The Open University s repository of research publications and other research outputs
|
|
|
- Lewis Hicks
- 8 years ago
- Views:
Transcription
1 Open Research Online The Open University s repository of research publications and other research outputs Patients, Professionals and the Internet: Renegotiating the Healthcare Encounter Other How to cite: Laing, Angus; Newholm, Terry; Keeling, Debbie; Spier, Diane; Hogg, Gill; Minocha, Shailey and Davies, Linda (2010). Patients, Professionals and the Internet: Renegotiating the Healthcare Encounter. National Institute of Health Research (NIHR), Service Delivery and Organisation (NIHR SDO) programme, UK. For guidance on citations see FAQs. c 2010 Queen s Printer and Controller of HMSO Version: Version of Record Link(s) to article on publisher s website: Copyright and Moral Rights for the articles on this site are retained by the individual authors and/or other copyright owners. For more information on Open Research Online s data policy on reuse of materials please consult the policies page. oro.open.ac.uk
2 EVALUATING MODELS OF HEALTH SERVICE DELIVERY PROGRAMME OF RESEARCH ON THE ACCEPTABILITY AND APPLICABILITY OF E-HEALTH STRATEGIES TO MEET THE AIMS OF THE NHS AND THE NATIONAL PROGRAMME FOR INFORMATION TECHNOLOGY Introduction The introduction of new technologies into NHS practice and service delivery has accelerated in the last six years. The term e-health was first used by the NHS in 1998 in the NHS Executive report, Information for Health: An Information Strategy for the Modern NHS (1). However, the term e-health has since been adopted and interpreted in many different ways. For example, a recent SDOcommissioned scoping exercise identified 51 unique definitions of e-health (2). Within the NHS, e-government has been contextualised within the NHS Plan which requires the use of new technology to design an NHS designed around the patient. Building the Information Core (3) contains specific targets that relate to the implementation of e-health systems, linked to the NHS core principles of a seamless service, and which are respectful of confidentiality of individual patients and open access to services, treatment and performance. Targets for the implementation of e-health technologies have been introduced and revisited over the years. Policy guidance from the Department of Health (4) reviewed these targets set out in the 1998 NHS Executive report and whilst the delivery dates of many have been pushed back, others have been brought forward. For example, the total coverage of all GPs to be using e-booking (now known as Choose and Book ) for some hospital appointments and out-of-hours remote access have been advanced from 2008 to Most recently the National Programme for Information Technology (NPfIT) has focused on procuring and implementing IT in the NHS to improve patient care. It is an essential element in delivering the NHS Plan since it aims to create an integrated 1 NHS Executive. Information for Health: An Information Strategy for the Modern NHS (September 1998) 2 Pagliari, C., and Gregor, P. Literature review of traditional research databases, draft report to SDO, 2004 ( 3 NHS Executive, Building the Information Core Implementing the NHS Plan, January Department of Health, Delivering 21st Century Support to the NHS: National Strategic Plan,2002
3 information infrastructure to improve patient care through empowering patients and improving the efficiency and effectiveness in the way clinicians and other NHS staff work. The programme has four particular goals: electronic appointment booking, an electronic care records service, electronic transmission of prescriptions, and fast, reliable underlying IT infrastructure. Its aim is to transform the way information flows around the health service, making it possible to deliver faster, safer and more convenient patient care. At the same time it's giving patients the information they need to look after their own health. (5) The value of e-health in the coming years needs to be placed in the context of the aims of NPfIT: to improve the health and well-being of the population. The appropriateness of any new approach must therefore be assessed in the following areas: Its acceptability to and usability by patients and carers; Its impact and contribution to improved health outcomes and enhanced quality of life; Its safety when it is used by those for whom it is intended, as well as by others Its cost-effectiveness and cost-efficiency (in financial and human resources terms); Its contribution to addressing health inequalities and promoting universal access to, and acceptability of, ICT systems amongst patients; and Its cross-sector accessibility/inclusiveness, including independent/private healthcare providers, local authority departments (such as social services, education, and housing), voluntary sector agencies, the police and other stakeholders committed to health improvement. Although there is excitement around perceived benefits and (the) rush forward with collaborative opportunities using advanced technologies in health information, research is needed in order to demonstrate the value of e-health in meeting the aims and goals of the NHS and to help inform the successful implementation of NPfIT and future IT policies. Current call for proposals This SDO research programme aims to investigate the value of e-health in meeting the aims and goals of the NHS and, in particular, is aimed at examining how e- Health can empower patients, the public and clinicians in making use of the internet or other electronic media in the access and use of health and lifestyle information or services. To this end, the SDO Programme is inviting research proposals in three topic areas under its programme of research on the acceptability and applicability of e-health in meeting the aims of the NHS. This programme of research cuts across, and relates closely to, the other themes within which the SDO programme works, for example, on continuity of care, access to health services, and change management (see ONE project will be funded in each of the following three topic areas: 5
4 EH93 - Harnessing the internet as an effective health information tool to empower patients, carers and members of the general public EH94 - The attitudes of health care professionals to e-health technologies and services, and the identification of strategies to support increased uptake EH95 - A study of the use of e-health solutions in the management and treatment of disease and in facilitating change in the organisation and delivery of services Applicants should familiarise themselves with relevant research already commissioned by other NHS R&D programmes (such as the Policy Research Programme and the Health Technology Assessment Programme) to ensure that they can demonstrate that their proposals do not duplicate other research. In particular, applicants should read and show familiarity with the results of the two SDOcommissioned scoping exercises which have been used to inform this call for proposals (Pagliari SDO/60/2003; Jones SDO/59/2003) ( Applicants should also refer to the general criteria for prioritising research topics, developed and agreed by the SDO Programme board, available on the SDO website ( Those interested in submitting a proposal for any of the topics should note that a two-stage commissioning process is being used and applicants are invited to submit outline research proposals by Wednesday 20 th April EH93: Harnessing the internet as an effective health information tool to empower patients, carers and members of the general public Research suggests there are around 70,000 internet sites worldwide disseminating health information issues (Pagliari and Gregor, 2004). In April 2004, some 49 per cent of UK households were connected to the internet (National Statistics estimate). Recent research has revealed how such web-based interventions have improved knowledge and/or behavioural outcomes amongst users (Dean et al, 2004). However, systematic literature reviews of the consumer use of online health information make clear that there is little evidence of the effect this may have on health outcomes (Bessell et al, 2002). Qualitative research has demonstrated that internet-users are most likely to assess the credibility of a website by considering its source, the professionalism of the design, the use of scientific or official language, and ease of use (Pagliari and Gregor, 2004). However, internet users are less likely to check the quality of the information being provided by, for example, examining the about us sections of the website, disclaimers or disclosure statements. Such evidence also suggests that the internet is used by patients and carers most often to retrieve information on a range of public health issues such as smoking cessation guidance, cardiac and nutritional advice. Reasons for using internet resources in this way appear to be that they are more convenient; timely; anonymous; compared with the information not readily available elsewhere (Pagliari and Gregor, 2004).
5 Although qualitative research has identified scepticism amongst internet users of some web-based information, many see it as an important source of health-related information. Access to internet resources has also been shown to be inequitable, with many potential users hindered by the lack of the necessary computer equipment, technophobia, problematic design features, off-putting technical language, and lack of permanence of some sites (Pagliari and Gregor, 2004). The purpose of this research is to: understand how and why consumers use the internet for health care information and services; examine what subsequent actions they take, and how this effects their behaviour and health status; review and assess the degree of inequity in access to, and acceptability of, the internet for health advice and information by people of different ages, gender, socio-economic class and ethnicity; assess the internet s value in improving patients self-management and health behaviour; examine methods of best practice in supporting the use of internet-based health advice by patients and the public; assess the extent to which patient use of the internet can and should be employed as part of the overall NPfIT in terms of its ability to empower patients, carers and members of the general public. Specific questions that need to be addressed include: What is the potential impact of internet-based health information resources on health outcomes? o What is the likely impact on outcomes in the primary care or secondary care sector? o What are the findings from the many pilots or projects exploring the use of the internet by patients/carers that have been conducted in the public health field? How do consumers use the internet for health care information and services? o What actions do consumers take after accessing health care information? o Do these actions have an impact upon health status and empowerment? What systems and structures exist by which internet information on health advice can be assessed for quality? o To what extent do UK-based health-related websites adhere to a set of quality standards? o To what extent is such information awarded a mark for quality assurance? o Are systems that introduce quality marks more effective and efficient at directing consumers toward worthwhile information? To what extent do inequities exist in access to and use of health-related internet sites?
6 o Examine this question in relation to age, gender, ethnicity, education, family income, social class and other relevant factors What is the role of the Public and Patient Involvement Groups and the Expert Patient Programme in supporting internet use? What can be learnt from projects within the NHS that encourage and support patients/carers in the use of the internet? What lessons can be learnt from outside the NHS, for example, from voluntary sector agencies working with age-, gender-, or ethnic communities? o Can models be applied from non-health related fields? What methods can best be employed to support patients and the general public to improve their search and appraisal skills in order to help them discern and select useful, or best-quality, health-related information. What is the potential for a partnership approach, including healthcare and public health professionals and e-health developers, to educate and guide patients and the general public in their search and appraisal skills? To what extent can and should patients use of the internet be integrated within wider strategies employed within the NPfIT? Methods Applicants for the study should provide a clear conceptual and theoretical grounding for this research, and should be encouraged to explore a variety of research methods to include both review and empirically-based approaches. Applicants should clearly outline their proposed methods for carrying out this research including a process for identifying and assessing internet-based health information resources. The nature of the research study may require the development of a variety of qualitative and quantitative research methods and may include the collection of statistical and other data where appropriate. Applicants should demonstrate that they have a research team in place with the appropriate research skills. Indication should be provided about how they will work with the SDO Programme and relevant stakeholders to build in an active programme for disseminating their research findings in policy, practice and research contexts. The methodology should clearly show how interim findings will be available to inform policy developments such as NPfIT. Outputs The principal output of this research project will be a detailed report containing details of the research and its findings. The report will also need to include: A short and coherent executive summary of no more than three pages; A full account of the methods used in the research project, including a critical appraisal of these methods; Rigorous and detailed conclusions that examine the use and acceptability of the internet for health advice, its value in improving self-management and health behaviour, and models of best practice; A commentary that indicates how these findings relate to current policy and practice in the NHS, and the key lessons to be learned; and
7 An agenda that establishes the key areas for further research and the appropriate methods that should be used in this research. Successful applicants may be required to present their completed work to the SDO Programme Board. Interim findings will be required on a yearly basis to inform policy developments. References Bessell, T., McDonald, S., Silagy, S., Anderson, J., Hiller, J. and Sansom, L. (2002), Do Internet interventions for consumers cause more harm than good? A systematic review, Health Expectations, 5 (1): Wantland, D, Portillo J, Holzemer W, Slaughter R and McGhee E (2004). The Effectiveness of Web-Based vs. Non-Web-Based Interventions: A Meta-Analysis of Behavioural Change Outcomes. J Med Internet Res, 11, 10; 6(4):e40 Pagliari, C. and Gregor, P (2004). Literature review of traditional research databases, report to SDO, EH94: The attitudes of health care professionals to e-health technologies and services and the identification of strategies to support increased uptake Studies have shown that the uptake of e-health clinical decision support systems and other computer-based systems by healthcare professionals has been variable (Pagliari and Gregor, 2004). This variability has been argued to be the result of a number of factors, including: the lack of involvement of healthcare professionals during the development and implementation phase; the perceived extra time required to use e-health systems; the varying quality of web-based medical information; incompatible systems across and between disciplines and institutions; and a lack of guaranteed patient privacy and confidentiality of data. Within primary care, a few systematic comparative studies have been done to assess the effect of web-based information resources on quality, accessibility or cost of the delivery of care (Pagliari and Gregor, 2004). A study of Scottish GPs in 1999, for example, found that few GPs used to communicate with patients, citing the lack of data privacy and additional workload as barriers to implementation. It suggested that GPs needed more training in the use of the internet and other computer-based systems and that this was not a core activity in GP practices. Nonetheless, the research showed the potential for electronic information to be used for accessing medical and patient data, supporting clinical and other staff, and for informing patients (see Pagliari and Gregor, 2004). A key challenge in the implementation of new e-health technologies is to ensure that clinicians are engaged and supportive of the process. This research study will examine the factors that influence professionals to use (and not to use) e-health systems and other computerised tools. Specific attention within the research should be placed on the attitudes of professionals to the use of new information systems,
8 particularly those being developed between organizational and professional boundaries (for example, Choose and Book) and systems such as shared clinical record systems. Specific questions for the research will include: To what extent are new e-health technologies challenging the cultural and structural norms in which professionals work? What is the attitude of professionals towards the use of new information systems and technologies? o What are the roots of resistance to the use of new e-health systems and how can they be overcome? o Are the factors that help and hinder the uptake of computer-based systems similar across the secondary and primary care sectors and in social care? To what extent is the impact of e-health tools and systems before, during and after the patient consultation positive or detrimental? o What impact does it have on the nature of patient-professional communications and relationships? What role should clinicians and other healthcare professionals play in the development and implementation of e-health systems? What kind of support and training is appropriate, acceptable and effective to healthcare professionals in the primary and secondary care sectors to increase utilisation? o What are the training and support needs in this area, and to what extent do these differ between the primary and secondary care sectors? What can be learnt from the strategies used to develop, implement and enhance the uptake of internet or computer-based tools for professionals in other fields? Methods Applicants for the study should provide a clear conceptual and theoretical grounding for this research, and will be encouraged to explore a variety of research methods. Applicants should clearly outline their proposed methods for carrying out this research including a process for identifying and assessing the attitudes of professionals in different sectors towards the use and development of clinical decision support systems. Where necessary, applicants are encouraged to develop innovative research methodologies. The nature of the research study may require a variety of qualitative and quantitative methods and the use of different case examples. Applicants should demonstrate that they have a research team in place with the appropriate research skills. Indication should be provided about how they will work with the SDO Programme and relevant stakeholders to build in an active programme for disseminating their research findings in policy, practice and research contexts. The methodology should clearly show how interim findings will be available to inform policy developments such as NPfIT.
9 Outputs The principal output of this research project will be a detailed report containing details of the research and its findings. The report will also need to include: A short and coherent executive summary of no more than three pages; A full account of the methods used in the research project, including a critical appraisal of these methods; Rigorous and detailed conclusions that examine the extent to which primary and secondary care clinicians use and/or resist e-health tools; support and training needs to improve utilisation; and the impact of such tools on the clinician-patient relationship. A commentary that indicates how these findings relate to current policy and practice in the NHS and the key lessons to be learned; and An agenda that establishes the key areas for further research and the appropriate methods that should be used in this research. Successful applicants may be required to present their completed work to the SDO Programme Board. Interim findings will be required on a yearly basis to inform policy developments. References Pagliari, C. and Gregor, P (2004). Literature review of traditional research databases, report to SDO ( EH95: A review of the use of e-health solutions in the management and treatment of diseases and in facilitating change in the organisation and delivery of services. There is optimism that the uptake of computer based systems and tools, including clinical decision support tools, telemedicine and internet-based tools, will facilitate improved use of medical records, improved detection of adverse incidents, better communication with patients and information-sharing with other professionals, and rapid access to medical information for both clinician and patient. E-Health solutions also have been promoted for their potential to support research activity and the management of health systems in general. However, little evidence currently exists of a positive impact on health outcomes in particular disease areas. Moreover, the ability of new information systems to bring about cultural and structural change has yet to be examined. A review of e-health systems in one or more disease or client-based areas where usage is relatively advanced has the potential to identify the generic factors that facilitate and hinder uptake and acceptance of information systems by both patients and healthcare professionals. Fruitful areas to study may be those disease areas where telemedicine and information technology have been well established and where applications supporting high quality treatment now exist in clinical management, education, decision support and modelling. Suggested disease areas for consideration, therefore, might include diabetes, stroke, coronary heart disease
10 and/or cancer. Consultations from distant locations have been made possible in these areas by the development of high-speed networks which enable transmission of good quality photographs and/or information. Since the conditions manifest themselves in acute and chronic scenarios, benefits can be achieved through regular patient monitoring, drug compliance monitoring, patient reassurance and selfmanagement all of which can be supported by the use of electronic and computerbased systems by patients and carers. However, e-health systems come at a cost to the local Primary Care Trust and acute Hospital Trust and the implementation of e- health solutions will require strict cost-effectiveness and outcome monitoring and analysis. This review will study e-health systems in specific areas of disease management and treatment to develop principles of good practice that can be used to inform practice in other disease areas and to help inform the successful development of NPfIT. This study will involve the identification of several examples in England of innovative practice in the use of e-health systems in the treatment and management of disease in order to explore the following questions: To what extent does the process through which e-health systems are introduced, developed and implemented have consequences for their effective use and implementation thereafter? o What are the generic lessons or best practice for the process of establishing new e-health systems? What are the key success factors and/or barriers in the development of new e-health systems? What can be learnt from the role of patients and carers in the development and implementation of the service? o To what extent has the Expert Patient Programme been influential? What are the additional training and support needs for patients/carers and different groups of healthcare professionals? o Have any programmes been evaluated? What different e-health systems have been used, by whom, with what degree of satisfaction and impact on health behaviours? o Where is there a need for improved technological systems, and what disease treatment and management needs are still unmet by e-health systems? Methods Applicants for the study should provide a clear conceptual and theoretical grounding for this research, and should be encouraged to explore a variety of research methods to include both review and empirically-based approaches. Applicants should clearly outline their proposed methods for carrying out this research including a process for identifying relevant disease areas and methods for assessing best practice. The nature of the research study may require the development of a variety of qualitative and quantitative research methods and may include the collection of statistical and other data where appropriate. In addition, applicants may consider the examination of different case examples.
11 Applicants should demonstrate that they have a research team in place with the appropriate research skills. Indication should be provided about how they will work with the SDO Programme and relevant stakeholders to build in an active programme for disseminating their research findings in policy, practice and research contexts. The methodology should clearly show how interim findings will be available to inform policy developments such as NPfIT. Outputs The principal output of this research project will be a detailed report containing details of the research and its findings. The report will also need to include: A short and coherent executive summary of no more than three pages; A full account of the methods used in the research project, including a critical appraisal of these methods; Rigorous and detailed conclusions that examine the use and effectiveness of e-health solutions in the management and treatment of the disease area(s) and their acceptability to patients and health-care professionals. A commentary that indicates how these findings relate to current policy and practice in the NHS and the key lessons to be learned including generic lessons for the use of e-health in other areas of chronic disease management; and An agenda that establishes the key areas for further research and the appropriate methods that should be used in this research. Successful applicants may be required to present their completed work to the SDO Programme Board. Interim findings will be required on a yearly basis to inform policy developments. Application process The process of commissioning each of these three studies will be in two stages and applicants should submit outline proposals. Applicants must submit proposals using the A4 Outline Proposal application form, which is available as a Word 97 file or Rich text format from: the SDO website: or by from: Donna.Cox@LSHTM.ac.uk Please do not use any previously obtained version of an SDO Programme application form.
12 Applicants are asked to submit proposals by Wednesday 20 th April 2005 at 1pm to: Donna Cox Commissioning Manager NCCSDO London School of Hygiene and Tropical Medicine 99 Gower Street London WC1E 6AZ AN ORIGINAL PLUS TWENTY-FIVE HARD COPIES (double sided) of the completed A4 Outline Proposal application form should be submitted together with a copy on disk or CD. Please note we will not accept electronic submissions or hand written proposals. No late applications will be considered. To ensure the efficient and equitable answering of additional queries, all questions about this new scheme should be sent by only to Donna.Cox@LSHTM.ac.uk with the words e-health Question in the subject header. Questions received by 11 th March 2005 will have generic answers posted on the SDO website ( by 18 th March No other correspondence about this call can be entered into. Guidance notes for the completion of the Outline Proposal application form can be found at the front of the application form. Funding of up to 300,000 is available for funding each of the three projects in this topic area. Applicants should note that value for money is an important consideration in respect of this research. Proposed costs of the project should not exceed the limits stated above. Following submission of outline proposals successful applicants will be notified no later than early June They will then be invited to submit full proposal by late July The outcome of the review of full proposals will be notified by late October The project should take no longer than 3 years to complete and start no later than December Please note that these dates are approximate and may be subject to change. In addition, applicants should indicate how they will work with the SDO Programme and relevant stakeholders to build in an active program for disseminating their research findings in policy, practice and research contexts. The SDO Programme will look favorably on proposals which include an element of research capacity building. Please clearly label the outside of the envelope in which you submit your proposal with the following: Tender Documents EH (Appropriate Reference Number). This will enable us to identify proposals and keep them aside so that they may all be opened together after the closing date and time.
13 Teams should ensure that their proposal complies with the Research Governance Framework, which can be found on the Department of Health website, or via a link on the SDO website under the Call for Proposals page. Before funding, successful teams will be required to provide proof of research ethics committee approval for their project, if this is required (information regarding this can be found on the SDO website under the Calls for Proposals page). We anticipate that there will be informal discussions with NCCSDO throughout the duration of the project regarding the final report. Applicants should visit the SDO website: to familiarise themselves with the work of the SDO Programme in general and with previous scoping exercises in other topic areas.
14 Addendum This document was published by the National Coordinating Centre for the Service Delivery and Organisation (NCCSDO) research programme, managed by the London School of Hygiene & Tropical Medicine. The management of the Service Delivery and Organisation (SDO) programme has now transferred to the National Institute for Health Research Evaluations, Trials and Studies Coordinating Centre (NETSCC) based at the University of Southampton. Prior to April 2009, NETSCC had no involvement in the commissioning or production of this document and therefore we may not be able to comment on the background or technical detail of this document. Should you have any queries please contact
PUBLIC HEALTH LIMITED OPEN CALL SCHEME (LOCS) PHA202 RESEARCH BRIEFING
 Introduction PUBLIC HEALTH LIMITED OPEN CALL SCHEME (LOCS) PHA202 RESEARCH BRIEFING Following publication of its new national health research strategy Best Research for Best Health (DH 2006a), the Department
Introduction PUBLIC HEALTH LIMITED OPEN CALL SCHEME (LOCS) PHA202 RESEARCH BRIEFING Following publication of its new national health research strategy Best Research for Best Health (DH 2006a), the Department
PROGRAMME OF RESEARCH ON EVALUATING MODELS OF SERVICE DELIVERY
 PROGRAMME OF RESEARCH ON EVALUATING MODELS OF SERVICE DELIVERY CALL FOR PROPOSALS FOR EMPIRICAL RESEARCH ON MATERNITY SERVICES: AN EVALUATION OF MIDWIFERY-LED UNITS As part of its programme of research
PROGRAMME OF RESEARCH ON EVALUATING MODELS OF SERVICE DELIVERY CALL FOR PROPOSALS FOR EMPIRICAL RESEARCH ON MATERNITY SERVICES: AN EVALUATION OF MIDWIFERY-LED UNITS As part of its programme of research
BriefingPaper. Towards faster treatment: reducing attendance and waits at emergency departments ACCESS TO HEALTH CARE OCTOBER 2005
 ACCESS TO HEALTH CARE OCTOBER 2005 BriefingPaper Towards faster treatment: reducing attendance and waits at emergency departments Key messages based on a literature review which investigated the organisational
ACCESS TO HEALTH CARE OCTOBER 2005 BriefingPaper Towards faster treatment: reducing attendance and waits at emergency departments Key messages based on a literature review which investigated the organisational
Consultation Response Medical profiling and online medicine: the ethics of 'personalised' healthcare in a consumer age Nuffield Council on Bioethics
 Consultation Response Medical profiling and online medicine: the ethics of 'personalised' healthcare in a consumer age Nuffield Council on Bioethics Response by the Genetic Interest Group Question 1: Health
Consultation Response Medical profiling and online medicine: the ethics of 'personalised' healthcare in a consumer age Nuffield Council on Bioethics Response by the Genetic Interest Group Question 1: Health
Specification Document (11/1023)
 Responsive funding in the NIHR SDO programme: open call (with special interest in studies with an economic/costing component) Closing date 1.00pm on 15 September 2011 1. Introduction This is the fifth
Responsive funding in the NIHR SDO programme: open call (with special interest in studies with an economic/costing component) Closing date 1.00pm on 15 September 2011 1. Introduction This is the fifth
CALL FOR PROPOSALS. 1 Introduction and overview
 EVALUATING A WHOLE SYSTEM TRANSFORMATION OF A GROUP OF HEALTHCARE PROVIDER AND COMMISSIONING ORGANISATIONS BASED ON TOYOTA PRODUCTION SYSTEM REF: LM257 1 Introduction and overview CALL FOR PROPOSALS The
EVALUATING A WHOLE SYSTEM TRANSFORMATION OF A GROUP OF HEALTHCARE PROVIDER AND COMMISSIONING ORGANISATIONS BASED ON TOYOTA PRODUCTION SYSTEM REF: LM257 1 Introduction and overview CALL FOR PROPOSALS The
National Assembly for Wales: Health and Social Care Committee
 2 Ashtree Court, Woodsy Close Cardiff Gate Business Park Cardiff CF23 8RW Tel: 029 2073 0310 wales@rpharms.com www.rpharms.com 18 th October 2011 Submission to: Call for Evidence: Response from: National
2 Ashtree Court, Woodsy Close Cardiff Gate Business Park Cardiff CF23 8RW Tel: 029 2073 0310 wales@rpharms.com www.rpharms.com 18 th October 2011 Submission to: Call for Evidence: Response from: National
Incident reporting policy National Chlamydia Screening Programme
 Incident reporting policy National Chlamydia Screening Programme Date of publication: November 2014 Date for review: November 2016 About Public Health England Public Health England exists to protect and
Incident reporting policy National Chlamydia Screening Programme Date of publication: November 2014 Date for review: November 2016 About Public Health England Public Health England exists to protect and
Evaluation of a Primary Care Dermatology Service: final report
 Evaluation of a Primary Care Dermatology Service: final report Report for the National Co-ordinating Centre for NHS Service Delivery and Organisation R&D (NCCSDO) December 2005 prepared by Chris Salisbury*
Evaluation of a Primary Care Dermatology Service: final report Report for the National Co-ordinating Centre for NHS Service Delivery and Organisation R&D (NCCSDO) December 2005 prepared by Chris Salisbury*
Better Skills Better Jobs Better Health. National occupational standards for the practice of public health guide
 Better Skills Better Jobs Better Health National occupational standards for the practice of public health guide March 2004 Acknowledgements These national occupational standards describe good practice
Better Skills Better Jobs Better Health National occupational standards for the practice of public health guide March 2004 Acknowledgements These national occupational standards describe good practice
JOINT DIRECTOR OF PUBLIC HEALTH JOB DESCRIPTION
 JOINT DIRECTOR OF PUBLIC HEALTH JOB DESCRIPTION Employing organisation: London Borough Waltham Forest Grade/Salary: 88-98,000 (permanent). Interim Daily Rate 910. Responsible to: Deputy Chief Executive
JOINT DIRECTOR OF PUBLIC HEALTH JOB DESCRIPTION Employing organisation: London Borough Waltham Forest Grade/Salary: 88-98,000 (permanent). Interim Daily Rate 910. Responsible to: Deputy Chief Executive
A literature review on the structure and performance of not-for-profit health care organisations
 A literature review on the structure and performance of not-for-profit health care organisations Report for the National Co-ordinating Centre for NHS Service Delivery and Organisation R & D (NCCSDO) February
A literature review on the structure and performance of not-for-profit health care organisations Report for the National Co-ordinating Centre for NHS Service Delivery and Organisation R & D (NCCSDO) February
Information systems in health care breaking down barriers or creating more?
 To be published in Dilemmas in Human Services 2010 Ed. J. Radcliffe and M. Dent Information systems in health care breaking down barriers or creating more? Ken Eason Emeritus Professor of Cognitive Ergonomics
To be published in Dilemmas in Human Services 2010 Ed. J. Radcliffe and M. Dent Information systems in health care breaking down barriers or creating more? Ken Eason Emeritus Professor of Cognitive Ergonomics
HEALTH SYSTEM. Introduction. The. jurisdictions and we. Health Protection. Health Improvement. Health Services. Academic Public
 FUNCTIONS OF THE LOCAL PUBLIC HEALTH SYSTEM Introduction This document sets out the local PH function in England. It was originally drafted by a working group led by Maggie Rae, FPH Local Board Member
FUNCTIONS OF THE LOCAL PUBLIC HEALTH SYSTEM Introduction This document sets out the local PH function in England. It was originally drafted by a working group led by Maggie Rae, FPH Local Board Member
BriefingPaper. The access/relationship trade off: how important is continuity of primary care to patients and their carers?
 CONTINUITY OF CARE SEPTEMBER 2006 BriefingPaper The access/relationship trade off: how important is continuity of primary care to patients and their carers? Key messages Patients want both quick access
CONTINUITY OF CARE SEPTEMBER 2006 BriefingPaper The access/relationship trade off: how important is continuity of primary care to patients and their carers? Key messages Patients want both quick access
Improving children s health can nurses, midwives and health visitors make a difference? Key messages
 NURSING AND MIDWIFERY MARCH 2007 ResearchSummary Improving children s health can nurses, midwives and health visitors make a difference? Children s health services in the UK are improving all the time,
NURSING AND MIDWIFERY MARCH 2007 ResearchSummary Improving children s health can nurses, midwives and health visitors make a difference? Children s health services in the UK are improving all the time,
A Health and Wellbeing Strategy for Bexley Listening to you, working for you
 A Health and Wellbeing Strategy for Bexley Listening to you, working for you www.bexley.gov.uk Introduction FOREWORD Health and wellbeing is everybody s business, and our joint aim is to improve the health
A Health and Wellbeing Strategy for Bexley Listening to you, working for you www.bexley.gov.uk Introduction FOREWORD Health and wellbeing is everybody s business, and our joint aim is to improve the health
JOB DESCRIPTION. Advanced Nurse Practitioner Professional Lead
 JOB DESCRIPTION JOB TITLE: RESPONSIBLE TO: LOCATION(S): JOB PROFILE: Advanced Nurse Practitioner Advanced Nurse Practitioner Professional Lead North Bristol Trust Southmead Hospital This role is to work
JOB DESCRIPTION JOB TITLE: RESPONSIBLE TO: LOCATION(S): JOB PROFILE: Advanced Nurse Practitioner Advanced Nurse Practitioner Professional Lead North Bristol Trust Southmead Hospital This role is to work
DIRECTOR OF PUBLIC HEALTH ROLE PROFILE
 Appendix A DIRECTOR OF PUBLIC HEALTH ROLE PROFILE Title: Employing Organisation: Accountable to: Hours: Work base: Key Relationships Director of Public Health London Borough of Tower Hamlets Professionally
Appendix A DIRECTOR OF PUBLIC HEALTH ROLE PROFILE Title: Employing Organisation: Accountable to: Hours: Work base: Key Relationships Director of Public Health London Borough of Tower Hamlets Professionally
Harness Care Cooperative Ltd Quality primary care services provided through local cooperation Company registration: 06584450
 Harness Care Cooperative Ltd Quality primary care services provided through local cooperation Company registration: 06584450 Job Description Job title: Nurse Practitioner /Lead Nurse ACCOUNTIBILITY The
Harness Care Cooperative Ltd Quality primary care services provided through local cooperation Company registration: 06584450 Job Description Job title: Nurse Practitioner /Lead Nurse ACCOUNTIBILITY The
Delivering Local Health Care
 Delivering Local Health Care Accelerating the pace of change Delivering Local Integrated Care Accelerating the Pace of Change WG 17711 Digital ISBN 978 1 0496 0 Crown copyright 2013 2 Contents Joint foreword
Delivering Local Health Care Accelerating the pace of change Delivering Local Integrated Care Accelerating the Pace of Change WG 17711 Digital ISBN 978 1 0496 0 Crown copyright 2013 2 Contents Joint foreword
Code of Conduct. Property of UKAPA 20/11/2009 1
 Code of Conduct A Physician Assistant (now associate) (PA) is defined as someone who is: a new healthcare professional who, while not a doctor, works to the medical model, with the attitudes, skills and
Code of Conduct A Physician Assistant (now associate) (PA) is defined as someone who is: a new healthcare professional who, while not a doctor, works to the medical model, with the attitudes, skills and
How To Improve Safety In The Nhs
 PS035 Original research completed in 2010 Briefing Paper Introduction: Principal Investigator: Professor John Clarkson Should the NHS adopt a new system for predicting possible risks to patient safety?
PS035 Original research completed in 2010 Briefing Paper Introduction: Principal Investigator: Professor John Clarkson Should the NHS adopt a new system for predicting possible risks to patient safety?
Supporting information for appraisal and revalidation: guidance for General Practitioners
 Supporting information for appraisal and revalidation: guidance for General Practitioners Based on the Academy of Medical Royal Colleges and Faculties Core for all doctors 2 Supporting information for
Supporting information for appraisal and revalidation: guidance for General Practitioners Based on the Academy of Medical Royal Colleges and Faculties Core for all doctors 2 Supporting information for
IMPROVING DENTAL CARE AND ORAL HEALTH A CALL TO ACTION. February 2014 Gateway reference: 01173
 1 IMPROVING DENTAL CARE AND ORAL HEALTH A CALL TO ACTION February 2014 Gateway reference: 01173 2 Background NHS dental services are provided in primary care and community settings, and in hospitals for
1 IMPROVING DENTAL CARE AND ORAL HEALTH A CALL TO ACTION February 2014 Gateway reference: 01173 2 Background NHS dental services are provided in primary care and community settings, and in hospitals for
Patient Choice at the Point of GP Referral
 DEPARTMENT OF HEALTH Patient Choice at the Point of GP Referral LONDON: The Stationery Office 9.25 Ordered by the House of Commons to be printed on 17 January 2005 REPORT BY THE COMPTROLLER AND AUDITOR
DEPARTMENT OF HEALTH Patient Choice at the Point of GP Referral LONDON: The Stationery Office 9.25 Ordered by the House of Commons to be printed on 17 January 2005 REPORT BY THE COMPTROLLER AND AUDITOR
Good Scientific Practice
 Section 1: The purpose of this document There are three key components to the Healthcare Science workforce in the UK: 1. Healthcare Science Associates and Assistants who perform a diverse range of task
Section 1: The purpose of this document There are three key components to the Healthcare Science workforce in the UK: 1. Healthcare Science Associates and Assistants who perform a diverse range of task
Systematic Reviews. knowledge to support evidence-informed health and social care
 Systematic Reviews knowledge to support evidence-informed health and social care By removing uncertainties in science and research, systematic reviews ensure that only the most effective and best-value
Systematic Reviews knowledge to support evidence-informed health and social care By removing uncertainties in science and research, systematic reviews ensure that only the most effective and best-value
Policy Statement 16/2006. Acute and Multidisciplinary Working
 RCN Policy Unit Policy Statement 16/2006 Acute and Multidisciplinary Working The Royal College of Nursing of the United Kingdom and the Royal College of Physicians (London) September 2006 Royal College
RCN Policy Unit Policy Statement 16/2006 Acute and Multidisciplinary Working The Royal College of Nursing of the United Kingdom and the Royal College of Physicians (London) September 2006 Royal College
Self Care in New Zealand
 Self Care in New Zealand A roadmap toward greater personal responsibility in managing health Prepared by the New Zealand Self Medication Industry Association. July 2009 What is Self Care? Self Care describes
Self Care in New Zealand A roadmap toward greater personal responsibility in managing health Prepared by the New Zealand Self Medication Industry Association. July 2009 What is Self Care? Self Care describes
Department of Health/ Royal College of General Practitioners. Implementing a scheme for General Practitioners with Special Interests
 Department of Health/ Royal College of General Practitioners Implementing a scheme for General Practitioners with Special Interests April 2002 Foreword Improved access and consistently high quality services
Department of Health/ Royal College of General Practitioners Implementing a scheme for General Practitioners with Special Interests April 2002 Foreword Improved access and consistently high quality services
Good Practice Guidelines for Appraisal
 Good Practice Guidelines for Appraisal Dr Laurence Mynors Wallis Dr David Fearnley February 2010 1 Contents Page Introduction 3 Link between appraisal and revalidation 4 Preparation for the appraisal meeting
Good Practice Guidelines for Appraisal Dr Laurence Mynors Wallis Dr David Fearnley February 2010 1 Contents Page Introduction 3 Link between appraisal and revalidation 4 Preparation for the appraisal meeting
Delivering Quality in Primary Care National Action Plan. implementing the Healthcare Quality Strategy for NHSScotland
 Delivering Quality in Primary Care National Action Plan implementing the Healthcare Quality Strategy for NHSScotland Delivering Quality in Primary Care National Action Plan implementing the Healthcare
Delivering Quality in Primary Care National Action Plan implementing the Healthcare Quality Strategy for NHSScotland Delivering Quality in Primary Care National Action Plan implementing the Healthcare
Improving Emergency Care in England
 Improving Emergency Care in England REPORT BY THE COMPTROLLER AND AUDITOR GENERAL HC 1075 Session 2003-2004: 13 October 2004 LONDON: The Stationery Office 11.25 Ordered by the House of Commons to be printed
Improving Emergency Care in England REPORT BY THE COMPTROLLER AND AUDITOR GENERAL HC 1075 Session 2003-2004: 13 October 2004 LONDON: The Stationery Office 11.25 Ordered by the House of Commons to be printed
Prime Minister s Challenge Fund (PMCF): Improving Access to General Practice. Innovation Showcase Series Using Technology to Improve Access
 Prime Minister s Challenge Fund (PMCF): Improving Access to General Practice Innovation Showcase Series Using Technology to Improve Access February 2015: Showcase Two About PMCF In October 2013, the Prime
Prime Minister s Challenge Fund (PMCF): Improving Access to General Practice Innovation Showcase Series Using Technology to Improve Access February 2015: Showcase Two About PMCF In October 2013, the Prime
JOB DESCRIPTION NURSE PRACTITIONER
 JOB DESCRIPTION NURSE PRACTITIONER TITLE OF POST: NURSE PRACTITIONER : GENERAL PRACTICE /OUT OF HOURS SALARY : To be negotiated HOURS OF EMPLOYMENT: To be agreed APPOINTMENT: Permanent contract RESPONSIBLE
JOB DESCRIPTION NURSE PRACTITIONER TITLE OF POST: NURSE PRACTITIONER : GENERAL PRACTICE /OUT OF HOURS SALARY : To be negotiated HOURS OF EMPLOYMENT: To be agreed APPOINTMENT: Permanent contract RESPONSIBLE
Submission by the Irish Pharmacy Union to the Department of Health on the Scope for Private Health Insurance to incorporate Additional Primary Care
 Submission by the Irish Pharmacy Union to the Department of Health on the Scope for Private Health Insurance to incorporate Additional Primary Care Services January 2015 1 IPU Submission to the Department
Submission by the Irish Pharmacy Union to the Department of Health on the Scope for Private Health Insurance to incorporate Additional Primary Care Services January 2015 1 IPU Submission to the Department
Information Governance and Management Standards for the Health Identifiers Operator in Ireland
 Information Governance and Management Standards for the Health Identifiers Operator in Ireland 30 July 2015 About the The (the Authority or HIQA) is the independent Authority established to drive high
Information Governance and Management Standards for the Health Identifiers Operator in Ireland 30 July 2015 About the The (the Authority or HIQA) is the independent Authority established to drive high
How To Share Your Health Records With The National Health Service
 HOW WE USE YOUR PERSONAL INFORMATION Information Leaflet Your Health. Our Priority. Page 2 of 9 Introduction This Leaflet explains why the NHS collects information about you and how it is used, your right
HOW WE USE YOUR PERSONAL INFORMATION Information Leaflet Your Health. Our Priority. Page 2 of 9 Introduction This Leaflet explains why the NHS collects information about you and how it is used, your right
NHS Innovator Accelerator. Guidance note - for completing the application form
 NHS Innovator Accelerator Guidance note - for completing the application form Guidance note - for completing the application form Please read the Call for Applications before completing the application
NHS Innovator Accelerator Guidance note - for completing the application form Guidance note - for completing the application form Please read the Call for Applications before completing the application
Industry Charter. Introduction. Context
 Industry Charter Introduction This short document is aimed at all industry that has an interest in working with the NHS. It sets out how Imperial College Health Partners, the Academic Health Science Network
Industry Charter Introduction This short document is aimed at all industry that has an interest in working with the NHS. It sets out how Imperial College Health Partners, the Academic Health Science Network
Governance. Information. Bulletin. Welcome to the nineteenth edition of the information governance bulletin
 Welcome to the nineteenth edition of the information governance bulletin Our regular bulletin about information governance and the work of the IG transition programme Publication Gateway Reference: 02465
Welcome to the nineteenth edition of the information governance bulletin Our regular bulletin about information governance and the work of the IG transition programme Publication Gateway Reference: 02465
ehealth Competencies for Undergraduate Medical Education
 ehealth Competencies for Undergraduate Medical Education Created by The Association of Faculties of Medicine of Canada in Partnership with Canada Health Infoway, May 2014 Contents Contents Acknowledgements...
ehealth Competencies for Undergraduate Medical Education Created by The Association of Faculties of Medicine of Canada in Partnership with Canada Health Infoway, May 2014 Contents Contents Acknowledgements...
SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST EXECUTIVE SUMMARY COUNCIL OF GOVERNORS 2 ND DECEMBER 2014
 SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST C EXECUTIVE SUMMARY COUNCIL OF GOVERNORS 2 ND DECEMBER 2014 Subject: Supporting Director: Author: Status 1 NHS England Five Year Forward View A Summary
SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST C EXECUTIVE SUMMARY COUNCIL OF GOVERNORS 2 ND DECEMBER 2014 Subject: Supporting Director: Author: Status 1 NHS England Five Year Forward View A Summary
Online Access to Electronic Medical Records and Service in Primary Care
 Online Access to Electronic Medical Records and Service in Primary Care Dr Freda Mold Professor Simon de Lusignan Wednesday, 29 April 2015 1 Contents Overview 1. Research Overview 2. Methods 3. Findings
Online Access to Electronic Medical Records and Service in Primary Care Dr Freda Mold Professor Simon de Lusignan Wednesday, 29 April 2015 1 Contents Overview 1. Research Overview 2. Methods 3. Findings
Connection with other policy areas and (How does it fit/support wider early years work and partnerships)
 Illness such as gastroenteritis and upper respiratory tract infections, along with injuries caused by accidents in the home, are the leading causes of attendances at Accident & Emergency and hospitalisation
Illness such as gastroenteritis and upper respiratory tract infections, along with injuries caused by accidents in the home, are the leading causes of attendances at Accident & Emergency and hospitalisation
Priorities and strategies for successful EHR adoption
 HIQA Electronic Health Records Workshop Priorities and strategies for successful EHR adoption Dr Dipak Kalra Centre for Health Informatics and Multiprofessional Education (CHIME) University College London
HIQA Electronic Health Records Workshop Priorities and strategies for successful EHR adoption Dr Dipak Kalra Centre for Health Informatics and Multiprofessional Education (CHIME) University College London
MANCHESTER MENTAL HEALTH AND SOCIAL CARE TRUST and DIVISION OF CLINICAL PSYCHOLOGY UNIVERSITY OF MANCHESTER
 MANCHESTER MENTAL HEALTH AND SOCIAL CARE TRUST and DIVISION OF CLINICAL PSYCHOLOGY UNIVERSITY OF MANCHESTER Doctorate of Clinical Psychology Post of Trainee Clinical Psychologist JOB DESCRIPTION Job Title
MANCHESTER MENTAL HEALTH AND SOCIAL CARE TRUST and DIVISION OF CLINICAL PSYCHOLOGY UNIVERSITY OF MANCHESTER Doctorate of Clinical Psychology Post of Trainee Clinical Psychologist JOB DESCRIPTION Job Title
Evaluation of the first year of the Inner North West London Integrated Care Pilot. Summary May 2013. In partnership with
 Evaluation of the first year of the Inner North West London Integrated Care Pilot Summary May 2013 In partnership with 2 The North West London Integrated Care Pilot is a large-scale programme incorporating
Evaluation of the first year of the Inner North West London Integrated Care Pilot Summary May 2013 In partnership with 2 The North West London Integrated Care Pilot is a large-scale programme incorporating
A Route Map to the 2020 Vision for Health and Social Care
 A Route Map to the 2020 Vision for Health and Social Care 02 A Route Map to the 2020 Vision for Health and Social Care Introduction This paper sets out a new and accelerated focus on a number of priority
A Route Map to the 2020 Vision for Health and Social Care 02 A Route Map to the 2020 Vision for Health and Social Care Introduction This paper sets out a new and accelerated focus on a number of priority
Information Governance Strategy
 Information Governance Strategy Document Status Draft Version: V2.1 DOCUMENT CHANGE HISTORY Initiated by Date Author Information Governance Requirements September 2007 Information Governance Group Version
Information Governance Strategy Document Status Draft Version: V2.1 DOCUMENT CHANGE HISTORY Initiated by Date Author Information Governance Requirements September 2007 Information Governance Group Version
The Evaluation of the Welsh Assembly Government Inequalities in Health Fund 2001-2007. Executive Summary. Welsh Institute for Health and Social Care
 The Evaluation of the Welsh Assembly Government Inequalities in Health Fund 2001-2007 Welsh Institute for Health and Social Care This document was produced as a joint publication between WIHSC and WAG
The Evaluation of the Welsh Assembly Government Inequalities in Health Fund 2001-2007 Welsh Institute for Health and Social Care This document was produced as a joint publication between WIHSC and WAG
NHS WIRRAL / METROPOLITAN BOROUGH OF WIRRAL JOINT DIRECTOR OF PUBLIC HEALTH JOB DESCRIPTION. Joint Director of Public Health (Full Time/Job Share)
 NHS WIRRAL / METROPOLITAN BOROUGH OF WIRRAL JOINT DIRECTOR OF PUBLIC HEALTH JOB DESCRIPTION Employing organisation: Title: Accountable to: Managerially responsible for: NHS Wirral Joint Director of Public
NHS WIRRAL / METROPOLITAN BOROUGH OF WIRRAL JOINT DIRECTOR OF PUBLIC HEALTH JOB DESCRIPTION Employing organisation: Title: Accountable to: Managerially responsible for: NHS Wirral Joint Director of Public
Sharing Healthcare Records
 Summary Care Record has been used by healthcare professionals for a number of years records a summary of key health information these records enable healthcare professionals to treat you safely if you
Summary Care Record has been used by healthcare professionals for a number of years records a summary of key health information these records enable healthcare professionals to treat you safely if you
NATIONAL STATISTICS TO MONITOR THE NHS CANCER PLAN - REPORT OF A PRE SCOPING STUDY
 NATIONAL STATISTICS TO MONITOR THE NHS CANCER PLAN - REPORT OF A PRE SCOPING STUDY Statistics Commission Report No 2 May Statistics Commission Statistics Commission Report No. 2 National Statistics to
NATIONAL STATISTICS TO MONITOR THE NHS CANCER PLAN - REPORT OF A PRE SCOPING STUDY Statistics Commission Report No 2 May Statistics Commission Statistics Commission Report No. 2 National Statistics to
Informatics: The future. An organisational summary
 Informatics: The future An organisational summary DH INFORMATION READER BOX Policy HR/Workforce Management Planning/Performance Clinical Document Purpose Commissioner Development Provider Development Improvement
Informatics: The future An organisational summary DH INFORMATION READER BOX Policy HR/Workforce Management Planning/Performance Clinical Document Purpose Commissioner Development Provider Development Improvement
Research is everybody s business
 Research and Development Strategy (DRAFT) 2013-2018 Research is everybody s business 1 Information Reader Box to be inserted for documents six pages and over. (To be inserted in final version, after consultation
Research and Development Strategy (DRAFT) 2013-2018 Research is everybody s business 1 Information Reader Box to be inserted for documents six pages and over. (To be inserted in final version, after consultation
Essentials of RESEARCH GOVERNANCE
 Promoting Good Practice in Research Essentials of RESEARCH GOVERNANCE Information for Researchers, Students and Support Staff involved in Health & Social Care Research 2005 Reproduced with the permission
Promoting Good Practice in Research Essentials of RESEARCH GOVERNANCE Information for Researchers, Students and Support Staff involved in Health & Social Care Research 2005 Reproduced with the permission
INFORMATION GOVERNANCE POLICY
 INFORMATION GOVERNANCE POLICY Issued by: Senior Information Risk Owner Policy Classification: Policy No: POLIG001 Information Governance Issue No: 1 Date Issued: 18/11/2013 Page No: 1 of 16 Review Date:
INFORMATION GOVERNANCE POLICY Issued by: Senior Information Risk Owner Policy Classification: Policy No: POLIG001 Information Governance Issue No: 1 Date Issued: 18/11/2013 Page No: 1 of 16 Review Date:
PROGRAMME SPECIFICATION
 PROGRAMME SPECIFICATION KEY FACTS Programme name Master of Public Health Award Master of Public Health (MPH) School Health Sciences Department or equivalent Health Services Research and Management Programme
PROGRAMME SPECIFICATION KEY FACTS Programme name Master of Public Health Award Master of Public Health (MPH) School Health Sciences Department or equivalent Health Services Research and Management Programme
ehealth: the future of health care Royal College of Nursing position statement
 ehealth: the future of health care Royal College of Nursing position statement EHEALTH: THE FUTURE OF HEALTH CARE 2 Nursing staff form the largest group of health care professionals, and because of their
ehealth: the future of health care Royal College of Nursing position statement EHEALTH: THE FUTURE OF HEALTH CARE 2 Nursing staff form the largest group of health care professionals, and because of their
Better Outcomes for People Living with Chronic and Complex Health Conditions through Primary Health Care
 Submission: Primary Health Care Advisory Group Discussion Paper (August 2015) Better Outcomes for People Living with Chronic and Complex Health Conditions through Primary Health Care August 2015 Contact
Submission: Primary Health Care Advisory Group Discussion Paper (August 2015) Better Outcomes for People Living with Chronic and Complex Health Conditions through Primary Health Care August 2015 Contact
Job Description. Line Management of a small team of staff administrating and managing patient and professional feedback and incidents.
 Job Description Job Title Pay Band Base Dept./Team Responsible to Accountable to Responsible for Complaints, Incidents and Governance Manager New Alderley House, Macclesfield Eastern Cheshire Clinical
Job Description Job Title Pay Band Base Dept./Team Responsible to Accountable to Responsible for Complaints, Incidents and Governance Manager New Alderley House, Macclesfield Eastern Cheshire Clinical
Balance of Care Inquiry Scottish Campaign for Cardiac Rehabilitation
 It may be surgery that brings you to the foothills of the Alps, but it's the Cardiac Rehabilitation Programme that gets you over them.' Heart patient, Ayrshire and Arran Introduction The was launched in
It may be surgery that brings you to the foothills of the Alps, but it's the Cardiac Rehabilitation Programme that gets you over them.' Heart patient, Ayrshire and Arran Introduction The was launched in
Diabetes: Factsheet. Tower Hamlets Joint Strategic Needs Assessment 2010-2011. Executive Summary. Recommendations
 Diabetes: Factsheet Tower Hamlets Joint Strategic Needs Assessment 2010-2011 Executive Summary Diabetes is a long term condition that affects 11,859 people in Tower Hamlets, as a result of high levels
Diabetes: Factsheet Tower Hamlets Joint Strategic Needs Assessment 2010-2011 Executive Summary Diabetes is a long term condition that affects 11,859 people in Tower Hamlets, as a result of high levels
Patient Choice Strategy
 Patient Choice Strategy Page 1 of 14 Contents Page 1 Background 4 2 Putting Patients and the Public at the Heart of Health and 5 Healthcare in West Lancashire 3 Where are we now and where do we need to
Patient Choice Strategy Page 1 of 14 Contents Page 1 Background 4 2 Putting Patients and the Public at the Heart of Health and 5 Healthcare in West Lancashire 3 Where are we now and where do we need to
Standards of proficiency. Occupational therapists
 Standards of proficiency Occupational therapists Contents Foreword 1 Introduction 3 Standards of proficiency 7 Foreword We are pleased to present the Health and Care Professions Council s standards of
Standards of proficiency Occupational therapists Contents Foreword 1 Introduction 3 Standards of proficiency 7 Foreword We are pleased to present the Health and Care Professions Council s standards of
Director of Communications. Ref: DC14/15. Candidate Brief
 Ref: DC14/15 Candidate Brief December 2015 Job Title: Reporting to: Salary: Location: Website: Director of Communications Chief Executive (Nigel Edwards) Competitive package London www.nuffieldtrust.org.uk
Ref: DC14/15 Candidate Brief December 2015 Job Title: Reporting to: Salary: Location: Website: Director of Communications Chief Executive (Nigel Edwards) Competitive package London www.nuffieldtrust.org.uk
Overview of the UK Health Sector: the NHS. Frances Pennell-Buck
 Overview of the UK Health Sector: the NHS Frances Pennell-Buck AGENDA Healthcare Sector in the UK Overview of the National Health Service (NHS) Recent transition where are we now? NHS England Five Year
Overview of the UK Health Sector: the NHS Frances Pennell-Buck AGENDA Healthcare Sector in the UK Overview of the National Health Service (NHS) Recent transition where are we now? NHS England Five Year
Guide for Clinical Audit Leads
 Guide for Clinical Audit Leads Nancy Dixon and Mary Pearce Healthcare Quality Quest March 2011 Clinical audit tool to promote quality for better health services Contents 1 Introduction 1 1.1 Who this
Guide for Clinical Audit Leads Nancy Dixon and Mary Pearce Healthcare Quality Quest March 2011 Clinical audit tool to promote quality for better health services Contents 1 Introduction 1 1.1 Who this
Doctor of Clinical Psychology
 Doctor of Clinical Psychology Programme of study for the degree of Doctor of Clinical Psychology 1. The following may be accepted as a candidate for the degree of Doctor of Clinical Psychology: Graduates
Doctor of Clinical Psychology Programme of study for the degree of Doctor of Clinical Psychology 1. The following may be accepted as a candidate for the degree of Doctor of Clinical Psychology: Graduates
One in Four Lives. The Future of Telehealth in Australia
 One in Four Lives The Future of Telehealth in Australia March 2014 Lisa Altman Shehaan Fernando Samuel Holt Anthony Maeder George Margelis Gary Morgan Suzanne Roche Contributing to a Sustainable Australian
One in Four Lives The Future of Telehealth in Australia March 2014 Lisa Altman Shehaan Fernando Samuel Holt Anthony Maeder George Margelis Gary Morgan Suzanne Roche Contributing to a Sustainable Australian
Event-based data dissemination control in healthcare
 Event-based data dissemination control in healthcare Jatinder Singh and Jean Bacon Computing Laboratory University of Cambridge firstname.lastname@cl.cam.ac.uk Abstract. There is a movement in healthcare
Event-based data dissemination control in healthcare Jatinder Singh and Jean Bacon Computing Laboratory University of Cambridge firstname.lastname@cl.cam.ac.uk Abstract. There is a movement in healthcare
NHS Leeds South and East CCG Governing Body Meeting
 Agenda Item: LSEGB2014/06 FOI Exempt: No NHS Leeds South and East CCG Governing Body Meeting Date of meeting: 23rd January 2014 Title: Primary Care Engagement Lead Board Member: Dr Jackie Campbell, Director
Agenda Item: LSEGB2014/06 FOI Exempt: No NHS Leeds South and East CCG Governing Body Meeting Date of meeting: 23rd January 2014 Title: Primary Care Engagement Lead Board Member: Dr Jackie Campbell, Director
How To Write The Joint Strategic Needs Assessment For Rutland
 Rutland JSNA Executive summary Aim of the JSNA This Joint Strategic Needs assessment is the means by which Leicestershire County and Rutland PCT and Rutland County Council will describe the current and
Rutland JSNA Executive summary Aim of the JSNA This Joint Strategic Needs assessment is the means by which Leicestershire County and Rutland PCT and Rutland County Council will describe the current and
Executive Summary and Recommendations: National Audit of Learning Disabilities Feasibility Study
 Executive Summary and Recommendations: National Audit of Learning Disabilities Feasibility Study Contents page Executive Summary 1 Rationale and potential impact of a future audit 2 Recommendations Standards
Executive Summary and Recommendations: National Audit of Learning Disabilities Feasibility Study Contents page Executive Summary 1 Rationale and potential impact of a future audit 2 Recommendations Standards
Job Description Psychology Services
 Job Description Psychology Services Job Title Accountable to - Trainee Clinical Psychologist - Clinical Tutor, Director of Clinical Practice and Course Director Grade - Trainee Psychologist, Agenda for
Job Description Psychology Services Job Title Accountable to - Trainee Clinical Psychologist - Clinical Tutor, Director of Clinical Practice and Course Director Grade - Trainee Psychologist, Agenda for
The National Health Service. Constitution. A draft for consultation, July 2008
 The National Health Service Constitution A draft for consultation, July 2008 NHS Constitution The NHS belongs to the people. It is there to improve our health, supporting us to keep mentally and physically
The National Health Service Constitution A draft for consultation, July 2008 NHS Constitution The NHS belongs to the people. It is there to improve our health, supporting us to keep mentally and physically
Socio-economic benefits of interoperable electronic health record systems in Europe the evidence -
 Socio-economic benefits of interoperable electronic health record systems in Europe the evidence - Karl A. Stroetmann FRSM PhD MBA with Alexander Dobrev, Tom Jones, Yvonne Vatter empirica Communication
Socio-economic benefits of interoperable electronic health record systems in Europe the evidence - Karl A. Stroetmann FRSM PhD MBA with Alexander Dobrev, Tom Jones, Yvonne Vatter empirica Communication
Map 1 Statutory specialist services and organisations in England
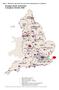 Map 1 Statutory specialist services and organisations in England Isle of Man 31 Neuro Rehab Units (YDU) Spinal Injury Centres Brain Injury Services - NHS Brain Injury Service non NHS Stroke Units Regional
Map 1 Statutory specialist services and organisations in England Isle of Man 31 Neuro Rehab Units (YDU) Spinal Injury Centres Brain Injury Services - NHS Brain Injury Service non NHS Stroke Units Regional
THE ROLE OF HEALTH INFORMATION TECHNOLOGY IN PATIENT-CENTERED CARE COLLABORATION. 2012 Louisiana HIPAA & EHR Conference Presenter: Chris Williams
 THE ROLE OF HEALTH INFORMATION TECHNOLOGY IN PATIENT-CENTERED CARE COLLABORATION 2012 Louisiana HIPAA & EHR Conference Presenter: Chris Williams Agenda Overview Impact of HIT on Patient-Centered Care (PCC)
THE ROLE OF HEALTH INFORMATION TECHNOLOGY IN PATIENT-CENTERED CARE COLLABORATION 2012 Louisiana HIPAA & EHR Conference Presenter: Chris Williams Agenda Overview Impact of HIT on Patient-Centered Care (PCC)
Dundee e-health Centre of Excellence
 Dundee e-health Centre of Excellence 1 Arthritis Research UK, British Heart Foundation Cancer Research UK Economic and Social Research Council Engineering and Physical Sciences Research Council National
Dundee e-health Centre of Excellence 1 Arthritis Research UK, British Heart Foundation Cancer Research UK Economic and Social Research Council Engineering and Physical Sciences Research Council National
NICE Implementation Collaborative Concordat
 NICE Implementation Collaborative Concordat Foreword Innovation has always been at the heart of the NHS. Access to innovative medicines, technologies, devices, diagnostics and treatments has transformed
NICE Implementation Collaborative Concordat Foreword Innovation has always been at the heart of the NHS. Access to innovative medicines, technologies, devices, diagnostics and treatments has transformed
Townsville NBN diabetes in-home monitoring trial Dr Karen Carlisle Townsville-Mackay Medicare Local
 Townsville NBN diabetes in-home monitoring trial Dr Karen Carlisle Townsville-Mackay Medicare Local The Trial is supported by funding from the Australian Government under the Digital Regions Initiative
Townsville NBN diabetes in-home monitoring trial Dr Karen Carlisle Townsville-Mackay Medicare Local The Trial is supported by funding from the Australian Government under the Digital Regions Initiative
WSIC Integrated Care Record FAQs
 WSIC Integrated Care Record FAQs How your information is shared now Today, all the places where you receive care keep records about you. They can usually only share information from your records by letter,
WSIC Integrated Care Record FAQs How your information is shared now Today, all the places where you receive care keep records about you. They can usually only share information from your records by letter,
Date of birth Gender NHS number (if known) Town/Country of birth. Home Telephone no. Work Telephone no.
 ADULT - FEB 15 Office use only Staff initials Date ID seen Welcome to Wokingham Medical Centre Thank you for completing this registration form. When registering in person at the surgery please supply two
ADULT - FEB 15 Office use only Staff initials Date ID seen Welcome to Wokingham Medical Centre Thank you for completing this registration form. When registering in person at the surgery please supply two
Doing Well, Doing Better. Standards for Health Services in Wales
 Doing Well, Doing Better Standards for Health Services in Wales April 2010 Foreword by the Assembly Minister for Health and Social Services The Healthcare Standards for Wales (2005) framework has been
Doing Well, Doing Better Standards for Health Services in Wales April 2010 Foreword by the Assembly Minister for Health and Social Services The Healthcare Standards for Wales (2005) framework has been
The National Occupational Standards. Social Work. Topss UK Partnership
 The National Occupational Standards for Social Work Topss UK Partnership May 2002.doc &.pdf files edition Every effort has been made to keep the file sizes of this document to a manageable size. This edition
The National Occupational Standards for Social Work Topss UK Partnership May 2002.doc &.pdf files edition Every effort has been made to keep the file sizes of this document to a manageable size. This edition
Chronic Disease Management Systems for the Treatment and Management of Diabetes in Primary Health Care Practices in Ontario: OHTAC Recommendation
 Chronic Disease Management Systems for the Treatment and Management of Diabetes in Primary Health Care Practices in Ontario: OHTAC Recommendation Ontario Health Technology Advisory Committee April 2014
Chronic Disease Management Systems for the Treatment and Management of Diabetes in Primary Health Care Practices in Ontario: OHTAC Recommendation Ontario Health Technology Advisory Committee April 2014
Process for reporting and learning from serious incidents requiring investigation
 Process for reporting and learning from serious incidents requiring investigation Date: 9 March 2012 NHS South of England Process for reporting and learning from serious incidents requiring investigation
Process for reporting and learning from serious incidents requiring investigation Date: 9 March 2012 NHS South of England Process for reporting and learning from serious incidents requiring investigation
JOB TITLE: Data Quality/IT Manager
 JOB DESCRIPTION JOB TITLE: Data Quality/IT Manager RESPONSIBLE TO: PRACTICE MANAGER PARTNERS SALARY: Starting From 25000 HOURS: 35 Hours The post-holder will need to become familiar with all functions
JOB DESCRIPTION JOB TITLE: Data Quality/IT Manager RESPONSIBLE TO: PRACTICE MANAGER PARTNERS SALARY: Starting From 25000 HOURS: 35 Hours The post-holder will need to become familiar with all functions
The White Paper Valuing People: A. Diabetes and Me: learning disabilities and diabetes. Julia Kelly
 Diabetes and Me: Learning disabilities and diabetes Julia Kelly Article points 1. There is very little comprehensive education material available regarding diabetes education for adults with learning disabilities.
Diabetes and Me: Learning disabilities and diabetes Julia Kelly Article points 1. There is very little comprehensive education material available regarding diabetes education for adults with learning disabilities.
Primary care drug and alcohol treatment: commissioning and provision against a backdrop of localism
 Primary care drug and alcohol treatment: commissioning and provision against a backdrop of localism This joint paper considers the future impact of the changing commissioning environment on primary care
Primary care drug and alcohol treatment: commissioning and provision against a backdrop of localism This joint paper considers the future impact of the changing commissioning environment on primary care
The Way Forward: Strategic clinical networks
 The Way Forward: Strategic clinical networks The Way Forward Strategic clinical networks First published: 26 July 2012 Prepared by NHS Commissioning Board, a special health authority Contents Foreword...
The Way Forward: Strategic clinical networks The Way Forward Strategic clinical networks First published: 26 July 2012 Prepared by NHS Commissioning Board, a special health authority Contents Foreword...
Standards of proficiency. Operating department practitioners
 Standards of proficiency Operating department practitioners Contents Foreword 1 Introduction 3 Standards of proficiency 7 Foreword We are pleased to present the Health and Care Professions Council s standards
Standards of proficiency Operating department practitioners Contents Foreword 1 Introduction 3 Standards of proficiency 7 Foreword We are pleased to present the Health and Care Professions Council s standards
Best Practice Policy
 Best Practice Policy Reference No: P_CIG_06 Version: Version 3 Ratified by: LCHS Trust Board Date ratified: 29 th July 2014 Name of originator/author: Name of responsible committee/individual: Deputy Chief
Best Practice Policy Reference No: P_CIG_06 Version: Version 3 Ratified by: LCHS Trust Board Date ratified: 29 th July 2014 Name of originator/author: Name of responsible committee/individual: Deputy Chief
Job Description. Wilson Health Centre, Cranmer Road, Mitcham, Surrey, CR4 4TP. Practice Manager / Clinical Manager (Clinical Matters)
 Job Description Job Title: Job Location: Responsible to: Hours of work: Salary: Nurse Practitioner (NP) Wilson Health Centre, Cranmer Road, Mitcham, Surrey, CR4 4TP Practice Manager / Clinical Manager
Job Description Job Title: Job Location: Responsible to: Hours of work: Salary: Nurse Practitioner (NP) Wilson Health Centre, Cranmer Road, Mitcham, Surrey, CR4 4TP Practice Manager / Clinical Manager
Standards of proficiency. Dietitians
 Standards of proficiency Dietitians Contents Foreword 1 Introduction 3 Standards of proficiency 7 Foreword We are pleased to present the Health and Care Professions Council s standards of proficiency for
Standards of proficiency Dietitians Contents Foreword 1 Introduction 3 Standards of proficiency 7 Foreword We are pleased to present the Health and Care Professions Council s standards of proficiency for
Big Chat 4. Strategy into action. NHS Southport and Formby CCG
 Big Chat 4 Strategy into action NHS Southport and Formby CCG Royal Clifton Hotel, Southport, 19 November 2014 Contents What is the Big Chat? 3 About Big Chat 4 4 How the event worked 4 Presentations 5
Big Chat 4 Strategy into action NHS Southport and Formby CCG Royal Clifton Hotel, Southport, 19 November 2014 Contents What is the Big Chat? 3 About Big Chat 4 4 How the event worked 4 Presentations 5
