual 2: EFAST Extended Focused Assessment with Sonography in Trauma JUSTIN BOWRA 1 The Questions: 1. Is there free fluid (FF) a. In the pleural space?
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
THORACIC DIAGNOSTIC ASSESMENT PROGRAM (DAP) PATIENT INFORMATION FOR:
 central east regional cancer program in partnership with cancer care ontario THORACIC DIAGNOSTIC ASSESMENT PROGRAM (DAP) PATIENT INFORMATION FOR: Thoracic dap booklet March2012.indd 1 SCHEDULED TESTS YOUR
central east regional cancer program in partnership with cancer care ontario THORACIC DIAGNOSTIC ASSESMENT PROGRAM (DAP) PATIENT INFORMATION FOR: Thoracic dap booklet March2012.indd 1 SCHEDULED TESTS YOUR
Health Care Careers in the Field of Imaging. Shari Workman, MSM,PHR,CIR MultiCare Health System Senior Recruiter/Employment Specialist
 Health Care Careers in the Field of Imaging Shari Workman, MSM,PHR,CIR MultiCare Health System Senior Recruiter/Employment Specialist What is Health Care Imaging? Technologists working with patients, using
Health Care Careers in the Field of Imaging Shari Workman, MSM,PHR,CIR MultiCare Health System Senior Recruiter/Employment Specialist What is Health Care Imaging? Technologists working with patients, using
Incidence of Incidental Thyroid Nodules on Computed Tomography (CT) Scan of the Chest Performed for Reasons Other than Thyroid Disease
 International Journal of Clinical Medicine, 2011, 2, 264-268 doi:10.4236/ijcm.2011.23042 Published Online July 2011 (http://www.scirp.org/journal/ijcm) Incidence of Incidental Thyroid Nodules on Computed
International Journal of Clinical Medicine, 2011, 2, 264-268 doi:10.4236/ijcm.2011.23042 Published Online July 2011 (http://www.scirp.org/journal/ijcm) Incidence of Incidental Thyroid Nodules on Computed
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM
 CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
CHAPTER 1: THE LUNGS AND RESPIRATORY SYSTEM INTRODUCTION Lung cancer affects a life-sustaining system of the body, the respiratory system. The respiratory system is responsible for one of the essential
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Simple Thoracostomy Avoids Chest Drain Insertion in Prehospital Trauma
 Simple Thoracostomy Avoids Chest Drain Insertion in Prehospital Trauma Deakin, C. D. MA, MRCP, FRCA; Davies, G. MRCP; Wilson, A. FRCS Author Information From the Helicopter Emergency Medical Service, Royal
Simple Thoracostomy Avoids Chest Drain Insertion in Prehospital Trauma Deakin, C. D. MA, MRCP, FRCA; Davies, G. MRCP; Wilson, A. FRCS Author Information From the Helicopter Emergency Medical Service, Royal
Preparation iagnostic Medical Sonographer Overview"
 Diagnostic Medical Sonographer Overview The Field - Preparation - Specialty Areas - Day in the Life - Earnings - Employment - Career Path Forecast - Professional Organizations The Field Diagnostic imaging
Diagnostic Medical Sonographer Overview The Field - Preparation - Specialty Areas - Day in the Life - Earnings - Employment - Career Path Forecast - Professional Organizations The Field Diagnostic imaging
Case III. Disscussion. the UHP ultrasound protocol. Novel Ultrasound Approach to the Empiric Evaluation of the Undifferentiated Hypotensive Patient
 The UHP Ultrasound Protocol: A Novel Ultrasound Approach to the Empiric Evaluation of the Undifferentiated Hypotensive Patient JOHN S. ROSE, MD,* AARON E. BAIR, MD,* DIKU MANDAVIA, MD, AND DONNA J. KINSER,
The UHP Ultrasound Protocol: A Novel Ultrasound Approach to the Empiric Evaluation of the Undifferentiated Hypotensive Patient JOHN S. ROSE, MD,* AARON E. BAIR, MD,* DIKU MANDAVIA, MD, AND DONNA J. KINSER,
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide
 What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Lung cancer is one of the most common cancers. About 170,000
What If I Have a Spot on My Lung? Do I Have Cancer? Patient Education Guide A M E R I C A N C O L L E G E O F C H E S T P H Y S I C I A N S Lung cancer is one of the most common cancers. About 170,000
Administrative. Patient name Date compare with previous Position markers R-L, upright, supine Technical quality
 CHEST X-RAY Administrative Patient name Date compare with previous Position markers R-L, upright, supine Technical quality AP or PA ( with x-ray beam entering from back of patient, taken at 6 feet) Good
CHEST X-RAY Administrative Patient name Date compare with previous Position markers R-L, upright, supine Technical quality AP or PA ( with x-ray beam entering from back of patient, taken at 6 feet) Good
The Practice Standards for Medical Imaging and Radiation Therapy. Sonography Practice Standards
 The Practice Standards for Medical Imaging and Radiation Therapy Sonography Practice Standards 2015 American Society of Radiologic Technologists. All rights reserved. Reprinting all or part of this document
The Practice Standards for Medical Imaging and Radiation Therapy Sonography Practice Standards 2015 American Society of Radiologic Technologists. All rights reserved. Reprinting all or part of this document
School of Diagnostic Medical Sonography
 Semester 1 Orientation - 101 This class is an introduction to sonography which includes a basic anatomy review, introduction to sonographic scanning techniques and physical principles. This curriculum
Semester 1 Orientation - 101 This class is an introduction to sonography which includes a basic anatomy review, introduction to sonographic scanning techniques and physical principles. This curriculum
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES
 APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
APPENDIX B SAMPLE PEDIATRIC CRITICAL CARE NURSE PRACTITIONER GOALS AND OBJECTIVES The critical care nurse practitioner orientation is an individualized process based on one s previous experiences and should
International Journal of Case Reports in Medicine
 International Journal of Case Reports in Medicine Vol. 2013 (2013), Article ID 409830, 15 minipages. DOI:10.5171/2013.409830 www.ibimapublishing.com Copyright 2013 Andrew Thomas Low, Iain Smith and Simon
International Journal of Case Reports in Medicine Vol. 2013 (2013), Article ID 409830, 15 minipages. DOI:10.5171/2013.409830 www.ibimapublishing.com Copyright 2013 Andrew Thomas Low, Iain Smith and Simon
How To Understand How Cancer Works
 Mesothelioma Understanding your diagnosis Mesothelioma Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount of
Mesothelioma Understanding your diagnosis Mesothelioma Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount of
Facing Lung Cancer? Learn why da Vinci Surgery may be your best treatment option for lung cancer.
 Facing Lung Cancer? Learn why da Vinci Surgery may be your best treatment option for lung cancer. The Condition: Lung Cancer The lung is the organ that moves oxygen through your body. You have two lungs
Facing Lung Cancer? Learn why da Vinci Surgery may be your best treatment option for lung cancer. The Condition: Lung Cancer The lung is the organ that moves oxygen through your body. You have two lungs
Duplication Images in Vascular Sonography
 Article Duplication Images in Vascular Sonography Jonathan M. Rubin, MD, PhD, Jing Gao, MD, Keith Hetel, MD, Robert Min, MD Objective. The purpose of this study was to determine the characteristics and
Article Duplication Images in Vascular Sonography Jonathan M. Rubin, MD, PhD, Jing Gao, MD, Keith Hetel, MD, Robert Min, MD Objective. The purpose of this study was to determine the characteristics and
Evaluation and treatment of emphysema in a preterm infant
 ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
U.S. Bureau of Labor Statistics. Radiology Tech
 From the: U.S. Bureau of Labor Statistics Radiology Tech What They Do Radiologic technologists (RTs) perform diagnostic imaging examinations, such as x rays, on patients. Duties RTs typically do the following:
From the: U.S. Bureau of Labor Statistics Radiology Tech What They Do Radiologic technologists (RTs) perform diagnostic imaging examinations, such as x rays, on patients. Duties RTs typically do the following:
Lung Cancer. This reference summary will help you better understand lung cancer and the treatment options that are available.
 Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
Lung Cancer Introduction Lung cancer is the number one cancer killer of men and women. Over 165,000 people die of lung cancer every year in the United States. Most cases of lung cancer are related to cigarette
How To Use An Ultrasound For Medical Research
 Scan for mobile link. General Ultrasound What is General Ultrasound Imaging? Ultrasound is safe and painless, and produces pictures of the inside of the body using sound waves. Ultrasound imaging, also
Scan for mobile link. General Ultrasound What is General Ultrasound Imaging? Ultrasound is safe and painless, and produces pictures of the inside of the body using sound waves. Ultrasound imaging, also
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Breast cancer Faculty of Clinical Radiology www.rcr.ac.uk Contents Breast cancer 2 Clinical background 2 Who
Pulmonary Ventilation
 Pulmonary Ventilation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Pulmonary ventilation, or breathing, is the
Pulmonary Ventilation Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) Page 1. Introduction Pulmonary ventilation, or breathing, is the
CHAPTER 4 QUALITY ASSURANCE AND TEST VALIDATION
 CHAPTER 4 QUALITY ASSURANCE AND TEST VALIDATION CINDY WEILAND AND SANDRA L. KATANICK Continued innovations in noninvasive testing equipment provide skilled sonographers and physicians with the technology
CHAPTER 4 QUALITY ASSURANCE AND TEST VALIDATION CINDY WEILAND AND SANDRA L. KATANICK Continued innovations in noninvasive testing equipment provide skilled sonographers and physicians with the technology
by joseph e. muscolino, DO photography by yanik chauvin
 by joseph e. muscolino, DO photography by yanik chauvin body mechanics palpation of the anterior neck ESOUCES For more information go to www.medlineplus.gov and search under anterior neck. The anterior
by joseph e. muscolino, DO photography by yanik chauvin body mechanics palpation of the anterior neck ESOUCES For more information go to www.medlineplus.gov and search under anterior neck. The anterior
Chapter 2 - Anatomy & Physiology of the Respiratory System
 Chapter 2 - Anatomy & Physiology of the Respiratory System Written by - AH Kendrick & C Newall 2.1 Introduction 2.2 Gross Anatomy of the Lungs, 2.3 Anatomy of the Thorax, 2.4 Anatomy and Histology of the
Chapter 2 - Anatomy & Physiology of the Respiratory System Written by - AH Kendrick & C Newall 2.1 Introduction 2.2 Gross Anatomy of the Lungs, 2.3 Anatomy of the Thorax, 2.4 Anatomy and Histology of the
Imaging Technology. Diagnostic Medical Sonographer, Dosimetrist, Nuclear Medicine Technologist, Radiation Therapist, Radiologic Technologist
 Imaging Technology Diagnostic Medical Sonographer, Dosimetrist, Nuclear Medicine Technologist, Radiation Therapist, Radiologic Technologist Diagnostic Medical Sonographer, Dosimetrist Diagnostic Medical
Imaging Technology Diagnostic Medical Sonographer, Dosimetrist, Nuclear Medicine Technologist, Radiation Therapist, Radiologic Technologist Diagnostic Medical Sonographer, Dosimetrist Diagnostic Medical
Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment.
 Dictionary Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment. Applicator A device used to hold a radioactive source
Dictionary Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment. Applicator A device used to hold a radioactive source
Jefferson College Transfer Guide to St. Louis Community College Forest Park Clinical Laboratory Technology
 Transfer Guide to St. Louis Community College Clinical Laboratory Technology STLCC- is required to complete the AAS Degree. The clinical laboratory technician analyzes human blood and tissue samples. These
Transfer Guide to St. Louis Community College Clinical Laboratory Technology STLCC- is required to complete the AAS Degree. The clinical laboratory technician analyzes human blood and tissue samples. These
Ultrasound. for Vascular Access and Regional Anesthesia. Brian A. Pollard, md, med
 Ultrasound Guidance for Vascular Access and Regional Anesthesia Brian A. Pollard, md, med ULTRASOUND GUIDANCE for Vascular Access and Regional Anesthesia Brian A. Pollard BSc, MD, MEd, FRCPC www.usrabook.com
Ultrasound Guidance for Vascular Access and Regional Anesthesia Brian A. Pollard, md, med ULTRASOUND GUIDANCE for Vascular Access and Regional Anesthesia Brian A. Pollard BSc, MD, MEd, FRCPC www.usrabook.com
Mesothelioma: Questions and Answers
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Mesothelioma: Questions
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Mesothelioma: Questions
2011 Radiology Diagnosis Coding Update Questions and Answers
 2011 Radiology Diagnosis Coding Update Questions and Answers How can we subscribe to the Coding Clinic for ICD-9 guidelines and updates? The American Hospital Association publishes this quarterly newsletter.
2011 Radiology Diagnosis Coding Update Questions and Answers How can we subscribe to the Coding Clinic for ICD-9 guidelines and updates? The American Hospital Association publishes this quarterly newsletter.
Department of Surgery
 What is emphysema? 2004 Regents of the University of Michigan Emphysema is a chronic disease of the lungs characterized by thinning and overexpansion of the lung-like blisters (bullae) in the lung tissue.
What is emphysema? 2004 Regents of the University of Michigan Emphysema is a chronic disease of the lungs characterized by thinning and overexpansion of the lung-like blisters (bullae) in the lung tissue.
Training in Clinical Radiology
 Training in Clinical Radiology What is Clinical Radiology? Clinical radiology relates to the diagnosis or treatment of a patient through the use of medical imaging. Diagnostic imaging uses plain X-ray
Training in Clinical Radiology What is Clinical Radiology? Clinical radiology relates to the diagnosis or treatment of a patient through the use of medical imaging. Diagnostic imaging uses plain X-ray
Lung Cancer Understanding your diagnosis
 Lung Cancer Understanding your diagnosis Lung Cancer Understanding your diagnosis When you first hear that you have cancer you may feel alone and afraid. You may be overwhelmed by the large amount of information
Lung Cancer Understanding your diagnosis Lung Cancer Understanding your diagnosis When you first hear that you have cancer you may feel alone and afraid. You may be overwhelmed by the large amount of information
Preoperative Laboratory and Diagnostic Studies
 Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Preoperative Laboratory and Diagnostic Studies Preoperative Labratorey and Diagnostic Studies The concept of standardized testing in all presurgical patients regardless of age or medical condition is no
Airways Resistance and Airflow through the Tracheobronchial Tree
 Airways Resistance and Airflow through the Tracheobronchial Tree Lecturer: Sally Osborne, Ph.D. Department of Cellular & Physiological Sciences Email: [email protected] Useful links: www.sallyosborne.com
Airways Resistance and Airflow through the Tracheobronchial Tree Lecturer: Sally Osborne, Ph.D. Department of Cellular & Physiological Sciences Email: [email protected] Useful links: www.sallyosborne.com
Integumentary System Individual Exercises
 Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
Integumentary System Individual Exercises 1. A physician performs an incision and drainage of a subcutaneous abscess in his office for a particularly uncooperative established patient. How should this
RESPIRATORY VENTILATION Page 1
 Page 1 VENTILATION PARAMETERS A. Lung Volumes 1. Basic volumes: elements a. Tidal Volume (V T, TV): volume of gas exchanged each breath; can change as ventilation pattern changes b. Inspiratory Reserve
Page 1 VENTILATION PARAMETERS A. Lung Volumes 1. Basic volumes: elements a. Tidal Volume (V T, TV): volume of gas exchanged each breath; can change as ventilation pattern changes b. Inspiratory Reserve
Inferior Vena Cava Filter Placement and Removal
 Scan for mobile link. Inferior Vena Cava Filter Placement and Removal What is Inferior Vena Cava Filter Placement and Removal? In an inferior vena cava filter placement procedure, interventional radiologists
Scan for mobile link. Inferior Vena Cava Filter Placement and Removal What is Inferior Vena Cava Filter Placement and Removal? In an inferior vena cava filter placement procedure, interventional radiologists
Test Request Tip Sheet
 With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely necessary. The study
With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely necessary. The study
Lung cancer forms in tissues of the lung, usually in the cells lining air passages.
 Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
Scan for mobile link. Lung Cancer Lung cancer usually forms in the tissue cells lining the air passages within the lungs. The two main types are small-cell lung cancer (usually found in cigarette smokers)
IONISING RADIATION. X-rays: benefit and risk
 IONISING RADIATION X-rays: benefit and risk Impress Federal Office for Radiation Protection Postfach 10 01 49 D - 38201 Salzgitter Telephone: + 49 (0) 30 18333-0 Fax: + 49 (0) 30 18333-1885 Website: www.bfs.de
IONISING RADIATION X-rays: benefit and risk Impress Federal Office for Radiation Protection Postfach 10 01 49 D - 38201 Salzgitter Telephone: + 49 (0) 30 18333-0 Fax: + 49 (0) 30 18333-1885 Website: www.bfs.de
HEALTH CARE FOR EXPOSURE TO ASBESTOS. 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.
 HEALTH CARE FOR PATIENTS WITH EXPOSURE TO ASBESTOS 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.ca HEALTH CARE FOR PATIENTS WITH EXPOSURE
HEALTH CARE FOR PATIENTS WITH EXPOSURE TO ASBESTOS 2010 The SafetyNet Centre for Occupational Health and Safety Research Memorial University www.safetynet.mun.ca HEALTH CARE FOR PATIENTS WITH EXPOSURE
Human Anatomy and Physiology The Respiratory System
 Human Anatomy and Physiology The Respiratory System Basic functions of the respiratory system: as a Gas exchange supply oxygen to aerobic tissues in the body and remove carbon dioxide waste product. in-
Human Anatomy and Physiology The Respiratory System Basic functions of the respiratory system: as a Gas exchange supply oxygen to aerobic tissues in the body and remove carbon dioxide waste product. in-
CT scans and IV contrast (radiographic iodinated contrast) utilization in adults
 CT scans and IV contrast (radiographic iodinated contrast) utilization in adults At United Radiology Group, a majority of CT exams are performed either with IV contrast or without while just a few exams
CT scans and IV contrast (radiographic iodinated contrast) utilization in adults At United Radiology Group, a majority of CT exams are performed either with IV contrast or without while just a few exams
PARAMEDIC TRAINING CLINICAL OBJECTIVES
 Page 1 of 21 GENERAL PATIENT UNIT When assigned to the General Patient unit paramedic student should gain knowledge and experience in the following: 1. Appropriate communication with patients and members
Page 1 of 21 GENERAL PATIENT UNIT When assigned to the General Patient unit paramedic student should gain knowledge and experience in the following: 1. Appropriate communication with patients and members
Chest Pain. Acute Myocardial Infarction: Differential Diagnosis and Patient Management. Common complaint in ED. Wide range of etiologies
 Acute Myocardial Infarction: Differential Diagnosis and Patient Management Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Chest Pain
Acute Myocardial Infarction: Differential Diagnosis and Patient Management Presented By: Barbara Furry, RN-BC, MS, CCRN, FAHA Director The Center of Excellence in Education Director of HERO Chest Pain
Basics of Ultrasound Imaging
 2 Basics of Ultrasound Imaging Vincent Chan and Anahi Perlas Introduction... Basic Principles of B-Mode US... Generation of Ultrasound Pulses... Ultrasound Wavelength and Frequency... Ultrasound Tissue
2 Basics of Ultrasound Imaging Vincent Chan and Anahi Perlas Introduction... Basic Principles of B-Mode US... Generation of Ultrasound Pulses... Ultrasound Wavelength and Frequency... Ultrasound Tissue
The importance of the initial assessment in trauma patients /in a prehospital setting: Therapeutic decisions Patient outcomes
 The importance of the initial assessment in trauma patients /in a prehospital setting: Therapeutic decisions Patient outcomes Reporter: Intern 鄭 琬 蓉 Supervisor: Dr. 朱 健 銘 Date: Sep. 16th, 2014 The nonspecific
The importance of the initial assessment in trauma patients /in a prehospital setting: Therapeutic decisions Patient outcomes Reporter: Intern 鄭 琬 蓉 Supervisor: Dr. 朱 健 銘 Date: Sep. 16th, 2014 The nonspecific
Pulmonary Patterns VMA 976
 Pulmonary Patterns VMA 976 PULMONARY PATTERNS Which pulmonary patterns are commonly described in veterinary medicine? PULMONARY PATTERNS Normal Alveolar Interstitial Structured/Nodular Unstructured Bronchial
Pulmonary Patterns VMA 976 PULMONARY PATTERNS Which pulmonary patterns are commonly described in veterinary medicine? PULMONARY PATTERNS Normal Alveolar Interstitial Structured/Nodular Unstructured Bronchial
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Thoracic Epidural Catheterization Using Ultrasound in Obese Patients for Bariatric Surgery
 IBIMA Publishing Journal of Research in Obesity http://www.ibimapublishing.com/journals/obes/obes.html Vol. 2014 (2014), Article ID 538833, 6 pages DOI: 10.5171/2014.538833 Research Article Thoracic Epidural
IBIMA Publishing Journal of Research in Obesity http://www.ibimapublishing.com/journals/obes/obes.html Vol. 2014 (2014), Article ID 538833, 6 pages DOI: 10.5171/2014.538833 Research Article Thoracic Epidural
The Field. Radiologic technologists take x-rays and administer nonradioactive materials into patients' bloodstreams for diagnostic purposes.
 Radiologic Technologist Overview The Field - Specialty Areas - Preparation - Day in the Life - Earnings - Employment - Career Path Forecast - Professional Organizations The Field Radiologic technologists
Radiologic Technologist Overview The Field - Specialty Areas - Preparation - Day in the Life - Earnings - Employment - Career Path Forecast - Professional Organizations The Field Radiologic technologists
The leader in ultrasound training models. Over 150 different ultrasound training models available at www.bluephantom.com
 The leader in ultrasound training models Over 150 different ultrasound training models available at www.bluephantom.com The most realistic, ultra-durable Ultrasound training models available anywhere realistic
The leader in ultrasound training models Over 150 different ultrasound training models available at www.bluephantom.com The most realistic, ultra-durable Ultrasound training models available anywhere realistic
Vascular Access. Chapter 3
 Vascular Access Chapter 3 Vascular Access Introduction Obtaining vascular access in infants and children can be difficult even under optimal conditions. Attempting emergent access in a hypotensive, struggling
Vascular Access Chapter 3 Vascular Access Introduction Obtaining vascular access in infants and children can be difficult even under optimal conditions. Attempting emergent access in a hypotensive, struggling
Emphysema. Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide.
 Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide. Emphysema involves damage to the air sacs in the lungs. This
Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects about 64 million people worldwide. Emphysema involves damage to the air sacs in the lungs. This
