PRO-CPR Guidelines: ACLS Algorithm Overview. (Non-AHA supplementary precourse material) Please read, print & bring to class
|
|
|
- Benedict Heath
- 9 years ago
- Views:
Transcription
1 PRO-CPR 2015 Guidelines: ACLS Algorithm Overview (Non-AHA supplementary precourse material) Please read, print & bring to class PRO-CPR 4/1/2016
2 Pulseless Rhythms (No Perfusion Despite Visible Cardiac Rhythm) Obtain: O2, IV, Monitor/Defibrillator/Emergency Cart Search for & treat underlying cause: PATCH up the patient! Pulmonary embolism Acute MI Acidosis Tension Pneumothorax Tablets/Toxins Cardiac Tamponade Hypo: volemia, oxia, glycemia, thermia, magnesemia Hyper & Hypo: kalemia Shockable Pulseless Rhythms: Ventricular Fibrillation, Ventricular Tachycardia, Torsades de Pointes. First Restore effective oxygenation, ventilation & circulation Begin high quality CPR asap: Compressions, Airway, Breathing Defibrillate asap. Resume CPR quickly after each shock, & give Epinephrine as soon as IV/IO in place. Continue. CPR x 2 min. (5 cycles of 30:2) & Drug > Shock Rotate compressors every 2 min. Keep rhythm checks to 10secs or <. V. Fib., V.Tach Torsades de Pointes with Long QT Interval Epinephrine then Epinephrine then Amiodarone or Magnesium sulfate and/or Lidocaine Lidocaine (if Magnesium ineffective) Remember: * Max out one antiarrythmic before going on to the next. 1 loading dose than, ½ following dose * Begin maintenance infusion of whichever antiarrythmic (above) resulted in conversion to perfusing rhythm. * High quality CPR, early defibrillation & early Epi is of primary importance! Clinical interventions should not significantly delay/interrupt defibrillation or CPR! Non-shockable Pulseless Rhythms: PEA (Pulseless Electrical Activity) & Asystole Find and treat an immediately correctable cause. Think PATCH! Begin high quality CPR asap! 5 cycles, of 30:2, /min or if intubated, deliver ventilations per minute with uninterrupted chest compressions. (no pause for breaths) This means ventilate until the chest rises, every 6 seconds. No Hyperventilation.
3 Bradycardia (Ventricular Rate <60/min.) Obtain: O2, Pulse Ox, IV, Monitor Search for & treat underlying cause: PATCH ~~~ Stable: Adequate Perfusion Observe: EKG, vital signs, report any change in status. Unstable: Poor Perfusion May be associated with symptoms such as: Chest pain, shortness of breath, decreased level of consciousness, hypotension, shock, ischemic chest pain, pulmonary congestion, or CHF. Regardless of pacemaker site (wide or narrow QRS complex, or regular or irregular rhythms), Rate enhancement is key! We must: Decrease vagal stimulus. Increase conduction through the AV Node. Provide regular & effective electrical stimulus to the Ventricles. Drug / Intervention: Atropine is recommended for the bradycardic patient with signs of poor perfusion. While effective on some Bradycardias, Atropine may not affect high degree, 2 nd Degree (Mobitz Type II), or 3 rd Degree AV block. It may not affect Idioventricular rhythms as well. Denervated (transplanted) hearts will not respond to Atropine, but may respond to Isuprel. In these cases, anticipate & prepare for Transcutaneous Pacing. Dopamine or Epinephrine infusions may be beneficial if there is a delay in pacing, or if pacing is ineffective. Remember, these drugs increase vasoconstriction, heart rate & B/P. Yet while aiding a slow heart rate, they can also cause myocardial ischemia. Use cautiously! Transvenous Pacing may be the ultimate solution!
4 Tachycardia (Ventricular Rate > 100 min.) Obtain: O2, Pulse Ox, IV, Monitor, Emergency Cart Seek expert consultation! Note: Most rate related symptoms are uncommon if heart rate is < 150. Seek expert consultation for any tachycardia in the presence of MI or poor perfusion. Search for & treat underlying cause: PATCH. ~~~ Unstable Tachycardia: Deliver Synchronized Cardioversion Inadequate Perfusion: Ventricular Rate > 150 = Immediate Synchronized Cardioversion. Sedate conscious patient; do not delay cardioversion! Atrial Flutter or SVT: J for monophasic or biphasic cardioversion. Increase 2 nd and subsequent joules in gradual increments. Atrial Fibrillation: 200J, with an end point of 360J for monophasic cardioversion, & J for biphasic cardioversion. Increase 2 nd and subsequent joules in gradual increments. Monomorphic Ventricular Tachycardia: 100J for monophasic or biphasic cardioversion. Increase 2 nd and subsequent joules in gradual increments. If patient develops pulseless VT, defibrillate immediately! Polymorphic Ventricular Tachycardia: Very unstable! Use defibrillation doses( j) for cardioversion. May require unsynchronized shock! Stable Tachycardia: Treat with Vagal Maneuvers &/ or Drugs Obtain: O2, Pulse Ox, IV, Monitor, 12 Lead EKG Supraventricular Tachycardia Narrow QRS: Regular Vagal Maneuvers Adenosine, then: Beta Blocker or Calcium Channel Blocker Ventricular Tachycardia Wide QRS: Regular & Monomorphic Adenosine, then: Procainamide or Amiodarone or Sotalol or Lidocaine
5 Tachycardia Additional thoughts. When is doubt, always seek expert consultation! Use heart rate, presence of P waves, and presenting signs & symptoms to differentiate between PSVT, SVT and Sinus Tachycardia. Remember, Sinus Tachycardia is a compensatory result of a body problem that can be easily treated by identifying the underlying cause (i.e. fever, dehydration, anemia), while PSVT & SVT is clearly a cardiac problem. Identify between Supraventricular (narrow QRS) & Ventricular Tachycardias (wide ORS). Supraventricular Tachycardia with Bundle Branch Block can appear as a Ventricular rhythm. For the stable patient, try vagal maneuvers &/or 12 Lead EKG to help differentiate between Ventricular & Supraventricular rhythms. Vagal maneuvers generally slow Supraventricular, but not Ventricular rhythms. Adenosine is recommended for both instances however, the rhythm MUST be monomorphic. With the exception of Adenosine, if the patient remains tachycardic after the next rate control drug is maxed out, do not give additional drugs. Compounding drugs may have a pro-arrhythmic effect on the heart. Let cardioversion be your 2 nd drug. Tachycardias caused by unstable re-entry (premature beat lands on preceding T wave) such as SVT & VT, respond well to synchronized cardioversion. Unstable Atrial Fibrillation & unstable Atrial Flutter may also respond well to synchronized cardioversion. Tachycardias caused by automatic pacemakers (pacemaker cells spontaneously depolarizing at a rapid rate ) such as Junctional Tachycardia, 2:1 Atrial Flutter, & Ectopic Atrial Tachycardia may respond better to drugs. Cardioversion is often ineffective & may actually increase the rate! One more time. When in doubt, always seek expert consultation!
6 Acute Coronary Syndromes Obtain: Oxygen, IV, Monitor, 12 Lead EKG, CXR, Emergency Cart Immediate Treatment Oxygen: If O2 sat < 94%, begin 4 liters/min. Titrate as needed (94 99%). Maintain a calm, reassuring atmosphere. Maintain patient in a comfortable position. May be detrimental to patients with ACS with O2 sat > 94%, who are not hypoxic. Aspirin: 160 to 325 mg (given by EMS, otherwise give asap), crush or have patient chew tablets. Decreases platelet aggregation (clumping), & arterial the site of ischemia or injury. ASA rectal suppository can be used for those who cannot tolerate ASA orally. Clopidogrel (Plavix) can be used by those with ASA allergy. Nitroglycerin: Sublingual, spray, or IV for ischemic syndromes. Dilates coronary arteries, allowing more blood (oxygen) to reach the heart muscle, thus decreasing pain from ischemia. Dilates peripheral vessels which decrease afterload, and work of the heart. Note: Contraindicated in Right Ventricular injury or infarction (as it causes an acute drop in pulmonary pressures). Use caution in patients with systolic B/P <90 mm Hg, and within 24 hours use of phosphodiesterase inhibitors (ie., Viagra). Morphine Sulfate: 2-4 mg. Acts as a pain & stress reliever. Dilates peripheral vessels which decrease afterload and work of the heart. Decreases acute cardiogenic pulmonary edema in normotensive patients. Use with caution for patients with Unstable Angina Immediate Assessment Perform a brief, targeted history & physical. Complete fibrinolytic checklist. Draw initial cardiac troponin, CRP, electrolytes and coagulation panels. Evaluate 12 Lead EKG, categorize according to results, begin adjunctive treatment: ST Elevation / New LBBB (Myocardial Ischemia) = STEMI. Reperfuse!!!! Use as indicated: Beta Blockers, Clopidogrel, Heparin (UFH, LMWH). If < 12 hrs from onset of symptoms, consider PCI (stent) within 90 mins., or fibrinolytics within 30 mins. (if fibrinolytic checklist is completed). Additional adjunctive support: ACE inhibitors or blockers & statin therapy. ST Depression / T wave inversion (Myocardial Injury) = UA/NSTEMI. High Risk!!!! Use as indicated: Nitroglycerin, Beta Blockers, Clopidogrel, Heparin (UFH or LMWH), Glycoprotein inhibitors. Monitor for homodynamic instability, ST changes, chest pain, V Tach. Perform Cardiac cath or stent placement as necessary within 48 hrs. of Acute MI. Additional support: Continue ASA, ACE inhibitors or blockers & statin therapy. Morphine should be given with caution for Unstable Angina, & if preload dependent.
7 No ST or T wave changes (Non-specific) = Intermediate low risk. Continue serial 12 lead EKG s & monitoring for ST changes. Continue serial Troponin. If changes occur, proceed to UA/NSTEMI algorithm. If unchanged and remains stable following Troponins & noninvasive imaging, patient may be discharged with cardiology follow up. Suspected Stroke & Immediate Post-Arrest Care Algorithms will be covered during class
8 Pulseless Rhythms (No Perfusion Despite Visible Cardiac Rhythm) Obtain: O2, IV, Monitor/Defibrillator/Emergency Cart Search for & treat underlying cause: PATCH up the patient! Pulmonary embolism Acute MI Acidosis Tension Pneumothorax Tablets/Toxins Cardiac Tamponade Hypo: volemia, oxia, glycemia, thermia, magnesemia Hyper & Hypo: kalemia Shockable Pulseless Rhythms: Think PATCH Ventricular Fibrillation, Ventricular Tachycardia, Torsades de Pointes. First Restore effective oxygenation, ventilation & circulation Begin high quality CPR asap: Compressions, Airway, Breathing Defibrillate asap! Resume CPR quickly after each shock, & give appropriate drug as soon as IV/IO in place. Continue. CPR x 2 min. {2 rescuer: Child - 5 cycles of 15:2 / Newborn - 15:2 compression to ventilation for arrest with cardiac etiology, or Newborn - 3:1 compression to ventilation for arrest due to asphyxia} & Drug > Shock. Rotate compressors every 2 min. Keep rhythm checks to 10secs or <. V. Fib., V.Tach Torsades de Pointes with Long QT Interval Epinephrine Epinephrine Amiodarone Magnesium sulfate Remember: * Max out one antiarrythmic before considering another. * Begin maintenance infusion of whichever antiarrythmic resulted in conversion to perfusing rhythm. * High quality CPR & early defibrillation is of primary importance! Clinical interventions should not significantly delay/interrupt defibrillation or CPR!
9 Non-shockable Pulseless Rhythms: PEA (Pulseless Electrical Activity) & Asystole Find and treat an immediately correctable cause. Think PATCH! Begin high quality CPR asap! 5 cycles, of 15:2, or if intubated, deliver 8-10 ventilations per minute with uninterrupted chest compressions. This means ventilate over 1 second, every 6 to 8 sec. Epinephrine Bradycardia (Ventricular Rate <60/min.) Obtain: O2, IV, Monitor, 12 Lead EKG, Emergency Cart Search for & treat underlying cause: PATCH ~~~ Stable: Adequate Pulse, Perfusion, & Respirations Observe: EKG, vital signs,02 as necessary, report any change in status. Unstable: Poor Perfusion, May be associated with symptoms such as: Shortness of breath, dyspnea, cyanosis, decreased level of consciousness, hypotension, & shock. Regardless of pacemaker site (wide or narrow QRS complex, or regular or irregular rhythms), rate enhancement with perfusion is key! We must: Provide O2, ventilation & perfusion as needed. Decrease vagal stimulus. Increase conduction through the AV Node. Provide regular & effective electrical stimulus to the Ventricles. Drug / Intervention: Begin CPR if heart rate <60/min., & showing no response to oxygenation & ventilation. Epinephrine IV/IO or ET is our drug of choice to increase vasoconstriction, heart rate & B/P. Atropine will be effective on Bradycardias secondary to increased vagal tone or 1 st & 2 nd Degree AV Blocks. It will have little or no effect on Complete AV Block, Idioventricular rhythms, or on denervated (transplanted) hearts. In these cases, anticipate & prepare for Trancutaneous Pacing. Transvenous Pacing may be the ultimate solution! Seek Expert Consultation!
10 Tachycardia (Ventricular Rate > 100 min.) Obtain: O2, IV, Monitor, 12 Lead EKG, Emergency Cart Seek expert consultation! Note: Most rate related symptoms are uncommon if heart rate is < 180 for children, or 220/min. for infants. Seek expert consultation for any tachycardia in the presence of poor perfusion. Rule out Sinus Tachycardia! Search for & treat underlying cause: PATCH. ~~~ Unstable Tachycardia: Inadequate Perfusion With Pulse. Ventricular Rate > 180/ min. for children, > 220 / min. for infants. May be associated with symptoms such as: Shortness of breath, dyspnea, cyanosis, delayed capillary refill, decrease level of consciousness, hyptotension, & shock. *Support patent airway & breathing. *Attempt Vagal maneuver while preparing for Adenosine administration. *If Adenosine delivery is delayed or unsuccessful, prepare for Synchronized Cardioversion. Sedate conscious patient; do not delay cardioversion. Stable Tachycardia: Adequate Perfusion With Pulse. Ventricular Rate > 180/ min. for children, > 220 / min. for infants. Obtain: O2, IV, Monitor, 12 Lead EKG *Support patent airway & breathing. *Observe: EKG, vital signs, report any changes. *Rule out Sinus Tachycardia! Use heart rate & presenting signs & symptoms to differentiate between SVT & Sinus Tachycardia. Remember, Sinus Tachycardia is a body problem, while SVT is clearly a cardiac problem. Narrow QRS (0.09 or <): Regular Supraventricular Tachycardia Wide QRS (0.09 or>): Regular & Monomorphic Possible Ventricular Tachycardia
11 Vagal Maneuvers Adenosine Adenosine, then: Amiodarone or Procainamide Again, seek expert consultation Tachycardia Additional thoughts. When is doubt, always seek expert consultation! Use heart rate, presence of P waves, and presenting signs & symptoms to differentiate between PSVT, SVT and Sinus Tachycardia. Remember, Sinus Tachycardia is a compensatory result of a body problem that can be easily treated by identifying the underlying cause (i.e. fever, dehydration, anemia), while PSVT & SVT is clearly a cardiac problem. Identify between Supraventricular (narrow QRS) & Ventricular Tachycardias (wide ORS). Supraventricular Tachycardia with Bundle Branch Block can appear as a Ventricular rhythm. For the stable patient, try vagal maneuvers &/or 12 Lead EKG to help differentiate between Ventricular & Supraventricular rhythms. Vagal maneuvers generally slow Supraventricular, but not Ventricular rhythms. Adenosine is recommended for both instances however, the rhythm MUST be monomorphic. With the exception of Adenosine, if the patient remains tachycardic after the next rate control drug is maxed out, do not give additional drugs. Compounding drugs may have a pro-arrhythmic effect on the heart. Let cardioversion be your 2 nd drug. Tachycardias caused by unstable re-entry (premature beat lands on preceding T wave) such as SVT & VT, respond well to synchronized cardioversion. Unstable Atrial Fibrillation & unstable Atrial Flutter may also respond well to synchronized cardioversion. Tachycardias caused by automatic pacemakers (pacemaker cells spontaneously depolarizing at a rapid rate ) such as Junctional Tachycardia, 2:1 Atrial Flutter, & Ectopic Atrial Tachycardia may respond better to drugs. Cardioversion is often ineffective & may actually increase the rate! One more time. When in doubt, always seek expert consultation!
12 Happy B- Day Karen R. Have a happy forever.
PRO-CPR. 2015 Guidelines: PALS Algorithm Overview. (Non-AHA supplementary precourse material)
 PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
ACLS PRE-TEST ANNOTATED ANSWER KEY
 ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
If you do not wish to print the entire pre-test you may print Page 2 only to write your answers, score your test, and turn in to your instructor.
 This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006. ECG Analysis. Name the following rhythms from the list below:
 American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
Cardiac Arrest VF/Pulseless VT Learning Station Checklist
 Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
ACLS Study Guide BLS Overview CAB
 ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
IU Health ACLS Study Guide
 IU Health ACLS Study Guide Preparing for your upcoming ACLS Class REVISED SEPTEMBER 2011 ON APRIL 1, 2011 WE BEGAN TEACHING THE 2010 AHA GUIDELINES. WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND
IU Health ACLS Study Guide Preparing for your upcoming ACLS Class REVISED SEPTEMBER 2011 ON APRIL 1, 2011 WE BEGAN TEACHING THE 2010 AHA GUIDELINES. WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC. BLS Changes
 ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
 ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109
 Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
www.cprtrainingfast.com
 ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Precourse Self-Assessment. May 2011. 2011 American Heart Association
 E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
Community Ambulance Service of Minot ALS Standing Orders Legend
 Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
8 Peri-arrest arrhythmias
 8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
Team Leader. Ensures high-quality CPR at all times Assigns team member roles Ensures that team members perform well. Bradycardia Management
 ACLS Megacode Case 1: Sinus Bradycardia (Bradycardia VF/Pulseless VT Asystole Out-of-Hospital Scenario You are a paramedic and arrive on the scene to find a 57-year-old woman complaining of indigestion.
ACLS Megacode Case 1: Sinus Bradycardia (Bradycardia VF/Pulseless VT Asystole Out-of-Hospital Scenario You are a paramedic and arrive on the scene to find a 57-year-old woman complaining of indigestion.
PEDIATRIC TREATMENT GUIDELINES
 P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
Adult Drug Reference. Dopamine Drip Chart. Pediatric Drug Reference. Pediatric Drug Dosage Charts DRUG REFERENCES
 Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
Normal Sinus Rhythm. Sinus Bradycardia. Sinus Tachycardia. Rhythm ECG Characteristics Example (NSR) & consistent. & consistent.
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
PALS Interim Study Guide
 PALS Interim Study Guide 2006 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released November 28, 2005! The new AHA Handbook of Emergency Cardiac Care (ECC)
PALS Interim Study Guide 2006 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released November 28, 2005! The new AHA Handbook of Emergency Cardiac Care (ECC)
ACLS RHYTHM TEST. 2. A 74-year-old woman with chest pain. Blood pressure 192/90 and rates her pain 9/10.
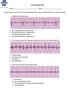 ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS. (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support)
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001
 BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
HTEC 91. Topic for Today: Atrial Rhythms. NSR with PAC. Nonconducted PAC. Nonconducted PAC. Premature Atrial Contractions (PACs)
 HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
HTEC 91 Medical Office Diagnostic Tests Week 4 Topic for Today: Atrial Rhythms PACs: Premature Atrial Contractions PAT: Paroxysmal Atrial Tachycardia AF: Atrial Fibrillation Atrial Flutter Premature Atrial
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
NAME OF THE HOSPITAL: 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3
 1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
1. Coronary Balloon Angioplasty: M7F1.1/ Angioplasty with Stent(PTCA with Stent): M7F1.3 1. Name of the Procedure: Coronary Balloon Angioplasty 2. Select the Indication from the drop down of various indications
table of contents drug reference
 table of contents drug reference ADULT DRUG REFERENCE...155 161 PEDIATRIC DRUG REFERENCE...162 164 PEDIATRIC WEIGHT-BASED DOSING CHARTS...165 180 Adenosine...165 Amiodarone...166 Atropine...167 Defibrillation...168
table of contents drug reference ADULT DRUG REFERENCE...155 161 PEDIATRIC DRUG REFERENCE...162 164 PEDIATRIC WEIGHT-BASED DOSING CHARTS...165 180 Adenosine...165 Amiodarone...166 Atropine...167 Defibrillation...168
New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010!
 ACLS Study Guide 2010 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010! The new AHA Handbook of Emergency Cardiac Care (ECC) contains
ACLS Study Guide 2010 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010! The new AHA Handbook of Emergency Cardiac Care (ECC) contains
Crash Cart Drugs Drugs used in CPR. Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University
 Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
Wilson County Emergency Management Agency Protocol Manual Protocols
 Asystole No pulse or respirations Confirm cardiac rhythm with combo pads or electrodes Record in two leads to confirm Asystole and to rule out fine V-Fib. Basic assessment and management (up to your scope
Asystole No pulse or respirations Confirm cardiac rhythm with combo pads or electrodes Record in two leads to confirm Asystole and to rule out fine V-Fib. Basic assessment and management (up to your scope
TO GET PAST THE 2 HARDEST STATIONS AT STATE PARAMEDIC BOARDS
 A REVIEW OF THE 2 CARDIOLOGY STATIONS: WHAT TO SAY & WHAT TO DO TO GET PAST THE 2 HARDEST STATIONS AT STATE PARAMEDIC BOARDS VERSION 8 AHA ECC 2005 STANDARD---BY JAMES ROFF PARAMEDIC GRADUATE PREPARATION
A REVIEW OF THE 2 CARDIOLOGY STATIONS: WHAT TO SAY & WHAT TO DO TO GET PAST THE 2 HARDEST STATIONS AT STATE PARAMEDIC BOARDS VERSION 8 AHA ECC 2005 STANDARD---BY JAMES ROFF PARAMEDIC GRADUATE PREPARATION
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Exams. May 2011
 E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
Advanced Cardiovascular Life Support Case Scenarios
 Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Advanced Cardiac Life Support
 Advanced Cardiac Life Support Dr Teo Wee Siong NATIONAL RESUSCITATION COUNCIL Singapore Guidelines 2006 Prof Anantharaman A/Prof Lim Swee Han Dr Chee Tek Siong A/Prof Peter Manning A/Prof Eillyne Seow
Advanced Cardiac Life Support Dr Teo Wee Siong NATIONAL RESUSCITATION COUNCIL Singapore Guidelines 2006 Prof Anantharaman A/Prof Lim Swee Han Dr Chee Tek Siong A/Prof Peter Manning A/Prof Eillyne Seow
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Current Management of Atrial Fibrillation DISCLOSURES. Heart Beat Anatomy. I have no financial conflicts to disclose
 Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Adult Cardiac Life Support (ACLS) Recertification Preparatory Materials
 Adult Cardiac Life Support (ACLS) Recertification Preparatory Materials 1 ADULT CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION TABLE OF CONTENTS PRIMARY AND SECONDARY ABCDs I. Primary ABCD s 03 II. Secondary
Adult Cardiac Life Support (ACLS) Recertification Preparatory Materials 1 ADULT CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION TABLE OF CONTENTS PRIMARY AND SECONDARY ABCDs I. Primary ABCD s 03 II. Secondary
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY. Guidelines for Use of Intravenous Isoproterenol
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
Bradycardia CHAPTER 12 CODE SCENARIO
 Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
Diagnosis Code Crosswalk : ICD-9-CM to ICD-10-CM Cardiac Rhythm and Heart Failure Diagnoses
 Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
Diagnosis Code Crosswalk : to 402.01 Hypertensive heart disease, malignant, with heart failure 402.11 Hypertensive heart disease, benign, with heart failure 402.91 Hypertensive heart disease, unspecified,
ACLS123.com 818.766.1111 2012. ACLS Study Guide. Critical Care Training Center
 ACLS123.com 818.766.1111 2012 ACLS Study Guide Critical Care Training Center 12/1/2012 Course Overview This study guide is an outline of content that will be taught in the American Heart Association Accredited
ACLS123.com 818.766.1111 2012 ACLS Study Guide Critical Care Training Center 12/1/2012 Course Overview This study guide is an outline of content that will be taught in the American Heart Association Accredited
Basic Cardiac Rhythms Identification and Response
 Basic Cardiac Rhythms Identification and Response Module 1 ANATOMY, PHYSIOLOGY, & ELECTRICAL CONDUCTION Objectives Describe the normal cardiac anatomy and physiology and normal electrical conduction through
Basic Cardiac Rhythms Identification and Response Module 1 ANATOMY, PHYSIOLOGY, & ELECTRICAL CONDUCTION Objectives Describe the normal cardiac anatomy and physiology and normal electrical conduction through
10. An infant with a history of vomiting and diarrhea arrives by ambulance. During your primary assessment the infant responds only to painful stimula
 1. You are called to help resuscitate an infant with severe symptomatic bradycardia associated with respiratory distress. The bradycardia persists despite establishment of an effective airway, oxygenation,
1. You are called to help resuscitate an infant with severe symptomatic bradycardia associated with respiratory distress. The bradycardia persists despite establishment of an effective airway, oxygenation,
American Heart Association. Pediatric Advanced Life Support. Written Precourse Self-Assessment. Questions and Answer Key for Students.
 E C C American Heart Association Pediatric Advanced Life Support Written Precourse Self-Assessment Questions and Answer Key for Students January 2012 PALS Written 2011 Precourse Self-Assessment ECG Rhythm
E C C American Heart Association Pediatric Advanced Life Support Written Precourse Self-Assessment Questions and Answer Key for Students January 2012 PALS Written 2011 Precourse Self-Assessment ECG Rhythm
Alabama Medications. Christopher J. Colvin January 2010
 Alabama Medications Christopher J. Colvin p January 2010 Activated Charcoal Used to absorb toxins ingested before they can be absorbed in the GI system. Contraindicated in AMS patients who cannot control
Alabama Medications Christopher J. Colvin p January 2010 Activated Charcoal Used to absorb toxins ingested before they can be absorbed in the GI system. Contraindicated in AMS patients who cannot control
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive.
 It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
NEONATAL & PEDIATRIC ECG BASICS RHYTHM INTERPRETATION
 NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
NEONATAL & PEDIATRIC ECG BASICS & RHYTHM INTERPRETATION VIKAS KOHLI MD FAAP FACC SENIOR CONSULATANT PEDIATRIC CARDIOLOGY APOLLO HOSPITAL MOB: 9891362233 ECG FAX LINE: 011-26941746 THE BASICS: GRAPH PAPER
RAPID INTERPRETATION OF. EKG s
 Personal Quick Reference Sheets 333 (pages 333 to 346) There is no need to remove these reference pages from your book. To download and print them in full color, go to: www.themdsite.com Reference Sheets
Personal Quick Reference Sheets 333 (pages 333 to 346) There is no need to remove these reference pages from your book. To download and print them in full color, go to: www.themdsite.com Reference Sheets
Procedure 17: Cardiopulmonary Resuscitation
 Cardiopulmonary Resuscitation 349 Procedure 17: Cardiopulmonary Resuscitation Introduction Cardiopulmonary arrest (CPA) occurs when a patient s heart and lungs stop functioning. In children, CPA usually
Cardiopulmonary Resuscitation 349 Procedure 17: Cardiopulmonary Resuscitation Introduction Cardiopulmonary arrest (CPA) occurs when a patient s heart and lungs stop functioning. In children, CPA usually
An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams
 Arrhythmias 1 An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams Things to keep in mind when analyzing arrhythmias: Electrical activity recorded in 12 and 15 leads Examine
Arrhythmias 1 An Introduction to Tachyarrhythmias R. A. Seyon MN, NP, CCN(C) & Dr. R. G. Williams Things to keep in mind when analyzing arrhythmias: Electrical activity recorded in 12 and 15 leads Examine
WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND IN THE 2010 ACLS Textbook available through AHA and other retail outlets.
 ACLS STUDY GUIDE 2015 WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND IN THE 2010 ACLS Textbook available through AHA and other retail outlets. The AHA also requests the following in preparation
ACLS STUDY GUIDE 2015 WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND IN THE 2010 ACLS Textbook available through AHA and other retail outlets. The AHA also requests the following in preparation
Purpose To guide registered nurses who may manage clients experiencing sudden or unexpected life-threatening cardiac emergencies.
 Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
OBJECTIVES. When the student has finished this module, he/she will be able to:
 Advanced Cardiac Life Support (ACLS) Review WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited
Advanced Cardiac Life Support (ACLS) Review WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited
The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010.
 ACLS Study Guide The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. Please read the below information carefully This letter is to confirm your
ACLS Study Guide The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. Please read the below information carefully This letter is to confirm your
By the end of this continuing education module the clinician will be able to:
 EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
EKG Interpretation WWW.RN.ORG Reviewed March, 2015, Expires April, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2015 RN.ORG, S.A., RN.ORG, LLC Developed
Practical ACLS Megacode Testing and Training Scenario Set for SimPad. Consolidated Instructor Manual. Frances Wickham Lee, DBA
 Practical ACLS Megacode Testing and Training Scenario Set for SimPad Consolidated Instructor Manual Frances Wickham Lee, DBA Scenario Authors: Frances Wickham Lee, DBA John Walker, BHS John Schaefer, MD
Practical ACLS Megacode Testing and Training Scenario Set for SimPad Consolidated Instructor Manual Frances Wickham Lee, DBA Scenario Authors: Frances Wickham Lee, DBA John Walker, BHS John Schaefer, MD
Department of Emergency and Disaster Medicine Medical University of LODZ
 Electrotherapy in emergency states Department of Emergency and Disaster Medicine Medical University of LODZ defibrillation defibrillation The purpous of defibrillation is to deliver a randomly timed high-energy
Electrotherapy in emergency states Department of Emergency and Disaster Medicine Medical University of LODZ defibrillation defibrillation The purpous of defibrillation is to deliver a randomly timed high-energy
Electrophysiology Daymar College. Lisa H. Young, RN, BSN, MAE 2011
 Electrophysiology Daymar College Lisa H. Young, RN, BSN, MAE 2011 Electrical Conduction Pathway Chemical Basis for Impulse Formation Cardiac Action Potential Phases http://www.youtube.com/watch?v=oqpffilde0e
Electrophysiology Daymar College Lisa H. Young, RN, BSN, MAE 2011 Electrical Conduction Pathway Chemical Basis for Impulse Formation Cardiac Action Potential Phases http://www.youtube.com/watch?v=oqpffilde0e
MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES. Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003.
 MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003. 1 ET Administration Atropine o First drug for symptomatic sinus bradycardia
MEDICATIONS USED IN ADULT CODE BLUE EMERGENCIES Source: ACLS Provider Manual. American Heart Association. 2001, 2002. Updated 2003. 1 ET Administration Atropine o First drug for symptomatic sinus bradycardia
Management of Adult Cardiac Arrest
 73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
ACLS Rhythms for the ACLS Algorithms
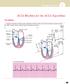 ACLS Rhythms for the ACLS Algorithms The Basics 1. Anatomy of the cardiac conduction system: relationship to the ECG cardiac cycle. A, Heart: anatomy of conduction system. B, P-QRS-T complex: lines to
ACLS Rhythms for the ACLS Algorithms The Basics 1. Anatomy of the cardiac conduction system: relationship to the ECG cardiac cycle. A, Heart: anatomy of conduction system. B, P-QRS-T complex: lines to
Banner Staff Service ECG Study Guide
 Banner Staff Service ECG Study Guide Edited by Larry H. Lybbert, MS, RN Table of Contents ECG STUDY GUIDE... 3 ECG INTERPRETATION BASICS... 4 EKG GRAPH PAPER...4 RATE MEASUREMENT...9 The Six Second Method...9
Banner Staff Service ECG Study Guide Edited by Larry H. Lybbert, MS, RN Table of Contents ECG STUDY GUIDE... 3 ECG INTERPRETATION BASICS... 4 EKG GRAPH PAPER...4 RATE MEASUREMENT...9 The Six Second Method...9
Guideline for the management of arrhythmias
 Guideline for the management of arrhythmias The following guideline is approved only for use at University College London Hospitals NHS Foundation Trust. It is provided as supporting information for the
Guideline for the management of arrhythmias The following guideline is approved only for use at University College London Hospitals NHS Foundation Trust. It is provided as supporting information for the
The American Heart Association Guidelines Including Pediatric Resuscitation
 Lesson 3 The American Heart Association Guidelines Including Pediatric Resuscitation Sharon E. Mace, MD, FACEP, FAAP Objectives On completion of this lesson, you should be able to: 1. List the correct
Lesson 3 The American Heart Association Guidelines Including Pediatric Resuscitation Sharon E. Mace, MD, FACEP, FAAP Objectives On completion of this lesson, you should be able to: 1. List the correct
Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations.
 INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
INTRODUCTION Coronary Artery Disease leading cause of morbidity & mortality in industrialised nations. Although decrease in cardiovascular mortality still major cause of morbidity & burden of disease.
Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials
 Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials 1 PEDIATRIC ADVANCED LIFE SUPPORT (PALS) RECERTIFICATION TABLE OF CONTENTS CYCLIC APPROACH 03 PEDIATRIC ASSESSMENT FLOWCHART
Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials 1 PEDIATRIC ADVANCED LIFE SUPPORT (PALS) RECERTIFICATION TABLE OF CONTENTS CYCLIC APPROACH 03 PEDIATRIC ASSESSMENT FLOWCHART
AMERICAN HEART ASSOCIATION 2010 ACLS GUIDELINES: WHAT EVERY CLINICIAN NEEDS TO KNOW
 AMERICAN HEART ASSOCIATION 2010 ACLS GUIDELINES: WHAT EVERY CLINICIAN NEEDS TO KNOW Joseph Heidenreich, MD Texas A&M Health Science Center Scott & White Memorial Hospital Scott & White Memorial Hospital
AMERICAN HEART ASSOCIATION 2010 ACLS GUIDELINES: WHAT EVERY CLINICIAN NEEDS TO KNOW Joseph Heidenreich, MD Texas A&M Health Science Center Scott & White Memorial Hospital Scott & White Memorial Hospital
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
Exam Name MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What term is used to refer to the process of electrical discharge and the flow of electrical
DEBRIEFING GUIDE. The key components of an optimal code response: 1. Early recognition that the patient is deteriorating or has become unresponsive.
 DEBRIEFING GUIDE I N T R O D U C T I O N Debriefing has been shown to improve clinical behavior during cardiac resuscitation and, as such, has become a recommended procedure in the 2010 American Heart
DEBRIEFING GUIDE I N T R O D U C T I O N Debriefing has been shown to improve clinical behavior during cardiac resuscitation and, as such, has become a recommended procedure in the 2010 American Heart
If you do not wish to print the entire pre-test you may print Page 2 only to write your answers, score your test, and turn in to your instructor.
 This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
Atrial Fibrillation Peter Santucci, MD Revised May, 2008
 Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
Atrial Fibrillation Peter Santucci, MD Revised May, 2008 Atrial fibrillation (AF) is an irregular, disorganized rhythm characterized by a lack of organized mechanical atrial activity. The atrial rate is
the basics Perfect Heart Institue, Piyavate Hospital
 ECG INTERPRETATION: the basics Damrong Sukitpunyaroj MD Damrong Sukitpunyaroj, MD Perfect Heart Institue, Piyavate Hospital Overview Conduction Pathways Systematic Interpretation Common abnormalities in
ECG INTERPRETATION: the basics Damrong Sukitpunyaroj MD Damrong Sukitpunyaroj, MD Perfect Heart Institue, Piyavate Hospital Overview Conduction Pathways Systematic Interpretation Common abnormalities in
Quiz 4 Arrhythmias summary statistics and question answers
 1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier
 Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier Most common dysrhythmia seen in ED, and incidence increasing with ageing population Presentation Common presentations: younger patients often
Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier Most common dysrhythmia seen in ED, and incidence increasing with ageing population Presentation Common presentations: younger patients often
Stimulates HR, BP, CO, and vasoconstriction. Stimulates renal, venous, mesenteric arterial. basic chart below) (alpha receptors) vasoconstriction
 Bolus Alternate Range Drip ACLS Drugs and Drips Amiodarone / Cordarone Lidocaine Procainamide / Pronestyl Dopamine / Intropin CARDIAC ARREST PULSELESS VT/VF Arrest Kit: (300mg bolus) Amiodarone 6 Vial
Bolus Alternate Range Drip ACLS Drugs and Drips Amiodarone / Cordarone Lidocaine Procainamide / Pronestyl Dopamine / Intropin CARDIAC ARREST PULSELESS VT/VF Arrest Kit: (300mg bolus) Amiodarone 6 Vial
Wide-Complex Tachycardias in the ED: Myths and Pitfalls
 Wide-Complex Tachycardias in the ED: Myths and Pitfalls, FACEP, FAAEM Professor and Vice Chair Director, Emergency Cardiology Fellowship Department of Emergency Medicine University of Maryland School of
Wide-Complex Tachycardias in the ED: Myths and Pitfalls, FACEP, FAAEM Professor and Vice Chair Director, Emergency Cardiology Fellowship Department of Emergency Medicine University of Maryland School of
Cardiac Arrest: General Considerations
 Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Megacode Testing Checklist 1/2 Bradycardia VF/Pulseless VT Asystole ROSC
 Megacode Testing Checklist 1/2 Bradycardia VF/Pulseless VT Asystole ROSC Student Name: Test Bradycardia Management Recognizes symptomatic bradycardia Administers correct dose of atropine Prepares for second-line
Megacode Testing Checklist 1/2 Bradycardia VF/Pulseless VT Asystole ROSC Student Name: Test Bradycardia Management Recognizes symptomatic bradycardia Administers correct dose of atropine Prepares for second-line
Michigan Adult Cardiac Protocols CARDIAC ARREST GENERAL. Date: May 31, 2012 Page 1 of 5
 Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
Atrial Fibrillation Management Across the Spectrum of Illness
 Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
School of Health Sciences
 School of Health Sciences Cardiology Teaching Package A Beginners Guide to Normal Heart Function, Sinus Rhythm & Common Cardiac Arrhythmias Welcome This document extends subjects covered in the Cardiology
School of Health Sciences Cardiology Teaching Package A Beginners Guide to Normal Heart Function, Sinus Rhythm & Common Cardiac Arrhythmias Welcome This document extends subjects covered in the Cardiology
The management of cardiac arrest
 CHAPTER 6 The management of cardiac arrest LEARNING OBJECTIVES In this chapter you will learn: How to assess the cardiac arrest rhythm and perform advanced life support 6.1. INTRODUCTION Cardiac arrest
CHAPTER 6 The management of cardiac arrest LEARNING OBJECTIVES In this chapter you will learn: How to assess the cardiac arrest rhythm and perform advanced life support 6.1. INTRODUCTION Cardiac arrest
ECG Findings. IV Access. 12 Lead Interpretation: STEMI and NSTEMI. ACLS Acute Coronary Syndrome Chest Pain Suggestive of Ischemia.
 12 Lead Interpretation: STEMI and NSTEMI Presented by Annmarie Keck, RN, BSN, CEN Northwest MedStar Clinical Outreach Educator ACLS Acute Coronary Syndrome Chest Pain Suggestive of Ischemia Immediate Assessment
12 Lead Interpretation: STEMI and NSTEMI Presented by Annmarie Keck, RN, BSN, CEN Northwest MedStar Clinical Outreach Educator ACLS Acute Coronary Syndrome Chest Pain Suggestive of Ischemia Immediate Assessment
Automatic External Defibrillators
 Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: May 27, 2016 Number: MG.MM.DM.10dC2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
CRNA ACLS, PALS, & BLS REFRESHER
 Attn: Certified Nurse Anesthetists (CRNA) CPR Consultants, Inc. 7404 G Chapel Hill Road, Raleigh, NC, 27607 CRNA ACLS, PALS, & BLS REFRESHER CRNA American Heart Association Triple Certification (BLS, ACLS,
Attn: Certified Nurse Anesthetists (CRNA) CPR Consultants, Inc. 7404 G Chapel Hill Road, Raleigh, NC, 27607 CRNA ACLS, PALS, & BLS REFRESHER CRNA American Heart Association Triple Certification (BLS, ACLS,
Chapter 16. Learning Objectives. Learning Objectives 9/11/2012. Shock. Explain difference between compensated and uncompensated shock
 Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
Chapter 16 Shock Learning Objectives Explain difference between compensated and uncompensated shock Differentiate among 5 causes and types of shock: Hypovolemic Cardiogenic Neurogenic Septic Anaphylactic
Introduction to Electrocardiography. The Genesis and Conduction of Cardiac Rhythm
 Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
Introduction to Electrocardiography Munther K. Homoud, M.D. Tufts-New England Medical Center Spring 2008 The Genesis and Conduction of Cardiac Rhythm Automaticity is the cardiac cell s ability to spontaneously
Recurrent AF: Choosing the Right Medication.
 In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
In the name of God Shiraz E-Medical Journal Vol. 11, No. 3, July 2010 http://semj.sums.ac.ir/vol11/jul2010/89015.htm Recurrent AF: Choosing the Right Medication. Basamad Z. * Assistant Professor, Department
2015 Interim Resources for HeartCode ACLS
 2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Precourse Self-Assessment. October 2006
 E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment Contents: Precourse Self-Assessment Memo Support Help for CD and FAQs Answer Sheet Self-Assessment
E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment Contents: Precourse Self-Assessment Memo Support Help for CD and FAQs Answer Sheet Self-Assessment
BLS: basic cardiac life support. ACLS: advanced cardiac life support. PALS: paediatric advanced life support. VF: ventricular fibrillation
 RN-Initiated Emergency Cardiac Care: Decision Support Tool #2 Emergency Cardiac Care in Areas Using Cardiac Monitoring, Defibrillation and Emergency Cardiac Drugs Decision support tools are evidenced-based
RN-Initiated Emergency Cardiac Care: Decision Support Tool #2 Emergency Cardiac Care in Areas Using Cardiac Monitoring, Defibrillation and Emergency Cardiac Drugs Decision support tools are evidenced-based
Here is a drug list that you need to know before taking the NREMT-P exam!! Taken from the book EMS NOTES.com
 Here is a drug list that you need to know before taking the NREMT-P exam!! Taken from the book EMS NOTES.com Special thanks to the number #1 internet training site id44.com and also to (NOTE) Please remember
Here is a drug list that you need to know before taking the NREMT-P exam!! Taken from the book EMS NOTES.com Special thanks to the number #1 internet training site id44.com and also to (NOTE) Please remember
Basic ECG rhythm interpretation skills (see our Six Second ECG Essentials or Mastery courses and our Six Second ECG Simulator online)
 SkillStat ACLS Precourse Package Thank you for choosing SkillStat Learning Inc. for your Advanced Life Support training needs. SkillStat Learning Inc. has delivered advanced practice programs to healthcare
SkillStat ACLS Precourse Package Thank you for choosing SkillStat Learning Inc. for your Advanced Life Support training needs. SkillStat Learning Inc. has delivered advanced practice programs to healthcare
The Pharmacist s Role in Advanced Cardiac Life Support (ACLS) Pharmacist Objectives. Pharmacists in the ER. Background
 The Pharmacist s Role in Advanced Cardiac Life Support (ACLS) I have no actual or potential conflict of interest in relation to this activity. it James Jensen B.S., Pharm.D., BCPS Pharmacist Objectives
The Pharmacist s Role in Advanced Cardiac Life Support (ACLS) I have no actual or potential conflict of interest in relation to this activity. it James Jensen B.S., Pharm.D., BCPS Pharmacist Objectives
