RESPIRATORY DISTRESS IN NEWBORN: TREATED WITH VENTILATION IN A LEVEL II NURSERY
|
|
|
- Marvin Leonard
- 7 years ago
- Views:
Transcription
1 RESPIRATORY DISTRESS IN NEWBORN: TREATED WITH VENTILATION IN A LEVEL II NURSERY A.K. Malhotra R. Nagpal R.K. Gupta D.S. Chhajta R.K. Arora ABSTRACT Fifty consecutive neonates with respiratory distress persisting beyond 6 h of age were studied during a 18 month period (total deliveries 2000/y). Twenty two neonates were managed with oxygen hood with increasing oxygen concentration, 28 with continuous positive airway pressure (CPAP) ventilation using a nasal cannula. Of these babies on CPAP, 10 were shifted to intermittent positive pressure ventilation (IPPV) on a pressure limited, time cycled ventilator (Neovent, Vickers). Babies were monitored with continuous hemoglobin oxygen saturation (SaO 2 ), hourly blood pressure and vital charting. Radial arterial blood gas analysis (ABG) was done when feasible and especially on clinical deterioration. Oxygen (FiO ) from an oxygen concentrator was used as a source of continuous supply of oxygen. Commonest cause of respiratory distress was hyaline membrane disease (18%), followed by wet lung syndromes (14%), meconium aspiration (12%), asphyxia (12%) and septicemia (8%). In 8 babies, a lung biopsy (postmortem) was done to confirm the diagnosis. Nineteen of the 50 babies with respiratory distress died, there was a survival of 50% on CPAP and 30% on IPPV. No case of oxygen toxicity or other major complications was encountered. Even with moderate resources, neonatal ventilation in a Level II nursery is a Respiratory distress is the most common problem in neonatal nurseries. It results from a variety of causes and an urgent work up is essential. Yet for hypoxemia some form of assisted ventilation is immediately warranted. The outlook of babies with respiratory distress syndrome has changed after the first use of continuous positive airway pressure (CPAP) by Gregory et al.(l). It is now an established modality for neonates for many years. In India, a survival of 100% in babies more than 1.5 Kg on CPAP mode is reported(2). It is also recommended that neonatal ventilation should be ventured in centres where basic facilities for Level II care already exist. Ours is a well equipped nursery recognized by the National Neonatology Forum (NNF). We treated 50 babies with respiratory distress, of which 31 survived. Material and Methods In a prospective study, we analyzed the causes of respiratory distress and indications for ventilation in newborns during a 18 month period (Jan '92-June '93). There were a total of 2931 booked deliveries during this period in our hospital which caters to a mixed Indian challenging task. Babies less than 1000g require aggressive measures which is not very economical in a special care baby unit (SCBU). Key words: Neonatal ventilation, Respiratory distress. From the Neonatal Unit, Department of Pediatrics, Command Hospital, Pune All 040. Reprint requests: Lt. Col. A.K. Malhotra, 174, Military Hospital C/o 56 A.P.O. Received for publication: October 2,1993; Accepted: June 8,1994
2 MALHOTRA ET AL. population. For the diagnosis of respiratory distress, the important signs are respiratory rate more than 60 per minute, grunt and sub-costal recessions. These signs being non-specific, we consider two out of three of these as confirmative of respiratory distress(3). Rarely, apneic attacks may present as a sole manifestation of ventilatory failure. As the spectrum of respiratory distress in newborns is large, we start a workup at four hours of age and give a provisional diagnosis at 6 hours of post natal life. The initial workup included a gastric aspirate shake test, chest X-ray and an arterial blood gas (ABG) analysis. Blood pressure and vital signs were recorded. Oxygen saturation (SaO 2 ) and heart rate were monitored using a pulse oximeter (Ohmeda Biox 3760). Oxygen from a oxygen concentrator (Air Sep Forlife) with FiO was used to supply oxygen. Intravenous fluids were started at the rate of 60 ml per kg body weight of 10% dextrose solution. If clinical condition warranted antibiotics, blood cultures were taken prior in 10 ml culture bottles. Downes RDS Score(4) was recorded and babies with a score of six or more were put on CPAP with a nasal cannula (Argyle). Babies with a score of five or less were managed with oxygen hood with increasing FiO 2 concentrations. The indication for giving CPAP were (i) Downes score of 6 or more; (ii) inability to maintain a SaO 2 of 87% with oxygen hood; (iii) PaO 2 of less than 50 mm Hg; and (iv) radiological evidence of severe hyaline membrane disease (HMD) with a negative shake test. CPAP is considered a failure if a baby has (i) inability to maintain a SaO 2 of VENTILATION FOR RDS 87% with CPAP of 12 cm H 2 O and FiO 2 of 0.9; (ii) PaO 2 <50 mm Hg with FiO 2 0.9; (iii) ph <7.25, PaCO 2 >60 mm Hg; and (iv) recurrent (more than 3) apneic attacks as a manifestation of respiratory failure. CPAP failures were shifted to intermittent positive pressure ventilation (IPPV) mode on a time cycled, pressure limited continuous flow neonatal ventilator (Neovent, Vickers). We use minimal ventilatory settings depending on the lung pathology to achieve a SaO 2 of 90±3% or PaO mm Hg. Subsequent ABG was done through repeated radial arterial punctures at 6-12 hourly intervals. The definitions suggested by NNF Group on Neonatal Nomenclature(3) were accepted. Babies delivered with a thick meconium stained liquor were intubated prior to first breath. Septicemia was diagnosed if the blood culture grew pathogenic organisms. Immaturity was labelled when a baby less than 1000 g had no other primary cause of death. Results Out of the 50 babies enrolled in the study, 26 were males and 24 females. There were 40 babies with low birth weight; of these 10 babies were less than 1000g. Mean birth weight was 1823 g (range g) and mean gestational. age 33 wk (range wk). The smallest baby a non survivor was 740 g with a gestational age of 26 weeks. Table I depicts the modes of oxygenation. Twenty two babies were managed with oxygen hood and 28 required CPAP ventilation. Of these 10 babies had a failure of CPAP ventilation and were shifted to IPPV mode. The mean duration of CPAP mode was 53 h (range h) and IPPV mode 46 h (range 7-74 h). 208
3 INDIAN PEDIATRICS Hyaline membrane disease (18%) was the commonest cause of respiratory distress, followed by wet lung syndromes (14%), meconium aspiration syndrome (12%), asphyxia (12%) and VOLUME 32-FEBRUARY 1995 septicemia (8%) (Table II). There was one baby 1000 g who developed chronic pulmonary insufficiency of prematurity (CPIP) and was discharged with a weight of 1750g. In 8 cases (birth weight
4 MALHOTRAETAL g) with a clinical diagnosis of HMD, the cause of death was confirmed by a postmortem lung biopsy. In all these cases, the histopathological features were consistent with hyaline membrane disease. Table III depicts the survival in relation to the birth weight and mode of ventilation. There was a 50% survival on CPAP and 30% on IPPV mode. Survival of babies less than 1000g was 30%. Three babies had a symptomatic ductus arteriosus (PDA) and were managed on standard lines. No baby developed pneumofhorax or other major complications of ventilation or oxygen therapy. Discussion Majority of the medical colleges in our country lack the basic infrastructure to ventilate babies(2). Ventilation has only been reported from tertiary centres and experience from Level II nurseries is lacking. We have the expertise but the resources are limited. At the same time, IPPV and aggressive monitoring results in a significant iatrogenic morbidity. Within the frame work of the physics of ventilation every nursery evolves its protocols and settings for ventilation. VENTILATION FOR RDS As oxygen is a drug, we choose a midline path whereby the complications are minimum. The CPAP mode with nasal cannula is an easy way to improve oxygenation. This makes the routine endotracheal intubation of infants requiring only continuous airway distending pressures no longer justifiable(5). Once oxygenation is adequate and signs of respiratory distress decrease, an optimal CPAP is achieved. CPAP failures appear to have an omnious prognosis regardless of the birth weight(5). In our series, we had 10 babies less than 1000g and the mortality in them was 70%. CPAP is not an ideal treatment for them and they may require IPPV at the outset(2). Chronic pulmonary insufficiency of prematurity is a distinct entity as these babies are less than 1000g and have a normal chest X-ray at birth but are oxygen dependent at 3-4 weeks of age. We agree with Singh et al. in considering a cut off of immaturity at 750 g(2). In a review of literature(5) the incidence of pneumothoraces was 0 to 14%. We had no case of pneumofhorax or other major complications of oxygen toxicity.
5 INDIAN PEDIATRICS Pulse oximetry is a reliable technique for monitoring of oxygenation in newborns(6,7). It is a handy tool in a Level II nursery as apart from SaO 2 it displays the heart rate. It obviates the use of an electrocardiograph and apnea monitors. In managing cases of respiratory distress, it has few limitations and the artifacts are avoidable. Fanconi et al.(8) constructed oxygen dissociation curves with pulse oximeter SaO 2, measured SaO 2 and calculated SaO 2 ; they were all similar. A pulse oximeter reading of 85% to 90% is a clinically safe target. We maintain a SaO 2 level of 90±3% and titrate FiO 2 to that level. On clinical deterioration and failure to maintain saturation, an ABG helps in correcting the acid base defect. As oxygen is always at a premium in a Level II nursery, oxygen (FiO ) from an oxygen concentrator is a useful equipment to supply oxygen. Getting a neonatal autopsy in India is a difficult task. We have found a lung biopsy done immediately after death an easy method to come to a diagnosis. In 8 of our babies, biopsy showed features suggesting HMD. Considering babies more than 1000g, we have a survival of 70% and only 30% in less than 1000g. These babies require aggressive measures which is not very economical in a Level II nursery. Acknowledgement The authors are grateful to Director General, Armed Forces Medical Services, New Delhi for financial assistance as part of AFMRC Project No 1912/92. REFERENCES VOLUME 32-FEBRUARY Gregory JZA, Kitterman JA, Phibbs RH, et al. Treatment of idiopathic respiratory distress syndrome with continuous positive airway pressure. N Engl J Med 1971, 284: Singh M, Deorari AK, Paul VK, et al. Three year experience with neonatal ventilation from a tertiary care hospital in Delhi. Indian Pediatr 1993, 30: Singh M, Paul VK, Bhakoo ON. Neonatal Nomenclature and Data Collection. New Delhi, National Neonatology Forum, Downes JJ, Vidyasagar D, Morrow GM, et al. Respiratory distress syndrome of infants I. New clinical scoring system (RDS Score) with acidbase and blood-gas correlction. Clin Pediatr 1970, 9: Boros SJ, Reynolds JW. Hyaline membrane disease treated with early nasal and expiratory pressure: One year's experience. Pediatrics 1975, 56:' Jennis MS, Peabody JL. Pulse oximetry: An alternative method of assessment of oxygenation in newborn infants. Pediatrics 1987, 79: Ramnathan R, Durand M, Larrazabal C. Pulse oximetry in very low birth weight infants with acute and chronic lung disease. Pediatrics 1978, 79: Fanconi S, Doherty P, Edmonds JF, et al. Pulse oximetry in pediatric intensive care: Comparison with measured saturations and transcutaneous oxygen tension. J Pediatr 1985, 107:
Oxygenation and Oxygen Therapy Michael Billow, D.O.
 Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
Accuracy and reliability of pulse oximetry in
 Accuracy and reliability of pulse oximetry in premature neonates with respiratory distress GINNY W. HENDERSON, CRNA, MS Concordville, Pennsylvania Continuous noninvasive monitoring of oxygenation in premature
Accuracy and reliability of pulse oximetry in premature neonates with respiratory distress GINNY W. HENDERSON, CRNA, MS Concordville, Pennsylvania Continuous noninvasive monitoring of oxygenation in premature
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline
 NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
From AARC Protocol Committee; Subcommittee Adult Critical Care Version 1.0a (Sept., 2003), Subcommittee Chair, Susan P. Pilbeam
 AARC - ADULT MECHANICAL VENTILATOR PROTOCOLS 1. Guidelines for Using Ventilator Protocols 2. Definition of Modes and Suggestions for Use of Modes 3. Adult Respiratory Ventilator Protocol - Guidelines for
AARC - ADULT MECHANICAL VENTILATOR PROTOCOLS 1. Guidelines for Using Ventilator Protocols 2. Definition of Modes and Suggestions for Use of Modes 3. Adult Respiratory Ventilator Protocol - Guidelines for
The patient s response to therapy within the first hour in the Emergency Room is one of the most reliable ways to predict need for hospitalization.
 Emergency Room Asthma Management Algorithm The Emergency Room Asthma Management Algorithm is to be used for any patient seen in the Emergency Room with the diagnosis of asthma. (The initial history should
Emergency Room Asthma Management Algorithm The Emergency Room Asthma Management Algorithm is to be used for any patient seen in the Emergency Room with the diagnosis of asthma. (The initial history should
 GUIDELINES FOR HOSPITALS WITH NEONATAL INTENSIVE CARE SERVICE : REGULATION 4 OF THE PRIVATE HOSPITALS AND MEDICAL CLINICS REGULATIONS [CAP 248, Rg 1] I Introduction 1. These Guidelines serve as a guide
GUIDELINES FOR HOSPITALS WITH NEONATAL INTENSIVE CARE SERVICE : REGULATION 4 OF THE PRIVATE HOSPITALS AND MEDICAL CLINICS REGULATIONS [CAP 248, Rg 1] I Introduction 1. These Guidelines serve as a guide
More detailed background information and references can be found at the end of this guideline
 Neonatal Intensive Care Unit Clinical Guideline Oxygen Over the past few years there have been significant changes, based on high quality research, in our understanding of how to give the right amount
Neonatal Intensive Care Unit Clinical Guideline Oxygen Over the past few years there have been significant changes, based on high quality research, in our understanding of how to give the right amount
How To Determine The Difference Between Long Versus Short Inspiratory Times In Neonates
 Long versus short inspiratory times in neonates receiving mechanical ventilation (Review) Kamlin COF, Davis PG This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Long versus short inspiratory times in neonates receiving mechanical ventilation (Review) Kamlin COF, Davis PG This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
CPT Pediatric Coding Updates 2009. The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009.
 CPT Pediatric Coding Updates 2009 The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009. NEW CODES Evaluation and Management Services Normal Newborn Care Codes 99431-99440
CPT Pediatric Coding Updates 2009 The 2009 Current Procedural Terminology (CPT) codes are effective as of January 1, 2009. NEW CODES Evaluation and Management Services Normal Newborn Care Codes 99431-99440
Common Ventilator Management Issues
 Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
The Heart Center Neonatology. Congenital Heart Disease Screening Program
 The Heart Center Neonatology Congenital Heart Disease Screening Program Our goal is simple. We want all infants with critical congenital heart disease to be identified before leaving the nursery. Together,
The Heart Center Neonatology Congenital Heart Disease Screening Program Our goal is simple. We want all infants with critical congenital heart disease to be identified before leaving the nursery. Together,
Evaluation and treatment of emphysema in a preterm infant
 ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
NURSING SERVICES DEPARTMENT
 NURSING SERVICES DEPARTMENT TITLE: Mechanical Ventilation PATIENT CARE PLAN DIAGNOSIS: DISCHARGE CRITERIA: 1 The patient will: Maintain adequate mechanics of PERTINENT INFORMATION:. ventilation as demonstrated
NURSING SERVICES DEPARTMENT TITLE: Mechanical Ventilation PATIENT CARE PLAN DIAGNOSIS: DISCHARGE CRITERIA: 1 The patient will: Maintain adequate mechanics of PERTINENT INFORMATION:. ventilation as demonstrated
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context
 Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
Addendum to the NRP Provider Textbook 6 th Edition Recommendations for specific modifications in the Canadian context A subcommittee of the Canadian Neonatal Resuscitation Program (NRP) Steering Committee
5/30/2014 OBJECTIVES THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM. Disclosure
 THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
MECHINICAL VENTILATION S. Kache, MD
 MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
2008 Coding Questions and Answers
 2008 Coding Questions and Answers 1. An infant is born at 29 wks gestation and has RDS. His birthweight is 1200 gms. He is admitted to the NICU. It is evident that he has severe RDS and a decision is made
2008 Coding Questions and Answers 1. An infant is born at 29 wks gestation and has RDS. His birthweight is 1200 gms. He is admitted to the NICU. It is evident that he has severe RDS and a decision is made
NICU Level of Care Criteria
 Introduction The NICU Criteria were developed to assist in the authorization for various levels of Neonatal Intensive Care Unit (NICU), as well as assistance in determining the appropriate level of care.
Introduction The NICU Criteria were developed to assist in the authorization for various levels of Neonatal Intensive Care Unit (NICU), as well as assistance in determining the appropriate level of care.
A8b. Resuscitation of a Term Infant with Meconium Staining. Session Summary. Session Objectives. References
 A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
A8b Resuscitation of a Term Infant with Meconium Staining Karen Wright, PhD, NNP-BC Assistant Professor and Coordinator, Neonatal Nurse Practitioner Program Dept. of Women, Children, and Family Nursing,
Safe Zone: CV PIP < 26; HFOV: MAP < 16; HFJV: MAP < 16 Dopamine infusion up to 20 mcg/kg/min Epinephrine infusion up to 0.1 mcg /kg/min.
 Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
DRG 475 Respiratory System Diagnosis with Ventilator Support. ICD-9-CM Coding Guidelines
 DRG 475 Respiratory System Diagnosis with Ventilator Support ICD-9-CM Coding G The below listed g are not inclusive. The coder should refer to the applicable Coding Clinic g for additional information.
DRG 475 Respiratory System Diagnosis with Ventilator Support ICD-9-CM Coding G The below listed g are not inclusive. The coder should refer to the applicable Coding Clinic g for additional information.
The Advantages of Transcutaneous Co 2 Over End-Tidal Co 2 for Sleep Studies PETCo 2 vs. TCPCo 2
 The Advantages of Transcutaneous Co 2 Over End-Tidal Co 2 for Sleep Studies PETCo 2 vs. TCPCo 2 Ramalinga P. Reddy, M.D., MBA, FCCP Director, Children s Pulmonary & Sleep Center Mercy Children s Hospital
The Advantages of Transcutaneous Co 2 Over End-Tidal Co 2 for Sleep Studies PETCo 2 vs. TCPCo 2 Ramalinga P. Reddy, M.D., MBA, FCCP Director, Children s Pulmonary & Sleep Center Mercy Children s Hospital
Lothian Guideline for Domiciliary Oxygen Therapy Service for COPD
 Lothian Guideline for Domiciliary Oxygen Therapy Service for COPD This document describes the standard for clinical assessment, prescription, optimal management and follow-up of patients receiving domiciliary
Lothian Guideline for Domiciliary Oxygen Therapy Service for COPD This document describes the standard for clinical assessment, prescription, optimal management and follow-up of patients receiving domiciliary
Oxygenation. Chapter 21. Anatomy and Physiology of Breathing. Anatomy and Physiology of Breathing*
 Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy
 The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
The Sepsis Puzzle: Identification, Monitoring and Early Goal Directed Therapy Cindy Goodrich RN, MS, CCRN Content Description Sepsis is caused by widespread tissue injury and systemic inflammation resulting
Respiratory failure and Oxygen Therapy
 Respiratory failure and Oxygen Therapy A patient with Hb 15 G % will carry 3X more O2 in his blood than someone with Hb 5G % Give Controlled O2 treatment in acute pulmonary oedema to avoid CO2 retention
Respiratory failure and Oxygen Therapy A patient with Hb 15 G % will carry 3X more O2 in his blood than someone with Hb 5G % Give Controlled O2 treatment in acute pulmonary oedema to avoid CO2 retention
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
Pulmonary Diseases. Lung Disease: Pathophysiology, Medical and Exercise Programming. Overview of Pathophysiology
 Lung Disease: Pathophysiology, Medical and Exercise Programming Overview of Pathophysiology Ventilatory Impairments Increased airway resistance Reduced compliance Increased work of breathing Ventilatory
Lung Disease: Pathophysiology, Medical and Exercise Programming Overview of Pathophysiology Ventilatory Impairments Increased airway resistance Reduced compliance Increased work of breathing Ventilatory
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings
 AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn
 Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn A presentation of Texas Pulse Oximetry Project: A Joint Educational Initiative of The University of Texas Health Science
Screening for Critical Congenital Heart Disease in the Apparently Healthy Newborn A presentation of Texas Pulse Oximetry Project: A Joint Educational Initiative of The University of Texas Health Science
Respiratory Distress Syndrome of the Newborn
 19 Respiratory Distress Syndrome of the Newborn Respiratory distress syndrome (RDS) of the newborn, also known as hyaline membrane disease, is a breathing disorder of premature babies. In healthy infants,
19 Respiratory Distress Syndrome of the Newborn Respiratory distress syndrome (RDS) of the newborn, also known as hyaline membrane disease, is a breathing disorder of premature babies. In healthy infants,
MECHANICAL VENTILATION IN THE NEONATE
 Supplemental Resources for the PICU/NICU MECHANICAL VENTILATION IN THE NEONATE I. GENERAL PRINCIPLES A. NEONATAL VENTILATORS We use three types of neonatal ventilators in the NICU: 1. SIMV (Synchronized
Supplemental Resources for the PICU/NICU MECHANICAL VENTILATION IN THE NEONATE I. GENERAL PRINCIPLES A. NEONATAL VENTILATORS We use three types of neonatal ventilators in the NICU: 1. SIMV (Synchronized
Mechanical Ventilation
 Mechanical Ventilation 127 Mechanical Ventilation William Benitz, M.D. Caring for a mechanically ventilated neonate continues to unnecessarily strike fear in the heart of many a resident. This fear is
Mechanical Ventilation 127 Mechanical Ventilation William Benitz, M.D. Caring for a mechanically ventilated neonate continues to unnecessarily strike fear in the heart of many a resident. This fear is
Milliman Guidelines NICU Levels*
 Milliman Guidelines NICU Levels* Neonatal Intensive Care Unit Level IV If the following conditions/procedures exist, in addition to the fulfillment of Level III Criteria, the approved inpatient days should
Milliman Guidelines NICU Levels* Neonatal Intensive Care Unit Level IV If the following conditions/procedures exist, in addition to the fulfillment of Level III Criteria, the approved inpatient days should
Eileen Whitehead 2010 East Lancashire HC NHS Trust
 Eileen Whitehead 2010 East Lancashire HC NHS Trust 1 Introduction: Arterial blood gas analysis is an essential part of diagnosing and managing a patient s oxygenation status and acid-base balance However,
Eileen Whitehead 2010 East Lancashire HC NHS Trust 1 Introduction: Arterial blood gas analysis is an essential part of diagnosing and managing a patient s oxygenation status and acid-base balance However,
NEONATAL RESPIRATORY CARE: CLINICAL APPLICATIONS
 By Kevin T. Martin BVE, RRT, RCP RC Educational Consulting Services, Inc. 16781 Van Buren Blvd, Suite B, Riverside, CA 92504-5798 (800) 441-LUNG / (877) 367-NURS www.rcecs.com BEHAVIORAL OBJECTIVES BY
By Kevin T. Martin BVE, RRT, RCP RC Educational Consulting Services, Inc. 16781 Van Buren Blvd, Suite B, Riverside, CA 92504-5798 (800) 441-LUNG / (877) 367-NURS www.rcecs.com BEHAVIORAL OBJECTIVES BY
ASSISTED VENTILATION IN NEONATES
 ASSISTED VENTILATION IN NEONATES CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Continuous Positive Airway Pressure or CPAP is a modality of respiratory support in which increased pulmonary pressure
ASSISTED VENTILATION IN NEONATES CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Continuous Positive Airway Pressure or CPAP is a modality of respiratory support in which increased pulmonary pressure
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire
 Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Congenital Diaphragmatic Hernia. Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate
 Congenital Diaphragmatic Hernia Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate Congenital Diaphragmatic Hernias Incidence 1 in 2000 to 5000 live births. 80% in the left side, 20%
Congenital Diaphragmatic Hernia Manuel A. Molina, M.D. University Hospital at Brooklyn SUNY Downstate Congenital Diaphragmatic Hernias Incidence 1 in 2000 to 5000 live births. 80% in the left side, 20%
Mechanical Ventilators
 University of Washington Academic Medical Center Copyright 2000 Disclaimer Children's Hospital and Regional Medical Center Copyright 2002 Disclaimer Mechanical Ventilators Authors Created 07/31/95 Reviewed
University of Washington Academic Medical Center Copyright 2000 Disclaimer Children's Hospital and Regional Medical Center Copyright 2002 Disclaimer Mechanical Ventilators Authors Created 07/31/95 Reviewed
COURSE SYLLABUS RC 223 CLINICAL-3
 COURSE SYLLABUS RC 223 CLINICAL-3 Class Hours: 0 Laboratory Hours: 24 Credit Hours: 4 Course Description: Entry Level Standards: This course will emphasize neonatal-pediatric intensive care, pulmonary
COURSE SYLLABUS RC 223 CLINICAL-3 Class Hours: 0 Laboratory Hours: 24 Credit Hours: 4 Course Description: Entry Level Standards: This course will emphasize neonatal-pediatric intensive care, pulmonary
OET: Listening Part A: Influenza
 Listening Test Part B Time allowed: 23 minutes In this part, you will hear a talk on critical illnesses due to A/H1N1 influenza in pregnant and postpartum women, given by a medical researcher. You will
Listening Test Part B Time allowed: 23 minutes In this part, you will hear a talk on critical illnesses due to A/H1N1 influenza in pregnant and postpartum women, given by a medical researcher. You will
Titration protocol reference guide
 Titration protocol reference guide Description Page Titration protocol goals 4 CPAP protocol CPAP protocol 6 CPAP titration protocol 7 CPAP reimbursement criteria 8 BiPAP S protocol BiPAP S protocol 10
Titration protocol reference guide Description Page Titration protocol goals 4 CPAP protocol CPAP protocol 6 CPAP titration protocol 7 CPAP reimbursement criteria 8 BiPAP S protocol BiPAP S protocol 10
From Children s National Medical Center. Congenital Heart Disease Screening Program Toolkit: A Toolkit for Implementing Screening.
 From Children s National Medical Center. Congenital Heart Disease Screening Program Toolkit: A Toolkit for Implementing Screening. Washington, DC: Children s National Medical Center; 2009. 1 Critical Congenital
From Children s National Medical Center. Congenital Heart Disease Screening Program Toolkit: A Toolkit for Implementing Screening. Washington, DC: Children s National Medical Center; 2009. 1 Critical Congenital
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
NRP 2012 Putting New Resuscitation Guidelines into Practice
 Outreach Education Online Video Library for Healthcare Professionals NRP 2012 Putting New Resuscitation Guidelines into Practice. Jeanette Zaichkin, RN, MN, NNP-BC December 2, 2010 Program Handouts This
Outreach Education Online Video Library for Healthcare Professionals NRP 2012 Putting New Resuscitation Guidelines into Practice. Jeanette Zaichkin, RN, MN, NNP-BC December 2, 2010 Program Handouts This
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
Using the Electronic Medical Record to Improve Evidence-based Medical Practice. P. Brian Smith Duke University Medical Center Durham, NC
 Using the Electronic Medical Record to Improve Evidence-based Medical Practice P. Brian Smith Duke University Medical Center Durham, NC Disclosure I have no relevant financial relationships with the manufacturer
Using the Electronic Medical Record to Improve Evidence-based Medical Practice P. Brian Smith Duke University Medical Center Durham, NC Disclosure I have no relevant financial relationships with the manufacturer
Critical Congenital Heart Disease (CCHD) Screening
 Critical Congenital Heart Disease (CCHD) Screening Screening The Florida Genetics and Newborn Screening Advisory Council recommended to the Department of Health that CCHD be added to the panel of disorders
Critical Congenital Heart Disease (CCHD) Screening Screening The Florida Genetics and Newborn Screening Advisory Council recommended to the Department of Health that CCHD be added to the panel of disorders
KING FAISAL SPECIALIST HOSPITAL AND RESEARCH CENTRE (GEN. ORG.) NURSING AFFAIRS. Scope of Service PEDIATRIC INTENSIVE CARE UNIT (PICU)
 PICU-Jan.2012 Page 1 of 7 Number of Beds: 18 Nurse Patient Ratio: 1:1-2 : The Pediatric Intensive Care Unit (PICU) provides 24 hour intensive nursing care for patients aged neonate through adolescence.
PICU-Jan.2012 Page 1 of 7 Number of Beds: 18 Nurse Patient Ratio: 1:1-2 : The Pediatric Intensive Care Unit (PICU) provides 24 hour intensive nursing care for patients aged neonate through adolescence.
COPD with Respiratory Failure Case Study #21. Molly McDonough
 COPD with Respiratory Failure Case Study #21 Molly McDonough Patient: Mr. Hayato 65 year old male Brought to ER with severe SOB Past History of emphysema Longstanding chronic obstruction pulmonary disease
COPD with Respiratory Failure Case Study #21 Molly McDonough Patient: Mr. Hayato 65 year old male Brought to ER with severe SOB Past History of emphysema Longstanding chronic obstruction pulmonary disease
Neonatal Emergencies. Care of the Neonate. Care of the Neonate. Care of the Neonate. Student Objectives. Student Objectives continued.
 Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
Student Objectives Neonatal Emergencies After completing this section the student will be able to: 1. Identify three physiologic and/or anatomic features unique to the newborn 2. List three perinatal factors
Understanding Hypoventilation and Its Treatment by Susan Agrawal
 www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
A. All cells need oxygen and release carbon dioxide why?
 I. Introduction: Describe how the cardiovascular and respiratory systems interact to supply O 2 and eliminate CO 2. A. All cells need oxygen and release carbon dioxide why? B. Two systems that help to
I. Introduction: Describe how the cardiovascular and respiratory systems interact to supply O 2 and eliminate CO 2. A. All cells need oxygen and release carbon dioxide why? B. Two systems that help to
High-Frequency Oscillatory Ventilation
 High-Frequency Oscillatory Ventilation Arthur Jones EdD, RRT Learning Objectives Describe the indications and rationale and monitoring for HFOV. Identify HFOV settings and describe the effects of their
High-Frequency Oscillatory Ventilation Arthur Jones EdD, RRT Learning Objectives Describe the indications and rationale and monitoring for HFOV. Identify HFOV settings and describe the effects of their
CORD BLOOD COLLECTION / ANALYSIS- AT BIRTH
 WOMEN AND NEWBORN HEALTH SERVICE King Edward Memorial Hospital CLINICAL GUIDELINES OBSTETRICS AND MIDWIFERY King Edward Memorial Hospital WOMEN AND NEWBORN HEALTH SERVICE INTRAPARTUM CARE SPECIMEN COLLECTION
WOMEN AND NEWBORN HEALTH SERVICE King Edward Memorial Hospital CLINICAL GUIDELINES OBSTETRICS AND MIDWIFERY King Edward Memorial Hospital WOMEN AND NEWBORN HEALTH SERVICE INTRAPARTUM CARE SPECIMEN COLLECTION
Perioperative Management of Patients with Obstructive Sleep Apnea. Kalpesh Ganatra,MD Diplomate, American Board of Sleep Medicine
 Perioperative Management of Patients with Obstructive Sleep Apnea Kalpesh Ganatra,MD Diplomate, American Board of Sleep Medicine Disclosures. This activity is supported by an education grant from Trivalley
Perioperative Management of Patients with Obstructive Sleep Apnea Kalpesh Ganatra,MD Diplomate, American Board of Sleep Medicine Disclosures. This activity is supported by an education grant from Trivalley
RESPIRATORY THERAPIST CLASSIFICATION SERIES
 STATE OF WISCONSIN CLASSIFICATION SPECIFICATION RESPIRATORY THERAPIST CLASSIFICATION SERIES Effective Date: June 16, 1985 Modified Effective: November 5, 2000 Modified Effective: May 6, 2001 I. INTRODUCTION
STATE OF WISCONSIN CLASSIFICATION SPECIFICATION RESPIRATORY THERAPIST CLASSIFICATION SERIES Effective Date: June 16, 1985 Modified Effective: November 5, 2000 Modified Effective: May 6, 2001 I. INTRODUCTION
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS
 NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION 4 TEMPERATURE CONTROL.4 CLEARING THE AIRWAY OF MECONIUM 5
NEONATAL RESUSCITATION PROVIDER (NRP) RECERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION 4 TEMPERATURE CONTROL.4 CLEARING THE AIRWAY OF MECONIUM 5
3100B Clinical Training Program. 3100B HFOV VIASYS Healthcare
 3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 PS1006 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: NEONATAL INTENSIVE CARE UNIT: ADMISSION AND TRANSFER PROCEDURE AND ACUITY GUIDELINES Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE:
PS1006 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: NEONATAL INTENSIVE CARE UNIT: ADMISSION AND TRANSFER PROCEDURE AND ACUITY GUIDELINES Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE:
BUNDLES IN 2013: SURVIVING SEPSIS CAMPAIGN
 BUNDLES IN 2013: SURVIVING SEPSIS CAMPAIGN R. Phillip Dellinger MD, MSc, MCCM Professor of Medicine Cooper Medical School of Rowan University Professor of Medicine University Medicine and Dentistry of
BUNDLES IN 2013: SURVIVING SEPSIS CAMPAIGN R. Phillip Dellinger MD, MSc, MCCM Professor of Medicine Cooper Medical School of Rowan University Professor of Medicine University Medicine and Dentistry of
Hospital Coding Making the Rounds
 Hospital Coding Making the Rounds Initial & Subsequent Care, Consults, Discharges, Observation and Critical Care Objectives Participants will be educated on the documentation requirements for Initial and
Hospital Coding Making the Rounds Initial & Subsequent Care, Consults, Discharges, Observation and Critical Care Objectives Participants will be educated on the documentation requirements for Initial and
James F. Kravec, M.D., F.A.C.P
 James F. Kravec, M.D., F.A.C.P Chairman, Department of Internal Medicine, St. Elizabeth Health Center Chair, General Internal Medicine, Northeast Ohio Medical University Associate Medical Director, Hospice
James F. Kravec, M.D., F.A.C.P Chairman, Department of Internal Medicine, St. Elizabeth Health Center Chair, General Internal Medicine, Northeast Ohio Medical University Associate Medical Director, Hospice
Air or oxygen as driving gas for nebulised salbutamol
 Archives of Disease in Childhood, 1988, 63, 9-94 Air or oxygen as driving gas for nebulised salbutamol J G A GLEESON, S GREEN, AND J F PRICE Paediatric Respiratory Laboratory, Department of Thoracic Medicine,
Archives of Disease in Childhood, 1988, 63, 9-94 Air or oxygen as driving gas for nebulised salbutamol J G A GLEESON, S GREEN, AND J F PRICE Paediatric Respiratory Laboratory, Department of Thoracic Medicine,
Neonatal Reference Guide
 Operated by REACH Air Medical Services Assessment Heart Rate (beats/min.) Age Rate
Operated by REACH Air Medical Services Assessment Heart Rate (beats/min.) Age Rate
Chapter 26. Assisting With Oxygen Needs. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 26 Assisting With Oxygen Needs Oxygen (O 2 ) is a gas. Oxygen It has no taste, odor, or color. It is a basic need required for life. Death occurs within minutes if breathing stops. Brain damage
Chapter 26 Assisting With Oxygen Needs Oxygen (O 2 ) is a gas. Oxygen It has no taste, odor, or color. It is a basic need required for life. Death occurs within minutes if breathing stops. Brain damage
Asthma in Infancy, Childhood and Adolescence. Presented by Frederick Lloyd, MD Palo Alto Medical Foundation Palo Alto, California
 Asthma in Infancy, Childhood and Adolescence Presented by Frederick Lloyd, MD Palo Alto Medical Foundation Palo Alto, California Major Health Problem in Childhood Afflicts 2.7 million children in the USA
Asthma in Infancy, Childhood and Adolescence Presented by Frederick Lloyd, MD Palo Alto Medical Foundation Palo Alto, California Major Health Problem in Childhood Afflicts 2.7 million children in the USA
Doppler Ultrasound in the Management of Fetal Growth Restriction Chukwuma I. Onyeije, M.D. Atlanta Perinatal Associates
 Doppler Ultrasound in the Management of Fetal Growth Restriction Chukwuma I. Onyeije, M.D. Atlanta Perinatal Associates 1 For your convenience a copy of this lecture is available for review and download
Doppler Ultrasound in the Management of Fetal Growth Restriction Chukwuma I. Onyeije, M.D. Atlanta Perinatal Associates 1 For your convenience a copy of this lecture is available for review and download
Midwestern State University Respiratory Care Program PRECEPTOR TRAINING WORKSHOP
 Midwestern State University Respiratory Care Program PRECEPTOR TRAINING WORKSHOP Class of 2012 The Purpose of this Presentation Commission on Accreditation For Respiratory Care Standard 3.11 The program
Midwestern State University Respiratory Care Program PRECEPTOR TRAINING WORKSHOP Class of 2012 The Purpose of this Presentation Commission on Accreditation For Respiratory Care Standard 3.11 The program
Importance of Protocols in the Decision to Use Noninvasive Ventilation
 Importance of Protocols in the Decision to Use Noninvasive Ventilation Janice L. Zimmerman, M.D. Weill Cornell Medical College The Methodist Hospital Houston, Texas Objectives Review application of protocols
Importance of Protocols in the Decision to Use Noninvasive Ventilation Janice L. Zimmerman, M.D. Weill Cornell Medical College The Methodist Hospital Houston, Texas Objectives Review application of protocols
Cord Blood Erythropoietin and Markers of Fetal Hypoxia
 July 21, 2011 By NeedsFixing [1] To investigating the relationship between cord blood erythropoietin and clinical markers of fetal hypoxia. Abstract Objective: To investigating the relationship between
July 21, 2011 By NeedsFixing [1] To investigating the relationship between cord blood erythropoietin and clinical markers of fetal hypoxia. Abstract Objective: To investigating the relationship between
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC. BLS Changes
 ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
Paul Seddon Royal Alexandra Children s Hospital, Brighton. David Wertheim Kingston University
 Paul Seddon Royal Alexandra Children s Hospital, Brighton David Wertheim Kingston University Respiratory problems account for almost half the cost of primary healthcare More premature infants are surviving,
Paul Seddon Royal Alexandra Children s Hospital, Brighton David Wertheim Kingston University Respiratory problems account for almost half the cost of primary healthcare More premature infants are surviving,
DME: Definition... 2 Life Sustaining DME... 3 Oxygen Use Policy... 4 Non-Life Sustaining DME... 7
 DME: Definition... 2 Life Sustaining DME... 3 Oxygen Use Policy... 4 Non-Life Sustaining DME... 7 A Division of Health Care Service Corporation, a Mutual Legal Reserve Company, an Independent Licensee
DME: Definition... 2 Life Sustaining DME... 3 Oxygen Use Policy... 4 Non-Life Sustaining DME... 7 A Division of Health Care Service Corporation, a Mutual Legal Reserve Company, an Independent Licensee
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD Definition ARDS is a clinical syndrome of lung injury with hypoxic respiratory failure caused by intense pulmonary inflammation that
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD Definition ARDS is a clinical syndrome of lung injury with hypoxic respiratory failure caused by intense pulmonary inflammation that
81 First Responder Respiratory
 81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
Idiopathic Pulmonary Fibrosis
 Idiopathic Pulmonary Fibrosis What is Idiopathic Pulmonary Fibrosis? Idiopathic pulmonary fibrosis (IPF) is a condition that causes persistent and progressive scarring of the tiny air sacs (alveoli) in
Idiopathic Pulmonary Fibrosis What is Idiopathic Pulmonary Fibrosis? Idiopathic pulmonary fibrosis (IPF) is a condition that causes persistent and progressive scarring of the tiny air sacs (alveoli) in
Original Article COPD and Hospital Stay Pak Armed Forces Med J 2014; 64 (1): 46-50. Ahmed Raza, Mahmood Iqbal Malik*, Yousaf Jamal**
 Original Article COPD and Hospital Stay Pak Armed Forces Med J 2014; 64 (1): 46-50 COMPARISON OF NIPPV WITH STANDARD TREATMENT IN PATIENTS WITH ACUTE EXACERBATIONS OF COPD IN TERMS OF IMPROVEMENT IN ABGS
Original Article COPD and Hospital Stay Pak Armed Forces Med J 2014; 64 (1): 46-50 COMPARISON OF NIPPV WITH STANDARD TREATMENT IN PATIENTS WITH ACUTE EXACERBATIONS OF COPD IN TERMS OF IMPROVEMENT IN ABGS
SWISS SOCIETY OF NEONATOLOGY. Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema
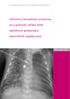 SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
GE Healthcare. Welcome to the future of anesthesia Aisys * Carestation *
 GE Healthcare Welcome to the future of anesthesia Aisys * Carestation * The way you practice today may be different from the past. Diverse patient types and co-morbidities make your world challenging.
GE Healthcare Welcome to the future of anesthesia Aisys * Carestation * The way you practice today may be different from the past. Diverse patient types and co-morbidities make your world challenging.
The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome
 Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Biomedical & Pharmacology Journal Vol. 6(2), 259-264 (2013) The Initial and 24 h (After the Patient Rehabilitation) Deficit of Arterial Blood Gases as Predictors of Patients Outcome Vadod Norouzi 1, Ali
Recommendations: Other Supportive Therapy of Severe Sepsis*
 Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Levels of Critical Care for Adult Patients
 LEVELS OF CARE 1 Levels of Critical Care for Adult Patients STANDARDS AND GUIDELINES LEVELS OF CARE 2 Intensive Care Society 2009 All rights reserved. No reproduction, copy or transmission of this publication
LEVELS OF CARE 1 Levels of Critical Care for Adult Patients STANDARDS AND GUIDELINES LEVELS OF CARE 2 Intensive Care Society 2009 All rights reserved. No reproduction, copy or transmission of this publication
9/12/2011 OBJECTIVES BREATH OF LIFE. Review the role that Potentially Better Practices (PBP s) play in clinical practice
 Ona. O. Fofah, MD, FAAP Director, Division of Neonatal Perinatal Medicine, Department of Pediatrics, UMDNJ/NJMS UMDNJ RESPIRATORY LECTURE SERIES SEPT 2011 OBJECTIVES Review the role that Potentially Better
Ona. O. Fofah, MD, FAAP Director, Division of Neonatal Perinatal Medicine, Department of Pediatrics, UMDNJ/NJMS UMDNJ RESPIRATORY LECTURE SERIES SEPT 2011 OBJECTIVES Review the role that Potentially Better
Fetal Acid Base Status and Umbilical Cord Sampling. David Acker, MD
 Fetal Acid Base Status and Umbilical Cord Sampling David Acker, MD Part I: Some Background Intra-uterine Event as Causative of CP Cord ph < 7.00 and base excess of > 12 Early onset neonatal encephalopathy
Fetal Acid Base Status and Umbilical Cord Sampling David Acker, MD Part I: Some Background Intra-uterine Event as Causative of CP Cord ph < 7.00 and base excess of > 12 Early onset neonatal encephalopathy
Principle of oxygen therapy in the newborn
 Principle of oxygen therapy in the newborn Thrathip Kolatat M.D. Neonatal Intensive Care Unit Department of Pediatrics Faculty of Medicine Siriraj Hospital Oxygen The most common drugs used in NICU Goal
Principle of oxygen therapy in the newborn Thrathip Kolatat M.D. Neonatal Intensive Care Unit Department of Pediatrics Faculty of Medicine Siriraj Hospital Oxygen The most common drugs used in NICU Goal
Regions Hospital Delineation of Privileges Nurse Practitioner
 Regions Hospital Delineation of Privileges Nurse Practitioner Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic
Regions Hospital Delineation of Privileges Nurse Practitioner Applicant s Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic
Medicare C/D Medical Coverage Policy
 Medicare C/D Medical Coverage Policy Oxygen and Oxygen Supplements Origination: April 10, 1992 Review Date: July 15, 2015 Next Review: July, 2017 DESCRIPTION OF PROCEDURE OR SERVICE USP Oxygen is a gaseous
Medicare C/D Medical Coverage Policy Oxygen and Oxygen Supplements Origination: April 10, 1992 Review Date: July 15, 2015 Next Review: July, 2017 DESCRIPTION OF PROCEDURE OR SERVICE USP Oxygen is a gaseous
MINI - COURSE On TEMPERATURE CONTROL IN THE NEWBORN
 MINI - COURSE On TEMPERATURE CONTROL IN THE NEWBORN Instructions: Read each sheet and answer any questions as honestly as possible The first sheets have four questions to allow you to give your thoughts
MINI - COURSE On TEMPERATURE CONTROL IN THE NEWBORN Instructions: Read each sheet and answer any questions as honestly as possible The first sheets have four questions to allow you to give your thoughts
NICU Reporting. Alyssa Yang CDC/CSTE Applied Epidemiology Fellow February 28, 2014
 NICU Reporting Alyssa Yang CDC/CSTE Applied Epidemiology Fellow February 28, 2014 NICU Definitions Level I nurseries are normal newborn nurseries. For this discussion, NICU will refer to Level II and III
NICU Reporting Alyssa Yang CDC/CSTE Applied Epidemiology Fellow February 28, 2014 NICU Definitions Level I nurseries are normal newborn nurseries. For this discussion, NICU will refer to Level II and III
Cardiac Arrest VF/Pulseless VT Learning Station Checklist
 Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Southern Stone County Fire Protection District Emergency Medical Protocols
 TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
1.4.4 Oxyhemoglobin desaturation
 Critical Care Therapy and Respiratory Care Section Category: Clinical Section: Clinical Monitoring Title: Monitoring of Patients Undergoing Conscious Sedation Policy #: 09 Revised: 05/00 1.0 DESCRIPTION
Critical Care Therapy and Respiratory Care Section Category: Clinical Section: Clinical Monitoring Title: Monitoring of Patients Undergoing Conscious Sedation Policy #: 09 Revised: 05/00 1.0 DESCRIPTION
MECHANICAL VENTILATION
 MECHANICAL VENTILATION INDICATIONS: Respiratory Failure Cardiopulmonary arrest Trauma (especially head, neck, and chest) Cardiovascular impairment (strokes, tumors, infection, emboli, trauma) Neurological
MECHANICAL VENTILATION INDICATIONS: Respiratory Failure Cardiopulmonary arrest Trauma (especially head, neck, and chest) Cardiovascular impairment (strokes, tumors, infection, emboli, trauma) Neurological
THE AIRWAY IN AEROMEDICAL EVACUATION. PBLD (Problem Based Learning Discussion)
 THE AIRWAY IN AEROMEDICAL EVACUATION PBLD (Problem Based Learning Discussion) D. John Doyle MD PhD 2012 Edition Image Credit: http://www.arabianaerospace.aero/media/images/stories/medevac%20services.jpg
THE AIRWAY IN AEROMEDICAL EVACUATION PBLD (Problem Based Learning Discussion) D. John Doyle MD PhD 2012 Edition Image Credit: http://www.arabianaerospace.aero/media/images/stories/medevac%20services.jpg
NRP Study Guide. This packet is intended for review only. Requirements to successfully complete NRP:
 This packet is intended for review only Requirements to successfully complete NRP: Completed NRP Pretest is required for admission to the course. Score 84% on the multiplechoice posttest. You may be allowed
This packet is intended for review only Requirements to successfully complete NRP: Completed NRP Pretest is required for admission to the course. Score 84% on the multiplechoice posttest. You may be allowed
