Care of Persons With Jejunostomy Tubes Or Gastrojejunal Tubes
|
|
|
- Aubrey Hudson
- 7 years ago
- Views:
Transcription
1 STATE OF CONNECTICUT DEPARTMENT OF DEVELOPMENTAL SERVICES NURSING PROTOCOL # NP 09-2 Care of Persons With Jejunostomy Tubes Or Gastrojejunal Tubes Issue Date: March 2009 Implementation Date: May 1, 2009 Author: DDS Health Services/Nursing Directors Contact Person: David Carlow DDS Director of Health and Clinical Services Purpose: This protocol is designed to establish the minimal best practice standards of nursing care for licensed nurses supporting persons served by the department who have jejunostomy or gastrojejunal tubes in place. Applicability: This protocol applies to all licensed nurses employed by the Department of Developmental Services (DDS). All private residential and/or day providers licensed or funded by DDS shall adopt this protocol or develop a substantively similar protocol that meets accepted standards of nursing practice. Introduction: An increasing number of persons with intellectual/ developmental disabilities have their nutritional needs met through the use of an enteral feeding tube that delivers nutrition, fluids, and/or medications into a section of the person s small intestine known as the jejunum. This method can be accomplished in a number of ways. The first is the surgical insertion of a balloon-tip jejunostomy tube or j-tube directly into the jejunum. The second method involves the use of an endoscope or fluoroscope to visualize the internal organs as a tube is percutaneously (through the skin) placed in the jejunum. This is referred to as a PEJ tube. Another method involves the insertion of a tube through a gastrostomy into the jejunum. This type of tube is referred to as a gastrojejunal or g/j tube. The last method, called the Roux-en-y jejunostomy involves the surgical creation of a limb or pouch in the jejunum that is appropriate for the intermittent insertion of a feeding tube for a small bolus feeding. Persons with enteral feeding tubes are at risk for the migration and malpositioning of those tubes. Several methods have been identified in the past to check tube placement such as the insertion of an air bolus followed by auscultation, the observation of aspirated jejunal contents and/or checking the ph of these contents. Current literature indicates that radiologic confirmation is the only reliable method to confirm jejunostomy tube and gastrojejunal tube placement. This confirmation of the placement of the tube shall be done following the initial insertion of the tube and when the tube is replaced. At these times, the baseline identification of the tube marking at the level of the skin or a baseline measurement of the tube length from the skin to the end of the tube shall be identified. Prior to each tube feeding or the administration of medication or water through a j-tube or g/j tube, the placement of the tube shall be checked. The DDS Health Services Directors have determined that the minimal standard method of checking j-tube or g/j- tube placement that shall be expected to be performed is by the visualization and comparison of tube markings or the measurement of tube length outside the skin if there are no markings on the tube. These methods were identified based upon best practice standards currently identified in literature to be more effective. These methods was may be combined with other measures as prescribed by the person s health care provider. It is important to mention at this juncture that RNs and LPNs are not permitted to replace/reinsert jejunostomy or gastrojejunal tubes as this responsibility has been identified to be outside the scope of practice for these nurses per the decision of the Connecticut Board of Examiners for Nursing. In the instance of a person with a Roux-en-y jejunostomy that requires frequent reinsertion of a feeding tube a waiver may be obtained from the Board that allows trained licensed nurses to perform this care. DDS Protocol #NP 09-2 Care of Persons with Jejunostomy Tubes or Gastrojejunal Tubes 1
2 This DDS protocol was developed with the assistance of Lisa Baker APRN who shared her expertise in gastroenterology and provided information resulting from an extensive review of the current literature on enteral access feeding tubes. This protocol incorporates evidence based practices that have been identified to promote optimal outcomes. Definitions: Balloon tip tube- a type of feeding tube that has a balloon on the distal end that is filled with water to keep it in place. It also has an external disk or bumper that allows for stabilization. Bolus feeding- the method of delivering enteral feedings using a limited amount of nutritional product that is administered over a span of minutes several times per day. This method of feeding is not usually recommended for persons with a jejunostomy tube as the intestine cannot hold the same volume that the stomach can. Continuous feeding- the method of delivering nourishment that involves the drip of formula by gravity or assisted by a pump in an ongoing manner over a specified number of hours into a gastrostomy, jejunostomy, or gastrojejunal tube Endoscopy: A procedure in which an instrument containing a camera is inserted into the gastrointestinal tract to visualize organs. This procedure is one of the methods used in the percutaneous placement of g-tubes, j-tubes and g/j tubes. Enteral feeding tube: a feeding device placed into the stomach or jejunum through which formula, fluids and/or medication are given to a person as an alternative to oral feeding. Gastrojejunal a type of tube for nutritional support that is inserted into the jejunum through an established gastrostomy. It is also referred to as a g/j-tube or transgastric tube. This type of tube has 2 or more lumen or openings. One port leads to the stomach, one to the jejunum and the third is for the insertion of water into the balloon to hold the tube in place. Percutaneous endoscopic jejunostomy - a type of j-tube placement for nutritional support that occurs with the aid of endoscopy to visualize the jejunum so that a tube can be threaded through a small opening made in the abdominal wall into the jejunum. It is also known as a PEJ tube. Roux-en-y jejunostomy- a type of j-tube placement for nutritional support that involves the surgical creation of a short limb or pouch in the jejenum that is sutured to an opening in the abdominal wall to create a stoma. This type of procedure allows for the eventual use of a skin level device such as a button feeding tube in place of a traditional tube. 1. COMPONENTS/ COMMON CAUSES NECESSITATING J-TUBE or G/J-TUBE PLACEMENT a. Dysphagia and/or medical conditions that compromise swallowing ability b. High risk aspiration c. Gastric dysfunction due to disease, trauma, or surgery d. Poor gastric motility, Gastroparesis, or impaired gastric emptying e. Gastroesophageal reflux 2. NURSING DIAGNOSES: a. Risk for imbalanced nutrition related to less than body requirements due to mechanical problems or dislodgement of tube b. Risk for infection related to impaired skin integrity 3. NURSING INTERVENTIONS/ PLAN: a. Immediate Post-operative period to Discharge DDS Protocol #NP 09-2 Care of Persons with Jejunostomy Tubes or Gastrojejunal Tubes 2
3 (1) Actively participate in the discharge planning for the person to understand needs of person, anticipated date of discharge, and to identify issues that impact may discharge (i.e., need for temporary skilled nursing facility placement) (2) Participate with the person s planning team in the modification of the person s individual plan that reflect changes in support/ resource needs (i.e., nursing, staff) and/or ability to return to the home (3) Identify supply needs and providers (e.g.,. nutritional product(s), feeding supplies, spare tubes, IV pole, syringes, dressings, measurement devices for abdominal girth measurement) (4) Identify training needs of nurses and/or staff and timeframe for addressing these needs Training Topics for LPNs and/or delegated staff as applicable to scope of practice and appropriate to consumer need Observational skills especially signs and symptoms that indicate change of condition, tube blockage/dislodgement/changes in tube integrity, and/or abnormal response/change in response to feeding) Reporting responsibilities Documentation/ data collection Universal precautions and Infection control considerations Type of tube, reason for tube, type of nutritional product, method of administration (i.e., continuous via pump or gravity), tube flushes, and safety considerations (e.g., NPO status, movement and transfer considerations, bathing considerations, aspiration precautions [head elevated at least 30 degrees], other positioning requirements and observing of tube integrity and/or presence of kinks in tube) Nursing and/or delegation procedures as applicable (e.g., checking tube placement [Refer to Appendix A and B], tube flushes, administration of fluids, and/or medication; pump operation including troubleshooting and connection/ disconnection, abdominal girth measurement, stoma care) Medication Administration concerns (e.g., use of liquid forms of medication, alteration of medication [dissolving tablets, opening capsules, crushing medications] and those that cannot be altered (i.e., enteric coated, time released), medication interactions with nutritional formulas and/or other medications) Oral hygiene needs Bowel monitoring Training specific to persons with Roux-en-y jejunostomy tubes as applicable (i.e, insertion of tube as prescribed, administration of feedings) b. Re-admission to home (Some of these tasks may be completed prior to person s discharge, delegated to trained staff as appropriate, or completed by the RN within 2 working days of discharge as per DDS Nursing Standard # 08-1, Nursing Process) (1) RN assessment of person following discharge to identify new baseline (e.g., identify skin integrity issues, note infections, measure abdominal girth, identify tolerance of prescribed nutritional support, document tube markings, determine current weight). At time of re-admission, the RN may direct trained staff to complete a body check to document presence of obvious skin alteration, measure abdominal girth/ document tube markings and/or check current weight until the nursing assessment is completed. (2) Document type of tube and manufacturer as well as amount of water in balloon (as appropriate) (3) Identify procedure for checking tube placement that utilizes tube markings and/or measuring length of tube to compare to baseline prior to administration of feedings, medications or water (Refer to Appendix A) (4) Identify procedure for addressing mechanical problems/tube clogging DDS Protocol #NP 09-2 Care of Persons with Jejunostomy Tubes or Gastrojejunal Tubes 3
4 (5) Identify actions and provider for reinsertion of tube as needed (Reinsertion of j-tubes and g/jtubes cannot be done by a licensed nurse per CT Board of Examiners for Nursing. Tube replacement must be done with radiologic verification) (6) Inform RN On Call of the person s change in status, the potential for concerns, and the planned responses that have been identified for the person (7) Obtain Dietary consult to ensure that nutritional needs are identified and met (8) Determine need for physical therapy consultation regarding positioning considerations and/or equipment needs (10) Contact PCP to determine blood work needs and frequency (11) Modify procedures, directions, etc. based on changes identified following discharge (12) Identify and provide additional training as appropriate to person Training Topics for LPNs and/or delegated staff as applicable to scope of practice and appropriate to consumer need Changes in person s baseline Additions and/or changes to previously provided trainings Baseline tube graduation markings/ tube length and abdominal girth Plan and provider for tube replacement c. Chronic Care Management (1) Periodic and PRN assessment by RN of skin integrity (2) Monitor response to prescribed treatment plan (3) Monitor tube function, changes to markings (4) Monitor stoma site for signs of infection, leakage (5) Monitor weight status (6) Monitor prescribed blood work (7) Identify schedule of tube replacements and process for scheduling these at the identified site (8) Record new baselines with change of tube as well as type, size, and amount of water in balloon (as applicable) (9) Review of documentation (e.g., medication administration, tube markings) (10) Obtain periodic Dietary consult as appropriate to needs of the person (11) Modify delegated procedures as necessary (12) Provide training/re-training as necessary Training Topics for LPNs and/or delegated staff as applicable to scope of practice and appropriate to consumer need Periodic required retraining (i.e., signs and symptoms that includes observational skills, infection control and universal precautions, documentation/ data collection) Periodic retraining/observation of nursing skills/ delegated responsibilities to ensure continued competence Training topics related to changes in prescribed care Frequency of planned tube replacements d. Management of Acute Issues related to (1) Compromised skin integrity (a) Sensitivity at site Signs include redness, itching without sign of infection Causes- Irritation from leakage at g-tube site, lack of hygiene, bumper too tight on skin, moisture retention due to dressing Action- good hygiene at site, monitor for infection, contact doctor if persists DDS Protocol #NP 09-2 Care of Persons with Jejunostomy Tubes or Gastrojejunal Tubes 4
5 (b) Infection Signs include redness, inflammation, heat at site, fever, discharge Causes- poor asepsis at insertion or contamination of tube or insertion site secondary to poor technique or hygiene, co-morbidities include: Diabetes, obesity, malnutrition, chronic steroid therapy Action- good hygiene at site, question need for wound culture, contact doctor for treatment (c) Excoriation Signs include: redness, irritation, skin damage Causes- leakage of gastric fluids at site Action- good hygiene, evaluation of amount of leakage, repositioning, consideration of need for change of tube, contact doctor for treatment, possible wound consult) (d) Overgranulation Signs- pink to red overgrown tissue, bleeding, Causes- friction or chaffing around stoma or tube dragging downwards causing the tissue to fill in/grow around the gastrostomy opening Action- good hygiene at site, handle tube gently and position above the stoma, contact doctor for treatment (e.g., acid blocking medication, ointments or cream to site, Silver nitrate around the stoma, possible wound consult, wound culture) (e) Buried Bumper Syndrome Signs- ulceration, bleeding, leakage, infection, catheter immobility, pain with infusion or resistance to infusion Causes- complete or partial growth of tissue over the internal bumper secondary to tight opposition of external bolster against abdominal wall, malnutrition, poor wound healing, significant weight gain Action- Medical attention to confirm condition and remove imbedded bumper; Prevent by rotate tube with regular site care, (2) Tube leakage (a) Signs- Enlarged stoma opening Excessive moisture at stoma site with or without skin redness or excoriation Saturated dressings requiring frequent changing (b) Causes- Weight changes (+/- 10 lb) can alter the tension on the bumper and can cause leakage. Underinflated balloon Incorrect positioning of g-tube Constipation that delays gastric emptying (c) Actions Re-position tube (above the stoma, not tucked in underwear as necessary Check balloon and inflate to prescribed level Administer treatment for constipation as prescribed Good hygiene to site; Apply absorbent dressing and change frequently, consider benefit of commercial clamping device to prevent side to side motion, removal of tube and replacement after stoma heals (3) Clogged or malfunctioning tube DDS Protocol #NP 09-2 Care of Persons with Jejunostomy Tubes or Gastrojejunal Tubes 5
6 (a) Signs Nutritional product, fluids, and/or medication unable to get into tube Not able to withdraw contents (b) Causes Medications that were not dissolved/ crushed small enough Inadequate flushing of tube Interactions of incompatible medications administered at the same time Deterioration of tube or balloon Burst balloon that is blocking the tube Kinking of tube (c) Action Administer medication one at a time and flush in between; flush between feeding and medications Use liquid medication form as possible; finely crush and/or melt medications Use of warm water, carbonated beverage such as Coke, or Pancreatic enzymes dissolved in bicarbonate solution Check for kinking of tube/tubing Send person to identified physician, radiologist, or emergency department for re-insertion or replacement of tube Flush J-tubes with warm water at least every 4 hours to help prevent future clogging (4) Loss of tube (a) Signs- tube fell out or was pulled out ; change in the appearance of gastric residuals (b) Causes- Balloon deflation/ deflation of internal fixation device Tube failure Tube accidentally lost due when positioning, etc. Person pulled tube out (c) Action- Transfer person to identified site for re-insertion Send replacement tube as appropriate to arrangement with facility If new tube less than 4 weeks since insertion, seek medical intervention (5) Migration of tube (a) Signs- Abdominal distention, vomiting, pain (b) Causes- Migration of the tube due to lack of being secured, too much (c) Actions- Measure abdominal girth to check against baseline; Check tube markings, Seek medical care Training Topics for LPNs and/or delegated staff as applicable to scope of practice and appropriate to consumer need Provide training on observational skills for issues noted above and action to be taken (emergent and non-emergent) 5. CRITERIA FOR MD REFERRAL: a. Changes in abdominal girth measurement significant for the person especially in combination with nausea, vomiting, abdominal pain, elevated temperature, and/or decreased bowel sounds b. Excoriation at stoma due to leakage c. Stoma infections d. Replacement of J-tube e. Suspicion of tube migration or buried bumper syndrome DDS Protocol #NP 09-2 Care of Persons with Jejunostomy Tubes or Gastrojejunal Tubes 6
7 6. CRITERIA FOR CONSULTATION: a. LPN to RN (1) All changes in the individual's baseline, condition, vital signs, behavior, and/ or response to treatment that alter the current health care plan shall promptly be reported to the primary RN or RN on call. (2) All changes to the prescribed orders/ treatment plan shall be communicated to the primary RN or RN on call prior to implementation. If immediate implementation of orders is indicated, the primary RN or RN on call must be notified as soon as possible. (3) Specific considerations to be reported for an individual with a j-tube include: Abdominal distention Vomiting Decreased or diminished bowel sounds Questionable migration of tube as evidenced by change in external graduation markings Evidence of infection at the stomal site Medication administration or nutritional feeding issues Loss of tube or tube blockage b. RN-to-RN Supervisor (1) When symptoms do not resolve with medical or nursing intervention (2) Emergency treatment, hospitalization, and/or change in condition that may impact the type and/ or frequency of nursing support provided to the individual (3) Presence of infectious condition (e.g., MRSA) (4) Programmatic difficulties that can t be resolved at the RN level (staff compliance, resource difficulties, etc.) 7. RELATED NURSING/DELEGATION PROCEDURES AS APPLICABLE a. Stoma Care b. Continuous tube feeding c. Checking placement of jejunostomy tube by tube markings and/or measurement d. Flushes e. Administration of medication through tube f. Tube blockages g. Intermittent insertion of Roux-en-y jejunostomy tube and administration of feeding 8. DOCUMENTATION: a. Documentation in the nursing notes should reflect: (1) The nurse s application of the nursing process specific to the needs of the person and the scope of practice of the nurse (2) The care/ interventions provided to the person and his/her response (3) Communications with others b. Documentation on records related to delegated responsibilities (e.g., medication administration records) c. Documentation of review of information related to delegated responsibilities performed by others E. Appendix Appendix A- Checking Feeding Tube Placement by Comparison of Tube Markings Appendix B- Checking Feeding Tube Placement by Measurement of Tube Length DDS Protocol #NP 09-2 Care of Persons with Jejunostomy Tubes or Gastrojejunal Tubes 7
8 F. References Coben R, Dimarino AJ. Percutaneous Endoscopic Gastrostomy and Jejunostomy. Gastrointestinal Disease: An endoscopic approach. 2004; 38: Carucci L, Levine M, Rubesin S, Laufer I, Assad S, Herlinger H. Evaluation of patients with jejunostomy tubes: Imaging findings. Gastrointestinal imaging. 2002: Conner TM, Carver O. The role of ph testing with small-bore feeding tubes: In the intensive care unit. Dimensions in critical care nursing. 2005; 24 (5): (Sept/Oct). E Medicine. Percutaneous gastrostomy and jejunostomy. Updated 2/2008 Disario J. Endoscopic approaches to enteral nutritional support. Best practice and research in Clinical Gastroenterology. 2006; 20 (3): Loeffler K, Bumgarner C. (Editors) Lipincott Manual. Seventh Edition Baker LS, Goglia S. Hartford Hospital tube feed procedure. revised 2006 Duszak, Richard Jr, MD, FACR, FSIR, Percutaneous Gastrostomy and Jejunostomy, emedicine from WebMD, Guenter, Peggi, RN, PhD, CNSN, Mechanical Complications in Long-Term Feeding Tubes, Nursing Spectrum Career Fitness Online, copyright Lynch, Christopher, MD, Fang, John C., MD, Prevention and Management of Complications of Percutaneous Endoscopic Gastrostomy (PEG) Tubes, Practical Gastroenterology, November 2004, page Reising, Deanna L. PhD, APRN, BC and Neal, Ronald Scott BSN, RN, Enteral Tube Flushing: What you think are the best practices may not be American Journal of Nursing, Volume 105-number 3, March 2005 page DDS Protocol #NP 09-2 Care of Persons with Jejunostomy Tubes or Gastrojejunal Tubes 8
My patient has a feeding tube
 My patient has a feeding tube What does that mean? Martha Kliebenstein, MSN, RN Clinical Educator (December, 2014) Types of tubes Gastrostomy (G-tube) Gastrostomy jejunostomy (G-J tube) Naso gastric (NG
My patient has a feeding tube What does that mean? Martha Kliebenstein, MSN, RN Clinical Educator (December, 2014) Types of tubes Gastrostomy (G-tube) Gastrostomy jejunostomy (G-J tube) Naso gastric (NG
Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role. Lillian Khalil, BSN, RN Volunteers of America, Chesapeake
 Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role Lillian Khalil, BSN, RN Volunteers of America, Chesapeake Objectives The participants will be able to identify the
Care of Gastrostomy Tubes for Adults with IDD in Community Settings: The Nurse s Role Lillian Khalil, BSN, RN Volunteers of America, Chesapeake Objectives The participants will be able to identify the
GJ TUBE (GASTROJEJUNOSTOMY TUBE) Daily Care
 GJ TUBE (GASTROJEJUNOSTOMY TUBE) Daily Care Your child has a Picture 1 The GJ Tube inside the body. gastrojejunostomy (GJ) tube Disc (Picture 1). This set of tubes lets food or medicine go into either
GJ TUBE (GASTROJEJUNOSTOMY TUBE) Daily Care Your child has a Picture 1 The GJ Tube inside the body. gastrojejunostomy (GJ) tube Disc (Picture 1). This set of tubes lets food or medicine go into either
Management of Gastrostomy Tube Complications for the Pediatric and Adult Patient
 Management of Gastrostomy Tube Complications for the Pediatric and Adult Patient Introduction Ideally, Gastrostomy Tube (GT) management should not be a problem. However, there may be underlying conditions
Management of Gastrostomy Tube Complications for the Pediatric and Adult Patient Introduction Ideally, Gastrostomy Tube (GT) management should not be a problem. However, there may be underlying conditions
Gastrostomy Feeding CARE GUIDELINES FOR PATIENTS & CARERS. Accessory items. Freka UK Funnel Adapter. Fixation Plate CH9. Male Luer Lock Adapter
 Accessory items Freka UK Funnel Adapter Fixation Plate CH9 Code: 7755681 Code: 7903002 Male Luer Lock Adapter CH9 Fixation Plate CH15 Code: 7981311 Code: 7904002 Male Luer Lock Adapter CH15 Code: 798137Y
Accessory items Freka UK Funnel Adapter Fixation Plate CH9 Code: 7755681 Code: 7903002 Male Luer Lock Adapter CH9 Fixation Plate CH15 Code: 7981311 Code: 7904002 Male Luer Lock Adapter CH15 Code: 798137Y
Delivering nutrition, fluids & medication via a PEG. By Julia Pointer & Caroline Ross, Staff Nurses, Hospice Day Service
 Delivering nutrition, fluids & medication via a PEG By Julia Pointer & Caroline Ross, Staff Nurses, Hospice Day Service Aims of this session? To give an explanation of the theory and practice of a Percutaneous
Delivering nutrition, fluids & medication via a PEG By Julia Pointer & Caroline Ross, Staff Nurses, Hospice Day Service Aims of this session? To give an explanation of the theory and practice of a Percutaneous
STAY-PUT Nasojejunal Feeding Tubes. Nursing Manual/ Patient Information
 SPECIALTY FEEDING TUBES STAY-PUT Nasojejunal Feeding Tubes Nursing Manual/ Patient Information Manual contains important care and maintenance information and should accompany patient NURSING CONSIDERATIONS
SPECIALTY FEEDING TUBES STAY-PUT Nasojejunal Feeding Tubes Nursing Manual/ Patient Information Manual contains important care and maintenance information and should accompany patient NURSING CONSIDERATIONS
Patients First. Tube Feeding Guidelines. Careful handwashing and a clean work surface help prevent infection. Patient Education CARE AND TREATMENT
 Patient Education CARE AND TREATMENT Careful handwashing and a clean work surface help prevent infection. Tube Feeding Guidelines This information will guide you in learning about the procedure for tube
Patient Education CARE AND TREATMENT Careful handwashing and a clean work surface help prevent infection. Tube Feeding Guidelines This information will guide you in learning about the procedure for tube
Chapter 6 Gastrointestinal Impairment
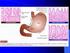 Chapter 6 Gastrointestinal This chapter consists of 2 parts: Part 6.1 Diseases of the digestive system Part 6.2 Abdominal wall hernias and obesity PART 6.1: DISEASES OF THE DIGESTIVE SYSTEM Diseases of
Chapter 6 Gastrointestinal This chapter consists of 2 parts: Part 6.1 Diseases of the digestive system Part 6.2 Abdominal wall hernias and obesity PART 6.1: DISEASES OF THE DIGESTIVE SYSTEM Diseases of
Acute Abdominal Pain following Bariatric Surgery. Disclosure. Objectives 8/17/2015. I have nothing to disclose
 Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Acute Abdominal Pain following Bariatric Surgery Kathy J. Morris, DNP, APRN, FNP C, FAANP University of Nebraska Medical Center College of Nursing Disclosure I have nothing to disclose Objectives Pathophysiology
Caring for Your Gastrostomy
 Caring for Your Gastrostomy Table of Contents What Is a Gastrostomy Tube (G-tube)?... 2 Types of Gastrostomy Tubes... 3 Cleaning the Gastrostomy Site... 4 Gastrostomy Feedings... 5 Giving Medicines...
Caring for Your Gastrostomy Table of Contents What Is a Gastrostomy Tube (G-tube)?... 2 Types of Gastrostomy Tubes... 3 Cleaning the Gastrostomy Site... 4 Gastrostomy Feedings... 5 Giving Medicines...
G E R D. (Gastroesophageal Reflux Disease)
 G E R D (Gastroesophageal Reflux Disease) What is GERD? Gastroesophageal reflux disease (GERD) is a disorder caused by gastric acid flowing from the stomach into the esophagus. What are the symptoms of
G E R D (Gastroesophageal Reflux Disease) What is GERD? Gastroesophageal reflux disease (GERD) is a disorder caused by gastric acid flowing from the stomach into the esophagus. What are the symptoms of
Tube Feeding at Home Gravity or Syringe Feeding
 Tube Feeding at Home Gravity or Syringe Feeding Adapted from the former Taming the Feeding Tube, North Shore Hospital. 1 Where do I find information in this booklet? Subject Page How do I contact my health
Tube Feeding at Home Gravity or Syringe Feeding Adapted from the former Taming the Feeding Tube, North Shore Hospital. 1 Where do I find information in this booklet? Subject Page How do I contact my health
Are any artificial parts used in the ACE Malone surgery?
 ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
ACE Malone (Antegrade Continence Enema) What is the ACE Malone? The Antegrade Continence Enema (ACE) is a type of surgery designed for the child who has chronic bowel problems with bouts of constipation,
Kimberly-Clark* MIC-KEY* Low-Profile Gastrostomy Feeding Tube
 Lock MIC Kimberly-Clark* MIC-KEY* Low-Profile Gastrostomy Feeding Tube Directions For Use The Kimberly-Clark* MIC* Gastrostomy feeding tube (figure A) and the Kimberly-Clark* MIC* Bolus Gastrostomy Feeding
Lock MIC Kimberly-Clark* MIC-KEY* Low-Profile Gastrostomy Feeding Tube Directions For Use The Kimberly-Clark* MIC* Gastrostomy feeding tube (figure A) and the Kimberly-Clark* MIC* Bolus Gastrostomy Feeding
TUBE FEEDING AT HOME
 TUBE FEEDING AT HOME Adapted from the former Taming the Feeding Tube, Royal North Shore Hospital. Revised 2005, 2007, Jan 2009 1 Where do I find information in this booklet? Only the pages that you need
TUBE FEEDING AT HOME Adapted from the former Taming the Feeding Tube, Royal North Shore Hospital. Revised 2005, 2007, Jan 2009 1 Where do I find information in this booklet? Only the pages that you need
PATIENT CONSENT TO PROCEDURE - ROUX-EN-Y GASTRIC BYPASS
 As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
As a patient you must be adequately informed about your condition and the recommended surgical procedure. Please read this document carefully and ask about anything you do not understand. Please initial
The Ins & Outs of Gastrostomy Tubes
 The Ins & Outs of Gastrostomy Tubes JULIA POND, RN(EC), MN, NP-PEDIATRIC PEDIATRIC SURGERY Today s Lesson: What is a gastrostomy tube Indication for tubes Types of tubes G-tube placement Post-operative
The Ins & Outs of Gastrostomy Tubes JULIA POND, RN(EC), MN, NP-PEDIATRIC PEDIATRIC SURGERY Today s Lesson: What is a gastrostomy tube Indication for tubes Types of tubes G-tube placement Post-operative
Emergencies in Post- Bariatric Surgery Patients
 Emergencies in Post- Patients Disclosures Dr. Birnbaumer has no financial disclosures Diane M. Birnbaumer, M.D., FACEP Professor of Medicine University of California, Los Angeles Senior Clinical Educator
Emergencies in Post- Patients Disclosures Dr. Birnbaumer has no financial disclosures Diane M. Birnbaumer, M.D., FACEP Professor of Medicine University of California, Los Angeles Senior Clinical Educator
Medicines & Enteral Feeding Tubes A DELA V IDICKI-MASTILOVICH C LINICAL P HARMACIST R OYAL C HILDREN S H OSPITAL
 Medicines & Enteral Feeding Tubes A DELA V IDICKI-MASTILOVICH C LINICAL P HARMACIST R OYAL C HILDREN S H OSPITAL Introduction Types of Tubes Choosing a formulation Crushing tablets/opening capsules Administration
Medicines & Enteral Feeding Tubes A DELA V IDICKI-MASTILOVICH C LINICAL P HARMACIST R OYAL C HILDREN S H OSPITAL Introduction Types of Tubes Choosing a formulation Crushing tablets/opening capsules Administration
Gastrointestinal Bleeding
 Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Gastrointestinal Bleeding Introduction Gastrointestinal bleeding is a symptom of many diseases rather than a disease itself. A number of different conditions can cause gastrointestinal bleeding. Some causes
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop
 Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Urinary Diversion: Ileovesicostomy/Ileal Loop/Colon Loop Why do I need this surgery? A urinary diversion is a surgical procedure that is performed to allow urine to safely pass from the kidneys into a
Caring for Your Child s Gastrostomy Tube
 Caring for Your Child s Gastrostomy Tube Table of Contents What Is a Gastrostomy Tube (G-tube)?... 2 Types of Feeding Tubes... 3 Cleaning the Gastrostomy Site... 5 Gastrostomy Feedings... 7 Giving Medicines...
Caring for Your Child s Gastrostomy Tube Table of Contents What Is a Gastrostomy Tube (G-tube)?... 2 Types of Feeding Tubes... 3 Cleaning the Gastrostomy Site... 5 Gastrostomy Feedings... 7 Giving Medicines...
11/10/2014. I have nothing to Disclose. Covered Stents discussed are NOT FDA approved for the indications covered in my presentation
 I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
I have nothing to Disclose Ramsey Dallal, MD, FACS Vice Chair Department of Surgery Chief Bariatric i and Minimally i Invasive Surgery Einstein Healthcare Network Nemacolin, PA 2014 Covered Stents discussed
Freka. Enteral Feeding Tube Product Range ENTERAL NUTRITION
 ENTERAL NUTRITION Freka Enteral Feeding Tube Product Range Fresenius Kabi Limited, Cestrian Court, Eastgate Way, Runcorn, Cheshire WA7 1NT tel: 01928 533533 fax: 01928 533520 email: nutrition.service@fresenius-kabi.com
ENTERAL NUTRITION Freka Enteral Feeding Tube Product Range Fresenius Kabi Limited, Cestrian Court, Eastgate Way, Runcorn, Cheshire WA7 1NT tel: 01928 533533 fax: 01928 533520 email: nutrition.service@fresenius-kabi.com
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS
 CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
CUESTA COLLEGE REGISTERED NURSING PROGRAM CRITICAL ELEMENTS LEVELS I through IV A. OVERRIDING CRITICAL ELEMENTS Violation of an overriding area will result in termination and failure of the particular
By Deanna L. Reising, PhD, APRN,BC, and Ronald Scott Neal, BSN, RN
 HOURS CE3 Continuing Education What you think are the best practices may not be. By Deanna L. Reising, PhD, APRN,BC, and Ronald Scott Neal, BSN, RN Flushing an enteral tube (in other words, keeping it
HOURS CE3 Continuing Education What you think are the best practices may not be. By Deanna L. Reising, PhD, APRN,BC, and Ronald Scott Neal, BSN, RN Flushing an enteral tube (in other words, keeping it
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter
 Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Patient Information Guide Morpheus CT Peripherally Inserted Central Catheter IC 192 Rev C A measure of flexibility and strength. Table of Contents 1. Introduction 2. What is the Morpheus CT PICC? 3. What
Having a PEG tube inserted?
 Having a PEG tube inserted? Information for Patients and Carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having a PEG tube inserted? Information for Patients and Carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery
 Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Program Overview The University of Hong Kong Department of Surgery Division of Esophageal and Upper Gastrointestinal Surgery Weight Control and Metabolic Surgery Program The Weight Control and Metabolic
Sleeve Gastrectomy Surgery & Follow Up Care
 Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Sleeve Gastrectomy Surgery & Follow Up Care Sleeve Gastrectomy Restrictive surgical weight loss procedure Able to eat a smaller amount of food to feel satiety, less than 6 ounces at a meal Surgery The
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
PATIENT GUIDE. Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL
 PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
PATIENT GUIDE Understand and care for your peripherally inserted central venous catheter (PICC). MEDICAL Introduction The following information is presented as a guideline for your reference. The best
Information for people being discharged with a naso-gastric (NG) feeding tube
 Information for people being discharged with a naso-gastric (NG) feeding tube The aim of this leaflet is to provide patients with the relevant information for the use of a nasogastric tube. It will include:
Information for people being discharged with a naso-gastric (NG) feeding tube The aim of this leaflet is to provide patients with the relevant information for the use of a nasogastric tube. It will include:
Surgical Weight Loss. Mission Bariatrics
 Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
Surgical Weight Loss Mission Bariatrics Obesity is a major health problem in the United States, with more than one in every three people suffering from this chronic condition. Obese adults are at an increased
PICCs and Midline Catheters
 Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Patient Education PICCs and Midline Catheters Patient s guide to PICC (peripherally inserted central catheter) and midline catheters What are PICCs and midline catheters used for? Any medicine given over
Overview of Bariatric Surgery
 Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
Overview of Bariatric Surgery To better understand how weight loss surgery works, it is helpful to know how the normal digestive process works. As food moves along the digestive tract, special digestive
INTERDISCIPLINARY CLINICAL MANUAL Policy & Procedure
 INTERDISCIPLINARY CLINICAL MANUAL Policy & Procedure TITLE: Section: Nasogastric Tube Insertion, Gastrointestinal/Nutrition NUMBER: CC 25-015 Date Issued: May 2007 Source: Distribution: Surgical Specialties
INTERDISCIPLINARY CLINICAL MANUAL Policy & Procedure TITLE: Section: Nasogastric Tube Insertion, Gastrointestinal/Nutrition NUMBER: CC 25-015 Date Issued: May 2007 Source: Distribution: Surgical Specialties
Having a RIG tube inserted
 Having a RIG tube inserted Information for patients and carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Having a RIG tube inserted Information for patients and carers Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
URINARY CATHETER CARE
 URINARY CATHETER CARE INTRODUCTION Urinary catheter care is a very important skill, and it is a skill that many certified nursing assistants (CNAs) must know. Competence at providing urinary catheter care
URINARY CATHETER CARE INTRODUCTION Urinary catheter care is a very important skill, and it is a skill that many certified nursing assistants (CNAs) must know. Competence at providing urinary catheter care
Peripherally Inserted Central Catheter (PICC) for Outpatient
 Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Peripherally Inserted Central Catheter (PICC) for Outpatient Introduction A Peripherally Inserted Central Catheter, or PICC line, is a thin, long, soft plastic tube inserted into a vein of the arm. It
Gastrostomy Tubes Home Care Manual (Corpak, Foley catheter, Genie, Malecot, Mic-G)
 Physician who placed the gastrostomy: Date placed: Type of gastrostomy tube: Size of the gastrostomy: Gastrostomy tubes are measured in French (Fr.) sizes. A size 16 Fr. gastrostomy is larger than a 14
Physician who placed the gastrostomy: Date placed: Type of gastrostomy tube: Size of the gastrostomy: Gastrostomy tubes are measured in French (Fr.) sizes. A size 16 Fr. gastrostomy is larger than a 14
Within the Scope of Practice/Role of APRN RN _ X_LPN CNA
 Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: wsbn-info-licensing@wyo.gov Home Page: https://nursing-online.state.wy.us/ OPINION:
Wyoming State Board of Nursing 130 Hobbs Avenue, Suite B Cheyenne, WY 82002 Phone (307) 777-7601 Fax (307) 777-3519 E-Mail: wsbn-info-licensing@wyo.gov Home Page: https://nursing-online.state.wy.us/ OPINION:
8.470 HOSPITAL BACK UP LEVEL OF CARE PAGE 1 OF 10. Complex wound care means that the client meets the following criteria:
 8.470 HOSPITAL BACK UP LEVEL OF CARE PAGE 1 OF 10 8.470 HOSPITAL BACK UP LEVEL OF CARE 8.470.1 DEFINITIONS Complex wound care means that the client meets the following criteria: 1. Has at least one of
8.470 HOSPITAL BACK UP LEVEL OF CARE PAGE 1 OF 10 8.470 HOSPITAL BACK UP LEVEL OF CARE 8.470.1 DEFINITIONS Complex wound care means that the client meets the following criteria: 1. Has at least one of
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter
 Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Guy s, King s and St Thomas Cancer Centre The Cancer Outpatient Clinic Central venous catheter: Peripherally inserted central catheter This information leaflet aims to help answer some of the questions
Guideline for the use of subcutaneous hydration in palliative care (hypodermoclysis)
 Guideline for the use of subcutaneous hydration in palliative care (hypodermoclysis) Date Approved by Network Governance September 2012 Date for Review September 2015 Page 1 of 7 1 Scope of Guideline 1.1
Guideline for the use of subcutaneous hydration in palliative care (hypodermoclysis) Date Approved by Network Governance September 2012 Date for Review September 2015 Page 1 of 7 1 Scope of Guideline 1.1
GASTRIC BYPASS SURGERY CONSENT FORM
 Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Page 1 of 6 I, have been asked to read carefully all of the (name of patient or substitute decision-maker) information contained in this consent form and to consent to the procedure described below on
Policies & Procedures. ID Number: 1118
 Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
Policies & Procedures Title: INTRAVENOUS AND/OR PERIPHERAL SALINE LOCK INSERTION AND MAINTENANCE ID Number: 1118 Authorization [X] SHR Nursing Practice Committee Source: Nursing Date Revised: September
III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004
 III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004 Purpose A. Allow for precise measurement of urine output. B. Collect a sterile urine specimen. C.
III-701 Urinary Catheterization/Bladder Irrigation Original Date: 3/1/1977 Last Review Date: 10/28/2004 Purpose A. Allow for precise measurement of urine output. B. Collect a sterile urine specimen. C.
VUMC Guidelines for Management of Indwelling Urinary Catheters. UC Access/ Maintenance
 VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
VUMC Guidelines for Management of Indwelling Urinary Catheters UC Insertion Preparation & Procedure Indications for insertion and continued use of indwelling urinary catheters include: Urinary retention
PICC & Midline Catheters Patient Information Guide
 PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
PICC & Midline Catheters Patient Information Guide medcompnet.com 1 table of contents Introduction 4 What is a PICC or Midline Catheter? 4 How is the PICC or Midline Catheter Inserted? 6 Catheter Care
TRACHEOSTOMY TUBE PARTS
 Page1 NR 33 TRACHEOSTOMY CARE AND SUCTIONING Review ATI Basic skills videos: Tracheostomy care and Endotracheal suction using a closed suction set. TRACHEOSTOMY TUBE PARTS Match the numbers on the diagram
Page1 NR 33 TRACHEOSTOMY CARE AND SUCTIONING Review ATI Basic skills videos: Tracheostomy care and Endotracheal suction using a closed suction set. TRACHEOSTOMY TUBE PARTS Match the numbers on the diagram
Information for Patients having a Colonic Stent Placement
 Information for Patients having a Colonic Stent Placement Information for Patients having a Colonic Stent Placement The Digestive System To understand the procedure you are about to have, it helps to have
Information for Patients having a Colonic Stent Placement Information for Patients having a Colonic Stent Placement The Digestive System To understand the procedure you are about to have, it helps to have
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES
 Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
Laparoscopic Gallbladder Removal (Cholecystectomy) Patient Information from SAGES Gallbladder removal is one of the most commonly performed surgical procedures. Gallbladder removal surgery is usually performed
A guide for adults with. Intestinal. Dysmotility
 A guide for adults with Intestinal Dysmotility This leaflet contains information for patients with dysmotility of the gut and discusses symptoms and management. page 2 Contents Introduction 4 Symptoms
A guide for adults with Intestinal Dysmotility This leaflet contains information for patients with dysmotility of the gut and discusses symptoms and management. page 2 Contents Introduction 4 Symptoms
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions
 Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Laparoscopic Surgery of the Colon and Rectum (Large Intestine) A Simple Guide to Help Answer Your Questions What are the Colon and Rectum? The colon and rectum together make up the large intestine. After
Cancer Treatment Centers of America Treating the Whole Patient. Presented by: Jill Schuman, RD, CNSC, CSP, LCN Date: Spring 2012
 Cancer Treatment Centers of America Treating the Whole Patient Presented by: Jill Schuman, RD, CNSC, CSP, LCN Date: Spring 2012 What is Cancer Two types of tumors Liquid tumor Leukemia Lymphoma Aplastic
Cancer Treatment Centers of America Treating the Whole Patient Presented by: Jill Schuman, RD, CNSC, CSP, LCN Date: Spring 2012 What is Cancer Two types of tumors Liquid tumor Leukemia Lymphoma Aplastic
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy. Patient Name
 Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
Informed Consent for Laparoscopic Vertical Sleeve Gastrectomy Patient Name Please read this form carefully and ask about anything you may not understand. I consent to have a laparoscopic Vertical Sleeve
A Guide for Families and Caregivers
 A Guide for Families and Caregivers May 2003 Fourth Edition, 2003 The practices of nutrition support are continually evolving with new knowledge and guidelines from expert authorities. This booklet is
A Guide for Families and Caregivers May 2003 Fourth Edition, 2003 The practices of nutrition support are continually evolving with new knowledge and guidelines from expert authorities. This booklet is
Colic is one of the most dreaded conditions horse owners and trainers encounter with
 Impaction Colic and Hydration Michele Frazer, DVM, DACVIM, DACVECC Impaction Colic Colic is one of the most dreaded conditions horse owners and trainers encounter with their horses. The term colic, however,
Impaction Colic and Hydration Michele Frazer, DVM, DACVIM, DACVECC Impaction Colic Colic is one of the most dreaded conditions horse owners and trainers encounter with their horses. The term colic, however,
After care following insertion of a suprapubic catheter
 Other formats After care following insertion of a suprapubic catheter If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign
Other formats After care following insertion of a suprapubic catheter If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign
Types of Bariatric Procedures. Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012
 Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
Types of Bariatric Procedures Tejal Brahmbhatt, MD General Surgery Teaching Conference April 18, 2012 A Brief History of Bariatric Surgery First seen in pts with short bowel syndrome weight loss First
Long Term Tube Feeding. Sunnybrook. A Guide for Patients and Substitute Decision Makers VETERANS & COMMUNITY
 Long Term Tube Feeding A Guide for Patients and Substitute Decision Makers Sunnybrook VETERANS & COMMUNITY Sunnybrook VETERANS & COMMUNITY This brochure has been produced by: Sunnybrook Health Sciences
Long Term Tube Feeding A Guide for Patients and Substitute Decision Makers Sunnybrook VETERANS & COMMUNITY Sunnybrook VETERANS & COMMUNITY This brochure has been produced by: Sunnybrook Health Sciences
BARD MEDICAL DIVISION UROLOGICAL DRAINAGE. Foley Catheter Care & Maintenance. Patient Education Guide
 BARD MEDICAL DIVISION Foley Catheter Care & Maintenance Patient Education Guide WHAT IS A FOLEY CATHETER? Because of your medical problem, your body is having trouble completely emptying your bladder of
BARD MEDICAL DIVISION Foley Catheter Care & Maintenance Patient Education Guide WHAT IS A FOLEY CATHETER? Because of your medical problem, your body is having trouble completely emptying your bladder of
Orthopaedic Spine Center. Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs
 Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
Orthopaedic Spine Center Graham Calvert MD James Woodall MD PhD Anterior Cervical Discectomy and Fusion (ACDF) Normal Discs The cervical spine consists of the bony vertebrae, discs, nerves and other structures.
V: Infusion Therapy. Alberta Licensed Practical Nurses Competency Profile 217
 V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
V: Infusion Therapy Alberta Licensed Practical Nurses Competency Profile 217 Competency: V-1 Knowledge of Intravenous Therapy V-1-1 V-1-2 V-1-3 V-1-4 V-1-5 Demonstrate knowledge and ability to apply critical
Individualized Care Plans Fully Developed
 Appendix Individualized Care Plans Fully Developed A Refer to Chapter 1 The Nursing Process: A Synopsis, p. 32: Two Individualized Care Plans Fully Developed; Care Plan 1 for Mr. John Walters, Care Plan
Appendix Individualized Care Plans Fully Developed A Refer to Chapter 1 The Nursing Process: A Synopsis, p. 32: Two Individualized Care Plans Fully Developed; Care Plan 1 for Mr. John Walters, Care Plan
Epidural Continuous Infusion. Patient information Leaflet
 Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
Epidural Continuous Infusion Patient information Leaflet April 2015 Introduction You may already know that epidural s are often used to treat pain during childbirth. This same technique can also used as
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary
 X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
X-Plain Subclavian Inserted Central Catheter (SICC Line) Reference Summary Introduction A Subclavian Inserted Central Catheter, or subclavian line, is a long thin hollow tube inserted in a vein under the
Goals and Objectives for the General Surgery Rotation Resident PGY1 Hamilton Health Sciences or St. Joseph Healthcare (2 four-week rotational blocks)
 Goals and Objectives for the General Surgery Rotation Resident PGY1 Hamilton Health Sciences or St. Joseph Healthcare (2 four-week rotational blocks) Overview During the first year of their residency training
Goals and Objectives for the General Surgery Rotation Resident PGY1 Hamilton Health Sciences or St. Joseph Healthcare (2 four-week rotational blocks) Overview During the first year of their residency training
Catheter Care. What you need to know. Jacinta Stewart Continence Nurse
 Catheter Care What you need to know Jacinta Stewart Continence Nurse Indications for Long Term Catheter Use Long term urinary catheters should only be used with clients who cannot satisfactorily be managed
Catheter Care What you need to know Jacinta Stewart Continence Nurse Indications for Long Term Catheter Use Long term urinary catheters should only be used with clients who cannot satisfactorily be managed
NORTH CAROLINA BOARD OF NURSING NURSE AIDE II TRAINING MODULE
 PART A: PREPARING FOR ADMINISTRATION OF IV FLUIDS All four parts of this module, including skills checklists must be successfully completed in order to complete this training module. This activity is a
PART A: PREPARING FOR ADMINISTRATION OF IV FLUIDS All four parts of this module, including skills checklists must be successfully completed in order to complete this training module. This activity is a
After your gastric banding
 After your gastric banding Exceptional healthcare, personally delivered 2 Please call J Ward at Southmead Hospital on 0117 323 5132 if you have any questions or concerns soon after discharge. You may be
After your gastric banding Exceptional healthcare, personally delivered 2 Please call J Ward at Southmead Hospital on 0117 323 5132 if you have any questions or concerns soon after discharge. You may be
Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed
 Page 1 of 6 Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed Title: Standard Procedure for the Irrigating (flushing) of
Page 1 of 6 Status: Standard Procedure: specifies the procedures to be followed, only in exceptional circumstances should these not be followed Title: Standard Procedure for the Irrigating (flushing) of
Vaxcel PICCs Valved and Non-Valved. A Patient s Guide
 Vaxcel PICCs Valved and Non-Valved A Patient s Guide Information about your Vaxcel PICC is available by calling the Navilyst Medical Vascular Access Information Line 800.513.6876 Vaxcel Peripherally Inserted
Vaxcel PICCs Valved and Non-Valved A Patient s Guide Information about your Vaxcel PICC is available by calling the Navilyst Medical Vascular Access Information Line 800.513.6876 Vaxcel Peripherally Inserted
TUBE-FEEDING INSTRUCTIONS FOR HOME
 Name Clinic Number Room: TUBE-FEEDING INSTRUCTIONS FOR HOME CENTER FOR HUMAN NUTRITION, M17/ DIGESTIVE DISEASE INSTITUTE 9500 Euclid Avenue Cleveland, OH 44195 1.800.CCF.CARE 1.216.444.3046 YOUR TUBE-FEEDING
Name Clinic Number Room: TUBE-FEEDING INSTRUCTIONS FOR HOME CENTER FOR HUMAN NUTRITION, M17/ DIGESTIVE DISEASE INSTITUTE 9500 Euclid Avenue Cleveland, OH 44195 1.800.CCF.CARE 1.216.444.3046 YOUR TUBE-FEEDING
Enteral Feeding Care and Maintenance of the Stoma Site and Feeding Tube. Kimberly-Clark Health Care Education
 Care and Maintenance of the Kimberly-Clark Health Care Education Technical Support Home Delivery Customer Service vygon@vygon.co.uk www.vygon.co.uk Notes 21 Post Test Answers 1. True. Enteral feeding is
Care and Maintenance of the Kimberly-Clark Health Care Education Technical Support Home Delivery Customer Service vygon@vygon.co.uk www.vygon.co.uk Notes 21 Post Test Answers 1. True. Enteral feeding is
online version Understanding Indwelling Urinary Catheters and Drainage Systems Useful information When to call for help
 When to call for help This will depend on the individual situation, but usually help should be sought if any of the following occurs: 1. The catheter does not start to drain, despite trying the problem
When to call for help This will depend on the individual situation, but usually help should be sought if any of the following occurs: 1. The catheter does not start to drain, despite trying the problem
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD
 St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone:314-997-EYES Fax: 314-997-3911 Toll Free: 866-869-3937 STRABISMUS SURGERY (Post-Op Strabismus
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone:314-997-EYES Fax: 314-997-3911 Toll Free: 866-869-3937 STRABISMUS SURGERY (Post-Op Strabismus
Pediatric Gastroenterology Fellowship Pediatric Nutrition Rotation Goals and Objectives - 1 st Year
 Pediatric Nutrition Rotation Goals and Objectives - 1 st Year Goal 1: Gain experience and competency in managing common and rare gastrointestinal, liver and nutritional problems. (Competencies: patient
Pediatric Nutrition Rotation Goals and Objectives - 1 st Year Goal 1: Gain experience and competency in managing common and rare gastrointestinal, liver and nutritional problems. (Competencies: patient
Biliary Drain. What is a biliary drain?
 Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Biliary Drain What is a biliary drain? A biliary drain is a tube to drain bile from your liver. It is put in by a doctor called an Interventional Radiologist. The tube or catheter is placed through your
Percutaneous Endoscopic Gastrostomy (PEG) removal
 Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Feedback We appreciate and encourage feedback. If you need advice or are concerned about any aspect of care or treatment please speak to a member of staff or contact the Patient Advice and Liaison Service
Policies & Procedures. Care of
 Policies & Procedures Title: SUPRAPUBIC CATHETER Care of Changing Removal Authorization: [x] SHR Nursing Practice Committee I.D. Number: 1021 Source: Nursing Date Revised: November 2014 Date Effective:
Policies & Procedures Title: SUPRAPUBIC CATHETER Care of Changing Removal Authorization: [x] SHR Nursing Practice Committee I.D. Number: 1021 Source: Nursing Date Revised: November 2014 Date Effective:
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH
 PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
PERIPHERALLY INSERTED CENTRAL CATHETERS (PICC) Fong So Kwan APN, Haematology unit Medical Department, QMH 1 What is a PICC catheter? Primary vascular access device since their introduction in the mid-1970s,
Spinal Cord and Bladder Management Male: Intermittent Catheter
 Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Spinal Cord and Bladder Management Male: Intermittent Catheter The 5 parts of the urinary system work together to get rid of waste and make urine. Urine is made in your kidneys and travels down 2 thin
Total Vaginal Hysterectomy with an Anterior and Posterior Repair
 Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
Total Vaginal Hysterectomy with an Anterior and Posterior Repair What is a total vaginal hysterectomy with an anterior and posterior repair? Total vaginal hysterectomy is the removal of the uterus and
483.25(i) Nutrition (F325) Surveyor Training: Interpretive Guidance Investigative Protocol
 483.25(i) Nutrition (F325) Surveyor Training: 1 With regard to the revised guidance F325 Nutrition, there have been significant changes. Specifically, F325 and F326 were merged. However, the regulatory
483.25(i) Nutrition (F325) Surveyor Training: 1 With regard to the revised guidance F325 Nutrition, there have been significant changes. Specifically, F325 and F326 were merged. However, the regulatory
Obesity Affects Quality of Life
 Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
Obesity Obesity is a serious health epidemic. Obesity is a condition characterized by excessive body fat, genetic and environmental factors. Obesity increases the likelihood of certain diseases and other
All About Your Peripherally Inserted Central Catheter (PICC)
 All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
All About Your Peripherally Inserted Central Catheter (PICC) General Information Intravenous (IV) therapy is the delivery of fluid directly into a vein. An intravenous catheter is a hollow tube that is
Gastroschisis and My Baby
 Patient and Family Education Gastroschisis and My Baby Gastroschisis is a condition where a baby is born with the intestine outside the body. Learning about the diagnosis What is gastroschisis? (pronounced
Patient and Family Education Gastroschisis and My Baby Gastroschisis is a condition where a baby is born with the intestine outside the body. Learning about the diagnosis What is gastroschisis? (pronounced
Nursing college, Second stage Microbiology Dr.Nada Khazal K. Hendi L14: Hospital acquired infection, nosocomial infection
 L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
L14: Hospital acquired infection, nosocomial infection Definition A hospital acquired infection, also called a nosocomial infection, is an infection that first appears between 48 hours and four days after
Intraperitoneal Chemotherapy
 Intraperitoneal Chemotherapy What is Intraperitoneal (IP) Chemotherapy? Intraperitoneal (IP) chemotherapy is a way to put some of your chemotherapy into your abdomen (also called the peritoneal cavity)
Intraperitoneal Chemotherapy What is Intraperitoneal (IP) Chemotherapy? Intraperitoneal (IP) chemotherapy is a way to put some of your chemotherapy into your abdomen (also called the peritoneal cavity)
UW MEDICINE PATIENT EDUCATION. Weight Loss Surgery. What is bariatric surgery?
 UW MEDICINE PATIENT EDUCATION Weight Loss Surgery Divided proximal roux-y-gastric bypass, laparoscopic adjustable gastric banding, and laparoscopic sleeve gastrectomy. This section of the Guide to Your
UW MEDICINE PATIENT EDUCATION Weight Loss Surgery Divided proximal roux-y-gastric bypass, laparoscopic adjustable gastric banding, and laparoscopic sleeve gastrectomy. This section of the Guide to Your
Having a Gastric Band
 Having a Gastric Band Hope Building Upper G.I. / Bariatrics 0161 206 5062 All Rights Reserved 2014. Document for issue as handout. This booklet aims to describe: l What is a gastric band page 2 l How is
Having a Gastric Band Hope Building Upper G.I. / Bariatrics 0161 206 5062 All Rights Reserved 2014. Document for issue as handout. This booklet aims to describe: l What is a gastric band page 2 l How is
Colonic Stenting Your Procedure Explained
 Colonic Stenting Your Procedure Explained Patient Information Introduction This leaflet tells you about the procedure known as colonic stenting. It explains what is involved and some of the common complications
Colonic Stenting Your Procedure Explained Patient Information Introduction This leaflet tells you about the procedure known as colonic stenting. It explains what is involved and some of the common complications
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters
 Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
Policy and Procedure Flushing and / or Blood withdrawal Aspiration Procedure For PICC Line and Midline Catheters Purpose: Blood Withdrawal: To obtain blood samples for laboratory evaluation, eliminating
Riesa Gusewelle, MNSc, RN, APRN, GNP-BC. OBJECTIVES Identify early warning signs of urinary tract
 Detection, Early Management & Prevention, of Urinary Tract Infections in Older Adults Riesa Gusewelle, MNSc, RN, APRN, GNP-BC OBJECTIVES Identify early warning signs of urinary tract infections (UTIs)
Detection, Early Management & Prevention, of Urinary Tract Infections in Older Adults Riesa Gusewelle, MNSc, RN, APRN, GNP-BC OBJECTIVES Identify early warning signs of urinary tract infections (UTIs)
What is Barrett s esophagus? How does Barrett s esophagus develop?
 Barrett s Esophagus What is Barrett s esophagus? Barrett s esophagus is a pre-cancerous condition affecting the lining of the esophagus, the swallowing tube that carries foods and liquids from the mouth
Barrett s Esophagus What is Barrett s esophagus? Barrett s esophagus is a pre-cancerous condition affecting the lining of the esophagus, the swallowing tube that carries foods and liquids from the mouth
YTTRIUM 90 MICROSPHERES THERAPY OF LIVER TUMORS
 YTTRIUM 90 MICROSPHERES THERAPY OF LIVER TUMORS The information regarding placement of Yttrium 90 microsphres for the management of liver tumors on the next several pages includes questions commonly asked
YTTRIUM 90 MICROSPHERES THERAPY OF LIVER TUMORS The information regarding placement of Yttrium 90 microsphres for the management of liver tumors on the next several pages includes questions commonly asked
Information and advice following placement of seton for anal fistula
 Oxford University Hospitals NHS Trust Information and advice following placement of seton for anal fistula page 2 What is a fistula? You can get an anal fistula as a result of an infection or a collection
Oxford University Hospitals NHS Trust Information and advice following placement of seton for anal fistula page 2 What is a fistula? You can get an anal fistula as a result of an infection or a collection
