Treatment of skin and soft tissue infections due to methicillin-resistant Staphylococcus aureus in adults
|
|
|
- Frank Bond
- 8 years ago
- Views:
Transcription
1 1 of 6 9/24/ :16 AM Official reprint from UpToDate UpToDate Treatment of skin and soft tissue infections due to methicillin-resistant Staphylococcus aureus in adults Author Franklin D Lowy, MD Section Editor Daniel J Sexton, MD Deputy Editor Elinor L Baron, MD, DTMH Last literature review version 18.2: May 2010 This topic last updated: December 31, 2009 INTRODUCTION Methicillin resistance in Staphylococcus aureus is defined as an oxacillin minimum inhibitory concentration (MIC) 4 mcg/ml. Isolates resistant to oxacillin or methicillin are also resistant to all beta-lactam agents including oxacillin, dicloxacillin, and cefazolin [1,2]. The treatment of MRSA skin and soft tissue infections in adults will be reviewed here. The treatment of invasive MRSA infections, the mechanisms of antibiotic resistance, epidemiology of MRSA infection, and general issues related to skin and soft tissue infections are discussed separately. (See "Treatment of invasive methicillin-resistant Staphylococcus aureus infections in adults" and "Microbiology of methicillin-resistant Staphylococcus aureus" and "Epidemiology of methicillin-resistant Staphylococcus aureus infection in adults" and "Cellulitis and erysipelas" and "Skin abscesses, furuncles, and carbuncles" and "Impetigo" and "Folliculitis".) APPROACH TO TREATMENT Given the increasing prevalence of methicillin-resistant Staphylococcus aureus (MRSA) as both a nosocomial and community-associated pathogen, beta-lactam antibiotics are no longer reliable empiric therapy for skin and soft tissue infections [3]. Familiarity with local antibiotic patterns is important for selecting empiric antibiotic therapy, and culture with susceptibility data is critical for tailoring treatment. (See "Epidemiology of methicillin-resistant Staphylococcus aureus infection in adults".) The approach to treatment is guided by the type of skin and soft tissue infection and the severity of clinical presentation. Empiric antibiotic therapy should include MRSA coverage if it is suspected based upon local epidemiology; risk factors or the clinical features are not sufficient to make this determination [4-6]. Although many patients with MRSA infection have nasal colonization with the same strain that is responsible for the infection, the predictive value of screening for colonization in the outpatient setting is not known [7]. Patients with fluctuant or purulent skin and soft tissue infections should undergo incision and drainage, and debrided material should be sent for culture and susceptibility testing [8]. Incision and drainage alone may be sufficient for abscesses smaller than 5 cm [9,10]. This was illustrated in a randomized trial of 166 patients with uncomplicated skin abscesses at risk for community-associated MRSA (CA-MRSA) who were managed with cephalexin or placebo following incision and drainage of skin and soft tissue abscesses; the cure rates were similar in the two groups (84 and 90 percent, respectively) [10]. Among the isolates tested, 88 percent were MRSA; because cephalexin does not have activity against MRSA, the cephalexin arm was also a functional placebo arm in this group. (See "Technique of incision and drainage for skin abscess".) Patients with larger abscesses and/or systemic signs of infection should be managed with incision and drainage plus antimicrobial therapy [9]. Important considerations in antibiotic selection include baseline susceptibility testing prior to antibiotic administration and individual patient circumstances including the type of infection, underlying comorbidities, and other concurrent medications [11]. Oral therapy The optimal oral antibiotic therapy for empiric treatment of skin and soft tissue infection when MRSA is known or suspected is unclear [12]. Reasonable antibiotics for treatment of MRSA include older agents (clindamycin, trimethoprimsulfamethoxazole, and tetracyclines such as doxycycline or minocycline) and a newer agent, linezolid (table 1). Use of the older agents is supported by susceptibility testing and clinical experience, but their efficacy for treatment of skin and soft tissue infections due to MRSA has not been rigorously evaluated or compared in clinical trials [13]. Clindamycin (300 to 450 mg every six to eight hours) has good activity against MRSA and is also capable of inhibiting bacterial production of toxins including Panton-Valentine leukocidin and other virulence factors [14]. Careful monitoring of local clindamycin resistance rates is important; some advocate avoiding empiric clindamycin therapy when local MRSA resistance rates exceed 10 to 15 percent [12]. In addition, isolates that appear susceptible to clindamycin and resistant to erythromycin by standard susceptibility testing techniques may be capable of inducing resistance to clindamycin in the presence of the drug [15]. Clinicians should confer with their microbiology laboratory to request evaluation of such isolates for inducible clindamycin resistance with D testing prior to treatment with clindamycin [16,17]. (See "Overview of antibacterial susceptibility testing", section on 'D test'.) Trimethoprim-sulfamethoxazole (two double-strength tablets twice daily) has been suggested for treatment of skin and soft tissue infections due to MRSA, although data for its efficacy are limited to observational and retrospective reports [18-22]. Trimethoprimsulfamethoxazole is a reasonable antibiotic choice in the setting of MRSA with known susceptibility to the drug, although it is not advisable for empiric management of soft tissue infections that may be due to group A streptococci [23]. In such cases, some favor combination therapy using a beta-lactam antibiotic with activity against streptococci together with trimethoprim-sulfamethoxazole for empiric MRSA coverage (figure 1) [12]. There is a theoretic concern that clinical failure with this agent may occur due to thymidine released from damaged host tissues, which may bypass the metabolic blockades of trimethoprim and sulfamethoxazole by acting downstream of their target enzymes in the folate synthesis pathway [24]. Data on the efficacy of long-acting tetracyclines for treatment of skin and soft tissue infections due to MRSA are limited to observational and retrospective reports [18-21]. As with trimethoprim-sulfamethoxazole, a tetracycline is a reasonable antibiotic choice in the setting of MRSA with known susceptibility to this agent, although it is not advisable for empiric management of soft tissue infections that may be due to group A streptococci [23]. In such cases, some favor combination therapy using a beta-lactam antibiotic with activity against streptococci together with a tetracycline for empiric MRSA coverage (figure 1) [12].
2 2 of 6 9/24/ :16 AM Linezolid has activity against both MRSA and streptococci and has been shown to be as effective as vancomycin for the treatment of skin and soft tissue infection [25]. Its use is limited by cost, toxicity, and potential for resistance. It should be reserved for those who do not respond to or cannot tolerate an older agent. (See "Treatment of invasive methicillin-resistant Staphylococcus aureus infections in adults", section on 'Linezolid'.) Fluoroquinolones should NOT be used to treat skin and soft tissue infections due to MRSA; resistance to ciprofloxacin has been observed to develop readily during therapy, and widespread MRSA fluoroquinolone resistance is already prevalent in many regions [18,26]. There is also concern that resistance may emerge during therapy even for fluoroquinolones with enhanced antistaphylococcal activity such as levofloxacin and moxifloxacin [26]. Rifampin has excellent activity against MRSA and may be used in combination with one of the above agents for treatment of skin and soft tissue infections due to MRSA, although data supporting this approach are lacking [12]. Use of rifampin alone is contraindicated given rapid development of resistance to this agent. Follow-up Repeat evaluation after 24 to 48 hours of outpatient empiric oral antibiotic therapy is prudent to verify clinical response [3]. The appropriate duration of therapy is one to two weeks; the clinical response to therapy should guide antibiotic duration. Lack of response may be due to infection with resistant pathogens or a deeper, more serious infection than previously realized. Parenteral therapy Parenteral therapy should be considered for patients with extensive soft tissue involvement, fever or other signs of systemic illness, or patients with diabetes or other immunodeficiency [12]. Such patients should also be evaluated for evidence of invasive disease. (See "Epidemiology of methicillin-resistant Staphylococcus aureus infection in adults" and "Treatment of invasive methicillin-resistant Staphylococcus aureus infections in adults" and "Treatment of Staphylococcus aureus bacteremia in adults" and "Complications of Staphylococcus aureus bacteremia".) Vancomycin remains the antibiotic of choice for treatment of invasive MRSA infection, although there is increasing concern regarding the rise in S. aureus MICs to this antibiotic [27]. Dosing is 30 mg/kg per 24 hours in two divided doses, not to exceed 2 g per 24 hours unless serum concentrations are inappropriately low. (See "Vancomycin dosing and serum concentration monitoring in adults".) For patients who fail to respond or cannot tolerate vancomycin, the optimal alternative parenteral agent is not known (table 1). Among the newer agents, linezolid, daptomycin, tigecycline, telavancin and quinupristin-dalfopristin all have FDA approval for treatment of skin and soft tissue infections. If continued outpatient antibiotic therapy is expected, linezolid (600 mg every 12 hours) is an appropriate choice given the capacity for parenteral or oral administration with good bioavailability [25]. Daptomycin (4 mg/kg once daily) and tigecycline (100 mg IV once, followed by 50 mg IV every 12 hours) are reasonable alternatives. Telavancin (10 mg/kg every 24 hours), although noninferior to vancomycin in clinical studies, has a higher rate of toxicity and substantially higher cost. Use of quinupristindalfopristin is limited by adverse effects. Supportive data for the use of these drugs in the management of MRSA infections are presented separately. (See "Treatment of invasive methicillin-resistant Staphylococcus aureus infections in adults".) Among the older agents, data on parenteral use for treatment of MRSA are limited. Parenteral clindamycin may be given in regions where the likelihood is resistance is low [12]. Parenteral trimethoprim-sulfamethoxazole was less effective than vancomycin in a randomized trial of intravenous drug users with serious S. aureus infections [28]. The appropriate duration of therapy is one to two weeks; clinical response to therapy may guide antibiotic duration. INFORMATION FOR PATIENTS Educational materials on this topic are available for patients. (See "Patient information: Methicillinresistant Staphylococcus aureus (MRSA)".) We encourage you to print or this topic review, or to refer patients to our public web site, which includes this and other topics. SUMMARY AND RECOMMENDATIONS Patients with skin and soft tissue infections amenable to debridement should undergo Incision and drainage with culture and susceptibility testing. Debridement alone may be sufficient for abscesses smaller than 5 cm. Patients with larger areas of infection and/or systemic signs of infection should be managed with antimicrobial therapy. Susceptibility testing should guide antibiotic selection. It is appropriate for empiric antibiotic therapy to include activity against MRSA. For the outpatient management of possible or proven MRSA infection, we suggest oral antibiotic therapy with clindamycin, trimethoprim-sulfamethoxazole or a long acting tetracycline such as minocycline or doxycycline (Grade 2B). Linezolid is an acceptable alternative agent; its use is limited by cost, toxicity, and potential for resistance. Appropriate dosing for these agents is as outlined in the Table (table 1). Parenteral therapy should be considered for patients with extensive soft tissue involvement, fever or other signs of systemic illness, or patients with diabetes or other immunodeficiency. We suggest parenteral antibiotic therapy with vancomycin (30 mg/kg per 24 h in two divided doses, not to exceed 2 g per 24 hours unless serum concentrations are inappropriately low) (Grade 2B). (See "Vancomycin dosing and serum concentration monitoring in adults".) For patients who fail to respond or cannot tolerate vancomycin, we suggest linezolid (600 mg every 12 hours) or daptomycin (4 mg/kg once daily) (Grade 2C). The duration of therapy is usually one to two weeks; the clinical response to therapy may guide antibiotic duration. Treatment may be switched from parenteral to oral therapy with clinical improvement. Use of UpToDate is subject to the Subscription and License Agreement.
3 3 of 6 9/24/ :16 AM REFERENCES 1. Karchmer, AW. Staphylococcus aureus and vancomycin: The sequel. Ann Intern Med 1991; 115: Lowy, FD. Staphylococcus aureus infections. N Engl J Med 1998; 339: Stevens, DL, Bisno, AL, Chambers, HF, et al. Practice guidelines for the diagnosis and management of skin and soft-tissue infections. Clin Infect Dis 2005; 41: Chambers, HF. The changing epidemiology of Staphylococcus aureus? Emerg Infect Dis 2001; 7: Charlebois, ED, Perdreau-Remington, F, Kreiswirth, B, et al. Origins of community strains of methicillin-resistant Staphylococcus aureus. Clin Infect Dis 2004; 39: Miller, LG, Perdreau-Remington, F, Bayer, AS, et al. Clinical and epidemiologic characteristics cannot distinguish communityassociated methicillin-resistant Staphylococcus aureus infection from methicillin-susceptible S. aureus infection: a prospective investigation. Clin Infect Dis 2007; 44: von Eiff, C, Becker, K, Machka, K, et al. Nasal carriage as a source of Staphylococcus aureus bacteremia. Study Group. N Engl J Med 2001; 344: Miller, LG, Quan, C, Shay, A, et al. A prospective investigation of outcomes after hospital discharge for endemic, communityacquired methicillin-resistant and -susceptible Staphylococcus aureus skin infection. Clin Infect Dis 2007; 44: Lee, MC, Rios, AM, Aten, MF, et al. Management and outcome of children with skin and soft tissue abscesses caused by communityacquired methicillin-resistant Staphylococcus aureus. Pediatr Infect Dis J 2004; 23: Rajendran, PM, Young, D, Maurer, T, et al. Randomized, double-blind, placebo-controlled trial of cephalexin for treatment of uncomplicated skin abscesses in a population at risk for community-acquired methicillin-resistant Staphylococcus aureus infection. Antimicrob Agents Chemother 2007; 51: Ruhe, JJ, Smith, N, Bradsher, RW, et al. Community-onset methicillin-resistant Staphylococcus aureus skin and soft tissue infections: Impact of antimicrobial therapy on outcome. Clin Infect Dis 2007; 44: Daum, RS. Clinical practice. Skin and soft-tissue infections caused by methicillin-resistant Staphylococcus aureus. N Engl J Med 2007; 357: Moellering, RC Jr. Current treatment options for community-acquired methicillin-resistant Staphylococcus aureus infection. Clin Infect Dis 2008; 46: Martinez-Aguilar, G, Hammerman, WA, Mason, EO Jr, Kaplan, SL. Clindamycin treatment of invasive infections caused by community-acquired, methicillin-resistant and methicillin-susceptible Staphylococcus aureus in children. Pediatr Infect Dis J 2003; 22: Siberry, GK, Tekle, T, Carroll, K, Dick, J. Failure of clindamycin treatment of methicillin-resistant Staphylococcus aureus expressing inducible clindamycin resistance in vitro. Clin Infect Dis 2003; 37: Panagea, S, Perry, JD, Gould, FK. Should clindamycin be used as treatment of patients with infections caused by erythromycinresistant staphylococci? J Antimicrob Chemother 1999; 44: Frank, AL, Marcinak, JF, Mangat, PD, et al. Clindamycin treatment of methicillin-resistant Staphylococcus aureus infections in children. Pediatr Infect Dis J 2002; 21: Moran, GJ, Krishnadasan, A, Gorwitz, RJ, et al. Methicillin-resistant S. aureus infections among patients in the emergency department. N Engl J Med 2006; 355: Szumowski, JD, Cohen, DE, Kanaya, F, Mayer, KH. Treatment and outcomes of infections by methicillin-resistant Staphylococcus aureus at an ambulatory clinic. Antimicrob Agents Chemother 2007; 51: Iyer, S, Jones, DH. Community-acquired methicillin-resistant Staphylococcus aureus skin infection: a retrospective analysis of clinical presentation and treatment of a local outbreak. J Am Acad Dermatol 2004; 50: Ruhe, JJ, Monson, T, Bradsher, RW, Menon, A. Use of long-acting tetracyclines for methicillin-resistant Staphylococcus aureus infections: case series and review of the literature. Clin Infect Dis 2005; 40: Kaka, AS, Rueda, AM, Shelburne SA, 3rd, et al. Bactericidal activity of orally available agents against methicillin-resistant Staphylococcus aureus. J Antimicrob Chemother 2006; 58: Swartz, MN. Clinical practice. Cellulitis. N Engl J Med 2004; 350: Proctor, RA. Role of folate antagonists in the treatment of methicillin-resistant Staphylococcus aureus infection. Clin Infect Dis 2008; 46: Stevens, DL, Herr, D, Lampiris, H, et al. Linezolid versus vancomycin for the treatment of methicillin-resistant Staphylococcus aureus infections. Clin Infect Dis 2002; 34: Trucksis, M, Hooper, DC, Wolfson, JS. Emerging resistance to fluoroquinolones in staphylococci: An alert. Ann Intern Med 1991; 114: Choice of antibacterial drugs. Treat Guidel Med Lett 2007; 5: Markowitz, N, Quinn, EL, Saravolatz, LD. Trimethoprim-sulfamethoxazole compared with vancomycin for the treatment of Staphylococcus aureus infection. Ann Intern Med 1992; 117:390.
4 4 of 6 9/24/ :16 AM GRAPHICS
5 Antimicrobial therapy for infections due to methicillin-resistant Staphylococcus aureus in adults Bacteremia Preferred Vancomycin (30 mg/kg IV every 24 hours in 2 equally divided doses; not to exceed 2 g/24 hours unless concentrations in serum are inappropriately low) Alternative Daptomycin (6 mg/kg IV once daily) Linezolid (600 mg IV or orally twice daily; IV preferred) Skin and soft tissue infections Parenteral therapy Vancomycin (30 mg/kg IV every 24 hours in 2 equally divided doses; not to exceed 2 g/24 hours unless concentrations in serum are inappropriately low) Daptomycin (4 mg/kg IV once daily) Linezolid (600 mg IV twice daily) Tigecycline (100 mg IV once, thereafter 50 mg IV every 12 hours) Oral therapy TMP-SMX (2 double-strength tablets orally twice daily) Doxycycline or minocycline (100 mg orally twice daily) Clindamycin* (300 to 450 mg orally every 6 to 8 hours) Linezolid (600 mg orally twice daily) IV: intravenously; TMP-SMX: trimethoprim-sulfamethoxazole. * D testing required to evaluate for inducible resistance; see text. 5 of 6 9/24/ :16 AM
6 Approach to outpatient management of soft tissue infections DS: double strength. * MSSA: methicillin-susceptible Staphylococcus aureus. Δ MRSA: methicillin-resistant Staphylococcus aureus. Note local prevalence of inducible clindamycin resistance UpToDate, Inc. All rights reserved. Subscription and License Agreement Support Tag: [ecapp1002p.utd.com bb ] Licensed to: Univ Of Nc At Chapel Hill 6 of 6 9/24/ :16 AM
Current Treatment Options for Community-Acquired Methicillin-Resistant Staphylococcus aureus Infection
 REVIEW ARTICLE Current Treatment Options for Community-Acquired Methicillin-Resistant Staphylococcus aureus Infection Robert C. Moellering, Jr. Beth Israel Deaconess Medical Center, Harvard Medical School,
REVIEW ARTICLE Current Treatment Options for Community-Acquired Methicillin-Resistant Staphylococcus aureus Infection Robert C. Moellering, Jr. Beth Israel Deaconess Medical Center, Harvard Medical School,
Randomized Controlled Trial of Cephalexin Versus Clindamycin for Uncomplicated Pediatric Skin Infections
 ARTICLES Randomized Controlled Trial of Cephalexin Versus Clindamycin for Uncomplicated Pediatric Skin Infections AUTHORS: Aaron E. Chen, MD, a Karen C. Carroll, MD, b Marie Diener-West, PhD, c Tracy Ross,
ARTICLES Randomized Controlled Trial of Cephalexin Versus Clindamycin for Uncomplicated Pediatric Skin Infections AUTHORS: Aaron E. Chen, MD, a Karen C. Carroll, MD, b Marie Diener-West, PhD, c Tracy Ross,
 Skin and Soft tissue Infections: new bugs, old drugs Disclosure Statement Sponsor: Goodman Photographic Presented by: Dr. Kristopher Wiebe, MD, CCFP (EM) Presented to: BC Chapter, Canadian Society of Hospital
Skin and Soft tissue Infections: new bugs, old drugs Disclosure Statement Sponsor: Goodman Photographic Presented by: Dr. Kristopher Wiebe, MD, CCFP (EM) Presented to: BC Chapter, Canadian Society of Hospital
Interim Guidelines for the Management of Community-Associated Methicillin-Resistant Staphylococcus aureus Infections in Primary Care February 2006
 Table of Contents 1. Background... 2 2. Diagnosis... 2 3. Susceptibility Patterns of MRSA... 3 4. Management... 3 5. Decolonization of the Patient... 4 6. Prevention and Control... 5 7. Information for
Table of Contents 1. Background... 2 2. Diagnosis... 2 3. Susceptibility Patterns of MRSA... 3 4. Management... 3 5. Decolonization of the Patient... 4 6. Prevention and Control... 5 7. Information for
Methicillin-resistant S taphylococcus
 Nevio Cimolai, MD, FRCPC Community-acquired MRSA infection: An emerging trend The use of culture as backup to empiric treatment of staphylococcal infection can help deal with widespread antibiotic resistance.
Nevio Cimolai, MD, FRCPC Community-acquired MRSA infection: An emerging trend The use of culture as backup to empiric treatment of staphylococcal infection can help deal with widespread antibiotic resistance.
Skin and soft tissue infections (SSTIs) are a frequent emergency
 Emergency Department Infections In The Era Of Community-Acquired MRSA A 45-year-old man presents to the ED complaining of a painful lump on his right thigh that appeared yesterday and has become progressively
Emergency Department Infections In The Era Of Community-Acquired MRSA A 45-year-old man presents to the ED complaining of a painful lump on his right thigh that appeared yesterday and has become progressively
Infectious Disease. Update. July 2008
 July 2008 Antibiotic eview ubcommittee of the Pharmacy & Therapeutics Committee Update Infectious Disease Community-Acquired Methicillin-esistant taphylococcus aureus (CA-MA) kin & oft Tissue Infections
July 2008 Antibiotic eview ubcommittee of the Pharmacy & Therapeutics Committee Update Infectious Disease Community-Acquired Methicillin-esistant taphylococcus aureus (CA-MA) kin & oft Tissue Infections
It s Not a Spider Bite, It s Community-Acquired
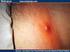 BRIEF REPORTS It s Not a Spider Bite, It s Community-Acquired Methicillin-Resistant Staphylococcus aureus Tamara J. Dominguez, MD Skin and soft tissue infections caused by hospitalacquired methicillin-resistant
BRIEF REPORTS It s Not a Spider Bite, It s Community-Acquired Methicillin-Resistant Staphylococcus aureus Tamara J. Dominguez, MD Skin and soft tissue infections caused by hospitalacquired methicillin-resistant
Cellulitis and Abscess: Emergency Department Clinical Practice Guideline (CPG)
 Cellulitis and Abscess: Emergency Department Clinical Practice Guideline (CPG) Clinical Practice Guideline Protocol Approved by: Division of Pediatric Emergency Medicine Date of Approval: 4/14 2013 SSM
Cellulitis and Abscess: Emergency Department Clinical Practice Guideline (CPG) Clinical Practice Guideline Protocol Approved by: Division of Pediatric Emergency Medicine Date of Approval: 4/14 2013 SSM
Clinical Infectious Diseases Advance Access published January 4, 2011
 Clinical Infectious Diseases Advance Access published January 4, 2011 IDSA GUIDELINES Clinical Practice Guidelines by the Infectious Diseases Society of America for the Treatment of Methicillin-Resistant
Clinical Infectious Diseases Advance Access published January 4, 2011 IDSA GUIDELINES Clinical Practice Guidelines by the Infectious Diseases Society of America for the Treatment of Methicillin-Resistant
Management of Methicillin-Resistant Staphylococcus aureus (MRSA) Infections
 Management of Methicillin-Resistant Staphylococcus aureus (MRSA) Infections Federal Bureau of Prisons Clinical Practice Guidelines April 2012 Clinical guidelines are made available to the public for informational
Management of Methicillin-Resistant Staphylococcus aureus (MRSA) Infections Federal Bureau of Prisons Clinical Practice Guidelines April 2012 Clinical guidelines are made available to the public for informational
Received 20 March 2007/Returned for modification 10 July 2007/Accepted 27 August 2007
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Nov. 2007, p. 4044 4048 Vol. 51, No. 11 0066-4804/07/$08.00 0 doi:10.1128/aac.00377-07 Copyright 2007, American Society for Microbiology. All Rights Reserved. Randomized,
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Nov. 2007, p. 4044 4048 Vol. 51, No. 11 0066-4804/07/$08.00 0 doi:10.1128/aac.00377-07 Copyright 2007, American Society for Microbiology. All Rights Reserved. Randomized,
Staphylococcus aureus Bloodstream Infection Treatment Guideline
 Staphylococcus aureus Bloodstream Infection Treatment Guideline Purpose: To provide a framework for the evaluation and management patients with Methicillin- Susceptible (MSSA) and Methicillin-Resistant
Staphylococcus aureus Bloodstream Infection Treatment Guideline Purpose: To provide a framework for the evaluation and management patients with Methicillin- Susceptible (MSSA) and Methicillin-Resistant
Methicillin-Resistant S. aureus Infections among Patients in the Emergency Department
 The new england journal of medicine original article Methicillin-Resistant S. aureus Infections among Patients in the Emergency Department Gregory J. Moran, M.D., Anusha Krishnadasan, Ph.D., Rachel J.
The new england journal of medicine original article Methicillin-Resistant S. aureus Infections among Patients in the Emergency Department Gregory J. Moran, M.D., Anusha Krishnadasan, Ph.D., Rachel J.
Urinary Tract Infections
 Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Urinary Tract Infections Overview A urine culture must ALWAYS be interpreted in the context of the urinalysis and patient symptoms. If a patient has no signs of infection on urinalysis, no symptoms of
Guidance for Industry Acute Bacterial Skin and Skin Structure Infections: Developing Drugs for Treatment
 Guidance for Industry Acute Bacterial Skin and Skin Structure Infections: Developing Drugs for Treatment U.S. Department of Health and Human Services Food and Drug Administration Center for Drug Evaluation
Guidance for Industry Acute Bacterial Skin and Skin Structure Infections: Developing Drugs for Treatment U.S. Department of Health and Human Services Food and Drug Administration Center for Drug Evaluation
Guidelines for the Management of Community-Acquired Methicillin-Resistant Staphylococcus aureus (CA-MRSA) Infections in the US Navy and Marine Corps
 Guidelines for the Management of Community-Acquired Methicillin-Resistant Staphylococcus aureus (CA-MRSA) Infections in the US Navy and Marine Corps AUGUST 2005 Navy Environmental Health Center 620 John
Guidelines for the Management of Community-Acquired Methicillin-Resistant Staphylococcus aureus (CA-MRSA) Infections in the US Navy and Marine Corps AUGUST 2005 Navy Environmental Health Center 620 John
Antimicrobe.org: An Online Reference for the Practicing Infectious Diseases Specialist
 INVITED ARTICLE SURFING THE WEB Victor L. Yu, Section Editor Antimicrobe.org: An Online Reference for the Practicing Infectious Diseases Specialist Steven D. Burdette and Thomas E. Herchline Department
INVITED ARTICLE SURFING THE WEB Victor L. Yu, Section Editor Antimicrobe.org: An Online Reference for the Practicing Infectious Diseases Specialist Steven D. Burdette and Thomas E. Herchline Department
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis
 Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
Antibiotic-Associated Diarrhea, Clostridium difficile- Associated Diarrhea and Colitis ANTIBIOTIC-ASSOCIATED DIARRHEA Disturbance of the normal colonic microflora Leading to alterations in bacterial degradation
METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COMMUNITY ACQUIRED vs. HEALTHCARE ASSOCIATED
 METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COMMUNITY ACQUIRED vs. HEALTHCARE ASSOCIATED Recently, there have been a number of reports about methicillin-resistant Staph aureus (MRSA) infections
METHICILLIN-RESISTANT STAPHYLOCOCCUS AUREUS (MRSA) COMMUNITY ACQUIRED vs. HEALTHCARE ASSOCIATED Recently, there have been a number of reports about methicillin-resistant Staph aureus (MRSA) infections
Fungal Infection in Total Joint Arthroplasty. Dr.Wismer Dr.Al-Sahan
 Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
Fungal Infection in Total Joint Arthroplasty Dr.Wismer Dr.Al-Sahan Delayed Reimplantation Arthroplasty for Candidal Prosthetic Joint Infection: A Report of 4 Cases and Review of the Literature David M.
Outpatient Parenteral Antimicrobial Therapy
 Outpatient Parenteral Antimicrobial Therapy Jason E. Bowling, MD a,b, *, James S. Lewis II, PharmD c,d, Aaron D. Owens, MD a,e KEYWORDS Outpatient parenteral antimicrobial therapy Antibiotics Adverse events
Outpatient Parenteral Antimicrobial Therapy Jason E. Bowling, MD a,b, *, James S. Lewis II, PharmD c,d, Aaron D. Owens, MD a,e KEYWORDS Outpatient parenteral antimicrobial therapy Antibiotics Adverse events
SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS
 Page 1 of 8 TITLE: SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS GUIDELINE: Antibiotics are administered prior to surgical procedures to prevent surgical site infections. PURPOSE:
Page 1 of 8 TITLE: SURGICAL PROPHYLAXIS: ANTIBIOTIC RECOMMENDATIONS FOR ADULT PATIENTS GUIDELINE: Antibiotics are administered prior to surgical procedures to prevent surgical site infections. PURPOSE:
Develop an understanding of the differential diagnosis of pseudomembranous colitis
 Update on Clostridium difficile Colitis Clostridium difficile infection has recently emerged in populations without any known risk factors. This presentation will focus on the historical background, diagnosis,
Update on Clostridium difficile Colitis Clostridium difficile infection has recently emerged in populations without any known risk factors. This presentation will focus on the historical background, diagnosis,
IDSA GUIDELINES EXECUTIVE SUMMARY
 IDSA GUIDELINES International Clinical Practice Guidelines for the Treatment of Acute Uncomplicated Cystitis and Pyelonephritis in Women: A 2010 Update by the Infectious Diseases Society of America and
IDSA GUIDELINES International Clinical Practice Guidelines for the Treatment of Acute Uncomplicated Cystitis and Pyelonephritis in Women: A 2010 Update by the Infectious Diseases Society of America and
Skin and Soft Tissue Infections
 Prim Care Clin Office Pract 33 (2006) 697 710 Skin and Soft Tissue Infections Robert L. Rogers, MD, FAAEM, FACEP, FACP*, Jack Perkins, MD Department of Emergency Medicine, The University of Maryland School
Prim Care Clin Office Pract 33 (2006) 697 710 Skin and Soft Tissue Infections Robert L. Rogers, MD, FAAEM, FACEP, FACP*, Jack Perkins, MD Department of Emergency Medicine, The University of Maryland School
SEVENTH EDITION BOOK 9 INFECTIOUS DISEASES
 SEVENTH EDITION BOOK 9 INFECTIOUS DISEASES Bone and Joint Infections By Jamie S. Winner, Pharm.D., BCPS (AQ Infectious Diseases) Reviewed by Michael B. Kays, Pharm.D., FCCP; Emilie L. Karpiuk, Pharm.D.,
SEVENTH EDITION BOOK 9 INFECTIOUS DISEASES Bone and Joint Infections By Jamie S. Winner, Pharm.D., BCPS (AQ Infectious Diseases) Reviewed by Michael B. Kays, Pharm.D., FCCP; Emilie L. Karpiuk, Pharm.D.,
CCHCS Care Guide: Skin & Soft Tissue Infections
 GOALS Early diagnosis and treatment of skin and soft tissue infections Infection control measures to prevent transmission to others Incision & drainage if abscess present Evidence based use of antibiotics
GOALS Early diagnosis and treatment of skin and soft tissue infections Infection control measures to prevent transmission to others Incision & drainage if abscess present Evidence based use of antibiotics
Skin and Soft Tissue Infections
 Skin and Soft Tissue Infections Cellulitis Note: The most common etiology of cellulitis with purulent drainage is S. aureus, although Group A streptococci and other streptococcal species can also present
Skin and Soft Tissue Infections Cellulitis Note: The most common etiology of cellulitis with purulent drainage is S. aureus, although Group A streptococci and other streptococcal species can also present
Hemodialysis catheter infection
 Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Hemodialysis catheter infection Scary facts In 2006, 82% of patients in the United States initiated dialysis via a catheter The overall likelihood of Tunneled cuffed catheters use was 35% greater in 2005
Bachir K. Younes, M.D., M.P.H.
 Work: 36923 Cook St. # 103 Palm Desert, CA 92211 Phone (760) 636-1336 Fax (760) 636-1335 Bachir K. Younes, M.D., M.P.H. Personal Born: Jan. 1 st, 1971 in Lebanon Marital Status: Married to Roula Sleilati
Work: 36923 Cook St. # 103 Palm Desert, CA 92211 Phone (760) 636-1336 Fax (760) 636-1335 Bachir K. Younes, M.D., M.P.H. Personal Born: Jan. 1 st, 1971 in Lebanon Marital Status: Married to Roula Sleilati
Molluscum BOTE Sign: A Predictor of Imminent Resolution
 Molluscum BOTE Sign: A Predictor of Imminent Resolution abstract Molluscum contagiosum is a common self-limited viral skin infection. The course of the infection often includes tender, crusted, erythematous
Molluscum BOTE Sign: A Predictor of Imminent Resolution abstract Molluscum contagiosum is a common self-limited viral skin infection. The course of the infection often includes tender, crusted, erythematous
COMPOUNDING PHARMACY SOLUTIONS PRESCRIPTION COMPOUNDING FOR DERMATOLOGY
 JUNE 2012 COMPOUNDING PHARMACY SOLUTIONS PRESCRIPTION COMPOUNDING WWW.CPSRXS. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Acne 2 Cutaneous Candidiasis
JUNE 2012 COMPOUNDING PHARMACY SOLUTIONS PRESCRIPTION COMPOUNDING WWW.CPSRXS. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Acne 2 Cutaneous Candidiasis
8/5/2014. We have no commercial or financial conflict of interest
 Erica Runningdeer, MSN, MPH, RN Illinois Department of Public Health Gail Itokazu, PharmD John H Storger Jr. Hospital of Cook County Sarah Becca Peglow, MD Rush University Medical Center John H Stroger,
Erica Runningdeer, MSN, MPH, RN Illinois Department of Public Health Gail Itokazu, PharmD John H Storger Jr. Hospital of Cook County Sarah Becca Peglow, MD Rush University Medical Center John H Stroger,
Practice Guidelines for the Diagnosis and Management of Skin and Soft Tissue Infections: 2014 Update by the Infectious Diseases Society of America
 Clinical Infectious Diseases Advance Access published June 18, 2014 IDSA GUIDELINE Practice Guidelines for the Diagnosis and Management of Skin and Soft Tissue Infections: 2014 Update by the Infectious
Clinical Infectious Diseases Advance Access published June 18, 2014 IDSA GUIDELINE Practice Guidelines for the Diagnosis and Management of Skin and Soft Tissue Infections: 2014 Update by the Infectious
Date: November 30, 2010
 Department of Health and Human Services Public Health Service Food and Drug Administration Center for Drug Evaluation and Research Date: November 30, 2010 To: Through: From: Subject: Drug Name(s): Application
Department of Health and Human Services Public Health Service Food and Drug Administration Center for Drug Evaluation and Research Date: November 30, 2010 To: Through: From: Subject: Drug Name(s): Application
Drug Use Review. Edward Cox, M.D. Director Office of Antimicrobial Products
 Department of Health and Human Services Public Health Service Food and Drug Administration Center for Drug Evaluation and Research Drug Use Review Date: April 5, 2012 To: Through: Edward Cox, M.D. Director
Department of Health and Human Services Public Health Service Food and Drug Administration Center for Drug Evaluation and Research Drug Use Review Date: April 5, 2012 To: Through: Edward Cox, M.D. Director
Practice Guidelines for the Diagnosis and Management of Skin and Soft-Tissue Infections
 IDSA GUIDELINES Practice Guidelines for the Diagnosis and Management of Skin and Soft-Tissue Infections Dennis L. Stevens, 1,3 Alan L. Bisno, 5 Henry F. Chambers, 6,7 E. Dale Everett, 13 Patchen Dellinger,
IDSA GUIDELINES Practice Guidelines for the Diagnosis and Management of Skin and Soft-Tissue Infections Dennis L. Stevens, 1,3 Alan L. Bisno, 5 Henry F. Chambers, 6,7 E. Dale Everett, 13 Patchen Dellinger,
Pertussis Whooping Cough Update
 May 3, 1 Dear Kitsap County Providers, This is an update about our current status of pertussis cases here in Kitsap County. We currently have 35 cases as outlined below. See the epidemiology curve (Figure
May 3, 1 Dear Kitsap County Providers, This is an update about our current status of pertussis cases here in Kitsap County. We currently have 35 cases as outlined below. See the epidemiology curve (Figure
Urinary Tract Infections
 Urinary Tract Infections Leading cause of morbidity and health care expenditures in persons of all ages. An estimated 50 % of women report having had a UTI at some point in their lives. 8.3 million office
Urinary Tract Infections Leading cause of morbidity and health care expenditures in persons of all ages. An estimated 50 % of women report having had a UTI at some point in their lives. 8.3 million office
How Common is MRSA in Adult Septic Arthritis?
 INFECTIOUS DISEASE/BRIEF RESEARCH REPORT How Common is MRSA in Adult Septic Arthritis? Bradley W. Frazee, MD Christopher Fee, MD Larry Lambert, MPH From the Department of Emergency Medicine, Alameda County
INFECTIOUS DISEASE/BRIEF RESEARCH REPORT How Common is MRSA in Adult Septic Arthritis? Bradley W. Frazee, MD Christopher Fee, MD Larry Lambert, MPH From the Department of Emergency Medicine, Alameda County
Practice Guidelines for the Diagnosis and Management of Skin and Soft-Tissue Infections
 IDSA GUIDELINES Practice Guidelines for the Diagnosis and Management of Skin and Soft-Tissue Infections Dennis L. Stevens, 1,3 Alan L. Bisno, 5 Henry F. Chambers, 6,7 E. Dale Everett, 13 Patchen Dellinger,
IDSA GUIDELINES Practice Guidelines for the Diagnosis and Management of Skin and Soft-Tissue Infections Dennis L. Stevens, 1,3 Alan L. Bisno, 5 Henry F. Chambers, 6,7 E. Dale Everett, 13 Patchen Dellinger,
ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM
 ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 77th Annual Meeting March 9-12, 2010 New Orleans, Louisiana COMMITTEE ON PATIENT SAFETY PREPARED
ORTHOPAEDIC INFECTION PREVENTION AND CONTROL: AN EMERGING NEW PARADIGM AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 77th Annual Meeting March 9-12, 2010 New Orleans, Louisiana COMMITTEE ON PATIENT SAFETY PREPARED
Vancomycin. Beta-lactams. Beta-lactams. Vancomycin (Glycopeptide) Rifamycins (rifampin) MID 4
 Antibiotic Classes Introduction to Antimicrobials Rachel J. Gordon, MD, MPH Assistant Professor of Clinical Medicine and Epidemiology Beta-lactams Inhibit cell wall synthesis Penicillins Cephalosporins
Antibiotic Classes Introduction to Antimicrobials Rachel J. Gordon, MD, MPH Assistant Professor of Clinical Medicine and Epidemiology Beta-lactams Inhibit cell wall synthesis Penicillins Cephalosporins
PRIORITY RESEARCH TOPICS
 PRIORITY RESEARCH TOPICS Understanding all the issues associated with antimicrobial resistance is probably impossible, but it is clear that there are a number of key issues about which we need more information.
PRIORITY RESEARCH TOPICS Understanding all the issues associated with antimicrobial resistance is probably impossible, but it is clear that there are a number of key issues about which we need more information.
Consequences of Discontinuing Rivaroxaban in Patients with Atrial Fibrillation
 A summary of current literature of interest to pharmacists. March 2013 Alan Hopefl, Pharm.D., Amerinet Clinical Manager Consequences of Discontinuing Rivaroxaban in Patients with Atrial Fibrillation Patients
A summary of current literature of interest to pharmacists. March 2013 Alan Hopefl, Pharm.D., Amerinet Clinical Manager Consequences of Discontinuing Rivaroxaban in Patients with Atrial Fibrillation Patients
Blue Team Teaching Module: Periorbital/Orbital Infections
 Blue Team Teaching Module: Periorbital/Orbital Infections Format: 1. Case 2. Topic Summary 3. Questions 4. References Case: A 3-year-old boy presents with 2 days of increasing redness, swelling, and pain
Blue Team Teaching Module: Periorbital/Orbital Infections Format: 1. Case 2. Topic Summary 3. Questions 4. References Case: A 3-year-old boy presents with 2 days of increasing redness, swelling, and pain
Introduction to Antimicrobial Therapy
 Introduction to Antimicrobial Therapy Christine Kubin, Pharm.D., BCPS Clinical Pharmacist, Infectious Diseases Case #1 L.G. is a 78 yo woman admitted for cardiac cath. 3-vessel disease was identified and
Introduction to Antimicrobial Therapy Christine Kubin, Pharm.D., BCPS Clinical Pharmacist, Infectious Diseases Case #1 L.G. is a 78 yo woman admitted for cardiac cath. 3-vessel disease was identified and
Staphyloccus aureus sepsis: follow- up practice guidelines
 Staphyloccus aureus sepsis: follow- up practice guidelines March 17, 2012 National Study Day Hospital Antibiotic Stewardship prof. dr. Dirk Vogelaers, Ghent University Hospital apr. Franky Buyle, Ghent
Staphyloccus aureus sepsis: follow- up practice guidelines March 17, 2012 National Study Day Hospital Antibiotic Stewardship prof. dr. Dirk Vogelaers, Ghent University Hospital apr. Franky Buyle, Ghent
The first report in Brazil of severe infection caused by community-acquired methicillin-resistant Staphylococcus aureus (CA-MRSA)
 ISSN 0100-879X Volume 42 (8) 692-775 August 2009 CLINICAL INVESTIGATION Braz J Med Biol Res, August 2009, Volume 42(8) 756-760 The first report in Brazil of severe infection caused by community-acquired
ISSN 0100-879X Volume 42 (8) 692-775 August 2009 CLINICAL INVESTIGATION Braz J Med Biol Res, August 2009, Volume 42(8) 756-760 The first report in Brazil of severe infection caused by community-acquired
Computer Decision Support for Antimicrobial Prescribing: Form Follows Function. Matthew Samore, MD University of Utah
 Computer Decision Support for Antimicrobial Prescribing: Form Follows Function Matthew Samore, MD University of Utah And it was so typically brilliant of you to have invited an epidemiologist Outline
Computer Decision Support for Antimicrobial Prescribing: Form Follows Function Matthew Samore, MD University of Utah And it was so typically brilliant of you to have invited an epidemiologist Outline
NewYork-Presbyterian Hospital Sites: Columbia University Medical Center Guideline: Medication Use Manual Page 1 of 12
 Page 1 of 12 TITLE: ANTIBIOTICS IN ADULT PATIENTS EMPIRIC USE GUIDELINES, COLUMBIA UNIVERSITY MEDICAL CENTER MEDICATION GUIDELINE PURPOSE: These are the 2011 guidelines for the empiric use of antibiotics
Page 1 of 12 TITLE: ANTIBIOTICS IN ADULT PATIENTS EMPIRIC USE GUIDELINES, COLUMBIA UNIVERSITY MEDICAL CENTER MEDICATION GUIDELINE PURPOSE: These are the 2011 guidelines for the empiric use of antibiotics
Taking the Bite out of Dog ma
 Taking the Bite out of Dog ma Dr. Michael Woo MD, CCFP(EM), RDMS Director, Emergency Medicine Ultrasonography Associate Professor, Department of Emergency Medicine Ultrasound uottawa DEM 25 May 2013 ACKNOWLEDGEMENTS
Taking the Bite out of Dog ma Dr. Michael Woo MD, CCFP(EM), RDMS Director, Emergency Medicine Ultrasonography Associate Professor, Department of Emergency Medicine Ultrasound uottawa DEM 25 May 2013 ACKNOWLEDGEMENTS
Why Do Some Antibiotics Fail?
 Why Do Some Antibiotics Fail? Patty W. Wright, M.D. April 2010 Objective To outline common reasons why antibiotic therapy is not successful and how this can be avoided. And to teach you a little bit about
Why Do Some Antibiotics Fail? Patty W. Wright, M.D. April 2010 Objective To outline common reasons why antibiotic therapy is not successful and how this can be avoided. And to teach you a little bit about
Intravenous cefazolin plus oral probenecid vs. oral cephalexin for the treatment of cellulitis: a randomized controlled trial STUDY PROTOCOL
 Intravenous cefazolin plus oral probenecid vs. oral cephalexin for the treatment of cellulitis: a randomized controlled trial STUDY PROTOCOL Co-Primary Investigators: Dawn Dalen, BSP, ACPR, PharmD Clinical
Intravenous cefazolin plus oral probenecid vs. oral cephalexin for the treatment of cellulitis: a randomized controlled trial STUDY PROTOCOL Co-Primary Investigators: Dawn Dalen, BSP, ACPR, PharmD Clinical
ANNUAL REPORT ON STAPHYLOCOCCUS AUREUS BACTERAEMIA CASES IN DENMARK 2009 (part I)
 ANNUAL REPORT ON STAPHYLOCOCCUS AUREUS BACTERAEMIA CASES IN DENMARK 2009 (part I) STAPHYLOCOCCUS LABORATORY, STATENS SERUM INSTITUT 1 Staphylococcus aureus Bacteraemia Annual Report, Part I The annual
ANNUAL REPORT ON STAPHYLOCOCCUS AUREUS BACTERAEMIA CASES IN DENMARK 2009 (part I) STAPHYLOCOCCUS LABORATORY, STATENS SERUM INSTITUT 1 Staphylococcus aureus Bacteraemia Annual Report, Part I The annual
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #65 (NQF 0069): Appropriate Treatment for Children with Upper Respiratory Infection (URI) National Quality Strategy Domain: Efficiency and Cost Reduction 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES:
Measure #65 (NQF 0069): Appropriate Treatment for Children with Upper Respiratory Infection (URI) National Quality Strategy Domain: Efficiency and Cost Reduction 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES:
BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC)
 BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC) September 2014 Review date: September 2017 Bulletin 203: Tocilizumab (subcutaneous) in combination with methotrexate or as monotherapy for the treatment
BEDFORDSHIRE AND LUTON JOINT PRESCRIBING COMMITTEE (JPC) September 2014 Review date: September 2017 Bulletin 203: Tocilizumab (subcutaneous) in combination with methotrexate or as monotherapy for the treatment
STAPHYLOCOCCUS AUREUS IS AN IMPORTANT AND
 Staphylococcus aureus Endophthalmitis: Antibiotic Susceptibilities, Methicillin Resistance, and Clinical Outcomes JAMES C. MAJOR, JR, MICHAEL ENGELBERT, HARRY W. FLYNN, JR, DARLENE MILLER, WILLIAM E. SMIDDY,
Staphylococcus aureus Endophthalmitis: Antibiotic Susceptibilities, Methicillin Resistance, and Clinical Outcomes JAMES C. MAJOR, JR, MICHAEL ENGELBERT, HARRY W. FLYNN, JR, DARLENE MILLER, WILLIAM E. SMIDDY,
Original Article Article original
 Original Article Article original Megan Bollinger, MD, CFPC Northern Ontario School of Medicine, Sioux Lookout, Ont. Marsha Hamilton, RN Sioux Lookout Meno Ya Win Health Centre, Sioux Lookout, Ont. Kurt
Original Article Article original Megan Bollinger, MD, CFPC Northern Ontario School of Medicine, Sioux Lookout, Ont. Marsha Hamilton, RN Sioux Lookout Meno Ya Win Health Centre, Sioux Lookout, Ont. Kurt
Clostridium Difficile Colitis. Presented by Mark Skains August 2003
 Clostridium Difficile Colitis Presented by Mark Skains August 2003 What is Clostridium Difficile Gram positive rod Produces spores (hang out in diverticula) Forms Endotoxin A + B which cause diarrhea.
Clostridium Difficile Colitis Presented by Mark Skains August 2003 What is Clostridium Difficile Gram positive rod Produces spores (hang out in diverticula) Forms Endotoxin A + B which cause diarrhea.
Clinical Review. Evidence-based approach to abscess management
 Clinical Review Evidence-based approach to abscess management Christina Korownyk MD CCFP G. Michael Allan MD CCFP ABSTRACT Objective To provide family physicians with an overview of the evidence for managing
Clinical Review Evidence-based approach to abscess management Christina Korownyk MD CCFP G. Michael Allan MD CCFP ABSTRACT Objective To provide family physicians with an overview of the evidence for managing
THIS IS AN OFFICIAL NH DHHS HEALTH ALERT
 THIS IS AN OFFICIAL NH DHHS HEALTH ALERT Distributed by the NH Health Alert Network Health.Alert@nh.gov August 13, 2015 1400 EDT (2:00 PM EDT) NH-HAN 20150813 Updated Centers for Disease Control (CDC)
THIS IS AN OFFICIAL NH DHHS HEALTH ALERT Distributed by the NH Health Alert Network Health.Alert@nh.gov August 13, 2015 1400 EDT (2:00 PM EDT) NH-HAN 20150813 Updated Centers for Disease Control (CDC)
PRMCE ANTI-INFECTIVES SELECTION GUIDELINE FOR ADULTS
 PRMCE ANTI-INFECTIVES SELECTION GUIDELINE FOR ADULTS SKIN AND SOFT TISSUE INFECTIONS: Mild A. Cellulitis: MRSA uncommonly causes cellulitis in the absence of a wound abscess. Add empiric anti-mrsa therapy
PRMCE ANTI-INFECTIVES SELECTION GUIDELINE FOR ADULTS SKIN AND SOFT TISSUE INFECTIONS: Mild A. Cellulitis: MRSA uncommonly causes cellulitis in the absence of a wound abscess. Add empiric anti-mrsa therapy
Post-surgical V.A.C. VeraFlo Therapy with Prontosan Instillation on Inpatient Infected Wounds * COLLECTION OF CASE STUDIES
 COLLECTION OF CASE STUDIES Post-surgical V.A.C. VeraFlo Therapy with Prontosan Instillation on Inpatient Infected Wounds * *All patients were treated with systemic antibiotics Post-surgical V.A.C. VeraFlo
COLLECTION OF CASE STUDIES Post-surgical V.A.C. VeraFlo Therapy with Prontosan Instillation on Inpatient Infected Wounds * *All patients were treated with systemic antibiotics Post-surgical V.A.C. VeraFlo
Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations. J. Stuart Wolf, Jr., M.D.
 Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations J. Stuart Wolf, Jr., M.D. Department of Urology University of Michigan Ann Arbor, MI Official Recommendations for
Antimicrobial Prophylaxis for Transrectal Prostate Biopsy: Organizational Recommendations J. Stuart Wolf, Jr., M.D. Department of Urology University of Michigan Ann Arbor, MI Official Recommendations for
Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection
 Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection Emi Minejima, PharmD Assistant Professor of Clinical Pharmacy USC School of Pharmacy minejima@usc.edu
Antimicrobial Stewardship for Hospital Acquired Infection Prevention: Focus on C. difficile infection Emi Minejima, PharmD Assistant Professor of Clinical Pharmacy USC School of Pharmacy minejima@usc.edu
Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD
 82 Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD Abstract Urinary tract infections are commonly treated in urgent care practice. Clinicians need to be aware of the advantages and limitations
82 Urinary Tract Infection Update Kim Gibson, MD Joseph Toscano, MD Abstract Urinary tract infections are commonly treated in urgent care practice. Clinicians need to be aware of the advantages and limitations
5.07.09. Aubagio. Aubagio (teriflunomide) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.07.09 Subject: Aubagio Page: 1 of 6 Last Review Date: December 5, 2014 Aubagio Description Aubagio (teriflunomide)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.07.09 Subject: Aubagio Page: 1 of 6 Last Review Date: December 5, 2014 Aubagio Description Aubagio (teriflunomide)
ANTIMICROBIAL AGENT CLASSES AND SUBCLASSES
 ANTIMICROBIAL AGENT CLASSES AND SUBCLASSES FOR USE WITH CLSI DOCUMENTS M2 AND M7 Beta-lactams: penicillins e penicillin a penicillin beta-lactam/beta-lactamase inhibitor combinations aminopenicillin a
ANTIMICROBIAL AGENT CLASSES AND SUBCLASSES FOR USE WITH CLSI DOCUMENTS M2 AND M7 Beta-lactams: penicillins e penicillin a penicillin beta-lactam/beta-lactamase inhibitor combinations aminopenicillin a
Appropriate Treatment for Children with Upper Respiratory Infection
 BCBS ACO Measure Appropriate Treatment for Children with Upper Respiratory Infection HEDIS Measure CPT II coding required: YES Click here to go to Table of Contents BCBS Measure: Page 50 of 234 Dated:
BCBS ACO Measure Appropriate Treatment for Children with Upper Respiratory Infection HEDIS Measure CPT II coding required: YES Click here to go to Table of Contents BCBS Measure: Page 50 of 234 Dated:
Use of Packing for Surgical Wounds. Maggie Benson Clinical Problem Solving II
 Use of Packing for Surgical Wounds Maggie Benson Clinical Problem Solving II Purpose Present patient management s/p Incision and Drainage in an outpatient setting Examine evidence for the use of wound
Use of Packing for Surgical Wounds Maggie Benson Clinical Problem Solving II Purpose Present patient management s/p Incision and Drainage in an outpatient setting Examine evidence for the use of wound
Surveillance cultures PRO. Kurt Espersen ICU 4131 Rigshospitalet Copenhagen
 Kurt Espersen ICU 4131 Rigshospitalet Copenhagen Difficult to Diagnose Systemic Candidal Infection Immunsuppression in critically ill patients Frequent manifestation of fungus in ICU Fungi were isolated
Kurt Espersen ICU 4131 Rigshospitalet Copenhagen Difficult to Diagnose Systemic Candidal Infection Immunsuppression in critically ill patients Frequent manifestation of fungus in ICU Fungi were isolated
Guidelines for Management of Patients with Methicillin-Resistant Staphylococcus aureus In Acute Care Hospitals and Long Term Care Facilities
 Guidelines for Management of Patients with Methicillin-Resistant Staphylococcus aureus In Acute Care Hospitals and Long Term Care Facilities Prepared By The MRSA Interagency Advisory Committee in conjunction
Guidelines for Management of Patients with Methicillin-Resistant Staphylococcus aureus In Acute Care Hospitals and Long Term Care Facilities Prepared By The MRSA Interagency Advisory Committee in conjunction
ANNUAL REPORT ON STAPHYLOCOCCUS AUREUS BACTERAEMIA CASES IN DENMARK 2008 (part I)
 ANNUAL REPORT ON STAPHYLOCOCCUS AUREUS BACTERAEMIA CASES IN DENMARK 2008 (part I) STAPHYLOCOCCUS LABORATORY, STATENS SERUM INSTITUT 1 Staphylococcus aureus bacteraemia annual report, part I The format
ANNUAL REPORT ON STAPHYLOCOCCUS AUREUS BACTERAEMIA CASES IN DENMARK 2008 (part I) STAPHYLOCOCCUS LABORATORY, STATENS SERUM INSTITUT 1 Staphylococcus aureus bacteraemia annual report, part I The format
Frequently Asked Questions
 Guidelines for Testing and Treatment of Gonorrhea in Ontario, 2013 Frequently Asked Questions Table of Contents Background... 1 Treatment Recommendations... 2 Treatment of Contacts... 4 Administration
Guidelines for Testing and Treatment of Gonorrhea in Ontario, 2013 Frequently Asked Questions Table of Contents Background... 1 Treatment Recommendations... 2 Treatment of Contacts... 4 Administration
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Contents
 Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
Antibiotic Guidelines: Ear Nose and Throat (ENT) Infections. Classification: Clinical Guideline Lead Author: Antibiotic Steering Committee Additional author(s): Authors Division: DCSS & Tertiary Medicine
Disease Site Breast. Less than 120 kg: Cefazolin 2 grams IV Greater than or equal to 120 kg: Cefazolin 3 grams IV. Head & Neck
 Patients scheduled for surgery should have the following antibiotics administered prior to their procedure Vancomycin and Ciprofloxacin are to be initiated 60 to 120 minutes prior to incision and all other
Patients scheduled for surgery should have the following antibiotics administered prior to their procedure Vancomycin and Ciprofloxacin are to be initiated 60 to 120 minutes prior to incision and all other
GEORGIA DEPARTMENT OF CORRECTIONS Floyd Veterans Memorial Building Room 952 - East Tower Atlanta, Georgia 30334
 Sonny Perdue Governor GEORGIA DEPARTMENT OF CORRECTIONS Floyd Veterans Memorial Building Room 952 - East Tower Atlanta, Georgia 30334 1 MEMORANDUM TO: FROM: Medical Directors, Medical Administrators, &
Sonny Perdue Governor GEORGIA DEPARTMENT OF CORRECTIONS Floyd Veterans Memorial Building Room 952 - East Tower Atlanta, Georgia 30334 1 MEMORANDUM TO: FROM: Medical Directors, Medical Administrators, &
C-Difficile Infection Control and Prevention Strategies
 C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer Adrienne.Mims@AlliantQuality.org 1/18/2016 1 Disclosure This educational activity does not have commercial
C-Difficile Infection Control and Prevention Strategies Adrienne Mims, MD MPH VP, Chief Medical Officer Adrienne.Mims@AlliantQuality.org 1/18/2016 1 Disclosure This educational activity does not have commercial
PERTUSSIS SURVEILLANCE AND RESPONSE PROTOCOL
 PERTUSSIS SURVEILLANCE AND RESPONSE PROTOCOL Public Health Action 1. Educate the public, particularly parents of infants, about the dangers of whooping cough and the advantages of initiating immunization
PERTUSSIS SURVEILLANCE AND RESPONSE PROTOCOL Public Health Action 1. Educate the public, particularly parents of infants, about the dangers of whooping cough and the advantages of initiating immunization
The 14th EURL-AR Proficiency Test - enterococci, staphylococci and E. coli 2013. Lina Cavaco Susanne Karlsmose Rene S. Hendriksen Frank M.
 The 14th EURL-AR Proficiency Test - enterococci, staphylococci and E. coli 2013 Lina Cavaco Susanne Karlsmose Rene S. Hendriksen Frank M. Aarestrup The 14TH EURL-AR Proficiency Test Enterococci, Staphylococci
The 14th EURL-AR Proficiency Test - enterococci, staphylococci and E. coli 2013 Lina Cavaco Susanne Karlsmose Rene S. Hendriksen Frank M. Aarestrup The 14TH EURL-AR Proficiency Test Enterococci, Staphylococci
Hematologic Malignancies/Stem Cell Transplantation Program Clinical Section UCLA Health System Los Angeles, CA 90095
 Clinical Section UCLA Health System Los Angeles, CA 90095 CS 6.2 DIAGNOSIS AND MANAGEMENT OF INTERSTITIAL PNEUMONIA Location: Clinical Section Supersedes/Replaces: B3.421g Document drive\path\name Effective
Clinical Section UCLA Health System Los Angeles, CA 90095 CS 6.2 DIAGNOSIS AND MANAGEMENT OF INTERSTITIAL PNEUMONIA Location: Clinical Section Supersedes/Replaces: B3.421g Document drive\path\name Effective
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Received 4 July 2010; returned 10 August 2010; revised 27 September 2010; accepted 30 September 2010
 J Antimicrob Chemother 2011; 66: 205 209 doi:10.1093/jac/dkq404 Advance Access publication 8 November 2010 Sustained reduction in antimicrobial use and decrease in methicillin-resistant Staphylococcus
J Antimicrob Chemother 2011; 66: 205 209 doi:10.1093/jac/dkq404 Advance Access publication 8 November 2010 Sustained reduction in antimicrobial use and decrease in methicillin-resistant Staphylococcus
WARNING LETTER. According to its approved product labeling (PI) (in pertinent part, emphasis original):
 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Silver Spring, MD 20993-0002 TRANSMITTED BY FACSIMILE Sapan A. Shah, Ph.D. President and Chief Executive Officer
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Silver Spring, MD 20993-0002 TRANSMITTED BY FACSIMILE Sapan A. Shah, Ph.D. President and Chief Executive Officer
A case of concurrent deep venous thrombosis, pseudoaneurysm, and extremity abscess in an intravenous methamphetamine abuser
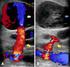 A case of concurrent deep venous thrombosis, pseudoaneurysm, and extremity abscess in an intravenous methamphetamine abuser BY MATTHEW L HARRISON Abstract Introduction. Intravenous drug abuse is a global
A case of concurrent deep venous thrombosis, pseudoaneurysm, and extremity abscess in an intravenous methamphetamine abuser BY MATTHEW L HARRISON Abstract Introduction. Intravenous drug abuse is a global
Title: Antibiotic Guideline for Acute Pelvic Inflammatory Disease
 Title: Antibiotic Guideline for Acute Pelvic Inflammatory Disease Version 3 Date ratified December 2007 Review date December 2009 Ratified by NUH Antimicrobial Guidelines Committee Gynaecology Directorate
Title: Antibiotic Guideline for Acute Pelvic Inflammatory Disease Version 3 Date ratified December 2007 Review date December 2009 Ratified by NUH Antimicrobial Guidelines Committee Gynaecology Directorate
Bacterial skin and soft tissue infections (SSTIs)
 C l i n i c a l R e v i e w A r t i c l e Bacterial Skin and Soft Tissue Infections Suzanne J. Templer, DO Maximo O. Brito, MD Bacterial skin and soft tissue infections (SSTIs) are a common problem encountered
C l i n i c a l R e v i e w A r t i c l e Bacterial Skin and Soft Tissue Infections Suzanne J. Templer, DO Maximo O. Brito, MD Bacterial skin and soft tissue infections (SSTIs) are a common problem encountered
CARRIAGE OF STAPHYLOCOCCUS AUREUS AMONG INJECTION DRUG USERS: LOWER PREVALENCE IN AN INJECTION HEROIN MAINTENANCE PROGRAM THAN IN
 Vol. 25 No. 2 INFECTION CONTROL AND HOSPITAL EPIDEMIOLOGY 133 CARRIAGE OF STAPHYLOCOCCUS AUREUS AMONG INJECTION DRUG USERS: LOWER PREVALENCE IN AN INJECTION HEROIN MAINTENANCE PROGRAM THAN IN AN ORAL METHADONE
Vol. 25 No. 2 INFECTION CONTROL AND HOSPITAL EPIDEMIOLOGY 133 CARRIAGE OF STAPHYLOCOCCUS AUREUS AMONG INJECTION DRUG USERS: LOWER PREVALENCE IN AN INJECTION HEROIN MAINTENANCE PROGRAM THAN IN AN ORAL METHADONE
Liofilchem - Antibiotic Disk Interpretative Criteria and Quality Control - F14013 - Rev.7 / 20.02.2013
 Liofilchem Antibiotic Disk Interpretative Criteria and Quality Control F0 Rev.7 /.02. Amikacin AK Amoxicillin + Clavulanic acid AUG (+) ATCC 352 Coagulasenegative staphylococci Amoxicillin + Clavulanic
Liofilchem Antibiotic Disk Interpretative Criteria and Quality Control F0 Rev.7 /.02. Amikacin AK Amoxicillin + Clavulanic acid AUG (+) ATCC 352 Coagulasenegative staphylococci Amoxicillin + Clavulanic
SURGICAL ANTIBIOTIC PROPHYLAXIS. Steve Johnson, PharmD, BCPS Prime Therapeutics, Inc
 SURGICAL ANTIBIOTIC PROPHYLAXIS Steve Johnson, PharmD, BCPS Prime Therapeutics, Inc OBJECTIVES Discuss antibiotic use as prophylaxis vs presumptive therapy vs treatment of infections. Discuss risk factors
SURGICAL ANTIBIOTIC PROPHYLAXIS Steve Johnson, PharmD, BCPS Prime Therapeutics, Inc OBJECTIVES Discuss antibiotic use as prophylaxis vs presumptive therapy vs treatment of infections. Discuss risk factors
Diagnosis and Management of Prosthetic Joint Infection: Clinical Practice Guidelines by the Infectious Diseases Society of America a
 Clinical Infectious Diseases Advance Access published December 6, 2012 IDSA GUIDELINES Diagnosis and Management of Prosthetic Joint Infection: Clinical Practice Guidelines by the Infectious Diseases Society
Clinical Infectious Diseases Advance Access published December 6, 2012 IDSA GUIDELINES Diagnosis and Management of Prosthetic Joint Infection: Clinical Practice Guidelines by the Infectious Diseases Society
Lecture Outline. Quinolones
 Lecture Outline Quinolones Trimethoprim/Sulfamethoxazole Miscellaneous antimicrobials - Metronidazole Daptomycin Cases Quinolones Bactericidal broad spectrum antibiotics Increasingly used because of their
Lecture Outline Quinolones Trimethoprim/Sulfamethoxazole Miscellaneous antimicrobials - Metronidazole Daptomycin Cases Quinolones Bactericidal broad spectrum antibiotics Increasingly used because of their
WHO Guidelines for Pharmacological Management of Pandemic (H1N1) 2009 Influenza and other Influenza Viruses
 WHO Guidelines for Pharmacological Management of Pandemic (H1N1) 2009 Influenza and other Influenza Viruses 20 August 2009 Table of contents EXECUTIVE SUMMARY... i Other recommendations...iii 1. INTRODUCTION...
WHO Guidelines for Pharmacological Management of Pandemic (H1N1) 2009 Influenza and other Influenza Viruses 20 August 2009 Table of contents EXECUTIVE SUMMARY... i Other recommendations...iii 1. INTRODUCTION...
Etiology and treatment of chronic bacterial prostatitis the Croatian experience
 Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
Etiology and treatment of chronic bacterial prostatitis the Croatian experience Višnja Škerk University Hospital for Infectious Diseases "Dr. Fran Mihaljevic" Zagreb Croatia Milano, Malpensa, 14 Nov 2008
Treating Clostridium difficile infection (CDI) the second time around
 Treating Clostridium difficile infection (CDI) the second time around Ciarán P. Kelly, MD Professor of Medicine Harvard Medical School. Beth Israel Deaconess Medical Center, Boston The difficult Clostridium
Treating Clostridium difficile infection (CDI) the second time around Ciarán P. Kelly, MD Professor of Medicine Harvard Medical School. Beth Israel Deaconess Medical Center, Boston The difficult Clostridium
NASAL COLONIZATION BY MICROORGANISMS IN NURSING PROFESSIONALS IN UNITS SPECIALIZING IN HIV/AIDS
 University of Sa o Paulo at Ribeira o Preto College of Nursing. WHO Collaborating Centre for Nursing Research Development. Ribeirão Preto (SP), Brazil. RENAIDST Rede Nacional NASAL COLONIZATION BY MICROORGANISMS
University of Sa o Paulo at Ribeira o Preto College of Nursing. WHO Collaborating Centre for Nursing Research Development. Ribeirão Preto (SP), Brazil. RENAIDST Rede Nacional NASAL COLONIZATION BY MICROORGANISMS
CURRICULUM VITAE. Jason Yamaki, Pharm.D., Ph.D.
 CURRICULUM VITAE Jason Yamaki, Pharm.D., Ph.D. Personal Information Business Address Chapman University School of Pharmacy 9401 Jeronimo Road Irvine, CA, 92618 Telephone 714-516-5482 E-mail address yamaki@chapman.edu
CURRICULUM VITAE Jason Yamaki, Pharm.D., Ph.D. Personal Information Business Address Chapman University School of Pharmacy 9401 Jeronimo Road Irvine, CA, 92618 Telephone 714-516-5482 E-mail address yamaki@chapman.edu
