Integra. Proximal Humeral Fracture Plate System SURGICAL TECHNIQUE
|
|
|
- Lizbeth Dennis
- 7 years ago
- Views:
Transcription
1 Integra Proximal Humeral Fracture Plate System SURGICAL TECHNIQUE
2 Table of Contents Introduction Product Description... 2 Indications... 3 Contraindications... 3 Warnings and Precautions... 4 Design Rationale LP (Low Profile) Plate... 5 (Greater Tuberosity) Plate... 6 LP Plate Surgical Technique Step 1: Patient Positioning... 7 Step 2: Exposure... 7 Step 3: Fracture Reduction and Debridement... 7 Step 4: Plate Positioning... 8 Step 5: Proximal 3.5mm Screw Insertion... 9 Step 6: 3.5mm Shaft Screw Insertion Step 7: Final Verification Plate Surgical Technique Step 1: Patient Positioning Step 2: Exposure Step 3: Fracture Reduction and Debridement Step 4: Plate Positioning Step 5: Proximal 3.5mm Screw Insertion Step 6: 2.7mm Proximal Holes ( Plate Only) Step 7: 3.5mm Shaft Screw Insertion Step 8: Final Verification Product Information Instrumentation... 19
3 Surgical Technique As the manufacturer of this device, Integra does not practice medicine and does not recommend this or any other surgical technique for use on a specific patient. The surgeon who performs any implant procedure is responsible for determining and using the appropriate techniques for implanting the device in each patient. Introduction Joseph Abboud, MD Philip Duke, MB.BS, FRACS, FA(ORTH)A William Geissler, MD Anand Murthi, MD Mark Ross, MB.BS, FRACS, FA (ORTH)A Caution: Federal law restricts this device to sale by or on the order of a physician or practitioner. Product Description The Integra Proximal Humeral Fracture Plate System is composed of left and right Humeral reconstruction plate implants in two options, Plate and LP Plate. The plate is designed to cover the greater tuberosity and is available in four-hole (91mm) and seven-hole (115mm), and ten-hole (138mm) lengths or sizes. The LP plate is designed to sit lower on the greater tuberosity and is available in three-hole (88mm), six-hole (112mm), and nine-hole (135mm) lengths or sizes. The system will feature 3.5mm locking screws (15-75mm lengths), non-locking compression screws (15-40mm lengths) and non-locking partial thread lag screws (40-75mm lengths)., In addition to, 2.7mm locking screws (10-25mm lengths) are also available. The Integra Proximal Humeral Fracture Plate is a single component made from stainless steel (SS 316L). The non-locking compression, locking and non-locking partial thread lag screws are made from stainless steel (SS 316L). 2
4 Indications The Integra Proximal Humeral Fracture Plate system is designed for fractures and fracture dislocations, osteotomies and non-unions of the proximal humerus. Indications Include: Dislocated two-, three-, and four-fragment fractures of the proximal humerus, including fractures involving osteopenic bone Pseudoarthroses in the proximal humerus Osteotomies in the proximal humerus Contraindications Not indicated for use with acute infections or for children during the growth phase Screws are contraindicated in: active infection, conditions which tend to retard healing such as blood supply limitations, previous infections, insufficient quantity or quality of bone to permit stabilization of the fracture complex, conditions that restrict the patient s ability or willingness to follow postoperative instructions during the healing process and foreign body sensitivity. Cases with malignant primary or metastatic tumors which preclude adequate bone support or screw fixations, unless supplemental fixation or stabilization methods are utilized. Foreign body sensitivity where material sensitivity is suspected, appropriate tests should be made and sensitivity ruled out prior to implementations. These implants are intended as a guide to normal healing, and are NOT intended to replace normal body structure or bear the weight of the body in the presence of incomplete bone healing. Delayed unions or non-unions in the presence of load bearing or weight bearing might eventually cause the implant to break due to metal fatigue. All metal surgical implants are subjected to repeated stress in use, which can result in metal fatigue. 3
5 Warnings and Precautions No metallic surgical implant should be reused. Any metal implant, once used, should be discarded. Even though it appears undamaged, it may already have small defects and internal stress patterns which may lead to fatigue failure. Correct handling of implant is extremely important. Avoid contouring metallic implants whenever possible. If necessary, or allowed by design, the device should not be bent sharply, reverse bent, notched or scratched. All of these operations can produce defects in the surface finish and internal stress concentrations, which may become the focal point for eventual failure of the appliance. If metal plates or other metallic devices are to be used together with the Integra Proximal Humeral Fracture Plates, all such devices should be manufactured from a metal that has a similar composition to avert possibility of galvanic corrosion or other metallic reactions. Correct selection of the implant is extremely important. The potential for success in fracture fixation is increased by the selection of the proper size of the implants. The patient s anatomy and indication will determine the size of the Integra Proximal Humeral Fracture Plate to be used. The size of the human bones presents limiting restrictions on the size and strength of implants. Postoperative care is extremely important. The patient must be warned that noncompliance with postoperative instructions could lead to breakage of the implant requiring revision surgery to remove the device. The use of Integra Proximal Humeral Fracture Plates provides the surgeon a means of bone fixation and helps generally in the management of fractures and reconstructive surgeries. The implants are intended as a guide to normal healing and are NOT intended to replace normal body structure. All metal surgical implants are subject to repeated stress in use which can result in metal fatigue. Failure to immobilize a delayed union or nonunion of bone will result in excessive and repeated stresses which are transmitted by the body to any temporary internal fixation device prior to the healing of the fracture. Due to normal metal fatigue, these stresses can cause eventual bending or breakage of the device. Therefore, it is important that immobilization of the fracture site is maintained until firm bony union (confirmed by clinical and roentgenographic examination) is established. Detailed written instructions on the use and limitations of the device should be given to the patient. While the surgeon must make the final decision on implant removal, whenever possible and practical for the individual patient, fixation devices should be removed once their service as an aid to healing is accomplished, particularly in younger more active patients. The MR environment presents risks to patients with metal implant. Review of the available literature documents that metal implants may heat resulting in tissue damage and may migrate out of position. They may also cause artifact affecting image quality. Physicians should take these risks into consideration when recommending MRI imaging for patients with metal implants. Note: The Integra Proximal Humeral Fracture Plate System has not been evaluated for safety and compatibility in the MR environment. The Integra Proximal Humeral Fracture Plate System has not been tested for heating or migration in the MR environment. 4
6 Design Rationale LP (Low Profile) Plate Designed to sit lower on the greater tuberosity to minimize subacromial impingement 9 proximal screw options 4 calcar screws to provide inferior medial support Slotted screw option for initial plate positioning Anatomic fit with right and left plates and different length plates 3-hole (89mm) 6-hole (112mm) 9-hole (135mm) 6 suture holes for tuberosity fixation Easy in-situ needle passing through angled and scalloped holes Also used as wire holes for initial plate fixation Multiple Screw Options 3.5mm Locking, Non-Locking and Lag Screw Options 5
7 Design Rationale (Greater Tuberosity) Plate Maximizes tuberosity coverage and humeral head bone purchase with 12 proximal screw options 4 calcar screws to provide inferior medial support Anterior tab for initial plate positioning and buttress option Anatomic fit with right and left plates and different length plate 4-hole (91mm) 7-hole (116mm) 10-hole (140mm) 5 suture holes for soft tuberosity fixation Easy in-situ needle passing through angled and scalloped holes Also used as wire holes for initial plate fixation Multiple Screw Options 2.7mm Proximal Locking Screws 3.5mm Locking, Non-Locking and Lag Screw Options 6
8 Surgical Technique: LP (Low Profile) Plate Step 1: Patient Positioning 1-1 Place the patient in beach chair position (1-1). Ensure that the involved shoulder extends laterally over the top corner of the table so that the arm can be brought into extension and abduction (this is essential for good exposure of the proximal humerus). 1-1 Step 2: Exposure 2-1 Deltopectoral approach Exposure is achieved through a 10-12cm incision that starts at the clavicle and proceeds over the coracoid toward the deltoid insertion. The incision should be in line with the deltoid-pectoral interval. Once the initial incision is made, develop the subcutaneous flap, locate and identify the cephalic vein. Gently retract the cephalic vein either laterally with the deltoid muscle or medially with the pectoralis major. Self-retaining retractors can be utilized to achieve this exposure. Release the fascia along the lateral border of the coracobrachialis and gently retract it medially. To help improve visualization and reduction find the pectoralis insertion and release the proximal third of the pectoralis tendon to expose the biceps. Take care to protect the biceps tendon which lies directly underneath. Step 3: Fracture Reduction and Debridement 3-1 Debride the fracture and keep any bone pieces to aid in the repair. After debridement of the fracture, reduction can be achieved by manual traction and indirect manipulation. Reduction clamps are also available in the tray. In cases of severe comminution reduction of the tuberosities can be achieved by suturing the rotator cuff together. To aid in healing, bone graft should be considered to fill any voids. 7
9 Step 4: Plate Positioning 4-1 Select the appropriate Integra Proximal Humeral plate, left or right, LP plate (4-1) in the appropriate length to stabilize the fracture. The LP plate is designed to sit lower on the proximal humerus which can help to prevent acromial impingement but does not allow full buttress of the greater tuberosity. 4-1 The LP plate is placed onto the humerus approximately 2cm distal to the rotator cuff attachment on the upper part of the greater tuberosity and 2-3mm lateral to the bicipital groove. Temporarily fix the plate with 2.0mm guide wires. 4-2 Place a PF Pin in the center of the slot on the plate(4-2). This will allow the plate to be translated up or down to achieve desired plate position. Once desired plate positioning has been achieved proceed with proximal screw insertion. 4-2 LP LP 8
10 Step 5: Proximal 3.5mm Screw Insertion Note: It is recommended to start with the screws that angle up into the head to secure the reduced humeral head fragments. 5-1 Place the appropriate LP Proximal Hole Targeting Guide onto the plate. Lock the targeting guide into place by inserting the 2.4mm Locking Drill Guide into the most proximal hole on the guide (5-1). 5-1 LP 5-2 Using the 2.4mm Drill Sleeve inside the 3.5mm Screw Guide place the guide into one of the four proximally angled holes on the targeting guide (5-2). Drill using the 2.4mm drill until resistance is felt. Use fluoroscopy to verify the tip of the drill is close to the subchondral bone. 5-2 Note: Care should be taken to ensure the subchondral bone is not penetrated. LP 5-3 Use the depth readings on the drill to determine screw length (close up of drill in drill guide showing laser marks on drill). The Standard Depth Gauge can be used at this point if necessary (5-3). Remove the drill and 2.4mm Drill Sleeve leaving the 3.5mm Screw Guide in place. 5-3 LP 9
11 5-4 Insert the determined length locking, non-locking compression, or non-locking partial thread 3.5mm screw through the Screw Guide using the TX15 Driver Shaft and Ratcheting Driver Handle (5-4). Repeat the above steps for the remaining angled screw holes on the targeting guide before proceeding to the additional proximal screw holes. 5-4 LP Step 6: 3.5mm Shaft Screw Insertion The shaft of the plate can be secured by either locking screws or multidirectional non-locking screws. 6-1 Locking Screws Thread the 2.4mm Locking Drill Guide into the most proximal shaft hole. Drill using the 2.4mm Drill until the far cortex is penetrated). Use the markings on the drill to determine screw length or remove the drill guide and use the Standard Depth Gauge (6-1a). 6-1a If power is used to insert the screw, use of a torque limiter is recommended. Start the power tool slowly, increase the speed and then reduce it again before the screw is fully tightened. Final tightening of Locking Screws should always be performed manually using a two finger tighten technique to prevent over-tightening of Locking Screws. Insert the corresponding 3.5mm locking screw using the TX15 Driver Shaft and Ratcheting Driver Handle (6-1b). Repeat for the remaining shaft holes ensuring the plate stays aligned with the humeral shaft as you work distally. 6-1b LP Note: Use of a torque limiter is required if inserting screws under power. Do not lock the screws under power as this risks damaging the screw recess, making implant removal difficult. LP 10
12 6-2 Non-Locking Compression Screws Place the 2.4mm drill sleeve into the 3.5mm Screw Guide, insert in the desired screw orientation and drill using the 2.4mm drill until the desired depth is achieved (6-2a). Use the Standard Depth Gauge to determine screw length (6-2b). 6-2a Insert the corresponding 3.5mm non-locking compression screw using the TX15 Driver Shaft and Ratcheting Driver Handle (6-2c). Repeat for the remaining shaft holes ensuring the plate stays aligned with the humeral shaft as you work distally. 6-2b LP LP 6-2c LP Step 7: Final Verification 7-1 Using Fluoroscopy evaluate the humerus to verify proper reduction and screw placement. 11
13 Surgical Technique: (Greater Tuberosity) Plate Step 1: Patient Positioning 1-1 Place the patient in beach chair position (1-1). Ensure that the involved shoulder extends laterally over the top corner of the table so that the arm can be brought into extension and abduction (this is essential for good exposure of the proximal humerus). 1-1 Step 2: Exposure 2-1 Deltopectoral approach Exposure is achieved through a 10-12cm incision that starts at the clavicle and proceeds over the coracoid toward the deltoid insertion. The incision should be in line with the deltoid-pectoral interval. Once the initial incision is made, develop the subcutaneous flap, locate and identify the cephalic vein. Gently retract the cephalic vein either laterally with the deltoid muscle or medially with the pectoralis major. Self-retaining retractors can be utilized to achieve this exposure. Release the fascia along the lateral border of the coracobrachialis and gently retract it medially. To help improve visualization and reduction find the pectoralis insertion and release the proximal third of the pectoralis tendon to expose the biceps. Take care to protect the biceps tendon which lies directly underneath. Step 3: Fracture Reduction and Debridement 3-1 Debride the fracture and keep any bone pieces to aid in the repair. After debridement of the fracture, reduction can be achieved by manual traction and indirect manipulation. Reduction clamps are also available in the tray. In cases of severe comminution reduction of the tuberosities can be achieved by suturing the rotator cuff together. To aid in healing, bone graft should be considered to fill any voids. 12
14 Step 4: Plate Positioning 4-1 Select the appropriate Integra Proximal Humeral plate, left or right, plate (4-1) in the appropriate length to stabilize the fracture. The Plate is designed to cover the greater tuberosity and should be utilized in fractures that require additional support or buttress of the greater tuberosity fragments. The plate is placed onto the humerus approximately 6-10mm distal to the rotator cuff attachment on the upper part of the greater tuberosity and 2-3mm lateral to the bicipital groove. Temporarily fix the plate with 2.0mm guide wires Place a PF Pin in the center of the slot on the plate(4-2). This will allow the plate to be translated up or down to achieve desired plate position. Once desired plate positioning has been achieved proceed with proximal screw insertion
15 Step 5: Proximal 3.5mm Screw Insertion Note: It is recommended to start with the screws that angle up into the head to secure the reduced humeral head fragments. 5-1 Place the appropriate Proximal Hole Targeting Guide onto the plate. Lock the targeting guide into place by inserting the 2.4mm Locking Drill Guide into the most proximal hole on the guide (5-1) Using the 2.4mm Drill Sleeve inside the 3.5mm Screw Guide place the guide into one of the four proximally angled holes on the targeting guide (5-2). 5-2 Drill using the 2.4mm drill until resistance is felt. Use fluoroscopy to verify the tip of the drill is close to the subchondral bone. Note: Care should be taken to ensure the subchondral bone is not penetrated Use the depth readings on the drill to determine screw length (close up of drill in drill guide showing laser marks on drill). The Standard Depth Gauge can be used at this point if necessary (5-3). Remove the drill and 2.4mm Drill Sleeve leaving the 3.5mm Screw Guide in place. 5-4 Insert the determined length locking, non-locking compression, or non-locking partial thread 3.5mm screw through the Screw Guide using the TX15 Driver Shaft and Mini Ratchet Driver Handle (5-4). Repeat the above steps for the remaining angled screw holes on the targeting guide before proceeding to the additional proximal screw holes
16 Step 6: 2.7mm Proximal holes ( Plate Only) These four most proximal holes can either be used for suture holes or 2.7mm locking screws or a combination of both to repair the tuberosity. 6-1 Suture Technique Place a heavy non absorbable suture through the tendon at the attachment to the tuberosity and then through the plate (6-1). There is a recess cut out of the back of the plate to allow the passing of suture after the plate is secured. 6-1 Note: Sutures may also be passed prior to the plate being secured for ease of insertion. Tighten the suture until appropriate tension is achieved mm Screw Technique Thread the 1.9mm Locking Drill Guide into the plate. Drill with the 1.9mm Drill until desired depth is achieved (6-2). Use either the markings on the drill to determine screw length or remove the drill guide and use the Standard Depth Gauge (6-3). Insert the corresponding 2.7mm locking screw using the TX8 Driver Shaft and Mini Ratchet Driver Handle (6-4). Repeat the above steps for the remaining 2.7mm screw holes. 6-3 If power is used to insert the screw, use of a torque limiter is recommended. Start the power tool slowly, increase the speed and then reduce it again before the screw is fully tightened. Final tightening of Locking Screws should always be performed manually using a two finger tighten technique to prevent over-tightening of Locking Screws. Note: Use of a torque limiter is required if inserting screws under power. Do not lock the screws under power as this risks damaging the screw recess, making implant removal difficult
17 Step 7: 3.5mm Shaft Screw Insertion The shaft of the plate can be secured by either locking screws or multidirectional non-locking screws. 7-1 Locking Screws Thread the 2.4mm Locking Drill Guide into the most proximal shaft hole. Drill using the 2.4mm Drill until the far cortex is penetrated). Use the markings on the drill to determine screw length or remove the drill guide and use the Standard Depth Gauge (7-1a). 7-1a If power is used to insert the screw, use of a torque limiter is recommended. Start the power tool slowly, increase the speed and then reduce it again before the screw is fully tightened. Final tightening of Locking Screws should always be performed manually using a two finger tighten technique to prevent over-tightening of Locking Screws. Insert the corresponding 3.5mm locking screw using the TX15 Driver Shaft and Mini Ratchet Driver Handle (7-1b). Repeat for the remaining shaft holes ensuring the plate stays aligned with the humeral shaft as you work distally. 7-1b Note: Use of a torque limiter is required if inserting screws under power. Do not lock the screws under power as this risks damaging the screw recess, making implant removal difficult. 16
18 7-2 Non-Locking Compression Screws Place the 2.4mm drill sleeve into the 3.5mm Screw Guide, insert in the desired screw orientation and drill using the 2.4mm drill until the desired depth is achieved (7-2a). Use the Standard Depth Gauge to determine screw length (7-2b). 7-2a Insert the corresponding 3.5mm non-locking compression screw using the TX15 Driver Shaft and Mini Ratchet Driver Handle (7-2c). Repeat for the remaining shaft holes ensuring the plate stays aligned with the humeral shaft as you work distally. 7-2b 7-2c Step 8: Final Verification 8-1 Using Fluoroscopy evaluate the humerus to verify proper reduction and screw placement. 17
19 Product Information Screws Plates Catalog Number Description Catalog Number Description 2.7mm Locking Screws PSS2710LS 2.7mm locking screw 10mm PSS2712LS 2.7mm locking screw 12.5mm PSS2715LS 2.7mm locking screw 15mm PSS2717LS 2.7mm locking screw 17.5mm PSS2720LS 2.7mm locking screw 20mm PSS2722LS 2.7mm locking screw 22.5mm PSS2725LS 2.7mm locking screw 25mm 3.5mm Locking Screws PSS3515LS 3.5mm locking screw 15mm PSS3517LS 3.5mm locking screw 17.5mm PSS3520LS 3.5mm locking screw 20mm PSS3522LS 3.5mm locking screw 22.5mm PSS3525LS 3.5mm locking screw 25mm PSS3527LS 3.5mm locking screw 27.5mm PSS3530LS 3.5mm locking screw 30mm PSS3532LS 3.5mm locking screw 32.5mm PSS3535LS 3.5mm locking screw 35mm PSS3537LS 3.5mm locking screw 37.5mm PSS3540LS 3.5mm locking screw 40mm PSS3545LS 3.5mm locking screw 45mm PSS3550LS 3.5mm locking screw 50mm PSS3555LS 3.5mm locking screw 55mm PSS3560LS 3.5mm locking screw 60mm PSS3565LS 3.5mm locking screw 65mm PSS3570LS 3.5mm locking screw 70mm PSS3575LS 3.5mm locking screw 75mm 3.5mm Compression Screws PSS3515CS 3.5mm compression screw 15mm PSS3517CS 3.5mm compression screw 17.5mm PSS3520CS 3.5mm compression screw 20mm PSS3522CS 3.5mm compression screw 22.5mm PSS3525CS 3.5mm compression screw 25mm PSS3527CS 3.5mm compression screw 27.5mm PSS3530CS 3.5mm compression screw 30mm PSS3532CS 3.5mm compression screw 32.5mm PSS3535CS 3.5mm compression screw 35mm PSS3537CS 3.5mm compression screw 37.5mm PSS3540CS 3.5mm compression screw 40mm 3.5mm Partially Treaded Screws PSS3540PS 3.5mm partially threaded screw 40mm PSS3545PS 3.5mm partially threaded screw 45mm PSS3550PS 3.5mm partially threaded screw 50mm PSS3555PS 3.5mm partially threaded screw 55mm PSS3560PS 3.5mm partially threaded screw 60mm PSS3565PS 3.5mm partially threaded screw 65mm PSS3570PS 3.5mm partially threaded screw 70mm PSS3575PS 3.5mm partially threaded screw 75mm HFP RS HFP LS HFP RS HFP LS HFP RS HFP LS HFP RS HFP LS HFP RS HFP LS HFP RS HFP LS Single Use Catalog Number Humeral Fracture Plate 4-Hole, Right Humeral Fracture Plate 4-Hole, Left Humeral Fracture Plate 7-Hole, Right Humeral Fracture Plate 7-Hole, Left Humeral Fracture Plate 10-Hole, Right Humeral Fracture Plate 10-Hole, Left Low Profile Humeral Fracture Plate 3-Hole, Right Low Profile Humeral Fracture Plate 3-Hole, Left Low Profile Humeral Fracture Plate 6-Hole, Right Low Profile Humeral Fracture Plate 6-Hole, Left Low Profile Humeral Fracture Plate 9-Hole, Right Low Profile Humeral Fracture Plate 9-Hole, Left Description DRL mm Drill Bit DRL mm Drill Bit DRL mm Drill Bit WIRE S 2.0mm K-wire Smooth WIRE T 2.0mm K-wire Threaded PFP mm Provisional Fixation Pin lb-in Single Use Torque Limiter lb-in Single Use Torque Limiter Instruments Catalog Number Description LDG mm Locking drill guide LDG mm Locking drill guide DDG mm Drill Guide DDG mm Screw Guide DDG mm Drill Guide Torx 15 Drive Shaft Torx 8 Drive Shaft PDG Plate Depth Gauge PDG Drill Guide Depth Gauge RM1011S03 Mini Ratchet Driver Handle AO to Trinkle adapter A Periosteal Elevator Bone Reduction Forceps Straight Bone Reduction Forceps Curved 8 HTG093003L Left Proximal Hole Targeting Guide Plate HTG093003R Right Proximal Hole Targeting Guide Plate HTG093001L Left Proximal Hole Targeting Guide LP Plate HTG093001R Right Proximal Hole Targeting Guide LP Plate CSA00014 Tray Lid CSA Tray Base CSA Tray Upper CSA Screw Caddy Base CSA Screw Caddy Lid 18
20 Instrumentation Bone Reduction Forceps Curved 2. Left/Right Plates 3. Left/Right LP Plates 4. Bone Reduction Forceps 19
21 Smooth/Threaded K-Wires mm Drill Guide mm Provisional Fixation Pin mm/2.4mm Locking and Non-Locking Drill Guides 5. Mini Ratchet Driver Handle 6. Left/Right Hole Targeting Guides 7. Drill Guide Depth Gauge 8. Plate Depth Gauge mm/2.4mm/3.5mm Drills 10. TORX 8/15 Drive Shafts 11. AO Trinkle Adaptor 12. Elevator 13. Screw Caddy 20
22 21
23 22
24 Integra Proximal Humeral Fracture Plate System For more information or to place an order, please contact: Integra n 311 Enterprise Drive, Plainsboro, NJ USA n outside USA n fax integralife.com Integra and the Integra logo are registered trademarks of Integra LifeSciences Corporation or its subsidiaries in the United States and/or other countries Integra LifeSciences Corporation All rights reserved. Printed in the USA. 0K LC
Zimmer Periarticular Proximal Tibial Locking Plate
 Zimmer Periarticular Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Tibial Locking Plate 1 Table of Contents Introduction 2 Locking Screw Technology
Zimmer Periarticular Proximal Tibial Locking Plate Surgical Technique The Science of the Landscape Zimmer Periarticular Proximal Tibial Locking Plate 1 Table of Contents Introduction 2 Locking Screw Technology
SALVATION. Fusion Bolts and Beams SURGICAL TECHNIQUE
 SALVATION Fusion Bolts and Beams SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 4 Intended Use Chapter 3 4 Device Description 4 Fusion Beams 5 Fusion Bolts Chapter 4 5 Preoperative Planning
SALVATION Fusion Bolts and Beams SURGICAL TECHNIQUE Contents Chapter 1 4 Introduction Chapter 2 4 Intended Use Chapter 3 4 Device Description 4 Fusion Beams 5 Fusion Bolts Chapter 4 5 Preoperative Planning
Zimmer Periarticular Elbow Locking Plate System
 Zimmer Periarticular Elbow Locking Plate System Surgical Technique The Right Solutions for Fractures Around the Elbow Disclaimer This document is intended exclusively for physicians and is not intended
Zimmer Periarticular Elbow Locking Plate System Surgical Technique The Right Solutions for Fractures Around the Elbow Disclaimer This document is intended exclusively for physicians and is not intended
V-TEK IVP System 2.7 System 4.0
 V-TEK IVP System Ankle 2.7 Fix System 4.0 Surgical Technique Surgical Technique Titanium osteosynthesis system for tibio-talar and tibio-talo-calcaneal fusion SECTION 1 Ankle Fix System 4.0 Titanium osteosynthesis
V-TEK IVP System Ankle 2.7 Fix System 4.0 Surgical Technique Surgical Technique Titanium osteosynthesis system for tibio-talar and tibio-talo-calcaneal fusion SECTION 1 Ankle Fix System 4.0 Titanium osteosynthesis
Achilles Tendon Repair, Operative Technique
 *smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
*smith&nephew ANKLE TECHNIQUE GUIDE Achilles Tendon Repair, Operative Technique Prepared in Consultation with: C. Niek van Dijk, MD, PhD KNEE HIP SHOULDER EXTREMITIES Achilles Tendon Repair, Operative
Zimmer Small Fragment Universal Locking System. Surgical Technique
 Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
Zimmer Small Fragment Universal Locking System Surgical Technique Zimmer Small Fragment Universal Locking System 1 Zimmer Small Fragment Universal Locking System Surgical Technique Table of Contents Introduction
How To Fix A Radial Head Plate
 Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Mayo Clinic CoNGRUENT RADIAL HEAD PLATE Since 1988 Acumed has been designing solutions to the demanding situations facing orthopedic surgeons, hospitals and their patients. Our strategy has been to know
Knotilus TM. Anchor Instability Repair. Technique Guide
 Knotilus TM Anchor Instability Repair Technique Guide Instability Repair Using the Knotilus TM Anchor Introduction While the shoulder has more mobility than any other joint in the body, it is also the
Knotilus TM Anchor Instability Repair Technique Guide Instability Repair Using the Knotilus TM Anchor Introduction While the shoulder has more mobility than any other joint in the body, it is also the
NCB Distal Femur System. Surgical Technique
 NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
NCB Distal Femur System Surgical Technique NCB Distal Femur System Surgical Technique 3 Surgical Technique NCB Distal Femur System Table of Contents Introduction 4 Indications 8 Preoperative Planning
Technique Guide. 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP). For minimally invasive osteosynthesis.
 Technique Guide 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP). For minimally invasive osteosynthesis. Table of Contents Introduction 3.5 mm and 4.5 mm Curved Locking Compression 2 Plates (LCP)
Technique Guide 3.5 mm and 4.5 mm Curved Locking Compression Plates (LCP). For minimally invasive osteosynthesis. Table of Contents Introduction 3.5 mm and 4.5 mm Curved Locking Compression 2 Plates (LCP)
Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery.
 Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by
Orthopedic Foot Instruments. Dedicated instruments for reconstructive foot surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by
OptiLock Periarticular Plating System For Proximal Tibial Fractures. Pre-Launch Surgical Technique
 OptiLock Periarticular Plating System For Proximal Tibial Fractures Pre-Launch Surgical Technique Contents Introduction... Page 1 Indications & Fracture Classifications... Page 4 Design Features... Page
OptiLock Periarticular Plating System For Proximal Tibial Fractures Pre-Launch Surgical Technique Contents Introduction... Page 1 Indications & Fracture Classifications... Page 4 Design Features... Page
CLAW II. Polyaxial Compression Plating System SURGIC A L T ECHNIQUE
 CLAW II Polyaxial Compression Plating System SURGIC A L T ECHNIQUE Contents Chapter 1 2 3 3 3 Chapter 2 4 4 7 Chapter 3 8 8 8 8 8 8 8 9 11 11 11 Chapter 4 12 Introduction Intended Use Indications Contraindications
CLAW II Polyaxial Compression Plating System SURGIC A L T ECHNIQUE Contents Chapter 1 2 3 3 3 Chapter 2 4 4 7 Chapter 3 8 8 8 8 8 8 8 9 11 11 11 Chapter 4 12 Introduction Intended Use Indications Contraindications
Technique Guide. Large Fragment LCP Instrument and Implant Set. Part of the Synthes locking compression plate (LCP) system.
 Technique Guide Large Fragment LCP Instrument and Implant Set. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction Large Fragment LCP Instrument and Implant Set
Technique Guide Large Fragment LCP Instrument and Implant Set. Part of the Synthes locking compression plate (LCP) system. Table of Contents Introduction Large Fragment LCP Instrument and Implant Set
PERIPROSTHETIC IMPLANTS
 PERIPROSTHETIC IMPLANTS PRODUCT OVERVIEW CLINICAL SOLUTIONS Periprosthetic fractures present unique challenges, such as how to gain fixation when the medullary canal is occupied. Special techniques and
PERIPROSTHETIC IMPLANTS PRODUCT OVERVIEW CLINICAL SOLUTIONS Periprosthetic fractures present unique challenges, such as how to gain fixation when the medullary canal is occupied. Special techniques and
The information contained in this document is intended for healthcare professionals only.
 The information contained in this document is intended for healthcare professionals only. Dall-Miles Cabling System Dall-Miles Recon and Trauma Cable System Trochanteric Reattachment Using the Trochanteric
The information contained in this document is intended for healthcare professionals only. Dall-Miles Cabling System Dall-Miles Recon and Trauma Cable System Trochanteric Reattachment Using the Trochanteric
Titanium Wire with Barb and Needle. For canthal tendon procedures.
 Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
Titanium Wire with Barb and Needle. For canthal tendon procedures. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Titanium Wire with Barb and Needle
LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle.
 LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for distribution
LCP Superior Clavicle Plate. The anatomically precontoured fixation system with angular stability for clavicle shaft and lateral clavicle. Surgical Technique This publication is not intended for distribution
TABLE OF CONTENTS. Surgical Technique 2. Indications 4. Product Information 5. 1. Patient Positioning and Approach 2
 Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
Surgical Technique TABLE OF CONTENTS Surgical Technique 2 1. Patient Positioning and Approach 2 2. Intervertebral Device Implanted 2 3. Buttress Plate Selection 2 4. Awl Insertion 2 5. Screw Insertion
Lentur Cable System. Surgical Technique
 Lentur Cable System Surgical Technique Contents Introduction... Page 1 System Design Features And Benefits... Page 2 Implants... Page 3 Instrumentation... Page 4 Surgical Technique... Page 5 Single Cable...
Lentur Cable System Surgical Technique Contents Introduction... Page 1 System Design Features And Benefits... Page 2 Implants... Page 3 Instrumentation... Page 4 Surgical Technique... Page 5 Single Cable...
Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System
 *smith&nephew SHOULDER TECHNIQUE GUIDE Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System KNEE HIP SHOULDER EXTREMITIES Arthroscopic
*smith&nephew SHOULDER TECHNIQUE GUIDE Arthroscopic Shoulder Instability Repair Using the SUTUREFIX ULTRA Suture Anchor and SUTUREFIX ULTRA Instrumentation System KNEE HIP SHOULDER EXTREMITIES Arthroscopic
Technique Guide. 2.7 mm/3.5 mm Variable Angle LCP Ankle Trauma System. Part of the Synthes variable angle locking compression plate (VA-LCP) system.
 Technique Guide 2.7 mm/3.5 mm Variable Angle LCP Ankle Trauma System. Part of the Synthes variable angle locking compression plate (VA-LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm Variable
Technique Guide 2.7 mm/3.5 mm Variable Angle LCP Ankle Trauma System. Part of the Synthes variable angle locking compression plate (VA-LCP) system. Table of Contents Introduction 2.7 mm/3.5 mm Variable
Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor
 Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Wrist and Hand. Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Fractures of the Wrist and Hand: Carpal bones
 Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
Patient Information Guide to Bone Fracture, Bone Reconstruction and Bone Fusion: Wrist and Hand Fractures of the Wrist and Hand: Fractures of the wrist The wrist joint is made up of the two bones in your
NCB Proximal Humerus System. Surgical Technique
 NCB Proximal Humerus System Surgical Technique NCB Proximal Humerus System Surgical Technique 3 Surgical Technique NCB Proximal Humerus System Table of Contents Introduction 4 Cable Fixation Options 5
NCB Proximal Humerus System Surgical Technique NCB Proximal Humerus System Surgical Technique 3 Surgical Technique NCB Proximal Humerus System Table of Contents Introduction 4 Cable Fixation Options 5
VariAx Distal Radius Locking Plate System. Anatomical & Universal Volar Plates Dorsal Plates Fragment Specific Plates
 VariAx Distal Radius Plate System Anatomical & Universal Volar Plates Dorsal Plates Fragment Specific Plates System Module The NEW VariAx Distal Radius Plating System represents the Next Generation of
VariAx Distal Radius Plate System Anatomical & Universal Volar Plates Dorsal Plates Fragment Specific Plates System Module The NEW VariAx Distal Radius Plating System represents the Next Generation of
4052 Slimplicity Tech final_layout 1 6/29/15 3:29 PM Page 2 Surgical Technique
 Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Surgical Technique TABLE OF CONTENTS Slimplicity Anterior Cervical Plate System Overview 2 Indications 2 Implants 3 Instruments 4 Surgical Technique 6 1. Patient Positioning and Approach 6 2. Plate Selection
Elbow System 2.0, 2.8
 SurgicAL TecHNiqUE STEP by step Elbow System 2.0, 2.8 APTUS Elbow 2 Elbow System 2.0, 2.8 Elbow System 2.0, 2.8 3 Elbow System 2.0, 2.8 Contents 4-5 Features, Technique 6-13 Introduction and Indications
SurgicAL TecHNiqUE STEP by step Elbow System 2.0, 2.8 APTUS Elbow 2 Elbow System 2.0, 2.8 Elbow System 2.0, 2.8 3 Elbow System 2.0, 2.8 Contents 4-5 Features, Technique 6-13 Introduction and Indications
Aesculap Veterinary Orthopaedics. Targon VET Interlocking Nail
 Aesculap Veterinary Orthopaedics Targon VET Interlocking Nail Flexibility Stability Dynamics The Targon VET is based on new, technology which reverses the known principles of interlocking nails. The rotation-stabilising
Aesculap Veterinary Orthopaedics Targon VET Interlocking Nail Flexibility Stability Dynamics The Targon VET is based on new, technology which reverses the known principles of interlocking nails. The rotation-stabilising
LCP Compact Foot/Compact Hand.
 LCP Compact Foot/Compact Hand. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of contents Indications 2
LCP Compact Foot/Compact Hand. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table of contents Indications 2
Mini TightRope CMC Surgical Technique
 Mini TightRope CMC Surgical Technique Mini TightRope CMC Mini TightRope CMC Fixation The Mini TightRope provides a unique means to suspend the thumb metacarpal after partial or complete trapezial resection
Mini TightRope CMC Surgical Technique Mini TightRope CMC Mini TightRope CMC Fixation The Mini TightRope provides a unique means to suspend the thumb metacarpal after partial or complete trapezial resection
DARCO MRS. Locked Plating System for Reconstructive Rearfoot Surgery
 DARCO MRS Locked Plating System for Reconstructive Rearfoot Surgery DARCO MRS Locked plating system for reconstructive rearfoot surgery System Basics The DARCO MRS plating system for the rearfoot has been
DARCO MRS Locked Plating System for Reconstructive Rearfoot Surgery DARCO MRS Locked plating system for reconstructive rearfoot surgery System Basics The DARCO MRS plating system for the rearfoot has been
TransFx External Fixation System Large and Intermediate Surgical Technique
 TransFx External Fixation System Large and Intermediate Surgical Technique TransFx External Fixation System Large and Intermediate Surgical Technique 1 Surgical Technique For TransFx External Fixation
TransFx External Fixation System Large and Intermediate Surgical Technique TransFx External Fixation System Large and Intermediate Surgical Technique 1 Surgical Technique For TransFx External Fixation
Technique Guide. 4.5 mm LCP Proximal Femur Plates. Part of the Synthes Periarticular LCP Plating System.
 Technique Guide 4.5 mm LCP Proximal Femur Plates. Part of the Synthes Periarticular LCP Plating System. Table of Contents Introduction 4.5 mm LCP Proximal Femur Plates 2 AO Principles 4 Indications 5 Surgical
Technique Guide 4.5 mm LCP Proximal Femur Plates. Part of the Synthes Periarticular LCP Plating System. Table of Contents Introduction 4.5 mm LCP Proximal Femur Plates 2 AO Principles 4 Indications 5 Surgical
the revo / mini-revo shoulder fixation system s u r g i c a l t e c h n i q u e
 the revo / mini-revo shoulder fixation system s u r g i c a l t e c h n i q u e REVO The following techniques are described by Stephen J. Snyder, M.D., Van Nuys, CA. Arthroscopic repair of the rotator
the revo / mini-revo shoulder fixation system s u r g i c a l t e c h n i q u e REVO The following techniques are described by Stephen J. Snyder, M.D., Van Nuys, CA. Arthroscopic repair of the rotator
Technique Guide. Orthopaedic Cable System. Cerclage solutions for general surgery.
 Technique Guide Orthopaedic Cable System. Cerclage solutions for general surgery. Table of Contents Introduction The Orthopaedic Cable System 2 Indications 4 Contraindications 4 Surgical Technique Cerclage
Technique Guide Orthopaedic Cable System. Cerclage solutions for general surgery. Table of Contents Introduction The Orthopaedic Cable System 2 Indications 4 Contraindications 4 Surgical Technique Cerclage
NCB Periprosthetic Femur Plate System. Surgical Technique
 NCB Periprosthetic Femur Plate System Surgical Technique NCB Periprosthetic Femur System Surgical Technique 3 Table of Contents Introduction 4 System Features and Benefits 9 Indications and Contraindications
NCB Periprosthetic Femur Plate System Surgical Technique NCB Periprosthetic Femur System Surgical Technique 3 Table of Contents Introduction 4 System Features and Benefits 9 Indications and Contraindications
Technique Guide. 2.4 mm LCP Distal Radius System. A comprehensive plating system to address a variety of fracture patterns.
 Technique Guide 2.4 mm LCP Distal Radius System. A comprehensive plating system to address a variety of fracture patterns. Table of Contents Introduction 2.4 mm LCP Distal Radius System 2 AO Principles
Technique Guide 2.4 mm LCP Distal Radius System. A comprehensive plating system to address a variety of fracture patterns. Table of Contents Introduction 2.4 mm LCP Distal Radius System 2 AO Principles
How To Use A Phoenix Retrograde Femoral Nail
 Phoenix Retrograde Femoral Nail System Featuring CoreLock Technology Surgical Technique Contents Introduction... Page 1 Indications... Page 2 Design Features... Page 3 Surgical Technique... Page 6 Product
Phoenix Retrograde Femoral Nail System Featuring CoreLock Technology Surgical Technique Contents Introduction... Page 1 Indications... Page 2 Design Features... Page 3 Surgical Technique... Page 6 Product
Comprehensive Reverse Shoulder System
 Comprehensive Reverse Shoulder System Surgical Technique Knees Hips Extremities Cement and Accessories PMI Trauma Technology One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon
Comprehensive Reverse Shoulder System Surgical Technique Knees Hips Extremities Cement and Accessories PMI Trauma Technology One Surgeon. One Patient. Over 1 million times per year, Biomet helps one surgeon
Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion
 Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Integra. Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE
 Integra Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE Table of contents Introduction Description... 2 Indications... 2 Contraindications... 2 Surgical Technique Step 1: Incision and Dissection...3
Integra Subtalar MBA and bioblock Implant SURGICAL TECHNIQUE Table of contents Introduction Description... 2 Indications... 2 Contraindications... 2 Surgical Technique Step 1: Incision and Dissection...3
Rotator Cuff Tears in Football
 Disclosures Rotator Cuff Tears in Football Roger Ostrander, MD Consultant: Mitek Consultant: On-Q Research Support: Arthrex Research Support: Breg Research Support: Arthrosurface 2 Anatomy 4 major muscles:
Disclosures Rotator Cuff Tears in Football Roger Ostrander, MD Consultant: Mitek Consultant: On-Q Research Support: Arthrex Research Support: Breg Research Support: Arthrosurface 2 Anatomy 4 major muscles:
Minimally Invasive Hip Replacement through the Direct Lateral Approach
 Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
Surgical Technique INNOVATIONS IN MINIMALLY INVASIVE JOINT SURGERY Minimally Invasive Hip Replacement through the Direct Lateral Approach *smith&nephew Introduction Prosthetic replacement of the hip joint
(English) NEXUS SPINE SPACER SYSTEM
 (English) NEXUS SPINE SPACER SYSTEM INDICATIONS FOR USE NEXUS Spine Spacer System, a GEO Structure is indicated for use in the thoraco-lumbar spine (i.e., T1 to L5) to replace a diseased vertebral body
(English) NEXUS SPINE SPACER SYSTEM INDICATIONS FOR USE NEXUS Spine Spacer System, a GEO Structure is indicated for use in the thoraco-lumbar spine (i.e., T1 to L5) to replace a diseased vertebral body
Technique Guide. DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation.
 Technique Guide DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation. Table of Contents Introduction Dynamic Hip Screw (DHS) 2 Dynamic Condylar Screw (DCS) 3 Indications
Technique Guide DHS/DCS Dynamic Hip and Condylar Screw System. Designed to provide stable internal fixation. Table of Contents Introduction Dynamic Hip Screw (DHS) 2 Dynamic Condylar Screw (DCS) 3 Indications
ZIMMER BIGLIANI/ FLATOW THE COMPLETE SHOULDER SOLUTION. Total Shoulder Arthroplasty Surgical Technique
 ZIMMER BIGLIANI/ FLATOW THE COMPLETE SHOULDER SOLUTION Total Shoulder Arthroplasty Surgical Technique BIGLIANI/FLATOW THE COMPLETE SHOULDER SOLUTION SURGICAL TECHNIQUE Instruments and surgical technique
ZIMMER BIGLIANI/ FLATOW THE COMPLETE SHOULDER SOLUTION Total Shoulder Arthroplasty Surgical Technique BIGLIANI/FLATOW THE COMPLETE SHOULDER SOLUTION SURGICAL TECHNIQUE Instruments and surgical technique
TriLock 1.5 Implants for the Phalanges
 P R O D U C T IN F O RM AT I O N TriLock 1.5 Implants for the Phalanges APTUS Hand 2 TriLock 1.5 Implants for the Phalanges TriLock 1.5 The Smallest Locking System Small, slender, strong Low profile and
P R O D U C T IN F O RM AT I O N TriLock 1.5 Implants for the Phalanges APTUS Hand 2 TriLock 1.5 Implants for the Phalanges TriLock 1.5 The Smallest Locking System Small, slender, strong Low profile and
Malleolar fractures Anna Ekman, Lena Brauer
 Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
Malleolar fractures Anna Ekman, Lena Brauer How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning
Bigliani/Flatow The Complete Shoulder Solution TSA
 Bigliani/Flatow The Complete Shoulder Solution TSA Surgical Technique Replicates natural shoulder mobility, balance, and stability Bigliani/Flatow The Complete Shoulder Solution Surgical Technique 1 Bigliani/Flatow
Bigliani/Flatow The Complete Shoulder Solution TSA Surgical Technique Replicates natural shoulder mobility, balance, and stability Bigliani/Flatow The Complete Shoulder Solution Surgical Technique 1 Bigliani/Flatow
Implant materials. Learning outcomes. Implant materials in trauma. How to use this handout? Functions of implants. Types of materials
 Implant materials How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning outcomes At the end of
Implant materials How to use this handout? The left column is the information as given during the lecture. The column at the right gives you space to make personal notes. Learning outcomes At the end of
Zimmer Natural Nail System. Cephalomedullary Nail Surgical Technique STANDARD
 Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique STANDARD Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique - Standard 1 Zimmer Natural Nail System Cephalomedullary
Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique STANDARD Zimmer Natural Nail System Cephalomedullary Nail Surgical Technique - Standard 1 Zimmer Natural Nail System Cephalomedullary
Shoulder Restoration System
 Shoulder Restoration System PopLok Knotless Suture Anchor Simple, Secure, Versatile all-peek knotless anchor system for rotator cuff and instability repairs CO M M I T T ED TO I N N OVATI O N SURGICAL
Shoulder Restoration System PopLok Knotless Suture Anchor Simple, Secure, Versatile all-peek knotless anchor system for rotator cuff and instability repairs CO M M I T T ED TO I N N OVATI O N SURGICAL
Stabilization of Acute Acromioclavicular Joint Dislocations using Dog Bone Button Technology Surgical Technique
 Stabilization of Acute Acromioclavicular Joint Dislocations using Dog Bone Button Technology Surgical Technique AC Repair - Dog Bone Button Stabilization of Acute Acromioclavicular Joint Dislocations using
Stabilization of Acute Acromioclavicular Joint Dislocations using Dog Bone Button Technology Surgical Technique AC Repair - Dog Bone Button Stabilization of Acute Acromioclavicular Joint Dislocations using
Scout Vessel Guard. A cover for vessels during anterior lumbar spine surgery.
 Scout Vessel Guard. A cover for vessels during anterior lumbar spine surgery. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Scout Vessel Guard 2
Scout Vessel Guard. A cover for vessels during anterior lumbar spine surgery. Technique Guide Instruments and implants approved by the AO Foundation Table of Contents Introduction Scout Vessel Guard 2
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL)
 Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Anatomic Percutaneous Ankle Reconstruction of Lateral Ligaments (A Percutaneous Anti ROLL) Mark Glazebrook James Stone Masato Takao Stephane Guillo Introduction Ankle stabilization is required when a patient
Posterior Referencing. Surgical Technique
 Posterior Referencing Surgical Technique Posterior Referencing Surgical Technique INTRO Introduction Instrumentation Successful total knee arthroplasty depends in part on re-establishment of normal lower
Posterior Referencing Surgical Technique Posterior Referencing Surgical Technique INTRO Introduction Instrumentation Successful total knee arthroplasty depends in part on re-establishment of normal lower
Adult Forearm Fractures
 Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
Adult Forearm Fractures Your forearm is made up of two bones, the radius and ulna. In most cases of adult forearm fractures, both bones are broken. Fractures of the forearm can occur near the wrist at
ACTIV ANKLE DISTAL AND DIAPHYSEAL FIBULA INNOVATION MEANS MOTION
 ACTIV ANKLE DISTAL AND DIAPHYSEAL FIBULA POLYAXIAL LOCKING FIXATION DUALTEC SYSTEM II Precontoured implants Polyaxiality of 20 2 surgical approaches : lateral and posterolateral ACTIV ANKLE The ACTIV ANKLE
ACTIV ANKLE DISTAL AND DIAPHYSEAL FIBULA POLYAXIAL LOCKING FIXATION DUALTEC SYSTEM II Precontoured implants Polyaxiality of 20 2 surgical approaches : lateral and posterolateral ACTIV ANKLE The ACTIV ANKLE
MINI FRAGMENT SYSTEM. Instruments and implants for 1.5 mm, 2.0 mm, and 2.4 mm plate fixation PRODUCT OVERVIEW
 MINI FRAGMENT SYSTEM Instruments and implants for 1.5 mm, 2.0 mm, and 2.4 mm plate fixation PRODUCT OVERVIEW TABLE OF CONTENTS INTRODUCTION Mini Fragment System 2 PRODUCT INFORMATION Plates 4 Screws 6
MINI FRAGMENT SYSTEM Instruments and implants for 1.5 mm, 2.0 mm, and 2.4 mm plate fixation PRODUCT OVERVIEW TABLE OF CONTENTS INTRODUCTION Mini Fragment System 2 PRODUCT INFORMATION Plates 4 Screws 6
Modular Sternal Cable System. Flexibility and strength in sternal closure and repair.
 Modular Sternal Cable System. Flexibility and strength in sternal closure and repair. Multiple closure options Stable fixation in all configurations Improved strength and flexibility compared to wire Modular
Modular Sternal Cable System. Flexibility and strength in sternal closure and repair. Multiple closure options Stable fixation in all configurations Improved strength and flexibility compared to wire Modular
Versa-Fx II Femoral Fixation System Surgical Techniques
 Versa-Fx II Femoral Fixation System Surgical Techniques Versa-Fx II Femoral Fixation System Surgical Techniques 1 Surgical Technique For Fixation Of Intertrochanteric and Supracondylar Fractures of the
Versa-Fx II Femoral Fixation System Surgical Techniques Versa-Fx II Femoral Fixation System Surgical Techniques 1 Surgical Technique For Fixation Of Intertrochanteric and Supracondylar Fractures of the
Total Shoulder System. Anatomic adaptability... simplified SURGICAL TECHNIQUE
 Total Shoulder System Anatomic adaptability... simplified SURGICAL TECHNIQUE Inclination Version Offset 125-140 +/- 10 3.5 mm A of Possibilities I III The Univers II Total Shoulder System was designed
Total Shoulder System Anatomic adaptability... simplified SURGICAL TECHNIQUE Inclination Version Offset 125-140 +/- 10 3.5 mm A of Possibilities I III The Univers II Total Shoulder System was designed
Technique Guide. Screw Removal Set. Instruments for removing Synthes screws.
 Technique Guide Screw Removal Set. Instruments for removing Synthes screws. Table of Contents Introduction Screw Removal Set 2 Surgical Technique Preoperative Planning and Preparation 6 Removal of Intact
Technique Guide Screw Removal Set. Instruments for removing Synthes screws. Table of Contents Introduction Screw Removal Set 2 Surgical Technique Preoperative Planning and Preparation 6 Removal of Intact
.org. Rotator Cuff Tears: Surgical Treatment Options. When Rotator Cuff Surgery is Recommended. Surgical Repair Options
 Rotator Cuff Tears: Surgical Treatment Options Page ( 1 ) The following article provides in-depth information about surgical treatment for rotator cuff injuries, and is a continuation of the article Rotator
Rotator Cuff Tears: Surgical Treatment Options Page ( 1 ) The following article provides in-depth information about surgical treatment for rotator cuff injuries, and is a continuation of the article Rotator
LCP Olecranon Plate. The anatomical fixation system with angular stability for olecranon and proximal ulnar fractures.
 LCP Olecranon Plate. The anatomical fixation system with angular stability for olecranon and proximal ulnar fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments
LCP Olecranon Plate. The anatomical fixation system with angular stability for olecranon and proximal ulnar fractures. Surgical Technique This publication is not intended for distribution in the USA. Instruments
Surgical Technique. Clavicle Plating System Acu-Sinch Repair System
 Surgical Technique Clavicle Plating System Acu-Sinch Repair System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and
Surgical Technique Clavicle Plating System Acu-Sinch Repair System Acumed is a global leader of innovative orthopaedic and medical solutions. We are dedicated to developing products, service methods, and
FUSEFORCE. Hand Fixation System SURGIC A L T ECHNIQUE
 FUSEFORCE Hand Fixation System SURGIC A L T ECHNIQUE Contents Chapter 1 3 Chapter 2 4 Appendix A 7 Intended Use Surgical Technique Ordering Information Indication Sizing Reference Proper surgical procedures
FUSEFORCE Hand Fixation System SURGIC A L T ECHNIQUE Contents Chapter 1 3 Chapter 2 4 Appendix A 7 Intended Use Surgical Technique Ordering Information Indication Sizing Reference Proper surgical procedures
Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy
 Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Anterior Capsule reconstruction is a surgical procedure utilized for anterior
Anterior Capsular Repair Rehabilitation Program Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy Anterior Capsule reconstruction is a surgical procedure utilized for anterior
Integra. MCP Joint Replacement PATIENT INFORMATION
 Integra MCP Joint Replacement PATIENT INFORMATION Integra MCP Patient Information This brochure summarizes information about the use, risks, and benefits of the Integra MCP finger implant. Be sure to discuss
Integra MCP Joint Replacement PATIENT INFORMATION Integra MCP Patient Information This brochure summarizes information about the use, risks, and benefits of the Integra MCP finger implant. Be sure to discuss
ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning. Orthodontics and Implantology
 ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning Orthodontics and Implantology 2 All rights are reserved. Any reproduction of the present publication is prohibited in whole or in part and by
ORTHODONTIC MINI IMPLANTS Clinical procedure for positioning Orthodontics and Implantology 2 All rights are reserved. Any reproduction of the present publication is prohibited in whole or in part and by
Cable System. For Orthopaedic Trauma Surgery.
 Cable System. For Orthopaedic Trauma Surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
Cable System. For Orthopaedic Trauma Surgery. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Image intensifier
TwinFix Cannulated Compression Screw
 TwinFix Cannulated Compression Screw Leibinger Solutions for Hand Surgery Procedural Guide TwinFix Sterilization, Organization, Storage 29-12020 Profyle MODULAR Sterilizing Container 29-40162 TwinFix Implant
TwinFix Cannulated Compression Screw Leibinger Solutions for Hand Surgery Procedural Guide TwinFix Sterilization, Organization, Storage 29-12020 Profyle MODULAR Sterilizing Container 29-40162 TwinFix Implant
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach.
 Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Anterior Lumbar Interbody Fusion (ALIF). Instrument set supports placement of ALIF spacers using anterior or anterolateral approach. Technique Guide Instruments and implants approved by the AO Foundation
Integra. Subtalar MBA Implant
 Integra Subtalar MBA Implant Patient EDUCATION Overview: What is Flatfoot? Flatfoot is a physical deformity where there is an absence of the arch that runs from the heel of the foot to the toes. A common
Integra Subtalar MBA Implant Patient EDUCATION Overview: What is Flatfoot? Flatfoot is a physical deformity where there is an absence of the arch that runs from the heel of the foot to the toes. A common
LOMAS / MONDEFIT ORTHODONTICS. The most innovative anchorage method for tooth correction
 LOMAS / MONDEFIT The most innovative anchorage method for tooth correction No extraction of healthy teeth Completion of tooth correction without gaps Symmetrical, beautiful smile For young people and young
LOMAS / MONDEFIT The most innovative anchorage method for tooth correction No extraction of healthy teeth Completion of tooth correction without gaps Symmetrical, beautiful smile For young people and young
Fracture Care Coding September 28, 2011
 Fracture Care Coding September 28, 2011 Julie Edens Leu, CPC, CPCO, CPMA, CPC-I 1 Disclaimer Every reasonable effort has been made to ensure that the educational material provided today is accurate and
Fracture Care Coding September 28, 2011 Julie Edens Leu, CPC, CPCO, CPMA, CPC-I 1 Disclaimer Every reasonable effort has been made to ensure that the educational material provided today is accurate and
Technique Guide. Norian SRS Fast Set Putty. Calcium phosphate bone void filler.
 Technique Guide Norian SRS Fast Set Putty. Calcium phosphate bone void filler. TableofContents Introduction Norian SRS Fast Set Putty 2 Indications and Contraindications 3 Basic Science 4 Surgical Technique
Technique Guide Norian SRS Fast Set Putty. Calcium phosphate bone void filler. TableofContents Introduction Norian SRS Fast Set Putty 2 Indications and Contraindications 3 Basic Science 4 Surgical Technique
TABLE OF CONTENTS. Indications and Contraindications 3. Features and Benefits 4. Ease of connection 4 Stable fixation concept 5
 Surgical Technique TABLE OF CONTENTS Indications and Contraindications 3 Features and Benefits 4 Ease of connection 4 Stable fixation concept 5 Surgical Technique Steps 6 Identification and preparation
Surgical Technique TABLE OF CONTENTS Indications and Contraindications 3 Features and Benefits 4 Ease of connection 4 Stable fixation concept 5 Surgical Technique Steps 6 Identification and preparation
INTRODUCTION Cerclage Cable Vs. Monofilament Wire
 B M P CABLE S Y S T E M S U R G I C A L TECHNIQUE INTRODUCTION The Biomet Medical Products (BMP ) Cable System provides a cost effective and simple method of trochanteric reattachment, fracture fixation,
B M P CABLE S Y S T E M S U R G I C A L TECHNIQUE INTRODUCTION The Biomet Medical Products (BMP ) Cable System provides a cost effective and simple method of trochanteric reattachment, fracture fixation,
ANTERIOR CERVICAL DISCECTOMY AND FUSION. Basic Anatomical Landmarks: Anterior Cervical Spine
 Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Anterior In the human anatomy, referring to the front surface of the body or position of one structure relative to another Cervical Relating to the neck, in the spine relating to the first seven vertebrae
Implant Extraction Guide Module One & Two
 Implant Extraction Set Implant Extraction Guide Module One & Two 1 Contents Page 1. Introduction 3 Introduction 3 Features and Benefits 3 Contraindications 3 2. Product Description 4 3. Technical Details
Implant Extraction Set Implant Extraction Guide Module One & Two 1 Contents Page 1. Introduction 3 Introduction 3 Features and Benefits 3 Contraindications 3 2. Product Description 4 3. Technical Details
A Simplified Approach to Common Shoulder Problems
 A Simplified Approach to Common Shoulder Problems Objectives: Understand the basic categories of common shoulder problems. Understand the common patient symptoms. Understand the basic exam findings. Understand
A Simplified Approach to Common Shoulder Problems Objectives: Understand the basic categories of common shoulder problems. Understand the common patient symptoms. Understand the basic exam findings. Understand
Ms. Ruth Delaney ROTATOR CUFF DISEASE Orthopaedic Surgeon, Shoulder Specialist
 WHAT DOES THE ROTATOR CUFF DO? WHAT DOES THE ROTATOR CUFF DO? WHO GETS ROTATOR CUFF TEARS? HOW DO I CLINICALLY DIAGNOSE A CUFF TEAR? WHO NEEDS AN MRI? DOES EVERY CUFF TEAR NEED TO BE FIXED? WHAT DOES ROTATOR
WHAT DOES THE ROTATOR CUFF DO? WHAT DOES THE ROTATOR CUFF DO? WHO GETS ROTATOR CUFF TEARS? HOW DO I CLINICALLY DIAGNOSE A CUFF TEAR? WHO NEEDS AN MRI? DOES EVERY CUFF TEAR NEED TO BE FIXED? WHAT DOES ROTATOR
Ankle Syndesmosis Surgical Protocol by Timothy Charlton, M.D.
 Featuring Ankle Syndesmosis Surgical Protocol by Timothy Charlton, M.D. ZipLoop Technology is a unique weave in which a single strand of braided polyethylene is woven through itself twice in opposite directions.
Featuring Ankle Syndesmosis Surgical Protocol by Timothy Charlton, M.D. ZipLoop Technology is a unique weave in which a single strand of braided polyethylene is woven through itself twice in opposite directions.
MatrixNEURO. The next generation cranial plating system.
 MatrixNEURO. The next generation cranial plating system. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table
MatrixNEURO. The next generation cranial plating system. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation. Table
.org. Shoulder Pain and Common Shoulder Problems. Anatomy. Cause
 Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Technique Guide. Reamer/Irrigator/Aspirator (RIA). For intramedullary reaming and bone harvesting.
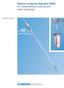 Technique Guide Reamer/Irrigator/Aspirator (RIA). For intramedullary reaming and bone harvesting. Table of Contents Introduction Reamer/ Irrigator/ Aspirator (RIA) 2 Indications 4 Surgical Technique Preparation
Technique Guide Reamer/Irrigator/Aspirator (RIA). For intramedullary reaming and bone harvesting. Table of Contents Introduction Reamer/ Irrigator/ Aspirator (RIA) 2 Indications 4 Surgical Technique Preparation
THE REVERSE SHOULDER REPLACEMENT
 THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
Information for the Patient About Surgical
 Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Information for the Patient About Surgical Decompression and Stabilization of the Spine Aging and the Spine Daily wear and tear, along with disc degeneration due to aging and injury, are common causes
Upper Limb QUESTIONS UPPER LIMB: QUESTIONS
 1 Upper Limb QUESTIONS 1.1 Which of the following statements best describes the scapula? a. It usually overlies the 2nd to 9th ribs. b. The spine continues laterally as the coracoid process. c. The suprascapular
1 Upper Limb QUESTIONS 1.1 Which of the following statements best describes the scapula? a. It usually overlies the 2nd to 9th ribs. b. The spine continues laterally as the coracoid process. c. The suprascapular
Chapter 5. The Shoulder Joint. The Shoulder Joint. Bones. Bones. Bones
 Copyright The McGraw-Hill Companies, Inc. Reprinted by permission. Chapter 5 The Shoulder Joint Structural Kinesiology R.T. Floyd, Ed.D, ATC, CSCS Structural Kinesiology The Shoulder Joint 5-1 The Shoulder
Copyright The McGraw-Hill Companies, Inc. Reprinted by permission. Chapter 5 The Shoulder Joint Structural Kinesiology R.T. Floyd, Ed.D, ATC, CSCS Structural Kinesiology The Shoulder Joint 5-1 The Shoulder
Labral Repair. Surgical Protocol by Ronald Glousman, M.D. and Nicholas Sgaglione, M.D.
 Labral Repair Surgical Protocol by Ronald Glousman, M.D. and Nicholas Sgaglione, M.D. It s small. It s strong. And it's all suture. The JuggerKnot Soft Anchor represents the next generation of suture anchor
Labral Repair Surgical Protocol by Ronald Glousman, M.D. and Nicholas Sgaglione, M.D. It s small. It s strong. And it's all suture. The JuggerKnot Soft Anchor represents the next generation of suture anchor
North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com
 North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com Physical Therapy Protocol for Patients Following Shoulder Surgery -Rotator Cuff
North Shore Shoulder Dr.Robert E. McLaughlin II 1-855-SHOULDER 978-969-3624 Fax: 978-921-7597 www.northshoreshoulder.com Physical Therapy Protocol for Patients Following Shoulder Surgery -Rotator Cuff
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T
 THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
THE SHOULDER JOINT T H E G L E N O H U M E R A L ( G H ) J O I N T CLARIFICATION OF TERMS Shoulder girdle = scapula and clavicle Shoulder joint (glenohumeral joint) = scapula and humerus Lippert, p115
Technique Guide. VersiTomic. Michael A. Rauh, MD. Anterior Cruciate Ligament Reconstruction
 Technique Guide VersiTomic Anterior Cruciate Ligament Reconstruction Michael A. Rauh, MD The opinions expressed are those of Dr. Rauh and are not necessarily those of Stryker VersiTomic Anterior Cruciate
Technique Guide VersiTomic Anterior Cruciate Ligament Reconstruction Michael A. Rauh, MD The opinions expressed are those of Dr. Rauh and are not necessarily those of Stryker VersiTomic Anterior Cruciate
Technique Guide. Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures.
 Technique Guide Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Table of Contents Introduction Titanium Trochanteric Fixation Nail System 2 Biomechanical
Technique Guide Titanium Trochanteric Fixation Nail System. For intramedullary fixation of proximal femur fractures. Table of Contents Introduction Titanium Trochanteric Fixation Nail System 2 Biomechanical
Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S.
 Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S. Global-HELP Publications Chapter Eight: TECHNICAL REQUIREMENTS FOR FORMATION OF A TUBED PEDICLE FLAP Creating a tube pedicle
Abdominal Pedicle Flaps To The Hand And Forearm John C. Kelleher M.D., F.A.C.S. Global-HELP Publications Chapter Eight: TECHNICAL REQUIREMENTS FOR FORMATION OF A TUBED PEDICLE FLAP Creating a tube pedicle
Lateral Ankle Instability Repair using TWINFIX Ti 3.5 mm Suture Anchors
 *smith&nephew ANKLE TECHNIQUE GUIDE Lateral Ankle Instability Repair using TWINFIX Ti 3.5 mm Suture Anchors Prepared in Consultation with: James Calder, MD KNEE HIP SHOULDER EXTREMITIES Lateral Ankle Instability
*smith&nephew ANKLE TECHNIQUE GUIDE Lateral Ankle Instability Repair using TWINFIX Ti 3.5 mm Suture Anchors Prepared in Consultation with: James Calder, MD KNEE HIP SHOULDER EXTREMITIES Lateral Ankle Instability
METAL HEMI. Great Toe Implant SURGICAL TECHNIQUE
 METAL HEMI Great Toe Implant SURGICAL TECHNIQUE Contents Chapter 1 4 Product Information 4 Device Description Chapter 2 5 Intended Use 5 Indications 5 Contraindications Chapter 3 6 Surgical Technique
METAL HEMI Great Toe Implant SURGICAL TECHNIQUE Contents Chapter 1 4 Product Information 4 Device Description Chapter 2 5 Intended Use 5 Indications 5 Contraindications Chapter 3 6 Surgical Technique
