Clinical Pathology: Odontogenic and Nonodontogenic Tumors of the Jaws
|
|
|
- Laurence Randolf Harrington
- 10 years ago
- Views:
Transcription
1 Ch23-F10053.qxd 5/15/06 6:00 PM Page C H A P T E R Clinical Pathology: Odontogenic and Nonodontogenic Tumors of the Jaws M. ANTHONY POGREL, BRIAN L. SCHMIDT, CHAD G. ROBERTSON KEY POINTS The differential diagnosis should be established early and should guide the diagnostic work-up, method of biopsy, and planned treatment of jaw tumors. Overall, odontogenic tumors are rare and form only a small proportion of the lesions found in the jaw. They are virtually all benign. Several tumors exist, which only appear to occur in the jaws. Although they do not normally contain odontogenic tissue, they are probably odontogenic because of their site of origin. Several lesions of the jaws contain giant cells, and their differentiation often presents a problem. The diagnosis of a lesion of the jaw containing giant cells often depends on a combination of histological examination, the clinical history, and ancillary laboratory tests. Treatment should be tailored to the biological behavior of the specific lesion. Obtaining a representative biopsy is of paramount importance. Many lesions are misdiagnosed on inadequate biopsy material. An adequate biopsy may require general anesthesia. ODONTOGENIC TUMORS OF THE JAW This rare group of tumors may derive from the toothforming elements of the jaws. In general, the more primitive the dental structures from which they are derived, the more aggressive they are thought to be, and the more mature the dental tissues, the less aggressive they are. The vast majority of these tumors are benign or locally aggressive with few malignant variants being reported. In many cases their relationship to the teeth is fairly clear-cut, both histologically and radiographically. In other cases, their relationship to teeth
2 Ch23-F10053.qxd 5/15/06 6:00 PM Page 491 PART II ONCOLOGY 491 and teeth-forming structures is less well defined in that tissues resembling dental tissues are rarely, if ever, found within them, and the assumption that they are odontogenic in origin derives from the fact that they are only found in the jaws and therefore may have a relation to teeth and teeth-bearing tissues. Conversely, tumors that are strongly thought to be odontogenic do have histologically similar lesions occurring in other parts of the body where teeth are not found (e.g., the relationship between the ameloblastoma and the adamantinoma of the tibia and the craniopharyngioma), and this sometimes causes confusion as to whether these tumors are truly odontogenic in origin. In general, odontogenic tumors only occur in the jaws, but they have been reported in tooth-bearing tissues in such structures as dermoid cysts and teratomas. CLASSIFICATION Odontogenic tumors are normally classified by their presumed tissue of origin, being epithelial, mesenchymal, or a mixed lesion (Box 23-1). Studies of odontogenic tumors reveal that there are often no clear divisions among many types of tumors, but rather a transition from one to another, and it is not unusual for tumors to show areas that resemble different types of tumors within the lesion. Because of this, there have been numerous attempts at reclassification of these lesions, as well as attempts to introduce new variants of lesions, which are generally extremely rare with only a handful of cases reported. In general these lesions have been avoided in this chapter. However, there are numerous reports of combined tumors, new tumors, and BOX 23-1 Odontogenic and Nonodontogenic Tumors of the Jaws ODONTOGENIC TUMORS EPITHELIAL TUMORS Benign: Ameloblastoma Calcifying epithelial odontogenic tumor Adenomatoid odontogenic tumor Squamous odontogenic tumor Malignant: Malignant ameloblastoma Clear cell odontogenic carcinoma Odontogenic carcinoma MESENCHYMAL TUMORS Benign: Odontogenic fibroma Cementoblastoma Odontogenic myxoma Cementifying fibroma Malignant: Ameloblastic fibrosarcoma MIXED EPITHELIAL AND MESENCHYMAL TUMORS (ALL BENIGN) Odontoma Ameloblastic fibroma Ameloblastic fibro-odontoma NONODONTOGENIC TUMORS OF THE JAWS Benign: Fibro-osseous tumors Ossifying fibroma Juvenile ossifying fibroma Langerhans cell disease Chronic localized Chronic disseminated Acute disseminated Lesions containing multinucleated giant cells Central giant cell granuloma Giant cell tumor Hyperparathyroidism Cherubism Aneurysmal bone cyst Neurogenic tumors Schwannoma Neurofibroma Osteoid osteoma and osteoblastoma Osteoma Chondroma Desmoplastic fibroma Malignant: Osteosarcoma Peripheral osteosarcoma Chondrosarcoma Mesenchymal chondrosarcoma Fibrosarcoma of bone Malignant fibrous histiocytoma Ewing s sarcoma Burkitt s lymphoma Multiple myeloma Solitary plasmacytoma of bone Malignant peripheral nerve sheath tumor Postradiation sarcoma of bone Metastatic carcinoma
3 Ch23-F10053.qxd 5/15/06 6:00 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS histological variants on established odontogenic tumors, and new classifications of these lesions will probably occur However, few of them have any clinical significance because the vast majority of these lesions are benign, and true malignant variants are extremely rare. BENIGN EPITHELIAL ODONTOGENIC TUMORS OF THE JAW AMELOBLASTOMA The ameloblastoma is a benign tumor located exclusively in the jaws. It has a distinctive histological appearance, and the diagnostic cells are columnar, basally staining cells arranged in a palisaded pattern along the basement membrane (Fig. 23-1). The name of this tumor derives from the fact that these cells closely resemble ameloblasts and are felt to be the cells of origin. Studies have almost certainly confirmed this hypothesis because it is now known that these cells are epithelial in origin and can express amelogenin, a precursor of enamel. 11,12 Histologically similar tumors seen in other parts of the body are now believed to be unrelated. The adamantinoma of the tibia is believed to be a locally malignant tumor of bone, 13,14 while the craniopharyngioma, which appears histologically similar, is felt to be a developmental anomaly arising from the remnants of Rathke s pouch. 15 Ameloblastomas are divided into three fairly distinct types: Solid ameloblastomas Cystic ameloblastomas Peripheral ameloblastomas Fig The typical histological appearance of a follicular ameloblastoma showing follicle of deeply staining basophilic cells in palisaded pattern on a basement membrane (hematoxylin and eosin, 40). Solid Ameloblastomas These tumors present with various histological patterns including follicular, plexiform, and granular cell variants. They are thought to be of histological interest only and do not affect the treatment or prognosis. 16 At one time the granular cell ameloblastoma was believed to be a more aggressive variant, but this is no longer the case. These tumors are benign but locally aggressive and can occasionally metastasize (see later). 17,18 They most commonly occur in the mandible, particularly around the angle of the mandible. They are most commonly found in the third to fifth decades of life. The male-to-female ratio is approximately equal. 19 The exact incidence is unknown, but there do appear to be geographical variations. In most studies they are the second commonest odontogenic lesions after odontomas. 20 However, studies from Africa suggest that they may represent more than 50% of all tumors of the head and neck, although this may be due to referral patterns and late presentation in these areas. 21,22 Larsson and Almeren 23 described an incidence of 0.3 cases per million people per year in Sweden. Imaging of these lesions is normally initially with plain radiography such as Panorex radiographs, reinforced by computed tomography (CT) scans, when there is any question of lingual or buccal expansion or perforation (Fig. 23-2). Although benign, these tumors are locally aggressive with a high recurrence rate when treated locally. Enucleation has been traditionally associated with a recurrence rate of between 60% and 80%, mandating that more aggressive treatment be performed. Histologically, cells have been shown to be present several millimeters from the radiographical margin of the lesion, 28 and this has led to a general principle that surgery should be performed with 1-centimeter bony margins around the radiographical limits of the lesion and a single tissue plane clearance in the case of soft tissue extension (e.g., a supraperiosteal dissection). Sometimes this can be carried out with a marginal mandibulectomy, but often a segmental resection is required. The inferior alveolar nerve is often sacrificed and can be reconstructed with a nerve graft if indicated. Techniques have been described for segmentally resecting the mandible with nerve preservation, but this does run the theoretical risk of recurrence around the nerve. 29 In the maxilla, wide margins can result in invasion of the sinus, nasal cavity, orbit, and infratemporal fossa. Intermediate techniques such as aggressive local curettage followed by liquid nitrogen cryotherapy have also been advocated These techniques have been associated with high levels of success and do deserve con-
4 Ch23-F10053.qxd 5/15/06 6:00 PM Page 493 PART II ONCOLOGY 493 A B C D Fig A large multilocular solid ameloblastoma of the right angle of the mandible and displacing teeth. A, Panorex. B, Axial computed tomography (CT) scan. C, Coronal CT scan. D, Resected specimen. sideration in treatment planning. Algorithms have been developed recommending curettage and cryotherapy for intrabony lesions and resection for lesions with an extraosseous component. 33 Maxillary Ameloblastomas. Maxillary ameloblastomas, although rarer, are often more troublesome than mandibular lesions. Histologically, they are identical and behave similarly except that their pathways to infiltrate are more numerous. Involvement of the maxillary sinus and nasal cavity tends to occur fairly early, and spread through the posterior wall of the maxilla into the pterygomaxillary space also occurs. Additionally, infiltration of the greater palatine canal up to the base of the skull is not unknown. Resection involving 1-cm margins is generally guided by CT or magnetic resonance imaging but often involves a maxillectomy, frequently with an incontinuity resection of the pterygoid plates (Fig. 23-3). Reconstruction of this area is normally by means of a skin graft and prosthetic obturator, although in some centers autogenous reconstruction of the palate with microvascular free flaps has been
5 Ch23-F10053.qxd 5/15/06 6:00 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS A B C D E Fig An ameloblastoma of the posterior maxilla extending to the pterygoid plates. A, Panorex (lesion arrowed). B, Axial computed tomography (CT) scan. C, Coronal CT scan. D, Weber-Fergusson incision for surgical access. E, Resected specimen. used. Ultimately, implants would be placed in any bone graft for the final prosthetic reconstruction. Cystic Ameloblastomas This is a difficult diagnosis because many ameloblastomas have cystic components within them (Fig. 23-4). A particular variant called a unicystic ameloblastoma was first described in 1977 by Robinson and Martinez. 34 They reported that the unicystic variant is a less aggressive type of ameloblastoma and suggested simple enucleation as treatment. The unicystic ameloblastoma has been reported to occur in a younger population (third decade) than its solid counterpart (fourth decade). It is most commonly encountered in the posterior mandible, followed by the parasymphysis region, anterior maxilla,
6 Ch23-F10053.qxd 5/15/06 6:00 PM Page 495 PART II ONCOLOGY 495 Fig mandible. Panorex radiograph of a multicystic ameloblastoma of the left posterior and posterior mandible (Fig. 23-5). It has also been reported that they commonly occur in association with an impacted tooth In 1988 unicystic ameloblastomas were classified into three histological subsets, 38 depending on whether they had a cystic lining composed of simple odontogenic epithelium or a cystic lesion showing intraluminal plexiform proliferation of the epithelial lining or a cystic lesion with epithelial invasion of the supporting connective tissue in either a follicular or plexiform form. At this time it was suggested that the first two groups were nonaggressive and may be treated by enucleation, whereas the third group would require more aggressive treatment. The problem with this philosophy is that in many cases the diagnosis can only be made retrospectively from the histological material. Clinical findings indicate that many lesions diagnosed radiographically as unicystic turn out to be multicystic on exploration, and it is quite likely that the prognosis for multicystic ameloblastomas is similar to solid ameloblastomas. Studies have also shown clinically that simple enucleation of so-called cystic ameloblastomas is actually associated with a high recurrence rate, which may be as high as 60%. 39 Therefore it would seem that simple enucleation is an inappropriate treatment for these lesions, and possibly a more aggressive treatment with peripheral ostectomy or liquid nitrogen cryotherapy, or both, may be more appropriate. 39 Peripheral Ameloblastoma The peripheral ameloblastoma is also known as the extraosseous ameloblastoma, or soft tissue ameloblastoma. It generally occurs in the gingiva, and there is no bony involvement. 40 Apparently, lesions that may previously have been reported as basal cell carcinoma of the gingiva may in fact be peripheral ameloblastomas. 41 The peripheral ameloblastoma is a painless, sessile, firm, exophytic growth that is usually relatively smooth or granular. It may also have a warty appearance. They are generally believed to represent between 2% and 10% of all ameloblastomas diagnosed. They have been reported in all age-groups between the ages of 9 and 92, with a mean age of Cases reported in males outnumber those in females 1.9 to 1. Seventy percent of peripheral ameloblastomas appear to occur in the mandible, with the body of the mandible anterior to the mental foramen being most frequently associated. Although histologically they appear identical to intraosseous ameloblastomas, palisading in the stellate reticulum is seldom conspicuous. Ghost cell formation is often present, and clear cells may be present. The cells of origin of these lesions are probably not ameloblasts, but they are more likely to arise directly from the surface epithelium or from residues from the dental lamina lying outside the bone. Some authors consider them to be hamartomas rather than neoplasms, and they appear to behave in a benign fashion and do not recur following simple complete excision. 40 CALCIFYING EPITHELIAL ODONTOGENIC TUMOR Pindborg first described this tumor in Earlier cases were probably classified as variants of ameloblastoma. This is a rare rumor, and fewer than 200 cases
7 Ch23-F10053.qxd 5/15/06 6:00 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS A B C Fig A unicystic ameloblastoma of the posterior right mandible. In all respects this appears like any other cystic lesion of the posterior mandible. A, Panorex. B, Axial computed tomography scan. C, Enucleated specimen. have been reported in the literature, so some aspects of its pathogenesis and behavior are still in doubt. The lesion has been reported in ages ranging from 13 to 80 with no gender predilection. The majority of cases occur in the mandible with a ratio of approximately 3:1. The mandibular premolar molar area appears to be the most common site for these lesions. They are slow growing and asymptomatic until they are either found by chance on routine radiography or they become large enough for the patient to be aware of them. Radiographically, they are classically described as being well defined, mixed radiolucent/radiopaque lesions, though radiolucent and radiopaque variants have been described. They can be unilocular or multilocular 43 (Fig. 23-6). Histologically, the calcifying epithelial odontogenic tumor (CEOT) is most characterized by sheets of large eosinophilic staining epithelial cells. The stroma is a hyaline-like homogenous material that has been identified as amyloid (Fig. 23-7). Liesegang rings are prominent calcifications in concentric shapes that can occur in the amyloid areas and account for the radiopacities seen radiographically. The lesion is thought to arise
8 Ch23-F10053.qxd 5/15/06 6:00 PM Page 497 PART II ONCOLOGY 497 A Fig Imaging studies of a calcifying epithelial odontogenic tumor. A, Panoral radiograph of a lesion of the posterior right mandible. B, Coronal computed tomography scan of lesion showing lingual perforation by the lesion. B reported following local enucleation. Malignant variants (odontogenic carcinoma) have been described rarely. 45 A prominent clear cell component (seen in 8% of lesions) may be associated with increased aggressiveness and cortical perforation. 46 In general the CEOT appears to be less aggressive than the solid ameloblastoma. Treatment is usually recommended as wide local excision with margins of 5 to 10 mm, which in the mandible may require a marginal resection or even segmental resection and subsequent reconstruction. Fig Typical histological appearance of a calcifying epithelial odontogenic tumor with sheets of darkly staining cells in a homogenous amyloid containing matrix (hematoxylin and eosin, 40). from the stratum intermedium tissue of the developing enamel organ. 44 The behavior of the calcifying epithelial odontogenic tumor remains in some doubt, but it is believed to be locally aggressive with recurrence rates of 14% to 20% ADENOMATOID ODONTOGENIC TUMOR The adenomatoid odontogenic tumor contains structures that resemble enamel formation. It is presumed to be of odontogenic origin, as it only occurs in the jaws. Immunohistochemical and ultrastructural findings have revealed that the eosinophilic deposits normally seen probably represent some form of enamel matrix and are positive for amelogenin in limited areas. 47 The adenomatoid odontogenic tumor is more common in females than males (1.9:1). It represents approximately 3% of odontogenic tumors and appears between the ages
9 Ch23-F10053.qxd 5/15/06 6:00 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS of 5 and 30 years. The most common site is the anterior maxilla, and this tumor is often found in association with impacted teeth (Fig. 23-8). Intraosseous follicular (70%), extrafollicular (26%), and peripheral variants (4%) have been described, but they are all histologically identical. 48 A subvariant of the extrafollicular type of adenomatoid odontogenic tumor may mimic periapical disease radiographically. 49 The classic radiographical appearance is of a pear-shaped radiolucency with speckled opaque foci distributed throughout the lesion, indicating calcification (Fig. 23-9). Magnetic resonance imaging findings correlate with radiography and histology. 50 Divergence of roots is not unusual. They are most often discovered as chance radiographical findings. Simple enucleation seems to be all that is necessary in the way of treatment (see Fig. 23-8), and although recurrences have been reported, they are usually because of incomplete primary excision. Clinically, they behave more like a hamartoma than a neoplasm. SQUAMOUS ODONTOGENIC TUMOR This rare odontogenic tumor was first described in It normally involves the alveolar process and appears to originate from the rests of Malassez in the periodontium. In the past it has been confused with other odontogenic entities such as ameloblastomas, carcinomas, and fibromas. 52 The tumor is often asymptomatic but can present with pain and tooth mobility. It appears to occur in the mandible and maxilla equally, though when in the maxilla it seems to favor the anterior maxilla. 53 When in the mandible, it favors the posterior mandible. Multiple lesions have been described, as have familial lesions. The age range appears to extend from the second to the seventh decade with a mean age of around 40. There is no gender predilection. The characteristic radiographical appearance is of a triangular shape or semilunar radiolucency associated with the roots of erupted or erupting teeth. 54 Histologically, the A B C Fig An adenomatoid odontogenic tumor. A, A firm swelling over the upper left canine and first premolar. B, Radiographical appearance showing a pearshaped lesion with speckled opaque foci. C, Clinical appearance of enucleated lesion.
10 Ch23-F10053.qxd 5/15/06 6:00 PM Page 499 PART II ONCOLOGY 499 A B C D Fig An ameloblastoma of the left posterior mandible. A, Presenting radiographical appearance as a well-developed radiolucency. B, Histological appearance of lesion showing plexiform appearance with some atypical and hyperchromatism (hematoxylin and eosin, 20). C, Axial computed tomography scan 3 years after initial resection showing a metastasis to the posterior orbit (arrow). D, Histological appearance of the metastasis showing dedifferentiation with hyperchromatism, pleomorphism, and mitotic figures. Lesion is now an ameloblastic carcinoma (hematoxylin and eosin, 80).
11 Ch23-F10053.qxd 5/15/06 6:00 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS tumor is characterized by the formation of variably sized nests and cores of uniform benign-appearing squamous epithelium with occasional vacuolization and keratinization. Treatment is by conservative surgical excision, which is normally curative, though recurrences have been reported. MALIGNANT EPITHELIAL ODONTOGENIC TUMORS OF THE JAW Malignant odontogenic tumors are rare and comprise only about 4% of all odontogenic tumors. 55 MALIGNANT VARIANTS OF AMELOBLASTOMA Malignancy in the ameloblastoma has been subdivided into two distant lesions. A malignant ameloblastoma is diagnosed when a seemingly histologically benign ameloblastoma produces a metastasis resembling the original lesion. Both lesions are microscopically well differentiated with the characteristic histological features of the ameloblastoma. The second lesion is the ameloblastic carcinoma, which is a term reserved for tumors that demonstrate a malignant morphological appearance regardless of whether metastasis is present at the time of discovery and treatment. Malignant Ameloblastoma As already stated, these cases are diagnosed retrospectively when a metastasis is discovered. These metastases generally only arise after many surgical attempts at treatment of the original lesion and are often isolated pulmonary metastases that can sometimes be treated surgically. 18,56-58 Lymph node metastases also occur. In some cases the metastasis may in fact be caused by aspiration or implantation at the time of surgery. Ameloblastic Carcinoma In this case, either the primary or metastatic lesion exhibits less microscopic differentiation showing cytologic atypia and mitotic figures. The lesion often has a spindle cell appearance, 58 though immunohistochemistry shows that the spindle cells are epithelial in origin, being positive for cytokeratin and negative for vimentin. 59,60 They metastasize locally to the lymph nodes but also have distant metastases in the lungs, bone, 61 and myocardium. Treatment of the primary site is essentially surgical and often includes a lymph node dissection of the neck. Radiation therapy has not been shown to be effective, but chemotherapy with paclitaxel and carboplatin and oral cyclophosphamide has been used with some effect. 62 Malignant variants of ameloblastoma occur in the same sites as the more frequent well-differentiated lesion and are therefore more common in the posterior mandible, although both mandibular and maxillary cases have been described. Most ameloblastic carcinomas are believed to arise de novo, although there are a few reports of apparent change from a normal well-differentiated ameloblastoma into an ameloblastic carcinoma, 63 and there are also reports of hybrid lesions histologically showing areas of normal ameloblastoma and areas of ameloblastic carcinoma, suggesting that extensive tissue sampling may be required in some cases (see Figs and 23-12). Death has been reported from ameloblastic carcinoma often due to extensive local recurrence involving the base of the skull and cranial cavity. CLEAR CELL ODONTOGENIC CARCINOMA This rare neoplasm has been described in both the mandible and maxilla and is of unknown etiology, but the fact that it has only been described in the jaws and has some resemblance to other odontogenic lesions suggests that it is probably odontogenic in origin. It appears to occur most commonly in females, often older than the age of 60. It appears as a locally aggressive lesion and is poorly circumscribed both clinically and radiographically. Histologically, it consists of clear cells, which are positive for cytokeratin and negative for vimentin and also negative for mucicarmine, which differentiates it from some of the other clear cell tumors such as mucoepidermoid carcinoma and renal carcinoma and CEOT. Metastases to the lungs 67 and neck have been described, necessitating a metastatic workup on these patients. ODONTOGENIC CARCINOMA 68,69 This is a central lesion occurring most often in the mandible and is felt to arise from remnants of the dental lamina or reduced enamel epithelium. 70 Histologically, it has all the appearances of a squamous cell carcinoma and usually appears to be well differentiated. Because the lesion cannot be differentiated histologically from any other squamous cell carcinoma, its odontogenic origin can only be assumed when there is no connection to the epithelium or any other site of a squamous cell carcinoma and there is no possibility of this being a metastatic lesion. If it is contiguous with the overlying mucosa, the perception is that it almost certainly arose in the mucosa and only involved the bone secondarily.
12 Ch23-F10053.qxd 5/15/06 6:00 PM Page 501 PART II ONCOLOGY 501 Radiographically, it normally appears as a poorly defined radiolucency and the diagnosis is often made from routine radiographs, although instances have been described where the presenting feature was involvement of the inferior alveolar nerve or a nonhealing socket following tooth removal (Fig ). 71 Odontogenic carcinoma is often found in conjunction with another odontogenic lesion 72,73 and may result from epithelial malignant change within the lesion. 74,75 Treatment is as for squamous cell carcinoma in other sites and involves a metastatic work-up followed by primary surgery, which can often involve a neck dissection followed by radiation therapy depending on the adequacy of the surgical margins, their histological appearance, and the presence or absence of metastatic spread. BENIGN MESENCHYMAL ODONTOGENIC TUMORS ODONTOGENIC FIBROMA The central odontogenic fibroma, a rare lesion that occurs in both males and females and in all age-groups, is found in both the mandible and maxilla. Fewer than 100 cases have been reported worldwide. 76 Radiographically, it appears as a radiolucent lesion that is often multilocular and can cause cortical expansion. It thus resembles a number of other odontogenic lesions. Histologically, two patterns have been described, one with a mass of mature fibrous tissue containing a few epithelial rests and the other a more mature connective tissue with abundant rests and calcific deposits of either dentin or cementum. 77 Clinically, the two subgroups appear to behave similarly. The lesions are normally well demarcated but nonencapsulated. Treatment is enucleation and excision. Recurrence is rare, although more aggressive variants have been described. 78 CEMENTOBLASTOMA The cementoblastoma is also known as the true cementoma and is a rare odontogenic lesion representing less than 1% of all odontogenic tumors. 79 It is most common in the second and third decades of life and typically affects the lower molar region. 80 It is intimately associated with the root of a tooth being formed from the cementum and is commonly associated with a lower molar tooth including the third molar. The tooth normally remains vital, and symptoms include cortical expansion and a low-grade intermittent pain. Radiographically, the lesion appears as a radiopaque lesion attached to and surrounding the root of a tooth. Classically, it is surrounded by a radiolucent ring that represents the periodontal ligament space around the tumor (Fig ). Histologically, cementum and bone are difficult to distinguish from each other, and this lesion is the cemental equivalent of the osteoblastoma. Radiographically, symptomatically, and histologically, they are almost identical, and it is difficult to differentiate the two if the causative tooth is not present. Radiographically, it must be distinguished from an odontoma, focal sclerosing osteomyelitis, and hypercementosis. Treatment is normally removal of the lesion and the associated tooth. Thorough curettage is required, and recurrence is rare but has been recorded. Peripheral ostectomy has also been recommended as a treatment Fig An odontogenic carcinoma involving the roots of the lower right second molar (arrow). No connection with the overlying mucosa existed at surgery.
13 Ch23-F10053.qxd 5/15/06 6:00 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS A B Fig A cementoma associated with the lower left first molar. A, A cementoblastoma associated with the roots of the first molar. Note the radiolucent ring around it representing the periodontal ligament. B, Resected and sutured specimen. for these lesions if recurrence is likely to be a problem (see Fig ). 81 ODONTOGENIC MYXOMA This odontogenic tumor may comprise 15% to 20% of odontogenic tumors. 82 It is the second most common odontogenic tumor with a possible incidence of 0.07 new cases/million people/year. 83 Odontogenic myxoma typically occurs between the second and fourth decades, is more common in females than males (male-to-female ratio 1:1.5), and two thirds of cases occur in the mandible and one third in the maxilla. 84 The tumor typically presents as either a swelling in the affected jaw or as an asymptomatic radiographical finding. Radiographically, more than 50% of these tumors are multilocular and somewhat less than 50% unilocular with fairly welldefined borders. Larger lesions are more likely to be multilocular. They are only rarely associated with unerupted teeth. The radiographical appearance of myxoma is similar to that of the ameloblastoma, but differences have been noted on dynamic magnetic resonance imaging scanning 85 with the center of the myxoma showing enhancement while the ameloblastoma did not (Fig ). Histologically, the lesion contains a loose mesenchymal fibrous tissue that lacks atypia. It has a bland histological appearance. Odontogenic epithelium is rarely found within the lesion, and its odontogenic origin is assumed from the fact that it does not appear to occur elsewhere in the body (see Fig ). Although lesions containing myxomatous tissue have been recorded in other parts of the body, they normally represent myxomatous degeneration in another type of lesion. The odontogenic myxoma is assumed to derive from primitive dental pulp or primitive dental papilla. In fact, the dental papilla and the tooth follicle of a mature individual is histologically similar to the myxoma, and errors have been made histologically in differentiating a normal dental follicle from a myxoma, which can result in overtreating some patients. 86 The odontogenic myxoma is a benign but locally aggressive lesion that is slightly less aggressive than the solid ameloblastoma. Normally it is treated by either enucleation and radical curettage or peripheral ostectomy. In larger lesions or lesions perforating the buccal or lingual plate, segmental resection of the mandible or a hemimaxillectomy in the maxilla may be required. Physicochemical adjuncts to treatment such as liquid nitrogen cryotherapy or Carnoy s solution have also been used in addition to enucleation. Recurrence rate is normally quoted as between 15% and 20%. CEMENTIFYING FIBROMA A cementifying fibroma is the odontogenic equivalent of the ossifying fibroma; these fibromas are clinically and histologically similar, if not identical. Lesions in the areas of the jaws where cementum could be found and which contain calcified spherules are normally believed to be cementifying fibromas (Fig ). They have been described in both the maxilla and mandible
14 Ch23-F10053.qxd 5/15/06 6:00 PM Page 503 PART II ONCOLOGY 503 A B Fig An odontogenic myxoma of the right mandible. A, Radiograph of an odontogenic myxoma of the right mandible. The myxoma appears as a moderately welldefined multilocular radiolucency. B, The mandible grossly sectioned through the myxoma. Despite its irregular borders, it is gelatinous in nature and fairly well defined. but are more frequent in the mandible, and they are classified as benign fibro-osseous lesions. Although histologically similar, differences have been found on immunohistochemical staining because ossifying fibromas show no significant immunoreactivity for keratin sulfate or chondroitin-4-sulfate, while the cementifying fibroma has significant immunoreactivity for keratin sulfate. Chondroitin-4-sulfate is also found to have intense immunostaining in the premineralized and poorly mineralized matrices of cementifying fibromas. 87 Maxillary lesions have been described in the maxillary antrum, 88 ethmoids, 89 and sphenoids 90 and have even caused proptosis. 91 Although cementifying fibromas are generally believed to be benign and they respond well to enucleation, recurrences have been described necessitating local resection. 92 Unlike the ossifying fibroma, a juvenile aggressive version has not been described. MALIGNANT MESENCHYMAL ODONTOGENIC TUMORS AMELOBLASTIC FIBROSARCOMA This represents the only well-described odontogenic mesenchymal malignant tumor. Malignant odontogenic tumors are rare and represent only about 4% of odontogenic tumors. The ameloblastic fibrosarcoma is one of the rarer variants with fewer than 80 cases in the literature. Clinically, two thirds arise de novo, while one third arise in preexisting benign odontogenic lesions. 93 Possible malignant transformation from ameloblastic fibroma (normally believed to be benign) has been described. 94 Histologically, the lesions are composed of a benign-appearing epithelial component consisting of epithelial islands and strands within a cellular mass of mesenchymal tissue with stellate- and spindle-shaped
15 Ch23-F10053.qxd 5/15/06 6:00 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS A B Fig A cementifying fibroma of the right posterior mandible. A, Radiographical appearance showing the lesion possibly arising from the mesial root of the lower right first molar. B, Histology of specimen. Note calcified spherules representing cementum (hematoxylin and eosin, 20). fibroblast-like cells with marked pleomorphism. The fibrous stroma is believed to be malignant. Occasional cementum-like calcification has been noted. 95 Immunohistochemically, the mesenchymal cells are positive for Ki 67, PCNA, p53, and vimentin, unlike the negativity of the ameloblastic fibroma. 96 They appear to be most frequently located in the posterior region of the mandible, and the average age of affected patients is The lesion is thought to be locally aggressive, and one study noted that 37% of reported cases had at least one metastasis. The overall prognosis is generally believed to be good, although one study showed that 19.3% of patients died of their disease. 93 Nevertheless, wide surgical excision remains the standard treatment, augmented if necessary by radiation therapy and chemotherapy. 96,97 MIXED EPITHELIAL AND MESENCHYMAL ODONTOGENIC TUMORS ODONTOMA The odontoma, or odontome, is the most common odontogenic tumor, representing approximately 22% of all odontogenic tumors, and consists of fully differentiated, irregularly arranged, mature dental tissues. Odontomas are mixed tumors, as they contain both epithelial and mesenchymal elements, and they are benign. They are developmental abnormalities found in young people and are most often found on routine radiographs, although they can present as a swelling or with an infected lesion, particularly if they erupt. Because they contain
16 Ch23-F10053.qxd 5/15/06 6:00 PM Page 505 PART II ONCOLOGY 505 mature dental tissue, they often replace a missing tooth. They can be found throughout the jaws but are most frequent in the mandibular molar region. Two distinct forms have been described, but the difference is of radiographical and histological interest only because the prognosis and treatment are the same for both. The compound odontome (Fig ), which is more commonly found in the anterior part of the mouth, contains numerous small denticles or tooth-like fragments within the lesion, each containing a denticle of enamel with dentin and pulp (see Fig ). In the complex odontome, most frequently found in the posterior part of the mouth (Fig ), there is an amorphous conglomeration of dental tissues consisting of enamel, dentin, cementum, pulp, and enamel organ. The compound odontone is twice as common as the complex odontome. 98 The epithelial cells have been shown to have the ability to keratinize, and keratin can sometimes be found in these lesions. Radiographically, the lesions appear as well-circumscribed radiopaque lesions, often surrounded by a small, clear margin that may represent a periodontal ligament. In a compound odontome, the small denticles can often be differentiated radiographically, whereas in the complex odontome radiographs show a more amorphous pattern with what looks like a multilobular appearance. The differential diagnosis of similar radiopaque lesions of the jaws would include the ossifying fibroma, cementoblastoma, and possibly focal sclerosing osteitis. A fine dividing line exists between a deformed tooth such as a geminated or dilacerated tooth and an odontome. Odontomes have limited growth potential, although they normally reach a certain size and then cease to grow. Enucleation is the curative treatment, and recurrences do not occur. AMELOBLASTIC FIBROMA This is a true mixed odontogenic lesion containing both epithelial and mesenchymal neoplastic components. It occurs in young people, often in the second or third decades of life, and is extremely rare after the age of 40. The ameloblastic fibroma has no gender predilection, and although it has been reported in all areas of the alveolus, it appears to be most frequent in the lower bicuspid region. This fibroma is often associated with an impacted tooth and may appear as a radiolucency either associated with the crown or the root of an impacted tooth. The associated teeth are vital. The ameloblastic fibroma may represent approximately 2% of all odontogenic tumors. 99 Radiographically, the ameloblastic fibroma appears as a well-defined radiolucency that can be either unilocular or multilocular. Teeth may be displaced but are not normally resorbed (Fig , A). Histologically, the lesion shows islands of odontogenic epithelium, often two cells thick in a loose or myxomatous connective tissue matrix (Fig , B). The lesion is encapsulated, and treatment consists of enucleation. Recurrences are rarely encountered (Fig , C and D). The ameloblastic fibrosarcoma (already described) may represent the malignant counterpart of the ameloblastic fibroma. A B Fig A compound odontome. A, Occlusal radiograph showing discrete and separate denticles. B, Histology of the specimen showing denticles with enamel, dentin, and pulp (hematoxylin and eosin, 10).
17 Ch23-F10053.qxd 5/15/06 6:00 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS A B Fig A complex odontome. A, Radiograph of an amorphous mass of enamel and dentin, a radiolucent border, and an embedded tooth. B, Enucleated specimen of odontome. AMELOBLASTIC FIBRO-ODONTOMA This lesion is best thought of as a combination of an ameloblastic fibroma with an odontoma, 99 which may be either compound or complex in type. Thus radiographically, it appears as a combined radiolucent/ radiopaque lesion and must be differentiated from other similar-appearing lesions such as the ossifying fibroma, the calcifying epithelial odontogenic tumor, the calcifying odontogenic cyst, an odontoma, and an adenomatoid odontogenic tumor. The age and gender predilection is the same as ameloblastic fibroma, as is treatment, which consists of enucleation. BENIGN NONODONTOGENIC TUMORS OF THE JAW FIBRO-OSSEOUS TUMORS Ossifying Fibroma (Cemento-Ossifying Fibroma) The ossifying fibroma is a benign neoplasm characterized by the replacement of normal bone by fibrous tissue and varying amounts of newly formed bone or cementum-like material, or both. As a result of histological similarities, ossifying fibroma, fibrous dysplasia, and cemento-osseous dysplasia are classified together as benign fibro-osseous lesions. The diagnosis of benign fibro-osseous lesions is based on clinical, radiographical, and histopathological correlation. Chromosomal abnormalities have been identified in the ossifying fibroma ; however, the molecular mechanisms that underlie the development of this tumor remain unknown. An ossifying fibroma usually presents as a painless, slow-growing, expansile lesion (Fig , A). Although these fibromas occur over a wide age range, most cases occur in the third and fourth decades of life. Female predilection is definite. Ossifying fibromas are believed to be confined to the jaws and craniofacial complex. 103 The mandible, particularly the premolar-molar region, is affected more commonly than the maxilla. Rare multicentric or familial ossifying fibromas, or both, have been reported. 104,105 The radiographical appearance is typically a welldefined radiolucency with a variable degree of internal calcification (Fig , B). The borders may be sclerotic. Larger mandibular lesions characteristically
18 Ch23-F10053.qxd 5/15/06 6:01 PM Page 507 PART II ONCOLOGY 507 A B D C Fig An ameloblastic fibroma in a 26-year-old female. A, Presenting on a panoral radiograph, as a well-defined radiolucency displacing teeth. B, Histological appearance. Note islands of odontogenic epithelium in a loose myxomatous matrix. C, After it has been de-roofed but before enucleation. D, As a cream-colored, lobulated specimen following enucleation.
19 Ch23-F10053.qxd 5/15/06 6:01 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS B A C Fig Ossifying fibroma. A, Frontal view of a 21-year-old female demonstrating expansion of the right side of the mandible. B, Mixed radiolucent-radiopaque lesion of the mandible extending from the first molar region on the right to the first premolar region on the left, producing a bowing of the inferior border. C, Submental three-dimensional reconstructed computed tomography demonstrating the expansion of the mandible. produce bowing of the inferior border (Fig , C). Root displacement and, less commonly, root resorption may be seen. Histologically, these fibromas are composed of a fibrous stroma with bony trabeculae or cementum-like spherules, or both, evenly distributed throughout the stroma. The microscopical appearance may be indistinguishable from fibrous dysplasia. The recommended treatment of ossifying fibromas is complete surgical excision. They characteristically shell out from the surrounding bone with ease. Reported rates of recurrence have ranged from less than 1% to 63% In light of the potential for recurrence, some authors advocate more extensive surgery for more aggressive lesions and lesions involving the craniofacial bones. 107,115,116 Ossifying fibromas do not display an infiltrative pattern into bone and therefore require smaller margins than the 1 cm typically required for an ameloblastoma, odontogenic myxoma, or a calcifying epithelial odontogenic tumor. Involved teeth with evidence of resorption should be removed with the lesion. Juvenile Ossifying Fibroma (Juvenile Aggressive Ossifying Fibroma; Juvenile Active Ossifying Fibroma) The juvenile ossifying fibroma is considered by many to be a unique lesion because of its reported tendency to occur in children and adolescents, its more complex histological features, and its tendency for more aggressive growth. However, there is no general agreement among pathologists with respect to the proper terminology, histopathological features, or criteria for separating
20 Ch23-F10053.qxd 5/15/06 6:01 PM Page 509 PART II ONCOLOGY 509 these lesions from conventional ossifying fibromas. 117 Adding to the controversy are the facts that these lesions have been noted in older patients and they are not always particularly aggressive. Two variants of the juvenile ossifying fibroma have been described the trabecular variant 118 and the psammomatoid variant. 119 The trabecular variant has strands of immature cellular osteoid within the lesion and usually occurs in childhood with a slight maxillary predilection. The psammomatoid variant has small spherical ossicles surrounded by osteoid rims within the lesion. It occurs over a wider age range than the trabecular variant and usually affects the orbit or paranasal sinuses (Fig ). A B Fig Juvenile ossifying fibroma. A, Axial computed tomography of a 6-year-old male with an expansile mass of the right maxilla. B, Spherical ossicles in a cellular fibroblastic stroma. Although it is considered more aggressive than the more common ossifying fibroma that generally occurs at a later age, conservative excision is recommended for the juvenile ossifying fibroma. However, lesions involving the craniofacial bones may require more extensive surgery. Recurrence rates of 20% to 58% have been reported. 117 Recurrences may be managed by local excision, and malignant transformation has not been reported. LANGERHANS CELL DISEASE Langerhans cell disease was formerly known as histiocytosis X and before that as three separate diseases: eosinophilic granuloma, Hand-Schüller-Christian disease, and Letterer-Siwe disease. The clinical manifestations of these diseases range from solitary or multiple bone lesions to disseminated visceral, skin, and bone lesions. Despite their diverse manner of clinical disease expression, these three diseases are characterized by proliferation of Langerhans cells accompanied by varying numbers of eosinophils, other chronic inflammatory cells, and multinucleated giant cells. Langerhans cells, which are derived from the monocytic series, are found in the epidermis, mucosa, lymph nodes, and bone marrow. They are dendritic cells that process and present antigens to T lymphocytes. The etiology and pathogenesis of Langerhans cell disease remains unknown. Evidence suggests a neoplastic process, 120 viral etiology, 121 and an overwhelming allergenic challenge. 122 Langerhans cell disease generally affects children and young adults, although it may affect older adults. Three forms exist. Chronic localized Langerhans cell disease, formerly known as eosinophilic granuloma, refers to solitary or multiple bone lesions only (Fig , A). Chronic disseminated Langerhans cell disease, formerly known as Hand-Schüller-Christian disease, is classically associated with a clinical triad of lytic bone lesions, exophthalmos, and diabetes insipidus (Fig , B). Acute disseminated Langerhans cell disease, formerly known as Letterer-Siwe disease, usually affects infants and is multisystem in nature, affecting the skin, bones, and internal organs, especially the lungs and liver. Bone lesions, either solitary or multiple, are the most common clinical presentation. Lesions most frequently involve the skull, mandible, ribs, and vertebrae, although almost any bone may be involved. Jaw lesions may produce pain and tenderness, tooth mobility, and expansion. Radiographically, jaw lesions usually appear as well-defined, punched-out radiolucencies, although they may be ill defined. Lesions often involve the alveolar bone, producing the classic appearance of floating teeth. The involved teeth remain vital; however, they
21 Ch23-F10053.qxd 5/15/06 6:01 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS A B Fig Langerhans cell disease. A, Chronic localized form of the disease producing a punched-out radiolucency seen at the mandibular alveolar crest in the region of the first premolar. B, Chronic disseminated form of the disease producing multiple mandibular radiolucencies. often do not have adequate support and should not prevent biopsy of the tissue deep in the jaws that will be required for diagnosis. The diagnosis of Langerhans cells disease may be confirmed using immunohistochemical studies. Langerhans cells stain positive for S-100 protein and CD1a antigen. In addition, Langerhans cells contain unique, rod-shaped cytoplasmic structures known as Birbeck granules, which are seen on electron microscopy. Accessible bone lesions of chronic localized Langerhans cell disease are usually treated with aggressive local curettage or resection with 5-mm margins where possible. Less accessible lesions may be treated with low-dose radiation therapy. Intralesional steroids have also been employed with some success, 122 and cases of spontaneous regression have also been reported. 123 It is necessary to evaluate these patients for additional bone or visceral involvement and to follow them for recurrence or disease progression. Individual lesions of chronic disseminated Langerhans cell disease may be treated as they are with the chronic localized form, but with widespread or visceral involvement, chemotherapy is often used. Acute disseminated Langerhans cell disease follows a rapidly progressive course and is treated with chemotherapy. The acute disseminated form is frequently fatal. LESIONS CONTAINING MULTINUCLEATED GIANT CELLS A number of lesions occur within the jaws, with multinucleated giant cells as a prominent histological feature; however, their relationship to one another is ill defined. The lesions in this group are similar, if not
22 Ch23-F10053.qxd 5/15/06 6:01 PM Page 511 PART II ONCOLOGY 511 identical, histologically, and they usually cannot be distinguished from one another solely on the basis of light microscopy. Clinical history, physical and radiographical examination, and serum biochemistry may be used to differentiate these lesions. Central Giant Cell Granuloma The central giant cell granuloma is a benign proliferation of fibroblasts and multinucleated giant cells. This lesion was initially thought to represent a reparative process thus it was termed a giant cell reparative granuloma. 124,125 It is no longer considered to be reparative, and if left untreated the lesion will progress. The precise nature of the central giant cell granuloma remains speculative. It has been suggested that it may be an inflammatory lesion, a reactive lesion, a neoplasm, or an endocrine lesion. The proliferating cell in this lesion is the fibroblast, which is thought to produce cytokines, resulting in the recruitment of monocytes, which subsequently transform into multinucleated giant cells. Immunohistochemistry has shown the giant cells to be osteoclasts. 126 Whether the central giant cell granuloma is unique to the jaws or whether it represents a continuum of the same disease process as giant cell tumors affecting the long bones is debatable and is discussed later. Central giant cell granulomas of the jaws are most often found in children and young adults, with up to 75% of cases occurring before 30 years of age. Females are affected twice as frequently as males. The lesion most often occurs anterior to the first permanent molar teeth. The mandible is affected three times more frequently than the maxilla, and the lesion may be seen to cross the midline. It most often produces painless expansion of the affected jaw; however, it may infrequently produce pain. Radiographically, central giant cell granulomas may present as a unilocular or multilocular radiolucency that is usually well delineated (Fig ). On the basis of clinical and radiographical features, there appear to be two types of central giant cell granulomas. The first is the more common, nonaggressive lesion, which is asymptomatic, grows slowly, and does not produce cortical perforation or root resorption. The second is an aggressive lesion, which presents with pain, rapid growth, cortical perforation, and root resorption. The aggressive type may have a higher recurrence rate. Presently, no histopathological methods of differentiating the aggressive from the nonaggressive type exist. Histologically, the central giant cell granuloma contains few to many multinucleated giant cells in a background of fibroblasts with varying amounts of collagen. The multinucleated giant cells are often focally aggregated; however, they may be evenly distributed. Hemosiderin-laden macrophages and extravasated erythrocytes are commonly seen. Foci of osteoid may be seen, particularly at the periphery of the lesion. These histopathological features are similar, if not identical, to those seen in the brown tumor of hyperparathyroidism and cherubism. For years surgical curettage has been the treatment of choice. Surgical treatment has generally been associated with a recurrence rate of 15% to 20%, although recurrence rates as high as 50% have been reported. Fig Central giant cell granuloma. Radiolucency of the anterior mandible seen to cross the midline in a 17-year-old male.
23 Ch23-F10053.qxd 5/15/06 6:01 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS Recurrence risk and the fact that with large lesions even conservative curettage may be associated with the loss of teeth, damage to the inferior alveolar nerve, and sinus and nasal implications has led to the development of several nonsurgical treatments. The first nonsurgical treatment proposed was intralesional corticosteroid injections. 127 Weekly injections of triamcinolone for 6 weeks have been shown to induce partial and in some cases complete resolution of the lesions The mode of action of this treatment remains unknown. Subcutaneous calcitonin injections have also been used with some success The injections are given daily for approximately 18 months. The mode of action of calcitonin remains speculative; however, some of the giant cells in these lesions have been shown to have calcitonin receptors. 133 Thus the therapeutic effect of calcitonin may be mediated through inhibition of osteoclastogenesis. Alpha-interferon given by subcutaneous injection has also been advocated. 135,136 The rationale for this therapy is that the antiangiogenic action of the alpha-interferon will suppress the angiogenic component of the lesion, resulting in resolution. In most cases surgery is still required after the alpha-interferon treatment; however, it may be less radical and there may be a reduced recurrence rate. Giant Cell Tumor The giant cell tumor normally found in long bones is an aggressive lesion that some people believe is a variant of low-grade osteosarcoma. This tumor is generally believed to be an entity that is separate from the central giant cell granuloma of the jaws, although some authorities report it rarely occurs in the jaws. Histologically, it is similar to the central giant cell granuloma, although the giant cells are larger with more nuclei, the giant cells are more evenly distributed, the stroma is more cellular, and there may be areas of necrosis. However, in any particular case it may be difficult to make a distinction. The recurrence rate of giant cell tumors in long bones following curettage is higher than for central giant cell granulomas of the jaws, leading some authorities to advocate resection. Hyperparathyroidism Hyperparathyroidism is characterized by the overproduction of parathyroid hormone (PTH). Primary hyperparathyroidism is the uncontrolled production of PTH as the result of a parathyroid adenoma, hyperplasia, or rarely an adenocarcinoma. Secondary hyperparathyroidism occurs in response to hypocalcemia, most often as a result of chronic renal failure. In both forms of hyperparathyroidism, excess PTH levels stimulate osteoclast-mediated bone resorption, which may produce a focal bone lesion known as a brown tumor of hyperparathyroidism. The lesion derives its name from the color of the tissue as seen on surgical exploration, which is a result of the erythrocyte extravasation and hemosiderin deposition within the lesion. Like the central giant cell granuloma, this lesion appears radiographically as a well-defined unilocular or multilocular radiolucency, and it commonly occurs in the jaws (Fig ). These lesions may be solitary or multiple. They are histologically identical to central giant cell granulomas. Patients with primary hyperparathyroidism are hypercalcemic, with associated signs and symptoms. In contrast, those with secondary hyperparathyroidism are hypocalcemic and those with central giant cell granulomas have normal serum calcium levels. Elevated serum PTH levels are associated with both forms of hyperparathyroidism. Additionally, laboratory studies in secondary hyperparathyroidism demonstrate impaired renal function. A 24-hour urinary calcium level can be measured to rule out benign familial hypocalciuric Fig Brown tumor of hyperparathyroidism. Multiple radiolucencies seen in the mandible of this patient with hyperparathyroidism.
24 Ch23-F10053.qxd 5/15/06 6:01 PM Page 513 PART II ONCOLOGY 513 hypercalcemia, which is a hereditary condition that leads to hyperparathyroidism secondary to low renal sensitivity to parathyroid hormone. Normal PTH levels are found in association with central giant cell granulomas. Therefore it is prudent to obtain serum calcium and PTH levels in patients with giant cell lesions in order to exclude hyperparathyroidism. If a diagnosis of hyperparathyroidism is confirmed, treatment must be aimed at the cause and the lesions will usually resolve without any further treatment. Cherubism Cherubism is a rare hereditary condition characterized by painless, bilateral, symmetrical expansion of the jaws. It was first described in 1933, when it was named familial multilocular cystic disease of the jaws. 137 It follows an autosomal dominant pattern of inheritance with 100% penetrance in males, 50% to 75% penetrance in females, and variable expressivity. A 2:1 male predominance exists. Sporadic cases have also been reported; these presumably represent spontaneous mutations. The genetic defect has been mapped to chromosome which encodes the binding protein SH3 4p16.3, 138,139 BP The lesions of cherubism commonly begin to manifest as painless, bilateral, symmetric expansion of the jaws between 2 and 5 years of age (Fig , A), although milder forms may not be detected until a later age. The lesions are confined to the mandible and maxilla. The regions most often affected are the mandibular angle, ascending ramus, retromolar region, and maxillary tuberosity; however, in severe cases the entire mandible and maxilla may become involved. The mandibular condyles are always spared. With involvement of the maxillary contribution to the orbital floor, the globes may be displaced upward, resulting in scleral show. With eyes that appear to be turned upward and a round face, children with a severe form of this condition appear like cherubs depicted in Renaissance paintings. Radiographically, the involved bones show multilocular radiolucencies with thin and expanded cortices (Fig , B). There may be premature exfoliation of primary teeth, as well as unerupted and displaced permanent teeth. Histologically, the lesions resemble the central giant cell granuloma. However, some lesions exhibit eosinophilic perivascular cuffing of collagen surrounding small capillaries throughout the lesion, allowing for differentiation between the two lesions. A B Fig Cherubism. A, Frontal view of a 6-year-old male with bilateral facial expansion. B, Multilocular radiolucencies seen in the maxilla and mandible bilaterally. Note the sparing of the mandibular condyles.
25 Ch23-F10053.qxd 5/15/06 6:01 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS The lesions of cherubism tend to enlarge until puberty, at which time they begin to regress. In the majority of cases, abnormal facial growth ceases and the lesions recalcify by age 30. Therefore treatment is usually conservative, allowing natural regression to occur. If surgical recontouring of expanded bone is necessary, it is best to defer it until after puberty. During childhood and early adolescence treatment should be directed toward assisting the eruption of teeth. As a result of the histologic similarity to central giant cell granuloma, calcitonin has been used in an attempt to cause resolution, but unlike the central giant cell granuloma it has not met with success, suggesting that cherubism lesions and central giant cell granuloma lesions are, in fact, different. 143 Aneurysmal Bone Cyst The aneurysmal bone cyst is a pseudocyst characterized by blood-filled spaces in a connective tissue stroma containing multinucleated giant cells. The lesion occurs most commonly in the long bones and vertebrae. Within the craniofacial complex it is most common in the mandible, followed by the maxilla. The etiology and pathogenesis of the lesion remains unknown, although the lesion is generally regarded as reactive. Controversy remains over whether the lesion occurs as a primary entity or results from the development of a dilated vascular bed in a preexisting intrabony lesion. The peak incidence occurs within the second decade of life, with most occurring before 30 years of age. There is a slight female predilection. Mandibular and maxillary lesions most frequently occur in the molar regions. Patients often present with facial swelling that may develop fairly rapidly and can be associated with pain. The lesion usually appears radiographically as a multilocular radiolucency, although it may be unilocular (Fig , A). There may be significant cortical expansion and thinning (Fig , B). Microscopically, A B C Fig Aneurysmal bone cyst. A, A radiolucent lesion seen to produce expansion of the mandibular left angle in a 13-year-old female. B, Coronal computed tomography demonstrating cortical expansion and thinning. C, Numerous small sinusoids surrounded by a connective tissue stroma and scattered multinucleated giant cells.
26 Ch23-F10053.qxd 5/15/06 6:01 PM Page 515 PART II ONCOLOGY 515 sinusoidal blood-filled spaces of varying size are seen. These spaces are not lined by endothelium but are surrounded by a fibrous connective tissue stroma with variable numbers of multinucleated giant cells (Fig , C). Osteoid and woven bone can often be seen within the lesion. Although some authors feel aneurysmal bone cysts are associated with a relatively high recurrence rate, curettage remains the treatment of choice. At the time of surgery lesional tissue appears like a blood-soaked sponge ; however, significant hemorrhage is usually not encountered. NEUROGENIC TUMORS Schwannoma (Neurilemmoma) The schwannoma is a slowly growing, benign neoplasm arising from Schwann cells of the nerve sheath (neurilemma). As this encapsulated tumor enlarges, it pushes the involved nerve aside without enveloping it. It most commonly occurs in the soft tissues of the head and neck, as well as the flexor surfaces of the upper and lower extremities. Intraosseous lesions are rare; however, the mandible is the most common site of occurrence for central lesions and maxillary lesions have been reported. Lesions may occur over a wide age range but are most common in young adults. Bony lesions may be asymptomatic or produce expansion, pain, paresthesia, tooth mobility, and tooth displacement. The usual radiographical appearance is that of a well-defined, unilocular radiolucency with a thin, sclerotic border. Histologically, this is an encapsulated spindle cell tumor that consists of variable amounts of two types of tissue, Antoni A and Antoni B. Antoni A tissue consists of spindle cells organized in palisaded whorls and waves around central acellular, eosinophilic areas termed Verocay bodies. Antoni B tissue consists of spindle cells randomly arranged within a loose, myxomatous stroma. The tumor is strongly S-100 protein positive. Intraosseous schwannomas can be treated by enucleation and curettage. When the lesion arises from an identifiable nerve such as the inferior alveolar nerve, it can be excised from the nerve while preserving the integrity of the nerve. Recurrences are rare. Neurofibroma Neurofibromas arise from a mixture of cell types including Schwann cells and perineural fibroblasts. They may occur as solitary lesions or in association with neurofibromatosis. Neurofibromatosis is an autosomal dominant condition in which 50% of cases result from spontaneous mutation. Two types of this genetic disorder exist, neurofibromatosis type 1 (von Recklinghausen s disease of skin) and neurofibromatosis type 2. Type 1 (Box 23-2) is characterized by multiple cutaneous neurofibromas and café-au-lait spots in addition to several other features. Type 2 (Box 23-3) is characterized by the development of bilateral vestibular schwannomas in more than 90% of individuals with the condition. Peripheral neurofibromas occur rarely in neurofibromatosis type 2. Although most commonly reported in soft tissues, neurofibromas do occur in bone and have been reported in association with the inferior alveolar nerve. Pain or paresthesia may result from lesions of the inferior alveolar nerve. Patients may also present with cortical expansion. Intraosseous lesions may produce a welldemarcated or poorly defined unilocular or multilocular BOX 23-2 Neurofibromatosis Type 1 A diagnosis is established when two or more of the following findings are present: 1. Six or more café-au-lait spots greater than 5 mm in diameter in prepubertal patients and greater than 15 mm in postpubertal patients 2. One plexiform neurofibroma or two or more neurofibromas of any type 3. Two or more pigmented iris hamartomas (Lisch nodules) 4. Axillary or inguinal region freckling 5. Optic nerve glioma 6. A distinctive osseous lesion such as dysplasia of the greater wing of the sphenoid or pseudoarthrosis 7. A first-degree relative with neurofibromatosis type 1 From National Institutes of Health Consensus Development Conference: Arch Neurol 45: , BOX 23-3 Neurofibromatosis Type 2 A diagnosis is established when one or more of the following findings are present: 1. Bilateral cranial nerve VIII masses 2. A first-degree relative with neurofibromatosis type 2 and either a single cranial nerve VIII mass or any of the following findings: Schwannoma Neurofibroma Meningioma Glioma Juvenile posterior subcapsular lens opacity From Consensus Development Panel: Arch Neurol 51: , 1994.
27 Ch23-F10053.qxd 5/15/06 6:01 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS radiolucency. Adjacent soft tissue neurofibromas may produce cortical erosion. Solitary neurofibromas and those found in association with neurofibromatosis share the same microscopic features. The tumor is composed of spindle-shaped cells with fusiform or wavy nuclei in a delicate connective tissue matrix. It is not encapsulated and may blend with the adjacent connective tissues. Mast cells are characteristically scattered throughout the lesion. A histological subtype known as a plexiform neurofibroma is highly characteristic of neurofibromatosis. The normally recommended treatment of solitary lesions following biopsy is localized excision. The lesions are often vascular, and extensive blood loss has been reported from surgical management of mandibular lesions; thus some authors have advocated mandibular resection. The number of neurofibromas that can occur with neurofibromatosis type 1 makes complete surgical therapy impractical. In these cases surgery is reserved for lesions that are large and symptomatic or compromise function, or both. Malignant transformation to neurogenic sarcoma occurs in 5% to 15% of neurofibromas associated with neurofibromatosis. Authorities believe that malignant transformation does not occur with solitary lesions. OSTEOID OSTEOMA AND OSTEOBLASTOMA The osteoid osteoma and osteoblastoma share the exact same histological features. They are distinguished from one another primarily by size, although there are also differences in sites of occurrence and associated symptoms. These are benign neoplasms, the etiology of which is unknown. Most cases occur in the second decade, with 85% to 90% occurring before 30 years of age. A 2:1 male predilection exists. The osteoid osteoma is less than 2 cm in diameter, occurring most frequently in the femur, tibia, and phalanges. Rarely it occurs in the jaws. An osteoid osteoma classically presents with nocturnal pain that is alleviated by aspirin. The osteoblastoma is greater than 2 cm in diameter, occurring most frequently in the vertebrae and long bones of the extremities. The craniofacial skeleton is the site of involvement in 15% of osteoblastomas. The mandible is affected more frequently than the maxilla. Within the jaws, the posterior tooth-bearing portion is the area most often involved. Clinically, it often develops relatively rapidly, producing swelling and pain. In contrast to osteoid osteomas, the pain is not typically nocturnal and it does not respond as well to aspirin. Radiographically, these lesions are usually well defined with a mixed radiolucent-radiopaque pattern (Fig ). A thin radiolucency may be noted surrounding a variably calcified central tumor mass. A zone of reactive sclerosis surrounding the lesion is a characteristic feature of the osteoid osteoma. Histologically, the osteoid osteoma and osteoblastoma are identical. Irregular trabeculae of osteoid and immature bone are seen within a cellular fibrovascular stroma. The osteoid trabeculae, which exhibit varying degrees of calcification, are surrounded by prominent osteoblasts. In some cases differentiation between osteoblastoma and low-grade osteosarcoma may be difficult. Fig Osteoblastoma. Well-defined calcified mass with a radiolucent rim in the posterior left mandible.
28 Ch23-F10053.qxd 5/15/06 6:01 PM Page 517 PART II ONCOLOGY 517 Treatment is generally confined to conservative surgical excision either with curettage or local excision. Reports have been made of some lesions regressing after incomplete excision or biopsy. 144 Recurrences are rare but have been reported and may necessitate more aggressive treatment such as en bloc resection. 145 Rare examples of malignant transformation have been reported. 146,147 However, due to the possible difficulty in differentiating some osteoblastomas from osteosarcomas, some of these may represent an incorrect initial diagnosis. OSTEOMA Osteomas are benign tumors composed of mature compact or cancellous bone. They are distinguished from the common palatal and mandibular tori, as well as buccal exostoses, despite identical histopathology. Tori and buccal exostoses are thought to be of developmental or reactive origin and not true neoplasms. Osteomas may arise from the surface of bone (periosteal osteoma), or they may be located in the medullary bone (endosteal osteoma). Osteomas may arise in the paranasal sinuses, skull bones, and facial bones including the maxilla and mandible. They most commonly develop in young adults. Periosteal osteomas most often present as slowgrowing, painless, discrete bony masses. Endosteal osteomas are usually asymptomatic and noted on routine radiographs. As a result of their location, some lesions may cause headaches, sinusitis, or ophthalmological complaints. Radiographically, osteomas appear as well-circumscribed, sclerotic masses. Two histological variants exist. One variant consists of normalappearing, dense, compact bone with sparse marrow tissue. The other form consists of lamellar trabeculae of cancellous bone with fibrofatty marrow. Osteoblastic activity is often prominent. Osteomas are usually solitary, except in cases of Gardner syndrome. This syndrome is an autosomal dominant condition in which patients have intestinal polyposis, multiple osteomas, fibromas of the skin, epidermal cysts, impacted permanent and supernumerary teeth, and odontomas. The genetic defect has been mapped to 5q21 where the familial adenomatous polyposis coli (APC) gene resides The majority of patients have an incomplete manifestation of the syndrome. Osteomas in association with Gardner syndrome are frequently seen at the mandibular angles, as well as other facial bones and long bones. Importantly, the development of osteomas precedes other manifestations of the syndrome. The most clinically important aspect of the syndrome is the high rate of malignant transformation of bowel polyps into invasive adenocarcinoma. In fact, the malignant transformation rate is 50% by age 30. As a result, patients with an established diagnosis of Gardner syndrome typically undergo a prophylactic colectomy. Osteomas are diagnosed and treated by local excision. Recurrences are rare. Small, asymptomatic cases may be followed clinically and radiographically. Patients with multiple osteomas should undergo investigation for Gardner syndrome. CHONDROMA The chondroma is a benign tumor composed of mature hyaline cartilage. It most commonly occurs in the bones of the hands and feet, with rare occurrences in the craniofacial complex. Within the maxillofacial region, chondromas most often occur in the nasal septum and anterior maxilla. They have also been reported in the mandibular condyle, coronoid process, body, and symphysis. Chondromas typically present as painless, slowly progressive swelling. They usually appear before 50 years of age. There is no sex predilection. Radiographically, they appear as a unilocular or multilocular radiolucency, which may have internal foci of calcification. The lesions are composed of well-defined lobules of mature hyaline cartilage containing small chondrocytes with regular nuclei. The microscopic distinction between a benign chondroma and low-grade chondrosarcoma is difficult. Considering the rarity with which chondromas occur in the craniofacial complex, the difficulty in differentiating between a chondroma and a low-grade chondrosarcoma, and the aggressive nature of chondrosarcomas, one should question the diagnosis of a benign chondroma in the jaws. To avoid the potential risk of undertreating a malignancy, some authors consider chondromas of the jaws as potentially malignant and manage them accordingly. 151,152 These authors recommend wide surgical excision with 1-cm margins. If the lesion recurs following more conservative surgical treatment, the lesion should certainly be considered a low-grade chondrosarcoma and treated with wide surgical excision. DESMOPLASTIC FIBROMA The desmoplastic fibroma is a benign, locally aggressive tumor of bone that is considered to be the osseous counterpart of soft tissue fibromatosis. The etiology and pathogenesis of this lesion remain unknown, although genetic, endocrine, and traumatic factors have been suggested. The lesion usually occurs in children and young adults, with most cases being discovered before 30
29 Ch23-F10053.qxd 5/15/06 6:01 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS years of age. It most commonly occurs in the long bones but may occasionally affect the jaws. Within the jaws, the posterior mandible is the area most frequently involved. Patients most often present with a painless, slow-growing, firm swelling of the affected jaw. Radiographically, the lesion produces a radiolucency, which may be unilocular or multilocular (Fig ). The margins may be well defined or poorly defined. Cortical perforation and root resorption may be seen. Microscopically, the lesion is composed of interlacing bundles and whorled aggregates of densely collagenous tissue with spindled and elongated fibroblasts. The degree of cellularity may vary from one area of the lesion to another. Cellular atypia and mitotic figures are not seen. This lesion does not produce bone. Recurrence rates following conservative surgical treatment such as curettage and local excision are high, while lesions treated by resection or wide excision do not tend to recur. 153,154 Thus despite a benign histology, the desmoplastic fibroma should be treated aggressively. Radiation 155 and chemotherapy 156,157 have been recommended for lesions involving vital structures and those located in areas where resection would be debilitating. MALIGNANT NONODONTOGENIC TUMORS OF THE JAWS OSTEOSARCOMA Osteosarcoma is a malignant tumor characterized by the direct production of osteoid by a sarcomatous stroma. It is the most common primary sarcoma of bone and second only to plasma cell neoplasms as the most common primary tumor of bone. It can develop in previously irradiated bone, as well as preexisting bone abnormalities such as Paget s disease, fibrous dysplasia, and giant cell tumors. Osteosarcomas may be classified into the more common central type, which arises from the medullary portion of the bone, and the less common peripheral (juxtacortical) type, which originates on the surface of the bone and initially grows outward. The molecular mechanisms associated with the pathogenesis of osteosarcoma appear to be related to a variety of genetic alterations resulting in inactivation of tumorsuppressor genes and overexpression of oncogenes. 158 In addition, cytogenetic studies have found that the majority of osteosarcomas are characterized by complex chromosomal abnormalities, often with pronounced cell-to-cell variation and heterogeneity. 158 Central osteosarcomas most often involve the distal femur and proximal tibia of patients in their second decade of life. Lesions involving the jaws account for 5% to 7% of all osteosarcomas and most commonly affect patients in their third and fourth decades of life, with a mean age of approximately 35 years. There is a slight male predilection. The mandible is affected more frequently than the maxilla. The most common symptoms of jaw lesions are swelling and pain. Depending on the location of the lesion, patients may also experience paresthesia, loosening of teeth, nasal obstruction, epistaxis, proptosis, or diplopia. Unfortunately, because some signs and symptoms may be associated with other nonmalignant conditions, there is often a delay in the diagnosis of osteosarcoma. Fig Desmoplastic fibroma. A multilocular radiolucency of the posterior left mandible in a 12-year-old male.
30 Ch23-F10053.qxd 5/15/06 6:01 PM Page 519 PART II ONCOLOGY 519 Depending on the degree of calcification, the radiographical appearance of a central osteosarcoma may vary from a dense radiopaque area to a mixed radiopaque and radiolucent lesion to a radiolucent process (Fig , A). The margins are usually irregular and poorly defined. Symmetric widening of the periodontal ligament and extracortical bone producing a sunburst appearance are radiographical features classically associated with osteosarcoma, although these features are not unique to this condition. Cortical destruction and root resorption may also be apparent on radiographical examination. The histological appearance is highly variable, although all osteosarcomas have a sarcomatous stroma that directly produces a variable amount of tumor osteoid (Fig , B). Lesions are histologically subdivided into osteoblastic, chondroblastic, and fibroblastic subtypes, depending on the relative amounts of osteoid, cartilage, or collagen produced by the stroma. The osteoblastic type is most common in the skeleton and the chondroblastic type most common in the jaws. The prognosis is not dependent on the histologic subtype; however, patients with high-grade lesions have a poorer prognosis in comparison with those with a low-grade lesion. A telangiectatic subtype of osteosarcoma contains numerous large blood-filled spaces and prominent multinucleated giant cells. In addition, there is a small cell variant of osteosarcoma, which resembles Ewing sarcoma; however, the small round cells produce osteoid, which does not occur in Ewing sarcoma. Rare examples of the telangiectatic and small cell variants have been reported in the jaws. 159,160 Wide surgical resection with negative margins is the only treatment that conclusively leads to increased survival. A bone margin of 3 cm from the radiographical margin is recommended. As a result of the limited numbers of patients in most studies and the lack of randomized controlled trials, the role of radiation therapy and chemotherapy in osteosarcoma of the jaws A B Fig Osteosarcoma. A, Poorly defined radiolucency of the posterior left mandible in a 28-year-old female complaining of pain in the area. B, Production of osteoid by a sarcomatous stroma.
31 Ch23-F10053.qxd 5/15/06 6:01 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS largely remains unproven. The vast majority of studies indicate radiation therapy has no beneficial effect on survival. Although chemotherapy in combination with surgery has improved the prognosis of osteosarcoma of the long bones, 161,162 the beneficial effects in the jaws are not as well established. Most studies have been unable to demonstrate a survival benefit with chemotherapy, while a couple of authors report some benefit to chemotherapy in combination with surgery. 167,168 At present, treatment protocols used in the treatment of osteosarcoma of the long bones, which include preoperative and postoperative chemotherapy and wide surgical resection, are commonly used to treat osteosarcomas of the jaws. Most reports state an overall 5-year survival rate for head and neck osteosarcomas of between 40% and 70%. 164,166, The main cause of death in osteosarcoma of the jaws is uncontrolled local recurrence. Metastasis occurs in approximately 18% of cases, 165 although rates as high as 50% 172 have been reported. The lungs are the most frequent site of metastasis. Because regional lymph node metastasis is rare, neck dissection is not advocated. Osteosarcomas of the jaws generally metastasize less frequently and have a better prognosis in comparison with lesions of the extremities. PERIPHERAL (JUXTACORTICAL) OSTEOSARCOMA In contrast to the central medullary osteosarcoma, which arises from the medullary surface of the bone, the peripheral osteosarcoma arises from the periosteal surface of the bone. The peripheral tumors have distinct clinical, histological, and radiographical features, in addition to a different biological behavior. Peripheral lesions are further divided into parosteal and periosteal subtypes. Peripheral osteosarcomas are much less common than the central medullary type. Reports of peripheral lesions affecting the jaws are rare, with the parosteal type occurring more frequently than the periosteal type. Radiographically, the parosteal osteosarcoma appears as a radiodense mass on the cortical surface of bone. The tumor arises from a broad pedicle and then grows along the cortical surface, outgrowing the base of origin. A radiolucent line may be seen between the tumor and the underlying cortex as a result of this mushroom-like pattern of growth. Daughter masses may be seen adjacent to the principle mass. In contrast, the periosteal osteosarcoma is not as radiodense or homogeneous and the periphery is not as well defined as with the parosteal type. It has a spiculated appearance and does not outgrow its base. The cortex of the underlying bone may be thickened, but the medullary space is not involved. Histologically, the parosteal osteosarcoma is well differentiated with a bland appearance. Irregular trabeculae of woven bone are seen in a spindle cell stroma with minimal atypia and rare mitotic figures. In contrast, the periosteal osteosarcoma is histopathologically a higher grade tumor that microscopically resembles a central chondroblastic osteosarcoma. The periosteal osteosarcoma typically does not infiltrate medullary bone, differentiating it from the central chondroblastic osteosarcoma that perforates the cortex and extends into the soft tissue. Knowledge of the biological behavior, treatment, and prognosis of peripheral osteosarcomas is limited by the rarity with which they occur in the jaws. On the basis of current knowledge, jaw lesions are best treated by en bloc resection. Peripheral tumors of the long bones are associated with a considerably better prognosis than intramedullary tumors. The periosteal subtype is thought to have both a higher recurrence rate and greater metastatic potential in comparison with the parosteal subtype. CHONDROSARCOMA A chondrosarcoma is a malignant tumor characterized by the formation of cartilage, but not of bone, by the tumor cells. It is second to osteosarcoma as the most common primary sarcoma of bone; however, only 1% to 2% of chondrosarcomas occur in the head and neck region. The maxilla is more frequently involved than the mandible. Maxillary lesions occur most often in the anterior region, and mandibular lesions occur most often in the molar-premolar region. This lesion occurs over a wide age range with a peak incidence in the third decade. There is no significant gender predilection. The most common presentation is that of a slow-growing, painless mass or swelling (Fig , A). A minority of lesions produce pain. Lesions involving the alveolar bone may result in displaced and mobile teeth. Depending on the location of the tumor, patients may also experience nasal symptoms, visual disturbances, and sensory alterations. The radiographical appearance may vary, although most lesions demonstrate features consistent with a malignant process. The majority of chondrosarcomas appear as an osteolytic lesion with poorly defined borders containing scattered and variable amounts of radiopaque foci (Fig , B, C, and D). The radiopacities represent calcification of the neoplastic cartilage. Some lesions develop significant calcification and appear as a densely calcified mass with irregular margins. Some
32 Ch23-F10053.qxd 5/15/06 6:01 PM Page 521 PART II ONCOLOGY 521 B A C D Fig Chondrosarcoma. A, Expansion of the maxillary left alveolus with mucosal ulceration laterally. B, Panoramic radiograph demonstrating a poorly defined mass causing expansion of the posterior left maxilla. C and D, Axial and coronal magnetic resonance images demonstrating the extent of the tumor. tumors grow in a lobular pattern with few or no foci of calcification, producing a multilocular radiolucency that appears more like a benign process. Similar to osteosarcoma, some lesions produce a peripheral sunburst pattern or symmetric widening of the periodontal ligament space around involved teeth. The tumor may extend well beyond radiographical margins. 173 The histological appearance of chondrosarcoma is variable, although all demonstrate the formation of cartilage, but not osteoid or bone, from a sarcomatous stroma. If the sarcomatous stroma is seen to produce osteoid or bone in any part of the lesion, the tumor is considered to be an osteosarcoma, regardless of the amount of cartilage produced. 174 However, calcification of the chondroid matrix does occur in chondrosarcomas. Additional histological features of a malignant tumor of cartilage include hypercellularity, particularly an increase in the number of cartilage cells with plump nuclei, binuclear or multinuclear cartilage cells, nuclear hyperchromatism, and both cellular and nuclear pleomorphism. Mitotic figures may be scarce or absent. Chondrosarcomas have been classified into grades I, II, and III on the basis of mitotic rate, cellularity, and nuclear size. 175 This grading system correlates well with
33 Ch23-F10053.qxd 5/15/06 6:01 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS prognosis. In the head and neck region, grade I and II chondrosarcomas predominate. Radical ablative surgery is the treatment of choice. Radiation therapy has generally not been shown to provide a significant survival benefit, 173,175,176 although there have been occasional reports of long-term benefits Thus radiation therapy may be considered in cases of unresectable, residual, or recurrent tumors. The vast majority of reports involving chemotherapy show no significant therapeutic benefit. 173,175,176,181 The prognosis for chondrosarcomas of the jaws is worse than that for extragnathic tumors. The overall 5-year survival rate for chondrosarcomas of the jaws ranges from 32% 173 to 81%. 176 Factors influencing the prognosis for chondrosarcomas of the jaws include the site of origin, histological grade, and therapeutic modality. Mandibular tumors have a more favorable prognosis than maxillary lesions. Grade III lesions have a higher rate of metastasis and a poorer prognosis than grade I and II lesions. The lung is the most common site of metastasis, while lymph node metastasis is rare; thus neck dissection is not advocated for chondrosarcomas of the jaws. The primary factor influencing the rate of recurrence is the adequacy of the surgical resection. The most common cause of death for jaw lesions is uncontrolled local recurrence and extension into adjacent vital structures. Recurrences may occur 10 to 20 years following surgery; thus long-term follow-up is required. MESENCHYMAL CHONDROSARCOMA Mesenchymal chondrosarcoma is a rare tumor that is clinically and histologically distinct in comparison with chondrosarcoma. Up to one third of cases arise in soft tissue. The maxilla and mandible are two of the more commonly involved bony sites. The tumor most commonly occurs between 10 and 30 years of age, with an equal distribution between genders. Patients most often present with swelling and occasionally pain. Radiographically, the lesion appears as a radiolucency with well or poorly demarcated borders. Stippled calcifications may be seen within the lesion. Histologically, the tumor displays a bimorphic pattern composed of islands of well-differentiated malignant cartilage surrounded by an anaplastic small, round cell malignancy. The cartilaginous component distinguishes mesenchymal chondrosarcoma from Ewing sarcoma and hemangiopericytoma, which resemble the undifferentiated small cell component. Surgical resection with wide margins is required to obtain local control. Information regarding the use of both radiation therapy and chemotherapy is limited; thus meaningful conclusions regarding adjuvant therapy cannot be made. The 5-year and 10-year survival rates for mesenchymal chondrosarcoma are approximately 50% and 28%, respectively. 182,183 Reports limited to mesenchymal chondrosarcomas of the jaws suggest the prognosis for jaw tumors may be better than that for extragnathic sites. 184,185 Mesenchymal chondrosarcoma has a propensity for recurrence and metastasis, with the lung being the most frequent site of metastasis. Recurrences and distant metastases may take up to 20 years to manifest following treatment of the primary tumor; therefore long-term follow-up is required. 182 FIBROSARCOMA OF BONE Fibrosarcoma is a soft tissue and bone malignancy that rarely occurs in the head and neck region. Following refinement of the diagnostic criteria for fibrosarcoma, many tumors formerly classified as such are now considered to be malignant fibrous histiocytomas or another type of spindle cell neoplasm. Tumors that originate in the bone may theoretically arise from the periosteum, endosteum, or periodontal ligament. Fibrosarcomas of bone occur over a wide age range with a relatively uniform incidence over the second to sixth decades. No gender predilection exists. Bone lesions most commonly occur in long bones, although a small proportion occur in the jaws. Patients with jaw lesions most often present with jaw expansion and tooth mobility (Fig , A). Some patients may also experience pain or paresthesia. Radiographically, tumors involving the jaws usually appear as an osteolytic process with an ill-defined, irregular pattern (Fig , B). Histopathologically, fibrosarcomas of soft tissue and bone are defined as malignant spindle cell tumors showing a herringbone or interlacing fascicular pattern and no expression of other connective tissue cell markers. Low-grade tumors demonstrate a herringbone pattern with rare mitoses and abundant collagen. Higher-grade tumors show increased mitotic activity, less collagen, and loss of the herringbone pattern. Surgical resection with wide margins is the recommended treatment for fibrosarcoma of bone. The efficacy of neither chemotherapy nor radiation therapy is well established. The tumor has minimal metastatic potential. Recurrences are not uncommon and are best managed with salvage surgery. Studies that have assessed survival for fibrosarcoma of bone generally include cases diagnosed before the refinement of the diagnostic criteria; as a result, cases of malignant fibrous histiocytoma, which are associated with a poor prognosis, are frequently included. Thus valid survival data for fibrosarcoma of the jaws is difficult to obtain. One report involving 14 patients with fibrosarcoma of the
34 Ch23-F10053.qxd 5/15/06 6:01 PM Page 523 PART II ONCOLOGY 523 A B Fig Fibrosarcoma of bone. A, Erythematous gingival lesion seen in the anterior right maxilla. B, Coronal computed tomography image demonstrating the extent of the tumor. jaws found a 5-year survival rate of 71%. 186 This suggests fibrosarcomas of the jaws may have a better prognosis than lesions located elsewhere in the skeleton because the estimated overall 5-year survival rate for fibrosarcoma of bone is between 34% and 45%. 187 Factors that negatively influence the prognosis include high-grade tumors and patients older than 40 years of age. MALIGNANT FIBROUS HISTIOCYTOMA The malignant fibrous histiocytoma is a malignant neoplasm of soft tissue and bone, which is composed of fibroblasts and pleomorphic cells with a prominent storiform pattern. It occurs most often in soft tissues and represents 2% to 6% of all primary bone malignancies. The long bones, particularly the femur, are the most frequently affected osseous sites. Lesions involving the jaws occur rarely. They may arise as a primary tumor of bone (70%) or secondary to a preexisting bone condition (30%) including previously irradiated bone, Paget s disease, or bone infarct. The tumor occurs over a wide age range, with most occurring older than 40 years of age. A male predilection exists. Patients most frequently present with jaw expansion and tooth mobility. The tumor may occasionally be associated with pain. Radiographically, the tumor typically appears as an ill-defined, irregular osteolytic lesion. Irregular root resorption may be seen. Several histological subtypes have been identified. Common to all subtypes is the proliferation of pleomorphic spindle cells, histiocyte-like cells, and varying numbers of multinucleated giant cells. The most common subtype is the storiform-pleomorphic type, in which bundles of spindle cells are arranged in a storiform or pinwheel pattern. The histological subtype does not affect the prognosis. Most malignant fibrous histiocytomas are high-grade malignancies. This is an aggressive tumor with a propensity for recurrence and distant metastasis, particularly to the lungs. Wide surgical resection is recommended for lesions of the jaws. The limited number of reported cases of malignant fibrous histiocytoma of the jaws precludes the formulation of meaningful conclusions regarding chemotherapy and radiation therapy. In patients with high-grade lesions of the long bones, chemotherapeutic regimens similar to those used in osteosarcoma, which involve preoperative chemotherapy, appear to provide a survival benefit The role of radiation therapy is limited to unresectable and incompletely resected tumors. The disease-free 5-year survival for malignant fibrous histiocytoma of the long bones with preoperative chemotherapy and surgical resection is greater than 50%. 189,190 The prognosis of tumors affecting the jaws, however, appears to be worse. EWING S SARCOMA Ewing s sarcoma is in a family of tumors including the primitive neuroectodermal tumors, defined as round cell sarcomas that show varying degrees of neuroectodermal origin. These tumors are characterized by a recurrent t(11;22)(q24;q12) chromosomal translocation, which is detectable in approximately 85% of cases. This family of tumors accounts for 6% to 8% of primary bone malignancies, although it is second to osteosarcoma as the most common sarcoma in bone and soft tissue in children. The bones of the lower extremity and pelvis are most commonly affected, with lesions of the jaws
35 Ch23-F10053.qxd 5/15/06 6:01 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS accounting for less than 3% of Ewing s sarcomas. In the jaws, the posterior mandible is most frequently affected, while maxillary lesions are rare. Ewing s sarcoma primarily affects children and young adults, with 80% of cases occurring in patients younger than 20 years of age. A male predilection exists, and black individuals are rarely affected. Pain and swelling are the most common presenting symptoms. A soft tissue mass, paresthesia, tooth mobility, and fever may also be present (Fig , A). Radiographically, an irregular osteolytic process with ill-defined borders is seen (Fig , B). Tooth displacement and root resorption may also be seen. Histologically, Ewing s sarcoma is composed of proliferation of uniform, closely packed cells that may be compartmentalized by fibrous bands. The nuclei are round to oval with finely dispersed chromatin (Fig , C). The cytoplasm of the tumor cells frequently stains with periodic acid Schiff stain, indicating the presence of glycogen. Necrosis is commonly seen with viable cells remaining in a perivascular distribution. The tumor typically grows rapidly with extensive destruction of bone and a propensity for metastasis, particularly to the lungs and other bones. Clinically apparent metastases are present in 15% of patients with nonpelvic tumors at the time of diagnosis. 191 Treatment protocols for Ewing s sarcoma vary; however, the introduction of multimodal therapy has dramatically improved the prognosis. Treatment protocols involve multiagent chemotherapy with either surgical resection or radiation therapy or a combination of surgery and radiation therapy. Surgery tends to offer slightly better local control compared with radiation therapy alone. 192 In addition, the incidence of secondary sarcomas following radiation therapy in Ewing s sarcoma patients is approximately 6.5%. 193 With multimodal therapy the 5-year survival for patients presenting without metastatic disease is now 60%, and for those with metastatic disease the 5-year survival is 30%. 191 Patients younger than 15 years tend to have a better prognosis than those older than 15 years of age. 191 Ewing s sarcoma of the mandible appears to have a prognosis that is more favorable than that for other sites of involvement. Additional research into the role of autologous hematopoietic stem cell transplantation, immunotherapy, and biologic modifiers may eventually lead to further A B C Fig Ewing s sarcoma. A, A mass visible in the posterior left mandible of a 4-year-old male complaining of facial swelling and a loose tooth. B, A poorly defined osteolytic lesion of the posterior left mandible. C, Densely packed cells with round nuclei.
36 Ch23-F10053.qxd 5/15/06 6:01 PM Page 525 PART II ONCOLOGY 525 improvement in the long-term survival of patients with Ewing s sarcoma. 192 BURKITT S LYMPHOMA Burkitt s lymphoma is a high-grade, non-hodgkin s B-cell lymphoma that occurs in several clinical forms. Dennis Burkitt originally described it in 1958 as a jaw tumor that occurred frequently in African children. 194 It was later identified to be a form of malignant lymphoma. 195 Burkitt s lymphoma has subsequently been recognized to occur sporadically outside of Africa. The endemic (African) and sporadic (American) forms of Burkitt s lymphoma are characterized by the activation of the c-myc oncogene through reciprocal chromosomal translocations, most commonly t(8:14). 196 The endemic form is associated with Epstein-Barr virus (EBV) in more than 95% of cases, whereas the sporadic form is mostly EBV negative. A third type of Burkitt s lymphoma is associated with human immunodeficiency virus infection in adults. The endemic form has a peak incidence between 3 and 8 years of age. Jaw involvement is common and related to age, with almost 90% of patients younger than 3 years of age and 25% of those older than 15 years of age having jaw lesions. The maxilla is involved more frequently than the mandible, although all four quadrants may be involved. In contrast, the sporadic form occurs in a slightly older age-group with a peak incidence between 10 and 12 years of age; the jaws are involved in just 16% of cases at the time of diagnosis; the lesions are more localized, most commonly involving one quadrant; and the mandible is affected more frequently than the maxilla. 197 Jaw lesions of Burkitt s lymphoma can progress rapidly, appearing as a facial swelling or exophytic mass. These tumors may be associated with mobility of teeth, pain, and paresthesia. Radiographically, an osteolytic process with ragged, ill-defined margins is seen. Histologically, Burkitt s lymphoma represents an undifferentiated small, noncleaved B-cell lymphoma. The tumor is composed of sheets of medium-sized B cells with round nuclei and multiple nucleoli. Interspersed throughout the tumor cells are macrophages that stain less intensely than the hyperchromatic neoplastic B cells, resulting in a starry sky appearance. Mitoses are numerous; in fact, this tumor is known to have the highest proliferation rate of any neoplasm in humans. This aggressive malignancy, if untreated, results in death within 4 to 6 months of diagnosis. Intensive chemotherapy has resulted in a dramatic improvement in the prognosis of Burkitt s lymphoma. Current treatment involves intensive, short-term, multi-agent chemotherapy including intrathecal drugs for central nervous system prophylaxis. For advanced-stage disease, survival rates of between 70% and 87% have been achieved using these regimens. 198,199 MULTIPLE MYELOMA Multiple myeloma is a monoclonal, malignant, neoplastic proliferation of plasma cells with multicentric bone marrow involvement. Extraskeletal sites may occasionally be involved. It accounts for 1% of all malignancies in whites and 2% of those in blacks. It is the most frequently occurring primary malignancy of bone. The bones most frequently involved are the vertebrae, ribs, skull, pelvis, femur, clavicle, and scapula. The mandible and maxilla may also be involved. The median age at diagnosis is 68 years with 90% of cases occurring in individuals older than 40 years of age. A male predilection exists. The signs and symptoms characteristic of multiple myeloma result from the uncontrolled proliferation of malignant plasma cells within the bone marrow and the uncontrolled manufacture of their protein products. These signs and symptoms include bone pain, pathological fracture, hypercalcemia, anemia, renal failure, and recurrent bacterial infections. Because these tumors are derived from a single neoplastic clone, they are associated with the production of monoclonal immunoglobulin components. This is demonstrated on serum protein electrophoresis as an abnormal monoclonal immunoglobulin protein spike, called the M component. The immunoglobulin is most frequently of the IgG or IgA class, with the light chain restricted to either the lambda or kappa type. Monoclonal light chain (Bence- Jones protein) is found in the urine of approximately 50% of patients. Bence-Jones protein is directly toxic to renal epithelial cells and is a major contributing factor in the development of renal failure in multiple myeloma. In up to 25% of patients the light chain protein also accumulates in soft tissues, resulting in the development of amyloidosis, which may manifest in the maxillofacial region as macroglossia. Approximately 1% of multiple myeloma patients do not have an identifiable M component in the serum or urine. This form of the disease is termed nonsecretory myeloma. The typical radiographical appearance is that of multiple well-defined, punched-out radiolucencies of bone, which are noncorticated. These may be particularly evident on views of the skull. Rather than having focal osteolytic lesions of bone, generalized osteoporosis or, more infrequently, osteosclerotic lesions may be seen in some patients. Bone lesions in multiple myeloma usually are not evident on a bone scan. Histologically, the lesional tissue is composed of monotonous sheets of neoplastic, variably differentiated plasma cells. With
37 Ch23-F10053.qxd 5/15/06 6:01 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS the use of immunohistochemistry, the monoclonal nature of the intracytoplasmic immunoglobulin light chain can be demonstrated. This may be used to differentiate multiple myeloma from reactive plasma cell infiltrates, which are uniformly polyclonal. The treatment of multiple myeloma involves systemic chemotherapy to control the progression of the disease and supportive care to prevent serious morbidity from the complications of the disease. High-dose chemotherapy with autologous stem cell transplantation has significantly improved complete remission rates, eventfree survival, and overall survival as compared with conventional chemotherapeutic regimens. 200 Improvements in the management of multiple myeloma have resulted in complete remission rates of 20% to 59% and median overall survival of 4.4 to 7.1 years, with a substantial proportion of patients surviving more than 10 years. 201 Despite improvements in survival, at present there is no cure and patients eventually relapse. Death is most commonly a result of infection, renal failure, or progressive myeloma. Recent research has led to the development of biological treatments such as thalidomide, thalidomide analogs, and proteasome inhibitors, which target the myeloma cell and the bone marrow microenvironment. 201,202 These agents have shown promise in the management of relapsed or refractory patients with multiple myeloma by overcoming resistance to conventional chemotherapy, yet they do not have the potential to cure. In addition to chemotherapy, localized radiation therapy may be used to treat painful bone lesions. Bisphosphonates, which inhibit osteoclastic resorption of bone and may also have direct antitumor effects, are routinely used in the management of multiple myeloma. Bisphosphonates have proven to be beneficial in preventing pathological vertebral fractures, hypercalcemia, and ameliorating bone pain. 54 A significant maxillofacial complication related to bisphosphonate therapy has recently been recognized. The use of intravenous pamidronate and zoledronate has been associated with the development of osteonecrosis of the jaws. 203,204 Definitive management of this complication has proven difficult. Débridement cannot be carried out to viable bleeding bone and may cause further exposure of bone as a result of the systemic effect of the bisphosphonate therapy. Furthermore, the effectiveness of hyperbaric oxygen therapy has been limited and discontinuation of bisphosphonate therapy has not proven beneficial. Palliative treatment limited to intermittent courses of antibiotics, chlorhexidine mouth rinses, wound irrigation, and if necessary minor débridement of superficial bony sequestrae is most appropriate. To reduce the risk of developing osteonecrosis, patients should have a thorough dental evaluation to identify and treat any dental pathology before initiation of bisphosphonate therapy. With patients on pamidronate or zoledronate, invasive dental procedures should be avoided when possible. SOLITARY PLASMACYTOMA OF BONE A solitary plasmacytoma is a unifocal, monoclonal, neoplastic proliferation of plasma cells that most often occurs within bone but may occasionally be found in soft tissue. To establish the diagnosis, a complete radiological skeletal survey and a bone marrow biopsy away from the solitary lesion must demonstrate no evidence of plasmacytosis in other areas. The lesion occurs at a mean age of 50 years with a male predilection. Although rarely found in the jaws, the mandible is affected more commonly than the maxilla. Presenting signs and symptoms include pain, swelling, and pathological fracture. Radiographically, the lesion appears as a well-defined radiolucency without sclerotic borders. The histological appearance is identical to that of multiple myeloma. An abnormal monoclonal immunoglobulin protein spike (M component) may be demonstrated in the serum or urine in up to 25% of cases of solitary plasmacytoma. Radiation therapy using 3500 cgy to 4500 cgy is the treatment of choice for solitary plasmacytomas. Unfortunately, approximately 70% of patients with solitary lesions develop multiple myeloma; however, it is not possible to predict which ones will do so. The overall mean survival of patients diagnosed with a solitary plasmacytoma is 10 years. MALIGNANT PERIPHERAL NERVE SHEATH TUMOR (NEUROFIBROSARCOMA, MALIGNANT SCHWANNOMA) The malignant peripheral nerve sheath tumor (MPNST) is a rare malignancy that may develop within a preexisting neurofibroma, de novo, or as a postradiation sarcoma. Fifty-two percent of cases develop in patients with neurofibromatosis type The Schwann cell and possibly other nerve sheath cells are believed to be the cell of origin. The lesion occurs most frequently in the soft tissues of the extremities and trunk, with intraosseous lesions occurring rarely. The most common site for intraosseous lesions is the mandible, where 55% of reported intraosseous lesions have occurred. In contrast to soft tissue MPNSTs, intraosseous lesions are infrequently associated with neurofibromatosis type 1. Intraosseous tumors have been reported in patients ranging in age from 4 to 76 years of age with no sex predilection. The tumor frequently produces paresthesia or anesthesia in the regional nerve distribution.
38 Ch23-F10053.qxd 5/15/06 6:01 PM Page 527 PART II ONCOLOGY 527 Within the jaws it may also produce bony expansion and tooth mobility. Radiographically, tumors of the mandible may produce widening of the inferior alveolar canal or the mental foramen or a diffuse, irregular radiolucency. Microscopically, the lesion consists of fascicles of spindle cells that closely resemble the cells of fibrosarcoma. The nuclei may be wavy or comma shaped, and nuclear pleomorphism may be prominent. Streaming and palisading of nuclei are often seen. Less cellular myxoid areas may also be present. Heterologous elements such as skeletal muscle, cartilage, or bone may be seen. The malignant Triton tumor is a highly aggressive variant that shows rhabdomyoblastic differentiation. Determining that the tumor arises from a nerve trunk or a neurofibroma aids in the differentiation between MPNST and fibrosarcoma. In addition, MPNSTs are S-100 protein positive in 50% of cases. The treatment of choice for intraosseous MPNSTs is surgical resection with wide margins. Due to the rarity of intraosseous tumors, the role of radiation and chemotherapy remains undetermined, although neither has been found to provide a survival benefit in soft tissue tumors. 205 Recurrence is common, and metastasis occurs via the hematogenous route. Survival data for intraosseous tumors is limited; however, the 5-year survival rate for soft tissue tumors in patients without neurofibromatosis is 53%, compared with 16% for those with neurofibromatosis. 205 POSTRADIATION SARCOMA OF BONE Postradiation sarcoma of bone, a sarcoma that develops in a bone within a previous irradiated field, is a rare tumor. Radiation-induced sarcomas occur more frequently in soft tissues than in bone. Postradiation sarcoma of bone is estimated to occur in 0.02% of irradiated patients. Postradiation sarcomas develop a mean of 14 years following the initial radiation therapy. Although there are reports of cases developing with less than 1-year latency, authors have proposed a minimum latency period that ranges between 3 and 5 years to make a diagnosis of postradiation sarcoma. 206,207 The risk of development of postradiation sarcoma is related to the dose of radiation received. The most common types of sarcomas that occur in a previously irradiated field are osteosarcoma, malignant fibrous histiocytoma, and fibrosarcoma. These tumors have clinical, radiographical, and histological features that are similar to their de novo counterparts. However, postradiation sarcomas tend to behave more aggressively and are less responsive to treatment. Wide surgical resection provides the best chance for cure. 208,209 Adjuvant chemotherapy has not provided encouraging results. 210 If the tissues in the site of the radiation-induced sarcoma have not previously been treated to tissue tolerance, radiation therapy may be considered, but its role is limited. The 5-year survival rate is approximately 30%. 208,209,211,212 METASTATIC CARCINOMA Metastatic carcinoma is the most common form of malignancy affecting bone. Bones with active marrow such as the vertebrae, ribs, pelvis, and skull are the preferential sites for metastasis. The jaws are relatively uncommon sites of metastasis. Approximately 1% of all oral malignancies represent malignancies that have metastasized from elsewhere in the body. 213 However, the incidence of metastasis to the jaws may be underestimated. A report involving autopsied carcinoma cases demonstrated 16% of the mandibles to have microscopic deposits of metastatic tumor cells, despite the lack of radiographical evidence of metastatic deposits in these mandibles. 214 The most common sites of the primary carcinoma are the breast and lung, followed by the kidney, prostate, thyroid, colon, and rectum. Metastatic spread of carcinoma to the jaws occurs by the hematogenous route. Emboli of primary carcinomas distant from the jaws may enter the venous circulation and bypass the lungs via the valveless paravertebral venous plexus of Batson to deposit into the jaws. 215 In patients with metastatic lesions in the jaws, the jaw lesions are the first indication of a malignancy in 30% of cases. 216 The majority of patients with metastatic carcinoma to the jaws are in their fifth to seventh decades, with a mean age of 45 years. Within the jaws, approximately 80% of the metastases are to the mandible, 14% to the maxilla, and 5% to both jaws. 216 The molar/premolar region is the area within both the mandible and the maxilla most frequently affected. Swelling, pain, and paresthesia are the most common presenting symptoms. Tooth mobility, trismus, and pathological fracture may also be clinically evident. Radiographically, a metastatic lesion in the jaws usually appears as an irregular radiolucency (Fig 23-30). However, metastatic prostate and breast lesions are often characterized by an osteoblastic process, resulting in either a radiopaque lesion or a mixed radiopaqueradiolucent lesion. The histological appearance of metastatic carcinoma is highly variable depending on the tumor type and the degree of differentiation. Some tumors may be sufficiently well differentiated and distinctive enough to provide a strong indication of the primary site. This most frequently occurs with renal cell carcinomas and thyroid tumors. However, metastatic carcinomas are more frequently poorly differentiated
39 Ch23-F10053.qxd 5/15/06 6:01 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS Fig Metastatic breast cancer. An irregular radiolucency of the mandibular right body. and provide little clue as to the site of the primary lesion. In such cases, immunohistochemistry can aid in determining the site of the primary carcinoma. Immunoperoxidase stain for cytokeratin will verify the presence of cells of epithelial origin in all carcinomas, and tissue-specific markers may be used to further characterize the tumor. However, the final diagnosis depends on a complete medical history, physical examination, and appropriate investigations. Management of metastatic carcinoma to the jaws begins with identification of the primary site and determining the extent of metastatic involvement. Jaw metastases are usually evidence of widely disseminated disease, and palliative treatment should be aimed at eliminating pain and preserving function. Depending on the type of carcinoma, its responsiveness to treatment, and the overall health status of the patient, palliation may involve surgical excision of the metastatic deposit, radiation therapy, chemotherapy, or chemoradiotherapy. If the metastatic lesion of the jaw represents the only site of metastasis, adequate surgical treatment or chemoradiotherapy may improve the prognosis. Overall, the prognosis of metastatic carcinoma of the jaws is poor, with a mean survival of 6 to 7 months. 213,216 PITFALLS The oral and maxillofacial pathologist should also be given a representative and large enough biopsy specimen. Diagnosis is often made by pattern recognition of the lesion, and the margins may not be important for diagnosis. For a lesion of the jaws, there may be debate regarding the order of investigations as to whether biopsy should precede three-dimensional imaging or not. If the biopsy is taken first, it may cause artifact on the three-dimensional imaging. If the imaging is done first, it may prove to have been unnecessary or inadequate once the diagnosis is established. Treatment of ameloblastoma should not vary on the basis of histological subtype. The histological subtype can easily be misdiagnosed because of sampling. Furthermore, the data regarding clinical behavior and histologic subtype are equivocal. Follow-up for aggressive odontogenic tumors (including ameloblastoma, odontogenic myxoma, and calcifying epithelial odontogenic tumor) should be at least 20 years and possibly for life. REFERENCES 1. Wakoh M, Harada T, Inoue T: Follicular/desmoplastic hybrid ameloblastoma with radiographic features of concomitant fibro-osseous and solitary cystic lesions, Oral Surg Oral Med Oral Pathol Oral Radiol Endod 94(6): , Ide F, Sakashita H, Kusama K: Ameloblastomatoid, central odontogenic fibroma: an epithelium-rich variant, J Oral Pathol Med 31(10): , Garcia-Pola Vallejo M, Gonzalez Garcia M, Lopez-Arranz JS et al: Adenomatoid odontogenic tumor arising in a dental cyst: report of unusual case, J Clin Pediatr Dent 23(1):55-58, Hisatomi M, Asaumi J, Konouchi H et al: A case of glandular odontogenic cyst associated with ameloblastoma: correlation of diagnostic imaging with histopathological features, Dentomaxillofac Radiol 29(4): , Braunshtein E, Vered M, Taicher S et al: Clear cell odontogenic carcinoma and clear cell ameloblastoma: a single clinicopathologic entity? A new case and comparative analysis of the literature, J Oral Maxillofac Surg 61(9): , Hirshberg A, Kaplan I, Buchner A: Calcifying odontogenic cyst associated with odontoma: a possible separate entity (odontocalcifying odontogenic cyst), J Oral Maxillofac Surg 52(6): , Aithal D, Reddy BS, Mahajan S et al: Ameloblastomatous calcifying odontogenic cyst: a rare histologic variant, J Oral Pathol Med 32(6): , Mosqueda-Taylor A, Carlos-Bregni R, Ramirez-Amador V et al: Odontoameloblastoma. Clinico-pathologic study of three cases and critical review of the literature, Oral Oncol 38(8): , Zeitoun IM, Dhanrajani PJ, Mosadomi HA: Adenomatoid odontogenic tumor arising in a calcifying odontogenic cyst, J Oral Maxillofac Surg 54(5): , Piattelli A, Scarano A, Piattelli M: Calcifying odontogenic cyst associated with compound odontoma: a study on
40 Ch23-F10053.qxd 5/15/06 6:01 PM Page 529 PART II ONCOLOGY 529 undemineralized material, Bull Group Int Rech Sci Stomatol Odontol 38(3-4): , Snead ML, Luo W, Hsu DD et al: Human ameloblastoma tumors express the amelogenin gene, Oral Surg Oral Med Oral Pathol 74(1):64-72, Kumamoto H, Yoshida M, Ooya K: Immunohistochemical detection of amelogenin and cytokeratin 19 in epithelial odontogenic tumors, Oral Dis 7(3): , Hazelbag HM, Laforga JB, Roels HJ et al: Dedifferentiated adamantinoma with revertant mesenchymal phenotype, Am J Surg Pathol 27(12): , Qureshi AA, Shott S, Mallin BA et al: Current trends in the management of adamantinoma of long bones. An international study, J Bone Joint Surg Am 82-A(8): , Van Effenterre R, Boch AL: Craniopharyngioma in adults and children: a study of 122 surgical cases, J Neurosurg 97(1):3-11, Regezi J, Sceulba JJ, Jordon RCK: Clinical pathologic correlations, ed 4, Philadelphia, 2003, Saunders. 17. Henderson JM, Sonnet JR, Schlesinger C et al: Pulmonary metastasis of ameloblastoma: case report and review of the literature, Oral Surg Oral Med Oral Pathol Oral Radiol Endod 88(2): , Campbell D, Jeffrey RR, Wallis F et al: Metastatic pulmonary ameloblastoma. An unusual case, Br J Oral Maxillofac Surg 41(3): , Reichart PA, Philipsen HP, Sonner S: Ameloblastoma: biological profile of 3677 cases, Eur J Cancer B Oral Oncol 31B(2):86-99, Daley TD, Wysocki GP, Pringle GA: Relative incidence of odontogenic tumors and oral and jaw cysts in a Canadian population, Oral Surg Oral Med Oral Pathol 77(3): , Arotiba JT, Ogunbiyi JO, Obiechina AE: Odontogenic tumours: a 15-year review from Ibadan, Nigeria, Br J Oral Maxillofac Surg 35(5): , Fregnani ER, Fillipi RZ, Oliveira CR et al: Odontomas and ameloblastomas: variable prevalences around the world? Oral Oncol 38(8): , Larsson A, Almeren H: Ameloblastoma of the jaws. An analysis of a consecutive series of all cases reported to the Swedish Cancer Registry during , Acta Pathol Microbiol Scand [A] 86A(5): , Sehdev MK, Huvos AG, Strong EW et al: Proceedings: ameloblastoma of maxilla and mandible, Cancer 33(2): , Shatkin S, Hoffmeister FS: Ameloblastoma: a rational approach to therapy, Oral Surg Oral Med Oral Pathol 20(4): , Waldron CA: Ameloblastoma in perspective, J Oral Surg 24(4): , Mehlisch DR, Dahlin DC, Masson JK: Ameloblastoma: a clinicopathologic report, J Oral Surg 30(1):9-22, Gardner DG, Pecak AM: The treatment of ameloblastoma based on pathologic and anatomic principles, Cancer 46(11): , Kuriakose MA, Lee JJ, DeLacure MD: Inferior alveolar nerve-preserving mandibulectomy for nonmalignant lesions, Laryngoscope 113(7): , Pogrel MA: The use of liquid nitrogen in the management of locally aggressive bone lesions, J Oral Maxillofac Surg 51:269, Pogrel MA: The management of lesions of the jaws with liquid nitrogen cryotherapy, J Calif Dent Assoc 23(12):54-57, Salmassy DA, Pogrel MA: Liquid nitrogen cryosurgery and immediate bone grafting in the management of aggressive primary jaw lesions, J Oral Maxillofac Surg 53(7): , Sampson DE, Pogrel MA: Management of mandibular ameloblastoma: the clinical basis for a treatment algorithm, J Oral Maxillofac Surg 57(9): ; discussion , Robinson L, Martinez MG: Unicystic ameloblastoma: a prognostically distinct entity, Cancer 40(5): , Philipsen HP, Reichart PA: Unicystic ameloblastoma. A review of 193 cases from the literature, Oral Oncol 34(5): , Eversole LR, Leider AS, Strub D: Radiographic characteristics of cystogenic ameloblastoma, Oral Surg Oral Med Oral Pathol 57(5): , Junquera L, Ascani G, Vicente JC et al: Ameloblastoma revisited, Ann Otol Rhinol Laryngol 112(12): , Ackermann GL, Altini M, Shear M: The unicystic ameloblastoma: a clinicopathological study of 57 cases, J Oral Pathol 17(9-10): , Rosenstein T, Pogrel MA, Smith RA et al: Cystic ameloblastoma behavior and treatment of 21 cases, J Oral Maxillofac Surg 59(11): ; discussion , Philipsen HP, Reichart PA, Nikai H et al: Peripheral ameloblastoma: biological profile based on 160 cases from the literature, Oral Oncol 37(1):17-27, Gardner DG: Peripheral ameloblastoma: a study of 21 cases, including 5 reported as basal cell carcinoma of the gingiva, Cancer 39(4): , Pindborg J: Calcifying epithelial odontogenic tumor, Acta Pathol Microbiol Scand [suppl] 111:71, Kaplan I, Buchner A, Calderon S et al: Radiological and clinical features of calcifying epithelial odontogenic tumour, Dentomaxillofac Radiol 30(1):22-28, Aviel-Ronen S, Liokumovich P, Rahima D et al: The amyloid deposit in calcifying epithelial odontogenic tumor is immunoreactive for cytokeratins, Arch Pathol Lab Med 124(6): , Veness MJ, Morgan G, Collins AP et al: Calcifying epithelial odontogenic (Pindborg) tumor with malignant transformation and metastatic spread, Head Neck 23(8): , Anavi Y, Kaplan I, Citir M et al: Clear-cell variant of calcifying epithelial odontogenic tumor: clinical and radiographic characteristics, Oral Surg Oral Med Oral Pathol Oral Radiol Endod 95(3): , Abiko Y, Murata M, Ito Y et al: Immunohistochemical localization of amelogenin in human odontogenic
41 Ch23-F10053.qxd 5/15/06 6:01 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS tumors, using a polyclonal antibody against bovine amelogenin, Med Electron Microsc 34(3): , Philipsen HP, Reichart PA: Adenomatoid odontogenic tumour: facts and figures, Oral Oncol 35(2): , Philipsen HP, Srisuwan T, Reichart PA: Adenomatoid odontogenic tumor mimicking a periapical (radicular) cyst: a case report, Oral Surg Oral Med Oral Pathol Oral Radiol Endod 94(2): , Konouchi H, Asaumi J, Yanagi Y et al: Adenomatoid odontogenic tumor: correlation of MRI with histopathological findings, Eur J Radiol 44(1):19-23, Pullon PA, Shafer WG, Elzay RP et al: Squamous odontogenic tumor. Report of six cases of a previously undescribed lesion, Oral Surg Oral Med Oral Pathol 40(5): , Haghighat K, Kalmar JR, Mariotti AJ: Squamous odontogenic tumor: diagnosis and management, J Periodontol 73(6): , Kusama K, Kawashima A, Nagai H et al: Squamous odontogenic tumor of the maxilla: report of a case, J Oral Sci 40(3): , Barrios TJ, Sudol JC, Cleveland DB: Squamous odontogenic tumor associated with an erupting maxillary canine: case report, J Oral Maxillofac Surg 62(6): , Eversole LR: Malignant epithelial odontogenic tumors, Semin Diagn Pathol 16(4): , Zwahlen RA, Vogt P, Fischer FS et al: Case report: myocardial metastasis of a maxillary malignant ameloblastoma, J Oral Maxillofac Surg 61(6): , Ciment LM, Ciment AJ: Malignant ameloblastoma metastatic to the lungs 29 years after primary resection: a case report, Chest 121(4): , Zarbo RJ, Marunick MT, Johns R: Malignant ameloblastoma, spindle cell variant, Arch Pathol Lab Med 127(3): , Avon SL, McComb J, Clokie C: Ameloblastic carcinoma: case report and literature review, J Can Dent Assoc 69(9): , Dhir K, Sciubba J, Tufano RP: Ameloblastic carcinoma of the maxilla, Oral Oncol 39(7): , Datta R, Winston JS, Diaz-Reyes G et al: Ameloblastic carcinoma: report of an aggressive case with multiple bony metastases, Am J Otolaryngol 24(1):64-69, Grunwald V, Le Blanc S, Karstens JH et al: Metastatic malignant ameloblastoma responding to chemotherapy with paclitaxel and carboplatin, Ann Oncol 12(10): , Cox DP, Muller S, Carlson GW et al: Ameloblastic carcinoma ex ameloblastoma of the mandible with malignancy-associated hypercalcemia, Oral Surg Oral Med Oral Pathol Oral Radiol Endod 90(6): , Kumar A, Loughran T, Alsina M et al: Management of multiple myeloma: a systematic review and critical appraisal of published studies, Lancet Oncol 4(5): , Iezzi G, Rubini C, Fioroni M et al: Clear cell odontogenic carcinoma, Oral Oncol 38(2): , Benton DC, Eisenberg E: Clear cell odontogenic carcinoma: report of a case, J Oral Maxillofac Surg 59(1):83-88, Brinck U, Gunawan B, Schulten HJ et al: Clear-cell odontogenic carcinoma with pulmonary metastases resembling pulmonary meningothelial-like nodules, Virchows Arch 438(4): , Thomas G, Pandey M, Mathew A et al: Primary intraosseous carcinoma of the jaw: pooled analysis of world literature and report of two new cases, Int J Oral Maxillofac Surg 30(4): , Thomas G, Sreelatha KT, Balan A et al: Primary intraosseous carcinoma of the mandible a case report and review of the literature, Eur J Surg Oncol 26(1):82-86, Ide F, Shimoyama T, Horie N et al: Primary intraosseous carcinoma of the mandible with probable origin from reduced enamel epithelium, J Oral Pathol Med 28(9): , Shimoyama T, Ide F, Horie N et al: Primary intraosseous carcinoma associated with impacted third molar of the mandible: review of the literature and report of a new case, J Oral Sci 43(4): , Ide F, Shimoyama T, Horie N et al: Intraosseous squamous cell carcinoma arising in association with a squamous odontogenic tumour of the mandible, Oral Oncol 35(4): , Hamakawa H, Kayahara H, Sumida T et al: Mandibular intraosseous carcinoma coexisting with ameloblastoma, J Oral Maxillofac Surg 58(4): , Murillo-Cortes J, Etayo-Perez A, Sebastian-Lopez C et al: Primary intraosseous carcinoma arising in a mandibular cyst, Med Oral 7(5): , Scheer M, Koch AM, Drebber U et al: Primary intraosseous carcinoma of the jaws arising from an odontogenic cyst a case report, J Craniomaxillofac Surg 32(3): , Ramer M, Buonocore P, Krost B: Central odontogenic fibroma report of a case and review of the literature, Periodontal Clin Investig 24(1):27-30, Gardner DG: Central odontogenic fibroma current concepts, J Oral Pathol Med 25(10): , Drebber U, Scheer M, Zoller JE et al: [The central odontogenic fibroma. A rare tumor]. Pathologe 24(2): , Piattelli A, Di Alberti L, Scarano A et al: Benign cementoblastoma associated with an unerupted third molar, Oral Oncol 34(3): , El-Mofty SK: Cemento-ossifying fibroma and benign cementoblastoma, Semin Diagn Pathol 16(4): , Brannon RB, Fowler CB, Carpenter WM et al: Cementoblastoma: an innocuous neoplasm? A clinicopathologic study of 44 cases and review of the literature with special emphasis on recurrence, Oral Surg Oral Med Oral Pathol Oral Radiol Endod 93(3): , Mosqueda-Taylor A, Ledesma-Montes C, Caballero- Sandoval S et al: Odontogenic tumors in Mexico: a collaborative retrospective study of 349 cases, Oral Surg
42 Ch23-F10053.qxd 5/15/06 6:01 PM Page 531 PART II ONCOLOGY 531 Oral Med Oral Pathol Oral Radiol Endod 84(6): , Simon EN, Merkx MA, Vuhahula E et al: Odontogenic myxoma: a clinicopathological study of 33 cases, Int J Oral Maxillofac Surg 33(4): , Kaffe I, Naor H, Buchner A: Clinical and radiological features of odontogenic myxoma of the jaws, Dentomaxillofac Radiol 26(5): , Asaumi J, Matsuzaki H, Hisatomi M et al: Application of dynamic MRI to differentiating odontogenic myxomas from ameloblastomas, Eur J Radiol 43(1):37-41, Barker BF: Odontogenic myxoma, Semin Diagn Pathol 16(4): , Endo Y, Uzawa K, Mochida Y et al: Differential distribution of glycosaminoglycans in human cementifying fibroma and fibro-osseous lesions, Oral Dis 9(2):73-76, Santos LD, Arianayagam S: Cementifying fibroma of the maxillary antrum, Pathology 26(4): , Akao I, Ohashi T, Imokawa H et al: Cementifying fibroma in the ethmoidal sinus extending to the anterior cranial base in an 11-year-old girl: a case report, Auris Nasus Larynx 30 (suppl):s , Molinari SP, Di Rocco A, Merchant C et al: An unusual sphenoid ridge tumor: cementifying fibroma, J Neurol 243(1): , Sigler SC, Wobig JL, Dierks EJ et al: Cementifying fibroma presenting as proptosis, Ophthal Plast Reconstr Surg 13(4): , Kreutziger KL, Weiss LS: Cementifying fibroma: resection of recurrent mandibular lesion with microsurgical preservation of inferior alveolar nerve and immediate reconstruction, South Med J 87(6): , Bregni RC, Taylor AM, Garcia AM: Ameloblastic fibrosarcoma of the mandible: report of two cases and review of the literature, J Oral Pathol Med 30(5): , Nogueira Tde O, Carvalho YR, Rosa LE et al: Possible malignant transformation of an ameloblastic fibroma to ameloblastic fibrosarcoma: a case report, J Oral Maxillofac Surg 55(2): , Tajima Y, Utsumi N, Suzuki S et al: Ameloblastic fibrosarcoma arising de novo in the maxilla, Pathol Int 47(8): , Huguet P, Castellvi J, Avila M et al: Ameloblastic fibrosarcoma: report of a case. Immunohistochemical study and review of the literature, Med Oral 6(3): , Stambaugh MD, DeNittis AS: Out of radiation field recurrence of an ameloblastic sarcoma of the maxilla, J Oral Maxillofac Surg 56(11):1364, Amado Cuesta S, Gargallo Albiol J, Berini Aytes L et al: Review of 61 cases of odontoma. Presentation of an erupted complex odontoma, Med Oral 8(5): , Martin-Granizo Lopez R, Ortega L, Gonzalez Corchon MA et al: Ameloblastic fibroma of the mandible. Report of two cases, Med Oral 8(2): , Parham DM, Bridge JA, Lukacs JL et al: Cytogenetic distinction among benign fibro-osseous lesions of bone in children and adolescents: value of karyotypic findings in differential diagnosis, Pediatr Dev Pathol 7(2): , Dal Cin P, Sciot R, Fossion E et al: Chromosome abnormalities in cementifying fibroma, Cancer Genet Cytogenet 71(2): , Gollin SM, Storto PD, Malone PS et al: Cytogenetic abnormalities in an ossifying fibroma from a patient with bilateral retinoblastoma, Genes Chromosomes Cancer 4(2): , Fletcher CDM, Unni KK, Mertens F: World Health Organization classification of tumors: pathology and genetics of soft tissue and bone, Lyon, France, 2002, IARC Press Yih WY, Pederson GT, Bartley MH Jr: Multiple familial ossifying fibromas: relationship to other osseous lesions of the jaws, Oral Surg Oral Med Oral Pathol 68(6): , Canger EM, Celenk P, Kayipmaz S et al: Familial ossifying fibromas: report of two cases, J Oral Sci 46(1):61-64, Sciubba JJ, Younai F: Ossifying fibroma of the mandible and maxilla: review of 18 cases, J Oral Pathol Med 18(6): , Eversole LR, Leider AS, Nelson K: Ossifying fibroma: a clinicopathologic study of sixty-four cases, Oral Surg Oral Med Oral Pathol 60(5): , Zachariades N, Vairaktaris E, Papanicolaou S et al: Ossifying fibroma of the jaws. Review of the literature and report of 16 cases, Int J Oral Surg 13(1):1-6, Sweet RM, Bryarly RC, Kornblut AD et al: Recurrent cementifying fibroma of the jaws, Laryngoscope 91(7): , Boysen ME, Olving JH, Vatne K et al: Fibro-osseous lesions of the cranio-facial bones, J Laryngol Otol 93(8): , Dehner LP: Tumors of the mandible and maxilla in children. I. Clinicopathologic study of 46 histologically benign lesions, Cancer 31(2): , Waldron CA, Giansanti JS: Benign fibro-osseous lesions of the jaws: a clinical-radiologic-histologic review of sixty-five cases. II. Benign fibro-osseous lesions of periodontal ligament origin, Oral Surg Oral Med Oral Pathol 35(3): , Hamner JE III, Scofield HH, Cornyn J: Benign fibroosseous jaw lesions of periodontal membrane origin. An analysis of 249 cases, Cancer 22(4): , Smith AG, Zavaleta A: Osteoma, ossifying fibroma, and fibrous dysplasia of facial and cranial bones, AMA Arch Pathol 54(6): , Said-al-Naief NA, Surwillo E: Florid osseous dysplasia of the mandible: report of a case. Compend Contin Educ Dent 20(11): , passim; quiz 1032, Commins DJ, Tolley NS, Milford CA: Fibrous dysplasia and ossifying fibroma of the paranasal sinuses, J Laryngol Otol 112(10): , Brannon RB, Fowler CB: Benign fibro-osseous lesions: a review of current concepts, Adv Anat Pathol 8(3): , 2001.
43 Ch23-F10053.qxd 5/15/06 6:01 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS 118. Kramer IR: The World Health Organization: histological typing of odontogenic tumours: an introduction to the second edition, J Dent Assoc S Afr 47(5): , Johnson LC, Yousefi M, Vinh TN et al: Juvenile active ossifying fibroma. Its nature, dynamics and origin, Acta Otolaryngol Suppl 488:1-40, Willman CL, Busque L, Griffith BB et al: Langerhans -cell histiocytosis (histiocytosis X) a clonal proliferative disease, N Engl J Med 331(3): , Kawakubo Y, Kishimoto H, Sato Y et al: Human cytomegalovirus infection in foci of Langerhans cell histiocytosis, Virchows Arch 434(2): , Arico M, Danesino C: Langerhans cell histiocytosis: is there a role for genetics? Haematologica 86(10): , Boutsen Y, Esselinckx W, Delos M et al: Adult onset of multifocal eosinophilic granuloma of bone: a long-term follow-up with evaluation of various treatment options and spontaneous healing, Clin Rheumatol 18(1):69-73, Jaffe HL: Giant-cell reparative granuloma, traumatic bone cyst, and fibrous (fibro-osseous) dysplasia of the jawbones, J Oral Surg (Chic) 6(1): , Bernier JL, Cahn LR: The peripheral giant cell reparative granuloma, J Am Dent Assoc 49(2): , Flanagan AM, Nui B, Tinkler SM et al: The multinucleate cells in giant cell granulomas of the jaw are osteoclasts, Cancer 62(6): , Jacoway J, Howell FV, Terry BC: Central giant cell granuloma: an alternative to surgical therapy, Oral Surg Oral Med Oral Pathol 66:572, Terry BJJ: Management of central giant cell lesions: an alternative to surgical therapy, Oral Maxillofac Surg Clin N Am 6: , Kermer C, Millesi W, Watzke IM: Local injection of corticosteroids for central giant cell granuloma. A case report, Int J Oral Maxillofac Surg 23(6 Pt 1): , Carlos R, Sedano HO: Intralesional corticosteroids as an alternative treatment for central giant cell granuloma, Oral Surg Oral Med Oral Pathol Oral Radiol Endod 93(2): , Harris M: Central giant cell granulomas of the jaws regress with calcitonin therapy, Br J Oral Maxillofac Surg 31(2):89-94, O Regan EM, Gibb DH, Odell EW: Rapid growth of giant cell granuloma in pregnancy treated with calcitonin, Oral Surg Oral Med Oral Pathol Oral Radiol Endod 92(5): , Pogrel MA, Regezi JA, Harris ST et al: Calcitonin treatment for central giant cell granulomas of the mandible: report of two cases, J Oral Maxillofac Surg 57(7): , Pogrel MA: Calcitonin therapy for central giant cell granuloma, J Oral Maxillofac Surg 61(6): ; discussion 53-54, Kaban LB, Mulliken JB, Ezekowitz RA et al: Antiangiogenic therapy of a recurrent giant cell tumor of the mandible with interferon alfa-2a, Pediatrics 103(6 Pt 1): , Kaban LB, Troulis MJ, Ebb D et al: Antiangiogenic therapy with interferon alpha for giant cell lesions of the jaws, J Oral Maxillofac Surg 60(10): ; discussion , Jones WA: Familial multi-locular cystic disease of the jaws, Am J Cancer 17: , Mangion J, Rahman N, Edkins S et al: The gene for cherubism maps to chromosome 4p16.3, Am J Hum Genet 65(1): , Tiziani V, Reichenberger E, Buzzo CL et al: The gene for cherubism maps to chromosome 4p16, Am J Hum Genet 65(1): , Ueki Y, Tiziani V, Santanna C et al: Mutations in the gene encoding c-abl-binding protein SH3BP2 cause cherubism, Nat Genet 28(2): , Lo B, Faiyaz-Ul-Haque M, Kennedy S et al: Novel mutation in the gene encoding c-abl-binding protein SH3BP2 causes cherubism, Am J Med Genet 121A(1):37-40, Imai Y, Kanno K, Moriya T et al: A missense mutation in the SH3BP2 gene on chromosome 4p16.3 found in a case of nonfamilial cherubism, Cleft Palate Craniofac J 40(6): , Southgate J, Sarma U, Townend JV et al: Study of the cell biology and biochemistry of cherubism, J Clin Pathol 51(11): , Eisenbud L, Kahn LB, Friedman E: Benign osteoblastoma of the mandible: fifteen year follow-up showing spontaneous regression after biopsy, J Oral Maxillofac Surg 45(1):53-57, Colm SJ, Abrams MB, Waldron CA: Recurrent osteoblastoma of the mandible: report of a case, J Oral Maxillofac Surg 46(10): , Ohkubo T, Hernandez JC, Ooya K et al: Aggressive osteoblastoma of the maxilla, Oral Surg Oral Med Oral Pathol 68(1):69-73, Benoist M: Experience with 220 cases of mandibular reconstruction, J Maxillofac Surg 6(1):40-49, Bodmer WF, Bailey CJ, Bodmer J et al: Localization of the gene for familial adenomatous polyposis on chromosome 5, Nature 328(6131): , Groden J, Thliveris A, Samowitz W et al: Identification and characterization of the familial adenomatous polyposis coli gene, Cell 66(3): , Nishisho I, Nakamura Y, Miyoshi Y et al: Mutations of chromosome 5q21 genes in FAP and colorectal cancer patients, Science 253(5020): , Hackney FL, Aragon SB, Aufdemorte TB et al: Chondrosarcoma of the jaws: clinical findings, histopathology, and treatment, Oral Surg Oral Med Oral Pathol 71(2): , Marx RE, Stern D, editors: Oral and maxillofacial pathology: a rationale for diagnosis and treatment, Carol Stream, Ill, 2003, Quintessence Publishing Bohm P, Krober S, Greschniok A et al: Desmoplastic fibroma of the bone. A report of two patients, review of the literature, and therapeutic implications, Cancer 78(5): , Kwon PH, Horswell BB, Gatto DJ: Desmoplastic fibroma of the jaws: surgical management and review of the literature, Head Neck 11(1):67-75, 1989.
44 Ch23-F10053.qxd 5/15/06 6:01 PM Page 533 PART II ONCOLOGY Sanfilippo NJ, Wang GJ, Larner JM: Desmoplastic fibroma: a role for radiotherapy? South Med J 88(12): , Ayala AG, Ro JY, Goepfert H et al: Desmoid fibromatosis: a clinicopathologic study of 25 children, Semin Diagn Pathol 3(2): , Goepfert H, Cangir A, Ayala AG et al: Chemotherapy of locally aggressive head and neck tumors in the pediatric age group. Desmoid fibromatosis and nasopharyngeal angiofibroma, Am J Surg 144(4): , Sandberg AA, Bridge JA: Updates on the cytogenetics and molecular genetics of bone and soft tissue tumors: osteosarcoma and related tumors, Cancer Genet Cytogenet 145(1):1-30, Chan CW, Kung TM, Ma L: Telangiectatic osteosarcoma of the mandible, Cancer 58(9): , Giangaspero F, Stracca V, Visona A et al: Small-cell osteosarcoma of the mandible. Case report, Appl Pathol 2(1):28-31, Eilber FR, Rosen G: Adjuvant chemotherapy for osteosarcoma, Semin Oncol 16(4): , Pratt CB, Champion JE, Fleming ID et al: Adjuvant chemotherapy for osteosarcoma of the extremity. Longterm results of two consecutive prospective protocol studies, Cancer 65(3): , Kassir RR, Rassekh CH, Kinsella JB et al: Osteosarcoma of the head and neck: meta-analysis of nonrandomized studies, Laryngoscope 107(1):56-61, Ha PK, Eisele DW, Frassica FJ et al: Osteosarcoma of the head and neck: a review of the Johns Hopkins experience, Laryngoscope 109(6): , Mardinger O, Givol N, Talmi YP et al: Osteosarcoma of the jaw. The Chaim Sheba Medical Center experience, Oral Surg Oral Med Oral Pathol Oral Radiol Endod 91(4): , Patel SG, Meyers P, Huvos AG et al: Improved outcomes in patients with osteogenic sarcoma of the head and neck, Cancer 95(7): , Smeele LE, Kostense PJ, van der Waal I et al: Effect of chemotherapy on survival of craniofacial osteosarcoma: a systematic review of 201 patients, J Clin Oncol 15(1): , August M, Magennis P, Dewitt D: Osteogenic sarcoma of the jaws: factors influencing prognosis, Int J Oral Maxillofac Surg 26(3): , Junior AT, de Abreu Alves F, Pinto CA et al: Clinicopathological and immunohistochemical analysis of twenty-five head and neck osteosarcomas, Oral Oncol 39(5): , Ryan RF, Eisenstadt S, Shambaugh EM: Osteogenic sarcoma of the mandible: a plea for radical initial surgery, Plast Reconstr Surg 78(1):41-44, Russ JE, Jesse RH: Management of osteosarcoma of the maxilla and mandible, Am J Surg 140(4): , Garrington GE, Scofield HH, Cornyn J, Hooker SP: Osteosarcoma of the jaws. Analysis of 56 cases, Cancer 20(3): , Garrington GE, Collett WK: Chondrosarcoma. II. Chondrosarcoma of the jaws: analysis of 37 cases, J Oral Pathol 17(1):12-20, Lichtenstein L, Jaffe HI: Chondrosarcoma of bone, Am J Pathol 19: , Evans HL, Ayala AG, Romsdahl MM: Prognostic factors in chondrosarcoma of bone: a clinicopathologic analysis with emphasis on histologic grading, Cancer 40(2): , Saito K, Unni KK, Wollan PC et al: Chondrosarcoma of the jaw and facial bones, Cancer 76(9): , Harwood AR, Krajbich JI, Fornasier VL: Radiotherapy of chondrosarcoma of bone, Cancer 45(11): , Krochak R, Harwood AR, Cummings BJ et al: Results of radical radiation for chondrosarcoma of bone, Radiother Oncol 1(2): , Sinkovics JG, Shirato E, Martin RG et al: Chondrosarcoma. I. A brief review of eighty-three patients, J Med 1(1):15-25, Kim RY, Salter MM, Brascho DJ: High-energy irradiation in the management of chondrosarcoma, South Med J 76(6): , 735, Garrington GE, Collett WK: Chondrosarcoma. I. A selected literature review, J Oral Pathol 17(1):1-11, Nakashima Y, Unni KK, Shives TC et al: Mesenchymal chondrosarcoma of bone and soft tissue. A review of 111 cases, Cancer 57(12): , Huvos AG, Rosen G, Dabska M et al: Mesenchymal chondrosarcoma. A clinicopathologic analysis of 35 patients with emphasis on treatment, Cancer 51(7): , Vencio EF, Reeve CM, Unni KK et al: Mesenchymal chondrosarcoma of the jaw bones: clinicopathologic study of 19 cases, Cancer 82(12): , Takahashi K, Sato K, Kanazawa H et al: Mesenchymal chondrosarcoma of the jaw report of a case and review of 41 cases in the literature, Head Neck 15(5): , Taconis WK, van Rijssel TG: Fibrosarcoma of the jaws, Skeletal Radiol 15(1):10-13, Papagelopoulos PJ, Galanis E, Frassica FJ et al: Primary fibrosarcoma of bone. Outcome after primary surgical treatment, Clin Orthop (373):88-103, Bielack SS, Schroeders A, Fuchs N et al: Malignant fibrous histiocytoma of bone: a retrospective EMSOS study of 125 cases. European Musculo-Skeletal Oncology Society, Acta Orthop Scand 70(4): , Bramwell VH, Steward WP, Nooij M et al: Neoadjuvant chemotherapy with doxorubicin and cisplatin in malignant fibrous histiocytoma of bone: a European Osteosarcoma Intergroup study, J Clin Oncol 17(10): , Bacci G, Picci P, Mercuri M et al: Neoadjuvant chemotherapy for high grade malignant fibrous histiocytoma of bone, Clin Orthop (346): , Cotterill SJ, Ahrens S, Paulussen M et al: Prognostic factors in Ewing s tumor of bone: analysis of 975 patients from the European Intergroup Cooperative Ewing s Sarcoma Study Group, J Clin Oncol 18(17): , 2000.
45 Ch23-F10053.qxd 5/15/06 6:01 PM Page CHAPTER 23 CLINICAL PATHOLOGY: ODONTOGENIC AND NONODONTOGENIC TUMORS OF THE JAWS 192. Rodriguez-Galindo C, Spunt SL, Pappo AS: Treatment of Ewing sarcoma family of tumors: current status and outlook for the future, Med Pediatr Oncol 40(5): , Kuttesch JF Jr, Wexler LH, Marcus RB et al: Second malignancies after Ewing s sarcoma: radiation dosedependency of secondary sarcomas, J Clin Oncol 14(10): , Burkitt DP: Sarcoma involving jaws in African children, Br J Surg 46: , O Connor GT: Malignant lymphoma in African Children. II. A pathologic entity, Cancer 14: , Lindstrom MS, Wiman KG: Role of genetic and epigenetic changes in Burkitt lymphoma, Semin Cancer Biol 12(5): , Sariban E, Donahue A, Magrath IT: Jaw involvement in American Burkitt s Lymphoma, Cancer 53(8): , Mead GM, Sydes MR, Walewski J et al: An international evaluation of CODOX-M and CODOX-M alternating with IVAC in adult Burkitt s lymphoma: results of United Kingdom Lymphoma Group LY06 study, Ann Oncol 13(8): , Spreafico F, Massimino M, Luksch R et al: Intensive, very short-term chemotherapy for advanced Burkitt s lymphoma in children, J Clin Oncol 20(12): , Attal M, Harousseau JL, Stoppa AM et al: A prospective, randomized trial of autologous bone marrow transplantation and chemotherapy in multiple myeloma. Intergroupe Francais du Myelome, N Engl J Med 335(2):91-97, Sirohi B, Powles R: Multiple myeloma, Lancet 363(9412): , Bruno B, Rotta M, Giaccone L et al: New drugs for treatment of multiple myeloma, Lancet Oncol 5(7): , Ruggiero SL, Mehrotra B, Rosenberg TJ et al: Osteonecrosis of the jaws associated with the use of bisphosphonates: a review of 63 cases, J Oral Maxillofac Surg 62(5): , Marx RE: Pamidronate (Aredia) and zoledronate (Zometa) induced avascular necrosis of the jaws: a growing epidemic, J Oral Maxillofac Surg 61(9): , Ducatman BS, Scheithauer BW, Piepgras DG et al: Malignant peripheral nerve sheath tumors. A clinicopathologic study of 120 cases, Cancer 57(10): , Cahan WG, Woodard HG, Higinbotham NL et al: Sarcoma arising in irradiated bone: report of 11 cases, Cancer 1:3-29, Arlen M, Higinbotham NL, Huvos AG et al: Radiationinduced sarcoma of bone, Cancer 28(5): , Pitcher ME, Davidson TI, Fisher C et al: Post irradiation sarcoma of soft tissue and bone, Eur J Surg Oncol 20(1):53-56, Lagrange JL, Ramaioli A, Chateau MC et al: Sarcoma after radiation therapy: retrospective multiinstitutional study of 80 histologically confirmed cases. Radiation Therapist and Pathologist Groups of the Federation Nationale des Centres de Lutte Contre le Cancer, Radiology 216(1): , Robinson E, Neugut AI, Wylie P: Clinical aspects of postirradiation sarcomas, J Natl Cancer Inst 80(4): , Weatherby RP, Dahlin DC, Ivins JC: Postradiation sarcoma of bone: review of 78 Mayo Clinic cases, Mayo Clin Proc 56(5): , Wiklund TA, Blomqvist CP, Raty J et al: Postirradiation sarcoma. Analysis of a nationwide cancer registry material, Cancer 68(3): , van der Waal RI, Buter J, van der Waal I: Oral metastases: report of 24 cases, Br J Oral Maxillofac Surg 41(1):3-6, Hashimoto N, Kurihara K, Yamasaki H et al: Pathological characteristics of metastatic carcinoma in the human mandible, J Oral Pathol 16(7): , Batson OV: The function of the vertebral veins and their role in the spread of metastases, Ann Surg 112: , Hirshberg A, Leibovich P, Buchner A: Metastatic tumors to the jawbones: analysis of 390 cases, J Oral Pathol Med 23(8): , 1994.
Odontogenic Cysts and Tumors
 Odontogenic Cysts and Tumors Michael Underbrink, MD Faculty Advisor: Anna Pou, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation February 13, 2002 Introduction
Odontogenic Cysts and Tumors Michael Underbrink, MD Faculty Advisor: Anna Pou, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation February 13, 2002 Introduction
CHAPTER 12 CYSTS OF THE JAWS ODONTOGENIC CYSTS
 CHAPTER 12 CYSTS OF THE JAWS ODONTOGENIC CYSTS Primordial cyst Dentigerous cyst (follicular) Radicular cyst (periodontal, dental, periapical, inflammatory, infected) Lateral periodontal cyst Residual cyst
CHAPTER 12 CYSTS OF THE JAWS ODONTOGENIC CYSTS Primordial cyst Dentigerous cyst (follicular) Radicular cyst (periodontal, dental, periapical, inflammatory, infected) Lateral periodontal cyst Residual cyst
Cysts of the Jaws. Cyst. Types. Effects on adjacent structures. Non-Odontogenic cysts. Odontogenic Cysts
 Cyst A Cyst is a benign pathologic cavity filled with fluid, lined by epithelium, and surrounded by a connective tissue wall A = connective tissue wall Cysts of the Jaws B = epithelium Effects on adjacent
Cyst A Cyst is a benign pathologic cavity filled with fluid, lined by epithelium, and surrounded by a connective tissue wall A = connective tissue wall Cysts of the Jaws B = epithelium Effects on adjacent
CHARACTERSTIC RADIOGRAPHIC APPEARANCE
 OSTEOLYTIC LESIONS APPROACH AGE Metastatic Neuroblastoma in infant and young child. Metastases and multiple myeloma in middle aged and elderly. Ewing s sarcoma and simple bone cyst in children and teens.
OSTEOLYTIC LESIONS APPROACH AGE Metastatic Neuroblastoma in infant and young child. Metastases and multiple myeloma in middle aged and elderly. Ewing s sarcoma and simple bone cyst in children and teens.
Development of Teeth
 Development of Teeth Dr. Khaldoun Darwich Specialist in Oral and Maxillo-Facial Surgery Hamburg University PhD Hamburg University Academic Teacher - Department of OMF Surgery in Damascus University Instructor
Development of Teeth Dr. Khaldoun Darwich Specialist in Oral and Maxillo-Facial Surgery Hamburg University PhD Hamburg University Academic Teacher - Department of OMF Surgery in Damascus University Instructor
Something Old, Something New.
 Something Old, Something New. Michelle A. Fajardo, D.O. Loma Linda University Medical Center Clinical Presentation 6 year old boy, presented with hematuria Renal mass demonstrated by ultrasound & CT scan
Something Old, Something New. Michelle A. Fajardo, D.O. Loma Linda University Medical Center Clinical Presentation 6 year old boy, presented with hematuria Renal mass demonstrated by ultrasound & CT scan
Prosthetic rehabilitation with dental implants after treatment of a keratocystic odontogenic tumor. case report
 Journal section: Oral Surgery Publication Types: Case Report doi:10.4317/jced.3.e360 Prosthetic rehabilitation with dental implants after treatment of a keratocystic odontogenic tumor. case report Amila
Journal section: Oral Surgery Publication Types: Case Report doi:10.4317/jced.3.e360 Prosthetic rehabilitation with dental implants after treatment of a keratocystic odontogenic tumor. case report Amila
Tooth Formation. Chapter 1
 Chapter Tooth Formation Teeth develop from epithelial cells from the mucosal lining of the oral cavity and cranial neural crest-derived ectomesenchymal cells. These latter cells originate at the ectodermal/neuroectodermal
Chapter Tooth Formation Teeth develop from epithelial cells from the mucosal lining of the oral cavity and cranial neural crest-derived ectomesenchymal cells. These latter cells originate at the ectodermal/neuroectodermal
1. Occlusal view 2. Pan 3. PA, OM, lateral oblique 4. CT - for bony lesions. 5. MRI - for soft tissue lesions
 1 IMAGING OF CYSTS OF THE JAWS. April 1999 N. Serman This is an area where radiology plays an important role in assisting with the diagnosis, determining the size of the lesion and the relationship to
1 IMAGING OF CYSTS OF THE JAWS. April 1999 N. Serman This is an area where radiology plays an important role in assisting with the diagnosis, determining the size of the lesion and the relationship to
Developmental Cysts. Non-odontogenic Cysts. Nasopalatine duct cyst. Palatal and gingival cysts of newborns
 Non-odontogenic Cysts Dr. Ioannis G. Koutlas Division of Oral Pathology Developmental Cysts a.k.a. fissural cysts Exact pathogenesis of some of them uncertain Generally, slow increase May be identified
Non-odontogenic Cysts Dr. Ioannis G. Koutlas Division of Oral Pathology Developmental Cysts a.k.a. fissural cysts Exact pathogenesis of some of them uncertain Generally, slow increase May be identified
Odontomas are considered to be developmental anomalies
 Oral Pathology Compound odontoma diagnosis and treatment: three case reports Branca Heloísa de Oliveira DDS, MS Vera Campos DDS, MS Sonia Marçal DDS, MS Dr. Oliveira and Dr. Campos are assistant professors,
Oral Pathology Compound odontoma diagnosis and treatment: three case reports Branca Heloísa de Oliveira DDS, MS Vera Campos DDS, MS Sonia Marçal DDS, MS Dr. Oliveira and Dr. Campos are assistant professors,
MANAGEMENT OF BENIGN BONE TUMORS
 MANAGEMENT OF BENIGN BONE TUMORS HISTORY AND EXAMINATION An adequate history and physical examination are the first and most important steps in evaluating a patient with a musculoskeletal tumor PRESENTING
MANAGEMENT OF BENIGN BONE TUMORS HISTORY AND EXAMINATION An adequate history and physical examination are the first and most important steps in evaluating a patient with a musculoskeletal tumor PRESENTING
ATLAS OF HEAD AND NECK PATHOLOGY THYROID PAPILLARY CARCINOMA
 Papillary carcinoma is the most common of thyroid malignancies and occurs in all age groups but particularly in women under 45 years of age. There is a high rate of cervical metastatic disease and yet
Papillary carcinoma is the most common of thyroid malignancies and occurs in all age groups but particularly in women under 45 years of age. There is a high rate of cervical metastatic disease and yet
Secondary dentition permanent teeth - 32. Primary dentition deciduous teeth - 20
 Department of Histology and Embryology, P. J. Šafárik University, Medical Faculty, Košice DEVELOPMENT OF TEETH: Sylabus for foreign students Dental medicine Author: doc. MVDr. Iveta Domoráková, PhD. Primary
Department of Histology and Embryology, P. J. Šafárik University, Medical Faculty, Košice DEVELOPMENT OF TEETH: Sylabus for foreign students Dental medicine Author: doc. MVDr. Iveta Domoráková, PhD. Primary
UNMH Oral and Maxillofacial Surgery Clinical Privileges
 All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 09/26/2014 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
All new applicants must meet the following requirements as approved by the UNMH Board of Trustees effective: 09/26/2014 INSTRUCTIONS Applicant: Check off the "Requested" box for each privilege requested.
Update on Mesothelioma
 November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
November 8, 2012 Update on Mesothelioma Intro incidence and nomenclature Update on Classification Diagnostic specimens Morphologic features Epithelioid Histology Biphasic Histology Immunohistochemical
Introduction: Tumor Swelling / new growth / mass. Two types of growth disorders: Non-Neoplastic. Secondary / adaptation due to other cause.
 Disorders of Growth Introduction: Tumor Swelling / new growth / mass Two types of growth disorders: Non-Neoplastic Secondary / adaptation due to other cause. Neoplastic. Primary growth abnormality. Non-Neoplastic
Disorders of Growth Introduction: Tumor Swelling / new growth / mass Two types of growth disorders: Non-Neoplastic Secondary / adaptation due to other cause. Neoplastic. Primary growth abnormality. Non-Neoplastic
05 - DENTAL SURGERY. (02) MS (Oral Surgery) Part II Examination
 05 - DENTAL SURGERY (02) MS (Oral Surgery) Part II Examination 01. October 1990 02. October 1991 03. October 1992 04. October 1993 05. October 1994 06. November 1995 07. October 1996 08. November 1997
05 - DENTAL SURGERY (02) MS (Oral Surgery) Part II Examination 01. October 1990 02. October 1991 03. October 1992 04. October 1993 05. October 1994 06. November 1995 07. October 1996 08. November 1997
Anatomic Anomalies. Anomalies. Anomalies. Anomalies. Supernumerary Teeth. Supernumerary Teeth. Steven R. Singer, DDS 212.305.5674 srs2@columbia.
 Anatomic Anomalies Steven R. Singer, DDS 212.305.5674 [email protected] Anomalies! Anomalies are variations in the:! Size! Morphology! Number! Eruption of the teeth Anomalies Anomalies There are two categories:!
Anatomic Anomalies Steven R. Singer, DDS 212.305.5674 [email protected] Anomalies! Anomalies are variations in the:! Size! Morphology! Number! Eruption of the teeth Anomalies Anomalies There are two categories:!
Male. Female. Death rates from lung cancer in USA
 Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Male Female Death rates from lung cancer in USA Smoking represents an interesting combination of an entrenched industry and a clearly drug-induced cancer Tobacco Use in the US, 1900-2000 5000 100 Per Capita
Radiologic Evaluation of Bone Tumors. Alan Laorr, MD Chief, Musculoskeletal Radiology Suburban Radiologic Consultants Minneapolis, Minnesota
 Radiologic Evaluation of Bone Tumors Alan Laorr, MD Chief, Musculoskeletal Radiology Suburban Radiologic Consultants Minneapolis, Minnesota Dx of Bone Tumors I. Clinical Information II. Location III. Morphology
Radiologic Evaluation of Bone Tumors Alan Laorr, MD Chief, Musculoskeletal Radiology Suburban Radiologic Consultants Minneapolis, Minnesota Dx of Bone Tumors I. Clinical Information II. Location III. Morphology
Primary -Benign - Malignant Secondary
 TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
TUMOURS OF THE LUNG Primary -Benign - Malignant Secondary The incidence of lung cancer has been increasing almost logarithmically and is now reaching epidemic levels. The overall cure rate is very low
Nuno Morais 1 José António Moreira da Costa 2
 Nuno Morais 1 José António Moreira da Costa 2 1 Neurosurgery Department, Hospital de Braga, Braga, Portugal 2 Private Practice, Clínica Neurológica e da Coluna Vertebral, Braga, Portugal Disclosure Funding
Nuno Morais 1 José António Moreira da Costa 2 1 Neurosurgery Department, Hospital de Braga, Braga, Portugal 2 Private Practice, Clínica Neurológica e da Coluna Vertebral, Braga, Portugal Disclosure Funding
Oncology. Objectives. Cancer Nomenclature. Cancer is a disease of the cell Cancer develops when certain cells begin to grow out of control
 Oncology Objectives Describe the etiology and pathophysiological mechanisms of cancer Discuss medical and family history findings relevant to cancer Identify general signs and symptoms associated with
Oncology Objectives Describe the etiology and pathophysiological mechanisms of cancer Discuss medical and family history findings relevant to cancer Identify general signs and symptoms associated with
.org. Osteochondroma. Solitary Osteochondroma
 Osteochondroma Page ( 1 ) An osteochondroma is a benign (noncancerous) tumor that develops during childhood or adolescence. It is an abnormal growth that forms on the surface of a bone near the growth
Osteochondroma Page ( 1 ) An osteochondroma is a benign (noncancerous) tumor that develops during childhood or adolescence. It is an abnormal growth that forms on the surface of a bone near the growth
Malignant Lymphomas and Plasma Cell Myeloma
 Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Diagnostic Challenge. Department of Pathology,
 Cytology of Pleural Fluid as a Diagnostic Challenge Paavo Pääkkö,, MD, PhD Chief Physician and Head of the Department Department of Pathology, Oulu University Hospital,, Finland Oulu University Hospital
Cytology of Pleural Fluid as a Diagnostic Challenge Paavo Pääkkö,, MD, PhD Chief Physician and Head of the Department Department of Pathology, Oulu University Hospital,, Finland Oulu University Hospital
Maxillary Sinus. (Antrum of Higmore)
 Maxillary Sinus (Antrum of Higmore) The maxillary sinus is a pneumatic space. It is the largest bilateral air sinus located in the body of the maxilla and opens in the middle nasal meatus of the nasal
Maxillary Sinus (Antrum of Higmore) The maxillary sinus is a pneumatic space. It is the largest bilateral air sinus located in the body of the maxilla and opens in the middle nasal meatus of the nasal
Cardiac Masses and Tumors
 Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
Cardiac Masses and Tumors Question: What is the diagnosis? A. Aortic valve myxoma B. Papillary fibroelastoma C. Vegetation from Infective endocarditis D. Thrombus in transit E. None of the above Answer:
Pediatric Oncology for Otolaryngologists
 Pediatric Oncology for Otolaryngologists Frederick S. Huang, M.D. Division of Hematology/Oncology Department of Pediatrics The University of Texas Medical Branch Grand Rounds Presentation to Department
Pediatric Oncology for Otolaryngologists Frederick S. Huang, M.D. Division of Hematology/Oncology Department of Pediatrics The University of Texas Medical Branch Grand Rounds Presentation to Department
DESMOPLASTIC SMALL ROUND CELL TUMOR: A RARE PATHOLOGY PUZZLE
 DESMOPLASTIC SMALL ROUND CELL TUMOR: A RARE PATHOLOGY PUZZLE Ryan Granger University of Rhode Island Cytotechnology program May 2, 2015 ASCT Annual Meeting Nashville, Tennessee DESMOPLASTIC SMALL ROUND
DESMOPLASTIC SMALL ROUND CELL TUMOR: A RARE PATHOLOGY PUZZLE Ryan Granger University of Rhode Island Cytotechnology program May 2, 2015 ASCT Annual Meeting Nashville, Tennessee DESMOPLASTIC SMALL ROUND
A Retrospective Review of Treatment of the Odontogenic Keratocyst
 A Retrospective Review of Treatment of the Odontogenic Keratocyst J Oral Maxillofac Surg 63:635-639, 2005 Teresa A. Morgan, DDS, MS,* Christopher C. Burton, DDS, MS, and Fang Qian, MA, PhD Purpose: The
A Retrospective Review of Treatment of the Odontogenic Keratocyst J Oral Maxillofac Surg 63:635-639, 2005 Teresa A. Morgan, DDS, MS,* Christopher C. Burton, DDS, MS, and Fang Qian, MA, PhD Purpose: The
TABLE OF DENTAL PROCEDURES PLEASE READ THE FOLLOWING INFORMATION CAREFULLY FOR YOUR PROCEDURE FREQUENCIES AND PROVISIONS.
 TABLE OF DENTAL PROCEDURES PLEASE READ THE FOLLOWING INFORMATION CAREFULLY FOR YOUR PROCEDURE FREQUENCIES AND PROVISIONS. The attached is a list of dental procedures for which benefits are payable under
TABLE OF DENTAL PROCEDURES PLEASE READ THE FOLLOWING INFORMATION CAREFULLY FOR YOUR PROCEDURE FREQUENCIES AND PROVISIONS. The attached is a list of dental procedures for which benefits are payable under
MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION
 MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION Effective for dates of service on and after November 1, 2005, the following dental coding, policy and related fee revisions
MEDICAID DENTAL PROGRAMS CODING, POLICY AND RELATED FEE REVISION INFORMATION Effective for dates of service on and after November 1, 2005, the following dental coding, policy and related fee revisions
Kidney Cancer OVERVIEW
 Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Kidney Cancer OVERVIEW Kidney cancer is the third most common genitourinary cancer in adults. There are approximately 54,000 new cancer cases each year in the United States, and the incidence of kidney
Contents. Introduction 1. Anatomy of the Spine 1. 2. Spinal Imaging 7. 3. Spinal Biomechanics 23. 4. History and Physical Examination of the Spine 33
 Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Complications Associated with Tooth Extraction
 1 Complications Associated with Tooth Extraction Mark M. Smith, VMD, DACVS, DAVDC Center for Veterinary Dentistry and Oral Surgery 9041 Gaither Road Gaithersburg, MD 20877 Introduction Tooth extraction
1 Complications Associated with Tooth Extraction Mark M. Smith, VMD, DACVS, DAVDC Center for Veterinary Dentistry and Oral Surgery 9041 Gaither Road Gaithersburg, MD 20877 Introduction Tooth extraction
Leukemias and Lymphomas: A primer
 Leukemias and Lymphomas: A primer Normal blood contains circulating white blood cells, red blood cells and platelets 700 red cells (oxygen) 1 white cell Neutrophils (60%) bacterial infection Lymphocytes
Leukemias and Lymphomas: A primer Normal blood contains circulating white blood cells, red blood cells and platelets 700 red cells (oxygen) 1 white cell Neutrophils (60%) bacterial infection Lymphocytes
The evolving pathology of solitary fibrous tumours. Luciane Dreher Irion MREH / CMFT / NSOPS
 The evolving pathology of solitary fibrous tumours Luciane Dreher Irion MREH / CMFT / NSOPS Historical review Haemangiopericytoma (HPC) first described primarily as a soft tissue vascular tumour of pericytic
The evolving pathology of solitary fibrous tumours Luciane Dreher Irion MREH / CMFT / NSOPS Historical review Haemangiopericytoma (HPC) first described primarily as a soft tissue vascular tumour of pericytic
CASE OF THE MONTH AUGUST-2015 DR. GURUDUTT GUPTA HEAD HISTOPATHOLOGY
 CASE OF THE MONTH AUGUST-2015 DR. GURUDUTT GUPTA HEAD HISTOPATHOLOGY CASE HISTORY 52Y MALE RIGHT RADICAL NEPHERECTOMY Case of right renal mass with IVC thrombus. History of surgery and RT for right occipital
CASE OF THE MONTH AUGUST-2015 DR. GURUDUTT GUPTA HEAD HISTOPATHOLOGY CASE HISTORY 52Y MALE RIGHT RADICAL NEPHERECTOMY Case of right renal mass with IVC thrombus. History of surgery and RT for right occipital
5 Localized Bone Lesions
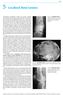 75 5 Localized Bone Lesions Conventional radiography remains the primary imaging modality for the evaluation of skeletal lesions. The combination of conventional radiography, which has a high specificity
75 5 Localized Bone Lesions Conventional radiography remains the primary imaging modality for the evaluation of skeletal lesions. The combination of conventional radiography, which has a high specificity
Report series: General cancer information
 Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Fighting cancer with information Report series: General cancer information Eastern Cancer Registration and Information Centre ECRIC report series: General cancer information Cancer is a general term for
Crosswalk of CPT Codes to CDT Codes
 Crosswalk of CPT Codes to CDT Codes Note: Given the sheer number of codes from which to draw, this CPT-CDT crosswalk should be viewed as a tool to assist states in reporting CPT codes on the dental lines
Crosswalk of CPT Codes to CDT Codes Note: Given the sheer number of codes from which to draw, this CPT-CDT crosswalk should be viewed as a tool to assist states in reporting CPT codes on the dental lines
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma
 Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
Rotation Specific Goals & Objectives: University Health Network-Princess Margaret Hospital/ Sunnybrook Breast/Melanoma Medical Expert: Breast Rotation Specific Competencies/Objectives 1.0 Medical History
TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD
 TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD Victor E. Reuter, MD Memorial Sloan-Kettering Cancer Center [email protected] 66 th Annual Pathology Seminar California Society of Pathologists Short
TUMORS OF THE TESTICULAR ADNEXA and SPERMATIC CORD Victor E. Reuter, MD Memorial Sloan-Kettering Cancer Center [email protected] 66 th Annual Pathology Seminar California Society of Pathologists Short
OBJECTIVES By the end of this segment, the community participant will be able to:
 Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Cancer 101: Cancer Diagnosis and Staging Linda U. Krebs, RN, PhD, AOCN, FAAN OCEAN Native Navigators and the Cancer Continuum (NNACC) (NCMHD R24MD002811) Cancer 101: Diagnosis & Staging (Watanabe-Galloway
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers
 Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Resorptive Changes of Maxillary and Mandibular Bone Structures in Removable Denture Wearers Dubravka KnezoviÊ-ZlatariÊ Asja»elebiÊ Biserka LaziÊ Department of Prosthodontics School of Dental Medicine University
Coding and Payment Guide for Dental Services. A comprehensive coding, billing, and reimbursement resource for dental services
 Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2011 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2011 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Basic modules: List of individual modules Basic Module 1 Basic principles of general and dental medicine
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Basic modules: List of individual modules Basic Module 1 Basic principles of general and dental medicine
Oncology Quarterly. Corky and Kaylee Smith
 Oncology Quarterly Volume 2 Winter 2007 Corky and Kaylee Smith For Richard and Monica Smith, it started simply as a small area of hair loss on their eight yearold Shetland Sheepdog, Corky s, left tarsus.
Oncology Quarterly Volume 2 Winter 2007 Corky and Kaylee Smith For Richard and Monica Smith, it started simply as a small area of hair loss on their eight yearold Shetland Sheepdog, Corky s, left tarsus.
A Diagnostic Chest XRay: Multiple Myeloma
 Daniela Marinho Tridente, VI FCMSCSP October 2013 A Diagnostic Chest XRay: Multiple Myeloma Daniela Marinho Tridente, VI FCMSCSP Our Learning Agenda Introduction of our patient His imaging data and findings
Daniela Marinho Tridente, VI FCMSCSP October 2013 A Diagnostic Chest XRay: Multiple Myeloma Daniela Marinho Tridente, VI FCMSCSP Our Learning Agenda Introduction of our patient His imaging data and findings
SECTION 2. Oral Maxillofacial Surgeon Services. Table of Contents
 SECTION 2 Table of Contents Table of Contents 1. GENERAL POLICY (Updated 4/1/12)... 3 1-1 Credentials... 3 1-2 Clients Enrolled in a Managed Care Plan... 3 1-3 Clients NOT Enrolled in a Managed Care Plan...
SECTION 2 Table of Contents Table of Contents 1. GENERAL POLICY (Updated 4/1/12)... 3 1-1 Credentials... 3 1-2 Clients Enrolled in a Managed Care Plan... 3 1-3 Clients NOT Enrolled in a Managed Care Plan...
RECURRENCE OF BENIGN OSTEOBLASTOMA OF THE MANDIBLE AND WITH A 4-YEAR-FOLLOW-UP: A CASE REPORT
 CLINICAL DENTISTRY AND RESEARCH 2013; 37(2): 50-54 Case Report RECURRENCE OF BENIGN OSTEOBLASTOMA OF THE MANDIBLE AND WITH A 4-YEAR-FOLLOW-UP: A CASE REPORT Alper Aktaş, DDS, PhD Associate Professor, Department
CLINICAL DENTISTRY AND RESEARCH 2013; 37(2): 50-54 Case Report RECURRENCE OF BENIGN OSTEOBLASTOMA OF THE MANDIBLE AND WITH A 4-YEAR-FOLLOW-UP: A CASE REPORT Alper Aktaş, DDS, PhD Associate Professor, Department
Attachment S: Benefits Covered - ADULTS - AGE 21 AND OVER
 Diagnostic services include the oral examinations and selected radiographs needed to assess the oral health, diagnose oral pathology and develop an adequate treatment plan for the Participant s oral health.
Diagnostic services include the oral examinations and selected radiographs needed to assess the oral health, diagnose oral pathology and develop an adequate treatment plan for the Participant s oral health.
LYMPHOMA. BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons
 LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
A. DEVELOPMENT OF THE DENTAL ORGAN (ENAMEL ORGAN):
 A. DEVELOPMENT OF THE DENTAL ORGAN (ENAMEL ORGAN): AS EARLY AS THE SECOND MONTH OF FETAL LIFE, THE DEVELOPMENT OF THE DECIDUOUS TEETH MAY FIRST BECOME EVIDENT. 1. Dental lamina and Bud stage At about six
A. DEVELOPMENT OF THE DENTAL ORGAN (ENAMEL ORGAN): AS EARLY AS THE SECOND MONTH OF FETAL LIFE, THE DEVELOPMENT OF THE DECIDUOUS TEETH MAY FIRST BECOME EVIDENT. 1. Dental lamina and Bud stage At about six
CHAPTER 2. Neoplasms (C00-D49) March 2014. 2014 MVP Health Care, Inc.
 Neoplasms (C00-D49) March 2014 2014 MVP Health Care, Inc. CHAPTER SPECIFIC CATEGORY CODE BLOCKS C00-C14 Malignant neoplasms of lip, oral cavity and pharynx C15-C26 Malignant neoplasms of digestive organs
Neoplasms (C00-D49) March 2014 2014 MVP Health Care, Inc. CHAPTER SPECIFIC CATEGORY CODE BLOCKS C00-C14 Malignant neoplasms of lip, oral cavity and pharynx C15-C26 Malignant neoplasms of digestive organs
chronic leukemia lymphoma myeloma differentiated 14 September 1999 Pre- Transformed Ig Surface Surface Secreted Myeloma Major malignant counterpart
 Disease Usual phenotype acute leukemia precursor chronic leukemia lymphoma myeloma differentiated Pre- B-cell B-cell Transformed B-cell Plasma cell Ig Surface Surface Secreted Major malignant counterpart
Disease Usual phenotype acute leukemia precursor chronic leukemia lymphoma myeloma differentiated Pre- B-cell B-cell Transformed B-cell Plasma cell Ig Surface Surface Secreted Major malignant counterpart
The Diagnosis of Cancer in the Pathology Laboratory
 The Diagnosis of Cancer in the Pathology Laboratory Dr Edward Sheffield Christmas Select 74 Meeting, Queen s Hotel Cheltenham, 3 rd December 2014 Agenda Overview of the pathology of cancer How specimens
The Diagnosis of Cancer in the Pathology Laboratory Dr Edward Sheffield Christmas Select 74 Meeting, Queen s Hotel Cheltenham, 3 rd December 2014 Agenda Overview of the pathology of cancer How specimens
Disease/Illness GUIDE TO ASBESTOS LUNG CANCER. What Is Asbestos Lung Cancer? www.simpsonmillar.co.uk Telephone 0844 858 3200
 GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
GUIDE TO ASBESTOS LUNG CANCER What Is Asbestos Lung Cancer? Like tobacco smoking, exposure to asbestos can result in the development of lung cancer. Similarly, the risk of developing asbestos induced lung
Cytology of Lymph Nodes
 Indications Cytology of Lymph Nodes Lymph node enlargement That was easy Mary Anna Thrall Don Meuten Indications Lymph node enlargement Suspect metastasis Normal sized lymph nodes are Normal Do NOT aspirate
Indications Cytology of Lymph Nodes Lymph node enlargement That was easy Mary Anna Thrall Don Meuten Indications Lymph node enlargement Suspect metastasis Normal sized lymph nodes are Normal Do NOT aspirate
INFUSE Bone Graft (rhbmp-2/acs)
 1 INFUSE Bone Graft (rhbmp-2/acs) For patients who need more bone to place dental implants Enjoy living with INFUSE Bone Graft. www.medtronic.com Medtronic Spinal and Biologics Business Worldwide Headquarters
1 INFUSE Bone Graft (rhbmp-2/acs) For patients who need more bone to place dental implants Enjoy living with INFUSE Bone Graft. www.medtronic.com Medtronic Spinal and Biologics Business Worldwide Headquarters
IMPLANT DENTISTRY EXAM BANK
 IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
IMPLANT DENTISTRY EXAM BANK 1. Define osseointegration. (4 points, 1/4 2. What are the critical components of an acceptable clinical trial? (10 points) 3. Compare the masticatory performance of individuals
LIST OF DENTAL PROCEDURES (LOW PLAN) PREVENTIVE PROCEDURES
 LIST OF DENTAL PROCEDURES (LOW PLAN) The following is a complete list of the dental procedures for which benefits are payable under this section. No benefits are payable for a procedure that is not listed.
LIST OF DENTAL PROCEDURES (LOW PLAN) The following is a complete list of the dental procedures for which benefits are payable under this section. No benefits are payable for a procedure that is not listed.
Lip Cancer: Treatment & Reconstruction
 Lip Cancer: Treatment & Reconstruction GBMC - Head & Neck Cancer Grand Rounds Elizabeth E. Redd, M.D. With the assistance of Ira Papel, M.D. Patrick Byrne, M.D. Lip Cancer: Treatment & Reconstruction Anatomic
Lip Cancer: Treatment & Reconstruction GBMC - Head & Neck Cancer Grand Rounds Elizabeth E. Redd, M.D. With the assistance of Ira Papel, M.D. Patrick Byrne, M.D. Lip Cancer: Treatment & Reconstruction Anatomic
MODERN IMMUNOHISTOCHEMISTRY
 MODERN IMMUNOHISTOCHEMISTRY Cambridge Illustrated Surgical Pathology Peiguo G. Chu City of Hope National Medical Center, Duarte, California Lawrence M. Weiss City of Hope National Medical Center, Duarte,
MODERN IMMUNOHISTOCHEMISTRY Cambridge Illustrated Surgical Pathology Peiguo G. Chu City of Hope National Medical Center, Duarte, California Lawrence M. Weiss City of Hope National Medical Center, Duarte,
Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium
 Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium Introduction 3 cavities with the same embryologic origin the mesoderme Pleura Exudates Pleura Peritoneum Pericardium 22%
Cytology : first alert of mesothelioma? Professor B. Weynand, UCL Yvoir, Belgium Introduction 3 cavities with the same embryologic origin the mesoderme Pleura Exudates Pleura Peritoneum Pericardium 22%
THYROID CANCER. I. Introduction
 THYROID CANCER I. Introduction There are over 11,000 new cases of thyroid cancer each year in the US. Females are more likely to have thyroid cancer than men by a ratio of 3:1, and it is more common in
THYROID CANCER I. Introduction There are over 11,000 new cases of thyroid cancer each year in the US. Females are more likely to have thyroid cancer than men by a ratio of 3:1, and it is more common in
Brain Cancer. This reference summary will help you understand how brain tumors are diagnosed and what options are available to treat them.
 Brain Cancer Introduction Brain tumors are not rare. Thousands of people are diagnosed every year with tumors of the brain and the rest of the nervous system. The diagnosis and treatment of brain tumors
Brain Cancer Introduction Brain tumors are not rare. Thousands of people are diagnosed every year with tumors of the brain and the rest of the nervous system. The diagnosis and treatment of brain tumors
Histopathology of Major Salivary Gland Neoplasms
 Histopathology of Major Salivary Gland Neoplasms Sam J. Cunningham, MD, PhD Faculty Advisor: Shawn D. Newlands, MD, PhD Faculty Advisor: David C. Teller, MD The University of Texas Medical Branch, Department
Histopathology of Major Salivary Gland Neoplasms Sam J. Cunningham, MD, PhD Faculty Advisor: Shawn D. Newlands, MD, PhD Faculty Advisor: David C. Teller, MD The University of Texas Medical Branch, Department
Tom Daley, DDS, MSc, FRCD(C) Mark Darling, BChD, MSc (Dent), MSc (Med), MChD
 C L I N I C A L P R A C T I C E Nonsquamous Cell Malignant Tumours of the Oral Cavity: An Overview Tom Daley, DDS, MSc, FRCD(C) Mark Darling, BChD, MSc (Dent), MSc (Med), MChD A b s t r a c t Many malignant
C L I N I C A L P R A C T I C E Nonsquamous Cell Malignant Tumours of the Oral Cavity: An Overview Tom Daley, DDS, MSc, FRCD(C) Mark Darling, BChD, MSc (Dent), MSc (Med), MChD A b s t r a c t Many malignant
21140 Closed treatment of reimplantation. mandibular or maxillary and/or stabilization. alveolar ridge fracture of accidentally
 Medical in Nature Oral Surgery CDT Code Description (CDT code) CPT Code Description (CPT Code) D7270 Tooth 21140 Closed treatment of reimplantation mandibular or maxillary and/or stabilization alveolar
Medical in Nature Oral Surgery CDT Code Description (CDT code) CPT Code Description (CPT Code) D7270 Tooth 21140 Closed treatment of reimplantation mandibular or maxillary and/or stabilization alveolar
4-1-2005. Dental Clinical Criteria and Documentation Requirements
 4-1-2005 Dental Clinical Criteria and Documentation Requirements Table of Contents Dental Clinical Criteria Cast Restorations and Veneer Procedures... Pages 1-3 Crown Repair... Page 3 Endodontic Procedures...
4-1-2005 Dental Clinical Criteria and Documentation Requirements Table of Contents Dental Clinical Criteria Cast Restorations and Veneer Procedures... Pages 1-3 Crown Repair... Page 3 Endodontic Procedures...
Objectives. Mylene T. Truong, MD. Malignant Pleural Mesothelioma Background
 Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Imaging of Pleural Tumors Mylene T. Truong, MD Imaging of Pleural Tumours Mylene T. Truong, M. D. University of Texas M.D. Anderson Cancer Center, Houston, TX Objectives To review tumors involving the
Introduction to Dental Anatomy
 Introduction to Dental Anatomy Vickie P. Overman, RDH, MEd Continuing Education Units: N/A This continuing education course is intended for dental students and dental hygiene students. Maintaining the
Introduction to Dental Anatomy Vickie P. Overman, RDH, MEd Continuing Education Units: N/A This continuing education course is intended for dental students and dental hygiene students. Maintaining the
Cervical Cancer The Importance of Cervical Screening and Vaccination
 Cervical Cancer The Importance of Cervical Screening and Vaccination Cancer Cells Cancer begins in cells, the building blocks that make up tissues. Tissues make up the organs of the body. Sometimes, this
Cervical Cancer The Importance of Cervical Screening and Vaccination Cancer Cells Cancer begins in cells, the building blocks that make up tissues. Tissues make up the organs of the body. Sometimes, this
Translocation Renal Cell Carcinomas
 Translocation Renal Cell Carcinomas Cora N. Sternberg, MD, FACP Chair, Department of Medical Oncology San Camillo and Forlanini Hospitals Rome, Italy Kidney cancer is not a single disease Clear cell (75%)
Translocation Renal Cell Carcinomas Cora N. Sternberg, MD, FACP Chair, Department of Medical Oncology San Camillo and Forlanini Hospitals Rome, Italy Kidney cancer is not a single disease Clear cell (75%)
Diagnosis and Treatment of Common Oral Lesions Causing Pain
 Diagnosis and Treatment of Common Oral Lesions Causing Pain John D. McDowell, DDS, MS University of Colorado School of Dentistry Chair, Oral Diagnosis, Medicine and Radiology Director, Oral Medicine and
Diagnosis and Treatment of Common Oral Lesions Causing Pain John D. McDowell, DDS, MS University of Colorado School of Dentistry Chair, Oral Diagnosis, Medicine and Radiology Director, Oral Medicine and
Residency Competency and Proficiency Statements
 Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
Residency Competency and Proficiency Statements 1. REQUEST AND RESPOND TO REQUESTS FOR CONSULTATIONS Identify needs and make referrals to appropriate health care providers for the treatment of physiologic,
95% of childhood kidney cancer cases are Wilms tumours. Childhood kidney cancer is extremely rare, with only 90 cases a year in
 James Whale Fund for Kidney Cancer Childhood kidney cancer factsheet Kidney cancer rarely afflicts children and about 90 paediatric cases are diagnosed in the UK each year. About 75% of childhood kidney
James Whale Fund for Kidney Cancer Childhood kidney cancer factsheet Kidney cancer rarely afflicts children and about 90 paediatric cases are diagnosed in the UK each year. About 75% of childhood kidney
TREATMENT REFUSAL FORMS
 TREATMENT REFUSAL FORMS These forms are intended to be used when a patient refuses the treatment. These forms help confirm that the patient is informed and aware of the risks involved with not proceeding
TREATMENT REFUSAL FORMS These forms are intended to be used when a patient refuses the treatment. These forms help confirm that the patient is informed and aware of the risks involved with not proceeding
Pathology of lung cancer
 Pathology of lung cancer EASO COURSE ON LUNG CANCER AND MESOTHELIOMA DAMASCUS (SYRIA), MAY 3-4, 2007 Gérard ABADJIAN MD Pathologist Associate Professor, Saint Joseph University Pathology Dept. Hôtel-Dieu
Pathology of lung cancer EASO COURSE ON LUNG CANCER AND MESOTHELIOMA DAMASCUS (SYRIA), MAY 3-4, 2007 Gérard ABADJIAN MD Pathologist Associate Professor, Saint Joseph University Pathology Dept. Hôtel-Dieu
4/15/2013. bi/o carcin/ chem/o immun/o onc/o radi/o sarc/o. anabrachydysectoendoneo- -ectomy -genesis -oma -plasia -sarcoma
 Chapter Sixteen Oncology bi/o carcin/ chem/o immun/o onc/o radi/o sarc/o Combining Forms Prefixes and Suffixes Carcinogenesis anabrachydysectoendoneo- -ectomy -genesis -oma -plasia -sarcoma Causes of cancer
Chapter Sixteen Oncology bi/o carcin/ chem/o immun/o onc/o radi/o sarc/o Combining Forms Prefixes and Suffixes Carcinogenesis anabrachydysectoendoneo- -ectomy -genesis -oma -plasia -sarcoma Causes of cancer
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
بسم هللا الرحمن الرحيم Updates in Mesothelioma By Samieh Amer, MD Professor of Cardiothoracic Surgery Faculty of Medicine, Cairo University History Wagner and his colleagues (1960) 33 cases of mesothelioma
Dental-based Injuries
 Dental-based Injuries LUXATIONS CROWN FRACTURE CROWN/ROOT FRACTURE ROOT FRACTURE ALVEOLAR BONE FRACTURE AVULSIONS LUXATIONS The tooth is loose, now what? 1. Concussive-not loose or displaced, but tender
Dental-based Injuries LUXATIONS CROWN FRACTURE CROWN/ROOT FRACTURE ROOT FRACTURE ALVEOLAR BONE FRACTURE AVULSIONS LUXATIONS The tooth is loose, now what? 1. Concussive-not loose or displaced, but tender
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout
 PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
PREPARATION OF MOUTH FOR REMOVABLE PARTIAL DENTURES Dr. Mazen kanout Mouth preparation includes procedures in four categories: 1. Oral Surgical Preparation. 2. Conditioning of Abused and Irritated Tissue.
MEDICAL ASSISTANCE PROGRAM DENTAL FEE SCHEDULE
 Dental General Payment Policies Children under 21 years of age are eligible for all medically necessary dental services. For children under 21 years of age who require medically necessary dental services
Dental General Payment Policies Children under 21 years of age are eligible for all medically necessary dental services. For children under 21 years of age who require medically necessary dental services
.org. Metastatic Bone Disease. Description
 Metastatic Bone Disease Page ( 1 ) Cancer that begins in an organ, such as the lungs, breast, or prostate, and then spreads to bone is called metastatic bone disease (MBD). More than 1.2 million new cancer
Metastatic Bone Disease Page ( 1 ) Cancer that begins in an organ, such as the lungs, breast, or prostate, and then spreads to bone is called metastatic bone disease (MBD). More than 1.2 million new cancer
RESEARCH EDUCATE ADVOCATE. Just Diagnosed with Melanoma Now What?
 RESEARCH EDUCATE ADVOCATE Just Diagnosed with Melanoma Now What? INTRODUCTION If you are reading this, you have undergone a biopsy (either of a skin lesion or a lymph node) or have had other tests in which
RESEARCH EDUCATE ADVOCATE Just Diagnosed with Melanoma Now What? INTRODUCTION If you are reading this, you have undergone a biopsy (either of a skin lesion or a lymph node) or have had other tests in which
Activity: Can You Identify the Age?
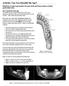 Activity: Can You Identify the Age? Skeletons are good age markers because teeth and bones mature at fairly predictable rates. How Teeth Reveal Age For toddler to age 21, teeth are the most accurate age
Activity: Can You Identify the Age? Skeletons are good age markers because teeth and bones mature at fairly predictable rates. How Teeth Reveal Age For toddler to age 21, teeth are the most accurate age
Position Classification Standard for Dental Officer Series, GS-0680
 Position Classification Standard for Dental Officer Series, GS-0680 Table of Contents SERIES DEFINITION... 2 BACKGROUND... 2 TITLES... 3 GRADE-LEVEL EVALUATION CRITERIA... 3 NOTES ON THE USE OF THE STANDARDS...
Position Classification Standard for Dental Officer Series, GS-0680 Table of Contents SERIES DEFINITION... 2 BACKGROUND... 2 TITLES... 3 GRADE-LEVEL EVALUATION CRITERIA... 3 NOTES ON THE USE OF THE STANDARDS...
THE PATHOLOGY OF MEDIASTINAL MASSES. Anatomic Distribution of Mediastinal Masses
 Page 1 of 5 THE PATHOLOGY OF MEDIASTINAL MASSES Dr. S. Boag 549-6666 Ext. 4190, mailto:%[email protected] 1. INTRODUCTION A wide range of process, neoplastic and non-neoplastic, can produce
Page 1 of 5 THE PATHOLOGY OF MEDIASTINAL MASSES Dr. S. Boag 549-6666 Ext. 4190, mailto:%[email protected] 1. INTRODUCTION A wide range of process, neoplastic and non-neoplastic, can produce
DEVELOPMENT AND GROWTH OF THE MANDIBLE
 2012-2013 ORAL BIOLOGY DEVELOPMENT AND GROWTH OF THE MANDIBLE Ass. Prof. Dr. Heba M. Elsabaa Development and Growth of the Mandible DEVELOPMENT OF THE MANDIBLE The Mandible Is the largest and strongest
2012-2013 ORAL BIOLOGY DEVELOPMENT AND GROWTH OF THE MANDIBLE Ass. Prof. Dr. Heba M. Elsabaa Development and Growth of the Mandible DEVELOPMENT OF THE MANDIBLE The Mandible Is the largest and strongest
SEMESTER VI 3 RD YEAR PATHOLOGY KIDNEY TUMORS
 SEMESTER VI 3 RD YEAR PATHOLOGY KIDNEY TUMORS LEARNING OBJECTIVES At the end of the lecture, students should be able to: Know the pathology of renal tumors. RENAL TUMORS RENAL PAPILLARY ADENOMA Common
SEMESTER VI 3 RD YEAR PATHOLOGY KIDNEY TUMORS LEARNING OBJECTIVES At the end of the lecture, students should be able to: Know the pathology of renal tumors. RENAL TUMORS RENAL PAPILLARY ADENOMA Common
Coding and Payment Guide for Dental Services. A comprehensive coding, billing, and reimbursement resource for dental services
 Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2014 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
Coding and Payment Guide for Dental Services A comprehensive coding, billing, and reimbursement resource for dental services 2014 Contents Introduction...1 Coding Systems... 1 Claim Forms... 2 Contents
LYMPHOMA IN DOGS. Diagnosis/Initial evaluation. Treatment and Prognosis
 LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
Ando A., Nakamura Y., Kanbara R., Kumano H., Miyata T., Masuda T., Ohno Y. and Tanaka Y.
 11. The Effect of Abutment Tooth Connection with Extracoronal Attachment using the Three Dimensional Finite Element Method - Part 2. The Construction of Finite Element Model from CT Data - Ando A., Nakamura
11. The Effect of Abutment Tooth Connection with Extracoronal Attachment using the Three Dimensional Finite Element Method - Part 2. The Construction of Finite Element Model from CT Data - Ando A., Nakamura
