The Ohio State University Department of Orthopaedics. Residency Curriculum. Sports Medicine
|
|
|
- Marvin Richardson
- 8 years ago
- Views:
Transcription
1 The Ohio State University Department of Orthopaedics Residency Curriculum Sports Medicine
2 About This Curriculum It is the responsibility of both the resident and the attending to go over the goals and guidelines included in this handbook o At the beginning of the rotation o At the conclusion of the rotation Additional materials and/or service handbooks may be provided by the attendings at the beginning of the rotation
3 The Ohio State University Department of Orthopaedics Orthopaedic Residency Program Revised 6/29/10 Sports Medicine Service Information - OSU Christopher C. Kaeding M.D. Director, Division of Sports Medicine Office: Office address: Martha Morehouse, 3 rd floor, Sports Medicine: OSU SMC 2050 Kenny Rd, Columbus, OH Grant Jones, MD Pager: grant.jones@osumc.edu Office: Martha Morehouse, 3 rd floor, Sports Medicine Dave Flanigan, MD Pager: david.flanigan@osumc.edu Office: Martha Morehouse, 3 rd floor, Sports Medicine Julie Bishop, MD Pager: Julie.bishop@osumc.edu Office: Martha Morehouse, 3 rd floor, Sports Medicine Rob Najarian, MD Pager: Robert.najarian@osumc.edu Office: Care Point Gahanna Amber Thompson, Administrative Assistant to Dr Kaeding Phone: Fax: amber.thompson2@osumc.edu Michelle Rogers, Administrative Assistant to Dr Jones Phone: office Fax: michelle.rogers@osumc.edu Yvonne Daugherty, Administrative Assistant to Dr Flanigan Phone: Fax:
4 Courtney Dalrymple, Administrative Assistant to Dr Bishop Phone: Fax: Rose Backs PA-C (Clinical Dr Kaeding) Cell: Melissa Bowlby, PA-C (Clinical Dr Jones) Cell: Pager: Stephanie Stradley, PA-C (Clinical Dr Flanigan) Cell: Pager: David Agbunag, PA-C (Clinical Dr Bishop) Cell: Pager: Schedules During the 2 month rotation, the PGY 4 sports resident will rotate with the attendings that do not have a sports fellow on their service. The goal is for the resident to have a near even split of sports knee and shoulder, thus you will spend time with several of the attendings throughout your work week and 2 months rotation. However, the schedules are flexible to allow the resident to participate in and see unique cases and also cover an attending that is in need of assistance. Dr Kaeding Monday am: Administrative / research meetings Monday noon 6pm Clinic (Stoneridge) Tuesday 7-3: surgery, OSU east Tuesday 4 7 training room Wednesday 7 3 surgery, OSU east Wednesday 4 7 training room Thursday 9 5 Clinic (Morehouse) Friday 7 5 education conferences, administrative / research meetings Dr Jones Monday: OR, OSU east, 7am Tuesday: clinic, Morehouse 2 nd Tuesday prison cases at Main Wednesday: clinic, Morehouse 3 rd Wednesday prison cases at Main Thursday: OR, OSU east, 8am Friday: academic time, except 3 rd Friday: clinic at Morehouse 38
5 Dr Flanigan Monday: office at Morehouse, 7:30 5pm Tuesday: OR, OSU east 7am First Tuesday of the month is prison cases at OSU main Wednesday: office at Morehouse, 7:30 5pm Thursday: OR, OSU east 8am Friday: academic day or multi-lig cases Dr Bishop Monday: Clinic at Martha Morehouse, 7:30 am 5pm Tuesday: OR at OSU east, 7am Wednesday: 1 st,2 nd,5 th : Clinic at Stoneridge: 8am 3 rd Wed: Clinic at Morehouse: 8am 3pm 4 th Wed: Prison cases at OSU Main Thursday: OR at OSU east, 8am Friday: 1-3 rd Friday: academic time versus add on cases 4 th Friday Prison cases after conference Dr Najarian Monday: OR at OSU east, 7am Tuesday: Clinic at Care Point Gahanna: 8:30 5pm Wednesday: OR at OSU east, 12-5pm Thursday: Clinic at Care Point Gahanna: 8:30 am 5pm Friday: academic day except 2 nd Friday: 1-4 pm clinic at Martha Morehouse 39
6 The Ohio State University Department of Orthopaedics Orthopaedic Residency Program Revised 6/29/10 Dilineation of Resident Resposnibilities: Sports Medicine Service: PGY4 I. Resident Responsibilites for Patient Care Rounding: During the course of your rotation, patients may be admitted before and or after surgery. The expectation is for the resident to know about and round on all inpatient surgical patients, even if you were not involved in the case. This is particularly important on the weekends. As of now, there is a rotating senior resident rounding on the weekends at OSU East. If you are not rounding for the weekend, please sign out all Sports Service patients to the resident rounding. Please have the resident call the attending after rounds to discuss issues and management. IF you go out of town, please arrange coverage for the rounding of inpatients. DO NOT make the attending find someone to round on their patients take care of this prior to leaving. Orders: Orders will be done via the current order entry system. There are order sets for UE postop orders and also for LE and sports cases. Consult MMT on all sports patients that were admitted. Order X-rays in the PACU on all patients that underwent any type of fixation or implant. Dictations: Most of the sports medicine attendings do dictate their own operative notes. However, there will be times when you are responsible for the dictation. Before the patient leaves the OR, the decision should be made as to who will be responsible for the dictation. You will be expected to dictate at least one operative report and review this with the attending prior to the conclusion of the service. Post-Op Radiographs: As above all patients that undergo any type of hardware fixation or implant will get radiographs in the PACU. If it is the last case of the day DO NOT LEAVE until you see the x-rays were completed and you view them. Dressings/drains: If the patients are still in the hospital all dressings are changed on POD 2 you do the dressing change and look at the wound NOT the nurse. If there is a drain check with that individual attending for when to pull the drain. Discharge: Most sports medicine patients will be outpatient surgeries. You will be responsible to coordinate with the PA s filling out the discharge paperwork, instruction sheets, rehab orders and pain medication scripts. Pain medication is unique to each attending and should be discussed with the attending staff for preferences. Discharge paperwork is unique to each attending and you should discuss with the respective attending how they approach this. If there are any inpatients for the service you will be responsible for the discharge summaries for all inpatients, whether or not you participated in their surgery. Please do this on the day of discharge. Communication: Many questions will certainly arise and should be addressed on an as needed basis. Constant communication between all members of the health care team is the best way to get an optimal educational experience and provide the best care possible for each patient. Clinic Notes: Resident should be able to create appropriate notes in EPIC for each patient encounter. They should discuss with each attending how to include the pertinent smart sets/phrases to help.
7 II. Resident Level of Responsibility for Patient Care Please understand that patients are real people whom have developed a relationship with the attending physician. They are not limbs or extremities for you to practice surgery skills. Please give the patient and your attending respect by your professionalism, preparation, and diligent hard work. You will in turn learn more and provide confidence in your attending physicians. Resident rotations are structured so that the residents have a one-on-one relationship with attendings. The level of responsibility given by the attending to the resident is determined by that attending, depending on the attendings assessment of the resident s knowledge and skills, and the complexity of the procedure. Residents will be expected to be prepared for clinic and OR Thorough knowledge of the surgery, surgical approach, and the reasoning, biomechanics, placement, and technique of the surgical reconstuctions/repair and implants used. Questions related to any case should be discussed with the attending prior to the case (preferably the day before) Residents should see and exam the patient prior to surgery and are EXPECTED to have reviewed all the patient office notes and radiographic studies. Lack of preparation will prevent participation III. Resident Supervision Attendings are responsible for the direct supervision of residents in both the clinic and the operating room, as well as in on-call situations. Attending physicians are available for consultation at all times. Senior residents (PGY4 and above) are also directly responsible for the supervision of junior residents (PGY1, PGY2, and PGY3). This applies to all of the above situations (i.e. on-call, in clinic, in the OR). Senior residents must be available for consultation at all times. Ultimately, chief residents (all PGY5 s) are responsible for the supervision of all residents, regardless of PGY year. IV. Performance Feedback Both attending staff members are available at any time if questions or concerns arise. At the end of each rotation, each attending on the service will evaluate each resident assigned to the service. A meeting should be scheduled at the conclusion of the rotation to discuss performance and provide written feedback on the rotation. Resident should arrange a mid-rotation meeting with the primary attendings that they are working with to discuss performance and assess if goals are being met.
8 Goals and Objectives Sports Medicine Rotation PGY3 I. Core Competency Areas By the end of the PGY3 rotation in Sports Medicine, the resident should demonstrate progress towards obtaining excellence in each of the following core competency areas. Patient Care 1. Demonstration of caring and respectful behaviors when interacting with patients and families 2. Procurement of thorough, logical, and concise patient histories with an emphasis on the musculoskeletal system 3. Responsiveness to the individual needs of patients and their families 4. Performance of physical examinations that are accurate, comprehensive, and directed to patient s problems. This applies to the clinic, emergency department, and in-patient settings. 5. Integration of medical facts and clinical data as the basis for diagnosis 6. Evaluation of risks, benefits, and alternative treatments 7. Formulation and carry out of a complete and effective treatment plan (operative and non-operative) 8. Counsel of patient and family in treatment procedure, options, and potential outcomes 9. Dissemination of education and services to the patient which are aimed at preventing treatment complications and maintaining health 10. Understanding of and performance of medical procedures related to treatment plan 11. Ability to work well with entire team of health care professionals and be involved in care of the patient Medical Knowledge 1. Exhibition of a fund of medical knowledge that is up-to-date and ability to cite literature appropriately 2. Investigation of topics as needed for clinical assignments 3. Understanding and use of basic science principles as related to medical practice Practice-Based Learning 1. Assessment of ones own patient management skills and ability to make appropriate changes in practice 2. Integration of evidence from scientific studies in the care of patient s problems 3. Demonstration of knowledge of study designs and statistical methods in order to evaluate scientific studies 4. Usage of available information technology to obtain and manage information 5. Willingness to take time to educate students and other health care professionals Interpersonal Skills 1. Fostering of a compassionate, therapeutic relationship with patients and their families 2. Ability to listen to patients and include them in treatment decisions 3. Ability to listen to information provided by other members of the health care team Professionalism 1. Respectfulness of patient wishes and ability to provide adequate counseling, education, and informed consent instructions to patients 2. Demonstration of an ethically sound practice of medicine 3. Demonstration of sensitivity to cultural, age, gender, and disability issues among patients
9 Systems-Based Practice 1. Knowledge of how to provide cost-effective care 2. Willingness to advocate for patients within the health care system 3. Referral of patient to appropriate practitioners and agencies within the health care system 4. Accessing of consultants appropriately and use of their assistance in the management of ongoing care II. Specialty Specific Knowledge By the end of the PGY3 rotation in Sports Medicine, the resident should: 1. Understand physical therapy modalities in general sports medicine 2. Understand and describe the pertinent clinical anatomy of the shoulder, elbow, knee, leg, ankle, and foot 3. Understand and weigh surgical risk and potential benefit for each patient for each surgical procedure considered. 4. Understand and describe the clinical anatomy and biomechanics of the shoulder 5. Understand and describe the mechanics of the throwing motion 6. Understand and describe the relationship between shoulder instability and rotator cuff tendinitis 7. Understand and describe the relationship between impingement and rotator cuff tears. 8. Describe the pathophysiology and the rationale for non-operative treatment of the following pathologic entities related to the shoulder: rotator cuff tendinitis/tear/impingement, Gleno-humeral instability, adhesive capsulitis 9. Describe the indications and rationale for the following procedures related to the shoulder (describe both open and arthroscopic variations of the procedure, indication for each, and rehabilitation protocol): Rotator cuff repair, subacromial decompression, stabilization procedures, Mumford procedure. 10. Understand the differential diagnosis and treatment for anterior knee pain and patellar instability. 11. Understand the typical history and presentation of Anterior or Posterior Cruciate Ligament Injuries 12. Be familiar with the various types of knee braces 13. Understand the healing potential and current treatment options of meniscal tears and chondral defects. 14. Understand the presentation and pathology of meniscal cysts and discoid menisci 15. Understand the non-operative treatment of patella tendinitis, saphenous neuritis, and MCL sprains 16. Understand the post-operative rehabilitation of meniscal repairs and ACL reconstructions 17. Understand the presentation, evaluation and treatment of common post-operative complications of infection and deep venous thrombosis 18. Understand and describe the pathophysiology of Compartment Syndrome 19. Understand and describe the pathophysiology of Stress Fracture 20. Be familiar with special radiographic examinations of the leg and thigh including MRI, CT, and nuclear medicine studies 21. Discuss the possible etiologies of peroneal nerve injury and recognize the signs of peroneal nerve injury. 22. Understand the pathophysiology and presentation of OCD of the talus 23. Understand the pertinent clinical anatomy and biomechanics of the ankle. 24. Understand the non-operative treatment of the following related to the ankle: Peroneal or posterior tibialis tendinitis, ankle sprains, achilles tendinitis, ankle instability 25. Understand the pathophysiology and presentation of the following related to the ankle: the different types of achilles tendinitis, the different types of ankle sprainos, and ankle instability. 26. Understand the presentation and the non-operative treatment of the following related to the elbow: lateral epicondylitis, medial epicondylitis, UCL sprains, ulnar neuritis, olecranon bursitis, and radial head fractures. 27. Understand the pertinent clinical anatomy and biomechanics of the elbow. 28. Understand the pathology and presentation of Panner s Disease (OCD capitellum) and Valgus extension overload
10 III. Specialty Specific Psychomotor Skills By the end of the PGY3 rotation in Sports Medicine, the resident should be able to: 1. Write a concise physical therapy prescription 2. Write a physical therapy prescription for the following related to the shoulder: Rotator cuff tendinitis/tear/impingement, gleno-humeral instability, adhesive capusulitis, rotator cuff repair, subacromial decompression, stabilization procedures, and the Mumford procedure. 3. Perform a physical examination of the shoulder and identify all pertinent anatomic landmarks, quantify range of motion, evaluate glenohumeral stability of the rotator cuff and the AC joint 4. Make a clinical diagnosis of the following: Adhesive capsulitis, anterior instability, posterior instability, rotator cuff tendinitis, impingement syndrome, AC joint arthrosis, AC joint separation and grade, and biceps rupture. 5. Identify all pertinent anatomic landmarks of the knee. 6. Evaluate knee range of motion. 7. Make a clinical diagnosis of the following related to the shoulder: labral tear and rotator cuff tear. 8. Know the indications for and perform the following procedures related to the shoulder: distal clavicle excision and open decompression. 9. Evaluate and grade knee stability in varus/valgus, anterior/posterior, and rotatory directions using appropriate clinical tests 10. Make a clinical diagnosis of the following: ACL tear, PCL ter, MCL injury/tear, LCL injury/tear, chondromalacia patella, patella instability, degenerative arthritis, pre-patella bursitis, tibial plateau fracture, quadriceps rupture, patellar tendon rupture, knee dislocation. 11. Make a clinical diagnosis of the following related to the knee: Posterior lateral corner injuries, meniscal tear, loose body, synovitis, plica syndrome, and VMO avulsion 12. Perform and ORIF patella procedure 13. Diagnose and describe the nonoperative treatment of the following related to the thigh/leg: quadriceps contusion, hamstring tear/strain, quadriceps strain/tear, hip flexor/adductor strain/tear, stress fracture of femur or tibia, shin splints, and gastrocnemius strain/tear. 14. Know the indication for and perform the following procedures related to the knee: diagnostic arthroscopy, arthroscopic debridement, partial meniscectomy, abrasion chondroplasty, and patellar tendon repair. 15. Diagnose and describe the non-operative treatment of exertional compartment syndrome, medial tibial stress syndrome, and stress and traumatic fractures of the tibia and fibula. 16. Diagnose the following related to the Leg and Thigh: Exertional compartment syndrome, medial tibial stress syndrome, shin splints, gastrocnemius strain/tear, and Maissoneuve fracture/syndesmosis injury. 17. Know the indications for and be able to perform the following procedures related to the leg/thigh: Compartment releases: Anterior, lateral, and posterior. 18. Be able to perform an intramedullary nailing of stress fracture of the tibia and femur 19. Know the indications for and perform the following procedures related to the ankle: diagnostic arthroscopy, ORIF Jones fracture. 20. Know the indications for and perform the following procedures related to the elbow: diagnostic arthroscopy, tennis elbow debridement, ORIF fractures, Olecranon bursa debridement/drainage. 21. Perform a physical examination of the elbow and identify all pertinent landmarks. 22. Evaluate range of motion and stability of the elbow joint. 23. Diagnose the following related to the elbow: Lateral epicondylitis, medial epicondylitis, ulnar nerve entrapment, valgus extension overload, UCL incompetence, biceps tendinitis or distal rupture, OCD of capitellum, and Olecranon bursitis. 24. Perform the following procedures related to the elbow: Decompression of the Ulnar nerve, reduction of dislocation, and saline arthrogram.
11 Goals and Objectives Sports Medicine Rotation PGY4 I. Core Competency Areas By the end of the PGY4 rotation in Sports Medicine, the resident should demonstrate progress towards obtaining excellence in each of the following core competency areas. Patient Care 1. Demonstration of caring and respectful behaviors when interacting with patients and families 2. Procurement of thorough, logical, and concise patient histories with an emphasis on the musculoskeletal system 3. Responsiveness to the individual needs of patients and their families 4. Performance of physical examinations that are accurate, comprehensive, and directed to patient s problems. This applies to the clinic, emergency department, and in-patient settings. 5. Integration of medical facts and clinical data as the basis for diagnosis 6. Evaluation of risks, benefits, and alternative treatments 7. Formulation and carry out of a complete and effective treatment plan (operative and nonoperative) 8. Counsel of patient and family in treatment procedure, options, and potential outcomes 9. Dissemination of education and services to the patient which are aimed at preventing treatment complications and maintaining health 10. Understanding of and performance of medical procedures related to treatment plan 11. Ability to work well with entire team of health care professionals and be involved in care of the patient Medical Knowledge 1. Exhibition of a fund of medical knowledge that is up-to-date and ability to cite literature appropriately 2. Investigation of topics as needed for clinical assignments 3. Understanding and use of basic science principles as related to medical practice Practice-Based Learning 1. Assessment of ones own patient management skills and ability to make appropriate changes in practice 2. Integration of evidence from scientific studies in the care of patient s problems 3. Demonstration of knowledge of study designs and statistical methods in order to evaluate scientific studies 4. Usage of available information technology to obtain and manage information 5. Willingness to take time to educate students and other health care professionals Interpersonal Skills 1. Fostering of a compassionate, therapeutic relationship with patients and their families 2. Ability to listen to patients and include them in treatment decisions
12 3. Ability to listen to information provided by other members of the health care team Professionalism 1. Respectfulness of patient wishes and ability to provide adequate counseling, education, and informed consent instructions to patients 2. Demonstration of an ethically sound practice of medicine 3. Demonstration of sensitivity to cultural, age, gender, and disability issues among patients Systems-Based Practice 1. Knowledge of how to provide cost-effective care 2. Willingness to advocate for patients within the health care system 3. Referral of patient to appropriate practitioners and agencies within the health care system 4. Accessing of consultants appropriately and use of their assistance in the management of ongoing care II. Specialty Specific Knowledge By the end of the PGY4 rotation in Sports Medicine and building upon the experiences from the PGY3 rotation, the resident should: Detailed knowledge of the anatomical structures of the shoulder, elbow, knee and ankle as it relates to sports injuries and surgical approaches and reconstructions Understand anatomy, physiology, and biomechanics as they relate to patients with sports related injuries and disease Understanding of the incidence, natural history, cause, historical features, exam findings, classification, non-operative and operative management of the following key sports related injuries: ankle sprains turf toe 5 th metatarsal fractures lisfranc injuries Achilles pathology Gastroc strains ACL injuries Mensical injuries Osteochondral defects and cartilage injuries Patellofemoral pain syndrome Patella dislocations and instability Quad mechanism injuries Hamstring injuries Stress fractures Multiligament injuries AC sprains and injuries Anterior instability
13 Multidirection instability Rotator cuff pathology and tears SLAP tears Throwing injuries Ulnar collateral ligament injuries Distal biceps ruptures Game keepers injury Mallet finger Jersey finger 4. Understanding of incidence, natural history, cause, historical features, exam findings, classification, and return to play issues with the following sports related injuries: Concussion C-spine injuries Stingers Ankle sprains Muscle injuries Stress fractures 5. Understanding the pre-participation examination and key medical issues in sports medicine: Concussion Ocular trauma Asthma Sudden cardiac death Visceral injury Key infections (Mono, HIV, MRSA, Herpes) Ergogenic aids 6. Be familiar with the various types of knee braces 7. Understand the post-operative protocols for various surgeries and decision making for return to full activities. 8. Understand the presentation, evaluation, and treatment of common post-op complications such as arthrofibrosis. 9. Resident should be able to take a detailed and appropriate injury specific history and formulate a differential of pathology, appropriate tests to order, and appropriate indications for surgery. III. Specialty Specific Psychomotor Skills The attendings do NOT expect PGY4 residents to be doing a complex knee (ie meniscal repair, ACL reconstruction) or complex shoulder (ie Bankart repair, RTC repair) skin to skin on their rotation. The goal is to provide learning the skills that will need to be put together for your prison experience as a PGY5, to know how to assist properly and understand the flow and thinking of these complex sports cases. By the end of the PGY4 rotation in Sports Medicine and building upon the experiences from the PGY3 rotation, the resident should:
14 1. Have a thorough knowledge of the surgery, surgical approach, and the reasoning, biomechanics, placement, and technique of the surgical reconstuctions/repair and implants used. 2. Interpret and synthesize patient history, clinical exam, and diagnostic tests into coherent diagnoses for each condition 3. Perform procedures necessary for the treatment of athletic-associated injuries, including performing the task with a clear understanding of surgical indications 4. In particular, the resident should feel confident in their ability to perform the following at the conclusion of their rotation: Perform a diagnostic knee arthroscopy Perform safely a partial meniscectomy Perform a microfracture Perform graft harvest and preparation in ACL Surgery Doing a notchplasty in ACL surgery Creation of bony tunnels for ACL reconstruction Performing an Achilles repair, patella tendon, or quad tendon repair Perform a diagnostic shoulder arthroscopy Perform a biceps tenotomy Placement of suture anchors in instability or SLAP lesions Passage of suture through the capsule and or labrum Tying arthroscopic suture knot Perform a subacromial decompression Performing a mumford Placement of suture anchors in Rotator cuff tears Understand rotator cuff repair suture management First assist and anticipate all steps of an arthroscopic RCR
15 The Ohio State University Department of Orthopaedics Orthopaedic Residency Program Revised 6/19/10 Physical Exam Competencies Sports Medicine Service: PGY3 and PGY4 By the end of the PGY 4 rotation in sports medicine, the resident should be able to demonstrate proficiency in the key physical examination tests Knee Exam: Normal examination of the knee, including: Inspection Gait Effusion Lower extremity alignment Palpation Medial/lateral joint line tenderness Crepitus Range of motion Flexion/extension Neurovascular testing Special Tests: Patellofemoral Tests: Q angle PF apprehension PF grind/compression PF quadrants J sign Patellar tilt test Meniscal Tests: McMurray s test Apley compression test Deep knee bend Other Tests: Palpable fluid wave Ballotable patella Wilson s test Ligament Stability Tests: Valgus stress test Varus stress test Lachman test Anterior drawer Posterior drawer Posterior sag Quadriceps-active test Pivot shift Reverse pivot shift Dial test External rotation recurvatum test Hughston posterolateral drawer sign Shoulder exam: Normal examination of the shoulder, including: Inspection: atrophy, deformity, skin changes, prior scars, etc.
16 Special Tests: Palpation: AC joint Greater tuberosity Bicipital groove Coracoid process Range of motion: Internal/external rotation Forward elevation Abduction/adduction Neurovascular testing Instability Testing: Load and shift test Apprehension test Relocation sign Posterior apprehension sign Sulcus sign (with and without external rotation) Generalized ligamentous laxity Rotator Cuff Testing: Jobe test (empty can test) External rotation lag sign Hornblower s sign Resisted external rotation at the side and at 90 abduction Lift off Belly press Drop arm Impingement Testing: Neer/Impingement sign Hawkin s test Neer Impingement test Other Tests: Cross body adduction Yergason s test Speed s test Active compression (O brien s test) Scapular winging/scapular stabilization Adson s test (thoracic outlet syndrome) Spurling s test (cervical spine involvement)
17 The Ohio State University Department of Orthopaedics Orthopaedic Residency Program Revised 6/10 Surgical Competencies Sports Medicine Service: PGY3 By the end of the PGY3 rotation in Sports Medicine, the resident should be able to perform the following procedures: 1. Perform a diagnostic knee arthroscopy 2. Perform safely a partial meniscectomy 3. Perform a microfracture 4. Perform graft harvest and preparation in ACL Surgery 5. Doing a notchplasty in ACL surgery 6. Creation of bony tunnels for ACL reconstruction 7. Performing an Achilles repair, patella tendon, or quad tendon repair 8. Perform a diagnostic shoulder arthroscopy 9. Perform a biceps tenotomy 10. Placement of suture anchors in instability or SLAP lesions 11. Passage of suture through the capsule and or labrum 12. Tying arthroscopic suture knot 13. Perform a subacromial decompression 14. Performing a mumford 15. Placement of suture anchors in Rotator cuff tears 16. Understand rotator cuff repair suture management 17. First assist and anticipate all steps of an arthroscopic RCR
18 The Ohio State University Department of Orthopaedics Orthopaedic Residency Program Revised 7/15/10 Surgical Competencies Sports Medicine Service: PGY4 By the end of the PGY4 rotation in Sports Medicine, the resident should be able to perform the following procedures: 1. Perform a diagnostic knee arthroscopy 2. Perform safely a partial meniscectomy 3. Perform a microfracture 4. Perform graft harvest and preparation in ACL Surgery 5. Doing a notchplasty in ACL surgery 6. Creation of bony tunnels for ACL reconstruction 7. Performing an Achilles repair, patella tendon, or quad tendon repair 8. Perform a diagnostic shoulder arthroscopy 9. Perform a biceps tenotomy 10. Placement of suture anchors in instability or SLAP lesions 11. Passage of suture through the capsule and or labrum 12. Tying arthroscopic suture knot 13. Perform a subacromial decompression 14. Performing a mumford 15. Placement of suture anchors in Rotator cuff tears 16. Understand rotator cuff repair suture management 17. First assist and anticipate all steps of an arthroscopic RCR
19 The Ohio State University Department of Orthopaedics Orthopaedic Residency Program Revised 9/10 Sports Medicine Reading Lists PGY4 1) Hoppenfeld s Orthopedic Surgical Anatomy 2) Deleze and Drez Sports Medicine 3) Cambell s operative orthopaedics 4) Miller s Techniques in Arthroscopy 5) OKU Sports Medicine Update 3
20 The Ohio State University Department of Orthopaedics Orthopaedic Residency Program Revised 6/19/10 Sports Medicine Service (OSU) Didactics Arthroscopy Labs: Residents also have 6 arthroscopy labs each year (basic knee, basic shoulder, advanced knee, advanced shoulder, hip, elbow): principles of surgical skills/repairs will be reviewed here. For all residents (Friday conference): 12 lectures over a 2-year period: 1) Traumatic Anterior Shoulder Instability/MDI/posterior instability (Jones) 2) Shoulder injuries in the throwing athlete (Jones) a. SLAP/Internal impingement/biceps injuries 3) Elbow injuries in the throwing athlete (Najarian) a. Throwing injuries/arthroscopy/distal biceps 4) Ankle Injuries in the athlete (Najarian) a. OCD/Impingement/sprains/arthroscopy 5) Quadriceps mechanism/ hamstrings and gastrocnemious injuries/ exertional compartment syndrome (Flanigan) 6) ACL Injuries (Kaeding) a. Adult and pediatric 7) PCL/Postero-lateral corner, MCL and Multi-Ligament knee injuries (Flanigan) 8) Patellofemoral joint injuries (Najarian) 9) Cartilage and meniscus injuries (Flanigan) 10) Hip Joint injuries/arthroscopy indications (Ellis) 11) Event coverage (Kaeding) a. Medical/ortho emergencies b. C spine emergencies c. Stingers return to play d. Concussion 12) Overuse injuries, tendinopathies, stress fractures (Kaeding) Additional Conferences: 1) Multidisciplinary sports medicine conference: Fridays 7 am 7:45 am a. Resident will be expected to research and present one topic at the conclusion of the 2 month rotation, working with the sports fellows to develop talk. 2) Rotating resident will be expected to attend monthly orthopaedic sports medicine journal club and will assist in preparing articles with the fellows for discussion. Faculty: Dr s Kaeding, Flanigan, Jones, Najarian, Ellis, Bishop
Administration ~ Education and Training (919) 684 3170
 The Accreditation Council for Graduate Medical Education requires the educational program to provide a curriculum that must contain the following educational components to its Trainees; overall educational
The Accreditation Council for Graduate Medical Education requires the educational program to provide a curriculum that must contain the following educational components to its Trainees; overall educational
o Understand the anatomy of the covered areas. This includes bony, muscular and ligamentous anatomy.
 COURSE TITLE Kin 505 Activities, Injuries Disease in the Larger Society On-Line offering Instructor Dr. John Miller John.Miller@unh.edu Course Description. Sports and exercise are a part of American society
COURSE TITLE Kin 505 Activities, Injuries Disease in the Larger Society On-Line offering Instructor Dr. John Miller John.Miller@unh.edu Course Description. Sports and exercise are a part of American society
A Simplified Approach to Common Shoulder Problems
 A Simplified Approach to Common Shoulder Problems Objectives: Understand the basic categories of common shoulder problems. Understand the common patient symptoms. Understand the basic exam findings. Understand
A Simplified Approach to Common Shoulder Problems Objectives: Understand the basic categories of common shoulder problems. Understand the common patient symptoms. Understand the basic exam findings. Understand
Notice of Independent Review Decision DESCRIPTION OF THE SERVICE OR SERVICES IN DISPUTE:
 Notice of Independent Review Decision DATE OF REVIEW: 12/10/10 IRO CASE #: NAME: DESCRIPTION OF THE SERVICE OR SERVICES IN DISPUTE: Determine the appropriateness of the previously denied request for right
Notice of Independent Review Decision DATE OF REVIEW: 12/10/10 IRO CASE #: NAME: DESCRIPTION OF THE SERVICE OR SERVICES IN DISPUTE: Determine the appropriateness of the previously denied request for right
Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions
 Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises Artwork and slides taken from the book Clinical
Integrated Manual Therapy & Orthopedic Massage For Complicated Knee Conditions Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises Artwork and slides taken from the book Clinical
A Patient s Guide to Shoulder Pain
 A Patient s Guide to Shoulder Pain Part 2 Evaluating the Patient James T. Mazzara, M.D. Shoulder and Elbow Surgery Sports Medicine Occupational Orthopedics Patient Education Disclaimer This presentation
A Patient s Guide to Shoulder Pain Part 2 Evaluating the Patient James T. Mazzara, M.D. Shoulder and Elbow Surgery Sports Medicine Occupational Orthopedics Patient Education Disclaimer This presentation
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS
 SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
SPINE SERVICE ROTATION ROTATION SPECIFIC OBJECTIVES (RSO) DEPT. OF ORTHOPEDICS AND PHYSICAL REHABILITATION UNIVERSITY OF MASSACHUSETTS The purpose of this RSO is to outline and clarify the objectives of
www.ghadialisurgery.com
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Michael K. McAdam, M.D. Orthopedic Surgeon Specializing in Arthroscopy and Sports Medicine
 Michael K. McAdam, M.D. Orthopedic Surgeon Specializing in Arthroscopy and Sports Medicine Anterior Cruciate Ligament Injury Injury to the anterior cruciate ligament (ACL) is common, especially in athletic
Michael K. McAdam, M.D. Orthopedic Surgeon Specializing in Arthroscopy and Sports Medicine Anterior Cruciate Ligament Injury Injury to the anterior cruciate ligament (ACL) is common, especially in athletic
Physician Assistant Post Graduate Orthopaedic Surgery Fellowship Program. Watauga Orthopaedics
 Physician Assistant Post Graduate Orthopaedic Surgery Fellowship Program Watauga Orthopaedics Physician Assistant Post-Graduate Fellowship Program in Orthopaedic Surgery Required Texts: 1. Backache Macnab,
Physician Assistant Post Graduate Orthopaedic Surgery Fellowship Program Watauga Orthopaedics Physician Assistant Post-Graduate Fellowship Program in Orthopaedic Surgery Required Texts: 1. Backache Macnab,
Goals. Our Real Goals. Michael H. Boothby, MD Southwest Orthopedic Associates Fort Worth, Texas. Perform a basic, logical, history and physical exam
 Michael H. Boothby, MD Southwest Orthopedic Associates Fort Worth, Texas Goals Our Real Goals Perform a basic, logical, history and physical exam on a patient with knee pain Learn through cases, some common
Michael H. Boothby, MD Southwest Orthopedic Associates Fort Worth, Texas Goals Our Real Goals Perform a basic, logical, history and physical exam on a patient with knee pain Learn through cases, some common
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY.
 QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
QUESTION I HAVE BEEN ASKED TO REHAB GRADE II AND III MCL INJURIES DIFFERENTLY BY DIFFERENT SURGEONS IN THE FIRST 6WEEKS FOLLOWING INJURY. SOME ARE HINGE BRACED 0-90 DEGREES AND ASKED TO REHAB INCLUDING
Hand and Upper Extremity Injuries in Outdoor Activities. John A. Schneider, M.D.
 Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Hand and Upper Extremity Injuries in Outdoor Activities John A. Schneider, M.D. Biographical Sketch Dr. Schneider is an orthopedic surgeon that specializes in the treatment of hand and upper extremity
Rotator Cuff Tears in Football
 Disclosures Rotator Cuff Tears in Football Roger Ostrander, MD Consultant: Mitek Consultant: On-Q Research Support: Arthrex Research Support: Breg Research Support: Arthrosurface 2 Anatomy 4 major muscles:
Disclosures Rotator Cuff Tears in Football Roger Ostrander, MD Consultant: Mitek Consultant: On-Q Research Support: Arthrex Research Support: Breg Research Support: Arthrosurface 2 Anatomy 4 major muscles:
DUKE ORTHOPAEDIC SURGERY GOALS AND OBJECTIVES SPINE SERVICE
 GOALS AND OBJECTIVES PATIENT CARE Able to perform a complete musculoskeletal and neurologic examination on the patient including cervical spine, thoracic spine, and lumbar spine. The neurologic examination
GOALS AND OBJECTIVES PATIENT CARE Able to perform a complete musculoskeletal and neurologic examination on the patient including cervical spine, thoracic spine, and lumbar spine. The neurologic examination
Dermatomes and Myotomes
 Dermatomes and Myotomes C1 C2 C3 C4 C5 C6 C7 C8 T1 Upper Cervical Flexion Upper Cervical Extension Cervical Lateral Flexion Shoulder Girdle Elevation Shoulder Abduction Elbow Flexion Elbow Extension Thumb
Dermatomes and Myotomes C1 C2 C3 C4 C5 C6 C7 C8 T1 Upper Cervical Flexion Upper Cervical Extension Cervical Lateral Flexion Shoulder Girdle Elevation Shoulder Abduction Elbow Flexion Elbow Extension Thumb
.org. Shoulder Pain and Common Shoulder Problems. Anatomy. Cause
 Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
Shoulder Pain and Common Shoulder Problems Page ( 1 ) What most people call the shoulder is really several joints that combine with tendons and muscles to allow a wide range of motion in the arm from scratching
ORTHOPAEDIC KNEE CONDITIONS AND INJURIES
 11. August 2014 ORTHOPAEDIC KNEE CONDITIONS AND INJURIES Presented by: Dr Vera Kinzel Knee, Shoulder and Trauma Specialist Macquarie University Norwest Private Hospital + Norwest Clinic Drummoyne Specialist
11. August 2014 ORTHOPAEDIC KNEE CONDITIONS AND INJURIES Presented by: Dr Vera Kinzel Knee, Shoulder and Trauma Specialist Macquarie University Norwest Private Hospital + Norwest Clinic Drummoyne Specialist
Arthroscopic Shoulder Procedures. David C. Neuschwander MD. Shoulder Instability. Allegheny Health Network Orthopedic Associates of Pittsburgh
 Arthroscopic Shoulder Procedures David C. Neuschwander MD Allegheny Health Network Orthopedic Associates of Pittsburgh Shoulder Instability Anterior Instability Posterior Instability Glenohumeral Joint
Arthroscopic Shoulder Procedures David C. Neuschwander MD Allegheny Health Network Orthopedic Associates of Pittsburgh Shoulder Instability Anterior Instability Posterior Instability Glenohumeral Joint
The Knee Internal derangement of the knee (IDK) The Knee. The Knee Anatomy of the anteromedial aspect. The Knee
 Orthopedics and Neurology James J. Lehman, DC, MBA, FACO University of Bridgeport College of Chiropractic Internal derangement of the knee (IDK) This a common provisional diagnosis for any patient with
Orthopedics and Neurology James J. Lehman, DC, MBA, FACO University of Bridgeport College of Chiropractic Internal derangement of the knee (IDK) This a common provisional diagnosis for any patient with
Sports Injuries of the Foot and Ankle. Dr. Travis Kieckbusch August 7, 2014
 Sports Injuries of the Foot and Ankle Dr. Travis Kieckbusch August 7, 2014 Foot and Ankle Injuries in Athletes Lateral ankle sprains Syndesmosis sprains high ankle sprain Achilles tendon injuries Lisfranc
Sports Injuries of the Foot and Ankle Dr. Travis Kieckbusch August 7, 2014 Foot and Ankle Injuries in Athletes Lateral ankle sprains Syndesmosis sprains high ankle sprain Achilles tendon injuries Lisfranc
Chapter 5. Objectives. Normal Ankle Range of Motion. Lateral Ankle Sprains. Lateral Ankle Sprains. Assessment of Lateral Ankle Sprains
 Objectives Chapter 5 Assessment of Ankle & Lower Leg Injuries Review the following components of injury assessment related to the ankle and lower leg Stress tests Special tests Normal Ankle Range of Motion
Objectives Chapter 5 Assessment of Ankle & Lower Leg Injuries Review the following components of injury assessment related to the ankle and lower leg Stress tests Special tests Normal Ankle Range of Motion
Anatomy and Physiology 101 for Attorneys
 Knee Injuries Anatomy and Physiology 101 for Attorneys Phil Davidson, MD Heiden-Davidson Orthopedics Salt Lake City, UT May 2011 Introduction Dr. Phil Davidson Park City and SLC clinics Education: Harvard,
Knee Injuries Anatomy and Physiology 101 for Attorneys Phil Davidson, MD Heiden-Davidson Orthopedics Salt Lake City, UT May 2011 Introduction Dr. Phil Davidson Park City and SLC clinics Education: Harvard,
Posttraumatic medial ankle instability
 Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Posttraumatic medial ankle instability Alexej Barg, Markus Knupp, Beat Hintermann Orthopaedic Department University Hospital of Basel, Switzerland Clinic of Orthopaedic Surgery, Kantonsspital Baselland
Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction
 UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
UW Health Sports Rehabilitation Rehabilitation Guidelines for Knee Multi-ligament Repair/Reconstruction The knee joint is comprised of an articulation of three bones: the femur (thigh bone), tibia (shin
Evaluating Knee Pain
 Evaluating Knee Pain Matthew T. Boes, M.D. Raleigh Orthopaedic Clinic September 24, 2011 Introduction Approach to patient with knee pain / injury History Examination Radiographs Guidelines for additional
Evaluating Knee Pain Matthew T. Boes, M.D. Raleigh Orthopaedic Clinic September 24, 2011 Introduction Approach to patient with knee pain / injury History Examination Radiographs Guidelines for additional
Musculoskeletal: Acute Lower Back Pain
 Musculoskeletal: Acute Lower Back Pain Acute Lower Back Pain Back Pain only Sciatica / Radiculopathy Possible Cord or Cauda Equina Compression Possible Spinal Canal Stenosis Red Flags Initial conservative
Musculoskeletal: Acute Lower Back Pain Acute Lower Back Pain Back Pain only Sciatica / Radiculopathy Possible Cord or Cauda Equina Compression Possible Spinal Canal Stenosis Red Flags Initial conservative
Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA
 Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA 2 offices 805 Sir Thomas Court Harrisburg 3 Walnut Street Lemoyne Mechanism of injury Repetitive overhead activities Falls to the ground Falls with
Eric M. Kutz, D.O. Arlington Orthopedics Harrisburg, PA 2 offices 805 Sir Thomas Court Harrisburg 3 Walnut Street Lemoyne Mechanism of injury Repetitive overhead activities Falls to the ground Falls with
Screening Examination of the Lower Extremities BUY THIS BOOK! Lower Extremity Screening Exam
 Screening Examination of the Lower Extremities Melvyn Harrington, MD Department of Orthopaedic Surgery & Rehabilitation Loyola University Medical Center BUY THIS BOOK! Essentials of Musculoskeletal Care
Screening Examination of the Lower Extremities Melvyn Harrington, MD Department of Orthopaedic Surgery & Rehabilitation Loyola University Medical Center BUY THIS BOOK! Essentials of Musculoskeletal Care
 ROTATOR CUFF SYNDROME Arbejds- og Miljømedicinsk Årsmøde 2008 ROTATOR CUFF SYNDROME = SHOULDER PAIN Steen Bo Kalms, Shoulder- and Elbow Surgeon ROTATOR CUFF SYNDROME VERY COMMON DIAGNOSIS ON REFERRED PTT
ROTATOR CUFF SYNDROME Arbejds- og Miljømedicinsk Årsmøde 2008 ROTATOR CUFF SYNDROME = SHOULDER PAIN Steen Bo Kalms, Shoulder- and Elbow Surgeon ROTATOR CUFF SYNDROME VERY COMMON DIAGNOSIS ON REFERRED PTT
SHOULDER INSTABILITY IN PATIENTS WITH EDS
 EDNF 2012 CONFERENCE LIVING WITH EDS SHOULDER INSTABILITY IN PATIENTS WITH EDS Keith Kenter, MD Associate Professor Sports Medicine & Shoulder Reconstruction Director, Orthopaedic Residency Program Department
EDNF 2012 CONFERENCE LIVING WITH EDS SHOULDER INSTABILITY IN PATIENTS WITH EDS Keith Kenter, MD Associate Professor Sports Medicine & Shoulder Reconstruction Director, Orthopaedic Residency Program Department
EFSUMB EUROPEAN FEDERATION OF SOCIETIES FOR ULTRASOUND IN MEDICINE AND BIOLOGY Building a European Ultrasound Community
 MINIMUM TRAINING REQUIREMENTS FOR THE PRACTICE OF MEDICAL ULTRASOUND IN EUROPE Appendix 12: Musculoskeletal Musculoskeletal ultrasound comprises a wide range of different examinations increasingly performed
MINIMUM TRAINING REQUIREMENTS FOR THE PRACTICE OF MEDICAL ULTRASOUND IN EUROPE Appendix 12: Musculoskeletal Musculoskeletal ultrasound comprises a wide range of different examinations increasingly performed
Knee Injuries What are the ligaments of the knee?
 As sporting participants or observers, we often hear a variety of terms used to describe sport-related injuries. Terms such as sprains, strains and tears are used to describe our aches and pains following
As sporting participants or observers, we often hear a variety of terms used to describe sport-related injuries. Terms such as sprains, strains and tears are used to describe our aches and pains following
Elbow Examination. Haroon Majeed
 Elbow Examination Haroon Majeed Key Points Inspection Palpation Movements Neurological Examination Special tests Joints above and below Before Starting Introduce yourself Explain to the patient what the
Elbow Examination Haroon Majeed Key Points Inspection Palpation Movements Neurological Examination Special tests Joints above and below Before Starting Introduce yourself Explain to the patient what the
9/7/14. I do not have a financial relationship with any orthopedic manufacturing organization
 I do not have a financial relationship with any orthopedic manufacturing organization Timothy M. Geib, MD Oklahoma Sports & Orthopedic Institute September 27, 2014 Despite what you may have heard, I am
I do not have a financial relationship with any orthopedic manufacturing organization Timothy M. Geib, MD Oklahoma Sports & Orthopedic Institute September 27, 2014 Despite what you may have heard, I am
Knee Microfracture Surgery Patient Information Leaflet
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Knee Microfracture Surgery Patient Information Leaflet Table of Contents 1. Introduction
SHOULDER INSTABILITY. E. Edward Khalfayan, MD
 SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
SHOULDER INSTABILITY E. Edward Khalfayan, MD Instability of the shoulder can occur from a single injury or as the result of repetitive activity such as overhead sports. Dislocations of the shoulder are
Treatment Guide Understanding Elbow Pain. Using this Guide. Choosing Your Care. Table of Contents:
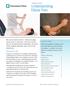 Treatment Guide Understanding Elbow Pain Elbow pain is extremely common whether due to aging, overuse, trauma or a sports injury. When elbow pain interferes with carrying the groceries, participating in
Treatment Guide Understanding Elbow Pain Elbow pain is extremely common whether due to aging, overuse, trauma or a sports injury. When elbow pain interferes with carrying the groceries, participating in
Rotator Cuff Pathophysiology. treatment program that will effectively treat it. The tricky part about the shoulder is that it is a ball and
 Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Rotator Cuff Pathophysiology Shoulder injuries occur to most people at least once in their life. This highly mobile and versatile joint is one of the most common reasons people visit their health care
Semmelweis University Department of Traumatology Dr. Gál Tamás
 Semmelweis University Department of Traumatology Dr. Gál Tamás Anatomy Ankle injuries DIRECT INDIRECT Vertical Compression (Tibia plafond Pilon) AO 43-A,B,C Suppination (adduction + inversion) AO 44-A
Semmelweis University Department of Traumatology Dr. Gál Tamás Anatomy Ankle injuries DIRECT INDIRECT Vertical Compression (Tibia plafond Pilon) AO 43-A,B,C Suppination (adduction + inversion) AO 44-A
COMMON ROWING INJURIES
 COMMON ROWING INJURIES Prevention and Treatment Jo A. Hannafin, MD, PhD Professor of Orthopaedic Surgery Hospital for Special Surgery, Cornell University Medical College Team Physician, US Rowing FISA
COMMON ROWING INJURIES Prevention and Treatment Jo A. Hannafin, MD, PhD Professor of Orthopaedic Surgery Hospital for Special Surgery, Cornell University Medical College Team Physician, US Rowing FISA
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION
 KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
KNEE LIGAMENT REPAIR AND RECONSTRUCTION INFORMED CONSENT INFORMATION The purpose of this document is to provide written information regarding the risks, benefits and alternatives of the procedure named
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction
 Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Pre - Operative Rehabilitation Program for Anterior Cruciate Ligament Reconstruction This protocol is designed to assist you with your preparation for surgery and should be followed under the direction
Foot and Ankle Injuries in the Adolescent Athlete
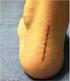 Foot and Ankle Injuries in the Adolescent Athlete Kevin Latz, MD Children s Mercy Hospital Center for Sports Medicine Foot and Ankle Injuries Very common Influenced by the unique properties of growth plates
Foot and Ankle Injuries in the Adolescent Athlete Kevin Latz, MD Children s Mercy Hospital Center for Sports Medicine Foot and Ankle Injuries Very common Influenced by the unique properties of growth plates
Competency Based Goals and Objectives:
 PEDIATRIC SPORTS MEDICINE FELLOWSHIP COMPETENCY-BASED GOALS AND OBJECTIVES & OVERALL EDUCATIONAL GOALS Competency Based Goals and Objectives: Mission: Train fellows to become sports medicine physicians
PEDIATRIC SPORTS MEDICINE FELLOWSHIP COMPETENCY-BASED GOALS AND OBJECTIVES & OVERALL EDUCATIONAL GOALS Competency Based Goals and Objectives: Mission: Train fellows to become sports medicine physicians
Field Evaluation and Management of Non-Battle Related Knee and Ankle Injuries by the ATP in the
 Field Evaluation and Management of Non-Battle Related Knee and Ankle Injuries by the ATP in the JF Rick Hammesfahr, MD Editor s Note: Part Three consists of ankle injury evaluation and taping. Part Two
Field Evaluation and Management of Non-Battle Related Knee and Ankle Injuries by the ATP in the JF Rick Hammesfahr, MD Editor s Note: Part Three consists of ankle injury evaluation and taping. Part Two
Clarification of Medicare Benefits Schedule rules for the Transport Accident Commission and WorkSafe Victoria
 Clarification of Medicare Benefits Schedule rules for the Transport Accident Commission and WorkSafe Victoria MAY 2013 When paying the reasonable costs of medical services, the TAC and WorkSafe pay in
Clarification of Medicare Benefits Schedule rules for the Transport Accident Commission and WorkSafe Victoria MAY 2013 When paying the reasonable costs of medical services, the TAC and WorkSafe pay in
A patient s s guide to: Arthroscopy of the Hip
 A patient s s guide to: Arthroscopy of the Hip Brian J. White MD Assistant Team Physician Denver Nuggets Western Orthopaedics - Denver, Colorado Introduction This is designed to provide you with a better
A patient s s guide to: Arthroscopy of the Hip Brian J. White MD Assistant Team Physician Denver Nuggets Western Orthopaedics - Denver, Colorado Introduction This is designed to provide you with a better
Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor
 Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
Shoulder Series Technique Guide *smith&nephew BIORAPTOR 2.9 Suture Anchor Bankart Repair using the Smith & Nephew BIORAPTOR 2.9 Suture Anchor Gary M. Gartsman, M.D. Introduction Arthroscopic studies of
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE
 ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
ACCELERATED REHABILITATION PROTOCOL FOR POST OPERATIVE POSTERIOR CRUCIATE LIGAMENT RECONSTRUCTION DR LEO PINCZEWSKI DR JUSTIN ROE January 2005 Rationale of Accelerated Rehabilitation Rehabilitation after
Mary LaBarre, PT, DPT,ATRIC
 Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
Aquatic Therapy and the ACL Current Concepts on Prevention and Rehab Mary LaBarre, PT, DPT,ATRIC Anterior Cruciate Ligament (ACL) tears are a common knee injury in athletic rehab. Each year, approximately
Ms. Ruth Delaney ROTATOR CUFF DISEASE Orthopaedic Surgeon, Shoulder Specialist
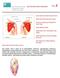 WHAT DOES THE ROTATOR CUFF DO? WHAT DOES THE ROTATOR CUFF DO? WHO GETS ROTATOR CUFF TEARS? HOW DO I CLINICALLY DIAGNOSE A CUFF TEAR? WHO NEEDS AN MRI? DOES EVERY CUFF TEAR NEED TO BE FIXED? WHAT DOES ROTATOR
WHAT DOES THE ROTATOR CUFF DO? WHAT DOES THE ROTATOR CUFF DO? WHO GETS ROTATOR CUFF TEARS? HOW DO I CLINICALLY DIAGNOSE A CUFF TEAR? WHO NEEDS AN MRI? DOES EVERY CUFF TEAR NEED TO BE FIXED? WHAT DOES ROTATOR
Abstract Objective: To review the mechanism, surgical procedures, and rehabilitation techniques used with an athlete suffering from chronic anterior
 Abstract Objective: To review the mechanism, surgical procedures, and rehabilitation techniques used with an athlete suffering from chronic anterior glenohumeral instability and glenoid labral tear. Background:
Abstract Objective: To review the mechanism, surgical procedures, and rehabilitation techniques used with an athlete suffering from chronic anterior glenohumeral instability and glenoid labral tear. Background:
Spinal Arthrodesis Group Exercises
 Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Spinal Arthrodesis Group Exercises 1. Two surgeons work together to perform an arthrodesis. Dr. Bonet, a general surgeon, makes the anterior incision to gain access to the spine for the arthrodesis procedure.
Shoulder Injuries. Why Bother? QAS Injury Prevalence. Screening Injury 29.2% 12 month cumulative injury prevalence. Dr Simon Locke
 Shoulder Injuries Dr Simon Locke Why Bother? Are shoulder and upper limb injuries common? Some anatomy What, where, what sports? How do they happen? Treatment, advances? QAS Injury Prevalence Screening
Shoulder Injuries Dr Simon Locke Why Bother? Are shoulder and upper limb injuries common? Some anatomy What, where, what sports? How do they happen? Treatment, advances? QAS Injury Prevalence Screening
Rehabilitation of Revision ACL Reconstruction
 Chapter 1 Rehabilitation of Revision ACL Reconstruction Michael B. Ellman, MD Rush University Medical Center, Chicago, Illinois Michael D. Rosenthal, PT, DSc, SCS, ECS, ATC, CSCS Naval Medical Center,
Chapter 1 Rehabilitation of Revision ACL Reconstruction Michael B. Ellman, MD Rush University Medical Center, Chicago, Illinois Michael D. Rosenthal, PT, DSc, SCS, ECS, ATC, CSCS Naval Medical Center,
Elbow Injuries and Disorders
 Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
Elbow Injuries and Disorders Introduction Your elbow joint is made up of bone, cartilage, ligaments and fluid. Muscles and tendons help the elbow joint move. There are many injuries and disorders that
3. Be able to perform a detailed clinical examination of the forearm and wrist.
 Patient Care: 1. Demonstrate appropriate evaluation and treatment of patients with hand/wrist surgery problems in the emergency room and as part of the inpatient consultation service, including application
Patient Care: 1. Demonstrate appropriate evaluation and treatment of patients with hand/wrist surgery problems in the emergency room and as part of the inpatient consultation service, including application
Anterior Cruciate Ligament Reconstruction
 1 Anterior Cruciate Ligament Reconstruction Surgical Indications and Considerations Anatomical Considerations: The anterior cruciate ligament (ACL) lies in the middle of the knee. It arises from the anterior
1 Anterior Cruciate Ligament Reconstruction Surgical Indications and Considerations Anatomical Considerations: The anterior cruciate ligament (ACL) lies in the middle of the knee. It arises from the anterior
Medial patellofemoral ligament (MPFL) reconstruction
 Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
Medial patellofemoral ligament (MPFL) reconstruction Introduction Mal-tracking (when the knee cap doesn t move smoothly in the grove below) and instability of the patella (knee Normal patella (above) on
P A T H W A Y S T O A. Career in. Sports Medicine
 P A T H W A Y S T O A Career in Sports Medicine P A T H W A Y S T O A Career in Sports Medicine What is sports medicine? Sports medicine is not a single career, but instead a widely varied group of professionals
P A T H W A Y S T O A Career in Sports Medicine P A T H W A Y S T O A Career in Sports Medicine What is sports medicine? Sports medicine is not a single career, but instead a widely varied group of professionals
PROTOCOLS FOR INJURIES TO THE FOOT AND ANKLE
 PROTOCOLS FOR INJURIES TO THE FOOT AND ANKLE I. DIGITAL FRACTURES A. Background Digital fractures commonly occur in the workplace and are usually the result of a crush injury from a falling object, or
PROTOCOLS FOR INJURIES TO THE FOOT AND ANKLE I. DIGITAL FRACTURES A. Background Digital fractures commonly occur in the workplace and are usually the result of a crush injury from a falling object, or
Shoulder Arthropathies. Crystal Skovly, PA-C Orthopedic Institute Yankton, SD
 Shoulder Arthropathies Crystal Skovly, PA-C Orthopedic Institute Yankton, SD Covered Glenohumeral Arthritis Impingement Syndrome Rotator Cuff Tears Rupture of the Long Head Biceps Tendon Shoulder Instability
Shoulder Arthropathies Crystal Skovly, PA-C Orthopedic Institute Yankton, SD Covered Glenohumeral Arthritis Impingement Syndrome Rotator Cuff Tears Rupture of the Long Head Biceps Tendon Shoulder Instability
Goals and Objectives Pediatric Surgery PGY 1 MCVH
 Goals and Objectives Pediatric Surgery PGY 1 MCVH PGY-1 Clinical Duties and Privileges Lines of Supervision During the PGY-1 each resident begins his/her clinical experience in the General Surgery Residency
Goals and Objectives Pediatric Surgery PGY 1 MCVH PGY-1 Clinical Duties and Privileges Lines of Supervision During the PGY-1 each resident begins his/her clinical experience in the General Surgery Residency
Chiropractic ICD 9 Code List
 Use of valid ICD 9 codes, billed with appropriate and corresponding CPT codes, benefits providers by facilitating treatment authorization and claims payment. The use of valid and appropriate codes also
Use of valid ICD 9 codes, billed with appropriate and corresponding CPT codes, benefits providers by facilitating treatment authorization and claims payment. The use of valid and appropriate codes also
History Inspection Palpation Range of motion Other Tests
 Diagnosis and Management of Common Shoulder and Hip Complaints UCSF Essentials of Primary Care August 8, 2013 Carlin Senter, M.D. At the end of this hour you will know 1. The differential diagnosis for
Diagnosis and Management of Common Shoulder and Hip Complaints UCSF Essentials of Primary Care August 8, 2013 Carlin Senter, M.D. At the end of this hour you will know 1. The differential diagnosis for
Internal Impingement in the Overhead Athlete: A Correlation of Findings on MRI and Arthroscopic Evaluation
 Internal Impingement in the Overhead Athlete: A Correlation of Findings on MRI and Arthroscopic Evaluation Lee D Kaplan, MD J Towers, MD PJ McMahon, MD CH Harner,, MD RW Rodosky,, MD Thrower s shoulder
Internal Impingement in the Overhead Athlete: A Correlation of Findings on MRI and Arthroscopic Evaluation Lee D Kaplan, MD J Towers, MD PJ McMahon, MD CH Harner,, MD RW Rodosky,, MD Thrower s shoulder
Refer to Specialist. The Diagnosis and Management of Shoulder Pain 1. SLAP lesions, types 1 through 4
 The Diagnosis Management of Shoulder Pain 1 Significant Hisry -Age -Extremity Dominance -Hisry of trauma, dislocation, subluxation -Weakness, numbness, paresthesias -Sports participation -Past medical
The Diagnosis Management of Shoulder Pain 1 Significant Hisry -Age -Extremity Dominance -Hisry of trauma, dislocation, subluxation -Weakness, numbness, paresthesias -Sports participation -Past medical
SURG 410/410s Orthopedic Surgery
 Kansas City University of Medicine and Biosciences College of Osteopathic Medicine SURG 410/410s Orthopedic Surgery Course Description: This elective clerkship is a four (4) week experience in the management
Kansas City University of Medicine and Biosciences College of Osteopathic Medicine SURG 410/410s Orthopedic Surgery Course Description: This elective clerkship is a four (4) week experience in the management
Patellofemoral/Chondromalacia Protocol
 Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
Patellofemoral/Chondromalacia Protocol Anatomy and Biomechanics The knee is composed of two joints, the tibiofemoral and the patellofemoral. The patellofemoral joint is made up of the patella (knee cap)
The Two Banditos: SLAP Lesion Shoulder and Labral Tear Hip. Dr. Arno Smit - WROSC Hazelmere Golf and Country Club April 11, 2013
 The Two Banditos: SLAP Lesion Shoulder and Labral Tear Hip Dr. Arno Smit - WROSC Hazelmere Golf and Country Club April 11, 2013 Hip is the new shoulder Increasing interest in non-arthroplasty hip issues.
The Two Banditos: SLAP Lesion Shoulder and Labral Tear Hip Dr. Arno Smit - WROSC Hazelmere Golf and Country Club April 11, 2013 Hip is the new shoulder Increasing interest in non-arthroplasty hip issues.
Clients w/ Orthopedic, Injury and Rehabilitation Concerns. Chapter 21
 Clients w/ Orthopedic, Injury and Rehabilitation Concerns Chapter 21 Terminology Macrotrauma A specific, sudden episode of overload injury to a given tissue, resulting in disrupted tissue integrity (Acute)
Clients w/ Orthopedic, Injury and Rehabilitation Concerns Chapter 21 Terminology Macrotrauma A specific, sudden episode of overload injury to a given tissue, resulting in disrupted tissue integrity (Acute)
Shoulder Instability. Fig 1: Intact labrum and biceps tendon
 Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
Shoulder Instability What is it? The shoulder joint is a ball and socket joint, with the humeral head (upper arm bone) as the ball and the glenoid as the socket. The glenoid (socket) is a shallow bone
.org. Ankle Fractures (Broken Ankle) Anatomy
 Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Ankle Fractures (Broken Ankle) Page ( 1 ) A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken. A fractured ankle can range
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Anterior Cruciate Ligament The anterior cruciate ligament or ACL is one of the major ligaments located in the knee joint. This ligament
ACL Injuries in Women Webcast December 17, 2007 Christina Allen, M.D. Introduction
 ACL Injuries in Women Webcast December 17, 2007 Christina Allen, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or
ACL Injuries in Women Webcast December 17, 2007 Christina Allen, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of UCSF Medical Center, its medical staff or
The Diagnosis-Driven Physical Exam of the Shoulder
 The Diagnosis-Driven Physical Exam of the Shoulder April 24, 2014 Carlin Senter MD, Natalie Voskanian MD, Veronica Jow MD Carlin Senter, MD Assistant Clinical Professor UCSF Sports Medicine 1 Natalie Voskanian,
The Diagnosis-Driven Physical Exam of the Shoulder April 24, 2014 Carlin Senter MD, Natalie Voskanian MD, Veronica Jow MD Carlin Senter, MD Assistant Clinical Professor UCSF Sports Medicine 1 Natalie Voskanian,
INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D.
 05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
05/05/2007 INJURIES OF THE HAND AND WRIST By Derya Dincer, M.D. Hand injuries, especially the fractures of metacarpals and phalanges, are the most common fractures in the skeletal system. Hand injuries
PATELLOFEMORAL TRACKING AND MCCONNELL TAPING. Minni Titicula
 PATELLOFEMORAL TRACKING AND MCCONNELL TAPING Minni Titicula PF tracking disorder PF tracking disorder occurs when patella shifts out of the femoral groove during joint motion. most common in the US. affects
PATELLOFEMORAL TRACKING AND MCCONNELL TAPING Minni Titicula PF tracking disorder PF tracking disorder occurs when patella shifts out of the femoral groove during joint motion. most common in the US. affects
5/7/2009 SHOULDER) CONDITIONS OF THE SHOULDER NOW IT TIME TO TEST YOU ICD-9 SKILLS: PLEASE APPEND THE APPROPRIATE DIAGNOSIS CODE FOR EACH:
 SHOULDER CONDITIONS OF THE SHOULDER AND THEIR TREATMENT Presented by Kevin Solinsky, CPC,CPC-I,CEDC, CEMC The is a major joint and plays a large part in daily life, particularly for athletes and those
SHOULDER CONDITIONS OF THE SHOULDER AND THEIR TREATMENT Presented by Kevin Solinsky, CPC,CPC-I,CEDC, CEMC The is a major joint and plays a large part in daily life, particularly for athletes and those
George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY
 George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY The Ankle Sprain That Won t Get Better With springtime in Louisville upon us, the primary care physician and the orthopaedist alike
George E. Quill, Jr., M.D. Louisville Orthopaedic Clinic Louisville, KY The Ankle Sprain That Won t Get Better With springtime in Louisville upon us, the primary care physician and the orthopaedist alike
Football Medicine Strategies for Knee Injuries FIRST ANNOUNCEMENT. and call for papers
 International Conference on Sports Rehabilitation and Traumatology FIRST ANNOUNCEMENT and call for papers Football Medicine Strategies for Knee Injuries In partnership with: 21 st -22 nd April, 2012 Stamford
International Conference on Sports Rehabilitation and Traumatology FIRST ANNOUNCEMENT and call for papers Football Medicine Strategies for Knee Injuries In partnership with: 21 st -22 nd April, 2012 Stamford
TOWN CENTER ORTHOPAEDIC ASSOCIATES P.C. Labral Tears
 Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Labral Tears The shoulder is your body s most flexible joint. It is designed to let the arm move in almost any direction. But this flexibility has a price, making the joint prone to injury. The shoulder
Adolescent Female Knee/ACL Injuries and Prevention. Camille Clinton, MD ProOrtho
 Adolescent Female Knee/ACL Injuries and Prevention Camille Clinton, MD ProOrtho Background Native Seattlelite Played most sports, but primarily soccer High school, select, ODP, college College at Notre
Adolescent Female Knee/ACL Injuries and Prevention Camille Clinton, MD ProOrtho Background Native Seattlelite Played most sports, but primarily soccer High school, select, ODP, college College at Notre
13. The Spurling Test for Cervical Radiculopathy Secondary to Herniated Disc or Cervical Spondylosis
 Table of Contents: 1. Functional Anatomy of the Bony Cervical Spine 2. Functional Anatomy of the Cervical Intervertebral Disc 3. Nomenclature of the Diseased Cervical Disc 4. Painful Conditions Emanating
Table of Contents: 1. Functional Anatomy of the Bony Cervical Spine 2. Functional Anatomy of the Cervical Intervertebral Disc 3. Nomenclature of the Diseased Cervical Disc 4. Painful Conditions Emanating
Imaging of Sports Injuries
 Imaging of Sports Injuries Capable of tremendous mobility Paradox Must be loose enough to function but stable enough to prevent symptoms Shoulder injuries occur when the balance between stability & mobility
Imaging of Sports Injuries Capable of tremendous mobility Paradox Must be loose enough to function but stable enough to prevent symptoms Shoulder injuries occur when the balance between stability & mobility
Shoulder Examination
 Shoulder Examination Summary Inspection Palpation Movement Special Tests Neurological examination Introduction Shoulder disorders are can be broadly classified into the following types: Pain Stiffness
Shoulder Examination Summary Inspection Palpation Movement Special Tests Neurological examination Introduction Shoulder disorders are can be broadly classified into the following types: Pain Stiffness
5/24/2010. The 10 Ways to Improve Coding
 10 WAYS TO IMPROVE an ASCs ORTHO & SPINE CODING Orthopedic, Spine & PM ASC Conference asc Communications/the ASC Assoc. Conference Speaker: Stephanie Ellis, R.N., CPC Ellis Medical Consulting, Inc. (615)
10 WAYS TO IMPROVE an ASCs ORTHO & SPINE CODING Orthopedic, Spine & PM ASC Conference asc Communications/the ASC Assoc. Conference Speaker: Stephanie Ellis, R.N., CPC Ellis Medical Consulting, Inc. (615)
Procedure. 2 29827 $ 3,560 $ 1,476 Arthroscopy, shoulder, surgical; with rotator cuff repair 5.5% 241.1%
 Exhibit 1 Top 50% of Payments for Surgical s (Physician costs) On average, Workers' payments for Surgical s in are 256% the average allowed claim costs for Healthcare in. $6,000 $5,000 $4,000 Allowed Claim
Exhibit 1 Top 50% of Payments for Surgical s (Physician costs) On average, Workers' payments for Surgical s in are 256% the average allowed claim costs for Healthcare in. $6,000 $5,000 $4,000 Allowed Claim
Anatomy for Workers Compensation Attorneys
 Anatomy for Workers Compensation Attorneys Donato J. Borrillo MD JD Plant Medical Advisor Chrysler/Jeep Assembly Toledo Zoll, Kranz, and Borgess May 16, 2015 Imaging studies neck 1 Bulge and herniation
Anatomy for Workers Compensation Attorneys Donato J. Borrillo MD JD Plant Medical Advisor Chrysler/Jeep Assembly Toledo Zoll, Kranz, and Borgess May 16, 2015 Imaging studies neck 1 Bulge and herniation
WINDY CITY ORTHOPEDICS & SPORTS MEDICINE
 WINDY CITY ORTHOPEDICS & SPORTS MEDICINE ACUTE KNEE AND CHRONIC LIGAMENT INJURIES G. KLAUD MILLER M.D. ASSISTANT PROFESSOR OF CLINICAL ORTHOPEDICS NORTHWESTERN UNIVERSITY MEDICAL SCHOOL ORTHOPEDIC SURGERY
WINDY CITY ORTHOPEDICS & SPORTS MEDICINE ACUTE KNEE AND CHRONIC LIGAMENT INJURIES G. KLAUD MILLER M.D. ASSISTANT PROFESSOR OF CLINICAL ORTHOPEDICS NORTHWESTERN UNIVERSITY MEDICAL SCHOOL ORTHOPEDIC SURGERY
Good morning, everyone! I m Sue Banta, a coding consultant for Amphion Medical. ambulatory knee and shoulder procedures.
 Copyright 2013 by the American Health Information Management Association. All rights reserved. No part of this publication may be reproduced, stored in a retrieval system, or transmitted in any form or
Copyright 2013 by the American Health Information Management Association. All rights reserved. No part of this publication may be reproduced, stored in a retrieval system, or transmitted in any form or
Curriculum Vitae Curtis R. Noel, MD
 Curriculum Vitae Curtis R. Noel, MD Education Fellowship: Steadman-Hawkins Clinic of the Carolinas 2005 2006 Spartanburg, SC Residency: Summa Health Systems 2000-2005 Akron, OH Medical School: University
Curriculum Vitae Curtis R. Noel, MD Education Fellowship: Steadman-Hawkins Clinic of the Carolinas 2005 2006 Spartanburg, SC Residency: Summa Health Systems 2000-2005 Akron, OH Medical School: University
Orthopedic Surgery. General Description
 Orthopedic Surgery Office for Clinical Affairs (515) 271-1629 FAX (515) 271-1727 General Description Elective Rotation This elective rotation in Orthopedic Surgery is a four (4) week experience in the
Orthopedic Surgery Office for Clinical Affairs (515) 271-1629 FAX (515) 271-1727 General Description Elective Rotation This elective rotation in Orthopedic Surgery is a four (4) week experience in the
Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee.
 Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee. The athlete is a defender/mid-fielder and has been involved in soccer
Introduction This case study presents a 24 year old male soccer player with an Anterior Cruciate Ligament (ACL) tear in his left knee. The athlete is a defender/mid-fielder and has been involved in soccer
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on Knee replacement or arthritis management. All decisions about
International Standards for the Classification of Spinal Cord Injury Motor Exam Guide
 C5 Elbow Flexors Biceps Brachii, Brachialis Patient Position: The shoulder is in neutral rotation, neutral flexion/extension, and adducted. The elbow is fully extended, with the forearm in full supination.
C5 Elbow Flexors Biceps Brachii, Brachialis Patient Position: The shoulder is in neutral rotation, neutral flexion/extension, and adducted. The elbow is fully extended, with the forearm in full supination.
Scope it Out! Arthroscopic Procedures. Disclaimer
 Scope it Out! Arthroscopic Procedures Julie A. Leu, eu,cpc, C,CPCO, CO,C CPMA, CPC-I 2009-2011 NAB Member, Region 7 Disclaimer Every reasonable effort has been made to ensure that the educational material
Scope it Out! Arthroscopic Procedures Julie A. Leu, eu,cpc, C,CPCO, CO,C CPMA, CPC-I 2009-2011 NAB Member, Region 7 Disclaimer Every reasonable effort has been made to ensure that the educational material
Shoulder Arthroscopy
 Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
Copyright 2011 American Academy of Orthopaedic Surgeons Shoulder Arthroscopy Arthroscopy is a procedure that orthopaedic surgeons use to inspect, diagnose, and repair problems inside a joint. The word
