INTERDISCIPLINARY CLINICAL MANUAL Policy & Procedure
|
|
|
- Frank Elliott
- 9 years ago
- Views:
Transcription
1 INTERDISCIPLINARY CLINICAL MANUAL Policy & Procedure TITLE: Section: Nasogastric Tube Insertion, Gastrointestinal/Nutrition NUMBER: CC Date Issued: May 2007 Source: Distribution: Surgical Specialties Capital Health Holders of Interdisciplinary Clinical Manuals Date To Be Reviewed: Issuing Authority: May 2010 Brian Butt Health Services Director COMPONENTS OF NASOGASTRIC TUBE INSERTION, MAINTENANCE AND REMOVAL ARE POST-ENTRY LEVEL COMPETENCIES FOR REGISTERED NURSES AND LICENSED PRACTICAL NURSES, AND WHICH REQUIRE ASSESSMENT OF COMPETENCY PRIOR TO PERFORMING. (Refer to Policy Statements # 1 and 2 for specifics). TABLE OF CONTENTS PAGE Policy Statements 2 Guiding Principles.. 4 Procedures: 1. Equipment required Procedure: Insertion of nasogastric tube Verification of placement, irrigation, and tube maintenance Administering enteral feeds Nasogastric tube removal Administering medications via nasogastric tube References 6 Nasogastric Tube Insertion, CC Page 1 of 7
2 POLICY 1. For Registered Nurses (RNs): 1.1. Insertion of a Nasogastric (NG) Tube is a post-entry level competency of NG tubes are basic entry level competencies. 2. For Licensed Practical Nurses (LPNs): 2.1. Insertion of a small-bore feeding tube is a post-entry level competency in approved practice settings only LPNs do not insert large bore NG tubes Removal of NG tubes is a post-entry level competency Maintenance of NG tubes is a basic entry level competency. 3. Insertion and removal of a nasogastric tube requires a physician s order. 4. Although the RN or LPN (approved practice settings only) may insert a small-bore weighted tube without stylet for the purpose of complete or supplemental nutritional support, prior to insertion the nurse should refer to their facility specific or unit specific protocols. 5. Nurses (RNs and LPNs) do not insert nasogastric tubes for the purpose of compression, to control bleeding. (i.e.: Esophageal Compression tubes such as a Blakemore tube). 6. Prior to inserting a nasogastric tube, the nurse should review the patient s history and blood work to assess the potential for and increased risk of bleeding during and following insertion. (e.g.: decreased platelets or increased INR). 7. No more than three attempts at nasogastric tube insertion should be made by any one nurse at any one time. 8. Following insertion of a nasogastric tube for enteral nutrition or medication administration, radiological (X-ray) verification of tube placement must be done prior to the initiation of enteral nutrition or medications. 9. Once tube placement is confirmed, the external length of the tube from point of entry at the nare to the tip of the tube is to be measured and documented on the patient s Kardex (or care plan). A mark or tape is to be placed on the tube at the entry point to the nare to use as an assessment indicator of possible tube migration. 10. Unless the physician orders state otherwise, the patient s head of the bed should be elevated 30 degrees while the nasogastric tube is in place. If the patient must have the bed in a flat position, it is possible to keep the bed flat yet elevate the head by placing the bed in reverse Trendelenburg position. 11. Due to the increased risk of perforation, do not place nasogastric tubes in the refrigerator or on ice prior to insertion. 12. Situations in which the nurse should not insert, reinsert, reposition or manipulate a nasogastric tube include patients with: nasal pharyngeal surgery Nasogastric Tube Insertion, CC Page 2 of 7
3 12.2. esophageal or upper gastrointestinal surgery in the past 30 days surgical procedures at the site of tube entry (i.e.: craniofacial surgery) esophageal or nasal pharyngeal obstruction severe maxillofacial trauma esophageal varices basal skull fractures thermal or chemical injury to the upper respiratory tract and esophagus 13. If a nasogastric tube is inadvertently removed, consideration should first be given to whether the patient continues to require therapy. If not, a physician s order is required to discontinue the therapy. 14. A physician order is required before irrigating a nasogastric tube in a patient who has had esophageal or gastrointestinal surgery within the past 30 days. 15. A nasogastric tube is not to be forced past resistance. This may cause damage to nasal mucosa or force the tube into a potentially dangerous position. 16. The end of the NG tube is never to be placed in a container of fluid while checking for placement. If the tube is in the trachea, the patient could inhale the water. 17. If using a large bore nasogastric tube for suction, the lowest suction that will effectively decompress the stomach is to be used. 18. If patient has a large bore Salem sump tube, saline or sterile water is never to be injected into the blue pigtail air vent tube. Only air is to be injected into this blue vent The blue air vent is never to be clamped or tied off, connected to suction, or used for irrigation. The air vent must remain patent to ensure proper sump function If the blue air vent is clamped or occluded by drainage, continuous suction may cause damage to the patient s gastric lining. 19. To prevent tube rupture, a 60mL syringe is to be used to check placement or instill fluid into large bore nasogastric tubes (i.e.: Salem sump). For small bore feeding tubes, a 30mL or larger syringe must be used (silastic, polyurethane). 20. At any time, if uncertainty of nasogastric tube placement exists, particularly in high-risk patients, x-ray verification is warranted. This is done to confirm correct tip placement prior to the administration of enteral nutrition or medication. High risk patients include those with: absent or diminished cough or gag reflexes, decreased level of consciousness, anatomical abnormalities along the placement pathway (i.e., tracheostomy, endotracheal intubation, or cardiomegaly), significant debilitation or difficult tube placement. (Bohnker, Artman, Hoskins, 1987) Return to TOC Nasogastric Tube Insertion, CC Page 3 of 7
4 GUIDING PRINCIPLES 1. A nurse may insert a nasogastric tube (as per policy statements 1 and 2) after it has been ordered by a physician for the purposes of: 1.1 decompression of the stomach by removal of flatus and liquid gastric contents (e.g., with full or partial obstruction due to a variety of causes) 1.2 prevention and relief of nausea and vomiting after surgery or a traumatic event by decompressing the stomach 1.3 administration of nutrition and/or medications when the oral route cannot be used 1.4 gastric irrigation 1.5 diagnostic or motility studies: ph monitoring; to determine the amount of pressure and motor activity in the GI tract 1.6 laboratory studies (to obtain a specimen of gastric contents for diagnostic purposes, i.e., when pyloric or intestinal obstruction is suspected) 2. Large bore nasogastric tubes (i.e.: Salem sump) are the most common type of tubes used for gastric decompression. This type of tube uses continuous low pressure to decompress the stomach and should not be used for administering enteral nutrition. 3. Small-bore nasogastric feeding tubes or Levine tubes are used to administer enteral nutrition and medications. They should be flushed with 30-50mL of sterile water when the feeding is stopped for any reason and at least every six hours during continuous infusions. 4. Medications should not be administered into a large-bore nasogastric tube that is inserted for decompression. In the event that this route of administration is required, the placement of the large-bore nasogastric tube should be verified by x-ray. 5. Irrigation of the large bore nasogastric tube with 30 ml of sterile water is done on a regular basis (every 2-4 hours): 5.1 if the tip of the tube rests against the stomach wall 5.2 with medication administration, or 5.3 if the tube becomes blocked with thick secretions. 6. To prevent the large bore nasogastric tube from becoming clogged or air-locked, the manufacturer recommends any irrigation into the main suction lumen be followed with an injection of approx 20 ml of air through the blue pigtail and then reinsert the anti-reflux valve. 7. If using Salem sump, the blue pigtail or air vent should be positioned above the level of the stomach to avoid back flow of stomach secretions. An anti-reflux valve is attached to the blue pigtail to prevent gastric contents from seeping out. Nasogastric Tube Insertion, CC Page 4 of 7
5 8. In the critical care areas, decompression tubes may be placed orally. Maintenance of these tubes is the same as nasogastric tubes; however once the patient is transferred out of the critical care area, consideration should be given to removing the oral tube and, if required, replacing it with a nasogastric tube. 9. If unsuccessful on the initial attempt to obtain a gastric aspirate from the small- bore tube: 9.1 Try injecting 10-20mL of air into the tube prior to aspirating. The air might be enough to dislodge the tip of the tube from the gastric mucosa. 9.2 Have the patient turn onto their left side or change position to see if the tube will move into the fluid pocket and away from the gastric mucosa. 9.3 Advance the tube 1-2 cm to ensure that the tip is sitting in a pool of fluid in the stomach. 10. Auscultation of an air bolus is no longer considered a reliable or safe method for verification of nasogastric tube position. This method cannot detect when a tube has inadvertently been placed into the respiratory tract and cannot distinguish between placement in the stomach versus the intestine. (Perry & Potter, 2006) Return to TOC EQUIPMENT See Perry & Potter, (2006). Clinical Nursing Skills and Techniques, Sixth edition: page 1015 (small-bore nasogastric feeding tubes) and page 1136 (large bore nasogastric tubes). See the Proficiency Standard Skills Checklist. PROCEDURE 1. INSERTION OF NG TUBE (RNs and - in approved practice settings only - LPNs) 1.1 Refer to Perry & Potter, (2006) Clinical Nursing Skills and Techniques, Sixth edition: pages (Intubating the Patient with a Nasogastric Feeding Tube) and pages (Inserting and Maintaining the Nasogastric tube for Gastric Decompression). See the Proficiency Standard Skills Checklist. 2. VERIFICATION OF NG TUBE PLACEMENT, IRRIGATION, AND MAINTENANCE OF PATENCY (RN and/or LPN) 2.1 Refer to Perry & Potter, (2006). Clinical Nursing Skills and Techniques, Sixth edition: (steps # inclusive) and pages (feeding tube). 2.2 Refer also to the Enteral Nutrition policies. (site-based policies pending distribution of CDHA policy) 3. CONTINUING ASSESSMENT (RN and/or LPN): 3.1 Perform assessment of placement/position and patency of the tube: upon initial insertion each shift, as part of physical assessment Nasogastric Tube Insertion, CC Page 5 of 7
6 3.1.3 prior to the instillation of fluid for the purpose of irrigation prior to the administration of nutrition and/or medications after vomiting, retching, or severe coughing if the tube is accidentally pulled if the mark on the tube is not visible or is in a different position if the patient feels the placement is in question if there is a change in the patient s condition, such as abdominal pain, cramping, bloating, fullness or burning with feedings if there is unusual leakage around the tube if the patient becomes suddenly short of breath 4. ADMINISTERING ENTERAL FEEDS VIA NASOGASTRIC TUBE (RN s and/or LPN s ) 4.1 Refer to Perry & Potter, (2006). Clinical Nursing Skills and Techniques, Sixth edition: pages Refer also to Enteral Nutrition policies (site-based policies pending distribution of CDHA policy). 5. REMOVAL OF NASOGASTRIC TUBE (RN s and/or LPN s): 5.1 Refer to Perry & Potter (2006), Clinical Nursing Skills and Techniques, Sixth edition: page ADMINISTERING MEDICATIONS VIA A NASOGASTRIC TUBE (RN s; LPN s in approved practice settings for medication administration): 6.1 Refer to Perry & Potter (2006), Clinical Nursing Skills and Techniques, Sixth edition: pages RELATED CAPITAL HEALTH DOCUMENTS Site-specific policies addressing enteral nutrition (pending distribution of CDHA policy) REFERENCES: Best, Carolyn, (2005, September) Caring for a Patient with a Nasogastric Tube. Nursing Standard. Volume 20, Number 3, Gallagher, John E., (2004, August) Nasogastric Tubes: Hard to Swallow. Annals of Emergency Medicine, Volume 44, Number 2. Cullen, Louise, Taylor, David, Taylor, Simone, Chu, Kevin, (2004, August) Nebulized Lidocaine Decreases the Discomfort of Nasogastric Tube Insertion: a Randomized, Double-blind Trial. Annals of Emergency Medicine, Volume 44, Number 2. Guenter, Peggy and Silkroski, Marcia, (2001). Tube Feeding Practical Guidelines and Nursing Protocols, Gaithersburg, Maryland, Aspen Publishers. Nasogastric Tube Insertion, CC Page 6 of 7
7 Lord, Linda, (2001, September). How to Insert a Large-Bore Nasogastric Tube. Nursing 2001: Volume 31, Number 9: Return to TOC Lynn-McHale, D.J. & Carlson, K.K. (editors), (2001) AACN Procedure Manual for Critical Care (4 th edition). Philadelphia: W.B. Saunders Company. McConnell, E.A., (1997, January). Clinical Do s and Don ts: Inserting a Nasogastric Tube. Nursing 97: Volume 27, Number 1. Metheny, Norma A. and Titler, Marita G. (2001, May) Assessing Placement of Feeding Tubes. American Journal of Nursing, Volume 101, Number 5: Perry, A.G. & Potter, P.A., (2002). Clinical Nursing Skills and Techniques, (6th Ed), St. Louis: Mosby, Inc., Harcourt Health Sciences Company. Potter, P.A. & Perry, A. G., (2001). Canadian Fundamentals of Nursing, (2nd Ed), Toronto: Mosby, Harcourt Canada Ltd. HISTORICAL DATES Integrated January, 2007{(Replaces December 1996 (DGH); August 1997 (Eastern Shore Memorial Hospital); October 2001 (QEII NC ); May 2002 (Hants Community Hospital); (Cobequid Community Health Center)} Nasogastric Tube Insertion, CC Page 7 of 7
LEARNING MODULE FOR NASOGASTRIC TUBE, INSERTION, MAINTENANCE & REMOVAL (POST ENTRY LEVEL COMPETENCY)
 LEARNING MODULE FOR NASOGASTRIC TUBE, INSERTION, MAINTENANCE & REMOVAL (POST ENTRY LEVEL COMPETENCY) Date: November, 2006 Developed by: Eleanor Griffiths, Nurse Educator Medical/ Surgical Resource Team
LEARNING MODULE FOR NASOGASTRIC TUBE, INSERTION, MAINTENANCE & REMOVAL (POST ENTRY LEVEL COMPETENCY) Date: November, 2006 Developed by: Eleanor Griffiths, Nurse Educator Medical/ Surgical Resource Team
Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role. Lillian Khalil, BSN, RN Volunteers of America, Chesapeake
 Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role Lillian Khalil, BSN, RN Volunteers of America, Chesapeake Objectives The participants will be able to identify the
Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role Lillian Khalil, BSN, RN Volunteers of America, Chesapeake Objectives The participants will be able to identify the
STAY-PUT Nasojejunal Feeding Tubes. Nursing Manual/ Patient Information
 SPECIALTY FEEDING TUBES STAY-PUT Nasojejunal Feeding Tubes Nursing Manual/ Patient Information Manual contains important care and maintenance information and should accompany patient NURSING CONSIDERATIONS
SPECIALTY FEEDING TUBES STAY-PUT Nasojejunal Feeding Tubes Nursing Manual/ Patient Information Manual contains important care and maintenance information and should accompany patient NURSING CONSIDERATIONS
Gastrostomy Feeding CARE GUIDELINES FOR PATIENTS & CARERS. Accessory items. Freka UK Funnel Adapter. Fixation Plate CH9. Male Luer Lock Adapter
 Accessory items Freka UK Funnel Adapter Fixation Plate CH9 Code: 7755681 Code: 7903002 Male Luer Lock Adapter CH9 Fixation Plate CH15 Code: 7981311 Code: 7904002 Male Luer Lock Adapter CH15 Code: 798137Y
Accessory items Freka UK Funnel Adapter Fixation Plate CH9 Code: 7755681 Code: 7903002 Male Luer Lock Adapter CH9 Fixation Plate CH15 Code: 7981311 Code: 7904002 Male Luer Lock Adapter CH15 Code: 798137Y
PICC & Midline Catheters Patient Information Guide
 PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
TRACHEOSTOMY TUBE PARTS
 Page1 NR 33 TRACHEOSTOMY CARE AND SUCTIONING Review ATI Basic skills videos: Tracheostomy care and Endotracheal suction using a closed suction set. TRACHEOSTOMY TUBE PARTS Match the numbers on the diagram
Page1 NR 33 TRACHEOSTOMY CARE AND SUCTIONING Review ATI Basic skills videos: Tracheostomy care and Endotracheal suction using a closed suction set. TRACHEOSTOMY TUBE PARTS Match the numbers on the diagram
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter
 Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Information for people being discharged with a naso-gastric (NG) feeding tube
 Information for people being discharged with a naso-gastric (NG) feeding tube The aim of this leaflet is to provide patients with the relevant information for the use of a nasogastric tube. It will include:
Information for people being discharged with a naso-gastric (NG) feeding tube The aim of this leaflet is to provide patients with the relevant information for the use of a nasogastric tube. It will include:
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH
 PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
REMOVAL OF A PICC. Possible Cause Nursing Actions Prevention
 REMOVAL OF A PICC PICC lines are removed following a physician order, when therapy is completed or complications such as line sepsis, thrombosis or phlebitis, require removal. The removal of a PICC line
REMOVAL OF A PICC PICC lines are removed following a physician order, when therapy is completed or complications such as line sepsis, thrombosis or phlebitis, require removal. The removal of a PICC line
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS
 CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters
 Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
NURSING 500.105 Effective Date Title: 6/12 SCOPE OF PRACTICE FOR STUDENT NURSES AND NURSING ASSISTANTS
 XXX DAYTONA XXX _OCEANSIDE HEALTH CARE PARTNERS Department: Page 1 of 5 POLICY & PROCEDURE Policy Number NURSING 500.105 Effective Date Title: 6/12 SCOPE OF PRACTICE FOR STUDENT NURSES AND NURSING ASSISTANTS
XXX DAYTONA XXX _OCEANSIDE HEALTH CARE PARTNERS Department: Page 1 of 5 POLICY & PROCEDURE Policy Number NURSING 500.105 Effective Date Title: 6/12 SCOPE OF PRACTICE FOR STUDENT NURSES AND NURSING ASSISTANTS
Peripherally Inserted Central Catheter (PICC) for Outpatient
 Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Long Term Tube Feeding. Sunnybrook. A Guide for Patients and Substitute Decision Makers VETERANS & COMMUNITY
 Long Term Tube Feeding A Guide for Patients and Substitute Decision Makers Sunnybrook VETERANS & COMMUNITY Sunnybrook VETERANS & COMMUNITY This brochure has been produced by: Sunnybrook Health Sciences
Long Term Tube Feeding A Guide for Patients and Substitute Decision Makers Sunnybrook VETERANS & COMMUNITY Sunnybrook VETERANS & COMMUNITY This brochure has been produced by: Sunnybrook Health Sciences
Freka. Enteral Feeding Tube Product Range ENTERAL NUTRITION
 ENTERAL NUTRITION Freka Enteral Feeding Tube Product Range Fresenius Kabi Limited, Cestrian Court, Eastgate Way, Runcorn, Cheshire WA7 1NT tel: 01928 533533 fax: 01928 533520 email: [email protected]
ENTERAL NUTRITION Freka Enteral Feeding Tube Product Range Fresenius Kabi Limited, Cestrian Court, Eastgate Way, Runcorn, Cheshire WA7 1NT tel: 01928 533533 fax: 01928 533520 email: [email protected]
PATIENT GUIDE. Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL
 PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
By Deanna L. Reising, PhD, APRN,BC, and Ronald Scott Neal, BSN, RN
 HOURS CE3 Continuing Education What you think are the best practices may not be. By Deanna L. Reising, PhD, APRN,BC, and Ronald Scott Neal, BSN, RN Flushing an enteral tube (in other words, keeping it
HOURS CE3 Continuing Education What you think are the best practices may not be. By Deanna L. Reising, PhD, APRN,BC, and Ronald Scott Neal, BSN, RN Flushing an enteral tube (in other words, keeping it
NURSING SERVICES DEPARTMENT
 NURSING SERVICES DEPARTMENT TITLE: Mechanical Ventilation PATIENT CARE PLAN DIAGNOSIS: DISCHARGE CRITERIA: 1 The patient will: Maintain adequate mechanics of PERTINENT INFORMATION:. ventilation as demonstrated
NURSING SERVICES DEPARTMENT TITLE: Mechanical Ventilation PATIENT CARE PLAN DIAGNOSIS: DISCHARGE CRITERIA: 1 The patient will: Maintain adequate mechanics of PERTINENT INFORMATION:. ventilation as demonstrated
My patient has a feeding tube
 My patient has a feeding tube What does that mean? Martha Kliebenstein, MSN, RN Clinical Educator (December, 2014) Types of tubes Gastrostomy (G-tube) Gastrostomy jejunostomy (G-J tube) Naso gastric (NG
My patient has a feeding tube What does that mean? Martha Kliebenstein, MSN, RN Clinical Educator (December, 2014) Types of tubes Gastrostomy (G-tube) Gastrostomy jejunostomy (G-J tube) Naso gastric (NG
INTERDISCIPLINARY CLINICAL MANUAL Policy & Procedure
 INTERDISCIPLINARY CLINICAL MANUAL Policy & Procedure TITLE: Section: Source: Distribution: Chest Drainage and Chest Tube Management Respiratory/Thoracic Joy Tarasuk, CNE, Thoracic Surgery Capital Health
INTERDISCIPLINARY CLINICAL MANUAL Policy & Procedure TITLE: Section: Source: Distribution: Chest Drainage and Chest Tube Management Respiratory/Thoracic Joy Tarasuk, CNE, Thoracic Surgery Capital Health
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO)
 A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO) Types of Catheter Related Thrombotic A catheter-related thrombus may be intraluminal (inside the catheter)
A4.7 Management of a totally occluded central catheter and persistent withdrawal occlusion (PWO) Types of Catheter Related Thrombotic A catheter-related thrombus may be intraluminal (inside the catheter)
2. Does the patient have one of the following appropriate indications for placing indwelling urinary catheters?
 A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
A. Decision to Insert a Urinary Catheter: 1. Before placing an indwelling catheter, please consider if these alternatives would be more appropriate: Bladder scanner: to assess and confirm urinary retention,
Nutritional Management in Esophageal Cancer. Kurt Boeykens Nutrition Nurse Specialist
 Nutritional Management in Esophageal Cancer Kurt Boeykens Nutrition Nurse Specialist 1 Are these patients nutritionally at risk? If surgery: Major surgery Preoperative treatment Chemotherapy and radiation
Nutritional Management in Esophageal Cancer Kurt Boeykens Nutrition Nurse Specialist 1 Are these patients nutritionally at risk? If surgery: Major surgery Preoperative treatment Chemotherapy and radiation
Emergency Medical Services Advanced Level Competency Checklist
 Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
Emergency Services Advanced Level Competency Checklist EMS Service: Current License in State of Nebraska: # (Copy of license kept in file at station) Date of joining EMS Service: EMS Service Member Name:
INTERDISCIPLINARY CLINICAL MANUAL Practice Guideline
 INTERDISCIPLINARY CLINICAL MANUAL Practice Guideline TITLE: Insertion of a curved tip Urinary Catheter (Coude/Tiemann) NUMBER: CC 50-013 Effective Date: August 2015 Page 1 of 5 Applies To: All Preamble:
INTERDISCIPLINARY CLINICAL MANUAL Practice Guideline TITLE: Insertion of a curved tip Urinary Catheter (Coude/Tiemann) NUMBER: CC 50-013 Effective Date: August 2015 Page 1 of 5 Applies To: All Preamble:
III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004
 III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004 Purpose A. Allow for precise measurement of urine output. B. Collect a sterile urine specimen. C.
III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004 Purpose A. Allow for precise measurement of urine output. B. Collect a sterile urine specimen. C.
Kimberly-Clark* MIC-KEY* Low-Profile Gastrostomy Feeding Tube
 Lock MIC Kimberly-Clark* MIC-KEY* Low-Profile Gastrostomy Feeding Tube Directions For Use The Kimberly-Clark* MIC* Gastrostomy feeding tube (figure A) and the Kimberly-Clark* MIC* Bolus Gastrostomy Feeding
Lock MIC Kimberly-Clark* MIC-KEY* Low-Profile Gastrostomy Feeding Tube Directions For Use The Kimberly-Clark* MIC* Gastrostomy feeding tube (figure A) and the Kimberly-Clark* MIC* Bolus Gastrostomy Feeding
Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider. www.umke.org
 Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider Objectives: Identify the indications, contraindications and side effects of LMA use. Identify the equipment necessary for
Laryngeal Mask Airways (LMA), Indications and Use for the Pre-Hospital Provider Objectives: Identify the indications, contraindications and side effects of LMA use. Identify the equipment necessary for
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter
 Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Licensed Vocational Nurse Scope of Practice Standards Health Care Services
 1BCHAPTER 5 2BLicensed Vocational Nurse Scope of Practice Standards I. POLICY: Licensed Vocational Nurses (LVNs) are NOT independent practitioners. It is not within the scope of LVN practice to function
1BCHAPTER 5 2BLicensed Vocational Nurse Scope of Practice Standards I. POLICY: Licensed Vocational Nurses (LVNs) are NOT independent practitioners. It is not within the scope of LVN practice to function
N26 Chest Tubes 5/9/2012
 Thoracic cavity, pleural space 1 Conditions requiring chest drainage_1 Air between the pleurae is a pneumothorax Occurs when there is an opening on the surface of the lung or in the airways, y, in the
Thoracic cavity, pleural space 1 Conditions requiring chest drainage_1 Air between the pleurae is a pneumothorax Occurs when there is an opening on the surface of the lung or in the airways, y, in the
Tube Feeding at Home Gravity or Syringe Feeding
 Tube Feeding at Home Gravity or Syringe Feeding Adapted from the former Taming the Feeding Tube, North Shore Hospital. 1 Where do I find information in this booklet? Subject Page How do I contact my health
Tube Feeding at Home Gravity or Syringe Feeding Adapted from the former Taming the Feeding Tube, North Shore Hospital. 1 Where do I find information in this booklet? Subject Page How do I contact my health
Caring for a Tenckhoff Catheter
 Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
Caring for a Tenckhoff Catheter UHN A Patient s Guide What is a Pleural Effusion? There is a small space between the outside of your lung and the chest wall (ribs). This space is called the pleural space.
RATIFIED BY NNPDG SEPTEMBER 2006 FOR REVIEW 2009
 NOTTINGHAM UNIVERSITY HOSPTIALS/RUSHCLIFFE PCT NURSING PRACTICE GUIDELINES GUIDELINES FOR CARE OF A PATIENT WITH A WOUND DRAINAGE SYSTEM CONTENTS PAGE Introduction and Types of Drains 1 Procedure for Applying
NOTTINGHAM UNIVERSITY HOSPTIALS/RUSHCLIFFE PCT NURSING PRACTICE GUIDELINES GUIDELINES FOR CARE OF A PATIENT WITH A WOUND DRAINAGE SYSTEM CONTENTS PAGE Introduction and Types of Drains 1 Procedure for Applying
Delivering nutrition, fluids & medication via a PEG. By Julia Pointer & Caroline Ross, Staff Nurses, Hospice Day Service
 Delivering nutrition, fluids & medication via a PEG By Julia Pointer & Caroline Ross, Staff Nurses, Hospice Day Service Aims of this session? To give an explanation of the theory and practice of a Percutaneous
Delivering nutrition, fluids & medication via a PEG By Julia Pointer & Caroline Ross, Staff Nurses, Hospice Day Service Aims of this session? To give an explanation of the theory and practice of a Percutaneous
MISSISSIPPI BOARD OF NURSING IV THERAPY COURSE FOR THE EXPANDED ROLE LICENSED PRACTICAL NURSE COURSE OUTLINE
 THEORY MINIMUM 40 HOURS COURSE OUTLINE UNIT TOPIC HOURS* I LEGAL ASPECTS AND PRACTICE OF IV THERAPY 1 II REVIEW OF ANATOMY AND PHYSIOLOGY 6 III FLUID AND ELECTROLYTE BALANCE 10 IV EQUIPMENT AND PROCEDURES
THEORY MINIMUM 40 HOURS COURSE OUTLINE UNIT TOPIC HOURS* I LEGAL ASPECTS AND PRACTICE OF IV THERAPY 1 II REVIEW OF ANATOMY AND PHYSIOLOGY 6 III FLUID AND ELECTROLYTE BALANCE 10 IV EQUIPMENT AND PROCEDURES
Care of Persons With Jejunostomy Tubes Or Gastrojejunal Tubes
 STATE OF CONNECTICUT DEPARTMENT OF DEVELOPMENTAL SERVICES NURSING PROTOCOL # NP 09-2 Care of Persons With Jejunostomy Tubes Or Gastrojejunal Tubes Issue Date: March 2009 Implementation Date: May 1, 2009
STATE OF CONNECTICUT DEPARTMENT OF DEVELOPMENTAL SERVICES NURSING PROTOCOL # NP 09-2 Care of Persons With Jejunostomy Tubes Or Gastrojejunal Tubes Issue Date: March 2009 Implementation Date: May 1, 2009
LESSON 4 ORAL, NASOPHARYNGEAL, AND NASOTRACHEAL SUCTIONING.
 LESSON 4 ORAL, NASOPHARYNGEAL, AND NASOTRACHEAL SUCTIONING. 4-1. SUCTIONING a. Suctioning is a common nursing activity performed for the purpose of removing accumulated secretions from the patient's nose,
LESSON 4 ORAL, NASOPHARYNGEAL, AND NASOTRACHEAL SUCTIONING. 4-1. SUCTIONING a. Suctioning is a common nursing activity performed for the purpose of removing accumulated secretions from the patient's nose,
BLS TREATMENT GUIDELINES - CARDIAC
 BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
Use of stents in esophageal cancer" Hans Gerdes, M.D. Director, GI Endoscopy Unit Memorial Sloan-Kettering Cancer Center
 Use of stents in esophageal cancer" Hans Gerdes, M.D. Director, GI Endoscopy Unit Memorial Sloan-Kettering Cancer Center Features of esophageal cancer Esophageal cancer is an abnormal growth that arises
Use of stents in esophageal cancer" Hans Gerdes, M.D. Director, GI Endoscopy Unit Memorial Sloan-Kettering Cancer Center Features of esophageal cancer Esophageal cancer is an abnormal growth that arises
Policies & Procedures. ID Number: 1118
 Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
Policies & Procedures. Care of
 Policies & Procedures Title: SUPRAPUBIC CATHETER Care of Changing Removal Authorization: [x] SHR Nursing Practice Committee I.D. Number: 1021 Source: Nursing Date Revised: November 2014 Date Effective:
Policies & Procedures Title: SUPRAPUBIC CATHETER Care of Changing Removal Authorization: [x] SHR Nursing Practice Committee I.D. Number: 1021 Source: Nursing Date Revised: November 2014 Date Effective:
Are any artificial parts used in the ACE Malone surgery?
 ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
PATIENT CARE MANUAL PROCEDURE
 PATIENT CARE MANUAL PROCEDURE NUMBER VII-E-5 PAGE 1 OF 7 APPROVED BY: CATEGORY: Tri-site Nursing Policy and Procedures Review Committee Body Systems; Genitourinary 1.0 GOALS To influence patient care providers
PATIENT CARE MANUAL PROCEDURE NUMBER VII-E-5 PAGE 1 OF 7 APPROVED BY: CATEGORY: Tri-site Nursing Policy and Procedures Review Committee Body Systems; Genitourinary 1.0 GOALS To influence patient care providers
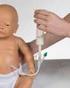
Parent Information for USING A NASOGASTRIC TUBE
 Parent Information for USING A NASOGASTRIC TUBE The information sheet has been written for parents whose baby / child requires a nasogastric tube for short or long term feeding. WHAT IS A NASOGRASTRIC
Parent Information for USING A NASOGASTRIC TUBE The information sheet has been written for parents whose baby / child requires a nasogastric tube for short or long term feeding. WHAT IS A NASOGRASTRIC
Motility Disorders that are Commonly Mistaken for Reflux by Susan Agrawal
 www.complexchild.com Motility Disorders that are Commonly Mistaken for Reflux by Susan Agrawal A surprisingly large number of children with motility disorders experience the same progression of events
www.complexchild.com Motility Disorders that are Commonly Mistaken for Reflux by Susan Agrawal A surprisingly large number of children with motility disorders experience the same progression of events
TUBE FEEDING AT HOME
 TUBE FEEDING AT HOME Adapted from the former Taming the Feeding Tube, Royal North Shore Hospital. Revised 2005, 2007, Jan 2009 1 Where do I find information in this booklet? Only the pages that you need
TUBE FEEDING AT HOME Adapted from the former Taming the Feeding Tube, Royal North Shore Hospital. Revised 2005, 2007, Jan 2009 1 Where do I find information in this booklet? Only the pages that you need
Scope of Practice Approved by the State Board of EMS (EMS Board), within the Division of EMS of the Ohio Department of Public Safety
 Scope of Practice Approved by the State Board of EMS (EMS Board), within the Division of EMS of the Ohio Department of Public Safety This document offers an at-a-glance view of the Scope of Practice for
Scope of Practice Approved by the State Board of EMS (EMS Board), within the Division of EMS of the Ohio Department of Public Safety This document offers an at-a-glance view of the Scope of Practice for
NORTH CAROLINA BOARD OF NURSING NURSE AIDE II TRAINING MODULE
 PART A: PREPARING FOR ADMINISTRATION OF IV FLUIDS All four parts of this module, including skills checklists must be successfully completed in order to complete this training module. This activity is a
PART A: PREPARING FOR ADMINISTRATION OF IV FLUIDS All four parts of this module, including skills checklists must be successfully completed in order to complete this training module. This activity is a
a guide to understanding pierre robin sequence
 a guide to understanding pierre robin sequence a publication of children s craniofacial association a guide to understanding pierre robin sequence this parent s guide to Pierre Robin Sequence is designed
a guide to understanding pierre robin sequence a publication of children s craniofacial association a guide to understanding pierre robin sequence this parent s guide to Pierre Robin Sequence is designed
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
PICC and Midline Catheters
 PICC and Midline Catheters Infusion RN s Deb Bucher RN BSN CRNI Dawn Finch RN CRNI Marianne Hansen RN BSN CRNI Karman Youngblood RN BS CRNI Infusion Pharmacist Kathy Cimakasky Pharm D Tamara Migut RPh
PICC and Midline Catheters Infusion RN s Deb Bucher RN BSN CRNI Dawn Finch RN CRNI Marianne Hansen RN BSN CRNI Karman Youngblood RN BS CRNI Infusion Pharmacist Kathy Cimakasky Pharm D Tamara Migut RPh
DELEGATION OF NURSING
 DELEGATION OF NURSING FUNCTIONS TO UNLICENSED DIRECT CARE PROVIDERS IN A SCHOOL SETTING MARYLAND STATE SCHOOL HEALTH SERVICES GUIDELINE JANUARY 2006 Maryland State Department of Education Maryland Department
DELEGATION OF NURSING FUNCTIONS TO UNLICENSED DIRECT CARE PROVIDERS IN A SCHOOL SETTING MARYLAND STATE SCHOOL HEALTH SERVICES GUIDELINE JANUARY 2006 Maryland State Department of Education Maryland Department
Procedure -8. Intraosseous Infusion Adult and Pediatric EZIO. Page 1 of 7 APPROVED:
 Page 1 of 7 Intraosseous Infusion Adult and Pediatric APPROVED: EMS Medical Director EMS Administrator 1. Goals/Introduction: 1.1 Intraosseous (IO) infusion provides an effective alternative means of providing
Page 1 of 7 Intraosseous Infusion Adult and Pediatric APPROVED: EMS Medical Director EMS Administrator 1. Goals/Introduction: 1.1 Intraosseous (IO) infusion provides an effective alternative means of providing
Within the Scope of Practice/Role of APRN RN _ X_LPN CNA
 Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: [email protected] Home Page: https://nursing-online.state.wy.us/ OPINION:
Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: [email protected] Home Page: https://nursing-online.state.wy.us/ OPINION:
The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery
 Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Contraindications: Malign or benign strictures in the upper part of esophagus close to the cricopharyngeal muscle.
 Manufactured by: ELLA CS, s.r.o. Milady Horákové 504 500 06 Hradec Králové 6 Czech Republic Phone: +420 49 527 91 11 Fax: +420 49 526 56 55 E-mail: [email protected] Instructions for Use FerX-ELLA Esophageal
Manufactured by: ELLA CS, s.r.o. Milady Horákové 504 500 06 Hradec Králové 6 Czech Republic Phone: +420 49 527 91 11 Fax: +420 49 526 56 55 E-mail: [email protected] Instructions for Use FerX-ELLA Esophageal
Caring for Your Gastrostomy
 Caring for Your Gastrostomy Table of Contents What Is a Gastrostomy Tube (G-tube)?... 2 Types of Gastrostomy Tubes... 3 Cleaning the Gastrostomy Site... 4 Gastrostomy Feedings... 5 Giving Medicines...
Caring for Your Gastrostomy Table of Contents What Is a Gastrostomy Tube (G-tube)?... 2 Types of Gastrostomy Tubes... 3 Cleaning the Gastrostomy Site... 4 Gastrostomy Feedings... 5 Giving Medicines...
Level 4 Trauma Hospital Criteria
 Level 4 Trauma Hospital Criteria Hospital Commitment The board of directors, administration, and medical, nursing and ancillary staff shall make a commitment to providing trauma care commensurate to the
Level 4 Trauma Hospital Criteria Hospital Commitment The board of directors, administration, and medical, nursing and ancillary staff shall make a commitment to providing trauma care commensurate to the
PICCs and Midline Catheters
 Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Emergencies in Post- Bariatric Surgery Patients
 Emergencies in Post- Patients Disclosures Dr. Birnbaumer has no financial disclosures Diane M. Birnbaumer, M.D., FACEP Professor of Medicine University of California, Los Angeles Senior Clinical Educator
Emergencies in Post- Patients Disclosures Dr. Birnbaumer has no financial disclosures Diane M. Birnbaumer, M.D., FACEP Professor of Medicine University of California, Los Angeles Senior Clinical Educator
Tracheostomy Care at Home
 Tracheostomy Care at Home Patient Education CARE AND TREATMENT This information will help you understand how to care for a person with a tracheostomy at home. It is a supplement to the teaching offered
Tracheostomy Care at Home Patient Education CARE AND TREATMENT This information will help you understand how to care for a person with a tracheostomy at home. It is a supplement to the teaching offered
LOS ANGELES COUNTY EMERGENCY MEDICAL SERVICES LOS ANGELES COUNTY EMT-I EXPANDED SCOPE OF PRACTICE
 LOS ANGELES COUNTY EMERGENCY MEDICAL SERVICES LOS ANGELES COUNTY EMT-I EXPANDED SCOPE OF PRACTICE Upon completion of this unit of instruction, the student will be able to: LEARNING OBJECTIVES LESSON CONTENT
LOS ANGELES COUNTY EMERGENCY MEDICAL SERVICES LOS ANGELES COUNTY EMT-I EXPANDED SCOPE OF PRACTICE Upon completion of this unit of instruction, the student will be able to: LEARNING OBJECTIVES LESSON CONTENT
Scope of Practice Approved by State Board of Emergency Medical, Fire and Transportation Services Division of EMS, Ohio Department of Public Safety
 Scope of Practice Approved by State Board of Emergency Medical, Fire and Transportation Services Division of EMS, Ohio Department of Public Safety This document offers an at-a-glance view of the Scope
Scope of Practice Approved by State Board of Emergency Medical, Fire and Transportation Services Division of EMS, Ohio Department of Public Safety This document offers an at-a-glance view of the Scope
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
CARE OF PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC LINES)
 LEARNING MODULE FOR CARE OF PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC LINES) CC 80-018 POST-ENTRY LEVEL COMPETENCY Date: July, 2004 Developed by: Maxine Young, RN Revised by: Central Venous Access
LEARNING MODULE FOR CARE OF PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC LINES) CC 80-018 POST-ENTRY LEVEL COMPETENCY Date: July, 2004 Developed by: Maxine Young, RN Revised by: Central Venous Access
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information
 Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
Understanding your Peripherally Inserted Central Catheter (PICC) Patient Information The Purpose of this Information Sheet This information sheet has been written by patients, members of the public and
How to care for a Midline Catheter
 How to care for a Midline Catheter Developed by the health care professionals of the IV Program with assistance from the Department of Learning and Development. All rights reserved. No part of this book
How to care for a Midline Catheter Developed by the health care professionals of the IV Program with assistance from the Department of Learning and Development. All rights reserved. No part of this book
X-Plain Sinus Surgery Reference Summary
 X-Plain Sinus Surgery Reference Summary Introduction Sinus surgery is a very common and safe operation. Your doctor may recommend that you have sinus surgery. The decision whether or not to have sinus
X-Plain Sinus Surgery Reference Summary Introduction Sinus surgery is a very common and safe operation. Your doctor may recommend that you have sinus surgery. The decision whether or not to have sinus
PACKAGE LEAFLET: INFORMATION FOR THE USER. PARACETAMOL MACOPHARMA 10 mg/ml, solution for infusion. Paracetamol
 PACKAGE LEAFLET: INFORMATION FOR THE USER PARACETAMOL MACOPHARMA 10 mg/ml, solution for infusion Paracetamol Read all of this leaflet carefully before you start using this medicine. Keep this leaflet.
PACKAGE LEAFLET: INFORMATION FOR THE USER PARACETAMOL MACOPHARMA 10 mg/ml, solution for infusion Paracetamol Read all of this leaflet carefully before you start using this medicine. Keep this leaflet.
The degree of liver inflammation or damage (grade) Presence and extent of fatty liver or other metabolic liver diseases
 ilearning about your health Liver Biopsy www.cpmc.org/learning What is a Liver Biopsy? A liver biopsy is a procedure where a specially trained doctor (typically a hepatologist, radiologist, or gastroenterologist)
ilearning about your health Liver Biopsy www.cpmc.org/learning What is a Liver Biopsy? A liver biopsy is a procedure where a specially trained doctor (typically a hepatologist, radiologist, or gastroenterologist)
Section Two: Arterial Pressure Monitoring
 Section Two: Arterial Pressure Monitoring Indications An arterial line is indicated for blood pressure monitoring for the patient with any medical or surgical condition that compromises cardiac output,
Section Two: Arterial Pressure Monitoring Indications An arterial line is indicated for blood pressure monitoring for the patient with any medical or surgical condition that compromises cardiac output,
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
V: Infusion Therapy. Alberta Licensed Practical Nurses Competency Profile 217
 V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
Enables MDA Medical Teams to categorize victims in mass casualty scenarios, in order to be able to triage and treat casualties
 MDA Disposable ALS + BLS Medical Ambulance Equipment Prices shown in CDN. Funds Items Description Picture Mass Casualty ID tag 1000 units = $350 Enables MDA Medical Teams to categorize victims in mass
MDA Disposable ALS + BLS Medical Ambulance Equipment Prices shown in CDN. Funds Items Description Picture Mass Casualty ID tag 1000 units = $350 Enables MDA Medical Teams to categorize victims in mass
Peripherally Inserted Central Catheter (PICC) Benefits Long-term access - dwell time varies (can be > one year) Decreased length of stay in hospital a
 Nursing Management of Venous Access Devices: Peripherally Inserted Central Catheter (PICC) Mimi Bartholomay, RN, MSN, AOCN Denise Dreher, RN, CRNI, VA-BC Theresa Evans, RN, MSN Susan Finn, RN, MSN, AOCNS
Nursing Management of Venous Access Devices: Peripherally Inserted Central Catheter (PICC) Mimi Bartholomay, RN, MSN, AOCN Denise Dreher, RN, CRNI, VA-BC Theresa Evans, RN, MSN Susan Finn, RN, MSN, AOCNS
Neonatal Intubation. Purpose. Scope. Indications. Equipment Cardiorespiratory monitor SaO 2 monitor. Anatomic Considerations.
 Page 1 of 5 Purpose Scope Indications Neonatal Intubation To assure proper placement of endotracheal tubes for maximum ventilation using proper intubation procedures. The policy applies to all Respiratory
Page 1 of 5 Purpose Scope Indications Neonatal Intubation To assure proper placement of endotracheal tubes for maximum ventilation using proper intubation procedures. The policy applies to all Respiratory
Prerequisites: None. Course Description: Studies principles and procedures essential to the basic nursing care of patients.
 Revised: Fall 2015 22TPNE 142 22TNursing Skills II Prerequisites: None Course Description: Studies principles and procedures essential to the basic nursing care of patients. Semester Credits: 3 Lecture
Revised: Fall 2015 22TPNE 142 22TNursing Skills II Prerequisites: None Course Description: Studies principles and procedures essential to the basic nursing care of patients. Semester Credits: 3 Lecture
Vaxcel PICCs Valved and Non-Valved. A Patient s Guide
 Vaxcel PICCs Valved and Non-Valved A Patient s Guide Information about your Vaxcel PICC is available by calling the Navilyst Medical Vascular Access Information Line 800.513.6876 Vaxcel Peripherally Inserted
Vaxcel PICCs Valved and Non-Valved A Patient s Guide Information about your Vaxcel PICC is available by calling the Navilyst Medical Vascular Access Information Line 800.513.6876 Vaxcel Peripherally Inserted
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Implanted Central Venous Access Devices (Ports)
 Nursing Management of Venous Access Devices: Implanted Central Venous Access Devices (Ports) Mimi Bartholomay, RN, MSN, AOCN Denise Dreher,, RN, CRNI, VA-BC Theresa Evans, RN, MSN Susan Finn, RN, MSN,
Nursing Management of Venous Access Devices: Implanted Central Venous Access Devices (Ports) Mimi Bartholomay, RN, MSN, AOCN Denise Dreher,, RN, CRNI, VA-BC Theresa Evans, RN, MSN Susan Finn, RN, MSN,
VIDEOFLUOROSCOPIC SWALLOWING EXAM
 VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/Medical record number, Date of birth, Date of exam, Referred by, Reason for referral HISTORY/SUBJECTIVE INFORMATION
VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/Medical record number, Date of birth, Date of exam, Referred by, Reason for referral HISTORY/SUBJECTIVE INFORMATION
Acute abdominal conditions Key Points
 7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
7 Acute abdominal conditions Key Points 7.1 ASSESSMENT AND DIAGNOSIS Referred abdominal pain Fore gut pain (stomach, duodenum, gall bladder) is referred to the upper abdomen Mid gut pain (small intestine,
PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS
 PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS Approved: February 2010 Date for review: February 2010 1 PROCEDURE
PROCEDURE FOR SUBCUTANEOUS INSERTION, REMOVAL, MEDICATION ADMINISTRATION AND FLUID ADMINISTRATION FOR COMMUNITY PALLIATIVE CARE PATIENTS Approved: February 2010 Date for review: February 2010 1 PROCEDURE
DISCHARGE CRITERIA FOR PHASE I & II- POST ANESTHESIA CARE
 REFERENCES: The Joint Commission Accreditation Manual for Hospitals American Society of Post Anesthesia Nurses: Standards of Post Anesthesia Nursing Practice (1991, 2002). RELATED DOCUMENTS: SHC Administrative
REFERENCES: The Joint Commission Accreditation Manual for Hospitals American Society of Post Anesthesia Nurses: Standards of Post Anesthesia Nursing Practice (1991, 2002). RELATED DOCUMENTS: SHC Administrative
Patients First. Tube Feeding Guidelines. Careful handwashing and a clean work surface help prevent infection. Patient Education CARE AND TREATMENT
 Patient Education CARE AND TREATMENT Careful handwashing and a clean work surface help prevent infection. Tube Feeding Guidelines This information will guide you in learning about the procedure for tube
Patient Education CARE AND TREATMENT Careful handwashing and a clean work surface help prevent infection. Tube Feeding Guidelines This information will guide you in learning about the procedure for tube
Managing Your Non-Tunneled (Percutaneous) Catheter: PICC, SICC, and JCC. What is a PICC catheter?
 Managing Your Non-Tunneled The staff of the Procedure, Vascular Access, Conscious Sedation Service has written this information to explain your new PICC (peripherally inserted central catheter), SICC (subclavian
Managing Your Non-Tunneled The staff of the Procedure, Vascular Access, Conscious Sedation Service has written this information to explain your new PICC (peripherally inserted central catheter), SICC (subclavian
Patient Information Guide for the ReShape Procedure
 Patient Information Guide for the ReShape Procedure Please review this information before your procedure. Please talk to your doctor if you have any questions or do not understand any of this information.
Patient Information Guide for the ReShape Procedure Please review this information before your procedure. Please talk to your doctor if you have any questions or do not understand any of this information.
SUCTION & TUBING YANKAUER, POOLE, FRAZIER AND SIGMOID INSTRUMENTS PREMIUM CONNECTORED AND ECONOMY ROLL TUBING
 SUCTION INSTRUMENTS & TUBING YANKAUER, POOLE, FRAZIER AND SIGMOID INSTRUMENTS PREMIUM CONNECTORED AND ECONOMY ROLL TUBING A complete line of quality, disposable Suction Instruments and Tubing to meet your
SUCTION INSTRUMENTS & TUBING YANKAUER, POOLE, FRAZIER AND SIGMOID INSTRUMENTS PREMIUM CONNECTORED AND ECONOMY ROLL TUBING A complete line of quality, disposable Suction Instruments and Tubing to meet your
ACI UROLOGY NETWORK - NURSING BLADDER IRRIGATION GUIDELINES
 ACI UROLOGY NETWORK - NURSING BLADDER IRRIGATION GUIDELINES The following pages provide examples of clinical guidelines to enable clinicians to develop their own resource material relevant to their hospital
ACI UROLOGY NETWORK - NURSING BLADDER IRRIGATION GUIDELINES The following pages provide examples of clinical guidelines to enable clinicians to develop their own resource material relevant to their hospital
Surgery for oesophageal cancer
 Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
Surgery for oesophageal cancer This information is an extract from the booklet Understanding oesophageal cancer (cancer of the gullet). You may find the full booklet helpful. We can send you a free copy
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND
 RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
RGN JOY LAUDE WATFORD GENERAL HOSPITAL, ENGLAND Monitor patient on the ward to detect trends in vital signs and to manage accordingly To recognise deteriorating trends and request relevant medical/out
Management of Chest Tubes and Air Leaks after Lung Resection
 Management of Chest Tubes and Air Leaks after Lung Resection Emily Kluck PA-C The Johns Hopkins Hospital Baltimore, MD AATS 2014, Toronto, CAN April 2014 Management of Chest Tubes 1 Overview Review the
Management of Chest Tubes and Air Leaks after Lung Resection Emily Kluck PA-C The Johns Hopkins Hospital Baltimore, MD AATS 2014, Toronto, CAN April 2014 Management of Chest Tubes 1 Overview Review the
