INSTRUCTOR GUIDE. TOPIC: Trauma Assessment and Patient Destination. TIME REQUIRED: 2-3 Hours
|
|
|
- Martin Johnson
- 10 years ago
- Views:
Transcription
1 INSTRUCTOR GUIDE TOPIC: Trauma Assessment and Patient Destination TIME REQUIRED: 2-3 Hours MATERIALS: Appropriate audio/visual materials and equipment REFERENCES: Prehospital Trauma Life Support, 5 th Edition, Mosby Maryland EMS Protocols PREPARATION: ATTENTION: MOTIVATION: Assessment and triage of a trauma patient can be a difficult task. The use of organized and consistent assessment techniques can assist the EMS provider in recognition of those patients who have sustained potentially life threatening injuries. This recognition helps the EMS provider to decide the type of medical treatment the patient receives and to differentiate between patients who require immediate transport ( Load and Go ) from those who would benefit from continued assessment and care on scene. Lastly, information gained from the assessment, along with knowledge of local trauma protocols, will help guide the EMS provider in transporting the patient to the most appropriate facility. OBJECTIVE (SPO): The student will be able to discuss the rationale for performing an organized assessment as well as describe the proper assessment, management and destination decision for the trauma patient. OVERVIEW: Trauma Assessment and Patient Destination * Introduction * Scene / Situation Survey * Primary Survey * Identification of the Critical Trauma Patient * On Scene Care of the Trauma Patient * Secondary Survey * Patient Destination
2 TRAUMA ASSESSMENT & PATIENT DESTINATION SPO EO 1-1 EO 1-2 EO 1-3 EO 1-4 EO 1-5 EO 1-6 EO 1-7 The student will be able to discuss the rationale for performing an organized assessment as well as describe the proper assessment, management and destination decision for the trauma patient. Discuss the rationale for performing an organized assessment on a trauma patient. List the components of the scene/situation survey. Describe the primary survey that is performed on every trauma patient. Explain the importance of identifying a patient with a critical injury and the impact it may have on patient management. Describe the difference in the on-scene care of a patient with critical injuries as opposed to a patient with non-critical injuries List and describe the components of the secondary survey on a trauma patient. Describe how to utilize the Maryland Medical Protocols to determine the appropriate destination for a trauma patient. 2
3 I. INTRODUCTION (EO 1-1) A.Epidemiology of trauma 1 Trauma is a disease of the young a. Leading cause of death in patients aged 1-44 years old 2 3 rd leading cause of death in all age groups 3 More than 60 million injuries occur annually in the United States a. It is also a major problem worldwide 4 Many of these injuries may cause significant disability 5 Major financial losses too a.direct costs b.lost tax income c.lost productivity d.lost years of life B.When do patients die from trauma? 1 Immediate (minutes to 1 hour) a.can only be prevented by injury prevention education 2 Early (within 4 hours) a.may be prevented through appropriate prehospital care 3 Late (2 to 5 weeks) a.may be prevented through prompt transport to a hospital appropriately staffed for trauma care. C.What is the Golden Hour 1 R Adams Cowley described the Golden Hour a.patients with major trauma had higher survival rates if surgical intervention occurred within one hour of injury. b.***there is no definitive research that validates the time frame of one hour (60 minutes)*** i. Some patients have more than an hour, some have less ii.the concept, though, is very important a) The sooner we can get a patient with major injuries to a trauma center, the better the chances of survival 2 The Golden Period is probably a better description D.What encompasses the Golden Period 1 7 different time periods a.time of injury to 911 call b.time of 911 call to EMS dispatch 3
4 c.time of EMS dispatch to Ambulance response d.time of Ambulance response to arrival on scene e.time spent on scene with the patient f.time of Ambulance transport to the hospital g.time the patient spends in the emergency room prior to surgery 2 EMS Providers can only truly affect one of these time periods a.on scene time i. ***Note: Some students may feel that we can significantly affect response time and transport time by driving the ambulance faster. Research in this matter does not support this notion except when driving over long distances (Greater than 60 miles)*** b.the American College of Surgeons and Prehospital Trauma Life Support (PHTLS) International have come to a consensus on the optimal on-scene time for major trauma i. 10 minutes a) K.A. The Platinum 10 Minutes E.The Platinum 10 Minutes 1 Factors that help EMS providers attain the 10 minute on-scene goal when treating the patient with critical trauma a.rapid & efficient assessment of the scene and patient i. Helps to identify patients with critical injuries b.limit on-scene care to addressing life threatening issues only c.effective teamwork to rapidly package the patient d.initiation of timely transport to an appropriate facility i. Performing additional assessment and care during transport F.Special Considerations with Helicopter Transport 1 Trauma Center accessible by ground (Approximate 25 minute transport time) a.transport should be initiated as soon as possible once in the ambulance 2 Trauma Center better accessed by helicopter a.because of the number of variables associated with calling a helicopter to a trauma scene, it is unlikely that the goal of transporting the patient within 10 minutes of ambulance arrival will be met. b.ground crews should, though, still work to meet the goal of having the patient in the ambulance within 10 minutes of arrival on scene 4
5 i. Increases the likelihood that all assessment and care that can be performed by the ground crew will be completed prior to the arrival of the helicopter. a) Facilitates a smoother and faster transfer of patient care. b) Decreases the amount of time the helicopter remains on scene c) Decreases the amount of time it takes to get the patient to the hospital (Which is our overall goal anyway!) II. SCENE / SITUATION SURVEY (EO 1-2) A.Scene situation survey encompasses two divisions 1 Scene Safety 2 Situation B.The survey begins upon dispatch prior to arrival 1 Information from dispatch can provide a.information about the incident b.information about known hazards c.information about available resources C.Scene Safety 1 What are the components for assessing scene safety a.ensure safety of rescuers and patients b.threatening situations may include i. Fire ii.electrical lines iii.hazardous materials iv.blood and body fluids v. Traffic vi.weapons vii.environmental conditions viii.***can students think of any others? D.Scene Situation 1 Survey of the situation helps to identify a.what really happened? b.what is the mechanism of injury to the patient? c.how many patients are involved. i. What are their ages a) Why is this important? 5
6 1) It may help to identify the need for pediatric specific resources or transport destinations d.are any additional resources needed? i. Examples include a) Fire Suppression b) Rescue & Extrication c) HazMat d) Tactical Rescue e) Shock Trauma Go Team e.how will the patients be transported? i. Examples include a) Ambulances b) Helicopters c) Buses (Mass Casualty) III. IV. BODY SUBSTANCE ISOLATION A.Prior to beginning any physical assessment, the EMS provider should take body substance isolation (BSI) precautions B.BSI precautions can include 1 Gloves 2 Eye protection a.especially if the patient has any potential for spurting fluids 3 Masks 4 Gowns PATIENT ASSESSMENT OVERVIEW A.The patient management for trauma is divided into 4 segments 1 Primary survey a.identifies life-threatening conditions b. Treat as you go i. It is recommended that when an EMS provider finds a life threatening condition, it is managed immediately a) ***Note-This can be performed by other providers as directed by the one performing the assessment 2 Resuscitation a.manage life threatening conditions on scene b.package the patient for rapid transport (if indicated) 3 Secondary survey a.more detailed assessment i. Head to toe 6
7 b.performed in ambulance for critical patient c.performed on scene for non-critical patient 4 Definitive care in the field a.address all injuries as time allows b.performed in ambulance for critical patient c.performed on scene for non-critical patient V. PRIMARY SURVEY (EO-1-3) A.The primary survey should be performed on every potential trauma patient 1 The information gathered in the primary survey will assist the EMS provider in deciding whether or not the patient is critical a.critical patients are managed differently than non-critical patients B.Performed in an A-B-C-D-E format 1 Airway with C-spine 2 Breathing 3 Circulation 4 Disability 5 Expose / Environment C.Airway 1 Assessment a.assess for patency b.open the airway while protecting cervical spine i. Utilize modified-jaw-thrust technique 2 Potential Life Threatening Airway Conditions a.obstruction i. Tongue ii.blood / Fluid iii.foreign Body 3 Potential Airway Treatments a.manual opening of the airway (Modified Jaw Thrust) b.bls Airway usage i. Oropharyngeal airway ii.nasopharyngeal airway c.suction d.endotracheal Intubation (Advanced Life Support) D.Breathing 1 Assessment 7
8 a.estimate rate of ventilations i. Does not require an exact number ii.should be thought of as Fast, Normal or Slow a) An exact number can be obtained later in the secondary survey b.assess depth of respirations i. Deep, Normal, Shallow c.listen to Lung Sounds i. ***VERY IMPORTANT*** a) Many students think of lung sounds as a secondary survey assessment. b) The sooner a deficiency can be identified in a patient s respiratory system, the sooner treatment can begin (May require ALS intervention) ii.listen at 5 th intercostal space, midclavicular line a) Armpits iii.assess for presence and sounds a) Does not require a detailed assessment. Just the two armpit locations 2 Potential Life Threatening Breathing Conditions a.shortness of Breath b.abnormal Breathing i. Apnea ii.shallow Tidal Volume iii.irregular Patterns c.diminished or Absent Lung Sounds i. Hemothroax ii.pneumothorax / Tension Pneumothorax d.crackles / Fluid in Lungs / Pulmonary Edema 3 Potential Breathing Treatments a.oxygen administration i. Nonrebreather Mask ii.nasal Cannula b.bag-valve-mask Ventilations with supplemental oxygen E. Circulation 1 Assessment a.is there any uncontrolled external hemorrhage? b.pulse i. Feel at the neck(carotid) and the wrist (radial) 8
9 ii.estimate rate a) Do not need exact number 1. Fast, Normal or Slow 2. Can get exact number in secondary survey iii.note quality (strength) a) Signs of shock include 1. Weak carotid pulse 2. Weak or absent radial pulses c.assess Skin i. Color a) Normal (pink mucosa), pale, flushed, cyanotic ii.temperature a) Hot, warm, cool, cold iii.moisture a) Normal (dry), diaphoretic iv.capillary refill time a) Normal, Delayed (> 2 seconds) 2 Potential Life Threatening Circulatory Conditions a.hemorrhage i. External ii.internal b.shock 3 Potential Circulatory Treatments a.control external hemorrhage i. Direct pressure/pressure dressing ii.elevation, pressure points, tourniquets as needed b.***no IV LINES*** i. While IV access may be performed by properly certified personnel, it should not be done in the primary survey. It should not be initiated until the patient is within the ambulance. F. Disability 1 Assessment a.assess Level of Consciousness i. Utilize the Glasgow Coma Scale a) Eye Opening 1. 4 open spontaneously 2. 3 open to verbal command 3. 2 open to painful stimuli 9
10 4. 1 no opening b) Verbal Response 1. 5 oriented 2. 4 confused, disoriented 3. 3 inappropriate words 4. 2 incomprehensible sounds 5. 1 no verbal response c) Motor Response 1. 6 follows commands 2. 5 localizes to pain 3. 4 withdraws to pain 4. 3 abnormal flexion (decorticate posturing) 5. 2 abnormal extension (decerebrate posturing) 6. 1 No motor response ii.a Quick Method to use the GCS a) Open your eyes 1. If eyes open already 4 2. If opens eyes to command 3 3. If no eye opening to command, administer nailbed pressure (pain). If eyes open to pain If eyes do not open to the pain 1 b) What happened to you 1. Note what the patient s verbal response is to your question c) Hold up two fingers 1. If the patient holds up two fingers, he/she receives a 6 for motor response 2. If the patient does not follow the command, administer nailbed pressure (pain) then record the patient s motor response. b.assess Pupils i. Reactivity ii.equality 2 Potential Life Threatening Disablity Conditions a.unconsciousness b.altered Mental Status c.suspected Head Injury with unequal pupils 10
11 3 Potential Treatments a.no specific treatments in the primary survey G.Exposure / Environment 1 Expose the patient as the environment allows to assess for other life threatening conditions a.may not be noticeable with clothing on b.clothing can absorb large amounts of blood 2 After exposure, cover to maintain body heat a.hypothermia can worsen outcome from shock. VI. IDENTIFICATION OF THE CRITICAL TRAUMA PATIENT (EO-1-4) A.Upon completion of the primary survey, the EMS provider has enough information to identify if the patient appears critical B.A critical trauma patient may present with one of the following 1 Inadequate or threatened airway a.for example coma, obstruction, airway burns 2 Impaired ventilations a.for example decreased tidal volume, decreased respirations 3 Hemorrhage a.for example significant external or suspected internal hemorrhage 4 Shock 5 Abnormal neurologic status a.for example GCS < 15 or neurologic deficits 6 Penetrating trauma to head, neck, torso or proximal to elbows/knees 7 Amputation or near amputation a.for example mangled extremity C.A critical trauma patient will be managed differently than a non-critical trauma patient 1 Platinum 10 minutes 2 Limited on scene care 3 Initiate rapid transport to a trauma center VII. ON SCENE CARE OF THE TRAUMA PATIENT (EO-1-5) A.For patients identified as critical: 1 EMS providers should attempt to begin transport within 10 minutes 2 Medical care should be limited on scene to addressing life threatening issues only 11
12 a.airway management i. BLS maneuvers, OPA/NPA, suction, intubation b.oxygen administration c.supplemental ventilations with BVM d.control external hemorrhage e.no IVs! Should be deferred until in ambulance i. May be appropriate if the patient is entrapped during extrication f.no BLOOD PRESSURES! Should be deferred until in ambulance i. This information is not necessary on scene and will only take time and resources away from moving the patient to the ambulance in a rapid fashion 3 Patients should be packaged rapidly a.may include C-spine immobilization if indicated 4 Secondary survey and definitive care should be deferred until transport has been initiated. a.see below for secondary survey format 5 Patient should be transported to a trauma center unless otherwise directed by protocol or on-line medical direction B.For patients identified as non-critical 1 There is no need to leave the scene rapidly unless other external factors create a hazard 2 Secondary survey can be performed on scene prior to transport a.see below for secondary survey format 3 Definitive care should be performed prior to transport 4 Patient comfort should be considered. 5 Patient should be transported to a medical facility as dictated by medical protocol or on-line medical direction a.may be a trauma center or a local hospital VIII. SECONDARY SURVEY (EO-1-6) A.There are 3 main components to the secondary survey 1 Vital Signs 2 AMPLE history 3 Head to toe assessment B.Obtain a full set of vital signs 1 Obtaining numerical values for vital signs in the primary survey was not necessary. Now the provider should obtain values for the following: 12
13 a.blood pressure b.pulse c.respirations d.oxygen Saturation e.ecg (if ALS) C.Obtain an AMPLE history 1 This includes: a.allergies b.medications c.past Medical History d.last Meal e.events Prior to Traumatic Incident 2 This information may be obtained by direct questioning of the patient, statements from family/friends/bystanders or by examining the patient s body for medical alert tags a.this information may be important to obtain early if the patient is at risk for losing consciousness. D.Head-to-Toe Exam 1 Body systems are generally assessed for DCAP-BTLS a.deformities b.contusions c.abrasions d.penetrations e.burns f.tenderness g.lacerations h.swelling 2 Head a.in addition to DCAP-BTLS i. Assess the ears, nose and mouth for blood/fluid ii.assess the pupils for equality and reactivity to light 3 Neck a.in addition to DCAP-BTLS i. Assess the neck for distended jugular veins ii.assess the trachea (is it midline or deviated at the sternal notch) iii.assess for subcutaneous emphysema a) Will feel like rice krispies under the skin 13
14 4 Chest a.in addition to DCAP-BTLS i. Look at the chest for symmetrical chest rise ii.look at the chest for paradoxical movement a) Indicates a possible flail chest 1. 3 or more ribs broken in two or more places iii.palpate the chest for crepitus or instability iv.listen to lung sounds a) Should be the 2 nd assessment of lung sounds b) Can be assessed in multiple locations 5 Abdomen a.in addition to DCAP-BTLS i. Look for abdominal distention ii.palpate for abdominal rigidity a) May indicate abdominal bleeding iii.do not listen for abdominal sounds a) Takes a number of minutes perform correctly b) Does not provide useful information to guide EMS treatment 6 Pelvis a.in addition to DCAP-BTLS i. Palpate straight down (anterior surface of pelvis) ii.palpate both areas where the femur attaches to the pelvis a) If instability is felt, the patient may have a fractured pelvis 1. 20% Mortality rate for untreated pelvic fractures. 7 Legs a.in addition to DCAP-BTLS i. Palpate both legs ii.assess distal neurologic function a) Distal pulse (dorsalis pedis) b) Sensation c) Motor function 8 Arms a.in addition to DCAP-BTLS i. Palpate both arms ii.assess distal neurologic function a) Distal pulse (radial pulse) b) Sensation 14
15 c) Motor function E. Remind students when to perform secondary surveys 1 Critical patients a.during transport, or b.in the ambulance awaiting helicopter transport 2 Non-critical patients a.on scene prior to transport i. May be performed in the ambulance if the environment does not allow for assessment in the field IX. DEFINITIVE CARE IN THE FIELD A.Definitive care in the field is treatment that generally addresses injuries that are not life threatening B.Usually performed after the secondary survey C.Definitive care includes 1 Spinal Immobilization a.may be performed earlier as part of patient packaging for a critical trauma patient 2 Establish IV access a.may be performed shortly after movement of patient to ambulance i. In conjunction with secondary survey 3 Splint musculoskeletal injuries a.helps to facilitate patient movement b.helps to decrease pain c.helps to decrease the incidence of fat embolisms after a fracture 4 Dress wounds a.apply sterile dressing to soft tissue injuries that were not life threatening X. PATIENT DESTINATION (EO-1-7) A.A decision has to be made as to where to transport a patient and what mode of transport to utilize B.Mode of Transport 1 Generally two types 15
16 a.ambulance i. Acceptable mode of transport if transport time is reasonable. a) Most experts agree that a transport time of minutes is acceptable for ground transport to a trauma center ii.no weight restrictions iii.generally little restriction on continued assessment and treatment b.helicopter i. Good mode of transport to cover long distances ii.smaller compartment size limits the number of rescuers iii.some compartment designs make certain patient treatment and assessment difficult in flight, requiring almost all treatment be performed prior to lift off. C.Destination 1 Critically injured patients should be transported to a designated trauma center with immediate surgical capabilities if available. 2 Maryland has created a triage decision tree to identify which patients should be transported to a trauma center. a.utilizes criteria based on physiology, anatomy, mechanism of injury and preexisting conditions. b.categorized as A, B, C or D 3 Category A Criteria a.these patients should be transported to a trauma center. Emergency transport should be considered as these situations are often potentially life threatening i. GCS < 8 ii.adult Blood Pressure < 90 systolic iii.pediatric Blood Pressure < 60 systolic iv.respiratory Rate less than 10 or greater than 29 v. Flail Chest vi.pelvic Fracture vii.rapidly declining GCS viii.penetrating injuries to head, neck or torso ix.two or more proximal long bone fractures a) Long bone = femur or humerus 4 Category B Criteria 16
17 a.these patients should be transported to a trauma center. Some of these conditions are potentially life threatening and some are potentially limb threatening. The decision for emergency vs non emergency transport should be made based upon the patient s condition i. GCS 8-14 ii.paralysis or vascular compromise of limb iii.penetrating injuries to extremities proximal to elbow & knee iv.amputation proximal to wrist and ankle v. Combination of trauma with burns 5 Category C Criteria a.these patients should be transported to a trauma center. The situations in this category describe mechanisms of injury that have been associated with significant injury. It is possible, though, that a patient involved in this situation may not be experiencing any critical injuries. Therefore, the mode of transport (ambulance vs. helicopter, emergency vs non-emergency) should be based upon the patient s condition i. Ejection from automobile ii.death in the same passenger compartment iii.extrication time greater than 20 minutes iv.fall greater than 3 times the patient s height v. Vehicular rollover vi.high speed auto crash vii.initial speed greater than 40 mph viii.major auto deformity greater than 20 inches ix.intrusion into passenger compartment greater than 12 inches x. Auto/pedestrian or Auto/bicycle injury with significant impact (>5 mph) xi.exposure to blast or explosion xii.pedestrian thrown or run over xiii.motorcycle crash > 20 mph xiv.motor cycle crash with separation of rider from motorcycle 6 Category D Criteria a.this category lists situations or medical conditions that a patient may have that make him/her more susceptible to traumatic injuries. They are referred to as Co-morbid factors. If a patient has experienced a traumatic incident and does not fall into Criteria A, B or C, you should check to see if they have any of those factors. If they do fall into Category D, you may consider transport to a 17
18 trauma center. It is recommended, though, that you consult with online medical direction as the local hospital may feel comfortable caring for the patient. In most circumstances, emergency transport is not warranted for these patients. i. Age less than 5 ii.age greater than 55 iii.cardiac disease iv.respiratory disease v. Insulin dependant diabetes vi.cirrhosis of the liver vii.morbid obesity viii.pregnancy ix.immunosuppressed patients x. Patient with a bleeding disorder or on anticoagulants 7 Always remember, though, that when in doubt, transport the patient to a trauma center. XI. PRACTICE PATIENT SCENARIOS A.Instructor should create patient care scenarios. These can be utilized, as time permits, to practice the trauma assessment presented in this drill. Information should be provided for the following patient assessment categories: 1 Scene Assessment 2 Mechanism of injury 3 Primary Survey 4 Critical vs. non-critical patient 5 Secondary Survey 6 Suggested management of patient care 7 Reassessment B.The best method of practicing this, is to encourage the students to be as hands-on as possible with their physical assessment of the patient and treatment of the patient. C.While moulage is not necessary, its use can enhance the learning experience and make training more realistic. 18
19 SUMMARY REVIEW: Trauma Assessment and Patient Destination * Introduction * Scene / Situation Survey * Primary Survey * Identification of the Critical Trauma Patient * On Scene Care of the Trauma Patient * Secondary Survey * Patient Destination REMOTIVATION: It has been said that the fate of the wounded lies in the hands of the one who applies the first bandage. Research has also shown that the care a trauma patient receives within the first hour after injury can have an affect on their outcome 2 to 20 days later. By performing good assessments, providing quality care and initiating transport to the most appropriate facility for the situation, we can give our trauma patients the best possible chances for recovery. ASSIGNMENT: EVALUATION: 19
20 20
21 21
22 22
23 23
National Registry of Emergency Medical Technicians Emergency Medical Technician Psychomotor Examination BLEEDING CONTROL/SHOCK MANAGEMENT
 BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
BLEEDING CONTROL/SHOCK MANAGEMENT Candidate: Examiner: Date: Signature: Possible Applies direct pressure to the wound 1 NOTE: The examiner must now inform the candidate that the wound continues to bleed.
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPORT State Form 54407 (R / 5-13)
 EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT State Form 54407 (R / 5-3) INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street,
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log
 First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
First Responder (FR) and Emergency Medical Responder (EMR) Progress Log Note: Those competencies that are for EMR only are denoted by boldface type. For further details on the National Occupational Competencies
404 Section 5 Shock and Resuscitation. Scene Size-up. Primary Assessment. History Taking
 404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
404 Section 5 and Resuscitation Scene Size-up Scene Safety Mechanism of Injury (MOI)/ Nature of Illness (NOI) Ensure scene safety and address hazards. Standard precautions should include a minimum of gloves
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination BVM VENTILATION OF AN APNEIC ADULT PATIENT
 BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
BVM VENTILATION OF AN APNEIC ADULT PATIENT Candidate: Examiner: Date: Signature: Possible Points Checks responsiveness NOTE: After checking responsiveness and breathing for at least 5 but no 1 Checks breathing
Patient Assessment/Management Trauma
 Patient Assessment/Management Trauma Date: / / Test Site Location: Station #: Takes or verbalizes standard precautions (BSI) if appropriate based on patient scenario SCENE SIZE-UP Determines the scene
Patient Assessment/Management Trauma Date: / / Test Site Location: Station #: Takes or verbalizes standard precautions (BSI) if appropriate based on patient scenario SCENE SIZE-UP Determines the scene
National Registry Skill Sheets
 Bleeding Control/Shock Management BVM Ventilation of an Apneic Adult Patient Cardiac Arrest Management/AED Joint Immobilization Long Bone Immobilization Oxygen Administration By Non-Rebreather Mask Patient
Bleeding Control/Shock Management BVM Ventilation of an Apneic Adult Patient Cardiac Arrest Management/AED Joint Immobilization Long Bone Immobilization Oxygen Administration By Non-Rebreather Mask Patient
National Registry of Emergency Medical Technicians Emergency Medical Responder Psychomotor Examination PATIENT ASSESSMENT/MANAGEMENT TRAUMA
 PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
PATIENT ASSESSMENT/MANAGEMENT TRAUMA Scenario # Note: Areas denoted by ** may be integrated within sequence of Primary Survey/Resuscitation SCENE SIZE-UP Determines the mechanism of injury/nature of illness
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT What to wear STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT ITLS is a practical course that stresses hands-on teaching. You should wear comfortable clothes that you
INTERNATIONAL TRAUMA LIFE SUPPORT What to wear STUDENT GUIDE TO INTERNATIONAL TRAUMA LIFE SUPPORT ITLS is a practical course that stresses hands-on teaching. You should wear comfortable clothes that you
(a) Glasgow coma scale less than or equal to thirteen; (b) Loss of consciousness greater than five minutes;
 ACTION: Original DATE: 09/11/2014 3:19 PM 4765-14-02 Determination of a trauma victim. Emergency medical service personnel shall use the criteria in this rule, consistent with their certification, to evaluate
ACTION: Original DATE: 09/11/2014 3:19 PM 4765-14-02 Determination of a trauma victim. Emergency medical service personnel shall use the criteria in this rule, consistent with their certification, to evaluate
EMS POLICIES AND PROCEDURES
 EMS POLICIES AND PROCEDURES POLICY #: 13 EFFECT DATE: xx/xx/05 PAGE: 1 of 4 *** DRAFT *** SUBJECT: TRIAGE OF TRAUMA PATIENTS *** DRAFT *** APPROVED BY: I. PURPOSE Art Lathrop, EMS Director Joseph A. Barger,
EMS POLICIES AND PROCEDURES POLICY #: 13 EFFECT DATE: xx/xx/05 PAGE: 1 of 4 *** DRAFT *** SUBJECT: TRIAGE OF TRAUMA PATIENTS *** DRAFT *** APPROVED BY: I. PURPOSE Art Lathrop, EMS Director Joseph A. Barger,
Frontline First Aid EMR Scenario Examples
 Course Type: Start Date: Instructors initial scenarios as they are completed CPR-AED Scenarios CPR with Hypothermia Load and Go CPR with Obstructed Airway Continue CPR after airway clears with NO obvious
Course Type: Start Date: Instructors initial scenarios as they are completed CPR-AED Scenarios CPR with Hypothermia Load and Go CPR with Obstructed Airway Continue CPR after airway clears with NO obvious
State of Indiana EMR Psychomotor Skills Examination
 SECONDARY ASSESSMENT (Detailed Exam) *Credit should be given to candidates that use a brief exam f life-threatening injuries in the Primary Survey so long as it does not delay appropriate care. Head Neck
SECONDARY ASSESSMENT (Detailed Exam) *Credit should be given to candidates that use a brief exam f life-threatening injuries in the Primary Survey so long as it does not delay appropriate care. Head Neck
EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPORT
 Reset Form EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street, Room E239 Indianapolis,
Reset Form EMERGENCY MEDICAL RESPONDER (EMR) PRACTICAL SKILLS EXAMINATION REPT INDIANA DEPARTMENT OF HOMELAND SECURITY EMERGENCY MEDICAL SERVICES CERTIFICATION 302 West Washington Street, Room E239 Indianapolis,
ITLS & PHTLS: A Comparison
 ITLS & PHTLS: A Comparison International Trauma Life Support (ITLS) is a global organization dedicated to preventing death and disability from trauma through education and emergency care. ITLS educates
ITLS & PHTLS: A Comparison International Trauma Life Support (ITLS) is a global organization dedicated to preventing death and disability from trauma through education and emergency care. ITLS educates
State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services
 State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services September 2013 PATIENT ASSESSMENT / MANAGEMENT - TRAUMA Time allowed: 10 minutes SCENARIO
State of New Hampshire Department of Safety Division of Fire Standards and Training & Emergency Medical Services September 2013 PATIENT ASSESSMENT / MANAGEMENT - TRAUMA Time allowed: 10 minutes SCENARIO
Emergency Medical Technician Basic. Practical Skills Examination Sheets
 New York State Department of Health Basic Practical Skills Examination Sheets Rev 07/12 Basic Practical Skills Examination Sheets Updates Included on this page are the changes or updates that have been
New York State Department of Health Basic Practical Skills Examination Sheets Rev 07/12 Basic Practical Skills Examination Sheets Updates Included on this page are the changes or updates that have been
RP0807 - PERFORM SPLINTING TECHNIQUES
 RP0807 - PERFORM SPLINTING TECHNIQUES TERMINAL LEARNING OBJECTIVE. 1. Without the aid of references, given a casualty and standard combat lifesaver medical equipment set, perform splinting techniques,
RP0807 - PERFORM SPLINTING TECHNIQUES TERMINAL LEARNING OBJECTIVE. 1. Without the aid of references, given a casualty and standard combat lifesaver medical equipment set, perform splinting techniques,
CENTRAL TEXAS COLLEGE EMSP 1305 EMERGENCY CARE ATTENDANT. Semester Hours Credit: 3
 CENTRAL TEXAS COLLEGE EMERGENCY CARE ATTENDANT INSTRUCTOR: Semester Hours Credit: 3 OFFICE HOURS: I. INTRODUCTION Course Description: First responder course in emergency medical care. Emphasis on requirements
CENTRAL TEXAS COLLEGE EMERGENCY CARE ATTENDANT INSTRUCTOR: Semester Hours Credit: 3 OFFICE HOURS: I. INTRODUCTION Course Description: First responder course in emergency medical care. Emphasis on requirements
TRAUMA PATIENT TRANSPORT
 TRAUMA PATIENT TRANSPORT I. Region XI EMS uses a pre-hospital scoring system (see Attachment 1, Trauma Field Triage Criteria) to assist with the identification of injured adult and pediatric patients and
TRAUMA PATIENT TRANSPORT I. Region XI EMS uses a pre-hospital scoring system (see Attachment 1, Trauma Field Triage Criteria) to assist with the identification of injured adult and pediatric patients and
EMR EMERGENCY MEDICAL RESPONDER Course Syllabus
 6111 E. Skelly Drive P. O. Box 477200 Tulsa, OK 74147-7200 EMR EMERGENCY MEDICAL RESPONDER Course Syllabus Course Number: HLTH-0009 OHLAP Credit: No OCAS Code: 9373 Course Length: 66 Hours Career Cluster:
6111 E. Skelly Drive P. O. Box 477200 Tulsa, OK 74147-7200 EMR EMERGENCY MEDICAL RESPONDER Course Syllabus Course Number: HLTH-0009 OHLAP Credit: No OCAS Code: 9373 Course Length: 66 Hours Career Cluster:
How To Treat A Heart Attack
 13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
13 Resuscitation and preparation for anaesthesia and surgery Key Points 13.1 MANAGEMENT OF EMERGENCIES AND CARDIOPULMONARY RESUSCITATION ESSENTIAL HEALTH TECHNOLOGIES The emergency measures that are familiar
Northwestern Health Sciences University. Basic Life Support for Healthcare Providers
 Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
Northwestern Health Sciences University Basic Life Support for Healthcare Providers Pretest May 2005 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses Based
EMERGENCY MEDICAL SERVICES TRAUMA TRANSPORT PROTOCOLS
 I. DISPATCH PROCEDURES: 1. The Okaloosa County EMS Communications Center is located in Okaloosa County Emergency Operations Complex in the City of Niceville. The Communications Center has enhanced 911
I. DISPATCH PROCEDURES: 1. The Okaloosa County EMS Communications Center is located in Okaloosa County Emergency Operations Complex in the City of Niceville. The Communications Center has enhanced 911
Pennsylvania Trauma Nursing Core Curriculum. Posted to PTSF Website: 10/30/2014
 Pennsylvania Trauma Nursing Core Curriculum Posted to PTSF Website: 10/30/2014 PREFACE Care of the trauma patient has evolved since 1985, when the Pennsylvania Trauma Systems Foundation (PTSF) Board of
Pennsylvania Trauma Nursing Core Curriculum Posted to PTSF Website: 10/30/2014 PREFACE Care of the trauma patient has evolved since 1985, when the Pennsylvania Trauma Systems Foundation (PTSF) Board of
Southern Stone County Fire Protection District Emergency Medical Protocols
 TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
TITLE Pediatric Medical Assessment PM 2.4 Confirm scene safety Appropriate body substance isolation procedures Number of patients Nature of illness Evaluate the need for assistance B.L.S ABC s & LOC Focused
Chapter 6. Hemorrhage Control UNDER FIRE KEEP YOUR HEAD DOWN
 Hemorrhage Control Chapter 6 Hemorrhage Control The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel
Hemorrhage Control Chapter 6 Hemorrhage Control The hemorrhage that take[s] place when a main artery is divided is usually so rapid and so copious that the wounded man dies before help can reach him. Colonel
TITLE 836 INDIANA EMERGENCY MEDICAL SERVICES COMMISSION. ARTICLE 1.5 Trauma Field Triage and Transport Destination Requirements
 TITLE 836 INDIANA EMERGENCY MEDICAL SERVICES COMMISSION ARTICLE 1.5 Trauma Field Triage and Transport Destination Requirements 836 IAC 1.5-1 Purpose Affected: [IC 10-14-3-12; IC 16-18; IC 16-21-2; IC 16-31-2-9;
TITLE 836 INDIANA EMERGENCY MEDICAL SERVICES COMMISSION ARTICLE 1.5 Trauma Field Triage and Transport Destination Requirements 836 IAC 1.5-1 Purpose Affected: [IC 10-14-3-12; IC 16-18; IC 16-21-2; IC 16-31-2-9;
1st Responder to Emergency Medical Responder Transition Course
 1st Responder to Emergency Medical Responder Transition Course Mandatory Training July 5, 2011 Authored by: Eddie Manley, Education Coordinator OSDH - EMS 1 st Responder to EMR Recommended Transition Course
1st Responder to Emergency Medical Responder Transition Course Mandatory Training July 5, 2011 Authored by: Eddie Manley, Education Coordinator OSDH - EMS 1 st Responder to EMR Recommended Transition Course
NORTH REGION EMS & TRAUMA CARE SYSTEM Operational Guidelines
 PATIENT CARE PROCEDURES #1 Access to Prehospital EMS Care To define elements of the Regional EMS and trauma system necessary to assure rapid universal access to 911 and E-911, rapid identification of emergent
PATIENT CARE PROCEDURES #1 Access to Prehospital EMS Care To define elements of the Regional EMS and trauma system necessary to assure rapid universal access to 911 and E-911, rapid identification of emergent
Nassau Regional EMS Council Basic Life Support Protocols and Supplements to State BLS Protocol Manual Table of Contents
 Nassau Regional EMS Council Basic Life Support Protocols and Supplements to State BLS Protocol Manual Table of Contents Approved/ Revised Effective BLS Adult Nerve Agent/Organophosphate Poisoning Antidote
Nassau Regional EMS Council Basic Life Support Protocols and Supplements to State BLS Protocol Manual Table of Contents Approved/ Revised Effective BLS Adult Nerve Agent/Organophosphate Poisoning Antidote
BLS TREATMENT GUIDELINES - CARDIAC
 BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
BLS TREATMENT GUIDELINES - CARDIAC CARDIOPULMONARY ARREST - NON-TRAUMATIC (SJ-B101) effective 07/01/99 Defibrillation CPR Apply S-AED and assess rhythm as trained. Defib as indicated Simultaneous OXYGEN:
TN Emergency Medical Services
 TN Emergency edical ODULES AND UNITS ES System ES Providers: ER and ET Safety and Wellness Body echanics System Communication Documentation Therapeutic Communication Legal and Ethical Issues Intro to Respiratory
TN Emergency edical ODULES AND UNITS ES System ES Providers: ER and ET Safety and Wellness Body echanics System Communication Documentation Therapeutic Communication Legal and Ethical Issues Intro to Respiratory
First Responder: The National EMS Scope of Practice changes the name to Emergency Medical Responder.
 APPROVED SCOPE 2/8/08 BOARD MTG First Responder: The National EMS Scope of Practice changes the name to Emergency Medical Responder. Emergency Medical Responder (EMR) Description of the Profession The
APPROVED SCOPE 2/8/08 BOARD MTG First Responder: The National EMS Scope of Practice changes the name to Emergency Medical Responder. Emergency Medical Responder (EMR) Description of the Profession The
Bleeding Control for the Injured
 Bleeding Control for the Injured Bleeding Control (1 of 2) The focus of this training is on recognition of life-threatening bleeding with appropriate medical treatment. This training will show you the
Bleeding Control for the Injured Bleeding Control (1 of 2) The focus of this training is on recognition of life-threatening bleeding with appropriate medical treatment. This training will show you the
Gunshot wounds. Warning: This presentation has extremely graphic pictures! Richard P. Kness, EMT- P
 Gunshot wounds Warning: This presentation has extremely graphic pictures! Richard P. Kness, EMT- P Objectives After this lesson the student will be able to: List scene safety issues Describe procedures
Gunshot wounds Warning: This presentation has extremely graphic pictures! Richard P. Kness, EMT- P Objectives After this lesson the student will be able to: List scene safety issues Describe procedures
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer
 Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
Adult, Child, and Infant Written Exam CPR Pro for the Professional Rescuer Instructions: Read each of the following questions carefully and then place an X over the correct answer on the separate answer
EMR Instructional Guidelines. Preparatory
 EMR Instructional Guidelines Preparatory EMS Systems Uses simple knowledge of the EMS system, safety/well being of the EMR, medical/legal issues at the scene of an emergency while awaiting a higher level
EMR Instructional Guidelines Preparatory EMS Systems Uses simple knowledge of the EMS system, safety/well being of the EMR, medical/legal issues at the scene of an emergency while awaiting a higher level
EYE, EAR, NOSE, and THROAT INJURIES
 T6 EYE, EAR, NOSE, and THROAT INJURIES Management of injuries of the eyes, ears, nose, and throat focuses on airway management and initial stabilization of the injury. Bilateral comparisons can assist
T6 EYE, EAR, NOSE, and THROAT INJURIES Management of injuries of the eyes, ears, nose, and throat focuses on airway management and initial stabilization of the injury. Bilateral comparisons can assist
Emergency Medical Technician - Basic
 Washington State Specific Objectives for Emergency Medical Technician - Basic OFFICE OF EMERGENCY MEDICAL AND TRAUMA PREVENTION September 1996 Emergency Medical Technician - Basic Definition: Emergency
Washington State Specific Objectives for Emergency Medical Technician - Basic OFFICE OF EMERGENCY MEDICAL AND TRAUMA PREVENTION September 1996 Emergency Medical Technician - Basic Definition: Emergency
Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
 Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
Overview Estimated scenario time: 10 15 minutes Estimated debriefing time: 10 minutes Target groups: Paramedics, nurses, respiratory therapists, physicians, and others who manage respiratory emergencies.
EPINEPHRINE AUTO-INJECTOR TRAINING POLICY ALLERGIC REACTION / ANAPHYLAXIS
 Page 1 of 1 EPINEPHRINE AUTO-INJECTOR TRAINING POLICY ALLERGIC REACTION / ANAPHYLAXIS All members/employees of (service) affiliate number must complete DOH training module #004124 and be familiar with
Page 1 of 1 EPINEPHRINE AUTO-INJECTOR TRAINING POLICY ALLERGIC REACTION / ANAPHYLAXIS All members/employees of (service) affiliate number must complete DOH training module #004124 and be familiar with
Confined Space Rescue
 Both the Building Code and Fire Code require us to have a suitable emergency response plan to get our workers to safety. The confined space legislation puts confined space rescue squarely on the shoulders
Both the Building Code and Fire Code require us to have a suitable emergency response plan to get our workers to safety. The confined space legislation puts confined space rescue squarely on the shoulders
3/24/2014. Waubonsee Community College Safety Day 2014. Why do we need a First Aid Program?
 Waubonsee Community College Safety Day 2014 Why do we need a First Aid Program? 4,383 workers were killed on the job in 2012 Total recordable non fatal cases: 2,976,400 in 2012 Cases involving days away
Waubonsee Community College Safety Day 2014 Why do we need a First Aid Program? 4,383 workers were killed on the job in 2012 Total recordable non fatal cases: 2,976,400 in 2012 Cases involving days away
Certified Athletic trainers should follow a 10-step process of evaluation for orthopedic injuries, which includes but is not limited to:
 Acute Care Policy Acute Care Policy and Procedures Athletic training students within Winona State University s Athletic Training Education Program have the opportunity to evaluate acute athletic injuries
Acute Care Policy Acute Care Policy and Procedures Athletic training students within Winona State University s Athletic Training Education Program have the opportunity to evaluate acute athletic injuries
Basic ATLS. The Primary Survey. Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon
 Basic ATLS The Primary Survey Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon Trauma - expression comprising a spectrum of severity of mechanical violation of tissues, from a little scratch to a multiply
Basic ATLS The Primary Survey Jason Smith MD DMI FRCS(Gen.Surg) Consultant Surgeon Trauma - expression comprising a spectrum of severity of mechanical violation of tissues, from a little scratch to a multiply
INTERNATIONAL TRAUMA LIFE SUPPORT
 INTERNATIONAL TRAUMA LIFE SUPPORT NEEDLE DECOMPRESSION OF TENSION PNEUMOTHORAX Roy Alson, MD, PhD, FACEP, FAAEM and Sabina Braithwaite, MD, MPH, FACEP INTRODUCTION The purpose of this document is to update
INTERNATIONAL TRAUMA LIFE SUPPORT NEEDLE DECOMPRESSION OF TENSION PNEUMOTHORAX Roy Alson, MD, PhD, FACEP, FAAEM and Sabina Braithwaite, MD, MPH, FACEP INTRODUCTION The purpose of this document is to update
CHAPTER 1 DISASTER FIRST AID INTRODUCTION
 CHAPTER 1 DISASTER FIRST AID INTRODUCTION This chapter will cover the following topics: Introduction: The basic concepts of providing disaster first aid and the equipment required to safely respond to
CHAPTER 1 DISASTER FIRST AID INTRODUCTION This chapter will cover the following topics: Introduction: The basic concepts of providing disaster first aid and the equipment required to safely respond to
OSDH EMS EMERGENCY MEDICAL RESPONDER
 OSDH EMS EMERGENCY MEDICAL RESPONDER Recommended Training Hours for National Education Standard OSDH 2011 Approved: Oklahoma Training and Licensure SubCommittee November 17 th, 2011 Approved: Oklahoma
OSDH EMS EMERGENCY MEDICAL RESPONDER Recommended Training Hours for National Education Standard OSDH 2011 Approved: Oklahoma Training and Licensure SubCommittee November 17 th, 2011 Approved: Oklahoma
COALINGA STATE HOSPITAL. Effective Date: August 31, 2006
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 715 Effective Date: August 31, 2006 SUBJECT: EMERGENCY CARE OF HEMORRHAGE 1. PURPOSE: The management
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 715 Effective Date: August 31, 2006 SUBJECT: EMERGENCY CARE OF HEMORRHAGE 1. PURPOSE: The management
.org. Fractures of the Thoracic and Lumbar Spine. Cause. Description
 Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Fractures of the Thoracic and Lumbar Spine Page ( 1 ) Spinal fractures can vary widely in severity. While some fractures are very serious injuries that require emergency treatment, other fractures can
Types of electrical injuries
 Types of electrical injuries Electrical injury is a term for all injuries caused by contact with electrical energy. Electrical contact can cause a wide variety of injuries involving most organ systems.
Types of electrical injuries Electrical injury is a term for all injuries caused by contact with electrical energy. Electrical contact can cause a wide variety of injuries involving most organ systems.
Obstetrical Emergencies
 Date: July 18, 2014 Page 1 of 5 Obstetrical Emergencies Purpose: To provide the process for the assessment and management of the patient with an obstetrical related emergency. Pre-Medical Control 1. Follow
Date: July 18, 2014 Page 1 of 5 Obstetrical Emergencies Purpose: To provide the process for the assessment and management of the patient with an obstetrical related emergency. Pre-Medical Control 1. Follow
6.0 Management of Head Injuries for Maxillofacial SHOs
 6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
6.0 Management of Head Injuries for Maxillofacial SHOs As a Maxillofacial SHO you are not required to manage established head injury, however an awareness of the process is essential when dealing with
Scenario 2 Is it ever safe enough?
 IRECA BLS Competition 2011 Scenario 2 Is it ever safe enough? Team Name Captain Name Judge 1 Judge 2 The Event: You are dispatched to a shooting for two injured at a local bar. Witnesses have told police
IRECA BLS Competition 2011 Scenario 2 Is it ever safe enough? Team Name Captain Name Judge 1 Judge 2 The Event: You are dispatched to a shooting for two injured at a local bar. Witnesses have told police
First Aid as a Life Skill. Training Requirements for Quality Provision of Unit Standard-based First Aid Training
 First Aid as a Life Skill Training Requirements for Quality Provision of Unit Standard-based First Aid Training New Zealand Qualifications Authority 2010 2 Index Introduction 3 Section One: Framework outline
First Aid as a Life Skill Training Requirements for Quality Provision of Unit Standard-based First Aid Training New Zealand Qualifications Authority 2010 2 Index Introduction 3 Section One: Framework outline
Emergency Medical Responder Mid-Course Knowledge Evaluation
 Emergency Medical Responder Mid-Course Knowledge Evaluation Please do not write on this sheet. Indicate your answers on the answer sheet provided. 1. Medical control is the process by which a physician
Emergency Medical Responder Mid-Course Knowledge Evaluation Please do not write on this sheet. Indicate your answers on the answer sheet provided. 1. Medical control is the process by which a physician
MODULE III PLANNING &TRIAGE
 MODULE III PLANNING &TRIAGE PLANNING By failing to prepare, you are preparing to fail Benjamin Franklin OBJECTIVES Discuss the components of disaster planning Review the levels of planning Discuss the
MODULE III PLANNING &TRIAGE PLANNING By failing to prepare, you are preparing to fail Benjamin Franklin OBJECTIVES Discuss the components of disaster planning Review the levels of planning Discuss the
How To Be A Medical Flight Specialist
 Job Class Profile: Medical Flight Specialist Pay Level: CG-36 Point Band: 790-813 Accountability & Decision Making Development and Leadership Environmental Working Conditions Factor Knowledge Interpersonal
Job Class Profile: Medical Flight Specialist Pay Level: CG-36 Point Band: 790-813 Accountability & Decision Making Development and Leadership Environmental Working Conditions Factor Knowledge Interpersonal
Emergency Medical Responder Course Syllabus
 Emergency Medical Responder Course Syllabus Instructor: Assistant Instructor: Instructor Office Hours and Location: One half hour before and after class or by appointment Course Meeting Days and Times:
Emergency Medical Responder Course Syllabus Instructor: Assistant Instructor: Instructor Office Hours and Location: One half hour before and after class or by appointment Course Meeting Days and Times:
ITLS Basic Pre-Test 7 th Edition
 1. Which of the following organs is contained in the retroperitoneal region of the abdomen? A. Stomach B. Liver C. Kidney D. Uterus 2. What is Sellick's maneuver? A. A method allowing the rescuer to hold
1. Which of the following organs is contained in the retroperitoneal region of the abdomen? A. Stomach B. Liver C. Kidney D. Uterus 2. What is Sellick's maneuver? A. A method allowing the rescuer to hold
American Heart Association. Basic Life Support for Healthcare Providers
 American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
American Heart Association Basic Life Support for Healthcare Providers Pretest February 2001 This examination to be used only as a PRECOURSE TEST for BLS for Healthcare Providers Courses 2001 American
EMERGENCY MEDICAL RESPONDER REFRESHER TRAINING PROGRAM Ohio Approved Curriculum
 EMERGENCY MEDICAL RESPONDER REFRESHER TRAINING PROGRAM Ohio Approved Curriculum Instructor Course Guide Ohio Approved EMR Refresher 5-16-2012 Page 1 OHIO APPROVED EMERGENCY MEDICAL RESPONDER REFRESHER
EMERGENCY MEDICAL RESPONDER REFRESHER TRAINING PROGRAM Ohio Approved Curriculum Instructor Course Guide Ohio Approved EMR Refresher 5-16-2012 Page 1 OHIO APPROVED EMERGENCY MEDICAL RESPONDER REFRESHER
S.T.A.R.T SIMPLE TRIAGE AND RAPID TREATMENT
 S.T.A.R.T SIMPLE TRIAGE AND RAPID TREATMENT Incidents which produce multiple human casualties are somewhat rare but do occur and must be planned for. A multiple or mass casualty incident can be defined
S.T.A.R.T SIMPLE TRIAGE AND RAPID TREATMENT Incidents which produce multiple human casualties are somewhat rare but do occur and must be planned for. A multiple or mass casualty incident can be defined
[This page is intentionally left blank]
![[This page is intentionally left blank] [This page is intentionally left blank]](/thumbs/27/11307501.jpg) Drill #3 [This page is intentionally left blank] CERT DRILLS AND EXERCISES: DRILL #3 Table of Contents CERT Drills and Exercises... 1 What is a Drill?... 1 Exercise Overview... 2 For Exercise Staff...
Drill #3 [This page is intentionally left blank] CERT DRILLS AND EXERCISES: DRILL #3 Table of Contents CERT Drills and Exercises... 1 What is a Drill?... 1 Exercise Overview... 2 For Exercise Staff...
American Heart Association
 American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
American Heart Association Basic Life Support for Healthcare Providers Pretest April 2006 This examination to be used only as a PRECOURSE TEST For BLS for Healthcare Providers Courses 2006 American Heart
CHAPTER 32 QUIZ. Handout 32-1. Write the letter of the best answer in the space provided.
 Handout 32-1 QUIZ Write the letter of the best answer in the space provided. 1. All of the following are signs and symptoms in patients with spinal injuries except A. paralysis. C. hyperglycemia. B. priapism.
Handout 32-1 QUIZ Write the letter of the best answer in the space provided. 1. All of the following are signs and symptoms in patients with spinal injuries except A. paralysis. C. hyperglycemia. B. priapism.
100018 100016 100017. Scope of Course Public Safety First Aid and CPR Course Content. (a) The initial course of instruction shall at a minimum
 100018 100016 100017. Scope of Course Public Safety First Aid and CPR Course Content. (a) The initial course of instruction shall at a minimum consist of not less than fifteen (15) hours in first aid and
100018 100016 100017. Scope of Course Public Safety First Aid and CPR Course Content. (a) The initial course of instruction shall at a minimum consist of not less than fifteen (15) hours in first aid and
Vanderbilt University Medical Center Division of Trauma & Surgical Critical Care. Clinical Management Guideline: Standard Trauma Resuscitation
 Vanderbilt University Medical Center Division of Trauma & Surgical Critical Care Clinical Management Guideline: Standard Trauma Resuscitation Global Communication is the key to a well organized and efficient
Vanderbilt University Medical Center Division of Trauma & Surgical Critical Care Clinical Management Guideline: Standard Trauma Resuscitation Global Communication is the key to a well organized and efficient
EMS Patient Care Report Navigation Logic for Record Creation
 EMS Patient Report Navigation Logic for Record Creation This document serves to provide specifications regarding data entry and data element completion requirements for PreMIS Version 2 web-based application
EMS Patient Report Navigation Logic for Record Creation This document serves to provide specifications regarding data entry and data element completion requirements for PreMIS Version 2 web-based application
Lassen Community College Course Outline. EMT-60 Emergency Medical Technician 1 (Basic)
 Lassen Community College Course Outline EMT-60 Emergency Medical Technician 1 (Basic) 6.5 units I. Catalog Description Covers all techniques of emergency medical care and transportation of the sick and
Lassen Community College Course Outline EMT-60 Emergency Medical Technician 1 (Basic) 6.5 units I. Catalog Description Covers all techniques of emergency medical care and transportation of the sick and
(ISBN:9781449604103) Preferred Package Digital Supplement
 College of DuPage Technology Center of DuPage 10 Semester Credit Hours E-mail: [email protected] Phone Number: 630-691-7561 Class meets on: Monday through Friday Morning Session Students: 8:00 am -10:50am
College of DuPage Technology Center of DuPage 10 Semester Credit Hours E-mail: [email protected] Phone Number: 630-691-7561 Class meets on: Monday through Friday Morning Session Students: 8:00 am -10:50am
Pediatric Airway Management
 Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
Pediatric Airway Management Dec 2003 Dr. Shapiro I., PICU Adult Chain of Survival EMS CPR ALS Early Defibrillation Pediatric Chain of Survival Prevention CPR EMS ALS Out-of-Hospital Cardiac Arrest SIDS
2 CHECKING AN INJURED OR ILL ATHLETE
 American Red Cross 2 CHECKING AN INJURED OR ILL ATHLETE ~~~'1'H ~.. 2 CHECKING AN INJURED OR III ATHLETE Checking the scene for safety and checking an injured or ill athlete is the first action to take,
American Red Cross 2 CHECKING AN INJURED OR ILL ATHLETE ~~~'1'H ~.. 2 CHECKING AN INJURED OR III ATHLETE Checking the scene for safety and checking an injured or ill athlete is the first action to take,
The Phoenix Document An Evolution from National Standard Curriculum to the Virginia EMS Education Standards
 The Phoenix Document An Evolution from National Standard Curriculum to the Virginia EMS Education Standards Training Levels Included: Emergency Medical Responder (EMR) Last Revised: January 19, 2011 Page
The Phoenix Document An Evolution from National Standard Curriculum to the Virginia EMS Education Standards Training Levels Included: Emergency Medical Responder (EMR) Last Revised: January 19, 2011 Page
ENT Emergencies. Injuries of the Neck. Registrar Dept Trauma and emergency Medicine Tygerberg Hospital
 ENT Emergencies Injuries of the Neck Registrar Dept Trauma and emergency Medicine Tygerberg Hospital Neck Injuries Blunt and Penetrating Trauma Blunt Injuries Blunt trauma direct/indirect Trauma to larynx
ENT Emergencies Injuries of the Neck Registrar Dept Trauma and emergency Medicine Tygerberg Hospital Neck Injuries Blunt and Penetrating Trauma Blunt Injuries Blunt trauma direct/indirect Trauma to larynx
Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma
 Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma Chapter 50 Abdominal Trauma 1 Describe the epidemiology, including morbidity, mortality rates, and prevention strategies,
Aehlert: Paramedic Practice Today PowerPoint Lecture Notes Chapter 50: Abdominal Trauma Chapter 50 Abdominal Trauma 1 Describe the epidemiology, including morbidity, mortality rates, and prevention strategies,
2. (U4C2L3:F2) If your friend received a deep cut on her wrist, what would you do?
 Cadet Name: Date: 1. (U4C2L3:F1) Your friend receives a deep cut on her wrist while washing dishes. She asks for your help. How confident are you that you could provide appropriate aid? A) My friend is
Cadet Name: Date: 1. (U4C2L3:F1) Your friend receives a deep cut on her wrist while washing dishes. She asks for your help. How confident are you that you could provide appropriate aid? A) My friend is
United States Department of Transportation National Highway Traffic Safety Administration Paramedic: National Standard Curriculum 1
 UNIT TERMINAL OBJECTIVE 4-8 At the completion of this unit, the paramedic student will be able to integrate pathophysiologic principles and the assessment findings to formulate a field impression and implement
UNIT TERMINAL OBJECTIVE 4-8 At the completion of this unit, the paramedic student will be able to integrate pathophysiologic principles and the assessment findings to formulate a field impression and implement
Emergency Medical Technician-I. Scenarios for Training
 Emergency Medical Technician-I Scenarios for Training Revised March 1, 1995 Alaska Emergency Medical Services Section Division of Public Health Department of Health and Social Services Box 110616 Juneau,
Emergency Medical Technician-I Scenarios for Training Revised March 1, 1995 Alaska Emergency Medical Services Section Division of Public Health Department of Health and Social Services Box 110616 Juneau,
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK
 CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
CPR/AED for Professional Rescuers and Health Care Providers HANDBOOK TABLE OF CONTENTS SECTION 1: THE PROFESSIONAL RESCUER The Duty to Respond 2 Preventing the Spread of Bloodborne Pathogens 3 Taking Action
Intermedix Inc. EMR 2006 Data Element Name. Compliant. Data Number. Elements
 D01_01 EMS Agency X D01_02 EMS Agency D01_03 EMS Agency State X D01_04 EMS Agency County X D01_05 Primary Type of Service D01_06 Other Types of Service D01_07 Level of Service X D01_08 Organizational Type
D01_01 EMS Agency X D01_02 EMS Agency D01_03 EMS Agency State X D01_04 EMS Agency County X D01_05 Primary Type of Service D01_06 Other Types of Service D01_07 Level of Service X D01_08 Organizational Type
CHAPTER 6 HEAD INJURY AND UNCONSCIOUSNESS
 CHAPTER 6 HEAD INJURY AND UNCONSCIOUSNESS BRAIN INJURY Injury to the brain is one of the more serious outcomes that occur due to injury or illness. The first aider plays a major role in limiting damage
CHAPTER 6 HEAD INJURY AND UNCONSCIOUSNESS BRAIN INJURY Injury to the brain is one of the more serious outcomes that occur due to injury or illness. The first aider plays a major role in limiting damage
STATE OF CONNECTICUT
 STATE OF CONNECTICUT DEPARTMENT OF PUBLIC HEALTH June 7, 2010 The Following Will Be Policy For Emergency Medical Service Care Providers: GUIDELINES FOR EMR, EMT, AEMT, and Paramedic DETERMINATION OF DEATH/DISCONTINUATION
STATE OF CONNECTICUT DEPARTMENT OF PUBLIC HEALTH June 7, 2010 The Following Will Be Policy For Emergency Medical Service Care Providers: GUIDELINES FOR EMR, EMT, AEMT, and Paramedic DETERMINATION OF DEATH/DISCONTINUATION
Emergency Action Plans
 Emergency Action Plans Clearly the most effective way to deal with an injury- emergency is to plan ahead and to practice the appropriate procedures. An emergency action plan is a written plan of action
Emergency Action Plans Clearly the most effective way to deal with an injury- emergency is to plan ahead and to practice the appropriate procedures. An emergency action plan is a written plan of action
81 First Responder Respiratory
 81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
81 First Responder Medical Scenarios Asthma Scenario: You are called to a local house for a woman with trouble breathing. You arrive to find a 67-year-old woman sitting upright in a chair. She states she
Module 5 ADULT RECOvERY POSITION STEP 1 POSITION ThE victim
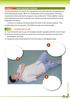 Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
Module 5 ADULT RECOVERY POSITION The recovery position is used in the management of victims who are unresponsive but have breathing and pulse. When an unresponsive victim is lying supine, the airway may
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course
 Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Success Manual and Cheat Sheet Notes to Pass Your Basic Life Support (BLS) Course Written by: Jay Snaric, MS And Kimberly Hickman, RN CPR St. Louis 44 Meramec Valley Plaza St. Louis MO 63088 www.stlcpr.com
Obstetric Emergencies
 Obstetric Emergencies Dr. Si Lay Khaing Senior Lecturer/ O&G Specialist Faculty of Medicine University of Malaya 15 th March 2014 Abstract Life Saving, The obstetric patient is unique in medicine as two
Obstetric Emergencies Dr. Si Lay Khaing Senior Lecturer/ O&G Specialist Faculty of Medicine University of Malaya 15 th March 2014 Abstract Life Saving, The obstetric patient is unique in medicine as two
Oxygen - update April 2009 OXG
 PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
PRESENTATION Oxygen (O 2 ) is a gas provided in compressed form in a cylinder. It is also available in liquid form, in a system adapted for ambulance use. It is fed via a regulator and flow meter to the
EMR Medical Directives and Guidelines
 EMR Medical Directives and Guidelines Central East Prehospital Care Program, May 1, 2009 Section One 1 USE OF MEDICAL DIRECTIVES / GUIDELINES These medical directives and guidelines are not intended to
EMR Medical Directives and Guidelines Central East Prehospital Care Program, May 1, 2009 Section One 1 USE OF MEDICAL DIRECTIVES / GUIDELINES These medical directives and guidelines are not intended to
New York State Department of Health Bureau of Emergency Medical Services
 New York State Department of Health Bureau of Emergency Medical Services Statewide Basic Life Support Adult & Pediatric Treatment Protocols EMT-B and AEMT 2008 Updated 11/20/08 = Preface and Acknowledgments
New York State Department of Health Bureau of Emergency Medical Services Statewide Basic Life Support Adult & Pediatric Treatment Protocols EMT-B and AEMT 2008 Updated 11/20/08 = Preface and Acknowledgments
By Accident. OEC Edition Fall 2012
 By Accident OEC Edition Fall 2012 As we get ready for the winter, it is time to think about refreshing our first aid training, dusting off our skills before the ski season starts and getting ready another
By Accident OEC Edition Fall 2012 As we get ready for the winter, it is time to think about refreshing our first aid training, dusting off our skills before the ski season starts and getting ready another
Contact your Doctor or Nurse for more information.
 A spinal cord injury is damage to your spinal cord that affects your movement, feeling, or the way your organs work. The injury can happen by cutting, stretching, or swelling of the spinal cord. Injury
A spinal cord injury is damage to your spinal cord that affects your movement, feeling, or the way your organs work. The injury can happen by cutting, stretching, or swelling of the spinal cord. Injury
ITLS Advanced Pre-Test 7 th Edition
 1. A 34 year old man is injured in a motor vehicle collision. Physical examination is normal except for diffuse abdominal tenderness. He is conscious and vital signs obtained enroute to the hospital are
1. A 34 year old man is injured in a motor vehicle collision. Physical examination is normal except for diffuse abdominal tenderness. He is conscious and vital signs obtained enroute to the hospital are
