Guidelines for Management of Joint Hypermobility Syndrome in Children and Young People.
|
|
|
- Margaret Payne
- 8 years ago
- Views:
Transcription
1 The British Society for Paediatric and Adolescent Rheumatology Guidelines for Management of Joint Hypermobility Syndrome in Children and Young People. A Guide for professionals managing young people with this condition These guidelines have been compiled by the Allied Health Professionals Group of the British Society for Paediatric and Adolescent Rheumatology (BSPAR, 2012). In order to cover the complexities of this condition some aspects of management have been divided into different professions, however there will be significant overlap as to who provides the intervention depending upon local teams. Introduction These guidelines are designed to help and support therapists working with children and young people with Joint Hypermobility and musculoskeletal pain. Objectives 1. To facilitate the development of specialised, expert consensus opinioned and holistic management programmes for children and young people with Joint Hypermobility Syndrome (JHS), using a bio psychosocial model which acknowledges the global impact of the condition. 2. To optimise the standard of care of children and young people with JHS by empowering them, their carers and other health professionals through the provision of treatment, education, information and support. 3. To enable children, young people and their parents to be active participants in their selfmanagement. 4. To ensure efficient, cost effective and evidence-based therapy management for children and young people with JHS. These guidelines will be reviewed in 2015 by the BSPAR AHP group. Page 1 of 16
2 Contents: Assessment a. Introduction b. Subjective Assessment I. Presenting Problems and Common Symptoms II. Pain and Fatigue III. Additional but rare symptomatology c. Objective Assessment Management I. Self-management II. Pain Management III. Physiotherapy IV. Occupational therapy V. Podiatry VI. Clinical Psychology VII. Pacing VIII. School/Education IX. Activity and Sport X. Sleep management XI. Weight management XII. Mood and Motivation XIII. Equipment i. Autonomic dysfunction The British Society for Paediatric and Adolescent Rheumatology 1. Gastrointestinal and urinary tract symptoms 2. Cardiovascular autonomic dysfunction ii. Other cardiac features Concerning symptoms and behaviours References a. Orthostatic hypotension b. Orthostatic intolerance c. Postural orthostatic tachycardia syndrome (POTS) Page 2 of 16
3 The British Society for Paediatric and Adolescent Rheumatology Therapy Management Guidelines Assessment a. Introduction Hypermobile joints are common in the general population and many individuals with hypermobility do not experience any significant difficulties. In fact in many situations (i.e. sportspeople, dancers etc.) hypermobility can have positive advantages. However some people experience difficulties and symptoms which are understood to be related to being hypermobile; commonly known as Joint Hypermobility syndrome (JHS) or Ehlers-Danlos syndrome Type III (Hypermobile EDS). It is sometimes unhelpful for a young person to have the label of EDS III because the significant risks associated with the other forms of EDS can mistakenly be assumed to also apply to this group. For this reason, the preferred term to use is Joint Hypermobility Syndrome (JHS). Assessing and managing this condition in children and young people requires specialist knowledge since for all the extra-articular symptoms including abdominal involvement, headaches, fatigue etc. there is a normal variance in the population. Care must be taken to ensure that appropriate importance is placed upon each symptom and the condition is not over-medicalised. In general hypermobility should be regarded as a connective tissue advantage providing the child is strong and fit, difficulties occur mainly when the body has become weak and deconditioned. Signs and Symptoms There can be considerable variability in the severity of JHS, even within the same family. The main features are: joint hypermobility associated with muscle and joint pains and some level of fatigue. Easy bruising and clicking of joints are common symptoms which should not cause concern. Much less commonly young people may have problems with abdominal pain with or without some levels of bladder and bowel dysfunction and even rarer, postural orthostatic tachycardia syndrome (POTS), hernia, uterine or rectal prolapse and joint dislocation (though subluxation is slightly more common). There may also be an overlap with Developmental Co-ordination Disorder (DCD) and it may be difficult to differentiate between the symptomatic aspects of both without considering the criteria/definitions within the latest DSM assessment; however JHS is not life threatening and much benefit can be achieved from proactive and positive self-management with the goal being full participation in all activities. Aims JHS is often under recognised, not well understood and poorly managed. These guidelines are to provide further information for health professionals involved in the management of children and young people diagnosed with JHS. Patients have often been seen by a number of health professionals before a diagnosis is reached and families frequently report feeling that they haven t been listened to. Therefore, an important part of management is to listen to the family s concerns and deal with the expectations of both patients and parents. The aims of treatment for JHS are to improve current symptoms, as well as avoiding future complications. Widespread and longstanding pain can result in a downward spiral of general physical Page 3 of 16
4 The British Society for Paediatric and Adolescent Rheumatology deconditioning, pain and fatigue. A multi-systemic approach is needed to deal with the variable symptoms that can present. Each person with JHS is affected differently and so has varying management needs. It is important to work together with patients and families to develop an appropriate individual management plan. It is also helpful to establish realistic expectations along the way. Management of JHS requires professionals, young people and their families to work together towards clearly defined and shared goals. The overall aim of any intervention is for the patient to gain a full understanding of hypermobility and the skills and knowledge to manage the condition themselves. The longer-term outlook for young people with JHS is very positive and with the correct management all young people should be able to participate in all activities they want to without ongoing professional support. Most treatment centres would usually provide advice/orthotics/selfmanagement programmes and would have limited resources for unlimited on-going treatment. These guidelines outline the main issues that may need to be considered when developing an individualised management plan. b. Subjective Assessment: The subjective assessment of a child or young person with JHS should include a clear and comprehensive history covering the following areas: Presenting Problems Past Medical History Drug History Social and Family History Mental health and well being Ethnic and cultural concerns Benefits Participation in Activities of Daily Living (ADL) including self-care, leisure and sleep Impact on learning and participation in school activities Career planning / development What information has been given? Level of understanding of problems Occupational / Physiotherapy / Other Professionals Page 4 of 16
5 I. Presenting problems and Common Symptoms: The British Society for Paediatric and Adolescent Rheumatology Joint and/or muscle aches and pains o Often occurring after activity or during the night more often lower limb than upper. Muscle and joint stiffness o Usually after exercise or increased activity, may occur for a few days after increased activity. Fatigue o o o Often associated with reduced walking distance and reduced exercise tolerance and /or difficulties attending fulltime education due to tiredness. This symptom is commonly linked to level of deconditioning of the child. Poor sleep will also impact upon fatigue levels. Fidgetiness, difficulty sitting still and poor organisation of movement etc Headaches o This is often related to muscle spasm of the Trapezius muscles. Poor sleep Easy bruising o This is benign and not of concern. Clicking joints o Joints can click spontaneously or be clicked deliberately, both are fine and can be performed safely many times a day. This only becomes a concern if it becomes habitual and obsessive impacting on QOL. Reduced co-ordination and balance o Poor proprioception leading to clumsiness and reduced balance. o Poor core stability leading to difficulties such as hand writing challenges and other issues with fine motor control. o Reduced fine motor control especially involving small grip function. o If these symptoms do not improve with improvement of strength and gross motor skills and have significant impact upon ADL s and are significantly below what is expected for chronological age and intelligence level an assessment for a Developmental Co-ordination Disorder (DCD) may be advisable. Response to local anaesthetic o There is very little evidence to support this concern, however it has been reported that some people with JHS may have a reduced effect of a local anaesthetic. Abdominal pain o This is common in childhood generally and the incidence may be slightly higher in children who are hypermobile. o Constipation is a common cause of abdominal pain. It is also important to remember that many of these symptoms have normal variants in the general population and care must be taken to ensure that there is a balance between medical investigation and effective symptom management. Page 5 of 16
6 The British Society for Paediatric and Adolescent Rheumatology II. Pain and Fatigue We usually understand pain to be a warning about damage to the body. When this is the case a reasonable response to the pain would be to withdraw or avoid activity. However in JHS pain is an indication that the body is not strong enough to do the task and that it requires strengthening. This means that the young person will need to keep engaging in everyday activities and exercise, not do less. Similarly fatigue is not necessarily an indication that more rest is required. Rather, it may signal that the body requires more fitness training, pacing of activities and better sleep hygiene. It is also important to recognise that normal sleep patterns change throughout childhood into adolescence and then into adulthood. It is important to consider this when assessing fatigue levels and abnormal sleeping patterns. Gradually pacing up activity levels and exercise is the most effective cure for fatigue during the day and often when there is a slump in energy levels a small snack and a brisk walk or other type of exercise will often rejuvenate the body in order to continue with the day s activities. III. Additional but rare Symptomatology: i. Autonomic dysfunction Some children with JHS have been found to have an increased frequency of problems relating to the autonomic nervous system. Symptoms of autonomic dysfunction can occur at any age. 1. Gastrointestinal and urinary tract symptoms Children and young people with JHS may have unspecific gastrointestinal symptoms, such as nausea, stomach ache, diarrhoea and constipation. Faecal and urinary incontinence can also be a feature of the condition. However these symptoms are also very common in children generally and may not be related to their hypermobility. In very rare cases a disease called eosinophilic collitis may be present. This is a condition that can cause constipation and difficulty maintaining a healthy weight and is often linked to food intolerances; however this condition can be well controlled with the guidance of a specialist gastroenterologist. Routine treatment of paediatric constipation is extremely effective with these symptoms. Advice about toilet habits can also be useful; such as having a stool to rest their feet on in front of the toilet to help optimise the position of the pelvis and enable effective bowel opening. If appropriate, arrange assessment of medical management of bowel symptoms through a paediatric gastroenterologist. Refer children or adolescents with significant urological problems for specialist assessment. Page 6 of 16
7 2. Cardiovascular autonomic dysfunction The British Society for Paediatric and Adolescent Rheumatology Patients with JHS may describe symptoms of cardiovascular autonomic dysfunction, which affects heart rate, blood pressure and blood flow. Again, these symptoms are very common throughout the general population especially during adolescence. a. Orthostatic hypotension A fall in blood pressure upon standing causes symptoms such as; venous pooling, dizziness, light headedness and syncope. b. Orthostatic intolerance Symptoms appear after periods of standing and can include; fatigue, light headedness, hyperventilation, sweating, paleness, anxiety, and acrocyanosis. c. Postural orthostatic tachycardia syndrome (POTS) POTS is characterised by a rapid rise in heart rate on standing (30 beats per minute above lying down heart rate). A common age of onset for POTS symptoms is during adolescence. Symptoms of POTS can include: Light-headedness and dizziness particularly on standing Fainting Heart palpitations or a racing heart beat Non -specific fatigue Diagnosis of POTS is not easy and though it is often done by performing a tilt table test (or standing and lying heart rate if tilt table unavailable) this not validated in children and adolescents so the results of the tilt table test have to be interpreted carefully. Treatment for POTS is available and usually involves simple measures such as increased fluid and salt intake. Exercise has been shown to be the most effective management for this aspect of JHS and medication should be used very carefully. ii. Those with severe symptoms of cardiac autonomic dysfunction should be referred to a specialist clinic, such as a POTS clinic, or a Cardiologist with a specialist interest in syncope and arrhythmias. Other cardiac features Increased aortic root size and mitral valve prolapse had been reported to be more common in patients with JHS, but current evidence suggests they are usually of little clinical consequence and is extremely rare. It is important to be careful not to alarm the child and their family and so referral for assessment of this should be carefully considered as increased anxiety about this condition is not helpful for the child. An echocardiogram may be recommended as a baseline assessment in extreme situations. Page 7 of 16
8 The British Society for Paediatric and Adolescent Rheumatology Objective Assessment: I. General wellbeing a. Patient VAS. A visual analogue scale for the perceived level of general wellbeing at the present time completed by the child if old enough. b. Parent VAS. II. Baseline measurements: a. Height /weight /centiles / blood pressure b. Pain (VAS may be used) c. Fatigue (VAS may be used) III. Joint range of movement a. Knowledge of where hypermobility is present is usually most effective in designing a management programme. b. Beighton Scale may be useful. IV. Muscle length a. Awareness of muscles that move over 2 joints may become tight despite generalised Hypermobility. V. Muscle strength a. A basic assessment of muscle strength is vital. Often scoring using the Kendal Scale (0-10) provided a score that easily monitors change over time. b. Specific muscles should always be assessed including: i. Inner Range Quads (Straight Leg Raise without a quadriceps lag) ii. Hip abductors specifically Gluteus Medius iii. Hip Extensors specifically Gluteus Maximus iv. Plantar Flexors v. Core central Stability VI. Posture and Gait a. Both should be assessed especially with the view to prescribe orthotics. VII. Stamina a. 6 min walk test may be useful. b. Subjective reporting of distance and time walked is also effective. VIII. Function a. The CHAQ may often demonstrate how significantly independent function is affected by this condition. (CHAQ is not formally validated for JHS). b. An objective assessment of occupational performance including self-care, leisure and activities at school such as handwriting, dextrous manipulation, activity organisation, dressing etc. Page 8 of 16
9 The Multi-Disciplinary Team: The British Society for Paediatric and Adolescent Rheumatology Management of JHS As some young people with JHS can present with a wide variety of difficulties, they may need to be seen by a number of different professionals who must ensure that they communicate with each other in order to provide a cohesive management programme. A thorough MDT assessment will help determine the most appropriate individualised treatment plan. I. Self management It is helpful for families to understand JHS and that this is a non life threatening condition and in many instances hypermobility can be advantageous. The aim for young people and their families is for them to develop the skills and knowledge in order to manage the symptoms and participate in all activities. For the best chance of success parents and adolescents should be fully involved in the treatment plan and age appropriate language must be used with children. People with JHS do benefit from maintaining a healthy everyday life. A well balanced diet, regular gentle exercise, full participation in school and activities as well as quality sleep all play their part. Children and adolescents may benefit from advice on best technique for carrying out tasks of daily living, to avoid placing unnecessary strain on their joints and minimising pain. Often encouragement is needed to include appropriate exercise into their daily routines. It is well recognised that significant periods of inactivity greatly exacerbate symptoms of JHS. A good understanding of pacing activities needs to be developed by children and adolescents with JHS in order to avoiding the boom and bust cycle (over exertion leading to pain and fatigue). As children and adolescents grow up, gaining an understanding themselves about JHS will help them develop the motivation needed to manage their condition and develop a healthy lifestyle incorporating regular exercise. II. Pain Management / Education Recognition and management of chronic pain is an important part of management for children with JHS. Pain can affect concentration, memory, mood and sleeping. If appropriate a referral to a unit that is confident with the management of chronic pain in children may be helpful as chronic pain is most effectively managed with a combination of physical and psychological techniques. Pain medications are often ineffective and the side effects should be carefully considered. Pain management interventions can be provided by physiotherapists, occupational therapists and psychologists depending upon the local service provision. The aim of pain management is to increase quality of life. Therefore patient-led goals will be an important part of boosting motivation to engage in the self-management programme. Fear of the unknown can be a big source of anxiety for both the young person and their family, so education and addressing the personal beliefs can be helpful in reducing such fears. Cognitive restructuring can help to recognise unhelpful behaviours, such as excessive rest, and establish new patterns of reasoning. It is important to identify any catastrophising and avoidance behaviours and to recognise their role in the fear cycle. Page 9 of 16
10 The British Society for Paediatric and Adolescent Rheumatology For children and young people with JHS it is helpful to consider their relationships with others. Parents can be hugely disempowered if their child is experiencing pain. It is therefore important to help parents to develop strategies that they can use to ensure they promote positive rather than unhelpful patterns of behaviour for their child. It is helpful to establish realistic expectations. There will be times of increased pain, for example after a lot of sport or injury and a management plan for dealing with these times should be discussed. It is really important to ensure that at these times rest is not promoted for long periods of time. In general, medical approaches to pain management are not thought to be particularly beneficial for JHS, with patients reporting that analgesics have limited effect and there is the disadvantage of side effects that come with certain medicines. COMFORT TOOL BOX: it is useful for the child and family to develop their own collection of activities and interventions that can be used to reduce the pain. These can be items that facilitate distraction as well as positive coping statements, relaxation scripts, aromatherapy oils, exercises, physical activities comforting objects and pictures etc. This may be a real box full of these things or a virtual box that have been created between the young person and their family. III. Physiotherapy A lifelong commitment to exercise is needed for all patients with JHS. Physiotherapy can help to promote this from a young age using specific exercises and encouraging activities that can be incorporated into daily life and, most importantly, be enjoyed! The plan: The goal: Restore and maintain full muscle strength and function throughout the full range of movement. Restore effective and efficient movement patterns. Improve general fitness. Restore normal range of movement, including into hypermobile range. Provide education, reassurance, advice, pain management and develop problem solving. Self-management. Patients with JHS often experience pain. Left unresolved, this may lead to fear of movement and decreased activity, resulting in muscle deconditioning. Core and specific muscular strength is vital for patients with JHS to help minimise pain, maintain good posture and reduce joint instability. Activities to maintain strength and stamina are vital for managing this condition. However, patients with JHS tend to have a poor tolerance of static, repetitive or excessive activity, often resulting in pain and fatigue the following day. This is due to having specific muscle imbalances resulting in delayed onset muscle pain (DOMS) and joint discomfort. This can cause worries about aggravating symptoms and result in a reluctance to exercise. However DOMS is a completely normal response to an increased level of exercise and is not an indication of damage. Page 10 of 16
11 The British Society for Paediatric and Adolescent Rheumatology Patients with JHS may have reduced proprioception, making it harder for them to carry out exercises correctly on their own. Incorrect positioning may result in exercises being ineffectual or damaging. Children with JHS are often hypersensitive and become more aware of the pain sensations and so this should be taken into consideration when using massage or manual treatment techniques. The physiotherapy will be most effective if targeted to the specific areas of difficulty the young person is experiencing. This may be a specific muscle weakness or a specific function that is difficult. Often a specific exercise programme will ensure that the muscles can protect the hypermobile joints enabling full inclusion in all activities. In order to engage children and young people, physical therapy should aim to be specific, effective, time efficient and if possible FUN! Consider the patient s goals and what will be achievable. Normal activities Encourage normal activities and a return to sport, providing individual advice on specific elements of activities as appropriate. Specific exercise programme The most effective exercise programme for the management of hypermobility will be a progressive resisted exercise programme that targets the specific muscles that are weak and that are required to control the joints into their hypermobile range. If the muscles are completely effective then posture and function will improve. The use of open chained exercises, non-weightbearing which build on the principal of high repetitions and low weights has been shown to be very effective. These exercises can be started at a very early age. Advise on postural alignment Good postural alignment protects supporting structures against injury, enables muscles to function most efficiently and provides optimum positions for thoracic and abdominal organs. Core Strengthening Exercises to build core strength, muscular strength and endurance improve stability, balance and coordination. Incorporate functional and everyday activities. Try balance boards, wobble cushions and gymnastic balls as well as specific exercises. Stretching Stretching can be used to maintain muscle length, joint range and to stretch out old injuries or muscle spasms. Stretching should not be to increase an already hypermobile range. Joint Subluxations Repeated self-subluxation of joints should be avoided, however resting in unusual postures i.e. W sitting is fine as this is in their normal range of movement. Goal setting Realistic goal setting (both short and long term) can help patients in making progress. Proprioception training Exercises to enhance proprioception can include the use of mirrors, bio feedback and balance boards may also be effective as well as the strengthening exercises. Programmes to enhance proprioception have been proven to show good results. Page 11 of 16
12 Sport specific assessment The British Society for Paediatric and Adolescent Rheumatology Assessment of swimming and other sports techniques may be helpful to enable to young person to participate fully. IV. Occupational Therapy Occupational therapists can assess a child s performance in a range of daily activities. This may be done in a clinic setting, in the home or school environment. Assessment will be holistic and will consider the child s skills, their motivation and their daily routine, as well as their environment. Comprehensive assessment will allow the OT to identify barriers to occupational performance and the design the most appropriate intervention. This may include building skills; suggesting strategies, educating the young person and others in order to enable independence in daily activities. Those with JHS have greater difficulty building up muscle strength and endurance and most will be familiar with the boom and bust cycle associated with overuse. Pain will often after activity which may lead to children avoiding particular activities which may have a marked impact on their selfconfidence and self esteem Pacing Pacing which refers to a systematic graded approach to participation in activity, along with energy conservation is vital so that young people learn to use their energy for the activities they need and want to do. An activity diary will shed light on the current level and pattern of activity. From this, an activity baseline which is easily manageable with minimal effort can be set. Over time the level of activity should be increased until they have enough stamina and coping strategies to manage all activities. Daily occupations Assessment of participation in daily activities will be important. Interventions are likely to include both physical and psycho social strategies. The chief focus should be on building skills and resilience. Rarely would assistive devices (such as splints) as a compensatory approach prove beneficial in the longer term. Simple adaptations such as pen grips may be very effective and there are a large variety of different styles and shapes of pen and pencil which can be found that will enable writing to be more efficient. Home, school and leisure should all be considered and close liaison with the school would be important to ensure the most appropriate support is provided in a school environment. Sleep and relaxation For those experiencing difficulties with sleep, sleep hygiene advice may be useful. A careful assessment of sleep patterns will be helpful in targeting other interventions such as distraction, stress management and relaxation techniques. Pain management The OT profession is founded on the principal that there is a direct link between activity, health and well-being, they are therefore well placed to also help the young person explore the inter relation between physical symptoms, feelings/emotions and activity and offer appropriate advice or intervention. Page 12 of 16
13 Self confidence The British Society for Paediatric and Adolescent Rheumatology In some instances pain and difficulty engaging in a full range of every -day activities may have impacted on a child/young person s self-esteem and motivation level. OT s will promote meaningful activities aimed at increasing this to ensure satisfactory participation in daily life. Splinting Splinting is generally avoided due to the risk of deconditioning, but occasionally for the hypermobile MCP of the writing hand a splint is useful to prevent the hyperextension therefore aiding writing, reducing pain and fatigue. V. Podiatry Podiatrists provide advice on suitable foot wear. Slip-on shoes should be avoided and supportive boots/ shoes that are purchased from appropriate shoe shops may be considered for children with weak ankles. Often boots with laces or high-top trainers are appropriate and comfortable footwear. Orthotics may be prescribed for those with flat feet where the positioning and function of the feet may contribute to symptoms. VI. Clinical Psychology Clinical psychology may be required to ensure that JHS does not prevent the young person fully participating in life. Psychology input may focus upon pain management skills and techniques or on thoughts, feelings and behaviours in response to symptoms. Cognitive behaviour therapy (CBT) may be useful in modifying unhelpful beliefs and behaviours, though many other approaches may also be utilised. If the young person is experiencing low mood and/or anxiety these may negatively impact upon their symptoms and their ability to self-manage. A clinical psychologist would be able to work with the young person and their family in order to help modify these feelings so that they are able to regain control of the symptoms and their life. VII. Pacing It is important for all young people with JHS to balance periods or activity and rest in order to maximise their ability to achieve physically, emotionally and intellectually. A good understanding of pacing can help avoid the boom and bust cycle (over exertion leading to pain and fatigue and consequent under-activity). It is also important to recognise that initially the balance between rest and exercise/activity may have more time spent resting but the goal will be to increase the activity levels and reduce the rest until the balance is tipped back to normal activity levels during the day and the majority of rest gained at night. Once a young person has recovered to this level, pacing can be reduced and in many cases stopped altogether as the young person is able to engage in everyday activities, including full time school, without an increase in symptoms. VIII. School/Education Children and young people with JHS need to be able to engage in regular education just like any other child. From time to time they may need extra support to achieve their best in school, and some minor modifications may be appropriate. Page 13 of 16
14 The British Society for Paediatric and Adolescent Rheumatology Guidance from health professionals working with the individual may help school staff understand the impact the child s condition. Most pupils do not like to feel different. It is important for emotional well-being to enable pupils with JHS to be included as much as possible in school activities, but with appropriate modifications. An OT assessment within school may be beneficial. Suitable sporting activities should be encouraged, with advice on the suitability of high impact activities and allowances made for reduced stamina. Appropriate seating may help with posture and comfort in the classroom and movement can help avoid discomfort and pain. It is often helpful to ensure that the child does not stay still for extended periods of time. For example asking the child to do small tasks that require getting up and walking about may prevent discomfort without disrupting the class. Pupils with JHS may need extra time to move between classes and travel around the school. For pupils with increased pain leaving classes early maybe helpful. After an OT assessment it may be appropriate to recommend that extra time is given during exams and that the use of typing the exam may help as well. Urinary urgency and bowel problems may be part of JHS so access to toilets should not be restricted. Storage may be helpful for books and bags so they don t have to be carried around school all day. A Hypermobility guide for schools booklet is available from the Hypermobility Syndrome Association (HMSA). IX. Activity and Sport Physical activity should be actively encouraged for all young people with JHS. However it is extremely important that the child is fit enough to engage in the sport they wish to do. If this is not the case, young people may need to gradually build up their strength and stamina before engaging in the new activity. Often the physiotherapy programme can be used to ensure that every muscle can do its job effectively. There are some sports that will need more preparation for than others such as contact sports. Care, however needs to be taken when considering trampolining and bouncy castles as these activities put significant stress on the joints and often involve several children at a time which can increase the risk of injury. With the correct preparation any sport can be considered. However in childhood it is often better to enjoy a variety of sports throughout the week rather than focus on just one. X. Sleep management Children and young people with JHS often describe poor and disturbed sleep which may be a result of pain or poor pacing skills resulting in too much rest during the day making it difficult to get to sleep at night. Parents can help to ensure routine and good sleep hygiene. Relaxation techniques may also help promote sleep. Additional professional advice is available if needed. Page 14 of 16
15 XI. Weight Management The British Society for Paediatric and Adolescent Rheumatology Maintaining optimum body weight is important. Extra weight can put significant strain on the joints and increase the symptoms of pain and fatigue. Advice may be provided about healthy diets and this may also help in the management of constipation. It is equally important not to become underweight as this can make maintaining adequate muscle strength difficult. In this instance, it may not be safe to engage in an intensive exercise programme until the young person is at a healthy weight. Weight should be monitored during any intervention. XII. Mood and Motivation Understandably, experiencing any of the symptoms described above can have a negative impact on mood, which can reduce the person s ability to engage in everyday activities and the recommended management programme. Lack of activity and participation, in turn can further exacerbate the symptoms. Low mood and anxiety are commonly experienced by people stuck in such a negative cycle and they may start to avoid activities such as a result of a fear of causing more pain and /or fatigue. A thorough MDT assessment will help to identify individuals/families that may benefit from further support in managing emotional distress associated with chronic symptoms. XIII. Equipment The general principal is that special equipment is not required. There should never be the provision of a wheelchair for a young person with JHS as this is very damaging to the requirement of maintaining full strength and function. Crutches can be equally unhelpful and should also be avoided in the management of JHS. The general philosophy applies to the provision of equipment in that the most effective solution to a physical challenge is to find a way to get stronger and fitter so that it can be done with minimum adaptations. Concerning Symptoms Unfortunately for some families the philosophy of self-management and maintaining strength and full independent function is very challenging and their fear of the pain and symptoms may be such that they find following the advice of the Professionals very difficult. These families may need more time and interventions in order to help them understand the condition and the real meaning of the pain messages and it may be that for these families the psychological input, in order to help them modify their beliefs, may be the first treatment required. At this time a Multidisciplinary assessment including a level 3 Child Protection trained Paediatric Rheumatologist or Paediatrician and a Psychologist would be appropriate.. Page 15 of 16
16 Peer Support The British Society for Paediatric and Adolescent Rheumatology Therapists should also ensure that families are aware of organisations, which may be able to offer emotional, financial and practical support. A number of organisations that provide such help are listed below. Resources include handbooks, newsletters, and family holidays. Hypermobility Association HMSA Phone: Web: The Hypermobility Syndrome Association 49 Orchard Crescent Oreston Plymouth PL9 7N Key / Audit points: Self management of the symptoms is vital for the long-term effective management of JHS in children and young people. This may include a specific exercise regime and active participation in non-pharmacological pain management techniques to ensure full participation in all activities. Pain management and education is an important role of any Allied Health Professional involved in the care of a child or young person with JHS. Liaison with school is an important role of the AHP in the care of young people with JHS. References The following texts were used as reference and may be helpful for further reading: Brad T. Tinkle, MD, PHD (2008). Issues and Management of Joint Hypermobility. A Guide for the Ehlers-Danlos Hypermobility Type and the Hypermobility Syndrome. Left Paw Press 2008 Rosemary Keer & Rodney Grahame (2003). Hypermobility Syndrome: Recognition and Management for Physiotherapists. Butterworth Heinemann Acknowledgements: Multi-disciplinary team members of the British Society for Paediatric and Adolescent Rheumatology. Produced by: Sue Maillard, Catherine Stott and Sue Kemp Issue number 1.1, Jan 2013 Ratified by BSPAR Executive Committee: To be reviewed 2015 Page 16 of 16
15 things you might not know about back pain
 15 things you might not know about back pain Mary O Keeffe (University of Limerick), Dr Kieran O Sullivan (University of Limerick), Dr Derek Griffin (Tralee Physiotherapy Clinic) Managing back pain costs
15 things you might not know about back pain Mary O Keeffe (University of Limerick), Dr Kieran O Sullivan (University of Limerick), Dr Derek Griffin (Tralee Physiotherapy Clinic) Managing back pain costs
National Hospital for Neurology and Neurosurgery. Managing Spasticity. Spasticity Service
 National Hospital for Neurology and Neurosurgery Managing Spasticity Spasticity Service If you would like this document in another language or format, or require the services of an interpreter please contact
National Hospital for Neurology and Neurosurgery Managing Spasticity Spasticity Service If you would like this document in another language or format, or require the services of an interpreter please contact
he American Physical Therapy Association would like to share a secret with you. It can help you do more with less effort breathe easier feel great.
 The Secret... T he American Physical Therapy Association would like to share a secret with you. It can help you do more with less effort breathe easier feel great. The secret is about good posture, which
The Secret... T he American Physical Therapy Association would like to share a secret with you. It can help you do more with less effort breathe easier feel great. The secret is about good posture, which
Fainting - Syncope. This reference summary explains fainting. It discusses the causes and treatment options for the condition.
 Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Fainting - Syncope Introduction Fainting, also known as syncope, is a temporary loss of consciousness. It is caused by a drop in blood flow to the brain. You may feel dizzy, lightheaded or nauseous before
Fact Sheet. Queensland Spinal Cord Injuries Service. Pain Management Following Spinal Cord Injury for Health Professionals
 Pain Management Following Injury for Health Professionals and Introduction Pain is a common problem following SCI. In the case where a person with SCI does have pain, there are treatments available that
Pain Management Following Injury for Health Professionals and Introduction Pain is a common problem following SCI. In the case where a person with SCI does have pain, there are treatments available that
Therapeutic Canine Massage
 Meet our Certified Canine Massage Therapist, Stevi Quick After years of competitive grooming and handling several breeds in conformation, I became interested in training and competing with my dogs in the
Meet our Certified Canine Massage Therapist, Stevi Quick After years of competitive grooming and handling several breeds in conformation, I became interested in training and competing with my dogs in the
Stem cell transplant, you and your rehabilitation Information for patients and their carers
 Oxford University Hospitals NHS Trust Physiotherapy department Stem cell transplant, you and your rehabilitation Information for patients and their carers Stem cell transplant exercise handout Thank you
Oxford University Hospitals NHS Trust Physiotherapy department Stem cell transplant, you and your rehabilitation Information for patients and their carers Stem cell transplant exercise handout Thank you
By Agnes Tan (PT) I-Sports Rehab Centre Island Hospital
 By Agnes Tan (PT) I-Sports Rehab Centre Island Hospital Physiotherapy Provides aids to people Deals with abrasion and dysfunction (muscles, joints, bones) To control and repair maximum movement potentials
By Agnes Tan (PT) I-Sports Rehab Centre Island Hospital Physiotherapy Provides aids to people Deals with abrasion and dysfunction (muscles, joints, bones) To control and repair maximum movement potentials
Registered Charity No. 5365
 THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: mscontact@ms-society.ie www.ms-society.ie
THE MULTIPLE SCLEROSIS SOCIETY OF IRELAND Dartmouth House, Grand Parade, Dublin 6. Telephone: (01) 269 4599. Fax: (01) 269 3746 MS Helpline: 1850 233 233 E-mail: mscontact@ms-society.ie www.ms-society.ie
12. Physical Therapy (PT)
 1 2. P H Y S I C A L T H E R A P Y ( P T ) 12. Physical Therapy (PT) Clinical presentation Interventions Precautions Activity guidelines Swimming Generally, physical therapy (PT) promotes health with a
1 2. P H Y S I C A L T H E R A P Y ( P T ) 12. Physical Therapy (PT) Clinical presentation Interventions Precautions Activity guidelines Swimming Generally, physical therapy (PT) promotes health with a
ACL Reconstruction Rehabilitation Program
 ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
ACL Reconstruction Rehabilitation Program 1. Introduction to Rehabilitation 2. The Keys to Successful Rehabilitation 3. Stage 1 (to the end of week 1) 4. Stage 2 (to the end of week 2) 5. Stage 3 (to the
How to treat your injured neck
 How to treat your injured neck Exceptional healthcare, personally delivered Your neck is made up of a number of bones bound together by strong discs and ligaments. It is also protected by strong muscles.
How to treat your injured neck Exceptional healthcare, personally delivered Your neck is made up of a number of bones bound together by strong discs and ligaments. It is also protected by strong muscles.
Exercise Principles and Guidelines for Persons with Cerebral Palsy and Neuromuscular Disorders
 Exercise Principles and Guidelines for Persons with Cerebral Palsy and Neuromuscular Disorders INTRODUCTION: Health and well being are the result of many factors: Physical activity is one of these factors.
Exercise Principles and Guidelines for Persons with Cerebral Palsy and Neuromuscular Disorders INTRODUCTION: Health and well being are the result of many factors: Physical activity is one of these factors.
Clinical Care Program
 Clinical Care Program Therapy for the Cardiac Patient What s CHF? Not a kind of heart disease o Heart disease is called cardiomyopathy o Heart failure occurs when the heart can t pump enough blood to meet
Clinical Care Program Therapy for the Cardiac Patient What s CHF? Not a kind of heart disease o Heart disease is called cardiomyopathy o Heart failure occurs when the heart can t pump enough blood to meet
PLANTAR FASCITIS (Heel Spur Syndrome)
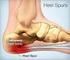 PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
PLANTAR FASCITIS (Heel Spur Syndrome) R. Amadeus Mason MD Description Plantar fascitis is characterized by stiffness and inflammation of the main fascia (fibrous connective [ligament-like] tissue) on the
Who We Serve Adults with severe and persistent mental illnesses such as schizophrenia, bipolar disorder and major depression.
 We Serve Adults with severe and persistent mental illnesses such as schizophrenia, bipolar disorder and major depression. We Do Provide a comprehensive individually tailored group treatment program in
We Serve Adults with severe and persistent mental illnesses such as schizophrenia, bipolar disorder and major depression. We Do Provide a comprehensive individually tailored group treatment program in
Injury Prevention for the Back and Neck
 Injury Prevention for the Back and Neck www.csmr.org We have created this brochure to provide you with information regarding: Common Causes of Back and Neck Injuries and Pain Tips for Avoiding Neck and
Injury Prevention for the Back and Neck www.csmr.org We have created this brochure to provide you with information regarding: Common Causes of Back and Neck Injuries and Pain Tips for Avoiding Neck and
INDEPENDENT MENTAL HEALTHCARE PROVIDER. Eating Disorders. Eating. Disorders. Information for Patients and their Families
 INDEPENDENT MENTAL HEALTHCARE PROVIDER Eating Disorders CARDINAL CLINIC Eating Disorders Information for Patients and their Families What are Eating Disorders? Eating Disorders are illnesses where there
INDEPENDENT MENTAL HEALTHCARE PROVIDER Eating Disorders CARDINAL CLINIC Eating Disorders Information for Patients and their Families What are Eating Disorders? Eating Disorders are illnesses where there
Document Author: Frances Hunt Date 03/03/2008. 1. Purpose of this document To standardise the treatment of whiplash associated disorder.
 Guideline Title: WHIPLASH ASSOCIATED DISORDER Document Author: Frances Hunt Date 03/03/2008 Ratified by: Frances Hunt, Head of Physiotherapy Date: 16.09.15 Review date: 16.09.17 Links to policies: All
Guideline Title: WHIPLASH ASSOCIATED DISORDER Document Author: Frances Hunt Date 03/03/2008 Ratified by: Frances Hunt, Head of Physiotherapy Date: 16.09.15 Review date: 16.09.17 Links to policies: All
COMMON OVERUSE INJURIES ATTRIBUTED TO CYCLING, AND WAYS TO MINIMIZE THESE INJURIES
 COMMON OVERUSE INJURIES ATTRIBUTED TO CYCLING, AND WAYS TO MINIMIZE THESE INJURIES Listed are a few of the most common overuse injuries associated with cycling long distances. 1. Cervical and upper back
COMMON OVERUSE INJURIES ATTRIBUTED TO CYCLING, AND WAYS TO MINIMIZE THESE INJURIES Listed are a few of the most common overuse injuries associated with cycling long distances. 1. Cervical and upper back
Fatigue Management in Neurology. Alison Nock MS Specialist Occupational Therapist
 Fatigue Management in Neurology Alison Nock MS Specialist Occupational Therapist Overview of Fatigue Common disabling symptom Some people rate fatigue as the worst symptom of their disease. Predominant
Fatigue Management in Neurology Alison Nock MS Specialist Occupational Therapist Overview of Fatigue Common disabling symptom Some people rate fatigue as the worst symptom of their disease. Predominant
Lumbar Disc Herniation/Bulge Protocol
 Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
Lumbar Disc Herniation/Bulge Protocol Anatomy and Biomechanics The lumbar spine is made up of 5 load transferring bones called vertebrae. They are stacked in a column with an intervertebral disc sandwiched
This is my information booklet: Introduction
 Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
Hip arthroscopy is a relatively new procedure which allows the surgeon to diagnose and treat hip disorders by providing a clear view of the inside of the hip with very small incisions. This is a more complicated
The type of cancer Your specific treatment Your pre training levels before diagnose (your current strength and fitness levels)
 Exercise and Breast Cancer: Things you can do! Cancer within the fire service is one of the most dangerous threats to our firefighter s health & wellness. According to the latest studies firefighters are
Exercise and Breast Cancer: Things you can do! Cancer within the fire service is one of the most dangerous threats to our firefighter s health & wellness. According to the latest studies firefighters are
Introduction. What is syncope?
 Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Syncope Introduction What is syncope? Syncope (SING-kuh-pee) is a medical term for fainting. When you faint, your brain is not receiving enough blood and oxygen, so you lose consciousness temporarily.
Rehabilitation Documentation and Proper Coding Guidelines
 Rehabilitation Documentation and Proper Coding Guidelines Purpose: 1) Develop a guide for doctors in South Dakota to follow when performing reviews on rehabilitation cases. 2) Provide doctors in South
Rehabilitation Documentation and Proper Coding Guidelines Purpose: 1) Develop a guide for doctors in South Dakota to follow when performing reviews on rehabilitation cases. 2) Provide doctors in South
Patient Information. and Physical Activity Diary. Wythenshawe Hospital Cardiac Rehabilitation. Name:... The ticker club Registered Charity No.
 Wythenshawe Hospital Cardiac Rehabilitation Patient Information Remember : Lifelong regular physical activity - 0 minutes, five times per week is important for your general health. I feel so much better
Wythenshawe Hospital Cardiac Rehabilitation Patient Information Remember : Lifelong regular physical activity - 0 minutes, five times per week is important for your general health. I feel so much better
Understanding. Depression. The Road to Feeling Better Helping Yourself. Your Treatment Options A Note for Family Members
 TM Understanding Depression The Road to Feeling Better Helping Yourself Your Treatment Options A Note for Family Members Understanding Depression Depression is a biological illness. It affects more than
TM Understanding Depression The Road to Feeling Better Helping Yourself Your Treatment Options A Note for Family Members Understanding Depression Depression is a biological illness. It affects more than
SYDNEY 22-24 August 2014
 SYDNEY 22-24 August 2014 Overview Most common injuries Injury prevention strategies - massage - posture advice - walking poles - stretching - strengthening - taping / bracing Hills Training Cross Training
SYDNEY 22-24 August 2014 Overview Most common injuries Injury prevention strategies - massage - posture advice - walking poles - stretching - strengthening - taping / bracing Hills Training Cross Training
How you will benefit by implementing an early reporting system
 Introduction How you will benefit by implementing an early reporting system Early reporting and action for musculoskeletal discomfort and pain directly assists workplaces wishing to prevent and manage
Introduction How you will benefit by implementing an early reporting system Early reporting and action for musculoskeletal discomfort and pain directly assists workplaces wishing to prevent and manage
What muscles do cyclists primarily use?
 Stress & Injury The following information has been taken from freely available articles from British Cycling and other Cycling organisations. Sources are noted at the end of this document. Please note
Stress & Injury The following information has been taken from freely available articles from British Cycling and other Cycling organisations. Sources are noted at the end of this document. Please note
Managing children and the young person with diabetes at school. A England September 2009
 Managing children and the young person with diabetes at school. A England September 2009 To establish the principles of managing Diabetes Mellitus Discuss the types of diabetes To inform/update staff of
Managing children and the young person with diabetes at school. A England September 2009 To establish the principles of managing Diabetes Mellitus Discuss the types of diabetes To inform/update staff of
WHAT 350 HEDS PATIENTS TAUGHT ME IN 2013! Professor Rodney Grahame University College London The Hypermobility Unit, London UK
 WHAT 350 HEDS PATIENTS TAUGHT ME IN 2013! Professor Rodney Grahame University College London The Hypermobility Unit, London UK 1967 1970 1980 1990 2000 MUSCULOSKELETAL PAIN/JOINT INSTABILITY OVERLAP WITH
WHAT 350 HEDS PATIENTS TAUGHT ME IN 2013! Professor Rodney Grahame University College London The Hypermobility Unit, London UK 1967 1970 1980 1990 2000 MUSCULOSKELETAL PAIN/JOINT INSTABILITY OVERLAP WITH
Sit stand desks and musculo skeletal health. Katharine Metters
 Sit stand desks and musculo skeletal health Katharine Metters Topics Sitting Standing Movement and activity Work and human change Sitting uses less energy Sitting provides support for the body to reduce
Sit stand desks and musculo skeletal health Katharine Metters Topics Sitting Standing Movement and activity Work and human change Sitting uses less energy Sitting provides support for the body to reduce
Rehabilitation after shoulder dislocation
 Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your shoulder dislocation. It is not a substitute
total hip replacement
 total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
total hip replacement EXCERCISE BOOKLET patient s name: date of surgery: physical therapist: www.jointpain.md Get Up and Go Joint Program Philosophy: With the development of newer and more sophisticated
Heart information. Cardiac rehabilitation
 Heart information Cardiac rehabilitation Contents 2 What is cardiac rehabilitation? 3 What are the benefits of cardiac rehabilitation? 4 Who should take part in cardiac rehabilitation? 4 When does cardiac
Heart information Cardiac rehabilitation Contents 2 What is cardiac rehabilitation? 3 What are the benefits of cardiac rehabilitation? 4 Who should take part in cardiac rehabilitation? 4 When does cardiac
Running Injury Prevention Tips & Return to Running Program
 Department of Rehabilitation Services Physical Therapy The intent of these guidelines is to provide the athlete with a framework for return to sports activity following injury. These guidelines should
Department of Rehabilitation Services Physical Therapy The intent of these guidelines is to provide the athlete with a framework for return to sports activity following injury. These guidelines should
Non-epileptic seizures
 Non-epileptic seizures a short guide for patients and families Information for patients Department of Neurology Royal Hallamshire Hospital What are non-epileptic seizures? In a seizure people lose control
Non-epileptic seizures a short guide for patients and families Information for patients Department of Neurology Royal Hallamshire Hospital What are non-epileptic seizures? In a seizure people lose control
The service. The OT role where do we fit in? The future?
 The service The OT role where do we fit in? The future? Medical Consultants Assistant Practitioner Therapy Assistant Dietitians SWMS Team Health Trainer Physiotherapists Psychologist Occupational Therapists
The service The OT role where do we fit in? The future? Medical Consultants Assistant Practitioner Therapy Assistant Dietitians SWMS Team Health Trainer Physiotherapists Psychologist Occupational Therapists
Musculoskeletal System
 CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
CHAPTER 3 Impact of SCI on the Musculoskeletal System Voluntary movement of the body is dependent on a number of systems. These include: The brain initiates the movement and receives feedback to assess
Knowledge of a generic model of adjustment to long-term health conditions
 Knowledge of a generic model of adjustment to long-term health conditions An ability to draw on knowledge that adjustment is not an end-point but a process of assimilation that takes place over time, and
Knowledge of a generic model of adjustment to long-term health conditions An ability to draw on knowledge that adjustment is not an end-point but a process of assimilation that takes place over time, and
The road to recovery. The support available to help you with your recovery after stroke
 The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Introduction Need to talk? Call our confidential Stroke Helpline
The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Introduction Need to talk? Call our confidential Stroke Helpline
Manage cancer related fatigue:
 Manage cancer related fatigue: For People Affected by Cancer In this pamphlet: What can I do to manage fatigue? What is cancer related fatigue? What causes cancer related fatigue? How can my health care
Manage cancer related fatigue: For People Affected by Cancer In this pamphlet: What can I do to manage fatigue? What is cancer related fatigue? What causes cancer related fatigue? How can my health care
St Gemma s Hospice Therapy Team
 St Gemma s Hospice Therapy Team Occupational Therapists Physiotherapists Dietitian Complementary Therapists Creative Arts Worker 0113 218 5500 www.st-gemma.co.uk St Gemma s Therapy Team The therapy team
St Gemma s Hospice Therapy Team Occupational Therapists Physiotherapists Dietitian Complementary Therapists Creative Arts Worker 0113 218 5500 www.st-gemma.co.uk St Gemma s Therapy Team The therapy team
Service Overview. and Pricing Guide
 Service Overview and Pricing Guide Millard Health s Service Overview and Pricing Guide Millard Health provides rehabilitation services for both work-related and non-work-related injuries. The rehabilitation
Service Overview and Pricing Guide Millard Health s Service Overview and Pricing Guide Millard Health provides rehabilitation services for both work-related and non-work-related injuries. The rehabilitation
Biomechanical Pain and Hypermobility Syndrome in Children and Adolescents. Verna Cuthbert May 2014
 Biomechanical Pain and Hypermobility Syndrome in Children and Adolescents Verna Cuthbert May 2014 Differential Diagnosis. BIOMECHANICAL ARTHRITIS/ INFLAMMATION JOINT PAIN MISC NON ORGANIC Prince et al
Biomechanical Pain and Hypermobility Syndrome in Children and Adolescents Verna Cuthbert May 2014 Differential Diagnosis. BIOMECHANICAL ARTHRITIS/ INFLAMMATION JOINT PAIN MISC NON ORGANIC Prince et al
Once the immune system is triggered, cells migrate from the blood into the joints and produce substances that cause inflammation.
 HealthExchange Points For Your Joints An Arthritis Talk Howard Epstein, MD Orthopaedic & Rheumatologic Institute Rheumatic & Immunologic Disease Cleveland Clinic Beachwood Family Health & Surgery Center
HealthExchange Points For Your Joints An Arthritis Talk Howard Epstein, MD Orthopaedic & Rheumatologic Institute Rheumatic & Immunologic Disease Cleveland Clinic Beachwood Family Health & Surgery Center
Falls and falls injury prevention activity audit for residential aged care facilities
 Falls and falls injury prevention activity audit for residential aged care facilities National Ageing Research Institute October 2009 www.nari.unimelb.edu.au This tool is based on a tool that was originally
Falls and falls injury prevention activity audit for residential aged care facilities National Ageing Research Institute October 2009 www.nari.unimelb.edu.au This tool is based on a tool that was originally
Anxiety and breathing difficulties
 Patient information factsheet Anxiety and breathing difficulties Breathing is something that we all automatically do and we often take this for granted. Some chronic health conditions, for example asthma
Patient information factsheet Anxiety and breathing difficulties Breathing is something that we all automatically do and we often take this for granted. Some chronic health conditions, for example asthma
The advanced back rehabilitation programme
 Physiotherapy Department The advanced back rehabilitation programme This booklet explains what happens during the advanced back rehabilitation programme and how the exercises may help your condition. We
Physiotherapy Department The advanced back rehabilitation programme This booklet explains what happens during the advanced back rehabilitation programme and how the exercises may help your condition. We
Sciatica Yuliya Mutsa PTA 236
 Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
Sciatica Yuliya Mutsa PTA 236 Sciatica is a common type of pain affecting the sciatic nerve, which extends from the lower back all the way through the back of the thigh and down through the leg. Depending
Recovery After Stroke: Bladder & Bowel Function
 Recovery After Stroke: Bladder & Bowel Function Problems with bladder and bowel function are common but distressing for stroke survivors. Going to the bathroom after suffering a stroke may be complicated
Recovery After Stroke: Bladder & Bowel Function Problems with bladder and bowel function are common but distressing for stroke survivors. Going to the bathroom after suffering a stroke may be complicated
New York State Workers' Comp Board. Mid and Lower Back Treatment Guidelines. Summary From 1st Edition, June 30, 2010. Effective December 1, 2010
 New York State Workers' Comp Board Mid and Lower Back Treatment Guidelines Summary From 1st Edition, June 30, 2010 Effective December 1, 2010 General Principles Treatment should be focused on restoring
New York State Workers' Comp Board Mid and Lower Back Treatment Guidelines Summary From 1st Edition, June 30, 2010 Effective December 1, 2010 General Principles Treatment should be focused on restoring
Primary Health-care, Adult Services and Children Services in Westminster
 Primary Health-care, Adult Services and Children Services in Westminster In Westminster over 4,000 people receive Supporting People services provided by 44 different organisations. The Supporting People
Primary Health-care, Adult Services and Children Services in Westminster In Westminster over 4,000 people receive Supporting People services provided by 44 different organisations. The Supporting People
Breathlessness. and anxiety. Being anxious can make breathlessness feel worse. Not being able to catch your breath can be very frightening
 Breathlessness and anxiety Being anxious can make breathlessness feel worse Not being able to catch your breath can be very frightening Learning to relax and slow down can help to build your confidence
Breathlessness and anxiety Being anxious can make breathlessness feel worse Not being able to catch your breath can be very frightening Learning to relax and slow down can help to build your confidence
SLEEP AND PARKINSON S DISEASE
 A Practical Guide on SLEEP AND PARKINSON S DISEASE MICHAELJFOX.ORG Introduction Many people with Parkinson s disease (PD) have trouble falling asleep or staying asleep at night. Some sleep problems are
A Practical Guide on SLEEP AND PARKINSON S DISEASE MICHAELJFOX.ORG Introduction Many people with Parkinson s disease (PD) have trouble falling asleep or staying asleep at night. Some sleep problems are
Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario
 Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Page 1 Closed Automobile Insurance Third Party Liability Bodily Injury Claim Study in Ontario Injury Descriptions Developed from Newfoundland claim study injury definitions No injury Death Psychological
Toilet Training Resource Pack
 This pack provides hints and tips to help you facilitate independence in toileting with the children you work with. Please use the advice and strategies contained in this pack before you make a referral
This pack provides hints and tips to help you facilitate independence in toileting with the children you work with. Please use the advice and strategies contained in this pack before you make a referral
SENIOR S HEALTH INFORMATION PACK. www.northsfitness.com.au
 SENIOR S HEALTH INFORMATION PACK www.northsfitness.com.au North Sydney Leagues Club 12 Abbott Street, Cammeray NSW 2062 T: 02 9245 3011 E: fitness@norths.com.au It s never too late to start... Seniors
SENIOR S HEALTH INFORMATION PACK www.northsfitness.com.au North Sydney Leagues Club 12 Abbott Street, Cammeray NSW 2062 T: 02 9245 3011 E: fitness@norths.com.au It s never too late to start... Seniors
National Hospital for Neurology and Neurosurgery. Migraine associated dizziness Department of Neuro-otology
 National Hospital for Neurology and Neurosurgery Migraine associated dizziness Department of Neuro-otology If you would like this document in another language or format or if you require the services of
National Hospital for Neurology and Neurosurgery Migraine associated dizziness Department of Neuro-otology If you would like this document in another language or format or if you require the services of
Helping you manage your pain
 Helping you manage your pain This booklet contains confidential personal information. If found, please mail to the address below. Personal details Name Address Telephone My health care team (please tick)
Helping you manage your pain This booklet contains confidential personal information. If found, please mail to the address below. Personal details Name Address Telephone My health care team (please tick)
Better Choices, Better Health
 PROGRAM BROCHURE Fall 2015 and Winter 2016 October 2015 March 2016 Education Classes Better Choices, Better Health Exercise Classes D isease-specific and general topics are offered in different formats
PROGRAM BROCHURE Fall 2015 and Winter 2016 October 2015 March 2016 Education Classes Better Choices, Better Health Exercise Classes D isease-specific and general topics are offered in different formats
Halloween Costume Ideas - The Ultimate Party Planning Formula
 Patient Type 2 Diabetes Aboriginal Health Workers Audiologists Chiropractors Diabetes Educators Dietitians Exercise Physiologists Mental Health Nurses Mental Health Social Workers Occupational Therapists
Patient Type 2 Diabetes Aboriginal Health Workers Audiologists Chiropractors Diabetes Educators Dietitians Exercise Physiologists Mental Health Nurses Mental Health Social Workers Occupational Therapists
Learning Disabilities Nursing: Field Specific Competencies
 Learning Disabilities Nursing: Field Specific Competencies Page 7 Learning Disabilities Nursing: Field Specific Competencies Competency (Learning disabilities) and application Domain and ESC Suitable items
Learning Disabilities Nursing: Field Specific Competencies Page 7 Learning Disabilities Nursing: Field Specific Competencies Competency (Learning disabilities) and application Domain and ESC Suitable items
in young people Management of depression in primary care Key recommendations: 1 Management
 Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
Management of depression in young people in primary care Key recommendations: 1 Management A young person with mild or moderate depression should typically be managed within primary care services A strength-based
Student Centred Appraisal of Need
 Student Centred Appraisal of Need Booklet for parents, carers and staff January 2010 INTRODUCTION The Student Centred Appraisal of Need provides a consistent approach in determining educational needs of
Student Centred Appraisal of Need Booklet for parents, carers and staff January 2010 INTRODUCTION The Student Centred Appraisal of Need provides a consistent approach in determining educational needs of
Understanding sport and physical activity as a therapy choice for young disabled people. Views and opinions of paediatric physiotherapists
 Understanding sport and physical activity as a therapy choice for young disabled people Views and opinions of paediatric physiotherapists 2 Contents Acknowledgements... 4 Executive Summary... 6 Section
Understanding sport and physical activity as a therapy choice for young disabled people Views and opinions of paediatric physiotherapists 2 Contents Acknowledgements... 4 Executive Summary... 6 Section
Presently, there are no means of preventing bipolar disorder. However, there are ways of preventing future episodes: 1
 What is bipolar disorder? There are two main types of bipolar illness: bipolar I and bipolar II. In bipolar I, the symptoms include at least one lifetime episode of mania a period of unusually elevated
What is bipolar disorder? There are two main types of bipolar illness: bipolar I and bipolar II. In bipolar I, the symptoms include at least one lifetime episode of mania a period of unusually elevated
Cerebral palsy can be classified according to the type of abnormal muscle tone or movement, and the distribution of these motor impairments.
 The Face of Cerebral Palsy Segment I Discovering Patterns What is Cerebral Palsy? Cerebral palsy (CP) is an umbrella term for a group of non-progressive but often changing motor impairment syndromes, which
The Face of Cerebral Palsy Segment I Discovering Patterns What is Cerebral Palsy? Cerebral palsy (CP) is an umbrella term for a group of non-progressive but often changing motor impairment syndromes, which
PERFORMANCE RUNNING. Piriformis Syndrome
 Piriformis Syndrome Have you started to experience pain in your hip or down your leg while beginning or advancing your fitness program? This pain may be stemming from the piriformis muscle in your hip.
Piriformis Syndrome Have you started to experience pain in your hip or down your leg while beginning or advancing your fitness program? This pain may be stemming from the piriformis muscle in your hip.
ABOUT US OUR VISION. ROWVILLE SPORTS MEDICINE CENTRE offers health services within the same high quality care model to our community.
 ABOUT US ROWVILLE PHYSIOTHERAPY was established in 2001 with the aim to provide quality physiotherapy services to our community. With an established reputation for clinical excellence we have rapidly grown
ABOUT US ROWVILLE PHYSIOTHERAPY was established in 2001 with the aim to provide quality physiotherapy services to our community. With an established reputation for clinical excellence we have rapidly grown
Cerebral Palsy. Causes
 Cerebral Palsy Cerebral Palsy (sera brul PAUL zee) (CP) is an injury or abnormality of the developing brain that affects movement. This means that something happened to the brain or the brain did not develop
Cerebral Palsy Cerebral Palsy (sera brul PAUL zee) (CP) is an injury or abnormality of the developing brain that affects movement. This means that something happened to the brain or the brain did not develop
A Guide To Our Family Services For Disabled Children
 Caudwell Children A Guide To Our Family Services For Disabled Children Supported by caudwellchildren caudwellchildren.com caudwellkids How We Can Help You may be reading this information because a child
Caudwell Children A Guide To Our Family Services For Disabled Children Supported by caudwellchildren caudwellchildren.com caudwellkids How We Can Help You may be reading this information because a child
ALL ABOUT SPASTICITY. www.almirall.com. Solutions with you in mind
 ALL ABOUT SPASTICITY www.almirall.com Solutions with you in mind WHAT IS SPASTICITY? The muscles of the body maintain what is called normal muscle tone, a level of muscle tension that allows us to hold
ALL ABOUT SPASTICITY www.almirall.com Solutions with you in mind WHAT IS SPASTICITY? The muscles of the body maintain what is called normal muscle tone, a level of muscle tension that allows us to hold
sleep handbook Keep this by your bedside to help you get straight to sleep.
 sleep handbook Keep this by your bedside to help you get straight to sleep. BEDSIDE BUDDY Chiropractic how can it help me get straight to sleep? Chiropractic is based on the scientific fact that the human
sleep handbook Keep this by your bedside to help you get straight to sleep. BEDSIDE BUDDY Chiropractic how can it help me get straight to sleep? Chiropractic is based on the scientific fact that the human
CP Factsheet An introduction to ageing and cerebral palsy
 An introduction to ageing and cerebral palsy The concept of ageing and cerebral palsy is now becoming more recognised and more research is being undertaken. However many people, including some professionals,
An introduction to ageing and cerebral palsy The concept of ageing and cerebral palsy is now becoming more recognised and more research is being undertaken. However many people, including some professionals,
Allied Conditions and rehabilitation
 Allied Conditions and rehabilitation Dr Helen Cohen Consultant Rheumatology & Chronic Pain, Royal National Orthopaedic Hospital Cmglee, Radially-symmetrical five-set Venn diagram devised by Branko Grünbaum,
Allied Conditions and rehabilitation Dr Helen Cohen Consultant Rheumatology & Chronic Pain, Royal National Orthopaedic Hospital Cmglee, Radially-symmetrical five-set Venn diagram devised by Branko Grünbaum,
Patient Guide. Sacroiliac Joint Pain
 Patient Guide Sacroiliac Joint Pain Anatomy Where is the Sacroiliac Joint? The sacroiliac joint (SIJ) is located at the bottom end of your spine, where the "tailbone" (sacrum) joins the pelvis (ilium).
Patient Guide Sacroiliac Joint Pain Anatomy Where is the Sacroiliac Joint? The sacroiliac joint (SIJ) is located at the bottom end of your spine, where the "tailbone" (sacrum) joins the pelvis (ilium).
Fitness Training A Sensible Guide to Preparing for Selection in the Gurkhas
 Fitness Training A Sensible Guide to Preparing for Selection in the Gurkhas Background Physical fitness has a number of components: aerobic endurance (stamina), strength, speed, flexibility, muscle endurance,
Fitness Training A Sensible Guide to Preparing for Selection in the Gurkhas Background Physical fitness has a number of components: aerobic endurance (stamina), strength, speed, flexibility, muscle endurance,
South Wilts Grammar School. When do teenage problems become Problems? A presentation by Dr. Anna Randle, Chartered Clinical Psychologist
 South Wilts Grammar School When do teenage problems become Problems? A presentation by Dr. Anna Randle, Chartered Clinical Psychologist Do you remember being a teenager? What were some of the dilemmas
South Wilts Grammar School When do teenage problems become Problems? A presentation by Dr. Anna Randle, Chartered Clinical Psychologist Do you remember being a teenager? What were some of the dilemmas
Helping your child with Non-verbal Learning Disability
 Helping your child with Non-verbal Learning Disability What is non-verbal learning disability? Non-verbal learning disability (NVLD) is a term used to describe a pattern of strengths and weaknesses in
Helping your child with Non-verbal Learning Disability What is non-verbal learning disability? Non-verbal learning disability (NVLD) is a term used to describe a pattern of strengths and weaknesses in
LUMBAR. Hips R L B R L B LUMBAR. Hips R L B R L B LUMBAR. Hips R L B R L B
 1 Patient Name In order to properly assess your condition, we must understand how much your BACK/LEG (SCIATIC) PAIN has affected your ability to manage everyday activities. For each item below, please
1 Patient Name In order to properly assess your condition, we must understand how much your BACK/LEG (SCIATIC) PAIN has affected your ability to manage everyday activities. For each item below, please
Wigan Educational Psychology Service
 Wigan Educational Psychology Service Therapeutic and Direct Intervention Approaches Assessment Staff and Whole School Support Training Service Overview Wigan Educational Psychology Service (EPS) offers
Wigan Educational Psychology Service Therapeutic and Direct Intervention Approaches Assessment Staff and Whole School Support Training Service Overview Wigan Educational Psychology Service (EPS) offers
Asthma, anxiety & depression
 Anxiety and are common in people with asthma. The good news is that there are effective treatments both for asthma and for anxiety and. With careful management, the symptoms of anxiety and can be treated
Anxiety and are common in people with asthma. The good news is that there are effective treatments both for asthma and for anxiety and. With careful management, the symptoms of anxiety and can be treated
Occupational therapy after stroke
 Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Occupational therapy after stroke After a stroke, you are likely to need help to regain your abilities, learn new skills and cope with any remaining
Stroke Helpline: 0303 3033 100 Website: stroke.org.uk Occupational therapy after stroke After a stroke, you are likely to need help to regain your abilities, learn new skills and cope with any remaining
Lewy body dementia Referral for a Diagnosis
 THE Lewy Body society The more people who know, the fewer people who suffer Lewy body dementia Referral for a Diagnosis Lewy Body Dementias REFERRAL FOR A DIAGNOSIS In the UK people with all forms of dementia
THE Lewy Body society The more people who know, the fewer people who suffer Lewy body dementia Referral for a Diagnosis Lewy Body Dementias REFERRAL FOR A DIAGNOSIS In the UK people with all forms of dementia
Fact Sheet: Occupational Overuse Syndrome (OOS)
 Fact Sheet: Occupational Overuse Syndrome (OOS) What is OOS? Occupational Overuse Syndrome (OOS) is the term given to a range of conditions characterised by discomfort or persistent pain in muscles, tendons
Fact Sheet: Occupational Overuse Syndrome (OOS) What is OOS? Occupational Overuse Syndrome (OOS) is the term given to a range of conditions characterised by discomfort or persistent pain in muscles, tendons
The Process of Strength and Conditioning for Golfers
 The Process of Strength and Conditioning for Golfers The use of different sporting activities and resistance work to develop a strength and conditioning program specific to golf. Many club golfers are
The Process of Strength and Conditioning for Golfers The use of different sporting activities and resistance work to develop a strength and conditioning program specific to golf. Many club golfers are
Meath School Occupational Therapy Department Professional Practice Policy Document
 Meath School Occupational Therapy Department Professional Practice Policy Document Principles of Delivery of Service by the Occupational Therapy Department at Meath School (to include Sensory Integration
Meath School Occupational Therapy Department Professional Practice Policy Document Principles of Delivery of Service by the Occupational Therapy Department at Meath School (to include Sensory Integration
Introduction: Anatomy of the spine and lower back:
 Castleknock GAA club member and Chartered Physiotherapist, James Sherry MISCP, has prepared an informative article on the common causes of back pain and how best it can be treated. To book a physiotherapy
Castleknock GAA club member and Chartered Physiotherapist, James Sherry MISCP, has prepared an informative article on the common causes of back pain and how best it can be treated. To book a physiotherapy
General Home Activity and Exercise Guidelines
 General Home Activity and Exercise Guidelines After a Heart Attack / Angina Angioplasty / Stent Heart Failure Heart Health Risk Reduction Program Vancouver Island Health Authority Created January 2002;
General Home Activity and Exercise Guidelines After a Heart Attack / Angina Angioplasty / Stent Heart Failure Heart Health Risk Reduction Program Vancouver Island Health Authority Created January 2002;
Eating Disorder Policy
 Eating Disorder Policy Safeguarding and Child Protection Information Date of publication: April 2015 Date of review: April 2016 Principal: Gillian May Senior Designated Safeguarding Person: (SDSP) Anne
Eating Disorder Policy Safeguarding and Child Protection Information Date of publication: April 2015 Date of review: April 2016 Principal: Gillian May Senior Designated Safeguarding Person: (SDSP) Anne
A BETTER TOMOR W. A balanced approach to Occupational Therapy & Case Management REHAB OPTIONS
 A BETTER TOMOR W Beech House, 54b High Street, Chapmanslade, Wiltshire, BA13 4AN T: 01373 832459 info@rehaboptions.co.uk www.rehaboptions.co.uk Registered in England & Wales No 5860678 Designed by Plum
A BETTER TOMOR W Beech House, 54b High Street, Chapmanslade, Wiltshire, BA13 4AN T: 01373 832459 info@rehaboptions.co.uk www.rehaboptions.co.uk Registered in England & Wales No 5860678 Designed by Plum
Eastman Dental Hospital. Temporomandibular disorder. Facial Pain Team
 Eastman Dental Hospital Temporomandibular disorder Facial Pain Team If you would like this document in another language or format or if you require the services of an interpreter contact us on 020 3456
Eastman Dental Hospital Temporomandibular disorder Facial Pain Team If you would like this document in another language or format or if you require the services of an interpreter contact us on 020 3456
Employee Assistance Programmes Manager s Guide
 March 2012 Employee Assistance Programmes Manager s Guide Support and assistance when you need it Vhi Corporate Solutions Employee Assistance Programme Confidential Professional Help Support Communicate
March 2012 Employee Assistance Programmes Manager s Guide Support and assistance when you need it Vhi Corporate Solutions Employee Assistance Programme Confidential Professional Help Support Communicate
Early Intervention, Injury Resolution & Sustainable RTW Outcomes. Presented by: Mr. Fred Cicchini, Chief Operations Manager September 2013
 Early Intervention, Injury Resolution & Sustainable RTW Outcomes. Presented by: Mr. Fred Cicchini, Chief Operations Manager September 2013 Session Objectives Early Intervention in the RTW Context Injury
Early Intervention, Injury Resolution & Sustainable RTW Outcomes. Presented by: Mr. Fred Cicchini, Chief Operations Manager September 2013 Session Objectives Early Intervention in the RTW Context Injury
Social Phobia. Fact sheet 39. What is Social Phobia? Signs and symptoms. How common is Social Phobia and who experiences it?
 Social Phobia Fact sheet 39 What is Social Phobia? It is normal to feel nervous in situations in which we could possibly come under the scrutiny of others, whether they are strangers or people we know.
Social Phobia Fact sheet 39 What is Social Phobia? It is normal to feel nervous in situations in which we could possibly come under the scrutiny of others, whether they are strangers or people we know.
Our Local Offer for Special Educational Needs and Disability (SEND)
 Our Local Offer for Special Educational Needs and Disability (SEND) Rosewood Free School is a maintained special school in Southampton for children with PMLD complex physical, medical and learning difficulties.
Our Local Offer for Special Educational Needs and Disability (SEND) Rosewood Free School is a maintained special school in Southampton for children with PMLD complex physical, medical and learning difficulties.
