The Evolving Role of Prostate Brachytherapy
|
|
|
- Wesley Higgins
- 8 years ago
- Views:
Transcription
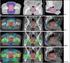
1 Brachytherapy is rapidly becoming a preferred choice by patients for the management of their localized prostate cancer. Faith Krucina. Power of Sound Acrylic on canvas, Courtesy of Artistic Images by Faith, Dunedin, Fla. The Evolving Role of Prostate Brachytherapy David C. Beyer, MD Background: The publication of several large studies with long-term results on the use of prostate brachytherapy has resulted in increased use of this option for patients with localized prostate cancer. Methods: A historical review of brachytherapy as an approach to prostate cancer management is provided, as well as a general summary of the implant technique and the results to date according to patient risk. The effects of combination therapies for specific patient groups are also reviewed. Results: A recent 12-year follow-up reported no failures after 10 years, and 75% of recurrences occurred within the first 5 years. Patients at low risk for failure based on stage, grade, and prostate-specific antigen (PSA) parameters are likely to have disease confined to the prostate. Those with more advanced disease are likely to have a lower probability of cure with brachytherapy as monotherapy. Complications involve primarily the urinary tract. Ideal candidates have a PSA of 10, Gleason score of 7, and low-volume/low-stage disease (stage T1c or T2a). Patients with more-advanced disease are candidates for brachytherapy combined with external-beam radiation therapy (EBRT). For high-risk men with multiple adverse prognostic features, consideration should be given to clinical trials investigating innovative treatment combinations (eg, the addition of androgen blockade, and EBRT). Conclusions: The rarity of failures after 5 years and the absence of recurrence after 10 years suggest a that brachytherapy for localized prostate cancer can provide durable disease control. Future improvements in pathologic tools may lead to selection of patients more likely to respond well to brachytherapy. Introduction From Arizona Oncology Services, Scottsdale, Ariz. Address reprint requests to David C. Beyer, MD, Arizona Oncology Services, 8994 E. Desert Cove Avenue, Suite 100, Scottsdale, AZ dbeyer@azoncology.com No significant relationship exists between the author and the companies/organizations whose products or services may be referenced in this article. Prostate cancer is a serious health concern, with approximately 180,000 new cases diagnosed each year in the United States and 396,000 reported worldwide. With the widespread use of prostate-specific antigen (PSA) screening over the past decade, patients are being seen with earlier-stage disease. Cure rates are March/April 2001, Vol.8, No.2 Cancer Control 163
2 steadily improving, with 5-year survival rising from 67% in 1976 to 93% in At the same time, the number of therapeutic options available has increased. Permanent brachytherapy, commonly called seed implantation, has become an accepted and standard means of therapy and is now a part of the therapeutic armamentarium available to radiation oncologists and urologists worldwide. In a patient care evaluation study conducted by the American College of Surgeons, 2 brachytherapy accounted for only 1.5% of treatments in Mettlin et al 3 reported a doubling of this rate to 3% by Significantly, by 1996, 5.8% of patients with T1c tumors (nonpalpable), which has accounted for a significant proportion of recent cancer diagnoses, received brachytherapy. Regional variations across the United States were also reported, with a higher probability of receiving brachytherapy in the East compared to the West and Midwest. Since 1996, the interest in brachytherapy has continued to grow exponentially as evidenced by the number of seeds sold, the plethora of publications, and the extensive meeting time devoted to this topic. When the statistics are compiled for 2000, brachytherapy will probably have reached the 19% predicted in the mid 1990s. This article provides a summary of the current status for professionals involved in prostate brachytherapy, as well as a guide to the state of the art for other allied physicians who provide care and guidance for patients with prostate cancer. In 1965, radioactive iodine ( 125 I) was introduced to clinical practice for permanent implantation. 4 With a half-life of just under 60 days and a relatively low energy radiation (average = 32 kv), it is well suited for permanent brachytherapy. During the 1970s and early 1980s, retropubic implants with 125 I were popular. 5 As with many innovations in medicine, the initial enthusiasm was dampened by reports of poor source and dose distribution and high recurrence rates. The technique proved to be difficult to reproduce widely, and many implants were judged to be inadequate, even by the comparatively primitive imaging and dosimetry capabilities available at that time. Most practitioners abandoned this procedure; however, a few understood that with improvements in case selection and technique, the fundamentals remain sound. Prostate brachytherapy came into the modern era with a preliminary report in 1983 by Holm et al, 6 who described the use of transrectal ultrasonography to guide transperineal insertion of needles into the prostate to permanently deposit 125 I sources into the gland. This concept was studied by a number of investigators, but Blasko et al 7,8 are generally credited for developing and popularizing the current techniques. With the passage of time and the publication of numerous large studies with long-term results, prostate brachytherapy is undergoing a worldwide renaissance, with more patients choosing this treatment each year. History Brachytherapy is the placement of radioactive sources in close proximity to any tumor. It takes advantage of the simplest physical properties of radiation. High doses of radiation are present in the vicinity of a radioactive material, and a rapid drop in dose occurs with increasing distance from the source. Brachytherapy has been in use worldwide since shortly after the introduction of radioactive materials. Intracavitary or surface applications are used in some human tumor types (eg, cervix, skin, and bronchus), while interstitial insertions are useful in other situations (eg, head and neck, gynecologic, prostate, and sarcoma). Prostate brachytherapy has been performed over the years with a variety of approaches and with stateof-the-art technology during each era. Implantation techniques have evolved from intraurethral insertion of a temporary source in the early decades of last century, to permanent interstitial implantation using a retropubic approach, and eventually to the current ultrasoundguided transperineal techniques (Fig 1). Fig 1. An AP radiograph of a typical 125 I implant. The sources can be seen as linear metallic wires within the pelvis. The extent of the prostate cannot be seen on such a film; however, the entire gland is treated and always confirmed on computed tomography. 164 Cancer Control March/April 2001, Vol.8, No.2
3 Description of the Procedure A variety of techniques have been developed and are in current practice for permanent prostate brachytherapy. It is beyond the scope of this review to catalog them all or to provide enough detail to perform any one technique. Nevertheless, a general understanding of the basic concepts is important to answer patient questions that may fall outside of a physician s field. In addition, certain biologic constraints are imposed on brachytherapists that must be understood to better guide case selection. Implantation is almost always performed as minor outpatient surgery under general or spinal anesthesia. An implant typically requires approximately 1 hour, and patients can return home after a brief recovery. A urinary catheter may be left in overnight or removed prior to discharge, depending on the individual. Most patients return to their normal routines within 1-2 days with minimal restrictions. Since the energy of the implanted sources is low, the radiation exposure surrounding the patient is low. This is measured postoperatively and compared to published radiation safety guidelines. Normal social interaction a few feet away should not be of concern, even for children and pregnant women who are generally considered to be more sensitive to the effects of radiation. In an effort to achieve optimal geometry of the implanted sources, templates are now almost universally used, in contrast to the freehand approach commonly used with retropubic implants. With the patient in the lithotomy position, these templates are held rigidly in place over the perineum and act as guides for needle placement. This allows for control over the entire prostate target volume and specification of source placement at any point within the gland. If the prostate is imagined as a three-dimensional ellipsoid within the pelvis, then any point within the prostate can be given a unique set of coordinates using the grid on the template to define the X and Y coordinates and using the distance from the plane of the template at the perineum to define the Z coordinate. For every 5-mm increment or step from the zero plane at the base of the prostate to the apex, transrectal ultrasonography can be used to map the area of the gland onto this grid. This creates a series of 2-dimensional images that can be totaled to create a 3-dimensional target volume. For a number of reasons, the treated area is slightly larger than the actual organ boundaries. While no absolute margin is applied, a general consensus has developed that 3-5 mm is generally adequate and can be achieved 9 (Fig 2). Fig 2. A portion of a preimplant ultrasound plan for a single axial plane through the gland. The prostate has been outlined in white. Radionuclides deposited in this plane are shown as solid green dots, while needles to be used only in adjacent planes are shown as open circles. The resultant dose is calculated and displayed as isodose lines. Everything within the red isodose line will receive 145 Gy (100% of the dose). Note that this is placed 3-5 mm beyond the edge of the gland. (The grid points are 5 mm apart.) All tissue within the blue line will receive 150% of the prescription dose. The central zone containing the urethra (faintly visible as a white enhanced signal) is spared from this higher-dose region. Modern treatment planning computers can use this planning target volume to develop a pattern for radioactive source placement that will deliver the desired dose. The position of each source is defined based on the grid coordinate system that follows from the chosen template and its depth or distance from the template. Generally, each needle is used to place multiple sources in a line. Historically, they have been placed every 1 cm along the path of a given needle from base to apex. However, with improvements in planning capabilities, irregular spacing is now commonly used along a needle path. Planning may take place weeks in advance of the implant procedure or may be performed intraoperatively. While most practitioners utilize computer optimization for planning, others have successfully developed a nomogram for estimating source requirements and placement. 10 Skill and experience are required with whichever approach is used. It is generally agreed that postoperative dosimetry must be performed to assess the adequacy of implantation and to determine the actual dose received by the prostate and normal tissues. 10 Historically,this dose calculation was performed using a pair of orthogonal radiographs. Even during the retropubic era, it was possible to identify those implants with significant dose inhomogeneity and recognize those patients at higher risk for treatment failure. Unfortunately, these plain March/April 2001, Vol.8, No.2 Cancer Control 165
4 dose of 140 Gy to at least 90% of the prostate using 125 I achieved a higher PSA-based tumor control rate than those with lower D90. Fig 3. A single axial CT image of a completed implant. The sources as metallic objects produce significant white artifact. The prostate, bladder, and rectal outlines are traced in white, yellow, and brown, respectively. As in the preplan, the isodose distribution is superimposed with the red line as 100% and dark blue as 150% of the dose. films fail to identify the prostate anatomy. With the more recent use of computed tomography scanning for dose calculation, it is now possible to calculate the dose received not only by the patient, but also by the prostate (Fig 3). Thus the planning and execution of the implant can be evaluated using 3-dimensional reconstruction of the prostate to optimally assess the dose coverage of the gland. Within the gland, some dose inhomogeneity is always created. Areas and structures in immediate proximity to a source will often receive more than the stated dose. As a result, the dose is generally defined to a volume rather than at some fixed point. In years past, this was termed the matched peripheral dose. Some practitioners have used the term minimum peripheral dose to indicate the lowest dose received within the prostate volume. More recently, a variety of dose measures have been recognized, such as the D90 (dose received by 90% of the prostate volume) or V100 (percent volume of the prostate receiving the prescription dose). These dose parameters are of increasing importance as a quality indicator for the brachytherapist and as a prognostic indicator for the patient. While controversy continues regarding many technical details, such as when to perform the computed tomography scan and how to define the prostate contour, there is general agreement that these parameters predict for outcomes. Stock et al 11 described a dose response curve for D90. Patients who achieved a Physicians have a variety of options in the choice of isotope. Radium, radon, cesium, and colloidal gold are interesting historical footnotes but are not of value to today s brachytherapists. Gold seeds remain available but are rarely used today. Iridium is often employed for temporary insertion at either low or high dose rates. For permanent implantation, 125 I has been in use for 35 years, and palladium ( 103 Pd) has been available for more than a decade. Despite differences in the half-lives and energies of these two isotopes, no differences have been established in clinical outcomes (eg, effectiveness or complications). As a result, both isotopes continue to be used for prostate brachytherapy with no clear consensus or rational schema for choosing one over the other. Studies often report mixed groups, since stratification by isotope has not shown any difference. No attempt has been made in this review to separate studies by the choice of source. To achieve equivalent biologic results when using the two isotopes, the prescribed doses must be different due to differences in the basic physics. Over the years, several advancements in physics and dose calculation have occurred. As a result, the initial dose specification of 160 Gy for 125 I from the early literature has been updated to 145 Gy as the most common current prescription (attempting to consistently achieve a dose of >140 Gy to 90% of the gland). For 103 Pd, the historical dose of Gy developed in the late 1980s has been updated to 125 Gy. 12 For both isotopes, the prescribed dose is reduced when combined with external-beam radiation (EBRT): 110 Gy for 125 I and 100 Gy for 103 Pd. Results Prostate cancer, with its long natural history and variable biology, is not well suited for evaluation using simple survival or local control endpoints. Many untreated patients with prostate cancer do not die of their disease for many years or even decades. Consequently, control of the prostate-specific antigen, or PSA, has become the surrogate endpoint used to evaluate treatments. While there are pitfalls with this strategy, better standard endpoints have not yet been developed, and all the studies reviewed in this article have used some form of this PSA endpoint. It is generally accepted that the American Society for Therapeutic Radiology and Oncology (ASTRO) definition of PSA failure (ie, three consecutive rising intervals) is suitable for brachytherapy as well as EBRT. 13 Much of the pub- 166 Cancer Control March/April 2001, Vol.8, No.2
5 NED Survival % 84% 54% Months Post-Implant Favorable Intermediate Unfavorable Fig 4. The actuarial PSA-based freedom from recurrence is shown for 403 patients treated with brachytherapy as monotherapy. Printed with permission from Peter D. Grimm, DO. lished literature that predated the ASTRO consensus statement used a variety of PSA cutoff points. Also,case selection has varied among institutions, making strict comparisons difficult. With these caveats, much can be learned from a review of the published results. In a large and well-documented report in 1995, Blasko et al 14 noted that the PSA normalized in 98% of treated patients. They also showed that long follow-up is required; at 2 years, only 82% had achieved a PSA nadir of <1.0, whereas 97% had done so by 4 years. These initial excellent results have been updated and carefully analyzed. In 1998, Radge et al 15 observed 10- year brachytherapy results in the treatment of 152 consecutive patients with clinically organ-confined prostate carcinoma. Ten-year disease-free survival was reported at 70% for the entire cohort, which compared favorably with surgical results. In a 2000 update, 16 no failures were seen after 10 years, and 75% of recurrences occurred within the first 5 years. Numerous other studies report 5-year results and have documented flattening of the survival curves. The rarity of failures after 5 years, which is demonstrated both in the biochemical no evidence of disease (bned) plots in Fig 4 and in the absence of recurrence after 10 years, suggests a true and durable cure from prostate brachytherapy. Nine-year follow-up for monotherapy using 103 Pd was separately reported by Blasko et al. 17 In 230 patients selected for implantation alone, 5-year PSAbased NED rates ranged from 65% to 94%, depending on the presence or absence of high-risk features. Risk groups have typically been developed depending on the presence of PSA at 10 or a Gleason score of 7. For the purposes of this study,low-risk patients had neither feature, while high-risk patients showed both. The presence of a single adverse feature was associated with an intermediate risk (82% NED). These optimistic results are mirrored in studies from other institutions. Our series of 1,463 implanted patients was recently updated. 18 With median followup of 61 months, 345 favorable-risk patients treated with implantation alone had 5-year bned rates of 85%. With shorter median follow-up, Stokes et al 19 reported 5-year bned rates of 100% and 86% for patients with initial PSA level 4 and , respectively. Grado et al, 20 with almost a 4-year median follow-up, described a bned rate of 88% overall for men presenting with a PSA <10. Dattoli 21 presents similar results of 93% for low-risk patients. Two studies have evaluated outcomes when different treatments are used. Brachman et al 22 compared a series of 695 brachytherapy patients with 1,527 treated with conventional (nonconformal) EBRT at our institution. Low-risk patients (PSA <10, Gleason score <7) have a 5-year bned of 89%, regardless of the treatment method. D Amico et al 23 report similar results of 85%- 90% when comparing brachytherapy, radical prostatectomy, and EBRT in several related institutions. These data also suggest that high-risk patients presenting with bulky disease, high initial PSA, or high Gleason score fare poorly (<50% bned) when managed with brachytherapy alone. In both series, either EBRT or surgery was superior to implant as monotherapy. Zelefsky et al 24 retrospectively stratified 248 patients with a median of 48 months of follow-up into favorable, unfavorable, and intermediate strata using PSA of 10, Gleason score of 6, and stage T2a. As in all similar studies, favorable-risk patients fared well with 88% NED at 5 years (Table). 17,18,23-26 Unfavorable-risk patients (showing 2 or more of these poor prognostic features) had roughly 50% PSA control at 5 years, while the intermediate group (a single adverse feature) was consistently in between. These high-risk patients are the same ones predicted by the Partin Tables 27 to have a high-risk of established capsular penetration and other indications of Comparisons of 5-Year PSA-Based Freedom From Cancer Following Brachytherapy Alone Author Favorable Intermediate Unfavorable Blasko et al 17 94% 82% 65% Beyer 18 88% 79% 65% D Amico et al 23 85% 33% 5% Zelefsky et al 24 88% 77% 38% Stock et al 25 88% 60% Potters et al 26 92% 74% 55% Adapted from Zelefsky et al. 24 March/April 2001, Vol.8, No.2 Cancer Control 167
6 more advanced disease. Independent studies by Davis et al 28 and Sohayda et al 29 confirm that patients generally considered at low risk for failure based on these parameters of stage, grade, and PSA level are likely to have all disease confined to the prostate plus a margin of no more than 3 mm. This is well within the range of implantation alone. Those with more advanced disease are likely to have more extraprostatic disease and a lower probability of cure with brachytherapy as monotherapy. This is supported in other brachytherapy and surgical series in which 5-year bned rates were consistently less than 50% in such patients. As a result, most practitioners now eschew brachytherapy as monotherapy for this population. Combination Therapies Brachytherapy has been combined with modest doses of EBRT for these high-risk subgroups in several reports. Some advocate combination therapy for all patients, 30 while most suggest the addition of EBRT for high-risk patients only. This remains controversial since no prospective studies have been designed to test this hypothesis. Retrospectively, Ragde et al 15 reported improved 12-year disease-free survival from 66% to 79% in those patients receiving EBRT. However, Grado et al 20 suggest no benefit with the addition of EBRT (80% vs 72%). However, both reports contain confounding variables that limit the value of the conclusions. Grimm et al 31 reported on 232 high-risk patients treated with 45 Gy EBRT followed by a reduced-dose implant showing 76% bned at 7 years. Dattoli 21 published similar results for 102 high-risk patients, with 79% bned at 5 years using EBRT followed by a 103 Pd implant. Critz et al 30 describe results for 1,020 patients treated with combination therapy, albeit with a much shorter median follow-up. All patients, including those with favorable prognostic features, received EBRT, and many of these early patients were treated with open retropubic implant techniques. While these series may not be truly comparable, 72% of patients at 10 years remain as bned. Hormonal therapies have been used in conjunction with prostate radiation therapy with increasing frequency over the past few years. Total androgen blockade has been used to downsize the prostate prior to brachytherapy, thus allowing for implantation of glands that might otherwise be too large for the technique and also to improve the therapeutic ratio with improved geometry. No long-term results have been reported to support its use based on survival or PSA endpoints. The use of total androgen blockade with EBRT has been established for high-risk patients based on just such endpoints in studies by both the Radiation Therapy Oncology Group (RTOG) 32 and the European Organization for Research and Treatment of Cancer (EORTC). 33 Further research is needed to determine whether this intervention will be of value with brachytherapy for more than purely technical reasons. It is important to recognize that using these same risk groupings, equivalent PSA relapse rates are obtained with brachytherapy as with conformal EBRT or surgery. Stage for stage and grade for grade, all therapies show increasing failures with increasing risk. It is often impossible to select one therapy over another based only on cure rates. Consequently, patient decisions are often guided by issues relating to quality of life and individual value judgments. Complications Early side effects and complications involve primarily the urinary tract. Irritative and obstructive lower urinary tract symptoms develop immediately as a result of implant trauma and over the first weeks as a result of the radiation. While some practitioners routinely choose to leave a urinary catheter in place overnight, retention may require more prolonged catheterization in 5%-22% of cases. Recent work suggests that it is possible to predict those patients at greatest risk of retention based on their response to a standardized survey of urinary symptoms (frequency, urgency, hesitancy, etc) and on their International Prostate Symptom Score (IPSS). 34 Less dramatic urinary symptoms are commonly managed with nonsteroidal anti-inflammatory drugs and alpha blockers. Merrick et al 35 reported that 85% of men required alpha blockers at 26 weeks, with 56% still using them at 50 weeks. Late grade 3 urinary complications (ie, requiring surgical intervention or altering functional status) may occur in approximately 2%-5% of patients, 36 with stricture reported in 2%-3% of patients. 37 Management of the occasional patient with significant or prolonged urinary symptoms requires patience. While incontinence following brachytherapy alone is rare (<1%),it occurs to some degree in 25%-48% of men who have a transurethral resection of the prostate (TURP) after implantation. Spontaneous relief of obstruction may occur many months after implant, with complete symptom relief occasionally occurring as long as 1 year away. Thus, early surgical intervention (eg,turp) after an implant should be avoided. Whether TURP performed prior to implantation poses a significant risk of incontinence remains controversial. The 168 Cancer Control March/April 2001, Vol.8, No.2
7 current consensus is that it probably does not so long as healing has been adequate and sufficient tissue remains for good implant geometry. 38 Late rectal complications, including proctitis with diarrhea, tenesmus, or rectal bleeding, may occur in 2%- 19% of patients. 39 There have been isolated reports of rectal fistula formations, particularly during the early years, with older implant techniques. Many of these were temporally correlated with aggressive rectal biopsies or laser therapies for minor bleeding. Conservative management of rectal radiation reactions is indicated with rectal steroids and other rectal preparations. Biopsy and laser rectal treatments should be used judiciously. Compared with other standard treatments, permanent brachytherapy has been reported to offer prostate cancer patients their best chance of preservation of potency. Radiation-induced erectile dysfunction develops over time, and strict comparisons among various reported rates are difficult. Stock et al 40 report impotence in 2.5% at 1 year and 6% at 2 years. However,39% report some decrease in sexual function. In our own series of 706 evaluable patients, 76% report preservation of potency at 5 years (actuarial rate). Quality-of-life issues have played a significant role in the emergence of prostate brachytherapy over the past decade. Recent work by Lee et al 41 addresses this question using the FACT-G and FACT-P questionnaires combined with the commonly used IPSS. Thirty-one patients were evaluated prior to treatment and at 1 month, 3 months, 6 months, and 1 year following treatment. Patients experienced a minor decrease in the general quality-of-life measure (FACT-G) that, while statistically significant, is clinically trivial. The instruments more specific for lower urinary tract symptoms, such as the IPSS and FACT-P, revealed a clinically significant increase in patient-reported symptoms within the first month. For the IPSS, there is more than a twofold increase from a baseline median of 8 to 18, suggesting moderate to severe lower urinary tract symptoms. Longitudinal measurements show that this decrease in health-related quality of life is transient; by the end of the first year, scores are indistinguishable from baseline measurements. Continued quality-of-life analysis is needed for all therapeutically equivalent cancer treatments. Case Selection Current recommendations for case selection generally require a clinically localized prostate cancer in a man with a reasonable life expectancy, suitable gland size (generally <60 cc), and limited underlying obstructive urinary symptoms. Ideal candidates have a low risk of significant extraprostatic extension beyond the first few millimeters from the capsule. The most favorable patients, and those often considered suitable for brachytherapy as monotherapy, are those with a PSA of 10, Gleason score of 7, and low-volume/low-stage disease (typically stage T1c or T2a). Patients with moreadvanced disease are candidates for brachytherapy in conjunction with a limited course of EBRT. For high-risk men with multiple adverse prognostic features, consideration should be given to clinical trials investigating innovative treatment combinations (eg, the addition of androgen blockade, EBRT) or new treatments, since results with standard therapy offer no better than a 50% of PSA control at 5 years. Future Prospects As the available pathologic tools improve, other factors such as DNA ploidy, number or percent of involved cores, perineural invasion, or newer blood markers may eventually play a role in selecting patients likely to respond well to brachytherapy. Better delineation of risk groups should help to determine the optimal use of adjuvant treatments such as EBRT or androgen deprivation. Advances in imaging technology are currently being exploited. Innovative uses of computed tomography and magnetic resonance imaging scanning with prostate brachytherapy are being studied to perform brachytherapy as well as to determine diagnostic staging. New devices to assist in implantation and to improve dose distribution and accuracy are being developed and should help to enhance the quality and consistency of implants. Brachytherapy is a rapidly evolving treatment option. Innovations are introduced on an ongoing basis as more practitioners devote time and energy to creating better ways to evaluate patients and execute implants. At all times, the basic underlying principle remains: to deliver more radiation dose to the tumor and less to the surrounding normal tissues in a ongoing effort to improve the therapeutic ratio in the battle against prostate cancer. References 1. Parkin DM, Pisani P, Ferlay J. Global cancer statistics. Cancer. 1999;49: Jones GW,Mettlin C,Murphy GP,et al. Patterns of care for carcinoma of the prostate gland: results of a national survey of 1984 and J Am Coll Surg. 1995;180: Mettlin CJ, Murphy GP, McDonald CJ, et al. The national cancer data base report on increased use of brachytherapy for the treatment of patients with prostate carcinoma in the U.S. Cancer. 1999; 86: Hilaris BS, Whitmore WF, Batata M, et al. Behavioral patterns of prostate adenocarcinoma following an 125I implant and pelvic node dissection. Int J Radiat Oncol Biol Phys. 1977;2: March/April 2001, Vol.8, No.2 Cancer Control 169
8 5. Whitmore WF. Interstitial radiation therapy for carcinoma of the prostate. Prostate. 1980;1: Holm HH, Juul N, Pedersen JF, et al. Transperineal 125iodine seed implantation in prostatic cancer guided by transrectal ultrasonography. J Urol. 1983;130: Blasko JC, Grimm PD, Ragde H. Brachytherapy and organ preservation in the management of carcinoma of the prostate. Semin Radiat Oncol. 1993;3: Blasko JC, Ragde H, Schumacher D. Transperineal percutaneous iodine-125 implantation for prostatic carcinoma using transrectal ultrasound and template guidance: endocurie/hypertherm. Oncology. 1987;3: Gray JR, Merrick GS, Beyer DC, et al. Comparative analysis of prostate brachytherapy pre-planning. Radiother Oncol. 2000;55: Prete JJ, Prestidge BR, Bice WS, et al. A survey of physics and dosimetry practice of permanent prostate brachytherapy in the United States. Int J Radiat Oncol Biol Phys. 1998;40: Stock RG, Stone NN,Tabert A, et al. A dose-response study for I-125 prostate implants. Int J Radiat Oncol Biol Phys. 1998;41: Beyer D, Nath R, Butler W, et al. American Brachytherapy Society recommendations for clinical implementation of NIST-1999 standards for (103)palladium brachytherapy: the clinical research committee of the American Brachytherapy Society. Int J Radiat Oncol Biol Phys. 2000;47: American Society for Therapeutic Radiology and Oncology Consensus Panel. Consensus statement: guidelines for PSA following radiation therapy. Int J Radiat Oncol Biol Phys. 1997;37: Blasko JC,Wallner K, Grimm PD, et al. Prostate specific antigen based disease control following ultrasound guided 125iodine implantation for stage T1/T2 prostatic carcinoma. J Urol. 1995;154: Ragde H, Elgamal AA, Snow PB, et al. Ten-year disease free survival after transperineal sonography-guided Iodine-125 brachytherapy with or without 45-gray external beam irradiation in the treatment of patients with clinically localized, low to high Gleason grade prostate carcinoma. Cancer. 1998;83: Ragde H, Korb LJ, Elgamal AA. Modern prostate brachytherapy: prostate specific antigen results in 219 patients with up to 12 years of observed follow-up. Cancer. 2000;89: Blasko JC, Grimm PD, Sylvester JE. Palladium-103 brachytherapy for prostate carcinoma. Int J Radiat Oncol Biol Phys. 2000; 46: Beyer D. Permanent prostate brachytherapy: the Arizona experience. Radiother Oncol. 2000;55: Stokes SH, Real JD,Adams PW, et al. Transperineal ultrasoundguided radioactive seed implantation for organ-confined carcinoma of the prostate. Int J Radiat Oncol Biol Phys. 1997;37: Grado GL, Larson TR, Balch CS. Actuarial disease-free survival after prostate cancer brachytherapy using interactive techniques with biplane ultrasound and fluoroscopic guidance. Int J Radiat Oncol Biol Phys. 1998;42: Dattoli M, Wallner K, Sorace R, et al. 103 Pd brachytherapy and external beam irradiation for clinically localized, high-risk prostatic carcinoma. Int J Radiat Oncol Biol Phys. 1996;35: Brachman DG,Thomas T,Hilbe J,et al. Failure-free survival following brachytherapy alone or external beam irradiation alone for T1-2 prostate tumors in 2222 patients: results from a single practice. Int J Radiat Oncol Biol Phys. 2000;48: D Amico AV,Whittington R, Malkowicz SB, et al. Biochemical outcome after radical prostatectomy, external beam radiation therapy, or interstitial radiation therapy for clinically localized prostate cancer. JAMA. 1998;280: Zelefsky MJ, Leibel SA, Burman CM, et al. Neoadjuvant hormonal therapy improves the therapeutic ratio in patients with bulky prostatic cancer treated with three-dimensional conformal radiation therapy. Int J Radiat Oncol Biol Phys. 1994;29: Stock RG, Stone NN. The effect of prognostic factors on therapeutic outcome following transperineal prostate brachytherapy. Semin Surg Oncol. 1997;13: Potters L, Cha C, Oshinsky G, et al. Risk profiles to predict PSA relapse-free survival for patients undergoing permanent prostate brachytherapy. Cancer J Sci Am. 1999;5: Partin AW, Kattan MW, Subong EN, et al. Combination of prostate-specific antigen, clinical stage, and Gleason score to predict pathological stage of localized prostate cancer: a multi-institutional update. JAMA. 1997;277: Davis BJ, Pisansky TM,Wilson TM, et al. The radial distance of extraprostatic extension of prostate carcinoma: implications for prostate brachytherapy Cancer. 1999;85: Sohayda C, Kupelian PA, Levin HS, et al. Extent of extracapsular extension in localized prostate cancer. Urology. 2000;55: Critz FA, Levinson AK,Williams WH, et al. Simultaneous radiotherapy for prostate cancer: 125 I prostate implant followed by external-beam radiation. Cancer J Sci Am. 1998;4: Grimm PD, Blasko J, Ragde H, et al. Transperineal ultrasound guided I125/Pd103 brachytherapy for early stage prostate cancer: update on clinical experience at seven years. Int J Radiat Oncol Biol Phys. 1997;39:219. Abstract. 32. Pilepich MV, Krall JM, al-sarraf M, et al. Androgen deprivation with radiation therapy compared with radiation therapy alone for locally advanced prostatic carcinoma: a randomized comparative trial of the Radiation Therapy Oncology Group. Urology. 1995;45: Bolla M, Gonzalez D, Warde P, et al. Improved survival in patients with locally advanced prostate cancer treated with radiotherapy and goserelin. N Engl J Med. 1997;337: Terk MD, Stock RG, Stone NN. Identification of patients at increased risk for prolonged urinary retention following radioactive seed implantation of the prostate. J Urol. 1998;160: Merrick GS, Butler WM, Lief JH, et al. Temporal resolution of urinary morbidity following prostate brachytherapy. Int J Radiat Oncol Biol Phys. 2000;47: Gelblum DY, Potters L,Ashley R, et al. Urinary morbidity following ultrasound-guided transperineal prostate seed implantation. Int J Radiat Oncol Biol Phys. 1999;45: Beyer D. Complications and late toxicity following permanent prostate brachytherapy. Int J Radiat Oncol Biol Phys. 1998;42(1 suppl): Wallner K, Lee H, Wasserman S, et al. Low risk of urinary incontinence following prostate brachytherapy in patients with a prior transurethral prostate resection. Int J Radiat Oncol Biol Phys. 1997;37: Hu K,Wallner K. Clinical course of rectal bleeding following I-125 prostate brachytherapy. Int J Radiat Oncol Biol Phys. 1998; 41: Stock RG, Stone NN, Iannuzzi C. Sexual potency following interactive ultrasound-guided brachytherapy for prostate cancer. Int J Radiat Oncol Biol Phys. 1996;35: Lee WR, McQuellon RP, Harris-Henderson K, et al. A preliminary analysis of health-related quality of life in the first year after permanent source interstitial brachytherapy (PIB) for clinically localized prostate cancer. Int J Radiat Oncol Biol Phys. 2000;46: Cancer Control March/April 2001, Vol.8, No.2
FIVE-YEAR BIOCHEMICAL OUTCOME FOLLOWING PERMANENT INTERSTITIAL BRACHYTHERAPY FOR CLINICAL T1 T3 PROSTATE CANCER
 PII S0360-3016(01)01594-2 Int. J. Radiation Oncology Biol. Phys., Vol. 51, No. 1, pp. 41 48, 2001 Copyright 2001 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/01/$ see front matter
PII S0360-3016(01)01594-2 Int. J. Radiation Oncology Biol. Phys., Vol. 51, No. 1, pp. 41 48, 2001 Copyright 2001 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/01/$ see front matter
NATURAL HISTORY OF CLINICALLY STAGED LOW- AND INTERMEDIATE-RISK PROSTATE CANCER TREATED WITH MONOTHERAPEUTIC PERMANENT INTERSTITIAL BRACHYTHERAPY
 doi:1.116/j.ijrobp.9..1 Int. J. Radiation Oncology Biol. Phys., Vol. 76, No., pp. 349 354, 1 Copyright Ó 1 Elsevier Inc. Printed in the USA. All rights reserved 36-316/1/$ see front matter CLINICAL INVESTIGATION
doi:1.116/j.ijrobp.9..1 Int. J. Radiation Oncology Biol. Phys., Vol. 76, No., pp. 349 354, 1 Copyright Ó 1 Elsevier Inc. Printed in the USA. All rights reserved 36-316/1/$ see front matter CLINICAL INVESTIGATION
PROSTATE CANCER WITH LARGE GLANDS TREATED WITH 3- DIMENSIONAL COMPUTERIZED TOMOGRAPHY GUIDED PARARECTAL BRACHYTHERAPY: UP TO 8 YEARS OF FOLLOWUP
 0022-5347/03/1694-1331/0 Vol. 169, 1331 1336, April 2003 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2003 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000055773.91290.e8 PROSTATE CANCER
0022-5347/03/1694-1331/0 Vol. 169, 1331 1336, April 2003 THE JOURNAL OF UROLOGY Printed in U.S.A. Copyright 2003 by AMERICAN UROLOGICAL ASSOCIATION DOI: 10.1097/01.ju.0000055773.91290.e8 PROSTATE CANCER
doi:10.1016/j.ijrobp.2006.07.1382 CLINICAL INVESTIGATION
 doi:10.1016/j.ijrobp.2006.07.1382 Int. J. Radiation Oncology Biol. Phys., Vol. 67, No. 1, pp. 57 64, 2007 Copyright 2007 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/07/$ see front matter
doi:10.1016/j.ijrobp.2006.07.1382 Int. J. Radiation Oncology Biol. Phys., Vol. 67, No. 1, pp. 57 64, 2007 Copyright 2007 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/07/$ see front matter
The optimal treatment for clinically localized
 REVIEW COMBINING EXTERNAL BEAM RADIOTHERAPY WITH PROSTATE BRACHYTHERAPY: ISSUES AND RATIONALE CLARISSA FEBLES AND RICHARD K. VALICENTI The optimal treatment for clinically localized prostate cancer remains
REVIEW COMBINING EXTERNAL BEAM RADIOTHERAPY WITH PROSTATE BRACHYTHERAPY: ISSUES AND RATIONALE CLARISSA FEBLES AND RICHARD K. VALICENTI The optimal treatment for clinically localized prostate cancer remains
7. Prostate cancer in PSA relapse
 7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
7. Prostate cancer in PSA relapse A patient with prostate cancer in PSA relapse is one who, having received a primary treatment with intent to cure, has a raised PSA (prostate-specific antigen) level defined
Radiation Therapy for Prostate Cancer: Treatment options and future directions
 Radiation Therapy for Prostate Cancer: Treatment options and future directions David Weksberg, M.D., Ph.D. PinnacleHealth Cancer Institute September 12, 2015 Radiation Therapy for Prostate Cancer: Treatment
Radiation Therapy for Prostate Cancer: Treatment options and future directions David Weksberg, M.D., Ph.D. PinnacleHealth Cancer Institute September 12, 2015 Radiation Therapy for Prostate Cancer: Treatment
These rare variants often act aggressively and may respond differently to therapy than the more common prostate adenocarcinoma.
 Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Brachytherapy for prostate cancer
 Brachytherapy for prostate cancer Findings by SBU Alert Published Jun 7, 2000 Version 1 Brachytherapy is not widely used in Sweden to treat localized prostate cancer. This treatment method has been available
Brachytherapy for prostate cancer Findings by SBU Alert Published Jun 7, 2000 Version 1 Brachytherapy is not widely used in Sweden to treat localized prostate cancer. This treatment method has been available
Prostatectomy, pelvic lymphadenect. Med age 63 years Mean followup 53 months No other cancer related therapy before recurrence. Negative.
 Adjuvante und Salvage Radiotherapie Ludwig Plasswilm Klinik für Radio-Onkologie, KSSG CANCER CONTROL WITH RADICAL PROSTATECTOMY ALONE IN 1,000 CONSECUTIVE PATIENTS 1983 1998 Clinical stage T1 and T2 Mean
Adjuvante und Salvage Radiotherapie Ludwig Plasswilm Klinik für Radio-Onkologie, KSSG CANCER CONTROL WITH RADICAL PROSTATECTOMY ALONE IN 1,000 CONSECUTIVE PATIENTS 1983 1998 Clinical stage T1 and T2 Mean
How To Know If You Should Get A Brachytherapy Or Radioactive Seed Implantation
 MEDICAL POLICY SUBJECT: BRACHYTHERAPY OR PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy
MEDICAL POLICY SUBJECT: BRACHYTHERAPY OR PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy
Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate
 Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_the_prostate
Corporate Medical Policy Intensity-Modulated Radiation Therapy (IMRT) of the Prostate File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_the_prostate
Bard: Prostate Cancer Treatment. Bard: Pelvic Organ Prolapse. Prostate Cancer. An overview of. Treatment. Prolapse. Information and Answers
 Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Medical Policy Brachytherapy for Clinically Localized Prostate Cancer Using Permanently Implanted Seeds
 Medical Policy Brachytherapy for Clinically Localized Prostate Cancer Using Permanently Implanted Seeds Table of Contents Policy: Commercial Coding Information Information Pertaining to All Policies Policy:
Medical Policy Brachytherapy for Clinically Localized Prostate Cancer Using Permanently Implanted Seeds Table of Contents Policy: Commercial Coding Information Information Pertaining to All Policies Policy:
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Prostate Cancer. Patient Information
 Prostate Cancer Patient Information 1 The Prostate & Prostate Cancer The prostate is a small gland in the male reproductive system, approximately the size and shape of a walnut. It is located directly
Prostate Cancer Patient Information 1 The Prostate & Prostate Cancer The prostate is a small gland in the male reproductive system, approximately the size and shape of a walnut. It is located directly
PROSTATE CANCER. Get the facts, know your options. Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology
 PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
Patient Selection for Prostate Brachytherapy
 Patient Selection for Prostate Brachytherapy a report by Gregory S Merrick, MD 1, Wayne M Butler, PhD 1 and K ent E Wallner, MD 2 1. Schiffler Cancer Center and Wheeling Jesuit University, 2. Puget Sound
Patient Selection for Prostate Brachytherapy a report by Gregory S Merrick, MD 1, Wayne M Butler, PhD 1 and K ent E Wallner, MD 2 1. Schiffler Cancer Center and Wheeling Jesuit University, 2. Puget Sound
LATE MORBIDITY PROFILES IN PROSTATE CANCER PATIENTS TREATED TO 79 84 GY BY A SIMPLE FOUR-FIELD COPLANAR BEAM ARRANGEMENT
 PII S0360-3016(02)03822-1 Int. J. Radiation Oncology Biol. Phys., Vol. 55, No. 1, pp. 71 77, 2003 Copyright 2003 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/03/$ see front matter
PII S0360-3016(02)03822-1 Int. J. Radiation Oncology Biol. Phys., Vol. 55, No. 1, pp. 71 77, 2003 Copyright 2003 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/03/$ see front matter
Brachytherapy for Prostate Cancer
 Urol Int 1999;63:87 91 Manfred P. Wirth Oliver W. Hakenberg Klinik und Poliklinik für Urologie, Universitätsklinikum Carl-Gustav-Carus der Technischen Universität Dresden, Deutschland Brachytherapy for
Urol Int 1999;63:87 91 Manfred P. Wirth Oliver W. Hakenberg Klinik und Poliklinik für Urologie, Universitätsklinikum Carl-Gustav-Carus der Technischen Universität Dresden, Deutschland Brachytherapy for
Prostate Cancer Treatment
 Scan for mobile link. Prostate Cancer Treatment Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam,
Scan for mobile link. Prostate Cancer Treatment Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam,
American College Of Radiology ACR Appropriateness Criteria PERMANENT SOURCE BRACHYTHERAPY FOR PROSTATE CANCER
 American College Of Radiology ACR Appropriateness Criteria PERMANENT SOURCE BRACHYTHERAPY FOR PROSTATE CANCER Expert Panel on Radiation Oncology Prostate Work Group: Louis Potters, MD 1 ; Carlos A. Perez,
American College Of Radiology ACR Appropriateness Criteria PERMANENT SOURCE BRACHYTHERAPY FOR PROSTATE CANCER Expert Panel on Radiation Oncology Prostate Work Group: Louis Potters, MD 1 ; Carlos A. Perez,
LONG-TERM URINARY TOXICITY AFTER 3-DIMENSIONAL CONFORMAL RADIOTHERAPY FOR PROSTATE CANCER IN PATIENTS WITH PRIOR HISTORY OF TRANSURETHRAL RESECTION
 PII S0360-3016(00)00714-8 Int. J. Radiation Oncology Biol. Phys., Vol. 48, No. 3, pp. 643 647, 2000 Copyright 2000 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/00/$ see front
PII S0360-3016(00)00714-8 Int. J. Radiation Oncology Biol. Phys., Vol. 48, No. 3, pp. 643 647, 2000 Copyright 2000 Elsevier Science Inc. Printed in the USA. All rights reserved 0360-3016/00/$ see front
FAQ About Prostate Cancer Treatment and SpaceOAR System
 FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
Clinical Trials and Radiation Treatment. Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto
 Clinical Trials and Radiation Treatment Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto What I will cover.. A little about radiation treatment The clinical trials
Clinical Trials and Radiation Treatment Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto What I will cover.. A little about radiation treatment The clinical trials
Prostate Cancer. What is prostate cancer?
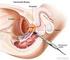 Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Implementation Date: April 2015 Clinical Operations
 National Imaging Associates, Inc. Clinical guideline PROSTATE CANCER Original Date: March 2011 Page 1 of 5 Radiation Oncology Last Review Date: March 2015 Guideline Number: NIA_CG_124 Last Revised Date:
National Imaging Associates, Inc. Clinical guideline PROSTATE CANCER Original Date: March 2011 Page 1 of 5 Radiation Oncology Last Review Date: March 2015 Guideline Number: NIA_CG_124 Last Revised Date:
Cyberknife Information Guide. Prostate Cancer Treatment
 Cyberknife Information Guide Prostate Cancer Treatment CYBERKNIFE INFORMATION GUIDE PROSTATE CANCER TREATMENT As a patient recently diagnosed with localized prostate cancer, it is important that you familiarize
Cyberknife Information Guide Prostate Cancer Treatment CYBERKNIFE INFORMATION GUIDE PROSTATE CANCER TREATMENT As a patient recently diagnosed with localized prostate cancer, it is important that you familiarize
Radiation Therapy in Prostate Cancer Current Status and New Advances
 Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Presentation Welcome Overview of UCSD, Moores
Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Presentation Welcome Overview of UCSD, Moores
BRACHYTHERAPY OR RADIOACTIVE SEED IMPLANTATION CANCER OF THE PROSTATE
 BRACHYTHERAPY OR RADIOACTIVE SEED IMPLANTATION CANCER OF THE PROSTATE Prostate cancer, like other cancers, is a disease of the body's cells. Normal cells reproduce themselves by dividing--facilitating
BRACHYTHERAPY OR RADIOACTIVE SEED IMPLANTATION CANCER OF THE PROSTATE Prostate cancer, like other cancers, is a disease of the body's cells. Normal cells reproduce themselves by dividing--facilitating
An Introduction to PROSTATE CANCER
 An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
CYBERKNIFE RADIOSURGERY FOR EARLY PROSTATE CANCER Rationale and Results. Alan Katz MD JD Flushing, NY USA
 CYBERKNIFE RADIOSURGERY FOR EARLY PROSTATE CANCER Rationale and Results Alan Katz MD JD Flushing, NY USA Prostate Ablative Therapy Over the last 10 years our therapy has improved bned rates for LDR/HDR
CYBERKNIFE RADIOSURGERY FOR EARLY PROSTATE CANCER Rationale and Results Alan Katz MD JD Flushing, NY USA Prostate Ablative Therapy Over the last 10 years our therapy has improved bned rates for LDR/HDR
Treatment Options After Failure of Radiation Therapy A Review Daniel B. Rukstalis, MD
 MANAGEMENT OF RADIATION FAILURE IN PROSTATE CANCER Treatment Options After Failure of Radiation Therapy A Review Daniel B. Rukstalis, MD Division of Urology, MCP Hahnemann University, Philadelphia, PA
MANAGEMENT OF RADIATION FAILURE IN PROSTATE CANCER Treatment Options After Failure of Radiation Therapy A Review Daniel B. Rukstalis, MD Division of Urology, MCP Hahnemann University, Philadelphia, PA
Prostate Cancer. Treatments as unique as you are
 Prostate Cancer Treatments as unique as you are UCLA Prostate Cancer Program Prostate cancer is the second most common cancer among men. The UCLA Prostate Cancer Program brings together the elements essential
Prostate Cancer Treatments as unique as you are UCLA Prostate Cancer Program Prostate cancer is the second most common cancer among men. The UCLA Prostate Cancer Program brings together the elements essential
radiotherapy in locally advanced prostatic cancer: A dosimetric point of view
 Radiotherapy and Oncology 78 (2006) 47 52 www.thegreenjournal.com Prostate brachytherapy 192 Ir or 125 I prostate brachytherapy as a boost to external beam radiotherapy in locally advanced prostatic cancer:
Radiotherapy and Oncology 78 (2006) 47 52 www.thegreenjournal.com Prostate brachytherapy 192 Ir or 125 I prostate brachytherapy as a boost to external beam radiotherapy in locally advanced prostatic cancer:
Prostate Cancer Treatment: What s Best for You?
 Prostate Cancer Treatment: What s Best for You? Prostate Cancer: Radiation Therapy Approaches I. Choices There is really a variety of options in prostate cancer management overall and in radiation therapy.
Prostate Cancer Treatment: What s Best for You? Prostate Cancer: Radiation Therapy Approaches I. Choices There is really a variety of options in prostate cancer management overall and in radiation therapy.
Thomas A. Kollmorgen, M.D. Oregon Urology Institute
 Thomas A. Kollmorgen, M.D. Oregon Urology Institute None 240,000 new diagnosis per year, and an estimated 28,100 deaths (2012) 2 nd leading cause of death from cancer in U.S.A. Approximately 1 in 6 men
Thomas A. Kollmorgen, M.D. Oregon Urology Institute None 240,000 new diagnosis per year, and an estimated 28,100 deaths (2012) 2 nd leading cause of death from cancer in U.S.A. Approximately 1 in 6 men
CMScript. Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014
 Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
External-Beam Radiotherapy in the Management of Carcinoma of the Prostate
 Technological advances in external-beam radiation therapy and the developments in equipment and computers allow for safer delivery of higher radiation doses to the prostate. Tina Sotis. The Tropic of Capricorn
Technological advances in external-beam radiation therapy and the developments in equipment and computers allow for safer delivery of higher radiation doses to the prostate. Tina Sotis. The Tropic of Capricorn
Analysis of Prostate Cancer at Easter Connecticut Health Network Using Cancer Registry Data
 The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
Prostate IMRT: Promises and Problems Chandra Burman, Ph.D. Memorial Sloan-Kettering Cancer Center, New York, NY 10021
 Prostate IMRT: Promises and Problems Chandra Burman, Ph.D. Memorial Sloan-Kettering Cancer Center, New York, NY 10021 Introduction Prostate is one of the treatment sites that is well suited for IMRT. For
Prostate IMRT: Promises and Problems Chandra Burman, Ph.D. Memorial Sloan-Kettering Cancer Center, New York, NY 10021 Introduction Prostate is one of the treatment sites that is well suited for IMRT. For
JAMA. 1998;280:969-974
 Original Contributions Biochemical Outcome After Radical Prostatectomy, Radiation Therapy, or Interstitial for Clinically Localized Prostate Cancer Anthony V. D Amico, MD, PhD; Richard Whittington, MD;
Original Contributions Biochemical Outcome After Radical Prostatectomy, Radiation Therapy, or Interstitial for Clinically Localized Prostate Cancer Anthony V. D Amico, MD, PhD; Richard Whittington, MD;
Radiation Therapy for Prostate Cancer
 Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Erectile function and quality of life after interstitial radiation therapy for prostate cancer
 (2000) 12, Suppl 3, S18±S24 ß 2000 Macmillan Publishers Ltd All rights reserved 0955-9930/00 $15.00 www.nature.com/ijir Erectile function and quality of life after interstitial radiation therapy for prostate
(2000) 12, Suppl 3, S18±S24 ß 2000 Macmillan Publishers Ltd All rights reserved 0955-9930/00 $15.00 www.nature.com/ijir Erectile function and quality of life after interstitial radiation therapy for prostate
Radiation Therapy in Prostate Cancer Current Status and New Advances
 Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Radiation Therapy Wilhelm Roentgen (1845-1923)
Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Radiation Therapy Wilhelm Roentgen (1845-1923)
PSA After Radiation for Prostate Cancer
 Review Article [1] May 01, 2004 By Deborah A. Kuban, MD [2], Howard D. Thames, PhD [3], and Larry B. Levy, MS [4] The introduction of prostate-specific antigen (PSA) as a reliable tumor marker for prostate
Review Article [1] May 01, 2004 By Deborah A. Kuban, MD [2], Howard D. Thames, PhD [3], and Larry B. Levy, MS [4] The introduction of prostate-specific antigen (PSA) as a reliable tumor marker for prostate
Role of Radiation after Radical Prostatectomy Review of Literature
 Vol. 9, No: 1 Jan - Jun 2013. Page 1-44 Role of Radiation after Radical Prostatectomy Review of Literature S.K. Raghunath, N. Srivatsa Abstract Biochemical relapse after radical prostatectomy occurs in
Vol. 9, No: 1 Jan - Jun 2013. Page 1-44 Role of Radiation after Radical Prostatectomy Review of Literature S.K. Raghunath, N. Srivatsa Abstract Biochemical relapse after radical prostatectomy occurs in
A918: Prostate: adenocarcinoma
 A918: Prostate: adenocarcinoma General facts of prostate cancer The prostate is about the size of a walnut. It is just below the bladder and in front of the rectum. The tube that carries urine (the urethra)
A918: Prostate: adenocarcinoma General facts of prostate cancer The prostate is about the size of a walnut. It is just below the bladder and in front of the rectum. The tube that carries urine (the urethra)
Us TOO University Presents: Understanding Diagnostic Testing
 Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Does my patient need more therapy after prostate cancer surgery?
 Does my patient need more therapy after prostate cancer surgery? Contact the GenomeDx Patient Care Team at: 1.888.792.1601 (toll-free) or e-mail: client.service@genomedx.com Prostate Cancer Classifier
Does my patient need more therapy after prostate cancer surgery? Contact the GenomeDx Patient Care Team at: 1.888.792.1601 (toll-free) or e-mail: client.service@genomedx.com Prostate Cancer Classifier
PROTON THERAPY FOR PROSTATE CANCER: THE INITIAL LOMA LINDA UNIVERSITY EXPERIENCE
 doi:10.1016/j.ijrobp.2003.10.011 Int. J. Radiation Oncology Biol. Phys., Vol. 59, No. 2, pp. 348 352, 2004 Copyright 2004 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/04/$ see front
doi:10.1016/j.ijrobp.2003.10.011 Int. J. Radiation Oncology Biol. Phys., Vol. 59, No. 2, pp. 348 352, 2004 Copyright 2004 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/04/$ see front
Therapies for Prostate Cancer and Treatment Selection
 Prostatic Diseases Therapies for Prostate Cancer and Treatment Selection JMAJ 47(12): 555 560, 2004 Yoichi ARAI Professor and Chairman, Department of Urology, Tohoku University Graduate School of Medicine
Prostatic Diseases Therapies for Prostate Cancer and Treatment Selection JMAJ 47(12): 555 560, 2004 Yoichi ARAI Professor and Chairman, Department of Urology, Tohoku University Graduate School of Medicine
150640_Brochure_B 4/12/07 2:58 PM Page 2. Patient Information. Freedom From an Enlarged Prostate
 150640_Brochure_B 4/12/07 2:58 PM Page 2 Patient Information Freedom From an Enlarged Prostate 150640_Brochure_B 4/12/07 2:58 PM Page 3 GreenLight Laser Therapy 1 150640_Brochure_B 4/12/07 2:58 PM Page
150640_Brochure_B 4/12/07 2:58 PM Page 2 Patient Information Freedom From an Enlarged Prostate 150640_Brochure_B 4/12/07 2:58 PM Page 3 GreenLight Laser Therapy 1 150640_Brochure_B 4/12/07 2:58 PM Page
Long-term outcomes and prognostic factors in patients treated with intraoperatively planned prostate brachytherapy
 Brachytherapy - (2012) - Long-term outcomes and prognostic factors in patients treated with intraoperatively planned prostate brachytherapy Carlos Vargas 1, *, Douglas Swartz 2, Apoorva Vashi 2, Mark Blasser
Brachytherapy - (2012) - Long-term outcomes and prognostic factors in patients treated with intraoperatively planned prostate brachytherapy Carlos Vargas 1, *, Douglas Swartz 2, Apoorva Vashi 2, Mark Blasser
Historical Basis for Concern
 Androgens After : Are We Ready? Mohit Khera, MD, MBA Assistant Professor of Urology Division of Male Reproductive Medicine and Surgery Scott Department of Urology Baylor College of Medicine Historical
Androgens After : Are We Ready? Mohit Khera, MD, MBA Assistant Professor of Urology Division of Male Reproductive Medicine and Surgery Scott Department of Urology Baylor College of Medicine Historical
馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引
 馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引 2009.12.02 修 訂 2013.05.13 四 版 前 言 新 竹 馬 偕 醫 院 放 射 腫 瘤 科 藉 由 跨 院 聯 合 會 議 機 制 進 行 討 論, 以 制 定 符 合 現 狀 之 前 列 腺 癌 放 射 治 療 指 引 本 院 前 列 腺 癌 放 射 治 療 指 引 的 建 立, 係 參 考 國 內
馬 偕 紀 念 醫 院 新 竹 分 院 前 列 腺 癌 放 射 治 療 指 引 2009.12.02 修 訂 2013.05.13 四 版 前 言 新 竹 馬 偕 醫 院 放 射 腫 瘤 科 藉 由 跨 院 聯 合 會 議 機 制 進 行 討 論, 以 制 定 符 合 現 狀 之 前 列 腺 癌 放 射 治 療 指 引 本 院 前 列 腺 癌 放 射 治 療 指 引 的 建 立, 係 參 考 國 內
HEALTH NEWS PROSTATE CANCER THE PROSTATE
 HEALTH NEWS PROSTATE CANCER THE PROSTATE Prostate comes from the Greek meaning to stand in front of ; this is very different than prostrate which means to lie down flat. The prostate is a walnut-sized
HEALTH NEWS PROSTATE CANCER THE PROSTATE Prostate comes from the Greek meaning to stand in front of ; this is very different than prostrate which means to lie down flat. The prostate is a walnut-sized
Newly Diagnosed Prostate Cancer: Understanding Your Risk
 Newly Diagnosed Prostate Cancer: Understanding Your Risk When the urologist calls with the life-changing news that your prostate biopsy is positive for prostate cancer, an office appointment is made to
Newly Diagnosed Prostate Cancer: Understanding Your Risk When the urologist calls with the life-changing news that your prostate biopsy is positive for prostate cancer, an office appointment is made to
Early Prostate Cancer: Questions and Answers. Key Points
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
Technical Advices for Prostate Needle Biopsy Under Transrectal Ultrasound Guidance
 Technical Advices for Prostate Needle Biopsy Under Transrectal Ultrasound Guidance Makoto Ohori 1 and Ayako Miyakawa 2 1 Dept. of Urology, Tokyo Medical University 2 Dept. of Molecular Medicine and Surgery,
Technical Advices for Prostate Needle Biopsy Under Transrectal Ultrasound Guidance Makoto Ohori 1 and Ayako Miyakawa 2 1 Dept. of Urology, Tokyo Medical University 2 Dept. of Molecular Medicine and Surgery,
Prostate Cancer. There is no known association with an enlarged prostate or benign prostatic hyperplasia (BPH).
 Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
PATIENT GUIDE. Localized Prostate Cancer
 PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
DIAGNOSIS OF PROSTATE CANCER
 DIAGNOSIS OF PROSTATE CANCER Determining the presence of prostate cancer generally involves a series of tests and exams. Before starting the testing process, the physician will ask questions about the
DIAGNOSIS OF PROSTATE CANCER Determining the presence of prostate cancer generally involves a series of tests and exams. Before starting the testing process, the physician will ask questions about the
Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment.
 Dictionary Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment. Applicator A device used to hold a radioactive source
Dictionary Radiation therapy involves using many terms you may have never heard before. Below is a list of words you could hear during your treatment. Applicator A device used to hold a radioactive source
A Woman s Guide to Prostate Cancer Treatment
 A Woman s Guide to Prostate Cancer Treatment Supporting the man in your life Providing prostate cancer support and resources for women and families WOMEN AGAINST PROSTATE CANCER A Woman s Guide to Prostate
A Woman s Guide to Prostate Cancer Treatment Supporting the man in your life Providing prostate cancer support and resources for women and families WOMEN AGAINST PROSTATE CANCER A Woman s Guide to Prostate
PSA Testing 101. Stanley H. Weiss, MD. Professor, UMDNJ-New Jersey Medical School. Director & PI, Essex County Cancer Coalition. weiss@umdnj.
 PSA Testing 101 Stanley H. Weiss, MD Professor, UMDNJ-New Jersey Medical School Director & PI, Essex County Cancer Coalition weiss@umdnj.edu September 23, 2010 Screening: 3 tests for PCa A good screening
PSA Testing 101 Stanley H. Weiss, MD Professor, UMDNJ-New Jersey Medical School Director & PI, Essex County Cancer Coalition weiss@umdnj.edu September 23, 2010 Screening: 3 tests for PCa A good screening
Prostate Cancer Guide. A resource to help answer your questions about prostate cancer
 Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Prostate Cancer Action Plan: Choosing the treatment that s right for you
 Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
American Brachytherapy Society consensus guidelines for transrectal ultrasound-guided permanent prostate brachytherapy
 Brachytherapy 11 (2012) 6e19 American Brachytherapy Society consensus guidelines for transrectal ultrasound-guided permanent prostate brachytherapy Brian J. Davis 1, *, Eric M. Horwitz 2, W. Robert Lee
Brachytherapy 11 (2012) 6e19 American Brachytherapy Society consensus guidelines for transrectal ultrasound-guided permanent prostate brachytherapy Brian J. Davis 1, *, Eric M. Horwitz 2, W. Robert Lee
Transperineal Permanent Brachytherapy of Localised Prostate Cancer
 european urology supplements 7 (2008) 732 741 available at www.sciencedirect.com journal homepage: www.europeanurology.com Transperineal Permanent Brachytherapy of Localised Prostate Cancer Nader Naderi
european urology supplements 7 (2008) 732 741 available at www.sciencedirect.com journal homepage: www.europeanurology.com Transperineal Permanent Brachytherapy of Localised Prostate Cancer Nader Naderi
HDR Brachytherapy. Patient Information
 HDR Brachytherapy Patient Information 1 About Brachytherapy Cancer is a term used for diseases in which abnormal cells divide without control and then invade other tissues. This disease can affect many
HDR Brachytherapy Patient Information 1 About Brachytherapy Cancer is a term used for diseases in which abnormal cells divide without control and then invade other tissues. This disease can affect many
Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical
 Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Summary. 111 Detection and staging of recurrent prostate cancer is still one of the important clinical problems in prostate cancer. A rise in PSA or biochemical recurrence (BCR) is the first sign of recurrent
Re irradiation Using HDR Interstitial Brachytherapy for Locally Recurrent. Disclosure
 Re irradiation Using HDR Interstitial Brachytherapy for Locally Recurrent Cervical lcancer Yasuo Yoshioka, MD Department of Radiation Oncology Osaka University Graduate School of Medicine Osaka, Japan
Re irradiation Using HDR Interstitial Brachytherapy for Locally Recurrent Cervical lcancer Yasuo Yoshioka, MD Department of Radiation Oncology Osaka University Graduate School of Medicine Osaka, Japan
Treating Prostate Cancer
 Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
1. What is the prostate-specific antigen (PSA) test?
 1. What is the prostate-specific antigen (PSA) test? Prostate-specific antigen (PSA) is a protein produced by the cells of the prostate gland. The PSA test measures the level of PSA in the blood. The doctor
1. What is the prostate-specific antigen (PSA) test? Prostate-specific antigen (PSA) is a protein produced by the cells of the prostate gland. The PSA test measures the level of PSA in the blood. The doctor
Prostate Cancer What Are the Outcomes of Radical Prostatectomy for High-risk Prostate Cancer?
 Prostate Cancer What Are the Outcomes of Radical Prostatectomy for High-risk Prostate Cancer? Stacy Loeb, Edward M. Schaeffer, Bruce J. Trock, Jonathan I. Epstein, Elizabeth B. Humphreys, and Patrick C.
Prostate Cancer What Are the Outcomes of Radical Prostatectomy for High-risk Prostate Cancer? Stacy Loeb, Edward M. Schaeffer, Bruce J. Trock, Jonathan I. Epstein, Elizabeth B. Humphreys, and Patrick C.
High Intensity Focused Ultrasound for Prostate Cancer
 High Intensity Focused Ultrasound for Prostate Cancer Patient Information Exploring a Minimally Invasive Prostate Cancer Therapy The Choice for HIFU Worldwide A Patient s Guide to Prostate Cancer and Sonablate
High Intensity Focused Ultrasound for Prostate Cancer Patient Information Exploring a Minimally Invasive Prostate Cancer Therapy The Choice for HIFU Worldwide A Patient s Guide to Prostate Cancer and Sonablate
Oncology Annual Report: Prostate Cancer 2005 Update By: John Konefal, MD, Radiation Oncology
 Oncology Annual Report: Prostate Cancer 25 Update By: John Konefal, MD, Radiation Oncology Prostate cancer is the most common cancer in men, with 232,9 new cases projected to be diagnosed in the U.S. in
Oncology Annual Report: Prostate Cancer 25 Update By: John Konefal, MD, Radiation Oncology Prostate cancer is the most common cancer in men, with 232,9 new cases projected to be diagnosed in the U.S. in
Protons vs. CyberKnife. Protons vs. CyberKnife. Page 1 UC SF. What are. Alexander R. Gottschalk, M.D., Ph.D.
 Protons vs. CyberKnife UC SF Protons vs. CyberKnife UC SF Alexander R. Gottschalk, M.D., Ph.D. Associate Professor and Director of the CyberKnife Radiosurgery Program Department of Radiation Oncology University
Protons vs. CyberKnife UC SF Protons vs. CyberKnife UC SF Alexander R. Gottschalk, M.D., Ph.D. Associate Professor and Director of the CyberKnife Radiosurgery Program Department of Radiation Oncology University
CURRICULUM VITAE. PETER D. GRIMM, D.O. Prostate Cancer Treatment Center 1-877-330-7722 Email: peter@grimm.com
 CURRICULUM VITAE PETER D. GRIMM, D.O. Prostate Cancer Treatment Center 1-877-330-7722 Email: peter@grimm.com CURRENT STATUS Executive Director (July 2009-present) Chief Executive Officer: Prostate Cancer
CURRICULUM VITAE PETER D. GRIMM, D.O. Prostate Cancer Treatment Center 1-877-330-7722 Email: peter@grimm.com CURRENT STATUS Executive Director (July 2009-present) Chief Executive Officer: Prostate Cancer
Proton Therapy for Prostate Cancer
 Proton Therapy for Prostate Cancer Andrew K. Lee, MD, MPH Director, Proton Therapy Center Associate Professor Department of Radiation Oncology M.D. Anderson Cancer Center Randomized studies showing benefit
Proton Therapy for Prostate Cancer Andrew K. Lee, MD, MPH Director, Proton Therapy Center Associate Professor Department of Radiation Oncology M.D. Anderson Cancer Center Randomized studies showing benefit
Forum. Advances in radiation therapy for prostate. cancer. Abstract. Radiation therapy for localised prostate. cancer
 Advances in radiation therapy for prostate cancer Nitya Patanjali 1 and Scott Williams 2 1. Radiation Oncology, Sydney Cancer Centre, Royal Prince Alfred Hospital, Sydney. 2. Radiation Oncology, Peter
Advances in radiation therapy for prostate cancer Nitya Patanjali 1 and Scott Williams 2 1. Radiation Oncology, Sydney Cancer Centre, Royal Prince Alfred Hospital, Sydney. 2. Radiation Oncology, Peter
Update on Prostate Cancer: Screening, Diagnosis, and Treatment Making Sense of the Noise and Directions Forward
 Update on Prostate Cancer: Screening, Diagnosis, and Treatment Making Sense of the Noise and Directions Forward 33 rd Annual Internal Medicine Update December 5, 2015 Ryan C. Hedgepeth, MD, MS Chief of
Update on Prostate Cancer: Screening, Diagnosis, and Treatment Making Sense of the Noise and Directions Forward 33 rd Annual Internal Medicine Update December 5, 2015 Ryan C. Hedgepeth, MD, MS Chief of
Effective for dates of service on or after May 1, 2015 refer to: Blue Cross and Blue Shield of Alabama Radiation Therapy Management RTM Policies
 Effective for dates of service on or after May 1, 2015 refer to: Blue Cross and Blue Shield of Alabama Radiation Therapy Management RTM Policies Name of Policy: Brachytherapy for Clinically Localized Prostate
Effective for dates of service on or after May 1, 2015 refer to: Blue Cross and Blue Shield of Alabama Radiation Therapy Management RTM Policies Name of Policy: Brachytherapy for Clinically Localized Prostate
Non-coronary Brachytherapy
 Non-coronary Brachytherapy I. Policy University Health Alliance (UHA) will reimburse for non-coronary brachytherapy when it is determined to be medically necessary and when it meets the medical criteria
Non-coronary Brachytherapy I. Policy University Health Alliance (UHA) will reimburse for non-coronary brachytherapy when it is determined to be medically necessary and when it meets the medical criteria
Local Salvage Therapies After Failed Radiation for Prostate Cancer. Biochemical Failure after Radiation
 Local Salvage Therapies After Failed Radiation for Prostate Cancer James Eastham, MD Memorial Sloan-Kettering Cancer Center New York, New York Biochemical Failure after Radiation ASTRO criteria 3 consecutive
Local Salvage Therapies After Failed Radiation for Prostate Cancer James Eastham, MD Memorial Sloan-Kettering Cancer Center New York, New York Biochemical Failure after Radiation ASTRO criteria 3 consecutive
Treating Localized Prostate Cancer A Review of the Research for Adults
 Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
ACTION PLAN. Choosing the treatment that s right for you. Endorsed by Kaiser Permanente Inter-regional Chiefs of Urology
 Prostate Cancer ACTION PLAN Choosing the treatment that s right for you Video Series Guidebook View videos at kpactionplans.org Endorsed by Kaiser Permanente Inter-regional Chiefs of Urology 2015 Kaiser
Prostate Cancer ACTION PLAN Choosing the treatment that s right for you Video Series Guidebook View videos at kpactionplans.org Endorsed by Kaiser Permanente Inter-regional Chiefs of Urology 2015 Kaiser
Prostate Cancer Screening in Taiwan: a must
 Prostate Cancer Screening in Taiwan: a must 吳 俊 德 基 隆 長 庚 醫 院 台 灣 醫 學 會 105 th What is the PSA test? The blood level of PSA is often elevated in men with prostate cancer, and the PSA test was originally
Prostate Cancer Screening in Taiwan: a must 吳 俊 德 基 隆 長 庚 醫 院 台 灣 醫 學 會 105 th What is the PSA test? The blood level of PSA is often elevated in men with prostate cancer, and the PSA test was originally
Current and Future Trends in Proton Treatment of Prostate Cancer
 Current and Future Trends in Proton Treatment of Prostate Cancer Reinhard W. Schulte Assistant Professor Department of Radiation Medicine Loma Linda University Medical Center Loma Linda, CA, USA Outline
Current and Future Trends in Proton Treatment of Prostate Cancer Reinhard W. Schulte Assistant Professor Department of Radiation Medicine Loma Linda University Medical Center Loma Linda, CA, USA Outline
For further information on screening and early detection of prostate cancer, see the Section entitled Screening for Prostate Cancer.
 Prostate Cancer For many older men, prostate cancer may be present but never cause symptoms or problems and many men will die with their prostate cancer rather than of their prostate cancer. Yet it remains
Prostate Cancer For many older men, prostate cancer may be present but never cause symptoms or problems and many men will die with their prostate cancer rather than of their prostate cancer. Yet it remains
TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software.
 SAMPLE CLINICAL RESEARCH APPLICATION ABSTRACT: TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software. Hypothesis:
SAMPLE CLINICAL RESEARCH APPLICATION ABSTRACT: TITLE: Comparison of the dosimetric planning of partial breast irradiation with and without the aid of 3D virtual reality simulation (VRS) software. Hypothesis:
Hyperthermia: a treatment possibility for prostate cancer
 Oncothermia Journal 6:47--53 (2012) Hyperthermia: a treatment possibility for prostate cancer Friedreich R. Douwes MD St. George Hospital, Bad Aibling, Germany Oncothermia Journal, September 2012 46 Hyperthermia:
Oncothermia Journal 6:47--53 (2012) Hyperthermia: a treatment possibility for prostate cancer Friedreich R. Douwes MD St. George Hospital, Bad Aibling, Germany Oncothermia Journal, September 2012 46 Hyperthermia:
PROSTATE CANCER. Diagnosis and Treatment
 Diagnosis and Treatment Table of Contents Introduction... 1 Patient and Coach Information... 1 About Your Prostate... 1 What You Should Know About Prostate Cancer... 2 Screening and Diagnosis... 2 Digital
Diagnosis and Treatment Table of Contents Introduction... 1 Patient and Coach Information... 1 About Your Prostate... 1 What You Should Know About Prostate Cancer... 2 Screening and Diagnosis... 2 Digital
Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Pre-authorization Required]
![Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Pre-authorization Required] Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Pre-authorization Required]](/thumbs/33/16383859.jpg) Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Pre-authorization Required] Medical Policy: MP-SU-01-11 Original Effective Date: February 24, 2011 Reviewed: February 24, 2012 Revised:
Accelerated Partial Breast Irradiation (APBI) for Breast Cancer [Pre-authorization Required] Medical Policy: MP-SU-01-11 Original Effective Date: February 24, 2011 Reviewed: February 24, 2012 Revised:
GYNECOLOGIC CANCERS Facts to Help Patients Make an Informed Decision
 RADIATION THERAPY FOR GYNECOLOGIC CANCERS Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY FACTS ABOUT GYNECOLOGIC CANCERS Gynecologic cancers
RADIATION THERAPY FOR GYNECOLOGIC CANCERS Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY FACTS ABOUT GYNECOLOGIC CANCERS Gynecologic cancers
Understanding the. Controversies of. testosterone replacement. therapy in hypogonadal men with prostate cancer. controversies surrounding
 Controversies of testosterone replacement therapy in hypogonadal men with prostate cancer Samuel Deem, DO CULTURA CREATIVE (RF) / ALAMY Understanding the controversies surrounding testosterone replacement
Controversies of testosterone replacement therapy in hypogonadal men with prostate cancer Samuel Deem, DO CULTURA CREATIVE (RF) / ALAMY Understanding the controversies surrounding testosterone replacement
BRACHYTHERAPY FOR TREATMENT OF BREAST CANCER
 BRACHYTHERAPY FOR TREATMENT OF BREAST CANCER Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
BRACHYTHERAPY FOR TREATMENT OF BREAST CANCER Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
Precise, Minimally Invasive Prostate Cancer Removal
 Precise, Minimally Invasive Prostate Cancer Removal Learn why da Vinci Surgery may be your best treatment option 1 Beyond Minimally Invasive For Prostate Cancer 1 Facing Prostate Cancer Prostate cancer
Precise, Minimally Invasive Prostate Cancer Removal Learn why da Vinci Surgery may be your best treatment option 1 Beyond Minimally Invasive For Prostate Cancer 1 Facing Prostate Cancer Prostate cancer
Understanding Prostate Cancer. The Urology Group Guide for Newly Diagnosed Patients. Advanced Care. Improving Lives.
 Understanding Prostate Cancer The Urology Group Guide for Newly Diagnosed Patients Advanced Care. Improving Lives. UNDERSTANDING PROSTATE CANCER The Urology Group has created this publication to provide
Understanding Prostate Cancer The Urology Group Guide for Newly Diagnosed Patients Advanced Care. Improving Lives. UNDERSTANDING PROSTATE CANCER The Urology Group has created this publication to provide
