DIFFERENTIATING INFLAMMATORY AND MECHANICAL BACK PAIN
|
|
|
- Silvia Robertson
- 10 years ago
- Views:
Transcription
1 DIFFERENTIATING INFLAMMATORY AND MECHANICAL BACK PAIN CHALLENGE YOUR DECISION MAKING Claire Harris, Senior Physiotherapist, The North West London Hospitals NHS Trust Susan Gurden, Advanced Physiotherapy Practitioner in Rheumatology, Aneurin Bevan Health Board, Wales Dr Jane Martindale, Clinical Specialist Physiotherapist, Wrightington, Wigan and Leigh NHS Foundation Trust Claire Jeffries, Physiotherapy Clinical Specialist in Hydrotherapy and Rheumatology, Solent NHS Trust, Portsmouth The development of this educational tool was funded by Abbott. Date of preparation: August 2012 AXHUR120968
2 Contents Introduction... 3 Back pain: inflammatory vs mechanical... 4 Subjective examination: the importance of assessing patient history... 5 Objective examination: indicators of inflammatory back pain... 6 Distinguishing back pain: further supporting questions... 7 Comparison of inflammatory back pain and chronic mechanical back pain... 8 The ASAS inflammatory back pain questionnaire...9 Assess your knowledge of differentiating inflammatory and mechanical back pain Useful contacts and further information Next module in this series
3 Introduction Welcome to this first module in a series of educational guides on inflammatory back pain. This module, Differentiating inflammatory and mechanical back pain, compares the key features of mechanical and inflammatory back pain and contains guidance and information to assist you in distinguishing inflammatory back pain in your patients. Back pain is very common; 60-80% of the UK population report back pain at some point in their life. 1 Back pain is not only a major source of pain and disability, but has other secondary effects on patients quality of life and is also detrimental to society as a whole: o Approximately 6-9% of UK adults consult their GP about lower back pain each year. 2,3 o Back pain is one of the main reasons for work loss and a major cost to Western society. 4 Recurrent and chronic pain account for 75-85% of total workers absenteeism. 5 o Over half of chronic back pain patients can suffer with insomnia. 6 o Individuals with back pain can suffer severe emotional stresses and relationship breakdowns as a result of their condition, including severe emotional distress to the partner and limitations in fulfilling their family role. 4 Chronic back pain is defined as pain which occurs for >3 months. 7 Identifying back pain as acute or chronic is one of the key processes in determining the source of the pain. o Mechanical back pain (MBP), which arises from structural changes which may be in the spinal joints, vertebrae or soft tissues, can be chronic but is usually acute in onset and often self-limiting. 7,8 o Inflammatory back pain (IBP), due to an underlying inflammatory disease such as inflammatory arthritis, results in chronic back pain lasting >3 months. 7 It is important to distinguish inflammatory from mechanical back pain as early as possible as the management and treatment of the two conditions is very different. 3
4 Back pain: inflammatory vs mechanical There are many different causes of back pain and these various sources can present with similar symptoms, often meaning it is difficult to distinguish the underlying pathology during musculoskeletal evaluation. Mechanical back pain is pain which arises from a structure within the spine, including the vertebral bodies, intervertebral discs, zygapophysial joints, sacroiliac (SI) joints, spinal ligaments, paraspinal muscles, dura, spinal cord, and nerves. 8 Inflammatory back pain is a symptom complex rather than a condition, and often indicates inflammation of the vertebrae, joints of the spine and entheses the sites of tendon and ligament attachment to bone. Possible sources which may present with mechanical back pain 9 Degenerative disc diseases Facet joint derangement Osteoarthritis Muscle imbalance Spinal stenosis Herniated disc Osteoporotic compression fracture Spondylolisthesis Traumatic fracture Severe kyphosis Severe scoliosis Transitional vertebrae Possible sources which may present with inflammatory back pain 7,9 Inflammatory arthritis Ankylosing spondylitis (AS) Psoriatic arthritis (PsA) Inflammatory bowel disease Other possible sources of back pain 9 Abdominal aortic aneurysm Tumours including metastases Renal diseases Gastrointestinal diseases Infections* such as: Epidural abscess Osteomyelitis Septic discitis Paraspinous abscess *Infections which result in back pain due to inflammatory sources can also lead to mechanical pain as a result of changes caused by the infection; for example, disc degeneration and collapse resulting from vertebral disc infection. The above table outlines several examples of different sources of back pain but the list is not exhaustive. 4
5 Subjective examination: the importance of assessing patient history In order to build an accurate picture of your patient s back pain and attain a hypothesis of underlying cause, it is important to assess the pattern of back pain in line with the patient s history. The following questions may help you to determine if your patient has, or has had, some of the clinical signs associated with inflammatory back pain: How long has the patient been experiencing back pain? o Chronic back pain of >3 months could indicate an inflammatory source. 7 Has the patient experienced back pain previous to this? o The current episode of back pain may be of a shorter duration, but the patient could have had previous episodes of back pain indicating chronicity. How old was the patient when the back pain started? o Inflammatory back pain due to inflammatory arthritis usually has an onset before the age of Is there a family history of inflammatory back pain such as ankylosing spondylitis, a type of inflammatory arthritis mainly affecting the spine? o Autoimmune inflammatory conditions such as inflammatory arthritis can have a strong hereditary component. 10 Does the patient have a history of other musculoskeletal problems? o Enthesitis, inflammation at sites where tendons and ligaments attach onto bone, at locations such as the heels, knees and ribs can be a histopathological characteristic of inflammatory arthritis affecting the spine. 12 Has the patient experienced any of the following: iritis, psoriasis, inflammatory bowel disease, peripheral joint inflammation? o Autoimmune inflammatory conditions such as these have a strong association with types of inflammatory arthritis which are a cause of back pain. 11 How does the patient describe the pain e.g. gnawing, throbbing, deep? o These descriptions are commonly used to depict pain caused by an inflammatory source within the spine. What is the usual pattern of back pain over a 24 hour period? For example, is the pain worse in the morning or during periods of inactivity? o Pain caused by inflammatory back pain does not improve with rest and can be associated with morning stiffness for >30 minutes after rising. 7 Does the pain improve with the use of non-steroidal anti-inflammatory drugs (NSAIDs)? o Patients with back pain due to inflammatory arthritis often respond well to NSAIDs. 7,11 5
6 Objective examination: indicators of inflammatory back pain During physical examination there are several key features to be aware of which may indicate inflammatory back pain. Tenderness over enthesis sites Observed postural changes Pain or tenderness over the sacroiliac joint, lumbar spine and/or thoracic spine Reduction in the range of movement in the lumbar spine Loss of hip abduction 6
7 Distinguishing inflammatory back pain: further supporting questions Once you have established your patient is suffering from back pain which may be inflammatory in nature, there are several key questions you can ask to help further classify if it is mechanical or inflammatory. The following five questions are from the ASAS (Assessment of SpondyloArthritis international Society) criteria for identifying inflammatory back pain: ONE Did your back pain start when you were aged younger than 40? Inflammatory back pain usually begins in the third decade of life and is unlikely to have an onset after 45 years. 7 It is important to ascertain the patient s age at the onset of the back pain as opposed to only recording their current age as they may have been experiencing back pain for several years. TWO Did your back pain develop gradually? Unlike inflammatory back pain, mechanical back pain, such as disc herniation, is frequently of a more sudden onset. IBP has an insidious onset and patients are likely to have been experiencing back pain for >3 months. 7 THREE Does your back pain improve with movement? Symptoms of musculoskeletal inflammation are often improved with movement and exercise. 7 FOUR Do you find there is no improvement in your back pain when you rest? Similar to the above, no improvement of the pain with rest is a classic feature of inflammatory back pain. FIVE Do you suffer from back pain at night which improves upon getting up? Patients with inflammatory back pain often experience a worsening of symptoms when resting at night, and waking during the second half of the night due to pain and discomfort is a key feature of inflammatory back pain. 7 Inflammatory back pain requiring further investigation is usually indicated if the answer is yes to 4 or more of these parameters. 7 In addition to these key distinguishing features, as outlined by the ASAS criteria for inflammatory back pain, other signs of inflammatory back pain to look out for include: Good response to NSAIDs 7 Alternating buttock pain 7,13 Waking during the second half of the night 13 Morning stiffness : pain and stiffness for >30 minutes after rising in the morning 7,13 7
8 Comparison of inflammatory back pain and chronic mechanical back pain IBP MBP Age of onset <40 years Age of onset: any age Insidious onset; less likely to be acute Variable onset; may be acute Pain improves with exercise Pain may worsen with movement Pain does not improve with rest Pain at night which may wake patient during second half of the night Pain often improves with rest Morning stiffness >30 minutes Morning stiffness <30 minutes Early recognition of IBP is important in order to facilitate effective management; increased awareness and improved classification should improve all outcomes for these patients. Susan Gurden, Advanced Physiotherapy Practitioner in Rheumatology, Aneurin Bevan Health Board, Wales 8
9 The ASAS inflammatory back pain questionnaire The ASAS inflammatory back pain questionnaire is a simple and useful tool, available as a tear-off pad, which you can use to assess your patients back pain. You can download this assessment questionnaire from the AStretch website at or from the NASS website at Patient name: Date of birth / hospital number: Have you suffered from back pain for more than 3 months? Yes No Inflammatory Back Pain Assessment ASAS experts' criteria 1. Did your back pain start when you were aged 40 or under? Yes No If you answered Yes, please complete the questions on the other side of this page and hand this to your healthcare professional. If you answered No, please hand this form back to your healthcare professional. 2. Did your back pain develop gradually? Yes No 3. Does your back pain improve with exercise? Yes No 4. Do you find there is no improvement in your back pain when you rest? Yes No 5. Do you suffer from back pain at night which improves upon getting up? Yes No For clinician use only The criteria are fulfilled if at least four out of five parameters are present. In this case, please refer the patient to a rheumatologist. Adapted from Sieper J et al. New criteria for inflammatory back pain in patients with chronic back pain: a real patient exercise by experts from the Assessment of SpondyloArthritis International Society (ASAS). Ann Rheum Dis 2009;68: The Assessment for Ankylosing Spondylitis initiative is led by the UK AS Assessment Academy and funded by Abbott Laboratories. AXHUR111757k Date of preparation: March 2012 What to do after you have recognised the possibility of inflammatory back pain: The next step is to refer the patient to a rheumatologist for further investigation as the pain could be due to a form of inflammatory arthritis. 9
10 Assess your knowledge of differentiating inflammatory and mechanical back pain Please complete the below multiple choice questions on inflammatory back pain. 1. Chronic back pain is usually defined as back pain occurring for (choose one answer): a. >3 weeks q b. >3 months q c. >6 weeks q d. >6 months q 2. The age of onset for inflammatory back pain caused by inflammatory arthritis is usually (choose one answer): a. <40 years of age q b q c. >60 q d. Any age q 3. The age of onset for mechanical back pain is more frequently (choose one answer): a. <30 years of age q b q c. >50 q d. Any age q 4. Inflammatory back pain is more frequently related to the following characteristics (tick all that apply): a. Morning stiffness pain and stiffness for >30 minutes after rising q b. Decreased pain with rest q c. Decreased pain with movement q d. Pain which disturbs sleep q e. Sudden onset q 5. Mechanical back pain is more frequently related to the following characteristics (tick all that apply): a. Sudden/acute onset q b. Insidious onset q c. Decreased pain with movement q d. Increased pain with rest q e. Morning stiffness pain and stiffness for >30 minutes after rising q 10
11 6. Which of the following cases presented do you think is most likely to be related to inflammatory back pain? (choose one answer) a. 60 year old male with back pain for less than 3 months, which causes pain at night and sleep disturbances q b. 34 year old male with back pain for 5 years which is worst at night q c. 25 year old female with chronic back pain which is eased with rest q d. 29 year old male with back pain for 3 months which is worsened by exercise q 7. Which of the following cases presented do you think is most likely to be related to inflammatory back pain? (choose one answer) a. 27 year old male with lower back pain for 2 weeks following a car accident q b. 30 year old female with back pain for 3 months which has not improved since she was prescribed NSAIDS q c. 40 year old male with back and buttock pain which came on suddenly while exercising a week ago q d. 28 year old female who has had increasingly severe lower back pain for 6 months but the pain has q improved since she has been taking NSAIDS 8. You have just assessed a patient you suspect may have inflammatory back pain, what do you do next? (choose one answer) a. Refer to a physiotherapist q b. Refer to a rheumatologist q c. Refer to a chiropractor q d. Tell patient to rest q Answers are provided on the back page. PERSONAL REFLECTION AND NEW KEY LEARNING POINTS PERSONAL ACTIONS 11
12 Useful contacts and further information British Health Professionals in Rheumatology (BHPR) NASS guide to inflammatory back pain The Chartered Society of Physiotherapy (CSP) AStretch ASAS Next module in this series Module 2: What is SpA? References 1. Waddel, G et al. Occup Med 2001; 51: Dunn, KM and Croft, PR. Spine 2005; 16: Cremin, MC and Finn, AM. Ir Med J 2002; 95: de Souza, L and Frank AO. Disability and rehabilitation 2011; 33: van Tulder M, et al. Eur Spine J 2006; 15 (Suppl. 2): S169-S Tang, NK et al. J Sleep Res 2007; 16: Sieper, J et al. Ann Rheum Dis 2009; 68: Chien, JJ and Bajwa, ZH. Current pain and headache reports 2008; 12: Deyo, RA and Weinstein, JN. N Eng J Med 2001; 344: Evnouchidou, I et al. J Immunol 2011; 186: Braun, A et al. Ann Rheum Dis 2011; 70: Mander, M et al. Annals of the Rheumatic Disease 1987; 46: Rudwaleit, M et al. Arthritis Rheum 2006; 54: Answers to questions 1: b; 2: a; 3: d; 4: a,c,d; 5: a; 6: b; 7: d; 8: b
RECOGNISING INFLAMMATORY BACK PAIN. This programme is supported and funded by Pfizer Date of preparation: December 2011 Project code: ENB 248
 RECOGNISING INFLAMMATORY BACK PAIN This programme is supported and funded by Pfizer Date of preparation: December 2011 Project code: ENB 248 Contents Inflammatory back pain: overview Spondyloarthropathies
RECOGNISING INFLAMMATORY BACK PAIN This programme is supported and funded by Pfizer Date of preparation: December 2011 Project code: ENB 248 Contents Inflammatory back pain: overview Spondyloarthropathies
Introduction: Anatomy of the spine and lower back:
 Castleknock GAA club member and Chartered Physiotherapist, James Sherry MISCP, has prepared an informative article on the common causes of back pain and how best it can be treated. To book a physiotherapy
Castleknock GAA club member and Chartered Physiotherapist, James Sherry MISCP, has prepared an informative article on the common causes of back pain and how best it can be treated. To book a physiotherapy
Low Back Injury in the Industrial Athlete: An Anatomic Approach
 Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Low Back Injury in the Industrial Athlete: An Anatomic Approach Earl J. Craig, M.D. Assistant Professor Indiana University School of Medicine Department of Physical Medicine and Rehabilitation Epidemiology
Stickler Syndrome and Arthritis
 Stickler Syndrome and Arthritis Arthritis Foundation Pacific Region, Nevada Office Presented by: Crystal Schulz, MPH Community Development Manager Arthritis Foundation Improving lives through leadership
Stickler Syndrome and Arthritis Arthritis Foundation Pacific Region, Nevada Office Presented by: Crystal Schulz, MPH Community Development Manager Arthritis Foundation Improving lives through leadership
BACK PAIN: WHAT YOU SHOULD KNOW
 BACK PAIN: WHAT YOU SHOULD KNOW Diane Metzer LOWER BACK PAIN Nearly everyone at some point has back pain that interferes with work, recreation and routine daily activities. Four out of five adults experience
BACK PAIN: WHAT YOU SHOULD KNOW Diane Metzer LOWER BACK PAIN Nearly everyone at some point has back pain that interferes with work, recreation and routine daily activities. Four out of five adults experience
How To Write An Icd10
 Crosswalk of Common Spine ICD-9-CM Codes to ICD-10 Codes As of October 1, 2015, all health care entities covered by the Health Insurance Portability and Accountability Act (HIPAA) will be required to use
Crosswalk of Common Spine ICD-9-CM Codes to ICD-10 Codes As of October 1, 2015, all health care entities covered by the Health Insurance Portability and Accountability Act (HIPAA) will be required to use
What s new in clinical assesment of ankylosing spondylitis?
 What s new in clinical assesment of ankylosing spondylitis? Désirée van der Heijde Professor of Rheumatology Leiden University Medical Center, the Netherlands Diakonhjemmet Hospital, Oslo, Norway Content
What s new in clinical assesment of ankylosing spondylitis? Désirée van der Heijde Professor of Rheumatology Leiden University Medical Center, the Netherlands Diakonhjemmet Hospital, Oslo, Norway Content
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) Introduction Diffuse Idiopathic Skeletal Hyperostosis (DISH) is a phenomenon that more commonly affects older males. It is associated
Pathophysiology of Acute and Chronic Low Back Pain
 Pathophysiology of Acute and Chronic Low Back Pain Mary Beth Partyka MSN APN Adult Nurse Practitioner Adult Pain Service Advocate Christ Medical Center Presentation Objectives Review the incidence of acute
Pathophysiology of Acute and Chronic Low Back Pain Mary Beth Partyka MSN APN Adult Nurse Practitioner Adult Pain Service Advocate Christ Medical Center Presentation Objectives Review the incidence of acute
6/3/2011. High Prevalence and Incidence. Low back pain is 5 th most common reason for all physician office visits in the U.S.
 High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
High Prevalence and Incidence Prevalence 85% of Americans will experience low back pain at some time in their life. Incidence 5% annual Timothy C. Shen, M.D. Physical Medicine and Rehabilitation Sub-specialty
(Intro to Arthritis with a. Arthritis) Manager of Education & Services for the Vancouver Island Region of The Arthritis Society
 Arthritis 101 (Intro to Arthritis with a Focus on Rheumatoid Arthritis) by Cari Taylor by Cari Taylor Manager of Education & Services for the Vancouver Island Region of The Arthritis Society What You Will
Arthritis 101 (Intro to Arthritis with a Focus on Rheumatoid Arthritis) by Cari Taylor by Cari Taylor Manager of Education & Services for the Vancouver Island Region of The Arthritis Society What You Will
LOW BACK PAIN; MECHANICAL
 1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
1 ORTHO 16 LOW BACK PAIN; MECHANICAL Background This case definition was developed by the Armed Forces Health Surveillance Center (AFHSC) for the purpose of epidemiological surveillance of a condition
NURS 821 Alterations in the Musculoskeletal System. Rheumatoid Arthritis. Type III Hypersensitivity Response
 NURS 821 Alterations in the Musculoskeletal System Margaret H. Birney PhD, RN Lecture 12 Part 2 Joint Disorders (cont d) Rheumatoid Arthritis Definition: Autoimmune disorder occurring in genetically sensitive
NURS 821 Alterations in the Musculoskeletal System Margaret H. Birney PhD, RN Lecture 12 Part 2 Joint Disorders (cont d) Rheumatoid Arthritis Definition: Autoimmune disorder occurring in genetically sensitive
Low Back Pain Protocols
 Low Back Pain Protocols Introduction: Diagnostic Triage And 1. Patient Group Adults aged 18 years and over with routine low back problems. Patients who have had recent surgery should be referred directly
Low Back Pain Protocols Introduction: Diagnostic Triage And 1. Patient Group Adults aged 18 years and over with routine low back problems. Patients who have had recent surgery should be referred directly
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN. Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA
 DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
DIFFERENTIAL DIAGNOSIS OF LOW BACK PAIN Arnold J. Weil, M.D., M.B.A. Non-Surgical Orthopaedics, P.C. Atlanta, GA MEDICAL ALGORITHM OF REALITY LOWER BACK PAIN Yes Patient will never get better until case
Psoriatic arthritis in practice : How to detect? How to diagnose? Pascal RICHETTE Hôpital Lariboisière, Paris. Copyright
 Psoriatic arthritis in practice : How to detect? How to diagnose? Pascal RICHETTE Hôpital Lariboisière, Paris The patient: a 57 year-old man, with a history of psoriatic nail dystrophy for 10 years Past
Psoriatic arthritis in practice : How to detect? How to diagnose? Pascal RICHETTE Hôpital Lariboisière, Paris The patient: a 57 year-old man, with a history of psoriatic nail dystrophy for 10 years Past
SPINE ANATOMY AND PROCEDURES. Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132
 SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
SPINE ANATOMY AND PROCEDURES Tulsa Spine & Specialty Hospital 6901 S. Olympia Avenue Tulsa, Oklahoma 74132 SPINE ANATOMY The spine consists of 33 bones called vertebrae. The top 7 are cervical, or neck
Temple Physical Therapy
 Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Temple Physical Therapy A General Overview of Common Neck Injuries For current information on Temple Physical Therapy related news and for a healthy and safe return to work, sport and recreation Like Us
Spinal Surgery 2. Teaching Aims. Common Spinal Pathologies. Disc Degeneration. Disc Degeneration. Causes of LBP 8/2/13. Common Spinal Conditions
 Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Teaching Aims Spinal Surgery 2 Mr Mushtaque A. Ishaque BSc(Hons) BChir(Cantab) DM FRCS FRCS(Ed) FRCS(Orth) Hunterian Professor at The Royal College of Surgeons of England Consultant Orthopaedic Spinal
Early Diagnosis of Rheumatoid Arthritis & Axial Spondyloarthritis
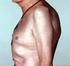 Early Diagnosis of Rheumatoid Arthritis & Axial Spondyloarthritis 奇 美 醫 院 過 敏 免 疫 風 濕 科 陳 宏 安 Rheumatoid arthritis Most common chronic inflammatory joint disease Multisystem autoimmune disease of unknown
Early Diagnosis of Rheumatoid Arthritis & Axial Spondyloarthritis 奇 美 醫 院 過 敏 免 疫 風 濕 科 陳 宏 安 Rheumatoid arthritis Most common chronic inflammatory joint disease Multisystem autoimmune disease of unknown
Advanced Practice Provider Academy
 (+)Dean T. Harrison, MPAS,PA C,DFAAPA Director of Mid Level Practitioners; Assistant Medical Director Clinical Evaluation Unit, Division of Emergency Medicine, Department of Surgery, Duke University Medical
(+)Dean T. Harrison, MPAS,PA C,DFAAPA Director of Mid Level Practitioners; Assistant Medical Director Clinical Evaluation Unit, Division of Emergency Medicine, Department of Surgery, Duke University Medical
Information on the Chiropractic Care of Lower Back Pain
 Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
Chiropractic Care of Lower Back Pain Lower back pain is probably the most common condition seen the the Chiropractic office. Each month it is estimated that up to one third of persons experience some type
There are four main regions of the back; the cervical (C), thoracic (T), lumbar (L), and sacral (S) regions
 Low Back Pain Overview Low back pain is one of the most common disorders in the United States. About 80 percent of people have at least one episode of low back pain during their lifetime. Factors that
Low Back Pain Overview Low back pain is one of the most common disorders in the United States. About 80 percent of people have at least one episode of low back pain during their lifetime. Factors that
Understanding Rheumatoid Arthritis
 Understanding Rheumatoid Arthritis Understanding Rheumatoid Arthritis What Is Rheumatoid Arthritis? 1,2 Rheumatoid arthritis (RA) is a chronic autoimmune disease. It causes joints to swell and can result
Understanding Rheumatoid Arthritis Understanding Rheumatoid Arthritis What Is Rheumatoid Arthritis? 1,2 Rheumatoid arthritis (RA) is a chronic autoimmune disease. It causes joints to swell and can result
Sample Treatment Protocol
 Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Sample Treatment Protocol 1 Adults with acute episode of LBP Definition: Acute episode Back pain lasting
Back & Neck Pain Survival Guide
 Back & Neck Pain Survival Guide www.kleinpeterpt.com Zachary - 225-658-7751 Baton Rouge - 225-768-7676 Kleinpeter Physical Therapy - Spine Care Program Finally! A Proven Assessment & Treatment Program
Back & Neck Pain Survival Guide www.kleinpeterpt.com Zachary - 225-658-7751 Baton Rouge - 225-768-7676 Kleinpeter Physical Therapy - Spine Care Program Finally! A Proven Assessment & Treatment Program
Clinical Signs of Low Back Pain
 Review of Clinical Signs Series Editor: Bernard Karnath, MD Clinical Signs of Low Back Pain Bernard Karnath, MD Back pain has been cited as the fifth most common reason that patients visit a physician.
Review of Clinical Signs Series Editor: Bernard Karnath, MD Clinical Signs of Low Back Pain Bernard Karnath, MD Back pain has been cited as the fifth most common reason that patients visit a physician.
It is worth noting that people with psoriasis can also develop other forms of arthritis such as rheumatoid arthritis and osteoarthritis.
 Psoriatic Arthritis Main Colour - pantone 2597u Research - pantone 206u Children - pantone 123 4 What is psoriatic arthritis? Psoriatic arthritis is an inflammatory joint disease associated with psoriasis.
Psoriatic Arthritis Main Colour - pantone 2597u Research - pantone 206u Children - pantone 123 4 What is psoriatic arthritis? Psoriatic arthritis is an inflammatory joint disease associated with psoriasis.
Cervical Spondylosis (Arthritis of the Neck)
 Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Copyright 2009 American Academy of Orthopaedic Surgeons Cervical Spondylosis (Arthritis of the Neck) Neck pain is extremely common. It can be caused by many things, and is most often related to getting
Whiplash Associated Disorder
 Whiplash Associated Disorder Bourassa & Associates Rehabilitation Centre What is Whiplash? Whiplash is a non-medical term used to describe neck pain following hyperflexion or hyperextension of the tissues
Whiplash Associated Disorder Bourassa & Associates Rehabilitation Centre What is Whiplash? Whiplash is a non-medical term used to describe neck pain following hyperflexion or hyperextension of the tissues
Medical Report Prepared for The Court on
 Medical Report Prepared for The Court on Mr Sample Report Claimant's Address Claimant's Date of Birth Instructing Party Instructing Party Address Instructing Party Ref Solicitors Ref Corex Ref 1 The Lane
Medical Report Prepared for The Court on Mr Sample Report Claimant's Address Claimant's Date of Birth Instructing Party Instructing Party Address Instructing Party Ref Solicitors Ref Corex Ref 1 The Lane
Standard of Care: Cervical Radiculopathy
 Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
Department of Rehabilitation Services Physical Therapy Diagnosis: Cervical radiculopathy, injury to one or more nerve roots, has multiple presentations. Symptoms may include pain in the cervical spine
DIVISION OF RHEUMATOLOGY DEPARTMENT OF MEDICINE UNIVERSITY OF WESTERN ONTARIO POSTGRADUATE EDUCTION ORTHOPAEDIC OFF-SERVICE GOALS & OBJECTIVES
 DIVISION OF RHEUMATOLOGY DEPARTMENT OF MEDICINE UNIVERSITY OF WESTERN ONTARIO POSTGRADUATE EDUCTION ORTHOPAEDIC OFF-SERVICE GOALS & OBJECTIVES GOAL #1 develop the ability to order and understand interpretation
DIVISION OF RHEUMATOLOGY DEPARTMENT OF MEDICINE UNIVERSITY OF WESTERN ONTARIO POSTGRADUATE EDUCTION ORTHOPAEDIC OFF-SERVICE GOALS & OBJECTIVES GOAL #1 develop the ability to order and understand interpretation
Clinical Guideline. Low Back Pain Orthopaedics. Princess Alexandra Hospital Emergency Department. 1 Purpose. 2 Background
 Princess Alexandra Hospital Emergency Department Clinical Guideline Orthopaedics Review Officer: Katherine Isoardi Version no: 1 Approval date: 18/03/2015 Review date: 18/03/2017 Approving Officer Dr James
Princess Alexandra Hospital Emergency Department Clinical Guideline Orthopaedics Review Officer: Katherine Isoardi Version no: 1 Approval date: 18/03/2015 Review date: 18/03/2017 Approving Officer Dr James
Musculoskeletal: Acute Lower Back Pain
 Musculoskeletal: Acute Lower Back Pain Acute Lower Back Pain Back Pain only Sciatica / Radiculopathy Possible Cord or Cauda Equina Compression Possible Spinal Canal Stenosis Red Flags Initial conservative
Musculoskeletal: Acute Lower Back Pain Acute Lower Back Pain Back Pain only Sciatica / Radiculopathy Possible Cord or Cauda Equina Compression Possible Spinal Canal Stenosis Red Flags Initial conservative
.org. Herniated Disk in the Lower Back. Anatomy. Description
 Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Herniated Disk in the Lower Back Page ( 1 ) Sometimes called a slipped or ruptured disk, a herniated disk most often occurs in your lower back. It is one of the most common causes of low back pain, as
Sciatica Yuliya Mutsa PTA 236
 Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
Low back pain. Quick reference guide. Issue date: May 2009. Early management of persistent non-specific low back pain
 Issue date: May 2009 Low back pain Early management of persistent non-specific low back pain Developed by the National Collaborating Centre for Primary Care About this booklet This is a quick reference
Issue date: May 2009 Low back pain Early management of persistent non-specific low back pain Developed by the National Collaborating Centre for Primary Care About this booklet This is a quick reference
Biomechanical Basis of Lumbar Pain. Prepared by S. Pollak. Introduction:
 Biomechanical Basis of Lumbar Pain Prepared by S. Pollak Introduction: The lumbar area of the back is made up of five movable L1-L5 vertebrae which have intervertebral discs in between them 1. The intervertebral
Biomechanical Basis of Lumbar Pain Prepared by S. Pollak Introduction: The lumbar area of the back is made up of five movable L1-L5 vertebrae which have intervertebral discs in between them 1. The intervertebral
Developing a National Audit for Rheumatoid and Early Inflammatory Arthritis Ian Rowe
 Developing a National Audit for Rheumatoid and Early Inflammatory Arthritis Ian Rowe Chair Clinical Affairs Committee, BSR Outline The British Society for Rheumatology Challenges in improving patient outcomes
Developing a National Audit for Rheumatoid and Early Inflammatory Arthritis Ian Rowe Chair Clinical Affairs Committee, BSR Outline The British Society for Rheumatology Challenges in improving patient outcomes
Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization
 Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Client HMSA: PQSR 2009 Measure Title X RAY PRIOR TO MRI OR CAT SCAN IN THE EVAULATION OF LOWER BACK PAIN Disease State Back pain Indicator Classification Utilization Strength of Recommendation Organizations
Whiplash and Whiplash- Associated Disorders
 Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
Whiplash and Whiplash- Associated Disorders North American Spine Society Public Education Series What Is Whiplash? The term whiplash might be confusing because it describes both a mechanism of injury and
Lower Back Pain An Educational Guide
 Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
Lower Back Pain An Educational Guide A publication from the Center of Pain Medicine and Physiatric Rehabilitation 2002 Medical Parkway Ste 150 1630 Main St Ste 215 Annapolis, MD 21401 Chester, MD 21619
ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015
 Presented by: Teri Romano, RN, MBA, CPC, CMDP ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015 Source: http://journal.ahima.org/2015/02/04/us house committee to hold hearing on icd 10 implementation/ 2 2015 Web_Non
Presented by: Teri Romano, RN, MBA, CPC, CMDP ICD 10 CM IMPLEMENTATION DATE OCT 1, 2015 Source: http://journal.ahima.org/2015/02/04/us house committee to hold hearing on icd 10 implementation/ 2 2015 Web_Non
.org. Cervical Spondylosis (Arthritis of the Neck) Anatomy. Cause
 Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Cervical Spondylosis (Arthritis of the Neck) Page ( 1 ) Neck pain can be caused by many things but is most often related to getting older. Like the rest of the body, the disks and joints in the neck (cervical
Patient Guide. Sacroiliac Joint Pain
 Patient Guide Sacroiliac Joint Pain Anatomy Where is the Sacroiliac Joint? The sacroiliac joint (SIJ) is located at the bottom end of your spine, where the "tailbone" (sacrum) joins the pelvis (ilium).
Patient Guide Sacroiliac Joint Pain Anatomy Where is the Sacroiliac Joint? The sacroiliac joint (SIJ) is located at the bottom end of your spine, where the "tailbone" (sacrum) joins the pelvis (ilium).
Helping you manage your pain
 Helping you manage your pain This booklet contains confidential personal information. If found, please mail to the address below. Personal details Name Address Telephone My health care team (please tick)
Helping you manage your pain This booklet contains confidential personal information. If found, please mail to the address below. Personal details Name Address Telephone My health care team (please tick)
LOW BACK PAIN. common of these conditions include: muscle strain ( pulled muscle ), weak core muscles
 LOW BACK PAIN Most episodes of low back pain are caused by relatively harmless conditions. The most common of these conditions include: muscle strain ( pulled muscle ), weak core muscles (abdominal and
LOW BACK PAIN Most episodes of low back pain are caused by relatively harmless conditions. The most common of these conditions include: muscle strain ( pulled muscle ), weak core muscles (abdominal and
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances?
 Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Does the pain radiating down your legs, buttocks or lower back prevent you from walking long distances? Do you experience weakness, tingling, numbness, stiffness, or cramping in your legs, buttocks or
Do I need a physician referral? Yes, we see patients on referral from a health care provider.
 FAQS FOR OFFICE POLICIES How do I get an appointment? New appointments are made by physician referral only. Your referring health care provided will call for the appointment for you. What do I need to
FAQS FOR OFFICE POLICIES How do I get an appointment? New appointments are made by physician referral only. Your referring health care provided will call for the appointment for you. What do I need to
Acute Low Back Pain. North American Spine Society Public Education Series
 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Psoriatic Arthritis www.arthritis.org.nz
 Psoriatic Arthritis www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Psoriatic arthritis usually appears in people between the ages of 30 to 50.
Psoriatic Arthritis www.arthritis.org.nz Did you know? Arthritis affects one in six New Zealanders over the age of 15 years. Psoriatic arthritis usually appears in people between the ages of 30 to 50.
Management of Low Back Pain: Physiotherapy Approaches
 Management of Low Back Pain: Physiotherapy Approaches Professor Sunday R.A. Akinbo PhD, FWSPC, FPC Consultant Physiotherapist; Department of Physiotherapy Lagos University Teaching Hospital, Idi-Araba,
Management of Low Back Pain: Physiotherapy Approaches Professor Sunday R.A. Akinbo PhD, FWSPC, FPC Consultant Physiotherapist; Department of Physiotherapy Lagos University Teaching Hospital, Idi-Araba,
Lumbar Laminectomy and Interspinous Process Fusion
 Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
Lumbar Laminectomy and Interspinous Process Fusion Introduction Low back and leg pain caused by pinched nerves in the back is a common condition that limits your ability to move, walk, and work. This condition
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN
 CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
CLINICAL PRACTICE GUIDELINES FOR MANAGEMENT OF LOW BACK PAIN Low back pain is very common, up to 90+% of people are affected by back pain at some time in their lives. Most often back pain is benign and
Appointment Types First outpatient. Clinic Types CATS Spine CATS Hip and Knee CATS General Orthopaedic Injection Clinic Podiatry/Foot and Ankle
 Clinic Types CATS Spine CATS Hip and Knee CATS General Orthopaedic Injection Clinic Podiatry/Foot and Ankle Conditions Treated Ankle & foot pain & stiffness Back pain & stiffness Carpal Tunnel/ Nerve impingement/entrapment
Clinic Types CATS Spine CATS Hip and Knee CATS General Orthopaedic Injection Clinic Podiatry/Foot and Ankle Conditions Treated Ankle & foot pain & stiffness Back pain & stiffness Carpal Tunnel/ Nerve impingement/entrapment
Herniated Lumbar Disc
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Psoriatic arthritis FACTSHEET
 1 What is psoriatic arthritis? Psoriatic arthritis (PsA) is a disease where joints around the body become inflamed and sore. It can make moving about difficult and painful. People who have PsA also have
1 What is psoriatic arthritis? Psoriatic arthritis (PsA) is a disease where joints around the body become inflamed and sore. It can make moving about difficult and painful. People who have PsA also have
Return to same game if sx s resolve within 15 minutes. Return to next game if sx s resolve within one week Return to Competition
 Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Assessment Skills of the Spine on the Field and in the Clinic Ron Burke, MD Cervical Spine Injuries Sprains and strains Stingers Transient quadriparesis Cervical Spine Injuries Result in critical loss
Clinical guidance for MRI referral
 MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
MRI for cervical radiculopathy Referral by a medical practitioner (excluding a specialist or consultant physician) for a scan of spine for a patient 16 years or older for suspected: cervical radiculopathy
ICD-9-CM coding for patients with Spinal Cord Injury*
 ICD-9-CM coding for patients with Spinal Cord Injury* indicates intervening codes have been left out of this list. OTHER DISORDERS OF THE CENTRAL NERVOUS SYSTEM (340-349) 344 Other paralytic syndromes
ICD-9-CM coding for patients with Spinal Cord Injury* indicates intervening codes have been left out of this list. OTHER DISORDERS OF THE CENTRAL NERVOUS SYSTEM (340-349) 344 Other paralytic syndromes
Neck Injuries and Disorders
 Neck Injuries and Disorders Introduction Any part of your neck can be affected by neck problems. These affect the muscles, bones, joints, tendons, ligaments or nerves in the neck. There are many common
Neck Injuries and Disorders Introduction Any part of your neck can be affected by neck problems. These affect the muscles, bones, joints, tendons, ligaments or nerves in the neck. There are many common
Diagnosis and Management for Chronic Back Pain: Critical for your Recovery
 Diagnosis and Management for Chronic Back Pain: Critical for your Recovery Dr. Connie D Astolfo, DC, PhD (candidate) In past articles I have stressed that the causes of back pain can be very complex. This
Diagnosis and Management for Chronic Back Pain: Critical for your Recovery Dr. Connie D Astolfo, DC, PhD (candidate) In past articles I have stressed that the causes of back pain can be very complex. This
Cervical Spondylosis. Understanding the neck
 Page 1 of 5 Cervical Spondylosis This leaflet is aimed at people who have been told they have cervical spondylosis as a cause of their neck symptoms. Cervical spondylosis is a 'wear and tear' of the vertebrae
Page 1 of 5 Cervical Spondylosis This leaflet is aimed at people who have been told they have cervical spondylosis as a cause of their neck symptoms. Cervical spondylosis is a 'wear and tear' of the vertebrae
Neck Pain Overview Causes, Diagnosis and Treatment Options
 Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
Neck Pain Overview Causes, Diagnosis and Treatment Options Neck pain is one of the most common forms of pain for which people seek treatment. Most individuals experience neck pain at some point during
The Lewin Group undertook the following steps to identify the guidelines relevant to the 11 targeted procedures:
 Guidelines The following is a list of proposed medical specialty guidelines that have been found for the 11 targeted procedures to be included in the Medicare Imaging Demonstration. The list includes only
Guidelines The following is a list of proposed medical specialty guidelines that have been found for the 11 targeted procedures to be included in the Medicare Imaging Demonstration. The list includes only
Guide to Claims against General Practitioners (GPs)
 Patients often build up a relationship of trust with their GP over a number of years. It can be devastating when a GP fails in his or her duty to a patient. Our medical negligence solicitors understand
Patients often build up a relationship of trust with their GP over a number of years. It can be devastating when a GP fails in his or her duty to a patient. Our medical negligence solicitors understand
Neck and Back Pain in VA Incidence and Prevalence in VA Users
 Neck and Back Pain in VA Incidence and Prevalence in VA Users Spotlight on Pain Management: Patsi Sinnott, PT, PhD, MPH Sharon Dally, MS, Tigran Avoundjian, MPH, Jody Trafton, PhD, Todd Wagner, PhD Dec.
Neck and Back Pain in VA Incidence and Prevalence in VA Users Spotlight on Pain Management: Patsi Sinnott, PT, PhD, MPH Sharon Dally, MS, Tigran Avoundjian, MPH, Jody Trafton, PhD, Todd Wagner, PhD Dec.
SPINE AND NECK SURGERY: MAKING A DECISION THAT S RIGHT FOR YOU
 1. GET THE FACTS: Back and neck pain affects 8 out of 10 people at some point in their life. Acute back and neck pain comes on suddenly and usually lasts from a few days to a few weeks. Chronic back and
1. GET THE FACTS: Back and neck pain affects 8 out of 10 people at some point in their life. Acute back and neck pain comes on suddenly and usually lasts from a few days to a few weeks. Chronic back and
Lumbar Spinal Stenosis
 Copyright 2009 American Academy of Orthopaedic Surgeons Lumbar Spinal Stenosis Almost everyone will experience low back pain at some point in their lives. A common cause of low back pain is lumbar spinal
Copyright 2009 American Academy of Orthopaedic Surgeons Lumbar Spinal Stenosis Almost everyone will experience low back pain at some point in their lives. A common cause of low back pain is lumbar spinal
Pain Management Top Diagnosis Codes (Crosswalk)
 Pain Management Top s (Crosswalk) 274.00 Gout arthropathy, M1000 Idiopathic gout, unspecified site unspecified M10011 Idiopathic gout, right shoulder M10012 Idiopathic gout, left shoulder M10019 Idiopathic
Pain Management Top s (Crosswalk) 274.00 Gout arthropathy, M1000 Idiopathic gout, unspecified site unspecified M10011 Idiopathic gout, right shoulder M10012 Idiopathic gout, left shoulder M10019 Idiopathic
Do you have Back Pain? Associated with:
 Do you have Back Pain? Associated with: Herniated Discs? Protruding Discs? Degenerative Disk Disease? Posterior Facet Syndrome? Sciatica? You may be a candidate for Decompression Therapy The Dynatronics
Do you have Back Pain? Associated with: Herniated Discs? Protruding Discs? Degenerative Disk Disease? Posterior Facet Syndrome? Sciatica? You may be a candidate for Decompression Therapy The Dynatronics
Thoracic and Chest Pain Anatomy Risk Factors and Prevention Posture: Increased thoracic curve
 Thoracic and Chest Pain The thoracic spine is the region of the spine least likely to be injured in sport when compared to the cervical and lumbar region. However, this region can contribute to lumbar
Thoracic and Chest Pain The thoracic spine is the region of the spine least likely to be injured in sport when compared to the cervical and lumbar region. However, this region can contribute to lumbar
Minimally Invasive Spine Surgery For Your Patients
 Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Minimally Invasive Spine Surgery For Your Patients Lukas P. Zebala, M.D. Assistant Professor Orthopaedic and Neurological Spine Surgery Department of Orthopaedic Surgery Washington University School of
Contents. Introduction 1. Anatomy of the Spine 1. 2. Spinal Imaging 7. 3. Spinal Biomechanics 23. 4. History and Physical Examination of the Spine 33
 Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Contents Introduction 1. Anatomy of the Spine 1 Vertebrae 1 Ligaments 3 Intervertebral Disk 4 Intervertebral Foramen 5 2. Spinal Imaging 7 Imaging Modalities 7 Conventional Radiographs 7 Myelography 9
Practice Guidelines For Low Back Pain
 Consumers Guide Practice Guidelines For Low Back Pain Copyright 2008 American Chronic Pain Association Page 1 Written by: Penney Cowan Founder Executive Director American Chronic Pain Association Editors:
Consumers Guide Practice Guidelines For Low Back Pain Copyright 2008 American Chronic Pain Association Page 1 Written by: Penney Cowan Founder Executive Director American Chronic Pain Association Editors:
SpineFAQs. Whiplash. What causes this condition?
 SpineFAQs Whiplash Whiplash is defined as a sudden extension of the cervical spine (backward movement of the neck) and flexion (forward movement of the neck). This type of trauma is also referred to as
SpineFAQs Whiplash Whiplash is defined as a sudden extension of the cervical spine (backward movement of the neck) and flexion (forward movement of the neck). This type of trauma is also referred to as
BACK PAIN BASICS COMMON QUESTIONS, UNCOMPLICATED ANSWERS
 BACK PAIN BASICS COMMON QUESTIONS, UNCOMPLICATED ANSWERS About the North American Spine Society The North American Spine Society (NASS) is the world s largest multidisciplinary organization that advances
BACK PAIN BASICS COMMON QUESTIONS, UNCOMPLICATED ANSWERS About the North American Spine Society The North American Spine Society (NASS) is the world s largest multidisciplinary organization that advances
Hitting a Nerve: The Triggers of Sciatica. Bruce Tranmer MD FRCS FACS
 Hitting a Nerve: The Triggers of Sciatica Bruce Tranmer MD FRCS FACS Disclosures I have no financial disclosures Objectives - Sciatica Historical Perspective What is Sciatica What can cause Sciatica Clinical
Hitting a Nerve: The Triggers of Sciatica Bruce Tranmer MD FRCS FACS Disclosures I have no financial disclosures Objectives - Sciatica Historical Perspective What is Sciatica What can cause Sciatica Clinical
Back Pain in Children and Adolescents: Clinically and Cost Effective Treatment
 Back Pain in Children and Adolescents: Clinically and Cost Effective Treatment Matthew E. Oetgen, MD Department of Orthopaedics and Sports Medicine Children s National Medical Center Children s National
Back Pain in Children and Adolescents: Clinically and Cost Effective Treatment Matthew E. Oetgen, MD Department of Orthopaedics and Sports Medicine Children s National Medical Center Children s National
Lower Back Pain HealthshareHull Information for Guided Patient Management
 HealthshareHull Information for Guided Patient Management Index Introduction 2 Lumbar spine anatomy 2 What is lower back pain? 3 Conditions that may be causing your back pain 3 When should I see my doctor?
HealthshareHull Information for Guided Patient Management Index Introduction 2 Lumbar spine anatomy 2 What is lower back pain? 3 Conditions that may be causing your back pain 3 When should I see my doctor?
A review of spinal problems
 Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
Dr Ulrich R Hähnle MD, FCS Orthopaedic Surgeon, Wits Facharzt für Orthopädie, Berlin Phone: +27 11 485 3236 Fax: +27 11 485 2446 Suite 102, Medical Centre, Linksfield Park Clinic P.O. Box 949, Johannesburg
RHEUMATOID ARTHRITIS. Dr Bruce Kirkham Rheumatology Clinical Lead
 RHEUMATOID ARTHRITIS Dr Bruce Kirkham Rheumatology Clinical Lead RHEUMATOID ARTHRITIS (RA) RA is a common disease: 0.8 per cent of the population RA more common in females: female to male ratio 3:1 RA
RHEUMATOID ARTHRITIS Dr Bruce Kirkham Rheumatology Clinical Lead RHEUMATOID ARTHRITIS (RA) RA is a common disease: 0.8 per cent of the population RA more common in females: female to male ratio 3:1 RA
Clarian Health Partners - Marketing Group. Procedure Code Listing by Specialty Report Prepared: February 11, 2011 at 8:50 AM
 IU Health Listing by Abdominal Diagnostic Ultrasound ABDOMDX All Aspects of Spine Care SPINE Amputations AMPUTATE Ankle Arthroscopy ANKLEART Ankle Pain ANKLEPAI Ankle Surgery ANKLESX Arthritic Recon. Proc.
IU Health Listing by Abdominal Diagnostic Ultrasound ABDOMDX All Aspects of Spine Care SPINE Amputations AMPUTATE Ankle Arthroscopy ANKLEART Ankle Pain ANKLEPAI Ankle Surgery ANKLESX Arthritic Recon. Proc.
Facet and Axial Spine Pain
 Facet and Axial Spine Pain Diane M. Rowles, MS, ACNP, BC, CRRN Nurse Practitioner, University Neurosurgery Rush University Medical Center Adjunct Assistant Professor, Feinberg School of Medicine Northwestern
Facet and Axial Spine Pain Diane M. Rowles, MS, ACNP, BC, CRRN Nurse Practitioner, University Neurosurgery Rush University Medical Center Adjunct Assistant Professor, Feinberg School of Medicine Northwestern
The Physiotherapy Pilot. 1.1 Purpose of the pilot
 The Physiotherapy Pilot 1.1 Purpose of the pilot The purpose of the physiotherapy pilot was to see if there were business benefits of fast tracking Network Rail employees who sustained injuries whilst
The Physiotherapy Pilot 1.1 Purpose of the pilot The purpose of the physiotherapy pilot was to see if there were business benefits of fast tracking Network Rail employees who sustained injuries whilst
Acute Oncology Service Patient Information Leaflet
 Spinal cord compression Acute Oncology Service Patient Information Leaflet Introduction If you have been diagnosed with cancer, you need to know about spinal cord compression and the warning signs. What
Spinal cord compression Acute Oncology Service Patient Information Leaflet Introduction If you have been diagnosed with cancer, you need to know about spinal cord compression and the warning signs. What
1 REVISOR 5223.0070. (4) Pain associated with rigidity (loss of motion or postural abnormality) or
 1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
1 REVISOR 5223.0070 5223.0070 MUSCULOSKELETAL SCHEDULE; BACK. Subpart 1. Lumbar spine. The spine rating is inclusive of leg symptoms except for gross motor weakness, bladder or bowel dysfunction, or sexual
INFORMATION FOR YOU. Lower Back Pain
 INFORMATION FOR YOU Lower Back Pain WHAT IS ACUTE LOWER BACK PAIN? Acute lower back pain is defined as low back pain present for up to six weeks. It may be experienced as aching, burning, stabbing, sharp
INFORMATION FOR YOU Lower Back Pain WHAT IS ACUTE LOWER BACK PAIN? Acute lower back pain is defined as low back pain present for up to six weeks. It may be experienced as aching, burning, stabbing, sharp
Osteoarthritis and osteoporosis
 Osteoarthritis and osteoporosis What is osteoporosis? Osteoporosis occurs when the struts which make up the mesh-like structure within bones become thin causing them to become fragile and break easily,
Osteoarthritis and osteoporosis What is osteoporosis? Osteoporosis occurs when the struts which make up the mesh-like structure within bones become thin causing them to become fragile and break easily,
Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario
 Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
The Newest Breakthrough In Non- Surgical Treatment of Herniated or Degenerative Discs
 The Newest Breakthrough In Non- Surgical Treatment of Herniated or Degenerative Discs The DRX 9000 is Your Answer To Persistent Back Pain To People Who Want To Be Rid Of Lower Back Pain But Think They
The Newest Breakthrough In Non- Surgical Treatment of Herniated or Degenerative Discs The DRX 9000 is Your Answer To Persistent Back Pain To People Who Want To Be Rid Of Lower Back Pain But Think They
Colossus Important Diagnoses. Instructions for How to List Diagnoses
 1 Colossus Important Diagnoses Instructions for How to List Diagnoses 1. Only list diagnoses on HCFA-1500 or CMS-1500 billing forms 2. Use as many billing forms/pages as necessary (4 diagnoses per billing
1 Colossus Important Diagnoses Instructions for How to List Diagnoses 1. Only list diagnoses on HCFA-1500 or CMS-1500 billing forms 2. Use as many billing forms/pages as necessary (4 diagnoses per billing

 More information >>> HERE
More information >>> HERE  More information >>> HERE
More information >>> HERE