Adult Cardiac Life Support (ACLS) Recertification Preparatory Materials
|
|
|
- Gloria Nelson
- 10 years ago
- Views:
Transcription
1 Adult Cardiac Life Support (ACLS) Recertification Preparatory Materials 1
2 ADULT CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION TABLE OF CONTENTS PRIMARY AND SECONDARY ABCDs I. Primary ABCD s 03 II. Secondary ABCD s 04 AIRWAY SKILLS I. Basic 04 II. Advanced 05 ARRHYTHMIAS 06 ELECTRICAL THERAPY 07 VASCULAR ACCESS 07 ACLS DRUGS 08 ACLS CORE CASES I. Respiratory Arrest Case 09 II. VF Treated with CPR and AED Case 09 III. Pulseless Arrest: VF / Pulseless VT Case 10 IV. Pulseless Arrest: Pulseless Electrical Activity (PEA) Case 11 V. Pulseless Arrest: Aystole Case 11 VI. Acute Coronary Symptoms (ACS) 13 VII. Bradycardia Case 14 VIII. Unstable Tachycardia 15 IX. Stable Tachycardia 15 X. Acute Stroke Case 17 2
3 What is ACLS? ACLS is an assess then manage approach for those at risk of or in cardiac arrest. Primary and Secondary ABCD s This is a methodical assess-then-manage approach used to treat adults in respiratory distress and failure, stable and unstable arrhythmias and pulseless arrest. Algorithms are menus that guide you through recommended treatment interventions. Know the following ABCD s approach because it begins all ACLS case scenarios. The information you gather during the assessment will determine which algorithm you choose for the patient s treatment. I. Primary ABCDs: these refer to CPR and the AED. A. A ssess: Tap and ask: Are you OK? A. send someone to call 911 and bring an AED B. if alone, call 911, get an AED and return to victim Airway: Open with the head-tilt/chin lift. B. B reathing: Assess for adequate breathing. 1. if inadequate: give 2 breaths over 1 second each 2. each breath should cause a visible chest rise 3. use mouth-to-mask or barrier, bag mask - ventilation (BMV) or mouth to mouth 4. give oxygen (O 2 ) as soon as it is available C. C irculation: Check carotid pulse for no more than 10 seconds 1. if not definitely felt, give 30 compressions in center of chest between the nipples 2. compress the chest wall 1½ - 2 inches 3. one cycle of CPR is 30 compressions and 2 breaths 4. give 5 cycles of CPR (about 2 minutes) 5. minimize interruptions to compressions 6. 2 rescuers: the compressor PAUSES while 2 breaths are given 7. change compressors after 5 cycles to avoid fatigue and ineffective compressions D. D efibrillation: When an AED arrives, immediately power it on! 1. follow the voice prompts 2. use adult pads on adults 3
4 II. Secondary ABCDs A. A irway: Use bag mask connected to 100% O 2 1. give each breath over 1 second each 2. compressor pauses to allow the 2 breaths to go in 3. consider inserting an advanced airway, (see Advanced Airway on page 5) B. B reathing: Look for visible chest rise during each breath 1. confirm advanced airway tube placement (see Advanced Airway on page 5) 2. secure the airway tube. 3. compressor now gives 100 continuous compressions per minute 4. ventilator gives 8-10 breaths per minute (one every 6-9 seconds) C. C irculation: Obtain vascular access with an IV(intravascular) or 10 (intraosseous) cannula 1) give drugs as recommended per algorithm. D. D iagnosis: Why is the patient in the rhythm? Look for any possible causes to treat: 6 Hs 5 Ts H ypoxia H ypovolemia H ypothermia H ypoglycemia H ypo / H yperkalemia H ydrogen ion (acidosis) T amponade T ension pneumothorax T oxins poisons, drugs T hrombosis coronary (AMI) pulmonary (PE) T rauma Airway Skills I. Basic Airway A. Oxygen B. Open the Airway 1. use the head - tilt chin lift when assessing for adequate breathing 2. use a jaw thrust for unresponsive unwitnessed, trauma or drowning victims if unable to open the airway with a jaw thrust, use head-tilt chin lift C. Maintain 1. insert an oropharyngeal airway when unconscious with no cough or gag reflex 2. insert a nasopharyngeal airway when a cough or gag reflex is present (better tolerated) D. Ventilate: give each breath over 1 second using enough volume to see the chest rise 1. 2-rescuer CPR: give 2 breaths during the pause following 30 compressions 2. Rescue breathing: when a pulse is present, give breaths/minute (one each 5-6 seconds) 4
5 II. Advanced Airway A. Laryngeal Mask Airway (LMA): requires the least training for insertion 1. inserts blindly into the hypopharynx 2. regurgitation and aspiration are reduced but not prevented 3. confirm placement: see chest rise and listen for breath sounds over lung fields 4. contraindications: gastric reflux, full stomach, pregnancy or morbid obesity B. Combitube: requires more training for insertion than the LMA 1. inserts blindly into esophagus (80% of the time) or the trachea 2. ventilation can occur whether the tube is the esophagus or the trachea 3. confirm placement: clinical exam and a confirmation device (see devices) 4. contraindications: gag reflex, esophageal disease, caustic ingestion, under 16 years of age or under 60 inches in height C. Endotracheal Tube (ETT): requires the most training, skill and frequent retraining for insertion 1. inserts by direct visualization of vocal chords 2. isolates the trachea, greatly reduces risk of aspiration and provides reliable ventilation 3. high risk of tube displacement or obstruction whenever patient is moved 4. confirm placement, clinical exam and a confirmation device (see devices) D. Confirm tube placement 1. Clinical Assessment a. look for bilateral chest rise b. listen for breath sounds over stomach and the 4 lung fields (left and right anterior and midaxillary) c. look for water vapor in the tube (if seen this is helpful but not definitive) 2. Devices a. End-Tidal CO 2 Detector (ETD): if weight > 2 kg i. attaches between the ET and Ambu bag; give 6 breaths with the Ambu bag ii. litmus paper center should change color with each inhalation and each exhalation original color on inhalation = OK O 2 is being exhaled: expected color change on exhalation = CO 2!! Tube is in trachea iii. Trouble shooting: original color on exhalation = litmus paper is wet replace ETD, or tube is not in trachea remove ET, or cardiac output is low during CPR b. Esophageal Detector (EDD): if weight > 20 kg and in a perfusing rhythm i. Resembles a turkey baster compress the bulb and attach to end of ET bulb inflates quickly - tube is in the trachea bulb inflates poorly - tube is in the esophagus ii. No recommendation for its use in cardiac arrest 5
6 Arrhythmias Pulseless Rhythms (Arrest Rhythms) Shockable VF (Ventricular Fibrillation) VT (Ventricular Tach Pulsless) Torsades de Pointes Non-Shockable PEA (Pulseless Electrical Activity) Asystole (Silent Heart) Perfusing Rhythms (Non-Arrest Rhythms) Bradycardia Sinus Bradycardia Junctional Rhythm Idioventricular Rhythm Artioventricular Block: 1 st Degree 2 nd Degree: Mobitz Type I (Wenckebach) Mobitz Type II 3 rd Degree (Complete Heart Block) Tachycardias: Narrow QRS Regular Rhythms: Sinus Tachycardias Atrial Flutter Supraventricular Tachycardia Junctional Tachycardia Irregular Rhythms: Atrial Flutter Atrial Fibrillation Multifocal Atrial Tachycardia Tachycardias: Wide QRS Regular Rhythm: Ventricular Tachycardia monomorphic Ventricular Tachycardia polymorphic Torsades des pointes 6
7 Electrical Therapy I. Defibrillation: high energy shocks with manual defibrillator: ECC handbook, p. 9 A. recommended shock dose: biphasic = J (per manufacturer) B. recommended shock dose: monophasic = 360 J II. Synchronized Cardioversion: timed low energy shocks: ECC handbook p. 14 A. timed to QRS to reduce risk of R-on-T : a shock that hits the T wave may cause VF III. Transcutaneous Pacer: noninvasive emergent bedside pacing: ECC handbook, p. 62 A. apply pacer pads B. verify pacer capture Vascular Access Peripheral: preferred in arrest due to easy access and no interruption in CPR A. use a large bore IV catheter B. attempt large veins: anticubital, external jugular, cephalic, femoral C. can take 1-2 minutes for IV drugs to reach the central circulation D. follow IV drugs with a 20 ml bolus of IV fluid and elevate extremity for seconds Intraosseous (IO): inserts into a large bone and accesses the venous plexus A. may use if unable to obtain intravascular access B. drug delivery is similar to that via a central line C. safe access for fluids, drugs, blood samples D. commercial kits are available for IO access E. drug doses are the same as when given IV Central Line: not needed in most resuscitations A. insertion requires interruption of CPR B. if a central line is already in place and patent, it can be used Endotracheal: some drugs may be given via the ETT in the absence of a IV/IO A. drug delivery is unpredictable thus IV/IO delivery is preferred B. drug blood concentration stay lower than when given IV C. increase dose given to times the recommended IV dose D. drugs that absorb via the trachea E. N aloxone A tropine V asopressin E pinephrine L idocaine 7
8 ACLS Drugs The primary focus in cardiac arrest is effective CPR and early defibrillation. Drug administration is secondary and should NOT interrupt CPR. Know the timing of drug administration in CPR as shown. The Class of Recommendation number denotes potential benefit versus risk. General Statements: Pulse arrest, all: give a vasopressor drug Epinephrine or Vasopressin Vasopressors cause peripheral vasoconstriction, which shunts increased blood flow to the heart and brain. Pulseless ventricular rhythms: consider antiarrhythmics Amiodarone, Lidocaine or Magnesium May make myocardium easier to defibrillate and/or more difficult for it to again fibrillate after conversion. Bradycardia: give a speed up drug Atropine Atropine blocks vagal input and stimulates the SA mode, which can increase heart rate. Consider dopamine and epinephrine infusions if unresponsive to atropine and waiting on a pacer. Dopamine and epinephrine may increase heart rate but also increase myocardial oxygen demand. Tachycardia, Reentry SVT: give a drug to interrupt the rhythm Adenosine Adenosine blocks the AV node for a few seconds, which may break the re-entry pattern. Tachycardia, Afib or Aflutter: to convert rhythm Amiodarone to slow rate beta blocker Dilitazem Tachycardia, VT, stable: to convert rhythm Amiodarone or Sync Cardiovert Acute Coronary Syndromes: first line treatment is MONA ECC M orphine decreases pain not relieved by nitroglycerin; also dilates peripheral vessels decreasing resistance against which the heart has to pump O xygen increases the oxygen available to the ischemic or injured heart muscle N itroglycerin dilates coronary arteries so more oxygenated blood can reach the muscle and decrease pain; also dilates peripheral vessels decreasing resistance against which the heart has to pump A spirin decreases platelet clumping, the first step in forming a new clot*** ***If allergic to Aspirin (ASA): give Clopidogrel (Plavix) affects platelet clumping similar to ASA 8
9 ACLS Core Cases I. Respiratory Arrest Case II. VF Treated with CPR and AED Case You are walking down the hall and the person in front of you suddenly collapses Assess: Tap, ask: Are you OK? No movement or response, call 911 and get the AED!!! or if a second person is present, send them to call and get the AED Primary ABCD Survey A irway: open and hold (head tilt chin lift or Jaw Thrust) Look, listen & feel B reathing: give 2 breaths (1 second each) that make the chest rise *avoid rapid or forceful breaths C irculation: check carotid pulse at least 5 but no longer than 10 seconds - begin CPR if a definite pulse is not felt - 30 compressions: 2 ventilations = 1 cycle - push hard: 1 ½ - 2 inches deep - push fast: 100 compressions per minute - allow the chest wall to completely recoil (take weight off hands) - minimize interruptions recheck pulse after 5 cycles of CPR (approximately 2 minutes) 2 rescuer CPR, basic airway: pause compressions to ventilate D efibrillation: Automated External Defibrillator 1. Power On turn power on (some AEDs automatically turn on) 2. Attachement select adult pads a. attach pads to patient (upper right sterna border and cardiac apex) b. attach cables to AED, if needed 3. Analysis a. announce analyzing rhythm stand clear! b. press analyze, if needed 4. Shock a. if shock indicated: announce Shock is indicated. Stand Clear! I m going to shock. verify no one is touching the patient press shock button when signaled to do so b. if no shock indicated, follow prompts from AED 9
10 Unacceptable actions: did not provide effective CPR did not follow AED s commands did not clear patient before shock (unsafe defibrillation) III. Pulseless Arrest: VF / Pulseless VT Case You respond to a patient monitor alarm, to find the patient is unresponsive. Call for help and begin CPR (primary ABCD survey). A team member arrives with the crash cart which has a manual defibrillator and advanced equipment. The patient is attached to the monitor and you identify and verify VT or PVT. Primary D: Defibrillation: Shock #1 1. After verifying the rhythm, resume CPR while the defibrillator is charging 2. once charged, Clear!!! ensure that no one is touching the patient or bed 3. give 1 shock: biphasic defibrillators = manufacturer s recommendation, if unknown 200J monophasic defibrillators = 360J 4. Immediately resume CPR for 5 cycles 5. After 5 cycles: check rhythm (shockable?), check pulse (5-10 seconds) Secondary ABCD Survey: conducted between 1 st and 2 nd shock and Ongoing 1. Airway a. BVM with 100% O 2 b. consider advanced airway placement: LMA, Combitube or ETT 2. Breathing a. check for visible chest rise with BVM b. confirm advanced airway placement by exam and confirmation device c. secure advanced airway in place with tape or a commercial device d. give 8-10 breaths/min and continuous compressions at 100 per minute 3. Circulation: establish vascular access via IV or IO a. do not interrupt CPR for access 4. Differential Diagnosis use the H s and T s mnemonic Defibrillation: Shock #2 1. after 5 cycles of CPR a. check rhythm (shockable?) b. check pulse (5-10 seconds) 2. resume CPR while defibrillator is charging 3. once charged, Clear!!! ensure no one is touching the patient or bed 4. give 1 shock: biphasic defibrillators = manufacturer s recommendation, if unknown 200J monophasic defibrillators = 360J 5. immediately resume CPR for 5 cycles 10
11 Medications: Administration either: give during CPR 1. epinephrine 1 mg IV/IO (every 3 5 minutes) or 2. vasopressin 4OU IV/IO to replace the first or second dose of epinephrine Defibrillation: Shock #3 1. after 5 cycles of CPR a. check rhythm (shockable?) b. check pulse (5-10 seconds) 2. resume CPR while defibrillator is charging 3. once charged, Clear!!! ensure no one is touching the patient or bed 4. give 1 shock: biphasic defibrillators = manufacturer s recommendation, if unknown 200J monophasic defibrillators = 360J 5. immediately resume CPR for 5 cycles Medications: Consider Antiarrhythmics: give during CPR 1. Amiodarone 300 mg IV/VO once, then consider additional 150 mg IV/VO once 2. Lidocaine mg/kg first dose then mg/kg IV/VO, max 3 doses or 3 mg/kg 3. Magnesium 1 2 g IV/VO loading doses for torsades de pointes Unacceptable actions: did not provide effective CPR did not clear before shock did not confirm advanced airway placement did not give a vassopressor IV. Pulseless Arrest: Pulseless Electrical Activity (PEA) Case V. Pulseless Arrest: Asystole Case You find that a patient is unresponsive. Call for help and begin CPR (primary ABCD survey). A team member arrives with a crash cart, which has a manual defibrillator and advanced equipment. The patient is attached to the monitor and you identify and verify Asystole or PEA. Primary D: Defibrillation: NO shock indicated for Asystole or PEA Secondary ABCD Survey: Ongoing 1. BVM with 100% O 2 2. consider advanced airway placement: LMA, Combitude or ETT Breathing 1. check for visible chest rise with BVM 2. confirm advanced airway placement by exam and confirmation device 3. secure advanced airway in place with tape or a commercial device 4. give 8-10 breaths/min and continuous compressions at 100 per minute Circulation: establish vascular access via IV or IO 1. do not interrupt CPR for access 11
12 Medication: give a vasopressor 1. Epinephrine 1 mg IV/VO (repeat every 3 5 minutes 2. Vasopressin 40 U IV/VO to replace first or second dose of epinephrine 3. consider Atropine 1 mg for Asystole or PEA rate less than check rhythm, check pulse after 2 minutes of CPR (5 cycles) Differential Diagnosis use the H s and T s mnemonic 6 Hs 5 Ts H ypoxia H ypovolemia H ypothermia H ypoglycemia H ypo / H yperkalemia H ydrogen ion (acidosis) T amponade T ension pneumothorax T oxins poisons, drugs T hrombosis coronary (AMI) pulmonary (PE) T rauma Consider family members Unacceptable actions: did not provide effective CPR did not confirm advanced airway placement did not give a vassopressor did not look for reversible causes to treat attempted defibrillation attempted transcutaneous pacing for asystole 12
13 VI. Acute Coronary Symptoms (ACS) Case Your neighbor complains of feeling weak and is sweaty, short of breath and slightly nauseated. You are worried this is an acute coronary problem can call 911. While waiting for their arrival, you ask if he can take aspirin. He says yes and you have him chew 2-3 baby aspirin (81 mg). EMS Arrival 1. Attach monitor, start IV 2. Give MONA 3. Obtain 12-lead ECG, if available 4. Notify hospital and transport 5. Begin fibrinolytic checklist Arrival at ED: Assess 12 Lead ECG ST segment Elevation (STEMI) ST Segment Depression (Non-STEMI or NSTEMI) ST- segment T wave Normal Injury Diagnostic Ischemia Non-Diagnostic Drug Therapy: Beta Blockers: myocardial work Clopidogrel: platelet clumping Heparin: fibrin so new clot doesn t form Goal is reperfusion by: Fibrinolytic: lyses fibrin in If <12 hours from onset If no contraindications ED door to drug goal = 30 Or PCI (percutaneous intervention: angioplasty and/or stents) If <12 hours from onset ED door to balloon goal = 90 min After reperfusion give: Resume above drugs ACE-inhibitor: myocardial work Statin: inflammation and arrhythmias Drug Therapy: Nitroglycerin: work Beta blockers Clopidogrel Heparin IIb / IIIa inhibitor: plateletfibrin bonding Goal is revascularization: PCI or possible surgery After revascularization give: Resume above drugs as needed ACE-inhibitor Statin 13 Consider admit to ED bed: Serial enzymes + Troponin: Repeat ECGs Monitor ST segment Consider stress test Admit to hospital bed if: Troponin positive ST segment deviates Refractory chest pain Ventricular Tachycardia Becomes unstable Discharge if: No ischemia / injury evolves Give follow-up directions
14 Unacceptable actions: did not give oxygen and aspirin to a suspected chest pain patient did not attempt to control chest pain did not obtain 12 - lead ECG VII. Bradycardia Case A patient appears pale and complains of dizziness and fatigue. The pulse rate is 56, blood pressure is 86/60 and on the monitor you identify a bradycardia rhythm. Primary ABCD Survey: 1. Maintain patient airway; assist breathing as needed 2. Give oxygen 3. Monitor ECG (identify rhythm), blood pressure, oximetry 4. Establish IV access Assess rhythm and perfusion: Is the heart rate <60 bpm or Inadequate for clinical condition Signs or symptoms of poor perfusion caused by the Bradycardia? (eg, acute altered mental status, ongoing chest pain, hypotension, or other signs of shock) Observe/Monitor Adequate Perfusion Prepare for transcutaenous pacing: use without delay for high-degree block (type II second-degree block or third-degree AV block) Consider Atropine 0.5 mg IV while awaiting pacer. May repeat to a total dose of 3 mg. If ineffective, begin pacing. Consider epinephrine (2 to 10 ug/min) or dopamine (2 to 10 ug/kg per min) infusion while awaiting pacer or if pacing ineffective 14
15 Poor Perfusion Reminders If pulseless arrest develops, go to Pulseless Arrest Algorithm Search for and treat possible contributing factors: - Hypovolemia - Toxins - Hypoxia - Tamponade, cardiac - Hydogen Ion (acidosis) - Tension pneumothorax - Hypo/hyperkalemia - Thrombosis (coronary or - Hypoglycemia pulmonary - Hypothemia - Trauma (hypovolemia, increased ICP) Prepare for transvenous pacing Treat contributing causes Consider expert consultation Unacceptable actions: did not identify a high-degree block did not initiate TCP immediately for high-degree block treated asymptomatic patient as if had poor perfusion VIII. IX. Unstable Tachycardia Case Stable Tachycardia Case A patient appears pale and complains of dizziness and fatigue. The pulse rate is 170, blood pressure is 100/60 and on the monitor you identify a tachycardia rhythm. Primary ABCD Survey 1. assess and support ABC s as needed 2. give Oxygen 3. monitor ECG (identify rhythm), blood pressure, oximetry 4. identify and treat reversible causes Is patient stable? 1. unstable signs include altered mental status, ongoing chest pain, hypotension, or other signs of shock 2. Note: rate-related symptoms uncommon if heart rate <150/min 3. Unstable perform Immediate Synchronized Cardioversion a. establish IV access and give sedation if patient is conscious: do not delay Cardioversion. b. consider expert consultation c. if pulseless arrest develops, see Pulseless Arrest Algorithm 15
16 4. Stable See chart below. a. establish IV access b. obtain 12-lead ECG (when available or rhythm strip) c. Is QRS narrow (<0.12 sec)? Narrow QRS: Is Rhythm regular? Wide QRS: Is Rhythm regular? Expert consultation advised Regular Irregular Regular Irregular Attempt vagal maneuvers Give Adenosine 6 mg rapid IV push. If no conversion, give 12 mg rapid IV push; may repeat 12 mg dose once Does rhythm convert? Note: Consider expert consultation Converts If rhythm converts, probable reentry SVT: - observe for recurrence - treat recurrence with adenosine or longer-acting AV nodal blocking agent Irregular Narrow-Complex Tachycardia Probable atrial fibrillation or possible atrial flutter or MAT (Multifocal atrial tachycardia) Consider expert consultation Control rate (eg, diltiazem, B-blockers, use B-blockers with caution in COPD and CHF Does Not Convert If rhythm does not convert, possible atrial flutter, ectopic atrial tachycardia, or Junctional tachycardia: - control rate - treat underlying cause - consider expert consultation If ventricular tachycardia or uncertain rhythm Amiodarone 150 mg IV over 10 min. Repeat as needed to max dose of 2.2 g/24 hr prepare for elective Synchronized Cardioversion If SVT with with aberrancy Give Adenosine 6 mg rapid IV push. If no conversion, give 12 mg rapid IV push, may repeat 12 mg dose once If atrial fibrillation with aberrancy See Irregular Narrow Complex tachycardia If pre-excited atrial fibrillation (AF + WPW) expert consultation advised avoid AV nodal blocking agents (eg, adenosine, digoxin, diltiazem, verapamil) consider antiarrhythmiacs (eg, amiodarone 150 mg IV over 10 min If recurrent polymorphic VT, seek expert consultation. If torsades de pointes, give magnesium (load with 1-2 g over 5-60 min, then infusion. 16
17 X. Acute Stroke Case You find a normally alert, active adult in a chair staring blankly at the television and leaning to one side. Identify signs of possible stroke 1. Critical EMS assessments and actions a. Support ABC s; give oxygen if needed b. Perform prehospital stroke assessment: The Cincinnati Prehospital Stroke Scale Facial Droop (have the patient show teeth or smile) Arm Drift (patient closes eyes and extends both arms straight out with palms up, for 10 seconds Abnormal Speech (have the patient say) you can t teach an old dog new tricks 2. establish time when patient last known normal (symptoms onset) 3. transport; consider triage to a center with a stroke unit if appropriate; consider bringing a witness, family member or caregiver 4. alert hospital 5. check glucose if possible ED Arrival: Immediate general assessment and stabilization 10 min 1. assess ABC s, vital signs 2. provide oxygen if hypoxemic 3. obtain IV access and blood samples 4. check glucose; treat if indicated 5. perform neurologic screening assessment 6. activate stroke team 7. order emergent Non-contrast CT scan of brain 8. obtain 12-lead ECG ED Arrival: Immediate neurologic assessment by stroke team 25 min 1. review patient history 2. establish symptom onset 3. perform neurologic examination (NIH Stroke Scale) Does CT scan show any hemorrhage? 45 min 1. Hemorrhage consult neurologist or neurosurgeon; consider transfer 2. No hemorrhage Probable acute ischemic stroke; consider fibrinolytic therapy a. check for fibrinolytic exclusions b. repeat neurologic exam: are deficits rapidly improving? 17
18 3. Patient remains candidate for fibrinolytic therapy? a. Not a candidate - administer aspirin b. Candidate 60 min - Review risks / benefits with patient and family: - If acceptable Give tpa No anticoagulants or antiplatelet treatment for 24 hours 18
Official Online ACLS Exam
 \ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
\ Official Online ACLS Exam Please fill out this form before you take the exam. Name : Email : Phone : 1. Hypovolemia initially produces which arrhythmia? A. PEA B. Sinus tachycardia C. Symptomatic bradyarrhythmia
ACLS Study Guide BLS Overview CAB
 ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS Study Guide The ACLS Provider exam is 50-mutiple choice questions. Passing score is 84%. Student may miss 8 questions. For students taking ACLS for the first time or renewing students with a current
ACLS PRE-TEST ANNOTATED ANSWER KEY
 ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
ACLS PRE-TEST ANNOTATED ANSWER KEY June, 2011 Question 1: Question 2: There is no pulse with this rhythm. Question 3: Question 4: Question 5: Question 6: Question 7: Question 8: Question 9: Question 10:
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006. ECG Analysis. Name the following rhythms from the list below:
 American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
American Heart Association ACLS Pre-Course Self Assessment Dec., 2006 ECG Analysis This pre-test is exactly the same as the pretest on the ACLS Provider manual CD. This paper version can be completed in
If you do not wish to print the entire pre-test you may print Page 2 only to write your answers, score your test, and turn in to your instructor.
 This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
This is a SAMPLE of the pretest you can access with your AHA PALS Course Manual at Heart.org/Eccstudent using your personal code that comes with your PALS Course Manual The American Heart Association strongly
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109
 Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Present : PGY 王 淳 峻 Supervisor: F1 王 德 皓 991109 Interventions to prevent cardiac arrest + Airway management + Ventilation support + Treatment of bradyarrhythmias & Tachyarrhythmias Treat cardiac arrest
Community Ambulance Service of Minot ALS Standing Orders Legend
 Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Legend Indicates General Information and Guidelines Indicates Procedures Indicates Medication Administration Indicates Referral to Other Protocol Indicates Referral to Online Medical Direction Pediatric
Cardiac Arrest VF/Pulseless VT Learning Station Checklist
 Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
Cardiac Arrest VF/Pulseless VT Learning Station Checklist VF/VT 00 American Heart Association Adult Cardiac Arrest Shout for Help/Activate Emergency Response Epinephrine every - min Amiodarone Start CPR
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC. BLS Changes
 ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
ACLS Provider Manual Comparison Sheet Based on 2010 AHA Guidelines for CPR and ECC CPR Chest compressions, Airway, Breathing (C-A-B) BLS Changes New Old Rationale New science indicates the following order:
PRO-CPR. 2015 Guidelines: PALS Algorithm Overview. (Non-AHA supplementary precourse material)
 PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
PRO-CPR 2015 Guidelines: PALS Algorithm Overview (Non-AHA supplementary precourse material) Please reference Circulation (from our website), the ECC Handbook, or the 2015 ACLS Course Manual for correct
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Precourse Self-Assessment. May 2011. 2011 American Heart Association
 E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
E C C American Heart Association Advanced Cardiovascular Life Support Written Precourse Self-Assessment May 2011 2011 American Heart Association 2011 ACLS Written Precourse Self-Assessment 1. Ten minutes
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
Cardiac Arrest Pediatric Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble In contrast to cardiac arrest in adults, cardiopulmonary arrest in pediatric
PALS Interim Study Guide
 PALS Interim Study Guide 2006 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released November 28, 2005! The new AHA Handbook of Emergency Cardiac Care (ECC)
PALS Interim Study Guide 2006 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released November 28, 2005! The new AHA Handbook of Emergency Cardiac Care (ECC)
IU Health ACLS Study Guide
 IU Health ACLS Study Guide Preparing for your upcoming ACLS Class REVISED SEPTEMBER 2011 ON APRIL 1, 2011 WE BEGAN TEACHING THE 2010 AHA GUIDELINES. WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND
IU Health ACLS Study Guide Preparing for your upcoming ACLS Class REVISED SEPTEMBER 2011 ON APRIL 1, 2011 WE BEGAN TEACHING THE 2010 AHA GUIDELINES. WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND
ACLS PHARMACOLOGY 2011 Guidelines
 ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
ACLS PHARMACOLOGY 2011 Guidelines ADENOSINE Narrow complex tachycardias or wide complex tachycardias that may be supraventricular in nature. It is effective in treating 90% of the reentry arrhythmias.
New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010!
 ACLS Study Guide 2010 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010! The new AHA Handbook of Emergency Cardiac Care (ECC) contains
ACLS Study Guide 2010 Bulletin: New resuscitation science and American Heart Association treatment guidelines were released October 28, 2010! The new AHA Handbook of Emergency Cardiac Care (ECC) contains
www.cprtrainingfast.com
 ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
ADVANCED CARDIAC LIFE SUPPORT (ACLS) RECERTIFICATION EXAMINATION 1. Ten minutes after an 85 year old woman collapses, paramedics arrive and start CPR for the first time. The monitor shows fine (low amplitude)
E C C. American Heart Association. Advanced Cardiovascular Life Support. Written Exams. May 2011
 E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
E C C American Heart Association Advanced Cardiovascular Life Support Written Exams Contents: Exam Memo Student Answer Sheet Version A Exam Version A Answer Key Version A Reference Sheet Version B Exam
Atrial & Junctional Dysrhythmias
 Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Atrial & Junctional Dysrhythmias Atrial & Junctional Dysrhythmias Atrial Premature Atrial Complex Wandering Atrial Pacemaker Atrial Tachycardia (ectopic) Multifocal Atrial Tachycardia Atrial Flutter Atrial
Team Leader. Ensures high-quality CPR at all times Assigns team member roles Ensures that team members perform well. Bradycardia Management
 ACLS Megacode Case 1: Sinus Bradycardia (Bradycardia VF/Pulseless VT Asystole Out-of-Hospital Scenario You are a paramedic and arrive on the scene to find a 57-year-old woman complaining of indigestion.
ACLS Megacode Case 1: Sinus Bradycardia (Bradycardia VF/Pulseless VT Asystole Out-of-Hospital Scenario You are a paramedic and arrive on the scene to find a 57-year-old woman complaining of indigestion.
8 Peri-arrest arrhythmias
 8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
8 Peri-arrest arrhythmias Introduction Cardiac arrhythmias are relatively common in the peri-arrest period. They are common in the setting of acute myocardial infarction and may precipitate ventricular
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008
 Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Cardiac Arrest - Ventricular Fibrillation / Pulseless Ventricular Tachycardia Protocol revised October 2008 Preamble Survival from cardiorespiratory arrest for patients who present with ventricular fibrillation
Crash Cart Drugs Drugs used in CPR. Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University
 Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
Crash Cart Drugs Drugs used in CPR Dr. Layla Borham Professor of Clinical Pharmacology Umm Al Qura University Introduction A list of the drugs kept in the crash carts. This list has been approved by the
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course
 Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
 ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
ACLS Cardiac Arrest Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767 Copyright 2010 American Heart Association ACLS Cardiac Arrest Circular Algorithm Neumar, R. W. et al. Circulation 2010;122:S729-S767
Advanced Cardiovascular Life Support Case Scenarios
 Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
Advanced Cardiovascular Life Support Case Scenarios ACLS Respiratory Arrest Case Out-of-Hospital Scenario You are a paramedic and respond to the scene of a possible cardiac arrest. A young man lies motionless
American Heart Association
 American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
2015 Interim Resources for HeartCode ACLS
 2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
2015 Interim Resources for HeartCode ACLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published
Advanced Cardiac Life Support
 Advanced Cardiac Life Support Dr Teo Wee Siong NATIONAL RESUSCITATION COUNCIL Singapore Guidelines 2006 Prof Anantharaman A/Prof Lim Swee Han Dr Chee Tek Siong A/Prof Peter Manning A/Prof Eillyne Seow
Advanced Cardiac Life Support Dr Teo Wee Siong NATIONAL RESUSCITATION COUNCIL Singapore Guidelines 2006 Prof Anantharaman A/Prof Lim Swee Han Dr Chee Tek Siong A/Prof Peter Manning A/Prof Eillyne Seow
GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS. (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support)
 AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
AUSTRALIAN RESUSCITATION COUNCIL GUIDELINE 11.9 MANAGING ACUTE DYSRHYTHMIAS (To be read in conjunction with Guideline 11.7 Post-Resuscitation Therapy in Adult Advanced Life Support) The term cardiac arrhythmia
The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010.
 ACLS Study Guide The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. Please read the below information carefully This letter is to confirm your
ACLS Study Guide The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. Please read the below information carefully This letter is to confirm your
Management of Adult Cardiac Arrest
 73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
73991_CH27_page68-73.qxd 6/6/11 3:54 PM Page 68 27.68 Section 5 Medical Guidelines for Performing a 12-Lead ECG The only way to learn how to obtain a 12-lead ECG is to practice with the equipment itself.
Northwestern Health Sciences University. Basic Life Support for Healthcare Providers
 Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Quiz 4 Arrhythmias summary statistics and question answers
 1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
1 Quiz 4 Arrhythmias summary statistics and question answers The correct answers to questions are indicated by *. All students were awarded 2 points for question #2 due to no appropriate responses for
2015 Interim Resources for BLS
 2015 Interim Resources for BLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published in the 2015
2015 Interim Resources for BLS Original Release: November 25, 2015 Starting in 2016, new versions of American Heart Association online courses will be released to reflect the changes published in the 2015
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new?
 Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
Update on Small Animal Cardiopulmonary Resuscitation (CPR)- is anything new? DVM, DACVA Objective: Update on the new Small animal guidelines for CPR and a discussion of the 2012 Reassessment Campaign on
ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE
 ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE An Advanced Care Paramedic will provide the treatment based on the randomization scheme and as prescribed in this
ROC CONTINUOUS CHEST COMPRESSIONS STUDY (CCC): MEDICAL CARDIAC ARREST MEDICAL DIRECTIVE An Advanced Care Paramedic will provide the treatment based on the randomization scheme and as prescribed in this
Procedure 17: Cardiopulmonary Resuscitation
 Cardiopulmonary Resuscitation 349 Procedure 17: Cardiopulmonary Resuscitation Introduction Cardiopulmonary arrest (CPA) occurs when a patient s heart and lungs stop functioning. In children, CPA usually
Cardiopulmonary Resuscitation 349 Procedure 17: Cardiopulmonary Resuscitation Introduction Cardiopulmonary arrest (CPA) occurs when a patient s heart and lungs stop functioning. In children, CPA usually
Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials
 Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials 1 PEDIATRIC ADVANCED LIFE SUPPORT (PALS) RECERTIFICATION TABLE OF CONTENTS CYCLIC APPROACH 03 PEDIATRIC ASSESSMENT FLOWCHART
Pediatric Advanced Life Support (PALS) Recertification Preparatory Materials 1 PEDIATRIC ADVANCED LIFE SUPPORT (PALS) RECERTIFICATION TABLE OF CONTENTS CYCLIC APPROACH 03 PEDIATRIC ASSESSMENT FLOWCHART
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY. Guidelines for Use of Intravenous Isoproterenol
 ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
ANNE ARUNDEL MEDICAL CENTER CRITICAL CARE MEDICATION MANUAL DEPARTMENT OF NURSING AND PHARMACY Guidelines for Use of Intravenous Isoproterenol Major Indications Status Asthmaticus As a last resort for
Michigan Adult Cardiac Protocols CARDIAC ARREST GENERAL. Date: May 31, 2012 Page 1 of 5
 Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
Date: May 31, 2012 Page 1 of 5 Cardiac Arrest General This protocol should be followed for all adult cardiac arrests. Medical cardiac arrest patients undergoing attempted resuscitation should not be transported
ACLS123.com 818.766.1111 2012. ACLS Study Guide. Critical Care Training Center
 ACLS123.com 818.766.1111 2012 ACLS Study Guide Critical Care Training Center 12/1/2012 Course Overview This study guide is an outline of content that will be taught in the American Heart Association Accredited
ACLS123.com 818.766.1111 2012 ACLS Study Guide Critical Care Training Center 12/1/2012 Course Overview This study guide is an outline of content that will be taught in the American Heart Association Accredited
Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
 Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
PEDIATRIC TREATMENT GUIDELINES
 P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
P1 Pediatric Patient Care P2 Cardiac Arrest Initial Care and CPR P3 Neonatal Resuscitation P4 Ventricular Fibrillation / Ventricular Tachycardia P5 PEA / Asystole P6 Symptomatic Bradycardia P7 Tachycardia
Wilson County Emergency Management Agency Protocol Manual Protocols
 Asystole No pulse or respirations Confirm cardiac rhythm with combo pads or electrodes Record in two leads to confirm Asystole and to rule out fine V-Fib. Basic assessment and management (up to your scope
Asystole No pulse or respirations Confirm cardiac rhythm with combo pads or electrodes Record in two leads to confirm Asystole and to rule out fine V-Fib. Basic assessment and management (up to your scope
Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010
 Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010 Q: What are the most significant changes in the 2010 AHA Guidelines for CPR & ECC? A: Major changes for all rescuers,
Question-and-Answer Document 2010 AHA Guidelines for CPR & ECC As of October 18, 2010 Q: What are the most significant changes in the 2010 AHA Guidelines for CPR & ECC? A: Major changes for all rescuers,
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
ACLS RHYTHM TEST. 2. A 74-year-old woman with chest pain. Blood pressure 192/90 and rates her pain 9/10.
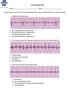 ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
ACLS RHYTHM TEST Name Date Choose the best answer for each of the following questions. Each of the following strips is 6 seconds in length. 1. Identify the following rhythm a. Sinus bradycardia with 2
Emergency Medical Services Advanced Level Competency Checklist
 Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer
 Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
Purpose To guide registered nurses who may manage clients experiencing sudden or unexpected life-threatening cardiac emergencies.
 Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
Emergency Cardiac Care: Decision Support Tool #1 RN-Initiated Emergency Cardiac Care Without Cardiac Monitoring/Manual Defibrillator or Emergency Cardiac Drugs Decision support tools are evidence-based
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive.
 It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
It is recommended that the reader review each medical directive presented in this presentation along with the actual PCP Core medical directive. This presentation will highlight the changes and any new
AMERICAN HEART ASSOCIATION 2010 ACLS GUIDELINES: WHAT EVERY CLINICIAN NEEDS TO KNOW
 AMERICAN HEART ASSOCIATION 2010 ACLS GUIDELINES: WHAT EVERY CLINICIAN NEEDS TO KNOW Joseph Heidenreich, MD Texas A&M Health Science Center Scott & White Memorial Hospital Scott & White Memorial Hospital
AMERICAN HEART ASSOCIATION 2010 ACLS GUIDELINES: WHAT EVERY CLINICIAN NEEDS TO KNOW Joseph Heidenreich, MD Texas A&M Health Science Center Scott & White Memorial Hospital Scott & White Memorial Hospital
American Heart Association. Basic Life Support for Healthcare Providers
 American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
Practical ACLS Megacode Testing and Training Scenario Set for SimPad. Consolidated Instructor Manual. Frances Wickham Lee, DBA
 Practical ACLS Megacode Testing and Training Scenario Set for SimPad Consolidated Instructor Manual Frances Wickham Lee, DBA Scenario Authors: Frances Wickham Lee, DBA John Walker, BHS John Schaefer, MD
Practical ACLS Megacode Testing and Training Scenario Set for SimPad Consolidated Instructor Manual Frances Wickham Lee, DBA Scenario Authors: Frances Wickham Lee, DBA John Walker, BHS John Schaefer, MD
PALS Study Guide. PALS Study Guide Revised August 2010, Page 1 [TCL]
![PALS Study Guide. PALS Study Guide Revised August 2010, Page 1 [TCL] PALS Study Guide. PALS Study Guide Revised August 2010, Page 1 [TCL]](/thumbs/26/7254148.jpg) PALS Study Guide Course Overview This Study Guide is an extensive outline of content that will be taught in the American Heart Association Accredited Pediatric Advanced Life Support (PALS) Course. It is
PALS Study Guide Course Overview This Study Guide is an extensive outline of content that will be taught in the American Heart Association Accredited Pediatric Advanced Life Support (PALS) Course. It is
DEBRIEFING GUIDE. The key components of an optimal code response: 1. Early recognition that the patient is deteriorating or has become unresponsive.
 DEBRIEFING GUIDE I N T R O D U C T I O N Debriefing has been shown to improve clinical behavior during cardiac resuscitation and, as such, has become a recommended procedure in the 2010 American Heart
DEBRIEFING GUIDE I N T R O D U C T I O N Debriefing has been shown to improve clinical behavior during cardiac resuscitation and, as such, has become a recommended procedure in the 2010 American Heart
Heart Attack: What You Need to Know
 A WorkLife4You Guide Heart Attack: What You Need to Know What is a Heart Attack? The heart works 24 hours a day, pumping oxygen and nutrient-rich blood to the body. Blood is supplied to the heart through
A WorkLife4You Guide Heart Attack: What You Need to Know What is a Heart Attack? The heart works 24 hours a day, pumping oxygen and nutrient-rich blood to the body. Blood is supplied to the heart through
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination BVM VENTILATION OF AN APNEIC ADULT PATIENT
 BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination PATIENT ASSESSMENT/MANAGEMENT TRAUMA
 PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
CRNA ACLS, PALS, & BLS REFRESHER
 Attn: Certified Nurse Anesthetists (CRNA) CPR Consultants, Inc. 7404 G Chapel Hill Road, Raleigh, NC, 27607 CRNA ACLS, PALS, & BLS REFRESHER CRNA American Heart Association Triple Certification (BLS, ACLS,
Attn: Certified Nurse Anesthetists (CRNA) CPR Consultants, Inc. 7404 G Chapel Hill Road, Raleigh, NC, 27607 CRNA ACLS, PALS, & BLS REFRESHER CRNA American Heart Association Triple Certification (BLS, ACLS,
BLS: basic cardiac life support. ACLS: advanced cardiac life support. PALS: paediatric advanced life support. VF: ventricular fibrillation
 RN-Initiated Emergency Cardiac Care: Decision Support Tool #2 Emergency Cardiac Care in Areas Using Cardiac Monitoring, Defibrillation and Emergency Cardiac Drugs Decision support tools are evidenced-based
RN-Initiated Emergency Cardiac Care: Decision Support Tool #2 Emergency Cardiac Care in Areas Using Cardiac Monitoring, Defibrillation and Emergency Cardiac Drugs Decision support tools are evidenced-based
National Registry of Emergency Medical Technicians Emergency Medical Technician Psychomotor Examination BLEEDING CONTROL/SHOCK MANAGEMENT
 BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
Alabama Medications. Christopher J. Colvin January 2010
 Alabama Medications Christopher J. Colvin p January 2010 Activated Charcoal Used to absorb toxins ingested before they can be absorbed in the GI system. Contraindicated in AMS patients who cannot control
Alabama Medications Christopher J. Colvin p January 2010 Activated Charcoal Used to absorb toxins ingested before they can be absorbed in the GI system. Contraindicated in AMS patients who cannot control
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001
 BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
BASIC CARDIAC ARRHYTHMIAS Revised 10/2001 A Basic Arrhythmia course is a recommended prerequisite for ACLS. A test will be given that will require you to recognize cardiac arrest rhythms and the most common
ACLS Provider Manual Supplementary Material
 ACLS Provider Manual Supplementary Material 2006 American Heart Association 1 Contents Airway Management...5 Part 1 Basic Airway Management...6 Devices to Provide Supplementary Oxygen...6 Overview...6
ACLS Provider Manual Supplementary Material 2006 American Heart Association 1 Contents Airway Management...5 Part 1 Basic Airway Management...6 Devices to Provide Supplementary Oxygen...6 Overview...6
Tachyarrhythmias (fast heart rhythms)
 Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
Patient information factsheet Tachyarrhythmias (fast heart rhythms) The normal electrical system of the heart The heart has its own electrical conduction system. The conduction system sends signals throughout
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
GENERAL HEART DISEASE KNOW THE FACTS
 GENERAL HEART DISEASE KNOW THE FACTS WHAT IS Heart disease is a broad term meaning any disease affecting the heart. It is commonly used to refer to coronary heart disease (CHD), a more specific term to
GENERAL HEART DISEASE KNOW THE FACTS WHAT IS Heart disease is a broad term meaning any disease affecting the heart. It is commonly used to refer to coronary heart disease (CHD), a more specific term to
American Heart Association. Pediatric Advanced Life Support. Written Precourse Self-Assessment. Questions and Answer Key for Students.
 E C C American Heart Association Pediatric Advanced Life Support Written Precourse Self-Assessment Questions and Answer Key for Students January 2012 PALS Written 2011 Precourse Self-Assessment ECG Rhythm
E C C American Heart Association Pediatric Advanced Life Support Written Precourse Self-Assessment Questions and Answer Key for Students January 2012 PALS Written 2011 Precourse Self-Assessment ECG Rhythm
Atrial Fibrillation Management Across the Spectrum of Illness
 Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
Disclosures Atrial Fibrillation Management Across the Spectrum of Illness NONE Barbara Birriel, MSN, ACNP-BC, FCCM The Pennsylvania State University Objectives AF Discuss the pathophysiology, diagnosis,
How you can help save lives
 How you can help save lives Through Life Support Training Courses with THE INTERNATIONAL LIFE SUPPORT TRAINING CENTER (ILSTC) TABLE OF CONTENTS Introduction Page 3 Basic Life Support for Healthcare Provider
How you can help save lives Through Life Support Training Courses with THE INTERNATIONAL LIFE SUPPORT TRAINING CENTER (ILSTC) TABLE OF CONTENTS Introduction Page 3 Basic Life Support for Healthcare Provider
WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND IN THE 2010 ACLS Textbook available through AHA and other retail outlets.
 ACLS STUDY GUIDE 2015 WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND IN THE 2010 ACLS Textbook available through AHA and other retail outlets. The AHA also requests the following in preparation
ACLS STUDY GUIDE 2015 WE HIGHLY RECOMMEND REVIEWING THE NEW ALGORYHMS FOUND IN THE 2010 ACLS Textbook available through AHA and other retail outlets. The AHA also requests the following in preparation
OBJECTIVES. When the student has finished this module, he/she will be able to:
 Advanced Cardiac Life Support (ACLS) Review WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited
Advanced Cardiac Life Support (ACLS) Review WWW.RN.ORG Reviewed September, 2015, Expires September, 2017 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited
Airway and Breathing Skills Levels Interpretive Guidelines
 Office of Emergency Medical Services and Trauma INDEX EFFECTIVE LAST REVIEW PAGES VERSION R-P11A 7/1/2011 7/1/2011 5 2011 Scope of Practice for EMS Personnel Emergency Medical Personnel are permitted to
Office of Emergency Medical Services and Trauma INDEX EFFECTIVE LAST REVIEW PAGES VERSION R-P11A 7/1/2011 7/1/2011 5 2011 Scope of Practice for EMS Personnel Emergency Medical Personnel are permitted to
Department of Emergency and Disaster Medicine Medical University of LODZ
 Electrotherapy in emergency states Department of Emergency and Disaster Medicine Medical University of LODZ defibrillation defibrillation The purpous of defibrillation is to deliver a randomly timed high-energy
Electrotherapy in emergency states Department of Emergency and Disaster Medicine Medical University of LODZ defibrillation defibrillation The purpous of defibrillation is to deliver a randomly timed high-energy
table of contents drug reference
 table of contents drug reference ADULT DRUG REFERENCE...155 161 PEDIATRIC DRUG REFERENCE...162 164 PEDIATRIC WEIGHT-BASED DOSING CHARTS...165 180 Adenosine...165 Amiodarone...166 Atropine...167 Defibrillation...168
table of contents drug reference ADULT DRUG REFERENCE...155 161 PEDIATRIC DRUG REFERENCE...162 164 PEDIATRIC WEIGHT-BASED DOSING CHARTS...165 180 Adenosine...165 Amiodarone...166 Atropine...167 Defibrillation...168
The management of cardiac arrest
 CHAPTER 6 The management of cardiac arrest LEARNING OBJECTIVES In this chapter you will learn: How to assess the cardiac arrest rhythm and perform advanced life support 6.1. INTRODUCTION Cardiac arrest
CHAPTER 6 The management of cardiac arrest LEARNING OBJECTIVES In this chapter you will learn: How to assess the cardiac arrest rhythm and perform advanced life support 6.1. INTRODUCTION Cardiac arrest
Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier
 Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier Most common dysrhythmia seen in ED, and incidence increasing with ageing population Presentation Common presentations: younger patients often
Episode 20 Atrial fibrillation Prepared by Dr. Lucas Chartier Most common dysrhythmia seen in ED, and incidence increasing with ageing population Presentation Common presentations: younger patients often
New Approaches for Prehospital Cardiac Arrest Management 2010 NCEMSF Conference
 New Approaches for Prehospital Cardiac Arrest Management 2010 NCEMSF Conference Mark E. Pinchalk, MS, EMT-P Paramedic Crew Chief City of Pittsburgh EMS Out of Hospital Cardiac Arrest Poor outcomes: Arizona
New Approaches for Prehospital Cardiac Arrest Management 2010 NCEMSF Conference Mark E. Pinchalk, MS, EMT-P Paramedic Crew Chief City of Pittsburgh EMS Out of Hospital Cardiac Arrest Poor outcomes: Arizona
Current Management of Atrial Fibrillation DISCLOSURES. Heart Beat Anatomy. I have no financial conflicts to disclose
 Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Current Management of Atrial Fibrillation Mary Macklin, MSN, APRN Concord Hospital Cardiac Associates DISCLOSURES I have no financial conflicts to disclose Book Women: Fit at Fifty. A Guide to Living Long.
Adult Drug Reference. Dopamine Drip Chart. Pediatric Drug Reference. Pediatric Drug Dosage Charts DRUG REFERENCES
 Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care
 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Presenter Name Disclosures
2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Presenter Name Disclosures
Cardiac Arrest: General Considerations
 Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
Andrea Gabrielli, MD, FCCM Cardiac Arrest: General Considerations Cardiopulmonary resuscitation (CPR) is described as a series of assessments and interventions performed during a variety of acute medical
EMS SKILL CARDIAC EMERGENCY: AUTOMATED EXTERNAL DEFIBRILLATION (AED)
 EMS SKILL CARDIAC EMERGENCY: AUTOMATED EXTERNAL DEFIBRILLATION (AED) PERFORMANCE OBJECTIVE Demonstrate competency in assessing signs of cardiopulmonary arrest and performing defibrillation using a semi-automated
EMS SKILL CARDIAC EMERGENCY: AUTOMATED EXTERNAL DEFIBRILLATION (AED) PERFORMANCE OBJECTIVE Demonstrate competency in assessing signs of cardiopulmonary arrest and performing defibrillation using a semi-automated
Paediatric Advanced Life Support
 Paediatric Advanced Life Support Introduction There is concern that resuscitation from cardiac arrest is not performed as well as it might because the variations in guidelines for different age groups
Paediatric Advanced Life Support Introduction There is concern that resuscitation from cardiac arrest is not performed as well as it might because the variations in guidelines for different age groups
Basic ECG rhythm interpretation skills (see our Six Second ECG Essentials or Mastery courses and our Six Second ECG Simulator online)
 SkillStat ACLS Precourse Package Thank you for choosing SkillStat Learning Inc. for your Advanced Life Support training needs. SkillStat Learning Inc. has delivered advanced practice programs to healthcare
SkillStat ACLS Precourse Package Thank you for choosing SkillStat Learning Inc. for your Advanced Life Support training needs. SkillStat Learning Inc. has delivered advanced practice programs to healthcare
Arrest. What s a Nurse to do?
 Benzo s, Blockers, Coma & Cardiac Arrest What s a Nurse to do? Objectives Review of ACLS Algorithms for Cardiac Arrest Management Discuss the toxicology of Beta Blocker Poisoning Describe the clinical
Benzo s, Blockers, Coma & Cardiac Arrest What s a Nurse to do? Objectives Review of ACLS Algorithms for Cardiac Arrest Management Discuss the toxicology of Beta Blocker Poisoning Describe the clinical
ADVANCED LIFE SUPPORT LEARNING PACKAGE
 SOUTH WEST HEALTHCARE WARRNAMBOOL ADVANCED LIFE SUPPORT LEARNING PACKAGE Prepared by: J. Brown, ICU Last revised February, 2010. C. Joseph, Nursing Education. CONTENTS: Page: Objectives 3-5 Basic Life
SOUTH WEST HEALTHCARE WARRNAMBOOL ADVANCED LIFE SUPPORT LEARNING PACKAGE Prepared by: J. Brown, ICU Last revised February, 2010. C. Joseph, Nursing Education. CONTENTS: Page: Objectives 3-5 Basic Life
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT
 Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Adding IV Amiodarone to the EMS Algorithm for Cardiac Arrest Due to VF/Pulseless VT Introduction Before the year 2000, the traditional antiarrhythmic agents (lidocaine, bretylium, magnesium sulfate, procainamide,
Normal Sinus Rhythm. Sinus Bradycardia. Sinus Tachycardia. Rhythm ECG Characteristics Example (NSR) & consistent. & consistent.
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Hypoxia
Anatomy and Physiology: Understanding the Importance of CPR
 Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Anatomy and Physiology: Understanding the Importance of CPR Overview This document gives you more information about the body s structure (anatomy) and function (physiology). This information will help
Emergency Scenario. Chest Pain
 Emergency Scenario Chest Pain This emergency scenario reviews chest pain in a primary care patient, and is set up for roleplay and case review with your staff. 1) The person facilitating scenarios can
Emergency Scenario Chest Pain This emergency scenario reviews chest pain in a primary care patient, and is set up for roleplay and case review with your staff. 1) The person facilitating scenarios can
ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY
 Care Pathway Triage category ATRIAL FIBRILLATION PATHWAY ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY AF/ FLUTTER IS PRIMARY REASON FOR PRESENTATION YES NO ONSET SYMPTOMS OF AF./../ TIME DURATION OF AF
Care Pathway Triage category ATRIAL FIBRILLATION PATHWAY ACCIDENT AND EMERGENCY DEPARTMENT/CARDIOLOGY AF/ FLUTTER IS PRIMARY REASON FOR PRESENTATION YES NO ONSET SYMPTOMS OF AF./../ TIME DURATION OF AF
Bradycardia CHAPTER 12 CODE SCENARIO
 Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
Senecal-12.qxd 14/04/2005 09:44 AM Page 69 CHAPTER 12 Bradycardia CODE SCENARIO A code is called for a 78-year-old man who was admitted to the hospital for syncope of unknown etiology. He was resting comfortably
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPORT State Form 54407 (R / 5-13)
 EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI)
 Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Novartis Gilenya FDO Program Clinical Protocol and Highlights from Prescribing Information (PI) Highlights from Prescribing Information - the link to the full text PI is as follows: http://www.pharma.us.novartis.com/product/pi/pdf/gilenya.pdf
Cardioversion for. Atrial Fibrillation. Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation
 Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
Cardioversion for Atrial Fibrillation Your Heart s Electrical System Cardioversion Living with Atrial Fibrillation When You Have Atrial Fibrillation You ve been told you have a heart condition called atrial
EMS Course Requirements
 EMS Course Requirements The following outlines should be followed when creating your course syllabi. The minimum course hours must be met, but they can be exceeded depending on the needs of your class.
EMS Course Requirements The following outlines should be followed when creating your course syllabi. The minimum course hours must be met, but they can be exceeded depending on the needs of your class.
10. An infant with a history of vomiting and diarrhea arrives by ambulance. During your primary assessment the infant responds only to painful stimula
 1. You are called to help resuscitate an infant with severe symptomatic bradycardia associated with respiratory distress. The bradycardia persists despite establishment of an effective airway, oxygenation,
1. You are called to help resuscitate an infant with severe symptomatic bradycardia associated with respiratory distress. The bradycardia persists despite establishment of an effective airway, oxygenation,
