Hospital readmissions contribute to the increasing. Deployment of Lean Six Sigma in Care Coordination An Improved Discharge Process
|
|
|
- Laurence Porter
- 10 years ago
- Views:
Transcription
1 Professional Case Management Vol. 19, No. 2, Copyright 2014 Wolters Kluwer Health Lippincott Williams & Wilkins Deployment of Lean Six Sigma in Care Coordination An Improved Discharge Process Susan Ellen Breslin, DNP, RN, NE-BC, Karen Marie Hamilton, PhD, RN, and Jacquelyn Paynter, MPH, RN ABSTRACT Purpose/Objectives: This article presents a quality improvement project to reduce readmissions in the Medicare population related to heart failure, acute myocardial infarction, and pneumonia. The article describes a systematic approach to the discharge process aimed at improving transitions of care from hospital to post acute care, utilizing Lean Six Sigma methodology. Primary Practice Setting: Inpatient acute care hospital. Findings/Conclusions: A coordinated discharge process, which includes postdischarge follow-up, can reduce avoidable readmissions. Implications for Case Management: The quality improvement project demonstrated the significant role case management plays in preventing costly readmissions and improving outcomes for patients through better transitions of care from the hospital to the community. By utilizing Lean Six Sigma methodology, hospitals can focus on eliminating waste in their current processes and build more sustainable improvements to deliver a safe, quality, discharge process for their patients. Case managers are leading this effort to improve care transitions and assure a smoother transition into the community postdischarge. Key words: care management, discharge process, Lean Six Sigma, readmissions Hospital readmissions contribute to the increasing cost of health care and are the focus of the Centers for Medicare & Medicaid Service s (CMS s) efforts to move toward a pay-forperformance payment methodology. The goal of the CMS strategy is to reduce hospital readmission rates by 20% by The three diagnoses currently selected by the CMS are acute myocardial infarction (AMI), heart failure (HF), and pneumonia. The plan is to develop and implement a discharge process that assures better compliance with the discharge plan of care and can result in better outcomes for the patients. To address readmissions, hospitals will be held accountable for better discharge programs and improved transitions across the continuum of care. The Institute for Healthcare Improvement has identified four processes shown to decrease readmissions: (1) improved assessment of discharge needs on admission, (2) more effective discharge teaching, (3) improved communication with the patient and family about the discharge plan, and (4) better posthospital follow-up. Through the use of a holistic approach, care management teams can impact this escalating problem with better discharge planning and improved postdischarge follow-up. Case management departments are at the center of the readmission prevention effort in acute care facilities. According to Askren-Gonzalez and Frater (2012), failed discharge plans are a major contributor to hospital readmissions. Lack of follow-up care postdischarge, with a primary care practitioner, was found to have the most influence on readmissions within 30 days. In addition to the concerns with the cost of readmissions, they are often associated with lower quality of care ( Askren-Gonzalez & Frater, 2012). Poor quality of care reflects on the hospital and can affect the choices patients make when seeking care. An improved discharge process based on effective coordination of postdischarge care can result in lower readmission rates and better outcomes for patients. SCOPE OF THE PROBLEM Since the publication of the Institute of Medicine s report in 2001, there has been increasing focus within Address correspondence to Susan Ellen Breslin, DNP, RN, NE-BC, Patient Care Services & CNO, DeKalb Regional Health System, 2701 North Decatur Road, Decatur, GA ( [email protected] ). The authors report no conflicts of interest. DOI: /NCM Vol. 19/No. 2 Professional Case Management 77
2 acute care hospitals on quality and safety ( Institute of Medicine, 2001). In today s pay-for-performance environment, hospitals are under increasing pressure to improve quality and safety, while containing cost. According to the 2005 Medicare Payment Advisory Commission, as many as 18% of all Medicare patients are readmitted within 30 days of discharge (Watkins, Hall, & Kring, 2012). This statistic suggests that patients are not adequately prepared at discharge to care for themselves at home. Four areas have been identified by IHI to decrease readmissions: (a) improved assessment of discharge needs on admission, (b) more effective discharge teaching, (c) improved communication with the patient and family about the discharge plan, and (d) better post hospital follow-up (Institute for Healthcare Improvement). Patients continue to experience the same or different symptoms related to their illness, requiring them to return to the hospital for treatment. Health reform is aimed at improving patient outcomes and increasing efficiency by decreasing preventable readmissions (Mulder, Tzeng, & Vecchioni, 2012). By better preparing patients at discharge and assuring adequate post acute care, patients can experience better outcomes. For hospitals to avoid penalties for readmissions, the focus needs to shift to the acute care setting for better discharge planning and post acute care follow-up. Today, HF is the most common diagnosis requiring frequent trips to the emergency department, resulting in readmissions. In some cases, HF readmissions have increased (Annema, Luttik, & Jaarsma, 2009). Despite the efforts by health care providers to address readmission through patient education and better discharge planning, there has been little improvement. Patients continue to return to emergency departments to relieve their symptoms, resulting in increased rehospitalizations. PURPOSE The quality improvement team developed a team charter and identified the purpose of the project. The team elected to use Lean Six Sigma as the model for this quality improvement effort. The need to reengineer the discharge process was the strategy chosen for this project, with the following initiatives: To create a comprehensive approach to dis charge that will reduce avoidable readmissions. To align inpatient and outpatient services to provide care across the continuum from acute care to post acute care. Through the application of Lean Six Sigma principles, eliminate waste in the current process. To avoid unnecessary rehospitalizations for this vulnerable population, the focus needs to shift to the acute care setting for better discharge planning and post acute care follow-up. Reduce rates of readmissions for three key diagnoses of HF, AMI, and pneumonia. Improve patient satisfaction with the discharge process. For hospitals to avoid payment penalties, more effective strategies need to be deployed to prevent excess readmissions. According to the Agency for Healthcare Research and Quality (2008), hospital costs for avoidable readmissions represent 20% of total health care spending in the United States. Hospital readmissions are a focus of the Patient Protection and Affordable Care Act of 2010 (CMS Office of the Actuary, 2010). The 2010 Affordable Care Act established a hospital readmission reduction program that would reduce Inpatient Prospective Payment System payments to hospitals that demonstrate excess readmissions on or after October 1, The excess readmission rates will be used to determine the payment adjustment for each eligible hospital. NEED FOR CHANGE To avoid unnecessary rehospitalizations for this vulnerable population, the focus needs to shift to the acute care setting for better discharge planning and post acute care follow-up. One of the outcome measures monitored and reported to the CMS is readmissions. Readmissions are costly to the hospital and the patient. Hospital readmissions are a health care concern that drive up costs and inefficiencies that are largely avoidable (Kocher & Adashi, 2011). The organization selected for an improved discharge program is a private not-forprofit health care system in Atlanta, GA. The threehospital system includes two acute care facilities and a long-term acute care hospital. Of the approximately 35,000 annual admissions to this health care system, the targeted population of Medicare patients represents 30% of total admissions. Efforts to improve outcomes and avoid readmissions have been ongoing for several years. Despite those efforts, readmissions continue to represent a challenge for the organization. Despite the efforts by health care providers to address readmission through patient education and better discharge planning, there has 78 Professional Case Management Vol. 19/No. 2
3 been little improvement. In some cases, heart failure readmissions have increased (Annema et al., 2009). It became evident to the team early in the project that the inpatient work was not sufficient to assure patients were compliant with the discharge plan. The inpatient team needed to address better transitions of care into the community. The need for post acute care follow-up would be a key factor in the success of the project. According to Jencks, Williams, and Coleman (2009), more than 50% of patients readmitted for a medical diagnosis had no record of an appointment with a post acute care provider between hospitalizations. The lack of follow-up care between hospitalizations contributed to the likelihood of a readmission. As part of the Affordable Care Act (2009), avoiding preventable readmissions has been identified as a measure that can improve quality and lower health care costs. The two most common reasons for readmission were congestive HF and pneumonia. Together, these two diagnoses were responsible for half of all hospital costs for preventable readmissions. This hospital s CMS pay-for-performance readmission rates for HF, AMI, and pneumonia are consistent with risk-adjusted national rates. However, as hospitals across the United States continue to reduce readmission rates, continuous improvement will be needed to stay competitive. Table 1 illustrates the publicly reported hospital data on readmissions for AMI, HF, and pneumonia. COST ANALYSIS To quantify the opportunity for improvement, an analysis of the current state of readmissions was conducted. This analysis found that the total number of patients readmitted in the identified diagnoses, over a 1-year period, was more than 1,500. Of the total patients readmitted in these diagnoses, 400 were within 30 days of discharge. The assessment included financial data, such as the cost of a readmission, the likely penalties incurred if readmissions were not reduced, and the cost to the health care system for repeated rehospitalizations. The unadjusted cost per case related to 30-day readmissions is $8,033 for HF, $10,549 for AMI, and $7,816 for pneumonia. This translates into an annual excess opportunity cost of $359,505. If the hospital is not successful in reducing 30-day readmissions, the penalties could be severe. The cost in reimbursement for the federal fiscal year 2013 is 1% of total Medicare reimbursements, increasing to 3% by federal fiscal year For this organization, $1.8 million is at risk annually. DEPLOYMENT OF LEAN SIX SIGMA TO CREATE A N EW DISCHARGE PROCESS The methodology chosen for this project was Lean Six Sigma. According to Lighter (2011), applying lean processes to health care environments has become a method by which hospitals can reduce the probability of errors and improve patient safety. The discharge improvement team (DIT) was led by a Lean Six Sigma Green Belt facilitator. The DIT included nurses, case managers, physicians, nurse practitioners, a discharge call center representative, clinic nurses, and key members of the patient care team. The DIT established a charter and problem statement to define the scope of the project as follows: Complexities of the discharge process results in higher than expected readmissions for Medicare pay-forperformance diagnoses, AMI, HF, and pneumonia and loss in revenue. TABLE 1 Federal Fiscal Year 2013 CMS Hospital Compare Results Pay-for-Performance Period: July 1, 2008, to June 30, 2011 National Average Crude Rate Eligible Discharges Number of Readmissions Predicted Risk Adjusted Hospital Rate Expected Risk Adjusted National Rate Excess Readmission Ratio North Decatur AMI HF CAP Hillandale AMI HF CAP Note. The hospital weighted readmission ratios for the CMS pay-for-performance measures will favorably impact on federal fiscal year 2013 Medicare reimbursement rates with the exception of the pneumonia excess readmission ratio at Hillandale. AMI = acute myocardial infarction; CMS = Centers for Medicare & Medicaid Service; CPA = community acquired pneumonia; HF = heart failure. Vol. 19/No. 2 Professional Case Management 79
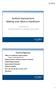
4 FIGURE 1 Fishbone diagram. Comm = communication; DC = discharge; diff = different; info = information; lab = laboratory; Med = medicine; MD = doctor of medicine; Pt. = patient; w/all = with all. Initially, the DIT developed a supplier, input, process, output, customer flow diagram, which was used to illustrate the key steps in the discharge process, beginning with admission and ending with discharge. The DIT created an Ishikawa or fishbone diagram (see Figure 1 ), which illustrates cause and effect relationships between processes, people, policy, and plan. Failure to address these components of the process can result in an ineffective discharge process resulting in increased 30-day readmissions. Risk assessments conducted for 150 readmitted patients included the voice of the customer interviews to learn about the customer s point of view regarding service issues and gaps that prompt readmission. A fullday kaizen event was held to identify the steps needed to correct waste, gaps, and barriers in the current process. The DIT created a failure mode and effect analysis for further validation and prioritization. Through the use of brainstorming techniques and multivoting, the process improvement action steps and tools were identified. The DIT used the failure mode and effect analysis to score the severity, probability, and detectability of the discharge process against the reengineered discharge. Reengineered discharge largely focuses on arranging postdischarge appointments, diagnostic testing and results, services, equipment, medication reconciliation, teach-back education, handover communication to post acute care providers, and postdischarge telephone calls (Jack et al., 2009). As a result, the DIT identified three priorities for improvement in the current discharge process. The key focus areas were (a) need to identify a primary care physician (PCP) for patients before discharge; (b) if the patient did not have a PCP, one would be assigned from the 80 Professional Case Management Vol. 19/No. 2
5 primary care network; and (c) patients would have a postdischarge appointment with the PCP or the discharge clinic before discharge. During the course of this project, a number of barriers were identified in implementing the new discharge process: The discharge clinic needed to be approved by administration, funded, and staffed. Case management would need to change the current discharge process to include scheduling the appointment with the PCP. The discharge call center would take responsibility for assigning a PCP if none was on record. Staff needed to be educated on the new process. REDESIGNED DISCHARGE PROCESS A key component of the redesigned discharge process was the ability to incorporate a postdischarge clinic. The clinic was designed to see patients discharged with or without a PCP who were cared for by the hospitalist service. The hospital already had a postdischarge clinic in place for patients requiring anticoagulation management. Although this clinic was successful in providing anticoagulation management, it was felt that a discharge clinic could continue to see patients on anticoagulants and provide postdischarge follow-up for a larger population of patients. The nurse practitioner was transitioned from the anticoagulation clinic to the discharge clinic. In addition to the nurse practitioner, a small office staff was hired, and a practice manager/case manager was transitioned from the hospital case management department. In addition, two nurse patient care coordinators were recruited to work closely with the hospitalists. These nurses serve a vital role in communicating the plan of care to the patients, assisting with the discharge plan and following up on any questions the patients might have about their care. They are also responsible for setting the discharge appointment with the discharge clinic. The clinic case manager calls patients who do not keep their appointment to arrange another appointment, refer them to a PCP, or refer them to community mental health services. To A key component of the redesigned discharge process was the ability to incorporate a postdischarge clinic. The clinic was designed to see patients discharged with or without a PCP who were cared for by the hospitalist service. assure continuity of care, the hospitalists have access to the patients record through the electronic medical record. The hospitalists have access to their patients record throughout the inpatient stay as well as postdischarge. Following the visit, the PCP is contacted directly by the case manager to provide information about the patient visit. In addition to the call, a note is faxed to the primary physician. Funding for the clinic comes from two sources. The clinic was set up as an outpatient clinic with billing capability. If the patient has insurance, the insurance company is billed for an office visit; however, no patient is turned away due to inability to pay. The hospital bears the cost of the inpatient care coordinators and provides a subsidy to the clinic for the office space and the personnel. RESULTS For this project, various Lean Six Sigma tools were used to outline the current process and identify areas for implementation of lean processes. Currently, discharge appointments are made for 6 to 8 patients per day, who are discharged from the pilot unit. In the first 30 days of the pilot, 86 patients have been referred to the discharge clinic with a 50% no-show rate. The discharge clinic staff calls all of the no-show patients to follow up on their status. As part of that phone call, the discharge plan is reviewed, including medications, and a follow-up visit is confirmed with either the discharge clinic or the PCP. In the first 30 days, the clinic contacted 40 patients, 20 of whom intended to keep their PCP appointment. Early results suggest that the new process is having an impact on readmissions. After 30 days, the readmission rate for the 46 patients seen in the clinic was 6.5%, compared with baseline readmissions rates for the pilot unit of 16.2%. It is still too early to predict the long-term effects of the new discharge process. If the project continues to show success, the plan is to deploy the same process across the organization. Another aim of the project was an increase in patient satisfaction with the discharge process. The pilot unit has achieved a significant improvement in patient satisfaction on the questions regarding satisfaction with discharge information. The patient satisfaction score for this indicator exceeded 90% during the second quarter of 2013, compared with 76% in the last quarter of FUTURE IMPLICATIONS FOR CASE MANAGEMENT Health care is rapidly moving from the 1990 s era of managed care to today s environment of care management. This project exemplifies the need for case Vol. 19/No. 2 Professional Case Management 81
6 managers to focus on disease-specific care across the continuum from acute care to post acute care. Inpatient case managers are charged with establishing connections in the outpatient arena to assure care is timely, effective, safe, and appropriate. According to the Health Care Advisory Board (2013), there are four key principles guiding the care management of the future: 1. Patient-centered care is matched to the individual patient population. 2. Care is provided across the continuum from hospital to post acute care provider. 3. Primary care is accessible. 4. Metrics are used to align cost and quality. Benchmarking is used to assure that the program is meeting national benchmarks for effectiveness. As case management evolves into an expanded role in managing patients through the transitions of care, resources need to be reallocated to match patient populations with the m ost appropriate care model. The discharge process is one area for more focused efforts to align care with the post acute care setting. The need to change current discharge processes or face penalties was the impetus for the change project. However, the frequency of readmissions reflects poorly on the care provided in an organization and can lead to a loss of trust within the community served. With the onset of public reporting of quality data, such as readmissions, the public has the information readily available to make decisions about care. The pressure on case management departments today to reduce cost by reducing length of stay and reducing avoidable readmissions has put this specialty on the forefront of the evolving health care arena. CONCLUSION The purpose of this quality improvement plan was to prevent patient harm and improve outcomes by implementation of a comprehensive discharge process aimed at avoiding readmissions. The level of patient education provided, implementation of the discharge plan and coordination of care following discharge can be predictors of whether a patient will be readmitted (Aspenson & Hazaray, 2012). The methodology chosen for this project was Lean Six Sigma. The decision to use Lean Six Sigma methodology was effective and provided the tools and structure for this project. The discipline and the tools resulted in a comprehensive approach to the problem of readmissions. The integration of acute care and post acute care providers on the team assured that patients received safe, timely, and effective care across the continuum. Readmissions can be reduced as the result of a discharge plan that assures follow-up postdischarge with a PCP or a transitional care clinic. REFERENCES Agency for Healthcare Research and Quality. ( 2008 ). Hospital readmissions: In search of potentially avoidable costs. Paper presented at the AHRQ 2008 Annual Conference. Retrieved from about/annualmtg08/090908slides/friedman.htm Annema, C., Luttik, M. L., & Jaarsma, T. ( 2009 ). Reasons for readmission in heart failure: Perspectives of patients, caregivers, cardiologists, and heart failure nurses. Heart Lung, 38 ( 5 ), Askren-Gonzalez, A., & Frater, J. ( 2012 ). Case management programs for hospital readmission prevention. Professional Case Management, 17 ( 5 ), Aspenson, M., & Hazaray, S. ( 2012, July ). The clock is ticking on readmission penalties. Healthcare Financial Management, 66, Centers for Medicare & Medicaid Services. Retrieved from CMS Office of the Actuary. ( 2010 ). Affordable Care Act update: Implementing Medicare cost strategies. Retrieved from Health Care Advisory Board. ( 2013, March) National Meeting Series. Risk and reward: Positioning your health system to deliver value in a transforming health care marketplace. Washington, DC: The Advisory Board Company. Institute for Healthcare Improvement. Reducing Avoidable Readmissions by Improving Transitions of Care. Retrieved from Institute of Medicine. ( 2001 ). Crossing the quality chasm: A new health system for the 2 1st century. Washington, DC : National Academies Press. Jack, B. W., Chetty, V. K., Anthony, D., Greenwald, J. L., Sanchez, G. M., Johnson, A. E., Culpepper, L. ( 2009 ). A reengineered hospital discharge program to decrease rehospitalizations: A randomized trial. Annals of Internal Medicine, 150 ( 3 ), Jencks, S. F., Williams, M. V., & Coleman, E. A. ( 2009 ). Rehospitalizations among patients in the Medicare fee-for-service program. The New England Journal of Medicine, 306 ( 14 ), Kocher, R. P., & Adashi, E. Y. ( 2011 ) Hospital readmissions and the Affordable Care Act: Paying for coordinated quality care. Journal of the American Medical Association, 306 ( 16 ), Lighter, D. E. ( 2011 ). Advanced performance improvement in health care. Sudbury, MA : Jones and Bartlett. Mulder, B. J., Tzeng, H., & Vecchioni, N. D. ( 2012 ). Preventing avoidable rehospitalizations by understanding the characteristics of frequent fliers. Journal of Nursing Care Quality, 27 ( 1 ), doi: / NCQ.0b013e31822fddc Watkins, L., Hall, C., & Kring, D. ( 2012 ). Hospital to home: A transition program for frail older adults. Professional Case Management, 17 ( 3 ), Susan Ellen Breslin, DNP, RN, NE-BC, is a health care professional and Nurse Executive with greater than 25 years of experience in operations and patient care. Dr. Breslin has her master of science in nursing from University of Cincinnati, her bachelor of science in nursing from 82 Professional Case Management Vol. 19/No. 2
7 George Mason University and has her Doctor of Nursing Practice from University of South Alabama. Susan is Board Certifi ed in Nursing Administration with the American Nurses Association. Karen Marie Hamilton, PhD, RN, is Clinical Associate Professor at the University of South Alabama College of Nursing. Dr. Hamilton s role includes Doctor of Nursing Practice advisor in the public health track and instructor in the Public Health Nursing Administration graduate program. Other areas of specialty include research and school health. She is an active member of the nursing Honor Society, Sigma Theta Tau International, and served as President of Zeta Gamma Chapter Jacquelyn Paynter, MPH, RN, Executive Director of Care Management at DeKalb Medical, oversees utilization management, discharge planning, and population-based programs. As a Certifi ed Lean Six Sigma Green Belt, Jackie has facilitated throughput and care coordination Lean projects. Vol. 19/No. 2 Professional Case Management 83
1. Executive Summary Problem/Opportunity: Evidence: Baseline Data: Intervention: Results:
 A Clinical Nurse Leader led multidisciplinary Heart Failure Program: Integrating best practice across the care continuum to reduce avoidable 30 day readmissions. 1. Executive Summary Problem/Opportunity:
A Clinical Nurse Leader led multidisciplinary Heart Failure Program: Integrating best practice across the care continuum to reduce avoidable 30 day readmissions. 1. Executive Summary Problem/Opportunity:
Presented by Kathleen S. Wyka, AAS, CRT, THE AFFORDABLE CA ACT AND ITS IMPACT ON THE RESPIRATORY C PROFESSION
 Presented by Kathleen S. Wyka, AAS, CRT, THE AFFORDABLE CA ACT AND ITS IMPACT ON THE RESPIRATORY C PROFESSION At the end of this session, you will be able to: Identify ways RT skills can be utilized for
Presented by Kathleen S. Wyka, AAS, CRT, THE AFFORDABLE CA ACT AND ITS IMPACT ON THE RESPIRATORY C PROFESSION At the end of this session, you will be able to: Identify ways RT skills can be utilized for
Nurse Transition Coach Model: Innovative, Evidence-based, and Cost Effective Solutions to Reduce Hospital Readmissions
 Nurse Transition Coach Model: Innovative, Evidence-based, and Cost Effective Solutions to Reduce Hospital Readmissions Leslie Becker RN, BS Jennifer Smith RN, MSN, MBA Leslie Frain MSN, RN Jan Machanis
Nurse Transition Coach Model: Innovative, Evidence-based, and Cost Effective Solutions to Reduce Hospital Readmissions Leslie Becker RN, BS Jennifer Smith RN, MSN, MBA Leslie Frain MSN, RN Jan Machanis
WHITE PAPER. How a multi-tiered strategy can reduce readmission rates and significantly enhance patient experience
 WHITE PAPER How a multi-tiered strategy can reduce readmission rates and significantly enhance patient experience Vocera Communications, Inc. June, 2014 SUMMARY Hospitals that reduce readmission rates
WHITE PAPER How a multi-tiered strategy can reduce readmission rates and significantly enhance patient experience Vocera Communications, Inc. June, 2014 SUMMARY Hospitals that reduce readmission rates
Avoiding Rehospitalizations in LTC Chris Osterberg, RN BSN Pathway Health Services
 Avoiding Rehospitalizations in LTC Chris Osterberg, RN BSN Pathway Health Services Objectives Understand the new consequences to hospitals for discharged clients being re-admitted within selected time
Avoiding Rehospitalizations in LTC Chris Osterberg, RN BSN Pathway Health Services Objectives Understand the new consequences to hospitals for discharged clients being re-admitted within selected time
hospital readmission rate reduction: building better interfaces within the community.
 hospital readmission rate reduction: building better interfaces within the community. Whitepaper By Ken Taverner, M.Sc. the issue of hospital readmission rates Leaving the hospital after being admitted
hospital readmission rate reduction: building better interfaces within the community. Whitepaper By Ken Taverner, M.Sc. the issue of hospital readmission rates Leaving the hospital after being admitted
Reducing Readmissions with Predictive Analytics
 Reducing Readmissions with Predictive Analytics Conway Regional Health System uses analytics and the LACE Index from Medisolv s RAPID business intelligence software to identify patients poised for early
Reducing Readmissions with Predictive Analytics Conway Regional Health System uses analytics and the LACE Index from Medisolv s RAPID business intelligence software to identify patients poised for early
Preventing Readmissions
 Emerging Topics in Healthcare Reform Preventing Readmissions Janssen Pharmaceuticals, Inc. Preventing Readmissions The Patient Protection and Affordable Care Act (ACA) contains several provisions intended
Emerging Topics in Healthcare Reform Preventing Readmissions Janssen Pharmaceuticals, Inc. Preventing Readmissions The Patient Protection and Affordable Care Act (ACA) contains several provisions intended
Transitions of Care: The need for collaboration across entire care continuum
 H O T T O P I C S I N H E A L T H C A R E, I S S U E # 2 Transitions of Care: The need for collaboration across entire care continuum Safe, quality Transitions Effective C o l l a b o r a t i v e S u c
H O T T O P I C S I N H E A L T H C A R E, I S S U E # 2 Transitions of Care: The need for collaboration across entire care continuum Safe, quality Transitions Effective C o l l a b o r a t i v e S u c
IMPROVING INPATIENT DISCHARGE PROCESS TO REDUCE READMISSION
 1 IMPROVING INPATIENT DISCHARGE PROCESS TO REDUCE READMISSION Vanda Ametlli; Industrial & Systems Engineering, Wayne State University, Detroit, Michigan Abstract The cost of a preventable readmission to
1 IMPROVING INPATIENT DISCHARGE PROCESS TO REDUCE READMISSION Vanda Ametlli; Industrial & Systems Engineering, Wayne State University, Detroit, Michigan Abstract The cost of a preventable readmission to
Readmissions as an Enterprise Priority. Presenters 4/17/2014
 Readmissions as an Enterprise Priority April 24, 2014 Presenters Vincent A. Maniscalco, MPA, LNHA Administrator Middletown Park Rehabilitation and Health Care Center [email protected] Eileen
Readmissions as an Enterprise Priority April 24, 2014 Presenters Vincent A. Maniscalco, MPA, LNHA Administrator Middletown Park Rehabilitation and Health Care Center [email protected] Eileen
Tool 6: How To Monitor Re-Engineered Discharge Implementation and Outcomes
 Tool 6: How To Monitor Re-Engineered Discharge Implementation and Outcomes 6.. Purpose of This Tool Monitoring the RED lets you know whether each component of RED is being successfully implemented and
Tool 6: How To Monitor Re-Engineered Discharge Implementation and Outcomes 6.. Purpose of This Tool Monitoring the RED lets you know whether each component of RED is being successfully implemented and
How Health Reform Will Affect Health Care Quality and the Delivery of Services
 Fact Sheet AARP Public Policy Institute How Health Reform Will Affect Health Care Quality and the Delivery of Services The recently enacted Affordable Care Act contains provisions to improve health care
Fact Sheet AARP Public Policy Institute How Health Reform Will Affect Health Care Quality and the Delivery of Services The recently enacted Affordable Care Act contains provisions to improve health care
How To Reduce Hospital Readmission
 Reducing Hospital Readmissions & The Affordable Care Act The Game Has Changed Drastically Reducing MSPB Measures Chuck Bongiovanni, MSW, MBA, NCRP, CSA, CFE Chuck Bongiovanni, MSW, MBA, NCRP, CSA, CFE
Reducing Hospital Readmissions & The Affordable Care Act The Game Has Changed Drastically Reducing MSPB Measures Chuck Bongiovanni, MSW, MBA, NCRP, CSA, CFE Chuck Bongiovanni, MSW, MBA, NCRP, CSA, CFE
FINANCIAL IMPLICATIONS OF EXCESS HOSPITAL READMISSIONS JOSESPH B. HENDERSON, J.D.
 FINANCIAL IMPLICATIONS OF EXCESS HOSPITAL READMISSIONS JOSESPH B. HENDERSON, J.D. Executive MHA Candidate, 2013 University of Southern California Sol Price School of Public Policy Abstract A 2007 Medicare
FINANCIAL IMPLICATIONS OF EXCESS HOSPITAL READMISSIONS JOSESPH B. HENDERSON, J.D. Executive MHA Candidate, 2013 University of Southern California Sol Price School of Public Policy Abstract A 2007 Medicare
Transitions of Care: The need for a more effective approach to continuing patient care
 H O T T O P I C S I N H E A L T H C A R E Transitions of Care: The need for a more effective approach to continuing patient care The need for a more effective approach to continuing patient care This paper
H O T T O P I C S I N H E A L T H C A R E Transitions of Care: The need for a more effective approach to continuing patient care The need for a more effective approach to continuing patient care This paper
Nancy L. Wilson Department of Medicine-Geriatrics Houston Center for Quality of Care& Utilization Studies Texas Consortium of Geriatric Education
 1 Nancy L. Wilson Department of Medicine-Geriatrics Houston Center for Quality of Care& Utilization Studies Texas Consortium of Geriatric Education Centers Care for Elders Governing Council Acknowledge
1 Nancy L. Wilson Department of Medicine-Geriatrics Houston Center for Quality of Care& Utilization Studies Texas Consortium of Geriatric Education Centers Care for Elders Governing Council Acknowledge
Discharge Planning. Home Care 1. Objectives. Where are they Going?
 Discharge Planning Heidi White, MD Associate Professor of Medicine Yvonne Spurney, RN Associate Chief Nurse Cristina C. Hendrix, DNS, GNP-BC Associate Professor of Nursing Objectives Describe challenges
Discharge Planning Heidi White, MD Associate Professor of Medicine Yvonne Spurney, RN Associate Chief Nurse Cristina C. Hendrix, DNS, GNP-BC Associate Professor of Nursing Objectives Describe challenges
From the Ground Up: The implementation of a Transition Care Program (TOC) and its impact in COPD 30-day readmissions
 From the Ground Up: The implementation of a Transition Care Program (TOC) and its impact in COPD 30-day readmissions Cristiane L. Fukuda RN, MSN, ANP-BC Email: [email protected] Office: 404-851-6914
From the Ground Up: The implementation of a Transition Care Program (TOC) and its impact in COPD 30-day readmissions Cristiane L. Fukuda RN, MSN, ANP-BC Email: [email protected] Office: 404-851-6914
Care Coordination and Transitions in Behavioral Health
 Care Coordination and Transitions in Behavioral Health Pam Pietruszewski Integrated Health Consultant The National Council for Behavioral Health This product is supported by the Florida Department of Children
Care Coordination and Transitions in Behavioral Health Pam Pietruszewski Integrated Health Consultant The National Council for Behavioral Health This product is supported by the Florida Department of Children
Journey to Excellence
 Journey to Excellence Kevin W. Sowers, MSN, RN, FAAN President, Duke University Hospital 2 Agenda Introduction to Duke Medicine Call to Action: The Jesica Santillan Story Duke University Hospital s Journey
Journey to Excellence Kevin W. Sowers, MSN, RN, FAAN President, Duke University Hospital 2 Agenda Introduction to Duke Medicine Call to Action: The Jesica Santillan Story Duke University Hospital s Journey
Reducing Readmissions Using Teach-Back: Enhancing Patient and Family Education.
 Lehigh Valley Health Network LVHN Scholarly Works Patient Care Services / Nursing Reducing Readmissions Using Teach-Back: Enhancing Patient and Family Education. Debra Peter MSN, RN-BC Lehigh Valley Health
Lehigh Valley Health Network LVHN Scholarly Works Patient Care Services / Nursing Reducing Readmissions Using Teach-Back: Enhancing Patient and Family Education. Debra Peter MSN, RN-BC Lehigh Valley Health
Providing and Billing Medicare for Transitional Care Management
 PYALeadership Briefing Providing and Billing Medicare for Transitional Care Management Updated November 2014 2014 Pershing Yoakley & Associates, PC (PYA). No portion of this white paper may be used or
PYALeadership Briefing Providing and Billing Medicare for Transitional Care Management Updated November 2014 2014 Pershing Yoakley & Associates, PC (PYA). No portion of this white paper may be used or
Kaiser Permanente: Transition Care Performance and Strategies
 Kaiser Permanente: Transition Care Performance and Strategies Carol Ann Barnes, PT, DPT, GCS [email protected] April 2009 Netta Conyers-Haynes, October, 2014 Principal Consultant, Communications Agenda
Kaiser Permanente: Transition Care Performance and Strategies Carol Ann Barnes, PT, DPT, GCS [email protected] April 2009 Netta Conyers-Haynes, October, 2014 Principal Consultant, Communications Agenda
Transitions of Care Management Coding (TCM Code) Tutorial. 1. Introduction Meaning of moderately and high complexity 2
 Transitions of Care Management Coding (TCM Code) Tutorial Index 1. Introduction Meaning of moderately and high complexity 2 2. SETMA s Tools for using TCM Code 3 Alert that patient is eligible for TCM
Transitions of Care Management Coding (TCM Code) Tutorial Index 1. Introduction Meaning of moderately and high complexity 2 2. SETMA s Tools for using TCM Code 3 Alert that patient is eligible for TCM
Population Health Management Helps Utica Park Clinic Ease the Transition to Value-Based Care
 CASE STUDY Utica Park Clinic Population Health Management Helps Utica Park Clinic Ease the Transition to Value-Based Care The transition from fee-for-service to value-based reimbursement has been a challenge
CASE STUDY Utica Park Clinic Population Health Management Helps Utica Park Clinic Ease the Transition to Value-Based Care The transition from fee-for-service to value-based reimbursement has been a challenge
Improving Care Transitions using PDSA Methodology
 Improving Care Transitions using PDSA Methodology Catherine Payne, MD, FHM Care Transitions Physician Champion Medical Director of Clinical Informatics Erlanger Medical Center Chattanooga, Tennessee Objectives
Improving Care Transitions using PDSA Methodology Catherine Payne, MD, FHM Care Transitions Physician Champion Medical Director of Clinical Informatics Erlanger Medical Center Chattanooga, Tennessee Objectives
Get With The Guidelines Best Practices: A look at reducing 30-day heart failure readmission rates
 Get With The Guidelines Best Practices: A look at reducing 30-day heart failure readmission rates Thank you for joining the webinar! The presentation will begin shortly. *Please make sure your computer
Get With The Guidelines Best Practices: A look at reducing 30-day heart failure readmission rates Thank you for joining the webinar! The presentation will begin shortly. *Please make sure your computer
Cheri Basso BSN, RN-BC,CHFN Hospital Initiatives to Improve Outcomes. FINANCIAL DISCLOSURE: No relevant financial relationship exists
 Cheri Basso BSN, RN-BC, CHFN Mary Washington Healthcare Fredericksburg, VA Cheri Basso BSN, RN-BC,CHFN Hospital Initiatives to Improve Outcomes FINANCIAL DISCLOSURE: No relevant financial relationship
Cheri Basso BSN, RN-BC, CHFN Mary Washington Healthcare Fredericksburg, VA Cheri Basso BSN, RN-BC,CHFN Hospital Initiatives to Improve Outcomes FINANCIAL DISCLOSURE: No relevant financial relationship
Taking Aim at Reducing Hospital Readmission Rates
 Taking Aim at Reducing Hospital Readmission Rates It has been three years since the Centers for Medicare & Medicaid Services (CMS) implemented progressive penalties to hospitals that have higher 30-day
Taking Aim at Reducing Hospital Readmission Rates It has been three years since the Centers for Medicare & Medicaid Services (CMS) implemented progressive penalties to hospitals that have higher 30-day
Reducing Hospital Readmissions With Enhanced Patient Education
 Published by FierceHealthcare Custom Publishing Reducing Hospital Readmissions With Enhanced Patient Education SPONSORED BY At least 20 percent of all patients who are admitted to a U.S. hospital make
Published by FierceHealthcare Custom Publishing Reducing Hospital Readmissions With Enhanced Patient Education SPONSORED BY At least 20 percent of all patients who are admitted to a U.S. hospital make
Project BOOST: A Return On Investment Analysis
 Project BOOST: A Return On Investment Analysis dsfjk Project BOOST: A Return On Investment Analysis SHM 2010 1 Reducing Hospital Readmissions: Who benefits? Who pays? The US Department of Health and Human
Project BOOST: A Return On Investment Analysis dsfjk Project BOOST: A Return On Investment Analysis SHM 2010 1 Reducing Hospital Readmissions: Who benefits? Who pays? The US Department of Health and Human
Understanding Care Transitions as a Patient Safety Issue
 Article reprinted from Patient Safety & Quality Healthcare, May/June 2011 Understanding Care Transitions as a Patient Safety Issue By Sara Butterfield RN, BSN, CPHQ, CCM; Christine Stegel, RN, MS, CPHQ;
Article reprinted from Patient Safety & Quality Healthcare, May/June 2011 Understanding Care Transitions as a Patient Safety Issue By Sara Butterfield RN, BSN, CPHQ, CCM; Christine Stegel, RN, MS, CPHQ;
A STRATIFIED APPROACH TO PATIENT SAFETY THROUGH HEALTH INFORMATION TECHNOLOGY
 A STRATIFIED APPROACH TO PATIENT SAFETY THROUGH HEALTH INFORMATION TECHNOLOGY Table of Contents I. Introduction... 2 II. Background... 2 III. Patient Safety... 3 IV. A Comprehensive Approach to Reducing
A STRATIFIED APPROACH TO PATIENT SAFETY THROUGH HEALTH INFORMATION TECHNOLOGY Table of Contents I. Introduction... 2 II. Background... 2 III. Patient Safety... 3 IV. A Comprehensive Approach to Reducing
Innovations@Home. Home Health Initiatives Reduce Avoidable Readmissions by Leveraging Innovation
 How Does CMS Measure the Rate of Acute Care Hospitalization (ACH)? Until January 2013, CMS measured Acute Care Hospitalization (ACH) through the Outcomes Assessment and Information Set (OASIS) reporting
How Does CMS Measure the Rate of Acute Care Hospitalization (ACH)? Until January 2013, CMS measured Acute Care Hospitalization (ACH) through the Outcomes Assessment and Information Set (OASIS) reporting
Implementing an Evidence Based Hospital Discharge Process
 Implementing an Evidence Based Hospital Discharge Process Learning from the experience of Project Re-Engineered Discharge (RED) Webinar January 14, 2013 Chris Manasseh, MD Director, Boston HealthNet Inpatient
Implementing an Evidence Based Hospital Discharge Process Learning from the experience of Project Re-Engineered Discharge (RED) Webinar January 14, 2013 Chris Manasseh, MD Director, Boston HealthNet Inpatient
A Project to Reengineer Discharges Reduces 30-Day Hospital Readmission Rates. April 11, 2014
 A Project to Reengineer Discharges Reduces 30-Day Hospital Readmission Rates April 11, 2014 About the QIO Program Leading rapid, large-scale change in health quality: Goals are bolder. The patient is at
A Project to Reengineer Discharges Reduces 30-Day Hospital Readmission Rates April 11, 2014 About the QIO Program Leading rapid, large-scale change in health quality: Goals are bolder. The patient is at
The Role of Telemedicine in Home Monitoring and Long Term Care June 7, 2012. Penny S. Milanovich President UPMC Visiting Nurses Association
 The Role of Telemedicine in Home Monitoring and Long Term Care June 7, 2012 Penny S. Milanovich President UPMC Visiting Nurses Association Cost of Chronic Conditions An average of 40-50% of healthcare
The Role of Telemedicine in Home Monitoring and Long Term Care June 7, 2012 Penny S. Milanovich President UPMC Visiting Nurses Association Cost of Chronic Conditions An average of 40-50% of healthcare
Accountable Care: Implications for Managing Health Information. Quality Healthcare Through Quality Information
 Accountable Care: Implications for Managing Health Information Quality Healthcare Through Quality Information Introduction Healthcare is currently experiencing a critical shift: away from the current the
Accountable Care: Implications for Managing Health Information Quality Healthcare Through Quality Information Introduction Healthcare is currently experiencing a critical shift: away from the current the
Value-Based Programs. Blue Plans Improving Healthcare Quality and Affordability through Innovative Partnerships with Clinicians
 Value-Based Programs Blue Plans Improving Healthcare Quality and Affordability through Innovative Partnerships with Clinicians Issue: U.S. healthcare spending exceeds $2.8 trillion annually. 1 With studies
Value-Based Programs Blue Plans Improving Healthcare Quality and Affordability through Innovative Partnerships with Clinicians Issue: U.S. healthcare spending exceeds $2.8 trillion annually. 1 With studies
Aiming for Fewer Hospital U-turns: The Medicare Hospital Readmission Reduction Program
 Aiming for Fewer Hospital U-turns: The Medicare Hospital Readmission Reduction Program Cristina Boccuti and Giselle Casillas For Medicare patients, hospitalizations can be stressful; even more so when
Aiming for Fewer Hospital U-turns: The Medicare Hospital Readmission Reduction Program Cristina Boccuti and Giselle Casillas For Medicare patients, hospitalizations can be stressful; even more so when
ACOs: Impacting the Past, Present and Future State of Healthcare
 ACOs: Impacting the Past, Present and Future State of Healthcare Article By Alan Cudney, RN, CPHQ, PMP, FACHE, Executive Consultant October 2012 What are Accountable Care Organizations? Can they help us
ACOs: Impacting the Past, Present and Future State of Healthcare Article By Alan Cudney, RN, CPHQ, PMP, FACHE, Executive Consultant October 2012 What are Accountable Care Organizations? Can they help us
Locking the Revolving Door of Readmissions
 Locking the Revolving Door of Readmissions The Pharmacist s Role in Keeping Patients Healthy, Happy and At Home Steve Riddle, BS Pharm, BCPS, FASHP VP of Clinical Affairs, Pharmacy OneSource Objectives
Locking the Revolving Door of Readmissions The Pharmacist s Role in Keeping Patients Healthy, Happy and At Home Steve Riddle, BS Pharm, BCPS, FASHP VP of Clinical Affairs, Pharmacy OneSource Objectives
THE 2015 QUALIS HEALTH AWARDS OF EXCELLENCE IN HEALTHCARE QUALITY
 THE 2015 QUALIS HEALTH AWARDS OF EXCELLENCE IN HEALTHCARE QUALITY Since 2002, Qualis Health has presented the annual Awards of Excellence in Healthcare Quality to outstanding organizations in Idaho and
THE 2015 QUALIS HEALTH AWARDS OF EXCELLENCE IN HEALTHCARE QUALITY Since 2002, Qualis Health has presented the annual Awards of Excellence in Healthcare Quality to outstanding organizations in Idaho and
Sanford Improvement Making Lean Work in Healthcare
 Sanford Improvement Making Lean Work in Healthcare David Peterson Enterprise Director of Continuous Improvement Outline/Agenda Office of Continuous Improvement Who are we and what do we do? History/Journey
Sanford Improvement Making Lean Work in Healthcare David Peterson Enterprise Director of Continuous Improvement Outline/Agenda Office of Continuous Improvement Who are we and what do we do? History/Journey
Home Health Care: A More Cost-Effective Approach to Medicaid in Illinois Illinois HomeCare & Hospice Council December 2010
 Home Health Care: A More Cost-Effective Approach to Medicaid in Illinois Illinois HomeCare & Hospice Council December 2010 As the Illinois Legislature prepares to act on the future of Medicaid, it is important
Home Health Care: A More Cost-Effective Approach to Medicaid in Illinois Illinois HomeCare & Hospice Council December 2010 As the Illinois Legislature prepares to act on the future of Medicaid, it is important
Optum s Role in Mycare Ohio
 Optum s Role in Mycare Ohio What is MyCare Ohio? New opportunities generated by the Affordable Care Act have allowed Ohio to implement the MyCare Ohio program. MyCare Ohio is a demonstration project that
Optum s Role in Mycare Ohio What is MyCare Ohio? New opportunities generated by the Affordable Care Act have allowed Ohio to implement the MyCare Ohio program. MyCare Ohio is a demonstration project that
Person-Centered Nurse Care Management in Home Based Care: Impact on Well-Being and Cost Containment
 Person-Centered Nurse Care Management in Home Based Care: Impact on Well-Being and Cost Containment Donna Zazworsky, RN, MS, CCM, FAAN Vice President: Community Health and Continuum Care Carondelet Health
Person-Centered Nurse Care Management in Home Based Care: Impact on Well-Being and Cost Containment Donna Zazworsky, RN, MS, CCM, FAAN Vice President: Community Health and Continuum Care Carondelet Health
Using Root Cause Analysis to Determine Why Readmissions are High. Presentation Objectives. Background Information 11/30/2011
 Using Root Cause Analysis to Determine Why Readmissions are High Nancy Seck RBN, BSN, MPH, CPHQ Director, Quality Management Glendale Memorial Hospital and Health Center Presentation Objectives Identify
Using Root Cause Analysis to Determine Why Readmissions are High Nancy Seck RBN, BSN, MPH, CPHQ Director, Quality Management Glendale Memorial Hospital and Health Center Presentation Objectives Identify
Connect4 Patients CCCM Primary Care Community. Presented By: Veronica Mansfield, DNP, APRN, AE-C, CCM Kit McKinnon, MBA, BSN, RN, CDE, CCM
 Connect4 Patients CCCM Primary Care Community Presented By: Veronica Mansfield, DNP, APRN, AE-C, CCM Kit McKinnon, MBA, BSN, RN, CDE, CCM September 17, 2015 Objectives: Describe innovative care management
Connect4 Patients CCCM Primary Care Community Presented By: Veronica Mansfield, DNP, APRN, AE-C, CCM Kit McKinnon, MBA, BSN, RN, CDE, CCM September 17, 2015 Objectives: Describe innovative care management
Proven Innovations in Primary Care Practice
 Proven Innovations in Primary Care Practice October 14, 2014 The opinions expressed are those of the presenter and do not necessarily state or reflect the views of SHSMD or the AHA. 2014 Society for Healthcare
Proven Innovations in Primary Care Practice October 14, 2014 The opinions expressed are those of the presenter and do not necessarily state or reflect the views of SHSMD or the AHA. 2014 Society for Healthcare
Medicare Psychiatric Patients & Readmissions in the Inpatient Psychiatric Facility Prospective Payment System
 Medicare Psychiatric Patients & Readmissions in the Inpatient Psychiatric Facility Prospective Payment System Prepared For: National Association of Psychiatric Health Systems May 2013 Table of Contents
Medicare Psychiatric Patients & Readmissions in the Inpatient Psychiatric Facility Prospective Payment System Prepared For: National Association of Psychiatric Health Systems May 2013 Table of Contents
Henry Ford Health System Care Coordination and Readmissions Update
 Henry Ford Health System Care Coordination and Readmissions Update September 2013 BACKGROUND Most hospital readmissions are viewed as avoidable, costly, and in some cases as a potential marker of poor
Henry Ford Health System Care Coordination and Readmissions Update September 2013 BACKGROUND Most hospital readmissions are viewed as avoidable, costly, and in some cases as a potential marker of poor
caresy caresync Chronic Care Management
 caresy Chronic Care Management THE PROBLEM Chronic diseases and conditions, including heart disease, diabetes, COPD and obesity, are among the most common, expensive, and preventable health problems in
caresy Chronic Care Management THE PROBLEM Chronic diseases and conditions, including heart disease, diabetes, COPD and obesity, are among the most common, expensive, and preventable health problems in
PIONEER ACO A REVIEW OF THE GRAND EXPERIMENT. Norris Vivatrat, MD Associate Medical Director Monarch HealthCare
 PIONEER ACO A REVIEW OF THE GRAND EXPERIMENT Norris Vivatrat, MD Associate Medical Director Monarch HealthCare 2 Agenda Pioneer ACO basics, performance and challenges Monarch HealthCare Post-acute network
PIONEER ACO A REVIEW OF THE GRAND EXPERIMENT Norris Vivatrat, MD Associate Medical Director Monarch HealthCare 2 Agenda Pioneer ACO basics, performance and challenges Monarch HealthCare Post-acute network
Transforming traditional case management through local provider partnerships
 Transforming traditional case management through local provider partnerships Introduction The dramatic changes sweeping the health care industry are driving a strong interest in engaging patients at the
Transforming traditional case management through local provider partnerships Introduction The dramatic changes sweeping the health care industry are driving a strong interest in engaging patients at the
ESSENTIA HEALTH AS AN ACO (ACCOUNTABLE CARE ORGANIZATION)
 ESSENTIA HEALTH AS AN ACO (ACCOUNTABLE CARE ORGANIZATION) Hello and welcome. Thank you for taking part in this presentation entitled "Essentia Health as an ACO or Accountable Care Organization -- What
ESSENTIA HEALTH AS AN ACO (ACCOUNTABLE CARE ORGANIZATION) Hello and welcome. Thank you for taking part in this presentation entitled "Essentia Health as an ACO or Accountable Care Organization -- What
HEDIS 2012 Results
 Capital District Physicians Health Plan, Inc. Nonprofit Health Plan Albany, New York Capital District Physicians Health Plan, Inc. (CDPHP ) is featured as a high performer in cardiovascular care, identified
Capital District Physicians Health Plan, Inc. Nonprofit Health Plan Albany, New York Capital District Physicians Health Plan, Inc. (CDPHP ) is featured as a high performer in cardiovascular care, identified
PCMH and Care Management: Where do we start?
 PCMH and Care Management: Where do we start? Patricia Bohs, RN, BSN Quality Assurance Manager Kelly McCloughan QA Data Manager Wayne Memorial Community Health Centers Honesdale, PA Wayne Memorial Community
PCMH and Care Management: Where do we start? Patricia Bohs, RN, BSN Quality Assurance Manager Kelly McCloughan QA Data Manager Wayne Memorial Community Health Centers Honesdale, PA Wayne Memorial Community
Health Care Leader Action Guide to Reduce Avoidable Readmissions
 Health Care Leader Action Guide to Reduce Avoidable Readmissions January 2010 TRANSFORMING HEALTH CARE THROUGH RESEARCH AND EDUCATION Osei-Anto A, Joshi M, Audet AM, Berman A, Jencks S. Health Care Leader
Health Care Leader Action Guide to Reduce Avoidable Readmissions January 2010 TRANSFORMING HEALTH CARE THROUGH RESEARCH AND EDUCATION Osei-Anto A, Joshi M, Audet AM, Berman A, Jencks S. Health Care Leader
RIH Transitions of Care Collaboration with Coastal Medical To Improve Transitions for Patients Discharged Hospital To Home
 RIH Transitions of Care Collaboration with Coastal Medical To Improve Transitions for Patients Discharged Hospital To Home Sergio Petrillo, PharmD Clinical Pharmacist Specialist, Rhode Island Hospital
RIH Transitions of Care Collaboration with Coastal Medical To Improve Transitions for Patients Discharged Hospital To Home Sergio Petrillo, PharmD Clinical Pharmacist Specialist, Rhode Island Hospital
BUNDLING ARE INPATIENT REHABILITATION FACILITIES PREPARED FOR THIS PAYMENT REFORM?
 BUNDLING ARE INPATIENT REHABILITATION FACILITIES PREPARED FOR THIS PAYMENT REFORM? Uniform Data System for Medical Rehabilitation Annual Conference August 10, 2012 Presented by: Donna Cameron Rich Bajner
BUNDLING ARE INPATIENT REHABILITATION FACILITIES PREPARED FOR THIS PAYMENT REFORM? Uniform Data System for Medical Rehabilitation Annual Conference August 10, 2012 Presented by: Donna Cameron Rich Bajner
INTRO TO THE MICHIGAN PIONEER ACO 101: THE BASICS. Karen Unholz, RN, BSN
 INTRO TO THE MICHIGAN PIONEER ACO 101: THE BASICS Karen Unholz, RN, BSN Origins of the Accountable Care Organization ACOs originated from the Patient Protection and Affordable Care Act (Healthcare Reform)
INTRO TO THE MICHIGAN PIONEER ACO 101: THE BASICS Karen Unholz, RN, BSN Origins of the Accountable Care Organization ACOs originated from the Patient Protection and Affordable Care Act (Healthcare Reform)
Leadership Summit for Hospital and Post-Acute Long Term Care Providers May 12, 2015
 Leveraging the Continuum to Avoid Unnecessary Utilization While Improving Quality Leadership Summit for Hospital and Post-Acute Long Term Care Providers May 12, 2015 Karim A. Habibi, FHFMA, MPH, MS Senior
Leveraging the Continuum to Avoid Unnecessary Utilization While Improving Quality Leadership Summit for Hospital and Post-Acute Long Term Care Providers May 12, 2015 Karim A. Habibi, FHFMA, MPH, MS Senior
Abstraction 101 An Introduction for New Abstractors
 California and Florida In the Know Webinar Series Abstraction 101 An Introduction for New Abstractors September 2011 Becky Ure, RN, BSN, MEd 1 Topics The driving forces behind abstraction and public reporting
California and Florida In the Know Webinar Series Abstraction 101 An Introduction for New Abstractors September 2011 Becky Ure, RN, BSN, MEd 1 Topics The driving forces behind abstraction and public reporting
2.b.vii Implementing the INTERACT Project (Inpatient Transfer Avoidance Program for SNF)
 2.b.vii Implementing the INTERACT Project (Inpatient Transfer Avoidance Program for SNF) Project Objective: Skilled nursing facilities (SNFs) will implement the evidence based INTERACT program developed
2.b.vii Implementing the INTERACT Project (Inpatient Transfer Avoidance Program for SNF) Project Objective: Skilled nursing facilities (SNFs) will implement the evidence based INTERACT program developed
Capacity Management: Patient Throughput and Case Management Improvement. February 25, 2015
 Capacity Management: Patient Throughput and Case Management Improvement February 25, 2015 Agenda Introduction Impetus for Change Approach to Improving Case and Capacity Management Client Case Study Key
Capacity Management: Patient Throughput and Case Management Improvement February 25, 2015 Agenda Introduction Impetus for Change Approach to Improving Case and Capacity Management Client Case Study Key
Research Brief. Physician Visits After Hospital Discharge: Implications for Reducing Readmissions. Readmissions, Not Just a Medicare Problem
 Research Brief NUMBER 6 DECEMBER 2011 Physician Visits After Hospital Discharge: Implications for Reducing Readmissions BY ANNA SOMMERS AND PETER J. CUNNINGHAM Public and private payers view reducing avoidable
Research Brief NUMBER 6 DECEMBER 2011 Physician Visits After Hospital Discharge: Implications for Reducing Readmissions BY ANNA SOMMERS AND PETER J. CUNNINGHAM Public and private payers view reducing avoidable
Value-Based Purchasing Program Overview. Maida Soghikian, MD Grand Rounds Scripps Green Hospital November 28, 2012
 Value-Based Purchasing Program Overview Maida Soghikian, MD Grand Rounds Scripps Green Hospital November 28, 2012 Presentation Overview Background and Introduction Inpatient Quality Reporting Program Value-Based
Value-Based Purchasing Program Overview Maida Soghikian, MD Grand Rounds Scripps Green Hospital November 28, 2012 Presentation Overview Background and Introduction Inpatient Quality Reporting Program Value-Based
Accountable Care Organizations: What Are They and Why Should I Care?
 Accountable Care Organizations: What Are They and Why Should I Care? Adrienne Green, MD Associate Chief Medical Officer, UCSF Medical Center Ami Parekh, MD, JD Med. Director, Health System Innovation,
Accountable Care Organizations: What Are They and Why Should I Care? Adrienne Green, MD Associate Chief Medical Officer, UCSF Medical Center Ami Parekh, MD, JD Med. Director, Health System Innovation,
Patient Navigators and Community Health Workers: The Evolving Role of Certification
 Patient Navigators and Community Health Workers: The Evolving Role of Certification Presented by: Jan Chamness, MPH, Public Health Director, Montgomery County Health Department Frances J. Feltner, DNP,
Patient Navigators and Community Health Workers: The Evolving Role of Certification Presented by: Jan Chamness, MPH, Public Health Director, Montgomery County Health Department Frances J. Feltner, DNP,
Nurse Practitioners: A Role in Evolution Past, Present and Future
 Nurse Practitioners: A Role in Evolution Past, Present and Future Jasmiry Bennett, RN, MS, ACNP-BC Acute Care Nurse Practitioner Department of Vascular Surgery Objectives Describe and discuss the evolution
Nurse Practitioners: A Role in Evolution Past, Present and Future Jasmiry Bennett, RN, MS, ACNP-BC Acute Care Nurse Practitioner Department of Vascular Surgery Objectives Describe and discuss the evolution
A white paper. Collaborative Accountable Care. CIGNA s Approach to Accountable Care Organizations. 841282 a 11/11
 A white paper Collaborative Accountable Care CIGNA s Approach to Accountable Care Organizations 841282 a 11/11 Transforming the Health Care System Successfully transforming the U.S. health care system
A white paper Collaborative Accountable Care CIGNA s Approach to Accountable Care Organizations 841282 a 11/11 Transforming the Health Care System Successfully transforming the U.S. health care system
HOW TO UNDERSTAND YOUR QUALITY AND RESOURCE USE REPORT
 HOW TO UNDERSTAND YOUR QUALITY AND RESOURCE USE REPORT CONTENTS A BACKGROUND AND PURPOSE OF THE MID-YEAR QUALITY AND RESOURCE USE REPORTS... 1 B EXHIBITS INCLUDED IN THE MID-YEAR QUALITY AND RESOURCE USE
HOW TO UNDERSTAND YOUR QUALITY AND RESOURCE USE REPORT CONTENTS A BACKGROUND AND PURPOSE OF THE MID-YEAR QUALITY AND RESOURCE USE REPORTS... 1 B EXHIBITS INCLUDED IN THE MID-YEAR QUALITY AND RESOURCE USE
Managing and Coordinating Non-Acute Care in an ACO Environment
 Managing and Coordinating Non-Acute Care in an ACO Environment By Glen Roebuck, Vice President of Business Development, Health Dimensions Group Hospital and health care systems across the country are engaging
Managing and Coordinating Non-Acute Care in an ACO Environment By Glen Roebuck, Vice President of Business Development, Health Dimensions Group Hospital and health care systems across the country are engaging
Community Paramedicine
 Community Paramedicine A New Approach to Integrated Healthcare Prepared by a committee of: 600 Wilson Lane Suite 101 Mechanicsburg, PA 17055 (717) 795-0740 800-243-2EMS (in PA) www.pehsc.org 1 P age Community
Community Paramedicine A New Approach to Integrated Healthcare Prepared by a committee of: 600 Wilson Lane Suite 101 Mechanicsburg, PA 17055 (717) 795-0740 800-243-2EMS (in PA) www.pehsc.org 1 P age Community
Assessing Risk of Readmission. NoCVA Preventing Avoidable Readmission Collaborative Laura Maynard, MDiv, NCQC Amanda Hobbs, NCQC July 31, 2013
 Assessing Risk of Readmission NoCVA Preventing Avoidable Readmission Collaborative Laura Maynard, MDiv, NCQC Amanda Hobbs, NCQC July 31, 2013 Collaborative Goals Reduce readmission rates by 20% Increase
Assessing Risk of Readmission NoCVA Preventing Avoidable Readmission Collaborative Laura Maynard, MDiv, NCQC Amanda Hobbs, NCQC July 31, 2013 Collaborative Goals Reduce readmission rates by 20% Increase
Quality and Performance Improvement PATRICK SCHULTZ MS RN ACNS BC DIRECTOR OF QUALITY AND PATIENT SAFETY SANFORD MEDICAL CENTER FARGO
 Quality and Performance Improvement PATRICK SCHULTZ MS RN ACNS BC DIRECTOR OF QUALITY AND PATIENT SAFETY SANFORD MEDICAL CENTER FARGO Crossing The Quality Chasm: A New Health System For The 21st Century
Quality and Performance Improvement PATRICK SCHULTZ MS RN ACNS BC DIRECTOR OF QUALITY AND PATIENT SAFETY SANFORD MEDICAL CENTER FARGO Crossing The Quality Chasm: A New Health System For The 21st Century
Preventing Avoidable Re-Hospitalizations: Where Do You Fit in the Quality Care Puzzle?
 Speaker Disclosures Care Transitions Interventions: The Sussex County Transitional Care Program Dr. Wang has disclosed that he has no relevant financial relationship(s). George C. Wang, MD, PhD Medical
Speaker Disclosures Care Transitions Interventions: The Sussex County Transitional Care Program Dr. Wang has disclosed that he has no relevant financial relationship(s). George C. Wang, MD, PhD Medical
