Blast crisis. Progressive relapsing (malignant) Primary progressive. Secondary progressive. Relapsing/remitting
|
|
|
- Alfred Beasley
- 7 years ago
- Views:
Transcription
1 Scroll right to see the database codes for Disease status and Response Diagnosis it refers to Disease status or response to treatment AML ALL CML CLL MDS or MD/MPN or acute leukaemia secondary to previous treatment of another disease Chronic phase Accelerated phase Blast crisis Progressive relapsing (malignant) None of the features of accelerated phase or blast crisis blasts 10-19% of WBCs in peripheral blood and/or nucleated bone marrow cells; peripheral blood basophils >=20%; persistent thrombocytopenia (<100 x 10 9 )/L unrelated to therapy; persistent thrombocytosis (>1000 x 10 9 /L) unresponsive to standard therapy; increasing spleen size and increasing WBC count unresponsive to standard therapy; cytogenetic evidence of clonal evolution blasts >=20% of peripheral blood white cells or nucleated bone marrow cells; extramedullary blast proliferation; large foci or clusters of blasts in the bone marrow biopsy Primary progressive Secondary progressive Relapsing/remitting Primary induction failure / Primary refractory Stable disease (no change, no response) Stringent Complete remission (scr) Despite treatment patient has never achieved a complete remission Patients who have not achieved a CR or a PR, and who have not exhibited progression, will be considered to have no change Treatment with intent to achieve remission was given, but no Complete remission was achieved Complete remission or response (CR) Haematological CR Cytogenetic CR Molecular CR CR confirmed No blast cells in peripheral blood and no more than 5% blasts in the bone marrow No blast cells in peripheral blood and no more than 5% blasts in the bone marrow Disappearance of cytogenetic anomalies if previously detected Disappearance of molecular anomalies if previously detected absence of clonal lymphocytes in the peripheral blood absence of significant lymphadenopathy (e.g. lymph nodes If unqualified, Complete remission is considered to be Haematological complete remission greater than 1,5 cm in diameter) absence of hepatomegaly or splenomegaly absence of constitutional symptoms WBC<10X10 9 /L; Hemoglobin>11.0gm/dL; platelet count<500x10 9 /L; normal differential (<1%precursor cells); no palpable splenomegaly; no extramedullary disease; Haematological remission 0% positive (t(9;22) metaphases Haematological remission Cytogenetic remission (if cytogenetics done) Cells with the BCR/ABL fusion protein are not detectable in the peripheral blood and /or the bone marrow, by an assay with a sensitivity to allow detection of one t(9;22) positive cell in 10 5 to 10 6 RT-PCR cells. The result should be confirmed by two consecutive tests done at least 4 weeks apart. Response must persist for a minimum duration of four weeks: Bone marrow with 5 percent myeloblasts with normal maturation of all cell lines. Dysplastic changes may be seen, but should be considered within the normal range of dysplastic changes. Peripheral blood demonstrates hemoglobin 11 g/dl, platelets 100 x 109/L, neutrophils 1 x 109/L, and no circulating blasts. CR unconfirmed
2 Disease status or response to treatment AML ALL CML CLL MDS or MD/MPN or acute leukaemia secondary to previous treatment of another disease First partial remission (PR1) Very good PR (VGPR) Partial remission or response Note: The specification (>1, without previous CR, if diagnosis Lym or Solid tumours) only applies to disease status in Lymphoma and Solid Tumours. For any other diagnosis, the disease status of PR can have been preceded by a relapsed CR Minimal respponse / Poor partial remission or response At leat one of the following: A decrease in the number of blood lymphocytes by below 50% or more from the value prior to therapy; A decrease in lymph node size by below 50% or more in the sum products of up to 6 lymph nodes, or in one lymph node diameter if only a single lymph node was present prior to therapy, without increase in any lymph node, and no new enlarged lymph node; A decrease in the size of the liver and/or spleen by 50% or more as defined by CT scan, palpation, or ultrasound. The blood count should show one of the following results if abnormal prior to therapy:. Polymorphonuclear leukocytes at 1.500/μL or more or 50% improvement over baseline without G-CSF support;?? Response / improvement (no CR) Relapse > 5% blasts in the bone marrow after a period of Complete remission. If unqualified, Relapse is considered to be Haematological relapse At least one Complete remission was achieved with a previous treatment but the patient has relapsed since then Haematological Relapse > 5% blasts in the bone marrow after a period of Complete remission. Cytological and/or histological evidence of the disease in the marrow-blood and/or in extramedullary sites (CNS, testis, skin, etc.) in a patient considered to have been in Haematological complete remission Cytogenetic Relapse Molecular Relapse Reappearance of chromosome anomalies detected earlier in the history of the disease. Presence of one or more t(9:22) positive metaphases with standard cytogenetics or Cytogenetic relapse can only hypermetaphase FISH and/or >2% cells with the BCR/ABL fusion gene by interphase FISH, in be determined if Cytogenetic a patient lacking any evidence of the disease at haematological/clinical level. remission has been previously demonstrated. Reappearance of molecular anomalies detected earlier in the history of the disease. Presence of one or more t(9:22) positive metaphases with standard cytogenetics or Molecular relapse can only be hypermetaphase FISH and/or >2% cells with the BCR/ABL fusion gene by interphase FISH, in determined if Molecular a patient lacking any evidence of the disease at haematological/clinical level. remission has been previously demonstrated.
3 Disease status or response to treatment AML ALL CML CLL MDS or MD/MPN or acute leukaemia secondary to previous treatment of another disease untreated relapse sensitive (responding) relapse resistant relapse Progression Never in CR Not in CR Untreated/Upfront [progression] resistant to chemotherapy [progression] sensitive to chemotherapy Patient has never been treated for this disease Progression of lymphadenopathy, defined as the occurrence of at least one of the following events...appearance of any new lesion such as enlarged lymph nodes (> 1.5 cm), splenomegaly, hepatomegaly or other organ infiltrates....an increase by 50% or more in greatest determined diameter of any previous site. More blasts in bone marrow than before treatment or...an increase of 50% or more in the sum of the product of leukaemic transformation diameters of multiple nodes. An increase in the liver or spleen size by 50% or more or the de novo appearance of hepatomegaly or splenomegaly. An increase in the number of blood lymphocytes by 50% or more with at least 5,000 B-cells per μl. Transformation to a more aggressive histology (e.g. Richter's syndrome). Patient received another treatment following progression but no remission of any type was achieved Patient received another treatment after progression and achieved some kind of remission Patient has never been treated for this disease use only if more precise evaluati use only if more precise evaluati Treatment is supportive or there has not been any treatment at all (blood transfusions are not considered as treatment in this context) Adjuvant Not evaluable unknown if pat. died within 100 days after if data cannot be obtain
4 Scroll right to see the database codes for Disease status and Response Disease status or response to treatment Myelofibrosis (MPN) Lymphoma Plasma cell disorders; mainly Multiple myeloma Solid Tumors Chronic phase Accelerated phase Blast crisis Progressive relapsing (malignant) Primary progressive Secondary progressive Relapsing/remitting Primary induction failure / Primary refractory Stable disease (no change, no response) Stringent Complete remission (scr) Doest not present any of the features of any type of remission after treatment Despite treatment patient has never achieved a Complete or a Partial remission Less than 50% reduction in the disease burden Does not meet the criteria for Complete remission, Very good partial remission, Partial remission or Progressive disease Complete remission as defined below normal free light chain ratio absence of clonal cells in bone marrow by immunohistochemistry or immunofluorescence The patient has not achieved any of the types of response described below until now with any type of therapy Less than 50% reduction in the disease Complete remission or response (CR) Haematological CR Resolution of disease related symptoms and signs including palpable hepatosplenomegaly. Hb >11gr/dl, Platelet >100 x109/l and neutrophils Complete absence of disease, no signs or >1 x 109/L. symptoms of the original disease normal bone marrow histology, and fibrosis grade no higher than 1 Absence of detectable monoclonal immunoglobulin in serum or monoclonal light chains in the urine by immunofixation. Detectable monoclonal immunoglobulin, even if impossible to quantify, is not a Complete remission. <5% of plasma cells in bone marrow aspirate Disappearance of any soft tissue plasmacytomas. No increase in size or number of lytic lesions if assessed (radiographic studies are not mandatory) The patient has achieved complete absence of disease prior to HSCT and the HSCT is not part of any adjuvant therapy Cytogenetic CR Molecular CR CR confirmed CR unconfirmed no abnormalities detected in any scan a negative PET scan if there is previous history of a positive PET scan, even in the presence of abnormalities in the CT scan Scan abnormalities of unknown significance in the absence of a negative PET scan No abnormalities detected in scan Persistent scan abnormalities of unknown significance
5 Disease status or response to treatment Myelofibrosis (MPN) Lymphoma Plasma cell disorders; mainly Multiple myeloma Solid Tumors First partial remission (PR1) Patient achieved a reduction in disease of 50% or more for the first time ever, but did not achieve Complete remission Patient achieved a reduction in disease of 50% or more for the first time ever, but did not achieve Complete remission Very good PR (VGPR) A reduction in disease of 90% or more Serum and urine M-protein detectable by immunofixation but not on electrophoresis >90% reduction in serum M-protein plus urine M-protein level <0.1 g/ per 24h Disease burden is reduced by at least Plus no increase in size or number of lytic lesions if assessed (radiographic studies 90% are not mandatory) Partial remission or response Note: The specification (>1, without previous CR, if diagnosis Lym or Solid tumours) only applies to disease status in Lymphoma and Solid Tumours. For any other diagnosis, the disease status of PR can have been preceded by a relapsed CR Minimal respponse / Poor partial remission or response Second or subsequent time a reduction in the Second or subsequent time a disease of 50% or more is achieved in patients >50% reduction in serum M-protein plus reduction in 24h urinary M-protein by >90% reduction in the disease of 50% or who have never achieved a Complete remission or to <0.2g/ per 24h In the absence of measurable serum and urine M-protein, the following criteria applies: more is achieved in patients who have never achieved a Complete remission... A decrease in the difference between involved and uninvolved free light chain (FLC) of more than 50% If the FLC assay cannot be measured, the following criteria applies:.- >50% reduction in plasma cells provided baseline bone marrow plasma cell percentage was >30% A reduction of more than 50% in the size of soft tissue plasmacytomas if present at pre-treatment. No increase in size or number of lytic lesions if assessed (radiographic studies are not mandatory) Response / improvement (no CR) Relapse At least one of the following in the absence of progression: Haemoglobin increase of 2 g/dl or transfusion independence Spleen reduction of 50% 100% increase in platelet count and an absolute platelet count of at least x 10 9 /L 100% increase in ANC and an ANC of at least 0.5 x Loss of Complete remission At least one of the following in a patient whose last disease status was a Complete remission which lasted for 3 months or more. See Progression if CR lasted less than 3 months: Occurrence of new sites of the disease Re-occurence of disease or systemic symptoms (B symptoms) At least one of the following for patients whose last disease status was Complete remission: - Reappearance of measurable monoclonal immunoglobulin in serum or urine by immunofixation or electrophoresis - Appearance of more than 5% plasma cells in the bone marrow - Increase of old/appearance of new osteolytic bone lesions on x-ray - Appearance of soft tissue plasmacytoma Reappearance of disease in patients whose last disease status was Complete remission Haematological Relapse Cytogenetic Relapse Molecular Relapse
6 Disease status or response to treatment Myelofibrosis (MPN) Lymphoma Plasma cell disorders; mainly Multiple myeloma Solid Tumors Progression untreated relapse sensitive (responding) relapse resistant relapse At least one of the following progressive splenomegaly leukemic transformation an increase of peripheral blood blast percentage of at least 20% No further treatment given from date of relapse Patient received another treatment after relapse and achieved a Partial remission Patient received another treatment following relapse but no remission of any type was achieved Worsening of the disease status in patients previously assessed as not in Complete remission or whose Complete remission has lasted less than 3 months - Increase of 25% or more in measurable monoclonal immunoglobulin in serum or urine (absolute increase must be >0.5g/dL) - Increase of 25% or more in urinary light chains (absolute increase must be >0.2g/ per 24h)...In the absence of measurable serum and urine M-protein, the following criteria applies:.. - An increase of 25% or more in the difference between involved and uninvolved free light chain (absolute increase must be >0.01g/dL) - An increase of 25% or more in bone marrow plasma cells (absolute % must be >10%) - Increase of old/appearance of new osteolytic bone lesions on x-ray - Appearance of soft tissue plasmacytoma - Development of hypercalcemia (corrected serum calcium >11.5 mg/dl or 2.65 mmol/l) that can be attributed solely to the plasma cell disorder Patient has not been treated for this relapse Patient achieves a reduction of >50% in the disease burden after treatment for this relapse Patient has not achieved a reduction of more than 50% in the disease burden after treatment for this relapse [progression] resistant to chemotherapy [progression] sensitive to chemotherapy Never in CR Not in CR Untreated/Upfront Adjuvant on is not possible on is not possible Treatment is supportive or there has not been any treatment at all (blood transfusions are not considered as treatment in this context) Patient has never been treated for this disease Patient has never been treated for this disease Patient has never been treated for this disease and the high dose therapy is part of the overall treatment strategy Patient has no residual disease and the HSCT is part of the consolidation treatment; metastatic patients can never be considered as adjuvant. Not evaluable unknown r transplant ned
7 Scroll right to see the database codes for Disease status and Response Disease status or response to treatment Chronic phase Accelerated phase Data base codes Severe Aplastic anaemia (SAA) non Severe Aplastic anaemia (nsaa) Multiple sclerosis Disease status Response 1 2 Blast crisis 3 Progressive relapsing (malignant) Primary progressive Secondary progressive Relapsing/remitting Primary induction failure / Primary refractory Continuous disease progression with clear acute disease exacerbation episodes Continuous disease progression without distinct acute disease exacerbation episodes Acute disease exacerbations periods where there is disease progression after the acute disease exacerbation Acute disease exacerbation periods that resolve completely without worsening of neurologic functions Stable disease (no change, no response) Stringent Complete remission (scr) Still meeting criteria of severe aplastic anaemia and transfusion dependence Not meeting criteria of partial or complete response Complete remission or response (CR) haemoglobin normal for age neutrophils >= 1.5 x 10 9 /L platelets >= 150 x 10 9 /L (21) (22) (23) Haematological CR Cytogenetic CR Molecular CR CR confirmed CR unconfirmed
8 Disease status or response to treatment Severe Aplastic anaemia (SAA) non Severe Aplastic anaemia (nsaa) Multiple sclerosis Disease status Response First partial remission (PR1) 40 Very good PR (VGPR) (36) (37) (38) Partial remission or response Note: The specification (>1, without previous CR, if diagnosis Lym or Solid tumours) only applies to disease status in Lymphoma and Solid Tumours. For any other diagnosis, the disease status of PR can have been preceded by a relapsed CR All of the following transfusion independent no longer meeting criteria for severe aplastic anaemia (see MED-AB Manual) transfusion independence (if previously required) doubling or normalization of at least one cell line increase above baseline* by. 3 g/dl hemoglobin and. 0.5x10 9 /L neutrophils and. 20x10 9 /L platelets (31) (32) (33) Minimal respponse / Poor partial remission or response Response / improvement (no CR) All of the following transfusion independent levels of hemoglobin, neutrophils and platelets still meeting criteria for severe aplastic anaemia (see MED-AB Manual ) Relapse Haematological Relapse Cytogenetic Relapse Molecular Relapse
9 Disease status or response to treatment Severe Aplastic anaemia (SAA) non Severe Aplastic anaemia (nsaa) Multiple sclerosis Disease status Response untreated relapse sensitive (responding) relapse resistant relapse Progression [progression] resistant to chemotherapy [progression] sensitive to chemotherapy Never in CR Not in CR Untreated/Upfront Adjuvant 75 Not evaluable unknown
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL VOLUME I RESPONSE ASSESSMENT LEUKEMIA CHAPTER 11A REVISED: OCTOBER 2015
 LEUKEMIA Response in Acute Myeloid Leukemia (AML) Response criteria in Acute Myeloid Leukemia for SWOG protocols is based on the review article Diagnosis and management of acute myeloid leukemia in adults:
LEUKEMIA Response in Acute Myeloid Leukemia (AML) Response criteria in Acute Myeloid Leukemia for SWOG protocols is based on the review article Diagnosis and management of acute myeloid leukemia in adults:
UNDERSTANDING MULTIPLE MYELOMA AND LABORATORY VALUES Benjamin Parsons, DO bmparson@gundersenhealth.org Gundersen Health System Center for Cancer and
 UNDERSTANDING MULTIPLE MYELOMA AND LABORATORY VALUES Benjamin Parsons, DO bmparson@gundersenhealth.org Gundersen Health System Center for Cancer and Blood Disorders La Crosse, WI UNDERSTANDING MULTIPLE
UNDERSTANDING MULTIPLE MYELOMA AND LABORATORY VALUES Benjamin Parsons, DO bmparson@gundersenhealth.org Gundersen Health System Center for Cancer and Blood Disorders La Crosse, WI UNDERSTANDING MULTIPLE
Multiple Myeloma Patient s Booklet
 1E Kent Ridge Road NUHS Tower Block, Level 7 Singapore 119228 Email : ncis@nuhs.edu.sg Website : www.ncis.com.sg LIKE US ON FACEBOOK www.facebook.com/ nationaluniversitycancerinstitutesingapore Multiple
1E Kent Ridge Road NUHS Tower Block, Level 7 Singapore 119228 Email : ncis@nuhs.edu.sg Website : www.ncis.com.sg LIKE US ON FACEBOOK www.facebook.com/ nationaluniversitycancerinstitutesingapore Multiple
Malignant Lymphomas and Plasma Cell Myeloma
 Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
Malignant Lymphomas and Plasma Cell Myeloma Dr. Bruce F. Burns Dept. of Pathology and Lab Medicine Overview definitions - lymphoma lymphoproliferative disorder plasma cell myeloma pathogenesis - translocations
TABLE OF CONTENTS. Multiple Myeloma / Plasma Cell Leukemia Pre-HSCT Data
 Instructions for Multiple Myeloma / Plasma Cell Leukemia Pre-HSCT Data (Form 2016) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Multiple Myeloma /
Instructions for Multiple Myeloma / Plasma Cell Leukemia Pre-HSCT Data (Form 2016) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Multiple Myeloma /
Adult Medical-Surgical Nursing H A E M A T O L O G Y M O D U L E : L E U K A E M I A 2
 Adult Medical-Surgical Nursing H A E M A T O L O G Y M O D U L E : L E U K A E M I A 2 Leukaemia: Description A group of malignant disorders affecting: White blood cells (lymphocytes or leucocytes) Bone
Adult Medical-Surgical Nursing H A E M A T O L O G Y M O D U L E : L E U K A E M I A 2 Leukaemia: Description A group of malignant disorders affecting: White blood cells (lymphocytes or leucocytes) Bone
Multiple Myeloma Workshop- Tandem 2014
 Multiple Myeloma Workshop- Tandem 2014 1) Review of Plasma Cell Disorders Asymptomatic (smoldering) myeloma M-protein in serum at myeloma levels (>3g/dL); and/or 10% or more clonal plasma cells in bone
Multiple Myeloma Workshop- Tandem 2014 1) Review of Plasma Cell Disorders Asymptomatic (smoldering) myeloma M-protein in serum at myeloma levels (>3g/dL); and/or 10% or more clonal plasma cells in bone
chronic leukemia lymphoma myeloma differentiated 14 September 1999 Pre- Transformed Ig Surface Surface Secreted Myeloma Major malignant counterpart
 Disease Usual phenotype acute leukemia precursor chronic leukemia lymphoma myeloma differentiated Pre- B-cell B-cell Transformed B-cell Plasma cell Ig Surface Surface Secreted Major malignant counterpart
Disease Usual phenotype acute leukemia precursor chronic leukemia lymphoma myeloma differentiated Pre- B-cell B-cell Transformed B-cell Plasma cell Ig Surface Surface Secreted Major malignant counterpart
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Farooqui MZH, Valdez J, Martyr S, et al. Ibrutinib
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Farooqui MZH, Valdez J, Martyr S, et al. Ibrutinib
An overview of CLL care and treatment. Dr Dean Smith Haematology Consultant City Hospital Nottingham
 An overview of CLL care and treatment Dr Dean Smith Haematology Consultant City Hospital Nottingham What is CLL? CLL (Chronic Lymphocytic Leukaemia) is a type of cancer in which the bone marrow makes too
An overview of CLL care and treatment Dr Dean Smith Haematology Consultant City Hospital Nottingham What is CLL? CLL (Chronic Lymphocytic Leukaemia) is a type of cancer in which the bone marrow makes too
Leukemias and Lymphomas: A primer
 Leukemias and Lymphomas: A primer Normal blood contains circulating white blood cells, red blood cells and platelets 700 red cells (oxygen) 1 white cell Neutrophils (60%) bacterial infection Lymphocytes
Leukemias and Lymphomas: A primer Normal blood contains circulating white blood cells, red blood cells and platelets 700 red cells (oxygen) 1 white cell Neutrophils (60%) bacterial infection Lymphocytes
Current Multiple Myeloma Treatment Adapted From the NCCN Guidelines
 Current Multiple Myeloma Treatment Adapted From the NCCN Guidelines Diagnosis Survival 3-5 yrs Survival
Current Multiple Myeloma Treatment Adapted From the NCCN Guidelines Diagnosis Survival 3-5 yrs Survival
Stem Cell Transplantation
 Harmony Behavioral Health, Inc. Harmony Behavioral Health of Florida, Inc. Harmony Health Plan of Illinois, Inc. HealthEase of Florida, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance
Harmony Behavioral Health, Inc. Harmony Behavioral Health of Florida, Inc. Harmony Health Plan of Illinois, Inc. HealthEase of Florida, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance
Things You Don t Want to Miss in Multiple Myeloma
 Things You Don t Want to Miss in Multiple Myeloma Sreenivasa Chandana, MD, PhD Attending Hematologist and Medical Oncologist West Michigan Cancer Center Assistant Professor, Western Michigan University
Things You Don t Want to Miss in Multiple Myeloma Sreenivasa Chandana, MD, PhD Attending Hematologist and Medical Oncologist West Michigan Cancer Center Assistant Professor, Western Michigan University
 MULTIPLE MYELOMA 1 PLASMA CELL DISORDERS Multiple l Myeloma Monoclonal Gammopathy of Undetermined Significance (MGUS) Smoldering Multiple Myeloma (SMM) Solitary Plasmacytoma Waldenstrom s Macroglobulinemia
MULTIPLE MYELOMA 1 PLASMA CELL DISORDERS Multiple l Myeloma Monoclonal Gammopathy of Undetermined Significance (MGUS) Smoldering Multiple Myeloma (SMM) Solitary Plasmacytoma Waldenstrom s Macroglobulinemia
Waldenström Macroglobulinemia: The Burning Questions. IWMF Ed Forum May 18 2014 Morie Gertz MD, MACP
 Waldenström Macroglobulinemia: The Burning Questions IWMF Ed Forum May 18 2014 Morie Gertz MD, MACP Are my kids going to get this? Familial seen in approximately 5 10% of all CLL patients and can be associated
Waldenström Macroglobulinemia: The Burning Questions IWMF Ed Forum May 18 2014 Morie Gertz MD, MACP Are my kids going to get this? Familial seen in approximately 5 10% of all CLL patients and can be associated
Interesting Case Review. Renuka Agrawal, MD Dept. of Pathology City of Hope National Medical Center Duarte, CA
 Interesting Case Review Renuka Agrawal, MD Dept. of Pathology City of Hope National Medical Center Duarte, CA History 63 y/o male with h/o CLL for 10 years Presents with worsening renal function and hypercalcemia
Interesting Case Review Renuka Agrawal, MD Dept. of Pathology City of Hope National Medical Center Duarte, CA History 63 y/o male with h/o CLL for 10 years Presents with worsening renal function and hypercalcemia
Response Criteria for Malignant Lymphoma 2007. Cheson Criteria. Quick Reference Guide
 Response Criteria for Malignant Lymphoma 2007 Cheson Criteria Quick Reference Guide Table of Contents Summary of Assessments...3 Baseline Lesion Burden...4 What isameasurable Lesion?...5 Choosing Target
Response Criteria for Malignant Lymphoma 2007 Cheson Criteria Quick Reference Guide Table of Contents Summary of Assessments...3 Baseline Lesion Burden...4 What isameasurable Lesion?...5 Choosing Target
Response Definition, Evaluation and Monitoring. Michele Baccarani
 Response Definition, Evaluation and Monitoring Michele Baccarani European LeukemiaNet EVOLVING CONCEPTS IN THE MANAGEMENT OF CHRONIC MYELOID LEUKEMIA VENICE 8 9 MAY 2006 Response definition, evaluation
Response Definition, Evaluation and Monitoring Michele Baccarani European LeukemiaNet EVOLVING CONCEPTS IN THE MANAGEMENT OF CHRONIC MYELOID LEUKEMIA VENICE 8 9 MAY 2006 Response definition, evaluation
FastTest. You ve read the book... ... now test yourself
 FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
FastTest You ve read the book...... now test yourself To ensure you have learned the key points that will improve your patient care, read the authors questions below. Please refer back to relevant sections
Cytogenetics for the Rest of Us: A Primer
 Cytogenetics for the Rest of Us: A Primer James J. Stark, MD, FACP Medical Director Cancer Program Maryview Medical Center Diane Maia, M.D. Pathologist, Bon Secours Hampton Roads Case #1 78 y.o. lady seen
Cytogenetics for the Rest of Us: A Primer James J. Stark, MD, FACP Medical Director Cancer Program Maryview Medical Center Diane Maia, M.D. Pathologist, Bon Secours Hampton Roads Case #1 78 y.o. lady seen
Lymphoma and Chronic Lymphocytic Leukemia Clinical Trials
 Recommendations for Implementing Assessment Criteria Guidelines in Lymphoma and Chronic Lymphocytic Leukemia Clinical Trials A PAREXEL Company Lymphoma Assessment Guidelines Standardized assessment criteria
Recommendations for Implementing Assessment Criteria Guidelines in Lymphoma and Chronic Lymphocytic Leukemia Clinical Trials A PAREXEL Company Lymphoma Assessment Guidelines Standardized assessment criteria
Introduction. About 10,500 new cases of acute myelogenous leukemia are diagnosed each
 Introduction 1.1 Introduction: About 10,500 new cases of acute myelogenous leukemia are diagnosed each year in the United States (Hope et al., 2003). Acute myelogenous leukemia has several names, including
Introduction 1.1 Introduction: About 10,500 new cases of acute myelogenous leukemia are diagnosed each year in the United States (Hope et al., 2003). Acute myelogenous leukemia has several names, including
Information Pathway. Myeloma tests and investigations. Paraprotein measurement
 Information Pathway Myeloma UK Broughton House 31 Dunedin Street Edinburgh EH7 4JG Tel: + 44 (0) 131 557 3332 Fax: + 44 (0) 131 557 9785 Myeloma Infoline 0800 980 3332 www.myeloma.org.uk Charity No. SC
Information Pathway Myeloma UK Broughton House 31 Dunedin Street Edinburgh EH7 4JG Tel: + 44 (0) 131 557 3332 Fax: + 44 (0) 131 557 9785 Myeloma Infoline 0800 980 3332 www.myeloma.org.uk Charity No. SC
SOUTHWEST ONCOLOGY GROUP CLINICAL RESEARCH ASSOCIATE (CRA) MANUAL. MYELOMA CHAPTER 10 REVISED: March 2008
 Introduction This disease site includes the following three malignancies: multiple myeloma, amyloidosis, and waldenstrom's macroglobulinemia. See pages 4 and 5 for descriptions of the latter two diseases.
Introduction This disease site includes the following three malignancies: multiple myeloma, amyloidosis, and waldenstrom's macroglobulinemia. See pages 4 and 5 for descriptions of the latter two diseases.
Whole Antibody and Free Light Chain Production by Plasma Cells
 MYELOMA Very Good ; Stringent or Complete Navigating the maze of Responses Parameswaran Hari Medical College of Wisconsin Milwaukee Increasing understanding of disease biology in the last few years Deeper
MYELOMA Very Good ; Stringent or Complete Navigating the maze of Responses Parameswaran Hari Medical College of Wisconsin Milwaukee Increasing understanding of disease biology in the last few years Deeper
HOVON Staging and Response Criteria for Non-Hodgkin s Lymphomas Page 1
 HOVON Staging and Response Criteria for Non-Hodgkin s Lymphomas Page 1 This document describes the minimally required staging and evaluation procedures and response criteria that will be applied in all
HOVON Staging and Response Criteria for Non-Hodgkin s Lymphomas Page 1 This document describes the minimally required staging and evaluation procedures and response criteria that will be applied in all
MULTIPLE MYELOMA Review & Update for Primary Care. Dr. Joseph Mignone 21st Century Oncology
 MULTIPLE MYELOMA Review & Update for Primary Care Dr. Joseph Mignone 21st Century Oncology OVERVIEW Identify the diagnostic criteria for multiple myeloma Compare first & second line therapies, using data
MULTIPLE MYELOMA Review & Update for Primary Care Dr. Joseph Mignone 21st Century Oncology OVERVIEW Identify the diagnostic criteria for multiple myeloma Compare first & second line therapies, using data
Acute Myelogenous Leukemia Pre-HSCT Data
 Instructions for Acute Myelogenous Leukemia Pre-HSCT Data (Form 2010) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the AML Pre-HSCT Data Form. E-mail
Instructions for Acute Myelogenous Leukemia Pre-HSCT Data (Form 2010) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the AML Pre-HSCT Data Form. E-mail
Acute myeloid leukemia (AML)
 Acute myeloid leukemia (AML) Adult acute myeloid leukemia (AML) is a type of cancer in which the bone marrow makes abnormal myeloblasts (a type of white blood cell), red blood cells, or platelets. Adult
Acute myeloid leukemia (AML) Adult acute myeloid leukemia (AML) is a type of cancer in which the bone marrow makes abnormal myeloblasts (a type of white blood cell), red blood cells, or platelets. Adult
Multiple Myeloma. The term multiple myeloma is considered to be synonymous with myeloma, plasma cell myeloma, active and symptomatic myeloma.
 Multiple Myeloma. The term multiple myeloma is considered to be synonymous with myeloma, plasma cell myeloma, active and symptomatic myeloma. The intent is to positively identify patients with active or
Multiple Myeloma. The term multiple myeloma is considered to be synonymous with myeloma, plasma cell myeloma, active and symptomatic myeloma. The intent is to positively identify patients with active or
Collaboration to collect Autologous transplant outcomes in Lymphoma and Myeloma (CALM) Additional Questionnaire (MED C) INCLUSION CRITERIA CALM STUDY
 Additional Questionnaire (MED C) CALM study Inclusion period: 01/01/2008 to 31/12/2011 PATIENT REGISTRATION FORM Disease Diagnosis Lymphoma S Non Hodgkin Lymphoma (NHL) Mature B-cell neoplasm Follicular
Additional Questionnaire (MED C) CALM study Inclusion period: 01/01/2008 to 31/12/2011 PATIENT REGISTRATION FORM Disease Diagnosis Lymphoma S Non Hodgkin Lymphoma (NHL) Mature B-cell neoplasm Follicular
Multiple Myeloma How to Evaluate Response To Treatment and Relapse
 Multiple Myeloma How to Evaluate Response To Treatment and Relapse D R L. G AR D E R E T Saint Antoine Hospital, Paris Haematology Department 1 What is Multiple Myeloma? 4 Diagnostic Tools 8 Response to
Multiple Myeloma How to Evaluate Response To Treatment and Relapse D R L. G AR D E R E T Saint Antoine Hospital, Paris Haematology Department 1 What is Multiple Myeloma? 4 Diagnostic Tools 8 Response to
ACUTE MYELOID LEUKEMIA (AML),
 1 ACUTE MYELOID LEUKEMIA (AML), ALSO KNOWN AS ACUTE MYELOGENOUS LEUKEMIA WHAT IS CANCER? The body is made up of hundreds of millions of living cells. Normal body cells grow, divide, and die in an orderly
1 ACUTE MYELOID LEUKEMIA (AML), ALSO KNOWN AS ACUTE MYELOGENOUS LEUKEMIA WHAT IS CANCER? The body is made up of hundreds of millions of living cells. Normal body cells grow, divide, and die in an orderly
Blood & Marrow Transplant Glossary. Pediatric Blood and Marrow Transplant Program Patient Guide
 Blood & Marrow Transplant Glossary Pediatric Blood and Marrow Transplant Program Patient Guide Glossary Absolute Neutrophil Count (ANC) -- Also called "absolute granulocyte count" amount of white blood
Blood & Marrow Transplant Glossary Pediatric Blood and Marrow Transplant Program Patient Guide Glossary Absolute Neutrophil Count (ANC) -- Also called "absolute granulocyte count" amount of white blood
NATIONAL CANCER INSTITUTE. Lenalidomide or Observation in Treating Patients With Asymptomatic High-Risk Smoldering Multiple Myeloma
 NATIONAL CANCER INSTITUTE Lenalidomide or Observation in Treating Patients With Asymptomatic High-Risk Smoldering Multiple Myeloma Basic Trial Information Phase Type Status Age Sponsor Protocol IDs Phase
NATIONAL CANCER INSTITUTE Lenalidomide or Observation in Treating Patients With Asymptomatic High-Risk Smoldering Multiple Myeloma Basic Trial Information Phase Type Status Age Sponsor Protocol IDs Phase
LYMPHOMA IN DOGS. Diagnosis/Initial evaluation. Treatment and Prognosis
 LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
LYMPHOMA IN DOGS Lymphoma is a relatively common cancer in dogs. It is a cancer of lymphocytes (a type of white blood cell) and lymphoid tissues. Lymphoid tissue is normally present in many places in the
MEDICAL COVERAGE POLICY
 Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms of your particular benefit plan. Each
Important note Even though this policy may indicate that a particular service or supply is considered covered, this conclusion is not necessarily based upon the terms of your particular benefit plan. Each
New diagnostic criteria for myeloma
 New diagnostic criteria for myeloma Dr Guy Pratt Senior Lecturer/Honorary Consultant Haematologist University of Birmingham/Heart of England NHS Trust International Myeloma Working Group (IMWG) define
New diagnostic criteria for myeloma Dr Guy Pratt Senior Lecturer/Honorary Consultant Haematologist University of Birmingham/Heart of England NHS Trust International Myeloma Working Group (IMWG) define
Hodgkin Lymphoma Disease Specific Biology and Treatment Options. John Kuruvilla
 Hodgkin Lymphoma Disease Specific Biology and Treatment Options John Kuruvilla My Disclaimer This is where I work Objectives Pathobiology what makes HL different Diagnosis Staging Treatment Philosophy
Hodgkin Lymphoma Disease Specific Biology and Treatment Options John Kuruvilla My Disclaimer This is where I work Objectives Pathobiology what makes HL different Diagnosis Staging Treatment Philosophy
PROGNOSIS IN ACUTE LYMPHOBLASTIC LEUKEMIA PROGNOSIS IN ACUTE MYELOID LEUKEMIA
 PROGNOSIS IN ACUTE LYMPHOBLASTIC LEUKEMIA UNFAVORABLE Advanced age High leukocyte count at diagnosis Presence of myeloid antigens Late achievement of CR Chromosomal abnormalities: t(9:22)(q34:q11) t(4;11)(q21;q23)
PROGNOSIS IN ACUTE LYMPHOBLASTIC LEUKEMIA UNFAVORABLE Advanced age High leukocyte count at diagnosis Presence of myeloid antigens Late achievement of CR Chromosomal abnormalities: t(9:22)(q34:q11) t(4;11)(q21;q23)
Acute myeloid leukaemia (AML) in children
 1 61.02 Acute myeloid leukaemia (AML) in children AML can affect children of any age, and girls and boys are equally affected. Leukaemia Acute myeloid leukaemia (AML) FAB classification of AML Causes of
1 61.02 Acute myeloid leukaemia (AML) in children AML can affect children of any age, and girls and boys are equally affected. Leukaemia Acute myeloid leukaemia (AML) FAB classification of AML Causes of
亞 東 紀 念 醫 院 Follicular Lymphoma 臨 床 指 引
 前 言 : 惡 性 淋 巴 瘤 ( 或 簡 稱 淋 巴 癌 ) 乃 由 體 內 淋 巴 系 統 包 括 淋 巴 細 胞 淋 巴 管 淋 巴 腺 及 一 些 淋 巴 器 官 或 組 織 如 脾 臟 胸 腺 及 扁 桃 腺 等 所 長 出 的 惡 性 腫 瘤 依 腫 瘤 病 理 組 織 型 態 的 不 同 可 分 為 何 杰 金 氏 淋 巴 瘤 (Hodgkin s disease) 與 非 何 杰 金
前 言 : 惡 性 淋 巴 瘤 ( 或 簡 稱 淋 巴 癌 ) 乃 由 體 內 淋 巴 系 統 包 括 淋 巴 細 胞 淋 巴 管 淋 巴 腺 及 一 些 淋 巴 器 官 或 組 織 如 脾 臟 胸 腺 及 扁 桃 腺 等 所 長 出 的 惡 性 腫 瘤 依 腫 瘤 病 理 組 織 型 態 的 不 同 可 分 為 何 杰 金 氏 淋 巴 瘤 (Hodgkin s disease) 與 非 何 杰 金
Estimated New Cases of Leukemia, Lymphoma, Myeloma 2014
 ABOUT BLOOD CANCERS Leukemia, Hodgkin lymphoma (HL), non-hodgkin lymphoma (NHL), myeloma, myelodysplastic syndromes (MDS) and myeloproliferative neoplasms (MPNs) are types of cancer that can affect the
ABOUT BLOOD CANCERS Leukemia, Hodgkin lymphoma (HL), non-hodgkin lymphoma (NHL), myeloma, myelodysplastic syndromes (MDS) and myeloproliferative neoplasms (MPNs) are types of cancer that can affect the
What is chronic lymphocytic leukaemia?
 Revised October 2011 What is chronic lymphocytic leukaemia? The diagnosis of a blood cancer can be a devastating event for patients, families and friends. It is therefore vital for everyone to have access
Revised October 2011 What is chronic lymphocytic leukaemia? The diagnosis of a blood cancer can be a devastating event for patients, families and friends. It is therefore vital for everyone to have access
Glossary of Multiple Myeloma Terms
 Some things that make multiple myeloma (MM) difficult to understand are the unfamiliar medical terms that some experts and healthcare providers use to explain it. You may come across words like these when
Some things that make multiple myeloma (MM) difficult to understand are the unfamiliar medical terms that some experts and healthcare providers use to explain it. You may come across words like these when
Acute Myeloid Leukemia
 Acute Myeloid Leukemia Introduction Leukemia is cancer of the white blood cells. The increased number of these cells leads to overcrowding of healthy blood cells. As a result, the healthy cells are not
Acute Myeloid Leukemia Introduction Leukemia is cancer of the white blood cells. The increased number of these cells leads to overcrowding of healthy blood cells. As a result, the healthy cells are not
CLL. Handheld record. Stockport NHS foundation trust
 CLL 2015 Handheld record Contains- Patient information booklet, details of haematology clinic assessment and ongoing clinical assessment at GP surgery Stockport NHS foundation trust You have been diagnosed
CLL 2015 Handheld record Contains- Patient information booklet, details of haematology clinic assessment and ongoing clinical assessment at GP surgery Stockport NHS foundation trust You have been diagnosed
A Science Writer s Guide to Multiple Myeloma
 A Science Writer s Guide to Multiple Myeloma 1 A Science Writer s Guide to Multiple Myeloma A Science Writer s Guide to Multiple Myeloma PREFACE Blood cancers and related disorders a serious health risk
A Science Writer s Guide to Multiple Myeloma 1 A Science Writer s Guide to Multiple Myeloma A Science Writer s Guide to Multiple Myeloma PREFACE Blood cancers and related disorders a serious health risk
Why discuss CLL? Common: 40% of US leukaemia. approx 100 pa in SJH / MWHB 3 inpatients in SJH at any time
 Why discuss CLL? Common: 40% of US leukaemia approx 100 pa in SJH / MWHB 3 inpatients in SJH at any time Median age of dx is 65 (30s. Incurable, survival 2-202 20 years Require ongoing supportive care
Why discuss CLL? Common: 40% of US leukaemia approx 100 pa in SJH / MWHB 3 inpatients in SJH at any time Median age of dx is 65 (30s. Incurable, survival 2-202 20 years Require ongoing supportive care
PROTOCOLS FOR TREATMENT OF MALIGNANT LYMPHOMA
 2012 1 31,, PROTOCOLS FOR TREATMENT OF MALIGNANT LYMPHOMA Version 1.0 2012 DIVISION OF HAEMATOLOGY / ONCOLOGY DEPARTMENT OF MEDICINE KAOHSING VETERAN GENERAL HOSPTIAL General Guide Diagnosis 1.Adequate
2012 1 31,, PROTOCOLS FOR TREATMENT OF MALIGNANT LYMPHOMA Version 1.0 2012 DIVISION OF HAEMATOLOGY / ONCOLOGY DEPARTMENT OF MEDICINE KAOHSING VETERAN GENERAL HOSPTIAL General Guide Diagnosis 1.Adequate
NON SECRETORY MULTIPLE MYELOMA A CASE REPORT
 NON SECRETORY MULTIPLE MYELOMA A CASE REPORT Golwilkar A.,*Saluja R., Mehendale A. and Jalnapurkar N. Department of Histopathology, Golwilkar Metropolis Health Services (India) Pvt Ltd *Author for Correspondence
NON SECRETORY MULTIPLE MYELOMA A CASE REPORT Golwilkar A.,*Saluja R., Mehendale A. and Jalnapurkar N. Department of Histopathology, Golwilkar Metropolis Health Services (India) Pvt Ltd *Author for Correspondence
Table of Contents Accelerate Your Research Introduction I. From the Real World to the Lab II. Research Challenges III. How Can Conversant Bio Help?
 Table of Contents Accelerate Your Research 2 Introduction 3 I. From the Real World to the Lab 4 A. Diagnosing Multiple Myeloma 4 1. Lab Tests 4 2. Bone Marrow Exams 6 3. Imaging Studies 7 B. Subtypes of
Table of Contents Accelerate Your Research 2 Introduction 3 I. From the Real World to the Lab 4 A. Diagnosing Multiple Myeloma 4 1. Lab Tests 4 2. Bone Marrow Exams 6 3. Imaging Studies 7 B. Subtypes of
Acute leukemias and myeloproliferative neoplasms
 Acute leukemias and myeloproliferative neoplasms GERGELY SZOMBATH SEMMELWEIS UNIVERSITY OF MEDICINE IIIRD. DEPARTMENT OF INTERNAL MEDICINE Basics of acute leukemia Neoplastic disease Cell of origin is
Acute leukemias and myeloproliferative neoplasms GERGELY SZOMBATH SEMMELWEIS UNIVERSITY OF MEDICINE IIIRD. DEPARTMENT OF INTERNAL MEDICINE Basics of acute leukemia Neoplastic disease Cell of origin is
Hematology Morphology Critique
 Survey Slide: History: 60-year-old female presenting with pneumonia Further Laboratory Data: Hgb : 90 g/l RBC : 2.92 10 12 /L Hct : 0.25 L/L MCV : 87 fl MCH : 30.8 pg MCHC : 355 g/l RDW : 17.7 % WBC :
Survey Slide: History: 60-year-old female presenting with pneumonia Further Laboratory Data: Hgb : 90 g/l RBC : 2.92 10 12 /L Hct : 0.25 L/L MCV : 87 fl MCH : 30.8 pg MCHC : 355 g/l RDW : 17.7 % WBC :
Haematopoietic Chimerism Analysis after Allogeneic Stem Cell Transplantation
 Haematopoietic Chimerism Analysis after Allogeneic Stem Cell Transplantation Dr Ros Ganderton, Ms Kate Parratt, Dr Debbie Richardson, Dr Kim Orchard and Dr Liz Hodges Departments of Molecular Pathology
Haematopoietic Chimerism Analysis after Allogeneic Stem Cell Transplantation Dr Ros Ganderton, Ms Kate Parratt, Dr Debbie Richardson, Dr Kim Orchard and Dr Liz Hodges Departments of Molecular Pathology
Hematopathology VII Acute Lymphoblastic Leukemia, Chronic Lymphocytic Leukemia, And Hairy Cell Leukemia
 John L. Kennedy, M.D. UIC College of Medicine Associate Professor of Clinical Pathology M2 Pathology Course Lead Pathologist, VA Chicago Health Care System Lecture #43 Phone: (312) 569-6690 Thursday, November
John L. Kennedy, M.D. UIC College of Medicine Associate Professor of Clinical Pathology M2 Pathology Course Lead Pathologist, VA Chicago Health Care System Lecture #43 Phone: (312) 569-6690 Thursday, November
MALIGNANT LYMPHOMAS. Dr. Olga Vujovic (Updated August 2010)
 MALIGNANT LYMPHOMAS Dr. Olga Vujovic (Updated August 2010) Malignant lymphomas consist of Hodgkin and non-hodgkin lymphomas. The current management of these diseases involves a multi-disciplinary approach.
MALIGNANT LYMPHOMAS Dr. Olga Vujovic (Updated August 2010) Malignant lymphomas consist of Hodgkin and non-hodgkin lymphomas. The current management of these diseases involves a multi-disciplinary approach.
Who is affected by HCL and what causes it?
 Freephone helpline 0808 808 5555 information@lymphomas.org.uk www.lymphomas.org.uk Hairy cell leukaemia Hairy cell leukaemia (HCL) is a rare and very distinctive cancer of blood cells called B lymphocytes
Freephone helpline 0808 808 5555 information@lymphomas.org.uk www.lymphomas.org.uk Hairy cell leukaemia Hairy cell leukaemia (HCL) is a rare and very distinctive cancer of blood cells called B lymphocytes
Emerging New Prognostic Scoring Systems in Myelodysplastic Syndromes 2012
 Emerging New Prognostic Scoring Systems in Myelodysplastic Syndromes 2012 Arjan A. van de Loosdrecht, MD, PhD Department of Hematology VU University Medical Center VU-Institute of Cancer and Immunology
Emerging New Prognostic Scoring Systems in Myelodysplastic Syndromes 2012 Arjan A. van de Loosdrecht, MD, PhD Department of Hematology VU University Medical Center VU-Institute of Cancer and Immunology
Pro Cure in Multiple Myeloma. Nicolaus Kröger Dept. of Stem Cell Transplantation University Hospital Hamburg Hamburg, Germany
 Pro Cure in Multiple Myeloma Nicolaus Kröger Dept. of Stem Cell Transplantation University Hospital Hamburg Hamburg, Germany Pro Cure in Multiple Myeloma Several hematological malignancies can be cured
Pro Cure in Multiple Myeloma Nicolaus Kröger Dept. of Stem Cell Transplantation University Hospital Hamburg Hamburg, Germany Pro Cure in Multiple Myeloma Several hematological malignancies can be cured
Aggressive lymphomas. Michael Crump Princess Margaret Hospital
 Aggressive lymphomas Michael Crump Princess Margaret Hospital What are the aggressive lymphomas? Diffuse large B cell Mediastinal large B cell Anaplastic large cell Burkitt lymphoma (transformed lymphoma:
Aggressive lymphomas Michael Crump Princess Margaret Hospital What are the aggressive lymphomas? Diffuse large B cell Mediastinal large B cell Anaplastic large cell Burkitt lymphoma (transformed lymphoma:
Oncology. Objectives. Cancer Nomenclature. Cancer is a disease of the cell Cancer develops when certain cells begin to grow out of control
 Oncology Objectives Describe the etiology and pathophysiological mechanisms of cancer Discuss medical and family history findings relevant to cancer Identify general signs and symptoms associated with
Oncology Objectives Describe the etiology and pathophysiological mechanisms of cancer Discuss medical and family history findings relevant to cancer Identify general signs and symptoms associated with
Controversies in the management of patients with PMF 0/1
 State of the art treatments of patients with MPNs Turracher Höhe 2010 Controversies in the management of patients with PMF 0/1 Heinz Gisslinger Medical University of Vienna Divison for Hematology, Vienna
State of the art treatments of patients with MPNs Turracher Höhe 2010 Controversies in the management of patients with PMF 0/1 Heinz Gisslinger Medical University of Vienna Divison for Hematology, Vienna
Treatment Recommendations for People Living with CML
 Treatment Recommendations for People Living with CML Foreword by CML Workgroup Chronic myeloid leukaemia (CML) is a disease of the blood and bone marrow that results when there is a cancerous transformation
Treatment Recommendations for People Living with CML Foreword by CML Workgroup Chronic myeloid leukaemia (CML) is a disease of the blood and bone marrow that results when there is a cancerous transformation
Corporate Medical Policy
 Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplantation_for_cll_and_sll
Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplantation_for_cll_and_sll
Outline. Question 1. Question 2. What is Multiple Myeloma? Andrew Eisenberger, MD
 Outline A Disease Overview June 3, 2013 Andrew Eisenberger, MD Assistant Professor of Medicine Hematology/Oncology Columbia Presbyterian Medical Center Introduction Epidemiology/Risk Factors Clinical Features/Diagnostic
Outline A Disease Overview June 3, 2013 Andrew Eisenberger, MD Assistant Professor of Medicine Hematology/Oncology Columbia Presbyterian Medical Center Introduction Epidemiology/Risk Factors Clinical Features/Diagnostic
Radiotherapy in Plasmacytoma and Myeloma. David Cutter Multiple Myeloma NSSG Annual Meeting 14 th September 2015
 Radiotherapy in Plasmacytoma and Myeloma David Cutter Multiple Myeloma NSSG Annual Meeting 14 th September 2015 Contents Indications for radiotherapy: Palliation in Multiple Myeloma Solitary Bone Plasmacytoma
Radiotherapy in Plasmacytoma and Myeloma David Cutter Multiple Myeloma NSSG Annual Meeting 14 th September 2015 Contents Indications for radiotherapy: Palliation in Multiple Myeloma Solitary Bone Plasmacytoma
New Evaluation Criteria for Response and Toxicity in Lung Cancer Treatment
 Lung Cancer New Evaluation Criteria for Response and Toxicity in Lung Cancer Treatment JMAJ 46(12): 554 558, 2003 Masahiko SHIBUYA Chief, Division of Respiratory Medicine, Tokyo Metropolitan Komagome Hospital
Lung Cancer New Evaluation Criteria for Response and Toxicity in Lung Cancer Treatment JMAJ 46(12): 554 558, 2003 Masahiko SHIBUYA Chief, Division of Respiratory Medicine, Tokyo Metropolitan Komagome Hospital
A 32 year old woman comes to your clinic with neck masses for the last several weeks. Masses are discrete, non matted, firm and rubbery on
 A 32 year old woman comes to your clinic with neck masses for the last several weeks. Masses are discrete, non matted, firm and rubbery on examination. She also has fever, weight loss, and sweats. What
A 32 year old woman comes to your clinic with neck masses for the last several weeks. Masses are discrete, non matted, firm and rubbery on examination. She also has fever, weight loss, and sweats. What
Pulling the Plug on Cancer Cell Communication. Stephen M. Ansell, MD, PhD Mayo Clinic
 Pulling the Plug on Cancer Cell Communication Stephen M. Ansell, MD, PhD Mayo Clinic Why do Waldenstrom s cells need to communicate? Waldenstrom s cells need activating signals to stay alive. WM cells
Pulling the Plug on Cancer Cell Communication Stephen M. Ansell, MD, PhD Mayo Clinic Why do Waldenstrom s cells need to communicate? Waldenstrom s cells need activating signals to stay alive. WM cells
Collect and label sample according to standard protocols. Gently invert tube 8-10 times immediately after draw. DO NOT SHAKE. Do not centrifuge.
 Complete Blood Count CPT Code: CBC with Differential: 85025 CBC without Differential: 85027 Order Code: CBC with Differential: C915 Includes: White blood cell, Red blood cell, Hematocrit, Hemoglobin, MCV,
Complete Blood Count CPT Code: CBC with Differential: 85025 CBC without Differential: 85027 Order Code: CBC with Differential: C915 Includes: White blood cell, Red blood cell, Hematocrit, Hemoglobin, MCV,
A Diagnostic Chest XRay: Multiple Myeloma
 Daniela Marinho Tridente, VI FCMSCSP October 2013 A Diagnostic Chest XRay: Multiple Myeloma Daniela Marinho Tridente, VI FCMSCSP Our Learning Agenda Introduction of our patient His imaging data and findings
Daniela Marinho Tridente, VI FCMSCSP October 2013 A Diagnostic Chest XRay: Multiple Myeloma Daniela Marinho Tridente, VI FCMSCSP Our Learning Agenda Introduction of our patient His imaging data and findings
Monoclonal Gammopathy of Undetermined Significance (MGUS) Facts
 Monoclonal Gammopathy of Undetermined Significance (MGUS) Facts Normal plasma cells (a type of white blood cell) produce antibodies (also known as immunoglobulins) which help fight infection. Each type
Monoclonal Gammopathy of Undetermined Significance (MGUS) Facts Normal plasma cells (a type of white blood cell) produce antibodies (also known as immunoglobulins) which help fight infection. Each type
MULTIPLE MYELOMA. Overview
 MULTIPLE MYELOMA Overview Steven R. Schuster, M.D. May 7, 2015 Objectives Give an overview of Multiple Myeloma Everything I know in 15 minutes Explain how genetic information can be used to personalize
MULTIPLE MYELOMA Overview Steven R. Schuster, M.D. May 7, 2015 Objectives Give an overview of Multiple Myeloma Everything I know in 15 minutes Explain how genetic information can be used to personalize
The CML Guide Information for Patients and Caregivers
 The CML Guide Information for Patients and Caregivers LEUKEMIA LYMPHOMA CHRONIC MYELOGENOUS LEUKEMIA MYELOMA Printing of this publication made possible by a grant from A Message from John Walter President
The CML Guide Information for Patients and Caregivers LEUKEMIA LYMPHOMA CHRONIC MYELOGENOUS LEUKEMIA MYELOMA Printing of this publication made possible by a grant from A Message from John Walter President
Update in Hematology Oncology Targeted Therapies. Mark Holguin
 Update in Hematology Oncology Targeted Therapies Mark Holguin 25 years ago Why I chose oncology People How to help people with possibly the most difficult thing they may have to deal with Science Turning
Update in Hematology Oncology Targeted Therapies Mark Holguin 25 years ago Why I chose oncology People How to help people with possibly the most difficult thing they may have to deal with Science Turning
Plasma cell dyscrasias Mark Drayson
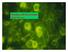 Plasma cell dyscrasias Mark Drayson Mortality statistics for England and Wales. Deaths attributed to multiple myeloma from 1988-1997 by age cohort as a percentage of total (21,257) deaths Deaths in age
Plasma cell dyscrasias Mark Drayson Mortality statistics for England and Wales. Deaths attributed to multiple myeloma from 1988-1997 by age cohort as a percentage of total (21,257) deaths Deaths in age
Leukaemia and lymphoma what s the difference?
 Freephone helpline 0808 808 5555 information@lymphomas.org.uk www.lymphomas.org.uk Leukaemia and lymphoma what s the difference? This is a difficult question to answer simply but it is one that is often
Freephone helpline 0808 808 5555 information@lymphomas.org.uk www.lymphomas.org.uk Leukaemia and lymphoma what s the difference? This is a difficult question to answer simply but it is one that is often
What is chronic myeloid leukaemia?
 Chronic Myeloid Leukaemia What is chronic myeloid leukaemia? Let us explain it to you. www.anticancerfund.org www.esmo.org ESMO/ACF Patient Guide Series based on the ESMO Clinical Practice Guidelines CHRONIC
Chronic Myeloid Leukaemia What is chronic myeloid leukaemia? Let us explain it to you. www.anticancerfund.org www.esmo.org ESMO/ACF Patient Guide Series based on the ESMO Clinical Practice Guidelines CHRONIC
General Rules SEER Summary Stage 2000. Objectives. What is Staging? 5/8/2014
 General Rules SEER Summary Stage 2000 Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
General Rules SEER Summary Stage 2000 Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
I've Just Been Diagnosed. with Multiple Myeloma, What s Next?
 I've Just Been Diagnosed with Multiple Myeloma, What s Next? Table of Contents Message from a Survivor Introduction What is Multiple Myeloma? What Causes Multiple Myeloma? Genes & Multiple Myeloma What
I've Just Been Diagnosed with Multiple Myeloma, What s Next? Table of Contents Message from a Survivor Introduction What is Multiple Myeloma? What Causes Multiple Myeloma? Genes & Multiple Myeloma What
Multiple Myeloma Understanding your diagnosis
 Multiple Myeloma Understanding your diagnosis Multiple Myeloma Understanding your diagnosis When you first hear that you have cancer you may feel alone and afraid. You may be overwhelmed by the large amount
Multiple Myeloma Understanding your diagnosis Multiple Myeloma Understanding your diagnosis When you first hear that you have cancer you may feel alone and afraid. You may be overwhelmed by the large amount
I was just diagnosed, so my doctor and I are deciding on treatment. My doctor said there are several
 Track 3: Goals of therapy I was just diagnosed, so my doctor and I are deciding on treatment. My doctor said there are several factors she ll use to decide what s best for me. Let s talk about making treatment
Track 3: Goals of therapy I was just diagnosed, so my doctor and I are deciding on treatment. My doctor said there are several factors she ll use to decide what s best for me. Let s talk about making treatment
Chronic Lymphocytic Leukemia. Case Study. AAIM Triennial October 2012 Susan Sokoloski, M.D.
 Chronic Lymphocytic Leukemia AAIM Triennial October 2012 Susan Sokoloski, M.D. Case Study 57 year old male, trial application for $1,000,000 Universal Life coverage Cover letter from sales agent indicates
Chronic Lymphocytic Leukemia AAIM Triennial October 2012 Susan Sokoloski, M.D. Case Study 57 year old male, trial application for $1,000,000 Universal Life coverage Cover letter from sales agent indicates
How CanCer becomes critical in the claims
 How CanCer becomes critical in the claims arena Cancer is a disease in which cells in your body grow in an uncontrolled way and form a lump called a tumour. In a healthy individual cells grow and reproduce
How CanCer becomes critical in the claims arena Cancer is a disease in which cells in your body grow in an uncontrolled way and form a lump called a tumour. In a healthy individual cells grow and reproduce
Appendix D- Monoclonal Gammopathy of Undetermined Significance (MGUS)
 Local Enhanced Service: Primary care management of stable haematological patients Monoclonal Gammopathy of Undetermined Significance (MGUS) 1. Introduction Monoclonal Gammopathy of Undetermined Significance
Local Enhanced Service: Primary care management of stable haematological patients Monoclonal Gammopathy of Undetermined Significance (MGUS) 1. Introduction Monoclonal Gammopathy of Undetermined Significance
Understanding Protein Electrophoresis
 Understanding Protein Electrophoresis International Myeloma Foundation 12650 Riverside Drive, Suite 206 North Hollywood, CA 91607 USA Telephone: 800-452-CURE (2873) (USA & Canada) 818-487-7455 Fax: 818-487-7454
Understanding Protein Electrophoresis International Myeloma Foundation 12650 Riverside Drive, Suite 206 North Hollywood, CA 91607 USA Telephone: 800-452-CURE (2873) (USA & Canada) 818-487-7455 Fax: 818-487-7454
Multiple Myeloma Making Sense of the Report Forms. Parameswaran Hari Medical College of Wisconsin Milwaukee
 Hodgkin CML MDS/Other Leuk CLL Neuroblastoma Multiple Myeloma Making Sense of the Report Forms Parameswaran Hari Medical College of Wisconsin Milwaukee Indications for Blood and Marrow Transplantation
Hodgkin CML MDS/Other Leuk CLL Neuroblastoma Multiple Myeloma Making Sense of the Report Forms Parameswaran Hari Medical College of Wisconsin Milwaukee Indications for Blood and Marrow Transplantation
Multiple Myeloma. This reference summary will help you understand multiple myeloma and its treatment options.
 Multiple Myeloma Introduction Multiple myeloma is a type of cancer that affects white blood cells. Each year, thousands of people find out that they have multiple myeloma. This reference summary will help
Multiple Myeloma Introduction Multiple myeloma is a type of cancer that affects white blood cells. Each year, thousands of people find out that they have multiple myeloma. This reference summary will help
CML. cure. A Patient s Guide. Molecular Biology Diagnosis Stem Cell Transplant Monitoring New Drugs Questions to Ask and More
 A Patient s Guide to CML Molecular Biology Diagnosis Stem Cell Transplant Monitoring New Drugs Questions to Ask and More cure C a n c e r U p d at e s, R e s e a r c h & E d u c at i o n Based on science,
A Patient s Guide to CML Molecular Biology Diagnosis Stem Cell Transplant Monitoring New Drugs Questions to Ask and More cure C a n c e r U p d at e s, R e s e a r c h & E d u c at i o n Based on science,
Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL)
 Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL) Version History Version Date Summary of Change/Process 2.0 08.05.08 Endorsed by the Governance Committee 2.1 16.02.11 Circulated at
Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL) Version History Version Date Summary of Change/Process 2.0 08.05.08 Endorsed by the Governance Committee 2.1 16.02.11 Circulated at
Multiple Myeloma. What is cancer?
 What is cancer? Multiple Myeloma The body is made up of trillions of living cells. Normal body cells grow, divide to make new cells, and die in an orderly way. During the early years of a person's life,
What is cancer? Multiple Myeloma The body is made up of trillions of living cells. Normal body cells grow, divide to make new cells, and die in an orderly way. During the early years of a person's life,
Understanding Leukemia
 Understanding Leukemia Ray, CML survivor Revised 2012 A Message from Louis J. DeGennaro, PhD President and CEO of The Leukemia & Lymphoma Society The Leukemia & Lymphoma Society (LLS) is the world s largest
Understanding Leukemia Ray, CML survivor Revised 2012 A Message from Louis J. DeGennaro, PhD President and CEO of The Leukemia & Lymphoma Society The Leukemia & Lymphoma Society (LLS) is the world s largest
Myeloma pathways to diagnosis UCLP audit
 Myeloma pathways to diagnosis UCLP audit Dr Neil Rabin Consultant Haematologist University College London Hospitals & North Middlesex University Hospital Myeloma Clinical Features Bone pain (70%) High
Myeloma pathways to diagnosis UCLP audit Dr Neil Rabin Consultant Haematologist University College London Hospitals & North Middlesex University Hospital Myeloma Clinical Features Bone pain (70%) High
Myelodysplasia. Dr John Barry
 Myelodysplasia Dr John Barry Myelodysplasia Group of heterogenouus bone marrow disorders that are due to a defect in stem cells. Increasing bone marrow failure leading to quan>ta>ve and qualita>ve abnormali>es
Myelodysplasia Dr John Barry Myelodysplasia Group of heterogenouus bone marrow disorders that are due to a defect in stem cells. Increasing bone marrow failure leading to quan>ta>ve and qualita>ve abnormali>es
Background Information Myeloma
 Myeloma FAST FACTS Myeloma, also known as multiple myeloma, is a type of cancer that develops from plasma cells which originate in the bone marrow 1 Myeloma is the second most common type of blood cancer
Myeloma FAST FACTS Myeloma, also known as multiple myeloma, is a type of cancer that develops from plasma cells which originate in the bone marrow 1 Myeloma is the second most common type of blood cancer
LYMPHOMA. BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons
 LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
LYMPHOMA BACHIR ALOBEID, M.D. HEMATOPATHOLOGY DIVISION PATHOLOGY DEPARTMENT Columbia University/ College of Physicians & Surgeons Normal development of lymphocytes Lymphocyte proliferation and differentiation:
Us TOO University Presents: Understanding Diagnostic Testing
 Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Bone Marrow Evaluation for Lymphoma. Faizi Ali, MD Hematopathology Fellow William Beaumont Hospital
 Bone Marrow Evaluation for Lymphoma Faizi Ali, MD Hematopathology Fellow William Beaumont Hospital Indications One of the most common indications for a bone marrow biopsy is to evaluate for malignant lymphoma.
Bone Marrow Evaluation for Lymphoma Faizi Ali, MD Hematopathology Fellow William Beaumont Hospital Indications One of the most common indications for a bone marrow biopsy is to evaluate for malignant lymphoma.
