TPLO HOME RECOVERY PROGRAM
|
|
|
- Marcia Robbins
- 10 years ago
- Views:
Transcription
1 TPLO HOME RECOVERY PROGRAM Crestwood Veterinary Centre Street Edmonton, AB T5P 1J
2 The Cranial Cruciate Ligament (CCL) There are a number of ligaments in a dog s stifle (knee) that contribute to joint stability. The Cranial Cruciate Ligament (CCL) is the primary ligament responsible for limiting cranial drawer motion (excessive forward and backward sliding of the femur on the tibia bone). When a dog has a partial tear or ruptures this ligament the joint instability causes inflammation and pain which is why your dog favours the leg. Osteoarthritis, also known as OA, degenerative joint disease, or degenerative arthritis, is a form of arthritis caused by inflammation, breakdown, and the eventual loss of cartilage in the joints. There are many factors that lead to the progression of osteoarthritis; failure to stabilize this joint will accelerate this process. What is a TPLO? The TPLO (Tibial Plateau Levelling Osteotomy) procedure neutralizes the effect of this drawer motion. A circular cut is made in the top of the tibia and the smaller portion of bone is rotated to reduce the slope of the tibia. A special surgical grade stainless steel plate is used to hold the two bone segments together. Over time the bone segments will heal together to provide life long stability. This booklet serves as a guide during the important post-operative healing period following your pet s TPLO surgery. Included in this booklet is a week-by-week recovery schedule along with visual aids and descriptions to help guide you through the various exercises. Please follow this program.
3 Preparing For your Pet s Recovery at Home Preparing your Home: Prior to your pet coming home, you should determine where you are going to confine your dog during this post-operative period. Making your dog as comfortable as possible is as important as having a good rehabilitation plan. As your dog s mobility is to be restricted, we recommend that you utilise the following: A dog crate that is large enough that he/she can stand up and turn around A gated off area such as the kitchen Confinement to a room Surfaces such as hardwood floors, tile, linoleum, etc. can be very slippery. We suggest that you place some throw rugs with rubber backing or yoga mats on these surfaces to make it easier for your dog to walk around. House Rules: No jumping at all! No jumping on/off the bed! No jumping on/off the couch! No jumping on you! Overextension of the knee could compromise the repair of your dog s leg and delay the healing time. Stairs: For the first 2 4 weeks following surgery, stairs should be limited to a short flight to get in or out of the house. Your pet needs to be on a short leash and slowly guided up and down 2 3 stairs (use the Thera-Band sling provided under their belly for support). If you have stairs in your home, limit your dog s access to them with something like a baby gate to prevent unsupervised use of stairs. Longer flights of stairs should not be used for strength training but are allowed with supervision after the 4 weeks post surgery as long as your dog is consistently using their leg and is not allowed to run or jump up the stairs. No active play! Refrain from active play with your dog and do not allow him/her to play with other dogs until your veterinarian tells you otherwise (likely after the 8 week post operative x-rays to confirm bone healing).
4 TPLO Home Recovery Program Uncontrolled pain can slow down the healing process and delay your pet s recovery. We have supplied medications to alleviate this post surgical pain. It is important that you give all medications as directed so that your pet is most comfortable. This does not mean that they should have free reign because they, Feel good. Your pet still needs to be restricted to avoid compromising the surgery which may lead to prolonged recovery and potentially additional surgeries. After the surgery your dog is going to limp on the surgically repaired leg for a period of time. This is because your dog has lost muscle and the leg is weaker and may get sore from building muscle as you progress through your program. Your dog should be placing some weight on the surgical leg (even just touching toes to the floor) within 7 days from the date of the surgery. Over the course of the next few weeks the degree of limping should decrease. If your pet is too active during recovery, his/her limp may become more severe. In this case, you should apply ice 3-4 times a day, allow 24 hours of rest and give any prescribed pain medication. Call your veterinarian if there is no improvement after the 24 hour period. No licking! Allowing your dog to lick at the incision will compromise the healing process. Licking introduces bacteria to the area and, in severe cases, can cause infection to not only the incision but to the bone itself. This type of complication can delay the healing significantly and potentially do permanent damage to the leg. Infection due to licking is the most common complication following TPLO surgery and is totally preventable. Monitor your pet s incision site NORMAL Swelling around the incision and the surgical leg for the first week Bruising on the leg A small amount of clear or blood tinged discharge from the incision (for first few days only) Mild discomfort around the incision and the leg itself Warm to the touch around the leg ABNORMAL Swelling that lasts longer than a week Discharge that is not clear, is blood tinged, or any discharge after the first few days Large amounts of discharge or bleeding Discomfort that continues after pain medications and icing Discomfort that causes your pet to cry out or bite ***NOTE*** If any of the abnormal signs appear, contact your veterinarian The incision should be healed days after the surgery. The sutures will need to be removed at this time. Please make an appointment so that we can assess the incision site and your dog s recovery/progress.
5 Week by Week Recovery Program The weekly recovery program described in the following pages is invaluable for ensuring your pet s recovery. This program has been designed to: Accelerate your pet s recovery to full function of the leg Reduce pain and muscle atrophy (muscle loss and weakness) Strengthen muscles to help stabilize and support the joint Enhance the healing of the affected bone and tissue due to increased blood flow Restore normal joint range of motion Decrease the risk for future injury Recognize when veterinarian intervention is required The physical therapy exercises should be started slowly and cautiously. It is best to time these approximately 30 minutes after you administer your dog s pain medications so that he/she is most comfortable. It is unfair to ask a dog to exercise when it hurts to do so. Watch for signs of discomfort such as struggling or significant resistance to the exercises. Signs of pain can include: decreased appetite, excessive panting, vocalization, aggression or decreased interaction with family members, altered posture (hunched posture), restlessness, flinching when touched, elevated heart rate and respiratory rate, and/or dilated pupils. If your dog is stiff and reluctant to allow further manipulation you may need to reduce the amount of physical activity and/or request additional pain medications from your Veterinarian. Your dog may be tentative at first but his/her comfort level will increase as you progress. Please remember: Adequate rest and physical therapy are the keys to obtaining and maintaining normal limb function. If your dog does not appear to be making positive progress, has any complications, or you have any questions, please contact us anytime. ***NOTE*** It is extremely important to follow this program guideline as closely as possible to ensure proper recovery. The exercises described in this package should be performed in the order they are listed. Please refer to our website for video examples of the described exercises:
6 Rehabilitation Plan: Day 0-14 after surgery The first hours following your dog s surgery he/she may have a bandage on the affected leg. This bandage has been applied to protect the incision as the skin is sealing and to provide some compression to minimize swelling. Manual therapy can begin as soon as the bandage is removed; 2 days following surgery. The following routine should be done daily until your pet is consistently using their leg and has full range of motion in the knee (when you can bend and straighten the surgical leg the same amount as the non-surgical leg). At that point, it is still recommended once to twice a week as he/she will be building muscle and compensating for the surgical leg (The other limbs and lower back will often have muscle tension and discomfort). 1) Massage and Passive Range of Motion (PROM) Massaging your dog s leg is important for relaxing the muscles prior to performing the exercises for rehabilitation. Lay your pet on his/her side on a comfortable surface with the surgical limb up. Target the muscles above and below the joint. Start the massage by pressing down on the muscles with the heel of your palm. You should not move your hand over the skin, but instead press down hard enough to move the skin over the tissues below. Using the heel of your palm, it s unlikely that you will press too hard and possibly injure healing tissue. If your dog shows no signs of discomfort, go back and massage the same areas with the balls of your fingers, where your fingerprints are, not the tips. This provides a deeper massage. Then run the flats of your hands over the whole massaged area. Finally, flex and extend the affected limb several times, gently, until a little resistance is felt. Support the joint while doing this to prevent any twisting of the limb. If you have time, your dog will also greatly benefit from this therapy on the other limbs as they have been compensating for the injured leg. It is also a great way to practice your technique on a healthy limb to build your confidence Frequency and Duration: 2 3 times daily for approximately 15 minutes
7 Rehabilitation Plan: Day 0-14 after surgery 3) Controlled leash walks This exercise requires your dog to be on a short lead very close to your body so that you have complete control of him/her. Leash walks must be done slowly and for short periods of time to build up strength in the leg. For the first few days any walks outside should be for urination or defecation only. By the end of the first week, your dog should be able to walk for 5 minutes per walk. The slower you walk your dog the more inclined he/she will be to place weight on the leg. Make sure to support the hind end under the belly with your Thera-Band sling if needed. This is particularly important on slippery surfaces. Your dog will benefit more from several short walks in one day rather than a single long walk. If your dog has been sent home with a bandage, please ensure the bandage does not get wet when he/she is outside. If this happens, it needs to be removed immediately. Placing a heavy plastic bag or dog bootie on to go outside should eliminate this possibility. Controlled leash walks benefit your dog by: Keeping the muscles strong and lubricating the joints Encouraging use of the affected limb Decreasing pain Positively rewarding your dog emotionally Frequency and Duration: 3-4 times daily up to 5 minutes per walk 4) Ice Therapy After completing the above exercises it is especially important to apply cold therapy to the affected knee to reduce pain and inflammation. You can use gel ice packs from the drugstore, frozen bags of popcorn kernels, or bags of crushed ice. Wrap the ice material in a towel before applying. Place the ice on both the inside and outside of the knee. Frequency and Duration: after exercise for minutes 5) Heat Therapy By the third day you can begin applying heat to the affected leg at the very start of your therapy session prior to massaging. Heat will draw blood to the area to enhance circulation at the surgical site, which aids the healing process. A variety of products are available such as Magic Bags or other heat products from the drugstore. Do not use topical products such as gels or creams. Check the temperature before applying heat to the area and make sure that you use a light towel in-between the product and the skin. Do not apply heat to the joint if it is inflamed (swollen) and warm to the touch. Frequency and Duration: prior to massage for 5 10 minutes
8 Activities to Build Strength and Body Awareness The following exercises will be incorporated into the next 12 weeks of recovery. The intent of this program is to gradually increase strength, balance, and body awareness so that your pet can return to normal activity. All of these exercises are demonstrated on our website for your reference at These two pages provide detailed descriptions of the exercises. Please follow the schedule indicated on the table on the following page. 1. Controlled Leash Walks: Walks should be on a 6 lead with the dog by your side. Up until this point, you have been walking up to 5 minutes per walk 3 4 times per day. From this point on, you can add 3 5 minutes per walk per week. This activity should only be increased if your pet is consistently using his/her leg at a walk. You can incorporate activities such as: Figure 8 patterns, walking up and down curbs in a S-pattern, gentle inclines (hills), stepping over obstacles/through long grass or snow, and short trotting intervals (10 steps) into these walks to make them more challenging and to increase muscle mass and strength. 2. Weight Shifting Exercise: Have your pet stand squarely on a non-slip surface and gently nudge the hind end from side to side for 10 repetitions. This will help with balance and core strength and will lay the groundwork for further core conditioning. For a further challenge, have your pet stand with the front legs elevated (first on a stable surface like some stairs, and then on an unstable one like a cushion, air mattress, or FitPAWS equipment). This will force more weight onto the hind end. 3. Exercises to increase body awareness: These exercises have you walking your dog on a leash in a figure 8 pattern and/or through a series of obstacles in a weave pattern. This exercise helps to encourage the use of the leg and increases proprioception (Proprioception is the knowledge of where all one s body parts are in space). Another great exercise to help with proprioception is walking slowing through the rungs of a ladder laid on the ground. As your pet walks slowly through this obstacle, they must carefully think about where they are putting their feet. Drop treats in between the rungs to make this an extra fun game
9 4. Cookie Stretches: Have your pet stand squarely on a non-slip surface and guide his nose to each hip, up, and then down for one repetition. Do this 5 times working up to 10 repetitions. Once he is comfortable with this exercise, you can place him on an unstable surface such as a couch cushion (on the floor), air mattress, or FitPAWS giant disc/balance pad/peanut (available for purchase) to further challenge him. This exercise will help with spinal mobility and core strengthening. 5. Sit-to-Stand: This exercise is a Doggy Squat. Have your pet sit squarely and then stand for 5-10 repetitions. They have a tendency to cheat and use their nonsurgical leg to push up so it is often helpful to have their surgical leg against a wall as you perform this exercise. This can also be incorporated into daily walks or, at feeding time, you can use part of his kibble to entice him to do this exercise. 6. Three Legged Standing: Have your pet stand squarely on a non-slip surface and then gently lift one leg off of the ground and hold for 5 10 seconds. Alternate with all but the surgical limb. Once your pet becomes good at this exercise, you can try two legged standing by lifting diagonal legs (left front and right hind) and vice versa. 7. Wading in water: Once your pet has their sutures removed, they are able to walk in water that is up to hip height. The buoyancy of the water will displace some of your pet s weight and take some pressure off of the joints. There is also resistance in the water so they are also working on strength and flexibility. IMPORTANT: If you pet will not walk in a controlled manner and likes to leap in water then this is not a good activity until after the 8 week x-ray is assessed by your Veterinarian. 8. Walking in deep snow or in long grass: Walking in deep snow and in longer grass will make your pet pick their legs up higher which will build strength. This should only be done if you have your dog on a short leash and have control of them. 9. Swimming: Swimming is allowed after the 8 week x-rays have been assessed and you have the go ahead from your Veterinarian. The uncontrolled kicking action can be harmful in the early stages of your pet s recovery so it is important to be aware of this. Swimming is a great cardiovascular workout and is great for weight loss. 10. Tug: Tug games are a great way to burn energy and to work on strength. The best tug toys have a bungee cord in the tug rope to prevent jarring to your dog s neck or your shoulders when the taut rope suddenly stops the dog.
10 Stage of Recovery Exercise/Manual Therapy 0 14 days post op Follow the manual therapy routine listed on pages 3 & 4 Daily Frequency Time/Repetitions 2 3 times per day for the first week or until range of motion is normal compared to the opposite limb AT THIS TIME YOU WILL NEED TO MAKE AN APPOINTMENT TO HAVE THE SUTURES REMOVED. WE WILL ALSO ASSESS YOUR PET S PROGRESS AND MAKE ADJUSTMENTS TO YOUR REHABILITATION PROGRAM AS NEEDED Weeks 3 & 4 post op (If patient is consistently using the leg) Weeks 5 8 post op Manual therapy as above 1 2 times per week ~ 30 minutes Ice Therapy As needed (after 15 minutes exercise or if your pet overdoes it and is sore) Controlled Leash Walks 3 times per day 10 minutes Weight Shifting Once a day 2 minutes Figure 8/weaves/ladder Once a day 2 minutes Cookie Stretches Once a day 5 repetitions working up to 10 Sit-to-stand Twice a day 5 repetitions working up to 10 Three legged standing Twice a day 2 repetitions working up to 4 Manual therapy as above Ice Therapy Controlled Leash Walks. Add in short trot intervals and hills into each walk to increase fitness Walking in water/snow/long grass Weight Shifting: add unstable footing (air mattress, couch cushion) for further challenge 1 2 times per week ~ 30 minutes As needed (after 15 minutes exercise or if your pet overdoes it and is sore) 3 times per day Add 3 5 minutes per walk per week to a maximum of 20 minutes per walk or 60 minutes total per day 3 times per week Incorporate into total walk time (up to 60 minutes for the day) 1 2 times per day 4 minutes, add 1 minute per session per week Cookie Stretches 1 2 times per day Add 3-5 repetitions per session per week up to 15 reps/session Sit-to-stand Twice a day Add 3-5 repetitions per session per week up to 15 reps/session Two legged standing Twice a day 30 seconds each side AT THIS TIME YOU WILL NEED TO MAKE AN APPOINTMENT FOR A FOLLOW UP X-RAY TO ASSESS BONE HEALING. YOUR VETERINARIAN WILL INFORM YOU IF YOU ARE OKAY TO PROGRESS TO THE FOLLOWING ACTIVITIES: Weeks 8 12 post op Activities can be continued as above with the addition of any of the following Off leash activity Daily 20 minutes working up TO 60 minutes Tug Daily 5 minutes Swimming Daily 5 minutes working up to 20 minutes over several weeks
11 ADDITIONAL RECOMMENDATIONS FOR LONG TERM JOINT HEALTH AND QUALITY OF LIFE 1. Weight Management: The number one way that you can extend the lifespan and quality of your pet s life is by maintaining a lean and fit body condition. Studies show that dogs that are maintained at an ideal weight for them will likely live 15% longer than dogs that are overfed. This translates to 2 years longer in a dog the size of a Labrador Retriever. We use a body condition scoring system that scores your pet out of 9 points where 5 out of 9 is ideal. A copy of this chart is included in this package. If your dog has a body condition score above 6, it is strongly recommended that you feed your dog a weight management diet. Increased body mass significantly increases your dog s risk of developing osteoarthritis. 2. Joint Health: We have stabilized your dog s stifle (knee) with this surgery but with any injury to a joint, there is an increased chance of developing osteoarthritis. Osteoarthritis develops over time with inflammation in joints and leads to the formation of osteophytes (bone spurs) around the joint, which can cause pain. There are a couple of ways to supplement your dog to provide the building blocks for preserving cartilage and increasing joint lubrication, shock absorption, and mobility: a. Disease Modifying Osteoarthritis Drug: Cartrophen VET is of plant origin and is administered as a series of subcutaneous injections (under the skin). The protocol is one injection weekly for 4 weeks and then once a month for maintenance. b. Oral joint supplements: These Nutraceuticals given orally as a tablet or powder on their food. There are many choices of joint supplements on the market. We recommend one that is formulated for dogs for best absorption, effect, and palatability. c. Joint Mobility Prescription Diets: We recommend a food that is specifically formulated to maintain joint health. Purina and Hill s have put significant research into their joint mobility diets and are highly recommended by our Veterinary team. Both diets have moderate protein to maintain lean body mass, high levels of omega 3 fatty acids, and natural sources of Glucosamine and Chondroitin. Note: If your dog has a Body Condition Score of 7/9 or higher, we recommend a weight management diet to reduce your pet s weight first and then switch to a joint mobility diet.
12 ADDITIONAL RECOMMENDATIONS FOR LONG TERM JOINT HEALTH AND QUALITY OF LIFE 3. Omega 3 Fatty Acids: Research is showing that omega-3 fatty acids, especially EPA, may be helpful in reducing the inflammation associated with arthritis. You may supplement these separately or choose one of the above joint mobility diets which have superior levels. 4. Life-long physical fitness: Physical activity is important for your dog s overall health and wellbeing. Dogs with regular physical activity live longer, healthier lives and have less behaviour problems. SPECIAL CASES We perform the TPLO surgery on a variety of dogs at different life stages. For most young healthy dogs, this program will be sufficient to get them back to the activity level they were at prior to their injury and surgery. Others may have other physical challenges and pre-existing conditions to deal with as they recover such as: Osteoarthritis Bilateral knee surgeries Hip dysplasia Back pain Muscle pain and Myofacial Trigger Points Chronic pain and muscle weakness Obesity (BCS >7/9) For these special cases, a consultation can be arranged with our Certified Canine Rehabilitation Practitioner (CCRP), Penny Radostits. Penny will work with our doctors to find the right combination of pain management pharmaceuticals and physical modalities (therapeutic laser, massage, Chiropractic, targeted exercises, etc) to help your pet s recovery and restore mobility and quality of life.
13 After 12 weeks... By now, your dog s repaired tibia should be healed completely as long as there have been no post-operative complications. Although the bone may have healed, there is still plenty of conditioning required for the muscles and tissues that support the knee joint. As a rule, it takes 2 4 times as long to build muscle as it does to lose it. This means that for every 1 week of inactivity leading to muscle atrophy, 2 4 weeks are needed to rebuild that muscle mass. It may take 6 months before your dog s hind legs have equal muscling. Studies show that there is a 60% chance that your dog will injure the cranial cruciate ligament in the OTHER leg. This is why it is so important to keep your dog lean and active for life. If you have any questions regarding your dog s level of fitness at this time, please discuss this with your Crestwood rehabilitation team. NOTES: GOOD LUCK!
Post Surgical Care of Patella Luxation Repair
 Post Surgical Care of Patella Luxation Repair Home patient care after orthopedic surgery is critical to the success of the surgery. Allowing your pet too much activity may alter the anticipated outcome
Post Surgical Care of Patella Luxation Repair Home patient care after orthopedic surgery is critical to the success of the surgery. Allowing your pet too much activity may alter the anticipated outcome
Ankle Sprain. Information and Rehabilitation. Grade II. Grade I. Grade III
 514-412-4400, ext. 23310 2300 Tupper street, C-831, Montreal (Quebec) H3H 1P3 Ankle Sprain Information and Rehabilitation An ankle sprain is a stretch or a tear of the ligaments (bands of tissue that hold
514-412-4400, ext. 23310 2300 Tupper street, C-831, Montreal (Quebec) H3H 1P3 Ankle Sprain Information and Rehabilitation An ankle sprain is a stretch or a tear of the ligaments (bands of tissue that hold
CRUCIATE STIFLE REHABILITATION PROGRAM TRIAL VERSION
 CRUCIATE STIFLE REHABILITATION PROGRAM TRIAL VERSION CRUCIATE STIFLE REHABILITATION PROGRAM DISCLAIMER: Please be aware that these notes are guidelines and are not intended to over-ride personal observation
CRUCIATE STIFLE REHABILITATION PROGRAM TRIAL VERSION CRUCIATE STIFLE REHABILITATION PROGRAM DISCLAIMER: Please be aware that these notes are guidelines and are not intended to over-ride personal observation
Goals of Rehabilitating Cranial Cruciate Ligament Rupture (CCL) (aka ACL in people)
 Goals of Rehabilitating Cranial Cruciate Ligament Rupture (CCL) (aka ACL in people) California Animal Rehabilitation (CARE) www.calanimalrehab.com Heather Oxford, DVM, MPH, CVA, CCRT Jessica H. Waldman,
Goals of Rehabilitating Cranial Cruciate Ligament Rupture (CCL) (aka ACL in people) California Animal Rehabilitation (CARE) www.calanimalrehab.com Heather Oxford, DVM, MPH, CVA, CCRT Jessica H. Waldman,
A resource for families of MedVet Surgery patients MEDVET. Home Recovery Guide. Use Only
 A resource for families of MedVet Surgery patients Home Recovery Guide TTA & TPLO Preparing the home for your pet s recovery after surgery Rehabilitation and strengthening exercises your family can perform
A resource for families of MedVet Surgery patients Home Recovery Guide TTA & TPLO Preparing the home for your pet s recovery after surgery Rehabilitation and strengthening exercises your family can perform
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
The Knee: Problems and Solutions
 The Knee: Problems and Solutions Animals, like people, may suffer a variety of disorders of the knee that weaken the joint and cause significant pain if left untreated. Two common knee problems in companion
The Knee: Problems and Solutions Animals, like people, may suffer a variety of disorders of the knee that weaken the joint and cause significant pain if left untreated. Two common knee problems in companion
Self Management Program. Ankle Sprains. Improving Care. Improving Business.
 Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Ankle Sprains Improving Care. Improving Business. What is an ankle sprain? Ligaments attach to the ankle bones and allow for normal movement and help prevent too much motion within the joint. Ankle sprains
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ARTHRITIS INTRODUCTION
 ARTHRITIS INTRODUCTION Arthritis is the most common disease affecting the joints. There are various forms of arthritis but the two that are the most common are osteoarthritis (OA), and rheumatoid arthritis
ARTHRITIS INTRODUCTION Arthritis is the most common disease affecting the joints. There are various forms of arthritis but the two that are the most common are osteoarthritis (OA), and rheumatoid arthritis
Knee Arthroscopy Exercise Programme
 Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: [email protected]
Chester Knee Clinic & Cartilage Repair Centre Nuffield Health, The Grosvenor Hospital Chester Wrexham Road Chester CH4 7QP Hospital Telephone: 01244 680 444 CKC Website: www.kneeclinic.info Email: [email protected]
Knee sprains. What is a knee strain? How do knee strains occur? what you ll find in this brochure
 what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
what you ll find in this brochure What is a knee strain? How do knee strains occur? What you should do if a knee strain occurs. What rehabilitation you should do. Example of a return to play strategy.
Home Therapy Booklet
 Step-by-Step Guide to Post- Surgical Home Therapy for Pet Owners TTA Tibial Tuberosity Advancement Home Therapy Booklet 1! www.topdoghealth.com Introduction to Home Therapy Program Booklets This booklet
Step-by-Step Guide to Post- Surgical Home Therapy for Pet Owners TTA Tibial Tuberosity Advancement Home Therapy Booklet 1! www.topdoghealth.com Introduction to Home Therapy Program Booklets This booklet
ACL Reconstruction Rehabilitation Program
 ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
.org. Achilles Tendinitis. Description. Cause. Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel.
 Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Achilles Tendinitis Page ( 1 ) Achilles tendinitis is a common condition that causes pain along the back of the leg near the heel. The Achilles tendon is the largest tendon in the body. It connects your
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Knee arthroscopy advice sheet
 Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Knee arthroscopy advice sheet During an arthroscopy, a camera is inserted into the knee through two or three small puncture wounds. It allows the surgeon to look at the joint surfaces, cartilage and the
Anterior Cruciate Ligament Reconstruction Rehabilitation Protocol
 The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
The First Two Weeks After Surgery You will go home with crutches and be advised to use ice. Goals 1. Protect reconstruction 2. Ensure wound healing 3. Maintain full knee extension 4. Gain knee flexion
Strength Training HEALTHY BONES, HEALTHY HEART
 Strength Training HEALTHY BONES, HEALTHY HEART No matter what your age, strength training can improve your bone health and your balance. As we age, our bones lose both tissue and strength. This condition
Strength Training HEALTHY BONES, HEALTHY HEART No matter what your age, strength training can improve your bone health and your balance. As we age, our bones lose both tissue and strength. This condition
Rehabilitation after shoulder dislocation
 Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Cast removal what to expect #3 Patient Information Leaflet
 Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
Cast removal what to expect #3 Patient Information Leaflet SM466 Now your cast is off, self help is the key! Follow the advice given to you by your doctor and the staff in the clinic. Your skin will be
.org. Arthritis of the Hand. Description
 Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
Arthritis of the Hand Page ( 1 ) The hand and wrist have multiple small joints that work together to produce motion, including the fine motion needed to thread a needle or tie a shoelace. When the joints
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME
 ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
ACL RECONSTRUCTION POST-OPERATIVE REHABILITATION PROGRAMME ABOUT THE OPERATION The aim of your operation is to reconstruct the Anterior Cruciate Ligament (ACL) to restore knee joint stability. A graft,
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Sports Injury Treatment
 Sports Injury Treatment Participating in a variety of sports is fun and healthy for children and adults. However, it's critical that before you participate in any sport, you are aware of the precautions
Sports Injury Treatment Participating in a variety of sports is fun and healthy for children and adults. However, it's critical that before you participate in any sport, you are aware of the precautions
A Patient s Guide to Post-Operative Physiotherapy. Following Anterior Cruciate Ligament Reconstruction of the Knee
 A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
A Patient s Guide to Post-Operative Physiotherapy Following Anterior Cruciate Ligament Reconstruction of the Knee Introduction The anterior cruciate ligament (ACL) is one of the main supporting ligaments
Bankart Repair For Shoulder Instability Rehabilitation Guidelines
 Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
Bankart Repair For Shoulder Instability Rehabilitation Guidelines Phase I: The first week after surgery. Goals:!! 1. Control pain and swelling! 2. Protect the repair! 3. Begin early shoulder motion Activities:
.org. Plantar Fasciitis and Bone Spurs. Anatomy. Cause
 Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Plantar Fasciitis and Bone Spurs Page ( 1 ) Plantar fasciitis (fashee-eye-tiss) is the most common cause of pain on the bottom of the heel. Approximately 2 million patients are treated for this condition
Rehabilitation. Rehabilitation. Walkers, Crutches, Canes
 Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Walkers, Crutches, Canes These devices provide support through your arms to limit the amount of weight on your operated hip. Initially, after a total hip replacement you will use a walker to get around.
Wrist Fracture. Please stick addressograph here
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS FOLLOWING WRIST FRACTURE Please stick addressograph
Shoulder Tendonitis. Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696
 Shoulder Tendonitis Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Shoulder tendinitis is a common overuse injury in sports (such as swimming,
Shoulder Tendonitis Brett Sanders, MD Center For Sports Medicine and Orthopaedic 2415 McCallie Ave. Chattanooga, TN (423) 624-2696 Shoulder tendinitis is a common overuse injury in sports (such as swimming,
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
Herniated Lumbar Disc
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Arthritis of the hip. Normal hip In an x-ray of a normal hip, the articular cartilage (the area labeled normal joint space ) is clearly visible.
 Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Arthritis of the hip Arthritis of the hip is a condition in which the smooth gliding surfaces of your hip joint (articular cartilage) have become damaged. This usually results in pain, stiffness, and reduced
Knee Arthroscopy Post-operative Instructions
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Knee Arthroscopy Post-operative Instructions PLEASE READ ALL OF THESE INSTRUCTIONS CAREFULLY. THEY WILL ANSWER MOST OF YOUR QUESTIONS. 1. You may walk
Knee Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Senior pets are not unlike senior citizens.
 P ro c e d u re s P ro G E R I A T R I C S / R E H A B I L I T A T I O N Peer Reviewed Christine Jurek, DVM, CCRT, & Laurie McCauley, DVM, CCRT TOPS Veterinary Rehab, Grayslake, Illinois Physical Rehabilitation
P ro c e d u re s P ro G E R I A T R I C S / R E H A B I L I T A T I O N Peer Reviewed Christine Jurek, DVM, CCRT, & Laurie McCauley, DVM, CCRT TOPS Veterinary Rehab, Grayslake, Illinois Physical Rehabilitation
PLANTAR FASCITIS (Heel Spur Syndrome)
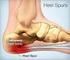 PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
SCRIPT NUMBER 82 SPRAINED ANKLE (TWO SPEAKERS)
 SCRIPT NUMBER 82 SPRAINED ANKLE (TWO SPEAKERS) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: SPRAINED ANKLE PROGRAM NUMBER: 82 SUBJECT: PATHOLOGY, CAUSES, DIAGNOSIS, TREATMENT, PREVENTION OF SPRAINED ANKLES
SCRIPT NUMBER 82 SPRAINED ANKLE (TWO SPEAKERS) PROGRAM NAME: HEALTH NUGGETS PROGRAM TITLE: SPRAINED ANKLE PROGRAM NUMBER: 82 SUBJECT: PATHOLOGY, CAUSES, DIAGNOSIS, TREATMENT, PREVENTION OF SPRAINED ANKLES
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
ILIOTIBIAL BAND SYNDROME Description The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon
Rehabilitation. Rehabilitation. Walking after Total Knee Replacement. Continuous Passive Motion Device
 Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
Walking after Total Knee Replacement After your TKR, continue using your walker or crutches until your surgeons tells you it is okay to stop using them. When turning with a walker or crutches DO NOT PIVOT
What is Osteoarthritis? Who gets Osteoarthritis? What can I do when I am diagnosed with Osteoarthritis? What can my doctor do to help me?
 Knee Osteoarthritis What is Osteoarthritis? Osteoarthritis is a disease process that affects the cartilage within a joint. Cartilage exists at the surface of the ends of the bones and provides joints with
Knee Osteoarthritis What is Osteoarthritis? Osteoarthritis is a disease process that affects the cartilage within a joint. Cartilage exists at the surface of the ends of the bones and provides joints with
Recent Injuries. www.physiofirst.org.uk
 Recent Injuries www.physiofirst.org.uk A recent or acute injury can occur suddenly during any activity, from tripping over the kerb, to making the bed, to playing sport. In some cases, an acute injury
Recent Injuries www.physiofirst.org.uk A recent or acute injury can occur suddenly during any activity, from tripping over the kerb, to making the bed, to playing sport. In some cases, an acute injury
We ve got your back. Physical Therapy After Lumbar Fusion Surgery
 We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
We ve got your back Physical Therapy After Lumbar Fusion Surgery Physical therapy is an extremely important part of you recovery after spinal surgery. This booklet, prepared by the therapists who specialize
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE
 ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
Rehabilitation of Sports Hernia
 Rehabilitation of Sports Hernia (Involving Adductor Tenotomy, Ilioinguinal Neurectomy and Osteitis Pubis) An appendix follows this protocol for examples of exercises in each phase of rehabilitation. There
Rehabilitation of Sports Hernia (Involving Adductor Tenotomy, Ilioinguinal Neurectomy and Osteitis Pubis) An appendix follows this protocol for examples of exercises in each phase of rehabilitation. There
Plantar Fascia Release
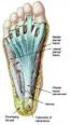 Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
Plantar Fascia Release Introduction Plantar fasciitis is a common condition that causes pain around the heel. It may be severe enough to affect regular activities. If other treatments are unsuccessful,
TOWN CENTER ORTHOPAEDIC ASSOCIATES P.C. Labral Tears
 Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Range of Motion. A guide for you after spinal cord injury. Spinal Cord Injury Rehabilitation Program
 Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Range of Motion A guide for you after spinal cord injury Spinal Cord Injury Rehabilitation Program This booklet has been written by the health care providers who provide care to people who have a spinal
Therapeutic Canine Massage
 Meet our Certified Canine Massage Therapist, Stevi Quick After years of competitive grooming and handling several breeds in conformation, I became interested in training and competing with my dogs in the
Meet our Certified Canine Massage Therapist, Stevi Quick After years of competitive grooming and handling several breeds in conformation, I became interested in training and competing with my dogs in the
X-Plain Rheumatoid Arthritis Reference Summary
 X-Plain Rheumatoid Arthritis Reference Summary Introduction Rheumatoid arthritis is a fairly common joint disease that affects up to 2 million Americans. Rheumatoid arthritis is one of the most debilitating
X-Plain Rheumatoid Arthritis Reference Summary Introduction Rheumatoid arthritis is a fairly common joint disease that affects up to 2 million Americans. Rheumatoid arthritis is one of the most debilitating
TIPS and EXERCISES for your knee stiffness. and pain
 TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
TIPS and EXERCISES for your knee stiffness and pain KNEE EXERCISES Range of motion exercise 3 Knee bending exercises 3 Knee straightening exercises 5 STRENGTHENING EXERCISES 6 AEROBIC EXERCISE 10 ADDITIONAL
ISOMETRIC EXERCISE HELPS REVERSE JOINT STIFFNESS, BUILDS MUSCLE, AND BOOSTS OVERALL FITNESS.
 ISOMETRIC EXERCISE HELPS REVERSE JOINT STIFFNESS, BUILDS MUSCLE, AND BOOSTS OVERALL FITNESS. By Askari A. Kazmi KazmisBioscienceLabs exercise helps reverse joint stiffness, builds muscle, and boosts overall
ISOMETRIC EXERCISE HELPS REVERSE JOINT STIFFNESS, BUILDS MUSCLE, AND BOOSTS OVERALL FITNESS. By Askari A. Kazmi KazmisBioscienceLabs exercise helps reverse joint stiffness, builds muscle, and boosts overall
A compressive dressing that you apply around your ankle, and
 Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
Ankle Injuries & Treatment The easiest way to remember this is: R.I.C.E. Each of these letters stands for: Rest. Rest your ankle. Do not place weight on it if it is very tender. Avoid walking long distances.
INTRODUCTION TO POSITIONING. MODULE 3: Positioning and Carrying
 MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
MODULE 3: Positioning and Carrying Blankets, pillows and towels, sandbags, carpet on the floor, a doll with floppy limbs that can be positioned i.e. not a hard plastic doll, display materials. Icebreaker
Predislocation syndrome
 Predislocation syndrome Sky Ridge Medical Center, Aspen Building Pre-dislocation syndrome, capsulitis, and metatarsalgia are all similar problems usually at the ball of the foot near the second and third
Predislocation syndrome Sky Ridge Medical Center, Aspen Building Pre-dislocation syndrome, capsulitis, and metatarsalgia are all similar problems usually at the ball of the foot near the second and third
Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery
 Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
Amon T. Ferry, MD Orthopedic Surgery Sports Medicine Achilles Tendon Repair Surgery Post-operative Instructions Phase One: The First Week After Surgery Amon T. Ferry, MD Orthopedic Surgery / Sports Medicine
General Guidelines. Neck Stretch: Side. Neck Stretch: Forward. Shoulder Rolls. Side Stretch
 Stretching Exercises General Guidelines Perform stretching exercises at least 2 3 days per week and preferably more Hold each stretch for 15 20 seconds Relax and breathe normally Stretching is most effective
Stretching Exercises General Guidelines Perform stretching exercises at least 2 3 days per week and preferably more Hold each stretch for 15 20 seconds Relax and breathe normally Stretching is most effective
Your knee: Rheumatoid arthritis or osteoarthritis?
 Your knee: Rheumatoid arthritis or osteoarthritis? Age Rheumatoid arthritis can come on at any age while osteoarthritis usually starts later in life. How does it start? Rheumatoid arthritis comes on rapidly
Your knee: Rheumatoid arthritis or osteoarthritis? Age Rheumatoid arthritis can come on at any age while osteoarthritis usually starts later in life. How does it start? Rheumatoid arthritis comes on rapidly
How To Stretch Your Body
 Exercise Module A New Leaf Choices for Healthy Living University of North Carolina at Chapel Hill 2007 Center for Health Promotion and Disease Prevention Physical Activity Exercises for Keeping Active
Exercise Module A New Leaf Choices for Healthy Living University of North Carolina at Chapel Hill 2007 Center for Health Promotion and Disease Prevention Physical Activity Exercises for Keeping Active
Otago Exercise Program
 Otago Exercise Program Edited Version Exercise Booklet Created by: Genesee County Coalition Supported by a grant from the Health Foundation for Western and Central New York Otago Exercise Program to Prevent
Otago Exercise Program Edited Version Exercise Booklet Created by: Genesee County Coalition Supported by a grant from the Health Foundation for Western and Central New York Otago Exercise Program to Prevent
Herniated Cervical Disc
 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Sue Schuerman, PT, GCS, PhD UNLVPT
 Sue Schuerman, PT, GCS, PhD UNLVPT Exercise & Physical Activity (Your Everyday Guide from the National Institute on Aging) Go4Life Retain our physical and mental health Continue to do the things we enjoy
Sue Schuerman, PT, GCS, PhD UNLVPT Exercise & Physical Activity (Your Everyday Guide from the National Institute on Aging) Go4Life Retain our physical and mental health Continue to do the things we enjoy
Range of Motion Exercises
 Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
Range of Motion Exercises Range of motion (ROM) exercises are done to preserve flexibility and mobility of the joints on which they are performed. These exercises reduce stiffness and will prevent or at
ACL Reconstruction Physiotherapy advice for patients
 Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Oxford University Hospitals NHS Trust ACL Reconstruction Physiotherapy advice for patients Introduction This booklet is designed to provide you with advice and guidance on your rehabilitation after reconstruction
Hip Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft
 ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
ACL Reconstruction: Patellar Tendon Graft/Hamstring Tendon Graft Patellar Tendon Graft/Hamstring Tendon Graft General Information: The intent of these guidelines is to provide the therapist with direction
YOUR GUIDE TO TOTAL HIP REPLACEMENT
 A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
A Partnership for Better Healthcare A Partnership for Better Healthcare YOUR GUIDE TO TOTAL HIP REPLACEMENT PEI Limited M50 Business Park Ballymount Road Upper Ballymount Dublin 12 Tel: 01-419 6900 Fax:
Adult Advisor: Plantar Fasciitis. Plantar Fasciitis
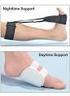 Adult Advisor: Plantar Fasciitis Page 1 of 3 Plantar Fasciitis What is plantar fasciitis? Plantar fasciitis is a painful inflammation of the bottom of the foot between the ball of the foot and the heel.
Adult Advisor: Plantar Fasciitis Page 1 of 3 Plantar Fasciitis What is plantar fasciitis? Plantar fasciitis is a painful inflammation of the bottom of the foot between the ball of the foot and the heel.
Endoscopic Plantar Fasciotomy
 Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
Endoscopic Plantar Fasciotomy Introduction Plantar fasciitis is a common condition that causes pain centralized around the heel. It may be severe enough to affect regular activities. Health care providers
HOPE EXERCISE RECOVERY RESOURCES RELATIONSHIPS INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RELATIONSHIPS MOVEMENT. A Stroke Recovery Guide
 INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RECOVERY HOPE A Stroke Recovery Guide RELATIONSHIPS MOVEMENT RESOURCES RELATIONSHIPS EXERCISE www.stroke.org CHAPTER FOUR Movement and Exercise Moving
INFORMATION REHABILITATION PREVENTION SELF ADVOCACY RECOVERY HOPE A Stroke Recovery Guide RELATIONSHIPS MOVEMENT RESOURCES RELATIONSHIPS EXERCISE www.stroke.org CHAPTER FOUR Movement and Exercise Moving
Why Back Safety is Important
 Back Safety Why Back Safety is Important Back injuries are considered by OSHA (the Occupational Safety and Health Administration) as the nation's #1 workplace safety problem. Back Injuries are often: Very
Back Safety Why Back Safety is Important Back injuries are considered by OSHA (the Occupational Safety and Health Administration) as the nation's #1 workplace safety problem. Back Injuries are often: Very
REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON
 175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
175 Cambridge Street, 4 th floor Boston, MA 02114 617-726-7500 REHABILITATION AFTER REPAIR OF THE PATELLAR AND QUADRICEPS TENDON The patellar tendon attaches to the tibial tubercle on the front of the
UK HealthCare Sports Medicine Patient Education December 09
 LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
LCL injury Description Lateral collateral knee ligament sprain is a sprain (stretch or tear) of one of the four major ligaments of the knee. The lateral collateral ligament (LCL) is a structure that helps
What Are Bursitis and Tendinitis?
 Bursitis and tendinitis are both common conditions that cause swelling around muscles and bones. They occur most often in the shoulder, elbow, wrist, hip, knee, or ankle. A bursa is a small, fluid-filled
Bursitis and tendinitis are both common conditions that cause swelling around muscles and bones. They occur most often in the shoulder, elbow, wrist, hip, knee, or ankle. A bursa is a small, fluid-filled
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW Health Sports Rehabilitation Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
world-class orthopedic care right in your own backyard.
 world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
world-class orthopedic care right in your own backyard. Patient Promise: At Adventist Hinsdale Hospital, our Patient Promise means we strive for continued excellence in everything we do. This means you
Exercises for Low Back Injury Prevention
 DIVISION OF AGRICULTURE RESEARCH & EXTENSION University of Arkansas System Family and Consumer Sciences Increasing Physical Activity as We Age Exercises for Low Back Injury Prevention FSFCS38 Lisa Washburn,
DIVISION OF AGRICULTURE RESEARCH & EXTENSION University of Arkansas System Family and Consumer Sciences Increasing Physical Activity as We Age Exercises for Low Back Injury Prevention FSFCS38 Lisa Washburn,
Physical Capability Strength Test: One Component of the Selection Process
 Physical Capability Strength Test: One Component of the Selection Process One aspect of the Power Systems Institute selection process is to successfully complete and achieve a passing score on a physical
Physical Capability Strength Test: One Component of the Selection Process One aspect of the Power Systems Institute selection process is to successfully complete and achieve a passing score on a physical
Exercises for older people
 Exercise for older people Exercises for older people Sitting Getting started If you ve not done much physical activity for a while, you may want to get the all-clear from a GP before starting. For the
Exercise for older people Exercises for older people Sitting Getting started If you ve not done much physical activity for a while, you may want to get the all-clear from a GP before starting. For the
Passive Range of Motion Exercises
 Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
Exercise and ALS The physical or occupational therapist will make recommendations for exercise based upon each patient s specific needs and abilities. Strengthening exercises are not generally recommended
TOTAL KNEE REPLACEMENT
 PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT Home Exercise Program PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT HOME EXERCISE PROGRAM To get the best results from your surgery, it is important that you do your
PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT Home Exercise Program PENN ORTHOPAEDICS TOTAL KNEE REPLACEMENT HOME EXERCISE PROGRAM To get the best results from your surgery, it is important that you do your
Otago Exercise Program Activity Booklet
 Head Movements Stand up tall and look ahead. Slowly turn your head as far as you can to the right. Slowly turn your head as far as you can to the left. Repeat five times to each side. 44 Neck Movements
Head Movements Stand up tall and look ahead. Slowly turn your head as far as you can to the right. Slowly turn your head as far as you can to the left. Repeat five times to each side. 44 Neck Movements
Shoulder Joint Replacement
 Shoulder Joint Replacement Many people know someone with an artificial knee or hip joint. Shoulder replacement is less common, but it is just as successful in relieving joint pain. Shoulder replacement
Shoulder Joint Replacement Many people know someone with an artificial knee or hip joint. Shoulder replacement is less common, but it is just as successful in relieving joint pain. Shoulder replacement
Foot and Ankle Conditioning Program. Purpose of Program
 Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Prepared for: Prepared by: OrthoInfo Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Preventing & Treating Low Back Pain
 Preventing & Treating Low Back Pain An Introduction to Low Back Pain Low back pain is the number two reason that Americans see a health care practitioner second only to colds and flu. While most people
Preventing & Treating Low Back Pain An Introduction to Low Back Pain Low back pain is the number two reason that Americans see a health care practitioner second only to colds and flu. While most people
Sciatica Yuliya Mutsa PTA 236
 Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
it s time for rubber to meet the road
 your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
your total knee replacement surgery Steps to returning to a Lifestyle You Deserve it s time for rubber to meet the road AGAIN The knee is the largest joint in the body. The knee is made up of the lower
Patient Guide. Sacroiliac Joint Pain
 Patient Guide Sacroiliac Joint Pain Anatomy Where is the Sacroiliac Joint? The sacroiliac joint (SIJ) is located at the bottom end of your spine, where the "tailbone" (sacrum) joins the pelvis (ilium).
Patient Guide Sacroiliac Joint Pain Anatomy Where is the Sacroiliac Joint? The sacroiliac joint (SIJ) is located at the bottom end of your spine, where the "tailbone" (sacrum) joins the pelvis (ilium).
let s talk bleeds a bleed checklist for haemophilia patients
 let s talk bleeds a bleed checklist for haemophilia patients Specific signs of a bleed Watch for Bruising, with or without lumps Difference in the size of arms/legs Difference in movement in arms/legs
let s talk bleeds a bleed checklist for haemophilia patients Specific signs of a bleed Watch for Bruising, with or without lumps Difference in the size of arms/legs Difference in movement in arms/legs
Lower Back Pain www.spireperform.com 01283 576333
 Lower Back Pain www.spireperform.com 01283 576333 Low back pain can be caused through deficiencies in movement, posture and your lower limbs or pelvis. The advice in this booklet aims to help with relieving
Lower Back Pain www.spireperform.com 01283 576333 Low back pain can be caused through deficiencies in movement, posture and your lower limbs or pelvis. The advice in this booklet aims to help with relieving
12 Week Do-it-Yourself Fitness Program
 12 Week Do-it-Yourself Fitness Program Created by Brad Awalt, MS, ACSM Assistant Manager, Health Plus [email protected] January 2011 Do you have a goal to begin an exercise routine, but not sure
12 Week Do-it-Yourself Fitness Program Created by Brad Awalt, MS, ACSM Assistant Manager, Health Plus [email protected] January 2011 Do you have a goal to begin an exercise routine, but not sure
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Shoulder Dislocation or Instability Surgery: A Guide to Recovery After Surgery
 What is Shoulder Instability? What is a Shoulder Dislocation? The shoulder joint is a ball in socket joint and is the most mobile joint in the human body. The socket, however, is quite shallow which means
What is Shoulder Instability? What is a Shoulder Dislocation? The shoulder joint is a ball in socket joint and is the most mobile joint in the human body. The socket, however, is quite shallow which means
UK HealthCare Sports Medicine Patient Education December 09
 Meniscus tear Description The meniscus is a C-shaped cartilage structure in the knee that sits on top of the lower leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The meniscus
Meniscus tear Description The meniscus is a C-shaped cartilage structure in the knee that sits on top of the lower leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The meniscus
Injury Prevention for the Back and Neck
 Injury Prevention for the Back and Neck www.csmr.org We have created this brochure to provide you with information regarding: Common Causes of Back and Neck Injuries and Pain Tips for Avoiding Neck and
Injury Prevention for the Back and Neck www.csmr.org We have created this brochure to provide you with information regarding: Common Causes of Back and Neck Injuries and Pain Tips for Avoiding Neck and
KNEES A Physical Therapist s Perspective American Physical Therapy Association
 Taking Care of Your KNEES A Physical Therapist s Perspective American Physical Therapy Association Taking Care of Your Knees When the mother of the hero Achilles dipped him in the river Styx, she held
Taking Care of Your KNEES A Physical Therapist s Perspective American Physical Therapy Association Taking Care of Your Knees When the mother of the hero Achilles dipped him in the river Styx, she held
Welcome to your LOW BACK PAIN treatment guide
 Welcome to your LOW BACK PAIN treatment guide You are receiving this guide because you have recently experienced low back pain. Back pain is one of the most common musculoskeletal problems treated in medicine
Welcome to your LOW BACK PAIN treatment guide You are receiving this guide because you have recently experienced low back pain. Back pain is one of the most common musculoskeletal problems treated in medicine
MOON SHOULDER GROUP. Rotator Cuff Home Exercise Program. MOON Shoulder Group
 MOON Shoulder Group For information regarding the MOON Shoulder Group, talk to your doctor or contact: Rosemary Sanders 1215 21 st Avenue South 6100 Medical Center East Vanderbilt University Medical Center
MOON Shoulder Group For information regarding the MOON Shoulder Group, talk to your doctor or contact: Rosemary Sanders 1215 21 st Avenue South 6100 Medical Center East Vanderbilt University Medical Center
