NEUROLOGICAL DISORDERS
|
|
|
- Daniella Harrington
- 10 years ago
- Views:
Transcription
1 The Great Diseases A collaborative approach to real world science in the classroom Infectious Diseases Neurological Disorders Metabolic Disease Cancer NEUROLOGICAL DISORDERS Katherine Malanson and Karina Meiri
2 Welcome to the Neurological Disorders Module! Outline This module focuses on how our brains work, as well as how disorders and our choices change our brains. The Neurological Disorders (ND) Module has five units, each of which builds upon the others that came before it. The goal of each unit is to answer a new question about how our brains function. Unit 1: What do our brains need to do? Unit 2: What are the building blocks of our brains? Unit 3: How do our neurons communicate with each other? Unit 4: How do our neurons work together to control behaviors? Unit 5: How do our choices change our brains? In Unit 1, we ll begin our discussion by investigating what it is that our brains need to do. From there, in Unit 2, we ll zoom in on the neuron, which is the basic building block of our brains. Then, in Unit 3, we ll focus on the synapse, which is how neurons communicate with each other. Next, in Unit 4, we ll take a larger approach and examine the circuit, which is how neurons work together to control behaviors. Finally, in Unit 5, using the example of drug addiction, we ll look at how our choices change our brains. To help orient you on how these topics relate to each other, we ve put together the following graphic that you ll see at the beginning of each unit. Notice how these topics relate to each other not only in content but also in size. Our brains are composed of circuits, which are composed of synapses, and synapses are the junctions between two neurons. Throughout this module, you ll have not only class lessons, but also this workbook to guide you through your exploration of Neurological Disorders. This workbook is designed to provide you with readings to complement your class lessons. We have helped make your reading of this workbook interactive by encouraging you to take notes and answer questions throughout.
3 LESSON 1.1 WORKBOOK How can we study our brains? This unit introduces you to how we can study our brains - both how they are built, and how they function. In this lesson, we will begin our exploration by examining how scientists and doctors have historically tried to study the behaving brain. Historically, how did scientists study the behaving brain? How can we study our brains? Your brain is the most important organ in your body. It controls your organs, your behavior and your memories and emotions. Without it, none of these would function and you wouldn t be aware of it, because the brain also controls the very basis for human consciousness. Perhaps the last frontier of biological science its ultimate challenge is to understand the exact mental processes within the brain that allow us to perceive and act, learn and remember the biological basis of consciousness. Until recently, most of what we could glean about the behaving brain came from comparing the behavior of people with brains that had been damaged, with people apparently behaving normally. As we shall see, this approach has provided some interesting clues, but doesn t give an insight into normal behavior. Today, we are at the beginning of a technological revolution. Scientists and engineers have developed instruments that have opened unprecedented windows into the living brain. Techniques that can visualize living neurons behaving in real time have allowed us to view the normal brain as we are thinking, feeling and acting. Researchers can now see which parts of the brain are activated when we eat, sleep, listen to music, dance, meditate or do any number of other activities. On top of this, advances in computing power have allowed us to build machines that are increasingly able to function like actual brains. As young people at the beginning of the 21st century you will be participating in the final frontier - as we gather the tools to ask the question What does it mean to be human? How can scientists study the brain in the present day? Lesson 1.1 3
4 LESSON READING What can we learn from studying cases of injury or disease? The first and most famous brain injury case that scientists used to investigate the relationship between the brain and behavior occurred in the mid-1800s. Phineas Gage was the foreman of a railway construction crew, and by all accounts was a model citizen, serious, industrious and energetic. One day, while using a steel rod to ram a charge of blasting powder into a hole, the charge suddenly exploded, sending the rod into Gage s cheek, through his brain, and out the top of his head! (Figure 1). Incredibly he survived, even walking away from the blast once he regained consciousness. But the Phineas that woke up after the accident was a very different man. He became childish and feckless, producing outbursts of temper that led some friends to remark that it looked as if Dr. Jekyll had become Mr. Hyde. The very fact that Gage had survived such a terrible accident put him under intense medical scrutiny. Add to that the dramatic changes in personality that resulted from the accident, and you have one of the most famous case studies in neuroscience history. After years of observing his new reactions to situations, his doctors came to the conclusion that the front portions of his brain that had been damaged must Figure 1: Phineas Gage ( ). Phineas Gage is perhaps the most famous brain injury patient. In 1848, a metal rod impaled his brain - entering just below the left eye socket and exiting at the top of his head. The injury caused a dramatic change in Gage s personality. be critical for controlling a rather subtle aspect of our personality that we now refer to as executive function which is basically a filter that stops you saying the things you think, but know you shouldn t say, or doing the things you d like to, but know aren t a good idea. Gage s accident destroyed this filter so he just blurted out whatever came to mind, and got tangled up in all kinds of ill-advised schemes. (You can see Phineas Gage s skull and the iron bar at the Warren Anatomical Museum at Harvard Medical School, 10 Shattuck St., Boston, MA it s open Monday Friday, 9-5.) How was Gage s behavior affected by his injury? What part of his brain was damaged? What did his doctors conclude about the part of his brain that was injured? Lesson 1.1 4
5 LESSON READING Another famous case of brain injury affecting totally different brain areas was that of Henry Gustav Molaison, known in the medical and scientific literature as Patient H.M.. Born in 1926, Molaison suffered from severe epilepsy that left him almost totally unable to function. In 1953, surgeons attempted to treat it by removing areas in both the right and left side of his brain just above the ears (Figure 2). The surgery was successful and H.M. s epilepsy disappeared. Unfortunately, the epilepsy was replaced by an equally debilitating memory impairment. H.M. woke up from the operation suffering from severe anterograde amnesia, meaning that although he could remember events from his past, he couldn t make any new memories and therefore couldn t learn anything new. As a result he wasn t able to remember people he met after the operation, and when his family moved to a new house, he was never able to learn how to get around in the new neighborhood. The famous Canadian neurologist, Brenda Milner, made it her life s work to study what exactly had happened when those parts of H.M. s brain had been removed. By painstakingly giving him many different kinds of memory and recall tasks, Milner was not only able to determine the parts of the brain that are critical for the formation of new memories, she was also able to figure out that there are several different kinds of memory and our brains process each kind differently. We ll talk more about this later. You can hear a fascinating interview with Dr. Milner and H.M. online - see this unit on the student website or click below: Figure 2: Henry Gustav Molaison ( ). Henry Gustav Molaison, known as patient H.M., became a very popular case study for learning and memory after he underwent surgery to treat his epilepsy. The surgery removed a portion of H.M. s brain just above the ears on both sides of his head. We later learned this area is critical for learning and memory. Audio: H.M. s Brain and the History of Memory Although no other patient has had the same surgery as H.M., similar cases of brain damage can occur after illness. One of the most striking is Clive Wearing who was an eminent musician who contracted viral encephalitis (an infection that destroyed part of his brain). Clive Wearing suffers from both anterograde and retrograde amnesia so he retains memories for less than a minute, which means he is in a constant state of believing he has just woken up. You can watch Clive Wearing and hear his wife and doctor describe what his life is like online - see this unit on the student website or click below: How was Patient H.M. affected by his surgery? What part of his brain was damaged? What did Dr. Milner and her team conclude about the part of the brain that was damaged? Lesson 1.1 Video: Life Without Memory: The Case of Clive Wearing 5
6 LESSON READING Can we only study the brain using cases of injury or disease? Much of what we know about the brain and how it functions has come from scientists and doctors who have studied cases of brain disease and injury, but we no longer have to rely on finding new cases in order to investigate how our brains work. Dramatic new advances in technology have given us a plethora of different tools that can be used to study the healthy, behaving brain. As we shall see, we are now able to literally eavesdrop on the brain while subjects are involved in any number of activities, from listening to music, reacting to a joke or watching a magic trick. Can we use what we know to control someone else s brain? How likely is it that once we know exactly how the brain functions that we will be able to control another person s brain? It sounds like science fiction, but we can actually do it right now, even with the limited knowledge we have. Transcranial magnetic stimulation (TMS) uses magnetic energy to send pulses of magnetic energy into the brain through the skull. In this way it can activate or disrupt the functioning of specific brain regions (Figure 3). TMS is noninvasive and extensive studies have shown it to be safe, so its been approved for use in humans by the Food and Drug Administration (FDA), which is the drug and medical appliance safety watchdog. TMS can be precisely aimed at specific brain regions and has been used to trigger ordinary people s inner mathematical genius and to invoke religious experiences. There are hopes it could be used to help people with depression and other brain disorders such as schizophrenia and bipolar disorder, which have all been linked to specific areas. Figure 3: Transcranial magnetic stimulation (TMS). TMS is a noninvasive procedure that uses magnetic pulses to stimulate different brain areas. While TMS has also been used to study the brain areas involved in moral decision making, it s far from the mind control displayed in science fiction movies, but it ll be an invaluable tool as we continue to study brain areas and their functions. In a later lesson, we ll look at other techniques to visualize specific brain areas involved in normal behaviors. How can TMS be used to control brain function? Can you envision any problems with using TMS therapy? What might they be? Lesson Magne&c field Wire coil Targeted brain region
7 STUDENT RESPONSES Remember to identify your sources What do you see as some of the disadvantages in trying to determine how the brain functions from studying cases of injury or disease? What are some of the advantages of using modern day technologies to investigate how the brain functions? Do you think we ll ever get to a stage where we will be able to completely control the brain? Why or why not? Lesson 1.1 7
8 DEFINITIONS OF TERMS Central nervous system (CNS) contains the brain and spinal cord. Peripheral nervous system (PNS) includes all the nerves outside the brain and spinal cord. For a complete list of defined terms, see the Glossary. LESSON 1.2 WORKBOOK How does brain structure impact its function? In this lesson, you ll be dissecting a sheep s brain. During the dissection you ll localize and identify major brain structures. By understanding where these structures are localized you ll begin to appreciate how the brain is organized spatially. Once you understand spatial organization we can begin to investigate how the different parts connect to control behavior. If you have an iphone or an ipad you can download a great free app that will allow you to look at the structures of the brain in 3D. These pictures are worth a thousand words as we examine more closely how the brain is organized. The app is available FREE from the itunes store. Just search 3D brain. How can we study our brains? Before we get too much further in our discussion of how the brain is organized, let s take a short tour of the nervous system as a whole to orient you on all the different parts, how they re classified and what their functions are. First of all we need to remember that your nervous system has basically three functions it receives information via our various sensory systems; it makes sense of these sensations and decides what an appropriate response should be; and it executes that response. To complete these three functions, our nervous system uses its two main branches - the central nervous system (CNS) and the peripheral nervous system (PNS). Sensations come in from the environment via the PNS. The PNS delivers this information to the CNS which then evaluates the information and decides how to respond. Finally, the CNS sends a signal the PNS in order to be able to execute the response. Your central nervous system (CNS) includes your brain and spinal cord while your peripheral nervous system includes all the nerves in your head, body and limbs that lie outside the brain and spinal cord (Figure 4). Let s start by briefly talking about the What are the three basic functions of your nervous system? What is the CNS? What is the PNS? peripheral nervous system and spinal cord, then we can concentrate on the brain for the remainder of Lesson 1.2 this lesson. 8
9 DEFINITIONS OF TERMS Peripheral nervous system (PNS) includes all the nerves outside the brain and spinal cord. Somatic nervous system - part of the PNS that controls voluntary movement. Autonomic nervous system part of the PNS that controls the function of organs and glands. For a complete list of defined terms, see the Glossary. LESSON READING Your Peripheral Nervous System (PNS) The PNS can be further divided into the somatic nervous system, which controls voluntary muscles, and the autonomic nervous system, which controls the function of organs and glands. The autonomic nervous system has two divisions: Sympathetic nervous system is nicknamed the fight-or-flight system because it prepares our body when energy expenditure is necessary, such as during times of stress or excitement. This system increases heart rate and blood pressure, stimulates secretion of adrenaline, and increases blood flow to the skeletal muscles. Parasympathetic nervous system helps our body conserve and store energy for later use. This system increases salivation, digestion, and storage of glucose and other nutrients, as well as slowing the heart and decreasing respiration. Overall, the peripheral nervous system connects with non-neuronal cells at one end and the central nervous system at the other. The neurons of the PNS can be divided into two classes: Sensory neurons bring sensations such as smell, touch, hearing, taste and pain to the CNS where they are evaluated to determine what response is needed. Motor neurons execute those responses. Motor neurons of the somatic nervous system control voluntary responses such as muscle contractions, whereas motor neurons of the autonomic nervous system control involuntary responses such as changes in heart rate. Peripheral nerves are protected by the organs they travel through, and in cases of injury or disease peripheral nerves are able to regenerate. Figure 4: Peripheral and central nervous systems. The CNS is in pink, and contains all neurons in the brain and spinal cord. The PNS is in blue, Are you aware of your somatic nervous system? What about your autonomic nervous system? Which part of your autonomic nervous system is working as you are reading this page? What about if you heard a fire alarm? and contains all neurons not in the Lesson 1.2 brain or spinal cord. 9
10 DEFINITIONS OF TERMS Cerebrospinal fluid (CSF) - the fluid that bathes the brain and spinal cord. Meninges protective membranes that cover the brain and spinal cord Ventricles - the spaces inside the hollow brain and spinal cord that are gilled with cerebro spinal fluid. For a complete list of defined terms, see the Glossary. LESSON READING Your Central Nervous System (CNS) The central nervous system (CNS) is also divided into different parts - the spinal cord and the brain. The sensations that are received in the periphery via sensory neurons first enter the spinal cord and then pass into the brain. Then once the brain has decided on a response, output from the brain passes into the spinal cord before it exits to the somatic or autonomic peripheral motor neurons in the periphery. The central nervous system is protected from damage by the bony skull and vertebrae. Both the brain and spinal cord are cushioned by sheets of protective membranes called meninges (Figure 5). The brain also contains a series of hollow, interconnected chambers called ventricles which are filled with cerebrospinal fluid (CSF). The largest of these chambers are the lateral ventricles which are located in the center of the brain (Figure 6). The CSF serves two main functions - it provides the brain with nutrients and it cushions the meninges to protect the brain. Fourth ventricle Lateral ventricles Third ventricle Figure 5: Meninges. The brain is protected in part by the meninges which are fluid filled membranes covering the brain. (A) The meninges have three layers: the pia mater, the arachnoid, and the dura mater. (B) Meningitis results from inflammation of the meninges. Despite these multiple levels of protection, in cases of injury or disease, the CNS is unable to regenerate. What is the role of the meninges? What are two functions of the cerebrospinal fluid? Figure 6: Ventricles. The ventricles are interconnected chambers that are filled with cerebro- Lesson 1.2 spinal fluid (CSF). 10
11 DEFINITIONS OF TERMS Myelin fatty substance that insluates most nerves. White matter portions of the nervous system that appear white in color because they are composed of myelinated axons. Grey matter portions of the nervous system that appear grey in color because they are composed of neuron cell bodies and unmyelinated axons. For a complete list of defined terms, see the Glossary. LESSON READING Your Spinal Cord (CNS) The spinal cord is a long, conical structure, approximately as thick as your little finger. Its main function is to act as a two-way track that collects the sensory information from the periphery to pass it onto the brain, and then to collects the motor responses from the brain to pass onto the somatic and autonomic nervous systems. We can divide the spinal cord into four regions, each controlling a specific region of the body. Starting from the top (Figure 7): The cervical region serves the neck and arms. The thoracic region serves the trunk. The lumbar region serves the legs. The sacral region serves the bowels and bladder. The spinal cord is arranged so the neurons traveling up into the brain and down out of the brain are arranged on the outside. These neurons are coated with a layer of fatty insulation that appears white, called myelin. As we will see later, myelin makes the signals that are transmitted along neurons move more efficiently. Because of this white appearance, this area of the spinal cord is referred to as white matter. The area where connections between the peripheral and central nervous system neurons are made is in the middle of the spinal cord, and lacks myelin. Because of this it appears grey in comparison to the white matter. So, this area is referred to as grey matter. Crossing over B. A. One interesting thing to note about the neurons traveling up and down the spinal cord is that they cross over from one side to another. Because of this cross, each side of the brain receives sensory information from the opposite side of the body. Similarly, the spinal cord output neurons also cross from one side of the body to the other so that each side of the brain also controls the responses of the opposite side of the body. What is the function of the spinal cord? What side of the brain controls the left side of the body? What side of the brain controls the right side of the body? Lesson Brainstem Spinal cord Vertebra Cervical Thoracic Lumbar Sacral Figure 7: The spinal cord. The spinal cord is segmentally arranged. The segments are grouped into 4 major divisions: cervical, thoracic, lumbar, and sacral. (A) The spinal cord is encased in vertebral bone. (B) The spinal cord has pathways along which sensory information can be conveyed to the brain (indicated in red), and motor information can be transmitted from the brain to the body (indicated in blue).
12 LESSON READING Your Brain The brain is also organized into areas of white matter where neurons travel and gray matter where connections between different neurons are made. In addition it can also be divided into distinct areas, each of which perform a specific function. Starting from the region where the spinal cord connects to the brain, these areas are called the brainstem, diencephalon, cerebellum, and cerebrum (Figure 8). We will take a look at each of these areas in turn. What is the function of the following brain structures? What symptoms would you see if they were damaged? Would the patient survive? Medulla The Brainstem Figure 8: Main brain areas. The brain can be subdivided into the brainstem, diencephalon, cerebellum, and cerebrum (or cerebral hemisphere). The brainstem is an evolutionarily old area of the brain where the spinal cord and the brain connect. Part of the brainstem consists of sensory neurons that are traveling into the brain, and motor neurons that are traveling out of the brain. But the brainstem also has its own functions, that divide it into 3 parts, from the bottom, closest to the spinal cord, to the top, closest to the brain itself. The medulla controls breathing, heart rate and digestion. As you can imagine these are critical functions, and it is difficult to survive when the medulla is damaged. The pons (from the Latin that means bridge) is a part of the brainstem that acts like a bus station connecting upper levels of the brain (the cortex) with the spinal cord and a part of the brain called the cerebellum. These connections allow the brain not only to give instructions about which movements to make, but also to monitor those movements as they are happening. Pons Midbrain The midbrain is also involved with coordinating movements. In this case it coordinates eye movement responses to visual and auditory stimulation. Lesson
13 LESSON READING The Diencephalon Moving on upwards, the diencephalon is located at the upper end of the brain stem. It has two parts that perform functions that are critical for life: What is the function of the following brain structures? What symptoms would you see if they were damaged? Would the patient survive? Thalamus The thalamus acts as a relay station (like a post office) where all the major ascending sensory pathways from spinal cord and brainstem connect to neurons destined for the upper parts of the brain in the cortex. There are also reciprocal connections from the cortex to the thalamus. The thalamus is thought to be the first area in the brain where consciousness can be experienced. We ll talk more about the thalamus and how important these connections are when we talk about epilepsy and seizures. The hypothalamus is tiny! Only 1 oz. in adult humans, yet it is the master regulator of homeostasis controlling heart rate, blood pressure, blood composition, eating behaviors, and body temperature to name but a few of its functions. It also links body responses to emotions. We ll talk more about the hypothalamus when we talk about sleep. The Cerebellum The cerebellum lies behind and on top of the pons (Figure 9). It communicates with both the spinal cord and the cortex. The cerebellum monitors how the intention to perform a motor movement compares with how well the movement is actually being executed. It can then adjust the response to make sure the intention is being executed accurately. Amazingly, you are completely unaware of the cerebellum as it works it functions below the level of consciousness. Figure 9:The cerebellum. The cerebellum lies just behind the pons Lesson 1.2 and is critical for controlling motor 13 Cerebellum movements. Hypothalamus Cerebellum
14 LESSON READING The Cerebrum The cerebrum forms the bulk of the CNS (Figure 10). The cerebrum consists the three deep-lying structures surrounded by the cerebral cortex. These three structures also have distinct functions. Cingulate cortex The basal ganglia are involved in the intention to move (like when you re lying in bed and then suddenly you re up, but you haven t consciously jumped out of bed and put your feet on the Hypothalamus floor). The hippocampus is involved with making memories, as we saw with H.M. The amygdala is involved in creating emotional states. It then works with the hippocampus to coordinate the emotional states with the correct hormonal responses (think fight or flight). Corpus callosum Amygdala Hippocampus Cingulate cortex Basal ganglia Hypothalamus Corpus callosum Amygdala Thalamus Hippocampus Cerebral cortex Basal ganglia Thalamus Cerebral cortex Figure 10: The Cerebrum. The cerebrum consists of the cerebral cortex and three deep-laying structures: basal ganglia, hippocampus, and amygdala. The two hemispheres of the cerebral cortex are connected via the corpus callosum. (The thalamus and hypothalamus, which together compose the diencephalon, are also shown for spatial reference.) The outer layer of the cerebrum is called the cerebral cortex. The cortex contains at least 30 billion individual cells. Approximately half are the neurons that transmit information around the nervous system. Just like in the spinal cord the neurons are arranged in layers of white matter where neurons are traveling, and grey matter where they are connecting. In the cortex these layers are alternating. The cerebral cortex is divided into two hemispheres, one on the left and one on the right. Although they superficially look the same they are neither structurally nor functionally symmetrical. Each hemisphere receives sensory information from, and sends motor instructions to, the opposite side of the body. Even though the two cerebral hemispheres perform somewhat different functions, our perceptions and our memories are unified. This unity is accomplished by the corpus callosum, a large band of neurons that travels between corresponding parts of the left and right hemispheres connecting them and providing both sides of the cortex with the same information one world through two eyes. What is the function of the following brain structures? What symptoms would you see if they were damaged? Would the patient survive? Basal ganglia Hippocampus Amygdala Corpus callosum Lesson
15 LESSON READING Each hemisphere of the cortex can be divided into 4 lobes, each of which has a different function (Figure 11): The frontal lobe is concerned with planning for future action and with control of movement. The parietal lobe is concerned with receiving sensory information and with body image. The occipital lobe is concerned with vision. The temporal lobe is concerned with hearing, learning and memory and emotion. What is the function of the following brain structures? What symptoms would you see if they were damaged? Would the patient survive? Frontal lobe Frontal lobe Planning, motor control Temporal lobe Hearing, memory, learning, emotion Brainstem Parietal lobe Sensation, body image Occipital lobe Vision Figure 11: The four lobes of the cerebral cortex. The cerebral cortex is divided into four lobes: frontal, temporal, parietal and occipital. Each lobe has many characteristic folds and grooves. The folds are called gyri (singular gyrus), and the grooves are called sulci (singular sulcus). Together the gyri and sulci increase the area of the cortex considerably increasing the amount of information it can handle. The two most prominent sulci are: The longitudinal sulcus (or fissure) which separates the left and right hemispheres The central sulcus which separates the frontal lobe from the parietal lobe Notably, mammals lower in the evolutionary scale than humans have many fewer sulci and gyri than humans. Parietal lobe Occipital lobe Temporal lobe Lesson Spinal cord Cerebellum
16 LESSON READING Getting information into and out of the brain As we saw before, the brain communicates with the rest of the body via the cranial nerves (that supply the head) and the spinal nerves (that supply the body). These nerves are part of the PNS. Since we ve not dealt with them before, let s end by taking a look at the cranial nerves. There are twelve pairs of cranial nerves that attach to the bottom surface of the brain before they enter it via the brainstem (Figure 12). Many of them deal with sensory and motor functions in the head and neck region in the same way that spinal neurons do. Others convey what we call the special senses (vision, smell and taste and hearing) to the brain. For example, the olfactory sensory neurons transmit olfactory information from receptors in the nose to the brain, while the optic nerve transmits visual signals from the eye to the brain. The optic nerves partially cross before entering the brain at the optic chiasm. Figure 12:The cranial nerves. Twelve pairs of cranial nerves attach to the bottom surface of the brain and innervate the head and neck region. The three we focus on are: olfactory (CNI), optic (CNII), and vagus (CNX). Finally, the vagus nerve is an important autonomic cranial nerve that regulates the functions of organs of the chest and abdomen such as the heart, lungs and digestive system. What are two functions of cranial nerves? If the vagus nerve was damaged what symptoms would you see? Lesson
17 STUDENT RESPONSES What differences are there between your central and peripheral nervous systems? (Be sure to address their overall functions, and ability to regenerate). Remember to identify your sources Given what you know about how your brain controls the function of your body, if you met a stroke patient who had difficulty moving his left leg, what half of his brain was affected by the stroke? Lesson
18 LESSON 1.3 WORKBOOK How can we study the behaving brain? We are in the middle of a technological revolution when it comes to how closely we can look at the behaving brain. Scientists and doctors now have many different options if they want to investigate which parts of the brain are linked with which function they no longer need to wait for a Phineas Gage to show up at their hospital with an iron spike protruding from his head! In this lesson, we ll take a closer look at the most common techniques used to study the behaving brain and investigate their advantages and limitations. How can we study the behaving brain? Two research areas had to come together to allow this technological revolution to occur. Firstly, noninvasive methods had to be developed to visualize the behaving brain. These methods use what doctors call markers chemicals that had some property that can be detected, either because they re radioactive or fluorescent or magnetic. The markers could be injected intravenously and then observed as they enter and accumulate in, specific brain areas. The second area was computing technology. It is only the development of computers with huge capacities for analyzing data that make it even possible to understand what we are seeing when we use the markers to observe the brains. The combination of these two areas into new technologies have allowed researchers to monitor brain function in a healthy patient, as well as to study the location and extent of brain damage while a patient is still living. What two technologies needed to be developed before we could start studying the living behaving brain/ Lesson
19 DEFINITIONS OF TERMS Glucose a simple sugar that is an important energy source throughout the body, but especially in the brain Gamma rays form of electromagnetic wave with shorter wavelength than X-rays For a complete list of defined terms, see the Glossary. LESSON READING Positron emission tomography (PET) Positron emission tomography, also called PET imaging or a PET scan, is a type of brain imaging that uses nuclear medicine. Nuclear medicine is a branch of medicine that uses small amounts of radioactive material to diagnose or treat a variety of diseases, including many types of cancers, heart disease and other abnormalities. PET imaging uses a radioactive chemical called a radiotracer as the marker. It is noninvasive, and with the exception of the intravenous injection that delivers the radiotracer to the bloodstream, is painless. When getting a PET scan, patients first receive an intravenous injection of the radiotracer usually radioactive glucose. After the injection, the radioactive glucose accumulates in tissues that are highly active, like the brain. Once the radiotracer becomes concentrated in these tissues, it gives off energy in the form of gamma rays. The assumption is that the tissues that are most active will accumulate the most tracer and therefore will show higher levels of radioactivity. Eventually the radioactive glucose is broken down and leaves the body. The dose of radiation given is harmless. To detect the varying levels of radioactivity in different parts of the brain, the patient s head is placed in a machine that contains a camera that can detect gamma rays (otherwise known as positron emission, hence PET scan). The camera is connected to a computer that collects information about which regions of the brain have taken up the most radioactive glucose. As the computer accumulates the information the camera scans different areas of the brain. Together the camera and computer produce a picture that looks like a slice through the brain, showing the level of radioactivity that have accumulated in the brain regions found in that slice, or section. Figure 13 shows a PET scan of a horizontal section through the brain of a resting 54-year-old man. The computer has colored the image to relate color directly to the tissue concentration of radioactivity: red indicates areas of higher concentrations, and blue indicates areas of lower concentrations. Notice that high levels of radioactivity are present in the cortex. Figure 13: PET scan taken from a normal brain. The areas indicated in red show high activity and the areas in blue show What does a PET scan measure and how? In a PET scan, what do the warm colors usually represent? What about cool colors? Lesson 1.3 low activity. 19
20 DEFINITIONS OF TERMS Glucose a simple sugar that is an important energy source throughout the body, but especially in the brain. Gamma rays form of electromagnetic wave with shorter wavelength than X-rays. Hemoglobin protein responsible for transporting oxygen in the blood. Deoxyhemoglobin hemoglobin once it has delivered oxygen to body tissues. For a complete list of defined terms, see the Glossary. LESSON READING Figure 14 shows a PET scan of a horizontal section through the brain of an Alzheimer s patient. This scan shows reduced activity in the parietal lobe compared to either the frontal lobe or the occipital lobe. Remember that the parietal lobe is involved in language, which suggests that this patient will have had difficulties in language processing. Figure 15: PET scan taken from a patient with brain cancer. Notice the areas of heightened metabolic activity (indicated with red arrows) and yellow/red coloration. PET scans are also able to detect the origins of seizures, which show up as areas where metabolic activity is low. In Figure 16 there is an area of low accumulation of radioactivity, and hence low metabolic activity, in the parietal lobe that could be due to a seizure. Figure 14: PET scan taken from a patient with Alzheimer s disease. Notice the reduced activity in the parietal lobe (indicated with red arrow) and blue coloration. PET scans are good at finding areas of high metabolic activity where it does not belong, and thus have been successfully used to detect cancer in the brain, since cancer cells, because they are dividing rapidly are very active. The yellow/red colors in Figure 15 indicate an area of high metabolic activity detected by the radioactive glucose, and unfortunately for the patient, the location of a brain tumor. Figure 16: PET scans taken from a patient with epilepsy. Notice the area of reduced activity in the parietal lobe (indicated with red arrow) and blue coloration. Why would an Alzheimer s patient have a PET scan with more areas colored in cool colors? Why would a brain tumor show up as a hot spot on a PET scan? Lesson
21 LESSON READING The major disadvantage of PET scans is what is known as spatial resolution, i.e. the ability to detect small areas of the brain. This means that very small abnormalities less than 1 mm in size may be difficult to distinguish from the blurs simply caused by the patient shifting position. As you can imagine, even 1mm of brain may contain thousands of neurons, hence certain abnormalities, such as small areas of damage causing seizures, can be missed. Another problem is false positives, i.e. areas that look like they have high areas of radioactivity, but are also artifacts. Finally, the amount of radiotracer that can be safely injected into the body is obviously limited, and this in turn can make it difficult to see different areas that have rather low metabolic rates. Other problems with PET scans are that they must be completed when patients are awake. The tracer takes between 30 and 60 minutes to reach the appropriate area in the body, and the scanning process, during which they patient has to stay still, takes an additional 45 and 60 minutes. Therefore, patients with limited mobility or difficulty remaining still for long periods of time may find the PET scan process uncomfortable or impossible. A final disadvantage of PET scans is their cost. For obvious reasons of safety, the radioactive tracers used need to be able to decay and lose their radioactivity very quickly. But because the chemicals decay so quickly, they must be produced fresh each time they are used, in an atomic particle accelerator called a cyclotron. Therefore, the cost of the cyclotron and the salaries of the personnel who operate it must all be added the cost of the PET scanner. List three disadvantages of PET scans. What is the major difference between the PET method and MRI? Magnetic resonance imaging (MRI) Magnetic resonance imaging, also called MRI, is another noninvasive method that is able to image internal structure in amazing detail. It is based on the principle that the body is largely composed of water molecules. Each of these water molecules has two hydrogen nuclei or protons. When a person is put inside a scanner with a powerful magnetic field, some of these protons align with the direction of the field. Then a radio frequency transmitter is briefly turned on, producing a second electromagnetic field. This radiofrequency (RF) field has just the right energy to flip the spin of the aligned protons in the body, so that after the RF field is turned off, those protons that absorbed its energy and flipped revert back to their original state by releasing a photon. The scanner detects the released photons as an electromagnetic signal, similar to radio waves. The protons in different tissues return to their original (equilibrium) state at different rates. These different rates can be detected by the MRI scanner. Figure 17 shows a What does MRI measure, can you explain how? picture of an MRI scanner. Because of the extremely Lesson 1.3 high magnetic fields, it is critical that no ferrous (mag- Figure 17: MRI scanner. 21 netizable) metal is near the scanner.
22 DEFINITIONS OF TERMS Hemoglobin protein responsible for transporting oxygen in the blood. Deoxyhemoglobin hemoglobin once it has delivered oxygen to body tissues. For a complete list of defined terms, see the Glossary. LESSON READING The computer uses the differences in when and where photons are released as the protons flip back at different rates to create an image of different tissues. While MRI can be used to image every part of the body, it is particularly useful for tissues with high concentrations of water and therefore many hydrogen nuclei, such as the brain, muscle, connective tissue and most tumors. These areas of low density show up as high contrast, while areas of high density, like bone, have much lower contrast. Because the brain in particular has a very high water concentration and low density, MRIs reveal brain structures at extremely high resolution. Figure 18 shows an MRI image of a sagittal section (slice) through the brain. The corpus callosum connecting the two hemispheres can be seen clearly. Functional MRI (fmri) Figure 18: MRI scan of brain. Structural MRI provides good contrast between the different soft tissues of the body, making it especially useful for brain imaging. Functional MRI (fmri) is a variation of the MRI principle that measures the magnetization of oxygenated hemoglobin and deoxyhemoglobin rather than water in order to study brain activity. When brain activity increases there is an increased demand for oxygen, and the vascular system responds by increasing the amount of oxygenated hemoglobin relative to deoxyhemoglobin. Oxygenated hemoglobin increases the MRI signal just like magnetized water does, while deoxyhemoglobin decreases the MRI signal relative to the oxygenized hemoglobin signal. Therefore if blood flow in a specific area is increased the MRI signal in that area is also increased proportionately to the neuronal activity in that area. This is called the BOLD signal (Blood-Oxygen-Level-Dependent) signal. To detect a BOLD signal an area of the brain is scanned very rapidly (typically once every 2 3 seconds). Figure 19 shows an fmri image of a horizontal section through the brain after a subject had been asked to read a single word. Why are MRIs not as useful to study bone as brain? What is the difference between MRI and fmri? What are is the main advantage of fmri compared to MRI? _ Figure 19: fmri scan. One fmri section through the brain of a person who had been Lesson 1.3 asked to read one word aloud. The regions 22 indicated in red are areas of high activity.
23 LESSON READING What are the benefits and drawbacks of using MRI/fMRI scans? MRI scans are good at detecting metabolic activity where it does not belong, and thus have been successfully used to detect cancer in the brain. Figure 20 shows images of a coronal section through the back of the brain, the light-colored regions show areas of high metabolic activity, and unfortunately for this patient, the location of a tumor. Note that MRIs show the left hand side of the brain on the right and vice versa. Like PET scans, MRI shows a composite picture of many thousands of neurons, and so its spatial resolution, like PET is also very low. Additionally, its temporal resolution (its resolution in time) is also slow and this is problematic. fmri measures brain activity indirectly, making the assumption that areas of highly oxygenated blood correlate with areas where neurons are very active is reasonable. However it may be difficult to pinpoint what those pictures of areas of high blood flow are really showing: The blood flow response to a specific area of the brain takes about two seconds to occur, but as we know a thought can happen in thousandths of a second. So it s difficult to say what a picture of a rush of blood to an area actually means. The timing issue comes up again and again when researchers attempt to study how brain regions involved in complex behaviors communicate. Communication between brain regions Figure 20: MRI scan of patient with brain cancer. The light colored areas indicate the presence of a tumor. can occur very quickly - within a hundredth of a thousandth of a second but the increased blood flow that this increased activity would occur far too sluggishly for MRI to detect it. So, what is the increased blood flow actually measuring the event itself or the brain s slower response to communication which happened a while ago, maybe somewhere else? The analogy that has been made is that it s like trying to understand the process of photosynthesis in plants by measuring how much sunlight a tree or plant is getting. You ll see the tree grow or plant shrink based upon sunlight, but you re still not really much closer to understanding how photosynthesis actually occurs. How do you think MRI scans detect areas of high metabolic activity? What is fmri actually measuring? What are the implications of this for investigating complex behaviors like reading? Lesson
24 DEFINITIONS OF TERMS Glucose a simple sugar that is an important energy source throughout the body, but especially in the brain Gamma rays form of electromagnetic wave with shorter wavelength than X-rays Hemoglobin protein responsible for transporting oxygen in the blood Deoxyhemoglobin hemoglobin once it has delivered oxygen to body tissues For a complete list of defined terms, see the Glossary. LESSON READING Electroencephalography (EEG) Electroencephalography (EEG) examines the brain much more directly. It involves applying a set of electrodes on the scalp and then detecting the electrical activity of brain beneath them. In conventional EEG, the electrodes are placed on the scalp with a conductive gel or paste that ensures a connection that will transmit the signal. Some systems use individual electrodes, others (Figure 21) use caps or nets into which the electrodes have been embedded. In most clinical applications the cap consists of 19 recording electrodes placed in standard positions (Figure 22) that are distributed over specific brain regions on the cortex such as frontal (F), parietal (P), temporal (T) and occipital (O) (plus ground and system reference). Brain activity between the pairs of electrodes is then detected. Figure 22: Placement of EEG electrodes. The electrodes are placed in stereotyped positions so that the current flow between specific regions in the cortex can be measured. Figure 21: EEG cap containing electrodes to record brain activity. Each electrode is connected to one input of an amplifier that can amplify the voltage between the active electrode and the reference electrode (typically 1, ,000 times voltage gain). The digital EEG signal is stored electronically and can be filtered for display. A typical adult human EEG signal is about 10 microvolts (µv) to 100 microvolts (µv) in amplitude when measured through the scalp and this is increased a thousand fold to about millivolts (mv) if a hole is drilled in the skull and the electrodes are placed directly on the cortex (this is sometimes necessary to detect epileptic seizures). You can watch an EEG being done online - see this unit on the student website or click below: What does EEG measure? What are two differences between EEG and PET scans? Between EEG and MRI? Lesson 1.3 Video: Measuring Brain Waves with an EEG (Electroencephalogram) 24
25 LESSON READING What does EEG actually measure? As we know, the brain is composed of billions of neurons that communicate electrically (we ll see how in more detail later). The communication between individual neurons is called the synaptic potential. The synaptic potentials generated by single cortical neurons are far too small to be picked up by the EEG. Rather the EEG reflects the sum of the communication between the thousands or millions of neurons between each pair of electrodes. This is why each EEG trace is reported directionally (P3 - T5 [parietal 3 - temporal 5] for example). Because each pair of electrodes samples the activity of a population of neurons between the electrodes in different brain regions, each of the individual EEG traces will be different (Figure 23). Figure 23: Normal EEG. An EEG taken from a healthy patient. Notice how each trace (wavy line) is coded as to what pair of electrodes it was recorded from we ll talk more about that later. Scalp EEGs show waves that have characteristic frequencies that correspond to different states of brain functioning (e.g., waking and the various sleep stages, Figure 24). The neurons that are communicating to cause some of these characteristic waves are well known - for example connections from the thalamus to the cortex are known to generate the so-called theta waves seen during sleep. Others are not for example the neurons that are responsible for the so-called occipital waves are not well understood at all. What are the two characteristics of and EEG scan? _ What behaviors do the following EEG brain waves detect? alpha (α) _ beta (β) _ theta (θ) _ Figure 24: Typical EEG waves. The EEG shows typical patterns of activity that can be correlated with various stages of sleep and wakefulness. α waves originate from occipital cortex when the eyes are closed, β waves are associated with intense mental activity, θ waves are associated Lesson 1.3 with drowsiness, δ waves are associated with 25 the deepest stages of sleep. delta (δ) _
26 DEFINITIONS OF TERMS Glucose a simple sugar that is an important energy source throughout the body, but especially in the brain Gamma rays form of electromagnetic wave with shorter wavelength than X-rays Hemoglobin protein responsible for transporting oxygen in the blood Deoxyhemoglobin hemoglobin once it has delivered oxygen to body tissues For a complete list of defined terms, see the Glossary. LESSON READING What are the benefits and drawbacks of EEG recordings? Clinically, EEGs are very commonly used to monitor for seizure activity, to evaluate depth of anesthesia or coma, and to test for brain death. The major advantage of the EEG is obviously how simple it is: EEG is totally non-invasive and unlike PET and MRI, EEG does actually directly measure the electrical behavior of populations of neurons. Moreover, EEGs can detect changes that occur over milliseconds, which is much closer to the time scale of actual neuronal communication and much faster than either PET or MRI. A major disadvantage of the EEG is its poor spatial resolution, which is worse than either PET or MRI. Placement of the electrodes means that each pair of electrodes may be measuring activity over several centimeters room enough for thousands if not millions of individual neurons. Another disadvantage is that the relationship between the activity of neurons and what is depicted on the EEG trace is quite complex: Not only does the trace between a pair of EEG electrodes represent the sum of the activities of thousands of neurons, but those electrodes will only detect neurons that are all communicating at the same time (synchronously) because it can t detect individual neurons. In order to communicate (fire) synchronously these neurons need to be to be aligned in the same direction, i.e. to have similar spatial orientation. If the neurons don t line up they won t create the waves of electrical activity that the EEC electrodes detect. Neurons connecting the thalamus and the cortex (thalamocortical neurons) have these characteristics, as do neurons extending from the cortex to the spinal cord, but many other neurons do not, and so they will never be detected by EEG. Another problem with EEG is that activity from deep within the brain is more difficult to detect than currents near the skull. This is because of the simple electrical principle of the square rule that voltage fields decline with the square of the distance. So in cases where activity deeper in the brain needs to be measured, a hole must be drilled in the skull, which is very invasive Could you measure the behavior of the basal ganglia with an EEG? If you wanted to measure H.M. s seizures using an EEG, what would you have had to do first? Lesson
27 STUDENT RESPONSES Which of the described imaging techniques (PET, MRI/fMRI, EEG) would you choose if you had to examine a new-born baby who you suspected had been born with structural abnormalities in their cerebellum? Remember to identify your sources Which of the described imaging techniques (PET, MRI/fMRI, EEG) would you choose if a patient came to your surgery with a bad headache, and you suspected they might have brain cancer? Which of the described imaging techniques (PET, MRI/fMRI, EEG) would you choose if a patient came to your research lab with a severe case of anterograde amnesia and you wanted to diagnose where the deficits originated from. What tests would you do? Would you completely trust the results? Lesson
28 DEFINITIONS OF TERMS Sensation immediate and basic experience generated as sensory stimuli fall on our sensory systems. Perception the higher-order process of integrating, recognizing, and interpreting complex patterns of sensations. For a complete list of defined terms, see the Glossary. LESSON 1.4 WORKBOOK How do our brains interpret the environment? Every day our brains are bombarded with simple and complex sensory stimuli that they need to process, interpret and filter. In this lesson you ll experience firsthand how the brain senses our environment, and also how sensations can be interpreted and processed, and in some cases, fool our brains. How do our brains interpret the environment? Ask someone what the ultimate function of the brain is, and they ll often answer with thinking or reasoning, or remembering, or sensing or perceiving. Certainly the nervous system performs all these functions, but they all support one fundamental function to control your body. So the basic goal of sensation and perception is to inform us of what is happening in our environment so that our behaviors can adapt in a useful way. Sensation and Perception As you read this text, you are demonstrating extraordinary sensory and perceptual abilities. Your eyes move along this page at a steady pace, identifying letters and words so fast as to defy explanation. If you re like most people, you tend to take sensation and perception for granted because you can see, hear, touch, smell and taste so naturally and automatically. You open your eyes and see; you put a morsel of food in your mouth and taste what could be simpler? Perception, however, is a complex puzzle that has intrigued researchers for centuries. Before we go any further we need to define our terms because they have different meanings that ultimately reflects how they are controlled: Sensation refers to the immediate and basic experiences generated as stimuli fall on our sensory systems: Perception involves the interpretation of those sensations, organizing them to give them meaning. If you had to describe what the ultimate function of your brain is, what would you say? What is the difference between sensation and perception? Lesson
29 DEFINITIONS OF TERMS Perceptual illusions perceptions that are inaccurate representations of sensory stimuli For a complete list of defined terms, see the Glossary. LESSON READING Our sensory systems Our five basic senses are vision, hearing, taste, smell and touch. All five sensory systems receive information from the environment through specialized cells at the surface of the body and then transmit this information along peripheral sensory nerves to the central nervous system. There the information is decoded to form a perception and used for three main functions: Controlling movement Regulating the function of internal organs Maintaining arousal. While we tend to think of sensation as a conscious experience, not all sensory information reaches consciousness. When we withdraw a hand after touching a hot surface, the sensory information drives the motor response automatically even before we are consciously aware that the surface is hot. Our sensory systems perform incredibly well at gathering information about our environments. All of the sensory systems are able to operate in a range of environments. For example, you can see in extremely bright sunlight and to a degree, in moonlight even though the light from the bright sun is 100 million times brighter than that from the moon! Our sensory systems are also well adapted to humans specific needs. For example, our visual system is especially competent at detecting motion by other humans, and our hearing is particular sensitive to the frequency range of the human voice. Perceptual Illusions As good as our senses are they can occasionally be led astray by particular stimuli. For example, look at Figure 25. Do the two horizontal lines appear to be equal in length, or is one longer than the other? We can learn about how our senses function by examining cases like this in which they fail to provide us with accurate information - perceptual illusions inaccurate perceptions. After measuring the length of the lines in Figure 26, does one still appear to be longer than the other? Why do you think that might be? Our perceptions cannot always be trusted because they can be distorted by the components of an object, or by its surroundings. In the case of the lines in Figure 25 the pairs of lines attached to the end fool the brain, which adds more length to the line where the ends diverge. So our brains are the final arbiter, deciding on the truth. Because of this we can learn about our brains by studying how different per- Lesson 1.4 ceptual illusions trick our brains into delivering an imaginary 29 truth. Figure 25: Mueller-Lyer illusion. The two horizontal lines seem to differ in length, but their length is actually the same. Don t believe us measure it yourself.
30 LESSON READING Optical Illusions Perhaps the most common perceptual illusions are optical. Optical illusions take advantage of basic weaknesses in the visual system. Until recently, visual perception was often compared to how a camera operates because, like the lens of a camera, the lens of the eye focuses an image on the retina. This analogy falls far short of what vision really does, which is to create a three-dimensional perception of the world that is significantly more complex than the two-dimensional image projected onto the retina. A. Ambiguous pa-ern B. Law of similarity C. Law of proximity Figure 26: Visual patterns. (A) The array of identical dots can be seen alternatively as columns or rows. (B) Similarities in appearance of some of the dots create a strong pattern of columns (top) or rows (bottom). (C) Spatial arrangement alone determines whether we see vertical (top) or horizontal (bottom) pattern. The visual system creates perceptions by following certain innate laws that govern how it recognizes pattern, shape, color, distance, and movement of objects in the visual field. These laws of perception can be illustrated with examples of visual patterning: Consider the array of dots in Figure 26A. The dots are equally spaced, yet the brain organizes them so that they look like they are either in rows or in columns. Whether we perceive one pattern rather than the other is due to the laws of similarity and proximity. Thus, if some of the dots in one direction look similar there is a tendency to apply a pattern to all the dots that takes that similarity into consideration (Figure 26B). Likewise, if some of the dots in one direction are brought closer together, the brain will apply a pattern that takes into consideration that proximity (Figure 26C). This process of perceptual organization is continuous and dynamic, as illustrated with the well-known picture showing figures on a background apparently alternating (Figure 27). The image can either be seen as two white profiles against a black background, or as a black vase against a white background, but it is almost impossible to see both images simultaneously. This winner-take-all strategy illustrates another principle of visual perception: only part of the image is selected as the focus of attention, while the rest becomes submerged into the background. Optical illusions, which misread the visual information sent to the brain, demonstrate how the brain imposes certain assumptions it has Figure 27: Face or vase illusion. We sometimes see a pair of faces, sometimes a vase. A perceptual decision must be made between what is the figure and what is the background. By focus on the figure (face or vase) What other illusions have you experienced? Why do you think it was that they tricked your brain? _ Lesson 1.4 about the visual world to the objective sensory information it receives. we cause the other to recede into 30 the background.
31 LESSON READING What brain areas are involved in creation of illusions? Many perceptual illusions are the result of our brains trying to reconcile conflicting sensory information. Two areas in particular are involved (Figure 28). The frontal lobe helps resolve conflicts between sensory inputs (such as the two figure illustration in Figure 27). The insular cortex (which is buried deep inside the cerebral cortex near the hippocampus) is responsive to discrepancies between what we see and what we touch (such as when we expect something to be light based on what it looks like, and then it turns out to be heavy). Are there any practical applications for sensation and perception? Sensation and perception also have numerous practical applications in schools, medicine and industries. Reading teachers can apply what we ve learned about eye movements and letter identification to help students learn to read. Physicians can use information about how to reduce the perception of pain to help their patients and designers can use information about color and size in home decoration. See this unit on the student website or click below to watch the following TED talk about how optical illusions help us learn how we see. Answer the question: It s an illusion or is it? Video: Beau Lotto: Optical illusions show how we see Figure 28: Processing conflicts. Our brains relay on the frontal lobe, located at the front of the brain, and insular cortex, located inside the brain, to help resolve conflicts between incoming sensory information. What brain areas are responsible for decoding sensory illusions? Lesson
32 DEFINITIONS OF TERMS Aphasia deficit in the ability to use or comprehend language caused by brain damage. Broca s area area of left frontal lobe that is critical for the production of speech. For a complete list of defined terms, see the Glossary. LESSON 1.5 WORKBOOK How do the parts of our brains work together? Now that we re becoming more familiar with all the different parts of the nervous system, let s turn our attention to one example of how all these different parts work together to create complex behaviors. Maybe one of the best illustrations is to analyze how the brain manages language, the highest and perhaps the most characteristically human mental function. Looking at language Much of what we know about language comes from the study of language disorders or aphasias most often found in patients who have suffered a stroke that has destroyed specific areas of their brains. The last half of the nineteenth century produced an explosion of research that gave us our most important discoveries about how and why aphasia occurs. When we look at all these studies together, they tell an exciting story of how we got our first insight into how complex mental function actually had a simple biological basis. Paul Broca In 1861, the neurologist Paul Broca (Figure 29) described one of his patients who could understand language perfectly, but could not speak. The patient had no defects to his tongue, mouth or vocal cords, but he could only utter isolated words (in fact his nickname was Tan because that was one of the few words he could say). He could whistle and sing a melody, but he could not use the isolated words grammatically, create complete sentences nor express his ideas in writing. After he died, postmortem examination of his brain showed damage in the posterior region of the frontal lobe. This region became known as Broca s area (Figure 30). Figure 29: Paul Broca ( ). Broca was the first neuroscientist to really examine how the structure of the Would a patient with Broca s aphasia be able to understand the question What is your name? How might they answer the question? Lesson 1.5 brain contributes to complex functions. 32
33 DEFINITIONS OF TERMS Wernicke s area area of the temporal lobe that is critical for understanding language For a complete list of defined terms, see the Glossary. LESSON READING Broca studied a further 8 patients, all of whom had the same symptoms, and all of whom had damage in the same area of the left cerebral hemisphere near the frontal cortex when their brains were autopsied. This discovery led Broca to state: We speak with the left hemisphere! You can watch a teenage girl, Srarah, with Broca s aphasia online - see this unit on the student website or click below: Video: Broca s aphasia - Sarah Scott - teenage stroke Figure 31: Carl Wernicke ( ). Wernicke noticed that not all language deficits were the result of damage to Broca s area. Carl Wernicke In this case the damage was located in the posterior part of the temporal lobe where it joins the parietal and occipital lobes. This region became known as Wernicke s area (Figure 32), and Wernicke might have said (but he didn t) We understand language at the back of the left Figure 30: Broca s area. Broca s area is situated next to the part of the frontal lobe that controls movement. The next step was taken in 1876 by Carl Wernicke (Figure 31). He described another kind of aphasia. Wernicke s aphasia involved a failure to understand what was being said or written, rather than speak. While Broca s patients could understand language but not speak, Wernicke s patients could speak, but could not understand the language they heard. Their conversations were fluent, but unintelligible. Would a patient with Wernicke s aphasia be able to understand the question What is your name? How might they answer the question? What does the part of the brain that Broca s area is found in control? What about Wernicke s area? Figure 32: Wernicke s area. Wernicke s area is located where the parietal and tem- hemisphere! poral lobes meet. It encircles the auditory Lesson cortex.
34 LESSON READING You can watch a patient with Wernicke s aphasia online - see this unit on the student website or click below: Video: Wernicke s aphasia Wernicke was the first to appreciate that different components of a single behavior are processed in different regions in the brain. His theory proposes that language involves separate motor and sensory programs, each governed by several regions of the cortex (Figure 33). A motor program that controls the movements of the mouth, tongue, palate and vocal cords is located in front of the motor area in Broca s area. Wernicke s area A sensory program that controls word perception is located in the temporal lobe area in Wernicke s Area. This area is surrounded by the auditory cortex, as well as the areas that integrate auditory, visual, and touch sensation into complex perceptions and that are therefore known as association cortex. Wernicke s model for the organization of language has been elaborated on over the years but is still in use today. According to the most up-to-date model, language is processed in a specialized pathway that involves several areas of the brain, as follows: The initial perceptions of language are formed in separate sensory areas of the cortex specialized for hearing words (auditory cortex) or reading words (visual cortex). These perceptions are then conveyed to an area of the association cortex called the angular gyrus that is able to transform auditory and visual information into a single code that is shared by both speech and the written word. From the angular gyrus this code is conveyed to Wernicke s area, where it is recognized as language and associated with meaning. Without that association, the ability to comprehend language is lost. The common neural code is then relayed from Wernicke s area to Broca s area, where it is transformed into a motor representation that can lead to either to spoken or written language. What pathways through the brain are activated when someone says Hi! to you and you reply. Draw them out. What pathways through the brain are activated when you read this message: Say Hi out loud. When this last stage, where the single code is transformed to a spoken or written motor representation cannot take place, the ability to express language is lost. Lesson Broca s area Motor cortex Figure 33: Language processing. Both Wernicke s and Broca s areas contribute when we hear a spoken word and then repeat it.
35 DEFINITIONS OF TERMS Distributed processing theory suggesting that information is processed in several different parts of the brain. Conduction aphasia language disorder in which patients can understand language, and speak without any problem, but they omit parts of words or substitute incorrect words. For a complete list of defined terms, see the Glossary. LESSON READING Using this reasoning and proposed neural pathway, Wernicke correctly deduced that a third type of aphasia must exist, that would result if the connection between Broca s and Wernicke s area is damaged. He predicted that patients with conduction aphasia would be able to understand language and would also be able to speak, but that they would not be able to use words correctly. Indeed patients with conduction aphasia can understand words they hear and read perfectly, and can also speak and write quite fluently, yet, they cannot speak coherently. They omit parts of words or substitute incorrect sounds. They are painfully aware of their errors, but unable to put them right. Our current understanding of language processing Figure 34: PET scans of language areas. PET scans taken while subjects were hearing, seeing, speaking and thinking about words. Only when patients were listening to words, did their Wernicke s areas show activity. The PET scans taken while the subject was seeing, speaking and thinking show activation of the occipital cortex, Broca s area and frontal lobes. Until recently, everything we knew about language came from studies of patients who had suffered brain damage. Now PET and fmri imaging let us look at language in behaving uninjured, healthy people. PET scans show where individual words are coded in the brain of healthy subjects when words are read or heard (Figure 34). The data shows that not only are reading and listening processed separately, but the mere act of thinking about a word s meaning activates still a different area in the frontal cortex. Thus, language processing occurs in parallel in a number of different areas as well as in serial via Wernicke s and Broca s areas. Wernicke s discoveries also provided the first evidence for distributed processing, which is the important concept that different types of information are routed to a number of different areas in the brain in order to organize a response. This evidence and studies using PET scans and fmri has led to the current thinking that our brains organize language using a modular format that consists of processing centers each having more or less independent functions, that are connected together in serial and in parallel. We now appreciate that all cognitive abilities, not just language, are constructed using a similar format. This means that while specific brain regions are concerned with simple processing operations, complex functions like perception, movement, thought, and memory are all made possible because several brain regions, each with their own specific function, are linked together in serial and in parallel. As a result, damage to a single area need not result in the loss of an entire behavior. Even if a behavior initially disappears, Would a patient with conduction aphasia be able to understand the question What is your name? How might they answer the question? If Wernicke s area wasn t activated when we read words, does that mean we need to hear words in order to understand them? Lesson 1.5 it may partially return as undamaged parts of the same functional module reorganize their linkages. 35
36 STUDENT RESPONSES Remember to identify your sources We have leearned that many areas of our brain are involved in complex behaviors. Do you consider that this is a good or a bad thing when you are thinking about cases of brain injury or disease? What could it mean in terms of patient recovery? Lesson
37 Unit 2: What are the building blocks of our brains? Overview In the last unit we discovered that complex brain functions occur as individual structures in the brain work together like an orchestra. We also discussed one of the limitations of our new visualization techniques that they only sample populations of hundreds or thousands of neurons, so they don t give us any information about how the individual cells of the nervous system work together. So now we re going to take another step back and dial down our focus to the primary building blocks of our brains, the neurons and the glial cells. In this unit we will explore how these basic cells are built and how they work, and importantly what can go wrong when these building blocks are diseased and their functions are compromised. Remember our graphic from the beginning of this workbook? This unit focuses on the neuron, which is the building block of our brains.
38 DEFINITIONS OF TERMS Neuron cells of the nervous system that are specialized for the reception, conduction and transmission of electrochemical signals. For a complete list of defined terms, see the Glossary. LESSON 2.1 WORKBOOK What is the structure of a neuron? This unit introduces you to the building blocks of our brains: neurons and glia cells. In this lesson, we will begin our exploration of how the brain is put together by investigating why neurons have such complex structures and how these structures allow the neurons to perform highly specialized functions What are neurons? Neurons are the most important functional cells in our nervous system. The adult human brain contains roughly 86 billion individual neurons. Each neuron is interconnected, forming a precise network. Within that network neurons are assembled into many different kinds of functionally distinct regions (like Broca s area for example). As we saw in the last lesson these regions interact with each other to produce our perception of the external world, to fix our attention on the responses that need to be made, and to control our bodily functions. Our first step in understanding the brain, therefore, has to be to understand the neuron how it is put together and how it works. Neurons are cells with highly complex structures, much more complex than any other cell in the body. Wiggle your big toe. The neuron that controls that wiggle starts off in the spinal cord somewhere in your upper chest and ends up at your big toe, a distance that would be tens of meters if you were a giraffe (which don t have toes, but whatever, you get the point). Neurons are different from other cells in a number of ways especially because, unlike most cells, neurons don t divide the number of neurons you had when you are born is the maximum you will ever have. This means that when a neuron is damaged the only possibility you have to restore its function is to fix it, you can t simply make another one to take its place, like you could in the liver. In the peripheral nervous system you can fix damaged neurons so that they ll grow slowly back to make their original connections. The central nervous system is different. When a CNS neuron is damaged it cannot regrow long distances to repair its connections. Why? No one really knows. (Interestingly, CNS neurons can grow in lower vertebrates like fish). One potential reason why our CNS neurons aren t able to regrow lays in the hypothesis that all of our complex behaviors demand a neuronal network with a very precise architecture. Meaning that, CNS neurons have had to trade off the ability to regrow, so Can neurons in the PNS repair themselves? What would this mean in regards to recovery after an injury to the PNS? _ Can neurons in the CNS repair themselves? What would this mean in regards to recovery after an injury to the CNS? _ that the network remains stable. Even so, some nervous system damage can be repaired if we can induce Lesson 2.1 neurons to rewire over short distances. 38
39 DEFINITIONS OF TERMS Cell body part of the neuron containing the nucleus, but not including the axon and dendrites. Also called the soma. Endoplasmic reticulum organelle in the cell that forms a network of tubules and vesicles. It functions to synthesize proteins and lipids as well as metabolize carbohydrates. Nucleus the DNA containing structures of cells. For a complete list of defined terms, see the Glossary. LESSON READING Neurons have three distinct functional regions The typical neuron contains three different regions, each of which looks different and each of which has its own specialized function (Figure 1). These regions are: The cell body The dendrites The axon The cell body The cell body (also sometimes called the soma) is the metabolic center of the neuron (Figure 2). It contains the nucleus, which stores the genes of the cell in chromosomes, and the smooth and rough endoplasmic reticulum, which are the sites where proteins are synthesized. It also contains the lysosomes that degrade proteins that have become old or damaged. Because the ribosomes are mostly concentrated in the cell body, protein synthesis primarily occurs there and in the dendrites that are closest to it. Because of this, a major role of the cell body is to package the proteins it has made so they can be transported over long distances down the leg and into the foot to our big toe (or our little finger etc.). Similarly, because the cell body is also the site were lysosomes are concentrated, any big toe protein that has reached its sell-by date needs to be transported back up the leg to the cell body for destruction. Keeping all the parts of the neuron supplied with protein is a major task carried out by the cell body. Dendrites What are the three functional regions of the neuron? Name two important functions carried out by the neuron s cell body. _ Lesson Cell Body Ini2al Segment Presynap2c cell Axon Synapse Postsynap2c cell Figure 1: Neuron structure. Neurons have three distinct regions: the dendrites, the cell body, and the axon. Figure 2: Cell body. The cell body is the metabolic center of the cell and contains all the cellular organelles required to support cell life: the nucleus, mitochondria, ribosomes, rough and smooth endoplasmic reticulum.
40 DEFINITIONS OF TERMS Dendrites branched projection(s) of a neuron that functions as the receptive area of a neuron. Dendritic spines tiny spikes of various shapes that are located on the surfaces of many dendrites and are the sites of synapses. For a complete list of defined terms, see the Glossary. LESSON READING We can identify two types of outgrowths sprouting off from the cell body, the dendrites and the axon. The dendrites Most neurons have several dendrites (Figure 3). These dendrites branch out from the cell body in a shape that makes them look like a tree. In fact the dendrites are often called the dendritic tree. The dendritic tree is the main region of the neuron that receives signals. These signals can come in the form of sensations from the environment. Alternatively, in the depths of the neuronal network they may come from other neurons. The role of the dendrites is to convert these signals, which may be in the form of physical signals if they are from the environment (such as light, sound or touch) or chemicals if they are from other neurons, into an electrical signal. Dendrites do this by changing the electrical properties of their membranes via depolarization or hyperpolarization. We will talk more about the important processes of depolarization and hyperpolarization later on in this unit. Each of our sensory systems contains unique neurons that are specialized to detect specific types of sensory stimuli in the environment. The dendrites from these neurons are able to convert these stimuli into a neural response that the brain can understand. For example, different types of sensory dendrites in our skin are uniquely tuned to detect changes in pressure. They then convert the physical sensation of pressure into a neural response by depolarizing or hyperpolarizing their membranes. Figure 4: Dendritic spines. Dendrites have small protuberances called spines. Each spine can contain a synapse. The branches of the dendritic tree often have many hundreds of thousands of little twigs that we call dendritic spines because they look like spikes (Figure 4). Each dendritic spine usually contains one synapse, which is an exact area where the dendrite can receive a signal, whether from the environment or from another neuron. You can appreciate that if a single dendritic tree has hundreds of thousands of spines, then it can have hundreds of thousands of different inputs. Remember that there are also 86 billion neurons makes you appreciate Lesson 2.1 that trying to understand how everything is connected is a massive task. No wonder neuroscientists were 40 excited by the development of supercomputers! Figure 3: Dendrites. The dendritic arbor of two neurons (a Purkinje neuron on the left, and a sensory neuron on the righ) illustrating the extensive branching of dendrites.. What is the function of the dendritic tree? Which kind of neuron has more inputs: a neuron without dendritic spines, or a neuron with dendiritc spines? Why? _
41 DEFINITIONS OF TERMS Action potential the electrical signal of the axon. Axon projection of a neuron that functions to conduct electrical impulses away from a neuron s cell body. Presynaptic cell neuron located before the synapse, and thus sending the signal Postsynaptic cell neuron located after the synapse, and thus receiving the signal For a complete list of defined terms, see the Glossary. LESSON READING The axon The other type of sprout we can detect coming off the cell body is the axon. Unlike the branches of the dendritic tree, which are tapered just like real branches, the axon can be identified because it looks just like a cylindrical tube. There is usually only one axon per neuron. The axon grows out from a specialized region of the cell body called the axon hillock or initial segment. This structure is important because the axon is the main transmitting or conducting unit of the neuron, conveying electrical signals from the dendritic tree down to its very tip. In our big toe analogy, the axon would convey the signal from dendrites in the spinal cord along your leg to tell your muscles to wiggle your toe. The axon hillock gathers together all the signals the neuron has received from the dendritic tree, converts them into the single output response and sends them down the axon. This output response is an electrical signal called the action potential. We will focus on how the action potential is made and transported in another lesson in this unit. Many axons split into several branches at their tips (like the roots of the tree). This means that the action potential can affect a larger area of its target cell, for example a muscle, than it could if it didn t have roots. Just as dendrites have specific points of contact called synapses, where they receive information from the environment or other cells, so too do axons. Axons form synapses with muscles, glands, or when located deep within a network of the CNS, with other neurons (Figure 5). In fact the synapse actually contains both the transmitting point of contact (axon) and the receiving point of contact (dendrite). The cell transmitting the signal is called the presynaptic cell for before the synapse, whereas the cell receiving the signal is the postsynaptic cell for after the synapse. Our neurons are classified into two main groups depending on what other cells they make connections with and what type of information they convey. Neurons that receive input from the environment, and transmit that input into the CNS are called sensory neurons. Whereas neurons that carry information out of the CNS and make connections with muscles and glands are called motor neurons. If we are going to be able to understand how neurons make functional networks it is going to be very important to understand exactly how the neurons connect together. Figure 5: Synapse. The end of the axon divides into fine branches that swell to form axon terminals. These axon terminals are separated from the postsynaptic cell by the synaptic cleft. What is the function of the axon? At a synapse, the cell sending a signal is called what? (Hint: It s the cell before the synapse.) At a synapse, the cell receiving the signal is called what? (Hint: It s the cell after the synapse.) Lesson Presynap)c cell Postsynap)c cell Axon terminal Synap)c cle4
42 DEFINITIONS OF TERMS Axon terminals/presynaptic terminals swellings at the end of the axon s branches that serve as the transmitting site of the presynaptic cell. Synaptic cleft small gap in the synapse that separates the presynaptic cell from postsynaptic cell. For a complete list of defined terms, see the Glossary. LESSON READING Within the depths of the network in the central nervous system, neurons connect to other neurons, so the presynaptic site is usually on an axon and the postsynaptic site is usually a dendrite (we may run into exceptions later, but for now don t worry about them). The points of contact on the axon are specialized swellings on the axon s branches called axon terminals or presynaptic terminals, while the points of contact on the dendrite are called, not surprisingly, postsynaptic terminals. It is an important characteristic of synapses that the pre- and postsynaptic terminals do not physically touch each other. Instead, they are separated by a space called the synaptic cleft. In order to get the signal across the synaptic cleft, and depolarize or hyperpolarize the dendritic membrane the presynaptic terminal turns the action potential into a chemical signal that can cross the physical space. We will talk about this process of transmitting a signal across the synapse called synaptic transmission in another lesson. As you might imagine, the function of the neuron critically depends on how long its axon is. Neurons with long axons are able to convey information over long distances to your big toe and so are called projection or relay neurons. Neurons with short axons are only able to convey information into a limited region and integrate information within a specific local area. Neuronal function So now we can classify neurons into three groups on the basis of their function: Sensory neurons carry information into the central nervous system for perception. Motor neurons carry commands out of the central nervous system to muscles and glands. Interneurons carry information from area to area within the nervous system. They are by far the largest class, consisting of all the neurons that are not specifically sensory or motor. In summary, although all neurons contain the same three functional components, they do not all look or behave the same (Figure 6). Figure 6: Examples of neurons. Neurons that perform different functions have different shapes. Sensory neurons receive input from a sensory organ, like the ear. Motor neurons control muscle information. Local interneurons integrate activity within a small area. Projection neurons convey information for long distances. Neuroendocrine cells release hormones into blood vessels. Model neurons show that each of What is the name of the site on the axon that connects to the dendrite? What is the name of the site on the dendrite that connects to the axon? Are the axons and dendrites in physical contact with each other? the different types have the same Lesson 2.1 functional components. 42
43 STUDENT RESPONSES Remember to identify your sources How are neurons specialized to complete their functions? Given what you know about the different types of neurons, what types of neurons do you predict to be involved in your ability to smell warm chocolate chip cookies? And then taste one after you eat it? What has to happen after you ve smelled the cookie, but before you make the first bite? Be as specific as you can. Lesson
44 LESSON 2.2 WORKBOOK How do our axons transmit electrical signals? This lesson introduces you to the action potential, which is the process by which axons signal electrically. In this lesson you will learn how our axons utilize energy stored in their membranes to send signals throughout our bodies. Signaling is organized in the same way in all neurons To produce a behavior, each participating neuron in a circuit produces, in the same sequence, four types of signals at different sites: The dendrites generate electrical input signals. The axon hillock (or initial segment) integrates the input signals into a single electrical signal the action potential. The axon transmits the electrical action potential down to the presynaptic terminal. The presynaptic terminals convert the electrical action potential into a chemical output signal. We will discuss each of these signals, but it s easiest to understand if we start with the action potential, even though it comes in the middle. Before we discuss any of the signals though, we need to review the electrical properties of the cell membrane that are important to understand how these signals are generated. What are the four types of signals generated within neurons and where are they generated? Lesson
45 DEFINITIONS OF TERMS Diffusion the net movement of molecules from areas of high concentration to areas of low concentration. Electrostatic Pressure the repulsion of like charges and the attraction of opposite charges Potential energy the energy a body has because of its position relative to others, electric charge and other factors. Resting membrane potential the steady membrane potential of a neuron at rest, usually about -70 mv. For a complete list of defined terms, see the Glossary. LESSON READING Neuronal membranes store energy in the form of membrane potentials Neuronal membranes are electrically charged. This means there is a difference in electrical charge across their cell membranes of about 70 millivolts (mv). As we shall see in a minute this difference in charge occurs because sodium (Na + ), and potassium (K + ) ions and organic anions (A - ) are unevenly distributed across the membrane so that the inside of the axon is negatively charged relative to the outside (Figure 7). This electrical charge is called the resting membrane potential. The term potential refers to the energy stored in the membrane or its potential energy. Because the outside of the axon is arbitrarily defined as zero, we say that the resting membrane potential of the axon is -70 mv. The resting membrane potential is produced as a result of the forces of diffusion and electrostatic pressure that the ions inside and outside the membrane experience. Remember that: Diffusion is the net movement of molecules (such as ions) down a concentration gradient Electrostatic pressure is the repulsion of like charges (positive is repulsed by positive and negative with negative) and the attraction of opposite charges Understanding what produces the membrane potential therefore requires that we know the concentration of various ions inside and outside the axon and what forces of diffusion and electrostatic pressure they are experiencing. Figure 7: Membrane potential. (A) When both electrodes are applied to the exterior of the axon in the extracellular fluid, no difference in potential is recorded. (B) When one electrode is inserted into the axon, a voltage difference between the inside and the outside is recorded. The graphs show the voltage change when one electrode is inside the axon. The force of diffusion, molecules moving down their concentration gradient, predicts the result of adding one drop of blue food coloring to a glass of water. Immediately after adding one drop of blue food coloring to a glass of water, that drop sits on the top of the water in an area of high concentration. What happens if you let the water sit for 5 minutes? _ The force of electrostatic pressure, attraction of opposite charges and repulsion of like charges, predicts what would happen if you had negatively charged ions at the top of a cup and positively charged ions at the bottom of a cup. Where do you predict the negatively charged ions will go? Lesson
46 LESSON READING Athough there are many types of ions inside and outside the axon, three are particularly important for the membrane potential (Figure 8): Organic anions (symbolized as A - ) Potassium ions (K + ) Sodium ions (Na + ) Let s now consider how each of these important ions experiences the forces of diffusion and electrostatic pressure. Once we know this we will understand why each ion is located where it is when the axon membrane is at rest. Organic anions are negatively charged proteins and intermediary products of a cell s metabolism. They are unable to pass through neuron s membrane and so they are only found inside the axon. Therefore, they make the interior of the axon more negative and contribute to the negative membrane potential. Potassium ions (K + ) are also concentrated within the axon, however they can move to the outside through special channels in the cell membrane. Thus, the force of diffusion will tend to push them out of the cell. However the high concentration of At rest negative organic anions makes the inside of the cell more negative relative to the outside. Because of this negative charge, electrostatic pressure tends to keep the potassium ions inside the cell. In the case of potassium ions the two forces of diffusion and electrostatic pressure oppose each other and balance each other out. As a result, potassium ions tend to remain where they are at high concentrations inside the axon. Sodium ions (Na + ) are concentrated outside the axon, in the extracellular fluid. Like potassium, there are sodium ion channels in the membrane. Therefore, the force of diffusion pushes these ions inwards. In addition, sodium ions are positively charged, so electrostatic pressure also attracts them into the negatively charged axon. However, if the sodium ions did enter the axon the charge difference across the membrane would break down and the potential energy in the membrane would be lost. Na + Figure 8: Distribution of ions at resting membrane potential. Na + ions (represented by blue circles) are more concentrated outside the neuron. K + ions (represented by red circles) and negatively charged proteins (represented by black stars) are more concentrated inside the neuron.axon, a voltage difference between the inside and the outside is recorded. What are organic anions, and where are they in highest concentration in our nervous systems? Where are potassium ions in highest concentration in our nervous systems? Where are sodium ions in highest concentration in our nervous systems? Lesson K Na + K + Na + Na+ - - Na + K + K +
47 DEFINITIONS OF TERMS Sodium-potassium pump active transport mechanism that pumps sodium (Na + ) ions out of neurons and potassium (K + ) ions into neurons. Voltage-gated channels channels that open or close in response to changes in voltage across the membrane. For a complete list of defined terms, see the Glossary. LESSON READING How then can Na + overcome the two forces of diffusion and electrostatic pressure and stay on the outside the axon, preserving the resting membrane potential? The answer is this: there is another force provided by a pump that continuously pushes Na + out of the axon, swapping an Na + ion that might have leaked inside for a K + ion that might have leaked outside. Because the membrane is not very permeable to Na + (there are fewer Na + channels) the sodium-potassium pump (Na + /K + pump) is very effective at keeping the intracellular concentration of Na + very low when the membrane is at rest. Just a quick side note: Sodium-potassium pumps use enormous amounts of energy up to 40% of a neuron s energy is used to operate them. The Action Potential We just saw that the forces of both diffusion and electrostatic pressure tend to attract Na + into the axon. However, we also saw that the membrane is not very permeable to Na + ions, and that the sodium/potassium pump continuously pumps Na + out of the axon, keeping intracellular Na + concentrations low. But imagine what would happen if the membrane suddenly became permeable to Na +. The forces of diffusion and electrostatic pressure would cause Na + to rush into the cell. This sudden influx of positively charged ions would drastically reduce the membrane potential. This is precisely what happens to cause the action potential: A brief increase in the permeability of the membrane to Na + (which allows Na + to enter the cell), is immediately followed by a transient increase in permeability of the membrane to K + (allowing K + to exit the cell). The question now is what is responsible for these transient increases in permeability? We already saw that there are two ways to move ions across the membrane, either through channels in the membrane or by hooking them up to pumps, like the sodium-potassium pump. Sometimes the passages or pores in the ion channels are always open, but usually they are closed and only open under specific conditions. When the channel pores are open they are only permeable to a particular type of ion, which can flow through the pore and thus enter or exit the cell. Some ion channels open or close depending on the cell s membrane potential. They are referred to as Voltage-gated ion Figure 9: The membrane s ion channels and pumps. Two ion channels are critical in the axon s conduction of the action potential: the voltage-gated Na + channel and the voltage-gated How does sodium remain in highest concentration outside the axon? How do sodium channels open in response to changes in the cell s membrane potential? _ channels. K Lesson channel. Additionally the Na + /K + pump plays a critical role as well. between the inside and the outside is recorded. 47
48 LESSON READING Two voltage-gated channels are critical in the action potential (Figure 9): Voltage-gated Na + channels open when the membrane potential reaches -50 mv, and close when the membrane potential reaches +40 mv. Voltage-gated K + channels open when the membrane potential reaches +40 mv, and close when the membrane potential reaches 70 mv. The following numbered paragraphs describe the movement of ions across the membrane through channels and pumps which underlies the action potential. The numbers in Figure 10 correspond to the numbers in the paragraphs below. Figure 10: Stage of the action potential. The opening and closing of voltage-gated Na + and K + channels is responsible for the characteristic shape of the action potential. Refer to Figures to see what is happening at each stage of the action potential. Describe the different types of voltage-gated ion channel. 1. The Resting Membrane potential: At rest the voltage-gated Na + channels and voltage-gated K + channels are closed and the Na + /K + pump is working hard, using ATP to sustain the resting membrane potential to move three Na + ions out of the axon for every two K + ions moved into the axon. As a result the concentration of Na + outside the axon is high, and the concentration of K + inside the axon is high (Figure 11). Because of the contribution of the organic cations (A - ) the inside of the axon is more negative than the outside, even though the K + is in high concentration there. As a result the membrane potential at rest is -70 mv, as we saw before. Na + Na + Na + Na + Na + Figure 11: Resting membrane potential (Stage 1 in Figure 10). The resting membrane potential is maintained by the Na + /K + pump. At rest, there is a slow leak of K + ions out of the cell, which the Na + /K + pump corrects by pumping 3 Na + ions out of the cell for every 2 K + ions it pumps into the cell. Describe where the Na + and K + ions are when the axon s membrane is at rest. Why are they located there? Lesson Na + Na + Na + K + K + K + K + Na + K + K +
49 DEFINITIONS OF TERMS Absolute refractory period a brief period after the initiation of an action potential during which it is impossible to elicit another action potential in the same neuron. Depolarize to decrease the resting membrane potential. Decreasing membrane potential means that the membrane potential is becoming more positive. Local potentials small changes in voltage (membrane potential) due to dendritic signaling. Threshold the level of depolarization needed to generate an action potential. For a complete list of defined terms, see the Glossary. LESSON READING 2. Reaching Threshold: When the dendrites receive a signal just a few voltage-gated Na + channels open and the charge across the dendritic membranes drops briefly causing small changes in voltage or local potentials. The forces of diffusion and electrostatic pressure then pull Na + ions into the cell through the open channels (Figure 12). This inward flow of positive sodium ions starts to reduce or depolarize the membrane potential, meaning that the inside of the cell is becoming more positive relative to the outside. If enough Na + channels open and enough Na + ions enter the cell, then the membrane potential will decrease to the threshold (-50 mv) at which all the Na + channels will open and large quantities of Na + ions will enter the cell. Threshold is the critical level of membrane depolarization at which the cell can actively generate an action potential. As we see, whether threshold is reached depends on the strength of the dendritic signal. If the dendritic signal is strong then we are more likely to reach threshold. 3. Depolarization: When a threshold of -50 mv is reached, many more voltage-gated Na + channels open allowing even more Na + ions to quickly flow into the axon (Figure 13). This inward flow of Na + Na + into the axon further depolarizes the membrane, Na reducing the membrane potential even more so + that eventually the inside of the axon becomes positive relative to the outside. 4. Hyperpolarization: When so many Na + ions have entered the axon that the interior has reached +40 mv (relative to the external value of 0 mv) the voltage-gated Na + channels close. This inactivates them, so they cannot open for a period of time. This is called the absolute refractory period. Describe where the Na + and K + ions are when the axon s membrane is reaching threshold. Why are they there? Describe where the Na + and K + ions are when the axon s membrane is depolarizing. Why are they there? Lesson Na + Na + Na + Na + Na + Na + Na + Na + Figure 12: Reaching threshold (Stage 2 in Figure 10). Local potentials open a few voltage-gated Na + channels, allowing Na + ions to enter the axon. Na + Na + Na + Na + Na+ Na + Na+ Figure 13: Depolarization (Stage 3 in Figure 10). Once the membrane reaches threshold (-50 mv), many more voltage-gated Na + channels open, allowing even more Na + ions to enter the axon. K + K + K + K + Na + K + K + K + K + K + K + K + K +
50 DEFINITIONS OF TERMS Hyperpolarize to increase the resting membrane potential. Increasing membrane potential means that the membrane potential is becoming more negative. Relative refractory period period after the absolute refractory period during which a higher-thannormal amount of stimulation is necessary to make a neuron fire For a complete list of defined terms, see the Glossary. LESSON READING Remember that voltage-gated K + channels also open at +40 mv. This opening of K + channels allows K + ions to flow out of the axon (Figure 14). The K + ions flow out of the axon because the prior passage of Na + ions into the cell has altered the forces of diffusion and electrostatic pressure that the K + ions now experience. First of all, K + is in higher concentrations inside the axon than outside the axon, so with the K + channel open the K + ion is forced down its concentration gradient and out of the cell by diffusion. Furthermore, with Na + ions now inside the axon, the inside is now positive relative to the outside. So, electrostatic pressure also forces the positive K + ions outside the axon. This flow of K + outside of the axon decreases the positive charge on the inside, and has the effect of hyperpolarizing the axon membrane meaning that the inside of the membrane becomes more negative relative to the outside. Due to the huge flow of K + out of the cell, the membrane potential becomes higher than it is at rest (the inside of the axon is more negative relative to the outside). This period of higher membrane potential is called the relative refractory period because the sodium channels are now able to open, so if enough positive charge came along the axon could potentially reach threshold and depolarize again. However if you think about it, because the membrane potential is higher, more positive ions would be needed to reach threshold than if the cell was at rest, so depolarization during the relative refractory period is less Na + Na + Na Na Na likely to occur Na + 5. Returning to rest: To return the membrane to its resting membrane potential of -70mV, the Na + /K + pump works hard and uses ATP to move three Na + ions out of the cell for every two K + ions moved into the cell (Figure 15). Na + Na+ Na + Na+ Figure 14: Hyperpolarization (Stage 4 in Figure 10). At +40 mv the voltage-gated Na + channels close and the voltage-gated K + channels open, allowing K + ions to exit the axon. Describe where the Na + and K + ions are when the axon s membrane is hyperpolarizing. Why are they there? _ Describe where the Na + and K + ions are when the axon s membrane is returning to rest. Why are they there? _ Lesson 2.2 ions out of the cell for every 2 K + ions it pumps into the cell. 50 Na + Na + K + Na + K + Na + Na + K + Figure 15: Returning to rest (Stage 5 in Figure 10). The voltage-gated K + channels close, and the Na + /K + pump returns the membrane to rest by pumping 3 Na + Na + K + K + K + K + K+ Na + Na + K + K + K + K +
51 DEFINITIONS OF TERMS Conduction of the action potential movement of the action potential down the length of the axon For a complete list of defined terms, see the Glossary. LESSON READING Conduction of the Action Potential along the Axon Now we have a basic understanding of what the resting membrane potential is and how the action potential is produced, we can turn our attention to how this electrical message moves down the length of the axon to the presynaptic terminal. Axons do this in a process called the conduction of the action potential. The membrane depolarization that occurs during the action potential is localized to a small area of membrane where the ions and channels are localized. Meaning, this electrical signal does not move very far down the axon. Axons therefore need to use another method, called active conduction, to prevent the electrical signal from decaying. It does this by repeatedly generating action potentials along the length of the axon. Axons can use active conduction by stacking many voltage-gated Na + channels along their membranes in close proximity to one another. When the dendrite signal causes the axon hillock to reach threshold and the Na + channels to open, the depolarization of the membrane will cause adjacent Na + channels to also open generating another action potential. This process is repeated until the action potential reaches the presynaptic terminal where it is converted to a chemical signal to cross the synaptic cleft (Figure 16). So, essentially conduction of an action potential down the length of the axon requires many individual action potentials along the length of the axon to be generated in sequence. Each individual action potential provides a depolarizing current which causes the next set of voltage-gated Na + channels to reach threshold and trigger another action potential, causing a domino effect down the length of the axon. It is important to note that in order for the action potential to be conducted efficiently it is critical that the voltage-gated Na + channels are stacked up along the entire length of the axon. If they are not, the depolarizing current from a single action potential will get smaller as it travels down the axon, either because the current leaks or because the proteins the axon is made of offer resistance to conduction. When voltagegated Na + channels are in close proximity, the depolarizing current does not have enough space to decline before the next set of Na + channels open and initiate a new action potential. You can watch a video about action potentials online see this unit on the student website or click below: Lesson Video: Action Potentials Figure 16: Conduction of the action potential. An action potential is generated as Na + ions flow in at one location along an axon. The depolarization spreads to the neighboring region of the membrane, initiating an action potential there. The original region repolarizes as K + ions flow out. The depolarization-repolarization process is repeated as the action potential is propagated down the length of the axon. How does an axon conduct the action potential down its length?
52 STUDENT RESPONSES Write a summary of what is happening at each stage of the action potential diagrammed below. Step 1: Remember to identify your sources Step 2: Step 3: Step 4: Step 5: Lesson
53 DEFINITIONS OF TERMS Glial cell several classes of non-neuronal cells of the nervous system. For a complete list of defined terms, see the Glossary. LESSON 2.3 WORKBOOK How fast do our neurons signal? Remember that winning goal you scored, that snowball you dodged or the cup of coffee you managed to catch before the cat knocked it all over your computer? Hundreds of times a day our quick reactions improve our performance or save us from disaster. Take a minute to think of something that happened to you this week. Often we react so quickly that we ve reacted before we even know what has happened. How can your neurons signal so quickly? In this lesson we will find out, and to do so we need to learn about the other important type of cell in our nervous systems the glial cell. Glial Cells There are actually far more glial cells (usually referred to as glia) than neurons in the CNS of vertebrates between 10 to 50 times more in fact. Nerve cell bodies and axons are surrounded by them and because of this they were named from the Greek word for glue. For a long time neuroscientists thought glial cells did behave like glue, and pretty much ignored them. Over the last few years though they have been found to be far more active than we thought, conducting their own signals and acting more as partners for neurons than the boring old structural cells we originally thought. Glia in fact have several vital roles in neuronal function: They provide firmness and structure to the brain. This isn t trivial. Remember from the lesson on neural imaging that the brain has very low density. Glia beef up the density and make the neurons more resistant to trauma. That s important because remember that if a brain neuron is damaged and dies it can t be replaced. Two different types of glial cells act as insulation, which as we shall see, allows the action potential to travel faster important if we want to move a signal quickly. When the brain is developing in the embryo, some glia act as guides so that the neural network forms its connections in the right place. What are glia cells, and what are some of their functions? Other glial cells help form an impermeable lining around the capillaries and venules of the brain that prevents toxic substances in the blood from entering the brain. This lining Lesson 2.3 is called the blood-brain barrier. 53
54 DEFINITIONS OF TERMS Nodes of Ranvier gaps between adjacent myelin segments on an axon. Demyelination the loss of myelin insulating neurons. For a complete list of defined terms, see the Glossary. LESSON READING Myelination increases the conduction speed of the action potential In the last lesson we saw that if only one action potential occurred at the beginning of the axon, the depolarizing current wouldn t reach the axon terminal. This happens because as it travels down the axon some of the current leaks out of the axon across the membrane, and also because the materials in the axon (chiefly protein) offer resistance to the current. We also learned that some axons solve this problem by lining up their voltage-gated Na + channels along the axon membrane, so multiple action potentials can occur in rapid succession, ensuring that the signal is transmitted all the way down the axon. This is not a great solution because the energy required to keep the Na + /K + pump working to repolarize the axon membrane is huge. So axons have come up with another strategy, which is to have the action potential jump along the axon rather than progress down it (think of the action potential pogo-sticking down the axon rather than walking down). This how it works. Remember that the problem with a single action potential was that the current would decay. To prevent that decay glial cells wrap around the axon like beads on a necklace covering the axon tightly except for the areas in between the beads called nodes of Ranvier which remain naked axon (Figure 17). Two things make this strategy work. First the glia make a substance called myelin, which acts as an insulator. Now the parts of Figure 17: Nodes of Ranvier. Myelin is formed the axon that are wrapped around by the myelin from membranes of glial cells wrapping tightly are insulated and the depolarizing current can t around the axon, like beads on a necklace. Between the beads of myelin are spaces of naked leak out. Second the sodium channels are concentrated in the small areas of naked axon in axon, called the nodes of Ranvier. between each myelin bead so the action potential can hop down the axon like a pogo stick. Let s have a look in a bit more detail: Figure 18: Cross section of myelinated axons. The glial cell membranes wrap so tightly around the axon that the cytoplasm is squeezed out of the glial cells. The glial cells wrap around the axon like paper wrapping around a pencil. The glial cell membrane attaches so tightly to the axon, and to itself that there is no extracellular fluid in contact with the axon in that area (Figure 18). The only place where the axon comes into contact with extracellular fluid is at a node of Ranvier, where the axon is naked. In the myelinated areas therefore, there can be no inward flow of Na + into the How does myelination increase the conduction velocity of the action potential? axon because the myelin insulates the axon from the Lesson 2.3 extracellular fluid. 54
55 DEFINITIONS OF TERMS Saltatory conduction conduction of the action potential from one node of Ranvier to the next along a myelinated axon. For a complete list of defined terms, see the Glossary. LESSON READING How then does the action potential travel along the area of an axon covered by a myelin sheath? The answer to this is by behaving like an electrical cable. Since the axon is covered in myelin, there is minimal leakage of depolarizing charge out of the axon so the depolarizing current is able to travel passively between the nodes of Ranvier. When the depolarizing current reaches the next node of Ranvier, it encounters both Na + ions and Na + channels, and so it can trigger another action potential at the node. The action potential gets retriggered, or repeated, at each node of Ranvier and the depolarizing current moves passively along the myelinated portions of the axon to the next node. This type of conduction, which appears to hop from node to node, is called saltatory conduction, from the Latin saltare, to leap, to dance (Figure 19). Figure 20: Comparing action potential conduction in unmyelinated and myelinated axons. The black arrows represent current flowing down an unmyelinated axon and the red arrows represent current flowing down Why is myelination an advantage for the axon? We can immediately see two advantages of saltatory conduction. The first is it saves energy. Sodium ions that enter axons during the action potential must eventually be removed. You ll remember that the Na + ions are removed by Na + /K + pumps, which use significant amounts of energy. As we mentioned before, in axons that aren t myelinated, these pumps must be located along the entire length of the axon, because Na + ions can enter everywhere. However, in a myelinated axon, where Na + ions can only enter at the nodes of Ranvier, much less Na + gets in, and consequently, much less needs to be pumped out. Therefore, in myelinated axons much less energy is needed to remove Na + ions and maintain the high extracellular Na + concentration. The second advantage of myelin is speed. The action potential is conducted much faster in a myelinated axon because transmission between the nodes, which occurs by means of the axon s cable properties, is very fast (Figure 20). Increased speed enables us to react faster and undoubtedly to think faster. In fact, the fastest myelinated axon, 20 micrometers (µm) in What are the advantages of myelination? Think about your big toe neuron. Imagine the axon starts under your armpit. How long will an action potential take to travel down to your big toe if is myelinated? Lesson 2.3 a myelinated axon. Notice how diameter, can conduct action potentials at speeds of 150 m/s, 55 much faster the myelinated current travels. or 335 mph! Figure 19: Saltatory conduction. Action potentials are conducted down the myelinated axon via saltatory conduction. The depolarization jumps from one node to the next without decaying.
56 DEFINITIONS OF TERMS Demyelination the loss of myelin insulating neurons. Saltatory conduction conduction of the action potential from one node of Ranvier to the next along a myelinated axon Demyelination the loss of myelin insulating neurons For a complete list of defined terms, see the Glossary. LESSON READING Why aren t all neurons myelinated? Since myelin provides such important benefits decreasing energy consumption and increasing speed why aren t all of our axons myelinated? In fact, most of our axons are myelinated, but later we ll argue that having some unmyelinated axons is important. Take for example the so-called C fibers (fibers is just another name for nerve). C fibers are sensory neurons located in the PNS and involved in the pain response. They are not myelinated and their conduction velocities are slow 2 m/s (or only 4.5 mph). But conducting pain information slowly, gives us an advantage because we can respond to the source of the pain before the pain sensation becomes intense. Sometimes it is actually beneficial for a signal to reach our brains more slowly. What happens when myelin gets damaged? Demyelination is the loss of the myelin sheath insulating neurons. As you might imagine, losing even a part of the myelin sheath disrupts action potential conduction. When myelin is disrupted, conduction along an axon may become desynchronized or even fail completely. Demyelination is the hallmark of some neurodegenerative diseases including multiple sclerosis, (MS) and Charcot-Marie-Tooth disease. Demyelination results in a set of symptoms that will depend on which neurons are affected. We ll talk more about demyelinating diseases in the last lesson of this unit, but for now remember that the myelin sheath insulates the axon increasing the conduction velocity of the action potential, as well conserving the axon s energy. When does myelination occur? Under what circumstances would it be beneficial not to have myelinated axons? What if your big toe neuron wasn t myelinated? How long would it take the action potantial to reach your toe then? Would this be an advantage or not? At what age does our frontal lobe become myelinated? Recently, research has shown that our brains Mostly grey ma-er gradually add myelin as we mature. Figure 21 is taken from one of the studies on which that statement is based. Remember, grey matter is where Mostly white ma-er neurons connect with each other and white matter is where the myelinated axons are. The study analyzed changes in grey matter relative to white Figure 21: Loss of grey matter and gain of white matter from 5 20 years. Notice that our frontal matter, so another way to look at the data is that lobes are the last areas to become heavily myelinated and thus be represented as mostly white not only does grey matter decrease, but white matter also increases as we mature. Take a look matter. specifically our frontal lobes, which do not become fully myelinated until we are about 20. Some scientists have taken this further to argue that teenag- ers show poor judgment because their frontal lobes aren t fully myelinated. This conclusion has been hotly Lesson 2.3 debated in the field, and might be one you d like to take a minute to think about. 56
57 STUDENT RESPONSES Remember to identify your sources You just read about research that shows that the human brain, specifically the frontal lobe, is not heavily myelinated until the age of 20. Some scientists argue that teenagers show poor judgment because their brains aren t fully myelinated. What do you think? Do you agree with the scientists arguments? Do you think there could be another explanation? Lesson
58 LESSON 2.4 WORKBOOK What do our neurons need to work efficiently? We ve learned that axons can be very long, and that most of the proteins that make up their structures are made in the cell body. We ve also learned that proteins don t last forever, they wear out and need to be replaced this includes all the channels and the Na + /K + pump that s so important for keeping the resting membrane potential stable, as well as everything that s needed to convert the action potential into a chemical signal to cross to the other side of the synapse. How can our neurons keep up with this relentless demand? As you can imagine getting what s needed to where it s needed, when it s needed is a task that requires a highly organized transport system that delivers cargo both into and out of the axon. When this transport goes wrong, it can be a big problem. This lesson will look at axonal transport. Axon structure underlies axonal transport We ve used our big toe axons in several examples, but in fact axons can be anything from a few millimeters to several meters long. The shortest axons belong to the interneurons that connect local areas within the brain and can be less than 0.1 mm; the longest axons are the big toe axons that would be several meters long if you were a giraffe. But all axons, short or long, have the same internal structure thanks to their cyto (from the word for cell) skeleton. The cytoskeleton is conveniently organized parallel to the length of the axon so it can provide the tracks that transport cargo to and from the presynaptic terminal just like a railroad. The axon s cytoskeleton has three main protein components microtubules, neurofilaments, and actin each of which play different roles. Neurofilaments are like filler that hold the mature axon rigid and determine its diameter. Actin is important when the axon is growing in the embryo and keep it flexible and able to move. Microtubules are important for axonal transport, so we ll focus on them here. What are the benefits of having both short and long axons? _ List one function for each component of the axon cytoskeleton: _ Lesson
59 DEFINITIONS OF TERMS Anterograde transport movement of materials from cell body to axon terminals. Minus-end end of microtubules oriented toward cell body. Minus-end directed motors molecular motors that travel toward the minus-end of microtubules, and thus carry cargo from the axon terminal to the cell body. Plus-end end of microtubules oriented toward axon terminal. Plus-end directed motors molecular motors that travel toward the plus-end of microtubules, and thus carry cargo from the cell body to the axon terminal. Retrograde transport movement of materials from axon terminals to the cell body. For a complete list of defined terms, see the Glossary. LESSON READING Microtubules provide the tracks on which cargo is transported Microtubules form the actual tracks that move cargo to and from the axon terminal. How do they do this? They are hollow cylindrical polymers that are made from two different forms of the tubulin protein called alpha and beta tubulin. These two tubulin isoforms polymerize together to form a hollow tube that is polarized, meaning that one end is different from the other. The two different ends are called the plus-end and the minus-end. In axons, all microtubules are oriented in the same way, with the plus-end toward the presynaptic terminal, and the minus-end toward the cell body (Figure 22). Motors can attach to the microtubules. If they are plus-end directed motors, they will move toward the presynaptic terminal. If they are minus-end directed motors, they will move towards the cell body. (Figure 23). We ll talk more about these motors in a minute. Cargo can attach directly to these motors and be transported from the cell body into the axon and the presynaptic terminal (anterograde transport) or from the presynaptic terminal and axon back to the cell body (retrograde transport). Figure 23: Axonal transport. The neuron provides its terminal with important structural proteins and organelles via axonal transport along the microtubule tracks. How does transport work? Figure 22: Microtubule structure. Microtubules are composed of two different forms of tubulin, α and β, that polymerize together to form a slightly polarized dimer. When the dimers assemble, they then have a plus-end that is oriented toward the axon terminal and a minus-end that is oriented toward the cell body. Scientists knew that most protein synthesis occurred in the cell body, and they deduced that there must be a system that can transport these items efficiently to where they were needed. Fortunately, major technological advances in microscopy occurred precisely at the time we began to question exactly how materials are transported in the axon. One of the previous problems had been in observing very small structures. New advances with lenses and computing allowed scientists to detect structures moving down the axons. Using the newly developed tools that allowed us to see the inside of living axons, scientists could observe the movement of materials in axons and then figure out exactly how transport works. What kind of motors carry cargo to the axon terminal? What motors carry cargo to the cell body? Why do neurons need such an elaborate transport system? Lesson
60 DEFINITIONS OF TERMS Anterograde transport movement of materials from cell body to axon terminals. For a complete list of defined terms, see the Glossary. LESSON READING Proteins are not transported down the axon individually. Instead the cell body organizes them into structures (organelles) like mitochondria or the spherical membrane vesicles that contain neurotransmitters. You can watch a video showing vesicles moving down an axon online see this unit on the student website or click the link below. In this case the particles have been tagged with a fluorescent marker that allows them to be detected with a fluorescent microscope. The upper image shows the fluorescent signal and the middle image shows the actual picture of the vesicles. In the bottom image they have been merged. Video: Axonal Transport We knew that cargo had to get to both the presynaptic terminal and back from it to the cell body. From many different kinds of experiments that used fluorescent and radioactive chemicals to tag transported proteins, we found out there are basically two different ways to transport material in the axon fast and slow. Fast axonal transport is used to get materials where they are needed quickly to the presynaptic terminal to be used in neurotransmission across the synapse (anterograde transport), or back to the cell body for recycling (retrograde transport). It s fast because it uses a lot of energy, and depends on the microtubule motors we talked about before (Figure 24). In contrast, slow axonal transport is used to rebuild the axonal cytoskeleton itself the microtubules, neurofilaments and actin polymers. Frankly, we are still unsure about how slow transport works and it is an active area of research. Its important though because a number of diseases affect slow transport and have serious consequences. Fast transport anterograde and retrograde Anterograde transport The presynaptic terminal needs a constant supply of membrane vesicles, because as we shall see in the next unit, it packages neurotransmitters into the vesicles so it can control their release into the synapse. It (and the axon) also requires a constant supply of energy in the form of ATP, which is delivered by mitochondria. Hence vesicles and mitochondria need to be transported rapidly and on time, so the axon has developed a sophisticated mechanism that directs them where they need to be. What types of materials do you think get transported via anterograde transport? What types of materials do you think get transported via anterograde transport? Lesson Microtubules Anterograde transport Retrograde transport Figure 24: Fast axonal transport. There are two types of fast axonal transport: anterograde and retrograde. Anterograde transports moves materials from the cell body towards the axon terminal. Retrograde transport moves materials from the axon terminal towards the cell body.
61 DEFINITIONS OF TERMS Kinesin plus-end directed motor that carries cargo from the cell body to the axon terminal along microtubules. Dynein minus-end directed motor that carries cargo from the axon terminal to the cell body along microtubules. Retrograde transport movement of materials from axon terminals to the cell body. For a complete list of defined terms, see the Glossary. LESSON READING Recall that fast transport uses microtubules and motors, and that anterograde transport (meaning going to the presynaptic terminal) uses plus-end directed motors. These motors work by attaching to and traveling along microtubles toward their plus-end which, again, is oriented towards the presynaptic terminal. So, the motors use the polarity of the microtubules as a cellular GPS. These plus-end directed motors are a family of proteins called kinesins (Figure 25). In the cell body, kinesins, which actually look exactly like legs and feet, attach to the cargo being transported down the axon. The kinesin molecule then walks down the microtubule toward the plus-end at the presynaptic terminal, carrying the cargo to its destination. Kinesin uses energy in the form of ATP to move itself and its cargo down the microtubule. In fact it hydrolyzes one molecule of ATP for each 8 nanometer (nm) step it takes down the microtubule. The vast amounts of energy needed to make this trip are supplied by the mitochondria, so its clear that mitochondria will be needed in the axon as well as the presynaptic terminal. You can watch a short video online showing how kinesin walks down the microtubule towards the plus end. The video was made using the actual structure of the kinesin molecule, and what is known about how its shape changes as it hydrolyzes ATP and attaches to microtubules. The cargo would attach to the two kinesin arms that are sticking up. Video: Kinesin Transport Protein Retrograde transport Rapid retrograde transport returns materials from the presynaptic terminal or the axon to the cell body for recycling. As in fast anterograde transport, cargo moves along microtubules attached to a motor protein. In this case the motor is the minus-end directed motor protein, dynein. Dynein works much the same way as kinesin, except it carries substances toward the cell body (Figure 26). The combination of the polarity of the microtubules, and the specificity of the motors for the microtubules and their cargo, ensures that cargo gets to the right place at the right time this is crucial if the axon terminal is going to function properly. While we ve told a simplified story here, keep in mind that the kinesins are actual a A. B. Figure 25: The plus-end directed motor protein: Kinesin. (A) Cartoon of kinesin protein carrying organelle down microtubule track from the cell body to the axon terminal. (B) Electron microscope photograph of kinesin carrying a vesicle. transport moves materials from the axon terminal towards the cell body. What motor protein is responsible for getting cargo from the cell body to the axon terminal? How does it work? What motor protein is responsible for getting cargo to the cell body from the axon terminal? How does it work? family of proteins with more than 40 different kinesin proteins, each axon terminal to the cell body Lesson 2.4 specific for a particular cargo or particular destination. along the microtubule tracks. 61 Vesicle Dynein Microtubule Figure 26: The minus end directed motor protein: Dynein. Dynein carries cargo from the
62 STUDENT RESPONSES Imagine you have nerve damage that affects your axonal transport systems, what symptoms would you have? Think about this question in the light of what you know about the roles of axonal transport, and how neurons function to transmit signals. Remember to identify your sources If kinesin uses one molecule of ATP for each 8 nm step, how much ATP is used to move one synaptic vesicle from a neuronal cell body at the base of your spine to your big toe? (Assume that the distance from your spine to big toe is 3 feet (or 1 meter). Lesson
63 LESSON 2.5 WORKBOOK What can go wrong? Throughout this unit, we ve discussed the basic structures and functions of the major cells that make our nervous systems: neurons and glia. In this lesson, we ll investigate what happens when these functions are compromised by disease or injury. What if there are problems conducting action potentials? We can make several predictions about when and how problems in conducting action potentials might occur. For example, action potential conduction will be affected if: The voltage-gated Na + channels don t function properly. Myelination is abnormal. If any of the above happens, we can predict what effect it will have on the neuron: If the voltage-gated Na + channels don t function properly, the axon will be unable to generate action potentials properly. If myelination is abnormal, then the axon will be unable to synchronize conduction of the action potential and signaling may fail completely. Diseases of axonal conduction Let s now investigate three diseases of action potential conduction in more depth: Congenital analgesia Multiple Sclerosis (MS) Charcot-Marie Tooth Disease (CMTD) Lesson
64 DEFINITIONS OF TERMS Congenital analgesia disease in which patients do not sense pain. For a complete list of defined terms, see the Glossary. LESSON READING Congenital Analgesia Case study of Gabby Gabby is 5 years old (Figure 27). Her parents have consulted with many specialists throughout their daughter s life in hopes of finding an explanation for why their daughter behaves so strangely. Gabby s parents first knew that something was wrong when Gabby was only a few months old. Like other babies her age, she was teething. But unlike other babies, who would cry in pain, Gabby never cried. One morning, her father noticed that she had been chewing Figure 27: Five year old Gabby. on her fingers so much that they were bleeding, but again, she never cried. Her mother described Gabby s hand as mangled and nasty, like raw hamburger. After consulting with several doctors, Gabby s parents had all of her baby teeth removed so that she could not further harm herself. When Gabby was a year old, her mother noticed a white spot on her left eye. She thought it was just something floating in Gabby s eye, but in fact Gabby had somehow scratched her cornea. The doctor who treated Gabby told her mother that In most patients, this type of wound would be so painful, they would not be able to open their eye. To prevent Gabby from scratching her eye any more, the doctor stitched that eye closed. But, unable to feel pain, Gabby ripped out the stitches. These are just two of the incidents that brought Gabby s parents into see a neurologist for further examination. The doctor diagnosed Gabby with congenital analgesia. Congenital analgesia is a very rare inherited disease in which children, usually from birth, cannot sense pain even though their other senses are normal. Like Gabby, children with this disease often suffer from oral damage, like biting off the tip of their tongue, and scratches to the cornea. Researchers have learned that the disease can be caused by a mutation in the gene that codes for a voltage-gated Na + channel. This voltage-gated Na + channel (called SCN9A) is found specifically in the specialized receptors that detect pain called nociceptors. In a normal person, when nociceptor dendrites detect a pain sensation, the SCN9A Na + channel will amplify the signal so it reaches threshold and allows an action potential to fire. However, in patients with congenital analgesia this voltage-gated sodium channel doesn t work and thus the input from the dendrites never reaches threshold so an action potential doesn t fire (Figure 28). Congenital analgesia is not fatal, but patients suffering from it will never lead a normal life. Because they can t detect pain, they need to closely monitor their bodies for injuries and infections. Even so, the Normal Pa)ent What are Gabby s symptoms? What did her doctor diagnose her with? What is the neuronal defect in congenital analgesia? _ What is the treatment for congenital analgesia? inability to feel pain causes complications that mean very few patients Lesson 2.5 the nociceptors never detect with this disease live to a normal life expectancy. 64 Congenital Analgesia X X Figure 28: Congenital analgesia. Patients do not feel pain because a mutation in the voltage-gated N a+ channels in their nociceptors means an action potential cannot fire, so any pain.
65 DEFINITIONS OF TERMS Multiple sclerosis (MS) disease in which myelin within the central nervous system is damaged. For a complete list of defined terms, see the Glossary. LESSON READING Multiple sclerosis (MS) Case study of Maria Maria is 37 years old (Figure 29). She has been having reoccurring episodes of muscle weakness in her arms and legs. The weakness lasts for a week or two and then subsides. At other times she noticed numbness in different parts of her body. Since the episodes came and went, she did not think much of it until she started having changes in her vision. First, she noticed that she was experiencing double vision, and then she noticed that she was having problems seeing out of her left eye. It was at this point that Maria called her doctor. Maria s doctor started the appointment by reviewing Maria s family history. Luckily, none of Maria s extended family had ever suffered from a neurological disease. She then gave Maria a thorough examination. First, she checked her eye reflexes and noted that her left eye had a decreased pupillary reflex, which means it didn t respond to a bright light by contracting. Next, she checked Maria s sensitivity to touch sensation and found it was decreased in different parts of her body. The doctor ordered both an MRI to see if there were any abnormalities in Maria s brain, and a spinal tap to see if there were any abnormal proteins in Maria s cerebrospinal fluid. The MRI showed a couple of small areas in Maria s brain where the myelin looked abnormal (called plaques), and the spinal tap detected a high level of antibodies in her cerebrospinal fluid. The doctor gave Maria a preliminary diagnosis of multiple sclerosis, but told her that to confirm the diagnosis; she would need to follow Maria s condition and rule out any other neurological abnormality. Multiple sclerosis (MS) can occur at any age, but is most commonly diagnosed between the ages of 20 and 40. The disease affects more women than men. MS is caused by damage to myelin within the central nervous system (Figure 30). The CNS myelin is damaged because the immune system makes antibodies against it, and the antibodies attack the myelin, causing inflammation. Repeat episodes of inflammation can occur anywhere in the brain, optic nerve and spinal cord. We think that some aspect of myelin s structure must resemble an infectious agent that previously infected the patient. The body first made antibodies against the infection, but those antibodies then become confused and attack the patient s own myelin. This is attack on self, causes an autoimmune disease. Figure 29: Maria, age 37. areas of damaged myelin, appearing here as Lesson 2.5 denser plagues. Regions close to the ventricles 65 A. B. Figure 30: Multiple sclerosis. (A) Multiple sclerosis is an autoimmune disease in which a patient s T cells destroy the glial cells that myelinate CNS neurons. (B) MRI scans of patients brains with multiple sclerosis show are commonly affected. What are Maria s symptoms? What did her doctor diagnose her with? What is the neuronal defect in multiple sclerosis? _ What does the treatment for multiple sclerosis hope to do?
66 LESSON READING The symptoms of MS can vary based on the location of inflammation. The most common symptoms include disturbances in vision, weakness, numbness or abnormal sensations in the arms or legs, muscle spasms and loss of balance. The intensity of any episode and how long it lasts depends on the severity of the inflammation in the CNS. However many patients experience even long periods without any symptoms, and during those stages they are said to be in remission. Most patients return near normal function while they are in remission. But over time and with more episodes, function gradually declines. Even so, most patients with MS remain able to walk and can function normally or with minor disability for 20 years or more after diagnosis. Patients at later stages of disease may require a wheelchair to get around. MS is a chronic disease that is currently incurable; treatment aims to slow the disease progression and lessen symptoms. Even so, patients with MS have normal, or almost normal, life expectancies. Charcot-Marie Tooth Disease (CMTD) Case study of Allison Figure 31: Allison, age 37. Concerned that Allison might be developing CMTD too, her doctor examined Allison s lower legs carefully. He noticed that Allison s legs look a bit like an inverted champagne bottle because she has lost a lot of muscle bulk in the lower legs (Figure 32). Allison s doctor also tested her tendon reflexes and sensory perception. Given Allison s family history and worried by her poor performance on these tests, the doctor also ordered electrodiagnostic tests to see how well Allison s peripheral nerves were able to conduct an action potential. Allison is sixteen years old (Figure 31). Recently she noticed that she is having a difficult time walking. Her feet and legs do not seem to be as strong as they were even just a year ago. Allison considers herself to be in good shape, but lately on her daily walks, she has been tripping frequently. She has also been having a hard time breathing. During her yearly physical she mentioned these difficulties to her doctor. Allison s doctor asked questions about her family history. Allison knew that her uncle has a disease called Charcot-Marie Tooth Disease (CMTD). Her uncle s disease was diagnosed when he was in his early 20s and it has made it difficult for him to walk and perform fine tasks with his fingers. The tests are done by placing electrodes on the skin. These electrodes produce a small electric shock which stimulates both sensory and motor nerves. A needle, inserted into the skin, measures the ability of Allison s nerves to conduct an action potential in response to the small electric shock. Unfortunately, Allison s readings on this test indicate that her axons are not conducting action potentials as quickly as they Lesson would in normal people. A. B. Figure 32: Charcot-Marie Tooth disease (CMTD). (A) CMTD is caused by damage to myelin in the peripheral nervous system. (B) Stork legs seen in CMTD are due to muscle wasting in the lower part of the leg because innervation of skeletal muscles is defective. What are Allisons symptoms? What did her doctor diagnose her with? _ What is the neuronal defect in CMTD?
67 DEFINITIONS OF TERMS Charcot-Marie Tooth Disease (CMTD) disease in which myelin within the peripheral nervous system is damaged. For a complete list of defined terms, see the Glossary. LESSON READING Given her family history, and her results on the electrodiagnostic test, Allison s doctor diagnosed her with Charcot-Marie Tooth Disease (CMTD). CMTD is the one of the most common inherited neurological disorders. CMTD is commonly diagnosed when patients are in their teens or early twenties. CMTD is caused by damage to the myelin sheath around peripheral nerves (Figure 32). Usually, the motor nerves in the legs are affected first, causing lower leg weakness and muscle atrophy, as Allison saw. Sensory nerve degeneration causes a reduced ability to sense heat, cold, and feel pain. In later stages of the disease, similar symptoms may appear in the arms and hands as well as the legs. The severity of the symptoms is variable between patients. CMTD is not fatal and patients with most forms of the disease have normal life expectancies. While there currently is no treatment, orthopedic shoes and braces may help patients to walk. Physical and occupational therapy are also helpful for many patients because therapy helps to maintain muscle strength. You can watch a video of patients with CMTD online click below or see this unit on the student website: Video: Charcot-Marie-Tooth Disease: A patient s perspective What if there are problems with axonal transport? We can make several predictions about when and how problems in transport will occur. For example, transport will be affected if: The transport motors don t function properly. The microtubule tracks are disturbed. The supply of ATP to the neuron is compromised or if mitochondria are defective. If any of the above happens, we can predict the effect on the neuron. If transport of organelles and mitochondria is affected, then the axon terminal will be unable to function. If transport of cytoskeleton is affected, then axonal structure and diameter will be abnormal. Diseases of axonal transport Let us now investigate three of these diseases in more depth: Hereditary spastic paraplegia (HSP) Diabetic neuropathy Alzheimer s disease For two of the three (diabetic neuropathy and Alzheimer s disease) the disruptions to axonal transport occur as a result of the disease, but are not its cause. Regardless, when axonal transport doesn t function Lesson properly, neurons degenerate in all three diseases. If you were going to design a drug to treat CMTD, what would you have that drug do?
68 DEFINITIONS OF TERMS Hereditary spastic paraplegia (HSP) group of inherited disorders that are characterized by progressive weakness and stiffness of the legs, can be caused by defects in axonal transport. For a complete list of defined terms, see the Glossary. LESSON READING Hereditary spastic paraplegia (HSP) Case study of Mitchell Mitchell is 17 years old and recently noticed that he has begun to trip up frequently (Figure 33). As he paid more attention to why, he noticed that he was having difficulty raising his legs to walk. Since he thought this was odd, he mentioned it to his doctor during his yearly physical. His doctor asked him to stand up, and then lift just his toes. Mitchell had a really difficult time with it. The doctor prescribed physical therapy and asked Mitchell to make another appointment if his symptoms got worse. A year later, Mitchell s problem had not got better. He felt the muscles in his legs were often weak and quite stiff. He also noticed that his sense of balance was not what it once had been. Sometimes his legs even felt numb. He called the doctor and went back for another appointment. After many tests, including an MRI, Mitchell s doctor diagnosed him with hereditary spastic paraplegia (HSP). HSP is characterized by progressive spasticity, defined as stiff or rigid muscles in the lower limbs. Patients can also experience bladder disturbances, and impaired sensations in the feet. HSP can develop at any age. Those patients who develop symptoms before the age of 35 have Type 1, and those patients who develop symptoms after 35 have Type 2. For Type 1 cases, spasticity of the lower limbs is greater than weakness of lower limbs so difficulty walking is not common. In Type 2 cases, muscle weakness, urinary symptoms and sensory loss are more severe. Mitchell s doctor referred him to a specialist who was studying the genetic causes of HSP. The specialist completed a genetic screen on Mitchell to determine if he was a carrier of the mutation his lab studied. As it turned out, Mitchell did carry a mutation within the specialist s gene of interest, KIF5A. Figure 34: Hereditary spastic paraplegia can be caused by mutations within the motor domain of kinesin proteins Figure 33: Mitchell, age 17. KIF5A is a member of the kinesin family. Remember that Kinesins are plus-end directed motor proteins that carry cargo from the cell body to the axon terminal. Research has demonstrated that mutations within the motor part of the KIF5A protein can cause HSP because fast anterograde axonal transport is disrupted, and this in turn disrupts axonal function (Figure 34). There are currently no treatments to slow or reverse HSP. However, regular physical therapy is important for muscle strength and to preserve range of motion. Lesson 2.5 that are responsible for transporting 68 cargo to the axon terminal. What are Mitchell s symptoms? What did his doctor diagnose him with? What is the neuronal defect in hereditary spastic paraplegia? _ What does the treatment for hereditary spastic paraplegia hope to do?
69 DEFINITIONS OF TERMS Diabetic neuropathy disorder in which nerves of the body are damaged due to high blood sugar levels resulting from diabetes For a complete list of defined terms, see the Glossary. LESSON READING Diabetic Neuropathy Case study of Albert Albert is 67 years old (Figure 35). He was diagnosed with type II diabetes almost 17 years ago. Despite going on a diet and exercising, Albert has never been able to successfully manage the levels of glucose in his blood, and get them under control, so they still remain high (hyperglycemia). During the last year, Albert noticed a tingling sensation in his feet. Since he is getting older, he did not think much of it. However, when the tingling sensation developed into an actual pain, he called his doctor. His doctor did a complete examination including testing Albert s ability to detect sensations in his feet. When Albert did not perform well on this test, she told him he has likely developed diabetic neuropathy, a condition that commonly occurs in patients who have had diabetes for 10 to 20 years. Diabetic neuropathy is a common complication of diabetes, in which nerves are damaged as a result of hyperglycemia. Diabetic neuropathy can present with any number of symptoms, including tingling or burning sensations in the feet, a deep pain in the arms or legs, muscle cramps, loss of sensitivity to warm or cold, loss of bladder control, and vision changes. The symptoms vary depending on which nerves are affected. Usually feet and legs are affected first, followed by hands and arms. While it is possible to slow diabetic neuropathy by strictly controlling blood glucose levels, diabetes itself is incurable. Figure 36: Diabetic neuropathy. Damage to blood vessels in diabetes results in transport defects because ATP supply to the axons is compromised. Figure 35: Albert, age 67. Researchers have learned that diabetic neuropathy occurs when the blood supply to nerves is reduced (Figure 36). Over an extended period of time, the high levels of glucose in the blood damage blood vessels. These damaged blood vessels are less able to deliver oxygen to peripheral neurons. Lack of oxygen to nerves reduces their ability to generate ATP. Since fast axonal transport is dependent on ATP, it is particularly vulnerable in diabetic neuropathy. When axonal transport is compromised, the terminal degenerates, resulting in decreased sensitivity and motor control. While there is no cure for diabetic neuropathy, the goal of treatment is to minimize the symptoms and prevent the disease from getting any worse. It is critically important to control blood glucose levels, and some medications can help reduce the symptoms in the arms and legs. What are Albert s symptoms? What did his doctor diagnose him with? What is the neuronal defect in diabetic neuropathy? Would you expect myelinated or unmyelinated nerves to be more affected? How does that explain the symptoms? _ What does the treatment for diabetic neuropathy hope to do? Lesson
70 DEFINITIONS OF TERMS Alzheimer s disease (AD) major cause of dementia in old age, characterized by neurofibrillary tangles, amyloid plagues and neuron loss. For a complete list of defined terms, see the Glossary. LESSON READING Alzheimer s disease (AD) Case study of Yumiko Yumiko is 66 years old and incredibly forgetful (Figure 37). Lately her family has become very concerned. At a recent family dinner, Yumiko could not remember the name of her favorite dessert chocolate mousse pie. She also had difficulty remembering how to get home from her son s house. Then, later that week she had to ask for help to balance her checkbook, something she used to do all the time, often without a calculator. When Yumiko saw her doctor, she described her symptoms and asked if her family s worries were reasonable that her forgetfulness was not normal, but instead something to be concerned about. The doctor asked her a series of questions about her memory, including whether or not she was having difficulty with language, misplacing things, and thinking about abstract topics. He also asked whether or not she had noticed any changes in her mood or behavior. Yumiko didn t want to admit it, but after being pressed by her daughter she reluctantly answered that yes in fact she had been experiencing all of those things to some degree. The doctor told Yumiko that yes, in fact these symptoms, together with her age were cause for further testing. He did a complete physical exam and ordered a thorough neurological exam. The test results ruled out a brain tumor, stroke, and thyroid disease, which all could also cause the symptoms Yumiko was experiencing, so the doctor gave the diagnosis of Alzheimer s disease (AD). Alzheimer s disease is the leading cause of dementia in the elderly. It is estimated that ten percent of people over 65 have AD, and that fifty percent of those over 85 have the disease. AD affects memory, thinking and behavior. Problems with memory, as well as impairments with language, decision-making ability, judgment and personality must be present for the diagnosis to be made. AD is caused by an increased buildup of tangles of neurofilaments within the cell bodies of neurons as well as increased numbers of protein clumps called amyloid plaques at the synapse (Figure 38). Researchers have discovered that when the plaques develop, neurons are not able to communicate with each other. Perhaps due to the accumulation of tangles within the neural cell body, or perhaps due to defects in neuronal signaling, neurons start to die. Patients with AD often die earlier than normal, although a patient may live anywhere from 3 to 20 years after the diagnosis. The final phase of the disease, in which patients no longer understand language, recognize family members, and are unable to perform basic activities of daily living, may last from a few months to several years. Death usually occurs from an infection or failure of other body systems. While there is no cure for AD, treatment focuses on slowing the progression of the disease. You can watch a video about the changes to neurons that we see in Alzheimer s disease online click below or see this unit on the student website: Lesson 2.5 Video: Inside the Brain: Unraveling the Mystery of within the synapse. 70 Alzheimer s Disease Figure 37: Yumiko, age 67. Figure 38: Alzheimer s disease. Alzheimer s disease results in an buildup of neurofibrillary tangles within f neurons as well as amyloid plaques What are Yumiko s symptoms? What did her doctor diagnose him with? What are the neuronal defects in Alzheimer s disease? _ If you were designing a drug to treat Alzheimer s disease, what would you have it do? When would you start giving the drug?
71 STUDENT RESPONSES Remember to identify your sources In the figure below, label the parts of the neuron and list a function for each part. Describe what could possibly go wrong within the different parts of a neuron. What symptoms might a patient display should these problems arise? Lesson
72 Unit 3: How do our neurons communicate with each other? Overview In the last unit we learned all about the main cells that make up our nervous system neurons and glia and how they work. This unit will build on our knowledge of the neuron by exploring how neurons are able to communicate with each other. This process, called synaptic transmission, enables neurons to send signals from one part of the brain to another and ultimately to control all of our behaviors. This unit uses the experience of pain (something we can all relate to!) as the framework we will use to investigate how synaptic transmission occurs. Remember our graphic from the beginning of this workbook? This unit focuses on the synapse, which is the connection zone between two neurons.
73 DEFINITIONS OF TERMS Pain unpleasant sensory and emotional experience associated with actual or potential tissue damage For a complete list of defined terms, see the Glossary. LESSON 3.1 WORKBOOK Why do we all experience different levels of pain? This unit introduces you to the process of synaptic transmission, which is how neurons are able to communicate with each other. We will frame our exploration in the context of how we experience pain (something we can all relate too). In this lesson we will begin by examining how many different factors influence how we perceive pain. What is pain? Pain is a curious phenomenon. It s more than a simple sensation like hearing, because of the highly charged emotions associated with it. Pain researchers define pain as an unpleasant sensory and emotional experience associated with actual or potential tissue damage. Note the tight linkage between the emotional and sensory components of pain, which is not always the case for our other senses. Both the emotional and sensory components are clearly crucial to our perception of pain. You might ask why we experience pain in the first place. The answer is that in most cases, pain plays a protective role. For example, inflammation, which often accompanies skin or muscle injuries, greatly increases how sensitive the inflamed region is to stimuli. This increase in sensitivity motivates us to minimize movement of the injured area and avoid banging it, which could cause pain. In the end, both of these behaviors work together to reduce the likelihood of further injury. There is a key distinction between the neural mechanisms by which we sense pain and pain itself which is our response to actual (or even perceived) tissue damage. The distinction is very important, both clinically and experimentally. Sensing pain does not necessarily lead to the perception of pain. In fact the intensity of the pain felt depends as much on the individual and the surrounding conditions as on the sensory stimulus itself. Hence there is no such thing as a painful stimulus that will always cause the perception of pain in everyone. This first lesson of this unit focuses on the many different factors that can influence how we perceive pain. But before we can dive into that discussion, we first need to review how the researchers who study pain What was your most physically painful experience? What happened? And how did you feel? _ Why do you think some people cringe at the idea of getting a shot and others voluntarily sign up for (and actually pay) to get tattoos? _ Lesson 3.1 know for sure that we each experience a painful stimulus differently. 73
74 DEFINITIONS OF TERMS Pain threshold the intensity of a stimulus at which a subject says, It s painful half of the time, and, It s not painful the other half of the time. Pain tolerance maximum level of pain people will voluntarily accept. For a complete list of defined terms, see the Glossary. LESSON READING How can we study pain? If you wanted to ask someone to describe the pain they are experiencing, how might you do it? The task is made difficult because we don t have a good vocabulary to describe the experience of pain it either hurts a lot, or it doesn t hurt a lot. On the other hand, we do provide good involuntary cues about the pain we are experiencing through our facial expressions and bodily reactions. We are very good at decoding facial expressions of pain, to the point of being able to distinguish between facial responses to genuine pain and facial expressions that feign pain (Figure 1). Although these involuntary responses to pain are useful, researchers have devoted a great deal of effort trying to provide people with a vocabulary to articulate how they perceive pain. The first thing researchers did was to determine what someone s pain threshold is. Pain threshold is the intensity of stimulation at which a person says, It s painful half of the time, and, It s not painful the other half of the time. Pain thresholds depend on many different factors. For instance, different parts of the body have different sensitivities to pain. The cornea, back of the knee, and neck region are particularly sensitive. On the other hand, tip of the nose, and the inside lining of the cheek are particularly insensitive. If you ve ever compared the pain you feel after a tiny paper cut on the tip of a finger to the pain you feel after a gash on the sole of your foot you re already well aware that different parts of your body have different sensitivities to pain. A term related to pain threshold is pain tolerance. Pain tolerance is the maximum pain level that people will voluntarily accept. As you might imagine, research on pain tolerance is even more difficult to conduct because of ethical considerations. We have found enormous variation in both the threshold and tolerance individuals have to pain. For instance, in one study in which researchers used an electrical shock to produce consistent painful stimuli in 40 participants, they found an eight-fold difference between the smallest to largest pain threshold and tolerance. That is to say any one stimulus could be perceived by one person as being below their pain threshold, whereas the same stimulus would be perceived as being above someone else s. Now, the question becomes what causes this difference in pain threshold and pain tolerance? Figure 1: Real and faked pain facial expressions. Can you tell which frame represents the one where the subject was actually in pain (hand submerged in ice water)? For both subjects, the frame on the left represents their face when they were actually in pain. The frame on the right represents their facial expression when Have you ever noticed circumstances that adjust your pain threshold? Meaning that in one circumstance a stimulus is painful and in another it s not as bad? (Attitude, expectations, etc.) Where do you think your pain tolerance is compared to other people? Do you think you can withstand more pain than most, and have a high tolerance? Or do you think you re fairly sensitive and have a low tolerance? Give an example. Lesson 3.1 they were asked to fake being in pain. (Image 74 taken from Littlewort et al. 2007)
75 LESSON READING Pain Modifiers Our perception of pain can be modified by opiate painkillers, sugar pills, past experiences, suggestion, hypnosis and even by activating other sensations at the same time, such as happens during acupuncture. Environmental events can also diminish pain perception. For example, one researcher noted that many wounded American soldiers returning from battles during World War II reported that they felt no pain from their wounds. They did not even want pain medication. It seemed that their perception of pain was reduced by the relief they felt that they had survived such a terrible ordeal. There are other examples in which people report that even though they can perceive pain they aren t bothered by it. Some tranquilizers have this effect, and they are often used during oral surgery. Some kinds of brain damage also have this effect. Does gender play a role? Any mother will tell you that if men needed to go through the excruciating pain of childbirth, the human race would have gone extinct long ago. According to feminine lore, men simply can t handle pain. The tiniest discomfort is enough to reduce most men into helpless, whimpering heaps. Women, on the other hand, can handle the tough stuff. The trouble with this theory is it s probably wrong, or at least it s not the whole story. Some research suggests that women actually have lower tolerance for many kinds but not all kinds of painful stimuli. Other research suggests that men and women may experience pain differently because women use estrogen to reduce how much pain they perceive. That same research is now investigating whether a woman s menstrual cycle plays a role in her perception of pain. So, the fact remains, no one really knows for sure if women and men perceive pain differently. Your brain itself has no pain Curiously enough, the outside of your brain doesn t feel a thing. Surgeons can, and do, touch the outer surface of brains during surgery. That s because the perception of any stimulus, including pain, depends on the presence of sensory neurons with receptors that respond to pain, and your brain (and other internal organs) don t have very many of these. In fact, your internal organs in total house only about 2 5 percent of any of the sensory neurons in the body. Because of this, while we can keep close touch (literally) with the world around us, we have limited conscious awareness of what s going on in our innards possibly we have evolved this way because most threats we need to deal with come from the external environment. Pain receptors (remember they re called nociceptors) do exist near your brain: they re in its blood vessels and in the meninges that surround it. In fact one of the likely sources of migraine headache pain is from the nociceptors that are found in the meninges. Do you think men and women have different tolerances for pain? From your own observations, would you expect that women have a lower tolerance for pain than men? Lesson
76 STUDENT RESPONSES Remember to identify your sources Why do you think so many different things are able to change our perception of pain? Why would and how could this be beneficial? Lesson
77 LESSON 3.2 WORKBOOK How do our neurons communicate with each other? This lesson introduces you to how one neuron communicates with another neuron during the process of synaptic transmission. In this lesson you will learn how the electrical signal of the action potential is converted into a chemical signal at the nerve terminal, and how this chemical signal crosses the small gap, the synapse, between the presynaptic and the postsynaptic neuron. Getting pain to the brain Pain pathways deliver information about painful stimuli (nociceptive information) using an ascending pathway that travels from the nociceptive receptors in the periphery to the brain. The pathway has four important neurons, each of which plays a different role in transmitting and interpreting the painful signal (Figure 2): The first, or primary, neuron is at the very beginning of the pathway. The end of its dendrites in the periphery is where the nociceptive stimulus is first encountered. Its presynaptic terminal is in the spinal cord and connects with.. The dendrites of the second neuron, which is located in the spinal cord. This neuron gathers nociceptive information from several primary neurons into distinct pathways that ascend in the white matter of the spinal cord. Their presynaptic terminals are in the thalamus and connect with The third neuron, which is located in the thalamus. The thalamus is like a post office that gathers information and sends it to the right place in the cortex. So their presynaptic terminals are in the cortex where they connect with Neurons in region of the cortex that deals with receiving sensory information about pain (somatosensory cortex). Within the cortex these neurons also communicate with cortical areas having other information about the environment and emotion, so that the body can initiate a response. Lesson 3.2 Now that we know about the four neurons involved in getting pain information to the brain, let s focus on 77 how the neurons communicate with each other at the synapses between them. What are the four neurons involved in getting pain to the brain? Where are they and what role do they play in the pathway?
78 DEFINITIONS OF TERMS Neurotransmitters chemicals that are released by the axon terminal and convey the message across the synapse to another cell. Postsynaptic potentials small changes in voltage (membrane potential) due to the binding of neurotransmitter. Receptors proteins that contain binding sites for particular neurotransmitters. For a complete list of defined terms, see the Glossary. LESSON READING An introduction to synaptic transmission Synaptic transmission is the major way that neurons communicate with each other across the small gap between the presynaptic site and postsynaptic site called the synaptic cleft. When we left the presynaptic terminal, an electrical signal the action potential had traveled down the axon. However the action potential, being electric, can t jump the synaptic cleft between the pre- and postsynaptic sites. To transmit the message to the postsynaptic site the neuron must convert the electrical signal to a chemical one. This chemical signal is carried by neurotransmitters chemicals that are released when the axon terminal is stimulated by the action potential. Motor neuron Sensory neuron Interneuron Projec'on neuron Figure 2: The synapses in the pain pathway. The synapses in the pain pathway allow for modulation of pain stimuli. The first synapse is in the periphery, where nociceptors are initially activated. The second synapse is in the spinal cord. The third synapse is in the thalamus (not shown here) and the fourth synapse is in the cortex. The neurotransmitters diffuse across the synaptic cleft to the postsynaptic site where they bind to specific receptors that recognize them on the postsynaptic membrane. Once the neurotransmitter has bound to the receptor it can produce a postsynaptic potential a brief depolarization or hyperpolarization in the postsynaptic membrane that happens because the neurotransmitter receptors themselves are associated with ion channels. If enough postsynaptic potentials occur, the membrane may be pushed toward or away from threshold, depending on whether the membrane has depolarized or hyperpolarized, increasing or decreasing the likelihood of the postsynaptic neuron firing an action potential and sending the signal down its axon to another synapse. Since there are obviously several steps involved in synaptic transmission, let s investigate each one in more detail. We ll start our more detailed discussion of synaptic transmission by taking a closer look at the synapse. How is synaptic transmission different from the action potential? Compare where the two signals occur and how the signal is sent. Lesson
79 DEFINITIONS OF TERMS Synaptic vesicles small spherical membranes that store neurotransmitters and release them into the synaptic cleft For a complete list of defined terms, see the Glossary. LESSON READING The Synapse The word synapse was coined in 1897 by the British physiologist Sir Charles Sherrington (Figure 3) from the Greek word synapo, which means to clasp. Using only a light microscope, Sherrington could not see the actual point of communication between neurons, but his experiments had shown that transmission can only occur in one direction (from what we now call the presynaptic cell to the postsynaptic cell). Sherrington even correctly inferred that the sending (presynaptic) and receiving (postsynaptic) cells do not actually touch each other. Presynap)c membrane Postsynap)c membrane Microtubule Mitochondrion The presynaptic terminal Presynap)c cell Postsynap)c cell Axon Figure 4: Structure of a typical synapse. The presynaptic membrane faces the postsynaptic membrane. Notice that the presynaptic cell contains both large and small synaptic vesicles, mitochondria and microtubules. Notice that the postsynaptic membrane contains receptors sites that will bind neurotransmitter. Figure 3: Sir Charles Sherrington ( ). For his work, he was awarded the Nobel Prize for Physiology or Medicine in Figure 4 illustrates a synapse. The presynaptic membrane, located at the end of the axon terminal, faces the postsynaptic membrane, located on the neuron receiving the information. These two membranes face each other across the synaptic cleft, a gap that varies in size from synapse to synapse but is usually around 20 nanometers (nm) wide. As you may have noticed in Figure 4, the axon terminal contains two prominent structures: mitochondria and synaptic vesicles. (We can also see the microtubules, which as you will remember are responsible for transporting the mitochondria and vesicles from the cell body where they are made to the terminal.) Because the terminal is often swollen to contain all this material it is often called the terminal button or more precisely bouton, which is simply button in French. Recall from Unit 2 that vesicles are small, hollow, beadlike structures that are transported down the axon from the cell body. In the synaptic terminal most of them are filled with neurotransmitters and become synaptic vesicles. Axon terminals can contain as few as a few hundred and as many as nearly a million Why do you think mitochondria are located in the presynaptic terminal? Lesson 3.2 synaptic vesicles. 79
80 LESSON READING The postsynaptic terminal The picture in Figure 5 was taken with a very high resolution electron microscope, and shows that the postsynaptic membrane appears somewhat thicker and more dense than the membrane elsewhere. This increased density occurs because the postsynpatic membrane is loaded with neurotransmitter receptors specialized proteins that detect the presence of neurotransmitter in the synaptic cleft because the neurotransmitters bind to them very specifically. What are neurotransmitters? Neurotransmitters are the chemicals neurons release in order to communicate with other cells. Scientists first thought that only a few chemicals were involved in neurotransmission, but we have now identified over 100 different neurotransmitters. Fortunately, most of them conveniently fall into a small number of chemical classes. See Box 3.1 for descriptions of your body s primary neurotransmitters. BOX 3.1: Your Neurotransmitters Figure 5: Electron micrography of an synapse. This photography shows a cross section of a synapse. The axon terminal is filled with synaptic vesicles (upper left corner). The postsynaptic membrane on the dendritic spine appears thicker and denser than the other membranes; this is due to the presence of receptors. There are more than a hundred different neurotransmitters, with more being discovered all the time. Scientists are finding that many hormones can also play the role of transmitter as well. Here are some the neurotransmitters your brain uses every day: Acetylcholine (ACh) gets us going. It excites cells, activates muscles, and is involved in wakefulness, attentiveness, anger, aggression, and sexuality. Alzheimer s disease is associated with a shortage of acetylcholine. Glutamate is a major neurotransmitter that excites other neurons. It is dispersed widely throughout the brain. It s involved in learning and memory. GABA (gamma-aminobutyric acid) is your brain s main inhibitory neurotransmitter. It slows everything down and helps keep your systems in balance. It helps regulate anxiety. Epinephrine, also known as adrenaline, keeps you alert and your blood pressure balanced, and it jumps in when you need energy. It s produced and released by the adrenal glands in times of stress. Too much can increase anxiety or tension. Norepinephrine (noradrenaline) is a precursor and has similar actions. Dopamine (DA) is vital for voluntary movement, attentiveness, motivation and pleasure. It s a key player in addiction, so we ll discuss it again in Unit 5. What neurotransmitters have you heard of before and in what context? Lesson 3.2 Serotonin helps regulate body temperature, memory, emotion, sleep, appetite, and mood. Many antidepressants work by regulating serotonin. 80
81 DEFINITIONS OF TERMS Exocytosis process by which the contents of membrane bound vesicle are released to the exterior through fusion of the vesicle membrane with the cell membrane. For a complete list of defined terms, see the Glossary. LESSON READING Release of neurotransmitter When action potentials are conducted down the axon and enter the presynaptic terminal, something happens inside the terminals a number of small synaptic vesicles spill their contents into the synaptic cleft (Figure 6) Figure 6: Steps involved in synaptic transmission. See text for descriptions, then write your own summary How does an action potential cause synaptic vesicles to release neurotransmitter into the synaptic cleft? The process begins when an action potential invades the presynaptic terminal (Figure 6: Step 1). Then, some of the synaptic vesicles closest to presynaptic membrane become docked at a region in the presynaptic terminal called the active zone. Docking happens when clusters of proteins on the outside of the synaptic vesicle attach to other proteins located on the inside of the active zone. Once they are docked, synaptic vesicles are ready to release their neurotransmitter into the synaptic cleft. Synaptic vesicles only release their neurotransmitter when the action potential tells them to. How does this happen? We need to introduce another player located at the presynaptic terminals the voltagegated calcium channel. Voltage-gated calcium channels are similar to voltage-gated sodium channels in that they only open when the membrane depolarizes. They are different from voltage-gated sodium channels because they are permeable to calcium ions (Ca 2+ ), not Na + ions. Like Na + ions, calcium ions (Ca 2+ ) are located in highest concentration in the extracellular fluid, so when an action potential arrives at the presynaptic terminal and depolarizes the membrane, the calcium channels open and Ca 2+ floods into the presynaptic terminal, propelled by the forces of diffusion and electrostatic pressure as we talked about in Lesson 2.2 (Figure 6: Step 2). The entry of Ca 2+ into the presynaptic terminal is an essential step in synaptic transmission because it gives the synaptic vesicles the signal to release their neurotransmitter into the synaptic cleft. The Ca 2+ ions bind with the cluster of proteins that docked the membrane of the synaptic vesicles with the active zone. The binding of Ca 2+ changes the shape of these proteins, making them move apart. As they move apart a hole or pore appears in both the synaptic vesicle and the active zone it is attached to. Both membranes then form a fusion pore so the synaptic vesicles can release their contents into the synaptic cleft. The arrival of an action potential triggers the release of neurotransmitters. How does it trigger this release? The entry calcium ions into the presynaptic terminal is another important step in the release of neurotransmitter. What happens after calcium levels rise? With synaptic vesicles fusing to the presynaptic membrane, how does the presynaptic membrane not just continually increase in size? Lesson 3.2 Another name for this process of fusion and release is exocytosis (Figure 6: Step 3). 81
82 DEFINITIONS OF TERMS Endocytosis process by which matter is taken in by a living cell by invagination of its membrane to form a vesicle. Postsynaptic potentials small changes in voltage (membrane potential) due to the binding of neurotransmitter. For a complete list of defined terms, see the Glossary. LESSON READING What happens to the membrane of the synaptic vesicles after they have broken open and released the neurotransmitter they contain? If the open vesicles have not completely collapsed onto the presynaptic membrane they can simply pinch off again and drift away to be filled once more with neurotransmitter. This has been called kiss and run. Other times the fusion pore becomes so large that the vesicles seem to flatten down and merge entirely with the presynaptic membrane. In these cases the little buds of the presynaptic membrane pinch off back into the terminal, effectively creating new synaptic vesicles. Another name for this process of pinching off and recovery is endocytosis. Activation of receptors How does the release of neurotransmitters from the presynaptic terminal into the synaptic cleft produce an effect in the postsynaptic cell? The answer to this question begins with the binding of neurotransmitters to their receptors on the postsynaptic cell membrane (Figure 6: Step 4). Once this binding occurs, the postsynaptic receptors too change their shapes, and in the process open ion channels located in the postsynaptic membrane. These ion channels, which are called receptor-gated ion channels, because they are activated by receptors, not by voltage, permit specific ions to pass into or out of the postsynaptic cell (Figure 6: Step 5). Thus, the neurotransmitter in the synaptic cleft, by binding to receptors, allows particular ions to pass through the postsynaptic cell s membrane, changing the membrane potential at the postsynaptic site and creating postsynaptic potentials. Termination of synaptic transmission Postsynaptic potentials are therefore brief changes in the postsynaptic membrane potential caused by the activation of postsynaptic receptors by neurotransmitters. They are kept brief because the neurotransmitter is rapidly removed from the synaptic cleft, and once it is removed it can no longer activate its receptors. Neurotransmitters can be removed by two mechanisms: Reuptake Degradation by enzymes Almost all central nervous system neurotransmitters are removed by reuptake (Figure 6: Step 6). This simply involves taking the neurotransmitter back into the presynaptic terminal again, using a special energy-dependent pump called a transporter. This means that from the time that an action potential stimulates release of neurotransmitter into the synaptic cleft, until the presynaptic terminal takes it back up again, the postsynaptic receptors only have a brief exposure to the neurotransmitter. The process of reuptake ensures that postsynaptic potentials are also quite brief. The binding of neurotransmitters to receptors causes ion channels to open, thus changing the membrane potential in the postsynaptic neuron. Can you predict how this change in membrane potential might affect the postsynaptic neuron? What might result from this change in membrane potential? Certain drugs inhibit the reuptake of neurotransmitter from the synaptic cleft. What would happen if this reuptake was blocked? Lesson
83 LESSON READING Neurotransmitters can also be broken down in the synaptic cleft by enzymes. As far as we know only one neurotransmitter is dealt with in this way, but it is an important one. Acetylcholine (ACh) is the neurotransmitter used at our neuromuscular junctions, where neurons instruct our muscles to contract. It is critical that the postsynaptic potentials produced by ACh be short-lived because the quick breakdown of ACh is important for us to have tight control over the timing of muscle contraction. So at the neuromuscular junction the synaptic cleft is awash with the specific enzyme that can chew up ACh, and stop it binding to its receptor. Summary In conclusion remember that the communication between neurons requires several steps. First the presynaptic cell must fire an action potential. Once the action potential invades the presynaptic axon terminal, the presynaptic cell releases neurotransmitters into the synaptic cleft. These neurotransmitters then cross the synapse and bind to receptors on the postsynaptic cell. After binding to receptors, neurotransmitters cause postsynaptic potentials in the postsynaptic cell. What do you predict would be the effect of drugs or toxins that stop the breakdown of ACh in the neuromuscular junction? Lesson
84 STUDENT RESPONSES On the diagram below, label and describe the steps of synaptic transmission. The goal of synaptic transmission is to send a signal from one neuron to another. Does it matter which ions channels open and which ions flow into the postsynaptic cell? (Hint: Think about the effect positive and negative ions would have on the chances of the postsynaptic neuron reaching threshold.) Lesson
85 DEFINITIONS OF TERMS Postsynaptic potentials small changes in voltage (membrane potential) due to the binding of neurotransmitter. Receptor-gated ion channels ion channels that open or close in response to the binding of a neurotransmitter. For a complete list of defined terms, see the Glossary. LESSON 3.3 WORKBOOK Why does applying pressure relieve pain? In the last lesson, we learned how neurons send signals across the synaptic cleft via synaptic transmission. But two questions remain how does this type of signaling result in an action potential in the postsynaptic cell? And thinking back to our pain framework, how does communication between neurons in the pain pathway allow us to control how we perceive painful stimuli? The answer to both questions lies in the specialized structure at the start of the axon where the action potential originates the axon hillock. Postsynaptic potentials Remember that the local changes in membrane potential created by neurotransmitters binding to their receptors at the synaptic cleft are referred to as postsynaptic potentials. Interestingly, the kind of postsynaptic potential a particular synapse produces does not depend on the neurotransmitter itself. Instead, it is determined by the characteristics of the postsynaptic receptors the neurotransmitter binds to in particular, by the specific type of ion channel they open. Receptor-gated ion channels in the postsynaptic membrane are much more versatile than the voltage-gated ion channels in the axon. First, the postsynaptic membrane contains more than just Na + and K + channels. The postsynaptic membrane contains anion channels (permeable to negatively charged ions) as well as other cation channels (permeable to positively charged ions). Second, receptor-gated ion channels can move ions out of the postsynaptic cell as well as into it. This means that the receptor-gated ion channels can have a varied range of effects on the postsynaptic cell, as we shall see. The end goal of all these effects is on the threshold that regulates whether an action potential will fire. We can identify two major types of receptor-gated ion channels in the postsynaptic membrane: cation channels (permeable to positively charged ions) and anion channels (permeable to negatively charged ions): Two cation channels permeable to: One anion channel permeable to: What causes receptor-gated ion channels to open? How is that different from the voltagegated channels we saw in the axon? _ Why does opening sodium or calcium ion channels cause a neuron to depolarize? _ Why does opening chloride ion channels cause a neuron to hyperpolarize? _ Lesson 3.3 Sodium (Na + ) Chloride (Cl - ) 85 Calcium (Ca 2+ )
86 DEFINITIONS OF TERMS Excitatory postsynaptic potentials (EPSP) graded postsynaptic depolarizations, which increase the likelihood that an action potential will be generated. Inhibitory postsynaptic potentials (IPSP) graded postsynaptic hyperpolarizations, which decrease the likelihood that an action potential will be generated. Integration adding or combining a number of individual signals into one overall signal. For a complete list of defined terms, see the Glossary. LESSON READING Note that these channels are different from the voltage-gated sodium and calcium channels we talked about on the axon and the presynaptic terminal because they are stimulated to open by a neurotransmitter binding to its receptor, and not by a change in voltage. When channels open that are permeable to either sodium or calcium, Na + or Ca 2+ ions can enter the cell, as we saw before. This entry of positive ions depolarizes the postsynaptic membrane, making the membrane potential more positive, or phrased another way, less negative. This is called an excitatory postsynaptic potential (EPSP) and it brings the postsynaptic cell closer to the threshold for firing an action potential. However, when channels that are permeable to chloride (Cl - ) open, the negatively charged Cl - ions that are in high concentration outside the cell, are pushed inside by the force of diffusion. This entry of negative ions hyperpolarizes the postsynaptic membrane, making the membrane potential more negative. This is called an inhibitory postsynaptic potential (IPSP) and it brings the postsynaptic cell farther away from the threshold to fire an action potential. Threshold Voltage at which Na + channels open Inhibitory Postsynap/c poten/als (IPSP) caused either by entry of Cl - ions, or exit of K + ions Excitatory Postsynap/c poten/als (EPSP) caused by entry of either Na + or Ca 2+ ions Figure 7: Getting to threshold. IPSPs decrease the chance of reaching threshold because they make the membrane potential more negative. EPSPs increase the chance of reaching threshold because they make the membrane potential more positive. Recall that an action potential is only initiated after the threshold that opens the axon s voltage-gated Na + channels is reached. Because EPSPs depolarize the postsynaptic membrane, they bring the membrane potential closer to threshold, increasing the likelihood that the voltage-gated Na + channels will open and the postsynaptic neuron will fire an action potential. Conversely because IPSPs hyperpolarize the postsynaptic membrane they move the membrane potential further away from threshold, decreasing the likelihood the voltage-gated Na + channels will open and the postsynaptic neuron will fire an action potential. (Figure 7). Remember though that a single dendritic tree may have hundreds of thousands of synapses, all of which receive inputs from presynaptic terminals. What happens when an EPSP and an IPSP arrive at the same time close to each other? Do they simply cancel each other out in the membrane? Obviously this isn t a good solution and each neuron has the job of integrating all these many different types of inputs into a coherent output. They do this through the process of integration. Why do EPSPs increase the likelihood of firing an action potential? Why do IPSPs decrease the likelihood of firing an action potential? Lesson
87 DEFINITIONS OF TERMS Axon hillock specialized part of a neuron s cell body that connects to the axon. As a result, the initial segment or axon hillock is the site where action potentials originate. For a complete list of defined terms, see the Glossary. LESSON READING The integration of all local postsynaptic potentials (EPSPs and IPSPs) occurs in the axon hillock (Figure 8). The goal of input integration is to put the neuron into a final electrical state whereby it can either fire an action potential or not. Generally: Excitatory Synapse: Neurotransmi4ers open Na + or Ca 2+ channels producing EPSPs. Inhibitory Synapse: Neurotransmi4ers open either K + or Cl - channels producing IPSPs. Axon hillock reaches threshold and acdon potendal is fired. IPSPs encounter EPSPs. Threshold is not reached and no acdon potendal is fired. Figure 8: Axon hillock. The axon hillock generates an action potential if the excitatory inputs reach threshold to open the voltage-gated Na + channels. The axon hillock will not generate an action potential if the inputs do not reach the threshold to open the voltage-gated Na + channels. The axon will only fire an action potential if the postsynaptic membrane reaches the threshold to open the axon s voltage-gated Na + channels. This can only happen when the excitatory inputs are greater than the inhibitory inputs. The axon will not fire an action potential if the postsynaptic membrane does not reach the threshold to open the axon s voltage-gated Na + channels. This happens when the excitatory inputs aren t great enough, and/or when the inhibitory inputs are greater than the excitatory inputs. The process of synaptic integration is in continuous operation in every neuron in the nervous system. Each cell integrates all of the synaptic information it receives at any one time, and depending on the balance of excitation and inhibition, it either fires an action potential or it doesn t. Under what circumstances will the axon hillock initiate an action potential? Under what circumstances will the axon hillock not initiate an action potential? Why? To further explore this idea let s examine how applying pressure can relieve pain, but before we dive into Lesson 3.3 that discussion, let s first remind ourselves of the pathway to get pain to the brain. 87
88 DEFINITIONS OF TERMS Projection neuron neuron whose axons make synapses in the brain. For a complete list of defined terms, see the Glossary. LESSON READING The pain synapse in the spinal cord Recall that the pain pathway has four neurons. The first is in the periphery, the second is in the spinal cord, the third is in the thalamus, and the fourth is in the somatosensory cortex. Let s take a closer look at the synapse between the first neuron and the second in the spinal cord. In the spinal cord, neurons carrying pain stimuli make synaptic connections within the grey matter in the area that deals with sensory information called the dorsal horn. Specifically, the first pain neurons connect to projection neurons that then project up the spinal cord, carrying pain information to the third neuron in the thalamus (Figure 9). But the first pain neurons aren t the only neurons that make connections with the projection neurons. A different type of neuron that is sensitive to pressure, not to pain, also connects with the same projection neuron (Figure 9). We call these connections between pain, pressure and projection neurons a circuit. This circuit is the first way we manage our responses to painful stimuli. We can diagram how the circuit is wired (Figure 10). How the circuit works Now that we know how the circuit is wired, let s look at how it works. Figure 9: Pain and pressure synapse in the spinal cord. Neurons carrying painful information, as well as neurons carrying pressure information both synapse on the same projection neuron that carries information to the brain. Remember, that the neurons carrying painful stimuli synapse on the projection neurons. These pain neurons make excitatory synapses with projection neurons. This means that when pain neurons are activated What is the benefit of having both pain and pressure sensitive neurons synapsing on the same projection neuron? How does applying pressure relieve some of our pain? by painful stimuli they will always excite the projection neurons to produce an action potential. Lesson Interneuron Pain neuron Pressure neuron Projec-on neuron To Brain Figure 10: Wiring of pain and pressure synapse in the spinal cord.
89 DEFINITIONS OF TERMS Behavioral inhibition inhibition of behavior. Neural inhibition inhibition of neural signaling. For a complete list of defined terms, see the Glossary. LESSON READING However, remember that the projection neurons are also connected to pressure sensitive neurons. But these neurons make inhibitory synapses with the projection neurons. This means that when pressuresensitive neurons are activated by pressure stimuli, they will always inhibit the projection neurons, preventing them from producing an action potential. We can see this circuit in action when we bang our elbow or stub our toe, and then immediately go to rub it. By rubbing the painful area we re applying pressure that will activate our pressure-sensitive neurons. These neurons will then communicate with the projection neurons in the spinal cord and inhibit them so they ll no longer tell the brain that they re getting painful information from the first pain neurons. It s all a matter of balancing excitatory and inhibitory inputs. It s not quite the same as No brain, no pain, but if the pain never gets to the brain, we certainly can t feel it. Excitation vs Inhibition It s just a bit more complicated Note that an inhibitory postsynaptic potential, which leads to neural inhibition, does not always produce behavioral inhibition. For example, suppose a group of neurons actually prevents a particular movement from taking place, for instance if they hold your head erect, preventing it from falling forward. If these neurons experience enough IPSPs they won t fire an action potential and will experience neural inhibition. But what effect will this have on your head? In fact if these neurons are inhibited, i.e. prevented from functioning, they will no longer be able to prevent your head falling onto your chest. Thus, inhibiting inhibitory neurons makes the behavior more likely to occur. If we think about neural excitation we can see that the same thing occurs: If we activate neurons that inhibit a behavior, we will tend to suppress that behavior. For example, when we are dreaming, a particular set of inhibitory neurons in the brains becomes active and prevents us from getting up and acting out our dreams. It is important to remember that all neurons need to reach threshold before they can fire an action potential and communicate with other neurons via synaptic transmission. Whether they will reach that threshold depends on how the axon hillock integrates the hundreds of thousands of excitatory and inhibitory inputs that fall onto the dendritic tree. If the action potential is fired, whether that neuron will have an excitatory or inhibitory effect on the postsynaptic cells it communicates with will depend on which neurotransmitters it releases, how they interact with their receptors on the postsynaptic side and which ion channels they open. In summary, an action potential always precedes synaptic transmission, and an action potential is always preceded by reaching threshold, and to reach threshold more excitatory inputs than inhibitory inputs are required (even if the neuron is inhibitory). Can you predict the effects of damage to our neurons that prevent us acting out our dreams? Lesson
90 STUDENT RESPONSES What must always precede the release of neurotransmitter? Remember to identify your sources What must always precede the firing of an action potential? Therefore, even in the case of an inhibitory neuron, what sequence of events must occur before it can release neurotransmitter to inhibit the postsynaptic cell? Lesson
91 LESSON 3.4 WORKBOOK What causes different pain phenomena? Now that we re familiar with the process of synaptic transmission and the pain pathway, let s turn our attention to how these can explain some of the most puzzling sensory perceptions we know pain phenomena. Types of Pain First and Second Pain: Why do we first feel a stabbing pain, and then later feel an aching pain? We ve talked about the pain receptors or nociceptors on the dendrites of the first pain neuron that recognize pain, or nociceptive, or noxious stimuli. Nociceptors are simply free nerve endings in the skin. They are activated after the inflammation that occurs following either pressure or extremes of temperature, so we can identify three different types of nociceptors. Thermal nociceptors are activated by extreme temperatures. They transmit information very quickly because their Aδ axons are myelinated. Mechanical nociceptors are activated by intense pressure. They also transmit information quickly via myelinated Aδ axons. Polymodal nociceptors are activated by thermal, pressure or chemical stimuli. They transmit information more slowly because their C axons are unmyelinated. Lesson
92 DEFINITIONS OF TERMS Anterograde transport movement of materials from cell body to axon terminals. Retrograde transport movement of materials from axon terminals to the cell body. Kinesin plus-end directed motor that carries cargo from the cell body to the axon terminal along microtubules. Dynein minus-end directed motor that carries cargo from the axon terminal to the cell body along microtubules. For a complete list of defined terms, see the Glossary. LESSON READING Nociceptors will transmit noxious information quickly if the myelinated Aδ neurons are activated and more slowly if the unmyelinated C neurons are activated (Figure 11). Because of this, the painful information carried by Aδ neurons is often referred to as first pain because it is felt first as a sharp sensation. The painful information carried by C neurons is often referred to as second pain because it occurs later and is felt as burning or aching (Figure 12). Figure 12: First versus second pain. First pain is felt as a stabbing pain, whereas second pain is felt more as a diffuse ache or throbbing pain. Figure 11: Fast versus slow pain. Fast pain is due to the activation of myelinated Aδ fibers. Slow pain is due to the activation of unmyelinated C fibers. Thus we can see that how pain is felt depends on which nerves transmit the pain information. If only Aδ neurons respond, then only a first pain is felt in a sharp sensation. If only C neurons respond, then only a second pain of burning or aching is felt. If both Aδ and C neurons signal, then a sharp sensation is felt first due to the Aδ neuron response, then a second burning or aching pain is felt due to the C neuron response. Referred Pain: Why do people feel pain in their arm when they are having a heart attack? Noxious information from the internal organs is detected by receptors that are activated by inflammation and chemicals, such as toxins released by bacteria or tainted food. We talked about the first pain neurons that make a synapse in the sensory region of the spinal cord (dorsal horn). It turns out that pain neurons from the internal organs synapse on the same neurons (Figure 13). However, pain sensation from the skin are usually more common than those from the internal organs. Therefore, when pain receptors from the internal organs are activated, our cortex tends to think the pain neurons in the skin have been affected and it localizes, or refers, the sensations to areas of the skin. What is first and second pain? Describe the phenomenon. Why does first and second pain occur? What is it about our nervous system that causes this phenomenon? Lesson
93 LESSON READING Thus we experience pain from an internal organ on predictable areas of the body surface. When you feel pain in the arm following a heart attack, this is because your brain is misinterpreting the source of the painful stimulus, not because your arm has also been damaged. Why are these areas so predictable? Pain neurons from the skin and the internal organs are always coupled in the same area of the spinal cord. Figure 14 shows the stereotyped distribution of referred pain used to diagnose damage to internal organs. As we already discussed, pain in the heart is often perceived on the left arm. Pain originating in the lung and diaphragm are similarly perceived on the left side of the neck and left shoulder. Figure 13: Synapse in referred pain. Nociceptive neurons from the skin (red) and the internal organs (green) synapse in the same place in the spinal cord. Since the brain cannot tell where the stimulus is coming from and sensations from the skin usually predominate, the brain incorrectly assumes the pain is in the skin. If a pateint described a pain in the center of his chest, but couldn t remember suffering any injury to his chest, what internal organs would you suspect might be injured? Phantom Limb Pain: Why do amputees feel pain in their missing limbs? Almost immediately following the amputation of a limb, 90-98% of patients report experiencing a sensation coming from their missing limb, called phantom sensation (Figure 15). For some lucky patients, the phantom limb experiences may fade, disappear or change over time, in others, not so lucky, the phantom limb experiences continue for Figure 14: Referred pain. The stereotyped distribution of referred pain is used to diagnose damage to internal organs. Why does referred pain occur? What is it about our nervous system that causes this phenomenon? Figure 15: Phantom limb. The solid lines show the site of the amputation, the dotted lines where the Lesson 3.4 years. phantom limbs were experienced. 93
94 LESSON READING This is how we explain this strange phantom limb phenomenon: When a limb is stimulated by any kind of sensation the appropriate part of the opposite parietal lobe is activated in the somatosensory cortex. If the limb is removed, this part of the brain no longer receives its normal input but continues to expect it, therefore it recreates a phantom limb where that limb used to be (Figure 16). In some cases the brain reorganizes so that the part of the brain that used to respond to the missing limb responds to other things instead. For example, it may respond to touch in a different part of the body. Some amputees have painless phantom limbs, whereas others experience excruciating phantom limb pain. Doctors do not completely understand why this is. One factor known to be important is whether the limb was in pain prior to amputation. If the real limb was in pain prior to amputation, then there is a high chance that the phantom limb will be painful too, presumably because the brain is still expecting that pain activation. Many patients experience pain because the phantom limb seems to be clenched. Since phantom limbs are obviously not under voluntary control, unclenching them is impossible. Neurologists have recently discovered the ability to use mirror boxes to trick the brain into perceiving the phantom limb is unclenched. By watching the mirror image of the intact limb, mirror box therapy provides the brain with visual stimuli showing the phantom limb being unclenched (Figure 17). If a patient who had just had his left leg amputated because of diabetes started feeling pain in that left leg, what would you diagnose? Why does phantom limb occur? What is it about our nervous system that causes this phenomenon? You can watch a video of Ramachandran talking about phantom pain online click below or see this unit on the student website: Lesson Figure 16: Phantom sensations in the somatosensory cortex. It is believed that the experience of a phantom limb occurs because the area of the cortex that used to receive input from the amputated limb starts responding to other sensations. For example, if the right arm was amputated, the pink line shows the area of the somatosensory cortex no longer receiving input. If this area were to respond to other sensations, the brain might mistake that as coming from the right arm. Figure 17: Mirror box therapy. Neurologists have discovered that mirror box therapy can provide relief for phantom limb pain. The theory is that if the brain receives visual feedback that the limb is not in pain, then the phantom limb pain will decrease. Video: VS Ramachandran: 3 clues to understanding your brain
95 LESSON READING Pain and Emotions: Why do our emotions play such a large role in how we perceive pain? Many areas of the brain collaborate in our experiences of pain, including some of the areas involved in dealing with our emotions. This overlap probably explains why emotion is such a large component of the pain response. We have seen how the sensory neurons in the pain pathway carry pain sensations to the somatosensory cortex located in the parietal lobe. The somatosensory cortex is responsible for processing all tactile sensations from the body, not just pain (Figure 18). However, pain does not simply arise from how information is processed in the somatosensory cortex. If it did, the sensation would reflect the small, well-defined areas of the skin that the pain receptors sample. Instead, as we have seen, most clinical pain involves aches that seem to spread around the whole body. These so-called diffuse aches occur because other areas of the cortex are also involved in pain perception, notably the insular cortex (Figure 19), and anterior cingulate cortex (ACC) (Figure 20). Figure 19: Insular cortex. The insular cortex is directly beneath the primary somatosensory cortex and is involved in emotional responses to pain. Figure 18: Somatosensory cortex. Sensory input from the body maps onto the parietal cortex at the somatosensory strip. The homunculus reflect the differences in sensory input from each area. The insular cortex is found directly underneath the primary somatosensory cortex. Its role is to deal with information about the internal state of the body and it also contributes to the emotional response to pain. Patients whose insular cortex is damaged don t have an appropriate emotional response to pain, they may know its occurring but they aren t affected by it. How do our emotions change the way we perceive pain? Lesson
96 DEFINITIONS OF TERMS Analgesics drugs that reduce pain. For a complete list of defined terms, see the Glossary. LESSON READING Figure 20: Cingulate cortex (also kown as Cingulate gyrus). The cingulate gyrus is part of the limbic system that is also important in the emotional responses to pain. The anterior cingulate cortex (ACC) is the front half of the cingulate gyrus. The anterior cingulate cortex (ACC) is important for processing emotion (Figure 20). It is part of an evolutionarily ancient area of the cortex called the limbic system. The emotional or affective component of pain that can be described by terms like sickening, terrifying and punishing, relates to activation of the ACC. The insular cortex and ACC work together to determine how we will respond emotionally to pain by associating the current painful sensations we are experiencing with our past experiences of pain. The insular cortex and ACC can also control how painful sensations are processed and thus change how we perceive pain. Interestingly, this is not just a one-way street with emotions affecting how we process pain. We have discovered that the converse also happens i.e. that pain also affects how we process our emotions. When volunteers were asked to play a gambling card game to study how they made decisions in risky, emotionally laden situations, those volunteers with chronic pain made 40 percent fewer good choices compared to those without pain. What s more, the amount of suffering correlated with how badly the volunteers played! Medications for Pain: How do medicines that relieve pain work? Analgesics are a group of drugs used to relieve pain. They work in a variety of ways, both within the brain and within the spinal cord. Their goal is to relieve pain without affecting any other sensation (Figure 21). How do they work? It turns out that the pain pathways that ascend up the spinal cord to the brain are mirrored by complementary pathways that descend from the brain to the spinal cord. These complementary pathways have an analgesic effect. How? They release chemicals called opioids onto the pain projection neuron in the spinal cord. The opioids inhibit the transmission of painful information to the cortex by blocking the firing of projection neurons. Descending pain pathway Opioids Local anesthe5cs Which parts of the brain are responsible for processing the emotions related to pain? Lesson 3.4 perception through actions in the periphery. 96 Ascending pain pathway Pain Receptors Opioids Local anesthe5cs An5- inflammatory drugs Figure 21: Descending and ascending pain pathways. The descending analgesia pathway modulates pain perception through actions of endogenous opioids in the brain and spinal cord. Local anesthetics and anti-inflammatory drugs modulate pain
97 LESSON READING Receptors for these analgesic opioids are found in all areas of the brain that play roles in pain regulation. The artificial opioid morphine works the same way it stimulates the descending pain pathway to inhibit the pain projection neurons within the spinal cord. Giving morphine systemically can cause addiction because of all the other opioid receptors in the brain (we ll talk about them in Unit 5). To avoid the complication of addiction, morphine is often injected directly into the spinal cord where it can directly inhibit the pain projection neurons without affecting receptors we want to avoid. Local anesthetics (like Novocain if you remember from Unit 1) directly affect pain neurons close to where they re injected or applied. Local anesthetics block synaptic transmission by blocking voltage-gated sodium channels. When voltage-gated sodium channels are unable to open, the neurons in the area are unable to fire an action potential. In addition to blocking neurons carrying pain information, local anesthetics also block neurons carrying other sensory information as well, which is why your whole jaw often feels numb when you go to the dentist. Anti-inflammatory drugs, like aspirin, block pain transmission by blocking inflammatory hormones. If you remember, most nociceptors are activated as a result of inflammation so these inflammatory hormones are critical for pain to be transmitted, so if they are blocked, much less pain is perceived. In summary, medications that relieve pain work at a variety of points along the pain pathway. Some medications work directly in the brain, while others work in the spinal cord, and finally some work right at the site of trauma. In Summary It is important to distinguish between a nociceptive (noxious) stimulus and the perception of pain. Nociceptive information is sensed in the periphery and then transmitted to the cortex by a multi-synaptic pathway that ascends through the spinal cord. Each ascending synapse is an important site for regulation of the response. A complementary descending pathway can inhibit the ascending pathway by releasing of analgesic opioids that directly inhibit the pain pathway. How do analgesics work? Lesson
98 STUDENT RESPONSES Remember to identify your sources A single neuron receives thousands of inputs which may be conflicting or overlapping. a. First, describe how neurons manage all of these inputs. b. Second, what is the benefit of having this many connections within our nervous systems? Lesson
99 Unit 4: How do our neurons work together to control behaviors? Overview In the previous unit we learned how neurons communicate with each other using the process of synaptic transmission. This unit further expands on that knowledge by examining how neurons work together in circuits to control behaviors. In this unit, we ll use the experience of sleep, something we all experience, as a guide to discuss neural circuits. Remember our graphic from the beginning of this workbook? This unit focuses on the circuit, which is how our neurons work together to control our behaviors.
100 LESSON 4.1 WORKBOOK What is sleep? This unit introduces you to the neural circuit, which is how neurons work together to control our behaviors. In this lesson, we ll learn about sleep, a behavior that is tightly controlled by a neural circuit. An introduction to sleep Sleep remains one of the great mysteries of modern neuroscience. We spend nearly one-third of our lives asleep, and we still don t really understand why (Figure 1). We do know that sleep occurs in all mammals and probably all vertebrates. Sleep is crucial for concentration, memory, and coordination. Without enough sleep, we have trouble focusing and responding quickly in fact, sleep loss can have as big an effect on performance as drinking alcohol. Getting enough sleep is also important for our emotional health. And growing evidence suggests that a lack of sleep increases the risk of a variety of health problems, including diabetes, cardiovascular disease and heart attacks, stroke, depression, high blood pressure, obesity, and infections. In animals sleep deprivation can be fatal. Disorders of sleep are among the nation s most common health problems, affecting up to 70 million people, most of whom are undiagnosed and untreated. These disorders are one of the least recognized sources of disease, disability, and even death, costing an estimated $100 billion annually in lost productivity, medical bills, and industrial accidents. Figure 1: Sleep. We spend nearly 1/3 of our life asleep and a considerable amount of our What do you notice about your own behaviors and feelings when you don t get enough sleep? Lack of sleep increases the risk of what? Lesson 4.1 time awake worrying about it, yet we still don t 100 understand what it s for.
101 DEFINITIONS OF TERMS Electroencephalogram (EEG) measure of gross electrical activity of the brain, commonly recorded through scalp electrodes. Non-rapid eye movement (NREM) sleep sleep stages 1 through 4, during which sleepers are still and EEG waves decrease in frequency and increase in amplitude. Rapid eye movement (REM) sleep the stage of sleep characterized by rapid eye movements, loss of muscle tone, and EEG waves similar to those seen when awake. For a complete list of defined terms, see the Glossary. LESSON READING Sleep is an active state For centuries up to the 1950 s in fact most people thought that the purpose of sleep was simply to give the brain a rest. This seemed to be confirmed when, in 1953, two researchers put electrodes onto the scalp of sleeping subjects, revealing slow waves of brain activity. The slowness of the waves was precisely what they expected a state of rest to look like. However, they were startled to find that their subjects actually spent much of their night in a wholly different form of sleep that did not look like the brain was resting at all. In fact it was characterized by the same kind of high frequency activity that it displayed when subjects were awake. Not only that, but the sleepers eyes were constantly moving rapidly. They called this type of sleep rapid eye movement or REM sleep. For contrast, they called slow wave activity sleep non-rapid eye movement or NREM sleep. Measuring brain activity during sleep Today we use the electroencephalogram (EEG) to measure the brain activity as people sleep. An electroencephalography involves applying a set of electrodes on the scalp. As we saw in Unit 1, EEGs use pairs of electrodes placed in 19 standard positions distributed over specific brain regions. (Figure 2). The encephalogram then records the voltage that flows through the brain tissue between each pair of electrodes (which is why each EEG trace is reported as a pair for example: P3 - T5 [parietal 3 - temporal 5]) (Figure 3). Because each pair of electrodes samples the activity of a population of neurons in a different brain region, each of the individual EEG traces will be different. If you didn t watch how EEGs are recorded in Unit 1, you may want to watch that video now at the student website or the link below: Video: Measuring Brain Waves with an EEG (Electroencephalogram) Figure 2: Placement of EEG electrodes. The electrodes are placed in stereotyped positions so that the current flow between specific regions in the cortex can be measured. Figure 3: An EEG from an awake subject. The EEG measures the current flow between a pair of electrodes. The electrodes are named for the part of the cortex they are over, hence F = frontal; P What are the two stages of sleep? How do scientists measure brain activity in people as they sleep? What are the two characteristics of EEG waves? Lesson 4.1 = parietal; T = temporal; O = 101 occipital.
102 DEFINITIONS OF TERMS Amplitude refers to how large (height) a wave is from peak to peak. Frequency refers to how long (length) a wave is from trough to trough. For a complete list of defined terms, see the Glossary. LESSON READING EEG rhythms have two characteristics the frequency of the electrical activity and its amplitude. The frequency refers to how long a wave is from trough to trough (length). Amplitude refers to how tall the wave is (height). Different rhythm characteristics are found during different behaviors. (For example see Figure 4.) High frequency, low amplitude waves occur when we are mentally alert with eyes open. Medium frequency, medium amplitude waves occur when we re drowsy. Low frequency, high amplitude waves occur when we re asleep. The EEG and sleep stages The awake EEG is characterized by waves that have high frequencies and low amplitudes. The waves slowly decrease in frequency and increase in amplitude as we fall asleep and progress through the night s sleep. That is, until we get to Stage 5 (Figure 5). At that point the EEG trace looks similar to the awake brain the waves have high frequencies and low amplitude. Can you predict what might be happening when you are in Stage 5 sleep that would cause your brain to show an EEG that looks like it s Mentally alert with eyes open Awake with eyes closed Drowsiness & sleep Epilepsy High frequency, low amplitude Medium frequency, medium amplitude Low frequency, high amplitude High frequency, high amplitude Figure 4: Typical EEG waves. The EEG shows typical patterns of activity that can be correlated with various stages of sleep and wakefulness. Non rapid eye movement (NREM) Rapid eye movement (REM) What happens to EEG waves as we progress through a night s sleep? What would cause the EEG during stage 5 sleep to be similar to the EEG during wakefulness? Lesson 4.1 awake? low amplitude waves. 102 Awake Stage 1 Stage 2 Stage 3 Stage 4 Stage 5 Figure 5: EEG changes during the stages of sleep. The awake EEG is characterized by high frequency, low amplitude waves, which slowly decrease in frequency and increase in amplitude as we progress through a night s sleep. That is, until we get to REM sleep, which again has an EEG with high frequency and
103 LESSON READING REM sleep, which occurs in Stage 5 is a very dynamic state. Our overall physiology is active. We experience changes in heart rate, respiration and blood pressure. But other than the muscles that control breathing and eye movements, all of our other muscles are paralyzed. As you might guess from its name, our eyes move rapidly in REM sleep. If sleepers are woken during REM sleep, they commonly report dreams (although they may forget them shortly thereafter). In contrast to REM sleep, non rapid eye movement (NREM) sleep is not dynamic. Our overall physiology is not active. We experience a decrease in heart rate, respiration and blood pressure. In NREM sleep, people are still, and their eyes don t move. If people are woken in this stage, they rarely describe dreams. During the night, the cycles of NREM slow wave sleep and REM sleep alternate, with the slow wave periods shortening and REM periods lengthening until we wake up (Figure 6). Figure 6: The stages of sleep cycle throughout the night. Deep sleep (stages 3 4) predominates during the beginning of the night. Later on, sleep is lighter and REM stages predominate. NREM Wake REM Stage 1 Stage 2 Stage 3 Stage 4 1 st 2 nd 3 rd 4 th 5 th Cycle Cycle Cycle Cycle Cycle 20min 30min 40min 50min 30min + REM Deep sleep Hours A<er Going to Bed Dreaming and the possible functions of REM sleep Thanks to the EEG we can describe the stages of sleep quite well, but we still don t really know what they are for, especially REM sleep. Most sleep researchers accept the idea that the purpose of REM sleep is at least in part to give the brain a rest, however we are still not at all sure how, so this idea is very controversial. We dream for about 2 hours every night, usually during REM sleep. On the other hand REM sleep doesn t always mean a dream is in progress, although it does act as one of the triggers for dreams. If you sleep for only 4 hours tonight, are you primarily missing your slow wave deep sleep or your REM sleep? As you well know REM dreams don t just recall a past experience they re more like a movie that can sometimes be quite lurid and surreal (Figure 7). Because of this, dreams have been intensely studied by psychoanalysts who think they can reveal our unconscious desires. Sigmund Freud s work The Interpretation of Dreams published in 1899 thought dreams had deep significance, but there is little scientific evidence to support his theory. Nonetheless many people consider the content of their dreams to be sig- Lesson 4.1 nificant. 103
104 LESSON READING However, the source of this content and how it becomes so vividly surreal is not known. One clue might come from functional MRI (fmri), which shows that the areas which regulate higher-order reasoning are inactive during dreaming. What is sleep for? Figure 7: Most dreams occur during REM sleep. Most people report dreams with a story-like description. We dream for about 2 hours each night, mostly during REM sleep. But no one knows where dreams come from or what they re for. The bottom line is we don t really know. We do know that if we can t sleep we suffer. In fact, rats can only survive three weeks if they aren t allowed to sleep at all. In humans sleep deprivation induces paranoia and hallucinations. Here are some current and not so current hypotheses on sleep function. None are proven and all are flawed. Sleep allows body systems to recover after consuming energy during the day. In fact as we saw previously, the brain is active during sleep and there s no evidence that more repair occurs during sleep than during rest or relaxed wakefulness. Sleep allows us to conserve energy. Our overall metabolic rate while we sleep is lower than while we re awake, but species with greater sleep times have higher metabolic rates. So, this theory doesn t hold up either. Sleep protects us from predators. But it also decreases sensitivity to external stimuli which surely increases vulnerability. Sleep allows us to consolidate our memories. Maybe. Studies have shown that people who get plenty of deep non-rem sleep in the first half of the night, and REM sleep in the second improve their ability to perform spatial memory tasks. Sleep is needed for discharging emotions. Maybe. Activity in the brain regions that control emotions, decision-making and social interactions is reduced during sleep, which may provide relief from stresses that occur during wakefulness. Do you think your dreams have meaning? Why or why not? Sleep is needed during brain development. Certainly babies and infants sleep more than adults. Lesson
105 STUDENT RESPONSES Remember to identify your sources Of the hypotheses listed above for the functions of sleep, which do you think is most accurate, and why? Lesson
106 LESSON 4.2 WORKBOOK Are you getting enough quality sleep? We all know how insistent the urge to sleep can be, and how bad we feel when we have to resist it and stay awake. With the exception of the effects of severe pain and the need to breathe, sleepiness is probably the most insistent drive that we experience. So, how much sleep do we actually need? How much sleep do we need? When was the last time you woke up feeling rested and refreshed? How much sleep did you get that night? Sleep experts say most of us aren t getting enough sleep. Here s what the National Sleep Foundation says we need. (But keep in mind that your sleep needs are as individual as you, your genetics, and your lifestyle. And a timely nap may mean you need less nighttime sleep). Babies take the sleep they need: sixteen to eighteen hours out of twenty-four. Toddlers need about fifteen hours, young children need eleven to thirteen hours. Teens need nine or more sleep hours, but seldom get it. Adults need eight hours, but generally get just around seven. Elders sleep a bit more, but have trouble falling asleep and staying asleep. (By the way, small animals require much more sleep than large animals, with opossums craving eighteen hours and elephants needing only three hours a day (Figure 8). Describe your bedroom. Is your bed comfortable? Do you sleep in the dark or the light? Do you text in bed? How long for? Lesson 4.2 Figure 8: Different animals need different amounts of sleep. 106
107 LESSON READING What are the effects of sleep deprivation? When we are forced to miss a night s sleep, we become very sleepy. The fact that sleepiness is so motivating suggests that sleep is a necessity of life. If so, it should be possible to deprive people or laboratory animals of sleep and see what functions are disrupted. From these studies we should be able to infer the roles that sleep plays. However, the results of sleep deprivation studies have not revealed as much as investigators had originally hoped. Adding to uncertainty about the purposes of REM sleep is the fact that depriving people of REM sleep for as much as 2 weeks has little effect on their behavior. They compensate by experiencing more of it after the period of deprivation, but suffer no obvious adverse effects. In contrast, total sleep deprivation has devastating effects. The longest documented period of voluntary sleeplessness is approximately 12 days, chalked up by a Californian who used coffee to keep him awake and spent his wakefulness in the window of a coffee shop. He recovered after a few days of getting sleep, apparently none the worse for wear. Most people who experience sleep deprivation know that it severely impacts both mental and motor functioning. Too little sleep has been linked with: Increased risk of motor vehicle accidents Increased body mass index greater likelihood of obesity due to an increased appetite caused by sleep deprivation Increased risk of diabetes and heart problems Increased risk for psychiatric conditions including depression and substance abuse Decreased ability to pay attention, react to and remember new information. If we don t get enough sleep, our sleep debt progressively accumulates and leads to decreased mental functioning. When the opportunity to sleep comes again, we will sleep much more, to repay the debt. Our slow wave sleep debt is usually paid off first. So it seems like we can get along without REM sleep, but need non-rem sleep in order to survive. Why is it important to get enough quality sleep? What happens if you don t get enough sleep? Lesson
108 DEFINITIONS OF TERMS Narcolepsy a disorder characterized by daytime sleep attacks and loss of muscle tone. Insomnia disorder of going to sleep and staying and asleep. For a complete list of defined terms, see the Glossary. LESSON READING How do sleep disorders affect our quality of sleep? Given the odds, it s likely that we ll each experience some form of sleep disorder in our lifetime. There are a range of sleep disorders, but we ll discuss the most common here. Sleep disorders affect our quality of sleep, and if you suspect that you have one, it is important to seek medical attention. So, how do sleep disorders affect our quality of sleep? Narcolepsy Narcolepsy is a neurological disorder characterized by falling asleep at inappropriate times. Since we ll be focusing on narcolepsy in the next section of this chapter, we ll save further description of this sleep disorder for then. Insomnia Most people are familiar with insomnia (Figure 9). Insomnia is said to affect approximately 25 percent of the population occasionally, and 9 percent regularly. But there is no single definition of insomnia that we can apply to all people. Insomnia must be defined in relation to a person s particular sleep needs, and the amount of sleep we need is quite variable between individuals. Some people may feel fine with 5 hours of sleep; others may still feel unrefreshed after 10 hours of sleep. Therefore, we ll define it simply as difficulty falling or staying asleep, such that when you do wake up, you don t feel rested. Some people have difficulty falling asleep initially, and others fall asleep and then awaken partway through the night and cannot fall asleep again. Insomnia is more common in women than men, and tends to increase with age. Short-term insomnia is often associated with stress, the environment (noise, light), jet lag, or medication. Long-term insomnia may be due to other sleep disorders or may be a secondary effect of other physical or mental problems. Unfortunately, the shortacting sedatives, and sedating antidepressant drugs that are available over the counter that many people use to help themselves sleep don t mimic truly natural and restful sleep, because they don t allow the deeper stages of slow wave sleep that are so necessary for a restful sleep. Figure 9: Insomnia. Insomnia is the difficulty falling or staying asleep, so that when you wake up, you don t feel rested. What is narcolepsy? How does narcolepsy affect our quality of sleep? _ What is insomnia? Is there only one definition of insomnia? Why or why not? Lesson
109 DEFINITIONS OF TERMS Obstructive sleep apnea condition in which breathing stops while you are asleep because the airway has become narrowed, blocked, or floppy. REM sleep behavior disorder disorder in which the paralysis that normally occurs during sleep is incomplete or absent, allowing people to act out his or her dreams. For a complete list of defined terms, see the Glossary. LESSON READING Obstructive sleep apnea (OSA) An estimated 12 million Americans have obstructive sleep apnea (OSA) and this number is expected to rise because OSA is made worse by the presence of excess fat. In children OSA is related to enlarged tonsils or adenoids. OSA is a major cause of inadequate sleep, and can be life-threatening. It occurs as sleep deepens. The airway muscles in the throat relax until collapse, closing the airway (Figure 10). This prevents breathing, which causes the sufferer to wake up and stops the sufferer from progressing to the deeper stages of slow wave sleep. Sleep apnea can cause high blood pressure, and may also increase the risk of heart attack. Treatment aims to stop the airway muscles collapsing and may include approaches like losing weight, avoiding alcohol and sedating drugs, and not sleeping on one s back. However, most people with sleep apnea require devices like a mask that provides continuous positive pressure to the airway, keeping it open. Figure 11: Sleep walking. Sleep walking is most common in children and often triggered by disturbances in sleep patterns. Parasomnias Figure 10: Obstructive sleep apnea (OSA) occurs when muscles at the back of the throat relax and obstruct airflow. Parasomnias include a range of behaviors that occur during sleep including sleepwalking (Figure 11), sleep talking, bed-wetting (enuresis) and sleep terrors. Many, including sleepwalking, talking and terrors are more common in children than adults. Sufferers usually have no memory of the events. Most suffers outgrow their parasomnias, so they don t require treatment. REM sleep behavior disorder occurs later in the night than the other sleep disorders and usually affects middle-aged and elderly people. REM sleep disorder appears because the muscle paralysis that normally occurs during REM sleep doesn t happen, which can result in sufferers acting out potentially violent dreams, even injuring themselves or their bed partners. What is obstructive sleep apnea? How does obstructive sleep apnea affect our quality of sleep? What are parasomnias? How do parasomnias affect our quality of sleep? Lesson
110 LESSON READING Restless leg syndrome About 10-15% of the population has unpleasant leg sensations and an almost irresistible urge to move their legs. Symptoms are usually worse in the evening and at night and often interfere with sleep. Mild cases can be treated with exercise, leg massages and eliminating alcohol and caffeine from the diet. What can you do to improve your sleep? First you need to begin by assessing what you yourself need. See how you respond to different amounts of sleep. Pay careful attention to your mood, energy and health after a poor night s sleep versus a good one. Ask yourself, How often do I wake up feeling well rested? If the answer is not often, then you may need to consider changing your sleep habits or consulting a physician or sleep specialist. To pave the way for better sleep, experts recommend that you and your family members follow these sleep tips: Establish consistent sleep and wake schedules, even on weekends. Create a regular, relaxing bedtime routine such as soaking in a hot bath or listening to soothing music begin an hour or more before the time you expect to fall asleep. Create a dark, quiet, comfortable and cool environment. Sleep on a comfortable mattress and pillow. Use your bedroom only for sleep (keep sleep stealers out of the bedroom avoid watching TV, using a laptop or iphone or reading in bed). Finish eating at least 2-3 hours before your regular bedtime. Exercise regularly during the day or at least a few hours before bedtime. Avoid caffeine and alcohol close to bedtime, and give up smoking. If you or a family member are experiencing symptoms such as excessive sleepiness during the day, snoring, leg cramps or tingling, gasping or difficulty breathing during sleep, prolonged insomnia or another symptom that is preventing you from sleeping well, you should consult your primary care physician or sleep specialist to determine the underlying cause. You may also try keeping a sleep diary to track your sleep habits over a one- or two-week period and bring the results to your physician. Most importantly, make sleep a priority. You must schedule sleep like any other daily activity, so put it on your to-do list and cross it off every night. But don t make it the thing you do only after everything else is What is restless leg syndrome? How does restless leg syndrome affect our quality of sleep? Is your bedroom a sleep-conducive environment? Lesson 4.2 done stop doing other things so you get the sleep you need. 110
111 STUDENT RESPONSES What could you do to improve the quality of sleep you get each night? Lesson
112 DEFINITIONS OF TERMS Arousal neurons neurons located in the brainstem that when active keep us awake and alert. Ventrolateral preoptic nucleus (VLPO) nucleus in the hypothalamus that when active, puts us to sleep. For a complete list of defined terms, see the Glossary. LESSON 4.3 WORKBOOK What makes us go to sleep, and what makes us wake up? So far we ve discussed the nature of sleep, its functions, and problems associated with it. Now, let s examine what researchers have discovered about the neural circuits that are responsible for sleep and its counterpart, alert wakefulness. Control of the sleep-wake cycle Our sleep-wake cycles are controlled by two main factors: The length of time we ve been awake and active The time of day The Flip-Flop Switch When we are awake and alert, most of the neurons in our brain especially those in our forebrain are active, which enables us to pay attention to sensory information, to think about what we are perceiving, to retrieve and think about memories, and to engage in the variety of behaviors that we have to do during the day. The level of brain activity is largely controlled by the arousal neurons located in our brainstem (Figure 12). A high level of activity of these neurons keeps us awake, and a low level puts us to sleep. Areas in the hypothalamus put us to sleep VLPO (Sleep neurons) Areas in the brainstem keep us awake Arousal Neurons What area of the brain is responsible for keeping us awake and alert? _ What area of the brain is responsible for putting us to sleep? But what controls the activity of the arousal neurons? What causes this activity to fall, and put us to sleep? We know that a region of the hypothalamus, usually referred to as the ventrolateral preoptic nucleus (VLPO), is critically important for controlling when we fall asleep (Figure 12). If this area is destroyed total insomnia results. On the other hand, stimulating this area electri- Figure 12: Neural control of sleep and wakefulness. cally can induce sleep. Arousal neurons in the brainstem keep us awake. VLPO Lesson 4.3 neurons in the hypothalamus put us to sleep. 112
113 DEFINITIONS OF TERMS Orexin neurons neurons located in the hypothalamus that use the neurotransmitter orexin. When active, these neurons activate the arousal neurons in our brainstem to keep us awake. Damage to these neurons has been implicated in narcolepsy. For a complete list of defined terms, see the Glossary. LESSON READING The VLPO contains sleep neurons. Their axons form inhibitory synaptic connections with the brain s arousal neurons, and inhibit them. When our VLPO sleep neurons become active and suppress the activity of our arousal neurons, we fall asleep. The sleep neurons in the VLPO themselves receive inhibitory inputs from some of the same regions they inhibit, including the arousal neurons in the brainstem. Thus, when arousal neurons are active, they inhibit the VLPO sleep neurons and we remain awake. It is important to understand that the VLPO sleep neurons need to be active to inhibit the arousal neurons and vice versa inhibition is an active process, just like excitation. The fact that the sleep neurons inhibit the arousal neurons and vice versa is called a flip-flop switch that sets periods of sleep and waking. As you might imagine the flip-flop switch can only be in one of two states on or off. If the sleep neurons are active and inhibit the arousal neurons we will be asleep. Conversely, if the arousal neurons are active and inhibit the sleep neurons, we are awake (Figure 13). Also because the two switches are mutually inhibitory, it is impossible for the neurons in both sets of regions to be active at the same time. A flip-flop switch has one important advantage when it switches from one state to another, it does so quickly. Clearly, it is to our advantage to be either asleep or awake. A state that has some of the characteristics of both sleep and wakefulness would be quite problematic! Controlling the switch A. During wakefulness B. During sleep Figure 13: The flip-flop switch. The VLPO and the arousal neurons are connected to each other by inhibitory neurons. (A) When the arousal neurons are active, they inhibit the VLPO and we remain awake. (B) When the VLPO neurons are active, they inhibit the arousal neurons and we fall asleep. There is one problem with flip-flop switches however they can be unstable. In fact, people with narcolepsy exhibit just this characteristic. They have difficulty staying awake and they also have trouble remaining asleep for an extended amount of time. We know from examining animals with narcolepsy that the problem lies in damage to a set of neurons called orexin neurons. The orexin neurons are located in the hypothalamus and are so named because they use the neurotransmitter orexin. Orexin neuron are connected to the arousal neurons in the brainstem and help stabilize the sleep-wake flip-flop switch (Figure 14). How do these two areas connect? What type of synapse do these two areas make with each other? What neurons help to stabilize the flip-flop switch? Lesson
114 LESSON READING But how do orexin neurons stabilize the flip-flop switch? Orexin neurons are activated by light, energy balance, and the limbic system (which you ll remember regulates emotion). These inputs cause the orexin neurons to activate the arousal neurons, tipping the activity of the flip-flop switch toward the waking state, thus promoting wakefulness and inhibiting sleep. When input to the orexin neurons from light, energy balance and limbic system stops, the orexin neurons stop activating the arousal neurons. Now the balance is shifted, allowing the VLPO sleep neurons to inhibit the arousal neurons, thus promoting sleep and inhibiting wakefulness (Figure 15). A. During wakefulness B. During sleep Figure 14: The orexin neurons. Orexin neurons in the hypothalamus send projections to the arousal neurons in the brainstem to further control the flipflop switch regulating our sleep-wake circuit. Figure 15: The orexin neurons are the actual switch between being awake and being asleep. (A) When orexin neurons are stimulated by light, emotional cues or energy balance they activate the arousal neurons, which in turn inhibit the VLPO and we remain awake. (B) When input to the orexin neurons from light, energy balance and limbic system stops, the orexin neurons stop activating the arousal neurons. Now the balance is shifted and the VLPO can inhibit the arousal neurons and we fall asleep. How do orexin neurons connect to the flipflop switch? What turns orexin neurons on? What turns them off? Lesson
115 LESSON READING So what causes narcolepsy? Narcolepsy is a relatively uncommon condition only one case per 2,500 people but it is a great example of a defect in the flip-flop switch that controls the transition between wakefulness and sleep, particularly REM sleep. Narcoleptics have sleep attacks during the day, in which they suddenly fall asleep. This is socially disruptive, as well as dangerous for example, if it strikes while they are driving. They tend to enter REM sleep very quickly, and may even enter a dreaming state while still partially awake. They also have attacks during which they lose muscle tone similar to what occurs during REM sleep only while they are awake. These attacks of paralysis, known as cataplexy, can be triggered by emotional experiences, even by hearing a funny joke. You can watch a profile of a patient with narcolepsy online see this unit on the student website or click below: Video: Narcolepsy Figure 16: Defects in orexin signaling cause narcolepsy. If orexin input to the arousal neurons doesn t occur, wakefulness and sleep are no longer carefully controlled and people transition uncontrollably from one to the next. Narcolepsy has been traced to defects in the orexin neurons (Figure 16). For instance, two dog species that have narcolepsy naturally have an abnormality in the gene that will make a receptor for the orexin neurotransmitter. Also, if we remove the gene for orexin from mice, they immediately become narcoleptic. These mice also move directly from wakefulness to REM sleep which is also a characteristic of patients with narcolepsy (Figure 17). Since signaling between the orexin neurons and the arousal neurons requires both the orexin neurotransmitter and the orexin receptors on the arousal neurons that recognize the transmitter, removing either of the two partners in orexin signaling between the neurons can cause narcolepsy. Figure 17: Narcoleptic mice. Normal mice are called wild-type (top). When they fall asleep they move through the stages of sleep until they enter REM sleep. When the orexin receptor is removed from the mice by genetic engineering, this is called Orexin-knockout (right). Orexin knockout mice become narcoleptic, transitioning from wakefulness to sleep many times a day. Sometimes they transition directly from wakefulness to REM sleep What causes narcolepsy? Lesson 4.3 (indicated by the small arrovheads). 115
116 LESSON READING Figure 18: Narcolepsy in humans is triggered by actual loss of orexin containing neurons in the hypothalamus. The pictures are data from normal patients (left panel) and narcoleptic patients (right panel). The pictures are of brain tissue after the orexin neurons have been marked with an antibody against them. Then the antibody itself is marked with a dark brown color. The dark brown spots represent neurons that contain orexin. The narcoleptic patient has far fewer orexin containing neurons than the control patient. Human cases of narcolepsy also show problems with the orexin signaling pathway, and have abnormally low orexin levels in the brain and spinal fluid. However human patients don t have the genetic defects we saw in the dogs. Humans develop the disorder in their teens or 20s, and we think its because the immune system attacks the orexin neurons (like we saw in multiple sclerosis). Using brain tissues postmortem (after people have died), researchers have shown that humans with narcolepsy have far fewer orexin neurons than humans without narcolepsy (Figure 18). How did scientists realize that the orexin neurons were affected in narcoleptic humans? You can watch a video of a narcoleptic dog online see this unit on the student website or click below: Video: Snoozy the Narcoleptic Dog! Lesson
117 STUDENT RESPONSES Remember to identify your sources Given what you know about the causes of narcolepsy, how do you think you could treat the disorder? Lesson
118 DEFINITIONS OF TERMS Adenosine neurotransmitter that accumulates in the brain during wakefulness, implicated as an important sleepiness factor. For a complete list of defined terms, see the Glossary. LESSON 4.4 WORKBOOK Can caffeine treat narcolepsy? Remember that sleepiness is controlled by two factors: length of time our brains have been awake and active, and the time of day. Let s turn our attention now to the first factor the length of time we ve been awake and active. Adenosine The longer we stay awake, the sleepier we become and the pressure to sleep is hard to resist. Why? What is responsible for the sleepiness that increases the longer we re awake and mentally active? The precise mechanism is unknown but it seems that the neurotransmitter adenosine is an important sleepiness factor (Figure 19). Researchers measured the levels of adenosine in the basal forebrain of cats during 6 hours of prolonged waking and during 3 hours of sleep afterwards. They found that adenosine levels rise during wakefulness and slowly decrease during sleep. They concluded that the accumulation of adenosine that occurs after we have been awake for a long period may be the most important cause of the sleepiness that follows periods of wakefulness (Figure 20). Adenosine What is adenosine? What happens to adenosine levels during wakefulness? by neurons and glial cells. Figure 20: Adenosine in the forebrain region of cats during 6 hours of waking followed by 3 hours of recov- Figure 19: Adenosine, the Lesson 4.4 sleepiness factor, is released ery (sleep). Levels of adenosine rise during wakeful- 118 ness and slowly decrease during sleep.
119 LESSON READING Another clue about adenosine s role in promoting sleep came from studying caffeine, which as we all know, decreases drowsiness and promotes wakefulness. Caffeine Caffeine is found in coffee, tea, cocoa beans, and other plants. It is a drug that produces excitatory effects (Figure 21). In much of the world, a majority of the adult population ingests caffeine every day fortunately, without apparent harm. Several studies have shown that caffeine prevents the normal drowsiness that occurs after being awake by binding to and interfering with the receptors that recognize adenosine. One study in particular used mice that didn t have any adenosine receptors. When these mice where given caffeine, it failed to keep them awake, unlike mice with adenosine receptors, showing that indeed you need adenosine receptors for caffeine to have its normal effect. Caffeine Figure 21: Caffeine molecular structure is similar to adenosine, so it can bind to adenosine receptors and also promote wakefulness. How much caffeine do you drink in an average day? When do you have it? Do you recognize any effects it s having? There is now overwhelming evidence that caffeine s effect as a stimulant occurs because it binds to adenosine receptors and blocks the action of adenosine (Figure 22). You can see now why that first cup of coffee in the morning helps shake off the lingering sleepiness of the previous night, how a midafternoon coffee break helps bring you back to an alert state during a post-lunch period of drowsiness, or how that late night cup of coffee keeps you awake (unless you ve already built up a tolerance to caffeine). A. Adenosine binds to its receptors. When levels are high enough, it promotes sleep Figure 22: Adenosine signaling. (A) When adenosine levels are high they bind to adenosine receptors and cause us to fall asleep. (B) Caffeine also binds to the adenosine How does caffeine keep us awake? Lesson 4.4 receptors, which stops adenosine from binding. By preventing adenosine from binding 119 to its receptors, caffeine keeps us awake. B. Caffeine also binds to adenosine receptors and stops adenosine binding. Sleep is prevented
120 DEFINITIONS OF TERMS Tolerance decreased response to a drug as a direct result of repeated drug exposure. Withdrawal the condition brought on by the elimination from the body of a drug on which the person has become physically dependent. For a complete list of defined terms, see the Glossary. LESSON READING Let s take a minute now to introduce the concepts of tolerance and withdrawal two topics we ll spend a lot more time talking about in Chapter 5. The concepts may make more sense in the context of a drug that probably everyone has used caffeine. We can define a drug as a chemical that changes behavior. So caffeine is a drug, but it does not produce the compulsive drug-seeking behavior that people who abuse amphetamine, cocaine or other opiates show. Therefore, it poses minimal risk and is not controlled by government laws and regulations so it s readily available, and legal, to consume. Now, let s look at tolerance and withdrawal with caffeine, our most popular drug. Tolerance is what happens when we are repeatedly exposed to a drug we become less susceptible to its effects. Prolonged use of caffeine does lead to a moderate amount of tolerance. Tolerance explains why those of us who consume caffeine regularly do not experience the same stimulating effects as nonusers, and why those of us who regularly use caffeine need more of the it to get the same effects. Withdrawal is what happens if we try to stop using a drug we ve become dependent on. People who suddenly stop taking caffeine often complain of headaches, drowsiness and difficulty concentrating. These withdrawal symptoms will stop after consuming more caffeine, but if the person continues to abstain, they ll disappear within a few days. Often, especially with drugs of abuse, these withdrawal symptoms are so severe that individuals continue to consume the drug simply to avoid the withdrawal symptoms. Could caffeine be used to treat narcolepsy? If caffeine is a stimulant that keeps us awake, could it be used to treat narcolepsy a disorder characterized by falling asleep at inappropriate times? Although, some patients with mild narcolepsy do report that caffeine helps them overcome their daytime fatigue, caffeine is not currently an approved treatment because it is not strong enough to override the defects in orexin signaling that cause narcolepsy. But, luckily other drugs have been developed that do. Not surprisingly one drug, modafinil, which has been used to treat narcolepsy, is thought to act on orexin neurons. Researchers found that giving modafinil increased orexin neuron activity, but whether this is a direct or indirect effect is still not clear. Other drugs used to treat narcolepsy include central nervous system stimulants and antidepressants that are much stronger than caffeine. The sleep attacks can be reduced by stimulants such as methylphenidate (Ritalin). The untimely episodes of REM sleep can be helped by antidepressant drugs. What is tolerance? How would you know if you ve developed tolerance to a drug? What is withdrawal? How would you know if you re experiencing withdrawal symptoms? Lesson
121 STUDENT RESPONSES Would caffeine be an adequate treatment for narcolepsy? Why or why not? Remember to identify your sources As caffeine wears off, we feel incredibly sleepy why is that? What has happened to our adenosine levels after we consume caffeine? Lesson
122 DEFINITIONS OF TERMS Homeostasis tendency to relatively stable equilibrium. Feed-forward inhibition control mechanism whereby the output of one pathway inhibits the activity of another pathway. Negative feedback/feedback inhibition control mechanism whereby activity of a circuit ends up inhibiting the activity of the circuit. For a complete list of defined terms, see the Glossary. Lesson 4.5 LESSON 4.5 WORKBOOK How do circuits regulate their output? Now that we have discussed an example of a neural circuit, let s take a closer look at how these circuits regulate their output. Circuits do this through the use of different arrangements of excitatory and inhibitory connections. The other sleep clue: time of day Recall that sleepiness is controlled by two factors: time of day and length of time our brains have been awake and active. We ve already discussed the first factor, so let s now explore the second time of day. Before we dive into our discussion of how time of day regulates sleep, let s first remind ourselves how our body regulates the activity of cells, tissues and organs. The activity of all of our bodies cells, tissues, and organs are regulated and integrated with each other. Homeostasis is the name given to the body s overall response to different stimuli. Because a number of different responses are integrated together the overall state is quite stable. For example, take a room whose temperature is regulated by a heater that is controlled by a thermostat. When the room is colder than the temperature the thermostat is set to, the thermostat turns the heater on, and the heater warms the room. Once the room reaches the set temperature, the thermostat turns the heater off. Because the production of heat feeds back to the thermostat and causes it to turn off, this process is called negative feedback or feedback inhibition. Negative feedback control systems are the most common homeostatic control mechanisms in our bodies, so it shouldn t come as a surprise that our nervous system uses negative feedback to control the output of neural circuits. Another type of regulatory process frequently used together with feedback inhibition is feed-forward inhibition. Feed-forward inhibition anticipates changes, improves the speed of the homeostatic responses, and minimizes fluctuations in the level of the variable being regulated. Feed-forward inhibition learns the meaning of cues from the external environment and responds to them. For example with our room analogy, feed forward control might learn that opening a particular door to the outside would make the temperature in the room drop faster than the opening an inside door. So it would learn to make the heater work faster if that door were opened. Not surprisingly, the first time the outside door were opened feed forward control would not know what the result would be, and the first fluctuations in temperature would be much larger than after it learns to anticipate the change. What are the two factors that control sleepiness? _ What is homeostasis? What are the two types of regulatory processes that our bodies use to control circuit activity? 122
123 DEFINITIONS OF TERMS Circadian recurring naturally on a twenty-four-hour cycle. Melatonin so-called ' hormone of darkness' released by the pineal gland. When light levels fall, melatonin levels rise. Preoptic nucleus (PON) nucleus in the hypothalamus that signals the pineal gland to release melatonin when light levels fall. Suprachiasmatic nucleus (SCN) nucleus in the hypothalamus that controls that circadian cycles of various body functions For a complete list of defined terms, see the Glossary. Lesson 4.5 LESSON READING One very well characterized negative feedback loop occurs within our biological clocks which keep track of the time of day and help control our sleep-wake cycles. The signals for sleep the biological clock Our internal biological clock regulates the timing for sleep, keeping us awake during the day and making us sleepy at night. The clock cycles with approximately a 24-hour period, and so it is called circadian (circa diem is the Latin for about the day ). The major brain structure regulating the clock is in the tiny hypothalamus. The hypothalamus has many different brain nuclei that control many aspects of homeostasis. One of these nuclei the suprachiasmatic nucleus (SCN) coordinates the timing of sleep with the light-dark cycle (Figure 23). The SCN consists of two pinhead structures, one on each side of the brain, and acts as a master clock. The SCN nucleus sets the pace for daily cycles of activity, sleep, hormone release, and other bodily functions The SCN is linked to many different brain regions. The SCN receives information about the outside world s light-dark cycle through direct input from the eye via the retina. The SCN then passes on this information to the following brain areas, each of which is also involved in controlling our sleep-wake cycles: The preoptic nucleus (PON) located in the hypothalamus. When it is active the PON stimulates the pineal gland to release melatonin. Melatonin has been called the hormone of darkness because its levels rise at night. It is responsible for causing drowsiness. Thus, when light levels fall, melatonin levels rise and we feel drowsy. Figure 23: The circadian clock in the hypothalamus. The suprachiasmatic nucleus (SCN) receives information about light levels from the retina. When light levels are high, output from the SCN that regulates the timing of sleep is switched off. The sleep neurons in the ventrolateral preoptic nucleus (VLPO) located in the hypothalamus. As we ve already seen, when active the VLPO sleep neurons inhibit arousal neurons, causing us to go to sleep. At times when light levels are high, such as during daylight, the retina signals to the SCN, which then inhibits the pineal gland, preventing it from secreting melatonin. Because the hormone of darkness is not present, we feel awake. How are these regulatory processes similar? How are they different? What is melatonin? How is it involved in our need for sleep? 123
124 Lesson 4.5 LESSON READING However, when light levels fall, the retina no longer signals to the SCN, and the SCN can no longer inhibit the pineal gland, which is now able to secrete melatonin (Figure 24). Because the hormone of darkness is present, we feel drowsy. A. During light B. During darkness Inhibits Figure 24: The SCN also controls the flip-flop switch. Light activates the SCN which inhibits the VLPO and prevents the pineal gland from secreting the hormone melatonin. However, in darkness, the SCN is not activated and therefore no longer inhibits either the VLPO or the pineal gland, which can now secrete melatonin. Together, the activity of the VLPO and the hormone melatonin promote sleepiness. SCN activity is regulated by genes that are called clock genes. The clock genes synthesize clock proteins. The clock proteins slowly enter the cell nucleus and stop the clock genes from synthesizing more clock proteins (Figure 25). But over a period of about 24 hours, these clock proteins break down and so the clock genes become active again and are able to synthesize more clock proteins. They slowly enter the nucleus etc. etc. This control of clock gene expression is a good example of feedback inhibition at the level of the individual cells in the SCN. Figure 25: Feedback inhibition controls the production of clock proteins. Clock genes express clock proteins which then affect behavior and other activities. When levels of clock proteins are high, they enter the nucleus and suppress the genes responsible for their production. Over time the levels of clock proteins fall, which removes the inhibition on the clock genes, so they can again synthesize more clock proteins. Inhibits The circadian clock in humans actually cycles at just over 24 hours, so the cellular clock must match the light-dark cycle. The cue for matching the cellular clock to the circadian clock is light. Neurons in the eye that are sensitive to light (photoreceptors) transmit signals to the SCN, which sets the clock genes so they match the environmental cues. If the clock genes fail to reset properly, the neurons in the SCN become out of sync with the environment and can produce various problems such as jet lag, seasonal affective disorder, and Monday morning blues. How does the SCN connect with the flip-flop switch? What is the biological clock? Where is it located? How does it control our need for sleep? _ 124
125 Lesson 4.5 LESSON READING Biological clock disorders Jet Lag Travelers who cross multiple time zones rapidly (such as by plane) often suffer from jet lag (Figure 26). Jet lag has many unwelcome effects, including disrupting sleep, causing loss of concentration, poor motor control, slowed reflexes, nausea, and irritability. Jet lag happens because our circadian clock can t immediately adjust to the changes in the light cues that result from crossing time zones quickly. So, the clock is out of step with the cues in the new time zone. This conflict between external and internal clocks affects more than just the sleep-wake cycle. All the rhythms are out of sync, and they take a number of days to re-match (also known as re-entrain to) the new time zone. Eastward travel generally causes more severe jet lag than westward travel, because traveling east requires that we shorten our day and adjust to time cues occurring earlier than our clock is used to. Seasonal affective disorder (SAD) Seasonal affective disorder (SAD) is a form of depression that occurs at a certain time of year, when the hours of daylight decrease i.e. winter (Figure 27). The change of seasons in the fall brings on both a loss of daylight savings time (fall back one hour) and a shortening of the daytime. During this season of short days and long nights, too little bright light reaching the biological clock in the SCN causes some individuals to develop symptoms similar to jet lag but more severe. These symptoms include decreased appetite, loss of concentration and focus, lack of energy, feelings of depression and despair, and excessive sleepiness. Treatment with light boxes that artificially increase the length of daylight are very effective. Figure 26: Jet lag is the bane of frequent travelers because our circadian clocks can t automatically readjust to changes in light-dark cycles that happen rapidly with modern day travel. Figure 27: Seasonal affective disorder (SAD) is caused by lack of sunlight to reset our biological clocks. It can be helped by light therapy to stimulate summer, or at least brighter light conditions. How does jet lag happen? How does jet lag affect our sleep-wake cycles? How does SAD happen? How does SAD affect our sleep-wake cycles? 125
126 Lesson 4.5 LESSON READING Monday morning blues By staying up later and sleeping in more than usual on the weekends, we provide our biological clocks with cues that push it toward a later nighttime phase. If we keep a late sleep schedule on both weekend nights, our internal clock can become two hours or more behind our usual weekday schedule. This delay in our clocks (not to mention facing another work week) makes it very difficult to wake up on Monday morning a condition called the Monday morning blues (Figure 28). To cure the Monday morning blues, it is recommended we stay on our weekday sleep schedules on the weekends. (We know it s hard, but it s what recommended in order to not throw off your biological clock.) Figure 29: People who work the night shift often encounter behavioral problems like jet lag and SAD. Shift work Figure 28: Monday morning blues. The circadian clock is not set exactly at 24 hours, so if we go to bed and sleep late on the weekends, our internal clock becomes behind schedule, making Monday mornings particularly miserable. Humans are normally active during daylight hours and sleep at night. This pattern is called diurnal activity. For humans and other diurnally active animals, light signals the time to awake, and sleep occurs during the dark. People who work the night shift may experience mental and physical difficulties similar to jet lag and SAD because their internal clocks and external daylight and darkness signals, are no longer synchronized (Figure 29). How do the Monday morning blues happen? How do they affect our sleep-wake cycles? How does shift work affect our sleep-wake cycles? 126
127 STUDENT RESPONSES What are the benefits of using feedback and feed-forward inhibition to control circuit activity? Remember to identify your sources How do our biological clocks use feedback and feed-forward inhibition to control our sleep-wake cycles? Lesson
128 DEFINITIONS OF TERMS Generalized seizures seizures that involve the entire brain. Partial seizures seizures that do not involve the entire brain. Positive symptom symptom in which one acquires an abnormal behavior. Negative symptom symptom in which one loses a normal behavior. For a complete list of defined terms, see the Glossary. Lesson 4.6 LESSON 4.6 WORKBOOK What causes epilepsy? So far in this unit we ve seen how the activity of circuits regulate behaviors, as well as how the activity of circuits can be regulated by feedback inhibition and feed-forward inhibition. In this lesson, we ll turn our attention to a disorder in which the control of circuit activity is abnormal epilepsy. When neuronal activity is unregulated All complex behaviors rely on precisely ordered communication between neurons in circuits. What happens to the circuit when the ordered communication between neurons breaks down? The result is called a seizure one of the most dramatic examples of disordered electrical behavior in the mammalian brain. Epilepsy is the chronic neurological condition that results from unprovoked seizures. It affects approximately 50 in every 1000 people in developed countries. In the US, about 3% of all people living to the age of 80 will be diagnosed with epilepsy. Three to four times that number will have epilepsy in developing countries why the discrepancy? No one knows. How seizures are classified Not all seizures are the same, and they must be sorted out according to their clinical features before any treatment program can begin. Seizures can include both positive and negative motor or sensory symptoms. A positive symptom involves acquiring an abnormal behavior like jerking an arm for instance. A negative symptom involves losing a normal behavior like briefly losing sight for instance. What symptoms appear depends on the effected region of the brain and the extent to which the normal brain tissue is involved. Seizures can be classified clinically into two categories: partial seizures and generalized seizures. This simple classification is very useful because the effectiveness of the treatment depends on the category of seizure being treated. What is a seizure? What is epilepsy? What are the two main types of symptoms associated with seizures? And what determines what types of symptoms will appear with a seizure? What are the two main types of seizures? 128
129 DEFINITIONS OF TERMS Complex partial seizures partial seizure in which patient loses consciousness. Seizure focus specific area of the brain where partial seizures begin. Simple partial seizures partial seizure without the loss of consciousness For a complete list of defined terms, see the Glossary. Lesson 4.6 LESSON READING Partial Seizures Partial seizures originate in a small group of neurons that are called the seizure focus. The seizure focus can be any small group of excitatory neurons that are damaged in some way for example because of a blood clot, a tumor, or a scar. The symptoms of a partial seizure depend on where the seizure focus is located (Figure 30). Somatosensory Visual If the activity in the focus is intense, the inhibitory neurons surrounding the area can t keep up with the excitation. The excitatory electrical activity then begins to spread to other brain regions (Figure 31). This spread follows the normal connections in the affected circuit. The cortex is heavily interconnected. Therefore seizure foci in the cortex are more likely to spread within that hemisphere of the cortex, then to the other hemisphere, and finally to the thalamus, which can redirect the seizure throughout the entire brain. Partial seizures are further classified into two categories: simple and complex. Simple partial seizures often cause changes in consciousness, but do not cause loss of consciousness. Simple partial seizures involve localized symptoms, such as jerking of the arm. The simple partial seizure becomes a complex partial seizure if it progresses so that the patient loses consciousness. A. B. People who experience partial seizures often describe symptoms that precede the actual seizure called auras. Common auras include a sense of fear, a rising feeling in the abdomen, or a specific odor. Auditory Motor in limbs Motor in face and head Figure 30: The symptoms of seizure depend on where the seizure focus is located. Symptoms may include visual, auditory, somatosensory and motor abnormalities depending on where the abnormal electrical activity is located. Figure 31: Secondary spread of the seizure. (A) Seizure activity may spread within the same lobe of the cortex, to the opposite lobe via the corpus callosum or throughout the entire brain via the thalamus. (B) Once the thalamus is involved, the seizure is likely to spread widely throughout the brain. This is known as secondary spread. What is the seizure focus? What causes the abnormal activity in a seizure focus to spread? What is the difference between simple and complex partial seizures? 129
130 DEFINITIONS OF TERMS Absence seizure seizure in which patients have a transient loss or impairment of consciousness. Convulsive seizure seizure involving uncontrollable jerking of the body. Grand mal seizure (also known as tonic-clonic seizure) type of generalize seizure that affects the entire brain. Non-convulsive seizure seizure without jerking. For a complete list of defined terms, see the Glossary. Lesson 4.6 LESSON READING Generalized seizures In contrast to partial seizures that originate in the cortex, generalized seizures involve connections to the cortex from subcortical structures like the thalamus, and connections from the cortex to subcortical structures like the thalamus (Figure 32). Generalized seizures begin without an aura or a seizure focus and involve both hemispheres of the brain from the onset. They can be divided into non-convulsive or convulsive. The best understood non-convulsive generalized seizure is the absence seizure (formerly called petit mal). These seizures begin abruptly, usually last less than 10 seconds and are characterized by repeated loss of attention or consciousness without any physical symptoms. Absence seizures can happen many times a day and are most common in children. In this case the issue is not a defective area in the brain but a sudden generalized cortical hyper-excitability. This hyper-excitability then synchronizes with the excitatory input from the thalamus to the cortex, which causes a massive depolarization. In response, the inhibitory neurons in the thalamus try to control the output. The resulting prolonged hyperpolarization causes the neurons to take a long time to repolarize, but once they do, the synchronized depolarization can happen again. Interestingly, the EEG in absence seizures is very similar to the EEG in the deep stages of sleep known as sleep spindles. The most common convulsive generalized seizure is the tonic-clonic or grand mal seizure. These seizures also begin abruptly, often with a grunt or a cry as the thorax and diaphragm contract suddenly. The patient may fall to the ground with a clenched jaw, lose bladder or bowel control, and become blue in the face (cyanotic). This tonic phase typically lasts 30 seconds before evolving into jerking of the extremities lasting 1-2 min. This active phase is followed by an ictal phase during which the patient is sleepy and may complain of headache and muscle soreness. Thalamus Figure 32: Generalized seizures involve connections both to and from the cortex via the thalamus and other subcortical structures. Since the thalamus is involved, the seizure activity immediately spreads to the entire brain. What is a generalized seizure? How is it different from a partial seizure? What is an absence seizure? What is a grand mal seizure? 130
131 LESSON READING You can imagine that it is often difficult to distinguish a generalized seizure from a complex partial seizure with a brief aura. The distinction isn t academic it s vital to choosing the proper treatment as well as pinpointing the underlying cause. Electrical activity and seizures As you can imagine, the most accurate way to pinpoint the region that initiates a seizure would be to impale the brain with electrodes and then measure where activity is defective. This is obviously not feasible in human patients. So, the EEG is called into service. The EEG provides a non-invasive way of examining brain activity. EEG recordings made during partial seizures show abnormal neuronal firing beginning first in a single region. This abnormal activity then may spread to other regions, but initially only one region is affected (Figure 33). Figure 33: EEG of partial seizure. Seizure activity shows up initially on only some the EEG leads, indicating that initially only one area is involved, but may recruit others if the seizure spreads. How do doctors diagnose the origin of a seizure? What would an EEG trace look like during a partial seizure? Lesson 4.6 Figure 33: EEG of generalized seizure. Seizure activity shows up simultaneously on all the leads of the EGG, indicating that the entire cortex is involved. Conversely, EEG recordings made during generalized seizures show abnormal neuronal firing beginning simultaneous throughout many, if not all, brain regions (Figure 33). What would an EEG trace look like during a generalized seizure? 131
132 Lesson 4.6 LESSON READING Treatments Seizure disorders are treated with anticonvulsant drugs, many of which work by increasing the effectiveness of inhibitory synapses. Most patients respond well enough to drugs that they can lead a normal life. In a few instances, drugs provide little or no help. Sometimes, seizure foci remain so irritable that despite drug treatment, brain surgery is required (Figure 34). In these cases, the surgeon removes the seizure foci and some of the region of the brain surrounding the focus. Most patients recover well from surgery, with their seizures eliminated or greatly reduced in frequency. Figure 35: Vagus nerve stimulation (VNS). VNS is a treatment option for patients who do not respond well to medications and are not considered good candidates for surgery. VNS involves the implantation of a pacemaker like device that provides electrical stimulation to the brain via the vagus nerve. Figure 34: Most patients with epilepsy respond well to anticonvulsant medications which increase the effectiveness of inhibitory synapses. In some cases surgery is required to remove a seizure focus. Surgery often means removing a considerable amount of brain tissue, but it can be extremely effective. For those patients who do not respond to anticonvulsant medications, and who are not considered good candidates for surgery (because their seizures are produced throughout the brain), vagus nerve stimulation (VNS) is another treatment option (Figure 35). VNS involves the implantation of a pacemaker device that generates pulses of electricity to stimulate the vagus nerve. While it is not exactly known how VNS works, it is thought that by stimulating the vagus nerve, electrical energy is discharged upward into a wide area of the brain, disrupting the abnormal activity that causes seizures. Another theory suggests that stimulating the vagus nerve causes the release of inhibitory neurotransmitters that decrease seizure activity. What treatments are available for epilepsy? 132
133 STUDENT RESPONSES If a friend of yours was diagnosed with epilepsy, what questions would you ask to find out whether it caused partial or general seizures? Remember to identify your sources How would you tell the difference between a partial seizure that has spread or a generalized seizure? Lesson
134 Unit 5: How do our choices change our brains? Overview In the previous units, we learned about the neuron, synaptic transmission, and neuronal circuits. In this key culminating unit, we ll bring all of that knowledge together with a discussion of drug addiction, to understand how our choices affect our brains, as well as how our brains affect our choices. Remember our graphic from the beginning of this workbook? This unit focuses on how our choices change our brains so we re pulling all the information from the previous units together.
135 DEFINITIONS OF TERMS Addiction chronic, relapsing brain disease that is characterized by compulsive drug seeking and use, despite harmful consequences Ventral tegmental area (VTA) brain region containing dopamine neurons that form connections with nucleus accumbens and prefrontal cortex Nucleus accumbens (NAc) brain structure that plays an important role in rewarding and reinforcing effects of many abused drugs Prefrontal cortex (PFC) part of the frontal lobe that receives emotional and motivational input and is necessary for logical decision making For a complete list of defined terms, see the Glossary. LESSON 5.1 WORKBOOK What circuit do drugs affect in our brains? To start our discussion of drug addiction, in this lesson you ll be introduced to the circuit that controls how we experience pleasure the neural reward circuit. What is drug addiction? Drug addiction poses a serious problem to our society. Consider the disastrous effects caused by the abuse of one of our oldest drugs, alcohol: automobile accidents, fetal alcohol syndrome, increase rate of liver disease, increased rate of heart disease, and increased rate of stroke. Or take smoking which causes addiction to nicotine. It greatly increases the chances of dying of lung cancer, heart attack, and stroke. The term addiction is derived from the Latin word addicere, to sentence. Someone who is addicted to a drug is, in a way, sentenced to a term of involuntary servitude, because they are shackled to their drug dependency, which defines how they live their lives. Addiction is defined as a chronic, relapsing brain disease that is characterized by compulsive drug seeking and use, despite harmful consequences. It is considered a brain disease because drug use changes brain structure and function. These changes can be long lasting, and can lead to the harmful behaviors seen in people who abuse drugs. How do drugs of abuse work in the brain? Drugs of abuse interfere with neurotransmission. They do this by altering signaling in the pathway that controls our feelings of reward and pleasure. This pathway is called the dopamine reward pathway. The dopamine reward pathway originates in a subcortical area of the brain near the midline called the ventral tegmental area (VTA). Dopamine neurons whose cell bodies are in the VTA end up in the nucleus accumbens (NAc) and the prefrontal cortex (PFC). What is drug addiction? It s important to be familiar with the complete definition. What brain pathway do drugs of abuse affect? What brain structures are involved in this pathway? Lesson
136 DEFINITIONS OF TERMS Reward pathway neural circuit that plays an important role in rewarding and reinforcing effects of behaviors, including the VTA, NAc, and PFC. Intracranial self-stimulation method that involves implanting electrodes into an animal s brain and then allowing the animal to electrically stimulate the electrode to activate that brain region. For a complete list of defined terms, see the Glossary. LESSON READING The connections between the VTA and the nucleus accumbens are called the reward pathway because the pathway is activated during pleasurable experiences such as eating, sex or receiving praise. Researchers have learned that this pathway is well conserved among animals, making the same connections in our brains as it does in a rodent s brain (Figure 1). Human Brain PFC NAc Since these structures are buried deep within the middle of the brain, you might want to take a look at a 3D model to get a better understanding of where these structures actually are. (We really like the free smart phone app called 3-D Brain.) Methods to study drug effects in the brain Rat Brain The reward pathway was discovered using the technique of intracranial self-stimulation (Figure 2). In these experiments, scientists implanted an electrode in different areas of rats brains, and then trained the rats to press a lever to active the electrode. When the electrode was implanted in the VTA, the rats spent their time compulsively pressing the lever, even at the expense of eating and drinking. The rats didn t behave like this if the electrode was implanted in areas other than the VTA. Knowing that rats only compulsively repeat behaviors that are pleasurable, the scientists concluded that stimulation of the VTA must activate a pathway that stimulates feelings of pleasure or reward. VTA Figure 1: Reward pathway. The reward pathway connects the ventral tegmental area (VTA) with the nucleus accumbens (NAc) and prefrontal cortex (PFC). This pathway is well conserved in animals, having the exact same connections in a rodent brain as it does in the human brain. Figure 2: Intracranial self-stimulation. When the animal presses the lever it receives an electrical shock directly to an area of its brain via an implanted electrode. Alternatively, the experiment can be setup so that the animal receives a drug after pressing the lever. This drug self-administration method predicts abuse potential. You can watch a video about intracranial self-stimulation online see this unit on the student website or click below: How did intracranial self-stimulation experiments help scientists discover the reward pathway? _ What do scientists use the drug self-administration method for? Lesson 5.1 Video: Brain Mechanisms of Pleasure and Addiction 136
137 DEFINITIONS OF TERMS Self-administration method test used to measure the abuse potential of a drug by allowing an animal to give itself doses of the drug. Breaking point the point at which an animal will no longer expend the effort required to receive a reward. For a complete list of defined terms, see the Glossary. LESSON READING A modification of intracranial self-stimulation has been used very effectively in identifying drugs that have the potential to be abused by humans. Based again on the idea that animals only compulsively repeat pleasurable behaviors, if an animal compulsively presses a lever in order to receive an injection of a drug into either their blood or their brain, we can conclude that the drug must have reinforcing properties (meaning that the drug activates the reward pathway and encourages animals to keep repeating the behavior). Using animals and this drug self-administration method, scientists have been able to very accurately predict whether or not a drug is likely to be addictive in humans. For example, rodents will readily self-administer morphine, cocaine and amphetamines, drugs that we know are readily abused by humans. In contrast, drugs like aspirin, antidepressants, and drugs that are used to treat psychoses like schizophrenia, are neither self-administered by animals nor abused by humans. We can also use this self-stimulation method to ask the animal which of several drugs it prefers by placing two levers in the chamber and training the animal to press lever A for one drug, and lever B for the alternative. Given free access to the levers, the animal s choice will indicate which drug the animal prefers, because that drug will have greater reinforcing properties. Additionally, we can ask how much the animal really likes a particular drug by varying how hard the animal needs to work to get the drug. For example, we can make the animal press the lever ten times for one injection or sixty-five times for one injection. We can tell how reinforcing the drug is by how many times the animal will press the level for a single injection. The point at which the effort required exceeds the reinforcing value is called the breaking point the higher the breaking point, the greater the reinforcement of the drug, and presumably the greater the abuse potential in humans. Drugs like cocaine sustain incredibly high rates of responding: animals will lever-press for drug reinforcement until exhaustion. Addicted to You ve probably suspected that addiction is not limited to drugs. Many brain parts are interlocking and overlapping, so the reward pathway can get turned on by well, just about anything. In addition to the usual physical suspects, you can get hooked on a feeling as well, and that includes (but is not limited to) compulsive behavior such as eating, gambling, shopping, risk taking, and sex. That s because these feelings, thoughts and sensations hijack our reward pathways. (See Box 5.1 for a description on how food effects our reward pathway.) Certainly many events and experiences register pleasure, but some things are much more potent than others. All drugs of abuse, for example, prompt a tsunami of dopamine signaling in the reward pathway a reaction much more powerful than any natural reward. Eventually these reactions overwhelm, capture, and change the reward pathway, leaving us craving more and more. Would you expect a rat to self-administer an antibiotic? Why or why not? Lesson
138 LESSON READING BOX 5.1 Controlling the desire to eat: The Reward Pathway Various feeding and satiety messages from the body do not single-handedly determine what we eat. Almost everyone has encountered a mouth-watering dessert and devoured it, even on a full stomach. We have an innate taste for sweet and acquire a taste for fat. We often eat because food confronts us. It smells good, tastes good, and looks good. We might eat because it is the right time of day, we are celebrating, or we are trying to overcome sadness. After a meal, memories of pleasant tastes and feelings reinforce appetite, our desire to eat. Our desire to eat is controlled by the dopamine reward pathway. Scientists have learned that the reward pathway is activated by all pleasurable stimuli, including food. Our reward pathways are particularly sensitive to high-calorie food, containing sugar and fat. This makes sense evolutionarily because as hunters, we did not always succeed in finding something to eat. So high-calorie foods, which contained a lot of energy, offered a survival advantage. In that environment, it was in our best interest to consume as many high-calorie foods as we could find. So our bodies adapted a mechanism to find high-calorie foods rewarding, which motivated us to consume them. But today, when we no longer need to hunt to find our food, our reward pathways are still guiding our food selection to high-calorie foods that are full of sugar and fat. The involvement of the reward pathway in food selection and consumption is an area of much scientific research. Research indicates that even in the absence of hunger, the sight, smell and even the thought of high-calorie foods can activate the reward pathway and motivate us to consume these foods. Consuming foods to please appetite but not hunger, is one reason why we intake more food than is needed to maintain an energy balance. What was the evolutionary advantage of having high calorie food stimulate the reward pathway, and how is that advantage actually maladaptive today? Lesson
139 STUDENT RESPONSES Remember to identify your sources Recently, different celebrities have blamed transgressions on addictions (i.e. Tiger Woods addicted to sex) to what extent do you believe that people get addicted to different behaviors? To what extent do you think people are using addiction as an excuse? Since anything that is pleasurable activates the reward pathway, it is technically possible to become addicted to anything that is pleasurable for example running. Describe how an addiction to running would occur. Lesson
140 DEFINITIONS OF TERMS Reuptake process that involves transport of neurotransmitter out of the synaptic cleft by the same cell that released the neurotransmitter. For a complete list of defined terms, see the Glossary. LESSON 5.2 WORKBOOK How do drugs alter synaptic transmission? Now that we know which neural pathway is activated in response to rewarding stimuli, let s take a closer look at the synapses in the pathway and see how different drugs of abuse change their synaptic signaling. Dopamine signaling All the natural reinforcers that have been studied so far (such as food for a hungry animal, water for a thirsty one, or sexual contact) have one physiological effect in common they cause the release of dopamine in the nucleus accumbens. The release of dopamine appears to be a necessary condition for positive reinforcement to take place. Addictive drugs including amphetamine, cocaine, opiates, nicotine, alcohol, PCP, and cannabis trigger the VTA to release dopamine in the nucleus accumbens. Different drugs stimulate the release of dopamine in different ways. Before we get into the specifics of how different drugs stimulate dopamine signaling, we need to mention one important feature of the dopamine synapse. Once dopamine has been released, moved across the synaptic cleft and interacted with its receptors, the dopamine synapse clears dopamine from the synaptic cleft by pumping it back into the presynaptic terminal using specific transporters. This process is known as reuptake (Figure 3). This means that any drug inhibiting the reuptake of dopamine from the synaptic cleft will cause dopamine levels to stay high, Lesson 5.2 and its effects to persist, because it can t be taken back up by the presynaptic terminal. Keep this in mind 140 as we discuss how specific drugs change dopamine signaling. Figure 3: Dopamine synapse. The dopamine synaptic cleft does not contain an inactivating enzyme, therefore in order to turn off dopamine signaling, dopamine must be recaptured and transported back into the presynaptic terminal by transporters in a process known as reuptake. What do all natural reinforcers have in common? How does the dopamine synapse clear dopamine from the synaptic cleft?
141 DEFINITIONS OF TERMS Agonist drug that facilitates the effects of a neurotransmitter on the postsynaptic cell. Stimulants class of drugs that increase the activity of the central nervous system. For a complete list of defined terms, see the Glossary. LESSON READING Stimulant drugs: Cocaine and Amphetamine Cocaine and amphetamine have similar behavioral effects: both are stimulants and both act as potent dopamine agonists. However, their sites of action are different. Cocaine binds with and inactivates the dopamine transporter proteins, thus blocking dopamine reuptake and keeping dopamine levels in the synaptic cleft high. Amphetamine has two effects: It also inhibits the reuptake of dopamine, but its most important effect is to directly stimulate the release of dopamine from axon terminals. Cocaine When people take cocaine (Figure 4), they become euphoric, active and talkative. They say that they feel powerful and alert. Some of them become addicted to the drug, and obtaining it becomes an obsession to which they devote more and more time and money. Laboratory animals, which quickly learn to self-administer cocaine, also act excited and show intense exploratory activity. If animals are given continuous access to self-inject cocaine, they often self-inject so much that they die from an overdose. Figure 4: Cocaine. When people take cocaine they become euphoric, active and talkative. Once addicted to cocaine, obtaining it becomes an obsession. One of the alarming effects seen in people who abuse either cocaine or amphetamine is psychotic behavior: hallucinations, delusions of persecution, mood disturbances, and repetitive behaviors. These behaviors so closely resemble those of paranoid schizophrenia that even trained mental health professionals cannot distinguish between them unless he or she knows about the person s history of drug abuse. These effects disappear once people stop taking the drug. As mentioned previously, cocaine use increases alertness, energy, motor activity and feelings of well-being. But feelings of anxiety, paranoia and restlessness are also common effects of cocaine. With excessive use, cocaine can cause tremors, convulsions, stroke and even death. Cocaine effects dopamine synaptic transmission by altering the way in which dopamine is removed from the synaptic cleft. Under normal conditions, the VTA releases dopamine onto the nucleus accumbens. Dopamine binds to receptors within the nucleus accumbens and this initiates downstream signaling in the nucleus accumbens neurons. As we saw before, dopamine signaling is normally stopped when the dopamine transporters (also known as pumps) in the dopamine reuptake system pump dopamine back into the presynaptic neurons, thus decreasing the levels of dopamine in the synaptic cleft. What are the psychological and behavioral effects of taking cocaine? Where does cocaine act within the reward pathway? Lesson
142 LESSON READING Compare the healthy brain at the top with the brain of a cocaine abuser at the bottom of Figure 6. Didn t we say cocaine is a stimulant? Why then does cocaine reduce brain activity if it increases the activity of dopamine neurotransmission at the nucleus accumbens synapse? This is because the output neurons from the nucleus accumbens are actually inhibitory. That is to say when they are activated they shut down signaling in the regions they synapse with. When they are stimulated by cocaine the inhibition is even more intense. Cocaine blocks the activity of dopamine transporters. Since dopamine transporters are responsible for removing excess dopamine from the synaptic cleft, when they are blocked, dopamine cannot be removed from the synaptic cleft, and dopamine levels increase which increases dopamine signaling at the nucleus accumbens (Figure 5). You can watch an animation describing how cocaine affects the brain online see this unit on the student website or click below: Cocaine Figure 5: Mechanism of cocaine action. Cocaine increases synaptic dopamine by binding to the dopamine transporter and inhibiting dopamine reuptake. Video: How Does Cocaine Affect the Brain? Figure 6: PET scans showing decreased activity in cocaine addict. Cocaine reduces brain activity because output from the nucleus accumbens is largely inhibitory. What is the effect of cocaine on dopamine levels in the nucleus accumbens? Lesson
143 LESSON READING Amphetamine Amphetamines include methamphetamine, crystal meth, and crack. Amphetamines are also central nervous system stimulants, increasing alertness and focus, while decreasing fatigue and appetite. They also produce hyperactivity and anxiety. With chronic use and/or high doses, amphetamines can also cause seizures, stroke, coma, and death. Figure 7: Amphetamines include methamphetamine, crystal meth and crank. Amphetamines are CNS stimulants. Amphetamine (Figure 7) has two effects on the VTA-nucleus accumbens synapse: The first effect is similar to cocaine it also prevents dopamine reuptake. The most important effect of amphetamine however is to stimulate release of dopamine into the synaptic cleft (Figure 8). Under normal conditions, the VTA releases moderate amounts of dopamine onto the nucleus accumbens. Dopamine then binds to receptors within the nucleus accumbens and effects downstream signaling, as we have seen before. Then, to stop dopamine signaling, dopamine transporters (also called dopamine reuptake pumps) pump dopamine back into the presynaptic neurons, which decreases the levels of dopamine in the synaptic cleft. Amphetamines can alter dopamine synaptic transmission by blocking dopamine transporters like cocaine does. When the dopamine transporters are blocked, dopamine cannot be removed from the synaptic cleft, and dopamine levels remain high, which increases dopamine signaling in the nucleus accumbens, just as we saw for cocaine. The second way amphetamines can alter synaptic transmission is by entering the presynaptic terminals of the VTA s neurons and causing dopamine to be released even in the absence of action potentials. This release also increases the level of dopamine signaling to the nucleus accumbens. Scientists are still trying to figure out exactly how amphetamines cause the release of dopamine in the absence of action potentials, but somehow this mechanism gives amphetamines another way to alter dopamine signaling in the reward pathway. Figure 8: Mechanism of amphetamine action. Amphetamine (AMPH) increases synaptic dopamine in two ways. First, it binds to the dopamine transporter and inhibits dopamine reuptake. Second, it enters the presynaptic terminal and stimulates dopamine release. The combined Lesson 5.2 effect is a massive increase in synaptic dopamine levels. 143 Amphetamine What are the psychological and behavioral effects of taking amphetamine? Where does amphetamine act within the reward pathway? How does amphetamine alter synaptic signaling of the reward pathway? What is the drug target? What is the effect of amphetamine on dopamine levels in the nucleus accumbens?
144 DEFINITIONS OF TERMS Opiates class of drugs with pain reducing qualities. For a complete list of defined terms, see the Glossary. LESSON READING Opiates: Heroin and Morphine Opium, derived from a sticky resin produced by the opium poppy, has been eaten and smoked for centuries, and in 1847 scientists figured out to make it themselves, producing heroin, the most commonly abused opiate. Addiction to opiates, like heroin, has several high personal and societal costs. First, because heroin (Figure 9) is an illegal drug is most countries, an addict becomes by definition, a criminal. Second, because of tolerance, a person must take increasing amount of the drug to achieve a high. The habit thus becomes more and more expensive, and the person often turns to crime to obtain enough money to support his or her habit. Figure 9: Heroin is the most commonly abused opiate. Third, addicts that inject opiates often don t have access to sterile one-use needles, so a substantial percentage of people who inject illicit drugs have been exposed to hepatitis or HIV. Fourth, if the addict is a pregnant woman, her infant will also become dependent on the drug, which easily crosses the placenta barrier. The infant must be given opiates right after birth, and then weaned off the drug with gradually decreasing doses. Fifth, the uncertainty about the strength of a given batch of heroin means that a user could unwittingly take an overdose, with possibly fatal consequences. Heroin and morphine are both opiates. They are analgesics, meaning they reduce pain without producing unconsciousness. Heroin and morphine produce a sense of relaxation and sleep, and at high doses can cause coma and death. Heroin and morphine increase the activity at the nucleus accumbens in two ways, both are different from how cocaine and amphetamines act. Both heroin and morphine work on a group of inhibitory neurons that normally inhibit the VTA. Under normal circumstances these neurons decrease the activity of the VTA. However when heroin and morphine bind to their receptors, they can no longer decrease the activity of the VTA. When the inhibition to the VTA is blocked, the VTA s activity is increased, which results in an increase in dopamine signaling to the nucleus accumbens. Thus when either heroin or morphine are present, more dopamine is released by the VTA to the nucleus accumbens because the VTA is no longer inhibited. Heroin and morphine can also affect the nucleus accumbens directly by binding to receptors for opiates found on the nucleus accumbens itself. The body itself produces natural opiates, which play an important role in reducing pain sensations and many neurons have receptors for these natural opiates. The nucleus What are the psychological and behavioral effects of taking heroin? Where does heroin act within the reward pathway? How does heroin alter synaptic signaling of the reward pathway? What is the drug target? What is the effect of heroin on dopamine levels in the nucleus accumbens? accumbens is no exception. Both heroin and morphine can bind to these receptors and in this way can Lesson 5.2 directly affect the activity of the nucleus accumbens. 144
145 LESSON READING Nicotine While nicotine (Figure 10) might seem rather tame in comparison to cocaine, amphetamine and opiates, it is still an addictive drug, and it accounts for more deaths than all the other so called hard drugs combined. The combination of nicotine and other substances in tobacco smoke is carcinogenic and leads to cancer in the lungs, mouth, throat and esophagus. The World Health Organization (WHO) estimates that 50% of people who begin to smoke as adolescents and continue to smoke will die from smoking-related diseases. Nicotine is extremely addictive; many people continue to smoke even when their health is seriously affected. Although tobacco companies and others with vested interests have tried to argue that smoking is a habit rather than an addiction, it is clear that people who regularly use tobacco behave like compulsive drug users. Smokers tend to smoke regularly or not at all; few smoke just a little. Male smokers smoke an average of 17 cigarettes per day, while female smokers smoke an average of 14. Nineteen out of twenty smokers smoke every day, and only 60 out of 3500 smokers surveyed smoke fewer than 5 cigarettes a day. Of those who attempt to quit smoking by enrolling in a special program, only 20% manage to abstain for one year. The record is much poorer for those Figure 10: Nicotine is the active ingredient in cigarettes and chewing tobacco. who try to quit on their own: one-third manage to stop for one day, one-fourth manage for one week, but only 4% manage to stop for six months. Ours is not the only species that will willingly self-administers nicotine, laboratory animals will too. Nicotine binds to and stimulates nicotinic acetylcholine receptors in the VTA. Once nicotine binds to these receptors, the neurons in the VTA fire action potentials. These action potentials cause the VTA to release dopamine onto the nucleus accumbens, thus increasing dopamine levels in the synaptic cleft. Scientists have also learned that nicotine can increase the actual amount of dopamine that the VTA releases, although they do not understand how. They do know that when nicotine binds to its receptors, the VTA releases more dopamine than normal. Thus nicotine binding to its receptor not only causes dopamine to be released in response to an action potential, but also the amount of dopamine released is greater. Through binding to nicotinic receptors, nicotine stimulates the central nervous system, causing increased alertness, and decreased appetite. Like other drugs nicotine also has unpleasant effects such as nausea, vomiting, diarrhea, and confusion. When people stop smoking, they often start overeating and gain weight. One lab discovered why: As you will see in the Metabolic Diseases module, eating and changes in metabolism are regulated by the activity of two different types of neurons whose cell bodies are located in the hypothalamus. One of these sets of neurons secretes the peptide called melanocyte-stimulating hormone (MSH). MSH affects neurons that normally increase appetite. When nicotine is present, it inhibits these neurons, suppressing appetite. However when nicotine is removed, such as when people try to stop smoking, this inhibition is removed and the MSH neurons can stimulate eating again so people overeat and gain weight. Lesson 5.2 You can watch a video about nicotine s effect on the brain online see the student website or click below: 145 Video: Visualization award winner in Science - Nicotine addiction and molecule diffusion What are the psychological and behavioral effects of taking nicotine? Where does nicotine act within the reward pathway? How does nicotine alter synaptic signaling of the reward pathway? What is the drug target? What is the effect of nicotine on dopamine levels in the nucleus accumbens?
146 DEFINITIONS OF TERMS Apoptosis type of cell death in which the cell uses specialized cellular machinery to kill itself. Depressant class of drugs that decrease the activity of the central nervous system. For a complete list of defined terms, see the Glossary. LESSON READING Alcohol Alcohol (Figure 11) also has enormous costs to society. A large percentage of deaths and injuries caused by car accidents are related to alcohol use. Additionally, alcohol contributes to violence and aggression. Chronic alcoholics often lose their jobs, homes, and families; and many die of cirrhosis of the liver, exposure, or diseases caused by poor living conditions Figure 11: Alcohol is the most commonly used drug in the United States. and abuse of their bodies. Alcohol consumption by pregnant women leads to fetal alcohol syndrome, one of the leading causes of mental retardation in the Western world today. Therefore, understanding the physiological and behavioral effects of alcohol is an imporant issue. Alcohol s serious effects on fetal development occur during the brain growth spurt period, which occurs during the last trimester of pregnancy and for several years after birth. One study found that exposure of an immature rat brain to alcohol triggered widespread death of neurons called apoptosis. This resulted in the death of various areas of the immature brain, and abnormal brain development. Alcohol acts as a depressant in the central nervous system. Alcohol consumption produces a decrease in anxiety, disinhibition, intoxication, memory impairment and sleep. At high doses, alcohol can cause vomiting, unconsciousness and even death due to the inhibition of the brain s breathing center. Alcohol is considered a sedative because it reduces the excitability of neurons. Alcohol has this effect by increasing the activity of the brain s main inhibitory neurotransmitter, GABA. Alcohol can bind to the GABA receptor and increasing its activity. When alcohol is present, GABA signaling is increased, thus increasing inhibition. Alcohol can also affects the brain s reward system. It does this by inhibiting the same inhibitory neurons that project to the VTA that opiates work on. Recall that when they are active these inhibitory neurons decrease the activity of the VTA, which decreases the levels of dopamine the VTA releases onto the nucleus accumbens. However, when alcohol is present, the activity of these inhibitory neurons is blocked which removes their inhibition of the VTA. This removal of inhibition increases the activity of the VTA. The VTA is then able to increase dopamine signaling to the nucleus accumbens. Thus when alcohol is present, more dopamine is released by the VTA onto the nucleus accumbens because inhibition is removed. What are the psychological and behavioral effects of taking alcohol? Where does alcohol act within the reward pathway? How does alcohol alter synaptic signaling of the reward pathway? What is the drug target? What is the effect of alcohol on dopamine levels in the nucleus accumbens? Lesson
147 LESSON READING Marijuana Another drug that people regularly self-administer is THC, the active ingredient in marijuana (Figure 12). THC comes from the flowering hemp plant, Cannabis sativa, and is a class of chemical called cannabinoids. THC is found in several different forms such as marijuana and hashish, both of which may be smoked or eaten. The consumption of cannabis for its intoxicating effects is thought to date back thousands of years to Eastern cultures. The practice of marijuana smoking was introduced in the United States in the early 1900s by Mexican and West Indian immigrants. Marijuana is the most heavily used illicit drug in the United States. Marijuana use causes euphoria, disinhibition, relaxation, altered sensations and increased appetite. Long-term use of marijuana has been associated with deficits in cognitive function, respiratory problems and impaired immune function. Studies with laboratory animals show that in rodents THC produces changes in motor activity, catalepsy (inability to move), hypothermia, and analgesia. Cannabinoids disrupt memory in several kinds of learning tasks, an effect that is thought to be related to activation of the hippocampus. Figure 12: Marijuana. The active ingredient in marijuana, THC is regularly self-administered, resulting in euphoria, disinhibition, relaxation, altered sensations and increased appetite. When marijuana is smoked, THC rapidly passes from the lungs into the bloodstream which carries THC into the brain. Once in the brain, THC binds to receptors, called cannabinoid receptors. These receptors are particularly concentrated on the VTA. The binding of THC to cannabinoid receptors on the VTA stimulates them to fire an action potential. These action potentials cause the VTA to release dopamine, thus increasing dopamine signaling at the nucleus accumbens. There are many concerns about the adverse effects of chronic cannabis use. In young people the amount of cannabis use directly correlates with poor educational performance, although whether this is a causal effect is not clear. Long-term use has been associated with at least temporary decrements in cognitive function, although whether these effects persist has been disputed. Likewise, it has been suggested that heavy cannabis use produces persistent cognitive deficits and/or apathy, loss of achievement motivation and decreased productivity, but the evidence supporting these suggestions is not strong. Because of this, researchers currently favor the hypothesis that early cannabis use is linked to lifestyles that devalue educational achievement. What are the psychological and behavioral effects of taking marijuana? _ Where does marijuana act within the reward pathway? How does marijuana alter synaptic signaling of the reward pathway? What is the drug target? What is the effect of marijuana on dopamine levels in the nucleus accumbens? On the other hand, there are real health risks associated with marijuana smoking that involve respiratory problems. Lesson
148 LESSON READING Drugs of abuse have similar effects All drugs of abuse increase dopamine activity at the synapse between the VTA and the NAc, but they do it in slightly different ways: Cocaine and amphetamine both inhibit dopamine reuptake transporters, thus increasing the amount of dopamine remaining in the synaptic cleft. Heroin and other synthetic opiates, like morphine, effect dopamine signaling in two ways. First, they inhibit inhibitory neurons projecting to the VTA. By removing this inhibition, the drugs increase VTA activity and the release of dopamine. Second, the drugs can also directly affect the nucleus accumbens by binding to opiate receptors. Alcohol, like the opiates, inhibits inhibitory projections to the VTA, thereby increasing VTA activity and its release of dopamine. Nicotine stimulates the VTA, where the dopamine neurons originate, directly, increasing dopamine release. THC the active ingredient in marijuana binds to cannabinoid receptors on the VTA which stimulates it to release dopamine. Drugs of abuse can increase the amount of dopamine in the synaptic cleft between 2-10 fold more than normal. In some cases, this occurs almost immediately (as when drugs are smoked or injected), and the effects can last much longer than those produced by natural rewards. Lesson
149 STUDENT RESPONSES On the diagram of the reward circuit below, draw in where each drug of abuse affects the pathway. Make sure to include: cocaine, amphetamine, heroin & morphine, nicotine, alcohol, and marijuana. Prefrontal Cortex What do all drugs of abuse have in common? In terms of their activity on the reward pathway? In terms of their abuse potential? Lesson NAc Inhibitory Neuron VTA
150 LESSON 5.3 WORKBOOK Should animals be used in scientific research? In the last couple of lessons we have referred to experiments in which laboratory animals have been used to test the adverse effects of drugs. The question of whether or not animals should be used in scientific research is one that triggers quite a debate. In this lesson, you will explore the issue as a class, reading various perspectives on the issue and debating the merits of each. Various perspectives The relationship of animals and humans has been the subject of differing philosophical views for thousands of years. The controversy continues today in many aspects of contemporary life. Some people believe that a vegan lifestyle is the only moral choice. Others believe that humans should treat animals humanely, but that we should be able to use animals and animal products at will, including for biomedical or other scientific research. Others believe that humans have no moral responsibilities to animals and we are free to treat animals however we want. Advocates of animal rights believe that animals have legal rights and are members of the moral community. Therefore, they believe that animals should not be used by humans for any purpose. Advocates of animal welfare believe that non-human animals should be treated humanely and without unnecessary suffering, but otherwise are available for humans to use for food, clothing, research and entertainment. To determine where you stand on the issue, you need to learn about the historical views on the relationship between humans and animals, current views, and in particular the role of animals in biomedical research. In groups, you will learn about these concerns from multiple perspectives, including: National Institutes of Health (NIH) People for the Ethical Treatment of Animals (PETA) Americans for Medical Progress (AMP) Understanding Animal Research Humane Society of the United States A brief summary of each perspective is included here, but you are encouraged to do your own research Lesson 5.3 to learn more about each perspective s stance on the use of animals in biomedical research. 150
151 LESSON READING National Institutes of Health (NIH) NIH is the steward of medical and behavioral research for the nation. Its mission is to support science in the pursuit of fundamental knowledge about the nature and behavior of living systems and the application of that knowledge to extend healthy life and reduce the burdens of illness and disability. NIH-supported scientists study diseases that cause pain and suffering and threaten the quality and length of life. NIH-supported scientists also study basic biological processes, expanding our knowledge of the origins and causes of disease. Through such research, involving both humans and animals, scientists identify new ways to treat illnesses, extend life, and improve health and well-being. Figure 13: National Institute of Health (NIH). Both people and animals have unique and important roles as research subjects. Many medical advances that enhance the lives of both humans and animals originate from animal studies. The types of animals used in research are chosen for their similarity to humans in anatomy, physiology, and/or genetics. Not only can we learn how to prevent, treat, and cure human diseases by studying animals, but often the treatments developed can also be used to improve the health of animals. When new thinking about diseases and treatments are developed from this research, they must be evaluated very carefully so that benefits and risks from the proposed approach are clear. When necessary, new hypotheses are tested in animals first in order to gather sufficient evidence of these benefits and risks before considering possible use in humans. We can study animals in ways that we cannot study people for many reasons. Animal studies conducted in the laboratory allow scientists to control factors that might affect the outcome of the experiments factors like temperature, humidity, light, diet, or medications. Even the genetic composition of many animal models can be known and understood completely. These rigorous controls allow for more precise understanding of biological factors at hand and provide greater certainty about experimental outcomes when developing treatments. All animals used in federally-funded research are protected by laws, regulations, and policies to ensure the smallest possible number of subjects and the greatest commitment to their welfare. Fulfilling these protections is a collaborative effort between NIH, federally-supported scientific investigators, and research institutions. You can learn more about the NIH s perspective on animal use in research at their website see this unit on the student website or click below: From the NIH s perspective, what historical precedents justify contemporary use or nonuse of animals in scientific research? From the NIH s perspective, what benefits and problems have developed because of the use or non-use of animals in scientific research? From the NIH s perspective, should animals be used in scientific research? If so, what considerations should be given to their care and well-being? If not, why not? Lesson 5.3 NIH Website: OER Animals in Research 151
152 LESSON READING People for the Ethical Treatment of Animals (PETA) Each year, more than 100 million animals including mice, rats, frogs, dogs, cats, rabbits, hamsters, guinea pigs, monkeys, fish, and birds are killed in U.S. laboratories for chemical, drug, food, and cosmetics testing; biology lessons; medical training; and curiosity-driven experimentation. Before their deaths, some are forced to inhale toxic fumes, others are immobilized in restraint devices for hours, some have holes drilled into their skulls, and others have their skin burned off or their spinal cords crushed. In addition to the torment of the actual experiments, animals in laboratories are deprived of everything that is natural and important to them they are confined to barren cages, socially isolated, and psychologically traumatized. The thinking, feeling animals who are used in experiments are treated like nothing more than disposable laboratory equipment. Human clinical, population, and in vitro studies are critical to the advancement of medicine; even animal experimenters need them if only to confirm or reject the validity of their experiments. However, research with human participants and other non-animal methods does require a different outlook, one that is creative and compassionate and embraces the underlying philosophy of ethical science. Animal experimenters artificially induce diseases; clinical investigators study people who are already ill or who have died. Animal experimenters want a disposable research subject who can be manipulated as desired and killed when convenient; clinicians must do no harm to their patients or study participants. Animal experimenters face the ultimate dilemma knowing that their artificially created animal model can never fully reflect the human condition, while clinical investigators know that the results of their work are directly relevant to people. Human health and well-being can also be promoted by adopting nonviolent methods of scientific investigation and concentrating on the prevention of disease before it occurs, through lifestyle modification and the prevention of further environmental pollution and degradation. The public needs to become more aware and more vocal about the cruelty and inadequacy of the current research system and must demand that its tax dollars and charitable donations not be used to fund experiments on animals. You can learn more about the PETA s perspective on animal use in research on their website see this unit on the student website or click below: PETA Website: Animals Used for Experimentation Figure 14: People for the Ethical Treatment of Animals (PETA). From PETA s perspective, what historical precedents justify contemporary use or nonuse of animals in scientific research? From PETA s perspective, what benefits and problems have developed because of the use or non-use of animals in scientific research? From PETA s perspective, should animals be used in scientific research? If so, what considerations should be given to their care and well-being? If not, why not? Lesson
153 LESSON READING Americans for Medical Progress Animal research plays a crucial role in scientists understanding of diseases and in the development of effective medical treatments. Research animals provide scientists with complex living systems consisting of cells, tissues and organs. Animal models can interact and react to stimuli, giving researchers a picture of a compound moving through a living system and an idea of how that stimuli might react in a human being. Animals are biologically similar to humans in many ways and they are vulnerable to over 200 of the same health problems. This makes Figure 15: Americans for Medical Progress (AMP). them an effective model for researchers to study. The majority of research animals are used in experiments focused on disease treatment and prevention, and the treatment of injuries. Laboratory animals are also used in basic medical research, breeding other research animals and diagnosis. Rats and mice account for about 95 percent of all animals used in research. Most of the remaining research animals are rabbits, guinea pigs, hamsters, farm animals, fish and insects. Combined, less than one percent of the remaining research animals are cats, dogs and non-human primates. The overwhelming majority of research animals are specifically bred for laboratories. Before conducting research on animals, most scientists make absolutely certain animals are needed for their experiments. For more than 50 years, scientists have relied on the 3Rs : refinement of tests so animal distress or pain is minimal, reduction of the number of animals used in one particular study, and the replacement, whenever possible, of animal experiments with non-animal experiments. As living beings with a conscience mind, we cannot ignore human or animal suffering. Each day scientists use their knowledge to minimize suffering in both humans and animals by conducting medical research that will benefit the greater good. They work to provide research animals with a clean environment, food, water and minimal pain and suffering. You can learn more about the perspective of Americans for Medical Progress on animal use in research on their website see this unit on the student website or click below: AMP Website: Animal Research Benefits From the perspective of Americans for Medical Progress, what historical precedents justify contemporary use or non-use of animals in scientific research? From the perspective of Americans for Medical Progress, what benefits and problems have developed because of the use or nonuse of animals in scientific research? From the perspective of Americans for Medical Progress, should animals be used in scientific research? If so, what considerations should be given to their care and well-being? If not, why not? Lesson
154 LESSON READING Understanding Animal Research Animals are essential in scientific research, medicine development and safety testing. They are necessary to understand the body in health and disease, and to develop new and improved medical treatments. But their use is not undertaken lightly. Both the potential scientific and medical benefits of the research, and the possible suffering of the animals used, are weighed up carefully before any animal research project can proceed. No one wants to use animals in research, and no one would use them unnecessarily. Animal research is considered a last resort, to be used only when there is no alternative method. Strict regulations and a licensing system mean that animals must be looked after properly and may not be used if there is any other way of doing a piece of research. Non-animal methods are used for the majority of biomedical research. Animal studies are used alongside these other types of research. Such alternative methods include the study of cells and tissues grown in the laboratory, computer-modeled systems, and human patients, volunteers or populations. You can learn more about the perspective of Understanding Animal Research on animal use in research on their website see this unit on the student website or click below: Website: Understanding Animal Research Figure 16: Understanding Animal Research. From the perspective of Understanding Animal Research, what historical precedents justify contemporary use or non-use of animals in scientific research? From the perspective of Understanding Animal Research, what benefits and problems have developed because of the use or nonuse of animals in scientific research? From the perspective of Understanding Animal Research, should animals be used in scientific research? if so, what considerations should be considered for their care and wellbeing? If not, why not? Lesson
155 LESSON READING Humane Society of the United States Picture the dog at your feet, the guinea pigs or mice you had as pets growing up, or the birds at the feeder in your yard. Now imagine 25 million animals just like these living in small laboratory cages and being deliberately sickened over the course of weeks, months, or even years and then killed. If animal experimentation was the hallmark of 20th century biomedical research, sophisticated non-animal methods are likely to characterize 21st century research. Many humane state-of-the-art alternatives to animal experiments have already been shown to be effective in advancing medical progress, cutting research costs, and eliminating animal suffering. The Humane Society of the United States (HSUS) is at the forefront of promoting these research methods and their continued development, as well as ending some of the most inhumane research practices. Until the day when animals are no longer used in harmful experiments, the HSUS, with your help, also strives to gain stronger legal protection for animals used in research, and seeks to limit animal use and suffering. Right now, approximately 95% of the animals used for research aren t afforded even the minimal protections of the Animal Welfare Act. You can learn more about the Humane Society s perspective on animal use in research on their website see this unit on the student website or click below: Humane Society Website: Biomedical Research Figure 17: Humane Society of the United States. From the perspective of the Humane Society, what historical precedents justify contemporary use or non-use of animals in scientific research? From the perspective of the Humane Society, what benefits and problems have developed because of the use or non-use of animals in scientific research? From the perspective of the Humane Society, should animals be used in scientific research? If so, what considerations should be given to their care and well-being? If not, why not? _ Lesson
156 STUDENT RESPONSES Do you think animals should be used in scientific research? If so, what considerations should be given to their care and wellbeing? If not, why not? Remember to identify your sources Do humans have moral responsibilities for animals or are animals destined to serve humanity? Lesson
157 DEFINITIONS OF TERMS Appetitive phase phase of motivated behavior where subject seeks out a goal. Consummatory phase phase of motivated behavior where subject actually consumes the goal, whether that goal be a drug, food, or sex. Intracranial self-stimulation a method that involves implanting electrodes into an animal s brain and then allowing the animal to electrically stimulate the electrode to activate that brain region. For a complete list of defined terms, see the Glossary. LESSON 5.4 WORKBOOK How is dopamine involved in addictive behaviors? Now that we re familiar with the reward pathway and how different drugs of abuse increase the levels of dopamine in the nucleus accumbens, let s turn our attention to new research indicating that dopamine is also involved in drug seeking behaviors. Two phases of motivated behaviors Motivated behaviors are any behavior directed toward receiving a reward or goal. The reward may be natural (food, sex, etc.) or artificial (electrical stimulation, drugs, etc.). Drug addiction, like sexual behavior, is a kind of motivated behavior. There are two phases of motivated behavior: Appetitive phase Consummatory phase During the appetitive phase, motivated behavior consists of those behaviors related to approaching the goal. In sexual behavior, for instance, the appetitive phase consists of behaviors that establish, maintain or promote sexual interaction. Generally speaking, appetitive behaviors allow an animal to come into contact with its goal. The consummatory phase represents the actually attaining the goal. In the case of sexual behavior, the consummatory phase is sexual intercourse. Collectively, appetitive and consummatory aspects characterize motivated behaviors. Neurobiology of motivated behaviors The neurobiology of motivation is a field that seeks to identify which neuronal circuits are responsible for motivated behavior. In the first section of this unit, we described the classic experiment of intracranial self-stimulation. This experiment was used to demonstrate the existence of the brain s reward pathway. The VTA and nucleus accumbens play central roles in this pathway. Through dopamine projections from the VTA to nucleus accumbens, this pathway carries signals about motivational and emotional information. Thus, dopamine neurons terminating in the nucleus accumbens play an important role in motivated What behaviors does the appetitive phase include? What behaviors does the consummatory phase include? Lesson 5.4 behavior. Not unexpectedly, the activity of these dopamine neurons changes as rewards are sought out 157 and consumed.
158 DEFINITIONS OF TERMS Microdialysis technique used to measure neurotransmitter release in the brain of an awake, freely moving animal by collecting samples of extracellular fluid and then analyzing the samples biochemically. For a complete list of defined terms, see the Glossary. LESSON READING Intracranial self-stimulation leads to dopamine increases in the nucleus accumbens Let s go back and take a second look at the classic experiment of intracranial self-stimulation. As we previously mentioned, intracranial self-stimulation helped researchers to identify and map the reward pathway. During the experiment, a stimulating electrode was implanted in the VTA to activate dopamine neurons using electrical pulses. The stimulating electrode and the instrument generating the electrical pulses were connected to a lever that the animal could press. When the animal pressed the lever, electrical pulses were delivered to the stimulating electrode. Thus, the animal controlled the stimulation of its dopamine neurons. To obtain the rewarding electrical stimulation, rats pressed the lever at astonishing rates, sometimes pressing continuously for hours. These early studies with intracranial self-stimulation were very informative. Indeed, the highest rates of lever pressing during intracranial self-stimulation occurred when the stimulating electrode activated dopamine neurons directly in the VTA. Collectively, these experiments led neuroscientists to conclude that dopamine was the transmitter responsible for reward. New experiments examine the appetitive and consummatory phase Recent studies challenge that traditional view. One of the key considerations is this to fully understand dopamine s role in each phase of motivated behavior (appetitive and consummatory), we must be able to monitor dopamine levels very quickly. The experiment we use to monitor dopamine levels must be able to distinguish between the appetitive and consummatory phases, which are separated by less than a second. The original studies used a technique called microdialysis (Figure 18). In this technique, samples of extracellular fluid are removed from the brain and analyzed biochemically to determine what neurotransmitters are present. These experiments showed that dopamine levels increased when animals pressed a lever and received a rewarding electrical stimulation. The problem is that animals will press the lever at rates of upwards of 5 times per second, and microdialysis is not able to sample at rates fast enough to detect what dopamine levels are doing with each press of the lever. Nor can it detect what happens to dopamine levels just before the animal presses the lever. Therefore, microdialysis is not an appropriate technique to distinguish between dopamine s role in the appetitive and consummatory phases of motivated behavior. A. B. Figure 18: Method of microdialysis. (A) Microdialysis allows the collection of samples from deep within the brain. The collected samples are identified and measured by one of several techniques, such as HPLC. (B) Typical microdialysis probe which uses flexible tubing that is sealed except at its tip, where it is semipermeable and is able to collect samples. What did the initial experiments using intracranial self-stimulation teach us about the involvement of the reward pathway and dopamine in addictive behaviors? _ Why is microdialysis an inappropriate tool to examine dopamine involvement in the appetitive and consummatory phases of motivated behavior? It is held in place by dental plastic on the animal s skull. Lesson
159 DEFINITIONS OF TERMS Fast-scan cyclic voltammetry technique used to measure neurotransmitter release in the brain of an awake, freely moving animal by inserting a microsensor that detects the presence of specific neurotransmitters at very fast rates. For a complete list of defined terms, see the Glossary. LESSON READING A. B. Figure 19: Method of in vivo voltammetry. (A) In vivo voltammetry uses implanted electrodes to measure chemicals in extracellular fluid. (B) In voltammetry, a very fine electrode is implanted and a small electrical potential is applied. Changes in the current flow at the electrode tip reflect changes in the concentration of electroactive substances such as neurotransmitters and their metabolites. A major advantage is that because the measurements are made continuously, researchers can evaluate neurotransmitter release as it s occurring in real time. Luckily, scientists developed a new technique that allowed more rapid sampling of dopamine levels in the brain. This chemical microsensor technique, called fastscan cyclic voltammetry uses carbonfiber electrodes and is able to measure dopamine levels 10 times per second (Figure 19). Finally, we have a suitable technique for monitoring dopamine levels during the appetitive and consummatory phases of motivated behavior. When researchers used voltammetry to monitor dopamine release during motivated behavior, some very interesting findings were obtained. The researchers found that dopamine levels increase at two different times first, at 5 seconds before the animal pressed the lever, and then again 36 seconds after the animal pressed the letter (Figure 20). The increase in dopamine 36 seconds after the animal pressed the lever was rapid and substantial. This time point coincides with the delivery of cocaine to the animals brains. So, it is consistent with previous studies showing that dopamine levels increase rapidly when cocaine is consumed (consummatory phase). The new and very interesting finding was that dopamine increased before the animal even pressed the lever. Approximately 5 seconds before the animal pressed the lever, researchers saw a small increase in dopamine levels. The dopamine levels then increased gradually until 2 seconds before the animal pressed the lever, and then there was a rapid and sizable increase. Approximately 10 seconds after a lever press, dopamine levels returned to normal, which was still 26 seconds before the researchers observed the very rapid and substantial increase due to cocaine consumption. Because dopamine levels rise while the rat was engaged in cocaine seeking behavior, but before it receives its cocaine reward, the researchers concluded that dopamine also plays a role in cocaine seeking (appetitive phase). A. B. Figure 20: Dopamine increases as measured by in vivo voltammetry during self-administration. (A) The solid blue trace represents dopamine concentrations during the experiment. Notice how dopamine levels increase as the animal approaches the bar (inverted red triangle). These levels drop as the animal presses the lever (inverted black triangle), and then sore after infusion of cocaine (light-blue bar). (B) The solid blue line is the mean dopamine changes across all animals around the lever press, and the dashed blue line is the mean plus standard error. Increases in dopamine before the lever press What new technique did scientists develop in order to be able to detect changes in dopamine quickly enough to distinguish between the appetitive and consummatory phases of motivated behaviors? What did scientist observe about dopamine levels during motivated behavior when using voltammetry? Lesson 5.4 are highlighted by the arrows. (Figure adapted from Phillips, et al ) 159
160 DEFINITIONS OF TERMS Remissions drug free periods. Relapses reoccurring drug use after periods of abstinence. For a complete list of defined terms, see the Glossary. LESSON READING You might be asking why would dopamine levels rise during the appetitive phase? The researchers hypothesized that before a cocaine-addicted animal receives cocaine, it thinks about its need for cocaine. Thinking about cocaine then activates the reward pathway, and stimulates the release of dopamine. Thus, the brain of the cocaine-addicted animal responds not only to the physical presence of cocaine in the brain, it also responds to any stimuli associated with seeking out cocaine. Dopamine signaling in appetitive phase may underlie relapse In terms of the reward pathway, a rat s brain is very similar to a human brain. Since the brain of a drugaddicted rat responds not only to the physical presence of the drug, but also to the activity of drug seeking, it is possible that human drug addicts react to drug seeking behavior with a spike in dopamine levels. If so, then breaking the addiction will be more difficult for addicts who spend time in activities and locations associated with past drug seeking behavior. Researchers have in fact shown that exposing addicts to stimuli associated with past drug use will lead to drug-like effects. These drug-like effects (that is, responses similar to those produced by the drug itself) may serve as primers, promoting subsequent drug seeking and drug consumption by reminding the individual of how the drug feels. This phenomenon may be what underlies the strong cravings addicts feel when presented with stimuli that remind them of the previous drug use. This also means that individuals stay addicted for long periods of time, and that drug-free periods (remissions) are often followed by relapses in which drug use recurs. Why would dopamine levels increase before receiving a reward (appetitive phase)? Lesson
161 STUDENT RESPONSES What do these findings about dopamine levels in the appetitive phase mean for addicts trying to break their addiction? Remember to identify your sources How could we use these findings to help people overcome their addictions? Lesson
162 Lesson 5.5 LESSON 5.5 WORKBOOK When does abuse become addiction? So far in this unit, we ve talked about how drugs affect our brains, including their effects on neural circuitry, synaptic signaling and neurons. In this lesson, we ll start getting to the bigger picture of drug abuse and addiction by talking about the different risk and protective factors that underlie addiction. Why do people start using drugs? People being taking drugs for a variety of reasons: To feel good As we ve already seen, drugs of abuse produce intense feelings of pleasure by activating the reward pathway. To feel better Some people who suffer from social anxiety, stress-related disorders, and depression begin abusing drugs in an attempt to lesson feelings of distress. Stress can play a major role in beginning drug use, continuing drug abuse, or relapse in patients recovering from addiction. To do better The increasing pressure that some individuals feel to chemically enhance or improve their athletic or cognitive performance can similarly play a role in initial experimentation and continued drug abuse. Curiosity and peer pressure In this respect, adolescents are particularly vulnerable because of the strong influence of peer pressure, they are more likely, for example to engage in thrilling and daring behaviors. If taking drugs makes people feel better, what s the problem? At first, people may perceive what seem to be positive effects with drug use. They also may believe that they can control their use. However, drugs can quickly take over their lives. Consider how a social drinker can become intoxicated, put himself behind a wheel and quickly turn a pleasurable activity into a tragedy for him and others. Over time, if drug use continues, pleasurable activities become less pleasurable, and drug use becomes necessary for abusers to simply feel normal. Drug abusers reach a point where they seek and take drugs, despite the tremendous problems they cause for themselves and their loved ones. You can watch two stories of young people who became addicted to cocaine online see this unit on the student website or click on the link below: Video: Council on Drug Abuse: Crossroads (Parts 1-2) What reason do you think is the most common for people to start using drugs? _ 162
163 DEFINITIONS OF TERMS Addiction the continued compulsive use of drugs despite adverse health or social consequences. Drug abuse overuse of a drug by an individual. Risk factors factors in a person s life that increase the risk of developing addiction. Protective factors factors in a person s life that reduce the risk of developing addiction. For a complete list of defined terms, see the Glossary. Lesson 5.5 LESSON READING Is continued drug abuse a voluntary behavior? The initial decision to take drugs is mostly voluntary. However, when drug abuse the overuse of a drug by an individual takes over, a person s ability to exert self-control can become seriously impaired. Brain imaging studies from drug-addicted individuals show physical changes in areas of the brain that are critical to judgment, decision-making, learning and memory, and behavior control. Scientists believe that these changes alter the way the brain works, and may help explain the compulsive and destructive behaviors of addiction. Remember that addiction is defined as the continued compulsive use of drugs in spite of adverse health or social consequences. Why do some people become addicted to drugs, while others do not? As with any other disease, vulnerability to addiction differs from person to person. There are many factors that can influence either the likelihood of someone becoming a drug addict, or the probability that they will be able to achieve stable abstinence once addicted. In general, the more risk factors an individual has, the greater the greater the chance that taking drugs will lead to abuse and addiction. Conversely, protective factors reduce a person s risk of developing addiction. No single factor determines whether a person will become addicted to drugs. The overall risk for addiction is impacted by the biological makeup of the individual, and it can be influenced by gender or ethnicity, his or her developmental stage, and the surrounding social environment (for example conditions at home, at school, and in the neighborhood). Risk factors can therefore be environmental, social, psychological or biological. Environmental, social, and psychological risk factors One important environmental risk factor is the occurrence of stress and the ability of the person to cope with such stress. The life histories of drug addicts often show instances in which stressful events either promoted increased drug use or triggered relapse from a previous period of abstinence. Numerous animal studies confirm that stress can increase self-stimulation of abused drugs, as well as trigger renewed drugtaking after periods of relapse. For this reason, many treatment providers teach their clients new coping skills to deal with life stresses without relapse. Family and socio-cultural influences also influence the risk of developing a pattern of drug abuse or addiction. Family factors have been studied most in conjunction with alcoholism. For example, adult children of alcoholics are at increased risk for having alcohol or other substance abuse problems. In the case of alcohol, this may be related in part to modeling (imitation) of the parent s drinking behavior or to a heightened expectancy that drinking will lead to positive mood changes. Socio-cultural studies have identified at least four different functions served by drug abuse. The first involves the ability to fit into a social situation. Alcohol and other drugs are often consumed in a group setting where the substance may appear to enhance social bonds like at a frat party where everyone is drinking. Is continued drug abuse a voluntary behavior? Why do some people become addicted to drugs, while others do not? How is stress involved in the development of drug addiction? 163
164 Lesson 5.5 LESSON READING The second function is to remove the user from normal social roles and responsibilities, thereby allowing an escape from the burdens associated with responsibilities. Third, substance use may promote group solidarity within a particular ethnic group. A good example of this phenomenon is the association of the Irish culture with heavy alcohol use and a high rate of alcoholism. Finally, substance abuse sometimes occurs with a drug subculture that embraces social rituals surrounding a particular subculture and rejects conventional social norms and lifestyles. Sociological studies have identified distinct subcultures for many different drugs of abuse, including heroin, cocaine, alcohol, marijuana, and methamphetamine. Biological risk factors While social and environmental factors contribute to the risk of addiction, the finding that several genes are linked to specific addictive behaviors indicates that there is also a genetic susceptibility (Figure 21). Scientists estimate that genetic factors account for between 40 and 60 percent of a person s vulnerability to addiction, including the effects of environment on gene expression and function. Fortunately the reward pathway is located in a part of the brain that is evolutionarily very old, so all aspects of the pathway are almost identical in mice, rats and humans. This means that mice, which are a valuable genetic tool, are also useful animal models to investigate genetic susceptibility. Mice have the same number of genes as humans (20,000 25,000) and each mouse gene is about 85% identical to its human counterpart (or homolog). Among the genes now identified to be involved in susceptibility to addictive behaviors are dopamine receptors. Figure 21: Addictive behaviors are associated with defects to a number of genes, indicating genetic susceptibilities. According to sociocultural studies, what are the four different functions served by drug abuse? _ Why are animal models useful tools in investigating the biological risk factors for addiction? _ 164
165 Lesson 5.5 LESSON READING Dopamine receptors Since all drugs of abuse modulate dopamine signaling, it is necessary to consider how dopamine receptors mediate drug effects and addiction potential. Intriguing results have come from studies involving dopamine receptors. These studies suggest that animals with higher the levels of dopamine receptors are more prone to addiction, presumably because they experience greater effects from dopamine binding. Levels of dopamine released The greater the high experienced by drug users, the more likely addiction will develop. In the case of cocaine, one biological factor that influences the experienced high is the baseline level of dopamine activity in the reward pathway. Imagine two subjects A and B. Due to individual differences in dopamine signaling, subject A starts with a relatively low level of baseline dopamine release, whereas subject B starts with a relatively high level of release. Both subjects are now given cocaine which inhibits dopamine transporters. Even with equivalent amounts of reuptake blocked, the effect of this blockage on stimulating postsynaptic dopamine receptors will be greater in subject B than in subject A because of the higher initial concentration of dopamine in the synaptic cleft (Figure 22). Protective factors Low baseline dopamine release Cocaine Cocaine High baseline dopamine release Figure 22: Role of baseline DA release. If baseline levels of dopamine release are low (left), then partial inhibition of dopamine transporters by cocaine or amphetamine has relatively little effect on synaptic levels of dopamine. However, if baseline dopamine release is high (right), then the same inhibition results in much greater synaptic levels and receptor activation. There are two different ways that we can think about protective factors in drug addiction. First, an absence of the various risk factors described previously would confer some protection in respect of developing a drug addiction. Put another way, individuals who do not suffer from preexisting personality or mood disorders, who come from a stable family without any substance abuse, who do not belong to an ethnic group that promotes substance use, and who do not become involved in social rituals surrounding drug use are at a reduced risk for becoming addicted. The second way that protective factors can operate is to help maintain a stable abstinence in previously drug-abusing or addicted individuals. Once the decision to abstain has been made, the risk of relapse is reduced by such actions as avoiding drug-associated cues (for example, moving to a new area and developing new social relationships with nonusers), and engaging in substitute activities like physical exercise or mediation. Why would having increased levels of dopamine receptors be a risk factor for developing addiction? Why would having a high baseline level of dopamine activity be a risk factor for developing an addiction to cocaine? What are protective factors and how do they help people remain drug free? 165
166 STUDENT RESPONSES Do you think these risk and protective factors tell the whole story of the development of drug addiction? Why or why not? Remember to identify your sources In addition to risk factors, one s motivation for taking drugs is a critical factor in the development of addiction. Why would your motivation to taking a drug play such a critical role? (Think about people who are prescribed drugs by doctors, versus people who take drugs for recreation.) Lesson
167 DEFINITIONS OF TERMS Tolerance decreased response to a drug as a direct result of repeated drug exposure. Dependence state of drug use in which user requires drug to maintain normal bodily function. Withdrawal symptoms the condition brought on by the elimination from the body of a drug on which the person has become physically dependent. For a complete list of defined terms, see the Glossary. LESSON 5.6 WORKBOOK What are the long-term effects of drug abuse and addiction? Now that we re familiar with the reasons why people start taking drugs, and the factors that can influence the likelihood of someone becoming addicted, let s turn our attention to the long-term effects of drug abuse and addiction. How does long-term drug abuse affect our brains? Just as we turn down the volume on a radio that is too loud, our brains adjust to the overwhelming surges in dopamine caused by drugs of abuse by producing less dopamine and/or reducing the numbers of dopamine receptors that receive the signals. As a result, dopamine s impact on the reward circuit can become abnormally low, and the ability to experience any pleasure is reduced. This is why abusers eventually feel flat, lifeless, and depressed, and why they are unable to enjoy things that previously brought them pleasure. Now, they need to take drugs just to try and bring their dopamine function back up to normal. And, they must take larger amounts of the drug than they first did to create the same dopamine high an effect known as tolerance. We know that the same sort of mechanisms involved in the development of tolerance can eventually lead to profound changes in neurons and brain circuits that can severely affect the brain s long-term health. The early stages of addiction are characterized by tolerance and dependence. After a drug binge, an addict needs more of a substance to get the same effect on mood. This increase in tolerance then provokes an escalation of drug use that develops into dependence needing a drug to function normally. Once dependent, if an addict abstains they face withdrawal symptoms painful emotional, and at times, physical reactions that result from stopping drug use (Figure 23). Both tolerance and dependence occur because frequent drug use can, ironically, suppress parts of the brain s reward circuit. How do our brains adjust to the overwhelming surges of dopamine in the case of drug addiction? What causes tolerance? What is dependence? Lesson
168 DEFINITIONS OF TERMS Transcription factors proteins that bind to DNA and influence the expression of particular genes. For a complete list of defined terms, see the Glossary. LESSON READING A. B. At the heart of this cruel suppression lie molecules known as transcription factors, proteins that regulate the expression, or activity of genes and thus the overall behavior of neurons. When drugs of abuse are consumed, specific transcription factors are switched on. After these transcription factors are switched on, they bind to a specific set of genes, triggering the production of the proteins those genes encode. What causes relapse? Figure 23: Model of tolerance and withdrawal. (A) Theoretical model suggesting that the nervous system adapts to the disturbing presence of a drug, so tolerance develops, but if the drug is suddenly stopped, the adaptive mechanisms continue to function, causing disturbed homeostasis characterized by withdrawal symptoms. (B) Application of model to morphine addiction. Morphine acutely inhibits camp, but the effect becomes less as tolerance develops and neural adaptation occurs. If morphine is suddenly withdrawn, a larger than normal amount of camp is produced, resulting in withdrawal effects and suggesting that the adaptive mechanism is still operating. With time, cells once again adapt, this time to the absence of the drug. Figure 24: Chronic exposure to drugs of abuse results in neurons changinf their structures, including increased dendritic spines, which increases the connections between neurons Chronic exposure to cocaine and other drugs of abuse is known to induce the dendrites of nucleus accumbens neurons to sprout more dendritic spines (Figure 24). Increasing the number of dendritic spines, bolsters the cell s connections to other neurons. In rodents, this sprouting can continue for months after drug use stops. It s suggested that specific transcription factors may be responsible for these added spines. It is speculated that the extra connections can amplify the signal in the nucleus accumbens for years and that the heightened signaling might cause the brain to overact to drug-related cues. These dendritic changes may, in the end, be the key to adaptation that accounts for how hard addiction is to break. These changes in dendritic spines and thus connections between neurons may also underlie relapse. What are withdrawal symptoms? What are transcription factors? How do neurons in the nucleus accumbens change in response to chronic exposure to drugs? Lesson
169 LESSON READING Additionally, learning may also be involved in relapse. Conditioning is one example of this type of learning and memory, in which environmental cues become associated with the drug experience and can trigger uncontrollable cravings if the individual is later exposed to these cues, even without the drug being available. This learned reflex is extremely robust and can emerge even after many years of abstinence, leading to relapse. Drugs of abuse change our brains In summary, researchers have discovered that long term drug abuse changes our brains. Drug abuse activates transcription factors, which in turn stimulate the production of different proteins that ultimately increase the number of dendritic spines, thus increasing the number of synapses and altering our synaptic connections. This response lasts long after drug use stops. The synaptic connections created are stable additions to our neural circuits, and may underlie relapse. How might these changes in NAc neurons explain relapse? Put the following in order: Protein, DNA, RNA. _ Lesson
170 STUDENT RESPONSES Remember to identify your sources How does drug abuse and addiction change our neurons and thus our brains? Lesson
171 DEFINITIONS OF TERMS Addiction is a disease idea that states drug addiction is no different from other chronic diseases, like diabetes and heart disease, and thus needs to be treated as a distinct medical disorder. For a complete list of defined terms, see the Glossary. LESSON 5.7 WORKBOOK Is addiction a chronic disease? In this last lesson, we will explore the idea of addiction as a chronic disease. Drug Addiction as a disease Throughout much of the last century, scientists studying drug abuse labored in the shadows of powerful myths and misconceptions about the nature of addiction. When scientists began studying addiction in the 1930s, people addicted to drugs were thought to be morally flawed and lacking in willpower. Those views shaped society s responses to drug abuse, treating it as a moral failing rather than a health problem, which led to an emphasis of punitive rather than preventative and therapeutic actions. Today, thanks to science, our views and responses to drug abuse have changed dramatically. Groundbreaking discoveries about the brain have revolutionized our understanding of drug addiction, enabling use to develop more effective responses to the problem. As a result of scientific research, we know that addiction is a disease that affects both the brain and behavior (Figure 25). We have identified many of the biological and environmental factors, and are beginning to search for the genetic variations that contribute to the development and progression of the disease. Using this knowledge, scientists are developing more effective prevention and treatment options that reduce the toll drug addiction takes on individuals, families and communities. Figure 25: Addiction is a disease. PET scans comparing decreased metabolism in diseased brain and diseased heart. Just as a heart attack causes decreased metabolism in the heart, Why would the myths and misconceptions about drug addiction in the 1930s hinder research on and treatment of drug addiction? Why is drug addiction considered a disease? Lesson 5.7 addiction causes decreased metabolism in the 171 brain.
172 LESSON READING Can addiction be treated? Yes. Addiction is a treatable disease. Discoveries in the science of addiction have led to advances in drug abuse treatment that help people stop abusing drugs and resume their productive lives. Like other chronic diseases, addiction can be managed successfully. Treatment enables people to counteract addiction s powerful disruptive effects on the brain and behavior and regain control of their lives. Figure 26: Comparison of relapse rates. Relapse rates for drug-addicted patients compared with those suffering from diabetes, hypertension and asthma. Relapse is a common and similar across these illness (as is adherence to medication). Thus, drug addiction should be treated like any other chronic illness, with relapse serving as a trigger for reinstated or adjusted treatment. Figure 27: Medications used to treat drug addiction. With scientific research, we ve been Relapse does not mean treatment has failed. The chronic nature of addiction means that relapsing back to drug abuse is not only possible, but likely. Relapse rates for drug addiction are similar to those for other well-characterized chronic medical illnesses, such as diabetes, hypertension, and asthma, which also have physiological and behavioral components (Figure 26). Treatment of chronic diseases involves changing deeply embedded behaviors, and relapse does not mean treatment failed. For the addicted patient, lapses back to drug abuse indicate that treatment needs to be reinstated or adjusted, or that alternative treatment is needed and again, not that treatment has failed. Research shows that combining treatment medication, where available, with behavioral therapy is the best way to ensure success for most patients. Treatment approaches must be tailored to address each patient s drug abuse patterns and drug-related medical, psychiatric and social problems. How can medications help treat drug addiction? Different types of medications may be useful at different stages of treatment to help a patient stop abusing drugs, stay in treatment, and avoid relapse (Figure 27). When patients first stop abusing drugs, they can experience a variety of physical and emotional symptoms, including depression, anxiety, and other mood disorders, restlessness, and sleeplessness. Certain treatment medications are designed to reduce these How can drug addiction be treated? How can medications be used to help treat drug addiction? able to develop a variety of medications to symptoms, which makes it easier to stop abuse. Lesson 5.7 aid in the treatment of addiction. 172
173 LESSON READING Some treatment medications are used to help the brain gradually adapt to the absence of the abused drug for example nicotine patches or gum in the case of cigarette smokers, or methadone in the case of heroin addicts. These medications act slowly to stave off drug cravings, and have a calming effect on body systems. They can help patients focus on counseling and other psychotherapies related to their drug treatment. Science has taught us that stress, cues linked to drug experience (for example people, places, things, moods), and exposure to drugs are the most common triggers for relapse. Medications are being developed to interfere with these triggers to help patients sustain recovery. How do behavioral treatments help drug addiction? Behavioral treatments help engage people in drug abuse treatment (Figure 28). Behavioral treatments aim to modify attitudes and behaviors related to drug abuse. They also focus on increasing life skills to handle stressful circumstances and combat environmental cues that may trigger intense drug cravings and prompt another cycle of compulsive abuse. Moreover, behavioral therapies can enhance the effectiveness of medications and help people remain in treatment longer. How do the best treatment programs help patients recover? Getting an addicted person to stop abusing drugs is just one part of a long and complex recovery process. When people enter treatment, addiction has often taken over their lives. The compulsion to get drugs, take drugs, and experience the effects of drugs has dominated their every waking moment, and drug abuse has taken the place of all the things they used to enjoy doing. It has disrupted how they function in their family lives, at work and in the community, and has made them more likely to suffer from other serious illnesses. Because addiction can affect so many aspects of a person s life, treatment must address the needs of the whole person to be successful. This is why the best programs incorporate a variety of rehabilitation services into their comprehensive treatment regimens. Treatment counselors select from a menu of services for meeting the individual medical, psychological, social, vocational, and legal needs of their patients to foster their recovery from addiction. Figure 28: Variety of behavioral therapies. A variety of behavioral therapies aim to help drug addicted patients beat their How do behavioral treatments help to treat drug addiction? Lesson 5.7 addictions. 173
174 LESSON READING Summary Research has shown that addiction is a disease that affects brain structure and impacts behavior. Many of the biological and environmental factors that contribute to addiction have been identified, and the search has begun to identify the underlying genetic variations that predispose and contribute to its development and progression. Addiction occurs when the activity of the reward pathway is disturbed. The reward pathway is composed of the connections between the ventral tegmental area (VTA) and the nucleus accumbens (NAc). Drugs of abuse act on this pathway in various ways to increase dopamine neurotransmission across this synapse. Dopamine neurotransmission can lead to transient effects on the postsynaptic cell membrane, but also effects gene transcription. Effects on gene transcription result in longer acting effects on neuronal structure, including building more synapses on the post-synaptic cell. Finally, addiction is considered a chronic disease because it causes long term changes in the brain, it is characterized by the compulsive, non-voluntary use of drugs, and people are never completely cured of their addictions. Lesson
175 STUDENT RESPONSES Remember to identify your sources Pretend you are an advisor to a government agency that needs to decide whether or not insurance companies should be required to cover treatment for addiction. Write an opinion piece to help the agency make the right choice. Lesson
Nervous System: PNS and CNS
 Nervous System: PNS and CNS Biology 105 Lecture 10 Chapter 8 Outline I. Central Nervous System vs Peripheral Nervous System II. Peripheral Nervous System A. Somatic Nervous System B. Autonomic Nervous
Nervous System: PNS and CNS Biology 105 Lecture 10 Chapter 8 Outline I. Central Nervous System vs Peripheral Nervous System II. Peripheral Nervous System A. Somatic Nervous System B. Autonomic Nervous
Parts of the Brain. Chapter 1
 Chapter 1 Parts of the Brain Living creatures are made up of cells. Groups of cells, similar in appearance and with the same function, form tissue. The brain is a soft mass of supportive tissues and nerve
Chapter 1 Parts of the Brain Living creatures are made up of cells. Groups of cells, similar in appearance and with the same function, form tissue. The brain is a soft mass of supportive tissues and nerve
Slide 4: Forebrain Structures. Slide 5: 4 Lobes of the Cerebral Cortex. Slide 6: The Cerebral Hemispheres (L & R)
 Slide 1: [Film Clip: The Brain #2- Phineas Gage] Integrated Bodily Communications Within Brain (Hemispheres and structures) The remaining Nervous System Endocrine System (Hormonal communication) Our bodies-
Slide 1: [Film Clip: The Brain #2- Phineas Gage] Integrated Bodily Communications Within Brain (Hemispheres and structures) The remaining Nervous System Endocrine System (Hormonal communication) Our bodies-
2401 : Anatomy/Physiology
 Dr. Chris Doumen Week 7 2401 : Anatomy/Physiology The Brain Central Nervous System TextBook Readings Pages 431 through 435 and 463-467 Make use of the figures in your textbook ; a picture is worth a thousand
Dr. Chris Doumen Week 7 2401 : Anatomy/Physiology The Brain Central Nervous System TextBook Readings Pages 431 through 435 and 463-467 Make use of the figures in your textbook ; a picture is worth a thousand
3) Cerebral Cortex & Functions of the 4 LOBES. 5) Cranial Nerves (Nerves In the Cranium, i.e., Head)
 Lecture 5 (Oct 8 th ): ANATOMY and FUNCTION OF THE NERVOUS SYSTEM Lecture Outline 1) Basic Divisions (CNS vs. PNS, Somatic vs. Autonomic) and Directional Terms 2) The Brain (Hindbrain/ Midbrain/ Forebrain)
Lecture 5 (Oct 8 th ): ANATOMY and FUNCTION OF THE NERVOUS SYSTEM Lecture Outline 1) Basic Divisions (CNS vs. PNS, Somatic vs. Autonomic) and Directional Terms 2) The Brain (Hindbrain/ Midbrain/ Forebrain)
Diagram 2(i): Structure of the Neuron
 Diagram 2(i): Structure of the Neuron Generally speaking, we can divide the nervous system into different parts, according to location and function. So far we have mentioned the central nervous system
Diagram 2(i): Structure of the Neuron Generally speaking, we can divide the nervous system into different parts, according to location and function. So far we have mentioned the central nervous system
Sheep Brain Dissection Picture Guide
 Sheep Brain Dissection Picture Guide Figure 1: Right Hemisphere of Sheep s Brain Figure 2: Underside of Sheep s Brain Figure 3: Saggital cut of Sheep s Brain to reveal subcortical structures Figure 4:
Sheep Brain Dissection Picture Guide Figure 1: Right Hemisphere of Sheep s Brain Figure 2: Underside of Sheep s Brain Figure 3: Saggital cut of Sheep s Brain to reveal subcortical structures Figure 4:
THE BRAIN AND CRANIAL NERVES
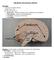 THE BRAIN AND CRANIAL NERVES The Brain - made up of a trillion neurons - weighs about 3 lbs - has four principle parts 1. Brain stem - medulla oblongata, pons, midbrain (mesencephalon) 2. Diencephalon
THE BRAIN AND CRANIAL NERVES The Brain - made up of a trillion neurons - weighs about 3 lbs - has four principle parts 1. Brain stem - medulla oblongata, pons, midbrain (mesencephalon) 2. Diencephalon
Brain Power. Counseling and Mental Health
 Brain Power Counseling and Mental Health TEA COPYRIGHT Copyright Texas Education Agency, 2012. These Materials are copyrighted and trademarked as the property of the Texas Education Agency (TEA) and may
Brain Power Counseling and Mental Health TEA COPYRIGHT Copyright Texas Education Agency, 2012. These Materials are copyrighted and trademarked as the property of the Texas Education Agency (TEA) and may
Vocabulary & General Concepts of Brain Organization
 Vocabulary & General Concepts of Brain Organization Jeanette J. Norden, Ph.D. Professor Emerita Vanderbilt University School of Medicine Course Outline Lecture 1: Vocabulary & General Concepts of Brain
Vocabulary & General Concepts of Brain Organization Jeanette J. Norden, Ph.D. Professor Emerita Vanderbilt University School of Medicine Course Outline Lecture 1: Vocabulary & General Concepts of Brain
Chapter 3 The Anatomy of the Nervous System
 Chapter 3 The Anatomy of the Nervous System Systems, Structures, and Cells That Make Up Your Nervous System 1 General Layout of the Nervous System Central Nervous System (CNS) Brain (in the skull) Spinal
Chapter 3 The Anatomy of the Nervous System Systems, Structures, and Cells That Make Up Your Nervous System 1 General Layout of the Nervous System Central Nervous System (CNS) Brain (in the skull) Spinal
DISSECTION OF THE SHEEP'S BRAIN
 DISSECTION OF THE SHEEP'S BRAIN Introduction The purpose of the sheep brain dissection is to familiarize you with the threedimensional structure of the brain and teach you one of the great methods of studying
DISSECTION OF THE SHEEP'S BRAIN Introduction The purpose of the sheep brain dissection is to familiarize you with the threedimensional structure of the brain and teach you one of the great methods of studying
Human Neuroanatomy. Grades 9-12. Driving Question: How did the evolution of the human brain impact the structure and function it has today?
 Human Neuroanatomy Grades 9-12 Driving Question: How did the evolution of the human brain impact the structure and function it has today? Objectives: Students will be able to Describe the basic parts and
Human Neuroanatomy Grades 9-12 Driving Question: How did the evolution of the human brain impact the structure and function it has today? Objectives: Students will be able to Describe the basic parts and
Integration and Coordination of the Human Body. Nervous System
 I. General Info Integration and Coordination of the Human Body A. Both the and system are responsible for maintaining 1. Homeostasis is the process by which organisms keep internal conditions despite changes
I. General Info Integration and Coordination of the Human Body A. Both the and system are responsible for maintaining 1. Homeostasis is the process by which organisms keep internal conditions despite changes
The brain structure and function
 The brain structure and function This information is an extract from the booklet Understanding brain tumours. You may find the full booklet helpful. We can send you a copy free see page 5. Contents Introduction
The brain structure and function This information is an extract from the booklet Understanding brain tumours. You may find the full booklet helpful. We can send you a copy free see page 5. Contents Introduction
Module 1: The Brain and the Central Nervous System (CNS)
 Module 1: The Brain and the Central Nervous System (CNS) By the end of this unit, the learner will be able to: Describe the anatomy of the brain and the central nervous system Identify regions of the brain
Module 1: The Brain and the Central Nervous System (CNS) By the end of this unit, the learner will be able to: Describe the anatomy of the brain and the central nervous system Identify regions of the brain
Basic Brain Information
 Basic Brain Information Brain facts Your brain weighs about 3lbs, or just under 1.5Kg It has the texture of blancmange Your brain is connected to your spinal cord by the brain stem Behind your brain stem
Basic Brain Information Brain facts Your brain weighs about 3lbs, or just under 1.5Kg It has the texture of blancmange Your brain is connected to your spinal cord by the brain stem Behind your brain stem
BIOLOGY STUDY PACKET THE BRAIN
 BIOLOGY STUDY PACKET THE BRAIN SC.912.L.14.26 AA Spring 2012 The intent of this packet is to supplement regular classroom instruction, not to replace it. This also supposes that the students have access
BIOLOGY STUDY PACKET THE BRAIN SC.912.L.14.26 AA Spring 2012 The intent of this packet is to supplement regular classroom instruction, not to replace it. This also supposes that the students have access
CSE511 Brain & Memory Modeling. Lect04: Brain & Spine Neuroanatomy
 CSE511 Brain & Memory Modeling CSE511 Brain & Memory Modeling Lect02: BOSS Discrete Event Simulator Lect04: Brain & Spine Neuroanatomy Appendix of Purves et al., 4e Larry Wittie Computer Science, StonyBrook
CSE511 Brain & Memory Modeling CSE511 Brain & Memory Modeling Lect02: BOSS Discrete Event Simulator Lect04: Brain & Spine Neuroanatomy Appendix of Purves et al., 4e Larry Wittie Computer Science, StonyBrook
What is the basic component of the brain and spinal cord communication system?
 EXPLORING PSYCHOLOGY David Myers The Biology of Mind Chapter 2 Neural Communication Neurons How Neurons Communicate How Neurotransmitters Influence Us The Nervous System The Peripheral Nervous System The
EXPLORING PSYCHOLOGY David Myers The Biology of Mind Chapter 2 Neural Communication Neurons How Neurons Communicate How Neurotransmitters Influence Us The Nervous System The Peripheral Nervous System The
Function (& other notes)
 LAB 8. ANATOMY OF THE HUMAN BRAIN In this exercise you each will map the human brain both anatomy and function so that you can develop a more accurate picture of what s going on in your head :-) EXTERNAL
LAB 8. ANATOMY OF THE HUMAN BRAIN In this exercise you each will map the human brain both anatomy and function so that you can develop a more accurate picture of what s going on in your head :-) EXTERNAL
31.1 The Neuron. BUILD Vocabulary. Lesson Objectives
 Name Class Date 31.1 The Neuron Lesson Objectives Identify the functions of the nervous system. Describe the function of neurons. Describe how a nerve impulse is transmitted. BUILD Vocabulary A. The chart
Name Class Date 31.1 The Neuron Lesson Objectives Identify the functions of the nervous system. Describe the function of neurons. Describe how a nerve impulse is transmitted. BUILD Vocabulary A. The chart
3. The neuron has many branch-like extensions called that receive input from other neurons. a. glia b. dendrites c. axons d.
 Chapter Test 1. A cell that receives information and transmits it to other cells via an electrochemical process is called a(n) a. neuron b. hormone c. glia d. endorphin Answer: A difficulty: 1 factual
Chapter Test 1. A cell that receives information and transmits it to other cells via an electrochemical process is called a(n) a. neuron b. hormone c. glia d. endorphin Answer: A difficulty: 1 factual
Student Academic Learning Services Page 1 of 8 Nervous System Quiz
 Student Academic Learning Services Page 1 of 8 Nervous System Quiz 1. The term central nervous system refers to the: A) autonomic and peripheral nervous systems B) brain, spinal cord, and cranial nerves
Student Academic Learning Services Page 1 of 8 Nervous System Quiz 1. The term central nervous system refers to the: A) autonomic and peripheral nervous systems B) brain, spinal cord, and cranial nerves
Chapter 7: The Nervous System
 Chapter 7: The Nervous System I. Organization of the Nervous System Objectives: List the general functions of the nervous system Explain the structural and functional classifications of the nervous system
Chapter 7: The Nervous System I. Organization of the Nervous System Objectives: List the general functions of the nervous system Explain the structural and functional classifications of the nervous system
THE SPINAL CORD AND THE INFLUENCE OF ITS DAMAGE ON THE HUMAN BODY
 THE SPINAL CORD AND THE INFLUENCE OF ITS DAMAGE ON THE HUMAN BODY THE SPINAL CORD. A part of the Central Nervous System The nervous system is a vast network of cells, which carry information in the form
THE SPINAL CORD AND THE INFLUENCE OF ITS DAMAGE ON THE HUMAN BODY THE SPINAL CORD. A part of the Central Nervous System The nervous system is a vast network of cells, which carry information in the form
Sheep Brain Dissection
 Sheep Brain Dissection http://www.carolina.com/product/preserved+organisms/preserved+animals+%28mammal s%29/sheep+organs/preserved+sheep+dissection.do Michigan State University Neuroscience Program Brain
Sheep Brain Dissection http://www.carolina.com/product/preserved+organisms/preserved+animals+%28mammal s%29/sheep+organs/preserved+sheep+dissection.do Michigan State University Neuroscience Program Brain
Brain & Mind. Bicester Community College Science Department
 B6 Brain & Mind B6 Key Questions How do animals respond to changes in their environment? How is information passed through the nervous system? What can we learn through conditioning? How do humans develop
B6 Brain & Mind B6 Key Questions How do animals respond to changes in their environment? How is information passed through the nervous system? What can we learn through conditioning? How do humans develop
CENTRAL NERVOUS SYSTEM. Sensory Pathway (PNS) OVERVIEW OF SPINAL CORD ANATOMY OF THE SPINAL CORD FUNCTIONS OF THE SPINAL CORD
 CENTRAL NERVOUS SYSTEM Central nervous system (CNS) brain and spinal cord enclosed in bony coverings Functions of the spinal cord spinal cord reflexes integration ti (summation of inhibitory and excitatory)
CENTRAL NERVOUS SYSTEM Central nervous system (CNS) brain and spinal cord enclosed in bony coverings Functions of the spinal cord spinal cord reflexes integration ti (summation of inhibitory and excitatory)
AP Biology I. Nervous System Notes
 AP Biology I. Nervous System Notes 1. General information: passage of information occurs in two ways: Nerves - process and send information fast (eg. stepping on a tack) Hormones - process and send information
AP Biology I. Nervous System Notes 1. General information: passage of information occurs in two ways: Nerves - process and send information fast (eg. stepping on a tack) Hormones - process and send information
Brain Computer Interfaces (BCI) Communication Training of brain activity
 Brain Computer Interfaces (BCI) Communication Training of brain activity Brain Computer Interfaces (BCI) picture rights: Gerwin Schalk, Wadsworth Center, NY Components of a Brain Computer Interface Applications
Brain Computer Interfaces (BCI) Communication Training of brain activity Brain Computer Interfaces (BCI) picture rights: Gerwin Schalk, Wadsworth Center, NY Components of a Brain Computer Interface Applications
Homework Help Stroke
 The Brain & Strokes Your brain is the most complex organ in your body. It is the command centre for everything you do, think, sense and say! It has over 100 billion special nerve cells called neurons.
The Brain & Strokes Your brain is the most complex organ in your body. It is the command centre for everything you do, think, sense and say! It has over 100 billion special nerve cells called neurons.
Chapter 9 Nervous System
 Chapter 9 Nervous System Nervous System function: The nervous system is composed of neurons and neuroglia. at the ends of peripheral nerves gather information and convert it into nerve impulses. When sensory
Chapter 9 Nervous System Nervous System function: The nervous system is composed of neurons and neuroglia. at the ends of peripheral nerves gather information and convert it into nerve impulses. When sensory
Functional neuroimaging. Imaging brain function in real time (not just the structure of the brain).
 Functional neuroimaging Imaging brain function in real time (not just the structure of the brain). The brain is bloody & electric Blood increase in neuronal activity increase in metabolic demand for glucose
Functional neuroimaging Imaging brain function in real time (not just the structure of the brain). The brain is bloody & electric Blood increase in neuronal activity increase in metabolic demand for glucose
Explore the Neuroscience for Kids Web Site (ANSWERS) Start at: http://faculty.washington.edu/chudler/neurok.html
 NAME Explore the Neuroscience for Kids Web Site (ANSWERS) Start at: http://faculty.washington.edu/chudler/neurok.html On the left side, click on Explore, then click on The Neuron, then click on Millions
NAME Explore the Neuroscience for Kids Web Site (ANSWERS) Start at: http://faculty.washington.edu/chudler/neurok.html On the left side, click on Explore, then click on The Neuron, then click on Millions
Chapter 4. The Brain
 Chapter 4 The Brain The Nervous System Central Nervous System (CNS) receives, processes, interprets and stores info (taste, sound, smell, color etc.) Sends information to muscles, glands and internal organs
Chapter 4 The Brain The Nervous System Central Nervous System (CNS) receives, processes, interprets and stores info (taste, sound, smell, color etc.) Sends information to muscles, glands and internal organs
What role does the nucleolus have in cell functioning? Glial cells
 Nervous System Lab The nervous system of vertebrates can be divided into the central nervous system, which consists of the brain and spinal cord, and the peripheral nervous system, which contains nerves,
Nervous System Lab The nervous system of vertebrates can be divided into the central nervous system, which consists of the brain and spinal cord, and the peripheral nervous system, which contains nerves,
How are Parts of the Brain Related to Brain Function?
 How are Parts of the Brain Related to Brain Function? Scientists have found That the basic anatomical components of brain function are related to brain size and shape. The brain is composed of two hemispheres.
How are Parts of the Brain Related to Brain Function? Scientists have found That the basic anatomical components of brain function are related to brain size and shape. The brain is composed of two hemispheres.
Brain Cancer. This reference summary will help you understand how brain tumors are diagnosed and what options are available to treat them.
 Brain Cancer Introduction Brain tumors are not rare. Thousands of people are diagnosed every year with tumors of the brain and the rest of the nervous system. The diagnosis and treatment of brain tumors
Brain Cancer Introduction Brain tumors are not rare. Thousands of people are diagnosed every year with tumors of the brain and the rest of the nervous system. The diagnosis and treatment of brain tumors
Adapted from Human Anatomy & Physiology by Marieb and Hoehn (9 th ed.)
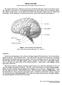 BRAIN ANATOMY Adapted from Human Anatomy & Physiology by Marieb and Hoehn (9 th ed.) The anatomy of the brain is often discussed in terms of either the embryonic scheme or the medical scheme. The embryonic
BRAIN ANATOMY Adapted from Human Anatomy & Physiology by Marieb and Hoehn (9 th ed.) The anatomy of the brain is often discussed in terms of either the embryonic scheme or the medical scheme. The embryonic
BIOL 1108 Vertebrate Anatomy Lab
 BIOL 1108 Vertebrate Anatomy Lab This lab explores major organs associated with the circulatory, excretory, and nervous systems of mammals. Circulatory System Vertebrates are among the organisms that have
BIOL 1108 Vertebrate Anatomy Lab This lab explores major organs associated with the circulatory, excretory, and nervous systems of mammals. Circulatory System Vertebrates are among the organisms that have
Nervous System Organization. PNS and CNS. Nerves. Peripheral Nervous System. Peripheral Nervous System. Motor Component.
 Nervous System Organization PNS and CNS Chapters 8 and 9 Peripheral Nervous System (PNS) connects CNS to sensory receptors, muscles and glands Central Nervous System (CNS) control/integrating center brain
Nervous System Organization PNS and CNS Chapters 8 and 9 Peripheral Nervous System (PNS) connects CNS to sensory receptors, muscles and glands Central Nervous System (CNS) control/integrating center brain
Nervous System sensor input integration motor output sensory organs central nervous system
 Nervous System Nervous system performs three overlapping functions of sensor input, integration, and motor output. This process is generally the same even at a very primitive level of nervous system, but
Nervous System Nervous system performs three overlapping functions of sensor input, integration, and motor output. This process is generally the same even at a very primitive level of nervous system, but
The Amazing Brain LEVELED BOOK Y. A Reading A Z Level Y Leveled Book Word Count: 1,470. www.readinga-z.com
 The Amazing Brain A Reading A Z Level Y Leveled Book Word Count: 1,470 LEVELED BOOK Y The Amazing Brain Visit for thousands of books and materials. Photo Photo Credits: Credits: Photo Credits: Front Front
The Amazing Brain A Reading A Z Level Y Leveled Book Word Count: 1,470 LEVELED BOOK Y The Amazing Brain Visit for thousands of books and materials. Photo Photo Credits: Credits: Photo Credits: Front Front
Andrew Rosen - Chapter 3: The Brain and Nervous System Intro:
 Intro: Brain is made up of numerous, complex parts Frontal lobes by forehead are the brain s executive center Parietal lobes wave sensory information together (maps feeling on body) Temporal lobes interpret
Intro: Brain is made up of numerous, complex parts Frontal lobes by forehead are the brain s executive center Parietal lobes wave sensory information together (maps feeling on body) Temporal lobes interpret
Name: Teacher: Olsen Hour:
 Name: Teacher: Olsen Hour: The Nervous System: Part 1 Textbook p216-225 41 In all exercises, quizzes and tests in this class, always answer in your own words. That is the only way that you can show that
Name: Teacher: Olsen Hour: The Nervous System: Part 1 Textbook p216-225 41 In all exercises, quizzes and tests in this class, always answer in your own words. That is the only way that you can show that
Chapter 7: The Nervous System
 Chapter 7: The Nervous System Objectives Discuss the general organization of the nervous system Describe the structure & function of a nerve Draw and label the pathways involved in a withdraw reflex Define
Chapter 7: The Nervous System Objectives Discuss the general organization of the nervous system Describe the structure & function of a nerve Draw and label the pathways involved in a withdraw reflex Define
What Is an Arteriovenous Malformation (AVM)?
 What Is an Arteriovenous Malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair 1 What
What Is an Arteriovenous Malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair 1 What
Related KidsHealth Links. Discussion Questions
 Grades 6 to 8 Human Body Series KidsHealth.org/classroom Teacher s Guide This guide includes: Standards Related Links Discussion Questions Activities for Students Reproducible Materials Standards This
Grades 6 to 8 Human Body Series KidsHealth.org/classroom Teacher s Guide This guide includes: Standards Related Links Discussion Questions Activities for Students Reproducible Materials Standards This
CHAPTER 6 PRINCIPLES OF NEURAL CIRCUITS.
 CHAPTER 6 PRINCIPLES OF NEURAL CIRCUITS. 6.1. CONNECTIONS AMONG NEURONS Neurons are interconnected with one another to form circuits, much as electronic components are wired together to form a functional
CHAPTER 6 PRINCIPLES OF NEURAL CIRCUITS. 6.1. CONNECTIONS AMONG NEURONS Neurons are interconnected with one another to form circuits, much as electronic components are wired together to form a functional
The Brain of a Normal Human
 The Brain of a Normal Human Your Brain Evolved Over Time Human Brain Logic and reasoning Mammalian Brain More complex feelings and reactions Lizard Brain Basic functions The Brain Stem or Hindbrain (The
The Brain of a Normal Human Your Brain Evolved Over Time Human Brain Logic and reasoning Mammalian Brain More complex feelings and reactions Lizard Brain Basic functions The Brain Stem or Hindbrain (The
CHAPTER 11: NERVOUS SYSTEM II: DIVISIONS OF THE NERVOUS SYSTEM OBJECTIVES: 1. Outline the major divisions of the nervous system.
 CHAPTER 11: NERVOUS II: DIVISIONS OF THE NERVOUS OBJECTIVES: 1. Outline the major divisions of the nervous system. NERVOUS CENTRAL NERVOUS (BRAIN & SPINAL CORD) (INTERNEURONS) PERIPHERAL NERVOUS (CRANIAL
CHAPTER 11: NERVOUS II: DIVISIONS OF THE NERVOUS OBJECTIVES: 1. Outline the major divisions of the nervous system. NERVOUS CENTRAL NERVOUS (BRAIN & SPINAL CORD) (INTERNEURONS) PERIPHERAL NERVOUS (CRANIAL
Reflex Physiology. Dr. Ali Ebneshahidi. 2009 Ebneshahidi
 Reflex Physiology Dr. Ali Ebneshahidi Reflex Physiology Reflexes are automatic, subconscious response to changes within or outside the body. a. Reflexes maintain homeostasis (autonomic reflexes) heart
Reflex Physiology Dr. Ali Ebneshahidi Reflex Physiology Reflexes are automatic, subconscious response to changes within or outside the body. a. Reflexes maintain homeostasis (autonomic reflexes) heart
North Bergen School District Benchmarks
 Grade: 10,11, and 12 Subject: Anatomy and Physiology First Marking Period Define anatomy and physiology, and describe various subspecialties of each discipline. Describe the five basic functions of living
Grade: 10,11, and 12 Subject: Anatomy and Physiology First Marking Period Define anatomy and physiology, and describe various subspecialties of each discipline. Describe the five basic functions of living
Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease.
 Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease. Memory loss and changes in mood and behavior are some signs that you or a family member may have Alzheimer s disease. If you have
Steps to getting a diagnosis: Finding out if it s Alzheimer s Disease. Memory loss and changes in mood and behavior are some signs that you or a family member may have Alzheimer s disease. If you have
D.U.C. Assist. Lec. Faculty of Dentistry General Physiology Ihsan Dhari. The Autonomic Nervous System
 The Autonomic Nervous System The portion of the nervous system that controls most visceral functions of the body is called the autonomic nervous system. This system helps to control arterial pressure,
The Autonomic Nervous System The portion of the nervous system that controls most visceral functions of the body is called the autonomic nervous system. This system helps to control arterial pressure,
Cognitive Neuroscience. Questions. Multiple Methods. Electrophysiology. Multiple Methods. Approaches to Thinking about the Mind
 Cognitive Neuroscience Approaches to Thinking about the Mind Cognitive Neuroscience Evolutionary Approach Sept 20-22, 2004 Interdisciplinary approach Rapidly changing How does the brain enable cognition?
Cognitive Neuroscience Approaches to Thinking about the Mind Cognitive Neuroscience Evolutionary Approach Sept 20-22, 2004 Interdisciplinary approach Rapidly changing How does the brain enable cognition?
Neurophysiology. 2.1 Equilibrium Potential
 2 Neurophysiology 2.1 Equilibrium Potential An understanding of the concepts of electrical and chemical forces that act on ions, electrochemical equilibrium, and equilibrium potential is a powerful tool
2 Neurophysiology 2.1 Equilibrium Potential An understanding of the concepts of electrical and chemical forces that act on ions, electrochemical equilibrium, and equilibrium potential is a powerful tool
Biology 141 Anatomy and Physiology I
 Fall 2016 Biology 141 Anatomy and Physiology I COURSE OUTLINE Faculty Name: Enter Faculty Name Here Program Head: Enter Program Head Here Dean s Review: Dean s Signature: Date Reviewed: / / Revised: Fall
Fall 2016 Biology 141 Anatomy and Physiology I COURSE OUTLINE Faculty Name: Enter Faculty Name Here Program Head: Enter Program Head Here Dean s Review: Dean s Signature: Date Reviewed: / / Revised: Fall
Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment.
 Dictionary Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment. Applicator A device used to hold a radioactive source
Dictionary Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment. Applicator A device used to hold a radioactive source
Lecture One: Brain Basics
 Lecture One: Brain Basics Brain Fractured Femur Bone Spinal Cord 1 How does pain get from here to here 2 How does the brain work? Every cell in your body is wired to send a signal to your brain The brain
Lecture One: Brain Basics Brain Fractured Femur Bone Spinal Cord 1 How does pain get from here to here 2 How does the brain work? Every cell in your body is wired to send a signal to your brain The brain
Norepinephrine Effects On the System
 Norepinephrine Effects On the System NE Conversion to Epinephrine in the Circulation Under stress, the increased norepinephrine produced is transmitted throughout the system. This increased level represents
Norepinephrine Effects On the System NE Conversion to Epinephrine in the Circulation Under stress, the increased norepinephrine produced is transmitted throughout the system. This increased level represents
Thymus Cancer. This reference summary will help you better understand what thymus cancer is and what treatment options are available.
 Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
Best Teaching Practices Conference. Teacher ID: BTPC07_07 SUBJECT: BIOLOGY. Class: X. TOPIC: Exploring our Nervous System
 Best Teaching Practices Conference Teacher ID: BTPC07_07 SUBJECT: BIOLOGY Class: X TOPIC: Exploring our Nervous System OBJECTIVES: Use Information Technology to enable the students to: Explain the general
Best Teaching Practices Conference Teacher ID: BTPC07_07 SUBJECT: BIOLOGY Class: X TOPIC: Exploring our Nervous System OBJECTIVES: Use Information Technology to enable the students to: Explain the general
Background on Brain Injury
 CHAPTER 1 Background on Brain Injury In this chapter, you will: Read about Alberta s definition of Acquired Brain Injury and how that affects which supports you will be able to access. Learn about the
CHAPTER 1 Background on Brain Injury In this chapter, you will: Read about Alberta s definition of Acquired Brain Injury and how that affects which supports you will be able to access. Learn about the
Chetek-Weyerhaeuser High School
 Chetek-Weyerhaeuser High School Anatomy and Physiology Units and Anatomy and Physiology A Unit 1 Introduction to Human Anatomy and Physiology (6 days) Essential Question: How do the systems of the human
Chetek-Weyerhaeuser High School Anatomy and Physiology Units and Anatomy and Physiology A Unit 1 Introduction to Human Anatomy and Physiology (6 days) Essential Question: How do the systems of the human
Hole s Human Anatomy and Physiology Eleventh Edition. Mrs. Hummer Hanover Area Jr./Sr. High School. Chapter 1 Introduction to Anatomy and Physiology
 Hole s Human Anatomy and Physiology Eleventh Edition Mrs. Hummer Hanover Area Jr./Sr. High School Chapter 1 Introduction to Anatomy and Physiology 1 Chapter 1 Introduction to Human Anatomy and Physiology
Hole s Human Anatomy and Physiology Eleventh Edition Mrs. Hummer Hanover Area Jr./Sr. High School Chapter 1 Introduction to Anatomy and Physiology 1 Chapter 1 Introduction to Human Anatomy and Physiology
Do I Have Epilepsy? Diagnosing Epilepsy and Seizures. Epilepsy & Seizures: Diagnosis
 Epilepsy & Seizures: Diagnosis Do I Have Epilepsy? Diagnosing Epilepsy and Seizures Artwork by Studio E participant Ashley N. (details on inside cover) About the Cover: Cover artwork was created by Ashley
Epilepsy & Seizures: Diagnosis Do I Have Epilepsy? Diagnosing Epilepsy and Seizures Artwork by Studio E participant Ashley N. (details on inside cover) About the Cover: Cover artwork was created by Ashley
WHEN PROSTATE CANCER RETURNS: ADVANCED PROSTATE CANCER. How Will I Know If My Prostate Cancer Returns?
 WHEN PROSTATE CANCER RETURNS: ADVANCED PROSTATE CANCER (The following information is based on the general experiences of many prostate cancer patients. Your experience may be different.) How Will I Know
WHEN PROSTATE CANCER RETURNS: ADVANCED PROSTATE CANCER (The following information is based on the general experiences of many prostate cancer patients. Your experience may be different.) How Will I Know
BIO130 Chapter 14 The Brain and Cranial Nerves Lecture Outline
 BIO130 Chapter 14 The Brain and Cranial Nerves Lecture Outline Brain structure 1. Cerebrum Hemispheres: left & right Cerebral cortex Gyri Sulci Fissures Longitudinal fissure Corpus callosum Lobes Central
BIO130 Chapter 14 The Brain and Cranial Nerves Lecture Outline Brain structure 1. Cerebrum Hemispheres: left & right Cerebral cortex Gyri Sulci Fissures Longitudinal fissure Corpus callosum Lobes Central
The Cranium Connection
 Your Brain! The brain is the command center of your body. It controls just about everything you do, even when you are sleeping. Weighing about 3 pounds, the brain is made up of many parts that all work
Your Brain! The brain is the command center of your body. It controls just about everything you do, even when you are sleeping. Weighing about 3 pounds, the brain is made up of many parts that all work
Functions of the Brain
 Objectives 0 Participants will be able to identify 4 characteristics of a healthy brain. 0 Participants will be able to state the functions of the brain. 0 Participants will be able to identify 3 types
Objectives 0 Participants will be able to identify 4 characteristics of a healthy brain. 0 Participants will be able to state the functions of the brain. 0 Participants will be able to identify 3 types
A LIFESPAN OF BRAIN DEVELOPMENT
 PURDUE UNIVERSITY COOPERATIVE EXTENSION SERVICE Crawford County A LIFESPAN OF BRAIN DEVELOPMENT Developed by Carol Judd Description: Brain architecture is a process that begins early in life and continues
PURDUE UNIVERSITY COOPERATIVE EXTENSION SERVICE Crawford County A LIFESPAN OF BRAIN DEVELOPMENT Developed by Carol Judd Description: Brain architecture is a process that begins early in life and continues
Brain Development. Genetic make-up... is not the major determiner
 Brain Development Presented by: Linda Alsop SKI-HI Institute Utah State University Genetic make-up... is not the major determiner Early experiences are so powerful that they can completely change the way
Brain Development Presented by: Linda Alsop SKI-HI Institute Utah State University Genetic make-up... is not the major determiner Early experiences are so powerful that they can completely change the way
Nuclear medicine. Answering your questions
 Nuclear medicine Answering your questions ANSTO s OPAL research reactor in Sydney What is nuclear medicine? This is a branch of medicine that uses radiation from radioactive tracers to provide information
Nuclear medicine Answering your questions ANSTO s OPAL research reactor in Sydney What is nuclear medicine? This is a branch of medicine that uses radiation from radioactive tracers to provide information
Nervous System. from the Human Body Systems Series. catalog # 2890. Published & Distributed by AGC/UNITED LEARNING
 Nervous System from the Human Body Systems Series catalog # 2890 Published & Distributed by AGC/UNITED LEARNING 1560 Sherman Avenue Suite 100 Evanston, IL 60201 1-800-323-9084 24-Hour Fax No. 847-328-6706
Nervous System from the Human Body Systems Series catalog # 2890 Published & Distributed by AGC/UNITED LEARNING 1560 Sherman Avenue Suite 100 Evanston, IL 60201 1-800-323-9084 24-Hour Fax No. 847-328-6706
THORACIC DIAGNOSTIC ASSESMENT PROGRAM (DAP) PATIENT INFORMATION FOR:
 central east regional cancer program in partnership with cancer care ontario THORACIC DIAGNOSTIC ASSESMENT PROGRAM (DAP) PATIENT INFORMATION FOR: Thoracic dap booklet March2012.indd 1 SCHEDULED TESTS YOUR
central east regional cancer program in partnership with cancer care ontario THORACIC DIAGNOSTIC ASSESMENT PROGRAM (DAP) PATIENT INFORMATION FOR: Thoracic dap booklet March2012.indd 1 SCHEDULED TESTS YOUR
U N IT 10 NE RVOUS SYS TE M REVIEW 1. Which of the following is controlled by the somatic nervous system? A. rate of heartbeat B.
 U N IT 10 NE RVOUS SYS TE M REVIEW 1. Which of the following is controlled by the somatic nervous system? A. rate of heartbeat B. contraction of skeletal muscles C. increased blood flow to muscle tissue
U N IT 10 NE RVOUS SYS TE M REVIEW 1. Which of the following is controlled by the somatic nervous system? A. rate of heartbeat B. contraction of skeletal muscles C. increased blood flow to muscle tissue
The Anatomy of Spinal Cord Injury (SCI)
 The Anatomy of Spinal Cord Injury (SCI) What is the Spinal Cord? The spinal cord is that part of your central nervous system that transmits messages between your brain and your body. The spinal cord has
The Anatomy of Spinal Cord Injury (SCI) What is the Spinal Cord? The spinal cord is that part of your central nervous system that transmits messages between your brain and your body. The spinal cord has
Vision: Receptors. Modes of Perception. Vision: Summary 9/28/2012. How do we perceive our environment? Sensation and Perception Terminology
 How do we perceive our environment? Complex stimuli are broken into individual features, relayed to the CNS, then reassembled as our perception Sensation and Perception Terminology Stimulus: physical agent
How do we perceive our environment? Complex stimuli are broken into individual features, relayed to the CNS, then reassembled as our perception Sensation and Perception Terminology Stimulus: physical agent
ANIMATED NEUROSCIENCE
 ANIMATED NEUROSCIENCE and the Action of Nicotine, Cocaine, and Marijuana in the Brain Te a c h e r s G u i d e Films for the Humanities & Sciences Background Information This program, made entirely of
ANIMATED NEUROSCIENCE and the Action of Nicotine, Cocaine, and Marijuana in the Brain Te a c h e r s G u i d e Films for the Humanities & Sciences Background Information This program, made entirely of
Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College
 Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Primary Sources for figures and content: Eastern Campus Marieb,
Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Primary Sources for figures and content: Eastern Campus Marieb,
Optic Neuritis. The optic nerve fibers are coated with myelin to help them conduct the electrical signals back to your brain.
 Optic Neuritis Your doctor thinks that you have had an episode of optic neuritis. This is the most common cause of sudden visual loss in a young patient. It is often associated with discomfort in or around
Optic Neuritis Your doctor thinks that you have had an episode of optic neuritis. This is the most common cause of sudden visual loss in a young patient. It is often associated with discomfort in or around
NEUROLOCALIZATION MADE EASY
 NEUROLOCALIZATION MADE EASY Jared B. Galle, DVM, Diplomate ACVIM (Neurology) Dogwood Veterinary Referral Center 4920 Ann Arbor-Saline Road Ann Arbor, MI 48103 Localizing a neurologic problem to an anatomical
NEUROLOCALIZATION MADE EASY Jared B. Galle, DVM, Diplomate ACVIM (Neurology) Dogwood Veterinary Referral Center 4920 Ann Arbor-Saline Road Ann Arbor, MI 48103 Localizing a neurologic problem to an anatomical
Brain Basics: A Brain in Sync
 Brain Basics: A Brain in Sync By: Dr. Robert Melillo The idea of a functional relationship between the left and right sides of the brain is hardly new. In 1949, Canadian neuropsychologist Donald O. Hebb,
Brain Basics: A Brain in Sync By: Dr. Robert Melillo The idea of a functional relationship between the left and right sides of the brain is hardly new. In 1949, Canadian neuropsychologist Donald O. Hebb,
Introduction to Neurophysiological Psychology (PSY 451)
 Portland State University Physiological Psychology Page 1 Introduction to Neurophysiological Psychology (PSY 451) Bill Griesar, Ph.D., Adjunct Instructor, [email protected] OFFICE HOURS: Mondays, 11:30
Portland State University Physiological Psychology Page 1 Introduction to Neurophysiological Psychology (PSY 451) Bill Griesar, Ph.D., Adjunct Instructor, [email protected] OFFICE HOURS: Mondays, 11:30
Please read chapter 15, The Autonomic Nervous System, complete this study guide, and study this material BEFORE coming to the first class.
 Please read chapter 15,, complete this study guide, and study this material BEFORE coming to the first class. I. Introduction to the autonomic nervous system: Briefly describe the autonomic nervous system.
Please read chapter 15,, complete this study guide, and study this material BEFORE coming to the first class. I. Introduction to the autonomic nervous system: Briefly describe the autonomic nervous system.
Anatomy & Physiology Bio 2401 Lecture. Instructor: Daryl Beatty Nervous System Introduction Part 1
 Anatomy & Physiology Bio 2401 Lecture Instructor: Daryl Beatty Nervous System Introduction Part 1 Nervous System Introduction Chapter 11 Section A Sequence 4.1 DB Nervous system 1 Intro Presentations 4.2,
Anatomy & Physiology Bio 2401 Lecture Instructor: Daryl Beatty Nervous System Introduction Part 1 Nervous System Introduction Chapter 11 Section A Sequence 4.1 DB Nervous system 1 Intro Presentations 4.2,
Chapter 9 - Nervous System
 Chapter 9 - Nervous System 9.1 Introduction (p. 215; Fig. 9.1) A. The nervous system is composed of neurons and neuroglia. 1. Neurons transmit nerve impulses along nerve fibers to other neurons. 2. Nerves
Chapter 9 - Nervous System 9.1 Introduction (p. 215; Fig. 9.1) A. The nervous system is composed of neurons and neuroglia. 1. Neurons transmit nerve impulses along nerve fibers to other neurons. 2. Nerves
Brain Tumor 101. Shanna Armstrong, RN Neuro Oncology Nurse Clinician UC Brain Tumor Center
 Brain Tumor 101 Shanna Armstrong, RN Neuro Oncology Nurse Clinician UC Brain Tumor Center Objectives Identify the different parts of the brain Describe how each part of the brain works Connect each part
Brain Tumor 101 Shanna Armstrong, RN Neuro Oncology Nurse Clinician UC Brain Tumor Center Objectives Identify the different parts of the brain Describe how each part of the brain works Connect each part
BRAIN storming Copyright, Poliakoff and Bee, 2000
 by Ellen Poliakoff and Sally Bee Illustrations by Serena Korda BRAIN storming The 1990 s was hailed as the decade of the brain. We ask, what do we really know about the elusive workings of the grey matter
by Ellen Poliakoff and Sally Bee Illustrations by Serena Korda BRAIN storming The 1990 s was hailed as the decade of the brain. We ask, what do we really know about the elusive workings of the grey matter
NERVOUS SYSTEM B 1. Which of the following is controlled by the somatic nervous system? A. rate of heartbeat B. contraction of skeletal muscles C.
 NERVOUS SYSTEM B 1. Which of the following is controlled by the somatic nervous system? A. rate of heartbeat B. contraction of skeletal muscles C. increased blood flow to muscle tissue D. movement of food
NERVOUS SYSTEM B 1. Which of the following is controlled by the somatic nervous system? A. rate of heartbeat B. contraction of skeletal muscles C. increased blood flow to muscle tissue D. movement of food
Reavis High School Anatomy and Physiology Curriculum Snapshot
 Reavis High School Anatomy and Physiology Curriculum Snapshot Unit 1: Introduction to the Human Body 10 days As part of this unit, students will define anatomy, physiology, and pathology. They will identify
Reavis High School Anatomy and Physiology Curriculum Snapshot Unit 1: Introduction to the Human Body 10 days As part of this unit, students will define anatomy, physiology, and pathology. They will identify
Introduction to Psychology, 7th Edition, Rod Plotnik Module 3: Brain s Building Blocks. Module 3. Brain s Building Blocks
 Module 3 Brain s Building Blocks Structure of the Brain Genes chains of chemicals that are arranged like rungs on a twisting ladder there are about 100,000 genes that contain chemical instructions that
Module 3 Brain s Building Blocks Structure of the Brain Genes chains of chemicals that are arranged like rungs on a twisting ladder there are about 100,000 genes that contain chemical instructions that
NEURO M203 & BIOMED M263 WINTER 2014
 NEURO M203 & BIOMED M263 WINTER 2014 MRI Lab 1: Structural and Functional Anatomy During today s lab, you will work with and view the structural and functional imaging data collected from the scanning
NEURO M203 & BIOMED M263 WINTER 2014 MRI Lab 1: Structural and Functional Anatomy During today s lab, you will work with and view the structural and functional imaging data collected from the scanning
Smoking and misuse of certain pain medicines can affect the risk of developing renal cell cancer.
 Renal cell cancer Renal cell cancer is a disease in which malignant (cancer) cells form in tubules of the kidney. Renal cell cancer (also called kidney cancer or renal adenocarcinoma) is a disease in which
Renal cell cancer Renal cell cancer is a disease in which malignant (cancer) cells form in tubules of the kidney. Renal cell cancer (also called kidney cancer or renal adenocarcinoma) is a disease in which
Chapter 13. The Nature of Somatic Reflexes
 Chapter 13 The Nature of Somatic Reflexes Nature of Reflexes (1 of 3) A reflex is an involuntary responses initiated by a sensory input resulting in a change in a gland or muscle tissue occur without our
Chapter 13 The Nature of Somatic Reflexes Nature of Reflexes (1 of 3) A reflex is an involuntary responses initiated by a sensory input resulting in a change in a gland or muscle tissue occur without our
