2015 OPEN ENROLLMENT MEDICAL PLANS
|
|
|
- Cynthia Merritt
- 8 years ago
- Views:
Transcription
1 2015 OPEN ENROLLMENT MEDICAL PLANS
2 Table of Contents Section I. Enrollment Guidelines Page 3 Health Plan Comparison Chart Page 4 Health Plan Premiums and Employee Cost-Sharing Page 5 Section II. Blue Shield Health Plans Blue Shield PPO Plan Page 7 10 Blue Shield HMO Plan Page Blue Shield Account Based Health Plan with HSA Page Section III. Kaiser Permanente Health Plans Kaiser Permanente HMO Plan Page Kaiser Chiropractic and Acupuncture Information Page Kaiser Permanente Account Based Health Plan with HSA Page Section IV. Wells Fargo HSA Frequently Asked Questions Page & Addition Information
3 2015 Enrollment Guidelines Enrollment in a health plan begins the first of the month following the date of hire or triggering event. Employees must provide proof of dependent eligibility when enrolling for the first time. The following documents must be provided along with completed enrollment forms: Copy of a Marriage Certificate to enroll a spouse Copy of a Domestic Partner Affidavit or State of California Registration to enroll a Domestic Partner Copy of Page 1 of your most recent Federal tax return (white out all income and first five numbers of all social security numbers) to add a spouse or domestic partner Copy of birth certificates for children up to age 26 The annual health plan open enrollment is the month of August. Any changes made to your medical plan become effective the following October 1 st. IMPORTANT: This year, there will be two open enrollment periods. This year SRJC will make three new health plans available to eligible employees. These plans will begin phasing in during our August 2015 Open Enrollment. The additional plans include a Blue Shield HMO, Blue Shield Account Based Health Plan (ABHP), and a Kaiser Permanente Account Based health Plan (ABHP) The ABHP plans are high deductible plans that are eligible for participation in a Health Savings Account (HSA). If you choose to switch from your existing plan to either the Blue Shield HMO, Blue Shield PPO, or Kaiser HMO you must do so during the August 2015 Open Enrollment. If you choose to switch from either the Blue Shield HMO, Blue Shield PPO, or Kaiser HMO plan to an ABHP plan, you must do so during the October 2015 open enrollment. The ABHP plans will become effective January 1, Please be aware, if you choose to enroll in an ABHP plan you are not eligible to participate in the Flexible Savings Account (FSA) for out of pocket medical expenses.
4 OPEN ENROLLMENT 2015 HEALTH PLAN OPTION COMPARISON CHART Blue Shield HMO Kaiser ABHP Blue Shield ABHP Kaiser HMO Blue Shield PPO CALENDAR YEAR OUT-OF-POCKET MAXIMUM (OOP) Member Pays Member Pays Member Pays Member Pays Member Pays Individual/Family Deductibles $0/$0 $0/$0 $1,500/$3,000 $1,500/$3,000 $0/$0 Individual/Family Out-of-Pocket Max (includes deductibles and co-pays) $1,500/$3,000 $2,000/$4,000 $3,000/$6,000 $4,000/$8,000 $1,000/$3,000 PROFESSIONAL SERVICES Office Visit co-pay $25 $25 10% 10% $30 Specialists/Consultants co-pay $25 $30 10% 10% $30 Prenatal, postnatal office visit co-pay $0 $0 $0 10% $30 Scans: CT, CAT, MRI, PET etc. $0 $0 10% 10% 0% Diagnostic X-ray & Laboratory Procedures $0 $0 10% 10% 0% Preventive Care Services (includes physical exams & screenings) $0 $0 0%, Ded Waived 0%, Ded Waived $0 HOSPITAL & SKILLED NURSING FACILITY SERVICES Emergency Room visit co-pay (waived if admitted) 10% $100 co pay $100 $100 $100 10% Inpatient Hospital co-pay $0 $500/admit 10% 10% 0% Outpatient Hospital co-pay $25 $500/admit 10% 10% 0% Surgery, Outpatient (performed in an Ambulatory Surgery Center) $25 $150 10% 10% 0% Surgery, Outpatient (performed in a Hospital) $25 $300 10% 10% 0% MENTAL HEALTH SERVICES & SUBSTANCE ABUSE TREATMENT INPATIENT CARE: Facility based care $0 $500/admit 10% 10% 0% OUTPATIENT CARE: Facility based care $25 $25 10% 10% $30 OTHER SERVICES Acupuncture - Limits may apply $10/30 visits $10/30 visits Limited coverage, combined w/chiro combined w/chiro if authorized 10% $0/12 visits Ambulance (Ground or Air) $50 $100 10% 10% 0% Chiropractic - Limits may apply $10/30 visits combined w/acu $10/30 visits combined w/acu Not covered 10% $0/20 visits Durable Medical Equipment (DME) $0 20% 10% 10% 0% Physical and Occupational Therapy - Limits may apply $25 $25 10% 10% 0% PRESCRIPTION DRUG PLANS Prescription Deductible $0 $200/$500 Part of Medical Deductible Part of Medical Deductible After $200/$500 Generic co-pay/days supply $10/100 day $10 / 30 day After deductible, $10 / 30 day deductible, $7/ After 30 day $10 / 30 day Brand co-pay/days supply $25/100 day After deductible, $35 / 30 day After deductible, $30 / 30 day deductible, $25/30 day After deductible, $35 / 30 day Mail Order (Generic-Brand co-pay/days supply) $10 25/100 day Brand - after deductible, $90/90 / Generic - $0/90 After deductible, $20 $60 / 100 day After deductible, $14 25/90 day Brand - after deductible, $90/90 / Generic - $0/90
5 OPEN ENROLLMENT 2015 HEALTH PLAN OPTION COMPARISON CHART Blue Shield HMO Kaiser ABHP Blue Shield ABHP Kaiser HMO Rates - Single $564 $617 $436 $527 $711 Rates - Double $1,210 $1,303 $954 $1,149 $1,510 Rates - Family $1,663 $1,813 $1,302 $1,616 $2,104 Health Savings Account District Contributions - Single / Double & Family $1200/$1800 $1200/$1800 Employee Monthly Portion 7/1/ /31/ Single Faculty amounts based on 10 months, Classified /Management based on 12 months $0 $0 N/A N/A Employee Monthly Portion 7/1/ /31/15 - Double Faculty amounts based on 10 months, Classified /Management based on 12 months $0 $0 N/A N/A Employee Monthly Portion 7/1/ /31/15 - Family Faculty amounts based on 10 months, Classified /Management based on 12 months $0 $0 N/A N/A Employee Monthly Portion 1/1/2016-9/30/ Single Faculty amounts based on 10 months, Classified /Management based on 12 months $0 Employee Monthly Portion 1/1/2016-9/30/ Double Faculty amounts based on 10 months, Classified /Management based on 12 months $0 Employee Monthly Portion 1/1/2016-9/30/ Family Faculty amounts based on 10 months, Classified /Management based on 12 months $0 Faculty $25, Classified and Management $21 $0 $0 Faculty $44, Classified and Management $37 $0 $0 Faculty $72, Classified and Management $60 $0 $0 Blue Shield PPO Faculty $22, Classified $18.33, Management $30 Faculty $48, Classified $40, Management $60 Faculty $66, Classified $55, Management $90 Faculty $71, Classified and Management $59 Faculty $144, Classified and Management $120 Faculty $211, Classified and Management $176 NOTATIONS: This is only a brief summary of benefits that reflects In-Network benefits. Please review the benefit summaries or plan booklets for details, limitations and exclusions. OOP maximum on Blue Shield plans with a Navitus pharmacy carve out does not include prescription drug co-pays. Health Savings Account Plans and Kaiser HMO or ABHP OOP maximum does include prescription drug co-pays. For plans with a deductible, co-insurance applies after the deductible has been met unless otherwise noted.
6 SISC BLUE SHIELD OF CALIFORNIA HEALTH PLANS SISC BLUE SHIELD OF CALIFORNIA PPO HEALTH PLAN SISC BLUE SHIELD OF CALIFORNIA HMO HEALTH PLAN SISC BLUE SHIELD OF CALIFORNIA ACCOUNT BASED HEALTH PLAN (ABHP) ELIGIBLE FOR PARTICIPATION IN A HEALTH SAVINGS ACCOUNT (HSA)
7 An independent member of the Blue Shield Association SISC ASO Blue Shield of California 100% Plan A $30 Copayment Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A SUMMARY ONLY. THE PLAN CONTRACT SHOULD BE CONSULTED FOR A DETAILED DESCRIPTION OF COVERAGE BENEFITS AND LIMITATIONS. Blue Shield of California Effective: October 1, 2015 Calendar Year Medical Deductible (All providers combined) Calendar Year Out-of-Pocket Maximum 2 (Includes the plan deductible) LIFETIME BENEFIT MAXIMUM Participating Providers 1 Non Participating Providers 1 None $1,000 per individual / $3,000 per family None Covered Services Member Copayment PROFESSIONAL SERVICES Participating Providers 1 Non Participating Providers 1 Professional (Physician) Benefits Physician and specialist office visits $30 per visit 50% 2 CT scans, MRIs, MRAs, PET scans, and cardiac diagnostic No Charge 50% 2 procedures utilizing nuclear medicine (prior authorization is required) 3 Other outpatient X-ray, pathology and laboratory (Diagnostic testing by No Charge Not Covered providers other than outpatient laboratory, pathology, and imaging departments of hospitals/facilities) 3 Allergy Testing and Treatment Benefits Office visits (includes visits for allergy serum injections) No Charge 50% 2 Preventive Health Benefits Preventive Health Services (As required by applicable federal law.) No Charge Not Covered OUTPATIENT SERVICES Hospital Benefits (Facility Services) Outpatient surgery performed at an Ambulatory Surgery Center 4 No Charge No Charge 5 Outpatient surgery in a hospital No Charge No Charge 5 Outpatient Services for treatment of illness or injury and No Charge 50% 2 necessary supplies (Except as described under "Rehabilitation Benefits") CT scans, MRIs, MRAs, PET scans, and cardiac diagnostic No Charge 50% 2, 5 procedures utilizing nuclear medicine performed in a hospital (prior authorization is required) 3 Other outpatient X-ray, pathology and laboratory performed in a No Charge Not Covered hospital 3 Bariatric Surgery (prior authorization required by the Plan; medically necessary surgery for weight loss, for morbid obesity only) 6 No Charge No Charge 5 HOSPITALIZATION SERVICES Hospital Benefits (Facility Services) 2, 15 Inpatient Physician Services No Charge 50% Inpatient Non-emergency Facility Services (Semi-private room and No Charge No Charge 7 board, and medically-necessary Services and supplies, including Subacute Care) Bariatric Surgery (prior authorization required by the Plan; medically necessary No Charge No Charge 7 surgery for weight loss, for morbid obesity only) 6 Skilled Nursing Facility Benefits 8 (Combined maximum of up to 100 prior authorized days per Calendar Year; semi-private accommodations) Services by a free-standing Skilled Nursing Facility No Charge No Charge 9 Skilled Nursing Unit of a Hospital No Charge No Charge 7 EMERGENCY HEALTH COVERAGE Emergency room Services not resulting in admission (The ER $100 per visit $100 per visit copayment does not apply if the member is directly admitted to the hospital for inpatient services) Emergency room Services resulting in admission (when the member is No Charge No Charge admitted directly from the ER) Emergency room Physician Services No Charge No Charge 15
8 AMBULANCE SERVICES Emergency or authorized transport No Charge No Charge PRESCRIPTION DRUG COVERAGE Outpatient Prescription Drug Benefits Administered by Navitus Health Solutions PROSTHETICS/ORTHOTICS Prosthetic equipment and devices (Separate office visit copay may apply) No Charge 50% 2 Orthotic equipment and devices (Separate office visit copay may apply) No Charge Not Covered DURABLE MEDICAL EQUIPMENT Breast pump No Charge Not Covered Other Durable Medical Equipment No Charge Not Covered 10, 11 MENTAL HEALTH AND SUBSTANCE ABUSE SERVICES Inpatient Hospital Services No Charge No Charge 7 Residential Care No Charge No Charge 7 Inpatient Physician Services No Charge 2, 15 50% Routine Outpatient Mental Health and Substance Abuse Services (includes professional/physician visits) $30 per visit 50% 2 Non-Routine Outpatient Mental Health and Substance Abuse Services (includes behavioral health treatment, electroconvulsive therapy, intensive outpatient programs, office-based opioid treatment, partial hospitalization programs, and transcranial magnetic stimulation. For partial hospitalization programs, a higher copayment and facility charges may apply per episode of care) No Charge 50% 2 HOME HEALTH SERVICES Home health care agency Services (up to 100 visits per Calendar Year) 8 No Charge Not Covered 12 Home infusion/home intravenous injectable therapy and infusion No Charge Not Covered 12 nursing visits provided by a Home Infusion Agency OTHER Hospice Program Benefits Routine home care No Charge Not Covered 12 Inpatient Respite Care No Charge Not Covered hour Continuous Home Care No Charge Not Covered 12 General Inpatient care No Charge Not Covered 12 Chiropractic Benefits 8 Chiropractic Services (up to 20 visits per Calendar Year) No Charge Not Covered Acupuncture Benefits 8 Acupuncture Services (up to 12 visits per Calendar Year) No Charge 50% 2 Rehabilitation Benefits (Physical, Occupational and Respiratory Therapy) Office location No Charge Not Covered Speech Therapy Benefits Office Visit No Charge 50% 2 Pregnancy and Maternity Care Benefits Prenatal and postnatal Physician office visits (For inpatient hospital services, see "Hospitalization Services") Abortion services (Facility charges may apply - see "Hospital Benefits (Facility Services)") $30 per visit 50% 2 No Charge Not Covered Family Planning Benefits Counseling and consulting 13 No Charge Not Covered Tubal ligation No Charge Not Covered Vasectomy 14 No Charge Not Covered Diabetes Care Benefits Devices, equipment, and non-testing supplies (for testing supplies see Outpatient Prescription Drug Benefits.) No Charge 50% 2 Diabetes self-management training $30 per visit 50% 2 Hearing Aid Benefits Audiological evaluations $30 per visit 50% 2 Hearing Aid Instrument and ancillary equipment (Up to a maximum combined benefit of $700 per person every 24 months for the hearing aid and ancillary equipment) No Charge No Charge Care Outside of Plan Service Area Benefits provided through BlueCard Program, for out-of-state emergency and non-emergency care, are provided at the Participating level of the local Blue Plan allowable amount when you use a Blue Cross/Blue Shield provider. Within US: BlueCard Program See Applicable Benefit See Applicable Benefit Outside of US: BlueCard Worldwide See Applicable Benefit See Applicable Benefit
9 1 Unless otherwise specified, copayments/coinsurance are calculated based on allowable amounts. Participating providers agree to accept Blue Shield's allowable amount plus the plan s and any applicable member s payment as full payment for covered services. Non Participating providers can charge more than these amounts. When members use Non Participating providers, they must pay the applicable deductibles, copayments or coinsurance plus any amount that exceeds Blue Shield's allowable amount. Charges above the allowable amount do not count toward the Calendar Year deductible or out-of-pocket maximum. 2 Copayments/Coinsurance marked with this footnote do not accrue to Calendar Year out-of-pocket maximum. Copayments/Coinsurance and charges for services not accruing to the member's Calendar Year out-of-pocket maximum continue to be the member's responsibility after the Calendar Year out-of-pocket maximum is reached. This amount could be substantial. Please refer to the Plan Contract for exact terms and conditions of coverage. 3 Participating non Hospital based ("freestanding") laboratory or radiology centers may not be available in all areas. Laboratory and radiology Services may also be obtained from a Hospital or from a laboratory and radiology center that is affiliated with a Hospital, and paid according to the benefit under your health plan's Hospital Benefits. 4 Participating Ambulatory Surgery Centers may not be available in all areas. Outpatient surgery Services may also be obtained from a Hospital or from an ambulatory surgery center that is affiliated with a Hospital, and paid according to the benefit under your health plan's Hospital Benefits. 5 The maximum allowed charges for non-emergency surgery performed in a Non Participating Ambulatory Surgery Center or outpatient unit of a Non Participating hospital is $350 per day. Members are responsible for all charges in excess of $ Bariatric surgery is covered when pre-authorized by the Plan. However, for members residing in Imperial, Kern, Los Angeles, Orange, Riverside, San Bernardino, San Diego, Santa Barbara and Ventura Counties ("Designated Counties"), bariatric surgery services are covered only when performed at designated contracting bariatric surgery facilities and by designated contracting surgeons; coverage is not available for bariatric services from any other Participating provider and there is no coverage for bariatric services from Non Participating providers. In addition, if prior authorized by the Plan, a member in a Designated County who is required to travel more than 50 miles to a designated bariatric surgery facility will be eligible for limited reimbursement for specified travel expenses for the member and one companion. Refer to the Plan Contract for further benefit details. 7 The maximum allowed charges for non-emergency hospital services received from a Non Participating hospital is $600 per day. Members are responsible for all charges in excess of $ For plans with a Calendar Year medical deductible amount, services with a day or visit limit accrue to the Calendar Year day or visit limit maximum regardless of whether the plan medical deductible has been met. 9 Services may require prior authorization by the Plan. When services are prior authorized, members pay the Participating provider amount. 10 Mental health and Substance Abuse services are accessed through Blue Shield s Participating and Non Participating providers. 11 Inpatient services for acute detoxification are covered under the medical benefit; see the Hospital Benefits (Facility Services) section of the Plan Contract for benefit details. Services for acute medical detoxification are accessed through Blue Shield using Blue Shield's Participating providers or with Non Participating providers. 12 Out of network home health care, home infusion and hospice services are not covered unless pre-authorized. When these services are pre-authorized, the member pays the Participating provider copayment. 13 Includes insertion of IUD, as well as injectable and implantable contraceptives for women. 14 Copayment shown is for physician's services. If the procedure is performed in a facility setting (hospital or outpatient surgery center), an additional facility copayment may apply. Services from Non Participating providers and Non Participating facilities are not covered under this benefit. 15 When these services are rendered by a Non Participating Radiologist, Anesthesiologist, Pathologist and Emergency Room Physicians in a Participating facility, the member pays the Participating Provider copayment. Plan designs may be modified to ensure compliance with federal requirements. ASO (1/15) RH ; DC ; ;
10 Self-Insured Schools of California (SISC) Pharmacy Benefit Schedule PLAN Walk-in 200DED/10-35 Mail Network Costco Costco Navitus Days Supply* Generic $10 Free Free Free Brand $35 $35 $90 $90 Specialty $35 Out-of-Pocket Maximum Brand/Specialty Deductible $2,500 Individual / $3,500 Family $200 Individual / $500 Family SISC urges members to use generic drugs when available. If you or your physician requests the brand name when a generic equivalent is available, you will pay the generic copay plus the difference in cost between the brand and generic. The difference in cost between the brand and generic will not count toward the Annual Out-of-Pocket Maximum. *Members may receive up to 30 days and/or up to 90 days supply of medication at participating pharmacies. Some narcotic pain and cough medications are not included in the Costco Free Generic or 90-day supply programs. Navitus contracts with most independent and chain pharmacies with the exception of Walgreens. Mail Order Service The Mail Order Service allows you to receive a 90-day supply of maintenance medications. This program is part of your pharmacy benefit and is voluntary. Specialty Pharmacy Navitus SpecialtyRx helps members who are taking medications for certain chronic illnesses or complex diseases by providing services that offer convenience and support. This program is part of your pharmacy benefit and is mandatory. Navi-Gate for Members allows you to access personalized pharmacy benefit information online at For information specific to your plan, visit Navi-Gate for Members. Activate your account online using the Member Login link and an activation will be sent to you. The site provides access to prescription benefits, pharmacy locator, drug search, drug interaction information, medication history, and mail order information. The site is available 24 hours a day, seven days a week. 2015_2016_RX_10_35_200_500_DED Navitus SISC 14
11 An independent member of the Blue Shield Association SISC Custom HMO Admit Inpatient Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Highlights: A description of the prescription drug coverage is provided separately THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A SUMMARY ONLY. THE EVIDENCE OF COVERAGE AND PLAN CONTRACT SHOULD BE CONSULTED FOR A DETAILED DESCRIPTION OF COVERAGE BENEFITS AND LIMITATIONS. Effective: October 1, 2015 Calendar Year Medical Deductible Calendar Year Out-of-Pocket Maximum LIFETIME BENEFIT MAXIMUM Covered Services None $2,000 per Individual / $4,000 per Family None Member Copayment PROFESSIONAL SERVICES Professional (Physician) Benefits Physician and specialist office visits $25 per visit (Note: A woman may self-refer to an OB/GYN or family practice physician in her Personal Physician's medical group or IPA for OB/GYN services) Outpatient X-ray, pathology and laboratory No Charge Allergy Testing and Treatment Benefits Office visits (includes visits for allergy serum injections) $25 per visit Access+ Specialist SM Benefits 1 Office visit, Examination or Other Consultation (Self-referred office visits and consultations $30 per visit only) Preventive Health Benefits Preventive Health Services (As required by applicable federal and California law.) No Charge OUTPATIENT SERVICES Hospital Benefits (Facility Services) Outpatient surgery performed at an Ambulatory Surgery Center 2 $150 per surgery Outpatient surgery in a hospital $300 per surgery Outpatient Services for treatment of illness or injury and necessary supplies (Except as described under "Rehabilitation Benefits" and "Speech Therapy Benefits") No Charge HOSPITALIZATION SERVICES Hospital Benefits (Facility Services) Inpatient Physician Services No Charge Inpatient Non-emergency Facility Services (Semi-private room and board, and medically $500 per admission necessary Services and supplies, including Subacute Care) Inpatient Medically Necessary skilled nursing Services including Subacute Care 3, 4 $100 per day EMERGENCY HEALTH COVERAGE Emergency room Services not resulting in admission (The ER copayment does not apply if $100 per visit the member is directly admitted to the hospital for inpatient services) Emergency room Physician Services No Charge AMBULANCE SERVICES Emergency or authorized transport $100 PRESCRIPTION DRUG COVERAGE Outpatient Prescription Drug Benefits Administered by Navitus Health Solutions PROSTHETICS/ORTHOTICS Prosthetic equipment and devices (Separate office visit copay may apply) No Charge Orthotic equipment and devices (Separate office visit copay may apply) No Charge DURABLE MEDICAL EQUIPMENT Breast pump No Charge Other Durable Medical Equipment (member share is based upon allowed charges) 20%
12 MENTAL HEALTH AND SUBSTANCE SERVICES 5, 6 Inpatient Hospital Services $500 per admission Residential Care $500 per admission Inpatient Physician Services No Charge Routine Outpatient Mental Health and Substance Abuse Services (includes professional/physician visits) Non-Routine Outpatient Mental Health and Substance Abuse Services (includes behavioral health treatment, electroconvulsive therapy, intensive outpatient programs, office-based opioid treatment, partial hospitalization programs and transcranial magnetic stimulation. For partial hospitalization programs, a higher copayment and facility charges may apply per episode of care) $25 per visit No Charge HOME HEALTH SERVICES Home health care agency Services (up to 100 visits per Calendar Year) $25 per visit Medical supplies (See "Prescription Drug Coverage" for specialty drugs) No Charge OTHER Hospice Program Benefits Routine home care No Charge Inpatient Respite Care No Charge 24-hour Continuous Home Care $250 per day General Inpatient care $250 per day Pregnancy and Maternity Care Benefits Prenatal and postnatal Physician office visits (For inpatient hospital services, see No Charge "Hospitalization Services") Abortion services 8 $100 per surgery Family Planning and Infertility Benefits Counseling and consulting 7 No Charge Infertility Services (member share is based upon allowed charges) 50% (Diagnosis and treatment of cause of infertility. Excludes in vitro fertilization, injectables for infertility, artificial insemination and GIFT). Tubal ligation No Charge Vasectomy 8 $75 per surgery Rehabilitation Benefits (Physical, Occupational and Respiratory Therapy) Office location (Copayment applies to all places of services, including professional and facility settings) $25 per visit Speech Therapy Benefits Office Visit (Copayment applies to all places of services, including professional and facility settings) $25 per visit Diabetes Care Benefits Devices, equipment, and non-testing supplies (member share is based upon allowed charges; 20% for testing supplies see Outpatient Prescription Drug Benefits.) Diabetes self-management training $25 per visit Hearing Aids Audiological evaluations $25 per visit Hearing Aid Instrument and ancillary equipment (every 24 months for the hearing aid and 50% ancillary equipment) Urgent Care Benefits (BlueCard Program) Urgent Services outside your Personal Physician Service Area $25 per visit Optional Benefits Optional dental, vision, hearing aid, infertility, chiropractic or chiropractic and acupuncture benefits are available. If your employer purchased any of these benefits, a description of the benefit is provided separately. 1 To use this option, members must select a personal physician who is affiliated with a medical group or IPA that is an Access+ provider group, which offers the Access+ Specialist feature. Members should then select a specialist within that medical group or IPA. Access+ Specialist visits for mental health services must be provided by a MHSA network Participating provider. 2 Participating Ambulatory Surgery Centers may not be available in all areas. Outpatient surgery Services may also be obtained from a Hospital or from an ambulatory surgery center that is affiliated with a Hospital, and paid according to the benefit under your health plan's Hospital Benefits. 3 For Plans with a facility deductible amount, services with a day or visit limit accrue to the Calendar Year day or visit limit maximum regardless of whether the plan deductible has been met. 4 Skilled nursing services are limited to 100 preauthorized days during a calendar year except when received through a hospice program provided by a Participating hospice agency. This 100 preauthorized day maximum on skilled nursing services is a combined maximum between SNF in a hospital unit and skilled nursing facilities. 5 Mental Health and Substance Abuse services are accessed through Blue Shield's Mental Health Service Administrator (MHSA) using Blue Shield's MHSA Participating providers. 6 Inpatient services for acute detoxification are covered under the medical benefit; see the Hospital Benefits (Facility Services) section of the Evidence of Coverage for benefit details. Services for acute medical detoxification are accessed through Blue Shield using Blue Shield Participating providers. 7 Includes insertion of IUD, as well as injectable and implantable contraceptives for women. 8 Copayment shown is for physician s services. If the procedure is performed in a facility setting (hospital or outpatient surgery center), an additional facility copayment may apply. Plan designs may be modified to ensure compliance with state and federal requirements. A15814 (1/15) RH ;
13 Chiropractic and Acupuncture Benefits Additional coverage for your HMO and POS plans Blue Shield Chiropractic and Acupuncture Care coverage lets you self-refer to a network of more than 3,310 licensed chiropractors and more than 1,245 licensed acupuncturists. Benefits are provided through a contract with American Specialty Health Plans of California, Inc. (ASH Plans). How the Program Works You can visit any participating chiropractors or acupuncturists in California from the ASH Plans network without a referral from your HMO or POS Personal Physician. Simply call a participating provider to schedule an initial exam. At the time of your first visit, you ll present your Blue Shield identification card and pay only your copayment. Because participating chiropractors and acupuncturists bill ASH Plans directly, you ll never have to file claim forms. If you need further treatment, the participating chiropractor or acupuncturist will submit a proposed treatment plan to ASH Plans and obtain the necessary authorization from ASH Plans to continue treatment up to the calendar-year maximum of 30 combined visits. What s Covered The plan covers medically necessary chiropractic and acupuncture services including: Initial and subsequent examinations Office visits and adjustments (subject to annual limits) Adjunctive therapies X-rays (chiropractic only) Benefit Plan Design Calendar-year Maximum 30 Combined Visits Calendar-year Deductible Calendar-year Chiropractic Appliances Benefit 1,2 $50 Covered Services Acupuncture Services Chiropractic Services Out-of-network Coverage 1. Chiropractic appliances are covered up to a maximum of $50 in a calendar-year as authorized by ASH Plans. None Member Copayment $10 per visit $10 per visit 2. As authorized by ASH Plans, this allowance is applied toward the purchase of items determined necessary, such as supports, collars, pillows, heel lifts, ice packs, cushions, orthotics, rib belts and home traction units. Friendly Customer Service Helpful ASH Plans Member Services representatives are available at (800) Monday through Friday from 6 a.m. to 5 p.m. to answer questions, assist with problems, or help locate a participating chiropractor or acupuncturist. This document is only a summary for informational purposes. It is not a contract. Please refer to the Evidence of Coverage and the Group Health Service Agreement for the exact terms and conditions of coverage. None An independent member of the Blue Shield Association A17273 (01/15
14 Self-Insured Schools of California (SISC) Pharmacy Benefit Schedule PLAN Walk-in 200DED/10-35 Mail Network Costco Costco Navitus Days Supply* Generic $10 Free Free Free Brand $35 $35 $90 $90 Specialty $35 Out-of-Pocket Maximum Brand/Specialty Deductible $2,500 Individual / $3,500 Family $200 Individual / $500 Family SISC urges members to use generic drugs when available. If you or your physician requests the brand name when a generic equivalent is available, you will pay the generic copay plus the difference in cost between the brand and generic. The difference in cost between the brand and generic will not count toward the Annual Out-of-Pocket Maximum. *Members may receive up to 30 days and/or up to 90 days supply of medication at participating pharmacies. Some narcotic pain and cough medications are not included in the Costco Free Generic or 90-day supply programs. Navitus contracts with most independent and chain pharmacies with the exception of Walgreens. Mail Order Service The Mail Order Service allows you to receive a 90-day supply of maintenance medications. This program is part of your pharmacy benefit and is voluntary. Specialty Pharmacy Navitus SpecialtyRx helps members who are taking medications for certain chronic illnesses or complex diseases by providing services that offer convenience and support. This program is part of your pharmacy benefit and is mandatory. Navi-Gate for Members allows you to access personalized pharmacy benefit information online at For information specific to your plan, visit Navi-Gate for Members. Activate your account online using the Member Login link and an activation will be sent to you. The site provides access to prescription benefits, pharmacy locator, drug search, drug interaction information, medication history, and mail order information. The site is available 24 hours a day, seven days a week. 2015_2016_RX_10_35_200_500_DED Navitus SISC 14
15 An independent member of the Blue Shield Association SISC ASO PPO HSA Plan A Benefit Summary Blue Shield of California Highlights: $1,500 individual coverage deductible or $3,000 family coverage deductible Effective: October 1, 2015 THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE COVERAGE BENEFITS AND IS A SUMMARY ONLY. THE PLAN CONTRACT SHOULD BE CONSULTED FOR A DETAILED DESCRIPTION OF COVERAGE BENEFITS AND LIMITATIONS. Participating Providers 1 Non Participating Providers 1 Calendar Year Deductible (All providers combined) $1,500 per Individual / $3,000 per Family (Note: For individual on family coverage plan, enrollee can receive benefits for covered services once individual deductible is met.) Calendar Year Out-of-Pocket Maximum 2 (Includes the plan deductible) $4,000 per Individual / $8,000 per Family (For individual on family coverage plan, enrollee can receive 100% benefits for covered services once individual out-of-pocket maximum is met.) LIFETIME BENEFIT MAXIMUM None Covered Services Member Copayment PROFESSIONAL SERVICES Participating Providers 1 Non Participating Providers 1 Professional (Physician) Benefits Physician and specialist office visits 10% 50% 2 CT scans, MRIs, MRAs, PET scans, and cardiac diagnostic 10% 50% 2 procedures utilizing nuclear medicine (prior authorization is required) 3 Other outpatient X-ray, pathology and laboratory (Diagnostic testing by providers other than outpatient laboratory, pathology, and imaging departments of hospitals/facilities) 3 10% Not Covered Allergy Testing and Treatment Benefits Office visits (includes visits for allergy serum injections) 10% 50% 2 Preventive Health Benefits Preventive Health Services (As required by applicable federal law.) No Charge (Not subject to the Calendar Year Deductible) OUTPATIENT SERVICES Not Covered Hospital Benefits (Facility Services) Outpatient surgery performed at an Ambulatory Surgery Center 4 10% No Charge 5 Outpatient surgery in a hospital 10% No Charge 5 Outpatient Services for treatment of illness or injury and 10% 50% 2 necessary supplies (Except as described under "Rehabilitation Benefits") CT scans, MRIs, MRAs, PET scans, and cardiac diagnostic 10% 50% 2, 5 procedures utilizing nuclear medicine performed in a hospital (prior authorization is required) 3 Other outpatient X-ray, pathology and laboratory performed in a 10% Not Covered hospital 3 Bariatric Surgery (prior authorization required by the Plan; medically necessary surgery for weight loss, for morbid obesity only) 6 10% No Charge 5 HOSPITALIZATION SERVICES Hospital Benefits (Facility Services) Inpatient Physician Services 10% 2, 10 50% Inpatient Non-emergency Facility Services (Semi-private room and board, and medically necessary Services and supplies, including Subacute Care) 10% No Charge 7 Bariatric Surgery (prior authorization required by the Plan; medically necessary 10% No Charge 7 surgery for weight loss, for morbid obesity only) 6 Skilled Nursing Facility Benefits 8 (Combined maximum of up to 100 days per Calendar Year; semi-private accommodations) Services by a free-standing Skilled Nursing Facility 10% 10% 9 Skilled Nursing Unit of a Hospital 10% No Charge 7 EMERGENCY HEALTH COVERAGE Emergency room Services not resulting in admission (The ER $100 per visit + 10% $100 per visit + 10% copayment does not apply if the member is directly admitted to the hospital for inpatient services) Emergency room Services resulting in admission (when the member is 10% 10% admitted directly from the ER) Emergency room Physician Services 10% 10% 11
16 AMBULANCE SERVICES Emergency or authorized transport 10% 10% 11, 12, 13, 14, 15 PRESCRIPTION DRUG COVERAGE Participating Pharmacy Non Participating Pharmacy (Subject to deductible) Outpatient Prescription Drug Benefits Retail Prescriptions (For up to a 30-day supply) Contraceptive Drugs and Devices 16 No Charge Not Covered Formulary Generic Drugs $7 per prescription $7 per prescription Formulary Brand Name Drugs $25 per prescription $25 per prescription Non-Formulary Brand Name Drugs $25 per prescription $25 per prescription Mail Service Prescriptions (For up to a 90-day supply) Contraceptive Drugs and Devices 16 No Charge Not Covered Formulary Generic Drugs $14 per prescription Not Covered Formulary Brand Name Drugs $60 per prescription Not Covered Non-Formulary Brand Name Drugs $60 per prescription Not Covered Specialty Pharmacies (up to a 30-day supply) Specialty Drugs $25 per prescription Not Covered PROSTHETICS/ORTHOTICS Prosthetic equipment and devices (Separate office visit copay may apply) 10% 50% 2 Orthotic equipment and devices (Separate office visit copay may apply) 10% Not Covered DURABLE MEDICAL EQUIPMENT Breast pump No Charge Not Covered (Not subject to the Calendar Year Deductible) Other Durable Medical Equipment 10% Not Covered 17, 18 MENTAL HEALTH AND SUBSTANCE ABUSE SERVICES Inpatient Hospital Services 10% No Charge 7 Residential Care 10% No Charge 7 Inpatient Physician Services 10% 50% 2 Routine Outpatient Mental Health and Substance Abuse Services (includes professional/physician visits) 10% 50% 2 Non-Routine Outpatient Mental Health and Substance Abuse Services (includes behavioral health treatment, electroconvulsive therapy, intensive outpatient programs, office-based opioid treatment, partial hospitalization programs, and transcranial magnetic stimulation. For partial hospitalization programs, a higher copayment and facility charges may apply per episode of care) 10% 50% 2 HOME HEALTH SERVICES Home health care agency Services (up to 100 visits per Calendar Year) 8 10% Not Covered 19 Home infusion/home intravenous injectable therapy and infusion 10% Not Covered 19 nursing visits provided by a Home Infusion Agency OTHER Hospice Program Benefits Routine home care 10% Not Covered 19 Inpatient Respite Care 10% Not Covered hour Continuous Home Care 10% Not Covered 19 General Inpatient care 10% Not Covered 19 Chiropractic Benefits 8 Chiropractic Services (up to 20 visits per Calendar Year) 10% Not Covered Acupuncture Benefits 8 Acupuncture Services (up to 12 visits per Calendar Year) 10% 50% 2 Rehabilitation Benefits (Physical, Occupational and Respiratory Therapy) Office location 10% Not Covered Speech Therapy Benefits Office Visit 10% 50% 2 Pregnancy and Maternity Care Benefits Prenatal and postnatal Physician office visits (For inpatient hospital services, see "Hospitalization Services") Abortion services (Facility charges may apply - see "Hospital Benefits (Facility Services)") 10% 50% 2 10% Not Covered
17 Family Planning Benefits Counseling and consulting 20 No Charge Not Covered (Not subject to the Calendar Year Deductible) Tubal ligation No Charge Not Covered (Not subject to the Calendar Year Deductible) Vasectomy 21 10% Not Covered Diabetes Care Benefits Devices, equipment, and non-testing supplies (for testing supplies see Outpatient Prescription Drug Benefits.) Plan designs may be modified to ensure compliance with federal requirements. ASO (1/15) DC ; ; ; % 50% 2 Diabetes self-management training 10% 50% 2 Hearing Aid Benefits Audiological evaluations 10% 50% 2 Hearing Aid Instrument and ancillary equipment (Up to a maximum combined benefit of $700 per person every 24 months for the hearing aid and ancillary equipment) 10% 10% Care Outside of Plan Service Area (Benefits provided through the BlueCard Program for out-of-state emergency and non-emergency care are provided at the Participating level of the local Blue Plan allowable amount when you use a Blue Cross/Blue Shield provider) Within US: BlueCard Program See Applicable Benefit See Applicable Benefit Outside of US: BlueCard Worldwide See Applicable Benefit See Applicable Benefit 1 Unless otherwise specified, copayments/coinsurance are calculated based on allowable amounts. Participating providers agree to accept Blue Shield's allowable amount plus the plan s and any applicable member s payment as full payment for covered services. Non Participating providers can charge more than these amounts. When members use Non Participating providers, they must pay the applicable deductibles, copayments or coinsurance plus any amount that exceeds Blue Shield's allowable amount. Charges in excess of the allowable amount do not count toward the Calendar Year deductible or out-of-pocket maximum. Payments applied to your Calendar Year deductible accrue towards the out-of-pocket maximum. 2 Copayments/Coinsurance marked with this footnote does not accrue to Calendar Year out-of pocket maximum. Copayments/Coinsurance and charges for services not accruing to the member's Calendar Year out-of-pocket maximum continue to be the member's responsibility after the Calendar Year out-of-pocket maximum is reached. This amount could be substantial. Please refer to the Plan Contract for exact terms and conditions of coverage. 3 Participating non Hospital based ("freestanding") laboratory or radiology centers may not be available in all areas. Laboratory and radiology Services may also be obtained from a Hospital or from a laboratory and radiology center that is affiliated with a Hospital, and paid according to the benefit under your health plan's Hospital Benefits. 4 Participating Ambulatory Surgery Centers may not be available in all areas. Outpatient surgery Services may also be obtained from a Hospital or from an ambulatory surgery center that is affiliated with a Hospital, and paid according to the benefit under your health plan's Hospital Benefits. 5 The maximum allowed charges for non-emergency surgery performed in a Non Participating Ambulatory Surgery Center or outpatient unit of a Non Participating hospital is $350 per day. Members are responsible for all charges in excess of $ Bariatric surgery is covered when pre-authorized by the Plan. However, for members residing in Imperial, Kern, Los Angeles, Orange, Riverside, San Bernardino, San Diego, Santa Barbara and Ventura Counties ("Designated Counties"), bariatric surgery services are covered only when performed at designated contracting bariatric surgery facilities and by designated contracting surgeons; coverage is not available for bariatric services from any other Participating provider and there is no coverage for bariatric services from Non Participating providers. In addition, if prior authorized by the Plan, a member in a Designated County who is required to travel more than 50 miles to a designated bariatric surgery facility will be eligible for limited reimbursement for specified travel expenses for the member and one companion. Refer to the Plan Contract for further benefit details. 7 The maximum allowed charge for non-emergency hospital services received from a Non Participating hospital is $600 per day. Members are responsible for all charges in excess of $600. Payments that exceed the allowed charge do not count toward the Calendar Year out-of-pocket maximum, and continue to be owed after the maximum is reached. 8 For plans with a Calendar Year deductible amount, services with a day or visit limit accrue to the Calendar Year day or visit limit maximum regardless of whether the plan deductible has been met. 9 Services may require prior authorization by the Plan. When services are prior authorized, members pay the Participating provider amount. 10 When these services are rendered by a Non Participating Radiologist, Anesthesiologist, Pathologist and Emergency Room Physicians in a Participating facility, the member pays the Participating Provider copayment. 11 If the member requests a Brand Name drug when a generic drug equivalent is available, the member is responsible for paying the difference between the cost to Blue Shield for the Brand Name Drug and its generic drug equivalent, as well as the applicable generic drug Copayment. This difference in cost that the member must pay is not applied to their Calendar Year deductible and is not included in the Calendar Year out-of-pocket maximum responsibility calculations. 12 Please note that if you switch from another plan, your prescription drug deductible credit from the previous plan during the Calendar Year, if applicable, will not carry forward to your new plan. 13 For the Outpatient Prescription Drugs Benefit, covered Drugs obtained from Non Participating Pharmacies will be subject to and accrue to the Calendar Year Deductible and the Calendar Year Out-of-Pocket Maximum for Participating providers. 14 Specialty drugs are covered only when dispensed by select pharmacies in the Specialty Pharmacy Network unless Medically Necessary for a covered emergency. 15 Specialty Drugs are specific Drugs used to treat complex or chronic conditions which usually require close monitoring such as multiple sclerosis, hepatitis, rheumatoid arthritis, cancers, and other conditions that are difficult to treat with traditional therapies. Specialty Drugs are listed in the Blue Shield Outpatient Drug Formulary. Specialty Drugs may be self-administered in the home by injection by the patient or family member (subcutaneously or intramuscularly), by inhalation, orally or topically. Specialty Drugs may also require special handling, special manufacturing processes, and may have limited prescribing or limited pharmacy availability. Specialty Drugs must be considered safe for self-administration by Blue Shield's Pharmacy & Therapeutics Committee, be obtained from a Blue Shield Specialty Pharmacy and may require prior authorization for Medical Necessity by Blue Shield. Infused or Intravenous (IV) medications are not included as Specialty Drugs. 16 Contraceptive Drugs and Devices covered under the outpatient prescription drug benefits will not be subject to the Calendar Year deductible. If a Brand Name contraceptive is requested when a generic equivalent is available, the member will be responsible for paying the difference between the cost to Blue Shield for the Brand Name contraceptive and its generic drug equivalent. In addition, select contraceptives may need prior authorization to be covered without a copayment. 17 Mental Health and Substance Abuse services are accessed through Blue Shield s Participating and Non Participating providers. 18 Inpatient services for acute detoxification are covered under the medical benefit; see the Hospital Benefits (Facility Services) section of the Plan Contract for benefit details. Services for acute medical detoxification are accessed through Blue Shield using Blue Shield's Participating providers or with Non Participating providers. 19 Out of network home health care, home infusion and hospice services are not covered unless pre-authorized. When these services are pre-authorized, the member pays the Participating provider Copayment. 20 Includes insertion of IUD, as well as injectable and implantable contraceptives for women. 21 Copayment shown is for physician's services. If the procedure is performed in a facility setting (hospital or outpatient surgery center), an additional facility copayment may apply. Services from Non Participating providers and Non Participating facilities are not covered under this benefit.
18 SISC KAISER PERMANENTE HEALTH PLANS SISC KAISER PERMANENTE HMO HEALTH PLAN SISC KAISER PERMANENTE ACCOUNT BASED HEALTH PLAN (ABHP) ELIGIBLE FOR PARTICIPATION IN A HEALTH SAVINGS ACCOUNT (HSA)
19 Benefit Summary SISC - SELF-INSURED SCHOOLS OF CALIFORNIA Principal Benefits for Kaiser Permanente Traditional Plan (10/1/15 9/30/16) The Services described below are covered only if all of the following conditions are satisfied: The Services are Medically Necessary The Services are provided, prescribed, authorized, or directed by a Plan Physician and you receive the Services from Plan Providers inside our Northern California Region Service Area (your Home Region), except where specifically noted to the contrary in the Evidence of Coverage (EOC) for authorized referrals, hospice care, Emergency Services, Post-Stabilization Care, Out-of- Area Urgent Care, and emergency ambulance Services Accumulation Period The Accumulation Period for this plan is 1/1/15 through 12/31/15 (calendar year). Plan Out-of-Pocket Maximum For Services subject to the maximum, you will not pay any more Cost Share for the rest of the calendar year if the Copayments and Coinsurance you pay for those Services add up to one of the following amounts: For self-only enrollment (a Family of one Member)... $1,500 per calendar year For any one Member in a Family of two or more Members... $1,500 per calendar year For an entire Family of two or more Members... $3,000 per calendar year Plan Deductible None Professional Services (Plan Provider office visits) Most Primary Care Visits for evaluations and treatment... $25 per visit Most Specialty Care Visits for consultations, evaluations, and treatment... $25 per visit Routine physical maintenance exams, including well-woman exams... No charge Well-child preventive exams (through age 23 months)... No charge Family planning counseling and consultations... No charge Scheduled prenatal care exams... No charge Routine eye exams with a Plan Optometrist... No charge Hearing exams... No charge Urgent care consultations, evaluations, and treatment... $25 per visit Most physical, occupational, and speech therapy... $25 per visit Outpatient Services Outpatient surgery and certain other outpatient procedures... $25 per procedure Allergy injections (including allergy serum)... $5 per visit Most immunizations (including the vaccine)... No charge Most X-rays and laboratory tests... No charge Covered individual health education counseling... No charge Covered health education programs... No charge Hospitalization Services Room and board, surgery, anesthesia, X-rays, laboratory tests, and drugs... No charge Emergency Health Coverage Emergency Department visits... $100 per visit Note: This Cost Share does not apply if admitted directly to the hospital as an inpatient for covered Services (see "Hospitalization Services" for inpatient Cost Share). Ambulance Services Ambulance Services... $50 per trip Prescription Drug Coverage Covered outpatient items in accord with our drug formulary guidelines at a Plan Pharmacy or through our mail-order service: Most generic items... $10 for up to a 100-day supply Most brand-name items... $25 for up to a 100-day supply Durable Medical Equipment (DME) DME items that are essential health benefits in accord with our DME formulary guidelines... No charge DME items that are not essential health benefits in accord with our DME formulary guidelines... No charge S SISC - Self-Insured Schools Of California (continues)
SISC Custom SaveNet Zero Admit 10 Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix)
 SISC Custom SaveNet Zero Admit 10 Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Highlights: A description of the prescription drug coverage is provided separately
SISC Custom SaveNet Zero Admit 10 Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Highlights: A description of the prescription drug coverage is provided separately
CSAC/EIA Health Small Group Access+ HMO 15-0 Inpatient Benefit Summary
 CSAC/EIA Health Small Group Access+ HMO 15-0 Inpatient Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE
CSAC/EIA Health Small Group Access+ HMO 15-0 Inpatient Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California THIS MATRIX IS INTENDED TO BE USED TO HELP YOU COMPARE
No Charge (Except as described under "Rehabilitation Benefits" and "Speech Therapy Benefits")
 An Independent Licensee of the Blue Shield Association Custom Access+ HMO Plan Certificated & Management Benefit Summary (For groups of 300 and above) (Uniform Health Plan Benefits and Coverage Matrix)
An Independent Licensee of the Blue Shield Association Custom Access+ HMO Plan Certificated & Management Benefit Summary (For groups of 300 and above) (Uniform Health Plan Benefits and Coverage Matrix)
Ultimate Full PPO for Small Business 0 Benefit Summary (For groups 1 to 50) (Uniform Health Plan Benefits and Coverage Matrix)
 Ultimate Full PPO for Small Business 0 Benefit Summary (For groups 1 to 50) (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Effective January 1, 2014 THIS MATRIX IS INTENDED
Ultimate Full PPO for Small Business 0 Benefit Summary (For groups 1 to 50) (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California Effective January 1, 2014 THIS MATRIX IS INTENDED
County of San Bernardino - Retiree Shield Signature High Option
 An Independent Member of the Blue Shield Association County of San Bernardino - Retiree Shield Signature High Option Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California
An Independent Member of the Blue Shield Association County of San Bernardino - Retiree Shield Signature High Option Benefit Summary (Uniform Health Plan Benefits and Coverage Matrix) Blue Shield of California
S c h o o l s I n s u r a n c e G r o u p Health Net Plan Comparison Fiscal Year 7/1/14-6/30/15
 S c h o o l s I n s u r a n c e G r o u p Health Net Plan Comparison Fiscal Year 7/1/14-6/30/15 This information sheet is for reference only. Please refer to Evidence of Coverage requirements, limitations
S c h o o l s I n s u r a n c e G r o u p Health Net Plan Comparison Fiscal Year 7/1/14-6/30/15 This information sheet is for reference only. Please refer to Evidence of Coverage requirements, limitations
S c h o o l s I n s u r a n c e G r o u p Health Net Plan Comparison Fiscal Year 7/1/15-6/30/16
 S c h o o l s I n s u r a n c e G r o u p Health Net Plan Comparison Fiscal Year 7/1/15-6/30/16 This information sheet is for reference only. Please refer to Evidence of Coverage requirements, limitations
S c h o o l s I n s u r a n c e G r o u p Health Net Plan Comparison Fiscal Year 7/1/15-6/30/16 This information sheet is for reference only. Please refer to Evidence of Coverage requirements, limitations
benefit summary guide
 benefit summary guide Group health plan information for small businesses with 1 to 50 eligible employees Effective January 1, 2014 blueshieldca.com Healthcare coverage that works for your business With
benefit summary guide Group health plan information for small businesses with 1 to 50 eligible employees Effective January 1, 2014 blueshieldca.com Healthcare coverage that works for your business With
go with ^ Health Savings PPO plan (paired with the Health Savings Account) Core plan (administered by Blue Shield of California)
 go with ^ Health Savings PPO plan (paired with the Health Savings Account) Core plan (administered by Blue Shield of California) Effective January 1, 2014 Go with the plan that s right for you When you
go with ^ Health Savings PPO plan (paired with the Health Savings Account) Core plan (administered by Blue Shield of California) Effective January 1, 2014 Go with the plan that s right for you When you
UC Care Plan. Benefit Booklet. University of California. Group Number: W0051612 Plan ID: PPOX0001 Effective Date: January 1, 2016
 UC Care Plan Benefit Booklet University of California Group Number: W0051612 Plan ID: PPOX0001 Effective Date: January 1, 2016 An independent member of the Blue Shield Association Claims Administered by
UC Care Plan Benefit Booklet University of California Group Number: W0051612 Plan ID: PPOX0001 Effective Date: January 1, 2016 An independent member of the Blue Shield Association Claims Administered by
Important Questions Answers Why this Matters:
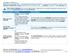 Minimum Coverage PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan
Minimum Coverage PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan
$0. See the chart starting on page 2 for your costs for services this plan covers.
 Access+ HMO Facility Coinsurance 15-20% Coverage Period: Beginning On or After 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan
Access+ HMO Facility Coinsurance 15-20% Coverage Period: Beginning On or After 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan
Western Health Advantage: City of Sacramento HSA ABHP Coverage Period: 1/1/2016-12/31/2016
 Coverage For: Self Plan Type: HMO This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.westernhealth.com or
Coverage For: Self Plan Type: HMO This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.westernhealth.com or
CIGNA HEALTH AND LIFE INSURANCE COMPANY, a Cigna company (hereinafter called Cigna)
 Home Office: Bloomfield, Connecticut Mailing Address: Hartford, Connecticut 06152 CIGNA HEALTH AND LIFE INSURANCE COMPANY, a Cigna company (hereinafter called Cigna) CERTIFICATE RIDER No CR7SI006-1 Policyholder:
Home Office: Bloomfield, Connecticut Mailing Address: Hartford, Connecticut 06152 CIGNA HEALTH AND LIFE INSURANCE COMPANY, a Cigna company (hereinafter called Cigna) CERTIFICATE RIDER No CR7SI006-1 Policyholder:
2015 Medical Plan Summary
 2015 Medical Plan Summary AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copayments for 2015. This is not a contract, it s a summary of the plan highlights and is
2015 Medical Plan Summary AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copayments for 2015. This is not a contract, it s a summary of the plan highlights and is
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 Gold 80 PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type:
Gold 80 PPO Network Name: Exclusive Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type:
AVMED POS PLAN. Allergy Injections No charge 30% co-insurance after deductible Allergy Skin Testing $30 per visit 30% co-insurance after deductible
 AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copays for 2015. This is not a contract, it s a summary of the plan highlights and is subject to change. For specific
AVMED POS PLAN This Schedule of Benefits reflects the higher provider and prescription copays for 2015. This is not a contract, it s a summary of the plan highlights and is subject to change. For specific
Summary of Services and Cost Shares
 Summary of Services and Cost Shares This summary does not describe benefits. For the description of a benefit, including any limitations or exclusions, please refer to the identical heading in the Benefits
Summary of Services and Cost Shares This summary does not describe benefits. For the description of a benefit, including any limitations or exclusions, please refer to the identical heading in the Benefits
$0. See the chart starting on page 2 for your costs for services this plan covers.
 City of Los Angeles Access+ HMO SaveNet (Narrow) Zero Admit 15 Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual +
City of Los Angeles Access+ HMO SaveNet (Narrow) Zero Admit 15 Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual +
$0. See the chart starting on page 2 for your costs for services this plan covers.
 County of San Mateo HMO Per Admit 15-100 Coverage Period: 01/01/2015 12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: HMO
County of San Mateo HMO Per Admit 15-100 Coverage Period: 01/01/2015 12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: HMO
Important Questions Answers Why this Matters:
 Bronze 60 EPO - Network Name: EPO Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: EPO
Bronze 60 EPO - Network Name: EPO Coverage Period: Beginning on or after 1/1/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: EPO
RETIREE OPEN ENROLLMENT 2014
 RETIREE OPEN ENROLLMENT 2014 The month of August 2014 is open enrollment for eligible retirees to switch from one retiree health plan to another. Open enrollment is also the time when you are allowed to
RETIREE OPEN ENROLLMENT 2014 The month of August 2014 is open enrollment for eligible retirees to switch from one retiree health plan to another. Open enrollment is also the time when you are allowed to
2015 Medical Plan Options Comparison of Benefit Coverages
 Member services 1-866-641-1689 1-866-641-1689 1-866-641-1689 1-866-641-1689 1-866-641-1689 1-800-464-4000 Web site www.anthem.com/ca/llns/ www.anthem.com/ca/llns/ www.anthem.com/ca/llns/ www.anthem.com/ca/llns/
Member services 1-866-641-1689 1-866-641-1689 1-866-641-1689 1-866-641-1689 1-866-641-1689 1-800-464-4000 Web site www.anthem.com/ca/llns/ www.anthem.com/ca/llns/ www.anthem.com/ca/llns/ www.anthem.com/ca/llns/
PLAN DESIGN AND BENEFITS POS Open Access Plan 1944
 PLAN FEATURES PARTICIPATING Deductible (per calendar year) $3,000 Individual $9,000 Family $4,000 Individual $12,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being
PLAN FEATURES PARTICIPATING Deductible (per calendar year) $3,000 Individual $9,000 Family $4,000 Individual $12,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being
$0. See the chart starting on page 2 for your costs for services this plan covers.
 San Francisco Electrical Workers Custom HMO Coverage Period: 08/01/2015-07/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: HMO
San Francisco Electrical Workers Custom HMO Coverage Period: 08/01/2015-07/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan Type: HMO
Are there other deductibles for specific services?
 Blue Shield of CA Life & Health Active Choice Plan 750 Coverage Period: 04/01/2015-03/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan
Blue Shield of CA Life & Health Active Choice Plan 750 Coverage Period: 04/01/2015-03/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual + Family Plan
PLAN DESIGN AND BENEFITS HMO Open Access Plan 912
 PLAN FEATURES Deductible (per calendar year) $1,000 Individual $2,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services
PLAN FEATURES Deductible (per calendar year) $1,000 Individual $2,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Member cost sharing for certain services
Your Plan: Value HMO 25/40/20% (RX $10/$30/$45/30%) Your Network: Select Plus HMO
 Your Plan: Value HMO 25/40/20% (RX $10/$30/$45/30%) Your Network: Select Plus HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
Your Plan: Value HMO 25/40/20% (RX $10/$30/$45/30%) Your Network: Select Plus HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary
go with ^ Access+ HMO blueshieldca.com blueshieldca.com/sfhss For active employees, early retirees, and Medicare Coordinated retirees
 go with ^ Access+ HMO For active employees, early retirees, and Medicare Coordinated retirees blueshieldca.com/sfhss blueshieldca.com Go with the plan that s right for you When you go with Blue Shield,
go with ^ Access+ HMO For active employees, early retirees, and Medicare Coordinated retirees blueshieldca.com/sfhss blueshieldca.com Go with the plan that s right for you When you go with Blue Shield,
Shield Savings 3500 - G. Blue Shield of California Life & Health Insurance Company
 Shield Savings 3500 - G Blue Shield of California Life & Health Insurance Company Policy Individual and Family Plan An independent licensee of the Blue Shield Association (Intentionally left blank) Shield
Shield Savings 3500 - G Blue Shield of California Life & Health Insurance Company Policy Individual and Family Plan An independent licensee of the Blue Shield Association (Intentionally left blank) Shield
Prescription Drugs and Vision Benefits
 Medical Plans Prescription Drugs and Vision Benefits Salaried Employees. may enroll for coverage in either the Cigna Open Access Plus Plan or the Cigna Choice Fund (Health Savings Account [HSA] Eligible)
Medical Plans Prescription Drugs and Vision Benefits Salaried Employees. may enroll for coverage in either the Cigna Open Access Plus Plan or the Cigna Choice Fund (Health Savings Account [HSA] Eligible)
Mental Health Services: University of California Custom Health Savings Plan 1300/2600
 Cover Letter for Summary of Benefits and Coverage Mental Health Services: University of California Custom Health Savings Plan 1300/2600 Coverage Period: 01/01/2015-12/31/2015 The enclosed Summary of Benefits
Cover Letter for Summary of Benefits and Coverage Mental Health Services: University of California Custom Health Savings Plan 1300/2600 Coverage Period: 01/01/2015-12/31/2015 The enclosed Summary of Benefits
Benefit Summary - A, G, C, E, Y, J and M
 Benefit Summary - A, G, C, E, Y, J and M Benefit Year: Calendar Year Payment for Services Deductible Individual $600 $1,200 Family (Embedded*) $1,200 $2,400 Coinsurance (the percentage amount the Covered
Benefit Summary - A, G, C, E, Y, J and M Benefit Year: Calendar Year Payment for Services Deductible Individual $600 $1,200 Family (Embedded*) $1,200 $2,400 Coinsurance (the percentage amount the Covered
Coverage for: Large Group Plan Type: HMO
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan
Summary of Benefits and Coverage: What this Plan Covers & What it Costs This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan
California Small Group MC Aetna Life Insurance Company
 PLAN FEATURES Deductible (per calendar year) $1,000 per member $1,000 per member Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate
PLAN FEATURES Deductible (per calendar year) $1,000 per member $1,000 per member Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate
LOCKHEED MARTIN AERONAUTICS COMPANY PALMDALE 2011 IAM NEGOTIATIONS UNDER AGE 65 LM HEALTHWORKS SUMMARY
 Annual Deductibles, Out-of-Pocket Maximums, Lifetime Maximum Benefits Calendar Year Deductible Calendar Year Out-of- Pocket Maximum Lifetime Maximum Per Individual Physician Office Visits Primary Care
Annual Deductibles, Out-of-Pocket Maximums, Lifetime Maximum Benefits Calendar Year Deductible Calendar Year Out-of- Pocket Maximum Lifetime Maximum Per Individual Physician Office Visits Primary Care
California Ironworkers Field Welfare Plan 1/1/2014 Open Enrollment Benefit Plan Comparison Non-Medicare Retired Participants Residing in Nevada
 Non- Choice of Providers Calendar Year Deductible *The Fund s Calendar Year Deductible is never waived. However, some services are not subject to the Deductible. If you live in Nevada, your network of
Non- Choice of Providers Calendar Year Deductible *The Fund s Calendar Year Deductible is never waived. However, some services are not subject to the Deductible. If you live in Nevada, your network of
PLAN DESIGN AND BENEFITS - PA Health Network Option AHF HRA 1.3. Fund Pays Member Responsibility
 HEALTHFUND PLAN FEATURES HealthFund Amount (Per plan year. Fund changes between tiers requires a life status change qualifying event.) Fund Coinsurance (Percentage at which the Fund will reimburse) Fund
HEALTHFUND PLAN FEATURES HealthFund Amount (Per plan year. Fund changes between tiers requires a life status change qualifying event.) Fund Coinsurance (Percentage at which the Fund will reimburse) Fund
Anthem Blue Cross Life and Health Insurance Company University of Southern California Custom Premier PPO 400/20%/20%
 Anthem Blue Cross Life and Health Insurance Company University of Southern California Custom Premier 400/20%/20% Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period:
Anthem Blue Cross Life and Health Insurance Company University of Southern California Custom Premier 400/20%/20% Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period:
Blue Shield of California Life & Health Insurance Company
 Active Start SM Plan 25 - G Blue Shield of California Life & Health Insurance Company Policy Individual Plan An independent licensee of the Blue Shield Association (Intentionally left blank) Active Start
Active Start SM Plan 25 - G Blue Shield of California Life & Health Insurance Company Policy Individual Plan An independent licensee of the Blue Shield Association (Intentionally left blank) Active Start
Vital Shield 2900. blueshieldca.com. New! Protect yourself with our lowest-priced PPO plan for individuals.
 Underwritten by Blue Shield of California Life & Health Insurance Company. Pending regulatory approval. Plan benefits are effective June 1, 2007. New! Protect yourself with our lowest-priced PPO plan for
Underwritten by Blue Shield of California Life & Health Insurance Company. Pending regulatory approval. Plan benefits are effective June 1, 2007. New! Protect yourself with our lowest-priced PPO plan for
Boston College Student Blue PPO Plan Coverage Period: 2015-2016
 Boston College Student Blue PPO Plan Coverage Period: 2015-2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: PPO This is only a
Boston College Student Blue PPO Plan Coverage Period: 2015-2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: PPO This is only a
National PPO 1000. PPO Schedule of Payments (Maryland Small Group)
 PPO Schedule of Payments (Maryland Small Group) National PPO 1000 The benefits outlined in this Schedule are in addition to the benefits offered under Coventry Health & Life Insurance Company Small Employer
PPO Schedule of Payments (Maryland Small Group) National PPO 1000 The benefits outlined in this Schedule are in addition to the benefits offered under Coventry Health & Life Insurance Company Small Employer
Important Questions Answers Why this Matters:
 Anthem Blue Cross Life and Health Insurance Company Unify: PPO Coverage Period: 01/01/2015 12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family
Anthem Blue Cross Life and Health Insurance Company Unify: PPO Coverage Period: 01/01/2015 12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family
How To Pay For Health Care With Bluecrossma
 PPO Student/Affiliate Plan MIT Student/Affiliate Extended Insurance Plan Coverage Period: 2014-2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual, Couple,
PPO Student/Affiliate Plan MIT Student/Affiliate Extended Insurance Plan Coverage Period: 2014-2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual, Couple,
HEALTH PLAN COMPARISON
 City of San José HEALTH PLAN COMPARISON For Employees Represented by AEA, AMSP, CAMP, CEO, IAFF, IBEW, MEF and OE#3 SERVICE Kaiser Permanente Blue Shield HMO QUESTIONS ABOUT PLAN DESIGN AND PROVIDER NETWORKS
City of San José HEALTH PLAN COMPARISON For Employees Represented by AEA, AMSP, CAMP, CEO, IAFF, IBEW, MEF and OE#3 SERVICE Kaiser Permanente Blue Shield HMO QUESTIONS ABOUT PLAN DESIGN AND PROVIDER NETWORKS
PPO Schedule of Payments (Maryland Large Group) Qualified High Deductible Health Plan National QA2000-20
 PPO Schedule of Payments (Maryland Large Group) Qualified High Health Plan National QA2000-20 Benefit Year Individual Family (Amounts for Participating and s services are separated in calculating when
PPO Schedule of Payments (Maryland Large Group) Qualified High Health Plan National QA2000-20 Benefit Year Individual Family (Amounts for Participating and s services are separated in calculating when
Coverage for: Individual/Family Plan Type: PPO. What is the overall deductible?
 Blue Cross Blue Shield Premier 101, a Multi-State Plan SM Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family
Blue Cross Blue Shield Premier 101, a Multi-State Plan SM Coverage Period: 01/01/2016-12/31/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family
Summary of PNM Resources Health Care Benefits Active Employees 2011
 of PNM Resources Health Care Benefits Active Employees 2011 The following charts show deductibles, limits, benefit levels and amounts for the PNM Resources medical, dental and vision programs. For more
of PNM Resources Health Care Benefits Active Employees 2011 The following charts show deductibles, limits, benefit levels and amounts for the PNM Resources medical, dental and vision programs. For more
What is the overall deductible? Are there other deductibles for specific services? Is there an out-ofpocket
 Regence BlueShield: Regence Direct Gold with Dental, Vision, Individual Assistance Program Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What
Regence BlueShield: Regence Direct Gold with Dental, Vision, Individual Assistance Program Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.cfhp.com or by calling 1-800-434-2347. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.cfhp.com or by calling 1-800-434-2347. Important Questions
Bates College Effective date: 01-01-2010 HMO - Maine PLAN DESIGN AND BENEFITS PROVIDED BY AETNA HEALTH INC. - FULL RISK PLAN FEATURES
 PLAN FEATURES Deductible (per calendar year) $500 Individual $1,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family Deductible is met, all family
PLAN FEATURES Deductible (per calendar year) $500 Individual $1,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. Once Family Deductible is met, all family
California Small Group MC Aetna Life Insurance Company
 PLAN FEATURES Deductible (per calendar year) $3,000 Individual $6,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate separately
PLAN FEATURES Deductible (per calendar year) $3,000 Individual $6,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable. All covered expenses accumulate separately
Large group benefit comparison
 Large group benefit comparison effective January 1, 2015 A guide to choosing the right plan for your business San Diegans choose Health Plan With a range of plans and provider networks, we have the right
Large group benefit comparison effective January 1, 2015 A guide to choosing the right plan for your business San Diegans choose Health Plan With a range of plans and provider networks, we have the right
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 : VIVA HEALTH Access Plan Coverage Period: 01/01/2015 12/31/2015 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document
: VIVA HEALTH Access Plan Coverage Period: 01/01/2015 12/31/2015 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document
SMALL GROUP PLAN DESIGN AND BENEFITS OPEN CHOICE OUT-OF-STATE PPO PLAN - $1,000
 PLAN FEATURES PREFERRED CARE NON-PREFERRED CARE Deductible (per calendar year; applies to all covered services) $1,000 Individual $3,000 Family $2,000 Individual $6,000 Family Plan Coinsurance ** 80% 60%
PLAN FEATURES PREFERRED CARE NON-PREFERRED CARE Deductible (per calendar year; applies to all covered services) $1,000 Individual $3,000 Family $2,000 Individual $6,000 Family Plan Coinsurance ** 80% 60%
Anthem Blue Cross Life and Health Insurance Company University of California San Francisco Custom Premier PPO 200/20 (200/20/80/60)
 Anthem Blue Cross Life and Health Insurance Company University of California San Francisco Custom Premier PPO 200/20 (200/20/80/60) Summary of Benefits and Coverage: What this Plan Covers & What it Costs
Anthem Blue Cross Life and Health Insurance Company University of California San Francisco Custom Premier PPO 200/20 (200/20/80/60) Summary of Benefits and Coverage: What this Plan Covers & What it Costs
Important Questions Answers Why this Matters:
 Anthem BlueCross Premier HMO 20 / $10/$25/$45/20% Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2014-12/31/2014 Coverage For: Individual/Family Plan Type:
Anthem BlueCross Premier HMO 20 / $10/$25/$45/20% Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage Period: 01/01/2014-12/31/2014 Coverage For: Individual/Family Plan Type:
Anthem Blue Cross Life and Health Insurance Company Your Plan: Solution PPO 1500/15/20 Your Network: Prudent Buyer PPO
 Anthem Blue Cross Life and Health Insurance Company Your Plan: Solution PPO 1500/15/20 Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with
Anthem Blue Cross Life and Health Insurance Company Your Plan: Solution PPO 1500/15/20 Your Network: Prudent Buyer PPO This summary of benefits is a brief outline of coverage, designed to help you with
Blue Care Elect Preferred 90 Copay Coverage Period: on or after 09/01/2015
 Blue Care Elect Preferred 90 Copay Coverage Period: on or after 09/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Only Plan Type: PPO This is only
Blue Care Elect Preferred 90 Copay Coverage Period: on or after 09/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual Only Plan Type: PPO This is only
Coverage level: Employee/Retiree Only Plan Type: EPO
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan documents at www.dbm.maryland.gov/benefits or by calling 410-767-4775
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan documents at www.dbm.maryland.gov/benefits or by calling 410-767-4775
Health Plans Comparison Chart
 Health Plans Comparison Chart PPO Deductible Coinsurance (Plan pays) Annual Out-of-Pocket Maximum (Medical) (all medical s, deductibles and coinsurance for covered services will apply. Once limit is met,
Health Plans Comparison Chart PPO Deductible Coinsurance (Plan pays) Annual Out-of-Pocket Maximum (Medical) (all medical s, deductibles and coinsurance for covered services will apply. Once limit is met,
Blue Care Elect Preferred Amherst College Coverage Period: on or after 07/01/2014
 Blue Care Elect Preferred Amherst College Coverage Period: on or after 07/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type:
Blue Care Elect Preferred Amherst College Coverage Period: on or after 07/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type:
California PCP Selected* Not Applicable
 PLAN FEATURES Deductible (per calendar ) Member Coinsurance * Not Applicable ** Not Applicable Copay Maximum (per calendar ) $3,000 per Individual $6,000 per Family All member copays accumulate toward
PLAN FEATURES Deductible (per calendar ) Member Coinsurance * Not Applicable ** Not Applicable Copay Maximum (per calendar ) $3,000 per Individual $6,000 per Family All member copays accumulate toward
How To Pay For Health Care Benefits
 Blue Shield PPO Plan Benefit Booklet Stanford University Group Number: 170292 Effective Date: January 1, 2013 An independent member of the Blue Shield Association Claims Administered by Blue Shield of
Blue Shield PPO Plan Benefit Booklet Stanford University Group Number: 170292 Effective Date: January 1, 2013 An independent member of the Blue Shield Association Claims Administered by Blue Shield of
PLAN DESIGN AND BENEFITS Basic HMO Copay Plan 1-10
 PLAN FEATURES Deductible (per calendar year) Member Coinsurance Not Applicable Not Applicable Out-of-Pocket Maximum $5,000 Individual (per calendar year) $10,000 Family Once the Family Out-of-Pocket Maximum
PLAN FEATURES Deductible (per calendar year) Member Coinsurance Not Applicable Not Applicable Out-of-Pocket Maximum $5,000 Individual (per calendar year) $10,000 Family Once the Family Out-of-Pocket Maximum
Blue Care Elect Saver with Coinsurance Northeastern University HDHP Coverage Period: on or after 01/01/2016
 Blue Care Elect Saver with Coinsurance Northeastern University HDHP Coverage Period: on or after 01/01/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual
Blue Care Elect Saver with Coinsurance Northeastern University HDHP Coverage Period: on or after 01/01/2016 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual
Medical Plan - Healthfund
 18 Medical Plan - Healthfund Oklahoma City Community College Effective Date: 07-01-2010 Aetna HealthFund Open Choice (PPO) - Oklahoma PLAN DESIGN AND BENEFITS PROVIDED BY AETNA LIFE INSURANCE COMPANY -
18 Medical Plan - Healthfund Oklahoma City Community College Effective Date: 07-01-2010 Aetna HealthFund Open Choice (PPO) - Oklahoma PLAN DESIGN AND BENEFITS PROVIDED BY AETNA LIFE INSURANCE COMPANY -
$500 member / $1,000 family Self- Referred. Does not apply to emergency room, emergency transportation, or acupuncture services.
 Blue Choice New England Plan 2 MIT Choice Coverage Period: on or after 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual, Ind.+Spouse, Ind.+Child(ren)
Blue Choice New England Plan 2 MIT Choice Coverage Period: on or after 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual, Ind.+Spouse, Ind.+Child(ren)
Land of Lincoln Health : Family Health Network LLH 3-Tier Bronze PPO Coverage Period: 01/01/2016 12/31/2016
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.landoflincolnhealth.org or by calling 1-844-FHN-4YOU.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.landoflincolnhealth.org or by calling 1-844-FHN-4YOU.
Blue Shield of California Life & Health Insurance: Active Start Plan 25 - G Coverage Period: Beginning on or after 1/1/2014
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.blueshieldca.com or by calling 1-800-431-2809. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.blueshieldca.com or by calling 1-800-431-2809. Important
Small group and CalChoice benefit comparison
 Small group and CalChoice benefit comparison effective July 1, 2015 We believe in choice. A guide to choosing the right plan for your business US health plan 1 San Diegans choose Sharp Health Plan With
Small group and CalChoice benefit comparison effective July 1, 2015 We believe in choice. A guide to choosing the right plan for your business US health plan 1 San Diegans choose Sharp Health Plan With
PLAN DESIGN AND BENEFITS AETNA LIFE INSURANCE COMPANY - Insured
 PLAN FEATURES Deductible (per calendar year) Individual $750 Individual $1,500 Family $2,250 Family $4,500 All covered expenses accumulate simultaneously toward both the preferred and non-preferred Deductible.
PLAN FEATURES Deductible (per calendar year) Individual $750 Individual $1,500 Family $2,250 Family $4,500 All covered expenses accumulate simultaneously toward both the preferred and non-preferred Deductible.
$0 See the chart starting on page 2 for your costs for services this plan covers.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/lausd or by calling 1-800-700-3739. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/lausd or by calling 1-800-700-3739. Important
Member s responsibility (deductibles, copays, coinsurance and dollar maximums)
 MICHIGAN CATHOLIC CONFERENCE January 2015 Benefit Summary This is intended as an easy-to-read summary and provides only a general overview of your benefits. It is not a contract. Additional limitations
MICHIGAN CATHOLIC CONFERENCE January 2015 Benefit Summary This is intended as an easy-to-read summary and provides only a general overview of your benefits. It is not a contract. Additional limitations
Why this Matters: Even though you pay these expenses, they don t count toward the outof-pocket limit.
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/sisc or by calling 1-855-333-5730. Important
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.anthem.com/ca/sisc or by calling 1-855-333-5730. Important
Important Questions Answers Why this Matters: $1,500 Individual/$3,000
 Anthem Blue Cross Life and Health Insurance Company Unify: Consumer Choice HSA Coverage Period: 01/01/2015 12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for:
Anthem Blue Cross Life and Health Insurance Company Unify: Consumer Choice HSA Coverage Period: 01/01/2015 12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for:
PLAN DESIGN AND BENEFITS - Tx OAMC 2500 08 PREFERRED CARE
 PLAN FEATURES Deductible (per calendar year) $2,500 Individual $5,000 Individual $7,500 3 Individuals per $15,000 3 Individuals per Unless otherwise indicated, the Deductible must be met prior to benefits
PLAN FEATURES Deductible (per calendar year) $2,500 Individual $5,000 Individual $7,500 3 Individuals per $15,000 3 Individuals per Unless otherwise indicated, the Deductible must be met prior to benefits
Banner Health - Choice Plus Coverage Period: 1/1/2015-12/31/2015
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the plan document at www.bannerbenefits.com by clicking on the Resources tab and then Plan
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the plan document at www.bannerbenefits.com by clicking on the Resources tab and then Plan
Blue Cross Premier Bronze Extra
 An individual PPO health plan from Blue Cross Blue Shield of Michigan. You will have a broad choice of doctors and hospitals within Blue Cross Blue Shield of Michigan s unsurpassed statewide PPO network
An individual PPO health plan from Blue Cross Blue Shield of Michigan. You will have a broad choice of doctors and hospitals within Blue Cross Blue Shield of Michigan s unsurpassed statewide PPO network
Cost Sharing Definitions
 SU Pro ( and ) Annual Deductible 1 Coinsurance Cost Sharing Definitions $200 per individual with a maximum of $400 for a family 5% of allowable amount for inpatient hospitalization - or - 50% of allowable
SU Pro ( and ) Annual Deductible 1 Coinsurance Cost Sharing Definitions $200 per individual with a maximum of $400 for a family 5% of allowable amount for inpatient hospitalization - or - 50% of allowable
HMO Blue Basic Coinsurance Coverage Period: on or after 01/01/2015
 HMO Blue Basic Coinsurance Coverage Period: on or after 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: HMO This is only
HMO Blue Basic Coinsurance Coverage Period: on or after 01/01/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual and Family Plan Type: HMO This is only
Your Plan: Premier HMO 20/200A/100 OP Your Network: California Care HMO
 Your Plan: Premier HMO 20/200A/100 OP Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not reflect
Your Plan: Premier HMO 20/200A/100 OP Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does not reflect
UMC Health Plan Operations Coverage Period: 01/01/2013-12/31/2013
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplanoperations@umchealthsystem.com or by calling
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.healthplanoperations@umchealthsystem.com or by calling
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.etf.wi.gov or by calling 1-877-533-5020. Important Questions
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the policy or plan document at www.etf.wi.gov or by calling 1-877-533-5020. Important Questions
Business Life Insurance - Health & Medical Billing Requirements
 PLAN FEATURES Deductible (per plan year) $2,000 Employee $2,000 Employee $3,000 Employee + Spouse $3,000 Employee + Spouse $3,000 Employee + Child(ren) $3,000 Employee + Child(ren) $4,000 Family $4,000
PLAN FEATURES Deductible (per plan year) $2,000 Employee $2,000 Employee $3,000 Employee + Spouse $3,000 Employee + Spouse $3,000 Employee + Child(ren) $3,000 Employee + Child(ren) $4,000 Family $4,000
$6,350 Individual $12,700 Individual
 PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible $5,000 Individual $10,000 Individual $10,000 Family $20,000 Family All covered expenses accumulate separately toward the preferred or non-preferred Deductible.
PLAN FEATURES IN-NETWORK OUT-OF-NETWORK Deductible $5,000 Individual $10,000 Individual $10,000 Family $20,000 Family All covered expenses accumulate separately toward the preferred or non-preferred Deductible.
PLAN DESIGN AND BENEFITS Georgia 2-100 HNOption 13-1000-80
 Georgia Health Network Option (POS Open Access) PLAN DESIGN AND BENEFITS Georgia 2-100 HNOption 13-1000-80 PLAN FEATURES PARTICIPATING PROVIDERS NON-PARTICIPATING PROVIDERS Deductible (per calendar year)
Georgia Health Network Option (POS Open Access) PLAN DESIGN AND BENEFITS Georgia 2-100 HNOption 13-1000-80 PLAN FEATURES PARTICIPATING PROVIDERS NON-PARTICIPATING PROVIDERS Deductible (per calendar year)
Important Questions Answers Why this Matters: What is the overall deductible? Are there other deductibles for specific services?
 Anthem Blue Cross Stanislaus County: Custom EPO Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type:
Anthem Blue Cross Stanislaus County: Custom EPO Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type:
SERVICES IN-NETWORK COVERAGE OUT-OF-NETWORK COVERAGE
 COVENTRY HEALTH AND LIFE INSURANCE COMPANY 3838 N. Causeway Blvd. Suite 3350 Metairie, LA 70002 1-800-341-6613 SCHEDULE OF BENEFITS BENEFITS AND PRIOR AUTHORIZATION REQUIREMENTS ARE SET FORTH IN ARTICLES
COVENTRY HEALTH AND LIFE INSURANCE COMPANY 3838 N. Causeway Blvd. Suite 3350 Metairie, LA 70002 1-800-341-6613 SCHEDULE OF BENEFITS BENEFITS AND PRIOR AUTHORIZATION REQUIREMENTS ARE SET FORTH IN ARTICLES
IL Small Group PPO Aetna Life Insurance Company Plan Effective Date: 04/01/2009 PLAN DESIGN AND BENEFITS- PPO HSA HDHP $2,500 100/80 (04/09)
 PLAN FEATURES OUT-OF- Deductible (per calendar ) $2,500 Individual $5,000 Individual $5,000 Family $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable.
PLAN FEATURES OUT-OF- Deductible (per calendar ) $2,500 Individual $5,000 Individual $5,000 Family $10,000 Family Unless otherwise indicated, the Deductible must be met prior to benefits being payable.
Your Plan: Anthem Silver HMO 1500/30%/6550 Your Network: California Care HMO
 Your Plan: Anthem Silver HMO 1500/30%/6550 Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does
Your Plan: Anthem Silver HMO 1500/30%/6550 Your Network: California Care HMO This summary of benefits is a brief outline of coverage, designed to help you with the selection process. This summary does
StudentBlue University of Nebraska
 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: PPO What is the overall deductible? This is only a summary. If you want more details about
Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual/Family Plan Type: PPO What is the overall deductible? This is only a summary. If you want more details about
!"#$%$&!"'()*+,-".-,/ &01*+("12"31+4156"$,+0"!*7("819".5(<(/4*<("&,5( :(()";(,-40"&,5( !"#$%$&!",/)"'()*+,5(
 submitted anytime during the year to your institution HR/Benefits Office, and the tobacco premium will be waived beginning the first of the month following submission of the form. Important: A member is
submitted anytime during the year to your institution HR/Benefits Office, and the tobacco premium will be waived beginning the first of the month following submission of the form. Important: A member is
MCPHS University Health Insurance Program Information
 MCPHS University Health Insurance Program Information Beginning September 1, 2014 Health Services MCPHS University students on the Boston campus have access to the Massachusetts College of Art and Design
MCPHS University Health Insurance Program Information Beginning September 1, 2014 Health Services MCPHS University students on the Boston campus have access to the Massachusetts College of Art and Design
Important Questions Answers Why this Matters:
 BridgeSpan Health Company: Exchange Silver Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Eligible
BridgeSpan Health Company: Exchange Silver Coverage Period: Beginning on or after 01/01/2014 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual & Eligible
Plans. Who is eligible to enroll in the Plan? Blue Care Network (BCN) Health Alliance Plan (HAP) Health Plus. McLaren Health Plan
 Who is eligible to enroll in the Plan? All State of Michigan Employees who reside in the coverage area determined by zip code. All State of Michigan Employees who reside in the coverage area determined
Who is eligible to enroll in the Plan? All State of Michigan Employees who reside in the coverage area determined by zip code. All State of Michigan Employees who reside in the coverage area determined
Important Questions Answers Why this Matters:
 This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the Summary Plan Description (SPD) or Plan Document at www.pebtf.org or by calling 1-800-522-7279.
This is only a summary. If you want more detail about your coverage and costs, you can get the complete terms in the Summary Plan Description (SPD) or Plan Document at www.pebtf.org or by calling 1-800-522-7279.
How To Pay For Health Care With A Health Care Plan With A Premium Rate Of $1,000 A Year
 Regence BlueCross BlueShield of Utah: Regence Direct Silver HSA Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual &
Regence BlueCross BlueShield of Utah: Regence Direct Silver HSA Coverage Period: 01/01/2015-12/31/2015 Summary of Benefits and Coverage: What this Plan Covers & What it Costs Coverage for: Individual &
