BRACHYTHERAPY OR RADIOACTIVE SEED IMPLANTATION CANCER OF THE PROSTATE
|
|
|
- Albert Robertson
- 8 years ago
- Views:
Transcription
1 BRACHYTHERAPY OR RADIOACTIVE SEED IMPLANTATION CANCER OF THE PROSTATE Prostate cancer, like other cancers, is a disease of the body's cells. Normal cells reproduce themselves by dividing--facilitating growth and replacing worn-out and injured tissue. Cancer is characterized by the uncontrolled growth of abnormal body cells. Occasionally, cells grow abnormally into a tumor mass. Some tumors are benign (non-cancerous); others are malignant, or cancerous. Cancers invade and destroy nearby tissues and organs or spread to other parts of the body. Prostate cancer is now the most common type of cancer of the male. If not treated early and effectively, however, prostate tumors can start to grow and spread into other tissues such as lymph nodes and bone. Although only a small proportion of prostate cancers progress to this severe stage, the ones that do can spread relatively quickly and are not easily treated or cured. The cancer can grow without symptoms for years, even decades. Prostate cancer is rare before the age of 40, and the risk increases with age. Its cause is unknown. GOALS OF PROSTATE CANCER TREATMENT Ideally, treatment for any cancer should cure the disease, be easily tolerated, and cause minimal or no problems. This concept is particularly important in prostate cancer for several reasons. Some men have an aggressive form of cancer that can lead to death from this disease. In other men, prostate cancers can grow so slowly that it causes few if any problems during a patient's natural lifetime. However, there is no absolute way to determine if prostate cancer will be aggressive or slow growing. Therefore, for most men whose disease is confined to the prostate, treatment is preferable to waiting and watching, especially since, as our life expectancies continue to increase, even slowgrowing cancers could in time become life-threatening. In other words, the ideal treatment for prostate cancer should effectively arrest or cure the disease particularly in men with aggressive cancer, but cause little if any problems, especially for men with slow-growing disease. Furthermore, since many men with prostate cancer are older or have other medical problems that make it impossible for them to undergo radical treatment, a treatment that minimizes trauma and complications is essential. CURRENT TREATMENT OPTIONS To ensure that prostate cancer does not develop further and is halted soon after diagnosis, physicians recommend early treatment to either remove or kill the tumor. The three main treatment options for early stage prostate cancer are
2 radical prostatectomy, external beam radiation therapy, and radioactive seed implants. Some physicians and patients will employ an observational strategy termed Watchful Waiting or Observation. This may be a good choice in older men (over 75 or in poor health) who have cancers that are slow-growing, meaning Gleason Score 2, 3, or 4. Evidence shows that younger men with Gleason Score cancers of 5-10 will require treatment for advanced prostate cancer about 65% of the time in less than 10 years if they don't die of something else. Since the hormonal treatment used for advanced cancers is not curative and still has side effects, most healthy younger men with more aggressive cancers prefer to be treated earlier when the potential for cure is higher. RADICAL PROSTATECTOMY Radical prostatectomy is currently the most common treatment for early-stage prostate cancer in the U.S. It is a major surgical procedure in which the surgeon removes the prostate gland, usually through an incision in the lower abdomen. Advantages: Surgery is a one-time procedure that may cure early prostate cancer. It has been considered the "gold standard" for treatment. However, this is not based on clinical studies comparing surgery to either external beam or brachytherapy. Cure rates for those who undergo surgery for early, localized cancer (T1-T2) are only roughly 75% at 5 years and roughly 60% at ten years after treatment. However, if the operation is done in men with advanced disease, only 35 to 50% might be cured with surgery alone. Disadvantages: Radical prostatectomy requires hospitalization and is not tolerated well in older men who are not in overall excellent health. The side effects from surgery include impotence (inability to have an erection) in a high percentage of patients (generally more than 75 to 80%) and incontinence (a loss of urinary control) in a small percentage (1-2% severe, up to 20% mild or moderate). Recovery from surgery takes 4 to 6 weeks, and a catheter is usually maintained in the bladder for two to three weeks after the operation. In virtually all series, even recent ones, the mortality of the surgery alone results in 1% of men dying, usually from blood clots to the lungs. Laparoscopic and Robot-assisted Laparoscopic Prostatectomy Some surgeons are learning to remove the prostate with less invasive procedures. Patients may return to activities more quickly. However, to date, failure to cure by having positive margins does not appear to be lessened with
3 either technique, occurring in as many as 25 to 28% of patients undergoing these forms of surgical treatment. Incontinence is still an issue after these approaches. What percentage of men are cured after radical surgery? A number of factors determine the outcome after surgery. Five and 10-year cure rates are shown in the table near the end of this file. The likelihood of cure goes down as PSA, Gleason Score, and extent of cancer go up. Other factors such as race and obesity may also have an impact. In a recent series of over 3,100 men undergoing surgery, Amling and associates showed that African-Americans and obese males had a worse outcome than Caucasians. However, among nonobese and Caucasian men, the cure rate after surgery was no better than 66-67% by 5 years, and only 51% at 10 years after surgery: Amling et al: Pathologic Variables and Recurrence Rates As Related to Obesity and Race in Men with Prostate Cancer Undergoing Radical Prostatectomy. J Clin Oncol 22: , Copyright American Society of Clinical Oncology. What percentage of patients undergoing surgery have an Optimal Outcome, that is, are cured, potent, and continent? In a landmark paper, Saranchuk studied 647 continent, potent men who underwent surgery. Cancer-free status with full continence and potency was achieved in 30% at 12 months, 42% at 24 months, 47% at 36 months, and only 53% at 48 months after surgery. 38% were impotent or incontinent, and 12% had a rising PSA at this early point:
4 Fig 5. Results of Markov model Saranchuk, J. W. et al. J Clin Oncol; 23: Copyright American Society of Clinical Oncology EXTERNAL BEAM RADIATION THERAPY or IMRT Radiation to stop the growth of cancer cells is delivered using a machine (usually a linear accelerator) that shoots a beam of radiation from outside the body through normal body tissue to reach the cancer. The radiation is given in short sessions over a long period, normally once a day, five days a week over a sevenor-eight-week period, to minimize damage to the normal tissue. Newer techniques may allow improved delivery and energy to the prostate, such as the Peacock device, Proton therapy, or IMRT. Advantages: External beam radiation therapy has a cure rate similar to surgery for early prostate cancer, perhaps 50 to 60% at ten years after treatment. Because it is not a surgical procedure, it is better tolerated, especially in older men. Hospitalization and anesthesia are not required and there are no life-threatening complications. When compared to radical prostatectomy, the risk of impotence is lower and the incidence of incontinence is approximately the same.
5 Disadvantages: Although hospitalization is not necessary, the patient must make daily visits to the radiation center for nearly two months. There is still a significant risk of impotence and external radiation damage to healthy tissue, such as the rectum and the bladder. While most of these are minor and disappear shortly after therapy stops, they include fatigue, skin reactions in the treated areas, frequent and painful urination, upset stomach, diarrhea and rectal irritation or bleeding. In some cases, damage to the rectum or bladder can be severe and permanent. BRACHYTHERAPY OR RADIOACTIVE SEED IMPLANTS In the early 1970s, a new approach was developed to confine radiation exposure to the prostate gland, increase radiation dosage to the tumor in order to kill the cancer, and minimize side effects. Cancer specialists began to implant radioactive iodine (I-125) seeds directly into the prostate, thereby providing internal radiation therapy exactly where it was needed. In these early attempts, surgery was performed to expose the prostate gland and the radioactive seeds were implanted freehand, without the aid of imaging techniques now available. This early method of prostate implantation began at New York's Memorial Sloan- Kettering Cancer Center. The results were not satisfactory due to incomplete coverage due to the uneven distribution of seeds placed in that fashion. In the 1980's, several groups began to use trans-rectal ultrasound to map the prostate, plan effective distribution of the seeds, and then do the implantation using ultrasound to guide seed placement in order to achieve an even distribution of radiation. Ten year data is now available from several centers, and results with this technique are at least as good as with surgery for prostate cancer (see table below). In addition to I-125, a newer agent, palladium or Pd-103 is now used. Both iodine and palladium appear to be well suited for prostate implantation. They give off very low energy radiation over several months which does not travel far outside the prostate and poses no threat to patients or those near them. This is termed low dose rate (LDR) permanent brachytherapy implantation. Using needles passed through the skin behind the scrotum (the perineum), pellets or seeds containing the radioactive iodine or palladium are permanently implanted directly into the prostate where they give off low-level radiation continuously for several months. Using trans-rectal ultrasound guidance, these seeds can be positioned so that radiation is distributed evenly throughout the prostate gland. Since only a small area is irradiated by each seed, relatively little radiation reaches the adjacent normal organs-the colon, which is directly under the prostate gland, or the bladder, lying on top of the gland. The entire prostate is radiated, since more than half the time, there are second or third cancers in addition to the one that might have been found on needle biopsy. The total dose
6 of radiation delivered to the prostate exceeds that which can be delivered by external beam therapy. The implant procedure does not require a surgical incision. Instead, the seeds are contained in thin needles which are passed into the prostate gland through the skin between the scrotum and rectum. The location of the needles can be seen on the screen of the ultrasound machine and can be accurately guided to the desired position. While the needles are being inserted, the ultrasound probe is in the rectum. When each needle is in its correct position in the prostate, the needle is slowly withdrawn and the individual seeds are injected into the prostate gland. The ultrasound probe and the needles are removed when the procedure has been completed. The numbers of needles and seeds required varies depending upon the size and shape of the prostate gland. Thus, treatment is truly tailored to each patient individually. Depending upon the size of the prostate and the extent of cancer in it, implant therapy may be performed as the only therapy used, or it may be used in combination with androgen blockade (hormonal) therapy or external beam radiation. In rare cases, all three modes of treatment might be combined. Most prostates are small enough to be implanted without needing to shrink them. However, big prostates may be hard to get the needles into because the pelvic bone blocks part of the gland. In such cases, hormonal treatment is used for several months to shrink the prostate and allow successful implantation. Advantages: Results from centers using I-125 and palladium since 1985 show a higher percentage of implant patients remaining disease-free than with either radical prostatectomy or external beam therapy. Seed implantation is normally done as an outpatient procedure taking about one hour to perform. The patient usually leaves the hospital the same day as the implant procedure or stays in the hospital for one night and then resumes normal activities within several days. Because they are placed inside the prostate, seeds actually deliver 2 to 4 times more radiation to the cancer than external radiation therapy or IMRT, which must use a lower dose because they may damage healthy tissue. This procedure is well suited to older patients because it is much easier to undergo than surgery or external radiation. It is well suited to younger patients who would prefer to avoid the rigors and potential complications of radical prostatectomy.
7 Disadvantages: There is little information yet on the effectiveness of the implant treatment after 10 years. While the current clinical data show good results through 10 years, younger men often are advised more strongly to consider radical prostatectomy. However, randomized comparisons of surgery to seed implant therapy are not underway, nor are they likely to take place. There is actually no factual basis on which to base the statement that younger men should undergo surgical removal of the prostate rather than seed implantation. It is common to experience problems with urination after seed implantation. Most are discharged without a catheter but 2-3% of men may need a bladder catheter to drain the urine for a few days after the procedure. Burning on urination as well as an ache from the prostate may occur as the radiation effect on the tissue occurs. Some increase in frequency of urination is to be expected. These symptoms will gradually disappear after a few weeks to 6 months, and by one year, most men are voiding at their pre-treatment levels. Incontinence occurs in less than 1% of patients who have not had prior surgery. If a patient has had a prior TURP or needs one later, some degree of urinary leakage may occur. Impotence occurs in less than 15% of patients under the age of 70. For patients over the age of 70, impotence occurs more often. Rectal irritation is frequent after an implant, but usually transient and self-limited. Bleeding from radiation changes can occur one or more years later and usually requires colonosopy and cauterization. Serious injury to the rectum can occur and may require colostomy. This is less common with brachytherapy seeds (less than 1%) than with external radiation alone (5%), but higher (3%) in patients receiving brachytherapy combined with external beam. Fortunately, the addition of external radiation to the seeds as combination therapy is necessary in only less than 5% of patients. WHO ARE BEST CANDIDATES FOR IMPLANTATION? Patients with early-stage and small prostate tumors are the best candidates for implant alone. That means that about 60 to 70% of men with prostate cancer will fit these criteria. The development of more sensitive tumor detection techniques means that prostate cancer patients are being diagnosed at earlier stages, permitting more patients to become potential candidates for seed implantation. More importantly, many men with low PSA and limited cancer will be found, after surgical removal of the prostate, to have extension of the cancer into the capsule, leading to "positive margins" with cancer left behind if the prostate is removed surgically. The Partin Tables can and should be used to help each patient understand his probability of having his cancer invade the capsule of the prostate
8 before a decision is made for surgery. This is the major reason for failure in most of those who fail to be cured by surgery. Even with positive margins, it may be several years after surgery before the PSA begins to rise again. That is why the percentage of patients cured by surgery averages only 75% five years after surgery, and drops further to 50 to 70% at 10 years, and a low 44% 15 years after surgery (see Table below). Since radiation with seeds alone or seeds with a low dose of external beam has the potential for killing the cancer that has invaded the capsule, many patients who would appear to be good candidates for surgery might be even better treated with brachytherapy. The fact that overall side effects with brachytherapy are less is an additional benefit of brachytherapy. The Radioactive Seed Implant Procedure: Before, During and After Before the Implant A volume study to determine the shape and size of the cancer will usually be performed about three weeks before the implant. Using a trans-rectal ultrasound unit, we will locate your prostate and a computer will make an exact 3-D model of the gland. This will allow the radiation physicist to determine the number of seeds needed to treat the prostate and exactly where they should be placed. A single slice (1 of 8 to 10) showing locations of seeds and the shape of the radiation field (yellow = 145 Gy, blue = 116 Gy) surrounding the prostate (green line): Approximately one week prior to the implant, you will have blood tests done and possibly an electrocardiogram (EKG) and chest X-ray. The test results are used to inform the anesthesiologist of your ability to tolerate anesthesia. You also will be given specific instructions regarding diet and enemas, and when to arrive at
9 the hospital. The enemas will help remove fecal material from your lower bowel and rectum so that the ultrasound image of your prostate will be optimal. During the Implant The implant procedure is performed in the operating room and lasts about 45 minutes. You will probably receive general anesthesia. You may also receive medication through an intravenous (I.V.) line, which will make you feel drowsy before the anesthetic takes over. An ultrasound probe will be inserted into the rectum to image the prostate on a television monitor. The seeds, usually numbering about 75 to 125, are then inserted into the prostate through 18 to 30 needles. The needles are inserted through the skin between the scrotum and the rectum and, with the transrectal ultrasound device, are guided with pin-point accuracy directly to their intended locations. After the seeds have been placed, a flexible scope is passed into the bladder to make sure that no seeds are loose in the urine channel or in the bladder itself. After that, a catheter is temporarily placed in your bladder to drain urine. After the Implant After the implant you will go to the recovery room for one to two hours, until you have awakened and are alert and medically stable for discharge. The urinary catheter is usually removed when you are alert and the urine is clear. Since seed implants are an outpatient procedure, you can go home or to your hotel after you have recovered from the anesthesia. Because you may feel a little weak, it is recommended that you do not drive for at least 12 hours. You may resume eating and have visitors as soon as you wish, but you should avoid heavy lifting or strenuous physical activity for the first two days you are home. After that, you will probably be ready to return to your normal activity
10 level. You will be placed on antibiotics for several days after the procedure. Most men return to work the next day. Possible Side Effects There is surprisingly little discomfort after the implant, although mild soreness is expected between the legs for one to two days. You may experience some slight bleeding or burning beneath the scrotum, or blood in the urine. These side effects are caused by the needles used to place the seeds. The seeds themselves, the catheter and other instruments used during the procedure also can contribute to these side effects. It is normal for some blood to appear in the urine draining from the catheter, which may continue for several days. While this slight bleeding is no cause for alarm, if it should become severe or there are large blood clots, call your urologist. Drinking plenty of water helps prevent blood clots and flushes the bladder. Other side effects that may occur after the implant, such as frequent urination or burning on urination, are generally due to the radiation from the seeds in the prostate. If severe, we will want to check your urine soon for infection. If not due to an infection, these symptoms will gradually decrease as the seeds lose their strength. Drinking plenty of fluids and avoiding caffeine may help to relieve these symptoms. If you have significant trouble urinating before or after the implant, you might be given medication to help, such as Hytrin or Flomax. As with all medical procedures, there is a small chance that there could be other longer term, or even permanent, side effects. Radiation Safety Many patients are concerned about whether an implant poses any potential dangers of radiation exposure to their family and friends. The seeds used in implant therapy emit a very low energy radiation that does not travel far; in fact, the vast majority of the radiation does not go beyond the prostate itself. Very small amounts of radiation, however, can reach other people either from a seed being passed in the urine or if a tiny amount of radiation escapes from the prostate and travels a short distance through the air. Because the amount that might escape is so small, it is not considered a risk for most people, and there are no restrictions on a patient's travel or physical contact with other adults. Small children and pregnant women, however, may be more sensitive to the effects of radiation. It is usually recommended that young children and pregnant women not be on the lap of the patient for the first two months following the implant. Suggested Follow-Up Schedule
11 After a seed implant, follow-up with your urologist and radiation oncologist should be done on a regular basis. Both of us will work together to provide you with the best care possible. The follow-up schedule usually includes a visit at 3 weeks to check for seed placement using a CAT scan. Further visits are then usually scheduled every three to six months for the first five years, to monitor treatment progress. Physical examination and blood tests will be performed periodically. BRACHYTHERAPY USING HIGH DOSE RATE AFTERLOADING WITH IRIDIUM A variation of brachytherapy is called HDR or High Dose Rate Afterloading. In this technique, which is used in only a few centers in the US, needles are placed into the prostate. The position of the needles is then checked with ultrasound or CAT scan and a dose plan is created. The patient is transferred to a special lead lined room that protects the staff from the radiation. A computer driven device then places a radioactive substance, usually Iridium-192, into the needles for a measured length of time. This appears to give a more exact dose of radiation to the prostate than external beam therapy. The patient will receive one to four treatments. External beam therapy must be added to this type of radiation. Data from HDR treated patients is much too early to determine how effective it might be. The major detraction is that the patient is awake and confined to a bed while the needles are held in place between the legs. For patients who need to have a pelvic lymph node dissection done prior to radiation, such bedrest and high dose therapy may not be unreasonable. However, most patients needing seed implants do not require lymph node dissection, so confinement to bed for this period to accomplish HDR therapy seems excessive compared to the ease of implant therapy. CRYOSURGERY OR FREEZING Freezing the prostate while it is still in the body is erroneously termed cryousurgery, since it is not a surgical procedure. It is being developed as a non-surgical method of treating prostate cancer. Under anesthesia, probes are placed into the prostate and it is frozen and thawed twice to literally turn the prostate into a ball of ice. Cell death occurs, and this can be effective in the short-term in controlling some cancers, though moderate morbidity and side effects may result. It may be useful to treat men who have failed external beam therapy. A major practical limitation is that the freeze line cannot be taken beyond the prostate for fear of causing damage to adjacent structures, and it is clear that most of the failures to surgery are due to disease that is already outside the prostate at the time of surgery. A clear role for cryo in the treatment of early, localized prostate cancer has not been defined clearly.
12 Percent of Patients With Undedetectable PSA after Surgery or < 0.5 after Brachytherapy Physician/Institution 5 years 10 years 15 years Radical Prostatectomy for T1-T2 Catalona/ Wash. U. 78% 68% n.a. Ohori / Baylor 76% 73% n.a. Partin / Hopkins 83% 70% n.a. Paulson / Duke 75% n.a. n.a. Trapasso / UCLA 69% 47% n.a. Zincke / Mayo 77% 54% 44% Amling et al, % 48% n.a. Brachtherapy for T1-T3 AVERAGE 75% 58% 44% Grimm / Northwest Inst. ( ) 91% 87% 84% Blasko et al, 2000 (Seeds only) 87% 85% Critz, 2002 (PSA < 0.2) 87% 84% adapted from Ragde et al, Cancer 83: , 1998
13 The Partin Table The Partin Table is a useful guide to predict the pathologic findings if a man were to have his prostate removed for cancer. It is based upon several thousand men who had cancer and underwent surgery. Ideally, the cancer would be contained or confined to the prostate, and not involve the capsule, seminal vesicles, or lymph nodes. We will fill this in when you visit with us. Based upon your Stage, Gleason Score, and PSA, the Partin Table predicts for you: - Organ-contained cancer in %; - Extension outside the prostate in %; - Seminal vesicle involvement in %; - Cancer in the lymph nodes in %.
PSA Screening for Prostate Cancer Information for Care Providers
 All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
All men should know they are having a PSA test and be informed of the implications prior to testing. This booklet was created to help primary care providers offer men information about the risks and benefits
Early Prostate Cancer: Questions and Answers. Key Points
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Early Prostate Cancer:
Bard: Prostate Cancer Treatment. Bard: Pelvic Organ Prolapse. Prostate Cancer. An overview of. Treatment. Prolapse. Information and Answers
 Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Bard: Prostate Cancer Treatment Bard: Pelvic Organ Prolapse Prostate Cancer An overview of Pelvic Treatment Organ Prolapse Information and Answers A Brief Overview Prostate Anatomy The prostate gland,
Prostate Cancer Screening. A Decision Guide
 Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Radiation Therapy for Prostate Cancer
 Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
Radiation Therapy for Prostate Cancer Introduction Cancer of the prostate is the most common form of cancer that affects men. About 240,000 American men are diagnosed with prostate cancer every year. Your
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options
 AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
Prostate Cancer Screening. A Decision Guide for African Americans
 Prostate Cancer Screening A Decision Guide for African Americans This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Published
Prostate Cancer Screening A Decision Guide for African Americans This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Published
Prostate Cancer. Patient Information
 Prostate Cancer Patient Information 1 The Prostate & Prostate Cancer The prostate is a small gland in the male reproductive system, approximately the size and shape of a walnut. It is located directly
Prostate Cancer Patient Information 1 The Prostate & Prostate Cancer The prostate is a small gland in the male reproductive system, approximately the size and shape of a walnut. It is located directly
A Woman s Guide to Prostate Cancer Treatment
 A Woman s Guide to Prostate Cancer Treatment Supporting the man in your life Providing prostate cancer support and resources for women and families WOMEN AGAINST PROSTATE CANCER A Woman s Guide to Prostate
A Woman s Guide to Prostate Cancer Treatment Supporting the man in your life Providing prostate cancer support and resources for women and families WOMEN AGAINST PROSTATE CANCER A Woman s Guide to Prostate
Treating Localized Prostate Cancer A Review of the Research for Adults
 Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
Treating Localized Prostate Cancer A Review of the Research for Adults Is this information right for me? Yes, this information is right for you if: Your doctor * said all tests show you have localized
Prostate Cancer. There is no known association with an enlarged prostate or benign prostatic hyperplasia (BPH).
 Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Prostate Cancer Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnut-sized structure that makes up part of a man's reproductive system. It wraps around
Radioactive Seed Implants for Prostate Cancer information for patients and their families
 UROLOGICAL CANCER Radioactive Seed Implants for Prostate Cancer information for patients and their families The Alvin J. Siteman Cancer Center 660 South Euclid Avenue, Box 8100 St. Louis, MO 63110-1093
UROLOGICAL CANCER Radioactive Seed Implants for Prostate Cancer information for patients and their families The Alvin J. Siteman Cancer Center 660 South Euclid Avenue, Box 8100 St. Louis, MO 63110-1093
Prostate Cancer. What is prostate cancer?
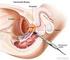 Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Scan for mobile link. Prostate Cancer Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam, prostate-specific
Prostate Cancer Action Plan: Choosing the treatment that s right for you
 Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
Prostate Cancer Action Plan: Choosing the treatment that s right for you Segment 1: Introduction Trust me, there's a better way to choose a treatment for your prostate cancer. Watching this program is
Prostate Cancer Treatment
 Scan for mobile link. Prostate Cancer Treatment Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam,
Scan for mobile link. Prostate Cancer Treatment Prostate cancer is a tumor of the prostate gland, which is located in front of the rectum and below the bladder. Your doctor may perform a physical exam,
An Introduction to PROSTATE CANCER
 An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
An Introduction to PROSTATE CANCER Being diagnosed with prostate cancer can be a life-altering experience. It requires making some very difficult decisions about treatments that can affect not only the
PATIENT GUIDE. Localized Prostate Cancer
 PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
PATIENT GUIDE Localized Prostate Cancer The prostate* is part of the male reproductive system. It is about the same size as a walnut and weighs about an ounce. As pictured in Figure 1, the prostate is
FAQ About Prostate Cancer Treatment and SpaceOAR System
 FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
FAQ About Prostate Cancer Treatment and SpaceOAR System P. 4 Prostate Cancer Background SpaceOAR Frequently Asked Questions (FAQ) 1. What is prostate cancer? The vast majority of prostate cancers develop
Understanding brachytherapy
 Understanding brachytherapy Brachytherapy Cancer Treatment Legacy Cancer Institute Your health care provider has requested that you receive a type of radiation treatment called brachytherapy as part of
Understanding brachytherapy Brachytherapy Cancer Treatment Legacy Cancer Institute Your health care provider has requested that you receive a type of radiation treatment called brachytherapy as part of
These rare variants often act aggressively and may respond differently to therapy than the more common prostate adenocarcinoma.
 Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
Prostate Cancer OVERVIEW Prostate cancer is the second most common cancer diagnosed among American men, accounting for nearly 200,000 new cancer cases in the United States each year. Greater than 65% of
PROSTATE CANCER. Get the facts, know your options. Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology
 PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
PROSTATE CANCER Get the facts, know your options Samay Jain, MD, Assistant Professor,The University of Toledo Chief, Division of Urologic Oncology i What is the Prostate? Unfortunately, you have prostate
Prostate Cancer Guide. A resource to help answer your questions about prostate cancer
 Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
Prostate Cancer Guide A resource to help answer your questions about prostate cancer Thank you for downloading this guide to prostate cancer treatment. We know that all the information provided online
A918: Prostate: adenocarcinoma
 A918: Prostate: adenocarcinoma General facts of prostate cancer The prostate is about the size of a walnut. It is just below the bladder and in front of the rectum. The tube that carries urine (the urethra)
A918: Prostate: adenocarcinoma General facts of prostate cancer The prostate is about the size of a walnut. It is just below the bladder and in front of the rectum. The tube that carries urine (the urethra)
Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE
 Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE Introduction This guide is designed to help you clarify and understand the decisions that need to be made about your care for the
Understanding Your Diagnosis of Endometrial Cancer A STEP-BY-STEP GUIDE Introduction This guide is designed to help you clarify and understand the decisions that need to be made about your care for the
LIvING WITH Prostate Cancer
 Living with Prostate Cancer A Common Cancer in Men If you ve been diagnosed with prostate cancer, it s normal to be concerned about your future. It may help you to know that this disease can often be cured
Living with Prostate Cancer A Common Cancer in Men If you ve been diagnosed with prostate cancer, it s normal to be concerned about your future. It may help you to know that this disease can often be cured
Treating Prostate Cancer
 Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
HEALTH NEWS PROSTATE CANCER THE PROSTATE
 HEALTH NEWS PROSTATE CANCER THE PROSTATE Prostate comes from the Greek meaning to stand in front of ; this is very different than prostrate which means to lie down flat. The prostate is a walnut-sized
HEALTH NEWS PROSTATE CANCER THE PROSTATE Prostate comes from the Greek meaning to stand in front of ; this is very different than prostrate which means to lie down flat. The prostate is a walnut-sized
Oncology Annual Report: Prostate Cancer 2005 Update By: John Konefal, MD, Radiation Oncology
 Oncology Annual Report: Prostate Cancer 25 Update By: John Konefal, MD, Radiation Oncology Prostate cancer is the most common cancer in men, with 232,9 new cases projected to be diagnosed in the U.S. in
Oncology Annual Report: Prostate Cancer 25 Update By: John Konefal, MD, Radiation Oncology Prostate cancer is the most common cancer in men, with 232,9 new cases projected to be diagnosed in the U.S. in
to Know About Your Partner s
 What You Need to Know About Your Partner s Prostate Cancer. A Guide for Wives, Partners, and the Men They Love. Providing Support for Your Partner Prostate cancer can be a physical and emotional challenge
What You Need to Know About Your Partner s Prostate Cancer. A Guide for Wives, Partners, and the Men They Love. Providing Support for Your Partner Prostate cancer can be a physical and emotional challenge
Prostate Cancer Treatment: What s Best for You?
 Prostate Cancer Treatment: What s Best for You? Prostate Cancer: Radiation Therapy Approaches I. Choices There is really a variety of options in prostate cancer management overall and in radiation therapy.
Prostate Cancer Treatment: What s Best for You? Prostate Cancer: Radiation Therapy Approaches I. Choices There is really a variety of options in prostate cancer management overall and in radiation therapy.
GYNECOLOGIC CANCERS Facts to Help Patients Make an Informed Decision
 RADIATION THERAPY FOR GYNECOLOGIC CANCERS Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY FACTS ABOUT GYNECOLOGIC CANCERS Gynecologic cancers
RADIATION THERAPY FOR GYNECOLOGIC CANCERS Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY FACTS ABOUT GYNECOLOGIC CANCERS Gynecologic cancers
Prostate Cancer Screening
 Prostate Cancer Screening The American Cancer Society and Congregational Health Ministry Team June Module To access this module via the Web, visit www.cancer.org and type in congregational health ministry
Prostate Cancer Screening The American Cancer Society and Congregational Health Ministry Team June Module To access this module via the Web, visit www.cancer.org and type in congregational health ministry
DIAGNOSIS OF PROSTATE CANCER
 DIAGNOSIS OF PROSTATE CANCER Determining the presence of prostate cancer generally involves a series of tests and exams. Before starting the testing process, the physician will ask questions about the
DIAGNOSIS OF PROSTATE CANCER Determining the presence of prostate cancer generally involves a series of tests and exams. Before starting the testing process, the physician will ask questions about the
Prostate Cancer. Understanding your diagnosis
 Prostate Cancer Understanding your diagnosis Prostate Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount
Prostate Cancer Understanding your diagnosis Prostate Cancer Understanding your diagnosis When you first hear that you have cancer, you may feel alone and afraid. You may be overwhelmed by the large amount
Cryosurgery in Cancer Treatment: Questions and Answers. Key Points
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Cryosurgery in Cancer
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Cryosurgery in Cancer
Laparoscopic Colectomy. What do I need to know about my laparoscopic colorectal surgery?
 Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
Laparoscopic Colectomy What do I need to know about my laparoscopic colorectal surgery? Traditionally, colon & rectal surgery requires a large, abdominal and/or pelvic incision, which often requires a
CONTENTS: WHAT S IN THIS BOOKLET
 Q Questions & A & Answers About Your Prostate Having a biopsy test to find out if you may have prostate cancer can bring up a lot of questions. This booklet will help answer those questions. CONTENTS:
Q Questions & A & Answers About Your Prostate Having a biopsy test to find out if you may have prostate cancer can bring up a lot of questions. This booklet will help answer those questions. CONTENTS:
Basics on Treatment for prostate cancer
 Basics on Treatment for prostate cancer SECTION 1: TREATMENTS This pamphlet provides information about different treatments for prostate cancer including what to expect and any risks and side-effects.
Basics on Treatment for prostate cancer SECTION 1: TREATMENTS This pamphlet provides information about different treatments for prostate cancer including what to expect and any risks and side-effects.
CMScript. Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014
 Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
Background CMScript Member of a medical scheme? Know your guaranteed benefits! Issue 7 of 2014 Prostate cancer is second only to lung cancer as the leading cause of cancer-related deaths in men. It is
Colorectal Cancer Treatment
 Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
Scan for mobile link. Colorectal Cancer Treatment Colorectal cancer overview Colorectal cancer, also called large bowel cancer, is the term used to describe malignant tumors found in the colon and rectum.
PROSTATE CANCER 101 WHAT IS PROSTATE CANCER?
 PROSTATE CANCER 101 WHAT IS PROSTATE CANCER? Prostate cancer is cancer that begins in the prostate. The prostate is a walnut-shaped gland in the male reproductive system located below the bladder and in
PROSTATE CANCER 101 WHAT IS PROSTATE CANCER? Prostate cancer is cancer that begins in the prostate. The prostate is a walnut-shaped gland in the male reproductive system located below the bladder and in
Making the Choice. Deciding What to Do About Early Stage Prostate Cancer
 Making the Choice Deciding What to Do About Early Stage Prostate Cancer We have all faced the same tough choices you face now. We talked with our doctors and others we love and trust. We each made our
Making the Choice Deciding What to Do About Early Stage Prostate Cancer We have all faced the same tough choices you face now. We talked with our doctors and others we love and trust. We each made our
Learning About Prostate Cancer
 Learning About Prostate Cancer Table of Contents Introduction... 1 Clinical services... 1 Appointment scheduling information... 1 Follow-up and support... 2 Prostatectomy... 2 External beam radiation...
Learning About Prostate Cancer Table of Contents Introduction... 1 Clinical services... 1 Appointment scheduling information... 1 Follow-up and support... 2 Prostatectomy... 2 External beam radiation...
Treatment Choices for Men
 National Cancer Institute Treatment Choices for Men With Early-Stage Prostate Cancer U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health Things to Remember Many men with prostate
National Cancer Institute Treatment Choices for Men With Early-Stage Prostate Cancer U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health Things to Remember Many men with prostate
dedicated to curing BREAST CANCER
 dedicated to curing BREAST CANCER When you are diagnosed with breast cancer, you need a team of specialists who will share their knowledge of breast disease and the latest treatments available. At Cancer
dedicated to curing BREAST CANCER When you are diagnosed with breast cancer, you need a team of specialists who will share their knowledge of breast disease and the latest treatments available. At Cancer
After Diagnosis: Prostate Cancer. Understanding Your Treatment Options
 After Diagnosis: Prostate Cancer Understanding Your Treatment Options What s inside How will this booklet help me?... 3 What is the prostate?... 4 What is prostate cancer?... 4 Who gets prostate cancer?...
After Diagnosis: Prostate Cancer Understanding Your Treatment Options What s inside How will this booklet help me?... 3 What is the prostate?... 4 What is prostate cancer?... 4 Who gets prostate cancer?...
Roswell Park scientists and clinicians:
 The Prostate Cancer Center at Roswell Park Connects You to Nationally Recognized Experts for State-of-the-Art Treatment Options and Compassionate, Evidence-based Care Founded in 1898, Roswell Park Cancer
The Prostate Cancer Center at Roswell Park Connects You to Nationally Recognized Experts for State-of-the-Art Treatment Options and Compassionate, Evidence-based Care Founded in 1898, Roswell Park Cancer
Thymus Cancer. This reference summary will help you better understand what thymus cancer is and what treatment options are available.
 Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
Thymus Cancer Introduction Thymus cancer is a rare cancer. It starts in the small organ that lies in the upper chest under the breastbone. The thymus makes white blood cells that protect the body against
The PSA Test for Prostate Cancer Screening:
 For more information, please contact your local VA Medical Center or Health Clinic. U.S. Department of Veterans Affairs Veterans Health Administration Patient Care Services Health Promotion and Disease
For more information, please contact your local VA Medical Center or Health Clinic. U.S. Department of Veterans Affairs Veterans Health Administration Patient Care Services Health Promotion and Disease
Brain Cancer. This reference summary will help you understand how brain tumors are diagnosed and what options are available to treat them.
 Brain Cancer Introduction Brain tumors are not rare. Thousands of people are diagnosed every year with tumors of the brain and the rest of the nervous system. The diagnosis and treatment of brain tumors
Brain Cancer Introduction Brain tumors are not rare. Thousands of people are diagnosed every year with tumors of the brain and the rest of the nervous system. The diagnosis and treatment of brain tumors
What to Expect While Receiving Radiation Therapy for Prostate Cancer
 What to Expect While Receiving Radiation Therapy for Prostate Cancer Princess Margaret Information for patients who are having radiation therapy Read this pamphlet to learn about: The main steps in planning
What to Expect While Receiving Radiation Therapy for Prostate Cancer Princess Margaret Information for patients who are having radiation therapy Read this pamphlet to learn about: The main steps in planning
Prostate Cancer. Treatments as unique as you are
 Prostate Cancer Treatments as unique as you are UCLA Prostate Cancer Program Prostate cancer is the second most common cancer among men. The UCLA Prostate Cancer Program brings together the elements essential
Prostate Cancer Treatments as unique as you are UCLA Prostate Cancer Program Prostate cancer is the second most common cancer among men. The UCLA Prostate Cancer Program brings together the elements essential
Understanding Prostate Cancer. The Urology Group Guide for Newly Diagnosed Patients. Advanced Care. Improving Lives.
 Understanding Prostate Cancer The Urology Group Guide for Newly Diagnosed Patients Advanced Care. Improving Lives. UNDERSTANDING PROSTATE CANCER The Urology Group has created this publication to provide
Understanding Prostate Cancer The Urology Group Guide for Newly Diagnosed Patients Advanced Care. Improving Lives. UNDERSTANDING PROSTATE CANCER The Urology Group has created this publication to provide
Multiple Myeloma. This reference summary will help you understand multiple myeloma and its treatment options.
 Multiple Myeloma Introduction Multiple myeloma is a type of cancer that affects white blood cells. Each year, thousands of people find out that they have multiple myeloma. This reference summary will help
Multiple Myeloma Introduction Multiple myeloma is a type of cancer that affects white blood cells. Each year, thousands of people find out that they have multiple myeloma. This reference summary will help
Prostate Cancer Information and Facts
 Prostate Cancer Information and Facts Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnutsized structure that makes up part of a man's reproductive system.
Prostate Cancer Information and Facts Definition Prostate cancer is cancer that starts in the prostate gland. The prostate is a small, walnutsized structure that makes up part of a man's reproductive system.
Prostate cancer screening. It s YOUR decision!
 Prostate cancer screening It s YOUR decision! For many years now, a test has been available to screen for. The test is called the prostate-specific antigen blood test (or PSA test). It is used in combination
Prostate cancer screening It s YOUR decision! For many years now, a test has been available to screen for. The test is called the prostate-specific antigen blood test (or PSA test). It is used in combination
For further information on screening and early detection of prostate cancer, see the Section entitled Screening for Prostate Cancer.
 Prostate Cancer For many older men, prostate cancer may be present but never cause symptoms or problems and many men will die with their prostate cancer rather than of their prostate cancer. Yet it remains
Prostate Cancer For many older men, prostate cancer may be present but never cause symptoms or problems and many men will die with their prostate cancer rather than of their prostate cancer. Yet it remains
Frequently Asked Questions About Ovarian Cancer
 Media Contact: Gerri Gomez Howard Cell: 303-748-3933 gerri@gomezhowardgroup.com Frequently Asked Questions About Ovarian Cancer What is ovarian cancer? Ovarian cancer is a cancer that forms in tissues
Media Contact: Gerri Gomez Howard Cell: 303-748-3933 gerri@gomezhowardgroup.com Frequently Asked Questions About Ovarian Cancer What is ovarian cancer? Ovarian cancer is a cancer that forms in tissues
male sexual dysfunction
 male sexual dysfunction lack of desire Both men and women often lose interest in sex during cancer treatment, at least for a time. At first, concern for survival is so overwhelming that sex is far down
male sexual dysfunction lack of desire Both men and women often lose interest in sex during cancer treatment, at least for a time. At first, concern for survival is so overwhelming that sex is far down
Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too.
 Male Breast Cancer Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too. Many people do not know that men can get breast
Male Breast Cancer Introduction Breast cancer is cancer that starts in the cells of the breast. Breast cancer happens mainly in women. But men can get it too. Many people do not know that men can get breast
Localised prostate cancer
 Diagnosis Specialist Nurses 0800 074 8383 prostatecanceruk.org 1 Localised prostate cancer In this fact sheet: What is localised prostate cancer? How is localised prostate cancer diagnosed? What do my
Diagnosis Specialist Nurses 0800 074 8383 prostatecanceruk.org 1 Localised prostate cancer In this fact sheet: What is localised prostate cancer? How is localised prostate cancer diagnosed? What do my
Brachytherapy: Low Dose Rate (LDR) Radiation Interstitial Implant
 Brachytherapy: Low Dose Rate (LDR) Radiation Interstitial Implant Goal of the Procedure Brachytherapy, or internal radiation therapy, is a way of giving a higher dose of radiation to the tumor area while
Brachytherapy: Low Dose Rate (LDR) Radiation Interstitial Implant Goal of the Procedure Brachytherapy, or internal radiation therapy, is a way of giving a higher dose of radiation to the tumor area while
Understanding Treatment Choices for Prostate Cancer
 Know Your Options A Prostate Cancer Education Program Understanding Treatment Choices for Prostate Cancer US TOO International, Inc. National Cancer Institute U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES
Know Your Options A Prostate Cancer Education Program Understanding Treatment Choices for Prostate Cancer US TOO International, Inc. National Cancer Institute U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES
Basic Radiation Therapy Terms
 Basic Radiation Therapy Terms accelerated radiation: radiation schedule in which the total dose is given over a shorter period of time. (Compare to hyperfractionated radiation.) adjuvant therapy (add-joo-vunt):
Basic Radiation Therapy Terms accelerated radiation: radiation schedule in which the total dose is given over a shorter period of time. (Compare to hyperfractionated radiation.) adjuvant therapy (add-joo-vunt):
Radiation Therapy and Prostate Cancer
 Radiation Therapy and Prostate Cancer The following information is based on the general experiences of many prostate cancer patients. Your experience may be different. If you have any questions about what
Radiation Therapy and Prostate Cancer The following information is based on the general experiences of many prostate cancer patients. Your experience may be different. If you have any questions about what
INTENSITY MODULATED RADIATION THERAPY (IMRT) FOR PROSTATE CANCER PATIENTS
 INTENSITY MODULATED RADIATION THERAPY (IMRT) FOR PROSTATE CANCER PATIENTS HOW DOES RADIATION THERAPY WORK? Cancer is the unrestrained growth of abnormal cells within the body. Radiation therapy kills both
INTENSITY MODULATED RADIATION THERAPY (IMRT) FOR PROSTATE CANCER PATIENTS HOW DOES RADIATION THERAPY WORK? Cancer is the unrestrained growth of abnormal cells within the body. Radiation therapy kills both
Questions to ask my doctor: About prostate cancer
 Questions to ask my doctor: About prostate cancer Being diagnosed with prostate cancer can be scary and stressful. You probably have a lot of questions and concerns. Learning about the disease, how it
Questions to ask my doctor: About prostate cancer Being diagnosed with prostate cancer can be scary and stressful. You probably have a lot of questions and concerns. Learning about the disease, how it
150640_Brochure_B 4/12/07 2:58 PM Page 2. Patient Information. Freedom From an Enlarged Prostate
 150640_Brochure_B 4/12/07 2:58 PM Page 2 Patient Information Freedom From an Enlarged Prostate 150640_Brochure_B 4/12/07 2:58 PM Page 3 GreenLight Laser Therapy 1 150640_Brochure_B 4/12/07 2:58 PM Page
150640_Brochure_B 4/12/07 2:58 PM Page 2 Patient Information Freedom From an Enlarged Prostate 150640_Brochure_B 4/12/07 2:58 PM Page 3 GreenLight Laser Therapy 1 150640_Brochure_B 4/12/07 2:58 PM Page
Stereotactic Radiotherapy for Prostate Cancer using CyberKnife
 Stereotactic Radiotherapy for Prostate Cancer using CyberKnife Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Stereotactic Radiotherapy for Prostate Cancer using CyberKnife Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Dynamic prostate brachytherapy
 Dynamic prostate brachytherapy a single visit treatment for prostate cancer This leaflet aims to answer your questions about having brachytherapy to treat your prostate cancer. It explains the benefits,
Dynamic prostate brachytherapy a single visit treatment for prostate cancer This leaflet aims to answer your questions about having brachytherapy to treat your prostate cancer. It explains the benefits,
About the Uterus. Hysterectomy may be done to treat conditions that affect the uterus. Some reasons a hysterectomy may be needed include:
 Hysterectomy removal of the uterus is a way of treating problems that affect the uterus. Many conditions can be cured with hysterectomy. Because it is major surgery, your doctor may suggest trying other
Hysterectomy removal of the uterus is a way of treating problems that affect the uterus. Many conditions can be cured with hysterectomy. Because it is major surgery, your doctor may suggest trying other
Understanding. Pancreatic Cancer
 Understanding Pancreatic Cancer Understanding Pancreatic Cancer The Pancreas The pancreas is an organ that is about 6 inches long. It s located deep in your belly between your stomach and backbone. Your
Understanding Pancreatic Cancer Understanding Pancreatic Cancer The Pancreas The pancreas is an organ that is about 6 inches long. It s located deep in your belly between your stomach and backbone. Your
There are many different types of cancer and sometimes cancer is diagnosed when in fact you are not suffering from the disease at all.
 About Cancer Cancer is a disease where there is a disturbance in the normal pattern of cell replacement. The cells mutate and become abnormal or grow uncontrollably. Not all tumours are cancerous (i.e.
About Cancer Cancer is a disease where there is a disturbance in the normal pattern of cell replacement. The cells mutate and become abnormal or grow uncontrollably. Not all tumours are cancerous (i.e.
How is Prostate Cancer Diagnosed?
 Prostate cancer: English Prostate cancer This fact sheet is about how prostate cancer is diagnosed and treated. We also have fact sheets in your language about chemotherapy, radiotherapy, surgery, side
Prostate cancer: English Prostate cancer This fact sheet is about how prostate cancer is diagnosed and treated. We also have fact sheets in your language about chemotherapy, radiotherapy, surgery, side
TheraSphere A Radiation Treatment Option for Liver Cancer
 TheraSphere A Radiation Treatment Option for Liver Cancer TheraSphere is a treatment which is done in the Interventional Radiology Clinic. If you have more questions after reading this handout, you can
TheraSphere A Radiation Treatment Option for Liver Cancer TheraSphere is a treatment which is done in the Interventional Radiology Clinic. If you have more questions after reading this handout, you can
1. What is the prostate-specific antigen (PSA) test?
 1. What is the prostate-specific antigen (PSA) test? Prostate-specific antigen (PSA) is a protein produced by the cells of the prostate gland. The PSA test measures the level of PSA in the blood. The doctor
1. What is the prostate-specific antigen (PSA) test? Prostate-specific antigen (PSA) is a protein produced by the cells of the prostate gland. The PSA test measures the level of PSA in the blood. The doctor
Cancer doesn t care but we do. 2010 Cancer Annual Report
 Cancer doesn t care but we do. 2010 Cancer Annual Report The Cancer Committee of CHRISTUS St. Patrick Hospital is proud to present its 2010 Annual Report. The Community Hospital Comprehensive Cancer Program
Cancer doesn t care but we do. 2010 Cancer Annual Report The Cancer Committee of CHRISTUS St. Patrick Hospital is proud to present its 2010 Annual Report. The Community Hospital Comprehensive Cancer Program
Patient Guide. Brachytherapy: The precise answer for tackling breast cancer. Because life is for living
 Patient Guide Brachytherapy: The precise answer for tackling breast cancer Because life is for living This booklet is designed to provide information that helps women who have been diagnosed with early
Patient Guide Brachytherapy: The precise answer for tackling breast cancer Because life is for living This booklet is designed to provide information that helps women who have been diagnosed with early
Us TOO University Presents: Understanding Diagnostic Testing
 Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Us TOO University Presents: Understanding Diagnostic Testing for Prostate Cancer Patients Today s speaker is Manish Bhandari, MD Program moderator is Pam Barrett, Us TOO International Made possible by
Making the Choice Deciding What to Do About Early Stage Prostate Cancer
 Making the Choice Deciding What to Do About Early Stage Prostate Cancer We have all faced the same tough choices you face now. We talked with our doctors and others we love and trust. We each made our
Making the Choice Deciding What to Do About Early Stage Prostate Cancer We have all faced the same tough choices you face now. We talked with our doctors and others we love and trust. We each made our
Possible Side Effects of Radiation Therapy on the Prostate Gland
 Possible Side Effects of Radiation Therapy on the Prostate Gland Information compiled by Daniel J. Faber, Coordinator of the Warriors+one, a Breakout Group of the Prostate Cancer Canada Network- Ottawa,
Possible Side Effects of Radiation Therapy on the Prostate Gland Information compiled by Daniel J. Faber, Coordinator of the Warriors+one, a Breakout Group of the Prostate Cancer Canada Network- Ottawa,
Screening for Prostate Cancer
 Screening for Prostate Cancer It is now clear that screening for Prostate Cancer discovers the disease at an earlier and more curable stage. It is not yet clear whether this translates into reduced mortality
Screening for Prostate Cancer It is now clear that screening for Prostate Cancer discovers the disease at an earlier and more curable stage. It is not yet clear whether this translates into reduced mortality
Mesothelioma. 1995-2013, The Patient Education Institute, Inc. www.x-plain.com ocft0101 Last reviewed: 03/21/2013 1
 Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Mesothelioma Introduction Mesothelioma is a type of cancer. It starts in the tissue that lines your lungs, stomach, heart, and other organs. This tissue is called mesothelium. Most people who get this
Questions to Ask My Doctor About Prostate Cancer
 Questions to Ask My Doctor Being told you have prostate cancer can be scary and stressful. You probably have a lot of questions and concerns. Learning about the disease, how it s treated, and how this
Questions to Ask My Doctor Being told you have prostate cancer can be scary and stressful. You probably have a lot of questions and concerns. Learning about the disease, how it s treated, and how this
Radiation Therapy in Prostate Cancer Current Status and New Advances
 Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Radiation Therapy Wilhelm Roentgen (1845-1923)
Radiation Therapy in Prostate Cancer Current Status and New Advances Arno J. Mundt MD Professor and Chairman Dept Radiation Oncology Moores Cancer Center UCSD Radiation Therapy Wilhelm Roentgen (1845-1923)
WHEN PROSTATE CANCER RETURNS: ADVANCED PROSTATE CANCER. How Will I Know If My Prostate Cancer Returns?
 WHEN PROSTATE CANCER RETURNS: ADVANCED PROSTATE CANCER (The following information is based on the general experiences of many prostate cancer patients. Your experience may be different.) How Will I Know
WHEN PROSTATE CANCER RETURNS: ADVANCED PROSTATE CANCER (The following information is based on the general experiences of many prostate cancer patients. Your experience may be different.) How Will I Know
RADIATION THERAPY FOR BLADDER CANCER. Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY
 RADIATION THERAPY FOR Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY FACTS ABOUT The bladder is located in the pelvis. It collects and stores
RADIATION THERAPY FOR Facts to Help Patients Make an Informed Decision TARGETING CANCER CARE AMERICAN SOCIETY FOR RADIATION ONCOLOGY FACTS ABOUT The bladder is located in the pelvis. It collects and stores
The following document includes information about:
 Patient information WHAT TO EXPECT WHILE RECEIVING RADIATION THERAPY FOR PROSTATE CANCER Oncology Vitalité Zone : 1B 4 5 6 Facility : Dr. Léon-Richard Oncology Centre The following document includes information
Patient information WHAT TO EXPECT WHILE RECEIVING RADIATION THERAPY FOR PROSTATE CANCER Oncology Vitalité Zone : 1B 4 5 6 Facility : Dr. Léon-Richard Oncology Centre The following document includes information
Smoking and misuse of certain pain medicines can affect the risk of developing renal cell cancer.
 Renal cell cancer Renal cell cancer is a disease in which malignant (cancer) cells form in tubules of the kidney. Renal cell cancer (also called kidney cancer or renal adenocarcinoma) is a disease in which
Renal cell cancer Renal cell cancer is a disease in which malignant (cancer) cells form in tubules of the kidney. Renal cell cancer (also called kidney cancer or renal adenocarcinoma) is a disease in which
Your Health Matters. Localized Prostate Cancer and Its Treatment
 Your Health Matters Localized Prostate Cancer and Its Treatment Greetings! Understanding prostate cancer and choosing among the various treatment options can be a difficult and anxiety-arousing process.
Your Health Matters Localized Prostate Cancer and Its Treatment Greetings! Understanding prostate cancer and choosing among the various treatment options can be a difficult and anxiety-arousing process.
Guide to Understanding Breast Cancer
 An estimated 220,000 women in the United States are diagnosed with breast cancer each year, and one in eight will be diagnosed during their lifetime. While breast cancer is a serious disease, most patients
An estimated 220,000 women in the United States are diagnosed with breast cancer each year, and one in eight will be diagnosed during their lifetime. While breast cancer is a serious disease, most patients
Colorectal Cancer Care A Cancer Care Map for Patients
 Colorectal Cancer Care A Cancer Care Map for Patients Understanding the process of care that a patient goes through in the diagnosis and treatment of colorectal cancer in BC. Colorectal Cancer Care Map
Colorectal Cancer Care A Cancer Care Map for Patients Understanding the process of care that a patient goes through in the diagnosis and treatment of colorectal cancer in BC. Colorectal Cancer Care Map
Breast Cancer. Sometimes cells keep dividing and growing without normal controls, causing an abnormal growth called a tumor.
 Breast Cancer Introduction Cancer of the breast is the most common form of cancer that affects women but is no longer the leading cause of cancer deaths. About 1 out of 8 women are diagnosed with breast
Breast Cancer Introduction Cancer of the breast is the most common form of cancer that affects women but is no longer the leading cause of cancer deaths. About 1 out of 8 women are diagnosed with breast
PROSTATE CANCER. Diagnosis and Treatment
 Diagnosis and Treatment Table of Contents Introduction... 1 Patient and Coach Information... 1 About Your Prostate... 1 What You Should Know About Prostate Cancer... 2 Screening and Diagnosis... 2 Digital
Diagnosis and Treatment Table of Contents Introduction... 1 Patient and Coach Information... 1 About Your Prostate... 1 What You Should Know About Prostate Cancer... 2 Screening and Diagnosis... 2 Digital
Colon and Rectal Cancer
 Colon and Rectal Cancer What is colon or rectal cancer? Colon or rectal cancer is the growth of abnormal cells in your large intestine, which is also called the large bowel. The colon is the last 5 feet
Colon and Rectal Cancer What is colon or rectal cancer? Colon or rectal cancer is the growth of abnormal cells in your large intestine, which is also called the large bowel. The colon is the last 5 feet
Clinical Trials and Radiation Treatment. Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto
 Clinical Trials and Radiation Treatment Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto What I will cover.. A little about radiation treatment The clinical trials
Clinical Trials and Radiation Treatment Gerard Morton Odette Cancer Centre Sunnybrook Research Institute University of Toronto What I will cover.. A little about radiation treatment The clinical trials
Jennifer Fournier, RN MSN AOCN CHPN on 6/16/2012 at Oncology Nursing Society
 SAMPLE This Survivorship Care Plan will facilitate cancer care following active treatment. It may include important contact information, a treatment summary, recommendations for follow-up care testing,
SAMPLE This Survivorship Care Plan will facilitate cancer care following active treatment. It may include important contact information, a treatment summary, recommendations for follow-up care testing,
Analysis of Prostate Cancer at Easter Connecticut Health Network Using Cancer Registry Data
 The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
The 2014 Cancer Program Annual Public Reporting of Outcomes/Annual Site Analysis Statistical Data from 2013 More than 70 percent of all newly diagnosed cancer patients are treated in the more than 1,500
Prostate Cancer & Its Treatment
 Your Health Matters Prostate Cancer & Its Treatment By the UCSF Medical Center Prostate Cancer Advocates Greetings! From our personal experience in dealing with our own prostate cancers, we UCSF Patient
Your Health Matters Prostate Cancer & Its Treatment By the UCSF Medical Center Prostate Cancer Advocates Greetings! From our personal experience in dealing with our own prostate cancers, we UCSF Patient
Locally advanced prostate cancer
 Diagnosis Specialist Nurses 0800 074 8383 prostatecanceruk.org 1 Locally advanced prostate cancer In this fact sheet: What is locally advanced prostate cancer? How is locally advanced prostate cancer diagnosed?
Diagnosis Specialist Nurses 0800 074 8383 prostatecanceruk.org 1 Locally advanced prostate cancer In this fact sheet: What is locally advanced prostate cancer? How is locally advanced prostate cancer diagnosed?
