Tracheostomy (trach) Tracheostomy 1
|
|
|
- Ernest Conley
- 9 years ago
- Views:
Transcription
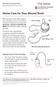
1 Tracheostomy (trach) Purpose of the tracheostomy A tracheostomy is an opening in the windpipe (trachea) that your baby breathes through instead of breathing through his nose and mouth. Often the tracheostomy is not permanent and can be removed after the problem has been corrected or the baby grows and no longer needs the tracheostomy. Babies with the following problems may get a tracheostomy: 1. Birth defects that affect the baby s breathing. 2. Noisy breathing caused by a soft or weak breathing tube. This causes him to have difficulty breathing. The noise is called stridor and the problem is called tracheomalacia. 3. Needs to be on a ventilator for a very long time. 4. BPD (Bronchopulmonary Dysplasia) with long term oxygen requirements. Anatomy 1. A small opening is made from the skin to the windpipe (trachea) by a cut in the neck for a tracheostomy. 2. A tracheostomy tube is a short piece of plastic that is placed into the trachea through a surgical hole in the neck. It does not reach into the lung. 3. The baby breathes through this plastic tube instead of through his nose and mouth. 4. You will not be able to hear the baby cry or talk with the tracheostomy tube in at first. He can learn to talk with the tube. Tracheostomy 1
2 Apnea monitor 1. The baby will go home on a home apnea and cardiac monitor. The monitor counts the baby s breathing rate and heart rate. 2. The monitor alarms to tell you if the baby is not breathing (apnea) or if the heart beat is too slow (bradycardia). Changing tracheostomy ties 1. Supplies twill tape or bias seam tape or shoe laces or velcro holder blanket roll for shoulders scissors blanket for mummy restraint-it may be necessary to wrap baby snugly to prevent wiggling 2. Changing the ties: do not change the tracheostomy ties by yourself unless absolutely necessary. change ties daily or when: ties become loose (should fit snugly when neck is bent forward). ties become wet or dirty. square knot causes pressure on your baby s skin. the trach is changed. suction before changing ties. Suctioning decreases chances of the baby s coughing while ties are off. Movement of the tube often causes the baby to cough and bring up mucus. changing ties requires two people one person to hold tube in place and position baby and the other person to change the ties. place blanket roll under shoulders to expose tracheostomy area. 2 Tracheostomy
3 slide old ties from center of hole to top on both sides of the tracheostomy tube. insert new ties under old ones. secure new ties with a square knot. Ties should be tight enough to easily slip one finger underneath the tape. cut off old ties and remove. Guard tips of scissors with your fingers. examine neck daily for redness, skin breakdown or rashes. If using trach holder: remove one side of velcro holder while holding the trach in place. Thread the clean holder in this side, then go to the other side and repeat the process. clean the dirty trach holder with warm soapy water and hang or lay flat to dry. It may be used for up to a month. Cleaning the tracheostomy opening (stoma) 1. Supplies: tap water Q-tips or cotton swab basin gauze trach dressing 2. Cleaning clean area around tracheostomy opening in neck (stoma) daily and when the area is soiled. support tracheostomy tube with a finger while cleaning. roll Q-tip dipped in water over skin under tracheostomy tube to remove crusted secretions. rinse with Q-tip dipped in clear water. Pat dry with gauze or clean cloth. wash skin around neck with clear water and a mild soap such as Basis Neutrogena. Tracheostomy 3
4 3. Place gauze trach dressing around trach tube. Change dressing as often as necessary to keep skin dry. may use pre-cut trach dressings (more expensive). may use 4x4 gauze without fiber filling. Fold to fit under trach tube. Do not cut gauze because small fibers can get in the trach and windpipe. 4. Clean stoma two or three times a day if an odor is present (or more often, if there is drainage present). 5. Powders and lotions must not be used around the trach stoma. 6. If ordered by the baby s doctor to treat irritations or rashes, apply ointments in a thin layer. (Ointments under the trach collar can make the skin irritation worse. Sometimes clean and dry is best.) Changing the tracheostomy tube 1. Equipment tracheostomy tube with obturator (guide) shoestring ties or twill tape scissors blanket roll to support shoulders blanket for mummy restraint-it may be necessary to wrap baby to prevent wiggling oxygen tank with Ambu bag attached 2. Changing the tracheostomy tube Do not change the tracheostomy tube by yourself unless absolutely necessary. WASH YOUR HANDS suction baby before changing trach tube. attach ties to new or clean trach tube with obturator in place. The obturator serves as a guide to provide easy insertion of the trach tube. Obturator out Obturator in place 4 Tracheostomy
5 lubricate the new trach with a small amount of water soluble lubricant or saline. place tube in the sterile tray until ready to insert new or cleaned tube. Keep tube portion sterile. place blanket roll under shoulders to expose neck area. a mummy restraint may be necessary to prevent baby from wiggling. cut old ties. Removing old trach Inserting new or cleaned trach remove old trach tube with one hand using an up-and-out motion (follow angle of tube). insert new or cleaned tube gently. Direct tube back and down. remove obturator as soon as the tube is in place. Your baby cannot breathe unless the guide (obturator) is removed. tie snugly in place. allow baby to breathe until calm (a few seconds), supporting trach tube with your finger. 3. Your baby may cough, cry, turn red, or sweat. He is OK. This does not hurt the baby. Calm him by talking and holding. Give him a few breaths with the Ambu bag or a little extra blow-by oxygen to calm him. A pacifier may help. 4. Change the trach tube every 1-2 weeks (as directed by your baby s doctor) or for: distressed infant who does not respond to suctioning or usual calming methods bleeding from tracheostomy tube. difficulty inserting suction catheter. whistling through trach which is not relieved by suctioning. Tracheostomy 5
6 5. Change tube before feeding or at least 2 hours after feeding. Avoid changing just before feeding if your baby is upset because of hunger. 6. Inspect the removed tube for color change, mucus plugs or odor. Cleaning the tracheostomy tube The medical equipment supply company will teach you how to clean the tracheostomy tubes and what to use for cleaning. Moisture requirements A nebulizer and tracheostomy collar (trach collar) are used to filter and moisten air entering the windpipe (trachea) because the baby does not breathe through his nose or mouth. 1. Supplies air compressor machine cascade humidifier with mounting bracket, nebulizer jar corrugated tubing and drip bag trach collar sterile, distilled water (boil distilled water for 10 minutes and let cool to room temperature) cleaning solution (recommended by home equipment company)large container with lid for cleaning solution spare valve for air compressor 2. How to use fill nebulizer jar with sterile water to line on jar. attach nebulizer jar to air compressor. connect trach collar to tubing with bag in place (corrugated tubing to bag to corrugated tubing) and attach to nebulizer. turn on machine and look for mist from trach collar. Cleaning equipment Daily 1. Change nebulizer jar and trach collar. 2. Fill clean nebulizer jar with sterile distilled water. 3. Check to make sure suction machine is working. 6 Tracheostomy
7 Every other day 1. Rinse tubing and drip bag with tap water. 2. Clean using solution recommended by the home equipment supply company. After use or weekly 1. Clean ambu bag and face mask in solution recommended by the home equipment supply company. More information 1. Your baby may have trach collar and humidity off during the day if allowed by your baby s doctor. 2. Use trach collar and humidity during naps and at night to keep trach moist and prevent mucus plugs. 3. If nebulizer is not available (during long trips or power failure), place one drop of saline every hour or two into the trach tube to moisten trach tube and windpipe. 4. The windpipe (trachea) of your baby is small and easily plugged with mucus so the nebulizer with trach collar provides a direct source of moisture that a vaporizer cannot. 5. If mucus becomes thick, move the numbered ring on the nebulizer to a lower number. The usual setting is 50%. Increasing the baby s fluid intake may help thin the mucus. Signs of breathing problems 1. Restlessness or increased irritability. 2. Increased breathing (respiratory) rate. 3. Heavy, hard breathing. 4. Grunting, noisy breathing. 5. Nasal flaring (sides of nostrils move in and out with breathing). 6. Retraction (sinking in of breastbone and skin between the ribs with each breath). 7. Blue or pale color. 8. Whistling from the trach tube. 9. Sweating. 10. Change in pattern of heart rate (less than 80 or more than 210 beats/minute). Tracheostomy 7
8 11. Bleeding from trach tube. report to doctor immediately. irrigate tube with saline and suction. if bleeding continues replace trach tube with a clean one. CPR (Cardiopulmonary resuscitation) You will take a basic CPR class. We will teach you how to do CPR with the trach and how to use an ambu bag to breathe for the baby. If the baby stops breathing: 1. SUCTION TRACH TUBE AT ONCE. 2. Replace trach tube if it has come out, is blocked with mucus or your baby does not improve with suctioning. Tie trach ties!!! 3. Begin CPR if baby does not breathe when trach tube is clear. CPR with a tracheostomy Call for help!! 1. Stimulate baby by gently shaking. 2. Position baby on a hard flat surface with his nose pointed straight up. 3. Suction tracheostomy. Replace if blocked. 4. Listen and feel for breath by placing ear over tracheostomy. Look at chest to see if baby is breathing. 5. Place mouth or attach ambu bag over trach tube to form seal. 6. Give 2 quick puffs. Observe to see if chest moves like an easy breath. 7. Feel for Brachial heart rate (pulse) in the bend of the arm for 5 seconds and check to see if baby is breathing on his own (look, feel and listen for air movement). 8 Tracheostomy
9 8. If you feel a pulse, breathe with mouth or ambu bag on tube. Count: 1-2-breathe; 1-2-breathe 9. If air is leaking from the nose and mouth, close them with your hand. 10. If you do not feel a heart rate in 5 seconds or if the heart rate is less than 60 bpm, do chest compressions and breathe for baby with mouth or ambu bag on trach tube. Press 1/2 to 1 inch with each compression. It is a little tricky to use the ambu bag and do chest compression, but you will learn how. Count: breathe (press) (press) (press) (press) (press) (breathe) This rate is about 100 times a minute. The breath is about 1 to 1-1/2 seconds long. 11. Check heart rate and breathing about every minute. Do what the baby is not doing. 12. Call your local Emergency number or ambulance team for help if your baby does not respond. 13. Have baby taken to nearest hospital. Call doctor if Food or liquid comes through the trach. 2. There is a rash, drainage or unusual odor around the trach opening. 3. Mucus becomes green or foul smelling (normal color is clear or whitish). 4. Bleeding occurs from the trach tube. 5. Difficult breathing not relieved by suctioning or changing trach. 6. Unable to replace trach tube. 7. Baby stops breathing. Emergencies and treatments 1. Plugged trach suction and use ambu bag. change trach if baby does not improve. 2. Coughing out trach tube insert new clean trach tube as soon as possible. reinsert old trach tube until clean trach tube available. Tracheostomy 9
10 3. Vomiting suction if you think vomit has gone down tube. observe for coughing, respiratory distress, fever. call doctor. 4. Unable to replace trach tube try to insert smaller trach tube. call Emergency Team 911 trach opening (stoma) will not close up suddenly. give mouth-to-trach opening CPR if not breathing OR block trach opening and use mouth-to-mouth CPR. General care Feeding 1. Your baby can be fed as a normal baby. 2. Burp well and place on right side or in infant seat after feeding. 3. DO NOT PROP THE BOTTLE. 4. Do not let your baby have a bottle unless you are present in case choking occurs. Bathing 1. Your baby can be bathed in tub, but do not let water get into the trach. 2. NEVER LEAVE YOUR BABY ALONE IN THE TUB. 3. Change the trach ties after the bath if they get wet. Clothing and bedding 1. You do not need to buy special clothing for your baby. 2. Clothing that covers the trach should not be worn. 3. Necklaces, strings, fuzzy clothing, fuzzy blankets and stuffed animals should be avoided. Tiny beads or fibers from these articles can get into the trach. 4. Purchasing a portable intercom system so you can hear the baby when you are in another room is often helpful. 10 Tracheostomy
11 Making sounds and talking 1. At first you will not be able to hear the baby cry or make sounds. This is because the air from the lungs does not pass through the vocal cords. 2. He will learn to talk around the trach tube. 3. It is important that you talk to him as you would any other baby. Baby-sitters 1. A baby with a trach needs to be watched closely all day. Plans must be made to teach another person how to care for the baby. 2. It is important that parents be able to rest and go out without the baby! Safety tips 1. Animals with fine hair should not be in the house. 2. Keep home as free from lint and dust as possible. 3. Do not use powders, chlorine bleach, ammonia or aerosol sprays in the same room as the baby. Particles and fumes get into the lungs through the trach. This will cause a burning feeling and breathing problems. 4. Do not smoke around your baby. Smoke is irritating to the baby s windpipe (trachea). 5. Watch play with other children so that toys, fingers and food are not put into trach tube. 6. Do not buy toys with small parts that can easily be removed. 7. Always carry your GO BAG supplies when you leave home. Weather 1. During freezing temperature, avoid allowing baby to breathe cold air directly into trach. This can cause tracheal spasm and form small ice particles in the mucus if exposed for long periods of time. Keep the baby s head and neck loosely covered with a blanket. Tie a scarf loosely around the neck of an older child. 2. Protect the tracheostomy on dusty windy days when dust particles may enter the trachea and cause drying or crusting mucus. Brothers and sisters 1. It is important to help older brothers/sisters to understand why and how the baby breathes through a trach. Tracheostomy 11
12 2. This is usually a frightening situation for older brothers/sisters and requires parents support and teaching to ease their initial discomfort and fear. 3. It may be helpful to involve brother and sister s help in small tasks such as holding the baby still, helping clean equipment, etc. 4. Watch young brothers and sisters around the baby! Counting baby s breathing 1. You may want to count the baby s breathing rate twice a day when the baby is quiet or asleep. You can write the number in a record book you bring to the doctor. 2. One count is a breath in and out. Sometimes the baby holds his breath briefly, breathes fast then slow, stretches or moves. Count the breathing as best you can. 3. Call the doctor if the breathing rate is counts higher than usual or your baby is working harder to breathe. Make sure the baby is not too warm or does not have mucus in his trach. 24-hour schedule 1. You will be very busy at home. 2. It helps to have a calendar with your day s activities clearly marked. 3. Some things you will do several times a day and some things you do several times a week. Organization and a schedule are important. So is help from family members. 4. It is important to teach several people to care for the baby so you can have a break and get out by yourself. Baby s weekly schedule Daily 1. Stoma care: 1-2 times a day, or more if necessary. do more often if skin breaks down, there is a large amount of secretions, or odor noticed. replace trach ties when wet (may use velcro trach holder, bias tape purchased at any sewing store, or shoelaces). 2. Wash suction bottle: hot soapy water. 12 Tracheostomy
13 3. CPT: 2-3 times a day (if recommended by the baby s doctor). before feeding or at least 2 hours after feeding. 4. Change trach collar and tubing. 5. Change water bottle for humidifier. 6. Check to make sure suction machine is working. Every other day 1. Clean humidifier in solution recommended by home equipment supply company. 2. Clean suction bottle and tubing in solution recommended by home equipment supply company. 3. Clean trach collar and tubing in solution recommended by home equipment supply company. Weekly to monthly (or as needed) 1. Change trach. always suction before changing trach. change before feeding or at least 2 hours after feeding. GO BAG for traveling 1. De Lee suction catheter. 2. Bulb syringe. 3. Suction catheters disposable. 4. Trach tube with tie and obturator (same size and size smaller). 5. Scissors. 6. Water soluble lubricant (sterile single use packets). 7. Saline (2-3 5-cc vials) X 4 s or trach sponges. 9. Portable suction machine. 10. Emergency phone numbers. Tracheostomy 13
14 Recipes Saline 1/2 teaspoon of table salt added to 8 ounces of boiled water. add salt when water is warm. cool before using. store in sterile bottle (bottle boiled in pan of water 10 minutes after water begins to roll). make new every day. Sterile distilled water boil tap or bottled water 10 minutes after the water begins to roll. store in sterile bottle. Hydrogen peroxide must buy. keep out of sunlight. do not use if cloudy or does not bubble when applied. Supplies 1. All of the home supplies you need will be provided through a home equipment and supply company. The hospital makes these arrangements with a company near where you live. 2. The supply company will contact you at home or while you room-in with your baby. 3. The supply company will tell you when and how to reorder supplies. They will give you a phone number to call if you have equipment problems. Call them if your equipment breaks or to reorder supplies. Help 1. Several programs are available to help provide medical and financial care of your baby. The Child Services Coordinator in your community or a social worker can help find out if you are eligible for the programs. Babies are eligible for different reasons and some may not be eligible or approved. Medicaid Children s Special Health Services SSI (Supplemental Security Income) 14 Tracheostomy
15 Medically Needy Program AFDC (Aid to Families with Dependent Children) 2. It is a lot of hard work to care for a baby with a trach. Yet most parents still prefer to have the baby at home. 3. We ask several family members to learn the care so everyone can get some rest. 4. Some insurance companies approve home-nursing care for a baby with a trach. We contact your insurance company to find out if they provide this service. 5. Home health agencies or public health services are used for short visits. These visits are an hour or less. The nurses answer questions, help with special treatments and help with medications. They may weigh the baby or watch a feeding. They work with your doctor to follow the baby s condition and progress. 6. Even though it is difficult to find people to babysit, it is important to teach other people to care for the baby so you can go out. 7. Respite services which provide relief for parents may not be available in all communities or for babies with trachs. 8. If you get too tired or frustrated, call the doctor or social worker. We will try to help. Doctor visits 1. Your baby returns to the hospital clinic to follow his breathing problems and trach. 2. If you see more than one doctor (eye, surgery, breathing, x-ray, lab, development), check to see if the appointment can be made for the same day. 3. At first it seems you spend most of your time going to the doctor. 4. As the baby s health gets better the visits become less frequent and some doctors will not need to see him. 5. You will take the baby to a local baby doctor for routine baby care and shots. Make an appointment to see him the first week the baby is home. 6. We mail your doctor a report of your visits to the hospital clinics. Emergency notification 1. The home equipment company will call and write the following agencies to inform them that your baby has a serious medical problem: Rescue squad Telephone company Electric/gas company 2. The letter asks that you be placed on the priority list for notification of anticipated interruptions of service. Tracheostomy 15
16 3. The letter asks that you be placed on the priority list for service restitution in the event of unexpected interruption of service. My equipment supply company is: Name Address Telephone 16 Tracheostomy
Tracheostomy Care at Home
 Tracheostomy Care at Home Patient Education CARE AND TREATMENT This information will help you understand how to care for a person with a tracheostomy at home. It is a supplement to the teaching offered
Tracheostomy Care at Home Patient Education CARE AND TREATMENT This information will help you understand how to care for a person with a tracheostomy at home. It is a supplement to the teaching offered
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
Pediatric Trach home care guide
 Pediatric Trach home care guide 2 Pages About This Book... 4 General Information... 5 Why I need my trach Emergency Equipment... 6 Always be prepared Types of Trachs... 7 Passy-Muir Speaking Valve... 9
Pediatric Trach home care guide 2 Pages About This Book... 4 General Information... 5 Why I need my trach Emergency Equipment... 6 Always be prepared Types of Trachs... 7 Passy-Muir Speaking Valve... 9
Dear Parent or Guardian:
 TABLE OF CONTENTS I II III IV V VI VII INTRODUCTION Letter from the ENT Team 2 Tracheotomy Introduction - Charles Myer III, M.D. 3 Message from the Nursing Staff 4 TRACHEOTOMY CARE Tracheotomy Care Learning
TABLE OF CONTENTS I II III IV V VI VII INTRODUCTION Letter from the ENT Team 2 Tracheotomy Introduction - Charles Myer III, M.D. 3 Message from the Nursing Staff 4 TRACHEOTOMY CARE Tracheotomy Care Learning
PROCEDURE FOR USING A NASAL CANNULA
 PROCEDURE FOR USING A NASAL CANNULA A nasal cannula is used to deliver a low to moderate concentration of oxygen. It can be used as long as nasal passages are open. A deviated septum, swelling of the nasal
PROCEDURE FOR USING A NASAL CANNULA A nasal cannula is used to deliver a low to moderate concentration of oxygen. It can be used as long as nasal passages are open. A deviated septum, swelling of the nasal
PROCEDURE FOR USING A NASAL CANNULA
 FOR USING A NASAL CANNULA A nasal cannula is used to deliver a low to moderate concentration of oxygen. It can be used as long as nasal passages are open. A deviated septum, swelling of the nasal passages,
FOR USING A NASAL CANNULA A nasal cannula is used to deliver a low to moderate concentration of oxygen. It can be used as long as nasal passages are open. A deviated septum, swelling of the nasal passages,
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
PICCs and Midline Catheters
 Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
X-Plain Foley Catheter Male Reference Summary
 X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
X-Plain Foley Catheter Male Reference Summary Introduction A Foley catheter is a tube that is put through the urinary opening and into your bladder to drain urine. Your doctor may have placed or may ask
Peripherally Inserted Central Catheter (PICC) Patient Instructions
 Patient Care Services 300 Pasteur Drive Stanford, CA 94305 Peripherally Inserted Central Catheter (PICC) Patient Instructions A Peripherally Inserted Central Catheter (PICC) is a soft flexible tube inserted
Patient Care Services 300 Pasteur Drive Stanford, CA 94305 Peripherally Inserted Central Catheter (PICC) Patient Instructions A Peripherally Inserted Central Catheter (PICC) is a soft flexible tube inserted
TRACHEOSTOMY TUBE PARTS
 Page1 NR 33 TRACHEOSTOMY CARE AND SUCTIONING Review ATI Basic skills videos: Tracheostomy care and Endotracheal suction using a closed suction set. TRACHEOSTOMY TUBE PARTS Match the numbers on the diagram
Page1 NR 33 TRACHEOSTOMY CARE AND SUCTIONING Review ATI Basic skills videos: Tracheostomy care and Endotracheal suction using a closed suction set. TRACHEOSTOMY TUBE PARTS Match the numbers on the diagram
HALO ORTHOSIS. 1. The ring and pins. 2. The vest. 3. The superstructure (uprights that connect the ring to the vest)
 UM Orthotics & Prosthetics Center UM Orthopaedics UM Neurosurgery HALO ORTHOSIS HALO Front View HALO Back View You have been placed in a halo vest. This orthosis (brace) is used to immobilize a neck fracture
UM Orthotics & Prosthetics Center UM Orthopaedics UM Neurosurgery HALO ORTHOSIS HALO Front View HALO Back View You have been placed in a halo vest. This orthosis (brace) is used to immobilize a neck fracture
Home Care for Your Nephrostomy Catheter
 Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Home Care for Your Nephrostomy Catheter This handout covers information about caring for your nephrostomy catheter right after placement and caring for it long term. If you have any questions, please call
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information
 Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
How to Care for Your Premature Baby s Skin
 The Emily Center How to Care for Your Premature Baby s Skin Child Care/Health Promotion Si usted desea esta información en español, por favor pídasela a su enfermero o doctor. Name of Child: Date: How
The Emily Center How to Care for Your Premature Baby s Skin Child Care/Health Promotion Si usted desea esta información en español, por favor pídasela a su enfermero o doctor. Name of Child: Date: How
Your Recovery After a Cesarean Delivery
 Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Your Recovery After a Cesarean Delivery It is normal to have many questions about your care after delivery. Cesarean delivery is surgery and your body needs time to heal and recover for the next 6 weeks,
Caring for Your PleurX Pleural Catheter
 Caring for Your PleurX Pleural Catheter A PleurX Pleural Catheter has been placed in your chest through a small incision in your skin into the pleural space (see picture below). This allows you to drain
Caring for Your PleurX Pleural Catheter A PleurX Pleural Catheter has been placed in your chest through a small incision in your skin into the pleural space (see picture below). This allows you to drain
Oxygen. Do not use flammable products, such as aerosol sprays, rubbing alcohol, paint thinners, and other oil-based lubricants near oxygen.
 Your doctor may have ordered oxygen to help you breathe easier. delivers oxygen to the blood and may help you move around, sleep or do other things you enjoy more comfortably. is highly flammable but safe
Your doctor may have ordered oxygen to help you breathe easier. delivers oxygen to the blood and may help you move around, sleep or do other things you enjoy more comfortably. is highly flammable but safe
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
- Woody Kageler, M.D.
 Dear Parent/Guardian, We all want our children with asthma to be healthy! Asthma can be a frightening experience for kids, as well as their parents. Let Darby BoIngg be your partner, along with your physician,
Dear Parent/Guardian, We all want our children with asthma to be healthy! Asthma can be a frightening experience for kids, as well as their parents. Let Darby BoIngg be your partner, along with your physician,
GJ TUBE (GASTROJEJUNOSTOMY TUBE) Daily Care
 GJ TUBE (GASTROJEJUNOSTOMY TUBE) Daily Care Your child has a Picture 1 The GJ Tube inside the body. gastrojejunostomy (GJ) tube Disc (Picture 1). This set of tubes lets food or medicine go into either
GJ TUBE (GASTROJEJUNOSTOMY TUBE) Daily Care Your child has a Picture 1 The GJ Tube inside the body. gastrojejunostomy (GJ) tube Disc (Picture 1). This set of tubes lets food or medicine go into either
Respiratory Syncytial Virus (RSV)
 Respiratory Syncytial Virus (RSV) What is? is a common virus that infects the linings of the airways - the nose, throat, windpipe, bronchi and bronchioles (the air passages of the lungs). RSV is found
Respiratory Syncytial Virus (RSV) What is? is a common virus that infects the linings of the airways - the nose, throat, windpipe, bronchi and bronchioles (the air passages of the lungs). RSV is found
Taking Care of Your Skin During Radiation Therapy
 Taking Care of Your Skin During Radiation Therapy Princess Margaret Information for patients who are having radiation therapy Read this pamphlet to learn about: What a radiation skin reaction is How to
Taking Care of Your Skin During Radiation Therapy Princess Margaret Information for patients who are having radiation therapy Read this pamphlet to learn about: What a radiation skin reaction is How to
Infant CPR. What You Need to Know. How to Do Infant CPR
 Infant CPR Infant CPR also called Cardiopulmonary resuscitation is emergency care given to a baby who has stopped breathing. This sheet has the steps for CPR for newborns or babies less than 1 year old.
Infant CPR Infant CPR also called Cardiopulmonary resuscitation is emergency care given to a baby who has stopped breathing. This sheet has the steps for CPR for newborns or babies less than 1 year old.
What You And Your Family Can Do About Asthma
 GLOBAL INITIATIVE FOR ASTHMA What You And Your Family Can Do About Asthma BASED ON THE GLOBAL STRATEGY FOR ASTHMA MANAGEMENT AND PREVENTION NHLBI/WHO WORKSHOP REPORT NATIONAL INSTITUTES OF HEALTH NATIONAL
GLOBAL INITIATIVE FOR ASTHMA What You And Your Family Can Do About Asthma BASED ON THE GLOBAL STRATEGY FOR ASTHMA MANAGEMENT AND PREVENTION NHLBI/WHO WORKSHOP REPORT NATIONAL INSTITUTES OF HEALTH NATIONAL
Gallbladder Surgery with an Incision (Cholecystectomy)
 Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
Gallbladder Surgery with an Incision (Cholecystectomy) It is normal to have questions about your surgery. This handout gives you information about what will happen to you before, during and after your
call 811 to get advice from a nurse, or have someone drive the patient to a hospital Emergency Department. Patients should NOT drive themselves.
 Taking Care at Home After Surgery This checklist is to help you and your support person know what to do after you go home following your surgery. If you are given instructions verbally or in writing by
Taking Care at Home After Surgery This checklist is to help you and your support person know what to do after you go home following your surgery. If you are given instructions verbally or in writing by
Home Care for Your Wound Drain
 PATIENT EDUCATION patienteducation.osumc.edu When you go home after surgery, you may have one or more drains in place to help your wounds heal. Hemovac, Jackson Pratt (JP) and Blake are common drains used
PATIENT EDUCATION patienteducation.osumc.edu When you go home after surgery, you may have one or more drains in place to help your wounds heal. Hemovac, Jackson Pratt (JP) and Blake are common drains used
National Hospital for Neurology and Neurosurgery. Continuous positive airway pressure (CPAP) Sleep Respiratory Unit
 National Hospital for Neurology and Neurosurgery Continuous positive airway pressure (CPAP) Sleep Respiratory Unit If you would like this document in another language or format or if you require the services
National Hospital for Neurology and Neurosurgery Continuous positive airway pressure (CPAP) Sleep Respiratory Unit If you would like this document in another language or format or if you require the services
In case of an urgent concern or emergency, call 911 or go to the nearest emergency department right away.
 Asthma Basics Patient and Family Education This teaching sheet contains general information only. Talk with your child s doctor or a member of your child s healthcare team about specific care of your child.
Asthma Basics Patient and Family Education This teaching sheet contains general information only. Talk with your child s doctor or a member of your child s healthcare team about specific care of your child.
Feeding. Baby. Your. Infant. Formula
 Feeding Your Infant Baby Formula 1 Feeding Your Baby Infant Formula There are many reasons why some mothers don t breastfeed. If you feel sad and/or disappointed that you are not fully breastfeeding your
Feeding Your Infant Baby Formula 1 Feeding Your Baby Infant Formula There are many reasons why some mothers don t breastfeed. If you feel sad and/or disappointed that you are not fully breastfeeding your
Section 4: Your Vascular Access. What is vascular access?
 Section 4: Your Vascular Access What is vascular access? What is a fistula? Taking care of a new fistula What is a graft? Taking care of a new graft What is a hemodialysis catheter? Taking care of a hemodialysis
Section 4: Your Vascular Access What is vascular access? What is a fistula? Taking care of a new fistula What is a graft? Taking care of a new graft What is a hemodialysis catheter? Taking care of a hemodialysis
Tracheostomy Journal
 Table of Contents Introduction to the Tracheostomy Home Care Program... i Anatomy and Physiology of the Airway... 1 Tracheostomy Care and Use... 3 Tracheostomy Home Care Equipment... 18 DME and Nursing
Table of Contents Introduction to the Tracheostomy Home Care Program... i Anatomy and Physiology of the Airway... 1 Tracheostomy Care and Use... 3 Tracheostomy Home Care Equipment... 18 DME and Nursing
Atrium Pneumostat Chest Drain Valve. Discharge Instructions
 Atrium Pneumostat Chest Drain Valve Discharge Instructions Your Physician Name: Contact Number for Emergencies: Introduction Your physician has decided to change your chest drainage system to a smaller
Atrium Pneumostat Chest Drain Valve Discharge Instructions Your Physician Name: Contact Number for Emergencies: Introduction Your physician has decided to change your chest drainage system to a smaller
Going home with your Tunneled Catheter
 Going home with your Tunneled Catheter Your Tunneled Catheter was put in by on Interventional Radiologist Date Your Tunneled Catheter was put in at: McMaster University Medical Centre Hamilton General
Going home with your Tunneled Catheter Your Tunneled Catheter was put in by on Interventional Radiologist Date Your Tunneled Catheter was put in at: McMaster University Medical Centre Hamilton General
Challenges of Foster Parents who Care for Infants with Neonatal Abstinence Syndrome
 Challenges of Foster Parents who Care for Infants with Neonatal Abstinence Syndrome All Health Care Providers are required by law to make a referral to the Department of Children s Services (DCS) Child
Challenges of Foster Parents who Care for Infants with Neonatal Abstinence Syndrome All Health Care Providers are required by law to make a referral to the Department of Children s Services (DCS) Child
PICC & Midline Catheters Patient Information Guide
 PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
There is no cure for COPD Chronic Bronchitis Emphysema
 Live Well With COPD Chronic Obstructive Pulmonary Disease, or COPD is a lung disease. People with COPD have a hard time getting air in and out of their lungs. There is no cure for COPD. COPD is also commonly
Live Well With COPD Chronic Obstructive Pulmonary Disease, or COPD is a lung disease. People with COPD have a hard time getting air in and out of their lungs. There is no cure for COPD. COPD is also commonly
Heart information. CPR cardiopulmonary resuscitation
 Heart information CPR cardiopulmonary resuscitation Contents 3 What is CPR? 3 What is cardiac arrest? 4 Heart attack and cardiac arrest 4 Cardiopulmonary resuscitation (CPR) 5 Danger 6 Response 7 Send
Heart information CPR cardiopulmonary resuscitation Contents 3 What is CPR? 3 What is cardiac arrest? 4 Heart attack and cardiac arrest 4 Cardiopulmonary resuscitation (CPR) 5 Danger 6 Response 7 Send
Adult Choking and CPR Manual
 Adult Choking and CPR Manual 2009 Breath of Life Home Medical Equipment and Respiratory Services CHOKING Description: Choking is the coughing spasm and sputtering that happen when liquids or solids get
Adult Choking and CPR Manual 2009 Breath of Life Home Medical Equipment and Respiratory Services CHOKING Description: Choking is the coughing spasm and sputtering that happen when liquids or solids get
Do not use soaps with added scents. We recommend plain Ivory liquid soap or baby shampoo. Rinse well and allow to air dry out of direct sunlight.
 ResMed CPAP Mask FAQ When and how should I clean my mask? Daily Wash the mask system with warm, soapy water. Do not use soaps with added scents. We recommend plain Ivory liquid soap or baby shampoo. Rinse
ResMed CPAP Mask FAQ When and how should I clean my mask? Daily Wash the mask system with warm, soapy water. Do not use soaps with added scents. We recommend plain Ivory liquid soap or baby shampoo. Rinse
Care for your child s Central Venous Catheter (CVC)
 Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
Care for your child s Central Venous Catheter (CVC) This booklet is intended for general informational purposes only. You should consult your doctor for medical advice. Please call the clinic or your home
Adult First Aid/CPR/AEd. Ready Reference
 Adult First Aid/CPR/AEd Ready Reference Contents Checking an Injured or Ill Adult 3 CPR 4 AED Adult or Child 5 Conscious Choking 7 Controlling External Bleeding 8 Burns 9 Poisoning 10 Head, Neck or Spinal
Adult First Aid/CPR/AEd Ready Reference Contents Checking an Injured or Ill Adult 3 CPR 4 AED Adult or Child 5 Conscious Choking 7 Controlling External Bleeding 8 Burns 9 Poisoning 10 Head, Neck or Spinal
PATIENT GUIDE. Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL
 PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
SELF-CATHETERISATION A Guide for Male Patients PATIENT EDUCATION
 SELF-CATHETERISATION A Guide for Male Patients PATIENT EDUCATION ADHB Urology Department; Reviewed JULY 2005 Ubix code NPEB2 1 This booklet has been designed to help you learn how to perform self-catheterisation.
SELF-CATHETERISATION A Guide for Male Patients PATIENT EDUCATION ADHB Urology Department; Reviewed JULY 2005 Ubix code NPEB2 1 This booklet has been designed to help you learn how to perform self-catheterisation.
Gastrostomy Tubes Home Care Manual (Corpak, Foley catheter, Genie, Malecot, Mic-G)
 Physician who placed the gastrostomy: Date placed: Type of gastrostomy tube: Size of the gastrostomy: Gastrostomy tubes are measured in French (Fr.) sizes. A size 16 Fr. gastrostomy is larger than a 14
Physician who placed the gastrostomy: Date placed: Type of gastrostomy tube: Size of the gastrostomy: Gastrostomy tubes are measured in French (Fr.) sizes. A size 16 Fr. gastrostomy is larger than a 14
Fact Sheet. Caring for and Changing your Supra-Pubic Catheter (SPC) Queensland Spinal Cord Injuries Service
 and Caring for and Changing your Supra-Pubic Catheter (SPC) What is a Suprapubic Catheter? A supra-pubic catheter is a tube that goes into your bladder through your abdominal wall which continuously drains
and Caring for and Changing your Supra-Pubic Catheter (SPC) What is a Suprapubic Catheter? A supra-pubic catheter is a tube that goes into your bladder through your abdominal wall which continuously drains
Radiation Therapy and Caring for Your Skin
 Patient Information Radiation Therapy and Caring for Your Skin Comments, Feedback? Contact Patient and Professional Education 519-685-8742 Email: [email protected] Reviewed by the LRCP Patient Education
Patient Information Radiation Therapy and Caring for Your Skin Comments, Feedback? Contact Patient and Professional Education 519-685-8742 Email: [email protected] Reviewed by the LRCP Patient Education
Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery.
 JP Drain Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery. This reference summary explains what a JP Drain is and discusses how to take
JP Drain Introduction A JP Drain is a soft tube and container used to drain fluids that build up under the skin after surgery. This reference summary explains what a JP Drain is and discusses how to take
PATIENT GUIDE. Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Clinician s Signature: Every drainage Weekly
 PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
PATIENT GUIDE Care and Maintenance Drainage Frequency: Max. Drainage Volume: Dressing Option: Every drainage Weekly Clinician s Signature: ACCESS SYSTEMS Pleural Space Insertion Site Cuff Exit Site Catheter
Procedure Code A4215 22 Insulin pen needles A4230 Infusion set for external insulin pump, non needle cannula type A4231 Infusion set for external
 A4215 22 Insulin pen needles A4230 Infusion set for external insulin pump, non needle cannula type A4231 Infusion set for external insulin pump, needle type A4232 Syringe with needle for external insulin
A4215 22 Insulin pen needles A4230 Infusion set for external insulin pump, non needle cannula type A4231 Infusion set for external insulin pump, needle type A4232 Syringe with needle for external insulin
Caring for Your Gastrostomy
 Caring for Your Gastrostomy Table of Contents What Is a Gastrostomy Tube (G-tube)?... 2 Types of Gastrostomy Tubes... 3 Cleaning the Gastrostomy Site... 4 Gastrostomy Feedings... 5 Giving Medicines...
Caring for Your Gastrostomy Table of Contents What Is a Gastrostomy Tube (G-tube)?... 2 Types of Gastrostomy Tubes... 3 Cleaning the Gastrostomy Site... 4 Gastrostomy Feedings... 5 Giving Medicines...
Keeping your lungs healthy
 Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
Keeping your lungs healthy A guide for you after spinal cord injury and other neurological conditions Regional Rehabilitation Program This booklet has been written by the health care providers who provide
MEASURING VITAL SIGNS TRAINING CHECKLIST
 Measuring Vital Signs A guide to help Direct Support Professionals learn how to measure, and report vital sign measurements. Outcomes: Know how to take each individual s vital signs. Demonstrate the correct
Measuring Vital Signs A guide to help Direct Support Professionals learn how to measure, and report vital sign measurements. Outcomes: Know how to take each individual s vital signs. Demonstrate the correct
Urinary Indwelling Catheter. The Urinary System
 Patient Education CARE AND TREATMENT Urinary Indwelling Catheter This information will help you care for a urinary indwelling catheter at home. It will answer many of your questions. Please ask your doctor
Patient Education CARE AND TREATMENT Urinary Indwelling Catheter This information will help you care for a urinary indwelling catheter at home. It will answer many of your questions. Please ask your doctor
American Heart Association
 American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
For the Patient: Paclitaxel injection Other names: TAXOL
 For the Patient: Paclitaxel injection Other names: TAXOL Paclitaxel (pak'' li tax' el) is a drug that is used to treat many types of cancer. It is a clear liquid that is injected into a vein. Tell your
For the Patient: Paclitaxel injection Other names: TAXOL Paclitaxel (pak'' li tax' el) is a drug that is used to treat many types of cancer. It is a clear liquid that is injected into a vein. Tell your
Caring for a Tenckhoff Catheter
 Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Things To Know Before You Go
 Things To Know Before You Go MUSCLE DEVELOPMENT AND MUSCULAR CONTROL What activities can I do to help normal development of muscle control in my baby? Listed below are things you can do with your baby
Things To Know Before You Go MUSCLE DEVELOPMENT AND MUSCULAR CONTROL What activities can I do to help normal development of muscle control in my baby? Listed below are things you can do with your baby
INSTRUCTIONS FOR USE HUMIRA 40 MG/0.8 ML, 20 MG/0.4 ML AND 10 MG/0.2 ML SINGLE-USE PREFILLED SYRINGE
 INSTRUCTIONS FOR USE HUMIRA (Hu-MARE-ah) (adalimumab) 40 MG/0.8 ML, 20 MG/0.4 ML AND 10 MG/0.2 ML SINGLE-USE PREFILLED SYRINGE Do not try to inject HUMIRA yourself until you have been shown the right way
INSTRUCTIONS FOR USE HUMIRA (Hu-MARE-ah) (adalimumab) 40 MG/0.8 ML, 20 MG/0.4 ML AND 10 MG/0.2 ML SINGLE-USE PREFILLED SYRINGE Do not try to inject HUMIRA yourself until you have been shown the right way
Care of a Foley Catheter
 Care of a Foley Catheter A Foley catheter is a tube that is put into the bladder to drain urine out of the body. A Foley catheter can stay in the bladder for hours or weeks. Having the catheter put in
Care of a Foley Catheter A Foley catheter is a tube that is put into the bladder to drain urine out of the body. A Foley catheter can stay in the bladder for hours or weeks. Having the catheter put in
How to care for a Midline Catheter
 How to care for a Midline Catheter Developed by the health care professionals of the IV Program with assistance from the Department of Learning and Development. All rights reserved. No part of this book
How to care for a Midline Catheter Developed by the health care professionals of the IV Program with assistance from the Department of Learning and Development. All rights reserved. No part of this book
A Guide to Help You Manage Your Catheter and Drainage Bags
 A Guide to Help You Manage Your Catheter and Drainage Bags A catheter can make a difference to your health and quality of life. We understand that it can be a big adjustment for you. This information will
A Guide to Help You Manage Your Catheter and Drainage Bags A catheter can make a difference to your health and quality of life. We understand that it can be a big adjustment for you. This information will
INSTRUCTIONS FOR USE HUMIRA 40 MG/0.8 ML SINGLE-USE PEN
 INSTRUCTIONS FOR USE HUMIRA (Hu-MARE-ah) (adalimumab) 40 MG/0.8 ML SINGLE-USE PEN Do not try to inject HUMIRA yourself until you have been shown the right way to give the injections and have read and understand
INSTRUCTIONS FOR USE HUMIRA (Hu-MARE-ah) (adalimumab) 40 MG/0.8 ML SINGLE-USE PEN Do not try to inject HUMIRA yourself until you have been shown the right way to give the injections and have read and understand
X-Plain Sinus Surgery Reference Summary
 X-Plain Sinus Surgery Reference Summary Introduction Sinus surgery is a very common and safe operation. Your doctor may recommend that you have sinus surgery. The decision whether or not to have sinus
X-Plain Sinus Surgery Reference Summary Introduction Sinus surgery is a very common and safe operation. Your doctor may recommend that you have sinus surgery. The decision whether or not to have sinus
WHEN COPD* SYMPTOMS GET WORSE
 WHEN COPD* SYMPTOMS GET WORSE *Includes chronic bronchitis, emphysema, or both. Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises or markets
WHEN COPD* SYMPTOMS GET WORSE *Includes chronic bronchitis, emphysema, or both. Boehringer Ingelheim Pharmaceuticals, Inc. has no ownership interest in any other organization that advertises or markets
GOING HOME AFTER YOUR TAVR PROCEDURE
 GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
GOING HOME AFTER YOUR TAVR PROCEDURE HENRY FORD HOSPITAL CENTER FOR STRUCTURAL HEART DISEASE GOING HOME After your TAVR procedure, you will need help when you go home. It is hard to predict how much help
Instructions for Use PROCRIT (PRO KRIT) (epoetin alfa)
 Instructions for Use PROCRIT (PROKRIT) (epoetin alfa) Use these Instructions for Use if you or your caregiver has been trained to give PROCRIT injections at home. Do not give yourself the injection unless
Instructions for Use PROCRIT (PROKRIT) (epoetin alfa) Use these Instructions for Use if you or your caregiver has been trained to give PROCRIT injections at home. Do not give yourself the injection unless
SECOND GRADE 1 WEEK LESSON PLANS AND ACTIVITIES
 SECOND GRADE 1 WEEK LESSON PLANS AND ACTIVITIES WATER CYCLE OVERVIEW OF SECOND GRADE WATER WEEK 1. PRE: Exploring the properties of water. LAB: Experimenting with different soap mixtures. POST: Analyzing
SECOND GRADE 1 WEEK LESSON PLANS AND ACTIVITIES WATER CYCLE OVERVIEW OF SECOND GRADE WATER WEEK 1. PRE: Exploring the properties of water. LAB: Experimenting with different soap mixtures. POST: Analyzing
Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions
 Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions No lifting greater than 10 15 lbs for the first three weeks following your surgery. Walking around the house, office
Abdominal Wall (Ventral, Incisional, Umbilical) Hernia Repair Postoperative Instructions No lifting greater than 10 15 lbs for the first three weeks following your surgery. Walking around the house, office
Achieving Independence
 Bard: Intermittent Self-Catheterization A Guide to Self-Catheterization Achieving Independence Introduction This brochure is provided by Bard, a leading provider of urology products since 1907. The best
Bard: Intermittent Self-Catheterization A Guide to Self-Catheterization Achieving Independence Introduction This brochure is provided by Bard, a leading provider of urology products since 1907. The best
Peripherally Inserted Central Catheter (PICC)
 Peripherally Inserted Central Catheter (PICC) Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified healthcare provider. Please
Peripherally Inserted Central Catheter (PICC) Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified healthcare provider. Please
Living with MRSA. Things to remember about living with MRSA: This is really serious. I need to do something about this now!
 Things to remember about living with MRSA: 1. Wash your hands often. 2. Take care of yourself: Eat right, exercise, quit smoking, and avoid stress. 3. Take good care of your skin. 4. Keep skin infections
Things to remember about living with MRSA: 1. Wash your hands often. 2. Take care of yourself: Eat right, exercise, quit smoking, and avoid stress. 3. Take good care of your skin. 4. Keep skin infections
Oxygen for Symptom Relief (Palliative Oxygen)
 Oxygen for Symptom Relief (Palliative Oxygen) Exceptional healthcare, personally delivered This leaflet has been written for patients starting, or who have just started, oxygen therapy and answers any
Oxygen for Symptom Relief (Palliative Oxygen) Exceptional healthcare, personally delivered This leaflet has been written for patients starting, or who have just started, oxygen therapy and answers any
Learning About MRSA. 6 How is MRSA treated? 7 When should I seek medical care?
 IMPORTANT MRSA is a serious infection that can become life-threatening if left untreated. If you or someone in your family has been diagnosed with MRSA, there are steps you need to take now to avoid spreading
IMPORTANT MRSA is a serious infection that can become life-threatening if left untreated. If you or someone in your family has been diagnosed with MRSA, there are steps you need to take now to avoid spreading
Going home after an AV Fistula or AV Graft
 Going home after an AV Fistula or AV Graft TGH Information for patients and families During your hospital stay, your surgeon created an: AV Fistula AV Graft Read this booklet to learn: how to care for
Going home after an AV Fistula or AV Graft TGH Information for patients and families During your hospital stay, your surgeon created an: AV Fistula AV Graft Read this booklet to learn: how to care for
Please Do Not Call 911
 The Last Hours of Life - What to Expect Names and Phone Numbers You May Need Name Phone Family Dr. Palliative Dr. After Hours Access Centre Visiting Nurse Hospice Clergy Funeral Contact Please Do Not Call
The Last Hours of Life - What to Expect Names and Phone Numbers You May Need Name Phone Family Dr. Palliative Dr. After Hours Access Centre Visiting Nurse Hospice Clergy Funeral Contact Please Do Not Call
Cholera Prevention and Control: Introduction and Community Engagement. Module 1
 Cholera Prevention and Control: Introduction and Community Engagement Module 1 Introduction This guide instructs how to prevent cholera illnesses and deaths in your communities. These slides and modules
Cholera Prevention and Control: Introduction and Community Engagement Module 1 Introduction This guide instructs how to prevent cholera illnesses and deaths in your communities. These slides and modules
Section 6: Your Hemodialysis Catheter
 Section 6: Your Hemodialysis Catheter What you should know about your dialysis catheter How to change your catheter TEGO connectors Starting dialysis using a catheter End of dialysis using a catheter Changing
Section 6: Your Hemodialysis Catheter What you should know about your dialysis catheter How to change your catheter TEGO connectors Starting dialysis using a catheter End of dialysis using a catheter Changing
Sterile Dressing Change with Tegaderm CHG for Central Venous Catheter (CVC)
 Sterile Dressing Change with Tegaderm CHG for Central Venous Catheter (CVC) The dressing protects your catheter site. It also helps prevent infection at the site. Keep your dressing clean and dry at all
Sterile Dressing Change with Tegaderm CHG for Central Venous Catheter (CVC) The dressing protects your catheter site. It also helps prevent infection at the site. Keep your dressing clean and dry at all
BLOOD BORNE PATHOGENS
 BLOOD BORNE PATHOGENS AIDS and other blood-borne pathogens such as Hepatitis B and C are deadly diseases that are present in today s society. All blood-borne pathogens are transmitted in blood and other
BLOOD BORNE PATHOGENS AIDS and other blood-borne pathogens such as Hepatitis B and C are deadly diseases that are present in today s society. All blood-borne pathogens are transmitted in blood and other
Enables MDA Medical Teams to categorize victims in mass casualty scenarios, in order to be able to triage and treat casualties
 MDA Disposable ALS + BLS Medical Ambulance Equipment Prices shown in CDN. Funds Items Description Picture Mass Casualty ID tag 1000 units = $350 Enables MDA Medical Teams to categorize victims in mass
MDA Disposable ALS + BLS Medical Ambulance Equipment Prices shown in CDN. Funds Items Description Picture Mass Casualty ID tag 1000 units = $350 Enables MDA Medical Teams to categorize victims in mass
CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery
 CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery For patients of Jeffrey Kramer, MD As you re discharged from the hospital, you may have questions about your continuing
CARDIAC REHABILITATION Follow-up Options & Dismissal Instructions Open Heart Surgery For patients of Jeffrey Kramer, MD As you re discharged from the hospital, you may have questions about your continuing
Using Oxygen at Home
 Using Oxygen at Home (2004, 2009) The Emily Center, Phoenix Children s Hospital 1 Contents 3 Important information 3 Who to call for help 5 The respiratory system 6 How to look at breathing problems 8
Using Oxygen at Home (2004, 2009) The Emily Center, Phoenix Children s Hospital 1 Contents 3 Important information 3 Who to call for help 5 The respiratory system 6 How to look at breathing problems 8
Clean Intermittent Catheterization (CIC) For Males
 The Emily Center Clean Intermittent Catheterization (CIC) For Males Procedure/Treatment/Home Care Si usted desea esta información en español, por favor pídasela a su enfermero o doctor. #200 male patient
The Emily Center Clean Intermittent Catheterization (CIC) For Males Procedure/Treatment/Home Care Si usted desea esta información en español, por favor pídasela a su enfermero o doctor. #200 male patient
Hysterectomy Vaginal hysterectomy Abdominal hysterectomy
 Hysterectomy A hysterectomy is a surgery to remove a woman s uterus. The uterus is one of the organs of the female reproductive system and is about the size of a closed hand. You can no longer have children
Hysterectomy A hysterectomy is a surgery to remove a woman s uterus. The uterus is one of the organs of the female reproductive system and is about the size of a closed hand. You can no longer have children
Better Breathing with COPD
 Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
Better Breathing with COPD People with Chronic Obstructive Pulmonary Disease (COPD) often benefit from learning different breathing techniques. Pursed Lip Breathing Pursed Lip Breathing (PLB) can be very
Going Home with a Urinary Catheter
 Going Home with a Urinary Catheter Doctor: Phone Number: About Your Catheter A urinary catheter is a small tube that goes through your urethra and into your bladder. This tube then drains the urine made
Going Home with a Urinary Catheter Doctor: Phone Number: About Your Catheter A urinary catheter is a small tube that goes through your urethra and into your bladder. This tube then drains the urine made
How to Prepare Formula for Bottle-Feeding at Home
 How to Prepare Formula for Bottle-Feeding at Home Printed in Ireland This document is published by the Department of Food Safety, Zoonoses and Foodborne Diseases, WHO, in collaboration with the Food and
How to Prepare Formula for Bottle-Feeding at Home Printed in Ireland This document is published by the Department of Food Safety, Zoonoses and Foodborne Diseases, WHO, in collaboration with the Food and
A GUIDE TO SPICA CAST CARE
 A GUIDE TO SPICA CAST CARE KAPI'OLANI ORTHOPAEDIC ASSOCIATES Pediatric Orthopaedics Spine Deformity Sports & Dance Medicine Young Adult Hip Preservation 1319 Punahou Street Suite #630 Honolulu, Hawaii
A GUIDE TO SPICA CAST CARE KAPI'OLANI ORTHOPAEDIC ASSOCIATES Pediatric Orthopaedics Spine Deformity Sports & Dance Medicine Young Adult Hip Preservation 1319 Punahou Street Suite #630 Honolulu, Hawaii
Heat Illnesses. Common Heat Rash Sites
 Heat Illnesses Introduction Heat illnesses happen when the body becomes too hot and cannot cool itself. There are several different types of heat-related illnesses. This includes heat cramps, heat exhaustion,
Heat Illnesses Introduction Heat illnesses happen when the body becomes too hot and cannot cool itself. There are several different types of heat-related illnesses. This includes heat cramps, heat exhaustion,
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY
 PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
PATIENT HANDBOOK AND JOURNAL DAY OF SURGERY PREPARING YOUR SKIN BEFORE SURGERY PRE-OP HIBICLENS BATHING INSTRUCTIONS: General Information: Because the skin is not sterile, it is important to make sure
How To Recover From A Surgical Wound From A Cast
 Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
Care of Your Wounds After Amputation Surgery by Paddy Rossbach, RN Depending on the reason for your amputation and the state of your limb at the time of surgery, definitive closure of the wound may take
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter
 Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Peripherally Inserted Central Catheter (PICC) for Outpatient
 Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Radiation Therapy To the Arms or Legs
 Radiation Therapy To the Arms or Legs You will be receiving two to six weeks of radiation to the arms or legs. It will describe how your treatments are given. It will also describe how to take care of
Radiation Therapy To the Arms or Legs You will be receiving two to six weeks of radiation to the arms or legs. It will describe how your treatments are given. It will also describe how to take care of
