Resident Manual of Trauma to the Face, Head, and Neck. First Edition
|
|
|
- Cornelius Hines
- 8 years ago
- Views:
Transcription
1 Resident Manual of Trauma to the Face, Head, and Neck First Edition
2 2012 All materials in this ebook are copyrighted by the American Academy of Otolaryngology Head and Neck Surgery Foundation, 1650 Diagonal Road, Alexandria, VA , and are strictly prohibited to be used for any purpose without prior express written authorizations from the American Academy of Otolaryngology Head and Neck Surgery Foundation. All rights reserved. For more information, visit our website at ebook Format: First Edition ISBN:
3 Preface The surgical care of trauma to the face, head, and neck that is an integral part of the modern practice of otolaryngology head and neck surgery has its origins in the early formation of the specialty over 100 years ago. Initially a combined specialty of eye, ear, nose, and throat (EENT), these early practitioners began to understand the inter-relations between neurological, osseous, and vascular pathology due to traumatic injuries. It also was very helpful to be able to treat eye as well as facial and neck trauma at that time. Over the past century technological advances have revolutionized the diagnosis and treatment of trauma to the face, head, and neck angiography, operating microscope, sophisticated bone drills, endoscopy, safer anesthesia, engineered instrumentation, and reconstructive materials, to name a few. As a resident physician in this specialty, you are aided in the care of trauma patients by these advances, for which we owe a great deal to our colleagues who have preceded us. Additionally, it has only been in the last years that the separation of ophthalmology and otolaryngology has become complete, although there remains a strong tradition of clinical collegiality. As with other surgical disciplines, significant advances in facial, head, and neck trauma care have occurred as a result of military conflict, where large numbers of combat-wounded patients require ingenuity, inspiration, and clinical experimentation to devise better ways to repair and reconstruct severe wounds. In good part, many of these same advances can be applied to the treatment of other, more civilian pathologies, including the conduct of head and neck oncologic surgery, facial plastic and reconstructive surgery, and otologic surgery. We are indebted to a great many otolaryngologists, such as Dr. John Conley s skills from World War II, who brought such surgical advances from previous wars back to our discipline to better care for patients in the civilian population. Many of the authors of this manual have served in Iraq and/or Afghanistan in a combat surgeon role, and their experiences are being passed on to you. So why develop a manual for resident physicians on the urgent and emergent care of traumatic injuries to the face, head, and neck? Usually the first responders to an academic medical center emergency department for evaluation of trauma patients with face, head, and neck injuries will be the otolaryngology head and neck surgery residents. Because there is often a need for urgent evaluation and treatment bleeding and 16 Resident Manual of Trauma to the Face, Head, and Neck
4 airway obstruction there is often little time for the resident to peruse a reference or comprehensive textbook on such trauma. Thus, a simple, concise, and easily accessible source of diagnostic and therapeutic guidelines for the examining/treating resident was felt to be an important tool, both educationally and clinically. This reference guide for residents was developed by a task force of the American Academy of Otolaryngology Head and Neck Surgery (AAO-HNS) Committee on Trauma. AAO-HNS recently established this standing committee to support the continued tradition of otolaryngology head and neck surgery in the care of trauma patients. An electronic, Portable Document Format (PDF), suitable for downloading to a smart phone, was chosen for this manual to facilitate its practical use by the resident physician in the emergency department and preoperative area. It should be used as a quick-reference tool in the evaluation of a trauma patient and in the planning of the surgical repair and/or reconstruction. This manual supplements, but does not replace, more comprehensive bodies of literature in the field. Use this manual well and often in the care of your patients. G. Richard Holt, MD, MSE, MPH, MABE Joseph A. Brennan, MD, Colonel, MC, USAF Editor and Chair Chair Task Force on Resident Trauma Manual AAO-HNS Committee on Trauma 17
5 Acknowledgments This quick reference guide for resident physicians in trauma management reflects the efforts of many individuals in the American Academy of Otolaryngology Head and Neck Surgery and a special task force of the AAO-HNS Committee on Trauma. The editors would like to thank all of the authors who generously gave their time and expertise to compose excellent chapters for this Resident Manual in the face of busy clinical and academic responsibilities and under a very narrow timeframe of production. These authors, experts in the care of patients who have sustained trauma to the face, head, and neck, have produced practical chapters that will guide resident physicians in their assessment and management of such trauma. The authors have a wide range of clinical expertise in trauma management, gained through community and military experience. A very special appreciation is extended to Audrey Shively, MSHSE, MCHES, CCMEP, Director, Education, of the AAO-HNS Foundation, for her unwavering efforts on behalf of this project, and her competent and patient management of the mechanics of the Resident Manual s production. Additionally, this manual could not have been produced without the expert copyediting and design of diverse educational chapters into a cohesive, concise, and practical format by Joan O Callaghan, Director, Communications Collective, of Bethesda, Maryland. The editors also wish to acknowledge the unwavering support and encouragement from: Rodney P. Lusk, MD, President; David R. Nielsen, MD, Executive Vice President and CEO; Sonya Malekzadeh, MD, Coordinator for Education; and Mary Pat Cornett, CAE, CMP, Senior Director, Education and Meetings, of the AAO-HNS/F. We also appreciate the administrative support of Rudy Anderson as AAO-HNS/F Staff Liaison for the Trauma Committee. Since it takes a group of dedicated professionals to produce an educational and clinical manual such as this, all have shared in the effort, and each individual s contribution has been outstanding. G. Richard Holt, MD, MSE, MPH, MABE Joseph A. Brennan, MD, Colonel, MC, USAF Editor and Chair Chair Task Force on Resident Trauma Manual AAO-HNS Committee on Trauma 18 Resident Manual of Trauma to the Face, Head, and Neck
6 Resident Trauma Manual Authors Joseph A. Brennan, MD, Colonel, MC, USAF Chair, AAO-HNS Committee on Trauma Chief, Department of Surgery San Antonio Military Medical Center Fort Sam Houston, Texas G. Richard Holt, MD, MSE, MPH, MABE Chair, Task Force on Resident Trauma Manual Professor Emeritus, Department of Otolaryngology Head and Neck Surgery University of Texas Health Science Center San Antonio, Texas Matthew P. Connor, MD, Captain, MC, USAF Resident Physician, Department of Otolaryngology Head and Neck Surgery San Antonio Uniformed Services Health Education Consortium Fort Sam Houston, Texas Paul J. Donald, MD Professor and Vice Chair, Department of Otolaryngology University of California-Davis Medical Center Sacramento, California Vincent D. Eusterman, MD, DDS Director, Otolaryngology Head and Neck Surgery Denver Health Medical Center Denver, Colorado David K. Hayes, MD, Colonel, MC, USA Chief of Clinical Operations, US Army Southern Regional Medical Command San Antonio Military Medical Center Fort Sam Houston, Texas Robert M. Kellman, MD Professor and Chair, Department of Otolaryngology and Communication Sciences State University of New York Upstate Medical Center Syracuse, New York John M. Morehead, MD Associate Professor and Program Director Department of Otolaryngology Head and Neck Surgery University of Texas Health Science Center San Antonio, Texas 19
7 Mark D. Packer, MD, Colonel (P), MC, FS, USAF Director, DOD Hearing Center of Excellence Chief, Neurotology, Cranial Base Surgery San Antonio Military Medical Center Fort Sam Houston, Texas Whitney A. Pafford, MD Resident Physician, Division of Otolaryngology New York University School of Medicine New York, New York Mitchell Jay Ramsey, MD, Lt Colonel, MC, USA Chief Otology/Neurotology Landstuhl Kaiserlautern Army Medical Center Germany Nathan L. Salinas, MD, Captain, MC, USA Chief, Department of Otolaryngology Bassett Army Community Hospital Ft. Wainwright, Alaska Joseph C. Sniezek, MD, Colonel, MC, USA Otolaryngology Consultant to the Surgeon General of the Army Tripler Army Medical Center Honolulu, Hawaii Christian L. Stallworth, MD Assistant Professor, Facial Plastic and Reconstructive Surgery Department of Otolaryngology Head and Neck Surgery University of Texas Health Science Center San Antonio, Texas Matthew Scott Stevens, MD Resident Physician, Department of Otolaryngology Head and Neck Surgery University of Texas Health Science Center San Antonio, Texas Richard W. Thomas, MD, DDS, Major General, MC, USA Otolaryngologist Head and Neck Surgeon Commanding General, Western Region Medical Command Joint Base Lewis-McChord, Washington 20 Resident Manual of Trauma to the Face, Head, and Neck
8 Chapter 7: Penetrating and Blunt Neck Trauma Nathan L. Salinas, MD, Captain, MC, USA Joseph A. Brennan, MD, Colonel, MC, USAF I. Penetrating Neck Trauma A. Introduction Penetrating neck trauma has historically carried a high mortality rate, ranging as high as 16 percent during World War I when nonsurgical management was performed. 1 During World War II, when mandatory neck exploration was instituted, the mortality fell to 7 percent and remained 4 7 percent during the Vietnam War. Surgical management has evolved over the last two decades, based on the advent of advanced radiographic studies and endoscopic techniques. Most civilian centers currently practice selective neck exploration, with mortality rates ranging 3 6 percent for low-velocity penetrating neck trauma (LVPNT). 2-6 Most recently, U.S. military surgeons have treated high-velocity penetrating neck trauma (HVPNT) patients with selective neck exploration and have reported mortality rates equivalent to civilian mortality rates for LVPNT. 6 B. Projectiles, BALLISTICS, and Mechanisms of Injury Different types of projectiles are associated with different ballistics and mechanisms of injury, since the severity of projectile injury is directly related to the kinetic energy that the missile imparts to the target tissue (Box 7.1). 7 Box 7.1. Formula for the Relationship Between Projectile Injury and Kinetic Energy The formula for the relationship between the severity of projectile injury and the kinetic energy that the missile imparts to the target tissue is as follows: KE = ½ M (v1-v2) 2 KE = kinetic energy of the missile M = missile mass V1 = entering velocity V2 = exiting velocity Resident Manual of Trauma to the Face, Head, and Neck
9 1. The Most Lethal Missiles The most lethal missiles are high-velocity projectiles that impart all of their energy into the tissues without exiting (V2 = 0). These types of projectiles include: y Tumbling missiles. y Expanding bullets. y Explosive bullets. 2. Temporary and Permanent Bullet Cavities Given the above understanding of kinetic energy of missiles, a single projectile will form two bullet cavities upon tissue impact: y The permanent cavity follows the injury tract due to the direct disruption of tissue from the missile. y The temporary cavity is proportional to the kinetic energy of the missile, and may be up to 30 times the cross-section of the missile along the injury tract Historical Categorization, Types, and Treatment of Penetrating Neck Wounds High-velocity projectiles cause significantly more damage and tissue destruction when compared to low-velocity projectiles. Table 7.1 presents the categories of missiles resulting in penetrating neck trauma and the types of wounds they cause. Historically, these wound types have been divided into low- and high-velocity trauma. Table 7.1. Historical Categories of Missiles and Types of Penetrating Neck Wounds Categories of Missiles Resulting in Penetrating Neck Wounds Knives Low Velocity (<610m/s) Single Projectiles Stab wounds Handguns Handgun wounds Rifles Long-range (>5 m Multiple Projectiles victim-to-weapon range) Shotgun pellets birdshot wounds Improvised explosive Long-range buckshot devices (IEDs) wounds Grenades Mortars Rocket < = less than; > = more than; m/s = meters per second. Types of Penetrating Neck Wounds High Velocity (>610m/s) Close-range (<5 m victim-to-weapon range) birdshot wounds Close-range buckshot wounds Rifle wounds Wounds from bombs, IEDs, grenades, mortars, and rockets 165
10 Chapter 7: Penetrating and Blunt Neck Trauma 4. Historical Treatment of Penetrating Neck Wounds Since World War II, surgeons have stratified management of penetrating neck trauma based on mortality rates and the rates of pathology discovered during neck exploration. 4 a. Low-Velocity Penetrating Neck Trauma LVPNT was typically managed with selective neck dissection, since the overall mortality rate was 3 6 percent with less than 50 percent of patients having major pathology found on neck exploration. b. High-Velocity Penetrating Neck Trauma On the other hand, HVPNT was historically treated with mandatory neck exploration, since those patients had mortality rates greater than 50 percent with percent major pathology found on neck exploration due to the tremendous amount of kinetic energy (up to 3,000 foot-pounds) imparted to the tissue. However, as previously discussed, selective neck dissection is currently used by combat surgeons to treat HVPNT in both Iraq and Afghanistan, with resulting low morbidity and mortality similar to rates seen in civilian trauma centers managing LVPNT. 6 C. Emergency Room Management 1. Initial Orderly Assessment Initial orderly assessment, using the Advanced Trauma Life Support protocol as developed by the American College of Surgeons, is appropriate in any trauma. This protocol includes rapid assessment of the A, B, Cs of trauma. Accordingly, airway management is the first priority in penetrating neck trauma. 8 a. Airway Management y Approximately 10 percent of patients present with airway compromise, with larynx or trachea injury. 5,9 While endotracheal intubation may be performed in these patients, nasotracheal intubation, cricothyroidotomy, or tracheostomy may be required in the presence of spinal instability. y To avoid air embolism, the patient should be supine or in Trendelenburg s position. y Direct pressure without indiscriminate clamping should be used to control active hemorrhage in the neck. y Deeply probing open neck wounds below the platysma muscle should be avoided in the emergency room, as this may lead to clot dislodgement and subsequent hemorrhage. y Two large-bore intravenous lines should be placed to establish access for fluid resuscitation. Subclavian vein injuries should be suspected in 166 Resident Manual of Trauma to the Face, Head, and Neck
11 Zone I injuries (as discussed below), and intravenous access should be placed on the contralateral side of the penetrating injury to avoid extravasation of fluids. y Spinal stabilization should be maintained until cleared clinically and/ or radiographically. y Tetanus toxoid should be administered if the status is unknown or outdated. y If possible, initial radiographic survey in the trauma bay should include chest x-ray and cervical spine x-rays. y Prophylactic antibiotics and nasogastric tube suction placement should also be considered. D. Anatomy 1. Vital Structures in the Neck To organize primary assessment, secondary survey, and surgical approaches to penetrating neck injuries, four types of vital structures in the neck must be considered: y Airway (pharynx, larynx, trachea, and lungs). y Blood vessels (carotid arteries, inominate artery, aortic arch vessels, jugular veins, and subclavian veins). y Nerves (spinal cord, brachial plexus, cranial nerves, and peripheral nerves). y Gastrointestinal tract (pharynx and esophagus). 2. Skeletal Anatomy Skeletal anatomy should be considered as well: y Mandible. y Hyoid. y Styloid process. y Cervical spine. 3. Muscular Landmarks Muscular landmarks are also important: y Platysma muscle Penetration of the platysma muscle defines a deep injury in contrast to a superficial injury. y Sternocleidomastoid muscle The sternocleidomastoid muscle also serves as a valuable landmark, since this large, obliquely oriented muscle divides each side of the neck into anterior and posterior triangles. y Anterior triangle The anterior triangle contains airway, major vasculature, nerves, and gastrointestinal structures, while the posterior triangle contains the spine and muscle
12 Chapter 7: Penetrating and Blunt Neck Trauma 4. Neck Zones The neck is commonly divided into three distinct zones, which facilitates initial assessment and management based on the limitations associated with surgical exploration and hemorrhage control unique to each zone (Figure 7.1). Figure 7.1 The neck is divided into Zones 1, 2 and 3. The axial computed tomographic (CT) images below correspond to Zone 1, Zone 2, and Zone 3. Zone 1 Zone 2 Zone Resident Manual of Trauma to the Face, Head, and Neck
13 a. Zone 1 Zone 1, the most caudal anatomic zone, is defined inferiorly by the clavicle/sternal notch and superiorly by the horizontal plane passing through the cricoid cartilage. Structures within this zone include the: y Proximal common carotid arteries. y Vertebral and subclavian arteries. y Subclavian, inominate, and jugular veins. y Trachea. y Recurrent laryngeal and vagus nerves. yesophagus. y Thoracic duct. Vascular injury management is challenging in Zone 1, and mortality is high. Due to the sternum, surgical access to Zone I may require sternotomy or thoracotomy to control hemorrhage. b. Zone 2 Zone 2, the middle anatomic zone, is between the horizontal plane passing through the cricoid cartilage and the horizontal plane passing through the angle of the mandible. Vertically or horizontally oriented neck exploration incisions provide straightforward surgical access to this zone, which contains the: y Carotid arteries. y Jugular and vertebral veins, pharynx, and larynx. y Proximal trachea. y Recurrent laryngeal and vagal nerves. y Spinal cord. c. Zone 3 Zone 3, the most cephalad anatomic zone, lies between the horizontal plane passing through the angle of the mandible and the skull base. Anatomic structures within Zone 3 include the: y Extracranial carotid and vertebral arteries. y Jugular veins. y Spinal cord. y Cranial nerves IX XII. y Sympathetic trunk. Because of the craniofacial skeleton, surgical access to Zone 3 is difficult, making surgical management of vascular injuries challenging with a high associated mortality at the skull base. Surgical access to Zone 3 may require craniotomy, as well as mandibulotomy or maneuvers to anteriorly displace the mandible
14 Chapter 7: Penetrating and Blunt Neck Trauma 5. Vascular Injuries The incidence of vascular injuries is higher in Zone 1 and Zone 3 penetrating neck trauma injuries. This occurs because the vessels are fixed to bony structures, larger feeding vessels, and muscles at the thoracic inlet and the skull base. Consequently, when the primary and temporary cavities are damaged, these vessels are less able to be displaced by the concussive force from the penetrating missile. However, in Zone 2, the vessels are not fixed; therefore, they are more easily displaced by concussive forces, and the rate of vascular injury is lower. Also, in Zone 1, the esophagus is at risk for injury. Missed esophageal injuries occur because up to 25 percent of penetrating esophageal injuries are occult and asymptomatic. 10 These missed esophageal injuries may be devastating, with reported mortality rates approaching 25 percent. 10 Therefore, for Zone 1 and for some Zone 2 penetrating neck injuries, it is imperative that esophageal injuries be ruled out with endoscopic examination and, possibly, swallow studies. E. Diagnostic Evaluation and Surgical Treatment 1. Selective Neck Exploration Selective neck exploration may be utilized to manage penetrating neck trauma when two important conditions are present at the trauma facility: reliable diagnostic tests that exclude injury and appropriate personnel to provide active observation. 6,11 In the setting of these two conditions, contemporary penetrating neck trauma management is selective neck exploration. a. Patient s Symptoms at Presentation The decision whether to explore the penetrating neck wound is determined based on the patient s symptoms at presentation, regardless of the missile velocity. y Symptomatic patients are explored in the operating room. If symptomatic patients are stable, computed tomographic angiography (CTA) may be obtained before exploration, since this study may better define anatomic approaches to Zone 1 and Zone 3 of the neck. y Asymptomatic patients are evaluated with diagnostic studies and, if pathologic findings are discovered during this workup, are taken to the operating room for neck exploration (Figure 7.2). If asymptomatic patients have a negative diagnostic workup showing no neck pathology, then they will be observed. Significant symptoms from penetrating neck trauma will occur, depending on which of the four groups of vital structures in the neck are injured. 170 Resident Manual of Trauma to the Face, Head, and Neck
15 Figure 7.2 Management algorithm based on symptoms if computed tomographic angiography (CTA), panendoscopy, and appropriate personnel are available. y Vascular injury may result in active hemorrhage, expanding hematoma, vascular bruit, and pulse deficit. y Airway injury may cause subcutaneous emphysema, hoarseness, stridor, and respiratory distress. y Esophageal injury is often asymptomatic and may result in leakage of saliva, subcutaneous emphysema, bleeding from the esophageal inlet, and ultimately neck or mediastinal abscess. y Nerve injury may result in cranial nerve deficits or hemiparesis. These fixed neurologic deficits may not require immediate neck exploration in an otherwise stable patient. 2. Mandatory Neck Exploration If appropriate diagnostic testing and personnel are not available, then penetrating neck trauma patients should undergo mandatory neck exploration, or if stable, should be immediately transferred to a facility with those capabilities. 3. Computed Tomographic Angiography Computed tomographic angiography (CTA) is generally considered the initial procedure of choice to evaluate cervical vasculature in asymptomatic penetrating neck trauma. In the past, formal neck angiography via groin catheters was the procedure of choice. However, since CTA 171
16 Chapter 7: Penetrating and Blunt Neck Trauma has a sensitivity ranging between 90 percent and 100 percent, along with a specificity ranging between 93 percent and 100 percent, this procedure is currently used to evaluate neck vessels. 3,12-14 a. Signs of Probable Injury on CTA Signs of probable injury on CTA include: y Hematoma. y Subcutaneous air adjacent to the carotid sheath. y Intravenous contrast extravasation. y Missile tracts in close proximity to vital structures. 14 b. Nondiagnostic Studies on CTA CTA may have a percent incidence of nondiagnostic studies due to the artifact from bullet fragments and metallic foreign bodies. 5,15 CTA is also useful in evaluating the trajectory of the missile tract and may help select patients who will benefit from further workup of the aerodigestive tract. 4. Evaluation of Aerodigestive Tract Injuries Aerodigestive tract injuries, especially those involving the cervical esophagus, should be identified and repaired within hours after injury to minimize associated morbidity and mortality. Evaluation of asymptomatic aerodigestive tract injuries includes contrast swallow studies and endoscopy (rigid and flexible esophagoscopy, bronchoscopy, and laryngosocpy). a. Endoscopy Endoscopy is more reliable than contrast swallow studies to identify injuries to the hypopharynx and cervical esophagus. Several authors have demonstrated that endoscopy will identify 100 percent of digestive tract injuries, whereas contrast swallow studies are less sensitive, especially for hypopharyngeal injuries. 16,17 b. Rigid and Flexible Esophagoscopy, Rigid and Flexible Bronchoscopy, and Rigid Direct Laryngoscopy Rigid and flexible esophagoscopy, rigid and flexible bronchoscopy and rigid direct laryngoscopy are performed in the operating room under general anesthesia. It is recommended that both rigid and flexible esophagoscopy be performed to rule out occult esophageal injuries. c. Rigid and Flexible Esophagoscopy Rigid esophagoscopy may provide a better view of the proximal esophagus near the cricopharyngeal muscle, while flexible esophagoscopy, with its magnification on the viewing screen and ability to insufflate, gives excellent visualization of more distal esophageal anatomy. 172 Resident Manual of Trauma to the Face, Head, and Neck
17 d. Swallow Studies Finally, swallow studies with either gastrograffin or barium may not be available in austere environments to rule out occult esophageal injuries and, as noted above, are less accurate than endoscopy. 6 Missed esophageal injuries, which may be occult in 25 percent of patients, can be devastating, with mortality rates ranging up to 25 percent. 10 F. CONCLUSION Penetrating neck trauma patients can be divided into two categories on presentation: symptomatic and asymptomatic. Symptomatic patients are taken to the operating room for neck exploration. Asymptomatic patients undergo workup with CTA, panendoscpy, and possibly swallow studies. If the workup shows occult neck pathology, then those patients are taken to the operating room for neck exploration. Asymptomatic patients with a negative diagnostic workup are observed. II. Blunt Neck Trauma A. Introduction Although the same anatomic structures described in penetrating neck trauma (airway, vascular structures, nerves, and gastrointestinal tract) may be impacted during blunt neck trauma. The laryngotracheal airway and cervical spine are the most clinically susceptible to injury. Vascular injuries are potentially devastating but are uncommon overall, occurring in percent of blunt neck trauma, depending on how aggressively asymptomatic patients are screened. 18,19 Despite the widespread use of advanced safety mechanisms, such as shoulder harness seatbelts and airbags, motor vehicle collisions remain the most common etiology for blunt neck trauma. Other mechanisms include blunt object impact sustained in assault, and sports injuries, crush injuries, and hanging or clothesline trauma. B. Presenting Signs and SyMPTOMS As in penetrating neck trauma, the presenting signs and symptoms of blunt neck trauma injuries are based on the dysfunction of the anatomic structures in the neck. Therefore, evaluation of the blunt neck trauma patient should follow the rapid, orderly process of trauma assessment, starting with the airway. 1. Initial Diagnostic Airway Evaluation Initial diagnostic airway evaluation with flexible laryngoscopy is helpful in documenting endolaryngeal findings as well as post-injury changes, since significant edema may occur during the first hours
18 Chapter 7: Penetrating and Blunt Neck Trauma y Computed tomographic (CT) imaging may be considered for surgical planning in symptomatic patients or in asymptomatic patients with suspected laryngeal injury. y Securing the airway is advocated in the setting of acute airway symptoms, such as stridor or respiratory distress, prior to considering imaging. 2. Hemodynamic Instability or Signs of Vascular Injury Hemodynamic instability or signs of vascular injury, such as bruit, expanding/pulsating hematoma, hemorrhage, or loss of pulse, warrant surgical exploration, as described in the Penetrating Neck Trauma section (Section I) of this chapter. 3. Hemodynamically Stable Patients Showing Risk Factors Hemodynamically stable patients should undergo initial diagnostic imaging with CTA if at-risk factors are present, including severe cervical injury, anoxic brain injury from hanging, closed head injury with diffuse axonal injury, midface or complex mandibular fractures, marked neck soft tissue swelling injury, high-risk cervical spine fractures (such as vertebral body subluxation, C1-3 vertebral body fracture, and any fracture extending into the transverse foramen), or basilar skull fractures involving the carotid canal Cervical Spine Injury Assessment After clinical examination, cervical spine injury assessment should include initial lateral and anteroposterior plain x-ray films if possible. Further evaluation with imaging should be based on the individual patient s musculoskeletal and neurologic complaints, as well as physical exam findings. C. CONCLUSION The laryngotracheal airway and the cervical spine are the two most integral structures that can be damaged in blunt trauma to the neck. Prior to any intervention, such as flexible fiberoptic evaluation of the airway, the neck must be stabilized securely in line. The status of the cervical spine takes evaluative precedence after the airway has been secured in a manner that does not compromise a potential cervical spine injury. Hemodynamic stability or instability will be an important guide to the urgency of intervention, including diagnostic CTA prior to exploration of the neck to control bleeding and secure the vascular elements. An excellent physical examination must always be performed and will be the clinical guide to the next steps in evaluation and treatment. 174 Resident Manual of Trauma to the Face, Head, and Neck
19 III. References 1. Obeid FN, Haddad GS, Horst HM, et al. A critical reappraisal of a mandatory exploration policy for penetrating wounds of the neck. Surg Gynecol Obstet. 1985;160: Brennan JA, Meyers AD, Jafek BW. Penetrating neck trauma: A 5-year review of the literature, 1983 to Am J Otolaryngol. 1990;11: Osborn TM, Bell RB, Qaisi W, Long WB. Computed tomographic angiography as an aid to clinical decision making in the selective management of penetrating injuries to the neck: A reduction in the need for operative exploration. J Trauma. 2008;64: Ordog GJ, Albin D, Wasserberger J, et al. Shotgun birdshot wounds to the neck. J Trauma. 1988;28: Carducci B, Lowe RA, Dalsey W. Penetrating neck trauma: Consensus and controversies. Ann Emerg Med.1986;15: Brennan J, Lopez M, Gibbons MD, et al. Penetrating neck trauma in Operation Iraqi Freedom. Otolaryngol Head Neck Surg. 2011; 144(2): Holt GR, Kostohryz G Jr. Wound ballistics of gunshot injuries to the head and neck. Arch Otolaryngol. 1983;109: Brennan J, Gibbons MD, Lopez M, et al. Traumatic airway management in Operation Iraqi Freedom. Otolaryngol Head Neck Surg. 2011;144(3): McConnell D, Trunkey D. Management of penetrating trauma to the neck. Adv Surg. 1994;27: Shama DM, Odell J. Penetrating neck trauma with tracheal and oesophageal injuries. Br J Surg. 1984;71: Biffl WL, Moore EE, Rehse DH, et al. Selective management of penetrating neck trauma based on cervical level of injury. Am J Surg. 1997;174: Munera F, Danton G, Rivas LA, Henry RP, Ferrari MG. Multidetector row computed tomography in the management of penetrating neck injuries. Semin Ultrasound CT MRI. 2009;30:
20 Chapter 7: Penetrating and Blunt Neck Trauma 13. Inaba K, Munera F, McKenney, et al. Prospective evaluation of screening multislice helical computed tomographic angiography in the initial evaluation of penetrating neck injuries. J Trauma. 2006;61: Mazolewski PJ, Curry J, Browder J, Fildes J. Computed tomographic scan can be used for surgical decision making in Zone II penetrating neck injuries. J Trauma. 2001;51: Jurkovich GJ, Zingarelli W, Wallace J, Curreri PW. Penetrating neck trauma: Diagnostic studies in the asymptomatic patient. J Trauma. 1985;25: Ahmed N, Massier C, Tassie J, Whalen J, Chung R. Diagnosis of penetrating injuries of the pharynx and esophagus in the severely injured patient. J Trauma. 2009;67: Armstrong WB, Detar TR, Stanley RB. Diagnosis and management of external penetrating cervical esophageal injuries. Ann Otol Rhinol Laryngol. 1994;103: Davis JW, Holbrook TL, Hoyt DB, et al. Blunt carotid artery dissection: Incidence, associated injuries, screening, and treatment. J Trauma. 1990;30: Kerwin AJ, Bynoe RP, Murray J, et al. Liberalized screening for blunt carotid and vertebral artery injuries is justified. J Trauma Inj Infect Crit Care. 2001;51: Stanley R, Hanson D. Manual strangulation injuries of the larynx. Arch Otolaryngol. 1983;109: Schroeder JW, Baskaran V, Aygun N. Imaging of traumatic arterial injuries in the neck with an emphasis on CTA. Emerg Radiol. 2010;17: Resident Manual of Trauma to the Face, Head, and Neck
21 The American Academy of Otolaryngology Head and Neck Surgery Foundation s education initiatives are aimed at increasing the quality of patient outcomes through knowledgeable, competent, and professional physicians. The goals of education are to provide activities and services for practicing otolaryngologists, physicians-in-training, and non-otolaryngologist health professionals. The Foundation s AcademyU serves as the primary resource for otolaryngology head and neck activities and events. These include an online library of expertdeveloped learning courses, learning platforms, and e-books, as well as Patient Management Perspectives in Otolaryngology and the Home Study Course. In addition, the AAO-HNSF Annual Meeting & OTO EXPO is the world s largest gathering of otolaryngologists, offering a variety of education seminars, courses, and posters. Many of the Foundation s activities are available for AMA PRA Category 1 Credit. Visit the Academy s Web site, to find out how AcademyU can assist you and your practice through quality professional development opportunities.
22 American Academy of Otolaryngology Head and Neck Surgery Foundation 1650 Diagonal Road Alexandria, VA USA T / F /
ENT Emergencies. Injuries of the Neck. Registrar Dept Trauma and emergency Medicine Tygerberg Hospital
 ENT Emergencies Injuries of the Neck Registrar Dept Trauma and emergency Medicine Tygerberg Hospital Neck Injuries Blunt and Penetrating Trauma Blunt Injuries Blunt trauma direct/indirect Trauma to larynx
ENT Emergencies Injuries of the Neck Registrar Dept Trauma and emergency Medicine Tygerberg Hospital Neck Injuries Blunt and Penetrating Trauma Blunt Injuries Blunt trauma direct/indirect Trauma to larynx
Resident Manual of Trauma to the Face, Head, and Neck. First Edition
 Resident Manual of Trauma to the Face, Head, and Neck First Edition 2012 All materials in this ebook are copyrighted by the American Academy of Otolaryngology Head and Neck Surgery Foundation, 1650 Diagonal
Resident Manual of Trauma to the Face, Head, and Neck First Edition 2012 All materials in this ebook are copyrighted by the American Academy of Otolaryngology Head and Neck Surgery Foundation, 1650 Diagonal
Neck Injuries. Penetrating Neck Injuries. Epidemiologic Features
 Neck Injuries Neck injuries are notoriously difficult to evaluate and treat because of the complex anatomy and the dense concentration of numerous vital structures in a small anatomical area. The clinical
Neck Injuries Neck injuries are notoriously difficult to evaluate and treat because of the complex anatomy and the dense concentration of numerous vital structures in a small anatomical area. The clinical
8_Neck Trauma STN E-Library 2012 1
 1 The evaluation and management of neck trauma has evolved over the past few decades. However, the challenges remain the same in that injuries to structures in the neck may cause life threatening situations
1 The evaluation and management of neck trauma has evolved over the past few decades. However, the challenges remain the same in that injuries to structures in the neck may cause life threatening situations
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
TNM Staging of Head and Neck Cancer and Neck Dissection Classification
 QUICK REFERENCE GUIDE TO TNM Staging of Head and Neck Cancer and Neck Dissection Classification Fourth Edition 2014 All materials in this ebook are copyrighted by the American Academy of Otolaryngology
QUICK REFERENCE GUIDE TO TNM Staging of Head and Neck Cancer and Neck Dissection Classification Fourth Edition 2014 All materials in this ebook are copyrighted by the American Academy of Otolaryngology
IV. DEFINITION OF LYMPH NODE GROUPS (FIGURE 1) Level IA: Submental Group
 IV. DEFINITION OF LYMPH NODE GROUPS (FIGURE 1) Fig. 1 The level system is used for describing the location of lymph nodes in the neck: Level I, submental and submandibular group; Level II, upper jugular
IV. DEFINITION OF LYMPH NODE GROUPS (FIGURE 1) Fig. 1 The level system is used for describing the location of lymph nodes in the neck: Level I, submental and submandibular group; Level II, upper jugular
Minimally Invasive Spine Surgery
 Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Chapter 1 Minimally Invasive Spine Surgery 1 H.M. Mayer Primum non nocere First do no harm In the long history of surgery it always has been a basic principle to restrict the iatrogenic trauma done to
Recurrent & Persistent Papillary Thyroid Cancer Central Nodal Dissection vs. Node-Picking Patterns of Nodal Metastases Recurrent Laryngeal Nerve,
 Recurrent & Persistent Papillary Thyroid Cancer Central Nodal Dissection vs. Node-Picking Patterns of Nodal Metastases Recurrent Laryngeal Nerve, Larynx, Trachea, & Esophageal Management Robert C. Wang,
Recurrent & Persistent Papillary Thyroid Cancer Central Nodal Dissection vs. Node-Picking Patterns of Nodal Metastases Recurrent Laryngeal Nerve, Larynx, Trachea, & Esophageal Management Robert C. Wang,
Anterior Approach Burn s Space Esophagus
 Cervical Complications Complications after Cervical Spine Surgery Dr. Rock Patel University of Michigan, Ann Arbor APPROACH RELATED Anterior Posterior PROCEDURE RELATED ACDF Disc Arthroplasty Laminectomy/Fusion
Cervical Complications Complications after Cervical Spine Surgery Dr. Rock Patel University of Michigan, Ann Arbor APPROACH RELATED Anterior Posterior PROCEDURE RELATED ACDF Disc Arthroplasty Laminectomy/Fusion
by joseph e. muscolino, DO photography by yanik chauvin
 by joseph e. muscolino, DO photography by yanik chauvin body mechanics palpation of the anterior neck ESOUCES For more information go to www.medlineplus.gov and search under anterior neck. The anterior
by joseph e. muscolino, DO photography by yanik chauvin body mechanics palpation of the anterior neck ESOUCES For more information go to www.medlineplus.gov and search under anterior neck. The anterior
Case 2. 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis
 Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
Case 2 30 year old involved in a MVA complaining of chest pain. Bruising over the right upper chest. Your Diagnosis Diagnosis: Posterior Sterno-clavicular dislocation [PSCD] A posterior sterno-clavicular
Gunshot wounds. Warning: This presentation has extremely graphic pictures! Richard P. Kness, EMT- P
 Gunshot wounds Warning: This presentation has extremely graphic pictures! Richard P. Kness, EMT- P Objectives After this lesson the student will be able to: List scene safety issues Describe procedures
Gunshot wounds Warning: This presentation has extremely graphic pictures! Richard P. Kness, EMT- P Objectives After this lesson the student will be able to: List scene safety issues Describe procedures
Chapter 7. Expose the Injured Area
 Chapter 7 GUNSHOT WOUNDS KEY FIGURES: Entrance/exit wounds This chapter describes how to treat the external, surface wounds caused by a bullet. The evaluation for underlying injury related to gunshot wounds
Chapter 7 GUNSHOT WOUNDS KEY FIGURES: Entrance/exit wounds This chapter describes how to treat the external, surface wounds caused by a bullet. The evaluation for underlying injury related to gunshot wounds
Management of spinal cord compression
 Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
Management of spinal cord compression (SUMMARY) Main points a) On diagnosis, all patients should receive dexamethasone 10mg IV one dose, then 4mg every 6h. then switched to oral dose and tapered as tolerated
6.0 Management of Head Injuries for Maxillofacial SHOs
 6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
Mechanism of Injury 1
 Mechanism of Injury 1 Objectives At the end of this lecture the participant will be able to: Describe the importance of the mechanism of injury in history taking of the trauma patient. Identify patterns
Mechanism of Injury 1 Objectives At the end of this lecture the participant will be able to: Describe the importance of the mechanism of injury in history taking of the trauma patient. Identify patterns
Posterior Cervical Decompression
 Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Posterior Cervical Decompression Spinal Unit Tel: 01473 702032 or 702097 Issue 2: January 2009 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed with a
Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain. Seth Cheatham, MD
 Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain Seth Cheatham, MD 236 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures Contact sports, specifically football, places
Cervical-Spine Injuries: Catastrophic Injury to Neck Sprain Seth Cheatham, MD 236 Seth A. Cheatham, MD VCU Sports Medicine I have no financial disclosures Contact sports, specifically football, places
Maricopa Integrated Health System: Administrative Policy & Procedure
 Maricopa Integrated Health System: Administrative Policy & Procedure Effective Date: 03/05 Reviewed Dates: 09/05, 9/08 Revision Dates: Policy #: 64500 S Policy Title: Cervical & Total Spine Clearance and
Maricopa Integrated Health System: Administrative Policy & Procedure Effective Date: 03/05 Reviewed Dates: 09/05, 9/08 Revision Dates: Policy #: 64500 S Policy Title: Cervical & Total Spine Clearance and
Diffuse Neck Swelling after Car Accident
 中 華 放 射 醫 誌 Chin J Radiol 2005; 30: 283-287 283 Diffuse Neck Swelling after Car Accident HUAN-WU CHEN SHENG-CHAU HUANG HUAN-WEN CHEN 2 KOU-MOU HUANG Departments of Medical Imaging, National Taiwan University
中 華 放 射 醫 誌 Chin J Radiol 2005; 30: 283-287 283 Diffuse Neck Swelling after Car Accident HUAN-WU CHEN SHENG-CHAU HUANG HUAN-WEN CHEN 2 KOU-MOU HUANG Departments of Medical Imaging, National Taiwan University
Discovery of an Aneurysm Following a Motorcycle Accident. Maya Babu, MSIII Gillian Lieberman, M.D.
 Discovery of an Aneurysm Following a Motorcycle Accident Maya Babu, MSIII Gillian Lieberman, M.D. Patient CC: July 2004 65 yo male transferred to the BI from an OSH s/p motorcycle crash w/o a helmet CC
Discovery of an Aneurysm Following a Motorcycle Accident Maya Babu, MSIII Gillian Lieberman, M.D. Patient CC: July 2004 65 yo male transferred to the BI from an OSH s/p motorcycle crash w/o a helmet CC
Cervical Spine Stabilization and Preventing Rapid Necessity Injuries
 Injury, Int. J. Care Injured 31 (2000) 305±309 www.elsevier.com/locate/injury Prehospital stabilization of the cervical spine for penetrating injuries of the neck Ð is it necessary? Y. Barkana a, *, M.
Injury, Int. J. Care Injured 31 (2000) 305±309 www.elsevier.com/locate/injury Prehospital stabilization of the cervical spine for penetrating injuries of the neck Ð is it necessary? Y. Barkana a, *, M.
Patient Information. Posterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
United States Department of Transportation National Highway Traffic Safety Administration Paramedic: National Standard Curriculum 1
 UNIT TERMINAL OBJECTIVE 4-8 At the completion of this unit, the paramedic student will be able to integrate pathophysiologic principles and the assessment findings to formulate a field impression and implement
UNIT TERMINAL OBJECTIVE 4-8 At the completion of this unit, the paramedic student will be able to integrate pathophysiologic principles and the assessment findings to formulate a field impression and implement
PRACTICE GUIDELINE TITLE: INTRAVENOUS LINE INSERTION: PERIPHERAL AND CENTRAL
 PRACTICE GUIDELINE Effective Date: 9-17-04 Manual Reference: Deaconess Trauma Services TITLE: INTRAVENOUS LINE INSERTION: PERIPHERAL AND CENTRAL PURPOSE: To outline the indications and options for intravenous
PRACTICE GUIDELINE Effective Date: 9-17-04 Manual Reference: Deaconess Trauma Services TITLE: INTRAVENOUS LINE INSERTION: PERIPHERAL AND CENTRAL PURPOSE: To outline the indications and options for intravenous
TRAUMA SURGERY Dr. Michal Cheatham Orlando Regional Health PGY-4
 ROTATION LIAISON: INSTITUTION: LEVEL(S): TRAUMA SURGERY Dr. Michal Cheatham Orlando Regional Health PGY-4 I. GENERAL INFORMATION The General Surgery Department at Orlando Regional Health has three full
ROTATION LIAISON: INSTITUTION: LEVEL(S): TRAUMA SURGERY Dr. Michal Cheatham Orlando Regional Health PGY-4 I. GENERAL INFORMATION The General Surgery Department at Orlando Regional Health has three full
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Imaging of Thoracic Endovascular Stent-Grafts
 Imaging of Thoracic Endovascular Stent-Grafts Tariq Hameed, M.D. Department of Radiology and Imaging Sciences, Indiana University School of Medicine, Indianapolis, Indiana Disclosures: No relevant financial
Imaging of Thoracic Endovascular Stent-Grafts Tariq Hameed, M.D. Department of Radiology and Imaging Sciences, Indiana University School of Medicine, Indianapolis, Indiana Disclosures: No relevant financial
ITLS & PHTLS: A Comparison
 ITLS & PHTLS: A Comparison International Trauma Life Support (ITLS) is a global organization dedicated to preventing death and disability from trauma through education and emergency care. ITLS educates
ITLS & PHTLS: A Comparison International Trauma Life Support (ITLS) is a global organization dedicated to preventing death and disability from trauma through education and emergency care. ITLS educates
Test Request Tip Sheet
 With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely necessary. The study
With/Without Contrast CT, MRI Studies should NOT be ordered simultaneously as dual studies (i.e., with and without contrast). Radiation exposure is doubled and both views are rarely necessary. The study
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
Patient Information. Anterior Cervical Surgery. Here to help. Respond Deliver & Enable
 Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Here to help Our Health Information Centre (HIC) provides advice and information on a wide range of health-related topics. We also offer: Services for people with disabilities. Information in large print,
Small cell lung cancer
 Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
Small cell lung cancer Small cell lung cancer is a disease in which malignant (cancer) cells form in the tissues of the lung. The lungs are a pair of cone-shaped breathing organs that are found within
ICD-9-CM coding for patients with Spinal Cord Injury*
 ICD-9-CM coding for patients with Spinal Cord Injury* indicates intervening codes have been left out of this list. OTHER DISORDERS OF THE CENTRAL NERVOUS SYSTEM (340-349) 344 Other paralytic syndromes
ICD-9-CM coding for patients with Spinal Cord Injury* indicates intervening codes have been left out of this list. OTHER DISORDERS OF THE CENTRAL NERVOUS SYSTEM (340-349) 344 Other paralytic syndromes
III./8.4.2: Spinal trauma. III./8.4.2.1 Injury of the spinal cord
 III./8.4.2: Spinal trauma Introduction Causes: motor vehicle accidents, falls, sport injuries, industrial accidents The prevalence of spinal column trauma is 64/100,000, associated with neurological dysfunction
III./8.4.2: Spinal trauma Introduction Causes: motor vehicle accidents, falls, sport injuries, industrial accidents The prevalence of spinal column trauma is 64/100,000, associated with neurological dysfunction
GENERAL OTOLARYNGOLOGY HEAD and NECK SURGICAL ONCOLOGY. MEE General ORL/Head and Neck Rotation - PGY 2,3,4,5 Longwood Rotation - PGY 2,3,4,5
 GENERAL OTOLARYNGOLOGY HEAD and NECK SURGICAL ONCOLOGY 1. BRIEF DESCRIPTION Training in general otolaryngology, upper aerodigestive tract endoscopy and head and neck oncologic surgery begins and continues
GENERAL OTOLARYNGOLOGY HEAD and NECK SURGICAL ONCOLOGY 1. BRIEF DESCRIPTION Training in general otolaryngology, upper aerodigestive tract endoscopy and head and neck oncologic surgery begins and continues
Evaluating muscle injuries and residuals of shell fragment and gunshot wounds
 Evaluating muscle injuries and residuals of shell fragment and gunshot wounds Training conducted by: Michael Fishman and Sandrine Fisher 1 Objectives To become familiar with the application of the rating
Evaluating muscle injuries and residuals of shell fragment and gunshot wounds Training conducted by: Michael Fishman and Sandrine Fisher 1 Objectives To become familiar with the application of the rating
ANTERIOR CERVICAL DISCECTOMY AND FUSION. Basic Anatomical Landmarks: Anterior Cervical Spine
 Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma
 Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma Chapter 50 Abdominal Trauma 1 Describe the epidemiology, including morbidity, mortality rates, and prevention strategies,
Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma Chapter 50 Abdominal Trauma 1 Describe the epidemiology, including morbidity, mortality rates, and prevention strategies,
Spine Injury and Back Pain in Sports
 Spine Injury and Back Pain in Sports DAVID W. GRAY, MD 1 Back Pain Increases with Age Girls>Boys in Teenage years Anywhere from 15 to 80% of children and adolescents have back pain depending on the studies
Spine Injury and Back Pain in Sports DAVID W. GRAY, MD 1 Back Pain Increases with Age Girls>Boys in Teenage years Anywhere from 15 to 80% of children and adolescents have back pain depending on the studies
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Vascular Access. Chapter 3
 Vascular Access Chapter 3 Vascular Access Introduction Obtaining vascular access in infants and children can be difficult even under optimal conditions. Attempting emergent access in a hypotensive, struggling
Vascular Access Chapter 3 Vascular Access Introduction Obtaining vascular access in infants and children can be difficult even under optimal conditions. Attempting emergent access in a hypotensive, struggling
Image. 3.11.3 SW Review the anatomy of the EAC and how this plays a role in the spread of tumors.
 Neoplasms of the Ear and Lateral Skull Base Image 3.11.1 SW What are the three most common neoplasms of the auricle? 3.11.2 SW What are the four most common neoplasms of the external auditory canal (EAC)
Neoplasms of the Ear and Lateral Skull Base Image 3.11.1 SW What are the three most common neoplasms of the auricle? 3.11.2 SW What are the four most common neoplasms of the external auditory canal (EAC)
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Cervical Spine Imaging
 March 20, 2006 Cervical Spine Imaging Johannes Kratz, Harvard Medical School Year IV 1 Overview Background Clinical Cases Diagnostic Tests and a Decision-Tree Algorithm Examples of Cervical Spine Evaluations
March 20, 2006 Cervical Spine Imaging Johannes Kratz, Harvard Medical School Year IV 1 Overview Background Clinical Cases Diagnostic Tests and a Decision-Tree Algorithm Examples of Cervical Spine Evaluations
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE:
 James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
James A. Sanfilippo, M.D. CONSENT FOR SPINAL SURGERY PATIENT: DATE: 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand
How To Learn To Perform An Ultrasound
 CAE ICCU E-Learning CAE VIMEDIX Ultrasound Simulator Master Ultrasonography of the Thoracic, Abdominal and Pelvic Cavities An Engaging Learning Solution for Ultrasound Hands-on Simulation, Multimedia Content,
CAE ICCU E-Learning CAE VIMEDIX Ultrasound Simulator Master Ultrasonography of the Thoracic, Abdominal and Pelvic Cavities An Engaging Learning Solution for Ultrasound Hands-on Simulation, Multimedia Content,
Autonomic Nervous System of the Neck. Adam Koleśnik, MD Department of Descriptive and Clinical Anatomy Center of Biostructure Research, MUW
 Autonomic Nervous System of the Neck Adam Koleśnik, MD Department of Descriptive and Clinical Anatomy Center of Biostructure Research, MUW Autonomic nervous system sympathetic parasympathetic enteric Autonomic
Autonomic Nervous System of the Neck Adam Koleśnik, MD Department of Descriptive and Clinical Anatomy Center of Biostructure Research, MUW Autonomic nervous system sympathetic parasympathetic enteric Autonomic
EYE, EAR, NOSE, and THROAT INJURIES
 T6 EYE, EAR, NOSE, and THROAT INJURIES Management of injuries of the eyes, ears, nose, and throat focuses on airway management and initial stabilization of the injury. Bilateral comparisons can assist
T6 EYE, EAR, NOSE, and THROAT INJURIES Management of injuries of the eyes, ears, nose, and throat focuses on airway management and initial stabilization of the injury. Bilateral comparisons can assist
Spinal Cord Injury Education. An Overview for Patients, Families, and Caregivers
 Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
Spinal Cord Injury Education An Overview for Patients, Families, and Caregivers Spinal Cord Anatomy A major component of the Central Nervous System (CNS) It is 15 to 16 inches long, and weighs 1 to 2 ounces
Upper Cervical Spine - Occult Injury and Trigger for CT Exam
 Upper Cervical Spine - Occult Injury and Trigger for CT Exam Bakman M, Chan K, Bang C, Basu A, Seo G, Monu JUV Department of Imaging Sciences University of Rochester Medical Center, Rochester, NY Introduction
Upper Cervical Spine - Occult Injury and Trigger for CT Exam Bakman M, Chan K, Bang C, Basu A, Seo G, Monu JUV Department of Imaging Sciences University of Rochester Medical Center, Rochester, NY Introduction
Program Specification for Master Degree Anesthesia, ICU and Pain Management
 Cairo University Faculty of Medicine Program type: Single Program Specification for Master Degree Anesthesia, ICU and Pain Management Department offering program: Anesthesia, intensive care and pain management
Cairo University Faculty of Medicine Program type: Single Program Specification for Master Degree Anesthesia, ICU and Pain Management Department offering program: Anesthesia, intensive care and pain management
Nursing. Management of Spinal Trauma. Content. Objectives. Objectives
 7 cervical vertebrae Content 12 thoracic vertebrae Nursing 5 sacral vertebrae Management of Spinal Trauma Kwai Fung Betty Siu Ward Manager O&T Dept TKOH Date : 22nd April 2007 5 lumbar vertebrae 4 coccygeal
7 cervical vertebrae Content 12 thoracic vertebrae Nursing 5 sacral vertebrae Management of Spinal Trauma Kwai Fung Betty Siu Ward Manager O&T Dept TKOH Date : 22nd April 2007 5 lumbar vertebrae 4 coccygeal
Case Report Chronic Neck Pain Associated with an Old Odontoid Fracture: A Rare Presentation
 Case Reports in Emergency Medicine Volume 2013, Article ID 372723, 4 pages http://dx.doi.org/10.1155/2013/372723 Case Report Chronic Neck Pain Associated with an Old Odontoid Fracture: A Rare Presentation
Case Reports in Emergency Medicine Volume 2013, Article ID 372723, 4 pages http://dx.doi.org/10.1155/2013/372723 Case Report Chronic Neck Pain Associated with an Old Odontoid Fracture: A Rare Presentation
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time.
 If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
If you or a loved one have suffered because of a negligent error during spinal surgery, you will be going through a difficult time. You may be worried about your future, both in respect of finances and
Electrical Burns 新 光 急 診 張 志 華
 Electrical Burns 新 光 急 診 張 志 華 Electrical Burns Definition Cellular damage due to electrical current High vs. low tension injuries 1,000 Volts dividing line Electrical Burns - Pathophysiology Joule Effect:
Electrical Burns 新 光 急 診 張 志 華 Electrical Burns Definition Cellular damage due to electrical current High vs. low tension injuries 1,000 Volts dividing line Electrical Burns - Pathophysiology Joule Effect:
Horizon Blue Cross Blue Shield of NJ Radiology Rules Bank
 Horizon Blue Cross Blue Shield of NJ Radiology Rules Bank * Rule added 05/30/13 Code Pay Code Do Not Pay Source 70010 Myelography, posterior fossa, radiological supervision and 76000 Fluoroscopy, up to
Horizon Blue Cross Blue Shield of NJ Radiology Rules Bank * Rule added 05/30/13 Code Pay Code Do Not Pay Source 70010 Myelography, posterior fossa, radiological supervision and 76000 Fluoroscopy, up to
Cervical Spine Surgery. Orthopaedic Nursing Seminar. Dr Michelle Atkinson. Friday October 21 st 2011. Cervical Disc Herniation
 Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Cervical Spine Surgery Dr Michelle Atkinson The Sydney and Dalcross Adventist Hospitals Orthopaedic Nursing Seminar Friday October 21 st 2011 Cervical disc herniation The most frequently treated surgical
Specific Standards of Accreditation for Residency Programs in General Surgery
 Specific Standards of Accreditation for Residency Programs in General Surgery 2010 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation of the
Specific Standards of Accreditation for Residency Programs in General Surgery 2010 INTRODUCTION The purpose of this document is to provide program directors and surveyors with an interpretation of the
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Medical Terminology, Anatompy & Physiology
 1. Which of the following BEST describes the anatomical position? a. Supine with arms crossed over the chest and knees slightly bent b. Standing, facing forward, with arms raised above the head c. Standing,
1. Which of the following BEST describes the anatomical position? a. Supine with arms crossed over the chest and knees slightly bent b. Standing, facing forward, with arms raised above the head c. Standing,
Fundamentals of Spine Surgery and Interventional Pain Management
 The North American Spine Society presents Fundamentals of Spine Surgery and Interventional Pain Management 9.5 Hours of Hands-on Cadaver Lab Sessions 15 AMA PRA Category 1 Credits TM A Surgical/Interventional
The North American Spine Society presents Fundamentals of Spine Surgery and Interventional Pain Management 9.5 Hours of Hands-on Cadaver Lab Sessions 15 AMA PRA Category 1 Credits TM A Surgical/Interventional
Traumatic injuries SPINAL CORD. Causes of Traumatic SCI SYMPTOMS. Spinal Cord trauma can be caused by:
 Traumatic injuries SPINAL CORD Jennie Trkulja RN, BScN, ENC (c) Causes of Traumatic SCI Spinal Cord trauma can be caused by: MVC (most injuries) Gunshots Falls Stabbings Assaults Industrial accidents Sports
Traumatic injuries SPINAL CORD Jennie Trkulja RN, BScN, ENC (c) Causes of Traumatic SCI Spinal Cord trauma can be caused by: MVC (most injuries) Gunshots Falls Stabbings Assaults Industrial accidents Sports
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS
 SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
THORACIC OUTLET SYNDROME & BRACHIAL PLEXUS INJURIES
 THORACIC OUTLET SYNDROME & BRACHIAL PLEXUS INJURIES I. THORACIC OUTLET SYNDROME TOS is a compression of nerves or blood vessels, or both, in the thoracic outlet region, which is the space between the collarbone
THORACIC OUTLET SYNDROME & BRACHIAL PLEXUS INJURIES I. THORACIC OUTLET SYNDROME TOS is a compression of nerves or blood vessels, or both, in the thoracic outlet region, which is the space between the collarbone
The Abbreviated Injury Scale (AIS) A brief introduction
 The Abbreviated Injury Scale (AIS) A brief introduction Abbreviated Injury Scale 1990 Revision Update 98 The Abbreviated Injury Scale produced by: Association for the Advancement of Automotive Medicine
The Abbreviated Injury Scale (AIS) A brief introduction Abbreviated Injury Scale 1990 Revision Update 98 The Abbreviated Injury Scale produced by: Association for the Advancement of Automotive Medicine
The Comprehensive Cancer Care Team at Penn Vet s Ryan Hospital CORE TEAM
 The Comprehensive Cancer Care Team at Penn Vet s Ryan Hospital Ryan Hospital s Comprehensive Cancer Care Program is led by a world- class team of board- certified veterinarians who each offer a unique
The Comprehensive Cancer Care Team at Penn Vet s Ryan Hospital Ryan Hospital s Comprehensive Cancer Care Program is led by a world- class team of board- certified veterinarians who each offer a unique
Pat Cox, CPC, CPC-H, CPMA, CPC-I, CEMC, CCS-P. Professional Medical Coding Education
 Pat Cox, CPC, CPC-H, CPMA, CPC-I, CEMC, CCS-P Professional Medical Coding Education Thank you for your interest in the upcoming Certified Professional Coder (CPC ) class. This session is a 16-week class
Pat Cox, CPC, CPC-H, CPMA, CPC-I, CEMC, CCS-P Professional Medical Coding Education Thank you for your interest in the upcoming Certified Professional Coder (CPC ) class. This session is a 16-week class
PLASTIC SURGERY RESIDENTS HANDBOOK
 PLASTIC SURGERY RESIDENTS HANDBOOK I. PLASTIC SURGERY REQUIREMENTS a. AACPS Post Interview Communication Guidelines b. General Competencies c. Plastic Surgery Goals & Objectives d. ACGME Required Index
PLASTIC SURGERY RESIDENTS HANDBOOK I. PLASTIC SURGERY REQUIREMENTS a. AACPS Post Interview Communication Guidelines b. General Competencies c. Plastic Surgery Goals & Objectives d. ACGME Required Index
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS?
 SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
SPINAL STENOSIS Information for Patients WHAT IS SPINAL STENOSIS? The spinal canal is best imagined as a bony tube through which nerve fibres pass. The tube is interrupted between each pair of adjacent
Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任
 Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任 Patient Data Name: 苏 XX Gender: Female Age:47 years old Admission date: 2010.06.09 Chief complaint Fell down from 4-54 5 meter tree and lead to lumbosacral
Thoracolumbar Fratures R1: 胡 家 瑞 指 导 老 师 : 吴 轲 主 任 Patient Data Name: 苏 XX Gender: Female Age:47 years old Admission date: 2010.06.09 Chief complaint Fell down from 4-54 5 meter tree and lead to lumbosacral
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 2 ORGANIZATION OF THE BODY
 ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 2 ORGANIZATION OF THE BODY Human beings are arguably the most complex organisms on this planet. Imagine billions of microscopic parts, each with its own identity,
ANATOMY & PHYSIOLOGY ONLINE COURSE - SESSION 2 ORGANIZATION OF THE BODY Human beings are arguably the most complex organisms on this planet. Imagine billions of microscopic parts, each with its own identity,
Physician Assistant Post Graduate Orthopaedic Surgery Fellowship Program. Watauga Orthopaedics
 Physician Assistant Post Graduate Orthopaedic Surgery Fellowship Program Watauga Orthopaedics Physician Assistant Post-Graduate Fellowship Program in Orthopaedic Surgery Required Texts: 1. Backache Macnab,
Physician Assistant Post Graduate Orthopaedic Surgery Fellowship Program Watauga Orthopaedics Physician Assistant Post-Graduate Fellowship Program in Orthopaedic Surgery Required Texts: 1. Backache Macnab,
1 of 6 1/22/2015 10:06 AM
 1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
1 of 6 1/22/2015 10:06 AM 2 of 6 1/22/2015 10:06 AM This cross-section view of the shoulder socket shows a typical SLAP tear. Injuries to the superior labrum can be caused by acute trauma or by repetitive
European Academy of DentoMaxilloFacial Radiology
 European Academy of DentoMaxilloFacial Radiology Framework for Specialist Training in Dental and Maxillofacial Radiology Background The scope of DentoMaxilloFacial Radiology DMFR (Dental and Maxillofacial
European Academy of DentoMaxilloFacial Radiology Framework for Specialist Training in Dental and Maxillofacial Radiology Background The scope of DentoMaxilloFacial Radiology DMFR (Dental and Maxillofacial
.org. Clavicle Fracture (Broken Collarbone) Anatomy. Description. Cause. Symptoms
 Clavicle Fracture (Broken Collarbone) Page ( 1 ) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages. Anatomy The collarbone (clavicle)
Clavicle Fracture (Broken Collarbone) Page ( 1 ) A broken collarbone is also known as a clavicle fracture. This is a very common fracture that occurs in people of all ages. Anatomy The collarbone (clavicle)
Endovascular Repair of an Axillary Artery Aneurysm: A Novel Approach
 Endovascular Repair of an Axillary Artery Aneurysm: A Novel Approach Bao- Thuy D. Hoang, MD 1, Jonathan- Hien Vu, MD 2, Jerry Matteo, MD 3 1 Department of Surgery, University of Florida College of Medicine,
Endovascular Repair of an Axillary Artery Aneurysm: A Novel Approach Bao- Thuy D. Hoang, MD 1, Jonathan- Hien Vu, MD 2, Jerry Matteo, MD 3 1 Department of Surgery, University of Florida College of Medicine,
Introduction. signs or symptoms. This approach may uncover subtle signs and symptoms that
 Introduction Even with today s understanding of the mechanisms that lead to spinal cord injury in athletics, some are still inclined to present these injuries as freak accidents1,2. The physics and mechanics
Introduction Even with today s understanding of the mechanisms that lead to spinal cord injury in athletics, some are still inclined to present these injuries as freak accidents1,2. The physics and mechanics
Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report
 Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report 1 Journal Of Whiplash & Related Disorders Vol. 1, No, 1, 2002 Gunilla Bring, Halldor Jonsson Jr.,
Pathoanatomical Changes of the Brachial Plexus and of C5-C6 Following Whiplash-Type Injury: A Case Report 1 Journal Of Whiplash & Related Disorders Vol. 1, No, 1, 2002 Gunilla Bring, Halldor Jonsson Jr.,
Guidelines for the Management of Patients Following Endoluminal Vein Dilation Procedures for the Treatment of Multiple Sclerosis
 Guidelines for the Management of Patients Following Endoluminal Vein Dilation Procedures for the Treatment of Multiple Sclerosis Report Submitted to the Minister of Health and Long-Term Care By the Ontario
Guidelines for the Management of Patients Following Endoluminal Vein Dilation Procedures for the Treatment of Multiple Sclerosis Report Submitted to the Minister of Health and Long-Term Care By the Ontario
Divisions of the Skeletal System
 OpenStax-CNX module: m46344 1 Divisions of the Skeletal System OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this
OpenStax-CNX module: m46344 1 Divisions of the Skeletal System OpenStax College This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this
All Intraosseous Sites Are Not Equal
 All Intraosseous Sites Are Not Equal Clinical Data Suggests the Sternal IO Route Improves Patient Outcomes Current Guidelines, (such as AHA) indicate that Intraosseous Infusion (IO) is a rapid, safe and
All Intraosseous Sites Are Not Equal Clinical Data Suggests the Sternal IO Route Improves Patient Outcomes Current Guidelines, (such as AHA) indicate that Intraosseous Infusion (IO) is a rapid, safe and
ORAL MAXILLO FACIAL SURGERY REFERRAL RECOMMENDATIONS
 ORAL MAXILLO FACIAL SURGERY REFERRAL RECOMMENDATIONS Diagnosis / Symptomatology Evaluation Management Options Referral Guidelines General problems include: Soft tissue conditions of the face and oral cavity
ORAL MAXILLO FACIAL SURGERY REFERRAL RECOMMENDATIONS Diagnosis / Symptomatology Evaluation Management Options Referral Guidelines General problems include: Soft tissue conditions of the face and oral cavity
Understanding. Spinal Cord Injury. Tasha, injured in 1997.
 Understanding Spinal Cord Injury Tasha, injured in 1997. What Is Spinal Cord Injury? The spinal cord is the part of the central nervous system that contains the body s longest nerve fibers. It serves as
Understanding Spinal Cord Injury Tasha, injured in 1997. What Is Spinal Cord Injury? The spinal cord is the part of the central nervous system that contains the body s longest nerve fibers. It serves as
BC Children s Hospital Emergency Room Clinical Practice Guidelines. Ingested Foreign Bodies
 BC Children s Hospital Emergency Room Clinical Practice Guidelines Ingested Foreign Bodies AUTHORS: Navid Dehghani, MD, FRCRC Division of Pediatric Emergency Medicine Department of Pediatrics, University
BC Children s Hospital Emergency Room Clinical Practice Guidelines Ingested Foreign Bodies AUTHORS: Navid Dehghani, MD, FRCRC Division of Pediatric Emergency Medicine Department of Pediatrics, University
Skeletal System. Axial Skeleton: Vertebral Column and Ribs
 Skeletal System Axial Skeleton: Vertebral Column and Ribs Functions Regions Cervical Thoracic Lumbar Sacral Primary & secondary curvatures There are three major functions of the vertebral column. First,
Skeletal System Axial Skeleton: Vertebral Column and Ribs Functions Regions Cervical Thoracic Lumbar Sacral Primary & secondary curvatures There are three major functions of the vertebral column. First,
Goals and Objectives for the General Surgery Rotation Resident PGY1 Hamilton Health Sciences or St. Joseph Healthcare (2 four-week rotational blocks)
 Goals and Objectives for the General Surgery Rotation Resident PGY1 Hamilton Health Sciences or St. Joseph Healthcare (2 four-week rotational blocks) Overview During the first year of their residency training
Goals and Objectives for the General Surgery Rotation Resident PGY1 Hamilton Health Sciences or St. Joseph Healthcare (2 four-week rotational blocks) Overview During the first year of their residency training
Her past medical history was non significant. She never had surgery, had no history or family history of cancer and was a nonsmoker.
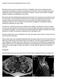 Surgical Technique Guide Debulking of Thoracic Tumor Metastatic spine tumors are rare (put article here). Metastatic spine tumors causing spinal cord compression and paralysis are almost non existent (put
Surgical Technique Guide Debulking of Thoracic Tumor Metastatic spine tumors are rare (put article here). Metastatic spine tumors causing spinal cord compression and paralysis are almost non existent (put
Spine Trauma: When to Transfer. Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU
 Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spine Trauma: When to Transfer Alexander Ching, MD Director, Orthopaedic Spine Trauma OHSU Disclosures Depuy Spine Consultant (teaching and courses) Department education and research funds Atlas Spine
Spinal Cord Injury. North American Spine Society Public Education Series
 Spinal Cord Injury North American Spine Society Public Education Series What Is a Spinal Cord Injury? A spinal cord injury is a condition that results from damage or trauma to the nerve tissue of the spine.
Spinal Cord Injury North American Spine Society Public Education Series What Is a Spinal Cord Injury? A spinal cord injury is a condition that results from damage or trauma to the nerve tissue of the spine.
Sample Learning Objectives for a Medical School Radiology Curriculum: Listed by Subjects
 Sample Learning Objectives for a Medical School Radiology Curriculum: Listed by Subjects This document lists sample learning objectives by subject matter The numerical ranking in parenthesis following
Sample Learning Objectives for a Medical School Radiology Curriculum: Listed by Subjects This document lists sample learning objectives by subject matter The numerical ranking in parenthesis following
Regions Hospital Delineation of Privileges Emergency Medicine
 Regions Hospital Delineation of Emergency Medicine Applicant s Name: Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic formal
Regions Hospital Delineation of Emergency Medicine Applicant s Name: Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic formal
Chapter 10. All chapters, full text, free download, available at http://www.divingmedicine.info SINUS BAROTRAUMA ANATOMY OF THE SINUSES
 Chapter 10 All chapters, full text, free download, available at http://www.divingmedicine.info SINUS BAROTRAUMA ANATOMY OF THE SINUSES The sinuses are air filled cavities contained within the bones of
Chapter 10 All chapters, full text, free download, available at http://www.divingmedicine.info SINUS BAROTRAUMA ANATOMY OF THE SINUSES The sinuses are air filled cavities contained within the bones of
CPT Code Changes for 2013
 CPT Code Changes for 2013 RADIOLOGY Cathy Woodall, CHC, CPC Nicholas Parish, CHC Compliance-Radiology McKesson Revenue Management Solutions This commentary is a summary prepared by McKesson s Revenue Management
CPT Code Changes for 2013 RADIOLOGY Cathy Woodall, CHC, CPC Nicholas Parish, CHC Compliance-Radiology McKesson Revenue Management Solutions This commentary is a summary prepared by McKesson s Revenue Management
(a) Glasgow coma scale less than or equal to thirteen; (b) Loss of consciousness greater than five minutes;
 ACTION: Original DATE: 09/11/2014 3:19 PM 4765-14-02 Determination of a trauma victim. Emergency medical service personnel shall use the criteria in this rule, consistent with their certification, to evaluate
ACTION: Original DATE: 09/11/2014 3:19 PM 4765-14-02 Determination of a trauma victim. Emergency medical service personnel shall use the criteria in this rule, consistent with their certification, to evaluate
What You Should Know About Cerebral Aneurysms
 What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council Randall T. Higashida, M.D.,
