Mechanical Ventilation
|
|
|
- Florence Green
- 7 years ago
- Views:
Transcription
1 Mechanical Ventilation 127 Mechanical Ventilation William Benitz, M.D. Caring for a mechanically ventilated neonate continues to unnecessarily strike fear in the heart of many a resident. This fear is only amplified by the fact that we nursery folk speak a language all our own, rich with three and four letter acronyms. By reviewing the physiology, and understanding the ventilator manipulations available, the task becomes much less intimidating, even manageable. After reading this chapter, I hope you ll find yourself more comfortable managing ventilated babies and talking the talk; and should a child not play by the rules, as preemies have been known to do, give your fellow a call. They will be happy to give you a hand. There are three main indications for the initiation of mechanical ventilation, and fortunately they re selfexplanatory: A. Apnea B. Inability to oxygenate C. Inability to ventilate The goal of mechanical ventilation is simply to assist the infant to maintain physiologic normalcy ; to keep arterial blood gas values in a desired range while minimizing iatrogenic lung injury. Desired ranges are provided in the section titled desired blood gas ranges. I. CPAP A. The simplest form of mechanical assistance (besides nasal cannula) is nasal CPAP (continuous positive airway pressure). CPAP is of benefit to children who have lungs prone to collapse, such as stiff lungs with RDS and pneumonia. By keeping the lung inflated, CPAP helps the lung to function in a happier part of the compliance curve. Using the analogy of the lung as a balloon, the hardest part of inflating it is overcoming the initial opening pressure (the first blow on the balloon), we usually start with a CPAP of 4-6 cm H 2O. Once it s open, distension becomes much easier. CPAP provides the opening pressure in a lung prone to collapse, decreasing the work of breathing for the infant and increasing functional residual capacity, improving both oxygenation and ventilation. II. Conventional Mechanical (Tidal) Ventilation A. Conventional mechanical ventilation is the primary mode of assisted ventilation used. Children on conventional ventilators look as though they are breathing, and as such are easily distinguished from their high-frequency ventilated counterparts. There are several modes of conventional ventilation; they differ primarily in how they interact with the infant s spontaneous respiratory efforts. B. IMV (intermittent mandatory ventilation): The set rate is delivered in a time-cycled manner regardless of where the baby is in their respiratory cycle. A child on an IMV rate of 30 gets a breath every two seconds, whether the infant is inhaling or exhaling. C. SIMV (synchronized IMV): The set rate is delivered in a time-cycled manner; however, the ventilator times breaths to coincide with baby s inspiratory effort. At a ventilator rate of 30 the ventilator assists a breath every two seconds. Should the infant not initiate a breath, the ventilator delivers an IMV breath. This is the primary mode of conventional ventilation used in the NICU.
2 128 Part 3-B Respiratory D. Assist control (A/C): In this mode, every breath the infant takes is assisted. The rate set is only an apnea backup rate. In this mode, you determine the size of the breath and the baby determines the rate. E. Pressure Support: 1. This term is most commonly used to describe a ventilation mode in which an infant s spontaneous effort is augmented by supplemental inspiratory pressure (short of that required to deliver a full tidal volume) with every breath. This is often delivered in combination with SIMV delivering full tidal augmenting volumes at a rate substantially lower than the infant s spontaneous rate. For example, an infant might be supported with SIMV at a rate of 15 and PIP of 20 along with pressure support of 8 for all other spontaneous breaths. In this mode, the baby contributes to ventilator breaths and sets the rate. 2. However, the pressure support mode on the Babylog ventilator does not provide that kind of pressure support. On the Babylog, pressure support simply means that the duration of inspiration is determined by the rate of gas flow into the lungs during inspiration, such that inspiration is terminated when the inspiratory flow rate drops below 15% of the peak inspiratory flow. For the Babylog, this mode is equivalent to A/C with patientcontrolled or flow-terminated inspiration. F. Volume guarantee: III. Settings 1. In this mode the ventilator assesses the pressure required to deliver a breath of the specific size that you choose. It can be used in the SIMV, A/C, or pressure support modes. You set the maximum pressure the ventilator can deliver, and should it require less it delivers less. For example, if you set a PIP maximum of 20 and the baby only requires a PIP of 12 to achieve your desired volumes it only delivers a PIP of If the maximum inspiratory pressure is not sufficient to deliver the desired tidal volume, the ventilator will display a low tidal volume alarm. Because the ventilator uses data from the last breath to set the pressure for the next one, which cannot guarantee delivery of the desired volume, this mode might be more accurately described as volume targeted ventilation. 3. This mode may produce ventilator behaviors that appear anomalous to the uninitiated. The Babylog will shorten the inspiratory time if the desired volume has already been delivered and it will often reduce the inspiratory pressure to equal the end expiratory pressure as the baby s lung function and respiratory effort improve. The latter will result in placement of the infant on CPAP via the endotracheal tube, which is usually not desirable. A. In any mode, conventional ventilation provides sustained inflation of the lung by delivering breaths of a set peak inspiratory pressure (PIP) above a baseline opening pressure (positive end expiratory pressure or PEEP) for an established inspiratory time (i-time). There are a number of variables you have at your disposal when ventilating an infant. The flow available to the ventilator (flow rate) determines how quickly you reach the PIP. The diagram to the right illustrates how these variables affect ventilator breaths. B. Ventilator changes: From this point forward, consider oxygenation and ventilation to be completely separate entities. As such, there are different ventilator manipulations you can make to enhance either oxygenation or ventilation and sometimes both. The following pointers are provided with the caveat that they all assume that you re ventilating the baby in the sweet spot of the compliance curve, and may not hold true if the baby is hyperinflated or atelectatic. If this is the case, call your fellow or attending.
3 Mechanical Ventilation 129 C. Oxygenation: For oxygenation to occur, you must provide lung expansion, particularly increasing the functional residual capacity, a by-product of your mean airway pressure. An easy way of remembering this is that any change that you make which increases the area under the curve above will increase oxygenation, assuming cardiac output can keep up. Considering the curve, the largest impact would be seen by changing the PEEP. Other maneuvers that would likely lead to an improvement in oxygenation include increasing PIP, increasing i-time, increasing the flow rate, or lastly increasing ventilator rate. 1. A recap to improve oxygenation: a. increase PEEP b. increase PIP c. increase i-time d. increase rate D. Ventilation 1. Minute ventilation is the product of tidal volume and respiratory rate. Tidal volume tends to be proportional to PIP-PEEP or P. So, to increase ventilation and lower your baby s PaCO2, you want to increase minute ventilation, probably by increasing the ventilator rate. You can also increase tidal volume by increasing PIP, decreasing PEEP, or increasing the i-time. 2. A recap to improve ventilation: a. increase rate b. increase PIP c. decrease PEEP d. increase i-time. Generally, lengthening your i-time increases your effective tidal volume. In some children, lengthening the i-time may lead to air trapping and a decrease in ventilation. e. increase tidal volume 3. Some tidal volume targets to keep in mind: a. Small baby (<1500 grams): 4-6 ml/kg b. Average baby: 6-8 ml/kg c. Big, sick PPHN types: 6-8 ml/kg
4 130 Part 3-B Respiratory IV. High Frequency Ventilation: A. At Packard, high frequency ventilation is used primarily as a rescue therapy, reserved for children in whom conventional mechanical ventilation has failed, or in whom ventilator pressures that are likely to result in significant lung injury are required. We use the high frequency oscillator (HFOV) exclusively, not the high frequency jet ventilator or high frequency flow interruptor. The mechanics of high frequency ventilation allow you to generate a higher mean airway pressure with a lower peak pressure than conventional ventilation (lower pressures, less lung injury). High frequency also allows for very effective ventilation with smaller tidal volumes than a conventional ventilator (lower volumes, less lung injury). B. When to use it 1. Unable to ventilate despite high ventilator rates and adequate tidal volumes, when this is caused by poor lung compliance. High frequency ventilation is not effective for high resistance respiratory failure. 2. Requiring very high mean airway pressures to oxygenate 3. Air leak (pneumothorax or pulmonary interstitial emphysema) C. How does it work? A high frequency ventilator provides a baseline distending pressure (mean airway pressure or Paw), and then delivers hundreds of tiny breaths (less than the anatomic dead space) per minute. It may not make any physiologic sense but it does work and is very effective at both oxygenating and ventilating infants. There are only three settings on a high frequency ventilator, and only two that you ll usually adjust. D. Ventilator changes: Think of oxygenation and ventilation as separate entities. Adjusting the mean airway pressure changes oxygenation, while changing the amplitude or P changes ventilation. E. Again: 1. Mean airway pressure = oxygenation 2. Amplitude ( P) = ventilation F. Special considerations with high frequency ventilation: 1. As effective as high frequency ventilation can be, it is not without its problems. Because babies being ventilated with high frequency aren t ventilated tidally, it is very difficult to clinically assess the adequacy of support being provided. For this reason frequent CXRs are obtained to evaluate lung distension (every 6-12 hours) and PaCO2 levels should be followed closely to avoid hypocarbia. It makes sense to have a transcutaneous CO2 monitor on any infant on a high frequency ventilator, as high frequency is extremely efficient at ventilating and can drop PaCO2 values to dangerously low levels very quickly. 2. Another consequence of non-tidal ventilation is its impact on cardiac function. The heart is able to compensate during conventional ventilation by refilling when intrathoracic pressures are at their low point (PEEP). By providing a higher continuous mean airway pressure, a high frequency ventilator can decrease venous return requiring more aggressive cardiovascular support including volume and at times pressors. It may not be well tolerated in a term infant with septic shock.
5 Mechanical Ventilation 131 V. Desired arterial blood gas ranges A. These are some ball park values to aim for, as each child will have their own targets for any given day. 1. Prematures: a. ph: b. PaCO2: c. PaO2: d. Sats: 88-92% 2. Terms: a. ph: b. PaCO2: c. PaO2: d. Sats: 92-97% 3. PPHN: a. ph: b. PaCO 2: c. PaO 2: >100 d. Sats: >95% VI. How to handle a bad blood gas (a systematic approach): A. So, you ve got a lousy blood gas: 1. Figure out what s going on (oxygenation, ventilation, or acid-base problem) 2. Evaluate the baby 3. Call for help if confused or unsure 4. Make an intervention if necessary B. As far as what s going on Is there acidosis, and if so is it metabolic or respiratory? 2. Look at the baby - Comfortable? Upset? Agitation is common in babies whose ventilation is sub-optimal. C. If you have a metabolic acidosis (i.e. base deficit with normal PaCO2) 1. Is baby dry? If so, consider a bolus. 2. Does baby need base? Some little babies do as their kidneys aren t very good at retaining base, consider acetate or sodium bicarbonate. 3. Could baby be septic? 4. You can make a ventilator change as respiratory compensation is faster than metabolic compensation, but you have to address the underlying metabolic acidosis. D. If you re dealing with a respiratory problem, troubleshoot first. 1. Tube s out 2. Tube s at the carina 3. Tube s occluded or needs suctioning 4. Recent vent change if you make a vent change and get a bad gas, undo that change! 5. Atelectasis 6. Pneumothorax - these kids will be sick a. Listen for decreased breath sounds
6 132 Part 3-B Respiratory b. Consider transillumination 7. Pulmonary intestinal emphysema (PIE) VII. Weaning Strategies VIII. A. The primary determinant in deciding to implement ventilator weaning strategies is the status of the disease being treated and its time course. Specifically, weaning infants with pneumonia will not usually occur until day three to four of life, whereby those with hyaline membrane disease can be weaned sooner on day two to three of life. In addition, if circulatory instability secondary to sepsis is ongoing, extubation efforts are inappropriate even if pulmonary dysfunction is minimal. B. Neonate must be in a state of physiologic homeostasis. C. Nutritional support is especially critical for successful weaning for chronic ventilator-dependent babies. D. When using conventional mechanical ventilation (CMV), gradual stepwise reductions in IMV should be instituted after FiO2 and mean airway pressure have been somewhat normalized. E. When using high frequency oscillatory ventilation (HFOV), FiO2 should be weaned to 60% before the MAP is decreased in 1 cm H2O increments. Lung expansion and PaCO2 levels will also influence weaning PaCO2. The lung inflation goal is 8-9 ribs. The amplitude is weaned as tolerated to keep PaCO2 in target range. Expiratory time and Hertz usually remain constant. If HFOV is being employed for treatment of air leaks, MAP should be weaned first and foremost and a lower degree of lung inflation is desirable. Suggestions for Weaning A. Weaning should be initiated after evidence that ventilatory support is decreasing. This evidence may include: 1. Improving compliance noted on your pressure/volume loops 2. Reduction in FiO2 requirements 3. Increased urine output (diuretic phase seen in RDS) 4. Low PaCO2 allows you to decrease your PIP, IMV, PEEP or i-time. B. Begin with the factors that are most toxic to the lung. Wean slowly, frequent small changes allow the infant to gradually assume responsibility for gas exchange. C. In the LPCH NICU we are focusing on extubating babies from a mean airway pressure (PAW) of 7 or less. Always note what your baby s PAW is. IX. Extubation 1. Weaning off support from the ventilator can be approached in numerous ways. Consider extubation when the PAW is <7, and work toward achieving these additional settings as you move toward this MAP. 2. These are suggestions. Your job as the baby s doctor is to carefully assess the changing compliance and to make suggestions to the team as to how they can improve your baby s outcome. Discuss your ideas with the respiratory therapists, senior residents, fellows, nurses, nurse practitioners, and attendings. By assuming responsibility for your patient, you can significantly reduce the damaging effects of positive pressure ventilation. A. When your baby meets extubation criteria, discuss the plan with the team. Are you extubating to NCPAP, NC, or RA? Consider placing on NCPAP prior to extubation to avoid atelectasis. B. At least four hours prior to extubation, feedings should be stopped or an NG tube should be inserted to evacuate the contents of the stomach in order to prevent aspiration.
7 Mechanical Ventilation 133 C. At the time of extubation you should be present at the bedside with a respiratory therapist and the infant s nurse. D. Your intubation supplies (the red box) should be available at the bedside in the event that infant requires immediate reintubation. Suction and oxygen via a bag and mask should also be available. E. Follow up with a CXR if infant appears to be in distress to check for atelectasis. F. Consider a follow up ABG, transcutaneous and/or end tidal CO2 monitoring, and follow oxygen saturations closely. G. Reassess throughout the following hours for signs of respiratory distress. H. Always sign out a recent extubation to the on call team. X. Signs of Respiratory Distress A. Tachypnea, retractions, cyanosis, agitation, lethargy, pallor, stridor, grunting, apnea XI. Long Inspiratory Time Strategy A. Time constants: A time constant is the product of the airway resistance and the compliance. Simply put, it is a measure of how quickly the patient s lungs can inflate or deflate: how long it takes for the pressure of air in the alveoli to equal the pressure of air in the proximal airway. B. Acute RDS: Near complete equilibration of alveolar pressures occurs in 3-5 time constants. The surfactant deficient, premature lung has low compliance and normal airway resistance, resulting in a short time constant; meaning it takes a short amount of time for the pressure to be equal between the proximal airway and the alveoli. The time constant may be as short as 0.05 seconds; this would mean that 95% of the applied pressure to the airway was delivered to the alveoli in 0.15 seconds (three time constants). C. Chronic Lung Disease: As the lung is healing from RDS, the airways develop increasing inflammation which leads to decreased bronchiolar diameter and increased resistance. Therefore, chronic lung disease (CLD) is a high resistance disease: as the resistance increases, the inspiratory time must increase in order to sufficiently inflate the alveoli. The goal of using a long i-time ( seconds) in a baby with high resistance disease is to allow ventilation of all lung units, even the alveoli connected to very inflamed, narrowed airways. We typically use low flow (<4 lpm) to create a slow ramp wave form. We also try to use the lowest flow that will meet the baby s own inspiratory flow demands.
8 134 Part 3-B Respiratory D. Using long i-times in babies can be quite dangerous if used improperly, therefore as a resident you should always consult the fellow or attending if you have questions about the i-time. Improper application of a long i-time can result in auto-peep if sufficient time for exhalation is not allowed. The inadvertent PEEP can lead to rupture of the alveoli, air leaks, and cardiopulmonary compromise. On the other hand, by the time an ex-preemie has made his or her way to a state of CLD in which long i-times are necessary, abruptly changing this strategy can result in acute hypoxia and alveolar collapse. Respect the long inspiratory time in these babies and ask for help before changing the strategy. XII. Ventilator Modes Mode Features Benefits Disadvantages Target For PSV All breaths supported with ventilatordriven breaths to set PIP. Patient-controlled i- time and RR. Operator-selected backup rate. WOB is lower for spontaneously breathing patients above operatorselected RR. Patient determines i- time and e-time; can vary from breath to breath based on patient demand. Patient can raise or lower V min as demand changes. Patient may hyperventilate or develop auto- PEEP. Fluctuations in patient RR and/or i-time may cause P aw to vary. Large ET air leaks may cause dysynchrony as breathending criteria may not be attainable. V T varies with changes in C&R. Patients who are spontaneously breathing. Patients who exhibit signs of raised WOB on non-vent supported breaths (e.g. SIMV) SIMV Patient can breathe spontaneously between set vent breaths. Fixed RR and I:E ratio for vent breaths. Set i-time. Complete clinician control of vent breath perimeters and vent-supported RR. Consistent P aw. Fixed i-time for infant unable to maintain adequate i-time in RR. WOB increased for patients breathing at rates above fixed rate. Spontaneous breaths not vent supported. Dysynchrony possible during inspiratory phase if patient i-times do not match vent. Patients who are not spontaneously breathing. Patients who develop uncorrectable respiratory alkalosis with PSV or A/C.
9 Mechanical Ventilation 135 Mode Features Benefits Disadvantages Target For A/C All breaths supported with ventilatordelivered breath to set PIP. Patient-controlled RR. Operatorselected backup rate. Set i-time. All patient breaths are vent supported. WOB is lower for patients spontaneously breathing above operatorselected RR. Patient can vary V min as demand changes. Fixed i-time for infants unable to maintain adequate i-time in PSV. Dysynchrony possible during inspiratory phase if patient i-times do not match vent. Patient may hyperventilate or inverse I:E ratio. Patients may develop auto-peep. Fluctuations in patient RR may cause P aw to vary. V T varies with changes in C&R. Patients who cannot maintain adequate i-times. Patients who exhibit signs of raised WOB on non-vent supported breaths (e.g. SIMV) VG Set V T. PIP adjusts to achieve target V T. V T constant with changes in C&R. PIP decreases as C&R improves. P aw may be affected when PIP varies. Patients who require a steady V T due to changes in C&R.
MECHINICAL VENTILATION S. Kache, MD
 MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
MECHINICAL VENTILATION S. Kache, MD Spontaneous respiration vs. Mechanical ventilation Natural spontaneous ventilation occurs when the respiratory muscles, diaphragm and intercostal muscles pull on the
Airway Pressure Release Ventilation
 Page: 1 Policy #: 25.01.153 Issued: 4-1-2006 Reviewed/ Revised: Section: 10-11-2006 Respiratory Care Airway Pressure Release Ventilation Description/Definition Airway Pressure Release Ventilation (APRV)
Page: 1 Policy #: 25.01.153 Issued: 4-1-2006 Reviewed/ Revised: Section: 10-11-2006 Respiratory Care Airway Pressure Release Ventilation Description/Definition Airway Pressure Release Ventilation (APRV)
Common Ventilator Management Issues
 Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
Common Ventilator Management Issues William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center You have just admitted a 28 year-old
MECHANICAL VENTILATION IN THE NEONATE
 Supplemental Resources for the PICU/NICU MECHANICAL VENTILATION IN THE NEONATE I. GENERAL PRINCIPLES A. NEONATAL VENTILATORS We use three types of neonatal ventilators in the NICU: 1. SIMV (Synchronized
Supplemental Resources for the PICU/NICU MECHANICAL VENTILATION IN THE NEONATE I. GENERAL PRINCIPLES A. NEONATAL VENTILATORS We use three types of neonatal ventilators in the NICU: 1. SIMV (Synchronized
3100B Clinical Training Program. 3100B HFOV VIASYS Healthcare
 3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
3100B Clinical Training Program 3100B HFOV VIASYS Healthcare HFOV at Alveolar Level Nieman,, G, SUNY 1999 Who DO We Treat? Only Pathology studied to date has been ARDS Questions about management of adults
Mechanical Ventilators
 University of Washington Academic Medical Center Copyright 2000 Disclaimer Children's Hospital and Regional Medical Center Copyright 2002 Disclaimer Mechanical Ventilators Authors Created 07/31/95 Reviewed
University of Washington Academic Medical Center Copyright 2000 Disclaimer Children's Hospital and Regional Medical Center Copyright 2002 Disclaimer Mechanical Ventilators Authors Created 07/31/95 Reviewed
Oxygenation and Oxygen Therapy Michael Billow, D.O.
 Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
Oxygenation and Oxygen Therapy Michael Billow, D.O. The delivery of oxygen to all body tissues is the essence of critical care. Patients in respiratory distress/failure come easily to mind as the ones
High-Frequency Oscillatory Ventilation
 High-Frequency Oscillatory Ventilation Arthur Jones EdD, RRT Learning Objectives Describe the indications and rationale and monitoring for HFOV. Identify HFOV settings and describe the effects of their
High-Frequency Oscillatory Ventilation Arthur Jones EdD, RRT Learning Objectives Describe the indications and rationale and monitoring for HFOV. Identify HFOV settings and describe the effects of their
Safe Zone: CV PIP < 26; HFOV: MAP < 16; HFJV: MAP < 16 Dopamine infusion up to 20 mcg/kg/min Epinephrine infusion up to 0.1 mcg /kg/min.
 Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
Congenital Diaphragmatic Hernia: Management Guidelines 5-2006 Issued By: Division of Neonatology Reviewed: Effective Date: Categories: Chronicity Document Congenital Diaphragmatic Hernia: Management Guidelines
Understanding Hypoventilation and Its Treatment by Susan Agrawal
 www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
www.complexchild.com Understanding Hypoventilation and Its Treatment by Susan Agrawal Most of us have a general understanding of what the term hyperventilation means, since hyperventilation, also called
Ventilator Application of the Passy-Muir Valve David A. Muir Course Outline Benefits Review of the Biased Closed Position No Leak Passy-Muir Valves
 Ventilator Application of the Passy-Muir Valve Michael S. Harrell, B.S., RRT Director of Clinical Education-Respiratory mharell@passy-muir.com (949) 833-8255 David A. Muir 23 year-old ventilator dependent
Ventilator Application of the Passy-Muir Valve Michael S. Harrell, B.S., RRT Director of Clinical Education-Respiratory mharell@passy-muir.com (949) 833-8255 David A. Muir 23 year-old ventilator dependent
Neurally Adjusted Ventilatory Assist: NAVA for Neonates
 Neurally Adjusted Ventilatory Assist: NAVA for Neonates Robert L. Chatburn, MHHS, RRT-NPS, FAARC Research Manager Respiratory Institute Cleveland Clinic Professor Department of Medicine Lerner College
Neurally Adjusted Ventilatory Assist: NAVA for Neonates Robert L. Chatburn, MHHS, RRT-NPS, FAARC Research Manager Respiratory Institute Cleveland Clinic Professor Department of Medicine Lerner College
ASSISTED VENTILATION IN NEONATES
 ASSISTED VENTILATION IN NEONATES CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Continuous Positive Airway Pressure or CPAP is a modality of respiratory support in which increased pulmonary pressure
ASSISTED VENTILATION IN NEONATES CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Continuous Positive Airway Pressure or CPAP is a modality of respiratory support in which increased pulmonary pressure
From AARC Protocol Committee; Subcommittee Adult Critical Care Version 1.0a (Sept., 2003), Subcommittee Chair, Susan P. Pilbeam
 AARC - ADULT MECHANICAL VENTILATOR PROTOCOLS 1. Guidelines for Using Ventilator Protocols 2. Definition of Modes and Suggestions for Use of Modes 3. Adult Respiratory Ventilator Protocol - Guidelines for
AARC - ADULT MECHANICAL VENTILATOR PROTOCOLS 1. Guidelines for Using Ventilator Protocols 2. Definition of Modes and Suggestions for Use of Modes 3. Adult Respiratory Ventilator Protocol - Guidelines for
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD Definition ARDS is a clinical syndrome of lung injury with hypoxic respiratory failure caused by intense pulmonary inflammation that
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) S. Agarwal, MD, S. Kache MD Definition ARDS is a clinical syndrome of lung injury with hypoxic respiratory failure caused by intense pulmonary inflammation that
Why is prematurity a concern?
 Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
Prematurity What is prematurity? A baby born before 37 weeks of pregnancy is considered premature. Approximately 12% of all babies are born prematurely. Terms that refer to premature babies are preterm
PULMONARY PHYSIOLOGY
 I. Lung volumes PULMONARY PHYSIOLOGY American College of Surgeons SCC Review Course Christopher P. Michetti, MD, FACS and Forrest O. Moore, MD, FACS A. Tidal volume (TV) is the volume of air entering and
I. Lung volumes PULMONARY PHYSIOLOGY American College of Surgeons SCC Review Course Christopher P. Michetti, MD, FACS and Forrest O. Moore, MD, FACS A. Tidal volume (TV) is the volume of air entering and
5/30/2014 OBJECTIVES THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM. Disclosure
 THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
THE ROLE OF A RESPIRATORY THERAPIST IN THE DELIVERY ROOM Ona Fofah, MD FAAP Assistant Professor of Pediatrics Director, Division of Neonatology Department of Pediatrics Rutgers- NJMS, Newark OBJECTIVES
Mechanical Ventilation for Dummies Keep It Simple Stupid
 Mechanical Ventilation for Dummies Keep It Simple Stupid Indications Airway Ventilation failure (CO2) Hypoxia Combination Airway obstruction Inability to protect airway Hypoxia (PaO 2 < 50) Hypercapnia
Mechanical Ventilation for Dummies Keep It Simple Stupid Indications Airway Ventilation failure (CO2) Hypoxia Combination Airway obstruction Inability to protect airway Hypoxia (PaO 2 < 50) Hypercapnia
A. All cells need oxygen and release carbon dioxide why?
 I. Introduction: Describe how the cardiovascular and respiratory systems interact to supply O 2 and eliminate CO 2. A. All cells need oxygen and release carbon dioxide why? B. Two systems that help to
I. Introduction: Describe how the cardiovascular and respiratory systems interact to supply O 2 and eliminate CO 2. A. All cells need oxygen and release carbon dioxide why? B. Two systems that help to
SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY
 PS1006 SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY TITLE: NON-INVASIVE POSITIVE PRESSURE (NPPV) VENTILATION (CPAP/BIPAP) Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: Director, Respiratory
PS1006 SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY TITLE: NON-INVASIVE POSITIVE PRESSURE (NPPV) VENTILATION (CPAP/BIPAP) Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE: POLICY TYPE: Director, Respiratory
MECHANICAL VENTILATION
 MECHANICAL VENTILATION INDICATIONS: Respiratory Failure Cardiopulmonary arrest Trauma (especially head, neck, and chest) Cardiovascular impairment (strokes, tumors, infection, emboli, trauma) Neurological
MECHANICAL VENTILATION INDICATIONS: Respiratory Failure Cardiopulmonary arrest Trauma (especially head, neck, and chest) Cardiovascular impairment (strokes, tumors, infection, emboli, trauma) Neurological
Principles of Mechanical Ventilation
 Principles of Mechanical Ventilation The Basics Presented by WANG, Tzong-Luen Professor, Medical School, FJU Director, ED, SKH President, SECCM, Taiwan Origins of mechanical ventilation The era of intensive
Principles of Mechanical Ventilation The Basics Presented by WANG, Tzong-Luen Professor, Medical School, FJU Director, ED, SKH President, SECCM, Taiwan Origins of mechanical ventilation The era of intensive
Comparison of the Rate of Improvement in Gas Exchange between Two High Frequency Ventilators in a Newborn Piglet Lung Injury Model
 Comparison of the Rate of Improvement in Gas Exchange between Two High Frequency Ventilators in a Newborn Piglet Lung Injury Model Kurt Gillette, MD, San Antonio Military Medical Center Background: High
Comparison of the Rate of Improvement in Gas Exchange between Two High Frequency Ventilators in a Newborn Piglet Lung Injury Model Kurt Gillette, MD, San Antonio Military Medical Center Background: High
How To Determine The Difference Between Long Versus Short Inspiratory Times In Neonates
 Long versus short inspiratory times in neonates receiving mechanical ventilation (Review) Kamlin COF, Davis PG This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Long versus short inspiratory times in neonates receiving mechanical ventilation (Review) Kamlin COF, Davis PG This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
OPTIMAL PEEP DETERMINATION
 by Kevin T. Martin BVE, RRT, RCP RC Educational Consulting Services, Inc. 16781 Van Buren Blvd, Suite B, Riverside, CA 92504-5798 (800) 441-LUNG / (877) 367-NURS www.rcecs.com BEHAVIORAL OBJECTIVES UPON
by Kevin T. Martin BVE, RRT, RCP RC Educational Consulting Services, Inc. 16781 Van Buren Blvd, Suite B, Riverside, CA 92504-5798 (800) 441-LUNG / (877) 367-NURS www.rcecs.com BEHAVIORAL OBJECTIVES UPON
RESPIRATORY VENTILATION Page 1
 Page 1 VENTILATION PARAMETERS A. Lung Volumes 1. Basic volumes: elements a. Tidal Volume (V T, TV): volume of gas exchanged each breath; can change as ventilation pattern changes b. Inspiratory Reserve
Page 1 VENTILATION PARAMETERS A. Lung Volumes 1. Basic volumes: elements a. Tidal Volume (V T, TV): volume of gas exchanged each breath; can change as ventilation pattern changes b. Inspiratory Reserve
Homeostasis. The body must maintain a delicate balance of acids and bases.
 Homeostasis The body must maintain a delicate balance of acids and bases. Metabolic and respiratory processes must work together to keep hydrogen ion (H+) levels normal and stable. ph of Blood The ph of
Homeostasis The body must maintain a delicate balance of acids and bases. Metabolic and respiratory processes must work together to keep hydrogen ion (H+) levels normal and stable. ph of Blood The ph of
Oxygenation. Chapter 21. Anatomy and Physiology of Breathing. Anatomy and Physiology of Breathing*
 Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Oxygenation Chapter 21 Anatomy and Physiology of Breathing Inspiration ~ breathing in Expiration ~ breathing out Ventilation ~ Movement of air in & out of the lungs Respiration ~ exchange of O2 & carbon
Ventilation Perfusion Relationships
 Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
Ventilation Perfusion Relationships VENTILATION PERFUSION RATIO Ideally, each alveolus in the lungs would receive the same amount of ventilation and pulmonary capillary blood flow (perfusion). In reality,
RES Non-Invasive Positive Pressure Ventilation Guideline Page 1 of 9
 Page 1 of 9 Scope: Respiratory Care Department, Physicians, Advanced Nurse Practitioners (APRN), Physician Assistants (PA) Population: Patients receiving rescue or non-rescue non-invasive positive pressure
Page 1 of 9 Scope: Respiratory Care Department, Physicians, Advanced Nurse Practitioners (APRN), Physician Assistants (PA) Population: Patients receiving rescue or non-rescue non-invasive positive pressure
Protocols for Early Extubation After Cardiothoracic Surgery
 Protocols for Early Extubation After Cardiothoracic Surgery AATS / STS CT Critical Care Symposium April 27, 2014 Toronto, Ontario Nevin M. Katz, M.D. Johns Hopkins University Foundation for the Advancement
Protocols for Early Extubation After Cardiothoracic Surgery AATS / STS CT Critical Care Symposium April 27, 2014 Toronto, Ontario Nevin M. Katz, M.D. Johns Hopkins University Foundation for the Advancement
Hospital of the University of Pennsylvania Physician Practice Guideline
 Page 1 of 5 KEY WORDS: Ventilator Respirator Weaning Extubation Liberation PURPOSE: To facilitate the liberation of patients from mechanical ventilation and provide a consistent approach to the ventilator
Page 1 of 5 KEY WORDS: Ventilator Respirator Weaning Extubation Liberation PURPOSE: To facilitate the liberation of patients from mechanical ventilation and provide a consistent approach to the ventilator
Artificial Ventilation Theory into practice
 Artificial Ventilation Theory into practice Keith Simpson BVSc MRCVS MIET(Electronics) www.vetronic.co.uk ksimpson@vetronic.co.uk June 13 th 2014 Today we will discuss the administration of IPPV to anaesthetised
Artificial Ventilation Theory into practice Keith Simpson BVSc MRCVS MIET(Electronics) www.vetronic.co.uk ksimpson@vetronic.co.uk June 13 th 2014 Today we will discuss the administration of IPPV to anaesthetised
GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY
 SOUTH DURHAM HEALTH CARE NHS TRUST GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY AIM To supplement oxygen intake using the appropriate equipment in order to correct hypoxia and relieve breathlessness.
SOUTH DURHAM HEALTH CARE NHS TRUST GUIDELINES FOR THE MANAGEMENT OF OXYGEN THERAPY AIM To supplement oxygen intake using the appropriate equipment in order to correct hypoxia and relieve breathlessness.
Nurses and Respiratory Therapists Working Together for Safe Alarm Systems Management
 Nurses and Respiratory Therapists Working Together for Safe Alarm Systems Management May 11, 2015 9/25/2013 1 AAMI Foundation Vision: To drive the safe adoption and use of healthcare technology Visit our
Nurses and Respiratory Therapists Working Together for Safe Alarm Systems Management May 11, 2015 9/25/2013 1 AAMI Foundation Vision: To drive the safe adoption and use of healthcare technology Visit our
Impact Uni-Vent 754 Portable Ventilator
 Impact Uni-Vent 754 Portable Ventilator Description - Indications- Contraindications- Side Effects- Special Considerations- The Uni-Vent 754 Portable Ventilator is a portable electronically controlled,
Impact Uni-Vent 754 Portable Ventilator Description - Indications- Contraindications- Side Effects- Special Considerations- The Uni-Vent 754 Portable Ventilator is a portable electronically controlled,
Volume Guarantee New Approaches in Volume Controlled Ventilation for Neonates. Jag Ahluwalia, Colin Morley, Hans Georg Wahle
 Volume Guarantee New Approaches in Volume Controlled Ventilation for Neonates Jag Ahluwalia, Colin Morley, Hans Georg Wahle Important Notice: Medical knowledge changes constantly as a result of new research
Volume Guarantee New Approaches in Volume Controlled Ventilation for Neonates Jag Ahluwalia, Colin Morley, Hans Georg Wahle Important Notice: Medical knowledge changes constantly as a result of new research
Critical Care Therapy and Respiratory Care Section
 Critical Care Therapy and Respiratory Care Section Category: Clinical Section: Special Procedures Title: Transport of Critically Ill Patients Policy #: 05 Revised: 04/00 1.0 DESCRIPTION 1.1 Definition:
Critical Care Therapy and Respiratory Care Section Category: Clinical Section: Special Procedures Title: Transport of Critically Ill Patients Policy #: 05 Revised: 04/00 1.0 DESCRIPTION 1.1 Definition:
NURSING SERVICES DEPARTMENT
 NURSING SERVICES DEPARTMENT TITLE: Mechanical Ventilation PATIENT CARE PLAN DIAGNOSIS: DISCHARGE CRITERIA: 1 The patient will: Maintain adequate mechanics of PERTINENT INFORMATION:. ventilation as demonstrated
NURSING SERVICES DEPARTMENT TITLE: Mechanical Ventilation PATIENT CARE PLAN DIAGNOSIS: DISCHARGE CRITERIA: 1 The patient will: Maintain adequate mechanics of PERTINENT INFORMATION:. ventilation as demonstrated
6 Easy Steps to ABG Analysis
 6 Easy Steps to ABG Analysis E-Booklet David W. Woodruff, MSN, RN- BC, CNS, CMSRN, CEN 571 Ledge Road, Macedonia, OH 44056 Telephone (800) 990-2629 Fax (800) 990-2585 1997-2012 Ed4Nurses, Inc. All rights
6 Easy Steps to ABG Analysis E-Booklet David W. Woodruff, MSN, RN- BC, CNS, CMSRN, CEN 571 Ledge Road, Macedonia, OH 44056 Telephone (800) 990-2629 Fax (800) 990-2585 1997-2012 Ed4Nurses, Inc. All rights
Home Ventilator. 2009 Breath of Life Home Medical Equipment and Respiratory Services
 Home Ventilator 2009 Breath of Life Home Medical Equipment and Respiratory Services 1 Your Prescription Your physician has prescribed a home ventilator system for your child. This book will help you to
Home Ventilator 2009 Breath of Life Home Medical Equipment and Respiratory Services 1 Your Prescription Your physician has prescribed a home ventilator system for your child. This book will help you to
COPD with Respiratory Failure Case Study #21. Molly McDonough
 COPD with Respiratory Failure Case Study #21 Molly McDonough Patient: Mr. Hayato 65 year old male Brought to ER with severe SOB Past History of emphysema Longstanding chronic obstruction pulmonary disease
COPD with Respiratory Failure Case Study #21 Molly McDonough Patient: Mr. Hayato 65 year old male Brought to ER with severe SOB Past History of emphysema Longstanding chronic obstruction pulmonary disease
High Frequency Ventilation Introductory Information
 High-Frequency Oscillatory Ventilation Learning Objectives: Explain the indications, rationale and monitoring for HFOV. Explain the effects of adjusting HFOV ventilator controls. Arthur Jones EdD, RRT
High-Frequency Oscillatory Ventilation Learning Objectives: Explain the indications, rationale and monitoring for HFOV. Explain the effects of adjusting HFOV ventilator controls. Arthur Jones EdD, RRT
Auto Flow 20 Questions 20 Answers. Joseph Fitzgerald
 Auto Flow 20 Questions 20 Answers Joseph Fitzgerald Important Notice: Medical knowledge changes constantly as a result of new research and clinical experience. The author of this introductory guide has
Auto Flow 20 Questions 20 Answers Joseph Fitzgerald Important Notice: Medical knowledge changes constantly as a result of new research and clinical experience. The author of this introductory guide has
NEONATAL RESPIRATORY CARE: CLINICAL APPLICATIONS
 By Kevin T. Martin BVE, RRT, RCP RC Educational Consulting Services, Inc. 16781 Van Buren Blvd, Suite B, Riverside, CA 92504-5798 (800) 441-LUNG / (877) 367-NURS www.rcecs.com BEHAVIORAL OBJECTIVES BY
By Kevin T. Martin BVE, RRT, RCP RC Educational Consulting Services, Inc. 16781 Van Buren Blvd, Suite B, Riverside, CA 92504-5798 (800) 441-LUNG / (877) 367-NURS www.rcecs.com BEHAVIORAL OBJECTIVES BY
COURSE SYLLABUS RC 223 CLINICAL-3
 COURSE SYLLABUS RC 223 CLINICAL-3 Class Hours: 0 Laboratory Hours: 24 Credit Hours: 4 Course Description: Entry Level Standards: This course will emphasize neonatal-pediatric intensive care, pulmonary
COURSE SYLLABUS RC 223 CLINICAL-3 Class Hours: 0 Laboratory Hours: 24 Credit Hours: 4 Course Description: Entry Level Standards: This course will emphasize neonatal-pediatric intensive care, pulmonary
WEANING PROTOCOL IMPORTANT NOTICE: THIS DOCUMENT IS PROVIDED BY FAIRVIEW SOUTHDALE HOSPITAL SOLELY FOR INSTRUCTIONAL PURPOSES.
 WEAIG PROTOCOL Contact: Ted Wawrzyniak, BS, RRT, CPS, tedwawrzyn@aol.com Fairview Southdale Hospital, Cardiopulmonary and eurology Services Department 6401 France Avenue South, Edina, M 55435-2199 Tel:
WEAIG PROTOCOL Contact: Ted Wawrzyniak, BS, RRT, CPS, tedwawrzyn@aol.com Fairview Southdale Hospital, Cardiopulmonary and eurology Services Department 6401 France Avenue South, Edina, M 55435-2199 Tel:
Management of airway burns and inhalation injury PAEDIATRIC
 Management of airway burns and inhalation injury PAEDIATRIC A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer to
Management of airway burns and inhalation injury PAEDIATRIC A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer to
DRG 475 Respiratory System Diagnosis with Ventilator Support. ICD-9-CM Coding Guidelines
 DRG 475 Respiratory System Diagnosis with Ventilator Support ICD-9-CM Coding G The below listed g are not inclusive. The coder should refer to the applicable Coding Clinic g for additional information.
DRG 475 Respiratory System Diagnosis with Ventilator Support ICD-9-CM Coding G The below listed g are not inclusive. The coder should refer to the applicable Coding Clinic g for additional information.
VENTILATION SERVO-s EASY AND RELIABLE PATIENT CARE
 VENTILATION SERVO-s EASY AND RELIABLE PATIENT CARE Critical Care SERVO-s 3 SERVO-s SIMPLY MAKES SENSE MAQUET THE GOLD STANDARD Leading the way: MAQUET is a premier international provider of medical products
VENTILATION SERVO-s EASY AND RELIABLE PATIENT CARE Critical Care SERVO-s 3 SERVO-s SIMPLY MAKES SENSE MAQUET THE GOLD STANDARD Leading the way: MAQUET is a premier international provider of medical products
Pulmonary Diseases. Lung Disease: Pathophysiology, Medical and Exercise Programming. Overview of Pathophysiology
 Lung Disease: Pathophysiology, Medical and Exercise Programming Overview of Pathophysiology Ventilatory Impairments Increased airway resistance Reduced compliance Increased work of breathing Ventilatory
Lung Disease: Pathophysiology, Medical and Exercise Programming Overview of Pathophysiology Ventilatory Impairments Increased airway resistance Reduced compliance Increased work of breathing Ventilatory
Evaluation and treatment of emphysema in a preterm infant
 ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
ISPUB.COM The Internet Journal of Pediatrics and Neonatology Volume 11 Number 1 Evaluation and treatment of emphysema in a preterm infant T Saad, P Chess, W Pegoli, P Katzman Citation T Saad, P Chess,
Tests. Pulmonary Functions
 Pulmonary Functions Tests Static lung functions volumes Dynamic lung functions volume and velocity Dynamic Tests Velocity dependent on Airway resistance Resistance of lung tissue to change in shape Dynamic
Pulmonary Functions Tests Static lung functions volumes Dynamic lung functions volume and velocity Dynamic Tests Velocity dependent on Airway resistance Resistance of lung tissue to change in shape Dynamic
Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support
 Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support Copyright by the SOCIETY OF CRITICAL CARE MEDICINE These guidelines can also be found in the
Guidelines for Standards of Care for Patients with Acute Respiratory Failure on Mechanical Ventilatory Support Copyright by the SOCIETY OF CRITICAL CARE MEDICINE These guidelines can also be found in the
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Neonatal Respiratory Failure Introduction This neonatal respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Importance of Protocols in the Decision to Use Noninvasive Ventilation
 Importance of Protocols in the Decision to Use Noninvasive Ventilation Janice L. Zimmerman, M.D. Weill Cornell Medical College The Methodist Hospital Houston, Texas Objectives Review application of protocols
Importance of Protocols in the Decision to Use Noninvasive Ventilation Janice L. Zimmerman, M.D. Weill Cornell Medical College The Methodist Hospital Houston, Texas Objectives Review application of protocols
Critical Care Therapy and Respiratory Care Section
 Category: Section: Title: Critical Care Therapy and Respiratory Care Section Policy #: 03 Revised: 5/02 1.0 DESCRIPTION Clinical Ventilator Management Invasive and Noninvasive Positive Pressure Ventilation
Category: Section: Title: Critical Care Therapy and Respiratory Care Section Policy #: 03 Revised: 5/02 1.0 DESCRIPTION Clinical Ventilator Management Invasive and Noninvasive Positive Pressure Ventilation
Respiratory failure. (Respiratory insuficiency) MUDr Radim Kukla KAR FN Motol
 Respiratory failure (Respiratory insuficiency) MUDr Radim Kukla KAR FN Motol Respiratory failure definition Failure of ability to secure the metabolic needs of organism i.e. proper oxygenation and excretion
Respiratory failure (Respiratory insuficiency) MUDr Radim Kukla KAR FN Motol Respiratory failure definition Failure of ability to secure the metabolic needs of organism i.e. proper oxygenation and excretion
Pathophysiology of hypercapnic and hypoxic respiratory failure and V/Q relationships. Dr.Alok Nath Department of Pulmonary Medicine PGIMER Chandigarh
 Pathophysiology of hypercapnic and hypoxic respiratory failure and V/Q relationships Dr.Alok Nath Department of Pulmonary Medicine PGIMER Chandigarh Jan 2006 Respiratory Failure inadequate blood oxygenation
Pathophysiology of hypercapnic and hypoxic respiratory failure and V/Q relationships Dr.Alok Nath Department of Pulmonary Medicine PGIMER Chandigarh Jan 2006 Respiratory Failure inadequate blood oxygenation
Acid/Base Homeostasis (Part 4)
 Acid/Base Homeostasis (Part 4) Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) 5. The newly formed bicarbonate moves into the plasma.
Acid/Base Homeostasis (Part 4) Graphics are used with permission of: Pearson Education Inc., publishing as Benjamin Cummings (http://www.aw-bc.com) 5. The newly formed bicarbonate moves into the plasma.
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire
 Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
Children's Medical Services (CMS) Regional Perinatal Intensive Care Center (RPICC) Neonatal Extracorporeal Life Support (ECLS) Centers Questionnaire Date: RPICC Facility: CMS use only Include the following
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline
 NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
NHS FORTH VALLEY Neonatal Oxygen Saturation Guideline Date of First Issue 11/07/2011 Approved 30/09/2011 Current Issue Date 07/09/2011 Review Date July 2013 Version 1 EQIA Yes 22/10/2011 Author / Contact
POCKET GUIDE. NAVA and NIV NAVA in neonatal settings
 POCKET GUIDE NAVA and NIV NAVA in neonatal settings Table of contents EMPTY 1 2 3 4 Introduction and background facts Invasive ventilation with NAVA Non invasive ventilation with NAVA NAVA and NIV NAVA
POCKET GUIDE NAVA and NIV NAVA in neonatal settings Table of contents EMPTY 1 2 3 4 Introduction and background facts Invasive ventilation with NAVA Non invasive ventilation with NAVA NAVA and NIV NAVA
Please answer the following questions before reading the tutorial. The answers are contained in the article.
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Author Dr D. Lacquiere Correspondence: david_lacquiere@hotmail.com Please answer the following questions before reading the tutorial. The answers are contained
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Author Dr D. Lacquiere Correspondence: david_lacquiere@hotmail.com Please answer the following questions before reading the tutorial. The answers are contained
GRADE 11F: Biology 3. UNIT 11FB.3 9 hours. Human gas exchange system and health. Resources. About this unit. Previous learning.
 GRADE 11F: Biology 3 Human gas exchange system and health UNIT 11FB.3 9 hours About this unit This unit is the third of six units on biology for Grade 11 foundation. The unit is designed to guide your
GRADE 11F: Biology 3 Human gas exchange system and health UNIT 11FB.3 9 hours About this unit This unit is the third of six units on biology for Grade 11 foundation. The unit is designed to guide your
9/12/2011 OBJECTIVES BREATH OF LIFE. Review the role that Potentially Better Practices (PBP s) play in clinical practice
 Ona. O. Fofah, MD, FAAP Director, Division of Neonatal Perinatal Medicine, Department of Pediatrics, UMDNJ/NJMS UMDNJ RESPIRATORY LECTURE SERIES SEPT 2011 OBJECTIVES Review the role that Potentially Better
Ona. O. Fofah, MD, FAAP Director, Division of Neonatal Perinatal Medicine, Department of Pediatrics, UMDNJ/NJMS UMDNJ RESPIRATORY LECTURE SERIES SEPT 2011 OBJECTIVES Review the role that Potentially Better
CHEST TUBES AND CHEST DRAINAGE SYSTEMS
 CHEST TUBES AND CHEST DRAINAGE SYSTEMS Central Nursing Orientation April 2008 Revised September 2011 OBJECTIVES Describe common tubes and indications for use at LHSC Review indications and contraindications,
CHEST TUBES AND CHEST DRAINAGE SYSTEMS Central Nursing Orientation April 2008 Revised September 2011 OBJECTIVES Describe common tubes and indications for use at LHSC Review indications and contraindications,
Recommendations: Other Supportive Therapy of Severe Sepsis*
 Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
Recommendations: Other Supportive Therapy of Severe Sepsis* K. Blood Product Administration 1. Once tissue hypoperfusion has resolved and in the absence of extenuating circumstances, such as myocardial
MECHANICAL VENTILATION: AN OVERVIEW
 MECHANICAL VENTILATION: AN OVERVIEW by Kevin T. Martin BVE, RRT, RCP V7117 HC 04 RC Educational Consulting Services, Inc. P.O. Box 1930, Brockton, MA 02303-1930 (800) 441-LUNG / (877) 367-NURS www.rcecs.com
MECHANICAL VENTILATION: AN OVERVIEW by Kevin T. Martin BVE, RRT, RCP V7117 HC 04 RC Educational Consulting Services, Inc. P.O. Box 1930, Brockton, MA 02303-1930 (800) 441-LUNG / (877) 367-NURS www.rcecs.com
SWISS SOCIETY OF NEONATOLOGY. Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema
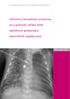 SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
SWISS SOCIETY OF NEONATOLOGY Selective bronchial occlusion in a preterm infant with unilateral pulmonary interstitial emphysema December 2002 2 Riedel T, Pfenninger J, Pediatric Intensive Care Unit, University
The Berlin definition of Severe ARDS includes assessment of which of the following?
 2013 ACS Critical Care Update ARDS, Ventilators MCQs August, 2013 (Berlin Definition of ARDS Question 1) The Berlin definition of Severe ARDS includes assessment of which of the following? A. Oxygenation:
2013 ACS Critical Care Update ARDS, Ventilators MCQs August, 2013 (Berlin Definition of ARDS Question 1) The Berlin definition of Severe ARDS includes assessment of which of the following? A. Oxygenation:
What, roughly, is the dividing line between the upper and lower respiratory tract? The larynx. What s the difference between the conducting zone and
 What, roughly, is the dividing line between the upper and lower respiratory tract? The larynx. What s the difference between the conducting zone and the respiratory zone? Conducting zone is passageways
What, roughly, is the dividing line between the upper and lower respiratory tract? The larynx. What s the difference between the conducting zone and the respiratory zone? Conducting zone is passageways
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings
 AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
AHA/AAP Neonatal Resuscitation Guidelines 2010: Summary of Major Changes and Comment on its Utility in Resource-Limited Settings Resuscitation step Recommendations (2005) Recommendations (2010) Comments/LOE
Eileen Whitehead 2010 East Lancashire HC NHS Trust
 Eileen Whitehead 2010 East Lancashire HC NHS Trust 1 Introduction: Arterial blood gas analysis is an essential part of diagnosing and managing a patient s oxygenation status and acid-base balance However,
Eileen Whitehead 2010 East Lancashire HC NHS Trust 1 Introduction: Arterial blood gas analysis is an essential part of diagnosing and managing a patient s oxygenation status and acid-base balance However,
Respiratory failure and Oxygen Therapy
 Respiratory failure and Oxygen Therapy A patient with Hb 15 G % will carry 3X more O2 in his blood than someone with Hb 5G % Give Controlled O2 treatment in acute pulmonary oedema to avoid CO2 retention
Respiratory failure and Oxygen Therapy A patient with Hb 15 G % will carry 3X more O2 in his blood than someone with Hb 5G % Give Controlled O2 treatment in acute pulmonary oedema to avoid CO2 retention
Airway Pressure Release Ventilation (APRV) for the Treatment of Severe Life-Threatening ARDS in a Morbidly Obese Patient
 Review Crit Care & Shock (2008) 11 : 132-136 Airway Pressure Release Ventilation (APRV) for the Treatment of Severe Life-Threatening ARDS in a Morbidly Obese Patient Amyn Hirani, Rodrigo Cavallazzi, Anastasia
Review Crit Care & Shock (2008) 11 : 132-136 Airway Pressure Release Ventilation (APRV) for the Treatment of Severe Life-Threatening ARDS in a Morbidly Obese Patient Amyn Hirani, Rodrigo Cavallazzi, Anastasia
Paediatric Intensive Care unit Nursing Procedure: Care of the ventilated child
 Paediatric Intensive Care unit Nursing Procedure: Care of the ventilated child All nursing staff should read this policy to inform themselves of relevant areas prior to undertaking any aspect of care related
Paediatric Intensive Care unit Nursing Procedure: Care of the ventilated child All nursing staff should read this policy to inform themselves of relevant areas prior to undertaking any aspect of care related
Two Steps forward in Ventilation. Ernst Bahns. Because you care
 Two Steps forward in Ventilation Ernst Bahns Because you care Important Note: Medical knowledge changes constantly as a result of new research and clinical experience. The author of this introductory guide
Two Steps forward in Ventilation Ernst Bahns Because you care Important Note: Medical knowledge changes constantly as a result of new research and clinical experience. The author of this introductory guide
240- PROBLEM SET INSERTION OF SWAN-GANZ SYSTEMIC VASCULAR RESISTANCE. Blood pressure = f(cardiac output and peripheral resistance)
 240- PROBLEM SET INSERTION OF SWAN-GANZ 50 kg Pig Rt Jugular 0 cm Rt Atrium 10 cm Rt ventricle 15 cm Wedge 20-25 cm SYSTEMIC VASCULAR RESISTANCE Blood pressure = f(cardiac output and peripheral resistance)
240- PROBLEM SET INSERTION OF SWAN-GANZ 50 kg Pig Rt Jugular 0 cm Rt Atrium 10 cm Rt ventricle 15 cm Wedge 20-25 cm SYSTEMIC VASCULAR RESISTANCE Blood pressure = f(cardiac output and peripheral resistance)
PULMONARY FUNCTION TESTS A Workshop on Simple Spirometry & Flow Volume Loops
 PULMONARY FUNCTION TESTS A Workshop on Simple Spirometry & Flow Volume Loops YOU SHOULD READ THE FOLLOWING MATERIAL BEFORE Tuesday March 30 Interpretation of PFTs Learning Objectives 1. Specify the indications
PULMONARY FUNCTION TESTS A Workshop on Simple Spirometry & Flow Volume Loops YOU SHOULD READ THE FOLLOWING MATERIAL BEFORE Tuesday March 30 Interpretation of PFTs Learning Objectives 1. Specify the indications
KING FAISAL SPECIALIST HOSPITAL AND RESEARCH CENTRE (GEN. ORG.) NURSING AFFAIRS. Scope of Service PEDIATRIC INTENSIVE CARE UNIT (PICU)
 PICU-Jan.2012 Page 1 of 7 Number of Beds: 18 Nurse Patient Ratio: 1:1-2 : The Pediatric Intensive Care Unit (PICU) provides 24 hour intensive nursing care for patients aged neonate through adolescence.
PICU-Jan.2012 Page 1 of 7 Number of Beds: 18 Nurse Patient Ratio: 1:1-2 : The Pediatric Intensive Care Unit (PICU) provides 24 hour intensive nursing care for patients aged neonate through adolescence.
Edwards FloTrac Sensor & Edwards Vigileo Monitor. Understanding Stroke Volume Variation and Its Clinical Application
 Edwards FloTrac Sensor & Edwards Vigileo Monitor Understanding Stroke Volume Variation and Its Clinical Application 1 Topics System Configuration Pulsus Paradoxes Reversed Pulsus Paradoxus What is Stroke
Edwards FloTrac Sensor & Edwards Vigileo Monitor Understanding Stroke Volume Variation and Its Clinical Application 1 Topics System Configuration Pulsus Paradoxes Reversed Pulsus Paradoxus What is Stroke
ACID- BASE and ELECTROLYTE BALANCE. MGHS School of EMT-Paramedic Program 2011
 ACID- BASE and ELECTROLYTE BALANCE MGHS School of EMT-Paramedic Program 2011 ACID- BASE BALANCE Ions balance themselves like a see-saw. Solutions turn into acids when concentration of hydrogen ions rises
ACID- BASE and ELECTROLYTE BALANCE MGHS School of EMT-Paramedic Program 2011 ACID- BASE BALANCE Ions balance themselves like a see-saw. Solutions turn into acids when concentration of hydrogen ions rises
Introduction to Cardiopulmonary Exercise Testing
 Introduction to Cardiopulmonary Exercise Testing 2 nd Edition Andrew M. Luks, MD Robb Glenny, MD H. Thomas Robertson, MD Division of Pulmonary and Critical Care Medicine University of Washington Section
Introduction to Cardiopulmonary Exercise Testing 2 nd Edition Andrew M. Luks, MD Robb Glenny, MD H. Thomas Robertson, MD Division of Pulmonary and Critical Care Medicine University of Washington Section
Interpretation of the Arterial Blood Gas Self-Learning Packet
 Interpretation of the Arterial Blood Gas Self-Learning Packet * See SWIFT for list of qualifying boards for continuing education hours. Table of Contents Purpose... 3 Objectives... 3 Instructions... 4
Interpretation of the Arterial Blood Gas Self-Learning Packet * See SWIFT for list of qualifying boards for continuing education hours. Table of Contents Purpose... 3 Objectives... 3 Instructions... 4
Titration protocol reference guide
 Titration protocol reference guide Description Page Titration protocol goals 4 CPAP protocol CPAP protocol 6 CPAP titration protocol 7 CPAP reimbursement criteria 8 BiPAP S protocol BiPAP S protocol 10
Titration protocol reference guide Description Page Titration protocol goals 4 CPAP protocol CPAP protocol 6 CPAP titration protocol 7 CPAP reimbursement criteria 8 BiPAP S protocol BiPAP S protocol 10
Bergen Community College Division of Health Professions Department of Respiratory Care RSP-231, Respiratory Care Clinical Externship IV
 Date of Most Recent Syllabus Revision: August 2014 Semester and Year: Fall 2014 Bergen Community College Division of Health Professions Department of Respiratory Care RSP-231, Respiratory Care Clinical
Date of Most Recent Syllabus Revision: August 2014 Semester and Year: Fall 2014 Bergen Community College Division of Health Professions Department of Respiratory Care RSP-231, Respiratory Care Clinical
More detailed background information and references can be found at the end of this guideline
 Neonatal Intensive Care Unit Clinical Guideline Oxygen Over the past few years there have been significant changes, based on high quality research, in our understanding of how to give the right amount
Neonatal Intensive Care Unit Clinical Guideline Oxygen Over the past few years there have been significant changes, based on high quality research, in our understanding of how to give the right amount
Lab #11: Respiratory Physiology
 Lab #11: Respiratory Physiology Background The respiratory system enables the exchange of O 2 and CO 2 between the cells and the atmosphere, thus enabling the intake of O 2 into the body for aerobic respiration
Lab #11: Respiratory Physiology Background The respiratory system enables the exchange of O 2 and CO 2 between the cells and the atmosphere, thus enabling the intake of O 2 into the body for aerobic respiration
Adult Ventilation Management
 Online Continuing Education for Nurses Linking Learning to Performance I NSIDE T HIS C OURSE: OJECTIVES... 1 ADULT VENTILATION MANAGEMENT... 2 AIRWAY MANAGEMENT AND MECHANICAL VENTILATION BASICS... 2 ARTIFICIAL
Online Continuing Education for Nurses Linking Learning to Performance I NSIDE T HIS C OURSE: OJECTIVES... 1 ADULT VENTILATION MANAGEMENT... 2 AIRWAY MANAGEMENT AND MECHANICAL VENTILATION BASICS... 2 ARTIFICIAL
2.06 Understand the functions and disorders of the respiratory system
 2.06 Understand the functions and disorders of the respiratory system 2.06 Understand the functions and disorders of the respiratory system Essential questions What are the functions of the respiratory
2.06 Understand the functions and disorders of the respiratory system 2.06 Understand the functions and disorders of the respiratory system Essential questions What are the functions of the respiratory
Acid-Base Balance and the Anion Gap
 Acid-Base Balance and the Anion Gap 1. The body strives for electrical neutrality. a. Cations = Anions b. One of the cations is very special, H +, and its concentration is monitored and regulated very
Acid-Base Balance and the Anion Gap 1. The body strives for electrical neutrality. a. Cations = Anions b. One of the cations is very special, H +, and its concentration is monitored and regulated very
Physiology of Ventilation
 Physiology of Ventilation Lecturer: Sally Osborne, Ph.D. Department of Cellular & Physiological Sciences Email: sosborne@interchange.ubc.ca Useful link: www.sallyosborne.com Required Reading: Respiratory
Physiology of Ventilation Lecturer: Sally Osborne, Ph.D. Department of Cellular & Physiological Sciences Email: sosborne@interchange.ubc.ca Useful link: www.sallyosborne.com Required Reading: Respiratory
Oxygen Therapy. Oxygen therapy quick guide V3 July 2012.
 PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
PRESENTATION Oxygen (O 2 ) is a gas provided in a compressed form in a cylinder. It is also available in a liquid form. It is fed via a regulator and flow meter to the patient by means of plastic tubing
Hypoxia and Oxygenation Hypoxia is a serious threat to patients and escorts alike when
 Chapter 4 2 71 Hypoxia and Oxygenation Hypoxia is a serious threat to patients and escorts alike when they fly. Air medical escorts need to understand what causes hypoxia, why some people are more likely
Chapter 4 2 71 Hypoxia and Oxygenation Hypoxia is a serious threat to patients and escorts alike when they fly. Air medical escorts need to understand what causes hypoxia, why some people are more likely
Nurses Competencies in Caring for Mechanically Ventilated Patients, What does the Evidence Say? Dr. Samah Anwar Dr. Noha El-Baz
 Nurses Competencies in Caring for Mechanically Ventilated Patients, What does the Evidence Say? Dr. Samah Anwar Dr. Noha El-Baz The mechanically ventilated patient presents many challenges for the intensive
Nurses Competencies in Caring for Mechanically Ventilated Patients, What does the Evidence Say? Dr. Samah Anwar Dr. Noha El-Baz The mechanically ventilated patient presents many challenges for the intensive
IMPAIRED BLOOD-GAS EXCHANGE. Intraoperative blood gas analysis
 IMPAIRED BLOOD-GAS EXCHANGE Intraoperative blood gas analysis When do you perform BGA Intraoperatively? Informe actual NEVER Routine:Thoracic Thoracic, Cardiac,Neurosurgery Emergency situation Drop in
IMPAIRED BLOOD-GAS EXCHANGE Intraoperative blood gas analysis When do you perform BGA Intraoperatively? Informe actual NEVER Routine:Thoracic Thoracic, Cardiac,Neurosurgery Emergency situation Drop in
Pediatric Respiratory System: Basic Anatomy & Physiology. Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City
 Pediatric Respiratory System: Basic Anatomy & Physiology Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City Outline Introduction Developmental Anatomy Developmental Mechanics of Breathing
Pediatric Respiratory System: Basic Anatomy & Physiology Jihad Zahraa Pediatric Intensivist Head of PICU, King Fahad Medical City Outline Introduction Developmental Anatomy Developmental Mechanics of Breathing
